2026 BENEFITS GUIDE
March 1, 2026 – February 28, 2027

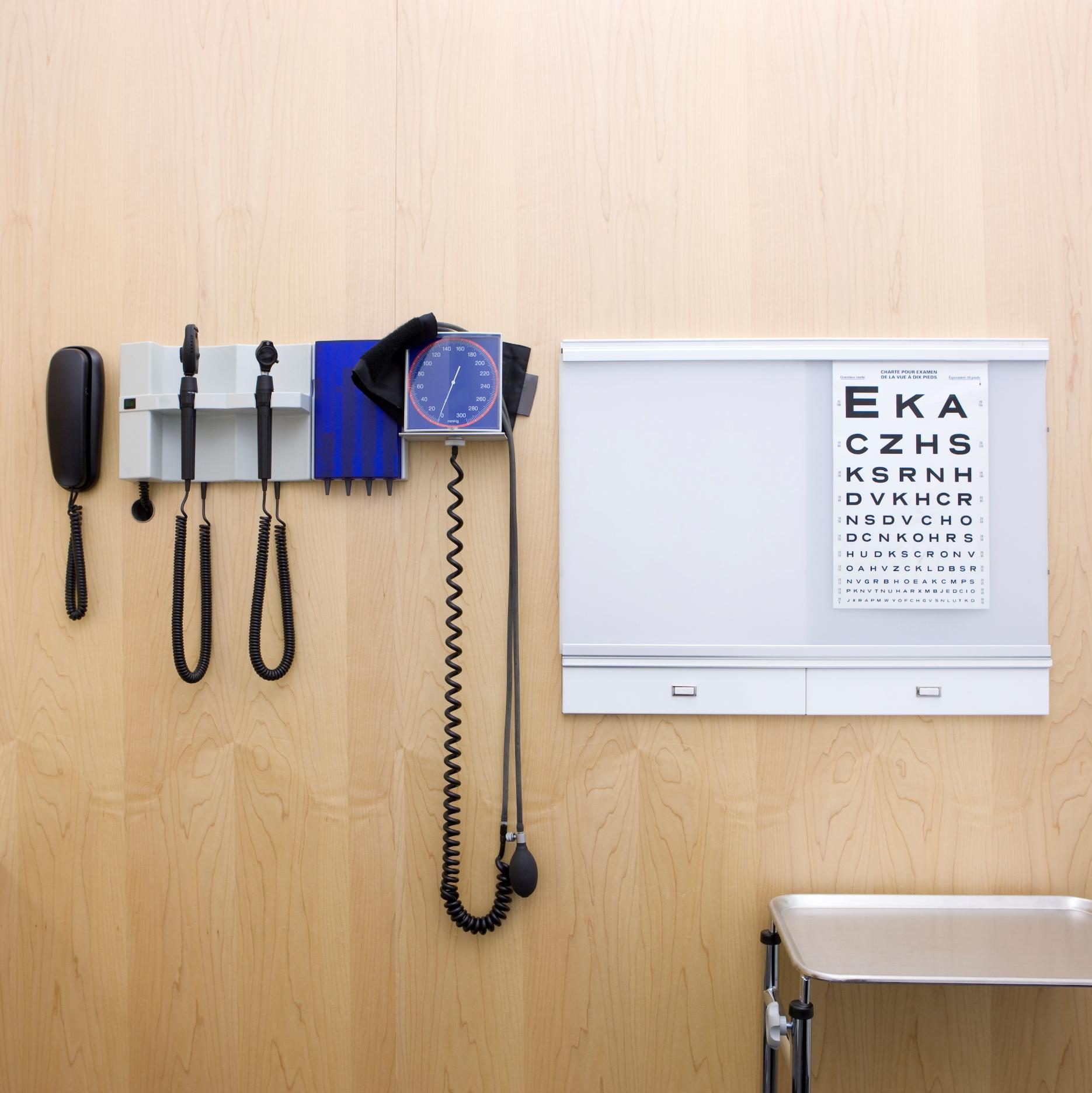



March 1, 2026 – February 28, 2027





It’s Your Health. Get Involved
Preventative Health Care Services
Your health is a work in progress that needs your consistent attention and support. Each choice you make for yourself, and your family is part of an ever-changing picture. Taking steps to improve your health such as going for annual physicals and living a healthy lifestyle can make a positive impact on your well-being.
It’s up to you to take responsibility and get involved, and we are pleased to offer programs that will support your efforts and help you reach goals.
Preventive care includes services like checkups, screenings and immunizations that can help you stay healthy and may help you avoid or delay health problems Many serious conditions such as heart disease, cancer, and diabetes are preventable and treatable if caught early It’s important for everyone to get the preventive care they need Some examples of preventive care services are:
o Blood pressure, diabetes, and cholesterol tests
o Certain cancer screenings, such as mammograms, colonoscopies
o Counseling, screenings and vaccines to help ensure healthy pregnancies
o Regular well-baby and well-child visits
Immunizations
Understanding What’s Covered
Some immunizations and vaccinations are also considered preventive care services Standard immunizations recommended by the Centers for Disease Control (CDC) Include: hepatitis A and B, diphtheria, polio, pneumonia, measles, mumps, rubella, tetanus and influenza although these may be subject to age and/or frequency restrictions.
Generally speaking, if a service is considered preventive care, it will be covered at 100% If it’s not, it may still be covered subject to a copay, deductible or coinsurance The Affordable Care Act (ACA) requires that services considered preventive care be covered by your health plan at 100% in- network, without a copay, deductible or coinsurance. To get specifics about your plan’s preventive care coverage, call the customer service number on your member ID card. You may want to ask your doctor if the services you’re receiving at a preventive care visit (such as an annual checkup) are all considered standard preventive care. If any service performed at an annual checkup is as a result of a prior diagnosed condition, the office visit may not be processed as preventive, and you may be responsible for a copay, coinsurance or deductible. To learn more about the ACA or preventive care and coverage, visit www.healthcare.gov.
Who is Eligible to Join the Benefit Plan?
You and your dependents are eligible to join the health and our company welfare benefit plans if you are a full-time employee regularly scheduled to work 30 hours per week. You must be enrolled in the plan to add dependent coverage.
Who is an Eligible Dependent?
•Your spouse to whom you are legally married
•Your domestic partner with whom you have shared a residence and financial obligations for 6 months or more
•Your dependent child under the maximum age specified in the Carriers’ plan documents including:
•Natural child
•Adopted child
•Stepchild
•Child for whom you have been appointed as the legal guardian
