Janna’s journey
One student’s determination to become a nurse

Watch and learn Strategies for engaging Gen Z students
Distinguished alum Meet the winner of the 47th annual award

Janna’s journey
One student’s determination to become a nurse

Watch and learn Strategies for engaging Gen Z students
Distinguished alum Meet the winner of the 47th annual award
How they led UI Health to Magnet® recognition for nursing excellence
TIESA HUGHES-DILLARD, DNP ’19
Chief Nursing Officer, UI HEALTH


SUSAN OKUNO-JONES, DNP ’10
Regional Chief Nursing Officer, ASCENSION
DALE BEATTY DNP ’17
Chief Nurse Executive and Senior Vice President, Patient Care Services, STANFORD HEALTH CARE

Our alumni prove what’s possible with a DNP in Health Systems Leadership from UIC. Learn more about the program that prepares you for the highest levels of executive leadership in health care. Visit go.uic.edu/DNP-HSL




A devastating diagnosis forced her to drop out of the BSN program. She didn’t know when, or if, she’d be able to return.
UIC Nursing alumni contributed in large and small ways to bring Magnet recognition to UI Health.
Around the State Updates from Peoria, Quad Cities, Rockford, Springfield and Urbana
The AACN chief education innovation officer is the 2025 UIC Nursing Distinguished Alumni Award winner.


Inthe face of a challenging climate for higher education, I’m proud to say that UIC Nursing’s programs are growing, and so is our enrollment.
For the first time ever, we’re the largest health sciences college at UIC, with more than 2,100 students enrolled across all campuses and programs. That record enrollment is driven by a few factors. One is a shift to freshmen admissions at our Chicago campus after decades of admitting undergraduate students as juniors. This makes us more competitive with our peers and allows us to seamlessly work with students from the moment they step foot on campus. We also launched two new academic programs this fall (see p. 3), welcomed the biggest BSN class ever in Springfield and continue to enjoy strong enrollment in our online RN to BSN program.
I’ve been so impressed with the way our faculty and staff have adapted to ensure that the quality of our programs remains as high as ever, even as we grow in size. Our BSN program was ranked No. 6 in the nation by U.S. News & World Report this fall, climbing seven spots from last year. This is a reflection of dedicated faculty, our rigorous coursework, state-of-the-art simulation and commitment to support each unique student. This is also a testament to our top-notch clinical partners, including UI Health, which earned its first Magnet designation for nursing excellence this summer (see p. 14).
And while we have so much to celebrate, I don’t want to downplay the ways that changes to the federal landscape have affected us. Some of our international students and visitors have been delayed — one PhD student was unable to enroll — due to visa difficulties. Some of our faculty have also been hit by cuts to federal research funding and have had to redefine their research to meet changing requirements.
These challenges make me all the more grateful to the donors who help us meet the needs of our college. We hope you’ll be inspired by the impact of these gifts on p. 20. Much of our ability to provide scholarships, supplement faculty research and projects, invest in facility upgrades and more is attributable to our generous donors.
I’m continually amazed by the drive and resilience of our students, faculty and staff, and I remain incredibly optimistic about the future of our college and the future of our beloved profession.

Eileen Collins, PhD, RN, FAAN, ATSF Professor and Dean UIC College of Nursing
Vital Signs is published for the alumni, faculty, staff, students and friends of the University of Illinois Chicago College of Nursing.
© 2025
DEAN
Eileen Collins , PhD, RN, FAAN, ATSF
EXECUTIVE
ASSOCIATE DEAN
Lauren Diegel-Vacek, DNP, FNP-BC, CNE, FAANP
CHIEF EDITOR
Liz Miller
MANAGING EDITOR & WRITER
Deborah Ziff Soriano
GRAPHIC
DESIGNER
Jennie
Ramazinski Miller
PHOTOGRAPHER
Jordyn Harrison
CONTRIBUTING PHOTOGRAPHERS
Joshua Clark
Jon Reyes
Diane Smutny
Brian Thomas
We welcome comments, suggestions and story ideas.
University of Illinois Chicago College of Nursing (MC 802)
845 S. Damen Ave. Chicago, IL 60612
Phone: 312.413.2337
Email: lhmiller@uic.edu
Web: nursing.uic.edu
Facebook: @uic.con
Twitter: @uicnursing
Instagram: @uicnursing
LinkedIn: @UICCollege-of-Nursing
Update your information and send us your news.




was a week of firsts.
During the first week of the fall 2025 semester, UIC Nursing welcomed its first class of freshmen (after decades of admitting BSN students as juniors), its first class of nurse anesthesia DNP students, and its first class of students enrolled in the MSN program for non-RNs on the Rockford campus (see p. 29).
Getting these three classes on campus for the first day of school meant the culmination of years of behind-thescenes work: curriculum development, administrative and accreditation approvals, facilities updates and shifting responsibilities for staff and faculty.
All three programs are mission-critical, giving students the highest quality nursing education
and providing the state of Illinois with RNs and APRNs prepared to practice in specialties and regions that need them most.
“Getting all three programs launched was no easy task, so it was incredibly gratifying to meet the students who will change their lives by earning these degrees,” says Dean Eileen Collins
(top to bottom)
Fifteen students make up the Rockford campus’s first-ever cohort in the MSN program for non-RNs.
Twenty students are in the first nurse anesthesia DNP class. The program was seeded with a $10 million gift from alumna M. Christine Schwartz.
The UIC Nursing BSN Class of 2029 gathered in front of the nursing building on the Chicago campus on Aug. 25. The freshmen class consists of 94 students.
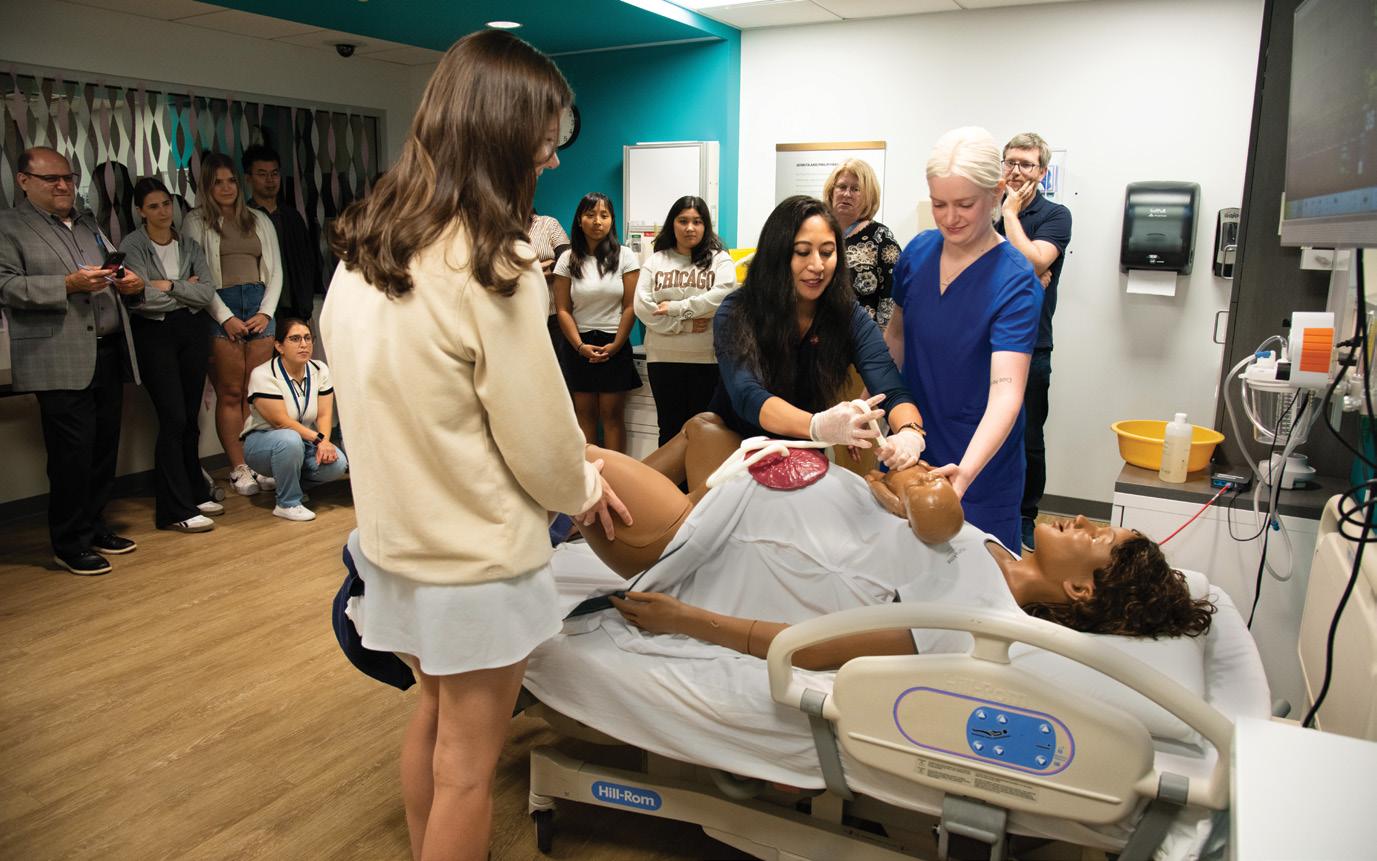
To celebrate Healthcare Simulation Week 2025, UIC Nursing threw a baby shower for the college’s newest, state-of-the-art birthing manikin.
There was food. There were games. There were suggestions for the new baby’s name.
And then things got really interesting. MamaAnne®, the high-fidelity simulator from Laerdal, went into labor.
Although it was a departure from what one might expect at a typical baby shower, it made perfect sense for this event, which was intended to showcase the capabilities of the newest addition to the M. Christine Schwartz Experiential Learning & Simulation Lab.
“Some of the key upgrades to this manikin include the improved realism of the skin and the ability to simulate obstetrical emergencies, such as a postpartum hemorrhage, without compromising the manikin’s
APPLAUSE!
Associate professor Janna Stephens, PhD, RN, was elected as a fellow of the American Heart Association, and associate dean for academic affairs Liz Aquino, PhD, RN, was appointed to the AHA’s Quality Oversight Committee.
mechanical system,” says Katie Vanderzwan, DNP ’17, MSN ’06, APRN-BC, CHSE, director of the Schwartz Lab.
The purchase of the upgraded manikin was made possible by additional funding from Nita and Phil Francis, who also made a gift in 2019 to name the birthing suite within the Schwartz Lab.
Healthcare Simulation Week is held annually each September to raise awareness about the vital role of simulation in improving the safety, effectiveness and efficiency of health care delivery.
Shower guests got to witness Vanderzwan and her staff instruct and care for MamaAnne through the birth, just as they would in a real situation. At the end of the party, Vanderzwan reached into the drop box of suggested baby names and picked one: Jena. The event was complete when the ID tag was placed on Jena’s tiny ankle.

