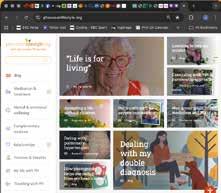
Cover star Emily, and mum Lorna, on their family’s journey




✓
✓
✓
✓









Cover star Emily, and mum Lorna, on their family’s journey




✓
✓
✓
✓










It’s great to see you here!
Thisis our first issue of 2026, and the team have really enjoyed putting these pages together. We hope you’ll find something in them that speaks to you.
We know how isolating it can be to live with PH, so we’re particularly pleased to share the details of our brand new service to make it easier to chat with other people affected by the condition. PH-CONNECT is also for family and caregivers, and it’s totally free for PHA UK members. You’ll find all the details on page 10
If you’re starting to think about summer holidays, you’ll enjoy our feature on page 54. PHA UK members Jayne and Cathy unknowingly booked the same cruise with their husbands –and what followed was a memorable European adventure! They share how they navigated travelling with oxygen and mobility equipment, proving that special trips are absolutely possible. It might just inspire you to take to the seas yourself.
Weight loss injections continue to make headlines, and we know that many of you have questions about whether they are safe to take with PH, and how they might help. That’s why we’ve
dedicated a bumper feature to the topic, which begins on page 24
As always, this issue is filled with personal stories from members of our PH community. We’re so grateful to everyone who shares their lived experience so openly and generously. There’s something really powerful about seeing your own thoughts and feelings reflected in someone else’s words.
On the topic of words, I’d urge you to take a look at the details of our new poetry competition on page 38. You definitely don’t need to be a ‘writer’ to benefit from getting creative!
The next issue of emPHAsis will be with you in the summer. 'In the meantime, enjoy the brighter days of spring. Until next time,
THERE’S SOMETHING REALLY POWERFUL ABOUT SEEING YOUR OWN THOUGHTS AND FEELINGS REFLECTED IN SOMEONE ELSE’S WORDS
Iain Armstrong Chair of the PHA UK hello@phauk.org
Introducing PH-CONNECT – our new free service to help you chat to others affected by PH
Emily and mum Lorna on their family’s journey
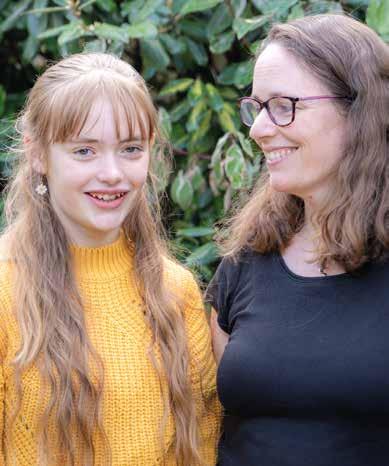
24
21 WEIGHT LOSS MEDICATIONS AND PH Facts, expert advice, and real experiences
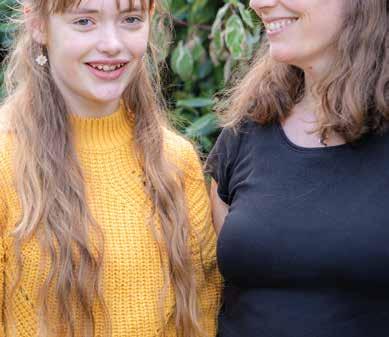
Tharuka’s


Coco’s
This
This
How
February saw some of the PHA UK team head to Dublin to showcase recent research by our charity. We were invited to present three of our original studies at the Pulmonary Vascular Research Institute Global Congress, which saw scientists and clinicians gather from around the world. UK patient voices were amplified through our poster presentations, where we shared the findings of our symptom severity survey, and our ongoing research into lived experiences of lung disease with PH.
Thank you to everyone who has been involved with these studies.
If you live in England, make sure you’re not missing out on savings!
Could a prescription pre-payment certificate save you money? Whilst your PH-specific medications are provided free on the NHS, all other prescriptions in England are charged at the standard rate of £9.90 per item. This includes medicines you may take to manage side effects from your PH medication.
A prescription pre-payment certificate (PPC) covers all your NHS prescriptions for a set price – either £32.05 for three months, or £114.50 for 12 months

This means you will save money if you need more than three items in three months, or 11 items in 12 months. You can pay by monthly direct debit for the 12-month certificate, making it even more affordable.
PPCs are available in-person from some pharmacies, and online at phauk.org/PPC
All prescriptions are free in Wales, Scotland, and Northern Ireland. Certain health conditions mean English patients pay for no prescriptions at all, but unfortunately pulmonary hypertension does not fall into this list. We hope that one day this will change, but until then, do consider a PPC to make things a little easier on your pocket.
Do you take hormone replacement therapy (HRT)? A specific HRT prescription pre-payment certificate is now available, covering certain HRT medicines for a set price of £19.80. This covers 12 months of prescriptions.

The beautiful Chelsea Physic Garden in London was the setting for another inspiring PH Research Forum at the end of last year, and it was our pleasure to support it once again.
This key annual event brings researchers, scientists and clinicians together from around the UK, and the twoday event in November saw fascinating presentations from across the specialist centre network.
Attendees shared study findings and learned from each other’s work, and the Alan Greenhalgh Award was given to the presentation voted ‘best of the event’ by delegates.
Awarded in memory of research nurse Alan, who died last year, the £1,000 grant was won by Dr Ruta Virsinskaite (pictured below) for her presentation titled: ‘CMR insights from sotatercept in PAH’.
Like everyone else, we left the event feeling hopeful, inspired, and proud to be part of such a special community.
Scan the code to see inside the event with our special video!

One of the most popular features in the last issue of this magazine was our interview with PHA UK member Nora Green, who explained how she makes the most of life with pulmonary hypertension. We shared the article on our Facebook page, and here’s what some of you said in reply:
Julie Royle
Perfectly put - let PH live with you and not the other way round☀
Angela Overton
I'm 82 and feel exactly the same way. Life is for living, do what you can now because tomorrow is not always guaranteed
Carol Taylor
Exactly how I feel. I don't let anyone or anything get in my way. I go out every day with my oxygen in tow. Enjoy life while you can, X X
Whilst this magazine was at print, we held our first Tea & Talk event of the year at our office space in Sheffield. This followed successful gatherings in 2025, bringing members together to chat, connect, and enjoy plenty of hot drinks and cake. More will be held throughout 2026, so do keep an eye on our social media channels. We understand not everyone can make it to Sheffield. We are planning other events held with specialist centres around the country, and in the meantime, turn to page 10 for news of an exciting new connection service that you can access wherever you live!









Developed by psychologists, and supported by the PHA UK, this is the world’s first self-help programme for people who live with pulmonary hypertension alongside depression or low mood.
✓ Complete the series of workbooks over four weeks in your own time from home
✓ Based on cognitive behavioural therapy (CBT) techniques
✓ Learn how to change your thinking habits and behaviours
Benefits Calculator
Find out what you might be able to apply for by answering questions about your personal circumstances. phauk.org/BenefitsCalculator
Grant Search
Discover what supportive grants may be available to you and your family. phauk.org/GrantsSearch
Personal Independence
Payment (PIP) Helper
Walk through the PIP application process step by step, access tips and checklists, and more. bit.ly/PIPhelper





All information was correct at the time of going to print, March 2026
After being licensed for use in the UK, the new PAH treatment sotatercept has been going through the commissioning process in both England and Scotland to see if it can be made available on the NHS. Here’s the current situation…
In August last year (2025), the National Institute for Health and Care Excellence (NICE) announced that sotatercept would not be commissioned for use by NHS England. Following a resubmission by the manufacturer, MSD, a second review took place in December. The process has since been paused while ‘commercial discussions’ take place between NHS England and MSD including negotiations over pricing, as sotatercept is significantly more expensive than existing PAH treatments.
The news of the pause was initially confidential, but here at the PHA UK we successfully pushed for a reconsideration of the confidentiality to allow patients - those at the heart of the process - to be kept updated. We will always stand up for what's right when it comes to our PH community.
It is unknown how long the commercial discussions will last for, and what they may lead to, but we will continue to bring you information as soon as we can.
In February this year, the Scottish Medicines Consortium (SMC) announced that sotatercept would not be commissioned for use by NHS Scotland at this stage. A further
meeting took place at the beginning of March, and an updated decision is expected in April. Please keep an eye on the PHA UK social media channels.
There have currently been no submissions to the commissioning bodies in these UK nations. We asked MSD about their plans, and they told us: “Access in Wales and NI are typically based on and follow the NICE decision, so we wouldn’t expect to see separate submissions for these regions.”
Whilst it has been disappointing news to see initial refusals in both England and Scotland, it has not unexpected. Initial refusal is common for new and specialised drugs, especially those as expensive as this one.
This is by no means the end in terms of securing UK access to sotatercept, which has been submitted under the brand name of Winrevair. We have had to fight for every drug that’s currently used to treat pulmonary hypertension, and we will continue to use your voices to secure equity of access.
Sotatercept is a totally new type of drug for pulmonary arterial hypertension. There are already a number of existing drugs that are known as ‘vasodilators’ – which work by opening up some of the arteries that have narrowed or closed down. But these drugs are treating the symptoms of PH, rather than what’s causing the disease. Rather than just opening up vessels, sotatercept works more directly on the underlying ‘problem proteins’ that are causing the disease in the first place. It’s the first time a PAH drug is getting to the root cause of the problem, rather than treating the consequences of it. It must be remembered though that this is not a cure, so it is not a life-saving drug. Sotatercept isn’t suitable for everyone. It is designed to be taken by some people alongside other medications, via an injection under the skin administered every three weeks.
Here at the PHA UK we have been key stakeholders in the review process for sotatercept, presenting evidence of the impact of pulmonary hypertension gathered via our surveys and research. When you share your voices in these ways, this is just one of the important ways we then make them heard.
Introducing PH-CONNECT, a FREE members-only space for one-to-one chats
Have you ever found yourself thinking, ‘I just wish I could talk to someone who truly understands this’? Living with pulmonary hypertension can feel isolating at times. It’s a rare condition, and sometimes it seems like the rest of the world carries on without quite realising what day-to-day life can look like for you. Here at the PHA UK, we hear this all the time – and that’s exactly why we’ve created this platform PH-CONNECT members-only service designed to help you find and chat one-to-one with other people affected by PH. Whether you’re living with the condition yourself, caring for someone who is, or supporting a loved one, this space is for you.
Maybe you’d like to speak to someone else who’s on IV medication. Maybe you’re about to go through transplant assessment and would value hearing from someone who’s been there. Or perhaps your partner, parent or child has PH, and you’d really appreciate talking to someone who understands what it’s like to love and support someone with the condition. Whatever
those conversations easier to start.
You can browse member profiles and search using different filters, such as type of PH, treatment, specialist centre, time since diagnosis, age, and more – helping you find someone whose experience feels close to yours. When you’re ready, simply click the ‘CONNECT’ button to start a private one-to-one chat.

Create your free my pha UK account
Visit my.phauk.org/register and sign up. This will allow you to access PH-CONNECT
Build your profile
Share as much or as little as you feel comfortable with. The more you include, the easier it is for others to find you.
Explore PH-CONNECT
Browse other members and use the search filters to narrow things down –by PH type, age, specialist centre and more.
Hit ‘CONNECT’

If you already have a My PHA UK account, simply sign in.

When you spot someone you’d like to talk to, simply press the button and start chatting. SCAN THE QR CODE OR

Because this is a brand new service, you may notice there are only a small number of profiles when you first join. Please don’t be discouraged – our community will grow as more members sign up. We’d encourage you to create your profile early and be part of building this supportive new space. The connections will come. 3 4 2 1

PH-CONNECT is accessed via our brand new online portal, My PHA UK. This innovative platform allows you to take control of your PHA UK membership by keeping your contact details updated, changing your preferences, setting up bespoke fundraising pages, and more. You can also use the portal to read back issues of this magazine and order our free publications and resources.
Check it out at my.phauk.org
If one-to-one chatting isn’t your thing, don’t worry– our private Facebook groups are still going strong and remain a valuable place for shared conversations and support (see page 36 for details).
This is an exclusive benefit for PHA UK members only. It’s free to join our charity – simply scan this code to become part of the family!
If you have any questions or comments about this new service, please email hello@phauk.org
How do you see yourself?
Last year, we supported trainee psychologist Jacob Pendrey to conduct a study into self-image and PH, and many of our members volunteered to be part of it. Here’s what he found out…
In terms of research, very little attention has been given to how PH changes a person’s sense of self: how they see themselves, their role in society, and their place in the world. Jacob’s study set out to explore these aspects of PH, and how that impacts self-image.
Self-image refers to how people think and feel about themselves, including their identity, their roles, their body, and their worth. For people with PH, everyday life is not only altered by
physical limitations but also by social and emotional changes. Understanding these changes is important, as they can affect mental health, quality of life, and even how well people manage their health condition.
what was already out there
The first section of the study saw Jacob review 23 existing pieces of research, as part of what’s known as a ‘literature review’.
The findings showed that pulmonary hypertension can strongly affect how people see themselves. It may lead to feelings such as low self-confidence, shame, or pulling away from social situations. These changes to a person’s sense of identity show why emotional and psychological support is just as important as medical treatment. When healthcare professionals understand how PH can affect identity, stigma, and changes in roles at work, home, or in relationships, they can offer more whole-person, person-centred care. This can help reduce emotional distress, support adjustment to living with PH, and improve quality of life.
The second part of the study saw Jacob conduct one-to-one interviews with PHA UK members, to understand how PH affects their self-image as individuals. To do this, Jacob used a method known as ‘photo elicitation’ – inviting members to submit photographs that represented their lived experience of PH from before
diagnosis, through to the present day. These photos were then discussed as part of the interviews, and Jacob was able to identify themes common to everyone who took part.
In their interviews, the 13 PHA UK members reported a disruption to self-image and wider self-concept (an overarching idea of who we are). They spoke of a loss of identity, a loss of control and ability, and described the
impact of living with PH on how they see themselves.
Analysis of the interviews also showed that self-image may be protected through acceptance and building resilience.
The findings backed up what the literature review in part one showed – that healthcare professionals may benefit from training that helps them understand how long-term illness can
Jacob Pendrey is studying psychology at Cardiff University in Wales, and this research formed the basis of his DClinPsy thesis – which he passed at the end of last year.
Q. Why did you choose pulmonary hypertension as the disease at the centre of this study?
A. “I chose PH because I have chronic health conditions myself, so the topic felt very relevant to me as a health psychology researcher. I felt I could bring a personal understanding that might be missing from existing research. When I realised that self-image in people with PH had not been studied before, it felt like an important and meaningful opportunity to explore this area and to help give a voice to people living with PH.”
Q. Did anything surprise you about the interviews you conducted with PHA UK members?
A. “In some ways, the interviews were what I expected. Using photos helped me understand why participants made certain choices and allowed for deeper conversations than I think would have been possible with more traditional research methods. What surprised me was how varied the photo submissions were. Some showed memories shaped by PH or by a time before diagnosis, while others used stock images to represent loss. Some images were abstract but explained things very literally, while others focused more on expressing emotions. This meant that people answered the same question in very different ways, which resulted in very rich and detailed data.”
affect how a person sees themselves. Providing this kind of support soon after diagnosis may help people hold on to their sense of self and avoid feeling defined only by their illness.
Jacob is now working to have the study results published in academic journals, to spread the reach of the findings and encourage self-image to be considered more widely as part of PH research.
Q. What did you personally learn about PH through this study?
A. “Like many people, I didn’t know much about PH before starting this project, so I had to learn a great deal from the beginning. Many of the themes that emerged were similar to those seen in other chronic health conditions.
However, what stood out was how these themes overlap and interact in PH. The experience of PH varies greatly between individuals and can also change over time. These differences strongly influence how people cope with the challenges of living with PH. This showed how important it is to look beyond standard measurements of quality of life and to understand each person’s individual experience. While PH requires people to make changes for their physical health, it is equally important to support them in living in ways that still reflect their personal values."

