










:

The title of the Lecture will be: Headwinds, Pandemics and the Rules of Golf - Tips for Delivering Your OH Strategy
For over 15 years, as VP for Health and CMO Dr Richard Heron led BP’s Global Health Agenda. This included wellbeing, occupational health, industrial hygiene and public health in over 65 countries.

Event open to Members/Non-Members, join the iOH Event details can be found on the iOH Website Tickets are limited to 60 and available at Eventbrite discount for members


Sponsored By :
 The Ruth Alston Memorial Lecture will be delivered by
Dr Richard Heron
The Ruth Alston Memorial Lecture will be delivered by
Dr Richard Heron

Clare qualified as a Physiotherapist in 2005 and quickly fell in love with musculoskeletal rehabilitation and occupational health and wellbeing (OH&W).

She has over 15 years of experience in delivering occupational health physiotherapy and workplace assessments in both the public and private sectors. She has also completed post-graduate training in Occupational Health via ACPOHE and an MSc in Occupational Health (Policy and Practice) in 2014.
Clare is the owner of Bespoke Wellbeing, which is a national provider of Occupational Health Physiotherapy, Workplace Assessments, and Functional Capacity Evaluations.
Her work in the field of Occupational Health has also been recognised in several awards and programmes, such as; ‘Best Musculoskeletal Initiative’ in the Occupational Health and Well-being Awards 2020, Natwest Accelerator Programme - "Scaling up Occupational Health Physiotherapy across the UK", Great British Entrepreneur Awards (GBEA) 2019, and the Zenith Global Health Award (Allied Health Professional) 2019.
Clare hopes her role at iOH will help to:
• Raise awareness and career opportunities in OH&W to AHPs.
• Break the silos within OH&W to create collaborative learning and services across clinical specialisms.
• Scope the specific OH&W learning needs AHPs may have and how this interlinks to wide iOH CPD programmes.
• Support member CPD for MSK, DSE/Ergonomics, Long Covid recovery, and functional capacity/physical capability testing to support a return to work.

 BY Phina Amahoro
BY Phina Amahoro
“Leadership in an occupational health (OH) context is defined as the ability to positively influence the working populations’ health and well-being while adapting to the ever-changing needs of the workplace”
There are numerous definitions of leadership across all healthcare disciplines, this may be because leadership has been observed to encompass various attributes and is often defined through the lens of an individual’s own perspective or experience of leadership. The literature available on leadership surmises that ultimately, leadership depends on the people and situation at hand (Syrett and Hogg, 1992).
Leadership in an occupational health (OH) context is defined as the ability to positively influence the working populations’ health and well-being while adapting to the ever-changing needs of the workplace. This is met by several challenges. For example, the ageing population, chronic conditions and the ever-increasing gap between demand and supply. Despite these challenges, clinical leaders within occupational health settings are tasked with the paramount responsibility of directing and influencing teams. (AlHabib, 2020; McCauley and Peterman, 2017; Dodd, 2012; Michaud, 1984).
OH Nurse (OHN) leadership differentiates itself from other nonclinical organisational leadership in a few ways. OHN leadership is rooted in delivering high-quality care and ensuring patient/client safety while maintaining traditional caring skills, with the addition of focusing on business outcomes and cost efficiency (Nieuwboer et al., 2019); Major, 2019).
Leadership styles:
Leadership was once thought to be exclusive to individuals that possessed innate leadership traits and/or qualities. More recently, however, researchers have theorised that leadership is a
trainable and transferable skill (Ancona et al., 2007).
Research reveals that there are several leadership styles evident in health care (See Table 1). To explore effective leadership in the OHN context, leaders should aim to understand the ways in which leadership skills can affect key OH stakeholders (See Table 2). Effective leadership skills are expected to be adopted and used interchangeably by the leader within an OH context. Knowing which skill to use and when is imperative.
The overall measure for effective leadership within OH, over and above the improved quality of workers’ health, is the positive organisational and societal implications. Effective OH leadership can aid in the building/ maintenance of team morale, positive & productive workplace culture, the retainment of OH staff and trust in OH services (Cai et al, 2021; Murray & Hill, 1992).
Several leadership approaches are evident across all nursing disciplines. Two approaches are explored for the purposes of this article.
Servant leadership:
Servant leadership, an approach introduced by Greenleaf (1997) sets the premise of serving others first. This leadership approach optimises the relational aspect of the leadersubordinate dynamic. The servant leader often possesses excellent listening skills, has a long-term vision, and inspires team members to reach said vision by leading by example and encouraging the heart. Within the
Transactional Leadership (directive/ delegative)
This leadership style is effective in clarifying followers’ roles and responsibilities. This leadership style can be used to achieve performance targets due to the incentives of rewards for high performers. conversely, those not achieving are at risk of consequences. This LS has been observed to possess more managerial traits than leadership ones. This is due to the reinforcement of tasks/goals and the exchanges in reward form following the completion of said task/goal. This LS has proved effective in a sales environment and is most effective in self-motivated individuals. However, it leaves little room for innovation and there is a risk of micromanagement and low staff morale.
Democratic (interactive) Group participation, discussions and shared decisions are often observed with this leadership style. This leadership style helps build organisational flexibility and often allows team members to generate innovative ideas.
Authoritarian / Autocratic Leadership (directive)
This leadership style has been defined as one where the leader makes every decision with little-no input from others. although evidence suggests that this leadership style is effective in managing the deliverance of high output from workers, it has often been observed to cause low staff morale, reduced autonomy & high staff turnover. This style has been theorised to be more of a management style than a leadership one, as it is task orientated and creates followers and not future leaders Despite the negative connotations associated with this style, it has been proven to be effective during a crisis/emergency or when a decision needs to be made immediately.
Laissez– faire (delegative) In contrast to the autocratic leadership style, the laissez-faire leader offers little to no direction/supervision to their subordinates, this style does very little to inspire/ motivate team members to achieve a mission/goal. Lack of role clarity encourages passivity in team members and fosters an environment of low accountability.
The patient – also known as the employee or client within the OH context.
These are the main stakeholders – those at the receiving end of the OHN’s care, advice, and support.
Healthcare Providers. This includes OH doctors, OH nurses, physiotherapists, psychologists, OH hygienists and OH technicians. These clinicians / allied healthcare professionals generally form the OH multidisciplinary team (MDT) and OHN’s are likely to work closely with a few - if not all these healthcare professionals, often. Payors. This can be business leaders in organisations that provide funding for OH services. This includes employers /shareholders in the local government, varying health boards or independent organisations. Policymakers. This includes accredited Health and safety organisations that focus on workers’ health. For example, the SEQOHS (Safe Effective Quality Occupational Health Service), aim to oversee the standards of care provided by occupational health services.
healthcare context, this leadership style can prove effective as it breeds an environment of trustworthiness and loyalty between the leader and fellow team members. (Trastek et al., 2014a).
Shared governance is essential in OH. This approach encourages shared leadership where decision-making is shared amongst the groups and others’ input is valid and welcomed. This allows for a culture of trust and empowerment within OH Nurses and other healthcare disciplines/partners. As a byproduct, servant leadership leads to cohesive interdisciplinary working, reduced staff turnover and high-value patient, or in the context of OH, employee care (Canavesi and Minelli, 2022; Cottey and McKimm, 2019; Gunnarsdóttir et al., 2018).
Despite a growing body of evidence indicating the effectiveness of servant leadership, this approach takes time to build due to the need for robust interpersonal relationships between a leader and team members. In addition, this approach relies heavily on the relational aspect of the leader-follower dynamic and collective decisionmaking, which will prove difficult in situations where decisions need to be made quickly such as a crisis (Aarum Andersen, 2009; Eva et al., 2019).

