





From your exemplary work to your continuous dedication. You reflect our world class care.
Congratulations to the nurses being recognized as the Faces of Care Award recipients. Thank you for the impact you’ve made in the nursing community.







From your exemplary work to your continuous dedication. You reflect our world class care.
Congratulations to the nurses being recognized as the Faces of Care Award recipients. Thank you for the impact you’ve made in the nursing community.
The Greater Cleveland Nurses Association empowers the nursing community and promotes the health and safety of residents in Northeast Ohio.
BY SARAH WEBBWithout nurses, there would be no health care, says Carol Sams, executive director of the Greater Cleveland Nurses Association (GCNA).
Penni-Lynn Rolen, past president of GCNA, agrees.
“Nurses protect and care for the public in unique and divergent ways to promote health, wellness and safety,” she adds. “There is a nursing shortage, and there is a great need for a dedicated and competent nursing workforce today for the future.”
Established in 1909, the Graduate Nurses Association of Cleveland was started to maintain and conduct a registry of trained private duty nurses, uphold standards of care and provide services for those unable to pay. In 1921, the group became District 4 of the Ohio State Nurses Association and an affiliate of the American Nurses Association. Today, GCNA continues to represent nurses by improving health care for all people, fostering high professional standards and promoting the professional development of nurses.
“GCNA collaborates with area schools of nursing in Cuyahoga and Geauga counties to promote professionalism in nursing, honor distinguished graduates and offer scholarships,” Rolen says.
She adds that GCNA offers continuing education programs at its quarterly membership meetings, which address current topics and issues in nursing. Some of the programs are tailored for members with specific interests, while others cover topics that apply to the general membership.
Held at various locations in the Cleveland area, the association’s district meetings engage members to meet and socialize with colleagues during dinner, learn about the organization’s activities, offer input to the board of directors and dive into topics of interest related to nursing, such as local disparities.
Involvement in GCNA can also include staying up to date on local and state policy issues that affect nurses and taking opportunities to influence local policy makers. Several GCNA members serve on state and local boards of health agencies and volunteer for various projects.
The GCNA is one of 13 local districts of the Ohio Nurses Association. Membership to the organization is open to all nurses who live or work in Cuyahoga and Geauga counties.

In addition to supporting the nursing community, the GCNA also supports the greater population. “GCNA has a long history of addressing various health-related needs in Cleveland and beyond,” Rolen says.
“We have a long history of dedicated, brilliant and courageous nurses working to promote the profession locally, regionally, nationally and internationally,” Rolen says. “Without the commitment of these women and men, nursing may not be what it is today.”
GCNA's current community initiatives include:
Many current GCNA members volunteer at MedWish International, a nonprofit organization that saves lives and the environment by repurposing surplus medical supplies and equipment to provide humanitarian aid to people in need, including people in Ukraine.
GCNA is recruiting volunteers to promote the Lead Safe Cleveland project, a collaboration between nursing organizations in Northeast Ohio and Concerned Citizens Organized Against Lead that strives to protect children, families and future generations from lead poisoning.
Various members of GCNA have volunteered to provide vaccinations and support public efforts throughout the COVID-19 pandemic.
In 2022, GCNA members participated in the Love A Nurse Walk to help raise funds for the Alice Flaherty Excellence in Nursing Scholarship Fund.
GCNA further supports scholarships with The Boys and Girls Club and the St. Luke's Nursing Alumni Foundation.
“Do we get to see surgeries?”
It was a question posed by a student in Laura Goliat’s Medical-Surgical Nursing I class that she wished she could answer with a resounding “Yes!” But the Ursuline College Breen School of Nursing and Health Professions, like many of its counterparts across the country, had dropped the clinical component dedicated specifically to perioperative nursing, which consists of patient care before, during and after surgery.
“A nursing student may go through their education and never see a surgery,” Goliat explains. “The focus, in the last years, has been a more generalist education.”
It’s just one of the things the Richfield resident has worked to change during her decade-plus at the college.
Goliat first experienced the love of nursing as a high-schooler performing nursing-assistant duties at Shaker Medical Center, where her mother was director of nursing. “It was beyond rewarding seeing a patient in their most vulnerable state and being able to help them regain health or be able to cope with something that is chronic,” she says of the appeal. An interest in teaching developed at Ursuline, where she served as a clinical instructor while earning her master’s degrees as a family nurse practitioner.
“I found it very valuable and very fulfilling, helping students understand the patient experience,” she explains. Her plans to work as a family nurse practitioner changed when the college asked her to stay on as a full-time clinical instructor and rounder after her 2012 graduation.
In 2017, Goliat, by then a tenured associate professor, contacted University
Hospitals, then the Cleveland Clinic, to arrange four-hour clinical “immersions” that would bring her perioperative-nursing lecture to life and place students right at the point-of-care at the hospitals to learn. For “class,” students don gowns and gloves, tour an operating room, collaborate with the interdisciplinary team from scrub technicians to surgeons and rotate through stations where they learn about preparing skin for an incision, providing oxygen to a patient, monitoring and assessing patients after surgery, etc.
A similar clinical immersion at University Hospitals designed to introduce Ursuline’s Medical-Surgical Nursing I students to radiological procedures such as CAT scans and MRIs as well as the patient prep, education and assessments required for them was added in 2019. That same year, two-day immersions in radiology and surgery for Medical-Surgical Nursing II students were introduced, involving one-on-one time with
“The reward [of nursing] is when you see healing, when you see acceptance, when you see all of those things that really help the human condition.”
—Laura Golianta perioperative and radiology nurse, actually placing each student into surgery and the radiology departments.
“We must work collaboratively and effectively in teams for the best patient outcomes,” she says.
To fully meet that need, in 2021 Ursuline named Goliat interprofessional education coordinator, a responsibility she took on in addition to those of her associate professorship.