See the results of another study with a trainee psychologist over the page >>
We all need rest to function, but many members reading this magazine will experience difficulties at night. Another student psychologist supported by the PHA UK last year was Jemma Green, who researched how PH affects sleep – and in turn, our mental health…
Problems with sleep can exacerbate PH symptoms and add to the burden of living with the condition – as so many of our PHA UK members know.
Previous studies have shown sleep difficulties to be common in PH, but this research is limited and lacks detail. Jemma set out to find out more by looking at the types of difficulties people experienced in their sleep, and examining how this then impacts levels of anxiety, depression, and overall quality of life.
PHA UK members were invited to take part, and over 100 volunteers put themselves forward. They completed a series of questionnaires, and as expected, sleeping difficulties were reported to be a very common issue.
80%
of participants reported having a poor quality of sleep
On average, they slept the same number of hours as people without PH but took a long time to nod off and were frequently disturbed during sleep. Breathing difficulties, anxiety, and other health conditions were among the reasons given for this.
One in three people said they experienced insomnia
84% said their poor sleep interfered with daily functioning
Jemma found that people who experienced insomnia, daytime sleepiness, or poor sleep quality also tended to report a lower health related quality of life, and anxiety and depression. However, when she looked more closely, this link appeared to be mainly connected to depression. In other words, sleep problems and lower health
One in three people said they fell asleep a lot during the day
Over 40%
of participants had levels of depression that would be clinically recognised and 29% of participants may have clinical levels of anxiety This supports the wider evidence suggesting people with PH are at a greater risk of anxiety and depression.
related quality of life often occurred alongside higher levels of depression. More research is needed to better understand how to support people with PH who experience sleep difficulties. The study is currently being prepared for publication in an open-access online journal, which means that the full findings will be available for anyone to read.
Jemma Green completed this study as part of her Master’s degree in Psychological Research Methods at The University

I was keen to study this disease area because I have family members living with long-term health conditions, so I am interested in research that aims to improve the quality of life of people living with conditions where there is not
necessarily a cure yet. Sleep quality particularly interested me as I feel it is sometimes taken for granted, but when we struggle to get to sleep, and to sleep well, its impact on our physical and mental health can feel huge. Also, research into sleep quality in PH, and its impact on psychological wellbeing and quality of life, is currently limited.
I was surprised by just how many people reported a poor quality of sleep (eight out of every ten people that took part).
I have really enjoyed working with the PHA UK on this research and valued them sharing their expertise and knowledge with me. I would like to thank everyone who took part in the study, sharing their experiences of sleep and living with pulmonary hypertension.
"We suggest that people with PH should be routinely asked whether they are experiencing sleep difficulties. It is worrying that we found such high rates of sleep problems."
"As we did not find sleep difficulties were strongly linked with demographics, such as age and gender, everyone with PH may be at risk and so should be asked."
"If someone does report sleep difficulties, they may be at a greater risk of experiencing depression and anxiety."
"Interventions looking to improve someone’s sleep with PH should also consider exploring whether they need help with symptoms of depression"
Both Jemma and Jacob were supervised by clinical psychologist Dr Gregg Rawlings, who led the development of our self-help programmes for those with PH experiencing anxiety or depression (see pages 8 and 67).
He said: “I would like to thank everyone who has supported our research into how living with PH affects mental health, and how mental health can, in turn, affect PH symptoms. What we learn from this research is essential for helping us develop better and more effective ways to support people living with the condition.”

COMING SOON!
Please keep an eye out for an upcoming study recruiting people to test a new self-help programme for those with PH who are experiencing sleep difficulties.
As the article on the page before shows, if you struggle to sleep with PH, you’re definitely not alone. There’s lots of advice out there, but not all of it is true. Here we set the record straight on common myths and misconceptions, to help you get your head down…
FACT: Most guidelines state that adults need seven to nine hours of sleep each night, but the truth is there is no magic number. Everyone is different; you may feel fine on seven, while someone else needs ten to feel functional. However, less than six hours a night, on a regular basis, is thought to be unhealthy.
FACT: Its sedative effects may help you fall asleep, but it makes it harder to stay there, as the liver works so hard to metabolise the alcohol. Alcohol is a diuretic, meaning you’ll probably wake up in the night needing the loo. Plus, excessive alcohol consumption means you spend more time in deep sleep and less time in Rapid Eye Movement (REM) sleep – which is why you can feel so exhausted after drinking, even if you’ve been in bed a long time.
FACT: You might feel like your daytime drowsiness stabilises after a few nights of reduced sleep, but the reality is that your sleep deprivation will continue to affect your metabolism, immune system, hormone production, cardiovascular system and mental health.
FACT: Daytime napping isn’t a substitute for proper night-time sleep. Firstly, you can’t get the same quality in short bursts, and secondly, it then makes it much harder to fall asleep at night. If fatigue means you need to nap, keep it to less than 30 minutes and take it before early afternoon.

“Sleeping
tablets are a sticking plaster, not a cure”
You may turn to tablets when insomnia kicks in, so it’s important to understand how they work, and what to consider when choosing them. Scan this code or visit phauk.org/SleepingPills for advice from Neil Hamilton, Consultant Pharmacist at the Sheffield Pulmonary Vascular Disease Unit.

If you’ve found something that has helped you sleep, we’d love to share it with our PH community. Email media@phauk.org and we’ll spread the word.
Join our panels and shape our work... GET INVOLVED IN YOUR OWN TIME, FROM THE COMFORT OF YOUR HOME!OWN
Members of our Feedback Forum and Research Forum panels play a key role in helping to guide PHA UK activities and contribute to important research work. We contact all forum members with

Singing in a local women’s choir has helped Christine Tabor come to terms with her diagnosis of chronic thromboembolic pulmonary hypertension (CTEPH) – and the group kindly raised money for our charity during their Christmas concert last year. Here Christine (pictured right) tells us more.

Iwas told I had pulmonary hypertension just before Christmas in 2024, at my local hospital in Stockport, Greater Manchester.
I had experienced recurring chest infections for a long time and then out of nowhere, I had quite a severe pain in the middle of my chest which took my breath away. I rang my GP, who advised I should go to casualty. Being December, it was bedlam and I was convinced I didn’t need to be there, but I stuck it out and underwent a series of tests.
The results showed high readings for blood clots and elevated pulmonary artery pressures. I was told that it was probably something called pulmonary hypertension and I would be referred to a specialist treatment centre.
I felt set adrift really, as nobody seemed to explain anything. The run up to Christmas that year was very hard because I felt really ill, very breathless, and I didn’t really understand what was wrong with me.
Whilst I was waiting for the specialist centre appointment, I came across the PHA UK online. I was in quite a low place at that time, because I’d made the classic mistake of reading everything I could find via Google, and it left me in bits. I felt devastated by what I read.
I arranged an appointment with the PHA UK’s Listening Line service and spoke to Paul, who helped me understand more about PH and the care that was available. It really helped. I’d say the PHA UK was a bit of a lifesaver for me then. If I’d been told about the charity when PH was first mentioned by my local hospital, it would have saved me a lot of heartache.
I was seen at the Sheffield Pulmonary Vascular Disease Unit in March 2025, and they confirmed it was chronic thromboembolic pulmonary hypertension (CTEPH).
The team there were fantastic and it was reassuring to know they were able to deal with what was wrong with me. I was started on medication and referred to Royal Papworth Hospital to talk about the specialist treatments procedures they provided for my type of PH.
I started singing with Great Moor Singers, a Stockport-based community ladies’ choir, about eight years ago, but I missed quite a few months when I was ill with my chest infections. I’ve tried to persevere with it though, especially since getting the CTEPH diagnosis, as I’m aware that singing is good for your lungs.
I’m not a great singer but it’s a really lovely group of women and I enjoy it. They are very supportive and friendly.
We have a concert three times a year and always donate the proceeds to charity. Last Christmas, I suggested the PHA UK because of the help they had given me, and everyone agreed. We raised £160 from selling raffle tickets on the night and I got up and said a few words about the charity, which prompted some people to put a little extra in. It all felt very supportive.
Lots of us in the choir have had health issues, and during the coffee breaks we all chat and check how each other is getting on. It’s partly about the singing, but it’s as much about the social aspect too.
The choir has helped me come to terms with the CTEPH diagnosis because there have definitely been evenings where I’ve not felt up to going, but when I’ve got there I’ve felt great. It feels like I’ve done something for myself and done something good. I get a sense of achievement from finding the energy to sing, and I think it helps me physically too.
We always start the sessions with breathing exercises as a warm-up, and although I can’t always hold the long notes, I don’t feel any pressure. The routine of attending each week helps, and I find it inspirational to see the other women who keep coming along despite their health conditions.
Christine recently underwent pioneering balloon pulmonary angioplasty treatment for her CTEPH. Hear about her experiences over the page...

In January of this year, Christine underwent her first balloon pulmonary angioplasty (BPA) procedure at Royal Papworth Hospital. We caught up with her three weeks afterwards to hear how it went…
“I was nervous when the BPA was first mentioned but the consultations I had with Papworth were very reassuring. It took around four months from the referral to having the procedure. They did my left lung this time, and my right lung will be done in my second session in four weeks’ time. They were able to clear five blockages, which they were pleased with, so that was a relief. I do know there are smaller blockages in inaccessible area of my lungs which they won’t be able to get to.
It’s been three weeks and I personally don’t feel any improvement yet, but it may just take more time for me.
I was in hospital for two nights. On the first day I had a series of tests, including an echocardiogram and a walking test, and the procedure took place around lunchtime on the second day. I expected it to be a bit more uncomfortable than it was to be honest. The whole thing took about an hour-and-a-half, and I had no bruising or problems with my groin, where the catheter was inserted. I felt fine afterwards.
The only problem I had was holding my breath. You have to hold your breath regularly when instructed by the doctor while the procedure is taking place and I kept taking big gasps which made it harder for me to hold onto my breath. Once I took smaller breaths, I could hold my breath for longer, which helped with the procedure.
The BPA wasn’t painful and I found it less uncomfortable than the right heart catheter procedures which I'd previously had via my neck.
Balloon pulmonary angioplasty is a treatment suitable for some people with chronic thromboembolic pulmonary hypertension (CTEPH), with the aim of clearing the clots that cause this type of PH.
The procedure is performed under local anaesthetic, with medication used to numb the area of the groin. A small tube called a catheter is inserted through a vein in the groin and guided up to the pulmonary arteries. A balloon is then inflated in the segments that require treatment. The vessels (clots) needing treatment are identified by injecting a contrast dye while using X-ray imaging.
The procedure typically requires between two and six sessions that each last approximately 90 minutes. A hospital visit with overnight stay is required for each session. Royal Papworth Hospital is the only hospital in UK that carries out the procedure, and it has only been available since 2018.
I had full trust in the team doing the procedure and I didn’t worry about things going wrong. They were wonderful the whole time I was in the hospital.
After the procedure I was taken back to the ward where I had to lay flat for an hour and have regular blood pressure and oxygen checks before being allowed to sit up.
My husband came to Cambridge with me and stayed in hospital accommodation in the grounds. It cost about £65 a night, and it was reassuring to know he was close.
I was discharged on the Friday night, the day after the procedure, and it was a four-hour journey back home to Stockport. I’ve felt tired since, but I think that’s to be expected. I rested for a few days when I got back, and I had to miss a choir session. Ultimately, the BPA wasn’t as frightening as it sounds on paper and to be honest, it’s probably one of the best hospital experiences I’ve had. I feel privileged to have been offered such a pioneering procedure.
I feel better about having the other lung done now that I know what to expect. I’m realistic, and I’m not expecting miracles, but I will be very happy if I see some
improvement with my symptoms. I’d love to feel a little bit more like I did before I got this diagnosis.”
Christine then sent us this update after the second procedure, at the end of February:
"My second BPA at Papworth took place exactly a month after my first one. I wasn't as nervous as the first time and I'm very happy to say that the doctors were able to successfully unblock five blockages in my right lung. Once any inflammation dies down, I'm hoping to feel some real benefits from the procedures. My third and final appointment at Papworth will be in three months’ time to check on my progress and I am feeling quite optimistic.
My main message to anyone who is experiencing something similar to me, is not to be fearful and have confidence in the professional teams at both Sheffield [my specialist centre] and Papworth hospitals."