Transformational Leadership:
Transformational leadership (TL) is a leadership approach that has been theorised to be the gold standard approach in nursing. Transformational leaders have been defined as individuals that are able to encourage and motivate their followers to meet a shared vision or goal. In addition, Transformational
leaders (TLs) provide opportunities for their followers/ subordinates to develop and often supersede their potential.
Transformational leadership assists employees or members of a group in meeting their needs for selfactualisation, as per Maslow’s hierarchy (Cope and Murray, 2017; Akilu and Junaidu, 2015; Mulla and Krishnan, 2011).
In addition to these characteristics, transformational leaders serve as role models for their followers/subordinates. This leadership style has been shown to improve patient (employee) outcomes, staff satisfaction, and safety culture (Specchia et al., 2021).
According to the evidence reviewed, both servant and transformational leadership have effective characteristics that can be applied in OH and other nursing settings. However, transformational leadership would benefit OH and all its stakeholders because it promotes both organisational success and the empowerment and growth of individual employees. (Collins
The World Health Organization declared the covid-19 outbreak a global pandemic in March 2020. Leaders in all healthcare disciplines faced multifaceted challenges because of this (Dadich and Mellick Lopes, 2022). Whether the crisis is physical, chemical, or biological in nature, OH plays a crucial role in crisis management. During the pandemic, OH played an important role in providing employers and employees with up-todate government guidelines, facilitating contact tracing, undertaking risk assessments, and being at the forefront of vaccination rollout (Ranka et al., 2020). The COVID-19 pandemic highlighted the importance of OH services acting as a link between health and workplaces more than ever. As a result, good leadership during the pandemic became critical in enabling OH services to provide adequate care and support to individuals in the
responsible for guiding their teams and patients through a global health crisis, restructuring healthcare systems and services, and ensuring quality patient care. According to the evidence, rather than focusing on specific leadership styles, nurse leaders adopted a variety of leadership approaches in response (Hwang et al., 2020; Nicola et al., 2020). Nurse leaders were tasked with adhering to a clear chain of command and being a visible leadership presence within healthcare settings in order to prevent disease transmission, keep up with rapidly changing guidance, and the direct and indirect impact of the virus on healthcare staff and patients (Sihvola et al., 2022). There is little research on the role of relational leadership in crisis response. Most of the research on crisis leadership is focused on authoritarian leadership styles, also known as the command-and-control approach. This approach is thought to work best in situations where there is little time for group decision-making or where the leader is the most knowledgeable member of the group (Boin et al., 2014; Cook, 2021; Webster et al., 2020).
A study by Smithson (2022) on leadership styles during the height of the covid 19 pandemic found that the command-and-control leadership style elicited mixed reactions among healthcare leaders. This leadership style was necessary for managing the uncertainty of the complex and prolonged covid crisis, but leaders in this study discovered that it was stifling, causing stress to the staff, and affecting team morale. As a result, leaders adopted a more relational approach, allowing for a dual leadership approach to the ongoing crisis, which appeared to

reduce staff anxiety.

This was consistent with the findings of a study conducted by Phillips et al., (2022) on the nursing workforce during the pandemic. According to this study, the command-and-control leadership style used during the pandemic clashes with nursing culture, where relational leadership produces the best results for staff satisfaction, team cohesion and quality patient care.

Conclusion:
OH Nurses must develop the necessary leadership skills to be successful change agents, ultimately improving employee satisfaction and nurse retention. Leadership is a role that all nurses, regardless of job title or experience, are expected to fulfil. The key to encouraging leadership is to have experienced nurse leaders act as mentors for other nurses. Mentors should encourage mentees to continue their formal and informal education by attending leadership conferences/
accredited training courses and obtaining a higher degree or certification. To maintain their own professional development, mentors should continue to learn tool (Cope and Murray, 2017; Major, 2019; Downey et al., 2011).
There are several healthcare leadership models and programmes that can be used to train and support healthcare leaders. The NHS compiled the healthcare leadership model which contains nine dimensions and was created to help healthcare workers from all backgrounds become better leaders. The dimensions include leading with care, sharing the vision, engaging the team, influencing for results, evaluating information, inspiring shared purpose, connecting our service, developing capability, and holding to account. These core concepts interlink with previously highlighted leadership styles/ approaches and are essential in effective OH leadership (Kumar and Khiljee, 2016; Pearce, 2004).
Phina is an experienced nurse who is currently studying for a specialist community public health nursing qualification, focusing on Occupational health. She is particularly passionate about community health and is a trustee of a charity centred on tackling mental ill-health within the African / Caribbean communities - Baba Yangu foundation. She works for PAM group which she says has been instrumental in her growth as an OH practitioner.









14-15 March 2023 NEC





As we evolve from a postpandemic world, we are quickly finding ourselves in one that will continue to challenge the psychological and physical wellbeing of our employees. As occupational health professionals continue to play a pivotal role in shaping the direction of travel for workforce health and wellbeing, they will need to be mindful of the world we now find ourselves in. According to Professor Dame Carol Black DBE, “few, if any of us have escaped the combined effect of Brexit, the pandemic, the war in Ukraine, the energy crisis and inflation. So much has changed recently, including the workplace. Emerging trends include the
increasing importance of mental health, flexibility, autonomy, financial wellbeing, compassionate leadership, the need for people-centered managers, personalised support, enhanced digital connectivity and the search for interventions that truly work. The Health and Wellbeing at Work event has never been more needed!”
And so as we move nearer to opening the doors of the 17th Health and Wellbeing at Work event, we take a look at some of the highlights enabling occupational health nurses and their colleagues to learn from best practice and address some of the burgeoning issues facing today’s workforce.

2023 sees the launch of a new Men’s Health programme run in partnership with the Mankind Initiative. Tackling some hard-hitting issues, Mankind’s founder Mark Brooks OBE wants “employers to better understand some of the pressing health issues affecting men in the workplace, offering easy to implement strategies that will create impact and engagement.” Programme Manager of Mental Health & Wellbeing, John Sidebotham BEM, shares his mission to improve men’s health at Network Rail. John’s work, complemented by occupational health and wellbeing professionals, encourages people to come together to share their feelings in a support network to combat the feeling of isolation. He uses his platform and in-person sessions to discuss big issues that can impact wider lives, finding solutions by working collaboratively.


Professor Nav Kapur, Professor of Psychiatry and Population Health at Manchester University discusses recent clinical guidelines and policy developments around suicide and self-harm, outlining evidence-based approaches to prevention and intervention. Actor Tommy Hatto shares his personal experience of battling eating disorders and how body image insecurities lead to low self-esteem and feeling inferior at work, “perfect is about being exactly who we are – flaws and all.” He wants employers to drive awareness and conversations around these issues to better support employees, especially in male-dominated work environments.


