Her Feet Back on
 PG. 8 Boone Babies Having Boone Babies
PG. 8 Boone Babies Having Boone Babies

 PG. 8 Boone Babies Having Boone Babies
PG. 8 Boone Babies Having Boone Babies

College of Distinction 2022-23

Experience the new vision of nursing education through our innovative partnership with Boone Hospital Center. Earn your Bachelor of Science in Nursing in just three years with early access to clinical experiences. We offer innovative, research-centric degrees in Integrative Human Biology, Health Science, Human Development and Psychology.


We believe that every American veteran deserves our gratitude, respect and support. But we know that women veterans, in particular, often face unique challenges. That’s why we’ve created Mission Promise Kept: to empower women veterans to earn a college degree through a coordinated network of academic, medical, legal, and social services.
Explore all that Stephens has to offer at stephens.edu.






Allow me to introduce myself: I’m Gene Meyer, the interim CEO for Boone Health, or as one employee called me, “The Transition Dude.” I received this nickname in 2020, when I first came to Columbia to serve as the interim CEO while Boone prepared to conclude its lease with BJC HealthCare and become an independent community healthcare organization.
My prior experience as the CEO of a community hospital has affirmed my belief that independent community healthcare organizations are vital. Their relationships with the people they serve and their ability to provide responsive and efficient care that meets their respective communities’ needs make a difference in the overall health of a community.
In my experience and analysis, I’ve observed that an independent health care organization benefits from having outstanding quality and safety scores, dedicated employees, committed leadership, a supportive medical staff, current technology, a strong market share, and financial strength.
In 2020, I witnessed Boone’s culture of quality, dedicated leadership, and commitment to improving the health of mid-Missouri. I was honored to work with their associates, physicians, and Board members and to see for myself why Boone Health has an outstanding reputation for a high standard of patient care.
Over a century ago, Boone County Hospital was built to serve the healthcare needs of this community. The first board members, physicians, nurses, leaders, and staff laid a solid foundation that successive generations have built upon.
Change is a constant in healthcare as technologies, knowledge, and populations change, but what hasn’t changed is Boone’s foundation of quality, tradition of service, and commitment to giving you and your loved ones the best care possible.
Change can be challenging but it can also be energizing. Change can present exciting opportunities for growth and stronger relationships. I’ve personally enjoyed the opportunity to support Boone Health’s outstanding leaders, medical staff, and Board of Directors with my leadership experience in community hospitals while they navigate changes in the healthcare system, review excellent candidates for a permanent CEO, and continue to provide high-quality services.
My experience has also taught me that when you ask anyone why they choose to receive care or work at Boone Health, almost without fail, the first thing they say is “It’s the people.” You’ll hear this at every level in every department.
And I’m no exception. When I was recently asked what I most looked forward to when I returned to Columbia, I said, “The friendly people.” (I also enjoy your restaurants and trails.) When I look at the history of this organization, it’s clear it’s always been the people. The people who work here are invested in providing a high standard of care to this community, and Boone Health invests in its people.
I’m looking forward to this opportunity to again work with the people here and help Boone Health continue to build upon a solid foundation of quality, dedication, and service. Thank you.
Gene Meyer Interim CEO, Boone Health
Change is a constant in healthcare as technologies, knowledge, and populations change, but what hasn’t changed is Boone’s foundation of quality, tradition of service, and commitment to giving you and your loved ones the best care possible.

On May 9, 2023, Boone Health honored its nurses and partners in caring at our annual Professional Excellence in Nursing Celebration. The event included the presentation of our 12th annual Professional Excellence in Nursing Awards. These peer-nominated awards celebrate individual nurses and nursing teams for their professional growth, teamwork, innovation, and overall excellence in providing a high standard of patient care.
Nursing Spirit Award
• Tyson Cason
• Kinna Cramer
Partner In Caring Award
• Alivia Forck
• Alayciah Hardin
Year One Wonder Award
• Josiah King
• Paige Beckerman
Excellence In Nursing Education Award
• Susan Lambert
• Sadie Brimer
Jake Petrosky, MD has joined the Boone Health Bariatric Team. Dr. Petrosky is board certified by the American Board of Surgery and a Fellow of the American College of Surgeons. Dr. Petrosky is a bariatric surgeon specializing in minimally invasive weight loss surgery using laparoscopic techniques and the robotic surgery platform. He performs bariatric endoscopy, sleeve gastrectomy, Roux-en-y gastric bypass, as well as revisional procedures.
Boone Health Bariatric Program is located at 1701 E. Broadway, Broadway Medical Plaza 3, Suite 204. For more information, call 573.815.6447 or visit www.boone.health/bariatrics.
Innovation in Nursing Award
• Addison Watson
Innovative Nursing Team Award
• ICU/T&D Competency Improvement Team
DAISY Nurse Team Award
• Emergency Department
DAISY Nurse Leader Award
• Andrea Primus
Transformational Leader Award
• Ashley Green
Dedicated Boone Nurse Award
• Sharon Everhart
LPN of the Year Award
• Andee Fielder
Excellence In Professional Nursing
• Jessica Fleshman
• Mika Schrimpf
• Molly Unterseher
Boone Health is happy to announce that we are once again an in-network provider for Aetna health insurance plans.

Spc. Michael Glosemeyer, 7228th Medical Support Unit and Boone Health Emergency Department Patient Care Technician, was recently recognized as the Best Warrior Soldier of the Year at the the 104th Training Division (Leader Training) Best Warrior Competition. The 104th Training Division is headquartered at Joint Base Lewis-McChord, Wash., with units and missions that stretch across the country, from coast to coast. The Timberwolves’ mission is to provide leader training support to the United States Army Cadet Command, United States Army Military Academy, United States Merchant Marine Academy and select Reserve Officer Training Corps universities across the nation to build future leaders of the Army.
Held at Fort Knox in Kentucky, competitors from across the division took part in the fourday event that tested their mental and physical abilities. Challenges included a fitness test, marksmanship, weapons qualification, water survival and a written exam.