*Your child’s spouse and a child for whom you are not the legal guardian are not eligible.
The Dependent Maximum Age Limits is up to age 26
The dependent does not need to be a full-time student; does not need to be an eligible dependent on parent’s tax return; is not required to live with you; and may be unmarried or married.
Once the dependent reaches age 26, coverage will terminate on the last day of the birth month
A totally disabled child who is physically or mentally disabled prior to age 26 may remain on the if the child is primarily dependent on the enrolled member for support and maintenance.
When Do Benefits Become Effective?
Your benefits become effective on the first day following 90 days of your full-time employment.
Annual Open Enrollment?
Each year during the annual Open Enrollment Period, you are given the opportunity to make changes to your current benefit elections. To find out when the annual Open Enrollment Period occurs, contact Human Resources.
You are allowed to make changes to your current benefit elections during the plan year if you experience an IRS- approved qualifying change in life status. The change to your benefit elections must be consistent with and on account of the change in life status
IRS-approved qualifying life status changes include:
•Marriage, divorce or legal separation
•Birth or adoption of a child or placement of a child for adoption
•Death of a dependent
•Change in employment status, including loss or gain of employment, for your spouse or a dependent
•Change in work schedule, including switching between full- time and part-time status, by you, your spouse or a dependent
•Change in residence or work site for you, your spouse, or a dependent that results in a change of eligibility
•If you or your dependents lose eligibility for Medicaid or the Children’s Health Insurance Program (CHIP) coverage
•If you or your dependents become eligible for a state’s premium assistance subsidy under Medicaid or CHIP
If you have a life status change, you must notify the company within 60 days for changes in life status due to a Medicare or CHIP event and within 31 days of the other events
If you do not notify the company during that time, you and/or your dependents must wait until the next annual open enrollment period to make a change in your benefit elections
Please note, loss of coverage due to non-pay mentor voluntary termination of other coverage outside a spouse’s or parent’s open enrollment is not an IRS-approved qualifying life event and you do not qualify for a special enrollment period.
For your convenience, Sterling Seacrest Pritchard uses the online benefits management system, Bernie Portal.
Through Bernie Portal, you can:
• View all your benefit information
• Compare plan information – which plan best suits your healthcare needs?
• Make your new-hire benefit elections
• Make your annual Open Enrollment benefit elections
• Make changes throughout the year (address updates, dependent information, etc.)
• Access a full document library, in which you will find complete benefit summaries, claim forms, prescription discount programs, and more!
PLEASE MAKE ALL ELECTIONS THROUGH BERNIE PORTAL BY FRIDAY, FEBRUARY 20th .

