




Empower yourself to help your patients
Dentists trust Great Lakes. And have trusted Great Lakes for sleep screening devices, appliances, and technical support for over 35 years. Whether you are new to sleep medicine or a veteran, we have the solutions to help your patient’s sleep disordered breathing.







When I began my career as an oral medicine specialist, I quickly realized that the mouth rarely keeps its secrets. It speaks volumes; not just in symptoms, but in signs of deeper, systemic disruptions. And nowhere is that more apparent than in the realm of sleeprelated breathing disorders.
As I step into the role of Editor in Chief at MedMark Media and Publisher of Dental Sleep Practice, I bring with me a deep belief that the future of healthcare lies not in further specialization or fragmentation but in bold and intentional integration. This is the work I have dedicated my career to: integrating medicine and dentistry, advancing personalized care, and reshaping the systems that too often keep our professions in parallel rather than in true collaborative partnership.
Our readers, clinicians like you, are already on the frontlines of that shift. You understand that managing sleep apnea is not just about mandibular advancement devices; it is about recognizing airway health as a cornerstone of whole-body wellness. You know that the success of our treatments not only improves sleep but improves health outcomes and saves lives.
That is why, starting now, we begin writing a new chapter in the story of Dental
Sleep Practice. In the coming months, you will see exciting changes unfold: a broader editorial scope, more medically grounded insight, expanded global perspective, and yes – a new name. This transformation will not just reflect where dental sleep medicine has been; it will illuminate where it is going. But our core mission remains unchanged: to equip and inspire a community of clinicians who are willing to think bigger, collaborate wider, and lead smarter. Together, we will explore what is next in diagnostics, therapeutics, patient engagement, precision medicine, and system-wide integration. Because the horizon is not just approaching, it is already here. Thank you for joining us in this moment of transformation. The journey ahead is not just about airway health; it is about breathing new life into how we practice, how we learn, and how we lead.
Let us take the bold and courageous next step. Together.
WATCH the DSP AADSM highlight reel by scanning the QR code or view more in-depth interviews and demos from the American Academy of Dental Sleep Medicine 2025 Annual Meeting. We didn’t miss anything!
While we hope to see you at Airway Palooza 2025 in October in Fort Lauderdale...
CONNECT with us on social media for more exclusive content.





Scott S. De Rossi, DMD, MBA Editor in Chief, Publisher, and Senior Strategic Advisor, MedMark Media

Cover Story
How Technology Enhances Patient Care and Your Financial Health by Dr. Mark Murphy
Read about why Dr. Murphy joined Restfull powered by IAOS


Continuing Education Healthcare as a Listening Exercise by Steve Carstensen, DDS
There are always two experts in the room.
2 CE CREDITS

Clinical Focus Tongue-Tie: Small Band, Big Problems by Bella Kavalerchik, PT
Physical Therapists add valuable insight to whole-body connection.


Medical Insight Obstructive Sleep Apnea During Pregnancy by Snigdhasmrithi Pusalavidyasagar, MD, FAASM
Pregnancy associated hormonal, physiological, and physical changes can all impact OSA.

Medical Insight
Congestive Heart Failure and Sleep Disordered Breathing by Alan D. Steljes, MD, FACC, FRCPC
Sleep disordered breathing is commonly associated with Congestive Heart Failure.







6 Publisher’s Perspective A Fresh Beginning and a Grateful Heart by Lisa
Moler, Founder, MedMark Media

12 In Memoriam John Remmers, MD He will be missed, but his enthusiasm lives on.
16 Cardio-Sleep Corner The Genetics of Sleep by Lee A. Surkin, MD, FACC, FCCP, FASNC, FAASM, and Robert J. Floro, MS, RRT
Every person’s unique genetics play a huge role in their sleep patterns.
30 Adjunctive Therapy Vibration Therapy and Orofacial Myofunctional Therapy: Enhancing Health Through Synergy by Angela Richwine, RDH, BAS, QOM Combination therapy improves results.
32 Product Spotlight Simplify Sleep Testing without Compromising Accuracy Scale with ease using WatchPAT Solutions.
34 Practice Management Unlocking Predictable Growth in Dental Sleep Medicine by Jon Nierman
Take the right steps to be successful.
37 Product Spotlight MediOX: Level 4 Overnight Pulse Oximetry and Body Position Recorder
Overnight pulse oximetry advances with more data.
38 Education Spotlight The Critical Need for Business and Leadership Excellence in the Dental Industry by Scott S. De Rossi, DMD, MBA Empowering the future through Serendequity Education.
43 Product Spotlight Great Lakes Can Help You Provide Solutions for Your Sleep and Airway Patients Support is merely a phone call away.
44 Product Spotlight Anaphylaxis Preparedness in Dental Practices by J. Wesley Sublett, MD, MPH, and Donald Cohen, DMD
What to know to be prepared.
48 Seek and Sleep DSP LetterBoxed
Fall 2025
Publisher | Scott S. De Rossi, DMD, MBA scott.derossi@nexusdentalsystems.com
Chief Dental Editor
Steve Carstensen, DDS, D.ABDSM stevec@medmarkmedia.com
Chief Medical Editor
Lee A. Surkin, MD, FACC, FCCP, FASNC drsurkin@n3sleep.com
Associate Editor | Lou Shuman, DMD, CAGS lou@medmarkmedia.com
Editorial Advisors
Jamila Battle, MD (Family/Sleep/Addiction)
Steven Bender, DDS
Jagdeep Bijwadia, MD (Pulmonary, Sleep)
Kevin Boyd, DDS
Saim Choudhry, DO (Internal Medicine, Sleep)
Alison Kole, MD, MPH, FCCP, FAASM (Sleep, Pulmonary, Critical Care)
Karen Parker Davidson, DHA, MSA, M.Ed., MSN, RN
Bertrand de Silva, MD, FCCP, D.ABSM
Daniel Gartenberg, PhD (Behavioral Sleep)
Kristie Gatto, MA, CCC-SLP, COM
Amalia Geller, MD (Neurology, Sleep)
William Hang, DDS, MSD
Steve Lamberg, DDS, D.ABDSM
Ian Lalich, MD (ENT, Sleep)
Christopher Lettieri, MD (Pulmonary, Critical Care, Sleep)
Pat McBride, PhD, CCSH
Jyotsna Sahni, MD (Internal Medicine, Sleep)
Ed Sall, MD (ENT, Sleep)
Alan D. Steljes, MD (Cardiology, Sleep)
Laura Sheppard, CDT, TE
DeWitt Wilkerson, DMD
Scott Williams, MD (Psychiatry, Sleep)
Gy Yatros, DMD

Director of Business Development
Adrienne Good | agood@medmarkmedia.com
Director of Operations
Melissa Minnick | melissa@medmarkmedia.com
Director of Publishing
Amanda Culver | amanda@medmarkmedia.com
Director of Marketing
Amzi Koury | amzi@medmarkmedia.com
eMedia Coordinator
Michelle Britzius | emedia@medmarkmedia.com
Social Media
Felicia Vaughn | felicia@medmarkmedia.com
Website Support
Eileen Kane | webmaster@medmarkmedia.com
MedMark, LLC
400 Crossing Blvd. Bridgewater, NJ 08807
Tel: (480) 621-8955
www.DentalSleepPractice.com
Subscription Rate: 1 year (4 issues) $149




Lisa Moler Founder, MedMark Media
American Poet T.S. Eliot wrote, “Every moment is a fresh beginning.” These words have become my North Star – my entire journey with MedMark has been a tapestry of transformative new beginnings, each one more meaningful than the last.
Looking back on these incredible 21 years, my heart is full thinking about how we’ve scaled our impact within the dental community. When I founded Doctor of Dentistry back in 2004, it felt like launching a passion project into the unknown. But watching it evolve, and then witnessing the game-changing expansion with Implant Practice US and Endodontic Practice US in 2007, followed by Orthodontic Practice US in 2009, and Dental Sleep Practice in 2014 – each launch was like watching my children take their first steps. Through this incredible journey, we’ve successfully published 297 publications to date since MedMark’s inception – that’s countless late nights, early mornings, weekend marathons, and probably tens of thousands of road-warrior travel hours poured into every single issue. Each publication represents not just content, but sleepless nights, endless revisions to ensure excellence, and the unwavering commitment to advancing our profession. The authentic connections I’ve built with some of the most visionary minds in dentistry have been nothing short of life-changing.
When MedMark became part of the Nexus Dental Systems family in 2020, it marked a pivotal moment in our growth story. Now, as I step into my next-level adventure as Chief Marketing Officer for Nexus Dental Systems, I’m overwhelmed with gratitude. I’ll still be championing the dental community, driving purpose-driven innovation at the intersection of dental and medical breakthroughs. And MedMark? Our publications will continue disrupting the status quo, empowering excellence across all specialties while scaling our content reach and finding new ways to innovate.
These 2 decades have been the most beautiful discovery – our dental community isn’t
just an industry, it’s a family of mission-driven change-makers, visionary innovators, and most importantly, treasured friends who have enriched my life beyond measure. The relationships I’ve built with these healthcare heroes, these brilliant minds determined to revolutionize patient care, have become some of the most meaningful friendships of my lifetime. Every revolutionary thought leader, inventor, and disruptor I’ve had the privilege to know personally hasn’t just shared their next-generation technologies with me – they’ve shared their hopes, their dreams, their breakthrough moments, and even their setbacks over countless conversations that turned strangers into lifelong friends.
Our publications became so much more than a showcase for disruptive innovations in imaging, instrumentation, equipment, patient communication, and practice management –they became the bridge that connected hearts and minds. We’ve amplified the voices of clinicians who became dear friends, brave souls willing to challenge outdated paradigms and pioneer bold new methodologies. Every single author who graced our pages didn’t just bring their expertise – they brought their authentic selves, their infectious passion, and often, their friendship. What started as professional relationships blossomed into an ecosystem where readers don’t just become industry leaders –they become mentors, collaborators, and genuinely cherished friends.
I’m tearing up just thinking about the incredible people I’ve encountered on this journey. Some of my closest confidants, the people I turn to for advice, the friends who celebrate my victories and support me through challenges – many of them came from this extraordinary profession. I have always said that I didn’t find my dental profession; it
found me. It has been a career built on divine alchemy and serendipitous moments. Twenty years of shared experiences, industry events that felt more like family reunions, deep conversations about life, work passions that turned into lifelong friendships, and a network of support that extends far beyond business cards and LinkedIn connections. This community has given me a chosen family I never expected to find. And for that, I am eternally grateful.
Our content strategy has always been laser-focused on real-time relevance and community impact. We survived even during the darkest chapter of the pandemic shutdown; our team’s resilience was extraordinary. We pivoted to address the moment’s most pressing challenges – how to continue serving patients with unwavering safety protocols for patients, staff, and doctors. Watching the rise of tele-dentistry and other innovative platforms during that time, seeing our community’s incredible adaptability of hope — it was a masterclass in transformation that redefined the entire profession, and one that I was proud to be a part of.
But never fear, MedMark publications will continue their exponential growth trajectory, serving our loyal community with cutting-edge topics, breakthrough innovations, and an unwavering commitment to helping you scale the successful businesses of your dreams. I’m thrilled to welcome our new Publisher/Editor in Chief Scott S. De Rossi, DMD, MBA, and I’m genuinely excited about the fresh perspective and seasoned expertise he’ll bring to our brand. Scott is a true professional and one of the best author/writers that I’ve had the pleasure to be associated with lately. Look for his contributions to be informative, smart, and engaging!
As I embark on this new adventure, my heart is filled with excitement while simultaneously overflowing with pride for what we’ve built together from the ground up. I’ll always be part of this incredible MedMark family, and my commitment remains rock-solid – I still remain in our industry to empower your journey to unprecedented success!
With endless gratitude, anticipation for the new journey, and always…to your best success!
Lisa Moler
“Our
publications will continue disrupting the status quo, empowering excellence across all specialties while scaling our content reach and finding new ways to innovate.”

by Dr. Mark Murphy
Throughout history, technological leaps have profoundly reshaped healthcare delivery, improving outcomes, patient experiences, and practitioner profitability. Time Magazine notably selected Johannes Gutenberg as the “Man of the Millennium,” underscoring technology’s enduring influence on humanity. In dental sleep medicine (DSM), this principle resonates deeply, emphasizing how technological advancements can not only elevate patient care but also ensure dentists receive predictable and timely reimbursement.
Despite approximately 100,000 dentists attending sleep courses, fewer than 2% (1,500–1,750) have successfully billed medical insurance. This staggering drop-off reveals the greatest barrier to DSM’s success: the complexity and inefficiency of reimbursement processes. We’ll return to this and discuss a predictable solution later in this article.
While about 7,500 dentists have delivered at least one appliance, inconsistent payments and extensive claim denials create frustration, discouraging ongoing engagement.

FDR’s famous sentiment – ”a fair day’s wage for a fair day’s work” – echoes deeply here, highlighting how vital predictable financial returns are to fostering sustainable growth and enthusiasm for DSM. It’s very difficult to stay on course if you cannot get paid. Chris Sager, the long-retired CEO of the Pankey Institute, reminded me of this delicate balance between patient care and financial viability. He preached that “unrewarded altruism ultimately fails.” Oral appliance therapy is a behaviorally rewarding service, but the warm fuzzies can’t pay the bills. The 20-year decline in dental reimbursement rates, and the subsequent challenge to our incomes, leaves little room for pro bono care.
According to industry data, only 450–500 practices nationwide consistently produce more than ten appliances monthly. Increasing that benchmark to fifteen cuts this number in half. The root cause? Inadequate and inconsistent reimbursement systems. The clinical procedures are easily mastered. But without predictable payment workflows, dentists struggle to scale beyond a handful of cash-paying cases, severely limiting their ability to provide the care patients deserve – and to grow their practices effectively.
This minuscule number of successful, and potentially sleep-only, practices reflects those who have “figured it out.” Although several medical billing services exist in this arena, timely financial reimbursement is still more illusion than reality. These ~500 practices have found a way to work with their billers and solve for reimbursement – perhaps not at the desired speed, but at least at a pace that allows for some financial success.
Albert Einstein cautioned, “It has become appallingly obvious that our technology has exceeded our humanity.” Yet, in the context of
DSM, technology enhances rather than diminishes our humanity. Consider CPAP machines and Inspire implants, two giants in the sleep treatment industry. CPAP manufacturers like ResMed achieve billions in revenue with impressive profit margins, thanks largely to structured reimbursement protocols.
Inspire, utilizing advanced medical technology, anticipates hitting nearly $1 billion in sales by 2025 with unprecedented margins. These successful financial models starkly contrast the struggles DSM faces –despite oral appliance therapy (OAT) demonstrating superior patient adherence and comparable or better clinical efficacy.
OAT offers significant advantages –patients prefer it, adherence rates are higher, and outcomes often surpass those of traditional CPAP. Yet DSM’s financial model has lagged, making widespread adoption elusive. The question remains: if OAT is clinically effective and financially sensible, why hasn’t it dominated the market?
Emerging platforms are now addressing reimbursement pain points by integrating AI-powered workflows, automated documentation prompts, and pre-auth accelerators. One such platform, Restfull powered by IAOS, has begun to address these gaps, offering features like reduced claim cycles and guided compliance. If technological advancements can bring oral appliances to the efficacy and adherence tables, why not bring predictable reimbursements as well?
Physician opinions on the effectiveness of oral appliance therapy are trending in our favor. It’s getting easier to get face time with them, discuss recent advances, and champion precision treatment as a viable, non-surgical alternative to CPAP. Understanding and managing the medical reimbursement environment will align oral appliances for prompt and improved reimbursement.
My passion for dental sleep medicine stems from helping dentists struggle with complex billing processes, unpredictable reimbursements, and compromised clinical protocols. After decades of learning it the hard

Understanding and managing the medical reimbursement environment will align oral appliances for prompt and improved reimbursement.
way – and witnessing talented professionals become discouraged by financial uncertainty – I realized we could leverage technology and coaching to remove these barriers.
I’ve worked through the difficult tasks of documentation and medical billing with external partners. Restfull provides the technological structure and predictable reimbursement we need – and this new generation of devices simplifies treatment.

