KIDNEY
The magazine of the National Kidney Federation

KDARS and the Brave Bean Awards
Kidney disease affects people of all ages – find out more about how children and their parents and carers manage and get support



Kidney disease affects people of all ages – find out more about how children and their parents and carers manage and get support

Hello and welcome…
Welcome to the second issue of Kidney Life for 2024. Officially our ‘Summer’ issue, at the time of writing it’s finally stopped raining so I hope you are able to enjoy the sunshine and all that the summer brings – holidays, gardening and enjoying being outside again.
This issue has varied content which I hope you find interesting. We have a number of articles about children and young people; we bring you some results from a recent clinical trial; reports about important events and the programme and booking form for the Annual Patients' Event in October. Also included with your copy of Kidney Life is the NKF’s third Impact Report for 2023 which details all the hard work and achievements over the last year as we continue to support millions of people living with kidney disease in the UK.
We also bring you an article on waiting times for kidney transplants across the country. Kirit and I have worked with clinical expert contacts to create this article. It's complex and complicated but carries an important message I believe.
I hope you enjoy reading this issue and please, as always get touch by emailing: kidneylife@kidney.org.uk if you'd like to tell your story or you have ideas for future articles.
Warmest wishes
Annie Taylor EditorNKF OFFICERS
Chairman – David Coyle
Co Vice Chair – Caryl Bryant
Co Vice Chair – Tarsem Paul
Treasurer – Mike Sinfield
Secretary – Brian Child
NKF TEAM
Andrea Brown – Chief Executive
Pete Revell – Head of Marketing & Fundraising
Donna Blizard – Office Manager
Sharney Warren – Communications and Marketing Officer
Fiona Broomhead – Senior Office Administrator
Chloe Ainsworth – Social Media and Website Coordinator
Heather Mooney – Accounts Administrator
Linda Pickering – Helpline Advisor
Stephen Emmerson – Helpline Advisor and Peer
Support Coordinator
On a surprisingly sunny day in April around 40 KPA chairs and members held their annual meeting in the rabbit warren at the Arden Hotel in Birmingham. The day was a great opportunity for networking, sharing and learning.
After a warm welcome from NKF Chairman, David Coyle and reflecting in a minute’s silence for family, friends and colleagues lost over the past year we were straight into the group sessions.
No time was wasted as we moved around in groups of 10 to each corner of the room where we considered:
• How to grow KPA membership
• Raising KPA profiles with your hospital and patients and how to support patients
• Organising social and fundraising events
• KPA’s understanding of the NKF
Lots of interesting discussions were generated in each group. All group discussions were facilitated and recorded by the NKF team. Collated comments were then fed back to the whole group and further questions were raised and information shared. In the next two issues of Kidney Life we will report in detail on two of the four topics discussed.
After lunch the annual general meeting was held followed by the council meeting.


The new NKF Officers and Executive Committee members were announced for 2024 as follows:
NKF Officers:
David Coyle – Chair
Tarsem Paul – Co Vice Chair
Caryl Bryant – Co Vice Chair
Mike Sinfield – Treasurer
Brian Child – Secretary
The following people have been elected as Executive Committee members:
Ros Aird – Lister Area KPA
Sarita Khurana – West London KPA
Charleen Sepede – Friends of Derriford KPA Soumeya Bouacida
Kirit Modi mbe – NKF Honorary President
Feedback from people attending the day was very positive with comments about the usefulness of sharing ideas and experiences, networking, the informality of the day, inspirational ideas for their own KPA. The food was good too, which always helps! In planning next year’s event we will take into account the comment that there were no guest speakers at the event.


Friday 25th and Saturday 26th October
Radisson Blu Hotel – East Midlands Airport


This year’s World Kidney Day (WKD) was held on Thursday 14th March. The NKF along with the other kidney charities in the UK – Kidney Charities Together - were actively raising awareness of kidney disease to anyone and everyone who would listen.
Many Kidney Patient Associations organised events with stands in their local units. Linda Pickering, our Helpline Advisor attended a renal patient education fair at Hull Hospital and we also had fundraisers supporting the NKF on the day at the Novotel Hotel in London.
The day was very busy and our social media was filled with people celebrating and spreading awareness. Here's an overview of some of the activities. Well done to everyone who took part.
Bristol Area KPA
Bristol Area Kidney Patients’ Association (BAKPA) had a table display in the atrium of Southmead Hospital where the renal department is situated, and had lots of interest from the public, staff and students of the University studying genetic diseases. Lots of information leaflets, pens and trolley token keyrings were given away. It was a great way of letting everyone know about the BAKPA and what it does.
Dorset KPA
At an entrance to Dorset County Hospital the Dorset Kidney Patients’ Association (DKPA) celebrated World Kidney Day by raising awareness about chronic kidney disease. The event was organised and run by the fabulous renal team, with a special mention to Leanne.
Dorset KPA were in Damers Restaurant promoting how to keep your kidneys healthy and what your kidneys do, as well as providing information about acute kidney injury.
Dorset KPA would like to say thank you to everyone involved including the cake bakers and cake buyers!


Royal London Hospital KPA
Our stall was set up on the Saturday morning following World Kidney Day at the Mercury Shopping Centre in Romford, East London. Saturday was chosen as it’s generally busier than weekdays. Staffed by two stalwarts of the Royal London Hospital KPA, Glenn Maloney and Marie Niven, it was a busy day as they handed out information leaflets and responded to a number of enquiries were. It was a pretty busy day.
Spreading the Word
Hattie Stiff was busy on WKD! NKF’s ambassador was interviewed by the BBC who followed up with an online article about her story which can be found here: www.bbc.co.uk/ news/uk-england-somerset-68439167

Hattie also did a live interview with BBC Points West and shared her story on BBC Radio Somerset.
Thank you to everyone who took part. WKD is a great annual event which increases awareness and understanding of kidney disease and its impact.