1. Visit Bernie Portal to begin your enrollment process.
2. Your username is your email address If you have forgotten your password, click “Forgot Password” to recover 3. Confirm your personal and contact information and add a photo if you would like to Then click “Save and Continue ”Note: the address listed is where your new ID cards will be sent Please ensure this information is correct
4. Add your Spouse/Dependent information Start by toggling the on switch for dependents that you wish to cover Make sure to provide legal names, correct birth dates, and social security numbers These are required to make elections with the carriers.
5. Note the benefits menu on the left, which tracks your plan election progress. Once you’ve made your election for that benefit type, a check mark will appear. A shopping cart on the right-hand side of the page will keep track of your coverage costs.
6. Scroll through benefit types and explore each plan option by using the “Select a Plan” dropdown. If you wish to waive coverage, use the “Waive” option to save and continue
7. Cost per pay period and coverage tiers will generate based on the plan you have selected and will show based on the dependents added If you were previously enrolled in coverage your current election will appear under each benefit type for your reference
8. Provide the requested beneficiary information for your basic life insurance coverage Adjust the percentage that each beneficiary should receive by sliding the distribution button to the desired percentage
9. Review your election sheet and complete any outstanding fields. Finally, move your mouse to sign the signature box and click “I Agree” to complete your enrollment.
PLEASE MAKE ALL ELECTIONS THROUGH BERNIE PORTAL BY FRIDAY, FEBRUARY 20th .

You pay either a copay &/or coinsurance per the assigned prescription drug tier. This plan meets the CMS standard for creditable prescription drug coverage. Prescription Drugs
Quantity Limits:
Retail = 30 day supply
Mail-Order = 90-day supply except Specialty
Retail: $15 copay
Tier 1 - Generic Drugs
Tier 2 - Preferred Brand-Name
Tier 3 - Non-Preferred BrandName
Tier 4 - Specialty Drug
Mail Order: $15 copay
Retail: $35 copay
Mail Order: $70 copay
Retail: $60 copay
Mail Order: $180 copay
Retail and Mail Order: 25% up to $350 30 day supply
$15 copay, retail only
$60 copay, retail only
$60 copay, retail only
up to $350, retail only









AsanAnthemmember,youqualify for discounts on products andservices that help promote better health and well-being.* Thesediscounts areavailable through SpecialOffersto help yousavemoney while taking care of yourhealth.
Vision,hearingand dental

Glasses.com and1-800-CONTACTS® Shopfor the latest brand-nameframesat afraction of the cost for similar framesat other retailers. Youarealsoentitled to anadditional $20 off orders of $100or more,free shipping andfreereturns.
EyeMed Take30%off anewpair of glasses,20% off non-prescription sunglassesand20% off all eyewear accessories.
PremierLASIK Save$800on LASIKwhenyou choose any“featured” Premier LASIKNetworkprovider.Save15% with all other in-networkproviders.
TruVision Saveup to 40%on LASIKeyesurgeryat more than 1,000locations.

NationsHearing Receivehearingscreenings and in-home service at no additional cost.All hearingaids start at $599each.
Hearing CareSolutions Digital instruments start at $500, and a hearing exam is free. Hearing Care Solutions has 3,100 locations and eight manufacturers, and offers a three-year warranty, batteries for two years and unlimited visits for oneyear.
Amplifon Take25%off,plusanextra $50off one hearingaid; $125offtwo.

ProClear Aligners Take$1,200off aset of custom aligners. Youcanimproveyour smile without metal braces andtime-consumingdental visits. Yourorder is 50%off andcomeswith afree whitening kit.



**DispatchHealth coverage area is limited to select zip codes throughout metro Atlanta and some neighboring suburbs. Reach out to Anthem member services for details.

