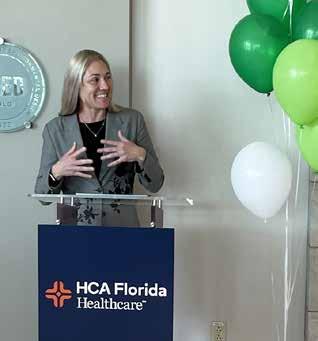UCF Lake Nona Hospital Setting the Standard for High-Quality, Patient-Centered Care MAY/JUNE 2024 • COVERING THE I-4 CORRIDOR

choose well.
A new name, for a new century of care. Three years ago, we welcomed Bayfront Health into the Orlando Health family of hospitals. Since that time, we’ve been making steady investments in Bayfront Health and the St. Petersburg community to improve the quality of care and your patient experience, with expanded services and access to more top specialists. And we are proud to add our name. Stay tuned for even more good news to come. OrlandoHealth.com/Bayfront Bayfront Health is now Orlando Health Bayfront Hospital.

Since opening two years ago, UCF Lake Nona Hospital has lived up to the high expectations that were set for Lake Nona’s only full-service hospital. Created through a unique partnership between the University of Central Florida and HCA Healthcare, the nation’s most extensive health system, UCF Lake Nona Hospital has established a new standard of healthcare for the whole family.
The technologically advanced hospital has been growing faster than projected, running ahead of expectations in all areas. The medical staff has grown to more than 450 affiliated physicians, including specialists in primary care, cardiology, colorectal surgery, thoracic surgery, general surgery, gastroenterology, orthopedic surgery, pulmonology, nephrology, OB/ GYN, gynecological oncology, infectious disease, neuro health sciences, spine and urology.
Before the hospital began construction in 2018, no other facilities in the Lake Nona area were designed to serve the adult patient population: Nemours Children’s Hospital and Orlando VA Medical Center, the two primary hospitals in the area, provided care for children and veterans respectively. To serve the region’s unmet need, the UCF Lake Nona facility opened with 64 inpatient beds and a 20-bed emergency department, with ample capacity for expansion in future years.

FLORIDA MD - MAY/JUNE 2024 1 DEPARTMENTS 2 FROM THE PUBLISHER 8 DERMATOLOGY 9 MARKETING YOUR PRACTICE 10 PULMONARY AND SLEEP DISORDERS 12 HEALTHCARE LAW 14 ORTHOPEDICS 16 PEDIATRICS contents MAY/JUNE 2024 COVERING THE I-4 CORRIDOR 18 WHY DEBUNKING THE MYTHS AROUND EPILEPSY IS CRUCIAL FOR OUR PATIENTS – AND CONSIDERATIONS FOR WOMEN WITH THE CONDITION 20 A NEW ERA IN SEVERE OBSTRUCTIVE SLEEP APNEA TREATMENT: FDA CLEARS INNOVATIVE ORAL MEDICAL DEVICES 19 CENTRAL FLORIDA REAL ESTATE MARKET REPORT 4 COVER STORY PHOTO: PROVIDED BY UCF LAKE NONA HOSPITAL
PROVIDED BY UCF LAKE NONA HOSPITAL
PHOTO:
ON THE COVER: UCF Lake Nona Hospital
Iam pleased to bring you another issue of Florida MD. Sometimes a patient may have the opportunity to participate in a clinical trial. Sometimes a patient may need specialized treatment that is not available in Central Florida. And sometimes there’s no money for that patient to get to those places. Fortunately there is Angel Flight Southeast to get those patients where they need to go. I asked them to tell us about their organization and how you, as physicians, can help. Please join me in supporting this truly wonderful organization.
Best regards,
 Donald B. Rauhofer Publisher
Donald B. Rauhofer Publisher


ANGELS ON EARTH HELP PATIENTS GET TO LIFESAVING MEDICAL TREATMENT
Everyone knows angels have wings! But did you know in Florida and many parts of the nation they have engines and tails with dedicated volunteers who donate lifesaving services every day? Leesburg, Fla.-based Angel Flight Southeast is a network of approximately 650 pilots who volunteer their time, personal airplanes and fuel to help passengers get to far-from-home medical care. A member of the national Air Charity Network, Angel Flight Southeast has been flying passengers since 1993.
Almost all of its passengers are chronic-needs patients who require multiple, sometimes 25-50 treatments. Passengers may be participating in clinical trials, may require post-transplant medical attention or are getting specialized treatment that is not available near home. Each passenger is vetted to confirm medical and financial need and is often referred to Angel Flight Southeast by medical personnel and social workers.
Angel Flight Southeast “Care Traffic Controllers” arrange flights 24 hours a day, 365 days a year. In the event of a transplant procedure, the Care Traffic Controllers have precious minutes to reach out to its list of volunteer pilots who have agreed to be prepared on a moment’s notice to fly a patient to receive his or her potentially lifesaving organ.
The organization is completely funded through donations by individuals and organizations. A typical Angel Flight Southeast pilot donates $400 to $500 in services-per-trip. In fact, Angel Flight Southeast has earned the Independent Charities of America Seal of Approval as a good steward of the funds it generates from the public. Each $1 donated generates more than $10 worth of contributed services by Angel Flight Southeast.
The charity always seeks prospective passengers, volunteer pilots and donations. For additional information, please visit https://www.angelflightse.org or call 1-888-744.8263.
ADVERTISE IN FLORIDA MD
For more information on advertising in Florida MD, call Publisher Donald Rauhofer at (407) 417-7400, fax (407) 977-7773 or info@floridamd www.floridamd.com
Email press releases and all other related information to: info@floridamd.com
PREMIUM REPRINTS
Reprints of cover articles or feature stories in Florida MD are ideal for promoting your company, practice, services and medical products. Increase your brand exposure with high quality, 4-color reprints to use as brochure inserts, promotional flyers, direct mail pieces, and trade show handouts. Call Florida MD for printing estimates.
Publisher: Donald Rauhofer
Photographer: Donald Rauhofer / Florida MD
Contributing Writers: JJohn “Lucky” Meisenheimer, MD, Daniel T. Layish, MD, John Meisenheimer, VII, MD, Sonda Eunus, MHA, Julie Tyk, JD, Bruce Levy, MD, Frank Ricci, Dipali Menade, MD, Tara M. Griffin, DMD, DBDSM, DASBA
Art Director/Designer: Ana Espinosa
Florida MD is published by Sea Notes Media,LLC, P.O. Box 621856, Oviedo, FL 32762. Call (407) 417-7400 for more information. Advertising rates upon request. Postmaster: Please send notices on Form 3579 to P.O. Box 621856, Oviedo, FL 32762.
Although every precaution is taken to ensure accuracy of published materials, Florida MD cannot be held responsible for opinions expressed or facts expressed by its authors. Copyright 2024 Sea Notes Media. All rights reserved. Reproduction in whole or in part without written permission is prohibited. Annual subscription rate $45.
FLORIDA MD - MAY/JUNE 2024 2
FROM THE PUBLISHER









FLORIDA MD - MAY/JUNE 2024 3 Scan here JOIN SLS NOW AND RECEIVE MEMBER DISCOUNTS TO ATTEND MISWEEK 2024 JOIN/RENEW ONLINE AT SLS.ORG/MEMBERSHIP Additional Member Benefits World-Class Conferences and Resources Tools and Opportunities to Advance Your Career Publications to Keep You at the Forefront of MIS Exclusive Member Interactions THE SOCIETY OF LAPAROSCOPIC & ROBOTIC SURGEONS REGISTRATION HAS OPENED JOIN US IN LAKE BUENA VISTA, FL SUBMIT YOUR ABSTRACT FOR PRESENTATION AT MIS WEEK 2024 Present your work to MIS and Robotic surgeons from around the globe Accepting submissions for Papers, Videos, and Posters. www.sls.org/mis2024/submit/
UCF Lake Nona Hospital – Setting the Standard for High-Quality, Patient-Centered Care
By Staff Writer
Since opening two years ago, UCF Lake Nona Hospital has lived up to the high expectations that were set for Lake Nona’s only full-service hospital. Created through a unique partnership between the University of Central Florida and HCA Healthcare, the nation’s most extensive health system, UCF Lake Nona Hospital has established a new standard of healthcare for the whole family.
The technologically advanced hospital has been growing faster than projected, running ahead of expectations in all areas. The medical staff has grown to more than 450 affiliated physicians, including specialists in primary care, cardiology, colorectal surgery, thoracic surgery, general surgery, gastroenterology, orthopedic surgery, pulmonology, nephrology, OB/GYN, gynecological oncology, infectious disease, neuro health sciences, spine and urology.
Before the hospital began construction in 2018, no other facilities in the Lake Nona area were designed to serve the adult patient population: Nemours Children’s Hospital and Orlando VA Medical Center, the two primary hospitals in the area, provided care for children and veterans respectively. To serve the
region’s unmet need, the UCF Lake Nona facility opened with 64 inpatient beds and a 20-bed emergency department, with ample capacity for expansion in future years.
The hospital benefits from the expertise, clinical knowledge and practices available across HCA Florida Healthcare’s network of 50 hospitals, 570 affiliated sites of care, 11,000 physicians and 77,000 colleagues and over 7 million patient encounters annually.
Overall the HCA Healthcare network encompasses to 182 hospitals supported by approximately 2,300 ambulatory sites of care in 20 states and the United Kingdom.
This enterprise supports the physical, mental, professional and financial health of its 294,000 colleagues and invests in a variety of benefits and resources to help improve their overall well-being, so they can provide comprehensive and compassionate patientcentered care for the communities it serves.
Sheila O’Ben’s health improved significantly following surgery with Dr. Keith Kim at UCF Lake Nona Hospital. “When I look in the mirror, I just can’t believe it’s me,” she said.

