

















It is not often in this sector that we find ourselves applauding the speed of government. Too frequently, good intentions dissolve into the familiar cycle of consultations, deferral and delay. So let us, on this occasion, give credit where it is genuinely due.
Health Secretary Wes Streeting has responded to Baroness Casey's urgent letter with unusual — and welcome — swiftness, and the commitments he has set out are, by any measure, bold.
The establishment of a new National Safeguarding Board, to be chaired by the Chief Social Worker and reporting directly to the Minister of State for Care, is a meaningful structural step.
The commitment to review Section 42 duty thresholds, consider powers of entry, and strengthen the link between Safeguarding Adults Reviews and CQC regulatory action are all areas that practitioners at the frontline have long flagged as in urgent need of attention.
Mr Streeting was frank in acknowledging what many of us have felt for years — that adult social care has been placed in the "too difficult" pile by successive administrations, and that the country has repeatedly lacked the political consensus needed to make reform stick. It is to his credit that he did not flinch from that honesty.
"Social care has been placed in the 'too difficult' pile for far too long. While there have been plenty of good ideas, we have lacked the broad political and national consensus
needed to ensure reforms stand the test of time."
But it is the commitment around dementia that caught my eye most keenly — and I confess it did so for deeply personal reasons.
My own mother first displayed symptoms of Alzheimer's disease when she was just sixty years old. Back then, the condition was barely spoken of in clinical, let alone public, discourse.
It was too often dismissed as simply part of growing old — something to be quietly endured rather than actively confronted.
The idea that it might one day be the subject of a dedicated national tsar, a Modern Service Framework, and a formal government strategy would have been almost unimaginable to the families living through it then, largely alone and largely without support.
Times and attitudes have changed, thankfully. But the scale of what still faces us is sobering.
DEMENTIA IN THE UK — THE SCALE OF THE CHALLENGE
76,000+
Deaths attributed to dementia in the UK in 2024
• £42bn
Estimated annual cost of dementia in 2024
£90bn
Projected annual cost by 2040
Analysis from Alzheimer's Research UK confirms that dementia remains the UK's single biggest killer. In 2024, more than 76,000 people across the country died from this devastating condition. The financial toll — already an estimated £42 billion annually — is projected to reach £90 billion by 2040 as the number of people affected continues to rise. These are not statistics that permit complacency.
The commitments from the Health Secretary — an interim Dementia and Frailty Modern Service Framework by September 2026, a full framework by year's end, and a new national dementia leadership role modelled on the Cancer Tsar — will be welcomed across the country, by professionals and families alike. The Alzheimer's Society described it as "a pivotal moment." I would not disagree.
Turning to a story closer to the daily rhythm of care home life, I read with great interest the new research from
the University of Stirling evaluating the danceSing Care digital platform across 78 care homes in Scotland. The findings — that residents reported lower loneliness and reduced fear of falling, while staff experienced higher wellbeing, lower stress and greater job satisfaction — are genuinely heartening.
The researchers rightly note that further controlled trials are needed, and we should be cautious about over-interpreting preliminary findings. But the direction of travel is clear, and the instinct behind the research feels profoundly right.
Because, frankly, none of this surprises me. We all love a good sing-song. At weddings, at birthdays, at anniversaries — and yes, at funerals too. Music reaches parts of us that words and clinical interventions simply cannot. It is one of the most human things we do.
My mother did not recognise me in the final stages of her illness. But she could still sing "Bye Bye Blackbird." I have recounted that story many times over the years, and I find I never tire of telling it — because it says something essential and hopeful about who we are.
For those of us who have sat with loved ones in the late stages of dementia, moments like those are not small. They are everything. And programmes that nurture those connections — for residents and for the staff who care so devotedly for them — deserve every encouragement and every pound of investment we can find.
We are delighted to be exhibitors and proud media partners at one of the sector's flagship events. The Care & Dementia Show at Birmingham's NEC brings together the sector's leading lights as keynote speakers, alongside a wonderful array of products, services and innovations from across the industry.
We here at The Carer always warmly welcome feedback and genuinely want to hear your thoughts, your challenges and your stories. Please do stop by — the kettle will be on and the conversation will be lively!!
Find us at Stand CD-B6
I can always be contacted at editor@thecareruk.com
The Carer is published by RBC Publishing Ltd, 3 Carlton Mount, 2 Cranborne Road, Bournemouth, Dorset BH2 5BR. Contributions are welcome for consideration, however, no responsibility will be accepted for loss or damage. Views expressed within this publication are not necessarily those of the publisher or the editorial team. Whilst every care is taken when compiling this publication to ensure accuracy, the publisher will assume no responsibility for any effects, errors or omissions therefrom. All rights reserved, reproduction is forbidden unless written permission is obtained. All material is assumed copyright free unless otherwise advised.


(CONTINUED FROM FRONT COVER)
In a formal letter of reply to Baroness Casey and published on GOV.UK, Health Secretary Wes Streeting MP set out his department's response to the recommendations Dame Louise had articulated in her own letter of 3 March and reiterated at the Nuffield Trust Summit just days later.
The most immediately consequential commitment for those running and working in care homes is the creation of a new national safeguarding board, to be established without delay and chaired by the Chief Social Worker, reporting directly to the Minister of State for Care. This body will be stood up ahead of any broader review, giving it an early mandate to drive coordinated national oversight of adult safeguarding.
GREATEST CHALLENGES
On dementia — which Mr Streeting described as "one of the greatest challenges of our time" — the Secretary of State has committed to publishing an interim version of the Dementia and Frailty Modern Service Framework (MSF) by September 2026, in time to feed into NHS and local government planning cycles. The full framework is committed for publication by the end of the 2026 calendar year.
For those caring for individuals with motor neurone disease in residential and nursing settings, the government has committed to developing a fast-track care 'passport' that will speed up assessments and access to care for people newly diagnosed with MND. Mr Streeting's letter acknowledged the "devastating impact" of the condition and the urgency of ensuring those affected can access support rapidly, without being subjected to assessments and processes designed for conditions with more gradual trajectories.
The Secretary of State indicated he would consider how best to safely implement the expedited process, including reviewing Dame Louise's own suggestions on delivery, signalling an intention to involve the commission in the design of the solution rather than simply announcing a pre-formed policy.
KEY COMMITMENTS AT A GLANCE:
New National Safeguarding Board-To be established immediately, chaired by the Chief Social Worker and reporting to the Minister of State for Care. Remit to include assessment of whether new statutory powers are needed.
Urgent Safeguarding Review-Will examine Section 42 duty thresholds, potential powers of entry, and strengthening links between Safeguarding Adults Reviews and CQC regulatory action.
Dementia & Frailty Framework-Interim product to be published September 2026. Full Modern Service Framework to follow by end of
calendar year 2026.
New Dementia Leadership Role-A new national post within DHSC to be created to drive dementia action across health and care. Cancer Tsar model cited as template for accountability and reach.
MND Care Passport-A fast-track assessment and access 'passport' for people diagnosed with MND to be developed, recognising the urgent and rapidly progressing nature of the condition.
ACCESS-AD Trial Review-Officials to report to the Secretary of State in April 2026 on merits of investment in this specific dementia trial, alongside wider clinical trial commitments.
UNACCEPTABLE
In his letter, Mr Streeting was unequivocal: "Any form of abuse or neglect is unacceptable. My department will create a new national safeguarding board and undertake an urgent review of adult safeguarding statutory duties and powers."
The Secretary of State confirmed that a central part of the new board's remit will be to assess whether it requires new statutory powers to operate most effectively — a direct response to one of Dame Louise's core recommendations. Critically, Mr Streeting stated that the government will not pre-judge this question but will allow it to be formally tested through the urgent review process.
The review itself will assess whether the existing legal framework provides sufficient "clarity and leverage" in high-risk situations — language drawn directly from Dame Louise's original recommendation — and is expected to examine three specific areas she identified in accompanying materials:
THREE AREAS UNDER REVIEW:
Section 42 threshold ambiguity — Clarifying what triggers the statutory duty on local authorities to make safeguarding enquiries, addressing inconsistency that may have left vulnerable adults without adequate protection.
Powers of entry — Considering whether mechanisms allowing practitioners to access a person suspected of being abused could strengthen outcomes, while remaining consistent with civil liberties.
Inspection and regulation linkage — Strengthening the feedback loop between Safeguarding Adults Reviews (SARs) and regulatory action, including the future focus of CQC inspections.
For care home providers, the proposed link between SARs and CQC inspection focus is likely to prove particularly significant, potentially creating a more direct pathway from lessons learned in serious cases to the regulatory environment within which providers operate.
LACKED CONSENSUS
In his letter, Mr Streeting was candid about the historic failures of successive administrations, acknowledging that adult social care had been placed in the "too difficult" pile for too long, and that, despite no shortage of good ideas, the country had consistently lacked the political consensus needed to make reforms stick. He framed Dame Louise's commission as central to breaking that impasse. “Social care has been placed in the 'too difficult' pile for far too long. While there have been plenty of good ideas for how to improve social care, we have lacked the broad political and national consensus needed to ensure reforms stand the test of time.” He said.
Michelle Dyson CB,Chief Executive Officer atAlzheimer’s Society said: “The announcement today from Wes Streeting, Secretary of State for Health and Social Care, that he is accepting the recommendations from Baroness Casey to prioritise dementia is a pivotal moment and brings hope that dementia will at last receive the attention that is so desperately needed and much overdue.
“At Alzheimer’s Society we are demanding better for everyone with dementia. We have worked alongside Baroness Casey to represent people with dementia and set out the change that needs to happen. We are confident that the introduction of a dementia tsar to lead the government’s plan on dementia is an important step in driving this change. The Modern Service Framework for Dementia and Frailty must now commit to an ambition to reduce the number of people dying from dementia, and ultimately set us on course towards a world in which dementia no longer devastates lives.
“Further commitments, including for the UK to lead the way on dementia trials and for the government to publish an interim version of the Modern Service Framework in September are welcome. People have waited long enough having a timeline for this progress is essential. It is vital that bold steps to improve diagnosis are central to these plans.
“We are grateful to Baroness Casey for being the voice of people with dementia and bringing dementia to the forefront, where it should be. We will continue to work tirelessly to ensure these plans come to fruition and change the lives of people with dementia now and in the future.”
Dame Louise's commission is expected to launch a national conversation later this year, giving the public — as well as professionals working at the frontline of care — the opportunity to contribute to the future shape of adult social care in England.


When communication breaks down in adult social care, the consequences go far beyond a difficult conversation. They affect staff retention, service quality, regulatory risk and, ultimately, the wellbeing of the people receiving care.
In a sector already facing chronic staff shortages, high turnover and increasing demand, communication problems can quietly amplify pressure on teams that are already stretched.
Ask any frontline social care worker what makes their job harder than it needs to be, and very few will say it is the care itself. More often they describe unclear instructions, last-minute changes, difficult conversations with families, or handovers that leave them without the information they need to keep someone safe.
These are not minor frustrations. They are early warning signs of a system under strain.
Poor communication in adult social care is not simply a management issue or a personality clash. It carries real organisational costs that often remain invisible until something goes wrong.
THE HIDDEN COSTS
The impact of poor communication tends to fall into three areas: operational pressure, workforce stress and financial cost.
Operationally, communication failures create duplication, delay and risk. Inadequate handovers can result in missed medications, overlooked changes in care routines or risk information not reaching the right person at the right time. These are not rare events — they appear repeatedly in safeguarding reviews and inspection findings.
In a sector where staffing levels are already tight, even small misun-
By Lynsey Flanagan, Mediator | Dispute Resolution, Conflict Management & Early Intervention
derstandings can create extra work for colleagues who are already covering gaps.
There is also a clear workforce impact. Social care staff frequently report that what drives them away is not the care itself but the working environment around it. Feeling unheard, unsupported or unclear about expectations contributes directly to stress and burnout.
When experienced staff leave, the effects ripple across the whole service. Remaining workers often carry additional responsibilities while new staff are recruited and trained. In a sector that increasingly relies on the knowledge and commitment of long-serving team members, this creates a difficult cycle.
Financially, the cost of turnover is significant. Research from Skills for Care estimates that replacing a single care worker can cost between £3,000 and £5,000 once recruitment, training and reduced productivity are considered. When staff leave because communication and management support have broken down, that becomes a preventable cost.
Communication pressures tend to appear in predictable places within care services.
Handovers and shift transitions are a common point of difficulty, particularly when teams are short-staffed and time is limited. Important details can be lost when information is rushed or inconsistently recorded.
Manager-to-staff communication can also become strained, particularly during periods of change. Staffing pressures, new policies or regulatory updates all require clear explanation. When information is incomplete or arrives too late, uncertainty grows.
Relationships with families can also be affected. When expectations are unclear or concerns are not addressed early, misunderstandings can escalate quickly, placing additional emotional pressure on staff.
Multi-agency work adds another layer of complexity. Differences in language, priorities and procedures between organisations can easily create confusion if communication is not handled carefully.
None of these challenges are new. But with services under increasing pressure, the margin for error is smaller than it once was. SUPPORTING COMMUNICATION IN STRETCHED TEAMS
Improving communication does not require expensive systems or

Welcome to Blue Rain - our activity store is built on over 14

complex frameworks. Often it is the small, consistent practices that make the greatest difference.
1. Keep handovers structured and simple
A clear handover does not need to be lengthy. A short, consistent structure covering key changes, current needs and potential risks can prevent vital information being missed, especially when staff are tired or covering additional shifts.
2. Create regular opportunities for staff to speak up
Psychological safety — the confidence that concerns can be raised without blame — develops through everyday interactions. Regular team check-ins, open one-to-one conversations and a calm response to feedback all help staff feel heard.
3. Address concerns early
Small tensions between colleagues or with families can quickly grow if they are ignored. Addressing issues early and respectfully can prevent them becoming formal complaints or safeguarding concerns later.
4. Communicate change clearly
In a workforce already under pressure, unclear messages about staffing, policies or inspections can quickly undermine trust. Even when information is incomplete, sharing what is known — and what is still uncertain — helps reduce anxiety.
Social care services operate in an environment where time, staff and resources are often in short supply. In that context, communication can easily be treated as a secondary issue.
In reality, it is part of the infrastructure that keeps services functioning.
When communication works well, experienced staff are better supported, teams collaborate more effectively and potential problems are identified earlier. For a sector navigating workforce shortages and increasing demand, strengthening everyday communication may be one of the most practical ways to support both staff wellbeing and quality of care.
Lynsey specialises in conflict, communication and workforce wellbeing, supporting adult social care providers to navigate difficult conversations and strengthen team resilience in high-pressure environments.

• We specialise in the sale and purchase of quality used wheelchair accessible vehicles and ambulances.
• They can be bought as seen or refurbished and sign-written to your own requirements.
• Fully serviced, new mot & warranty
• Engineers inspection supplied if required.
• Free delivery service
•


A new report released by carehome.co.uk, Caring Britain: How the care home landscape is changing, has revealed how the UK’s care home market is evolving amid rising costs, growing demand and increasing complexity of care needs.
The data shows that average weekly care home self-funded fees increased by 10% in the year to December 2025, as providers responded to rising wage costs, energy prices and broader inflationary pressures.
Fee growth for self-funders varied by region, ranging from 7.8% in the East of England to 11.3% in the North West.
Scotland and London are the most expensive regions in the UK, with average weekly self-funded fees exceeding £1,500. By contrast, the North East of England is the most affordable region at approximately £1,100 per week.
At the same time, the structure of the sector is shifting towards larger providers.
The average care home now provides 47 beds, with the strongest growth among homes with 60-79 beds (3.6%). Meanwhile, the number of smaller homes offering fewer than 20 beds declined by around 6% in the year to December 2025.
The data shows that purpose-built homes make up 57% of provision, underlining a shift towards modern, accessible environments designed to accommodate increasingly complex care needs.
Regionally, bed growth was strongest in the South East and West Midlands (1.8% and 1.5% respectively), while London and Scotland saw slight declines in overall capacity, reflecting limited opportunities for new development in dense or constrained markets.
The report also highlights uneven access to specialist services, particularly for people living with dementia.
While many homes are equipped to support residents in the early stages of dementia, provision reduces significantly for advanced and complex dementia care.
In London, 57% of care homes meet higher-level dementia needs. In comparison, just 33% of homes in Wales and 34% in the North West of England offer this level of support.
The report from carehome.co.uk also analyses regulator ratings, showing regional variations and gaps in inspections.
While just under 70% of homes in England are rated as ‘Good’ or ‘Outstanding by the Care Quality Commission (CQC), this rises to 80% for London and the North East. In comparison, this figure stands at 63% for the West Midlands and 66% for Yorkshire and the East of England.
Importantly, the report also looks at the frequency of inspections, and finds that around one in seven care homes are currently unrated in England, and over half of care homes have not been rated in the last four years. In some cases, this reflects changes in ownership, as ratings do not transfer when a care home is sold and providers must be re-rated under their new registration.
Will Blackwell, CEO of Tomorrow’s Guides which operates carehome.co.uk, said: “Our new report highlights a sector in transition. Growing demand from an ageing population, increasing complexity of need, workforce shortages and sustained cost pressures are fundamentally reshaping how care is delivered across the UK.
“Our data shows care homes are changing in structure with a shift towards large, purpose-built homes that can cater for increasingly complex care needs. At the same time, access to specialist care such as dementia care is dictated by a postcode lottery, leaving those affected not getting the support they desperately need.
“At a time when regulatory ratings may not always reflect the most up-to-date reality, trusted reviews and transparent provider information play an increasingly important role. Early planning and access to clear, reliable information can make a significant difference in helping families navigate what is often one of the most important and emotional decisions they will ever face.”
Professor Martin Green OBE, Chief Executive of Care England, said: “This report clearly shows that the lack of a strategic approach by the Government is delivering a significant financial and geographical divide across the country.
“Public under-funding is driving smaller care homes out of the sector and the only way to stay viable is to increase the size and scale of each home. There is clearly a need for high-quality care, but Government policy is denying access and choice to publicly funded citizens.
“The fact that care home fees have risen by 10% shows the enormous financial pressures that are placed on care home providers. These increases are levied reluctantly, but they are necessary to sustain care homes and the care they provide.”
To mark International Day of Happiness, residents at RMBI Care Co. Home Albert Edward Prince of Wales Court, in Porthcawl, picked up their guitars and enjoyed a cheerful musical session with volunteer Paul Harvey.
Observed each year on 20 March, the day highlights the importance of happiness, wellbeing and kindness in our daily lives. At the Home, the occasion was marked with music, laughter and plenty of positive energy as residents gathered for an uplifting jam session.
Volunteer Paul brought along his guitar and encouraged residents to

join in. Together, they strummed along, shared their favourite tunes and enjoyed the simple pleasure of making music together. Music has long been a popular activity at Albert Edward Prince of Wales Court, bringing residents together and creating moments of connection.
Paul says: “We had a wonderful time playing together. Music is such a great way to bring people together, and it was wonderful to see everyone enjoying themselves and having a laugh. It really felt like the perfect way to celebrate the International Day of Happiness.”

Choosing a care home is one of the most important and emotional decisions a family will make. Unlike many other sectors, marketing in the care industry isn’t simply about promoting a service – it’s about building trust, demonstrating compassion, and helping families feel confident they are making the right choice for their loved one.
In today’s competitive landscape, care homes need a balanced marketing approach that combines targeted digital strategies with
By Melissa Cooper, digital marketing specialist and the founder of Beanie Media
strong local reputation building. When done well, marketing becomes less about “selling” and more about clearly demonstrating the quality of care and community that residents and families can expect.
UNDERSTANDING THE CARE HOME DECISION JOURNEY
Before focusing on tactics, it’s important to understand how families make decisions.

The journey often begins when a family member starts researching care options following a change in circumstances. At this stage, people are looking for reassurance, information, and signs that a home will provide genuine care and dignity.
From there, families will compare providers, read reviews, explore websites and social media pages, and often ask people within their community for recommendations before arranging visits.
Because of this, marketing needs to support three key stages:
Awareness – ensuring your care home appears when people begin searching online.
Consideration – providing useful information, reviews and content that reassures families.
Decision – reinforcing trust through testimonials, recommendations and personal experiences.
Understanding this journey helps care homes focus their marketing on answering the questions families are actually asking.
The Importance of SEO and Local Search
Search engines are often the first place families go when researching care options, which makes search engine optimisation (SEO) essential.
A well-optimised website helps ensure your care home appears when people search for phrases such as “care homes near me” or “residential care in [town name]”. This includes clearly explaining the services you provide, using location-based keywords naturally, and publishing helpful information that answers common questions about care.
Equally important is your Google Business Profile, which often appears before websites in local searches. Care homes should ensure their profile includes accurate contact details, high-quality images, and up-to-date information. Encouraging families to leave reviews can also make a significant difference, as prospective residents often rely heavily on the experiences of others.
Your online presence should reflect the warmth and pro-

fessionalism of the care you provide.
High-quality photography and video are particularly powerful in the care sector. Families want to see real environments and genuine interactions between staff and residents. Images of activities, communal spaces and daily life help people visualise what living in the home would actually feel like.

