Research Education Innovation
ESCRS’s vision is to educate and help our peers excel in our field. Together, we are driving the field of ophthalmology forward.

Publishers
Therese Dolan, Operations Director ESCRS
Barbara Calderwood, Divisional Director Engagement Associations and Communities MCI UK
Mark Wheeler, Finance Director MCI UK
Editor-in-Chief
Sean Henahan
Senior Content Editor
Kelsey Ingram
Design Director
Kelsy McCarthy
Designer
Jen Basel
Circulation Manager
Vanessa McCourt
Contributing Editors
Cheryl Guttman-Krader
Howard Larkin
Dermot McGrath
Roibeard Ó hÉineacháin
Contributors
Cheryl Guttman-Krader
Leigh Spielberg
Gearóid Tuohy
Priscilla Lynch
Soosan Jacob
Colour and Print
W&G Baird Printers
Advertising Sales
Matthew Clapham
MCI UK Tel: +44 7342887969






email: matthew.clapham@mci-group. com

Published by the European Society of Cataract and Refractive Surgeons, Suite 7 - 9 The Hop Exchange, 24 Southwark St, London SE1 1TY. No part of this publication may be reproduced without the permission of the managing editor. Letters to the editor and other unsolicited contributions are assumed intended for this publication and are subject to editorial review and acceptance.
ESCRS EuroTimes is not responsible for statements made by any contributor. These contributions are presented for review and comment and not as a statement on the standard of care. Although all advertising material is expected to conform to ethical medical standards, acceptance does not imply endorsement by ESCRS EuroTimes.

MEDICAL EDITORS
INTERNATIONAL EDITORIAL BOARD


Noel Alpins (Australia), Bekir Aslan (Turkey), Roberto Bellucci (Italy), Hiroko Bissen-Miyajima (Japan), John Chang (China), Béatrice Cochener-Lamard (France), Oliver Findl (Austria), Nino Hirnschall (Austria), Soosan Jacob (India), Vikentia Katsanevaki (Greece), Daniel Kook (Germany), Boris Malyugin (Russia), Marguerite McDonald (USA), Cyres Mehta (India), Sorcha Ní Dhubhghaill (Ireland)
Rudy Nuijts (The Netherlands), Leigh Spielberg (The Netherlands), Sathish Srinivasan (UK), Robert Stegmann (South Africa), Ulf Stenevi (Sweden), Marie-José Tassignon (Belgium), Manfred Tetz (Germany), Carlo Enrico Traverso (Italy)
MDMaking Choices
Life is like riding a bicycle, in order to keep your balance, you must keep moving forward.
Albert EinsteinIam delighted to be invited to write this editorial for the July/August issue of EuroTimes. The COVID-19 pandemic brought cataract surgery to a near standstill. Now that we are in the early stages of re-opening in Europe we face a number of additional challenges not least of which is catching up on the backlog of cataract cases, while maintaining proper protocols to protect everyone involved.
The theme of this issue is choosing the right IOL for your patient. This has always been a complex, multifactorial process that gets more interesting every year as the selection of IOLs increases. The COVID-19 pandemic has not slowed the arrival of an ever increasing array of new lens designs in the clinic.
In the cover article, Dr Soosan Jacobs walks us through the current IOL choices, reminding us to base our decision on our patients’ needs. The article takes us through the complex decision matrix, looking at everything from lifestyle requirements, anatomic considerations, even costs and personality considerations.



A companion article features a recent presentation by Prof Beatrice Cochener at the French Implant and Refractive Surgery Association (SAFIR) annual meeting highlighting some of the latest advanced optic IOLs. She emphasizes how important patient selection issues are when deciding who might benefit from an EDOF lens or trifocal IOL, and who would be better served with another option. The patient’s age, lifestyle, and expectations all must be taken into account.
A report from our winter congress in Krakow from Dermot McGrath provides some early clinical study results on some of the new premium IOLs now entering the market.
As COVID vaccination rates increase in some areas, some of us can breathe a sigh of relief, with the feeling that the pandemic will be controlled eventually. However, the pandemic still rages in many parts of the world, as a special exclusive report from India confirms, where eye surgeons are faced with an epidemic of Mucor in the midst of the COVID pandemic.
The pandemic kept us from convening in person last year for the annual ESCRS Congress. We adapted, providing what turned out to be a very successful virtual conference. This year, the 39th Congress of the ESCRS will take place in Amsterdam, October 8 through 11. The Congress programme has been designed to allow delegates to participate fully, either in person or virtually. Due to COVID-19 safety regulations, only a limited number of seats will be available in Amsterdam. For those who are unable or unwilling to travel, virtual seating will be available. The Congress offers us not only the opportunity to take advantage of education and training, but also a long awaited chance to reconnect with friends and colleagues. Priority registration is now available at escrs.org. EuroTimes, as always, will provide comprehensive coverage of the Congress.
Finally, we also have choices to make of the democratic sort regarding the ESCRS board elections. I encourage all ESCRS members to see the section in this issue for more information on nominated candidates. That information is also available online at escrs.org/about-escrs/elections-2021.asp.
I’m looking forward to the day when we can meet in person and prepare for better times.
The COVID-19 panic has not slowed the arrival of an ever increasing array of new lens designs in the clinic.A WORD FROM OLIVER FINDL Oliver Findl MD, Incoming President of the ESCRS, Chief of the Department of Ophthalmology, Hanusch Hospital, and the Vienna Institute for Research in Ocular Surgery (VIROS), Vienna
Choosing the Right Lens
Every patient aspires to be able to see crystal clear at all distances and it is therefore imperative to set realistic expectations. Choosing an IOL is a combined decision involving both surgeon and patient. Factors needing consideration include visual requirements of the patient, preference for distance dominated, intermediate or near dominated work, previous prescription, spectacle or contact lens wearing habits and satisfaction with the same, actual reading distance, ocular dominance, anatomy of the eye, refractive state including higher order aberrations (HOA). Ocular and systemic co-morbidities, personality and spending ability of the patient, and options for insurance coverage/co-payment also must be considered.
Dr. Soosan Jacob, MS, FRCS, DNB reports
CHOOSING IOL TYPE:
Pre-operative assessment of visual needs: Once cataract surgery is decided on, it is important to have a discussion with the patient. The Dell questionnaire developed by Steven Dell has many advantages: it easily and rapidly facilitates dialogue with the patient, establishes common vocabulary, helps explain that optical compromises are often required, and sets patient’s expectations. It also reduces preand post-operative chair time and helps avoid dissatisfied patients. Pre-operative contact lens trials, images showing expected photic phenomena and contrast levels, and simulations such as SimVis (2EyesVision) can also help the patient understand what might be expected after surgery.
Monofocal IOLs may be used in patients who do not mind wearing spectacles. Monovision and micromonovision are useful strategies adopted with monofocals to attain reasonable freedom from glasses for many activities. Good distance visual acuity in dominant eye and either intermediate or near vision in nondominant eye can be aimed for depending on the patient’s requirements.

Monofocals are also useful in patients with ocular comorbidities such as macular pathology or glaucoma where they provide good optical quality without photic phenomena or loss of light/contrast sensitivity. They have also been used successfully in middle to lower income economies for high volume camp based surgeries as they provide an inexpensive means to get good visual quality, albeit relying on spectacles for an uninterrupted range of vision.
Monofocal aspheric IOLs are helpful in various situations. Negative spherical aberration IOLs may be used in patients with large pupils, nighttime driving needs, or post-myopic LASIK. Corneal positive aberrations are neutralized completely by Tecnis®, AMO (-0.27microns of spherical aberration) and partially by AcrySof IQ Aspheric®, Alcon (-0.20microns). Zero spherical aberration IOLs (Akreos AO®, B&L) are useful with subluxated cataracts and decentred pupils. Traditional spherical IOLs with positive spherical aberrations are preferred in post-hyperopic LASIK cases. The newer TECNIS Eyhance® IOL (J&J Vision) has a larger landing zone giving good distance and some amount of intermediate vision.
Pseudoaccommodative IOLs are a popular choice for patients who want greater freedom from glasses. The new trifocals provide good intermediate and near vision with fewer side effects. Trifocals such as the AT Lisa (Zeiss), FineVision (PhysIOL), Alsafit (Alsanza) and Acriva Reviol (VSY Biotechnology) have two add powers at 40 and 80 cm in addition to distance. The quadrifocal, PanOptix (Alcon) has add powers at 40, 60, and 120 cm. Redistribution of intermediate focal point at 120 cm to distance results in its behaving as a trifocal with higher transmission of light (88%) with a 3mm pupil, unlike other trifocals, thereby improving contrast sensitivity and quality of distance vision.
The extended depth of focus (EDOF) IOLs such as Tecnis Symfony (AMO) and AT LARA 829MP (Zeiss) provide an elongated area of focus that extends depth. EDOF IOLs cause less glare, halos, and loss of contrast and give reasonably clear vision at all distances though slightly less for near than trifocals. A micromonovision strategy may be used with EDOFs to attain good binocular vision at all distances. The Tecnis® Synergy is a far to near continuous range of vision IOL that eliminates visual gaps present in trifocal and other multifocals. These IOLs are preferred over multifocals in eyes with maculopathy, irregular corneas, large angle kappa, glaucoma, and in those patients with greater night driving needs.
Newer accommodative IOLs both in-thebag and sulcus placed, such as Synchrony dual-optic accommodating IOL (Visiogen, Alcon), Tetraflex (Lenstec), 1CU IOL (HumanOptics), Dynacurve IOL (Nulens) may become popular if they can provide
The Dell questionnaire developed by Steven Dell has many advantages: it easily and rapidly facilitates dialogue with the patient, establishes common vocabulary, helps explain that optical compromises are often required, and sets patient’s expectations.
safety as well as long term, continuous range of high quality vision without photic phenomena.
Toric IOLs are suitable for patients with astigmatism above 1 D on topography. Since uncorrected astigmatism degrades visual quality, toric versions of pseudoaccommodative IOLs should be used for best results. For less than 1 D of astigmatism, steep axis incision, limbal relaxing incisions, astigmatic keratotomies, or opposite clear corneal incisions work.
CHOOSING IOL POWER
IOL power calculation is crucial when implanting premium IOLs. Multiple, repeatable measurements with different instruments and devices help avoid errors. Variable measurements, irregular patterns on topography, and ocular staining may be indicative of dry eyes and measurements should be repeated after treatment of the dry eye. Consistent IOL power with different newer IOL formulae helps decrease error. Type and magnitude of astigmatism, amount of posterior corneal astigmatism, accurate biometry, and appropriate IOL formulae are all important for toric IOLs. Astigmatism from 0.75 D to 4.75 DC can be corrected using standard toric IOLs, which are available in the range of 1.5 D to 6.0 D cylinder, while higher powers may be made-to-order.
Post refractive surgery IOL power calculation is prone to errors using standard methods. Laser vision correction alters normal anterior/posterior curvature ratio causing errors. Radial keratotomy results in overestimation of routine keratometry value and with 2-variable formulae, also underestimates effective lens position. Various power calculation methods are described for these difficult eyes. Multi-component IOLs with changeable optic component such as Precisight (IVO) and Harmoni (ClarVista Medical), capsular devices allowing IOL position adjustment like the Gemini Refractive Capsule (Omega), and small aperture IOLs using pin-hole principle—the IC-8™ IOL (AcuFocus) and XtraFocus Pinhole implant (Morcher), the pinhole pupilloplasty technique, Light Adjustable Lens (LAL –Calhoun Vision) and post-operative LIRIC (laser induced refractive index changing (Perfect lens, Perfect Lens LLC) are useful for these and other conditions such as ectatic corneas where IOL power calculation is difficult and has less predictability. Intra-operative aberrometry can also help select power. A technique for ectatic corneas that I personally prefer is two-stage: CAIRS (Corneal Allogenic Intrastromal Ring Segments), a technique described by me to flatten the cornea followed later by cataract surgery.
CHOOSING IOL MATERIAL AND DESIGN
A square edge design helps prevent posterior capsular opacification. Threepiece IOLs are preferred for sulcus placement. Truncated edges, surface reflectivity, and refractive index affect the incidence of positive and negative dysphotopsias, which are reported to be higher with acrylic than silicone or copolymer IOLs. Hydrophobic acrylic IOLs give controlled unfolding. However, all hydrophobic acrylic IOLs are not the same and many properties such as biocompatibility, glistening formation, etc. are affected by component monomers and manufacturing conditions such as thermal history.
Patients with complex pathologies require careful selection of IOL material. Hydrophilic acrylic IOLs should be avoided in patients who may require endothelial keratoplasty or pars plana vitrectomy as intra-cameral/intravitreal gas can cause IOL anterior surface/sub-surface opacification. Similarly, silicone IOLs should be avoided in patients who may require posterior segment surgery to prevent fogging during fluid-air exchange and to avoid persistent silicone oil droplets on the posterior IOL surface even after oil removal. Silicone IOLs may develop calcification of the posterior surface in eyes with asteroid hyalosis even without a broken PC. In-the-bag acrylic and heparin surface modified PMMA IOLs cause lower post-operative inflammation in patients with uveitis.
Blue and violet blocking chromophore IOLs may help prevent retinal phototoxicity. Since blue light is also needed for colour vision, night vision, sleep and circadian rhythms, selective violetlight filtering chromophore IOL combined with sunglasses worn during the day may decrease the risk of macular degeneration. Photochromatic IOLs (Matrix Aurium; Medennium) have also been developed which remains colourless indoors but turn yellow in the sunlight.
Finally, it will be interesting to see how the newer technology IOLs such as SmartIOL (Medennium), FluidVision (PowerVision), Juvene (LensGen), Sapphire IOL (Elenza), Dynacurve IOL (NuLens), Lumina lens (Akkolens/Oculentis) play out in the future.
Dr Soosan Jacob is Director and Chief of Dr Agarwal's Refractive and Cornea Foundation at Dr. Agarwal's Eye Hospital, Chennai, India, and can be reached at dr_soosanj@hotmail.com.
Adapting to Evolving Vision Needs of Patients
Patient selection key to success with advanced optic IOLs.
Dermot McGrath reports
The latest generation of advanced optic IOLs, a category that includes multifocal, extended range of focus (EDOF) and monofocal-plus lenses, should be a standard part of every cataract surgeon’s toolkit even though they are not necessarily adapted for every patient, according to Beatrice Cochener-Lamard MD.
“Advanced optic IOLs are definitely an option for all surgeons because there is an obligation on us to progress with technology and to offer a full choice of options to our patients. But they are not for all patients and we need to make our choices based on biometry, corneal regularity, topography, slit-lamp examination, with a specific focus on ocular surface, and the patient’s age, lifestyle, and expectations,” she said at the online annual meeting of the French Implant and Refractive Surgery Association (SAFIR).
Dr Cochener-Lamard, Professor and Chairman of the ophthalmology department at the University Hospital of Brest, said she prefers to use the term “advanced optic IOLs” rather than “premium IOLs” or “refractive IOls” for these types of implant.
“These lenses are the culmination of technological advances in optical design in recent years, with features such as asphericity, toricity, and multifocality all integrated into the IOL design. Progress in cataract surgery has also played a role thanks to phacoemulsification, microincisions, improved biometry, and more accurate IOL power calculations. This has meant enhanced safety and comfort for the patient, with no induced astigmatism, rapid visual recovery, and the possibility of attaining emmetropia,” she said.
The boundaries between cataract and refractive surgery have dissipated over recent years, noted Dr Cochener-Lamard, with increased emphasis on the quality of vision obtained after cataract surgery.
“It is no longer enough to attain 20/20 vision under optimal conditions, but to deliver a high quality and continuous range of vision at all distances with a maximum of light reaching the retina. Patient expectations, however, should be realistic and the advantages and downsides of each lens type should be discussed. With
careful selection, correct biometry, and rigorous surgery, we can obtain consistent outcomes and a high level of patient satisfaction,” she said.
Delivering patient satisfaction increasingly depends on obtaining satisfactory intermediate vision, noted Dr Cochener-Lamard. Which actually represents a range of vision “social vision.”
“Our visual needs have evolved in recent decades. A high percentage of patients now use smartphones, computers, and other digital devices and many of our activities depend on good functional vision in the 40 cm to 1 metre range,” she said.
The frontiers between multifocal, EDOF, and monofocal-plus lenses are not always easy to determine, said Dr CochenerLamard, but important that surgeons understand the concepts behind each category of IOL in order to tailor their choice for each individual patient.
“The days of conventional cataract surgery using the same monofocal implant for all patients are over. Implantation nowadays is performed according to the age, condition of the eye, comorbidities, and lifestyle needs. We need to provide more than the minimum best-corrected visual acuity for our patients, by improving quality of vision at all distances and especially in the intermediate range which is so important today,” she said. We need to offer the best to patients according to state of art.
CONSIDER COMORBIDITIES FIRST
Lens choice will be oriented first and foremost by the presence of any ocular comorbidities such as dry eye, corneal anomalies, previous anterior segment surgery, glaucoma, and retinal disease, explained Dr Cochener-Lamard.
“The presence of a comorbidity does not automatically rule out advanced optic IOls for these patients, but it really needs to be assessed on a case-by-case basis in order to make an informed choice,” she said.
Discussing these conditions in greater detail, Dr Cochener-Lamard said dry eye is frequently underestimated.
“Around 50% to 60% of cataract patients have meibomian gland dysfunction which may not be apparent preoperatively but which will be exacerbated by surgery. The
consequences postoperatively can be visual symptoms such as halos and glare which may lead to anxiety and depression, and the implant will be unfairly blamed for these problems,” she said. It can produce inappropriate results because of a wrong calculation (especially toric IOL) induced by unstable tear film.
The goal should be, therefore, to diagnose and treat the patient using the full arsenal of dry eye treatments available. If it can be controlled preoperatively, an advanced optic IOL may be considered, otherwise a monofocal-plus lens might be the best option,” she said.
Other contraindications for advanced lenses include corneal anomalies such as opacities, pterygium, leucomas, and anterior dystrophies, as well as eyes with keratoconus and corneal grafts. For glaucoma, an EDOF IOL may be considered if the IOP is controlled and the benefit-risk profile is favourable. For retinal diseases such as AMD or diabetic retinopathy, refractive IOLs should be avoided if disease is progressing and OCT is not normal, she advised.
Dr Cochener-Lamard also said that special attention should be paid to patients presenting for cataract surgery who have previously undergone refractive surgery.
“These patients, which represent a growing population, typically have high expectations as they have already paid to be spectacle independent. Their quality of vision may be impacted by their previous surgery and dry eye may be present. We need to decide on a case-by-case basis and proceed with caution as IOL power calculations in these patients are also more problematic.”
The boundaries between cataract and refractive surgery have dissipated over recent years
New Meniscus IOL
Patients implanted with a new meniscus-shaped intraocular lens (ArtIOL, Voptica SL) appear to have a reduced amount of peripheral astigmatism compared to patients implanted with standard lenses, according to a study presented by Pablo Artal PhD at the ARVO 2021 Congress.
“This new intraocular lens provides reduced astigmatism and better contrast detection in the peripheral retina. This may have a positive impact in everyday tasks in patients after cataract surgery,” said Artal, Laboratorio de Óptica, Universidad de Murcia, Murcia, Spain.
The study involved 87 cataract patients who underwent implantation of the ArtIOL and a control group of 38 patients who were implanted with a standard monofocal IOL. Dr Pedro Taña and Dr José María Marín of the Oftalvist clinic in Spain performed the surgeries. Prof Artal noted the new meniscusshaped IOLs’ optics mimic that of the natural lens to provide optimised field curvature and then better vision. Composed of a hydrophobic acrylic material with UV-protection, the lenses have an optic diameter of 6.0 mm and a total diameter of 13 mm and range in power from 18.0 D to 24.5 D.
Prof Artal and his associates measured the patients’ peripheral refraction on the horizontal meridian using a scanning Hartmann-Shack wavefront sensor and measured the contrast detection threshold at 45 degrees of visual angle (both horizontally and vertically) psychophysically by means
of an adaptive staircase technique, using a 30-arc min. round stimulus 1 m in front of the patient’s eyes and a green LED for foveal fixation.
REDUCED PERIPHERAL ASTIGMATISM AND IMPROVED CONTRAST SENSITIVITY
The researchers found that eyes implanted with ArtIOLs had a reduced amount of peripheral astigmatism compared to eyes in the control group. At 30 degrees, the average cylinder in the control group was 3.0 D, compared to 2.0 D in the ArtIOL group. At 45 degrees, mean cylinder values were 6.0 D and 3.5 D respectively.

