NE UR OSCIENCE
Hearing, balance & the brain
University of Rochester | Ernest J. Del Monte Institute for Neuroscience Vol. 21 - 2024
PG 2

John J. Foxe, PhD
Kilian J. and Caroline F. Schmitt Chair in Neuroscience
Director, Ernest J. Del Monte Institute for Neuroscience
Professor & Chair, Department of Neuroscience
FROM THE DIRECTOR’S DESK
I amoften struck by the central and often outsized role that simple geography can play in the scientific enterprise, and here at the University of Rochester, we are blessed with excellent geography. What’s he talking about, I hear you ask? Well, I am referring to the fact that absent a full-scale blizzard, we are all within easy walking distance of each other. That our Neuroscience community on the River Campus is just across the road from the Neuroscience community at the Medical Center.
Neuroscience Diversity Commission series is in its third season. It brings postdoctoral fellows from across the country to Rochester to present their research, give chalk talks, and meet with faculty and students. This program, designed with inclusivity in mind, elevates early career investigators and allows them to practice and receive feedback on skills they will likely use to interview for a future faculty position. NEUROYES is also supported by Neuroscience and the Brain and Cognitive Sciences Departments.
ON THE COVER
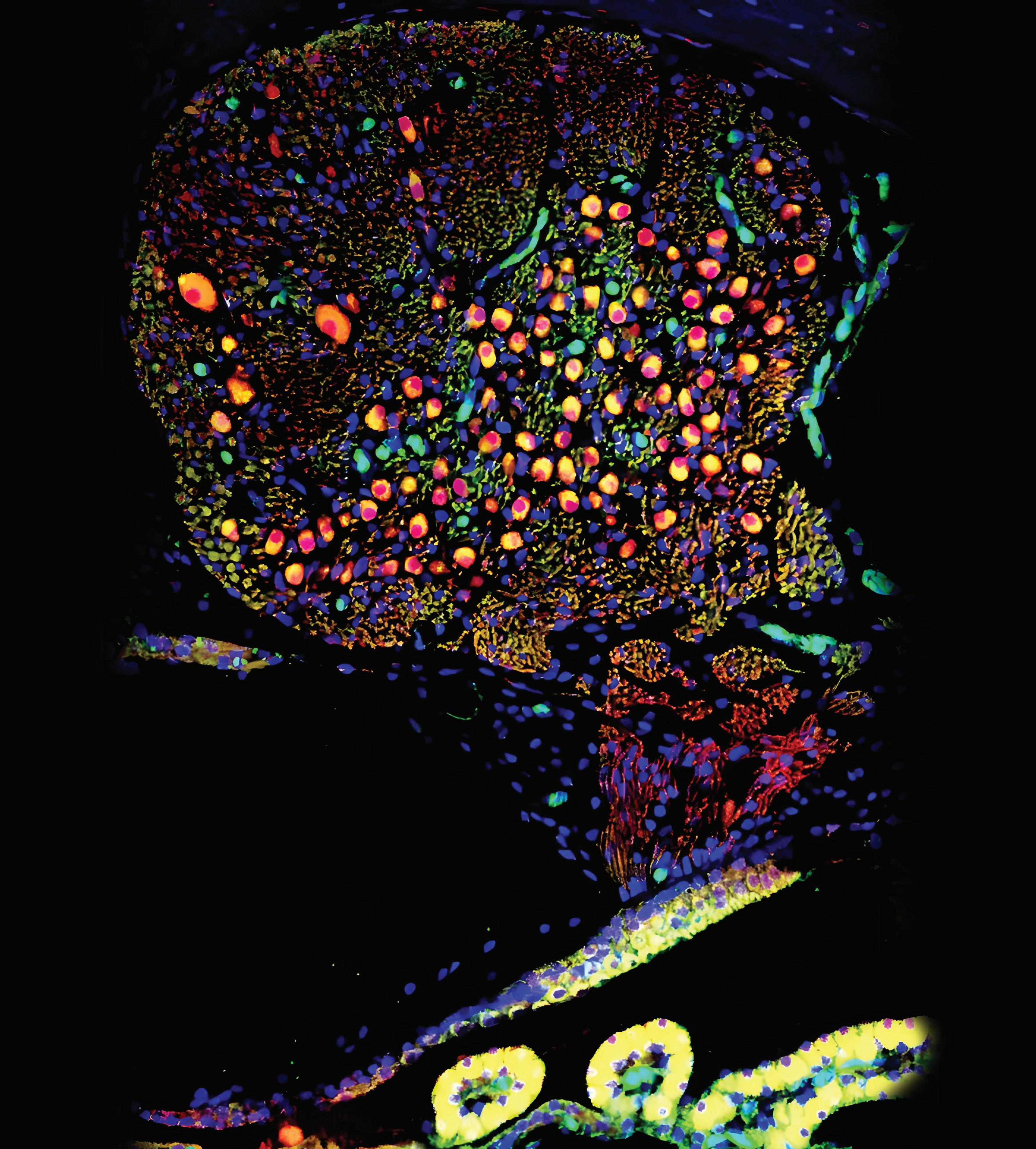
Photo cross section of cochlea showing hair cells and auditory nerve cell bodies. Image provided by the Henry Lab.