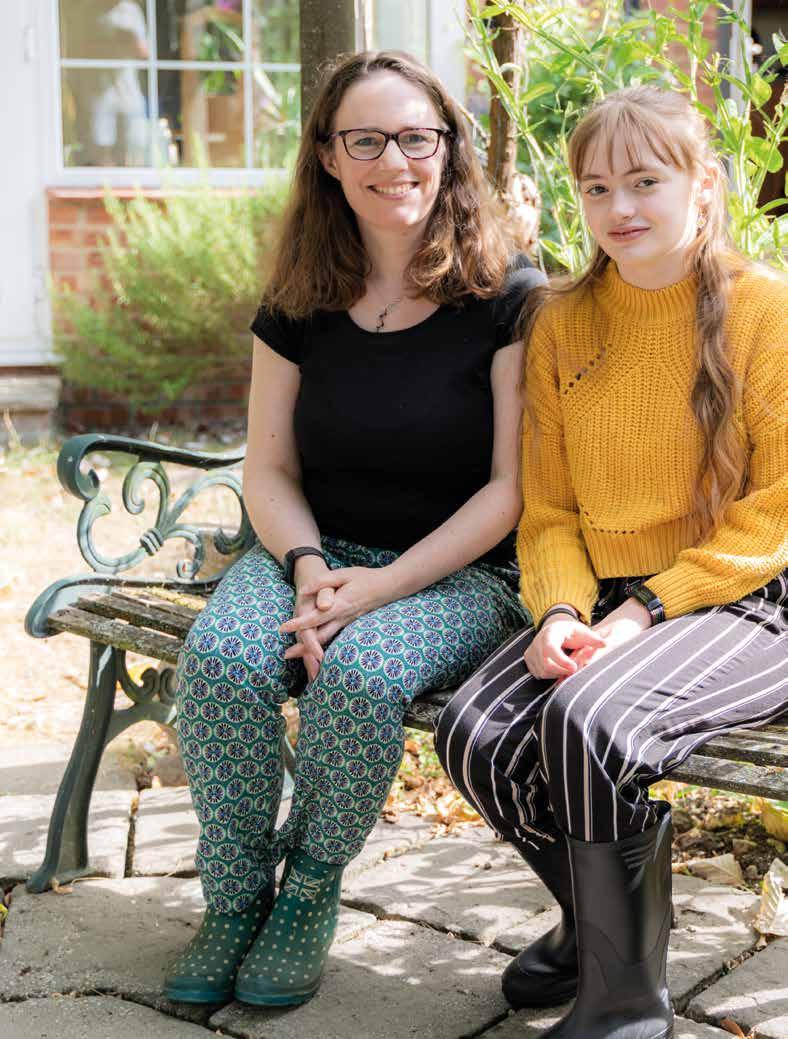
Emily Gravenstede, now 15, was diagnosed with pulmonary hypertension as a toddler. Her family have learned a lot about living alongside the disease since, and we caught up with her and mum Lorna to hear their reflections and advice…

When Emily first got her diagnosis at three, I couldn't imagine as far ahead as 11 years later. PH has made our lives different, but in a sense, I can't even think how things would have been instead – because it’s just been ‘life’. It’s meant a lot of medical appointments that wouldn't have been, a lot of dealing with medicines that wouldn't have been,

and advocating for Emily in ways that wouldn’t have been needed. It’s also meant a lot of learning.
Emily is amazing and I'm hugely proud of her. The PH has never stopped her doing anything she wants to do, and she's really confident and very mature With or without PH, she’d be a performer. I remember her giving a full-on performance as Elsa from Frozen during her visit to Great Ormond Street Children’s Hospital (GOSH), right there on Walrus Ward.
Emily has always loved going to GOSH. After so many years, it’s like meeting friends when we see the team there. She’s always been really good at telling the doctors what she's feeling and what her symptoms are, so they've loved that because they've gained insights they didn't have.
If you are a parent of a child who's just been diagnosed, my number one piece of advice is to trust your medical team, especially if it's the PH team at GOSH, because they really know what they're talking about.
If you've got any questions, just email or phone them. They'll get back to you, they'll explain, and they really know what they're talking about. Don’t trust the internet; trust the specialists, because they can guide you through.
Hope has got to be really important because if you've got no hope, that's going to change how you are with your child, and how you are in general. I appreciate that everybody's journey is different and the outcome isn't always good, but no-one knows at the start what that will be.
It’s not always easy to live with hope when you’re dealing with something like this, but it is true that no one knows what's going to happen to anybody tomorrow. My family have been really lucky, and equally there will be people who won’t be so lucky. But without hope, what is there?
It’s a bit of a cliche, but when you’re faced with PH in your family, it's all about living your best life and making the best of every opportunity.
“My advice to another young person with PH would be not to compare yourself to others”

People don't always understand what it's like to have PH. They'll understand that I will get a bit more breathless, but they don’t always understand how hard it can be to manage that.
I feel like when you can't see the fact that there's a disability, it automatically becomes less ‘severe’ in other people's eyes. When I damaged my knee and had to walk with a crutch, I found that people were being a lot more careful around me and were a lot more aware than they would be if I didn't have an accessory to

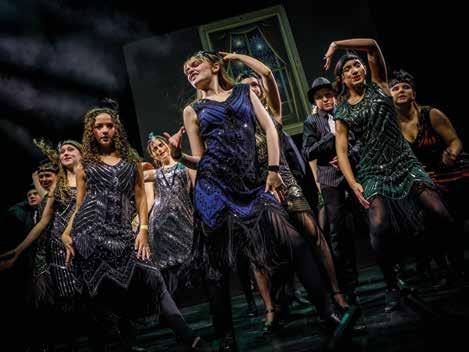
At the end of last year, Emily took to a West End stage in London as part of a show by her performing arts club. The Great Gatsby performance saw her dance and sing solo, and she described the experience as ‘thrilling’.
show. There was a really big difference. I like to be quite active and sometimes the breathlessness does get in my way. I find it stops me doing as much as other people, and overall, my PH symptoms mean that I often have to think a lot harder about what I'm doing.
But even though I've got PH I can still enjoy loads of things, such as Stagecoach (performing arts coaching), singing, acting, and dancing. I play the piano and violin and I really enjoy my music because it's a creative outlet for me that isn't affected by my health condition.
My advice to another young person with PH would be not to compare yourself to others, because everyone is different. I find comparing yourself

often leads to certain expectations, such as thinking you should be able to do something just because they can. I think it's really important for people with PH to find what makes them happy, because it gives them a life outside of the disease.
They’re rarely out of the headlines, and we know these injections are of interest to many in our PH community. This special feature brings you the facts, expert insight, and real experiences from people living with pulmonary hypertension who have taken this route for weight loss…
You probably hear them referred to as ‘weight loss jabs’, but the official name for these medications is glucagon-like peptide-1 receptor agonists (or GLP1-s, which is much less of a mouthful!)
There are a few different types of GLP-1 medications, but they all work in a similar way by mimicking a natural hormone your body releases after you eat, helping you feel fuller for longer. Some also act on a second hormone (glucose-dependent insulinotropic polypeptide – or 'GIP') which is involved in appetite and blood sugar control, and can further support weight management.
GLP-1s are usually taken as a once-weekly injection using a pen device that you administer yourself at home. In the UK, there are strict criteria about who can access them through the NHS. A higher BMI* on its own isn’t
always enough – you also need to meet certain additional health criteria linked to weight.
Some people choose to access GLP-1 medications through online pharmacies, where the eligibility criteria may be different. Even so, you’ll need to show that your BMI is over 30. This is because there is not yet enough evidence to confirm that these medications are safe and appropriate for people with a lower BMI.
Whilst there are no direct interactions between PH medications and GLP-1s (meaning your PH drugs will not react to the GLP-1s in the body) there is still lots to consider.
This feature aims to bring you tailored advice and information, to help you decide whether these medications might be worth exploring for you.
GLP-1s are prescription-only medicines, meaning they can only be prescribed by a healthcare professional. It can be dangerous to purchase these drugs through unregulated sellers such as beauty salons or via social media. All licensed GLP-1 medications are provided as pre-filled injection pens, so if it is any other form, it is
If you have PH, you must speak to your specialist team before starting GLP-1 medications
What you need to know...
likely to be counterfeit and potentially unsafe.
In addition, there is an increasing amount of marketing now around ‘natural’ alternatives to GLP-1 medications, available without prescription. Please be mindful of spending a lot of money on something that claims to be as effective – because it won’t be!
*BMI stands for Body Mass Index, a numerical value derived from someone’s weight and height to categorise them as underweight, at a healthy weight, overweight, or obese.
The following advice has been put together by the PHA UK with Emma Russell, an Advanced Pharmacist at the Scottish Pulmonary Vascular Unit.
Side effects need to be considered – especially if you have PH
There are no direct interactions between PH medications and GLP-1s, but there may be interactions with other drugs you are taking so this should always be discussed with your prescriber.
If you have PH, it is very important to consider the side effects of GLP-1s – especially as many of them overlap with the side effects of some PH medications.
Some people experience intense nausea, vomiting or diarrhoea with GLP-1s and this can lead to dehydration. This is especially risky if you are prescribed diuretics as part of your PH treatment as it could lead to kidney injury. The elderly are at a higher risk of dehydration in this way. Plus, vomiting may risk you bringing up PH medication you have taken.
Nausea, vomiting and diarrhoea are all really common side effects of PH medications. So, if you are experiencing them from GLP-1s at the same time, this may limit your specialist team progressing the dosage increases of
The injections can cause:
• Nausea
• Vomiting
• Diarrhoea
• Constipation
• Stomach pain
• Indigestion
• Tiredness
• Dizziness
• Hair loss
• A fast heart rate
• Headache
• Low blood pressure
your PH medications – compromising the impact of your PH treatment.
Your PH team will be able to provide anti-sickness medications, but ideally these wouldn’t be prescribed long-term. Adding more drugs into your regime to combat side effects, known as ‘polypharmacy’, is not ideal.
Ultimately, if you can't stomach your PH medicines because of this injection, then it probably isn’t right for you. If you develop side effects on weight loss injections, then report these to your local GP.
Weight loss injections should not be used on their own. Lifestyle changes, such as a reduced calorie diet and staying physically active, should also be adopted while taking - and after stoppingthese medications. You can find advice on this at nhs.uk/live-well
Some of the weight loss injection medications can very rarely cause sudden changes in vision, usually occurring in one eye at a time. This is also a known rare side effect of the PH drugs sildenafil and tadalafil. Always contact your specialist centre if you have a change in vision.
As weight loss is the desired outcome of GLP-1s, your blood pressure will naturally come down with your weight. People living with PH tend to already have low blood pressure, caused by the drug treatments – so there is a risk of it falling so low that you increase the risk of dizziness, falls, and even perfusion of certain organs.
Some drugs that you take for your PH will need to be taken with food. If your appetite is limited through the GLP-1 medication, you should take extra care to plan your eating around the PH treatments to ensure you can take them.
If you live with diabetes alongside your PH, it is vital that you speak to your
diabetes team before starting a GLP-1 medication. This is because you are at a higher risk of hypoglycaemia – where your blood sugar falls dangerously low – and this can be caused by not eating enough. Common symptoms of hypoglycaemia include sudden dizziness, sweating, shaking, increased heart rate, anxiety, confusion, tingling lips, and pale skin.
There is a risk of patients taking weight loss injections being at an increased risk of an inflamed pancreas.
If you experience the signs of pancreatitis - severe sudden abdominal pain (particularly after eating), nausea and vomiting, fever, and increased heart rate - you should seek urgent medical attention.
If you are taking GLP-1 medication, you must always inform your medical team if you are undergoing a procedure than involves anaesthetic – particularly general anaesthetic.
For safety reasons, you are always advised to fast before general anaesthetic to ensure your stomach is empty. GLP-1s are known to cause ‘delayed gastric emptying’, which may mean your stomach still contains food at the time of administering the anaesthetic, even if you have fasted for the advised period.
It can be dangerous to purchase these drugs through unregulated sellers Accessing
If you're lying down for a long time for the procedure, there's a high risk that you can aspirate (bring up what's left in your stomach) into your lungs – and that’s particularly dangerous for people with pulmonary hypertension.
GLP-1 medication can reduce the effectiveness of oral contraceptives, so it is advised to use an additional method (such as condoms), especially following a dosage increase. This is especially important for women with PH, where pregnancy is deemed very high risk.
GLP-1 medications should not be taken if you are pregnant or breastfeeding.
GLP-1 medication is injected via a pen, so if you take subcutaneous medication for your PH (such as Treprostinil) you should make sure you inject into a different area to avoid site pain. This is also the case if you inject any other subcutaneous drugs, such as insulin for diabetes.
It is not easy to access these medications via the NHS, so many people choose to obtain them privately
GLP-1s are prescription-only medicines, meaning they can only be prescribed by a healthcare professional. It can be dangerous to purchase these drugs through unregulated sellers such as beauty salons or via social media. All licensed GLP-1 medications are provided as pre-filled injection pens, so if it is any other form, it is likely to be counterfeit and potentially unsafe.
All online pharmacies must be registered with the General Pharmaceutical Council (GPHC) and their registration number can be found on their website, usually at the bottom. You can use this number to check they are registered by visiting pharmacyregulation.org/registers
It is vital that you consult with your PH team before making a decision to start these medications. It’s also
important to let the prescriber know you have pulmonary hypertension – this could be your GP, or the online pharmacy you obtain the treatment through. Be aware they may not know what pulmonary hypertension is, which is why it’s even more important that you talk to your specialist team too. When completing forms and questionnaires to access the medication through an online pharmacy, always be honest with your answers. These prescribers do not have access to your medical files, so your truthful answers are essential to ensure safe prescribing.
There is emerging evidence that GLP-1 medications may have a positive impact on vascular function, cardiac efficiency, and inflammation – but at the moment this evidence is limited. We will bring you a follow-up feature on this as more data is collected and published.
All information in this feature was correct at the time of going to print, March 2026
Further information on GLP-1 medications can be found at gov.uk, which is a trusted source of online information.

