What Makes Us Happy

FROM SACRIFICE TO SUCCESS MEDICAL OFFICE MANAGEMENT
LEGISLATIVE UPDATES



FROM SACRIFICE TO SUCCESS MEDICAL OFFICE MANAGEMENT
LEGISLATIVE UPDATES












www.doreyrealestate.com / (610) 346-8800
BELLE TERRE... A gated entrance & long drive is introduction to the 13,000 sqft stone manor house on 22 acres. 5 bedrooms, 10 garages, stone pool house, caretaker’s apartment, barn, tennis court, pool, waterfall, spa & greenhouse are just a few luxuries. Offered for $7,950,000

PREMIERE BUILDING LOTS... Wide curving roads lead to 2 culde-sacs in this enclave. Expansive lots, from 2 to 6 acres, have been created to provide room for sprawling landscapes and extraordinary homes by top custom home builder, Myron R. Haydt. Starting at $2,700,000
OLD WORLD VILLA... Set on three private acres, with views over pristine Cooks Creek, this stunning European style villa is one of the finest properties in Bucks County. 6 beds, 5 full baths, radiant heat floors, in-ground pool, Offered for $2,500,000

FAIRWAY VISTAS... Elegant, sophisticated & beautiful, this home with its lovely architectural design is perfectly positioned on 1.2 acres on a private golf course. Westerly views provide exquisite sunsets. Approximately 8,100 sqft, 4 beds, 4 full baths. Offered for $2,295,000
OVERBROOK MANOR... It’s love at first sight when you turn down the gravel driveway, cross the wooden bridge over Rapp creek, and peek around the corner at a fairy tale come to life. 5 beds, 4 full baths, guest cottage, 7.55 acres. Offered for $1,250,000
TIOGA MANOR... Tioga Manor stands proudly on a flat half acre corner lot in desirable downtown Bethlehem. Stately trees and meandering sidewalks are woven throughout Old Rosemont, a quintessential neighborhood of custom crafted homes. Offered for $1,195,000

GARDEN MANOR... Tucked away at the end of a cul-de-sac and bordered by tall trees is this elegant Bucks County home. More than 6,000 square feet of living space includes a fully finished walkout lower level. 5 beds, 4 full baths. Offered for $1,150,000

HOUSE BEAUTIFUL...Built in 1926 and lovingly updated over the years, this cheery home offers 3,200 square feet of living space over three finished floors. Tree lined sidewalks weave through the picturesque Bethlehem neighborhood. Offered for $650,000

2022-23 LCMS BOARD OF DIRECTORS
Rajender S. Totlani, MD President
Oscar A. Morffi, MD Treasurer


Charles J. Scagliotti, MD, FACS Secretary
William Tuffiash
Immediate Past President
CENSORS

Howard E. Hudson, Jr., MD
Edward F. Guarino, MD TRUSTEES
Wayne E. Dubov, MD
Kenneth J. Toff, DO
Well, fall is upon us. School is back in session, and you see pumpkin things everywhere. So welcome to the fall issue of the Lehigh County Medical Society magazine, Lehigh County Health & Medicine. Our goal is to offer you insightful information, helpful statistics, and tips and tools to consider using in your own lives and practices.
In this edition we’re offering articles centered around health. We have an article “Uterine Surprises” which covers the topic of uterine fibroids. This is a must-read that delves into the most common type of female pelvic tumor.
We offer a wonderful story “From Sacrifice to Success,” first brought to you by Physician Family magazine. The author writes of her family’s journey as an immigrants to the United States. You are sure to enjoy this family story.
What goes on behind the scenes at the doctor’s office? Please read the article “Medical Office Management in an Era of Administration Overload.” This piece covers what goes on from private practices to health network-employed practices.
We hope you enjoy this edition; we hope we can add to the conversation about how medicine and wellness can help us form strong communities in Lehigh County. If you are interested in back issues, or just want to read Lehigh County Health & Medicine online, please visit our website at https://lcmedsoc.org/our-publication.


As a black-haired girl with facial features distinct from other children, I was aware I was different. There were times when others made fun of how I dressed or the lunch my mom packed. However, I felt most self-conscious speaking to others. I couldn’t express myself as easily as before, so I had a difficult time fitting in. I wanted to speak as easily as the people in American movies.
So, our family taught each other how to say specific words. We played the game “Taboo” with one strict rule: no Tagalog (the language of the Philippines). “It’s a form of transportation!” my brother exclaimed.
“Car! Bus! Taxi! Bicycle!” we guessed with aggressive enthusiasm.
“Yes, bicycle, but just one tire!” my brother replied.
“One…ONE-cycle!” exclaimed my mom, the family English tutor, with conviction as we all roared with laughter.
While overcoming a language barrier was my biggest worry, my parents had bigger concerns: how our family could survive in this new environment.
I was 12 when we immigrated to the United States from Manila, Philippines in 2005. With only one month’s notice, we left our family, friends and a world that brought us comfort and happiness. We brought nothing but the clothes we owned, and a sliver of hope that we could make it in a new country. With money tight and anxiety for future expenses, we lived in one bedroom of a small apartment with a distant relative in Niles, Illinois. Five of us slept together in one bed.

