Empowering patient participation fosters continuous innovation in cataract surgery.
B eyond the Numbers

The Philosophy of Innovation
What one famous ophthalmologist learned from a Buddhist lesson.
Femtosecond Keratoplasty
Comes of Age
Intraoperative OCT and other innovations improve safety and efficacy.
Need to Know: HOAs
A comprehensive guide to understanding visual metrics.

14 Cover
Beyond the Numbers
Empowering patient participation fosters continuous innovation in cataract surgery.
24 Avoiding Posterior Capsule Rupture
Namrata Sharma MD, FRCOphth, FRCS(Ed) and Abhay R Vasavada MS, FRCS(Eng)
26 Picture This: Photo Contest Winners
28 Should Fuchs’ Dystrophy Patients Get Premium Lenses?
Pavel Studeny MD, PhD
29 AI in IOL Power Selection
Nambi Nallasamy MD
30 The Philosophy of Innovation
Reay H Brown MD
32 Interpreting OCT Changes in Glaucoma Patient Care
Sanjay G Asrani MD

34 Exploring Best Practices in Fungal Keratitis Treatment
Namrata Sharma MD, FRCOphth, FRCS(Ed)
35 Keratitis: Suggested Protocols by Evidence
Mor Dickman MD, PhD
36 Has Femtosecond Keratoplasty Come of Age?
Jod Mehta MBBS, FRCOphth, FRCS(Ed), FAMS, PhD
38 Need to Know: Visual Metrics
Soosan Jacob MS, FRCS, DNB
40 Autograft Hunting in LSCD
Marc Muraine MD
42 Corneal Surgery’s Contribution to Climate Change
Matteo Airaldi MD and Alfredo Borgia MD, FEBO
43 Systemised AI for Surfer’s Disease
Carolin Elhardt MD
DIGITAL OPHTHALMOLOGY
44 Four AI Applications Ready for Practice
Gregory A Eippert MD; Mark Packer MD, FACS; Grayson Armstrong MD, MPH; and Mitchell P Weikert MD, MS
46 AI-Assisted Cataract Surgery
Ryan G Smith MD
PAEDIATRIC OPHTHALMOLOGY
48 Making Myopia Consensus Accessible
Ken K Nischal MD, FAAP, FRCOphth and Dominique Brémond-Gignac MD, PhD, FEBO
US UPDATE
50 Aid Cuts Threaten Global Eye Care Progress


Publisher
Filomena Ribeiro
Executive Editor
Stuart Hales
Editor-In-Chief
Sean Henahan
Senior Content Editor
Kelsey Ingram
Creative Director
Kelsy McCarthy
Graphic Designer
Jennifer Lacey
Circulation Manager
Lucy Matthews


Contributing Editors
Cheryl Guttman Krader
Howard Larkin Roibeárd O’hÉineacháin
Contributors
Laura Gaspari
Soosan Jacob
Priscilla Lynch
Timothy Norris
Andrew Sweeney
Colour and Print
CitiPost

Advertising Sales
Roo Khan
MCI UK
Tel: +44 203 530 0100 | roo.khan@wearemci.com
EuroTimes® is registered with the European Union Intellectual Property Office and the US Patent and Trademark Office.
Published by the European Society of Cataract and Refractive Surgeons, Suite 7–9 The Hop Exchange, 24 Southwark Street, London, SE1 1TY, UK. No part of this publication may be reproduced without the permission of the executive editor. Letters to the editor and other unsolicited contributions are assumed intended for this publication and are subject to editorial review and acceptance.

ESCRS EuroTimes is not responsible for statements made by any contributor. These contributions are presented for review and comment and not as a statement on the standard of care. Although all advertising material is expected to conform to ethical medical standards, acceptance does not imply endorsement by ESCRS EuroTimes. ISSN 1393-8983


Learn more about EuroTimes or connect with ESCRS at ESCRS.org


Centre of Attention
What does patient-centred care mean? Surely all care is patient centred. It means considering the patient’s perspective—their fears, questions, needs, and expectations.
In our cover story, Laura Gaspari delves into the important role patient-reported outcome measures (PROMs) play in helping understand patients’ experiences. PROMs have become a key tool in evaluating the quality of surgical procedures, benchmarking, and researching and developing new techniques and technologies to further improve cataract surgery.
Cataract surgery was among the first areas of medicine to use PROMs to improve vision care under the guidance of Professor Mats Lundström in Sweden, who designed the standard Catquest patient questionnaire, used in conjunction with the Swedish National Cataract Registry. This then expanded to the European Registry of Quality Outcomes for Cataract and Refractive Surgery (EUREQUO), developed by the ESCRS and guided by Anders Behndig MD, PhD. Free to ESCRS members, EUREQUO allows surgeons to upload their own cases, compare results, and develop benchmarks using the ever-expanding online database.
PROMS surveys revealed there is more to patient satisfaction than a 20/20 result. Early on, they underscored the importance of dysphotopsia and other adverse effects, variable reading ability, and careful patient selection. PROMs continue to improve patient safety and best practices. They have also helped underscore the importance of patient counselling. Lessons learned from PROMs have since trickled down to clinical practice, with increasing efforts to integrate them into
the daily flow using standardised questionnaires to gather patient feedback.
PROMS also serve as a reminder to maintain human connections with patients—the innate skill of bedside manner. As Robert Ang MD noted in a recent ESCRS webinar, “We need to know how our patients see the world. [I’m] not just talking about their vision: we need to know what patients want. We will get higher patient satisfaction if we address their needs.”
The ESCRS has developed an online Patient Portal (www. escrs.org/patient-portal) to educate patients about their conditions relating to upcoming or recent cataract or refractive surgery. The portal is a good first step on the patient’s journey to improved vision.
The 2025 ESCRS Annual Congress in Copenhagen will celebrate the remarkable evolution of vision correction technology: as IOLs have celebrated 75 years, femtosecond lasers have been in use for 25 years, LASIK for 35, and penetrating keratoplasty for 120. The ESCRS programme will include discussions of robotics, artificial intelligence, and the digital OR, with the patient experience as the common thread for all. As surgery becomes more automated, remembering the human element becomes even more important.
The Congress includes sessions covering the many ways of improving patient care, from AI chatbots to personalising care via insights learned from registries such as EUREQUO. If you miss those sessions, don’t worry—EuroTimes will report on them in future issues.
Sean Henahan Editor-in-Chief
EDITORIAL BOARD

Adi Abulafia (Israel)
Bruce Allan (UK)
Noel Alpins (Australia)
Juan Alvarez de Toledo (Spain)
Gerd Auffarth (Germany)
Başak Bostanci (Turkey)
John Chang (Hong Kong SAR, China)
Béatrice Cochener-Lamard (France)
Burkhard Dick (Germany)
Mor Dickman (The Netherlands)


Joaquín Fernández (Spain)
Oliver Findl (Austria)
Nicole Fram (US)
Sri Ganesh (India)
Farhad Hafezi (Switzerland)
Nino Hirnschall (Austria)
Soosan Jacob (India)
Jack Kane (Australia)
Yao Ke (China)
Mika Kotimäki (Finland)
David Lockington (UK)
Artemis Matsou (Greece)
Cyres Mehta (India)
Jod Mehta (Singapore)
Sorcha Ní Dhubhghaill (Belgium)
Rudy Nuijts (The Netherlands)
Catarina Pedrosa (Portugal)
Konrad Pesudovs (Australia)
Nic Reus (The Netherlands)
Filomena Ribeiro (Portugal)
Andreia Rosa (Portugal)
Giacomo Savini (Italy)
Julie Schallhorn (US)
Sathish Srinivasan (UK)
Paola Vinciguerra (Italy)
Shin Yamane (Japan)
Ron Yeoh (Singapore)
Mihail Zemba (Romania)
See the Unseen Experience Cornea Layer Segmentation
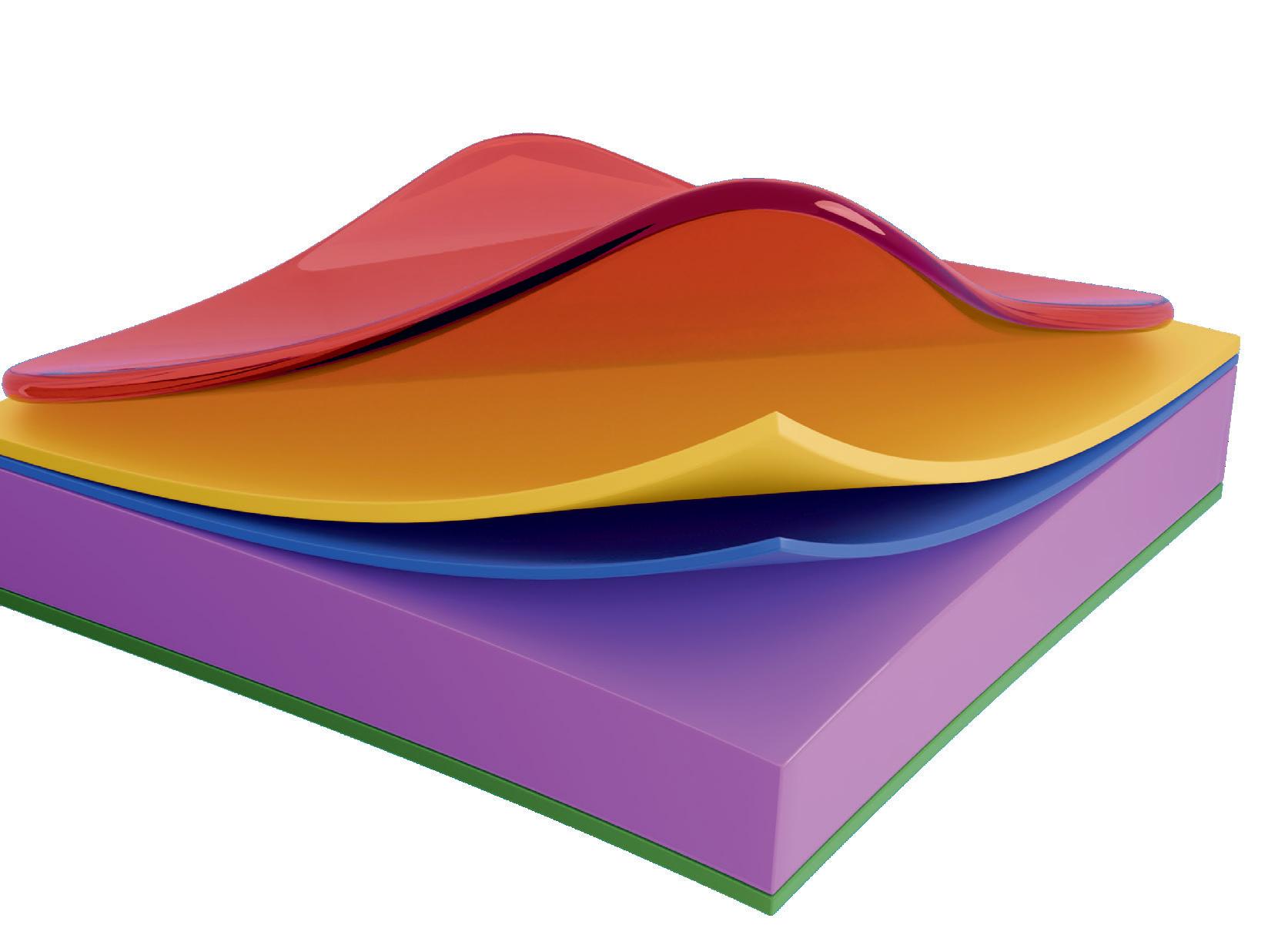

Detailed Sub-Layer Assessment
Combining the proven power of Scheimpflug imaging with the precision of ultra high-resolution OCT enables the detection of previously unseen corneal pathologies with unprecedented clarity.
Diagnose earlier. Treat smarter. Care deeper.
TEAR FILM
EPITHELIUM
BOWMAN’S LAYER
STROMAL LAYER
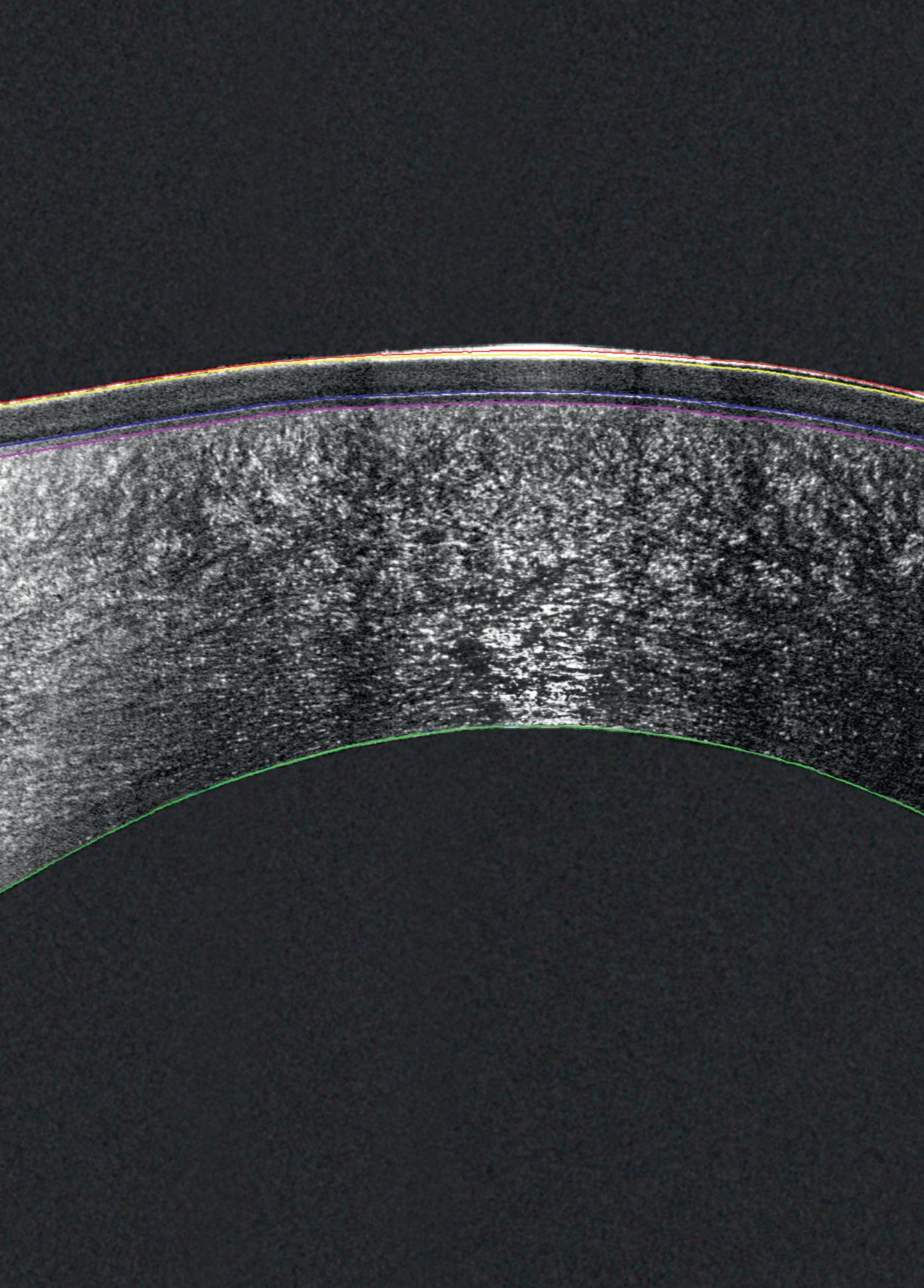

The Pentacam® Cornea OCT can increase the confidence that your diagnosis is correct.
ESCRS 2025 | Booth C2.017
Lunch Symposium I Room A3 Sat, 13 September 2025, 13-14 h Integrating key modalities for a complete refractive work-up
iStent infinite® –Finding the Right Patient
INTRODUCTION
The iStent infinite represents the latest advancement in trabecular micro-bypass technology, building on the proven safety and performance of the established iStent® platform. Recently granted MDR approval in Europe, it is designed to maintain a truly microinvasive approach while offering the flexibility to be used either with or without cataract surgery. With a redesigned injector that allows controlled, predictable stent placement and an unlimited number of deployment clicks, the system offers surgeons greater precision and confidence during implantation, all without compromising the trusted safety profile of earlier iStent® devices.
Dr. Sultan Aldrees is a consultant ophthalmologist and Cataract, Glaucoma and Advanced Anterior Segment surgeon in Riyadh Saudi Arabia. He holds a master’s degree in Sciences from McGill University in Montreal, Canada. Dr. Aldrees did his residency training in ophthalmology at the University of Toronto followed by 2-year subspecialty training in Cataract, Glaucoma and Advanced Anterior Segment Surgery (GAASS) under the mentorship of Ike Ahmed, MD FRCSC in Toronto, Canada. Dr. Aldrees currently works as an assistant professor at King Saud University in Riyadh, Saudi Arabia where he also serves as the director of cataract and glaucoma fellowship and deputy residency program director. His practice focuses on all types of glaucoma procedures including minimally invasive glaucoma surgeries in addition to complex cataract and advanced anterior segment surgery. We asked him to share a recent iStent infinte® case:
Dr. Sultan Aldrees MD, Ms, FRCSC
Dr Sultan Aldrees is a paid consultant of Glaukos
CASE PRESENTATION
A 70 year-old female referred for combined cataract and glaucoma surgery. At the time of presentation, she was complaining of mild decreased vision in addition to symptoms of glare in both eyes mainly at night. She was diagnosed with primary open angle glaucoma in her 50s and she reported that her intraocular pressures at the time of diagnosis were 31 mmHg in the right and 27 mmHg in the left. Since then, she has been using topical glaucoma treatment and escalation of medical treatment was done by her general ophthalmologist as needed. She does not have family history of glaucoma and she denied using all types of corticosteroids in the past. She also denied history of trauma to either eye.
EXAMINATION
Her examination showed best corrected visual acuity (BCVA) of 20/40 in the right eye and 20/30 in the left eye. She did have right relative afferent pupillary defect. Her intraocular pressures were 17 mmhg in the right (on Brinzolamide, Brimonidine, Alphagan and Timolol) eye and 15 mmhg in the left eye (On Brinzolamide, Brimonidine and Timolol). Her slit lamp examination was showed clear corneas with deep and quiet anterior chamber. She had moderate nuclear sclerosis with some cortical changes in both eyes. Gonioscopic exam showed open angles in both eyes with moderate pigmentation. There were no iris changes including any transillumination defects nor pseudoexfoliative material deposits in either eye. Fundus examination shows flat retina with large glaucomatous cupped disc in both eyes.
ANCILLARY TESTING
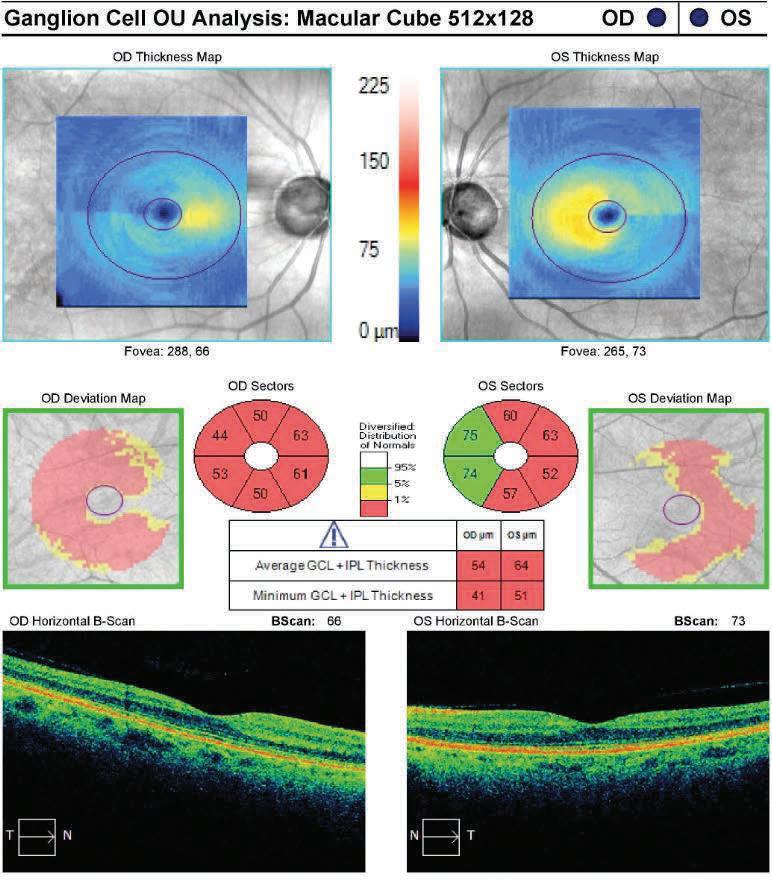
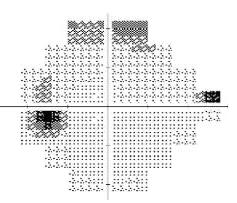
As part of our assessment, she did have optical coherence tomography of the retinal nerve fiber layer (OCTRNFL) analysis and ganglion cell complex (GCC) analysis for both eyes, which showed significant RNFL and GCC loss in the right eye more than the left. Those structural changes, corroborate with her functional changes on her visual fields where the right eye showed shows advanced visual field loss compared to milder changer in the left eye.
OPERATIVE AND POST OPERATIVE COURSE
Given her cataracts and the need for cataract surgery, we decided to combine cataract surgery with minimally invasive glaucoma surgery (MIGS) in the form of implanting an iStent infinite®. She had right then left eye phacoemulsification with monofocal intraocular lens implantation and three G2-W stents implanted in each eye around 2 clock-hours apart. Her operative and post operative courses were unremarkable for both eyes with no intraocular pressure spikes. Her follow up extended until 1 year after surgery and at that time, her BCVA was 20/20 in either eye and her intraocular pressures were maintained at 11 mmHg in the right and 10 mmHg in the left while using only one classes in both eyes (prostaglandin analogue). There was no evidence of structural or functional progression on her last follow up with us.
DISCUSSION
Though our patient was referred with above target IOP in the right on maximal topical treatment, performing traditional bleb forming surgery on her can give rare but serious side effects1. MIGS on the other hand redefined how we treat glaucoma where in addition to lowering IOP, it addresses many issues including medication compliance and ocular surface disease while avoiding many of the risks associated with traditional bleb-based procedures2. On the spectrum of MIGS procedures and devices, cost and the degree of invasiveness play an important role when choosing a specific procedure for a specific patient. While significantly reducing IOP and medication burden in both standalone and combine cases4, the safety profile of both iStent® and iStent inject® in combined cases is similar to cataract surgery alone5 Our patient had significant IOP reduction after her combined right eye surgery. This encouraged us to proceed with the same approach for her left eye. During her follow ups, she reported better quality of life with better vision and less ocular surface symptoms. Moreover, she is happier that she is using one drop at her bedtime compared to having to use multiple bottles with multiple drops per day before her surgery.