Social media should focus less on sales messaging and more on storytelling. Sharing resident activities, staff achievements and community involvement helps demonstrate the personality of your home and reinforces the human side of care. Social platforms also allow care homes to reach families within their local area through targeted content.
Trust is the single most important factor in care home marketing.
Testimonials and reviews are extremely influential because families naturally seek reassurance from people who have already experienced your care. Encouraging families to leave reviews on Google or care directories can strengthen your online reputation, while written testimonials and case studies help bring real experiences to life.
Offline reputation remains equally important. Word-of-mouth referrals from GPs, local community groups, charities and existing families continue to be one of the strongest drivers of new enquiries.
Ultimately, successful marketing for care homes is about authenticity.
Families are not simply choosing a facility – they are choosing the people who will care for someone they love. The most effective marketing therefore, focuses on showing the compassion, professionalism and community that exists within the home.
By combining strong local reputation building with thoughtful digital marketing, care homes can ensure that when families begin their search, they find reassurance, transparency, and a clear sense of the care they can expect.
And in an industry built on trust, that is what truly makes the difference.
In April 2025, the Supporting the Provider Market (STPM) team in County Durham published a new report evaluating the use of pobroll® — a waterproof bed-bathing wrap designed to improve dignity, comfort, and ease during personal care.
Written by Pat O’Brien of pobroll

This evaluation was carried out across 10 care homes with high numbers of residents living with dementia. Each setting was given one or more pobroll® units and invited to share feedback through a structured survey. The findings reveal how even simple tools can make a significant difference in everyday care.
How was pobroll® used?
Most care homes used pobroll® daily or several times per week, showing it quickly became part of regular practice. Staff noted that one of the biggest challenges was not having enough units — all homes requested additional stock after the trial, highlighting a clear appetite for wider adoption.
What did care teams think?
Feedback from the care homes showed strong support for the tool:
Ease of use was rated highly, with an average score of 4.4 out of 5. Staff found pobroll® straightforward to incorporate into care routines.
Training was rated slightly lower, at 3.8 out of 5, suggesting that while the wrap is easy to use, additional training resources could improve onboarding for new users.
Resident response was positive. Three in ten care homes reported improved mood or behaviour dur-
ing bed bathing for dementia patients.
• Key benefits included greater warmth, coverage, and dignity for residents, especially those who might find conventional methods distressing. Some teams also found it particularly useful for end-of-life care Would they recommend pobroll® for bed bathing for dementia patients?
Absolutely. Homes rated their likelihood to recommend pobroll® at 4.3 out of 5, with half of respondents giving it a full 5 out of 5. The overall feedback was clear: this is a valued, meaningful addition to personal care.
Would they recommend pobroll® for bed bathing for dementia patients?
The results of this trial reinforce what many professionals already believe — that small, thoughtful design changes can significantly improve care. For residents who are bedbound or living with dementia, personal care can often be a distressing experience. But with the right tools, it doesn’t have to be.
The pobroll® isn’t a complex device. It’s a simple, dual-layered cotton towelling wrap. But its thoughtful design — offering full coverage, comfort, and support — makes a real difference where it matters most.
If you’re part of a care home, hospice, or hospital and would like to explore how pobroll® could benefit your residents or service users, get in touch. We’re here to support compassionate, dignified care — one small change at a time.
See the advert on the facing page for details, or
Scientists in the United States have identified a blood-based protein marker capable of indicating a woman’s likelihood of developing dementia up to 25 years before any cognitive symptoms become apparent, according to research published in the journal JAMA Network Open in March 2026.
The study, conducted by researchers at the University of California San Diego, centred on a protein known as phosphorylated tau 217 — commonly referred to as p-tau217 — which reflects early biological changes in the brain associated with Alzheimer’s disease. Crucially, elevated levels of this protein were detectable in blood samples taken from women who were cognitively healthy at the time, suggesting the marker may serve as a very early warning signal long before memory difficulties emerge.
The research drew on data from 2,766 women aged between 65 and 79, all of whom were enrolled in the Women’s Health Initiative Memory Study during the late 1990s. Participants were tracked for up to 25 years, and blood samples collected at the outset of the study were later analysed for p-tau217 levels. Over the course of the follow-up period, researchers identified which participants went on to develop mild cognitive impairment or dementia, and cross-referenced these outcomes against their initial biomarker readings.
The findings showed a clear pattern: women with higher concentrations of p-tau217 in their blood at the start of the study were significantly more likely to develop dementia in later life, with the greatest
risk observed in those with the highest recorded levels.
However, researchers also found that the predictive strength of the biomarker varied between different groups. Women over the age of 70 at the time of enrolment showed a stronger association between elevated p-tau217 and subsequent cognitive decline than their younger counterparts.
The link was also more pronounced among women carrying the APOE 4 gene variant — a known genetic risk factor for Alzheimer’s disease — and among those who had received combined oestrogen and progestin hormone therapy. The study further noted differences between white and Black participants, though combining the biomarker with age improved predictive accuracy across both groups.
For care home operators and nursing staff, the implications of this research are significant. With an ageing residential population, any advance that could allow earlier identification of individuals at heightened dementia risk offers the potential for more proactive care planning, lifestyle interventions, and family discussions to take place well ahead of a formal diagnosis.
A key practical advantage highlighted by the researchers is that blood-based testing is far less invasive than existing methods such as brain imaging or lumbar puncture to collect cerebrospinal fluid — procedures that are costly, uncomfortable, and not readily available in community or residential care settings. A straightforward blood test could, in principle, be incorporated into routine clinical assessment,
though the researchers are clear that considerably more work is needed before that becomes a reality.
At present, blood biomarker testing of this kind is not recommended for use in people who show no symptoms of cognitive impairment. The research team stressed that further studies are required to establish how p-tau217 measurement might be integrated into clinical practice, and whether acting on early identification genuinely improves longterm outcomes for patients.
Future investigations will also examine how factors including hormone therapy, genetics, and age-related health conditions interact with p-tau217 levels throughout a person’s lifetime, potentially refining the picture of who is most at risk and when intervention would be most effective.
Michelle Dyson CB, Chief Executive Officer at Alzheimer’s Society, said: ‘Blood tests could transform how dementia is diagnosed and research we’re funding aims to make a blood test routinely available on the NHS for symptomatic Alzheimer’s disease within the next few years.
‘This study suggests that there may be a correlation for women between having a higher level of the p-tau127 biomarker earlier in life with an increased risk of developing dementia 25 years later. These findings are promising, but of course more research is needed to understand whether early identification of biomarkers can affect whether people will go on to develop dementia later on.”
At Gibraltar Nursing Home in Monmouthshire, supporting people living on a cognitive journey often means stepping into a reality that differs from our own. In these moments, emotional reassurance can sometimes be more important than ‘telling the truth’.
This approach, sometimes known as therapeutic lying, involves responding with compassion to reduce anxiety and protect a person’s sense of comfort and safety. If a person asks for their mother, father or loved one who has passed away, forgetting that they are no longer with us, correcting them may re-open grief or make the loss feel as though it is happening for the first time. This is why a therapeutic lie may be emotionally kinder in the moment.
One family member (resident) who lives at the care home, Audrey – known as Jingy – finds great comfort in caring for her soft toy dogs, which in her reality are beloved rescued pets. Rather than correcting her, the team support Jingy in this world she has created, speaking about the dogs with her and using them to help reassure her during moments where she may feel anxious or unsettled.
For Jingy, the dogs provide companionship, purpose and a sense of calm. For the team, it is a reminder that person-centred care is about meeting people where they are and protecting their emotional wellbeing.

By Sara-Michelle Colvin, Senior Associate in the

The UK care sector is currently facing one of the toughest periods of immigration related enforcement it has ever experienced. Recent Home Office figures reveal the scale of the shift: from July 2024 to June 2025, 1,948 sponsor licences were revoked – more than double the 937 revoked the year before, and dramatically higher than the 261 and 247 revocations issued in 2021–22 and 2022–23.
The Home Office continues to identify recurring weaknesses across parts of the sector, including: underpayment of sponsored workers
• mismatches between the job roles listed on Certificates of Sponsorship and the duties carried out
• attempts to use sponsorship as a means of bypassing immigration controls
• roles that do not constitute genuine vacancies
the increased vulnerability of migrant workers who are tied to their sponsoring employer.
Given the sector’s reliance on overseas recruitment and long standing staffing challenges, adult social care remains a central focus for enforcement activity.
A move toward digital, intelligence led monitoring
As part of this intensified scrutiny, the Home Office has largely replaced onsite compliance visits with a more sophisticated, data driven approach. Increasing integration of HMRC/PAYE information, Sponsorship Management System activity and other government intelligence allows caseworkers to highlight concerns quickly and with
greater accuracy.
This desk based model is supported by enhanced analytical tools –including AI – which provide faster processing and more reliable detection of anomalies or patterns of non compliance.
The government has also adopted a far more uncompromising approach to compliance failings. Issues previously regarded as technical or low level – late sponsor notifications, incomplete HR files, inconsistent Right to Work checks, or weak absence management – can now lead to immediate suspension or even revocation.
These stricter consequences sit alongside wider efforts to combat illegal working. Civil penalties now reach £45,000 for a first breach and £60,000 for subsequent breaches, and enforcement activity increased sharply in 2025 thanks to expanded capacity and automated systems.
In recent months, many care providers have been contacted unexpectedly by the Home Office seeking additional information, typically regarding pay. This stems from increased data sharing between HMRC and the Home Office, which is surfacing discrepancies that may point to reporting failures.
REQUESTS FOR INFORMATION
When the Home Office issues a Request for Information, sponsors usually have 10 working days to respond. The volume of evidence required can be substantial, often needing input from multiple departments. A long standing concern among organisations is the need to send sensitive employee information without encryption, as the Home Office’s current systems are limited to email attachments and do not support secure alternatives.
SUSPENSION AND REVOCATION
Where the Home Office identifies breaches, it may take one of the following actions:
SUSPENSION
• The licence may be suspended and the sponsor placed on an Action Plan.
• A fee must be paid within 10 working days to accept the Action Plan. The Action Plan can run for up to three months, during which the sponsor must demonstrate significant improvement to regain full compliance.
Failure to meet the required standard typically results in revocation.
REVOCATION
In serious cases, the Home Office may bypass suspension and move directly to revocation – something officials have indicated is increasingly common.
• Before revoking, the Home Office issues a notice of intention, giving the sponsor 20 working days to make representations.
• Although the Home Office is expected to respond within a further 20 working days, delays are frequent.
• In most cases, the outcome is ultimately revocation.
If revocation occurs, sponsored employees may continue working for 60 days from the date of their cancellation letter (or until their visa expiry date, if earlier). During this period, they must find a new sponsor or switch to another immigration route to remain lawfully in the UK. Revocation takes effect immediately for the organisation: it loses the ability to sponsor workers or assign Certificates of Sponsorship and cannot apply for a new licence for at least 12 months, a period that can be extended where civil penalties or criminal matters are involved. Legal challenges within the sector have centred on arguments relating to: risks to continuity of care for service users the impact on a business’s ability to operate and the effect on its domestic workforce the Home Office’s alleged failure to apply discretion or consider lesser sanctions.
STRENGTHENING COMPLIANCE IN A HIGH RISK ENVIRONMENT
In this climate, it is vital for care sector sponsors to adopt a proactive and rigorous compliance strategy. The rise in licence revocations, coupled with more sophisticated data monitoring and severe penalties for even minor breaches, demonstrates the Home Office’s determination to drive structural reform.
Organisations relying on sponsored workers must therefore ensure their HR systems, reporting procedures and governance arrangements are robust, transparent and consistently applied. Some groups are also exploring multi licence structures to spread risk across subsidiaries. Although revocation does not stop a business from trading, the operational disruption, staffing challenges and 12 month bar on reapplying can be highly damaging. Strong compliance is no longer a matter of good practice – it is essential for ensuring continuity of care, protecting vulnerable workers, and maintaining future access to skilled international labour.
Leading independent healthcare waste management specialist Anenta, which acts on behalf care homes and nursing homes throughout England, has been named UK Healthcare Waste Management Services Company of the Year for the second year running at the international Healthcare Business Review Europe Awards 2026.
The back-to-back win reinforces Anenta’s position as the UK’s leading independent healthcare waste management company, recognising the continued impact of its technology-led approach, sector expertise and commitment to driving efficiency, compliance and cost control across healthcare estates.
Anenta was selected following a rigorous evaluation by a panel of C-suite executives, industry experts, and the editorial board of Healthcare Business Review. Judges highlighted the continued evolution of Anenta’s proprietary Vector platform, alongside the company’s proven ability to deliver measurable financial and operational benefits for healthcare organisations.
SAVING CLIENTS MILLIONS
Highlights identified by the judges include Anenta’s work to save primary care clients over £13m in charges and the equivalent of £35m in efficiencies by cutting the amount of client staff time spent handling waste administration, auditing and dispute resolution.

This has been made possible through Anenta’s use of its proprietary Vector technology, which analyses hundreds of thousands of data points each month to identify any instances of waste collection or disposal partner billing inaccuracies so that these can be addressed before payment.
This rigorous yet collaborative approach, which identifies and addresses cases of overbilling, contract non-compliance or inefficiencies, was described by the judges as ‘setting a benchmark for best practice, valued by both healthcare providers and waste contractors for its focus on transparency, accuracy and continuous improvement.’
Alex D’Souza, Managing Editor of Healthcare Business Review Europe, commented on the award, saying: “Anenta continues to stand head and shoulders above other healthcare waste management service providers. Retaining this award reflects both Anenta’s consistency and outstanding leadership, as it continues to set itself apart through innovation, depth of sector knowledge and a clear focus on delivering tangi-
ble outcomes for healthcare organisations.”
D’Souza added: “The 2026 award recognises Anenta’s continued leadership in supporting NHS Integrated Care Boards (ICBs), helping unify complex waste arrangements under a single service specification, with consistent contract terms and a common environmental model. This scalable approach is raising standards across the healthcare waste management landscape, setting the bar for efficiency and collaboration.”
Graham Flynn, Managing Director of Anenta, commented: “This is a tremendous endorsement of our team, our technology and our approach. It is particularly meaningful because recognition comes from senior decision-makers who understand the operational and compliance pressures facing healthcare providers.”
Graham added: “As we move through 2026, we look forward to making a significant difference to an increasing number of businesses in the healthcare sector, enhancing levels of efficiency, compliance and cost control for healthcare estates, private healthcare businesses, dentists and care homes. Our focus remains on being a trusted partner — helping organisations operate with confidence, while continuously raising standards of healthcare waste management across the sector.”
Looking ahead, Anenta aims to build strong growth across its client base, with care homes and dental practices identified as key expansion areas. This reflects increasing regulatory scrutiny and risk in these environments, where correct segregation and management of clinical and healthcare waste is critical and time-consuming.
Anenta currently acts on behalf of more than 9,000 GP practices and 9,000 pharmacies across England, handling in excess of 39,000 healthcare waste management queries each year. It supports NHS organisations, GP practices, pharmacies, laboratories, dental practices and care homes. Its services include the provision of remote duty of care, and pre-acceptance audits, supported by free, standardised e-learning programmes. This approach helps clients meet their compliance obligations while reducing risk, enabling healthcare organisations to focus frontline teams on patient and resident care rather than administrative burdens associated with waste management.
For more information about Anenta, visit www.anentawaste.com or call 033 0122 2143.
The 53,000 sole traders in health and social work with a turnover of more than £50,000 from self-employment and property have just weeks left to prepare for MTD for Income Tax.
From 6 April 2026, those with income above the threshold must use compatible software to keep digital records, send four simple quarterly updates of their income and expenses and submit their tax return to HM Revenue and Customs (HMRC).
tistics released by HMRC show an estimated 40,000 sole traders in health and social work, and a further 14,000 who work in the sector and are also landlords will be required to use MTD for the 2026 to 2027 tax year.
Most customers will receive a letter from HMRC confirming they need to join, which also explains what they need to do and includes a QR code linking to GOV.UK guidance.
Craig Ogilvie, HMRC’s Director of Making Tax Digital, said: “MTD for Income Tax is a generational change and support is there for everyone who needs it.
“The quarterly updates aren’t tax returns – they’re simple summaries your software auto-populates, spreading the admin throughout the year, rather than leaving it all towards the January Self Assessment deadline.
“Go to GOV.UK – choose your software, read the guidance and get ready now.”
About 100,000 sole traders and landlords have already signed up for MTD for Income Tax, with more than 15,000 quarterly updates successfully submitted through a voluntary testing programme.
For most, the first quarterly update under MTD for Income Tax will cover the period from 6 April to 5 July 2026 and will need to be submitted by 7 August 2026.
A new points-based system for late submissions applies, where a £200 fine is only triggered once four points are reached, meaning the occasional slip-up will not result in an immediate fine. No penalty points will be issued for late quarterly updates for the 2026 to 2027 tax year –though points will still apply to late tax returns.
Free software options are available, with a range of paid packages also on offer to suit different needs. Once all your digital records of income and expenses have been created, the software will use them to generate your quarterly update.
Those joining MTD for Income Tax in April 2026 will still file their Self Assessment return for the 2025 to 2026 tax year in the usual way by 31 January 2027. The first tax return that most customers will submit using their MTD compatible software, covering 2026 to 2027, will be due by 31 January 2028.
HMRC is urging anyone else in scope of MTD for Income Tax to act now: read the guidance, choose software and sign up on GOV.UK. Those who genuinely cannot use digital tools can apply for an exemption.
The Social Care Institute for Excellence (SCIE) has appointed Baroness Glenys Thornton as Chair-Elect.
Baroness Thornton brings extensive experience of leadership across social care, health, public service and civil society. A member of the House of Lords for more than 25 years, she has held senior ministerial roles, including as a Parliamentary Under-Secretary of Health, as well as various Shadow Spokesperson roles, and has led organisations focused on social innovation, co-production and community impact. She will work alongside the current Chair, Rt. Hon. Paul Burstow, during a planned handover period ahead of the end of his term in June.
Rt. Hon. Paul Burstow said: “I am delighted that Baroness Thornton will be joining SCIE as Chair-Elect. She brings deep experience, sound judgement and a strong commitment to the values that underpin our work. We

have deliberately planned a transition period to ensure continuity, stability and alignment as SCIE continues to support innovation, improvement and reform across social care to achieve better lives for adults and children and help shape the National Care Service to come.”
Baroness Thornton said: “SCIE plays a vital role in collaborating and innovating across social care with a wide range of partners to change lives, grounded in evidence and lived experience. I am very much looking forward to working with colleagues across the organisation to build on our strong foundations and support the next phase of our impact.”
Mr Burstow will continue as Chair until the end of June, working closely with Baroness Thornton and Interim Chief Executive Gerard CroftonMartin, who stepped into the role earlier this year from within SCIE’s existing senior leadership team.







