
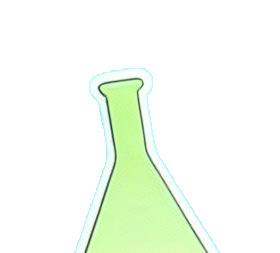
11 days after appendectomy, tests for acute abdominal pain revealed a



11 days after appendectomy, tests for acute abdominal pain revealed a
left inside the patient.
Surgical miscounts are considered never events because they are usually preventable by following established procedures.
ProAssurance offers risk assessments designed to help practices minimize errors by establishing and evaluating safety procedures and communication protocols.
With reliable procedures in place, our insureds are more likely to reduce errors in their medical practice, avoid claims, and make claims more defensible if they do occur.


PRESIDENT Sujeeth Punnam, MD
PRESIDENT ELECT Stephen Tsang, MD
TREASURER Sanjeev Goswami, MD
BOARD MEMBERS Maggie Park, MD, Alain Flores, MD, Manreet Basra, MD, Kinnari Parikh, MD, Bhagya Nakka, MD, Sunny Philip, MD, Rahuljit Bajwa, MD, Neelesh Bangalore, MD and Dheeraj Nandanoor, MD
MEDICAL SOCIETY STAFF
EXECUTIVE DIRECTOR Lisa Richmond
MEMBERSHIP COORDINATOR Jessica Peluso
COMMITTEE CHAIRPERSONS
CMA AFFAIRS COMMITTEE James Halderman, MD
CMA TRUSTEE Ramin Manshadi, MD
DECISION MEDICINE Kwabena Adubofour, MD
MEDICAL EDUCATION PROGRAMS Kelly Savage, MD
SCHOLARSHIP LOAN FUND Alexander Fodor, MD
CMA HOUSE OF DELEGATES REPRESENTATIVES
Aisha Chaudhry, MD, Dheeraj Nandanoor, MD, James R. Halderman, MD, Raissa Hill, DO, Richelle Marasigan, DO, Philip Edington, MD, Sujeeth Punnam, MD, Ripudaman Munjal, MD, Stephen Tsang, MD, Alberto Del Pilar, MD
SAN JOAQUIN PHYSICIAN MAGAZINE
EDITOR Lisa Richmond
EDITORIAL COMMITTEE Lisa Richmond, Sujeeth Punnam, MD
MANAGING EDITOR Lisa Richmond
CREATIVE DIRECTOR Sherry Lavone Design
CONTRIBUTING WRITERS Sujeeth Punnam, MD, Shadi Barfjani, MD, MS, Harmeet Kaur PhD, HCLD(ABB), M(ASCP) CM, Steven Stewart, B.S. PHM
THE SAN JOAQUIN PHYSICIAN MAGAZINE is produced by the San Joaquin Medical Society
SUGGESTIONS, story ideas are welcome and will be reviewed by the Editorial Committee.
PLEASE DIRECT ALL INQUIRIES AND SUBMISSIONS TO: San Joaquin Physician Magazine 3031 W. March Lane, Suite 222W Stockton, CA 95219
Phone: (209) 952-5299 Fax: (209) 952-5298
E-mail Address: lisa@sjcms.org
MEDICAL SOCIETY OFFICE HOURS: Monday through Friday 8:00am - 4:00pm
















As I write this, I have just returned from a Medical Executives Conference with my colleagues from medical societies across the state. These meetings provide a valuable opportunity to share ideas and best practices and to hear timely updates from Dustin Corcoran, CEO of the California Medical Association (CMA), and CMA President Dr. Rene Bravo. Our close partnership with CMA remains one of the key reasons the San Joaquin Medical Society continues to be effective in supporting our members and advancing the practice of medicine in our region.
The 2025 legislative session brought significant changes affecting health care across California, with a strong focus on reproductive care, public health, health care funding, prescription drug coverage and prescribing, and the growing role of private equity. CMA successfully sponsored several important bills that were signed into law by the Governor. These include SB 306, which eliminates prior authorization requirements for services insurers routinely approve; SB 351, which strengthens the corporate bar by allowing the Attorney General to hold private equity groups accountable when they interfere with the practice of medicine; and AB 489, which prohibits companies from marketing artificial intelligence chatbots as licensed medical professionals. Together, these victories reduce administrative burden, protect physician autonomy, and safeguard patient trust.
Another important development is the announcement by Physicians for a Healthy California of $85 million in CalMedForce and CalMedForce+ grants to expand graduate medical education opportunities across California. In this eighth round of funding, programs in San Joaquin County were awarded more than $4.6 million! We know that physicians who train here are far more likely to stay and practice locally, an outcome that directly improves access to care for patients in our community.
We encourage you to get involved in SJMS. Whether your interests include leadership, advocacy, governance, or supporting future physicians through our Decision Medicine and Bridge to Medicine pipeline programs, there are meaningful ways to contribute. Watch for an email this spring with opportunities to nominate yourself or others for open positions on the SJMS Board of Directors and the CMA House of Delegates.
Please also consider joining colleagues at CMA’s 52nd Legislative Advocacy Day on Wednesday, April 8, in Sacramento. This important event brings together more than 400 physicians and medical students from across specialties and practice settings to meet with legislators and advocate on priority health care issues. Registration is now open at www.cmadocs.org. For questions, please contact Lisa@sjcms.org
Finally, save the date for our Annual Awards Dinner on Sunday, June 7, at the Stockton Golf and Country Club. We look forward to celebrating our 2026 Young Physician and Lifetime Achievement Award recipients.
Best wishes, Lisa Richmond