References
1. Gedde SJ, Herndon LW, Brandt JD, et al. Postoperative complications in the Tube Versus Trabeculectomy (TVT) study during five years of follow-up. Am J Ophthalmol. 2012;153: 804–814.e1.
2. Saheb H, Ahmed IIK. Micro-invasive glaucoma surgery: current perspectives and future directions. Curr Opin Ophthalmol. 2012;23:96–104.
3. Paletta Guedes RA, Gravina DM, Paletta Guedes VM. Standalone implantation of 2-3 trabecular micro-bypass Stents (iStent inject ± iStent) as an alternative to trabeculectomy for moderateto-severe glaucoma. Ophthalmol Ther. 2022;11:271–292
4. Hengerer FH, Auffarth GU, Conrad-Hengerer I. iStent inject trabecular micro-bypass with or without cataract surgery yields sustained 5-year glaucoma control. Adv Ther. 2022;39: 1417–1431.
5. Samuelson TW, Sarkisian SRJ, Lubeck DM, et al. Prospective, randomized, controlled pivotal trial of an Ab interno implanted trabecular micro-bypass in primary open-angle glaucoma and cataract: two-year results. Ophthalmology. 2019;126:811–821
INDICATION FOR USE. The iStent infinite System is intended to reduce intraocular pressure safely and effectively in adult patients diagnosed with primary open-angle glaucoma, pseudo-exfoliative glaucoma or pigmentary glaucoma. The device is safe and effective when implanted in combination with or without cataract surgery in those subjects who require intraocular pressure reduction and/or would benefit from glaucoma medication reduction. The device may also be implanted in patients who continue to have elevated intraocular pressure despite prior treatment with glaucoma medications and/or conventional glaucoma surgery. CONTRAINDICATIONS: The iStent infinite System is contraindicated under the following circumstances or conditions: •In eyes with primary angle closure glaucoma, or secondary angle-closure glaucoma, including neovascular glaucoma, because the device would not be expected to work in such situations.• In patients with retrobulbar tumor, thyroid eye disease, Sturge-Weber Syndrome or any other type of condition that may cause elevated episcleral venous pressure WARNINGS/PRECAUTIONS: • For prescription use only. • Intended users are trained ophthalmologists only. • This device has not been studied in patients with uveitic glaucoma. • Do not use the device if the Tyvek® lid has been opened or the packaging appears damaged. In such cases, the sterility of the device may be compromised. • Due to the sharpness of certain injector components (i.e., the insertion sleeve and trocar), care should be exercised to grasp the injector body. Dispose of device in a sharps container. • iStent infinite is MR-Conditional • Physician training is required prior to use of the iStent infinite System. • Do not re-use the stent(s) or injector, as this may result in infection and/or intraocular inflammation, as well as occurrence of potential postoperative adverse events
• There are no known compatibility issues with theiStent infinite and other intraoperative devices (e.g., viscoelastics) or glaucoma medications. • Unused product & packaging may be disposed of in accordance with facility procedures. Implanted medical devices and contaminated products must be disposed of as medical waste. • The surgeon should monitor the patient postoperatively for proper maintenance of intraocular pressure. If intraocular pressure is not adequately maintained after surgery, the surgeon should consider an appropriate treatment regimen to reduce intraocular pressure. • Patients should be informed that placement of the stents, without concomitant cataract surgery in phakic patients can enhance the formation or progression of cataract. ADVERSE EVENTS: The most common postoperative adverse events reported in the iStent infinite pivotal trial included IOP increase ≥ 10 mmHg vs. baseline IOP (8.2%), loss of BSCVA ≥ 2 lines (11.5%), ocular surface disease (11.5%), perioperative inflammation (6.6%) and visual field loss ≥ 2.5 dB (6.6%). CAUTION: Please see DFU for a complete list of contraindications, warnings, precautions, and adverse events. For additional safety information on iStent products, see here: www.glaukos.com Glaukos®, iStent®,
Thinking Beyond the Surgery Room
Practice management workshop focuses on financial operations and AI business applications.
Clinical trial spotlights. Surgical pearls. Skills labs. Visual optics courses.
ESCRS Congresses encompass a wide variety of approaches to exploring the clinical aspects of anterior segment surgery. From hands-on training to panel presentations to expert symposia, these annual meetings offer something for ophthalmologists at all stages of their medical careers.
For surgeons interested in the operational success of their practice or department, ESCRS has a more focused solution: the ESCRS Leadership, Business, and Innovation (LBI) initiative. The latest LBI offering was a practice management workshop in June in Zurich, Switzerland, devoted to financial operations and artificial intelligence applications. The workshop was conducted in partnership with the Trinity College (Dublin) Business School Executive Education Programme, which is consistently ranked as a leader in executive education by the Financial Times.
The workshop attendees included not just doctors but also staff whose roles are essential to improving operational efficiency, streamlining processes, and achieving better patient outcomes.
“I decided to participate because, as a manager, I’m always looking to learn more about healthcare management,” said Vera Rodrigues, operational director at Clinica Oftalmologica Dr Miguel Sousa Neves in Portugal. “This opportunity was good to learn a little bit about finances and a lot about AI. I learned how to use and create images with AI, which is very important nowadays when working with social media.”
Interaction and engagement
One key to the success of the workshop was the interaction between presenters and attendees. Another key was the mindset of those in attendance—a mindset characterised by curiosity, pragmatism, and cautious optimism.












































































This opportunity was good to learn a little bit about finances and a lot about AI.
— Vera Rodrigues
“In Zurich, I engaged with decision makers—owners of private practices and department heads—who think beyond the surgery room,” said Vanessa Foser, a co-founder of the AI Business School, who presented at the workshop. “They saw AI not as a diagnostic revolution, but as a practical assistant in daily workflows, from automating doctor letters to multilingual patient communication via avatars. Their questions were often managerial: ‘How do I integrate this with my PMS?’ or ‘How do I train staff and maintain data safety?’ That mindset is different from a pure clinical AI curiosity—it’s business transformation with a medical compass.”
Paul Rosen, chair of the ESCRS LBI Committee and one of the organisers of the workshop, said he was especially pleased with the interaction between presenters and attendees.
“It worked extremely well because everyone was engaged,” he said. “People were asking questions of each other
and contributing, and the speakers were very interactive.”
The LBI Committee is helping organise another workshop in November that will focus on marketing. In the meantime, the committee is offering a day-long “LBI Bootcamp” at the 2025 Annual Congress in Copenhagen, comprising three sessions: (1) Podium Presentation Skills, (2) The Foundation of Success: Your Team, and (3) Strategies for Success.
The committee also produces occasional videos/podcasts on business topics. The latest, “Marketing Your Services,” is available on the ESCRS website along with other LBI resources.
Creating immediate value Rodrigues said she would be interested in attending another LBI workshop if the topics are pertinent to her job and career. “I would like to learn more about leadership and financial topics but especially specifics for healthcare management, human resource
Tips for Implementing AI Tools
management, and possibilities of growing,” she said.
The desire to grow—and to incorporate AI tools into practices and processes to help spur growth—was common among workshop attendees.
“There was a strong interest in use cases that create immediate value, especially for overworked admin teams,” Foser said. “Risks like data privacy were discussed, but the overall tone was, ‘We need to start using it and at the same time minimise company risks.’ That’s a very healthy, entrepreneurial attitude.”
Given the rapid evolution of AI and its potential uses (and misuses), Foser tried to strike a balance between current capabilities and enduring lessons.
“While the tools evolve rapidly, some principles remain timeless,” she said. “Ultimately, the timeless truth is this: Practices that embrace AI as a strategic enabler, not just a tech experiment, will shape the future of patient care and practice leadership.”
At the Practice Management Workshop in Zurich, Vanessa Foser shared these simple tips for implementing AI tools in surgical practices:
• Start small, but smart. Begin with low-risk, high-impact use cases like documentation or translation. Learn from those before scaling.
• Build literacy across your team. AI doesn’t replace your staff; it empowers them—but only if they understand how to use it responsibly.
• Don’t outsource your judgement. Always question AI output, especially in medical environments. Think of AI as a co-pilot, not an autopilot.
• Create governance early. Even for small pilots, set clear guidelines for data use, validation, and communication. This builds trust and reduces risk later.
Annual Report Shows Breadth of Society’s Impact Communicating the full impact of a professional society whose members deliver care to patients in a variety of cultural and economic settings is an ambitious task, but the 2024 Annual Report from ESCRS manages to capture the essence of that mission and paint a compelling picture of an organisation dedicated to advancing the science and practice of anterior eye surgery.
The online report, available on the ESCRS website, covers a wide range of topics, including educational opportunities, charity programmes, and social responsibility projects. It contains brief summaries of ESCRS initiatives, infographics that illustrate the diversity of the Society’s members and meeting attendees, and links to programmes and projects such as the ESCRS 100 video series, the three ESCRS registries, and results of research awards and grants.
Of particular note are videos of members describing how ESCRS has made an impact on their early careers. In one such video, Dr Alexander Gonzales explains why he chose to become an ESCRS member and what the Society offers him; in another, Dr Myriam Böhm talks about winning the ESCRS Peter Barry Fellowship, which allows a trainee to work abroad at a centre of excellence for clinical experience or research in the field of cataract and refractive surgery, anywhere in the world, for one year.
Four pages of the report are dedicated to ESCRS’s efforts in the areas of sustainability and social responsibility. These pages describe the BoSS (Building Our Sustainable Society) initiative, Mission Zero (an effort to deliver events with zero waste to landfills and net-zero carbon emissions), SIDICS (an initiative to create metrics to help cataract surgeons evaluate the overall sustainability of cataract packs), and EyeSustain (a global consortium co-sponsored by ESCRS that works to make ophthalmology more economically and environmentally sustainable).
Another four pages are devoted to research and address topics such as awards granted in 2024, research projects completed during the year, and the status of the three ESCRS registries. Overall, the ESCRS registries contain data on more than 4 million surgeries, making them one of the most comprehensive ophthalmology data sets in Europe.
Webinars Examine Postoperative Complications, Digital Operating Room
Education has long been a pillar of ESCRS, and a recent webinar and podcast attest to the Society’s commitment to raising the practice level of its members.
An ESCRS eConnect webinar, “Tackling Postoperative Complications in Corneal Surgery,” explored some of the key challenges faced after corneal refractive procedures, including visual quality concerns, the stability of results over time, healing complications, and the management of intracorneal implants. The one-hour video, featuring Vladimir Suvajac, Sara Sella, Kristina Mikak, and Tiago Monteiro, provided valuable guidance on how to recognise, prevent, and address these complications in everyday practice.
Discover the insights of this and other eConnect webinars by scanning the QR code.
A Leadership, Business, and Innovation podcast, “Marketing Your Services,” debated the need to market medical services in the field of ophthalmology and how to select the best tools for your needs. Europe has different regulations regarding medical marketing, and cataract and refractive surgery mostly belong to the premium eye services category, which complicates the marketing approach. Moreover, there are significant differences between academic, non-academic public, and private services. The interview shares the position of key opinion leaders from differing backgrounds who describe their approaches, special considerations, and ways to achieve success.
Scan the code to watch or listen to the episode on the ESCRS website.
Access the full report and member testimonials with the QR code.
Redefining Vision with the Galaxy Spiral IOL
What do patients expect from cataract surgery?
Patients undergoing cataract surgery often expect spectacle independence not only for distance but also for near and intermediate activities such as reading and using digital devices. Trifocal intraocular lenses (IOLs) have helped meet this demand by offering vision at all distances. However, they can cause side effects such as glare, halos, and light loss which negatively impacts contrast sensitivity, especially in dim-light conditions. Therefore, careful patient selection and thorough counselling are essential – and only those who can tolerate some visual disturbances are suitable candidates for diffractive trifocal IOLs.
A ground-breaking approach: The spiral IOL
At the 2024 ESCRS Congress, Rayner launched the world’s first spiral IOL – RayOne Galaxy. Developed in partnership with Prof. João Marcelo Lyra, the Galaxy IOL features a novel non-diffractive spiral optic designed with a proprietary AI engine tuned for optimal patient outcomes. The Galaxy IOL introduces a continuous and progressive variance of power along the spiral tracks on the IOL optic, focusing light at every position along the defocus curve for a smooth and continuous full range of vision, from distance to near.
Designed with AI – The future of IOL technology
The Galaxy IOL was engineered with the assistance of proprietary machine learning techniques to obtain the optimum IOL design needed to achieve a full range of vision while minimizing dysphotopsia. By systematically modelling millions of design iterations, the complex spiral optic was realized, accelerating the development

process of the new lens. Consequently, surgeons can offer their patients a lens technology that might not have otherwise been available for several years.
Testing the RayOne Galaxy IOL
A preclinical study using the Real Artificial Lens Vision (RALV) device evaluated the Galaxy IOL in 30 healthy subjects. Compared to traditional trifocal IOLs, the Galaxy IOL provided superior intermediate vision, comparable near and distance acuity, improved contrast sensitivity, and reduced halos.
Early clinical insights
In July 2024, a multicentre study began across 10 sites in Europe, Turkey, and New Zealand, involving 91 patients. Results at 3 months post-implantation showed strong visual outcomes, stable defocus curves, and reduced halo and glare compared to leading trifocal IOLs.
What this means for patients
The RayOne Galaxy is a FROF (full range of focus) IOL with minimal visual side effects, offering spectacle independence across all distances. It delivers high optical quality with fewer compromises, supporting active lifestyles and enhancing patient satisfaction after cataract surgery.
Learn more at rayner.com/Galaxy Full

Empowering patient participation fosters continuous innovation in cataract surgery.
B eyond the Numbers
BY LAURA GASPARI

Modern healthcare is undergoing a significant transformation towards patient-centred care, redefining the delivery of medical services by prioritising the patient’s voice in every clinical decision. Patient-reported outcome measures (PROMs) play a key role—simple and standardised questionnaires that give patients the chance to share how they really feel about a given treatment, in their own words. PROMs help specialists understand what truly matters to each person, linking medical care more closely to real-life experiences.
Ophthalmology is not an exception: patients’ direct and subjective evaluations have been recognised as an essential part of the overall assessment of ophthalmic care, with some consolidated tools in place for quite some time, especially for cataract surgery.
Initially a powerful tool in research, PROMs now feature more often in dayto-day care, and there is hope that they could be increasingly integrated into the clinical workflow as an important part of the patient journey in ophthalmic care. Additionally, all the data gathered and filed could be useful to evaluate future surgical techniques or medical treatments.
Yet challenges are always just around the corner, and this integration will not be an easy task for those who advocate a more patient-centred approach—even if technologies may help in overcoming problems and difficulties.
A consolidated but recent history
In ophthalmology, cataract surgery was the first field where PROMs began to make an impact because they give patients rather predictable outcomes, Anders Behndig MD, PhD recalled. His country, Sweden, began using PROMs in cataract surgery in the 1990s thanks to the efforts of Professor Mats Lundström, who designed the first Catquest—a questionnaire with four alternative answers per question. Each one of them has a score, evaluated using Rasch analysis, a psychometric model designed to analyse categorical data, to ensure all the data gathered can be statistically analysed. PROMs use in cataract surgery later expanded to all of Europe when ESCRS developed the European Registry of Quality Outcomes for Cataract and Refractive Surgery (EUREQUO) in 2007 to benchmark surgical outcomes, and Prof Lundström and Konrad Pesudovs met to design Catquest-9SF. This iteration is a set of nine questions and is used for cataract patients in EUREQUO. “Although it is quite an old form, it is still considered state of the art and has been demonstrated to be stable over time,” Prof Behndig reported. The goal is to assess patients’ preoperative and postoperative subjective experiences and outcomes, which can be a real asset.
What PROMs has taught us so far
The strength of PROMs derives from their broad yet comprehensive approach to medicine, considering all aspects of patients’ humanity. “It is a biopsychosocial model of healthcare, which considers the human being much more than just physical parts. PROMs help patients to ultimately dictate what they think is important to their own healthcare,” Yarrow Scantling-Birch MD stated. This kind of 360-degree perspective has proven to give ophthalmologists an additional tool to further improve surgical and treatment outcomes for their patients.
Since their introduction, the ophthalmic community has learned some lessons from PROMs. According to Prof Behndig, PROMs results generally align rather well with results achieved using the usual measurement values (e.g., visual acuity). However, this is not always the case. “Patients’ satisfaction is not always consistent with clinical metrics. For instance, a patient with 20/20 vision may still experience dissatisfaction due to dysphotopsia or trouble with near vision,” Burkhard Dick MD, PhD confirmed. For example, PROMs highlighted the importance of patients’ preoperative expectations, which are sometimes unrealistic, and the discomfort posed by some visual phenomena, such as halos and glares.
Moreover, as Prof Behndig pointed out, PROMs in Sweden have provided insight into the timing of cataract surgeries, revealing that these procedures are now performed earlier than they were 10 to 20 years ago, offering patients different perceptions of improvement and helping surgeons better understand the optimal
timing for surgery. Prof Dick noted PROMs data made it possible to benchmark across clinics and enhance patient communication regarding likely outcomes, thereby assisting in diagnosing different cases, from those with minimal visual impairment to those with comorbidities, who are more likely to be dissatisfied with the surgery.
The need for a more integrated approach
Although they have gained popularity over time, PROMs are still not fully used in clinical practice, despite the goal for integration into the clinical workflow, especially in a public context, according to Dr Scantling-Birch. In public healthcare settings, the volume of surgeries is often so high that it becomes difficult to fully capture each patient’s needs. PROMs can help streamline this process by using standardised questionnaires to gather important patient feedback.
PROMs’ potential is especially high when it comes to identifying patients who may have suboptimal outcomes in ophthalmic surgery. Prof Dick added they serve as a highly effective instrument to aid clinical decision-making for specialists, such as selecting the best IOL according to the patient’s need. In fact, surgeons can use aggregated PROMs data from platforms to counsel their patients on expected satisfaction rates. According to Prof Behndig, this becomes especially effective when the subjective data gathered through PROMs are combined with gathered objective clinical information— helping doctors gain the most complete picture of a patient’s condition and expected outcomes.
PROMs could also aid in assessing the entire patient pathway, from referral to postoperative assessment, as demonstrated in a study presented at the ESCRS Winter Meeting in Athens by Dr Scantling-Birch. This would allow surgeons to have a more comprehensive understanding of patients’ journeys and evaluate their feedback.
What could lead to an increasing integration of PROMs in clinical practice is the use of new technologies and digitalisation, which can help process the data more quickly and compare it with previous assessments.
Identifying the challenges ahead
Using PROMs comes with its own set of problems and challenges. First, PROMs questionnaires need to be unidimensional, not merging all the symptoms and issues. They must be meticulous and avoid repetitive questions that could lead to the same answer.
PROMs need to be clear and comprehensible, especially for elderly people or non-native speakers of a certain language. The digital integration of PROMs could also lead to some difficulties for those who are not particularly tech savvy. Such challenges pose a risk of low response rates from patients or of answers being influenced by other factors—such as mood, personal character, expectations, socioeconomic disadvantages, or unrelated health issues.
Additional complications arise from misinterpreting the data or from how PROMs questionnaires are distributed and processed. As Prof Behndig highlighted, even a well-established tool such as Catquest-9SF has some gaps, as it does not consider spectacle independence, uncorrected near or inter-
mediate vision, and optical phenomena associated with some types of IOLs, like multifocal lenses.
Hopes for the future
Overall, the hope for the future is that PROMs will be increasingly used in everyday ophthalmic practice, even beyond cataract surgery and ophthalmic surgery in general.
“What the patient thinks and feels is really what should matter most in healthcare, at least when it comes to visual impairment,” Prof Behndig said. “I hope that we will be able to work out some nice PROMs also for spectacle independence, uncorrected visual acuity, or symptoms not directly related to cataract.”
Building on this vision, PROMs data could guide more reimbursement, IOL selection, and surgical planning. “Their predictive power could be enhanced through AI-based analytics,” Prof Dick suggested, adding this brings the world of medicine even closer to its patients. “PROMs will help ophthalmologists deliver care that aligns closely with what patients value most: real-world visual function and quality of life.”
What the patient thinks and feels is really what should matter most in healthcare, at least when it comes to visual impairment. — Prof Anders Behndig
AI, machine learning, and digitalisation can further streamline a future of PROMs by potentially reducing the burden or limitations of filling out traditional checkbox questionnaires—within the boundaries of proper regulations and ethical approvals, of course. “Maybe it is controversial, but I see the future as not having PROMs but [a] software able to record and transcribe our consultations with patients, read the way they talk, or the tone of their voices, their mood, how they interact with the space, and integrate these data with the biological markers we collected,” Dr Scantling-Birch argued. “I imagine the future potentially all integrated electronically as part of our workflow.”
Anders Behndig MD, PhD is the co-chair of EUREQUO, former Head of the Swedish National Cataract Register and Swedish Ophthalmological Society, and Professor at Umeå University Hospital, Sweden. anders.behndig@umu.se
H Burkhard Dick MD, PhD, FEBOS-CR is professor and chairman of the Ruhr University Eye Hospital in Bochum, Germany, and ESCRS president elect. dickburkhard@aol.com
Yarrow Scantling-Birch MD is an ophthalmologist trainee at Moorfields Eye Hospital, London, UK. yarrow.scantling-birch@nhs.net
Meet us at the ESCRS 2025 in Copenhagen:
Booth C4.045

