TIPS FOR SECURING PHI WHEN USING LAPTOPS, PHONES, AND TABLETS 14
TRANSFORMATIONS: HOW ONE PROSTHETIST PREPARED A PATIENT FOR ‘SURVIVOR’ COMPETITION 26
O&P LEGISLATION: NEW AND PROPOSED BILLS IN INDIANA, NEW YORK, AND OHIO 40

TIPS FOR SECURING PHI WHEN USING LAPTOPS, PHONES, AND TABLETS 14
TRANSFORMATIONS: HOW ONE PROSTHETIST PREPARED A PATIENT FOR ‘SURVIVOR’ COMPETITION 26
O&P LEGISLATION: NEW AND PROPOSED BILLS IN INDIANA, NEW YORK, AND OHIO 40
While tech advancements abound, industry disruption may be many more years away

































































































































CUSTOM: FOOT ORTHOTICS • AFO’S • RICHIES
At Hersco, our first priority is to fabricate custom orthotics accurately and precisely. We have mastered the art of accepting scans and 3D printing to deliver better orthotics for your patients and the environment. 3D printing is not only environmentally friendly, but allows us to specify modifications that were not possible before.


 MICHAEL COLEMAN
MICHAEL COLEMAN
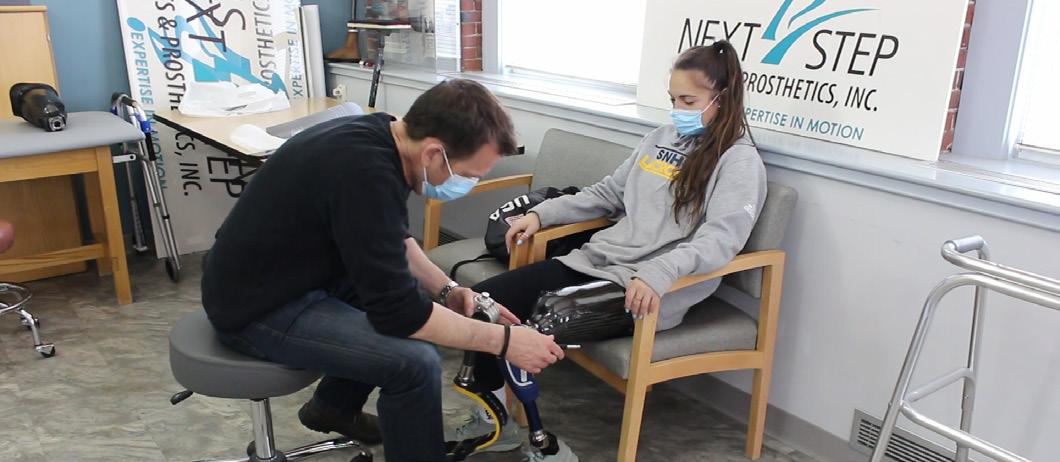
In the second installment of O&P Almanac’s new
column, we introduce you to Jason Lalla, CP. Lalla—clinical director of Next Step Bionics & Prosthetics and a former Paralympic athlete—played a key role in preparing Noelle Lambert for the challenges of participating in the “Survivor” reality TV show last fall.

Experience more with QUATTRO, scan now.

MORE INTUITIVE
MORE ADAPTABLE
Greetings to all! AOPA recognizes the critical impact research and outcomes have on practices and individuals living with limb loss and limb difference. This can be seen in various AOPA initiatives, including the creation and support of the Center for Orthotic and Prosthetic Learning and Outcomes/Evidence-Based Practice (COPL), the establishment of the Medical Advisory Board, and the support of legislation that drives money to orthotic and prosthetic research and institutions.
On Oct. 1, 2022, an exciting and important next step for how the profession supports research took place. Two organizations dedicated to improving O&P patient outcomes—COPL and the Orthotic and Prosthetic Education and Research Foundation (OPERF), managed by the American Academy of Orthotists and Prosthetists (AAOP)—merged into one entity under the name and management of The Orthotic and Prosthetic Foundation for Education and Research (The Foundation). AOPA worked in collaboration with AAOP to plan and execute this merger.
The Foundation’s vision is to achieve the highest quality of orthotic and prosthetic care through excellence in education and research. The mission is to advance the art and science of orthotic and prosthetic rehabilitation by:
• Enhancing clinical practices through professional training awards
• Promoting educational opportunities through academic scholarships
• Strengthening the body of knowledge through research grants and fellowships
• Inspiring excellence through the recognition of scholarly achievements.
The OPERF and COPL boards of directors went into The Foundation merger discussions in 2022 recognizing the value of their respective histories and missions. Under one unified research organization, the plan is to create synergies, reduce future O&P research redundancy, further the evolution toward a unified voice for the profession, and increase the value proposition to subscribers by enhancing and leveraging investments.
AOPA is in full support of The Foundation. AOPA Board Member and Research Director Shane Wurdeman, PhD, CPO, FAAOP(D), is currently serving as a co-chair of the transition board, along with Don Katz, MHA, CO, LO, FAAOP. Additionally, AOPA has allocated $40,000 to The Foundation in 2023.
I spoke with both Shane and Don, and here is what they asked me to relay:
Shane: “The purpose of research in healthcare is to advance the knowledge and future of patient care. If we as an industry are not advancing our research, then we are not in control of our future. The Foundation will catapult education and research forward to position all members of the O&P community to better serve our patients in the most effective and efficient manner.”
Don: “The establishment of this Foundation sets the stage for so many exciting opportunities. Not only do we see it as the perfect vehicle to support much needed research-grant funding for meritorious and clinically relevant investigations, O&P student scholarships, and other opportunities to increase awareness of so much that can be accomplished within our field, but also to enhance awareness of O&P to a much broader audience to support our mission.”
To learn more about The Foundation, please visit oandpfoundation.org. How can you get involved? You can spread the word, and you can support The Foundation. Please scan the QR code below.

The creation of The Foundation is a beautiful example of our O&P organizations strengthening connections and working together to make our O&P profession stronger. We look forward to continuing on this path through the year and into the future.
Very truly yours,
 Teri Kuffel, JD
Teri Kuffel, JD
Teri Kuffel, JD, is president of AOPA.
OFFICERS
President
Teri Kuffel, JD
Arise Orthotics & Prosthetics, Spring Lake Park, MN
President-Elect
Mitchell Dobson, CPO, FAAOP Hanger Clinic, Austin, TX
Vice President
Jeffrey M. Brandt, CPO Brandt Ventures, Exton, PA
Immediate Past President
Dave McGill Össur Americas, Foothill Ranch, CA
Treasurer
Rick Riley Bakersfield, CA
Executive Director/Secretary
Eve Lee, MBA, CAE AOPA, Alexandria, VA
Arlene Gillis, MEd, CP, LPO International Institute of Orthotics and Prosthetics, Tampa, FL
Elizabeth Ginzel, MHA, CPO Össur, Fort Worth, TX
Kimberly Hanson, CPRH Ottobock, Austin, TX
John “Mo” Kenney, CPO, FAAOP Kenney Orthopedics, Lexington, KY
James Kingsley Hanger Clinic, Oakbrook Terrace, IL
Lesleigh Sisson, CFo, CFm Prosthetic Center of Excellence, Las Vegas, NV

Linda Wise Fillauer Companies, Chattanooga, TN
Shane Wurdeman, MSPO, PhD, CP, FAAOP(D) Research Chair Hanger Clinic, Houston Medical Center, Houston, TX
A world where orthotic and prosthetic care transforms lives.

AOPA staff and volunteers are committed to our mission of being a trusted partner, advocating for and serving the orthotic and prosthetic community by:
• Fostering relationships with decision makers to ensure equitable access.
• Providing education that promotes professional excellence.
• Supporting research that informs innovative care.
• Advancing equality to strengthen the orthotic and prosthetic profession and improve the lives of patients.
A world where orthotic and prosthetic care transforms lives.
330 John Carlyle St., Ste. 200, Alexandria, VA 22314
AOPA Main Number: 571-431-0876 | AOPA Fax: 571-431-0899 | AOPAnet.org
Eve Lee, MBA, CAE, executive director, 571-431-0807, elee@AOPAnet.org
Akilah Williams, MBA, SHRM-CP, director of finance and strategic operations, 571-431-0819, awilliams@AOPAnet.org
Joe McTernan, director of health policy and advocacy, 571-431-0811, jmcternan@AOPAnet.org
Devon Bernard, assistant director of coding and reimbursement services, education, and programming, 571-431-0854, dbernard@AOPAnet.org
Sam Miller, manager, state and federal advocacy, 571-431-0814, smiller@AOPAnet.org
Susannah Engdahl, PhD, manager, health policy and research, 571-431-0843, sengdahl@AOPAnet.org
Tina Carlson, CMP, senior director, education and meetings, 571-431-0808, tcarlson@AOPAnet.org
Kelly O’Neill, CEM, senior manager of meetings and exhibition, 571-431-0852, kelly.oneill@AOPAnet.org
Kristen Bean, digital meetings specialist, 571-431-0876, kbean@AOPAnet.org
Joy Burwell, director of communications and membership, 571-431-0817, jburwell@AOPAnet.org
Betty Leppin, senior manager of member services, 571-431-0810, bleppin@AOPAnet.org
Nicole Ver Kuilen, manager of public engagement, 571-431-0836, nverkuilen@AOPAnet.org
AOPA Bookstore: 571-431-0876
Reimbursement/Coding: 571-431-0833, LCodeSearch.com
Eve Lee, MBA, CAE, executive director/publisher, 571-431-0807, elee@AOPAnet.org
Josephine Rossi, editor, 703-662-5828, jrossi@contentcommunicators.com
Catherine Marinoff, art director, 786-252-1667, catherine@marinoffdesign.com
Bob Heiman, director of sales, 856-520-9632, bob.rhmedia@comcast.net
Christine Umbrell, editorial/production associate and contributing writer, 703-662-5828, cumbrell@contentcommunicators.com
PUBLISHER EVE LEE, MBA, CAE
EDITORIAL MANAGEMENT CONTENT
COMMUNICATORS LLC
ADVERTISING SALES RH MEDIA LLC
DESIGN & PRODUCTION MARINOFF DESIGN LLC
PRINTING SHERIDAN
O&P Almanac (ISSN: 1061-4621) is published monthly, except for combined issues in June/July and November/ December, by the American Orthotic & Prosthetic Association, 330 John Carlyle St., Ste. 200, Alexandria, VA 22314. To subscribe, contact 571-431-0876, fax 571-431-0899, or email info@aopanet.org. Yearly subscription rates: $59 domestic, $99 foreign. All foreign subscriptions must be prepaid in U.S. currency, and payment should come from a U.S. affiliate bank. A $35 processing fee must be added for non-affiliate bank checks. O&P Almanac does not issue refunds. Periodical postage paid at Alexandria, VA, and additional mailing offices.
Postmaster: Send address changes to: O&P Almanac, 330 John Carlyle St., Ste. 200, Alexandria, VA 22314.
Copyright © 2023 American Orthotic and Prosthetic Association. All rights reserved. This publication may not be copied in part or in whole without written permission from the publisher. The opinions expressed by authors do not necessarily reflect the official views of AOPA, nor does the association necessarily endorse products shown in the O&P Almanac. The O&P Almanac is not responsible for returning any unsolicited materials. All letters, press releases, announcements, and articles submitted to the O&P Almanac may be edited for space and content. The magazine is meant to provide accurate, authoritative information about the subject matter covered. It is provided and disseminated with the understanding that the publisher is not engaged in rendering legal or other professional services. If legal advice and/or expert assistance is required, a competent professional should be consulted.
Engage the profession today. Reach AOPA’s membership with more than 10,694 subscribers. Contact Bob Heiman at 856-520-9632 or email bob.rhmedia@comcast.net
Learn more at bit.ly/23AlmanacMediaKit




The waterproof Terrain foot was created to achieve anatomical ankle motion and energy return in a low profile. College Park uses its tri-axial technology expertise in a new way. With a versatile and service-free design, the Terrain features a carbon fiber base and permanent bumpers inside the ankle housing for a progressive, comfortable response during low to high impact activities.




