CLINICAL IMMUNOLOGY
Edited by NIMA REZAEI
Professor of Clinical Immunology, Research Center for Immunodeficiencies, Children’s Medical Center and Department of Immunology, School of Medicine, Tehran University of Medical Sciences, Iran; Network of Immunity in Infection, Malignancy and Autoimmunity (NIIMA), Universal Scientific Education and Research Network (USERN), Tehran, Iran
Academic Press is an imprint of Elsevier
125 London Wall, London EC2Y 5AS, United Kingdom
525 B Street, Suite 1650, San Diego, CA 92101, United States
50 Hampshire Street, 5th Floor, Cambridge, MA 02139, United States
The Boulevard, Langford Lane, Kidlington, Oxford OX5 1GB, United Kingdom
Copyright © 2023 Elsevier Inc. All rights reserved.
No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopying, recording, or any information storage and retrieval system, without permission in writing from the publisher. Details on how to seek permission, further information about the Publisher’s permissions policies and our arrangements with organizations such as the Copyright Clearance Center and the Copyright Licensing Agency, can be found at our website: www.elsevier.com/permissions.
This book and the individual contributions contained in it are protected under copyright by the Publisher (other than as may be noted herein).
Notices
Knowledge and best practice in this field are constantly changing. As new research and experience broaden our understanding, changes in research methods, professional practices, or medical treatment may become necessary.
Practitioners and researchers must always rely on their own experience and knowledge in evaluating and using any information, methods, compounds, or experiments described herein. In using such information or methods they should be mindful of their own safety and the safety of others, including parties for whom they have a professional responsibility.
To the fullest extent of the law, neither the Publisher nor the authors, contributors, or editors, assume any liability for any injury and/or damage to persons or property as a matter of products liability, negligence or otherwise, or from any use or operation of any methods, products, instructions, or ideas contained in the material herein.
ISBN: 978-0-12-818006-8
For Information on all Academic Press publications visit our website at https://www.elsevier.com/books-and-journals
Publisher: Stacy Masucci
Acquisitions Editor: Linda Versteeg-Buschman
Editorial Project Manager: Sam W. Young
Production Project Manager: Sreejith Viswanathan
Cover Designer: Greg Harris
Cover design image by: Dr. Yousef Fattahi
Typeset by Aptara, New Delhi, India
This book would not have been possible without the continuous encouragement by my family. I wish to dedicate it to my daughters, Ariana and Arnika, with the hope that increasing the knowledge will lead to health to all and provide a brighter future for next generations. Whatever I have learnt, comes from my mentors. This book is therefore dedicated also to all of them, but most importantly to the patients and their families whose continuous support has guided me during all these years.
Harsini, Nima Rezaei
4.
Pouya Mahdavi Sharif, Amin Pastaki Khoshbin, Elaheh Nasrollahzadeh, Mahsa Keshavarz-Fathi,
Contributors
Melina Farshbafnadi
School of Medicine, Tehran University of Medical Sciences, Tehran, Iran; Cancer Immunology Project (CIP), Universal Scientific Education and Research Network (USERN), Tehran, Iran
Sara Harsini
Research Center for Immunodeficiencies, Children’s Medical Center, Tehran University of Medical Sciences, Tehran, Iran; Association of Nuclear Medicine and Molecular Imaging (ANMMI), Universal Scientific Education and Research Network (USERN), Tehran, Iran; BC Cancer, Vancouver, BC, Canada
Mahsa Keshavarz-Fathi
School of Medicine, Tehran University of Medical Sciences, Tehran, Iran; Cancer Immunology Project (CIP), Universal Scientific Education and Research Network (USERN), Tehran, Iran; Research Center for Immunodeficiencies, Children’s Medical Center, Tehran University of Medical Sciences, Tehran, Iran
Amin Pastaki Khoshbin
School of Medicine, Tehran University of Medical Sciences, Tehran, Iran; Cancer Immunology Project (CIP), Universal Scientific Education and Research Network (USERN), Tehran, Iran
Farimah Masoumi
School of Medicine, Tonekabon Branch, Islamic Azad University, Tonekabon, Iran
Elaheh Nasrollahzadeh
Cancer Immunology Project (CIP), Universal Scientific Education and Research Network (USERN), Tehran, Iran; School of Medicine, Guilan University of Medical Sciences, Rasht, Iran
Ali Nowroozi
School of Medicine, Tehran University of Medical Sciences, Tehran, Iran; Cancer Immunology Project (CIP), Universal Scientific Education and Research Network (USERN), Tehran, Iran
Parmida sadat Pezeshki
