

Fecal transplants are saving lives and their potential is flush with possibility. But there's a desperate need for donors. The Super Power of Poop
The Future is Bright
In my 25-year career at St. Joseph’s Health Care London, I’ve had the privilege of witnessing astounding creativity and innovation in real time. Nothing is more exhilarating than seeing an idea take shape, transformed and perfected through research, and then take flight to improve care and the patient experience.

Discovery is an essential part of who we are and what we do. We are proud to have people in our organization, like Dr. Michael Silverman, who push the boundaries of science every day to make the impossible possible. You can read more in this issue about his groundbreaking work in saving lives through fecal microbial transplantation.
Our people are our greatest asset and as we continue to navigate through year three of the COVID-19 pandemic, we are focused on ways to strengthen our workforce. We will continue to rely on leaders like Dr. Laura Lyons for their commitment to care, the dedication of our many volunteers, and new ways to welcome internationally trained health care workers like Jasmine Devassy to our ranks.
These stories are just a glimpse into the exciting work taking place at St. Joseph’s each day. We are energized and inspired by the possibilities – those known and those yet to be discovered. The future is bright.
Roy Butler President and CEO St. Joseph’s Health Care London

2 A publication of St. Joseph’s Health Care London Fall 2022 | Issue 06 St. Joseph’s welcomes your comments. For online or print publication contact: ComDept@sjhc.london.on.ca Copyright ©2022 by St. Joseph’s Health Care London. The publishers assume no responsibility for any effects from errors or omissions. All material published in My St. Joseph’s magazine is copyright and reproduction is forbidden without the permission of the publishers. Disclaimer: All photos were taken either before the COVID-19 pandemic or following appropriate physical distancing guidelines. CONTACT US PO BOX 5777 268 Grosvenor Street London, ON. N6A 4V2 519 646-6100 ext. 66034 www.sjhc.london.on.ca stjosephslondon stjosephslondon CONTRIBUTORS Allison Hansen Celine Zadorsky Dahlia Reich Kelsi Break Krista Devries Matthew Overall Renee Sweeney PHOTOGRAPHY Colleen MacDonald MY ST. JOSEPH'S IS Mount Hope Centre for Long Term Care Teams, clinics and programs in our community and beyond. Southwest Centre for Forensic Mental Health Care St. Joseph’s Hospital Parkwood Institute
What's Up Doc?
Top
Joseph’s Health
series hosted by London journalist Ian Gillespie.
Taking Control
Pace at a Time
Gearing Up for Mental Health
The
A Taste of Indigenous Culture
A Passion for Our Past
An
Realizing a Dream in a New Land
A
Hope Beyond Hospital Walls

The
at
and Slow –The Speeds of a Stroke Journey
initiative,
is
Pushing Boundaries in Stroke Rehabilitation
Dr. Robert Teasell's
with
in
ISSUE 05 | www.sjhc.london.on.ca FALL 2022 06
experts hit the airwaves this fall with DocTalks Podcast, a new St.
Care London
16
One
innovative online tool gives people with mild traumatic brain injuries the opportunity to take charge of their symptoms to enhance recovery. 07
Forest City Cycling Challenge sped past its fundraising goal on the path to support youth mental health. 17
new program is helping internationally trained nurses join the province’s health care team. 12
A piping hot and meaningful new item is now on the menu at St. Joseph’s Health Care London. 18 Fast
Specialized rehabilitation helps stroke survivors return to living life fully. 14
Zero Suicide
which began
St. Joseph’s Health Care London,
spreading across the province. 20
legacy
stroke rehabilitation research will continue
a new fellowship in his honour. CONTENTS Exemplary Physician, Compassionate Cheerleader Dr. Laura Lyons is filling a great need as an expert in the care of pregnant women who are struggling with addiction. COVER STORY 22
The artifacts on display at St. Joseph's Hospital each tell a story, as do the efforts taken to preserve them. FEATURES The Super Power of Poop Fecal transplants are saving lives and their potential is flush with possibility. But there's a desperate need for donors. 04 08 08. 3
EXEMPLARY PHYSICIAN, compassionate cheerleader
Dr. Laura Lyons is filling a great need, regionally and nationally, as an expert in the care of pregnant women who are struggling with addiction.
Alife of trauma would describe Jodi’s turbulent childhood. Repeatedly sexually assaulted, she would go on to be victimized many times in different ways, and become trapped in addiction.
Caught in the grips of alcohol, cocaine and ecstasy in high school, Jodi’s world evolved into a whirlwind of drugs, partying and destructive relationships. An attempt at methadone treatment failed and her addiction to opioids led to injecting hydromorphone.
“The first time I injected, it was either going to be a suicide attempt or the needle. After my first shot of hydromorph, there was no turning back.”
Jodi was just 28 years old when her hydromorph use became constant. She began to use all day, everyday, her life swirling around the next shot.
Eventually, Jodi was able to extricate herself from her circle of addicted companions. She was using less but still using when, in 2012, she became pregnant with her partner’s child. It was the impetus she needed to seek help.
“The morning after I got the positive test, I went to the emergency department and said ‘I don’t know what to do. I don’t want to use. I want this baby.’”
It was only with Dr. Lyons at my side could I face the neonatal intensive care experience while continuing to detox.
– JODI
Dr. Laura Lyons would become Jodi’s guide, inspiration and anchor, providing support and compassion she had never experienced before and that continues today.