My years at ProSomnus taught me how to build solutions that met the unmet needs of customers. Those devices – scientifically designed, supported by countless studies, and made from superior materials – transformed the market and helped create the country’s largest medical device manufacturer of oral appliances. Patients, dental providers, and physicians embraced better design, comfort, safety, and performance.
Because we’ve addressed how to meet payers needs with scientifically designed software and predictable reimbursement workflows, “not getting paid” and “the hassle of working with medical insurance” will no longer be excuses for giving up on DSM.
Joining Restfull powered by IAOS means more than just adopting cutting-edge software – it’s about reclaiming your ability to practice the dentistry you love with financial confidence. Restfull doesn’t just offer you a tool; it provides you with freedom – freedom from claim denials, cash flow uncertainty, and administrative overload. Coaching is even
included in our basic package, because your success is our success.
I couldn’t be more excited for this new role, leading a team dedicated to member success. Dental sleep medicine, teaching at Pankey, consulting with practices, helping develop better devices, and now fitting the final puzzle piece – reimbursement – together, have all been deeply rewarding… both spiritually and financially. I am leading a blessed life.
At Restfull, our guiding principle is that predictable, fast payments create sustainable, successful DSM practices. Our proprietary suite finally clears the hurdles that previously kept us from interfacing seamlessly with insurance providers. We reduce the pre-auth approval timeline, dramatically shorten the reimbursement cycle to under 30 days, and get claims paid at the full reimbursable rate.
Restfull ensures thorough, accurate claim submissions by prompting complete documentation through our software. Each necessary detail is captured precisely and designed to follow the exact compliant steps required – preventing denials due to incomplete information before they occur. This software-driven guidance is essential to helping more dentists experience financial success in dental sleep medicine.
But the power of Restfull goes beyond billing. We understand dentists’ daily challenges because Restfull was designed by sleep dentists, for sleep dentists, drawing from 12+ years of helping DSM providers through the IAOS.
We’ve streamlined every step – from telemedicine and automated patient communication to digital referral management – ensuring reduced chair time (often just 7–10 minutes) and an efficient, seamless workflow.
Ultimately, embracing technology like Restfull ensures dentists are fairly compensated for their vital work – positively impacting countless lives. As the proverb wisely says, “Give a man a fish, and you feed him for a day. Teach him to fish, and you feed him for a lifetime.” Restfull powered by IAOS equips dentists with the technological tools they need – not just to treat patients better, but to ensure predictable, reliable payments that allow their practices and professional satisfaction to flourish.




It is with deep sadness that we announce the passing of John Remmers, MD. In memory of his tremendous legacy, a couple of community members have reflected on the impact he has left on our field.
Dr. Gy Yatros:
It’s hard to find the right words to truly capture the impact that Dr. John Remmers had on my life and the lives of so many others in the field of sleep medicine. When I first met John nearly 25 years ago, I was a young and inexperienced dentist with only a vague understanding of sleep apnea. Yet he went out of his way, without hesitation, to help and inspire me. Barely knowing me, he spent an entire day in my office, generously sharing his knowledge, his passion, and his time. That day changed the course of my career and helped set me on the path toward dental sleep medicine. And he did it all with such sincerity and grace.
Beyond his incredible accomplishments, what stood out most about John was his kindness and selflessness. In every conversation, he had a way of turning the spotlight away from himself and toward others, always looking for ways to support, encourage, or uplift them. It was never about him; it was about people, and always, the science.
There’s no doubt the world is a better place because of Dr. John Remmers. He touched thousands of lives personally and through his groundbreaking contributions to sleep medicine. On a more personal note, we shared a special connection through our Kentucky roots.
John, I wish we had the chance to share one more bourbon toast. You are deeply missed.
John Remmers was nothing less than a legend; an iconoclast; a pulmonologist; a physiologist; a scientist; a father; a husband; a mentor; a colleague; an educator; a pioneer. And I consider myself lucky to have called John a dear friend.
John was the force of nature who discovered, evaluated, and characterized the pathophysiology of Obstructive Sleep Apnea, a chronic disease that afflicts 1 billion people worldwide. He subsequently directed his considerable talents, intellect, and work ethic to neutralizing this disease. He was the yin to Sleep Apnea’s yang. Sleep Apnea posed questions, John developed answers. John published more than 100 peer-reviewed articles on respiratory physiology and served two terms as the Editor-in-Chief of the Journal of Applied Physiology. During


his celebrated career, John invented and championed multiple technologies and clinical procedures that enabled more effective treatment of Obstructive Sleep Apnea. John successfully licensed his inventions to some of the biggest companies in sleep medicine, was a co-founder of Zephyr Sleep Technologies, and, most recently, Chief Scientist for ProSomnus Sleep Technologies where he provided the clinical and scientific inputs that defined the forthcoming, next generation of sleep apnea devices. John was generous with his knowledge, making it a priority to train, mentor and inspire thought leaders in the field of sleep medicine. As clinical professor of internal medicine at the University of Calgary, he founded the Foothills Medical Centre and Sleep Lab.
Yet awards and accolades do not begin to describe John’s contributions. He was a truly extraordinary human being. When my father-in-law fell ill with a respiratory disease, John interacted with the medical team in San Francisco and offered suggestions that likely extended my father in-law’s life by many months. But that was John. He spent time pondering the big, tough, public health questions. But he also kept it focused. Kept it personal. Kept it tangible. He always had time for the patient and the physician.
When you think on him, please know that John left the Earth doing exactly what he loved most, spending time with family, writing manuscripts, and developing innovative medical devices.
Words cannot describe the loss of John, an exceedingly unique and exceptional human being. Which is probably why, in a final demonstration of his sagacity, he aimed

“Beyond his incredible accomplishments, what stood out most about John was his kindness and selflessness.”
to ease my burden by suggesting I share his favorite poem.
By Robert Frost
Two roads diverged in a yellow wood, And sorry I could not travel both And be one traveler, long I stood And looked down one as far as I could To where it bent in the undergrowth;
Then took the other, as just as fair, And having perhaps the better claim, Because it was grassy and wanted wear; Though as for that the passing there Had worn them really about the same,
And both that morning equally lay In leaves no step had trodden black. Oh, I kept the first for another day! Yet knowing how way leads on to way, I doubted if I should ever come back.
I shall be telling this with a sigh Somewhere ages and ages hence: Two roads diverged in a wood, and I— I took the one less traveled by, And that has made all the difference.
More From Dr. Remmers
Dr. Remmers was featured in a DSP interview for our Fall 2022 issue. You can read it here: https://dentalsleeppractice.com/in2000-everything-changed/.
by Bella Kavalerchik, PT, myofunctional therapist
Did you know that the foundations of your baby’s oral health begin forming as early as 4 months into pregnancy? By birth, the tongue and oral tissues continue to play a crucial role in essential functions like breathing, feeding, and swallowing. Yet one common condition – tongue-tie (ankyloglossia) – often goes unnoticed at birth, and then during routine pediatrician’s check-ups.

• Jaw alignment: tension and imbalance of the oral cavity muscles and joints may lead to jaw misalignment and pain
Tongue-tie occurs when the band of tissue under the tongue is too tight, restricting tongue movement. While some cases are obvious, others – especially posterior tongue-ties – can be deceptively difficult to detect. In such cases, the tip of the tongue might move freely, while the deeper part of tongue remains restricted, causing significant challenges for the infant and the family.
Countries like Brazil have made tonguetie screening a standard part of newborn assessments. Unfortunately, there is no such standard procedure in the United States. This important condition remains underdiagnosed, often leading to a cascade of avoidable issues.
Tongue-tie can interfere with:
• Breastfeeding: difficulty latching, poor milk transfer, nipple pain
• Swallowing and digestion: leading to colic, gas, and reflux-like symptoms
• Sleep quality: mouth breathing and poor tongue posture can disrupt restful sleep
• Speech development: tongue movement restrictions interfere with certain sound pronunciation
• Body alignment: Fascial tension caused by a restricted tongue can extend throughout the body, contributing to what is often referred to as a midline defect. Torticollis, forward head posture, and overall muscular imbalances are some examples of such issues.
Many babies struggling with poor latch and suction swallow excessive air – a condition called aerophagia. This can mimic symptoms of reflux, leading to a misdiagnosis and unnecessary treatment with proton pump inhibitors (PPIs). Unfortunately, these medications often don’t help and can cause serious side effects such as disrupted gut flora and impaired nutrient absorption to name a few.
Instead of medicating the symptoms, addressing tongue function and oral muscle development can often resolve the root problem – naturally and effectively.
As a physical and myofunctional therapist, I work with infants facing these challenges. Using a specialized approach known as oral motor therapy, I apply myofascial release
techniques to work inside and outside the oral cavity. This gentle, hands-on treatment helps improve tongue mobility, encourages proper oral posture, and supports healthy swallowing and feeding patterns.
I also train parents to continue the work with targeted stretches and exercises at home. Empowering families is a vital part of the healing process.
In many cases, a frenotomy – a simple procedure performed by a pediatric dentist or ENT – is required to release the tongue restriction. But for best results, oral motor therapy before and after the procedure is essential:
• Before the release: To prepare the tongue and surrounding muscles, improving surgical outcomes.
• After the release: To prevent tongue reattachment and supports full functional recovery.
I feel truly fortunate to work as both a Pelvic Floor Physical Therapist and a Myofunctional Therapist. In my role as a pelvic floor PT, I often work with postpartum moms. Naturally, our conversations extend beyond recovery and often touch on challenges new moms are facing with their babies – such as breastfeeding difficulties, sleep issues, and more.
When a baby struggles with breastfeeding, it’s often a sign of an underlying ankyloglossia issue. I make it a priority to educate new moms about these potential concerns and offer compassionate, evidence-based support. Many of these moms choose to bring their babies to me for further evaluation and treatment.
In addition to hands-on care, I provide educational resources, including posters and a small library of parent-friendly books that explore topics like tongue ties and their impact on breathing, swallowing, brain development, and sleep.
Helping infants with myofunctional issues has become one of the most fulfilling parts of my journey as a Physical Therapist. It’s an honor to support families during such a formative time in their lives.
As a Physical Therapist trained in myofunctional therapy, my role differs from that of a lactation consultant or feeding therapist (such as
SLPs or OTs). Each profession plays a vital role in treating infants for myofunctional issues. A collaborative team approach ensures that each baby receives well-rounded, comprehensive care. After all, it truly does take a village.
Some parents of my little patients with myofunctional issues find me through a Google search – but most come to me because I treat their mothers for postpartum concerns.
What if those mothers had never become my patients? Would their babies still have the opportunity for a healthier start in life? Sadly, I’m not sure – and that’s what needs to change.
We must integrate myofunctional education into the core training of medical and dental schools, as well as into physical therapy, occupational therapy, and speech-language pathology programs. Every child deserves the chance to thrive.
Tongue-tie is not just a feeding issue. It can shape a child’s entire developmental trajector – from breathing and sleeping to posture, speech, and beyond. Raising awareness among parents, pediatricians, and policymakers is essential. Screening and therapy should not be privileges; they should be covered by insurance as standard care.
Early identification and intervention can transform a child’s future. Let’s work together to give every baby the best possible start in life.