School of Medicine, Tehran University of Medical Sciences, Tehran, Iran; Cancer Immunology Project (CIP), Universal Scientific Education and Research Network (USERN), Tehran, Iran; Network of Immunity in Infection, Malignancy and Autoimmunity (NIIMA), Universal Scientific Education and Research Network (USERN), Tehran, Iran
Sepideh Razi
Cancer Immunology Project (CIP), Universal Scientific Education and Research Network (USERN), Tehran, Iran; School of Medicine, Iran University of Medical Sciences, Tehran, Iran; Research Center for Immunodeficiencies, Children’s Medical Center, Tehran University of Medical Sciences, Tehran, Iran
Nima Rezaei
Research Center for Immunodeficiencies, Children’s Medical Center, Tehran University of Medical Sciences, Tehran, Iran; Network of Immunity in Infection, Malignancy and Autoimmunity (NIIMA), Universal Scientific Education and Research Network (USERN), Tehran, Iran; Department of Immunology, School of Medicine, Tehran University of Medical Sciences, Tehran, Iran
Mona Sadeghalvad
Department of Immunology, School of Medicine, Tehran University of Medical Sciences, Tehran, Iran; Research Center for Immunodeficiencies, Children’s Medical Center, Tehran University of Medical Sciences, Tehran, Iran; Network of Immunity in Infection, Malignancy and Autoimmunity (NIIMA), Universal Scientific Education and Research Network (USERN), Tehran, Iran
Kiarash Saleki
Student Research Committee, Babol University of Medical Sciences, Babol, Iran; USERN Office, Babol University of Medical Sciences, Babol, Iran
Pouya Mahdavi Sharif
School of Medicine, Tehran University of Medical Sciences, Tehran, Iran; Cancer Immunology Project (CIP), Universal Scientific Education and Research Network (USERN), Tehran, Iran
Samaneh Zoghi
Ludwig Boltzmann Institute for Rare and Undiagnosed Diseases (LBI-RUD), Vienna, Austria; St. Anna Children’s Cancer Research Institute (CCRI), Vienna, Austria; CeMM Research Center for Molecular Medicine of the Austrian Academy of Sciences, Vienna, Austria; Network of Immunity in Infection, Malignancy and Autoimmunity (NIIMA), Universal Scientific Education and Research Network (USERN), Vienna, Austria
Preface

Imagine that you are an ancient being and probably a distant ancestor of all mammals. Your life relies on an elementary defense system. If you are attacked by a parasite or microbe, you stop it from harming you by releasing phagocytic cells or producing and unleashing chemicals against it. Now, imagine that during evolution, you become a more sophisticated being, and soon you realize that you need a more complex defense system in order to protect you against all pathogens. Also, this defense system must not invade your own tissues or harm your cohabitants. This defense system is called “Immune system.” The immune system is one of the most incredible systems of the human body. It is made up of a vast network of cells, chemicals, tissues, and organs that protects our body from pathogenic invaders such as bacteria, fungi, viruses, and parasites, and it can keep a memory of the invaders to defend the host from any further encounters. In addition, the immune system plays a key role in the pathogenesis of cancer and controlling the growth of cancer cells. Various immunotherapeutic approaches have been approved for cancer treatment, and some of them, namely immune checkpoint inhibitors for solid tumors and CAR T-cell therapy for hematologic malignancies, are breakthroughs in cancer treatment. Any aberration from normal function of the immune system leads to the development of immune system disorders, which can be characterized by abnormally low activity or overactivity of the immune system. Immunodeficiencies are a group of immune system diseases in which the host is incapable of responding to the pathogens, properly and in a protective fashion, and they are divided into primary and secondary based on genetic and environmental causes of the disease, respectively. Any functional, developmental, proliferative, or differentiation defect of one or more components of the immune system results in the development of immunodeficiencies. Other types of immune system disorders, including autoimmune diseases and allergies, are characterized by activation of the immune system in the absence of any pathogens or tumor, or activation of innate immune response and releasing of inflammatory mediators without any evidence of an antigen-immune response in the case of autoimmune diseases or development of unfavorable immune responses against allergens in the case of allergies. Besides the development of immune system diseases, as a result of abnormal immune responses, these inappropriate responses can also lead to the rejection of the transplanted cells, tissues, and organs. Transplantation is a procedure in which cells, tissues, or organs of an individual are replaced by those of another individual or the same person. The immune system, which is designed to defend the host against foreign antigens, may act against the transplanted cells, tissue, or organ and cause rejection.
