, C H
B E R N





PAGE 3
PROGRAM OVERVIEW
An overview of CMFDE fellowship at the Trauma & Mental Health Lab
PAGE 5
ENHANCING MENTAL HEALTH SERVICES AT WELCOME CORPS
Keti Akhalbedashvili and Valantina Zeremariam
PAGE 11
INTEGRATING PSYCHOLOGICAL FIRST AID AT BARD COLLEGE
Maya Gjonbalaj and Natasha Bashore-Walker
PAGE 16
TELENOVELAS AND LATINX IMMIGRANT COMMUNITIES
Karina Gonzalez Perez
PAGE 21
BUILDING PIPELINES INTO MENTAL HEALTH CAREERS FOR ASIAN IMMIGRANT YOUTH
Abigail Wang
PAGE 27
PSYCHOLOGICAL INTERVENTION PROJECT: GRACE CHURCH– HOUSTON, TX
Andrea Morantes
PAGE 30
EVALUATING THE POTENTIAL BENEFITS OF INTEGRATING PROBLEM MANAGEMENT PLUS (PM+) AND PSYCHOLOGICAL FIRST AID (PFA) TO ADDRESS MENTAL HEALTH CHALLENGES AMONG COMMUNITY COLLEGE STUDENTS ON CUNY CAMPUSES
Engers Polanco

The New School for Social Research in partnership with The Consortium of Forced Migration, Displacement, and Education
FORCED MIGRATION AND GLOBAL MENTAL HEALTH

About the CFMDE Consortium
The Consortium of Forced Migration, Displacement, and Education (CFMDE) is a collaboration of The New School and Bard, Bennington, Sarah Lawrence, and Vassar Colleges. The CFMDE program in Bern, Switzerland offers undergraduate students the unique opportunity to learn about the field of Global Mental Health and strategies used to build capacities for mental health care, especially in the context of forcibly displaced individuals.
Over the course of four weeks, students had the opportunity to integrate academic discussions with field visits to key stakeholders in mental health and humanitarian efforts throughout Switzerland to gain insights into the lived experiences of individuals at the frontlines of global mental health. Finally, this report serves as an emblem of the value of this program in strengthening the capacities of the mental health workforce to address the psychosocial needs of their respective local communities.






V I S I T S
Bürgerspital, Solothurn 7.17.24
Inselspital, Bern 7 8 24
World Health Organization 7.9.24
Winterthur Vocational School 7 11 24
University of Zurich 7 11 24
International Organization of Migration 7.16.24
Basel Asylum Center 7.18.24
Swiss Federal Office of Public Health 7.22.24
Zurich Asylum Center 7.24.24
Asylex 7.25.24
U.S. Embassy 7.25.24
ENHANCING MENTAL HEALTH SERVICES AT WELCOME CORPS
IDENTIFYING NEEDS AND IMPLEMENTING EFFECTIVE INTERVENTIONS
by Valantina Zeremarian and Keti Akhalbedashvili
Throughout our experience in Switzerland, we have had the opportunity to closely examine mental health resources for migrants and displaced communities through surveying research and meeting directly with stakeholders, identifying strengths and significant gaps in mental health support systems As of May 2024, globally, more than 120 million people have been forcibly displaced (UNHCR, 2024)

Although the purpose of the United Nations Refugee Agency is to protect and support refugees, there are other programs like Welcome Corps working alongside other international agencies seeking to address some of these challenges by making it far easier to have a refugee or refugee family come into the United States Such programs must provide adequate mental health interventions to best support incoming refugees.
Welcome Corps is an initiative introduced in 2023 under the United States Refugee Admission Program (USRAP). The private refugee sponsorship program allows at least five US adult citizens or lawful permanent resident adults living in the same community to sponsor refugees This group of sponsors can either sponsor one refugee or a refugee family of up to ten members. They’re either assigned a refugee/refugee family or apply to sponsor someone they know. Welcome Corps engages everyday Americans in the resettlement process for refugees According to the United States Department of State, Welcome Corps plays a key role in the U.S. refugee resettlement system, providing a "lifesaving lifeline to vulnerable people in need of resettlement” (USDS, 2023)
The idea behind the initiative is to make it easier for refugees to enter and resettle in the United States by receiving support from their community members. Welcome Corps sponsors receive training, which is mandatory for at least one of the five sponsors participating in the refugee resettlement process.

However, the program strongly encourages all sponsors to be trained The training consists of in-depth information regarding the role of the sponsor and the resources needed to adequately prepare for welcoming refugees. Sponsors learn about the legal process of applying for refugee status, refugee rights in the United States, and commitments to being part of a private sponsor group The training also includes detailed modules on what sponsorship duties may look like.
The five sponsors must prepare for the refugees' first 90 days in the United States and provide ongoing support. The main goal is to provide resources and support so that, by the end of the 90 days, refugees are independent and well-integrated. During the preparation for the refugees' arrival, the sponsors must provide financial support of at least $2,425 per refugee for expenses, housing, and transportation. Upon the refugees' arrival, the sponsors must pick them up from the airport, take them to their initial housing, and orient them to their new community and the U.S. generally Sponsors must also connect them to English learning programs, secure essential documentation to obtain employment, and connect them to local hospitals for health services.
For refugee children, the sponsors must support in arranging childcare and education services. Although the sponsors work towards integrating the refugees into their community and the U.S., they should also connect the refugees to communities that align with their identities, such as their houses of worship, cultural food, and other people who have relocated from the same country. Sponsors provide 1, 3, 6, and 12month reports and surveys post-arrival to communicate any support needed or issues regarding the refugees' safety and well-being.