NEUROSCIENCE
Editor/Writer
Kelsie Smith Hayduk
Kelsie_Smith-Hayduk@ urmc.rochester.edu
Contributors
Mark Michaud Kelly Webster
Feature Photography
John Schlia Photography
J. Adam Fenster
It matters, and it matters a lot. Having been at institutions in New York City in my early career, where undergraduate, graduate, and medical school campuses were often flung across the five boroughs, collaboration between folks was next to impossible. So much of what we do depends on personal contact, the quick chat after a seminar, a cup of coffee, and a culture of friendship and collaboration. Thankfully, in the wake of COVID, we are back to interacting personally, and the remarkable collaborative spirit that marks the University apart is back in full swing. At the heart of this great institution is its people and their willingness to lift each other up. This collaborative environment has a major impact on our research. In these pages, we feature one such group. The Hearing and Balance Collective is a superb example of how a concerted effort, helped in no small part by our University Medical Center geography, has afforded investigators across our campuses the opportunity to transform science (pg 2).
I’d also like to call out another successful series of NEUROYES speakers. This
Del Monte Institute for Neuroscience Executive Committee
John Foxe, PhD, Chair, Department of Neuroscience
Bradford Berk MD, PhD, Professor of Medicine, Cardiology
Robert Dirksen, PhD, Chair, Department of Pharmacology & Physiology
Diane Dalecki, PhD, Chair, Department of Biomedical Engineering
Jennifer Harvey, MD, Chair, Department of Imaging Sciences
Robert Holloway, MD, MPH, Chair, Department of Neurology
It has been a month, and I am still energized by our Batten Disease Research Day, hosted by the University of Rochester Intellectual and Developmental Disabilities Research Center (UR-IDDRC) and the University of Rochester Batten Center (URBC). Being able to spend the day sharing science, asking each other questions, and getting real-time feedback and input from families on the frontlines of this wicked disease is how I believe we will truly make the biggest impact on a rare disease that could also shed light on many other neurodevelopmental disorders.
With a dozen new Del Monte Institute for Neuroscience pilot program grants on their way to investigators, a new group of Neuroscience Graduate Program trainees in the wings, and discoveries forthcoming, we have much to be grateful for and much to look forward to.