This reduction in astigmatism had a positive impact in contrast sensitivity, Prof Artal noted. In the horizontal meridian, average sensitivity values were 0.07 (SD=0.04) and 0.10 (SD=0.05) for the control and ArtIOL groups respectively. In the vertical meridian, average sensitivity values were 0.06 (SD=0.03) and 0.08 (SD=0.03) for the control and ArtIOL groups respectively.
Prof Artal noted the clinical results obtained thus far with the ArtIOL mirror those obtained with bench testing, showing superior optical quality compared to standard IOLs.
“Further research would be required to evaluate how this IOL may also have an impact in the patient’s functional vision,” he concluded.
Pablo Artal: pablo@um.esNew meniscus-shaped IOL may improve peripheral contrast and astigmatism. Roibeard Ó hÉineacháin reportsImages of letter chart recorded in a model eye at 40 degrees in an eye with a standard IOL and with ArtIOL. The image quality is clearly superior with the meniscus lens.
Growth in the Premium Lens Market
New IOLs jostle for space in crowded premium market. Dermot McGrath reports
Enhanced quality of vision at all distances with an increased depth of focus and a reduced incidence of visual side-effects are just some of the features that characterise the latest generation of premium IOLs coming onto the market, according to a number of speakers at the ESCRS Winter Meeting online.
“The good news is the premium lens market is growing and all the market indicators are that this is a global phenomenon,” said Kieren Darcy FRCOphth of the Bristol Eye Hospital, Bristol, United Kingdom.
Dr Darcy noted the categorisation of a “premium” lens is hotly debated and often confusing for surgeons and patients alike.
“In reality, this is only relevant to the patients in terms of will they be fully spectacle independent, will they need reading glasses for some tasks, or will they remain reliant on glasses for a lot of activities. Trifocal IOLs that offer a full range of focus and very good outcomes currently predominate in the premium lens market. However, there are certain factors such as vocational and lifestyle requirements and personality traits that can make these lenses unsuitable for some patients,” he said.
Dr Darcy presented his early clinical impressions of the AcrySof IQ Vivity (Alcon), a non-diffractive extended depth of focus (EDOF) lens. “This lens aims to improve on earlier model EDOF IOLs by offering an increased range of focus but with the visual disturbance profile we would normally only expect in a monofocal lens,” he said.
The IQ Vivity consists of two smooth-surface transition elements that stretch and shift the wavefront across the entire optic without splitting the light, explained Dr Darcy.
“The result of this technology is no light splitting and a monofocal visual disturbance profile, which was borne out by the results of two clinical trials,” he said.
Summing up, Dr Darcy said that while more real-world data is needed, his initial clinical impression of the lens has been largely positive.
“I think blended vision with a -0.50 D difference in the nondominant eye offers really good potential with this lens. It is best to try to avoid hyperopic outcomes as near and distance vision are disproportionately affected. I would also advise to minimise residual cylinder similar to other platforms as it compromises the distance vision,” he said.
TRANSITION ZONE
Promising results have also been obtained with another premium lens, the LuxSmart EDOF preloaded IOL (Bausch + Lomb), a onepiece hydrophobic acrylic lens with a four-point fixation and a 360-degree square-edge design.
Presenting his initial clinical experience with the lens, Pavel Stodulka MD, PhD, Gemini Eye Clinic, Zlin, Czech Republic, explained the IOL has a biconvex, aspheric optic with an EDOF centre, a patented transition zone, and a monofocal periphery. The lens creates a continuous area of vision and has no diffractive rings.
“The 2.0mm central part of the lens contains a pure refractive optic that combines sixth-order and fourth-order spherical aberration (SA6 and SA4) of opposite signs to optimise the depth of focus,” said Dr Stodulka.
The lens comes preloaded and is injected into the capsular bag through a 2.2 mm incision.
“The IOL unfolds smoothly and is easy to rotate and centre with the support of its four haptics. In our first patients we noticed a slight tendency towards a myopic outcome so we have since adjusted the A-constant from 119.2 to 118.6 in order to attain emmetropia in most eyes,” he said.
While longer follow-up is needed to confirm the initial results, Dr Stodulka said LuxSmart lens offers high-quality distance and intermediate vision and even some improvement in near vision and a significantly lower risk of dysphotopsias compared to trifocal lenses.
PUPIL INDEPENDENCE
In a separate presentation, Rafael Bilbao-Calabuig MD, PhD, FEBOS-CR Baviera Clinic, Madrid, Spain, said he has been impressed with the clinical performance of the ISOPURE (PhysIOL) lens, a premium monofocal IOL with extended depth of field.
The optic of the ISOPURE lens uses polynomial complex surface design parameters to extend the depth of focus compared to standard monofocal IOLs.

“The lens is purely refractive and fine-tuned for pupil independence and is made of a hydrophobic glistening-free material with a four-closed haptic design for stable positioning and comfortable insertion,” he said.
In initial results, the ISOPURE provided very good distance vision quality combined with a visual improvement in intermediate vision by accentuating the EDOF effect without inducing photic effects, he said.
“Compared to its monofocal predecessor, it offers similar distance vision, similar photopic and mesopic contrast sensitivity curves, a clear improvement in defocus curve, and better tolerance to residual ametropia,” he said.
Dr Bilbao-Calabuig said employing a mini-monovision strategy with the lens improves binocular intermediate vision without significantly altering the binocular distance and near vision.
“We have achieved a high level of patient satisfaction with very reasonable levels of spectacle independence using this approach. This IOL could also possibly be used in some ocular conditions considered contraindications for other multifocal IOLs,” he said.
Contrast sensitivity curves obtained between 3–6 months postoperatively in this pilot prospective study show values within the normal range for the group age and are similar to those obtained with a classic aspheric monofocal IOL.

Cataract Surgery Outcomes in Patients with Type 2 Diabetes
Study characterises risk factors for posterior capsule rupture in higher risk patients. Cheryl Guttman Krader reports

Previous studies show patients with type 2 diabetes mellitus undergoing cataract surgery are at increased risk for posterior capsule rupture (PCR). However, according to a study investigating this issue on a more granular level, the risk for these patients depends on diabetic retinopathy status and history of intravitreal injection (IVI).
“According to our study, the main driver of increased rates of PCR in eyes with diabetic retinopathy is a history of intravitreal injection,” reported Valerie J Dawson MD, at ARVO 2021.
She presented findings from a single institution retrospective study including 10,893 eyes of 6,636 patients. Eyes of patients without type 2 diabetes mellitus accounted for 76.8% of the cohort, while 17.8% had diabetes without retinopathy, and 5.5% had diabetes with retinopathy. The rate of PCR was 0.4% in eyes of patients without diabetes and significantly higher in those with diabetes and retinopathy (1.8%). This was not the case in eyes with type 2 diabetes who did not have retinopathy.
Results of a multivariate analysis adjusting for a host of confounders and with eyes categorised into six groups based on presence/absence of type 2 diabetes, diabetic retinopathy, and intravitreal injection showed that a history of intravitreal injections, regardless of diabetes status, was an independent risk factor for PCR. Relative to eyes without T2DM/DR and IVI, eyes with T2DM and neither DR nor IVI were not at increased risk of PCR while the risk was increased more than twofold in eyes with T2DM and DR but no IVI.
Eyes of patients with type 2 diabetes but no retinopathy or history of injections did not appear to be at increased risk of PCR. However, the risk was increased more than twofold in eyes with diabetic retinopathy with no history of injections. The p-value for the latter comparison achieved only borderline significance, which was felt to be due to the relatively small sample size, said Dr Dawson, ophthalmology resident, University of Colorado, Denver, Colorado, USA. Her team is planning to incorporate another year of data from the University of Colorado Cataract Database and expects to see this group reach statistical significance on re-analysis.
“Advancements in technology and knowledge have led to a decrease in posterior capsule complications during phacoemulsification, but it is prudent to understand the risk factors and identify subgroups of susceptible patients,” she said.
“We feel that patients who have undergone IVI and those with DR should be offered preoperative counselling, and surgeons operating on these patients should use caution to avoid surgical manoeuvres that may place unnecessary stress on the lens capsule.”
Dr Dawson suggested that the association between DR and PCR risk is likely explained by pathological changes in the lens capsule induced by prolonged exposure to elevated glucose levels that may predispose to capsule rupture by reducing tensile strength. She noted evidence that bevacizumab injections decrease lens epithelial cell viability and proliferation that leads to mechanical changes from decreased cell density and capsular bag confluence.
Valerie J Dawson MD valerie.dawson@cuanschutz.eduResident-performed ISBCS
Senior residents performing immediate sequential bilateral cataract surgery (ISBCS) is as safe and effective an approach as delayed sequential bilateral cataract surgery (DSBCS) with significantly fewer clinic visits, Tiffany A Chen MD told the Association for Research in Vision and Ophthalmology 2021 Annual Meeting.

The findings of the retrospective cohort study she conducted with her twin sister and fellow ophthalmology resident Stephanie P Chen MD and other colleagues at the University of California –San Francisco (UCSF), USA, suggest that offering senior residentperformed ISBCS for select patients may offer significant benefits. These include reducing potential exposure events for patients and providers during the COVID-19 pandemic, and lowering overall costs while improving patient satisfaction, Dr Chen said.
Bilateral cataracts were traditionally treated in a delayed sequential approach to avoid complications such as refractive surprise and bilateral endophthalmitis, Dr Chen noted. However, advances in cataract diagnostics and surgical procedures have greatly reduced the risk of such adverse events, and several large studies have shown similar safety and visual outcomes for ISBCS and DSBCS in appropriately selected patient populations, she emphasised.
The current pilot study examined the safety and visual outcomes, patient satisfaction, and number of perioperative visits, of 22 eyes in 14 patients and 56 eyes in 28 patients who underwent senior resident-performed ISBCS and DSBCS, respectively. In 6 of the ISBCS patients, senior residents performed one eye surgery and attending surgeons the other, and only the resident-operated eyes were included in the analysis. The study included patients aged 18 or older with no active ocular or medical comorbidities with the ability to lie flat for both procedures and the ability to tolerate topical anaesthesia in one eye.
Thirty days after the second surgery, 21, or 95%, of ISBCS eyes and 51, or 91%, of DSBCS eyes achieved corrected distance visual acuity of 20/25 or better while 77% and 84%, respectively, were
within 0.50 D of target refraction. There was no significant difference in the overall visual function score and no difference in preoperative or postoperative complications.
ISBCS patients averaged 3.5 fewer visits than DSBCS patients, 5.9 vs. 9.5, a significant difference. All ISBCS and 20 DSBCS patients, or 87%, reported they were overall “very satisfied” or “satisfied” (p=0.701). In addition, 5 of the 6 senior residents who performed the ISBCS cases reported they preferred performing ISBCS over DSBCS.
Further study is indicated, Dr Chen said. However, she believes that “residency programs should consider offering senior resident-performed ISBCS to select patients during the COVID-19 pandemic.”


