Medical Missions & Volunteerism





Volume 91 • Number 6 Published
December 2022
worcester WDMS.ORG
by Worcester District Medical Society
medicine
Your skills are in demand at many health systems. But only Reliant Medical Group offers you the right care culture in which to flourish. To collaborate and share your expertise. To give patients the attention they deserve. To leverage the latest treatment advances, information technologies and analytics to push the boundaries of medicine. Join us and there’s only one thing to do — your life’s best work. SM Reliant is a proud member of the Optum family of businesses.

www.practiceatreliant.org
ONE PLACE TO DELIVER YOUR BEST CARE.
ONLY
Contents
Medical Missions & Volunteerism
Medical Missions & Volunteerism
Editorial 4
Jane Lochrie, MD
President’s Message 6 Giles Whalen, MD
Ah, The Places You Will Go! 7 Nandana Kansra, MD, MPH, FACP Medicine in the Amazon 8
Nancy DeTora, MD
Volunteer Mission to El Salvador, 2023 11 James Umlas, MD
The Boy With the Blue Sweater 12
David C. Kim, MD, FACS
Preparing Today’s Students for Tomorrow’s Global Health Workforce: What they Need to Know 13
Michele Pugnaire, MD and Jean Boucher, PhD, NP
Where You Live Should Not Determine Whether You Live, or Whether You Die 15
Heidi K. Leftwich, DO
Responding to the Call: The Pharmacist’s Role in Disaster Responses and Medical Missions 17
Stephanie L. Conway-Allen, PharmD. RPh and Sheila M. Seed, PharmD, MPH, CTH, RCPS AFTM (Glasg), RPh
published by
Worcester District Medical Society
321 Main Street, Worcester, MA 01608 wdms.org | mwright@wdms.org | 508-753-1579
wdms officers
President Giles Whalen, MD
Vice President Alwyn Rapose, MD
Secretary Michelle Hadley, DO
Treasurer B. Dale Magee, MD
wdms administration
Martha Wright, MBA, Executive Director
Melissa Boucher, Administrative Assistant
wdms editorial board
Lisa Beittel, MBA
Sonia Chimenti, MD
Anthony L. Esposito, MD
Larry Garber, MD
Rebecca Kowaloff, DO
Susan Krantz, MD
Julianne Lauring, MD
Anna Morin, PharmD
Nancy Morris, PhD, NP
Thoru Pederson, PhD
Joel Popkin, MD
Alwyn Rapose, MD
Parul Sarwal, MD
Akil Sherif, MD (SVH Cardiology Fellow)
Reaching Out: What An Experience! 19 Marjorie Silva Rapose, DMD
El Medico Cubano 19 Warren Johnson, MD
A Night at St. Anne’s: Filling the Gap in Worcester’s Healthcare System 21 Madeline Schwartz
Cold, Displaced, and Diabetic: Lessons Learned While Caring for the Refugee Population of Worcester 22 Akanksha Nagarkar, BS, BA
Calendar of Events 18
In Memoriam 22 Richard Edward Hunter, MD Legal Consult Physician, Curb Thyself! 23 Peter Martin, Esq. Society Snippets 26
Robert Sorrenti, MD
Ram Upadhyay, MD
Martha Wright, MBA
Peter Zacharia, MD
Alex Newbury, MD, Resident Representative
Arunava Saha, MD, Resident Representative
Olivia Buckle, Student Representative
produced by Hana Lasell
advertising Inquiries to Martha Wright mwright@wdms.org 508-753-1579
thank you to The Reliant Medical Group, UMass Memorial Health
Music Worcester Physicians Insurance Carr Financial
Worcester Medicine does not hold itself responsible for statements made by any contributor. Statements or opinions expressed in Worcester Medicine reflect the views of the author(s) and not the official policy of the Worcester District Medical Society unless so stated. Although all advertising material is expected to conform to ethical standards, acceptance does not imply endorsement by Worcester Medicine unless stated. Material printed in Worcester Medicine is covered by copyright. No copyright is claimed to any work of the U.S. government. No part of this publication may be reproduced or transmitted in any form without written permission. For information on subscriptions, permissions, reprints and other services contact the Worcester District Medical Society.
DECEMBER 2022 WORCESTER MEDICINE 3
DECEMBER 2022
Jane Lochrie, MD
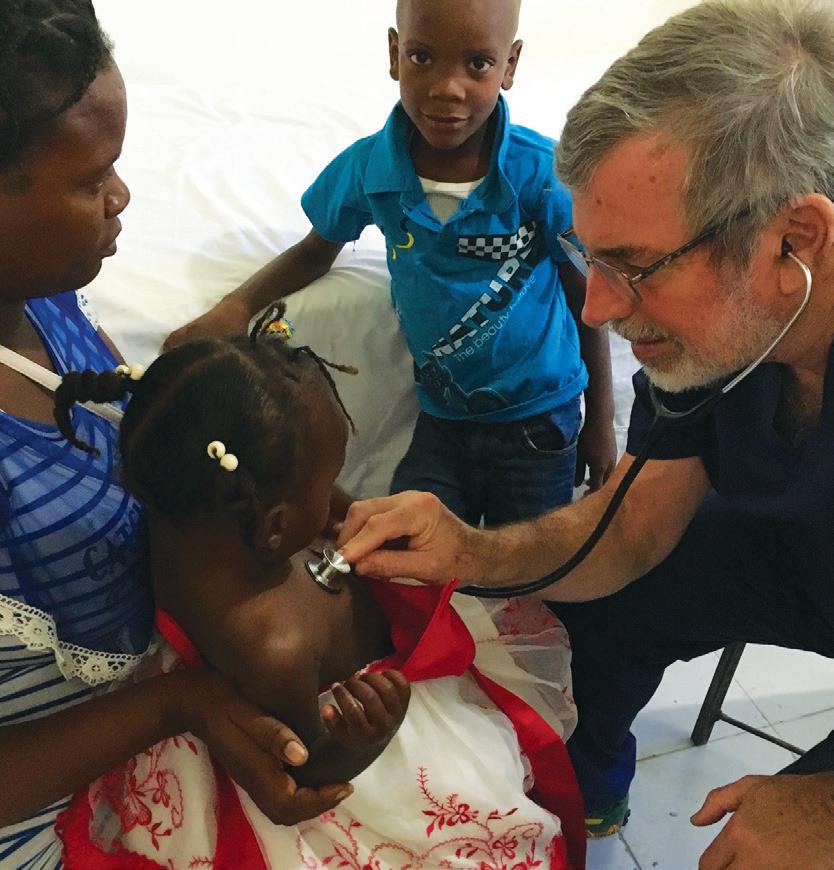
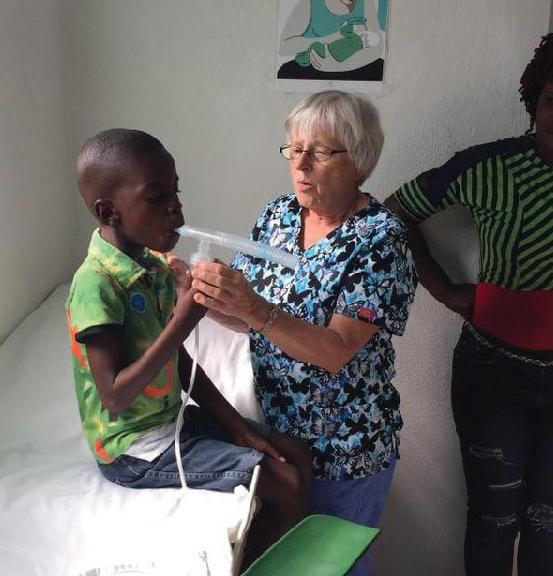
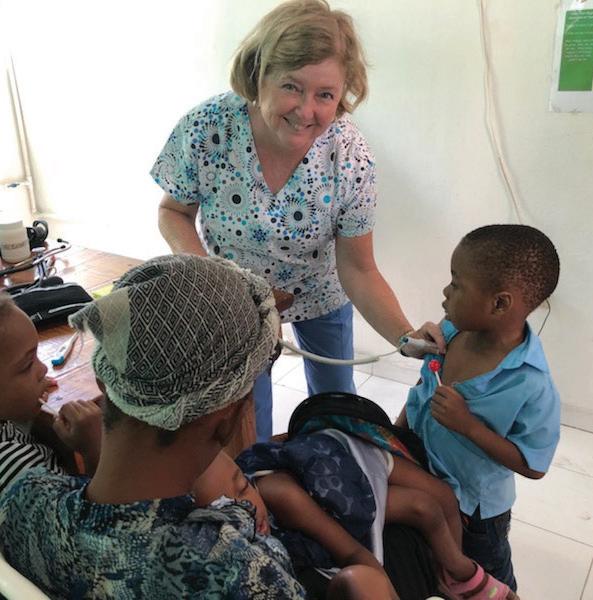
While I was in Haiti with my colleague, Dr. Nandana Kansra, I sponsored a child, as did all the volunteers in our group. I recently received this note from the five-year-old child I sponsored: “How are you? I hope you are well in the name of Jesus. Thank you for helping me. We are not very safe because the gangs are giving us trouble. May God help us.” This is so painful to read. No child should feel unsafe, especially in their own home. In this issue of Worcester Medicine, you will read the stories of some of our awe-inspiring volunteers and why they continue their work.
In the her article, “Ah the Places You Will Go” (page 7), Dr. Kansra describes her trip to Haiti where she and the team saw 600 patients in a week, “each one a story of resilience and courage.” Hunger was a pervasive symptom, with many patients forgoing their own meals to feed their children. She ends by stating “in that healing lies the greatest healing for the healer.”
In her article, “Medicine in the Amazon” (page 8), Dr. Nancy DeTora details how she chaperoned her child’s school trip to the Ecuadorian Amazon and spent the next 22 years going back once a year to care for the indigenous population, which had very limited healthcare. She gives a delightful description of some of the patients that she treated.
The desperate need for eye care in El Salvador is demonstrated in Dr. James Umlas’s article, “Volunteer Mission to El Salvador, 2023” (page 11). He has participated in 25 eye campaigns there. In addition to surgery, he and his team examined 2,000 patients and most received eye glasses.
Dr. David Kim gives a very powerful account of a young boy with a cleft lip that showed up unexpectedly to his clinic after all the equipment was packed to go home in “Boy With the Blue Sweater” (page 12). He unpacked and completed surgery under local anesthesia because his team had exhausted their anesthesia supplies. He reminds us that even though we may not be able to supply exactly what the patient needs, just listening, understanding, and holding their hand is enough to make them feel better.
In “Preparing Today’s Students for Tomorrow’s Global Health Workforce: What they Need to Know” (page 13), Drs. Michele Boucher and Jean Pugnaire tell us that student participation in global health at UMass Chan Medical School has risen exponentially to 67% and is now being offered to the graduate school of nursing. They describe the interprofessional program being offered there and relate the challenges and lessons learned over the years.
Dr. Heidi Leftwich explains, in “Where You Live Should Not Determine Whether You Live, or Whether You Die” (page 15), the hardships she encountered while sharing her knowledge of hypertensive disorder of
pregnancy to the faculty at Kenya Medical Research Institute. Most important is the gestational age of a viable fetus in Kenya being 28 weeks as compared to 22 weeks in the United States.
In “Reaching Out. What and Experience!” (page 19) Dr. Silva Rapose, a dentist, tells us about her trip to Meghalaya, India to conduct an oral hygiene awareness camp for the village children, some of whom never had the opportunity to learn to brush their teeth. On her way home she noted that she left a “transformed person.”
Pharmacists have been actively involved in responding to public health emergencies in Haiti. In “Responding to the Call: The Pharmacist’s Role in Disaster Response and Medical Missions” (page 17),Drs. Conway-Allen and Seed describe their experiences serving for Disaster Medical Assistance Teams and Medical Reserve Corps providing access to safe products, reviewing treatment plans, and making appropriate medication substitutions if drugs are not available.
Two medical students relate their experience working as case managers in two of the free medical programs. In “A Night at St. Anne’s: Filling the Gap in Worcester’s Healthcare System” (page 21) Madeline Schwartz writes that patients are the experts of their own bodies and circumstances, and they are truly our best teachers. Her experience deepened her knowledge of the barriers that patients face with the lack of access to healthcare.
In “Cold, Displaced, and Diabetic” (page 22), Akanksha Nagarkar was “blown away at the resilience of the patients” who visited the free clinical who were facing a multitude of adversities. She describes her experience as 30% frustration and 70% joy.
Please don’t leave this issue of Worcester Medicine without reading the president’s message, Legal Consult, and Society Snippets. +
Jane Lochrie, MD is Medical Director at St Anne’s and St. Peter’s Free Medical Programs and is a Professor of Medicine at UMass Chan Medical School.