UIC Nursing PhD student Eric Peprah Osei, RN, was selected as a recipient of the 2025-2026 Schweitzer Fellowship Program. He is one of 26 students throughout Chicago who will design and implement projects to improve the health and well-being of underserved Chicago communities.
During the course of his Schweitzer project, Peprah Osei plans to initiate interactive, culturally focused educational seminars in Chicago for Black individuals with Type 2 diabetes or pre-diabetes.
“We are going to talk about real-life strategies, things like reading food labels, understanding sugar labels and improving physical activity in a way that feels achievable and relatable,” he says. “The goal is to make the information not only accessible, but also meaningful to the people we see.”
Peprah Osei was inspired to pursue diabetes research and education after seeing his grandparents suffer complications from diabetes in his home country of Ghana. His interest was reinforced when he began working as a nurse and saw the challenges patients faced in managing the disease.
Clinical associate professors Robin Shannon (retired), DNP ’17, MSN ’09, RN, PHNA-BC, and Catherine Yonkaitis, DNP ’17, RN, PHNA-BC, are senior editors on the 4th edition of “School Nursing: A Comprehensive Text.” Clinical assistant professor Karen Madura, DNP ’22, RN, PEL-CSN, is an associate editor and chapter co-author.
Clinical assistant professors Afrodita Salievska, DNP, FNP-BC, and Susan Tracy, DNP ’23, RN, have been selected as 2025 Nurse Educator Fellows by the Illinois Board of Higher Education.
Associate dean for practice and community partnerships
Carolyn Dickens, PhD ’17, ACNP, believes that a video series she is producing will help promote empathy between nurses and patients and curb rising incivility in health care settings.
The first two videos in the animated series, called The Silent Exchange, depict opposite perspectives on a single, fraught nurse-patient interaction. One video, intended for viewing by nursing staff, reminds them of the fear and frustration patients and their families feel. The second video is intended for patients and families; it highlights the pressures and demands on nurses. Because the videos have no dialogue, the messages are accessible to everyone, regardless of language.
The videos are for use by any health care practice, anywhere in the world; they’ve been downloaded from California to Finland.
Dickens’ partner on the project is Eileen Knightly, MHA, RN, vice president and chief nursing officer at OSF HealthCare Little Company of Mary Medical Center in Evergreen Park, Illinois. The project had grant funding from the Community Health Advocacy program.
Both videos end with the same message: “Everyone’s stressed. Let’s help each other.”
“Our goal is for hospitals and clinics to download and disseminate these videos widely — to nurses, patients and their families,” Dickens says. “We’ve seen a rise in incivility between patients and staff in hospital settings, and we know this has led to staff burnout and nursing shortages. It’s detrimental not only to the well-being of nurses, but also to patient care and outcomes.”
The Power of Nursing Leadership event is still going strong after 28 years! Every November, UIC Nursing hosts the annual luncheon celebrating the impact and achievements of nurse leaders. Recent events featured keynotes by Jarrett Payton, son of the late NFL Hall of Famer Walter Payton, and Jennifer Mensik Kennedy, president of the American Nurses Association. Save the date for next year’s event: Nov. 6, 2026!


With more than 2,100 students enrolled for fall 2025, UIC Nursing had record enrollment for the second year in a row, and the College of Nursing became the largest health sciences college at UIC for the first time.



assistant professor Lexxie Gramke, PhD, MSN, PMHNP-BC, AGPCNP-BC, teaching assistant professor Jennifer Maffucci, EdD, RN, ACNS-BC, and visiting clinical instructor Michael Solomon, DNP ’21, MSN ’18, PMHNP-BC, were included in the Illinois Nurses Foundation 2025 class of 40 Under 40 Emerging Nurse Leaders.
of Science in Nursing (MSN) degree
School Nurse Certificate Program director Eileen Moss, DNP ’19, MSN ’11, RN, PEL-CSN, was installed as the president of the Illinois Association of School Nurses.
Clinical practice nurse educator Mitch Kordzikowski, DNP, MBA, PMHNP-BC, PMH-BC, NE-BC, and clinical associate professor Cynthia Taylor Handrup, DNP, PMHCNS-BC, each have a chapter in the new edition of Psychiatric Mental Health Management for Nurse Practitioners.
Helen Grace, PhD, MSN ’65, FAAN, the fourth dean of the UIC College of Nursing, died in August at the age of 90.
Grace, who was dean from 1977 to 1982, was instrumental in establishing the college’s PhD program, and, indeed, the first PhD was awarded during her tenure. The Quad Cities campus was also created during her time as dean.

Grace grew up on a farm in South Dakota and trained to be a nurse at West Suburban Hospital in Oak Park, Illinois. She got her bachelor’s degree in nursing at Loyola University of Chicago, her master’s degree in nursing at UIC in 1965 and her PhD at Northwestern University.
She articulated her view of the importance of doctoral education in nursing in a 1978 paper published in the Journal of Nursing Education: “Conflicts within administrative hierarchy, the effects of sexism, and circumscribed roles for women are but
a few of the constraints. Cast within this framework, doctoral education for nurses and in nursing is but another step within an overall struggle for independence and recognition of worth.”
Grace was the recipient of the first Distinguished Alumni Award given by the college in 1978 and was selected as a Living Legend by the American Academy of Nursing in 2008.
“As I reflect on her many accomplishments, what stands out to me is how she was always ahead of the curve and setting the trends — a true trailblazer,” wrote former UIC faculty colleague Kathleen Knafl.

Clinical assistant professor Leah Burt, PhD ’20, MSN ’10, ANP-BC, is one of five scholars nationwide to be chosen for the 2025 class of Macy Faculty Scholars, a highly selective program designed to identify and nurture the careers of promising educators in nursing and medicine.
Burt is the first faculty member from the UIC College of Nursing, and only the third from UIC, to be selected for the program since it launched in 2010.
The program provides scholars with resources — protected time, mentorship and a professional network of colleagues — to help them become leaders in health professions education.
They did it!
During her two years in the program, Burt will work on a project called Lead-Dx (Learning Equity, Addressing Disparities in Diagnosis). She’ll develop a simulation-based curriculum to teach health professions students to better understand and mitigate diagnostic disparities (see p. 28).
This year, Burt was also selected as a fellow of the American Association of Nurse Practitioners.

Six UIC College of Nursing faculty members were inducted as fellows of the American Academy of Nursing at the academy’s annual Health Policy Conference in Washington, D.C., in October.
Induction into the academy is one of the highest honors in nursing. Fellows are recognized for their substantial contributions to health and health care.

(l to r)
Associate professor and director of the PhD program Mary Dawn Koenig, PhD, RN, CNM, investigates how inflammation, the iron regulatory hormone hepcidin, and genetic factors in the placenta determine iron flow in both maternal and fetal systems.
(Read more on Koenig, p. 26.)
Clinical associate professor Rebecca Singer, DNP ’18, RN, has almost two decades of experience in global health and community partnerships. She co-leads UIC’s Outbreak Response Team, which works with the Chicago Department of Public Health to provide testing, vaccination and infection-control to Chicago residents.
Associate dean for practice and community partnerships
Carolyn Dickens, PhD ’17, ACNP-BC, is a board certified nurse practitioner who specializes in heart failure and cardiovascular disease in the cardiology department at UI Health.
(Read more on Dickens, p. 5.)
Associate professor Mark Lockwood, PhD, RN, is the lead researcher on a National Institutes of Health grant to study the relationship between the gut microbiome and pain and other distressing symptoms experienced by some kidney transplant recipients. (Read more on Lockwood, p. 8.)
Associate professor Sarah Abboud, PhD, RN, focuses her research on interventions to improve health outcomes among first- and second-generation Arab immigrants in the U.S., specifically at the intersections of immigration, gender, sexual orientation and ethnic identity.
Clinical professor of psychiatry and nursing Julie Carbray, PhD, FMHNP-BS, PMHCNS-BC, is a nationally recognized clinical expert in the area of children and adolescents with mood disorders and the director of the Pediatric Mood Disorder Clinic at UIC’s Institute for Juvenile Research.
NEW RANKINGS

