SPRING 2022
Supporting maternal and child health
 The University of Iowa College of Public Health
The University of Iowa College of Public Health
FROM THE

 The University of Iowa College of Public Health
The University of Iowa College of Public Health
FROM THE
As I write this, the spring semester is wrapping up and the College of Public Health Building is filled with the buzz of student poster sessions, the intensity of preparing for finals week, and the excitement surrounding graduation.
The rhythms of this academic year have been much closer to those of pre-COVID times, but with notable differences. We’ve learned to blend virtual events, remote and hybrid work, and in-person classes and activities, as well as to navigate the day-to-day decisions and complexities that accompany an evolving pandemic.
In this issue of the magazine, we look back at the two-plus years that have passed since COVID-19 arrived in Iowa. We asked a variety of faculty, students, and alumni to share some of their experiences of living and working through the turbulence of the pandemic. Their answers touch on challenges, strengths, and a few silver linings. Another story explores how the pandemic affected the health, well-being, and work arrangements of University of Iowa employees. The research, conducted by investigators from the Healthier Workforce Center of the Midwest, provides an illuminating look into the experiences of clinical, on-site, and remote workers, supervisors, caregivers, and other groups, and how work might be structured going forward.
You’ll learn about the college’s new Maternal and Child Health (MCH) Training Program that strengthens our MCH curriculum and prepares students for careers in the field. You’ll also meet Gul Rukh Mehboob, a doctoral student in health management and policy who is also a Fulbright scholar and artist. Gul’s artwork was selected to commemorate the University of Iowa’s 175th anniversary. We also have updates on several new leadership appointments in the college, research news, awards and honors, and class notes.
I’m extremely proud of our college’s accomplishments and of the people—students, staff, faculty, alumni, and friends—who make it all happen. Thank you for your support, and best wishes for a healthy and happy summer.
Edith ParkerInSight is published twice a year for alumni and friends of the University of Iowa College of Public Health.
Director of Communications and External Relations Dan McMillan, daniel-mcmillan@uiowa.edu
Editor Debra Venzke

Designer Leigh Bradford
Marketing and Community Outreach
Coordinator Mitch Overton
Alumni and Constituent Relations
Coordinator Tara McKee
Webmaster Patrick Riepe
Creative Media Specialist Joey Loboda
Correspondence, including requests to be added to or removed from the mailing list, should be directed to:

Debra Venzke
University of Iowa College of Public Health 145 N. Riverside Dr. 100 College of Public Health Bldg., Rm S257 Iowa City, Iowa 52242-2007 debra-venzke@uiowa.edu
Visit our website cph.uiowa.edu
Follow us
The University of Iowa prohibits discrimination in employment, educational programs, and activities on the basis of race, creed, color, religion, national origin, age, sex, pregnancy, disability, genetic information, status as a U.S. veteran, service in the U.S. military, sexual orientation, gender identity, associational preferences, or any other classification that deprives the person of consideration as an individual.
The university also affirms its commitment to providing equal opportunities and equal access to university facilities. For additional information on nondiscrimination policies, contact the Director, Office of Equal Opportunity and Diversity, the University of Iowa, 202 Jessup Hall, Iowa City, IA, 52242-1316,319-335-0705 (voice), 319-335-0697 (TDD), diversity@uiowa.edu. W 00 4749/5 - 2022

A new program prepares students for careers in maternal and child health. 6 WORKING

Iowa research shows how the pandemic affected employee health and well-being. 10 SILVER

Reflections on two years of COVID-19.
A painting by HMP student Gul Rukh Mehboob was selected to commemorate the University of Iowa’s 175th anniversary. 16 COLLEGE

Diane Rohlman has been named associate dean for research in the UI College of Public Health.
Stephen Corbeil (84MA) was honored with the Hancher-Finkbine Alumni Medallion.
A new program prepares students for careers in maternal and child health.
 BY DEBRA VENZKE
BY DEBRA VENZKE
Despite massive spending on health care, the United States continues to experience poor maternal and child health outcomes. Compared to other high-income nations, mortality rates for U.S. infants are higher and life expectancy at birth is lower. And although an estimated 60% of maternal deaths are preventable, about 700 women nationwide die each year from complications of pregnancy.

“Across the nation, and in Iowa as well, we’re seeing a rise in the maternal mortality rate. We’re also seeing a decrease in the maternal and child health workforce,” says Kelli Ryckman, College of Public Health professor of epidemiology. “In Iowa, more delivery hospitals have been closing in the last few years, and that creates obstetrics deserts. Women have to travel longer distances
In response to these needs, the College of Public Health established a new Maternal and Child Health Training Program in fall 2020. Funded by a five-year grant from the Health Resources & Services Administration (HRSA), the program is directed by Ryckman along with associate director William Story, associate professor of community and behavioral health.
The HRSA grants are intended to develop or expand maternal and child health (MCH) curriculum, competencies, and degree offerings within schools of public health where there is currently a lack of or limited MCH offerings; strengthen the public health graduate student competencies in

