Although doctors are trained to make difficult decisions in challenging situations, it doesn’t necessarily mean it gets any easier. This is especially true for ophthalmologists — who hold patients’ vision in their hands. On the last day of the virtual EURETINA 2020 congress (October 4), a panel of experts shared insights from their own experience in diagnosis and treatment, during the Decision Making in Challenging Cases session, chaired by Drs. Giuseppe Querques and Reinier Schlingemann.
by Brooke Herron
Use en face OCT to diagnose


versus AMN
Kicking off the session was Dr. David Sarraf (USA) with his presentation on differentiating between PAMM (paracentral acute middle maculopathy), AMN (acute macular neuroretinopathy), and cotton-wool spots (CWS).
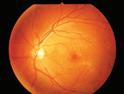
PAMM can be identified by its characteristic hyperreflective bands within the middle retina,





CAKE AND PIE MAGAZINES’ DAILY CONGRESS NEWS ON THE ANTERIOR AND POSTERIOR SEGMENTS 05 | 10 | 20 cataract • anterior segment • kudos • enlightenment 4ISSUE posterior segment • innovation • enlightenment & Decision
Overcoming Challenges in Retinopathy
Making and
J o i n u s f o r t h e v i r t u a l e x p e r i e n ce a n d l e a r n m o r e a b o u t t h e l a t e s t t e c h n o l o g i e s i n e y ec a r e We h a v e a n e x c i t i n g p r o gr a m l i n e d u p, i n c l u di n g t h e u n v e il i n g o f o u r a l l - n e w v i r t u a l s h o w r o o m ! R e g i s t e r he r e: ww w. z e i s s .c o m /e sc r s - e u r et i n a - r e g is t r a t i o n Z EISS O p ht hal m i c V i r tu al E x p e r i e n ce E S C R S - E U R E T I N A S p o t l i g h t 2020 O c t o ber 1 – 4, 2020 Join us for the virtual experience and learn more about the latest technologies in eyecare. We have an exciting program lined up, including the unveiling of our all-new virtual showroom! Register here: ZEISS Ophthalmic Virtual Experience ESCRS-EURETINA Spotlight 2020 October 1 – 4, 2020 Join us for the virtual experience and learn more about the latest technologies in eyecare. We have an exciting program lined up, including the unveiling of our all-new virtual showroom! Register here: www.zeiss.com/escrs-euretina-registration ZEISS Ophthalmic Virtual Experience ESCRS-EURETINA Spotlight 2020 October 1 – 4, 2020 Published by piemagazine.org cakemagazine.org Matt Young CEO & Publisher Robert Anderson Media Director Hannah Nguyen Production & Circulation Manager Gloria D. Gamat Chief Editor Brooke Herron Editor International Business Development Ruchi Mahajan Ranga Brandon Winkeler Writers Andrew Sweeney Hazlin Hassan Joanna Lee Olawale Salami Sam McCommon Tan Sher Lynn Maricel Salvador Graphic Designer Media MICE Pte. Ltd. 6001 Beach Road, #19-06 Golden Mile Tower, Singapore 199589 Tel: +65 8186 7677 | +1 302 261 5379 Email: enquiry@mediamice.com www.mediaMICE.com
Cont. on Page 3 >>
PAMM
EURETINA 2020 Virtual Congress
Missed our EURETINA 2020 symposia? Watch the video recordings to hear our global experts talk about optimizing outcomes in patients with nAMD and DME.
Optimizing patient outcomes in nAMD: The key principles



Chair: Prof. Paolo Lanzetta
Hear from Dr. Michael Stewart, Dr. Nancy Holekamp, and Prof. Nicole Eter as they present the latest evidence and discuss hot topics in nAMD management.
Video recording
Vision in focus: Delivering optimized patient outcomes in DME in the real world





Chair: Prof. Ian Pearce


Listen to Prof. Jean-François Korobelnik, Dr. Varun Chaudhary, and Prof. Francine Behar-Cohen as they share expert guidance for optimizing management of patients with retinal vascular diseases.


Video recording
“Join us as we examine the latest evidence from clinical trials and realworld practice to address key challenges in retinal disease management and ensure we are optimizing outcomes for our patients.”
Prof. Paolo Lanzetta
Additionally, we warmly welcome you to the Bayer Networking Lounge, which will provide you with an opportunity to connect with experts in the treatment of retinal diseases.
Learn more about Bayer Ophthalmology by visiting our online channels:

05 Oct 2020 | Issue #4 2 &
DME, diabetic macular edema; nAMD, neovascular age-related macular degeneration. The summary of product characteristics (SPC) of aflibercept solution for injection as approved by the European Commission can be found here BAYER and the Bayer Cross are registered trademarks of Bayer. © Bayer AG 2020. All rights reserved. Bayer (South East Asia) Pte Ltd, 2 Tanjong Katong Road Paya Lebar Quarter 3 #07-01, Singapore 437161. September 2020 | PP-PF-OPHT-ALL-0047-1 | PP-EYL-SG-0185-1 (09/20)
explained Dr. Sarraf. PAMM lesions can be difficult to detect on examination; they are differentiated from CWS, which are superficial, fluffy and chalk-white.
“PAMM lesions are more subtle, deep and grey,” he continued, adding that these differences can be clearly seen on OCT.
On near infrared, PAMM has a characteristic hyperreflective pattern, which can be confused with AMN. However, he says that with OCT, it is possible to appreciate the differences between PAMM and AMN lesions. “PAMM lesions have levels of abnormality in the middle retina, whereas AMN lesions represent abnormalities in the outer retina,” explained Dr. Sarraf.
“It’s interesting that PAMM and AMN lesions can coexist,” he continued. He then showed a patient case who had all three, including CWS.
While it’s important to understand that CWS, PAMM and AMN are related, they can be easily differentiated with multimodal imaging including en face OCT and OCT-A, which demonstrates their characteristic anatomy and mechanism of injury, concluded Dr. Sarraf.
Anti-VEGF typically not effective in PEVAC
Next, Dr. SriniVas Sadda (USA) presented on PEVAC or perifoveal exudative vascular complex. Citing literature, he described the condition as “a perifoveal, isolated, aneurysmal abnormality.”
“It occurs in otherwise healthy patients, and they may manifest other macular diseases,” he continued, noting that it typically doesn’t respond to anti-VEGF therapy. He says to use caution because sometimes there can be a response, but not because of the PEVAC, but because there could be associated type 3 neovascularization.
He also explained that now, PEVAC is also called ePVAC when there is exudation. “This can be preceded by the preclinical phase of (non-exudative) nePVAC and needs monitoring for conversion to exudation,” said Dr.
Sadda. Since it tends not to respond to anti-VEGF, he suggested focal laser as a treatment option (if it’s far enough away from the foveal center), as well as steroids.
Decision making in rare hereditary retinal disease
In his presentation, Dr. Bart LeRoy (Belgium) provided an overview of how ophthalmic genetics are becoming more complex — but also, a lot of fun. “Molecular analyses are evolving rapidly, and genotyping and phenotyping are inseparable. Genotyping may provide insight into patients’ problems, whereas phenotyping is sometimes crucial to make sense of molecular data,” he began.
To illustrate this, he presented two cases, one of which was a 49-yearold male with subnormal BCVA since childhood. The patient has noticed a progressive loss of vision since age 30 and his color vision was normal. His history showed that several males on the maternal side of his family had visual impairment since childhood. Dr. LeRoy employed several imaging modalities to aid in diagnosis.
However, it was an ERG (electroretinogram) that finally showed a very specific sign: “Electronegativity in the combined rod cone response to an intense flash in the dark-adapted patient, with all the rest being fairly normal” he stated.
Regarding the diagnosis, Dr. LeRoy said: “This is typical of X-linked retinoschisis at a later age; the cystoid lesions that are
normally seen at a younger age go away over time and an age-specific atrophy ensues. The diagnosis was proven with a RS1 mutation on the X chromosome.”

Subtle symptoms and subtle signs
The final presentation was by Dr. Thomas Wolfensberger (Switzerland), who discussed conditions like unilateral paracentral visual disturbances, unilateral diplopia after visual loss, and bilateral intermittent central blurriness.
His first case study was a healthy 40-year-old female who was referred with a visually debilitating paracentral floater. The referring physician was unable to locate any vitreous opacities on fundoscopy. Dr. Wolfensberger also noted that slit-lamp, fundoscopy and OCT were all normal; however, patient history showed that her complaints were consistent and credible.
So, Dr. Wolfensberger decided to dig deeper. On high-definition OCT with multiple scans, there was a small prefoveal vitreous detachment with opacity trapped adjacent nasally to the foveal surface in a space delineated by the posterior hyaloid and the vitreoretinal interface, he shared.
“Patients complaining of floaters in the absence of any clinical signs need to be examined at depth using high-definition OCT, lest their symptoms be branded psychological,” he explained. “Even in a busy vitreoretinal clinic, take the time to listen to the patient and dig down a little bit in their history.”
3 CAKE and PIE magazines’ Daily Congress News on the Anterior and Posterior Segments
>> Cont. from Page 1
One small slip can have devastating consequences in both free climbing and treating vitreoretinal disease.











2 18 November 2022 | Issue #1 SHOW DAILY by DIGITAL MARKETING + ADVERTISING + VIDEO PRODUCTION + MEDICAL WRITING + EVENTS Request our 2023 Media Kit Now! Write enquiry@mediamice.com for a copy HQ Office: 6001 Beach Road, #09-09 Golden Mile Tower, Singapore 199589 Phone: +65 8186 7677 Satellite Office: 2 Nuoc Man 2 Street, Da Nang City, Vietnam 50506 Phone: +84 868 063 773 E-mail: enquiry@mediamice.com Web: www.mediamice.com
Tackling Trauma
by Tan Sher Lynn
Experts shared their views on trauma management during the Forlini Trauma School session on the last day of the virtual EURETINA 2020 congress on October 4.
Dr. Wolfgang Schrader from Germany offers advice on managing severe ocular trauma. The first case he presented involves a perforating injury caused by a rocket in which the posterior segment reconstruction was not attempted for 10 weeks. When the case was referred to him, the attempt to open the posterior funnel with healon failed, and no light perception (NLP) persisted. The second case involved a boy with ocular forklift injury. As the case was promptly referred, he and his colleagues were able to unfold the funnel through the use of viscoelastics. After 2 hours of surgery, they were able to secure the retina with the endolaser. Four weeks later, VA was 6/200 and six months later, VA was 10/200.
The cases show that there is a limited window of time for successful reconstruction. “NLP is no contraindication for attempting reconstruction. Evaluate OTS score and have extensive counseling with the patient and his/her family, as often, repeated surgeries for months are necessary. For early secondary vitreoretinal reconstruction, it is beneficial to do it within 100 hours. If you fail, there might be someone else who is able to reconstruct, but this should be done quickly within days rather than waiting for months or years,” he said.

