Guidelines for Teaching Evidence-Based Medicine in Your Practice

 Linda L. Carr, Ph.D. CEO, Faculty Ed Solutions, LLC
Linda L. Carr, Ph.D. CEO, Faculty Ed Solutions, LLC
DOCTOR (skills and clinical experience)





EXTERN AL EVIDENC E (knowledge from studies)
E B M
PATIENT (individual experiences & preferences)
Know Do

Learning Objectives


• How to use and teach principles of EBM.
• How to use a variety of medical information resources in self-directed learning activities.
• Encouraged to promote learner self-assessment of learning needs as a prerequisite for selfdirected learning.
• Incorporate principles of EBM to assist learners in critically evaluating sources of medical information.

Feel
Ryan
Learner Scenario

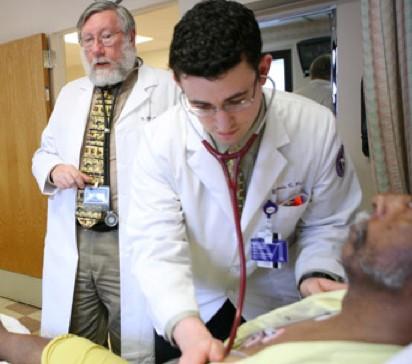
Ryan is a first-year resident beginning the 2nd month of an internal medicine rotation with Dr. Waters at the Feel Good Health Center. Together each day Dr. Waters and Ryan identify a clinical problem related to a specific patient seen that day, which Ryan is then assigned to research and present his findings to Dr. Waters and other clinical staff the next day.
While Ryan appeared to make an effort with his initial presentations, they lacked depth and lacked any references to appropriate medical literature.
After presenting for the third time, Dr. Waters asked Ryan to describe his approach to research the clinical problems assigned to him. Ryan glibly responded, “I don’t see what the big deal is. I find using Up-to-Date to research things just makes sense and is the most efficient use of my time.”
How can you encourage Ryan to be more self-directed?

A Self-Directed Learner
… is a proactive advocate for his/her own learning:
identifies what s/he needs to do (acquire knowledge, skills, or attitudes),
develops and executes a plan for responding to those needs, and

Ideally, a CLINICALEXPERIENCE will serve as a catalyst for the student’s personalassessment of his/her learning needs.
reviews the outcomes of that plan.
PEP2 Facilitator’s Module 9 (Teaching & Learning Collaboratively), p. 9.15.
PEP2
Learner reflects on a clinical experience




3
Learner reviews outcomes
Module
(Teaching
Facilitator’s
The Self-Directed Learning Process 9
1 & Learning
2 4 p. 9.15.
Learner completes a self-assessment Learner develops/impl ements a plan
Collaboratively),
Comparison of SDL with EBM
Make sure the learner understands the process and expectations for selfdirected learning
Role model how to do the process (complete the elements of the form)
Identify the “stage” of learner’s professional development and work accordingly
Can learner frame an answerable question?
Does learner lack knowledge of epidemiologic principles & research design
Assign an article on EBM

SDL EBM


Exposure Application Integration Where is Ryan on this vector? Novice Mature PROFESSIONAL DEVELOPMENT Stritter’s Learning Vector Independent
INSTRUCTION
PEP2 Facilitator’s Module 4 (Assessment), p. 4.8. Adapted from Stritter FT, Baker RM, Shahady EJ. Clinical instruction. In: McGahie WC, Frey JJ, eds. Handbook for the academic physician. New York: Springer-Verlag, 1986:102.
Professional Development of the Learner
CLINICAL
Dependent
How do Roles of Trainee and Preceptor Change in SDL?

SDL becomes prominent in the 2nd & 3rd stages of Stritter’s Professional Development

LEARNERS seek articles on conditions of the patients, ask questions
FACULTY/PRECEPTORS give learners opportunities to interact with patients and feel a part of the practice

SDL Activities for Learners
Use Clinical Guidelines (e.g., Asthma, COPD, Coronary Artery Disease, Diabetes, Heart Failure)
Understand Principles of Efficient Resource Utilization
Develop Skills in Patient Education
PEP2 Facilitator’s Module 9 (Teaching & Learning Collaboratively), p. 9.19.