Meet nurses who are working hard to uphold the profession's quality of care.
BY LYNNE THOMPSON
Dorothy Hamilton initially rejected a mentor’s suggestion that she consider teaching full time at Cleveland State University (CSU). She was happily employed as an acute care nurse practitioner at University Hospitals (UH) Cleveland Medical Center — a job that provided a bigger paycheck. And she already enjoyed the satisfaction of teaching part-time on the adjunct clinical faculty of the Case Western Reserve University (CWRU) Frances Payne Bolton School of Nursing. But the South Euclid resident had observed that some clinical instructors just didn’t seem to be able to convey their vast experiential knowledge to students and help them apply it.

“Just being at the bedside is not enough to teach people going into nursing, going into healthcare. … [Teaching] is a science of its own,” she says.
Hamilton has spent the last 16 years at CSU, first as a clinical assistant professor then as a clinical associate professor. In the early years of her tenure, she took teaching-education classes — something she continues to do — and became a certified nurse educator. At the same time, she’s helped develop a diverse nursing workforce. She talks to young people about the profession at high schools, churches and health fairs in racially and ethnically diverse inner-city communities. She says just seeing a person of color succeeding in the nursing and teaching professions can inspire someone to do the same, make it seem possible.
Teaching is the latest iteration of a career Hamilton discovered as an 8-yearold accompanying her mother to the hospital to visit her father, who suffered from diabetes. She still remembers how they interacted with him, “the touching, the stroking of his arms and his hands.” She served as a preceptor for recently graduated nurses as a staff nurse in the cardiac telemetry unit, then as an assistant nurse manager in the cardiothoracic intensive-care unit, at the Cleveland Clinic. She decided against pursuing a nurse manager position, instead opting to earn a master’s degree in nursing from CWRU so she could work as a nurse practitioner.
During her tenure at CSU, Hamilton continued working as a per diem acutecare nurse practitioner at UH Cleveland Medical Center until June 2021. “I still maintain my certification,” she points out. “And I can always go back.” She completed a doctorate in nursing at Kent State University in 2020; her research was on how homeless individuals manage Type 2 diabetes. Some might question why a 68-year-old would want to continue teaching, let alone earn an advanced degree.
“This is my lifelong dream, to be a nurse and to help people,” she explains. “So throughout the various changes of my life, that’s what I want to do.”
“My biggest challenge, I would say, particularly post-pandemic, is helping the students succeed and maintain their focus. [Nursing] is a people skill. You can’t learn it remotely through Zoom classes. Some of the students that graduated within the last two years, their skills really are not there like they should be as far as their study skills and having the ability to apply certain concepts.”
—Dorothy Hamilton“I feel like students keep me on my game. There’s a lot of times they’ll ask me questions and, even with a master’s degree, I’m like, ‘Hmmm. That’s a good question. I don’t know that. That’s why we’re lifelong learners. So let’s look it up together.”
“What a gift it has been to be with people in the two most vulnerable moments of someone’s life. How many times I’ve been there when people have come into the world and when they’ve left! How many people can say that?”
—Kristina LesterThe nursing care Kristina Lester’s father received in the hospital as a cancer patient wasn’t what a loving child would wish for a parent. The Chardon resident, then a labor-and-delivery staff nurse at University Hospitals Geauga Medical Center, remembers nurses talking about her father instead of to him when he was confused, not taking the time to coach the family in discussing end-oflife issues or explain what palliative care (also known as supportive oncology) was when it was offered.
It wasn’t until the last 24 hours of her father’s life that he got what she thought
he’d deserved all along: a nurse who talked to him even though he was confused, asked family members about his life, provided updates honestly yet sensitively and gave the ideal combination of care and privacy. Watching her work changed Lester’s career path.
“I was going to do this for somebody else,” she says.
In 2022, six years after her father’s death, Lester received a master’s degree in nursing from Ursuline College and landed a job as a nurse practitioner in Supportive Oncology at University Hospitals Seidman Cancer Center. She helps patients manage