Dr. Marco Zarbin from the USA agreed that loss of light perception after open globe injury does not necessarily mean the patient will have permanent visual loss. “Reported visual recovery rates from NLP to LP or better after open globe injury range from 4% to 33%. Unfortunately, there is no set of findings (except optic nerve avulsion, optic nerve transection, or profound loss of intraocular contents) that allows clinicians to be certain that NLP status is permanent,” he said.
“As such, we focus on identifying anatomic findings that are amendable with surgical repair. B-scan echography is best to identify retinal detachment, subretinal hemorrhage and suprachoroidal hemorrhage. We also try to identify findings that are consistent with irreversible loss of vision. Enucleation is considered for open globe injuries with NLP and major loss of retinal tissue or optic nerve avulsion/ transection. But for eyes with NLP after open globe injury that undergo successful primary closure with intact optic nerve should be considered for additional surgery, particularly if there is recovery of LP on postoperative day-1 after primary repair; treatable pathology underlying NLP status, such as extensive choroidal hemorrhage, extremely dense vitreous hemorrhage with RD, and/or subretinal hemorrhage; NLP in fellow eye; and if the patient is a child.
Meanwhile, Dr. Robert Rejdak from the Medical University of Lublin, Poland, said that post-traumatic endophthalmitis is fairly common (25-30%) and usually carries a worse prognosis if
it’s caused by virulent pathogens (Bacillus, Staphylococcus), or soil contamination, and if the patient is younger and male. “The primary line of treatment for the vast majority of eyes with endophthalmitis should be early vitrectomy with vancomycin in infusion fluid, ceftazidime and, if appropriate, voriconazole,” he advised.
Endoscopy can be an excellent option for optimal visualization in ocular trauma. According to Dr. Khalid Sabti from Kuwait, even though endoscope has a longer learning curve, it can assist in performing challenging maneuvers, such as ILM peeling for traumatic macular holes and repair of retinal detachment.
“Endoscopy allows excellent view to the posterior segment in selected trauma cases when getting a good view with conventional viewing systems is difficult or impossible. It gives us the chance to visualize the vitreous base and area behind the iris. It also provides a closer view to the retina. It helps to minimize surgical trauma and has fewer limitations than many surgeons believe,” he said.
5 CAKE and PIE magazines’ Daily Congress News on the Anterior and Posterior Segments
Opening Eyes
Highlights from the Research Session
by Sam McCommon
Ophthalmic research always draws a keen eye, and the October 4 session at the virtual EURETINA 2020 congress was no outlier. Some fascinating research results were presented, ranging from the tiny bacteria that make up our microbiome to larger concepts like artificial intelligence.
Gut microbiome and AMD

Many branches of science have been paying more attention to the microbiome and its effects on the larger human organism. We each have something to the tune of 100 trillion bacteria living in our gut, and upwards of 10,000 gut bacteria species have been identified — many of which are beneficial. But when the microbiome is out of whack, larger biological systems can go haywire as well.
Dr. Martin Zinkernagel explored the link between a person’s gut microbiome and age-related macular degeneration (AMD). In bad news for mice — and potentially humans — mice who were deficient in Complement Component 3 (C3) had significantly altered gut microbiomes compared to healthy mice.
There were similar discrepancies when patients with AMD were studied. Essentially, certain types of bacteria were more prevalent in those with AMD than those without. For example, Fermicutes was not more prevalent in those with AMD, but bacteroides were significantly
over-represented in patients with AMD.
There’s still lots of room for research in this field, to be sure, but even linking the gut microbiome to AMD is a significant step and one that should be explored further — especially as the gut microbiome has been so closely linked to inflammation.
Geographic atrophy and age