Tiffany Chen: tiffany.chen2@ucsf.edu
Stephanie Chen: stephanie.chen2@ucsf.edu
Fewer visits, better satisfaction, equal outcomes compared to separate procedures. Howard Larkin reports
“Residency programs should consider offering senior resident-performed ISBCS to select patients during the COVID-19 pandemic.”Stephanie P Chen MD
Automating Cataract Detection and Care Decisions
AI algorithms for image analysis hold promise for the future. Cheryl Guttman Krader reports
Artificial intelligence (AI) with enhanced computing power and the increasing availability of big data brings new opportunities for developing novel systems and strategies for cataract detection, grading, and management, said Sheila John PhD, at the ARVO 2021 virtual meeting.
“Cataract is the leading cause of preventable blindness. Early detection and treatment can alleviate the suffering of cataract patients and prevent visual impairment from turning into blindness. AI deployed to diagnose cataract would also reduce ophthalmologists’ current workload and potentially enable them to serve more patients,” said Dr Sheila John, Head of Teleophthalmology and E-learning, Sankara Nethralaya, Chennai, India.
“Artificial intelligence is still relatively underexplored in cataract-related clinical practice and services, but it is poised to introduce a paradigm shift in the future. Despite the hype, however, it is important to keep our mind and focus grounded on the ultimate goal of implementation and patient safety.”
In her presentation, Dr John discussed studies of AI-based algorithms for automated cataract assessment using slit-lamp or fundus photographs. Researchers from China utilised deep learning via a residual neural network to create a three-step, sequential AI algorithm for cataract diagnosis and referral. The first step involves capture mode recognition. Next, lens state is diagnosed as normal, cataract, or postoperative intraocular lens. Last, detected cataracts are categorised by type and severity and
management, either follow-up or referral for tertiary care, is determined. In their evaluation, the researcher found that the system performed robustly for completing all three tasks.
Recognising the increasing use of retinal imaging for diabetic retinopathy screening in primary care settings, another group of Chinese researchers developed an algorithm for cataract detection and severity grading based on classification of retinal image visibility. With ratings by experienced ophthalmologists serving as the ground truth, the algorithm correctly classified 94% of images for cataract detection and 91% of images for cataract severity.
Dr John noted that retinal imaging of patients who reside in rural communities without access to eye care providers is an opportunistic screening tool for automatic cataract detection as digital images of the lens may be acquired at the same session and transferred to a remote reading centre for automatic cataract detection and grading.

“In the future new AI systems can potentially provide better outreach for cataract screening, especially in rural or less resourced areas. With the increasing availability of ocular imaging modalities, including handheld retinal cameras or slit lamp adapters attached to smart phones, these imaging modalities are increasingly cheaper, easy to use, and can be used by trained technicians.”
Sheila John PhD: sheilajohn24@gmail.comMaking the Case for PRK
Back to the surface with trans-PRK approach. Dermot McGrath reports
Although LASIK or SMILE procedures remain the principal focus of most refractive surgery practices, there is still a viable place for surface ablations using the latest laser platforms, according to Alexandre Denoyer MD.
“I have been performing more and more surface ablations in my practice and I believe there are some compelling arguments to justify it in terms of safety and patient satisfaction,” Prof Denoyer said at the online annual meeting of the French Implant and Refractive Surgery Association (SAFIR).

Prof Denoyer, head of department of anterior eye surgery at University Hospital of Reims, France, noted surface treatments respect the biomechanical integrity of the cornea, unlike LASIK or lenticule extraction procedures.
“The sub‐basal nerve fibres are not affected by a surface procedure, and we know that the nerve re-composition in LASIK is not always total even if there is a reorganisation of the corneal nerve bundles in the months after surgery,” he said.





Problems of haze, often highlighted as one of the main reasons why PRK fell out of favour, are far less of an issue with the optimised surface ablation profiles used by today’s laser platforms, added Prof Denoyer.
Several excimer laser platforms now propose trans-PRK software options including SmartSurf (Schwind Amaris), TransEpi PRK (Bausch + Lomb Technolas), cTen (iVis Technologies) and Streamlight (Alcon Wavelight).
The basic concept is to employ an all-laser “no touch” surgery with trans-PRK, explained Alexandre Denoyer.
“It is one procedure with three key steps: an epithelial photoablation, a stromal photoablation, and a complementary photoablation for 'smoothing' the corneal surface. It’s a totally non-contact surgery in the sense that no instruments are used apart from the laser, and it has been shown that the healing with trans-PRK is even faster than after a standard surface ablation procedure,” he said.

In terms of outcomes, Prof Denoyer said that the results have been shown to be equivalent to traditional PRK treatments or LASIK and SMILE.
“For mild or moderate myopia with or without astigmatism the results are comparable to LASIK and SMILE. For hyperopia and severe astigmatism, there is a widespread perception that LASIK will perform better,” he said.
Another compelling reason to use trans-PRK is the issue of retreatments after LASIK or SMILE: “The efficacy of surface ablation retreatments is another advantage as it gives the same results as re-lifting the flap in LASIK without the risk of epithelial ingrowth which has been shown to be as high as 13% after flap re-lift,” he said.
Prof Denoyer added that further studies are needed to determine if postoperative pain is less than with traditional PRK. Issues of transient haze may still occur with trans-PRK due to laser heating the corneal surface when ablating the epithelial layer, but the effect can be attenuated by ensuring a brief pause between the epithelial ablation and the stromal ablation to allow the surface to cool, he concluded.
adenoyer@chu-reims.fr – alexandredenoyer.com
Measure, visualize, understand
And more to come...
All swept-source OCT precision measurements and imaging for greater » EYESTAR 900 Precision OCT


safety and improved outcomes.

A Rare but Serious Risk
Banishing the nightmare of postoperative endophthalmitis. Dermot McGrath reports
Postoperative endophthalmitis (POE) remains the most feared and devastating complication of intraocular procedures, but there are clear measures cataract surgeons can take to reduce the risk of its occurrence in the first place, according to Steve A Arshinoff MD, FRCSC, associate professor at the University of Toronto, Canada.
“Reports in the scientific literature identify the risk of endophthalmitis after cataract surgery as between one-in-2,000 and one-in-5,000 cases,” said Dr Arshinoff. Factors that increase the risk include diabetes, use of tamsulosin (Flomax), surgeon inexperience, duration of surgery, secondary lens procedures, contaminated devices such as irrigating solution, OVD, or other, vitreous loss, use of 2% xylocaine gel, and vitreous incarceration into the wound.
The good news is even bilateral simultaneous postoperative endophthalmitis (BSPOE) after immediately sequential bilateral cataract surgery (ISBCS) is extremely rare. “We estimate that the chance is less than one in 100 million. That means the chances of dying from general anaesthetic is 1,000 times higher, and the chances of winning the biggest lottery in Canada is seven times more likely,” Dr Arshinoff said at the 38th Virtual Congress of the ESCRS.
When dealing with suspect POE, Dr Arshinoff advised carefully reviewing the circumstances of the case to determine the odds that it really is endophthalmitis and not an inflammatory disorder. “We need to ask ourselves a battery of questions. Was this case bilateral surgery? If so, how is the other eye? Was it a phaco, femtosecond, or a manual small-incision cataract surgery? How long has it been since the surgery? Did we give antibiotics, and if so, which one and what was the amount and route of administration? Is the patient immunocompromised, does he or she have blepharitis, or wear contact lenses? Did anything go wrong in surgery? Was the capsule broken and was the incision sealed well? Were hooks or capsular tension rings used? Was it a black or white cataract? Were pseudoexfoliation, phacodonesis, or floppy iris or other small pupil problem present? What incision type was used?”
Answering these kinds of questions will change the risk profile and how you look at the patient to arrive at a diagnosis. “Perhaps it was a 95-year-old diabetic male who doesn’t take his eye drops reliably and is therefore a high-risk patient? Consider all these factors as you examine the eye,” said Dr Arshinoff.
The typical characteristics of POE to watch for include a mean time to onset of about two weeks postoperatively, presence of hypopyon, marked inflammation, variable pain, reduced vision, and cloudy vitreous said Dr Arshinoff.
Before settling on a firm diagnosis, it is important to rule out other possible causes, such as TASS. “Toxic anterior segment syndrome (TASS) begins quickly, usually the first day postoperatively, and presents with moderate pain, diffuse
limbal to limbal corneal oedema, and minimal posterior segment inflammation. The retina and media should look fairly clear once the pupil is dilated and checked with an indirect ophthalmoscope,” he said.
Other more unusual possibilities include inflammation due to retained lens material, a flare-up of pre-existing uveitis in patients with sarcoidosis, ankylosing spondylitis or other inflammatory disorder, or endogenous endophthalmitis.
To treat POE, Dr Arshinoff advised handing over to a retina surgeon or one who frequently deals with such cases.
“The goal is to begin treatment as soon as possible. Perform culture and sensitivity tests, and administer intravitreal vancomycin and ceftazidime and repeat if the patient does not respond quickly. For fungal infections, treat with agents such as amphotericin B, miconazole, or voriconazole. For refractory cases with very severe inflammation throughout the eye, and lightperception visual acuity, the patient should undergo a complete pars plana vitrectomy,” he said.
For cases of delayed onset endophthalmitis, the time to onset and clinical presentation will help to identify the most likely responsible organism, said Dr Arshinoff.
To reduce the risk of POE, Dr Arshinoff advised using intracameral antibiotics such as cefuroxime or moxifloxacin, which have been proven to decrease the risk of POE in studies encompassing 8 to 10 million eyes, with an eightfold reduction of infection.
Dr Arshinoff said that he routinely uses intracameral moxifloxacin 600 micrograms in 0.4ml in his simultaneous bilateral cataract surgeries. He also prescribes a course of topical moxifloxacin, prednisolone acetate, and ketorolac six times a day for the first four days after surgery and then four times a day until the bottles are finished.
“If you give postoperative topical drops of moxifloxacin, you actually obtain a high enough level in the anterior chamber to kill the most common bacteria that usually cause endophthalmitis, although not high enough to kill the most resistant (CoNS and MRSA) strains. I also give a drop of pilocarpine at the end of surgery, which reduces the incidence and severity of postoperative pressure spikes and brings the pupil down, allowing the patients to have very good vision within an hour of surgery,” he said.
There are clear measures that cataract surgeons can take to reduce the risk of its occurrence in the first place.
Steve A Arshinoff MD, FRCSC
IOL TERMINOLOGY
Anew rotationally asymmetrical multifocal IOL with +1.5 D near addition provides patients with excellent distance and intermediate visual acuity, with high contrast sensitivity and a low number of photic side-effects, according to Florian Kretz MD, FEBO.
Discussing the properties of the Lentis Comfort (Teleon GmbH, Berlin, Germany) lens at the 25th Winter Meeting of the ESCRS, Dr Kretz, medical director of the Precise Vision Augenärzte in multiple locations in Germany, said that the concept of the IOL is to offer an enhanced depth of focus with enhanced near and intermediate vision at a range up to 60 cm.
“We have evaluated the Comfort for a long time and have found that it offers several advantages over a lot of other competing IOLs. It shows similar-to-less incidence of dysphotopic phenomena compared to an aberration-neutral monofocal lens such as CT Asphina 409 IOL (Carl Zeiss Meditec). The rotational asymmetric optics also demonstrate better near-intermediate values compared to mini EDoF IOLs as they are less pupil dependent,” he said.
In comparison simulation studies with the Eyehance (Johnson & Johnson Vision) monofocal EDoF IOL, the Comfort lens offered a better overall defocus capacity because of the higher add power, with closer usable intermediate vision, less pupil dependence and very low photic side-effects, he said.
The Comfort also compares favourably with the new Vivity lens (Alcon), which uses wavefront-shaping design to provide a continuous range of focus with minimal halos and glare.
“If we compare it to the Comfort data in the recent trial conducted by Dr Oshika (Oshika, T. et al, Sci Rep 9, 13117 (2019)), the Comfort lens gives even more stable outcomes for intermediate distance and is also less pupil-dependent because it is rotationally asymmetric,” he said.

In a panel discussion after his presentation, Dr Kretz remarked on the need to provide greater clarity in terms of the terminology used to describe many of these newgeneration IOLs.
“It is very confusing. I personally don’t like this nomenclature with ‘monofocal plus’, ‘mini EDoF’ and so forth, which doesn’t tell us anything about the lens. I think the physical properties of the IOL are much more important. This is a rotational asymmetric lens with +1.5 D add, which gives enhanced vision in a range up to about 60 cm and more if the patient has higher spherical aberration on the cornea and less if the cornea is more neutral,” he said.
There is a need to provide greater clarity for the terminology used to describe many of new-generation IOLs.
Dermot McGrath reports
Surface Ablation Still Useful
Corneal session at Refractive Surgery Course discusses development of surface ablation. Priscilla Lynch reports
There is still room for surface ablation, despite the rise of LASIK in recent decades, Jesper Hjortdal MD, PhD, Denmark, told the 25th ESCRS Winter Meeting Virtual 2021.
Speaking during the Refractive Surgery Course— Corneal Session, Prof Hjortdal outlined the development of surface ablation; the first excimer laser-based procedure for changing the refractive power of the cornea.
The original photorefractive keratectomy (PRK) technique had issues with slow wound healing and visual recovery, pain until the epithelium had healed, and haze, however, he noted.
There was a shift towards LASIK in the mid-1990s, with its faster healing and visual recovery benefits, but refinements of the original surface ablation technique have improved outcomes as well as pharmacological modification, i.e. the addition of mitomycin-C, which reduces haze risk, Prof Hjortdal explained.
The surgical improvements are mainly due to technological perfection of the excimer lasers with respect to optimising the ablation profiles and eye-tracking during treatment.
“There are certain advantages of surface ablation compared to LASIK; there is no flap so that is the main advantage, you don’t have surgical complications—no flap folds, epithelial ingrowth, trauma, late dislocation, or ectasia, which can happen after LASIK,” he said.
Concluding, he said it is still worth considering surface ablation in thin corneas, irregular corneas, dry eyes, young
patients, lower range of refractive errors, and Epithelial Basement Membrane Dystrophy.
BEST PROFILE FOR STANDARD LASIK
Also speaking during this session, Dr Roberto Bellucci MD, Italy, said that a wavefront-optimised profile should be the standard ablation technique for LASIK in corneal refractive surgery.
While newer technology and more advanced protocols of ablation (wavefront optimised, wavefront guided, ray tracing, etc.) have improved some of the inconveniences with the original ‘Munnerlyn’s ablation protocol’, they consume more tissue, and are exposed to factors limiting their precision and efficacy: laser/tissue interaction, micro eye movements, epithelial healing, etc., he noted. “They are complex and frequently require complex and expensive devices, and confounding factors include dry eye, corneal, and epithelial variation. The cornea may not be thick enough because the ablation depth increases with all advanced profiles.”
However, the original protocol just achieves good results in certain situations; “so should only be used for specific eyes and conditions like thin cornea, low defects, and small pupils,” Dr Bellucci maintained.
He concluded that “wavefront-optimised profiles should be the standard, while wavefront-guided profiles can be used in eyes with high order aberrations above 0.3 microns at 7mm optical zone.”
Incremental Improvements












Patient safety the winner as cataract surgery continues to innovate.