Illinois has one of the highest volumes of out-of-state abortion patients in the country. Associate professor Kylea Liese, PhD, CNM, is leading an effort to make sure they have access to safe and skilled providers.
Fueled by a grant from the Illinois Department of Public Health in 2024, the Reproductive Advocacy and Diversity in Advanced Nursing Training (RADIANT) Fellowship trained and mentored 32 clinicians to provide safe abortion care in its first year. In addition, there were more than 100 participants who attended one of four one-day workshops on abortion topics in Chicago or Urbana.
In its second year, the fellowship will expand to include emergency department providers, particularly those in rural areas that are considered maternity care deserts. The RADIANT ED fellowship will target providers from emergency departments
that don’t have an OB unit on site and will help them to work with their facility’s administrators to become access points for medication abortions.
The program is also partnering with Carafem, an international abortion provider with a clinic in Skokie. The

Professor Pamela MartynNemeth, PhD, RN, was one of 15 worldrenowned nurse researchers inducted into the International Nurse Researcher Hall of Fame in Seattle on July 19.
Induction by the Sigma Theta Tau International Honor Society of Nursing is a recognition of Martyn-Nemeth’s significant and sustained program of research. Martyn-Nemeth’s area of scholarship is focused on cardiovascular disease risk reduction and improvement of quality of life in people with Type 1 diabetes. People with the disease experience two to four times the risk of cardiovascular disease.
Over the course of her career, Martyn-Nemeth has received 14 grants supporting her work

Get to know twins Ava and Mia Maglaya. Hailing from the southwest suburb of Romeoville, they are both juniors in the UIC Nursing BSN program and track & field athletes for the UIC Flames.
Why did you pick UIC?
Ava: Our mom [Elaine Maglaya] has always been a big inspiration as a UIC alum and now a UI Health nurse.
Mia: UIC was always on our radar after seeing her success, not only academically and professionally, but also, she was on the dance team at UIC and then went on to dance professionally for the Chicago Bulls as a Luvabull.
Ava: Mia decided to take a chance and directly reach out to UIC, and thankfully [UIC Track & Field] Coach Paul [Zavala] invited both of us on an official visit.
Mia: Meeting many different coaches and seeing so many different colleges, there was no other school that offered all of the opportunities that UIC did.
Were you surprised when your sister decided on the same career?
Ava: It wasn’t very surprising. We have historically always gone down the same general path, but we have always been able to put our own personal spin on whatever we do to make it our own.
What appeals to you most about working as a nurse?
Mia: What appeals to me is the bond and trust that grows between nurses and their patients. I can make a positive impact by seeing my patients as whole people, learning about their backgrounds and then delivering care and interventions.
Ava: Being able to have a direct effect on someone’s life, or even just their day, is something I always strive to do, and nursing gives me that opportunity and so much more. Also, I’ve always flourished in fast-paced environments and while working under pressure.
As nursing students and track athletes at the same school, how much time do you spend together?
Mia: We spend a huge amount of time together, sometimes upwards of 12 hours a day. We go from 7 a.m. practice, to our first morning class, to our lifting session, and then back to the College of Nursing for afternoon classes together again.
How would you describe your relationship with your sister?

Ava: It’s complex and unlike any other relationship I have in my life. Growing up with a sibling is one thing, but to have a twin is to have someone who has seen every part of your day, your growth and your life.
What’s your favorite and least favorite thing about being a twin?
Mia: My favorite thing about having a twin is having someone who deeply understands me as a person and is going through the same challenges I am facing. My least favorite thing is feeling like less of my own individual person at times. And wearing matching clothes!
Where do you hope your nursing journey ultimately takes you?
Mia: My goal is to become either a nurse practitioner or CRNA. I want to spend my life doing something I truly love and having a positive impact.
Ava: I want to find a specialty that I truly enjoy. Nursing has so many opportunities, which is why I chose it as a career, and I know that I can always change parts of my career as I grow and change as a person.
[Edited for print version]
Watch the Maglayas test their knowledge of each other and read the full Q&A.



In January 2023, Janna Janthapaiboonkajon, BSN ’25, was diagnosed with stage 4 non-Hodgkin lymphoma and dropped out of nursing school to endure a grueling chemotherapy treatment. She didn’t know when, or if, she’d be able to return to school.
Janna Janthapaiboonkajon is someone who maps out her future. At 20 years old — a junior in the UIC Nursing bachelor’s program — she knew what she wanted to do for the next 10 years. She’d graduate, work as a nurse, then return to UIC Nursing to get her DNP and become an advanced practice provider.
Then, all her plans were thrown into disarray.
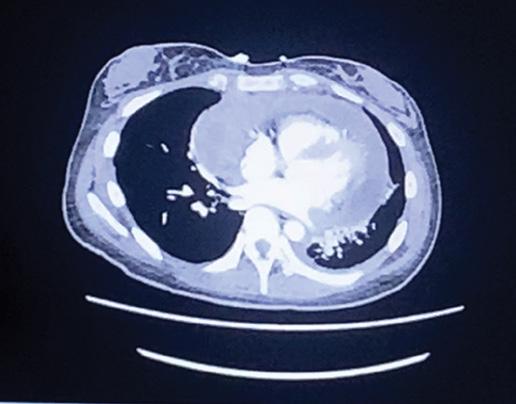
It was January 2023, and Janthapaiboonkajon was beginning the second semester of her junior year. She had been experiencing chest pain for months, but had chalked it up to asthma, a condition she’s had since childhood. When the pain overtook her ability to sleep, she finally went to urgent care and was admitted to Cook County Hospital.
There, imaging revealed a 7-inch tumor. It had grown so large that it was putting tremendous pressure on her chest and was leaking fluid into her lungs and kidneys.
Her diagnosis and prognosis were sobering. The cancer had metastasized to her lungs, lymph nodes and kidneys. Physicians told her she might have only 10 years to live.
Suddenly, instead of worrying about her next exam or preparing for her next clinical rotation, she was writing a will and outlining a power of attorney document.
“I just didn’t know how to adjust my timeline,” Janthapaiboonkajon says. “It wasn’t like, ‘You only have 10 years to do all this stuff.’ It was like, ‘You only have 10 years and that’s it.’ I didn’t really know how to process that.”
Determined to continue
Janthapaiboonkajon talked to UIC Nursing’s then-BSN program director Maripat King, DNP ’16, about a plan to stay in school during treatment.
“She was very sweet because she saw how stubborn I was about continuing school,” Janthapaiboonkajon says.
For two weeks, she tried it. Friends brought her from her dorm room to class in a wheelchair because the weight of the tumor was so heavy that she couldn’t stand up without losing consciousness.
When she went in to get a port placed for chemotherapy later that January, the tumor compressed her lungs so much that she couldn’t breathe on her own. She was intubated and put on a ventilator.
“That was when I wrote on a notepad, ‘I’m dropping out of nursing school,’” she recalls. “Being intubated and on a ventilator at 20 years old was so difficult.”
The treatment plan called for six cycles of intensive chemotherapy, with each cycle involving five days of inpatient treatment. Even with outpatient infusions to boost her immune system, Janthapaiboonkajon fought infection after infection, and was a frequent visitor to the hospital with high fevers.
She moved back in with her mom, who had recently retired from a 30-year career as a nurse at Cook


County Hospital and was a constant companion at her daughter’s appointments.
“It was really grueling, especially the halfway point through the cycles of treatment,”
Janthapaiboonkajon says. “The mental toll and the fatigue. The thing that threw me off the most was the brain fog. You get really confused. You forget things. You’re really slow. You don’t feel like yourself.”
She was in the hospital for treatment when she turned 21 that March. She recalls the nurses organizing a surprise celebration in her hospital room, toasting her with ginger ale cocktails to ward off nausea.
She also struggled with peripheral neuropathy, tingling in her hands and feet, which prevented her from doing daily tasks.
“I feel like I’m barely just existing at that point,” she recalls. “I can’t draw. I can’t really think. I’m just on bed rest the whole time. That was the part where it was really taking a mental toll on me.”
By the final cycle of chemo in May 2023, the tumor had shrunk down significantly, and her treatment was considered a success. Her tumor would always be there, providers said, but it was stable and no longer growing. By August, biopsies and tests confirmed she didn’t need radiation.
Janthapaiboonkajon was ready to return to nursing school, but because many required courses are
only offered once a year, she needed to wait until January 2024 to pick up where she left off. By that time, her classmates had moved on and were then in their final semester as seniors.
Janthapaiboonkajon would be returning as a second-semester junior, joining a completely new cohort of students.
“Re-entering nursing school was so scary for me,” she says. “I was really scared of the brain fog. [I was thinking,] ‘No one knows why I’m here. They’re just going to think I didn’t pass a class. What if I can’t catch up to everyone?’”
But Janthapaiboonkajon, an extrovert, jumped right back in. After months of being immunocompromised, she reveled in being around people — asking questions of her teachers and talking to her research advisor. She offered to share her study guides with classmates and was elected president of the College of Nursing Student Council.
Ivory Lau, BSN ’25, who served as vice president of the Student Council, soon became Janthapaiboonkajon’s best friend. Lau says she was surprised that Janthapaiboonkajon was so nervous to return.
“Now, looking back, I’m like, ‘girl, you’re being so silly,’” Lau says. “Everyone knows Janna. Everyone loves Janna. She’s known for her study guides, for her generosity, for sharing flowers and candy during Valentine’s Day, and for her uplifting, warm energy. I just think she’s an integral part of our cohort. I just hope she knows she’s so important to us.”