In Science,

John J. Foxe, PhD
Paige Lawrence, PhD, Chair, Department of Environmental Medicine
Hochang (Ben) Lee, MD, Chair, Department of Psychiatry
Shawn Newlands, MD, PhD, MBA, Chair, Department of Otolaryngology
Webster Pilcher, MD, PhD, Chair, Department of Neurosurgery
Steven Silverstein, PhD, Professor, Department of Psychiatry
Duje Tadin, PhD, Chair, Department of Brain & Cognitive Sciences
UNIVERSITY OF ROCHESTER | ERNEST J. DEL MONTE INSTITUTE FOR NEUROSCIENCE
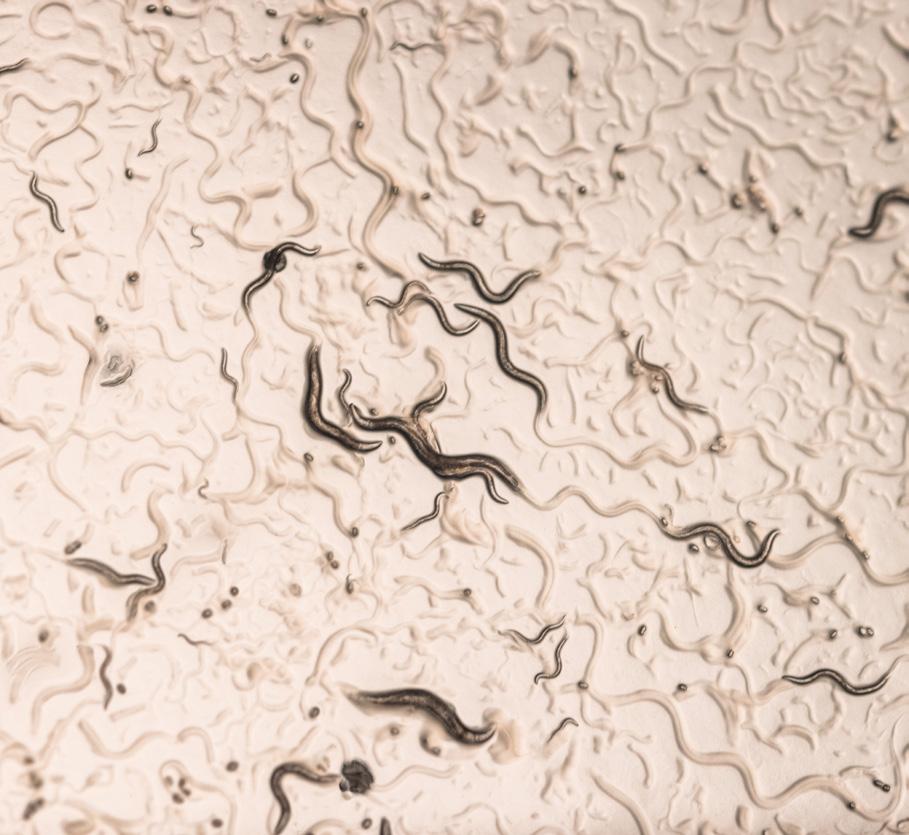
Turns out—male roundworms are picky when choosing a mate, research finds
It is well understood that mating is a priority for male roundworms or C. elegans. Previous research out of the lab of Douglas Portman, PhD, professor of Biomedical Genetics, found male C. elegans will suppress the ability to locate food in order to find a mate. In a study out today in Current Biology, the Portman lab discovered that the male worms used diverse chemical (pheromones) and physical (touch) signals to determine the sex, age, nutritional health, and mating history of the hermaphrodites. Researchers found male worms can determine a hermaphrodite’s nutritional status— whether it is healthy or food-deprived—and whether it has previously mated. When given a choice, the males showed preference toward hermaphrodites that have not previously mated with another male and are nutritionally healthy. However, once a hermaphrodite is a few days old—approaching middle age for a worm—it puts out a powerful sex pheromone that attracts males over long distances. That is because it starts to run out of its own sperm, so finding a mate becomes more important..
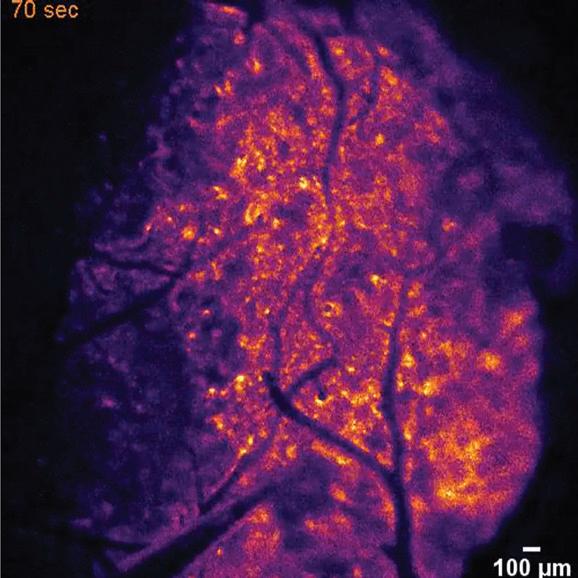
New imaging method illuminates oxygen's journey in the brain
The brain cannot survive long without oxygen, a concept demonstrated by the neurological damage that quickly follows a stroke or heart attack. But what happens when very small parts of the brain are denied oxygen for brief periods? A new method, published in Science and discovered by the lab of Maiken Nedergaard, MD, DMSc, co-director of the Center for Translation Neuromedicine (CTN), which is based at both the University of Rochester and the University of Copenhagen, has found a way to 'light-up' the oxygen in the brain by using luminescent proteins, chemical cousins of the bioluminescent proteins found in fireflies. The method, which can be easily replicated by other labs, will enable researchers to more precisely study hypoxia, the denial of oxygen to parts of the brain that occurs during a stroke or heart attack. It is already providing insight into why a sedentary lifestyle increases risk for diseases like Alzheimer’s.