Dermot McGrath reports
Aspectrum of ongoing incremental improvements to technologies and surgical techniques has completely transformed cataract surgery and improved outcomes and patient safety over the past decade, according to Ewa Mrukwa-Kominek MD, PhD.
Speaking during a special session organised by the Cataract and Refractive Surgery Section of the Polish Ophthalmological Society at the 25th ESCRS Winter Meeting, Dr Mrukwa-Kominek said advances in phacoemulsification equipment allied to improved intraocular lens design and implantation devices have taken cataract surgery to new levels of safety and comfort.
“All of these advances in technology have enabled us to perform surgery with greater precision, efficiency, and with a reduced risk of complications for patients. More recent innovations such as intraoperative OCT and 3D visualisation systems will further enhance our outcomes and raise the bar for safer and more efficient surgery,” she said.
The postoperative visual acuity attained by a patient depends not only on surgical experience but also on the available equipment and rigorous preoperative assessment of the eye, noted Dr Mrukwa-Kominek.
“Phacoemulsification technology has evolved over time with improvements in phacodynamics and advanced fluidics to reduce the amount of energy being delivered into the eye. The goal is to minimise trauma to the cornea and ocular tissues. Other developments in viscoelastics, torsional phacoemulsification, and enhanced tip design have also helped to enhance efficiency,” she said.

Dr Mrukwa-Kominek highlighted some of the recent enhancements to phacoemulsifcation systems such as the Centurion Vision System (Alcon), which enables surgeons to maintain anterior chamber stability and dynamically control intraocular pressure.
“The innovative design and occlusion surge reduction supports safety, consistency, and control. There is also improved responsiveness as the handpiece is equipped with a fluidics pressure sensor and the tip incorporates polymer technology to reduce damage to the capsular bag and other tissues,” she said.
In terms of intraocular lens design, Dr Mrukwa-Kominek said preloaded IOL systems have made life easier for surgeons.
“Fully preloaded and disposable IOL systems have enhanced safety as there is no need to touch or manipulate the lens. We can deliver the IOL quickly and easily into the capsular bag with less pressure on the eye. The market trend towards fully preloaded disposable IOL systems will account for up to 40% of all IOLs for the western European market by 2022 compared to 23% in 2018,” she said.
Other recent advances highlighted by Dr Mrukwa-Kominek included intraoperative guidance systems for toric lenses, as well as 3D visualisation devices, intraoperative OCT imaging, and digital microscopes for enhanced surgical comfort.
“As well as allowing us to perform surgery with greater precision and efficiency, many of these new tools are also excellent for training young ophthalmologists, which is very important in university centres,” she concluded.
l
l




• ESCRS Research Study
Intraocular NSAID
New
Intraocular delivery of ketorolac with the haptic-affixed OcuRingKTM (Layerbio, Inc.) reduces inflammation and pain from cataract surgery without untoward effects and without modification of surgical technique, according to the results of a Phase 1I open-label trial presented by Kenneth J. Mandell MD, PhD at the ARVO 2021 Congress.
“These findings support the potential of the OcuRing-K implant as a safe and effective alternative to NSAID eye drops for use in cataract surgery,” said Dr Mandell, founder and CEO of Layerbio Inc., Lexington, Massachusetts, United States.
• ESCRS Podcasts
• EyeJC (The ESCRS Journal Club)
• Case Studies
• EBO – ESCRS Examination
• ESCRS Media Player
• ESCRS On Demand
• ESCRS iLearn
• Astigmatism Double Angle Plot Tool and more...
The study involved five patients who underwent cataract extraction and implantation of an intraocular lens (IOL) with the OcuRing-K. Dr Mandell and his associates evaluated the patients postoperatively on day one, day seven, and day 28. They assessed inflammation using the standardisation of uveitis nomenclature (SUN) scale anterior chamber cell (ACC) score and postoperative pain using a visual analogue scale.
He noted that the new bio-erodible ring is designed for attachment to an IOL’s haptic just prior to loading the lens into its injection cartridge. The ring’s elastic properties enable its use with any standard IOL. The implant releases the nonsteroidal anti-inflammatory drug (NSAID) ketorolac for 14 days.
Dr Mandell pointed out that ketorolac is the active ingredient of several ophthalmic medications currently FDA-approved for use after cataract surgery. Moreover, the OcuRing-K’s intraocular mode of drug delivery avoids the risk of corneal complications that may occur with the topical administration of NSAIDs in certain high-risk patients.
SAFE EFFECTIVE AND EASY TO USE
In their study, the surgeon successfully implanted the IOL with the OcuRing-K in five patients without complication. In addition, slit lamp examination showed that in all five patients the IOLs were centred on the visual axis without tilt. There was also no evidence of contact between the NSAID implant the iris, Dr Mandell said.
Furthermore, the mean postoperative ACC scores were 0.6 and 0.4 at days one and day seven, respectively, and no ACC was observed in any subjects by day 28. Moreover, all patients were pain-free at all follow-up assessments, and none of the patients required rescue therapy with topical anti-inflammatory medication. There were no treatmentrelated adverse events.
Among the surgeon’s observations were that the OcuRing-K was compatible with the standard IOLs and injector systems most commonly used in cataract surgery. In addition, the OcuRing-K’s presence on the IOL’s haptic did not interfere with the insertion or unfolding of the IOL within the capsular bag or with the rotation and centring of the IOL, he emphasised.
 Kenneth J. Mandell MD, PhD: ken@layerbio.com
Kenneth J. Mandell MD, PhD: ken@layerbio.com
haptic-affixed bioerodible ring delivers NSAID intraocularly after cataract surgery. Roibeard Ó hÉineacháin reports
JCRS HIGHLIGHTS

AEROSOLIZATION DURING PHACOEMULSIFICATION

With COVID-19 a continuing risk, understanding whether ophthalmic procedures generate aerosols that may promote infection is essential. According to a study of 25 eyes in 23 patients, phacoemulsification does not. The study used an optical particle counter to measure aerosol particles ranging from less than 0.3 μm to 10.0 μm in the air surrounding a cataract surgical field. No significant differences were found in aerosol particles present before surgery, during the pre-phacoemulsification phase of cataract surgery, or during phacoemulsification. Use of a mobile laminar air flow (LAF) machine significantly reduced all sizes of aerosol particles, while the use of a 2% solution of hydroxypropyl methylcellulose during phacoemulsification had no effect. Aerosol particles of less than 10 μm are not produced during phacoemulsification in a live patient setting, the authors concluded. Kaur S et al., “Aerosol generation during phacoemulsification in live patient cataract surgery environment”, Vol 47, Issue 6, 695–701.

PRIORITISING PHACO CASES AFTER COVID-19 EMERGENCY
Faced with a backlog of more than 700 patients, a protocol that prioritised cataract surgery patients allowed surgeons to operate on all priority cases within three months. The protocol was implemented at a large tertiary referral centre and gave highest priority to white and brunescent cataracts, binocular patients with visual acuity of 20/200 or less, and monocular patients with VA of 20/63 or less. Medium priority was given to patients with anisometropia, glaucoma, and low to moderate risk for angle closure. Time waiting for surgery was considered a separate and over-riding factor. Median waiting time for all patients was 3.51 ± 1.57 months, with 191 patients waiting 4.5 months or more. The protocol proved effective, providing a timely surgical opportunity for priority cases, the authors said. Vieira R et al., “Return of phacoemulsification after emergency status related to COVID-19: experience of a tertiary referral centre”, Vol 47, Issue 6, 691–694.


LOOKING BACK ON THE LANDMARK FLOMAX STUDY
“A single study that leads to a profound change in practice and to a better and safer operation is a rare event,” writes David J Spalton FRCS in June’s guest editorial. The landmark 2005 study by Chang and Campbell describing intraoperative floppy-iris syndrome (IFIS) and its principal cause – use of the α-blocker tamsulosin (Flomax) – is one, he argues. Tamsulosin use even years before cataract surgery can result in iris billowing, prolapse, and progressive constriction, leading to serious complications during cataract surgery. Pharmaceutical management with phenylephrine or Mydrane can help, as can a soft-shell surgical technique and careful chamber management. “We must congratulate Chang and Campbell on their ability to think outside the box (and the eye!),” he concluded. Spalton DS, “Taking the flow out of Flomax”, Vol 47, Issue 6, 689–90.











Board Election 2021
Dear Member,
Please read the following instructions carefully before completing the enclosed ballot paper. The following 18 full members of the ESCRS have been nominated for election to the Board. There are six vacant positions on the Board so you can vote for up to 16 full members. You may vote for fewer than six candidates but if you vote for more than six, your ballot will not be valid.
Please follow the instructions on your Ballot Paper. Alternatively, this year you may also vote online if you prefer, personalised emails have been sent with online voting instructions. Voting is now open and will close on Monday 30 August 2021.
The result of the election will be announced at the Annual General Meeting of the ESCRS which will be held during the Annual Congress in Amsterdam in October.
Yours sincerely,
Filomena Ribeiro Secretary, ESCRSNominated Candidates
Burkhard Dick GERMANY
As a proud member of the ESCRS, I relished seeing our society grow and gain in importance as well as in global outreach. It is definitely not a wheel that has to be reinvented but a gem that will continue to grow. If elected, I would work hard to keep the ESCRS on this successful course with a focus on the society’s educational endeavours and on its meetings that have attracted participants not only from Europe but from all over the world. It will be a challenge—though definitely a pleasant one—to get back on this track after the pandemic.
I had the honour to work on numerous scientific boards, establishing contacts all over Europe and in the US and planning large meetings. To name just a few: I have been president of AECOS Europe and was president of the German Society of Cataract and Refractive Surgery (DGII), a society on whose executive board I am still serving. During the upcoming AAO/ISRS meeting, I am in charge of the program commission for the Refractive Surgery Subspecialty Day. It would be a great privilege to share my experience and enthusiasm with the distinguished ESCRS Board members.
Hirnschall AUSTRIAProfessor of Ophthalmology, University of Warmia and Mazury, Olsztyn, Poland; Head of Institute for Research in Ophthalmology, Poznan, Poland. Present scientific interests: artificial intelligence, ocular infections prevention and treatment, economization of health care. Active in AAO (the Global ONE Advisory Board and Museum of Vision’s Program Committee), EVER (chair of lens/cataract section 2018–2023), ISRS (member of the ISRS International Council), International Council of Ophthalmology (Programme Coordinator for WCO in 2011–2018), Euretina (co-opted board member 2016-2018), and APAO (Programme Coordinator 2017–2019), Polish Presbyopia Club (chairman). Ophthalmic History passionate: co-founder of ESCRS Archive (present co-curator), and ESCRS

Ihad the pleasure of visiting my first ESCRS meeting as a medical student at the age of 22. Since then, I have never missed an annual meeting and I have participated with free papers, courses, and moderations for more than 15 years. Furthermore, I was part of the Young Ophthalmologists committee and I continue to be part of the ESCRS research committee.
After my MD, I worked at the Moorfields Eye Hospital in London for 1.5 years, supervised by Prof Findl. Once back in Vienna, I finished my PhD in medical physics and started courses in advanced statistical modelling. At the end of my ophthalmology residency programme, I took the FEBO exam. I was very honoured when I was granted the Peter Barry fellowship from the ESCRS that allowed me to start a surgical cornea fellowship at the Sydney Eye Hospital in
Heritage Lecture; editor-in-chief Historia Ophthalmologica Internationalis (www.histoph.com).
Authored more than 500 articles, and over 50 book chapters; reviewer for more than 20 journals. Editorial board member: AJO, Acta Ophthalmologica, PLOS One, Graefe’s Archive, TVST (ARVO journal). Only Polish ophthalmologist included in TOP 2% ranking of world-best scientists prepared by Stanford University for 2019. Expertscape worldwide ranking: No. 1 in cataract field and No. 4 in cataract extraction field. Future work in ESCRS: practical evidenced-based recommendations (like AAO, ASCRS, etc.), educational programmes in less-developed parts of Europe, and ESCRS Surveys (like ASCRS, ASRS)—help us better understand trends in clinical practice and educational needs.

Australia in 2018. After returning to Vienna, I continued as a consultant at the Hanusch hospital, where I am still working in the cornea and cataract unit. My “habilitation” (associate Professor) topic was on biometry. Recently, I finished the MBA specialising in team management and motivation. My own motivation in research resulted in 100 accepted peer reviewed manuscripts, 9 published book chapters, and more than 150 talks in 65 meetings.
The ESCRS has always been a source of motivation for me and a chance to meet and learn from inspiring people. It would be an honour for me to use my background and skills as a researcher as well as a surgeon to participate in this exceptional society, thereby continuing the meaningful work in the form of deeper research, optimising clinical standards, and expanding the network.
Andrzej Grzybowski POLAND Nino Florian Kretz GERMANYBorn 1976. After medical school at the University of ErlangenNuremberg and Duke University Durham, North Carolina, USA, Daniel Kook completed his residency at the University Eye Hospital in Munich. His path into refractive surgery started with a fellowship at the University Eye Hospital in Frankfurt under the supervision of Professor Thomas Kohnen. During his years as senior physician at the University Eye Hospital Munich he was Head of the Division of Refractive Surgery dedicating his research on femtosecondlaser-assisted corneal surgery which resulted in his promotion to become a full professor. He authored more than 80 peer-reviewed publications, with more than 2,500 citations.
In 2020, he founded Prof Kook & Partner private practice, which specializes in Cataract and Refractive Surgery in

ESCRS Board Election 2021
Graefelfing, Munich district. Daniel Kook was part of the first ESCRS Young Ophthalmologists Committee, Programme Committee, and Practice Management and Development Committee.
“In times of transnationally growing influence of private equity in our entire profession I am convinced that a strong collaboration between ourselves as ophthalmologists is crucial for mastering this challenge together. With your support, my contribution to the ESCRS as your elected Board member will be enforcing our network strengthening intercollegiate exchange between us ophthalmologists in order to keep ophthalmology and Cataract and Refractive Surgery to the only place where it belongs—in the quality of our own hands.”
My name is Florian Kretz and I am honoured to have been selected to stand on the board of the ESCRS. My career started at the renowned University of Heidelberg. As a Cataract and Refractive Surgeon, I am currently CEO, Owner, and Lead Surgeon of Precise Vision Augenärzte with four medical centers across Germany. We strive to redefine the highest standard of patient care. My experience and passion for ophthalmology is continuously developing. At 38 years of age, I am delighted to share my knowledge and experience with other ophthalmologists across the
Iam Professor of Ophthalmology (MD, PhD, FEBO-CR), Head of the Department of Ophthalmology, Head of the Postgraduate Education College of the Medical University of Silesia, Katowice (Poland), Chair of the Department in the University Clinical Center where before I was medical director.

In the Polish Society of Ophthalmology I have been a board member since 2010, president of Cataract and Refractive Surgery Section. I am the national delegate in EBO and UEMS.
My activities include cataract, refractive, and corneal surgery, presbyopia, IOLs, and diagnostics. I am the author/ co-author of 230 published scientific papers, two books, four book chapters, and more than 550 presentations. I am
Danson currently serves as the chair of the Danish Cataract and Refractive Society. He is known for his skills in complex anterior segment surgery and his interest in cataract surgery education across the Nordics. He is a strong believer in providing better access to eye-care through innovation and digitalization, thus he co-founded a successful e-health company that provides novel e-health solutions for governments and industries alike.
Furthermore he is engaged in various NGO projects providing cataract surgery in various developing countries.
As a potential candidate for the ESCRS Board Danson wants to use his experience towards the following:
Ihave been working in ophthalmology since 1986. At present, I am Head of the Department of Ophthalmology Semmelweis University, Budapest and serve also as Dean of the Faculty of Health Sciences. My main interests are cataract and refractive surgery.


I started refractive surgery in Hungary in 1992 and have performed all kinds of refractive procedures. In 1997, I discovered the harmful role of ultraviolet-B during corneal avascular wound healing, which was published in Ophthalmology in 1997.
In 2008, I was the first to perform femtolaser-assisted cataract surgery in the world. In 2010, I was awarded the
world. In our clinics our teams are conducting clinical research and support further developments of the latest innovations. Our research findings and study results a re recognized in many publications and educational events. I regularly join international congresses to exchange and network with my colleagues’ and fellow researchers across the globe. To become an ESCRS Board member would be a great honour which would allow me to share my knowledge, experience, and passion in the field of ophthalmology.
a member of Advisory Board CRSToday Europe, editor of several issues and ophthalmology journals, and a reviewer in more than 10 ophthalmology journals.
In ESCRS I was member of the Focus Group, co-opted Board Member (2014–2016), and Board Member (2016–2019). I am still active in Education and Charity Committees, EBO-ESCRS Exam Board, ESCRS-Academy speaker, and Wetlab instructor during ESCRS Congresses.