This activates GLP-1
Brand name: Wegovy
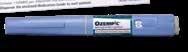
Brand name: Ozempic
Also a semaglutide but it is not licensed for weight loss in the UK

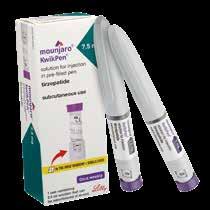
This activates GLP-1 and GIP (glucose-dependent insulinotropic polypeptide)
Brand name: Mounjaro
In the UK, there are several licensed GLP-1 medicines, outlined below. ‘Licensed’ means they have been assessed carefully by the UK medicines regulator, the Medicines and Healthcare Products Regulatory Agency (MHRA), and approved as safe and effective for certain use.
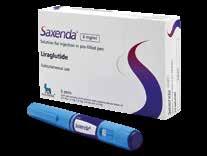
This activates GLP-1
Brand name: Nevolet

Brand name: Saxenda

Weight loss injections and PH
Four PHA UK members share their stories of taking different weight loss injections…
Cathy is 60 and lives in Wolverhampton. She was diagnosed with PH in 2020. Cathy has Type 2 diabetes and began taking Mounjaro on NHS prescription in June 2024, after being referred to a diabetic weight management clinic.
“Everyone kept telling me I’d feel better if I lost weight, but I can’t be very active with having PH, congenital heart disease, and being on oxygen – so I had no idea what I could do.
The minute I try to do any exercise I struggle. So, the only way I could make a difference was with diet, which was why my hospital specialists suggested the Mounjaro.
The first thing I noticed was the change in my appetite. It wasn’t huge beforehand because of my health and the menopause, but it got smaller when I started with the weekly injections.
I’ve still been able to enjoy food, but just in smaller portions, and I’ve had to get my head around the idea of not wasting it.
I did have side effects to begin with, which was mainly an upset stomach. Last year I started taking probiotics each day as capsules, and that’s definitely helped.
The Mounjaro helped me feel fuller more quickly, and I didn’t want sweet things so much, but that has died off a little now.
I didn’t want to lose weight too quickly as I don’t think it’s good for you. In the first year I lost 8-9kg (around one-and-a-half stones) but then it plateaued and it’s crept up a little recently. So I pushed for a review, saw the specialist last month, and I’m due to pick up a slightly increased prescription – so fingers crossed.
Even though I’m feeling a little frumpy from gaining a few kilograms back, I do feel better than before I started it.
Losing weight has improved my mobility, given me a bit more get-up-and-go, and enabled me to listen to what my body is telling me when I eat.”
Claire is 45 and lives near Liverpool. She was diagnosed with PH in November 2023 and started taking Wegovy in September last year, with the goal of losing enough weight to be considered for a double lung transplant.
“I weighed 138kg (21 stones) when I started with Wegovy, and was advised by my PH team that I needed to get down to 80kg to be eligible for assessment for a double lung transplant. They suggested trying Wegovy to get there.
Over 50kg is a lot to lose but I wasn’t fazed as I’m quite a stubborn person. I was determined to do it as I’m only young, and it broke my heart to think about having to tell my nieces and nephews that I wouldn’t survive.
I lost 25kg (four stones) on my own before starting the Wegovy, and since then I’ve lost another 12-13kg (two stones). I’ve had some horrible side effects from it though, so have now stopped taking it.
I was sick pretty much every time I ate, even though it was just a small amount of food, and I had terrible stomach pains. Trying to get to the bathroom quickly was difficult, especially because I’m on oxygen 24/7 and have to use the stairlift to get up there. My head felt heavy, and I generally just never felt well on it.
I used to dread injection day each week, as the side effects were always worse just afterwards. I’d inject at 10pm so I was asleep for the first few hours, but as soon as I tried to even drink water the next morning it would come straight back up.
I see all these people on social media doing so well on it, and losing loads of weight, but it just hasn’t agreed with me. My PH team have been really supportive through it all, and my specialist nurses would call regularly to check up on me and offer anti-sickness medication if I needed it.
I did consider trying Mounjaro instead, but the dosage is higher and I just don’t want to risk feeling even worse. When I started on the Flolan for my PH it took a long time to get to the dose I needed so I think I’m sensitive to medications.
I wasn’t able to get the Wegovy on prescription, so I had to pay for it privately, which wasn’t easy as I can’t work. The price went up as the dosage increased, so the first month was £79 and it was over £200 by the final month.
Although I’ve lost 41kg (six stones) in total I don’t think I look that different. I do feel better though; I’d say my breathing is a bit better and I can walk a little bit further.
I’ve set myself a goal of September to get down to the weight needed for a transplant assessment and I’m determined to do it. Going back to the Wegovy will be a last resort though.”
Jo is 53 and lives in the Shetland Islands. She was diagnosed with PH in 2019 and started taking Mounjaro in June 2024.
“I weighed around 184kg (29-and-a-half stones) when I began the Mounjaro. I’ve always had a big appetite, and I’m an emotional eater. I put a lot of weight on as an adult when I had my five children, and because of my health issues too.
I had tried slimming groups, and accessed hospital dietician and weight loss services, but nothing seemed to work for me. I’ve always found it difficult sticking to diets, as I always felt hungry. I’d lose a little bit but then go back to my old habits – and it would go back on again.
I’d heard about Mounjaro through the media, although it wasn’t talked about then as much as it is now. I assumed you’d get them from your GP, but weight loss injections are still not available on the NHS in my part of Scotland - even now - so I had to get it on a private prescription online.
As soon as I started taking it my appetite was cut completely. I wasn’t thinking about food at all, and at times back then I was living on just three chicken breasts and a bowl of soup a day.
Within a month of starting the injection, even though I hadn’t lost a huge amount of weight by that point, I was able to walk further than I had done in years. The difference it's made for my mobility is just amazing.
I had a few side effects at first, including constipation and a bit of nausea, but it was all manageable - nothing compared to pregnancy - and the benefits totally outweighed any discomfort.
The dosage was increased each month, and by the end of each month I’d start getting my appetite back, but it would then go again with the bigger dose. I’m on the highest dosage now and the food suppression has eased off a bit, but I can still control it. I can definitely sit and eat more now then when I started the Mounjaro back in 2024, but I don’t have the raging appetite I did before.
I make better food choices now too. Before the medication, breakfast would always be two slices of
toast with loads of butter, but I just don’t fancy things like that anymore. Instead, breakfast is lean chicken sausages with tomatoes, or eggs.
I used to really crave crisps and could eat a whole box of them at night. I still have them occasionally, but now I take a few from a packet and then put them down. I certainly couldn’t do that before! I still enjoy food, just not the stodgy and fatty things from before.

It’s not that I’ve learned more about nutrition –I always knew what I should be eating, but I just couldn’t do it. That’s the thing that’s changed.
I’ve lost 51kg (eight stones) so far, and I’d like to lose another 63kg (ten stones). But I’m paying around £300 a month for the Mounjaro now. It’s gone up quite a lot, and I don’t know how I’m going to continue paying for it. I’m just really hoping I’ll be able to access it on the NHS up here soon.
I’d describe the medication as life-changing. It means I can go out for a walk, go and meet friends, and do ‘normal’ things.
I couldn’t do anything before, and it dragged me down. I struggled to even walk the flat two minutes to my local shop without stopping at least two or three times due to breathlessness and pain in my back. I struggled with stairs and had to rest on my bed a lot. Now I manage fine; I’m just a bit breathless, but I can do it.
My doctor is really impressed with the improvements in my overall health, and I hope things get even better as I lose more weight.
A lot of people don’t like to talk about taking weight loss medication, and I know that everyone is different and it doesn’t work as well for all. But I’ve been shouting from the rooftops because it’s made such a difference for me.”
Maxine* is 44 and lives between the UK and the United Arab Emirates. She was diagnosed with PAH in September 2021 and began taking Ozempic in August last year.
“I started low-dose Ozempic after discussion with my PAH team. By the time I started, I had already lost a significant amount of weight through gradual lifestyle changes, so this was not about rapid weight loss.
From a PAH perspective, the most important thing is that I have remained clinically stable, with no worsening of breathlessness, chest symptoms, dizziness, or exercise tolerance, and I have stayed on my full PAH treatment throughout.
What feels most significant to me, though, is that I have genuinely felt better since starting it. My energy levels are better, day-to-day life feels easier, and my overall sense of wellbeing has improved. While it is always difficult to tease apart cause and
*Name has been changed on request
effect, I personally do believe Ozempic has played a role. That may be directly, indirectly through weight loss and improved metabolic health, or as part of a wider positive shift in cardiovascular efficiency. It may well be a combination of all of these, but the improvement I feel is very real.
I am very aware that PAH is a condition where symptoms alone do not tell the full story, so my medical team and I are focused on objective monitoring. I had a right heart catheterisation in July 2025, before starting Ozempic, and I am scheduled to have another one soon – which should provide a useful comparison to see whether there have been any measurable haemodynamic changes over time.”

It was another fundraising win for Gareth Davies, who helped his local football club organise a match in aid of our charity. It was the second time that Gareth, who has PH and regularly volunteers at Ton Pentre AFC in South-East Wales, has supported us in this special way.
The team may have lost the match, but they hit the back-of-the-net when it came to support for us!
An engagement party doubled up as a fundraiser for supporter Daniel Lerche and his fiancée. The kind pair gathered donations during their celebration, and they are pictured here with one of the collection boxes.

A year ago, Shane Double and Gabrielle Morley couldn’t run a kilometre, but they recently completed 13.1 miles at the Brighton Half Marathon – raising thousands for our charity. The pair completed the challenge in support of family member Marie, who lives with PH.
Marie’s daughter Alice, who is wife to Shane and cousin to Gabrielle, said: “Mum is doing so well now, and this will be her eighth year since her diagnosis, which we are all so incredibly grateful for. We are so proud of Shane and Gabs, especially because the running conditions were really rough.”

Dog trainer Jessica Burrows had the help of some four-legged friends when she held a raffle at her Christmas canine competition. Jessica’s aunt Julie Bestwick lives with PH, and she was motivated to support us after watching the video of her and husband Stephen speaking with others at our anniversary event in Birmingham. Jessica, who runs For The DOG Woodhall Spa, said: “I was very moved by how a disease I had never heard of affected so many different people. After talking to Julie and Stephen about all the amazing work by the PHA UK, I wanted to hold our raffle for them.”


�� Daniel Rowley-Thorne is taking on the upcoming Manchester Marathon, and Libby Burton will breathe in the sea air at April’s Brighton Marathon.
James Thomas is taking to the saddle for a 107-mile bike ride in May, in support of his young niece who lives with PH.
�� Craig Burton plans to tackle an epic 100-mile run in just 30 hours in September, following his Dad’s diagnosis. Good to luck to everyone planning challenges for us!


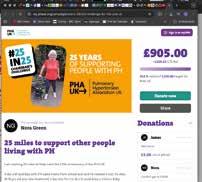
If you’re planning a fundraiser this year, you can now set up your very own My PHA UK page to collect sponsorship or donations online. Commercial platforms like Just Giving take a fee, so this way, every penny from your hard efforts will come directly to our charity. Check it out at my.phauk.org
Your kindness makes a difference.
We are an independent charity with no government funding, so we rely on the kindness of our fundraisers to help us support people affected by pulmonary hypertension. From bake sales to bike rides, marathons to motor racingand everything you’ve seen in this feature - we’re constantly amazed by the lengths our supporters go to in our name. We are so grateful for every penny raised, and with summer in full swing there couldn’t be a better time to support us. Find out more, get inspired, or request your free fundraising kit, by scanning the code
Don’t have Facebook?
We now have a NEW one-to-one online chat platform for PHA UK members. Turn to page 10 for details!



Our private Facebook groups are a valuable source of support and advice from people who truly understand. They are safe spaces to talk to other people with lived experiences of pulmonary hypertension. You need to have a Facebook profile in order to join these groups. Sign up at www.facebook.com. It’s free and easy!

We have dedicated groups for patients, carers, and loved ones too.
Scan the code to access the groups, or visit phauk.org/SafeSpaces
Last year, student mental health nurse Philip Donovan spent four weeks shadowing the PH team at London’s Hammersmith Hospital – and his time there made a lasting impression. These are his reflections of a placement that gave him valuable insight into what it means to live with pulmonary hypertension.
Ichose to complete my placement in a pulmonary hypertension unit because of my personal experiences with long-term health conditions. I was born with congenital heart disease, so I’ve been under a cardiologist all my life and had quite a few heart operations. I’ve always had an interest in how long-term conditions can affect patients and their mental health.
I spent 95 hours across four weeks within the service at the Hammersmith, predominantly shadowing the specialist nursing team while gradually building my assessment, communication, and clinical skills.
A lot of the assessments that I saw on the PH unit were fantastic for my learning. For example, it was helpful to see how using the emPHasis-10 quality of life questionnaire helped assess the impact of PH on someone’s quality of life. When patients open up to us as nurses, we can start treating them more holistically.
Some patients were very open, and they spoke to me about their mental health and problems they were experiencing – or experienced in the past. I learned a lot about the different types of PH and how people’s individual journeys with the condition can be so different.
I enjoyed some really good conversations with the nursing
teams about how to approach situations differently, and discover more about what is going on in a patient’s life to help understand them better.
I also learned a lot about how some of the recent PH treatments are making such a difference to people’s lives. And yet whilst seeing the improvement in their health, some were still stuck, mentally, in where they were with the disease previously. That’s where I felt a lot of the tears I saw came from.
Whilst trying to learn more about PH, I have found some of the research by the PHA UK really helpful, particularly the survey in 2019 which assessed the emotional impact on patients*. Seeing the percentages and the facts in the report really brought home that there is so much more than the physical side of this disease.

