A SHARED CARE APPROACH TO










16 Q&A Health and wellness questions asked and answered!
Dr Mark Resty Rivera put his medical skills to good use while on a biking trail
21 LIVE WELL From Clueless Student to Mentor & Guide
While nursing is clearly her calling, Senior Nurse Manager Manjit Kaur harboured other ambitions when she was deciding on a career
Tips to recognise the signs of stroke, and ways to support recovering patients
Yishun Health is leveraging collaborations between primary care doctors and hospital specialists to deliver seamless care flows, regardless of where patients are in the spectrum of care. Under a shared care model, suitable outpatients at Admiralty Medical Centre’s Diabetes Centre are referred to a community-based General Practitioner (GP) or Family Physician, who takes over part of their follow-up care. Apart from convenience for patients, this approach optimises the control of chronic conditions and provides a holistic approach to disease treatment and healthcare.

10COVER STORY A Shared Care Approach to Managing Diabetes Primary care doctors and hospital specialists collaborate to better manage patients with chronic conditions
PUTTING PATIENTS IN THE CENTRE OF CARE

Our Patient Care Officers deal with the nitty-gritty of hospital stays, giving inpatients a more pleasant and holistic experience

Find out what these two beanshaped organs do for your body
Steamed Sea Bass Belly with Teochew Sauce
This dish comes with a tasty sauce that goes well with rice and veggies
It’s a ‘Pole’ Lotta Fun Pole workouts require serious strength, flexibility and stamina
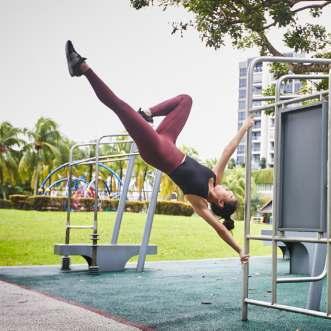
Maskless photos in this issue were taken before COVID-19 or with safe management measures in place
The name aha holds much significance for us at Yishun Health. In part, it is a nod to our history; it also stands for ‘Advocates for Health in Action’. Through these pages, we hope to empower you to take charge of your own health and discover those ‘aha!’ moments that lead to a healthier, happier you.
Yishun Health is a network of medical institutions and health facilities in the north of Singapore, under the National Healthcare Group. It comprises Admiralty Medical Centre, Khoo Teck Puat Hospital and Yishun Community Hospital. It also includes community extensions such as Wellness Kampung.
The editorial committee — made up of clinical, nursing, allied health, population health & community transformation, and administrative heads of department — advises aha’s direction.
A/Prof Tan Kok Yang Bastari Irwan Caroline Tan Fatimah Moideen Kutty Shirley Heng Teresa Foong
Hannah Wong Jack Lau Sabrina Ng Sharon Ng Albert Foo www.ktph.com.sg/ about-us/media/publications aha@ktph.com.sg
THINKFARM PTE LTD www.thinkfarm.sg
MANAGING DIRECTOR Christopher Tay
HEAD, EDITORIAL Chua Kim Beng
CONTRIBUTING EDITOR Sheralyn Tay EDITOR Dang Hui Ling
HEAD, CREATIVE Sean Lee
HEAD, CLIENT RELATIONSHIP Jessie Kek
CONTRIBUTORS Lee Lily Gina Ang Justin Loh
aha is the official bi-monthly publication of Khoo Teck Puat Hospital (Co. Reg. No. 200717564H) and is produced by ThinkFarm Pte Ltd. All rights to this publication are reserved and no part may be reproduced without the expressed written consent of the publishers. While every effort has been made to ensure that the information in this newsletter is accurate and up to date, the editorial team will not be responsible for errors due to information received. Opinions expressed are that of the writers and do not necessarily represent the views and opinions of the publishers. Printed by Mainland Press Pte Ltd. MCI (P) 062/07/2022
On 20 September 2022, Yishun Health’s Population Health and Community Transformation (PHCT) launched the book CaringCommunities at its Caring Communities Carnival at Wellness Kampung @ 765 Nee Soon Central.

The publication documents PHCT’s various community projects that have kept the community healthy since 2011. It showcases the asset-based approach to building community resilience, which is underpinned by the belief that individuals not only have the capability to take charge of their health, but contribute to keeping other residents in the community healthy as well. These programmes have benefited approximately 10,000 participants.
Minister for Health Ong Ye Kung and Yishun Health CEO Prof Chua Hong Choon officiated the book launch. Together with resident Mr Lim Kim Na, a calligrapher, they each wrote the Chinese character “人” (person) with a large calligraphy brush, cumulatively forming the Chinese character “众” (community), symbolising how individuals come together to form caring communities. The character “众” also forms part of the book’s Chinese title, 众心荟聚

In his address to the participants, Minister Ong emphasised, “Health happens with yourself, your family and friends, and out in the community. Even in the
community, it is not about the healthcare workers, but the residents working together to keep each other healthy.”
Prof Chua also shared that the CaringCommunities book is an important way to show how health can be practised beyond the hospital. “The projects featured are a testament to Yishun Health’s contribution to the national HealthierSG programme, where collaborations with community partners and residents form the foundation for a thriving preventive care health ecosystem,” he said.
The main author of the book, Dr Wong Sweet Fun, Deputy Chairman, Medical Board (Community Care & Population Health) & Clinical Director, PHCT, Yishun Health, noted that PHCT’s long-running approach to community health makes for a resilient health system that focuses on factors that keep our residents well, rather than what makes them ill. “It has been heartening for us to see these projects bear fruit, especially when our residents take over the ownership and grow them. Even when there were restrictions brought on by the COVID-19 pandemic, most of these resident-led projects could successfully adapt and continue running to benefit the community.”
More than 200 residents and community partners celebrated PHCT’s journey and achievements by participating in the Carnival and book launch.
Personalised Care and Support Planning (PCSP) is a form of relationship-based care that builds trust between patients and healthcare providers. Rather than a prescriptive approach, people are encouraged and supported by their care team to take full ownership and initiative of their health and other life goals. The care team acts in partnership with their patients by building confidence, supporting autonomy, and guiding them in independent self-management.
To raise awareness of PCSP as well as share best practices and on-ground insights into this care approach, a Zoom-based masterclass was held over two days (20 May and 9 June 2022). During the sessions, more than 600 participants were given a broadranging look into how PCSP is delivered
in different settings, including in the community, outpatient, and community health arenas.
Building on this masterclass,
Yishun Health will go on to train more clinicians in PCSP in the coming months so as to further inculcate the approach across our campus.
The Population Health and Community Transformation (PHCT) team held a masterclass on 15 August 2022 on Local Area Coordination (LAC), a framework that has been in use since 2018.
LAC is an upstream capability- and capacity-building approach that enables residents to stay strong and connected as valued members of the community. Almost 200 professionals in the health, social and community care sectors in Singapore attended the session.