Sujeeth Punnam, MD is the current president of the San Joaquin Medical Society and practices interventional cardiology at Sutter Gould Medical Group
Esteemed colleagues,
I hope you and your loved ones are doing well. It was wonderful connecting with many of you at the SJMS Winter Gala in December. As we move into a new season, I’d like to share important updates shaping our profession — from the evolving role of Artificial Intelligence in medicine to major developments in telehealth and graduate medical education funding.
Artificial Intelligence continues to dominate conversations in health care, and for good reason. With great power comes great responsibility — and AI’s potential to reshape our workflows is significant.
What’s important to remember is this: AI works best when you barely notice it.
Physicians and staff lose 2–3 hours every day to administrative tasks unrelated to patient care — documentation, phone tag, fax follow-up, billing corrections, and scheduling issues. Modern AI tools don’t add more work; they remove it by:
• Documenting encounters in real time
• Surfacing clinical evidence during patient conversations
• Suggesting accurate coding
• Consolidating patient communication into a single, secure channel
• Answering routine questions before your team picks up the phone
For larger groups, AI now streamlines compensation workflows as well — enabling billing within minutes of a shift and providing real-time visibility into earnings and incentives.
The best part is that you don’t need to “learn AI.” You simply adopt platforms that save time, reduce costs, and improve the patient experience. If you need guidance on implementation, our team is here to support you.
The federal shutdown on September 30, 2025, resulted in the temporary expiration of Medicare telehealth waivers. However, Congress has since reaffirmed what providers have demonstrated since the early pandemic: telehealth is now a core component of modern health care delivery.
On February 3, 2026, the President signed H.R. 7148 — the Consolidated Appropriations Act, 2026, extending key Medicare telehealth flexibilities through December 31, 2027.
• Medicare-enrolled providers may continue delivering authorized telehealth services
• No geographic restrictions on patient or provider location within the U.S.
• RHCs and FQHCs remain eligible distant sites for nonbehavioral telehealth
• Audio-only visits remain reimbursable
• Hospice recertification may be completed via audio-visual telehealth
• No in-person requirement within six months for behavioral health telehealth
Please note: These waivers apply only to Medicare. Medicaid and commercial plans may differ, and state licensure requirements remain unchanged.
California is now implementing voter-approved Proposition 35 measures, including approximately $85 million in Graduate Medical Education funding through CalMedForce (Physicians for Healthy California).
For the 2025–2026 cycle, $4.6 million in grants were awarded to SJMS service-area programs in the Central Valley:
Adventist Health Central Valley Network Hanford (Sonora) Family Medicine Residency Program — $1,260,000
St. Joseph Medical Center Family Medicine, Internal Medicine, Neurology, Orthopedic Surgery, Psychiatry, Urology Residency Programs; Cardiovascular Disease & Critical Care Medicine Fellowships — $2,885,000
San Joaquin General Hospital Family Medicine and Internal Medicine Programs — $510,000
These investments strengthen our region’s physician pipeline and support the future of health care in the Central Valley.
SJMS remains committed to working with CMA to address the rising cost of ACA premiums and advocate for sustainable solutions. As spring approaches, I look forward to gathering again and celebrating with you at our Summer Awards Gala.
The California State Legislature passed several new laws in 2025 affecting health care. In particular, there was a strong focus on reproductive care, public health, health care funding, prescription drug coverage and prescribing, and the role of private equity. Below is a list of the most significant new health laws of interest to physicians.
AB 460 – Radiologic technologists: venipuncture: direct supervision
CMA Position: Support
Authorizes remote supervision of radiologic technologist by revising the definition of “direct supervision” to require a licensed physician to be either physically present within the facility and immediately available to intervene, or available immediately via audio and video communication with access to patient’s medical imaging records and have ability to intervene by directing other onsite personnel, in relation to a radiologic technologist’s ability to perform upper extremity venipuncture under the direct supervision of a licensed physician. Requires facility to have safety protocols and either a licensed physician who is physically present, or onsite personnel with the appropriate license to respond to adverse events at the physician’s direction.
AB 876 – Nurse anesthetists: scope of practice
Authorizes a nurse anesthetist to perform anesthesia services. Defines “anesthesia services” to mean preoperative, intraoperative, and postoperative care and pain management provided by a nurse anesthetist for patients receiving anesthesia pursuant to an order by a physician, dentist or podiatrist. Deems an order by a physician, dentist, or podiatrist for anesthesia services for a specific patient as authorization for a nurse anesthetist to select and implement the modality of anesthesia for the patient and to abort or modify the modality during care. Clarifies that selection and administration of medication by a nurse anesthetist for purposes of anesthesia services, as defined, does not constitute a prescription.
1501
Increases number of physician assistants that a physician and surgeon may supervise at any one time to eight PAs. Adds “podiatric surgeon” to list of terms that cannot be used by anyone who is not a licensed podiatrist. Establishes state policy that doctors of podiatric medicine shall not be classified or treated as ancillary providers or allied health professionals in any health care setting or insurance reimbursement structure. Extends operations of Physician Assistant Board and Podiatric Medical Board until Jan. 1, 2030.
1503
Transitions aspects of pharmacy practice to a standard of care model. Streamlines and expands pharmacist authority to furnish preventive medications, and order and interpret tests. Authorizes pharmacists to furnish dangerous devices and FDA-approved or authorized medications as part of preventive health care services that do not require a diagnosis, and to complete missing information on a prescription for noncontrolled medication if there is evidence to support the change. Allows pharmacists to provide clinical advice and consultation to patient’s agent. Removes requirement that pharmacists make “every reasonable effort” to contact prescriber before refilling prescriptions in certain emergency cases. Deletes restriction preventing pharmacists from
dispensing 90-day supply if prescriber indicated “no change” to refill quantity. Deletes 2026 repeal date for pharmacist test-to-treat authority for COVID-19 oral therapeutics after positive test. Requires pharmacists to provide specified services or activities consistent with accepted standard of care, defined as degree of care a prudent and reasonable licensed pharmacist, with similar education, training, experience, resources, and setting, would use in similar situation. Extends operation of Board of Pharmacy to Jan. 1, 2030.
CMA Position: Support
Prohibits a pharmacy benefit manager (PBM) from requiring use of an affiliated pharmacy, and from imposing requirements, conditions, or exclusions that discriminate against a nonaffiliated pharmacy in connection with dispensing drugs. Limits a PBM’s income to a defined management fee for services provided and requires use of passthrough pricing model. Requires a contract between a health insurer and PBM issued, amended, or renewed on or after Jan. 1, 2027, or the date on which the Department of Managed Health Care has established the licensure process, to require PBMs to be licensed and in good standing. Authorizes Attorney General enforcement and specified legal remedies for a violation.
AB 316 – Intelligence: defenses
In a civil action alleging harm caused by artificial intelligence (AI), prohibits a developer, modifier, or user of AI from asserting a defense that the AI’s autonomous actions caused plaintiff’s harm. Does not limit or preclude a defendant from presenting any other affirmative defense, including evidence relevant to causation or foreseeability, or other evidence relevant to comparative fault of any other person or entity
AB 489 – Health care professions: deceptive terms or letters: artificial intelligence
CMA Position: Sponsor
Prohibits artificial intelligence (AI) or generative artificial intelligence (GenAI) technology from using certain terms, letters, or phrases that indicate or imply that the advice, care, reports, or assessments being provided through AI or GenAI is being provided by a natural person with the appropriate health care license or certificate. Makes existing prohibition on the use of specified terms, letters, or phrases to falsely indicate or imply possession of a professional practice license or certificate enforceable against an entity who develops or deploys AI or GenAI technology that uses those terms or phrases in its advertising or functionality. Makes a violation subject to the jurisdiction of the appropriate healing arts board, and makes each use of prohibited term or phrase a separate violation.
AB 45 – Privacy: health data: location and research
CMA Position: Support
Updates existing prohibitions on the collection, use, disclosure, sale, sharing, or retention of the personal information of a person who is physically located at, or near, a family planning center except under certain circumstances, including for the collection or use as necessary to perform or provide the requested services or goods. Prohibits geofencing, or selling or sharing personal information with a third party to geofence, an entity that provides in-person health care services in California. Does not alter applicable law regarding law enforcement agency use of personal information generated by an electronic monitoring device. Authorizes an aggrieved person to institute and prosecute a civil action against any organization or group of people acting in concert for a violation of these provisions.
81
CMA Position: Support
Revises definition of “medical information,” for purposes of the Confidentiality of Medical Information Act, to include immigration status and place of birth, if known or collected, and defines “immigration enforcement” to mean any and all efforts to investigate, enforce, or assist in investigation or enforcement of any federal civil immigration law, and also includes efforts to investigate, enforce, or assist in the investigation or enforcement of
any federal criminal immigration law that penalizes a person’s presence in, entry or reentry to, or employment in, the United States. Specifies that a provider, health plan, or contractor shall disclose medical information regarding a patient, enrollee, or subscriber, pursuant to a valid search warrant issued by a judicial officer to a government law enforcement agency, or pursuant to a court order issued by a California state court or federal court. Prohibits a health care provider, health care service plan, contractor, or corporation and its subsidiaries and affiliates from disclosing medical information for immigration enforcement, except to the extent authorized by a patient, enrollee, or subscriber, or as otherwise permitted or required.
Authorizes a health care provider to disclose the results of an HIV test that identifies or provides identifying characteristics of a Medi-Cal beneficiary without written authorization of the test subject or their representative, to the beneficiary’s Medi-Cal managed care plan, and to external quality review organizations conducting external quality reviews of Medi-Cal managed care plans, for the purpose of administering quality improvement programs designed to improve HIV care for Medi-Cal beneficiaries.
CMA Position: Support
Urgency measure effective Oct. 13, 2025. Prohibits a health care provider, health plan, or contractor from: (1) releasing medical information related to a person seeking or obtaining gender-affirming health care or genderaffirming mental health care in response to a criminal or civil action based on another state’s law that interferes with the right to such care; (2) cooperating with or providing medical information to an individual, agency, or department from another state, or to a federal law enforcement agency, identifying a person seeking or obtaining genderaffirming health care; or (3) releasing medical information related to sensitive services in response to foreign subpoena based on violation of another state’s laws authorizing criminal action against a person for providing or receiving legally protected health care. Prohibits issuance of subpoena based on violation of another state’s law that interferes with right to gender-affirming care.
Requires the Department of Health Care Access and Information (HCAI), on or before Jan. 1, 2026, to take over all functions of the California Health and Human Services Data Exchange Framework. Expands the entities required to execute data sharing agreements with the Data Exchange Framework to expressly include emergency medical services and additional types of physician organizations and group practices as specified. Requires HCAI to establish, by no later than July 1, 2026, a process to designate qualified health information organizations as data sharing intermediaries that have demonstrated their ability to meet Data Exchange Framework requirements. Requires HCAI, in collaboration with the stakeholder advisory group, to report on the Data Exchange Framework to the Legislature by July 1, 2027. Expands membership of stakeholder advisory group to also include representatives from skilled nursing facilities, physician organizations, medical groups, and management services organizations.
SB
CMA Position: Sponsor
Prohibits a private equity group or hedge fund involved in any manner with a physician or dental practice doing business in this state from interfering with the professional judgment of physicians or dentists in making health care decisions, or exercising control or being delegated power over specified actions involving the business of the practice. Prohibits a private equity or hedge fund from entering into an agreement with a physician or dental practice that would enable a person or entity to engage in prohibited actions, and makes such provisions void and unenforceable. Prohibits contracts between a private equity group or hedge fund and a physician or dental practice from including any clause barring a provider in that practice from competing with the practice in the event of termination or resignation, or from commenting on that practice as to any issues involving care, ethical or professional challenges in the practice of medicine or dentistry, or revenue-increasing strategies employed by the private equity group or hedge fund, and makes such provisions void and unenforceable.
AB 82 – Health care: legally protected health care activity
CMA Position: Support
Prohibits the reporting of a prescription for or the dispensing of testosterone or mifepristone to the CURES database, Department of Justice (DOJ), or contractor, as specified. Requires DOJ, by Jan. 1, 2027, to remove certain existing records created or maintained prior to Jan. 1, 2026. Strengthens existing laws protecting confidentiality of personal information of providers of gender-affirming or reproductive health care services, their employees, volunteers, and patients, and individuals who face threats of violence or harassment due to their affiliation with such facilities. Expands prohibitions on disclosure of the image or personal information of such individuals with intent of inciting or causing bodily harm to that person or individuals residing at the same home address to expressly include gender-affirming care, and raises legal penalties for violations
AB 309 – Hypodermic needles and syringes
CMA Position: Support
Deletes Jan. 1, 2026 repeal date of, and makes permanent, existing laws allowing the nonprescription furnishing or sale, by a physician or pharmacist, of hypodermic needles and syringes for human use to persons aged 18 years or older, and authorizing persons aged 18 years or older to obtain hypodermic needles and syringes solely for personal use from a physician or pharmacist, without a prescription or license, as a public health measure.
CMA Position: Support
Authorizes a prescriber to dispense an unused portion of a dangerous drug acquired by the hospital pharmacy to an emergency room patient upon discharge under certain conditions. Exempts from licensure the use of an automated unit dose system if used to dispense dangerous drugs to ER patients.
CMA Position: Support
Requires Research Advisory Panel of California to review research projects to be conducted in-state that require the administration of Schedule I or Schedule II controlled substances. Authorizes panel, until Jan. 1, 2028, to expedite review of projects that satisfy certain criteria, including, among other things, that have sought or received certain federal approvals and have proof of independent peer review of the study. Authorizes panel chairperson to deputize two or more panel members to review and approve research project without a vote by the entire panel. Authorizes panel to withdraw its approval for reasonable cause; requires panel to provide notice for the concern to be cured by the project before withdrawing approval.
The following are health budget trailer bills that consist of numerous provisions covering a broad range of health topics. The summaries below highlight only the most significant provisions of each bill.
Urgency measure effective June 30, 2025, except as noted below. Requires pharmacy benefit managers (PBMs) contracting with health plans or insurers to obtain a state license from the Department of Managed Health Care beginning Jan. 1, 2027 or the date a licensure process is established, if later. Also requires PBMs to report drug pricing and related data to HCAI, and adds PBMs to the advisory committee for the Health Care Payments Data Program.
Delays the effective date of the infertility coverage mandate for group health coverage under SB 729 (2024) to Jan. 1, 2026, and grants state regulators guidance authority until Jan. 1, 2027.
Authorizes the California Health and Human Services Agency to enter into partnerships to increase competition, lower prices, and address supply shortages for generic or brand name drugs for the development, production, procurement, or distribution of vaccines, and for the manufacture, purchase, or distribution of medical supplies or medical devices.
Revises Medi-Cal coverage requirements for COVID-19 testing, screening, vaccines, and treatment, requiring MediCal managed care plans to cover services in accordance with Medi-Cal rules, and deleting prohibition on cost sharing and utilization management for COVID-19 diagnostic and screening testing.
Increases state rebate requirements for pharmaceutical manufacturers participating in Medi-Cal and changes how beneficiaries continue receiving drugs when a manufacturer is placed on prior authorization status. Starting Jan. 1, 2026, patients may keep getting their prescribed medication only if a prior authorization request is submitted and approved. Raises minimum rebate percentages, increases the minimum rebate for manufacturers without supplemental agreements, among other program changes.
Eliminates the training requirement for Medi-Cal providers to be paid for annual cognitive health assessments for beneficiaries aged 65 and older, and removes the state’s obligation to collect and publicly report data on the use and payments for this benefit.
Beginning July 1, 2026, requires Medi-Cal to reimburse federally qualified health centers and rural health clinics for services eligible for federal funding and expands the definition of a reimbursable visit to include certain telehealth encounters when they meet standards of care.
Limits Medi-Cal benefits for adults without satisfactory immigration status to pregnancy-related and emergency services, and eliminates dental coverage, subject to a $30 monthly premium starting no sooner than July 1, 2027. Delays implementation of certain provisions until specified administrative actions are completed.
CMA Position: Support
Urgency measure effective Sep. 17, 2025, except as noted below. Directs CDPH to use federal immunization and preventive service guidelines from Jan. 1, 2025, as a baseline and authorizes CDPH to adopt and publish updated or expanded guidelines and recommendations without formal rulemaking. Authorizes certain healing arts licensees to prescribe, administer, or initiate immunizations based on CDPH recommendations instead of federal guidelines.
Replaces references to federal Advisory Committee on Immunization Practices (ACIP) with CDPH for purposes of school immunization requirements and medical exemption procedures effective in part July 1, 2026, and for CalWORKs childhood immunization requirements and notifications. Shifts authority from ACIP to CDPH for senior immunization requirements in health facilities and for posting influenza educational materials online. Revises coverage requirements for health plans and insurance policies to follow U.S. Preventive Services Task Force recommendations as of Jan. 1, 2025, and replaces ACIP references with CDPH. Mandates Medi-Cal coverage of vaccines and immunizations according to federal and professional medical recommendations and any updates adopted by CDPH, contingent on federal funding and approvals.
Exempts certain nonminor dependents and foster youth from Medi-Cal service limits and monthly premiums for adults without satisfactory immigration status.
AB 951 – Health care coverage: behavioral diagnoses
CMA Position: Support
Prohibits a health care service plan contract or health insurance policy issued, amended, or renewed on or after Jan. 1, 2026, from requiring an enrollee or insured previously diagnosed with pervasive developmental disorder or autism to receive a rediagnosis to maintain coverage for behavioral health treatment for their condition. Requires a treatment plan to be made available upon request.
AB 1041 – Health care coverage: health care provider credentials
Beginning Jan. 1, 2027, requires health plans and insurers to make a determination regarding a provider’s credentialing application within 90 days of receiving a completed application. Provides an applicant a 120-day provisional approval if a health plan or insurer does not meet the 90-day timeline, except as specified. Requires every health care service plan or health insurer to activate the provider upon successful approval and notify the applicant of the activation. Requires every full-service health care service plan and health insurer, or its delegate, to
subscribe to and use the Council for Affordable Quality Healthcare credentialing form on and after Jan. 1, 2028. Does not apply to Medi-Cal managed care plans.
CMA Position: Support
Prohibits a large group health care service plan contract or health insurance policy issued, amended, delivered, or renewed on or after Jan. 1, 2026, or an individual or small group health care service plan contract or health insurance policy on or after Jan. 1, 2027, from imposing a cost sharing of more than $35 for a 30-day supply of an insulin prescription drug. On and after Jan. 1, 2026, prohibits a health care service plan or health insurer from imposing step therapy as a prerequisite to authorizing coverage of insulin, and, for a large group health care service plan contract or health insurance policy, requires at least one insulin for a given drug type in all forms to be on the prescription drug formulary. Limits the $35 cap for an individual or small group health care service plan contract or health insurance policy to only Tier 1 and Tier 2 insulin if the drug formulary is tiered.
Expresses the intent of the Legislature to review California’s essential health benefits benchmark plan and establish a new benchmark plan for the 2027 plan year for health care service plans and health insurers. Beginning Jan. 1, 2027, if the U.S. Department of Health and Human Services approves the state’s new essential health benefits benchmark plan, requires the benchmark plan for health care service plans and health insurers to include certain additional benefits, including coverage for specified fertility services and specified durable medical equipment.
CMA Position: Sponsor