In this book, after an introduction to the immune system (Chapter 1), the definition, epidemiology, pathogenesis, clinical features, diagnosis, and treatment of allergic diseases, including asthma, allergic rhinitis, allergic conjunctivitis, urticaria and angioedema, atopic dermatitis, and allergic contact dermatitis, food allergy and gastrointestinal syndromes, drug allergy, and anaphylaxis are discussed (Chapter 2). Afterward, the immune cells and immune responses, which are involved in autoimmune reaction, initiation, and facilitation of autoimmunity, human multisystem autoimmune diseases, and some more common system-specific autoimmune diseases, are reviewed (Chapter 3). This book discusses the interaction between the immune system and transformed cells and provides an updated review on the application of immunotherapy for different cancer types, combination therapy, and immunoediting after other therapeutic approaches (Chapter 4). Then, it presents the types of immunodeficiency diseases, their possible diagnosis, and treatment (Chapter 5). Also, the definition and epidemiology, molecular mechanisms, diagnosis, and treatment of infectious diseases (Chapter 6) and different types of transplantations, the immunopathogenesis of transplantation, the process of matching the donor and the recipient, pretransplantation conditioning, and complications after transplant, and ways to manage them (Chapter 7) are reviewed in this book.
I hope that this book will be welcomed by basic scientists and clinicians who wish to extend their knowledge in the field of clinical immunology.
Nima Rezaei, MD, PhD
Acknowledgment
I would like to express my gratitude to the Editorial Assistant of this book, Dr. Sepideh Razi. With no doubt, the book would not have been completed without her contribution. Indeed, I am so thankful to Dr.Yousef Fatahi for his contribution in designing the book cover and a few illustrations for some chapters.
Nima Rezaei,
MD, PhD
The immune system
Samaneh Zoghia,b,c,d, Farimah Masoumie, Nima Rezaeif,g,h
aLudwig Boltzmann Institute for Rare and Undiagnosed Diseases (LBI-RUD),Vienna, Austria
bSt. Anna Children’s Cancer Research Institute (CCRI),Vienna, Austria
cCeMM Research Center for Molecular Medicine of the Austrian Academy of Sciences,Vienna, Austria
dNetwork of Immunity in Infection, Malignancy and Autoimmunity (NIIMA), Universal Scientific Education and Research Network (USERN),Vienna, Austria
eSchool of Medicine, Tonekabon Branch, Islamic Azad University, Tonekabon, Iran
fResearch Center for Immunodeficiencies, Children’s Medical Center, Tehran University of Medical Sciences, Tehran, Iran
gNetwork of Immunity in Infection, Malignancy and Autoimmunity (NIIMA), Universal Scientific Education and Research Network (USERN), Tehran, Iran
hDepartment of Immunology, School of Medicine, Tehran University of Medical Sciences, Tehran, Iran
Introduction
The Human immune system has two major components of Innate (natural) and adaptive (specific) immunity. Both compartments work together to protect the host against diseasecausing agents, which we are exposed to continuously.1 While even metazoans have innate immunity, adaptive immunity is specific to vertebrates.2 The cells and components of each of these immune systems are explained in the following sections.
Although the function of the immune system is to defend against infectious agents, non-infectious agents can also elicit an immune response.3 This process can injure tissues and cause diseases such as allergy and autoimmunity. In this chapter, we are going to explain the principles and functions of the human immune system briefly.
The main characteristics and drivers of the innate and adaptive immune systems are summarized in Table 1.1 4 In summary, innate immunity is the first and fast responder against pathogens (in a few hours to days), which recognize some common molecular patterns that are presented exclusively in microorganisms, and its function is nonspecific. In contrast, the adaptive immune system reacts specifically to each antigen, and therefore, it takes longer after the infection (days to weeks) for this type of immunity to function. Antigens are microbial or nonmicrobial agents that can elicit an immune response. A very important characteristic of the immune system is to differentiate selfantigens from non-self, and any deviation from this capability can cause a pathogenic complication.4
Humoral and cellular immunity
The adaptive immune system divides into two types: humoral and cellular immunity. Both are highly cooperating to defend the host against a wide range of infectious agents.5 Humoral immunity refers to antibody molecules that are secreted to the blood
https://doi.org/10.1016/B978-0-12-818006-8.00005-0
Table 1.1 Major characteristic of Innate and adaptive immunity.