When adjusting the alignment of transtibial prostheses, adjustment of coronal alignment should be performed last, according to a study published January in Nature. A team of researchers from Japan, China, and the United States investigated the appropriate sequence of dynamic alignment adjustment, noting that data-driven information on this topic would be helpful to prosthetists.
The researchers studied 10 participants with unilateral transtibial amputation and compared the effects of various socket and foot alignment changes. Results indicated that only the alignment changes of the socket in the sagittal plane significantly increased the varus moment in the coronal plane. They also noted that alignment changes of the foot in the coronal and sagittal planes did not show significant changes in socket reaction moments in the out-of-plane trials.
Investigators concluded that “the appropriate sequence of adjusting the alignment of transtibial prostheses should be first in the transverse plane in static alignment (i.e., adjustment of toe-in/toe-out angles for standing symmetry), followed by dynamic alignment (i.e., adjustment of toe-in/toe-out angles for gait symmetry), then in the sagittal alignment in dynamic alignment procedure, and lastly in the coronal plane.” They suggested these findings be used as a clinical guideline for alignment processes in transtibial prostheses, and recommended further studies with a larger sample size.
Nearly half (43%) of working-age adults were inadequately insured in 2022. Forty-six percent skipped or delayed care due to cost, and 42% reported problems paying medical bills or medical debt
Researchers from Vrije University in Brussels conducted a systematic review of the therapeutic benefits of performing daily activities using three categories of lower-limb prostheses: passive, quasi-passive, and active. They analyzed 34 previously published studies involving more than 4,000 records of individuals with a unilateral transfemoral or transtibial amputation.
The research team, led by Elke Lathouwers, synthesized study participants’ characteristics, types of prostheses, intervention, outcome, and main results, and conducted a risk of bias assessment to compare therapeutic benefits of the three types of prostheses.
The Belgian researchers concluded that, compared to passive ankle-foot prostheses, quasi-passive and active prostheses “significantly enhance quality of life.” They recommend that further research be completed to investigate the long-term therapeutic benefits of different types of prostheses. The research was published January in Journal of Neuroengineering and Rehabilitation

Brain-computer interface (BCI) technologies, which leverage implanted brain sensors, are increasingly being integrated into prostheses to assist in restoring communication, mobility, and independence. A new study demonstrates that BCI is associated with a low rate of adverse events.
A BrainGate clinical trial, run by a collaborative of investigators from several institutions, including Massachusetts General Hospital (MGH), demonstrates that the safety of implanted sensors is similar to the safety of other chronologically implanted neurologic devices. The researchers examined data from 14 adults with quadriparesis from spinal cord injury, brainstem stroke, or ALS over the course of seven years. Subjects had undergone surgical implantation of one or two Utah microelectrode arrays in the section of their brains that control limb movement. Average duration of device implantation was 872 days, for a combined total of 12,203 days of study.
Among participants, 68 device-related adverse events occurred during the study period, with skin irritation around the percutaneous pedestal found to be the most common event. Six events were deemed “serious,” but there were no reports of safety events that required removal of the device, infections of the brain or nervous system, or events causing permanent increased disability.
“The BrainGate Neural Interface system has a safety record comparable to other chronically implanted medical devices,” reported the authors. “Given rapid recent advances in this technology and continued performance gains, these data suggest a favorable risk/benefit ratio in appropriately selected individuals to support ongoing research and development.” The study was published January in Neurology.

Several prosthetic measurement tools were identified by the Consensus Outcome Measures for Prosthetic and Amputation Services (COMPASS) Committee from the International Society of Prosthetics and Orthotics (ISPO) as “recommended” when treating individuals with lower-limb amputation. The COMPASS group, composed of 46 users, clinicians, managers, and policymakers, met and identified several recommendations for routine use in episodes of rehabilitation care, to be administered before and after treatment to measure change in functioning.
It was recommended that the ISPO COMPASS, or main outcome measurement protocol, include six measurement instruments: the Amputee Mobility Predictor, the Timed Up and Go, the Two-Minute Walk Test, the Prosthetic Evaluation Questionnaire— Residual Limb Health, the Prosthetic Evaluation Questionnaire—Utility, and the Trinity Amputation and Prosthesis Experience Scales—Revised.
The committee made several additional recommendations:
• The COMPASS+, composed of two additional tests—the
Comprehensive High-Level Activity Mobility Predictor and the Six-Minute Walk Test—should be leveraged for higher activity-level individuals.
• The COMPASS Adjunct comprises the Patient-Specific Function Scale; it is an option that can be added, due to the clinical utility and focus on patients defining their own goals.
• A generic health-related quality of life outcome measure instrument, such as the European Quality of Life-5D-5L or Patient-Reported Outcomes Measurement Information System-29, can be used to supplement the COMPASS.
• Outcomes measures should be identified or developed specifically for low- and middle-income countries, with a focus on activities such as sitting cross-legged, kneeling, squatting, and other culturally important mobility-related activities.
• Translation, validation, and open sharing of translated outcome measures included in the COMPASS, COMPASS+, and COMPASS Adjunct should occur.
The full COMPASS report was published January in Prosthetics and Orthotics International


The 2023 DMEPOS Medicare fee schedule has increased by 8.7% for 2023, the largest increase in several decades.
SOURCE: CMS


Team USA Hockey, the defending Paralympic gold medal-winning team, participated in the first-ever Hanger LIVE Sled Hockey Classic in January as part of Hanger Inc.’s annual conference. With this year’s conference theme of “ShiftMoveGo,” the hockey game served as an integral part of Hanger LIVE’s Opening Ceremony and was broadcast live Jan. 23.

“We are grateful for the opportunity to bring our players together for this unique teambuilding event,” said Dan Brennan, general manager of the U.S. National Sled Hockey Team. The team comprises 17 players, including medalists Josh Pauls and Declan Farmer, who helped the team win gold at the 2022 Paralympic Winter Games. Members of the U.S. Women’s and Men’s Development Sled Hockey Teams also participated in the game.

This year’s in-person Hanger LIVE event drew more than 1,000 Hanger employees and 370 exhibitors. Participants chose from 80 educational courses, including a popular presentation on improving health outcomes by Scott Wallace, JD, MBA, co-founder and managing director of the Value Institute for Health and Care at the University of Texas at Austin’s Dell Medical School, and a “Women in Leadership” workshop session led by motivational speaker Tia Banks.
The Amputee Coalition has launched a Youth Engagement Program (YEP) to support the estimated 25,000-70,000 people under 18 living with limb loss and limb difference. YEP will focus on providing year-round resources and creating a community for youth and teens ages 10 to 17.
“YEP will advance the organization’s youth outreach beyond the annual Youth Camp and find new ways to engage black youth and teens with limb loss or limb difference,” according to a press statement.

As part of the program, the Amputee Coaltion will launch an app will launch this year. Other benefits of YEP include resources and programming in life skills, education and training, youth camp, workforce development, and mentorship. “We wanted to take a holistic approach to support young people under 18, and to create a space where they can be who they are and feel a sense of belonging,” said Alicia Straughter, MD, vice president of human resources, diversity and inclusion, and YEP. “We are building this program for them as a place where they know they can feel comfortable. Our efforts are focused on building everything from the ground up around what they want and need, and with their involvement in the initial development.” Find details on the Amputee Coalition website
Hanger has awarded its 10th annual Partner Awards. The Rising Star, Collaboration, Innovation, and Operational Performance Partner Award winners were selected by members of Hanger’s clinical and operational teams, while the Clinicians’ Choice Award winner was chosen by Hanger clinicians.
• Trendline was awarded the Rising Star Award, which recognizes an emerging leader driving industry change.
• OssKin received the Collaboration Award, which is granted to a partner that made outstanding contributions resulting in shared success.
• Fillauer was honored with the Innovation Award, which recognizes a partner that has exhibited expansive thinking in product innovation and technology, resulting in positive clinical outcomes. Fillauer was selected for providing prosthetic feet that feature adjustable torsion and vertical shock reduction.
• Anclote received the Operational Performance Award, which is granted to a partner that outperformed industry benchmarks in quality, efficiency, and cost containment.
• Blatchford was honored with the Clinicians’ Choice Award, which recognizes an exceptional partner that went above and beyond to support Hanger clinicians and their patients. Blatchford was recognized for the third year in a row due to excellent customer service, supportive education efforts, postdelivery technical support, and always going above and beyond to help clinicians provide superior patient outcomes.
MORE YOUNG PEOPLE AT RISK OF DIABETES
As many as 220,000 young people in the United States under the age of 20 could have Type 2 diabetes in 2060, which would represent a nearly eight-fold increase. Type 1 diabetes cases could increase by as much as 65% in the next 40 years.






Hanger Inc. Chairman and Chief Executive Officer (CEO) Vinit Asar will retire from the role of CEO effective May 1. In line with a multiyear succession plan, Hanger’s chief operating officer (COO), Pete Stoy, has been named president and COO, and will assume the role of CEO upon Asar’s retirement, in addition to serving on Hanger’s Board of Directors. At that time, Asar’s role will transition to executive chairman of Hanger’s board, where he will assist with strategic initiatives, including mergers and acquisitions, and provide support for Stoy and the board.

“It has been my absolute honor to serve as Hanger’s CEO over the past 11 years,” said Asar. “Each day I have been fueled by the passion our team brings to fulfilling our shared purpose of empowering human potential together, and I’m eternally grateful for what we have achieved together throughout these years. After making the decision to retire, I have been able to put in place a succession plan over the past couple of years to ensure I leave Hanger in excellent hands. Pete’s background, style, and experiences have more than adequately prepared him to be a fabulous leader for Hanger, and I know the future is bright with Pete at the helm.”
Asar joined Hanger as executive vice president and chief growth officer in December 2008 and served as Hanger’s president and COO from September 2011 through May 2012 before becoming CEO. “Vinit has made an indelible impact on Hanger throughout his storied tenure,” said Stoy. “He will leave behind an impressive legacy that will continue to live as part of Hanger’s extensive history, and we applaud and thank him for his exceptional leadership.”
Stoy has more than 20 years of healthcare experience with leadership in large, complex organizations. Prior to joining Hanger in November 2020, Stoy served as East Region president for the healthcare business of Sodexo. Prior to that role, Stoy served in leadership positions at McKesson and Cardinal Health.

Cassandra “Cass” Isidro has joined the Amputee Coalition as CEO and president and is expected to advance the Amputee Coalition mission to support, educate, and advocate for people impacted by limb loss and limb difference.