A new theory emerges on Parkinson’s disease origins and spread
The nose or the gut? For the past two decades, the scientific community has debated the wellspring of the toxic proteins at the source of Parkinson’s disease. In 2003, a German pathologist, Heiko Braak, MD, first proposed that the disease begins outside the brain. More recently, Per Borghammer, MD, and his colleagues argue that the disease is the result of processes that start in either the brain’s smell center (brain-first) or the body’s intestinal tract (body-first).
A new hypothesis paper appearing in the Journal of Parkinson’s Disease on World Parkinson’s Day unites the brain- and body-first models with some of the likely causes of the disease–environmental toxicants that are either inhaled or ingested. The authors of the new study, who include Borghammer, argue that certain pesticides, common dry-cleaning chemicals, and air pollution inhaled predispose to a brain-first model of the disease. Other ingested toxicants, such as tainted food and contaminated drinking water, lead to a body-first model of the disease.
“In both the brain-first and body-first scenarios the pathology arises in structures in the body closely connected to the outside world,” said Ray Dorsey, MD, professor of Neurology at the University of Rochester Medical Center and co-author of the piece. “Here we propose that Parkinson’s is a systemic disease and that its initial roots likely begin in the nose and in the gut and are tied to environmental factors increasingly recognized as major contributors if not the cause of the disease. This further reinforces the idea that Parkinson’s, the world’s fastest-growing brain disease, may be fueled by toxicants and is therefore largely preventable.”
NEWS BRIEFS NE UR OSCIENCE | VOL 21 | 2024 1
Hearing, balance & the brain
How collaboration is transforming research at the University of Rochester
It is not much bigger than a dime. Made up of a meticulous maze of anatomic loops and tubes, hair cells and neurons, and other signaling mechanisms, the ear and vestibular system take in information about the world around us and deliver it to the brain quickly. It is a system that is full of mystery, leaving much for science to explore and explain. However, it is well understood that it does not age gracefully—for adults aged 75 and older, imbalance is the number one cause of doctor visits, and 40 percent experience hearing loss.

Establishing a group to advance science
Researchers at the University of Rochester and Medical Center (URMC) have long been on the quest to understand this system and its parts. Faculty from an array of disciplines, such as Neuroscience, Otolaryngology, Biomedical Engineering, Linguistics, and Brain and Cognitive Sciences, all aim to discover better drug-delivery methods and improve mechanistic and functional understandings of the hearing, balance, and brain connection. The University of Rochester is among the top 20 institutions in the United States in funding for hearing—and balance—related research from the National Institute on Deafness and Communication Disorders (NIDCD). It is one of the few institutions on that list that does not have a designated center for the group.
“Collaboration has been really key,” said Laurel Carney, PhD, professor of Biomedical Engineering and Neuroscience. “There are no barriers between different groups to get funding that crosses departmental or school boundaries. That is important.”
In 2022, Carney led the group that formally organized nearly 20 faculty members and labs from across the University and Medical Center who study hearing and balance. Known as the Hearing & Balance Research Collective—the group has benefited from its concerted efforts to foster collaboration. It consists of a grant-writing group that has helped faculty secure millions of dollars in funding, a journal club organized by postdoctoral fellows Dana Boebinger, PhD, and Daniel Guest, PhD, that meets weekly to share and discuss new developments and innovations in the field or the research of an upcoming seminar speaker, which is the third component of the Collective. “Our goals are to teach each other about the various sub-fields within auditory science, and foster community and build relationships,” said Boebinger.