Requires the Department of Managed Health Care and Department of Insurance to issue instructions by July 1, 2026, to health care service plans and health insurers to report statistics regarding covered health care services subject to prior authorization and the percentage rate at which they are approved or modified. Requires health plans and insurers to report those statistics to the appropriate department by Dec. 31, 2026. Requires the departments to evaluate these reports, identify the health care services approved at a rate that meets or exceeds the threshold rate of 90%, and, by July 1, 2027, publish a list of the most frequently approved services. Beginning on the date specified by the departments, but no later than Jan. 1, 2028, requires plans and insurers to cease requiring prior authorization for the most frequently approved covered health care services. Authorizes a plan or insurer to reinstate prior authorization for a specific health care provider if it determines that the provider has engaged in fraudulent activity or clinically inappropriate care. No later than four years after cessation of prior authorization, requires departments to publish reports regarding the impact of that cessation using information reported by plans and insurers, including data on reinstatements of prior authorization for specific providers. Repeals these provisions on Jan. 1, 2034.
CMA Position: Support
Extends the operation of the California Health Benefit Review Program and the Health Care Benefits Fund through July 1, 2033, and authorizes the continued assessment of the annual charge on health care service plans and health insurers for that purpose for the 2026–27 to 2032–33 fiscal years. Increases the allowable total annual assessment on health plans and insurers to $3,200,000. Removes the Healthy Families Program as an example of the publicly funded state health insurance programs within an analysis of financial impacts of legislation.
AB 251 – Elders and dependent adults: abuse or neglect
Authorizes courts to apply preponderance of evidence standard in cases against residential care facilities for elderly, adult community care facilities, or skilled nursing facilities if defendant has engaged in spoliation of evidence.
AB 894
Beginning July 1, 2026, requires general acute care hospitals to inform patients or their representatives, at time of admission or as soon as reasonably possible, that patient or their representative may restrict or prohibit use or
disclosure of protected health information in hospital’s patient directory. Requires hospitals to provide patients or their representatives acknowledgment of hospital’s privacy practices by using a separate document and having hospital personnel verbally inform them of this right.
Requires general acute care hospitals to allow patients with physical, intellectual, or developmental disabilities, cognitive impairment, or another specified disability to have a family or friend caregiver with them as needed, including outside standard visiting hours, unless hospital reasonably determines that the presence of a particular visitor would endanger the health or safety of the visitor, a patient, staff, or another visitor, or would significantly disrupt hospital operations. Does not prohibit otherwise establishing reasonable visitation restrictions. Authorizes imposing legitimate health and safety requirements on visitors. Does not prohibit restrictions on patient visitation implemented during a state of emergency.
Authorizes administrators or authorized volunteers of licensed adult residential facilities or adult day programs (licensees) to administer intranasal emergency antiseizure medication to a client during a seizure emergency, if the client has been diagnosed with seizures, a seizure disorder, or epilepsy and has been prescribed intranasal emergency antiseizure medication. Licensees must first have a seizure action plan for the client containing specified information, including signed written authorization verifying that a seizure experienced by the client may be responded to by a nonmedical professional, including through administration of emergency antiseizure medication. Prohibits administrators and authorized volunteers from administering intranasal emergency antiseizure medication unless they have received specified training. Requires Department of Social Services to establish minimum training standards by Jan. 1, 2028. Prohibits professional review, civil liability, or criminal prosecution for acts or omissions of an administrator or authorized volunteer who administers intranasal emergency antiseizure medication, any person who provides training to an in good faith and not for compensation. Requires licensees to provide specified notice to administrators and authorized volunteers.
Expands the scope of material change transaction notices under the Office of Health Care Affordability (OHCA), by additionally requiring management services organizations (MSOs), hedge funds, and private equity groups, as defined, to provide notice to OHCA of specified transactions with a health care entity, as defined, or another MSO. Directs OHCA to establish data submission requirements for MSOs.
Establishes a framework for Medi-Cal coverage of services provided by field medicine providers to persons experiencing homelessness. Authorizes Medi-Cal managed care plans to elect to offer Medi-Cal covered services through field medicine providers. Managed care plans that elects to do so must allow Medi-Cal members experiencing homelessness to receive those services directly from in-network, contracted field medicine providers, regardless of the member’s in-network assignment. Requires managed care plans to allow an innetwork, contracted field medicine provider enrolled in Medi-Cal to directly refer a member who is experiencing homelessness for covered services within the appropriate network.
CMA Position: Support
Requires DHCS, starting in 2028 and every two years thereafter, to use Medi-Cal and other data sources to produce analyses in a publicly available Medi-Cal telehealth utilization report, addressing telehealth access and utilization data disaggregated by geographic, demographic, and social determinants of health to identify disparities. Requires DHCS to identify additional data elements for inclusion in future reports to help identify and address access-to-care issues or provide insight into utilization of telehealth modalities.
SB 246 – Medi- Cal: graduate medical education payments
CMA Position: Support
Requires the DHCS to make additional Medi-Cal payments to district and municipal public hospitals (DMPHs) and to their affiliated government entities in recognition of the Medi-Cal managed care share of graduate medical education (GME) costs. Payments must be made in a manner consistent with the methodology for GME payments to designated public hospitals and their affiliated government entities, consisting of direct and indirect GME payment components. Authorizes DHCS to seek federal approval for other forms of GME payments to DMPHs and their affiliated government entities.
SB 530 – Medi- Cal: time and distance standards
Extends the operation of time and distance and appointment time standards for Medi-Cal managed care covered services to Jan. 1, 2029. Requires Medi-Cal managed care plans to ensure that each subcontractor network complies with appointment time standards. Requires managed care plans, effective no sooner than contract periods commencing on or after Jan. 1, 2026, to inform enrollees of their option to use or not use telehealth, covered transportation services, or out-of-network providers to access covered services if a health care provider is located outside of the time or distance standards. Requires plans to demonstrate to DHCS each subcontractor network’s compliance with time or distance and appointment time standards.
AB 849 – Health providers: medical chaperones
Effective Jan. 1, 2027, clinics that offer sensitive examinations, defined as an ultrasound exam by a sonography technician of genitalia, breast, rectum, or pubic or groin region, must notify patients that a medical chaperone will be made available upon request to assist or observe. Notice must be delivered in hard copy, electronic transmission, or verbally to patient or their legal guardian. For sensitive exams provided to a patient receiving emergency care, clinics must inform patient of availability of a medical chaperone when feasible. A provider also has the right to decline performing a sensitive exam without a medical chaperone if the provider determines, for any reason, that a chaperone must be present. If a medical chaperone is unavailable at time of sensitive exam, clinic must coordinate with patient to find acceptable alternative, including but not limited to waiting without undue delay for a medical chaperone to become available. Clinics must document a medical chaperone’s presence in patient’s health record. Clinics must educate sonographers and staff who may serve as medical chaperones on specified topics such as appropriate observational and intervention techniques. Does not apply to correctional facilities.
SB 403 – End of Life Option Act: sunset
Repeals the Jan. 1, 2031, expiration date of the End of Life Option Act, making the act permanent.
AB 348 – Full- service partnerships
CMA Position: Support
Effective Jan. 1, 2027, makes individuals with a serious mental illness presumptively eligible for full-service partnership programs under the Behavioral Health Services Act, which provide specified behavioral health services and housing interventions. Classifies individual as having a serious mental illness if experiencing unsheltered homelessness, transitioning to the community after six months or more in a secured treatment or residential setting, has been detained five or more times over the last five years, or is transitioning to the community after six months or more in the state prison or county jail.
AB 416 – Involuntary commitment
CMA Position: Support
Requires county behavioral health directors to include an emergency physician as one of the practice disciplines eligible to be designated by the county when developing and implementing procedures for the designation and training of professionals to perform functions under Section 5150 regarding involuntary commitment and
treatment. Exempts an emergency physician responsible for the detainment of a person under those provisions from criminal and civil liability.
SB 820 – Inmates: mental health
CMA Position: Support
Establishes a legal process that allows antipsychotic medication to be administered involuntarily to misdemeanor defendants in county jail who have been found incompetent to stand trial, but only in emergencies or with a court order after a due-process hearing. Establishes strict criteria, patient rights, monitoring requirements, time limits, and review procedures for any involuntary medication order, while clarifying that the order cannot extend a person’s confinement. Remains in effect until Jan. 1, 2030.
AB 848 – Sexual Battery
In the case of a felony conviction for sexual battery where the defendant fraudulently represented that the touching served a professional purpose, requires the fact that the defendant was employed at a hospital where the offense occurred and the victim was in the defendant’s care or seeking medical care at the hospital to be a factor in aggravation in sentencing
SB 387 – Physicians and surgeons: special faculty permits: academic medical centers
CMA Position: Support
Allows a National Cancer Institute-designated comprehensive cancer center to be classified as an academic medical center if it is accredited by the Accreditation Council for Graduate Medical Education (ACGME) and trains a minimum of 25 resident or fellow physicians in ACGME-accredited residencies annually
AB
CMA Position: Support
Beginning Jan. 1, 2027, requires a covered platform, or addictive internet-based service or application, to display a black box warning to users under the age of 17 each day the user initially accesses the social media platform, again after three hours of cumulative active use, and thereafter at least once per hour of cumulative active use.
AB 366 – Ignition interlock devices
CMA Position: Support
Extends the operation of laws governing ignition interlock devices for motor vehicles to Jan. 1, 2033.
369
CMA Position: Support
Excuses a person who is otherwise not licensed to administer anti-seizure rescue medication, but who administers anti-seizure rescue medication at the scene of an emergency, in good faith and not for compensation, from professional review, liability in a civil action, or criminal prosecution so long as the person’s conduct is not grossly negligent and does not constitute willful or wanton misconduct.
544
CMA Position: Support
Requires an electric bicycle during all hours to be equipped with a red reflector or a solid or flashing red light with a built-in reflector on the rear that is visible from 500 feet to the rear when directly in front of lawful upper beams of headlamps on a motor vehicle
AB 965
Prohibits a person from selling a class 3 electric bicycle to a person under 16 years of age, and makes a violation punishable by a fine of up to $250.
CMA Position: Support
Expands authorizations to distribute, receive, possess, or administer an opioid antagonist to include those who are at risk of an overdose or who may be able to assist a person experiencing an overdose. Eliminates the training requirement for those who receive and possess opioid antagonists. Exempts a person who administers an opioid antagonist in good faith from liability for civil damages. Exempts health care providers who act with reasonable care from liability in a civil action resulting from administering the opioid antagonist in good faith. Also revises and modernizes requirements for drug- or alcohol-related programs to remove outdated and stigmatizing requirements for state funding eligibility, including eliminating references to “no lawful use” messaging, and prohibiting DHCS from requiring an admission agreement to require a person to be abstinent and not intoxicated in order to be admitted to care or continue treatment at DHCS-licensed residential treatment facilities.
CMA Position: Support
Prohibits a licensing authority from issuing a license to carry a concealed firearm if an applicant was convicted of contempt of court or specified criminal statutes in the 10 years prior to the completed application, was subject to any restraining order, protective order, or other type of court order, or is an unlawful user of, or addicted to, any controlled substance. Upon determining that an applicant is a disqualified person, requires the licensing authority to, within 5 days, submit specified information of the disqualified person and supporting documentation to the National Instant Criminal Background Check System Index. Requires a licensing authority to review the California Restraining and Protective Order System for information concerning whether the applicant is reasonably likely to be a danger to self, others, or the community at large.
CMA Position: Support
Beginning July 1, 2026, prohibits a licensed firearms dealer to sell, offer for sale, exchange, give, transfer, or deliver any semiautomatic machinegun-convertible pistol, as defined, with some exceptions
CMA Position: Support
Prohibits a person from knowingly or willfully causing another person to engage in the unlawful manufacture of firearms or knowingly or willfully aiding, abetting, prompting, or facilitating the unlawful manufacture of firearms, including the manufacture of any firearm using a 3D printer or CNC milling machine. Sets stricter standards for firearm industry members to follow when manufacturing a firearm for the purpose of selling, loaning, or transferring ownership of that firearm to another person. Makes a violation of these provisions a misdemeanor.
CMA Position: Support
Defines “ultraprocessed food” for specified school-related purposes and requires the California Department of Public Health (CDPH) to adopt regulations by June 1, 2028, defining “ultraprocessed foods of concern” and “restricted school foods,” taking into account specified factors, including whether a substance or group of substances is linked to health harms or adverse health consequences.
Requires schools to begin phasing out restricted school foods and ultraprocessed foods of concern no later than July 1, 2029, and beginning July 1, 2032, prohibits a vendor from offering those foods to a school.
On or before February 1, 2028, and on or before February 1 of each year thereafter through 2032, requires a vendor to report specified information to CDPH for each food product sold to a school in the prior calendar year, including the total quantity sold and whether the product is an ultraprocessed food, a restricted school food, or an ultraprocessed food of concern.
By July 1, 2028, and by July 1 of each year thereafter through 2032, requires CDPH, in consultation with the State Department of Education, to submit a summary and analysis of vendor-reported information and
recommendations for state and local legislative actions to reduce consumption of ultraprocessed foods, restricted school foods, and ultraprocessed foods of concern in schools.
SB 704 – Firearms: firearm barrels
CMA Position: Support
Prohibits the sale or transfer of a firearm barrel unless the transaction is completed in person by a licensed firearms dealer. Prohibits a person from possessing a firearm barrel with the intent to sell, or offering to sell, unless the person is a licensed firearms dealer. Beginning July 1, 2027, requires licensed firearms dealers to conduct an eligibility check of a purchaser or transferee and to record specified information pertaining to the transaction. Establishes penalties for violation of these prohibitions. Requires the Department of Justice to require the licensed firearms dealer to charge a fee up to $5 for each firearm barrel eligibility check.
AB 583 – Death certificates
Commencing July 1, 2026, authorizes to the medical and health section data and the time of death on death and fetal death certificates to be completed and attested by a nurse practitioner last in attendance, or, under specified circumstances, by a physician assistant under the supervision of a physician and surgeon in last attendance. Also authorizes a nurse practitioner to amend a record of death, fetal death, or live birth. Applies existing obligations to report to a coroner in specific circumstances to nurse practitioners and physician assistants who complete or amend such certificates or records.
SB 504 – Communicable diseases: HIV reporting
CMA Position: Support
Authorizes a health care provider of a patient with an HIV infection that has already been reported to a local health officer to disclose identifying information about the patient to a local health jurisdiction or CDPH if the disclosure is necessary to complete or supplement an HIV case report or for the local health jurisdiction or CDPH to carry out its duties in the investigation, control, or surveillance of disease, or the coordination of, linkage to, or reengagement in a person’s care.
AB 50 – Pharmacists: furnishing contraceptives.
Authorizes pharmacists to furnish OTC self-administered hormonal contraceptives without following standardized procedures or protocols required for prescription-only self-administered hormonal contraceptives, and to dispense up to a 12-month supply of OTC contraceptives at patient’s request.
AB 55 – Alternative birth centers: licensing and Medi -Cal reimbursement
CMA Position: Co-sponsor
Revises the criteria for facility licensure and Medi-Cal reimbursement of alternative birth centers. Deletes requirement that alternative birthing centers be a provider of comprehensive perinatal services under Medi-Cal, and replaces it with a list of specific services that must be offered. Requires licensed centers to meet other specified standards, including written policies for hospital transfers and arrangements for the referral of a complication to a physician and surgeon, which must be shared with patients.
AB 260 – Sexual and reproductive health care
CMA Position: Co-sponsor
Authorizes pharmacists to dispense mifepristone and other medication abortion drugs without patient or prescriber name, or pharmacy name or address. Prohibits disciplinary, civil, or criminal action as well as adverse licensing or other administrative action against licensed practitioners for prescribing or administering mifepristone and other medication abortion drugs for uses that differ from FDA-approved labeling or an approved federal risk evaluation and mitigation strategy (REMS). Requires plans that cover prescription drugs to cover brand name or generic mifepristone, even if not approved by FDA, and prohibits limiting or excluding coverage
solely on basis that drug is prescribed for off-label use, except if the state deems it necessary to address an imminent health or safety concern. Extends enforcement safe harbor for health care providers who are working to comply with state abortion-related medical privacy law (AB 352 (2023)) to Jan. 31, 2027.
SB
Temporarily exempts, until Jan. 1, 2035, vaginal suppositories containing intentionally added boric acid from a preexisting ban, set to take effect Jan. 1, 2027, on the manufacture, offer, sale, or delivery of cosmetic products containing specified, intentionally added ingredients. Beginning Jan. 1, 2027, requires vaginal suppository products containing intentionally added boric acid to include a medical warning label, as specified, and bans these products beginning Jan. 1, 2035.
CMA Position: Support
Starting Jan. 1, 2027, requires manufacturers of bulk or packaged prenatal multivitamin products sold, manufactured, delivered, held, or offered for sale in the state to test a representative sample of each lot of their products for heavy metals. Defines “heavy metals” to mean arsenic, cadmium, lead, and mercury. Requires both manufacturers and brand owners to provide test results to an authorized agent of CDPH upon request. Starting Jan. 1, 2027, requires brand owners of packaged prenatal multivitamin products sold, manufactured, delivered, held, or offered for sale in the state to disclose specified product information to the public. Starting Jan. 1, 2027, for products shipped to retailers or consumers, requires the outermost package of a packaged prenatal vitamin product and the product details page on a website where the product is sold to include a statement on heavy metal testing. Prohibits the sale, manufacture, delivery, holding, or offering for sale, of a prenatal multivitamin in the state that does not comply with these provisions.
SB 669 – Rural hospitals: standby
CMA Position: Support
Requires CDPH, by July 1, 2026, to establish a 10-year pilot project within up to five critical access hospitals to allow participating hospitals, on an application basis, to establish standby perinatal services, as defined. The first two hospitals selected, if qualified, would be nonprofit and located in the County of Humboldt and the County of Plumas. Up to three more critical access hospitals may be added to the pilot program, as long as the application either includes a labor union agreement confirming project won’t harm employees or a statement verifying that the hospital has no unionized workforce. Establishes standards and criteria regarding facility resources, services, and staffing for participating hospitals Requires CDPH to develop a template to collect and evaluate data on safety, outcomes, utilization, and populations served under the pilot project. Requires CDPH to prepare and submit an evaluation to the Legislature on or before two years after completion of the pilot project, and make the evaluation publicly available.
AB
For contracts entered into, on, or after Jan. 1, 2026, prohibits the inclusion of any terms in an employment contract that require the worker to pay an employer, training provider, or debt collector for a debt if the worker’s employment or work relationship with a specific employer terminates. Declares these contracts to be contracts that restrain a person from engaging in a lawful profession, and void under state law. Prohibition does not apply to certain contracts involving government loan repayment assistance or loan forgiveness programs, tuition repayment under specified requirements, enrollment in an apprenticeship program approved by the Division of Apprenticeship Standards, non-performance-based signing bonuses that meet specified conditions, or the lease, financing, or purchase of residential property. Authorizes a private right of action by or on behalf of a worker who has been subjected to a prohibited contract term, and authorizes specified civil penalties and relief.
Providing staff, physicians, and patients with relevant & up to date information