New research commissioned by Healthwatch England has revealed a significant and accelerating shift in how people in England are accessing healthcare, with the proportion of adults turning to private services having nearly doubled in just one year.
The consumer polling organisation Savanta surveyed 2,593 adults aged 18 and over to assess their use of NHS and private healthcare and to gauge confidence levels in NHS services. The findings paint a concerning picture of a health system under sustained pressure, with growing numbers of patients seeking alternatives outside the public sector.
Nearly one in seven people — 16 per cent — reported using private services such as non-urgent treatment and diagnostic tests in the past year. This represents a near-doubling of the nine per cent recorded in 2023, marking one of the most striking year-on-year shifts in healthcare consumption seen in recent years.
The research also reveals a meaningful shift in the reasons people are opting for private care. Long waiting times have emerged as the leading motivation, cited by nearly four in ten respondents (39 per cent) as their main reason for going private. This is a notable change from 2023, when perceived better quality of care — at 37 per cent — was the most commonly cited driver.
Other reasons given by respondents included better quality of care (31 per cent), convenience (30 per cent), and ineligibility for the procedure on the NHS (20 per cent). Together, these findings suggest that for a growing share of the population, private healthcare is less a lifestyle choice and more a perceived necessity driven by system-level constraints.
The data underscores that access to private care remains far from universal. Income is a powerful determinant: only ten per cent of those earning under £20,000 used private healthcare in the past year, compared with 35 per cent of those earning £80,000 or more. This three-and-a-half-fold difference points to a widening two-tier healthcare divide, with those on lower incomes effectively locked into an NHS whose services they are less able to access in a timely manner.
The shift towards private care comes against a backdrop of persistently low public confidence in NHS services. Just 32 per cent of respondents said they were confident in receiving timely hospital outpatient treatment — a modest improvement on the 28 per cent recorded in 2023, but still deeply underwhelming.
Confidence is particularly low when it comes to non-urgent operations, where just 22 per cent of people expressed confidence in timely access. Confidence in scans and diagnostics stood at 28 per cent, while mental health care (22 per cent) and GP appointments (31 per cent) also attracted low scores.
National data corroborates the public’s concerns. Although the elective waiting list has fallen slightly over the past year, an estimated 6.13 million people remained waiting for planned care at the end of January 2026. Of those, 2.7 million had been waiting longer than the NHS target of 18 weeks — a figure that reinforces why public confidence in timely treatment remains so fragile.
Chris McCann, Acting Chief Executive, Healthwatch England said: “The NHS 10-Year Plan aims to tackle long waits for elective care. However, this work needs to move faster if we want to boost patient confidence, stop the move towards two-tier healthcare, and restore the NHS as a truly universal service for all.
“The Government must keep its pledge to make sure most people are seen and treated within 18 weeks of referral, including meeting the interim target of 65 per cent of people by the end of this month.
“To build people’s confidence, the Government should introduce the promised minimum patient experience standards for elective care. Everyone waiting for hospital care, no matter where they live or which hospital they were referred to, should get the same level of service and communication.”
Healthwatch England is calling on the Government to introduce promised minimum patient experience standards for elective care — standards that would apply regardless of where a patient lives or to which hospital they have been referred. Such standards would include timely confirmation that referrals have been received and accepted, rather than lost in administrative processes, as well as information to help patients manage their symptoms whilst they await treatment.
The organisation is also pressing for hospitals to provide patients with regular updates confirming their continued place on the waiting list, and to give adequate notice of any planned cancellations. Critically, Healthwatch England is urging that these standards be tracked and progress shared publicly, to rebuild confidence in the NHS’s ability to reduce backlogs.
Customers from four of Stonewater’s retirement living schemes in Bedford have come together to celebrate culture, heritage and community through a new cookbook created in partnership with The Higgins Bedford art gallery and museum.
The Food for Thought project ran from November 2023 to August 2025 and brought together customers who shared cherished family recipes alongside the memories connected to them.
Through reminiscence workshops led by The Higgins Bedford, participants explored dishes that formed part of their childhoods, family milestones and cultural traditions.
The recipes have been combined into an illustrated recipe booklet featuring dishes from around the world, including India, Pakistan and Ukraine.
As part of the creative process, customers from Presentation House, the Lodge, Warwick House and Raglan Court were photographed and sketched, helping to share not only recipes but the memories connected to them.
Stories of cooking in clay ovens, childhood delicacies and celebrating family occasions with traditional sweets were documented alongside recollections of Bedfordshire heritage.
Among the contributors were Mrs Banti and her Mrs Devi, who shared their family recipe for chickpea curry and an Indian flatbread called puri. Mrs Banti said, “I learned this recipe from my mother in India and have passed it on to my daughter. We make this meal to enjoy with our loved ones and I am happy that other people can try the recipe.”

Mrs Bibi, a customer from Stonewater’s Presentation House, shared her recipe for gogian cookies, a traditional sweet from northern Pakistan. She said: “We use make these for weddings and celebrations. It is tradition that when a daughter returns to her in-laws, she takes freshly made gogian to share. I am so happy to have taken part and very glad that children in the future can use the recipe I shared.” For Mrs Kaur, contributing her recipe for khichri brought back vivid memories of her childhood in India. “Khichri is a food that everyone can enjoy,” she said. “I am very happy to have taken part in the recipe book
project. It helped me remember the memories of my past and it feels nice to be valued for it.”
Mrs Randova, who grew up in Ukraine, contributed her family’s borscht recipe.
“There are 200 recipes of borscht in Ukraine,” she said. “Every woman has her own recipe. I want to express my gratitude to everyone who took part in this project.”
The project concluded with a celebratory event where residents tasted dishes from the book and received certificates recognising their contribution.
Copies of the cookbook will be kept at the retirement living schemes and added to The Higgins Bedford Social History Collection to preserve residents’ experiences for future generations.
Cynthia Knight, Scheme Manager - Central East, Presentation House who led the project for Stonewater, said: “We began with a simple idea to bring people together, engage with customers, help them feel valued and facilitate sharing something meaningful from their lives. Food is such a powerful way of connecting people because it carries memories of childhood, family, celebration and comfort.
“What has been so special is seeing customers from different backgrounds come together, listen to and respect each other’s stories and feel proud of where they come from. The cookbook is not just about recipes, it is about identity, belonging and reminding people that their experiences matter.”
Lydia McDonald, Keeper of Social History from The Higgins Bedford added: “It has been a privilege to work alongside Stonewater and customers on this project. The reminiscence workshops created a space for people to reflect, share and connect through memories of food and family. These stories are an important part of Bedford’s social history and we are proud that the cookbook will form part of our collection for future generations. The project was funded by Arts Council England as part of The Higgins Bedford’s community outreach programme. The Higgins Bedford is part of Bedford Borough Council’s Leisure and Culture Services.”
At Broomy Hill Nursing Home, innovation and compassion come together in the most inspiring way. Residents at the home are stepping into a whole new world with the introduction of virtual reality headsets. It is an exciting innovation with the power to create uplifting and meaningful moments for the residents under our care.
Virtual reality is becoming an exciting innovation in care homes and at Broomy Hill Nursing Home it is making a meaningful impact. VR is more than just a tool; it allows residents to relive cherished memories and experience activities they may no longer be physically able to do.
For residents with dementia or complex mental health needs, VR stimulates memories, sparks conversations, and provides relaxation through immersive experiences. Using headsets to create digital 3D environments, VR acts as a tool for cognitive stimulation, pain relief, and wellbeing, enabling individuals to safely revisit familiar places or explore new worlds.
We were thrilled at the opportunity to be a part of the Recreo VR experience. It was something new for the residents and us. However, it is not only something new; it is a learning experience for the entire staff at the home.
Our Wellbeing Lead, Lauren, is currently working on a list of available experiences that our residents can choose from to do something different each time they use the headset. This way, our residents will have something new to look forward to each time they use the headset, as new content is added every eight weeks.

One of the new experiences that our residents will enjoy in the near future is a seated safari, where they will have the opportunity to come face to face with a rhino from the comfort of their chair.
Recently, our residents travelled through time to the 1950s, where they had a virtual visit to a traditional house, cinema, and a high street. In the house, our residents travelled from room to room, exploring the food pantry and admiring the decorations of the house. In the cinema, our residents explored the ticket office, the reel room, and the cinema itself. In the high street, our residents visited an electronics shop, a record shop, and a toy shop, enjoying the experience of each of these different stores.
Many of our residents commented on how real the experience felt, almost like stepping into a memory. Some were actually looking at their hands to get used to the virtual world. As the shops, toys, and songs from the period were brought up, the experience naturally evolved into memories and stories. The dialogue was effortless as the resident's shared memories from their own lives to each other and staff. Virtual reality is more than just an activity at Broomy Hill. It is another meaningful way we promote wellbeing and engagement for our residents. By using Recreo VR, we encourage conversation and reflection, while continuing to look for ways to enhance quality of life within our home. For further information visit www.recreovr.co.uk
A digital music and movement programme has been shown to improve wellbeing for both care home residents and staff, according to new research led by the University of Stirling.
The evaluation assessed the danceSing Care digital platform over a 12month period in 78 care homes across all Scottish health boards. The platform combines online music and movement group sessions which are led in-person by care home staff.
Researchers found that residents taking part in the activities reported lower levels of loneliness and reduced fear of falling, while staff delivering the sessions reported higher wellbeing, lower stress levels and improved job satisfaction.
Residents and staff completed surveys at the start of the programme and again at six and 12 months.

The evaluation was led by Professor Anna Whittaker of the University of Stirling’s Centre for Health and Innovation in Sport (CRIS), part of the Faculty of Health Sciences and Sport.
Professor Whittaker said: “Physical activity is widely recognised as a key factor in maintaining health and quality of life among older adults. However, delivering consistent exercise opportunities in residential care settings can be challenging due to staffing pressures, varying resident abilities and limited access to specialist instructors.
“Digital platforms such as danceSing Care aim to address these barriers by providing flexible, accessible
resources designed specifically for older adults.
“Our research found that danceSing Care can contribute to improved wellbeing metrics for both care home residents and staff.
“This suggests it would be beneficial to implement an evidence-based resource like this more widely to support physical, mental and social activity and improve the health of older people and their carers.”
The danceSing Care platform provides pre-recorded sessions of around 20 minutes, delivered by care home staff. Activities include chair-based exercise, strength and balance training, and dance styles such as salsa and ballroom. Staff receive training to deliver the sessions safely and adapt movements to residents’ individual abilities.
Researchers note that the evaluation was designed as a programme assessment rather than a controlled research trial, meaning the findings should be interpreted as preliminary. The team recommends further investigation through a larger clusterrandomised controlled trial to assess a broader range of health outcomes.
The paper Evaluation of the Impact of Digital Music and Movement on Care Home Staff and Resident Outcomes was published in the journal Advances in Geriatric Medicine and Research.
The research was funded by the Scottish Government Digital Directorate, which awarded £125,000 to danceSing to support the project. Of this, £15,000 was allocated to the University of Stirling for consultancy on methodology and analysis.
TLC’s Kailash Manor care home in Hatch End celebrated the Hindu festival of Holi which took place on Wednesday 4th March. Holi is celebrated as the festival of colours, love and spring. It celebrates the eternal and divine love between the deities Radha and Krishna. Additionally, the day signifies the triumph of good over evil as it commemorates the victory of Vishnu over Hiranyakashipu.
Hotel Services Manager, Sagar Joshi commented “Holi is such an important event in the Hindu calendar, we all enjoyed the spirit of celebration welcoming in the colours of the new season by throwing bright powder colours at each other.”
The home was filled with laughter and music as joyous songs were sung to celebrate the beginning of spring. Residents, families and the care team alike tenderly coated one another in powder mak-

ing sure no one left the celebration clean.
In the evening, after a thorough clean up, an Iftar dinner was hosted for our Muslim team members who are often still at work at the time of breaking fast. Iftar is the fast-breaking evening meal of Muslims in Ramadan at the time of adhan (call to prayer) of the Maghrib prayer. It is a time where families and communities often gather to share food, prayer and conversation.
Support Manager, Ruth Kigaa said: ““It was really interesting to find out all about Eid and how it is celebrated and it was really lovely to see everyone participate in the Iftar meal. We have people of all religions here and it is wonderful to be able to take part in different religious festivities.”
Residents from Wilton Manor Care Home, part of the Sanders Senior Living Group, recently enjoyed a day on the ice after a resident wish initiative brought a long-loved pastime back to life.
On 9 March 2026, the team at Wilton Manor organised a special outing to the National Ice Centre, taking six residents ice skating so they could experience the activity together and recreate happy memories from earlier in their lives.
The trip was inspired by two residents, Christine and Jean, who shared that they used to love skating regularly in the past and wished they could do it again. With support from the Wilton Manor team, the residents travelled to the rink where they were able to enjoy time on the ice and relive a favourite hobby.
The experience proved especially meaningful for Christine and Jean, who both revealed that they used to go ice skating every Saturday years ago. During the visit, they realised that they had very

likely been skating at the same rink at the same time in the past, long before they ever met.
Commenting on the day, Christine said: “It was absolutely wonderful to get back out on the ice again. I used to get the bus every Saturday and come skating, so being able to do it again brought back so many lovely memories. It felt magical to be there, and I felt very lucky to have the opportunity. It was such a special morning and I would absolutely love to do it again.”
Beth, Customer Relations Manager at Wilton Manor, said: “We’re so lucky to be able to do this sort of thing with our residents and take them on such lovely trips. It was heartwarming to see everyone so happy and enjoying themselves. Louise, our Lifestyle Lead, arranges such amazing trips and activities and I know that this one will be one to remember.”
The law is changing for care homes, but understanding your obligations has never been easier
Providing both comfort and dignity to those in your care is at the core of the Care homes profession, but when it comes to both residents and their families, one of the most important things you can offer is trust.
Moving to a care home can be an emotional time for some and transparency and fairness are key in reassuring prospective residents and their families that they will be cared for with compassion and respect - This, and compliance with the law.
Earlier this year we saw the introduction of the Digital Markets, Competition and Consumers Act 2024 (DMCCA) - a landmark piece of legislation that affects business and how they are required by law to safeguard their customer with fair trading practices. These changes may sound like legal jargon, but they directly impact how care homes operate, communicate, and contract with residents.
Compliance can be complex and that’s why the Business Companion Care Homes Guidance is essential reading for anyone working in the Care Homes sector. Written by legal experts this free and easy-to-read guide will walk you through all the steps to ensure you are safeguarding your customers and operating within the law.
WHAT’S CHANGED UNDER THE DMCCA?
The introduction of the DMCCA represents one of the biggest shifts in consumer law in over a decade. It replaces the old Consumer Protection from Unfair Trading Regulations and introduces stricter rules to protect consumers from misleading or unfair practices across almost all sectors. For care homes, this means:

Clearer Pricing and Transparency: The Act bans “drip pricing” which is when unavoidable fees are hidden until late in the process. Care homes must now present the full cost of services upfront, including any mandatory charges.
Fake Reviews and Misleading Endorsements: The DMCCA prohibits the use of fabricated or manipulated reviews. With care homes increasingly relying on their online reputation, ensuring authenticity is now a legal obligation.
Stronger Enforcement Powers: The Competition and Markets Authority (CMA) can now impose fines of up to £300,000 - or 10% of global turnover - for breaches. Compliance isn’t optional; it’s critical. • and much more!
These changes underline the importance of reviewing your policies, contracts, and marketing materials. The Care Homes Guidance on Business Companion provides practical steps to help you stay compliant and avoid costly mistakes.
KEEPING CONSUMER VULNERABILITY IN MIND
Vulnerability can arise from a number of different situations and factors throughout a person’s life, such as age, health, bereavement, or financial stress. As someone working in the Care homes sector,
you’re dealing with vulnerable individuals on a daily basis and recognising these factors isn’t just good practice; it’s a legal and ethical responsibility.
The Business Companion Consumer Vulnerability Guide offers checklists and practical advice to help you identify and support your residents who may be vulnerable when it comes to things like decision making and communication, ensuring your care home delivers not only compliance but compassion.
Your Go-To Resource for Compliance
Business Companion is more than just a care home resource - it’s a comprehensive hub for businesses across a broad range of sectors. From selling online to handling complaints, delivery charges, and even net zero strategies, the platform covers hundreds of topics delivered to you through clear, easy-to-read guidance. Backed by the Chartered Trading Standards Institute and the Department for Business & Trade, Business Companion is free, authoritative, and regularly updated by legal experts.
Act Now
The DMCCA is already in force, and enforcement powers are live. Don’t wait for a compliance issue to arise - visit Business Companion’s Care Homes Guidance today. Review your contracts, pricing structures, and communication strategies and explore the wider resources available to future-proof your business against legal pitfalls.
In a sector built on trust, staying informed isn’t just smart - it’s essential.
To find out more, visit: www.businesscompanion.info

By Barry Price, Content Operations and Delivery Manager of QCS,

The Social Care sector remains stuck at a crossroads. Workforce shortages, regulatory uncertainty and rising financial pressures continue to provide unprecedented challenges for providers. According to Skills for Care, around 111,000 posts remain unfilled, representing an 7.0% vacancy rate, these figures are still high compared to other UK sectors. At the same time, providers face constrained fee rates, surging costs: utility bills and water rates have risen by up to 50%, alongside increases in the living wage and National Insurance contributions. Smaller operators are disproportionately affected, accelerating consolidation across the sector.
In this environment, the question is clear: how can providers maintain quality services whilst navigating these pressures? The answer partly lies in connected technology, joined-up data and intelligent systems that support teams to work smarter, not harder.
Recruitment and retention have become critical pain points. With vacancy rates at historic highs, care and support teams are stretched thin, leading to burnout, increased risk and contract hand backs. Traditional approaches, manual processes, fragmented systems, and siloed data only compound the problem. Staff waste valuable time searching for compliance information or duplicating tasks, time that could be spent delivering face to face support.
Connected technology changes this dynamic. By integrating care management, compliance, and learning into one ecosystem, providers can streamline workflows and reduce administrative burden. Intelligent solutions like Lyra, our latest AI innovation, gives teams instant access to the information they need, whether it’s a compliance update, a care and support plan or a learning resource at the point of need.
According to the Department of Health and Social Care an estimated 30 million administrative hours will be saved per year through this digital-first approach so carers can spend more time looking after those with care needs, giving back at least 20 minutes per care worker per shift.
FINANCIAL PRESSURES: DOING MORE WITH LESS
The financial strain on providers is intensifying. Many local authorities are increasing fees paid to providers, but only by modest amounts (typically mid-single digit % increases), Rising utility costs, wage increases and NI contributions are squeezing margins, particularly for smaller operators. Many are forced to
consider consolidation or exit the market altogether. In this climate, efficiency isn’t optional, it’s essential. Connected systems deliver measurable cost savings by reducing duplication, minimising risk and improving resource allocation. For example:
Compliance automation reduces time spent on audits and inspections.
• Integrated learning tools cut training costs while improving staff capability.
Real-time insights help managers make informed decisions, avoiding costly errors.
Minister of State for Care, Stephen Kinnock, has said “A one-stop shop for a person’s care informationsecurely available to carers - cuts paperwork, helps reduce errors and gives carers more time to care”. Our one system approach exemplifies this. By bringing care management, compliance, and learning data together in a single platform, powered by Lyra’s intelligence, providers can unlock efficiencies that directly impact the bottom line. Instead of juggling multiple logins and disconnected tools, teams have one secure login, one source of truth and one partner committed to raising the standard of care everywhere.
The future of health and social care is connected, intelligent and human. Technology isn’t replacing people, it’s empowering them. When data flows seamlessly across systems, providers gain clarity and control. Risks are reduced, compliance is strengthened and staff are freed to focus on delivering compassionate person centred care.
AI technology like our own AI advisor Lyra, transforms how teams engage with content. Instead of searching through policies, they can simply ask questions and receive precise answers instantly. This not only saves time but builds confidence and capability, creating a more knowledgeable and resilient workforce.
As Skills for Care highlights, investment in workforce development and digital tools is key to sustainability. Providers who adopt connected technology today will be better positioned to thrive tomorrow.
The challenges facing the social care sector are real and urgent. Regulatory uncertainty, Workforce shortages and financial pressures won’t disappear overnight. But by embracing connected technology, joined-up data, and intelligent systems, providers can navigate complexity, protect margins and deliver consistently better outcomes for those who use our services.
At QCS, we believe in a better future. One where social care is connected, intelligent and human. With Lyra and our One System approach, we’re helping providers turn data into insights, insights into action and action into better outcomes for every person, every day.
For more information see the advert on page 15.
Henbrook House care home in St Neots, recently helped make a resident’s dream come true after taking Joyce (83-years-old) to see her favourite band, Collabro, perform live at Ely Cathedral. Events Manager Brian Moore even secured the ‘red carpet’ treatment for Joyce, who was invited backstage after the show to meet the band herself.
Collabro are a UK-based musical theatre group who rose to fame after winning the eighth series of Britain’s Got Talent in 2014. Joyce has been a devoted fan ever since. After tragically losing her best friend in 2022, Joyce found genuine comfort in Collabro’s music, especially their powerful recreations of musical theatre classics which she remembers listening to as a young woman.
Watching their performances on YouTube helped lift her spirits during the grieving process, and she soon became one of the group’s many loyal fans –known affectionately as “Collaborators”.
Brian Moore, Events Manager at Henbrook House said: “We believe music plays a vital role in exceptional later-life care, often helping people reconnect with memories and emotions from years gone by. When we saw how much Collabro’s music meant to Joyce, the team was determined to do everything we could to help her see them perform live. It was incredibly spe-

cial to watch Joyce meet the band and experience their performance after everything she had been through.”
Joyce had originally planned to see the band in 2024, after securing tickets to their 10th Anniversary Reunion Concert at Birmingham Symphony Hall. However, shortly before the concert she suffered a setback when she broke her hip, meaning she was unable to attend and had to pass her tickets on to another fan.
Determined not to let Joyce’s dream slip away, Henbrook House’s Events Manager Brian Moore reached out to Jamie Lambert, lead singer of Collabro, to share her story. To his delight, the band was so moved by Joyce’s passion that they invited her as a special guest to their show at Ely Cathedral, complete with a meet-and-greet alongside her daughter, Kirsty Hazell.
Michael Zinaka, General Manager at Henbrook House, shares his thoughts: “From the beginning, our vision for Henbrook House has been to create more than just a care home – we want it to feel like a true home where residents’ interests and passions are celebrated. Experiences like this, where we can honour a resident’s dreams and create lasting memories with their loved ones, are exactly what we had in mind. I am incredibly proud of the team for going the extra mile to make this happen for Joyce.”
Care & Dementia is the UK’s leading event for transforming social care and improving the lives of people living with dementia. Building on the successful foundation of The Alzheimer’s & Dementia Show and UK Care Week, it creates an essential, dedicated platform for both care professionals and the public. Taking place on 25-26 March at the NEC in Birmingham, this event represents a powerful evolution in the sector. Combined with the incredible momentum of Naidex, it creates a vibrant environment where vital communities meet to explore best practices, support services, and innovative products.
A WORLD-CLASS SPEAKER PROGRAMME
Carefully curated CPD sessions bridge the gap between industry innovation and personal care. The full programme is now live, featuring expert voices designed to provide actionable insights for every attendee.
CARE KEYNOTE THEATRE