EAPA’s Eugene Farrell teams up with Rugby Player Tony Underwood to discuss why men find it difficult to talk about their emotions and mental health. They profile examples from aviation as well as Tony’s personal experience within sport and its relevance to building resilience on an individual and business level. Other sessions deal with fatherhood and mental health, a lived experience from a victim of male domestic abuse and techniques to get men to open-up.
We are delighted to once again be working with iOH (don’t forget to meet up with colleagues on stand 47!) and there are several OHNs to look out for this year. Specialist Occupational Health Nurse Libby Morley-Hassanali will be explaining the practical skills required by OH practitioners for writing mental health assessment and consultation reports. She identifies key risks that could affect mental fitness and workability, offers guidance on how to ask and talk about high-risk feelings and behaviours, how and where to signpost and improving skills in creating an actionable report back to the employer. iOH’s Director of CPD Janet O’Neill looks at the future of OH and wellbeing education and training. Facilitating an interactive discussion, think of this as an opportunity to explore new ideas, better understand what does and doesn’t work and find out what colleagues want in terms of support, training and education.










There are more clinical sessions than ever this year, with a real focus on the management of long-term conditions as well as self-care. Over half of us are connected to someone close who has dementia. Alzheimer’s Research UK’s Tim Parry believes “the condition should be high priority for any workplace when it comes to looking after its employee’s brain health and wellbeing, as well as supporting them if they might be caring for someone affected.” With symptoms including memory loss, behavioural changes and difficulties in communicating, they seriously affect job performance and often force those in work to give up their careers. Those juggling caring and work roles are more likely to experience stress and depression. Tim explains how employers have a duty to support those affected by dementia, but they can also help reduce their employees’ risk of developing dementia in the future through simple lifestyle changes that can improve our brain health. Join Tim and find out how you can put brain health on the wellbeing agenda.



Exeter University’s Professor Helen Dawes examines the impact of Parkinson’s on employment potential, offering some practical interventions that can support people to stay in work. Other sessions include cognitive fatigue, ENT conditions, diabetes and occupational lung disease with a rare insight into a factory outbreak investigation.








Probably one of the busiest programmes last year focused on women’s health so we are delighted that we have such strong sessions once again.
Psycho-oncology Nurse Specialist Dr Alison Farmer explains how OH professionals support employees in managing the impact of gynaecological cancers. Diagnosed with ovarian cancer back in 2001, she shares her own experience of surgery and chemotherapy, offering valuable insight into the physical and psychological consequences of the disease.
Health and Wellbeing Lead at EY, Dr Sally Hemming teams up with colleague Emma Nasralla to profile EY’s pioneering work around managing the menopause at work. They share some great case studies and examples of best practice that can be implemented in any setting.

In addition to being able to source new products and ideas from over 150 exhibitors, look out for some new show features, including a Spotlight on Health Conditions theatre, round table discussion groups which you can join for smaller group networking and idea sharing, and skills workshops including spirometry updates from Vitalograph.
Health and Wellbeing at Work takes place at Birmingham’s NEC 1415 March. Join friends and colleagues on the iOH stand 47, always one of the busiest at the event! Make sure to visit www.healthwellbeingwork.co.uk to see the full programme and use code IOH2 to save up to 15% when registering. We look forward to welcoming you back in March.
In 2021 the HSE issued guidance to employers on buying cost-effective and competent support from Occupational Health (OH) professionals. This does not yet embrace the wider multi-disciplinary team (MDT) that I have seen emerging over the last 6 years as professional educator for the NHS National Performance Advisory Group, and subsequently being truly embedded in the wake of COVID-19. I am a passionate advocate for the opportunities afforded to us by the skills

and approaches exemplified by our MDT colleagues.
I hope that sharing my learnings and experience as an independent practitioner operating as a microbusiness, will generate some lively discussions and debates on our professional networking groups about the information and observations that I have shared in this article.
Questions that I find myself regularly contemplating include:
By Lucy Kenyon• How do you feel about the pace of change in the OH landscape?
• How do you get early notification of changes that might have an impact on your practice? Do you have a junk email box full of notifications that might contain important news?
• Do you feel confident of your evaluation and recommendations?
While preparing for my forthcoming course modules, I have reviewed the OH landscape and evidence to update my
materials and practical sessions.
New and updated standards relevant to OH NHS - Self-management programmes should include:
• Structured education;
• Defined relevant outcomes that can be demonstrated and achieved.
NICE - Standard operating policies and procedures (SOPs) can be a challenge for sole practitioners and micro-businesses.