The most rewarding aspect of the placement was spending time with patients, listening to their stories, and understanding how pulmonary hypertension has altered or reshaped their lives. Hearing family members’ perspectives was

particularly valuable, as it highlighted how PH creates a ‘new normal’ that significantly affects both physical well-being and mental health.
This experience reinforced the importance of holistic, person-centred care and strengthened my understanding of the close relationship between physical illness and psychological well-being. I’m grateful to the team at the Hammersmith for their time and insights, and for allowing me to have this experience.
I’d particularly like to express my gratitude to Clinical Nurse Specialist Margaret Hickey, who supported me throughout the process. She consistently prioritised my learning, facilitated valuable learning opportunities, and took the time to actively involve me in the service. She also encouraged other team members to support my learning, allowing me to shadow them and gain a broader understanding of pulmonary hypertension.
Through this experience, I gained meaningful exposure to the PHA UK and the fantastic support it provides to patients, which has been a highly valuable learning experience.
*92% of those who responded to the survey said PH has affected their emotional wellbeing, with 53% having experienced or been diagnosed with anxiety or depression.
You can see the full report at phauk.org/EmotionalImpact
This free competition is open to everyone in our PH community – patients, caregivers, family members, friends, and healthcare professionals too.
Your poem doesn’t have to be anything to do with pulmonary hypertension. If you do choose to focus on this, perhaps you could write about being diagnosed, how it feels to live with the condition, or how you overcome challenges?
Here are some ideas of what else you could write about:
• A holiday or experience (real or imaginary!)
• Animals and nature
• Childhood memories
• Love
• Gratitude – what are you grateful for, and why are these things important to you?
• Your favourite place
• Hope and what it means to you
• A time when you felt happy, a time when you felt sad, a time when you felt scared, or a time when you felt safe …the possibilities are endless and your poem can be as long, or as short, as you’d like.
You do not need to be a talented write to enter this competition. Anyone can be a poet! Please do not use AI tools to write your poem, it needs to be your own work ��

£50 Love2shop voucher
Redeemable with over 50 retailers
All six titles in the ’Women of Steel’ series
Written by head judge Michelle Rawlins
£30 Love2shop voucher
There will be separate prizes for children. The winner in each of these age categories will receive a £30 Love2shop voucher: 10 & under / 11-16
The top 10 poems will be published in a future issue of this magazine, and all will be published on our website.
Our ‘head judge’ for this competition is published author and award-winning journalist Michelle Rawlins, who has written a series of popular historical fiction books about the women who helped win World War Two.
You’ll find all six titles in the ‛Women of Steel’ series at michellerawlins.co.uk/books – and the winner of this competition will receive the full set as part of their prize. Michelle, who is also a lecturer in journalism at The University of
“Getting creative can be really helpful, especially when you live with a challenging health condition like PH. Putting words down can be both soothing and satisfying, and I personally use poetry to help with challenging times. Don’t be afraid to enter if you think you’re not a ‘good’ writer. This isn’t about being technical; it’s about expressing yourself in a way that means something to you.”
Dr Iain Armstrong, PHA UK Chair

Submit your poem online by scanning this code or visiting phauk.org/poetry. The closing date for entries is 31st August 2026, and the winners will be contacted in September.
Sheffield, said: "It’s an honour and a privilege to judge a competition that allows people to express themselves through the power of words. The written word has the ability to transport readers to a new place or give meaning to something that they also have a deep connection with, creating an often much needed and inclusive sense of belonging and community."
Michelle will be assisted by PHA UK Chair Iain Armstrong and emPHAsis editor Mary Ferguson in choosing the winning entries.

Columnist Raya was initially worried about travelling between her own family home and her fiancée’s – but the support she’s been shown has made all the difference. This issue Raya, who has lived with PH since she was a baby, shares how they all make it work around her health…


Meeting my fiancée Jade online through a hobby we both enjoyed meant that we did not get to choose how close to each other we lived. Ultimately, two-and-a-half hours isn’t the worst, however, when you have a condition like PH, even the smallest travel distance takes a lot of planning.
Jade decided to move to my family home in London seven months after we got together. Moving to London meant frequent visits back up to Warwick to visit her family. For the first few months I was just way too nervous to travel and stay up there with Jade, so she always went on her own. After seeing how easy it was to travel up to Warwick on the coach, it made me feel more at ease. Being around Jade's family more also made me want to travel too, as weeks without seeing them got harder the closer our relationship got.
Travelling to Jade’s means I must bring my oxygen concentrator, my portable oxygen, all my medications (and extra just in case), my saturation monitor, and spare cannulas for my oxygen. Then of course, all the other normal items you pack for a couple of nights away.
My mum is able to drop us right into the coach station and help us on the coach. We have a suitcase, the oxygen (which is so heavy!), our two backpacks, and the portable oxygen. The coach company are really good and handle my big oxygen concentrator with care. Then we sit at the front on the priority seats, so I don’t have to walk to find a seat. Then once we get to Warwick, Jade’s mum or dad is there to help us off and drive to the house which is literally only five minutes away.
At Jade’s we used to have her big brother Josh’s bedroom since Jades bedroom was super tiny and had only a single bed. However, Jade and her family have recently redone her whole room just for us. We have much more room, and it also means Josh gets his bed back (thanks again Josh for always letting us stay in it!)
Although I already felt comfortable there before, having our own space put my mind at ease even more. I always felt bad when I got a migraine and had to take up Josh’s room during the day, and
having the oxygen taking up space in his room was a worry too. Now I also leave my big oxygen concentrator at their house – it just slides down by the bed and is there ready for when I come. I also have a drawer with spare cannulas in too. We also have an emergency stash of my medicine in their kitchen in case I forget any and it runs out whilst I am there.
When I’m at Jades her family are amazing – they make me feel so much a part of the family and don’t treat me any differently because of my PH. Jenny (Jade’s mum) is always getting in my favourite safe snacks, and Coca Cola in case I get a headache too.

Josh always keeps me topped up with hot chocolate and cherry Lucozade (my ultimate favourite).
One time I was stressing because I forgot to charge my little oxygen and we were going out shopping, but Jamie (Jade’s dad) didn’t even think twice and got my big oxygen from upstairs and put

it in the boot of the car. It was so quick, and so calm, that it didn’t even give me a chance to panic.
Joel (Jade’s youngest brother) reminds me of my own little brother Max, as he’s so considerate and understanding of everything. I met him when he was still in high school. I was worried having a chronic condition would affect our relationship, because I know PH can be complex to understand and he was still young. However, I was incredibly wrong. Even right at the start of when we met and when we wanted to go to Thorpe Park together, he knew I would need my wheelchair and took it into consideration in all our plans.
That day was one of my favourites; Joel
didn’t even acknowledge my wheelchair, and he included me in everything he spoke about – even though he was walking and I was wheeling! We even went to a Billie Eilish concert together recently and we had to be in the wheelchair section; he was so happy with how close our seats were there.
I’ve grown so close with Joel over the last couple of years, even though he has a habit of stealing all the Domino’s garlic and herb sauce when we get pizza!
I’m also never short on cuddles when I’m at Jade’s house as their dog Pepsi loves a good snuggle under the blanket with me. We love our daytime naps together.
We always make sure that we visit Jade’s Nanny when we are there, and that’s truly one of my favourite places to be. I feel so incredibly blessed to still have both of my Nans – they are my favourite people ever, and I cherish every second I have with them. But now to also have Jade’s Nanny in my life makes me feel so grateful. I feel so loved and welcomed when I’m around her.
We also get to see our baby cousin Louie when we go there, as his parents Matt and Hattie always make sure we get to spend some time with him before we have to go home. He’s one already and always has a new milestone to show us. He will be walking next time we see him!
Jades' family truly are the best and I really do miss them so much when we aren’t with them, I feel so lucky to have such an amazing second family. I know you're all reading this – and I just want to thank every single one of you for welcoming me into your beautiful family. I love you all so much.
Data shows standards of PH care remain high, despite the rising demand on services
The UK’s specialist PH service is the envy of the world, and the latest National Audit of Pulmonary Hypertension has once again confirmed that it delivers high standards of care for patients.
Each year, the audit measures the quality of care across the network of specialist centres by asking them to provide data that is then measured against a set of 15 agreed standards.
All of the adult UK centres, plus Great Ormond Street Children’s Hospital, take part – and the 16th Annual Report shows that the services are busier than ever. Between April 2024 and March 2025 (the period covered by the audit), more patients were managed than at any time since its inception. Centres saw a 20% increase in new patients being referred with suspected PH compared to the year before, but despite these rising demands, performance against the national standards remained strong.
4469
people were referred to a PH centre last year (786 more than the year before)

The number of new referrals to PH centres has increased year-on-year, except in 2020-21 (during the COVID-19 pandemic). They have risen from 1,860 in 2009-10 (the first year of the Audit) to 4,469 in 2024-25.

“We should take comfort from a UK pulmonary
hypertension
service that continues to perform well against national standards despite the challenges we face in the NHS ”
Professor David G Kiely National Audit of PH Clinical Lead
1194 people started PH treatments last year (55 more than the year before)
1,194 people started treatment for PH in 2024-25. This has increased from 766 people in 2009-10, the first year of the audit.

These are some of the key findings from the 16th National Audit of Pulmonary Hypertension, based on the standards PHA UK members told us they were most interested in hearing about. The findings are based on data gathered between 1st April 2024 and 31st March 2025.
88% OF PATIENTS WHO HAVE HAD AT LEAST ONE CONSULTATION IN THE LAST YEAR HAVE HAD AN EMPHA SIS-10 QUALITY OF LIFE SCORE RECORDED. (90% TARGET)
Here at the PHA UK we championed the introduction of this standard because quality of life is so important.

8 OF THE 15 NATIONAL STANDARDS WERE MET AT NATIONAL LEVEL IN 2024-25.
99% OF PATIENTS REFERRED TO A SPECIALIST CENTRE WERE DIAGNOSED WITHIN 6 MONTHS. (95% TARGET)
93% OF PATIENTS RECEIVED A RIGHT HEART CATHETERISATION BEFORE BEING GIVEN DRUGS TO TREAT PH. (95% TARGET)
97% OF PATIENTS TAKING PH MEDICATION HAVE HAD AT LEAST ONE CONSULTATION WITHIN THE LAST 13 MONTHS. (95% TARGET)
All consultation types, including those not in-person, are included in this standard and statistic.
THE NATIONAL AUDIT OF PH SETS OUT TO ANSWER THE FOLLOWING QUESTIONS:
• Are pulmonary hypertension services appropriate?
• Are patients receiving the right treatment in a timely manner?
• What are the outcomes for patients with pulmonary hypertension?
“Although PH services across the UK differ in patient populations, geography, and staffing, all meet the international specifications required of expert centres. We work together with a shared goal: to optimise patient experience, survival, and quality of life. The national audit identifies areas for improvement and continues to drive high-quality, specialist care. Looking ahead, as our understanding of current and emerging treatments grows, we will be better equipped to deliver personalised medicine, offering tailored therapies with fewer side effects, longer life expectancy, and an improved quality of life for people living with PH.”
Wendy Gin-Sing Pulmonary Hypertension Nurse Consultant Hammersmith Hospital
Information from the audit is used by clinicians and commissioners to inform clinical practice, service development, improvement, and commissioning activities.
The audit is commissioned by NHS England, and supported by NHS Scotland, NHS Wales, and the National Pulmonary Hypertension Centres of United Kingdom and Ireland Physicians’ Committee.
The PHA UK also plays a key role in the audit. We funded its first year in 2009, and every year we bring our community the key findings in a clear and accessible way – in the form of this report. We continue to provide input into the development of the audit, influencing it to be of maximum benefit to patients.