If re-elected to the Board, I would like to continue these activities to extend the role of ESCRS in transferring knowledge to ophthalmologists across Europe. I intend to participate in the training of European YO and support clinical research.
Bridging young ophthalmologists across the European Continent and ESCRS society in order to improve educational content based on his experience as the past national YO Chair and represent in SOE.
Cataract is still a leading course of blindness in the global world. Danson wants to engage ESCRS society towards the needs in the global ophthalmic community in order to eradicate needless blindness.
The fourth industrial era goes along further digitalization and automatization. The impact and change related to big data, cloud, blockchain, VR, and AI are inevitable for refractive and cataract surgeons. Danson wants to engage ESCRS in this transition.
Waring Medal. In 2012 I received the Casebeer Award from the ISRS. In 2019 started the journal Developments in Health Sciences in English as a chief editor.
Within the ESCRS Board I would like to contribute to the scientific programme of the meetings and to the educational programme of the Young Ophthalmologists as being an active teacher of Semmelweis University. ESCRS is a strong society in ophthalmology, and I have a strong commitment for education and scientific work. One of the key factors for success is personal commitment, I would like to work together with the ESCRS Board members.
Ewa MrukwaKominek POLAND Daniel Kook GERMANY Danson Muttuvelu DENMARK Zoltan Nagy HUNGARYNominated Candidates
My name is Sorcha Ní Dhubhghaill (MBBCh, PhD, FEBO, FEBOS-CR). I hail from Ireland where I trained under the late Peter Barry before moving to Antwerp University Hospital (UZA) to work with Marie-José Tassignon. Apart from a side-quest to learn DMEK and collaborate with the Melles Clinic in Rotterdam, I’ve been in Antwerp ever since working in anterior segment surgery and research.

 Sorcha Ní Dhubhghaill BELGIUM
Sorcha Ní Dhubhghaill BELGIUM
As an ophthalmologist who practiced surgery in three different countries, international cooperation is a matter close to my heart. I’m a firm believer in the goals and values of the ESCRS. I am on the board of the Belgian Society for
Matteo Piovella, MD, is an internationally acclaimed cataract and refractive surgery expert and has a private practice in Monza (Milan), Italy.


Dr Piovella is the president of the Italian Ophthalmological Society – SOI, that represents 7,000 Italian eye doctors, his institutional role includes updating Guidelines for Ophthalmology. He is the recipient of the highest international awards for cataract and refractive surgery.

Cataract and Refractive Surgery (BSCRS), and a co-opted member to the EBO exam board educational committee.
I was the first woman to succeed in the ESCRS-EBO exam and I now sit on the exam board.
My academic research focuses on visual optics, lens techniques, and innovative corneal surgery. I also have a particular interest in training and education.
I am enthusiastic, driven, and not afraid of hard work. It would mean a lot to me to be able to count on your support, and I invite you to reach out to me with any questions you might have.
After many years of service in the ESCRS Scientific Committee, today he is acting as judge for the ESCRS Video Competition. He considered the possibility of applying to make available to ESCRS the opportunity to support the requests of ophthalmologists to promote efficient clinical organizational models throughout the European community. If elected he will focus on high-quality education, particularly for younger colleagues.
ESCRS has been my source of reliable and up-to-date information since I was a resident, so I would be honoured to contribute to improving the role of ESCRS as a global reference in corneal, cataract, and refractive surgery.
I work at the Cornea and Refractive Surgery section of the University Hospital of Coimbra and as an assistant professor of Ophthalmology at the University of Coimbra, Portugal.
I have been involved in clinical research for many years, particularly in studies involving functional magnetic resonance and neuroadaptation. Our group was awarded the ESCRS Clinical Research Awards in 2016, which enabled the work that received the ESCRS Obstbaum Award for the
Cédric Schweitzer MD, PhD, FEBO is professor in ophthalmology at Bordeaux University Hospital, France. He is specialised in cataract surgery, femtosecond lasers, IOL biomaterials and optics, and glaucoma. He led several clinical trials including the FEMCAT trial, recently released in The Lancet, which compared FLACS and phacoemulsification cataract surgery. He did a research fellowship at Moorfields Eye Hospital (London, UK), and has been involved in international research and educational programme for the ESCRS and the EBO.
“ I feel very honoured to be nominated for the ESCRS Board election. Keeping with my previous educational and research
Born in Latvia of Spanish ancestry, raised in Germany and trained in Germany, UK, and USA, I have always considered myself a true European with the ESCRS being my “home society”, professionally and intellectually.
I’ve been practising ophthalmology for 30 years. Since 2008, I am the medical director, professor, and Chairman of the department of ophthalmology at Philipps University of Marburg, Germany. While many refractive surgeons naturally associate my name with the development of SMILE, I am in fact a comprehensive ophthalmic surgeon. Of my 30,000 procedures performed, two-thirds were anterior and one-third posterior segment surgeries. I was fortunate to accomplish three fellowships: Eye Pathology (Tennents
best clinical research paper published in the Journal of Cataract and Refractive Surgery in 2017.
I am the current president of the Portuguese Group of Cataract and Refractive Surgery (CIRP). I also represented the Portuguese Society of Ophthalmology in the Leadership Course of 2018–2019 of the Pan-American Association of Ophthalmology, held in conjunction with the American Academy of Ophthalmology.
I am willing to work hard towards serving the ESCRS and providing our society with the tools to perform meaningful research and education, which will lead to the best care for our patients.
commitment, I will be a very engaged board member for the strength and the success of our European Society. Our specialty is at a milestone with challenges triggered by the pandemic, and new opportunities offered in ophthalmology with AI, telemedicine, new lasers, and IOLs to help improve the standard of care. I will be very willing to support scientific research and innovations, to promote relevant evidencebased recommendations for an optimised clinical practice and the best visual care for patients. I will also be very engaged to enhance education and training of our young colleagues across Europe. I would be very grateful and honoured to have your vote and support for this election.”
Institute, Glasgow, UK), Corneal & Refractive Surgery (Moorfields Eye Hospital, London, UK) and Vitreoretinal Surgery (University of Marburg, Germany). Many young ophthalmologists, PhD, and MD students have reached their goals under my guidance. I have published 170 original papers, 45 book chapters, and edited a book on SMILE. I also gave innumerable lectures and papers at local, national, and international venues, many of which at the ESCRS meetings. As a fully trilingual person with a broad expertise, I see my role in the ESCRS as a promoter for close scientific relationships between different subspecialties in ophthalmology and among east and west European members alike.
Matteo Piovella ITALY Andreia Rosa PORTUGAL Cédric Schweitzer FRANCE Walter Sekundo GERMANYThis nomination is an honour. As high-volume cataract, refractive, and DMEK surgeon I also like to innovate. In my country I performed the first lasik, femtolasik, MICS, FLACS, DMEK, Boston KPRO, synthetic endothelium, Avastin injection, and several other surgeries. I was the first Victus femtosecond laser European user. My world-firsts: presbyopic phakic IOL implantation, bio-synthetic corneal inlay, femtomatrix FLACS, and CapsuLaser capsulotomy as its co-inventor. My current research is focused on bio-synthetic collagen corneal inlay and synthetic endothelium. I am the founder and chief eye surgeon of Gemini Eye Clinics in the Czech Republic and Austria.
After gaining experience in clinical research and the pharmaceutical industry, Kristof found his ultimate challenge: ophthalmology! Since founding the Vista Alpina Eye Clinic in 2008, he has been working and teaching there, living out his passion for quality and innovation, and successfully mastering the many challenges that eye surgeons face every day.

Kristof is an experienced surgeon (2,000 surgeries annually). Although not pursuing an academic career, he has a strong interest in clinical research, with a special focus on refractive cataract surgery and phakic lenses. In 2014, he received the “Best Presentation Award” at the ESCRS Congress for his work on improving toric IOL design.
Prof Paolo Vinciguerra obtained his medica degree at the University of Milan in March 1982 and then his ophthalmology degree (1982 – 1986). Associate Professor of Ophthalmology (2016 – 2019), Full Professor (2020), Director of Residency Program in Ophthalmology at Humanitas University – Rozzano (Milan) and Director of Eye Center – Istituto Clinico Humanitas since November 1999. He is Coordinator of the Eye and Neck Department –Humanitas University. He has been appointed as professor at the Milan University, Chieti University, and visiting professor at the Ohio State University.
Pioneer of numerous ophthalmic surgery procedures, since 1989 Prof Vinciguerra MD, PhD, has contributed to countless Italian and international research projects studying refractive surgery and corneal topography. He is

I gave more than 900 presentations in Europe and beyond and I have been teaching young residents at phaco courses at ESCRS and SOE meetings for several years and run surgical simulator courses.
If re-elected I would like to contribute to the ESCRS Board according to the needs of this society at online ESCRS educational activities and annual meetings after the pandemic is over to keep growing ESCRS's educational impact on European eye surgeons. I would be grateful for your vote of support and you can contact me with any questions or suggestions regarding ESCRS.
He has an MBA and is fluent in English, German, French, and Flemish.
Since 2018, he has tirelessly defended the interests of Swiss ophthalmologists as president of the Tariff Committee and board member of the Swiss Society of Ophthalmology, successfully introducing innovative flat fees for ophthalmic surgery.
“To find out where my focus as a future board member should be, I conducted a mini-survey among ESCRS members. Clinical guidelines came first, followed by member advocacy and services (e.g., secretariat, website, video library, patient information). I am a typical ESCRS member. I am hardworking and ready to defend our interests.
Suggestions? Contact me on LinkedIn!”
president of the Italian Cataract and Refractive Surgery Society (AICCER), past president of the Italian Association of Private Hospitals (OPI), board member of the Italian Society of Cornea, Stem Cells, and Ocular Surface (SICSSO). He has been an Honorary Member of the Italian Ophthalmology Society since 1995 and an Honorary Member of the Italian Society for Corneal Transplants (SITRAC) since 2004. He has been a member of the International Council of the International Society of Refractive Surgery – American Academy (ISRS – AAO) since 2004.
As a pioneer of refractive surgery working with scientific institutes and ophthalmology companies engaged in development and research into technological innovations, Prof Vinciguerra MD has registered numerous patents in both Europe and the rest of the world.

Determining Progression After CXL
The latest version of the Belin ABCD keratoconus progression display has been updated to include data to objectively evaluate progression after corneal crosslinking (CXL) treatment.



Speaking at the 25th ESCRS Winter Meeting, Michael W Belin MD, professor of ophthalmology and vision science at the University of Arizona, said the software enhancement should prove a valuable addition to the standard Pentacam software that incorporates the Belin ABCD progression display.

“We recently tested this new version of the software in a study carried out in Switzerland and Germany and concluded that post CXL measurement variance or ‘noise’ can be used to determine progressive change in patients after their cross-linking treatment. The noise measurements were consistent across different centres and over the course of the follow-up period,” he said.
The Belin ABCD system utilises four key parameters to determine keratoconus progression: Anterior (“A”) and posterior (“B” for Back) radius of curvature taken from a 3.0 mm optical zone centred on the thinnest point, “C” is minimal Corneal thickness, and “D” best spectacle Distance visual acuity. The first three parameters (A, B, C) are machine-generated objective measurements that can be used to determine progressive change.
The ABCD Progression Display graphically displays each parameter and shows when statistical change above measurement noise is reached using colour-coded maps.
Prior to this upgrade, progression parameters after CXL were largely unknown, noted Dr Belin.
“There is not much known about post-CXL progression and the possible need for repeat treatments. All the confidence interval gates on the Belin ABCD progression display were removed once a CXL treatment was performed in earlier versions of the software,” he said.
In the study carried out in conjunction with the ELZA Institute in Zurich, Switzerland, and the Homburg Keratoconus Centre in Germany, Dr Belin and co-workers evaluated a group of 60 patients aged 11 to 66 years in a time span from 12 to 115 months after CXL treatment.
Three separate and consecutive Pentacam measurements were taken, removing the patient from the device between each measurement. A minimum of 7.5 mm of corneal coverage and an acceptable Pentacam quality score was required for inclusion. Both pooled variance and one-sided confidence intervals were then computed. The two populations had similar ABC values and similar noise measurements, noted Dr Belin.
From now on, the confidence intervals for post-CXL changes will be shown by blue gates in the Belin ABCD keratoconus progression display.


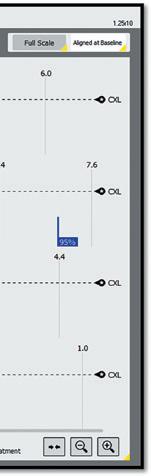
“These gates will only appear if a CXL treatment is marked and will only appear for the examinations 12 months after the treatment date to allow for epithelial healing and stromal haze to resolve,” he concluded.

The confidence intervals for post-CXL changes will be shown by blue gates in the Belin ABCD keratoconus progression display. Dermot McGrath reportsNOTE: Photo is of the Belin ABCD Progression Display. The crosslinking treatment is indicated by the dashed line (1/27/15). The post CXL confidence gates appear at exams one year post treatment and later. The patient shows a good response to CXL and there is no indication for a need for retreatment (all parameters are well below the 80% confidence interval). Michael W Belin MD
Automated Keratoconus Detection

OS 4TM THE NEXT GENERATION
Adeep learning programme using convolutional neural networks (CNN) to assess Pentacam (Oculus) images correctly identified keratoconic and normal corneas more than 99% of the time in a validation test, Henry Liu MD told the Association for Research in Vision and Ophthalmology 2021 Annual Meeting.
The same program displayed accuracy exceeding 87% in staging cases when manifest refraction was added to four Pentacam parameters. However, it was unable to predict progression, possibly due to a limited number of progressing cases to train the system, said Dr Liu, who is a first-year ophthalmology resident at the University of Ottawa, Canada.
TRAINING AND OUTCOMES
Deep learning is a type of machine learning in which a system is exposed to a large set of labelled training images, and develops its own rules for classifying them based on features it detects, rather than having identifying features predetermined by an expert programmer. CNNs act as filters within the deep learning network that identify specific abstract features, progressively increasing accuracy as the image is processed, Dr Liu explained.
Deep learning has been used extensively to automate detection of retinal diseases and glaucoma, but very little research has been done in the field of cornea, Dr Liu noted. This CNN program harnesses widely used Pentacam images, rather than OCT images, for automating keratoconus assessment.
In Dr Liu’s three-stage study with colleagues at Ottawa, a CNN was developed and trained with a dataset of corneal topographies, which included all patients with a diagnosis of keratoconus seen between January 2007 and June 2019, and patients assessed for refractive surgery as controls. A full 80% were used for training and 20% for validation. In all, 2,450 scans, with 1,215 keratoconus and 1,235 controls, were included for stage 1; 985 graded keratoconus scans for stage 2; and 144 keratoconus scans, 72 progressed, and 72 stabilized, for stage 3.
For stage 1 cases, the deep learning model with data from four Pentacam parameters showed an accuracy of 99.3% in discriminating keratoconic from normal corneas. Using individual parameters, anterior elevation, posterior elevation, and anterior curvature yielded accuracy of 98.7%, 98.4%, and 97.6% respectively, with pachymetry maps lagging at 77.1%. For study stage 2, the four parameters yielded 73.5% accuracy grading keratoconus on the four-stage AmslerKrumeich scale, increasing to 87.8% when manifest refraction was added. For study stage 3, progression was predicted with an accuracy of 53.6%.
“Even though it was not able to predict keratoconus progression, applications of CNNs are encouraging and can be used to solve practical clinical problems, and serve as an adjunct tool in clinical decision-making in the near future,”
Dr Liu concluded.
Henry Liu: hliu114@uottawa.caThe new OS 4 marks the beginning of the next generation of retina, glaucoma and cataract surgery. The all-in-one platform has received numerous exciting features that provide even more comfort, precision and safety.
Laser integration: More safety, fully automated user protection filter
Light: 45% more power*, maximum visibility



Pedal: Multifunctional with over 100 setting options
Phaco: Speedier readiness, greater controllability
User comfort: Even more userfriendly and communicative
Make the difference –with the new OS 4: www.oertli-instruments.com

Deep learning model more than 99% accurate, but fails to predict progression.
Howard Larkin reports
Right on the Mark
“Precision treatments with the YAG/SLT laser”
NIDEK, a leading manufacturer of modern YAG lasers, introduces the advanced YAG and SLT combination laser, YC-200 S plus, and the enhanced YAG laser, YC-200.