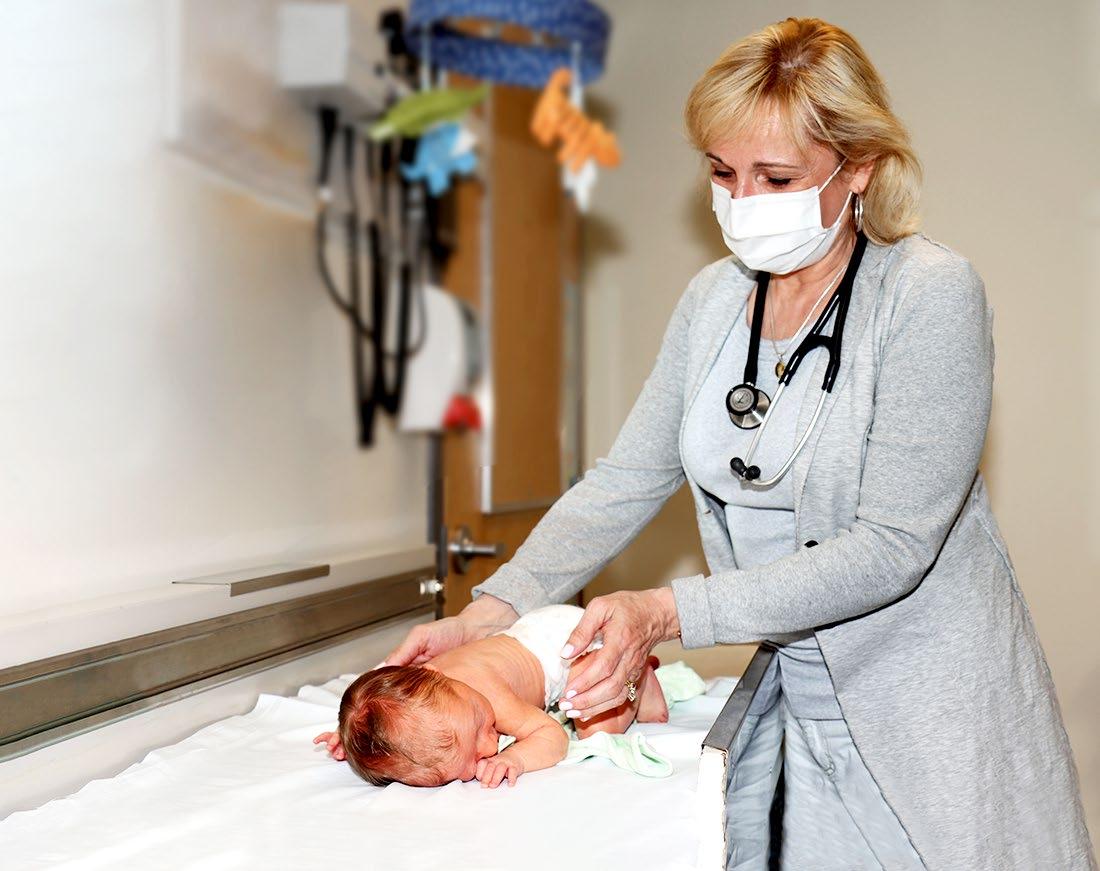
Dr. Laura Lyons
is an expert in the care of pregnant women who are struggling with substance dependence and addiction.
Regionally and nationally, Dr. Lyons has carved out a niche as an expert in the care of pregnant women who are struggling with substance dependence and addiction. She sees women in her practice at St. Joseph’s Family Medical and Dental Centre and as clinic lead with the Obstetrical Self-Referral Outpatient Clinic at London Health Sciences Centre serving women without a family doctor who need prenatal care. It was at the clinic she uncovered a need to care for many of these patients differently.
“I encountered a number of women struggling with substance use disorder,” says Dr. Lyons. “These women were often angry, likely scared, and distrustful during their visits at the hospital. I came to realize they all had a history of being treated poorly by people of authority and institutions. I also knew we weren’t serving them in the best way possible. There were not the resources in London that met their unique needs, which requires treating addictions while simultaneously providing prenatal care.”
4
“
Dr. Laura Lyons
at St. Joseph’s Family Medical and Dental Centre chose family medicine because of the opportunity it gives her to create continuous relationships with patients of all ages and generations of families, from birth to end-of-life care.
Pregnancy is “a wonderful window of opportunity” for recovery as women are highly motivated for the health and well-being of their child, adds Dr. Lyons. Wanting to take full advantage of that window, she became certified in addiction medicine and has taken a leading role in training clinicians to provide non-judgmental support for pregnant women in recovery, and in the development of policies to promote best care practices for these mothers and babies post-partum.
Under Dr. Lyons expert care, a pregnant Jodi began receiving medication to treat her opioid addiction and was making good progress coming off drugs. She was hoping to be clean by her due date but it wasn’t to be. Unforeseen complications led to her son being born at 28 weeks and a whole new ordeal began. The baby, however, did not suffer withdrawal symptoms because of the treatment Jodi received leading up to his birth.
“It was only with Dr. Lyons at my side could I face the neonatal intensive care experience while continuing to detox,” says Jodi, who becomes emotional talking about the importance of Dr. Lyons in her life.
“There is no way one human could treat all of her patients the way she accommodates me – but she probably does.”
Today, Jodi is a mom of two beautiful children with her partner, and owns her own business. Her oldest is now nine, her youngest almost one. She calls them “my reasons” – for staying the course, staying healthy. She admits that life is still hard and she will forever be an addict in recovery, but Dr. Lyons remains her “biggest cheerleader.”
“Without her I don’t know that I’d even be alive today. If I was, my life most certainly wouldn’t look the way it does. While I still have my struggles, life only keeps moving in a positive direction.”
Scan to read more about Dr. Laura Lyons or visit sjhc.london.on.ca.

ISSUE 05 | www.sjhc.london.on.ca 5
What's up, DOC?
Top experts from St. Joseph’s Health Care London hit the airwaves this fall with DocTalks Podcast, a new series hosted by London journalist Ian Gillespie.