MCH; and recruit graduate student trainees from underrepresented racial/ethnic backgrounds to complete MCH coursework.
The training program consists of two foundational courses; opportunities for research and practice experiences; workshops and training in MCH leadership, cultural humility, and health equity; membership in an MCH student interest group; and guest lectures by experts in the field.
“We really envision this as a pipeline to train maternal and child health professionals that can then go out to rural areas of the state to work with local departments of public health or the state department of public health. Nationally, agencies like the CDC and NIH have a lot of opportunities,” says Ryckman. “Maternal and child health really spans a wide range of areas, so I think individuals who get this training will be able to move into different arenas.”
Story also points to job opportunities at national organizations like HRSA’s Maternal & Child Health Bureau or the Association of Maternal & Child Health Programs (AMCHP). Other areas include working with Title V programming (a federal-state grant program that supports maternal and child health services), developmental disabilities, newborn screening, and adolescent, sexual, and reproductive health.
“We train across the life course, from preconception all the way through adolescence. We have students who are interested in things all along that life course, so there are a lot of opportunities,” he says.
A specific goal of the training program is to increase diversity in the MCH workforce to reflect an increasingly diverse population in the U.S. and Iowa. “Iowa has changing demographics with an increase in refugee and immigrant populations and Hispanic populations,” says Ryckman. “The changing demographics really create the potential for disparities in outcomes.”
The COVID-19 pandemic, in addition to magnifying existing MCH workforce challenges, also “intensified inequities for MCH populations that are rooted in the social determinants of health, including discrimination, health care access, education, and housing,” notes a recent journal commentary by a
team of authors from HRSA’s Maternal & Child Health Bureau.
Racial disparities in maternal and child health are well documented. Nationally, low birthweight among infants born to Black mothers is more than 2 times higher than among infants born to white mothers. Black women are 3 to 4 times more likely than white women to die from a pregnancy-related cause, while American Indian and Alaska Native women are 2.5 times more likely to suffer a pregnancyrelated death.
William Story, associate professor of community and behavioral health.
Depending on where women live, these rates can be even higher. In Iowa, non-Hispanic Black women are 6 times more likely to die from a pregnancy-related cause than white women, according to a 2020 report from the state’s Maternal Mortality Review Committee.
“As a student, I grew tired of hearing [these statistics] and wanted to do something about it,” says Kuann Fawkes, who graduated from Iowa with an MPH in community and behavioral health in 2021. She was in the first cohort of students to complete the MCH Training Program.
“Since maternal health outcomes are the clearest indicator of the health of a nation, addressing the challenges in the field forces us to deconstruct our past and hold ourselves accountable to creating a healthier future for all,” Fawkes continues. “I always found myself in spaces where it was healthy to unpack that statistic, and where I could talk freely about intersectionality, life course theory, racism, bias, discrimination, and their collective impact on health outcomes. I quickly learned that everything in public health starts with maternal and child health. It is so important for public health to prioritize birthing/parenting people and children.”
“I feel like our students, regardless of their identity, are being trained in how to address systemic barriers to equitable care for mothers and children.”
Fawkes completed a practicum experience at AMCHP, then a few months after finishing her MPH was hired full-time as a perinatal health research associate at AMCHP. She is now a CDC-assigned program manager at the Massachusetts Department of Public Health, where she supports the state’s Maternal, Infant, and Early Childhood Home Visiting Initiative housed in the Bureau of Family Health and Nutrition.
“Our program is designed to recruit a diverse student body, which will hopefully lead to a diverse workforce, which can certainly address some of the gaps we’re seeing in maternal mortality,” says Story. “But it’s not just the diversity of identities and perspectives that we bring in, but also the fact that our courses hit at the core component of what is driving these disparities. I feel like our students, regardless of their identity, are being trained in how to address systemic barriers to equitable care for mothers and children.”
So far, student interest in the MCH Training Program has been enthusiastic and the courses have had robust enrollment. “The response exceeded my
expectations,” says Story. “It really surprised me how many students want this type of training, so it’d be great to continue to meet that need.”
The development of additional courses is a possibility but would be tied to an increase in the grant, Ryckman says, noting that the HRSA funding comes out in five-year cycles. “There are three funding tracks, and we’re in Track 1,” she explains, “so we’ll be eligible for Track 2 at the end of our five years.”
The goal of Track 2 would be to offer a certificate program in MCH. For now, Ryckman and Story are waiting to see how the current cycle of funding goes.
“If we keep this traction and interest, then it would be worth exploring a certificate program,” Ryckman says. “I’ve talked to a lot of faculty in our college and they seem to be interested in offering different courses, and I think we could come up with a really nice track.”
Fawkes encourages students interested in maternal and child health to follow their passion. “It’s an incredibly broad field and there is room for so much innovation, diversity, and creativity,” she says.

 BY DEBRA VENZKE
BY DEBRA VENZKE
When the COVID-19 pandemic swept into the Midwest in March 2020, the University of Iowa quickly directed its non-essential employees to work from home. Jill Wiley, a research development coordinator at the university, was five months pregnant when she began working remotely.
By the time her daughter was born in July, the U.S. had surpassed 3 million COVID cases and many employees continued to work from home. As the months ticked by, Wiley and her husband faced the daily challenges of combining at-home childcare with remote work.