In her final semester, Janthapaiboonkajon spearheaded a Student Council fundraiser for the University of Illinois Cancer Center on “Pi Day,” March 14, 2025. She called it Pi-ing it Forward.
Janthapaiboonkajon’s experience helped her put things in perspective to better manage school stress.
“When I came back to nursing school, students would say, ‘this assignment is the worst thing ever.’ In my mind, nothing is as bad as going through cancer,” she says. “I take a deep breath. I just need to do this assignment. If I need help, I’ll ask for help.”
Her experience also made her want to be an oncology nurse, so she applied to work as a nurse tech on the oncology floor at UI Health. She got the job.
She recalls telling her manager, “You’re not going to find anyone who’s more enthusiastic to clean up after oncology patients. I’ve been there. I know how anxious, terrible and embarrassing it feels to have to use a bed pan.”
Janthapaiboonkajon spoke at the Class of 2025’s pinning ceremony and was selected by faculty to receive the Graduating Student Recognition Award, which honors academic excellence and initiative in actively supporting the College of Nursing.

“Janna is the embodiment of what we want our students to be,” says Julie Schwind, DNP ’17, MSN ’06, BSN ’00, her professor for pathophysiology and pharmacology. “It’s not just being smart. It’s being kind. It’s being a leader. It’s being tenacious. It is making sure you are checking on your peers as well.”
Lau says that it’s not just Janthapaiboonkajon’s story that is inspiring to other students, but her energy and ideas. She says she’s always planning her next move in life.
“Knowing Janna’s story, knowing what she’s been through, I think she’s so resilient,” Lau says. “I’m so proud of her for making it this far. And I know she’ll continue to do great things. She always has the most amazing ideas. I really hope she achieves all of them.”
Although Janthapaiboonkajon still carries some side effects from treatment — she was in the hospital for chest pain in early May 2025 — she says graduation was particularly meaningful because it coincided with the two-year anniversary of completing treatment. She passed the NCLEX in June and started working as an oncology nurse at UI Health in September.
“The past two years, I’ve been trying to navigate my life and my identity and how to go back to normal,” she says. “And now, all those experiences have built that resilience — along with the education — to be able to take care of someone and to be able to advocate for someone.”



UIC Nursing alumni played instrumental roles in helping UI Health achieve Magnet® recognition this summer.
Itcould be said that she manifested it.
Tiesa Hughes-Dillard, DNP ’19, MBA, RN, had been chief nursing officer at the University of Illinois Hospital and Clinics for about two years when she told the Board of Trustees, the governing body of the University of Illinois System, that she “promised” the hospital system would achieve Magnet recognition.
It was a bold statement. Only 10% of hospitals in the world have Magnet status, a recognition from the American Nurses Credentialing Center that exemplifies the best in nursing care. As a public, safety-net hospital — one that provides significant services to uninsured Medicaid and vulnerable populations — UI Health faced a steep climb to the achievement.
About 18 months later, Hughes-Dillard was standing on a stage, along with other hospital and university officials, in front of a packed auditorium, receiving the scheduled Zoom call from the credentialing center. UI Health had achieved the designation.
“We did everything in rapid fire because I knew now was the time to do it,” she says. “It was our time. What I promised was simply that the Magnet recognition would follow the excellence our nurses were already living.”
At that Magnet announcement in July, UI Health CEO Mark Rosenblatt described achieving the recognition as “a defining moment in the arc and history of UI Health” — and he made sure to give credit where it was due.
“I’d be remiss if I didn’t acknowledge the irresistible force that is Dr. Tye Hughes-Dillard,” he said. “She embodies UI Health and she embodies the Magnet process.”
Hughes-Dillard takes a humbler view. She says the story of Magnet recognition has been in the making for 16 years, and she is quick to recognize her predecessors in the CNO role, most recently, Shelly Major, and before Major, UIC Nursing alums Dale Beatty, DNP ’17, and Jan Spunt, MSN ’83, BSN ’74.
“I was the anchor leg,” says HughesDillard, who completed her DNP at UIC Nursing in Health Systems Leadership. “I picked up the baton from Jan, Dale
and Shelly and I just ran. I ran to the finish line.”
The recognition from the American Nurses Credentialing Center is considered the gold standard for clinical outcomes, nursing engagement and patient satisfaction.
“Keep in mind, this is extremely uncommon for a state, unionized hospital,” Hughes-Dillard says. “Many public hospitals struggle with staffing and resources, but what the Magnet appraisers observed at UI Health was very different. They saw a system designed to support nurses so they can deliver the best possible care.”
While many hospitals rely on agency staff, UI Health uses less than 1%, meaning their patients are cared for by permanent staff who are deeply invested in the hospital system’s patients, mission and culture. UI Health also provides free-floating charge nurses on every unit, offering an extra layer of support and coordination, and a resource nurse is available in critical care areas who can be deployed immediately in the event of an emergency or surge.
When Osei Omoike, MSN ’03, MBA, BSN ’00, RN, came on board as interim Magnet program director in April 2023, she was filling a temporary role left by a departing staff member.
She didn’t expect to stay in the role longer than a few months, but soon, she was digging into patient satisfaction and nurse engagement data to ensure the hospital system was meeting required
benchmarks. She analyzed and graphed data specific to quality outcomes. Omoike also collected 84 stories from nurses at all levels of the organization that illustrated UI Health’s adherence to the tenets of Magnet, which include transformational leadership, structural empowerment, professional practice and new knowledge and innovation.
Knee-deep in the application process, Omoike decided to stay on as the permanent Magnet director. After spending 17 years at UI Health, and before that, five years as a grant project manager at UIC Nursing, she had a personal stake in seeing it through.
“I was proud to be able to showcase the work of our nurses,” Omoike says. “We wanted to show all the hard work that we have been doing all these years to continuously improve at UI Health. Being able to connect all the dots was such an honor.”
Expediting a process that typically takes two years, Omoike pulled the documentation together in eight months. Hughes-Dillard told Omoike to stay the course during negotiations with unionized nurses and two strikes in 2024.
When Magnet officials came for a three-day site visit, they met with more than 700 people at multiple sessions, including nurses representing the union.
During the Zoom call in July, David Marshall, chair of ANCC’s Commission on Magnet Recognition, delivered the good news about UI Health achieving Magnet status. He highlighted a few exemplars, including: the implementation of a situational aggression screening tool
(see p. 17) and critical markers where UI Health outperformed the benchmark, such as surgical errors, data for pain, and patient education.
He also highlighted the high proportion of professional nurses with a baccalaureate or higher degree: 91%.
As the academic health enterprise of UIC, UI Health is inexorably linked to UIC Nursing. The college’s students complete many of their clinical rotations there. Faculty have joint appointments. Alumni populate the floors and leadership teams. UI Health actively recruits bachelor’s-prepared nurses from UIC and offers tuition reimbursement to nurses seeking a degree at UIC or any state university.
“Our relationship with the hospital is symbiotic,” says Dean Eileen Collins, PhD, RN. “Our students benefit from training at an organization with such a high standard of nursing and patient care, and the hospital benefits from the expertise in research and evidence-based practice that our faculty and alumni bring.”
Hughes-Dillard agrees.
“Together, we’re preparing the next generation of nurses in a real-world academic health setting while advancing evidence-based care,” she says. “This collaboration strengthens both institutions — enhancing patient outcomes, fostering innovation and ensuring a strong pipeline of nursing talent for the future.”

ANCC informing them that UI Health had achieved Magnet recognition.
To apply for Magnet recognition, UI Health had to submit stories from nurses. Eighty-four stories featuring nurses from all levels of the organization focused on transformational leadership, structural empowerment, professional practice and new knowledge and innovation. Here are the stories of just a few UIC Nursing alumni who took part.

Janelle Paguiligan, BSN ’18, RN
Staff nurse II (educator), Post-anesthesia care unit
Multiple attempts to insert an IV had been made by anesthesiologists, CRNAs and experienced nurses.
And then Janelle Paguiligan was called in.
The patient had lost consciousness due to low blood sugar and needed an IV to give her dextrose, a simple sugar. Paguiligan, who had been trained in ultrasound-guided IV insertion, was able to locate the patient’s vein with the ultrasound machine, insert the IV and help her regain consciousness.
Paguiligan received the DAISY award for that case, but her work didn’t end there. She became an integral part of a train-the-trainer initiative
to certify nurses in the ultrasound-guided peripheral intravenous insertion technique, leading to wider use of the practice in her unit.
Patients with difficult IV access can require multiple insertion attempts, resulting in added prep time, delays for surgery start and reduced patient satisfaction.
“When a patient needs multiple IV sticks, it can be very anxiety-inducing during a stressful time when patients are preparing for surgery,” Paguiligan says.
After the intervention was implemented, patient satisfaction scores increased in response to the question: “Does the staff treat patients with courtesy and respect?”
Sunu Punnoose, DNP ’24, RN
Clinical nursing consultant II, Pediatrics
Sunu Punnoose was working as a night nurse in the pediatric intensive care unit (PICU) as she pursued her DNP at UIC Nursing. She noticed that the hospital had no tool to assess whether pediatric patients who are younger than 19 months old were at risk for falling, even though they used one for older children.
“We see falls in the younger populations and mostly people disregard them as developmental because they’re learning to walk,
but based on the evidence, a developmental fall can still cause a lot of injury,” Punnoose says.
Punnoose adds that 80% of the time, the falls happen in the presence of a parent, making education an important step in prevention.
Working closely with her DNP advisor, clinical assistant professor Susan Vonderheid, Punnoose created a plan to implement the CHAMPS fall risk assessment tool for patients
Nicholas Dotson, DNP ’23, MSN ’18, RN Senior director of adult and adolescent inpatient psychiatry
Nicholas Dotson has years of experience working with patients with mental illness, not to mention a doctorate in nursing practice with a focus on psychiatric and mental health.
So when he reviewed an incident where a patient brutally assaulted a technician, Dotson immediately recognized the warning signs indicating the patient was at risk for becoming violent.
But how could he give that same insight to techs, nurses and providers across the hospital?
Dotson set out to find a tool that could help nurses assess the risk of their patients becoming violent. He found the Dynamic Appraisal of Situational Aggression (DASA), which allows providers to
use seven metrics to gauge how likely a patient is to be an “imminent violent risk.”
The tool was successfully rolled out in the emergency department first, then across all inpatient hospital units. Under the new protocol, each patient is assessed every eight hours. Door signage and icons in the medical record indicate whether a patient is at high or imminent risk for violence.
Most importantly, Dotson helped implement Safe Management Plan Huddles, bringing together a multidisciplinary team to discuss violence prevention and mitigation techniques for every patient at high or imminent risk for violence. By July 2025, one year after implementation, incidents with injury were down 65%.

under 19 months of age. As part of her project, she created a nursing staff education presentation.
Pediatrics and PICU clinical nurses were instructed to use the assessment scale on admission and to provide education to parents using a leaflet that Punnoose created.
Since it was implemented in November 2023, only one child under the age of 19 months has experienced a fall.