During the session, various speakers — including guest speaker Mr Ralph Broad, Director, Inclusive
Neighbourhoods and Founder, Local Area Coordination Network — shared how to take an asset-based community development approach. This empowering approach moves away from fixing problems for people to identifying people’s innate skills, experiences and aspirations that enable them to solve and manage problems on their own, supported by their family, friends and community. It is a more personalised and strengths-based approach that increases self-sufficiency and reduces the demand for and dependency on formal health and social services for a more sustainable healthcare model.
Mdm Chia Kwee Lee is no stranger to leading from the front and undertaking big tasks. In her 20 years in public healthcare, she has steered Yishun Health’s Specialist Outpatient Clinic operations and led several patient service improvement projects. One of these is a ‘one-queue’ system, which consolidates patient visit timings to multiple clinics on the same day into a single easyto-read chit.
In the last two years, she has also led COVID-19 vaccination and swabbing exercises, and managed business continuity plans, bed flows, and manpower resources to optimise patient care. Most
recently, she took on the role of Project Office Director, furthering Yishun Health’s digitalisation transformation and training staff in our Next Generation Electronic Medical Records system.

Mdm Chia has pursued these commendable efforts while

Whatever her role within Yishun Health, Mdm Chia has always pursued her tasks while wearing her trademark smile and exuding warmth
wearing her trademark smile and exuding warmth. For her dedication in upholding safety and service standards, she received the Exemplary Service Excellence Award at the recent Public Sector Transformation Awards, held on 29 July 2022.
Seven Yishun Health nurses were awarded the prestigious Nurses’ Merit Award on 6 July 2022. They received their prize at the first in-person ceremony in two years. Presenting the awards, Minister for Health Ong Ye Kung expressed his appreciation and paid tribute to nurses for their outstanding performance and commitment to duty. To celebrate their win, large posters featuring their portraits were installed on the pillars at the KTPH lobby. The winners are as follows:

• Low Sing Ee, Nurse Manager, Community Nursing, PHCT
• Tan Sok Keng, Nurse Clinician, A&E, KTPH
• Meriani Chen, Nurse Clinician, Ward B85, KTPH
• Goh Soon Pang, Nurse Clinician, APN & Specialty Nurse, KTPH
• Aisyah Binte Nasir, Assistant Nurse Clinician, Ward B86, KTPH
• Yvonne Tan, Assistant Director of Nursing, Nursing Administration, YCH

• Sreevidya d/o Jayacopalan, Principal Enrolled Nurse, Ward D87, KTPH
The award winners sharing a candid moment with Yishun Health CEO Prof Chua Hong Choon, Yishun Health Chief Nurse Ms Shirley Heng, and YCH Director of Nursing Mdm Chua Gek Choo
This year’s Nurses’ Day was extra special, as we returned to in-person festivities after two years of remote celebrations. A number of events were held to commemorate the day, including performances and heartfelt speeches at the KTPH auditorium.




The session was graced by Minister for Health Ong Ye Kung, Senior Parliamentary Secretary (Health) Rahayu Mahzam, Director of Medical Services A/Prof Kenneth Mak, and NHG Group Chief Nurse A/Prof Yong Keng Kwang.
CEO Prof Chua Hong Choon saluted nurses by wearing the nursing uniform, and shared a moving recollection about his days as a young House Officer. He spoke about how — when he was the only doctor in the ward — it was the nurses who taught him what to do. This not only revealed to him the importance of practical knowledge versus theory, but also the important role of nurses, who, beyond their technical competencies, act as role models for person-centred care. Minister Ong also offered his profound gratitude to nurses and healthcare workers for continuing to carry the
burden of care as Singapore opens up so that the rest of us can go about our daily lives. On an inspiring note, Chief Nurse Ms Shirley Heng encouraged nurses to upgrade themselves, and view learning as opportunities to build their capabilities so that they continue to shine and reflect the profession in positive ways. The programme also included a series of engaging performances by staff and senior management, some of which were in line with this year’s theme: Shine Bright Like a Diamond.
Beyond this event, a series of activities were also held. One involved members of senior management living a day in the life of a nurse by serving in the subsidised wards as Nurse Buddies.
As they served meals, showered patients, assisted in dressing wounds, and sent patients for procedures, they gained a deeper appreciation of our nurses’ daily work. Another was a small carnival, held on 25 and 26 July 2022: the KTPH Learning Centre was transformed into a space that hosted carnival games and a photo booth, with plenty of drinks and snacks as a treat for nurses.



As Singapore makes a national shift towards a Healthier SG, community-based efforts will become increasingly important to support population health. To this end, Yishun Health partnered the Rotary Club of Singapore and Sembawang Grassroots Organisation (GRO) to start the Interact Club of Sembawang (ICS), the first of its kind in Singapore to serve public health needs in the community.
ICS was launched on 15 June 2022 at Admiralty Medical Centre during a ceremony graced by Mr Ong Ye Kung, Minister for Health and Grassroots Adviser to Sembawang Central GRO. Its goal: to act as a platform for youths aged 15 to 19 to participate in community health promotion and education. Guided by Yishun Health’s Population Health and Community
Transformation (PHCT) team, ICS youth leadership and members will run programmes focusing on four areas: metabolic, mental, social and environmental health.
To ensure ICS members are equipped with appropriate skills, the PHCT team facilitated attachments to familiarise them with community health posts and support resources. The youths also conducted door-to-door outreach to connect with residents and learn about their needs, strengths and concerns.
With the insights gained, ICS will synergise efforts to encourage, educate and empower residents to take more ownership of their health and build a healthy and resilient community in the North.


This year’s Mini Medical School (MMS) welcomed more than 300 participants, who ‘graduated’ on 4 June 2022 after completing a series of three webinars on the topic of metabolic syndrome.
During these sessions, participants, many of whom were members of the public, learned about the complex relationship between obesity and diabetes, as well as the science behind weight loss and diet. They were also introduced to a new evolving frontier of diabetes remission. In this engaging learning experience, ‘students’ participated in Q&As, chat sessions, and even shared personal experiences in managing their chronic illness. They also completed an assignment and sent in responses that were showcased to the class.
Held since 2013, MMS aims to make medical science education publicly accessible, thus raising the health literacy and self-sufficiency of the community.

This year’s Patient Safety Month (PSM) was a reminder that zero patient harm is ‘Mission Possible’, an outcome that is the responsibility of everyone at Yishun Health. To drive home the message, a series of virtual webinars was




held throughout the month of July 2022, covering common safety concerns and best practices in areas such as pressure injuries and medication safety.
During the closing on 29 July 2022, Yishun Health staff were recognised
for being role models for medication safety and Speaking Up for Safety (SUFS). In his address, CEO Prof Chua Hong Choon encouraged all staff to take ownership of safety and make it an ongoing quest and priority. He also shared that he was pleased to see staff’s strong commitment to safety during a ward walkabout just the day before.