ICL Sizing with CASIA2
The CASIA2 ICL Sizing application delivers precise, OCT-based phakic ICL sizing using the trusted NK and KS formulas. High-resolution tomographic imaging combined with real-time anatomical measurements enables precise ICL size recommendations for both horizontal and vertical fixation. Now with improved crystalline lens tracing and exportable ICL sizing reports – all within an intuitive workflow.
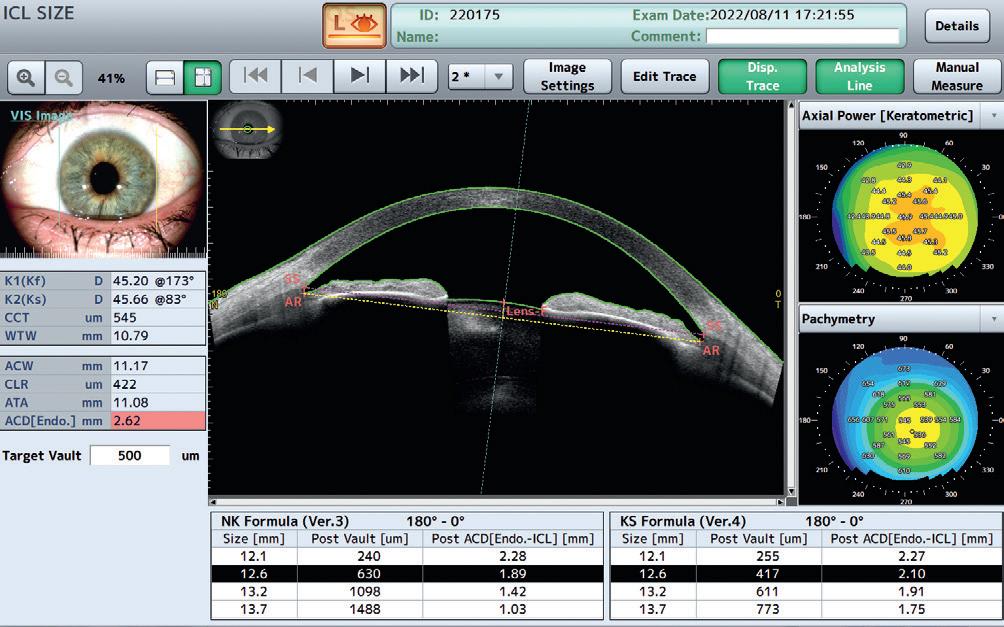
Pre-OP: Confirm the correct ICL size using WTW, ACW, ATA, CLR, and other key parameters.
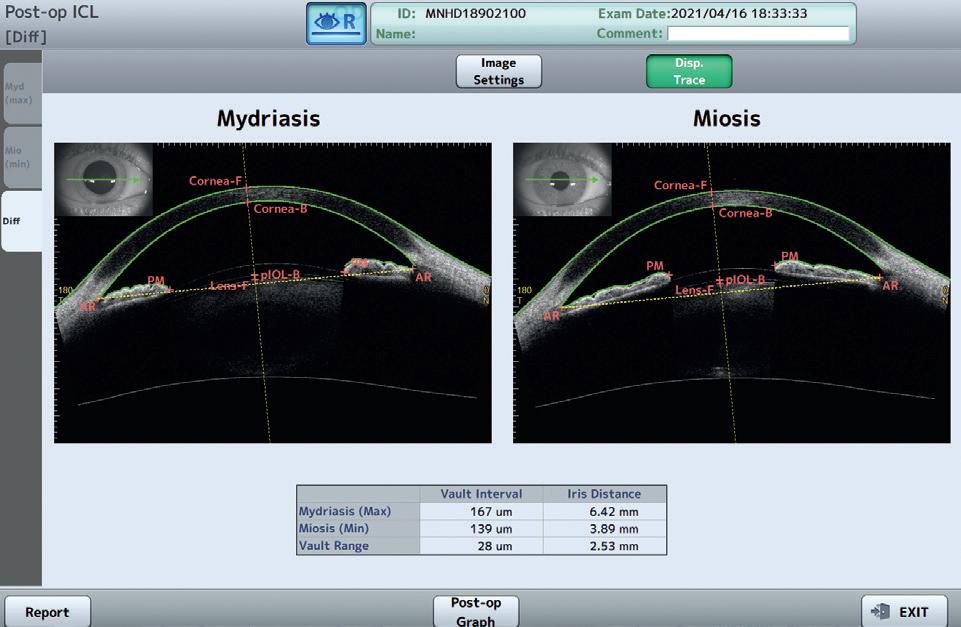
Post-OP: Visualize dynamic vaulting under mydriasis and miosis for quality control and outcome validation.

Presbyopic Phakic IOLs
EDOF and EDOF toric ICL preserve cornea and lens for future IOLs.
An extended depth of focus (EDOF) phakic intraocular lens (IOL) in both spherical and toric versions significantly improves overall vision and patient satisfaction with vision.
“It is the only refractive and presbyopia correction that allows us to preserve the cornea and lens for future IOL innovations,” said Robert E Ang MD.
Implanted behind the iris, the EDOF and EDOF toric versions of the implantable collamer lens (ICL, Staar Surgical) feature refractive optics with a slightly myopic central region, providing additional depth of focus without diffractive rings that split the wavefront. They can correct myopia, astigmatism, and presbyopia simultaneously, Dr Ang noted.
Good refractive results
In a prospective, open-label clinical study, Dr Ang implanted the EDOF ICL in 47 patients, of which 46 completed 6 months of follow-up. Overall, 26 eyes received spherical EDOF ICLs and 66 received the toric version. All but one patient were Asian, and mean age was 49.2 years, ranging from 42 to 57. Mean preoperative manifest refraction spherical equivalent was -4.87 D, ranging from -10.75 to -1.37 D. The study was supported by Staar Surgical.
At the 6-month follow-up, refractive results were good, with a mean spherical equivalent of -0.02 ± -0.33 D and similar results in toric and non-toric eyes. Results were stable from 1 week to 6 months of follow-up. Dr Ang reported 81.0% of eyes achieved uncorrected distance visual acuity of 20/32 or
better—93.0% achieving the same at intermediate distance and 77.0% at near. Rotational stability was also good, with 93.9% of eyes within 10 degrees of axis placement at 6 months. Patients showed a wider defocus curve after surgery than preoperatively, with similar contrast sensitivity. Several may have retained some accommodation, Dr Ang observed. Mean binocular corrected distance visual acuity was -0.00 before surgery and 0.01 at 6 months.
High patient satisfaction
On a scale of 1.0 to 5.0, mean satisfaction with near vision was 3.5, with 4.1 for intermediate, 4.3 for far, and 4.0 overall. All scores were higher than preoperative values. The lower satisfaction scores for near vision may reflect the fact that the patients were myopic to begin with and possibly used to near vision without spectacles before surgery, Dr Ang said.
No new safety risks were reported, demonstrating the safety of the EDOF and EDOF toric ICL models, Dr Ang said. The EDOF lenses are a great option to meet patient expectations, he concluded.
Dr Ang spoke at the 2025 ASCRS annual meeting in Los Angeles.
Robert Edward Ang MD is a senior consultant, head of cornea and refractive surgery, and head of research and training at the Asian Eye Institute, Makati City, Philippines. angbobby@hotmail.com
Perioperative Medication Regimens for Cataract Surgery
Randomised controlled clinical trial results provide evidence-based guidance.
CHERYL GUTTMAN KRADER REPORTS
Evidence-based recommendations on anaesthesia, endophthalmitis prophylaxis, and inflammation control in the European Society of Cataract and Refractive Surgeons (ESCRS) Cataract Surgery Guidelines should promote high-quality care and reduce existing unwanted practice variations in perioperative medication protocols, according to Thomas Kohnen MD, PhD.
Summarising the guideline’s key recommendations on these topics, Professor Kohnen discussed some of the underlying evidence and shared some details about the regimens followed at the Department of Ophthalmology, Goethe University, Frankfurt, Germany.
Per the ESCRS Guidelines, topical anaesthesia appears to be the most commonly used technique for anaesthesia. If needed, surgeons can consider adding intracameral lidocaine to reduce pain. An intracameral antibiotic (e.g., cefuroxime 1 mg/0.1 mL) injected at the end of surgery is recommended to reduce the risk of endophthalmitis. Postoperatively, a combination of a topical nonsteroidal anti-inflammatory drug (NSAID) plus a corticosteroid is recommended to prevent inflammation and cystoid macular oedema (CME) after routine cataract surgery. However, a depot of triamcinolone should also be considered in patients with diabetic retinopathy, and intraocular pressure monitored postoperatively.
The ESCRS Guidelines are grounded in high-level
evidence and aim to reduce practice variation while promoting better perioperative care.
“We stopped routine postoperative use of a topical antibiotic five years ago and have not seen any increase in infectious complications,” Prof Kohnen said.
The recommendation for intracameral cefuroxime is based on results of the prospective, randomised ESCRS Endophthalmitis Study showing intracameral cefuroxime decreased the risk of postoperative endophthalmitis by approximately fivefold.1 The preference for intracameral versus topical antibiotic treatment also reflects the need for antibiotic stewardship in the face of rising antimicrobial resistance and its benefits in reducing the burden and compliance issues accompanying topical drops. However, Prof Kohnen acknowledged that not all surgeons have access to a commercially available antibiotic approved for intracameral injection and compounded alternatives carry a risk of toxic anterior segment syndrome.
Prof Kohnen said povidone-iodine is used for antisepsis at his centre. It is applied three times—10 minutes before the start of surgery, after inserting the eyelid retractor, and at the end of the procedure—and left on for 40 seconds each time. Consistent with the ESCRS Guidelines recommendation, intracameral cefuroxime saline (1 mg/0.1 mL) is injected at the end of the procedure, and patients are prescribed a topical corticosteroid to use on a tapering schedule for 4 to 6 weeks, along with a topical NSAID for 6 weeks. A 1-week course of a topical antibiotic is prescribed only if an intraoperative complication occurs.
The recommended regimens for controlling inflammation and reducing the risk of CME are supported by findings of prospective, randomised ESCRS PREMED studies that compared different regimens in non-diabetic and diabetic patient cohorts.2,3 The study enrolling non-diabetics found the incidence of CME within 6 weeks after surgery was significantly reduced among patients treated with topical bromfenac and dexamethasone compared to those receiving the NSAID or corticosteroid as monotherapy (1.9% versus 4.1% and 8.1%, respectively). In the diabetic cohort, a single subconjunctival injection of triamcinolone acetonide added to a topical NSAID/corticosteroid regimen effectively prevented the development of CME, Prof Kohnen said.
Prof Kohnen spoke at the 2025 ASCRS annual meeting in Los Angeles.
For citation notes, see page 54.
Thomas Kohnen MD, PhD, FEBO is professor and chair of the Department of Ophthalmology, Goethe University, Frankfurt, Germany. kohnen@em.uni-frankfurt.de
Debate: FS-LASIK or KLEx for Hyperopia?
FS-LASIK has more of a track record, but KLEx offers advantages.
HOWARD LARKIN REPORTS
Which is the better corneal refractive treatment for hyperopia up to 4.00 D, femtosecond laser-assisted in situ keratomileusis (FS-LASIK) or keratorefractive lenticule extraction (KLEx)? Two experts debated the question in a symposium at the ASCRS 2025 annual meeting in Los Angeles.
In this corner, FS-LASIK
Arguing for FS-LASIK, Michael Mimouni MD noted it is faster to heal, has a lower regression risk, is more comfortable, and has a quicker vision recovery time than KLEx. “When it comes to what patients care about, FS-LASIK is ahead in every category,” he said.
Focusing on SMILE, the first KLEx technique to reach the market, Dr Mimouni noted a 2022 study by Dr Dan Z Reinstein and colleagues found that in hyperopic patients, 83% achieved 20/20 uncorrected vision or better, with 81% within 0.50 D of target, and 93% within 1.00 D, with good predictability and safety—not terrible, but still slightly inferior to hyperopic LASIK, he said.1
As far as the theoretical advantages of KLEx, a study comparing patients with FS-LASIK in one eye and SMILE in the other found they preferred LASIK.2 Another study found that, when measured by decrease in corneal stiffness, biomechanics were in fact worse with SMILE than LASIK or PRK, with residual stromal bed thickness apparently the biggest factor.3
For dry eye, yet another study found that, though SMILE initially resulted in less corneal denervation, there was no difference at 12 months, and self-reported dry eye symptoms were similar, Dr Mimouni argued.4
Dr Mimouni even asked ChatGPT and got this response: “In the hands of equally skilled surgeons, I’d go with what’s tried, true, and time-tested: FS-LASIK.”
KLEx comes out swinging
Sri Ganesh MBBS countered that Dr Mimouni’s arguments about corneal biomechanics and denervation mainly cited studies of myopic procedures, and cherry-picked them at that. Acknowledging even his own experience with SMILE is limited, Dr Ganesh, who participated in a multicentre approval study for hyperopic SMILE, sees great promise in the procedure. “If you look at hyperopia, SMILE has not even opened its eyes. Let’s see how the new baby performs.”
An early study of femtosecond lenticule extraction (FLEx) in 40 eyes with hyperopia found 70% within 0.50 D of target 9 months after surgery, Dr Ganesh noted.5 Another early study found good centration and optical zones effectively larger than LASIK with hyperopic SMILE.6
In the multicentre approval trial involving 374 eyes of 199 patients with up to +6.00 D hyperopia, 5.00 D cylinder, and 7.00 spherical equivalent, 80% achieved 20/25 or better uncorrected vision and 100% 20/40 or better 12 months after treatment.

Predictability was also good, with 81% within 0.50 D of target and 93% within 1.00 D. Results varied by the magnitude of correction. Astigmatic correction was good as well, with 75% within 0.50 D of target and 93% within 1.00 D.
When it comes to what patients care about, FS-LASIK is ahead in every category.
“Within 4.00 D, the results were excellent and stable,” Dr Ganesh said. However, corrections of more than 3.00 spherical equivalent showed increasing undercorrection, which may be due to healing factors. These results may be improved by modifying the nomogram, he added.
Safety was similarly encouraging, with 11% losing up to one line of vision, 1.3% losing up to two lines, and 10% gaining one line. The safety index rose from about 0.83 at one day after surgery to about 1.00 at 12 months, possibly reflecting the effects of healing over time, Dr Ganesh said. Stability was also good, though there was some regression even after 9 months, possibly due to late epithelial healing. However, this was less than typically seen with LASIK, possibly due to smaller optical zones, he added.
Overall, the results were better than in previous FLEx and SMILE studies, and refractive outcomes were marginally better than hyperopic LASIK with the MEL 90 (Zeiss), Dr Ganesh noted. Yet visual recovery was slower compared with FS-LASIK.
“The advantage is [KLEx] is more stable and there is less regression than with hyperopic LASIK,” though some issues remain, such as long treatment time and potential suction loss, Dr Ganesh said. However, the newer VISUMAX 800 laser should somewhat address these issues, as treatment times are expected to decrease from about 35 seconds to 12 seconds, making it an excellent option for hyperopia and hyperopic astigmatism, he concluded.
For citation notes, see page 54.
Michael Mimouni MD is associate professor at Technion-Israel Institute of Technology and director of the cornea unit at Rambam Health Care Campus, both in Haifa, Israel. michael@intername.co.il
Sri Ganesh MBBS, MS, DNB, DSC(Hon), FRCS(Gla), FWCRS is chairman and managing director of Nethradhama Hospitals in Bangalore, India. care@nethradhama.org
Apply Now for the Pioneer Research Award!
True innovation comes from good research. That’s the impetus for the ESCRS Pioneer Research Award (PRA).
The PRA aims to support and encourage independent clinical research in the field of cataract and refractive surgery. It can fund a variety of new initiatives, which may include—
• A novel research idea for the development of clinical trial studies;
• A non-interventional or observational study; or
• A natural history/epidemiological study.
An award of €25,000 is available for one grant. The competition is open to ophthalmologists up to the age of 45 (at the application deadline). Eligible participants must hold a full-time clinical or research position at a clinical or academic centre within the European region.
Applications are due by 31 October 2025.
Fulfilling AI’s Promise
As eye care uses expand, data collection and algorithm design are critical.
HOWARD LARKIN REPORTS
After the development of molecular biology in the 1950s and genomics in the 1980s, the current convergence of microelectronics and artificial intelligence (AI) marks the third great revolution in medical technology since the Flexner Report refocused medical education on science in the US in 1910, said Dimitri T Azar MD. However, while AI promises great strides in virtually every aspect of medicine, steps must be taken to ensure it does not introduce systemic biases, he added.
Multiple uses
In ophthalmology, actual and potential AI applications include analysis of corneal topography for ectasia signs, collagen cross-linking guidance, and cataract and refractive surgery planning, including topography analysis and IOL power calculation, Professor Azar said. Automated Fuchs’ dystrophy and glaucoma diagnosis and analysis of fundus photography and OCT for identifying retinal lesions, diabetic retinopathy, retinopathy of prematurity, and age-related macular degeneration exist or are in development.
Other potential AI applications include developing new dry eye diagnostic criteria, predicting Fuchs’ dystrophy progression, smart IOLs, guiding refractive surgery, and even robotic cataract surgery, Prof Azar said. And as miniaturization and AI converge, new, more economical diagnostic and monitoring devices will be available for clinical and home use. “There [will] be personalized refractive surgery based on knowledge that you [must] combine from many machines. You cannot rely on one device only.”
Regarding its role in ophthalmic education, he noted AI can supplement medical examination questions, provide multilingual translations, and create unique learning strategies. It has many roles in research, such as finding new treatments and targets, conducting literature reviews, drafting manuscripts, and recruiting patients.
AI is going to be your virtual assistant.
In the office, AI can help synthesize diverse pieces of information to improve clinical management and patient consultations, taking notes and filing claims. “AI is going to be your virtual assistant,” Prof Azar said.
Addressing hurdles
Achieving the promise of AI requires addressing significant challenges, Prof Azar said. Bias in training data sets is one.
Because AI produces empirical models based on connections it finds among data points, its reliability depends on data that are accurate and representative of the target population. For example, an AI algorithm based primarily on eyes from European populations may not work as well or at all in an Asian population. Rather than try to correct bias in algorithms after their creation, Prof Azar said efforts should focus on ensuring data quality, representative sampling, and how algorithms interpret data.
And since AI models are constructed using self-generated rules, they present the question of how the user can know if the output is correct. Regulators grapple with AI’s reliability, and the guidelines they adopt to ensure it will heavily influence how and what kind of systems are developed.
Still, there is no reason to fear the unknown, Prof Azar said. “We need to ensure that AI will be a helpful tool, rather than a competitor, for early referrals and diagnosis.”
Prof Azar presented in the JCRS Symposium at the 2025 ASCRS annual meeting in Los Angeles.
Dimitri T Azar MD, MBA is CEO of LACRISTAT.AI and distinguished university professor, BA field chair of ophthalmological research, professor of ophthalmology, pharmacology, and bioengineering, and executive dean emeritus at the University of Illinois College of Medicine, Chicago, US. dazar@uic.edu

Breathe New Life into Your Friday!