In the two years since it began serving the Lake Nona community, UCF Lake Nona Hospital has earned high marks for quality patient satisfaction. Since opening in March 2021, hospital departments have consistently ranked among the nation’s top 10 percent in patient satisfaction scores. Currently the hospital’s surgical services department is ranked first out of all HCA Healthcare hospitals for patient experience, and in the 99th percentile in Press Ganey, the industry’s leading human experience platform.
“This feedback reflects the voices of our patients,” said Wendy H. Brandon, FACHE, CEO of UCF Lake Nona Hospital. “These high scores are simply unheard of in healthcare.”
INNOVATIVE AND AT THE FOREFRONT OF CHANGE
UCF Lake Nona Hospital is transforming medical care by providing some of the most advanced technological tools and procedures. Recently, the learning-focused hospital became HCA Healthcare’s first Care Transformation and Innovation Hub (CT&I) to change how care is delivered to meet today’s demand for better, more efficient, and more effective patient care.
“The uptick of demand for healthcare services, coupled with accelerated progress in the digital space, creates an opportunity to transform the way we deliver care for the ultimate benefit of our patients,” Brandon said. “The designation as an Innovation Hub through HCA Healthcare is
FLORIDA MD - MAY/JUNE 2024 4 COVER STORY
PHOTO: PROVIDED BY UCF LAKE NONA HOSPITAL
a great honor, and our team is ready for the challenge of taking the delivery of healthcare excellence to the next level.”
CT&I builds on HCA Healthcare’s legacy of innovation and aims to transform the future of patient-centered care. The CT&I team is working to identify, build and roll out new technology solutions and process innovations that will create better outcomes and experiences for care teams and patients.
The work being done is designed to enhance the patient experience, create more face time between providers and patients, and improve both quality and safety in the delivery of healthcare. CT&I also works alongside HCA Healthcare nurses to better understand current processes and help generate insights to inform future innovations.
FLORIDA’S ONLY LEED GOLD HOSPITAL
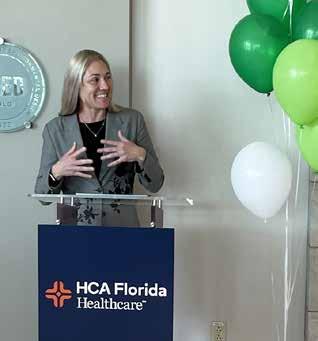
This spring UCF Lake Nona Hospital earned LEED Gold certification, the first and only hospital in Florida to achieve this green building designation. LEED (Leadership in Energy and Environmental Design), developed by the U.S. Green Building Council, (USGBC), is the most widely used green building rating system in the world and an international symbol of excellence.
“Sustainability is a growing priority and we are excited about this recognition by the USGBC,” Brandon said. “It’s a major milestone and testimony to the cumulative efforts and innovative work of our HCA Healthcare project team.”
The designation recognizes the hospital’s commitment to sustainable building products and energy-saving operations, including:
• Systems that reduce water use, including sinks, toilets and showers, that conserve 767,908 gallons of water per year –equivalent to nearly 6 million bottles of drinking water
• Native landscaping that reduces water consumption by nearly 600,000 gallons of water each year
• High efficiency LED lighting and other systems that save over 21% in annual energy costs, as compared to standard design and construction practices
• On-site recycling, recycled and sustainable building materials, and the fact that 75% of the building waste during the hospital’s construction was recycled
Through design, construction and operations practices that improve environmental and human health, LEED-certified buildings are helping to make the world more sustainable. In the U.S. alone, building account for almost 40% of national CO2 emissions, but LEED-certified buildings have 34 % lower CO2 emissions, consume 25% less energy and 11% less water, and have diverted more than 80 million tons of waste from landfills.

“This is an exceptional accomplishment for both UCF and HCA,” said Amy Pastor, USGBC Central Florida Board chair. “You are among the best and you will be known worldwide for this.”
“LEED was created to make the world a better place and revolutionize our buildings and communities by providing everyone with access to healthy, green and high performing buildings,” said Peter Templeton, president and CEO of USGBC. “UCF Lake Nona Hospital is a prime example of how the innovative work of project teams can create local solutions that contribute to making a global difference.”
CARING FOR FAMILIES FROM DAY ONE
In just two years since opening its state-of-the-art Family Birthing Unit, UCF Lake Nona Hospital has welcomed 2,000 babies to Lake Nona. Featuring modern, suite-style facilities, the new unit is designed to provide a more comfortable, supportive, and private experience for expecting parents and their families.
At the Family Birthing Unit, mothers can labor, deliver and recover in boutique specialty birthing suites, which come equipped with everything the family needs for a safe birth. The spacious rooms feature a range of amenities for patients and visitors, room service, WiFi, 55-inch smart TVs with streaming services, and space for one guest to stay overnight.
For overnight births and those requiring around-the-clock care, the Family Birthing Unit is staffed 24 hours a day and seven days a week by a dedicated obstetric team who can provide care until the patient’s personal physician arrives. Parents with specific birth preferences, including low-intervention births, can be accommodated as well.
As part of UCF Lake Nona Hospital’s commitment to supporting parents before, during and after a birth, the Family
FLORIDA MD - MAY/JUNE 2024 5 COVER STORY
PHOTO: PROVIDED BY UCF LAKE NONA HOSPITAL
On Earth Day U.S. Green Building Council’s Amy Pastor awarded UCF Lake Nona Hospital Florida’s only LEED Gold hospital certification. “You are among the best and you will be known worldwide for this,” she said.
Birthing Unit offers maternity, childbirth, breastfeeding and newborn care classes for the whole family, including siblings.
LIFE-CHANGING WEIGHT LOSS SURGERY
The hospital is also the site of life-changing care for bariatric patients who qualify for weight loss surgery. Sheila O’Ben went from 289 pounds to just 145 after undergoing gastric bypass surgery a year ago at UCF Lake Nona Hospital.
Obesity, characterized by a BMI of 30.0 or higher, is a common disease that impacts more than one in four adults statewide. This widespread public health risk is expected to become more prevalent over time, according to the Florida Department of Health.
Living with obesity can be limiting and isolating in daily life, and it can also lead to a range of related complications, such as joint pain, difficulty breathing, cholesterol problems, hypertension, sleep apnea and fatigue. Adults with obesity are at a higher risk for severe weight-related illnesses like type 2 diabetes, heart disease and cancer, as well as an increased risk of premature death.
Surgery is not a stand-alone treatment for obesity, and UCF Lake Nona Hospital’s bariatric team works collaboratively with the patient to select an appropriate treatment option based on health and lifestyle needs. As part of the treatment process, patients are screened for eligibility and counseled extensively about nutrition, exercise and supplementation requirements to ensure a safe procedure and a healthy recovery.
After visiting her primary care physician recently, O’Ben said her doctor couldn’t believe the change in her health. She has been
able to discontinue multiple prescriptions, including cholesterol and acid reflux medications, due to her successful weight loss.
“I’m doing fantastic and living a normal life. It’s awesome to see family members who haven’t seen me in a while. They have to look twice and barely recognize me,” she said.
LIFE-CHANGING AND TRANSFORMATIVE MEDICINE
The hospital has brought life-changing technological advancements to Central Florida for many patients. It was the first Orlando-area facility to offer MRI-guided focused ultrasound for the advanced treatment of essential tremor (ET).
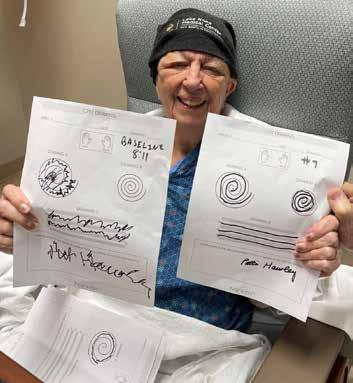
Central Florida’s first focused ultrasound patient Patricia Hawley was one of the more than 10 million Americans (an estimated 3% of the population) who live with ET, making it the most common movement disorder in the nation. Her involuntary shaking posed substantial hurdles in the normal activities of her daily life. As a school teacher Hawley had lost the ability to write years earlier and was no longer able to keep her daily journal.
“For patients who qualify, MRI-guided focused ultrasound provides an incision-less treatment option, performed on an outpatient basis with short recovery time and often immediate results,” said Dr. Nizam Razack, a neurosurgeon at UCF Lake Nona Hospital who performs the procedure. “This procedure can help restore independence and provide relief for individuals suffering from debilitating and progressive tremors within hours of treatment.”
The procedure, which was approved by the FDA in 2016 and by the Centers for Medicare and Medicaid Services (CMS) in July 2020, presents minimal risks, making it a strong alternative to existing surgical treatment options. Lake Nona is home to a large population of older adults, who are at a higher risk of being diagnosed with ET or Parkinson’s tremor, and noninvasive treatment options such as focused ultrasound can significantly improve independence, ability and quality of life.
“I am so happy and cannot believe the difference! After 15 years, I can write again,” Hawley said.
Innovation in medicine is a driving principle for UCF Lake Nona Hospital, and another new advancement is needle knee arthroscopy. Pioneered by orthopedic surgeon Dr. Vonda Wright and other UCF Lake Nona Hospital orthopedic surgeons, this new technology uses imaging sensors, LED light and image management to allow patients a less invasive arthroscopic surgery, during which they can stay awake under local anesthesia.
“This technology allows the patient to be a partner in their medical care as they see their joints in real-time and understand the treatment, minimizing patient risk and optimizing recovery in musculoskeletal surgery,” said Dr. Wright. “Needle arthroscopy is a game changer using only small points of entry, no general anesthesia, very little pain medications, no need for opioids, the procedure leads to extremely rapid recovery.”
Shorter downtime, less scars and fast recovery means returning to normal activity sooner, and in some instances, patients walk out of the hospital following the procedure.
FLORIDA MD - MAY/JUNE 2024 6 COVER STORY
PHOTO: PROVIDED BY UCF LAKE NONA HOSPITAL
Above, essential tremor patient Patricia Hawley holds her pre- and post-operative, before/after writing samples. These images were taken two hours apart from the incisionless surgery, and Hawley left the hospital shortly after this outpatient procedure.