“As a scientist, our journal club has really improved my understanding of a few areas of research that are related to my own but are not in my immediate comfort zone. One good example is physics,” Guest said. “The inner ear is a very complex mechanical system and there is a lot of exciting research, including here at UR and URMC, that is applying new techniques to provide better data on how this system works.”
The Collective’s seminar series has brought several leaders in the field from around the world to Rochester. “The seminar component is key for building our reputation and relationships with some of the leading hearing and balance research,” Kenneth Henry, PhD, associate professor of Otolaryngology and Neuroscience and co-leader of the Collective. “And so far, it has been a great success.”
2 UNIVERSITY OF ROCHESTER | ERNEST J. DEL MONTE INSTITUTE FOR NEUROSCIENCE FEATURE

POSTDOCTORAL SPOTLIGHT
DANA BOEBINGER, PHD, is a postdoctoral fellow in the Norman-Haignere lab at the University of Rochester Medical Center (URMC). She received her doctoral degree from Harvard University’s Speech and Hearing Bioscience and Technology program, her master’s degree in Cognitive Neuroscience from University College London as a Fulbright Scholar, and her undergraduate degrees in Psychology and Music at Florida State University. She was recently awarded an F32 from the NIH to study how the brain integrates information about speech over time, in both silent and noisy environments.

“As a musician, I’ve always been fascinated by sound and the profound effect it has on people,” said Boebinger. “The results of these experiments will further our knowledge of the computations that enable speech recognition in noisy real-world conditions, as well as how the auditory cortex flexibly adapts to changing environments. Answering these questions is a critical step towards understanding the deficits in listening in noises that are present in auditory neurodevelopmental and attentional disorders.”
DANIEL GUEST, PHD, is a postdoctoral fellow in the Carney lab at URMC. He completed his PhD in Psychology at the University of Minnesota, and his undergraduate studies in Psychology at the University of Texas at Dallas. His research focuses on building computer models of the auditory system to better understand how the auditory system works, including the role of feedback connections. He was recently awarded an F32 from the NIH to investigate the role of efferent pathways in the auditory system.
Guest has always been interested in science, but it was a research opportunity in a speech perception lab during undergrad that he saw a career path for himself. “I enjoyed the work, and I was intrigued by the scientific questions we were asking. One thing led to another, like a chain of dominos, and here I am!”

NE UR OSCIENCE | VOL 21 | 2024 3
NE UR OSCIENCE | VOL 21 | 2024 3
Grant writing group meets weekly on the University of Rochester campus. From front left: Eric Anson, PhD, Kenneth Henry, PhD. From back left: Jong-Hoon Nam, PhD, J. Chris Holt, PhD, Sarah Hayes, AuD, PhD.

Meeting unites three labs to ask one question
Mechanical Engineering Professor and co-leader of the Collective Jong-Hoon Nam, PhD, had a question but not all the tools he needed. Because of the Collective grant-writing meetings, he knew who may be able to help. Both Carney and Henry immediately responded to the opportunity to collaborate. “Jong-Hoon needed to use some neural measurements to assess the effectiveness of the drug delivery in the inner ear. It is something he could not do in his fluid-dynamics lab,” said Carney. “But we could create the experiments.” Henry and Carney helped develop in-vivo experiments for him to advance his hypothesis. Today, the three are investigators on a project funded by the NIDCD that is looking at whether the inner-ear fluid, which is isolated from all other body fluids, could be a target for drug delivery.
“This project is not trivial,” Nam said, “and it is a great example of the connections built by the Hearing and Balance Research Collective. We need more contact with scientists for this kind of collaboration, and as we mingle, new ideas come. Initially, I did not know if I could begin this experiment, but when I talked to Ken and Laurel, they said this is a feasible experiment and we can start right away. This is a success story.”
Many questions, many labs, one system
The questions being asked by nearly two dozen labs associated with the Collective are sprawling. From the prospect of regenerating hair cells, to treating motion sickness, to how neurons in our brain respond to music.