A must-attend for those looking to stay ahead of industry trends. Featuring leading voices from the CQC, Alzheimer's Society, Dementia UK, National Care Forum, and Care England, these sessions explore policy changes, funding models, and the future of the care sector. Sessions include Where is Social Care on the Political Agenda? with Damien Green from the Social Care Foundation. This is followed by a collaborative discussion titled Building Knowledge of the Sector - One Mind at a Time, featuring Amrit Dhaliwal (Walfinch), Samantha Crawley (EQ Care Group), and Sam Monaghan (Chief Executive at Methodist Homes MHA).
DEMENTIA MATTERS THEATRE
This theatre provides practical support for both professionals and family carers. The programme features
Dementia devastates lives, innovation transforms them: Alzheimer’s Society Innovation Team (Alzheimer’s Society) and Dementia and SafeguardingProtecting Rights, Reducing Risks: Kirsty Dallison-Perry (Dementia UK). These are complemented by In Conversation: A Carer’s Perspective: Frances Lawrence (Dementia Carers Count) & Rosie Brooks (Dementia Carers Count) and a highly informative Learn about dementia from people living with dementia Q&A: Ronnie Dean, Beth Britton MBE & George Rook (Dementia campaigner). INTERACTIVE FEATURES & PRACTICAL SUPPORT
Alongside the conference sessions, the event features a range of interactive experiences designed to provide practical support. Professionals can earn up to 12 CPD points through the accredited programme while accessing tailored advice at the CQC Inspector Hub. New for 2026, visitors can access a complimentary, confidential consultation to explore available options for early dementia or mild cognitive impairment at the Re:Cognition Health Assessment Clinic. For families and caregivers, the event offers 1-to-1 Advice Clinics with Admiral Nurses from Dementia UK, the Dementia Interpreters Workshop, and immersive training experiences like the Virtual Dementia Tour and the Autism Reality Experience. Visitors can also explore the Innovation Hub to discover the latest technologies and solutions for social care and rehabilitation.
Attendance is free. Ensure you are part of the UK’s most significant gathering for the care community. For more information and tickets visit www.naidex.co.uk/careanddementia


Springbank Care Home has announced the success of its recent ‘Through Our Eyes’ exhibition, which brought together residents, families, and the local community for a moving celebration of life and history. The project used technology to merge current portraits of residents living with dementia into photographs from their past, creating evocative scenes that highlight the vibrant person behind the diagnosis.
The event featured composite artwork that placed residents as they are in 2026 directly into historical settings, celebrating their lifelong journeys and cherished hobbies.
The atmosphere was further enhanced by the cheerful tunes of Richard and Honey, one of the home’s much loved visiting singer and dog duos, who performed hits ranging from "Blue Skies" to the Beatles. Following the exhibition's success, these meaningful photographs will now go on to be given to families and displayed in residents' rooms where appropriate.
A significant highlight of the exhibition was the presence of multiple generations of families to read about their loved one and view their composite portrait. One relative shared their experience:
“It was so lovely to see mum and her friends in their younger days. It’s such a great idea to show how these people were once young and so interesting and very hard working. They really were the generation that changed the world. I loved reading about each and every one of the residents. I particularly loved seeing one resident, who was my old art teacher.
I think we do forget the story behind their faces and it’s good for us to be reminded of the life they had before and what a brilliant way to portray this.”
Another relative added…
“As a relative be prepared for a very emotional experience in looking at photographs that chart the ageing process. It reminded me of the sometimes-forgotten young man I once knew. A big thank you for the hard work putting together the ‘Through Our Eyes’ exhibition.”
The exhibition's impact was further reflected in the glowing feedback shared on social media, with one guest commenting, "What a lovely afternoon, thank you for putting so much effort into making it such a nostalgic occasion. What a wonderful idea, the food was delicious too, you really are so hard working and the best care home." Others noted that they "thoroughly enjoyed ourselves and appreciated the effort put into organising the event," and described the presentation as "very moving" and "thoroughly enjoyable."
While the original images remain private to protect the dignity of the residents, the exhibition featured
several powerful scenes that illustrated the deep connection between past and present. One piece featured a lifelong fan as they appear today, seated alongside their younger self in the stands at Keighley Cougars. Another depicted a resident watching from the sidelines as their past self played a match on the football pitch.
The collection also included poignant professional tributes, such as a resident—as they appeared in the past—treating their presentday self as an NHS nurse at Harrogate Hospital. In another evocative scene, a lady looked into a mirror to see her past self: a fashionable woman balancing the demands of work, family, and style. The exhibition further captured moments of lifelong learning and industry, showing a resident sitting in a classroom being taught by their younger self, and another gazing through a window into the past to watch themselves at work in a wartime munitions factory.
The exhibition also focused on reconnecting residents with their personal histories and former friends. A representative from the local football club attended to spend the afternoon reminiscing with a resident over historical club photographs, sharing stories from their time as former teammates.

April Howie, Deputy Manager at Springbank Care Home, shared their pride in the event’s impact:
"This project has been a deeply moving journey for everyone involved. By merging the present with the past, we aren't just creating art; we are creating a powerful tool for empathy that reminds us all of the incredible lives our residents have led. It was a privilege to work alongside our fantastic corporate partners to make this event even bigger and better for our residents and guests. Specifically, working with Snuggle, who provided a wide variety of foods to complement the event as part of their initiative to give back to the health and social care industry, helped create a truly celebratory environment. We are so pleased to have been able to show the person behind the diagnosis."
Ollie Bellerby, representing Snuggle added:
“Snuggle Staffing were proud to support Spellman Care and the team at Springbank Care Home for such a meaningful event. The ‘Through Their Eyes’ exhibition was a wonderful celebration of residents’ stories, seen from a unique perspective and we were delighted to contribute by providing some nibbles that helped bring friends and family together.”
Lisa and April would be more than happy to speak to any other care homes or professionals interested in learning more about the project and its benefits. The ‘Through Our Eyes’ exhibition represents the latest in a line of innovative initiatives at Springbank Care Home, reflecting the forward-thinking philosophy of the Spellman Care group.
For more information, please contact the home directly at deputy@springbanksilsden.co.uk or 01535 282424.
A care home provider has strengthened its commitment to inclusivity and staff wellbeing by hosting a communal Iftar dinner for its team during the holy month of Ramadan.
Mauricare Homes recently hosted a special Iftar gathering for staff at its Old Vicarage Residential Home in Worksop.
The evening brought colleagues together to break the Ramadan fast, share a meal, and celebrate the rich cultural diversity that defines the Mauricare Homes team.
The event was warmly received by staff across all roles, with the gathering serving as an opportunity to foster connection, mutual
respect, and a shared sense of belonging in the workplace. Iftar — the meal that breaks the daily fast observed during Ramadan holds deep spiritual and social significance, and the team at Old Vicarage were delighted to come together in this spirit.
Umar Boodhoo, Managing Director, Mauricare Homes commented, “At Mauricare Homes, our people are our greatest strength. Events like this remind us of the importance of celebrating one another’s cultures and traditions, it brings us closer as a team and ultimately means we can provide better, more compassionate care to our residents.”

By Kevin Groombridge • Chief Executive, Care Inspections

In today’s highly regulated health and social care environment, providers face the dual challenge of ensuring compliance while striving to deliver safe, high-quality, and commercially sustainable services. Care Inspections UK Limited (CiUK) has emerged as a trusted partner in this landscape, providing a professional and independent inspection service that goes beyond the standard requirements of the Care Quality Commission (CQC), The Care Inspectorate Wales (CIW) and the Care Inspectorate (Scotland), collectively “The Inspectorates” What sets CiUK apart is its status as a registered inspection body, operating with the highest levels of professionalism and governance. This official recognition imbues care providers with confidence that inspections are carried out with rigour, objectivity, and an unwavering focus on evidence. Every report is underpinned by validated, researchbased methodology, ensuring the outcomes are credible, balanced, and practical.
BEYOND CQC/ CIW/ CI STANDARDS
While CQC/ CIW/ CI inspections focus on fundamental areas such as safety, effectiveness, responsiveness, and leadership, CiUK’s
approach extends further. Each CiUK inspection covers all the domains CQC/ CIW/ CI would expect, but also incorporates additional layers of analysis essential for continuous improvement. This Includes:
• Operational risk management involves identifying risks before they become incidents, reducing exposure for service users and providers.
• Quality enhancement: Assessing opportunities to raise standards in care delivery, staff engagement, and governance.
• Commercial sustainability: Offering insight into how operational practices influence financial performance, helping providers balance compliance with business viability.
The result is an inspection report that is not only regulatory-ready but also a strategic tool for improvement.
A PROFESSIONAL AND INDEPENDENT EYE
Professionalism is at the heart of CiUK’s ethos. Inspections are conducted by highly experienced professionals who bring frontline expertise from clinical, managerial, and governance roles in the care sector. This depth of knowledge allows CiUK to deliver meaningful feedback that resonates with staff at every level, from frontline carers to boardroom directors.
Independence is equally vital. As an external registered inspection body, CiUK reassures providers that its findings are unbiased and transparent. In a sector where credibility matters, this impartiality is invaluable in preparing for CQC inspections and demonstrating accountability to commissioners, investors, and the wider community.
DRIVING IMPROVEMENT AND REDUCING RISK
Care providers today operate in an environment of heightened
scrutiny and rising expectations. CIUK’s inspections do more than highlight compliance gaps; they provide a clear roadmap for reducing risk, enhancing quality, and driving organisational improvement.
By identifying weaknesses early, providers can take corrective action before issues escalate. At the same time, CiUK’s focus on strengths and opportunities supports a culture of positive development. This balanced approach ensures that inspection outcomes are constructive, not punitive, fostering continuous organisational improvement.
SUPPORTING COMMERCIAL PERFORMANCE
One of the most overlooked aspects of care provision is its commercial dimension. Poor compliance and weak governance inevitably carry financial consequences, from reputational damage to contract loss. CiUK recognises this and integrates commercial insight into every inspection. CiUK helps providers achieve operational excellence and commercial resilience by aligning care quality with business performance.
THE CIUK DIFFERENCE
Choosing Care Inspections UK Limited means selecting a partner committed to professionalism, independence, and comprehensive excellence. CiUK inspections do more than prepare organisations for regulatory visits—they empower providers to deliver safer, higher-quality care while protecting their reputation and commercial future. CiUK delivers evidence-based assurance and actionable insight for providers who want more than compliance.

THE WEIGHT CARE TEAMS CARRY, OFTEN SILENTLY
There is a moment in every care professional’s life that stays with them. For me, it was a late evening on the unit, years ago, when a nurse quietly said, “I hope everything was done right today. Sometimes I fear what I do not see.” Her words were simple, but they held the unspoken truth of our sector. Care is built on love, but it stands on safety. And safety, in the real world, is fragile. It lives in the seconds we do not have, the pressures we do not voice, the documentation that steals time from the people we came to serve.
Medication rounds, audits, handovers, stock checks, and incident reviews are essential but relentless. Behind every one of them is a carer trying to do the right thing, a senior hoping they have not missed a detail, and a manager carrying the weight of an entire home on their shoulders. For years, I watched this tension unfold. The intention was always pure, but the systems were not always kind. And that is where Empathika began.
It was never just a technological project. It was a response to the tired eyes of the night nurse, the rushed signatures at the end of a shift, the quiet fear of missing a dose, and the pressure to be perfect in a world that gives little room for human error. As a pharmacist, my world has always been accuracy, governance, and risk. But as a human being raised in a family dedicated to care, my world has also been empathy, dignity, and service. Empathika is where those two worlds meet.
TURNING PRESSURE INTO CLARITY, AND FEAR INTO CONFIDENCE
By Sibtain Nandjy, Chief Medical Officer, Empathika (www.empathika.com)
Medication is one of the most sacred responsibilities in care. It is where mistakes can cause harm, where delays can cause distress, and where oversight can save lives. Yet traditional approaches relied on memory, paper trails, and hope. Empathika was created to take the weight off people’s shoulders, not add to it. She records every dose in real time. She alerts before errors happen. She tracks stock, expiry dates, and changes in treatment. She protects controlled drug processes with dual witnessing and biometric verification. She gives managers visibility before problems even surface. Above all, she protects carers from carrying fear into their work. She holds the details so they can hold the residents.
One of the greatest challenges in care is not the work itself, but the constant interruption of it. A senior searching for stock. A carer chasing signatures. A manager preparing for an unannounced inspection. Empathika brings calm into the noise. Live dashboards show managers exactly where the home stands. Incidents, handovers, and reviews are captured without confusion. Compliance becomes a natural outcome of daily practice, not a monthly marathon. Families feel the difference because they see teams who are present, not pressured.
People often ask what makes Empathika different from other systems. The answer is simple. She was not built from a boardroom. She was built from lived experience. Every feature has a why. Every process has a story. Every safeguard has a person behind it. And that is why she feels different. She listens. She steadies. She gives time back to the floor.
The future of care will not depend on technology alone. It will depend on how well technology honours the people who use it. Empathika exists for that purpose. To make safety feel gentle. To make compliance feel natural. To make care feel like care again. Because at its core, Empathika is not equipment. She is a commitment. A promise that no carer will stand alone under the weight of responsibility, and no resident will be cared for in fear or uncertainty.
When Bristol resident Tacey Bain's husband David received a sudden cancer diagnosis, the final two weeks of his life were spent in the compassionate hands of specialist staff at St Peter's Hospice — a experience that left a lasting impression on their whole family.
Now Tacey is sharing their story in support of the Hospice's poignant new '44 Days' fundraising campaign, which draws attention to the average time a patient spends under the charity's care, and poses a question that will resonate deeply with everyone working in end-of-life care: what would you do with 44 days left?
For those on the frontline of caring for people in their final chapter, it is a reminder of just how profoundly specialist palliative support — and the people who deliver it — can shape a family's most precious and painful memories.
“David was a lovely man,” she said. “He was a very good family man – he regarded his greatest achievement as our three children and was enormously proud of them. He worked as a family law solicitor, supporting people during some of the hardest moments in their lives, which made him appreciate all the things that were good in life.
“He loved sport. At the age of 71 he was still playing hockey at Masters’ level. His team won the European Spirit of Masters Gold Cup in Valencia a year before he died.”

Cycling was another of David’s great passions. He completed Land’s End to John O’Groats with a friend and regularly took part in charity rides, including the St Peter’s Hospice Tour de Bristol. In 2024 the couple walked the Camino de Santiago, but towards the end of the trip David began suffering from stomach pain. At first, they assumed it was caused by something he had eaten but by the time they returned home, the pain had worsened significantly. After several hospital visits and scans, the couple received devastating news.
“Just one month after coming home David was diagnosed with cancer and we were told there were no treatment options available,” said Tacey.
When David’s pain became too difficult to manage at home, he was referred to St Peter’s Hospice directly from hospital.
“The diagnosis was entirely unforeseen and a big shock to us all, especially as David kept so fit and healthy,” she said. “It was a very overwhelming time but being at the Hospice felt completely different.
“When David arrived he was extremely uncomfortable and unable even to use his phone. But the Hospice let him relax and managed his pain,” Tacey explained. “Everything ran so smoothly once we were there. They know what they’re doing and they’re good at it. There was no moving between beds and wards, we could really settle.
“We found great comfort in the calm environment and the time it gave us together. The room was hotel standard and the food was brilliant. Even though it was hard for David to eat we felt nourished by the generosity. The whole set up made things we might usually take for granted, like being together and holding hands, far easier.”
David spent his final days at St Peter’s Hospice, just 100 metres from his childhood home, and died peacefully on 6 June 2024, less than two months after returning from holiday.
This sense of giving quality time to patients at their end-of-life, is central to the new 44 Days campaign the Hospice is running to raise vital funds.
Their aim is to fill those precious days with love and light, taking on the paperwork, the medication and the practical aspects of care, so that families can simply enjoy being together.
The 44 Days campaign also holds a special significance for Tacey and her family.
She said: “Forty-four was David’s lucky number. It was the number on his school locker, he used it when he raced Clubman’s cars in his 40s and it was in his email address.
“We feel so lucky that he was referred to the Hospice and would encourage everyone to donate to this amazing campaign. Even now the Hospice are supporting me through bereavement support, it is such a vital community resource.”
A fall- the F word- is massively on the increase: among older people, up 57% last year!(1). More than 40,000 people are hospitalised each year because of a fall on stairs(2)
Falls cost on many levels: ambulance call-outs, stays in hospital, admission into care, provision of home care. There is the psychological cost too: people become wary doing everyday activities.
Yet, with prescription of appropriate equipment, many of those could be avoided.
AAT’s S-Max Sella stairclimbing wheelchair is proven over 20 years to make traversing stairs safe for people with mobility issues/ a disability(3). Battery powered, Sella not only travels up and down stairs, but outside steps too. It removes the barrier(s) that prevents someone- young or old- being able to fully access their home environment.
Unlike alternative solutions, it is completely mobile/portable. The Sella stairclimber requires no installation nor electric supply to function. It is not limited to the staircase, meaning it can be used to move its passenger anywhere in the property and beyond without them needing to transfer off it.
Sella has an impeccable safety record and is the stairclimbing choice for virtually every local authority in the UK. As a result, it has the unique capability to be re-prescribed (re-issued) multiple times, giving the council best value and use of equipment resources.
The Nelson family demonstrates Sella’s value. They were prescribed one by their OT Fran Richardson after numerous “near misses” carrying their disabled son on the stairs. Fran commented,” “The stairclimber eliminates the risks associated with using the stairs for the family. Its versatility ensures it effectively addresses their current challenges and supports their long-term needs. The Sella cost less than half of the alternative options.”
Full details of the Sella stairclimber, including video of it in action, and how to book a free no obligation assessment, can be found @ www.aatgb.com/s-maxsella/ (1) https://operabeds.com/blogs/knowledge-hub/falls-in-the-elderly-uk-65-injury-and-accident-statistics


Wes Streeting, Secretary of State for Health, has delivered a statement to the House of Commons in which he confirmed that funding for mental health has fallen as a proportion of NHS spending in England. While there has been a real terms increase of £140m, this amounts a 3.2% reduction in share of spend from last year.
This reduction comes despite it being confirmed that one in five people aged 16-64 (22.6%) in England now have a common mental health condition, a 20% increase since 2014. This rises to one in four among young people. Mental health problems are the leading health condition among of young people out of work.
Mark Rowland, Chief Executive at the Mental Health Foundation, said: “Poor mental health is at record highs, including millions of children and young people on waiting lists for treatment or out of work with mental health problems without adequate support to return to the workforce. This is a human and economic

catastrophe, costing the UK at least £118 billion a year. In the midst of a national mental health crisis, a cut to the share of spend for mental health raises real concerns about the government’s commitment to mental health.
“We support essential NHS reforms to focus on early intervention and prevention (such as Mental Health in School Teams) as well as a focus on Neighbourhood health centres. However, a reduction in spend relative to other areas of health spend undermines this effort. We wouldn’t accept rising cancer rates and falling share of spend and we shouldn’t for mental health.
“Without an effective, co-ordinated ‘invest to save approach’, the mental health crisis will only get worse. It will continue to cost the UK billions of pounds, and millions of people will continue to suffer the consequences of preventable mental health problems.”
Nellsar Care Homes, a family-run group of Care Homes across Kent, Surrey and Essex has marked Food Waste Action Week throughout its 13 Homes – encouraging team members to think more carefully about how food waste can be reduced both at home and in professional care settings.
This year, the UK’s biggest annual food waste reduction campaign was built around the theme of making food go further, targeting preventing waste, using leftovers, and recycling.
Across Nellsar, the organisation looked to broaden the conversation beyond household habits, linking everyday actions people can take at home with the practical steps that can help reduce waste in Care Home kitchens and dining services. Areas of focus include efficient stock management, thoughtful menu planning, portion awareness, and the appropriate reuse of surplus food.