Innate immunity
Reacts to Common pathogenic determinants
Diversity of reactions
Restricted
Memory No
Differentiation of self from foreign antigen
Cellular components
Proteins
Other components
Yes
Macrophages, neutrophils, NK cells, and DCs
Blood proteins such as the complement system and lectins
Skin and mucosal barriers
NK, Natural killer; DCs, Dendritic cells.
Adaptive immunity
Any microbial and nonmicrobial antigen
Very diverse due to specificity
Yes
Yes
Lymphocytes
Antibodies
Tissue-resident lymphocytes and antibodies
or mucosa by B lymphocytes. Antibodies are very important proteins in defense against extra-cellular pathogenic agents such as microbes and their toxins. They can neutralize the toxins and specifically recognize the microbes and flag them to be phagocytosed by phagocytic cells.4
Cellular immunity refers to another type of defense mechanism that is mainly conducted by T lymphocytes against intracellular pathogens, where they cannot be accessed by antibodies. In this situation, T cells function to kill the infected cell, directly by the help of cytotoxic T cells or indirectly by activation of macrophages and neutrophils to stop the spread of infection.1,4
Lymphocytes and their specific receptors
B lymphocytes (B cells) and T lymphocytes (T cells) are major cellular components of the adaptive immune system. These cells can recognize antigens specifically, which occurs through their specific receptors. We will explain in the following sections the generation of these receptors with high diversity. B and T Lymphocytes present as different and distinct clones, which are the population of cells that express the same receptor with similar specificity, and each clone is unique.6 Lymphocytes differentiate in the primary lymphoid organs, and they circulate in the blood and lymphoid organs while they are mature. However, they considered naïve cells before an antigen encounter. After recognition of their specific antigen, which they express the specific receptor against, these cells undergo several changes through signal transduction and intracellular signaling pathways, and they become an effector lymphocyte. We will further explain in the following sections how the process of lymphocyte activation takes place in B and T cells. The specific receptor on the surface of B cell is called B cell receptor (BCR),
which is the same as antibody molecule, but a membrane-bound form of it. T cell receptor (TCR) is the specific receptor expressed on the surface of a T cell. Both BCR and TCR molecules have clonal differentiation and distribution.7 We will explain more about these receptors in the T cell and B cell development sections. As mentioned in Table 1.1, an important characteristic of TCR and BCR molecules is their diversity, which enables the adaptive immune system to recognize 107 to 109 different antigens.
