PAINMEDICINE ACASE-BASED LEARNINGSERIES
TheSpine
STEVEND.WALDMAN,MD,JD
Elsevier
1600JohnF.KennedyBlvd. Ste1800 Philadelphia,PA19103-2899
PAINMEDICINE:ACASE-BASEDLEARNINGSERIES THESPINE
Copyright © 2022byElsevier,Inc.Allrightsreserved
ISBN:978-0-323-75636-5
Allunnumberedfiguresare ©ShutterstockCh1#450846769,Ch2#119077213,Ch3#523752955, Ch4#1029126937,Ch5#797324008,Ch6#682553182,Ch7#51781282,Ch8#1080607136, Ch9#1145461898,Ch10#561008035,Ch11#1491945620,Ch12#514912501,Ch13#725790448, Ch14#1362404147,Ch15#278451497.
Nopartofthispublicationmaybereproducedortransmittedinanyformorbyanymeans, electronicormechanical,includingphotocopying,recording,oranyinformationstorageand retrievalsystem,withoutpermissioninwritingfromthepublisher.Detailsonhowtoseek permission,furtherinformationaboutthePublisher’spermissionspoliciesandourarrangements withorganizationssuchastheCopyrightClearanceCenterandtheCopyrightLicensingAgency, canbefoundatourwebsite: www.elsevier.com/permissions
Thisbookandtheindividualcontributionscontainedinitareprotectedundercopyrightbythe Publisher(otherthanasmaybenotedherein).
Notice
Practitionersandresearchersmustalwaysrelyontheirownexperienceandknowledgein evaluatingandusinganyinformation,methods,compoundsorexperimentsdescribedherein. Becauseofrapidadvancesinthemedicalsciences,inparticular,independentverificationof diagnosesanddrugdosagesshouldbemade.Tothefullestextentofthelaw,noresponsibility isassumedbyElsevier,authors,editorsorcontributorsforanyinjuryand/ordamageto personsorpropertyasamatterofproductsliability,negligenceorotherwise,orfromanyuse oroperationofanymethods,products,instructions,orideascontainedinthematerialherein.
LibraryofCongressControlNumber:2020950564
ExecutiveContentStrategist: MichaelHouston
ContentDevelopmentSpecialist: JeannineCarrado/LauraKlien
Director,ContentDevelopment: EllenWurm-Cutter
PublishingServicesManager: ShereenJameel
SeniorProjectManager: KarthikeyanMurthy
DesignDirection: AmyBuxton
PrintedinIndia.
Lastdigitistheprintnumber: 987654321
It’s Harder Than It Looks
MAKING THE CASE FOR CASE-BASED LEARNING
For sake of full disclosure, I was one of those guys. You know, the ones who wax poetic about how hard it is to teach our students how to do procedures. Let me tell you, teaching folks how to do epidurals on women in labor certainly takes its toll on the coronary arteries. It’ s true, I am amazing. . .I am great. . .I have nerves of steel. Yes, I could go on like this for hours. . .but you have heard it all before. But, it’ s again that time of year when our new students sit eagerly before us, full of hope and dreams. . .and that harsh reality comes slamming home. . .it is a lot harder to teach beginning medical students “doctoring” than it looks.
A few years ago, I was asked to teach first-year medical and physician assistant students how to take a history and perform a basic physical exam. In my mind I thought “this should be easy. . .no big deal” . I won ’t have to do much more than show up. After all, I was the guy who wrote that amazing book on physical diagnosis. After all, I had been teaching medical students, residents, and fellows how to do highly technical (and dangerous, I might add) interventional pain management procedures since right after the Civil War. Seriously, it was no big deal...I could do it in my sleep with one arm tied behind my back blah blah blah.
For those of you who have had the privilege of teaching “doctoring,” you already know what I am going to say next. It’s harder than it looks! Let me repeat this to disabuse any of you who, like me, didn’t get it the first time. It is harder than it looks! I only had to meet with my first-year medical and physician assistant students a couple of times to get it through my thick skull: It really is harder than it looks. In case you are wondering, the reason that our students look back at us with those blank, confused, bored, and ultimately dismissive looks is simple: They lack context. That’ s right, they lack the context to understand what we are talking about.
It’ s really that simple. . .or hard. . .depending on your point of view or stubbornness, as the case may be. To understand why context is king, you have to look only as far as something as basic as the Review of Systems. The Review of Systems is about as basic as it gets, yet why is it so perplexing to our students? Context. I guess it should come as no surprise to anyone that the student is completely lost when you talk about let’ s say the “constitutional” portion of the Review of Systems, without the context of what a specific constitutional finding, say a fever or chills, might mean to a patient who is suffering from the acute onset of headaches. If you tell the student that you need to ask about fever, chills, and the other “constitutional” stuff and you take it no further, you might as well be talking about the
InternationalSpaceStation.Justsaveyourbreath;itmakesabsolutelynosenseto yourstudents.Yes,theywanttoplease,sotheywillmemorizetheelementsofthe ReviewofSystems,butthatisaboutasfarasitgoes.Ontheotherhand,ifyoupresentthecaseofJannettePatton,a28-year-oldfirst-yearmedicalresidentwithafever andheadache,youcanseethelightsstarttocomeon.Bytheway,thisiswhat Jannettelookslike,andasyoucansee,Jannetteissickerthanadog.This,atitsmost basiclevel,iswhat Case-BasedLearning isallabout.