the physical, psychological and spiritual symptoms of their cancer and serves as an advocate for them.
It’s a radical change from the world of labor and delivery, which Lester first entered in 1997 as a float nurse in the Cleveland Clinic health system. Lester went on to teach as a clinical instructor at Ursuline College, Cuyahoga Community College, Kent State University, Lakeland Community College and Cleveland State University. In each contracted role, she strived to make the clinical experience a more positive one by making a point of welcoming students’ questions; planning activities such as student presentations of patient cases to their peers; and providing resources such as YouTube videos, Zoom tutoring sessions, charts and graphs, even old-fashioned flash cards.
“Nobody learns the same way,” she says. “I found that when I went back to school as an older person.”
Lester, now 49, anticipates completing her doctorate at Ursuline next year. She wants to use it to educate people about the importance of palliative care.
“[Treatment for] every chronic health condition should have palliative care in it,” she declares.
In 1999, Deb Lindell enrolled at the Case Western Reserve University (CWRU) Frances Payne Bolton School of Nursing to finish what she’d started years ago, before the birth of her children and multiple moves necessitated by her husband’s career: work on a doctorate of nursing practice in public health. As a visiting nurse she’d discovered she belonged out in the community rather than by a hospital bed.
“It involved promoting health and helping people stay healthy, preventing disease,” the Solon resident remembers. “I liked looking beyond individual patients to looking at groups and communities.”
The decision is one that has kept Lindell at CWRU for over two decades — and taken her around the globe. Wherever she’s gone, she’s helped improve public health and furthered nursing both as a profession and a discipline.

“I want to help build the next generation of nurses, whether it’s one on one, working with students in small clinical groups, teaching in a classroom setting or running a program,” she says.
Lindell’s climb up the academic ladder began in 2004. She applied for and was granted the rank of assistant professor. She led the development of a master of nursing degree for students who had a bachelor’s degree in another area of study and were returning to school to become nurses. In 2015, she became an associate
professor. After becoming a full professor in 2020, she served as faculty-development coordinator.
At the same time, Lindell was helping advance nursing practices internationally. In 2000, while still a doctoral student working at CWRU as an instructor, she was assigned to lead a project in which her team collaborated with University of Mexico faculty in developing public-health sessions for residents of a village outside Mexico City. She went on to teach nursing theory and advanced public health nursing once or twice a year, two weeks at a time, at a university in Ho Chi Minh City, Vietnam, then Wuhan University in China. In September 2021, she landed at a public college in a remote area of northwest Kenya on a Fulbright Scholarship. Over the next seven-plus months, she helped the two-yearold institution plan a nursing program.
“It gave me an opportunity to help nurses everywhere progress in their practice, in their education, in moving these countries’ discipline and profession of nursing forward,” Lindell says of the motivation to continue her international work.
At 76, Lindell continues working parttime as a professor. She also is coordinating the nursing school’s Curriculum Transformation Initiative to align four of its five programs (all but the Ph.D. course of study) with the American Association of Colleges of Nursing’s “The Essentials: Core Competencies for Professional Nursing Education” for curricula that better assess and evaluate students’ ability to meet specific competencies.
“Nursing is very key, is very critical, to our healthcare system and to the health of all the individuals who engage in our healthcare system. Without nurses, it couldn’t function. It’s very important, at least for me, in working with people of other countries, other cultures, even within the U.S., that I’m a collaborator. But it has to be in a way that works for you in your values, your beliefs, your goals, your healthcare system.”
—Deb LindellAs a young woman graduating from a Michigan high school in 1950, Jane F. Mahowald believed she had two career options: teaching and nursing. She chose nursing for the same reason so many enter the profession: “I thought I wanted to help people.” That thought was confirmed after she entered the St. Luke’s Hospital School of Nursing in Marquette, Michigan. She remembers caring for an elderly man recovering from a retinal detachment.
“When you took care of patients who had retinal detachments when I was in school, they had to stay in bed for weeks, have sandbags on both sides of their head,” she recalls. “They could hardly move. I thought, Oh, my goodness! To be able to see this fellow through this illness is really quite worth it.”
Mahowald stepped down as executive director of the Ohio League for Nursing, the Rocky River-based nonprofit dedicated to supporting nurse educators and nursing education, in late 2022 — at the age of 90.