Friday is often a day to wrap things up and get ready for a relaxing weekend. At the ESCRS 2025 Annual Congress, Friday is the day to expand your mind and take your imagination and education to a higher level!
Here’s just some of what’s in store for you on Friday, 12 September:
ESCRS iNovation Day
See how the latest technology innovations might address the most urgent clinical needs and barriers to success in anterior segment care. Presentations include the following topics:
• The Innovators Den
• Artificial intelligence and digital visualisation
• Keys to expanding refractive and corneal markets
• Leadership visions for the next five years
Glaucoma Day
Organised jointly by ESCRS and the European Glaucoma Society. Sessions include the following:
• Clinical cases in glaucoma management
• Navigating cataract and glaucoma together
• Choose your future: laser, surgery, meds, or AI
Cornea Day
Organised jointly by ESCRS and EuCornea. Sessions include the following:
• Infections and the ocular surface
• New developments in keratoconus and cross-linking
• Cataract surgery in the patient with cornea pathology
Independent Medical Education Forum: The Digital Operating Room
Topics to be addressed include the following:
• Workflow integration
• 3D visualisation
• Case studies: cataract surgery outcomes
Other highlights include the Global Refractive Summit, WSPOS Day, and instructional courses on performing a primary posterior capsulorhexis and complex cataract cases from the FEBOS-CR exam.
Some events require pre-registration and an additional fee. Check the online programme for more details.

Avoiding Posterior Capsule Rupture
Imaging may help, but surgical technique is key for managing posterior polar cataracts.
HOWARD LARKIN REPORTS
Avoiding posterior capsule (PC) rupture is a major concern with posterior polar cataracts. But the role of anterior segment optical coherence tomography (AS-OCT) in managing it is an open question, as two experts recently debated.
Advantages of preoperative AS-OCT
Absent a ‘fish tail’ sign or a visible PC opening, it is not always possible to determine at the slit lamp whether there is a PC defect, said Namrata Sharma MD. Therefore, preoperative imaging is beneficial.
Although ultrasound biomicroscopy can help, it is a contact procedure limited to examining a single axis. So Dr Sharma recommends swept-source AS-OCT, as it is non-contact and provides 360 degrees of coverage with better resolution.1
She also noted some advantages of preoperative sweptsource AS-OCT over intraoperative OCT: Compared with intraoperative imaging, preoperative imaging has a deeper and wider imaging range, allowing visualisation of the entire lens; it offers magnification and reassessment; and it supports preoperative patient counselling.
“Preoperative imaging with AS-OCT in posterior polar cataracts helps in delineating PC integrity, helps surgeons customise their techniques and tools, and aids in patient counselling in case of change of plans regarding IOL options,” Dr Sharma said. It also provides opportunities to inform patients about the risk of PC rupture and the possible need for vitrectomy, multiple procedures, and prolonged visual
recovery.2,3 However, intraoperative OCT is also useful, especially combined with femtosecond laser-assisted surgery. Dr Sharma cited several studies demonstrating the accuracy of preoperative AS-OCT. One involving 44 eyes found it identified intraoperative PC dehiscence with 97% sensitivity and 87% specificity as well as 97% positive predictive and 77% negative predictive value for a total diagnostic accuracy of 95.4%.4 Another involving 100 eyes found similar accuracy.5
Which other tool can predict posterior capsule rupture that accurately?
An AS-OCT study she and her colleagues published examining posterior polar cataract morphology found that those with a conical or moth-eaten appearance had a 100% PC rupture rate and those with ectatic appearance, 66%.6
“I think it’s a great tool to have because which other tool can predict PC rupture that accurately?”
Preoperative imaging is not necessary
Arguing the opposing side, Abhay R Vasavada noted that a good clinical examination and proper surgical technique and tools—potentially including femtosecond lasers— can cut the incidence of PC rupture with posterior polar
cataracts to 4–8%, which he said renders preoperative imaging superfluous.
Many posterior opacities seen in the real world are actually localised plaque cataracts, but are mistaken for posterior polar cataracts, Dr Vasavada noted. “You need to look on the slit lamp—you don’t need any other thing.” He advised looking around the posterior polar area for a ‘punched out’ area, which often indicates a capsular defect.
A sinking cortex is another sign that a capsular defect is present, Dr Vasavada said.7 The ‘fish tail’ sign is yet another. “It is very obvious; it doesn’t need any imaging.”
Identifying fragile capsules is important because they can rupture at any point in the surgery, Dr Vasavada noted. Any manipulation near a posterior polar cataract can cause a rupture because it is not only fragile, but very adherent.
Once identified, imaging does not help manage a fragile capsule, Dr Vasavada emphasised, but proper surgical technique does. Crediting Dr Robert Osher, he outlined a standardised technique for avoiding rupturing fragile capsules. Principles include:
• Avoid rapid build-up of hydraulic pressure.
• Create a mechanical cushion effect.
• Avoid forward bulge of the capsule-zonule diaphragm.
• Create a communication between anterior and posterior compartments.
• Use femtodelineation.
• Counsel the patient and family.
Dr Vasavada noted that using conventional hydrodelineation resulted in a 36% capsular rupture rate in his clinic.8 Switching to inside-out delineation lowered the rate to 8%, which dropped further to 3.8% with femtodelineation.9,10 His current rates are similar, he said.
“If you can reduce [PC rupture] to about 4%, is it really necessary to use intraoperative OCT? Preoperatively, I think all the detailed examination is a good thing, but generally it is not necessary,” Dr Vasavada said, adding imaging does not replace the need for proper surgical technique.
Yet ruptures still occur, so he advises being ready to manage them through the very end of the case. “Posterior polar cataract is not over until it is over,” Dr Vasavada said. “So, if your nurses and assistants start packing up [before you are finished], don’t let them do it.”
Drs Sharma and Vasavada debated this topic during the JCRS Symposium at the 2025 ASCRS annual meeting in Los Angeles.
For citation notes, see page 54
Namrata Sharma MD, FRCOphth, FRCS(Ed) is professor of ophthalmology at the All India Institute of Medical Sciences, N ew Delhi, India. namrata.sharma@gmail.com
Abhay R Vasavada MS, FRCS(Eng) is founder and director at Raghudeep Eye Hospital, Ahmedabad and Jaipur, India. icirc@abhayvasavada.com

Apply for the New Sustainability Research Award!
Ophthalmologists and researchers (MD and/or PhD) as well as experienced ophthalmic nurses are encouraged to apply for the new ESCRS Sustainability Research (SURE) Award, which will fund projects that investigate meaningful, practical ways to promote environmental responsibility in ophthalmic care.
Two awards will be granted; each award will provide up to €10,000 per project. Applicants must be active ESCRS members at the time of application and must hold a current full- or part-time clinical or research position at a clinical or academic institution. Early-career researchers and young ophthalmologists are especially encouraged to apply.
The application period opens 28 July and closes 01 November. Award recipients must submit an article to a peer-reviewed journal within six months after the research period concludes. The article should be made open access if accepted and submitted to the Journal of Cataract & Refractive Surgery in the first instance.
Get funding for projects to promote environmental responsibility in ophthalmic care.
Picture This: Photo Contest Winners
ESCRS 2025 Refractive and Cataract Photo Contest winners.
In anticipation of the ESCRS Congress in Copenhagen, ESCRS members were invited to capture and share special moments experienced in refractive or cataract surgery environments. The winners were offered free registration to next year’s Congress. The top three winners reflect the art and science of cataract and refractive surgery. You can see the winning photos displayed at the Annual Congress in Copenhagen.
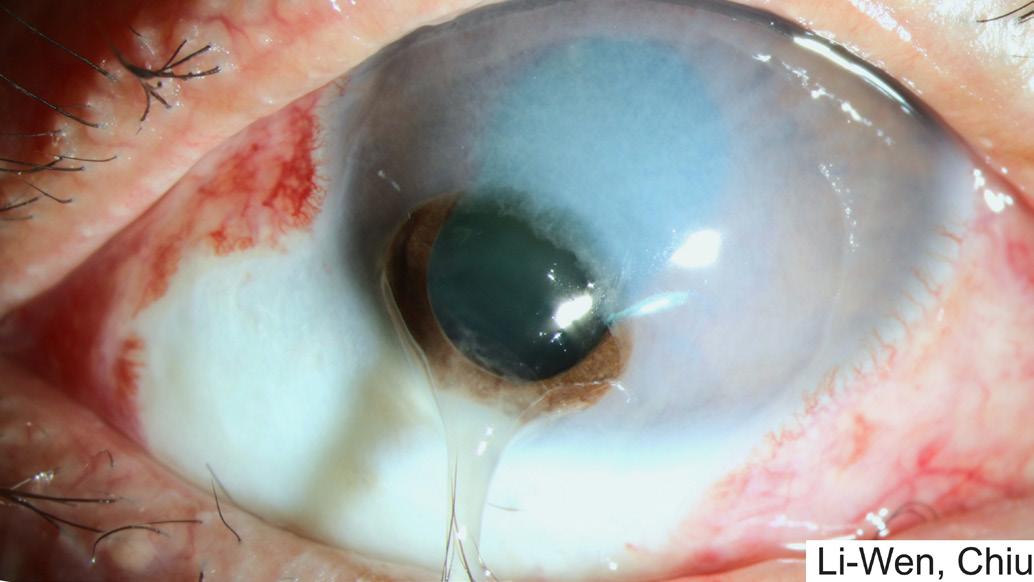
Corneal Rupture with Lens and Vitreous Protrusion Following NaOH Exposure
Li-Wen Chiu, Department of Ophthalmology, Kaohsiung Chang
Gung Memorial Hospital, Taiwan, Kaohsiung City, Taiwan
A 50-year-old male presented to the ophthalmology clinic with acute eye pain and headache following sodium hydroxide (NaOH) exposure to his left eye. Diagnosis of chemical burn, grade 2 (OS), with ocular hypertension as initial impression was made based on elevated intraocular pressure (IOP) of 49 mmHg, inferior limbal ischemia, and an epithelial defect with haze in the inferonasal cornea noted in ophthalmic examination.
Treatment consisted of auto serum eye drops, topical betamethasone eye drops, amniotic membrane graft, and vitamin C supplementation. However, the ocular condition worsened, with progressive corneal melting, eventually leading to corneal rupture and protrusion of intraocular contents, including the uvea, lens, and vitreous. Immediate primary repair was performed using a scleral patch, and follow-up evaluations indicated stable ocular condition.
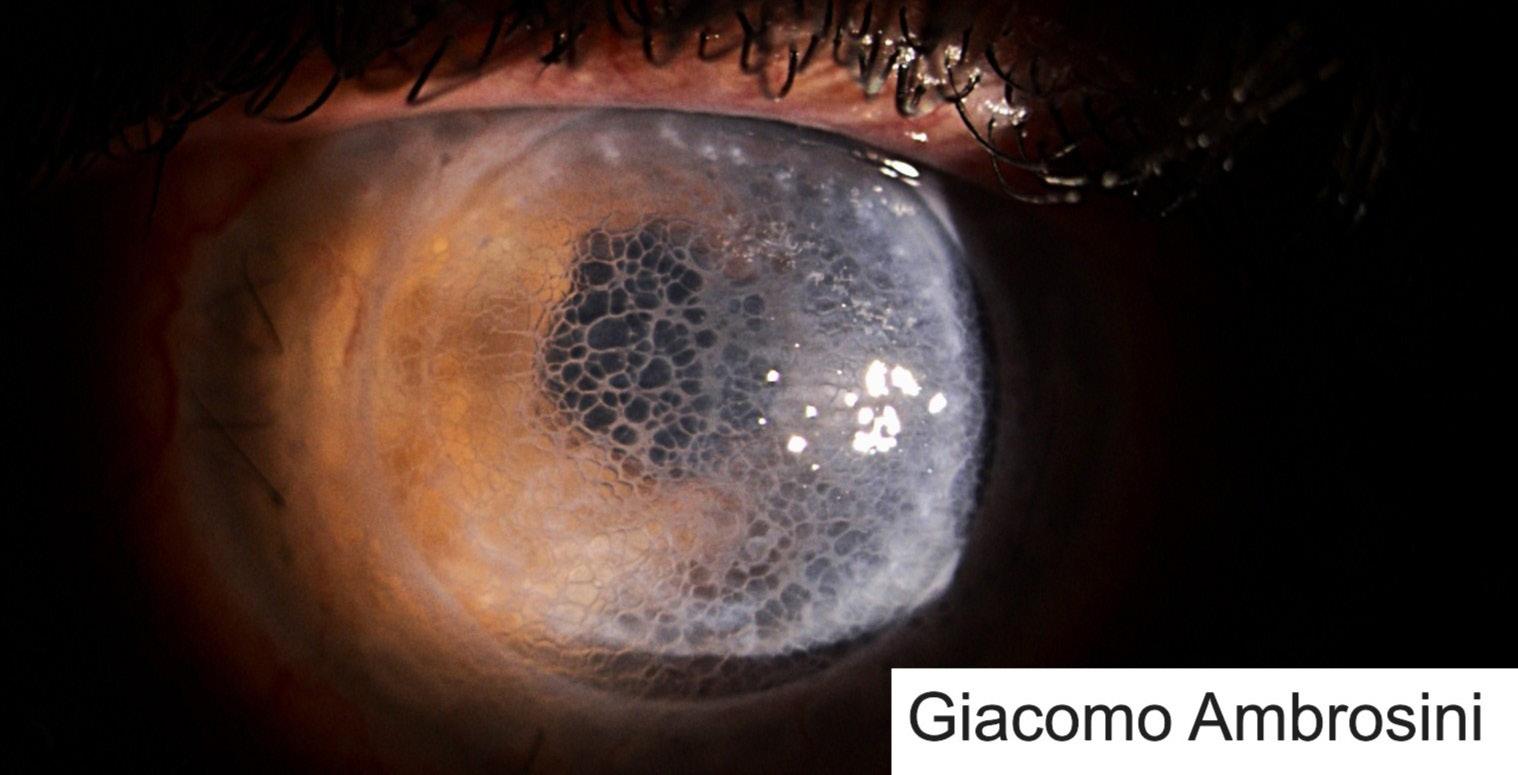
Honeycomb Epithelial Oedema Associated with Rho Kinase Inhibition
Giacomo Ambrosini, Eye Unit, University Hospital Southampton NHS Foundation Trust, Southampton, United Kingdom
Reversible reticular corneal epithelial oedema developed after 1 week of treatment with netarsudil and latanoprost in a patient with a history of keratoplasty. It presented as moderate-sized superficial epithelial bullae in a honeycomb pattern. The oedema fully resolved within 10 days of discontinuation.
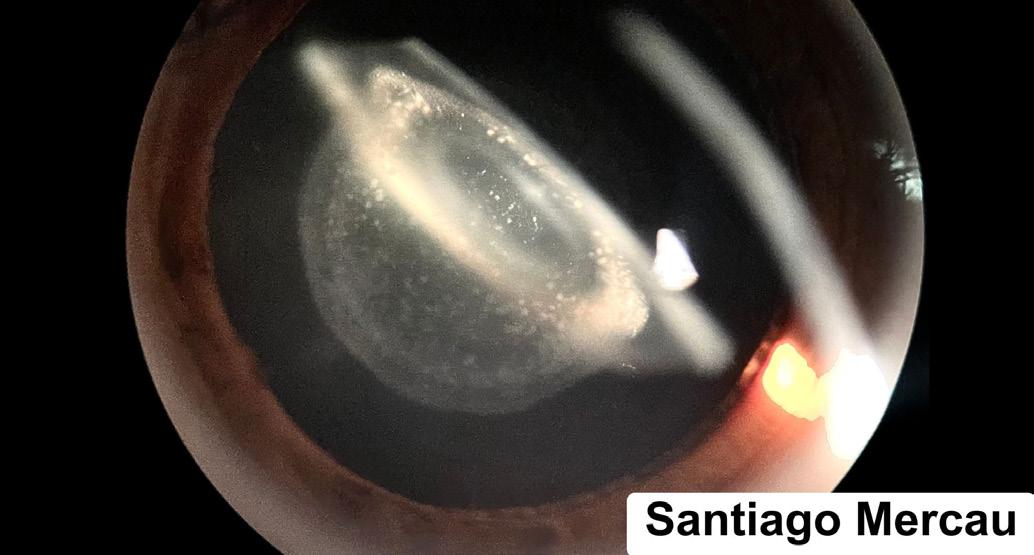
Unusual Congenital Cataract Presenting as a Saturn Ring Structure
Santiago Mercau, Dr Pedro Lagleyze Ophthalmology Hospital, Buenos Aires, Argentina
I decided to submit this picture because it illustrates a rare and visually striking presentation of a congenital cataract with annular opacities resembling planetary rings. The slit lamp image not only highlights the structural features of the lens abnormality but also provides an opportunity to capture the beauty and complexity of ocular pathology. It serves as a reminder that even in clinical findings, there is room for observation, teaching, and visual storytelling.
Get Ahead of Bias and Burnout and Build Your Career!
Are you concerned about burning out early? Wondering what you can do to help promote equitable eye care for all patients? Looking for advice on building your career?
The ESCRS BoSS (Building Our Sustainable Society) initiative is addressing these questions by sponsoring a symposium and courses as well as a speed mentoring programme at the ESCRS Annual Congress in Copenhagen.
Check out the details below and make plans to attend.
BoSS Symposium:
Are you satisfied? From burned out to burning bright
Date: 14 September
Time: 11:00–12:30
Location: Hall B2-M1 (300 seats)
Speed Mentoring Sessions
(Held at the ESCRS membership booth)
BoSS Course: Implicit bias
Date: 14 September
Time: 16:45–18:15
Location: Hall D2 (450 seats)
Speaker: Amy Johnson

Speed mentoring is a dynamic and interactive session where mentees have the opportunity to engage with experienced mentors in short, focused conversations. This format allows for the exchange of knowledge, guidance, and networking in a time-efficient manner. It also offers an excellent opportunity to build your professional network by meeting mentors and fellow mentees, fostering connections that could benefit your career for years to come.