Isidro is the former president and executive director of the Safe Routes Partnership, an organization focused on advancing policy and programs related to walking and biking in the community. She also previously worked with SHAPE America.
“I appreciate the warm welcome I have received from Amputee Coalition’s members and leaders. We have much to accomplish as we grow our reach and increase our services for all who are impacted by limb loss or limb difference,” said Isidro. “I look forward to connecting deeply and supporting a community that thrives.”

Isidro will lead the organization’s strategic direction, grow partnerships with key stakeholders, and increase funding opportunities. She will work closely with John Register, who has served as the acting CEO and president since June 2022 and will reassume his position on the Amputee Coalition Board of Directors. Register becomes the new board chair this month.
Jane Webster, MBA, has joined the Board of Certification/Accreditation (BOC) as vice president of strategy, growth, and regulatory affairs. Webster will develop strategic priorities for BOC’s next phase of growth and will oversee BOC’s business development and sales functions, as well as regulatory compliance operations to ensure the organization continues to fulfill its mission. She also will manage BOC’s contracted site surveyors and relationships with payors to ensure recognition of BOC credentials.
Webster joins BOC with decades of expertise in business strategy and implementation, product and operational planning, fiscal budget management, workforce optimization, and business analytics, most recently serving as managing director for Upward Associates. Her prior roles include serving as vice president of Erickson Advantage Health Plan Operations for Erickson Living and holding senior management roles at the Utilization Review Accreditation Commission and United States Pharmacopeia.
“Jane is a strong leader with experience in strategic planning and managing diverse departments with strong results,” said Judi Knott, MA, MBA, president and CEO of BOC. “We are pleased to welcome her to BOC’s leadership team and look forward to leveraging her professional experience and insights.”

quality orthotic, prosthetic, and pedorthic education and CE credits from the organization that knows O&P.Vinit Asar Pete Stoy Cassandra “Cass” Isidro
The Amputee Coalition has announced it will partner with the American Diabetes Association to support the Amputation Prevention Alliance (APA). The Amputee Coalition will collaborate with diverse stakeholders to reduce the number of “avoidable, diabetes-related amputations that take place every year in the United States.” Through policy change advocacy, raising awareness, and community empowerment, the Amputee Coalition, in cooperation with APA, will work to reduce the number of Americans who lose a limb due to diabetes complications each year.
“We applaud the American Diabetes Association for developing a meaningful alliance of organizations coming together to address this health crisis that is so disproportionately impacting communities of color,” said Ashlie White, chief programs officer of the Amputee Coalition. White will provide strategic vision, energy, leadership, and accountability for the program’s, strategies, plans, goals, and outcomes, with a focus on continual improvement and development to meet the needs of the limb loss and limb difference community.
BData, a healthcare data science company, is the new analytic partner to the National Quality Limb Loss & Preservation Registry, which collects universal data elements and links hospital, provider, and patient-reported O&P outcomes over time. “BData is excited to work with the vibrant community of individuals and organizations driving the Limb Loss & Preservation Registry,” said CEO Bart Phillips. “BData is looking forward to applying its healthcare data science capabilities and tools to maximize the value of the high-quality data being organized in the registry for the numerous stakeholders in this clinical space.” The company has built clinical data networks in adjacent clinical areas, including burn care.
PrimeFare Central in Tulsa meeting dates have been updated. The event will take place Friday and Saturday, Oct. 13-14, 2023.
CE credits accepted by certifying boards:


Under the Health Insurance Portability and Accountability Act (HIPAA) and the Breach Notification Rule, you are obligated to notify and report all breaches to Medicare. Breaches may include the access, use, and/or disclosure of unsecured protected health information (PHI) in a manner not permitted by HIPAA, which poses a significant risk of harm to the affected individual(s). How and when you must notify Medicare depends on the number of individuals affected by the breach.
If a breach affects fewer than 500 individuals, you must notify Medicare of the breach within 60 days of the end of the calendar year in which the breach was discovered. This means that any breaches involving fewer than 500 individuals that occurred and were discovered in 2022 must be reported to Medicare by March 1, 2023.
If a breach affects more than 500 individuals, you must notify Medicare immediately and without any unreasonable delay, but in no case later than 60 calendar days from the discovery of the breach. The notification must be completed electronically
via the breach portal on the website of the Department of Health & Human Services (HHS) Office of Civil Rights (OCR): ocrportal.hhs.gov/ocr/breach/wizard_breach.jsf
portal listed 876 separate incidents over a 24-month period.
With the yearly reporting deadline fast approaching, this month’s Reimbursement Page examines some of the more common reasons for breaches and provides tips to help you avoid them. The examples come from OCR, the entity in charge of enforcing HIPAA, in its publication, “Breach Portal: Notice to the Secretary of HHS Breach of Unsecured Protected Health Information.” This document offers a complete list of all breaches affecting 500 or more individuals. At the time this article was written, the
Thirty-four incidents in the OCR publication were listed as lost or stolen devices, and 19 of those indicated the lost or stolen item was a laptop or other portable/mobile device, such as a phone or tablet. This number is much lower than with previous breach portal listings; however, the issue of lost and stolen laptops and portable devices remains important, given the rise in the use of smartphones and tablets in the O&P fabrication/scanning process and in patient interactions.
HHS, through the Office of the National Coordinator of Health Information Technology, has created a list of 11 tips to help protect and secure PHI when using a portable device:
1. Use strong passwords and/or other forms of authentication to gain access to the device and to the files located on the device. It is suggested that your password comprise at least six characters. However, the longer it
Any breaches involving fewer than 500 individuals that occurred and were discovered in 2022 must be reported to Medicare by March 1, 2023.
is, the stronger it is—so consider using up to eight characters and include a combination of upper- and lowercase letters, numbers, and symbols. Also plan to change your passwords on a routine basis. Other forms of authentication to access your device include facial recognition and fingerprint recognition.
2. Install and enable some form of encryption software/apps or features on your devices. This means encrypting any data you store on your devices, as well as any information that you may send from your devices—for example, by using secured internet browsers or virtual private networks. If your devices don’t have encryption capabilities and you need to download and install software or apps, ensure they are from reputable vendors.
3. Be sure you have the ability to activate remote disabling and/or wiping. Remote disablement—a security feature that enables remote locking of data stored on a mobile device—and remote wiping—a security feature that enables remote erasure of the data—are helpful if your device is lost or stolen. Most current portable devices already include these features, but you must ensure the features are activated and being used.
4. Consider disabling, not installing, or limiting file sharing applications, as these can be a way for others to access your files without your knowledge.
5. Install and activate a firewall. Most devices and operating systems will come with some type of firewall, but you must be sure it has been activated and is being used.
6. Be sure you are using some type of security software.
7. In line with Tip 6, update your security software on a regular basis.
8. Before you download and use any new apps or programs, research them and understand how they work. For, example some apps may need to copy your files or access your contacts in order to work; this could jeopardize any PHI stored on your devices.
9. Maintain physical control of your devices. This is especially important for mobile/portable devices, including phones and tablets, as they can easily be misplaced. Some methods of maintaining control include securing the device when it is not in use (via a locker, secure room, or locking the screen) and making sure no one else can use it—for example, by following Tip 1. Also, don’t share
or allow others to use or access your tablet, phone, or laptop.
10. Take precautions when using Wi-Fi networks. Use only secured networks when transmitting PHI—do not use public Wi-Fi or unsecured hotspots to send or receive protected health information.
11. Finally, be sure to delete all stored PHI. This is particularly important when you are replacing or upgrading devices. It is suggested that you use some type of overwriting software rather than rely on the “delete” button, or empty your trash.
For more information on these tips and other suggestions about protecting and securing electronic health information, including how to conduct a complete and thorough risk analysis, visit healthit.gov
Of the 867 listed instances of breaches on the OCR website, 699 were self-reported as being related to hacking/IT issues, and the locations of these breaches were predominantly on network servers or in emails (639 out of the 699). As with using portable devices, healthit.gov has put together a list of tips to assist with cybersecurity.
To combat hacking issues, employ some of the same guidance given for protecting mobile devices: Use strong passwords and change passwords regularly; use firewalls and ensure all firewalls are
maintained, updated, and adequate for your needs; update your security software on a regular basis, and make sure it is capable of searching out the newest versions of malware and viruses; and ensure information is encrypted to a standard acceptable under HIPAA.

Note that encryption is not necessarily a HIPAA requirement; your data or other health information is not required to be encrypted as long as you have other safeguards in place. However, HIPAA regulations are clear that one of the only ways information is considered absolutely secured (unusable, unreadable, etc.) is if it is encrypted. So, if the health information you are using is encrypted, then you have a good level of protection—especially when it comes to possible breaches. Thus, you should make sure that your data is being encrypted during all phases of usage: transmission, rest, and storage.
It’s also important to implement training and protocols at your facility to promote a culture of security and compliance. Training doesn’t need to be too technical or intense but should focus on educating staff regarding potential threats and malicious software so they are able to identify and report these events. Also, make sure employees know which links and attachments are secure and valid, and understand what to do if they realize they have opened a link or attachment that should not have been opened.
In addition, ensure that employees practice proper computer habits, such as not installing games or software that is not needed for your daily operations, and ensuring that operating systems and necessary software, including antivirus and malware software, are updated regularly.
Finally, to prevent or limit the effects of hacking, talk to your IT department to verify that, at a bare minimum, the above steps are being taken. If you don’t have an IT department, consider contacting an IT consultant who is knowledgeable about HIPAA, and request an assessment of your vulnerabilities and risks. The OCR has some tools that can help you conduct your own risk assessments.
Improper disposal accounted for five of the 876 breaches listed on the OCR website. When disposing of records, ensure that the information is made unreadable/indecipherable and is unable to be reconstructed.
For paper files or records, this means instituting measures such as shredding or burning, or another means that ensures total destruction. Besides encryption, destruction is the only other way, under
HIPAA, to ensure that health information is considered secured.

For electronic records and files, proper disposal would include using software to overwrite the files or physically destroying the hard drive. This is especially important when disposing of old laptops, computers, thumb drives, or other external storage devices, but you should check other equipment as well. For example, if your copiers and scanners store copies, ensure these are erased on a regular basis, especially if you are leasing or renting the equipment.
Unauthorized access and/or disclosures accounted for 138 of the 867 breaches listed on the OCR website.
“Disclosures” are the means in which you communicate PHI to an outside entity and are normally allowed under HIPAA when necessary for daily operations— for example, emailing PHI to a physician for treatment, or to your billing company for billing. “Access” is the physical act of obtaining and looking at the PHI; under HIPAA, only certain people are allowed to access the data.
Some examples of unauthorized access or disclosures include the following:
• Not obtaining proper authorization to use patient videos or testimonials for your website or marketing materials
• Staff within your company looking at patients’ charts when they have no need to view the charts as part of their daily duties
• Not having or using business associate agreements (BAAs), when required.

It’s critical to ascertain that no one can access a patient’s medical records without proper authorization or approval, as directed by your policy and procedure manuals or under an employee’s job description and duties. If you use electronic health records, consider instituting tracking systems and/or clearance-level passwords to prevent unauthorized access. Also, be sure to review your current BAAs to make sure they are current and valid, and review your interactions with other individuals and companies to determine if you need a BAA.
These are just some examples of HIPAA breaches and compliance issues that have caused companies problems—and could cause problems for your facility. To view additional examples and tips, visit the OCR website and search under HIPAA Compliance and Enforcement, and then Case Examples. There, you may review sample case examples organized by topic. You also will find some current resolution agreements. If you review a case example or resolution agreement, or the issues addressed above, and you identify a similar issue within your organization, be sure to address the issue and, if necessary, update your training practices and procedures.
Implementing a strong and reliable training program, maintaining proof that all staff have received proper training, and demonstrating that you are doing your due diligence can drastically reduce your risk of a breach—and possibly lessen the fine if a breach does occur.



