“When you commit your whole life to something and you believe in it, it’s fun,” the longtime North Olmsted resident says.
Mahowald arrived in Cleveland in 1974 as Lutheran Medical Center’s director of nursing education. “[I liked] helping people understand what nursing is all about,” she explains.
At Lutheran Medical Center, Mahowald designed a marketing approach to increase student enrollment in its school of nursing and spearheaded a curriculum revision focused on utilization of the nursing process and meeting patient needs throughout the life span. After the school closed in 1984, she served as director of a resources-management program she developed and implemented, then head nurse in a chronic pain-management program she helped establish — work that was cut short in 1986 by a breast-cancer diagnosis and treatment. The experience reinforced the importance of treating each patient as an individual rather than a diagnosis.
“Because I had breast cancer — and that was at the time when you often didn’t recover from it — they weren’t treating me
like an individual who could live again!” she exclaims.
Just as Mahowald was recovering from surgery, the Cleveland Area League for Nursing began looking for a new executive director. “One of the major focuses of that job at that time was to recruit people into nursing, to speak to students,” she remembers. She applied for and got the job, one she kept after the league merged with the Ohio League for Nursing in 1987.
Among Mahowald’s achievements during her tenure was participating in a project that helped establish an Ohio Board of Nursing system that facilitated data collection about the number of different kinds of licensed nurses in the workforce — hospital staff nurses, public-health nurses, etc.
Mahowald still truly hasn’t experienced retirement. Now she’s reviewing
applications for continuing education programs for the league — the organization is one of the Ohio Board of Nursing’s “approvers” — as a volunteer.
“When you like and love your work, it’s never work; it’s just something you enjoy,” she says.
“Being certain that we have qualified nurses to care for patients, providing education in such a way that [nurses] are doing what I think is necessary and what other people think is necessary, like helping the individual through a time in their life when they can’t do things for themselves — that’s what challenges me.”
Graduate nurses start on a path of service and caring for others.


 BY CHRISSY KADLECK
BY CHRISSY KADLECK
75 Years
Taking care of people has always been the real attraction to nursing for Natasha Dumas.
“In the healthcare world, nurses are looked at as angels,” says Dumas. “You're able to help people in their worst times and make them feel better.”
Dumas, a member of the National Society of Leadership and Success and a driven mentor to help other nursing students be successful, recently accepted an RN position at Cleveland Clinic on the cardiovascular intensive care unit.