As the hospital begins its third year of caring for the Lake Nona community, its leader reflects with gratitude for all her team has accomplished together.
“It has been exciting to see UCF Lake Nona Hospital achieve the vision we all had from the beginning of the hospital of the future, delivering high-quality, patient-centered care with the latest technology,” Brandon said.
“A new era of healthcare has arrived, and I couldn’t be prouder of our colleagues who made it possible.”

CARDIOLOGY
COLORECTAL
GASTROENTEROLOGY
GENERAL
GYNOCOLOGIC
FLORIDA MD - MAY/JUNE 2024 7 UCF LAKE NONA HOSPITAL SERVICES: 6700 LAKE NONA BOULEVARD ORLANDO, FL 32827 689-216-8000 HCAFloridaHealthcare.com/ UCFLakeNonaHospital NEPHROLOGY NEUROHEALTH SCIENCES ORTHOPEDICS PULMONOLOGY
SURGERY
CARE
CARE
ULTRASOUND
ROBOTIC
SPINE
UROLOGY WOMEN’S
ONCOLOGY FOCUSED
SURGERY 24/7 EMERGENCY CARE
SURGERY
ONCOLOGY
DISEASE
IMAGING INFECTIOUS
MATERNITY BARIATRICS
COVER STORY
HCA Healthcare’s legacy of innovation continues at UCF Lake Nona Hospital as CT&I teams identify, build and roll out solutions and process innovations to create better outcomes for patients and care teams.
PHOTO: PROVIDED BY UCF LAKE NONA HOSPITAL
The $8500 Tube of Cream
By John “Lucky” Meisenheimer, MD and John Meisenheimer, VII, MD
Several years ago, a patient came back to my office for a return visit. She had been seen earlier that week for a small amount of intertrigo underneath her breasts. Intertrigo is a common inflammatory condition of the skin folds, and it is aggravated by heat, moisture, and friction. Occasionally a patient might get a minor secondary yeast infection in the area as well. The treatment is keeping the area dry and using a topical cream to clear the yeast and decrease the inflammation.
The patient said, “doctor, I am worse.” I asked how she was using the cream, and she responded that she had not filled her prescription. Now I have lived through this scenario before with other patients. I am always amazed when people seem surprised that their condition has not improved when they have either not filled their prescription or filled the prescription and never used the medicine.
Now, if they filled the prescription and didn’t use the medicine, I am flummoxed as I am not sure how to respond. So, I usually say “oh” and stop talking, leaving a long moment of uncomfortable silence that eventually forces the patient to speak. Then the response comes, “so you think I should use the medicine you prescribed?” I reply, “Well, yes, as we have tried not using the medicine, and that plan is not working so good.” Amazingly, the patient seems okay with this response and goes happily on his or her way. Yes, this very conversation has happened on more than one occasion.
Now, in this case, since this patient had not filled her prescription, I wanted to know why. In the past, the cream I prescribed called Alcortin sold for about $35 a tube, so I didn’t think the cost was a concern. She then told me that the pharmacist wanted to charge her $8500.00 for a tube of the cream. I laughed out loud because I knew there had been some gross misunderstanding regarding the cost, and I said there must have been a decimal put in the wrong place. I was confident she didn’t understand the pharmacist correctly.
one lousy 60-gram tube. At the time, that cream was selling for four times its weight in gold! The pharmacist had no explanation for why the medicine went up so much in price; all he knew was that was the price.

Since that bit of medical-cultural shock, other medicine prices have skyrocketed as well as everyone reading this knows. Nobody seems to know why, but I suspect this is due to our government meddling with the free market system. When the last big round of Medicare laws changed the way Medicare buys
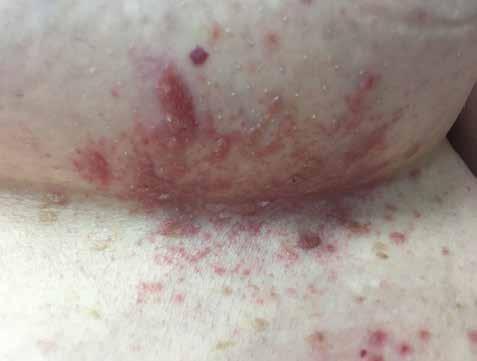
- Would you spend $8500.00 on a tube of cream to treat this eruption?
drugs, and this had bipartisan support I might add, this is when the chaos started. Drug companies loved the clause that they could name their price without any negotiation on price, and we are all now living the outcome.
The patient was very adamant that she had spoken with the pharmacist in person, and there was no question that the price was $8500.00. I asked her for her pharmacy, and I contacted the pharmacist myself. I started by saying, “well, I am just clearing up a misunderstanding. There is a patient here that is trying to tell me that Alcortin is $8500.00 a tube. I am sure the decimal point has been put in the wrong place, or you mistakenly thought I ordered a tractor-trailer full of the cream. There was a long pause, and the pharmacist said, “no, $8500 is correct,” and it wasn’t for a flatbed truck loaded with cream; it was for
Just recently, a study showed that worldwide, when several first world countries were compared for the average cost spent on nineteen different conventional medicines, the United States was paying 300% more than the average price paid by other countries. Iceland, for example, was paying approximately 50% the average cost, which means that we are spending six times as much as the Icelanders for the same medication. So why don’t we go to Iceland and buy all our medicines straight from Iceland? The answer is the drug companies have convinced the government that reimportation should be illegal. Therefore, it is unlawful to
Continued on page 15
FLORIDA MD - MAY/JUNE 2024
8
PHOTO: JOHN MEISENHEIMER,
DERMATOLOGY
VII, MD
Intertrigo
Is Your Online Reputation Costing You Patients?
By Sonda Eunus, MHA, CMPE
What does your online reputation say about your practice? If you have a negative online reputation, you are missing out on new patients every day. Most medical practices now get the majority of their new patients through Google and other search engine queries, such as “Pediatrician in Orlando”. If your practice appears in these searches, the most common next step for a potential new patient would be to check out your reviews – what are other patients saying about your practice? It has been reported that 90% of consumers read online reviews before visiting a business and that online reviews influence 67% of purchasing decisions (Bright Local). For this reason, it is incredibly important to pay attention to the rating and reviews that your practice has on search engines, social media platforms, and local online business directories.
However, despite the importance of cultivating a positive online reputation, only 33% of businesses report actively collecting and asking for reviews (1). One great process to set in place at your practice is asking for patient reviews after each patient visit. It can be as simple as training your front office staff to ask each patient how their visit went while checking them out, and if they receive favorable feedback then they can ask the patient to please leave a review on Google or Facebook about their experience. If they receive negative feedback, this feedback should be taken very seriously, and management should be notified as soon as possible so that the issue can be mitigated before the patient decides to post a negative review.