BoSS Course: Combatting unconscious gender bias in ophthalmology, industry, and research Date: 15 September
Time: 09:00–11:00
Location: Hall B1-M5 (300 seats)
Friday, 12 September, 14:00–15:00
Saturday, 13 September, 10:00–11:00
Saturday, 13 September, 14:00–15:00
Sunday, 14 September, 10:00–11:00
Sunday, 14 September, 14:00–15:00
Monday, 15 September, 10:00–11:00 Monday, 15 September, 14:00–15:00

Should Fuchs’ Dystrophy Patients Get Premium Lenses?
Patients’ demand for premium IOLs despite contraindications pose a challenge in Fuchs’ dystrophy treatment.
ANDREW SWEENEY
REPORTS
Finding the right lens for triple procedures is tricky enough without patients weighing in, according to Pavel Studeny MD, PhD.
Professor Studeny highlighted how Fuchs’ dystrophy is the most common cause of corneal transplantation (at around 41% of all cases), with a global prevalence of 7.33%. As risk increases with age, and considering it is often undiagnosed, the demand for treatment is likely to rise.
During 2023 and 2024, Prof Studeny found that 2,804 patients at his clinic had Fuchs’ dystrophy, representing approximately 30% of all patients. Each was graded according to the severity of their disease, and 3% found to have grade 3 Fuchs’ dystrophy or above.
In these cases, he recommends a combined approach, especially towards patients with epithelial cell density of less than or equal to 1,000 cells/mm², pachymetry greater than 640 µm, significant guttae, and morning foggy vision. He emphasised applying this to patients with a hard nucleus and a shallow anterior chamber.
After opting for the combined approach, the next decision is which IOL to use as part of the triple procedure. In the age of Google, this can present issues.
“Normally, we use monofocal IOLs, but some patients know about premium IOLs and want them, but they are contraindicated [in severe Fuchs’ dystrophy],” Prof Studeny noted. “The main problems are calculation errors caused by corneal oedema and hyperopic shift between +0.5 and +1.0.”
In search of a way to mitigate patients’ concerns, Prof Studeny examined whether Vivity (Alcon) extended depth of focus (EDOF) lenses have a higher chance of achieving emmetropia in triple procedures than monofocal lenses. He also wanted to discover whether this lens could extend focus.
The study examined 48 eyes, all of which had cataract and Fuchs’ dystrophy at grade 3 or above. Twenty-six were given the Vivity IOL, and 22 received an IQ monofocal lens (Alcon), as both “have the same lens material and shape.” The Barrett formula target was -0.50 D to -0.75 D.
Some patients know about premium IOLs and want them, but they are contraindicated.
After six months, both uncorrected distance visual acuity was “a little bit higher in the Vivity group,” with 10 eyes achieving ≥ 0.8 and 24 eyes ≥ -0.5. This compares with 8 and 19 eyes achieving the same results with the IQ lens, he reported.
For close distance visual acuity, 25 eyes in the Vivity group achieved ≥ 0.8 and 26 eyes ≥ -0.5. In the IQ lens group, 20 eyes reached ≥ 0.8 and 22 eyes ≥ 0.5. Regarding the defocus curve, the findings were broadly similar, with the monofocal lens being “slightly flatter,” he said.
Concluding, Prof Studeny said the results highlight the safety of using the Vivity EDOF lens during triple procedures. However, he did add that the lens did not produce “statistically significant” results in the study.
Prof Studeny spoke at the 2025 EuCornea conference in Prague.
Pavel Studeny MD, PhD is the head of the department of ophthalmology at the Charles University in Prague, Czech Republic. studenypavel@seznam.cz

AI in IOL Power Selection
Machine learning can improve IOL calculation accuracy but should be optimised.
HOWARD LARKIN REPORTS
Substituting a machine learning (ML)-derived prediction of postoperative anterior chamber depth (ACD) for effective lens position (ELP) estimates can improve the accuracy of many existing intraocular lens (IOL) power formulas.
However, with power formulas that are primarily ML-derived, there is a trade-off between generalisability and customisation. Ideally, they should be optimised for specific patient populations and lenses. New measures are also needed to evaluate their performance, said Nambi Nallasamy MD.
ML and existing formulas
ACD is a measure of the true IOL position after surgery that can be predicted based on preoperative biometry using ML-derived algorithms, Dr Nallasamy said. By contrast, ELP is the distance between the anterior surface of the cornea and the plane of the IOL, if it were infinitely thin. As such, ELP is a theoretical estimate that is back-calculated based on postoperative refractive error, or a “fudge factor,” Dr Nallasamy explained. “[ELP estimates] are really not accurate in existing formulas.”
To test whether using ML-derived ACD predictions could improve IOL power prediction accuracy, Dr Nallasamy directly measured the ACD in 1,205 eyes of 678 patients implanted with AcrySof IQ SN60WF (Alcon) monofocal IOLs. Measured by mean absolute error (MAE), the resulting base model and the base plus a model that included IOL data both predicted the final IOL position significantly more accurately than the Haigis, Hoffer Q, Holladay 1, Olsen, and SRK/T formulas, as well as a linear regression model, Dr Nallasamy reported. A model not considering keratometry for use in ectatic and post-refractive surgery patients also outperformed the existing formulas.1
In a related study, Dr Nallasamy and colleagues substituted their ML-derived ACD predictions for ELP in four existing vergence formulas. The ML-modified ELP significantly improved the performance of the Haigis, Hoffer Q, Holladay, and SRK/T as measured by MAE. The study was based on a training set of 5,761 eyes (80%) and a test set of 961 eyes (20%) of 4,806 patients.2 Similarly, the MLpowered ACD prediction improved the performance of the OKULIX raytracing formula.3
ML-derived IOL formulas
Several currently available IOL power formulas are based primarily on ML-derived algorithms, including the Pearl-DGS, Hill-RBF, Kane, and Nallasamy formulas. However, Dr Nallasamy stressed the trade-off between accuracy and generalisability must be addressed for them to be reliable in the real world. Though ML-derived formulas can be very accurate within their training sets and similar populations, they also tend to
take on the biases of these sets. For example, medium axial lengths and 0.0 D to -3.0 D refractive targets are generally over-represented, resulting in formulas that are less accurate for patients with shorter or longer eyes or unusual refractive targets. “If a machine sees that data and only that data, it’s going to start thinking that predicting zero all the time would make a pretty good formula, and that’s really a problem,” Dr Nallasamy said.
Dr Nallasamy reviewed several methods to address this ‘overfitting.’ One method uses an ensemble approach to derive the formula, in which the first step produces multiple models based on raw biometric and postoperative refractive data, and the second step produces a model based on the predictions of the first-step models plus postoperative refraction. This resulting second-step model tends to even out the biases the first-stage models may pick up from the raw data. Cross-validation further ensures a less biased model.4
Even so, ML models may need further optimisation for different lenses and patient populations, Dr Nallasamy said. IOL constants and transfer learning, in which the ML model is applied to a data set from the targeted population, can markedly improve performance. For example, using transfer learning to optimise the Nallasamy formula helped it outperform several existing formulas using IOL constant optimisation when applied to data from the Aravind eye system in India, as measured by MAE, he reported. Incorporating detailed modelling of the properties of the IOL and the eye can also improve ML formula performance without further optimisation.
However, MAE and median absolute error alone—which measure refraction errors—are not reliable for evaluating the generalisability of ML-based formulas, Dr Nallasamy said. Alongside them, he proposes using mean absolute error of the prediction of the IOL (MAEPI), which measures IOL power prediction errors rather than refractive error, and the correct IOL rate (CIR), which measures the proportion of IOL power prediction errors within 0.5 D of target. A high MAEPI and a low CIR suggest an overfit model.5 “We want to be very careful with our imbalanced data sets,” he said.
Dr Nallasamy presented in the JCRS Symposium at the 2025 ASCRS annual meeting in Los Angeles.
For citation notes, see page 54.
Nambi Nallasamy MD is assistant professor of ophthalmology and visual science and of computational medicine and bioinformatics at the University of Michigan Kellogg Eye Center, Ann Arbor, Michigan, US. nnallasa@med.umich.edu
The Philosophy of Innovation
Deluded personality essential for initiating and completing the journey.
CHERYL GUTTMAN KRADER REPORTS
One key to successful innovation is to have what Buddhists might call a ‘deluded personality,’ says Reay H Brown MD, noted cataract and glaucoma surgeon and innovator.
“Being deluded is a secret weapon for innovation,” he stated.
He traced the origin of this idea to a surprising moment during a university visit with his daughter, Annie. He recounted a conversation with one of Annie’s professors, a renowned neuroscientist and expert in Buddhism. The professor turned to Annie and said, “Your dad is so deluded.”
“The comment was startling at first, but the professor quickly clarified: in Buddhist psychology, there are only three basic personality types—aversive, greedy, and deluded. Given the options, ‘deluded’ did not sound so bad,” Dr Brown reflected.
He has since embraced the label—not as a flaw, but as a mindset essential for innovation.
“For me, being deluded means having irrational optimism, divergent thinking, believing things others don’t,” Dr Brown explained. “[It’s] thinking you can make a difference and not giving up.”
He proposed that innovation often requires two deluded steps: identifying an unmet need others have missed and believing you are the one who can fix it.
A basic, uncomplicated ‘why’ question can outline the unmet need. As an example, Dr Brown described his development of a triple post lid speculum.
“As a new surgeon, I wondered why lid speculums exposed the circular-shaped eye with a rectangular opening,” he said. “Featuring a central post, the speculum I designed and patented created a better, more rounded exposure.”
Nevertheless, having a good idea to solve a problem does not always lead to successful innovation. Timing is also important, Dr Brown said, and he quoted futurist and inventor Ray Kurzweil: “Most inventions fail not because they don’t work, but because the timing is wrong—not all the enabling factors are in place. Invention is like surfing: you have to catch the wave at the right time.”
Some things have to be seen to be believed—but others have to be believed to be seen.
Illustrating this factor, Dr Brown described his work to develop internal sclerectomy as an easier and safer alternative to trabeculectomy. This 15-year project led to the introduction of trabecuphine, which had very limited commercial success because viscoelastic, mitomycin-C, and other necessary tools were lacking at the time, and no companies sought to invest.
“So, imagine my surprise when at the 2019 ESCRS Congress, I saw my movie,” he said. “Sanoculis had brought back my idea as MIMS (minimally invasive microsclerostomy). Now, 35 years after initial conception, the trabecuphine is back because it is still a great idea.”
A big market is another fundamental element for successful innovation, Dr Brown said. Collaborative work with his wife, Mary Lynch MD, for example, led to the EyePass, a T-tube joining Schlemm’s canal to the anterior chamber. However, the FDA required testing in a costly blind eye study, and the sponsoring company went bankrupt during the phase 3 pivotal trial.
“Our goal was to help patients at risk of blindness, but they represented too small of a market,” he noted. “With the iStent, Glaukos created the engine of success for MIGS because it targeted mild to moderate glaucoma that accounts for 95% of the market.”
The long journey from idea to market
Beyond market size, success of independent innovation faces more challenges, as illustrated by the history of the Light Adjustable Lens. First conceived in 1995 by Dan Schwartz MD, a retina specialist at the University of California, San Francisco, the implant did not receive FDA approval until 2017. The years-long journey was possible because Dr Schwartz’s great idea was enabled through his collaboration with scientists at the California Institute of Technology (Caltech) University and company funding, Dr Brown said.
belief that future disruptive innovations will not come from large companies or from inventive surgeons who consult for many companies. Yet Dr Brown remained optimistic, observing there are still many independent innovators, who he described as deluded people with courage who want to solve big problems.
to prevent blindness. Each project felt like an adven ture,” he observed. “Innovators need to see things dif ferently. It is like a belief about seeing the future before it is visible. Some things have to be seen to be believed but others have to be believed to be seen. Most innova tions don’t begin with evidence—there is none. They begin with belief.
innovate you may fail, be discouraged, ignored, want to give up, see others more successful with your ideas, and see your contributions disregarded. But I hope you do it anyway,” he concluded.
Dr Brown spoke at an innovation session during the 2025 ASCRS annual meeting in Los Angeles.
Reay H Brown MD is in private practice in Atlanta, Georgia, US, where he specializes in cataract and glaucoma surgery. reaymary@comcast.net
LEADERSHIP AND BUSINESS RESOURCES
at Your Fingertips
What is the one leadership skill you would like to improve? What is the one business management challenge you would like to overcome?
The ESCRS Leadership, Business, and Innovation (LBI) programme provides ophthalmologists, clinic managers, and administrators and their teams with a variety of content to enable both online and in-person learning. Podcasts, webinars, video interviews, and more are available in the LBI library to help answer questions about topics such as selling a practice, finding a good work-life balance, facilitating patient decision making, and more.
Interpreting OCT Changes in Glaucoma Patient Care
Clinicians cautioned to beware many conditions that can mimic glaucoma.
CHERYL GUTTMAN KRADER REPORTS
Advances in optical coherence tomography (OCT) hardware and software are enabling detection of glaucoma and its progression, but ophthalmologists need not worry that these developments put their jobs at risk.
Sanjay Asrani MD underscored the need for clinical judgement. “OCT machines have no brain. So, please use your own and consider that the structural findings might be associated with another condition.”
Dr Asrani emphasised that a decrease in retinal nerve fibre layer (RNFL) thickness is not specific to glaucoma. Among the possible entities that can masquerade as glaucoma progression, posterior vitreous separation is the most common. Illustrating this situation, he presented an OCT report from a patient with glaucoma that showed a statistically significant negative slope of the RNFL. However, the apparent generalised loss of RNFL thickness occurred in the absence of any change in macular thickness.
“It was not glaucoma that caused the RNFL thickness to change in this case. Instead, it was due to traction caused by vitreous detachment,” he said.
“Glaucomatous OCT changes, on the other hand, are typically seen in the supero- and inferotemporal quadrants in earlier stages of glaucoma. Thus, a review of the raw OCT scans is necessary to make an accurate diagnosis.”
OCT machines have no brain. So, please use your own.

He also underscored the need to examine for symmetry in RNFL and macular thickness or a lack thereof. Highlighting that asymmetry is the hallmark of glaucoma, Dr Asrani added the finding of extreme symmetry or extreme asymmetry in structural changes should also raise suspicion about glaucoma as the cause.
Expounding on this consideration, he discussed a case of a patient with segmental optic nerve hypoplasia whose macular thickness, RNFL thickness, and visual fields showed extreme symmetry. Images from a patient with homonymous hemianopia were presented as an example of a case with high asymmetry, where glaucoma was not the cause. The finding of a vertical cut-off in macular thickness in both eyes led to the correct diagnosis, Dr Asrani said.
Structural changes noted on OCT that follow effective treatment of uveitis might also be misinterpreted as glaucoma progression. Dr Asrani explained that if a patient has RNFL oedema and subclinical oedema associated with active uveitis, resolution of the oedema following treatment for the uveitis will result in a dramatic decrease in RNFL and macular thickness along with cup enlargement. The example he presented was from a patient whose OCT showed these structural changes, suggesting severe glaucoma progression. However, they occurred in the absence of any changes in visual field testing.
Vascular events, like non-arteritic ischemic optic neuropathy, also cause RNFL thinning that can be misinterpreted as glaucoma progression. With vascular events, however, the loss typically occurs inferiorly or superiorly and the other half of the RNFL can be completely normal, Dr Asrani said.
Other conditions causing OCT changes that can be misinterpreted as glaucoma or its progression include cotton wool spots, cancer-associated retinopathy, neurosyphilis, and various common systemic diseases.
“RNFL losses and progressive thinning of the inner retinal layers could be due to hypertension, diabetes, and chronic kidney disease,” Dr Asrani said. “All three of these conditions are present in most patients with glaucoma.”
Dr Asrani presented at the 2025 ASCRS Glaucoma Subspecialty Day in Los Angeles.
Sanjay G Asrani MD is Professor of Ophthalmology and Head of the Glaucoma OCT Reading Center, Duke University School of Medicine, Durham, North Carolina, US. asran002@mc.duke.edu

Need a quick introduction or refresher about a surgical procedure? Have a tip to share about a technique or approach you use that makes surgery easier?
The ESCRS 100 is the place to go. It’s a library of short (roughly 100 seconds), high-quality instructional videos about all fields of cataract and refractive surgery.
More than 40 videos have already been created, and additional videos are being uploaded each month. Current videos include the following topics:
• Primary posterior capsulorhexis in the presence of a posterior capsule plaque
• Endoilluminator-assisted cataract surgery
• Hydrodissection
MAKE EVERY SECOND COUNT
—PUT THE ESCRS 100 VIDEO SERIES ON YOUR LIST OF MUST-WATCH EDUCATIONAL RESOURCES ! ESCRS 100
Exploring Best Practices in Fungal Keratitis Treatment
A leading expert on ocular fungal infections underscores importance of regional considerations.
ANDREW SWEENEY REPORTS
Namrata Sharma MD emphasised the importance of geographical awareness when considering the best treatment approach to fungal keratitis. For example, in north and west India, Aspergillus fumigatus and flavus are more present, whereas in south and east India, Fusarium solani, oxysporum, and moniliforme are more common, dictating which medication and level of aggression should be used in treatment.
Her preferred course of treatment for fungal keratitis is to use topical antifungals, particularly 5% natamycin, administered every hour during the day and twice hourly closer to the patient’s bedtime.
This treatment should be tapered at 4- to 7-day intervals, and overall therapy should take between 3 and 4 weeks. If the patient is initially unresponsive, or if symptoms worsen, Dr Sharma recommended adding 0.15% amphotericin B shots or 1% voriconazole if Candida is present.
For those truly recalcitrant cases, however, Dr Sharma recommended using intrastromal or intracorneal injections. She particularly emphasised that these injections should be used in cases involving deep mycotic keratitis, non-perforated corneal ulcers, and patients failing to respond to conventional topical and systemic antifungal therapy after 4 weeks.
Regarding pharmacological treatments, she noted that, unlike bacterial keratitis, topical steroids cannot treat inflammation in these cases.
Instead, Dr Sharma recommended using topical cyclosporine and tacrolimus, which she added can be combined with antifungal agents to treat the infection itself.
To demonstrate, she pointed to the results of a study she carried out to evaluate the role of cyclosporine as an adjuvant in fungal keratitis cases involving 40 eyes. Visual acuity was reported to be significantly better after 21 days in those patients treated with the topical medication, and there was a comparable difference in ulcer size between the treated patients and the untreated control group.
Lastly, Dr Sharma shared her investigation into the use of corneal cross-linking as a treatment for fungal keratitis via a retrospective study. In the 41 cases examined, she reported there was no advantage offered through cross-linking compared with conventional intervention, but it requires further investigation. Similarly, she believes photodynamic therapy for fungal keratitis requires more research.
Dr Sharma presented at the 2025 EuCornea conference in Prague.
Namrata Sharma MD, FRCOphth, FRCS(Ed) is a professor of ophthalmology at the All India Institute of Medical Sciences, New Delhi, India. namrata.sharma@gmail.com