A discovery in the lab of Neuroscience Associate Professor Patricia White, PhD, also a member of the Collective, is bringing us closer to possibly understanding how and if hair cells can be regenerated.
These are the primary cells that detect sound waves and cannot regenerate if damaged or lost in mammals. Her lab found how the

4 UNIVERSITY OF ROCHESTER | ERNEST J. DEL MONTE INSTITUTE FOR NEUROSCIENCE
Kenneth Henry, PhD, left, and Neuroscience graduate student Leslie Gonzales work together in the Henry Lab in the Medical Center.
Jong-Hoon Nam, PhD, (right) and Mechanical Engineering graduate student Wei-Ching Lin (left) discuss acquired data of colloquial vibrations in the Nam Lab at the University of Rochester.
activation of the active growth gene, the ERBB2 pathway, happens in mice, which in turn triggers a cascading series of cellular events by which cochlear support cells begin to multiply and activate other neighboring stem cells to become new sensory hair cells. Her lab’s current research is investigating this phenomenon from a mechanistic perspective to determine whether it can improve auditory function after damage in mammals.
J. Christopher Holt, PhD, associate professor of Otolaryngology and Neuroscience, expanded our understanding of how balance stimuli are received by the brain while also offering insights into potential drug targets in the ear, which may be leveraged for treating motion sickness and balance disorders. His study in the efferent vestibular system (EVS) which begins as a small collection of neurons that travel from the brainstem out to the ear where our sense of balance begins, was done in mice. Researchers recorded an increase in the activity of vestibular afferent neurons in mice during stimulation of the EVS system. The excitatory effects of EVS stimulation were diminished by the application of scopolamine, a drug widely used to treat motion sickness in humans, demonstrating for the first time that EVS mechanisms in the ear are also targeted by this drug.
Biomedical Engineering and Neuroscience Associate Professor Edmund Lalor, PhD, uses EEG to understand how the brain allows us to focus on one speaker out of many. His lab discovered the brain is taking an extra step in this processing phenomena. EEG brainwave recordings indicated the sounds coming from the person being listened to were converted into linguistic units known as phonemes, units of sound that can distinguish one word from another, while the other speaker’s sound was not.


“The grant writing meetings have been extremely beneficial. They can be tough but are constructive," said J. Chris Holt, PhD. Holt (left) is
Center.
NE UR OSCIENCE | VOL 21 | 2024 5
pictured with Choongheon Lee, PhD, in the Holt Lab at the Medical
Laurel Carney, PhD, professor of Biomedical Engineering and Neuroscience. Photo: J. Adam Fenster / University of Rochester
Anne Luebke, PhD, associate professor of Neuroscience and Biomedical Engineering at URMC, and Adam Dziorny, MD, PhD, assistant professor of Pediatrics and Biomedical Engineering, considered the role silence may play in hearing preservation. In a 2021 study, they found that a combination of sound and silence may be a key to helping slow the progression of permanent hearing loss. Using intermittent broadband sound, played over an extended period they were able to preserve sensory cells in the ear of mice, while also rewiring some of the central auditory system in the brain, helping preserve the ability to sense the timing of sounds.
The sound of music has a unique relationship to how humans hear. It turns out, there are neurons in the brain that “light up” only to the sound of singing. Samuel Norman-Haignere, PhD, assistant professor of Biostatistics and Neuroscience, was part of this research and helped develop a novel method of measuring the timescale over which different brain regions integrate information. This method is important for understanding the timing and location of how the auditory cortex responds to different sounds. This is integral to learning more about the relationship neurons have to speech and music.

rare opportunity to record neural activity from inside the human brain.”
6 UNIVERSITY OF ROCHESTER | ERNEST J. DEL MONTE INSTITUTE FOR NEUROSCIENCE
Samuel Norman-Haignere, PhD, (right) and Dana Boebinger, PhD, postdoctoral fellow, work together in the lab. The Norman-Haignere lab collaborates with neurosurgeons and neurologists in the Epilepsy Monitoring Unit at the Medical Center to work with patients who are in the hospital to have their brain activity monitored to localize seizures. The willing patients listen to sounds like speech and music, as well as simpler sounds like tones and noise. “We can monitor how their brain responds to the sounds,” said Boeginer. “It is an incredibly
Chair of Otolaryngology Shawn Newlands, MD, PhD, has spent much of his career at the Medical Center. He points to the faculty recruiting under the leadership of Gary Paige, PhD, professor emeritus and former chair of the Neuroscience Department, as the initial push that put Rochester on track to becoming a leader in hearing and balance research. “And we kept building from there,” said Newlands. “We continue to recruit faculty from multiple departments and now with the Collective, we are bringing faculty together regularly in the grant-writing group and engaging with students in a new way through the journal club.”