DECEMBER 2022 WORCESTER MEDICINE 4 Editorial
The trusted professionals at Carr Financial have eighty years of combined experience helping people, like you, navigate today's economy towards a healthier financial future. Call our local Certified Financial Planners™ today for a no-obligation discussion about we can guide you towards a life of success, as you define it.



Carr Financial Group is a Registered Investment Adviser located in Worcester, MA CarrFinancial.com | 508-795-0264 | 20 Park Avenue, Worcester, MA 01605 Wealth Management | Financial & Retirement Planning
You work to care for others. We
your
work to care for
finances.
Proud Sponsor
President’s Message
Giles Whalen, MD
Dear Colleagues,
Volunteerism is a selfless act that provides a sense of accomplishment and brings people together. It helps to change the lives of others, compensate for poverty, address environmental issues and improve education. I’m very proud of our many physician and medical student members who demonstrate what volunteerism means here and in other countries around the world. These individuals work tirelessly and voluntarily, sometimes funding their own projects, in efforts to help those in need who do not have regular access to many medical resources.
This issue focuses on just a few examples of these efforts led by our members and others. I’d like to thank our guest editor, Dr. Jane Lochrie, past recipient of the Massachusetts Medical Society’s Volunteer of the Year Award (2020). Here in Worcester, she is the Medical Director of both the St. Anne’s and St. Peter’s Free medical Programs. If you wish to volunteer, please contact Dr. Lochrie at: jane.lochrie@stvincenthospital.com.
As we reflect upon 2022 and begin 2023, please think of those in need and consider supporting some of these projects either by donating dollars, resources or your time. If you wish to get more involved, please be sure to read this issue, where you will find links to some of these organizations and/or the authors leading these very important efforts.
We hope to see you at one of these upcoming events:
• 227th Oration February 8, 2023, 5:30 pm, Beechwood Hotel
• Annual Business Meeting, April 11, 2023, Beechwood Hotel
All the best,
Giles Whalen, MD President, WDMS


DECEMBER 2022 WORCESTER MEDICINE 6
Ah, the Places You Will Go!
Oh, this is just feels just like home,” I said to myself, comparing the landscape of Haiti with India as I got into a rickety bus that took my team and me from the airport to our clinic in Port-au-Prince. We were going to be here for a week on a medical service trip and I was full of excitement.
However, as we traveled down the dusty streets, I gazed at first in delight at the vendors selling their wares at the side of the road, then had a growing realization that there was not much to sell. The fruit on the carts was meager and dull, while other carts sold rusted wires and broken automotive parts. The vendors looked listless as they sat by their wares apparently without much hope of making a sale. In a sharp contrast, the children in the streets played happily, splashing in the puddles that collected in the damaged roads.
It was my first time in Haiti, as I led a group of three doctors, three nurses, and three students into a land that had never known peace for very long. Haiti has a complex, rich, fascinating, and tumultuous culture and history filled with stories of resistance, revolt, and instability. But one of the fundamental aspects of Haiti is its resilience. Despite slavery, multiple coups, various foreign occupations, and militarization, Haiti continuously fights to remain strong. Haiti’s very existence is inscribed in its many proverbs, such as “Dèyè mòn, gen mòn,” which translates in English to “Behind the mountains there are mountains.”
Prior to this trip, I spent years volunteering in my community, spending Tuesday evenings at St. Anne’s Free Medical Program clinic in Shrewsbury seeing patients who lacked health insurance. However, the service trip to Haiti was my biggest leap of faith in leading a team to provide medical services and supplies in a country that was challenged by a sparse and rudimentary medical system.
Every physician who sets out on the journey of medicine likely asks themselves: Am I doing enough? Have I given back in a meaningful way to my community outside of my work? Have I made myself worthy of being able to heal and alleviate suffering with the training I have received? My one week in Haiti would be a humbling lesson on how little I knew and how much there was to learn.
After a simple meal on my team’s first night in Haiti, we all gathered around in the kitchen with our local guide, Emily who briefed us on what to expect in the one week we would be there. We had to wake up early, as lines to see the “d octor team from the U.S.” started to form around 4:30 a.m. People often rode two-to-three hours in a tuk tuk, sometimes bringing their entire family to be seen. The doctor- topatient ratio is Haiti is one doctor per 4,000 patients, the local clinics could not keep up with the demand for healthcare.
We slept in bunkbeds with mosquito nets draped over them to protect us from the frequent outbreaks of malaria and dengue. The tap water was not safe for consumption, so we only drank filtered or boiled water. Our showers were mostly cold, depending on the weather. Quietly, we began to understand that the luxuries we took for granted in
the United States were a rarity here, and how the simple act of drinking a glass of life- sustaining water was not something all Haitians could do safely.
The next morning, we were all ready by 7:30 a.m. to see the patients. When the doors opened, we realized that the line extended for about a mile- anda- half into the street, and that people had indeed gathered in the wee hours of the morning to be evaluated. We were equipped with nothing but the simple tools of our trade: A stethoscope, an otoscope, a flashlight, a nebulizer, and the medications and food packs we had secured thanks to the generous donations of our local community in the United States.
As my colleague and I started seeing patients that day, one thing became apparent: Stomach pain would be the most common complaint we would hear about all week. It did not matter if it was a child or an adult. What we didn’t realize that it wasn’t just parasitosis that was causing abdominal pain.

“I wake up at 2:00 every morning,” said one patient. I made a mental checklist of all the questions that usually follow this complaint: How much caffeine do you drink ? How much alcohol do you consume? Do you drink fluids close to bedtime ? Then, I asked: “What wakes you up?”
“I wake up thinking about food,” he said .
On further questioning, the patient had not eaten a proper meal in days. He had five children and an unreliable job in construction. We loaded his bag with protein bars, biscuits, dry cereal, and the donations we had brought from home. As he left the clinic for his long journey back home, he flashed a smile of gratitude, promising to return with his children later in the week. None had received any childhood immunizations.
DECEMBER 2022 WORCESTER MEDICINE 7
Medical Missions & Volunteerism
Nandana Kansra, MD, MPH, FACP
“
Every physician who sets out on the journey of medicine likely asks themselves: Am I doing enough?
Medical Missions & Volunteerism
Ah, The Places You Will Go! Continued
In the one week we were in Haiti we saw close to 600 patients, each one of them a story of resilience and courage. There was a 60-year-old grandmother raising the eight-month-old twins of her daughter, who died as a result of a post-partum hemorrhage.She carefully balanced one child on each hip, and when we asked her how she was coping, she said, with a smile, “I don’t have a choice. I am now their mama.”
There was a gentleman in his 50s whose face lit up in a smile as for the first time in his life, he wore eyeglasses which corrected his presbyopia. There were children who presented with severe dehydration and smoke inhalation injuries for which we used
basic oral re-hydration solution to hydrate, or we relied on solar electricity and our only nebulizer machine to give them respiratory treatments.
On our last day, we all gathered in the kitchen one final time, some of us breaking down in tears knowing that while we were returning to a life of comfort back in the United States, a lot more work needed to be done. We knew that the one week we spent there was just a minuscule Band-Aid on the colossal problem at hand.
When I look back on that trip and the many others I’ve taken since, I realize that what volunteerism really taught me is that it is easier to give from a state of relative abundance. However, those who give when they themselves are suffering are some of the most generous beings of all. My travels with my team over the next several years took us to different countries and to rural parts of America, each experience searing itself into our minds and hearts and teaching us invaluable lessons in humanity and the resilience of the human spirit. It showed us how easy it is to be trapped by the zip code of one’s existence, and how much work needed to be done to fight for basic equality and universal access to healthcare. Volunteerism is the essence of medicine—it’s when all transactions between a physician and a patient cease and one’s desire to help another human being is at its purest intention. In that healing lies the greatest gift for the healer. +
Nandana Kansra, MD, MPH, FACP Internal Medicine
Medicine in the Amazon
Nancy DeTora, MD
Sometime in my forties, I accompanied my son’s eighth-grade class to the Ecuadorian Amazon, not realizing that it was the start of a 22-year adventure. After flying into the capitol city of Quito and spending a day in the Andes Mountains, we took a short flight to Coca--an outpost military station--then traveled in a motorized boat for 60 miles down the Rio Napo. Finally, after a hike and a ride in a small dugout canoe, we finally arrived in our home for the week, Sani Isla. Sani Isla is an indigenous Quechuan community in Ecuador with 400-500 residents. They live in family units along the river in traditional thatchedroof huts with a kitchen fire pit and a gathering space. Furniture consists of split log benches around the perimeter. There is no electricity or running water, and there is a “bathroom trail.” At bedtime hammocks are pulled down from the rafters for sleeping, and bathing and laundry are done in the river. The community is not a monetary-based society and the Residents are hunters and gatherers. Tourism is the main source of income for the village, and profits are shared by all in the village.