Bella Kavalerchik, PT, is the founder of Bella Physical Therapy, a private outpatient practice dedicated to providing personalized and comprehensive care. With over 25 years of experience as a licensed Physical Therapist, Bella brings deep clinical expertise and a compassionate approach to her work. She graduated Magna Cum Laude from the Physical Therapy Program at Hunter College in 1996. Throughout her career, Bella has treated a wide range of conditions, including orthopedic, pediatric, and neurological disorders. Her specialties also include the treatment of TMJ dysfunction, headaches, tinnitus, vestibular disorders, and pelvic floor conditions in both adults and children. In 2014, Bella expanded her expertise by becoming a certified orofacial myofunctional therapist—a field that has since become her greatest professional passion. She now works with patients of all ages to address a full spectrum of myofunctional disorders, combining evidence-based care with individualized treatment strategies.

by Lee A. Surkin, MD, FACC, FCCP, FASNC, FAASM, and Robert J. Floro, MS, RRT
Sleep is a universal, natural, easily reversible periodic state with similar processes and rhythms across the human species. However, although it follows a recognizable pattern, sleep presents many differences among healthy individuals. Some of these differences are considered to be environmental as they relate to meal times, work routines, travel schedules, etc,. but many are inherited as well.
That said, every person’s unique genetics play a huge role in their sleep patterns, no matter if they are an early bird, a night owl, or something in between. To be more precise, your genes are linked with the amount of sleep you need, your sleep quality, and even the likelihood of sleepwalking or other sleep disorders.
Now, let’s dig deeper into the genetics of sleep.
Even though it may sound surprising, some people can get by on four hours of sleep per night, whereas others need six, eight, or nine. Sleep genetics research has shown that genetic factors have a significant impact on how long most living organisms need to sleep.1
One study conducted on thirteen generations of fruit flies found that each generation of short-sleepers slept less than the previous generation. Similarly, each generation of
long-sleepers slept longer than the previous generation. Hence, the study concluded that the genetic influence on sleep is quite strong, i.e. that genetics influence sleep duration, at least for some organisms.2
Another sleep genetics research on twelve-year-old twins identified similar sleep patterns in genetically identical siblings. The time the twins decided to go to bed and the time they woke up was particularly influenced by genetic factors. What’s more, sleep architecture, i.e. the amount of time spent in each sleep stage, was also similar in identical siblings.3
Sleep quality, as well as sleep duration, can be reduced significantly as a result of stress since it influences vulnerable genes. Namely, stress stimulates certain neurons which sets the stage for many sleeping issues such as difficulty falling asleep, staying asleep, and falling back to sleep after waking up in the middle of the night.
According to Japanese researchers, specific molecular pathway mutations can lead to fragmented sleep, resulting in poor sleep quality and quantity.4 Another study found that mutation of the circadian rhythm gene, called CRY1, can result in delayed sleep phase disorder in families. As a consequence of this mutation, there are generations of night owls with extended circadian rhythms. If people with such genetic sleep traits try
to fit into the usual societal sleep patterns, they experience fragmented sleep and sleep deprivation.5
However, one study conducted on night owls proved that delayed sleep patterns can be changed under specific environmental conditions that affect the circadian rhythm. This was shown after studying a night owl subject who was exposed to bright early morning regularly and was able to conform to typical sleep patterns.
Finally, due to lifestyle and behavioral factors, certain medical conditions, or genetic factors, some people may develop sleep disorders. But, they can also be idiopathic meaning that the cause of the disorder cannot be explained or identified. And, although there are about eighty sleep disorders affecting about seventy million Americans, some of them have a close connection with genetics.
So, here’s a brief list of the most commonly diagnosed sleep disorders with a genetic association:
• Restless legs syndrome
• Insomnia
• Kleine-Levin syndrome

• Sleep Paralysis
• Sleepwalking
• Nocturnal Bruxism (Teeth grinding)
• Sleep apnea
The bottom line, many factors can affect sleep including personal lifestyle, stress, environmental, and genetic factors. Hence, sleep requirements differ from person to person, but are strongly influenced by genetic sleep traits.
1. Parish, J. M. (2013, May). Genetic and immunologic aspects of sleep and sleep disorders. Chest. https://www.ncbi.nlm.nih.gov/ pmc/articles/PMC3734884/
2. Panchin, Y., & Kovalzon, V. M. (2021, April 7). Total wake: Natural, pathological, and experimental limits to sleep reduction. Frontiers in neuroscience. https://www.ncbi.nlm.nih.gov/pmc/ articles/PMC8058214/
3. Sletten, T. L., Rajaratnam, S. M. W., Wright, M. J., Zhu, G., Naismith, S., Martin, N. G., & Hickie, I. (2013, November 1). Genetic and environmental contributions to sleep-wake behavior in 12-year-old twins. Sleep. https://www.ncbi.nlm.nih.gov/pmc/ articles/PMC3792390/
4. Sharma, S., & Kavuru, M. (2010). Sleep and metabolism: An overview. International journal of endocrinology. https://www. ncbi.nlm.nih.gov/pmc/articles/PMC2929498/
5. Patke, A., Murphy, P. J., Onat, O. E., Krieger, A. C., Özçelik, T., Campbell, S. S., & Young, M. W. (2017, April 6). Mutation of the human circadian clock gene CRY1 in familial delayed sleep phase disorder. Cell. https://www.ncbi.nlm.nih.gov/pmc/ articles/PMC5479574/
6. AP;, F.-C. E. B. D. (n.d.). Resetting the late timing of “night owls” has a positive impact on mental health and performance. Sleep medicine. https://pubmed.ncbi.nlm.nih.gov/31202686/
Lee A. Surkin, MD, is the Chief Medical Officer of Nexus Dental Systems. A private practitioner in cardiology, sleep medicine, and obesity medicine, he is one of a small group of physicians to be triple board certified in cardiology, sleep medicine, and nuclear cardiology. In 2009, he created Carolina Sleep – the only dedicated sleep medicine practice in eastern NC. Dr. Surkin has created a cardiovascular and sleep healthcare model that includes a multi-faceted diagnostic and treatment approach that is enhanced by a network of relationships with physicians, dentists, respiratory therapists, sleep technologists, and public officials who recognize the important role that sleep medicine has in our daily life. In 2012, Dr. Surkin founded the American Academy of Cardiovascular Sleep Medicine which is a not-for-profit academic organization dedicated to educating healthcare providers, supporting research, and increasing public awareness of the convergence between cardiovascular disease and sleep disorders. In 2014, Dr. Surkin created a new multi-specialty practice called Carolina Clinic for Health and Wellness which combines his specialties with primary care, gynecology, behavioral health and a medical spa. Dr. Surkin is married with three daughters and a golden retriever and resides in Greenville, NC.

Robert J. Floro, MS, RRT, is the managing partner at Respiratoryedu.org and Sleepedu.org. He is also the managing Partner for HME Professional, a consulting firm working with home care organizations to develop business, manage human resources, and comply with accreditation standards, and federal and State regulatory standards. Bob has over forty years of experience in health care. He has a strong background in respiratory care and the durable medical equipment industry, including previous DME ownership and leadership positions. Prior to his position with HME Professional, Bob served as the Director of Home Care Accreditation Program at The Joint Commission. He has owned and managed medical equipment businesses, taught at the university level, and held board and membership positions in AARC, ALA of KY, AHA, ISRC, KSRC, KMESA, IAMES, and is currently an advisor to the Sleep Center Management Institute in Atlanta. Bob holds a Master of Science in Leadership from the Ken Blanchard College of Business and is a Registered Respiratory Therapist.

by Snigdhasmrithi Pusalavidyasagar, MD, FAASM

The prevalence of obstructive sleep apnea (OSA) during pregnancy is increasing worldwide. Pre-pregnancy obesity and the gestational weight gain increase the risk for OSA in pregnant women. In a recent meta-analysis, the estimated prevalence of OSA in pregnant women was 15%.1 Pregnancy associated hormonal, physiological, and physical changes can all impact OSA. In a large cohort study using level 3 home sleep apnea testing, the prevalence of OSA increased from 3.6% in early pregnancy to 8.3% in mid-pregnancy.2 A prospective study of 105 pregnant patients who completed polysomnography showed an increase in the prevalence of OSA from 10.5% in the first trimester to 26.7% in the third trimester.3 Despite the increasing prevalence, OSA during pregnancy is underdiagnosed due to barriers in identifying OSA.4 Sensitivity and specificity of the screening tools (Berlin questionnaire, Epworth Sleepiness Scale, and STOP-BANG) are suboptimal for pregnant women.5 Variables such as advanced maternal age, higher BMI, and frequent snoring can be used to predict OSA.6
OSA involves repetitive episodes of complete and partial upper airway obstruction, with intermittent hypoxemia/reoxygenation, causing sleep fragmentation, oxidative stress, increase in sympathetic activity, and endothelial dysfunction. All these factors increase risk for cardiovascular disease and can adversely impact maternal and fetal
health. Hypertensive disorders of pregnancy (gestational hypertension, chronic hypertension, pre-eclampsia, and eclampsia), cardiomyopathy, gestational diabetes, and preterm delivery are maternal complications associated with OSA.7 Moderate to severe OSA is one of the risk factors for maternal cardiovascular disease. OSA has been shown as a risk factor for anesthesia-related maternal complications.8 Delivery rates by cesarean section are higher in pregnant patients with OSA compared to pregnant patients without OSA.9 OSA during pregnancy has been associated with growth retardation, pre-term birth, congenital anomalies, and small for gestational age.10
There are no current guidelines from the American Academy of Sleep Medicine for optimal timing of screening for OSA and management of OSA during pregnancy. Some researchers recommend prenatal OSA screening between 12 and 18 weeks. Facco and colleagues found a dose response between AHI severity and cardiometabolic risk at both early and mid-pregnancy indicating that OSA evaluation should be considered as early as the first trimester.11 Women with suspected OSA during pregnancy should be referred to a sleep clinic for further evaluation and management. While polysomnography (PSG) remains the gold standard test for diagnosing OSA, testing is expensive, and scheduling can be delayed in
some centers due to capacity and demand. Home sleep apnea testing (HSAT) is convenient, less expensive and can be helpful in diagnosing OSA in pregnant women, who are at moderate to high risk.12 If the HSAT does not show evidence of OSA, PSG must be considered in pregnant women with high clinical suspicion.
Continuous positive airway pressure (CPAP) is the best treatment option for OSA during pregnancy and is safe. Women with a history of previously diagnosed OSA managed with CPAP should continue CPAP therapy during their pregnancy. Auto titrating CPAP therapy is more practical and helpful for treating OSA during pregnancy compared to CPAP with fixed pressure settings, since the severity of the OSA is subject to increase as the pregnancy progresses with gradual weight gain and hormonal changes.13 Close follow up after initiating CPAP therapy is important to assess the adherence to treatment. CPAP therapy has been shown to be helpful in specific high-risk obstetric populations. CPAP treated OSA women had lower incidence of severe forms of hypertensive disorders of pregnancy.14 Oral appliance therapy is often not practical for OSA during pregnancy, because it can take a few months to achieve adequate adjustment of the appliance to control the OSA.
OSA can persist in some women who do not return to their pre-pregnancy weight. CPAP therapy should continue until their BMI returns to 10% to 15% of their baseline BMI. A prospective observational study by Street and colleagues identified gestational OSA continued 2-3 months after delivery and estimated postpartum OSA prevalence at 20% at 6-8 months after delivery.15 Given the continuation of OSA in a subset of this population and the potential adverse effects to women’s overall health, effective OSA screening and treatment modalities for postpartum women need to be identified. OSA can be associated with postpartum depression (PPD). In a prospective study, Bourjeily et al showed a higher prevalence of PPD in women with OSA.16 Sleep apnea treatment can improve depression in postpartum women. However, adherence to CPAP therapy can be difficult for some new mothers attending to an infant. In these cases, positional therapy or mandibular advancement device may be considered. Further research is needed to develop
screening tools and treatment guidelines for OSA during pregnancy and postpartum periods to improve both maternal and fetal outcomes.
1. Liu, L., Su, G., Wang, S., & Zhu, B. (2019). The prevalence of obstructive sleep apnea and its association with pregnancy-related health outcomes: a systematic review and meta-analysis. Sleep and Breathing, 23, 399-412.
2. Facco, F. L., Parker, C. B., Reddy, U. M., Silver, R. M., Koch, M. A., Louis, J. M., ... & Zee, P. C. (2017). Association between sleep-disordered breathing and hypertensive disorders of pregnancy and gestational diabetes mellitus. Obstetrics & Gynecology, 129(1), 31-41.
3. Pien, G. W., Pack, A. I., Jackson, N., Maislin, G., Macones, G. A., & Schwab, R. J. (2014). Risk factors for sleep-disordered breathing in pregnancy. Thorax, 69(4), 371-377.
4. Farid, S., Giunio-Zorkin, M., Schust, D. J., & Cortese, R. (2024). Obstructive sleep apnea in pregnancy: A review of the literature from the obstetrics practitioner’s view and a proposed clinical approach. European Journal of Obstetrics & Gynecology and Reproductive Biology, 300, 29-34.
5. Amra, B., Mansouri, M., Soltaninejad, F., Feizi, A., & Kaminska, M. (2024). Screening Tools for Obstructive Sleep Apnea in Pregnant Women: An Extended and Updated Systematic Review and Meta-analysis. International Journal of Preventive Medicine, 15, 31.
6. Louis, J. M., Koch, M. A., Reddy, U. M., Silver, R. M., Parker, C. B., Facco, F. L., ... & Zee, P. C. (2018). Predictors of sleep-disordered breathing in pregnancy. American Journal of Obstetrics and Gynecology, 218(5), 521-e1.
7. Bourjeily, G., Danilack, V. A., Bublitz, M. H., Lipkind, H., Muri, J., Caldwell, D., ... & Rosene-Montella, K. (2017). Obstructive sleep apnea in pregnancy is associated with adverse maternal outcomes: a national cohort. Sleep Medicine, 38, 50-57.
8. Dominguez, J. E., & Habib, A. S. (2022). Obstructive sleep apnea in pregnant women. International Anesthesiology Clinics, 60(2), 59-65.
9. Louis, J., Auckley, D., Miladinovic, B., Shepherd, A., Mencin, P., Kumar, D., ... & Redline, S. (2012). Perinatal outcomes associated with obstructive sleep apnea in obese pregnant women. Obstetrics & Gynecology, 120(5), 1085-1092.
10. Brown, N. T., Turner, J. M., & Kumar, S. (2018). The intrapartum and perinatal risks of sleep-disordered breathing in pregnancy: a systematic review and metaanalysis. American Journal of Obstetrics and Gynecology, 219(2), 147-161.
11. Facco, F. L., Parker, C. B., Reddy, U. M., Silver, R. M., Koch, M. A., Louis, J. M., ... & Zee, P. C. (2017). Association between sleep-disordered breathing and hypertensive disorders of pregnancy and gestational diabetes mellitus. Obstetrics & Gynecology, 129(1), 31-41.
12. Facco, F. L., Lopata, V., Wolsk, J. M., Patel, S., & Wisniewski, S. R. (2019). Can we use home sleep testing for the evaluation of sleep apnea in obese pregnant women?. Sleep Disorders, 2019(1), 3827579.
13. Richardson, K., & Collop, N. (2024). Sleep medicine clinical pearls: understanding the dynamic changes in sleep apnea during pregnancy due to hormonal shifts. Journal of Clinical Sleep Medicine, 20(4), 663-666.
14. Stajić, D., Ilić, D., Vuković, J., Baturan, B., Ilić, A., & Milovančev, A. (2022). The effect of continuous positive airway pressure treatment on hypertensive disorder in pregnant women with obstructive sleep apnea. Sleep and Breathing, 26(1), 297-305.
15. Street, L. M., Aschenbrenner, C. A., Houle, T. T., Pinyan, C. W., & Eisenach, J. C. (2018). Gestational obstructive sleep apnea: biomarker screening models and lack of postpartum resolution. Journal of Clinical Sleep Medicine, 14(4), 549-555.
16. Bourjeily, G., Raker, C. A., Chalhoub, M., & Miller, M. A. (2010). Pregnancy and fetal outcomes of symptoms of sleep-disordered breathing. European Respiratory Journal, 36(4), 849-855.