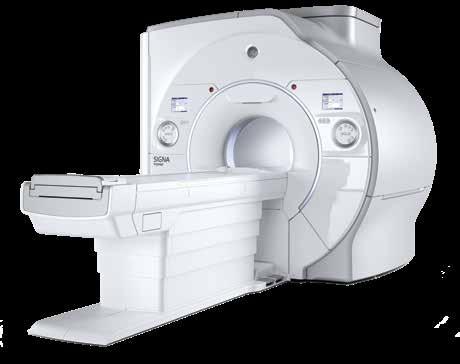
Boone Health recently upgraded their imaging capabilities with a new, state-of-the-art 3T widebore MRI machine at Boone Hospital Center. The new MRI features updated coil technology and enhanced patient movement reduction software, which will directly result in better image quality. The new software also allows for much faster scan times, which along with the wider table and more room inside the scanner, provides a more enjoyable patient experience.
I t was more than 100 years ago, on Christmas Eve 1921, when the first baby was born at the newly opened Boone County Hospital. David Etheridge, son of William and Fannie Etheridge, became the first Boone baby - and the babies have been arriving ever since.

Four Boone babies entered the world in March 1987, August 1988, May 1991 and June 1994, all children of Grant “Van” Dyke Darkow, MD and his wife, Caryl. When their son Andrew arrived in 1987, Dr. Darkow was immersed in a post-sophomore fellowship in pathology at the University of Missouri School of Medicine. He was a fourth-year student when Erik arrived in 1988 and a resident when their daughter Courtney appeared on the scene in 1991. By the time their son Blake showed up in 1994, Dr. Darkow was working as a pathologist for Boyce and Bynum. In 1995, he was stationed at Boone Hospital where he has remained for nearly 30 years.
Parents are always choosing which hospital they want their children to be born in. Doctors who become parents are no exception. You could say that those who choose where they work, like Dr. Darkow, might have a little insider information that inspires confidence.
“Boone has always provided excellent medical care. That starts with the OBGYNs that we’ve had the pleasure of knowing and working with over the years. Also, the staff is top-notch. The nurses, assistants, and everyone involved are so knowledgeable, experienced, and very caring,” Dr. Darkow says. “Boone has an excellent neonatal intensive care unit (NICU). The neonatologists are so
knowledgeable. Most anything you can think of that might happen in delivery they can take care of.”
Boone Hospital offers a Level III NICU. Only Level IV units offer a higher level of care. There are only three Level IV NICU’s in Missouri. Boone and Women’s and Children’s hospitals are among the 16 Level III NICUs in the state.
Dr. Darkow’s father was an atmospheric science professor at Mizzou, but his parents always went to Boone when they needed care. Caryl’s father, Dr. Lenard Politte, also a graduate of Mizzou School of Medicine, was instrumental in starting an interventional cardiology program at Boone in 1969. Boone Hospital runs deep in this family – especially where babies are concerned.
Van and Caryl recently became grandparents for the first time — actually, three times in rapid succession. Daughter Courtney and husband, Tom, delivered baby girl Cooper, on October 14, 2022, followed quickly by Erik and wife, Lynley’s, daughter, Nell, who arrived on December 15, 2022. About a month later, on January 14, 2023, Andrew and his wife, Katie, a physical therapist at Boone, brought their son Grant into the world. All three babies took their first breaths at Boone.

“When my husband and I found out we were expecting, we made the move back to Columbia. And I knew there was only one choice when it came to care and delivery. I wanted our sweet girl to be a Boone Baby,” Courtney says. “I felt so confident and comfortable knowing that my needs and wishes would be met and that’s exactly what I experienced. The team of doctors and nurses at Boone are the epitome of professionalism while, at the same time, incredible communicators with the best bedside manners. Boone will always be our number-one choice!”
Erik and Lynley also give Boone high marks for their major event.
“We had a great experience back in December when our daughter, Nell, was born at Boone,” Erik says. “From the moment we walked through the doors, from check-in to discharge, we received exceptional care. Nell spent her first couple of days in the NICU. We were comforted knowing that she was under the supervision of a skilled, knowledgeable, and compassionate staff to get her healthy.”
Sibling rivalry aside, Andrew and Katie were touched by those who went above and beyond.


“The amount of care, compassion, and and dedication during our experience was extraordinary,” says Andrew. “From the physicians to the nurses to techs, everyone went above and beyond to get to know us as patients and people as we went through this process of expanding our family. One of our nurses, Teresa, stayed past the end of her scheduled shift to help us through our last part of labor. She even came down the following morning to check on us, even though we had moved to a different unit. That is just one example of the outstanding care we received during our stay. We could probably write a similar story about all the staff we encountered.”
It takes a village to deliver a child. Moms and dads, grandparents, physicians, nurses, and other staff create a united front for their Boone babies.

David Etheridge might have been the first baby delivered at Boone Hospital, but he has been far from the last. Thousands of Boone babies — including the Darkow children and grandchildren — have been welcomed to the world from here. The tradition of Boone babies having Boone babies is bound to continue! By Michelle
Terhune Andrew and Katie Darkow w/ son Grant Courtney & Tom Morgan w/ daughter, Cooper Erik & Lynley Darkow w/ daughter, Nell Dr. Lenard & Mary Lu Politte (L to R) Cooper, Nell & GrantUnit nurse Skylar Gooch, RN, BSN may be young, but she is a skilled and valued member of the Boone Health team.
Skylar first began planning for her career in nursing during her junior year of high school.
“I was thinking about what I wanted to do and where I wanted to go to college, and I just really wanted to have a job that aligned with my faith. I liked the idea of being a nurse because it meant that I could serve and help others,” says Skylar.
Skylar decided to go to Mizzou after seeing how much her sister enjoyed the university.

