




•
•
•





1. Examine cancer in the fire service

2. Discuss how to reduce the risk
3. Discuss early diagnosis and detection
4. Discuss various screening methods
5. Understand the recommended screening program
6. Understand the importance of a patient doctor relationship.
7. Learn how to be an advocate with your health
8. Sign up to help further research



Fallen Firefighters
Memorial 75% of the names honored were Cancer related deaths






Firefighters have a Nine Percent higher risk being diagnosed.




Wear Full PPE …. Hood (Particulate Preferred) Gloves, Helmet No Exposed Skin !!
SCBA…… be on air anytime products of combustion are present whether inside or outside



Use SCBA from initial attack to finish of overhaul. (Not wearing SCBA in both active and post-fire environments is the most dangerous voluntary activity in the fire service today.)




Respect your gear (maintain PPE, isolate PPE when you can, wear only when necessary, clean station and gear room)
Reduce the exposures you can.
Decontaminate what you can’t eliminate. (on scene decon should be the standard)
Clean what you can when you can (doffing/donning, equipment, shower, etc.)




Every day asks ….
Eat real food and drink water.
Move. (Adopt physical fitness as a priority)
Connect. (Connect with others to reduce stress and maintain healthyrelationships)
Prioritize your sleep. (Rest and rejuvenate with a minimum of 7 hours each night)
Limit substance use. (stop tobacco use, limit alcohol consumption)
Access healthcare regularly (build relationship with provider you trust, get annual exams, get screened when recommended)






Firefighters have a Fourteen Percent higher mortality rate than the general population.




• Early diagnosis of cancer focuses on detecting symptomatic patients as early as possible, so they have the best chance for successfultreatment.
• When cancer care is delayed or inaccessible there is a lower chance of survival, greater problems associated with treatment and higher costs of care.
• 70% of all cancer deaths come from cancers for which there are currently no proven screening tests.



Screening is a different strategy than early diagnosis. It is defined as the presumptive identification of unrecognized disease in an apparently healthy, asymptomatic population by means of tests, examinations or other procedures that can be applied rapidly and easily to the target population.





The U.S. Preventive Services Task Force (USPSTF) sets cancer screening guidelines. The task force is a volunteer panel of experts. The panel makes recommendations about cancer screening and other ways to prevent many medical conditions.



•Biennial screening mammography for women aged 50 to 74 years
•Women who place a higher value on the potential benefit than the potential harms may choose to begin biennial screening between the ages of 40 and 49 years.
• Screening for cervical cancer every 3 years with cervical cytology alone age 21 to 29.
•30 to 65 years, every 3 years with cervical cytology alone, every 5 years with high-risk humanpa pillomavirus (hrHPV) testing alone, or every 5 years with hrHPV testing in combination with cytology (cotesting).
• Adults age 45 to 75 be screened for colorectal cancer. The decision to be screened between ages 76 and 85 should be made on an individual basis. If you are older than 75, talk to your doctor about screening.
• Annual screening for lung cancer with lowdose computed tomography (LDCT) in adults aged 50 to 80 years who have a 20 pack-year smoking history and currently smoke or have quit within the past 15 years.
• The decision to undergo periodic prostate-specific antigen (PSA)based screening for prostate cancer should be an individual one for men aged 55 to 69 years,.


Physical examinations
• Healthcare Provider Exam or Self
• Direct Observation Laboratory tests
• Blood
• Urine
• Tissue Imaging tests
• X -ray

• Ultrasound
• Computed Tomography (CT)
• Magnetic Resonance Imaging (MRI)



• Healthcare Provider Physical Exam focuses on overall health:
• Skin
• Eyes & Ears
• Heart and Lungs
• Abdomen
• Prostate
• Nervous system
• Mental Wellness
• Direct observationtests
• Colonoscopy
• Self Exams
• Breast
• Skin
• Testes


• Most important screening to have annually.
• During a physical exam, your physician may look for abnormalities, such as changes in skin color or enlargement of an organ, that may indicate the presence of cancer.
• Dentist examinefor oral cancers during checkups.
• Skin screenings check for melanoma and other skin cancers and diseases.
• Self checks of breasts and testis are simple and effective tools and should be done monthly .
• Cost: Free - $200