Yishun Health is improving outcomes for patients with stable and manageable chronic conditions by driving deeper collaborations between primary care doctors and hospital specialists. This shared care model also benefits patients — with greater convenience and the opportunity to see a doctor closer to home.

Evidence shows that a sustained regime of follow-ups, tests, screenings and engagement leads to better outcomes for those who have chronic illnesses, such as diabetes. While complex cases are conventionally seen in the specialist outpatient setting within hospitals, moves are being made towards a shared care model, where specialists co-manage patients with primary care providers in the community for holistic, convenient and accessible care.
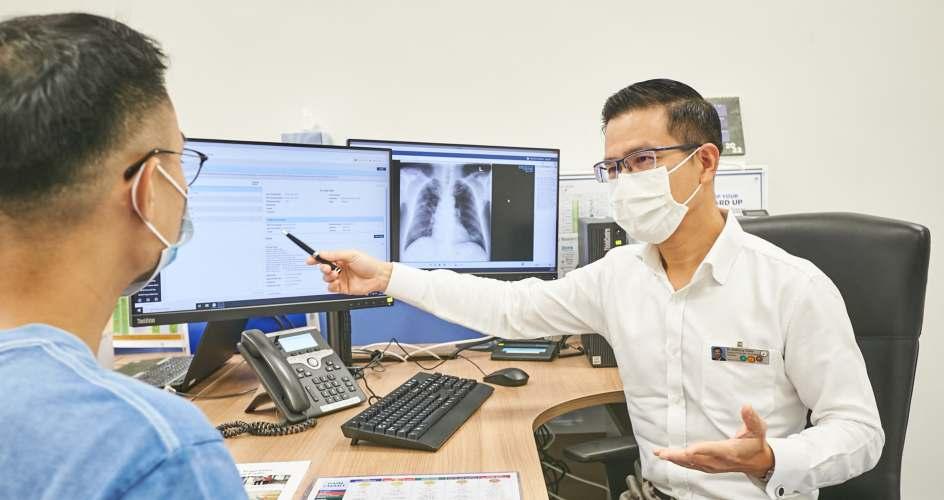
At Admiralty Medical Centre (AdMC), this idea was conceptualised in 2019, and has resulted in the launch of the Diabetes Mellitus (DM) Shared Care Programme. Dr Anthony Chao, Clinical Lead, Shared Care Partnership Office (SCPO), and Consultant, General Medicine, explains that the programme identifies suitable outpatients from the AdMC Diabetes Centre and co-manages them with partnering General Practitioners (GPs) or Family Physicians, who are the
patients’ existing primary care doctors or located near the patients’ residential addresses.

It was a timely move. When the COVID-19 pandemic started to take hold in early 2020, this programme began to take on greater relevance and urgency, shares Dr Chao. Due to restrictions, patient safety, and limited resources, many outpatient appointments in AdMC had to be suspended or rescheduled. This caused a longer window between specialist follow-ups, and affected diabetes patients to varying degrees.
For patients who were more stable, they were able to keep their DM condition under control. However, those with difficulties managing their insulin and blood sugar on their own developed complications and needed to be admitted to the hospital. This experience, notes Dr Chao, made it clear that having an extra layer of medical support was an important way forward not only to prevent complications, but to right-site patients to receive appropriate levels of care.
Dr Anthony Chao, Clinical Lead, SCPO, is one of the specialists under the DM Shared Care Programme run by AdMC

on CHAS and/or Medisave for GP consultation fees/investigations
medication delivered to home by AdMC Pharmacy



All these exigencies ramped up enrolment for the DM Shared Care Programme. According to Foo Yan Ci, Senior Executive, SCPO, this saw AdMC’s Diabetes Centre specialists deepening collaborations with private primary care doctors in the community to co-manage patients with stable diabetes conditions. “Under the DM Shared Care Programme, enrolled patients alternate visits between partner GPs and their specialist at AdMC,” Yan Ci explains. Typically, she says, a patient has three to four regular appointments a year with their specialist. With this new collaboration, they will instead see a doctor in the community between visits to the specialist.
A channel of clear and constant communication underpins this arrangement, says Dr Chao. For more seamless integration and
to ensure both the specialist and GP have all the information needed to ensure smooth care continuity, both parties have to make the effort to build and maintain a collaborative relationship.
Dr Chao, who used to be in charge of the Diabetes Education Programme for GPs for about a decade, highlights that this involves writing comprehensive case summaries, holding case discussions, and keeping open other forms of communication, such as messages or phone calls.
While patients benefit from the convenience and accessibility of the DM Shared Care Programme, getting this programme up and running was a matter involving much coordination, collaboration and workflow reorganisation.
The team shares that it was thanks to management support and clinical leadership, as well as strong partnership with the AdMC Pharmacy, that it all panned out. “We took about six months to iron out the workflow, legal framework, pharmacy logistics, and financing,” Dr Chao recalls. Despite these challenges, those involved persevered. Their mission was clear: to put patients in the centre of care for better outcomes. “We knew it would benefit patients,” says Yan Ci. “One of these benefits is definitely greater convenience, because they are able to see a doctor closer to home without a long wait, and have more flexibility in terms of timing.”
This means being able to see a doctor or take blood tests after working hours or on the weekends — a huge boon for working adults. The ability to use the Community Health Assist Scheme (CHAS) card for payment, as well as still
Dr Grace Ong, of Frontier Medical Associates, is one of numerous GPs who are partnering AdMC under the DM Shared Care Programme

being able to receive subsidised medication delivered to their homes, add to the affordability of the programme.
From a clinical perspective, patients also receive more holistic care, adds Dr Chao. Family Physicians in the community are in an advantageous and unique position to play a more active role in delivering comprehensive chronic disease management because they have broad-based medical training. This means that, apart from disease-specific care, they are able to focus on preventive care, screenings, and health promotion. One of the primary care doctors involved in the programme, Dr Grace Ong of Frontier Medical Associates, shares that this involves discussing lifestyle issues, such as weight management, diet, exercise, and more. She also ensures that patients are up-to-date with their screenings and vaccinations [see box story].
Apart from enhancing Yishun Health’s overall mission of healthcare delivery, shared care programmes such as the DM Shared Care Programme are aligned with the national drive known as Healthier SG, reveals Rachel Yeong, Deputy Director, SCPO.
Under this initiative, residents are encouraged to enrol with a primary care doctor at a private clinic or polyclinic. This major reform of the healthcare sector will see greater integration of GPs into the public healthcare ecosystem, and enhance the shift to preventive care.
The goal for shared care programmes, Rachel adds, is to ensure that care delivery flows seamlessly for patients, regardless of where they are on the spectrum of care. In summary, it brings together three factors: • provide comprehensive care for patients;
• right-site patients in the community; and • establish collaborations between GPs in the community and specialists in acute hospitals.
This team-based approach optimises the control of chronic conditions in partnership with a Family Physician, who provides preventive care for a holistic approach to disease management and healthcare.
Ultimately, Dr Chao says, this is all about the patients. “Whether you are a primary care doctor or a specialist, we are all working together because our patients and their overall wellness matter to us. This shared care approach puts the patient at the centre of care, so we can address their needs as a whole person and not just treat around the disease.”