Setting up an automated text or email campaign that asks each patient for their feedback after their appointment is also a great way to improve your online reputation as well as to correct any issues that may be occurring at your practice. When you receive feedback from patients, you are then able to prompt them to leave a public review on Facebook, Google, Yelp, Healthgrades, or other applicable review platforms. However, you must be aware that legally, you are not allowed to only direct people with favorable feedback to leave reviews, which is known as review-gating – so if you are implementing an automated system like this, just make sure that you are aware of this limitation. There are online reputation management platforms which allow you to customize the messages that people see when they leave negative feedback as opposed to positive feedback, but both of those messages must still offer the option to leave a public review. However, if you create your message in such a way as to communicate to the patient who may leave negative feedback that you are working hard on resolving the issue and that someone will be in touch shortly, that may prevent them from leaving a public negative review.
When you receive a public review on Google, Facebook, or other review sites, make sure that you respond to it – either by thanking them for a good review or by asking them to contact you to discuss how you can improve their experience. Do not argue or try to defend yourself online – try to speak about it with them privately, fix the issue, and ask them to remove the review if possible. When you receive great reviews, make sure to cross-share them on your various social media platforms. You should also create a “Reviews” page on your website and add all great reviews to this page. This instantly adds credibility to your website.
Finally, make sure that when you look over the feedback and reviews that you receive, you are paying attention to what the negative reviews are saying – this is a great opportunity to identify current process challenges and improve your patients’ experience at your practice. Need help managing your practice’s online reputation? Visit www.lms-plus.com to see how Leading Marketing Solutions can help.
Sonda Eunus is the CEO of Leading Marketing Solutions, a Marketing Agency working with Medical Practices and other Businesses to help them identify the best marketing strategies for their business, create a strong online presence, and automate their marketing processes for a better return on their Marketing budget. Learn more about Leading Marketing Solutions at www.lms-plus.com.
FLORIDA MD - MAY/JUNE 2024 9 MARKETING YOUR PRACTICE
Halotherapy
By Daniel T. Layish, MD, FACP, FCCP, FAASM
The word Halotherapy comes from the Greek word “halos” meaning salt. While the potential benefits and therapeutic nature of salt has been known for centuries, it was not until the early 1800’s that the underground salt mines throughout Eastern Europe were noted to benefit various respiratory conditions. As the workers were mining the salt in these climate-enriched chambers, dry salt particles would be inhaled into the respiratory system. The dry salt was discovered to be super absorbent, anti-bacterial and anti-inflammatory. Soon people with various conditions were spending time in these salt mines. In the mid-1900’s the Russians began working on a technology to replicate the dry salt particles in the air and developed the first halogenerator, a device that grinds pure sodium chloride into precise particles (several microns in diameter) and disperses the dry salt into a climate controlled room or chamber. This was the start of modern Halotherapy, which has been utilized for several decades throughout Eastern Europe and has begun to expand into many other countries including the United States and Canada. The small particle size is felt to be important to allow penetration deep into the lungs, since larger particles will simply be deposited in the nose, throat or large airways. The air in a halotherapy chamber is also filtered to remove contaminants and the temperature and humidity are well controlled.
As a pulmonologist, I initially became familiar with halotherapy through my care of individuals with Cystic Fibrosis. Cystic Fibrosis is a genetic disorder characterized by dehydration of the respiratory epithelial surface, resulting in impaired mucociliary clearance. In this disorder, thick tenacious secretions obstruct the lower airway and sinuses and provide an environment for chronic infection. Nebulized hypertonic saline has been shown (in well done randomized clinical trials) to improve pulmonary function and respiratory symptoms as well as reduce pulmonary exacerbation rate in individuals with cystic fibrosis. This may be referred to as “wet” salt therapy as opposed to halotherapy which is “dry” salt therapy. Nebulized hypertonic saline can sometimes cause bronchospasm, and not all patients can tolerate this therapy even when premedicated with a bronchodilator. In cystic fibrosis, halotherapy has some theoretical advantages over nebulized hypertonic saline. The prolonged duration of therapy (typically a 45-minute session) appears to be associated with a much lower incidence of bronchospasm then is seen in the setting of nebulized hypertonic saline. In addition, in the halotherapy mode of administration the salt particles are delivered to both the sinuses and the lower respiratory tract. After seeing anecdotal benefit in our patients with cystic fibrosis, we performed a clinical study, which confirmed that this therapy was well tolerated and the patients derived symptomatic benefit in terms of their sinus complaints. Other studies are planned to study this therapy further in individuals with cystic fibrosis.
The fundamental defect in cystic fibrosis is related to chloride transport and therefore there is a strong rationale for halotherapy in this particular disease. Anecdotally, I have seen patients with other respiratory diseases derive significant benefit from

Halotherapy including bronchiectasis, chronic bronchitis, chronic sinusitis and allergic rhinitis. The hypothesis is that Halotherapy may help with respiratory illnesses by liquefaction of airway secretions thereby enhancing expectoration. There seems to be very little risk to this therapy other than the financial and time investment. There is certainly a theoretical basis for the possible benefit of halotherapy, given the known antiinflammatory and anti-infective properties of salt. Currently, halotherapy is not covered by medical insurance companies. However, it is hoped that this may change as research is planned to try to prove the benefits that many patients have reported. Many halotherapy institutions offer a monthly pass that can make therapy more affordable than purchasing individual sessions. There is also an effort to develop systems that can deliver halotherapy in the home setting, avoiding the need to travel to a salt room. This is important since many people do not live close to a halotherapy center. It is worth noting that many patients have also noticed benefits in non-respiratory conditions, particularly dermatalogic conditions such as acne and psoriasis and research is planned in this area as well.
References available upon request. I would like to thank Leo Tonkin and Ulle Pukk for reviewing this manuscript.
Daniel Layish, MD, graduated magna cum laude from Boston University Medical School in 1990. He then completed an Internal Medicine Residency at Barnes Hospital (Washington University) in St.Louis, Missouri and a Pulmonary/Critical Care/Sleep Medicine Fellowship at Duke University in Durham, North Carolina. Since 1997, he has been a member of the Central Florida Pulmonary Group in Orlando. He serves as Co-director of the Adult Cystic Fibrosis Program in Orlando. Dr. Layish serves as the medical advisor for the Just Breathe Salt Therapy Wellness Spa and also sits on the board of the Salt Therapy Association. He may be contacted at 407841-1100 or by visiting www.cfpulmonary.com.

FLORIDA MD - MAY/JUNE 2024 10
PULMONARY AND SLEEP DISORDERS

Social Media – Five Things Physicians Should Never Post
By Julie A. Tyk, JD
Last year, Alaska dentist, Seth Lookhart, made national headlines for filming a video of himself riding a hoverboard while extracting a patient’s tooth. Dr. Lookhart filmed the procedure on a sedated patient without authorization and forwarded the video to several people. A lawsuit was filed by the State of Alaska in 2017 charging Dr. Lookhart with “unlawful dental acts”, saying his patient care did not meet professional standards. The lawsuit goes on to further allege Dr. Lookhart joked that performing oral surgery on a hoverboard was a “new standard of care,” citing phone records that were obtained. Dr. Lookhart has also been charged with medical assistance fraud for billing Medicaid for procedures that were not justified, unnecessary, and theft of $25,000 or more by diverting funds from Alaska Dental Arts. On Friday, January 17, 2020, Dr. Lookhart was convicted on 46 counts of felony medical assistance fraud, scheming to defraud, misdemeanor counts of illegally practicing dentistry and reckless endangerment. Dr. Lookhart is expected to be sentenced on April 30, 2020. He faces the possibility of up to 10 years in prison.
A doctor in Rhode Island was fired from a hospital and reprimanded by the state medical board. The hospital took away her privileges to work in the emergency room for posting information online about a trauma patient. The doctor’s post did not include the patient’s name, but she wrote enough that others in the community could identify the patient, according to a board filing.
The popularity of social media has exploded in recent years. According to a recent PEW report, 70% of Americans use social media. Before jumping on the bandwagon, healthcare professionals are advised to be mindful of the possible ramifications of posting information on social media sites. There are numerous legal issues that can arise when healthcare providers use social media, including issues related to patient privacy, fraud and abuse, tax-exempt status, and physician licensing. The Federation of State Medical Boards has issued the Model Guidelines for the Appropriate Use of Social Media and Social Networking in Medical Practice, which contains the “industry standards” for cyber security, online behavior, and patient privacy. Physicians should familiarize themselves with these guidelines.
Five things which physicians should never post to social media.
1. Inaccurate Medical Information: Medical professionals should avoid republishing, sharing, “liking,” or “retweeting” news stories about medical treatments unless they have completely read the story and have verified its accuracy. If a user finds inaccurate medical information through your social media channel, it can reflect very poorly upon you and your practice. Healthcare professionals also need to be careful about providing medical advice to patients using social media. If a patient receiving the medical advice from a doctor through social media is located in a state in which the doctor is not licensed, the doctor giving the advice risks liability under state licensing laws.
2. Do Not Post Anything that Violates Patient Confidentiality: Friending patients on social media sites may pose risks under Health Insurance Portability and Accountability Act (HIPAA) and state privacy laws. The fact that an individual is a patient of a healthcare provider falls within the types of health information