“My husband and I gave each other coverage to have focused work time, but otherwise trying to juggle a baby or toddler while on Zoom was really hard,” says Wiley.
The pandemic caused major disruptions in the professional and personal lives of millions of people. Researchers with the Healthier Workforce Center of the Midwest (HWC) are exploring how the pandemic affected the work arrangements, health, and wellbeing of University of Iowa employees.
The center, housed in the College of Public Health and directed by Diane Rohlman, professor of occupational and environmental health, is one of ten Total Worker Health Centers of Excellence funded by the National Institute for Occupational Safety and Health.
Early in the pandemic, HWC researchers recognized that the University of Iowa presented a unique opportunity for studying how the COVID crisis affected workers’ well-being.
“We have a major university hospital that has had to bear a huge brunt of Iowa’s COVID response. We have students and employees. It’s such a complex organizational structure with lots of different policy goals,” says Beth Livingston, HWC team member and assistant professor of management and entrepreneurship in the UI Tippie College of Business. By gathering local data, the team could compare the results to global and national trends in employee well-being.
Iowa research details how the pandemic affected employee health and well-being.
The HWC surveyed University of Iowa employees four times between May 2020 and April 2021. The web-based surveys were sent to faculty, staff, and postdoctoral researchers. Across the surveys, about half of all UI employees responded (11,755 unique participants).
The researchers looked at four different well-being outcomes over time: overall well-being, professional fulfillment, emotional exhaustion, and depression/ anxiety/stress. Workers were grouped into one of three categories: on-site clinical (health care workers), on-site non-clinical (facilities, student services, and other in-person employees), and remote workers.
The first survey conducted May to June 2020 showed that changes due to COVID-19 had a strong negative impact overall on employees’ well-being. As the pandemic disruptions dragged on, the second survey conducted August to September 2020 showed employees’ ratings of their wellbeing sank even lower.
“That was the roughest time period for university employees,” says Livingston. “People were scrambling to figure out school, childcare, and teaching.”
Workers’ well-being improved slightly around December 2020 to January 2021 when the third survey was conducted. COVID-19 vaccines became more widely available in early 2021, and the fourth survey in April 2021 showed that well-being had increased.
“There was a lot of hopefulness as we approached spring 2021,” Livingston says. “There was much less stress and better well-being. Then the Delta variant happened.”
The research team found that remote employees consistently reported better well-being overall than both clinical and non-clinical on-site workers.
“We’re currently doing follow-up research, but the reason for that better well-being is likely because remote and hybrid workers felt a better sense of control over the situation than on-site workers,” says Livingston.
The researchers also looked at demographic factors and outcomes. Women reported significantly worse depression, anxiety, and stress than men and significantly higher emotional exhaustion, but there were no differences between men and women in overall well-being or professional fulfillment scores. The surveys found no significant differences among racial and ethnic groups in well-being outcomes.
Across the surveys, workers under 40 reported worse well-being than other age groups. Conflict from work interfering with family was most strongly associated with emotional exhaustion among workers under 40, but increased workload was also critical.
The surveys also revealed that workers with caregiving responsibilities fared worse than their non-caregiving counterparts.
“People with children at home or who were taking care of elders more frequently identified with negative emotional states,” says Jonathan Davis, HWC team member and research assistant professor of occupational and environmental health. “Specifically, people with children had higher levels of stress, and people taking care of elders had higher levels of anxiety. Having to take care of their family members and worry about their well-being was impacting how they were personally feeling.”
Davis also explored the effect of alternative work arrangements on the well-being of workers with children. “They overwhelmingly had better experiences,” he says. “We saw a measurable improvement in stress, anxiety, and depression by having these alternative arrangements that allowed people to have some flexibility and control over their work.”
“Supervisors were struggling with an additional on top of everything else, which was, How do I figure out how to manage people remotely?”
S R O
Wiley, the university employee juggling work and parenting duties, found this to be true. “Kids introduce a lot of chaos into a typical schedule,” she says. “I was given a lot of support and flexibility by my supervisor to work off hours and weekends, which really helped.”
The survey data showed that people with remote management responsibilities reported lower wellbeing than non-supervisors who worked remotely.
“Supervisors were struggling with an additional stressor on top of everything else, which was, How do I figure out how to manage people remotely?” says Livingston. “How do I know employees are working?”
In response, the HWC and Tippie College of Business hosted two webinars on managing remote workers, one geared toward the UI community and another aimed at a regional audience.
“Research has shown that supervisor well-being and worker well-being are really linked together,” says Rohlman. Some key lessons for managers, she says, are having trust in your employees and creating a structure that supports different employees.
“We all work differently,” she says. “Some people want a more hands-on approach, so they may need more check-ins. Others don’t want to have as much of that.”
The information gathered from the surveys has provided a jumping-off point for additional research.
“It’s inspired a lot of important research questions that our team is trying to look at, whether it’s caregiving burden, remote management, or other components around age and professional development,” says Livingston.
One such endeavor is already underway. A project addressing supervisors of remote workers was included in the HWC renewal application. Livingston is the principal investigator of the $1.1 million grant funded by the Centers for Disease Control and Prevention to investigate better methods of training supervisors to manage remote workers, focusing on both productivity and worker well-being.
The survey results were also shared with University of Iowa leadership and human resources. The information helped inform The Future of Work@Iowa project, which aims to reimagine how and where University of Iowa employees work after COVID-19. It’s focused largely on understanding the long-term potential for remote and hybrid work, flexible schedules, and other types of work arrangements.
“The university has recognized that for recruitment and retention issues, it’s important that we allow hybrid or remote work,” says Rohlman. “In order to be competitive and attract people, that’s a really important factor.”
The pandemic accelerated changes in how and where we work, as well as how we think about our jobs and what matters to us.
“People want more work-life balance,” says Rohlman. “Allowing remote work or some flexibility in where, how, and when employees do their work benefits people and gives them a sense of control.
“We’ve always known that work organization and the environment of work impacts health and safety, which in turn impacts well-being, but the pandemic forced us into rethinking all of that,” she continues. “We now need to think about what we learned that we can apply going forward, and not just fall back into what we did because it’s the way we’ve always done it.”