“I’m from Wentzville, so I wasn’t going too far,” says Skylar.
While in her Mizzou nursing school program she did her clinicals at Boone Hospital Center.
Boone Health welcomes hundreds of student nurses each year for their clinicals. Clinical Education Supervisor Deanna Powers, BSN, RN, NE-BC oversees the program.
“Fundamentally students will have objective based clinical hours to match the theory they are learning in class. As they progress through school, their objectives change to hands-on experiences where they are caring for the patients and enhancing their knowledge, critical thinking, and skills. We offer all areas of the hospital for clinicals. I try to think outside of the box and may include a variety of experiences as well. Allowing students to be exposed to multiple areas, helps them not only understand the continuum of care and how each department works with another, but they get to see how nurses function in a variety of roles like inpatient, procedural, clinic, and home care,” says Deanna.
Skylar chose to spend most of her clinicals in postpartum and the ICU.
“I really liked the teamwork at Boone Hospital and how friendly and helpful everyone was, so I decided to apply after graduation,” says Skylar.
Skylar was hired as an ICU nurse following her graduation and became a part of Boone Health’s Nurse Residency Program.
The Nurse Residency Program supports new grad nurses during their entire first year of work through classroom learning and on-the-job assistance. The program focuses on leadership, patient outcomes, and developing in a professional role. It also gives new grads the opportunity to bond and share their experiences with other new graduate nurses.
“I was able to really get to know people and find community in nurse residency. There were even some nurses in it that I already knew from Mizzou nursing school,” says Skylar.

After working in the ICU for about a year, Skylar found she was interested in surgery patients.
“I shadowed the PACU and really liked it. I knew I would enjoy working with surgery patients. I transferred there, and I received great training and support,” says Skylar.
Skylar says she finds the work very fulfilling. “My favorite days are when I get to stay with the same patient post-op, pre-op, and then help them go home. I really feel like I get to know and help them,” says Skylar.
Skylar says she would recommend a career at Boone to any new nurses. “There is a wonderful atmosphere here. It’s like a big family. Everyone’s really supportive and helpful,” says Skylar.
When Skylar is not at work she enjoys reading, working out, and being outdoors. She also loves to travel and is always thinking of her next trip. “It’s just fun to have something planned and to look forward to,” says Skylar. By
Madison LoethenShelly Weter’s nurse practitioner in Milan, Mo., was the first to tell her she had a heart murmur. In 2008, Shelly had an echocardiogram performed at Sullivan County Memorial Hospital and was diagnosed with bicuspid aortic valve, a common congenital heart defect affecting roughly 2% of the population.
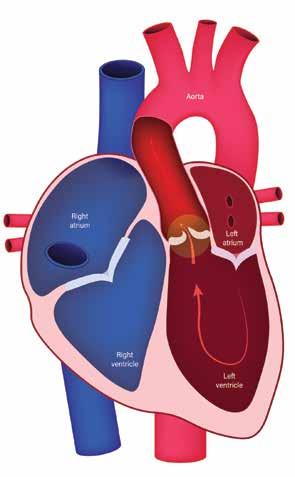
When the aortic valve doesn’t function properly, blood flow in to and out of the chambers of the heart is abnormal. It forces the heart to work far harder than it should, placing individuals at high risk for heart attack, stroke, heart failure, and sudden cardiac arrest. Shelly was told that when the condition of her valve worsened, she would need to have it replaced.
Sometime later, Shelly’s cousin was diagnosed with the same condition and was referred to Mozow Zuidema, MD at Missouri Heart Center. Unlike Shelly’s heart defect, her cousin’s valve deterioration was progressing quickly. Her cousin underwent aortic valve replacement surgery at Boone Hospital in March 2022.


“I got a little bit scared because I was supposed to be keeping an eye on mine and I wasn’t,” Shelly says. “So, I went to see Dr. Zuidema, and thank God I did.”
Shelly says she hadn’t really been feeling good and had a lack of energy – both symptoms of heart dysfunction – but she thought it might have something to do with putting on some weight during the pandemic. As it turned out, she needed surgery.
On Tuesday, Nov. 8, 2022, Richard Mellitt, MD, a thoracic surgeon with Boone Health Heart Surgery, performed an aortic valve replacement on Shelly. During the open-heart procedure, Shelly’s faulty valve was removed and replaced with a biological valve – in her case, a cow heart valve.

Replacement valves can be biological – from cows, pigs, or human donors – or mechanical. Although mechanical valves may last longer, they increase the risk of blood clots, which means patients are typically required to take blood thinners throughout their lifetime.
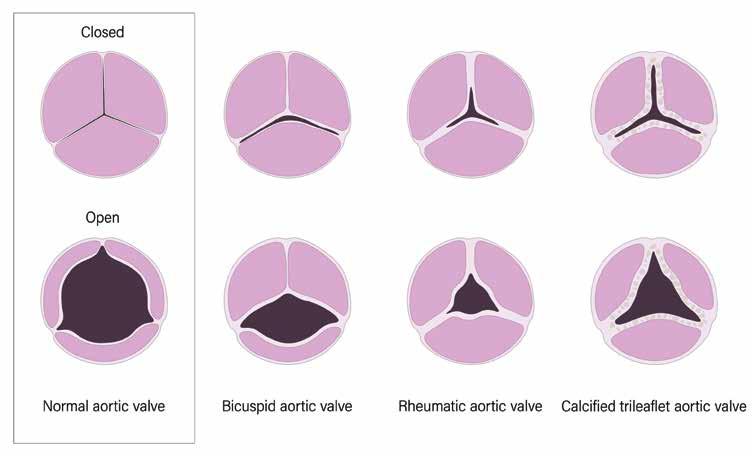
If Shelly’s valve wears out down the road, a new one can be inserted via a transcatheter aortic valve replacement (TAVR), which is a minimally invasive procedure. Dr. Mellitt’s surgical aortic valve replacement (SAVR) has left her TAVR-ready, should she need it in the future.
Shelly was discharged on Sunday, Nov. 13, and returned home to Milan with her husband, Terry, to rest up and take it easy. She was released from follow-up care in early December 2022.
“I just cannot say enough good things about the nurses and doctors about my care,” Shelly says. “I had one nurse named Theo, who was fantastic. They all were absolutely great. Even when I was in critical care, I could not have asked for anything better.”
Shelly says she loved Dr. Zuidema, Dr. Mellitt, and their nurses, Jennifer, Lisa, and Grace. They have made her experience with Boone a believer in the hospital, and that’s a long way from where Shelly was when she was choosing a hospital for the lifesaving procedure.
Years before, Shelly had a bad experience with someone at Boone who was caring for her dad who passed away while he was there. Such a loss can make it difficult to put faith in a
place with sad memories. But Shelly says she prayed about it. Now, she couldn’t be more pleased with the people and her care at Boone.
Lisa and Grace with Boone Health Heart Surgery even helped Shelly get answers for her billing questions – just another example of how Boone went above and beyond to deliver excellent patient care before, during, and after Shelly’s lifesaving procedure.
Shelly was a hairstylist for 40 years. Her finances were challenged since she couldn’t earn an income while she was recovering. Not knowing how that recovery would go, Shelly retired from her career.
“That way, I wouldn’t leave my clients hanging out there, not knowing what I was going to do, and if I was going to be able to come back or not,” Shelly says. “I didn’t want to, but I just felt like I needed to.”
These days, Shelly is focusing on getting more exercise, watching her diet, and trying to lower her stress levels. She is grateful for her new lease on life.
“If I ever know of anybody who needs to have this done or open-heart surgery, or bypass, I will talk until I’m blue in the face about going to Boone,” Shelly says. “And I already have, because I have family getting themselves checked for valve issues with Dr. Zuidema.”
When you’re dealing with matters of the heart, figuratively or literally, contentment may be all that matters.
By Michelle TerhuneChronic high blood pressure can sneak up on your heart – here’s how to catch it!