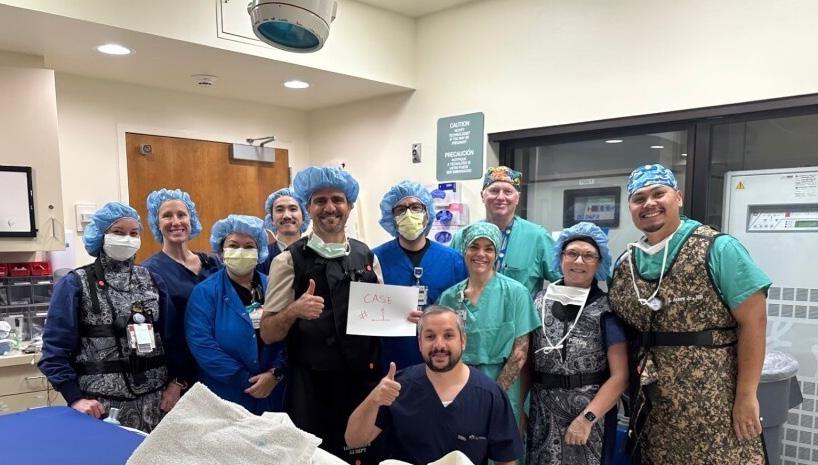
Dignity Health St. Joseph’s Medical Center Expands Robotic Surgery Capabilities with New Robotic System
Dignity Health St. Joseph’s Medical Center is proud to announce the successful completion of its first surgical procedure using the hospital’s newly acquired robotic-assisted surgical system. This latest addition enhances the medical center’s existing robotic surgery program, further supporting its commitment to advanced, patient-centered care.
The first procedure marks an important expansion of St. Joseph’s capabilities in minimally invasive surgery. The new robotic system will complement the hospital’s current robotic system, enabling a wide range of procedures across multiple specialties, including urology, gynecology, general surgery, and surgical oncology.
“This milestone reflects our commitment to bringing the
most advanced surgical technology to the patients we serve,” said St. Joseph’s Medical Center President and Chief Executive Officer David P. Ziolkowski. “The addition of the latest robotic system allows our surgeons to perform complex procedures with enhanced precision while offering patients the potential benefits of smaller incisions, less pain, and faster recovery times.”
Robotic-assisted surgery using this new system enables surgeons to operate through a few small incisions using advanced instruments and highdefinition, 3D visualization. The technology is designed to support greater surgical precision and control, which may lead to less invasive procedures, reduced blood loss, shorter hospital stays, and quicker healing for many patients. In many cases, roboticassisted surgery can also offer improved outcomes compared to traditional laparoscopy or open surgery.
“It was a privilege and pleasure to be one of the first surgeons to use the newest robotic surgical system. The introduction of this new technology has transformed our surgical capabilities. It makes complex operations possible through minimally invasive techniques, resulting in safer outcomes, less pain after surgery, and shorter recovery for patients,” said Dr. Param Gill, MD OB/GYN. “This new technology truly enhances patient outcomes, and I am excited to offer this to patients in our community.”
Among the first patients to benefit from the new roboticassisted surgical system was Suzanne Ledbetter, who recently underwent a procedure at St. Joseph’s Medical Center.
“Once again, St. Joseph’s Medical Center delivered exceptional care for my recent medical procedure. When I learned I
would need a hysterectomy, I was thrilled to learn the hospital acquired a brand new, state-of-the-art robot for laparoscopic surgeries. As I was rolled into the operating room, I was in awe of the sleek, impressive machinery surrounding me. The robot, combined with my dedicated surgeon, Dr. Param Gill, gave me peace of mind to undergo such a procedure locally. My surgery and recovery were smooth and successful! For the second time in my life, I find myself filled with gratitude to the hospital’s generous donors for bringing this life-changing technology to our community,” said Suzanne Ledbetter.
As additional surgeons complete training and procedures are introduced, St. Joseph’s Medical Center anticipates expanding robotic-assisted surgery across multiple service lines, further strengthening its comprehensive surgical program.
For more information about robotic-assisted surgery at Dignity Health St. Joseph’s Medical Center, visit https://www. dignityhealth.org/central-california/locations/stjosephsstockton
Adventist Health Lodi Memorial Completes Its First PCI Procedure
Adventist Health Lodi Memorial has reached a significant milestone in cardiac care. In early February, the hospital’s Cardiovascular team successfully performed its first Percutaneous Coronary Intervention (PCI), marking a major advancement in the level of heart care now available to patients in the Lodi community.
This achievement reflects months of coordinated preparation across multiple departments. The Cath Lab , Nursing, Emergency, Imaging, Registration, and Support Services
teams all played essential roles. Cardiologists Dr. Haytham Aljoudi and Dr. Alaa Gabi led the clinical effort, bringing this specialized procedure to fruition through multi-disciplinary collaboration and rigorous readiness planning.
The inaugural procedure was completed smoothly with a positive patient outcome. More importantly, the successful launch of PCI services means patients can now receive timesensitive, lifesaving intervention locally while reducing the need for transfers during cardiac emergencies.
This accomplishment highlights Adventist Health Lodi Memorial’s commitment to raising the standard of care in its community with excellence and compassion.
With this milestone as a starting point, the hospital looks forward to expanding access to life-saving care in Lodi for patients in the years ahead.
Adventist Health Lodi Memorial and Adventist Health Sonora Earn ASTRO APEx Accreditation
The radiation oncology programs at Adventist Health Lodi Memorial and the Diana J. White Cancer Institute at Adventist Health Sonora have earned accreditation from the American Society for Radiation Oncology (ASTRO) APEx –Accreditation Program for Excellence®, recognizing radiation oncology practices that meet nationally established standards for safety and quality.
“Adventist Health is thrilled to receive APEx accreditation from ASTRO, the largest radiation oncology society in the world,” said Christy Casey, Administrative Director of Oncology for Adventist Health Sonora and Lodi Memorial. “Our teams work hard every day to deliver safe, patientcentered cancer care. I am incredibly proud of their dedication.”
APEx is the fastestgrowing radiation oncology accreditation program in the country and involves a rigorous, multistep evaluation including a selfassessment and an external review by a radiation oncologist and medical physicist. The Lodi and Sonora teams prepared for nearly two years, culminating in an onsite survey in August 2025.
Lodi Memorial and Sonora are the first Adventist Health facilities to achieve APEx accreditation, joining leading centers in California such as City of