The National Kidney Federation recently organised and sponsored the KDARS for Kids Brave Bean Awards, an event bringing families together for a day of connection and entertainment at the Radisson Blu Hotel, East Midlands.
The day included a certificate ceremony for the children, recognising their bravery and resilience in the face of their kidney-related challenges. Following lunch, attendees were re-energised by a talented magician who mesmerised the children with his tricks, and to conclude the day there was a disco. It was a great gathering for families to come together, a chance to connect and finally meet each other face to face. Attendees had the opportunity to purchase NKF’s 'Brave Kidney Bean' children's t-shirts and 'Proud Parent' t-shirts, showing their support for the cause in style.
Overall, the event was a success with a sense of community and solidarity among all who attended.
Andrea Brown, NKF Chief Executive commented: “It was great to support the day and chat with the families offering NKF’s support and informing them of our patient support services when in need. KDARS for Kids is an incredible support group that has brought a lot of families together.”
To find out how one family has benefited hugely from the support of KDARS Facebook Group turn to page 12.

Heather Davis, Founder of KDARS for Kids Facebook Group said:
“As a parent of a young person who suffered acute kidney injury, secondary to antepartum haemorrhage during the new born period, and would, a few years later be diagnosed with chronic kidney disease stage 3b, we know how isolating and lonely this journey is. CKD doesn't just affect the "patient", it affects everyone around them, none more so than their siblings. Brothers and sisters often feel pushed out and a sense of responsibility in many ways.
The whole idea of the Brave Beans Award ceremony was to celebrate not only the courage of KDARS kidney beans, but that of their siblings and friends.
While the day began with the children receiving their certificates and medals, it was so much more than that, friendships were formed, not just for the children but parents too, the lunch buffet was a hit and Dave the magician went down a storm, he kept everyone laughing and the children were enthralled by his performance.
For Stephen and me, as the founding members of KDARS (Kidney Disease And Renal Support Group), it was a day we had envisioned for many years. It was everything we had dreamt of, and exceeded all of our expectations, we are itching to make it happen again.”








For those interested in purchasing our range of merchandise, including the 'brave kidney bean' children's t-shirts and 'proud parent' t-shirts, check out our shop:
www.kidney.org.uk/pages/shop/ department/tshirts





To join KDARS for Kids Facebook Group please visit:
www.facebook.com/ groups/750940214926395

Variation in waiting times currently exist for most, if not all, planned surgical activity in the NHS. Waiting times make the headlines almost every week with recognition that long waits can cause misery, pain and frustration which is often accompanied by a sense that life is on hold. This is nowhere more evident than in the wait for organ transplantation.
Around 5,500 adults are on the waiting list for a kidney transplant each year. Figures for 2022/23 (the latest available from NHS Blood & Transplant) show that 3,272 kidney transplants took place, of which 923 were from living donors. So why do people often have to wait longer in some parts of the UK before they get their kidney transplant?
The variation of waiting times for kidney transplantation
NHS Blood and Transplant (NHSBT) (www.nhsbt.nhs.uk) provides information for patients, their families and carers about organ transplants and specifically about kidney transplants. Their clinical site (odt.nhs.uk) provides further detailed statistics about organ transplantation.
They raise some key facts about the reasons why people have to wait. The average wait for a kidney transplant in the UK is around 2 years.
Factors that can influence how long the wait is for a kidney transplant from a deceased-donor for all transplant centres include:
• Blood type of the recipient (with blood group B relatively rare in UK kidney donors compared to the waiting list)
• HLA (Human leucocyte antigens) type of the recipient (otherwise known as tissue type). HLAs are present on most of the cells in your body. People inherit HLA antigens from their parents.
– Some ethnic groups have more complex and rarer tissue types than others.
• If a recipient has anti-HLA antibodies. HLA antibodies (either from previous blood transfusions, transplants or pregnancies) can be a major impediment to transplantation as it reduces the chances of finding a suitable donor.
The transplant waiting list is not a queuing system, where the first person in the queue is offered the next available organ. It is more a matching system based on a computer programme that considers several factors (e.g. blood type compatibility with the donor, similarity of HLA-type between donor and recipient, length of time a recipient has been on the waiting-list or on dialysis, and similarity of the recipient age with the donor), and deciding which patient is most suitable.
This allocation of donor kidneys is performed by NHS Blood and Transplant and will be similar across all the different transplant units in the UK. While it may appear that choosing where you are listed for transplantation may impact how long you wait for a kidney transplant, this may not always be the case and other factors influence waiting time.
Why variation in waiting times exist and what patients need to know
There are many reasons why people wait longer in some areas of the country for a kidney. While there are significant differences in waiting times between transplant units in the UK, most of these differences relate to local population demographics, rather than factors related to the individual transplant units.
Choosing where to have your transplant involves weighing up many factors, with geography a key issue. In more rural areas it’s likely that travel to an alternative centre would be impossible but in denser areas where there are several transplant centres serving a large urban population, there may be many local options.
The issue is that many patients are not aware that they have a choice about where their transplant might take place. And at the very least it might be helpful to know more about what’s possible and the variation in waiting times that exist between centres.
Patient Choice is a government initiative introduced into the NHS in the early 2000s. It is a legal right allowing people greater choice and control over how they receive their healthcare, enabling an individual to choose where and to some extent by whom their care is given.
In line with this, kidney patients going on to a waiting list for transplant can in fact choose where they have their surgery. While a renal unit may have arrangements in place with one or two transplant centres and they will guide their patients on this, an individual can choose where they go.
In conversation with a nephrologist colleague their concern was that referral for a transplant was not just about the surgery but about the care provided in the intervening period (after being listed) and post-surgery by both multidisciplinary care teams which in their view is hugely important in enhancing the quality of care. Moving out of an area where relationships are not necessarily in place and care shared and understood might not be in the patient’s best interest. It was however confirmed that there is almost always plenty of support available from the renal team to enable people to make informed decisions about where they might go – and plenty of time to make that decision.
Guidance for kidney patients waiting for transplant
There are many complex factors which affect waiting times at different transplant centres. It is most important that patients discuss these factors with their nephrologists when considering kidney transplantation. It should also be discussed with family members and support sought from NKF’s Helpline. Some hospitals have peer support services and having conversations with patients who have had a kidney transplant at the same hospital can be most helpful.
Some factors patients should consider include:
• Patients can only pick one transplant centre for their surgery.
• The impact of travel time, costs and arrangements for multiple visits – particularly post-transplant surgery –it needs to be a practical decision and a workable option for all concerned.
• Consider the waiting time as well as survival rates and outcomes for kidney transplants at the centre and talk with your nephrologist about these. People from ethnic minority backgrounds generally have longer waiting times compared to white patients.
• Always consider living donor transplantation as the fastest and most effective way of receiving a kidney transplant.
• Join your local Kidney Patients' Association if one exists. KPAs provide valuable opportunities to meet other kidney patients, and many have well established relationships with local renal department staff.
For more information
Visit How long is the wait for a kidney?Organ transplantation - NHS Blood and Transplant (nhsbt.nhs.uk) where there is lots of information but nothing about the choice of transplant centre or indeed patient choice.