that these laws are designed to protect. As a rule, healthcare providers should not use social media to share any health information that could be linked to an individual patient, such as names, pictures, and physical descriptions, without the patient’s consent. The American College of Physicians recommends that doctors be especially aware of the implications for patient confidentiality when using social media. There have been cases of physicians losing their medical license after posting an image on social media that violated patient confidentiality. Always obtain permission from the patient in writing if you intend to use an image featuring any body part. Avoid talking about specific patients at all on social media unless you have permission to do so. Even if there is no chance that a patient could be identified by what you write on social media, it is considered unprofessional to discuss the specifics of their condition. Also be careful when taking photographs of yourself while in your practice. There have been cases where medical professionals have accidentally included the image of the patient behind them while taking a ‘selfie’. Make sure there are no patient health records on display when taking photos in the medical practice and no patients are included in photographs unless they want to be.
3. Your Personal Information: The American College of Physicians (ACP) and the Federation of State Medical Boards (FSMB) recommend that doctors create separate social media accounts for their professional and personal lives. They also suggest that the professional profile be more visible than any personal one.
4. Opinions on Controversial Issues: Any controversial topic or “hot button” topic should be avoided as much as possible, including anything to do with religion, politics, racism, abortion, and gun control. Moreover, healthcare providers that are exempt from taxation under Section 501(c)(3) of the Internal Revenue Code are prohibited from intervening in political campaigns and from seeking to influence legislation as a substantial part of their activities. This restriction may extend to advertising on or sponsoring social media sites that support a political candidate or particular pieces of legislation.
5. Complaints or Rants: It is unprofessional to use social media platforms to complain or rant about your professional situation. Everything you write on social media may one day come back to haunt you. A patient might realize that you were complaining about them on social media.
A medical malpractice claim can have far reaching implications. The Health Care Practice Group at Pearson Doyle Mohre and Pastis, LLP, is committed to assisting Clients in navigating and defending medical malpractice claims. For more information and assistance, please contact David Doyle and Julie Tyk at Pearson Doyle Mohre & Pastis, LLP.
Julie A. Tyk, JD, is a Partner with Pearson Doyle Mohre & Pastis, LLP. Julie concentrates her practice in medical practice defense litigation, insurance defense litigation and health care law. She has represented physicians, hospitals, ambulatory surgical centers, nurses and other health care providers across the state of Florida, and may be contacted by calling (407) 951-8523; jtyk@pdmplaw.com.

FLORIDA MD - MAY/JUNE 2024 12 HEALTHCARE LAW
ORTHOPEDICS CARE
Just for kids.

Kids and teens need prompt and innovative care specifically designed for their growing bodies. We offer family-centered, kid-friendly care right here in Central Florida. Our expert team, including board-certified and fellowship-trained physicians, uses advanced technologies to diagnose and treat an extensive range of conditions through our highly specialized pediatric orthopedics programs.
From common to rare, we treat disorders and injuries involving bones, joints, muscles and nerves at Nemours Children’s Hospital, as well as our other specialty locations in: Call 407.650.7715 to refer a patient. Well Beyond Medicine
• Downtown Orlando
• Lakeland
• Lake Mary
• Melbourne
• Narcoosee Road
• Winter Garden
FLORIDA MD - MAY/JUNE 2024
© 2021. The Nemours Foundation. ® Nemours is a registered trademark of The Nemours Foundation. J7676 (08/21)
Many Floridians Suffer From Arthrofibrotic Knees That Can Be Treated Successfully With
Minimally Invasive
By Bruce Levy, MD
Since arriving at Orlando Health Jewett Orthopedic Institute, I have seen numerous patients referred to us who are dealing with a relatively uncommon condition: arthrofibrosis of the knee. This debilitating condition can be seen following knee ligament reconstruction, trauma fracture surgery and after knee replacements to name a few. This condition can cause significant functional limitations to a patient, resulting in extreme stiffness in the joint, decreased range of motion, and even chronic pain. Surgical treatment in the form of arthroscopic releases and removal of scar tissue can offer patients a minimally invasive approach with published successful patient reported outcomes.
The causes of arthrofibrosis vary and the susceptibility of some patients over others is not fully understood. Usually, it develops following a traumatic insult to the joint, an infection, or with surgery; for example, following anterior cruciate ligament (ACL) surgery. ACL reconstruction is one of the most common orthopedic surgeries in the United States; by some estimates there are more than 250,000 such procedures performed every year. Although complications following ACL surgery are rare, at this volume, even a small percentage can mean a significant number.
Once arthrofibrosis begins, it can initiate a cascade of proinflammatory mediators which then drives the proliferation of fibroblasts. These fibroblasts secrete Transforming Growth Factor Beta (TGF-β), a crucial cytokine, that begins a positive feedback loop that generates more fibroblasts, which then generates more TGF- β, and so on. This in turn forms an extra-cellular matrix, causing more adhesions to form inside the joint, which in turn causes bursa (the little pouches and fluid pockets in the knee) to contract. The results are pain, stiffness and decreased range of motion.
During my time at the Mayo Clinic, along with my colleagues Abhinav Lamba BS, Charles L. Holliday MD, Erick M. Marigi MD, Anna K. Reinholz MD, Ryan R. Wilbur MD, Bryant M. Song MD, Mario Hevesi MD, PhD, Aaron J. Krych MD, and Michael J. Stuart MD, we published “Arthroscopic Lysis of Adhesions for Arthrofibrosis After Anterior Cruciate Ligament Reconstruction” (https://journals.sagepub.com/doi/abs/10.1177 /03635465231195366).
We showed that with a minimally invasive arthroscopic approach combined with medications to inhibit TGF- β and physical therapy, people can have very successful outcomes with regards to pain relief, improvement to range of motion, and overall improvement of function. We had a mean follow-up of 10 years, so this was a long-term study. The protocols we developed were the result of a lot of dedicated work and study by medical students, research fellows, and lead by my orthopedic partners at Mayo Dr. Matthew Abdel and Dr. Mark Morrey. These protocols
Surgery
have been shown to be effective in reducing the recurrence, at least, in people who are being treated for this disease.

The article was published in the American Journal of Sports Medicine (AJSM) and the AJSM editors followed it with an extensive podcast.
Because we saw a large number of referrals at Mayo and now at Orlando Health Jewett Orthopedic Institute, our techniques have continued to evolve. With these advancements we are now able to reach even the posterior aspects of the knee (back of the knee) joint and release the scar tissue trapped there.
Although we are encouraged by the results of these techniques, this surgery presents a number of significant risk factors, such as the potential for neurovascular injury in particular when in these posterior recesses of the knee joint. The joint spaces behind the knee in which we are making incisions to release the scar tissue tend to be very contracted and very narrow. The popliteal neurovascular structures are sometimes within millimeters of where we are operating.
To help mitigate these risks, in addition to the techniques we’ve developed, we need a team of other specialists. Earlier this spring, I took care of a young man from Pittsburgh who had already had several operations to help with his arthrofibrosis. Unfortunately, even after months of therapy he was unable to straighten his knee and walked with his knee bent the whole time. He was so scarred in the back of the knee that the popliteal artery (the main artery giving blood supply to the lower leg) was within millimeters from where we needed to work. After thoroughly discussing the risks with the patient and his family, we developed a plan that included having a vascular surgeon from Orlando Health on standby and all their necessary equipment ready to go in the operating room. It is imperative to be prepared for as many potential complications as possible.
And, of course, this is one of the advantages of having a dedicated orthopedic institute that is directly adjoined to a leading multi-disciplinary healthcare system like Orlando Health. Throughout the patient’s treatment, we are able to align a team of all of the specialists and care providers who are within steps of each other: orthopedic, vascular, neurological, anesthesia, radiology, physical therapy, and all of the support staff. Fortunately, we were able to remove all the scar tissue in his knee through our minimally invasive techniques and he is now able to fully straighten his knee and walk with a completely normal gait.
FLORIDA MD - MAY/JUNE 2024 14
ORTHOPEDICS
The most important thing for prospective patients to know is that there is help available. The decision to have surgery is certainly not one to be made lightly. You want to begin with all of the non-surgical modalities first. And then only consider surgery as a last resort. That said, we have clearly shown with data from several published studies that people with arthrofibrosis after knee surgery can be successfully helped with these minimally invasive techniques, and the results appear to be sustainable overtime.
Seven of our most recent published studies on arthrofibrosis are collected by the National Library of Medicine at this link: https:// pubmed.ncbi.nlm.nih.gov/?term=levy+ba+arthrofibrosis.
Our podcast on arthroscopic lysis of adhesions for arthrofibrosis is available at this link: https://sageorthopaedics.libsyn.com/ajsmoctober-podcast-arthroscopic-lysis-of-adhesions-for-arthrofibrosis-after-anterior-cruciate-ligament-reconstruction
Bruce Levy, MD, is a board-certified orthopedic and sports medicine surgeon with Orlando Health Jewett Orthopedic Institute. He also serves as the academic chief of sports medicine and the director of the Sports Medicine Surgical Fellowship program. Previously he was a professor of orthopedics and surgeon at the Mayo Clinic in Rochester, Minnesota. He is an editorial board member for numerous medical journals and has published more than 300 scientific papers.
DERMATOLOGY Continued from page 12
reimport medicines (a bill has been passed in Florida to allow reimportation, but it still faces an uphill battle for implementation). In other words, the United States is subsidizing the healthcare of the rest of the world by paying outrageous prices, allowing other countries to continue paying bargain-basement prices. Yet, we wonder why our healthcare costs so much here in America.
So how did I resolve the problem of the $8500 cream? Well, we sent the prescription to the local compounding pharmacy and had virtually the same medicine compounded up for $75. The patient did well and saved $8425 along the way. And what happened to the company that made Alcortin and raised the price thousands of dollars? Well, they went bankrupt. What goes around comes around.
Lucky Meisenheimer, M.D. is a board-certified dermatologist specializing in Mohs Surgery. He is the director of the Meisenheimer Clinic – Dermatology and Mohs Surgery. John Meisenheimer, VII is an MD practicing in Orlando.