Memory
One of the key aspects of the adaptive immune system is the ability to keep a memory of the infection and to be able to recall it much faster in the next encounter. Therefore, lymphocytes undergo changes such as growing in number and transforming from an effector cell to a memory cell, which is a very long-lived cell. The first exposure of an immune cell to its specific antigen is called the primary immune response, which also primes lymphocytes and prepares them for memory cell formation. The second encounter of memory cells with the specific antigen is called the secondary immune response, which is not only faster but also more extensive than the primary immune response.8
Self-tolerance
Non-reactivity to self-antigens is a fundamental aspect of the immune system, which guarantees a successful and effective defense against foreign intruders without harming the self-tissues. This non-responsiveness of the immune system is called tolerance. Tolerance mechanisms are explained in the tolerance section, but in summary, all the self-reactive clones of lymphocytes are being eliminated or suppressed to become tolerant against self-antigens. Defects in the tolerance mechanisms and loss of self-reactivity causes autoimmunity.9
Cells of the immune system
The function of the immune system is coordinated by a variety of cells, playing role in the innate and adaptive immune responses (Fig. 1.1). Most of these cells are white blood cells that arise from pluripotent hematopoietic stem cells in bone marrow.10 Hematopoietic stem cells differentiate into two lineage precursors: common myeloid progenitor (CMP) and common lymphoid progenitor (CLP). Most of the innate immune system cells, including macrophages, granulocytes (such as neutrophils, eosinophils, and basophils), mast cells, and dendritic cells (DCs), differentiate from CMP. In contrast, specialized cells of the adaptive immune response, including B and T lymphocytes, generate from CLP.11 Most of the immune system cells are found in the blood,
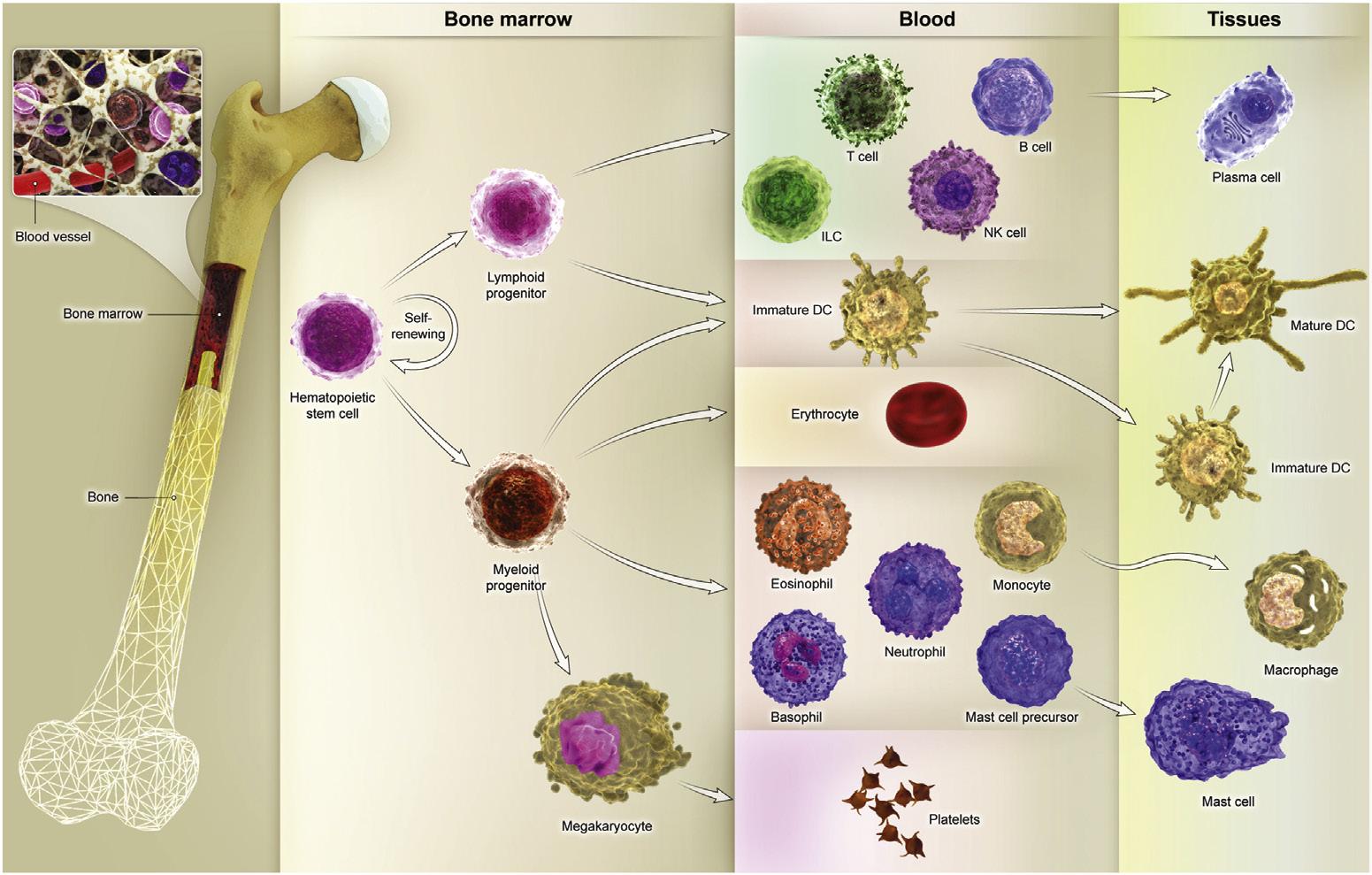
Fig. 1.1 Almost all cells of the immune system cells arise from a pluripotent hematopoietic stem cell in the bone marrow. Hematopoietic stem cells divide into common lymphoid progenitor (CLP) and common myeloid progenitor (CMP), which gives rise to the lymphoid and myeloid lineage, respectively.