Snigdhasmrithi Pusalavidyasagar (“Sagar”), MD, FAASM, is an associate professor of medicine in the Division of Pulmonary, Allergy, Critical Care and Sleep Medicine in the Department of Medicine at the University of Minnesota in Minneapolis. She serves as the University of Minnesota Medial Center Site Director for the Sleep Medicine Fellowship Program. She is board certified in internal medicine and sleep medicine. Her research interests include the role of sleep in women’s health and sleep disordered breathing as it related to cardiovascular disease. She is active with the American Academy of Sleep Medicine and was recognized with Fellow status in 2013. She serves on the Sleep Advisory Committee for the American Board of Internal Medicine, the Advisory Board of the American Academy of Cardiovascular Sleep Medicine, and is president-elect for the Minnesota Sleep Society. She completed her internal medicine residency at Howard University, Washington, DC, and sleep medicine fellowship at the Mayo Clinic, Rochester, Minnesota. Before her sleep medicine fellowship, she was a research fellow in cardiovascular physiology also at the Mayo Clinic.


by Alan D. Steljes, MD, FACC, FRCPC
A 68 year-old male complains of progressively limiting shortness of breath with exertion. He is occasionally awakened at night with shortness of breath which forces him to sit up. On exam, he is obese. Neck veins are distended. Heart sounds are slightly muffled. Fine crackles are heard at both lung bases. Mild swelling in both ankles. Ultrasound of the heart shows mild dilatation of the left ventricle with global reduction of systolic function. Ejection fraction: 35% (normal is 50 to 70%). The clinical diagnosis is congestive heart failure with reduced ejection fraction.
Congestive heart failure (CHF) is a common disorder which leads to progressive disability and ultimately death. Medical management of CHF is one of the big success stories in cardiology. However, even optimally managed patients may have untreated sleep disordered breathing (SDB) which adversely affects their prognosis. Effective evaluation and management of SDB unlocks significant gains.
There are two components to the syndrome. Congestion from excessive fluid retention is
responsible for most of the patients’ symptoms. Systemic congestion causes swelling in the legs but may later progress to the abdomen or liver. Congestion in the lungs causes shortness of breath which worsens when the patient lies down due to a shift of fluid from the legs to the chest.
Heart failure is the second component and refers to the impairment of the heart’s ability to deliver sufficient blood flow to the other organs. Exertion is limited due to fatigue or shortness of breath.
The function of the heart is to circulate blood (with nutrients and oxygen) to the skeletal muscles and to other organs. Any of several diverse conditions can cause CHF. Most commonly these are conditions that affect the left ventricle (LV), the main pumping chamber in the heart. With each heartbeat, the LV fills with oxygenated blood from the lungs, then it squeezes or contracts to eject blood into the bloodstream. Damage to the heart muscle (due to heart attack or a muscle disease

• Whole-Team Training
• Ongoing Coaching
• Streamlined Protocols
• Precision Bite Technology
• Patient Ed ucation
• In-Network Medical Billing




Untreated
OSA
leads to significant drops in oxygen levels and secondary activation of the sympathetic nervous system, both of which may provoke CHF.
known as cardiomyopathy) impairs the ability of the chamber to contract and eject blood. The “ejection fraction” of the left ventricle is reduced leading to the designation of CHF with reduced ejection fraction (HFrEF.)
Other patients may have CHF with preserved ejection fraction (HFpEF.) Pumping of the heart is normal but refilling of the LV between heartbeats is impaired.
Once CHF is established, it tends to be progressive due to activation of various neural and hormonal pathways.
About 50% of patients have moderate to severe obstructive sleep apnea (OSA). Untreated OSA leads to significant drops in oxygen levels and secondary activation of the sympathetic nervous system, both of which may provoke CHF.
However, CHF can also provoke OSA. Congestion within the pulmonary veins diminishes the upper airway size. This effect worsens when the patient is supine, due to fluid shifts from the lower extremities.
Many patients with reduced ejection fraction additionally have central sleep apnea (CSA). The mechanisms are complex and involve deficiencies in the negative feedback system which controls breathing. It is important for physicians who report sleep studies to characterize apneas as either central or obstructive in origin. Failing to do so may underestimate the severity of central sleep apnea and lead to errors in therapy.
General measures include dietary changes and exercise; avoidance of alcohol and smoking.

Alan D. Steljes, MD, FACC, FRCPC was trained as an interventional cardiologist. Since fellowship, he has obtained additional certification in nuclear cardiology, echocardiography, CT coronary angiography and finally sleep medicine. In 2010, he opened a two bed sleep lab, recognizing the heart-sleep apnea interaction. The initial 2 beds have been scaled up to 12 beds since associating with the Nevada Heart & Vascular Center. He has since retired from the cardiology practice but continues to oversee the sleep program. He remains passionate about spreading the word about sleep disordered breathing and the heart. He currently shares his time between Las Vegas, NV and Mount Pleasant, SC.
Commonly prescribed medications include furosemide, spironolactone, carvedilol, and Sacubitril/valsartan in addition to a SGLT2 inhibitor such as empagliflozin.
The aim of medical therapy is to control congestion and relieve symptoms but also to block those deleterious neural and hormonal pathways which lead to progression of CHF. Pacemakers or defibrillators may be needed for advanced CHF patients to coordinate the function of the left and right ventricles and to prevent sudden death.
Once medical therapy is optimized, patients should be screened for sleep apnea, recognizing that identifying and treating coexistent sleep apnea can have a major impact on patients’ well-being.
The treatment of choice for CHF with obstructive sleep apnea is CPAP. The benefits are well documented. Patients typically feel better. Objectively, there may be improvement in left ventricular function, reduced need for hospitalization, and potentially improved survival. Patients who are intolerant of CPAP may be managed with oral appliance or a hypoglossal nerve stimulator (may not be indicated if a pacemaker or defibrillator is in place).
The optimal management of central sleep apnea remains unclear.
Therapy generally starts with a trial of CPAP which can be effective for both OSA and CSA in some patients.
Persistent central sleep apnea is problematic. More advanced positive airway pressure protocols can be effective. However, the Serve-HF randomized trial of Adaptive Servo Ventilation (ASV) versus optimal medical therapy indicated excess cardiovascular mortality within the treatment group. This unexpected outcome may have been related to the particular algorithm used in the trial. However, we remain cautious about this therapy in patients with an ejection fraction < 45%.
Low flow nocturnal oxygen is another option.
More recently, an implanted phrenic nerve stimulator has had impressive results and may be used more frequently as clinical experience increases.
The frequency of congestive heart failure is increasing steadily. It is estimated that by 2030 there will be 8 million patients afflicted in the United States – equivalent to almost 3% of the adult population. Earlier management of sleep apnea could be helpful to slow this trend.
For example, there are an estimated 20 million people in the US who have a reduced left ventricular ejection fraction but who have not yet developed CHF. Half of these patients have undiagnosed OSA. Current protocols correctly emphasize management of hypertension to prevent progression to CHF but do not address sleep apnea.
Undertreatment of OSA is not just an issue with CHF but is true for other cardiovascular diseases. The problem is that sleep medicine has not yet proven the value of treatment of sleep apnea to the standard required for inclusion in cardiology clinical guidelines. In fairness, randomized clinical trials have been notoriously difficult to perform. The biggest challenge is the underwhelming adherence rates with
CPAP, our most commonly prescribed therapy. Adherence should improve with better patient follow-up in specialized clinics. New technologies including remote patient monitoring and improved comfort of PAP therapy (perhaps KPAP) should have an impact. Oral appliances tend to have better long-term compliance but are also lacking in long-term efficacy studies.
Sleep disordered breathing is commonly associated with CHF. There is likely a bidirectional relationship between the two conditions with congestive heart failure exacerbating upper airway obstruction and obstructive sleep apnea, in turn, exacerbating cardiac function.
CPAP is an effective therapy which may improve heart function beyond medication alone. Oral appliance therapy is a good alternative for patients who do not tolerate CPAP.
Central sleep apnea may also be seen in patients with CHF. Mechanisms are complex and optimal management of CSA remains to be determined.
Attending World Sleep 2025 Singapore? Join our bronze sponsored symposium, “Beyond Mandibular Advancement: Science, Innovation and Outcomes” September 8th, 2025 • Visit
airway collapse involves the velopharynx1. Protruding the mandible dilates the oropharynx but has only indirect effects on the velopharynx.
The Solution
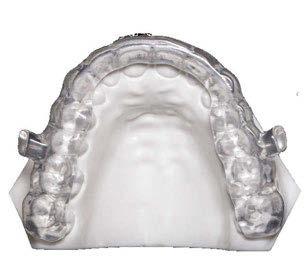
EVO Guided is bioengineered to prevent airway collapse by repositioning the hyo-glossal complex through guided jaw positioning, tongue posture support, and mouth closure—customized from your prescription. Lingual-less design offers up to 14x more tongue space than predicate devices
Why EVO Guided?
Prescribe ProSomnus EVO Guided as your frontline device to optimize efficacy, satisfaction, referrals, and adherence. Mitigate side effects. Boost practice economics by reducing non-responders


by Steve Carstensen, DDS
This self-instructional course for dentists is to empower the clinician to improve patient understanding and acceptance of the choices they have once diagnosed with a medical problem. By drawing out their story, the healthcare provider can match scientific expertise with what matters to the person they serve. Techniques for achieving this preferred outcome have been described for many years; putting them to work enhances our community health.
Dental Sleep Practice subscribers can answer the CE questions online at https://dentalsleeppractice.com/continuing-education/ to earn 2 hours of CE from reading the article. Correctly answering the questions will demonstrate the reader can:
1. Use lessons from Improv acting to connect with patients
2. Enhance listening skills for themselves and their team
3. Consider how science and human connection must both be used in today’s medicine
Betty looked at me expectantly. I sensed her curiosity about how I, a dentist, could help with what her physician said was a serious problem putting her health at risk: sleep apnea.
My objective is to provide therapy unique to dentistry that mitigates risk diagnosed by a colleague and to empower the suffering human to be involved in their own health solutions.
You may find yourself in a similar situation. This essay will show you how experts in communication, teaching, and making connections between people advise us to narrow the gap between the curious people we serve and the experts we have trained ourselves to become.
For thousands of years, healers used intuition and thoughtfulness about what they could observe to guide their ministrations. They used techniques such as bloodletting and trephination that seem barbaric today. People put themselves in the hands of those healers because they trusted their decision-making and recommendations. There were connections between those who put themselves out as learned thinkers and those who needed someone to give them hope for healing their afflictions.
It remains so, today. Advancements in science have given healers more and better tools. With information comes a different perspective. Increasing knowledge in a narrow field allows the healthcare expert to comprehend much more about potential troubles and the implications
of every treatment choice. It’s still a matter of building a trust relationship.
Our patients have not studied what we have; their expertise, no less important than ours, lies with their own lives and how disruptions to homeostasis have affected them.
Peter Atila, MD, writes in Outlive about the concept of ‘Medicine 3.0.’ He labels the early days of medicine as ‘1.0,’ informed only by what was observable by the eye and guessed at by the healers. Some of it was right – Hippocrates told us that both excellent medicine and bad medicine can be found in food. Other teachings, such as opening holes in skulls to let out the bad spirits, would be set aside as science produced ‘Medicine 2.0.’
As germ theory became widely known in the 19th century, (2000 years after Hippocrates!), it became possible to fully implement Sir Francis Bacon’s 1628 description of the scientific method. Observe, form a hypothesis, test, then consider what you’ve learned. For the first time, physicians could point to a cause of many diseases of the day, such as polio, and develop treatments aimed at the reason for the affliction, moving upstream from treating symptoms only. Medicine 2.0 describes the use of this method, with its highest form being randomized control trials (RCT). Once a patient, or a test subject, has a disease, it is easy to design an experiment where placebo is compared to an active treatment and see which has the most effect. This works very well when an organism, such as a bacteria or virus, is the acute cause of the disease. Healthcare professionals prescribe the same drug to everyone with the conditions detailed in the RCT.
Cardiovascular problems, writes Atila, are chronic diseases that build over years and decades, and, once they become entrenched, are hard to make go away. Medicine’s attention is turning toward prevention of the conditions from which chronic disease arise.
Medicine 3.0 places a far greater emphasis on prevention rather than treatment. It considers each person as a unique individual and shifts how both patient and provider assess the disease. New thinking leads the professionals and the patients to honestly assess risk and accept that no choice is risk free, including doing nothing.
Betty, (remember Betty? This is a story about Betty) waiting for me to say something,
has a chronic disease. I know from the literature (Medicine 2.0) that CPAP is considered the ‘gold standard’ for treating sleep apnea and is recommended as first line therapy for nearly everyone diagnosed with the disease. Medicine 3.0, however, complicates this simple diagnose-treat-assess pattern with curiosity about Betty, how she suffers from the chronic disease, and what she is willing to do to lower her risk.
As the sleep expert, I am qualified to study the facts of the diagnosis, follow the prescription by the physician, and choose which dental device is the best match for the patient’s condition. (It may change because insurance won’t pay for the ‘best’ one, but that’s another matter entirely.) None of these decisions are based on the patient’s input about what they want. I’m as likely to choose poorly as wisely.
Betty has her own story. She may not want to have any metal in her mouth. She may be focused on keeping medical devices exceptionally clean. Many years ago, a new patient in my office was adamant that they needed help keeping their mouth closed at night and asked for a device that would manage that for them. Later the same day, a different patient insisted their new oral appliance must allow them freedom to open their mouth easily.
Inviting the patient’s story to be part of the encounter has been taught since ancient times, documented by Aristotle and popularized by Dr. L.D. Pankey in his Philosophy of the Practice of Dentistry. Dr. Pankey taught that we must get to ‘Know our Patient’ prior to developing a treatment plan. In his day he provided a list of questions, not for the patient to fill out but to begin a conversation.
Inviting the patient’s story to be part of the encounter has been taught since ancient times, documented by Aristotle and popularized by Dr. L.D. Pankey.