On our third trip to Sani, we brought the students into the community to meet other school children and experience the local culture. During the soccer game (which instantly became a tradition) I took a walk and ended up in a kitchen area where some women were cooking lunch for the community children. I realized that they all had many burns on their hands and forearms, so I shared some ointments I had
with me to help soothe and heal their burns. That was the beginning of the community clinic.
With the help of our guides, we consulted with the Sani elders and the shaman and were granted permission to establish the clinic. Our initial team included Helen Blazis for Spanish translation, Blanca the amazing community midwife, Quechua translation, and me. Together we developed a successful working system for triage, treatment, and pharmacy.
Once the clinic was established, I would spend the year prior to each trip gathering supplies, which included suture sets, antibiotics, skin and eye ointments, ibuprofen and Tylenol, electrolyte powder, antacids, antiparasitics, anti-diarrheal meds, and vitamins. Sani does not have electricity, so the only diagnostic tests I could bring were urine dip sticks and pregnancy tests. I always appreciated donations from medical offices back in the United States, and I even received donations from my patients. On many trips, I was fortunate to have other health care providers and parent volunteers. Even on the trips I could not participate in, we were able to assemble a health care team and supplies for Sani.
Clinic day was always busy, starting by 8 a.m. and finishing long after sunset. Year after year, increasing numbers of families from Sani and surrounding
DECEMBER 2022 WORCESTER MEDICINE 8
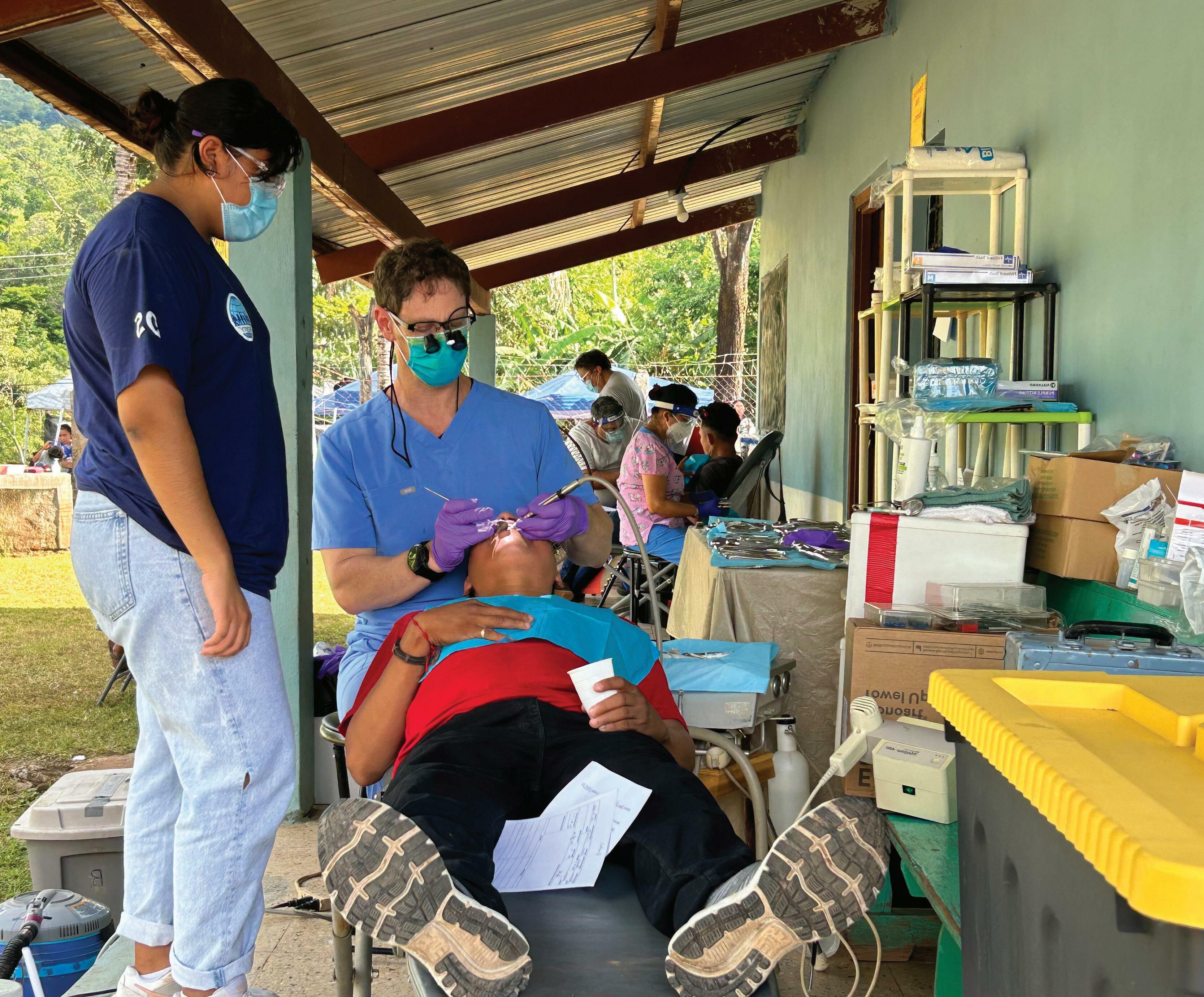




DECEMBER 2022 9 CAPE CARES CENTRAL AMERICAN RELIEF EFFORTS Join Our Volunteer Team We’re looking for: • Dentists • Doctors • Educators • Hygienists • Medical Assistants • Nurses • Pharmacists • Students • All other healthcare professionals Volunteer with Cape CARES for one week and rejuvenate your love for healthcare for a lifetime. If you’re ready to work hard, learn from the cultural differences in people, use skills you’ve forgotten about, and motivate people to help themselves, join us! Can’t join us? Donate! Contribute to growth and health in rural Hondurans WWW.CAPECARES.ORG
Medical Missions & Volunteerism
Medicine in the Amazon Continued
communities came to the clinic. Initially, we saw mostly children, but after a year or so, more women began coming to the clinic with OB/GYN issues. The next year, we had everyone--men, women, and children, and all body parts. I was truly humbled by my patients’ trust.
The most common issues we encountered were aches and pains, gastritis, grippe, machete injuries, conjunctivitis, soft tissue infections, and pneumonias. The most worrisome issues in the jungle environment were the pulmonary illnesses and soft tissue infections, since those issues can quickly become life-threatening. Some of the other issues were congenital heart disease, tumors, menstrual/ fertility issues, benign prostatic hyperplasia (BH), cutaneous Leishmaniasis, Type 2 diabetes, tuberculosis (TB) (very common in the jungle and the leader in mortality). We were always working on wound care and dental hygiene. We also tried to provide other educational information on topics like puberty and STI prevention. With improved communication technology I was able to bring along specific meds for individuals with specific needs. The youngest patient we saw was two hours old, the oldest an 85-1/2 year-old gentleman.
Throughout our time at the clinic, we were regularly reminded that we were not providing medical care in the luxurious clinical setting we were used to in Massachusetts, but rather in an extreme environment with Indigenous population that had very limited health care rights. The people of Sani were only allowed to go to indigenous clinics and were required to pay for their care before being seen, even though they are not part of a monetary society. They could access the occasional government doctor or oil company doctors, who both charged for care. The oil companies even held them hostage for money or oil rights on their property. We were lucky in that if we needed to transport someone, the village would provide some funds for transportation and care.
I wanted to include a few notable stories from my time at the clinic in Sani:
Around 2005, my friend Rosa started having syncopal episodes after the birth of her last child. She made her way through the indigenous health care system, where she was diagnosed with cardiac syncope and sent home. One day while at the river doing laundry, she had an episode and drowned.One morning a petite older woman was led into the clinic with respiratory distress due to massive ascites. She also had large purpuric lesions from her umbilicus to her toes, but had no history of jaundice or parasites.
In order to determine if this was tubercular, we were able to transport her to a medical facility with support from the community.A somnolent nine-month-old arrived at the clinic febrile and in severe respiratory distress. We worked on fever reduction and improvised an Albuterol treatment. By some miracle a doctor and transport boat arrived and the baby was able to be hospitalized and lived.
One evening, a man was brought to the lodge with a machete injury. He lacerated his entire posterior thigh--vertically, thank goodness. We stitched him up by flashlight, gave him supplies, and “signed him out” to the lodge manager, who would later take out his stitches.
On my last trip to Sani, a three-month-old infant with sepsis and apnea was brought in. We had to keep tapping her to keep her breathing. We worked on fever reduction by Tylenol and sponging, but at one point I thought she was going to die, so we moved to a private area and kept sponging. We were able to get her transported upriver and the only news I received was that she was still alive when they got there.
Now to end on some lighter notes:How do you take care of an anaconda bite? First, you have to get the anaconda off of the patient’s hand! During birdbanding research at a friend’s hut an anaconda was brought in for us to see. There was a bit of missed timing, and my physician colleague was bitten. We left the anaconda issue to Luis, who showed us how to thoroughly clean the snake bite with soap and clean water. The entire family watched closely.
One day, while examining a toddler, there was a roar and then an earthquake. The structure we were working in quickly emptied but for Dr. Gail Ryan, my child health partner. She continued to examine the toddler with her stethoscope, not realizing that the shaking was from an earthquake, not the toddler kicking the table! We were all fine.
Clinic day was always a big celebration that included a soccer tournament. One day, a young man (who happened to be the oh-so-important goalie) was gently and slowly led into my exam room, explaining that he had small a tumor, squeezed it, and “tumor juice” came out. I was worried about the jungle version of Burkett lymphoma, but as he came out of the shadows I was so glad to see a pimple and a facial cellulitis!
Our adventure in Sani continued for 22 years, paused for the time being due to the COVID-19 pandemic. Throughout the years we tried to provide good medical care and knowledge. We also received knowledge and great appreciation from the incredible people of Sani. It was a gift I gave to myself. +
Nancy DeTora, MD is a retired pediatrician.
DECEMBER 2022 WORCESTER MEDICINE 10
“
Year after year, increasing numbers of families came to the clinic.
Medical Missions & Volunteerism
Volunteer Eye Mission to El Salvador, 2023
James Umlas, MD
At the end of January 2023, I will have the good fortune to participate in my twenty-fifth annual eye campaign in Santa Ana, El Salvador. As a senior Tufts ophthalmology resident in 1995, I became involved with ASAPROSAR (Salvadoran Association for Rural Health), which is a multifaceted clinic serving the medical and socioeconomic needs of underserved populations in El Salvador. This experience has been one of the most rewarding and satisfying of my professional and personal life. I look forward to the annual ten-day excursion all year long and I have formed great friendships in the process. Through my experience, it has become clear that the medical knowledge, skills, and resources that we have available here in the United States are extremely valuable and applicable across the world.
ASAPROSAR, which is based in Santa Ana, with satellite clinics in San Miguel and other locations, was founded by internist Dr. Vicky Guzman in the 1970s, before the Salvadoran Civil War (1979-1992). She has dedicated her life to bringing quality healthcare and social services to people in El Salvador. Dr. Guzman saw a great need for eye care, which was beyond the reach of most people in her country. She initially made connections with congregants of the United Church of Christ in Norwell and then with Dr. Joseph Bowlds, a now-retired Lahey Clinic ophthalmologist, who organized the first eye campaigns in the late 1980s. We have formed a 501c3 partner organization to ASAPROSAR, which is called Partners for Visual Health (PVH ).

The earliest mission trips were conducted in church halls and community buildings, and frequently involved house calls through difficult terrain during time of war. Eventually, surgical services were added.