as we see their frequency in Table 1.2, but immune responses to antigens take place in lymphoid tissues.12
Granulocytes
Based on morphologic differences, polymorphonuclear leukocytes or granulocytes include neutrophils, eosinophils, and basophils. Neutrophils are the most frequent granulocytes of the blood circulation, and together with monocytes/macrophages perform phagocytosis in host defense.13 The process of phagocytosis includes entering the site of infection, capturing microorganisms or products of necrotic cells using innate immune system receptors, and ingesting and killing microorganisms within specialized cytoplasmic vacuoles called phagolysosomes.14 Neutrophils have a short lifespan, but
Neutrophils 40–60 percent
Lymphocytes 20–40 percent
Monocytes 2–8 percent
Eosinophils
Basophils
1–4 percent
<1 percent
Table 1.2 Normal White Blood Cells Percentage.
their response to pathogens is relatively rapid due to their cytoskeletal movements and enzymatic activity in pathogen destruction. Neutrophils also produce antimicrobial peptides that kill extracellular microbes.15 Eosinophils contain granules mainly with basic proteins that are toxic for helminths. These cells also can be found in mucosal tissues.16 Although mast cells derive from different bone marrow precursors, blood basophils have morphological and structural similarities to tissue mast cells. Moreover, mast cells and basophils have an important role in defense against parasites by degranulation of their biological mediators. With a similar mechanism, these cells bind to allergens through high affinity immunoglobulin (Ig) E specific FC receptor (FcεR) and mediate allergic reactions.17
Monocytes/macrophages
Monocytes and macrophages are recognized as mononuclear phagocytes. Monocytes derive from bone marrow precursors and circulate in the blood, but when they migrate into tissues, they mature into macrophages and are called inflammatory macrophages. Besides, there are long-lived tissue-resident macrophages in different tissues that have developed during fetal development, like Kupffer cells in the liver or alveolar macrophages in the lung.18
Based on the functional aspect, there are two main groups of monocytes: the most well-known type are inflammatory or classic monocytes, which have phagocytic activity and produce inflammatory mediators, and can quickly migrate to sites of infection or tissue injury. There are also nonclassical monocytes that mainly take part in tissue repair.19 Similarly, macrophages can gain different functional abilities and are divided into two groups: M1 macrophages, which are classically activated and mainly take part in phagocytosis, and M2 macrophages, which are alternatively activated and have tissue repair properties. Skewing toward M1 or M2 subtypes depends on cytokine milieu and activating stimuli that these cells are exposed to them.20
The major function of macrophages is phagocytosis and the killing of ingested microorganisms. Macrophages also ingest apoptotic cells, including neutrophils, that die at the sites of infection.21 Through phagocytosis, macrophages are stimulated by microbial products and produce different cytokines that enhance the recruitment of monocytes and other leukocytes into the site of infection. Furthermore, phagocytized microbes are presented to lymphocytes as the antigen-presenting capacity of macrophages and activate T lymphocytes during a cellular immune response.22
Antigen-presenting cells
Antigen-presenting cells (APCs) are a diverse group of immune system cells that are specialized for the presentation of antigens to lymphocytes, particularly T cells. Among APCs, there are monocytes, macrophages, B lymphocytes, cutaneous Langerhans cells, and most importantly, DCs.23
The main feature of APCs are the expression of class I and class II major histocompatibility complex (MHC) molecules for the presentation of antigenic peptides to cluster of differentiation (CD)8+ and CD4+ T cells, respectively, as well as other co-stimulatory molecules such as B7-1 (CD80), B7-2 (CD86), required for T cell activation. APCs capture and present antigens, along with providing cytokines that induce specific responses in cells to which they are presenting antigens.24
Different APCs uptake antigens and drive their specific effector functions, for example, monocytes and macrophages phagocyte opsonized antigens, and present them to T cells in the cellular immune response. T cells produce cytokines when become activated that help phagocytes to kill the ingested microorganisms.25
B cells antigenic presenting capacity for T cells seems to provide a mutual benefit for both sides during the humoral immune response. B cells capture antigens by their BCRs through endocytosis and present them to specific T cells by their surface MHC molecules. T cells activated by B cells also produce cytokines necessary for antibody production and B cell differentiation.26
Dendritic cells (DCs)