The unwelcome intrusion of COVID-19 has been part of our lives for more than two years, the disruptions forcing us to rethink and revise our routines in countless ways. We all have certain moments—the day we were told to work remotely, the results of a COVID test, the return to in-person classes—that flood us with memories and emotions. We asked College of Public Health students, faculty, and alumni to reflect on the past two years of living and working through the unpredictable twists and turns of the pandemic. Here’s a sample of their experiences and lessons learned.
In addition to the trials faced by the general population (i.e. loneliness, confusion, a heated political climate), there are a few challenges that students have faced in particular. I am a strong believer that college isn’t simply about coursework— extracurriculars, connections formed, and other experiences shape students immensely, and these learning opportunities just aren’t the same in a virtual format.
For example, I was slated to intern at a research lab in Florida during the summer of 2020 to gain valuable genetic laboratory experience, but due to the COVID-19 shutdown, I pursued a virtual internship locally. I am fortunate that I made the connection with a research lab (which I continue to work in), but I know many other students who were not able to gain experiences that could have guided their career choices.
A silver lining, however, is how we were all going through this together. Faculty, administrators, and other students were more accommodating than ever for people with health issues and unstable employment/living conditions, and mental health recognition has been on the rise. This disruption on a global scale is something everyone has in common, and although it showed how our society needs to be improved, it also displayed how supportive we are already in the face of adversity.
Radha Velamuri, BS/MPH undergraduate-to-graduate student
Among successes, we can point to the rapid development of highly effective vaccines, life-saving innovations in treatment, and the adoption of new technologies that support telework, increased collaboration, and expanded health services. Greater recognition of the critical roles of public health professionals, public health science, and health policy should be acknowledged as well—even though this heightened attention has sometimes felt harsh or even resentful.
Not surprisingly, the list of problems connected with the COVID response to date seems lengthier and easier to recount. Inequitable vaccine distribution. Communications miscues and polarizing political arguments, often grounded in misinformation. Widening health disparities, including notably those impacting rural populations. Worsened health status resulting from delayed health care. And the
devastating toll on mental health, especially among young people and other vulnerable populations.
The severe breakdown in trust—particularly the distrust of scientists, health officials, and other leaders at the local, state, and national levels—may stand out as one of the most serious problems emerging from the COVID-19 pandemic. Public health leaders, including those of us in academic public health, need to take the lead in restoring the social connections and sense of shared purpose that have long been the underpinnings of our profession.
Public health has prided itself on being non-partisan, a bridge between various sectors of society, with the unique capacity to bring together various stakeholders to work on shared challenges. Now, more than ever, this convener role may be public health’s most urgent mission.
Edith Parker, dean of the UI College of Public Health
The pandemic has provided many insights related to health behavior change. First, our ability to modify health behaviors is impacted tremendously by what is going on in our lives. Stressful and difficult emotional circumstances, such as those brought about by COVID-19, make it much harder to change behavior and maintain our resolve. This is partially because we often engage in unhealthy behaviors such as tobacco and alcohol use, snacking, and pleasurable sedentary activities to cope with stress and negative emotions. The self-control necessary to persist in sustaining behavior changes is also a finite resource that can become depleted from managing the many daily challenges imposed by the pandemic.
The impact of our physical and social environments has also become more evident. Our health behaviors—both positive and negative—are closely tied to where, how, and with whom we spend our time. Lockdowns, remote working conditions, and other mitigation efforts dramatically altered our routines and social interactions. This can mean spending greater (or lesser) amounts of time with people and in places that may either support or interfere with health promoting behaviors. This may be why we have seen such highly varied behavioral responses to the pandemic. Although increases in body mass, tobacco, and alcohol use have been widely reported, it is also true that many individuals made very positive changes. It is important for us to learn more about the ways in which these disruptions to our daily lives have the potential to both facilitate and undermine health behavior change.
Mark Vander Weg, professor and head of community and behavioral health
THE PANDEMIC HAS DEMONSTRATED HOW DIFFICULT IT CAN BE TO CHANGE PEOPLE’S HEALTH BEHAVIORS. WHAT ARE ONE OR TWO KEY LESSONS BEHAVIORAL HEALTH RESEARCHERS CAN GLEAN FROM THE PAST FEW YEARS?
Combined, MercyOne Elkader Medical Center and MercyOne Elkader Ambulance employ approximately 100 colleagues. When the pandemic started, the amount of preparedness planning needed for our hospital and ambulance teams seemed like an insurmountable task with such a small staff. However, we quickly discovered that our small, nimble, and mighty team is actually our greatest strength, and we were able to accomplish big things! With keeping the patient and community as our priority and applying an innovation mindset combined with undeniable determination, our team could tackle any challenge. There were many times that our team would already have processes underway or implemented before guidance would come out from trusted resources. This would infuse our team with motivation to keep going because we knew we were capable and prepared to meet the needs of our patients and communities. Having resources and partners that we could tap into was critical when COVID cases were peaking and we had to keep patients that we would normally transfer to a higher level of care. We are grateful for the expertise of our MercyOne providers and colleagues across the state and nation in various clinical and public health roles. We were stronger because of the innovation and teamwork across the county, state, region, country, and world!
Brooke Kensinger (05MHA), CEO of MercyOne Elkader (Iowa) Medical CenterAS SOMEONE WHO WAS HOSPITALIZED FOR MORE THAN A MONTH WITH SEVERE COVID IN 2020, WHAT IS ONE THING YOU’D LIKE PEOPLE TO KNOW ABOUT THE DISEASE OR COVID SURVIVORS?
People should know that our COVID battle is not over—for patients, survivors, and for our public health profession. As a survivor, I continue to manage respiratory and neuropathic issues, and I’ve been prescribed respiratory therapy for the unforeseen future to optimize quality of life. Research shows that more than one in four COVID survivors continues to live with symptoms related to this disease over
the longer term. While the science of diagnosing, treating, and mitigating COVID has come a long way since 2020, there are still many mysteries. For me, those mysteries about my longer-term health status can create stress.

It’s not over for public health professionals. Our College of Public Health is faced with many challenges—to investigate the origin and distribution of COVID, figure out its underlying determinants, and more effectively communicate prevention strategies to the public. The infrastructure of local, state, national, and global health organizations has been greatly challenged to deliver consistent and effective messaging. As a result, the prevalence of COVID and new variants seem to remain too high and for too long.
I’m most thankful for the remarkable care that I received during these uncertain times. Nurses, doctors, scientists, and all health care workers continue to deliver high performance medical care. Despite these victories, the health care system is under a great deal of stress. And it’s not over.
Kirk T. Phillips (05PhD, 02MS), adjunct associate professor of epidemiology
AS A STUDENT WHO GRADUATED THIS SPRING, HOW DO YOU THINK THE PANDEMIC HAS FOREVER CHANGED THE WORLD?
This is a hard question and to some degree I think we will continue to learn how the world has changed as we become farther removed from the beginning of the pandemic. However, changes have already occurred. In a professional capacity, I think the world now knows what public health is. When I tell people that I am a graduate student studying public health, most know what my field is now. I hope this improved understanding solidifies the importance and necessity of public health work on the local, state, and federal level.
Additionally, I think we all became more aware of the many cracks in our systems that were exposed during the pandemic, which I hope will inform how we engage with solutions to public health issues.
Sofie Dollison, 22MPH
A painting by HMP student Gul Rukh Mehboob was selected to commemorate the University of Iowa’s 175th anniversary.
BY EMILY NELSONGul Rukh Mehboob, a PhD student in the Department of Health Management and Policy studying health economics, has ensured that a part of herself will remain on the University of Iowa campus after she leaves.
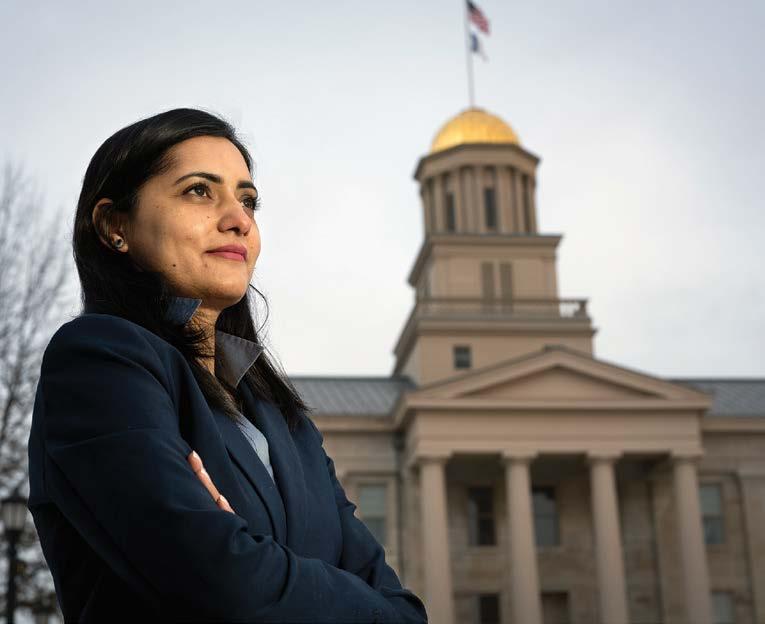
“I believe that wherever you go, you leave a part of yourself there,” says the Fulbright scholar from Peshawar, Pakistan.
Her watercolor painting of Old Capitol was selected to celebrate the university’s 175 years as an institution and to commemorate the installation of Barbara Wilson as UI’s 22nd president.
Mehboob’s concept for the piece was to illustrate the university’s rich history and transformation to a contemporary campus. The base of the work resembles a black-and-white photo of the Old Capitol to reflect the university’s long history with strategic color elements added in.