In the next issue of Kidney Life we will feature the work of NHS England’s Organ Utilisation Group and its plans.
Written by Kirit Modi, Honorary President of the NKF and Annie Taylor with expert input from Dr Gareth Jones, Consultant Nephrologist & Clinical Service Lead for Renal Transplantation, Royal Free London. Professor Reza Motallebzadeh, Consultant Renal Transplant Surgeon, Royal Free Hospital. Dr Richard Fluck, Consultant Renal Physician, at Derby Royal
and Clinical Director for Internal Medicine National Programme of
at NHS England.
in
Tracey Wells gives us an honest and heartfelt view of how she faced dialysis and coped with the changes it brought about.
I knew it was coming. Well, I half knew it was coming. I had a 50% chance of inheriting Polycystic Kidney Disease (PKD) and 50% chance of it leading to kidney failure. I have to say I’m not fully accurate with the actual statistics and percentages, but this is what I had stuck in my head.
I was diagnosed in my 40s (now 55), I knew I’d drawn the short straw with PKD. Initially my kidney function was good and there was still hope that the cysts on my kidneys wouldn’t get so bad that I would end up in renal failure. So, I didn’t give it much thought. I was fine. It wouldn’t happen to me.
My Mum had the same illness as did her dad. Still, I thought I was in with a chance of not following in their footsteps. In my head, I was invincible. I think a lot of people feel like this as they get older and begin to face some of life’s changes and challenges to their health. We all still somehow feel like we did in our twenties. Young, vibrant, fit, healthy. Nothing could get to us. It won’t happen to me.
And then it did and it came as such a huge shock. Even though I knew it might be coming... I simply could not believe it was happening to me.
In part, of course, the fact that I didn’t feel ill made me think it couldn’t be true. I was going about my daily business. Not a single symptom. “But I feel fine” is all I kept thinking as my dangerously high blood pressure put me in hospital and my other blood results kept me there for further tests. A brain scan? Really? But, I'm fine…
So the leap I had to make from feeling “fine” and “invincible” to having a chronic, life threatening illness was pretty damn quick. My brain felt like a flooded car engine. How to describe it? A fog? People were telling me things and their words floated away from me. It sounded as though they were talking in slow motion, underwater. And then the rage. I don’t know how I contained it, maybe I didn’t on occasion. I was so angry. At the time I thought the anger was to do with “Why me?”. I should have been prepared. But I wasn’t at all ready, and it came as the biggest shock of my life.
The first day after I was diagnosed I was in the hospital and the renal specialist nurse came to see me. She told
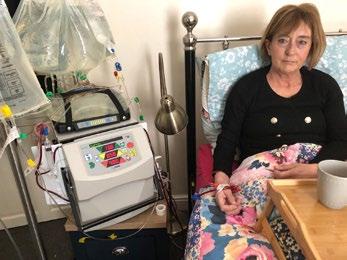
me I would need dialysis in the coming months. I just stared at the bottom of my hospital bed.
Dialysis? But I’m only in my 50s. I should have years yet. My Mum was much older than me when this happened to her. My life will never be normal again. And I felt guilty that I had perhaps wasted time not making the most of every minute up till now. Not making the most of normal life.
The woman in the next bed was a very ill kidney patient. She was younger than me. She was in excruciating pain and could not even sit up in bed. She lay there quietly, asking the nurses for something stronger for the pain. She looked so small in the bed, like a broken bird. I was terrified. Ashamed to say, horrified.
A porter arrived at her bed with a chair to take her down for dialysis. She looked up from her pillow and said there was no way she could get out of bed and into the chair due to the pain she was in.
Was this what I’ve got to look forward to? Having to receive lifesaving treatment for maybe years to come and not being well enough to get into a chair to get to dialysis. Later, when she returned to the ward, I couldn’t stop staring at her, my first glimpse of a renal patient. I wanted to run. Discharge myself, pull out the drip and wipe my name from the white board above my bed - no longer a patient. This was all a terrible mistake, a mix up.
They’d got the wrong person. I’m fine, I thought, of course I’m fine. Just go and they won’t be able to do any of this to you. You’ll be free like before. This can’t be real. Hot tears were forcing themselves into my eyes. I was desperate not to cry, not to show weakness. Not to invite sympathy, empathy, attention. I couldn’t tell anyone how this was making me feel. I must be the only person on the planet to react like this, to feel like this. Surely other patients took this diagnosis in their stride, they expected it, didn’t they? They were relieved that now they knew it was happening something could be done about it. Dialysis would keep them alive and all would be well. Surely. The fact that I wasn’t feeling like that meant there was something wrong with me. It’s my ‘poor coping mechanisms’ that mean I can’t see the bright side. My depressive personality that is usually oh-so-wellcontrolled by medication. I’m all over the place. I sit up and wipe my eyes. Phew, no-one saw, thankfully. I run my fingers through my hair, rub my face and throw my legs off the side of the bed. Cigarette. I need a cigarette.
Outside, in the cool November air I glance around me briefly. Usually, I’m really nosey and love a bit of people watching. Today I only see patients. But I’m not like them with their dressing gowns and slippers, their drip stands and walking frames, sitting in wheelchairs with lower limbs missing. I am still in my own clothes. I don’t want to get into pyjamas and dressing gowns. Somehow that means I’ve given in and let them be right. I don’t want to be ‘a patient’. Now or ever, and if keeping my own clothes on for as long as possible makes me feel I am delaying that, then so be it.
I knew deep down I couldn’t hide from this. I knew enough to know that my blood pressure was dangerously high and without continued inpatient treatment to bring it down, I was putting my life at risk from a stroke. I took a deep breath and went back to the ward.
Feeling a little lighter for some fresh air, I caught the eye of the lady in the next bed to me and we shared a small