Sacrifice is a word that I learned as a child. My parents left their practices as physicians in the Philippines; my father was an orthopedic surgeon. Even more of a sacrifice, my mother left her practice as a dermatologist and started a new career as a registered nurse so our family could qualify for a special program to recruit nurses from the Philippines to the United States.
While my father focused on passing licensure exams and residency, my mother was the breadwinner. Of course, we wouldn’t have been here at all if she hadn’t sacrificed her medical career.
She took a position as a registered nurse at a local nursing home, working as much as she could to make ends meet, sometimes backto-back shifts, while my father was studying and tending to home responsibilities. Later, she took another nursing job and juggled both. She was and continues to be a force to be reckoned with.
As my father prepared for the physical examination portion of the US Medical License Exam (USMLE), he often used my mother or me as patient actors, to hone his physical examination skills and master what Americans call “small talk.” While other medical graduates could focus on polishing their assessment skills, my father had to learn this extra piece of American culture.
Passing the USMLE was only the first step, though. Someone told my father he shouldn’t hope to become a doctor again; his

background was against him: a middle-aged non-U.S. citizen, and international medical graduate. While his years in practice as an orthopedic surgeon helped, he worried it wouldn’t be enough to match into any specialty in competition with American students. He decided to opt for the specialty he thought would be the best chance – family medicine.
Luckily, my father was accepted into a family medicine residency in Champagne, Illinois. Adjusting quickly became second nature; two years later my father accepted a sports medicine fellowship in Wilmington, Delaware.
I witnessed my father leave family events for emergency phone calls and my mother come home from 16-hour shifts, always inspired by their passion to serve the sick and their incredible work ethic despite the adversities of raising a family in a foreign country. I knew early on I wanted to be a health care professional, too.
Continued on page 8
As the eldest and first to attend college in America, I started out in nursing before realizing my passion for medicine during my junior year. Ironically, that passion developed during an externship back in the Philippines; being in the same environment they were as medical students made me feel closer to my parents.
After graduating, I worked part-time as a nurse while completing a master’s degree at the Philadelphia College of Osteopathic Medicine (PCOM), which led to my acceptance into PCOM’s medical school, where I am in my fourth year of studies.



My brothers are also pursuing medical careers, our decisions all inspired by our parents’ love of healing others. My oldest brother is an anesthesia resident, and my younger brother recently completed the same



Seventeen years ago, our family began new lives in the land of the free. As my brothers and I continue our journeys to become physicians, the pride of being Filipino has never faltered in us and is still very much alive.
Asked why they made the sacrifice to immigrate to the US if they had stable careers in the Philippines, my parents’ answer will always be that they were willing to make those sacrifices to provide greater opportunities for their children.
Sacrifice is the very love language of my parents, so my brothers and I strive to become people who will let them know that their sacrifices were not in vain.
With our native tongue preserved, hearts that yearn to care for others, and an ambition

Bianca Lacay is a fourth-year medical student in Philadelphia College of Osteopathic Medicine’s class of 2024. She is currently serving on clinical rotations, several of which she has spent in the Lehigh Valley where she will likely apply for residency programs. She has participated in numerous educational and research opportunities. She continues to be a mentor and teaching assistant to share her knowledge and guidance about obstacles she has faced as a medical student and as an Asian-American. Whenever possible, she sets aside time to spend with her family.
This article was originally published in the Winter 2022 edition of Physician Family magazine. It has been updated.

What makes us happy? It is highly doubtful that there is one clear answer to that question and that it is the same for each of us. There is clearly a degree of subjectivity to happiness and our experience verifies that some people are happier than others. As we ask ourselves “What makes us happy?” this may be a particularly relevant topic for the present. We have just lived through the worst pandemic in 100 years, spending nearly two years in social isolation. Our political climate is infused with suspicion, misinformation, and vitriol, and too many of our communities are marked by violence, especially from guns.
Continued on page 10