Keratitis: Suggested Protocols by Evidence
Knowing when and how to run diagnostics is an art and a science.
ANDREW SWEENEY REPORTS
When can bacterial keratitis be treated empirically by a generalist, and when should a specialist be consulted for more advanced diagnostics? Mor Dickman MD, PhD addressed this question at a recent conference.
“We need to make a distinction between what we see as cornea specialists and what is seen by general ophthalmologists,” he said. “When it comes to bacterial keratitis, most infections can be treated empirically and don’t really need diagnostics.”
However, Professor Dickman said that diagnostics should be considered when faced with the following factors: central corneal infiltrate within 3 mm of the centre and ≥ 2 mm in size, ≥ 2 adjacent infiltrates, significant stromal involvement or melting, and ≥ 1+ anterior cells.
A history of corneal surgery, atypical clinical features suggesting fungus, amoeba, or mycobacteria, a poor response to initial empiric therapy, and risk factors (like contact lens contamination in hot tubs) should also be considered.
When it comes to actually performing diagnostics, Prof Dickman advised caution for patients who have already been treated with antibiotics, as the process could have “a lower yield.” He noted that if the treatment fails, it’s still recommended to halt treatment for 12 to 24 hours, if possible. Proparacaine 0.5% can inhibit polymerase chain reactions (PCR), so he advocates using another anaesthetic, “scraping the periphery to reduce the risk of perforation,” adding that culturing contact lenses is not recommended due to the presence of normal flora, unless Acanthamoeba is suspected.
“It’s good to consider Giemsa staining for amoeba and chlamydia, KOH/Calcofluor for fungal testing, and acid fast for Nocardia and Mycobacteria. You should also consider non-nutrient agar seeded with E coli for Acanthamoeba keratitis,” Prof Dickman said. “Just be careful with your technique to avoid contamination.”
Growing HSV-1 resistance in the Netherlands
Prof Dickman then provided an interesting example of when materials should be taken for further diagnosis, in the form of herpes simplex (HSV-1) infectious epithelial keratitis. He said diagnostics should be collected during the patient’s first presentation, in recurring cases where the pathogen was not previously identified, and if the disease is severe enough to rule out acyclovir resistance.
“This is something we do in the Netherlands. I know this is not common practice elsewhere, but we have seen an increase in cases of resistant herpes,” Prof Dickman said.
“It’s important to distinguish between HSV-1 and herpes zoster (VZV). In some settings, up to a quarter of cases that we think
are HSV-1 are zoster, and that requires a different approach.”
Regarding the material that should be gathered in this case, Prof Dickman recommended a swab of the affected epithelium for PCR testing, which applies to both HSV-1 and VZV.
Discussing immune stromal keratitis HSV-1, Prof Dickman said that while there are generally no indications for diagnostics, they should be collected if HSV-1 infection is not confirmed and if there’s no response to therapy. In these cases, he said clinicians should consider corneal biopsy to identify other infectious causes and communicate consistently with the labs while doing so.
“Don’t just send and forget [your samples]. Discuss [with the lab] the reasoning why you’ve taken a biopsy and what kind of diagnostics you need from them,” Prof Dickman said.
Diagnostics are also recommended in all cases of necrotising stromal keratitis associated with HSV-1, he said, as the condition has a severe clinical presentation that carries a high risk of superinfection in addition to viral infection.
Be aware of contact lens wearers
Noting up to 23% of Acanthamoeba keratitis cases may be polymicrobial or co-infected with HSV-1, Prof Dickman emphasised the importance of considering contact lens wearers—especially in cases of corneal trauma complicated by exposure to soil or contaminated water when testing for Acanthamoeba keratitis, which is just as important from a legal perspective as it is good practice.
“If you miss Acanthamoeba keratitis in a contact lens wearer and there’s a [legal] claim from a patient, it would most likely be justified,” Prof Dickman said.
Finally, Prof Dickman also recommended taking a combined approach in testing for the condition as no single test is 100% sensitive and specific in detecting it. The culture eye swab test remains the gold standard, but he said this method is still slow and has low sensitivity, although PCR testing has its limitations too.
“You need to understand that the results of a PCR test are also a statistical function. You need to have internal controls,” Prof Dickman said. “That’s why it makes sense to concentrate all these tests in select centres—you can get a continuous flow of samples.”
Prof Dickman spoke at the 2025 EuCornea conference in Prague.
Mor Dickman MD, PhD is the Head of the Department of Ophthalmology at University Medical Center Utrecht, Netherlands. m.m.dickman@umcutrecht.nl

Has Femtosecond Keratoplasty Come of Age?
Lecture outlines femto surgery benefits.
ANDREW SWEENEY REPORTS
Ophthalmology has come a long way over the years, and “Femtosecond Keratoplasty, Coming of Age?” highlighted how this journey appears most evident in the evolutionary advances in laser technology within the discipline. Professor Jod Mehta’s medal lecture at EuCornea 2025 claimed inspiration from his personal journey as much as ophthalmology’s. Expressing his appreciation for the work of Donna Strickland, the Canadian optical physicist known for her work developing the chirped pulse amplification technique for lasers, he provided a comprehensive overview of the benefits of femtosecond lasers.
Femtosecond lasers work by emitting ultrashort pulses of light with durations measured in femtoseconds (10-¹⁵ s), the second shortest measurable unit of time currently known to science, which allows them to generate an extreme amount of power with relatively little energy expended.
These lasers cut tissue through photodisruption, involving plasma and shock wave formation to create a non-thermal ablation known as laser-induced optical breakdown (LIOB), during which plasma is generated by the laser pulse that expands to displace surrounding tissue.
“Femtosecond technology has been around since 2003, with first-generation devices like the AMO IntraLase 15/30 kHz proving effective. However, they were slow and prone to breaking down,” Prof Mehta said. “In 2007, technicians would
regularly be flown into Singapore from Germany to fix them.”
The third-generation devices represent a significant improvement, Prof Mehta said. The AMO IntraLase 60 kHz, Alcon Wavelight FS200, and others are more powerful and can perform extra functions previously unavailable, such as keratoplasty.
The benefits of femtosecond lasers in keratoplasty are obvious according to Prof Mehta, especially when compared with manual keratoplasty. He said the manual approach involves mechanical straight trephination, which can cause potential misalignment due to divergent recipient cut angles, something femtosecond lasers can avoid.
“With femtosecond, you also have the advantage of a faster healing time and better wound strength thanks to the increased surgical wound area, plus resistance to leaking,” he said. “The technique also provides for earlier visual rehabilitation due to quicker suture removal and less postoperative astigmatism.”
Lasers and mushrooms rolled into one
The femtosecond laser’s journey towards its coming of age didn’t finish with the third generation, however. Prof Mehta said two innovations have allowed it to complete this process: liquid interface and intraoperative-guided tunnel creation (iOCT) combined with deep anterior lamellar keratoplasty (DALK).
“Liquid interface keratoplasty enables real-time intraoperative adjustment of trephination to tackle difficult posterior stromal scar cases. This causes less endothelial cell damage to the recipient, with a lower intraocular pressure rise and no corneal distortion,” Prof Mehta said.
Femtosecond lasers have transformed keratoplasty.
“iOCT-guided mushroom tunnel DALK offers the advantage of tunnel creation with an optimal morphological and topographical profile, which provides improved safety and efficacy as a result.”
Prof Mehta pointed to several studies to verify their effectiveness, including one involving a 17-year-old girl with full-thickness corneal perforation related to paediatric keratitis. She was first treated with DALK in 2017 but withdrew from treatment until returning in 2020 with corneal scarring.1
“I took off the first DALK and repeated it again, and after doing the intraoperative-guided, femto[second laser]-assisted DMEK, the scar was removed from the inside of the eye. She’s now 22 and we never had to do a full-thickness penetrating graft for her. She had smaller endothelial cell replacement and best-corrected visual acuity (BCVA) of 6/9,” Prof Mehta said.
Regarding the iOCT mushroom tunnelling technique, Prof Mehta described a case study involving one patient with granular corneal dystrophy. He carried out a mushroom configuration graft on one eye, having previously opted for a conventional straight DALK procedure for the other several years earlier.
On the ‘mushroom eye,’ visual acuity reached +2.50/-1.75 x 90 6/6, whereas the eye treated more conventionally achieved +2.50/-6.50 x 74 6/6. However, Prof Mehta noted what was particularly important was that he was able to achieve these results within four months in the ‘mushroom eye,’ but it took “the best part of a year and a half” to achieve the results he recorded for the first eye treated with conventional DALK.
“Femtosecond laser-assisted mushroom DALK tunnel has the refractive advantage of large keratoplasty,” he said. “The larger anterior surface reduces the chance of perforations in suturing, and the mushroom configuration provides a mechanical advantage that supports better wound healing.”
Prof Mehta delivered the 2025 EuCornea Medal Lecture in Prague.
For citation notes, see page 54.
Jod Mehta MBBS, FRCOphth, FRCS(Ed), FAMS, PhD is a senior consultant at the Singapore Eye Centre. jodmehta@gmail.com

ESCRS Patient Portal
Patients are understandably curious to learn as much as they can about their upcoming cataract or refractive surgery. ESCRS has developed a Patient Portal on its website to help inform patients about these surgeries.
The Portal is split into two sections: Cataract and Refractive. Each section provides an easy-to-understand summary of the different types of conditions, including the benefits, risks, procedures, and aftercare of common conditions. Each section is easily navigable, with clear diagrams and a glossary to convey all the information patients might need to help prepare for surgery or during aftercare.
Need to Know: Visual Metrics
An ophthalmologist’s comprehensive guide to understanding visual metrics.
BY SOOSAN JACOB MS, FRCS, DNB
Optical quality of the images formed in the human eye can be assessed using key optical quality metrics. These include the modulation transfer function (MTF), optical transfer function (OTF), phase transfer function (PTF), point spread function (PSF), and the Strehl ratio. Visual perception or visual transfer function (VTF) is contributed to by the optical transfer function (OTF) and the neural transfer function (NTF). Let us understand each of these terms.
The optical transfer function describes how details or different spatial frequencies are transferred by the human eye’s optical system. It consists of the MTF and the PTF and is the Fourier transform of the PSF. A reduction in OTF results in loss of high spatial frequencies or fine details.
OTF = MTF (amplitude/magnitude) + PTF (phase shift).
Modulation transfer function
Image performance is characterized by resolution and contrast. Resolution is the ability to distinguish object detail and is measured in terms of line pairs per millimetre (lp/ mm), cycles per millimetre, or frequency. Inverse of frequency gives the spacing between two resolved line pairs. Contrast is the difference in light intensity between an object and its background. It can be degraded by diffraction effects, optical aberrations, and vignetting. Contrast = (Imax − Imin)/(Imax + Imin), where ‘I’ refers to intensity.
MTF is a performance metric that measures the ability of an optical system to transfer all the various levels of detail (spatial frequencies) from object to image. Thus, it describes contrast loss/preservation (how much image contrast is degraded as compared to object contrast) at different spatial frequencies. It is the optical contribution to contrast sensitivity function (CSF) and refers to the ratio of image contrast to object contrast as a function of spatial frequency.
To determine MTF, a sinusoidal pattern with 100% contrast is used as the object, and MTF is plotted on the y-axis (representing contrast transfer) with spatial frequency on the x-axis. It is also often plotted in comparison to that of a perfect, aberration-free, diffraction-limited system.
As spatial frequency of the lines increases (i.e., line spacing decreases), the contrast of the image decreases due to optical limitations such as diffraction, aberrations (both lower and higher order), and scatter (e.g., media abnormalities, such as corneal haze or cataracts). A high MTF allows contrast in fine details while a low MTF diminishes contrast, resulting in blurry, washed-out images. Degradation makes distinguishing small features in the image more difficult. Low illumination can affect MTF; therefore, testing is generally set to photopic conditions, although charts may also be plotted at different illumination levels.
MTF is the absolute value or magnitude of OTF, derived from the Fourier transform of the PSF. The human eye has low MTF and consequently a low OTF for high spatial frequencies, so very fine details are not perfectly transmitted, thus limiting resolution of vision.
PTF describes phase distortions across different spatial frequencies—the light waves that shift in phase affecting sharpness and alignment of details. This is especially necessary to describe aberrations (like coma and astigmatism) where MTF alone is not sufficient, as these create a shift in image features without decreasing contrast. Symptoms of phase distortions include ghosting, diplopia, and asymmetrical blur.
Point spread function
The PSF is the image of the point source formed by the human eye or any other optical system. A point source constitutes the most fundamental object and is the basis for more complex objects. A perfect optical system should image a point source of light as a single point. However, aberrations, diffraction, and imperfections spread the image into a blurry spot. The PSF for a perfect optical system is the Airy disc, which is the Fraunhofer diffraction pattern for a circular pupil. PSF is the inverse Fourier transform of the OTF; A larger PSF implies a poorer image quality.
A Strehl ratio is the ratio between peak intensity of the real PSF and a theoretically perfect, diffraction-limited PSF. A higher Strehl ratio indicates sharper vision, while a lower ratio indicates worse PSF and lower MTF. The average value for the human eye is approximately 0.1–0.3, which is secondary to aberrations.
NTF refers to the processing of spatial frequency information within the retina and the brain that further refines visual perception. Factors affecting NTF include:
Photoreceptor sampling: The cone density of the fovea limits the amount of detail perception. The Nyquist sampling theorem states that the maximum resolvable spatial frequency is half the photoreceptor sampling rate. The Nyquist limit refers to the highest frequency the retina can process without aliasing artefacts (false patterns). In the fovea, cone spacing allows a theoretical Nyquist limit of approximately 60 cycles per degree (cpd). However, the actual perceived limit is slightly lower (approximately 40–50 cpd) due to neural optimization.
Neural contrast enhancement: This works through lateral inhibition and cortical processing. Lateral inhibition reduces the activity of neighbouring neurons when one neuron is stimulated. In the visual process, surrounding signals are suppressed by horizontal and amacrine cells to enhance contrast and colour discrimination. It sharpens edges via the Mach band effect—an optical illusion of
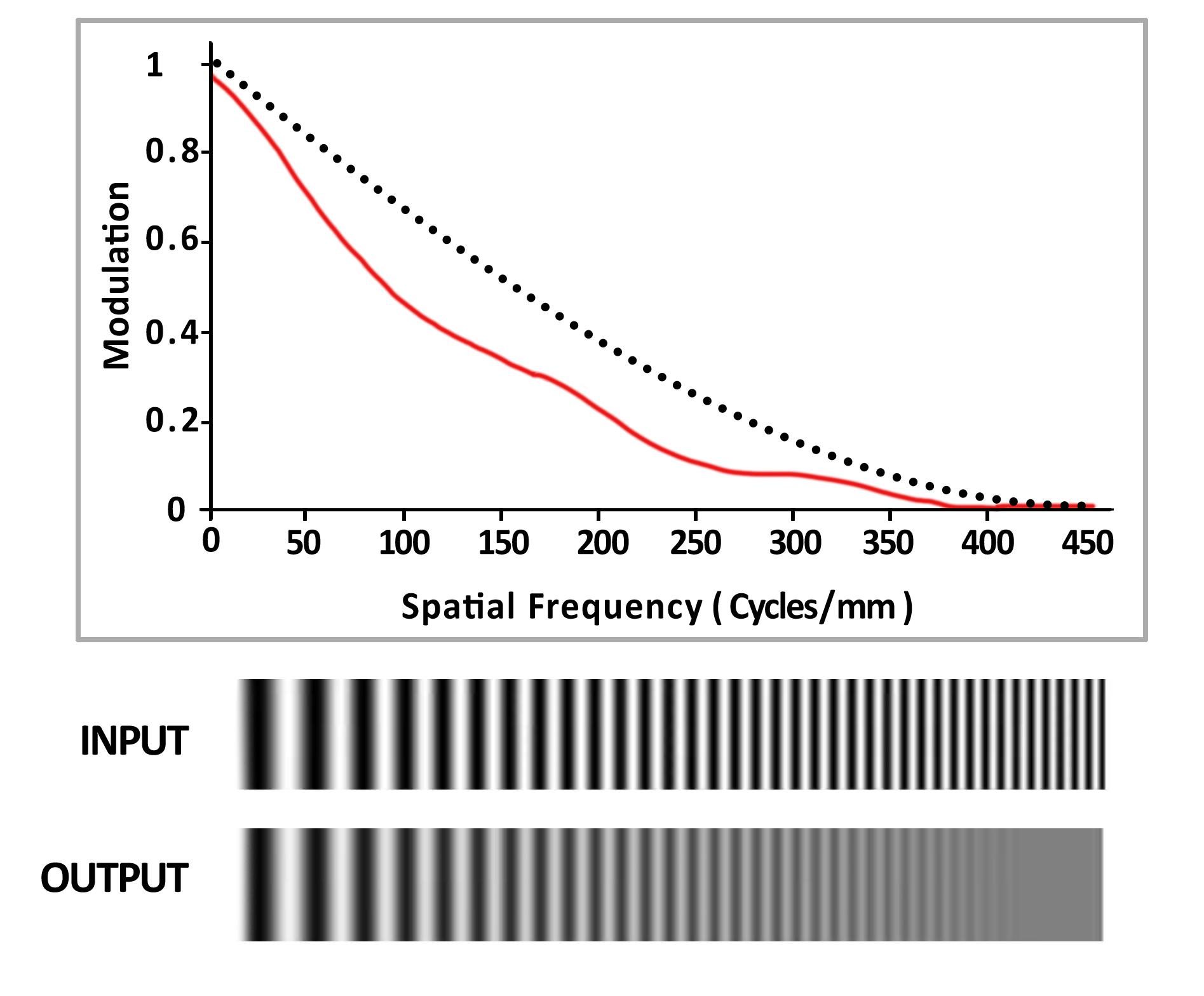
edges appearing darker or lighter than in reality. Cortical processing by the visual cortex is responsible for further enhancement and higher-level interpretation via edge detection, orientation sensitivity, and motion perception. NTF enhances mid-spatial frequencies, improving edge detection. It also suppresses very high spatial frequencies (above 60 cpd) to filter out noise and aliasing and reduce the perceptual impact of optical aberrations.
While neural processing can compensate for some optical aberrations, an excess decline in MTF, and consequently OTF and VTF (explained later), can cause loss of detail. Wavefront-guided, wavefront-optimized, and topography-guided LASIK, intracorneal ring segments, CAIRS, and aberration-modifying IOLs, among others, are all attempts to improve the optical transfer function of the eye. Adaptive optics aid in researching wavefront modification.
Stiles–Crawford effect
The Stiles–Crawford effect (SCE) is an optical and retinal phenomenon that gives different weightage to light entering the eye through different pupil locations. Cones are 200-fold more tightly packed in the foveal region. Foveal cones are also taller and thinner than peripheral cones (1.5–2.0 µm at the fovea versus 4.0–10.0 µm in the peripheral retina). The shape and high refractive index of the foveal cones compared to the surrounding intercellular medium give them optical waveguide-like properties.
Similar to an optical fibre, foveal cones guide and preferentially transmit axial light entering at angles closer to their optical axis. SCE-I explains how light rays entering at the
centre of the pupil are perceived as brighter and more effective for vision than those entering near the periphery of the pupil, even if their physical intensities are the same. SCE-I therefore pre-filters retinal input, providing a better optical signal to the retina by suppressing peripheral rays that are more affected by aberrations. SCE-II refers to the perceived colour of light changing slightly depending on the pupil entry location. This effect is greatest for red and blue light where chromatic dispersion is maximum. SCE-II compensates for chromatic aberration by altering neural perception of colour differences.
VTF describes the final perceived visual quality and is secondary to the combined effect of OTF and NTF.
Adaptive optics
In visual research, adaptive optics (AO) help to correct aberrations using a combination of wavefront sensors, real-time feedback control systems, and deformable mirrors or liquid crystal spatial light modulators that correct distortions. AO is used to study higher-order aberrations, design and simulate the effect of custom corrections, and understand neural adaptations. It is also used in retinal imaging to compensate for image distortion secondary to ocular aberrations.
This is the fourth in a multipart tutorial on higher-order aberrations. Previous articles in the series can be found at escrs.org/eurotimes.
Dr Soosan Jacob is Director and Chief of Dr Agarwal’s Refractive and Cornea Foundation at Dr Agarwal’s Eye Hospital, Chennai, India, and can be reached at dr_soosanj@hotmail.com.
Autograft Hunting in LSCD
Knowing when to perform LSCD surgery is as crucial as how.
ANDREW SWEENEY REPORTS
Some people may be autograph hunters, but in ophthalmology, autografts are more interesting, according to Marc Muraine MD.
Professor Muraine provided a comprehensive overview of limbal autografts as they pertain to the management of unilateral limbal stem cell deficiency (LSCD). The condition is serious, as it can result in the corneal epithelium becoming unable to heal itself.
“Limbal autografts are indicated for treatment because, in case of the destruction of the limbus—from a chemical burn, for example—you will have limbal stem cell deficiency with a corneal conjunctivalisation and a decrease in visual acuity,” he said. “Most of the time, this is unilateral, but it can be bilateral following a genetic or inflammatory disorder.”
Current protocols indicate surgery should be utilised in stages IIB and III of LSCD, in which the central axis is involved, and the complete vascularisation of the cornea is present, respectively. In unilateral cases, treatment usually involves harvesting stem cells from the unaffected eye.
However, in patients with severe conjunctival inflammation, this treatment is ineffective, and LSCD can reappear. This means a different approach is required, said Prof Muraine.
“The corneal epithelium [could be] represented by the flower, which can only bloom if it’s planted in fertile soil and watered regularly. Do you think it will grow in dry soil?”
To ensure the eye can therefore flourish, he recommended observing the patient for up to two years in cases of unilateral deficiency. If the conjunctiva, corneal sensitivity, and tear film are prepared, it’s time for surgery. If not, the ocular surface
needs to be optimised step by step, including conjunctival reconstruction and anti-inflammatory treatment.
While there are several surgical strategies for repairing LSCD, he highlighted one for particular attention: simple limbal epithelial transplantation (SLET). This technique achieves a stable epithelium of the avascular surface in 78% of cases, compared with 61.4% achieved by cultivated limbal epithelial transplantation (CLET).
Other limbal autografts Prof Muraine discussed involved taking a graft from the oral mucosa and placing it into the eye. However, he noted procedures involving the oral mucosa are contraindicated if attempts to improve the ocular surface previously failed.
Even with many surgical options available, Prof Muraine said LSCD remains “a condition with an uncertain prognosis,” while adding SLET does have the advantage of being simple and effective at low cost. The key factor for clinicians to remember when it comes to LSCD and limbal autografts is to ensure the proper groundwork is in place before proceeding with surgery.
“None of these techniques can be considered without prior normalisation of the conjunctiva, tear film, and the cornea,” he said. “Also, don’t forget scleral lens oxygen.”
Prof Muraine presented at the 2025 EuCornea conference in Prague.
Marc Muraine MD is Professor and Head of the Ophthalmology Department at the Charles Nicolle Hospital Rouen, France. marc.muraine@chu-rouen.fr


https://escrs.org/special-interest-groups/yos/
Corneal Surgery’s Contribution to Climate Change
Keratoplasty’s impact on greenhouse gases is greater than many might suspect.
ANDREW SWEENEY REPORTS
The fight against climate change involves ophthalmology as much as, or more than, other medical specialties. The effect of fluorinated gases used in keratoplasty procedures may have a greater impact than many might suspect, according to Matteo Airaldi MD.
“We know that healthcare contributes significantly to greenhouse gas emissions. In particular, in the UK, 5.5% of the country’s emissions are attributed to the national healthcare system,” said Dr Airaldi, presenting on behalf of Alfredo Borgia MD.
“In ophthalmology, fluorinated gases used during surgery are the main contributors to greenhouse gases. These include sulphur hexafluoride (SF6), hexafluoroethane (C2F6), and octafluoropropane (C3F8).”
Describing these gases as having a “high global warming potential,” he said they are used in routine procedures, including vitreoretinal surgery and endothelial keratoplasty. To understand their full impact on the environment, Drs Borgia and Airaldi evaluated the carbon emissions originating from the latter procedure.
Their research was organised as a retrospective singlecentre study at the Royal Liverpool University Hospital between 2022 and 2024 and involved 357 endothelial keratoplasty cases. These included Descemet membrane endothelial keratoplasty (DMEK), ultrathin Descemet stripping automated endothelial keratoplasty (UT-DSAEK), and rebubbling.