Dr Grace Ong, of Frontier Medical Associates, is one of the GPs participating in the shared care partnership. Currently, she sees patients under the AdMC DM Shared Care Programme and KTPH Psychiatric Shared Care Programme.
She recalls her first patient, a teenage boy she diagnosed with diabetes. After referring him to AdMC for specialist assessment and treatment, the boy was referred back to her for follow-up. “This was the first time I had encountered the DM Shared Care Programme; it was meaningful to be involved in the continuation of care of someone I had initially diagnosed with diabetes mellitus,” she shares. She has also gone on to look after this boy’s mother, who has hypertension and hyperlipidaemia in addition to diabetes.
As a Family Physician, Dr Ong believes in taking a multipronged approach when it comes to diabetes, such as managing patients’ weight, diet and exercise, as well as keeping track of their vaccinations and annual screenings. “I also believe in empowering patients to manage their conditions by teaching them to monitor their blood pressure and glucose level at home.”
Being part of the programme allows primary care doctors such as Dr Ong to practise at the top of their licence, and keeps them connected with fellow doctors. For instance, when needed, Dr Ong can reach out and confer with specialists at AdMC on patients with other conditions, such as fatty liver or diabetic retinopathy.


“Many shared care patients are on multiple and newer medications, and this challenges me to keep up-to-date with the newer drugs available in the market for diabetic patients. I am also able to keep in touch with colleagues in AdMC via memos; this makes general practice less ‘solo’ and thus different from the traditional GP model of care.”
Being a family doctor, Dr Ong values the rapport she builds with patients over time. “I look after their entire family, am privy to their social dynamics, and any personal or work issues that may adversely affect the control of their diabetes and other chronic diseases,” she says. This insight also lends itself to better diagnoses. “With a good understanding of their chronic diseases, I am better able to manage my patients’ acute episodes when they consult me for conditions such as headaches, gastroenteritis, or upper respiratory tract infections.”
Both specialists and GPs have to make the effort to build and maintain a collaborative relationship with each other as well as their shared patients
Yishun Health experts answer your frequently asked questions about health, well-being and medical conditions. In this issue, we answer questions from people coping with the aftermath of a COVID-19 infection.
Contributed by Adon Chan, Principal Physiotherapist, Lenis Phoa, Senior Physiotherapist, and the YCHCOVID-19TreatmentFacilityRehabilitation Services Team
After COVID-19, I feel breathless even at rest. What can I do to alleviate this? When should I see a doctor about the symptoms I’m experiencing?
Returning to your daily activities after recovering from COVID-19 may be a different experience for everyone, as some may encounter more serious symptoms than others. It would be important to take a gradual approach when returning to your previous lifestyle, including exercise. Start by asking yourself whether you are still experiencing any of the following common side effects: • breathlessness
• feeling very tired and weak, and/or • problems with attention, memory and thinking clearly
One main side effect of COVID-19 is reduced stamina. Losing strength and fitness while you were unwell can also mean you become breathless easily. Breathlessness is a common symptom of COVID-19, and some people experience this symptom for a while — even after the infection is over.
Your breathlessness should improve as you gradually increase your activities and exercise but, in the meantime, the positions and techniques on the right can help to manage it.
You can also practise breathing techniques to manage your breathlessness [see box story]. If your breathlessness persists or worsens to a point that
> Standing forward lean: Lean your elbows on the back of a chair or on a wall or railing.
High side lying: Lie on your side and prop yourself up on pillows so that your head is higher than your hips.
Seated forward lean: Lean forward and rest your elbows on your knees. If you have a table, rest your elbows and arms flat to form a cradle on which you can lie your head; use a cushion for more comfort.

Controlled breathing: Breathe in slowly through the nose and breathe out through your mouth.
> Standing with back support: Lean against a wall for support.
you start having to limit your indoor walking, or you grow increasingly anxious about it, seek advice from a healthcare professional or your primary care provider.
After recovering from COVID-19, I now realise that my memory has been affected, and I regularly experience ‘brain fog’. Is this normal? What can I do?
Some people find themselves experiencing new difficulties with attention, remembering things, and thinking clearly. This is also known as ‘brain fog’. These difficulties may resolve within weeks or months but, for some people, the symptoms can persist for longer. If you are experiencing brain fog, you can try the following strategies to help manage your symptoms:
• Gradually introduce gentle exercise into your daily routine — exercise can facilitate recovery of brain function and improve learning outcomes
• Take part in activities that are mentally stimulating, such as reading, puzzles and memory games
• Use memory aids, such as writing notes and setting reminders on your phone
• Break down tasks into steps and focus on one thing at a time
• Ask for help and adjust your expectations so that you are better able to cope with tasks, especially more complex ones
I recently recovered from COVID-19 and wish to resume exercise. What will I need to take note of?
Do take precautions if you are resuming exercise after recovering from COVID-19. It is important to exercise safely, even if you were physically active and exercised independently prior to falling ill. It is important to exercise with someone else for safety if you:
• are experiencing difficulties in mobility
• have a history of falls or near-falls
• have any other health condition(s) that may pose as risks during exercise
• are currently on supplemental oxygen after discharge from hospital (if so, seek recommendations from your healthcare professional)
It is important to pace your activity and start with gentle exercise. The intensity of exercise can gradually be increased over time. Keep in mind that it is common to experience a loss in fitness and stamina. You may also feel breathless, tired or weak. It is important to listen to your body and monitor your progress and tolerance as you gradually build up your fitness.
Always warm up before exercise, and cool down after you have completed your workout. Your exercise routine should comprise both cardiovascular and strengthening exercises to build up your heart, lungs and muscles. It is normal to feel a little breathless when exercising as long as the level of breathlessness is proportional to the intensity of the exercise. You can use the Rate of Perceived Exertion (RPE) scale [see table] to monitor the intensity of your workout.
Stop your exercise routine if you experience:
• nausea or sick feeling
• dizziness
• severe shortness of breath
• cold sweats
• chest tightness
• pain
If these symptoms persist, seek medical attention.
Scale
Level Talk Test
Very light Normal breathing, can talk normally
Light
Moderate no sweat
Moderate sweat
Can carry on a conversation; moderate breathing
Can carry on a conversation; moderate breathing
vigorous sweat
Can carry on a conversation; heavy breathing
Only able to complete 1–2 sentences; heavier breathing
strenuous
sentences; heavy breathing
Only able to speak in syllables; heavy breathing
severe
Can’t talk; very heavy breathing
Can’t talk; gasping for breath
Being a Resident Physician at Yishun Health’s Cardiology department, Dr Mark Resty Rivera has seen his share of cardiac emergencies. But he never expected that his medical training would one day be a decisive factor in the middle of a tropical jungle.
It was a typical Saturday morning for Dr Mark Resty Rivera back in August 2021. He and his friends were out on their bikes on a trail off Mandai Track 15. “I picked up mountain biking during the pandemic,” he explains. For him, it was a way to get out, exercise and explore Singapore, even amid the Circuit Breaker. That morning, he was biking through the trail when he spotted two men to his left. The older man appeared to be distressed and trying to help the younger one. Dr Rivera stopped to find out what was going on, and realised that the younger man was semi-conscious — it turned out that he had collapsed while cycling with his father-in-law!
Recognising the severity of the situation, Dr Rivera’s medical experience and lifesaving instinct immediately kicked in. “I saw that the younger man was very pale; so, with the help of my friends, we started basic checks on his vital signs,” Dr Rivera recalls. His initial gut feeling was that the man could have suffered a cardiac event, as he was not responding and did not have a discernible pulse. Dr Rivera and his friends quickly lay the man down on the ground and started cardiopulmonary resuscitation (CPR). Meanwhile, one of Dr Rivera’s friends dialled 995 for an ambulance.
The next half an hour or so was extremely intense and stressful as Dr Rivera continued to perform
A weekly mountain bike ride turned into an emergency situation for Dr Mark Resty Rivera one Saturday morning when he came upon a fellow biker in distress. Acting quickly, Dr Rivera put his training to the test, stabilising the medical situation while awaiting more help to arrive