NICE have a published guide to selecting and prioritising quality standards, which I have adapted for my own business as follows:
1 Create a long-list of topics from the published quality standards and accredited guidelines;
2 Review and update existing SOPs for updates based on 1 above;
3 Shortlist to:
• Align with national priorities;
• Impact outcomes for employees and their employers;
• Reduce impact of impairment(s) for occupational health, safety and wellbeing;
• Reduce premature disability and mortality;
• Improve quality of life and worklife balance;
4 Discuss with stakeholders;
5 Communicate feedback versions to stakeholders.
relevant to OH
GOV.UK
A new online employer’s Employee health and disability tool was released by the government last year.
HSE
Code of Practice (COP) on the prevention and control of infections and related guidance on the prevention and control of infections and related guidance
All commissioners and service users of a registered healthcare provider will have access to information and guidance on the standards they should expect. This is particularly relevant to OH services
providing health screening and surveillance tests involving equipment.
Effective communication6
ICO
Triage protocols and automated decisionmaking
Since the advent of the NHS 111 service, this has become a fascinating area of digital health that will be developing organically and rapidly. If you use any automated triage systems, set up an alert to notify you of updates and changes to the ICO’s guidance.
GDPR and consent are common hotpotatoes in discussion threads and I would refer you to the excellent articles that Diana Kloss has compiled on these matters.
NHS
Supported self-management
OH health records need to document encouragement, support and empowerment provided during the consultation to enable employees “to manage their ongoing physical and mental health conditions themselves.”
Fitness certificates - Ambiguities that lead to confusion
The term ‘certificate’ can imply confidence that a specific fitness threshold has been met. How many of us have had a frustrated employer on the line about an employee’s health-related problem within the first 6 months of employment? This confusion can be avoided by using the terms ‘statement’ and ‘guidance’ or ‘recommendations’.
Those of you who know me personally
will recognise the importance I attach to the Gallop v Newport City Council when it comes to supporting employers who might have “constructive knowledge” of a disability even though they have no “direct knowledge”.
A recent review of this case9, highlighted the importance of employee cooperation with adjustments, and this highlights the importance of delivering supported self-management within OH consultations, to ensure that the individual has sufficient information to understand and manage workplace health risks.
Since 2019, employers have had to consider whether OH reports contain sufficient information and evidence to support any decision that the Equality Act does not apply and, therefore, whether they can rely on the report when deciding that adjustments are not reasonably practicable. The report therefore needs to contain an evaluation of the individual’s ability to selfadvocate and recommendations for the support they need to manage workplace risks to their health.
OH outcomes need to closely aligned to those of our Occupational Therapy colleagues and advice should:
• Communicate how the employee’s condition affects them4;
• Aspects of daily work activities that they do not currently need support or help with4;
• Help the employee “to overcome challenges completing every day work tasks or activities”9;
• Provide “a plan of goals and adjustments targeted at achieving a specific set of activities”9;
• Give the employee “a renewed sense of purpose”9;
Key features that employers will now be looking for in reports4 include:
• Information to help them consider any circumstances which suggest that they may be disabled and need support;
• Advice on talking to the employee about their health condition or disability;
When compiling a report, uppermost in my mind is how I can support and assist employers to meet their legal duty to “consider reasonable adjustments”. Employers can, of course, only consider which adjustments are reasonable if they have received from us clear recommendations from us on the arrangements that are likely to:
a. reduce the impact of work demands or increase capacity to cope with them, and
b. reduce adverse physical forces and demands.
OH reports therefore must contain the following information:
• Identify changes at work:
• Aspects of the job or workplace might need changes4;
• Ways of working;
• Work environment;
• Extra help or support;
• Provide guidance on
• Any specific communication needs to support the employee and let the conversation develop gradually4;
• Words or vocabulary that the employee understands or prefers to use4;
• The type and frequency of monitoring by the manager to make sure any support is still working4 .
Finally, with the majority of OH professionals
operating as independent practitioners, the new and updated standards and guidance outlined above is invaluable to help us to create robust systems and enable us to inform individuals about the information we are processing and documenting and why, alongside the information we are retaining and offer simple ways for them to access the information and challenge our professional opinion.
1. HSE. (2021). Occupational health - Buying support from occupational health professionals. Retrieved 9 January 2023, from https://www.hse.gov.uk/health-surveillance/occupational-health/buying-support-fromprofessionals.htm
2. QISMET. (2020). Supporting the self-management sector to achieve excellent quality. Retrieved 9 January 2023, from https://www.qismet.org.uk/qis-2020/
3. NICE. Selecting and prioritising quality standard topics. Retrieved 9 January 2023, from https:// www.nice.org.uk/standards-and-indicators/selecting-and-prioritising-quality-standard-topics#review
4. GOV.UK. (2021) Support with employee health and disability Retrieved 9 January 2023, from https:// www.support-with-employee-health-and-disability.dwp.gov.uk/is-employee-currently-at-work
5. GOV.UK. (2021) Support with employee health and disability Retrieved 9 January 2023, from https:// www.support-with-employee-health-and-disability.dwp.gov.uk/is-employee-currently-at-work
6. DHSC. (2022). Health and Social Care Act 2008: code of practice on the prevention and control of infections and related guidance. Retrieved 9 January 2023, from https://www.gov.uk/government/publications/the-health -and-social-care-act-2008-code-of-practice-on-the-prevention-and-control-of-infections-and-relatedguidance/health-and-social-care-act-2008-code-of-practice-on-the-prevention-and-control-of-infectionsand-related-guidance
7. Rights related to automated decision-making including profiling. (2023). Retrieved 9 January 2023, from https://ico.org.uk/for-organisations/guide-to-data-protection/guide-to-the-general-data-protectionregulation-gdpr/individual-rights/rights-related-to-automated-decision-making-including-profiling/
8. NHS England (2020). Supported self-management. Retrieved 9 January 2023, from https:// www.england.nhs.uk/personalisedcare/social-prescribing/supported-self-management/
9. Gallop v Newport City Council [2013] EWCA Civ. 1583 https://assets.publishing.service.gov.uk/ media/618a5142d3bf7f56077ce880/Mr_A_Thomas_-v-_Quad_Recruitment_Ltd___Others_1601506.2019___Judgment_with_reasons_..pdf
10.Kelly v Royal Mail Group Ltd UKEAT/0262/18/RN (2019). Retrieved 9 January 2023, from https://www.gov.uk/ employment-appeal-tribunal-decisions/mr-r-kelly-v-royal-mail-group-ltd-ukeat-0262-18-rn
ACAS. (2023). Using occupational health at work. https://www.acas.org.uk/using-occupational-health-at-work
CIPD. (2023). Occupational Health | Factsheets | Retrieved 9 January 2023, from https://www.cipd.co.uk/ knowledge/culture/well-being/occupational-health-factsheet#gref
HSE Occupational health - Overview. (2023). Retrieved 9 January 2023, from https://www.hse.gov.uk/healthsurveillance/occupational-health/index.htm
ILO. (2023). International Labour Standards on Occupational Safety and Health . Retrieved 9 January 2023, from https://www.ilo.org/global/standards/subjects-covered-by-international-labour-standards/occupational-safetyand-health/lang en/index.htm
ISO (2018). Occupational health and safety management systems Requirements with guidance for use. Retrieved 9 January 2023, from https://www.iso.org/standard/63787.html

NHSE (2022). Workplace health and safety standards. (2023). Retrieved 9 January 2023, from https:// www.nhsemployers.org/publications/workplace-health-and-safety-standards
Lucy Kenyon is a Nurse Consultant, educator and entrepreneur. She has an active research profile and specialist experience in service transformation and developing protocols to respond to emerging evidence. Her roles include international crisis response, planning and management and has been actively involved in employee health protection and business continuity of frontline services during Swine flu, COVID and Orthopox outbreaks. Alongside her business, Workability Solutions, supporting and advising SME employers, she is a Clinical trainer for NHS NPAG and her voluntary work includes roles as NED and immediate past-president of iOH and more recently supporting refugees to build cultural understanding and employability skills.

For some years the Occupational Health (OH) Workforce has been slowly dying. Dr Yogarajah published the 2019 SOM report The Future of the OH Workforce, detailing a reduction in the OH Workforce. Not very auspicious, considering that 4 years before, in 2016, an All-party parliamentary group paper, called the diminishing Occupational Medical workforce, “a crisis of capability”, despite OH becoming more multidisciplinary.
Anecdotally, at a recent training session of 11 NHS senior leaders, the OH workforce crisis dominated the conversation.
As far back as the Black Report of 2008, OH has been considered key to the health of the working-age population; a position reiterated a number of times since then, accelerating during the pandemic and culminating in the Response to the Government paper; Health is everyone’s business in 2021.
In today’s UK employment market, significant numbers of people are leaving due to ill health, costing £150 billion and restricting economic growth (Times 2023). Yet, workplaces can influence health positively (CBI Nov 2022). According to the CBI, a new Work -health index (WHI) is being launched which will benchmark UK private sector

organisations’ health provision. That health position must include OH. OH is seen as essential in influencing health at work and supporting people back into work (DWP 2021). The Welsh Conservatives recently asked Labour to encourage businesses to engage Occupational Health services to support economic growth and reduce the impact on the NHS.
The NHS are “Growing OH and wellbeing” services as they see a direct benefit, not only to their workforce but to patient care. It is wonderful that so many resources and financial support is being made available for this project.
It is not enough to increase the OH population!
An effective and important solution is for OH to host pre-registration student placements. OH is not part of the
curriculum and of OH as a specialism Nurses and Allied When needing nursing population, published a 10
Occupational Health workforce – a crisis of capability?
and there is little awareness specialism for Doctors, Allied Health Professionals. needing to build the practice population, NHS England 10-point plan that identified
pre-registration placements as being key; substantiated by the BMC 2019 research project, exploring student views.
This will be a culture change, but the benefits go beyond increasing the workforce. Pre-registration placements support awareness and understanding of the profession; improve the understanding of work as a health

outcome and therefore will also be part of the solution in keeping the workforce at work. It is a win-win situation.
Should any OH providers wish to have further information, please contact Janet O’Neill. You may wish to view our YouTube video describing the lived experience of pre-registration placements. A further case study can be found here in this Occupational Medicine Journal article.
Deputy Head NSOH
janet.oneill@hee.nhs.uk