Recent recruit, Sarah Hayes, AuD, PhD, is an assistant professor of Otolaryngology and co-leader of the Collective, whose research interest aims to understand the adverse effects hearing loss can have on the brain. Specifically, she is investigating the relationship between brain plasticity caused by hearing loss and pathologies such as tinnitus and hyperacusis or the reduced tolerance of sound. “The Medical Center is a very unique setting where I can combine both my passion for helping patients with hearing loss, tinnitus, and hyperacusis, and join a collaborative and vibrant group of hearing and balance researchers,” said Hayes. “As a new faculty member, having the support and guidance from my colleagues in the Hearing and Balance Research Collective has been invaluable as I navigate my career as an early-stage clinician-scientist.”


Above: Shawn Newlands, MD, PhD, is a neuroscientist and cancer surgeon. His medical practice specializes in head and neck cancers, while his research focuses primarily on the vestibular system, particularly in recovery from injuries to the inner ear.
NE UR OSCIENCE | VOL 21 | 2024 7
Left: Sarah Hayes, AuD, PhD, works in an audio testing booth in the Medical Center.
Q&A with Manoela V. Fogaça, PhD
Manoela V. Fogaça, PhD, is an assistant professor of Pharmacology & Physiology at the University of Rochester Medical Center. She received her undergraduate degree in Biomedical Sciences at the State University of Londrina and completed her master’s and PhD in Pharmacology at the University of Sao Paulo. She went on to complete her postdoctoral fellowship at Yale University where she investigated molecular, cellular, and synaptic mechanisms underlying the actions of fast-acting antidepressants. She joined URMC in 2023 where her research focuses on understanding the molecular basis of behaviors relevant to stress and identifying how specific circuits are impacted by pharmaceuticals.
Please summarize your research.
Exposure to chronic stress can result in functional changes in the brain that contribute to the onset of neuropsychiatric disorders, such as Major Depressive Disorder (MDD), which impacts one in five individuals over their lifetime. Therefore, my research focuses on understanding the molecular basis of behaviors relevant to stress disorders and the actions of novel rapid antidepressant drugs, including compounds that target the glutamatergic and/or the GABAergic systems in the brain (ketamine, ketamine-like drugs, and GABA receptor modulators), aiming to identify specific circuits, neuronal subpopulations, and synaptic mechanisms involved in these responses. To this goal, we combine molecular neuropharmacology, genetic approaches, and circuit-level studies of neurobiological systems to investigate how specific subpopulations of GABAergic and glutamatergic neurons crosstalk to modulate excitation and inhibition network dynamics that lead to phenotypes relevant to MDD. In addition, we are interested in understanding how neuromodulators contribute to these responses, including endogenous opioids, endocannabinoids, and neuropeptides.
How did you become interested in your field?
When I started my undergraduate studies in Biomedical Sciences, I initially aimed to become a genetic engineer. However, in the early years of my academic journey, I faced

significant challenges due to chronic stress and high selfexpectations, leading to severe anxiety symptoms. At school, I underwent a sudden shift in behavior, transitioning from being sociable and outgoing to constantly introspective and worrying. This internal struggle prompted me to question: "How does a stressful environment shape my behavior, and how can I overcome it?" Motivated by my innate curiosity and a desire to address my challenges, I delved into neuroscience and fell in love with neuropsychopharmacology. The more I immersed myself in this field, the more I longed for knowledge. However, I soon realized that molecular psychiatry, while incredibly captivating, was relatively nascent compared to other fields, particularly over a decade ago.
Recognizing the need for advancement in this area, I made a conscious decision to dedicate my career to investigating the neurobiology of stress and pharmacological interventions.