Hope, Stanford, and UCLA.
“By undergoing this comprehensive review, these facilities demonstrated a strong commitment to delivering highquality radiation oncology services,” said Howard M. Sandler, MD, FASTRO, Chair of the ASTRO Board of Directors.
Accreditation is valid through August 2028 for Adventist Health Sonora and August 2029 for Adventist Health Lodi Memorial. This achievement underscores Adventist Health’s commitment to advancing safe, highquality cancer care across the region.


This year brought nonstop battles to protect health care. We started the year facing devastating fires in Southern California that disrupted physician practices, patients, and communities. CMA worked with local component medical societies to ease regulatory burdens on physicians, support members who were personally impacted and provide information to patients to ensure they had continuous care.
CMA engaged at the federal level throughout the year – pushing back against a series of efforts that threatened to undermine core public health protections, including the removal of all Advisory Committee on Immunization Practices (ACIP) members and proposals that would weaken evidencebased public health policy. CMA also challenged the sharing of Medicaid patients’ sensitive data with Homeland Security, and pushed back against broader federal proposals to weaken key physician and patient safeguards – from attempts to scale back the Public Service Loan Forgiveness (PSLF) program and lower federal loan maximums to new restrictions on gender-affirming care. At the same time, CMA continued pushing for policies that would protect coverage and access, including extending telehealth coverage, preserving ACA premium tax credits and protecting Medicaid funding.
The year’s challenges were also felt at the state level. Governor Newsom’s May budget diverted critical Prop 35 funds to address budget shortfalls. After significant pressure from CMA, the first bucket of Prop 35 funding was released in the late summer.
It has been one battle after another, but CMA remains steadfast. We will continue fighting for physicians, patients and the communities we serve.
PROP 35: Successfully pressed the state to begin implementing Prop 35 – securing a commitment to fund emergency department physician payments, family planning and abortion services, graduate medical education programs and emergency medical transport services.
Federal Advocacy: CMA repeatedly brought physician leaders to lobby Members of Congress to protect the health care safety net. We organized a 50-state coalition and worked with national specialty societies, who joined California physicians in lobbying against H.R. 1. We also formed Physicians for Medicaid and a grassroots texting operation through which physicians sent text messages about the health care harms of H.R. 1 to 6 million voters in targeted districts across the country. While Medicaid was significantly cut and premiums for many are increasing, Medicaid was protected as an entitlement program for pregnant women, kids, seniors and veterans.
CMA also successfully advocated for several telehealth provisions to be made permanent including: lifting frequency limits for hospital and skilled nursing facility telehealth visits, allowing virtual direct supervision for most services, and continuing pandemic-era policies allowing virtual supervision of residents providing telehealth care. These policies play a critical role in expanding access to care, particularly for patients in rural and underserved communities.
Our efforts on the Medicare Physician Fee Schedule resulted in gains for some primary care physicians, though the schedule included cuts for many specialists.
Legislative Victories: Three of CMA’s sponsored bills were signed by the Governor.
+ Prior Authorization (SB 306 - Becker): Eliminates prior authorization requirements for services that insurers routinely approve.
+ Strengthening the Corporate Bar (SB 351Cabaldon): Gives the Attorney General authority to hold private equity groups accountable when they interfere with the practice of medicine, protecting physician autonomy in patient care.
+ Artificial Intelligence (AB 489 - Bonta): Bans companies from marketing artificial intelligence (AI) chatbots as licensed medical professionals.
Stopping Problematic Legislation: CMA protected physicians and patients by blocking harmful bills that would have increased medical malpractice insurance costs, imposed mandatory continuing medical education without clear benefit, created new administrative burdens for clinicians using AI in care delivery, and infringed on physicians’ independent control of medical staffs.
Medway Launch: CMA’s Physician Services Organization launched MedWay, a new administrative support service that helps independent practices manage essential nonclinical operations. Providing hands-on support with HR, payroll and staffing, as well as access to practice insurance, employee benefits, and recruiting services, Medway allows physicians to focus on patient care while maintaining full ownership and operational control of their practices.
Medical Group Symposium: CMA’s popular Medical Group Advocacy Symposium was attended by more than 200 medical group and health system executives, clinical leaders, physicians across multiple specialties, and policy and advocacy professionals.
Public Health: CMA successfully passed AB 144, which allows California to continue to require health coverage for vaccines in California-regulated health plans if the federal recommendations no longer align with science.
Practice Advocacy: CMA successfully demanded that Cigna pause its automatic downcoding policy for commercial HMO and PPO products and continues to advocate for the pause to apply to self-insured plans. CMA also joined a federal antitrust lawsuit against MultiPlan (now Claritev) and major insurers alleging they conspired to depress out-of-network physician payments.
Empowering Physician Practices: CMA expanded its educational offerings to support small and independent practices, including new webinars on efficiencies, the regulator complaint process, and a “Know Your Rights” training series. In 2025, CMA reached a significant milestone, hitting $50 million recovered for physician members through one-on-one practice management assistance and direct intervention with payors and regulators.
GME: Physicians for a Healthy California (PHC) awarded nearly $84 million to 231 residency programs, to fund 270 physician training positions with a focus on growth in regions serving high Medi-Cal populations. The demand was significant, with almost $465 million in requests.
Supporting Students: PHC’s MedStudentsServe awarded more than $30,000 to 13 medical-student projects statewide, supporting initiatives such as free clinics, mobile health fairs and outreach for underserved populations. Students reached more than 2,300 people facing access barriers, while gaining hands-on experience in public health, cultural competence, and community service.
2026 AND BEYOND: CMA will advocate to strengthen the business of health care while defending the safety net, protecting patients and ensuring physicians—and their voices—are strongly represented in a critical election year.

Doctors Increasingly See AI Scribes in a Positive Light. BUT HICCUPS PERSIST.
By Michelle Andrews
When Jeannine Urban went in for a checkup in November, she had her doctor’s full attention.
Instead of typing on her computer keyboard during the exam, Urban’s primary care physician at the Penn Internal Medicine practice in Media, Pennsylvania, had an ambient artificial intelligence scribe take notes. At the end of the 30-minute visit, Urban’s doctor showed her the AI summary of the appointment, neatly organized into sections for her medical history, the physical exam findings, and an assessment and treatment plan for her rheumatoid arthritis and hot flashes, among other details.
“pajama time” catching up on work in the evening.
The potential of AI to transform every aspect of the health care system — from patient care to clinical efficiency to medical innovation — is an area of intense focus, including by the Trump administration.
Health tech experts estimate that a third of providers have access to ambient AI scribe technology. As adoption looks likely to grow rapidly over the next few years.
The clinical note, which Urban could also review on the patient portal at home, was incredibly thorough, she said. It summarized all of her questions and concerns and the doctor’s responses. The scribe “made sure we didn’t miss anything,” Urban said.
Ambient AI scribes are being hailed by physicians as a game changer that helps free them to focus on their patients rather than their computer keyboard. By releasing doctors from the onerous and time-consuming task of documenting what happens during every patient encounter, early studies show, AI scribes may help reduce physician burnout and after-hours
Last January, President Donald Trump issued an executive order to remove barriers to American leadership in AI. Later in the year, a press release from the federal Department of Health and Human Services invited stakeholders to weigh in on how the department can accelerate the adoption of AI in health care.
Several startup vendors in recent years have introduced ambient AI scribe products that can be integrated into electronic health records. EHR market leader Epic is piloting its own AI scribe technology, which it expects to release widely early this year, according to Jackie Gerhart, a family medicine physician who is chief medical officer and vice president of clinical informatics at Epic.
Health tech experts estimate that a third of providers have access to ambient AI scribe technology. As adoption looks

likely to grow rapidly over the next few years, many expect it to become more of a recruiting tool, a minimum requirement for incoming clinicians, who reports indicate are increasingly prioritizing work-life balance.
“It’s part of keeping doctors happy,” said Robert Wachter, a professor and the chair of the Department of Medicine at the University of California-San Francisco, whose forthcoming book, A Giant Leap, explores how AI is transforming health care. “Health systems that initially might have done a hardnosed return-on-investment calculation — many are softening on that and realizing that the cost of recruiting and retaining doctors is pretty high.”
But many questions remain. Does the use of ambient AI scribes improve patient care and health outcomes? Will doctors use time they gain by employing an AI scribe to improve the quality of the time they spend with their patients or just boost the number of patients they see? To what extent will expanding the amount of detail available from a patient visit lead to bigger bills if the AI scribe is integrated with a coding app that optimizes provider charges?
For now, these questions remain mostly unanswered.
Urban said that the AI scribe didn’t change her experience as a patient very much. Typically, after a patient gives verbal permission, the AI scribe records the visit on a phone and organizes the conversation into the structure of a clinical note, filtering out small talk that isn’t pertinent to the medical visit but incorporating relevant details about a family member’s recent cancer diagnosis, for example. The scribe’s note is often then integrated into the provider’s EHR. The doctor later reviews the note and signs off on it.
Even though the visit may not feel very different to patients, some clinicians report that ambient AI scribes are changing patient encounters in unanticipated ways.
“Now, when I’m doing a physical exam, I have to say what I’m doing and what I’m finding out loud in order for the AI scribe to document it,” said Dina Capalongo, Urban’s primary care doctor. “People find that very interesting,” she said.
When Capalongo places her stethoscope over the carotid artery under a patient’s jaw, for example, she might say that she doesn’t hear a “bruit,” or vascular murmur, whose presence could indicate atherosclerosis. Patients have told her, “I never knew why a doctor would listen there,” she said.
Saying things out loud for the AI scribe that would typically appear only in a clinical note can create its own set of challenges, particularly during sensitive physical exams. Doctors may feel it’s important to adjust their conversation accordingly.
“Sometimes patients are anxious and scared and my saying things that they don’t understand or they may worry about during an uncomfortable examination does not help the situation and honestly is insensitive to what the patient is going through,” said Genevieve Melton-Meaux, a professor in the Division of Colon and Rectal Surgery at the University of Minnesota, who is also chief health informatics and AI officer at Fairview Health Services in Minneapolis. “I’ll keep that top of mind and make sure I record it” after the visit.
“How we have conversations with patients about these tools
is really important, in particular for maintaining trust and ensuring accurate information,” Melton-Meaux said.
Studies have found that, across a range of measures such as completeness, timeliness, and coherence, the notes created by ambient AI scribes are generally at least as good as, and sometimes better than, traditional documentation, said Kevin Johnson, a pediatrician who is vice president for applied informatics at the University of Pennsylvania Health System.
An ongoing concern is around AI “hallucinations,” in which false, sometimes fabricated information appears in an AI output.
Kaiser Permanente, an early adopter of ambient AI scribe technology, provides it to more than 25,000 doctors, advanced practice providers, and pharmacists systemwide. It has found hallucinations to be “quite rare,” said Daniel Yang, an internist who is vice president of AI and emerging technologies at Kaiser Permanente.
But they happen. An AI-scribe-generated note, for instance, might say that the doctor planned to refer someone to a neurologist or to follow up in two weeks. The problem? The doctor might not have said that.
technology, Melton-Meaux said. But what about critical access hospitals or small private practices? “There need to be more resources,” she said.
Physicians’ enthusiasm for ambient AI scribes stands in sharp contrast to their negative reaction to electronic health record systems that have become widely adopted in recent years to replace paper charts.
“During the last 10 years, when EHRs became a thing, we all became very grumpy, overworked data scribes,” Wachter said.
The introduction of AI scribes makes physicians feel like technology is working for them rather than the other way around, health care AI experts said.
To improve health care value and save costs, Wachter said, we need a system that makes it more likely that physicians will practice evidence-based medicine to order the right tests and prescribe the right medications.
“The technology is not perfect, and that’s why physicians are reviewing it,” Yang said. It’s learning from regular physician visits as it goes, he said. That’s why having a person check the work product is critical.
Still, even such a “human-in-the-loop” system is fraught, Wachter said. “Humans stink at maintaining vigilance over time,” he said.
As the use of ambient AI scribes becomes routine, some clinicians worry that the technology will widen the divide between health care haves and have-nots.
Large health systems are able to move forward with the
And AI scribes are “training wheels” for more consequential adoption of AI in health care, Wachter said.
To improve health care value and save costs, Wachter said, we need a system that makes it more likely that physicians will practice evidence-based medicine to order the right tests and prescribe the right medications.
“It’s a few years away, but it’s all AI-dependent,” he said.
Epic has introduced roughly 60 AI use cases for patients, clinicians, and administration, with over 100 more in the works.
“It’s so much bigger than a scribe,” said Epic’s Gerhart. “It’s literally listening and acting in a way that tees things up for me so that I can take action.”
KFF Health News is a national newsroom that produces indepth journalism about health issues and is one of the core operating programs at KFF—an independent source of health policy research, polling, and journalism.