“I knew it was a critical moment; that, at this point, his brain was not getting enough blood and oxygen. I was also worried he would enter cardiac arrest.”

chest compressions and assess the man’s status. He noted that, during this time, the man’s circulation would occasionally resume on its own, and he would regain some consciousness and ask what was happening, before passing out again. This happened two or three times.
“At one point, we were able to help him to sit up,” Dr Rivera says. “While talking to him, I observed that his face began to skew to the side, as if he was having a stroke. I knew it was a critical moment; that, at this point, his brain was not getting enough blood and oxygen. I was also worried he would enter cardiac arrest.”
Meanwhile, Dr Rivera’s friends were communicating with the Singapore Civil Defence Force (SCDF) team on how to get to where they were — after all, they were in the middle of the forest, and thus had difficulty conveying their exact location. “We were so deep in the wilderness that the nearest automated external defibrillator (AED) or access point was over a kilometre away. Even trying to send a GPS pin was difficult because of poor signal strength.”
Eventually — much to everyone’s relief — the SCDF team found them, running the whole distance despite the challenges of the trail. The stricken man was stabilised and transferred to the stretcher semi-conscious and with a weak pulse. “I didn’t want to leave him, so I helped the SCDF team carry him on the hike back,” Dr Rivera shares. In all, eight people were involved in transporting the man and all the equipment to the ambulance. It was only after the man had been safely
For his quick thinking and heroic efforts, Dr Rivera was awarded the SCDF’s Community Lifesaver Award on 25 February 2022, and the Ministry of Home Affairs’ National Day Award for Public Spiritedness on 4 August 2022


loaded onto the ambulance and on his way to the hospital that Dr Rivera could fully process what had happened that morning.
A week or so later, Dr Rivera received a surprise call from the man whose life he had saved. The good news was that — thanks to timely efforts — he had recovered fully from the ordeal. The even better news was that the cardiac incident was not due to a blockage and no stroke had occurred.
Looking back at the events of that day, Dr Rivera feels a strong sense of gratitude that he was there at that exact moment, armed with the skills to help. “It was a very challenging situation, unlike in the hospital, where it’s a controlled setting, and we have access to all our resources and equipment. Out there in the jungle, we just did our best and let our training take over. It was my duty, and I am just glad I was there to help.”
A leader, mentor and example to many Yishun Health nurses, Senior Nurse Manager Manjit Kaur has made nursing her career and passion — though it was not the profession she wanted to pursue when she was young. This alternative path has proven to be her true calling, as testified by the Long Service Award she recently received for 50 years of dedication.
As a young woman about to make big decisions about her career, Manjit Kaur had a dream job in mind. She liked the idea of service, discipline and working for the greater good. The smart uniforms were a bonus, too.



The job in question, however, was not nursing — it was the army!
But her family dissuaded her from joining the military and advised her to take up another career.
“Being a conservative Punjabi family, they wanted me to take up nursing, which was more femaledominated,” she shares. She recalls fondly that it was her brother who had gotten her the application form and escorted her to the interview
and back, sensing that her strength and caring personality would serve her well on the job.
Thrown into nursing without a clue as to what to expect, Manjit took some time to adapt to the demands and duties of nursing school. In those days, she recalls, nursing involved a lot more manual work and rather menial and mundane tasks that were nevertheless a necessary part of patient care. For one, nursing students learnt more through handson experiences than through theory and technology. Nurses also had to undertake a lot of additional tasks over and beyond patient care.
“We didn’t have any disposable items back then,” Manjit explains.
“Everything was re-useable, so we had to not only perform our nursing duties, but also take care of all sorts of supplies, like washing syringes, cloths and masks, autoclaving them ourselves, and even sharpening needles used for procedures.” Even items that we take for granted today, such as bandages and gauze, had to be manually cut to size, packed and sterilised.
Her challenges did not just stem from picking up clinical skills and other duties. Manjit also had to get used to the confronting nature of disease, wounds, and the human body. In her days as a young and innocent nurse, she recounts how she fainted after seeing a festering