High blood pressure is known as the silent killer because people often do not show any symptoms, but the longer their blood pressure goes unmanaged, the greater chance they’ll have of a heart attack or stroke.
High blood pressure, also called hypertension, is a common condition that affects the body’s arteries. The force of the blood pushing against the artery walls is consistently too high, which makes the heart work harder to pump blood. Untreated high blood pressure increases the risk of heart attack, stroke, and other serious health problems.
Over time, high blood pressure can cause damage to arteries throughout the body. Undetected or uncontrolled high blood pressure can lead to:
• Heart attack: Damaged arteries can become blocked and prevent blood flow to the heart muscle.
• Stroke: Blood vessels that supply blood and oxygen to the brain can become blocked or burst.
• Heart failure: Working harder can cause the heart to enlarge and make it harder to supply blood to the body.
• Kidney disease or failure: Damaged arteries around the kidneys affect their ability to filter blood effectively.
• Vision loss: Strained or damaged blood vessels in the eyes can affect vision.
• Sexual dysfunction: Artery damage can lead to erectile dysfunction in men and may contribute to lower libido in women.
• Angina: High blood pressure can lead to heart disease including microvascular disease. Angina, or chest pain, is a common symptom.
• Peripheral artery disease: Atherosclerosis caused by high blood pressure can lead to narrowed arteries in the legs, arms, stomach, and head, causing pain or fatigue.
Stress can have a change on your blood pressure – and you may not even know it.
We experience two types of stress: acute stress and chronic stress. Both can cause your blood pressure to go up but have different long-term effects.
Acute stress is temporary stress caused by a specific event. When we experience acute stress, our bodies respond by increasing our heart rate and activating the sympathetic nervous system, which can temporarily raise our blood pressure. These symptoms ease up when the stressor is removed.
Medical researchers are still studying the physiological effects of chronic stress on blood pressure, but we do know that chronic stress can affect our lifestyle.
Unhealthy lifestyle habits like eating a diet with fewer healthy choices, getting poor or not enough sleep, not exercising, smoking, or alcohol and substance abuse can lead to chronically higher blood pressure and a higher risk for cardiovascular health concerns
All of these habits can lead to higher blood pressure and increase your risk of stroke or other heart issues.
So what can you do?
1. Know your numbers. Get your blood pressure checked. If you’re concerned, talk to your primary healthcare provider.
2. Understand the symptoms and risks. What are your risk factors for high blood pressure and serious medical conditions?
3. Make meaningful changes. We can all take steps to manage our blood pressure. Make hearthealthy lifestyle changes, take any medication as prescribed, and share any questions or concerns with your primary care provider.
4. Find ways to manage stress. Be open to trying new techniques and finding out what works for you.
Being in the health and wellness field for over 25 years, I’ve had the opportunity to educate many people with high blood pressure. After lifestyle changes or medication, I frequently hear, “I didn’t know how bad I felt until I felt good.” Please take your blood pressure results seriously. If you don’t do it for yourself, do it for those who care about you! By Jenny
L. Workman
120 mm Hg or lower/ 80 mm Hg or lower
120 to 129 mm Hg/ 80 mm Hg or lower
130 to 139 mm Hg/ 80 to 89 mm Hg
140 mm Hg or higher/ 90 mm Hg or higher
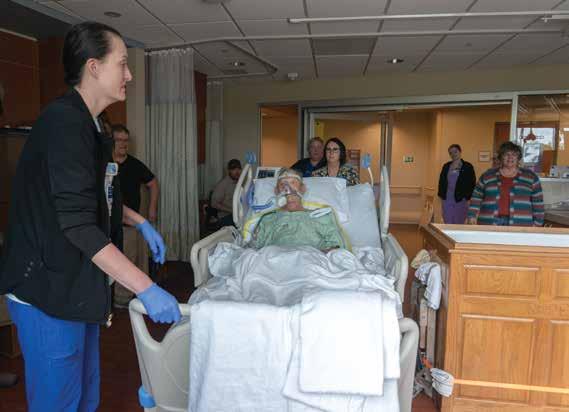
Martin Griffithis was wheeled in his ICU bed to a room that had been prepared to help fulfill his greatest wish: a full submersion baptism. The baptism tank had been delivered from his church earlier that day just for the occasion.