Through donations and grants, Dr. Guzman was able to build her own surgical suite, which is used by our group each winter, but is utilized by local Salvadoran ophthalmologists throughout the year. During a typical PVH eye campaign, more than 150 procedures are performed, including cataract extractions, corneal transplants, pterygium excisions, eye muscle surgeries, and laser treatments for glaucoma.
A large medical eye clinic runs in parallel to the surgical campaign. Each year, approximately 2,000 patients are examined and most receive donated eyeglasses. The Lions Club of Lexington, Massachusetts has been especially generous in providing eyeglasses, but many individuals have contributed as well. Most volunteers are from the Boston area, but many areas of the United States and other countries are represented annually. The volunteers include ophthalmologists, optometrists, nurses, anesthesiologists, ophthalmic technicians, Spanish interpreters, and other lay people without specific medical expertise. We set up a “pop-up” dispensary to give out eyeglasses, which have been cataloged in a computer program and are accessible when the patient receives a prescription. When glaucoma is diagnosed, we attempt to give patients six-to-twelve months of glaucoma eye drops.
Although PVH has been able to make significant contributions to eye care in El Salvador, it has been crucial to partner with a local organization that is familiar with and entrenched in El Salvador. Local health promoters and eye doctors screen for surgical and medical eye issues that need attention and refer the patients to the PVH clinic. They have community outreach to alert the local population about the upcoming eye campaign. Patients travel from local communities, but also from the entire country of El Salvador, as well as from Guatemala and Honduras. Many patients travel for hours on local buses or packed in the beds of open pickup trucks. Upon arrival, the wait to see a doctor can be many hours but there are rarely complaints.
As with many clinics in the developing world, ASAPROSAR charges small sliding scale fees for surgical services provided, based on economic status. Patients with higher means pay approximately $25 for a cataract surgery to offset patients who are more indigent and have no resources to pay. No patient left
DECEMBER 2022 WORCESTER MEDICINE 11
A patient at the ASAPROSAR clinic.
Medical Missions & Volunteerism
The Boy With the Blue Sweater
David C. Kim, MD, FACS

is turned away. Our PVH services and supplies are completely free of charge, but the ASAPROSAR clinic needs to pay staff, and provide food and dormitory services for some patients… It has been felt by our hosts that requiring small fees for those who can contribute is a more equitable solution and helps ensure sustainability of their programs throughout the year.
Each year, upon arrival, the team of PVH volunteers unpacks equipment and supplies within a matter of hours and is ready to start work the next day. The campaign is intense, but the esprit de corps keeps everybody focused and motivated during 12–14-hour workdays in the operating room and clinic. The pathology is often severe, so the surgeries are sometimes challenging, but the rewards can be life altering. People who are blind from cataracts frequently walk out with vastly improved vision. Children and adults with strabismus (eye muscle imbalance) emerge with straight eyes, which can not only help them functionally, but also emotionally. Having crossed eyes is frequently a huge social stigma and can limit a person’s life prospects.
Although the work is hard, the group has time for relaxation in the evenings and at the end of the journey. Our hosts treat us extremely well and the Salvadoran delicacies served daily keep us well nourished. Many of the volunteers have logged more than ten missions because of the unity of purpose and joy involved in serving the patients. The group has no religious or political agenda. We work tirelessly throughout the year to acquire medications, glasses, and ophthalmic equipment to keep the mission going and to help the local doctors who staff the clinic for the rest of the year. We are always looking to recruit interested volunteers, especially those with medical, nursing, or anesthesia skills, but also lay people who want to help raise funds, pack supplies, or learn how to dispense glasses. In addition, donations continue to be crucial to maintain our mission.
The ultimate goal is to make our services obsolete, but the reality is that with economic inequities, PVH’s efforts will likely be needed for the near future. I look forward to participating for many years to come. +
James Umlas, MD, Lexington Eye Associates; Secretary, Partners for Visual Health. https://partnersforvisualhealth.org.
Iam often asked if there is one memorable patient or operative case that has impacted my career. Indeed there is: The the boy with the blue sweater.
Several years ago, two days prior to departing from a surgical mission in Bhutan, I decided to walk from the hospital to my hotel rather than traveling on the Surgicorps team bus. I wanted to enjoy the views of the Himalayan mountains since our days were relegated to the hospital and hotel. On an isolated road, I passed a boy wearing a blue sweater who appeared 17 or 18 years old. I immediately noticed he had an extremely wide cleft lip, so wide his front teeth were exposed and his nose deformed. Clinically, his situation was rather unusual, not only because of the extent of his deformity, but also due to the rarity of an untreated cleft lip at his age. Cleft lips and palates are typically repaired during infancy. I was shocked by his condition. He passed so quickly, stopping him wasn’t even a thought.
Continuing my trek to the hotel, I rationalized my hesitation by convincing myself that I didn’t know the language and didn’t want to offend him by addressing his condition. That night I regretted my inaction. I questioned why I wasn’t more proactive. I agonized, imagining him enduring the deformity through his childhood and teenage years, its impact personally and socially as a young man. During my travels abroad, I learned that some societies marginalize and ostracize people with deformities, especially disfiguring ones.
The next day I walked the same route, desperately and selfishly hoping I might see him. But no such luck. Miraculously on the final day at the hospital, he showed up by himself—still wearing the blue sweater. Unfortunately, my team and I had already packed our supplies and were ready to leave the hospital. The team graciously agreed to unpack and assist me with the surgery. Because we had exhausted our anesthesia supplies, I operated on his lip using only local anesthesia. He didn’t flinch and tolerated the procedure without any emotion. I wondered
DECEMBER 2022 WORCESTER MEDICINE 12
“
By just listening, understanding, and sometimes holding their hands, patients appreciate our intentions, even if we cannot help.
Volunteer Mission to El Salvador
Continued
Medical Missions & Volunteerism
how he even knew to present to the hospital, why he was by himself, and if his stoicism was from years of hardship. In the end, it didn’t matter. After the surgery, I gave him a mirror. He smiled, and I cried.
I have had the honor of participating in 40 international surgical missions. They serve as continual reinforcement of providing medical care in its simplest form to people who are in dire situations. Where I have traveled, there are no overseeing agencies dictating care, no
secondary gains to manage, and no impending threats of liability. Even with the best of intentions, there are patients that we just cannot help. Sometimes their conditions are too extensive to treat. My team and I transport surgical equipment and supplies, but hospital resources and support are scarce or non-existent. And sometimes we just do not have enough time or staff to handle the droves of patients. But by just listening, understanding, and sometimes holding their hands, patients appreciate our intentions, even if we cannot help. Being a father myself, I cannot fathom how desperate parents can be so gracious with our inability to provide care.
I still believe medicine is one of the noblest professions known to humankind. Each of us is graced with the opportunity to help others who do not have access to the care and resources they need. I encourage you to nurture, embrace, and extend your talents without hesitation. While this notion was instilled in me by my parents, mentors, and family, I learned this lesson from the boy with the blue sweater. +
David C. Kim, MD, FACS is Chief of Plastic Surgery at St. Vincent Hospital and Reliant Medical Group.
Preparing Today’s Students for Tomorrow’s Global Health Workforce: What they Need to Know
Jean Boucher PhD, RN, ANP-BC Michele P. Pugnaire, MD


With the rise of the globally interconnected millennial generation, it’s no surprise that today’s health profession students are increasingly engaged in global health as part of their studies, and for some, their future career plans. Nation wide, about one-third of students entering pre-medical programs have participated in an international volunteer experience, with two-thirds of enrolled medical students expecting to participate in global health experiences during medical school.(1) At UMass Chan Medical School, student participation in global health programs rose two-fold from 33.8 percent in 2004 to 67percent in 2011.(2) Not unexpectedly, Tan Chingfen Graduate School of Nursing students are increasingly seeking out opportunities to participate in global health initiatives . This rising demand for international programs has fueled the expansion of UMass Chan’s global health offerings for School of Medicine and Graduate School of Nursing students and has accelerated the development of high-quality experiences consistent with educational standards in global health.(2,3,4,5,6,7)
Our contribution to this issue of Worcester Medicine offers an evolutionary perspective on global health education and how UMass Chan is best preparing today’s students for our future global health workforce. Our featured program is the Dominican Republic Batey Health Initia-
tive (DR-BHI), an interprofessional global health program for UMass Chan students and faculty in the School of Medicine and Graduate School of Nursing. Our DR-BHI overview describes four examples of challenges and lessons learned in global health education that illustrate how our students are actively learning four core precepts of best-practice global health:
• community engagement and empowerment
• cross cultural awareness and humility
• interprofessional teamwork and collaborative practice
• advocacy for sustainable development of communities being served
challenge: limitations of the shortterm medical mission model
Like many global health experiences, the DR-BHI, based in La Romana, Dominican Republic, is a short-term (one week) experience in global health (STEGH). Like other STEGH’s, our twice-yearly visits to the Dominican Republic initially focused on “mobile” ambulatory clinics based in remote communities know as bateyes (home to underserved Haitian migrant cane workers and families) with a key goal of hypertension control. With twice-yearly visits, our team experienced the shortfalls of STEGH models with limited continuity, follow-up and longitudinal engagement, and the risk of doing more harm than good for the communities we served. Addressing these limitations, we partnered with our host partner to designate two bateyes that we would
DECEMBER 2022 WORCESTER MEDICINE 13
Medical Missions & Volunteerism
Preparing Today’s Students... Continued
serve long-term to promote continuity and community engagement. We also partnered with a local La Romana-based NGO (non-governmental organization) to support two additional hypertension clinics per year, so clinics were offered on both bateyes every three months rather than twice yearly. To assess the effectiveness of our continuity-based model, DR-BHI medical and nursing students collaborated with the bateyes, host sponsor, and partner NGO to study hypertension control. Study outcomes demonstrated improved systolic blood-pressure control following implementation of the continuity model. Lesson learned: Establishing continuity of care and longitudinal engagement with communities requires community-based partnerships and collaborative practice with local healthcare organizations.
challenge: building local community workforce capacity to best serve the needs of local populations
With our continuity-based hypertension program in place, our batey-based health workers (or “promotoras”) were empowered to participate more actively in blood-pressure monitoring and batey-based care of their hypertensive patients. To advance the promotoras’ skills, the DR-BHI and our local sponsor overseeing the promotora program jointly established a promotora blood-pressure training program to build capacity in the promotora workforce and empower them as active partners in our hypertension management program. Both the promotoras and host sponsor endorsed the program, with the sponsor now supplying the promotoras with blood-pressure cuffs and ongoing training. Building on the success of this training model, additional promotora training has been offered in malnutrition screening, HIV prevention, and wound care. This training model was a collaborative effort with promotoras, the host sponsor, and DR-BHI medical and nursing students, with all sessions featuring interprofessional teambased care. Lesson learned: Building local community capacity is best achieved when responding to the host community’s needs through relationship building, empowerment, and interprofessional teamwork.
challenge: unanticipated roadblocks limiting on-the-ground service commitments abroad
Pandemic-related travel shutdowns threatened the sustainability of the DR-BHI’s hypertension program and promotora training. To sustain the clinics,
during the pandemnic funds for DR-BHI travel were reallocated to our NGO partner to support hypertension clinics every three months . For on-the-ground promotora training sessions, we partnered with our host to support real-time DR-BHI training sessions via Zoom. Our sponsor provided technology infrastructure and safe transport for promotoras to attend hospital-based Zoom sessions. We also recognized the reliance of promotora training on DR-BHI support. To promote long-term sustainability, we forged a new partnership with our host and two other affiliated organizations serving the bateyes to establish a train-the-trainers program, empowering local physicians to provide promotora training, thereby establishing a sustainable model for long-term promotora training without reliance on ongoing DR-BHI support. Lesson learned: Sustainability of on-the-ground service commitments requires partnerships, capacity-building, and empowering local individuals, programs, and organizations.
challenge: cultural effectiveness and humility as core values and skills for global health teams
It is widely recognized that ethical principles of cultural awareness and humility are foundational in preparing for global health experiences. Consistent with this understanding, DR-BHI requires cross-cultural awareness and humility training as part of pre-departure preparation. Our training in this area continues to evolve and is informed by the experiences of our students and feedback from DR-BHI participants including, our local partners. Through this iterative process, peer-topeer engagement has emerged as the backbone of our cross-cultural awareness training. With an increasingly diverse student body, DR-BHI students represent an expanding range of cultural, racial, ethnic, economic, and linguistic backgrounds. Given this rich diversity, students directly experience cross-cultural awareness through group interactions, allowing them to both inform and teach each other. Structuring time for peer-to-peer interaction as part of pre-travel preparation and through daily debrief sessions while in the Dominican Republic, have proven effective in promoting both cross-cultural awareness and humility among our learners. Another important contributor to cross-cultural development has been our local DR-BHI program advisor, a Haitian Dominican from La Romana who is now a United States citizen residing in Worcester. He serves many roles: guest lecturer, consultant on Dominican Republic-based initiatives, and reviewer of project materials to ensure cultural and linguistic alignment with our local based partners. Our advisor also serves as “culture broker,” assisting us in better understanding and collaborating with our Dominican Republic-based colleagues. Lesson learned: Cultural awareness and humility training can be promoted through the diversity of representation among student learners, along with the engagement of individuals representing the communities and cultures being served.
Building on these lessons learned, we continue to expand and enrich global health education to best prepare today’s students for tomorrow’s global health challenges. Now is also the time to nurture and support today’s students as the teachers and role models for future global health education who will teach the rising generation of new student learners. The need for high-quality, best-practice global health education has
DECEMBER 2022 WORCESTER MEDICINE 14
Medical Missions & Volunteerism
never been greater as we prepare to pass the baton to today’s students as our global health educators, workforce, and leaders of the future. +
Jean Boucher PhD, RN, ANP-BC is professor of nursing and medicine and director of the nursing practice PhD program in the Tan Chingfen Graduate School of Nursing at UMass Chan Medical School.
Michele P. Pugnaire, MD isprofessor emeritus, Office of Educational Affairs in the T.H. Chan School of Medicine atUMass Chan Medical School
References
1. Melby, Melissa K., et al. “Beyond medical “missions” to impact-driven short-term experiences in global health (STEGHs): ethical principles to optimize community benefit and learner experience.” Academic Medicine 91.5 (2016): 633-638.
2. 2011 GQ Medical School Graduation Questionnaire Individual School Report University of Massachusetts Medical © 2011, Association of American Medical Colleges.
3. Guidelines for Premedical and Medical Students Providing Patient Care During Clinical Experiences Abroad. Approved by the AAMC GSA Steering Committee on February 25, 2011 available at https://www.aamc.org/news-insights/packing-ethicsmedical-students-global-health-trips. Accessed as of November 11, 2022.
4. Jogerst, Kristen, et al. “Identifying interprofessional global health competencies for 21st-century health professionals.” Annals of global health 81.2 (2015): 239-247.
5. DeCamp, Matthew, et al. “Ethical obligations regarding short-term global health clinical experiences: an American College of Physicians position paper.” Annals of Internal Medicine 168.9 (2018): 651-657.
Where You Live Should Not Determine Whether You Live, or Whether You Die
Heidi K. Leftwich, DO