In a 2022 survey by the opinion research group Ipsos, fewer than 20% of Americans reported that they were “very happy” and in that same year 25% of adults in the U.S. told an American Psychological Association poll that they were too stressed to function. These have been anything but “happy times.”
Although our subjective experiences may describe our individual definition of what makes us happy, there is good evidence that there are factors which we can control that can influence our happiness. The search for these has been a focus of attention throughout history including the attention of many of the greatest Greek philosophers. The Greek word eudaimonia literally means “good spirit,” but is more readily translated as “happiness.” In ancient Greek philosophy it was recognized as the highest human good and closely linked with other terms e.g., virtue, prudence, and justice. Aristotle described eudaimonia not as a pursuit of pleasurable experiences, but rather as an ethical way of living. More recent philosophers, e.g., John Locke, Samuel Johnson, and of course, Thomas Jefferson, wrote of “the pursuit of happiness” building on those earlier philosophical traditions which emphasized civic virtues, e.g., courage, moderation, and justice as the basis of a life of happiness.
More recently, the subject of happiness has been the focus of scientific research. For example, beginning in 1938, a group of Harvard University researchers gathered health records and interviewed hundreds of individuals. In addition to answers to the question of “What makes us happy,” their work has produced a wealth of information (including evidence that happiness helps us live longer) emphasizing the importance of establishing quality relationships and finding meaning in what one does with their life experiences as sources of happiness. They found that wealth alone does not create happiness, but neither does the absence of money. Pleasure-seeking also does not have a lasting impact on one’s happiness. Indeed, the pursuit of pleasure, whether riches, power, sex, substances, or a myriad of other such
interests, often leads to destructive forces which create sorrow and tragedy, not the “happiness” one may be seeking.
In this article we will move beyond the philosophical and explore the most recent scientific research exploring the biologic, psychologic, social, and even genetic factors that influence our happiness. The message is clear: We have the capacity to control our own happiness.
,
In July 2004, something curious happened in the discipline of psychology. People gathered in Verbania Pallanza, Italy, for the first International Conference on Positive Psychology. Lead by psychologist and consummate researcher Martin Seligman, known widely for his landmark work Authentic Happiness, a collaboration began among an international community of scholars from a variety of disciplines, including psychologists, business leaders, clinicians, and educators, to establish the science of happiness and human flourishing. It was here that the Positive Psychology movement germinated and took the world of mental health by storm. In contrast to the illness model that had characterized psychology to that point, the scientific study of positive psychology focuses on investigating and isolating human strengths and virtues that help individuals use their innate gifts to thrive and live with meaning and purpose and thus greater happiness. In a small town in the lovely Italian countryside, a blueprint for happiness, human thriving, and well-being was born to the scientific community.
Seligman and Mihalik Csikszentmihalyi (noted for his work on “flow”) are the founding fathers of the Positive Psychology movement. They were among the first to demonstrate the building blocks of the science of happiness and human flourishing. The collaboration of scholars furthered the growth of Positive Psychology research focusing on topics such as character traits, personal strengths, optimism, well-being, positive emotions, gratitude, compassion,
and hope, to better understand human flourishing and happiness.
Humans have long been curious about the emotional, biologic, social, and personal basis for happiness. Aristotle wrote that happiness was the ultimate goal of the individual. William James in his 1890 book, The Principles of Psychology, wrote that positive emotions led to well-being. Einstein noted that a calm and modest life brings more happiness than the pursuit of success combined with constant restlessness. Though not psychology researchers, these great scholars of history were keen to understand what confers the simple yet elusive feelings of utter contentment, happiness, and well-being.
So how do we know we are happy, content, or thriving? According to related research, our body informs us through a complex alchemy of biologic, psychologic, and genetic forces. Have you ever had an unexpected feeling that things are “just right”? Like all the atoms are lined up and we move through the day with joy and ease? We all would agree that our brain functions better when we feel this way.
Many years ago, Barbara Fredrickson, PhD, introduced her simple yet profound research on positive emotions, a focus of study previously ignored by the psychiatric community. Fredrickson, a colleague and ardent supporter of Seligman’s work, studied the deepening and broadening effect of positive emotions on the brain. After forty years of research, she found that positive emotions such as happiness have a butterfly effect that lead to other positive emotions through complex brain connections, pathways, and neurotransmitters. Through some mysterious, yet concrete, chemical processes, positive emotions seem to be able to broaden our scope of attention and increase cognition, which in turn builds physical, intellectual, social, and psychological resources. Cultivating our positive emotions, such as happiness, seems a worthy pursuit toward well-being and a good life. Multiple studies have also shown that happiness has a positive impact
on immunologic function, cardiac wellness, and overall improved health.
Drilling down even further, we come to the question of genetics. According to some studies, genes account for 40% of differences between people’s happiness. This is partly due to a predisposition to neurotransmitters and chemicals related to the emotional states of happiness, such as dopamine, serotonin, endorphins, and oxytocin. For a variety of reasons some individuals have varying levels of these chemicals which affect their individual levels of happiness and well-being. We now know there are numerous ways to activate and boost these chemicals. Exercise increases endorphins. Positive relationships produce oxytocin. Meditation produces dopamine. And walking in morning sunlight produces serotonin.
In addition to genes and biology, personality influences happiness. The Big Five Personality cross cultural model identifies traits that influence our happiness and sense of well-being. These personality traits include an openness to experience, conscientiousness, agreeableness, extraversion, and neuroticism. Studies have found that these traits are important predictors of well-being. Both our personality traits and experiences can impact thoughts and beliefs about ourselves, others, and the world that will positively or negatively impact our happiness. Thus, being curious about how our thinking impacts our sense of happiness may be a valuable tool.
Perhaps the most important question to ask is – given that our genes, biology, and personality play a significant role in our sense of happiness and well-being, can we learn to enhance our happiness and flourish with a sense of purpose and meaning? The good news is a resounding yes. It once seemed naive to think we could alter our gene expression, change our biology, improve our mood, or lessen our anxiety. Today we know that there are positive epigenetic effects of mind-body therapies such as mindfulness, self-exploration, gratitude
1
Connect closely and honestly to those most important in your life, especially family and friends.
2
Find meaning and joy in what you do, especially work and hobbies, and keep doing it.
3
Fret less about yesterday, worry less about tomorrow, and live fully in the moment. 4
Practice self-care— emphasizing good mental and physical health.
5
Live a life of integrity, kindness, and generosity, while expressing gratitude for what you have, not craving what you don’t have
practice, thought monitoring, meditation, yoga, journaling, exercise, tai chi, positive thinking, and positive social connections that can change how we move through the world. This means that we as individuals, families, and communities are in the driver’s seat on the road to happiness.
The Seligmans and Fredricksons of the scientific community have given us an excellent roadmap to human flourishing. Positive Psychology invites us to change our mind and behavior, and by doing so, we might even be able to change our genes. And what is it all for in the end? Certainly, for each of us to be happy, but more than that, it is to share that happiness to create a more just, peaceful, and healthful world.
There is a science of happiness including the more recent research into Positive Psychology that describes the biologic, psychologic, social, and even genetic factors which contribute to our feelings of happiness. Perhaps most critical, science shows us that we can control our own happiness as well as contribute to the happiness of others. And our level of happiness can directly affect our state of health and the quality of our lives. This is especially important information for us as physicians and other health care providers. Too often we see psychologically as well as physically impaired patients who are overcome with the negative factors in their lives. Their search for happiness can be distorted by individual circumstances such as disease, poverty, or social disturbances, and may lead to a self-destructive path for far too many. Understanding the research will assist us in our role as healers for our suffering patients.
Continued on page 12
hoffpubs.com