In total, 160 DMEK procedures (44.8%) were performed, 118 (33.1%) UT-DSAEK, and 79 (22.1%) rebubbling. Equivalent CO2 was calculated according to data provided by the Intergovernmental Panel on Climate Change (IPCC),
and both 15 mL and 30 mL canisters of fluorinated gases were used. SF6 gas at a concentration of 20% was used during the DMEK and UT-DSAEK procedures; however, the rebubbling procedures used a combination, including air.
SF₆ has a significant carbon footprint despite its clinical benefits.
The study found that the total number of procedures in the study emitted 1.5 tonnes of CO2 over three years, equivalent to approximately “14,000 kilometres driven by an average car.” SF6 30 mL emitted 4.93 kg of CO2 per canister over the same period, equivalent to four times that of C2F6 or C3F8 15-mL canisters, whereas 15-mL canisters of SF6 emitted 2.46 kg of CO2
“SF6 has a significant carbon footprint despite its clinical benefits; it’s responsible for four times as many emissions as other fluorinated gases we considered. The smaller, 15-mL canisters are more efficient, especially C2F6 and C3F8,” Dr Airaldi said.
“Using an air tamponade for rebubbling may be sustainable in low-risk cases. Reusing canisters that have undergone filtration could be considered, where safe and permitted.”
The researchers concluded with a call to action to ophthalmic surgeons to consider how they can integrate eco-conscious choices in corneal surgery without compromising patient care. They highlighted the current policy of utilising disposable, single-use canisters as being particularly problematic, as alluded to in their study’s findings.
“We can reduce the environmental impact of corneal surgery by preferring smaller canisters, choosing alternative gases or air, and by advocating for more sustainable packaging. We might also have the possibility of reusing gases from larger cylinders,” Dr Airaldi said.
Dr Airaldi presented on behalf of Dr Borgia at the 2025 EuCornea conference in Prague.
Matteo Airaldi MD is a doctoral candidate at the University of Brescia, Italy. matteo.airaldi@unibs.it
Alfredo Borgia MD, FEBO is a cornea consultant at the “Mons. Dimiccoli” Teaching Hospital, Barletta, Italy. alfredo.borgia@aslbat.it

Systemised AI for Surfer’s Disease
A lack of a standardised process for pterygium surgery could change thanks to AI deep learning.
ANDREW SWEENEY REPORTS
Artificial intelligence is frequently used while surfing the web, but it’s now being applied to a condition associated with surfing—pterygium—according to Carolin Elhardt MD.
While the condition usually occurs in the corner of the eye, in severe cases it can grow to cover the cornea. It is commonly known as ‘surfer’s eye’ due to prolonged exposure to UV radiation as its primary cause.
As pterygium can present a variety of symptoms and clinical features, Dr Elhardt said the decision regarding whether to perform surgery is not standardised. The decision is ultimately based on the surgeon’s judgement, other factors, and their experience.
An AI-driven deep learning model uses multilayered neural networks to simulate the complex decision-making power of the human brain. This system can identify and analyse key patterns in complex, high-dimensional data, thus streamlining the diagnostic process of a disease like pterygium.
Dr Elhardt and her colleagues developed a deep learning model that processed information on 328 pterygium patients who were then split into two categories based on corneal specialist analysis: surgery indicated and surgery not indicated. Clinical information included in the model were age, artificial tear use, presence of symptoms, ocular surface irritation, sphere shape, astigmatism, and visual acuity.
The clinical raw data was entered into a deep learning model and fed through a rectified linear unit multilayer perceptron neural network. To act as a control, images based on the Scheimpflug principle were fed through a ResNet-18 multilayer neural net as part of the same process. Both data sets were then connected in a final layer of analysis to create a binary result.
95%
Our deep learning model reached 95% accuracy in aligning with specialist decisions—offering real potential to support more consistent, evidence-based care in pterygium surgery.
The independent corneal specialists placed 55% of the patients in the ‘surgery indicated’ category and 45% in the ‘surgery not indicated’ category. Dr Elhardt reported that the deep learning model achieved a top mark of 95% accuracy compared to the specialist findings when it combined the analysis of both the raw clinical data and Scheimpflug principle control images.
Data processed solely via the deep learning model achieved a 90% accuracy rate, and the information processed via the Scheimpflug principle control images achieved an 82% accuracy rate. Dr Elhardt also found that different factors were prioritised by the deep learning model during its decision-making process, with both sphere size and astigmatism weighed more heavily than other considerations.
In her concluding remarks, Dr Elhardt said the deep learning model they created is capable of assisting physicians in the decision-making process. It should particularly help in achieving higher rates of patient satisfaction by supporting well-considered, evidence-based decisions, which can affect pterygium surgery by a wide variety of factors.
Dr Elhardt presented at the 2025 EuCornea conference in Prague.
Carolin Elhardt MD is an ophthalmology resident at Ulm University Hospital, Germany. carolin.elhardt@uniklinik-ulm.de

Four AI Applications Ready for Practice
Artificial intelligence (AI) is entering the mainstream of ophthalmology. At the 2025 American Society of Cataract and Refractive Surgery annual meeting, four companies outlined currently available AI-powered platforms designed to increase the speed and reliability of everything from surgical planning and diagnostics to clinical research, patient flow, and inventory control.
Adi from Alcon
Developed by Alcon, the Adi platform helps manage all the moving parts that go into surgery, said Gregory A Eippert MD. It is designed to address supply chain problems such as guessing which supplies are available and when ordered supplies will arrive; time-consuming manual checks; and trouble getting complete patient data from the clinic to the surgical centre—all of which can delay procedures.
Adi helps ensure products are available on time every time, said Dr Eippert, who helped beta test the system. The platform fits in with Alcon’s Vision Suite. Two Adi modules, Clinic Connect and Inventory Manager, were released at the meeting.
Clinic Connect gathers and shares surgery information from clinics and surgery centres through a central database updated in real time for scheduling and ordering supplies. It is connected to Inventory Manager, which automatically tracks Alcon IOLs using RFID, monitors supply usage and upcoming need, and reserves and orders needed supplies online.
All this helps ensure a smooth, successful surgery day, Dr Eippert said. “It’s going to reduce miscommunications, reduce potential mistakes, and really reduce last-minute surprises.”
Amaros precision intelligence
The Amaros AI platform unifies fragmented clinical and research data into real-time insights to drive efficient and effective operations, said Mark Packer MD.
For example, the system can sift through thousands of records to identify patients with cataracts who have not been seen recently so they can be contacted. For research, it can quickly sift electronic records to identify patients meeting specific study inclusion and exclusion criteria, making it possible to find a dozen eligible candidates out of thousands. Amaros AI also seamlessly answers business questions, such as how much revenue premium lenses bring into the organisation.
“It’s machine learning, but it’s not the machine that is learning; it is helping us learn,” Dr Packer said.
AVTR for admin
AVTR Med creates AI assistants that reduce administrative costs in ophthalmic practices by 50%, said Grayson Armstrong MD—a significant reduction because, on average, physicians spend more than 15 hours per week on paperwork and administration, which is a major factor in provider burnout.
AI can help with tasks including scheduling, insurance verification, patient follow-up, and staff education, Dr Armstrong said. For example, patient calls to schedule or reschedule appointments can be done by an AI avatar. If the patient has questions, the system can switch them to a human staff member, which he said vastly boosts staff productivity. “You can call all of your patients simultaneously and
get the responses in a matter of minutes, not [through] a full day of work.”
Zeiss for precision surgery
Carl Zeiss Meditec has three AI initiatives focused on improving cataract surgery outcomes, said Mitchell P Weikert MD.
First is an IOL power calculation formula that replaces IOL constants with an AI formula optimised for each unique IOL model to better predict refractive outcomes in real eyes. So far, the system can be used with 13 lenses from Zeiss, Alcon, Bausch + Lomb, and Johnson & Johnson. It is available on the VERACITY surgical planning system.
In tests, the Zeiss AI formula equalled some of the best available IOL formulas—both conventional and AI derived—in all eyes and often did better in difficult cases. For example, in short eyes, the Zeiss formula was with 0.5 D of target refraction in 73% of eyes, compared with 67–69% for some of the best performing rivals.1 In post-LASIK/PRK eyes, Zeiss achieved 76% within 0.5 D of target, bettering Barret True-K and Oculix competitors.2
Second, Zeiss offers a surgical video analysis program that uses AI to segment and assess each step of the surgical process, which can help improve surgical speed, efficiency, and accuracy, Professor Weikert said. Simply upload the videos to the cloud for analysis.
Third, Zeiss is developing an AI-powered tool for preoperative macular OCT analysis, which may help select patients for premium lenses and improve outcomes. The system is designed to spot and offer preliminary diagnoses for a range of macular conditions that may interfere. It is currently in use in Europe and South America. “These are all very exciting,” Prof Weikert said.
All comments were made in an AI Symposium at the 2025 ASCRS annual meeting in Los Angeles.
For citation notes, see page 54.
Gregory A Eippert MD is an ophthalmologist in private practice in Mentor, Ohio, US.
Mark Packer MD, FACS heads Packer Research Associates, a consulting group specialising in ophthalmology in Fort Collins, Colorado, US. mark@markpackerconsulting.com
Grayson Armstrong MD, MPH is an ophthalmologist and medical director of Ophthalmic Emergency Services at Massachusetts Eye and Ear, and instructor associate director of medical student education at Harvard University, both in Boston, US. grayson_armstrong@meei.harvard.edu
Mitchell P Weikert MD, MS is a professor at the Cullen Eye Institute, Baylor College of Medicine, Houston, Texas, US. mweikert@bcm.edu
GLOBAL REACH
As a renowned authority in the field of cataract and refractive surgery, ESCRS facilitates global connections amongst ophthalmic professionals, fostering collaboration and the exchange of knowledge.
Our events span across continents, providing a platform for pioneering research, advanced surgical techniques, and continuous professional development.
Using the interactive map on our website, we invite you to explore our global presence by viewing upcoming events and academies.
Join us to network with esteemed experts, access the latest advancements, and contribute to the enhancement of eye care on a worldwide scale.
AI-Assisted Cataract Surgery
Emerging programs may enhance cataract grading and IOL power calculation.
HOWARD LARKIN REPORTS
Artificial intelligence-powered (AI) programs are developing rapidly and could improve cataract surgery outcomes, said Ryan G Smith MD. Intraocular lens (IOL) power calculation and cataract grading are among the promising applications.
AI in IOL calculation
The recent rise in AI and machine learning in diagnostics and surgical planning is driven by supervised learning using large data sets to create powerful predictive models, Dr Smith said. Deep learning models can interpret biometry, predict refractive error, and even incorporate intraoperative aberrometry, with the ORA device (Alcon) drawing on data from more than 2 million cases. Moreover, these can be updated as more postoperative data becomes available, further improving accuracy over time.
“The hope is we will get improved accuracy, especially in atypical eyes.”
Still, little data exists to show how much more accurate AI formulas may be, Dr Smith said. One study of 7 AI IOL formulas involving 214 Caucasian eyes with axial lengths from 24.50 mm to 25.97 mm found the Hill-RBF formula most accurate, with 86% within 0.5 D of target, followed by the LSI AI and PEARL-DGS, both above 85%.1
Another meta-analysis comparing 21 formulas across 12 studies involving 2,430 myopic eyes with axial lengths of 26.00 mm or more found a statistical difference between AI formulas and newer generation traditional formulas, with a trend towards AI superiority.2 A third study showed some AI formula accuracy exceeding 90%.3
“We’re getting better, but so are traditional formulas,” Dr Smith said.
On the horizon, the Precision Ladas Universal Super algorithm (PLUS) can train itself using just a few hundred eyes, yielding accuracy up to 94%. The model has the advantages of constantly updating itself and adding new parameters without creating a new model, Dr Smith said. It is customisable to the needs of one surgeon or groups.
AI cataract grading
Grading cataracts is crucial for surgical planning, and AI can help, Dr Smith said. Programs learn by analysing slit lamp and fundus images, allowing them to quantify nuclear sclerosis, cortical opacity, and posterior subcapsular opacity, which helps suggest optimal timing for surgery, as well as technique and approach, and reduces inter-observer variability, he noted. Benefits include better accuracy and better patient satisfaction.
Yet he did note several limitations on using AI for surgery, including data bias, poor generalisability, ‘black box’ concerns on AI decision making, and regulatory and medical-legal
issues. He stressed the importance of human oversight and the need for larger, unbiased studies to guide best practices.
Nonetheless, Dr Smith sees a big future for AI in cataract surgery. Integration into biometry devices and EHRs, AIassisted IOL formula options, and real-time prediction tools in the OR are all available or close to it.
“Ultimately, we will see personalised surgery planning using AI customised to individual surgeon preferences and outcomes,” he concluded.
Dr Smith spoke in an AI Symposium at the 2025 ASCRS annual meeting in Los Angeles.
For citation notes, see page 54.
Ryan G Smith MD is an ophthalmologist at Pacific Eye Institute in Upland, California, and assistant clinical professor at the University of California, Irvine, US. ryangsmithMD@gmail.com



Making Myopia Consensus Accessible
Digestible tool alerts all to myopia in children.
General ophthalmologists, eye care professionals, paediatricians, and all key figures involved in children’s health need practical and effective tools to recognise and manage myopia in children. This year’s Myopia Consensus Statement by the World Society of Paediatric Ophthalmology & Strabismus (WSPOS) helped fulfil this need, summarising everything essential about myopia management and treatment, as highlighted by both Ken K Nischal MD and Dominique Brémond-Gignac MD, PhD.
Myopia has become more of a public health concern, with a rise in the prevalence of nearsightedness globally. Experts are talking about a myopia pandemic, and by 2050, half of the global population may be myopic, with more than 740 million children and adolescents affected.1
Understanding the risks
The need to control myopia progression stems from the risks associated with high myopia, which can increase the
chances of retinal detachment, glaucoma, cataracts, and other eye conditions.
“The longer your eyeball, the [more] nearsighted you are, and as the eyeball becomes longer, it starts to affect the function and the outcomes of eye health,” Professor Nischal explained. “When the eyeball gets beyond 26 millimetres, the retina does not function properly.”
Several solutions with at least two years of follow-up and solid scientific evidence are now available to control myopia progression, including defocus lenses and contact lenses, lowdose atropine eye drops, orthokeratology, low-level red light therapy, and combination treatments. The WSPOS Consensus Statement presents all these options in an accessible and easyto-understand format, while also explaining their mechanisms of action and potential side effects.
By 2050, half of the global population may be myopic— including more than 740 million children and adolescents.
“The consensus statement provides new data for practitioners, and it is very important to update it regularly, because it is essential to keep children away from high myopia,” Professor Brémond-Gignac noted. “Every dioptre increases the risk of maculopathy, so every dioptre counts.”
However, as the statement highlights, prevention and behavioural interventions remain key in the fight against myopia progression. Daily exposure to natural light, for example, has strong scientific support in protecting children from myopia. Good habits—such as managing screen time and near work, taking breaks every 30 minutes, and avoiding reading in dim light—are also essential. In this context, the role of parents is pivotal, especially in ensuring children adhere to the prescribed treatment to support progress and prevent worsening, as both specialists emphasised. It is also important to consider customised solutions according to what the child and family need, especially financial ones, which must be thoroughly discussed, according to Prof Brémond-Gignac.
A multidisciplinary approach
Myopia management requires a comprehensive approach and understanding to become increasingly effective. For example, as Prof Nischal pointed out, paediatricians and general practitioners—not ophthalmologists—are often the first to respond to children’s health needs. As such, myopia management involves a multidisciplinary group of professionals, including physicians, optometrists, nurses, and opticians, which is why teamwork is essential. Education and awareness for everyone, therefore, play a fundamental role. WSPOS is fully committed to this through webinars, podcasts, and the broad dissemination of the consensus statement’s content, with plans to translate the WSPOS statement into multiple languages to reach a global audience.
Collaboration with public health institutions and schools should also be effective in educating the public about the risks of myopia, as Prof Nischal wrote in an editorial published in Eye 2 Some countries, such as France, dedicate an entire week each year to national myopia campaigns, featuring free screening programmes and advertisements on social media, TV, and newspapers.
Within the ophthalmic community, general ophthalmologists can play a vital role by staying updated and performing initial patient screenings to identify cases that require referral to a myopia specialist, as Prof Brémond-Gignac emphasised timing is a crucial element. Only patients with high myopia or associated conditions—such as glaucoma, retinal dystrophies, or retinopathies—should be referred to a paediatric ophthalmologist. As Prof Nischal suggested, it is important to establish a workflow within one’s clinic, which may include having a myopia specialist or a nurse practitioner who can counsel parents.
Windows to the soul
Spreading awareness about how to control and manage myopia is essential not only for children’s eye health but also for their overall and mental well-being. In an increasingly digital world, the ophthalmological community remains integral in helping children and families understand the importance of preventive strategies such as spending time outdoors and limiting screen time. “As leaders in ophthalmology, we can be the windows to the soul of the entire human race and influence the generations to come, improve their health, and control myopia. Children are our future, and their vision must be saved,” Prof Nischal said. For Prof Brémond-Gignac, early detection and prevention are among the most important strategies in myopia management.
“There are many existing myopia control systems that we can prescribe, and they need to be known by everybody. The Myopia Consensus Statement is an incredibly good system of guidelines to be disseminated globally,” she concluded.
The WSPOS Consensus Statement is available online at https://wspos.org/myopia-consensus-statement-2025/
For citation notes, see page 54.
Ken K Nischal MD, FAAP, FRCOphth is professor and chief of paediatric ophthalmology and strabismus at UPMC Children’s Hospital of Pittsburgh, Pennsylvania, US. nischalkk@upmc.edu
Dominique Brémond-Gignac MD, PhD, FEBO is professor and head of the ophthalmology department at University Hospital Necker-Enfants-malades and Paris University, Paris, France. dominique.bremond@aphp.fr