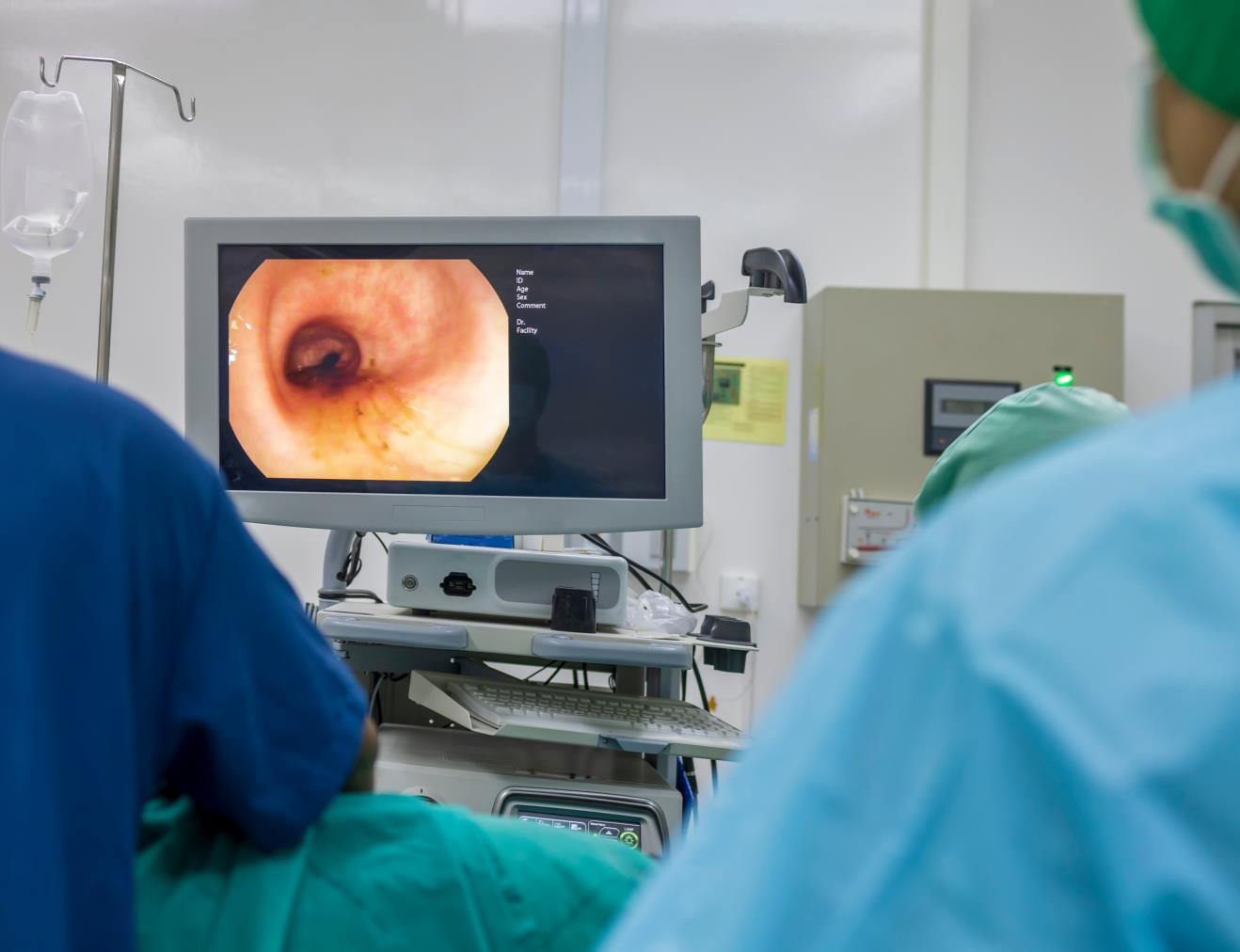
Direct observation tests involve visual examination of tissue for abnormal growths.
• A colonoscopy is a direct observation test for colorectal cancer.
• In this test, the rectum and colon are examined using a flexible lighted tube with a lens for viewing.
• Recommended for firefighters to have a colonoscopy starting at age 40.
• Cost: Free - $4800




High or low levels of certain substances can be a sign of cancer. Lab test results are used along with the results of other tests, such as biopsies and imaging, to help diagnose and learn more about a person’s cancer. Lab tests can include:
• Blood Chemistry Test
• Complete Blood Count (CBC)
• Cytogenetic Analysis
• Immunophenotyping
• Sputum Cytology
• Tumor Marker Tests
• Urinalysis
• Urine Cytology
• Multi-cancer early detection (MCED)



Multi-cancer detection (MCD) tests, also referred to as MCD assays or liquid biopsy tests.
• Measure different biological signals in blood plasma
• Does not diagnose cancer.
• Looks many types of cancer markers
• To date, no professional medical societies nor the U.S. Preventive Services Task Force have issued recommendations on the use of MCD.
• Health insurance programs are not routinely covering MCD testing.




• Have not received approval from the Food and Drug Administration
• Results should be interpreted by a healthcare provider
• Results require additional testing
• False positives or false negatives can result in emotional,financial,and resource risks associated with additional testing.
• Making an informed decision is essential when considering ultrasoundsfor early cancer detection.
• Cost $100 - $1000

OneTest is a prospective MCED test that uses machine learning algorithms to predict an individual’srisk of developingcancer in the coming 12-month period.
The Galleri test is an MCED test that can detect more than 50 cancers by scanning over 100,000 DNA regions. As cancer cells die, they shed DNA into the bloodstream known as cell-free DNA. Using DNA sequencing and machine learning, the test can determine if a cancer signal is present and potentiallyfrom where the cancer started


• Firefighters have elevated risk for developingand dying from esophageal cancer.
• To be eligiblefor screening, you must have 3 of the following risk factors:
• Heartburn/acid reflux and/or take any medication for heartburn/acid reflux
• Age 50+
• Male
• Caucasian race
• BMI of 30 or greater
• Smoke or a history of smoking
• Family history of Barrett’s Esophagus or Esophageal cancer
• Firefighter for 10+ years OR > age 35
• Cost: EsoGuard will bill insurance if the claim is deemed denied, we consider that claim adjudicated, meaning we do not follow up further with the patient.