Iwouldliketotell youthat,smartguy thatIam,Iimmediatelysawthelight andbecameaconvert to Case-BasedLearning. Buttruthbetold,it wasCOVID-19that reallygotmethinkingabout Case-Based Learning.Beforethe COVID-19pandemic, Icouldjustdragthestudentsdowntothemed/surgwardsandwalkintoa patientroomandriff.Everyonewasawinner.Forthemostpart,thepatients lovedtoplayalongandthoughtitwascool.ThepatientandthebedsidewasallI neededtoprovidethecontextthatwasnecessarytoillustratewhatIwastrying toteach thewhyheadacheandfeverdon’tmixkindofstuff.HadCOVID-19 notrudelydisruptedmyabilitytoteachatthebedside,Isuspectthatyouwould notbereadingthis Preface,asIwouldnothavehadtowriteit.Withinaveryfew daysaftertheCOVID-19pandemichit,mydaysofbedsideteachingdisappeared,butmystudentsstillneededcontext.Thisgotmefocusedonhowto providethecontexttheyneeded.Theanswerwas,ofcourse, Case-BasedLearning. Whatstartedasadesiretoprovidecontext becauseitreallywas harderthanit looked ledmetobeginworkonthiseight-volume Case-BasedLearning textbookseries.Whatyouwillfindwithinthesevolumesareabunchoffun,real-life casesthathelpmakeeachpatientcomealiveforthestudent.Thesecasesprovide thecontextualteachingpointsthatmakeiteasyfortheteachertoexplainwhy, whenJannette’schiefcomplaintis, “MyheadiskillingmeandI’vegotafever,” itis abigdeal.
Havefun!
StevenD.Waldman,MD,JD
Spring2021
Averyspecialthankstomyeditors,MichaelHouston,PhD,JeannineCarrado, andKarthikeyanMurthy,foralloftheirhardworkandperseveranceintheface ofdisaster.GreateditorssuchasMichael,Jeannine,andKarthikeyanmaketheir authorslookgreat,fortheynotonlyunderstandhowtobringtheThreeCsof greatwriting...Clarity 1 Consistency 1 Conciseness...totheauthor’swork,but unlikeme,theycanactuallypunctuateandspell!
StevenD.Waldman,MD,JD
P.S. ...Sorryforalltheellipses,guys!
MimiBraverman
A68-Year-OldFemaleWith AcuteWorseningNeckand OccipitalPain
LEARNINGOBJECTIVES
• Learnhowrheumatoidarthritisaffectsthecervicalspine.
• Developahighindexofsuspicionforthepotentialforlife-threatening complicationsofunrecognizedrheumatoidarthritis-inducedatlantoaxial instability.
• Learntoidentifyriskfactorsassociatedwithanincreasedincidenceof rheumatoidarthritisaffectingthecervicalspine.
• Learntheclinicalpresentationofatlantoaxialinstabilitysecondarytorheumatoid arthritis.
• Learntheclassicclinicalpresentationofrheumatoidarthritisaffectingthehands.
• Understandtheroleoflaboratorytestingandimagingintheevaluationof rheumatoidarthritis-inducedatlantoaxialinstability.
• Learntoidentifytheneurologicfindingsassociatedwithcervicalmyelopathy.
• Developanunderstandingoftheroleofdisease-modifyingdrugsinthe preventionofrheumatoidarthritis-induceddamagetothecervicalspine.
MimiBraverman
MimiBravermanisa68-year-old femalewiththechiefcomplaintof, “IknowthatyouwillthinkI’ mcrazy, butitfeelslikemyheadisgoingtofall off.” Mrs.Bravermansaidthatshe knew “somethingwasn’trightwith herhead” forseveralmonths.Shehad attributedtheheadandneckdiscomfortto “oldage” andshechoseto “justlivewiththepain.” Anavidknitter,itwasn’tuntilacoupleofweeks ago,whenshelookeddownather knitting,thatshefeltandhearda “clunk” inherneck.Thepatientnotedthatthe “clunk” reallyscaredherandshewasworriedthat “somethingwasreally wrong. ” Shesaidthatthe “clunk” happenedacoupleofmoretimesanditscared hersomuchthatnowshewasafraidtoknit...eventhoughtheoccupational therapisttoldherthat “knittingwasgoodforherhands.”
Whenthepatientwasaskedtouseonefingertopointtotheareawherethe “clunk” camefrom,shepointedtotheposteriorocciput.Thepatientnotedthat whenshelookeddown,painshotupintothebackofherheadaswellasintoher faceandear.Shealsonotedthatshefeltsuddenelectricshocksthatwentfrom thebackofherheaddownintoherarms.Thepainwentawayassoonasshe raisedherhead.Whenaskedtodescribethecharacterofthepain,thepatient statedthatthepaininthebackofherheadfeltlikewhenyourleggoestosleep,a kindofpinsandneedlessensation.Shenotedthatthepaindownherarmswas different...thatitwaslikeanelectricshock.Whenaskedwhatmadeherpain worse,shestatedemphaticallythatitonlyoccurredwhenshelookeddown. Whenaskedwhatmadeherpainbetter,shesaid, “lookingup.” Thepatientrated herpainasa5ona1to10verbalanaloguescalewith10beingtheworstand 1beingthemildest.