A suite of technologies has been incorporated in these lasers to achieve seamless function and greater precision. Features for targeting pathology, accurate energy delivery, and operative assist functions allow the surgeon to deliver treatments “Right on the Mark”.
CME After Keratoplasty
DMEK may carry a higher risk of postoperative CME compared to DSAEK.
Roibeard Ó hÉineacháin reports
Eyes that undergo Descemet’s membrane endothelial keratoplasty (DMEK) appear to have a higher rate of cystoid macular oedema (CME) compared to eyes that undergo Descemet-stripping automated endothelial keratoplasty, following endothelial keratoplasty, according to a study presented by Luca Furiosi MD at the 25th ESCRS Winter Meeting.
“Ages older than 67 years, diabetes, and DMEK are independent risk factors for CME following endothelial keratoplasty. Close observation is necessary, especially during the first postoperative year after EK—particularly in patients with a risk for CME,” said Dr Furiosi, University of Ferrara, Ferrara, Italy.
The study reviewed outcomes of 2,233 patients who underwent endothelial keratoplasty at Ospedali Privati Forlì “Villa Igea”, Forlì, Italy. Of that group, 1,909 patients underwent DSAEK from January 2005 to October 2018 and 324 patients underwent DMEK from June 2014 to August 2018. All had a minimum follow-up of 18 months. In patients undergoing keratoplasty bilaterally, a single eye was chosen at random for inclusion in the analysis, Dr Furiosi said.
Defining CME as the presence of intraretinal fluid spaces with or without subretinal fluid that impairs vision, the researchers found the overall incidence of postoperative CME was 2.82% (63 patients). However, CME occurred in only 2.36% of DSAEK-treated eyes compared to 5.56% of DMEK eyes (p=0.001). There was an average of 4.27 months (range 1–34 months) between the keratoplasty procedure and the onset of CME postoperatively.
Dr Furiosi noted that compared to those who did not develop CME, patients who developed CME were significantly older (70.5 vs. 67.1, p=0.01), the group had a significantly higher proportion of diabetic patients (24.2% vs. 9.8%, p<0.001), and a significantly higher proportion of patients that underwent DMEK rather than DSAEK (28.6% vs. 14.1%, p=0.001). However, there was no significant difference between the non-CME group and the CME group in terms of gender, surgical indication, lens status, rebubbling, concurrent glaucoma, or combined procedures.
A receiving operator curve analysis indicated that the age of more than 67 years was the ideal cut-off point for separating non-CME cases from CME cases. A patient with all three risk factors—age, diabetes, and DMEK—had an odds ratio of 16.75 of developing CME with a fitted probability of 18%, Dr Furiosi said.
He added that despite the inclusion of all indications for surgery such as previous grafts, the post-DMEK CME rate of 5.56% is in the lower end of range of the 0.7 to 15.6% rates reported in the literature, but was roughly in line with CME rates reported in other studies.
Treating Angle Closure Glaucoma
Patients with primary angle-closure glaucoma (PACG) or primary angle closure and high intraocular pressure (IOP) are less likely to need medication or surgery if they start with cataract surgery than if they start with a peripheral laser iridotomy, said Prof David S Friedman MD, MPH, PhD, Massachusetts Eye and Ear Infirmary, Boston, Massachusetts, USA.
“Other important predictors of good eye pressure control with either treatment included having a lower presenting eye pressure, not requiring eye drops initially to control the eye pressure, and being Chinese,” said Prof Friedman, who presented a review and analysis of the three-year results of the early lens extraction for the treatment of primary angle-closure glaucoma (EAGLE) trial at the ARVO 2021 Congress.
He noted that the EAGLE trial was a multicentre randomised controlled study comparing clear lens extraction (CLE) to laser peripheral iridotomy (LPI) in 419 patients who had newly diagnosed PAC or PACG and did not have cataract. The trial was conducted in Europe, Asia, and Australia, with most participants originating from the UK.
The target IOP in the study was 15–20 mmHg and the need for an increase or decrease in IOP-lowering medications was determined by the physician. Those whose IOP was not adequately controlled by medication could be offered surgery. Their baseline characteristics were a mean age of 67 years, a diagnosis of PAC in 37% and of PACG in 62%, a mean baseline IOP of 28.9 mmHg and a mean deviation (MD) of -4.2 dB. In addition, 29% of patients were of Chinese ethnicity.
BETTER IOP CONTROL WITH CLEAR LENS EXCHANGE
Prof Friedman noted that at 36-month follow-up the mean IOP was lower among eyes in the CLE group, having decreased from a mean baseline of 29.5 mmHg to 16.6 mmHg, compared to a decrease from 30.3 mmHg to 17.9 mmHg in the LPI group. That was despite the fact that 66% in the CLE group were using no IOP-lowering medication throughout follow-up, compared to only 18% in the LPI group. In addition, only one study eye randomised to CLE underwent trabeculectomy, compared to six study eyes (2.8%) in the LPI arm.
Furthermore, compared to the LPI group, patients in the CLE group reported a better quality of life in their responses to the EQ-5D questionnaire, which measures problems in five qualityof-life domains. Moreover, incremental cost analysis showed a benefit of ELE in terms of quality-adjusted life years (QALY), Prof Friedman said.
WHICH PATIENTS DO BEST?
Using data from the EAGLE trial, Prof Friedman and his associates conducted a study to assess the baseline parameters associated with better long-term IOP control. In their analysis, they defined “good responders” as those having an IOP lower
than 21 mmHg at the 36-month follow up without any further surgery and they defined “great responders” as those who maintained an IOP lower than 21 mmHg after the same follow-up period without requiring medication or further surgery.
Their analysis showed 89.6% of the patients in the CLE group had a good response compared to 66.8% of eyes in the LPI group. In addition, 63.9% in the CLE group were great responders, compared to only 17.7% in the LPI group. Furthermore, multivariate logistic regression analysis showed undergoing CLE rather than LPI was the strongest factor predicting a good response, with an odds ratio of 4.5, and was an even stronger predictor of a great response, with an odds ratio of 10.1.
Another predictive factor for a good response were low baseline IOP, with an odds ratio of 1.2 for every 5 mmHg lower of IOP baseline. Predictors of a great response included Chinese nationality, with an odds ratio of 2.3, and not using glaucoma medications at baseline, with an odds ratio of 2.8. A diagnosis of PAC vs. PACG was also a predictor of a great response, with an odds ratio of 2.1, as was a good baseline visual field which increased the odds ratio for a great response by 1.06 for every for decibel better.
Looking at the two treatments separately, the main predictor of a good response after LPI was lower IOP at baseline. LPI had the same predictive factors for a great response as the study group overall. In eyes that underwent CLE the odds ratio of a good response increased by 1.2 for every 1.0 mm of shallowness of the anterior chamber depth. The strongest predictor of a great response was not receiving glaucoma medications at baseline.
“The take home messages is that after clear lens extraction, IOP was controlled in nearly 90% without further surgery at three years, and almost two-thirds required no medications. On the other hand, those already requiring medications, those with PACG, and those undergoing laser iridotomy are less likely to be free of medications long-term and are also more likely to require additional surgery,” Prof Friedman said.
Prof David S Friedman MD, MPH, PhD: friedman@meei.harvard.eduGood preoperative IOP control without medication, Chinese nationality are predictors of good outcome for both lensectomy and iridotomy.
Roibeard Ó hÉineacháin reports
“Other important predictors of good eye pressure control with either treatment included having a lower presenting eye pressure, not requiring eye drops initially to control the eye pressure, and being Chinese,”
Prof David S Friedman MD, MPH, PhD
MIGS Jumps in USA
6-year study finds use doubles as standard glaucoma surgeries decline. Howard Larkin reports
Use of minimally invasive glaucoma surgery (MIGS)—including trabecular bypass, suprachoroidal outflow, subconjunctival drainage, and aqueous production-reducing procedures—more than doubled from 2013 through 2018 in the USA, despite limited evidence of their long-term safety or effectiveness.
Over the same period, standard glaucoma procedure volume—including trabeculectomy and glaucoma drainage devices (GDD)—declined by a smaller amount, reported Shuang-An Yang MD, MPH at the Association for Research in Vision and Ophthalmology 2021 Annual Meeting.

The findings highlight the need for trials comparing the safety and outcomes of novel MIGS with traditional glaucoma treatments known to be sight-saving, said Dr Yang, who is an ophthalmology research fellow from Taiwan at the Harvard TH Chan School of Public Health and the Massachusetts Eye and Ear Infirmary, Boston, Massachusetts, USA.
IRIS STUDY
The study is based on a review of 510,577 MIGS and standard glaucoma procedures recorded in the American Academy of Ophthalmology’s Intelligent Research in Sight (IRIS) database. During the six years examined, annual adjusted volume of MIGS procedures more than doubled, from 31,059 to 69,420. iStent (Glaukos) use grew most, from 14% to 40% of all glaucoma procedures. Traditional glaucoma surgeries declined from 46,385 to 22,347 annually over the same period.
About 10% of 203,332 eyes with a glaucoma diagnosis underwent multiple glaucoma procedures, with about 36% on the same day and 64% on subsequent days. iStent and endoscopic cyclophotocoagulation (ECP) were the most common concurrent procedures, accounting for 55%. Trabeculectomy and GDD were most often followed by another standard glaucoma surgery, but when followed by MIGS, ECP, and goniotomy were most common. Nearly two-thirds of eyes underwent concurrent phacoemulsification. Significant demographic differences among procedure types also were found. Females were more likely to receive iStent or ECP, while younger males were more likely to receive GDDs. Whites were more likely to receive iStent or Xen Gel Stent (Allergan), while Blacks more often received GDD, goniotomy, or trabeculectomy.

The trend towards MIGS is driven by the desire for intraocular pressure-lowering procedures that are less risky and uncomfortable for patients, Dr Yang said. During the study period more MIGS procedures were approved, and they are easy to combine with phaco. Changes in the USA’s Medicare insurance programme discouraging traditional glaucoma surgery may also be a factor.
Still, research is needed to better understand MIGS outcomes and guide their use, Dr Yang said.
“It is unclear whether MIGS can replace trabeculectomy as sight-saving surgery, and whether the expense of MIGS can be justified by their effectiveness, longevity, and safety.”
Durable Intravitreal Treatment of DME: Phase 3 YOSEMITE and RHINE Trials
Bispecific antibody demonstrates promising efficacy and safety at one year in ongoing pivotal trials.
The two pivotal phase three studies investigating two different dosing regimens of faricimab (Roche) for treatment of centre-involved diabetic macular oedema (DME) met their primary endpoints at one year. The studies showed mean BCVA gains were noninferior in eyes treated with the novel bispecific antibody inhibitor of VEGF-A and angiopoietin-2 (Ang-2) compared to aflibercept (Eylea, Regeneron) injected every eight weeks.
The one-year results also showed durability of the faricimab treatment benefit with a dosing interval of up to 16 weeks, better anatomic outcomes with faricimab versus aflibercept, and no safety signals for faricimab, said John A Wells MD, reporting findings from the YOSEMITE and RHINE trials at the virtual ARVO 2021 meeting.
“YOSEMITE and RHINE are ongoing, 2-year studies, and an additional two-year extension study, RHONE-X, will give us up to four years of data in the future. It will be important to see how many eyes that have achieved a 16-week dosing interval at one year maintain a durable response,” explained Dr Wells, a retina specialist in West Columbia, South Carolina, USA.
Together YOSEMITE and RHINE enrolled a total of 1,891 patients at 353 sites worldwide. Eligible patients were adults with centre-involved DME (central subfield thickness [CST] ≥ 325 µm) and BCVA ranging from 73 to 25 ETDRS letters (Snellen equivalent ~20/40 to 20/320).
Patients with either treatment naïve or previously treated DME were eligible, although the latter patients had to undergo a three-month washout period and were capped at 25% of the total enrolment.
Patients in each study were randomised equally into three groups to receive faricimab 6 mg every eight weeks (Q8W) after six monthly doses, faricimab 6 mg administered on a personalised treatment interval (PTI), or aflibercept 2 mg Q8W after five monthly doses. Dr Wells explained PTI is a treat and extend concept
Cheryl Guttman Krader reportsIn both studies, faricimab-treated eyes showed greater decreases in mean CST compared with aflibercept-treated eyes.
in which patients receive monthly dosing (minimum of four doses) until DME resolves (CST <325 microns). Then the dosing interval is increased in four-week increments up to Q16W as long as the CST and vision are stable. The interval is maintained if CST worsens and reduced if both CST and BCVA worsen.
The three arms in both studies were well-balanced at baseline with respect to both patient and ocular characteristics. Mean BCVA was about 62 letters (Snellen 20/63), mean CST ranged from 465 to 495 µm. Some 50% of eyes had mild to moderate nonproliferative diabetic retinopathy and less than 10% had proliferative diabetic retinopathy.
The primary endpoint for the two studies analysed mean change in BCVA from baseline averaged over weeks 48, 52, and 56. More than 90% of patients in all treatment arms completed the primary endpoint. The results showed mean BCVA gains in the faricimab Q8W, faricimab PTI, and aflibercept arms were 10.7, 11.6, and 10.9 letters, respectively, in YOSEMITE and 11.8, 10.8, and 10.3 letters, respectively, in RHINE.
In both studies, approximately 30% to 35% of eyes in all groups showed a BCVA gain at least 15 letters while just 1% to 2% of eyes lost 15 letters or more.
“Importantly, a similar proportion of eyes in the PTI arms gained at least 15 letters despite receiving less frequent dosing. In addition, the data showing that very few patients on PTI lost more than 15 letters indicates that less frequent dosing with faricimab was not harmful,” Dr Wells said.
The durability of the response to faricimab was assessed based on the proportion of patients being dosed at 4-, 8-, 12-, and 16-week intervals at week 52. The results were similar in both studies and showed that just over 50% of eyes
achieved the Q16W dosing interval and another 20% were being maintained with faricimab dosing Q12W.
“Approximately two-thirds of patients in the PTI arms achieved Q12W week or Q16W dosing without dropping below Q12W dosing through week 52,” Dr Wells added.
In both studies, faricimab-treated eyes showed greater decreases in mean CST compared with aflibercept-treated eyes. More eyes treated with faricimab than with aflibercept achieved CST < 325 microns (80% vs. 70%), and more faricimab-treated eyes had resolution of intraretinal fluid at week 56 (~45% vs. ~25%). Subretinal fluid was present at baseline in about one-third of eyes in all treatment arms and was completely resolved at week 56 in nearly all eyes.
“Less frequent dosing of faricimab was not associated with a lesser anatomic effect,” Dr Wells said.
A key secondary endpoint analysis of Diabetic Retinopathy Severity Scores showed that approximately 45% of eyes in all faricimab arms achieved a two-step or better improvement from baseline.
Rates of ocular and systemic adverse events, including Anti-Platelet Trialists Collaboration events, were similar in all groups in both studies, and serious ocular adverse events were infrequent.
“In the wake of brolucizumab, it is notable that the rate of inflammatory adverse events with faricimab was less than 1%, and the rate of endophthalmitis was also less than 1%. No cases of retinal vasculitis were reported and five cases of retinal venous or arterial obstruction were reported across all study arms at one year,” Dr Wells said.
Jack Wells: (803) 931-0077 (Office); jackwells@palmettoretina.comAt-Home Monitoring for Early Detection of Wet AMD
Cheryl Guttman Krader reports

Anovel investigational handheld device (KalEYEdoscope) intended for at-home use to identify conversion from dry to wet age-related macular degeneration (AMD) provides a rapid, comfortable, and easy testing solution for a range of patients, according to the findings of a clinical validation study.
The digital device, which was developed by researchers at the University of Michigan, Ann Arbor, Michigan, USA, uses the concept of shape discrimination hyperacuity (SDH) to exploit the fact that patients with wet AMD are able to distinguish distortions, explained Yannis Paulus MD, Assistant Professor, Departments of Ophthalmology and Visual Sciences and Biomedical Engineering.