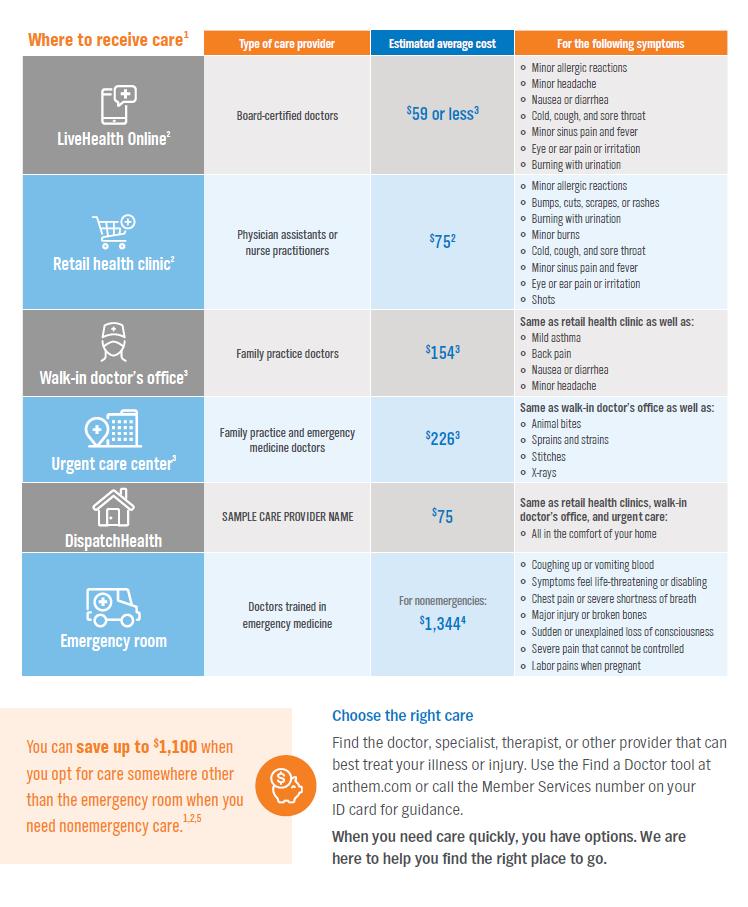
NOTE: The above costs are examples of what you might incur and may not be representative of your specific medical plan.

ENT of GA dental benefits are offered by Anthem Benefits provide access to coverage for dental care raging from routine cleanings to Orthodontia for children Through Anthem you have access to thousands of unique providers Out of network benefits are available, however, using in-network dentists will provide negotiated rates on services, as well as no balance billing. The network is the Anthem Blue Cross Blue Sheild Dental Complete.
Your Deductible paid once a year for Basic and/or Major Services
to preventive, basic, and major
Preventive & Diagnostic Services Exams, Cleanings & Bitewing X-Rays, Fluoride, Sealants
Basic Services Filings, Simple Extractions, Oral Surgery
Major Services Crowns, Endodontics, Periodontics
(Children up to age 19)
(Deductible waived)
Anthem pays 80% after youpay the deductible
Anthem pays 50% after youpay the deductible
Anthem pays 80% after you paythe deductible
Anthem pays 50% after you paythe deductible

ENT of GA vision benefits are offered through the Anthem Blue View Vision Network. You may elect vision coverage, whether you participate in the medical or dental plans. Many retail chains are included in the Anthem network as well as independent providers. To search for a provider near you, visit Anthem.vsp.com/find-eye-doctors.com.

To help you control your costs and reduce your out-of-pocket exposure, ENT of GA offers a Health Reimbursement Arrangement as part of our health plan!
ENT of GA is committed to reimbursing deductible expenses, the last $2,000 if you are enrolled in the Traditional Health Plan
Once you have paid any expenses towards your deductible you will receive an Explanation of Benefits (EOB) from Anthem. When you have received your EOB in the mail, all you need to do is submit the EOB and a claim form to Human Resources. At that point you will receive a tax-free reimbursement! This arrangement covers Employees Only. Reimbursement does not cover expenses paid for a dependent
ENT of GA provides all Full-Time employees a $25,000 basic life and Accidental Death & Dismemberment (AD&D) benefit. Life insurance pays your named beneficiary in the event of your death AD&D insurance will provide a benefit to your beneficiary if your death is the result of an accident AD&D insurance can provide a benefit to you if you suffer certain accidental injuries, such as the loss of limb (arm/leg), loss of eyesight or permanent paralysis This coverage is provided through Mutual of Omaha and is paid for by ENT of GA
All benefit eligible employees can purchase Short and or Long-Term Disability coverage
Voluntary Short-Term and Long-Term Disability plans are available through MetLife If you did not enroll in the disability coverage when it was first made available to you as a new hire, you will be required to complete an Evidence of Insurability form for MetLife. This form will ask questions about your own health and family medical history. For more information, please reach out to Tammy Meyer at: tmeyer@entofga.com.