What brought you to the University of Rochester?
The University community shares a vibrant scientific and institutional environment, fostering scientific progress, collaboration, and a wide array of resources for career development. With my background in Pharmacology and Neuroscience, URMC provides the perfect setting for advancing my studies. I am amazed by the friendly culture and high level of collaboration within the department, as well
8 UNIVERSITY OF ROCHESTER | ERNEST J. DEL MONTE INSTITUTE FOR NEUROSCIENCE
FACULTY PROFILE
as, the University’s strong dedication to inclusion and diversity. The "open doors" policy encourages the continuous exchange of ideas and knowledge among colleagues whom I’ve already begun collaborating with, including Drs. MacLean, Orlandi, Bidlack, and Wojtovich.
What is your favorite piece of advice?
Some advice I always share with my students: always try,
even when that inner voice of doubt tells you otherwise. Opportunities come and go, and it is important to be prepared to welcome them when they arise. Sometimes, all it takes is the courage to open a door, take a deep breath, and embrace the risks. To achieve your goals, trying is just as important as gaining knowledge.
Batten Research Day fosters collaboration and growth
The University of Rochester Intellectual and Developmental Disabilities Research Center (UR-IDDRC) and the University of Rochester Batten Center (URBC) hosted a Batten Research Day in March. The event brought basic scientists and clinical researchers from across the University of Rochester Medical Center together to share their latest research to advance knowledge about CLN3 Batten disease. CLN3 Batten is a neuronal ceroid lipofuscinosis (NCL) disorder, which are inherited neurodegenerative disorders that cause vision loss, motor and cognitive decline, seizures, and premature death. Most NCL disorders, including CLN3 Batten disease, begin during childhood. Parents of children with CLN3 Batten disease and Amy Fenton Parker, president and CEO of the Batten Disease Support and Research Association (BDSRA), also participated. They offered firsthand experiences and insight into the lived experiences of children and families impacted by Batten disease, and the research priorities for them and the community at large.
“This meeting is to continue to foster and grow the collaboration that exists between people across the University,” said Jennifer Vermilion, MD, assistant professor of Neurology, Child Neurology, and Pediatrics. “This will ultimately help us to move forward in our science.”
“Having families here and being a part of the process is key to our ability to grow our understanding of this devastating disease and improve care,” said John Foxe, PhD, director of the Del Monte Institute for Neuroscience and co-director of the UR-IDDRC. “It is always an important reminder of who we are doing this research for.”
The University has been at the forefront of research and care for CLN3 Batten disease and other NCLs. The URBC is a recognized leader in the research and treatment of this condition. It is a designated Center of Excellence by the BDSRA. In 2020, when the National Institute of Child Health and Human Development (NICHD) designated the University as an IDDRC, the disease became the Center’s principal project, and researchers identifying biomarkers to evaluate the effectiveness of experimental treatments became a renewed focus for faculty at the Medical Center.
Along with the IDDRC, the University has long been a University Center of Excellence in Developmental Disabilities Education, Research, and Service (UCEDD) and Leadership Education in Neurodevelopmental and Related Disabilities (LEND). The University is one of eight institutions with the trifecta of federal awards related to IDDs.

A group of trainees, faculty, clinicians, families, and advocates participate in a round-table discussion at the Batten Research Day event hosted by URIDDRC and URBC. This discussion followed a morning of presentations where researchers and clinicians shared their most recent projects and families of children living with Batten disease shared their journey and perspective.
NE UR OSCIENCE | VOL 21 | 2024 9
NEWS BRIEF




John Foxe, PhD, (left) host of NeURoscience Perspectives, interviews Nathan A. Smith, PhD, associate dean for Equity and Inclusion in Research and Research Education and associate professor of Neuroscience at the University of Rochester School of Medicine and Dentistry.
University of Rochester Medical Center 601 Elmwood Avenue, Box 603 Rochester, New York 14642 Visit us online: delmonte.urmc.edu Follow us @URNeuroscience Scan to receive the Neuroscience Newsletter giveto.urmc.edu/delmonte Watch and listen to new episodes of NeURoscience Perspectives.






