Where you live should not determine whether you live, or whether you die.” -Bono
According to 2021 statistics from the World Health Organization, 16 percent of maternal deaths in sub-Saharan Africa are attributable to hypertensive disorders of pregnancy. As a maternal-fetal medicine physician, I have spent my career caring for women with medical complications that impact pregnancy, with a focus on hypertensive disorders of pregnancy, including preeclampsia. Even in the United States, preeclampsia is a condition affecting approximately four to eight percent of pregnancies and a leading cause of maternal mortality.
Since the beginning of the pandemic, I have been working on a large research study looking at the link between the immunologic and histologic changes in the placenta from SARS-CoV-2 virus (the
6. Douglas MK, Reencounter M, Pacquiao DF, et al. Guidelines for Implementing Culturally Competent Nursing Care. J of Transcultural Nurs. 2014; 25(2): 109–121.
7. National Academy of Medicine. A framework for educating health professionals to address the social determinants of health; 2016. Available at: https://www. nationalacademies.org/ hmd/~/media/Files/ Report%20Files/2016/ SDH-Resources/ SDHeducation-RiB.pdf. Accessed December 26, 2018.
virus causing COVID-19) and its similarities to preeclampsia. When I was asked by a colleague and the Kenya Medical Research Institute (KEMRI) to come share my work and discuss ways to expand our research to collaboration in Kenya, I immediately thought it was an amazing opportunity to have the chance to impact care outside the United States. An avid traveler, I had never been to Africa, and I was excited about this opportunity. I quickly began making plans, as I did not have much time between accepting the offer and traveling. My colleagues were incredibly supportive, and they were instrumental in allowing me to participate in this incredible experience.
Since I would be in Kenya discussing research proposals, my schedule was starting to fill with meeting international researchers and going into the hospitals to talk with the local doctors about their needs and desires. I also reached out to the teaching hospital--which had three maternal-fetal medicine fellows--and was invited to give two days of lectures
DECEMBER 2022 WORCESTER MEDICINE 15
Medical Missions & Volunteerism
during my visit. While there, I found out that there are only three people in the whole of Kenya who are fellowship trained maternal-fetal medicine physicians. My participation in the training of these three fellows would help Kenya actually double that number once they finished their training and graduated. I will say that I had incredible help from my mentor, who has been traveling to Kenya for 20 years and was therefore able to set up a full schedule for me to be truly immersed in both the culture and hospital system.
What I learned is hard to describe in a short narrative. I was so incredibly welcomed in the three hospitals I had the opportunity to visit, locally by the community, and in the medical training college in Eldoret where I taught the maternal-fetal medicine fellows, obstetrics, and gynecology residents and students. I was warned they may not ask questions out of respect for seniority but I was pleasantly surprised as our time led on that we had an amazing interactive teaching and learning model, where we all learned from one another.
One of my lectures focused on hypertensive disorders of pregnancy. I discussed the changes in guidelines that have helped decrease morbidity and mortality in the United States, and the standard of care and practice management. When asking questions regarding these guidelines and how they are managing similar patients, I quickly learned some of the barriers for their patients to adhere to such management, including access to the hospital, limited bed space, and refusal of inpatient care by patients because of family needs. A very important factor in offering management was that the gestational age at which a fetus was considered viable (able to survive) was closer to 28 weeks in their hospitals, compared to 22 weeks in the United States. This difference meant that, if a pregnant patient before 28 weeks came to the hospital for preeclampsia with severe features--a condition that can cause life-threatening hemorrhage, liver and/or kidney failure, seizures, and strokes-- the choice would only be termination of the pregnancy and not preterm delivery, something I recommend frequently for the sickest of my patients. This knowledge helped me better understand the culture and struggle in healthcare, so I could better formulate a research project that had a better chance of successfully making an impact.
In visiting three separate hospitals in Kenya, I realized also that all hospitals are not created equal. The amount of funds allocated to hospitals was somewhat dependent on the tribe and location; The teaching hospital in Eldoret had far more resources than the other hospitals I visited. As I discussed a proposal to test for preeclampsia, one smaller community hospital told me their chemistry machine had been broken “for a while” and they did not have the ability to check liver or kidney function tests on their hypertensive patients. This would be a barrier to a research protocol, but more importantly is a scary reality that hypertensive pregnant patients who present to this facility have less care than at other facilities. With so many life-altering experiences from my time there, this one sticks with me as the most memorable. How could this be? How could we help? Their option was to send “whoever appeared the sickest” as a transfer to another hospital to obtain these tests, but by then they may already be in liver or kidney failure. I saw transports when visiting the hospital that accepted such patients, with three cases of preeclampsia in one day, with two having stillbirths, two having renal failure, and one in the ICU after a seizure. If caught earlier, these outcomes could have been largely avoided.
Now that I have returned from Kenya, my next steps are to apply for grant funding to assess the need from a research study, showing what I clearly witnessed: a need for earlier, easier access to diagnosis and treatment, including helping to staff the centers with the equipment needed to take care of their patients. I hope to be back next year if my funding is successful and will pursue getting a full medical license next time so that I can help with patient care as well, not just from a teaching/research perspective. I am hopeful that I can fund the new chemistry machine from a grant, but, if not, I have plans to set up a fundraiser to buy the hospital the chemistry machine needed to help their healthcare providers have access to the equipment they so desperately need and desire. The words of one physician there will never leave me. I cannot imagine being in that position and making the decisions he is forced to make daily. I am forever changed by my experience in Kenya. The country and its people are forever in my heart.
+
Heidi K. Leftwich, DO is Assistant Professor, Obstetrics and Gynecology and Associate Fellowship Director in the Division of Maternal-Fetal Medicine at UMass Chan Medical School and UMass Memorial Health.
DECEMBER 2022 WORCESTER MEDICINE 16
“
In visiting three separate hospitals in Kenya, I realized that all hospitals are not created equal.
Where You Live Should Not Determine... Continued
Medical Missions & Volunteerism
Responding to the Call: The Pharmacist’s Role in Disaster Responses and Medical Missions
Stephanie L. Conway-Allen, PharmD, RPh Sheila M. Seed, PharmD, MPH, CTH®, RCPS AFTM (Glasg), RPh