Users are shown a series of circle-like images on a 1.5-inch OLED screen, and after each is displayed, they are asked to indicate whether the image represents a perfect circle by pushing a button. The test concludes when enough data are obtained to establish the user’s minimum distortion-detection threshold. Data from the testing are collected longitudinally and statistically analysed to determine a change in condition.

The clinical validation trial was designed to evaluate testing duration and user impressions. It included 15 patients with refractive errors ranging from +1.25 D to -7.0 D. The device is designed to accommodate refractive errors of +5.0 D to -10.0 D.

The testing, which was done with a prototype device, was completed by all participants in an average test time of 70 seconds (standard deviation, 9.1 seconds, range 32 to 143 seconds). All of the patients rated the device as comfortable to hold, and they found the testing easy. Asked to rate the difficulty on a Likert scale of 1 (easiest) to 5 (hardest), the average rating was 1.5.
“The average duration of the testing with our device is 67% shorter than for the ForeseeHome monitoring system that is based on Vernier acuity. Furthermore, our device has been meticulously designed and redesigned with patient comfort in mind to facilitate its acceptance and use,” said Dr Paulus.
“We believe the shorter testing time along with the smaller, handheld nature of our device will be valuable for improving patient compliance with the testing.”
Larger prospective clinical trials to target regulatory (US FDA) approval are being planned.
The wide range in testing time documented in the validation study is being looked at in an ongoing larger trial to see if test duration is related to any particular patient characteristics.
Further trials are also necessary to demonstrate that use of the device results in improved outcomes for patients with dry AMD.
Yannis Paulus: ypaulus@med.umich.eduInvestigational device using shape discrimination hyperacuity shows promise in clinical validation study.Yannis Paulus MD
Addressing the Burden of Vision Loss from Diabetic Eye Disease
Friedenwald lecturer outlines past accomplishments and anticipated advances. Cheryl Guttman Krader reports
Lloyd P Aiello MD, PhD, was honoured as the Friedenwald Awardee at the virtual ARVO 2021 meeting for his work that has transformed the treatment of diabetic eye disease. His lecture provided a historical overview of developments that have changed the global paradigm for the evaluation, management, and treatment of diabetic retinopathy (DR) and diabetic macular oedema (DME) and offered a glimpse into what he believes will be an exciting future.
In beginning and ending his talk, Dr Aiello emphasised the advances he described could not have been realised without the participation of a host of researchers around the world.
“To me, this award is not so much a recognition of the work that our laboratory has been fortunate to be a part of, but rather a testament to the incredible efforts of so many exceptionally talented individuals worldwide to reduce the visual loss and alleviate the suffering associated with diabetes,” said Dr Aiello, Professor of Ophthalmology and Director of the Beetham Eye Institute, Joslin Diabetes Center, Harvard Medical School, Boston, Massachusetts, USA.
THE BEGINNING OF THE ANTI-VEGF ERA
In the mid-1960s, work by Dr Aiello’s father, Lloyd M Aiello MD, and grandfather, William P Beetham MD, introducing panretinal photocoagulation (PRP) for the treatment of proliferative DR (PDR) was the first paradigm shift in the management of diabetic eye disease. However, the discovery of VEGF led to an even more transformative change. Research by Dr Lloyd P Aiello and colleagues providing evidence that VEGF in the vitreous of eyes with PDR was directly responsible for retinal endothelial cell growth, and animal studies from his group and others showing that VEGF inhibition could block hyperoxia-induced retinal neovascularisation was a major step in DR research.
The ability to bring anti-VEGF therapy into the clinical arena was greatly facilitated by work of the DR Clinical Research Network (now known as the DRCR Retina Network), of which Dr Aiello was the founding chair. DRCR.net Protocol I was the first large scale randomised clinical trial to evaluate the effect of VEGF inhibition on vision loss from DME, and its findings together with those of other studies initiated the paradigm shift for the treatment of centre-involved DME with reduced vision.
Subsequent studies sought to expand the role of anti-VEGF therapy by investigating its use for treating PDR and nonproliferative DR (NPDR). DRCR.net Protocol S showed noninferiority of intravitreal ranibizumab compared to PRP for improving VA after two and five years in eyes with PDR. It also
demonstrated that anti-VEGF therapy had some advantages. Two-year results from DRCR.net Protocol W showed that compared to sham, aflibercept treatment in eyes with moderate to severe NPDR reduced the rates of PDR or centre involvedDME development. Preventive treatment with aflibercept did not confer a VA benefit compared with treatment initiated after the development of PDR or CME.
“Thus, with regards to NPDR, there are factors favouring use of anti-VEGF and those favouring monitoring,” Dr Aiello said.
EXPANDING FOCUS
While research investigating treatments for diabetic eye disease is continuing, the therapeutic advances are supporting interest in strategies for optimising outcomes.
“A major hurdle for DR therapy is lack of patient awareness because it is a major contributing factor for nonadherence to eye care guidelines and poor visual outcomes,” said Dr Aiello. He discussed findings from a recent study that showed the extent of this problem.
The limitations associated with use of ETDRS 7-field photography to evaluate retinopathy severity are being overcome with the availability of ultrawide field (UWF) cameras. Dr Aiello described research looking for prognostic markers identified from UWF retinal imaging and investigating UWF angiography.
“Overall, the retina periphery appears to hold substantial, possibly unique, information that may permit better assessment of retinopathy progression risk. Furthermore, evolving technologies, such as artificial intelligence, peripheral OCT, UWF fluorescein angiography, and others may yield additional predictive value if they are used to assess the retinal periphery,” Dr Aiello said.
“If such findings are confirmed, current standard DR severity grading approaches may require modification to include these parameters for optimal risk assessment. Indeed, the Diabetic Retinal Disease Staging Project of the Restoring Vision Moonshot is already underway.”
The goal of the latter project is to provide an updated diabetic retinal staging system, to incorporate relevant advances, and provide prognostic information necessary to better address early disease, disease progression, development and use of therapeutic interventions, and treatment effectiveness.
UPCOMING RESEARCH
Dr Aiello ended his talk with a brief description of some ongoing DRCR.net protocols. In addition to Protocol AA and W, these include AE, investigating photobiomodulation for DME; AC, comparing initial aflibercept vs bevacizumab with aflibercept as needed for centre involved-DME and VA 20/50 or worse; and AF, evaluating effects of fenofibrate on contrast sensitivity, OCT angiography, visual field, and DR severity.
Further into the future, studies are expected investigating recently discovered protective factors and non-VEGFA dependent pathological pathways. Meanwhile artificial intelligence and deep learning approaches for detecting diabetic eye disease are being increasingly pursued and some are already FDA-approved.
lpaiello@joslin.harvard.eduLloyd Paul Aiello MD, PhD, FARVO
“A major hurdle for DR therapy is lack of patient awareness because it is a major contributing factor for nonadherence to eye care guidelines and poor visual outcomes,”
Dr Lloyd R Aiello MD, PhD
PROMs for Kids
How do you make health care more patient-centred for children? Just as with any other group—ask them, and their parents. The recently developed PedEyeQ provides a structured assessment tool for doing just that for a wide range of paediatric ophthalmic conditions, said Jonathan M Holmes BM, BCh at the Association for Research in Vision and Ophthalmology 2021 Annual Meeting.
“The PedEyeQ now allows assessment of functional vision and quality-of-life domains in paediatric eye conditions from infants to teenagers, and may thereby prove useful in the management of these conditions and as an outcome measure in research,” Dr Holmes, professor and chair of ophthalmology and vision science at the University of Arizona, Tucson, Arizona, USA.
The key questions for developing effective patient-reported outcome measures (PROMs) are “what bothers you about your condition?” and “how does it affect your everyday life?” said Dr Holmes. Having patients answer such questions without clinician interpretation can give deep insight into issues ranging from functional vision, that is what the patient can or cannot do because of their vision (what the patient can and cannot do because of their vision), health-related quality-of-life (what bothers the patient), and symptoms.
GO TO THE SOURCE
"In developing the PedEyeQ questionnaire, we avoided the traditional process of experts coming up with PROM questions and testing them. Instead, we interviewed parents and children," Dr Holmes said. Semi-structured interviews captured three perspectives— the children’s; the parents’ perception of the child’s experience, known as a proxy assessment; and the effect on the parents themselves. Altogether, 204 children aged 5 to 17 years and 328 parents were interviewed across 10 diagnostic groups ranging from amblyopia to retina/optic nerve.
The open-ended interviews were transcribed and coded, resulting in 614 candidate questions for child and proxy,
and 589 for parents. A literature review to ensure completeness added no questions. For the PedEyeQ, questions pertaining to symptoms were removed, focusing on functional vision and quality-of-life.
The process included development of parallel questions, reflecting functional vision, for example, “are you unable to play with Buzz Lightyear because of your eyes?” and quality-of-life related to that aspect of functional vision, for example, “does it bother you that you are unable to play with Buzz Lightyear because of your eyes?”
The next step was grouping similar questions and coming up with general questions to cover them. For example, “are you unable to do things that you want to do because of your eyes?” rather than a specific Buzz Lightyear question.
The resulting 63 items were then combined into master child and proxy questionnaires, which were tested on a new cohort of children and parents, with separate questionnaires for children aged 5 to 11 years and 12 to 17 years; proxy questionnaires for children 0 to 4 years, 5 to 11 years, and 12 to 17 years; and a parent questionnaire.
WINNOWING QUESTIONS
Factor analysis revealed distinct groups of questions, and each group was assessed for unidimensionality to ensure that unlike concepts were not combined in scoring. Each group of questions was then labelled as a domain, with a descriptive title such as “functional vision.” Another child domain was labelled “social,” with questions such as “do you get teased?”, and a further domain was labelled “bothered by eyes and vision” with questions such as “does it bother you that you have a hard time seeing the board at school?” Frustration and worry was the fourth and final child domain. Proxy questions were analysed separately by age, 0 to 4, 5 to 11, and 12 to 17 yearolds, and the same domains as the child questionnaire emerged, with the addition of an eyecare domain.
The parent questionnaire was found to have four separate domains—impact on parent and family; worry regarding child’s eye condition; worry regarding child’s selfperception and interactions; and worry
Dr Jonathan M Holmes BM, BChregarding child’s visual function. For scoring, Rasch analysis was used to convert nonlinear question scores to linear measures. For each domain, a Rasch map was created to separate questions according to severity. For example, in the functional vision domain, the question “do you have a hard time seeing?” is answered affirmatively by more children than “do you run into things because of your eyes?” indicating a higher severity score for the second question. Rasch analysis was also used to eliminate items that did not fit or resulted in poorer questionnaire performance. The aim was to have 10 or fewer questions per domain.
Dr Holmes highlighted recent studies using the PedEyeQ that have found children with a wide range of ocular conditions, including amblyopia, cataract, refractive error, and strabismus, score lower than controls across functional vision and quality-of-life domains. (Hatt SR et al. AJO 2020. Leske DA et al. JAAPOS 2021.) The development of the PedEyeQ and subsequent validation studies have been a joint collaboration between Dr Holmes’ team at Mayo Clinic, Rochester, Minnesota, and Dr Eileen Birch’s team at the Retina Foundation of the Southwest, Dallas, Texas. The questionnaires and scoring sheets are available for download at the Paediatric Eye Disease Investigator Website www.pedig.net. and the development of the questionnaire has been published as Hatt SR et al, AJO 2019.
Jonathan Holmes: jmholmes@arizona.eduPedEyeQ offers outcome measures for assessing impact of ophthalmic conditions in childhood. Howard Larkin reports
The key questions for developing effective patient-reported outcome measures (PROMs) are “what bothers you about your condition?” and “how does it affect your everyday life?”
Amblyopia Screening and Treatment
Better early detection and new treatments could improve visual outcomes. Howard Larkin reports


Early screening has been shown to reduce amblyopia prevalence by 60% and residual amblyopia by 70% by the time children start school. Together with recent advances in theoretical understanding and new treatment options, emerging tools for detecting amblyopia and strabismus in preschool children may help further improve visual outcomes, Eileen Birch PhD said at the Association for Research in Vision and Ophthalmology 2021 Annual Meeting. Only about one-quarter of children are successfully screened for amblyopia at age three, as recommended by the American Academy of Pediatrics, said Dr Birch, who is a Senior Research Scientist and Director of the Pediatric Vision Laboratory at the Retina Foundation of the Southwest, Dallas, Texas, USA. High false positive rates are the major barrier, resulting in higher costs, parental anxiety and lack of confidence in results, and reducing the likelihood of referrals for eye care.
NEW DEVICES AND TREATMENTS
A recently developed retinal birefringence scanning device could help, Dr Birch said. The device scans in a circle centred on the fovea at 100Hz. If fixation on the central fovea holds steady, this produces a reflected signal doubling of 200Hz due to the regular birefringent nature of the tissues surrounding the central fovea. If fixation does not remain steady or is off
centre, due to amblyopia or some other ocular defect, there is little or no birefringence, so the reflected signal contains little or no 200Hz signal.








In a study involving 400 preschool children evaluating the device against blinded comprehensive eye examinations by a paediatric ophthalmologist, the device showed 97% sensitivity to detect amblyopia/strabismus, and 90% specificity to identify those with neither, Dr Birch said. (Jost et al. 2014, 2015) The device won FDA the PVS won FDA de novo clearance, with indications for screening young children for amblyopia and strabismus, as the blinq (Rebion) in 2016, she noted.
Dr Birch and colleagues are currently developing a device that measures visual acuity in preschool children with eye tracking. It features a stimulus on a screen that fades into the background if the child’s visual acuity is below age-normal. A camera records the child’s eye movement to detect when the shrinking dots are too small to be seen. The current device uses an iPad pro and clip on camera for maximum versatility.
“We are evaluating how accurate this approach is for screening preschool children,” she said.
Dr Birch also noted development of a device to monitor eye patch use that sticks to the inside of the patch to ensure accurate placement and comfort. Such monitoring may help improve adherence with patching and assessment of its effectiveness, which varies significantly.
Eileen Birch: ebirch@retinafoundation.orgWhat about my future?
OCULUS Myopia Master ®
For early myopia detection and management

Myopia in children and young people is increasing worldwide. Early detection and treatment can slow or stop the progression of myopia. The new Myopia Master® combines all important parameters for myopia management in a myopia analysis software.