So, tell me more about insulin”, DocTalks host Ian Gillespie asks as he leans intently towards the microphone. He’s interviewing Dr. Tamara Spaic, an endocrinologist at St. Joseph’s Health Care London (St. Joseph’s) and the topic of conversation today is diabetes. Informative conversations like this, plus many others, will be coming through your speakers this fall with the launch of St. Joseph’s all new DocTalks Podcast.
“We are fortunate to have many world-renowned expert physicians at St. Joseph’s who are leaders in treatment and research,” says President and CEO, Roy Butler. “These specialists have a wealth of medical knowledge to share and our DocTalks Podcast is a great way to connect these experts with our community as well as a broader audience. It’s a new facet of online education in health care and St. Joseph’s is proud to offer this accessible and engaging medium to the public.”
A growing number of Canadians are turning to podcasts for their news, entertainment and even their health information.
Podcast industry experts predict there will be more than 160 million podcast listeners worldwide by 2023. Among them is a burgeoning number of older adults. According to Statista, 26 per cent of the podcast audience are age 55 and above.
Listeners can tune into the DocTalks Podcast for free on their computer or smart device through established platforms like Apple Podcast and Spotify. Award winning London journalist Ian Gillespie hosts each episode, which features a trending health care conversation, including insights on leading-edge treatment and research. Season one focuses on a wide variety of topics, from the latest in erectile dysfunction, dementia and diabetes, to what’s new in prostate cancer and urinary incontinence in women.
Listen and subscribe to DocTalks Podcast wherever you get your podcasts or visit sjhc.london.on.ca. Have an idea for a DocTalks Podcast episode topic? Email comdept@sjhc.london.on.ca.

6
Ian Gillespie, London journalist and host of St. Joseph's Health Care London's new DocTalks Podcast.
Gearing up for Mental Health
For the second year in a row, the Forest City Cycling Challenge sped past its fundraising goal to support youth mental health research and purchase exercise bikes for patients of St. Joseph’s Health Care London.

It was the sound of celebration as the spinning wheels of hundreds of bicycles raced or coasted during the Forest City Cycling Challenge. The final destination was an important one – enhancing care for those living with mental illness.
The second annual event held in June was open to cyclists of all skill levels, with routes ranging from 25 km to 160 km. The ride began and ended at the Lerners Lawyers building, where riders were greeted by music, food trucks, and scores of volunteers.
Prizes were awarded to participants who raised the most money. Fittingly, Dr. Gillian Kernaghan, recently retired President and CEO of St. Joseph’s Health Care London (St. Joseph’s) earned bragging rights as the top fundraiser.
Event founders Joe DiBrita, Tim Mason and Alfonso Campos Reales hoped to match the $40,000 raised at their inaugural event. But their hard work, paired with enthusiastic riders and dedicated fundraising supporters, turned the event into a runaway success that brought in more than $60,000.
“We are totally blown away by the love and support people have shown for the Forest City Cycling Challenge,” says Alfonso, who also sits on St. Joseph’s Health Care Foundation’s Board of Directors. “Mental illness affects so many people in our community, so it’s been an honour to give back to this important cause in such a meaningful way.”
Proceeds from the event support mental health care at St. Joseph’s and the purchase of exercise bikes for patients living with severe and persistent mental illness. From the moment they arrived, the bikes have been a hit with inpatients at St. Joseph’s Parkwood Institute Mental Health Care Building.
“It’s been a huge benefit to our patients to be able to jump onto the bike whenever they feel like it,” says Kerrie Dewachter, Coordinator of the Treatment and Rehabilitation Program. “Their clinicians can even hop on with them for one-to-one connection while they’re enjoying physical activity.”
Event proceeds also support the Mental Health INcubator for Disruptive Solutions (MINDS), a social innovation lab addressing youth mental illness and addiction.
Joe, Tim and Alfonso are grateful for the outpouring of support for this year’s event and planning is already underway for next year.
2022 Forest City Cycling Challenge organizers present proceeds of the event to St. Joseph's Health Care Foundation and St. Joseph's Health Care London.
7
THE OF POOP
Fecal transplants are saving lives and their potential is flush with possibility. But there’s a desperate need for donors.
It’s quite the conversation starter. At parties or gatherings, when someone asks John Chmiel what he does, he gets a kick out of telling them “I sell poop for money.”
It’s true. He does. His own poop. John is a poop donor. Instead of slowly backing away, people are intrigued, says John. They want to know why and how. They quickly discover it has nothing to do with the money and everything to do with saving lives.
At St. Joseph’s Health Care London, fecal transplants are now routine treatment for debilitating and life-threatening Clostridioides difficile (C. difficile) – the major cause of antibiotic-associated diarrhea. The treatment makes it possible for people to recover from this destructive infection and holds tremendous potential in the care of various other serious diseases.
John is fascinated by this exciting new frontier in medicine and is invested – both as a donor and as a microbiology and immunology graduate student at Western University, training in Lawson Health Research Institute’s Canadian Centre for Human Microbiome and Probiotics at St. Joseph’s Hospital.
“As a grad student, when I heard how effective fecal transplants are for C. difficile and how many trials are going on related directly to patient care for various illnesses, I thought I had to help out,” says John, who became a donor in 2018.

For many patients struggling with C. difficile, fecal transplants are critical, explains Dr. Michael Silverman, Medical Director of St. Joseph’s Infectious Diseases Care Program who has been performing the procedure since 2003 and was one of the first in North America to do so. He and his team have played a key role in the treatment, becoming the standard of best practice for C. difficile across Canada and the USA.
Most cases of C. difficile occur in individuals who are taking antibiotics and some acquire it while hospitalized. Antibiotics can destroy the normal bacteria found in the gut, causing C. difficile bacteria to overgrow. When this occurs, the C. difficile bacteria produce toxins, which can damage the bowel and cause diarrhea and other severe complications. Treating C. difficile with antibiotics kills even more of the helpful normal gut bacteria, and when antibiotic treatment stops the C. difficile returns. This can happen over and over again, making relapsing C. difficile a significant challenge to treat.
COVER STORY
Continued...
John Chmiel is a microbiology and immunology graduate student at Western University, training at Lawson Health Research Institute. He is also a poop donor.