Currently our Chief Dental Editor, Dr. Carstensen co-founded DSP in 2014. He sees clinic patients in Bellevue, WA and is the Liaison to the American Dental Association for Sleep Related Breathing Disorders. As a Diplomate of the American Board of Dental Sleep Medicine, he lectures internationally and is Co-Author of The Clinician’s Handbook for Dental Sleep Medicine, in its second edition by Quintessence Publishing.
The challenge of such conversations is to keep the two experts, one professional, one suffering, from talking over each other and failing to exchange the important details that lead to mutual decision making. This necessary process has been called Co-Discovery. Perhaps first noted by Dr. Bob Barkley in his book Successful Preventive Dental Practices, Co-Discovery involves asking the patient questions about their history and why they are seeking care now. The dental auxiliary dutifully records the answers and guides the patient through the process. When the interview is nearly complete, the dentist joins to reinforce what is becoming known, invite corrections, and draw out details important to be said.
The critical skill for the professional staff in this scenario is listening. One of Dr. Barkley’s students, hygienist Mary Osborne, has been teaching for many years a listening exercise for dental teams called “Staying in the Question.” Here is a summary; more can be found at her website, listed in the references below. The dental team separates into partners. One is designated the first speaker, the other the first interviewer, asking questions. They sit knee to knee for better focus. First question: ‘So that we can work well together, what would you like me to know about you?” This begins a 6 –7-minute dialog between the partners that has a critically important feature: Once the first speaker answers, all subsequent questions must be directly connected

to the partner’s response to the previous question. If they talk about a health goal, the next question cannot be about their family. Interviewers cannot talk about themselves.
After 6 – 7 minutes, the pair thank each other, stand, switch chairs, and assume the other role. Same first question, same process.
At the end of the second interval, the team reassembles and the leader invites comments about ‘What did you notice?’ and ‘How was that for you?’ Mary Osborne instructs us to stay in the question, asking ‘What else?’ until there are no more ‘elses’ to be revealed. An important learning point often expressed is how difficult it was, at first, to not talk about themselves when the task was to stay focused on the partner. Ask: “What did you notice when you were able to refrain from interjecting something about yourself?” Someone almost always says they learned something more about their partner that they did not know. This allows your team to feel the usefulness in clinic situations with patients.
Betty wants me to know what is important to her. If I am focused, I will provide her the space and freedom to tell me. I will ask questions and gather critical insight about what she thinks about her health, diagnosis, risk, and willingness to participate in treatment.
There are plenty of questionnaires developed to collect data about medical conditions, symptoms, comorbid conditions, and other details necessary for the healthcare professional to consider. None of them were developed with an individual person in mind, so their efficiency is diminished by their lack of specificity.
Edgar Schein wrote Humble Inquiry to explain ‘the fine art of drawing someone out, of asking questions to which you do not know the answer, of building a relationship on curiosity and interest in the other person.’ He has the perspective of a businessman with insights easily applied in a healthcare setting. Inquiry takes four forms, he writes: Humble, Diagnostic, Confrontational, and Process-Oriented.
1. Humble Inquiry acknowledges ignorance on one side of the dialog and uses curiosity to fill the gap. Questions are designed to not influence the result nor to provoke a socially acceptable response. An example for a healthcare office is ‘What brings you here?”
2. Diagnostic Inquiry intends to steer the other to provide more information about something they said. It influences their mental process to come up with something of a justification of the comment. Examples include: “How did you feel about that?” “Why do you suppose that happened?” and “What are you going to do next?”
3. Confrontational Inquiry inserts the interviewer’s ideas into the conversation, sometimes making assumptions about the speaker’s emotions or thoughts. It takes discipline and proper body language to maintain an equal relationship using this form of inquiry. An example (and contrast) would be the confrontational “Have you thought about going on a diet?” vs. the humbler “What are you doing about your weight?”
4. Process-Oriented Inquiry checks in about how the conversation is going; is it achieving the objective of sharing important information. This is often helpful if the interviewer senses confusion in the conversational partner and sharing goes off track. Asking “What else should we be talking about” or “Is there something I haven’t asked that you would like me to know?” are examples of this type of inquiry.
Humble inquiry helps the interviewer to avoid shutting down the person who wants to tell their story by maintaining a more equal relationship in situations where power is often perceived to be unequal. We want our recommendations to be helpful, to solve a problem for the patient. We are not trying to get them to buy a device, we want them to ask for a solution that may include a device as part of the process. It is humbling to accept that the patient has information we need to be successful.
Betty has power, because she possesses that information. Sitting in the doctor’s office, she may not realize that power. Humble In-
quiry helps her claim her place and enhances her chance of successful therapy as she sees her shared insights considered and incorporated into her personal treatment plan.
Jim Pride, DDS, was a winemaker, dental school dean, office designer, and efficiency expert. He and his leaders at Pride Institute taught dentists and their teams how to organize their practices into systems to provide optimum patient care and improve business outcomes. While I was in dental school, I went to an ADA meeting and became a Pride fan while he drew diagrams on an overhead projector. (Old, I am) I was later honored to be invited to teach alongside Amy Morgan, who succeeded Dr. Pride as CEO of the company.
Humans are entrained to pay attention to what matters to them. Dale Carnegie said, “When dealing with people, remember you are not dealing with creatures of logic, but creatures of emotion.” And “People do things for their reasons, not ours. So, find their reasons.”
As we consider how to present the information the patient expects from us, using what we know about them has a big influence on what they hear.
These two sentences say the same thing: “Our custom oral devices are precision made and serve as retainers for your teeth”
“So that your teeth can’t move during treatment, I recommend a precision-made custom device that works like a retainer”
Dr. Pride taught that leading a sentence with something important to the patient will keep their attention through the part where you name the thing and describe its features. He called this a “Benefit Statement.” Notice the first sentence leads with the thing, while the second speaks about a patient concern. Benefit first. What is being proposed, or Procedure, comes next, followed by Features of the procedure/device/service. The patient focuses on ‘what’s in it for them’ with the benefit, endures the procedure (which they probably don’t want), and is emotionally supported by the features of the choice they feel they must make. B + P + F = acceptance. Put the same words in another order, and you lose
Dale Carnegie said, “People do things for their reasons, not ours. So, find their reasons.”
control. If you begin with the device, you risk the patient distracting themselves with what they think they know about oral appliances, what their friends and family have told them, or what it looks like. You say this isn’t possible in the time it takes for you to complete a sentence? Do you think, or talk, faster? So do they.
Betty is interested in what’s good for Betty, and she wants to stop the symptoms that drove her to get diagnosed with sleep apnea. She sees the oral device only to achieve that outcome, not as the goal itself. If we focus on the process of getting the device perfect, it may mean a lot to us, but not so much to Betty.
David McCarty, MD, is a sleep specialist who was an English major in college. His clinical work has always included challenging himself to improve communications with his patients. He’s also a writer/cartoonist and co-author of Empowered Sleep Apnea, A Handbook for Patients and the People Who Care About Them. Alan Alda, the actor, wrote a book: If I Understood You, Would I Have This Look on My Face? after a dental encounter that went wrong due to lack of communication by the dentist. Both provide resources for taking complex information and making it accessible for people who are experts only in themselves.

Dr. McCarty includes in his book this lesson: once a person is diagnosed with a sleep related breathing disorder, there are 5 reasons to treat it:
1. Risk – what level of health risk to that individual does the SRBD hold, such as a major adverse cardiovascular event?
2. Snoring – does snoring decrease quality of life for the snorer or another person?
3. Wake – how does the SRBD impact activities during wakefulness – drowsy driving, for example?
4. Sleep – what happens to keep sleep from being restful – frequently waking, poor sleep quality, gasping and choking?
5. Comorbidities – what chronic disease is the patient struggling with that may be impacted by SRBD?
Alan Alda promotes the tools of Improv to enhance the exchange of information. On stage, improv actors are trained to listen carefully to their scene partners to build the story for the audience. A scene only works when the actors connect, accept each other’s contributions, and add the next layer. This “Yes, and…” technical expertise is invisible because ‘how it works’ is not important; what matters is ‘how it plays.’ Consider each encounter in your office a scene and every patient a partner.
Betty has a medical history that I studied before she arrived. I know what’s bothering her because I asked appropriate questions and listened carefully. When it’s time for me to provide the advice she came for, I draw upon everything I’ve learned about my science and her humanness. I link her story (emotion and self-interest) to a good reason to treat (Medicine 3.0), and together we decide what treatment will give her the best chance of an outcome that solves the problems she feels. End scene. That’s good medicine.
1. Schein, Edgar H. Humble Inquiry: The Gentle Art of Asking Instead of Telling. Berrett-Koehler Publishers, 2013.
2. Attia, Peter, MD Outlive: The Science and Art of Longevity. Harmony, 2023.
3. Alda, Alan. If I Understood You, Would I Have This Look on My Face? Random House, 2017.
4. McCarty, David and Stothard, Ellen. Empowered Sleep Apnea, A Handbook for Patients and the People Who Care About Them. BookBaby, 2024
5. Mary Osborne RDH. https://maryosborne.com/
Each article is equivalent to two CE credits. Available only to paid subscribers. Free subscriptions do not qualify for the CE credits. Subscribe and receive up to 8 CE credits for only $149 by visiting https://dentalsleeppractice.com/subscribe/.
AGD Code: 730
Date Published: August 15, 2025 Course Expires: August 15, 2028
Legal disclaimer: Course expires 3 years after publication date. The CE provider uses reasonable care in selecting and providing accurate content. The CE provider, however, does not independently verify the content or materials. Any opinions expressed in the materials are those of the author and not the CE provider. The instructional materials are intended to supplement, but are not a substitute for, the knowledge, skills, expertise and judgement of a trained healthcare professional.
by Steve Carstensen, DDS
1. We learn from Edgar Schein’s “Humble Inquiry” the value of ___________.
a. Enlightened leadership
b. Teamwork as a goal
c. The art of asking questions
d. Using innovative technology
2. In “Outlive,” Peter Attia emphasize ______________ as crucial for today’s healthcare?
a. Dependence on scientific method
b. Traditional medical practice
c. Preventive healthcare
d. Social determinants of health
3. Alan Alda’s book “If I Understood You, Would I Have This Look on My Face?” teaches us about ________.
a. Public speaking
b. Listening skills
c. Facial Recognition
d. Written communication
4. _____________ is a key strategy discussed in “Empowered Sleep Apnea” by David McCarty?
a. Medication as the best answer for most people
b. Connecting patients with reasons to treat their disease
c. Cartooning is a fun way to communicate
d. Experts need to step back and claim their status
5. In “Humble Inquiry,” Edgar Schein suggests that asking questions can lead to _______________ in a professional setting?
a. Easier completion of necessary paperwork
b. Clearer understanding of the patient’s story
c. Establishing proper boundaries between doctor and patient
d. The patient feeling appreciative of the doctor’s time and attention
n To receive credit: Go online to dentalsleeppractice.com/continuing-education/, click on the article, then click on the take quiz button, and enter your test answers
To provide feedback on this article and CE, email us at education@medmarkmedia.com.
6. A listening skill exercise should lead your team to discover
a. How hard it is to stay focused on the person speaking
b. Their own strengths as interviewers
c. How much they enjoy role-playing
d. When team meetings are a good day to call in sick
7. Jim Pride taught about the Benefit Statement. __________ is a key feature?
a. Giving advice
b. Being very clear on the features of the product or service
c. Making sure the benefit matches a patient concern they have shared
d. Describing your expertise as the biggest benefit
8. David McCarty’s “Empowered Sleep Apnea” highlights which reasons to treat?
a. SpO2, AHI, ODI, HB, CSA
b. PSG, HSAT, CST, BMI
c. Snoring, Anxiety, CV Risk, Obesity, Excessive Daytime Sleepiness
d. Risk, Snoring, Sleep, Wake, Comorbidities
9. Mary Osborne teaches that a good way to focus a conversation is to _______________.
a. Stay in the Question
b. Close the door
c. Maintain steady eye contact
d. Take careful notes
10. A key teaching that Dr. L.D. Pankey brought forward is to first
_____________.
a. Master your craft
b. Get your ducks in a row
c. Assemble the right team
d. Know your Patient

by Angela Richwine, RDH, BAS, QOM
Vibration therapy has emerged as a versatile tool in healthcare, offering benefits ranging from improved circulation to enhanced neuromuscular function. When combined with orofacial myofunctional therapy (OMT), vibration therapy can target critical physiological systems, including nasal cilia function, nitric oxide production, vagus nerve stimulation, and lymphatic drainage. This synergy presents a holistic approach to optimizing respiratory, neurological, and immune health.

The Mechanisms of Vibration Therapy
Vibration therapy involves the application of mechanical oscillations to stimulate tissues and systems within the body. This modality enhances circulation, reduces inflammation, and improves neuromuscular coordination. In the context of OMT, vibration therapy amplifies the benefits of targeted muscle retraining and functional rehabilitation by addressing:
1. Nasal Cilia Function: Vibration therapy supports the natural clearance mechanisms of the nasal passages by stimulating cilia movement. This helps to remove mucus, allergens, and pathogens, promoting clear nasal airways and reducing the risk of sinus infections.

2. Nitric Oxide Production: Nitric oxide, a potent vasodilator and antimicrobial agent, is produced in the paranasal sinuses and released during nasal breathing. Vibration therapy enhances nitric oxide release, supporting improved oxygen delivery, immune function, and cardiovascular health.
3. Vagus Nerve Stimulation: The vagus nerve plays a central role in the para-
sympathetic nervous system, regulating stress responses, digestion, and inflammation. Vibration therapy applied to areas like the neck or face stimulates the vagus nerve, promoting relaxation, reducing inflammation, and improving overall autonomic balance.
4. Lymphatic Drainage: The gentle oscillations of vibration therapy stimulate lymphatic flow, aiding in the removal of toxins and waste products. This is particularly beneficial in reducing swelling and supporting the immune system.
OMT focuses on optimizing the function of orofacial muscles, including the tongue, lips, and cheeks. Proper oral posture, nasal breathing, and muscle coordination are key goals of OMT. Combining OMT with vibration therapy can:
• Enhance the efficiency of exercises by improving neuromuscular activation.
• Facilitate nasal breathing by clearing nasal passages and stimulating nitric oxide production.
• Reduce tension in orofacial muscles, supporting better posture and function.
• Accelerate recovery and functional improvements by promoting lymphatic drainage and reducing inflammation.
1. Improving Nasal Breathing: Vibration therapy clears nasal passages and enhances cilia function, while OMT retrains breathing patterns to prioritize nasal breathing. This combination reduces mouth breathing and its associated risks, such as dental malocclusions and airway issues.
2. Enhancing Airway Health: By increasing nitric oxide production and stimulating the vagus nerve, this approach supports better airway tone and reduces the risk of obstructive sleep apnea.
3. Reducing Inflammation and Swelling: Lymphatic drainage facilitated by vibration therapy complements OMT exercises, reducing orofacial tension and promoting healing after interventions like frenectomies or orthodontic treatments.
4. Promoting Relaxation and Stress Reduction: Vagus nerve stimulation via vibration therapy helps patients achieve better autonomic balance, enhancing the therapeutic outcomes of OMT.
• Guilleminault et al.3: Demonstrated the role of OMT in improving airway health and reducing sleep apnea severity, highlighting the importance of nasal breathing and nitric oxide.
• Brunton et al.1: Found that vibration therapy enhances lymphatic flow and reduces inflammation, supporting recovery in orofacial and respiratory conditions.
• Yin et al.4: Showed that vagus nerve stimulation improves autonomic function and reduces systemic inflammation, underscoring its relevance in conjunction with OMT.
• Elad et al.2: Highlighted the role of nasal nitric oxide in airway health, showing how therapies that enhance its production benefit respiratory function.
The combination of vibration therapy and orofacial myofunctional therapy offers a comprehensive approach to improving respiratory, neurological, and immune health. By targeting nasal cilia function, nitric oxide production, vagus nerve stimulation, and lymphatic drainage, this integrated strategy addresses both structural and functional aspects of well-being. As research continues to evolve, the synergy between these modalities promises to unlock new possibilities for enhancing patient care and quality of life.
1. Brunton, L., Parker, K., & Blumenthal, D. (2020). Vibration therapy and its impact on lymphatic drainage and inflammation. Journal of Physical Medicine and Rehabilitation, 12(3), 145154. https://doi.org/10.1234/jpmr.2020.0345
2. Elad, D., Wolf, M., Keck, T., & Bleicher, A. (2006). The generation of nitric oxide in paranasal sinuses and its role in airway health. American Journal of Respiratory and Critical Care Medicine, 174(7), 768-774. https://doi.org/10.1164/rccm.200510-1660OC
3. Guilleminault, C., Huang, Y. S., Monteyrol, P. J., Sato, R., & Quo, S. (2013). Myofunctional therapy as an adjunctive treatment for airway dysfunction: A preliminary report. Sleep Medicine, 14(6), 518-525. https://doi.org/10.1016/j.sleep.2012.11.017
4. Yin, J., Chen, J. D., & Jiang, Z. (2018). Vagus nerve stimulation: Clinical applications and future possibilities. Journal of Clinical Investigation, 128(6), 2564-2572. https://doi.org/10.1172/ JCI96060