American Association of Colleges of Nursing Chief Education
Innovation Officer Susan Corbridge is the UIC College of Nursing’s 2025 Distinguished Alumni Award recipient. This is the 47th year the college has conferred the award.
Whenever Susan Corbridge, PhD ’09, APRN, considers a career move, she always makes sure it checks three boxes.
“I want to make an impact; I have to continue to learn; and I want to have fun,” she says. “Life is short.”
Those parameters brought Corbridge to her current position as chief education innovation officer for the American Association of Colleges of Nursing (AACN), where she’s at the forefront of shaping national nursing education. She’s also leading the implementation of the 2021 AACN Essentials, a major shift for professional nursing schools nationwide from a content-based model to a competency-based education model.
“If you’ve been to a major nursing conference in the past three years, chances are you’ve seen Susan on the stage,” wrote Charles Yingling, DNP ’12, MSN ’05, FNP-BC, dean of the University of Nevada-Reno Orvis School of Nursing, in his nominating letter. “It’s no surprise — Susan’s fingerprints are on nearly every national conversation about the future of nursing education.”
23
Corbridge is now a clinical professor emerita at UIC Nursing, but she first came to UIC Nursing in 1998 to serve as director of the Acute Care Nurse Practitioner program.
At the time, nurse practitioners were just beginning to work in acute care settings such as hospitals and ICUs. Corbridge was working as a pulmonary and critical care nurse practitioner at Michael Reese Hospital when then-UIC Nursing faculty member Julie Zerwic, PhD, RN, recruited her to teach in UIC Nursing’s program.
“That’s when I just completely fell in love with education,” Corbridge says. “Education is a way to make a huge impact. I’ve always had so much joy in everything I do as a nurse practitioner, and I wanted to share that with students because that’s the way you can really multiply your impact.”
Corbridge served as the director of the ACNP program for 14 years and was an early adopter of simulation as a part of nursing education.
While still in that role, she enrolled in the PhD program at UIC Nursing, studying the effect of nicotine addiction in an animal model with her advisor, Mariann Piano, PhD ’88, MSN ’84, RN (2019 Distinguished Alumni Award winner). She valued the research strength at UIC, including the ability to take courses across the university in other disciplines.
Corbridge went on to serve in more leadership positions at UIC Nursing, including associate dean
for practice and community partnerships and executive associate dean until 2021. In those roles, she provided oversight as the college took a leading role in providing COVID-19 vaccinations and led the transition of the Peoria campus to a virtual campus.
Throughout Corbridge’s career, she has deliberately maintained her commitment to clinical practice, even while climbing the ladder in nursing education. From 2002 to 2022, she practiced as a pulmonary and critical care nurse practitioner at UI Health.
“My connection to practice was really several-fold,” she says. “It was my love for being a patient advocate and making change for the better in health care. It also made me a better educator because I could provide real-world cases, and it helped our college be connected with clinical opportunities and practice partnerships.”
Her work has led to her induction as a fellow of the American Academy of Nursing, the American Association of Nurse Practitioners, the National Academies of Practice and the American College of Chest Physicians.
Now, in her role at AACN, Corbridge represents nursing education nationally and is a sought-after speaker. She influences workforce development, sits on a national regulatory panel for advanced practice nursing, and leads academic-practice partnership initiatives, including collaborative work with the American Organization for Nursing Leadership.
In her work implementing the 2021 AACN Essentials, Corbridge designed and launched a national faculty coaching program and a series of educational workshops, which have reached over 4,000 faculty members. She delivered a national webinar and conference series and leads national direction and decision-making for the transition to the new Essentials.
Corbridge says one of the things she’s enjoyed most in her career is being a mentor — finding leadership opportunities for colleagues and encouraging them to pursue them. In 2022, Corbridge was recognized for her mentorship with the SAGE Award at the UIC Nursing Power of Nursing Leadership event, and in 2024, she was awarded Rush University College of Nursing’s Distinguished Alumni Award.
“How can we, as nurses, have the largest voice?” Corbridge asks. “We are the ones who are with patients. We’re the largest health care profession. Patients trust us. We are smart, innovative and can and should be leading change. We are such a valuable voice for patients.”
I’ve always had so much joy in everything I do as a nurse practitioner, and I wanted to share that with students because that’s the way you can really multiply your impact.”
– SUSAN CORBRIDGE
Know someone who should be the next Distinguished Alumni Award winner? Nominate them here.


The largest lecture hall in UIC Nursing’s Chicago campus building got a gut rehab this year thanks to a gift from Carolyn Jarvis, PhD ’05, FNP-C.

They may not recognize her face, but nursing students everywhere know her name.
As in, “get out your Jarvis,” or, “Look it up in Jarvis.”
The bible for many nursing students, “Physical Examination & Health Assessment,” is often referred to simply by the last name of its author, Carolyn Jarvis, PhD ’05, FNP-C.
Now, students at the UIC College of Nursing know her name for another reason. The alumna made a major gift to fund a gut rehab of the first-floor auditorium on the Chicago campus. The fully modernized and updated space is named the Carolyn Jarvis Auditorium and hosted its first lectures this fall.
It was while taking a tour of the building that Jarvis says she was “sold” on making a gift to update the auditorium. It was original to the 55-year-old building and the space no longer met the needs of the college, especially as enrollment has grown in recent years.
“While we were walking through the auditorium, students came and sat down. They said they had to come [to class] early because there weren’t enough seats,” Jarvis says. “They were using folding chairs.”
Jarvis spent much of her career teaching pathophysiology, pharmacology — and, of course, health assessment — at Illinois Wesleyan University School of Nursing and Health Sciences in Bloomington,
Illinois. Those same classes will be taught in the new auditorium, and she says she saw “huge possibilities” in the renovation.
“My idea of teaching pathophysiology and pharmacology is asking a lot of questions and getting students engaged and talking,” Jarvis says. “If the students were more comfortable in their seating and had more space … I thought it would be more conducive to those critical professor-student interactions.”
Jarvis’ gift allowed the college to remove a stage, bring the capacity from 92 to 160 seats, make it accessible for those with disabilities, and upgrade AV equipment to improve instructional capabilities.
Jarvis authored the first edition of “Physical Examination” in 1992 after being approached by the publisher, Elsevier, who had worked with her previously on chapters of other books. With crisp, vivid writing, and photos and art that perfectly complemented the topics, it was immediately a hit.
Jarvis has revised it every four years — the most recent edition, the 9th, with co-author Ann Eckhardt. (Her daughter, Sarah Jarvis, DNP, RN, a nurse practitioner in Ann Arbor, Michigan, contributed to a chapter in the 9th edition). It’s been translated into nearly a dozen languages and has maintained a
high market share of health assessment textbooks. Now 79, Jarvis is ready to hand off future revisions to new authors.
She was already a successful textbook author when she decided to get her PhD at UIC Nursing in the early 2000s. In addition to her work revising the textbook and her teaching position at Illinois Wesleyan, she was also working as a nurse practitioner at an alcohol treatment facility in Bloomington.
To better understand behaviors that she was seeing at the alcohol treatment facility, she wanted to increase her knowledge of basic sciences through research.
“I love the basic sciences,” she says. “I need to know how things work, and UIC was the only [nursing school] that was going to give me a grounding in the basic sciences.”
The decision to make a gift to UIC Nursing was in part to acknowledge the impact of her experience there, and in part to ensure the future success of students. She says she admires the diversity among UIC Nursing students and wants to continue to encourage diversity within the nursing profession.
“It was a goal of mine to pay back UIC,” she says. “Really, UIC was the capstone of my learning.”

Linda McCreary’s work in nursing research and education took her all over the world, including Malawi, Rwanda, Eswatini, India and the Caribbean. But there was a time when an international career was not on her radar.
“I lived internationally as a child because I was an ‘Army brat,’ and my dad was stationed in early post-war Japan,” says McCreary, PhD ’00, MSN ’93, BSN ’73, RN, who retired from the UIC College of Nursing in 2021 as associate dean for global health. “I was always interested in international issues but I’d never, ever dreamed that my career would go in that direction.”
McCreary credits mentors and role
career and literally opening up a world of opportunities. To show her gratitude, she made a gift of $50,000 to the college, splitting the money equally into five existing funds, four of which are named in honor of those individuals. The fifth is the general UIC Nursing Scholarship Fund.
“I was lucky to be mentored by several really wonderful, important nurse leaders in the area of global health,” McCreary says. “I wanted to honor these leaders who have meant so much to me and given me the opportunity to experience what I did in my career.”
McCreary says she hopes her gift will help support students and faculty, particularly to be able to afford experiences studying abroad or
“We’re often limited by what we imagine we could do,” she says. “I just want to widen the scope of what [students and faculty] can imagine.”
Read more about the women honored.