It’s simple and rewarding to offer placements.
Why?
• To prevent a reduction in the OH workforce affecting our ability to deliver services.
• To build awareness of occupational health as a profession through pre-registration placements. Evidence demonstrates that graduates select their first jobs based on placement experiences.
• To raise awareness of work as a health outcome to future health care workers
• To raise awareness of workforce wellbeing to future managers

• To give your team an opportunity to teach and supervise.
• To help your team to remain up to date with the latest knowledge, practice skills, evidence-based, and guidelines.
• To obtain different perspectives on service delivery from students of alternate backgrounds such as allied health
• To support your organisation’s social value strategy.
• It’s the right thing to do!
What can students do?
• Carry out quality improvement projects, audits, and research.
• Assist with service delivery as appropriate.
• Work remotely and in person.
How often and for how long?

• From 1 to 12 weeks depending on circumstances.
What do I have to do?
• Every university has a placement lead that will take you through every step and provide ongoing support.
• You will be supported through the learning environment audit.
• Name a trained supervisor. Training can be accessed freely (PEAP via E-lfh) or online via Anglia Ruskin University and takes one to two days. Most universities also provide support with training.



• Build a program of learning which can be with all team members and can be reused with the next students.
• Training via the university on the learning outcomes assessment log for students.

• A key contact is the Practice Learning Leader at the university and from your ICS Practice Learning Facilitator if NHS.
• A placement tariff that is paid for each student that you take, £132 per student per 37.5-hour week.
Please watch our YouTube video which takes you through lived experience. Contact janet.oneill@hee.nhs.uk for more information or to be put in contact with occupational health departments/providers already supporting placement

Hearing loss, deafness, tinnitus and sight loss affect 14 million UK people so being fully aware and catering for the requirements of any staff members with additional needs is essential for inclusive employers.
As these disabilities are often invisible, employers need to be aware of the barriers colleagues may be facing, so speaking openly about how hearing or sight loss affects their ability to work is vital.
This may cause inhibition, embarrassment and anxiety and as a result, pretending all is fine and understating the effects is common so encouraging employees to speak out in a relaxed face-to-face environment helps.

Ideally, hearing and sight checks should accompany regular staff health reviews in a reassuring way to communicate that support is available. If any changes to hearing levels or sight are identified, employees may need to be granted time off to attend
When conducting online or face-to-face DSE assessments, do you ask employees if they experience hearing or sight difficulties? With hearing loss, these may include problems with background noise, hearing on the phone or in meetings and not hearing the fire alarm when in isolated areas such as bathrooms and stairwells. Sight loss challenges may include difficulties with reading small print or text on the screen, glare, dry eyes and increased instances of trips and falls.


For most employees with one or more of the above conditions, there should be no need to change jobs as extensive support and adjustments are available.

A workplace assessment will identify any issues that may be worrying an employee and the follow-up report will recommend implementing often quite simple adjustments to ensure employees can perform their roles more effectively.
As you’ll know, employers are under a
legal obligation to make reasonable adjustments to ensure that employees with health-related barriers can perform their roles without unfair disadvantages.
Employers are sometimes concerned about this, expecting dramatic change and huge costs, yet a few easy-toimplement adjustments which are often free or relatively low cost can make a significant difference.
With today’s assistive technology, there is an excellent range of devices designed to facilitate accessibility and communication for colleagues.
Visualise has produced two videos to highlight the barriers and potential solutions:
Hearing Loss, Deafness and Tinnitus Needn’t Mean Job Loss https://youtu.be/eqYK0DSCHSY

Struggling to see at work? A Workplace Assessment will help... https://youtu.be/Mna7b__Ib1A



As well as helping employees successfully develop their careers, workplace assessments can also help colleagues to feel included and valued as part of the team.
Staff awareness training is also a key element in promoting accessibility and inclusion. Explore the options at https://visualisetrainingandconsultancy.com/training
Hearing loss, deafness, tinnitus and sight loss needn’t mean job loss, so to find out more or to make a referral, please visit https://visualisetrainingandconsultancy.com/workplace-assessments


 By Mandy Whalley, Specialist
By Mandy Whalley, Specialist
The Empowerment Passport™ is a secure web application, built to facilitate communication between an individual with a disability or long-term health condition and their line manager or tutor. It can be used in both education and employment and can act as a bridge to communicate adjustment needs in different
does the employer follow up on a disability declaration to explore adjustments needed for an interview and where is this documented?
How can individuals be empowered to normalise and lead inclusive conversations and prevent employers from being placed at a disadvantage if they are unaware of the adjustment needs of the individual (CIPD
environments and during transition e.g., between education and employment for students with disabilities entering work. It is currently being trialled in the NHS.
There are many different types of employment passports in circulation. Many of them are similar to the Empowerment Passport and most are provided by employers. Nearly all are paper-based, and many are only presented to an employee once a problem has been identified, or following a disclosure.
Much work has still to be done to ensure recruitment processes are inclusive. How often
Disability)? This process can be fraught with anxiety on both sides.
Occupational Health (OH) is often the first service where disabled candidates can confidently discuss their reasonable adjustment needs. Occupational Health reports, guide the employer to consider adjustments, or services such as Access to Work, etc but what about the small/discreet non-cost adjustments that can assist with a greater impact on productivity for the employee? The comprehensive questionnaire tool within the Empowerment Passport™ facilitates such conversations. Each licence allows individuals to build their adjustment
profile and provides an Empowerment Passport™ Action Plan for the employer to record and document all agreed adjustments. A copy is then kept with the employer and a copy is uploaded to the individual's Empowerment Passport™ ready for any updates, reviews or amendments when required.