His pastor Josh was waiting, along with his family, friends, and care team. His wife Vicky remained right by his side.
Once he was in the room, a medical lift picked Martin up out of his bed and then put him inside the baptism tank.
He repeated after his pastor; “I believe that Jesus is the Christ, the Son of the living God.”
After that confession of faith, he was slowly lowered into the water with just his mouth and nose left above the water, per doctor’s orders. When he emerged, he was applauded happily by the room.
Martin moved to Missouri 13 years ago after his Northern Indiana home burned down. He was looking to relocate and fell in love with a farm in Callao, Mo. A horse raiser by trade, he set up a horse farm once he bought his land in Callao. And it was in Callao that he met his wife Vickie through a mutual friend.
Last year, he was diagnosed with lung cancer but was eventually pronounced cancer free.
“I’ve had several problems after that though including a problem with circulation in my leg, needing a vein replaced, and heart trouble,” says Martin.
This past Easter weekend, Martin had a near-fainting spell. He went to his primary care physician the following Monday, who immediately recommended he be airlifted to Boone Hospital Center.
“I was helicoptered here, and they found I had a large blood clot in my lungs and my heart was out of rhythm on both sides,” says Martin.
Martin’s care team worked hard to help him.
“Everyone is very kind here. It makes me glad that I am here. The food’s not bad either,” says Martin.
Still Martin says being hospitalized isn’t easy.
“I’m someone who has been pretty self-sufficient my whole life. It’s hard to be in this position,” says Martin.
Something Martin and Vicky both say they appreciate is Martin’s nurses involving Vickie in Martin’s care.
“They let me help take care of him which provides comfort to both of us,” says Vicky.
When Martin’s pastor and church members visited him in the hospital, Martin began talking about his baptism wishes.
“I had been baptized in the Catholic church as a baby, but as I have gone to my non-denominational church and read the Bible, I have learned about believer baptism and being baptized through submersion. It’s something I had wanted to do for years,” says Martin
Right away, Lead Chaplain Kim Leon got to work to see if an ICU baptism could be arraigned.
“I coordinated with the patient’s nurse, Kara, the Respiratory Therapy Manager, Jennifer, the patient’s physician, Dr. Hernandez, ICU Manager Lindsay, and the patient, his wife, and his pastor. The interdisciplinary team discussed the possibility of baptism with the patient’s physician, Dr. Hernandez, who gave his approval on the condition that the patient’s mouth and nose not be submerged,” says Kim.
Because the hospital did not have a baptismal tank on site, the medical team worked with Martin’s pastor to come up with a solution.
“The pastor offered to bring a submersion tank from his church so everyone made sure that it would be safely transported through the hospital, and I cleaned it when it got here,” says Lindsay Divins, BSN, RN, ICU Nurse Supervisor.
When everything was set, Martin was brought to the room with the baptism tub. The baptism went beautifully and
everyone in the room was touched by the sweet moment.
“We had some new nurses that came and watched, and they were so moved,” says Lindsay.
“It was incredibly moving to witness this special and meaningful moment for Mr. Griffiths and his wife. It was inspiring to see the way that everyone involved was willing to do what they could to honor this patient’s wishes and to care for his spiritual health as well as his physical health. The way the entire team came together to make this happen is what makes Boone such a great place to work. I am grateful that I was able to be part of it,” says Kim.
Both Vickie and Martin say they have been so blessed by kindness and compassion while at Boone Hospital Center.
“We could never repay their kindness. Everyone here is so incredibly talented. Even nurses who aren’t on their shift will come by and check on him. You can’t train that kind of compassion. It’s just in their hearts,” says Vickie. By Madison Loethen

-year-old Sadie Hoyt of Mexico, Mo. was preparing for her job as a certified nurse assistant at the Missouri Veterans Home when pain in her foot nearly took her breath away.

21
“It was so bad that I could barely walk,” says Sadie.
Sadie immediately started worrying that it could be a bunion. She knew how painful and serious bunions could be because her dad suffered from them.
“I was worried but I decided to go to work anyway. After a couple of hours, the pain was so bad that I had to leave,” says Sadie.
Sadie got an x-ray locally that confirmed that the cause of the pain was in fact a bunion.
Bunions happen when some of the bones in the front of the foot move out of place causing the tip of the big toe to get pulled towards the smaller toes and the joint at the base of the big toe to stick out. This can cause pain and trouble walking.
Sadie was referred to Jason Blanchard, DPM of Boone Health Foot & Ankle.

“I met with Dr. Blanchard, and we talked about my options. We agreed that Lapiplasty 3D Bunion Correction was the way to go,” says Sadie.
Lapiplasty 3D Bunion Correction is a surgical procedure that addresses the bunion in three dimensions to correct the unstable joint. It uses fixation technology to secure the correction in place, which gets patients back on their feet faster than alternative bunion procedures.

“Lapiplasty bunion correction is a beautiful option we employ for patients
with moderate to severe bunions and pain. It allows people to bear minimal weight on day 1 after surgery, where other alternative treatment modalities for bunion surgery frequently require at least 1 month of no weight bearing on the surgical foot. This method is also one of the most sure-fire ways to make sure the bunion should not return,” says Dr. Blanchard.
Sadie had her surgery at Boone Hospital Center and says everything went well.
“The nurses were really sweet, and I was able to go home the same day. I was nervous about the pain because I had heard that it would be rough, but I only had to take the pain medicine three days before I didn’t feel like I needed it anymore,” says Sadie.
Sadie wore a boot to recover for a couple of weeks but was soon able to return to work.
“I didn’t mind the boot much. I was just happy not to be in pain from the bunion anymore.”
Now Sadie says she is back to normal and enjoying life.
“The veterans always ask me how my foot is feeling, and I can tell them it doesn’t hurt anymore!” says Sadie. By Madison Loethen
If your child or teen has trouble falling asleep, have them try these fun techniques.
 BY BLAKE BARNES, MD, TIGER PEDIATRICS
BY BLAKE BARNES, MD, TIGER PEDIATRICS
Oh, blessed sleep! There is something glorious about getting a full night’s rest without interruption and that wonderful feeling of rejuvenation in the morning. Unfortunately, sleep can be thrown off at many points.
For many of us, getting our brains to quiet down so that we can enter dreamland is a struggle – and that includes children and teens. But I’ve found some strategies helpful for my patients who don’t find it easy to fall asleep.
Stress keeps the mind awake. As we lie in bed, we think about things we should do or shouldn’t have done. We worry about future assignments or anxieties. The solution is to get your mind to focus on something interesting but not stressful – something fun that doesn’t require anything of you.
A classic example is counting sheep. You can try to count sheep in a pasture, but this is too boring to keep our attention long enough to enter slumber.
Here are some more fun and engaging techniques you can recommend your child try to help them fall asleep. (You can also try them yourself!)
Imagine walking through the woods or riding your bike through your favorite street. Imagine the things you would see and the people you’d wave to. Imagine the smell of the air and the sounds of nature all around you.
Think about a favorite story. Try to recall the main characters and what happened from the beginning all the way through the end. Where did the heroes come from? How did they end up on their adventure? What steps led them to all the other characters? Think through the entire story. If you finish it, fill in details or try this with another story.
Make up your own story with new characters. Imagine how the story progresses and how characters develop. Hopefully, sleep will come long before the story is finished. The next night, pick up the story wherever you left off and try to continue. This is my personal nightly habit. I spent months thinking through a Hobbit-esque fantasy adventure story. Now I’m working on a space dystopia. Each night when I lie down, I enjoy picking up the story and moving forward with it.
These techniques may be too abstract for younger children, but they can easily be simplified. Ask them to imagine their next LEGO build or drawing. They can plan their next Minecraft construction or invent a new game with new rules and imagine other kids playing it.
Sometimes when my daughter is struggling to fall asleep, I’ll give her an assignment like, “Think of a story with a cat and an apple and tell me the story in the morning,” or “Imagine you find yourself in a castle then tell me tomorrow what happens!”
Use your imagination to occupy your mind with something other than stressful thoughts while your brain drifts into sleep. I hope these tips help your child — or maybe you — to get a blessed night of rest.