bedsore on a patient’s lower back. She fainted yet again on another occasion, when she and fellow student nurses begged a staff nurse to let them observe a baby being delivered. “We were not supposed to be there as we were young student nurses, so we got the poor staff nurse into big trouble!” Manjit remembers sheepishly.
The memory of these incidents is a constant reminder to her of how far she has come on her nursing journey. From a clueless, naïve and inexperienced nursing student, Manjit has grown greatly in her skills and knowledge. More significantly, she has grown to love her ‘second choice’ career deeply. The turning
point came when she qualified to be a nurse and started to work independently. While it is a big responsibility to take on, Manjit also sees it as a privilege.
Even after five decades, she still feels a sense of excitement every day when she clocks in on her shift. “There is always lots to do and learn, and every day is different,” she says. There is also a sense of appreciation and gratitude in the air every time a patient recovers. “Every patient is someone’s loved one; it is our duty to care for them like our own,” she emphasises.
Manjit adds that it is not all roses and rainbows — there are also hard days, especially when patients do not do well or pass away. “In my junior days, I would not always take it well and would hide to secretly cry and grieve the loss,” Manjit shares. But with time, she has come to handle such emotions better. While she still feels the loss, she is able to process them as part and parcel of her work. “Nursing has made me stronger both emotionally and spiritually,” she says.
The challenges and demands also make it very rewarding because, despite them, experiencing intangible successes — like the

delight or gratitude of patients — is priceless. “I think nursing is noble and special because, in our work, our patients trust us with their lives. As nurses, we have a responsibility to ensure safe and efficient care,” Manjit reflects, viewing the onus of learning and betterment to be on the individual.
Plus, she adds, the skills learnt can be applied to daily life — be it patients, family or the public at large who are in need. “I have no regrets being a nurse, as it allowed me to attend to my late parents at the end of their lives, and they were able to pass on in the comfort of their own home.”
It is also a career that reminds her of what it means to live a fulfilling life in service to others, and where she can improve and grow personally. As nurses, she says, it is about more than providing care in the ward. “We are health advocates for our patients and colleagues.”
Manjit literally walks the talk, as she makes it a point to keep fit, and encourages her nurses to make exercise a way of life. In fact, she is the ‘face’ of Yishun Health’s ‘Take the Stairs’ signages, and often chides nurses for taking the lift, especially if their destination is just a few floors up or down. She continues her regular exercise routine, and has a varied range of hobbies — reading the classics, watching TV, as well as exploring Singapore in search of tasty food.
Building a satisfying life — with a balance of work, personal and social aspects — is important to Manjit, as it keeps her going and energises her in the pursuit of being the best nurse that she can be. Apart from self-care, she also reaches out to care for her colleagues. “Offering support to each other is vital to keep us going. It is important to take care of our nurses and teach, guide, mentor and mould them to be excellent nurses.”

“In my junior days, I would not always take it well and would hide to secretly cry and grieve the loss.
Nursing has made me stronger both emotionally and spiritually.”SNM Manjit appears around the hospital, encouraging others to step up to health SNM Manjit standing proud in the National Day Parade contingent in 2019
Stroke is a serious and life-threatening condition that happens when blood and oxygen supply to the brain is cut off or limited because of a blocked or bleeding artery. It requires fast action and immediate medical treatment, as well as sustained support during the road to recovery.
Contributed by Farhana Binte Salim, Nurse Clinician, Acute Stroke Unit, KTPHA sedentary lifestyle, having an unhealthy diet, smoking, obesity and excessive alcohol consumption can increase the risk of heart disease and recurrent strokes. You can reduce the risk of a stroke by managing your risk factors and making healthy lifestyle choices, such as:
• Monitor your blood pressure and blood sugar level










• Lower your cholesterol level
• Quit smoking
• Exercise regularly
• Eat healthy and have a well-balanced diet



When it comes to recognising the signs and symptoms of stroke, think ‘FAST’!
Stroke is an emergency! Early detection and treatment will improve outcomes.












When recovering from stroke, strong support from family and loved ones is important. To help your loved one journey towards better health, provide them with emotional support and encouragement, and partner them to be physically active and capable as much as possible.







The care and management plan after a stroke is an important part of recovery to help stroke survivors return to their best function and achieve quality of life. Help your loved one to keep up with their follow-up appointments to see the doctor or rehabilitation team.
To reduce the risk of subsequent strokes, medications will be prescribed. It is important to follow the medication schedule for the best outcomes. If it is hard to remember or keep track of what medications to take, try to come up with a plan to help your loved one. Try keeping reminders on a smartphone or put up sticky notes that can be easily seen and referred to. To access a resource guide for stroke survivors and their caregivers, scan the QR code on the left or go to www.healthhub.sg/strokehub
caRING & DELIGHTING:

A hospital stay may not be the most enjoyable of experiences, but attentive care that goes above and beyond day-to-day treatment needs can definitely make recovery more comfortable. At Yishun Health, Patient Care Officers work alongside ward nurses to deliver this valueadded service to care for and engage patients and their family members, thus delivering a more holistic, person-centred experience.
Each day, as dawn breaks and the early-morning sunlight spills through the many large windows of KTPH, the routine of the day begins. Each day in the ward revolves around a standard schedule of meals, doctors’ ward rounds, visiting hours, and bedtime, interspersed with tests, scans, therapies, treatments, as well as medication. With hundreds of patients to care for, each with individual needs and treatment plans, this regime is a busy one that is often made more complex by the unexpected.
Working alongside ward nurses and the care team in tackling these
challenges are Yishun Health’s Patient Care Officers (PCOs). Trained with caregiving skills, PCOs not only contribute to patient care, but also enhance the patient experience by engaging and meeting their needs.