A key aspect of providing holistic support for the successful resettlement of refugees is focusing on the overall physical and mental well-being of both sponsors and refugees. The mental health of refugees is especially relevant, as they are at increased risk of developing mental health problems due to traumatic experiences during migration and the stressful reasons for their migration. During their training, Welcome Corps sponsors are made aware that some refugees may have experienced trauma. Sponsors are advised to be compassionate when talking to refugees about their mental health, noting that some refugees might not be open to the idea of counseling. Further, sponsors are trained to check for local mobile crisis units and local mental health professionals. For further mental health support, Welcome Corps sponsors are directed to the Substance Abuse and Mental Health Services Administration (SAMHSA) Although SAMHSA offers strong behavioral health resources and the Welcome Corps acknowledges mental health, there is a notable lack of specific mental health training for sponsors dealing with vulnerable people and generally not enough direct service mental health interventions accessible to both sponsors and recently arriving individuals.
The field of Global Mental Health may offer some helpful strategies and frameworks that can complement the goals of Welcome Corps. Specifically, there has been a rapidly growing number of low-intensity mental health interventions that can be delivered by non-mental health specialists to help increase capacity and
accessibility to care This concept is sometimes referred to as "task-sharing" because those who receive training and deliver care are not mental health specialists. But their work benefits through the integration of care into other roles.
The World Health Organization has developed numerous scalable mental health interventions, such as Problem Management Plus (PM+) (WHO, 2018). Additionally, Psychological First Aid (PFA) (Red Cross and Red Crescent Societies, 2018), is an intervention first developed by the Red Cross. These interventions have been developed with a task-sharing principle in mind, aiming to fill the gaps in mental health access in countries where access is limited. Scalable mental health interventions serve as templates that can and have been adopted in various cultural contexts. Additionally, they offer a novel means of increasing access to care as they can be delivered by individuals who are not mental health specialists.
A stepped-care approach is an effective approach to implementing such mental health interventions, as it refers to a system of delivering mental health in a timely and cost-effective way. Looking at implementing these low-intensity scalable mental health interventions in the Welcome Corps mission, we suggest adhering to the stepped-care approach where the most effective yet least resource-intensive treatment is delivered first, while more intensive interventions would be considered the next step in providing care.
Psychological First Aid (PFA)
Psychological First Aid (PFA) is an approach designed to help individuals in the immediate aftermath of a traumatic event. It was originally intended to be used in humanitarian settings to provide support for individuals immediately after disastrous events, however, it has since been adapted to be used on university campuses, asylum centers, workplaces, and even community organizations and faith-based organizations. Psychological first aid aims to reduce initial distress, foster short-term and long-term adaptive functioning, and provide a supportive environment that can aid in recovery. PFA trains individuals to understand signs of common distress and respond appropriately. Pillars of PFA include promoting a sense of safety, providing a sense of calm when an individual is feeling anxious, promoting a sense of self and collective efficacy by helping regain a sense of competency and belief in one’s self, providing opportunities for further emotional support, and instilling a sense of hope and positivity after difficult experiences.

The key principle of PFA is to look for common signs of distress, listen to the needs of the person in distress, and link them to resources that will allow the distressed individual to healthily cope. PFA is designed to be flexible and culturally sensitive, allowing responders to adapt their approach based on the specific context and needs of the individuals they are assisting. Anyone can provide PFA, and it can be provided in an emergency or non-emergency setting
The intervention can be delivered faceto-face through phone calls, video calls, or even texts Clinical studies suggest that PFA intervention following trauma exposure shows a positive effect for reducing anxiety and facilitating adaptive functioning in the immediate and intermediate term (Wang et al , 2024) Depressive symptoms were reported to have a significant reduction postintervention even 3 and 6 months after the intervention, in a study done on the effectiveness of PFA done immediately after a traumatic event (Wang et al., 2024). The same study also reported a significant reduction in anxiety after the intervention. We strongly recommend that PFA training be the basis of the mental health support provided by the Welcome Corps, with all sponsors having to complete mandatory training to be adequately equipped to provide basic support to people in distress.
Problem Management Plus (PM+)
Problem Managament Plus (PM+) is a WHO transdiagnostic psychological intervention for mental health problems (Dawson et al., 2015), applying the same underlying principles across mental disorders without tailoring them to specific diagnoses. The intervention has been developed to deal with the mental health needs of individuals who have been affected by adversities or experience continuous trauma in low-income settings
PM+ is meant for adults suffering from symptoms of common mental health problems such as anxiety, depression, stress, grief, and self-identified practical problems such as unemployment and interpersonal conflict. It is intended to be delivered by lay helpers and meant to be an affordable, low-cost low-intensity intervention teaching individuals useful skills to alleviate daily symptoms of stress.
PM+ consists of five weekly 90-minute face-to-face sessions with a lay helper. The intervention utilizes some core strategies: managing stress & problems, get going keep doing, strengthening social support, and relapse prevention In order to help individuals develop skills to manage stress and relieve anxiety, techniques such as slow breathing are taught. For the managing problems component of PM+, individuals are taught to categorize problems as solvable, unsolvable, and unimportant to effectively deal with problems and alleviate stress
Since the intervention considers that some problems cannot be solved, the focus is on managing an issue Furthermore, PM+ incorporates positive
reinforcement and behavioral activation as a way to re-engage in activities that alleviate symptoms of depression. Strengthening social support is another pillar of PM+, which encourages people to engage in their existing support networks and communities For the relapse prevention component of the training, individuals are taught to identify personal warning signs of relapse and are tested on their knowledge of the strategies learned throughout the training and their ability to apply them to specific problems.
The strength of the intervention lies in its cultural adaptability PM+ training can be performed in a group setting, which would be most appropriate for implementing the intervention at Welcome Corps as there is a group of sponsors. Considering that the Welcome Corps sponsor training is conducted virtually, the cultural adaptability aspect of the intervention is important PM+ has been previously adapted to virtual settings for a study during COVID-19 in New York City, Europe, and East Africa (McBride et al., 2021). The study shows that the adaptation was successful with a hybrid of asynchronous recorded practice and incorporating role plays into the online training, which reduced the trainer's workload between the sessions.
Ongoing randomized controlled trials have shown PM+ to be effective in communities exposed to adversity. In a study done on Syrian refugees in the Netherlands, Problem Management Plus has been proven to have positive results (Graaff et al , 2020) Another research