Scan this code to access the full audit findings
By Sophie Papageorgis, a psychotherapist who has lived alongside pulmonary hypertension for 20 years.
Being diagnosed with PH doesn’t just impact the individual – it’s fair to say it ripples out to those around us too. Whether it’s family, friends, healthcare professionals, co-workers, or even passers-by, there can be a variety of different responses. While much of it comes from a place of care, managing those

like an additional weight you didn’t
People’s responses can be confusing, they may change over time, and sometimes they might even contradict each other. One minute you might feel smothered from concern and worry, and the next misunderstood or dismissed. You may find loved ones checking in, panicking about your symptoms, or sharing alarming things from Dr Google. While it’s comforting to know people care, this level of concern can feel overwhelming. Added to feelings of being a burden, it can be quite exhausting having to reassure others (particularly when internally you might be panicking from Google!) At the other end of the scale, you might find those who don’t seem worried enough. You might hear
Setting boundaries, being honest about our physical limitations, and stepping back from overwhelming conversations isn’t selfish – it’s necessary self-care.
'You don’t look ill,' or find people expecting you to keep the same pace as them. Because PH is often invisible, others may forget your limitations or compare it to conditions they understand better. While it can be nice not to have PH constantly as the focus of interactions with others, this can leave you feeling
!invalidated, lonely, or doubting your own symptoms.
Medical professionals often present similar challenges. Although our specialist centres have a great understanding, outside of there, medical staff can be unfamiliar with PH. They may confuse it with general high blood pressure or assume that you look well so you must be alright. When I was a teenager, any mention of breathing difficulties was put down to panic attacks, and I remember how much this made me question my sanity, chipping away at my mental health.
On the other hand, medics may panic when they see low oxygen levels without understanding that we have a
different baseline. Both responses can be equally exhausting, leading to repeated explanations and the constant need to advocate for yourself. And then on yet another hand (we don’t have three hands!), sometimes medics will understand, which can end up with them putting everything down to PH, overlooking other symptoms. It can be a tricky balance for sure!
Also, a brief mention needs to go to the passers-by. The ones who might notice that you’re a bit breathless and kindly check in with you (which personally causes me a mass amount of panic and 'Why?! What’s wrong with me?!'); the ones who may give you side-eye for waiting for a lift up one floor instead of taking the stairs; and the ones who might challenge you for using a disabled bay even though your badge is nicely on show. These can be reminders that not every struggle is visible, and when it is, we might not want to be asked about it – even when it comes from a place of good intentions.
While we can’t control how others react, it’s so important that we focus on what we can control and protect our own wellbeing. Although it can feel like an extra thing to navigate, trying to have open conversations about what is and isn’t helpful with those around us, can help us manage their reactions.
Setting boundaries, being honest about our physical limitations, and stepping back from overwhelming conversations isn’t selfish – it’s necessary self-care. If someone we loved had PH, or a similar condition, I bet we would want to support them in the way that works best for them. That means communicating openly, trying to understand life through their experiences, and listening to what actually helps. While these conversations can feel uncomfortable at first, in the long run they often make things easier for everyone involved.
Connecting with others who truly understand, through peer support, patient groups, or organisations like the PHA UK, can help ease isolation and be a good reminder that you don’t have to carry this alone.
Living with PH can be hard enough without holding everyone else’s reactions and emotions too, and the more open we become around potentially difficult conversations, the more comfortable it will begin to feel.
While we can’t control how others react, it’s so important that we focus on what we can control and protect our own wellbeing.
Sophie is a regular contributor to emPHAsis, combining her professional expertise and lived experience to bring advice to others affected by PH. You can read her personal story at phauk.org/SophiesJourney
Our free supportive call service gives you dedicated time with a PHA UK team member to talk through worries or concerns.
The Listening Line is for people living with PH and their family and friends too. It can help with:
• Adapting to a diagnosis of PH
• Coping with changes
• Concerns about the future
• Worries about loved ones

• How to access supportive palliative care
• Overcoming challenges
• Loss due to PH
...and much more! Please note we are unable to offer personalised medical advice or make or expedite NHS referrals.
Find out more at phauk.org/ListeningLine
Book your call online, at a date and time to suit you. Scan this code to find the next available appointment.
Please note: Our Listening Line and e-support services are not formal counselling services and are not designed to replace clinical advice from your specialist centre team.

“I can’t thank
the PHA UK
enough for providing this service. I’d have really struggled over the last couple of months without someone to talk to who understands PH.”
Listening Line user
Calls take place with Paul Sephton or Sian Richardson, who both have many years of experience working in pulmonary hypertension.


Would you prefer support by email?
Our e-support service provides advice and signposting, or ongoing emails to help you through a difficult time. Contact us at support@phauk.org at any time of day or night, and we’ll get back to you within two working days. You’re not on your own.


Here at the PHA UK we’ve teamed up with Great Ormond Street Children’s Hospital (GOSH) to build a special network to help the paediatric pulmonary hypertension service and paediatric research. Our dedicated young people’s advisory group, and separate group for parents and guardians, meet online every few months to share ideas and opinions.
These groups are for you if:
✓ You are a young person currently receiving PH treatment at GOSH
✓ You have received treatment from GOSH in the past, but are now cared for in adult services
✓ You are a parent, guardian, or carer of a child currently receiving, or who has received, PH treatment at GOSH
Your voice can influence future projects, keep research relevant to young people, and help GOSH receive funding to turn ideas into action.
Scan this code or visit phauk.org/GOSHgroup to complete the form. If you have any questions, please email annabelle.barnes@gosh.nhs.uk
Feedback from our first meetings:
“I liked that everyone was included in the discussions”
“It was good to hear about the new research which is happening to help improve young people's experiences and possible medical advances around PH”
“I enjoyed meeting others in a similar situation and hearing their stories /thoughts”

Our regular space for children with PH

If you are child or young person reading this page, the chances are you’re into Lego! It’s more popular than ever, and our Kids Corner columnist Coco had a special treat when she visited Lego House in Denmark a few months ago. This is what went on…
In December 2025, my family and I went to Denmark to see far’s dad farfar (far means dad in Danish and farfar is dad’s dad) for Christmas. After almost a week of seeing family and friends, my parents had one more present for us. We were going to go to Lego House, to do a Lego Masters Academy course! Known as the “home of the brick”, it first opened its doors in 2017 and has had many exciting events since, including the Lego Masters Academy.
Coco Praest is 11 years old and has been treated for PH since she was a baby. She has a twin sister, Aika, and they live with their parents in London.
Lego Masters is a competition where many teams of two people compete to build the best models, face tough “Elimination builds” and battle in the final to become The Lego Masters. By the way, my family are big fans of Lego Masters. We love the Australian version because it’s really funny and combines our two cultures. We enjoy curling up on the sofa together to watch the awesome models being
going to the Lego Masters Academy, to learn how to be the next Lego Masters.
The day we were due to leave Denmark, we drove the hour-long journey to Lego House. We were going to do the course and then explore the rest of Lego house. Afterwards, we were going to go to Billund airport, to catch our flight home.
We arrived at the Lego Masters Academy, ready to do our course. The course was called “aROUND the bricks we go” and it was all about the S.N.O.T (Studs Not On Top) technique, and making objects look more realistic. We had to make an apple, a pineapple, a pear and a half-circle.

With my twin sister Aika
We had front-row seats so we could see the instructor clearly. The course was awesome because we learnt how to make our models more curved, and we saw a brick-built Lego Masters trophy, a brick pit and the minifig wall. My favourite part was all of it but mostly building and playing Lego with my family. After the course, we were allowed to take our builds with us. Now the course was finished, we could go back to exploring the rest of Lego House!

Some of my favourite experience zones were the Blue zone, where you could engineer Lego cars, develop and improve them and race them on a racetrack, and the Green zone, where you could make a short Lego stop-motion brick film with special effects and music for 15 minutes. Both of these were really fun!
I would definitely recommend Lego House and the Lego Masters Academy to kids (and grown-ups) who have watched Lego Masters, want to start a career in Lego one day, or generally just love the world-building, imagination inspiring and creative toy, Lego!
Meet GOSH nurse Emma over the page...

We’re giving away one of these fantastic Lego bundles, kindly donated by Coco’s mum Michelle, to two lucky Kids Corner readers. All you have to do is answer this question (the answer can be found on this page!):
Q. Which three fruits did Coco and her sister build during the Lego Masters course?

Ask an adult to email your answer, name and address, to media@phauk.org before 30th June 2026. Two winners will be drawn at random after this date. Don’t forget to tell us whether you’d prefer the dinosaur or unicorn set!


Over the next few issues, we’ll be finding out more about the team at Great Ormond Street Children’s Hospital. This time, meet nurse Emma Ketteringham…
Q. How long have you been working with children at GOSH for?
A. I have been a nurse in the PH team at GOSH for three-and-a-half years, but I’ve worked as a nurse at GOSH for over 12 years in total, with lots of that time being spent on Bear Ward (one of the wards that cares for children and young people with PH).
Q. What does your job involve?
A. My job mainly involves keeping you out of hospital, which may sound strange for a nurse! I might see you for a clinic appointment at GOSH, or at another hospital closer to your home in one of our ‘outreach clinics’. If you need to take medicines for you PH I help train you or your parents to manage these at home, and sometimes I come and visit your schools to talk to your teachers about PH and your medicines. I also help teach you and your parents about PH and how to keep your heart and lungs as healthy and strong as possible.
Q. Why did you want to train to be a nurse?
A. Being a children’s nurse is something I have always wanted to be, right from when I was very young. I knew I wanted to do something that would help people feel better, and I can’t imagine myself doing anything else.
Q. What’s the best thing about being a nurse in the GOSH PH service?
A. It’s definitely getting to know all of the amazing children, young people and families who are looked after by our service. I learn so much from you all!
Q. Where can children have the most fun at GOSH?
A. There are lots of places to have fun at GOSH! If you are staying on the wards there are playrooms and play specialists who can provide lots of fun activities, crafts and games to help keep you entertained. In the Lagoon (restaurant) there is usually some arts and crafts and there is the Disney Reef you can visit if the weather is nice. Across the road is a big park which is a great place to go if you have some free time between appointments. My favourite place at GOSH is wherever the therapy dogs are!
Q. What’s your favourite treat from the hospital vending machine?
A. Anything that's chocolate!
Q. What do you like to do when you’re not being a nurse?
A. When I’m not at work I enjoy running and watching sports – particularly football. I also enjoy playing games with my friends and family, and my favourite card games are Phase 10 and Skyjo.
“It’s very normal to feel worried about coming to hospital, especially if it is a new environment for you. Remember that the doctors, nurses and everyone you meet during your appointments are there to help you feel safe, and keep you feeling healthy and strong, so you
can carry on doing all the things you enjoy doing at home with your family and friends. If there are things you are unsure about, you or your parents can ask as many questions as you need to so that we can help you understand what is happening.” Emma

By Shaun Clayton, Certified Nutritionist and Operations and Finance Director at the PHA UK
Remember when everyone suddenly started talking about protein? Gym-goers tracked it obsessively. Health magazines dedicated entire features to it. Supermarkets launched high-protein everything – yoghurts, cereals, even water. Now, science is shining the spotlight on another nutrient that's been quietly working away in the background: fibre. This is why it’s important to pay attention to it if you have PH…
Fibre is the part of plant foods your body can't fully digest.
Instead of being absorbed like other nutrients, it travels through your digestive system where your gut bacteria feed on it.
This might sound unimportant, but here's where it gets interesting: when your gut bacteria break down fibre, they create special substances called short-chain fatty acids. Think of these as tiny messengers that travel around your body, helping to reduce inflammation and support your immune system.
Scientists have discovered something fascinating: your gut and lungs communicate with each other. They call it the ‘gut-lung axis.’
Research shows that people with pulmonary hypertension often have different gut bacteria compared to healthy people. Specifically, they have fewer of the helpful bacteria that produce those inflammation-fighting substances from fibre.
Animal studies have shown that when researchers give animals with PH-like conditions either more fibre or those beneficial fatty acids directly, several things improve:
• Reduced pressure in the lungs
• Less inflammation
• Better heart function
These are early-stage studies in animals, not humans yet.
But they show genuine biological mechanisms – real ways that fibre might help support your health.
Large studies tracking thousands of people show that those eating more fibre have:
• Better lung function
• Lower rates of breathing problems like COPD
• Healthier blood pressure
• Better cholesterol levels
• Easier weight management
All of these matter when you're managing a condition affecting your heart and lungs.
Like protein's journey from boring to beloved, fibre is proving to be far more sophisticated than anyone realised. It's not just about keeping you regular – it actively influences inflammation, Continued overleaf...
immune function and cardiovascular health throughout your entire body. The problem? Most of us aren't eating nearly enough. UK adults typically eat around 18g of fibre daily. The recommendation is 30g. That's a significant gap.
Forget complicated meal plans. Focus on small, sustainable swaps: Breakfast
• Swap white toast → wholemeal or seeded bread
• Choose porridge or Weetabix → instead of Corn Flakes
• Add berries or banana → to cereal or yoghurt
Lunch & dinner
• White rice → brown rice or quinoa
• White pasta → wholegrain pasta
• Regular potatoes → keep the skins on (wash them well)
• Add beans to soup, casseroles or chilli Snacks that count
• Apple slices with peanut butter
• Carrot sticks with hummus
• Handful of nuts or dried fruit
• Wholegrain crackers Easy additions
• Throw frozen vegetables into pasta sauces
• Add a tin of chickpeas to salads
• Keep frozen berries in stock for smoothies
• Sprinkle seeds on soup or yoghurt Aim for five-a-day (at least)
• Fresh, frozen or tinned all count
• Variety matters – different colours provide different benefits
• A portion is roughly a handful
Go slowly: Increase fibre gradually over two to three weeks. Your gut needs time to adjust. Adding too much too quickly can cause bloating or discomfort. Drink plenty of water: Fibre works best with adequate fluids. Aim for six to
eight glasses daily (unless your specialist has advised fluid restrictions).
Check with your team: If you have other medical conditions, take multiple medications or have specific dietary requirements, discuss changes with your PH specialist or dietitian first.
Think of fibre like regular exercise or getting enough sleep: it's one piece of your overall health picture. It supports your body's natural processes and may help reduce inflammation, but it doesn't replace medical treatment.
Here's what we know and what we don't:
We know: Animal studies show fibre can reduce lung inflammation and improve heart function in PH-like conditions. Large human studies link higher fibre intake to better lung function and lower rates of breathing problems.
We don't know yet: Whether eating more fibre directly improves outcomes for people with PH. Those specific studies haven't been done yet.
This is exactly where protein research was 15 years ago - strong biological evidence showing how it works, needing larger trials to prove specific benefits.
Don't try to overhaul everything overnight. Pick one or two changes this week:
• This week: Switch to wholemeal bread
• Next week: Add beans to one meal
• Week after: Include an extra portion of vegetables daily
Small changes add up. If you add 3-4g of fibre daily through simple swaps, you'll reach that 30g target within weeks.
We're learning that nutrition isn't just about calories and basic nutrients. The food you eat actively
communicates with your body, influencing inflammation, immune function and how well your cardiovascular system works.
Fibre is emerging as a key player in these conversations - particularly the dialogue between your gut and your lungs. As someone living with PH, supporting your body's natural antiinflammatory processes makes sense alongside your prescribed treatments. The beauty of fibre is its simplicity. No expensive supplements. No complicated protocols. Just real food: vegetables, fruits, whole grains, beans and nuts.
1. Look at what you're eating now – where could you make simple swaps?
2. Pick one or two easy changes to start this week
3. Increase gradually as your body adjusts
4. Discuss your plan with your PH team at your next appointment Remember: this isn't about perfection. It's about progress. Even small increases in fibre intake bring benefits.
Important reminder: Always discuss dietary changes with your PH specialist team, particularly if you have other medical conditions or concerns about how changes might affect your medications.
Find more advice on nutrition and PH by scanning below. In this dedicated area of our website, you’ll find information on:
Eating to manage the side effects of PH medication... Ultra-processed food... Managing a reduced appetite... Making one-pan meals with PH... Understanding calories... and much more!