At St. Joseph’s, however, C. difficile patients are being cured thanks to poop donors like John. The success rate of fecal transplants performed by the Infectious Diseases Care Program is a staggering 96 per cent. The program is one of few performing the procedure as part of routine care for C. difficile, and the only program in Ontario – one of two in Canada – administering the treatment via capsules.
The diarrhea would make a raging return with every attempt to reduce the medication. After six months with crippling C. difficile and little hope, Katharine came to St. Joseph’s, the only centre in Ontario offering the procedure during the height of the pandemic.
It took one treatment.
“Within three days, I started to feel better. My life is now back on track. I had a normal poop today – I’m so stoked! I’m good every day. Hallelujah!
Such life-changing stories are common for C. difficile patients who undergo fecal transplants, yet others are left suffering. There is a serious shortage of donors. Criteria requiring only very healthy, local donors, the ‘ick factor’ often associated with donating poop, and the pandemic has created a poop supply crisis.
– KATHARINE GORJUP
“Many patients we treat have been ill with multiple episodes of diarrhea or chronic unremitting diarrhea for many months to years, with multiple hospitalizations,” explains Dr. Silverman. “Many have lost weight and become malnourished and frail. They often are fearful that they could die and indeed, 15 per cent of hospitalized patients with C. difficile do succumb to the illness.”
Patients are “delighted” when they see a dramatic improvement after one dose of capsules, adds Dr. Silverman. “For many patients there is really no other alternative except lifelong antibiotics.”

Katharine Gorjup, 62, is among those delighted patients. In October 2021, a dental infection requiring intravenous antibiotics triggered C. difficile so severe her weight dropped to 90 pounds. At 5’ 8”, she became skeletal and unable to care for herself.
“I looked like I was dying and that’s how I felt. I couldn’t cope. It was never-ending. I thought I might poop myself to death,” says the Etobicoke woman, whose bathroom humour is intact despite her ordeal.
Katharine ended up on antibiotics that had to be continually increased, caused various side effects, and was costing $300 a month even with drug coverage.
“Our need for London donors is great,” says Dr. Silverman. “COVID-19 has made the maintenance of donors in the program extremely difficult. When a donor gets COVID they cannot safely donate for three months. Donations also have to be put on hold after donors travel to tropical countries where bowel infections are common, until we can retest their stool and assure it is safe to donate again.”
HOW POOP SAVES LIVES
Fecal Transplant Step By Step
Poop Collection
Feces, also called stool or poop, is collected from a carefully screened, healthy donor.
2
Processing of Donor Poop In the lab, the donor poop is mixed with saline solution, then filtered. The finished product contains the good bacteria in a liquid or capsule format.
St. Joseph’s Health Care
London is the only hospital in Ontario – and one of only two in Canada – administering life-saving fecal transplants via capsules.
Fecal Transplant
The healthy fecal sample is transplanted into the intestines of the patient with C. difficile through either an oral route using capsules swallowed by the patient, or the rectal route via enema.
Healthy Gut
The organisms from the donor sample restores the healthy gut bacteria in the patient.
My life is now back on track. I had a normal poop today – I'm so stoked!
“
At times, there have been no eligible donors and the team has had to stop treating vulnerable patients, says Dr. Silverman.
John usually donates a few times a month and more often when clinical trials are underway. While he is currently on hold due to a recent bout of COVID-19, John says the donation process is easy and people need to get past the optics.
“It’s mind boggling for most people but the more donors we have, the more we can do. We need donors to fuel this exciting and expanding area of research, and to save lives.”
It's in you to become a poop donor

Just like blood transfusions, fecal transplants save lives. Currently there is a critical need for poop donors. To find out about eligibility and how to donate, call 519 646-6100, ext. 61726 or email Seema Nair Parvathy (PhD), Research Coordinator, at SeemaNair.Parvathy@sjhc.london.on.ca. Donors should reside in London.
You can also read how fecal transplants are done and their promising potential to treat an array of illnesses at sjhc.london.on.ca.

ISSUE 05 | www.sjhc.london.on.ca 11
Seema Nair Parvathy (PhD), Research Coordinator with Lawson Health Research Institute, holds up fecal transplant capsules being used at St. Joseph’s Health Care London.
A taste of Indigenous Culture
A piping hot and meaningful addition to the menu at St. Joseph’s Health Care London is nourishing patients and residents – body and soul.
Deep in the kitchen at St. Joseph’s Health Care London’s Parkwood Institute, certified chef Fred Cousins stirs a fragrant batch of freshly made soup for residents and patients to enjoy. It’s not just any soup – but one made from a traditional Indigenous recipe, which has become a staple and a favourite on the menu.
The soup, called Three Sisters Soup, was developed in collaboration by St. Joseph’s Food and Nutritional Services (FNS) team and Chef Bruno Antone from the Oneida Nation of the Thames Community Centre. The recipe includes a trio of beans, corn and squash and was prepared in keeping with the traditions and sacred practices of the Indigenous culture.
The soup originates from a traditional recipe of the Haudenosaunee (Iroquois) nation. The term “Three Sisters” refers to the three main crops of some North American tribes: maize (corn), squash, and beans.

The FNS team connected with Chef Bruno through Bill Hill (Ro'nikonkatste), project lead of St. Joseph’s Biigajiiskaan: Indigenous Pathways to Mental Wellness Program – a referral-based program in partnership with Atlohsa Family Healing Services that provides specialized care for Indigenous people living with a mental illness. In addition, Bill provides Indigenous education and mentoring opportunities for health care professionals and students.