With 29 years of experience in the dental field, Angela Richwine, RDH, BASc, QOM, discovered her passion for improving smiles as an orthodontic assistant in 1996. Graduating with a dental hygiene certificate in 2000, she later earned a bachelor’s degree in applied sciences with a business focus. As the founder of Central Virginia OMT LLC, she provides virtual and in-office myofunctional therapy, collaborating with healthcare professionals for comprehensive client care, and teaching dental hygiene students. Angela also serves as the Director of Operations for Airway Circle, volunteering to moderate educational discussions, and shares her expertise globally, educating dentists and dental hygienists, speech and language pathologists, occupational therapists, and lactation consultants, on identifying signs and symptoms of myofunctional disorders.


Dentists can play a pivotal role in helping to diagnose and treat sleep apnea. Like many of your colleagues, you can advance your practice and patient care with home sleep apnea testing.*
Zoll Itamar offers WatchPAT® Solutions.1 It’s as easy as 1-2-3. You can simply screen and order a home sleep apnea test, and the WatchPAT Solutions team can do the rest.
Screen your patients for OSA, and if they are at risk, place the order on our cloud platform. The WatchPAT Solutions team will ship the device to your patient, provide patient education and promote test completion. After test completion, home sleep study results are securely uploaded to the cloud for interpretation, interpreted by a sleep physician, and provided for your review. WatchPAT Solutions provides a highly accurate,2 reassuringly reliable,3 easy to use, and scalable home sleep apnea test to fit the needs of your practice. WatchPAT is clinically validated with an 89%
correlation to PSG in AHI2 and its ease-to-use design provides a 98% test success rate.3
For nearly 30 years, ZOLL Itamar has led in home sleep testing. WatchPAT delivers clinical-grade data and smart features for fast, accurate, reliable results. Our flexible service models – from full-service to fast, patientready testing – fit your workflow and help you scale with ease.
For more information, please contact Robin. Koster@zoll.com or Mary.Boros@zoll.com
*You should not act upon any information provided in this article without seeking professional legal counsel from an attorney licensed to practice law in your jurisdiction. No representations are being made as to the completeness or accuracy of the information contained herein
1. Empowered by ZOLL Laboratory Services LLC (“ZOLL”), the provider and operator of the Independent Diagnostic Testing Facility service.
2. Yalamanchali et al. JAMA Otolaryngnol Head Neck Surg, 2013, Diagnosis of Obstructive Sleep Apnea by Peripheral Arterial Tonometry (Meta-Analysis).
3. Carey, Sandra A., et al. “The utility of home sleep apnea testing in the advanced heart failure populations.” The American Journal of Cardiology, vol. 191, Mar. 2023, pp. 8–13
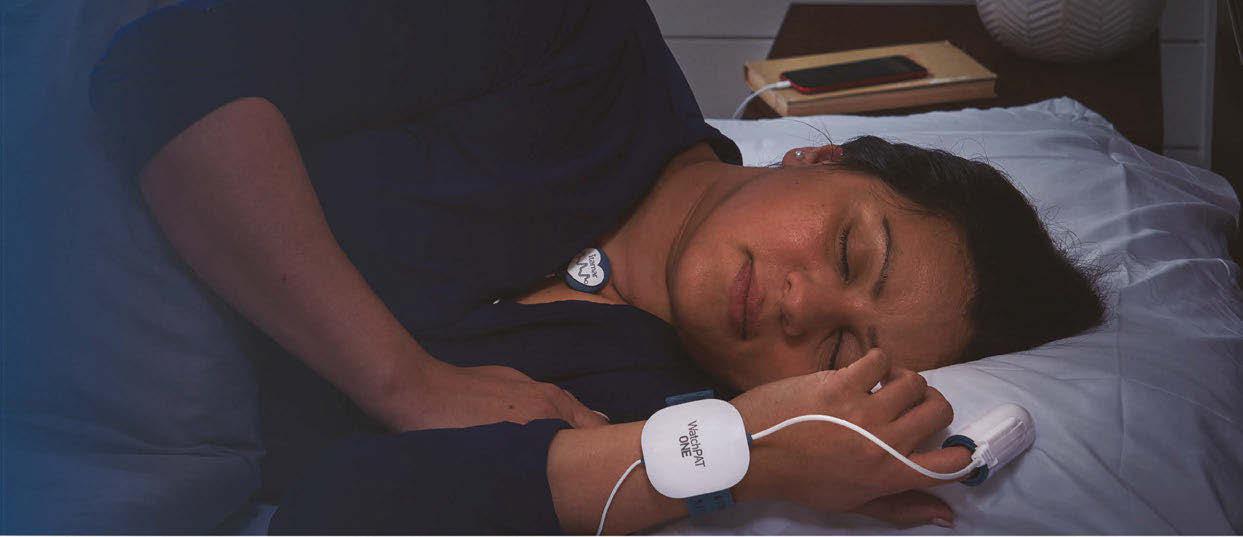









by Jon Nierman
s your DSM practice taking longer to take off than you thought it would? You’re not alone. Many dentists start with enthusiasm, invest in great training, and choose a high-quality appliance, only to find growth slower than expected. The reason? Success in dental sleep medicine isn’t just about clinical skills, hopes and dreams. The practices that truly thrive master three core systems: Medical Billing, Referrals, and Case Acceptance.
While clinical excellence is essential, the real foundation of a successful dental sleep medicine (DSM) practice lies in three core systems: Medical Billing, Referrals, and Case Acceptance.
Whether you handle medical billing inhouse or outsource it, your team must understand the workflow from a dental practice perspective. This goes beyond submitting claims. It is about preparing, documenting, and communicating.
Two guiding principles from Rose Nierman can help your team master this process:
“It’s what you do upfront that counts.”
Every successful dental sleep case starts with a strong medical Verification of Benefits (VOB). Knowing the policy criteria, deductible status, and coverage limitations allows you to present clear financial expectations to the patient from the start. This transparency
builds trust, reduces surprises, and sets the tone for smoother case acceptance and treatment success.
“Get your ducks in a row.”
Proper documentation is your golden ticket to not only medical billing, but also referrals. The sleep study, physician records, exam findings, narrative reports, and meeting the insurance policy criteria is the key to showing medical necessity. When documentation is incomplete, claims get denied or delayed. A software designed for DSM can streamline this process and help you generate accurate, professional SOAP reports.
Ask yourself:
• Is your team confident in the DSM billing process?
• Are you setting accurate expectations with patients regarding coverage?
• Are you finding that insurers are frequently asking for more documentation?
Referrals are the engine that drives patient flow in a dental sleep practice. Yet many dental teams hesitate to pursue these partnerships.
There are two key groups to focus on when building your referral network: the sleep community and the broader physician community. Both are essential components of a strong dental sleep medicine growth strategy.

Shift the conversation from clinical details to emotional benefits. Your patients will be far more motivated to move forward with treatment
when
they can clearly picture the life they want after resolving their sleep issues.
1. The Sleep World. While it may feel intimidating at first to engage with sleep professionals as a dentist, the reality is that many sleep providers are actively seeking alternatives for their CPAP-intolerant patients. Your outreach should go beyond sleep physicians. Look to connect with RPSGTs, sleep lab directors, and sleep technologists, they often play a vital role in guiding patients toward follow-up care and oral appliance therapy.
2. The Physician World. There is tremendous opportunity in building relationships with local primary care physicians, ENTs, cardiologists, pulmonologists, and even other general dentists. A practical starting point is to compile a list of your sleep patients’ shared providers. From there, implement a system for consistent communication.
Tools like DentalWriter Plus make this easy by generating narrative reports and SOAP notes that can be sent directly to each provider involved in the patient’s care. This not only strengthens the referral loop but positions your practice as the trusted local expert in dental sleep medicine.
When you present yourself as a collaborative partner focused on patient outcomes, you open the door to strong, long-term referral relationships.
Here are some ways to build a reliable referral system:
• Screen and refer dental patients you suspect of having a sleep disorder to local sleep labs
• Send SOAP reports to the patient’s primary care provider and specialists, including progress updates

Jon Nierman, President of Nierman Practice Management (NPM), is recognized for his contributions to continuing education, medical billing, and technology in the field of dental sleep medicine and TMD. Since 2010, Jon has led and expanded NPM’s renowned continuing education programs. His leadership at Nierman Practice Management drove the development of the next-generation dental sleep medicine platform DentalWriter Plus. A graduate of the Georgia Institute of Technology and an avid pianist, Jon brings a unique blend of technical expertise and creativity to the field.
• Provide a DSM packet that includes a cover letter, literature, patient brochures, and an oral appliance Rx template for sleep labs and medical offices
• Host short educational lunch-andlearns for local medical offices
Not every provider will refer immediately, but when you keep showing up and offering value, your credibility will grow along with your network.
Your team must be trained to connect treatment to outcomes that matter to each individual patient.
This starts with:
• Building trust and rapport from the very first interaction
• Verifying benefits ahead of the visit so patients are prepared
• Asking questions to uncover the patient’s priorities and daily struggles
• Helping patients envision how treatment can improve their life
Patient: “I wake up exhausted every morning.”
Team member: “That must be frustrating. How would your day look if you woke up feeling refreshed?”
Shift the conversation from clinical details to emotional benefits. Your patients will be far more motivated to move forward with treatment when they can clearly picture the life they want after resolving their sleep issues.
Strong clinical skills will always matter, but they are not enough on their own. Your practice will only reach its full potential when your systems are just as strong as your clinical protocols.
• Review one recent case for documentation quality and completeness
• Make sending SOAP reports a non-negotiable part of your workflow
• Role-play case presentations that focus on the patient’s goals
Clinical excellence sets the foundation. But your systems are what will allow your practice to grow, scale, and serve more patients at a higher level.
Sleep healthcare professionals require reliable, efficient screening devices that capture both oxygenation and positional data. The all new MediOX from BRAEBON Medical Corporation is a cloud-based overnight pulse oximeter and body position recorder ideal for the screening and management of sleep apnea.
Small, comfortable, and accurate, the MediOX is optimized for ease of use for screening and management of sleep disordered breathing.
MediOX houses a pulse oximeter alongside a body position sensor in a single, lightweight enclosure. The locking connector secures the SpO2 finger probe throughout the night, reducing lead-off events and preserving data integrity. Its low profile and minimal cabling enhance patient compliance, lower repeat study rates, and save valuable clinic resources.
MediOX continuously records peripheral oxygen saturation (SpO2), pulse rate, and body position. The PPG sensor detects subtle blood-volume changes, enabling precise heart-rate variability analysis. Simultaneously, accelerometry differentiates supine versus non-supine postures – critical for identifying positional OSA and guiding targeted therapies, particularly important for oral appliance therapy.
Unlike popular ring-based oximeters that capture only SpO2 and pulse rate, MediOX’s integrated accelerometer provides real-time body-position data. Without positional context, ring devices can obscure whether desaturation events occur primarily in the supine position – potentially distorting oral appliance titration efficacy and underestimating positional apnea’s contribution to overall disease burden.
Beyond standard desaturation indices, MediOX computes hypoxic burden index (HBI) that quantifies the frequency, depth, and duration of oxygen dips to better identify cardiovascular risk. All recordings upload securely to BRAEBON’s BridgeBuilder cloud platform, where clinicians can review comparative reports – baseline versus intervention nights – with side-by-side SpO2 waveforms, oxygen desaturation indices (ODI), and other metrics.
MediOX supports multiple care pathways:
• Primary screening of undiagnosed patients in primary care, cardiology, or ENT settings