• Checks for Barrett’s esophagus a premalignant condition of the distal esophagus that increases the risk of esophageal cancer.
• Test involvesswallowinga small capsule (with sips of water) to swab a sample of cells from the esophagus.
• Results come from epigenetic changes occurring within the cells of the distal esophagus that need to be further evaluated with an upper endoscopy if found to be positive



• PFAS Blood serum home test utilizing a finger stick.
• Results are based on the newest technology for whole blood. The serum equivalent is the conversion from whole blood to serum to allow comparison to national averages generated by the CDC.
• Results come with informational test guide, to show if your exposures are at, below, or above the average American’s exposure levels
• Cost: $249
• Nearly all Americans have PFAS in their blood due to their persistence in the body and the environment.
• PFAS blood serum testing can provide a baseline and repeated testing can demonstrate additoal exposure or reduction in levels.
• While research is still emerging on the impact of PFAS, these chemicals have been linked to health conditions like higher levels of cholesterol, reproductive health, complications for pregnant women and their infants, and increased risk of certain kinds of cancer




• Uses data from breath analysis, along with custom wearables to identify potential health risks from exposure.
• Uses AI models to provide a risk assessment from exposure or toxin levels in breath
• Provides baseline and toxin evolution though breath testing.
• Has APP, provides reports and links to health record
• Cost : $480 Per Person (5000 tests annually)
• Available in only a few areas (CA, NV, SC)






• Cancer sometimes appears to “run in families”, genetic testing looks for specific hereditary cancer syndromes.
• Personal or family medical history that may suggest a hereditary cancer syndrome are:
• Cancer at an unusuallyyoung age
• Several different types of cancer occurred in the same person
• Cancer in both organs in a set of paired organs
• Several first-degree relatives with same cancer
• Unusual cases of a specific cancer type
• The presence of birth defects that are known to be associated with inherited cancer syndromes
• Being a member of a racial or ethnic group that is known to have an increased risk of having a certain inherited cancer
• Several family members with cancer