Whenaskedaboutassociatedsymptoms,Mrs.Bravermannotedthatsince shebeganhavingthe “clunking” sensation,thatshewasalso “losingurine” and hadhadseveralaccidentswhenshedidn’tmakeittothebathroom.Whenquestioned,sheadmittedthatshenoticedthatherbottomwasnumbwhenshewiped aftergoingtothebathroom.
Onphysicalexamination,thepatientwasnormotensiveandafebrile.Hercognitionwasnormal,aswashernutritionalstatus.Bilateralcataractswerenotedin bothofhereyes.Hercardiopulmonaryexaminationwasunremarkable,aswas herabdominalexaminationTherewasnoperipheraledema.
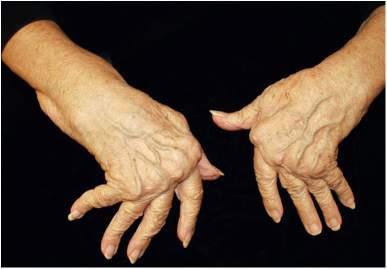
Fig.1.1 Ulnardrift.(FromChungKC,PushmanAG.Currentconceptsinthemanagementofthe rheumatoidhand. JHandSurg.2011;36(4):736 747,Fig.4.)
Examinationofthehandsrevealedsevereulnardriftbilaterally(Fig.1.1).No activesynovitiswasnoted.Examinationofherfeetrevealedseverearthritis. Carefulexaminationofthecervicalspinerevealedcrepituswithflexion.At about30degreesofflexion,anaudibleandpalpableclunkwasappreciated.This clunkelicitedapositiveLhermitte’ssign.Whenthecervicalspinewasreturned totheneutralposition,thepatientnotedthattheshocklikepaincompletely disappeared.
Thepatient’sneurologicexaminationrevealedthatthepatienthadan unsteadygait.Examinationofthedeeptendonreflexesoftheupperandlower extremitiesrevealedhyperreflexiathroughout.Babinskisignwaspresent,as wasHoffman’ssign(Videos1.1 and 1.2 onExpertConsult).Clonuswasnotpresent.Sensoryexaminationrevealednoevidenceofperipheralorentrapmentneuropathy,buttherewasdecreasedrectalsphinctertoneandperinealnumbness.
KeyClinicalPoints
THEHISTORY
’ Chiefcomplaintof “itfeelslikemyheadisgoingtofalloff”
’ Recentonsetofa “clunking” sensationandsoundinMimi’suppercervicalspine
’ Pinsandneedles-likepaininposteriorocciput
’ Electricshocklikepainradiatingdownupperextremitiesbilaterally
’ Shortdurationofsymptomsassociatedwithflexionofcervicalspine
’ Symptomstriggeredbyflexionofcervicalspine
’ Symptomsrelievedbyreturningcervicalspinetoneutralposition
’ Urinaryandfecalincontinence
’ Perinealnumbness
’ Handclumsiness
Video1.1 DemonstrationoftheBabinskisign.
Video1.2 TheHoffman’sreflex.ThevideodemonstratesapositiveHoffman’sreflex.
THEPHYSICALEXAMINATION
’ Thepatientisscaredandupset
’ Patientthoughtshehadcancer
’ Bilateralhanddeformities ulnardrift(see Fig.1.1)
’ Decreasedrangeofmotionofaffectedjoints
’ Bilateralfootdeformities
’ Decreasedrangeofmotionofwristandfingers
’ Crepitusonflexionofcervicalspine
’ Suddenpalpableandaudible “clunk” withflexionofthecervicalspine
’ ElicitationofLhermitte’ssignwithflexionofthecervicalspine
’ Unsteadygait
’ Hyperreflexicdeeptendonreflexesthroughout
’ Babinskisignpresent(see Video1.1 onExpertConsult)
’ Hoffmansignpresent(see Video1.2 onExpertConsult)
’ Perinealnumbness
’ Decreasedsphinctertone
OTHERFINDINGSOFNOTE
’ Bilateralcataracts
’ Normalcardiovascularexamination
’ Normalpulmonaryexamination
’ Normalabdominalexamination
’ Noperipheraledema
WhatTestsWouldYouOrder?
Thefollowingtestswereordered:
’ Rheumatoidfactorandanticitrullinatedproteinantibodytiters
’ Plainflexionandextensionradiographsofthecervicalspinewithopen mouthviewstoevaluatetheodontoid.Iaskedthattheradiologytechnician usegreatcarewhenflexingandextendingthecervicalspine.
’ Computedtomography(CT)scanofthecervicalspinetodocumentpreciselythe relativepositionoftheodontoidrelativetotheforamenmagnumandtoidentify thepresenceofotherbonyabnormalities,includingsubaxialsubluxation,that mightbecontributingtotheneurologic symptoms.Ialsohopedtodefinebetter whatwascausingcompromise ofthesubarachnoidspace.
’ Magneticresonanceimaging(MRI)ofthecervicalspinetoidentifyretroodontoidpseudotumorthatmightbecompromisingthecervicalspinal cord.Ialsowantedtotryandevaluatetheconditionofthetransverse ligamentandidentifyanyedemaand/orerosionoftheodontoidprocess,
aswellasidentifyanyofthejoints.Ialsohopedtoascertaintheappearance ofthecervicalspinalcord.