Dr. Barnes is a pediatrician with Tiger Pediatrics and sees patients in Columbia. He is currently accepting new patients.


I’m very local. I attended Rock Bridge High School and Mizzou for undergrad, and I plan to stay in Columbia for my entire career! I love what I do, where I work, and who I work for. When I was looking for a job out of residency, my #1 factor was to lay roots and build something that will last. Three years into being with Boone Health, I feel like I’ve made the right decision.
Why did you get into the health care field? To help people! The chance to be a beacon for people who are struggling and helping them make the right healthcare choices drew me to medicine. That and just about everybody in my family has a medical background. Dinner table conversations about medicine definitely sparked my interest at a young age.
What interested you in your particular specialty? I think of primary care providers as jacks of all trades. I was interested in helping many different people in many different ways and building long-term relationships with my patients and their families. I enjoy getting to know my patients, understanding their motivations and goals, and letting them get to know me. My goal is to empower my patients to make an informed decision. My patients often hear me say, “I make suggestions, you make decisions!”
What is the most rewarding part of your job? When a new patient returns as an established patient. When a patient comes back for a second, third or fourth visit, it’s a sign they feel comfortable with me and trust me. Knowing that a patient values my opinion when making critical or life-altering decisions is something I never take for granted.
What is the most challenging aspect of your job? Not having enough hours in the day to see more patients. I’m always interested in building relationships with new and established patients and think about how to make myself more available to people who need care.
What do you see changing in health care in the next 5 to 10 years? Telehealth has been taking off over the last few years, which I think is great. For some patients and conditions, personalized healthcare through telehealth can be more cost-effective and efficient. Streamlining these encounters is something I think will continue to grow. I think we’ll also see more direct patient and provider communication. Providers being accessible after hours and patients being well-versed in their own healthcare through technology like
wearable medical devices can lead to stimulating conversations and decisions made jointly between patients and providers.
What advice would you give someone looking to become a doctor? Get a taste of everything medicine has to offer. Knowing you want to be a doctor is great but there are many levels on any path. Most importantly, remember why you wanted to be a physician in the first place. Putting yourself in your patient’s shoes is necessary and leads to better care.
What do you enjoy doing outside of work? I love the outdoors. Fishing and scuba diving are my favorites. Water can be peaceful, but Mother Nature can also remind you that you’re not the one in control. If you ever see me, ask me to show you my album of fishing trips. I have fun stories that end with my freezer loaded with lots of fish!
What advice would you give to someone who is going to be a patient in a hospital for a period of time? Get to know and appreciate the many people involved in your care: care coordinators, patient service reps, pharmacists, paramedics, therapists, housekeepers, volunteers, and many others work with your provider to give you the best care possible. Nurses are patients’ true champions. Take a moment and thank these people. And make sure you ask questions. As a provider, I want my patients to understand their care plan and make an informed decision they are comfortable with.