BY JO ANN KIRBY
Today’s patients are taking an active role in managing their own health, armed with access to a growing amount of medical information.
Patients may follow social media health influencers or be swayed by pharmaceutical advertising. They might sport wearable fitness tracking devices that give them data on their sleep, steps, heart health and calories. Their entire medical history is often available to them via online healthcare provider portals. Patients can access the latest medical research findings on the Internet. And then there is Dr. Google! Patients simply search the Internet to find a cure for their symptoms. Now, artificial intelligence has entered the chat to offer a diagnosis.
KFF, a leading health policy research nonprofit, released a survey in July 2025, that found 55 percent of respondents use social media “to find health information and advice” at least occasionally. The Annenberg Public Policy Center’s April 2025 health survey finds that 79% of those surveyed say they’re likely to look online for the answer to a question about a health symptom or condition, while most 63% think AI-generated health information is somewhat or very reliable.\
The days when health care providers solely made medical decisions for a patient are long gone. Patients increasingly feel empowered to foster shared decision-making with their physicians based on their own personal priorities and goals. Some doctors are responding by staying at the forefront of patient education and health information technology while remaining open to what their patients want to achieve.
“Patients come to an appointment hoping I’m fully aware of the trends,” Ruby Gill, M.D., who is double-board certified in family medicine and integrative medicine, said. “I will start by asking what stood out to them, why did it resonate with them so that I can use that to help them.”
Dr. Gill, who started out practicing medicine in the Bay Area but now has her own practices in Lodi, said she quickly became accustomed to those in the tech industry coming into appointments with a plethora of information and questions.
She said that it’s important to listen to patients when they have seen something on social media


that mirrors their own experience. For example, women experiencing menopause symptoms are finding a wealth of information on social media about hormone replacement therapy that can help them to start a conversation with their healthcare provider. “Social media is empowering women,” said Dr. Gill, a certified Menopause Society Practitioner and fellowship-trained aesthetic physician. “They come in prepared with questions.”
One physician said the prevalence of information readily available to patients has changed the way he interacts with patients over the course of his career, but that can be a good thing because patients who are more invested in their care are often better about compliance. “Patients want to feel seen. They want to feel heard,” Brijinder Oberai, M.D., a hospitalist with Kaiser Permanente, said. “We can’t reject what they are saying, we can’t tell them they are wrong.”
Brijinder

" Patients want to feel seen. They want to feel heard. We can't reject what they are saying, we can't tell them they are wrong."
- Dr. Oberai
Dr. Gill agrees and says that she feels that physicians should never dismiss the patient’s thought process but rather use it as an opportunity to understand why they feel the need to explore what they did and then meet them with a plan that aligns with what they want to achieve in their wellness journey.
Social media has strongly influenced patient expectations and decision-making by increasing health awareness and patient engagement, said Hanadi Abou Dargham, M.D, who serves as program director for St. Joseph’s Family Residency Program and is an associate professor of family medicine for Touro University of California. “Patients may arrive with pre-formed diagnoses or treatment requests based on online content, requiring clinicians to spend time correcting myths and rebuilding trust,” she wrote in response to a San Joaquin Medical Society survey on the topic. “Overall, while social
media can empower patients and reduce stigma, it highlights the need for physicians to guide discussions with empathy and reinforce evidence-based, shared decision-making.”
But Dr. Dargham cautions that social media can spread misinformation, heighten anxiety, and create unrealistic expectations. “I advise patients to approach online health information with healthy skepticism and a structured way to evaluate credibility,” she said.
In times when the internet hasn’t delivered, patient education is vital. Dr. Oberai said that he had a recent patient who came in convinced by his Internet searches that he was suffering from pneumonia, even going so far as to demand a list of treatments and prescriptions from the receptionist at check-in desk. The patient had a long history of heart disease, having had several bypass operations and other procedures. After evaluating the patient and analyzing test results, the patient was found to be suffering from heart failure — not pneumonia. He said that when patients have misdiagnosed themselves, he will make it a teachable moment, empathetically explaining that in their particular case, what they suspected is not the issue because of so many other factors and underlying health issues unique to them.

Some doctors are joining social media to help inform and shape the conversation. When physicians engage on social media, they have the opportunity to share valuable medical news, dispel dangerous health disinformation, provide context to health trends, share information about their practice, post reminders about vaccination clinics and screenings or simply engage with their followers.
Dr. Dargham cautions that social media can spread heightenmisinformation, anxiety, and create unrealistic expectations
Dr. Gill has a marketing team that is helping her with her social media platforms. She said it’s important for physicians to get comfortable with social media. “I have a whole content calendar,” she said.
A Gill Aesthetic Institute Facebook post featuring Dr. Gill on January 29, 2025 read, in part:
“Mood swings you didn’t order? You’re not “being dramatic” perimenopause can be an emotional rollercoaster, and yes… it’s hormonal. Listen as Dr. Gill breaks down why emotions can feel so unpredictable during perimenopause and how HRT can help bring things back into balance — mentally and physically.” The emoji-filled post served as an introduction to a video of Dr. Gill breaking down the topic. She said equally important to the post, is the discussion that follows because it gives insight into what the thinking is on a particular topic.
“I think it can be used so positively,” she said of social media platforms such as Instagram, Facebook, TikTok and podcasts.



Funds 270 residency and fellowship positions statewide
Physicians for a Healthy California (PHC) today announced $85 million in CalMedForce and CalMedForce+ grants to expand graduate medical education (GME) opportunities across California. For the first time, all specialties were eligible for funding, compared to just five in previous cycles.
In this cycle, programs submitted record requests totaling more than $460 million, underscoring the need for additional training positions to keep pace with California’s growing patient population.
This is the first cycle to include CalMedForce+, which uses voter-approved Proposition 35 funds—passed in 2024 with 67.9% of the vote—to broaden eligibility and expand support for GME programs. Prop. 35 provides $75 million in GME investments. CalMedForce, now in its eighth year, continues to be funded through the Proposition 56 tobacco tax. Together, the programs will support 270 residency and fellowship positions across 231 GME programs in this cycle, directing resources to California’s most medically underserved regions.
“The demand we saw this year reflects what communities have been telling us for years—California must train more physicians to meet the health care needs of its growing population,” said PHC President and CEO Lupe Alonzo-Diaz, MPA. “CalMedForce and CalMedForce+ are essential to expanding access to care and building the workforce Californians will rely on for years to come.”
This year’s awards are nearly four times last year’s total, underscoring both the magnitude of need and the critical role these programs play in supporting access to care across California. As the state faces a projected shortfall of 4,100 primary care clinicians by 2030, sustained investment in GME will be essential to ensuring Californians can get the care they need.
“By supporting impactful programs that expand medical education, California can grow its physician workforce in high-need areas and specialties—making care more accessible for patients with Medi-Cal coverage and those without insurance,” said Deena McRae, M.D., associate vice president for Academic Health Sciences in the UC Office of the President. “I’m pleased that CalMedForce+ will offer additional impactful grants, helping to strengthen our health care workforce and advancing a healthier future for all Californians.”
Proposition 35 funding also enabled PHC to support fellowship programs for the first time, expanding subspecialty training opportunities critical to California’s future workforce. This approach balanced broad distribution with the need to provide adequate support where it is most critical.
About CalMedForce and CalMedForce+
PHC administers the CalMedForce and CalMedForce+ grant programs in partnership with the University of California (UC). As a state public institution, UC oversees the distribution of Proposition 56 and Proposition 35 funds to support GME programs statewide. Any accredited GME program is eligible for funding, with priority for programs serving under-resourced populations and communities with significant shortages. UC contracts with PHC to administer the award cycles.
Since its launch, CalMedForce has awarded over $275 million for 855 grants to 181 GME programs throughout California, supporting the retention and expansion of residency slots in primary care—including family medicine, internal medicine, pediatrics, and obstetrics and gynecology—as well as emergency medicine. CalMedForce+ begins its inaugural year with $64 million to 162 GME programs, expanding both residency and fellowship positions across the state.
For more information, visit phcdocs.org/CalMedForce. (@ PHCdocs / #CalMedForce)












A PLACE FOR ALL NEWS HIGHLIGHTING RESIDENTS AND GRADUATE MEDICAL EDUCATION
The Resident’s Report is dedicated to all the good news related to our hard-working residents training at San Joaquin General Hospital and St. Joseph’s Medical Center. Please email your submissions, written in third person with accompanying photo to Lisa@sjcms.org.
San Joaquin General Hospital’s Internal Medicine Residency Program congratulates Drs. Uzun and Ibrahim

Intern Dilek Uzun, MD’s abstract has been accepted to the 2026 Tandem Meetings (ASTCT/ CIBMTR). “Impact of IMWG Frailty and Nutritional Biomarkers on Outcomes in Multiple Myeloma Patients Undergoing Autologous Stem Cell Transplantation.”

Intern Ahmed Ibrahim
MD’s paper was published in the Journal of Diabetes & Metabolic Disorders. https://link.springer.com/ article/10.1007/s40200025-01737-y
As graduation approaches, our St. Joseph’s Family Medicine residents are preparing to take their next exciting steps carrying with them a deep commitment to patient care, service, and lifelong learning. From California to the East Coast, from outpatient clinics, hospital medicine to fellowship training, their paths reflect both diversity of interests and a shared foundation rooted in comprehensive, compassionate care.



Dr. Johnny Fu will be heading to Los Angeles to begin a Sports Medicine fellowship at the AltaMed Health Services where he will focus on musculoskeletal pathologies and team coverage.
Dr. Simerjit Gill will be staying in Stockton at Community Medical Centers (CMC), where she plans to focus on maternal health, gynecologic procedures, and comprehensive adult care while serving an underserved population.
Dr. Thomas Brokaw will be relocating to the East Coast with his partner, where he plans to focus on urgent care medicine while also exploring part-time hospitalist work.


Dr. Navdip Bhangoo looks forward to continuing her career in California as an outpatient Family Medicine physician, with the possibility of incorporating part-time hospitalist practice.

Dr. Benjamin Lee will be relocating to Southern California to begin his career as an outpatient Family Medicine physician.

Dr. Jaspreet Pandher is returning to her hometown in Southern California to practice outpatient Family Medicine, with a special passion for pediatrics and women’s health.

Dr. Noor Sandhu will be returning home to Napa Valley to provide outpatient Family Medicine care with a plan to focus on lifestyle based medicine and women’s health.

Dr. Tarek Fatahi, on the brink of graduation, is thoughtfully exploring all options (Hospital Medicine, Outpatient) as he applies broadly and considers the many paths ahead.

Dr. Dan Nguyen will tentatively be practicing locum Family Medicine in the Greater Sacramento area over the coming year while his wife completes her residency.
We are incredibly proud of each of these physicians and the unique journeys they are embarking on. Their dedication to patients and communities, near and far, reflects the very best of Family Medicine and the enduring impact of training rooted in service, excellence, and heart.

At St. Joseph’s Medical Center, we’ve grown alongside you and your family for generations with an unparalleled commitment to the health of our community. We’re proud to be named in some of health care’s top medical rankings, reflecting our team’s commitment to quality patient care. From advanced cardiac and cancer care, to emergency services, maternity, orthopedics, neurology and more, we are here to support you on your path to wellness. Learn more about us at DignityHealth.org/Stockton



Free to SJMS/CMA Members!

The Office Managers Forum empowers physicians and their practice manager staff with valuable tools via expert led education sessions from industry professionals who are committed to delivering quality healthcare. This quarterly forum is normally held on the second Wednesday of March, June, September and December at Papapavlo's in Stockton.
Registration is required!
If you don’t receive an invitation via E-Mail, please email Jessica@sjcms.org

March 11th, 2026: 11:00AM to 1:00PM
Discover how to navigate complex employment law changes and stay on track for a successful year. This will help businesses navigate California’s challenging employment and labor laws.
Jamie Bossuat, a shareholder and employment lawyer at Kroloff will present an update on the most pressing issues in employment law and will offer practical suggestions for reducing liability. Issues will include recent changes in wage and hour requirements, updates to leave of absence laws, and current litigation trends.