McCreary (foreground, color) is splitting her gift among the following funds named for her mentors and role models, (pictured l-r in black and white): Beverly J. McElmurry Endowed Scholarship Fund, which supports PhD students doing work in Primary Health Care; Heung Soo and Mi Ja Kim Endowed Faculty Scholar, which supports scholarly research; Carrol A.M. Smith Global Health Fund, which supports undergraduate students to study abroad; Virginia Ohlson International Studies Endowment Fund, which supports international students studying at UIC and UIC students who want to study abroad

Memorial Health has been with UIC Nursing-Springfield since even before the start, helping seed the launch of the campus in 2016. With the latest gift of $5 million, which will extend from 2025 to 2027, the Springfield-based health system has given $13.5 million over the course of the 10-year partnership.
The newest gift also extends scholarships to pre-nursing students enrolled at the University of Illinois
Springfield. Those who are eligible can receive seamless support from freshman year at UIS through graduation from UIC.
Besides scholarships, Memorial’s new gift also supports “program funds.”
Academic, enrichment and recruitment initiatives — such as Memorial Health Research Day, Back-to-School Lunch and Nurse for a Day (which invites high school students to campus) — benefit from that funding.
2025-2027 | $5 MILLION
As nurse manager of the (Advocate) Illinois Masonic Medical Center AIDS unit from 1989 to 2001, alumna Karen Coleman, BSN ’65, saw the arc of the epidemic in Chicago, from 30 deaths per month to the advent of life-saving medications.
She credits UIC Nursing with her “fabulous” career and wants to give back by earmarking a portion of her estate to the UIC College of Nursing Scholarship Fund.
“I had help along the way,” she says. “I had scholarships to help me pay for school, based on need. I want other young people who want to be in nursing to have some help.”
Growing up in Chicago’s North Side neighborhood of Rogers Park, Coleman knew she wanted to be a nurse. At UIC, she could get a bachelor’s degree in nursing for the in-state rate, which was “very inexpensive,” she recalls. It was a no-brainer. She recalls “wonderful instructors” and making good friends in the program.
After graduating, she took a job at Cedars-Sinai Medical Center in Los Angeles, where her degree from UIC Nursing helped her advance to the role of assistant director of nursing in the cardiac unit.
She worked with physicians William Ganz and Jeremy Swan as they developed the intravenous Swan-Ganz catheter. The unit housed a wall-to-wall, floor-to-ceiling computer to measure cardiac output for patients in cardiogenic shock. Now, the same data is measured by a small transistor at the end of a catheter.
By 1978, Coleman was looking for her next move. She decided to join
the U.S. Air Force, barely making the then-maximum age cut-off of 37.
Because of her bachelor’s degree, she was commissioned as a captain and assigned to the obstetrical unit at the base in Dover, Delaware. She remained in the Air Force Reserve even as she moved back to Chicago.
In 1989, she heard that Illinois Masonic needed a head nurse for its dedicated AIDS unit. The average survival time from diagnosis in the early days was about 18 months.
“I describe it as the good, the bad and the ugly,” she says. “The ugly was obviously 30 deaths a month. The good came in 1996 when the new cocktails were developed and our patients were getting healthier.”
Coleman recalls that local restaurants would provide food to the unit three days a week. The hospital hired a psychologist to help nurses and staff process the tremendous losses, and there was a cadre of volunteers to share the overwhelming workload.
I had help along the way ... I had scholarships to help me pay for school, based on need. I want other young people who want to be in nursing to have some help.
– KAREN COLEMAN
Thirteen years later, in 1991, she was deployed during Operation Desert Storm to a medical evacuation unit in Spain, but the unit didn’t see any casualties.
During the 1980s in Chicago, Coleman wanted to do her part to help fight the AIDS epidemic. The first case in Illinois was reported in 1981.
“My brother, who is gay, had a circle of friends who were getting sick and dying from AIDS,” she says. “I thought, well, I’m a nurse. There’s got to be something I can do.”
“The main devotion of the volunteers was that no patient was ever going to die alone,” she says. “If we knew somebody was at death’s door, either a staff member or volunteer would be sitting with them.”
By 2001, with the success of the new drugs, the unit was disbanded, Coleman says. She ended her career at the outpatient HIV center at Northwestern Medicine and conducted clinical research on patients who were on the new HIV/ AIDS drugs. She retired in 2013.
Coleman says she hopes her gift


MORE STUDENTS. MORE ANXIETY. HOW PROF JENNIFER MAFFUCCI IS MEETING THE NEEDS OF TODAY’S STUDENTS.
Standing in front of an audience that included UIC Chancellor Marie Lynn Miranda and faculty from across the university, assistant professor Jennifer Maffucci, EdD, RN, ACNS-BC, described her class this way.
“It’s like a Netflix watch party, with learning as the main event, and almost always less drama.”
The line elicited a big laugh when Maffucci delivered it last year at SparkTalks, UIC’s faculty lightning talks, where UIC’s changemakers are invited to share their innovative work in talks of about three minutes.
But behind Maffucci’s relatable analogy is an innovative teaching methodology that she has developed through extensive research.
Recognizing that both class sizes and anxiety are on the rise, Maffucci set out to invigorate her didactic classes with strategies that would keep her Gen Z students engaged while learning complex nursing skills.
“As educators, we know that active participation is key to learning, but it’s a little intimidating,” she says. “For students who already feel anxious, it’s even tougher. They might hold back, not wanting to speak up in a big group.”
Maffucci teaches Health Assessment and Adult Health Nursing, foundational courses where pre-licensure students

are expected to master skills such as clinical decision making, prioritization, assessment and communication. In recent years, UIC Nursing has had record enrollment to meet the demand for baccalaureate-prepared nurses, meaning her classes are now larger than ever before (see p. 5).
“Enrollment continues to increase each year, which is awesome, but it also reinforces the need to be more intentional to make sure everyone actively participates,” she says.
Maffucci’s approach involves several steps. First, the class watches videos of real-world scenarios together. Maffucci asks follow-up questions, and the students reflect and respond individually through live polls accessed via their smartphones.
“Everyone, even the quietest students, get a voice this way,” she says.
Next, Maffucci uses a strategy she calls, “think, pair, share.” After the students think independently and respond to the polls, they pair up with a partner to compare perspectives. Then, the class comes back together to share their perspectives while Maffucci guides the discussion.
The tech is free (she uses a polling software offered by UIC called Echo360), and through the live polls

and discussions, Maffucci can get an instant sense of whether the class is understanding the material. In course evaluations and conversations, students say the strategies help them remember the content better, too, Maffucci says.
Maffucci has a doctorate in education with a focus on teaching and curriculum, and she keeps up with the latest literature in the field. That’s great news, and not only for the students she teaches. Maffucci is also UIC Nursing’s student success coordinator for the Chicago campus. In that role, she helps lead “student success huddles” to share strategies with faculty that will help ensure UIC Nursing students are succeeding.
That’s what Maffucci was doing at the SparkTalks presentation, too: spreading the word on the educational strategies she’s pioneering in her classroom.
“I see my role as both a teacher and an amplifier,” she says. “If I can develop a strategy that reduces anxiety and addresses the modern challenges of teaching, then my responsibility is to share it far and wide, turning one classroom’s success into a blueprint for many.”

Could the path to curbing the spread of HIV in Indonesia be through the prisons?
UIC College of Nursing associate professor Gabriel Culbert, PhD ’12, BSN ’04, RN, is a principal investigator on a $3 million NIH grant that seeks to curb the spread of HIV through a prison-based partner-notification system. The grant will allow Culbert and co-principal investigator Agung Waluyo, PhD ’11, a professor at the University of Indonesia, to test the program in eight prisons in Indonesia.
The number of Indonesian adults and children with HIV is estimated at more than half a million. In 2023, an estimated 24,000 new infections occurred, and 26,000 people lost their lives due to AIDS-related illness.
The program, called Impart, uses health workers to confidentially notify and offer testing to partners of HIV-positive prisoners. The program is for inmates’ partners who are
(l-r)
outside of prison — those who shared an exposure, such as sex or needle-sharing, before incarceration, Culbert says.
“Partner notification is gradually being adopted in lots of countries but … no one has ever done this in a prison or a jail or other criminal legal settings, which is shocking when you think about how
Rohan Jeremiah, PhD, MPH, associate dean for global health, was one of two guest editors of “A Case for Achieving Refugee Health Equity,” a special issue of the journal Health Education & Behavior. Published in October 2025, the collection brings together diverse voices, rigorous research and community-centered insights to challenge systemic inequities that shape refugee health across contexts.
Researchers may have a “duty to warn” participants of abnormal heart failure test results that are discovered during the course of a research study, but clinicians did not agree on when immediate action is needed, according to a paper published in August 2025 by lead author and assistant professor Denise Kent, PhD, APRN, in the journal of Clinical and Translational Science.

How did the COVID-19 pandemic affect the outlook of patients with ischemic heart disease? Perhaps not surprisingly, the worse these patients perceived the pandemic’s impact on their lives, the more they felt acutely or chronically hopeless, and this relationship was explained in part by anxiety, according to a paper published online in the Journal of Cardiopulmonary Rehabilitation and Prevention in August 2025. UIC Nursing professor emerita Susan Dunn, PhD, RN, was lead author on the paper.