“I chose the golden dome because that represents hope,” Mehboob says. “And the autumn trees are colored to show inclusion—all the people who come here to study and the peace and prosperity and colors they take with them back to their homes and spread there. That was something in my mind that I wanted to tell through my art.”
Mehboob says her parents are big believers in education as a catalyst for social change and their house was always filled with books. While she grew up loving art, her family encouraged her to go in a different direction. She received bachelor’s and master’s degrees in economics. After being diagnosed with an autoimmune disease and experiencing the health care system from a patient perspective, Mehboob developed an interest in health economics and decided to devote herself professionally to that field. But she never abandoned her love of art.
“I kept on doing it as a hobby,” Mehboob says. “I see art as creativity of the soul, and it became a good form of inner growth and expression for me.” While she was a faculty member at a business school in Peshawar, Mehboob established an initiative called Arts, Creativity and Freedom, through which artists were invited to conduct workshops for the business students and faculty and were provided venues to exhibit art.
Mehboob also uses her art to help fund two volunteer projects that help education in Pakistan. All money she makes from selling her art—including the commission she received for the UI 175th anniversary artwork—goes to funding Ujala School initiative (which means “light of hope”) and Kitab Dost
(Friends of Books). Both initiatives were established under the umbrella of the Association for Business, Professional, and Agricultural Women, a nongovernmental volunteer organization with which Mehboob is heavily involved.
As Pakistan begins to roll out a universal health coverage program, health care financing experts are needed. Mehboob was already working with the ministry on the effort, but says she needed to improve some of her skills so she could contribute even more.
“I wanted to go for my PhD because of my strong belief in education as a tool that really can be used to make a difference at various levels,” Mehboob says.
Mehboob began applying for scholarships and earned a Fulbright—the second person in her family after her sister also studied in the United States on a Fulbright award.
As she started looking at where she wanted to study, Mehboob says she was impressed with Iowa’s College of Public Health—but something else stood out to her.
“The University of Iowa looked like a sort of mini world because it’s home to more than 130 nationalities and 2,800 international students,” Mehboob says. “That fascinated me and it said to me that they really welcome people from other countries. It felt like home before I even got here.”
Mehboob saw the call for artists for the 175th celebration near the end of her first semester at Iowa. She says it was perfect timing.
“When I came here, I was totally out of touch from my art because I was struggling to settle down and set up a home and learn the new system here and everything, so I missed my art,” Mehboob says. “When I’m away from my art, I feel that I’m just not in touch with myself, so I was craving for it.”

Mehboob says it’s amazing to think that when she returns to Pakistan after earning a PhD, her artwork will remain permanently on display—with the original in the Office of the President and a print in the Vice President’s office suite in the Iowa Memorial Union.
“For something artistic of mine to remain here means a lot to me,” Mehboob says.
Diane Rohlman has been named associate dean for research in the University of Iowa College of Public Health. Her appointment began March 1, 2022.
Rohlman is a professor in the Department of Occupational and Environmental Health where she is the Endowed Chair in Rural Health and Safety. She directs the Healthier Workforce Center of the Midwest and leads the Agricultural Safety and Health Training Program within the Heartland Center for Occupational Health and Safety.
Rohlman’s research interests include occupational and environmental exposures and their impact on neurobehavioral function, and the development of safety and health interventions to prevent workplace exposures, reduce injuries, and promote healthy behaviors. Her research has focused on vulnerable populations, including children, young workers, and those working in hazardous industries, which often include immigrant workers.
dean of the College of Public Health. “In addition to developing and leading her own diverse portfolio consisting of basic and applied research, Diane has mentored junior faculty and students, collaborated across disciplinary and institutional boundaries, led international research teams, and competed successfully for funding at the highest levels. Her expertise will help ensure that our research enterprise remains at the forefront of public health discovery nationally and continues as one of the most productive research units on campus.”
As associate dean for research, Rohlman will be responsible for providing leadership to establish and nurture interdisciplinary research collaboration within and outside the College of Public Health. The role includes identifying and promoting funding sources to support research and training programs, shaping the college’s research policies and practices, sustaining research standards, and developing effective working relationships with the college and the university in support of research success. Rohlman also will collaborate with department heads and faculty to promote new research initiatives, promote career development opportunities, and succession planning within CPH research centers.
“Diane brings an impressive combination of outstanding scholarship, high-level research experience, and strategic vision to this critical collegiate leadership position,” says Edith Parker,
Rohlman received both a master’s degree and PhD in experimental psychology from Bowling Green State University in Ohio. After completing a postdoctoral fellowship at the Center for Research on Occupational and Environmental Toxicology at Oregon Health & Science University, she joined the faculty at OHSU. In 2012, she became a member of the UI faculty in the Department of Occupational and Environmental Health before joining the UI Interdisciplinary Graduate Program in Human Toxicology in 2013. In 2016, she was named the Endowed Chair in Rural Health and Safety.
Rohlman, who also chairs the college’s Global Public Health committee, has led research studies examining pesticide exposures in agricultural workers in the United States and internationally. Over the course of her career, she has been involved in research on five continents and in more than 10 countries.
“I’m excited about the new opportunities,” says Rohlman. “The college has a strong research portfolio, and I look forward to promoting the great research from our faculty, building new collaborations, and helping to support student and faculty research.”
Her expertise will help ensure that our research enterprise remains at the forefront of public health discovery nationally and continues as one of the most productive research units on campus.
University of Iowa students, faculty, staff, and alumni received some of the institution’s highest honors on April 12, 2022, at the 105th Hancher-Finkbine Dinner.