’ Somatosensory-evokedpotentialstoquantifythepresenceandextentof cervicalmyelopathy
TESTRESULTS
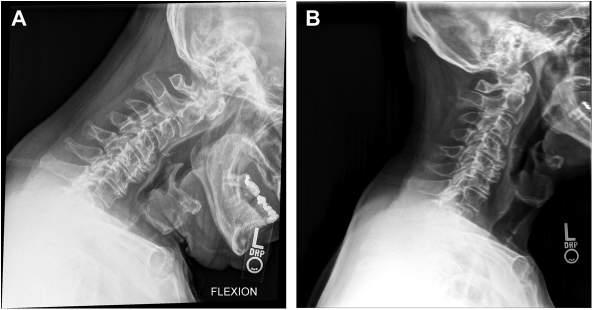
Asexpected,Mimi ’ srheumatoidfactorandantici trullinatedproteinantibody titersweremarkedlyelevated,confirmi ngmyclinicaldiagnosisofrheumatoid arthritis.GiventhedurationandextentofMimi ’ sdisease,itwasnotsurprisingthatallofherimagingresultswerem arkedlyabnormal.FlexionandextensioncervicalspineradiographsrevealedsignificantanteriorsubluxationofC1 onC2withananterioratlantodentali ntervalof5mm.Therewasextensive subaxialdiseasewithsubluxationofC3onC4anddiscspacenarrowing,anteriorosteophytosis,andfacetjointdiseaseofthelowercervicalspine( Fig.1.2 ).
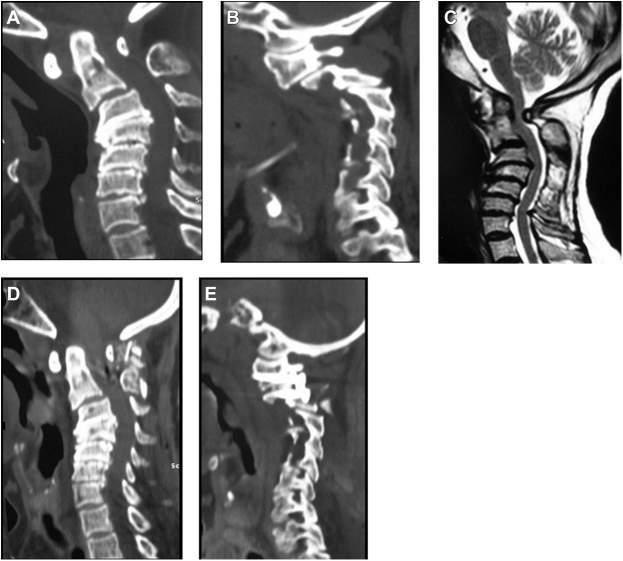
HerCTscanrevealedatlantoaxialdislocationandcervicalkyphosis( Fig.1.3 ).
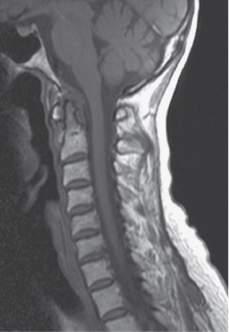
MRIscanofthecervicalspinerevealedatlantoaxialinstabilitywithproximal migrationoftheodontoidprocessandseverespinalcordcompressionat C3-C4.Thespinalcorddrapedovertheodontoidprocess( Fig.1.4 ). Somatosensory-evokedpotentialswereconsistentwithsignificantcervical myelopathy( Fig.1.5 ).
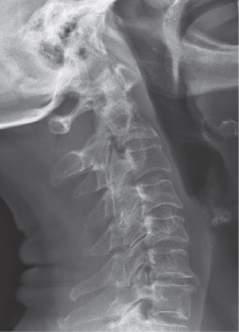
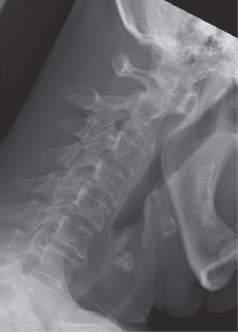
Fig.1.2 Plainlateralradiographsofthecervicalspineinflexion(A)andextension(B)revealsignificant anteriorsubluxationofC1onC2withananterioratlantodentalintervalof5mm.Thereisextensive subaxialdiseasewithsubluxationofC3onC4anddiscspacenarrowing,anteriorosteophytosis,and facetjointdiseaseofthelowercervicalspine.(FromDeQuattroK,ImbodenJB.Neurologicmanifestationsofrheumatoidarthritis. RheumDisClinNorthAm.2017;43(4):561 571,Fig.1.)
Fig.1.3 Computedtomography(CT)scanofthecervicalspineinanelderlyfemale.(A)Sagittalimage ofCTscanshowingatlantoaxialdislocationandcervicalkyphosis.(B)SagittalCTscanwithcutpassingthroughthefacets.Itshowstype1atlantoaxialfacetaldislocation.(FromGoelA,KaswaA,Shah A.Roleofatlantoaxialandsubaxialspinalinstabilityinpathogenesisofspinal “degeneration”—related cervicalkyphosis. WorldNeurosurg.2017;101:702 709,Fig.1A&B.)