For Mdm Lim, the warm and compassionate presence of our PCOs made a difference to her during her hospital stay. “They always checked in on me, asking if I’m okay. They also kept me company when my hospital stay got lonesome and I needed someone to talk to,” she shares. Another patient recalls how the helpfulness and cheerful demeanour of our PCOs made her feel well looked after. “They were always attentive and would often check to make sure I was not in pain and had what I needed during my rest.”
The PCOs are new service professionals providing caregiving and service management, and are envisioned to augment nurses in providing end-to-end care coordination to patients. This new role started in August 2020, and was an evolution of the Care Ambassador (CA) role that was created in May 2020 in response to the COVID-19 pandemic. During the pandemic, flight crew seconded to hospitals to become CAs were trained in simple caregiving roles to supplement the manpower in the wards. It was from this model that the core team from Operations, Nursing and Human Resource started the PCO role.
Today Yishun Health’s PCOs are a full-fledged job role that continues to add value to inpatient wards, undertaking numerous tasks
that go beyond basic caregiving. Currently, PCOs are supporting five inpatient wards (general medicine and geriatric medicine), and there are plans to have them assigned to more wards going forward.
According to Regina Yeoh, Senior Executive, Patient Care Unit, “Aside from providing caregiving, PCOs provide service management to patients.” By closely partnering and working in collaboration with ward nurses and care teams, PCOs are able to enhance care so that nurses can focus on their clinical duties. For instance, PCOs are trained to address and anticipate the needs of patients, provide general management of patients’ bedside and ward environment, and ensure that a patient’s stay is comfortable. This may involve attending to patient calls, relaying their requests to the
relevant people, or reporting any adverse patient conditions to the nurse-in-charge.
To complement the work of nurses, PCOs work hand-in-hand with the ward nurses for the smooth running of the ward and upholding patient safety. Regina elaborates, “PCOs ensure that ward equipment are in good working order, supplies are sufficient, and — in partnership with nurses — support in the organisation of the ward according to the principle of 5S: Sort, Set in Order, Shine, Standardise, Sustain. This maintains the efficiency and safety of wards.”
The main goal, she continues, is to “care and delight” our patients.
“It is a meaningful job because PCOs can be there for patients and care for them like our own family.”
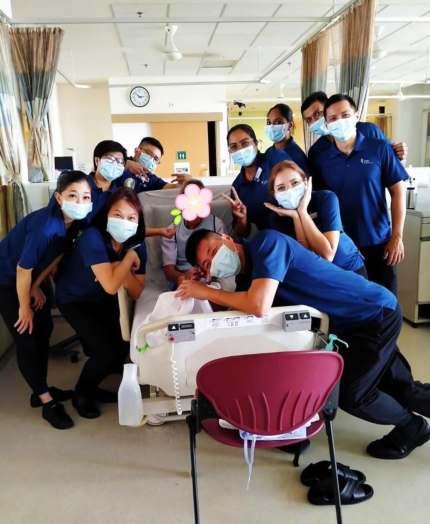
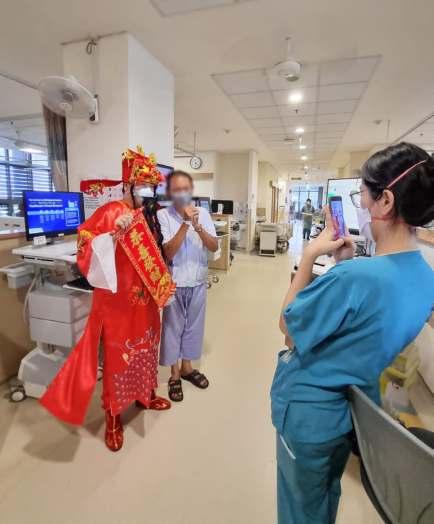
PCOs enhance the inpatient care experience by performing caregiving duties, delivering service management, and engaging patients, thus providing added value to person-centred care:
• Build rapport with patients, family and next-of-kin to understand their needs and manage their expectations in service delivery
• Engage patients and see to their non-clinical needs
• Help to contact and update family members as needed
• Perform inventory checks on commonly used ward equipment and supplies
• Provide clerical and logistical support to wards
• Report faulty equipment to ensure speedy repair
I came from a commission-based retail job. The industry was badly hit by the pandemic, but this crisis provided the opportunity for me to re-think my future, and I decided to step into healthcare.

I feel great satisfaction when patients and their families appreciate my work. Co-workers also recognise my work as I am new to healthcare and have lots to learn. The stable income improved my standard of living as well.
We had a 98-year-old patient who exhibited signs of dying. After a week of care and treatment, he improved so much that he could communicate clearly, captivating us with stories of past glories. He eventually deteriorated and passed away. As I served warm water to his family who had gathered around his bedside, they thanked us for not giving up, and reminded us to cheer up. The patient’s daughter said that although their father had begun mumbling incomprehensibly in the last few days, we still took good care of him and listened to him intently — the family appreciated this very much. Hearing her words lifted our spirits immediately!
I was a fashion sales associate. I left due to the long working hours and commute.
I enjoy caring for the elderly and assisting them with their daily activities.
We had a long-staying patient who had underlying family problems. She became uncommunicative with the ward staff, only blinking her eyes or nodding at us. I often


reassured her through my words that we are caring for her even though she never responded. I also frequently found her in tears.
I would always play Hokkien songs when I fed her. One day, after three months with us, I saw her sitting out of bed. As some of us approached her, she seemed happy to see us and said in a loud and clear voice, “I want Milo!” After getting over our initial shock, we fulfilled her request immediately. Many patients come and go, but we hope to make every patient’s experience a comfortable one.
Wherever she is right now, she is always in my thoughts and I am praying for her best well-being.
Our kidneys — two bean-shaped organs located in the lower back — are considered the ‘water treatment plant’ of the body. But they don’t only filter waste products and toxins; they also produce hormones and regulate key bodily functions. That’s why it’s important to care for them and keep them disease-free.
In consultation with DrLimEngKuang Senior Consultant, General Medicine, and ChongSinTzun, Senior Dietitian, Nutrition & Dietetics
Good kidney health starts with a good understanding of risk factors and how kidney health can be preserved through lifestyle and diet choices.
Diabetes is the leading risk factor for kidney disease, and the most common cause of kidney failure. Uncontrolled high blood sugar due to diabetes damages the kidneys and lowers their ability to filter waste and fluid.
High blood pressure is the second most common cause of kidney failure after diabetes. The force of high blood pressure damages the tiny blood vessels in the kidneys. High blood pressure is also an indicator of kidney disease.
Glomerulonephritis, or the inflammation of the tiny filters in the kidneys, can also lead to kidney disease.
Other factors that can increase the risk of kidney disease are smoking, obesity, genetic predisposition, overuse of medications that can damage the kidneys, and certain auto-immune disorders.

Kidney diseases often progress slowly, with signs and symptoms of chronic kidney disease developing over time. Some symptoms to look out for are:
• Urinary symptoms, such as bloody or bubbly urine
• Nausea, vomiting
• Loss of appetite
• Drastic changes in urination patterns, such as peeing a lot more or a lot less
• Swelling in the feet and ankles
• Loss of mental sharpness and an inability to focus
• High blood pressure that is hard to control
Other issues, such as incontinence (inability to hold in urine), are usually a sign of bladder and not kidney problems. However, incontinence may cause infections and the backflow of urine into the kidneys that could damage them. Contrary to popular belief, back pain is not a symptom of kidney disease, but could be a sign of kidney stones. If you suffer from any of these conditions, see a doctor to manage them and prevent complications from arising.

Use non-prescription pain medications or non-steroidal anti-inflammatory drugs (such as aspirin or paracetamol) in moderation — excessive use of these medications may lead to kidney damage.
A healthy diet can help keep the risk factors of obesity, high blood pressure, and high blood sugar in check — and thus prevent or slow the progress of kidney disease.
Eat a balanced diet by following the ‘quarter, quarter, half’ guide.