FLORIDA MD - MAY/JUNE 2024 15
ORTHOPEDICS
FloridaMDMagazine.com Your Medical Business Resource Practice Management Advice
A Dream Recovery: Avyn’s Story – Giving Them Back Comfort, Confidence and a Chance to Soar
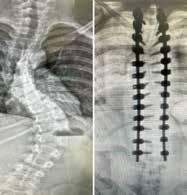
CAt just four years old, Avyn was diagnosed with a severe 60º curvature of Early Onset Scoliosis. Her local physicians recommended Mehta casting, prompting her family to begin searching for the best pediatric orthopedic specialists in the nation. Their search led them to Dr. Joseph Khoury in Florida and Dr. Alec Stall in Texas. The decision to choose between these two esteemed doctors wasn’t easy, but ultimately, Avyn’s family placed their trust in Dr. Khoury at Nemours Children’s Hospital, Florida.
“Avyn has been extremely resilient throughout her scoliosis journey,” says her mother, Sarah. Thanks to her treatments, Avyn’s curve progression slowed, allowing her to maintain her normal life, participating in athletics and daily activities with minimal discomfort. However, as she grew older, her family knew she would need a spinal fusion surgery at age 10.
“When it was time to schedule Avyn’s spinal fusion surgery, Dr. Khoury explained that Nemours required two surgeons to be present. Little did we know Dr. Alec Stall had transferred from Texas since our contact six years prior and would be the second surgeon taking care of our girl!” says Sarah. “Turns out we didn’t have to choose between the best of the best after all! Talk about peace of mind for us as parents!”
Avyn’s family’s experience at Nemours Children’s was nothing short of superb. “Dr. Khoury and his entire staff have been amazing since day one,” says Sarah. “On surgery day everyone was extremely knowledgeable, attentive, kind and overlyaccommodating, to Avyn and to us as two anxious parents. They kept our family informed and assured during our entire stay. Nurse Laura was especially wonderful to us.”
Avyn’s recovery from spinal fusion surgery exceeded expectations. Requiring minimal pain management postsurgery, she has seamlessly returned to school on schedule. “You’d never know she has two rods and 26 screws in her spine,” says Sarah.
Looking ahead, Avyn is optimistic about the future. Her plans include resuming normal activities like softball, dancing, gymnastics, and more after her six-month release. Avyn wants other patients to know, “Don’t be afraid. Keep your head up, and recovery will be here before you know it.” Her parents encourage others to know that their child is in the best hands at Nemours Children’s. “They will stop at nothing to take the very best care of your little one,” says Sarah.
In a testament to Avyn’s compassionate nature, she organized a tab drive for Ronald McDonald House, collecting an astonishing 4,196,160 tabs in a few months. This generous contribution resulted in a $3,162 donation, marking the largest tab donation the Ronald McDonald House of Central Florida had ever received.
By: Staff Writer
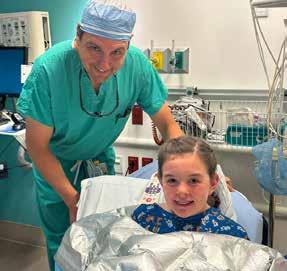
Avyn’s journey is an inspiration to all, reminding us that with faith and the right team, every challenge can be overcome. Call 407.650.7715 to refer a patient to the scoliosis experts at Nemours Children’s Health.

FLORIDA MD - MAY/JUNE 2024 16 PEDIATRICS NEMOURS CHILDREN’S HEALTH IS REDEFINING SCOLIOSIS CARE ONE PATIENT AT A TIME
Nemours Children’s orthopedic surgeon, Dr. Joseph Khoury, visits scoliosis patient, Avyn.
Nemours Children’s scoliosis patient, Avyn, is all smiles following her surgery.
Scoliosis patient, Avyn, underwent successful spine surgery at Nemours Children’s to address her severe curvature.
Why Debunking the Myths Around Epilepsy is Crucial for Our Patients –and Considerations For Women With the Condition
By Dipali Nemade, MD
For years, we as neurologists and physicians have seen discouragingly consistent reporting on widespread misperceptions, misunderstandings, and complete myths when it comes to epilepsy. These misconceptions impede our ability to offer all the three million Americans who suffer from some form of seizure disorder the help they need to lead their best lives.
A recent survey conducted by Orlando Health found that seizure misperceptions are widespread and that many people don’t recognize the lesser-known signs of seizures. Even though it is, as we know, a relatively common condition that can afflict anyone, we continue to see a social stigma and lack of basic understanding about it.
Let’s take a look at some of the most common misconceptions surrounding epilepsy and seizures that perhaps our patients and their families have brought to us:
1. People with epilepsy have lower-than-average IQs.
2. Epilepsy can be contagious.
3. Women with epilepsy should not become pregnant.
4. Flashing or strobing lights are a very common trigger of seizures in people with epilepsy.
5. If someone is having an epileptic seizure, there is nothing you can do.
6. Epilepsy is incurable.
These misperceptions are largely responsible for the stigmatization that surrounds the disease, and they sometimes interfere with patients getting the treatment they need and even assistance from bystanders when they are experiencing a seizure.
In light of this, I believe we as physicians need to conduct a more concerted effort to educate the public about epilepsy and seizure disorders so our patients can get the treatment they need and also decrease sudden unexpected deaths in epilepsy, or SUDEP, which claims about 3,000 lives in the U.S. each year.
Epilepsy is the fourth most common neurological disease after migraines, stroke, and Alzheimer’s. According to a 2021 National Health Interview Survey (NHIS), it affects about 3.4 million Americans, with about 150,000 Americans diagnosed each year. Over a lifetime, 1 in 26 people in the United States will be diagnosed with epilepsy.
Popular movies and television programs often show what I call “cinema seizures” when depicting epilepsy – people experiencing severe convulsions, foaming at the mouth, and other dramatic displays. Many television programs carry warnings that they contain flashing light sequences that may affect some people, but we know flashing lights trigger seizures in only about three percent of people with epilepsy.
EPILEPSY IN WOMEN

As a specialist in women with epilepsy, there is a misconception I frequently come across –and that is that people believe women with epilepsy shouldn’t become pregnant.
Although we know epilepsy does not discriminate by age or sex, there are some special considerations for women. Half of our total epilepsy patients – around 1.5 million – are women.
We should encourage all women in the reproductive age group who have epilepsy to see a neurologist or epileptologist before they plan to become pregnant so that a proper pathway can be laid to ensure the safety of the mother and baby during and after the pregnancy.
We need to have conversations with women of reproductive age groups and pregnant patients about what having epilepsy means for them during and after pregnancy. I emphasize the importance of taking anti-seizure medication before, during, and after the pregnancy for the safety of the mother and baby. With the whirlwind that comes along with being pregnant and having a baby (preparation, sleep deprivation, newborn care, etc.), I encourage my patients who are expecting to put measures in place that will ensure they do not forget to take their anti-seizure medication. One way I tell them to do this is to set a reminder or alarm on their phones to take it so it’s one less thing they have to remember on their own. I also advise them to make their obstetrician and prenatal care team aware of their epilepsy.
Another concern I hear from pregnant patients is about passing epilepsy to their children. After I evaluate the patient, I refer the patient to genetics testing and counseling if the genetic cause is suspected as we know certain types of epilepsy can be transmitted to children.
EDUCATING OUR PATIENTS ON HOW PEOPLE CAN HELP THEM
When someone appears to be having a heart attack or stroke, people around them are often quite good about rushing to help them. It should be no different with epilepsy. If our patients are having a seizure, people can help them.
Educating my patients on how to speak about their condition and inform their family, friends, coworkers, and neighbors about how to help them is a critical step in my care. This is another reason why working to debunk the myths around epilepsy and spread awareness about the symptoms is so vital in helping our patients and preventing SUDEP.
FLORIDA MD - MAY/JUNE 2024 17 Continued on page 18
WHY WE FOCUS ON COLLABORATIVE CARE
Our new Orlando Health Neuroscience Institute facility is adjacent to Orlando Health Orlando Regional Medical Center, which for over 100 years has provided the most advanced options available for surgical, medical, rehabilitative, and emergency care, including serving as Central Florida’s only Level 1 Trauma Center. Our multidisciplinary team at the Orlando Health Neuroscience Institute includes more than 45 physicians and more than 20 advanced care providers who offer next-level treatments and technology tailored to patients’ unique needs. At our institute, we are focused on collaborative care among our specialists, particularly our epileptologists.
With a new medical office building in the heart of downtown Orlando, our neurologists, neurosurgeons, and interventional spine and pain management specialists now work under one roof. This makes it easy for us to consult with each other, and for example in cases of epilepsy when neurosurgery may be needed, we can come together to determine the best course of action for our patients.
Most importantly for us, we are a level 4 epilepsy center. That means we provide more complex forms of intensive neurodiagnostic monitoring, as well as more extensive medical, neuropsychological, and psychosocial treatment. We also offer a complete evaluation for epilepsy surgery, including intracranial electrodes, cortical mapping/ functional mapping, and a broad range of surgical procedures for epilepsy (resection, ablation (LITT), and neuromodulation
(RNS, DBS, and VNS), etc. Orlando Health ORMC houses our Epilepsy Monitoring Unit (neurodiagnostic monitoring unit), where we work with our team to observe patients’ brain activity (EEG) and record what happens before, during, and after a seizure. This greatly helps us determine the most effective treatment plan as efficiently as possible as noted before.
Dr. Dipali Nemade is a board-certified epileptologist and neurologist at the Orlando Health Neuroscience Institute.
Dr. Nemade believes in providing high-quality and individualized care with the latest advanced epilepsy treatments. Her comprehensive approach toward epilepsy management includes EEG, sEEG, and brain mapping, diagnostic neuroimaging, and collaboration with neurosurgeons, neuropsychologists, and neuroradiologists.
76 W. Underwood St., 2nd Floor • Orlando, FL 32806
Call: (321) 841-2800
Fax: (321) 843-8777
Office Hours:
Monday - Thursday, 8:00 am - 5:00 pm Friday, 8:00 am - 2:00 pm