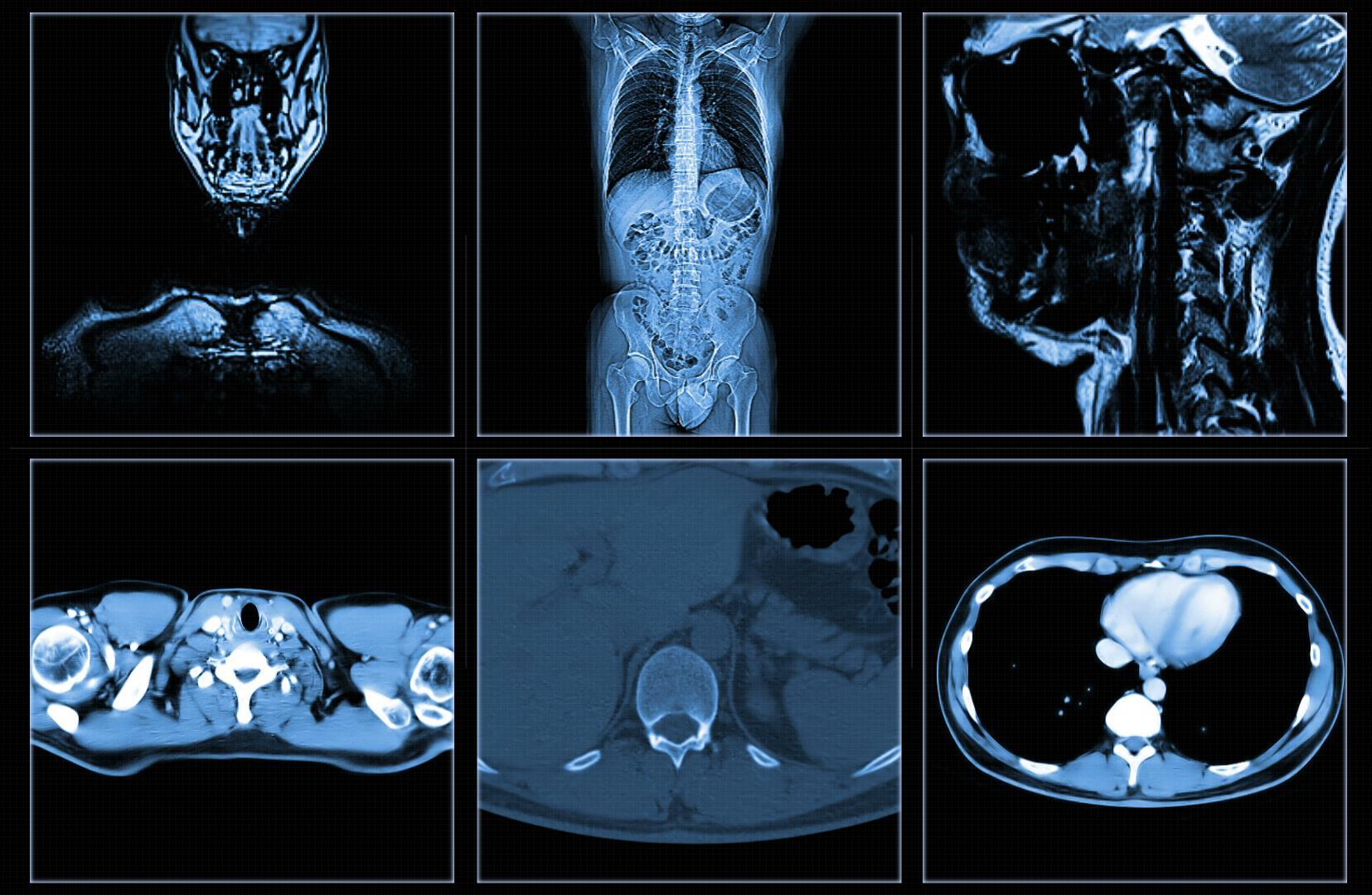

Imaging tests create pictures of areas inside your body that help the doctor see whether a tumor is present. These pictures can be made in several ways.
• X -ray
• Ultrasound
• Computed Tomography (CT)
• Magnetic Resonance Imaging (MRI)
• Nuclear scan
• Bone scan
• PET scan




• X-rays use low doses of radiation to create pictures of the inside of the body.
• Chest radiographs and mammograms are often used for early cancer detection.
• Risks:
• Radiation risk to you as a patient is similar adding 10 days of natural exposure or smoking a few cigarettes.
• allergic reactions to the contrast agent


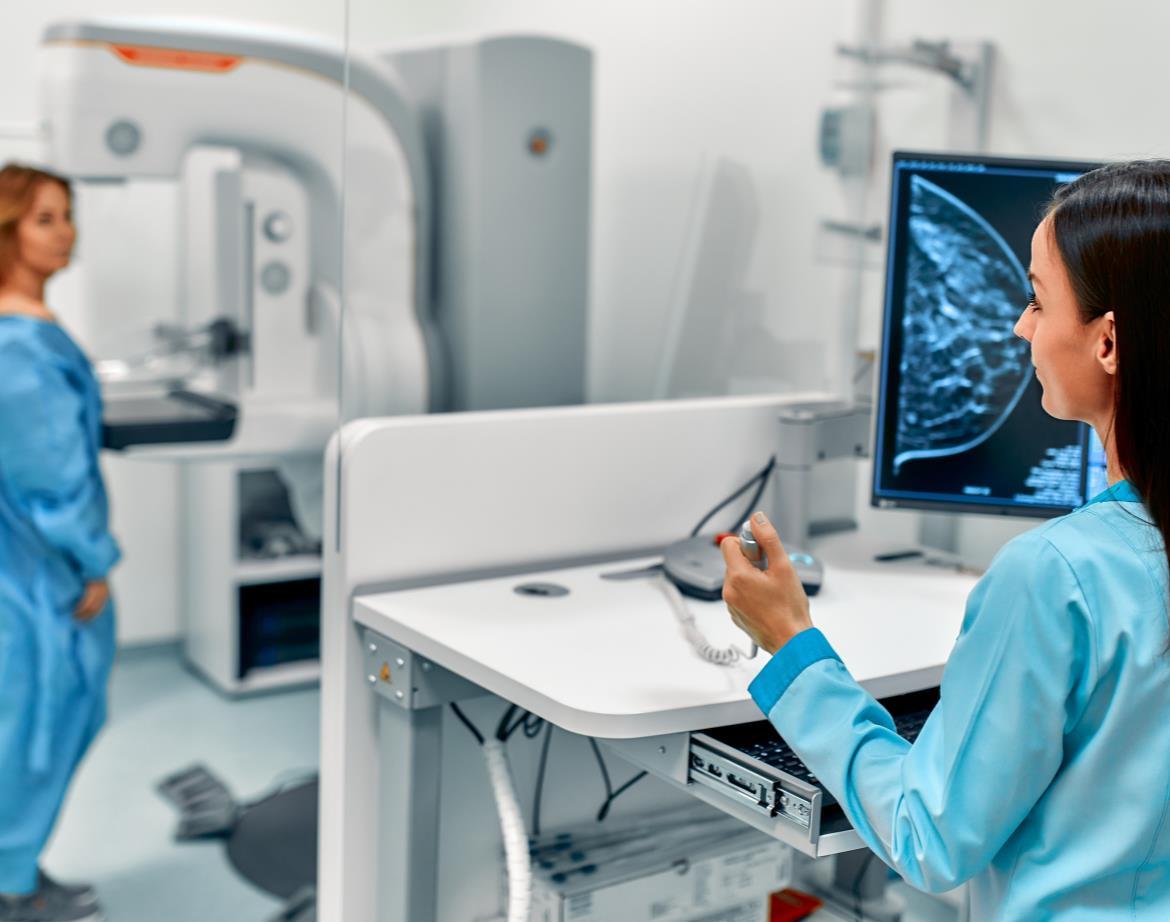

• Mammography has been shown to decrease the risk of dying from breast cancer by detecting it earlier when it is usually easier to treat.
• Obtain a baseline chest x-ray Repeat chest x-rays every 5 years or sooner if medically indicated
• Cost $100 - $400