Geographic atrophy (GA) — otherwise known as advanced dry AMD — was a topic presented by Dr. Caroline Klaver. A central focus of her presentation was on age, notably the age of onset and the remaining years of life a patient had before they passed on.
Perhaps one of the most interesting questions was raised in the postpresentation discussion. After the effects of GA truly set in, a patient had on average 6.4 years left to live. Of those who suffered GA, around 44% studied ended their lives significantly visually impaired towards the end of their lives.
A question raised in the discussion was just how valuable treatment was given GA usually occurs so late in life. Of course, no one would choose to have their eyes deteriorate — but expensive and risky treatments may not be worth it for those who have very limited time left. For those with significant time left, treatment may indeed be well worth it.
What is a trustworthy AI?
Artificial intelligence (AI) is becoming more important in, well, just about everything. That includes ophthalmology. But how can a practitioner, researcher, or patient know when an AI is trustworthy? Indeed, what makes a trustworthy AI, and how do you manage it?
Such a topic was brought up yesterday in the context of imaging: AI graders for conditions like diabetic retinopathy require higher-quality images than human graders do. However, when given higher-quality images, they can do excellent work.
A reliable AI needs to be able to handle different parameters, create reproducible results, and have a fall-back plan in case things go wrong. So what happens when it goes wrong, and you can’t trust the results?
Dr. Clarisa Sanchez discussed how to manage AI to make it trustworthy — and gave it a human touch as well. In the discussion, when asked if an ineffective algorithm should be thrown out, she displayed an almost maternal protectiveness. Essentially, she said, rather than throw out an algorithm that isn’t working perfectly, it needs to be guided like a child. It needs to be fed more information, and guided towards the correct answers more frequently — so that, when the time comes for it to be independent, it can be trusted.
AI is far from independent yet, but given the rate of technological development — combined with the fact that this software can learn — it likely won’t be long before AI is one of the most valuable tools any medical practitioner has.
05 Oct 2020 | Issue #4 6 &
Unraveling the Black Hole in Myopic Macular Diseases
Highlights from the EURETINA Myopia Update Session
by Olawale Salami
seen in patients with inner segment/ outer segment defects and foveal detachment,” noted Dr. Ikuno, commenting on risks.
Furthermore, Dr. Ikuno shared a new technique known as a foveal non-peeling technique, which was developed by a group in Taiwan. “In this technique, you peel the ILM in a donut fashion to limit the fovea’s damage,” he said.
PICs in OCT imaging: Look closer
“Hyperreflective material in spectral domain optical coherence tomography (SD-OCT) images of high myopes with acute blurred vision is often seen in patients with punctate inner choroidopathy (PIC), choroidal neovascularization (CNV), and myopic CNV ( M-CNV),” reported Dr. Xiao-Xin Li.
“These three different lesions look very similar on SD-OCT, but the treatment is different, as M-CNV, PIC-CNV and CNV need treatment with anti VEGFs, while PIC is self-limiting, “said Dr. Li. Discussing the design of clinical studies, Dr. Li shared that her team conducted a retrospective study aimed at evaluating SD-OCT images in PIC, PIC-CNV, and M-CNV. They observed hypo and hyper transmission and analyzed the integrity of the RPE/ Bruch’s membrane, she said.
—
During the Myopia Update 2020: Pathogenesis, Diagnosis & Treatment session at the virtual EURETINA 2020 congress on October 4, Dr. Yasushi Ikuno discussed current approaches to the surgical management of myopic macular diseases.
Myopic foveoschisis (MF) is one of the major causes of visual loss in highly myopic eyes, and optical coherence tomography (OCT) imaging shows the splitting of the inner and outer retinal layers, and sometimes, retinal detachment, highlighted Dr. Ikuno.
On the general principles of surgical management, Dr. Ikuno stated that: “The surgical approach to management involves vitreous cortex removal, internal limiting membrane peeling. Others have proposed a gas tamponade, but it remains controversial.”
According to Dr. Ikuno, there are three subtypes of myopic foveoschisis: Retinoschisis, foveal detachment, and macular hole. “And these subtypes have different surgical outcomes, with a macular hole having the worst prognosis of them,” he explained.
“Vitreoretinal surgery represents a major risk factor for the development of macular holes, and higher risks are
Dr. Ikuno and his team sought to confirm the effectiveness and safety of this fovea sparing ILM peeling technique. “We conducted a retrospective study, where we reviewed the data from 58 patients/ eyes at Osaka University. We concluded no significant differences in anatomical or visual functions between patients who underwent the foveal sparing compared to the standard technique. These results could be limited because of our small sample size,” he shared.
“With other studies, my take-home message is that in patients with foveoschisis, vitrectomy should be considered after retinoschisis. However, post-perative macular hole remains a significant complication, but foveal sparing ILM peeling may be an option in these cases,” concluded Dr. Ikuno.
ILM flap method remains a promising technique for surgical closure of macular holes.
“OCT imaging showed no disruption of RPE/ Bruch’s membrane in eyes with punctate inner choroidopathy”
— Dr. Xiao-Xin Li
“We defined PIC as a single or multiple lesion at the outer retina or RPE level, and no CNV. Next, we defined PIC-CNV as a neovascular lesion at the outer retina level that involves choroidal and retinal pigment epithelium, identified by OCT-A. Myopic CNV was defined as neovascularization at the outer retina level, involving the choroidal and RPE, identified by OCTA,” explained Dr. Li.
According to Dr. Li, all patients in the study had an acute blurred vision or distorted vision within 4 weeks, with myopia of at least -5D. SD-OCT showed an active, hyperreflective lesion, and patients were followed up for a minimum of 2 months.
“Hyper transmission was found in PICCNV patients. Our OCT imaging results showed no disruption of RPE/Bruch’s membrane in PIC, while RPE/ Bruch’s membrane is a definite sign of choroidal neovascularization and all patients showed features of ellipsoid zone disruption,” she concluded.
7 CAKE and PIE magazines’ Daily Congress News on the Anterior and Posterior Segments
“In patients with foveoschisis, vitrectomy should be considered after retinoschisis . However, Post-operative macular hole remains a significant complication, but foveal sparing ILM peeling may be an option in these cases.”
Dr. Yasushi Ikuno
Beyond
New Frontiers in Retina Innovation
by Brooke Herron
Today, we have numerous imaging modalities to visualize the eye’s posterior segment — and certainly this number grows along with innovation. Therefore, on the last day of virtual EURETINA 2020 congress (October 4), future advances in optical coherence tomography (OCT), tele-ophthalmology and artificial intelligence (AI) were among the topics discussed during the Beyond 2020: New Frontiers in Retina Innovation session, chaired by Drs. Judy Kim and Daniel Ting.
See more with high-resolution OCTA
“With OCT angiography (OCTA), we make multiple OCT scans. We compare those scans and look for differences — and from that, we can derive flow information,” said Dr. Rick Spaide (USA).
He says that when you look at OCTA, the information is relatively sparse: There are areas where the blood vessels are discontinuous and other where they are very faint. He then showed scans from a new, high-resolution OCTA prototype by Heidelberg Engineering (Heidelberg, Germany), with a 2.3 µm axial resolution and easy-to-see capillaries.
Dr. Spaide says that “this is an OCT that’s coming up and allows for imaging details that we couldn’t see before.”
The Future of OCT imaging
During his presentation, Dr. SriniVas Sadda (USA) provided a succinct overview of upcoming innovations in OCT imaging.
Ultra high-speed: “We’ve seen dramatic progress . . . but we can go a lot faster — and a lot faster matters when we’re talking about millions of A-scans per second, because we’re able to do much denser, transverse high-resolution en face imaging.”
He emphasized that ultimately, in both spectral domain OCT (SD-OCT) and swept-source OCT (SS-OCT), the limits of speed may not be the light source, but actually the processing speed. “There are new processing approaches that may overcome these limitations,” said Dr. Sadda.
Ultra high-resolution: “If you want to further improve the transverse resolution of OCT, you really have to correct for ocular aberrations in the eye — and that requires adaptive optics.”