study uses a cluster randomized controlled trial done in Nepal suggests that adults who obtained Group PM + training show a significant reduction in psychological distress after 3 months in comparison to adults who were only provided with reference options for mental health services. Moreover, 1 out of 3 adults who completed Group PM + training saw a 50 % decrease in depression symptoms whereas only 1 out of 6 adults who had the referral option saw the same decrease in depression using a referral option (Jordans, M J D , 2021) Group PM + has shown effectivness in the reduction of psychological distress and depression symptoms. Within the stepped-care approach of providing mental health services to refugees in the Welcome Corps resettlement program, we suggest that PM+ be treated as the second "step” to providing mental support. We suggest that at least one of the five sponsors be trained in PM+ as part of the mandatory training to become a sponsor. This would ensure that the sponsor has the tools to adequately support the refugee(s) they are hosting if stressful situations arise and intensive and specialized services are not immediately available or not necessarily needed
Integrating these WHO-developed interventions into programs like Welcome Corps can significantly enhance the support provided to refugees. By equipping sponsors with the necessary mental health training and resources, we can better address the complex needs of displaced individuals and foster their successful integration into new communities.
INTEGRATING PSYCHOLOGICAL FIRST AID INTO EXISTING HEALTH CARE SERVICES AT BARD COLLEGE
In recent years, the field of Global Mental Health has received increased attention from a wide range of stakeholders worldwide, including government agencies, NGOs, healthcare institutions, academics, and community groups This has occurred in response to an overwhelmed healthcare force faced with an abundance of individuals in need of services and a lack of appropriate care structures. In higher income countries this translates to extremely long wait lists for mental health care, and in low or middle income countries a single psychiatrist may serve the needs of over 200,000 people (WHO, 2022). Decentralizing low-intensity mental health care by training community members in mental health and psychosocial support (MHPSS) interventions could help address these significant gaps in care. Furthermore, integrating MHPSS into communities mitigates the harmful effects of culturallyinsensitive care and increases the effectiveness of interventions (Perera et al., 2020). This paper argues for the implementation of one such intervention, Psychological First Aid (PFA), into existing health-oriented services on Bard College’s campus. The proposed project would double as a valuable opportunity to strengthen existing mental health systems at Bard and to collect data on the
effectiveness of PFA, given the intervention’s current lack of a research base (Shultz & Forbes, 2013).

PFA seeks to reduce people’s symptoms of distress and address any of their practical needs (Hansen, 2018) It adheres to the principles of look, listen, and link, which refer to initial information gathering, how the PFA helper communicates with the distressed person, and the process of connecting the distressed person with formal and informal support, respectively. The intervention champions positive engagement with distressed individuals that recognizes their autonomy, validates
their struggles, and equips them with tools to address their problems and poor mental health.
The International Federation of Red Cross and Red Crescent Societies outlines several scenarios suited to PFA, including but not limited to personal crises, social challenges, health challenges, natural disasters, man-made disasters, violence, armed conflict, and forced migration. Although the specifics of the intervention vary based on context, the core principle of doing no harm by promoting the safety, dignity, and rights of distressed individuals remains. The widespread applicability of PFA enables trained individuals to utilize the intervention outside of crisis situations and in their everyday lives.
PFA’s relative simplicity as a preliminary mental health intervention makes it suitable to non-specialists. This may enable increased engagement among communities and bolstered training of competent responders during mental health crises. PFA has been adapted to different situations, like PFA for children and PFA in groups, so training time and content will vary. An introduction to PFA lasts only four to five hours and lays out basic helping skills, whereas basic PFA lasts eight and a half hours and includes example situations, reactions by distressed people, and helper responses during training (Hansen, 2018).

Bard College currently includes several mental health services intended to serve the needs of its student population. Bard Counseling Services employs psychologists, a psychiatrist, social workers, and mental health counselors, and the Bard Wellness Education Office deals with general topics of stress, student care and relaxation techniques, and maintaining a balance between personal and academic life (Bard HealthCounseling-Wellness, n.d.). However, given the college’s distance from major cities and cultural hubs, large campus, and diverse student population, it could benefit from low-scale mental health interventions to simultaneously address the needs of distressed individuals and facilitate connections among students. The integration of PFA into three existing health programs at Bard College – Bard Emergency Medical Services (BEMS), BRAVE counselors, and peer counselors –would enable efficient introduction and application of services Furthermore, these three services are student led, which may benefit campus-wide reception of the technique BEMS provides free, confidential, and on-site emergency
medical service 24/7 on Bard’s campus, with a focus on initial care and stabilizations of patients who require basic or further care (Bard EMS, n.d.). BEMS members have previously testified to situations in which they dealt with distressed individuals or experienced distress themselves during service. Considering the program's apparent emphasis on physical first-response, PFA could cater to any simultaneous symptoms of distress among injured individuals or BEMS members.