smile. I went around the side of my bed to my locker and started tidying my belongings. As I turned, I caught her eye again and found myself asking;
“What’s it like?”
She seemed calmer than before so maybe she’d had some pain relief. She didn’t press me for specifics.
She just said,
“It’s ok, y’know.”
I stayed silent as I felt there was more to come.
“It doesn’t stop you doing anything.” she said, with a warm smile.
I didn’t know what to say. Then she said,
“You just get on with it, really. I’ve been on dialysis 3 years now and I’ve got a great life. I’ve had three brilliant holidays abroad in that time, funded by a charity. You just work around it.”
She pulled herself into a part sitting position as she continued.
“Oh, and this?” she said, waving her arm down over her body. “This isn’t the usual state of affairs. I’ve never been like this before. I’m usually the one running around after everyone else. I’ve got an infection at the moment; I’ve been in so much pain. But now they are on to it thankfully. I’ll be fine in a day or two.”
I stayed silent. My brain just hearing the words; “It’s ok y’know. It doesn’t stop you doing anything.” Over and over in my head. Like a mantra.
Two and a half years later a lot has happened. Some good, but mostly a downward slide into deteriorating renal failure and becoming a dialysis patient myself. I’ve kept those words that she said with me. I thought if someone could go through all she’d been through and still come out like the cat that got the cream, then, as they say, there was hope for me yet…
After receiving devastating news at a growth scan during pregnancy, a journey of heartache and resilience began for mother, Mikayla Hiller and her unborn baby. With each pregnancy scan unveiling challenges, Mikayla’s determination to fight for her little girl shines through. Amidst the uncertainty and fear, the support and guidance provided by the KDARS for Kids Facebook group became a beacon of light for Mikayla, connecting her with people facing similar struggles and offering a sense of community in the face of hardship.
This is Mikayla and Natalia’s story:
The world feels like it has shattered when you attend a growth scan at 21 weeks pregnant to find out that something is wrong. It is hard to put into words. I was told half of the amniotic fluid was stuck in my baby’s kidneys and the kidneys were bright and enlarged. With this news, our care was transferred to Princess Anne Hospital.
At 28 weeks we went for our next scan, this was when we found the baby was growing at a normal rate, however, there was no amniotic fluid around my little girl anymore. Instead, her kidneys were huge, bright, cystic and effectively dead. My head would spin at the conversations to follow. Being told I could lose my baby when she hadn’t even graced the earth with her presence yet broke my heart completely.
Following this news I had weekly scans, I never took for granted seeing her or feeling her movements as I knew the brutal reality as it was repeated to me every appointment as was the offer of termination. Whatever the outcome, I would not give up on my little bean, I could feel she was a fighter.
I was recommended to join the KDARS Facebook group by the consultant we saw at every visit, she said it would help answer any questions and help to support me. For a while, I sat quietly in this group shocked at how many people were on this scary journey just as we were. I felt as if we were all in the ocean of kidney problems and failure but we all had separate boats and situations. Everyone was so kind and helpful to everyone else.
The day of my c-section came, this was the safest way to get her out, as I was told if you contract with a baby
which isn’t surrounded by fluid you would starve them of oxygen and blood flow with every contraction, so the option was a no brainer. Out came my beautiful baby girl who I was told would not cry because her lungs hadn’t had the amniotic fluid to develop. But she did, my little warrior screamed so hard to show me she was ready to fight that her lungs collapsed. She was intubated so they could use machinery to help her breathe and as they whizzed her to the NICU, they asked if I wanted to name her. Of course, I did, even if her life was short, she deserved a name. The name Natalia was etched into my heart and it couldn’t suit anyone better!
Hours passed before I got word I could go and see my baby. I was wheeled in my bed to this very quiet but overwhelming room of mums with their tiny babies, and there was my angel.
She was covered in tubes, and asleep but her strong heart was beating and ready for the fight ahead.