Back in 1997, I had the privilege of setting up and working in an innovative new role as a Disability Adviser for my local NHS Hospital Trust. The Occupational Therapy Service lead managed to write a successful business case to secure temporary funding for a pilot to assist the Trust in supporting its disabled staff in light of the new legislation of the Disability
With over 37 years of experience as a state registered Occupational Therapist (OT), I have been one of the lucky few OTs to work in the field of Occupational Health. I hold a voluntary role as a representative of the OT/OH speciality on the National Executive Committee for the Royal College of Occupational Therapists (RCOT): Specialist Section for Work. Growing a multidisciplinary approach within Occupational Health services (SOM 23) is important for all, as many realise OTs are perfectly positioned to use their dual training skill set, (physical and mental health) enabling full holistic analysis of the functional impact of health conditions or disabilities.
My colleagues in OH had long identified a gap in the provision for staff with long-term health conditions and disabilities, to stay well at work and to promote self-management through identifying reasonable adjustments. Referrals came from OH, HR, managers and individual staff members. All are seeking support for work capacity assessments, jobtask analysis, return to work planning, ergonomic assessments, dyslexia screening, etc, ensuring the Trust was compliant in its employment activities under DDA legislation.
The pilot was successful and became a
permanent position in 1999, however, it required additional training to achieve a thorough working knowledge of specific legislation and emerging discrimination cases.
The Equality Act 2010 came into force. The Disability Advisory service continued to develop and became the central hub for coordinating all staff Access to Work applications. This service was ahead of its time in providing practical and effective solutions for staff health and wellbeing. Fast forward to 2020, I left the NHS with over 21 years of accumulative experience working in the field of disability employment and OH. Working with a variety of individuals with physical, mental, neurodiverse and sensory issues, my focus was always on the interplay of person, environment and task. One major lesson learnt throughout that time was the importance of truly listening to the experts: the staff member with lived experience of disability.
My experience also taught me 2 things: - firstly, “Never assume” because surprises and workarounds are always an option. Secondly, Everyone is an individual, meaning how we learn, how we cope and how we operate as human beings are all different, even if you have
the same health condition or disability. These are essential ingredients that have helped shape the creation of the Empowerment Passport™.
I have also joined several people with the lived experience of disability after having been diagnosed with Dyslexia in my early 40s and currently awaiting a diagnosis of ADHD, in addition to an endocrine disorder. Therefore, I have transitioned from being a provider to a recipient.
I am the main carer to 2 of my 3 children who have disabilities; Autism and learning disability and ADHD and Dyslexia. I understand how challenging it can be to have to repeatedly explain what works well and what doesn’t in the work /educational environment. Diagnosis is not as important as the impact of the condition and how to communicate this to others can be extremely tricky.
Each Empowerment Passport™ has enough storage space to host up to 5 scanned documents, stored securely as supplementary evidence when requesting reasonable adjustments e.g., a consultant/specialist letter, a wellness recovery action plan, a previous Access to Work report, or a disabled student allowance (DSA) plan.

At the press of a button, the passport

holder can choose to share this information which may be particularly helpful at times of change, such as a new manager, new role or new employer. From an Occupational Health point of view, the Empowerment Passport™ can become a supplementary source of information to reinforce recommendations of reasonable adjustments, saving time not just for OH clinicians but also for the employer. The Empowerment Passport™ Action plan provides an important audit trail, should any disputes arise.
The effectiveness of the Empowerment Passport™ is being tested in 2 NHS pilots: One for existing staff with disabilities and one focusing on disabled students attending placements in NHS or entering employment. These pilots
will be concluded in March 2023.
Early feedback indicates some quick wins:
• Improvement in disability disclosure rates
• Greater confidence in communication between an employee and their manager
• Improvement in the speed of implementation of reasonable adjustments
• Creation of a centralised budget for all Access to work claims. Areas for improvement and development:
• To produce a “light touch/strength-based version of the Empowerment Passport™ To enable all action plans to be fully digital instead of PDF documents.


Choice and control are vital ingredients when embarking on any new service initiative particularly if it involves conducting sensitive conversations regarding disability in the workplace. Therefore, using the Empowerment Passport™ should always be an opt-in process and never enforced.
 Mandy Whalley, Specialist Occupational Therapist
DipCOT CACDP OCN LEVEL 4
Mandy Whalley, Specialist Occupational Therapist
DipCOT CACDP OCN LEVEL 4

 and Director of the Empowerment Passport™️ Ltd and Independent Occupational Therapist for Tailored Employment Solutions specialising in Staff health and well-being. Dyslexic
and Director of the Empowerment Passport™️ Ltd and Independent Occupational Therapist for Tailored Employment Solutions specialising in Staff health and well-being. Dyslexic

Founder
https://www.linkedin.com/in/mandy-whalley-ba8b6124/
thinking
Chronic obstructive pulmonary disease COPD is an umbrella term for obstructive lung diseases characterized by chronic respiratory symptoms such as shortness of breath, chronic cough, and increased sputum production) due to damage of the airways (bronchitis, bronchiolitis) and/or alveoli
(emphysema) which cause persistent, often progressive, airflow obstruction that is not reversible.1 In the UK an estimated 1.2 million people are living with diagnosed COPD –considerably more than the 835,000 the Department of Health estimated in 2011. In terms of diagnosed cases, this makes COPD the second most common lung disease in the
UK, after asthma. The number of people who have ever had a diagnosis of COPD has increased by 27% in the last decade, from under 1,600 to nearly 2,000 per 100,000. This could mean more undiagnosed cases are being diagnosed and the disease is becoming more common however changes in record-keeping could also be a factor2
The overall statistics for the prevalence of COPD in workers in the UK are difficult to pinpoint, however, the HSE states that 21.9 million working days across the population were lost due to COPD between 1994 – 19957 . COPD in workers tends to gradually develop, and the onset of COPD is most common in long-term smokers aged 40 years and older. The European Respiratory Society carried out research into occupational exposures and their relation to COPD, their latest research in 2020 named ‘Occupational exposures and 20-year incidence of COPD: the European Community Respiratory Health Survey’ observed workers who had normal spirometry initially, and then a follow-up spirometry test was performed 20 years later. They tested 3343 workers and 89 of the workers had COPD 20 years later, the workers exposed to biological dust had a higher prevalence of COPD than those not, as with those exposed to gases, fumes, and pesticides. The researchers summarised the results strengthen the evidence for occupational exposures as an important risk factor for COPD3 .