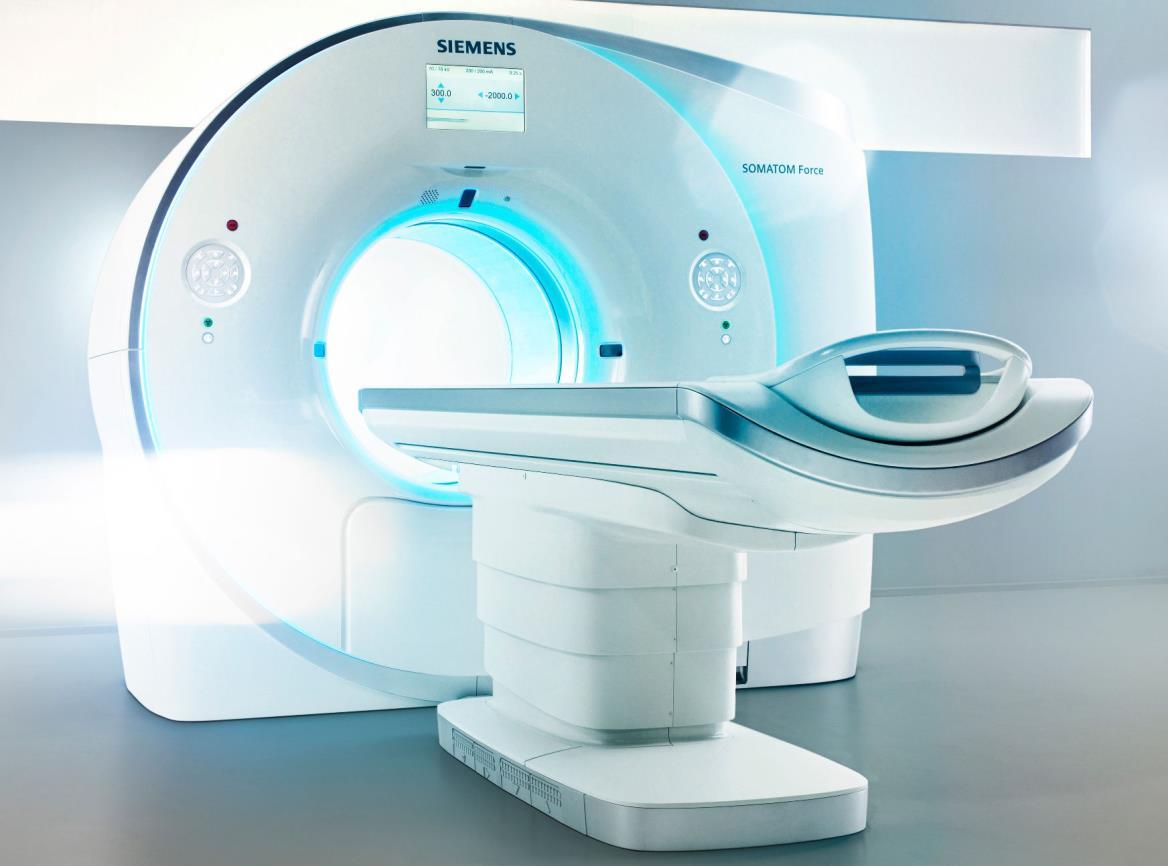

• A computed tomography scan CT scan, or CAT scan uses computer-controlled X-rays to create images of the body
• More vivid than a plain X-ray.
• May be given a contrast agent to more clearly show the boundaries between organs and potential tumors.
• Risks:
• Radiation risk to you depends on the amount of body scanned and can range from the equaling of 2 months to 10 years of background radiation.
• allergic reactions to the contrast agent


• CT scans are effective means of screening for colorectal and lung.
• Low-dose Helical Chest CT (LDCT) starting at age 50 is recommended for firefighters.
• Findings need follow up and additional testing or a biopsy which come with additional risk.
• Cost $100 - $400
• Low Dose Lung CT is being used in several studies on firefighter cancer and cardiac risks and the benefit.