Practitioners trust us most because we know your business and we know insurance unlike any other program.

































O&P technology continues to make breathtaking advancements: Clinicians who once wrapped body parts in plaster to make molds, now assess limb shapes and take measurements with smartphones. Highly trained technicians use computers and 3D printers to individually tailor highly precise prostheses made of carbon fiber and advanced plastics, with quality and consistency fabricators deemed impossible even a decade ago. Biomechanical engineers are devising technology that allows the brain to send signals to artificial limbs, creating a futuristic frontier previously
f New technologies abound in O&P facilities and manufacturing firms, but it can be a long road from the research lab to the marketplace.
f For most high-tech manufacturers, the path to successful commercialization includes developing a new product, completing several rounds of prototypes, and generating quality data.
imagined in science fiction, while computer scientists are developing digital tools for collecting information so that research and patient care decisions can be based on reliable pools of data.
“The industry is now leaning more on the science and less on the art,” says Jonathan Naft, CPO, and a mechanical engineer who founded Comb O&P, a 3D scanning company, and Geauga Rehabilitation Engineering, an advanced O&P equipment manufacturer, both in the Cleveland area.

But as new O&P technologies develop, it can be a long road from the research lab to the marketplace.
f Some facilities are reluctant to test new processes or test new devices unless they anticipate the benefits will be clear and significant.
f Two of the biggest challenges in adopting the latest and greatest technology are a lack of new billing codes from CMS and convincing payors to reimburse for new devices.
f Some O&P innovators believe that research can be leveraged to help convince payors that spending on technology is warranted.
True disruption requires diligence, hard work, and plenty of patienceJonathan Naft, CPO
Prostheses tricked out with microprocessors, high-powered batteries, and other cutting-edge accessories cost more, raising reimbursement and coding challenges for clinicians and innovators hoping to penetrate the marketplace. However, these digitally crafted devices also tend to fit patients better, in many cases helping them to lead more active and fulfilling lives.
While the technology is exciting, the “cutting edge” poses perils for O&P clinic owners who naively jump in without understanding the complexities and frustrations of introducing disruptive technology into an established practice. Meanwhile, some of the brightest minds emerging from elite science and engineering schools are eager to bring exciting ideas for improving O&P devices to the marketplace, but the path is beset by a lack of investment and job opportunities.
Experts in O&P innovation are excited about the possibilities as new technologies develop but caution that early adoption, especially in the relatively small O&P sector of the healthcare industry, requires patience, diligence, and hard work. The chal lenges mean true disruption of the industry has not fully materialized and could be many more years in the making.
Mark Ford, founder and CEO of Ohio-based Catdaddy Consulting Services, has worked the O&P industry from multiple angles, having run clinical practices, directed sales for a prosthetic manufacturer, and served as chief business developer and president of the OPIE Choice Network. Today, Ford connects technology companies that have developed new O&P products with universities, the Department of Defense (DOD), and the Veterans Administration (VA), which provide seed funding for commercialization and pay for expensive clinical trials. Ford also works with distributors and clinic owners on data analytics, process improvements, and strategy planning. His work often reveals reticence by many to adopt advanced technology.
“The average O&P practice is a busy place, and taking the time to learn a new process and change an exist ing process that [owners and clinicians] believe is good and effective takes time and effort,” Ford says. “The practice really has to be convinced that this is going to be a signifi cant change for them, and not a small change. If it’s just a
small change, it becomes a more difficult question as to whether it’s worth their time and effort to do it.”
Naft agrees but notes that practice owners and clinicians who embrace the technology and accept the expense and challenge of learning about it are rewarded with time to see more patients—often many more—in a day because they are no longer involved with fabrication.
“Today, the field has really shifted more toward technicians, and now practitioners are able to be in rooms all day seeing patients one after the other,” Naft explains. “It’s a really big difference.”
Many O&P clinic owners and manufacturers might be slow to welcome the latest technology, but universities and government institutions are helping to generate momentum. A 25-year veteran of the O&P industry, Ford estimates that the number of universities involved in O&P research has tripled over the past decade. And the VA has established O&P-specific research centers that didn’t exist 25 years ago. Today, VA’s Prosthetics and Sensory Aids Service is the largest and most comprehensive provider of prosthetic devices and sensory aids in the world.
As most O&P professionals know, two of the biggest challenges in adopting the latest and greatest technology are a lack of new billing codes for specific technologies from CMS, and convincing payors to reimburse for expensive new devices.



CMS is reportedly working to improve the reimbursement process by making it more transparent, offering the ability for practitioners to submit coding applications more frequently, and providing more feedback. But the challenges and frustrations remain, especially when the request involves expensive new devices.

“CMS will tell you all day long, they love new technology,” Ford says.
“But the system they’ve created to evaluate new technology and to potentially create new coding for new technology doesn’t support that theory.”
“The average O&P practice is a busy place, and taking the time to learn a new process and change an existing process that [owners and clinicians] believe is good and effective takes time and effort.”
Mark Ford



Josh Caputo, PhD, a Carnegie Mellon-educated mechanical engineer, is using research to help convince payors that spending on technology is warranted. He has created a new paradigm for assistive device technologies at Humotech, a Pittsburgh company he spun off from his research at CMU’s Experimental Biomechatronics Laboratory. Today, Caputo’s company develops robotic prostheses and exoskeletons and provides a platform for clinical trials in wearable robotics that aims to convince CMS and payors of their real-world benefits. Humotech has established 20 research centers across the United States, Canada, and Europe, working primarily with DOD and VA to conduct O&P research that recruits patients to test various devices and componentry.
want to contribute and innovate in this space. “There’s just not the level of investment from the commercial, and the financial end, to support that.”
Aman Haque, PhD, a mechanical engineering professor at Penn State University, launched Impulse Technology in 2017 with his business partner, Kamrun Nahar, PhD, a research faculty member in the university’s engineering science and mechanics department. During their spare time after hours teaching college students, the duo devised a six-degree-of-freedom ankle prosthesis that can be mounted on most commercially available prosthetic feet. The Goralign ankle “extends” the range of dynamic alignment performed by a prosthetist. The device is innovative but somewhat unusual in today’s O&P space because it doesn’t rely on microprocessors or batteries. It also sells for $1,500 to $2,500, compared to similar electrical devices that can cost anywhere from $10,000 to $45,000.
“My vision is to see a shift in how products, codes, and reimbursement develop, so we can consider the efficacy of the products handin-hand with the reimbursement of those products,” Caputo says. For most high-tech manufacturers, the road to successful commercialization includes developing a new product, several rounds of prototypes to bring it to market, and then generating enough quality data for CMS to justify adequate reimbursements.
“This takes years and years and years, and if the government decides they don’t want to pay for your product, or not the amount that you think it’s worth, it can be ruinous for the technology,” Caputo explains. “With a platform like ours, you can begin to assess how well the product is going to impact function, and, you can also assess what that improvement in function might be worth.”

Caputo says these daunting hurdles no doubt discourage investment in the next new thing, as well as bright minds from entering the field. He is deeply enmeshed in the O&P research-to-technology pipeline, and says promising young graduate students frequently approach him about careers in O&P. “I deal with a deluge of eager undergraduate students who want to get into this field, and they’re wondering where the jobs are,” he says. “I have to tell them I don’t see a lot of job openings” for technologists who
Haque and Nahar have been collaborating with Ability Prosthetics and Orthotics to run clinical trials and test the marketplace, and have attended conferences such as the AOPA National Assembly to showcase their product. But Haque says navigating the cutthroat business world isn’t easy. “We’re doing all the necessary steps, but commercialization is a new skill we’re learning,” he says. “If it doesn’t go well, you have to grind it out; you must believe in yourself and start at the grassroots level, talk to as many practitioners at as many clinics as you can. And slowly, you kind of get confidence from all these practitioners and all your customers, and gradually make it to the market and you get some credibility.”
Patience is key. “If it takes some time to win the appreciation of actual end users, clinics, and practitioners, so be it,” Haque says. “If you create a value for your customers, it may take some time, but they will come.”

Many innovators in the O&P space aren’t necessarily looking for a big payoff—they’re looking to help improve lives with technology they devised. If they can do both, all the better. But altruism is often

“My vision is to see a shift in how products, codes, and reimbursement develop, so we can consider the efficacy of the products hand-in-hand with the reimbursement of those products.”Josh Caputo, PhD






the guiding principle. “We wish to create a difference; we wish to impact people’s lives,” Haque explains.
Inventors and investors who are looking for a payoff must be highly exacting and strategic as they seek venture capital and success in the marketplace. First versions of new products often aren’t the best versions. A new company on a tight budget must work as hard as possible to get it right the first or second time, or they may not have enough money to get to the third time. That’s because big O&P manufacturers rarely acquire early-stage companies; they usually want them selling at least $3 to $5 million a year before they’ll even look at them, Ford says. They also spend a lot of money on internal research and product development but don’t make it public until it’s ready for the marketplace, which poses challenges for startups looking to enhance those companies’ offerings.
“It doesn’t happen in a year for a new young technology company,” Ford explains. “That’s usually a five- to seven-year journey. That’s the challenge— having the funds to get far enough that it’s something that legitimately the big boys will look at.”
Ralph Nobbe, CPO, is a second-generation practitioner whose father raised him in the business. Until a few years ago, Nobbe ran a practice with 23 employees and a registered nurse on staff and became proficient in several generations of advanced technologies, including early C-leg fittings, functional electrical stimulation, drop foot stimulators, and pain management through stimulation. He watched the business evolve from relying on paper charts in the office to entirely electronic records. Nobbe sold his practice in May 2019 but maintains a small consulting practice.
Nobbe predicts that practitioners will increasingly specialize in specific, highly specialized technologies—for example, upper extremity. He likens the experience of adopting expensive and complicated new technology to purchasing a Ferrari.
“A Ferrari is an awesome car, but it is not a daily driver,” Nobbe says. “And if you’re going to have a Ferrari with that kind of technology, you also need to have the support infrastructure to maintain it [and] keep it operational, as well as the programming to optimize the utilization of it.”

Jeff Brandt, CPO, an industry veteran and former Ottobock executive now in private consulting, says it’s important not to underestimate the emergence of highly advanced data in the development of technologies and the clinical evaluation of patient progress.