Ultra widefield/Far peripheral: “We can also go extra wide, and that’s something that’s at the forefront of OCT technology these days. I don’t think it’s a huge leap of faith to say that we can expect ora-to-ora scanning and whole eye OCT scanning in the near future.”
Home/Miniature OCT: “Another huge trend that is just around the corner is

doing home or miniaturized OCT . . . these kinds of devices can be married with AI algorithms, so you can imagine the patient doing the test at home, some fluid is detected, and then coming in for an assessment.”
Tele-ophthalmology: Where are we headed?
“Tele-ophthalmology, by definition, is eye care carried out remotely, using audiovisual telecommunications technology,” began Dr. Judy Kim (USA). “Telemedicine has been used around the world to provide access to eye care and to increase eye screening.”
However, she says that to establish a successful tele-ophthalmology system, there are many factors to consider. “This includes, firstly, the camera, where much effort is being made to design a good quality camera,” she said, adding the combination of imaging devices, with a low-cost and small footprint may allow for greater screening and diagnosis.
“The future of tele-ophthalmology will also be immensely improved by the incorporation of artificial intelligence,” she said.
Dr. Kim says that “given our current circumstances around the world, and as newer treatment modalities are developed, I believe that teleophthalmology will play a greater role.”
Can AI answer the unanswerable?
During the final presentation on AI, Dr. Daniel Ting (Singapore) brought up an important point during his presentation: “Can AI now unravel some of the unknown OCT parameters that humans or retina specialists don’t know?”
He shared that this year, Google and Moorfleld’s Eye Hospital jointly published a paper to “predict in patients with nAMD, the risk of conversion from dry to wet in the fellow eye.” The paper found that the AI algorithm has a superior performance to ophthalmologists and optometrists in gauging the risk of conversion.
With all of these innovations . . . the future is certainly looking “clearer” than ever before.

05 Oct 2020 | Issue #4 8 &
You Make the Call Highlights from the ESCRS Video Symposium on Surgical Complications
by Olawale Salami
Iridodialysis repair: Don’t rock the boat
you can define only the extension of the zonular dialysis in the area with no iris, but you don’t know if this area is more extensive. The ultrasound microscopy could also be useful here,” he explained.
Based on the polling results, 70% of conference attendees identified zonular instability as a major issue.
decided that iridodialysis repair is not necessary, given its long history and its position, which did not disturb the patient’s vision,” he said.
When the lens gets wobbly
If you have a case of a very wobbly lens with a cohesive viscoelastic device in the anterior chamber, what would you do? That’s the question Dr. Nick Reus asked during his case presentation, further in the session.
During the video symposium on surgical complications on the last day of the virtual ESCRS 2020 congress (October 4), Dr. Boris Malyugin from Russia presented an iridodialysis case of a 70 year-old patient who required an IOL implantation.
“The patient had a history of blunt trauma to the left eye as a child. His IOP was unremarkable, and astigmatism was moderate. An IOL implant of 22D was planned. On examination, there was an area of iridodialysis which occurred due to the blunt trauma,” shared Dr. Malyugin.
The possible complications in this eye, according to Dr. Malyugin, could be IOP fluctuation, zonular instability, or iris damage. “However, with the OCT,
“I decided to make a femtosecond laser capsulotomy, which is a good option for patients where we expect zonular issues. Then I performed hydro dissection, which was done gently to avoid excess pressure on the anterior capsule and utilized intraoperative OCT to ensure the nucleus and cortical materials were removed completely,” explained Dr. Malyugin on how he treated the case.
Tackling surgical complications, Dr. Malyugin noted: “From the OCT, I saw a bulge in the posterior capsule, and so the next question was: could this be a case of infusion misdirection syndrome? Indeed this was the case.”
Regarding the final treatment decision, Dr. Malyugin highlighted that due to the zonular defect, a conventional capsular tension ring was the preferred device in this case to support the IOL. “Finally, I
Dr. Reus then described the surgical approach that was taken in the management of this case. “My opinion here is that if the lens is wobbly, it is important to have a good view of the capsulorrhexis, so I put in some trypan blue and left the cohesive viscoelastic in place,” he shared.
“With the trypan blue, you can see that the entire lens was moving during the capsulorrhexis, which was more visible at the 6 o’clock position, “ Dr. Reus said.
Talking about zonulolysis, Dr. Reus highlighted that he and his team pondered on what to do with an inferior zonulolysis. “In such a case, there is a risk of vitreous prolapse into the anterior chamber through the zone of dehiscence. Therefore, as a precautionary measure, I usually insert a dispersive viscoelastic device in the sulcus,” he explained.
“I then performed a careful hydro dissection to ensure that the lens was rotating freely in the bag and there was no stress on the zonules,” he added.
Removing the lens came with complications as expected. Dr. Reus said: “To remove the lens, I used a divide-and-conquer technique, and there were some difficulties with handling the lens around the equator. For proper lens removal in such a case, it is crucial to avoid injuries to the zonular regions to keep the bag open and avoid possible posterior capsule rupture. So I recommend the use of dispersive OVD.”
“Then, to remove the cortex, I used a bimanual irrigation and aspiration cannula with a polymer tip, and low flow settings as an extra precaution to prevent capsule rupture. Finally, I inserted a 30-piece lens in the sulcus with optic capture,” concluded Dr. Reus.
9 CAKE and PIE magazines’ Daily Congress News on the Anterior and Posterior Segments
“In cases like this, an intraoperative OCT is very useful to fully assess the margins on the zonular area.“
— Dr. Boris Malyugin
The Cornea Nothing
Corny about 20/20 in 2020
by Sam McCommon
The final day of the virtual ESCRS 2020 congress (October 4) featured a two-hour discussion on corneal techniques cleverly titled 20/20 in 2020. It featured some wonderful speakers going on deep dives into all things cornea, and likely could be a conference all of its own.