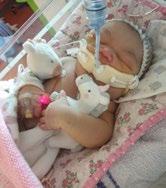
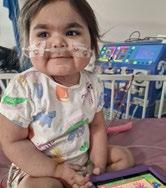
On the second day, I met with our lovely consultant who told me that Natalia was not passing any urine and that she needed to start peritoneal dialysis treatment. I had no idea what this entailed, but it was that or make her comfortable and hold her until she faded away. I would fight for her just as she fought with all her might to be here.
The surgery was a success and a nurse was at her side at all times. It was interesting to learn how the peritoneum can be the key to keeping my baby alive and how toxins and her levels were all kept safe by this mix of sodium and glucose fluid pulling all the toxins from her body.
Her body went from swollen and yellow to eventually this tiny pale bundle which was my whole world. During the start of the COVID-19 pandemic in 2020 I was on my own but I never felt lonely with her there.
After two weeks, Natalia was extubated and then by week four she was stable enough and ready to go over to the main hospital and go on a peritoneal dialysis machine. This was when my baby blues hit and I was a mess, I felt so isolated and I couldn’t stop crying.
Having the support from the Facebook group KDARS for Kids, and Natalia’s chances looking better, made it feel like the ground was gradually returning under my feet and I could breathe and let my guard down just a little without feeling selfish to take a minute to compose myself and allow these completely normal feelings given the circumstances.
KDARS for Kids helped me with everything, from asking advice regarding household bills, to hospital queries and asking if things with Natalia are normal or okay. I got guidance on which was better - a gastrostomy button or a peg, and not from a medical point of view but from parents who have experience. Overall, it was healing to read all the stories similar to ours.
By three months, Natalia’s Dad and I had learned how to set up Natalia’s PD machine, oxygen machine and feeds so we were able to take her home. At home, I had more questions which I just didn’t think we’re valid enough to call the nurse specialist or the ward. But I was never alone as KDARS for Kids was the perfect place to ask my questions.
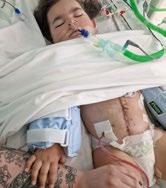
Sometimes others’ experience is better to learn from, sometimes clinical things aren’t always the best call. As a parent you learn little nifty tricks, so anything from Natalia pulling out her ng tube or being sick, I could ask about and I’d have such a heart-warming response.
Natalia is now nearly 4 years old and she has been through a journey which has involved peritoneal and haemodialysis treatment. She has experienced her lines being colonised, has had sepsis and peritonitis and has had a kidney transplant and many other ups and downs.
I cannot begin to thank Heather (the creator of KDARS for Kids) enough for giving me that safe space to be able to rant, ask questions or just get guidance from the group and feel no judgement. It’s a family where, without needing to know anything about each other, everyone has each other’s backs and will help in any way that they can.
Heather is brilliant at bringing people together and planning meet ups for all the families to meet others who actually understand the madness that is life with kidney failure or being a family member affected by kidney disease.
I cannot stress enough how earth moving it is to have true support without other intentions. The Facebook group is just there for pure unconditional care and I cannot put into words how grateful I am of it. Thank you to KDARS for Kids and all who are involved with the group. You have helped us through so much and we will always treasure you!
This article highlights the contents of a newly created NKF information leaflet – this one written by the Helpline Team especially for the carers of people living with kidney disease.
What does providing unpaid care mean?
A carer is someone who, informally and without payment, cares for a friend, family member, neighbour, or in fact anybody who could not manage without their help. This could be due to age, physical or mental health issues, substance misuse or disability. Carers come from all walks of life, can be all ages and are in different caring situations; often they have other commitments such as work, family and study.
This support might include:
• Helping with medication, reminding them, collecting it or helping to give medication.
• Providing daily support such as helping them move around the house, making meals, cleaning or other chores.
• Emotional support like helping someone manage anxiety.
• Helping manage money, paid care or other services.
• Making appointments, arranging care.
• Helping someone to wash, dress, bathe or helping someone to eat.
• Or it could be providing much more complex care such as supporting them to record observations such as pulse, blood pressure or sugar levels.
• It could be assisting in home dialysis.
If you do not receive payment for doing any of these things then that means you are an unpaid carer.
Helping your loved one to manage their renal condition:
The routine of home or hospital-based dialysis might mean limits for your lifestyle and the things you can enjoy together. Speak to your renal team about options and support for managing this and things such as going on holiday.
Your loved one might need to manage the types of foods they eat, how much fluid they drink, or need to take routine medications to manage their kidney failure or transplanted kidney. It may be a source of tension if your loved one struggles to keep up with these requirements, and you may feel the need to remind them where you can.
CARER’S HELPINGINFORMATION YOUR LOVED ONE MANAGE THEIR RENAL CONDITION