I remember one remarkable experience. Running late for work, I caught a red light. Annoyed by the delay, I sat impatiently waiting and noticed an elderly gentleman, likely in his 80s, sweeping his sidewalk. I immediately had a “good” feeling about how conscientious he was in caring for his environs. Then seconds later an elderly woman appeared and kissed him on the cheek. My heart swelled and I felt numerous positive feelings, many indescribable. Those positive feelings seemed to linger for the entire day and impacted my work and working relationships. Occasionally, I would find myself smiling when I thought of the incident. I now consider red lights full of possibility. DB

As we contemplate our own quest for happiness, research and experience shows us that our thoughts and behaviors can contribute significantly to the quality of our lives, to a sense of contentment, fulfillment, and yes, that sense of well-being that we perceive as happiness. Finding a sense of meaningfulness in who we are and what we do, establishing a commitment to the achievement of eudaimonia, living in a just and virtuous way, and honestly connecting to one another, especially those family, friends, co-workers, and others who are at the center of our lives, are the steps to a happiness that is attainable for each of us.
Dr. Baxter is the retired Chair of the Department of Family and Community Medicine at Reading Hospital and serves as the editor of the Medical Record.

“Looking to grow your business? Connect with our engaged, communityminded readers.”




The changes that affect medical practices keep coming. Pressures range from new technology, remote work, and an aging patient population to more administrative requirements and metrics from insurers. While the concerns are many, administrative duties tend to top the list when speaking of physicians and the chronic fatigue they’re feeling. Results from a recent
Continued on page 14
Doximity poll show that 46% of physicians believe decreasing administrative burden would be the most effective intervention in reducing exhaustion, followed by improving work-life balance (27%), and reducing clinical caseload (21%). (1)
As health care systems continue the largescale task of morphing themselves into more streamlined organizations, employed and independent practices have exercised innovation to make improvements in their own offices. It’s no longer just a smart thing to do; supreme efficiency has become a matter of survival. In this overview of what’s been changing, we’ll start with a look at some general steps any practice can take to increase office efficiency, but these mostly apply to private practices that are operating autonomously.
THE BASICS
Independent, private practices need to work smarter to meet requirements and keep everything running smoothly. These clinicians may not have supportive organizations with economies of scale that can make it easier to handle administrative tasks, maintain adequate IT support, reduce costs, or deal with other challenges. However, certain basic actions can benefit the independent – or employed – physician in ways that are simple yet effective. For example:
Map out the Patient Journey. Sketch out how a patient moves through the practice and note every point of contact and documentation requirement. Look for bottlenecks, unnecessary actions, and steps that fail or that require rework. These are the areas you’ll need to expend effort on to find better, faster, or more successful approaches.
Match Capacity with Demand. When your practice team knows its capacity constraints and demand patterns, it can make changes to align with demand. When both are matched, delays in care can be reduced. Having the right staff to handle all aspects of the practice, and ensuring accurate training, will help things flow more efficiently.