Chicken, fish, prawn, tofu, tempeh and legumes
Brown rice, wholemeal beehoon, chapati, wholemeal bread, or wholemeal pasta will keep you feeling full longer
Obesity is one of the major risk factors for kidney disease, so it is important to maintain a healthy weight with regular physical activity. If you need to lose weight, consult your doctor about how to achieve weight loss sustainably and healthily.
Leafy greens and colourful vegetables are high in fibre and rich in antioxidants; eat two servings of fresh fruit daily

Cigarette smoking damages the kidneys and can worsen existing kidney damage.
The recommended intake of salt per day is less than 1 teaspoon (5g), equivalent to 2,000mg of sodium. To reduce salt intake, limit intake of seasonings and processed, preserved and canned foods. Be mindful that there is a lot of hidden salt in commercially available soups, gravies and condiments such as ketchup and sambals. Table, sea, Himalayan or Celtic salt all contain about the same amount of sodium.
Beware of high-fructose corn syrup in processed foods and drinks. Also be wary of fruit juices, which are high in sugar and contain little to no fibre.
The danger of kidney diseases lies in the fact that there are few symptoms until the last stages. The best method of detection is regular screening. This is important, because many kidney diseases are reversible if detected early.

This savoury dish upcycles the belly of a sea bass to ensure nothing goes to waste. It is topped with a flavourful sauce that goes well with rice and vegetables.
Recipeprovidedby MokJeyLun, Demi Chef de Partie, Food Services, in consultation with Nutrition & Dietetics, KTPH
4
• 3tsp sesame oil, divided

150g onion, sliced
150g ginger, sliced
30g fermented soybean paste
3tsp sugar
6g white pepper powder

480g sea bass belly
1 medium red chilli, sliced, for garnish
1. In a wok, heat 2tsp sesame oil and saute onion and ginger slices till fragrant
2. Add 400ml of water and bring to a boil
3. Add fermented soybean paste, sugar, white pepper and the remaining 1tsp of sesame oil; stir to mix well
4. Arrange sea bass belly on a steaming plate and heat up the steamer
5. Pour the sauce over the fish belly and steam for 15 minutes
6. Garnish with red chili
Requiring strength, flexibility and stamina, pole workouts are gaining popularity as a dynamic, whole-body exercise that also trains coordination and develops the mind-body connection.
 In consultation with NatashaGoh,Physiotherapist,RehabilitationServices
In consultation with NatashaGoh,Physiotherapist,RehabilitationServices
alternative avenue for fitness and health. It has even been recognised as a sport, with many competitions held all over the world.
One reason for pole dancing’s rising popularity is the physical benefits it provides. Relying solely on a person’s own bodyweight, pole dancing offers a whole-body workout that trains one’s:
• Cardiovascular system
• Vestibular system
• Strength and flexibility
Every pole dancing class includes a pole routine, a three- to fiveminute choreography that combines various pole tricks and moves into a seamless whole. The pace of the routine is dependent on the sub-genre, as each has a distinctive style.
Pole dancing started around the 1920s and 1930s during the Great Depression in America, when travelling fairs would move from place to place, entertaining audiences in large tents. Many of these acts included dancing, which often involved the tall poles that held up these tents.
Over the years, pole dancing evolved from a sideshow act into performance art. It has expanded into numerous sub-genres that focus on different movements, music and
tricks. Depending on the sub-genre, the choreography may differ, with some focusing on the explosiveness of flips and tricks, while others emphasise grace and fluidity.
As with any dance form, pole dancing provides individuals with a means of self-expression, and allows them to hone their musicality and coordination. In recent years, pole dancing has gone beyond the boundaries of just being a form of artistic expression and entertainment, gaining mainstream popularity as an
Within a dance class, the choreography will also be repeated many times for participants to gain familiarity. This results in it being an intense cardiovascular workout! This in turn releases endorphins, the ‘happy’ hormone that helps relieve stress and anxiety.
Pole dancing requires one to spin around the pole at varying heights and speeds. This tests the vestibular system, the body’s
• Push ups
• Shoulder shrugs while hanging on pull-up bar
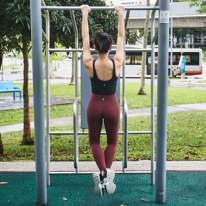


The Handspring is a move that many newcomers to pole dancing aspire to master. Learning this progression will open up one’s repertoire to many other moves.

Bridges
Hamstring curls
Heel raises
sensory mechanism responsible for providing the brain with information about movement, the position of our head, and spatial orientation. The vestibular system is also part of our motor function, and plays a role in maintaining posture and helping us keep our balance and stabilise our body during movement.
The spinning movements can cause
newcomers to feel uncomfortable in the beginning, but as the vestibular system becomes conditioned, faster spins can be achieved.
Pole dancing is also perfect for improving strength and flexibility throughout the body. Even though


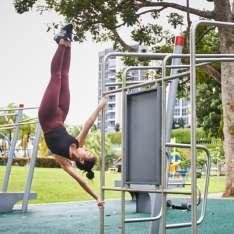

Planks and side planks

Russian twists
Sit-ups
there are strength-based and flexibility-based tricks, most require a combination of the two for seamless, effortless execution.
The various movements engage the arms, back, core, and leg muscles, but also require tendons and joints to move and stretch. At the same time, learning these movements trains coordination and muscle memory.

Wellness Kampung is an initiative comprising three wellness and care centres for residents in the N orth. They provide a suite of health and social programmes, creating a support network for residents to inspire each other to adopt healthier lifestyles in a close-knit 'kampung' setting.
Opening hours: Mondays to Fridays, 8.30am to 5.30pm (closed on Saturdays, Sundays and all Public Holidays)*


Blk 115 Yishun Ring Road #01-495, Singapore 760115 6257 4702


Blk 260 Yishun Street 22 #01-87, Singapore 760260 6257 4802

Blk 765 Yishun Street 72 #01-366, Singapore 760765 6257 4842
*In light of COVID-19 safe management measures, please check the KTPH website for the centre schedule and call in advance to see if there are vacancies for group activities.
AdMC is a one-stop medical centre for specialist outpatient consultation, day surgery, rehabilitation and diagnostic services, as well as community health outreach activities.



KTPH is a 795-bed general and acute care hospital serving more than 800,000 people living in the north of Singapore. It combines medical expertise with high standards of personalised care in a healing environment, to provide care good enough for our own loved ones.
YCH provides intermediate care for recuperating patients who do not require the intensive services of an acute care hospital. Situated beside KTPH, the two hospitals provide an integrated care experience for patients.
676 Woodlands Drive 71, #03-01 Kampung Admiralty, Singapore 730676 6807 8000
www.admiraltymedicalcentre.com.sg www.fb.com/admiraltymedicalcentre
90 Yishun Central Singapore 768828 6555 8000 www.ktph.com.sg www.fb.com/khooteckpuathospital
2 Yishun Central 2 Singapore 768024 6807 8800

www.yishuncommunityhospital.com.sg www.fb.com/yishuncommunityhospital