Aid Cuts Threaten Global Eye Care Progress
USAID closure leads retreat in development assistance.
The past 35 years marked steady progress towards reducing blindness and vision impairment worldwide. While absolute numbers climbed due to population growth, global blindness prevalence declined by half, and moderate to severe vision impairment prevalence rose slightly, driven largely by untreated presbyopia and other age-related diseases in ageing populations.1
Supporting these gains was a coincidental increase in donor governments’ official foreign development aid to lower-income countries, which more than doubled worldwide from less than $100 billion in 2000 to about $220 billion in 2023. That trend has now reversed. After a 9% drop in 2024, the Organisation for Economic Co-operation and Development (OECD) projects a further decrease of 9–17% in 2025, with more cuts announced through 2027.
The sharpest cuts are from the US, which accounted for about one-quarter of the total contributions over the past decade. And while several donor countries, including Ireland, Korea, and Spain, plan increases, 10 others, including France, Germany, and the UK, are also pulling back. Indeed, the 4 largest donors, which together account for nearly two-thirds of all government donations, all cut aid in 2024, and 2025 may mark the first time they all declined for 2 consecutive years.
As a result, total official development aid is likely to fall
to 2020 levels by 2027. “While still above 2019 pre-pandemic levels, the projected cuts risk undoing recent gains at a time of growing needs across countries and territories that receive [official development aid],” according to a June OECD report.2
Looming health crisis
The impact on global health could be devastating. Regarding cuts to programmes funded by the now-dissolved US Agency for International Development (USAID) alone, “[f]orecasting models predicted that the current steep funding cuts could result in more than 14 051 750 (uncertainty interval 8 475 990–19 662 191) additional all-age deaths, including 4 537 157 (3 124 796–5 910 791) in children younger than age 5 years, by 2030,” according to a June study in The Lancet.3
The study also estimated that USAID-funded programmes cut all-cause mortality for all age groups by 15%, and 32% for children aged less than 5 years, saving about 92 million lives from 2001 through 2021. “USAID funding has significantly contributed to the reduction in adult and child mortality across low-income and middle-income countries over the past two decades. […] Unless the abrupt funding cuts announced and implemented in the first half of 2025 are reversed, a staggering number of avoidable deaths could occur.”
Funding for some programmes initially cut has been re-
stored, though mostly for humanitarian aid. And overall cuts remain steep, leaving a fragmented and uncoordinated system.4
Though death due to sickness and starvation, particularly AIDS and malaria, is the most severe outcome, funding cuts also significantly harm global eye care. The cuts interfere with the treatment of blinding neglected tropical diseases, including trachoma, onchocerciasis (river blindness), and lymphatic filariasis, leading at least one affected agency to pause anti-blindness and other medication and health support campaigns.
“[T]he suspension of US funding now means this essential work is on pause. Even temporarily suspending mass drug administration means millions of people in vulnerable communities will miss life-saving treatments. These diseases don’t pause—every missed round of mass drug distribution allows them to spread, increasing suffering and disabling pain. Currently 100 million people across 6 African countries that Helen Keller serves are now at risk,” according to a statement on the Helen Keller International website.5
More broadly, cutting support for primary care, including vaccinations, leads not only to increased mortality but increased ocular disease related to infections, including malaria, herpes, and measles—which in the first half of 2025 hit a 25year record for new cases in, of all places, the US, where the disease was considered eradicated in 2000, and vaccination rates have been falling.
Prevention cuts
Funding for health clinics has already led to the closure of some outposts in lower-income countries, particularly in rural areas, according to aid agency reports. Eye screening, access to eyeglasses, and support for hospitals and clinics offering medical and surgical treatment for cataracts, glaucoma, and retinal disease are among the casualties.6 Malnutrition and treatable vitamin A deficiencies also contribute to poorer eye health, as do deep cuts in sanitation and clean water assistance.
The cuts have pushed many groups to step up private fundraising as well as advocacy efforts, including Helen Keller International.
“We are fighting for the lives and well-being of our communities. We are in Washington DC, speaking with elected officials to help them understand the full impact of funding pauses. We are rallying together with like-minded partners who don’t want to turn away from children and families. We are speaking with journalists to put a face to those bearing the brunt of US government funding pauses and cuts. And we are working around the clock to invite new donors and trusted friends to act with courage and generosity,” the organisation said in a statement.
We can wish them well—and help with donations and advocacy.
For citation notes, see page 54.

iLEARN
ESCRS iLearn is an online learning platform, free for ESCRS members.
Visit elearning.escrs.org to access over 30 hours of interactive, assessed, and accredited e-learning content, including surgical videos, diagrams, animations, quizzes, and forums.
EU MDR certification for Glaukos MIGS devices
Glaukos Corporation has received European Union Medical Device Regulation (EU MDR) certification for several minimally invasive glaucoma surgery (MIGS) devices, including the Trabecular Micro-Bypass iStent infinite and iStent inject W—its first approval under the new EU regulations. The iStent infinite (Model iS3) is approved as a standalone treatment for primary open-angle glaucoma unresponsive to other therapies, featuring three heparin-coated titanium stents that can be placed across up to six clock hours of Schlemm’s canal using an auto-injection mechanism. glaukos.com
EU approval for extended treatment intervals with EYLEA
The European Commission (EC) has approved an extension of the label for EYLEA 8 mg in the European Union (EU), allowing for treatment intervals of up to six months in patients with wet age-related macular degeneration (AMD) and diabetic macular oedema (DME). Previously, EYLEA 8 mg was authorised for administration at intervals of up to four months. It is now the first and only anti-vascular endothelial growth factor (VEGF) therapy in the EU that permits treatment intervals of up to six months for both wet AMD and DME. regeneron.com
Tecnis Odyssey multifocal IOL launched in Europe
Johnson & Johnson announced it has launched the Tecnis Odyssey intraocular lens (IOL) in Europe, the Middle East, and Canada. First launched in the US in October 2024 and built on the TECNIS platform, the lens is designed to deliver continuous vision—from near to far—using a freeform diffractive surface for seamless transitions. jnj.com
Alcon acquires LumiThera
Alcon has acquired LumiThera and its Valeda Light Delivery System, which is intended for the treatment of dry age-related macular degeneration (AMD) through photobiomodulation (PBM). The device uses specific wavelengths of red, near-infrared, and yellow light to stimulate mitochondrial energy production in the retina, aiming to reduce retinal inflammation and oxidative stress. In the LIGHTSITE III study, the device demonstrated positive results over two years compared to a control light therapy. It received De Novo marketing authorisation from the FDA in 2024. alcon.com
Heidelberg launches innovation hub
Heidelberg Engineering has announced the introduction of ZinserLab, an innovation hub dedicated to advancing imaging technologies for eye care. Named after the company’s late co-founder, Gerhard Zinser PhD, its purpose is to facilitate the transition from research to practical applications in ophthalmic imaging. Heidelberg Engineering is also expanding its collaboration with Orbis to support global training initiatives through Orbis’s telemedicine and e-learning platform, Cybersight. heidelbergengineering.com
Oral DME treatment shows promise
Breye Therapeutics has completed a phase 1b trial of danegaptide, an oral small molecule developed for early-stage non-proliferative diabetic retinopathy (NPDR) and diabetic macular oedema (DME). The multicentre dose-escalation study found danegaptide was well tolerated at all doses with no dose-limiting toxicities and showed preliminary clinical activity, such as reduced vascular leakage and improved retinal anatomy. breye.com

RIDLEY REAPPRAISED
To commemorate the 75th anniversary of Harold Ridley’s first intraocular lens (IOL) implantation in 1950, Robert K Maloney MD and Sloan Mahone DPhil offer a reassessment of Ridley’s legacy. They question the standard narrative—popularised by Ridley’s biographer David Apple—that portrays Ridley as a misunderstood innovator vindicated over time. The authors argue this view unfairly maligns Ridley’s critics, particularly Stewart DukeElder, who raised valid concerns about insufficient preclinical testing, high complication rates, patient safety, and Ridley’s secretive methods. Ultimately, they noted the historical debate highlights the tension between rapid innovation and prudent oversight, emphasising the importance of scepticism to protect against unsafe advances.
RK Maloney, et al. “Harold Ridley and the invention of the intraocular lens: a reappraisal,” 51(7): 629–634.
‘HOLE-IN-THE
CARD’ TESTING FOR OCULAR DOMINANCE CAN BE MISLEADING
Assignment of ocular dominance with the commonly used ‘hole-in-the card’ test often does not align with the patient’s preferred eye when using sensory testing with a visual simulator simulating monovision, a new study indicates. In the prospective double-masked study, 326 participants underwent ocular dominance testing using a ‘hole-in-thecard’ method through distance refraction and sensory testing using a wearable, head-mounted, binocular, see-through visual simulator to both identify and quantify the eye dominance strength at near and far. The study showed strong ocular dominance for far vision in 50% of participants and 56% for near vision, with a roughly equal percentage of the remaining distributed between weak and equidominance. The eye chosen as the dominant eye with the ‘hole-in-thecard’ sighting method did not match the results from the sensory dominance test for 41% of patients. In addition, 26% of participants changed from right eye dominance with the ‘hole-in-the-card’ to left eye dominance with the sensory EDS test, and 15% changed from left to right.
JS Pepose, et al. “Assessing ocular dominance: rethinking the current paradigm,” 51(7): 592–599.
MONOVISION WITH EDOF IOL ACHIEVES HIGH PATIENT SATISFACTION
Monovision correction with the Vivity® non-diffractive EDOF IOL (Alcon) provides good to excellent visual acuity at all distances, high spectacle independence, and strong satisfaction with minimal visual disturbances after cataract and refractive lens exchange (RLE) surgeries, according to a Vivity registry subgroup analysis. Among 200 patients (179 with cataracts, 24 with RLE), all showed excellent uncorrected distance and intermediate visual acuity at three to six months, as well as good near vision. Excellent distance acuity was maintained across low and medium monovision levels, while better near vision was seen with medium and high monovision. Spectacle independence for distance and intermediate was highest with medium monovision. Satisfaction and minimal visual issues were consistent across all monovision levels.
M Teus, et al. “Visual and participant-reported outcomes of a wavefront-shaping EDOF intraocular lens implanted bilaterally with monovision,” 51(7): 549–556.

Cited in this Issue
Perioperative Medication Regimens for Cataract Surgery
Page 19
1. Barry P, Seal DV, Gettinby G, Lees F, Peterson M, Revie CW; ESCRS Endophthalmitis Study Group. J Cataract Refract Surg, 2006; 32(3): 407–410. Erratum in: J Cataract Refract Surg, 2006; 32(5): 709.
2. Wielders LHP, Schouten JSAG, Winkens B, et al; ESCRS PREMED Study Group. J Cataract Refract Surg, 2018; 44(4): 429–439. Erratum in: J Cataract Refract Surg, 2018 Sep; 44(9): 1166.
3. Wielders LHP, Schouten JSAG, Winkens B, et al; ESCRS PREMED study group. J Cataract Refract Surg, 2018; 44(7): 836–847.
Debate: FS-LASIK or KLEx for Hyperopia?
Page 20
1. Reinstein DZ, Sekundo W, Archer TJ, et al. J Refract Surg, 2022 Dec; 38(12): 760–769.
2. Ma KK, Manche EE. J Cataract Refract Surg, 2023 Apr 1; 49(4): 348–353.
3. Hashemi H, Roberts CJ, Elsheikh A, et al. Trans Vis Sci Technol, Mar 1; 12(3): 12.
4. Ma KK, Manche EE. Am J Ophthalmol, 2022 Sep; 241: 248–253.
5. Sekundo W, Messerschmidt-Roth A, Reinstein DZ, et al. J Refract Surg, 2018 Jan 1; 34(1): 6–10.
6. J Refract Surg, 2017 Mar; 33(3) and 2017 Jun; 33(6).
Avoiding Posterior Capsule Rupture
Page 24
1. Chan TCY, et al. J Cataract Refract Surg, 2014; 40: 2076–2081.
2. Pujari A, et al. Semin Ophthalmol, 2021 Nov 17; 36(8): 684–691.
3. Pujari A, et al. Clin Ophthalmol, 2021 Feb 3; 15: 389–401.
4. Sarkar S, Das S. Oman J Ophthalmol, 2023 Jun 27; 16(2): 244–251.
5. Thamizhselvi D, et al. Indian J Ophthalmol, 2023 May; 71(5): 1913–1917.
6. J Cataract Refract Surg, 2020 Sep; 46(9): 1260–1265.
7. Nanavaty MA, Mehta PA, Raj SM, et al. Eye, 2006; 20: 949–951.
8. J Cataract Refract Surg, 1999; 25: 238–235.
9. Vasavada AT, Raj SM. J Cataract Refract Surg, 2004; 30: 1167–1169.
10. Vasavada AR, et al. J Cataract Refract Surg, 2015; 41: 702–707.
AI in IOL Power Selection
Page 29
1. Li T, Yang K, Stein JD, et al. Transl Vis Sci Technol, 2020 Dec 21; 9(13): 38.
2. Li T, Stein J, Nallasamy N. Br J Ophthalmol, 2021 Apr 9; 106(9): 1222–1226.
3. Li T, Reddy A, Stein JD, et al. Br J Ophthalmol, 2023 Apr; 107(4): 483–487.
4. Li T, Stein J, Nallasamy N. Br J Ophthalmol, 2022 Apr 4; 107(8): 1066–1071.
5. Li T, Stein JD, Nallasamy N. Transl Vis Sci Technol, 2023 Mar 28; 12(3): 29.
Has Femtosecond Keratoplasty Come of Age?
Page 36
1. Lim J, Abusayf MM, Liu YC, Mehta JS. Bioengineering (Basel), 2024 Nov 25; 11(12): 1192.
Four AI Applications Ready for Practice
Page 44
1. Kenny PI, et al. J Cataract Refract Surg, 2023; 49(7): 697–703.
2. Chen E, et al. Presentation at the American Society of Cataract and Refractive Surgeons annual meeting, 25–28 April 2025, Los Angeles, California, US.
AI-Assisted Cataract Surgery
Page 46
1. Stopyra W, et al. J Clin Med, 2024 Jan 16; 13(2): 498.
2. Zhou Y, et al. Front Public Health, 2023 Nov 9; 11: 1279718.
3. Tsessler M, et al. J Cataract Refract Surg, 2022 Jan 1; 48(1): 37–43.
Making Myopia Consensus Accessible
Page 48
1. Liang J, Pu Y, Chen J, et al. Br J Ophthalmol, 2025; 109: 362–371.
2. Nischal KK. Eye, 2025; 39: 1–3. doi:https://doi.org/10.1038/ s41433-024-03406-5
Aid Cuts Threaten Global Eye Care Progress
Page 50
1. The Lancet Global Health, 2021 Feb; 9(2): e130-e14.
2. “Cuts in official development assistance: OECD projections for 2025 and the near term,” OECD Policy Briefs. 26 June 2025. https://www.oecd.org/en/publications/cuts-in-official-development-assistance_8c530629-en.html
3. Cavalcanti DM, et al. The Lancet, Online first. 30 Jun 2025. doi:https://doi.org/10.1016/S0140-6736(25)01186-9
4. Walker AS, Khurana M, Zhang C. “What remains of USAID?,” New York Times, 22 Jun 2025.
5. Helen Keller International. www.helenkellerintl.org
6. Cure Blindness Project. www.cureblindness.org


ESCRS Educational Forum is supported by multiple industry partners to provide independent didactic education on selected therapeutic areas. The platform combines presentations from ESCRS Winter and Annual Congresses, selected EuroTimes articles, videos, and webinars to provide an in-depth overview on current clinical outlooks.
Upcoming Events
September 4–7
EURETINA
Paris, France
September 12–16
2025 ESCRS Congress Copenhagen, Denmark
September 12
ESCRS iNovation Day Copenhagen, Denmark
September 25–28
German Ophthalmology Society Berlin, Germany
October 18–20
American Academy of Ophthalmology
Orlando, Florida, US


4 Sept
12 Sept 25 Sept


18 Oct

Research. Education. Innovation.
ESCRS’s vision is to educate and help our peers excel in our field. Together, we are driving the field of ophthalmology forward.


YOU DON’T WANT TO MISS THIS!
Learn about iStent inject® W and the new iStent infinite® trabecular micro-bypass, the only truly microinvasive technologies offering safe interventional glaucoma helping delay disease progression.
Glaukos Speakers Corner
iStent infinite® IMPORTANT SAFETY INFORMATION: INDICATION FOR USE. The iStent infinite System is intended to reduce intraocular pressure safely and effectively in adult patients diagnosed with primary open-angle glaucoma, pseudo- exfoliative glaucoma or pigmentary glaucoma. The device is safe and effective when implanted in combination with or without cataract surgery in those subjects who require intraocular pressure reduction and/or would benefit from glaucoma medication reduction. The device may also be implanted in patients who continue to have elevated intraocular pressure despite prior treatment with glaucoma medications and/or conventional glaucoma surgery. CONTRAINDICATIONS: The iStent infinite System is contraindicated under the following circumstances or conditions: •In eyes with primary angle closure glaucoma, or secondary angle-closure glaucoma, including neovascular glaucoma, because the device would not be expected to work in such situations.• In patients with retrobulbar tumor, thyroid eye disease, Sturge-Weber Syndrome or any other type of condition that may cause elevated episcleral venous pressure WARNINGS/PRECAUTIONS:
• For prescription use only.
• Intended users are trained ophthalmologists only.
• This device has not been studied in patients with uveitic glaucoma.
• Do not use the device if the Tyvek® lid has been opened or the packaging appears damaged. In such cases, the sterility of the device may be compromised.
• iStent infinite is MR-Conditional
• Due to the sharpness of certain injector components (i.e., the insertion sleeve and trocar), care should be exercised to grasp the injector body. Dispose of device in a sharps container.
• Physician training is required prior to use of the iStent infinite System.
• Do not re-use the stent(s) or injector, as this may result in infection and/or intraocular inflammation, as well as occurrence of potential postoperative adverse events
• There are no known compatibility issues with theiStent infinite and other intraoperative devices (e.g., viscoelastics) or glaucoma medications.
• Unused product & packaging may be disposed of in accordance with facility procedures. Implanted medical devices and contaminated products must be disposed of as medical waste.
• The surgeon should monitor the patient postoperatively for proper maintenance of intraocular pressure. If intraocular pressure is not adequately maintained after surgery, the surgeon should consider an appropriate treatment regimen to reduce intraocular pressure.
• Patients should be informed that placement of the stents, without concomitant cataract surgery in phakic patients can enhance the formation or progression of cataract. ADVERSE EVENTS: The most common postoperative adverse events reported in the iStent infinite pivotal trial included IOP increase ≥ 10 mmHg vs. baseline IOP (8.2%), loss of BSCVA ≥ 2 lines (11.5%), ocular surface disease (11.5%), perioperative inflammation (6.6%) and visual field loss ≥ 2.5 dB (6.6%). CAUTION: Please see DFU for a complete list of contraindications, warnings, precautions, and adverse events. iStent inject® W IMPORTANT SAFETY INFORMATION: INDICATIONS FOR USE: The iStent inject® W, is intended to reduce intraocular pressure safely and effectively in patients diagnosed with primary openangle glaucoma, pseudo- exfoliative glaucoma or pigmentary glaucoma. The iStent inject® W, can deliver two (2) stents on a single pass, through a single incision. The implant is designed to stent open a passage through the trabecular meshwork to allow for an increase in the facility of outflow and a subsequent reduction in intraocular pressure. The device is safe and effective when implanted in combination with cataract surgery in those subjects who require intraocular pressure reduction and/or would benefit from glaucoma medication reduction. The device may also be implanted in patients who continue to have elevated intraocular pressure despite prior treatment with glaucoma medications and conventional glaucoma surgery. CONTRAINDICATIONS: The iStent inject® W System is contraindicated under the following circumstances or conditions: • In eyes with primary angle closure glaucoma, or secondary angleclosure glaucoma, including neovascular glaucoma, because the device would not be expected to work in such situations. • In patients with retrobulbar tumor, thyroid eye disease, Sturge-Weber Syndrome or any other type of condition that may cause elevated episcleral venous pressure. WARNINGS/PRECAUTIONS:• For prescription use only. • This device has not been studied in patients with uveitic glaucoma. • Do not use the device if the Tyvek® lid has been opened or the packaging appears damaged. In such cases, the sterility of the device may be compromised. • Due to the sharpness of certain injector components (i.e. the insertion sleeve and trocar), care should be exercised to grasp the injector body. Dispose of device in a sharps container. • iStent inject® W is MRConditional.• Physician training is required prior to use of the iStent inject® W System. • Do not re-use the stent(s) or injector, as this may result in