BRAVE counselors provide general counseling to students either in person or over the phone Students may request anonymity, facilitated by over-the-phone services, and counselors are trained to deal with numerous topics, including sexual violence and harassment, depression, anxiety, eating disorders, stress, sexuality and sexual orientation, and suicide (BRAVE Menu, n.d.).
Considering that BRAVE counselors already undergo extensive training in aspects of PFA like information gathering and linkage with relevant institutions, they
may serve as potential PFA trainers on campus for any interested individuals. Their firsthand experience with mental health intervention would complement PFA instruction well.
Peer counselors live in residence halls with students to provide direction and answer any questions These individuals also strive to create a unified community by hosting events and connecting with students beyond a superficial level (Engage in the Halls, n.d.). However, providing more structure to how PCs interact with students may increase their confidence when dealing with stressful situations and make distressed students feel heard.
An online study by Yorgasen et al (2008) sought to determine whether students knew about and utilized campus mental health services. Results revealed that 37% of respondents did not know how to contact such services, 30% had no knowledge of the services offered, and 38% knew of the services’ existence, but not their nature Thirty-three percent of students also cited that they did not use campus mental health services because they lacked time (Yorgasen et al., 2008). Increased interactions with students trained in PFA could help bolster mental health literacy among college communities. The efficient nature of PFA training and administration would also respond to time concerns.
The creation of a tangible reference including potential mental health services could give BEMS, BRAVE counselors, and
13|
PCs the tools necessary to help distressed students seek further care. By adhering to a stepped model of care, this document could cater to the needs of students facing varying levels of distress (Ho FY et al , 2016; WHO, 2022) These would be available in every residence hall, the library, the dining hall, and the campus center to enable widespread accessibility
Bard College’s campus includes a significant refugee population, with students hailing from Afghanistan, Ukraine, and Eurasia (Bard Institute for International Liberal Education, 2022). This warrants further attention since migrants, refugees and asylum seekers face an increased risk of developing or exacerbating existing mental health issues due to the precariousness of their situations (WHO, 2022). To effectively address student mental health, any interventions must cater to the specific needs of a distressed person. This necessitates the cultural adaptation of PFA to the language, culture, and context of those it intends to serve. Perera et al. (2020) proposes four steps – information gathering, adaptation hypotheses, local consultation with focus groups and community members, and external evaluations by specialists from the adaptation context – to achieve this Building a genuine understanding of different cultures requires the presence and input of those with lived experience in them. Therefore, the implementation of PFA in Bard student services must include workshops, with representatives from the diverse student population, with the goal of developing cultural sensitivity
Finally, Bard College may benefit from conducting training in PFA with students and interested community members in surrounding towns, such as Red Hook, Tivoli, and Kingston. The Bard Center for Civic Engagement (CCE) emphasizes the importance of interactions between students and community members through opportunities like volunteering, internships, research, and conferences (Bard CCE Community Partners, n d ) With Bard CCE’s aid and the willingness of community organizations – such as the Dutchess Stabilization Center of Family of Woodstock Crisis – students could introduce low-level mental health interventions to other relevant stakeholders. Many of the mental health resources listed on the Village of Red Hook’s crisis support website are hotlines or texting services, so the introduction of in-person strategies may prove valuable (Crisis Support, n.d.). The experience of undergoing training in PFA itself would serve as a valuable opportunity to interact with and form connections between trainees from Bard College and local communities alike. This may result in stronger relationships that would encourage continued cooperation regarding mental health education and services in the future.
Bard’s Trustee Leader Scholar Program (TLS) could potentially facilitate any attempts to introduce PFA to community organizations (Jorrin, n.d.). TLS scholars submit proposals that outline their plan, identify necessary resources and potential budgets, and explain how the project would have a positive impact. Students
attend workshops and one-one-ones with program administrators to cultivate their skills in public speaking, group work, communication, fundraising, and project organization Students also receive stipends to aid their work. Although these programs originate as student-led, many are later adopted as Bard College programs, their work continuing in perpetuity (Jorrin, n d )
Pending the outcome of this communitybased, student-led mental health project in Bard College, it could serve as a model for other college campuses in supporting student and community mental health Training non-specialists in low-intensity MHPSS interventions could lower stigma, cater to the lack of time or continued interest of potential trainees, lighten the burden on mental health professionals, address deficits in culturally appropriate care, and hopefully motivate future efforts at improving the spectrum of care in Global Mental Health.
Maya Gjonbalaj
Natasha Bashore-Walker

TELENOVELAS AND LATINX IMMIGRANT COMMUNITIES
: a way to intersect low-intensity interventions with worldwide mental health challenges
USING PM+ AND SH+ AS SCALABLE MENTAL HEALTH STRATEGIES
by Karina Gonzalez Perez
The Latinx immigration population is constantly growing, and therefore, the challenges they face grow in complexity every day. The mental health of any human being is likely affected in the context of migration, especially in the context of forced migration. Latinxs are particularly vulnerable to intergenerational trauma due to legacies of colonialism, political violence, and migration-related stressors (Cerdeña et al , 2021) The toll on mental health associated with immigrating to a new place, where you have to find a home, education, remake social ties, adapt to a new culture, and deal with economic insecurity (plus many other things) is a big one The lack of access to mental health care in migrant communities is a constant challenge that affects individuals involved. Some of the barriers Latinx immigrants have in regards to health care include: lack of culturally and language adapted services, discrimination by providers, external resource constraints (even worse if uninsured or underinsured), limited access to care (Ayón et al., 2020), plus dealing with the constant fear of deportation.
Given these challenges and mental health risks there is a need to develop novel strategies to fill gaps in care, in ways that are culturally responsive. One idea that has received little attention is the idea of integrating Mental Health and Psychosocial Support (MHPSS) strategies into digital media. There is considerable work from public health fields showing that television and radio can serve as a powerful tool for promoting positive health strategies but less has been examined in the context of mental health. A new pilot project, Tangling & Untangling: A Telenovela-based Adaptation of Manualized Transdiagnostic Scalable Mental Health Interventions for Displaced Spanish-Speaking Populations Globally, however, seeks to shed light on this idea It just had its first launch meeting this past Thursday, and I was incredibly lucky to be a part of it
We had a brief introduction to what the telenovela will look like, got some tips from the telenovela writing experts, and both of the interventions that we will be adapting: Problem Management Plus (PM+) and SelfHelp Plus (SH+) were introduced to the writers and the rest of the team. More conversations about how to culturally adapt this telenovela to the migrant Latinx community are meant to take place.
Culturally adapting any sort of intervention should be a priority of those in charge of it. The process of culturally adapting any intervention, treatment or even some sort of entertainment show takes time and resources, but the positive effects this can have on the targeted population make it worth it. As Grinner & Smith (2006) share in their article, when their interventions where culturally adapted and targeted to a specific cultural group they were four times more effective than the interventions they provided to groups from a variety of cultural backgrounds. In this same study, it was also shown how adaptations which were translated to the clients’ native language were twice as effective than those who were conducted in English only Culturally adapted interventions effectiveness can be explained by more openness to understanding from the client's side, better understanding of the intervention and sustained fidelity throughout intervention (Ferrer-Wreder et al., 2012; Bernal et al., 1995).
As the demographics in the United States change with the constant (often forced) migration of Latinx communities, entertainment like TV shows is forced to adapt to new communities and cultures who are watching A huge shift in digital media


that has been growing yearly are telenovelas (also known as soap operas). Telenovelas are a huge part of Latinx culture. They have emerged as a notable shift that Latinx scholars have identified as a long-lasting cultural force (Castañeda, 2020). Some put these shows into the same category of importance as fútbol or bachata for the culture’s heritage. The accessibility of mobile phones has made watching telenovelas a much easier activity, and one that can also create a sense of community when other people around you are also watching the same show. Suddenly, before commenting on the fútbol match from the day before, teenagers talk about the new episode that just came out and how they can identify with the characters When it comes to teenage and family telenovela watching, it is important to note that the impact some telenovelas can have on the population can be negative. This is why it is important to hold conversations with peers, friends and family, to clarify any questions or doubts that came with the show (Pérez, 2013), and therefore, this is another way to have a family conversation about important topics that might really help someone who is struggling Knowing this, having a telenovela geared towards mental health can be of great benefit to the population if community and family based conversations also take place to enhance the long-lasting impact the show can have