This comes from Paul Sephton, a PHA UK team member and a former Clinical Nurse Specialist in PH. He recently batch-cooked this dish for a friend going through a tough time, separating it into individual portions to be heated up when needed. It can also be frozen and kept for those days when the symptoms of PH mean cooking just isn’t an option.
This recipe is taken from The Medicinal Chef by Dale Pinnock. It’s full of goodness – including beta carotene, quercetine, inulin, sulphur, phyto-oestrogens, and zinc. These are fancy names for what are known as phytonutrients – natural chemicals in certain plants which are believed to be beneficial to human health and help prevent certain diseases. It’s also full of fibre and protein, so it ticks lots of boxes when it comes to good nutrition!
This is a vegetarian recipe, but it can be made vegan by removing or substituting the cheese.
PHA UK team member Mary tried this recipe out, leaving off the cheese. Her verdict?

• Two large sweet potatoes cut into large chunks, with the skin on
• Olive oil for cooking
• One garlic clove, finely chopped
• One red onion, finely chopped
• Two handfuls baby spinach
• 1 x 400g can cooked chickpeas (drained)
• Four tablespoons sun-dried tomato paste
• Danish blue cheese to taste (leave it out or substitute if preferred)
• Sea salt and black pepper

This is a satisfying dish – perfect comfort food, easy to make, low cost, and it’s even better knowing that it’s packed with nutrients. I chose to leave the cheese off, and served it with tenderstem broccoli, but any green veg would go well. I also added frozen peas to the bake mix for extra nutrients and texture, and I think sliced carrots or sweetcorn would work equally well.
Don’t be afraid to experiment!
1 Put the sweet potatoes in a pan, cover with boiling water and simmer for eight to ten minutes or until soft. Drain well, season with salt and pepper and mash into a smooth orange puree.
2 Preheat the oven to 200 degrees celsius. Heat a little olive oil in a pan and add the garlic and red onion. Cook for four to five minutes, or until softened.
3 Add the spinach to the onion and garlic and cook for a few minutes more until the spinach has wilted. Add the chickpeas, stir well, then add the sun-dried tomato paste. Season with salt and pepper.
4 Transfer the chickpea mixture to a baking dish. Put the sweet potato mash on top of this, as though you were making a shepherd's pie. Crumble the blue cheese over the top, if using, and bake in the oven


After a long cold winter, many of us will be looking ahead to holidays – but if you’re on oxygen therapy, you may be wondering what’s possible. PHA UK members Cathy and Jayne, who unknowingly booked the same trip at the same time, share how they made their 2025 European cruise work for them…
It was only when they were seated together at the PHA UK Together25 event in Birmingham that Cathy Jack and Jayne Venables realised they would be on the same ship just a few weeks later. Along with their husbands, they enjoyed a rewarding holiday that suited their health needs – making special memories along the way.
ICathyposted in the PHA UK private Facebook last year to get guidance and help on cruising with PH and oxygen, as I wanted to book a cruise for my 60th. Jayne was among the members who commented and said she was cruising later in the year. At that point I didn't know we would all end up on the same cruise.
I’ve been on oxygen since my PH diagnosis at the end of 2020 and have four litres whilst sitting, for up to 16 hours. I also use a portable concentrator and a mobility scooter.
I’ve cruised before, but this was my husband Jeff’s first time. I originally tried booking directly with P&O, but as I use a mobility scooter, they said that we couldn't do the cruise I chose as I’d need an accessible cabin and evacuation chair. I tried to explain I didn’t need either of these, but they wouldn’t budge and only offered a cruise to somewhere I wasn't interested in visiting. Jeff suggested I speak to a travel agent we knew, and she listened to what I was looking for and found the Celebrity Cruise for us.
It sounded perfect, as we’d be away for my birthday and would visit places I’d not been, plus Celebrity offered luxury but relaxed cruises which suited us.

Cathy and Jayne enjoyed plenty of excursions with their wheels

We sailed for two weeks and visited Gibraltar, Villefranche, Pisa, Portofino, Rome, Sardinia and Cadiz.
I didn’t realise we had booked the same cruise as Jayne and Liam until we randomly chose to sit next to them at the PHA UK event in Birmingham – as Jeff saw their dog Molly and wanted to fuss her. We introduced ourselves, got chatting and found not only were we on the same cruise, but our cabins were on the same deck area on opposite sides of the ship.
I guess my main concern was travelling with oxygen, but my travel agent reassured me that Celebrity had a good reputation for looking after travellers with additional needs.
I didn’t have any issues as the concentrator I hired was smaller than the one I have at home and fitted fine in our cabin. I hired it from The Oxygen Store They delivered it five days before we sailed in a hard-shelled case with wheels and handle and they collected it the Monday afterwards.


They can also deliver it directly to your cabin if needed, but this costs more.
I connected with Celebrity’s accessibility team in the run-up to the holiday and we chatted via email to ensure everything I needed was in place for me, including a fridge and extension leads. On the cruise itself, the on-board team were really helpful – from helping me up and down ramps on my scooter and onto tenders, to carrying my plate in the cafe.

When I cruised with my mum in 2012 before my diagnosis, she was in a wheelchair and not mobile which meant that excursion options were limited, but I hoped that as disabilities are now viewed differently that it would be more do-able for me.
There was plenty of room in the cabin for my scooter, plus as it folds up really small it could easily be put in the bag

hold on the minibuses that took us on excursions. Despite this, the excursions team thought the tour companies wouldn't be able to – or wouldn't want to – transport it, and wanted to cancel a couple of my trips, but I argued my case and showed them how it folded. Part of me thinks they just wanted to push us to buy the accessible tours which were way more expensive.
When I’ve travelled before in Europe and the UK, I’ve found many resorts are hilly, so even with a scooter it can be difficult to explore. On the cruise I had similar problems in some ports, but we explored what we could, then spent time on the ship as there was always plenty to do, or somewhere to sit, to people-watch and try the latest cocktail on offer.
My favourite excursion was wine pairing in Italy, which we did with Jayne and Liam. We initially booked to go into Rome but changed this as we decided it would be too hot and busy there on a Sunday with a festival happening.
Continued overleaf...
I’m glad we did as the tour guide was knowledgeable during the coach journey, and we got to spend some time by a lake, wandering and drinking coffee, before going to the winery. Here we did a tour then had wines paired with a tasty meal.
I loved our cabin. It had what they called an ‘infinity veranda’ and the balcony area was part of the room, though you could shut it off. It had a floor to ceiling / wall to wall window so you had a view from anywhere in the room. The top half of the window lowered to let fresh air into the room or went right down to make a balcony rail. It was lovely as if I was tired, I’d sit and cross-stitch or lay on the bed and chill.
it covered us for a year and was cheaper than for a single trip, which made it better value as I also ended up visiting my sister in Florida – a long-haul flight that I’ve done a few times with oxygen. I’d say cruising is much easier, as you just put everything in the car, drive to the docks and it’s transferred onto the ship. There’s no hanging around at airports. Everything we needed was there on the cruise – amazing food, excellent entertainment, and the opportunity to socialise with people. It was a trip of a lifetime – a wonderful way to celebrate my 60th birthday, and it was lovely that Jayne and Liam were there.

an added bonus to be able to spend time with them, which made the whole experience extra special.

A highlight of the cruise was a seven-course taster menu in one of the speciality restaurants for my birthday. Jayne and Liam by chance had booked the same restaurant on the same day and they arrived whilst we were still eating – so when a birthday cake was brought out for me, I was able to give half to them to enjoy (it was huge!)
Travel insurance cost me £1,500 with Co-op, for Jeff and I combined. It’s expensive, but




that you can still go on holiday if you have PH
seen Cathy’s name pop up on the Facebook group but I’d never met her and Jeff before the PHA UK event in Birmingham. We all got on really well on the holiday and although we did some things together, we also did things on our own.
My husband Liam and I had cruised before, about seven years ago, with Royal Caribbean. I had PH back then too, and it was so easy, which is why we decided to cruise again last year. The biggest benefit is that there is no flying involved. I probably could do it and would be able to get a fit-to-fly letter, but I just can’t face it – not with all my IV medication and oxygen.
With a cruise, I never lose sight of my meds as I take them straight onto the ship, and I find that reassuring.
Celebrity Cruises, who we went with last year, have a team called ‘Special needs at sea’ and I contacted them to explain I have PH, use a scooter, and am on oxygen therapy. They were great.
I’ve got an implantable loop recorder (which monitors my heart rhythm) and because of that they gave us upgraded Wi-Fi for free. I was also put in touch with a team called ‘Accessible excursions’ and they checked that all the trips I wanted to go on would be suitable, on my behalf. I was really impressed.

I hired the oxygen concentrator from The Oxygen Store
That was for three weeks, as although the holiday was for two, I needed time either side to allow for delivery and collection. We didn’t book an accessible cabin, as we didn’t think we needed one, and it was fine. We had more than enough room for all the equipment, and to move around. There was a fridge to store my IV meds, and we paid extra to have a balcony, which made a big difference. I would often go back to the cabin for a sleep in the afternoons, and it meant Liam had somewhere to sit and enjoy the view while I rested.

JayneandLiam makingthemostof thewineatatasting lunch in Rome
Jayne's highlight was getting in the ocean with a dry bag protecting her pump
My travel insurance cost £725 with PayingTooMuch. A lot of companies refused to cover me, and although it was a lot of money, I saw it as a necessary evil. Both Cathy and I would get asked about our oxygen by other passengers, and I got questions about my pump and IV line too. They were curious, and I didn’t mind – I never do. There were quite a lot of other people on board with scooters, and wheelchairs too, which helped me feel less ‘different’. By far the biggest highlight of the trip for me was being able to go into the sea for the first time since having my pump. I got myself an inflatable dry bag and took it along to an excursion to Nice in France. It’s completely watertight, so it held my pump safely and enabled me to go in up to my knees and then sit in the shallows for an hour. After ten years, I can’t tell you how amazing it felt to be able to do that. I took my spare pump to the beach with me just in case it all went

wrong, but it was absolutely fine. [You can find the bag at Amazon for £12.99 by searching for ‘Swim Buoy Tow Float Dry Bag’]
If anyone reading this article is thinking about cruising, just do it. Research it all first, and bear in mind that you don’ t necessarily need an accessible cabin. It’s so much simpler than flying. You don’t need a fit-to-fly letter – just turn up at the port, and half an hour later you’re on the ship.
Remember that you can still go on holiday if you have PH. It’s important to get away and it makes you feel like a ‘normal person’.
If you would like to share your own travel experiences and recommendations with other PHA UK members, please email media@phauk.org



and I’d only last three weeks, but look what it led to!
So how did you go from cleaning to nursing, and specifically to PH?
One of the areas I had to clean was the surgical unit, and I’d help

and there was no specialist PH service back then, but I learned a huge amount on the ward at that time.
I continued later with my nurse training, I became a staff nurse and eventually joined the specialist PH nurses team in 2010 – covering a sabbatical. I realised that was truly
My job is to lead the nursing teams, which are split between medical PH services, pulmonary endarterectomy (PEA) services, and balloon pulmonary angioplasty (BPA) services. Royal Papworth is the only hospital in the UK to offer PEA and BPA for people with chronic thromboembolic


“I feel really optimistic about what can be achieved for patients over the next decade or so”
career for this interview because when things are busy, you tend to navigate your way through each day and not look behind you.
I never want to get to a stage where I become too removed from patient contact. It’s what I truly love about my work.
You’ve been at Royal Papworth for almost four decades now. What are the biggest changes you’ve seen in PH care over that time?
There were no specialist PH nurses at all when I started as a ward nurse, so I’ve seen the service build from nothing, to what it is today. When all the treatments started coming along, including the IV medications, the specialist nurses really came into their own. And things then grew even further with the introduction of the PEA
We’ve gone from doing very little research into PH to having a huge research facility, so there have been some wonderful changes. When I look at how far things have come since I started, I feel really optimistic about what can be achieved for patients over the next decade or so.
What are you most proud of when you look back at your career?
I'm honestly really proud of becoming a nurse in the first place. When I started university I was petrified, but it was worth every single second and every tear shed. I'm also proud of helping the PH service at Royal Papworth develop into what it is today – to think that I’ve been a small cog in that process is fantastic.
It's been really nice to sit and reflect over my
If you had just one piece of advice for someone newly diagnosed with PH, who may be reading this, what would it be?
Never give up. Keep looking forward, because you never know when something new will come along to help you. Also, don’t forget the PH service is there to help you – not the other way around. Ask for help when you need it.
Finally, how do you like to relax away from work?
I’m someone who likes to keep busy, and my nine grandchildren definitely keep me on my toes. I absolutely love that time with them; it’s very precious. I also enjoy spending time with my husband, and our lurcher Elkie, who is named after the singer Elkie Brooks. When I do sit down, I enjoy watching anything to do with crime on TV. It’s very good escapism! .