“For me, data is innovation,” Brandt says, citing the National Quality Limb Loss & Preservation Registry unveiled at the AOPA National Assembly in September. The registry allows practitioners to submit and access data about patient prognosis and progress based on what types of care and devices they receive. O&P research shows that patients who can measure their progress against others with similar physical challenges tend to be more motivated and change behaviors based on that information.
“In a few years [when the registry is more populated with data], we’re going to be able to look back and say, ‘Hey, this person’s been in a really advanced knee for three years,’ and look at other metrics around their life, and assess their highs and lows,” Brandt says.
A former clinician, Naft is an inventor who developed and commercialized the innovative MyoPro arm brace that helps patients with partially paralyzed or weakened arms carry out everyday tasks more easily. He says certain types of high-tech devices are finding exceptional success with patients and commercial vendors: Lower-extremity exoskeletons are now manufactured by more than 30 companies, and prostheses with microprocessors that can control the artificial limbs are commonplace. Meanwhile, batteries are steadily becoming more advanced, allowing for greater longevity of use before these devices need to be recharged.
“When battery technology gets better, they get lighter, stronger, and smaller, and then we can put them in [O&P] devices, which power these motors throughout the day,” Naft explains, predicting that the next five to 10 years will see the industry adopting even more bionics and devices implanted inside the body. Crossing this technological threshold can be daunting, especially for some older practitioners and late adopters.
Naft predicts the entire industry will eventually embrace today’s most advanced technology—and profit from it—but, at least for now, patients are the ones benefiting most.
“Streamlining the way that devices work and fit their bodies allows patients to manage their average day much more efficiently,” he says. “When the [devices] fit better, the patients wear them more and have a better outcome. On a good day, a good month, a good quarter, we really can point to the impact that we have on patients. And that’s really satisfying.”
“In a few years [when the registry is more populated with data], we’re going to be able to look back and say, ‘Hey, this person’s been in a really advanced knee for three years,’ and look at other metrics around their life, and assess their highs and lows.”Jeff Brandt, CPO Ralph Nobbe, CPO
100% dynamic AFO
No skin contact
Symmetrical design that fits left and right shoes
Conforms to eneven grounds and slopes
Lace clip technology that allows fast installation from shoe to shoe












Included lace clips
Warranty on plastic and\or carbon fiber par ts
insurance coverage such as VA, Medicare and MedicAid
HCPCS PDAC approved
Turbomedusa.com
2 years
3 years
See through design that is almost invisible when worn

25% lighter**
18% more dorsi-flexion power**
35% more medio-lateral strength**
2 years
Designed for patients with reduced dexterit y and hand mobility such as stroke patients
Unique front suppor t design
Easy rear entry thanks to revolutionary frontal design
Magnetized velcro strap is easily attached with one hand




25% more medio-lateral stability**

New for 2023, O&P Almanac debuts the Transformations column. Each month, you will meet an O&P clinician who will share the success story of one inspiring or challenging patient. This month, we speak with Jason Lalla, CP, who helped prepare Noelle Lambert to compete on “Survivor ”

If you’re a fan of the “Survivor” reality TV series, you probably remember the dramatic come-from-behind moment from Season 43 in November: Noelle Lambert, a 25-year-old with above-knee limb loss, won an obstacle course reward challenge—after falling far behind all of the other contestants during the balance beam portion of the course.
From his TV, Jason Lalla, CP, Lambert’s prosthetist of several years, watched her complete the difficult task of navigating a balance beam while wearing a running blade. “Her everyday foot would have been better than her blade,” he notes, “but she was not able to switch prostheses during the challenge.”
Lambert spent several extra minutes
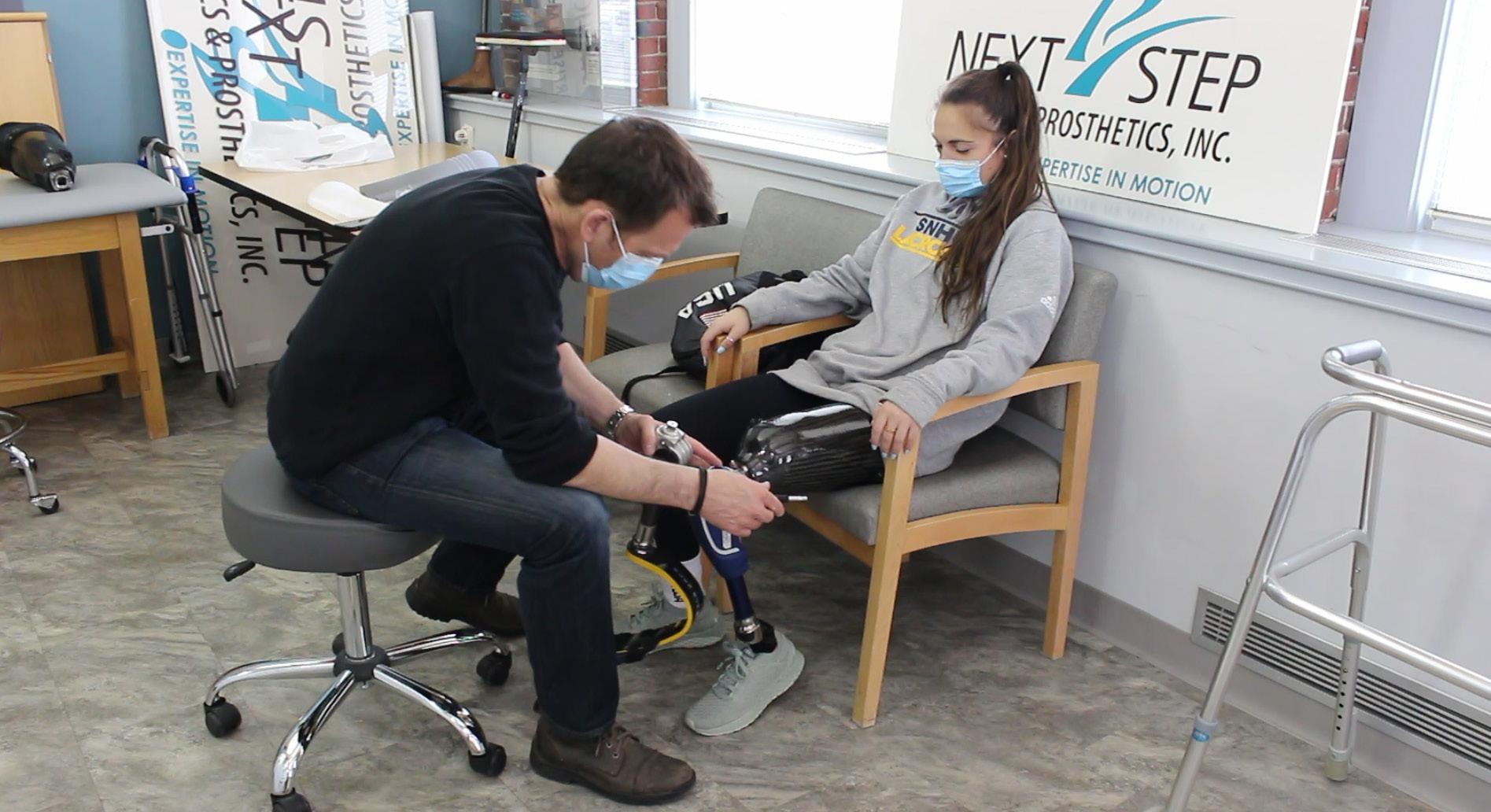
trying to get across the beam, falling many times and becoming very emotional— but she never stopped trying. She finally changed tactics and successfully crossed the beam by hopping on one leg. She was in last place when, in the final portion of the obstacle course, she threw a sandbag to land perfectly flat on top of a raised platform—and won the challenge.
Lalla, who is clinical director of Next Step Bionics & Prosthetics and works at the Manchester, New Hampshire, location, has been Lambert’s prosthetist since she lost her left leg above the knee in a moped accident in 2016. He helped her return to full mobility, which includes playing Division 1 lacrosse and participating in the Paralympic Games. But preparing Lambert to take part in the grueling reality show—where she would live on a sandy beach next to an ocean, undergo rapid weight loss due to lack of food, and test her athletic abilities in extreme heat—was perhaps Lalla’s biggest challenge yet.
Lalla first met Lambert six years ago, soon after her traumatic amputation. She had just completed her first year of college at UMass-Lowell, where she had been the leading scorer on the women’s lacrosse

team, when a moped she was driving was hit by a dump truck during a summer trip to Martha’s Vineyard.
An avid athlete himself, Lalla was a great match as a prosthetist for Lambert. He also is an above-knee amputee, having lost his leg in an eerily similar way to Lambert— in a motorcycle accident when he was 18 years old. After his amputation, Lalla went on to participate in two Paralympic Games, winning a gold medal in men’s giant slalom in 1998, a silver in men’s giant slalom in 2002, and a bronze in men’s downhill in 2002. He continues to participate in multiple sports in his free time.
“When I first asked Noelle what her goals were, she said she wanted to play lacrosse” again, Lalla recalls. “I’ve played lacrosse, my son plays, and I coach lacrosse, so I understand what’s involved.” He was confident he could help her return to running, but the quick stops and cuts required of the sport would be challenging. “I had doubts about whether she would return as a collegiate player.”
Lambert worked hard on her recovery, determined to return to competitive play. “She got up and walking at the start of her sophomore year of college, then progressed to running,” Lalla says. She was fit with an Össur Cheetah knee and Flex-Run foot; at
first, she was out of shape, and her running was labored. However, her dedication to rehab and physical therapy paid off. “During Noelle’s initial rehabilitation, I would attend some of her outpatient physical therapy appointments,” recalls Lalla, who spent many hours ensuring Lambert’s rehab went smoothly. “Sometimes, it was just passing a lacrosse ball around, watching and assessing how she moved and how her alignment may affect how the prosthesis performed for her in an outdoor, nonclinical environment. It was incredible to see how hard she worked.”
After a year of close work with Lalla and a team of physical therapists, Lambert returned to play lacrosse both her junior and senior years. “She even scored a goal in her first game back—that was a moment of joy and accomplishment,” says Lalla.
Once Lambert graduated, she dreamt of competing in track-and-field in the 2020 Paralympic Games. Lalla was happy to help her prepare, although her prosthetic needs had changed. At that point, Lambert was wearing a skin-fit suction socket and a Cheetah foot, but Lalla had to adjust her alignment to run straight in a full sprint.

He spent hours at a local track evaluating her gait pattern and making adjustments in that environment—”which is quite different than working at your office,” Lalla says. He also reached out to other clinicians to have them assess and evaluate her running videos. “I’m not opposed to being told that I could do better, or that I missed something,” he explains. “I think it just promotes the best clinical outcome, and that is what is important.”
Lalla accompanied Lambert to her first track meet, the Desert Challenge in Arizona, “because she was traveling without a coach or any type of support,” he recalls. He wanted to ensure that if Lambert had any issues with her prosthesis, she wouldn’t be stranded without options.
All of the hard work from both Lambert and Lalla paid off: Despite the fact that the Desert Challenge was the first time Lambert ever heard a training pistol, she beat the top U.S. above-knee female sprinter. She joined the U.S. Paralympic team, found a training partner, and proceeded to break the U.S. record in the 100-meter run during the qualifying event. She traveled to Tokyo in 2021 and placed fourth in 100-meter event at the 2020 Paralympic Games.
After the Paralympics, Lambert was invited to participate in “Survivor ” She had a few months to get ready for the competition, which would take place in Fiji May 2-27, 2022, in advance of the fall TV premiere date. She immediately turned to Lalla for assistance in preparing her prostheses— and herself—for the arduous competition.
Normally, Lambert wears a microprocessor knee—but because that component
requires an electric charger and there’s no power on the island, she wouldn’t be able to bring that device. In addition, “we knew she would not be eating the same and would lose weight,” explains Lalla. “And we knew she would be exposed to the elements,” including mud, sand, and ocean water. These factors would make Lambert’s experience on the show, as an individual with limb loss, particularly challenging.
Before joining “Survivor,” Lambert was using a skin-fit suction socket, “but it was not very adjustable,” says Lalla. “We needed to make sure the socket would still fit” if Lambert lost 10 or more pounds on the island. “For an above-knee amputee, there are a lot of different ways” to adjust for weight loss, says Lalla, “but I didn’t want to pile on too many socks,” given the mud and sand that could get stuck in between layers. “I didn’t think a Boa system would be reliable in sand and water,” he adds. Lalla suggested that Lambert wear a belt with her socket to make sure it wouldn’t fall off— but Lambert refused this option for aesthetic reasons. “So, we switched to a seal-in liner,” equipped with Velcro compression straps that she could use to tighten her socket and