Volunteerism is embedded in the makeup of a healthcare professional; we desire to assist others in times of need. Many healthcare professionals volunteer their services in response to a natural disaster or on medical mission trips. Pharmacists have long had a role in disaster response teams and medical missions. The International Pharmaceutical Federation (FIP) issued a Statement of Professional Standards on the role of the pharmacist on humanmade and natural disasters in 2006 (1) and developed the Responding to Disaster Guidelines for Pharmacy in 2016. (2)
Pharmacists have been involved for several years in the response to public health emergencies and disasters, such as pandemics, medical missions, serving on Disaster Medical Assistance Teams (DMAT), or as part of the Medical Reserve Corps (MRC). Proper training is essential and is provided for both DMAT and MRC response team members. The role of the pharmacist in these settings has traditionally consisted of dispensing medications and ensuring individuals have access to safe products, providing continuity of medical care. In addition to dispensing, pharmacists often need to review treatment plans and appropriate medication substitutions if a particular drug is not available. They are responsible for the proper storage of medications and must ensure a level of quality assurance for medications purchased locally. Recently, pharmacists have expanded their traditional roles to include screening patients for triage purposes, point-of-care testing, administering first aid, and providing immunizations. (1,2,3) When providing clinical pharmacy services, it is important to consider the needs of the local population and the available resources. This is true when responding to a disaster situation or while on a medical mission.
Responding to a natural disaster or public health emergency can either be either a local response with organizations such as the Worcester Regional Medical Reserve Corps (MRC) (https:// worcesterregionalmrc. org), or a federal response, such as with a DMAT unit when local resources are overwhelmed. The MRC is composed of both non-medical and healthcare profes-
sional volunteers, including pharmacists. During Hurricane Katrina, the response required both federal and local assistance to aid victims. In a combined effort of federal resources, chain pharmacies, and drug companies, a pharmacy was set up in the Houston Astrodome. The pharmaceutical needs for approximately 7,000 victims were met as hundreds of volunteer pharmacists filled more than 20,000 prescriptions. (4) In addition to responding to disasters, many healthcare professionals volunteer to assist on medical missions. One of the many advantages to volunteering for a medical mission is the opportunity to assist and implement healthcare needs in underserved communities, both domestically and internationally. You are able to provide care to individuals that may not have access to medical care, or it may be beyond their means to get medical care. There are a number of logistical issues with planning a medical mission, such as transportation of medications and supplies out of the country, lodging, proper travel documentation, and safety.
Both of us have had the opportunity to participate on mission trips. One mission trip was to the village of Roche-a-Bateau, located on the southwest coast of Haiti. There, we assisted a clinic run by the Sisters of Saint Anne. The mission team contacted the Sisters ahead of the trip to determine which medications and supplies the clinic needed the most. The greatest needs were over-the-counter medications for children and adults, including vitamins, analgesics, heartburn medications, basic first aid supplies, nebulizers, and a centrifuge. Donation bins were set up and five full suitcases were brought to Haiti--retrieving all the bags at the airport was an adventure in itself.
The clinic provided service to those within the village and the surrounding mountainous villages. Travel from some communities required over a two-hour walk down a mountainside and across rivers to reach the clinic. Access was limited to the remote mountainside village, so
DECEMBER 2022 WORCESTER MEDICINE 17
“
When providing clinical pharmacy services, it is important to consider the needs of the local population and the available resources.
Medical Missions & Volunteerism
Responding to the Call... Continued
we brought the supplies to the village by donkey. The supplies allowed for a nurse in the village to administer over-the-counter medications for mild ailments. Luckily, Haiti has the same electrical current as the United States, so the equipment was immediately operational in the clinic. The trip was a success! It filled up the empty medicine cabinets, allowed the nuns to provide some medical treatments, and for many individuals, prevented the need for travel to the nearest city for a breathing treatment that was well over an hour away by car.
In Honduras, the need for medical missions is extensive and year-round. Many communities exist in rural or mountain areas where access to healthcare is limited while the need is great. Through the Cape Cod, Massachusetts-based Central American Relief Efforts (Cape CARES) organization (https://capecares.org), several trips are made each year to areas of Honduras where medical services are not readily available. Los Encinitos sits far into the mountains of Honduras and is at least an hour drive (through the mountains and only with the assistance of very experienced drivers) from the country’s capital, Tegucigalpa. Each year, three teams set up both adult and pediatric medical and dental clinics for one week. The work required to prepare for each trip is extensive, and the role of the pharmacist is especially imperative in the preparation. Inventories are pertinent in both the medical and dental clinics to ensure that the adequate amount of medicine, supplies, and maintenance materials are available to those unable to journey to the nearest clinic (which for many is a day or more on foot). Pharmacists work with the team to obtain donated and purchased medications for various health issues such as blood pressure, diabetes, cardiovascular health, pain, gastrointestinal-related ailments, allergies, and numerous types of infections. The pharmacist works to prepare medication orders with complete Spanish-language label instructions and conducts medication patient counseling. The pharmacist is responsible for maintaining a running inventory of medications, making recommendations and adjustments to treatment plans based on evidence-based medicine and supply, and assisting in blood glucose and other point-ofcare testing. In Honduras, the pharmacist’s role is substantial and an absolute necessity.
While volunteering in response to either a disaster situation or a medical mission has its r own unique challenges and opportunities, both are professionally and personally fulfilling. +
Stephanie L. Conway-Allen, PharmD, RPh is Associate Professor of Pharmacy Practice at Massachusetts College of Pharmacy and Health Sciences School of Pharmacy.
Sheila M. Seed, PharmD, MPH, CTH®, RCPS AFTM (Glasg), RPh is Professor and Chair of Pharmacy Practice at Massachusetts College of Pharmacy School of Pharmacy.
References:
1. International Pharmaceutical Federation. FIP Statement of Professional Standards: The Role of the Pharmacist in Crisis Management: Including Manmade and Natural Disasters and Pandemics. Available at: https://www.fip.org/file/1472 Accessed October 20, 2022
2. International Pharmaceutical Federation. FIP Responding to Disasters: Guidelines for Pharmacy 2016. Available at https://www.fip.org/files/content/pharmacy-practice/militaryemergency-pharmacy/emergency-activities/2016-07-respondingto-disasters-guideline.pdf. Accessed October 20, 2022.
3. Ahmer Raza M, Aziz S, Noreen M, Masood Raza S. Role of Pharmacist in Disaster Management: A Quantitative Content Analysis Approach. Innov Pharm. 2021 Sep 22;12(4):10.24926/ iip.v12i4.4359. doi: 10.24926/iip.v12i4.4359. PMID: 36033125; PMCID: PMC9401375.
4. Koutnik-Fotopoulou, E. In the Wake of Katrina, Chain Pharmacies and Drug Companies Join Forces. Pharmacy Times, Oct 1, 2005. Available at: https://www.pharmacytimes.com/ view/2005-10-9919 Accessed October 20,2022.
Calendar of Events
Annual Business Meeting
April 11, 2023, 5:30 p.m., Beechwood Hotel Meeting includes presentation of the 2023-2024 Slate of Officers, the WDMS President’s Award, WDMS Career Achievement Award and 2022 MMS/WDMS Community Clinician of the Year.
Women in Medicine Leadership Forum: The Power of Food, The Power of the Pause May 3, 2023, 5:30 p.m., Mechanics Hall
Speaker: Michelle Dalal, MD and Harikirin Khalsa, MD How lifestyle medicine, plant based nutrition, and biological self-awareness build stronger selves, and help us empower our patients.
Author Event: The Heart of Caring May 24, 2023, 5:30 p.m., UMass Faculty Conference Room Mark Vonnegut, MD will review his latest book “The Heart of Caring: A Life in Pediatrics.”
DECEMBER 2022 WORCESTER MEDICINE 18
Medical Missions & Volunteerism
Reaching Out: What an Experience!
Marjorie Silva Rapose, DMD
In January 2020 I traveled to Patharlyndan in the hills of Meghalaya, India to conduct an Oral Hygiene Awareness camp for village children. My brother and his religious congregation run a small mission, teaching children to read. When he invited me to help with dental care, I felt the calling: “Whatever you do to the least of your brethren, you do unto me.” (Matthew 25:40)

Reaching Patharlyndan was a three-hour car ride from the airport, winding up and down mountains with no proper roads. On arriving, I was immediately struck by profound poverty. With temperatures below 40 degrees Fahrenheit and no electricity, locals lit fires to keep warm through the night. With no grocery stores, they ate what they produced. There was no television or radio, and literacy rate was very low. The nearest medical facility was two hours away. Most children could not attend school as they needed to work. Every morning I saw older kids going to the fields carrying younger siblings and returning in the evening with grain on their backs.
On the day of the dental camp, I will never forget the smiling faces, but the dental hygiene was beyond terrible. They never brushed, and forget the floss! As I handed them toothbrushes and toothpaste, I had to explain (my brother translating in Khasi) what the brush and paste were, and how to use them (including which side goes into the mouth).
At the end of the camp, they invited me into their homes. It was an amazing experience visiting them. Though they had very little to eat themselves, they wanted to share that with me. The kids played with stones and sticks and danced around the fire. The elders gathered every evening to smoke and chat. They lacked materially, but they were so happy and content.
El Medico Cubano
Warren Johnson, MD

As I sit on the sweltering back porch of the clinic, my own sweat blinds me while I struggle with a bullet in a buttock. I can’t wipe the salty water away with both hands in the sterile gloves I am wearing. The porch is the only clean location where there is sufficient light for a surgical procedure. My hands are struggling, probing several inches deep through several layers of muscle into Adrien’s adolescent thigh, fishing for the bullet that I can feel with my long-handled hemostats, but I can’t see the target. I shoo chickens away
As my flight took off from Guwahati, I realized that though I came here on a mission trip, I left a transformed person myself. I realized that disadvantaged communities have so much to teach the world. There is no depression or anxiety on those Khasi hills. They do not worry about a tomorrow but just live a happy today.

Now every morning when I pick my toothbrush I say, “I am blessed more than I can imagine.” +
Marjorie Silva Rapose, DMD graduated from Boston University Henry M. Goldman School of Dental Medicine and practices as General Dentist in the Sterling/ Leominster area.
from under my feet. We don’t evict the chickens from the clinic compound because they love to eat the biting flies and ants that I cannot swat away with my sweaty, sterile-gloved hands. Seven people standing nearby wince at the clicking sound the surgical instrument makes against the bullet. It makes me a little nervous to have this audience, but Adrien had invited them all, glad to have his neighbors witness the surgery being performed by “El Medico Cubano”--“The Cuban Doctor” (my local nickname) in the afternoon heat of Southern Honduras. Besides, this surgery is the only entertainment in town today.
I was known in the clinic as “El Medico Cubano,” a doctor with the American medical relief group, Cape CARES (https://capecares.org). Each year, Cape CARES brings dentists, doctors, and educators to a few small communities in the jungles of southern Honduras. Our four brigades per year last one week each, bringing 20 volunteers from across the United States. We work on young smiles, old teeth, aching bodies, and rarely, bullet wounds. Each clinic is located in an open-sided brick building, standing tall amidst humble adobe houses. For decades we had
DECEMBER 2022 WORCESTER MEDICINE 19
Medical Missions & Volunteerism
no electricity and no running water, but things are better now.
Cape CARES began in 1991 to fill the gaps created by Honduras’s struggling healthcare system, and those left after the end of emergency disaster relief initiatives. Cape CARES’s humanitarian work has no political or religious agenda. In the two communities where we run clinics, dental care has evolved from just extractions to restoration and prevention. Medical care has grown from first aid and acute disease care to ongoing primary care, well-child care, and health maintenance.
Adrien had high hopes of making a new and better life in Honduras’s capitol city of Tegucigalpa. He is good-looking, well spoken, and literate in his native Spanish. He is also a good soccer player. Sadly, there is no work for him in the small village of San Marcos, and no level ground on which to play soccer. The only professional job that existed in San Marcos— rope-making--was already taken by Adrien’s older brother. The historic industry of making rope from fibrous local plants was crushed under the weight of plastic fibers and cheaper Asian labor. Adrien’s only two options were to swing a machete all day in sugar cane fields, or go to work in a factory in the city where he had been shot twice in the back for his bus fare. A third option would be for Adrien to make the trip from southern Honduras, through Guatemala, to the wealthy countries of Mexico or the U.S. Even the poorest urban neighborhoods in the U.S. and Mexico are safe and opulent by Honduran standards.
shipwrecks on the Caribbean coast. But poor and uneducated Garufina rarely venture into southern Honduras where Cape CARES clinics operate. Years ago, the Cuban government sent health professionals throughout Honduras to help the rural underserved. Some were blackskinned. Thus, the San Marcos community assumed I was Cuban and so was born my alter ego, “El Medico Cubano.” It was on my second trip to San Marcos that I realized how some Hondurans truly did not believe that “El Medico Cubano” was one of the North American “Fat pink ones.” They would whisper to me in Spanish, “We like The Fat pink Ones, but they don’t understand us.” It was said with such tenderness, meant as endearment, not as insult. They told me things like, “They dress funny.” “They have strange ideas of money and land.” “They offer to buy things that we would have given for free.”
Dawn breaks in San Marcos with roosters crowing and dogs barking. At first light, shoeless children walk livestock from bare clay yard to green pasture. They run home, bathe, and dress in white shirts for school before they climb the narrow foot path to basic schoolrooms. School breaks at midday and, if the teachers are not on strike, they will have an afternoon school session before herding the cattle back to the yard. Life will go on like this from first grade to sixth grade. At that time the boys are old enough and strong enough to get jobs cutting sugar cane or harvesting melons. Some will go to work in one of the major cities: Tegucigalpa or San Pedro Sula. We employ a few local people during our brigades, and they gain a few non-agriculture job skills.
In 2014--the year when I removed that bullet--I was the only Black man to have come with Cape CARES to San Marcos, a community populated by brown-skinned Mayan people who did not immediately understand that this black man was American. Honduras is also home to the Garufina people; those coal black-skinned descendants of enslaved Africans who were stranded by sixteenth-century