June 10th, 2026: 11:00AM to 1:00PM
This presentation outlines the make-up of, and challenges associated with, the effective management of accounts receivable (A/R) in the physician practice. Presented by one of CMA’s experienced practice management experts, the presentation will cover areas that significantly impact a practice’s A/R and suggestions on how to address those A/R challenges.
Mark Lane, Associate Director in the CMA’s Center for Economic Services , began his career as a claims processor for plans such as Blue Shield and Health Net. Over the next 18 years, his experiences in claim operations, customer service, provider relations and contracting have allowed him to get a unique vantage point on the relationship between physicians and payors. Having experienced the physician-payor relationship from both ends, Mark is able to understand the needs and positions of the respective sides, making him an ideal candidate to educate providers on overcoming the ever-changing challenges of the healthcare landscape.
Under California’s unfair payment practices law, payors are required to establish a fast, fair and cost-effective dispute resolution mechanism (i.e., “appeal process”) to resolve provider disputes. Anytime a payor contests, adjusts or denies a claim, they are required to notify the physician of the availability of the dispute process and instructions for submitting the appeal.
California regulations establish clear requirements to ensure that provider appeals are received and reviewed promptly by payors, including payor acknowledgement of receipt of a written appeal within two working days for electronically submitted appeals or within 15 working days for paper appeals. Payors are also required to i ssue a written determination within 45 working days of receiving a provider’s appeal and must also report annually to the California Department of Managed Health Care on the nature and volume of provider appeals received.
Despite these safeguards, the appeals process can still be difficult to navigate. To help improve your chances of success, CMA recommends the following:
Clearly identify your submission as an appeal. Include the word “APPEAL” in the subject line and opening sentence of your submission. Avoid using the term “inquiry” since clearly labeling your submission as an appeal will ensure it is routed to the appropriate department and will be responded to in writing within the required timeframes.
Submit through the correct appeals channel.
Many payors maintain separate mailing addresses or electronic portals for the submission of an appeal. If you are unsure where or how to submit an appeal, review the payor’s website, provider manual, contract language, or online provider portal for appeal instructions.
Clearly state your “ask.”
Your appeal should clearly explain the specific action being requested, such as a re-review of coding or bundling edits, a medical necessity review by a physician of the same or similar specialty, or a correction of eligibility or authorization determinations. Simply venting about your frustration with how a claim was denied incorrectly or underpaid isn’t enough to communicate why you believe the claim was processed incorrectly or what action you are requesting in your appeal.
Track acknowledgements and responses. Look out for the acknowledgement of receipt of your appeal from the payor. If you don’t receive the acknowledgement of receipt, within two working days for electronic submissions and 15 working days for paper appeals, there is likely a
problem and a prompt follow-up with the payor may be in order. Remember the payor has 45 working days from the receipt of the appeal to issue a written determination explaining the reasons for its determination.
Pursue additional appeal levels when available. If a payor upholds its decision at the first level, review the determination carefully and consider whether to pursue second- or final-level appeals when available, submitting any additional documentation that supports your position.
File a complaint with the regulator. Practices that believe they have been paid improperly or that a payor is engaging in an unfair payment pattern, should file a complaint through the Department of Managed Health Care (DMHC) Provider Complaint Portal or by calling the DMHC Provider Complaint line at (877) 525-1295. To be eligible to file a formal complaint with the regulator, practices must first attempt to resolve the issue utilizing the payor’s formal appeal process. For more information about the DMHC complaint process, please review the DMHC FAQ and CMA’s on-demand webinar, “Navigating the DMHC’s Provider Complaint Process.”
Need help?
CMA members and their staff can access step-by-step appeals guidance through the CMA Know Your Rights series at cmadocs.org/kyr, which includes Quick Guide for Appeals and Timeframes to Appeal. For additional support, contact CMA’s practice management experts at (800) 786-4262 or economicservices@cmadocs.org
Covered California sees big shifts in enrollments: Why verifying eligibility is critical in 2026
With the expiration of the enhanced Affordable Care Act (ACA) premium tax credits, Covered California is seeing a marked increase in enrollee-generated plan cancellations and enrollees moving toward lowerpremium Bronze plans, which carry higher deductibles and cost-sharing responsibilities.
Given these developments, the California Medical Association (CMA) is advising physician practices to exercise diligence in verifying patient eligibility and benefits prior to visits.
Covered California shifts in cancellations and plan enrollments
The start of a new calendar year resets deductibles, but the shift in enrollment caused by the expiring ACA credits makes this particularly impactful in 2026. This year, Covered California reports a 57% increase in enrollee-generated plan cancellations (not counting consumers who will be cancelled for nonpayment). Additionally, a significant share of Covered California enrollees are choosing Bronze plans with significantly higher deductibles; for example, the 2026 Standard Bronze plan features a $5,800 deductible for individuals and $11,600 deductible for families.
Because open enrollment may have brought changes to your patients’ benefit plans or coverage options, practices should not assume coverage status has remained the same. Failing to verify these details can lead to uncompensated care, particularly if a patient has unknowingly entered the federal three-month grace period for non-payment of premiums.
To help practices adapt to these changes, CMA has published Navigating Covered California: Preparing for Changes in 2026, a comprehensive guide (available free to members) to managing the current exchange environment. The guide highlights two critical strategies for addressing changes in enrollees’ status:
• Ensure Staff Clarity and Proactive Communication: It is critical that all front office staff clearly understand the physician’s participation status with each plan offered in the area. Ideally, staff should discuss participation status and potential out-of-network costs with patients before scheduling appointments. This proactive approach avoids potential out-of-network costs and patient frustration from unexpected bills.
• Re-verify patient eligibility: Best practice is to remind patients upon scheduling that their plan deductible may have reset on January 1 and that, if that is the case, payment will be due at the time of service. Failure to collect deductibles, copays, and coinsurance at the time of service can be costly, as a practice’s ability to successfully collect decreases significantly once the patient leaves the office.





Now hiring primary care physicians and anesthesiologists
UC Davis Health is an extraordinary place to further your career. You’ll experience being part of an academic medical center that’s committed to advancing pioneering research, promoting a sense of belonging through an inclusive work environment, and fostering continuous learning to develop health care leaders.
UC Davis Health offers robust benefits, including:
■ Competitive compensation
■ Retirement and savings investment plans, including UC’s defined-benefit pension plan
■ An emphasis on work-life balance
■ Access to wellness programs, state-of-the-art facilities, and more
SHADI BARFJANI, MD, MS
HARMEET
KAUR PHD, HCLD(ABB), M(ASCP)CM
STEVEN
STEWART, B.S. PHM
Mycoplasma genitalium (M. genitalium) is a sexually transmitted bacterium that has increasingly drawn attention from clinicians and public health officials across the United States. Though less well known than infections such as chlamydia or gonorrhea, M. genitalium has been linked to urethritis in men and cervicitis, pelvic inflammatory disease, and reproductive complications in women.
Centers for Disease Control and Prevention (2021). Public Health image Library https://npwomenshealthcare.com/clinical-presentation-diagnosis-and-management-of-mycoplasma-genitalium/
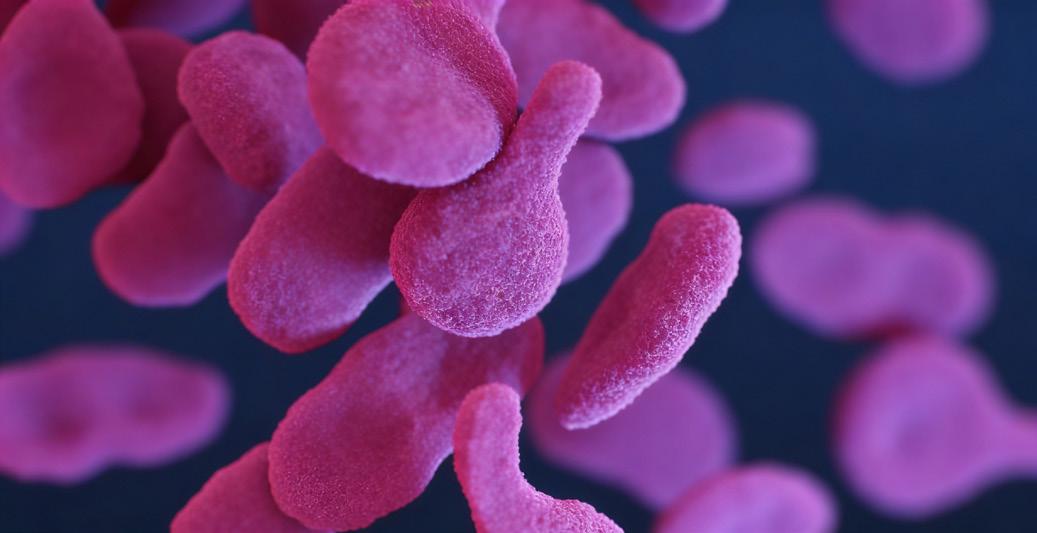
One of the challenges in addressing M. genitalium is that it often causes mild or no symptoms, allowing infections to go undetected. When symptoms do occur, they can closely resemble those of other sexually transmitted infections (STIs), making diagnosis difficult without specific laboratory testing. Unlike more common STIs, routine screening for M. genitalium is not yet widespread, and testing typically requires specialized molecular assays.
Another significant challenge is the lack of accurate and widely available diagnostic tests for M. genitalium. This organism is extremely slow-growing, and culturing for M. genitalium can take up to six months and is limited to only a handful of laboratories worldwide. As a result, the Centers for Disease Control and Prevention (CDC) recommends Nucleic Acid Amplification Testing (NAAT) for detection.
When selecting an appropriate NAAT, sensitivity and accuracy are critical. RNA-based assays offer a substantial advantage because they target ribosomal RNA (rRNA), which is present in thousands of copies per organism, compared to the single-copy DNA target used in DNA-based assays. This makes rRNA-based NAATs significantly more sensitive and better suited for detecting low-level infections.
To better understand the presence of this emerging infection in the local community, the San Joaquin County Public Health Lab (SJCPHL) conducted a limited retrospective random screening study between 2023 and 2024 using deidentified urine samples received from a local hospital. A total of 638 specimens submitted for routine NAAT screening for Chlamydia trachomatis (CT), Neisseria gonorrhoeae (NG), or Trichomonas vaginalis (TV) were included.
For this study, the SJCPHL validated and utilized the Aptima Mycoplasma genitalium Assay on a fully automated Panther® system. This assay qualitatively detects rRNA from M. genitalium, providing a highly sensitive and reliable method for identifying infection in clinical specimens.
Notably, 26.7% of M. genitalium–positive specimens demonstrated co-infection with another STI.
These findings underscore the clinical importance of considering M. genitalium in patients who test positive for other STIs, particularly in symptomatic individuals or those with persistent infections, as well as reproductive age population.
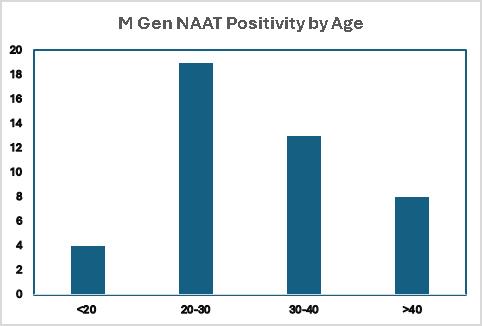
Efforts like this limited study reflect a growing need among public health agencies in assessing the burden of M. genitalium to inform future testing and treatment strategies. Of particular concern is the bacterium’s increasing resistance
to commonly used antibiotics, which complicate treatment and heightens the importance of early and accurate detection.
Understanding infections that often remain underdiagnosed is a critical step in protecting community health and ensuring that prevention and treatment strategies keep pace with evolving public health challenges. Effective M. Genitalium surveillance does require broader prevalence studies with larger and more diverse patient samples and multiple data sources to establish accurate and actionable positivity rates in the population.
Acknowledgement: The authors wish to thank the public health lab microbiologists M. Paniagua- Alexander, Joan Bernal, Marcela Bown, Kelli Hartley- Lawrence for their assistance in this project.