“It is heartwarming to see the partnership between Atlohsa and St. Joseph’s continue to thrive,” says Bill. “The FNS team is also working collaboratively with community partners to grow a garden on the grounds of Parkwood Institute. The food is grown in planter boxes built by Indigenous youth.
These kind and honest partnerships build bridges of health that start from a simple seed and grow into sustainable sources of nourishment for generations to come.”
During the summer months, the FNS team grew a variety of vegetables and herbs, including some of the ingredients used in Three Sisters Soup.
Fred Cousins, Chef at Parkwood Institute, serves up Three Sisters Soup, a new menu item developed as part of St. Joseph’s Health Care London’s Nourish Project.
The garden space was maintained by Urban Roots London, a non-profit organization that revitalizes underused land in London for agriculture. The designated area provides an opportunity to test growing conditions for future initiatives.
Three plants used in the making of the Three Sisters Soup – corn, squash and beans – are often planted tightly together and, like close sisters, aid one another in their respective growing processes.
Both the soup and pilot garden are part of a two-year program at St. Joseph’s called the Nourish Project, which aims to reduce negative impacts on the environment, strengthen community partnerships and develop more sustainable food practices, specifically within food services.
12
“By shaping food and nutrition for human and planetary health in a health care setting, St. Joseph’s is leveraging the power of food to propel us towards a healthier and better future,” says Lori Higgs, Nourish Project committee member and St. Joseph's Vice President of Clinical Support and Chief Financial Officer.
“The project will examine how we source our food, reduce food waste and packaging, and even the possibility of growing food onsite so that we can do a better job for our environment,” adds Lori.

Back in the kitchen, Chef Fred finishes prepping the soup and double-checks to ensure it’s at just the right temperature.
“Patients and residents are loving the soup and it’s now become part of our regular menus,” he explains. “I think it might be around and enjoyed for a long time to come.”

ISSUE 05 | www.sjhc.london.on.ca
Dick Haenni, a resident in the Veterans Care Program of St. Joseph’s Health Care London, enjoys a bowl of Three Sisters Soup.
Patients and residents are loving the soup and it’s now become part of our regular menus.
– CHEF FRED COUSINS
“
Urban Roots London staff and members of St. Joseph’s Nourish Project construct a pilot garden at Parkwood Institute.
13
For
Crisis
Hope Beyond Hospital Walls
St. Joseph’s Health Care London was the first organization in Canada to implement the Zero Suicide initiative. Today, it is spreading across the province.
hat started as a lofty goal to reduce suicides and attempted suicides within a health care setting is taking flight in communities across Ontario. A suicide prevention toolkit is generating hope well beyond hospital walls.
A leader in suicide prevention, St. Joseph’s Health Care London was the first organization in Canada to implement Zero Suicide, a patient safety initiative that strives for system-wide transformation by wrapping care around those at risk of suicide so that fewer people fall through gaps along their care journey.
Now, the framework is available to any community organization, large or small, via the Zero Suicide Community Implementation Toolkit. The toolkit has been specifically designed to support organizations that are not a formal part of the health care sector by providing them with tools to create their own suicide prevention initiative.

The Zero Suicide program at St. Joseph’s was shaped by those who have experienced a suicide attempt or suicidal thoughts – either personally or
•
•
at 648 Huron
519
•
•
Among them is Thomas Telfer, a professor in Western University’s Faculty of Law, who was a member of the Zero Suicide Implementation Committee when the program was first launched at St. Joseph’s.
“I am a survivor of two suicide attempts,” says Thomas. “That the hospital included someone with personal lived experience was really important.”
In 2016, St. Joseph’s began implementing the Zero Suicide initiative in phases within the Mental Health Care Program. Today, the framework is embedded within additional care areas across the organization. It includes processes to assess an individual’s suicide risk, helping them to stay safe, and providing evidence-based follow-up and treatment. The program’s implementation was funded entirely through donations to St. Joseph’s Health Care Foundation.
Through his role on the committee, Thomas shared experiences from his past hospitalizations, allowing him to provide a very important patient perspective. He was also involved in developing a ‘coping plan’ tool for patients. The tool helps patients identify, together with their care provider, types of situations that may cause stress and to determine healthy coping behaviours, as well as who they can connect with when
The Zero Suicide Community Implementation Toolkit
provides organizations
better
and assist those who may be
thoughts
with resources to
identify, support
experiencing
of suicide.
Mental Health
Support in London-Middlesex:
Contact Reach Out crisis response line – Call 519-433-2023 or 1-866-933-2023 (The crisis response line and web chat are both available 24/7 and confidential)
Go to the Canadian Mental Health Association Crisis Centre, located
St, London, ON,
434-9191
Go to your nearest emergency department
WCall 911 14
It’s a plan for wellness focusing on the positive steps to stay healthy – both physically and mentally. In addition, patients at higher risk work with their care provider to develop a suicide management plan and receive extra support until they feel safe again.
Many of these resources are now part of the Zero Suicide Community Implementation Toolkit.
“Our goal is to decrease suicide rates within our region by providing organizations and their staff members with the tools they need to better identify, support and assist those who may be experiencing thoughts of suicide,” explains Shauna Graf, project lead for St. Joseph’s Zero Suicide initiative.
Created in collaboration with Niagara Region Public Health (NRPH), which has also implemented the Zero Suicide model, the toolkit includes the experiences and successes of both St. Joseph’s and NRPH.
Thomas considers the toolkit “an amazing accomplishment” that provides all organizations with a vital guide to help care for the psychological health and well-being of their employees.
“It’s really about improving the quality of life of people,” he explains.
“The toolkit should be used as part of a larger conversation about mental health and to encourage open-dialogue, allowing people to be more open about their own personal thoughts, feelings and experiences so we can continue to break down the stigma that still surrounds mental illness and suicide awareness.”
As a registered nurse who has worked within the mental health field for eight years, Shauna feels the goal of zero suicide is indeed a community responsibility.

“We can all take part in suicide awareness and prevention," encourages Shauna. “From the way we individually think and talk about suicide to how we prioritize and commit to safer communities, action to prevent suicide is a collective responsibility. Working together to create and share resources are truly actions that generate ripples of hope.”
Scan to learn more about the Zero Suicide initiative or to request information on the Zero Suicide Community Implementation Toolkit, visit sjhc.london.on.ca
 Shauna Graf
Shauna Graf
at St. Joseph’s Health Care London led the development of the Zero Suicide Community Implementation Toolkit – a free resource to guide organizations in their suicide prevention plans.
15
Taking Control One Pace at a Time
An innovative online tool gives people living with mild traumatic brain injuries the opportunity to take charge of their symptoms to enhance recovery.
After an intense workout two years ago, Cindy Vanderveen began noticing an array of debilitating symptoms she thought were signs of a stroke.
“I had issues with my vision, problems speaking and couldn’t eat or drink without choking on my food,” explains Cindy. “Everything I used to enjoy doing – gardening, cycling, working – it just stopped and my entire life was put on hold.”