Culturally adapting an intervention can be seen through different actions by facilitators, which include translating it to the target language (and also adding specific phrases that are more accurate for the region or group), changing the illustrations on the materials used for the intervention to illustrations that might be more physically similar to the client and their environment, taking into account socioeconomic status and age of participants, and including existent issues or key cultural components that are part of the community Adam et al , (2023) share that in their research called Adapting Group Problem Management Plus (Group PM+) for Venezuelan Refugees and Migrants in Colombia, one of the cultural adaptations they did when giving PM+ to a group of Venezuelan refugees in Colombia was changing the word dificultades psicológicas (psychological difficulties) to problemas (problems) so that the intended audience could understand the statement better. These small changes can go a long way when it comes to the understanding of the intervention from the client, and therefore, this can have more positive impacts on the implementation of the intervention.
One of the interventions that we will focus on for the telenovela is Problem Management Plus (PM+) PM+ is a lowintensity psychological intervention for adults impaired by distress in communities who are exposed to adversity (World Health Organization, 2016) and it was created by the World Health Organization (WHO) in 2018, which originated in response to the urgent need of affordable and evidencebased interventions that can be adapted to a low-income setting. It started as an individual intervention, where there was one-on-one attention of the facilitator and the client but it has evolved to having a group option as well. It was designed to be delivered by lay helpers that do not have any sort of formal mental health care training, which helps address the lack of professionals in the area and the ongoing growth in the need for mental health care. It is based on 4 different strategies that are divided between the different sessions. PM+ is made up of five 90-minute sessions. The intervention also includes a pre and post-assessment session. The first strategy is Managing Stress It involves a series of breathing exercises and techniques to calm down at the peak moment of stress. Managing Problems is the second strategy, where they teach the client to make big problems seem smaller and to choose the solutions that make the most sense depending on their situation. The third strategy is Get Going, Keep Doing. The client is encouraged to try out activities that used to bring the most joy, which can directly impact their mood positively And the last strategy, Strengthening Social Support, helps clients reconnect with their support system that can go from friends, family members, to co-workers and community organizations.
The other intervention to be used for the telenovela is Self Help + (SH+). SH+ is another low-intensity intervention designed for adults who are experiencing stress, which was first published in 2021 This intervention is given by a facilitator (who does not need to be a mental health specialist) through five audio files, which the person can listen to while going about their day. There is also an illustration book that is followed as a complement to the audios. This intervention has been shown to reduce psychological distress and prevent the onset of mental disorders (World Health Organization, 2021) and it teaches a series of stress management skills.
Same as PM+, SH+ teaches clients a set of core skills they can develop through this intervention. The first skill is Grounding and it refers to bringing the attention back to the present moment, instead of staying stuck in an emotional storm, which can be very distressing The second skill is Unhooking This is a continuation of grounding skills. It involves separating from difficult thoughts and feelings by noticing and naming them, and after, going back to the present moment The third skill is Acting On Your Values. This skill involves identifying personal values and staying true to these values through your actions The fourth skill is Being Kind. As the name says, it involves being kind towards oneself and towards others And the last skill is called Making Room. This is the continuation of Unhooking but more advanced, which helps with noticing and naming difficult thoughts and allowing them to come and go, instead of just trying to fight them (World Health Organization, 2021).