Tharuka Kossinna is based in Brisbane, Australia, and has been navigating life with pulmonary arterial hypertension since the age of 11. Now 27, he is more active than ever – working full time, playing sports, and even taking snowboarding holidays with his Hickman line. He told emPHAsis how it wasn’t always this way, and why it’s important not to give up…

In the years leading up to when I got diagnosed, I started to notice
I was getting out of breath and getting tired really quickly, but it never resulted in much when my parents took me to the doctor.
When I was 11, I had a seizure whilst at the beach with my family and this led me to a hospital visit which resulted in getting my diagnosis.
Life didn’t change a lot at first; I started taking some tablets and being 11, I didn’t think too much into it. But things changed when at the age of 12 I was started on epoprostenol, delivered intravenously through a PICC line in my arm.
I transitioned into high school, and walking around with this thing hanging out of my arm, and a backpack on at all times, wasn’t ‘normal’. People kept asking what was wrong with me, and over time I started to feel like a bit of an ‘outcast’.
None of it was malicious; it was just curiosity because I was different. But at that age, everyone’s trying to fit in and I was clearly different. It was rough for a few years but my escape from it all was playing video games.
I would wake up, jump on the X-box with my headphones on, and play games all day. Granted, I did meet a few people via playing online – people I’m still friends with today – but it meant I wasn’t doing much physical activity, and over time there were concerns about whether my bones would start to get weak.
“Finding my voice again and coming out of my shell opened everything up to me”
When I was 15, my family started to push me a little bit more to get outdoors, and because I used to love cricket as a kid, one day they managed to persuade me to go and have a hit at the nets. It just happened that on this day, two friends who I grew up with where there. This led to us meeting up weekly to have a hit or to just hang out.
Over time, this started to show me that I wasn't as incapable as I thought I was,


and that I could slowly go back to living the life that I did by being more active and playing a bit of sport.
Also, by deepening my friendship with these two friends and getting some normalcy back in my life, it really helped me come out of my shell again and feel more like my old self.
Finding my voice again and coming out of my shell opened everything up to me. I started to try a little bit harder at school and set some proper goals for what I wanted to do after high school. Since then, I’ve achieved so much and ended up getting two Bachelor’s degrees from university - one in computer science, and one in finance - which has led to an exciting career that allowed me to move to a different state on my own for a year. That was huge.
I now work in investment management at a company here in Brisbane. There are occasional days when I don’t feel great, or when I have to take time off for a medical appointment, but I’m really lucky to have great employers who are flexible and understanding.
Right now, I’m on Veletri through a Hickman line for my PAH, as well as oral medication. And honestly, at the moment everything feels quite good. I’ve progressed so well over the past few years that I’m now down titrating down on the Veletri with the hopes of coming off soon. While it’s exciting, I do still get a little short of breath here and there, but it doesn’t stop me from living life – I’m still playing football, going to the gym, and

Undergoing tests at hospital
doing everything I normally do.
I've even been on three different snowboarding trips - including one in Japan - and I’ve taken part in a group triathlon and run in a 10km race.
I would say the biggest challenge with any of these things is just making sure I have my medications organised and on hand, but other than that, I don’t feel any real constraints. Over the years, I’ve found my limits and I try not to go beyond them, but this took years of slowly pushing my boundaries to figure out what those limits are, and to increase them over time. They will be different for everyone, so you need to be patient while you find yours.
People are always a little shocked when I tell them how much I am able to do with PAH, and I do know my story isn’t common. But I think it’s important that people keep their head up and make the most of life within their limits. Mindset is really the key.
Now that I've found a bit more confidence in who I am, I do find it a little bit easier to speak to other people about my condition, so I am pretty forthcoming about it.
Most of the time people are receptive
“ People are always a little shocked when I tell them how much I am able to do with PAH, and I do know my story isn’t common”



when I tell them about my PAH, and I don’t think I’ve ever come across someone with something negative to say. If they did have something negative to say, they’re probably not the people I want to be talking to anyway! Most people are just curious and interested to find out more. I actually think talking about my PAH is a really good way to break the ice with new people. They probably don’t have any experience around pulmonary hypertension, but most people have been impacted by health situations at some point, and I think it’s a good way of
“I think the biggest thing I’ve learned is how important it is to live in the moment more”
finding common ground that can quickly deepen and build relationships. Having PAH certainly doesn't stop me from meeting people or having a social life.
I’ve built really good relationships with my medical team, and I’ve never felt like ‘just a patient’. Right from the start I’ve felt able to contact them straight away with any questions or worries, and I’ve spoken to them about everything from school life to university and work. They always have good advice to guide me down the right path.
My medical team have gone above and beyond many times over the years – not just for me, but for my family too. I feel extremely lucky to have such great support.
It’s been 16 years since I was diagnosed with PAH and I think the biggest thing I’ve learned is how important it is to live in the moment more. Don’t ruminate, or get caught up in the negatives, because it doesn’t help you in any way. You need to keep your head up and do what makes you happy, and live as fully as you can within your limits.






When 53-year-old Dawn Sheffield was diagnosed with PH, it came amid a mental health crisis that saw her confined to the house. Discovering a love of music has helped her come to terms with the disease, find her voice and her confidence, and expand her world in a way she never could have imagined.
I’ve always kept all my emotions in, locking them inside, along with any stress I experienced. I would never show how I was feeling – I’d just push it all down, dust myself off, and keep on going.
The COVID-19 lockdown was the first time I didn’t have responsibility for somebody, or expectations to do something for somebody, so I let all my walls down that I’ve had up since I was a child. It was September 2021 and I had a breakdown. My anxiety and depression were off the chart, to the extent that for the first time I asked for help.
I was a few months into my therapy when in February 2022 I was taken ill with a chest infection. I couldn’t get rid of it, even after three courses of antibiotics, and I could hardly breathe – I couldn’t walk two steps without gasping for air. I already live with a disability caused by an accident in 2007, so I walk with a stick and live with a lot of pain. It made things very difficult.
In the June of 2022 I ended up being sent for a chest X-ray and an echocardiogram at my local hospital, and at this point I was unable to go anywhere on my own as my anxiety and depression levels were so high.
My friend came to all my medical appointments with me. She asked the questions, because I always felt unable to. I didn’t have a voice; I was unable to make decisions.
I had never heard of pulmonary hypertension when the doctor told me it was what they suspected. I was already spinning, just from being in the hospital. I was sent home and I spent a lot of time looking it up on the internet and reading about a life expectancy of five years. I fell right down that rabbit hole. I was told the PH diagnosis could only be confirmed after a right heart

I kept it on and I didn’t have a panic attack; in fact, I ended up spending an hour in the shop – which for me was amazing. When I got back in the car and turned the radio on, the same song played again. It was ‘Bigger than me’ by Louis Tomlinson, who used to be in One Direction, and that track changed everything for me.
catheter at a specialist centre in London, which felt a long way from my home in Eastbourne.
Whilst I was waiting for the appointment for this test, and waiting to start treatment, I started to do a couple of things just for me, on the advice of my therapist. I started violin lessons and decided to take care of my diet and nutrition. It was my first step towards taking control.

I started doing chair yoga and meditation, and I stopped the volunteering I did that was causing me stress. All of this helped – I had more energy, and my breathing felt easier.
My mental health problems were still there, but the biggest change for me came out of nowhere, and all because I pushed the wrong button on my phone.
It was September 2022, and I had started trying to do some things on my own. To help me while shopping alone, I’d wear earphones to enable me to speak to friends or family on the phone to help keep me calm. I was in the supermarket one day, and I accidentally pressed the wrong button on my phone – meaning music played through the earphones instead.
I had no idea who Louis was, but I immediately needed to find out everything about him and his music. I downloaded every song Louis had released, both as a solo artist and as part of the band. That one song changed the entire course of my life.
I signed up for singing lessons, as I thought singing would help my lungs too. And I was encouraged by my singing teacher to start writing my own songs, which was like journalling, and it enabled me to get things out.
By the time I had the appointment for my right heart catheter, I had started using music regularly to help me get through things.
I had it playing low through my earphones as I entered the hospital building, accompanied by my friend. I was feeling very anxious and agitated, and I had a long wait, so the music helped.
The time for me to go in for the procedure came, and I was told by the doctor who prepped me that it would be fine for me to wear my earphones whilst it was happening. However, when it came to it, the nurse told me to remove them. I lay waiting for the procedure in silence, with no music on, and my anxiety went through the roof.
Continued overleaf >

Waitingaroundathospital in December 2025

with tears running down my cheeks, and I couldn’t even speak. I was like a jelly on a plate, and it was impossible for them to administer the anaesthetic. The doctor ordered them to give the earphones back and by the end of the song that was playing, I was as calm as anything. It was a switch being flicked.
The PH was confirmed in November 2022, and I was started on medication. Music started to become an even bigger part of my life, as it helped me come to terms with the diagnosis.
In 2023 I decided I would go and see Louis in concert; the first concert of my life, on my 50th birthday. I then heard that Harry Styles was performing at Wembley so I booked tickets for that too.
In 2024 I started learning the piano and guitar too, and I agreed to perform at a concert organised by my singing and piano teachers. I sang ‘This town’ by Niall Horan. He was also a member of One Direction, and I discovered him through researching Louis Tomlinson. I discovered the other members too, including Harry Styles – and learning about him taught me to express myself more through my clothing, because that’s what he does. I changed my wardrobe and it changed the way I saw myself.
I stood up at that concert and sang in front of the other students and their families, and it was a long way from not being able to leave the house alone. I then did a piano performance - after only five lessons - and although I was trembling head to toe, I got through it.
I carried on songwriting and playing and listening to music, and despite some setbacks in my personal life, my confidence continued to grow.
I went to my first music festival
in 2024, a progression from just a concert. I went alone, because my (former) friends said I wouldn’t cope with it, and I wanted to prove them wrong. I connected with other fans on social media and met up with them there, and they looked after me for the whole day. They were so supportive.
I met Louis Tomlinson at the festival that day, and all I could say was ‘thank you for your music’.
I thought I would hurt the next day. I thought I would be tired, and ache, and have to rest. But all I felt was free – because I had done it. I had gone to a music festival alone. I might have PH, another physical disability with the pain in my leg, and anxiety and depression, but I had done it.
When former One Direction member Liam Payne died towards the end of 2024 it helped me understand feelings. It hit me hard, because I had never let myself ‘feel’ when people close to me had died before. It made me understand the death of family over the years and a lot of things started to make sense.
I started to listen to other bands and went to see one of them – The Mercians –perform in Brighton (again, on my own). I got to chat with them, and it seemed to spark something in me, inspiring me to go back to college and take courses in confidence-building and podcasting.
My music became my passion, and that helped me to set a goal. Because I’m unable to work, and I don’t know how long my health will last, I set short-term goals. I want to start my own podcast and YouTube channel to help give singers and musicians a voice – just like music gave me a voice too.
It will involve me travelling around the country to visit them, which will push me out of my comfort zone. But it’s a challenge, and that’s what PH is too. It’s a challenge every day, because you don’t know what’s going to happen. You can medicate it, but you can’t control how it makes you feel.
In November 2025, I went one step further with my singing and performed a song I had written myself at a concert organised by my teacher. I now take piano and guitar lessons weekly, and music helps me deal with both my PH and other issues, such as the poor health of my father. I try not to overload myself though.
Music has helped me deal with everything. It’s helped me realise what I can control, and what I can’t. It’s opened my horizons. It’s helped me find people that are more accepting and supportive of me – the real me.
Previously, the only way I could attend medical appointments was to have music constantly playing in my ears. Now, I don’t need it on all the time. I’m able to talk to people in the waiting room, and engage with medical staff, and that’s a big progression. Music really is a healer.
One doctor did one X-ray and saved my life. Louis Tomlinson did one song and changed my life. The little things we do in this world make the biggest difference. Music helped me come to terms with PH and find my identity. It has helped to me to see PH as an opportunity to live with clarity and focus, not just fear. It’s encouraged me to live intentionally and look up rather than down.

Me with the band 'The Merchants' at Pattern Festival in April 2025 - I attended on my own
I fight every day. I fight to get up, I fight my PH, I fight my disability, I fight my mental health, and I fight what’s going on around me. But I keep doing it; and that’s all because of music and because of the support I now have around me.
I’ve come a long way and my PH team at the Royal Free Hospital have been a really important part of that journey. I can’t thank them enough for persevering with me, encouraging me, and being there for me. It was their suggestion to share my story in this way. Recently, I’ve re-connected with others in my life and they have also helped me grow stronger within myself, regain my confidence, and find my voice. I couldn’t ask for a better support system now.
Our free self-help programme has been developed with psychologists specifically for people with pulmonary hypertension – and 100% of those who tested it said it helped with their anxiety.
Based on Cognitive Behavioural Therapy (CBT)
Complete the workbooks at home
Work through them in your own time



























We’re here to support people like you. Join the PHA UK today and benefit from:
• Support and advice
• Helpful printed information & resources
• emPHAsis magazine delivered to your door
• Free access to financial advice from qualified professionals via our partnership with Turn2Us
• Fundraising ideas and guidance
Being part of the PHA UK also enables you to participate in important research, and our friendly office staff are just one call away when you need advice. Join our PH family and you’ll be joining 4,500 members in a unique network of support and inspiration.

We welcome your thoughts on everything we do as a charity, to ensure we are the best we can be for our members.
Scan this code to leave your feedback via our online form (where you can remain anonymous if you wish). You can also email feedback@phauk.org
Please email media@phauk.org if you’d like to contribute to your member magazine.
✓ Share your PH story
✓ Tell us your tips
✓ Submit a letter
✓ Send us your poems, pictures or photographs
✓ Pass on a feature idea
✓ Give your feedback on this issue
WOULD YOU LIKE TO CHANGE HOW YOU RECEIVE THIS MAGAZINE?
Scan below to receive your copy by email instead, change your address, or cancel your subscription. You can also email hello@phauk.org
Contact us here at emPHAsis by emailing media@phauk.org or writing to emPHAsis, PHA UK Resource Centre, Unit 1, Newton Chambers Road, Thorncliffe Park, Chapeltown, Sheffield S35 2PH
Keeping you informed and helping you to live well with PH
Our wide range of titles cover topics from medication to menopause, palliative care to pregnancy – and much more.










Scan to see the full library and order your copies, or visit phauk.org/publications