At the event, alumnus Stephen Corbeil was presented with a Hancher-Finkbine Medallion in recognition of his leadership, learning, and loyalty.
Corbeil is an innovative leader of hospitals and health care systems who has charted a steady course through the industry’s turbulent changes. He earned a master’s degree in hospital and health administration (now the Department of Health Management and Policy) in 1984. He remains an avid supporter of the college and generously offers his time, resources, and expertise for the enrichment of today’s students.
For more than 30 years, Corbeil successfully managed multiple health care organizations within Tenet Healthcare and Hospital Corporation of America (HCA) in numerous states. Most recently,
as president of TriStar Health, a multi-billion-dollar division of HCA, he oversaw 22 hospitals, 9 ambulatory surgery centers, and over 12,000 employees in Tennessee, Georgia, and Kentucky.
After retirement in 2016, he served as a consultant with HCA engaged with its executive development program. He now serves as Executive Chairman at LucidHealth and on the Board of Trustees at Tennessee State University. He is an American College of Healthcare Executives Fellow and has served on numerous professional and community service boards.
Corbeil’s loyalty to the University of Iowa and College of Public Health has been exceptional. Throughout his career, he has been a professional and personal mentor to many students and served as preceptor for summer interns and postgraduate fellows. He served on the alumni board for the Department of Health Management and Policy from 2000-2012 and was president in 2007. He received the college’s
Outstanding Alumni Award in 2011, the UI Distinguished Alumni Achievement Award in 2016, and is recognized as a Founding Partner for the key role he played in the inception of the College of Public Health.
In addition, Corbeil and his wife, Mary Kay, are among the college’s most generous supporters. They have established an endowed scholarship, a graduate assistant scholarship, and provided funding for a pilot program in partnership with Tennessee State University.
He is among the most active and devoted alumni of the college’s MHA program. Despite his many commitments and accolades, he has consistently maintained a high level of engagement, leveraging his own network and expertise to ensure the continued excellence of the program. Corbeil is a member of the UI Foundation’s President’s Club and has served on the CPH Campaign Committee. Though not from Iowa, the Corbeils’ strong Hawkeye ties have been carried on through their three children who all earned UI degrees.

Dr. George Wehby has been named head of the University of Iowa Department of Health Management and Policy. His appointment begins July 1, 2022.
Wehby is currently a professor and the John W. Colloton Chair in the Department of Health Management and Policy. He holds secondary appointments in the Department of Economics, the Department of Preventive and Community Dentistry, and the Public Policy Center at the UI, as well as a research associate appointment in the National Bureau of Economic Research.
His research examines social, economic, and policy impacts on health, especially among children. From 2015 to 2019, he served as the PhD program director for the Department of Health Management and Policy before becoming director of graduate studies in 2019. He was awarded the CPH Faculty Teaching Award in 2013.
Wehby earned a Master of Public Health degree from American University of Beirut, followed by a PhD in health management and policy with a concentration in health economics from the University of Iowa in 2006. He joined the College of Public Health faculty in 2008 and attained the rank of full professor with tenure in 2017.
He will succeed Dr. Keith Mueller, Gerhard Hartman Professor of Health Management and Policy, who has served as department head since 2010. Mueller will remain on the faculty and will continue to direct the Rural Policy Research Institute (RUPRI).
“Dr. Wehby is a distinguished academic leader with a sustained record of achievement as a researcher, teacher, and mentor,” says Edith Parker, dean of the College of Public Health. “His dedication to students and to the excellence of our educational programs, his diverse portfolio of national and international research, and his vision for future growth and development will ensure the continued success and national prominence of our outstanding Department of Health Management and Policy.”
The University of Iowa Department of Health Management and Policy is pleased to welcome Dr. Kristin Wilson as the director of its Master of Health Administration (MHA) Program effective July 1, 2022. Wilson will be appointed as an associate professor in the clinical track.

Wilson earned a PhD in public health sciences with a concentration in health management and policy in 2008 from St. Louis University College for Public Health and Social Justice. She earned an MHA degree from the same institution in 1993.
Wilson joined the St. Louis University (SLU) faculty in 2005 and was promoted to associate professor in 2015. She directed the SLU Health Management and Policy Master of Public Health degree program from 2013 to 2017, and she directed the MHA degree program from 2016 to 2018. During her time as MHA director, she led the program through the accreditation process with the Commission on Accreditation of Healthcare Management Education and maintained the program’s No. 7 national ranking.
Wilson brings a wide variety of academic and practical leadership experience in health administration, including her current role as the executive director of the Heartland Center for Population Health and Community System Development at St. Louis University. In addition, since 2018 she has been the principal investigator of the Missouri subcontract to the HRSA-funded Midwestern Public Health Training Center for Workforce Development.
Wilson will succeed Dan Shane, associate professor of health management and policy, who has served as MHA program director for two years. Shane will continue as a member of the faculty.
Jim Torner, professor of epidemiology, was one of six UI faculty members honored by the Board of Regents, State of Iowa, with a 2022 Faculty Excellence Award. The award recognizes exceptional contributions and a sustained record of excellence. Each recipient received $1,000 and will be honored at a special awards celebration in the fall.

The University of Iowa College of Public Health is the No. 19 school of public health in the nation, according to the 2023 Best Graduate School rankings from U.S. News & World Report. Among publicly supported schools, the college ranks No. 10.
For the first time, U.S. News published a ranking of the Best Biostatistics Programs. The UI College of Public Health’s Department of Biostatistics is No. 20 in the nation.
Although it was not assessed this year, the college’s Department of Health Management and Policy was most recently ranked at No. 8 among health care management programs.