hopefully would reduce chafing. They also stocked up on thin gel socks to add circumference, if needed.
In lieu of her microprocessor, Lalla fit Lambert with a waterproof Ottobock hydraulic knee, coupled with an Össur ProFlex XC foot that is rated to be waterproof. Lambert also brought her running prosthesis, which is “technically not waterproof—but she risked exposure to the elements” to leverage the component for challenges.
Fortunately, Lambert would have access to a cleaning kit, replacement valves, and extra sealing rings, so she would be able to make some self-adjustments. With her devices in tow, Lambert set off for Fiji.
Lalla tuned into his TV every Wednesday night last fall, rooting for his patient as she competed on “Survivor,” and hoping her prosthetic equipment would serve her well. He was thrilled—but not surprised— to learn that she made it 19 out of the 26 days. She was voted out during episode 10, but not before she made many friends and admirers.
Lambert’s prosthetic equipment held up well, even in the elements. Her “disadvantage” on the reality show wasn’t that she was a prosthesis user, but that she was likable and inspirational, as well as a fierce competitor. The other contestants believed that if Lambert made it to the “Final Three,” no one could beat her in the last vote.
Lalla believes that when Lambert won the balance beam challenge, she “sealed her fate” on the show. “The other competitors realized she has unbelievable determination and is very popular,” he says. She was voted off at the next Tribal Council—but went home proud of her public accomplishment, and grateful to promote the Born To Run Foundation she founded to provide prostheses to children with limb loss to help them run again.
Back in the U.S., Lambert called Next Step Bionics and Prosthetics right away to make adjustments to her everyday prosthesis since she had lost so much weight. Lambert’s participation in the difficult reality series is “inspiring,” Lalla says. As an amputee himself, Lalla recognizes the important role prosthetists play in helping patients achieve their goals. “Aside from their family,

the prosthetist is one of the most important people in the amputee’s life,” he explains. “If a prosthesis doesn’t fit, it can affect their mood, their work, and their livelihood.”
Lalla’s intervention helped propel Lambert to the national spotlight. When the series aired, Lalla helped host a viewing party, to which several Born To Run grant recipients were invited. Lambert may not have won the $1 million prize, but she has motivated a new generation of children with limb loss, says Lalla. Seeing Lambert compete on “Survivor ” “It gives kids who have lost a limb hope,” he says, “and it opens up their world to the possibilities.”

Next up for Lambert, hopefully, is snowboarding at the 2024 Paralympic Games, and Lalla will be there to prepare and support her on the new journey. “When Noelle decided to pursue snowboarding, I went out on the hill with her to once again evaluate her stance and alignment to ensure the prosthesis was set up properly,”
says Lalla. “Years of evaluating video as a Paralympic skier really has helped in picking up nuances during normal ambulation and sport-related activity. Besides, having the ski hill as the office every now and then isn’t a bad thing!”

Lalla reiterates the importance of prosthetists and other healthcare professionals in returning athletes to competition. As a former Paralympic athlete, he recognizes “the fact that I did not achieve those successes on my own,” he says. “I thoroughly enjoy giving back, and watching someone succeed through determination and hard work is inspiring.” He has even helped coach other up-andcoming Paralympic athletes who were not his patients. “Sometimes that was because of the demographics of where they lived, and other times it was because their disability did not require a prosthetist’s intervention. Either way, I still gained a lot of satisfaction in feeling like I was able to give back in a similar way to those who helped me out when I was in that position.
“As prosthetists, we don’t get reimbursed for [patient care],” says Lalla, who notes that going above-and-beyond is standard procedure for some O&P clinicians. “We form relationships with our patients, and they become more than a name, or a limb, or a claim,” he says. “Sometimes, they become family, and friends, and inspirations to work harder and do better. Sometimes you do things, not because you are getting paid to do it, but because it is the right thing to do.
“Noelle’s journey has been an absolute joy to watch and be a part of,” Lalla adds. “And now she is doing the same by giving back with her Born To Run foundation. I think she is just getting started!”
DO YOU HAVE A TRANSFORMATIVE PATIENT-CARE EXPERIENCE YOU’D LIKE TO SHARE WITH O&P ALMANAC READERS? Contact Editor Josephine Rossi, jrossi@contentcommunicators.com, with your story to be considered for an upcoming profile.

Examination rooms at Great Steps Orthotics & Prosthetics feature patient-friendly themes, including a Disney-themed room, an entertainer-themed room, and a garage-themed room.



HISTORY: 22 years
After beginning his career as an orthotist in a small facility in Fargo, North Dakota, John Held, CO, decided he wanted a new challenge and joined a facility in Minnesota that was part of a large, national group. He spent three years there, then sought an even more ambitious venture: launching his own O&P practice. In August 2000, he opened the doors to Great Steps Orthotics & Prosthetics, and he’s spent more than 22 years leading the facility.
“I’m very independently minded, and I like to make my own decisions,” he says. “At the same time, I didn’t want to stay a very small facility because I appreciate the resources a large company can bring to patient care. We’ve hit the sweet spot at Great Steps, where we are small enough to be responsive and make quick decisions, but large enough to provide the services our patients need.”
Great Steps staffs 11 clinicians, 11 administrative staff members, and six technicians. Kristie Held, John’s wife, transferred her experience in manufacturing administration to healthcare to oversee billing and scheduling functions, working with a staff operations manager.
The facility occupies a two-story building that was constructed to order in 2006; the main floor houses 10,000 square feet, with the second floor dedicated to a few offices and storage space. In addition, the company rents space in hospitals, physical therapy practices, and local clinics to provide services throughout the surrounding rural area. Each practitioner normally devotes a day each week to outreach.
The practice provides upper- and lower-extremity orthoses and prostheses. In addition, Great Steps is one of the few facilities still offering a diabetic shoe program, and also specializes in cranial remolding helmets, according to Held. Practitioners work with many athletes, including professional Minnesota sports teams.
The community also is home to many Somali immigrants, who bring their own set of challenges to the practice. “We see folks who had poor healthcare to begin with, some with bomb injuries, and even an injury from a donkey kick,” says Held.
The facility fabricates roughly 95 percent of devices in house, although it outsources carbon orthoses,
custom thoracic lumbosacral orthoses, CROW boots, and leather and metal components. Staff members leverage some new technologies, including a three-spindle CNC milling machine with podiatric software and 3D scanning for cranial orthoses.
Held notes that practitioners have no financial quotas, allowing them to focus on patient care and the patient experience. “Our clinicians can treat patients as they see fit, rather than having to put them in a standard ‘box,’” he says. That approach, as well as a proactive administrative process that gets a head start on paperwork before the clinician ever sees the patient, enables the practice to get to patient delivery more quickly, according to Held.
Another feature that differentiates the facility is its décor. Each patient room has its own theme, including a Disney playhouse room, a sports room, a parlor, a beach room, and a dog room. “Our décor is very family oriented and homey; it’s not a medical environment,” he says.

One of the practice’s notable patient stories is that of Eve, who lost her fingertips and both legs below the knee in 2019 due to complications from lupus. Eve’s situation was challenging to her prosthetist: She experienced chronic pain and fatigue and significant lower-limb muscles weakness, as well as volume fluctuations in her residual limbs. Her prosthetist persevered, and Eve worked with a personal trainer at the Anytime Fitness gym in her community. To help meet Eve’s increasingly ambitious fitness goals, the prosthetist used Harmony elevated vacuum pumps to manage the residual limb volume and incorporated vertical shock and torsion units to reduce shear forces and her susceptibility to chronic joint pain. She wears a dynamic response foot to accommodate her improved functional level, and an adjustable heel height foot allows Eve to wear shoes from her vast and beloved collection. In December 2021, Anytime Fitness selected Eve as one of the year’s most inspirational members.
“Great Steps continues to manage Eve’s prosthetic care,” says Held. “We are excited to see where she’ll go next!”
Minnesota facility is small enough to be responsive, yet large enough to provide a range of services


When Samantha Payne first met Joel Gibbard, a robotics engineer who had just finished two years of research in prosthetics, she knew their interests would align.


“I was focused on technology that would improve lives,” she says. “Prosthetics was a natural fit.”
Gibbard and Payne set out to develop a more accessible multifunction prosthetic arm. The result was the Hero Arm, a lightweight, multigrip prosthesis that, Payne says, is an extremely affordable advanced prosthetic arm. The hand has six separate grips, including fist, hook, pinch, and tripod, as well as a manually posable thumb and wrist.
“We did a huge amount of research among upperextremity amputees, and we found that the vast majority had abandoned their devices. Some found their prostheses too heavy or too limited in their functionality, while others had a [poorly] fitting socket,” Payne says. “Many amputees hated the way their prostheses looked. They didn’t like cosmetic arms, which made them feel not brilliant about their own bodies. They wanted more futuristic and personal designs.”
The Hero Arm was the first to have a 3D-printed socket, and it features a ventilated liner that is soft and flexible. User feedback led to changes in the socket liner that offer improved donning and doffing for people with bulbous residual limbs, better ventilation, better suspension, and more surface contact.
Payne notes the hand is extremely lightweight. “We also have the smallest hand available,” says Payne, “so it’s suitable for children. Our youngest user is 7 years old; the oldest are in their 70s,” she says.

Open Bionics spent five years within the limb loss community testing and refining its designs. Key to the Hero Arm’s success is that patients are central to the process, and they play a major role in customizing the look of the arm. The company has partnered with Disney, Marvel, Lucasfilm, and others to offer pop-culture prosthetic covers as well as a wide range of other designs and bold colors. Covers are magnetically attached, allowing users to change their style as they please.
The Hero Arm was designed and is manufactured in Bristol, England, but the company, now with nearly
50 employees, is expanding its presence in the United States with a home base in Denver. Open Bionics has a patient-care clinic there, in addition to working with prosthetists and medical systems in every state.
The company has a strong relationship with Shriners Hospitals for Children. “We work closely with prosthetists and get a lot of feedback from them,” says Payne. “If they are unfamiliar with our product, our folks are available on video or in person to work with them one-on-one.”
Based on feedback from the limb loss community, Open Bionics continued its research and development efforts and devised a new arm with Bluetooth capabilities. “Normally, patients have to go to the clinic to customize the settings, but now users can get feedback and advice, and then use their smartphone to change the setup,” says Payne.
The company welcomes technological advances, and Payne expects 3D printing and scanning to become even more important in the O&P industry. “We also know that the industry has to develop more best practice standards and report on standardized outcomes. Data collection and analysis will play a huge role in that,” she notes. “Companies are investing in automating parts of the design process so that we can enable lower price points and bring assistive technology to more people around the world.”
Open Bionics recently hired a fundraising manager, Sara Locke, to help provide assistance to families who don’t have insurance. “Her full-time job is to help families afford their devices,” explains Payne. “She’ll do press, fundraising events—whatever it takes to help them pay for services at whatever clinic they choose.”
Looking ahead, Open Bionics plans to strengthen its presence in the United States. The company is looking at a range of assistive devices and expects to add to its offerings, with several new projects in the pipeline. As with the Hero Arm, the goal is to create greater functionality and maximum affordability, to improve the lives of individuals with limb loss.
Deborah Conn is a contributing writer to O&P Almanac. Reach her at deborahconn@verizon.net
It’s given that the AFO should fit and follow the shape of the leg and fit and adapt well to the shoe, for a comfortable wear for each individual. But fit should also mean a good dynamic function for the individual, and
We offer different models for different needs of support and stability. Our 25 years experience and development of composite AFO confirms the necessity of variety to meet and fulfill the need from patients in the best possible way, not only one way!
for control, safety and comfort. Within each model we offer 4-5 different sizes (XS-XL) to match different foot sizes and heights of users. All sizes have

especially of the important footplate. (Both build height and footplate length can also be adjusted, 1-1.5 cm).