As a labor and delivery nurse and later as a nurse-midwife, Mary Dawn Koenig, PhD, RN, CNM, frequently saw patients who suffered from iron deficiency anemia. Many of the mothers also complained that the prenatal iron supplements they were prescribed gave them unpleasant side effects, including nausea, vomiting and constipation.
“Iron is really important for both mom and baby, but particularly for the baby for neurocognitive development, and it’s something you can’t recoup later,” she says. “All that neurocognitive development happens in utero.”
With a nearly $3.5 million grant from the National Institutes of Health for a five-year study, Koenig will test whether a probiotic can enhance dietary iron absorption and improve iron status in pregnancy.
Participants in Koenig’s study will be given the probiotic Lactiplantibacillus
plantarum 299v (LP299V®), which has been shown to change the gut microbiome and increase the absorption of iron.
In the study of about 200 individuals, one group will take the commercially available oral LP299V® supplement twice daily with a standard prenatal supplement containing iron, starting from 10 to 16 weeks gestational age, until the time of labor. The other group, the control group, will take the regular prenatal vitamin and a placebo pill in place of the probiotic.
Koenig’s team will test the gut microbiome to see if the probiotic produces changes that could help with iron absorption. They will also collect placenta and cord blood and conduct neurocognitive developmental tests on the babies to see if the changes in the mother’s iron levels were transferred to the baby.
UIC ranks among top 10 nursing schools for NIH grants.
2024 $10.1 MILLION in NIH Funding

UIC COLLEGE OF NURSING UIC COLLEGE OF NURSING
2023
$7.7 MILLION in NIH Funding
Is there a formula for living that could help stave off dementia?
Associate professor Shannon Halloway, PhD, RN, is exploring whether changes to lifestyle health behaviors could be the key to preventing dementia with a $2.3 million grant from the National Institute on Aging.
The study, called InLife, will pool existing data from 12 U.S.-based trials with a sample of about 10,000 participants, says Halloway, who is the Heung Soo & Mi Ja Kim Endowed Faculty Scholar at UIC Nursing.


Two UIC Nursing postdocs received competitive grants to fund their research.
Michelle Villegas-Downs, PhD ’24, RN, was one of only 30 postdocs from across the country — in disciplines spanning the sciences — to receive a Postdoctoral Diversity Enrichment Program grant from the Burroughs Wellcome Fund.
The three-year, $60,000 award for research will allow Villegas-Downs to remotely monitor the health of mothers who are at risk for severe health complications by following them from delivery through the first six weeks at home. She’ll do this through the use of with Fitbits and other wearable devices.
Dahee Wi, PhD, RN, has been awarded $1 million from the National Institute of Nursing Research through the highly competitive NIH Pathway to Independence Award.
Wi’s project, “Mindfulness-based intervention for pain and sleep in adolescents and young adults with sickle cell disease,” will develop and test a digital, mindfulness-based intervention designed to reduce pain and improve sleep in young people with the disease. The intervention will be delivered via an app that combines short, educational modules with guided practices.
“This is the first project of this size that’s pooling U.S.-based trials, focusing on lifestyle health behaviors for cognitive health,” Halloway says.
The study will include data from adults who are at least 50 years old, although the average age of participants is in the early 70s.
In a smaller, preliminary study, Halloway found four lifestyle behaviors that benefited cognitive health: physical activity, cognitive activity (such as brain games, reading and crossword puzzles), social activity (spending time or talking with others in any setting) and a healthy diet (a Mediterranean diet that emphasizes foods that support brain health).
Halloway’s hypothesis is that small changes to those four lifestyle health behaviors could help prevent dementia, like Alzheimer’s disease, and that “the most powerful combination of behaviors”

BEING BISEXUAL AND OUT
What effect does coming out as a bisexual have on one’s mental health? There was no direct association between “outness” and anxiety or depression among a racially diverse sample of bisexual adults, according to a study published by assistant professor Ariel Smith Malonga, PhD, RN, and associate professor Wendy Bostwick, PhD, MPH, in the journal Self and Identity in June 2025.
A “how to” on integrating nurse practitioners and physician assistants into medical ICU teams, was the topic of a paper in the journal CHEST, the journal of the American College of Chest Physicians. UIC Nursing associate dean for practice and community partnerships Carolyn Dickens, PhD ’17, ACNP, was lead author on the paper, published in March 2025.
Clinical associate professor Shannon Simonovich, PhD, RN, was the lead guest editor on a special issue of the Journal of Obstetric, Gynecologic and Neonatal Nursing, titled “Women’s Mental Health Across the Life Course.” The journal is the flagship publication of the Association of Women’s Health, Obstetric and Neonatal Nurses. The issue contained 13 publications, including research articles, editorials, columns, and reviews, and was published in January 2025.


Why are improvements needed in the way NPs and other providers learn to make diagnoses?
Unfortunately, most of us will experience a diagnostic error in our lifetimes as patients. For nurse practitioners, making diagnoses is one of the most common tasks we engage in. And while making well-reasoned diagnoses is a critical skill, it is an area that has not received enough attention in nursing and medical education. In terms of educating our students, this is critically important because the stakes are so high for our patients.
What got you interested in this?
I was inspired to work on this while completing a fellowship through the Society to Improve Diagnosis in Medicine in 2021 and 2022. While there is ample

evidence demonstrating that NPs provide excellent patient care, we also know that each year an estimated 40,000 to 80,000 people die from diagnostic failures in U.S. hospitals.
What are you doing to help improve diagnostic competency?
I’ve created a tool to help improve diagnostic competency within the context of health care simulation.
The Diagnostic Competency During Simulation-based Learning Tool assesses individual diagnostic competencies. Using the tool, faculty observe students during an encounter with a standardized patient (an actor trained to portray a patient) and assign individual scores to observed behaviors reflecting each of the competencies. That allows them to identify areas where the student may

Clinical assistant professor
PhD ’20, MSN ’10, ANP-BC, CHSE, FAANP
2025 Macy Faculty Scholar
need additional practice and coaching to achieve competency.
For your Macy Faculty Scholars project, you’re creating a program to help future clinicians better understand and mitigate diagnostic disparities. What are some of those disparities?
The project is called Lead-Dx, and it’s a simulation-based educational program to address diagnostic inequality. There have been disparities identified based on race, ethnicity, gender, socioeconomic status, etc. For instance, Black Americans are 35% less likely to be diagnosed with dementia compared to white Americans. However, they are almost twice as likely to develop this condition.
How are you proposing to address this issue?
What’s innovative about Lead-Dx is that I’m collaborating with a diverse group of standardized patients who have experienced diagnostic inequity. They’ll be able to draw from their own experiences to co-design simulation scenarios that include patient perspectives and challenge provider assumptions.
What advice do you have for working NPs to mitigate diagnostic disparities?
Both communication and cultural humility are key. NPs should prioritize asking patients about their experiences, concerns, and life context — rather than assuming or telling — thereby fostering trust and shared understanding throughout the diagnostic process.