After reviewing these two strategies and connecting the dots from the first team meeting, I am now constantly thinking about ways we can implement these strategies in a telenovela, where it is not seen as a class or as if the characters are trying to teach a lesson, but it is seen as something that can genuinely help watchers feel better. Even though these two interventions have proved to be effective in the short-term, there is still a need to find an intervention that can help people stay engaged and remember the strategies they just acquired for a longer period of time. This is where internet-based interventions, like the telenovela we are writing, play a key role in communities like Latinx immigrants. Not only will it help address external barriers (accessibility, transportation, costs, finding child care, language barrier) that can affect someone when seeking for care but it can also help dealing with internal barriers (stigma, discrimination, cultural beliefs, health literacy) the person has.
Telenovela interventions have had a positive effect on symptoms of depression through adopting positive thinking/coping skills (Kajiyama et al., 2017). A study done by Rosy Chavez-Najera as her dissertation for the University of Nevada, Reno called “Necesito Un Psicólogo” A Behavioral Activation Telenovela Intervention for Depressed Latinas had positive results. With the ongoing migration of Latinxs to the U.S., telenovelas provide cultural relevance important for maintaining cultural connectedness The participants in her study specified that some components of the intervention they found satisfactory were the fact that it was in Spanish, their engagement with the storyline, and their ability to identify with the characters (Chavez-Najera, 2023) which suggests how important it is to culturally adapt an intervention to receive more positive results. Another study done related to the one before, called ¡Yo no Estoy Loca! A Behavioral Health Telenovela Style Entertainment Education Video: Increasing Mental Health Literacy Among Latinas also showed that a video based intervention experienced statistically significant increases in mental health literacy as compared to the participants in the flier condition and that both the video and the flier contributed to shifts in stigma, (Gonzalez & Benuto, 2022) which also proves how an everyday entertainment can also have an impact on your mental health. Connecting this to the past month I spent in Bern, Switzerland, a topic that came up constantly in our discussions is the fact that the lack of professionals in the mental health area is a worldwide issue Taskshifting, a strategy that involves training
non-health specialists to be able to do a series of tasks, is a great way to ensure an effective use of available resources. By using a telenovela, a digital media that is usually watched by millions of people worldwide, to transmit a message of mental health and possible strategies to use when in distress, gives me hope It makes me think that even though understaffing issues are a constant conversation topic and oftentimes the source of burnout in many organizations, using something Latinx communities connect to their culture, like telenovelas, to help with an issue that affects many individuals, can have a great impact on this population
Going forward, I think this project can go a long way By making a telenovela about mental health and migration, it can help families who are struggling daily with the challenges faced when migration occurs by helping them feel supported and seen. It can also open the eyes of those communities around immigrants to offer help and be more understanding about the situation I think it could fill the current gaps of lack of information and consciousness around the migration experience and Latinx communities can be seen benefited by more awareness of the topic. I also think that with the fast-paced and growing world we live in, there must be constant change in interventions that can adapt to what is currently having an impact. Whether that is seen as a podcast, a movie, a radio show, or even a theatrical play, there must be different ways to implement MHPSS through low-intensity interventions that can leave long-lasting effects on the population.
I am excited to see where this project is going and I am ready to give my best to help as many people as possible.
CULTURAL CONSIDERATIONS OF BUILDING PIPELINES INTO THE MENTAL
HEALTH INDUSTRY FOR ASIAN IMMIGRANT YOUTH
Investigations of intergenerational community building and apprenticeships in community-based organizations
Youth mental health is a critical issue, with rising rates of anxiety, depression, and other mental health disorders (WHO, 2022). The pressures faced by the youth today are diverse, encompassing academic, social, and personal challenges. For adolescents, microsystems such as families, schools, and communities can profoundly impact acculturation and development. Secure attachment to school and parental support systems, for instance, may be key protective factors for mental and physical health during a developmental period when distress is high. These concerns are compounded for immigrant youth, who must also learn to integrate home and host cultures and learn to form positive attachments to diverse individuals (Patel et al., 2022).
These issues are particularly acute for Asian American immigrant youth, who encounter unique cultural barriers and stigmas surrounding mental health As Asian American patients reported greater satisfaction with care if their doctor was of the same race or ethnic background than if their doctor was of a different background (Hopkins-Tanne, 2002),
the underrepresentation of Asian American clinicians can also present additional barriers to trust in service providers by immigrants and perceptions of mental health careers
Namely, clients of color being treated by a white therapist assumed that their provider lacked understanding of their racialized experience, and may decide to avoid topics related to race in their sessions (Kormendi & Brown, 2021). In order to effectively address these gaps in mental health care in the Asian American community, it is imperative to increase both the capacity and representation of mental health care Addressing these shortages, however, is a matter that extends beyond practical concerns and is instead deeply intertwined with
historical and systemic issues in the U S that contribute to internalized stigma and other cultural aspects of identity-related mental health These factors, some of which will be highlighted in the next section, emphasize the importance of culturally competent care and the need for the involvement of community members who understand the unique challenges faced by Asian Americans.
The relative invisibility of Asian American history within educational systems can leave behind lingering social and psychological effects of unresolved legacies of imperialism and colonialism (Cai & Lee, 2022). Thus, for younger generations of Asian Americans, understandings of themselves, their cultures, and their ethnic-racial identities largely depend on intergenerational communication within families and communities about these histories and experiences. However, the desire of immigrant families to fit in or to avoid burdening the next generation can also overshadow the importance of preserving cultural connections. Prolonged unresolved distress, especially regarding one’s cultural history, can create an accumulating stressinduced burden on overall systemic functioning due to demands of cognitive energy that can have spillover effects on long-term well-being, academic performance, and one’s general selfefficacy (Suh et al., 2022), one’s belief in their ability to succeed
Family-oriented interdependence can also mean that any decision-making process, including career decisions, is influenced by the interests of the family. Additionally, cultural stigma surrounding mental health is a significant barrier. Values emphasizing
family honor, self-reliance, and the avoidance of shame contribute to viewing mental health issues as personal weaknesses, discouraging individuals from seeking help. This stigma is often reinforced by parental and community expectations that prioritize academic and career success over mental well-being.
A pervasive negative consequence of internalizations of the model minority stereotype (MMS) – the perception that Asian Americans are “living examples of advancement” because of their racial or cultural differences – has been its infiltration into mental and physical health research and practice (Walton & Truong, 2023).
Namely, the perception that Asian immigrants in Western countries are successful and thus do not need research or clinical attention may also contribute to reduced resource allocation to this group in research, clinical care, and outreach (Gao et al., 2024). While the MMS may affect the quality of care experienced by immigrant youth, it can also indirectly affect the quality of mental health care in these communities by fragmenting potential pipelines into mental health careers In other words, as a consequence, the representation and perception of the need for research into the specific cultural needs of the Asian immigrant youth populations to support mental health become limited
Furthermore, dependence and obedience to authority exhibited by individuals with a collectivistic value orientation can also increase the desire to consider the needs and expectations of family members for important life decisions such as career choices (Leong & Tang, 2002). While Asian Americans exhibited lower levels of career maturity – readiness for career decisionmaking – than white Americans,
they did not differ in terms of vocational identity – the formation and consolidation of career goals and self-concepts (Leong & Tang, 2002). Trusted by parents to make informed decisions regarding the success of their children, career counselors often play a crucial role in shaping the professional aspirations of Asian American youth. However, these counselors can sometimes exhibit biases that inadvertently steer students away from careers such as those in mental health by prioritizing STEM (Science, Technology, Engineering, and Mathematics) fields due to perceived stability, prestige, and financial security associated with these careers. In other words, due to cultural influences of deference and trust in authority figures to make important decisions, individuals may defer their career decisions to others in the family and trusted sources despite their own interest in other careers. Counselors themselves may also lack awareness or understanding of the mental health field's importance and potential, further perpetuating the underrepresentation of Asian Americans in this sector. Altogether, long-standing stereotypes, discrimination, and marginalization contribute to a cycle that limits self-efficacy and reduces transparency about pathways for mental health careers for this population. Addressing structural limitations requires proactive strategies to foster interest and create more transparent pathways for individuals in these underrepresented communities.
Building capacities toward a more inclusive mental health workforce
One promising initiative that may be used to address workforce shortages is the Swiss Apprenticeship Model to create more transparent career pathways in the mental health field for Asian American youth. In Switzerland, approximately 70% of students chose to do an apprenticeship. The apprenticeship system is highly valued for the opportunity to transition from basic compulsory education to employment through a dual system that combines classroom instruction with onthe-job training to prepare them for highdemand, high-skilled jobs in rapidly evolving industries. For individuals of lower socio-economic status, it provides a safe route to stable employment following education, as apprenticeships are coordinated with market demands by both the government and companies. Apprenticeships follow a specialized program created in collaboration with vocational schools and organizations including targeted critical competencies, soft skills such as communication, problem-solving, and teamwork, and to gain a holistic understanding of the organizational structure. This model may be applied to address pipelines for mental health, specifically for Asian American populations as it reduces the lack of transparency that may be created by biases against these careers. While the educational model of Switzerland may be too expansive and costly to implement on a national scale in the U.S., smaller public-private collaborations such as the Youth Mental Health Corps can help to address the
growing mental health needs of young people by making career pathways to mental health more accessible (AmeriCorps, 2024). Members serve middle and high school students in schools and community-based organizations. They gain valuable on-the-job experience, receive a stipend, and earn credentials to advance their careers. Additionally, members are eligible for awards to pursue higher education or pay back qualifying student loans to support their education and development The integration and placement of members within schools and local organizations can also help make pathways into mental health careers more accessible and transparent to Asian American immigrant youth, where financial burdens can often pose significant challenges to obtaining further degrees that are required to obtain clinical licensing Another initiative in the U.S. that serves to address Asian American youth mental health, Let’s Talk, may provide additional insight into reducing stigmatized attitudes toward mental health through the combination of discussions with students, parents, mental health professionals, and other community members to invoke a more intergenerational, community-based approach to addressing the mental health needs of the community (Kim et al , 2020) This one-day conference, organized by 30 college students, graduate students, and alumni, focused on equipping parents of Asian and Asian American high school students with strategies to better support their children's emotional well-being (Kim et al, 2020). Social contact through peer-led networks and organizations, such as the Let’s Talk conference, is suggested to
be among the most effective types of intervention to improve stigma-related knowledge and attitudes (WHO, 2022), emphasizing the social, cross-cultural, and intergenerational nature of mental health risks among Asian American students with a culturally specific content and a culturallyspecific approach can be transformative in transforming attitudes on mental health by empowering the community as a whole in a collective effort towards greater advocacy. Leveraging the conference as an opportunity for learning and sharing of community members, the conference sought to challenge both professionalacademic and familial-generational deference by highlighting student voices in panel sessions, engaging parents in perspective-taking exercises, and providing mental health professionals with a platform to share their expertise Participants were equipped with skills to address emotional expression and communication differences, especially across familial and immigration generational gaps.