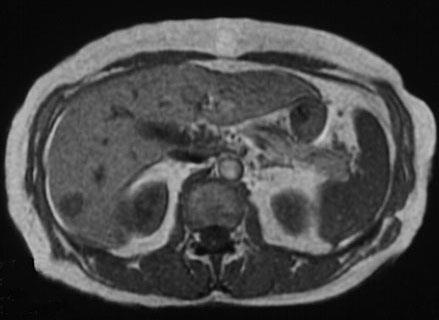
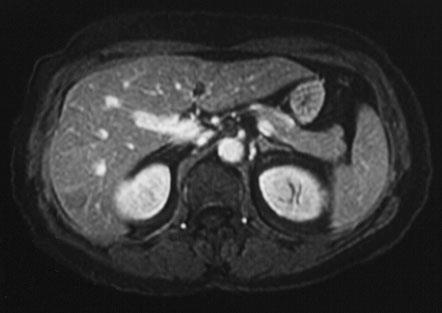
• Uses radio waves in the presence of a strong magnetic field that surrounds the opening of the MRI machine where the patient lies to get tissues to emit radio waves of their own.
• Different tissues emit a signal based on their chemical makeup, so a picture of the body organs is created.
• Risks:

• Generally Safe — so long as there is no metal in your body, there is no harmful radiation.
• Allergic reactions to the contrast agent


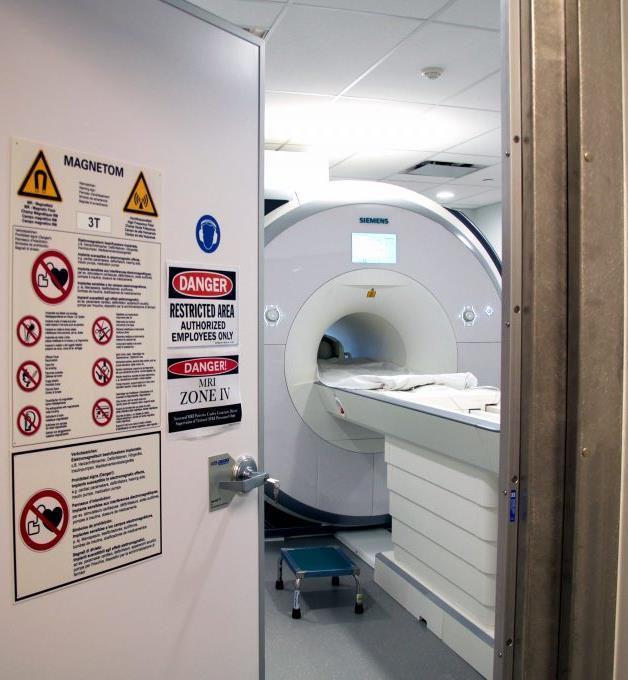
• The use of whole-body MRI is not recommended in asymptomatic patients who don’t have a genetic predisposition for cancer.
• Cost $400 - $12,000
• Varying rates of false positive results, additional testing can be resource exhaustive.
• Without the use of contrast in the MRI, it can overlook several cancers including colon, thyroid, and breast.



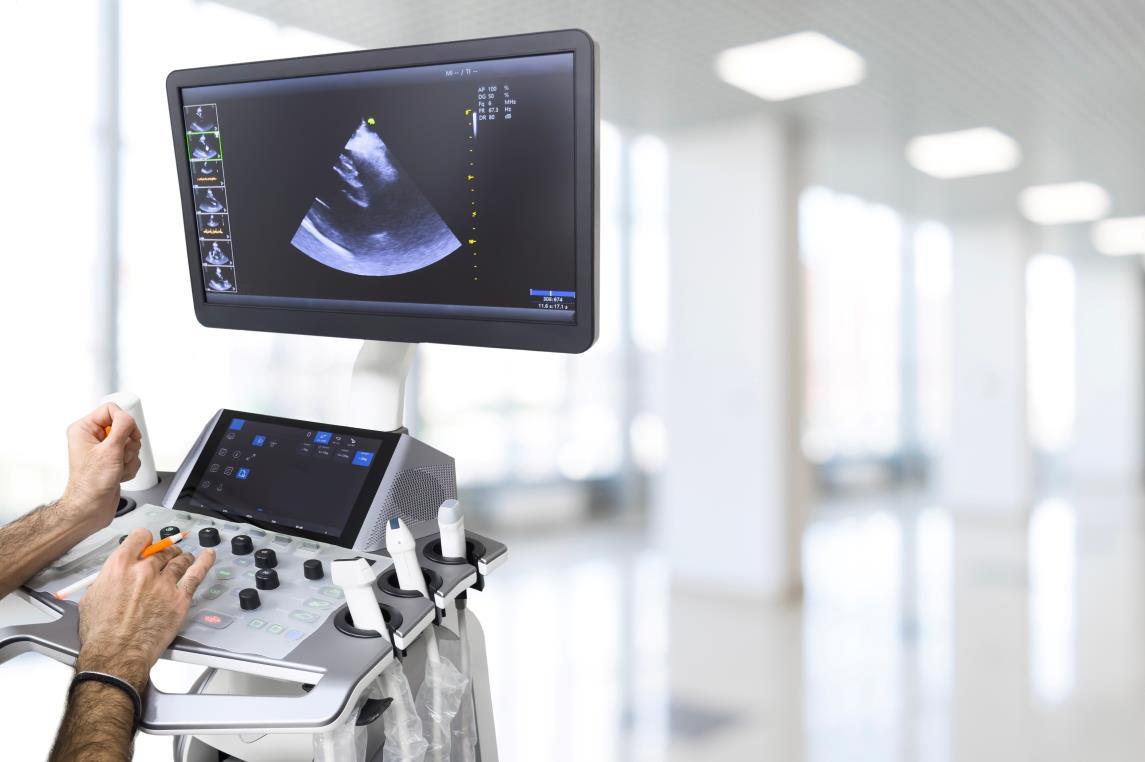
Use high-frequency sound waves to create picture of organs, blood vessels, and tissue.
• Used to examinemultiple organs, including the kidneys, stomach, uterus, liver, spleen, pancreas, thyroid, testes, and ovaries.
• Able to locate potential tumors
• Unable to determine if a tumor is cancerous
• Ultrasound is frequently used to guide physicians during biopsies