ClinicalCorrelation—PuttingItAllTogether
Whatisthediagnosis?
’ Atlantoaxialinstabilitysecondarytorheumatoidarthritisinvolvingthe cervicalspine
TheScienceBehindtheDiagnosis
Theexactpathophysiologyofrheumatoidarthritisremainselusive,but recentresearchthathasledtothedevelopmentofnewerdisease-modifying agentssuggeststhatabnormalantigensproducedbysynovialcellselicitthe productionofmultipleautoantibodies.Themostimportantoftheseautoantibodiesappearstoberheumatoidfactorandanticitrullinatedproteinantibodies.Someinvestigatorsbelievethattheseantiautoantibodiesmayact synergisticallytocausethejointandorgansystemdamageassociatedwith rheumatoidarthritis(Fig.1.6).
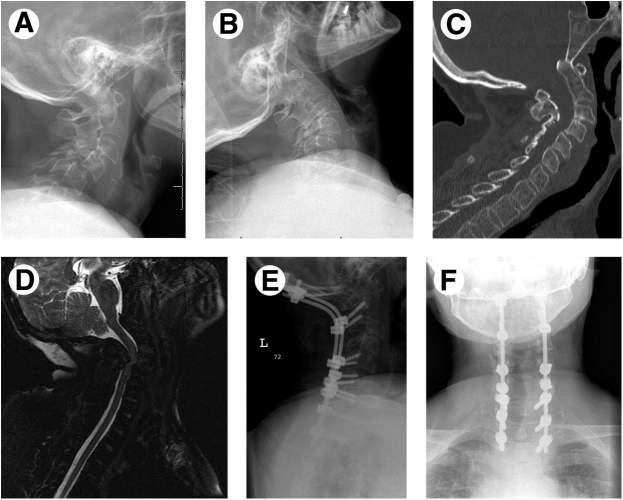
Fig.1.4 Treatmentofcombineddeformity:AIandsubaxialinstability.This39-year-oldwomanwith RAhadadvancedinvolvementofthecervicalspinewithAIandsubaxialinstabilitythatledtorapidprogressivemyelopathywithquadriparesis.(A)Flexionand(B)extensionviewsdemonstratesubaxial instabilityatC4andC5.(C)AIisshownmoreclearly,withproximalmigrationoftheodontoidprocess. (D)AnMRIT2sagittalview,depictingseverecordcompressionatC3-C4withthecorddrapedover theodontoidprocess.ThispatientwastreatedwithanocciputtoT2fusionwithC2-C6laminectomy (E,lateralview;F,anteroposteriorview).Sherecoveredenoughstrengthinherupperandlower extremitiestobeabletowalk30feetwithawalker.(FromHohlJB,GrabowskiG,DonaldsonWF. Cervicaldeformityinrheumatoidarthritis. SeminSpineSurg.2011;23(3):181 187,Fig.3C&D.)
Approximately80%ofpatientssufferingfromrheumatoidarthritiswillhave involvementofthecervicalspine.Riskfactorsforcervicalspineinvolvement, whicharelistedin Box1.1,includefemalegender,presenceofmarkersindicatinghigherdiseaseactivity,longdurationofdisease,delayinuseofdiseasemodifyingdrugs,andyoungerageatdiseaseonset.Theclinicalsignificanceof thisinvolvementcanrangefromasymptomatictolifethreatening.Although rheumatoidarthritishasthepotentialtoaffectallelementsofthecervicalspine, theatlantoaxialjoint(C1-C2)ismostcommonlyaffected(Figs.1.7,1.8,and 1.9). Ifthepatient’srheumatoidarthritisispoorlymanaged,inflammatorydestructionofthejoint,transverseligament,anderosionoftheodontoidprocess mayoccurwithresultantatlantoaxialjointinstability(Figs.1.10 and 1.11). Rheumatoidarthritis-inducedretro-odontoidpseudotumorformationcanexacerbatecompressionofthecervicalspinalcordatthislevelbycausingdirectcompressionofthespinalcordandbyweakeningthetransverseandalarligaments,
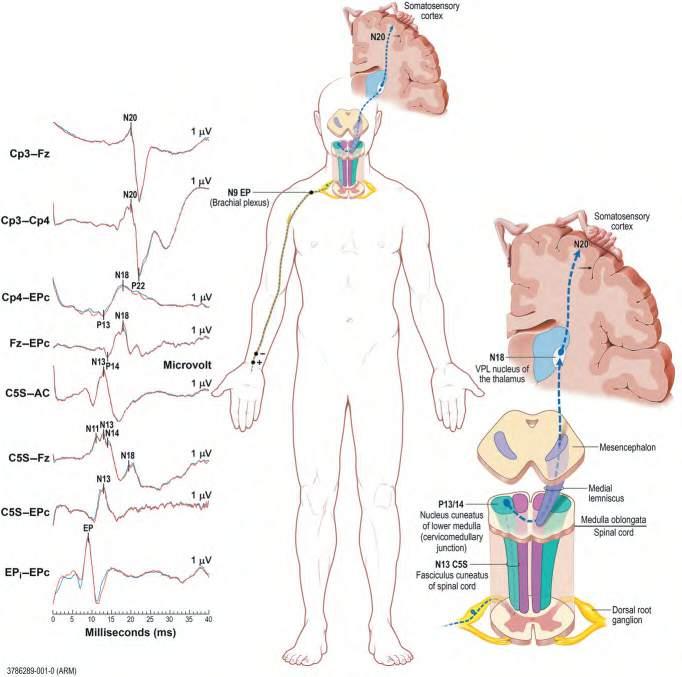
Fig.1.5 Cervicalsomatosensory-evokedresponsetesting. (FromLevinK,ChauvelP. Handbook ofClinicalNeurology.Vol.160.Amsterdam:Elsevier;2019:Fig.35.1.)