It’s helpful if you connect with other families of renal patients to understand the shared frustrations. There may be a local Kidney Patient Association in your area, the National Kidney Federation has details.
Lots of people provide care but the vast majority do not see themselves as carers. Many see the care they provide as a normal part of their role as a husband, wife, partner, etc. It is important to look after yourself, not only for you but also for your loved one. You cannot give to others if you are not taking care of yourself.
Caring can be very rewarding but also very demanding, it can affect your physical and mental health and emotional wellbeing. Many carers are trying to work, study, look after other family members in addition to their caring responsibilities.
Carers Act
The Care Act 2014 came into effect in April 2015. Under the Care Act, you are entitled to a carers assessment where you appear to have needs for support and if you meet the national eligibility criteria. Your local authority will have a website giving information about where to find advice and local support resources.
Carers and Work
If you’re working as well as caring for someone, it can seem like there simply aren’t enough hours in the day. But there are lots of adjustments you can make to ensure that you can continue working and be a carer. The first step is to think about how you’d like to balance working with your caring responsibilities. It’s good to have a clear idea about this if you need to have a conversation with your employer about flexible working.
A new piece of legislation, which came into force on 6th April 2024 is The Carers Leave Act, designed to support employees who are also unpaid carers. It creates an entitlement for employees to take five days of unpaid leave per year to support their caring responsibilities.
If you are looking after someone who has a disability, mental health condition, or long-term illness, you can register as a carer with your GP, DWP, local council, local carers service, employer, schools, university or colleges and your energy provider.
Carers Allowance Benefit
If you spend a lot of time looking after someone you may be entitled to extra money in the form of a benefit called Carer’s Allowance. You do not have to be related to, or live with, the person you care for.
Carers Discounts
Registering as a carer can open many doors to discounts for travel, days out, leisure activities, educational courses, local business discounts depending on where you live. Your local council website will have details.
Psychological effects
The impact and implications of caring for our partner varies depending on our age, life stage, our own health, their diagnosis (and impact) and many more factors. Taking on the responsibility of caring for our partner can feel different to looking after a parent, child or other relative. It can shift the balance in our relationship, change our anticipated future plans and dreams, and bring a strange duality to our role, as we shift between partner and carer.
Managing Care
Caring for a partner often involves managing personal tasks like bathing or toileting, this can be challenging for both parties as the partner may feel embarrassed needing help, and the caregiver may need time to adjust. Mutual understanding can ease the process. It’s not uncommon to use a touch of humour to help lighten the mood.
Many chronic illnesses cause problems with sexual function and disrupt how we connect with our partner. The transition from caregiving tasks to intimate moments can be challenging, and it’s normal to feel exhausted or still be processing the situation. Communicate openly about these feelings with your partner and seek support if needed.
When a loved one receives a life-changing diagnosis, they experience a range of emotions, including grief, denial, and anger. It’s common for individuals to vent these feelings on those closest to them. It’s important to remember that their words may reflect their fear and anger, or even a symptom of their illness, rather than a personal attack.
Adjusting to new roles following a loved one’s lifechanging diagnosis can initially be challenging. However, this situation also presents an opportunity to reframe our perspective and view it as a new challenge. We might find satisfaction in accomplishing different tasks and may even enjoy acquiring new skills. It’s normal if we don’t feel positive about these changes - fatigue and emotional exhaustion can make it difficult to think clearly.
Financial concerns can significantly strain our relationships. Anxiety may arise from potential income loss if our partner becomes unable to work. We might also have to quit our jobs or cut down our working hours to concentrate on caregiving, which can cause tension.
If our partner is affected by a health issue that hinders their work capacity, they might qualify for certain benefits.
Depending on the nature of our relationship and the diagnosis we’re facing, feelings of loneliness can certainly emerge. Some of us might feel as though we’re losing our closest companion. In some cases, we may become so engrossed in caregiving and adjusting to the new circumstances that we distance ourselves from our friends and family, or we might perceive them as distancing themselves from us.
Resentment is a common feeling experienced by unpaid carers. It is important to acknowledge these feelings as they can lead to poor outcomes for both the carer and the person being cared for.
Doing something enjoyable or relaxing can be very helpful when you have a caring responsibility. If you’re able to, make time for something like an exercise group or an evening class. Taking a break, also known as respite, is essential for your physical and mental wellbeing.
For more information on our NKF Helpline information leaflets, please visit our website: www.kidney.org.uk/helpline-leaflets
Our free to call confidential Helpline is available on: 0800 169 09 36
Available from: Mon-Thurs: 08:30am – 5:00pm, Fri: 08:30am – 12:30pm
Or alternatively email: helpline@kidney.org.uk

Continuing our reports on current kidney research – PLUTO is a paediatric kidney transplant study. It was funded by the National Institute for Health and Care Research (NIHR), sponsored by Great Ormond Street Hospital and supported by the NHS Blood and Transplant Clinical Trials Unit. Dr Wesley Hayes, a Consultant Paediatric Nephrologist, was the Chief Investigator and had the overall responsibility of the study. A large team of clinical experts in the field of paediatric kidney transplantation and clinical trials helped with the design and management of the study. The study started in February 2020 and concluded in February 2023.
Kidney transplantation is the best treatment for children with kidney failure and transforms the lives of children those with severe kidney disease, allowing many to return to a life without very frequent hospital visits or dialysis treatment. Approximately 130 children receive a kidney transplant each year in the UK. However, the transplant itself is a big operation.
During the operation and in the first few days after a kidney transplant, large volumes of fluid are given to maintain blood flow to the donor kidney. However, this increases the risk of abnormal levels of electrolytes in the blood. Electrolytes are salts and minerals, such as sodium, potassium, and chloride. These need to be maintained in an even balance for the body to function properly. As a result of the large amounts of fluid given by the doctors, many children develop dangerous changes in the amount of salt, water, and acid balance in the bloodstream. Therefore, children have blood tests every 2 to 4 hours to detect and correct these abnormalities, as severe electrolyte changes can cause serious problems like seizures (fits), coma, or death in extreme cases.
We aimed to compare the standard fluids used after a kidney transplant operation with an alternative called Plasma-Lyte. Plasma-Lyte is already used in adult kidney transplant patients and in children in intensive care and contains a similar level of salts which closely matches those in the bloodstream. The study team believed that its use would reduce the irregularity of salt levels in children following kidney transplant, in particular the proportion of children with abnormally low sodium levels’.
One hundred and forty-four (144) children from nine (9) hospitals took part in the PLUTO research study. Half of them had standard fluids, and half of them had PlasmaLyte. Patients and their care team knew which fluid they received. We compared the number of children who developed abnormal levels of salts and acid balance in their bloodstream after their transplants.
The number of children who had low levels of sodium (the main salt in the blood) was similar in those who had standard fluids and Plasma-Lyte. More of the children who had standard fluids developed high levels of chloride and acid imbalance in their blood. Children allocated to standard fluids also had more adjustments to their fluid prescriptions made by doctors. For these reasons, doctors may now change to giving Plasma-Lyte to children having a kidney transplant.
We will tell other doctors, nurses, surgeons, and professional teams about these results at conferences. We have published the results in a medical journal for everyone to access (www.kidney-international.org/ article/S0085-2538(23)00760-3/fulltext).
The Patient and Public Involvement (PPI) members’ contribution has been invaluable throughout the trial. We are working with our patient and parent team members who helped to design this research and our Trial Steering Committee independent lay member, to inform patients and the public of the results more widely.