The University of Iowa College of Public Health has named Brett Faine and Kenneth Saag the recipients of its 2022 Outstanding Alumni Awards.
Faine received a Doctor of Pharmacy degree in 2007 from the University of Iowa College of Pharmacy and a Master of Science degree in epidemiology from the UI College of Public Health in 2016. He is currently a clinical associate professor of pharmacy practice and emergency medicine at the University of Iowa.

Saag earned a Master of Science degree from the UI Department of Preventive Medicine and Environmental Health
(now part of the Department of Epidemiology in the UI College of Public Health) in 1993. He also received an MD degree from Northwestern University in 1986. He is currently the Jane Knight Lowe Endowed Chair in the Department of Medicine and professor of clinical immunology and rheumatology at the University of Alabama at Birmingham. The award recognizes College of Public Health alumni who have made distinguished contributions to the field of public health and demonstrated a strong interest and commitment to the mission, vision, and values of the college. The recipients will be honored at an event this fall.

A team of University of Iowa researchers will pool their talents to tackle climate change and related health concerns through a new initiative that uses a “collaboratory” approach. The project, titled “Illuminating the Nexus Between Climate Change and Public Health,” is led by Peter Thorne, professor of occupational and environmental health in the College of Public Health.
A collaboratory brings together team members from different backgrounds and disciplines within and outside the University of Iowa to solve complex problems. The Iowa Institute of Public Health Research and Policy (IIPHRP), based in the UI College of Public Health, selects and funds the interdisciplinary projects through a competitive application process.
“This project is an important initiative to help the University of Iowa respond to new funding opportunities that address climate change and public health,” says Vickie Miene, interim director of the IIPHRP.
Growing recognition of the extensive consequences of climate change has led the Biden administration to emphasize climate action and increase funding for climate change research through the National Institutes of Health and other federal agencies.
“The overarching goal of this collaboratory is to assemble multidisciplinary teams of climate scientists and public health experts to develop innovative proposals that will attract new funding for research that addresses the nexus between climate change and public health, with a focus on climate challenges in the heartland,” says Thorne.
A new study led by College of Public Health students examines the role that usergenerated content on the social media platform TikTok plays in promoting Puff Bar culture. Puff Bar is a brand of disposable e-cigarette available in flavors that appeal to youth.



Published in the International Journal of Environmental Research and Public Health, the study revealed seven genres of Puff Bar-related video content on TikTok: skits and stories, shared vaper experiences, product reviews, product unboxing, promotion of Puff Bar, videos to show off, and crafts. By classifying this content, the researchers hope that the information will be used by prevention organizations to better understand youth e-cigarette use and trends.
“I think it will be beneficial for these organizations to see what young e-cigarette users are saying about the nicotine products they use and develop subsequent messaging from it,” says Makayla Morales, an undergraduate public health student and lead author of the paper.
Lexi Fahrion, a Master of Public Health student and co-author of the study, says that there were some surprises that emerged from the study. “Many e-cigarette users seemed to express their awareness of the potential dangers of e-cigarette use in their videos, but ultimately didn’t let that stop them from vaping,” she says. “I had previously assumed that more people would be unaware of potential risks.”
Fahrion also noted the lack of regulation of e-cigarette content on TikTok, despite the community guidelines on substance use.
Shannon Lea Watkins, assistant professor of community and behavioral health, served as senior author of the study. The research was funded by the American Cancer Society, administered through the Holden Comprehensive Cancer Center at the University of Iowa and by the University of Iowa College of Public Health.

Anna Correa (22MPH) was awarded a Fulbright study/research grant in public health to India for 2022-23. Working with colleagues at St. John’s Medical College, she will facilitate interviews and focus groups with migrant workers in Bangalore, India.
“This research will help us explore the mental health landscape and needs of the migrant laborer community that faces many systematic challenges to daily life, overall health, and mental well-being,” Correa says. “The goal is that this study helps inform future educational campaigns, health programming, and policy changes to support migrant worker mental health.”