2023
Mark Your Calendar!
Submit Your Proposal by March 31
Share your knowledge and expertise with attendees at the 2023 National Assembly in Indianapolis in September! Submit your proposal to the appropriate Workgroup: Clinical Education, Business Education, Postmastectomy Education, Technical, Technical Tips and Tricks, or Digital O&P Care. Visit the AOPA website for details, and plan to submit your proposal before the March 31 deadline.
SAVE THE DATE
SEPTEMBER 6-9
Mark your 2023 calendar now and start making plans to travel to Indianapolis September 6-9 for the 106th AOPA National Assembly! Visit AOPAassembly.org
Stay up to speed on all of the rules and regulations for 2023— join AOPA’s regulatory staff and guest speakers for the 2023 monthly webinar series. Webinars provide relevant content and the opportunity to earn 1.5 continuing education credits each month. They are a great way to promote team building, providing an opportunity for your staff to come together and refresh their skills. One registration provides access for five staff members at your office location. (Contact Kristen Bean at kbean@AOPAnet.org to register more than one person from your facility—maximum of five per facility.)
New this year, and in response to feedback on preferred ways to access the webinars, all 2023 webinars will be available on demand (asynchronous) instead of live. Topics will be announced at the beginning of the month, and the webinars will be automatically delivered to AOPAversity accounts by the end of the month—then remain available. The popular Clinician’s Corner session will be featured in several webinars.
The January topic—Standard Documentation Policy Article Review—is now available.
The February topic—Urban Myths—will be available soon.
The full-year series is $790 for AOPA members—a great value at 12 for the price of 10! Nonmembers may purchase the series for $1,999. Individual webinars may be purchased at $79 for AOPA members and $199 for nonmembers.
Register for the series at My AOPA Connection. You also may register for just the January webinar or just the February webinar
Note that AOPA experts and guest speakers will be available to answer questions should they arise after you view the webinar. Contact AOPA’s experts with suggested webinar topics or questions: Email jmcternan@aopanet.org or dbernard@aopanet.org
Certificate in O&P Business Management
AOPA will offer several elective courses in 2023 for credit in the Certificate in O&P Business Management, brought to you by AOPA and the University of Hartford.
March 22, Noon – 2 p.m. ET
Join Chris Doerger, PT, CP, March 22 for a new online elective in AOPA’s Certificate in O&P Business Management Program. Doerger, who is senior manager, education strategy and development, at Ottobock’s Professional and Clinical Services, will offer an in-depth discussion on proper clinical documentation and evaluation.

Brought to you by AOPA and the University of Hartford, the Certificate
in O&P Business Management is a comprehensive certificate program that offers a series of business and management courses to provide business owners, managers, and practitioners of O&P patient-care facilities, O&P manufacturers, and distributors an opportunity to explore crucial business challenges—from finance, sales, and marketing to business operations, reimbursement policies, and management. Visit the AOPA website for details and register for courses on My AOPA Connection














Next Step
Prosthetics
2826 Randolph Road Charlotte, NC 28211-1386 980-215-9600



nextstepcharlotte.com






Scott Schall, CP Patient-Care Facility
Total Care Orthotics & Prosthetics LLC


6565 S. Yale, Ste. 909 Kelly Medical Bldg. Tulsa, OK 74136 918-502-5975







totalcareop.com















John Brestovansky, CO, CPed Patient-Care Facility
The officers and directors of the American Orthotic & Prosthetic Association (AOPA) are pleased to present these applicants for membership. Each company will become an official member of AOPA if, within 30 days of publication, no objections are made regarding the company’s ability to meet the qualifications and requirements of membership.
The O&P PAC Update provides information on the activities of the O&P PAC, including the names of individuals who have made recent donations to the O&P PAC and the names of candidates the O&P PAC has recently supported. The O&P PAC recently received donations from the following AOPA member*:





George Breece
The purpose of the O&P PAC is to advocate for legislative or political interests at the federal level that have an impact on the orthotic and prosthetic community. The O&P PAC achieves this goal by working closely with members of the House and Senate and other officials running for office to educate them about the issues, and help elect those individuals who support the orthotic and prosthetic community.
* To participate in, support, and receive additional information about the O&P PAC, federal law mandates that eligible individuals must first sign an authorization form, which may be completed online: bit.ly/aopapac




Now offering more Allard AFOs with half the heel height. All 2 ½ models include choice of wrap-around or D-Ring straps, shorter wings, and a Starter SoftKIT ™ included. It is easier to adapt ToeOFF® 2 ½ and BlueROCKER® 2 ½ to shoes with lower heel heights because there is a lower forefoot curvature and more space in the shoe toe box. ToeOFF® 2 ½ Addition models available in camouflage, birch, and black. Call 888-678-6548 or email info@allardusa.com to receive your free Product Selection Guide.


ALPS® Superior Performance Liner, made with either GripGel or HD Gel, features a black fabric with limited vertical stretch to improve control and stability of the prosthetic leg by reducing pistoning. The GripGel version combines softness, strength, and cushioning to deliver the greatest possible protection to the residual limb, making it beneficial for users with low to medium activity levels. The HD Gel version minimizes the movement of soft tissue and provides a high level of control of the prosthetic leg, resulting in a comfortable and durable liner that can keep up with your most active patients.

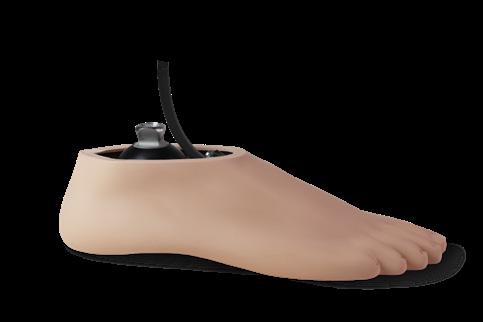
To learn more about the Superior Performance Liner, visit easyliner.com or call 727-528-8566 or 800-574-5426.
Spinner, Expandable Wall, Dynamic Socket System

• Expandable wall up to 3/8-inch
• Dynamic socket system
• Variable pressure application
• Enhanced skeletal stability
• Fine tune socket fit
• Socket suspension mechanism
• Easy fabrication
• Laminated or thermoplastic
• Waterproof
• AK, BK, and Upper Extremity
• L code L5630 (BK) or L5653 (AK).
For more information, contact BlackFin Biomechatronics LLC at 970-440-3244 or visit blackfinmt.com
Low-impact patients deserve lightweight, high-function products that enhance comfort for daily life. The new Celsus iVT offers efficient, integrated vacuum technology designed to reduce limb volume fluctuation and pistoning, as well as improve symmetrical gait. Users can achieve up to 20 inHg in fewer steps!* The Celsus iVT also features Intelliweave® composites for energy return, strength, and flexibility. If you’re seeking vacuum benefits with a higher weight limit, check out the Tempo iVT! Visit college-park.com

Newly designed children’s foot orthotics feature a semirigid extended heel cup in UCBL style for extra ankle control and support. The orthotic is covered with an antimicrobial fabric top liner for effective moisture and odor control. They come in W width and sizes starting at T4-T13, Y1-Y6. Retail packaging and all sizes are in stock for immediate delivery. For free display samples, call 888-937-2747. Wholesale accounts only.


• Costs less than carbon fiber
• Little to no itch
• Tougher than carbon fiber.
Coyote Composite is a natural fiber made of Basalt Braid (lava rock), a nontoxic and noncarcinogenic alternative to carbon fiber. Contact Coyote at 208-429-0026 or visit coyote.us
Light Weight
Durable
Rigid
The Cyclone™ Bike Foot was designed without compromising durability and to minimize foot weight. While pedaling, the Cyclone™ gives unmatched energy transfer. The short foot length design increases pedal stroke efficiency. The innovative design eliminates energy lost to weight caused by a foot shell and shoe. It also eliminates energy loss to deflection caused by the flex in a shoe and foot shell. The adjustable pyramid allows the foot to be either a right or a left. The cleat bracket can be used with two or three hole cleats.
Contact Coyote at 208-429-0026 or visit coyote.us

ESP created the Flexi family of suspension sleeves as a comfortable, durable, and cost-effective alternative to traditional suspension sleeves. Preflexed at 43 degrees for maximum comfort and natural unrestricted movement.

For more information, call ESP LLC at 888-932-7377 or visit wearesp.com
Hersco is delighted to offer HP’s advanced 3D-printing technology for custom orthotics. 3D printing has unique design capabilities not possible with other methods—reducing landfill waste by 90%! The accuracy of 3D is unparalleled, specs exceed direct-milled polypro, and manual plaster fabrication. Among the benefits: a 90% reduction in landfill waste, many new design possibilities for posting, and the ability to vary thickness and flexibility across the shell. The PA-11 polymer is a biobased renewable material that has been tested and proven in research and industry.

Call today, 800-301-8275, for a free sample.
It’s all about function. We are the manufacturers of durable prosthetic devices specifically for finger and partial-hand amputations. Our aim is to positively impact our wearers’ lives by providing high-quality finger prostheses. We offer four devices: MCPDriver (shown in rose gold), PIPDriver, ThumbDriver, and our newest device, the GripLock Finger. Our devices help to restore length, pinch, grasp, stability, and protection for sensitive residuum. Robust device engineering and their ability to withstand harsh environments help get people back to performing activities of daily living, and back to work. All are available in a dozen color coatings to match our wearers’ preferences and styles. To learn more, visit npdevices.com
Unique Liners from Ottobock are highly customized, so you can achieve innovative fitting results. The silicone Skeo Unique custom liner is recommended when high stability and durability are required. This liner:
• Is appropriate for very conical or scarred residual limbs
• Stabilizes residual limbs, even those with significant soft tissue
• Skin-friendly silicone enables a superior connection with the residual limb
• Easy handling, easy cleaning.
Utilize the new Ottobock EasyScanner or the free Custom4U iPad app with a Structure scanner to digitally capture the limb. STL files from any scanner can be uploaded into our iFab Customer Center (iCC) for easy digital ordering without shipping casts.
Learn more at shop.ottobock.us
Unique Liners from Ottobock are highly customized, so you can achieve innovative fitting results. The urethane Uneo Unique custom liner achieves an exact and comfortable fit thanks to the extraordinary flow characteristics. Other qualities include:

• Polyurethane gel to cushion highly sensitive or scarred residual limbs
• Good pressure distribution within the socket
• Comfortable impact absorption
• Skinguard antibacterial or fresh scent options available.
Utilize the new Ottobock EasyScanner or the free Custom4U iPad app with a Structure scanner to digitally capture the limb. STL files from any scanner can be uploaded into our iFab Customer Center (iCC) for easy digital ordering without shipping casts.