New Procedures
QuigleyDoing new procedures is fun. I had observed this one many times, either watching through the assistant arm of the microscope, or looking at the screen in theatre. Recently, I had logged in for a webinar on the technical aspects of how to do it. Implanting a stent into the trabecular meshwork, as an adjunct to cataract surgery, seemed like a neat thing to do for patients with glaucoma. In theatre I practiced; after a stent had been implanted, I took the left-over injector, sliding back and forward the guard over the trocar, getting a feel for the grip and the injector button. And then finally, one afternoon there was a suitable patient.
Operating from the temporal side was a little awkward, compared to my default superior seat. The operating tables in the cataract unit have a bulky underside, so my left leg had to be stretched out straight and over to the side to reach the microscope pedal. My right knee was tucked tight against the table, a snug fit at best.
Doing new procedures is fun.
I had observed this one many times, either watching through the assistant arm of the microscope, or looking at the screen in theatre.
I started. My Consultant Barry Quill scrubbed, ready to swap in if necessary. Phaco finished and lens in, I injected a good fill of viscoelastic. Then the novel steps began. The circulating nurse started to turn the microscope, slowly angling it, and I tilted the patient's head. It seemed to take forever for the microscope to be turned to the right angle, and finally I took the goniolens, pressing just enough to coat its under-surface with the viscoelastic that sat in a blob on the cornea, not so hard as to indent or cause shallowing. Focusing down, the view into the angle sharpened, and its details emerged.
“That's a hypopigmented angle,” Mr Quill observed.
“Yes,” I hesitated, disappointed. What were the chances, on my first trabecular stent surgery?
Gonioscopy is a skill that takes time to learn. At the start, I found it difficult. Among all the different examination techniques that we had to master, in that steep early learning curve, it was tricky. One of my first Consultant trainers, Gerry Fahy, observed me having trouble. He advised me to buy my own gonio-lens,
his rationale being that I would be more likely to do gonio regularly for my patients if I had a lens to hand with me all the time. If I was going to stick with ophthalmology as a specialty, I might as well invest in my own lenses, he said. It worked out—I realised that the only way for me to become proficient at gonioscopy was to do it regularly—and with my own lens I never had the excuse to forgo it because there was no lens available in clinic.
After years of practice, I could judge angle depth, and pick up other signs. But that was not helping me right now. How was I supposed to implant a stent into a trabecular meshwork that was not pigmented, and was therefore pretty much invisible?
“You see that red line? That line is Schlemm's canal,' Mr Quill said. 'You can see that when the eye pressure has been a little lowered. That's your target.”
“Oh, perfect,” I sighed in relief. I could see the red band. It did not matter then that the angle was hypo-pigmented. I asked the scrub nurse to open the injector.
Not accustomed to operating under a gonio-lens, it took a moment for me to adjust my perception of angles and correct the trajectory of the injector. I pulled back the guard and exposed the trocar. Advancing right across the chamber, I gently indented the trabecular meshwork. Tip in position, apposed, but not too firmly, I pressed the button—the loud click was palpable—and wispy strands of blood refluxed into view, showing that the implant was in the right place. Conscious that I did not want to waste time and lose my clear view, while blood steadily swirled into the anterior chamber through that first stent, I swung the trocar a few clock hours away—click—the second stent was in.
During this case, and the other cases on the list, we had music playing. For some time, I have been having trouble getting my phone to connect to the cataract units Bluetooth speaker, so lately, instead of Spotify, I bring up a playlist on YouTube on the theatre PC. This is usually fine. Until I pick an innocuous sounding playlist, “easy 90s”, which starts promisingly. Then suddenly the theatre is filled with the noise of “Barbie Girl” by Aqua and I realise I've made a mistake. Mid-phaco I call out to the circulating nurse, and she moves quickly to the computer in the corner of the room, switching for “acoustic 90s”. I resolve to figure out how to get my phone connected to the theatre speaker.
Multipurpose Femtosecond Laser

Ziemer have announced their newest femtosecond laser, the FEMTO Z8 NEO, successor to the multipurpose femtosecond laser LDV Z8. Featuring a new laser source and monitoring system to optimise precision and reliability, the new laser enhances usability with a slim handpiece and improved docking system to ensure perfect eye fit for even the most challenging cases. New software provides more intuitive user guidance, improving workflow, and offers new surgical applications. “The new FEMTO Z8 NEO continues a long-standing Ziemer tradition of raising the bar for ourselves and the entire ophthalmic industry,” explains Frank Ziemer, CEO and President of Ziemer Ophthalmic Systems.

NEWS IN BRIEF
PRESBYOPIC IOLS
OPHTEC have introduced a new pair of presbyopia-correcting lens, the Precizon Toric and Precizon Presbyopic IOL. For the correction of presbyopia, the lenses have multiple-segment optics with patented Continuous Transitional Focus for a smooth transition between the far and near segments, delivering excellent intermediate vision. A Transitional Conic Toric optic makes the lenses tolerant of misalignment by calculating different conic constants not only on the horizontal and vertical axis, but also between 0 and 90 degrees.
SUBRETINAL INJECTOR APPROVED
MedOne have received 510(k) pre-market approval from the US Food and Drug Administration (FDA) for their MicroDose Injector. The device adapts vitrectomy console viscous fluid injection sets to use a 1mL syringe, enabling full surgeon control for administering subretinal injections with minimal fluid loss. It can be attached to the VFI tubing set from Constellation®, Stellaris®, and EVA® systems.
ALL-IN-ONE SURGERY PLATFORM
Oertli have launched the newest generation of OS 4, their retina, glaucoma, and cataract surgery platform. Two LED light sources increase power by 45% while an extended control range provides for more applications, as well as high-resolution contrast viewing. The integrated endo laser offers a fully automated user protection filter. A multifunctional pedal with over 100 setting options offers precise control according to each surgeon’s preference. The unique three-pump fluidics system maintains control in a wide range of surgical scenarios. “The Oertil OS 4 is the only platform worldwide which serves three ophthalmic key disciplines in one device,” said Thomas Bossard, co-owner, board member, and head of marketing and sales.
CELL THERAPY ALLIANCE
BlueRock Therapeutics, FUJIFILM Cellular Dynamics, and Opsis Therapeutics have entered into a strategic alliance to discover and develop off-the-shelf induced pluripotent stem (iPS) cell technologies for ocular diseases. “We believe deeply that authentic cells are the breakthrough approach needed to treat degenerative retinal diseases like AMD and IRDs,” said Emile Nuwaysir PhD, president and CEO of BlueRock, a wholly owned subsidiary of Bayer. “Bringing together the expertise of our partners with Opsis Therapeutics’ innovation in generating authentic iPS cell-derived human retinal cells, we have the potential to develop life-changing treatments for patients and their families,” said Nick Manusos, CEO of Opsis.

COVID Associated Mucormycosis
BLACK FUNGUS INFECTION—an epidemic during a pandemic in India. Dr Soosan Jacob reports from India
Asecond COVID-19 wave of unprecedented ferocity in India brought back COVIDrelated morbidity and mortality, lockdowns, and economic slowdown. Ophthalmology has gone back to emergency-only practice with a sudden cessation of the increased number of elective surgeries that were just beginning to happen.
The second wave also brought a new fear of a different type—mucormycosis (colloquially called “Black Fungus”), an angioinvasive, potentially lethal fungal infection. Much like the history of COVID and the Chinese ophthalmologist, Li Wenliang, health authorities realised cases of mucormycosis were surging following informal chats between ophthalmologists and ENT surgeons. Cases had increased from a few cases per year to, unexpectedly, many cases a month.
Mucor is a ubiquitous saprophytic fungus seen rarely in the past, mostly in uncontrolled diabetics, immunosuppressed, and post road accidents. There has been an explosion of COVID-associated mucormycosis (CAM) in India with close to 12,000 cases being reported over a period of few months creating an epidemic within a pandemic. The first wave showed a 2.1-fold increase in prevalence. Current predictions during the second wave stand at a 50-fold increase. Causes include uncontrolled diabetes, new onset COVID related diabetes, immunosuppressed state, excessive use of steroids, and other immunosuppressives such as tocilizumab as part of COVID therapy, altered iron metabolism in COVID-19 causing a hyperferritinemic state, and probably new COVID variants. The panic created by mucor caused other factors to also be proposed, rightly or wrongly, but without clear evidencecontamination of nasal oxygen, humidifiers, and tubes; exposure to soil and organic matter, and increased consumption of prophylactic zinc.
The common presentation, rhino-orbito-cerebral mucormycosis progresses rapidly from nose to sinuses, orbit, and finally intra-cranially. Increased suspicion, early diagnosis, and aggressive treatment are a must to avoid fatal consequences. Two recent meta-analysis on CAM from India showed between 39–49% mortality. Warning symptoms include nasal stuffiness, black or blood-tinged discharge, black crusting in nostrils, foul smell that progress on to eschars, facial oedema, numbness, pain, fever, and malaise.

Orbital invasion presents with pain, ptosis, proptosis, diplopia, restricted ocular motility, loss of vision, artery and vein occlusions, and V1, V2, IIIrd, IVth, and VIth nerve palsies indicating superior orbital fissure/orbital apex involvement. In the final stages, cribriform plate and/or cavernous sinus involvement progresses on to the skull base and diffuse/ multifocal CNS involvement.
Microbiological diagnosis from deep nasal swabs and nasal or orbital biopsy and contrast enhanced MRI/CT help in diagnosis. Management is multi-disciplinary involving the ophthalmologist, ENT surgeon, neurosurgeon, neurologist, infectious disease specialist, intensive care specialist, diabetologist, microbiologist, radiologist, etc.
Medical management is with systemic liposomal amphotericin-B, in the shortage of which, less expensive but also less effective and more toxic forms such as amphotericin-B deoxycholate and amphotericin-B lipid complex may be considered acceptable under close monitoring in patients with good renal function. Prolonged treatment for even up to six months is required.
The second wave also brought a new fear of a different type—mucormycosis (colloquially called “Black Fungus”), an angio-invasive, potentially lethal fungal infection.
Surgical management includes aggressive debridement until clean margins of paranasal sinuses. If required, surgical management can also include turbinectomy, palatal, and orbital medial wall resection with local amphotericin-B and orbital exenteration for advanced disease. Only supportive treatment may be possible with advanced CNS disease.
Prophylaxis includes avoiding risk factors, well controlled blood sugar, judicious usage of steroids as per well-defined protocols, close monitoring, and mask usage especially in areas with potential high contamination (such as construction sites). With fungal infections on the rise, COVID-associated Aspergillosis and Candidiasis should also not be forgotten.
Legend for figure: A-C: Rapid progression of CAM requiring extensive sinus and orbital surgery; D: Microbiological study showing Mucor on LPCB mount (Image courtesy Dr. Rita Hepsi Rani, MS, DNB, Tamil Nadu, India).
Dr Soosan Jacob is director and chief of Dr Agarwal's Refractive and Cornea Foundation at Dr. Agarwal's Eye Hospital, Chennai, India and, can be reached at dr_soosanj@hotmail.com.
↙
LAST CALL
JULY 2021
2021 ASCRS Annual Meeting

23 – 27 July
Las Vegas, Nevada, USA
https://annualmeeting.ascrs.org/
33rd APACRS SNEC 30th Anniversary Joint Meeting
30 – 31 July
Virtual Meeting
https://apacrs-snec2021.org
AUGUST
Virtual Congress on Global Controversies in Ophthalmology: Global (COPHy GLOBAL)
20 – 21 August
Virual Meeting
https://cophy-global.comtecmd.com/
SEPTEMBER
12th EuCornea Congress
25 September Virtual Meeting
https://www.eucornea.org/
EURETINA 2021 Virtual 9 – 12 September
Virtual Meeting
https://www.euretina.org/
OCTOBER
39th Congress of the ESCRS 8 – 11 October
Amsterdam, the Netherlands
https://www.escrs.org/
NOVEMBER
SFO Autumn E-Congress
6 November
Virtual Meeting
https://www.sfo.asso.fr/
AAO 2021: Re/Create
12 – 15 November
New Orleans, Louisiana USA
https://www.aao.org/annual-meeting
2021/2022 ESCRS Pioneer Awards
Support, encourage and fund individuals interested to start clinical research activities in the eld of cataract and refractive surgery
Introduce and develop a body of clinical research work, addressing a challenging “problem” in order to devise a practical “solution”
Facilitate and support an independent culture of study for the ultimate bene t of patients.
Announcement of 2021/2022 Pioneer Award
http://pioneeraward.escrs.org
THE LATEST PRESERVATIVE-FREE OPTIONS FOR
Dry Eye Relief
HP-Guar is a gelling agent increasing viscosity allowing protection of the ocular surface.4,6,7

HA acts as a lubricating agent in joint tissue and has been shown in preclinical studies to promote anti-inflammation and wound healing.3

Tailoring symptom relief for a patient with dry eye disease demands consideration of many factors, including the causes, manifestations, and severity of symptoms, as well as a patient’s lifestyle and individual preferences. Patients rely on their Eye Care Professional’s recommendations and require professional guidance to properly manage their dry eye symptoms with the right eye drops that targets their specific needs.
Of course, air quality and screen time contribute to dry eye symptoms such as irritation, burning, blurriness, and eye fatigue, while factors such as postmenopausal estrogen use and cataract surgery may play an increasing role in symptoms.1,2
Another key factor in symptom management is whether a patient needs periodic, fast symptom relief or long-lasting relief of more severe, chronic symptoms. Finally, some patients may prefer or require preservative-free options.
Alcon has been a leader in supporting Eye Care Professionals in managing dry eye symptoms through its growing family of SYSTANE® artificial tears. The latest members of this family are SYSTANE® ULTRA and SYSTANE® HYDRATION Lubricant Eye Drops — preservative-free formulations each provided in a multi-dose bottle. The patented bottle design has a oneway valve that avoids contamination.
Relief from dry eye that is wholly or mainly aqueous deficient calls for increased hydration and lubrication.3 In addition to polyethylene glycol (PEG) and propylene glycol (PG), which spread across and moisturize the damaged ocular surface,4 SYSTANE® ULTRA contains HP-guar a gelling agent, which covers the ocular surface by forming a structured polymer network, which lubricates the eye during blinking.5 This mechanism reduces the blinking friction.6,* As a result, it provides fast-acting protection for the aqueous-deficient dry eye.4,7
In addition to HP-guar, SYSTANE® HYDRATION contains Hyaluronic Acid (HA), resulting in a dual-polymer formula that provides longlasting hydration protection and relief for those suffering from moderate, chronic dry eye.4,6,8
As part of the full SYSTANE family of artificial tears, these formulations reflect the continual innovation you expect from Alcon products and enable you to customize dry eye relief to serve your patients’ individual needs and sustain their loyalty.
15(2017):802-812. 3. Jones L,
LE,
D, et
TFOS DEWS II management and
report. Ocul Surf. 2017;15:575-628. 4.
M, Christensen M,
AE. Efficacy in patients with dry eye after treatment with a new lubricant eye drop formulation. J Ocul Pharmacol Ther. 2010;26(4):347-353. 5.

C.L.
for treatment of dry eye. Adv Therapy 27, 681–690 (2010). 6. Rangarajan R, Kraybill B, Ogundele A, Ketelson H. Effects of a hyaluronic acid/hydroxypropyl guar artificial tear solution on protection, recovery, and lubricity in models of corneal epithelium. J. Ocul. Pharmacol. Ther. 2015;31(8):491-497. 7. Christensen MT, Martin AE, Bloomenstein M. A comparison of efficacy between Systane Ultra and Optive lubricant eye drops

ocular surface and
SYSTANE® ULTRA AND SYSTANE® HYDRATION LUBRICANT EYE DROPS, NOW IN CONVENIENT MULTI-DOSE PRESERVATIVE-FREE BOTTLES, EXPAND THE WAYS YOU CAN MEET THE NEEDS AND PREFERENCES OF YOUR DRY EYE PATIENTS. ©2021 Alcon
Downie
Korb
al.
therapy
Davitt, WF, Bloomenstein
Martin
Springs,
Novel hydroxypropyl-guar gellable lubricant eye drops