euromedica-rhodes.gr

Thank you to everyone who took part in our spring draw, the winners were picked on Wednesday, May 8th May at the NKF Head office. The list of winners can be found on our website at www.kidney.org.uk/nkf-draw

It's going to be BIGGER, BOUNCIER, and BETTER than ever before! And events take place in Wolverhampton, Southampton, Altrincham, Newbury and Norwich. Dates for these inflatable events are from June to October depending on which venue you pick. The excitement has been pumped up to the MAX, you'll be jumping, sliding, and bouncing your way to the finish line like never before. So grab your friends, lace up your trainers, and get ready for the ultimate inflatable adventure! For more details please visit www.kidney.org.uk/Event/ inflatable-events
It's that time of the year to get your walking boots or trainers on and join our challenge. This June we would love you to take part in Best Foot Forward, our step challenge, walk or run 70,951 steps in June to represent the 70,951 people on dialysis or transplanted in the UK. This is an increase of steps on last year's challenge as more people are on dialysis or transplanted. It's very simple to sign up, visit www.kidney.org.uk/ BFF24 and once you have raised £10 or more we will send you a Best Foot Forward t-shirt, so you can join hundreds of other people as we step into summer to support kidney patients and their families.
If you would prefer to sign up over the phone please call the NKF office on 01909 544999.




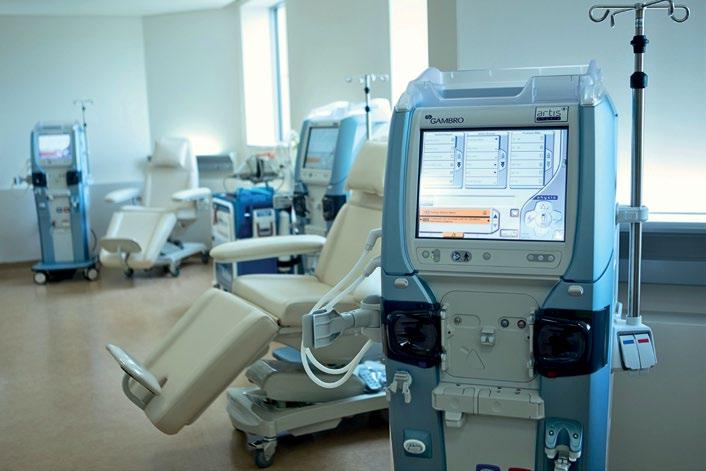
Look forward to a great holiday in the stunning Lake District whilst letting Lakeland Dialysis cater for all your haemodialysis needs in a relaxed and professional atmosphere.

Situated on the Northwest edge of the Lake District National Park, adjacent to the Cumbrian market town of Cockermouth we have been specialists in holiday dialysis since 2004. Things to do include taking in the majestic fell views, visiting the steam railway, cruising on a lake or just relaxing and enjoying the rich and local hospitality on offer.
Regulated by the CQC we pride ourselves in offering: personal and professional care, individual appointment times, disabled parking facilities and ground floor access.

COSTS ARE COVERED BY THE NHS
For more information, please speak with your Renal Team, contact us on 01900 822 888, e-mail info@lakelanddialysis.co.uk or visit our website www.lakelanddialysis.co.uk where you can make a booking enquiry, as well as access lists of locally available accommodation recommended by previous visitors to the clinic.
LakelandDialysisinCockermouth
Lakeland Dialysis Ltd, Unit 7E, Lakeland Business Park, Lamplugh Road, Cockermouth, Cumbria, CA13 0QT www.lakelanddialysis.co.uk

Anyone receiving care on a regular basis knows the importance and the impact individual carers can have on one’s experience. Sometimes an individual team member stands out from the crowd for their commitment to their patients – we’ve all experienced this. Vicki Furniss, a Healthcare Support Worker who has devoted her 26 year career to helping patients with kidney failure to live a ‘normal’ life, has won a national award from NHS England.
Vicki, who works at Sheffield Teaching Hospitals NHS Foundation Trust, was presented with the prestigious Chief Nursing Officer Healthcare Support Worker Award during a surprise ceremony at the Northern General Hospital in February.
NHS England’s Chief Nursing Officer Healthcare Support Worker Awards recognise the vital contribution of Healthcare Support Workers in England and their exceptional support of nursing and midwifery practice.
Vicki, who has worked at the Sheffield Teaching Hospitals NHS Foundation Trust within the haemodialysis care setting for the past 26 years, was nominated for the award for going above and beyond to ensure patients can continue to live a ‘normal’ life whilst receiving dialysis. Vicki works hard liaising with dialysis units both within the UK and abroad to make the necessary arrangements for patients to have dialysis away from their base unit, allowing them to enjoy holidays and special events whilst continuing to receive treatment.
Professor Chris Morley, Chief Nurse at Sheffield Teaching Hospitals NHS Foundation Trust said: “Vicki is an exceptionally motivated member of the team who constantly exceeds all expectations. For many patients and their families, without the support of Vicky in helping them arrange their much-needed holiday, it would not be a possibility. She is passionate about patient experience, and I am thrilled that she is being recognised in this way for the incredible work that she does.”
Vicki said: “I'm very honoured to have won the award, if not a bit overwhelmed by it all. To me I am just doing my job and not doing anything special. Seeing the same patients up to six days a week means I get to know them, not just on a medical
level but on a personal level too. We can have a laugh and some banter with each other which not only makes the patient’s treatment seem to go quicker, but also makes my job feel so rewarding.”
Vicki received a certificate signed by Dame Ruth May, the Chief Nursing Officer for England to recognise her incredible achievement.