A research team led by George Wehby, professor of health management and policy, found that expanding public coverage of dental care was linked to narrowed racial and ethnic disparities in use of dental services. The NIDCRfunded research was published in Health Affairs
The 2010 passage of the Affordable Care Act (ACA) expanded eligibility for Medicaid. As a result, many people became newly eligible for medical and dental coverage in states that
adopted Medicaid expansions in 2014. To find out if the eligibility changes affected disparities in dental care, the scientists analyzed responses from a nationally representative survey that asks U.S. adults about their health care, including their use of dental services. Among those adults who became newly eligible for Medicaid in 2014 based on income, the researchers compared responses from the three-year period before (2011-2013) and the five-year period after (2014-2018) states broadened eligibility.
Based on survey responses from about 5,700 adults in states that expanded Medicaid eligibility and offered extensive dental benefits (coverage of at least 100 dental procedures), rates of dental visits by Hispanic and non-Hispanic Black adults increased from 14% to 21% and from 20% to 26%, respectively, while rates among non-Hispanic white adults remained unchanged at about 30%. The researchers found a similar narrowing in disparities in these states for use of preventive services like oral exams and teeth cleaning, and for dental treatments like fillings and root canals. But survey responses from a separate group of about 3,500 adults indicated that disparities did not diminish in states that expanded Medicaid coverage yet offered more limited dental benefits.
Despite the improvements, the authors noted that use of dental services remained low across all three racial and ethnic groups, regardless of states’ expansion status or the extent of dental benefits offered.
“Insurance coverage is only one factor that affects access to care,” Wehby says. “There are many factors that are important for increasing access, enabling adequate use of services, and meeting dental care needs, particularly among low-income populations.”
Jessica Allen (21BA) is a COVID-19 health educator for the State of North Dakota Department of Health, contracted through the CDC Foundation’s COVID-19 Workforce and Vaccine Initiative.
Dianna Appelgate (05MS) is a patient experience specialist at PeaceHealth in Springfield, Oregon.
Carol Ayangbile (13MHA) is vice president, patient experience at Children’s Health in Dallas, Texas.
Jennifer Bernstein (09MPH) is Earth Class Mail privacy and compliance lead, associate corporate counsel at LegalZoom in Ann Arbor, Michigan.
Christian Cota (21MHA) is manager of the employee occupational health and safety program at Fairview Health Services in Minneapolis, Minnesota.
Kaitlin Emrich (09MPH) was named deputy director of the Black Hawk County Health Department in Waterloo, Iowa.
Brittany Erickson (13MHA) has been named vice president at MercyOne Medical Group in Mason City, Iowa.
Lauren Erickson (12MPH) is senior managing consultant at Berkeley Research Group LLC in Washington, DC.
Emma Hau (21BA) has joined the rotational assignment program, personal care product management at Medline Industries in Northfield, Illinois.
Sarah Henize (09MPH) is senior director, client success at Raziel Health in New York, New York.
Lucas Johnson (13MHA) is director of product management, value-based care at Clarify Health in Kansas City, Missouri.
Brooke Kensinger (05MHA) was awarded the Iowa Hospital Association 2021 Young Executive Achievement Award, which is presented to a hospital CEO under 40 who has significantly affected the community hospital or health system. Kensinger is CEO of MercyOne Elkader Medical Center in Elkader, Iowa.
Brita Kilburg-Basnyat (15PhD) is a senior scientist at Arcus Biosciences in Madison, Wisconsin.
Christopher Klitgaard (99MHA) is co-founder and CEO of Revology in Iowa City, Iowa.
Stephanie Kraft Sheley (16MHA) is the founder and director of Right By You, an all-options text line that helps Missouri youth navigate access to birth control, abortion care, birth care, and support for parenting and adoption. Kraft Sheley is also principal attorney of Kraft Sheley Law, LLC, an Illinois and Missouri firm focused on birth justice and safe access to abortion care.
Stephanie Lim (11MHA) has been named group chief strategy officer of Palm Beach Health Network in Palm Beach County, Florida.
Larissa Luckel (13MPH, 13MHA) is director, revenue cycle services at MediRevv in Coralville, Iowa.
Ryan Peterson (19PhD, 16MS) received the Journal of Applied Statistics 2020 Best Paper Prize for his first-authored paper “Ordered quantile normalization: a semiparametric transformation built for the cross-validation era.” Peterson is an assistant professor, Department of Biostatistics and Informatics at the Colorado School of Public Health in Aurora, Colorado.
Megan Pospisil (21MPH) is an epidemiologist, COVID-19 response for Thurston County Public Health and Social Services in Olympia, Washington.
Lawrence “Larry” Prybil (70PhD, 64MA) has been honored as a Public Health Legend by the University of Kentucky College of Public Health, which recognizes individuals who have achieved sustained success in their field and made an outstanding contribution toward the goal of health improvement for the state of Kentucky.
Casi Roethler (14MHA) is chief of staff to CMO at Brightline in New Orleans, Louisiana.
Alan Schultz (06MPH) is a UX researcher at Google in San Francisco, California.
Madison Snitker (21MPH, 20BA) is the Iowa service area 1-C education and exercise coordinator at Marion County Public Health Department in Knoxville, Iowa.
Kenni Sterns (19MPH) is a registered nurse at Wellpath in Fort Lauderdale, Florida.
Ni Sung (21BA) is a clinic services specialist at University of Iowa Hospitals and Clinics in Iowa City, Iowa.
Rachel Trevizo (10MHA) is co-founder and chief solutions officer at Revology in Iowa City, Iowa.
Greg Woods (15MPH) is the Alzheimer’s disease and related dementias program coordinator at Iowa Department of Public Health in Des Moines, Iowa.
George
Students in the course Zoonotic Diseases taught by Christine Petersen collect ticks at a local park.

means more outdoor activities—and a disease-carrying pest: the Ixodes tick. Commonly known as the black-legged tick or deer tick, Ixodes species begin searching for blood meals during spring and early summer, and humans are on the menu. A bite by one of these infected arachnids can transmit a variety of pathogens including Lyme disease, the most widely reported vector-borne disease in the United States.
To help protect against these nearly invisible ectoparasites, a team of University of Iowa epidemiologists has developed new disease surveillance strategies that couple historical data with information drawn from internet search terms to predict current trends in Lyme disease. The researchers say their innovative models are tools that local health agencies can use to tap free, up-to-date information—in this case, search history data from Google—to better understand Lyme disease patterns and make more timely, targeted interventions to battle the steadily rising incidence of the disease.
The team, led by Professor of Epidemiology Christine Petersen, set out to develop these “nowcasting” models—so-called because they’re designed to “predict the present”—to address reporting lags of up to two years that hamper current public health surveillance and mitigation efforts.
The research team built statistical models capable of predicting Lyme disease incidence in five regions of the United States: Northeast, Midwest, Southeast,
Southwest, and West. Two different models were developed for each geographic region—one model using only search terms related to the name, symptoms, and ticks that carry Lyme disease, and another model using those same disease-specific terms plus a broader list of terms, identified by Google Correlate, that an average person would be searching for during internet browsing. The researchers reviewed internet search data between 2004 and 2019, collected at monthly intervals to match against Lyme disease incidence data from the CDC.
When fit to the CDC data, the researchers found that both models provided accurate estimates of Lyme disease incidence in four of the five geographic regions; however, the model that included colloquial search terms resulted in more accurate predictions.
“Using web-based data from Google or social media sites to predict health outcomes is gaining popularity and credibility from a variety of public health audiences,” observes first author Eric Kontowicz (20PhD). The combination of “strong surveillance efforts and data coupled with computational modeling techniques can generate models that produce accurate predictions of disease trends,” he says.
The study was published in the open-access journal PLOS ONE and also included UI faculty researchers Kelly Baker, Grant Brown, Margaret Carrel, and Jim Torner.
145 N. Riverside Dr. 100 College of Public Health Bldg., Room S257 Iowa City, Iowa 52242-2007
We have a lot of reasons to be proud of our public health students. They’re scholars, researchers, travelers, teachers, creators, volunteers, and so much more! They are the future of public health.
 Students (from left) Alexis Clark, Alex Murra, Lexi Fahrion, and Emma Meador show their Iowa spirit.
Students (from left) Alexis Clark, Alex Murra, Lexi Fahrion, and Emma Meador show their Iowa spirit.