ENT of GA contributes to the cost of medical coverage for all eligible employees. For an additional premium employees can add dependent coverage. Please refer to the chart below for your payroll deductions.


Subscriber ID #
Date of Service
Name of Patient
Name of Doctor, Facility or Hospital
Copy of Bill or Explanation of
(EOB)
d: 678-553-8293 jrakestraw@sspins.com
The right to COBRA continuation coverage was created by a federal law, the Consolidated Omnibus Budget Reconciliation Act of 1985 (COBRA) COBRA continuation coverage can become available to you and other members of your family when group health coverage would otherwise end For more information about your rights and obligations under the Plan and under federal law, you should review the Plan’s Summary Plan Description or contact the Plan Administrator For additional information regarding COBRA qualifying events, how coverage is provided and actions required to participate in COBRA coverage, please see your Human Resources department.
The group health coverage provided complies with the Newborns’ and Mothers’ Health Protection Act of 1996 Under this law group health plans and health insurance issuers generally may not, under federal law, restrict benefits for any hospital length of stay in connection with childbirth for the mother or newborn to less than 48 hours following a vaginal delivery, or less than 96 hours following a cesarean section. However, Federal law generally does not prohibit the mother’s or newborn’s attending provider, after consulting with the mother, from discharging the mother or her newborn earlier than 48 hours (or 96 hours as applicable.) In any case, plans and issuers may not, under federal law, require that a provider obtain authorization from the plan or the insurance issuer for prescribing a length of stay not in excess of 48 hours (or 96 hours)
If you or your children are eligible for Medicaid or CHIP (Children’s Health Insurance Program) and you are eligible for health coverage from your employer, your State may have a premium assistance program that can help you pay for coverage. These States use funds from their Medicaid or CHIP programs to help people who are eligible for employersponsored health coverage but need assistance in paying their health premiums. If you or your dependents are already enrolled in Medicaid or CHIP you can contact your State Medicaid or CHIP office to find out if premium assistance is available If you or your dependents are NOT currently enrolled in Medicaid or CHIP, and you think you or any of your dependents might be eligible for either of these programs, you can contact your State Medicaid or CHIP office or dial 1877-KIDS NOW or www insurekidsnow gov to find out how to apply If you qualify, you can ask the State if it has a program that might help you pay the premiums for an employer-sponsored plan. Please see Human Resources for a list of state Medicaid or CHIP offices to find out more about premium assistance.
An Eligible Person and/or Dependent may also be able to enroll during a special enrollment period A special enrollment period is not available to an Eligible Person and his or her dependents if coverage under the prior plan was terminated for cause, or because premiums were not paid on a timely basis.
An Eligible Person and/or Dependent does not need to elect COBRA continuation coverage to preserve special enrollment rights Special enrollment is available to an Eligible Person and/or Dependent even if COBRA is elected Please be aware that most special enrollment events require action within 30 days of the event Please see Human Resources for a list of special enrollment opportunities and procedures.
If you have had or are going to have a mastectomy , you may be entitled to certain benefits under the Women’s Health and Cancer Rights Act of 1998 (WHCRA) For individuals receiving mastectomy-related benefits, coverage will be provided in a manner determined in consultation with the attending physician and the patient, for: All stages of reconstruction of the breast on which the mastectomy has been performed; Surgery and reconstruction of the other breast to produce a symmetrical appearance; and Prostheses and treatment of physical complications of the mastectomy, including lymphedemas. These benefits will be provided subject to deductibles and coinsurance applicable to other medical and surgical benefits provided under this plan. If you would like more information on WHCRA benefits, call your plan administrator
The Genetic Information Nondiscrimination Act (GINA) prohibits health benefit plans from discriminating on the basis of genetic information in regards to eligibility, premium and contributions This generally also means that private employers with more than 15 employees, its health plan or “business associate” of the employer, cannot collect or use genetic information, (including family medical history information) The once exception would be that a minimum amount of genetic testing results make be used to make a determination regarding a claim You should know that GINA is treated as protected health information (PHI) under HIPAA The plan must provide that an employer cannot request or require that you reveal whether or not you have had genetic testing; nor can your employer require that you participate in a genetic test. An employer cannot use any genetic information to set contribution rates or premiums.