Dictate Whatever You Can. Technology has lent a hand when it comes to taking time to write everything down. There’s no need to with the digital tools available today. Make it normal practice to dictate exam notes – ideally when you’re still in the exam room with the patient so you can remember every detail – as well as notes made during hospital rounds. The more you can dictate, the less work later.
Create a Team Culture (Even with a Few Employees). Communication among the
practice team is essential. Meet regularly, at a consistent time, with clear focus, frequency, and format. Use agenda templates to keep the conversation on point. An assigned recorder for each meeting can keep track of action items, assigned point persons, and due dates that come out in discussion.
Manage Pharmaceuticals. Drug purchasing contracts should be aggressively negotiated for the best available prices, making sure that you are not paying more than what’s reimbursed according to the average sales price. Because these amounts can change every quarter, contracts for drugs should be reviewed quarterly and may need to be negotiated more than once a year.
Lengthen Prescriptions for Chronic Medications. If you’re in the habit of authorizing prescriptions for 90 days, consider a one-year authorization instead. (Continue to see your patients at the same frequency so you can monitor their care and medication use.) By extending prescriptions, you will cut down on phone calls and messages related to refill requests.
Get Clear on Coding. Practices that utilize EMRs have assistance with coding and documentation, with alerts and notifications that will pop up and provide information. Even if you don’t, practitioners need to be up to speed on how to code accurately and with specificity, as this makes everything from patient exams to reimbursement more efficient. For assistance: https://www.cdc. gov/nchs/icd/Comprehensive-Listing-ofICD-10-CM-Files.htm
Focus on Patient Satisfaction. Independent practices can make it easy for patients to leave feedback by automatically sending survey requests via text or email. Surveys capture patient input and allow medical practices to make continual improvements in the care they provide. Making changes that relate directly to the patient experience will add to efficiency.
Join a Physician Organization. Larger entities like PHOs, ACOs, and IPAs can help small and medium-sized, physician-owned
practices in areas such as network access, timely receipt of performance data, and sustainable and fair payment rates. Some organizations provide education on the business of running a practice. Being part of an organization also aids in the ability to assemble a cache of legal, financial, real estate, and marketing advisors.(2)
The advantages of being an employed practitioner and part of a large health system mirror the age-old notion of “It takes a village.” The upside is you always have backup, resources, and assistance when you need it and everything doesn’t fall in your lap. This “community” concept is also the basis for changes that are currently being made across many health systems in the name of efficiency and necessity.
In the traditional ambulatory practice, most office tasks and general patient care duties are handled within the individual practice. However, some health systems are turning to what is referred to as the “Patient Partnership Model (PPM),” which takes a big-picture view of practice activity. This model consists of remote regional roles that form interdisciplinary support teams that can take on administrative tasks that do not need to be done in the practice setting. This allows more evenly distributed “indirect work” and creates a centralized workflow.
“We found that when remote teams supported a region of practices, workflow efficiencies were gained,” says Molly Thompson Chavez, MHL, Administrator of Operational Excellence and Director of Relationship Centered Communication at Lehigh Valley Health Network. “Internal staff were not being pulled to perform priority tasks for patients present in the office; they therefore had the time to extend the reach and scope of their efforts into connecting with patients outside the practice walls.”
After COVID changed working styles to hybrid and remote, the PPM model
Continued on page 16
Independent, private practices need to work smarter to meet requirements and keep everything running smoothly.
made perfect sense as a solution to maximize efficiency among separated personnel. When newly adopted, the first component was a welcome video or telephone visit. It came about considering the onboarding patient questionnaires and basic practice information could easily be completed by a central staff. Intake includes a template, developed along with the clinician, so that the information gathered is pertinent to a particular patient.
The process begins when a new patient makes a call to a practice which rings at a regional hub. They are directed by a phone tree to select the type of visit they are requesting. Choices might be new patient, hospital follow-up, acute visit, patient care, or scheduling future appointments. If the call is from a new patient, the patient call representative shares information about the practice and schedules a telephone or video visit with the intake team. The intake call can take anywhere from 10 to 45 minutes depending on the patient’s medical history and is conducted one to two weeks before a visit is scheduled.
“Patient engagement is so important, so we also ask what the patient would like to address with the doctor,” says Thompson Chavez. “We want patients to feel warmly welcomed and convey that we can assist with whatever their needs might be. This regional welcome call strategy helps the practice tremendously by taking those preliminary activities out of the office mix.”
This same concept is applied when evaluating care gaps: those routine screenings and visits that patients may have skipped from year to year, or health care for those with diabetes. Through “met” and “not-met” reports, the team finds out if, for example, diabetic patients missed their appointment or didn’t show positive lab results at their last appointment. The team will call the patient and follow up with key questions, perhaps bringing the patient back for care sooner. Sometimes an RN on the team can order the labs and save the clinician more time.
Along similar lines, pre-authorizations (PAs) required by insurance companies have historically been a huge consumer of time
inside a practice. Before PPM, the internal staff would try to complete them in between rooming patients and all the other activities for which they are responsible. PAs can take anywhere from 15 minutes to 1 hour because they entail a number of steps: calling the insurance company, making sure you have the information you need, getting the information you need if you don’t have it, and often waiting on hold on the phone for long periods of time. This kind of juggle for internal staff was universally unsustainable.
Under PPM, someone – or several people – are entirely devoted to PAs. They can be on hold with an insurance company and still complete other desk-oriented tasks while waiting. It’s estimated that handling PAs in this manner can save medical assistants six to eight hours of phone time.