Fig.1.6 Overviewofthefactorsthatmaycontributetothedevelopmentofrheumatoidarthritis.(From vanDelftMAM,HuizingaWJ.Anoverviewofautoantibodiesinrheumatoidarthritis. JAutoimmun. 2020;110.)
BOX1.1 ’ RiskFactorsforCervicalSpineInvolvementinRheumatoid Arthritis
’ Femalegender
’ Presenceofmarkersindicatinghigherdiseaseactivity
’ Positiverheumatoidfactor
’ Significantlyelevatederythrocytesedimentationrate
’ HighC-reactiveproteinlevel
’ Highdiseaseactivityscore
’ Longdurationofdisease
’ Delayinuseofdisease-modifyingagents
’ Youngerageatdiseaseonset
Transverse ligament
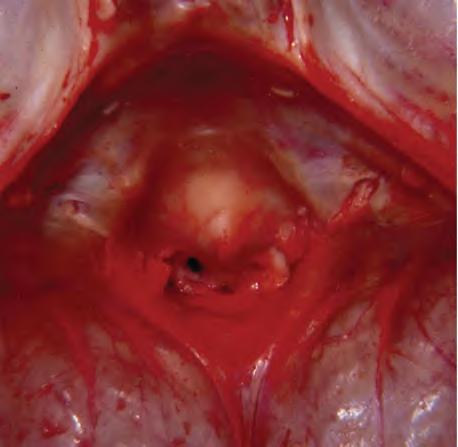
causingadditionalC1-C2instability(Figs.1.12 and 1.13).IftheC1-C2instability worsens,theodontoidprocessmaymigratesuperiorlyandimpingeonthe medullaandspinalcord(Fig.1.14).Complicatingtheclinicalpictureisthefact thatotherrheumatoidarthritis-inducedcervicalspineabnormalities,including subaxialsubluxationandfacetjointabnormalities,maycontributetothe patient’ssymptoms(see Figs.1.4 and 1.5).
Thephysicalfindingofulnardriftispathognomonicforrheumatoidarthritis (see Fig.1.1).Ulnardriftisthetermofartusedtodescribetwoseparaterheumatoidarthritis-inducedchangesofthemetacarpophalangealjoint:(1)ulnarrotationand(2)ulnarshift(Fig.1.15).Ulnarrotationistheresultofrotationofthe proximalphalanxintheulnaraxisrelativetothemetacarpalhead.Ulnarshiftis theresultofulnartranslationofthebaseoftheproximalphalanxrelativetothe metacarpalheads(see Fig.1.15).
Atlantoaxial joint
Dens
Articular facet for dens of axis
Atlas (C1) Axis (C2)
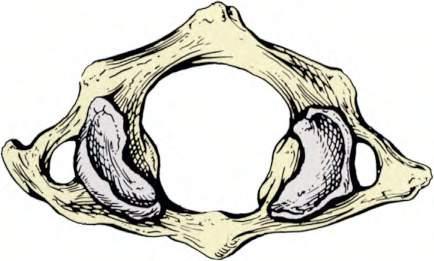
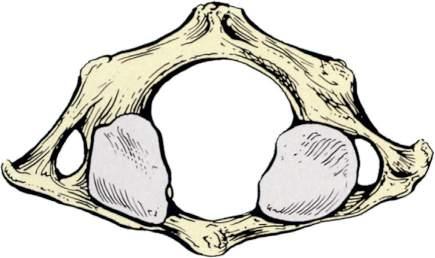
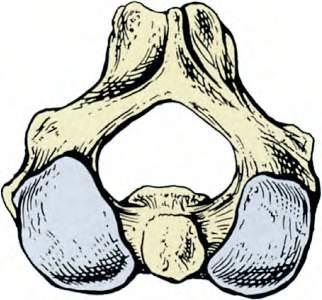
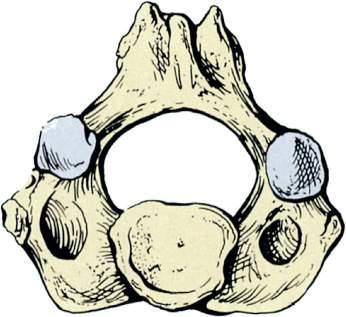
Fig.1.7 Anatomyoftheatlantoaxialjoint.