“Cardiovascular health has been something that has been a demise for my family as a black family,” she says. “I’ve had three people in my family that have passed on due to cardiac related death. I wanted to have that specialty in order to help others and their loved ones because I have a lot of understanding and empathy for my experiences with my family.”
Dumas, whose dream job is to become a perfusionist, aspires to eventually obtain
her critical care certificate and become a flight nurse.
Faith Geho had a long list of career goals as a child and nursing was not one of them.
“But when I was a young teenager, I got sick for several years and I spent a lot of time in and out of the hospital,” she says. “Some of the nurses I had made a huge impact on me, and I wanted to be able to do that for other people. I decided to become a nurse when I was 15.”
Geho, who works as an aide at Cleveland Clinic, accepted an RN job in an emergency department at a hospital system in Columbus, Ohio.
A community of faculty and students advancing the nursing discipline.
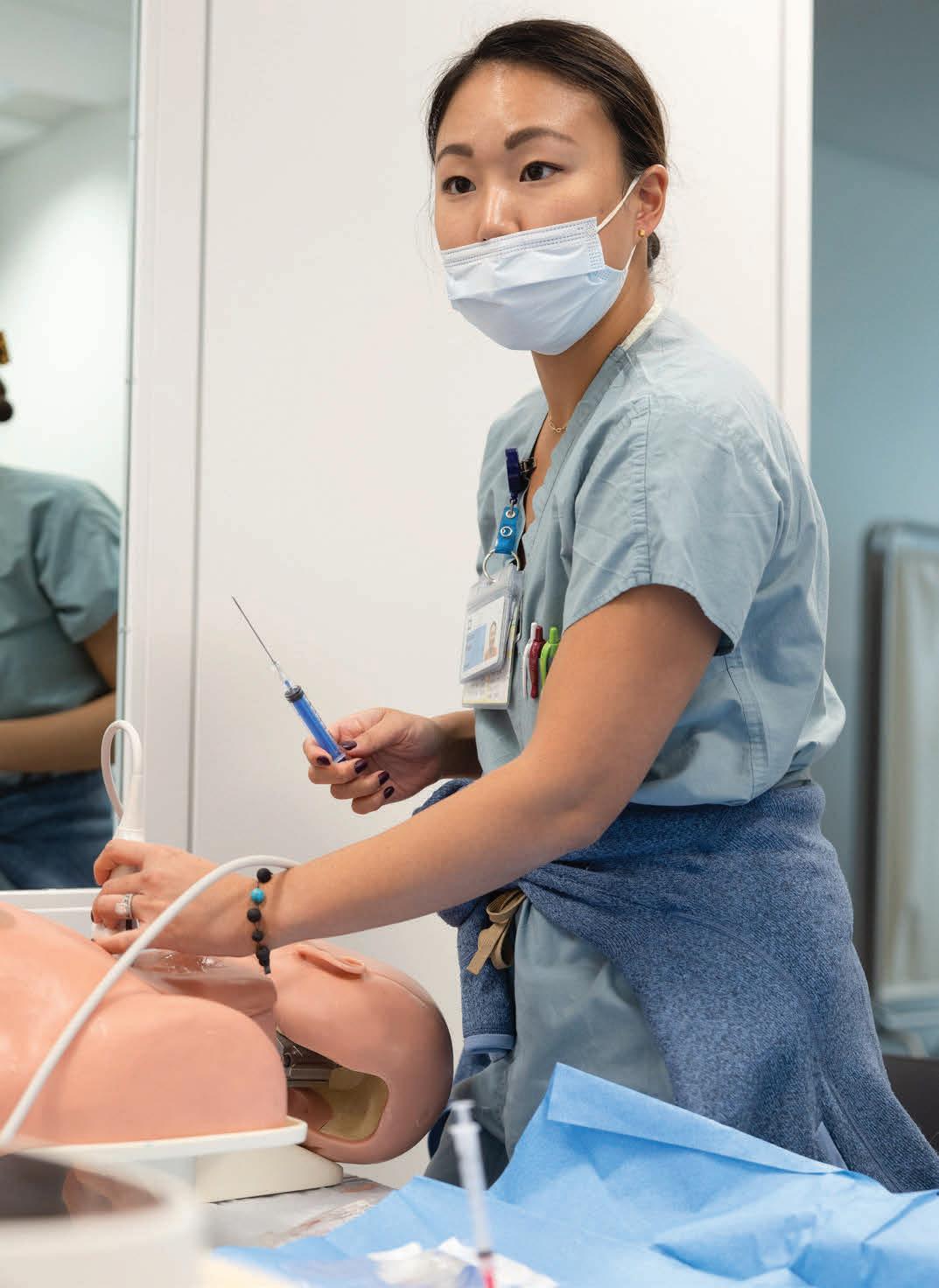
• #10 Bachelor of Science in Nursing*
• Master of Nursing
• #11 Master of Science in Nursing*
• #15 Doctor of Nursing Practice* (DNP)
• DNP Nurse Anesthesia