About5,000newstudies arepublisheddaily! 15-foldincrease inmedicaljournalsover last4decades!
Medical Information Overload!
What strategies do you use to keep current with medical knowledge and clinical practices?


Do you teach this to your learners?

What is Evidence-based Medicine?
Evidence-based Medicine (EBM) involves the integration of individual clinical expertise with the prudent use of the current best external evidence in making decisions about the care of individual patients.

EXTERNA




EVIDENC
EBM Defined Video (4:26)
(knowledge from studies)
DOCTOR (skills and clinical experience)
EBM
PATIENT (individual experiences and preferences)
PEP2 Facilitator’s Module 9 (Teaching & Learning Collaboratively), p. 9.25. Sackett, D.L., Rosenberg, W.M., Gray, J.A., Haynes, R.B., Richardson, W.S. Evidence-based medicine: what it is and what it isn’t. BMJ 1996;312:71-2.
L
E
5 Steps of Evidence Based Practice

1 Ask question


5 Evalua te
2 Search
4 Impleme


3 Critically appraise

nt
Strauss, S. E., et al,
it. New York: Elsevier/Churchill Livingstone.
(2005). Evidence-based medicine: how to practice and teach
ASSESS the Patient & ASK a Searchable Question

P – Patient, Population, or Problem
(The disease and the patient characteristics, if pertinent)
I – Intervention, Prognostic Factor, or Exposure
(Drug, procedure, diagnostic test, exposure)
C – Comparison or Intervention (if appropriate)
(Main alternative to the intervention)
O – Outcome you would like to measure or achieve
(Measurable i.e., Rather than “more effective”, use something that can be measured like “decreases all-cause mortality”)
EBM STEP 1
Researchguides.uic.edu
ACQUIRE the Evidence
Filtered VS Unfiltered Resources
Unfiltered: ALL studies are included:
MEDLINE & PubMed
Prefiltered: Critical appraisal consistently used to select studies
Cochrane Library (systematic reviews)
Essential Evidence Plus

EBM STEP 2
Researchguides.uic.edu
APPRAISE the Evidence (Using JAMA Guides)

Are the results valid?
Will the results help me in patient care?
EBM STEP 3
EMB Step 4: APPLY the Evidence
EBM Step 5: ASSESS the Outcome;
Communication

EBM STEPs 4-5
Components of Clinical Questions (can be applied to tx, dx, or risk)
In patients with acute MI
does early treatment with a statin
compared to placebo
In women with suspected coronary disease
In postmenopausal women
what is the accuracy of exercise ECHO does hormone replacement therapy

compared to exercise ECG compared to no HRT
decrease cardiovascular mortality? for diagnosing significant CAD? increase the risk of breast cancer?
Here are 3 examples of PICO questions.
Patient/ Population Outcome Intervention/ Exposure Comparison
A Typical PICO Question
Emma is a 6-week-old baby at her routine follow-up. She was born prematurely at 35 weeks. You want to tell the parents about her chances of developing hearing problems

Question: In infants born premature, compared to those born at full term, what is the subsequent lifetime prevalence of sensory deafness?

P Population / patient = ?
I Intervention / indicator = ?
C Comparator / control = ?
O Outcome = ?
.
PICO Answer
Emma is a 6-week-old baby at her routine follow-up. She was born prematurely at 35 weeks. You want to tell the parents about her chances of developing hearing problems.

Question: In infants born prematurely, compared to those born at full term, what is the subsequent lifetime prevalence of sensory deafness?

P Population / patient = Infants
I Intervention / indicator = Premature
C Comparator / control = Full-term
O Outcome
= Sensorial deafness
Major Barrier to Practice EBM?


Nonadherence
Why?
Timmermans, S., & Mauck, A. (2005). The Promises and Pitfalls of Evidence-Based Medicine. Health Affairs, 24(1):18-28.
to practice guidelines remains the major barrier to successful practice of EBM.


Select at least one of the ideas shared about EBM to implement.
LEARN – REFLECT - TEACH

What will you keep the same?
What will you do more of?
What will you do less of?
What will you stop doing?
What will you do differently & how will you do it?
What will you add?

 Linda L. Carr, Ph.D. CEO, Faculty Ed Solutions, LLC
Linda L. Carr, Ph.D. CEO, Faculty Ed Solutions, LLC



