The initiative is being supported by Nellsar’s Head of Nutrition and Head of Catering, working collaboratively with members of the Senior Management Team to help embed sustainable food practices across the organisation. It also complements wider efforts to reduce plastic use and unnecessary packaging, work with environmentally responsible suppliers and strengthen sustainable food sourcing and preparation across the group.
Luminita Mandache, Quality Development and Innovation Manager at Nellsar, said: “We believe good care, hospitality and sustainability should go hand-in-hand. Food Waste Action Week provides a valuable opportunity to reflect on how small, practical changes, both at home and within our Care Homes, can make a meaningful difference.
“This is not simply about reducing disposal. It is about strengthening the full journey of food, from plan-
ning and procurement through to preparation, presentation and dining experience. By helping our team members understand how thoughtful food practices support both environmental responsibility and resident wellbeing, we can create lasting change across our Homes.”
To coincide with Food Waste Action Week, Nellsar has also introduced a reviewed food waste management log across its Homes. The new system has been designed to help teams record food surplus, reuse, and disposal more consistently, enabling the group to build a clearer picture of where waste occurs and where improvements can be made.
Although this year’s campaign is primarily focused on team member awareness, residents continue to play an important role in shaping Nellsar’s catering and dining services. Across its Homes, residents are regularly invited to share feedback through pictorial meal satisfaction surveys and mealtime feedback tools, helping teams to review menus, portion sizes and dining experiences.
Nellsar’s wider approach also recognises the close link between food sustainability and resident wellbeing. Recent developments such as the introduction of a Development Chef role and dedicated Resident Mealtime Experience Lead are helping to raise standards in menu development, presentation, flavour and dining support, ensuring meals remain enjoyable, meaningful and tailored to individual needs.
Luminita added: “Our aim is to create systems that reduce waste while enhancing the quality, enjoyment and nutritional value of meals for residents. We know that environmental, social and financial sustainability are closely connected and by working together across our Homes, we can build practices that are both responsible and lasting.”
Technology decisions in adult social care are no longer confined to IT teams or procurement processes. They shape everyday experiences. They influence how people are supported, how staff work, and how services demonstrate that they are safe, effective and accountable. At the same time, the sector is under immense strain. Demand is rising. Workforces are stretched. Regulation is intensifying. Digital tools are increasingly positioned as part of the solution, expected to stabilise systems that are already under pressure.
It is no surprise, then, that social care has leaned heavily on frameworks, standards and guidance to help make sense of risk, data and technology. These are important. But they are not enough on their own. When you step away from policy documents and listen to lived experience, a more complicated picture emerges.
Families may experience monitoring tools as reassuring. People drawing on care can experience those same tools as intrusive, empowering, or something in between. Care leaders are often focused on accountability, liability and safety. All of these perspectives are valid, yet they rarely point in the same direction.
The danger is not disagreement. It is pretending these tensions do not exist.
SAFETY,
Safety often becomes the organising principle for digital decisions. Sensors, alerts and data sharing systems are introduced to reduce risk and provide reassurance in a system where staffing is limited and time is scarce.
For some people, this technology creates freedom and confidence. For others, it feels like constant visibility. Even where consent is given, the emotional experience of being monitored is not always fully
explored.
These decisions may be made in assessments and meetings, but their impact is felt in bedrooms and living rooms. Dignity and privacy are not technical concepts. They are personal, value-based, and deeply contextual.
How often do we revisit these choices?
How clear are we about what data is collected and why? What happens when one person’s sense of safety conflicts with another’s sense of dignity?
Consent in digital care is often treated as a single action. A form signed. A box ticked. A decision made.
In reality, consent is fragile and changeable. Technologies are frequently introduced during moments of transition, or gradually become part of daily routines before anyone has time to reflect. What starts as a choice can quietly become the default.
As systems grow more complex, understanding becomes harder too. Many people, including professionals, are still learning how data is stored, shared and analysed. That makes meaningful consent difficult to sustain over time.
True consent requires revisiting, re-explaining and re-negotiating. It also requires making refusal possible, even when doing so feels uncomfortable or increases perceived risk.
WHO BENEFITS, AND WHO CARRIES THE COST?
Technology is often discussed in terms of efficiency and innovation. For care workers, the experience can be mixed. New systems promise time savings, but sometimes introduce extra steps, new pressures and new forms of oversight.
At the same time, when tools are designed and introduced well, they can reduce duplication, improve coordination and support better care. The difference is rarely the technology itself. It is whether people were involved in shaping it, and whether their expertise was respected. When systems fail, it is frontline staff who absorb the impact. They manage workarounds, late alerts and broken workflows. How organisations acknowledge that reality shapes trust far more than any digital strategy document.
Having honest conversations about technology in care is uncomfortable. It forces us to confront trade-offs rather than hiding behind process or policy. But discomfort is not failure. It is a signal that something important is being examined.
Throughout March, Digital Care Hub is creating space for these difficult conversations, from privacy and consent to robotics and the future of care work. Because comfort is easy. But courage is what leads to better decisions.
Technology is the topic, but dignity, safety and relationships are what’s truly at stake.
Join the conversation at www.digitalcarehub.co.uk/digital-care-in-focus #DigitalCareInFocus #DifficultConversations


Specialist business property adviser, Christie & Co, has launched its ‘Scottish Healthcare Market Review 2026’ report, which analyses the supply and demand for new build and development across Scotland’s elderly care market.
The report begins with an analysis of the elderly care home sector in Scotland. According to Christie & Co, there are 772 care homes across Scotland, with an average size of 47 beds, which equates to circa 36,000 beds in total. Only 55 per cent of these homes are purposebuilt, 87 per cent have en suite facilities, and just 36 per cent have wetrooms.
However, the Care Inspectorate’s Care Homes for Adults – The Design Guide 2026 confirms that all new developments must incorporate full wetroom provision, meaning much of the existing provision will struggle to meet required standards.
The Care Inspectorate has also confirmed that new registrations and newly built care homes can now be brought forward at capacities of up to 100 beds, which is a positive and enabling clarification for largerscale developments. However, while this provides welcome flexibility in design and master planning, there remain important operational considerations around staffing models, including the need to maintain appropriate staffing ratios per unit to ensure safe, high-quality care. Developers and operators will therefore still need to demonstrate that workforce planning, unit configuration, and care delivery structures are robust and sustainable at this scale.
With an average house price in Scotland of £194,000, 34 per cent of the country’s population owns their home outright. Despite this, there are pronounced regional disparities in affluence, reflected in the wide range of average house prices across local authorities, with more affluent areas such as East Renfrewshire, the City of Edinburgh, and East Dunbartonshire commanding prices well above £280,000, compared with more economically-challenged regions like Inverclyde, North Ayrshire, and West Dunbartonshire, where values sit closer to between £120,000 and £150,000. These differences not only highlight concentrations of wealth around the Central Belt and major employment hubs, but also signal a stronger potential for private pay care resident demand in higher value markets, where household wealth and property equity are typically greater.
CLOSURES & OPENINGS
Between 2021 and 2025, 81 care homes closed across Scotland, totalling 2,637 beds lost. The average size of these homes was 33 beds, with 69 per cent having en suite provision.
Meanwhile, 55 care homes opened across Scotland, totalling 1,999 new beds, which indicates a net loss of 638 beds over the four years. 14 of the homes that opened were purpose-built – equating to an average
of 3.5 new schemes per year – which typically offer full wetroom provision and have an average registration capacity of around 65 beds. The remaining openings comprised newly registered services, including reopened care homes and facilities converted for care use.
Between 2021 and 2025, 47 new care home development schemes were approved across Scotland, representing a pipeline of 2,489 additional beds. This development activity remains heavily concentrated in Scotland’s Central Belt, with smaller clusters of activity emerging in the northeast and parts of the Highlands and Islands, where schemes typically aim to address gaps in provision within more rural or remote communities.
Most new care home projects are being advanced by private operators and developers. However, an increasing number of mixed-use housing schemes now include care provision, and several local authorities are also bringing forward their own developments. This reflects a growing blend of public and private sector activity across the market. Following the removal of the 60-bed cap on care home developments, Christie & Co expects renewed momentum in the Scottish pipeline as operators gain greater flexibility to progress larger, more commercially viable schemes. This policy shift is likely to stimulate further investment across both urban centres and underserved rural areas, helping to deliver a broader range of modern, purpose-built facilities.
Under the revised guidance, homes accommodating 61 to 80 residents must appoint a deputy manager with 100 per cent supernumerary time. For developments hosting 81 to 100 residents, each unit must have a dedicated unit manager with at least 50 per cent supernumerary time. In practical terms, these requirements may influence how developers structure and phase larger schemes.
CHRISTIE & CO FORECASTING
While 21 per cent of Scotland’s current population is over 65, it is anticipated to grow to 25 per cent over the next 10 years. Similarly, Christie & Co data suggests that the demand for elderly care beds will increase by 12 per cent by 2031 and 32 per cent by 2036. There will also be a substantial rise in the prevalence of specialist chronic, age-related conditions like dementia, which will not only increase overall demand for care but will also heighten the need for high acuity, specialist dementia care facilities capable of supporting individuals with advanced and complex needs.
Christie & Co also assessed future bed requirements based on the number of en suite beds (the minimum market standard) and the need for wetroom provision (full-market standard beds), and highlighted a current undersupply of 19,793 wetroom beds across Scotland, which is
forecasted to increase to a shortfall of 21,434 by 2031 and a staggering 27,683 by 2036.

Martin Daw, Regional Director –Scotland at Christie & Co, outlines the opportunities for operators and developers in the market, “Unlike many parts of the UK, Scotland has, in recent years, been overlooked from a new-build development perspective, primarily due to the 60-bed limit. The underlying demand from the ageing demographic in Scotland is, however, growing rapidly. There is a current undersupply of 19,793 wetroom beds across Scotland, and projections indicate that this shortage of market-standard provision will only worsen in the coming years.
“This growing deficit underscores the urgent need for strategic planning and investment to ensure that future demand can be met effectively. A large proportion of the existing providers report strong occupancy levels in assets, which may not necessarily be future-proof, highlighting the robust demand trend in the region.
“In many instances, smaller, converted homes are well-placed to cater for their local markets, particularly in areas of lower population density. Based on the undeniable increase in demand and general lack of existing modern wetroom facilities, we believe there is a significant opportunity for both regional and corporate care operators to capitalise on the early mover advantage by investing in new developments across Scotland.
“Additionally, operators have the opportunity to retrofit or reconfigure older stock that may not currently align with the latest market standards, thereby enhancing their competitiveness and future-proofing their homes. With the sector evolving to meet growing demand, strategic investment in high-quality care facilities will not only address existing gaps but also position operators for long-term success in an increasingly competitive market.”
To find out more about the challenges and opportunities within Scotland’s care market, read the report here:
www.christie.com/sectors/care/scottish-healthcare-market-review2026/
This week, Marie Curie ambassador Paul Chuckle MBE completed his ‘Thank you’ tour of the UK to celebrate 40 years of the Great Daffodil Appeal at Land’s End.
Between 3rd-11th March, Paul has been travelling from John O’Groats to Land’s End, stopping to meet Marie Curie supporters, staff and fans with the ‘Daff bike’, a Marie Curie-branded ‘Chuckle bike’.
Along the way, Paul joined charity collections in Glasgow, Bradford, Birmingham, Penarth, Exeter and Plymouth before completing his tour in Land’s End in Cornwall. At his final stop, Paul was met by a local Sea Shanty choir Bryher’s Boys who performed at the iconic landmark.
Paul has raised over £6,000 so far at collections across the UK and through online donations. He is aiming to hit a fundraising target of £40,000 for the charity’s flagship annual appeal by the end of the month.

Paul Chuckle and his brother Barry became official Marie Curie ambassadors in 2016, and Paul has continued to be an active supporter of the charity after experiencing the care and support that Barry received from Marie Curie at the end of his life in 2018.
The Great Daffodil Appeal is Marie Curie’s flagship fundraiser which happens once a year, with 2026 being the 40th anniversary of the appeal. The fundraiser raises much needed funds by encouraging the
public to wear a daffodil pin and donate. The money raised as part of the Great Daffodil Appeal will fund vital and expert care to more people at the end of their life.
Paul Chuckle MBE, Marie Curie ambassador, said: “I want to say a huge thank you to everyone who joined me along the way, sat with me on the ‘Daff bike’ and donated to the Great Daffodil Appeal. Travelling from John O’Groats to Land’s End has been a brilliant experience and I’ve loved meeting the Marie Curie volunteers, supporters and staff who give their time to help more people have the best possible end of life.
“It’s been a wonderful chance for me to give back to Marie Curie after they helped care for my brother Barry at the end of his life in 2018.”
Matthew Reed, Chief Executive Officer at Marie Curie said: “Every three minutes, someone dies without the end of life care they need. The Great Daffodil Appeal gives Marie Curie the chance to provide expert end of life care and support to more people, whatever their illness. Care that protects someone’s dignity – instead of leaving them alone or in avoidable pain.
“A huge thank you to Paul for taking on this mammoth tour of the UK and thank you to our loyal supporters and volunteers for the last 40 years of support for the Great Daffodil Appeal.”


New figures have revealed the number people attending A&E between November and February topped 9 million (9,110 591) this winter for the first time in NHS history – along with almost 130,000 more patients handed over by ambulances compared with winter 3 years ago.
Waiting times for patients this winter were the shortest in 4 years as NHS planning paid off for patients.
The number of patients attending A&E who were admitted, transferred, or discharged within 4 hours of arrival at emergency departments was at its highest rate this winter (73.6%) since 2021/22, when it was 73.8%.
While the number of ambulance call outs this winter were the highest on record, topping 3.2 million (3,223,778), figures show almost 130,000 more ambulances handovers at A&E where the handover time was known this winter (1,640,783) compared with 2 years ago (1,511,758).
Despite high 999 demand, ambulance responded faster to the most serious call outs, including for strokes and heart attacks, than they have for half a decade (2020/21) – with average Cat 2 ambulance waits down to 32:29.
Despite the record winter, the waiting list has continued to fall and decreased to 7.25 million in January 2026, dropping by 43,666 compared to the previous month.
This represents an estimated 6.13 million unique patients. Overall, the waiting list has decreased by more than 370,000 (374,083) since June 2024.
NHS National Medical Director Professor Meghana Pandit said: “The NHS was ready to tackle winter head on this year, which is why despite facing record-breaking demand, staff have delivered the shortest winter waiting times for 4 years – while waiting lists have continued to fall.
“This is proof that the NHS is starting to turn a corner for patients – but we know the job is far from done.
“For too long, too many patients have faced the indignity of being treated in hospital corridors. That’s why we’re taking a zero-tolerance approach – with hospital leaders out on the wards and corridors making sure patients are treated with the dignity they deserve.
“I also want to thank the public for their role in supporting the NHS this winter – these figures show the huge impact of the public getting vital winter jabs.”
Health and Social Care Secretary Wes Streeting said: “After years of rising waiting times, patients are finally starting to see things move in the right direction – with waiting lists at their lowest level for almost 3 years and more people getting treated within 18 weeks.“Despite record demand this winter, A&E and ambulance services improved – meaning patients are getting help faster when they need it most, thanks to the hard work of NHS staff, better planning and modernisation.
“But we won’t take our foot off the gas. We’ll keep cutting waiting times, backing NHS staff and making sure patients get the high-quality care they deserve.”
A Somerset home celebrated the work service of its colleagues combining to an excellent 323 years.
23 colleagues from MHA Torrwood, ranging from 10 years’ service to 29 across various roles were part of the celebrations.
MHA Torrwood provides residential, dementia and nursing care for 82 residents.
The colleagues are listed below
Beverley Davies (11 years), Anca Serediuc (10 years),Tracey Holloway(10 years), Iustina Mihai (10 years), Fiona Lane(10 years), Tom Randall, (25 years), Nicola Dicker(12 years), Joanna Withers(13 years), Rachael Bartlett (17 years),Lee Griffiths (10 years), Aileen Viles (18 years), Rebecca Yates (15 years), Hannah Vilensky (11 years), Louise Tallon (29 years), Sue Root (16 years), Ben Sinclair (12 years), Joan Carthy (10 years), Camelia Dumea (12 years), Lucy England (18 years), Monica Jaskowska (10 years), Katarzyna Kmieciak-
EDGE Services is one of the leading providers of people handling training in the UK today.
EDGE will train you to deliver moving and handling, dementia care, and challenging behaviour courses to your colleagues, providing you with the resources, techniques, and skills to make a real difference to the health and safety of both your colleagues and your clients.
Our courses:

Nowakowska (20 years), Laura Lazar (11 years) and Mark O’Callaghan (13 years).
Bevereley Davies, home manager said: “ Having an experienced workforce goes a long way in providing stability and consistent quality care.
“A stable workforce is always a good sign for a home and it’s definitely something we use when we are doing our show arounds for new residents and their family members.
“We feel it is something that adds a lot of comfort to our residents and their loved ones and it is something we are all very proud of here at MHA Torrwood.
“The home is a truly special place, everyone who knows the home comments on how warm and caring it feels, and together with our residents and their families, there is a real sense that we are one big family.
“I believe that’s why so many of our team members have stayed with us for a long time, and we hope to have plenty more doing the same.”

People Handling and Risk Assessment Key Trainer's certificate (4 consecutive days, includes a written assignment)
Children Handling and Risk Assessment Key Trainer's certificate (4 consecutive days, includes a written assignment)
People Handling and Risk Assessment Key Trainer's certificate Refresher/Update (2 consecutive days)
Children Handling and Risk Assessment Key Trainer's certificate Refresher/Update (2 consecutive days)
Understanding and Managing Behaviour that Challenges Key Trainer's certificate (2 consecutive days)
Dementia Care Key Trainer's certificate (2 consecutive days)
Our Key Trainer's certificate lasts for 2 years. Delegates are then given a 3-month grace period to renew their training though we don’t recommend they deliver any training during this interim period.
EDGE understands that the continued success of the company is down to us consistently providing highquality training that is received well by those attending the event and by those procuring it. We are committed to ensuring this success continues.
There’s a lot that makes EDGE different from your average training provider:
Healthcare Professionals: All EDGE trainers are nurses, occupational therapists or physiotherapists with over ten years’ clinical experience. Fully Accredited: All our’ People/Children Handling and Risk Assessment Key Trainer’s Certificate’ courses are accredited by RoSPA Qualifications to Level 4 or Advanced Level 4. They are recognised for providing continuous professional development by the CPD Certification Service.
Compliance with Professional Training Standards: All EDGE Manual Handling ‘Key Trainer’ events comply with the National Back Exchange Training Standards (2010); The All Wales NHS Manual Handling Training Passport and Information Scheme (2010); and The Scottish Manual Handling Passport Scheme (2014). Invaluable Training Resources: All delegates are given a fully illustrated and comprehensive textbook; professionally printed and produced by EDGE. Plus, proposed documents to assist and support in onward training delivery. These include course agendas, hand-outs, Power-Point slides, filmed practical techniques and tips for staff training and assessing.
Online Resources Library and E-Learning: Our Manual Handling ‘Key Trainer’ training is supported by an extensive, informative online resources library offering use of an exclusive e-learning module plus additional training tips and tools to develop and enhance onward training.
EDGE offers both public courses and in-house courses, the dates for which can be found on our website: https://edgeservices.co.uk
Alternatively, call: 01904 677853 or e-mail: enquiries@edgeservices.co.uk to see how EDGE Services can help you.
A maintenance professional at Manor Park Care Home in Old Malton, part of Sandstone Care Group, has been recognised for his outstanding contribution after being named a Sandstone Star. Marc Richardson, who works as a maintenance operative at the home, received the accolade in recognition of his commitment, reliability and the key role he has played in supporting the home during its construction and opening. The Sandstone Star award recognises exceptional staff members from across Sandstone Care Group’s homes. To be eligible, colleagues must first be named Employee of the Month at their respective home before being considered for the overall accolade. The final decision is made by The Sandstone Care Group directors.
Marc was recognised for his dedication and willingness to ensure the home opened, and now operates, safely and smoothly.
Laura Clegg, registered commissioning manager at Manor Park Care

Home, said: “Marc consistently goes above and beyond to ensure every task is completed to an exceptionally high standard, never giving up even in challenging situations. He has shown outstanding commitment to supporting the whole team, including coming in overnight to assist the night staff with fire alarms and safety tests. His dedication, attention to detail, and willingness to go the extra mile played a vital role in supporting the home to open its doors safely, making him a great asset to Sandstone Care Group.
“Marc has been an incredibly important part of the team as Manor Park has established itself. His positive attitude, practical skills and willingness to help wherever needed make a real difference every day. This recognition is very well deserved.”
Marc said he was delighted to receive the award. He said: “It’s a real honour to be recognised in this way. I enjoy being part of the team at Manor Park and helping to make sure everything runs smoothly for residents and colleagues. It means a lot to know the work I do is appreciated.”

The House of Lords Delegated Powers and Regulatory Reform Committee has published its second report on the Terminally Ill Adults (End of Life) Bill.
The report considers the implications for delegated powers in the Bill following amendments proposed by the Bill’s sponsor in the Lords Lord Falconer of Thoroton.
The report is available online here.
The DPRRC scrutinises proposals in bills to delegate legislative power from Parliament to Ministers or other bodies. Bills will often include clauses delegating the power to make future changes to the law through secondary legislation, limiting the level of scrutiny Parliament can apply to those future changes.
In its reports, the DPRRC draws the attention of the House of Lords to clauses where these delegated legislative powers are proposed and highlights when it believes the proposed delegations to be inappropriate. The Committee does not take a view on the possible merits or disadvantages of any policy or change to the law.