• Assessment of positional apnea before prescribing positional therapy
• Two-night comparative studies for CPAP or oral appliance therapy efficacy
Its robust design and automated reporting reduce manual scoring, streamline workflow, and improve patient throughput – crucial for busy sleep clinics and hospitals.
• Unique combination of pulse oximetry and body position
• Simple to use and cost-effective method to screen for sleep apnea
• Reliable and built on decades of dependable BRAEBON technology
• Auto cloud analysis and reporting –no manual scoring
• Monitor CPAP & oral appliance effectiveness and the benefit of OAT on positional apnea
• Comprehensive pulse oximeter and position report with ODI, HBI, detailed SpO2 graphs, and more
MediOX distinguishes itself by merging oximetry with position sensing, delivering robust HBI analytics, and offering seamless cloud-based reporting. This integrated approach enables rapid detection of OSA, optimized treatment titrations, and enhanced patient adherence.
To bring the benefits of MediOX into your clinic, hospital, or practice, contact BRAEBON today at 1-888-462-4841 x218 or customer.service@braebon.com to arrange a demonstration or place your first order.
by Scott S. De Rossi, DMD, MBA
The modern healthcare landscape is undergoing a profound transformation. Technological advancements, shifting patient expectations, regulatory complexities, and the rise of corporate delivery models have converged to redefine what it takes to succeed – not only as a clinician but as a leader. Nowhere is this evolution more evident than in the dental industry, where the traditional solo-practitioner model is rapidly giving way to Dental Support Organizations (DSOs), group practices, and dental education models that demand far more than clinical competency. In this changing environment, the value of business and leadership excellence is not ancillary – it is foundational.
To thrive in the future of healthcare, every member of the dental team must be equipped with knowledge, skills, abilities, and judgment that transcend the operatory. Business acumen, strategic thinking, and people leadership are no longer optional soft skills; they are essential survival traits. Serendequity Education’s Mini MBA for Dentistry and Leadership Excellence to Advance Practice (LEAP) certificates respond to this need with urgency, clarity, and action. These programs are not just academic exercises; they are transformational platforms that bridge the long-standing gap between clinical mastery and business and leadership excellence.
For decades, dental education has produced competent clinicians who were expected to “figure out” business on their own. As a result, thousands of private practitioners found themselves unprepared for the
financial, operational, and strategic realities of running a dental practice. Today, with declining insurance reimbursements, rising operating costs, and patient expectations shaped by consumer-centric industries, the challenge is even greater.
Meanwhile, DSOs have surged in influence, offering dentists opportunities for support, stability, and scale. Yet the success of these organizations hinges on local leaders who can manage P&Ls, build high-performing teams, and deliver exceptional patient experiences. Even the best DSO infrastructure fails without empowered clinicians who understand how to run their practices as businesses and lead their teams effectively.
At the same time, dental education must also evolve. Schools are increasingly recognizing the need to graduate dentists who are not only clinically competent but also strategically agile and prepared for multifaceted roles – as clinicians, managers, educators, entrepreneurs, and change agents. However, few institutions offer meaningful and practical structured business or leadership development integrated into their core curriculum.
Leadership in dentistry is not confined to owners or executives. It manifests in every interaction that shapes a patient’s experience and every decision that influences a team’s culture. From the front office administrator who manages scheduling efficiency, to the hygienist who educates patients and supports treatment acceptance, to the associate dentist managing chairside dynamics – every team member impacts the overall success of a practice.
Yet these professionals are rarely given formal training in conflict resolution, change
management, communication strategy, or operational improvement. This lack of leadership development is a missed opportunity not just for individual growth, but for organizational excellence.
By embedding leadership training across all team levels, practices and DSOs can build a culture of shared accountability, continuous improvement, and adaptive problem-solving. Empowered teams are resilient teams – and resilient teams are those that can navigate staffing shortages, integrate new technologies, respond to shifting payer models, and deliver better outcomes under pressure.
The Serendequity Solution: Mini MBA and LEAP Certificates
Serendequity Education’s Mini MBA and LEAP programs were created to address this urgent gap with precision and practicality.
This intensive, modular online program is designed for dentists and staff, specialists, practice owners, and DSO executives seeking a comprehensive foundation in business disciplines essential to healthcare leadership. With 12 interactive modules – including financial management, marketing strategy, team dynamics, operations, legal compliance, and strategic planning – the Mini MBA provides realworld tools rooted in dental practice realities. Through capstone projects and case-based learning, participants do not merely absorb knowledge, they apply it – building business plans, operational improvements, and leadership strategies that can be deployed immediately in their settings.
The Serendequity Education Mini MBA for Dentistry is an innovative, industry-tailored certificate program designed to equip dentists, hygienists, and dental leaders with core business competencies to thrive in today’s rapidly evolving dental landscape. This online, self-paced curriculum offers a practical, highimpact educational experience and essential tools to lead, grow, and future-proof dental practices and organizations.
At its core, this Mini MBA bridges the long-standing gap between clinical training and business knowledge in dental education. With deep roots in real-world practice scenarios and trends, this program empowers dental professionals to make data-informed decisions, navigate competitive pressures, and cre-

ate scalable, patient-centered businesses. It is a critical step forward in redefining how dentistry prepares its current and future leaders.
Targeted toward all dental professionals – dentists, hygienists, assistants, and administrative leaders – LEAP focuses on elevating leadership capacity within teams. These shorter, focused certificates develop core skills in emotional intelligence, decision-making, team building, coaching, and adaptability. LEAP cultivates confident, collaborative professionals who understand how to inspire others, align around vision, and foster cultures of trust, innovation, and excellence.
Both programs are designed with flexibility in mind: online, asynchronous, and accessible to working professionals. They combine world-

Scott S. De Rossi, DMD, MBA, Vice President of Strategic Growth and Innovation of Nexus Dental Systems, is passionate about driving strategic growth and innovation in healthcare. He has led initiatives to improve access, quality, outcomes, efficiency, patient satisfaction, and affordability by integrating medicine and dentistry. He has integrated cutting-edge technology and resources to optimize clinical and academic sectors, solving long-term issues and driving exponential growth. He has prioritized and communicated the importance of oral-systemic connections in patient-centered care, increasing endowment funds and ensuring compliance with accreditation and regulations. Dr. De Rossi has fostered innovative cultures by mobilizing cross-functional teams, balancing optimism with transparency and trust, and inspiring continuous improvement.
“To thrive in the future of healthcare, every member of the dental team must be equipped with knowledge, skills, abilities, and judgment that transcend the operatory.”
class faculty with evidence-based frameworks ensuring that content is both cutting-edge and grounded in dental practice.
Bridging the Business Education Gap in Dentistry
Most dental curricula prioritize clinical expertise but neglect business acumen. As a result, many dentists enter practice ownership or leadership roles ill-equipped to manage operations, finances, or strategy. The Serendequity Mini MBA directly addresses this gap by offering business and management education specifically contextualized for the dental industry. Unlike traditional MBA programs, this certificate is lean, focused, and immediately applicable – helping participants lead with confidence from day one.
The dental profession is undergoing significant transformation:
• Consolidation and the rise of DSOs: The Mini MBA offers insights into how to collaborate with, compete against, or even build a DSO, including practical tools for assessing affiliation and acquisition opportunities.
• Technology-driven disruption: From teledentistry to AI, participants learn how to evaluate, adopt, and leverage technologies that enhance productivity, reduce overhead, and elevate the patient experience.
• Consumer expectations and patientcentered care: The curriculum trains participants to develop marketing strategies, service excellence frameworks, and patient feedback systems that drive retention and satisfaction.
The modules on financial management,
team dynamics, operations, and marketing help practitioners:
• Analyze P&L statements and manage cash flow
• Build and retain high-performing teams
• Streamline workflows using lean principles
• Attract and retain patients using datadriven marketing
• Increase profitability while delivering high-quality care
These are not theoretical skills; they are mission-critical for any practice owner, associate, or DSO leader aiming for sustainable growth and resilience.
The Mini MBA cultivates leadership capacity by introducing proven frameworks in change management, organizational behavior, and strategic planning. Participants learn how to adapt their leadership styles to different situations, manage conflict, align teams around a shared vision, and drive performance in a clinical setting.
The Mini MBA spans 12 core modules delivered in a dynamic, flexible online format. Each module features video lectures by dental and business experts, interactive tools, real-world case studies, assessments, and peer discussion forums.
Highlights include:
Modules 1–3: Foundation in Business, Finance, and Leadership
• Business Foundations for Dental Practices
• Financial Management Essentials
• Leadership in Dental Practice
Modules 4–6: Team, Communication, and Marketing
• Team Management and Communication
• Marketing Strategies for Dental Practices and DSOs
• Patient Experience and Relationship Management
Modules 7–9: Operations, Legal, and Strategy
• Operational Excellence in Dental Practices and DSOs
• Legal and Ethical Considerations
• Strategic Planning in Dental Practices and DSOs

Whether you’re an owner looking to sharpen your business acumen, a practice manager striving for operational excellence, or an aspiring leader eager to make an impact, this Mini MBA for Dental Professionals lays out a step-by-step roadmap. In the 12 modules, you’ll gain hands-on templates, real-world case studies, and actionable frameworks that translate immediately into your day-to-day—and long-term—success.
Modules 1–3: Foundation in Business, Finance, and Leadership Modules 4–6: Team, Communication, and Marketing
Modules 7–9: Operations, Legal, and Strategy
Modules 10–12: Financial Planning and Capstone Project




Modules 10–12: Financial Planning and Capstone Project
• Financial Planning and Investment
• Capstone Business Plan Project
• Professional Reflection and Integration
The Capstone Project is a distinctive feature, allowing learners to develop and present a real-world business plan addressing a current challenge or opportunity within their own practice or the broader industry.
Differentiators and Innovation
• Dental-specific, practitioner-focused: Unlike generic business programs, every topic is translated for dental application – using dental-specific examples, case studies, and metrics.
• Expert-led and evidence-based: Instruction draws from Harvard Business Review, McKinsey, ADA policy, and successful DSO operators. This ensures that learners receive best-in-class thinking tailored to their world.
• Flexible, asynchronous learning: Designed for busy professionals, this online model supports learning on-demand while still enabling community interaction through discussion forums and coaching sessions.
• Scalable across roles and organizations: The program is valuable not only for private practitioners and owners but also for emerging leaders in DSOs, group practices, and even dental schools seeking to embed leadership into predoctoral curricula.
Professional Impact and Career Relevance
Graduates of the Serendequity Mini MBA will be equipped to:
• Launch or expand successful private practices or DSOs
• Increase efficiency, profitability, and patient satisfaction
• Lead multidisciplinary teams with clarity and purpose
• Make strategic financial and operational decisions
• Explore new career paths in executive leadership, consulting, or education
In a field where business illiteracy can hinder career progression, this program becomes a strategic enabler of growth, security, and fulfillment.
Equipping the Profession for the Future
As we enter an era of precision health, artificial intelligence, value-based care, and growing integration between oral and systemic health, the expectations placed on dental professionals will only increase. To lead in this new age, our profession must rethink how we define excellence.
• Excellence is no longer just about clinical outcomes; it is about organizational agility.
• Success is no longer just about solo achievement; it is about team empowerment.
• Impact is no longer limited to the dental chair; it is measured by systems thinking, strategic foresight, and the ability to lead change.
The Serendequity Mini MBA and LEAP programs offer a clear path forward. They democratize access to elite business and leadership education and bring it into the hands of those who need it most – practicing dental professionals and staff navigating real-world complexity.
The dental industry stands at an inflection point. Clinical skill will always be the foundation of dental medicine, but it is no longer sufficient to ensure success. Business literacy and leadership excellence must now be core competencies for every member of the dental team. Whether navigating the complexities of private practice, driving performance in a DSO, or preparing students in dental education, the need for strategic, empowered, and adaptive leaders has never been greater.
Serendequity Education’s Mini MBA and LEAP certificates are more than programs –they are movements. They represent a shift in how we prepare dental professionals for impact, resilience, and sustainable success. By embracing business and leadership education, the dental profession will not only meet the demands of today; it will shape the healthcare systems of tomorrow. As the profession evolves, so too must the way we prepare our clinicians – not just to drill, fill, and bill – but to lead, build, and grow.
This is not optional education – it is essential. Serendequity Education prepares people not only to survive the future of dentistry but to shape it.
From identifying patients with a sleep disorder or an airway issue to appliance selection to delivery and follow-up, Great Lakes can provide expert insight, extensive appliance knowledge, and more than 35 years of fabrication experience.

For experienced dentists who recognize patients who can benefit from sleep or airway therapy, Great Lakes can assist in all phases of treatment, from screening and identifying the appropriate appliance therapy to delivery, follow-up, and a secondary post-wear screening.
For a doctor new to sleep/airway, Great Lakes can help implement sleep/airway therapy into their practice and train both the doctor and staff.
Great Lakes helps office staff to understand the proper use of sleep screeners and interpret the results, offering both the 3D SleepSat screener and the Nonin sleep screener. Reporting from both home sleep screeners provides excellent insight into the severity of sleep or airway issues, ranging from mild to moderate to severe.

Taking a protrusive bite position is an essential step in patient therapy. This ‘bite position’ effectively opens the airway to improve breathing and facilitate obstruction-free sleep. Ideal for mandibular repositioning, the George Gauge® allows the clinician to capture the protrusive bite registration and vertical opening without relying on the patient to achieve proper positioning. The George Gauge eliminates the guesswork, is exceptionally accurate, and easy to use.
The George Gauge single-use bite fork with the bite registration in place is sent to the Lab. Great Lakes will generate models, and sleep specialists and designers can help determine the ideal appliance for the patient and their specific needs. An intra-oral scan of the protrusive bite position can also be sent electronically to the Lab.
Great Lakes’ sleep and airway team will walk through a series of questions to help
recommend the most effective appliance. These include:
1. Where is the ideal position for the advancement mechanism – buccal or anterior? Different appliances are suitable based on the position of the advancement mechanism. Herbst and Panthera feature buccal placement, while TAP appliances feature anterior placement.
2. What material is preferred?
• Basic, thin Biocryl: EMAs
• Nylon: Nylon Herbst®, Panthera Classic & X3™, OrthoApnea NOA
• Hard/Soft: Medleys and TAPs
• Hard: Herbst® and Medley
3. What patient habits should be considered?
• Clenching
• Grinding
• Bruxing
4. What patient anatomy considerations are there?
• Edentulous
• Partials/Dentures/Implants
• Short clinical crowns
• Orthodontic therapy
• Dental changes
The answers to these questions will help determine the ideal appliance type for your patient.
Once the patient has been screened for a baseline, the issue is identified, and an appliance has been fabricated, delivered, and worn, a subsequent screening is required. Screening during titration is imperative to see if the patient achieves optimal results. Great Lakes trains the practice to evaluate the screening, reporting, and effectiveness of the sleep appliance.
Great Lakes Sleep team has years of skill and experience, and the Lab has decades of fabrication expertise. Great Lakes can help you and your patients achieve better sleep and airway health outcomes.
Great Lakes is located in Tonawanda, New York, a suburb of Buffalo.
by J. Wesley Sublett, MD, MPH, Board-Certified Allergist in Louisville, Kentucky, and Donald Cohen, DMD, from New York State
One of the most dangerous emergencies you may encounter in a dental office is anaphylaxis, a severe allergic reaction that can happen within minutes and can be fatal if not treated immediately with epinephrine. The American Dental Association (ADA) recommends that dental practices have plans in place for responding to allergic emergencies, including using epinephrine auto-injectors to treat anaphylaxis. We asked J. Wesley Sublett, MD, and Donald Cohen, DMD, about the key facts every dental practice should know about anaphylaxis and how to prepare for it.
Q: What are common triggers for anaphylaxis in a dental office?
Dr. Cohen: The most common triggers of anaphylaxis in dental practice are antibiotics, antiseptics, and latex-containing products, such as gloves, bite-wing tabs, adhesive tape, and rubber dams. But these are not the only possible triggers.1 Medications, such as NSAIDs, local anesthetics, sedatives, and the materials used in endodontics and impressions can also cause anaphylaxis.1
Q: What are the symptoms of anaphylaxis?
Dr. Sublett: Because anaphylaxis is life-threatening and can occur quickly, it’s critical for dentists and their staff to recognize symptoms and respond immediately. Symptoms can occur in a number of different systems in the body.2 For example, there may be skin changes, including rash, hives, redness, itching, or swelling below the skin surface. The patient’s mouth, throat, or tongue can become swollen, causing swallowing or breathing difficulties such as wheezing or rapid breathing. The patient may experience nausea, vomiting, or other gastrointestinal symptoms. Cardiac symptoms, such as rapid heartbeat and a drop in blood pressure, can also occur.
Q: How can dentists and their staff treat anaphylaxis when it happens in the office?
Dr. Sublett: Epinephrine is the first-line treatment for anaphylaxis,4 and administering epinephrine early has been shown to reduce the risk of hospitalization and life-threatening consequences.5,6 A dose of epinephrine appropriate to the patient’s weight class should be given immediately.7 I recommend Intramuscular Injection (IM), as it is a proven route of administration that reliably delivers the full dose of epinephrine and whose effects have a rapid onset.8 The ADA recommends that practices have a plan in place,