What the 42-year-old knows now is she was experiencing symptoms of a mild traumatic brain injury (mTBI).
After multiple concussions over the years, she was struggling with post-concussion syndrome.
Although a person with a mTBI may appear fine on the outside, many have to pace their day-to-day activities in order to allow the time needed for the brain to properly heal.
Cindy was referred to the Acquired Brain Injury (ABI) Rehabilitation Program at St. Joseph’s Health Care London (St. Joseph’s) where she was encouraged to try a new research tool called MyBrainPacer™App.
Developed by scientists at Lawson Health Research Institute –the research institute of St. Joseph’s – the app was made possible by funding from the Cowan Foundation and other community supporters through St. Joseph’s Health Care Foundation.
“By documenting activity levels over time, patients and their clinicians can better understand what activities are linked to worsening symptoms,” explains Lawson scientist Dalton Wolfe (PhD), whose team is currently studying the efficacy of the app.
The MyBrainPacerTM App promotes recovery by helping individuals plan and pace their daily activity.
Much like point tracking used by dieters to monitor food choices, those using MyBrainPacer™ App can assign values to tasks like driving, grocery shopping, screen use and exercise so they can plan and pace their daily activity. Individual users are given a total number of points per day that will keep their persisting symptoms in the ‘safe range’. As users track their symptoms through the app, the app adjusts the daily point value to what is best for the user. After using the app for some time, Cindy has noticed some significant changes.
“In the beginning I wasn’t able to drive farther than five minutes at a time,” she explains. “Once I began to use the app to plan and track my activities, my symptoms dramatically decreased.”
Currently, anyone with a mTBI can enrol as a study participant on the MyBrainPacer™ App and use the tool.
Hoping to enrol about 5,000 users, Dalton says information gathered by the app “is vital to understand what is working for future therapeutic approaches.”
Anyone interested in using the MyBrainPacerTM App can do so by visiting mybrainpacer.ca.
 Cindy Vanderveen, who has suffered several concussions, uses the MyBrainPacerTM App to manage her brain injury.
Cindy Vanderveen, who has suffered several concussions, uses the MyBrainPacerTM App to manage her brain injury.
Realizing a Dream in a New Land
At St. Joseph’s Health Care London, internationally trained nurses are receiving the training they need to work in Ontario at a time of critical nursing shortages across the province.
Ever since she can remember, Jasmine Devassy has dreamed of being a nurse. She’s even chased that dream across the world.

“I grew up in India, in a family of nurses,” says Jasmine. “My mom is a nurse, and so are two of my sisters.”
Jasmine completed her registered nurse (RN) training in India in 2005 and went on to work as an RN in Singapore for 12 years. While working, she completed her RN degree through distance learning at a university in Australia. In 2018, Jasmine and her husband made the decision to move to Canada. With the move came a new set of challenges. Before working as an RN in Ontario, Jasmine needed to be certified with the College of Nurses of Ontario (CNO), the governing body of all nurses in the province. The rigorous certification process includes passing a written exam and demonstrating knowledge in both education and nursing practice.
“The training provided to nurses in other countries is not parallel to what’s provided in Canada,” explains Angela Reid, professional practice consultant at St. Joseph’s Health Care London (St. Joseph’s).
“These individuals often need to upgrade their skills, but proving they have the practical competencies needed without having worked in the Ontario health care system is difficult.”

In January 2022, Ontario Health and the CNO collaborated to develop the Supervised Practice Experience Partnership Program (SPEP), which provides internationally educated nurses the opportunity to demonstrate their competency to practice while being supervised and mentored by a CNO member.
At St. Joseph’s, the SPEP has been implemented across the organization and several applicants have been matched with registered practical nurse (RPN) or RN preceptors in various clinical areas.
“The applicants get the experience and clinical hours they need in a safe environment while our health care system gains the unique perspectives of care these individuals learned in their home countries,” says Angela. The SPEP is also a way for St. Joseph’s to recruit, retain and grow our nursing workforce.”
Creating new opportunities for nurses to join the system is especially important considering the current shortage of nurses across the province. Through the SPEP, Ontario Health and the CNO are tapping into a new pool of candidates willing to step in and fill these roles.
For Jasmine, the SPEP has meant she can stay with her family while reaching her career goals.
“At one point, I considered moving back to Singapore so I could continue working while my husband and children stayed here in Canada. Through the SPEP, St. Joseph’s has provided me the opportunity to once again work in the profession I love.”
Potential candidates and organizations interested in the Supervised Practice Experience Partnership Program can find more information on cno.org.
Jasmine Devassy
is gaining the practical skills and competencies needed to become a certified nurse in Ontario through the Supervised Practice Experience Partnership Program at St. Joseph’s Health Care London.
ISSUE 05 | www.sjhc.london.on.ca 17
Fast and Slow
The speeds of a stroke journey
Specialized rehabilitation at St. Joseph’s Health Care London helps stroke survivors return to living life fully.
It was the middle of the night in January 2022 when Michael woke up with a strange feeling. After tossing and turning, unable to get comfortable, Michael’s wife woke to ask if he was OK.
“When I replied, she noticed I was slurring my words,” Michael recalls. “Then she quickly asked me to squeeze her hands with mine and when I couldn’t, she called 911.”
Michael was having a stroke and his wife’s quick action and knowledge most likely saved his life.
Paramedics rushed Michael to hospital where he was diagnosed with a stroke caused by a blood clot in his brain.
After two surgeries – one to remove the clot and place a stint and a second to repair internal bleeding – Michael began the long road to recovery, which would include a transfer to St. Joseph’s Health Care London for specialized rehabilitation after his initial treatment.