The same is true for in-basket or messaging management since practices can get thousands of messages, requests, and questions in the course of one day, either from the patient portal or from phone calls. PPM has been able to successfully pull this activity from the practices to give the health care providers breathing room. A regional team triages inquiries: those that can be answered by looking at the medical charts or through research are handled by the team; those that require input from the provider are sent on. The physician may communicate back to the team or answer those inquiries independently. Either way, this approach cuts down substantially on time spent.
The concept of a scribe is nothing new. However, in the past, a scribe was an actual person who was in the exam room taking notes, saving the doctor from “pajama time,” transcribing the notes he or she compiled that day after hours at home. Now, virtual scribes are fairly common. Rather than joining the clinician onsite, they listen into patient encounters via video conferencing or phone from an offsite location.
This comes with a number of advantages over traditional medical scribes, including a smaller price tag, greater sense of privacy,
and increased flexibility even in rural areas. There can also be drawbacks. One is that virtual scribe services are delayed 12 to 24 hours and many times, providers want their notes right away. In addition, the “voice” of the scribe’s notes will be different than that of the physician. However, the bottom line is that scribes have been shown to increase efficiency and allow more direct provider-to-patient opportunity.
“Of course, we have to edit the notes but virtual scribes still save time,” says one physician. “I estimate they save me 30 to 40 minutes a day. That might not seem like much until you realize that could mean taking a lunch versus not taking a lunch or making it to my kid’s baseball practice in time.”
Also staking its claim in efficiency is using AI to capture patient visit information. As this technology ramps up, manufacturers say these products can “filter out small talk, identify key medical information, and generate complete, EHR-ready notes.” This industry-wide intentional move toward more reliance on technology, which includes the efficiency of the patient portal to collect information pre-visit, accomplishes another goal that is equally important for health care providers, both independent and employed.
“Finding ways to increase efficiency reflects the changing nature of access to health care,” says the physician quoted above. “If we can improve efficiency, we can compete against virtual, direct-to-consumer health care practices: the ones where you simply call a number and get medical advice. We can be successful by adopting a digital front door yet have a community presence and knowledge about local resources and expectations. We will certainly be more successful than a virtual company in California telling us how to do things in Allentown.”
(1) https://opmed.doximity.com/articles/ administrative-burden-remains-biggest-driver-of-burnout-doctors-say
(2) https://www.ama-assn.org/system/files/mathematica-ama-white-paper.pdf
 PATRICIA MARAN, MD, FACOG
LEHIGH VALLEY HOSPITAL AND HEALTH NETWORK
CHRISTINE PENG, BS, MS2 UNIVERSITY OF SOUTH FLORIDA MEDICAL SCHOOL
PATRICIA MARAN, MD, FACOG
LEHIGH VALLEY HOSPITAL AND HEALTH NETWORK
CHRISTINE PENG, BS, MS2 UNIVERSITY OF SOUTH FLORIDA MEDICAL SCHOOL
September is a busy month as a gynecologist. Women who have been ignoring their own self care trying to juggle children’s activities, camps, playdates, sports, and family summer vacations always seem to catch up on their own health care as autumn comes. Often I hear patients concerns such as:
Oh, my period was horrible this summer. It ruined my shore vacation. I couldn’t even swim because I was bleeding so heavily. I couldn’t even wear my summer clothes for fear of my menstrual coming on.
Continued on page 18
I don’t know why, but it always seems like the truth comes out once the children are back to school. Just like newborns are inevitably born 9 months after snowstorms, hurricanes, and national holidays, so too gynecology woes always seem to be a frequent topic of conversation in early fall.
While there are many reasons for a woman to begin having very heavy, crampy periods in their late 30s and early 40s, one of the most common reasons is that they may have developed a fibroid. Fibroids, otherwise known as leiomyomas, are benign masses in the uterus which can cause once tolerable menses to become more painful, heavier, and protracted. A woman may start to notice pressure, fullness, or even a change in frequency of bladder or bowel movements due to compressive symptoms of fibroids. Sometimes the bleeding pattern changes or the side effects from bleeding become problematic for patients. Often, women’s symptoms correlate with the location of the fibroids. The diagram indicates where fibroids may be positioned in the uterus.
People may feel light-headed, dizzy, or become winded performing activities of daily living including going up and down stairs. This is typically a sign that fibroids have caused menses to be so heavy that a woman becomes anemic. While all of these symptoms are relatively common, they certainly are something that signals a woman needs an exam and an ultrasound.
Fibroids are benign tumors of the smooth muscle of the uterus. They do not become cancerous.
Uterine fibroids can vary in size from very small, less than a centimeter in diameter, to large enough to cause pronounced abdominal distension. They change in size throughout a person’s life, and are somewhat correlated with estrogen levels – fibroids often grow slowly with age during the reproductive years.
While we don’t know exactly why a woman gets fibroids, we do know that they are the most common female pelvic tumor. The occurrence of leiomyomas is more frequent in folks with hypertension, obesity, family members having had them, and also African-American patients.
It’s important to note that if symptoms above describe your own menstrual patterns, control of the untoward side effects of heavy menstruation from fibroids can be managed well with common medical interventions.
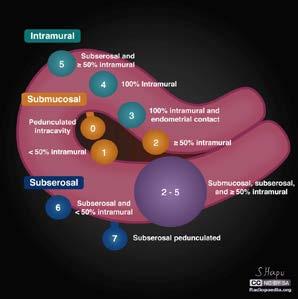
Fortunately, a multitude of treatments have become available for fibroids. Newer forms of medical management help women avoid surgery and preserve fertility. For the mildest cases, treatment may not be required at all. For cases with few or no symptoms, a physician may recommend watchful waiting, as it is possible for fibroids to remain stable or regress spontaneously. As for the cases that do cause excessive symptoms or pronounced anemia, many drug options exist. Ordinary birth control pills, IUDs, or nonhormonal medications can control heavy bleeding. Certain drugs known as GnRH agonists and antagonists may also be effective at shrinking existing fibroids and stopping bleeding altogether.
Minimally invasive procedures are available as well. Uterine artery embolization cuts off the blood supply to fibroids. Focused ultrasound surgery uses ultrasound to target fibroids. A surgeon may also remove the fibroids directly in a myomectomy, a procedure that spares fertility and the rest of the uterus. This is done minimally invasively as well, through a small hole in the abdominal wall (laparoscopically) or through the vagina (hysteroscopically). All these procedures have been proven effective at shrinking or completely removing fibroids. Finally, hysterectomy, the complete removal of the uterus, is definitive treatment available as a last resort.
Fibroids can be debilitating, yet they are common, and treatable. So often as women, we are taught to “just deal with our period.” But if just dealing seems to be getting harder and harder to do, there might be a logical explanation, and an even more simple solution. It starts with calling your local ob-gyn for evaluation.