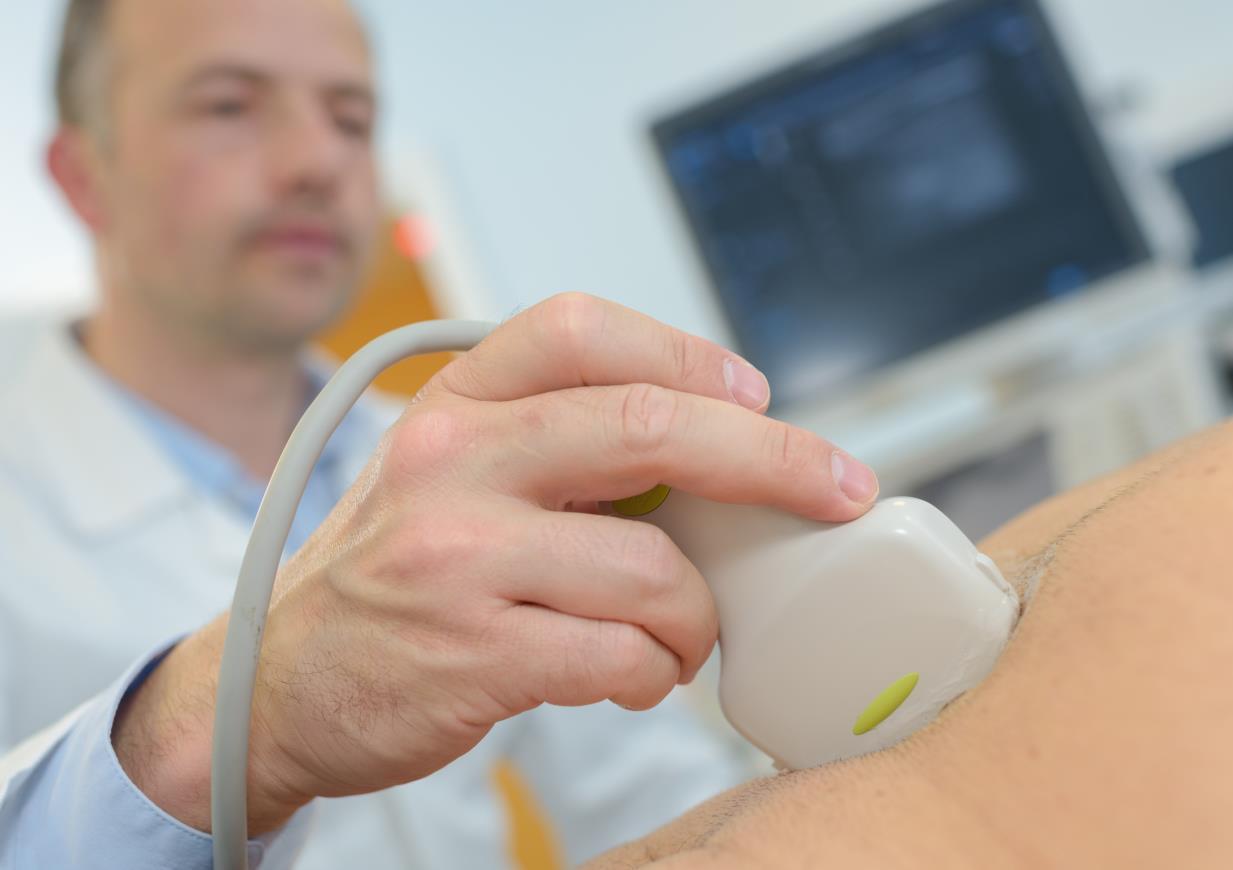
• Ultrasounds are a viable method for cancer screening, although results should be verified with a second method.
• Cost $300-$2000
• False positives or false negatives can result in emotional, financial, and resource risks associated with additional testing.
• Making an informed decision is essential when considering ultrasounds for early cancer detection
• Examines other potential conditions outside of cancer.