“The first four hours after a stroke are crucial,” explains Dr. Ricardo Viana, a physiatrist at St. Joseph’s Parkwood Institute. “In that timeframe a patient can receive lifesaving care that reduces the severity of damage a stroke can cause to the brain.”
Minimizing the damage also means a better chance at recovery through rehabilitation.
Blood clots are the most common cause of strokes and treatment includes a special type of drugs called thrombolytic medicines that work to break up or dissolve clots in the body. But administering drugs within that fourhour time frame is critical.
Dr. Viana encourages everyone to know the FAST signs of stroke, which stands for Facial drooping, Arm weakness, Speech difficulties and Time to call emergency services.
“Don’t drive to the hospital, he urges. “Call 911 right away.”
ON THE ROAD TO RECOVERY
While the stroke paralyzed the left side of his body, Michael quickly regained his ability to walk with the help of the inpatient rehabilitation team in the Stroke/ Neurological Rehabilitation Program at Parkwood Institute.
“I had intensive physio two to three hours a day. The team provided amazing support, especially the physiotherapists, who kept me motivated, focused and helped build my confidence to keep going.”
Recovery has been slower than Michael would like, but he’s determined to keep pushing forward.
“I want to get back to who I used to be. I’ve learned the harder I work at therapy, the faster I meet my goals.”
18
ONE STEP AT A TIME
On April 22, 2020, Roger Oatman awoke not feeling well. His last clear memory is picking up the phone and falling to the floor. The next thing he remembers is overhearing his wife on the phone and knowing something was wrong.
“The ambulance drivers wheeled me out the door, then… I can’t remember the next three weeks.”
Roger’s stroke affected his right arm and leg and he struggles to get words out due to Broca’s aphasia, an acquired language disorder caused by injury to the speech and language areas of the brain.
After a hospital stay, Roger was connected with Parkwood Institute’s Community Stroke Rehabilitation Team, a specialized program that provides rehabilitation for stroke survivors at home or in the community. The team includes health care providers from various specialties such as physiotherapy, occupational therapy, social work, nursing, speech language pathology and theraputic recreation. The team, in partnership with other community care providers, helped Roger return to living life fully. His advice to other stroke survivors is not to compare their progress to others.

“Just get up, every day. Remember, even one or two steps is an accomplishment. Don’t give up. It will get better.”
LEARN THE SIGNS OF A STROKE
SPEECH
9-1-1
ISSUE 05 | www.sjhc.london.on.ca 19
FA S T
ARMS Can you raise both? FACE Is it dropping?
Is it slurred or jumbled? TIME To call
right away.
Act FAST because the quicker you act, the better the chance of recovery.
Boundaries in Stroke Rehabilitation Pushing
Dr. Robert Teasell is an international leader in stroke rehabilitation research. Now his legacy will continue with the introduction of a new fellowship in his honour.
Dr. Robert Teasell remembers visiting veterans in the large open wards at the old Westminster Hospital when he was a medical student.
“The most popular person was a lady who went around twice a day and handed out free cigarettes,” he says with a laugh, “Times have changed!” They certainly have, and Dr. Teasell’s illustrious career in stroke rehabilitation at St. Joseph’s Health Care London (St. Joseph’s) has contributed significantly to those health care changes. He is considered the “godfather of stroke rehabilitation in Canada,” says Dr. Keith Sequeira, Interim Chief of Physical Medicine and Rehabilitation in London. It’s a legacy now inspiring others to make their own mark in stroke research and care with the creation of the Dr. Robert Teasell Fellowship in Stroke Rehabilitation Care & Research.
Dr. Teasell began his career at University Hospital (UH), a leading neurology hospital now part of London Health Sciences Centre. Alongside advances in acute care at UH, stroke rehabilitation began to change. With this shift, UH became one of the first centres to create a team to treat patients after stroke.
In the late 1990s the Ontario government developed a comprehensive stroke strategy and Dr. Teasell played a key role in the group assigned to improve and standardize stroke rehabilitation, and establish outcome measures.
In 2001, as part of health care restructuring in London, Dr. Teasell, then Chair of Physical Medicine and Rehabilitation, led the process of consolidating the city’s four stroke rehabilitation units into one, which was then relocated to Parkwood Hospital (now St. Joseph’s Parkwood Institute).
In 2002, he and his team produced the first Stroke Rehabilitation Evidence-Based Review (SREBR), a comprehensive analysis of existing research data with implications for patient care. The study shone a light on key principles that Dr. Teasell calls the “Big Five” – essential elements of rehabilitation that make the biggest difference.
They call for stroke therapy that is specialized, intense, task-specific, provided quickly after a stroke, and continued on an outpatient basis.
With these ground-breaking findings and Dr. Teasell’s expert guidance, Parkwood Institute made a major investment in outpatient post-stroke therapy to support the new, specialized stroke rehabilitation inpatient unit.
Dr. Jamie Fleet
is the inaugural recipient of the Dr. Robert Teasell Fellowship in Stroke Rehabilitation Care & Research, awarded to a scientist who is carving a promising new path in the field of stroke rehabilitation.