Posterior arch
Transverse process
Superior articular facet of superior articular process
Foramen of the transverse process
Groove for the vertebral artery
mass
Anterior arch
Inferior articular process (lateral surface)
articular process
Inferior articular facet of inferior articular process
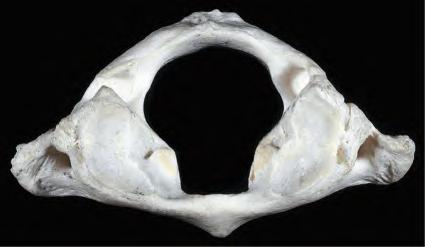
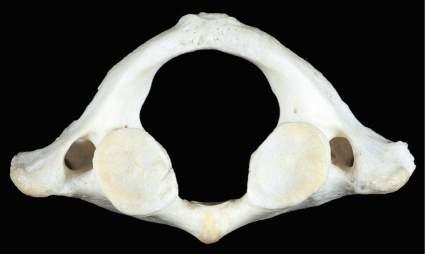
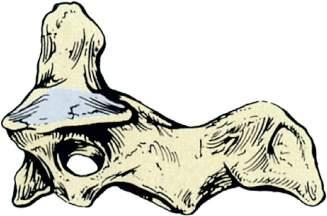
Fig.1.8 Atlas thefirstcervicalvertebra. Superior(A),inferior(B),and,lateral(C)viewsofthefirst cervicalvertebra theatlas.Superior(D),inferior(E),and,lateral(F)viewsofthefirstcervicalvertebra theatlas.(G)Close-up(superiorview)ofthelateralmassoftheatlas.Noticethecolliculusatlantisandsulcus(foveola)onthemedialsurfaceofthelateralmass.(FromCramerG,DarbyS. ClinicalAnatomyofthe Spine,SpinalCordandANS.3rded.St.Louis:Mosby;2014:135 209.)
Lateral
Posterior tubercle
Anterior tubercle
Superior
Posterior tubercle
Groove for the vertebral artery
Foramen of the transverse process
Foramen of the transverse process
Transverse process
(Continued).
Superior articular facet Transverse process
Inferior articular facet
Posterior ponticle
Arcuate (arcual) foramen
Posterior arch
Posterior tubercle
Anterior tubercle
Anterior tubercle
Anterior tubercle
Fig.1.8
MANAGEMENTANDTREATMENT
Posterior ponticle Transverse process
Superior articular facet
Oncethedamagecausedtotheatlantoaxialjointhasoccurred,thereisno effectivemedicationmanagement.Corticosteroidsmayprovidesome short-termsymptomaticrelief,butthereisnoevidencethattheycanprevent progressionofneurologicdeficitsoverthelongterm.Theuseofphysical modalitiesmayhelpprovidesymptomaticrelief.Asoftcervicalcollarmay helplimitflexionofthecervicalspine.Localheatmayprovidereliefofmusclespasms.Icepacksmayalsoprovidesymptomaticreliefoflocalizedpain andmusclespasm.
Onceatlantoaxialinstabilitysecond arytorheumatoidarthritis-induced damagetothecervicalspinehasoccurred,surgicalstabilizationisindicated. Studieshaveshownthatsurgicalstabi lizationnotonlyimprovesqualityof lifeandfunction,butalsoincreaseslifeexpectancyinthispatientpopulation. Surgicaloptionsavailableforthetreatm entofatlantoaxialinstabilityinclude (1)posteriortransarticularscrews,(2) posteriorsublaminarwiring,(3)Halifax clamping,and(4)screw-rodconstructs( Fig.1.16 ).Thechoiceofsurgical
Sulcus (foveola) atlantis Colliculus atlantis
Groove for the vertebral artery
Fig.1.8 (Continued).
Transverse process
Spinous process
Inferior articular facet
Lamina
Superior articular facet
Odontoid process
Superior articular facet
Groove for articulation with transverse ligament
Foramen of the transverse process
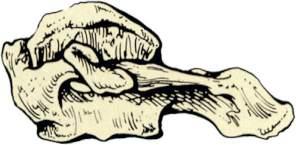
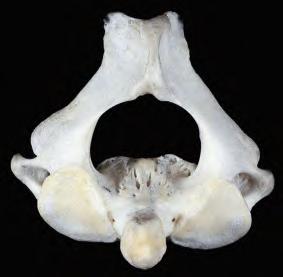
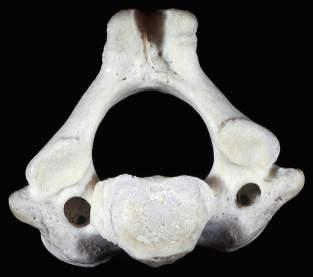
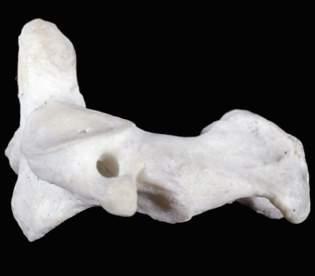
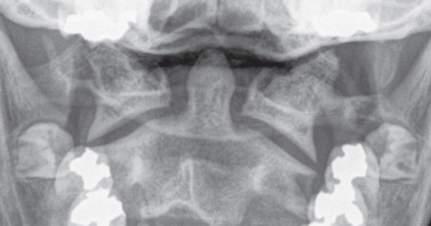
Fig.1.9 Axis thesecondcervicalvertebra. Superior(A),inferior(B),and,lateral(C)viewsofthe secondcervicalvertebra theaxis.Superior(D),inferior(E),and,lateral(F)viewsofthesecondcervicalvertebra theaxis.(G)Anterior-posterior “openmouth” viewoftheuppercervicalregionshowing theatlas,axis,andrelatedbonystructures.(FromCramerG,DarbyS. ClinicalAnatomyoftheSpine, SpinalCordandANS.3rded.St.Louis:Mosby;2014.)