Since key parts of the health care law took effect in 2014, there is a new way to buy health insurance: the Health Insurance Marketplace To assist you as you evaluate options for you and your family, this notice provides some basic information about the new Marketplace and employment based health coverage offered by your employer. If your employer offers health coverage that meets the “minimum value” plan standard, you will not be eligible for a tax credit through the Marketplace and may wish to enroll in your employer’s health plan. The “minimum value” plan standard is set by the Affordable Care Act. Your health plans offered by [Company] are ACA compliant plans (surpassing the “minimum value” standard), thus you would not be eligible for the tax credit offered to those who do not have access to such a plan
NOTE: If you purchase a health plan through the marketplace instead of accepting health coverage offered by your employer, then you will lose the employer contribution to the employer offered coverage Also, this employer contribution, as well as your employee contribution to employer offered coverage, is excluded from income for Federal and State income tax purposed
The Uniformed Services Employment and Reemployment Rights Act of 1994 (USERRA) established requirements that employers must meet for certain employees who are involved in the uniformed services In addition to the rights that you have under COBRA, you (the employee) are entitled under USERRA lo continue the coverage that you (and your covered dependents, if any) had under the [Company] plan.
You Have Rights Under Both COBRA and USERRA. Your rights under COBRA and USERRA are similar but not identical. Any election that you make pursuant to COBRA will also be an election under USERRA, and COBRA and USERRA will both apply with respect to the continuation coverage elected If COBRA and USERRA give you different rights or protections, the law that provides the greater benefit will apply The administrative policies and procedures described in the attached COBRA Election Notice also apply to USERRA coverage, unless compliance with the procedures is precluded by military necessity or is otherwise impossible or unreasonable under the circumstances
Definitions
"Uniformed services" means the Armed Forces, the Army National Guard, and the Air National Guard when an individual is engaged in active duty for training, inactive duty training, or full-time National Guard duty (i e , pursuant to orders issued under federal law), the commissioned corps of the Public Health Service, and any other category of persons designated by the President in time of war or national emergency
"Service in the uniformed services" or "service" means the performance of duty on a voluntary or involuntary basis in the uniformed services under competent authority, including active duty, active and inactive duty for training, National Guard duty under federal statute, a period for which a person is absent from employment for an examination to determine his or her fitness to perform any of these duties, and a period for which a person is absent from employment to perform certain funeral honors duty It also includes certain service by intermittent disaster response appointees of the National Disaster Medical System
Duration of USERRA Coverage
General Rule: 24-Month Maximum When a covered employee takes a leave for service in the uniformed services, USERRA coverage for the employee (and covered dependents for whom coverage is elected) can continue until up to 24 months from the date on which the employee's leave for uniformed service began. However, USERRA coverage will end earlier if one of the following events takes place:
A premium payment is not made within the required time; You fail to return to work or to apply for reemployment within the time required under USERRA (see below) following the completion of your service in the uniformed services; You lose your rights under USERRA as a result of a dishonorable discharge or other conduct specified in USERRA.
This Notice of Privacy Practices (the "Notice") describes the legal obligations of [Company] (the "Plan") and your legal rights regarding your protected health information held by the Plan under the Health Insurance Portability and Accountability Act of 1996 (HIPAA) and the Health Information Technology for Economic and Clinical Health Act (HITECH Act) Among other things, this Notice describes how your protected health information may be used or disclosed to carry out treatment, payment, or health care operations, or for any other purposes that are permitted or required by law. We are required to provide this Notice of Privacy Practices to you pursuant to HIPAA.
The HIPAA Privacy Rule protects only certain medical information known as "protected health information " Generally, protected health information is health information, including demographic information, collected from you or created or received by a health care provider, a health care clearinghouse, a health plan, or your employer on behalf of a group health plan, from which it is possible to individually identify you and that relates to:
•Your past, present, or future physical or mental health or condition;
•The provision of health care to you; or
•The past, present, or future payment for the provision of health care to you.
If you have any questions about this Notice or about our privacy practices, please contact your Human Resources department The full privacy notice is available with your Human Resources Department