Rock Bridge! Bruins! I’m from right here in midMissouri. I went to RBHS and graduated from Columbia College in 2010. I’ve been married to my husband Jeremy for 13 years, and between us we have four kids: Hannah, Keaton, Hailey, and Josh.
Why did you get into the health care field? Originally, I wanted to be an archeologist, but I got pregnant with my daughter, so my plans had to be changed. I had a job taking care of developmentally delayed adults and loved that work, so I decided I would investigate nursing. And here we are – with a career I could have never imagined would be this fulfilling.
What interested you in your particular specialty? I’m a thrill-seeker, and I thrive on the adrenaline roller coaster of the Emergency Room. Every day is wildly different, and I feel like I truly get to make a difference in my patients’ lives. I get to help people on what could be the worst day of their lives.
What is the most rewarding part of your job? Sometimes there will be a patient that nobody seems to be able to make a connection with. They may be scared, in pain, or altered – regardless of the cause, they’re at odds with the rest of staff. The most rewarding thing for me is being able to establish a rapport with these patients so we can get to the bottom of their health emergency and get them the treatment they need.
What is the most challenging aspect of your job? The one thing I absolutely dread about my job are the rare occasions when I need to deliver difficult news to a family. I wear my heart on my sleeve.
What has changed in your field since you started practicing? The relationship between nurses and providers is always evolving, and it looks completely different than it did just a decade ago.
What do you see changing in the next 5 to 10 years?
The technology we’ll have in the next 5 to 10 years will be remarkable. Just since COVID, we have expanded access to telehealth, which provides patients more timely outpatient care.
What do you enjoy doing outside of work? CROSSFIT! It has helped me become a healthier version of myself and has given me a chance to develop relationships outside of the hospital. I’ve even competed in a couple of events representing Boone! I also enjoy spending time with my husband and our kids. I love to travel, go to concerts, and in the occasional quiet moment I like to crochet… or take a nap. And did I mention CrossFit Aggregate in Columbia?
What advice would you give someone looking to become a nurse? Be open-minded. Nursing is an everchanging field, and the quickest way to fall out of touch is to close yourself off to new ideas. You can absolutely have a rewarding career as a bedside nurse. Don’t be afraid to ask questions and seek out learning opportunities. But the most important advice I can give you is to maintain your work-life balance.
Tanning “Safely?” Not a Thing! So, can you enjoy all the pleasures of summertime and tan “safely?” I’ll be the first to admit, I love having that sunkissed glow! In the past, I’ve been guilty of all the things I tell my patients not to do! But now I practice what I preach because I’ve seen the impact of the sun on my own skin and hated it.
First and foremost, stop using the tanning bed! The tanning bed is not your friend. I won’t even go into the cancer statistics on tanning beds, but they’re shocking. Tanning beds will NOT protect you from burning. Tanning beds are NOT needed for a “base tan.” There is NO safe amount of tanning bed use. The statistics and studies don’t lie!
But skipping vacations or swimming to avoid the sun isn’t realistic or fun. Enjoy lounging by the pool or beach, but make sure to wear your SPF and reapply often, wear a hat and sunglasses to cover your face, and spend time under the umbrella. If all else fails and you get a sunburn, make sure to care for that delicate skin. Keep the skin cool – stay out of the sun and avoid hot showers. Keep the skin moisturized with aloecontaining products, take ibuprofen or another NSAID if approved by your doctor for discomfort, and wear loose fitting clothing.
It’s June in Missouri – time for flip-flops, tan lines, summer vacations, and fun outdoors. What do these things have in common? Sun exposure. Start planning to adjust your skin care regimens and stock up on quality sunscreen. Don’t let all the work – and money – you’ve put in to improve your skin in the fall and winter go to waste. Protect your investment!
A suntan is actually a sign of sun damage to the skin. Sun damage is cumulative, meaning it adds up over your lifespan. Think about every time you’ve had a sunburn as a kid all the way through adulthood. Now, add every time your skin was exposed to the sun but didn’t get a sunburn. It all adds up! UVA and UVB rays enter and change skin cells and underlying tissues. Repeated exposure over time can result in a loss of elasticity, brown spots (hyperpigmentation), wrinkles, or worst of all, skin cancer. Skin cancer is currently the most common cancer diagnosis in the United States (American Academy of Dermatology, 2023). Each sunburn increases your risk of developing skin cancer in your lifetime.
Find a good sunless tanner that works well with your natural skin tone! The sunless tanner options have grown exponentially and improved. There are so many great brands, tones, and application types. With a little trial and error, I am sure you can find one.
I’ve also found a professional who does spray tans by hand. Her work is seamless and looks amazing. I get a beautiful glowing tan, with ZERO risk. Yes, please!

Sunscreen seems self-explanatory, right? Not always.
I get a lot of questions from my patients about sunscreen: specific concerns like acne-prone skin, body vs. face, brand, SPF, and sensitivity. SkinBetter Sunscreen and EltaMD UV
Clear are two of my favorites. They are gentle, moisturizing and won’t clog pores on the skin. Most people can use these for the face. They’re available in tinted, sheer and stick options. They can be a tad pricy compared to your average sunscreens, so if you’re looking for a new facial sunscreen, ask your aesthetic provider or dermatologist for samples. Try them to ensure you like how they feel on the skin and tolerate it well before buying.

I’m slightly less picky with sunscreen brands for the body as long as it’s safe and effective. My most used and recommended include Blue Lizard, Neutrogena, and Sun Bum. These brands are mineral-based, gentle on skin, come in SPF 50 or higher, and can be found in many stores. The American Academy of Dermatology recommends an SPF of at least 30 or higher for daily use (2023).

And remember: reapply sunscreen and reapply it frequently! This is the most important and most overlooked step.

Daily SPF isn’t just for sunny, summer months – your skin needs it year-round! Proper SPF protects all your other treatments such as neurotoxin (ex. Botox), chemical peels, Microneedling, dermal fillers, and medical-grade skin care. Don’t waste those results by not protecting your skin.


Skin can change with the seasons. During summer months, some patients complain that their skin feels oilier than normal. Don’t stop your moisturizer –rather, switch to something slightly less heavy. Moisture is very important with increased heat and sun exposure.

Don’t forget to exfoliate! Our skin is exposed to more sunscreen, sweat, dirt
and debris more in the summer, all of which can irritate skin and clog pores, leading to more frequent breakouts and buildup on the skin. Mechanical or chemical exfoliation are both acceptable. Just keep in mind that, with any form of exfoliation, your skin is more susceptible to sunburns.
Start thinking about suntan as a sign of sun damage to the skin. Adjustments to your daily and summertime regimen can make long-standing, positive impacts on your skin health. Find ways to get that summer glow without the risks. If you need recommendations, come see us for a consult! And enjoy your summer, but do it safely! By Tiffany Carmichael, FNP, Aesthetic Nurse Practitioner.

INGREDIENTS
(makes two servings)
Salmon
• Two 7oz salmon fillets
• 4 tbsp Montreal steak seasoning
• 4 tbsp olive oil
Cream Sauce
• ½ cup dry white wine
• 4 cloves garlic, minced
• 1 onion or shallots, minced
• 2 cups heavy cream
• salt & pepper, to taste
• 4 tbsp Italian seasoning
• 1 bunch fresh parsley
• 1 tbsp olive oil
Garlic Herb Risotto
• 1 cup arborio rice
• 4 tbsp butter
• 4 cloves garlic, minced
• 1 onion or shallots, minced
• 2 cups chicken stock
• ½ cup heavy cream
• ¼ cup parmesan
Asparagus
• 1 bunch asparagus
• 8 oz grape tomatoes, halved
• 2 tbsp olive oil
• 2 tbsp Montreal steak seasoning
Sweet Potato Haystack (optional)
• 1 whole sweet potato, julienned on a mandolin
Risotto
1. Sauté 4 cloves of minced garlic and the minced shallot in 4 tbsp of butter until translucent.
2. Add arborio rice and cook until toasted.
3. Once rice is toasted, add the chicken stock and cook until rice is al dente.

4. Turn off the heat and stir in ½ cup heavy cream and parmesan.
Asparagus
1. Season the asparagus with 4 tbsp olive oil and 4 tbsp Montreal steak seasoning.
2. In a skillet over medium-high heat, cook asparagus, turning often to ensure even cooking, about 10 minutes. Asparagus is done when it is fork tender.