Adrien is still in San Marcos. His teeth and body are in good repair because of Cape CARES dentists and doctors. He still has that second bullet deep in his buttock. When I last talked to Adrien, he was no longer contemplating a trip to the U.S. Working for Cape CARES for one week twice a year, he acquired some employment skills. He no longer calls me “El Medico Cubano.” I am one of the Americans now--tall and fat, just not pink. +
Warren Johnson, MD is a family physician in Colorado has volunteered with Cape CARES for 25 years.
DECEMBER 2022 WORCESTER MEDICINE 20
“
Adrien’s only two options were to swing a machete all day in sugar cane fields, or go to work in a factory in the city where he had been shot twice in the back for his bus fare.
El Medico Cubano
Continued
A Night at St. Anne’s: Filling the Gap in Worcester’s Healthcare System
Madeline Schwartz
Every other Tuesday, around 5:45 p.m., I hop in my car and make the seven-and-a-half-minute commute to St. Anne’s church on Route 9 right outside Worcester. I park around the periphery of a bustling parking lot, tucked away behind the church. Usually around 6:00 p.m. as I’m showing up for my case management shift, I hear the church bells ring. This familiar sound has signified a night I dedicate solely to sitting with and listening to patients from the greater Worcester community.
I was cloaked with my white coat within weeks of arriving at medical school, after I had completed a mere two exams out of the dozens I would be taking during my first year. I had little to no medical knowledge, yet this profession had already decided to dress my classmates and me with a symbol of power. As the initial months of first year wore on, the glory and pomp of the white coat wore off. I spent long nights in the library, learning the ins and outs of the human body. Never had I felt so disconnected to the reason why medicine called my name in the first place. I had half-heartedly signed up for an optional enrichment elective (OEE) titled “Case Management.” Having no idea what case management was, but knowing it sounded “less science-y” than the other classes I was taking, I decided to continue with it.
We learned how to sign patients up for MassHealth, connect them with primary care providers, and even offer resources such as housing support, legal counseling, free baby formula and supplies, and car seats-all the tasks that would traditionally be delegated to other members of the healthcare team. It felt rewarding and unique to be able to step out of the student-doctor position and into the case manager role.
Part of earning credit for the OEE was completing two volunteer case management shifts at the free clinics with current second-year student (M2) volunteers. My volunteer shifts were at St. Peter’s (the sibling clinic to St. Anne’s) with AJ, an M2. As I walked into the church building that evening, it was as if I had peered behind the curtain of UMass’s medical presence in Worcester. Children laughed on gym bleachers, mothers spoke with medical students earnestly, and veteran clinic liaisons joked and poked fun at each other, like a family reunion. Immediately I was hooked by this glorious underbelly of Worcester’s healthcare system. I applied to become a case management lead for the 2022 year, and in January I happily accepted the case management lead position at St. Anne’s. Now every other Tuesday, I make the familiar drive down Route 9 and practice my case management skills with community members.
Working at the free clinics has taught me many things as a medical student. I am extremely grateful for the opportunity to be a part of the well-oiled machine that is WFCC. My experience has been 30 percent frustration and 70 percent joy. I will begin by explaining the frustration so that we can end with joy.
During each shift at St. Anne’s, I am confronted with very familiar, almost identical problems and patient concerns. The most common is
health insurance. We are lucky to live in a state that provides universal health insurance for residents, depending on citizenship status.
I have met countless patients that have recently immigrated to the United States, lost a job, or have received a devastating diagnosis who are blown away by the option of MassHealth. However, this joy only lasts a short while. Primary care physicians, especially those who speak other languages, who accept MassHealth, and provide culturally competent care, are in such high demand in the Worcester area. Wait times to see a pediatrician or family physician can be months--time that families and patients do not have in the midst of starting school or taking care of a pressing health need. While it is frustrating to operate in a healthcare system that fails to serve so many, I am thankful that WFCC exists so that these patients can see a provider in a pinch.
The joy is hard to miss. Case management at St. Anne’s is an opt-in service. This means I get to sit and observe the patient interactions that are taking place for a large proportion of the night. When I see my classmates--just first and second-year medical students--eloquently taking histories, providing compassionate and trustworthy care, and even making patients laugh and smile during difficult conversations, I could not be prouder to be in this profession. Similarly, I have been blown away by the resilience of patients that visit the free clinics.
Most patients diligently take notes, listen to the physician’s advice, and report their own concerns and hesitancies. When I speak with patients at case management, I often hear of the multitude of adversities they are facing; whether it is a difficult divorce, applying for a green card, finding employment, or figuring out how to feed four young children, I am stunned at their ability to advocate for themselves and ask for help.
Medicine is community, and WFCC shows up for the greater Worcester community each day of the week. I am proud to have served as the case management lead at St. Anne’s this past year, and I look forward to handing over the honor to the next, somewhat naive, first-year medical student. +
Madeline Schwartz is a second-year medical student at UMass Chan Medical School and is on the Population Based Urban and Rural Health (PURCH) track.

DECEMBER 2022 WORCESTER MEDICINE 21 Medical
Missions & Volunteerism
Medical Missions & Volunteerism
Cold, Displaced and Diabetic: Lessons Learned While Caring for the Refugee
Population of Worcester
Akanksha Nagarkar, BS, BA
During my time working as an EMT prior to medical school, I was continually fascinated by how vast medicine is. Not only is it scientifically complex, but there are also many socioeconomic and logistical factors that impact medical care. I often wondered how it was possible to study and learn all that medicine encompasses.
When I entered medical school last year, I quickly became immersed in the lectures and resources that most medical students use to grasp the basics of this multifaceted field. However, it was not until my experience as a care coordinator at the Indian Society of Worcester Free Health Stop that I realized that medicine is best learned from the people for whom we have the opportunity to care. The patients we have the privilege to work with are the experts of their own bodies and circumstances, and they are truly our best teachers. Every patient I have had the opportunity to work with at the free clinic has taught me something about medicine that I will not forget. I would like to share one of these lessons with you.
One of the unique aspects of Worcester is that it is home to many refugee populations. These are resilient people who are fleeing some of the most unimaginable circumstances, and they bring with them a wealth of knowledge. One family, who had quite literally just landed in the United States, arrived at the clinic on a frigid winter evening. As I completed their intake, I noticed they were wearing shorts and T-shirts. When I offered to help them get warmer clothes, they told me the cold was not as bad as it had been in Europe, where they lived outside for months before arriving here. They told me about their life in their home country and how several of their family members had been killed in the civil unrest. Through their life stories, I learned how political unrest impacts families physically and mentally, and how such unrest
In Memoriam
Dr. Richard Edward Hunter

Richard Hunter passed away on October 11, 2022, at the age of 103. Those who knew him were lucky. His patients and colleagues were luckier still.
Dr. Hunter was the inaugural department chair of Obstetrics and Gynecology at UMass Chan Medical School. He was particu-
can have short-term and long-term effects on health outcomes. As I listened to the plight of one of the family members, I was confronted with a series of troubling questions: How is one supposed to carry insulin--which must be refrigerated--across country borders? What do they do if they run out of insulin and are in a different country? How does this impact the patient’s health long-term, and how can we anticipate and prevent the negative effects? Overall, this interaction deepened my knowledge of the barriers that some patients face to adequate healthcare.
As a medical student and physician-in-training, it is easy to get caught up in the academic aspect of medicine. It is easy to forget that we are not studying for hours upon hours for an exam, but rather we are building a strong knowledge base so we can provide the best care possible for our patients. We are working hard so that we can advance medicine and improve the systems through which it is delivered. I am incredibly grateful to the free clinics for reminding me of this every Wednesday. +
Akanksha Nagarkar, BS, BA, is a second-year medical student at UMass Chan Medical School on the Population Urban and Rural Community Health Track and the Clinical and Translational Research Pathway. She is a clinic coordinator at the Indian Society of Worcester Free Health Stop.

larly well suited for this position, having come from private practice and knowing virtually all who were in the practice of his specialty in the community. He initially practiced general OB-GYN later subspecializing in GYN Oncology. From the start, the new department was designed to harmonize with the community. Perinatology services delivered at UMass Memorial Medical Center and subspecialty GYN services at UMass Memorial’s University campus were designed to complement what was already being delivered at community hospitals. He created an atmosphere of collaboration and built a department designed to help practitioners in the community keep up with changes in the specialty.
Dr. Hunter earned his undergraduate degree from Clark Univer-
DECEMBER 2022 WORCESTER MEDICINE 22
sity in Biology and Chemistry and his medical degree from Boston University. He served a rotating internship at Worcester City Hospital and Residencies at Fort George Meade Hospital (OB/GYN), Framingham Union Hospital (General Surgery), and Mercy Hospital, Baltimore (OB/ GYN). He was a member of the American board of OB/GYN and a Diplomat of the National Board of Medical Examiners.
He married his sweetheart, Eleanor Harrington Hunter in 1944 (widowed in 1991). He enjoyed being Dad to their 4 children, Todd Hunter (spouse Julianne Spitz), Elayne Hunter (David Johnson), Jill Keil (Nicholas) and Amy Brown (Douglas). He leaves nine grandchildren and five great-grandchildren.
In 1993, he became a loving and dedicated husband to M. Minta Cowan (Shaw), who predeceased him in 2006.
In addition to the American Medical Association, the Massachusetts Medical Society, and the Worcester District, Dr. Hunter was an active member in the following societies: Fellow of the American College of OB/GYN, Fellow of the American College of Surgeons, New England Cancer Society, New England OB/GYN Society, Boston Obstetrical Society, New England Association of Gynecologic Oncologists, Society of Gynecologic Oncology, Royal Society of Medicine, International Gynecologic Cancer Society, and American Society of Clinical Oncologists.
Calm and affable, his leadership and clinical skill were responsible for building careers as well as a department all while delivering excellent care to thousands of patients. +
B. Dale Magee, MD