The initiative also underscored the importance of families and social connections in understanding intergenerational and cross-cultural differences. More specifically, fostering opportunities for open communication between parents and children about past experiences and adversities can also help children see their parents and ethnic connections as resilient and empowering (Cai & Lee, 2022), fostering closer relationships between parents and children and reinforcing the need for dialogue about dismantling systemic barriers that can interfere with adolescent identity development and wellbeing. At the culmination of the conference, participants expressed a desire for more direct dialogue and discussion, highlighting the continued need for iterative learning through cycles of exposure, reflection, and behavioral integration. While the conference primarily sought to expose participants to imminent mental health challenges and provide a safe space for diverse perspectives on mental health, an expansion could include inviting leaders of community-based organizations with similar goals to discuss opportunities for students passionate about Asian American mental health outreach and advocacy. The adaptation of the apprenticeship model to the field of community mental health is critical as cultural adaptation of mental health is dynamic, nuanced, and often situationbased, and thus cannot always be taught in classroom settings. Additionally, collaboration between educational institutions and community mental health organizations can ensure that training programs are aligned with industry needs
and that students gain relevant, hands-on experience. For instance, by incorporating discussions about challenges experienced at placements in schools and community centers, individuals can build on interests and connections established at conferences to increase the depth of learning about the practical adaptation and implementation of mental health interventions.
Programs would also provide training for diverse peer specialists who have experienced mental health challenges, and who can lend insight into personal experiences related to their culture and history. Early exposure to careers in mental health through paid apprenticeships at community mental health centers can not only increase interest in mental health careers but also instill leadership competencies in the next generation, as these experiences can also help high school students jump-start their careers. Social services, such as Garden of Hope, offer a comprehensive range of programs that can serve as a model for building additional pipelines to increase awareness of mental health careers and enhance selfefficacy through greater mental well-being and social connection. Garden of Hope’s community centers in the Queens and Brooklyn Family Justice Centers in New York City provide critical care for serving and rebuilding the lives of survivors of domestic violence, sexual assault, and human trafficking, specifically targeting the growing NYC-area Chinese community.
The framing of mental health as a community issue within discussions of mental health is of particular importance for collectivistic-value individuals, as cultural beliefs and internalized stereotypes can