Odontoid process (dens)
Lamina
Pedicle
Vertebral body A B
Odontoid process Superior articular facet
Odontoid process
Spinous process
Transverse process
Superior articular facet
Bifid spinous process
Inferior articular facet
Transverse process
Foramen of the transverse process
Vertebral body Foramen of the transverse process Inferior articular facet
(Continued).
Pedicle
Vertebral body
Fig.1.9
Fig.1.9 (Continued).
1. Odontoid process (dens)
2. C1 Lateral mass
3. C1 Transverse process
4. C1 Posterior arch
5. C2 Vertebral body
6. C2 Pedicle
7. C2 Spinous process
8. Odontoid-lateral mass space
9. Lateral atlanto-axial articulation
10. Styloid process
11. Unerupted third molar
A B C
Fig.1.10 (A)LateralradiographofthecervicalspineinextensionshowsnormalC1-C2alignment. (B)Oncervicalflexion,however,thereiswideningofthepredentalspaceowingtoC1-C2instability (double-headedarrow).(C)ThesagittalT1-weightedmagneticresonanceimageshowserosionofthe dorsalaspectoftheodontoidpeg.(FromWaldmanSD,CampbellRSD. ImagingofPain.Philadelphia: Saunders;2011:Fig24.1.)
techniquewillbedrivenbytheexperienceoftheoperatoraswellasthequality ofvertebralboneascorticosteroid-inducedosteoporosisisoftenpresent. Otherfactorsaffectingthechoiceofsurgicaltechniqueincludecoexistentsubaxialandatlanto-occipitalinstability.
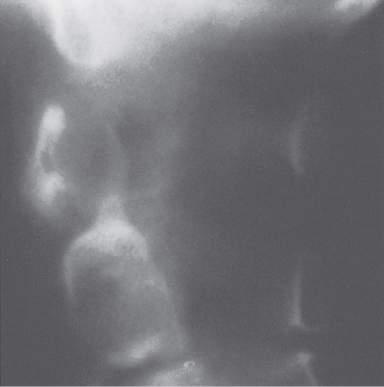
Fig.1.11 Abnormalitiesofthecervicalspine:odontoidprocesserosions. Lateralconventional tomogramrevealsseveredestructionoftheodontoidprocess (arrows),whichhasbeenreducedtoan irregular,pointedprotuberance.(FromResnickD,KransdorfMJ. BoneandJointImaging.3rded. Philadelphia:Saunders;2004:244.)
Retro-odontoid pseudotumor formation
Anterior arch of atlas
Base of skull
Posterior arch of atlas
Odontoid process
Fig.1.12 Rheumatoidarthritis-inducedretro-odontoidpseudotumorformationcanexacerbate compressionofthecervicalspinalcordatthislevelbydirectcompressionofthespinalcordandby weakeningthetransverseandalarligaments,causingadditionalC1-C2instability.
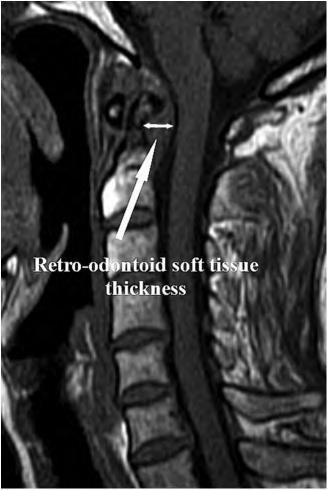
Fig.1.13 MidsagittalT1-weightedmagneticresonanceimagingshowingpresenceofretro-odontoid softtissue.(FromRyuJII,HanMH,CheongJH,etal.Theeffectsofclinicalfactorsandretroodontoidsofttissuethicknessonatlantoaxialinstabilityinpatientswithrheumatoidarthritis. World Neurosurg.2017;103:364 370,Fig.2.)
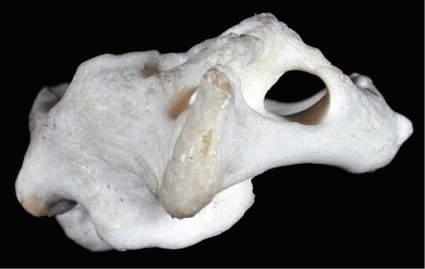
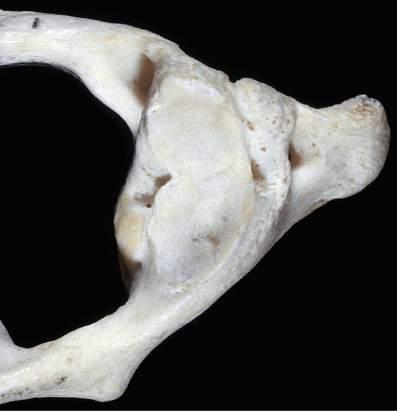
Fig. 1.14 Gross anatomic specimen of the base of the skull of a patient with severe rhematoid arthritis. Looking down into the foramen magnum from above, a bony protuberance can be seen. This upward dislocation of the odontoid process of the axis pushes the medulla and spinal cord backward. (From Kovacs G, Alafuzoff I. Handbook of Clinical Neurology. Vol. 145. Amsterdam: Elsevier; 2017: Fig. 29.9.)