But we should appreciate it being condensed into what it was, because there were some remarkable takeaways.
Supervision: Better than 20/20?
Denmark’s Dr. Jesper Hjortdal began the discussion with the question of supervision. The retina can do better than it currently is, he says — after all, eagles supposedly have a visual acuity of 20/5! At the very least, this means it’s physically possible for eyes to be better.
The 20th century goal, he pointed out, was to eliminate sphero-cylindrical blur with spectacles, contact lenses,


intraocular lenses, or refractive surgery. And that was indeed a lofty goal — but we’re not in the 20th century anymore. So what’s next?
The 21st-century goal should be to eliminate all traces of natural optical blur due to higher-order aberrations of the eye. Ultimately, this should create perfect retinal images and perfect vision.
The first twenty years of the 21st-century have not yet produced this perfect vision, unfortunately. Wavefront-guided corneal refractive surgery is not superior to wavefront-optimized corneal refractive surgery and wavefront-guided spectacles don’t provide perfect vision either. The same is true for contact lenses.
One of the main problems barring patients from achieving perfect vision is that visual aberrations are unstable over time. Tear fluid differs even between blinks, for example, not to mention between individuals. On top of that, pupil size limits maximum retinal visual acuity — the smaller the pupil, the less
visual acuity possible. So, unfortunately, super vision can’t be achieved in strong sunlight.
Dr. Hjortdal noted that astronomers have adopted adaptive optics (say that five times fast) to account for aberrations in the atmosphere. Unfortunately, according to data presented by Dr. Hjortdal, using adaptive optics for humans leads to worse visual acuity. Unfortunately — or fortunately, depending on your perspective — our eyes are not telescopes.
The real, most important question presented by Dr. Hjortdal was this: Is super vision worth aiming for? The answer is a resounding “not really.” Visual quality, he argues, is far more important than visual acuity. Reducing aberrations can make the effects of presbyopia worse, for example, so maintaining the soft lines rather than the jagged edges of imperfect images actually makes it easier to see. The goal should be the normalization of refractive errors rather than simply aiming for perfect visual acuity.
SLAK surgery: New options
Dr. Mario Nubile featured a presentation on stromal lenticule addition keratoplasty (SLAK), which is valuable in advanced keratoconus as well as refractive conditions. It can also be used in stromal loss to increase corneal thickness and curvature.
This procedure is still under development, and plenty more needs to be done. For example, according to Dr. Nubile, lenticule profiles and implantation depths need to be refined to achieve better predictability and stability.
In the discussion that followed Dr. Nubile’s presentation, a valuable point was raised. In the current procedure, the lenticules implanted are standardized, and are best for central keratoconus. In the near future, customized lenticules may be able to be made that can be adjusted to fit the individual patient. Once that’s possible, the world of opportunities for SLAK will likely open wide up, since many keratoconus patients have irregular corneal structures.
05 Oct 2020 | Issue #4 10 &
Get Ready for ISCBS Cataract Surgery, Says ESCRS President
by Andrew Sweeney
Imagine a world without blindness, it’s easy if you try, imagine all the people, livin’ for today… John Lennon sadly didn’t include a verse about curing global blindness in his song Imagine, but perhaps he should have. It is a dream of ophthalmologists throughout time, imagine a world where not a single child goes blind.
Could such a utopian goal ever be reached by the ophthalmological community? That was part of the discussion of the European Society of Cataract & Refractive Surgeons’ main seminar on its final day (October 4), Main Symposium: The Next Decade of Cataract Surgery. Offering an in depth examination of cataract surgery’s progress, the seminar was a fitting end to ESCRS 2020.
Prof. Dr. Serge Resnikoff of the Brian Holden Vision Institute in Sydney, began the symposium by setting out his belief in achieving an ambitious goal; the complete global elimination of blindness. He reported that there are an estimated 17 million unoperated cases of blindness in the world, primarily in Asia. Prof. Dr. Resnikoff views this as a long term but achievable goal.
a cause of blindness. However, while his optimism was met with enthusiasm, several of the participants of the symposium reported their skepticism about drawing a comparison. They argued that eliminating blindness via surgery was a far more lofty goal, and relies far more on high quality surgical training.
President of the ESCRS Prof. Dr. Rudy MMA Nuijts then presented his research on bilateral cataract surgery becoming the norm over the coming decade. Pointing to practical experience during the coronavirus pandemic, Prof. Dr. Nuijts said that immediately sequential bilateral cataract surgery (ISCBS) was more beneficial for patients and cost effective. Pointing to an ESCRS survey of Dutch doctors, nearly 50% of those polled said they were considering carrying out ISBCS.
“There is certainly a cost benefit in relation to ISBCS. The current guidelines in the Netherlands don’t allow it to be performed of course, but ISCBS is clearly
non-inferior to delayed sequential bilateral surgery at the predefined 10% noninferiority margin,” Prof. Dr. Nuijts said.
“There is no difference in effectiveness and significant lower costs. The potential cost savings in the Netherlands alone is €37 million from a health perspective, and €64 million from a societal perspective,” he said.
Following on was Prof. Dr. Thomas Olsen from the University of Aarhus in Denmark, who presented on improved ocular biometry imaging. He showed that the number of papers and research on the issue has been increasing exponentially, and that intraocular lens accuracy is rising exponentially. Prof. Dr. Olsen made his feelings clear; ‘biometry is no longer a significant source of error.’
According to the professor, new developments in biometry will use artificial intelligence and deep learning algorithms to achieve significant benefits for patients. Prof Dr. Olsen believes his own accuracy presidential model, the Olsen Method, can eliminate the main cause of error affecting biometry, namely lens placement.
Throughout the symposium the participants were optimistic about the overall direction of ophthalmology, despite any specific disagreements they may have had with individual findings. Such positivity is a sentiment we can really get on board with.
He pointed to the global ophthalmological community’s success in significantly depressing trachoma as
11 CAKE and PIE magazines’ Daily Congress News on the Anterior and Posterior Segments
“There is no difference in effectiveness and significant lower costs. The potential cost savings in the Netherlands alone is €37 million from a health perspective, and €64 million from a societal perspective,”
— Prof. Dr. Rudy MMA Nuijts
Simplifying Complexities in Cataract Surgery
Highlights from the ZEISS Satellite Symposium
by Hazlin Hassan
In cataract surgery, identifying possible complexities preoperatively is important.
Thus preoperative screening is essential, and diagnostic devices and surgical tools play important roles in clinical exams.
Using swept source biometry, which offers better accuracy and speed of measurements, can help surgeons to eliminate potential sources of errors and the risk of refractive surprises.