Legal Consult: Physician, Curb Thyself!
Physicians are special. Because they are special, they are held to higher standards than non-physicians. Two recent Massachusetts Supreme Judicial Court decisions serve to remind us of this fact. In one case, Welter v. Board of Registration in Medicine, misleading advertising was punishable without a showing that the physician had a fraudulent intent. In the other case, Schwartz v. Board of Registration in Medicine, a physician’s disruptive behavior led to discipline in the absence of proof that behavior had an adverse effect on patient care. Without condoning the physician’s behavior in either case, the decisions remind us that what might be considered acceptable in other walks of life is not permitted to physicians.
The Welter case arose out of the operation of a hair restoration practice. Dr. Welter hired Clark Tan, a foreign medical graduate with an MD but not a Massachusetts license, as a “nonprofessional assistant.” Prior to doing so, Dr. Welter consulted with the Massachusetts Medical Society and believed he could delegate work to Dr. Tan as a non-licensee. The practice’s website referred to Dr. Tan as a “surgeon” and mentioned him on a par with Dr. Welter. Nowhere on the site was it disclosed that Dr. Tan’s medical degree was from a foreign medical school, or that he was not licensed to practice medicine anywhere in the United States. Dr. Tan was issued business cards as “Clark Tan, MD,” introduced himself to patients as Dr. Tan, and consent forms used by the practice suggested that Dr. Tan’s services were those of a “doctor.”
Two physician patients of the practice learned Dr. Tan was not a licensed physician and complained to the Board of Registration in Medicine (BRM). After the complaint was filed, Dr. Welter “removed all references to Tan from [the practice’s] website and changed Tan’s position so that he would no longer conduct consultations, assist with procedures, or have contact with patients.” The BRM found that Dr. Welter had violated BRM regulations that prohibit advertising that is false, deceptive, or misleading; and that he was practicing medicine “deceitfully, or engaging in conduct which has the capacity to deceive or defraud.” Dr. Welter’s license to practice was suspended, but this suspension was stayed upon Dr. Welter entering into a probation agreement under which his credentialing applications, advertising, and media communications would be monitored.
Dr. Welter argued that he should not be disciplined if the BRM could not prove he committed fraud. The common law elements of fraud are: misrepresentation of a material fact, with knowledge of its falsity, for purposes of inducing another to act in reliance on the
DECEMBER 2022 WORCESTER MEDICINE 23 Legal
Consult
In Memoriam Continued
Peter Martin, Esq.
“
What might be considered acceptable conduct in the ‘rough and tumble’ of the marketplace is not permitted in a highly regulated learned profession.
Medical Missions & Volunteerism
misrepresentation, and the plaintiff relied upon the misrepresentation as true, and acted in reliance on it to his/her damage. The court noted that the specific language of the BRM regulations did not require a finding of fraudulent intent in misleading advertising: the regulations prohibit advertising that is false, deceptive, or misleading, and physicians may not engage in conduct that “has the capacity to deceive or defraud.” Those regulations impose an objective standard on physician advertisements, without requiring the BRM to show that the physician had an intent to deceive, or that a particular patient relied on any misleading statements to their detriment. In other words, a physician’s partial statements of fact, without proof of fraudulent intent, reliance, or patient harm, can lead to physician discipline.
The court also agreed with the BRM’s more general point--that it had broad authority to “protect the image of the medical profession” and “sanction physicians for conduct which undermines public confidence in the integrity of the medical profession,” the exercise of which is not limited to cases involving patient care, criminal activity, or deceit. This broad authority is based on the constitutional doctrine that the right to engage in a particular occupation is not a fundamental right, infringement of which deserves strict judicial scrutiny. Rather, a license to practice medicine is a non-fundamental right, regulation of which only requires a reasonable relation to a permissible legislative objective. The court noted that specifically with respect to advertising, physicians, like other practitioners of learned professions, are held to a higher standard of honesty than is prevalent in the general marketplace.
The Welter decision imposes higher standards on advertising by physicians than apply to non-professionals: commercial puffery is inappropriate in professional advertisements. The Schwartz decision supports disciplining physicians for their behavior even if that behavior does not necessarily have an adverse impact on patient care. In the Schwartz case, the physician became “upset, agitated, and loud” when he had difficulty accessing patient records while the hospital’s computerized medical record system was off line for maintenance. In another incident, the physician was trying to complete medical records in a treatment room that doubled as his office and refused when asked to leave the room so it could be used to examine a patient. He was then observed
arguing loudly with another physician in the hallway outside the treatment room about a medication issue, and when told that the patient in the treatment room could hear them, Dr. Schwartz said “I don’t care.”
When Dr. Schwartz admitted to the hospital’s CEO that he had been disruptive, he was suspended from the hospital and subsequently resigned. In a subsequent BRM action, the BRM alleged that Dr. Schwartz committed misconduct in the practice of medicine, lacked good moral character, engaged in conduct that undermines public confidence in the integrity of the medical profession, and finally, that he violated the BRM’s disruptive physician behavior policy. The BRM indefinitely suspended Dr. Schwartz’ license. In reaching that decision, the BRM magistrate noted that Schwartz was “good with patients” and that some other hospital staff agreed with him about patient care at the hospital and appreciated his efforts to improve patient safety. At the same time, it was noted that Dr. Schwartz had an earlier incident in which he was reprimanded by the BRM for violating the disruptive physician policy.
The BRM’s decision was affirmed by a single justice at the Supreme Judicial Court. On appeal, the Court re-affirmed that decision. It disagreed with Dr. Schwartz’s argument that violations of the disruptive physician policy required an impact on patient care. The court stated that he could be subject to discipline without violation of that policy on the grounds of his having committed “misconduct in the practice of medicine.” In any event, the Court disagreed that Dr. Schwartz’s conduct had no impact on patient care. “When a patient overhears doctors arguing with each other, and hears a doctor state that he does not care that patients can hear the argument, there is an impact on patient care.” Moreover, the court stated that Dr. Schwartz’s conduct impacted his relationship with his colleagues, “and it is not hard to imagine that this, in turn, can have an impact on patient care.” The court did not choose to describe exactly what impact on patient care these incidents might have had and seems not to have entertained the possibility that vigorous patient advocacy, even if conducted rudely, might have a positive impact on patient care.
The two decisions read together paint a picture of a profession being held to high standards of commercial and personal conduct. What might be considered acceptable conduct in the “rough and tumble” of the marketplace is not permitted in a highly regulated learned profession. This calls to mind Chief Judge Cardozo’s description of fiduciary duties: “A trustee is held to something stricter than the morals of the marketplace. Not honesty alone, but the punctilio of an honor the most sensitive, is then the standard of behavior.” (1) In dealing with patients, colleagues, and the public, physicians must keep in mind these higher standards and pause before giving into the temptation to engage in behavior the wider public might condone. +
Peter Martin, Esq., is a partner at Bowditch and Dewey.
References
1. Meinhard v. Salmon, 249 N.Y. 458, 464 (1928).
DECEMBER 2022 WORCESTER MEDICINE 24
Legal Consult Continued

Society Snippets
On November 5, 2022 the WDMS Student Committee sponsored a day of caring where UMass Chan students got together to clean up Bell Hill Park in Worcester, MA.



Thank you to the WDMS Medical Student Committee and the UMass Gold Humanism Honor Society

Over 35 bags of trash and other items were collected.
WDMS Annual Fall District Meeting and Awards Ceremony was held Virually on Tuesday, November 15, 2022

Click Here To View The Event or go to our website: www.wdms.org
Faculty Award
Dr. A. Jane Fitzpatrick Community Service Award Award Recipient: James J. Ledwith, Jr., MD, FAAFP

Worcester Medical Library Medical Student Achievement Award Award Recipient: Vanya Zvonar
Danae G. Alexandrou- Class of 2025
Loyola University Chicago - Stritch School of Medicine
Natasha A. Bitar- Class of 2025 UMass Chan Medical School
Arpan Bose- Class of 2025 UMass Chan Medical School
Kendall J. Burdick- Class of 2023 UMass Chan Medical School
Kimberly P. Burke- Class of 2023 UMass Chan Medical School
Allison L. Chevalier- Class of 2024 New York Institute College of Osteopathic Medicine
Margaret M. Desmond- Class of 2025
Loyola University Chicago - Stritch School of Medicine
Arianna S. Gray- Class of 2024 Philadelphia College of Osteopathic Medicine
Tara A. Hebert- Class of 2024 University of New England College of Osteopathic Medicine

Cindy A. Le- Class of 2023 UMass Chan Medical School
Siena E. Romano- Class of 2023 Georgetown University School of Medicine
Nathan B. Taber- Class of 2023 UMass Chan Medical School
WDMSA Nursing Student Scholarship Award Recipient Catherine Jones- Class of 2023 Assumption University
Congratulations to all of the recipients!
DECEMBER 2022 WORCESTER MEDICINE 26
WDMS Medical Student Scholarship Award Recipients
2023 SCHOLARSHIP FUND DRIVE
The Scholarship Fund of the Worcester District Medical Society
Thanks to the generous support from our 2021-2022 donors, we were able to award 16 medical student scholarships and book awards at our 2022 Fall District Meeting.
The recipients may hail from various medical schools in the country, but all are from Central Massachusetts, and they share one common pressing burden, student debt. The median debt upon graduation in 2022 was $202,526. Please consider supporting the next generation of physicians by donating. Your tax-deductible contribution, in whatever amount, will allow us to continue this tradition of honoring our donors and recipients.
Opportunities to Support The Scholarship Fund of the Worcester District Medical Society:
1. Flat donation:
a. Click on QR Code
b. Use PayPal on our website: WDMS Scholarship Fund
c.Send in a check payable to: The Scholarship Fund of the Worcester District Medical Society 321 Main Street, 2nd Floor Worcester, MA 01608
2.Named Scholarship or Book Award (one time donation)
3.Name Scholarship or Book Award (in perpetuity)
4.Establish Trust/Include in Will
5. Employer matching program
To inquire further please contact Martha Wright: mwright@wdms.org or call 508-753-1579
A special thank you to our 2021-2022 donors!
Dr. Janet Abrahamian and Arzoon Abrahamian
Dr. Eric Alper
Dr. Edward Amaral
Ms. Melissa Boucher
Dr. Lucy Candib
Ms. Joyce Carigilia and Mr. David Williams
Drs. Lynn Eckhert and Louis Fazen
Dr. Michael Hirsh
Dr. Sidney Kadish
Dr. Kenneth Kronlund and Mrs. Susan Kronlund
Dr. Anne Larkin
Dr. Jeffrey Levine
Dr. Lillian A. Luksis Charitable Giving Fund
Dr. Jane Lochrie
Dr. Gordon Manning and Karen Rothman
Milford Regional Medical Center
Dr. June O’Connor
Dr. Sahdev Passey and Mrs. Carolyn Passey Dr. Michele Pugnaire
Reliant Medical Group





Dr. Joyce Rosenfeld and Ms. Jill DeBender Dr. Sara Shields
Drs. Robert Sorrenti and Lynda Young
Dr. Spiro Spanakis
Saint Vincent Hospital Medical Staff
Dr. Paul Steen and Mrs. Donna Steen
UMass Memorial Health Care Dr. Giles Whalen
DECEMBER 2022 WORCESTER MEDICINE 27
THIS IS TOTAL HEALTH CARE FOR YOUR EYES.
The health of your eyes requires several things. Like easy access to exams and contact fittings. But it also requires access to specialists who provide breakthrough care for sight-threatening conditions like cataracts, macular degeneration, glaucoma and diabetes-related vision problems. So, we created one place for your patients to receive the very best in specialized eye care.
Locations in Northborough and Worcester ummhealth.org/eye-care | 800-431-5151

THE RELENTLESS PURSUIT OF HEALING




















