DCs are professional APCs that efficiently sense and capture microbial antigens in innate immune responses and display them as peptides to T cells resulting in T cells activation leading to the development of adaptive immune responses and thus, linking two arms of immune response together. In comparison to monocytes/macrophages, these cells have lesser phagocytic capacity, but due to the expression of a wide range of innate immune response receptors, including toll-like receptors (TLRs), they recognize microbial molecules and become activated.27 Following activation, these cells produce cytokines that recruit and activate innate cells at the infection sites. The innate immune response itself enhances the ability of DCs to migrate to and activate T cells during antigen presentation.28
DCs are recognized by having membranous projections and are divided into two main functional distinctive populations. Most DCs arise from bone marrow myeloid precursors and are commonly distributed in lymphoid tissues and mucosal epithelium. These DCs are called classical DCs and have the most potency in capturing protein antigens entered from epithelial barriers and stimulating strong T cell responses. A group of these populations is called Langerhans cells, which are located in the epithelial layer of skin and sense microbial antigens entered through cutaneous barriers. Similarly, resident DCs are found in lymphoid and nonlymphoid tissues that sample antigens of their residence and potently exert CD4+ T cell responses.29 The second group of DCs, Plasmacytoid DCs, are involved in innate anti-viral defense and production of type I interferon (IFN) in response to viruses. These cells develop from bone marrow precursors and normally are found in blood.30 There is also a third population of DCs called follicular dendritic cells (FDCs). These cells are not derived from bone marrow
precursors and do not present antigens to T cells. However, they are involved in B cell activation during the humoral immune response.31
Lymphocytes
Based on differences in cell surface markers, there are four categories of lymphocytes, including T, B, NK (natural killer), and NKT (natural killer T) cells. 32 All lymphocytes differentiate from CLP cells in the bone marrow and are morphologically similar. B and T lymphocytes have a pivotal role in specific antigen recognition by expression of clonally distributed cell surface receptors with single specificity for each antigenic determinant. So, millions of clones of B and T cells can respond to their specific antigens using their unique BCRs (Ig receptor) and TCRs, respectively. 12
B lymphocytes originate and become mature in the bone marrow. Follicular B cells, B-1 cells, and marginal zone B (MZB) cells are the main classes of B cells. Follicular B cells (B-2) have the most frequency and are found in the follicles of lymphoid organs and blood. They express a diverse set of Ig receptors and are differentiated to high affinity antibody-producing cells upon activation. B-2 cells differentiate into memory B cells after infection, which results in host protection against repeated exposure to the same antigen.33 B-1 and MZB cells express less diverse Ig receptors and produce natural antibodies (mainly IgM) with limited diversity.34
T lymphocytes are divided into two main groups of helper (CD4+) and cytotoxic (CD8+) cells. TCRs expressed on lymphocytes are consisted of either α and β chains (αβ T cells) or γ and δ chains (γδ T cells). αβ helper T cells mainly release cytokines upon antigen recognition and activation, which also help other cells such as other T cells, B cells, and macrophages in cellular and humoral immune responses while cytotoxic T cells mostly kill virus-infected cells and cancerous cells.35 Regulatory T cells (Tregs) are the third group of CD4+ αβ T cells, which are involved in immune response suppression.36 Moreover, NKT cells, γδ T cells, and mucosa-associated invariant T (MAIT) cells are a smaller group of T cells, which carry receptors with limited diversity. NKT cells exhibit both NK-like cytotoxicity and antigen-specific T-cell responsiveness.37,38
Lymphocytes are functionally inactive when they just become mature in generative lymphoid organs and are called naïve lymphocytes. After maturation, they migrate to secondary lymphoid tissues, where they first recognize their specific antigens and go through changes in phenotype and function. Subsequent to activation and proliferation, lymphocytes differentiate into effector cells, which eradicate antigens. Also, a small number of activated lymphocytes differentiate to memory cells, which then mediate rapid and enhanced responses in secondary exposures to specific antigens.39
NK cells originate from lymphoid precursors in the bone marrow and are categorized as effector cells of the innate immune response. NK cells do not express clonally
distributed TCRs and are important in the early elimination of virus-infected and damaged cells. Therefore, they are known as counterparts for cytotoxic T lymphocytes (CTLs) in adaptive immune response.40
Primary lymphoid organs
Primary lymphoid organs or generative lymphoid organs, including bone marrow and thymus, are the site of maturation of B cells and T cells, respectively. In fact, growth factors necessary for the early stages of lymphocyte development and also self-antigens required for selection and maturation of non-self-reactive lymphocytes are provided in primary lymphoid organs.41