In today’s report the Committee particularly draw the attention of the House to clauses 37 – which deals with substances that could legally be administered to cause death and devices for their administration and clauses 41 and 42 – which provide for the regulation of voluntary assisted dying services in England and Wales.
Proposed delegated powers within these clauses would allow future governments to use regulations to make any provision that could be made by an Act of Parliament without being subject to the Parliamentary scrutiny required of an Act. The Committee says this is ‘highly inappropriate” and the provisions allowing this should be removed from the Bill.
Whilst the report reiterates some concerns made in the Committee’s first report on the bill published in September 2025, the Committee have also welcomed in their new report steps taken by the Sponsor to address other concerns made in the initial report. The Sponsor’s memorandum to the Committee is enclosed in their report as an annex.
John, 91, a resident of Glastonbury Care Home, has dedicated more than 1,200 hours to handcrafting over 300 wooden monkey toys in a heartfelt effort to raise funds for the home and for a local Men’s Shed, where he creates the toys.
John, who moved to Glastonbury Care Home in September 2025, has dedicated his time and talent to whittling the charming wooden monkeys at Men’s Shed in Walton, a dedicated community workshop helping people who may feel isolated or lonely.
Attending twice a week, every Tuesday and Thursday, John spends around four hours carefully crafting each monkey. With over 300 completed so far, that equates to more than 1,200 hours of woodworking, the equivalent of 100 full days devoted to his craft.
John is transported to and from Men’s Shed by his son-in-law each week, enabling him to continue a hobby he has enjoyed for more than three years.
John said: “I really enjoy going to Men’s Shed, it keeps my mind and hands busy and I love the banter. I go every Tuesday and Thursday, and the home always makes sure I have a big, packed lunch to take with me. The team at Glastonbury Care Home are fantastic, so kind and caring. I can’t fault them. I’ve been going to the Men’s Shed for more than three years now and I absolutely love it!”

John sells his wooden monkey toys for £2 each at Glastonbury Care Home, he also sells them at Men’s Shed, and donates some to local charity shops, ensuring his creations spread smiles far and wide while supporting good causes.
Before retiring, John enjoyed a varied career that saw him move around the country, working within the Police Force, the Air Force, and later in accountancy. John has three children, seven grandchildren, and four great-grandchildren who regularly visit him at Glastonbury Care Home.
This remarkable effort highlights not only John’s dedication and creativity, but also the vibrant community spirit at Glastonbury Care Home, where residents are encouraged to continue pursuing the hobbies they love.
Nisha Binumon, Glastonbury Care Home Manager said: "It’s wonderful having John with us. He’s kind, caring, and always checking if any of his monkeys have sold. He often gives them to carers with children because he wants to bring joy to everyone. We make sure he gets to Men’s Shed and never forget his big, packed lunch. We always look forward to his return, and the bag of monkeys we display at the front desk for people to buy. He’s truly a joy to care for."
Care Show London 2026 running on 29-30 April at Excel London, will be opening its doors for the third consecutive year to the whole care community. Matthew Moore, Show Manager highlights what is on offer at Care Show London as well as key speakers and sessions to look out for.
KEY THEMES AND GOALS FOR CARE SHOW LONDON THIS YEAR
Care Show London is the meeting place for the social care community, united by a shared commitment to delivering the highest standards of care. The show provides a platform to learn best practice, explore innovative products and services, and develop practical skills to support day-to-day work.
The focus this year is on helping you confidently navigate the future of care. Through expert-led sessions and sector insight, you’ll gain the clarity, support, and direction needed to prepare for what’s next, with key themes including workforce, regulation, policy, AI and technology, business sustainability, palliative care, and more.
CONFERENCE PROGRAMME
Care Show London conference programme covers key challenges within the sector, matching these with established care professionals who are able to provide solutions to these. With over 180 experts in the sector speaking at the show, we'll cover everything from strategic business support to specialised dementia care, to sustainability wins and so much more!
With seven dedicated theatres hosting sessions across the two days and over 60 hours of world-class education, attending this event will provide you with the tools and solutions to improve the quality of care you provide.
Must see sessions:
• Keynote Theatre – CQC update: our journey, priorities, and what’s next for adult social care
People & Business Theatre - Winning self-funded clients through strategic marketing and sales
Technology Theatre - What's happening internationally? How social

care across the globe is using technology to improve outcomes
Catering, Hydration and Nutrition Theatre - Cognition-supporting Vitamin B12 needs our attention: how to incorporate more into meals with ease
IHSCM Leadership in Tough Times Theatre - How to build an effective team
Care Providers’ Voice Masterclasses - What will the care workforce look like in 2030?
The Outstanding Society Learning Lounge - Safe medicines management: complex medication and reporting
Key speakers: Chris Badger, Chief Inspector of Adult Social Care & Integrated Care, CQC
Isaac Samuels OBE, Co-Chair, NCAG & TLAP
Fran Vandelli, Dementia Lead, Bupa Care UK
Aneurin Brown, CEO, Hallmark Luxury Care Homes
Emma Jane Tinkler, Programme Manager, HC-One
Kevin Humphrys, CEO, Oakland Care Group
• Michelle Corrigan, Programme Director, Digital Care Hub
Clare Jefferies, Business Director, Home Instead Wimbledon & Kingston
Giuseppe Di Martino, Learning Disability and Autism Commissioner, Slough Borough Council
Katy Hague, Chief of Staff, Crystal Care Homes
Lucy Campbell, CEO, Right at Home UK
Sarah Sabater, CEO, CareYourWay
Charles Taylor, Owner, Taylor & Taylor Care Group
Alyson Vale, Business & Operations Director, Abbotsford Care Ltd TOP SUPPLIERS
Alongside the dedicated conference programme, Care Show London hosts over 200 top suppliers from the sector, offering a wide range of products and solutions to help improve your business. From catering suppliers to software providers, you’re sure to find an exhibitor with what you’re looking for.
With so much happening at the show, don’t forget to make time to connect with sector peers. With over 3,750 care professionals expected at Care Show London, it’s a great opportunity to meet like-minded professionals who understand your challenges and desire to build strong relationships.
Care Show London 2026 is your opportunity to confidently navigate the future of social care. With expert-led sessions, innovative suppliers, and thousands of professionals under one roof, the show provides the knowledge, connections, and tools you need to stay ahead and succeed in a changing landscape.
Register now to join your community for two days of learning, networking and inspiration. Visit the Care Show London website or click visit https://forms.reg.buzz/care-show-london-2026/carer To view the conference programme, visit: https://www.careshowlondon.co.uk/thecarer26

Construction is continuing on two flagship Extra Care developments in South Tyneside.
Together, the schemes will provide more than 200 affordable, modern homes designed for older people and those with additional support needs.
The developments are being delivered in partnership between South Tyneside Council and Karbon Homes to help address the need for specialist accommodation in the borough.
Construction of Griffin Court in Hebburn town centre is on schedule to complete this Autumn, with the roof now in place and the building becoming watertight ahead of the next phase of internal and external works starting.
Once finished, Griffin Court will offer 95 high quality apartments, including 17 specialist homes designed for people living with dementia, alongside communal lounges, activity spaces and a bistro café open to the public –all designed to support independence, reduce isolation and create a vibrant community hub.

Work is also progressing well on the second Extra Care development at Benton Road, South Shields following its start on site late last year.
Over the winter months, earthworks and stone pile installation were completed, followed by foundations and sub structure blockwork. Installation of the structural steel frame for the single-storey sections of the building is almost complete.
This second scheme will provide 124 modern apartments across four storeys and set around a central
courtyard. 25 of the homes are designed specifically for people with dementia.
Both developments are being delivered by Robertson Construction North East.
Cllr Ruth Berkley, Lead Member for Adults, Health and Independence at South Tyneside Council, said: “It’s fantastic to see such strong progress on these two major developments.
“Extra Care plays a vital role in our Adult Social Care and Commissioning strategy, reducing reliance on residential care by giving people the support they need to retain their independence, stay connected to their communities and enjoy a better quality of life.
“These schemes will make a real difference to local people, offering modern, affordable homes alongside facilities that promote wellbeing, social connection and dignity.”Both schemes are available to those over the age of 18 with additional needs for independent living.
Jon McDonald, Head of Supported Housing at Karbon Homes, said: “It’s great to see the Hebburn development taking shape, a scheme right at the heart of the community that will help local residents with additional support needs to live independently for as long as possible.
“Supported housing schemes like these are a vital part of the wider housing system, and the strong partnership we’ve formed with South Tyneside Council has enabled us to understand the needs of the local area and delivery a scheme that fills that gap.
“I’m looking forward to seeing the scheme complete towards the end of the year.”
Two Milewood services in Whitby have undergone significant refurbishment following a £150,000 investment aimed at improving living spaces for the people they support.
The investment has been made across Caedmon House and Hudson House, creating calmer, more modern environments designed to help individuals live comfortably and continue developing their independence.
The refurbishment programme has included improvements to both private bedrooms and communal areas, with the people supported by the services playing an active role in shaping the changes. Individuals helped select colour schemes and contributed ideas for the layout and design of shared spaces, creating environments that reflect their preferences and needs.
A new snug area and an additional living and meeting space have also been created, alongside a fully refurbished dining room.
Sandra Rolfe, home manager at the Whitby services, said: “We’ve

created really nice calm spaces for the individuals we support to live, grow and thrive in.
“The refurbishment means we can continue improving the care and support that people receive. Creating the right environment has a huge impact on wellbeing and independence.”
Sam Hunt, regional manager at Milewood, added: “It’s been great having the people we support involved in the refurbishment. People have chosen colour schemes for their bedrooms and helped shape the communal spaces which has made everything feel fresh, modern and much more usable.”
Martyn Heginbotham, chief executive of Milewood, said: “Investing in our services is essential to ensuring the people we support have the best possible environment to live in. The improvements made at our Whitby homes reflect our commitment to creating high-quality spaces where individuals feel comfortable, supported and able to thrive.”
Three Bridges Nursing Home in Warrington is celebrating a remarkable milestone as resident Irene “Rene” Chorley marks her 102nd birthday, continuing to inspire those around her with her sharp wit, resilience and refreshing approach to life.
Born on 10th March 1924 in Hollywood, South Birmingham, Rene looks back on her childhood as “wonderful”, filled with laughter, family adventures and life alongside her two brothers and two sisters. Among her fondest memories are family outings, which often included jumping out to push the car up hills when it stalled. Now at 102, Rene credits her long life to a simple and balanced approach: “I have always looked after myself, and I eat well, as many fruits and vegetables as possible… and I apply moisturiser to my face every day.”
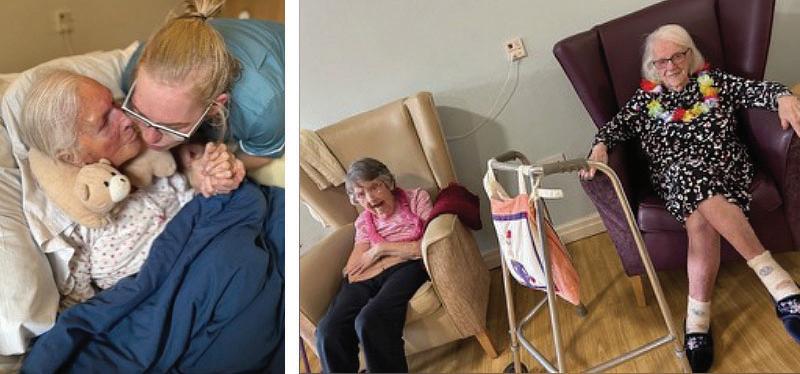
Her advice to younger generations is just as straightforward: “Learn and have fun in equal measure. And
be kind. It is very important to be kind to people.”
Reflecting on her younger years, she adds: “I would enjoy myself more and work a little less.”
To mark Rene’s birthday, the team at Three Bridges hosted a birthday celebration fit for a queen, complete with live music from a saxophonist and plenty of festivities for residents, friends and colleagues to enjoy together.
Whitney Sampson, Home Manager at Three Bridges Nursing Home, said: “Rene is as sharp as a pin. Her dry wit is legendary, and her memory is incredible. Residents and colleagues adore her. She’s feisty, caring and always makes us laugh.”
Whitney added, “Residents like Rene bring a lifetime of knowledge and experience. Take the time to listen to them, and you’ll be amazed at what you can learn.”
New friendships are blossoming at Sandwood care home in Sherwood, where babies, toddlers and older residents are coming together each week for a heart-warming intergenerational playgroup.
Launched in February, Sandwood Seedlings welcomes young families into the home’s bright, open-plan lounge and dining space for songs, arts and crafts, themed activities and plenty of playtime alongside Sandwood’s residents.
For a small £1 donation, parents can enjoy a relaxed and welcoming session where their children share stories, toys and laughter with their older friends. Cerron, who attends with her young child, said: “We love coming to playgroup – it’s the highlight of our week.”
Another parent, Ingrid, added: “It’s lovely to mix with other parents and for the children to spend time with the residents.”
Sandwood’s residents eagerly look forward to Thursdays just as much.
“I think we’re lucky to have it,” said resident Connie.

Each week at Sandwood Seedlings features a different theme – from dinosaurs to under-the-sea adventures, Chinese New Year celebrations and a World Book Day Mad Hatter’s tea party – with related toys and
storybooks laid out to encourage shared engagement and memory-making.
The playgroup was created by Sandwood’s activities coordinator, Mel Spouge, who joined the home’s staff team in September 2025 and has already introduced a packed programme of entertainment, outings, and collaborations with the local community.
“Creating an intergenerational playgroup was really a no-brainer,” Mel said.
“My predecessor had run a stay and play session for children in the past, so I knew there would be interest in the local area.
“Our residents always enjoy visits from local schools and nurseries, so this playgroup gives them the chance to interact with young people more often.
“For those residents without regular visits from their grandchildren, and for children who don’t see their grandparents much, it also provides a family-style experience that we know can provide comfort and emotional support both in young and old age.
Mel continued, “We’ve done a little publicity, but word of mouth has been the best promotion. Parents can see how much their children enjoy it – and some have brought friends along the following week.”
Researchers from the EMPOWER Dementia Network+ recently held an event in Parliament to launch a new co-produced policy briefing addressing inequalities in dementia care for adults needing greater support.
The network is co-led by Professor Catherine Evans and Professor Emma Wolverson and funded by the ESRC, NIHR and Alzheimer’s Society, and is based at the Cicely Saunders Institute, part of the Faculty of Nursing, Midwifery and Palliative Care at King’s and is co-led with the University of West London.
The briefing has five core calls to action to reduce inequalities in dementia care:
1. Establish a National Dementia Strategy with a clear ‘home’ for dementia in the health system
2. Build a dementia-aware society
3. Provide better care to people who live alone
4. Promote ‘relationship-centred’ care
5. Address the economic case to support integrated and equitable dementia care.
By 2040, it is estimated that 1.4m people in the UK will live with dementia; people living with dementia experience significant inequalities in health and social care provision.
Furthermore, access to dementia care for those who need it is not equally distributed or accessible for those from ethnically diverse communities, economically deprived areas, those living alone or with severe dementia and with multiple long-term conditions.
The policy briefing launched at Parliament was co-created with over 170 people from across the UK affected by dementia.
The launch was attended by people across local and national government, as well as representatives from the Department of Health and Social Care and colleagues from across community organisations and
charities from up and down the UK.
Professor Catherine Evans, Interim Director of the Cicely Saunders Institute and Professor of Palliative Care, said, “The network has created a shared platform for us all to work together to realise much needed change in the care and support for people with dementia and their families. As a network we work to connect diverse voices to amplify the impact of our shared vision and create the foundations for meaningful change. Our five calls for action address the very worst inequalities in dementia care for people needing greater support and their families.”

Jim Dickson MP also said on the day, “What EMPOWER’s work reminds us is that improving dementia care is not only about clinical pathways or organisational structures. It is about people – their dignity, their connections, and their ability to live well, whatever the stage of their condition. Reducing inequalities is essential to achieve this aim for all.
“I want to thank the EMPOWER Dementia Network and everyone who contributed their experience, evidence and insight to this brief. It offers a clear and constructive path forward. I hope colleagues across Parliament – and across the health and care system – will take this work to heart and help turn its recommendations into action.”
Brownscombe Care Residences, part of CHD Living, has once again been recognised in the Knight Frank Luxury Care Home Guide 2026, marking the fifth consecutive year the Haslemere home has been featured. The annual guide highlights care homes across the UK that are recognised for exceptional environments, high quality provision and an outstanding resident experience. Brownscombe Care Residences’ continued inclusion reflects its commitment to delivering warm, person centred residential, nursing and palliative care, alongside a setting designed for comfort, dignity and reassurance.
Shaleeza Hasham, Commercial Director at CHD Living, said: “Being named in the Knight Frank Luxury Care Home Guide for a fifth consecutive year is a significant achievement, and it speaks volumes about the consistency and quality of care delivered at Brownscombe Care Residences. We never take recognition like this for granted, because behind it is the daily commitment of our team members and the trust families place in us.
A 100-year-old has returned to her old school – for the first time since the outbreak of WWII.

Maureen Smith visited Tolworth Girls’ School & Sixth Form 86 years after her education was abruptly halted in September 1939. She was 14 at the time and went on to play an important role in the war effort.
The centenarian shared her memories of school life and WWII with staff and Year 12 students during the visit on 11 March. She was also given a tour of the school during her trip down memory lane, and looked at vintage photos, where she spotted her headteacher.
The visit was arranged by staff at Royal Star & Garter in Surbiton, where Maureen now lives. She was accompanied by her niece Jacqui, also an ex-Tolworth Girls’ School pupil who attended in the 1960s.
“Brownscombe Care Residences is a beautiful setting, but what truly defines it is the feeling inside, a home where people are known, respected and supported with real dignity. That is what ‘luxury’ should mean in care, and it is exactly what Brownscombe Care Residences strives to deliver every single day.”

Maureen said: “I remember feeling quite relieved when I discovered I didn’t have to return to school in 1939. It’s great to be back all these years later. Returning brought back so many happy memories, and I thoroughly enjoyed chatting with the current pupils and teachers. Thank you to staff at Royal Star & Garter and Tolworth Girls’ School for making this wonderful visit happen.”
Niece Jacqui added: “You could see how much my aunt enjoyed her time back at Tolworth Girls’ School, and so did I! I’m grateful to Royal Star & Garter and Tolworth Girls’ School for working together and making it a very special day for both of us.”
Sam Dixon is Subject Lead for History at the school. He said: “It has been a privilege to welcome Maureen back to Tolworth Girls’ School for the first time since 1939. To return more than eight decades after the outbreak of war is truly extraordinary. Our pupils and staff were captivated as she shared vivid memories of her school days and her experiences during wartime Britain. Her visit has brought history to life in the most powerful way, and we would very much love to welcome her back again soon.”
Yasmin Rogers, Deputy Home Manager at Royal Star & Garter in Surbiton, said: “Being able to reconnect Maureen to such an important place from her past is truly special and a privilege for everyone involved. It is heartwarming to help create such a meaningful experience, reflecting our commitment to person-centred care and to going above and beyond for our residents.”
Ghyll Royd Care Home has announced the appointment of Robee Gelido as its new Home Manager.
Robee’s vision for Ghyll Royd is to further enhance the home’s established “residentsfirst” philosophy by deepening its roots within the local community. While Ghyll Royd has always been a warm and welcoming hub, Robee aims to expand these connections even further into the heart of Guiseley and Yeadon. By opening doors to local groups and nurturing ties with neighbours, he intends to create even more meaningful opportunities for residents to engage with the local area. This includes enriching the home’s vibrant schedule with new collaborative activities, guest talks, and social links with visiting volunteers, ensuring residents continue to feel active, valued, and connected.
Robee’s journey is a shining example of the professional growth nurtured within the Spellman Care family. Joining the team in June 2022 from the Philippines, Robee arrived as part of the group’s highly successful international recruitment programme. Starting as a Senior Care Assistant progressing to Registered Nurse and subsequently Unit Manager of Beech, the home’s specialist dementia community.
“I am so honoured to lead the incredible team here at Ghyll Royd,” says Robee Gelido,

Home Manager. “My goal is to be a reliable, steady hand for our residents and their families. At Ghyll Royd, our residents have always come first, and I am committed to upholding that standard every single day. I believe in maintaining a service that is modern and proactive, but most importantly, transparent. I am incredibly keen to build even stronger connections within our local community so that everyone—whether they are a current resident or a neighbour—feels supported and at home here.”
“As a family-run company, we are so proud of Robee’s dedication,” says Steven Spellman, Director of Spellman Care. “Our recruitment initiative was designed to find the very best talent and provide the support needed to flourish. Robee’s journey from Senior Carer to Home Manager is a testament to how this programme allows staff to develop their professional training and build a lasting career with us, all while maintaining the highest standard of care for our residents.”
To meet the community personally, Robee will host his first ‘Resident and Relative’ meeting this Thursday, 19th March. With an ‘Open Door Policy,’ he also welcomes any members of the Ghyll Royd family to come forward at any time with ideas, questions, or just a friendly hello.
Ready-to-use activity products designed to support meaningful engagement in everyday life.
Everything you need to inspire connection, stimulation and wellbeing CREATIVE & SENSORY ACTIVITIES
Art, craft and sensory products designed to engage, calm and inspire. COGNITIVE & REMINISCENCE
Memory-based activities and conversation starters that encourage connection. GAMES & GROUP ACTIVITIES
Inclusive games and group activities suitable for a wide range of abilities. ONE-TO-ONE & MEANINGFUL ENGAGEMENT
Personalised activity products that support wellbeing and individual needs. Thoughtfully selected to be accessible, inclusive and easy to use in busy care environments.
Explore our full activity range - www.bluerain.store where you will also find our informative blogs and contact form as friendly advice is always on hand.
See thee advert on page 4.
HipSaver Soft Hip Protectors protect the elderly and disabled people from fallrelated hip fractures.
Designed to protect elderly people from fall related hip fractures, HipSavers are a leading brand of soft hip protectors. Used in the NHS since 2002, HipSaver Soft Hip Protectors are user friendly, affordable and cost-effective personal protective garments.
Soft, comfortable, effective and compatible with incontinence protection, HipSaver Soft Hip Protectors are perfect for use in care homes and by elderly people living independently.
HipSavers should be worn day and night for 24 hour protection and especially during physical and recreational activities, when accidental falls, slips and trips can lead to hip fractures.
Available as comfortable underwear or long casual pants in several sizes for men and women, HipSavers feature soft protective airPads permanently sewn into the garments over the hip areas prone to injuries and fractures. HipSaver TailBone models have an
additional protective airPad over the coccyx on lower back for protection during swaying, accidental knocks, bumps and backward falling.
Machine washable at high temperature and tumble drier friendly, HipSavers are practical, hygienic and durable.
HipSaver Soft Hip Protectors - affordable protective garments for the elderly and disabled people! For more information, contact Win Health Medical Ltd - 01835 864866 - www.win-health.com
See the advert on page 3 for further products.
MAG Laundry
Equipment is a multiaward-winning supplier of commercial washing machines & tumble dryers that supports over 10,000 care homes across the UK.
Clean laundry and bedding is critical for care homes, hospices, nursing homes, hospitals and other healthcare organisations. With a nationwide fleet of accredited engineers MAG Laundry Equipment has successfully assisted over ten thousand care homes with their products, services, information and support.
affordable machines on the market. Care homes have peace-of-mind that their laundry machines can quickly be maintained and repaired as MAG Laundry Equipment supply, install and service equipment across England, Scotland and Wales.
If you are looking for high quality wash results that remove stubborn stains then speak with MAG for their recommendations. Complete thermal disinfection is a standard feature on their washing machines for nursing homes.
MAG’s product range includes commercial washing machines, tumble dryers, ironers, presses and detergents. For 100 years, since 1922, MAG’s products have been developed and improved to become some of the most reliable, energy-efficient and
To find out more about how MAG can support your care home telephone 01353 883025 or visit www.maglaundryequipment.co.uk. See the advert onthe back cover of this issue.