Learn more at shop.ottobock.us


The RUSH ROGUE 2 provides an optimal vertical shock experience, axial rotation for improved comfort, predictable performance, ultimate fiberglass strength, and flexibility for daily life and highimpact activities.
And now, patients will no longer have to choose performance over sandal toe availability. With the RUSH ROGUE2 & EVAQ8 models, patients can choose optimal performance with the freedom to express themselves in their preferred daily footwear. Walk Your Way with RUSH Sandal Toe by PROTEOR. Visit Proteor.com


Turbomed has extended its line of AFOs to include 3 models: Xtern Classic, Summit and Frontier. The Xterns will allow running, walking and even hiking as long and far as you want without discomfort. Their unique design acts as an exoskeleton to the impaired limb, keeps the foot at 90 degrees and provides the user with unparalleled levels of function.
The Xtern Summit is lighter than the Classic, has more dorsi-flexion power, and features a see-through design. The Xtern Frontier was designed for patients with reduced hand dexterity and requiring front leg support. Visit turbomedusa.com, and think outside the shoe!
ProComp® Carbon-Infused Polypropylene Composite Composite Material Science = Improved Fabrication Processing = Enhanced Clinical Performance. ProComp® is produced in a high-pressure laminating process that infuses discontinuous carbon fiber into homopolymer propylene. The patented prepreg composite sheeting is compatible with standard drape-encapsulation or bubble vacuum thermoforming. Finishing techniques are standard. Four standard gauges are available for both orthotic and prosthetic applications. Eligible for double L2755 application in thermoplastic AFOs and appropriate prosthetic addition codes. For more information, visit fabwithprocomp.com. Contact Gary G. Bedard, CO, FAAOP(D), managing principal, Rhode 401 LLC, at 650-773-3730 or email garyb@fabwithprocomp.com

“I designed this composite to allow you to transition from plastic to composite thermoforming.”
GARY G. BEDARD, CO, FAAOP(D)
Contact Bob Heiman at bob.rhmedia@comcast.net
March 1–31
ABC: Application Deadlines, Exams Dates, O&P Conferences, and More! Check out ABC’s Calendar of Events at ABCop.org/calendar for the latest dates and event details, so you can plan ahead and be in the know. Questions? Contact us at info@abcop.org or visit ABCop.org/contact-us
March 22
Certificate in O&P Business Management—Clinical Documentation and Evaluation. Virtual, Noon – 2 p.m. ET. Register on My AOPA Connection

March 31
Deadline to Submit Proposal for AOPA National Assembly. Visit aopanet.org/2023-national-assembly
March 31–April 1

Ohio Chapter AAOP Meeting. Hyatt Regency Columbus, Columbus, OH. Visit ohaaop.attendease.com
April 13–15
Georgia Society of Orthotists & Prosthetists Annual Meeting. The Hotel at Avalon, Alpharetta, GA. Visit georgiaop.attendease.com
April 24–27
ISPO World Congress. Guadalajara, Mexico. Visit ispo-congress.com/en
May 5–6
Tennessee Society of Orthotics & Prosthetics Meeting. Nashville. Visit tennsop.org

May 10–11
AOPA Policy Forum. Washington Marriott Capitol Hill, Washington, DC. Visit aopanet.org
May 12
Kentucky Orthotic & Prosthetic Association Meeting. Castle & Key Distillery. Frankfort, KY. Visit kyopa.net
May 17–19
New York Chapter AAOP Annual Meeting. The Rivers Casino & Resort, Schenectady, NY. Visit nysaaop.com
Orthotic & Prosthetic Innovative Technologies Minneapolis. For updates, check our cme@gilletteto be added to conference mailing list.
June 23–24
PrimeFare East. Nashville Renaissance Hotel and Conference Center. In-Person Meeting. Contact Cathie Pruitt at 901-359-3936, pruittprimecare@gmail.com; or Jane Edwards at 901-487-6770, jledwards88@att.net. For more information, visit primecareop.com
July 27–29
Alabama Prosthetic & Orthotic Association Meeting. Birmingham, AL. Visit alabamapoa.org

August 24–26
Texas Society of Orthotic & Prosthetic Professionals Meeting. San Antonio. Visit txsop.org.

November 8–10
New Jersey AAOP Annual Meeting. Harran’s Resort, Atlantic City, NJ. Visit njaaop.org


September 6–9
AOPA National Assembly. Indianapolis. For more information, visit aopanet.org
AOPA Monthly Webinar Series— Now On Demand!
January: Standard Documentation Policy Article Review

February: Urban Myths
Full-year series: AOPA member $790; Nonmember $1,999
Individual webinar: AOPA member $79: Nonmember $199 Register for the series at My AOPA Connection
Advertise O&P events for maximum exposure with O&P Almanac Contact Bob Heiman at bob@rhmedia.comcast.net or learn more at bit.ly/23AlmanacMediaKit. Announcement and payment may also be sent to O&P Almanac, Calendar, P.O. Box 34711, Alexandria, VA 223340711 or emailed to jburwell@AOPAnet.org along with VISA or MasterCard number, cardholder name, and expiration date. Make checks payable in U.S. currency to AOPA. Note: AOPA reserves the right to edit calendar listings for space and style considerations.
If you are interested in participating in the AOPA State Reps network, email smiller@AOPAnet.org
Each month, State By State features news from O&P professionals about the most important state and local issues affecting their businesses and the patients they serve. This section includes information about medical policy updates, fee schedule adjustments, state association announcements, and more. These reports are accurate at press time, but constantly evolve. For up-to-date information about what is happening in your state, visit the Co-OP at AOPAnet.org/resources/co-op.
Indiana House Bill 1018, introduced Jan. 9, removes medical equipment and supplies from the list of items or services for which Medicaid may seek competitive bids; specifies that traditional Medicaid, managed care organizations, subcontractors, and third-party administrators must reimburse durable medical equipment, complex rehabilitation technology, and supplies at a rate that is at least 100% of the rate in specified fee schedules; and requires Medicaid to develop and implement a tool to assist in the determination of capped rental payments for certain items. To read the full text of the bill, visit the Indiana page of the AOPA Co-OP.
New York Assembly Bill 00337, introduced Jan. 4, directs the chair of the New York Workers’ Compensation Board to create a committee to establish the state’s workers’ compensation fee schedule. The committee must comprise the president of the Medical Society of the State of New York, the president of the New York State Osteopathic Medical Society, the president of the New York State Society of Orthopedists, the president of the New York State AFL-CIO, the president of the Business Council of the State of New York, an individual designated by the Senate majority leader, an individual designated by the speaker of the Assembly, and the chair of the board.
Previously, the chair established the fee schedule with the help of reports submitted
by the president of the Medical Society of the State of New York and the president of the New York State Osteopathic Medical Society, along with the input of other interested parties. To read the full text of the bill, visit the New York page of the AOPA Co-OP.
The Ohio Occupational Therapy, Physical Therapy, and Athletic Trainers Board has approved regulations establishing a confidential, nondisciplinary program for the evaluation and treatment of eligible practitioners who need assistance with a potential or existing impairment due to substance abuse, medical condition, or illness, known as the board’s “safe haven” program. Services provided by this program include screening and evaluation, referral to treatment providers, individualized monitoring, and case management.
Ohio Senate Bill 131, which passed into law in December, amends Sections 4779.17 and 4779.18 of the Ohio Revised Code to allow the Occupational Therapy, Physical Therapy, and Athletic Trainers Board to issue full or temporary O&P licenses if an
applicant holds a license from another state or has satisfactory experience or certification in a state that does not have licensure. Previously, applicants with out-of-state certification were unable to receive a full license under Section 4779.17, and applicants with either an out-of-state license or out-of-state certification were unable to receive a temporary license under Section 4779.18.
For the full texts of both policy developments, visit the Ohio page of the AOPA Co-OP.
The Pennsylvania Independent Regulatory Review Commission has approved new regulations related to orthotic fitter trainee requirements. Specifically, this regulation increases the time period during which an individual may practice as an orthotic fitter trainee under a temporary practice permit, identifies circumstances when an individual may apply for a second temporary practice permit, requires that an orthotic fitter trainee complete 1,000 hours of training, and allows for board approval of other entry-level education programs specific to orthotic fitting. To learn more about these regulations, visit the Pennsylvania page of the AOPA Co-OP.
For more information on these and other state developments, visit the AOPA Co-OP or contact Sam Miller at smiller@AOPAnet.org
So Kids Can Move is a new policy and advocacy initiative working to expand access to prostheses and orthoses utilized for physical activity as medically necessary healthcare for children and youth on a state-by-state basis. It is the result of a collaboration between AOPA, the National Association for the Advancement of Orthotics and Prosthetics, the Amputee Coalition, and the American Academy of Orthotists and Prosthetists.
To learn more or inquire about bringing the initiative to your state, contact Sam Miller, AOPA state and federal advocacy manager, at smiller@AOPAnet.org

• Basic business acumen

• Practical knowledge to apply immediately to your work
• Techniques for developing better business practices


• How to think about improving your company’s returns



To complete the certificate program, you must register and complete one core course and one elective course from each of the four areas of learning within a four-year period
LEARNING CORE ELECTIVES
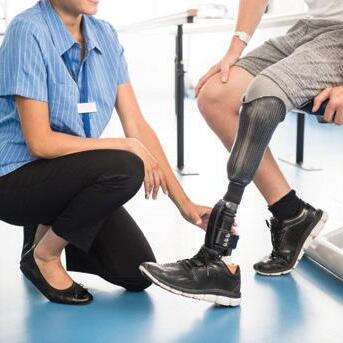
O&P
MANAGEMENT Increase
knowledge and skills to better manage multiple, individual, and team priorities.
HEALTHCARE SALES AND MARKETING Learn the functions of marketing along with a variety of tools and approaches to personal selling along with the many digital marketing tools available. 5
concepts and perspectives
Since the introduction of C-Leg and its groundbreaking control technology, Ottobock has never stopped inventing new ways to take your patients as far as they want to go. With a portfolio including the Kenevo, Genium, X3, and now the latest iteration of C-Leg 4, every microprocessor knee supports a journey toward a limitless future.





22
The Kenevo is designed specifically for users with mobility limitations who need a high level of stability. State-of-the-art technology allows users to feel safer and more independent in their everyday life.
An IP 22 rating protects from dripping water or dust.
67
The C-Leg 4 provides exceptional reliability and dynamically adapts to a wide variety of everyday situations. The legacy lives on with the new C-Leg 4 Update with over 10 new features including supported descent on ramps and stairs. The C-Leg 4 is easier and more intuitive than ever before.
An IP 67 rating provides protection from damage due to casual contact or temporary submersion in fresh water up to 1 meter for 30 minutes.
67

The Genium provides the highest degree of intuitive function to individuals who need to adapt to changing environments, move quickly over short distances, or require more than 2 days of battery life.
An IP 67 rating provides protection from damage due to casual contact or temporary submersion in fresh water up to 1 meter for 30 minutes.
The Genium X3 is the most durable, intuitive and technologically advanced microprocessor knee available. With features that support activities like running, swimming and ascending stairs step-overstep, X3 supports individuals who push the boundaries of mobility.
With an IP 68 rating, Genium also offers the highest level of water protection offered in a microprocessor knee.