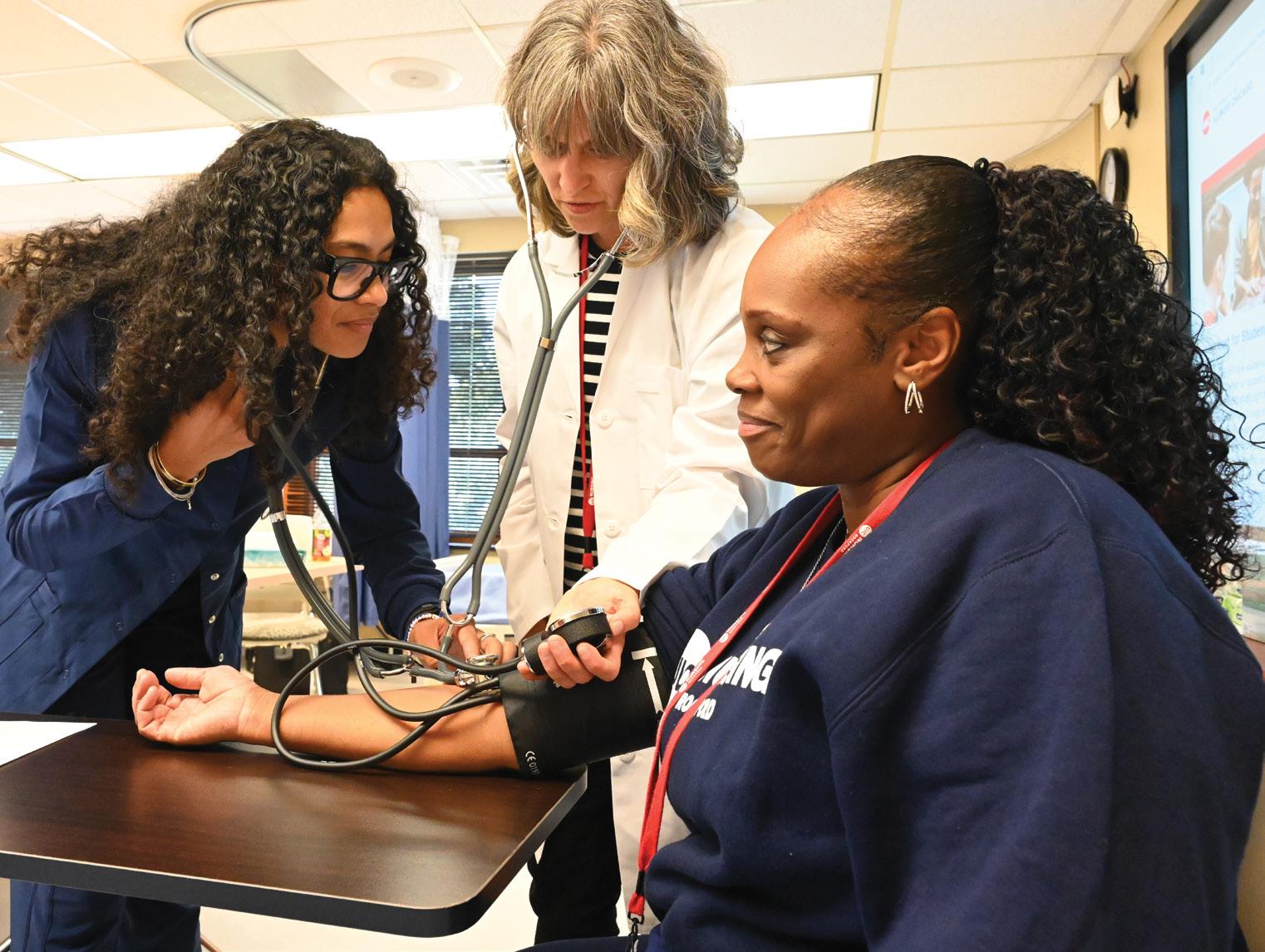

In August, UIC Nursing-Rockford welcomed its first class of students in the Master of Science in Nursing program for non-RNs, which will make it easier for career changers in northern Illinois to join the nursing profession.
Sometimes referred to as the “graduateentry program,” it is designed for students who already hold a bachelor’s degree in a field other than nursing. Graduates are prepared to pass the NCLEX, and they also enter the field with an MSN degree, positioning them for advanced RN roles.
“This is really a great opportunity for people in the Rockford area because our local hospitals are in great need of nurses, especially in the rural areas,” says campus director Laura Monahan, DNP ’16, MSN ’12, RN, MBA, OSF.
While more than half of the 15 students in the first class have backgrounds in health care fields, others come from more far-flung fields. Kyalisha McCall is transitioning to nursing after 15 years working as a security officer. Just a few weeks into the program, she said, “It’s like a close-knit family. You feel like you get that one-on-one attention.”

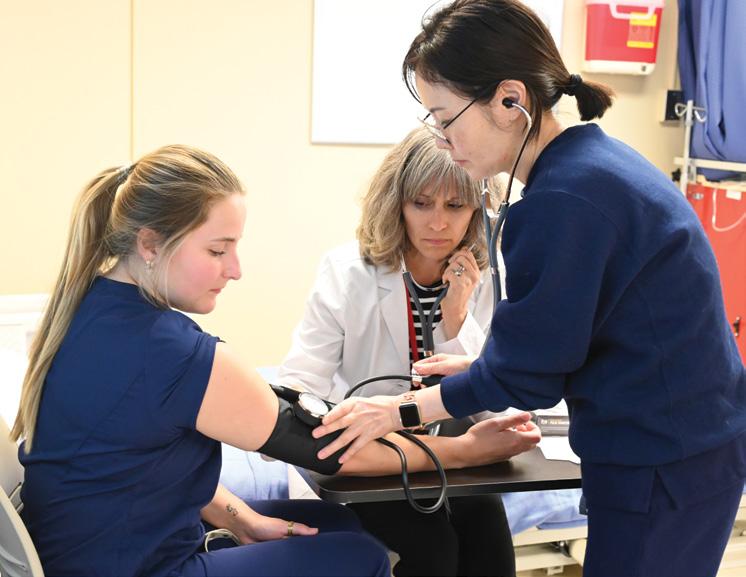
(clockwise from top left) 1. Melita Inthabandith, Samantha Como and Ciara King in class. 2. Milia Harris checks the blood pressure of Kyalisha McCall as instructed by instructor Jennifer Klein Colella, FNP-BC. 3. Yazmin Morales-Acevedo in class. 4. The inaugural cohort of prelicensure MSN students at Rockford. 5. Hwa Lee checks the blood pressure of Skylar Savage
Ciara King is returning to school five years after finishing her bachelor’s degree. She still holds a job outside of school, but says, “I’m managing just fine. And my 12-year-old [son] likes to say, ‘Now I get to ask you how your day at school was.’”
URBANA, ROCKFORD


UIC Nursing-Urbana campus director Krista Jones, DNP ’11, MSN ’07, RN, PHNA-BC (above), was inducted in the 2025 class of Distinguished Scholar Fellows of the National Academies of Practice.
In addition to Jones’ honor, Laura Monahan, DNP ’16, MSN ’12, RN, OSF, MBA, director of UIC Nursing’s Rockford campus, was accepted as a professional member of the National Academies of Practice.
The National Academies of Practice is an interprofessional group of health care practitioners and scholars dedicated to supporting affordable, accessible, coordinated health care for all. Distinguished practitioners and scholars are elected by their peers from multiple health professions.
The Hispanic Student Nursing Association wants to help future nurses appreciate cultural diversity.
If you were walking through the University of Illinois Urbana-Champaign’s Illini Union in March, you might have noticed students selling homemade esquites (Mexican street corn salad) and elotes (grilled Mexican street corn) next to a colorful poster with the letters “HSNA.”
This was the first fundraiser for the Hispanic Student Nursing Association at UIC Nursing’s Urbana campus. The group was founded in December 2024 and quickly grew from five to 60 members in its first semester alone.
An extension of UIC Nursing’s Urban Health Program, HSNA was spearheaded
future nurses are equipped to care for diverse communities with empathy and understanding,” she says.
Although the number of Hispanic nurses in the U.S. is growing, it still lags behind the general population at around 7%, according to the American Association of Colleges of Nursing.
“HSNA was founded to help bridge that gap,” says BSN student Mayra Ortega, current president, “by cultivating future health care leaders who honor Hispanic culture.”
In its first semester, the group focused on outreach efforts and hosted a slate of events — not just the fundraiser, but also a nursing faculty panel, a time-management workshop and an Abuelita hot chocolate-fueled Loteria Night social.
Ortega says the events give students the chance to connect, ask questions about pre-nursing and nursing life, and learn more about HSNA’s mission.
“Our patients are more diverse than ever,” says Vega, “and to care for them well, we

It’s no mystery why our Springfield campus welcomed a record-setting 145 new and continuing students in August. Year-round, they’re giving their all, having fun and building a strong community. AUGUST


It all starts with the Welcome Back Lunch. Students and faculty welcomed 400-plus students from 33 high schools over two days at “Nurse for a Day.”

Students joined the Sangamon County Department of Public Health to give flu shots in the community.


Seniors presented their poster projects to peers and to professionals at Memorial Health — and some won the People’s Choice Award!

Recipients of the notable Memorial Health Scholarship were honored at a luncheon (not all scholars shown).



Miniature horses help students “de-stress before the test” in advance of final exams.
Seniors helped local Scouts earn their first aid badge at the 2025 Merit Badge University, hosted by UIS.

In summer 2025, UIC Nursing-Urbana faculty members Krista Jones, DNP ’11, MSN ’07, PHNA-BC, and Amanda Sperry, DNP ’23, BSN ’97, RN, PEL-CSN, led thirteen UIC students on an inaugural summer study abroad course in Ireland.
“Traveling to Ireland gave students insights into opportunities and challenges present within the Irish health care system, and new insights into the U.S. health care system by comparison,” Jones says.
The three-week elective introduced students to the concept of community as a health system — or the idea that health is affected by societal factors such as
schools, housing, transportation, nutrition, employment and social networks. They also learned about the roles and responsibilities of health professionals in population health.
The trip — which included cultural experiences and travel across Ireland — culminated in a community assessment project to develop an intervention to address an identified health need.
“The experience offered both professional insight and personal growth that will undoubtedly shape my approach to nursing moving forward,” says BSN student Roshni Lotwala.
In a strategic alignment that considered students’ needs and program offerings, UIC Nursing’s Quad Cities campus went fully virtual at the start of the 2025-26 academic year.
Since 2021, nearly all nonclinical courses in the DNP program — the only degree offered at the Quad Cities campus — have been delivered 100% online.
“We saw that we could still offer the programs and support that students want [in Quad Cities],” says Dean Eileen Collins, noting also that students increasingly choose to meet with faculty and advisors virtually.
“We honor that our Quad Cities campus has been the academic home to many respected faculty and successful students over the years,” Collins adds. “Now, aligning it with today’s educational technologies and trends is the responsible decision for the future.”
We honor that our Quad Cities campus has been the academic home to many respected faculty and successful students.
– DEAN EILEEN COLLINS
419 5,874
Number of clinical visits

359
Number of individual patients served
The college’s Mobile Health & Wellness Services (MHWS) RV has been on the road for about a year, reaching underserved patients in central Illinois’ Peoria and Tazewell counties. Part of the federally funded ENRICH Project, the vehicle meets patients at the locations of community partners or at community events.
30
Number of community partners who regularly host the MHWS unit
14 50%
Percentage of patients who earn <$15K per year
Join UIC’s exclusive virtual networking platform, UIC Connected. It is a place for alumni and students to connect and grow.
• Create connections, build networks.
• Mentor students.
• Seek advice or expertise.
• Customize involvement to meet your needs.
This benefit is open to all UIC alumni. Join today to help our students succeed at: go.uic.edu/connected.
Number of DNP students named as ENRICH scholars, who are committed to serving rural populations and who have the opportunity to do rotations in the mobile clinic.

845 S Damen Ave, MC 802

A gift from alumna Carolyn Jarvis, PhD ’05, FNP-C, allowed the UIC College of Nursing to undertake a gut rehab of the main auditorium on the Chicago campus.
Now called the Carolyn Jarvis Auditorium, the upgraded lecture hall is accessible for individuals with disabilities, equipped with the latest technology, and seats nearly double the number of students — critical changes for this year’s record-setting enrollment.