Vicki is an exceptionally motivated member of the team who constantly exceeds all expectations.

Your donations help us to make a difference to
The National Kidney Federation (NKF) relies entirely on your support and donations to continue its vital work supporting kidney patients and their families.
Your regular donations will help support every kidney patient in the UK
£20 Helps us with printing and postage costs to distribute our free of charge Helpline leaflets
£10 Helps towards our campaign to increase patients on home dialysis
£5 Helps us make Government changes in Parliament
£2 Covers the cost of your Kidney Life magazine
Donate by PHONE
You can call us on 0800 169 0936 for a chat and to make a donation.

Donate by POST Donate


Given we have the Olympics in Paris soon I thought an Olympic themed wordsearch would be appropriate for this issue reminding us of the sports we’ll have the chance to watch. Apologies if you’re not sporty – but there’s usually something interesting to spot. Good luck!

WORDS TO FIND:
ARCHERY
BOXING
CANOESPRINT
CYCLINGBMX
DISCUS
DIVING
GOLF
GYMNASTICS
HOCKEY
JUDO
LACROSSE
LONGJUMP
SAILING
SQUASH
SURFING
SWIMMING
TAEKWONDO
TENNIS
TRAMPOLINING
TRIATHLON
VOLLEYBALL
WATER POLO (on 2 lines)
WEIGHT LIFTING (on 2 lines)

a recipe on p71 from TASTE!
This recipe is really lovely and zingy with the lemon and mint flavours, and the tartar sauce is great. Not only that, it was super quick to make. It was commented on that a portion of chips might have gone down well but I enjoyed fresh bread as suggested to accompany the dish. Enjoy!
Roasted salmon and peas are a classic combination. The peas are just crushed with a little lemon and mint to make a super quick 'fish supper'
4 x 120g boneless skinless salmon fillet
320g frozen peas
1 lemon, zested
2 tbsp finely chopped mint leaves
40g 0% fat natural yoghurt
2 tbsp finely chopped chives
80g gherkins, roughly chopped
Freshly ground black pepper
4 medium slices wholemeal bread
20g butter, softened
1. Preheat the oven to 200°C, fan 180°C, gas mark 6.
2. Place the salmon fillets onto a roasting tray then place in the oven to roast for 15 minutes until golden and cooked through. The fish should be opaque and flake when pressed gently.
3. Meanwhile, bring a pan of water to the boil, add the peas and simmer for 2 minutes until hot through. Drain and return to the pan.

Ready in about 20 minutes
Serves 4
4. Stir in the lemon zest and mint, then crush with a potato masher until a rough puree.
5. Spoon the natural yoghurt into a bowl, add the chives and gherkins and mix well, then season with black pepper.
6. Spread the bread with the butter.
7. Divide the roasted salmon and 'mushy' peas between serving plates, then spoon the tartare alongside. Serve with the buttered bread.

Friday 25th and Saturday 26th October
Radisson Blu Hotel, East Midlands Airport
STANDARD PRICES
Friday Evening 2-Course Supper Dialysis/Transplant patient* FREE
Friday Evening 2-Course Supper
Friday Bed and Breakfast
Saturday Day Delegate (event only) (includes entry to the event, tea/coffee breaks, full buffet lunch)
Saturday 3-Course Evening Dinner
Saturday Bed and Breakfast
Saturday Special Package (includes Saturday day delegate, plus 3-course evening dinner and Saturday bed and breakfast)
* Please delete as appropriate
Title: First Name(s):
Surname:
Address:
£16.00
Single £89.00
Double/Twin*
£99.00
£55.00
£30.00
Single £89.00
Double/Twin* £99.00
Single £140.00
Double/Twin* £190.00
My donation to the work of the NKF £
Total £
Title: First Name(s):
Surname:
Address:
Postcode:
Tel: Email:
I am a member of KPA
Special Requirements (subject to availability) please TICK as appropriate
FULLY DISABLED IMMOBILE VEGETARIAN
OTHER (Please state)
Tel:
Postcode:
Email:
I am a member of KPA
Special Requirements (subject to availability) please TICK as appropriate
FULLY DISABLED IMMOBILE VEGETARIAN
OTHER (Please state)
Please be advised that photographs may be taken at the event for promotional and documentation purposes. If you do not wish to have your photo taken, please inform a member of the staff or the photographer present. Please send the booking form with a cheque made payable to NKF and return to: NKF, The Point, Coach Road, Shireoaks, Worksop, Notts, S81 8BW. You can also book online at www.kidney.org.uk or by calling 01909 544999.
Any event booking cancellation must be confirmed in writing. The NKF is unable to offer refunds on bookings cancelled after 12th September 2024 and recommends cancellation insurance is purchased.