B lymphocytes partially mature in the bone marrow and complete their final stages of maturation in the spleen, where they recognize specific antigens for the first time.11 Bone marrow is also the main site of hematopoiesis-production of all blood cells after birth. As mentioned earlier, red blood cells, granulocytes, monocytes, DCs, mast cells, platelets, B and T lymphocytes, and innate lymphoid cells (ILCs) all originate from a common hematopoietic stem cell in the bone marrow.10 Stromal cells and hematopoietic stem cells are located in specific niches in the bone marrow providing contactdependent signals and growth factors required for hematopoiesis.42 Hematopoietic stem cells are self-renewing cells that give rise to two multipotent precursors, CMP and CLP. CMP then generates mature red blood cells, platelets, granulocytes (neutrophils, eosinophils, and basophils), and the main part of DCs. CLP gives rise to T cells, B cells, and ILC lineages. The generation of blood cells from bone marrow precursors is stimulated by a group of cytokines called colony-stimulating factors (CSFs).32
Besides hematopoiesis, bone marrow is also populated by long-lived plasma cells, which are activated in secondary lymphoid tissues and migrate to bone marrow.43
T lymphocytes mature in the thymus and then enter the circulation and migrate to secondary lymphoid organs where they develop an immune response to their specific antigens.44 The thymus is located in the anterior mediastinum and is the main site of T cells maturation from fetal developmental stages until puberty, and after that, the thymus undergoes hypertrophy. The thymus is a bilobed organ, each lobe is divided into multiple lobules by fibrous septa, and each lobule consists of a cortex and a medulla.45 T cell precursors are called thymocytes and migrate to the thymus from bone marrow. Thymocytes start their maturation in the cortex and migrate toward the medulla as they mature. There are thymic cortical epithelial cells in the cortex, which secrete interleukin (IL)−7, a cytokine necessary for the early development of T cells. The medulla is less populated with thymocytes in comparison with the cortex. DCs, macrophages, and thymic medullary epithelial cells are found in the medulla and are crucial for the maturation and selection of non-self-reactive T cells that finally leave the thymus and migrate toward secondary lymphoid organs. A chromosomal deletion that causes failure
of thymus development results in DeGeorge syndrome in patients, and these patients lack T cells. We will describe DeGeorge syndrome in detail later as a primary immunodeficiency.46
Secondary lymphoid organs
Secondary lymphoid organs or peripheral lymphoid tissues, including the spleen, lymph nodes, and mucosal-associated lymphoid tissues (MALT), are the sites of recognition and initiation of the immune response toward foreign antigens. Furthermore, APCs, B cells, and T cells are located in the distinct anatomic location in secondary lymphoid tissues. Transportation of foreign antigens to these sites guarantees the generation and development of specific adaptive immune response.47
Lymph nodes are a part of the lymphatic system, which also includes lymphatic vessels that collect interstitial fluid or lymph (including invaded microbes in case of infections) from all vascularized tissues and discharge it into their draining lymph nodes. Lymph collected from all over the human body is finally released to a large lymphatic vessel called the thoracic duct. Lymph from the thoracic duct is discharged into the superior vena cava, thus returning the lymph to the blood.48
Lymph nodes are capsular tissues, which are located along lymphatic vessels throughout the body. Microbial antigens entered through epithelial surfaces are entered lymph nodes through afferent lymphatic vessels as a free form or captured by DCs. Each lymph node consists of a cortex and a medulla. B cells and FDCs mainly are located in the follicles in the cortex, whereas DCs and T cells mainly migrate to paracortical regions below follicles. This anatomic isolation of cells is mediated by the secretion of special cytokines called chemokines from lymph node stromal cells, which binds to their specific ligands on B and T cells and direct their migration. This anatomic segregation ensures B and T cells, which are located near their stimulating APCs, FDCs, and DCs, respectively.49 It is also important to note that lymphoid tissue-inducer cells (a type of ILCs) stimulate the development of secondary lymphoid tissues by secretion of cytokines known as lymphotoxins.50
Spleen is another capsular secondary lymphoid organ, which mainly functions as a site for initiation of the adaptive immune response against microbial antigens entered through blood. Spleen has an important role in the removal of aging and damaged blood cells, immune complexes, and opsonized microbes by splenic macrophages. Spleen is divided into red pulp and white pulp. Red pulp consists of blood-filled vascular sinusoids, and white pulp is a lymphocyte rich region with similar B cells and T cells anatomic segregation to lymph nodes. B cells are mainly located in follicles, whereas T cells reside in regions near artery branches called periarteriolar lymphoid sheaths (PALS). The space between red and white pulp is called marginal zone, which is a region of specialized cells (especially MZB cells) surrounding the marginal sinus.51