The legislative session comes to an end with a victory! PAMED was successful in restoring money in the 2023-2024 state budget for the Primary Care Loan Repayment Program. The program provides loan repayment, up to $80,000, for a health care provider who commits to practicing in a rural or underserved area for three years. Gov. Shapiro’s initial budget proposal “zeroed out” the funding for this program. However, PAMED was successful in not only having these funds restored but also securing a one million dollar increase in the overall funding, bringing the program’s budget line to a little over eight million dollars.
Continued on page 20
PAMED continues to actively push for venue reform. The Pennsylvania Coalition for Civil Justice Reform (PCCJR) made a formal request to the Supreme Court’s Civil Procedural Rules Committee to conduct an immediate review of the impact of the medical liability venue rule that returned forum shopping to medical malpractice cases. Data from the first six months of the venue rule change shows a significant increase in medical liability cases in Philadelphia. These cases are seeing substantially higher settlements than similar cases throughout the Commonwealth.
The new venue rule imposes a requirement on the committee to review the impact of the venue rule change after two years. However, PAMED and PCCJR are asking for a review now before irreparable damage is done to physicians and the health care system over the next two years. PAMED is a founding member of the PCCJR and continues to lead the way on venue rule review. We will continue to update members on news regarding venue as this continues to develop.
Recently, at the annual meeting of the American Medical Association (AMA), PAMED leadership drove the passage of a
resolution to address the need for permanent and meaningful Medicare payment reform. Leadership from the Pennsylvania AMA Delegation, in partnership with the leaders of the Florida and Texas state delegations, presented the resolution at the AMA meeting, stating that this type of reform is critical for physicians’ practice sustainability and to protect senior citizens’ access to care. The passage of the resolution empowers the AMA to build a multipronged campaign addressing the issue on a national level.
Below are details on legislation that PAMED has been following.
Primary Care Loan Repayment Program (PCLRP) – As it currently stands, the program provides loan forgiveness, presently up to $80,000, for physicians who choose to practice in a rural or underserved community for two years. Next year’s proposed budget does not include the PCLRP line item — providing no student loan forgiveness. PAMED was successful in advocating to not only keep the Primary Care Loan Repayment Program in the 2023-2024 state budget, but also in advocating for a one million dollar increase in the overall funding.
Senate Bill 631 on POLST – Senator Gene Yaw (R-23rd District) introduced Senate Bill 631 for the codification of Pennsylvania Orders for Life Sustaining Treatment (POLST) to be used by medical professionals across all health care settings for patients who voluntarily wish to execute a POLST order. PAMED has supported previous legislative proposals on POLST and applauds Senator Yaw for introducing this most recent proposal.
Senate Bill 25 on Scope of Practice
Expansion – Legislation was introduced that would enable the independent practice of certified registered nurse practitioners (CRNP) and remove the collaborative agreement currently required to practice independently from physicians. PAMED opposes this legislation and supports the need for physician oversight of all non-physician practitioners.