“One of the remarkable advantages of swept-source biometry is the superior repeatability,” said Dr. Douglas Koch from the Baylor College of Medicine, USA. It also has a very rapid acquisition time.
In a study comparing the efficiency of a swept-source optical coherence tomography biometer, IOLMaster 700 (IOLM700), and a low-coherence optical reflectometry biometer, LENSTAR LS 900 (LS900), when acquiring biometry measurements during cataract evaluation, the IOLMaster was 73% faster than LENSTAR said Dr. Koch, who is a co-developer of IOLMaster 700’s Central Topography software feature.
In busy clinics, the use of the IOLM700 for biometry measures may save time and prove to be more efficient.
It also achieves a cataract penetration rate of 99% and reduces the number of A-scans even in dense cataracts, resulting in an improved workflow.
In a study of 1226 eyes, 99.5% cataract penetration rate was recorded in all but 6 eyes.

Further, 91.3% (21/23) of the eyes that were unsuccessful with IOLMaster 500 were measurable with the IOLMaster 700.

The IOLMaster 700 may also detect some macular holes and intraretinal fluid.
There is a fixation check to reduce the risk of refractive surprises. See the foveal pit? Good fixation! No foveal pit visible: Poor fixation!
In conclusion there are multiple advantages of swept-source biometry including improved accuracy of measurements and high repeatability and reproducibility.

Professor Oliver Findl, from the Vienna Institute for Research in Ocular Surgery (VIROS) Vienna, Austria, presented on how ZEISS helps to simplify and streamline patient workflow, thanks to paperless data transfers.
He uses the IOLMaster 700, FORUM with EQ Workplace, EQ Mobile, LUMERA 700 ophthalmic microscope with CALLISTO eye computer-assisted cataract surgery.
The EQ Workplace software from ZEISS streamlines the refractive cataract workflow and helps surgeons to save time during the preoperative processes.
05 Oct 2020 | Issue #4 12 &
With the EQ Workplace, surgeons can get access to their biometry data anytime, anywhere, and calculate IOLs without interrupting the measurement workflow.
In Prof. Findl’s cataract workflow, there is no manual entry for IOL power calculation which helps to avoid errors.
IOLMaster data is transferred automatically to the EQ Workplace. Data is also transferred smoothly to CALLISTO eye, saving time and boosting efficiency.
“All this data has been uploaded into the cloud, and I have it on my iPhone, I can access the cloud from my iPhone. I can choose several patients, and all I need to do is open the CALLISTO system which is connected to the LUMERA 700 microscope,” he said.

“The great thing about this workflow is that there is no manual entry for IOL power calculation, as we used to do it, where you had to use online calculators which can cause errors. You can choose the IOL during patient informed consent, you can order the IOL straight away through the email, and that really increases efficiency, and you can close the loop and audit your results afterwards.”
The miLOOP ® from ZEISS is a microinterventional lens fragmentation device which is designed to remove the challenges of hard cataracts.
Using micro-thin super-elastic, selfexpanding nitinol filament technology, the miLOOP allows cataract surgeons to achieve zero-energy lens fragmentation for any grade cataract.
Dr Gerald Roper, from the USA, shared his experience using the miLOOP.
“Microinterventional lens fragmentation with the miLOOP device reduces residual refractive error and has the potential to improve visual acuity outcomes,” he said.
“Less trauma to the capsule and zonules during the fragmentation
improves predictive accuracy of IOL power calculation formulas,” he said adding that further studies are needed to validate these findings.
Complications during cataract surgery occur at a higher rate in eyes with pseudoexfoliation syndrome than in standard cataract cases. This is a challenge.
Using the CT Lucia 621P, a newgeneration aspheric monofocal c-loop IOL, helps to provide fast and safe implantation using a new fully preloaded injector system, said Dr. Andreas F. Borkenstein, co-founder of Borkenstein & Borkenstein, private practice at the Clinic of Kreuzschwestern Graz, Austria.
Combining the benefits of aspheric and neutral IOLs makes the IOL less sensitive to decentration.
Its optic-haptic junction design ensures stability intra- and postoperatively.
The fully preloaded injector system is easy, fast and smooth to ensure good OR workflow with high reproducibility and safety.
“I’m choosing CT Lucia 621P because it is easy to use, it provides safe implantation in PXF eyes (undilated, phacodonesis, Malyugin), there is a smooth unfolding process without sticking, good IOL centration, optical quality, less sensitive to decentration, excellent clinical results after 1 year follow-up (BCVA), refractive predictability and stability,” said Dr Bokenstein.
There are also encouraging preliminary results in posterior capsule opacification (PCO) rates, he reported.
Editor’s Note:
The ZEISS Satellite Symposium was held at the virtual ESCRS 2020 congress on October 4, 2020. Reporting for this story also took place at the said conference.
13 CAKE and PIE magazines’ Daily Congress News on the Anterior and Posterior Segments
Highlights from the ESCRS-EURETINA Symposium on Cataract Surgery in AMD Patients
by Olawale Salami
Retinal dystrophy: The great masquerader in AMD