Spirometry is accepted as the gold standard diagnostic test to assess airflow obstruction and classify disease severity based on specific cut-off points. Spirometry is a safe, practical, and reproducible maximum breathing test that can be used in Occupational Health to get a baseline test for the worker and to monitor workers who may work with hazardous chemicals and substances to see whether the PPE is efficient. The test is relatively quick to perform and well tolerated by most people. It is important to appreciate that the clinical value of spirometry is critically dependent on the correct operation and accuracy of the
spirometer, performance of the correct maximal breathing manoeuvre, selection of the best test results to use, and correct interpretation.
In 2019 the American Thoracic Society (ATS) and European Respiratory Society (ERS) updated the previous 2005 standards for performing spirometry. The standards provide guidance on technical specifications in equipment and pre-test considerations on how to perform quality-assured spirometry. They have updated various elements of spirometry within the document, with the technique being one of the main updates. The importance of these guidelines is that they are evidence-
based which increases accuracy. They stated that ‘improvements in instrumentation and computational capabilities, together with new research studies and enhanced quality assurance approaches, have led to the need to update the 2005 technical standards for spirometry to take full advantage of current technical capabilities’. Spirometry within Occupational Health is utilized in various ways mentioned earlier in this article. Therefore, the importance of obtaining good techniques is important so that those with COPD can be detected at any stage of their working life using spirometry. It is important to note that spirometry is just one piece of the puzzle in the diagnosis of COPD which requires additional tests and investigations.
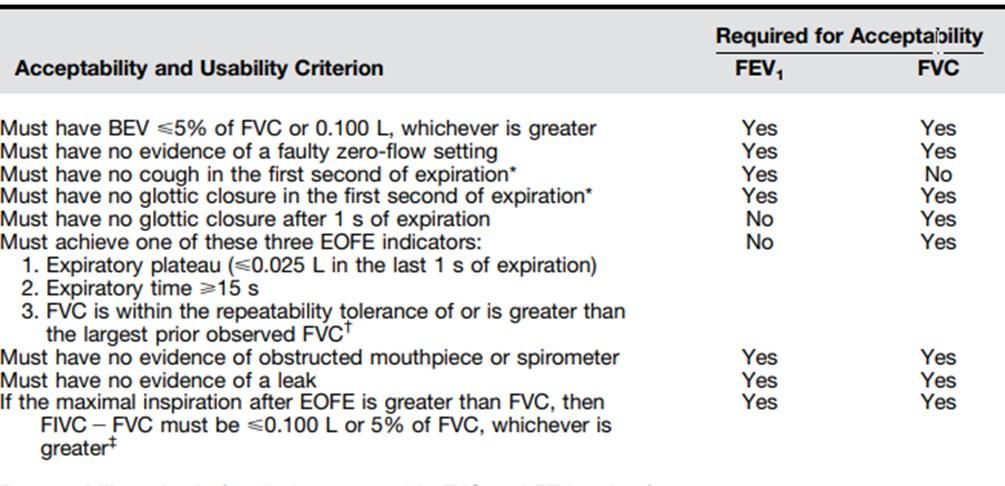
It is important to note good technique begins with the preparation of the patient, this involves a clear explanation and demonstration of the test. Figure 1 shows the new criterion for acceptability and usability.
Spirometry is commonly seen as a simple physiological test but it can be challenging to perform and interpret, particularly for those with COPD. The ATS and ERS have done research looking at factors that may contribute to COPD misdiagnosis. Researchers looked at the evidence from different literature on errors in the diagnostic process to determine what factors may be causing misdiagnosis and they looked at 73 papers and investigated various factors that contribute to the misdiagnosis of COPD, spirometry technique error was identified as the third leading potential cause of COPD misdiagnosis. Technique factors included poor testing quality, technological errors, patient errors, and test administration and interpreting errors. Therefore, this highlights that improved spirometry quality may limit misdiagnosis6. Although in
Occupational Health diagnosis is not routine early detection of any obstruction in the occupational setting may beneficial for the worker’s disease pathway.
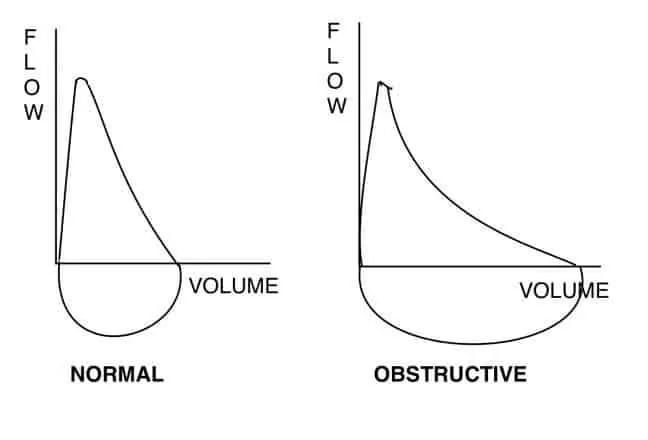
An important criterion in spirometry is getting the person to completely empty their lungs to reach the plateau, however, people with COPD tend to have a reduced expiratory rate, so they tend to breathe out slower because of the airway narrowing. When spirometry is performed in someone with COPD distinctive pattern comes up showing a concaved loop that differs from a healthy person’s flowvolume loop. This is because the maximum flow achieved during forced expiration decreases progressively as lung volume falls and is most evident in the expiratory flowvolume curve where flow is plotted as a function of volume Figure 2. The more concaved the flow volume is the more severe the obstruction present.
When testing someone with COPD they are likely to get fatigued easily. A minimum of 30s should be left between repeat attempts to allow the patient to recover, be aware not to make the person repeat the test before they have recovered.
In patients with airflow obstruction exhalation, either forced or relaxed can be more than 10 s and never achieve a plateau. In the past, people with COPD would fail the test because they couldn’t meet the criteria due to the long exhalation time. The 2019 Spirometry guidelines have replaced the previously termed ‘End of Test (EOT)’ criteria with ‘End of forced
expiration criteria (EOFE)’ also shown in figure 1. The EOFE criteria included exhalation ≥ 15 seconds. Research showed that any volume obtained past 15 seconds is unlikely to change clinical decisions and that multiple prolonged expirations are seldom justified and may cause light-headedness, syncope, undue fatigue, and unnecessary discomfort.
Obtaining good techniques in workers who may have COPD will be beneficial as having technically acceptable results will lead to a more accurate representation of the person’s obstruction and may lead to a better prognosis.
1. Johns DP, Walters JA, Walters EH. Diagnosis and early detection of COPD using spirometry. J Thorac Dis 2014;6(11):1557-1569. doi: 10.3978/j.issn.2072-1439.2014.08.18
2. Chronic obstructive pulmonary disease (COPD) statistics (no date) Chronic obstructive pulmonary disease (COPD) statistics | British Lung Foundation. Available at: https://statistics.blf.org.uk/copd (Accessed: January 30, 2023).
3. Lytras, T. et al. (2018) “Occupational exposures and 20-year incidence of COPD: The European Community Respiratory Health Survey,” Thorax, 73(11), pp. 1008–1015. Available at: https://doi.org/10.1136/thoraxjnl2017-211158.
4. Minov, Jordan et al "Chronic obstructive pulmonary disease in workers from different sectors." European Respiratory Journal 56.suppl 64 (2020)
5. Johns DP, Walters JA, Walters EH. Diagnosis and early detection of COPD using spirometry. J Thorac Dis. 2014 Nov;6(11):1557-69. doi: 10.3978/j.issn.2072-1439.2014.08.18. PMID: 25478197; PMCID: PMC4255165.
Figure 1 . Graham, B.L. et al. (2019) “Standardization of spirometry 2019 update. an official American Thoracic Society and European Respiratory Society Technical Statement,” American Journal of Respiratory and Critical Care Medicine, 200(8). Available at: https://doi.org/10.1164/rccm.201908-1590st.
6. Christopher Chalk, D.C. (2022) Errors in spirometry, primary care contribute to COPD misdiagnosis, Pulmonology Advisor. Available at: https://www.pulmonologyadvisor.com/home/topics/copd/errors-inspirometry-primary-care-contribute-to-copd-misdiagnosis/ (Accessed: January 15, 2023).
7. https://www.hse.gov.uk/copd/employers.htm (Accessed: January 18, 2023).
Figure2 . https://respiratorycram.com/flow-volume-loops/(Accessed: January 18, 2023).