Salmon
1. Rub each salmon fillet with 2 tbsp olive oil and then sprinkle each with 2 tbsp Montreal steak seasoning.
2. In a skillet on medium-high heat, add the salmon skin-side down and cook 1-2 minutes on each side until the internal temperature reached 145 degrees.

3. Remove from pan.
Cream Sauce
1. Using your salmon skillet, on medium-high heat, add 1 tbsp olive oil, 4 cloves minced garlic and the minced shallot and sauté until translucent.

2. Add white wine and Italian seasoning and simmer until the wine is reduced by about half — about 3 minutes.
3. Add 2 cups heavy cream and stir until the cream sauce thickens.
4. Finish with parsley and salt and pepper to taste.
5. Deep fry sweet potato until crispy or it starts to turn color.
1. Spoon risotto in the center of the plate.
2. Top with salmon and drizzle cream sauce on top.
3. Shape asparagus and tomatoes around the salmon.
4. Add sweet potato haystack if desired.
By Jason Anderson, Boone Health Chef

If you are looking for a new sport to try, consider disc golf. It’s a sport that’s easy to learn and fun for the whole family – and it could help you get your 10,000 steps in for the day!
Disc golf was introduced in the 1960s as a new way to get outdoor aerobic exercise. It’s similar to golf, but instead of a golf club and golf ball, the golfer uses specialized discs similar to a Frisbee.
Disc golf courses are found on rougher terrain than traditional golf courses. e courses are often designed in wooded areas and may include hills, rocky terrain, creeks, muddy elds, ponds, and lots of trees. Trees are not a disc golfer’s best friend – trying to throw a disc through a wooded area can be di cult for even the most experienced golfer. But they also o er shade on a hot summer’s day and, as with any sport, practice leads to better technique!
e 18 “holes” on a disc golf course are tall baskets with chains around the top. e average golfer can nish a round of 18 holes in 1 or 2 hours. Playing time can depend on how many people are playing and how much time you spend looking for a lost disc in the bushes and tall grass. Most disc golf courses are free and allow you to stay for as long as you want to, as long as you’re not disturbing other golfers.
Like traditional golf, disc golfers start at the #1 hole and end their round at the 18th hole. Traditional golf etiquette is expected – you may ask to play through if your group is smaller and faster than the one in front of you. ere is no dress code for disc golf, although proper clothing for the weather and supportive, athletic shoes are encouraged. Make sure you bring plenty of water to stay hydrated during the round of golf.
Disc golfers use a variety of throwing techniques. e two most common throws are forehand and backhand. A typical drive can be 150 to 300 feet to the basket.

Disc golf is scored just like traditional golf. Each basket has its own par, or number of throws expected for an expert to get a disc into the basket. A birdie is 1 point under par, an eagle is 2 points under par, and a bogey is 1 point over par. e golfer with the lowest score wins. e discs – called drivers, midranges, and putters – come in a variety of shapes, weights, and colors. Experienced golfers may have up to 30 or 40 discs in their golf bag. A starter set of discs includes a driver, a midrange, and a putter for about $30.
Disc golf competitions started in the 1970s. Today, there are national and international tournaments for recreational, amateur, and professional golfers, with di erent classes based on gender and age – some are even televised. e jackpots aren’t as large as they are in traditional golf tournaments, but they’re just as satisfying. Every disc golfer receives a rating based on how well they performed at the tournaments. Some of the top-rated disc golfers can have sponsors who support their tournament participation.
Columbia has several excellent disc golf courses including Albert-Oakland Park, Indian Hills Park, A.L. Gustin Golf Course, and the Harmony Bends Championship Disc Golf Course at Strawn Park, which hosted a national competition in August 2022. With thousands more disc golf courses across the country, it’s easy to pack your discs when you go on vacation.
To learn more about disc golf, including rules, courses, and tournament information, visit the Professional Disc Golf Association website at pdga.com.
Happy throwing! By Gretchen
Holmes, MS, Boone Health Exercise PhysiologistScrubs on Site Sale
July 26 & 27 in Boone Hospital Center Lobby
Scrubs on Site Sale
November 1 & 2 in Boone Hospital Center Lobby
Linen Sale
December 14 & 15 in Boone Hospital Center Lobby
Board Members
Leadership
Board President: Betsy Vicente
Board Vice-President: Dr. James Roller
Board Secretary: Sara Jeffrey
Board Treasurer: Paul Mehrle
Representatives
Board of Trustees Representative: Jan Beckett
Board of Trustees Representative: Randy Morrow
Boone Health Representative: Drew Wilkinson
Active Boone Physician Representative: Dr. Joss Fernandez

Community Members
• Arlene Heins
• Genie Rogers
• Jolene Schulz
• Larry Swindle
• Nancy Thomas
• Becky Willard
The Boone Hospital Foundation held their annual golf tournament on May 8, 2023 at The Club at Old Hawthorne. A huge thank you to the 45 teams and our many sponsors for supporting our massage therapy program benefiting Boone Hospital Center’s neurology and stroke patients. We raised nearly $78,000 and are so grateful for the community support.


A HUGE thank you to our hole sponsors and in-kind sponsors.

In-Kind
• Maca doodles
• Logboat Brewing Company
• Waves Cider Company
• Shelter Insurance
• American Document Soluti ons
Hole Sponsors
• Woodrail C entre
• Orscheln Products
• Septagon Construction
• Columbia Landcare
• Break Time
• MFA Oil
• Meyer Electric
• Feeler S. Architects
• Working Spaces
• Schindler Elevator
• Dr. Andrew and Mrs. Kim Getzoff
Boone Hospital Center
1600 East Broadway
Columbia, MO 65201
573-815-8000
Boone Health has been awarded a portion of a federal workforce development grant geared toward industries impacted most by the pandemic, which includes healthcare.

Funds will be awarded to candidates who are interested in becoming a:
• Paramedic
• Certified Surgical Technologist
• Certified Nurse Assistant
• Certified Medical Assistant
• Licensed Practical Nurse

Funds will cover the costs of certification, including:
• Application fees
• Tuition costs
• Text/curriculum books
• Entrance and certification exam fees
For more information, visit: boone.health/bbim-scholarship