FLORIDA MD - MAY/JUNE 2024 18
Central Florida Real Estate Market Report
By Frank Ricci, Medical/Dental Real Estate Specialist, Licensed Broker & Building Contractor
Welcome to our third installment in a series about medical/dental real estate in Central Florida. Today we are going to review the fastest growing areas of Central Florida. This region encompasses Orange, Seminole, Osceola, Lake, Brevard and Volusia counties. Each of these counties has seen a surge in housing development driven by various demographic trends and economic factors.
For medical/dental professionals looking to start a new practice, expand their existing practice or considering going out on their own, this article will highlight areas around central Florida to consider where a considerable number of new homes are being built, thereby creating new markets with fewer competitors. However, this does NOT preclude significant opportunities in already established neighborhoods where many practitioners are retiring or scaling back their practices.
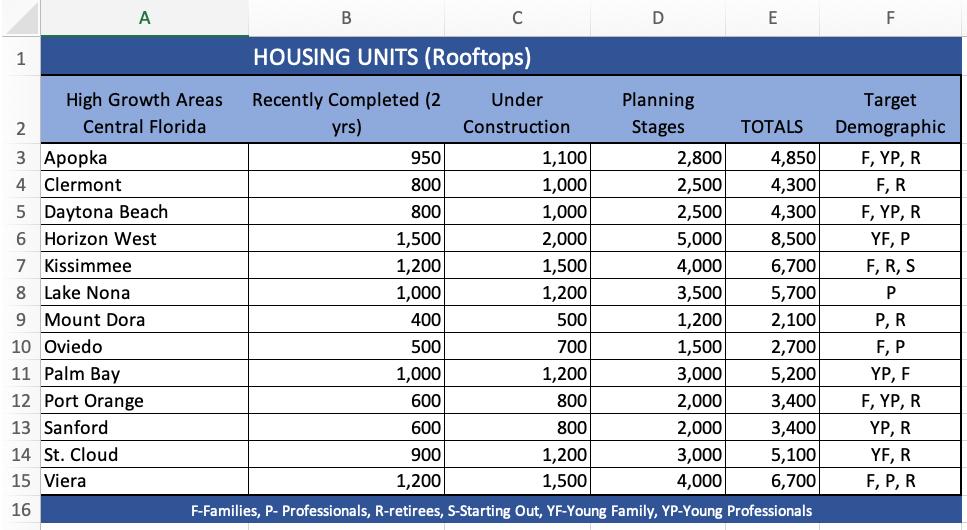
This article delves into the fastest-growing areas in Central Florida by housing units and explores the targeted homebuyer and renter demographics shaping these communities. By understanding the targeted demographics, we are better able to determine the types of practices that would benefit the most by locating there.
ORANGE COUNTY: Key Areas of Growth:
1. Lake Nona:
• Planned Housing Units: Approximately 3,500 units are planned.
• Under Construction: Around 1,200 units are currently under construction.
• Recently Completed: Over 1,000 units have been completed in the last two years.
• Target Demographic: Professionals, particularly those in the medical and tech industries, due to the proximity to the Lake Nona Medical City and the burgeoning tech hub.
2. Apopka:
• Planned Housing Units: Approximately 2,800 units are planned.
• Under Construction: Around 1,100 units are currently under construction.
• Recently Completed: Over 9500 units have been completed in the last two years.
• Target Demographic: Families, retirees and young professionals enjoy access to good schools, parks and excellent transportation.to major employers and attractions.
3. Horizon West:
• Planned Housing Units: Approximately 5,000 units are planned.
• Under Construction: About 2,000 units are currently under
construction.
• Recently Completed: Over 1,500 units have been completed in the last two years.
• Target Demographic: Young families and professionals, attracted by high-quality schools, recreational facilities, and convenient access to Orlando.

Demographic Trends: Orange County’s growth is fueled by its economy, anchored by the tourism sector and a growing tech industry. The area attracts young professionals and families seeking employment opportunities and a high quality of life.
SEMINOLE COUNTY: Key Areas of Growth:
1. Sanford:
• Planned Housing Units: Around 2,000 units are planned.
• Under Construction: Approximately 800 units are currently under construction.
• Recently Completed: About 600 units have been completed in the last two years.
• Target Demographic: Retirees and young professionals drawn by the mix of historic charm and modern amenities.
2. Oviedo:
• Planned Housing Units: Around 1,500 units are planned.
• Under Construction: About 700 units are currently under construction.
• Recently Completed: Approximately 500 units have been completed in the last two years.
• Target Demographic: Families and professionals, attracted by top-rated schools and family-friendly neighborhoods. Demographic Trends: Seminole County appeals to those seeking a balance between suburban living and proximity to Orlando’s urban amenities. Its excellent school system, access to parks and recreational areas make it a prime location for families.
OSCEOLA COUNTY: Key Areas of Growth:
1. Kissimmee:
• Planned Housing Units: Approximately 4,000 units are planned.
• Under Construction: Around 1,500 units are currently under construction.
• Recently Completed: Over 1,200 units have been completed in the last two years.
• Target Demographic: A diverse mix of families, retirees, and hospitality industry workers, benefiting from the area’s affordability and proximity to major attractions.
Continued on page 20
FLORIDA MD - MAY/JUNE 2024 19
2. St. Cloud:
• Planned Housing Units: Approximately 3,000 units are planned.
• Under Construction: About 1,200 units are currently under construction.
• Recently Completed: Around 900 units have been completed in the last two years.
• Target Demographic: Young families and retirees, attracted by the small-town feel and affordable housing options.
Demographic Trends: Osceola County’s growth is driven by its affordability and diverse population. The county attracts a wide range of residents, including those working in nearby Orlando and the tourism sector.
LAKE COUNTY: Key Areas of Growth:
1. Clermont:
• Planned Housing Units: Approximately 2,500 units are planned.
• Under Construction: Around 1,000 units are currently under construction.
• Recently Completed: About 800 units have been completed in the last two years.
• Target Demographic: Families and retirees, drawn by the scenic landscapes, recreational opportunities, and growing retail sector.
2. Mount Dora:
• Planned Housing Units: Around 1,200 units are planned.
• Under Construction: Approximately 500 units are currently under construction.
• Recently Completed: About 400 units have been completed in the last two years.
• Target Demographic: Retirees and professionals seeking a picturesque, small-town atmosphere with modern amenities.
Demographic Trends: Lake County appeals to those looking for a blend of natural beauty and modern living. The area’s lakes and rolling hills making it attractive to both retirees and active families.
BREVARD COUNTY: Key Areas of Growth:
1. Viera:
• Planned Housing Units: Approximately 4,000 units are planned.
• Under Construction: Around 1,500 units are currently under construction.
• Recently Completed: About 1,200 units have been completed in the last two years.
• Target Demographic: Families, professionals, and retirees, attracted by the area’s planned communities, recreational facilities, and proximity to the Space Coast.
2. Palm Bay:
• Planned Housing Units: Approximately 3,000 units are planned.
• Under Construction: Around 1,200 units are currently under construction.
• Recently Completed: Over 1,000 units have been completed in the last two years.
• Target Demographic: Young professionals and families, drawn by affordable housing and job opportunities in the tech and aerospace sectors.
Demographic Trends: Brevard County’s growth is closely tied to the aerospace industry and the Space Coast. The county attracts a mix of young professionals, families, and retirees, offering a unique blend of high-tech job opportunities and coastal living.
VOLUSIA COUNTY: Key Areas of Growth:
1. Daytona Beach:
o Planned Housing Units: Approximately 2,500 units are planned.
o Under Construction: Around 1,000 units are currently under construction.
o Recently Completed: About 800 units have been completed in the last two years.
o Target Demographic: A mix of retirees, young professionals, and families attracted by the coastal lifestyle and relatively affordable housing.
2. Port Orange:
o Planned Housing Units: Approximately 2,000 units are planned.
o Under Construction: About 800 units are currently under construction.
o Recently Completed: Around 600 units have been completed in the last two years.
o Target Demographic: Families, young professionals, and retirees, drawn by the proximity to beaches and recreational activities.
Demographic Trends: Volusia County’s growth is driven by its coastal location, abundant undeveloped property and a diverse range of residents. The county offers a mix of urban and suburban living with access to beautiful beaches, making it an appealing destination for retirees, families, and young professionals.
CONCLUSION
Central Florida’s rapid growth offers unparalleled opportunities to start/expand your practice and capture a significant and growing market share. However, to invest in these high growth areas will require diligence, expertise and careful analysis as appropriate sized land parcels are becoming more difficult to find and secure, especially for those looking to purchase and own their own facility. Add an experienced healthcare broker to your team to help you select and secure the best property available.
FLORIDA MD - MAY/JUNE 2024 20
Frank Ricci is president of Healthcare Realty & Development LLC and H R & D Construction Inc. and has over 30 years of medical real estate brokerage, construction and development experience. He can be reached at (407) 947-5074, or FrankR@HealthcareRealtyOnline.com or visit the company website at: www.HealthcareRealtyOnline.com. .