 By Libby Morley-Hassanali Mindshift Consultancy
By Libby Morley-Hassanali Mindshift Consultancy
Now, more than ever, employees may need additional psychological or financial support. It’s not our role to fix individuals problems but we can certainly signpost. Employees can access sector-specific support via the organisations below. Not all provide a 24-hour service, and some provide financial support via grants to those who are eligible. Phone numbers are included where available and it will be helpful to add these to your contacts in your own phone.
• The Charity for Civil Servants Home (foryoubyyou.org.uk)
• Nurse Lifeline, 0808 801 0455
Supporting Mental And Emotional Wellbeing | Nurse Lifeline
• The Ambulance Staff Charity Caring For Those Who Care For Us | TASC (theasc.org.uk)
• The Firefighters Charity 0800 389 8820 The Fire Fighters Charity - Changing The Lives Of Our Fire Fighting Heroes!
• The Care Workers Charity Home - The Care Workers Charity
• Police Care UK Rebuilding lives for a brighter future | UK police charity for serving and former police officers, police staff, volunteers, and the police familyPolice Care UK
• Hospitality Action 0808 802 2111 Get Help | Hospitality Action
• Ben, the Automotive support service 08081 311 333 Here for the automotive industry | Ben support for life
• The Bank Workers Charity Bank Workers Charity Bank Workers Charity (bwcharity.org.uk)
• The Retail Trust 0808 801 0808 About us | Retail Trust
• The Construction Industry Charity 0345 605 1956 Lighthouse Club - The Construction Industry Charity

• Foothold, supporting engineers Home - Foothold (myfoothold.org)
• Farming Help 03000 111 999 Farming Community Network - Farming Community Network (fcn.org.uk) and 0800 188 4444 About The Royal Agricultural Benevolent Institution | RABI
• The Insurance Charity 020 7606 3763 The charity for insurance industry employees - The Insurance Charities
• Education Support 08000 562 561 About Education Support UK charity for education staff
This article was kindly provided by Libby Morley-Hassanali and is an excerpt from her practical guide for OH practitioners on mental health consultation and report writing. For more information and to purchase your copy please head to Home - Mindshift Consultancy

I had the pleasure of catching up with Dr Vaughan Parsons, Senior research fellow at King's College London to discuss his role in Occupational Health.
What’s your background?


I am the centre manager of the recently launched London Centre for Work and Health and a senior research fellow. I am based in the Occupational Health Service at Guy’s and St Thomas’ NHS Foundation Trust / King’s College London. An experienced medical writer e.g., journal articles, clinical practice guidelines, health promotion material, web content and intergovernmental correspondence. I’m also a selfconfessed gym and fitness junkie, and budding urban gardener.
After graduating in the UK in 2000, I returned to my native home (Australia) and worked in a number of clinical roles in community and acute mental health services before changing career direction and moving into an employee
mental health and wellbeing lead role for a state-wide emergency service. During this time, I completed postgraduate training in public health and health management, and from this, I was particularly interested in developing my research skills. This led me to pursue a part-time PhD examining clinical decision making in relation to use of mental health legislation in clinical practice. My first research job was as a senior research officer for the Justice and Forensic Mental Health Service in NSW. In 2013, I returned to the UK to take up a trial manager post at King’s College London where I worked alongside Professor Ira Madan (chief investigator) in the Occupational Health Service at Guy’s and St Thomas’ NHS Foundation Trust. This study (the ‘SCIN trial’) was large multi-centre randomised controlled trial which tested the effectiveness of a bespoke behaviour change intervention to prevent hand dermatitis in at-risk nurses. Detailed

information about the trial can be found at: https:// www.journalslibrary.nihr.ac.uk/hta/ hta23580/#/abstract
Following completion of the SCIN trial, our programme of OH research has continued to grow and evolve, and it’s fair to say our research work is quite varied. Generally speaking, our research focuses on examining the relationship and interaction between work and health, and we have a particular interest in mental disorders, long-term health conditions and hidden disabilities, workplace health surveillance and vocational rehabilitation to name a few. We draw upon existing scientific knowledge and research to help us develop new work-orientated interventions e.g. those designed to support people to remain in work or return to work following sickness absence, interventions which prevent occupational diseases (e.g. occupational dermatitis) as well as workplace health promotion interventions. We’ve recently been commissioned by the Growing OH and Wellbeing Team at NHS England to explore future opportunities for growing the multidisciplinary OH and Wellbeing clinical workforce, and this exciting work means that we, in consultation with many NHS OH departments, will be contributing to the future strategic OH and Wellbeing workforce planning work which is now underway.
We launched in Mid-2022. Essentially, this was borne out of a keen desire
among a small group of senior clinical academic researchers in London (lead by Professors Ira Madan and Paul Cullinan) to improve the future capacity for work and health research in the UK, by investing in and supporting the junior and early career researchers and clinicians who have an interest in pursuing OH research but who require mentoring support and guidance. Since our launch, we’ve focused our energies on forging closer collaborations with existing researchers and clinicians from different biomedical and allied health specialties and across different academic institutions (King’s College London, Imperial College, University College London) and NHS organisations in London and beyond as well as establishing new partnerships. The new centre also complements the work of other specialist OH academic research groups in the UK which includes, the Centre for Musculoskeletal Health and Work (Aberdeen), Occupational and Environmental Health research group (Manchester) and the Healthy Working Lives Group (Glasgow).
Our purpose is simple- we want to establish a centre of excellence for research in work and health, and to use our research to facilitate working-age people to have and maintain healthy, fulfilling work through a multidisciplinary research centre focusing on work and health. You can check us out at www.lcwh.org or partner with us on twitter: @LCWH5
We are confident the centre will have influence by generating and building our specialty’s scientific evidence-base and using our research findings to inform and underpin evidence-based medicine in OH clinical practice. Given the nature of OH clinical practice, our programme of research responds directly to the government’s priority agenda to improve the health outcomes of the working-age population and so is also particularly relevant to policy makers and employers.
OH clinical practice is a diverse field and covers a broad range of health conditions and disabilities which can affect the working age population. It is also important to point out that OH researchers do not work in isolation. In fact, our work relies heavily on establishing multidisciplinary research collaborations with other of researchers and clinicians from different specialties and disciplines. Crucially, patient, public and employer (including Trade Unions) representatives are an important component of multidisciplinary research teams, and this ensures their voices and experiences help to shape and inform
our work. As such, we work in close collaboration with our research partners so we can draw upon and exchange our collective expertise and specialist knowledge to inform and guide our work.
The research team responsible for developing and implementing the largescale ‘NHS Check study’ (a study exploring the psychosocial impact of Covid-19 on NHS staff performance and wellbeing) comprises clinical academic experts from occupational medicine, occupational psychiatry, psychiatric epidemiology, public health, biostatistics, social science and policy. In addition, we are also in the early stages of developing, in collaboration with clinicians from dermatology, nursing and occupational health, a new research project aimed at testing the effectiveness of a digital screening tool for workplace skin surveillance.
Historically, two factors have presented particular challenges for us. First, relates to limited funding opportunities to support work and health research in the UK. However, encouragingly this situation has improved in recent years. In late 2022, the National Institute of Health Research (NIHR) reinforced their commitment to increase investment in multidisciplinary OH research by releasing two dedicated ‘work and health’ funding calls (‘Workforce Health’ and ‘Work and Health Research Development Awards) designed to mobilise and strengthen multidisciplinary OH collaborations and to
support the OH research community to develop plans for ambitious future research. This enhancement in funding for work and health research complements existing research funding opportunities available from the Colt Foundation (a main funder of occupational and environment research in the UK).

The second major challenge, is engendering a research culture in OH and identifying ‘practical’ opportunities to embed ‘research’ activity as a core
and routine function of OH clinical practice. This will only be achieved if we all recognise the benefits of OH research and the value and importance of growing our own specialty’s scientific evidence-base. We encourage readers who are interested in OH research to get in touch.
For further information on Dr Vaughan Parsons https:// www.linkedin.com/in/vaughan-parsons893a82b0/