Repose Furniture is one of the UK’s leading manufacturers of bespoke seating solutions, with a reputation built on craftsmanship, innovation, and a strong commitment to improving the quality of life for its customers. Established in 1999 and based in the West Midlands, the company has grown from a small family business into a trusted supplier to both the domestic and healthcare markets. Every chair produced by Repose is handmade in the UK, with an emphasis on quality, durability, and comfort, ensuring that each product meets the specific needs of its user. Whether for home use or demanding healthcare environments, Repose combines skilled upholstery techniques with modern engineering to create chairs that provide postural support, pressure management, and ease of use. Their wide product portfolio includes rise and recline chairs, hospital and care home seating, bariatric solutions, and specialist products designed to address particular medical and lifestyle needs. An essential element of their offering is flexibility: customers can choose from a range of back styles, seat cushions, mechanisms, and fabrics, allowing each chair to be tailored to the individual. Interchangeable parts mean that a chair can adapt as a user’s requirements change, extending the product’s longevity and ensuring value for money. The healthcare sector is a particular area of expertise for Repose. They strive to design chairs that balance comfort with clinical functionality. Features such as tilt-in-space mechanisms, adjustable cushioning, and pressure relief options make their healthcare seating particularly suited to long-term use in hospitals, hospices, and


Addressing postural care should be a pre-requisite of occupational therapy yet is a postcode lottery, says RCOT(1).
The problem is further complicated by lack of awareness among professionals, the breadth of issues posture management affects resulting in multiple disciplines being involved, and the diversity of equipment required to achieve round-the-clock support and correction and thus funding streams.
AAT is aiming to simplify the process.
Its Grande vacuum posture cushion delivers almost all sedentary and supine positioning support required day or night.

So just one health professional need prescribe.
Caregivers can precisely mould and fix the mattress-sized cushion to correctly support whether sitting or lying in the day or sleeping at night. Grande can be used as a mattress for resting, sleeping or physiotherapy, or folded to create a seat- standalone, on a chair, on a sofa.
Its construction also means it is tactile and easily transmits sound waves, so it can double as a conductor for sensory stimulation.
The technology Grande uses is based round the principles of a bean bag, giving the precise shaping inherent in the concept. The beans contour precisely to the required body shape. By attaching a pump, the air between the beans is extracted, fixing that shape
with the preferred degree of firmness. The shaping can be as detailed as required, providing correct stabilisation with minimal pressure and even allowing for pommels, wedges, hollows for feeding tubes. There is no need for restraint, even during dystonic episodes or hyperactivity.
Frequent re-plumping/ positioning of conventional cushion-type posture systems becomes a thing of the past.
To re-shape, simply allow air back into the Grande and mould as necessary, be it a simple adjustment for body position and comfort or a complete reconfiguration.
“The role postural care plays in the health and wellbeing of disabled people and their carers is acknowledged, but the way our health service is structured, delivery is fragmented. Yet addressing it would have a huge impact not only on the people who need it, but on the demand for associated NHS services,” says Peter Wingrave, AAT Director.
“If just one healthcare professional thinks outside the box and looks at something like Grande, that answers the specific issue they have for a client but simultaneously could answer other issues for that client, surely it must be considered?”
More details about Grande and its role in 24-hour postural management can be found @ www.aatgb.com/grande/.

care homes. The company’s bariatric range demonstrates the same careful attention to detail, offering robust yet comfortable solutions for larger users.
While customisation is the centre of the Repose offering, they also recognise the urgency often faced in healthcare settings. To address this, Repose have developed their Healthcare Express Chairs, designed to deliver high-quality healthcare seating at speed. The models in this range can be despatched within just five working days. The Multi Bari Express and bestselling Boston Express, for example, are available on this five-day lead time, offering
continues to be a trusted partner in multiple sectors throughout the country and beyond.
In combining bespoke design with reliable express options, Repose Furniture stands out as a manufacturer that truly understands the diverse needs of its customers. For over 25 years, it has delivered not just chairs, but comfort, dignity and independence
By Charlotte McKay, Head Chef at St Quentin Care Homes

In a care home, catering can be the difference between mealtimes that are anticipated with pleasure and those that are simply endured. Care itself is rightly personalised, tailored to the needs and preferences of each resident. The same principle should apply to the food they eat. Residents and their families are entitled to expect meals which reflect dietary needs, medical conditions, and personal tastes. But delivering that level of personalisation at scale, within budget, is no small task.
The Healthcare Management Trust acquired St Quentin Care Homes almost a year ago and has made significant improvements in care delivery, infrastructure, and leadership. Catering was a big area of focus and has brought tangible results: residents returning for second helpings, heartfelt thanks from families, and a noticeable reduction in food waste. These results haven’t happened by chance; they are the outcome of deliberate choices in how we source ingredients, design menus, and create the overall dining experience.
The value of using fresh ingredients over pre-packaged or heavily pro-
cessed alternatives cannot be overstated. Fresh produce boosts nutritional quality, enhances flavour, and increases the likelihood that residents will eat and enjoy their meals.
Variety is equally important. A repetitive or bland menu fails to tempt people to the dining room. Similarly, introducing a rotating weekly menu with diverse flavours and textures, including vegetarian and vegan options, will create something for everyone, which is especially important where care homes support residents of varying ages and cultural backgrounds.
Style should never overtake substance, but presentation matters and plays a vital role in whether a meal is eaten. An unappealing plate can lead to food being left untouched, no matter how nutritious it is.
Small touches make a big difference. Balancing colours on the plate, arranging food attractively, and serving it on crockery that complements the meal will encourage meals to be finished. Even something as simple as offering a platter of sandwiches with varied fillings, so residents first see vibrant colours rather than just bread, can boost appetite and engagement.
Many care home residents are unable to visit restaurants, and for them, mealtimes are often the closest equivalent to dining out. Recreating elements of that experience can lift the mood and turn a necessary routine into a highlight of the day.
Printed menus with clear, attractive typography help residents feel they have real choice and control. For some, reading a menu may even stir fond memories of past outings and family meals. This small detail rein-
forces the dignity and pleasure of the dining experience.
Sharing food is a social occasion. In care homes, shared meals can foster community spirit, reduce loneliness, and spark conversation. Making mealtimes engaging and enjoyable benefits both emotional wellbeing and nutritional intake.
This means paying attention to more than just the food. Lighting, music, table layout, and staff interaction all contribute to the atmosphere. A team that works seamlessly from kitchen to dining room by greeting residents warmly, knowing their preferences, and encouraging participation can transform mealtime into a joyful daily event.
Great catering doesn’t happen in isolation. It relies on strong collaboration between chefs, care staff, activities teams, administrators, residents, and families. Open communication ensures dietary needs are met, allergies are avoided, and preferences are respected.
When everyone takes shared responsibility, residents benefit from meals that are not only safe and nourishing, but also deeply satisfying. The catering team gains valuable insight from care staff who know residents well, while residents themselves feel heard and valued.
Ultimately, catering in a care home is about far more than providing three meals a day. It’s about respecting individuality, supporting health, and creating moments of joy. When meals are thoughtfully planned, beautifully presented, and shared in a warm environment, they nourish the body and the mind.

Harrison Carr is a national provider of commercial catering equipment, design, installation, and fabrication services and HVAC. Based in the Midlands, we support care homes, local authorities, charities, and specialist care providers with both day-today operational requirements and larger project-based developments.
A key advantage of working with us is our independence. We are not tied to any single manufacturer, enabling us to source the most suitable, reliable, and cost-effective equipment for each care environment. This ensures solutions that prioritise safety, energy efficiency, long-term value, and consistent performance.
Our team includes experienced designers, project managers, ventilation specialists, installation engineers, and in-house fabrication experts
all working under one roof. This ensures we can deliver a genuine endto-end service: from concept and planning through to supply, installation, and ongoing support.
CATERING EQUIPMENT SUPPLY & TRAINING
• Access to all major catering equipment brands
• Energy-efficient, sustainability-focused solutions compliant with caresector standards
• Fast delivery from our own on-site stock
• Competitive pricing and comparison quotes to support budget decisions
FULL KITCHEN DESIGN & INSTALLATION
• Complete kitchen and servery redesigns
• Workflow optimisation to support safe, efficient meal production
• CAD layouts and 3D visuals
• Compliance-led ventilation and extraction solutions
BESPOKE FABRICATION
• Custom counters, serveries, prep areas, and storage
• Bespoke servery and hydration stations for care settings REACTIVE & PLANNED SUPPORT
• 24/7 support with rapid turnaround for urgent equipment needs
• Standby and loan equipment for emergencies
• Assistance with refurbishments and operational upgrades
CAFÉ, SOCIAL & RESIDENT-FACING SPACES
• Coffee areas for staff and visitors
• Hydration and snack counters
• Modular and mobile units suitable for multi-use care environments Our approach is always centred around understanding each site’s workflow, resident needs, staffing pressures, and long-term operational goals ensuring the solutions we deliver enhance quality of service, safety, and overall dining experience.
Visit our website www.harrison-carr.co.uk

Sustainability and efficiency are top priorities for UK healthcare providers. With the government’s Net Zero 2050 target and NHS contracts requiring Carbon Reduction Plans that include Scope 3 emissions, kitchens must reduce food and plastic waste while controlling costs and protecting service users. It’s a challenging balancing act made much easier with the right tools. The Speedwrap Pro is the perfect example of a tool that delivers small, practical improvements that add up to major gains in productivity, safety, and sustainability.
It uses a patented safety blade that only unsheathes once the lid is pressed, reducing accidental cuts and lost time injuries. BioCote® antimicrobial protection inhibits harmful microbes, simplifying hygiene routines. And its intuitive design enables staff of all abilities to work efficiently, reducing food waste and ensuring proper storage and wrapping practices.
Hospitals like Stepping Hill in Stockport have already enjoyed all of these benefits, as well as the benefits of Ecocling - a PVC-free, recyclable film

exclusively compatible with Speedwrap Pro. It allows food waste and cling film to be separated for recycling; with food helping to power the national grid, and film being converted to refuse-derived fuel.
Erica Bell from Stepping Hill says: “As a trust, we love that Ecocling is recycle-ready and works with our food waste recycling process. The dispensers and refill rolls are modern, easy to clean, and safer to use. They make a real difference to our day-to-day operations."
Speedwrap Pro’s new refill rolls for cling film, foil, and parchment are plastic-free, replacing old adapters with cardboard cores. One catering service saved over 27,000 plastic adapters annually, cutting 178kg of plastic and enough CO2 to charge 1.2 million smartphones.
For healthcare kitchens, Speedwrap Pro is more than a dispenser – it’s a vital tool that cuts waste, improves staff safety, and reduces costs, all while maintaining the quality and hygiene standards critical to patient care.
Learn more at www.prowrap.co.uk or email sales@wrapex.co.uk
Mobile Kitchens Ltd specialises in the hire or sale of temporary catering facilities and foodservice equipment.
Ideal for events or to provide temporary catering facilities during your kitchen refurbishment, our versatile units and equipment offer an efficient and economic solution to the caterers’ needs.
Production Kitchens, Preparation Kitchens, Ware-washing Units, Dry Store Units, Cold Rooms and Restaurant Units are available as individual units in their own right or they can be linked together on site to form a complete complex. Alternatively, we can offer modular, open-plan facilities, usually for larger, longer-term hires.
We offer a free design service, and project management from concept through to delivery and installation on site, plus full technical support throughout the hire period.

We have many tried and tested design layouts and would be pleased to put forward our recommendations for your project.
So if you’re planning a refurbishment or need to cater for an event then why not give us a call and we’ll be happy to provide advice and put forward a competitive proposal.
For further information or to arrange a site visit, email: sales@mk-hire.co.uk or call us on 0345 812 0800, or visit our website: www.mk-hire.co.uk

Disease-related malnutrition remains one of the most persistent challenges in UK residential and nursing care. It affects millions, increases vulnerability to illness, slows recovery, drives hospital admissions, and places strain on already stretched care teams. Yet despite the scale of the problem, the tools available to homes have not kept pace with the needs of increasingly complex residents.
Hiquid Food, a Norwegian medical nutrition company, is entering the UK market with a clear mission: to make effective nutritional support simpler, more acceptable for residents, and easier for staff to deliver.
Simple, seamless meal enrichment
Many residents struggle to consume enough calories and protein, even with carefully prepared meals.
Hiquid Food’s freeze-dried powders, made from organic whole foods, allow caregivers to enrich everyday dishes like porridge, soups, puddings, purees, and drinks. This discreet approach reduces refusals and preserves dignity, helping residents receive the nutrition they need through meals they already enjoy.
ORAL NUTRITIONAL SUPPLEMENTS WITH HIGH ACCEPTANCE
For individuals at greater nutritional risk, Hiquid Food offers compact, nutrient-dense oral nutritional supplements designed for those with low appetite or increased medical demands. They are easy to consume, well tolerated, and provide balanced support in small volumes.
WHOLE FOOD GASTROSTOMY NUTRITION
For residents requiring enteral feeding, Hiquid Food’s whole-food gastrostomy products offer a

gentle, reliable option created with a focus on tolerance, safety, and long-term stability.
Better outcomes and operational efficiency
Care providers face rising acuity and workforce pressure. Hiquid Food products reduce complexity through easy mixing, no additives, and no large volumes while supporting improved resident strength, immunity, and recovery. Better nutritional status means improved wellbeing and lower overall care costs. With long shelf-life, low weight, and high versatility, the products are also environmentally responsible and easily integrated into a wide variety of meals.
As Hiquid Food launches in the UK through Food Untethered, they look forward to working closely with care homes, clinicians, and NHS commissioners to strengthen nutritional care in a practical, residentcentred way.
For more
information: contact@fooduntethered.com
See the advert below for further information.


Effective hygiene and odour management forms the cornerstone of quality care in residential and nursing home settings. Beyond mere cleanliness, these practices directly impact resident dignity, health outcomes, and the overall therapeutic environment that supports recovery and wellbeing.
THE FOUNDATION OF DIGNIFIED CARE
Personal hygiene represents far more than basic cleanliness—it embodies respect for the individual and recognition of their inherent worth. When residents feel clean and comfortable, their self-esteem improves, social interactions flourish, and psychological wellbeing strengthens. Conversely, poor hygiene practices can lead to social isolation, depression, and a profound loss of personal dignity.
HEALTH AND SAFETY IMPERATIVES
Proper hygiene protocols serve as the first line of defence against healthcare-associated infections. In residential settings where vulnerable populations live in close proximity, maintaining rigorous standards becomes critical for preventing cross-contamination and protecting community health.
Poor odour control often signals underlying health issues requiring immediate attention. Persistent odours may indicate skin breakdown, urinary tract infections, or inadequate wound care management. Staff trained to recognise these warning signs can intervene early, preventing minor concerns from escalating into serious medical complications.
Regular hygiene assessments should form part of comprehensive care planning, with individualised approaches reflecting each resident's preferences, cultural background, and physical capabilities.
BEST PRACTICE FRAMEWORK
Person-Centred Approach: Every hygiene intervention should begin with respectful communication. Explain procedures clearly, seek consent where possible, and honour personal preferences regarding timing, prod-
ucts, and assistance levels. This collaborative approach maintains autonomy whilst ensuring necessary care delivery.
Environmental Management: Maintain optimal room ventilation, use appropriate air fresheners sparingly, and address sources of odour promptly rather than masking them. Regular deep cleaning schedules, combined with immediate response to accidents, create pleasant living environments for all residents.
Product Selection: Choose gentle, pH-balanced cleansing products suitable for sensitive or compromised skin. Avoid harsh chemicals that may cause irritation or allergic reactions. Consider fragrance-free options for residents with respiratory sensitivities or cognitive conditions that may cause distress with strong scents.
Staff Training and Support: Comprehensive training programmes should cover infection control principles, dignity preservation techniques, and proper use of personal protective equipment. Regular refresher sessions ensure consistent standards across all care teams.
DIGNITY-PRESERVING
Maintaining privacy during personal care represents a fundamental aspect of dignified treatment. Use privacy screens, ensure doors remain closed, and limit the number of staff present to those directly involved in care delivery. Explain each step of the process and pause if residents express discomfort or distress.
Timing considerations prove equally important. Schedule hygiene activities around residents' natural rhythms and preferences where possible. Some individuals prefer morning care, whilst others feel more comfortable with evening routines. Flexibility demonstrates respect for individual choices and promotes cooperation.
Cultural sensitivity requires ongoing attention. Some residents may have specific religious or cultural requirements regarding personal care practices. Understanding and accommodating these needs shows respect
for diversity and supports emotional wellbeing.
When residents resist hygiene care, often due to cognitive impairment or past traumatic experiences, staff require specialised approaches. Gentle persistence, distraction techniques, and breaking tasks into smaller steps can reduce anxiety and promote acceptance.
For residents with dementia, maintaining familiar routines and using consistent caregivers helps reduce confusion and resistance. Simple, clear instructions and positive reinforcement encourage participation and preserve remaining independence.
BUILDING SUSTAINABLE SYSTEMS
Effective hygiene programmes require robust documentation, regular auditing, and continuous quality improvement processes. Track infection rates, resident satisfaction scores, and family feedback to identify areas for enhancement.
Invest in appropriate equipment and supplies to support best practice implementation. This includes adequate changing facilities, proper lifting equipment, and sufficient staffing levels to avoid rushing through personal care tasks.
CONCLUSION
Excellence in hygiene and odour control represents a fundamental expression of caring that extends far beyond basic cleanliness. When implemented thoughtfully, these practices preserve dignity, protect health, and create environments where residents can thrive with confidence and comfort.
The investment in comprehensive hygiene programmes yields dividends in improved health outcomes, enhanced resident satisfaction, and strengthened family relationships. Most importantly, it affirms the value and worth of every individual in our care, supporting their right to live with dignity and respect throughout their residential care journey.
Chiltern Water & Environment was established in 1991 by Robert Hunt after gaining 25 years' experience as an operational and analytical scientist in the water supply industry. The company gained engineering and further management knowledge when David Hunt joined in 2012. Since then, other water industry professionals have added to the breadth of
We have always provided high-quality consultancy, testing and remedial services in a professional but personable manner. Our steady growth has reflected our clients' trust in our services. Our current clients include large housing associations, pharmaceutical companies and facilities management companies, as well as individual landlords and small busi-

nesses. We ensure all our customers receive the same level of care and attention to detail.
Duty Holders of all commercial and public building premises are legally required to assess the risk from legionella to anyone using the water systems and put in place legionella control measures if required. The HSE has produced ACoP L8 and HSG274 as guidance for Duty Holders obligations. We have clients throughout the South East, London and the Midlands, and carry out water tests nationally and internationally. We currently provide regular water sampling and testing for over 500 sites.
Tel: 01844 347678. Email: info@chilternwater.co.uk Web: www.chilternwater.co.uk