Co-Sponsorship on Reforming Insurer
Credentialing – Legislation was introduced that would modernize the health insurer credentialing process. Senator Ryan Aument (R-Lancaster) has agreed to sponsor legislation that will, among other things, limit the time afforded to insurers to complete a physician’s application to participate in each health plan, though the bill does not require insurers to accept every applicant. PAMED supports this co-sponsorship memo.
PAMPAC plays a critical role in helping to advance PAMED’s legislative agenda. Although PAMPAC does not engage directly in legislative advocacy, PAMPAC’s support of legislative candidates helps to open doors for our members by developing positive and productive relationships with legislators and legislative candidates. Physicians are encouraged to support PAMPAC.
Contributions can be made here: pamedsoc.org/laws-advocacy/PAMPAC.
30,000+ TOTAL READERSHIP



Babatunde Babalola, MD Physical Medicine And Rehabilitation
Sohil Bhagat, DO Resident - Physical Medicine And Rehabilitation
Anna Bondonese Medical Student
Brittany Cataldo, DO Nephrology (Internal Medicine)
David Chandler Clark Medical Student
Jacob Feiertag Medical Student
Timothy Hartigan, MD Internal Medicine/Pediatrics

Carly A. Shaffer Medical Student
Sarah Kaitlyn Wong, DO Resident - Pediatrics

Experience the ultimate lifestyle in this stunning Weyhill Woods home with nearly 7000 sqft of living space situated on 2 lush acres in park-like setting. Features an in-ground pool & spa surrounded by breathtaking professional landscaping. Lower level completely finished with rec, lounge, fitness rooms + a fifth BR ensuite. 5 bedrooms, 6 full/2 half bath. $1,481,000
Many original features remain in this incredible 3-story Federal Style Georgian Colonial mansion, a reflection of the architectural brilliance of the 1920’s. Stunning gourmet kitchen and sumptuous primary suite. Outdoor private oasis with inground pool, meticulous landscaping & gardens. 2 attached + 4 car detached garage. 7 bedrooms, 4 full/1 half bath. $1,095,000

UPPER SAUCON TWP
Make this house your forever home. Nestled in a serene neighbor-hood in Brentwood Manor, this home features considerable living space. Primary w/ensuite bathroom, generously sized bedrooms, family room w/wood stove, spacious living room that flows into dining room, kitchen w/ample cabinet space & a breakfast bar. Full sized lower level w/ large recreation room, built-in bar & workroom/ storage rooms. 3 bedroom, 2 full/1 half bath. $395,000

UPPER SAUCON TWP
Charming 1880 farmhouse sits on just under 3 acres of land with a large bank barn and organic fruit orchard. This elegant home is a mixture of old and new, with original wide plank pumpkin pine floors and modern amenities throughout. Enjoy backyard privacy with a spacious, covered back porch and outdoor kitchen area - a perfect spot for entertaining. 3 bedroom/3 full bath. $975,000

Specializing in the Lehigh Valley and Upper Bucks County luxury home market, The Rebecca Francis Team delivers expert guidance, professional marketing expertise, and unrivaled market knowledge of the region’s finest homes and neighborhoods Recognized in the top half of 1% of Berkshire Hathaway HomeServices agents nationwide we are the Exceptional Choice for YOUR Exceptional Property


D o yo u h ave q u e st io n s a b o u t t h e ho m e b uyi n g o r sell i n g p ro ce s s? A s yo u r t r u ste d a dvi so r s , we o e r exp e r t k n owl e d g e a n d d i st i n g u i s h e d c a r e a s we h e l p g u i d e yo u t h rou g h yo u r h o m e jo u r n ey. C a l l to d ay.
LOWER SAUCON TWP

HANOVER TWP
Spacious living and backyard sanctuary are sure to impress. An outside oasis features an inground pool and spa with a gorgeous waterfall, koi pond, outdoor kitchen with built-in grill, granite counter seating and extensive landscaping...just perfect for entertaining. Inside, a gourmet kitchen, luxurious primary suite with vaulted ceilings and an extensive lower level recreation and entertainment area. 4 bedrooms, 4 full/1 half bath.
$975,000
Magnificent 7+ acre, flat, wooded residential lot, positioned in the heart of the Lehigh Valley, perfect for the home of your dreams. Choose your own builder and bring your vision to life. Public water, sewer, and natural gas are all available to the discerning buyer. Close to all major routes, shopping, and LVIA.

$475,000
© B H H Af fi li a te s L LC A n d nd e p e nd e n tl y o p e r a te d s u b s d a y of H o m e S er vce s of A m e r i c a n c a B e k s h e H a t h aw ay a f fi li a e a n d a a n c h i s e e o B H H A fi li a e s L LC B e r k s h re H a t h aw ay H o m e S e r v ce s a n d h e B e r k s h re H a t h aw ay H o m e S e v ce s s y m b o a re re g s te re d s e r v ce m a k s of H o m e S e r v ce s of A m eri c a I n c E q u a l H o u s i n g O p p o r u n t y n fo r m a t o n n o t ve ri fi e d o r g u a r a n te e d I yo u r ho m e s c u r e n y li s e d w h a B ro ke r h s s n o t i n te n d e d a s a s o i c a o n
2 8 0 6212 direc t • 6 1 0 2 82 444 4 of fi ce Reb ecc a Fra ncisTea m Info @ gm ail com Rebecc a Fra ncis Realtors .com











Now the region has more choices than ever for children’s health care. You’ll find everything from routine primary care to a long list of pediatric specialists as well as pediatric emergency, surgical, inpatient and critical care. Kids staying in our hospital are treated with leading-edge expertise and a big dose of compassion. Our complete range of pediatric care is convenient to home, close to family and easy to access. St. Luke’s Children’s Hospital. Just another example of how we‘re caring more for kids, parents and the community. sluhn.org/childrenshospital