• Use low doses of radioactive substances or compounds that attach to tumor cells.
• Traced in the body to see where and when they concentrate.
• PET scans play a role in determining whether a mass is cancerous, reoccurring or to check if a treatment is working.
• Not recommended for screening, but can be used as follow up to screenings
• Cost $1000-$8000





Get back to basics with your health first!

• Before opting for a screening make sure to have a therapeutic relationship with a primary care physician.
• Get annual physicals, they play a crucial role in preventive healthcare, early disease detection, and the overall maintenance of health.
• Have a conversation about the risks from firefighting.
• Make necessary adjustments to lifestyle to reduce risks.


Make a plan & follow it!


• Talk to your physician about what screenings and tests can identify the early signs of various diseases, such as diabetes, high blood pressure, and certain cancers.
• Make a plan that focuses on your health and wellness.
• Follow the plan!



Designedto ensure the firefighteris ready for duty and to catch potential health issues early on.

NFPA 1582 physicalsinclude:
• Health history and physical exam
• Blood analysis
• Urinalysis
• Infectious disease screening (tuberculosis and hepatitis)
• Pulmonary function test (spirometry)
• Chest X-ray
• EKG and cardiac risk assessment
• Cancer screening
• Audiometric exam
• Vision testing
• Clinical guidanceon sleep apnea
• Vaccination review/update
• Medical clearance to wear a respirator.


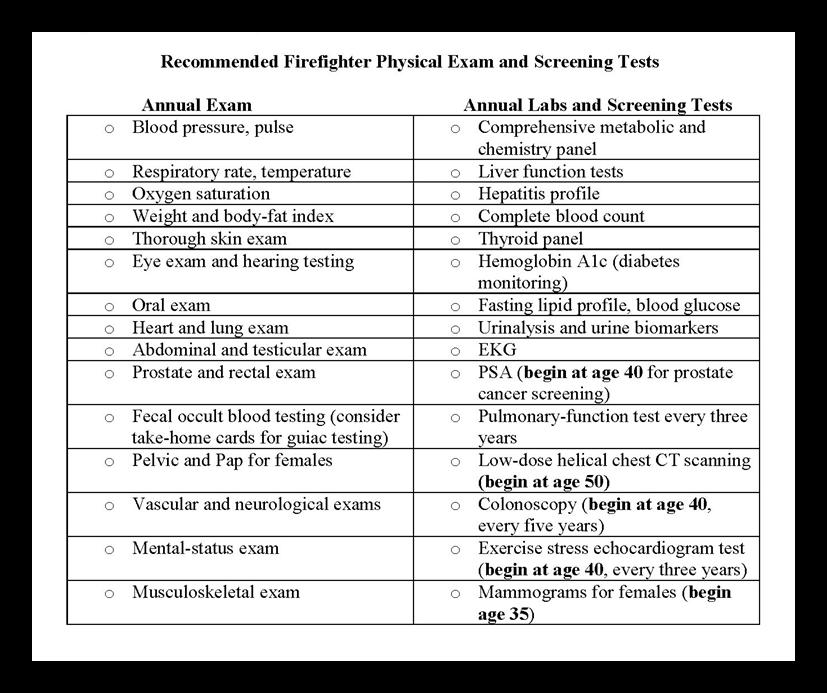




• Evidence-based screening programs have great potential to improve health outcome. they can prevent disease, reduce disability and cut mortality.
• Your healthcare provider should be involved in the process.
• False positives or false negatives can result in emotional, financial, and resource risks associated with additional testing.
• Firefighters must understand that a screening is not a replacement for a therapeutic relationship with a physician.




“Much like arriving on-scene to an incipient stage fire. Cancer is easier to manage, uses less resources and has less of a damaging impact when found early”. Heather Makel, DetecTogether








1 Remember what GREAT feels like.

2 Use the 2-WEEK rule.


3Share with your DOCTOR.





Pain Energy Level




Use the 2-Week Rule the same way you track other important dates and information.

STEP 2
Use the 2-Week rule.






• Firefighters must complete annual physicals as the foundation to a health program.
• Firefighters must work with their physician to develop a risk reduction plan and follow through both at home and on the fireground. Then can consider adding a screening to their regiment. Screening test alone cannot diagnose cancer.
• The risks and benefits of cancer screening depend on the individual and the type of screening. It is important to discuss the risks and benefits of cancer screening with a healthcare provider to make an informed decision.
• Use these tools to reduce the risk of developing cancer. Understand that early detection is the key to deducing death from cancer and that screenings are one portion of the overall program.




• Used to track and analyze cancer trends and risk factors among the U.S. fire service.
• All firefighters- active and retired should consider participating. This includes firefighters who have never received a cancer diagnosis, previously had cancer, or currently have cancer
• Firefighters who register for the NFR will play a critical role in helping to better understand the health risks this profession faces



We hope you found this presentation to be valuable for you and your brother and sister firefighters and EMS providers.

If you did, please consider making a small donation to help FCSN continue to spread the word nationwide about the dangers firefighters face and the precautions they can take to reduce their chances of getting cancer
THANK YOU!