Dr. Bob Teasell

at St. Joseph’s Health Care London is considered the godfather of stroke rehabilitation having made significant contributions to the field of stroke rehabilitation over the course of his illustrious career.
While unique at the time, outpatient therapy soon became a standard of care. In 2009, the team developed the community stroke rehabilitation teams in conjunction with the South West Local Health Integration Network.
“Introducing outpatient therapy resulted in significant changes in outcomes and reduced costs for patients and the system,” says Dr. Teasell.
Today, Dr. Teasell and his team are focused on the future of stroke rehabilitation. Enthused as ever, he predicts “a second transformation in stroke rehabilitation” is on the horizon.
With more than 375 peer-reviewed articles, 22 book chapters, and 60 monographs, Dr. Teasell’s contributions to research and patient care are exceptional. Equally important has been his mentorship of a new generation of rehabilitation scientists. He believes in hiring motivated people, giving them top billing on publications, and fostering collaboration.
– DR KEITH SEQUEIRA
To honour Dr. Teasell’s dedication to ensure a future generation of committed scientists and his many contributions to the field of stroke rehabilitation, St. Joseph’s and St. Joseph’s Health Care Foundation have partnered to create the fellowship in his name, which will provide salary and research support to a promising young researcher.
Dr. Jamie Fleet is such a researcher. With a focus on bone health and stroke, she is the inaugural Teasell Fellow. Her goal is to build a more complete understanding of bone health after stroke, identify gaps in screening and treatment, and study the safety and efficacy of potential treatments. Dr. Fleet is also working to shed light on the effect of aerobic exercise on brain activation and fatigue levels after a stroke, and to identify and address potential barriers to exercise recommendations.
“This will be huge for the future of stroke rehab research and patient care outcomes,” says Dr. Sequeira of the fellowship. “It will ensure our patients continue to receive the best quality of care.”
ISSUE 05 | www.sjhc.london.on.ca 21
This will be huge for the future of stroke rehab research and patient care outcomes.
“
A Passion For OurPast
Artifacts displayed at St. Joseph's Hospital each tell a story, as do the efforts taken to preserve them. The exhibit changes regularly to highlight the hospital’s fascinating history.
The history of St. Joseph’s Hospital is rich with more than 130 years of compassionate care, innovative research and teaching the next generation of care providers. This illustrious legacy is almost palpable within the halls and care areas, and tangible in the artifacts on display in the hospital’s heritage exhibit space. Here, the St. Joseph’s Hospital and Nursing School Artifact Collection is showcased to bring the past to life.
From needle-sharpening stones to portable electrocardiographs, the collection highlights the painstaking and pioneering efforts of St. Joseph’s physicians, scientists and nurses to put their patients first. Among the items hinting at bygone times is a complicated metal intubation set (circa 1915), which required assembly and sterilization prior and after use, and a 1930s drying oven used to remove moisture from chemicals during the lengthy process of medication preparation.
The laborious efforts to ensure the wellbeing of the sick are evident not only in the artifacts, but in the care taken with these intriguing items and their stories.
“There have always been people interested in preserving the history of St. Joseph’s over the decades,” says Noelle Tangredi, an eLearning developer and graphic designer with Organizational Development and Learning Services at St. Joseph’s Health Care London. “I happened to find out about boxes full of artifacts in storage and made it my mission to get them organized and have a way to share them with the staff and community.”
Noelle and a few other employees – now retired – worked to get an


A note on the back of a framed print speaks of a young patient’s battle with strep throat and rheumatic fever after being admitted in 1936 to St. Joseph’s Hospital, where she spent nearly a year recovering.

She receives invaluable assistance from Mary Kosta, Congregational Archivist for the Congregation of The Sisters of St. Joseph in Canada, along with Mary’s practicum students, to clean, catalogue, photograph, research and properly store the artifacts.


Since older documents and photographs require a special environment to be maintained, they become part of the congregation archives. The rest of the artifact collection is housed in a storage room at St. Joseph’s Hospital, which also contains a work area. A few times a year, Noelle curates an exhibit using the artifacts and research for her inspiration.
“Our collection only contains artifacts that have a direct connection to St. Joseph’s Hospital or St. Joseph’s Nursing School,” explains Noelle. “Many of the collection items come from donations from the community, but some come from our Environmental Services or Facilities Management teams having found things left behind in treatment rooms or offices.”
Not all artifacts are care or research tools. The collection also features a set of postcards and notes from former patients and residents of St. Joseph’s Hospital from the first half of the 20th century.
A note on the back of a framed print speaks of a young patient’s harrowing battle with illness in the hospital prior to World War II. The patient was only 10 years old when she was admitted to St. Joseph’s Hospital in 1936 for strep throat and rheumatic fever. She spent nearly a year recovering at the hospital under the care of Dr. Hubert Loughlin, a well-respected paediatrician who would later serve as Chief of Paediatrics from 1948 to 1963.
The patient's sentiments about her illness and her “year spent in bed” are noted in ink. “A terrible experience for a 10-year-old. Missed a lot of school, which I loved. Perhaps made me a special person, as I came through it all.”
Those coming to St. Joseph’s Hospital for a medical appointment are invited to view the history of St. Joseph’s on display while they are in the building. The exhibit space can be found in Zone A, Level 1, off the main corridor closest to Richmond Street. Have you uncovered any intriguing artifacts or stories related to the history of St. Joseph’s Hospital or the St. Joseph’s Nursing School in London? Interested in donating to the collection? Please email Noelle.Tangredi@sjhc.london.on.ca.
Noelle Tangredi, volunteer keeper of the historical artifacts at St. Joseph's Hospital, shows off the microscope that belonged to Dr. Frederick Luney, who set up the hospital's first pathology and biochemistry lab in 1927.
23
ISSUE 05 | www.sjhc.london.on.ca
St. Joseph’s Health Care London provides care through a unique mix of clinical settings – making us one of the most complex health care organizations in Ontario. In a continual effort to bring the best
possible to those we serve, we constantly engage patients and their families, leaders, physicians, staff, volunteers, donors and many partners to ensure St. Joseph’s takes innovative steps in addressing the health


MY
of our community, now and in the future.
JOSEPH’S
St.
Parkwood
Southwest
Teams,
SHARE
St.
N6A
24
care
care needs
YOUR FEEDBACK OR STORY WITH US
Joseph’s Health Care London PO BOX 5777, STN B London, ON
4V2 519 646-6100 ext. 66034 ComDept@sjhc.london.on.ca Mount Hope Centre for Long Term Care
clinics and programs in our community and beyond.
Centre for Forensic Mental Health Care
Joseph’s Hospital
Institute
ST.
IS























 Shauna Graf
Shauna Graf

 Cindy Vanderveen, who has suffered several concussions, uses the MyBrainPacerTM App to manage her brain injury.
Cindy Vanderveen, who has suffered several concussions, uses the MyBrainPacerTM App to manage her brain injury.