Remedial works
• Swimming and spa pool testing
Tel: 01844 347678
Email: info@chilternwater.co.uk www.chilternwater.co.uk
Angloplas are a UK manufacturer who specialise in producing dispensers for the health and hygiene industry. Although these are designed to keep the workplace tidy and uncluttered they are, more importantly, built knowing the control of healthcare-associated infections (HCAIs) are a priority for healthcare providers, and who are employing a combination of infection prevention and control strategies, including hand hygiene, cleaning, training and the adoption of new technologies, to tackle the problem.
As a result, a wide range of infection control products and technologies are emerging on the market, including antimicrobial technology. Angloplas’ range of dispensers are produced in the world’s first proven Antimicrobial PVC with silver ion technology and which is exclusive to Angloplas. This helps reduce the risk of cross infection by stopping the growth of bacteria and mould and works continuously for the lifetime of the product, reducing levels of bacteria such as MRSA, E Coli, Legionella, Salmonella and mould by up to 99.99%. For non-clinical environments Angloplas has recently launched its new Budget Range of products which are made to the same exacting standards as the antimicrobial protected ones but with lower price tags.
You can order Angloplas products directly from its website at www.angloplas.co.uk

by Lorcan Meikitarian, Chair of the CHSA

The world is changing, becoming more complex and challenging. It’s easy for business ethics to be a casualty but at the CHSA, we argue they have never been more important.
Ethical businesses operate with integrity, fairness and respect for people, communities and the environment. Rooted in the oganisation’s publicly stated core values, an ethical approach provides a framework for decision-making that brings with it reliability and accountability. These businesses are transparent in their dealings. They do not mislead, and they provide evidence that justifies the claims they make. This approach also fosters integrity and fairness, which inspires confidence and loyalty. It can also be a powerful motivator, attracting new talent and fostering commitment amongst the existing workforce. Ultimately, it underpins long term relationships, which in turn generate a better financial performance.
The words are meaningless if not backed up with the right action. For us at the CHSA, putting the talk about ethics into practice means five things:
1. adhering to national and international laws;
2. respecting human rights;
3. treading lightly environmentally;
4. cutting no corners when it comes to giving the customer what they believe they are paying for; and
5. and finally, being truthful, meaningful and transparent in all sales and marketing claims.
Adhering to the law is a given. Respect for human rights may be more complex. UK businesses in our

sector are likely to have it baked into their day-to-day operations. The challenge may come when examining their supply chains. In response we introduced a preference for an ethical audit for all CHSA manufacturing members. For CHSA Accredited Product, the manufacturer, whether based in the UK or overseas, must provide a copy of their most recent official ethical audit report. The report must meet the CHSA’s minimum requirement, and encompass labour standards, and health and safety. Compliance will be compulsory by the end of 2027. It will be a requirement of membership for those who fall within the Scope.
We all need to tread lightly environmentally. In 2022 we developed our Roadmap to Sustainability. It provides members with a framework for moving to sustainable solutions. Key to making a substantive, long term change is a thorough assessment of the corporate environmental impact. This requires a detailed understanding of carbon emissions at the product and corporate level. Calculating these emissions is complex. To support members, we delivered a webinar with a panel of experts able to provide guidance on overall approaches and the pros and cons of the different methodologies.
An ethical business supplies what it sells, without cutting corners. Setting and maintaining standards is in our DNA. We set up our Accreditation Schemes to tackle the problem of businesses selling product short or not fit for purpose. The Schemes have been incredibly successful. The logo for each Accreditation Scheme is a formally registered Trademark. It means every company displaying one must comply with the relevant standard and technical regulations. We audit accordingly and act wherever we find an infringement.
The fifth and final strand of our approach to ethics in business is honesty in sales and marketing. Our members do not play fast and loose with their sales and marketing messages and product claims, and they want their suppliers and the wider industry to know and understand this. This is why they introduced


a commitment to ethical marketing. It has four ethical principles:
1. All statements and claims are truthful.
2. Supporting evidence, such as data sheets, reports and certificates is available on request to substantiate all product and service claims.
3. All statements and claims are transparent. For example, it is clearly indicated if the claim applies to the product, the packaging or both.
4. All statements and claims are meaningful. For example, the term eco-friendly must be defined in relation to all aspects of the product and substantiated across the full lifecycle.
We are in the process of getting every member to sign this commitment.
Our Code of Practice underpins our entire ethical approach at the CHSA. Every member joining the CHSA makes a commitment to live by the Code; signing it is a requirement of membership. At its heart is a commitment made by every member to “maintain a high standard in the conduct of its business”.
In more detail it requires every member to conduct business dealings ‘in an open honest, fair and proper manner’, to ‘ensure all public statements made by and on behalf of the member are decent, honest and truthful’, to ‘hold and provide evidence on request for product and service claims’, and to ‘refrain from making inaccurate, misleading or malicious statements’. In essence it demands members trade ethically.
Our goal at the CHSA is always to advocate an ethical approach. Over recent years we have introduced many initiatives designed to bring this approach to life in very practical ways. This means our members’ customers and suppliers can trust them to trade honestly and fairly.


Care homes across the UK are transforming how they deliver care thanks to SyndoraAlto, the newly rebranded name behind CHARIS, the UK’s most advanced digital nurse call system.
Fully supplied, installed, and maintained from just £6.40 per bed, per month, CHARIS delivers smarter, safer, and more connected care through real-time alerts, mobile integration, and intuitive smart displays that help staff respond faster when residents need them most.
Every CHARIS system comes fully inclusive with 15” smart displays, help buttons, pull cords, guaranteed radio coverage, and 24/7 UK technical support, all backed by SyndoraAlto’s trusted installation and maintenance team.

For care providers not yet ready to replace their existing nurse call system, AltoEnhance offers the perfect first step into digital care.
Available from just £129.00 per month, AltoEnhance seamlessly connects to your current nurse call system, bringing digital reporting, mobile alerts, and actionable insights without the need for a full system upgrade.
“Technology should make care easier, not harder,” says Louis Johnson, Managing Director. “CHARIS and AltoEnhance connect people, information, and action empowering care teams to deliver truly person-centred care.”
Meet the team & learn more at www.syndoraalto.com
See the advert on the front cover for more information.
Alarm Radio Monitoring is the market leader in the design, manufacture and installation of bespoke, end-to-end, wireless alarm systems and solutions for the healthcare, leisure, custodial and education industries.
We have been providing wireless alarm and nurse call systems for over 30 years. Supplying care homes and hospitals with an essential lifeline that supports the delivery of outstanding care.
We believe in excellence which translates into: Advanced Technology Industry-leading wireless alarm technologies and software
Bespoke Solutions
We design systems to your needs rather than your team having to work around
Falls are a significant concern for vulnerable individuals, especially seniors and patients at risk. Medpage, a leader in assistive technology, offers a range of cuttingedge products designed to enhance safety and provide peace of mind for caregivers and families. Here’s an in-depth look at some of their standout solutions:
MPRCG1 (2023) BED LEAVING DETECTION ALARM WITH CAREGIVER RADIO PAGER
The MPRCG1 is a comprehensive system tailored for fall prevention in domestic, commercial, and NHS care settings. This all-inclusive kit includes a bed pressure mat sensor, a BTX21-MP alarm sensor transmitter, and an MP-PAG31 radio pager. The system is designed to alert caregivers when a patient leaves their bed, reducing the risk of falls.
HDKMB2 HOSPITAL DISCHARGE KIT FOR FALLS RISK PATIENTS
The HDKMB2 is a thoughtfully curated kit aimed at supporting patients transitioning from hospital to home care. It includes essential tools to mitigate fall risks and promote recovery. This kit is ideal for caregivers seeking a comprehensive solution to enhance patient safety during the critical post-discharge period.

CMEX-21 MULTI-PORT WIRELESS SENSOR INPUT EXPANDER FOR NURSE CALL CONNECTION
The CMEX-21 is Medpage’s latest innovation, designed to integrate seamlessly with existing nurse call systems. This multi-port expander allows for the connection of multiple wireless sensors, enhancing the monitoring capabilities of healthcare facilities. Its versatility makes it a valuable addition to any care environment, ensuring timely responses to patient needs. RON-WC2 WATERPROOF DISABLED PULL CORD ALARM TRANSMITTER WITH WIRELESS ALARM RECEIVER
The RON-WC2 is a robust solution for disabled individuals requiring immediate assistance. This waterproof pull cord alarm is ideal for use in bathrooms and other high-risk areas. Paired with a wireless alarm receiver, it ensures that help is just a pull away.
For more information, visit Medpage’s official website or contact their team to explore these products further. Safety starts with the right tools, and Medpage delivers just that. www.easylinkuk.co.uk
T: 01536 264 869

The wireless ARM Nurse Call system has been developed over 30 years with both the client and user in mind.
It enables staff to efficiently answer calls, making the management of resources more flexible and provides the functionality you would expect of any nurse call system.
The system is quick and easy to install and works wirelessly, using radio communication between both the call points and the system infrastructure. Call messages can be sent direct to staff to speed up response times and can also be integrated to work with smart phones & messaging. Data Analysis software provides a full audit trail of events
The all-new call logging software from ARM enhances the functionality of your care call system dramatically.
• It can help you track the quality of your service to your residents.
• It can help you demonstrate compliance with your aims and best practices, both to relatives and to authorities.
• It can help you find bottlenecks in service provision, track staffing requirements, and allow you to ensure staff are meeting expectations.
• Most importantly, it provides assurance that you know and can demonstrate what is happening in your care home.
Courtney Thorne, a long-standing innovator in healthcare communication systems, is setting new standards in the care home sector with its advanced wireless nurse call technology—designed to improve resident safety, enhance staff efficiency, and support a more responsive care environment.
With over 30 years of experience serving the UK healthcare market, Courtney Thorne’s systems are now trusted by thousands of care homes nationwide. Unlike traditional hardwired solutions, their wireless nurse call systems offer non-invasive installation, scalability, and smart analytics—making them ideal for both new builds and retrofit projects.
“At the heart of our technology is the belief that better communication leads to better care,” says Graham Vickrage, Managing Director at Courtney Thorne. “Our wireless systems not only reduce response times but also empower staff with the tools they need to deliver safe, person-centred care.”
Care providers are increasingly choosing wireless systems for their flexibility, reliability, and cost-effectiveness. With a full suite of accessories—including neck pendants, door monitors, fall detection, and
bed sensors—Courtney Thorne systems can be tailored to meet the specific needs of each home and resident.
In an industry where compliance, safety, and staff pressures are always front of mind, Courtney Thorne provides more than just products—they offer ongoing support, training, and a commitment to innovation that helps care homes future-proof their operations.
For more information or to book a free demo, visit www.c-t.co.uk or contact info@c-t.co.uk.

We here at Edison Telecom Ltd have been providing specialist solutions to your call system requirements tailor-made to each customers needs for over 25 years, says director Bob Johnson. Is your current Nurse Call “legacy”, obsolete, so full of software bugs or commercially not viable for your current supplier/maintainer to maintain?

We may have just the part and expertise that you are looking for to give your nurse call a further extension to life, adds Bob, “Edison will treat your nurse call with the same compassion that you give to those in your care. There will come a time when your equipment is beyond repair but Edison are experts in extending the life of obsolete systems.” www.edisontelecom.co.uk




Every day, care organisations are working tirelessly to deliver essential support in the face of growing needs and rising costs. However, too many providers are stuck balancing tight budgets, having ‘just enough’ to stay afloat. The hard truth is, just enough isn’t enough—not for the providers, not for the employees, and certainly not for the clients who depend on them.
Rising operational costs—from wages and the Fair Pay Agreement to energy bills—compound historic underfunding and financial pressures. And demand for care continues to increase, creating a widening gap that organisations are often forced to fill with limited resources.
Providers then end up in survival mode, unable to invest in improving their services for today and the future.
THE NEED TO RETHINK FINANCIAL STABILITY
Care providers need to have healthy finances in social care, and that doesn’t come at odds with delivering compassionate care.
A financially strong organisation has the breathing room to improve services, retain employees, and innovate to make a meaningful difference to the lives of people they support. And having this financial security means providers can actually plan for the future rather than constantly reacting to the present.
BENEATH THE SURFACE
Social care organisations face a web of financial intricacies. Local authori-

ty support often comes with layers of red tape. Managing aged debt and resolving invoicing errors take a significant amount of time that few organisations can spare. Regulation and compliance require meticulous reporting, and the sheer volume of admin work to manage all these leaves teams stretched thin.
At the same time, there’s an expectation for providers to keep doing more. But without the right tools and systems in place, these compounded financial struggles threaten to overwhelm this indispensable sector.
PAVING A SUSTAINABLE WAY FORWARD
Social care providers aren’t just keeping their organisations alive; they’re safeguarding the wellbeing of countless individuals and families.
Providers need to be able to prioritise long-term financial resilience. And part of this means having the tools—including robust financial management softwaresimplify manual processes, optimise resources, and reduce inefficiencies.
By championing financial sustainability, we’re creating conditions where employees can thrive, where clients receive the quality of care they deserve, and where the sector can confidently meet future challenges.
Find out more at: www.oneadvanced.com/ai
See the advert on the facing page.
FALL SAVERS ® WIRELESS MONITOR
Eliminate all cables with our new generation falls management solutions!
Upgrade your falls programme with the latest technology from Fall Savers®. The NEW Fall Savers® Wireless eliminates the cord between the monitor and sensor pad. This results in less work for nursing staff, improved safety for patients and reduced wear and tear on sensor pads. Wireless advantages include the ability to use one monitor with two sensor pads simultaneously and support for many new wireless devices.

BENEFITS INCLUDE:
Safer for patients; less work for staff
Bed and chair pads available
One monitor works with two sensor pads
Integrates with most nurse call systems
A variety of options, including: Call button Pager
The TreadNought® Floor Sensor Pad is built to last with a durable construction that far out lasts the competition. Our anti-bacterial floor sensor pad is compatible with most nurse call systems or can be used with a portable pager to sound an alert when a person steps on to the sensor pad. Caregivers typically place the sensor pad at the bedside, in a doorway or other locations to monitor persons at risk for falls or wandering. An optional anti-slip mesh reduces the potential for slippage on hard surface floors.
FEATURES INCLUDE:
Connects directly to most nurse call systems
High Quality anti-bacterial Floor Sensor Pad
Large Size Pad: Measures (L) 91cm x (H) 61cm
Options (sold separately):
Anti-slip mesh for hard surface floors
See the advert on this page for further details or visit www.fallsavers.co.uk.



Working in social care is demanding. It is one of the most heavily regulated yet underfunded sectors, with providers expected to comply with regulations, meet Quality Statements, follow good practice guidance, respond to local authority monitoring, and operate under constant scrutiny.
Regulation itself isn’t the problem — it protects people and improves standards. The challenge is capacity. Larger organisations may have in-house quality assurance teams, but smaller providers rarely have the time or budget to review compliance in depth. Many owners and managers tell us they feel overwhelmed and unsure how well their service is really performing, especially since the introduction of the Single Assessment Framework.
For many, confidence in compliance is the number one concern — not because standards are poor, but because there simply isn’t time to step back and take a full, objective view.
CAN AN EXTERNAL AUDIT HELP?
In short, yes — when it’s done properly. A high-quality external audit provides:
• A clear snapshot of current performance
• Identification of good practice and priority risks

• Practical advice on how to improve
• Evidence to support action plans and improvement journeys
• Demonstration of good governance and continuous improvement — a key CQC focus
• Reassurance for owners, directors, and managers
HOW W&P CAN HELP
W&P have supported health and social care providers for nearly 25 years, completing hundreds of audits across a wide range of services. This experience gives us deep insight into what regulators look for — and what genuinely improves outcomes.
Our audits are supportive, non-judgmental, and practical. They typically include around six hours on-site, followed by a detailed report that links evidence to regulations and Quality Statements. Reports also include clear guidance, tips, and sources to help you respond confidently.
Every audit is tailored to your needs — whether that’s safeguarding, medication management, or overall governance — ensuring it is truly fit for purpose.
If you would like to know more, then please contact us on audits@wandptrainng.co.uk or call 01305
767104 for a no-obligation chat on how our audits can help you. See the advert on page 2 for details.
Competency assessment might not be anyone’s favourite phrase, but in domiciliary, residential, and specialist care, it is the backbone of safe, highquality support. The challenge is making it genuinely useful, not just another hoop to jump through.
Care staff need more than theory. They need time to learn, practise, and make mistakes in a safe environment before they are expected to apply new skills with real people. That is where a blended learning approach truly shines. High quality eLearning builds consistent knowledge. Virtual sessions keep teams connected and engaged. Face to face training gives carers the chance to try techniques, ask questions, and build confidence before working directly with residents and service users in their homes or care settings.
But learning does not stop in the classroom. Competency assessments in real care environments provide the feedback carers need to know they are using best practice techniques, communicating well, and delivering safe, person-centred care. It is the


bridge between “I know it” and “I can do it.”
This balance of learning plus real world assessment creates confident, capable staff who trust their own skills and feel supported rather than judged. Managers also get clear, reliable evidence for CQC and Skills for Care requirements without drowning in admin.
At myAko, we have developed tools with our long term partners, that make this process simple and sustainable. Better learning, better practice, better competency. It is a straightforward formula that leads to stronger teams and better outcomes for residents and service users.
Because when staff feel skilled, supported, and confident, the quality of care speaks for itself.
Kevin Ashley
Founder I CEO, myAko
myako.online/care

"23 years, operating 4 Devon Nursing homes, has been pretty tough, as anyone in social care, knows, only too well. And if it was hard already, after 2024 budget, it's just got harder.
Anyway, at heart, I am just customer of Eden Alternative, and it was a stroke of luck to come across this whilst on holiday in New Zealand in 2009. It started in USA in 1994 and now runs in 22 countries.
The fact that I am now involved with this not-for-profit organisation (in the UK area) came about when one of the 2 main UK directors died suddenly just before Covid. But it's something I have run with for 11 years to help make 'vision' a reality, not a struggle. So, being both a customer and helping the admin seems quite natural.
It is a modern philosophy of care, but moreover, it's a programme that is straight forward, tried and tested for 30 years and really works.

Its member care organisations generally become trainers for their own teams, and run it themselves.
The programme is run in person over 2-3 days or online 1 hr a wk for 7 weeks. You choose.
It addresses loneliness, helplessness and boredom and operates through 10 principles to underpin 7 critical domains of wellbeing.
Moreover, it's effective, transformational and really works. As residents, and team members wellbeing, matter so much , it's a must, in my opinion.
Geoffrey Cox
Southernhealthcare.co.uk
eden-alternative.co.uk"
Restrictive practices such as physical restraint, bed rails, or lap belts remain one of the most challenging aspects of health and social care. Intended to keep patients safe, they can also cause harm, distress, and loss of dignity when used unnecessarily. Across the UK, the principle is clear: care must always use the least restrictive option.
Legislation provides the framework, but culture and staff behaviour shape daily practice. Nurses, carers, and clinicians often make quick decisions balancing safety with autonomy. Without training, restrictive practices risk becoming routine. To change this, staff need better understanding of the human impact and confidence to use alternatives.

That’s where Restrictive Practice makes a difference. Developed through codesign workshops with patients and carers, this gamified e-resource gives a voice to those most affected by restraint. Their lived experiences shaped the learning, helping staff see restraint
not as a neutral safety tool, but often as something frightening or disempowering.
The results are powerful. Staff trained with the resource led Quality Improvement projects, achieving measurable reductions:
- Bed rails dropped from 360 to 277 incidents
- Bed bumpers from 303 to 227
- Lap belt use halved, from 46 to 22
These improvements represent safer, more compassionate care and reassurance for families.
Restrictive practices may never disappear entirely, but they should be the exception, not the rule. With the right knowledge and tools, staff can choose safer alternatives and build a culture of dignity, compassion, and respect across UK care services.
See our advert on the front cover or visit
Global assists clients throughout the U.K. who specialise in the healthcare sector to achieve their objectives of purchase, development and refinance.
We have organised over £1.8bn for clients in the past 30 years, providing clients with competitively priced funding to refinance existing debt, ease cashflow and develop businesses further.

From helping clients make their first purchase through to allowing groups to grow significantly in size we