SJMS MEMBERS THIS WINTER! ...and even more on the way.
Lindsay Burton, MD
OB/GYN
900 Greenley Road, Ste 922 Sonora, CA 95370
Washington University School of Medicine
Tamara Chambless, MD
Psychiatry
193 Fairview Ln., Ste K Sonora, CA 95370
Weill Cornell Medical CollegeNew York Hospital
Jessica Nash, DO Gastroenterology
680 Guzzi Ln., Ste 206 Sonora, CA 95370
Pacific Northwest University of Health Services
Ashley Bedi, DO
Physical Medicine and Rehabilitation
515 S Fairmont Ave Lodi, CA 95240
Des Moines University, 2018
Quoc Tran, DO
Family Practice
12811 Covey Cir. Sonora, CA 95370
West Virginia School of Osteopathic Medicine, 2019
Gordon Fahey, MD
General Surgery
999 S. Fairmont Ave, Ste 100 Lodi, CA 95240
Medical College of Georgia, 2000
Jonathan Lu, MD
General Surgery
975 S. Fairmont Ave. Lodi, CA 95240
Loma Linda University School of Medicine, 2009
Khaleeq Siddiqui, MD
Gastroenterology
2415 W Vine St., Ste 103 Lodi, CA 95242
Nishtar Medical College and Hospital, 2007
Mayline Nambela-Barlow, MD
Family Practice
900 Mono Way Sonora, CA 95370
Loma Linda University School of Medicine, 2018
Ayaz Khan, MD
Physical Medicine and Rehabilitation
680 Guzzi Ln., Ste 102 Sonora, CA 95370
Michigan State University College of Human Medicine
Nedaa Issa, MD
Pediatrics
1901 W Kettleman Ln., Ste 200 Lodi, CA 95242
AL-QUDS University Faculty of Medicine, 2004
Brandon Painter, MD
General Surgery
680 Guzzi Ln., Ste 106 Sonora, CA 95370
Loma Linda University School of Medicine
Chrystal Bradley, MD OB/GYN
900 Greenley Rd., Ste 922 Sonora, CA 95370
University of Southern California Keck School of Medicine, 2011
Zachary Barlow, MD
Family Practice
193 S Fairview Ln. Sonora, CA 95370
Loma Linda University School of Medicine, 2021
James Boozer, MD
Internal Medicine
18661 Highway 120 Groveland, CA 95321
Loma Linda University School of Medicine, 1984
Kashan Rizvi, MD
Family Practice
1335 S Fairmont Ave Lodi, CA 95240
St George’s University College of Medicine, 2011
Muhtada Kamal Aldin, MD
Radiology
4722 Quail Lakes Dr Ste B Stockton, CA 95207
UC Davis School of Medicine, 2020
Vincent Trung Ngo, MD
Family Practice
2545 W. Hammer Ln Stockton, CA 95209
A.T. Still University of Health Sciences, 2018
Yoon Ko, DO
Family Practice
599 E. Valpico Rd Tracy, CA 95376
Touro College of Osteopathic Medicine – Harlem, 2019
Natasha Bir, MD, FACS General Surgery
100 Mission Boulevard Jackson, CA 95642
UC Davis School of Medicine, 2004
Steven Lalliss, MD Orthopedic Surgery
100 Mission Boulevard Jackson, CA 95642
Uniformed Services University of the Health Sciences, F. Edward Hebert School of Medicine, 1998
Steven Siegal, MD
Orthopedic Surgery
100 Mission Boulevard Jackson, CA 95642
Elisabeth Siegler, MD
Orthopedic Surgery
100 Mission Boulevard Jackson, CA 95642
Keck School of Medicine of USC, 1992
Donald Van Fossan, MD
Neurology
100 Mission Boulevard Suite 2200 Jackson, CA 95642
St. Louis University School of Medicine, 1985
Bess Brackett, MD
Orthopedic Surgery
100 Mission Boulevard Suite 2800
Jackson, CA 95642
Univ of Cincinnati College of Medicine, 1988
Jeffrey Meter, MD
Orthopedic Surgery
100 Mission Boulevard Suite 2800
Jackson, CA 95642
Hahnemann University School of Medicine, 1989
Maria Carla Krissel Badiola, MD
Hospital Medicine
200 Mission Boulevard Jackson, CA 95642
Hashim Chaudhry, DO
Internal Medicine
200 Mission Boulevard Jackson, CA 95642
Gurjant Singh, MD
Family Practice
1026 Lifestyle Street
Manteca, CA 95337
Ross University School of Medicine, 2020
Christy Behnam, MD
Dermatology
2505 West Hammer Lane
Stockton, CA 95209
Ogechukwu Etudo, MD
Family Practice
2505 West Hammer Lane
Stockton, CA 95209
Venkatramana Srinivasan, MD
Anesthesiology
2505 West Hammer Lane
Stockton, CA 95209
Stanley Medical Coll, Madras University, 1992
Sweet Gerlie Smith, MD
Internal Medicine
2545 West Hammer Lane
Stockton, CA 95209
Cebu Institute of Medicine, 2016
Yuchen You, DO
General Surgery
2545 West Hammer Lane
Stockton, CA 95209
Western University of Health Sciences/Coll of Osteopathic Medicine Pacific, 2019
Ahmad Ahmadzia, MD
Internal Medicine
445 West Eaton Avenue Tracy, CA 95376
Shayiq Ahmadzia, MD
Internal Medicine
445 West Eaton Avenue Tracy, CA 95376
Laurena Dongmo Fotsing, MD
Family Practice
445 West Eaton Avenue Tracy, CA 95376
Tabish Jalal, MD
Internal Medicine
445 West Eaton Avenue Tracy, CA 95376
Satinder Singh, DO
Internal Medicine
445 West Eaton Avenue Tracy, CA 95376
Touro University College of Osteopathic Medicine, 2006
Kavan Ramachandran, MD
Internal Medicine
4601 Dale Rd Modesto, CA 95356
Yu Cheng, MD
Hospital Medicine
4601 Dale Road Modesto, CA 95356
Tianjin Medical University, 2000
Jorge Kurek, MD
Anesthesiology
4601 Dale Road Modesto, CA 95357
Pearl Chan, MD
Urgent Care
599 East Valpico Road Tracy, CA 95376
Ross University School of Medicine, 2022
Susan Okpara, MD
Pediatrics
599 East Valpico Road Tracy, CA 95376
Kaylee Potter, DO OB/GYN
999 South Fairmont Avenue Suite 200 Lodi, CA 95240
New York Institute Technology, 2021

1939-2025
Dr. Jack L. Gilliland, a beloved pediatrician, passed peacefully to his rest on December 31, 2025, awaiting the second Advent and resurrection. He joins his beloved wife Jaquilyn, and we hope they are lovingly reunited.
Born on June 18, 1939, at Buchanan Hospital in Lodi to Cleo Litchfield Gilliland and Virgil Gilliland, Jack was delivered by Dr. Samuel Leiske, a 1925 graduate of the College of Medical Evangelists.
Jack’s education was entirely within the Seventh-day Adventist school system. He graduated from Lodi Academy in 1957, Pacific Union College in 1961, and Loma Linda University School of Medicine in 1965. His pediatric training was completed at the University of Washington and Children’s Orthopedic Hospital. Jack then served two years in the U.S. Navy as Chief of Pediatrics at Lemoore Naval Hospital.
In 1970, Jack returned to Lodi to assume the practice of the late Dr. Cecil Ramsel, M.D. Soon after, he and Dr. Roy Ishi founded the Lodi Pediatric Medical Group. Together with Drs. Denis Swanson and Wayne McFarland, they built the medical clinic across from Lodi Memorial Hospital, which served generations of local families.
In 1985, Jack joined the newly formed Stockton Kaiser Permanente Medical Clinic as one of its first 11 physicians. He served as Chief of Pediatrics for seven years before being elected the first Stockton Physician in Chief (PIC) in 1992, a role he held for 12 years. The North Tower of the Stockton Medical Office Building has been formally recognized as the Gilliland Tower. During his tenure, Jack oversaw the acquisition of St. Dominic’s Hospital and Medical Complex in Manteca, oversaw the construction of the Manteca Medical office followed by the construction of a new medical clinic in Tracy, and began the development of the Kaiser Foundation Hospital and Clinics in Modesto (also known as “the house that Jack built”). He was a treasured colleague, a ‘pediatrician’s pediatrician’, and a leader
who treated everyone he encountered with respect and dignity.
He also served as President of the San Joaquin Medical Society and on the board of the Hospice of San Joaquin. Jack wanted to acknowledge a few people he worked with, including Jose Rivera MGA, Mike Geronio MOC, Henry Illaga, Kristen Spracher Birtwhistle for her many roles within the community and the clinic, and his executive secretary Marsha MacDonald, whom he warmly noted worked alongside him for 12 years “without a harsh word.” Jack retired in 2006, surrounded by the friendship of colleagues, family, and the community he had cared for over decades. He maintained a long-standing commitment to the Lodi Boys and Girls Club and served on the boards of Lodi Academy and Fairmont Seventh-day Adventist Church.

The greatest blessing of Jack’s life came during a newborn exam at Dameron Hospital, where he met Jaquilyn Trent and her fourmonth-old second son, Ryan. After a couple years of courtship, they were married on January 9, 1981, at their home in Acampo.
Jacque enjoyed a distinguished 35-year teaching career with the Stockton Unified School District, retiring in 2004. Jacque lovingly raised her two sons and Jack’s daughter and son from his previous marriage. Jacque passed away in 2023 after a courageous battle with Parkinson’s and dementia.
Jacque and Jack especially cherished time with their
grandchildren. No matter where the family lived - Connecticut, London, Galt, Lodi, or Los Angeles - they made it a point to visit often, enthusiastically showing up to babysit, teach, mentor, and share adventures together. They took special pride in being present grandparents, whether offering guidance, encouragement, or introducing the children to travel and new experiences, always lavishing them with affection and gifts.
Jack and Jacque found great joy in travel and adventure. Their favorite destination was Turkey, whose rich history and blend of East and West deeply inspired them. Jacque encouraged Jack to take up scuba diving, and together they explored many remarkable underwater sites, including shipwrecks off Sharm El Sheikh, where they welcomed the new millennium together. They had many travel adventures with dear friends Tom and Sandi Stokes. The two couples shared countless memories, laughter, and Pinochle games (which the ladies usually won, to the gentlemen’s cheating protest).
Jack enjoyed a special group of friends – the ROMEOs (Retired
Old Men Eating Out). They met for a regular Friday lunch with dear friends – Sandi and Tom Stokes, Orlene and Al Dentone, Carol and Bob Romans, Ram Rao, and Ruthie, Jerry, and Mike Heminger.
Jack’s parents Cleo and Virgil, his brother Darrel (Bub), and his close friend C. Robert Breckenridge DDS preceded him in death. Jack is survived by his daughter Melissa Gilliland Frank, grandchildren Caitlin and Brendan; son Geoffrey Gilliland, grandchildren Steven and Megan; son Michael Schenone and wife Saret, grandchildren Michelle and Melissa; and son Ryan Schenone and wife Sherri, grandchild Nathan; and his dear dog Chloe. Jack was deeply grateful for the extraordinary care and devotion Ryan and Sherri provided during the past six years, enabling both Jacque and Jack to remain comfortably at home.
As Jack would say, “Old dogs never die, they just sleep in your heart.”


Hearing the words “you have cancer” can be overwhelming. At St. Joseph’s Cancer Institute, our patient navigators can answer questions, explain treatment options, and help guide you through your cancer journey. St. Joseph’s is the only accredited cancer center and NAPBC®-accredited breast center in San Joaquin County. With certified oncology specialists, state-of-the-art technology, and comprehensive support services, you can be assured St. Joseph’s is the right place for care.
Learn more at dignityhealth.org/stockton/cancercare or call our Cancer Patient Navigator at (209) 939-4526.


We'll Empower You to Defend Against Ransomware and Cyber Attacks

staying insurable. We created the Cyber Risk Initiative (CRI) to give you a clear picture of your vulnerabilities, so you have time to fix them before something breaks. It is a streamlined process designed to be low-impact for you, but high-impact for your practice.
Complementary: This is a free benefit for all current SJMS members.
Complete our brief, high-level security questionnaire any time of day, on your own schedule. Scan the QR code to get started.
Full Control: Make data security improvements with anyone you choose.
Stay Insurable: Verify you meet the security standards carriers require.
No Disruption: No downtime, no changes to your system, and no outside access to your data.
Verified Protection: Move from "hoping" you're secure to having a clear, documented plan.

Scan the code or visit the website below to take the first steps!
https://ce-technology.com/cyber-risk-initiative
We will email you a secure link to initiate a third-party external scan. This identifies vulnerabilities hackers see from the outside without ever touching your internal network.
A standard NDA is provided upfront. Your data privacy is our first priority.
Your custom report will show exactly where you’re secure and what to do to stay protected and insured— no tech jargon needed. We’ll review this together and answer any questions you may have.
San
Stockton, California 95219-6568