FLORIDA MD - MAY/JUNE 2024 21
A New Era in Severe Obstructive Sleep Apnea Treatment: FDA Clears Innovative Oral Medical Devices
By Tara M. Griffin, DMD, DBDSM, DASBA
At Sleep Solution Centers, we are here to provide safe, effective alternative treatment solutions to chronic sleep breathing disorders such as obstructive sleep apnea (OSA), and other related conditions. These options are ideal for patients who can’t tolerate traditional treatment methods such as a CPAP machine with low compliance and fear of having to endure a lifetime of wearing a mask while sleeping, or those not keen on invasive surgeries such as tonsil and adenoid removal or neurostimulation implant devices. Our goal is to bring a new dawn in treatment for such disorders that is safe, convenient, and non-invasive.
The recent FDA granting of the first-ever 510(k) clearance permitting the use of unique oral medical devices for the treatment of Severe OSA reflects an exceptional moment in the field of dentistry and medicine. It marks a grand stride towards a more integrative approach between the medical and dental communities, aiming to effectively and holistically treat OSA in patients across all severity levels.
For over 40 years, professionals in both the medical and dental industries have eagerly envisaged this momentous development. The recent FDA clearance implies that advanced oral medical devices, such as Vivos CARE devices, can cater to OSA patients with ground-breaking success rates—a blend of innovation and convenience that perfectly aligns with our philosophy at Sleep Solution Centers.
A study published in the esteemed Journal of Sleep Medicine substantiates the impressive efficacy of such oral medical devices. In the study, Vivos CARE demonstrated substantial reduction in apnea hypnopnea index (AHI) scores in a majority of OSA patients. Remarkably, 61% of the patients saw significant improvements in their OSA, with a full 26% experiencing complete resolution of their OSA symptoms and diagnosis–

an unprecedented breakthrough in OSA treatment! The resolution of OSA occurred when a sleep test was taken without any oral device in the patient’s mouth and the patient had an AHI < 5 with no diagnosis of OSA after treatment.

As the medical community scales up its understanding of the complex nature of OSA, the structure and functionality of the oral vault have emerged as paramount factors to this condition. This realization helps establish why collaboration with Sleep Solution Centers and airway-centered dentistry approaches like Vivos, is evolving as a unique game-changer providing transformative therapeutic alternatives for this condition that transcends traditional CPAP treatment.

The FDA’s decision to corroborate the application of oral medical devices for the treatment of mild to severe obstructive sleep apnea is surely a beacon of progress in the realm of patient care. Besides chronic OSA sufferers who have struggled to attain relief through traditional treatment methods, patients who prefer non-invasive treatments stand to benefit immensely from this development.
In light of this significant advancement, we urge physicians to consider these alternative treatment solutions to traditional CPAP, particularly for patients who are averse to a lifetime of continuous treatment or invasive surgeries. By referring them to specialized facilities such as Sleep Solution Centers, equipped with state-of-the-art advancements in oral appliance therapy as well as non-invasive adjunctive therapies, we can collectively contribute to a revolution in holistic and sustainable OSA management and/or resolution.
The FDA’s clearance of breakthrough oral medical devices for the treatment of mild to severe OSA marks the onset of a new
Continued on page 24
FLORIDA MD - MAY/JUNE 2024 22
The Vivos mRNA appliance
Sleep Solution Centers

era in OSA therapy. Our obligation is to ensure patients enjoy access to these transformative treatments and advance a sustainable and cross-disciplinary treatment outcome that holistically caters to OSA. This innovative approach bridges science and patient comfort to offer relief to patients in their long-standing battle against obstructive sleep apnea. Together, we can write a new chapter in the narrative of OSA treatment.
Sleep Solution Centers located in the heart of Medical City, Lake Nona, was co-founded by Dr’s Rupal Thakkar DMD and Tara M. Griffin DMD in March, 2024. We are both dentists by trade that have focused on treating sleep breathing disorders for the past 14 years of practice. The recent grand opening of Sleep Solution Centers marks our flagship medical center that solely treats the root cause of sleep breathing disorders and TMJ disorders for children and adults. With direct collaboration with our medical community, we aim to help revolutionize healthcare through early detection, prevention and treatment ensuring good quality sleep for a lifetime!
If you are interested in learning more about our practice, contact us at 407-502-0110 www.sleepsolutioncenters.com or info@sscln. com. References available upon request.
Tara M. Griffin, DMD, DBDSM, DASBA, graduated from Nova Southeastern University in 2006, with a doctorate in Dental Medicine. She became passionate about helping her patients breathe and sleep better and completed her Diplomate with the American Academy of Dental Sleep Medicine in 2011. In 2015, she completed her Diplomate with American Sleep and Breathing Academy. In 2016, she became a Clinical Advisor with Vivos Therapeutics to help educate and mentor doctors interested in the treatment of OSA with oral medical devices. She owned a private practice focused on sleep, TMD and general dentistry in the panhandle of Florida for 17 years before becoming the co-founder of Sleep Solution Centers in Medical City, Orlando in 2024. She may be contacted at 407-502-0110 or by visiting www.sleepsolutioncenters.com


FLORIDA MD - MAY/JUNE 2024 24

JANUARY – Digestive Disorders
Diabetes
2024
EDITORIAL CALENDAR
Florida MD is a monthly medical/business digital magazine for physicians..
Florida MD is emailed directly to healthcare providers in Orange, Seminole, Flagler, Volusia, Osceola, Polk, Brevard, Lake and Indian River counties. Cover stories spotlight extraordinary physicians affiliated with local clinics and hospitals. Special feature stories focus on new hospital programs or facilities, and other professional and healthcare related business topics. Local physician specialists and other professionals, affiliated with local businesses and organizations, write all other columns or articles about their respective specialty or profession. This local informative and interesting format is the main reason physicians take the time to read Florida MD.
It is hard to be aware of everything happening in the rapidly changing medical profession and doctors want to know more about new medical developments and technology, procedures, techniques, case studies, research, etc. in the different specialties. Especially when the information comes from a local physician specialist who they can call and discuss the column with or refer a patient. They also want to read about wealth management, financial issues, healthcare law, insurance issues and real estate opportunities. Again, they prefer it when that information comes from a local professional they can call and do business with. All advertisers have the opportunity to have a column or article related to their specialty or profession.
FEBRUARY – Cardiology
Heart Disease & Stroke
MARCH – Orthopaedics
Men’s Health
APRIL – Surgery
Scoliosis
MAY – Women’s Health
Advances in Cosmetic Surgery
JUNE – Allergies
Pulmonary & Sleep Disorders
JULY – Neurology / Neuroscience
Advances in Rehabilitation
AUGUST – Sports Medicine
Robotic Surgery
SEPTEMBER – Pediatrics & Advances in NICUs
Autism
OCTOBER – Cancer
Dermatology
NOVEMBER – Urology
Geriatric Medicine / Glaucoma
DECEMBER – Pain Management
Occupational Therapy
Please call 407.417.7400 for additional materials or information.

It’s not about counting the days.
It’s about making the days count.
18Hospice Palliative Care Grief Support
Featuring specialized programs and services for children to seniors, and a proud Level 5 We Honor Veterans program provider. (866) 269-4240 I reflectionslsc.org





 Donald B. Rauhofer Publisher
Donald B. Rauhofer Publisher