• Doctor of Philosophy in Nursing (PhD)
*U.S. News & World Report, 2023
“As I went through all my rotations, I really liked labor and delivery and women's health but it can be difficult to find a position as a new grad,” she says. “I think a nursing position in the emergency department will be better for general experience. I don’t know that I’ll stay in that department forever, but I'm excited to start there as my first job.
For Gojko Majerle, he points to his mother as the role model who led him to enter the healthcare field. First a nutritionist and now in HR, her three decades of caring for others at The MetroHealth System were inspirational as well as aspirational.
“I just saw the care and compassion that she had for all of her patients, and not even only limiting it to that, but to all the people that she connected with outside of the hospital,” he says. “It was a huge catalyst for me. It helped me decide that this was the path that I wanted to choose for myself.
And I'm happy to say that it's the right fit.”
Majerle currently works in the medical intensive care unit at MetroHealth, and he hopes to pursue additional training to become a nurse anesthetist.

“My faith is also something that has helped shape my path and allowed me the ability to provide compassionate care to those I am serving,” he says.
Coming from a medical family, Alisha McAteer initially fought the idea of following their footsteps into the scrub life.
But the draw was strong. Her mother is a registered nurse. Her father is a former
surgical technologist and his wife is a registered nurse. Even McAteer’s brother is a licensed practical nurse.
“As I've gotten older and understood what the job entailed and what it was actually about, I saw how much they were helping people and the good they did for the community, it just blew my mind,” she says.
Once it finally clicked, McAteer knew it was what she wanted to do with her professional life.
“I want to help people, that’s the real goal,” says McAteer, who graduates in May and has accepted a RN position in the OR at Hillcrest Hospital, where she has been working as a surgical technologist for six years. “My short-term goal is to stay in the OR and achieve an advanced CNOR
HONORING NURSES MAKING AN IMPACT IN THE NURSING COMMUNITY THE FACULTY AND STAFF OF CUYAHOGA COMMUNITY COLLEGE CONGRATULATE ALL OF THIS YEAR’S RECIPIENTS AND NOMINEES!
certification. Blood and guts are kind of my thing.”
Early on, Megan Rodriguez gravitated to the idea of a unique hands-on job that would harness her social skills.
“I really love learning about people through my work,” she says. “Throughout my time in college, I realized that I really wanted to focus on areas involving women and women’s health.”
In the summer of 2022, she had an internship on a postpartum unit, and earlier this spring she accepted a job in labor and delivery at a health system in Virginia.


“I always thought the woman's body and pregnancy was incredibly interesting to me as a physiological process,” she says. “I loved making those relationships with families and new moms, and all of the education that come with having a child and going through that entire experience. Nurses are special everywhere, but this area reminds me of how special the connection between a nurse and a patient is.”

Ever since she was in preschool, Anya Wu wanted to be a pediatrician and even has vivid memories of drawing pictures of herself wearing a white coat. In fact, it was a professional destiny without question until she started volunteering at a hospital as a sophomore in college and she saw firsthand the roles of doctors and nurses.

“The more I shadowed and the more I volunteered, I really saw the differences. It was the nurses who were at the bedside. It was the nurses who patients were asking for



and it was that patient-nurse relationship that I really desired,” says Wu, a local of Hawaii who earned a bachelor’s degree in molecular cell biology from the University of Hawaii.

She is most interested in specializing as a labor and delivery nurse. “It’s such a special relationship that I haven't seen in any other setting,” she says. “The nurse really gets to know the mom and the family. That’s why I wanted to go into healthcare.”


As a young person, Asa Zoeckler saw the way their newborn brother and their mother were taken care of in the neonatal intensive care unit (NICU) at Rainbow Babies and












Children’s Hospital and it set their career trajectory in motion.

“I kind of fell in love with how the nurses took care of my little brother and also how they took care of my mom,” Zoeckler says. “Then I was lucky; my high school had an internship program where it gave me the opportunity to be trained as a patient care assistant when I was 15 years old.”
Zoeckler’s brother is now a happy and healthy 11-year-old, and Zoeckler accepted a job at Akron Children’s NICU.
“I always knew I wanted to work with kids. I looked at pediatric nursing and for a long time I’ve been working in pediatric behavioral health,” Zoeckler says. “My goal is to be a pediatric psychiatric and mental health nurse practitioner.”
We salute our remarkable nurses, who make sure nothing stands in the way of caring for kids and their families.
Compassionate. Courageous. Unstoppable.