which includes using epinephrine to deliver a premeasured dose to treat anaphylaxis.7
In addition, the World Allergy Organization Anaphylaxis Guidance recommends implementing the following protocol immediately if anaphylaxis is suspected:5
1. If the trigger can be identified, remove it immediately (if feasible).
2. Activate emergency medical services.
3. Assess the patient’s vitals and weight.
4. And, simultaneously, give the weightappropriate dose of epinephrine.
5. If necessary, give the patient high-flow supplemental oxygen via a face mask.
Q: What are considerations during surgery for administering epinephrine to respond to anaphylaxis?
Dr. Cohen: Since use of a nasal cannula is common during dental surgery,10 I recommend IM epinephrine since it can easily be given during use of a nasal cannula and IV.
Q: When choosing an epinephrine device, what features should dental practices consider?
Dr. Sublett: Epinephrine auto-injectors, like AUVI-Q, simplify administration during an emergency because they can be administered through clothing and are pre-measured with a weight-appropriate dose to keep anaphylaxis symptoms from progressing. AUVI-Q is the only epinephrine device
It’s critical to recognize the symptoms of anaphylaxis and to respond quickly.
• Can administer epinephrine through clothing
• Features voice instructions to help users confidently administer epinephrine
• Is the only epinephrine device available in three weight-appropriate doses
• Common adverse reactions to epinephrine include anxiety, apprehensiveness, restlessness, tremor, weakness, dizziness, sweating, palpitations, pallor, nausea and vomiting, headache, and/or respiratory difficulties.


AUVI-Q (epinephrine injection, USP) is indicated in the emergency treatment of allergic reactions (Type I) including anaphylaxis to allergens, idiopathic and exercise-induced anaphylaxis. AUVI-Q is intended for patients with a history of anaphylactic reactions or who are at increased risk for anaphylaxis.
AUVI-Q is intended for immediate self-administration as emergency supportive therapy only and is not a substitute for immediate medical care. In conjunction with the administration of epinephrine, the patient should seek immediate medical or hospital care. Each AUVI-Q contains a single dose of epinephrine for single-use injection. More than two sequential doses of epinephrine should only be administered under direct medical supervision. Since the doses of epinephrine delivered from AUVI-Q are fixed, consider using other forms of injectable epinephrine if doses lower than 0.1 mg are deemed necessary.
Please see additional Important Safety Information on next page, and full Prescribing Information and Patient Information available at www.auvi-q.com.
Designed to provide confidence from start to finish—no experience required.1-3
A calm voice in a moment of anxiety
Voice instructions guide users through administration during anaphylaxis.
Simply press and hold
For 2-second administration that patients may not even feel.

Important Safety Information (continued)


Hear the voice instructions for yourself

Reassuring dose delivery confirmation LED lights flash red and voice instructions confirm administration.
AUVI-Q should ONLY be injected into the anterolateral aspect of the thigh. Do not inject intravenously, or into buttock, digits, hands, or feet. Instruct caregivers to hold the leg of young children and infants firmly in place and limit movement prior to and during injection to minimize the risk of injection-related injury.
Rare cases of serious skin and soft tissue infections have been reported following epinephrine injection. Advise patients to seek medical care if they develop any of the following symptoms at an injection site: redness that does not go away, swelling, tenderness, or the area feels warm to the touch.
Epinephrine should be administered with caution to patients with certain heart diseases, and in patients who are on medications that may sensitize the heart to arrhythmias, because it may precipitate or aggravate angina pectoris and produce ventricular arrhythmias. Arrhythmias, including fatal ventricular fibrillation, have been reported in patients with underlying cardiac disease or taking cardiac glycosides or diuretics. Patients with certain medical conditions or who take certain medications for allergies, depression, thyroid disorders, diabetes, and hypertension, may be at greater risk for adverse reactions. Common adverse reactions to epinephrine include anxiety, apprehensiveness, restlessness, tremor, weakness, dizziness, sweating, palpitations, pallor, nausea and vomiting, headache, and/or respiratory difficulties.
Please see the full Prescribing Information and the Patient Information available at www.auvi-q.com.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch or call 1-800-FDA-1088
References: 1. Kessler C, et al. Usability and preference of epinephrine auto-injectors: Auvi-Q and EpiPen Jr. Ann Allergy Asthma Immunol. 2019;123(3):256-262. 2. Turner P, et al. Pharmacokinetics of adrenaline autoinjectors. Clin Exp Allergy. 2022;52(1):18-28. 3. Camargo CA Jr, et al. Auvi-Q versus EpiPen: preferences of adults, caregivers, and children. J Allergy Clin Immunol Pract. 2013;1(3):266-272. e1-e3.
and
available in three weight-appropriate doses: 0.1 mg for young children weighing 16.5-33 pounds, 0.15 mg for children weighing 33 to 66 pounds, and 0.3 mg for adults and children weighing 66 pounds and above.
In addition, AUVI-Q has voice instructions that guide untrained users through administration during a moment of anxiety. In a recent usability study, users of AUVI-Q were significantly more likely to correctly demonstrate its use compared to other epinephrine auto-injectors.14
Q: What other steps can dental practices take to ensure their anaphylaxis preparedness?
Dr. Cohen: It’s critical to ensure the dental team is always prepared and confident in their ability to respond to allergic emergencies. To this end, regular team training in recognizing anaphylaxis and how to properly use emergency devices, like AUVI-Q, is essential.15
Dental practices should also keep emergency medical kits on hand.15 The ADA Member Advantage program has endorsed HealthFirst as its exclusive provider of dental emergency medical kits for ADA members. Dental professionals can learn more about emergency kits from HealthFirst that include AUVI-Q by visiting healthfirst.com/EMK.
Disclosure: Dr. Sublett is a paid advisor of Kaléo This information was provided by Kaléo.
Indication
AUVI-Q® (epinephrine injection, USP) is indicated in the emergency treatment of allergic reactions (Type I) including anaphylaxis to allergens, idiopathic and exercise-induced anaphylaxis. AUVI-Q is intended for patients with a history of anaphylactic reactions or who are at increased risk for anaphylaxis.
Important Safety Information
AUVI-Q is intended for immediate self-administration as emergency supportive therapy only and is not a substitute for immediate medical care. In conjunction with the administration of epinephrine, the patient should seek immediate medical or hospital care. Each AUVI-Q contains a single dose of epinephrine for single-use injection. More than two sequential doses of epinephrine should only be administered under direct medical supervision. Since the doses of epinephrine delivered from AUVI-Q are fixed, consider using other forms of injectable epinephrine if doses lower than 0.1 mg are deemed necessary.
AUVI-Q should ONLY be injected into the anterolateral aspect of the thigh. Do not inject intravenously, or into buttock, digits, hands, or feet. Instruct caregivers to hold the leg of young children and infants firmly in place and limit movement prior to and during injection to minimize the risk of injection-related injury.
Rare cases of serious skin and soft tissue infections have been reported following epinephrine injection. Advise patients

Emergency dental kits from HealthFirst
to seek medical care if they develop any of the following symptoms at an injection site: redness that does not go away, swelling, tenderness, or the area feels warm to the touch.
Epinephrine should be administered with caution to patients with certain heart diseases, and in patients who are on medications that may sensitize the heart to arrhythmias, because it may precipitate or aggravate angina pectoris and produce ventricular arrhythmias. Arrhythmias, including fatal ventricular fibrillation, have been reported in patients with underlying cardiac disease or taking cardiac glycosides or diuretics. Patients with certain medical conditions or who take certain medications for allergies, depression, thyroid disorders, diabetes, and hypertension, may be at greater risk for adverse reactions. Common adverse reactions to epinephrine include anxiety, apprehensiveness, restlessness, tremor, weakness, dizziness, sweating, palpitations, pallor, nausea and vomiting, headache, and/or respiratory difficulties.
Please see the full Prescribing Information (https://bit.ly/4j9fPAQ) and the Patient Information (https:// bit.ly/4iZ2o6o).
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/ medwatch or call 1-800-FDA-1088.
References
1. Goto T. Management of Anaphylaxis in Dental Practice. Anesth Prog. 2023;70(2):93-105. doi: 10.2344/anpr-70-0216. Epub 2023 Jun 28.
2. Jevon P, Shamsi S. Management of anaphylaxis in the dental practice: an update. Br Dent J. 2020 Dec;229(11):721728. doi: 10.1038/s41415-020-2454-1. Epub 2020 Dec 11.
3. Asthma and Allergy Foundation of America (AAFA). Food Allergy Anaphylaxis in Infants and Toddlers. https://aafa.org/ asthma-allergy-research/our-research/food-allergy-anaphylaxis-in-infants/. Accessed March 24, 2025.
4. Brown JC, Simons E, Rudders SA. Epinephrine in the Management of Anaphylaxis. J Allergy Clin Immunol Pract. 2020 Apr;8(4):1186-1195. doi: 10.1016/j.jaip.2019.12.015. Erratum in: J Allergy Clin Immunol Pract. 2021 Jan;9(1):604. doi: 10.1016/j.jaip.2020.11.035.
5. Bock SA, Muñoz-Furlong A, Sampson HA. Further fatalities caused by anaphylactic reactions to food, 2001-2006. J Allergy Clin Immunol. 2007 Apr;119(4):1016-1018. doi: 10.1016/j.jaci.2006.12.622. Epub 2007 Feb 15.
6. Fleming JT, Clark S, Camargo CA Jr, Rudders SA. Early treatment of food-induced anaphylaxis with epinephrine is associated with a lower risk of hospitalization. J Allergy Clin Immunol Pract. 2015 Jan-Feb;3(1):57-62. doi: 10.1016/j. jaip.2014.07.004. Epub 2014 Sep 8.
7. Cardona V, Ansotegui IJ, Ebisawa M, El-Gamal Y, Fernandez Rivas M, Fineman S, Geller M, Gonzalez-Estrada A, Greenberger PA, Sanchez Borges M, Senna G, Sheikh A, Tanno LK, Thong BY, Turner PJ, Worm M. World allergy organization anaphylaxis guidance 2020. World Allergy Organ J. 2020 Oct 30;13(10):100472. doi: 10.1016/j. waojou.2020.100472.
8. HealthFirst. Dr. Malamed: The Importance of Epinephrine Auto-Injectors. https://www.healthfirst.com/videos/dr-stanley-malamed-the-importance-of-epinephrine-auto-injectors/. Accessed March 24, 2025.
9. American Academy of Pediatric Dentistry. Managing Professional Risks, ADA Guidelines for Practice Success™ (GPS™), ADA Tip Sheet on Managing Patients’ Medical Emergencies. https://www.aapd.org/globalassets/media/ safety-toolkit-2.0/tip-sheet-on-managing-patients-medical-emergencies.pdf. Accessed March 24, 2025.
10. Becker DE, Rosenberg MB, Phero JC. Essentials of airway management, oxygenation, and ventilation: part 1: basic equipment and devices. Anesth Prog. 2014 Summer;61(2):78-83. doi: 10.2344/0003-3006-61.2.78.
11. Krishnamurthy M, Venugopal NK, Leburu A, Kasiswamy Elangovan S, Nehrudhas P. Knowledge and attitude toward anaphylaxis during local anesthesia among dental practitioners in Chennai - a cross-sectional study. Clin Cosmet Investig Dent. 2018 Jun 28;10:117-121. doi: 10.2147/CCIDE.S159341.
12. Çetinkaya F, Sezgin G, Aslan OM. Dentists’ knowledge about anaphylaxis caused by local anaesthetics. Allergol Immunopathol (Madr). 2011 Jul-Aug;39(4):228-231. doi: 10.1016/j.aller.2010.07.009. Epub 2011 Jan 13.
13. Smereka J, Aluchna M, Aluchna A, Szarpak Ł. Preparedness and attitudes towards medical emergencies in the dental office among Polish dentists. Int Dent J. 2019 Aug;69(4):321-328. doi: 10.1111/idj.12473. Epub 2019 Mar 7.
14. Zhang E, Sicherer S, Agyemang A. Proper use of epinephrine autoinjectors is related to device type, prior physical demonstration, and sociodemographic factors. J Allergy Clin Immunol Pract. 2025 Feb;13(2):418-420.e1. doi: 10.1016/j.jaip.2024.11.006. Epub 2024 Nov 19.
15. Rosenberg M. Preparing for medical emergencies: the essential drugs and equipment for the dental office. J Am Dent Assoc. 2010 May;141 Suppl 1:14S-19S. doi: 10.14219/jada.archive.2010.0351.
AUVI-Q® and AUVI-q® are registered trademarks of Kaléo, Inc. Other referenced trademarks are owned by their respective third-party owners. © 2025 Kaléo, Inc. CM-US-AQ-3704.
Spell words by connecting letters around the square. Words must be at least 3 letters long. The last letter of a word becomes the first letter of the next word. Letters can be reused, but consecutive letters cannot be from the same side. Use all of the letters in as few words as possible to solve; this puzzle is solvable with 2 words. E L I N U X R C O B A V S T G H

For the solution, visit www.dentalsleeppractice.com.
• In-Network options with major payors and plans
• Out-of-Network when appropriate
• Reliable, timely, predictable results with best rates
• Access to the Nexus Specialty Physician Network
• Nexus billing por tal ensures error-free claim submission and tracking
• Personal billing representative
• Complete solution for:
º Sleep Medicine
º Airway Expansion
º TMJ/TMD
º Botox
º CBCT

Getting reimbursement from medical insurance can be a nightmare for dentists. With the Nexus Bill system, you can avoid the common pitfalls of inconsistent payments, endless delays, constantly fighting with insurance companies, and patients refusing care because you are not “In-Network” for medical.