Are there other diseases often diagnosed as age related macular degeneration (AMD)? Dr. Carel Hoyng asked this question at the joint ESCRS/EURETINA symposium on the second day of the virtual EURETINA 2020 congress (October 3).
According to Dr. Hoyng, in a region of about 500,000 people around our hospital, we found 150 cases of sporadic cases of central areolar choroidal dystrophy, a hereditary disorder associated with a pathological mutation in the PRPHP2 gene. Most of these patients were diagnosed by their ophthalmologists as having AMD.
“In a database of 800 patients with AMD, we found 19 cases of patients with 2 mutations in the ABCA4 gene, which is the gene responsible for juvenile macular dystrophy (Stargardt’s disease),” reported Dr. Hoyng.
On the prevalence of dystrophies, Dr. Hoyng explained: “We found that these dystrophies can present as AMD, and in a genome-wide analysis that we performed, we discovered about 59 cases of monogenetic diseases in our cohort of 800 patients. This means that about 5% to 10% of cases of AMD result from monogenetic diseases.”
What are the distinguishing features of these dystrophies? Dr. Hoyng noted that they are characterized by early disease onset and positive family history. “When you examine, you are likely to find abnormalities on autofluorescence,
marked symmetry, and abnormal fundoscopy findings, such as yellow flecks, drusen, and drusen-like deposits in the retina,” explained Dr. Hoyng.
05 Oct 2020 | Issue #4 14 &
Examples of the most common dystrophies, according to Dr. Hoyng, include late onset Stargardt’s disease, adult-onset foveo-macular vitelliform dystrophy and pattern dystrophy. And that these diagnoses can only be confirmed by genetic testing.
Intravitreal injections and lens capsular rupture: Keeping it safe
“Dealing with a compromised lens capsule after intravitreal injections is a subject that many cataract surgeons are concerned about during surgery because there is a higher risk of posterior capsular rupture after many injections,” said Dr. Oliver Findl of the Vienna Institute for Research in Ocular Surgery.
“In fact, after about after 10 injections, the risk of a lens capsule rupture is more than doubled,” he added.
According to Dr. Findl, the widespread use of anti-VEGFs has changed how we manage sightthreatening diseases. Because multiple injections are needed due to the short half-lives of the anti-VEGF, this comes with associated risks’.
“Posterior capsular rupture occurs as a complication in about 2% of cases, and can lead to dropped nucleus, inflammation, endophthalmitis, retinal detachment and ultimately, poor visual outcome,” explained Dr. Findl.
“It appears that capsular rupture is even possible without visible damage (lens touch) to the posterior capsule,” he said.
And there is evidence to show this, noted Dr. Findl, who shared some data to support this statement. For example: “In a recent study of 4047 eyes, 108 eyes (2.7%) received anti-VEGFs. We saw that the capsular rupture rate was significantly higher (9.3% Vs. 1.9%) in those eyes that received anti-VEGFs compared to the control group.” “‘This risk of posterior capsular rupture was dose-dependent, with a relative risk of 8.6% per injection,” reported Dr. Findl.
estimate the effect of cataract surgery alone and special IOLs,” explained Dr. Scharioth. “However, if we find that the preoperative BCVA is worse than the cataract suggests, then immediate implantation of special IOLs could be indicated,” he said.
Dr. Scharioth identified gaps in currently available products. He highlighted that there are various special, magnifying IOLs on the market, with differences in their methods of action. However, many of these magnifying IOLs have not been well adapted because of large incisions and difficult Surgery and could affect distance vision and/or visual field. Besides, these IOLs are sensitive to decentration and tilt, affect retinal diagnostics, and can only be used in combination with cataract surgery. Some magnifying IOLs have unpredictable postoperative refraction, are very expensive with limited reversibility, and are contraindicated in single eye patients.
— Dr. Oliver Findl
On imaging in suspected cases, Dr. Findl stated that OCT can be beneficial in identifying posterior capsular ruptures that may be linked with intravitreal injections, and this is an area where published literature is lacking.
“The management requires a nearperfect Continuous Curvilinear Capsulorrhexis (CCC) with no hydrodissection and careful hydrolineation to reduce the risk of lens dislocation into the posterior segment,” said Dr. Findl. Also, careful phacoemulsification, with anterior vitrectomy (using 23G) and 3-piece IOL in sulcus.
In search of the best IOLs for patients with advanced macular disease
Finding the right IOLs in patients with the advanced macular disease remains a subject of intense debate among surgeons. “In patients with mild to moderate AMD, I don’t think there is a need for special IOLs, and standard technique and implants can be used,” said Dr. Gabor Scharioth of Germany. “The problem is that it is difficult to

“My choice of an IOL in AMD patients is a single piece, hydrophobic acrylic, made of clear material and in-the-bag implantation. Special lenses like the Scharioth Macular lens (SML), which we developed, can be used for patients with visual acuity <0.3 and advanced AMD, in the better eye,” shared Dr. Scharioth.
The Scharioth Macular Lens (SML) has now been implanted in more than 1000 eyes worldwide, and can potentially help patients with any macular disease. According to Dr. Scharioth, it provides sufficient magnification with no negative impact on the visual field or distance vision. “It also has highly predictable postoperative refraction, is affordable and can be reversed where necessary. Several studies have shown improved near vision in patients with advanced maculopathy,” he reported.
15 CAKE and PIE magazines’ Daily Congress News on the Anterior and Posterior Segments
“The question that has always lingered is ‘what is the impact of anti-VEGF injection on the posterior capsule’? Are there biochemical effects of this chronic application of anti-VEGFs on the posterior capsule?”
“In patients with mild to moderate AMD, I don’t think there is a need for special IOLs, and standard technique and implants can be used,”
— Dr. Gabor Scharioth
CONTENT MARKETING + ADVERTISING + MEDICAL WRITING







05 Oct 2020 | Issue #4 16 & 6001
Road, #19-06 Golden Mile Tower,
199589 magazine posterior segment innovation enlightenment
Beach
Singapore









