have negative impacts on social, educational, and health outcomes. While aforementioned community efforts may not completely eradicate racial and systemic inequities, structured multi-stakeholder partnerships can help to fund and support the Asian American youth in creating pathways of leadership and empowerment within the communities to which they feel most personally connected.
Extending the efforts of both youth-led conferences and placements of students in paid apprenticeships at community centers, especially those with lived experiences of mental health challenges, can pave a new path for the youth to become more actively involved in the work of grassroots community organizations. In addition to collaborative team building through a social justice framework, the inclusion of culturally relevant psychoeducation delivered by peer mentors of similar backgrounds, such as education about the effects of internalized MMS and racial stress may be instrumental in not only expanding outreach on the diversity of the Asian American immigrant experience from a youth perspective, but also to reverse the impacts of internalization of negative stereotypes on self-efficacy, starting from the communities most impacted by the stigmatization of mental health.
Abigail Wang
PSYCHOLOGICAL INTERVENTION PROJECT: GRACE CHURCH– HOUSTON, TX
by Andrea Morantes
According to the WHO, mental health and mental disorders continue to impact individuals in vulnerable communities drastically; such experiences can cause various difficulties in one’s daily life tasks and relationships i.e. family, friends, and communities (World Health Organization, 2024). The field of global mental health (GMH) aims to address such challenges to promote mental health equity and human rights (Moitra et al., 2023). Additionally, psychologists and researchers in the WHO have created action plans such as the “WHO Special Initiative for Mental Health (2019–2023): Universal Health Coverage for Mental Health” to promote quality and affordable mental health care among 100 million people in 12 different countries (World Health Organization, 2024). Despite the various action programs to address mental health challenges, barriers continue to prevent low-income communities from accessing mental health resources as it may relate to a lack of mental health education, economic resources, cultural experiences, etc For example, CDC and psychological researchers have identified that mental disorders begin in early childhood and the most prevalent diagnosis among U S children and adolescents ages 3-17 years were attention-deficit/hyperactivity disorder and anxiety, affecting one in 11 children (CDC, 2024). In 2019, 36.7% reported persistently feeling sad or hopeless in the past year and 18.8% considered attempting suicide; approximately seven in 100,000 adolescents 1019 years old died by suicide in 2018 and 2019 (Bitsko et al , 2022) Such mental health challenges among children and adolescents have been associated with immediate and long-
term physical health risks, social relationships, education, and employment (Bitsko et al., 2022).
To potentially address such barriers, the WHO has created various low-intensity psychological intervention manuals that allow non-specialists to deliver and assist individuals in distress or experiencing depression and anxiety (World Health Organization, 2024). Additionally, the WHO also suggests utilizing a self-guided stepped model that essentially guides individuals to support themselves as they experience manageable forms of psychological distress (World Health Organization, 2024). Early Adolescent Skills for Emotion (EASE) created by the WHO allows for interactive psychological support for a group of young adolescents experiencing forms of mental distress such as anxiety, depression, and stress (World Health Organization, 2024) Particularly focusing on young adolescents ages 10-15, the group session will allow the adolescents to collectively work together to develop healthy coping mechanisms as they experience forms of psychological distress. Current research and trials in low-income countries with vulnerable populations such as Syrian refugees and Lebanon communities highlight the effectiveness of EASE as young adolescents experience forms of psychological distress (Jordans et al., 2023). Incorporating low-intensity psychological interventions among adolescents and children such as EASE may assist them and their families to understand and manage psychological distress. Although self-guided step modules may be as beneficial, intervention programs that require community engagement may promote greater benefits by assisting adolescents, their communities, families, etc
To continue, low-intensity psychological intervention programs highlight the importance of community engagement, which permits individuals with similar cultural backgrounds and experiences to provide psychological support. Researchers have identified that community engagement is vital in addressing the barriers that prevent lowincome communities and individuals from accessing mental health resources and education (Fancourt et al , 2021) Community engagement refers to the relationships between individuals' social, cultural, and community engagement to address mental health barriers; particularly focusing on the mode of engagement, the process of engagement, and the structure that implicates engagement (Fancourt et al., 2021). To appropriately incorporate community engagement researchers and psychologists should consider cultural adaptions to support communities; cultural adaptation enhances the acceptability and effectiveness of psychological interventions among culturally diverse communities (Heim & Kohrt, 2019) The cultural adaption framework consists of three elements–cultural concepts of distress, treatment components, and treatment delivery to appropriately support diverse communities and enhance their willingness for psychological support (Heim & Kohrt, 2019)
The U.S. Census has statistically identified Houston, TX as the number one most diverse city in the United States (Bureau, 2024). Based on the current research and issues that continue to prevent individuals from seeking mental health services, implementing psychological interventions such as EASE can effectively support communities in Houston, TX. The diverse populations that reside in Houston, TX will greatly benefit from psychological
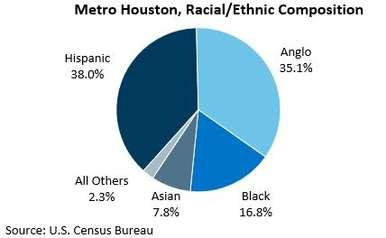
interventions as it permits nonspecialist individuals in the community to support one another Although Houston has various organizations that provide services, mental health remains unaddressed which emphasizes the need to collaborate with an organization to begin supporting the communities as they experience mental health challenges. Grace church located in Houston, TX aims to support individuals in various ways; volunteers and leaders provide support and resources for the community by supporting foster care children, Bridge Over Troubled Waters (women's shelter for domestic and sexual violence survivors), and vulnerable individuals. Despite offering various community engagement programs no psychological or mental health resources are available at Grace church Developing a partnership with Grace church will allow volunteers and leaders to deliver a psychological intervention– EASE to support future generations. Before implementing an intervention that requires clinical support, financial sponsorship, and efficient time by all members, psychological first aid can introduce the great benefits of mental health services. Psychological firstaid, PFA will introduce various forms of mental health services that aim to support psychological needs I aim to train leaders and volunteers while they complete the connect track requirement, which essentially connects volunteers to different ways to serve and support the community.
In closing, this project may currently not require an introduction to upcoming research, but the on-field work will allow me to support my community members and address the barriers to mental health services As I continue working on this project, I aim to introduce and start conversations with Grace church leaders to train volunteers in psychological first aid. The introduction of PFA will permit me to consider the communities’ approach to advanced material in lowintensity interventions such as EASE During that time, I will develop a partnership with a licensed psychologist who will oversee this project and potential donors interested in supporting the church and local community Lastly, I will consider the benefits of adopting other forms of psychological support for younger children under 10 and their caregivers to provide mental health education and support Grace church members and I are eager and willing to provide mental health support to all community members and the future generations of Houston, TX, and around the United States

EVALUATING THE POTENTIAL BENEFITS OF INTEGRATING PM+ AND PFA TO ADDRESS MENTAL HEALTH CHALLENGES AMONG
COMMUNITY COLLEGE STUDENTS
FOCUSING ON CUNY CAMPUS & STUDENTS
Problem management plus (PM+) is a psychological intervention designed to help adults manage symptoms of depression, anxiety and burnout (Dawson et al., 2015). Additionally, PM+ aims to assist individuals in handling practical problems, such as unemployment, displacement and interpersonal conflict Studies have shown that PM+ effectively minimizes symptoms of mild depression and anxiety (Dawson et al , 2015) PM+ was developed by the World Health Organization (WHO) in response to global shortages of mental health specialists, promising to increase accessibility to psychological care services (Dawson et al , 2015) This intervention consists of five weekly in-person sessions that expose participants to various problem-solving, stress management and behavioral treatment techniques (Dawson et al., 2015).
Psychological first aid (PFA) is another mental health intervention with similarities to PM+, but with a distinct approach Initially developed by the National Child Traumatic Stress Network (NCTSN) and the National Center for PTSD, PFA provides immediate assistance and support to individuals in distress following natural disasters, humanitarian crises and trauma (NCTSN, n.d.). This paper review will focus

on a specific manual adapted by the Red Cross and Red Crescent Societies, which offers simple guidelines that anyone can use to help reduce psychological distress in times of uncertainty (Minihan et al., 2020). PFA is not therapy or professional counseling; it is a series of actions aimed at alleviating human suffering (IFRC Psychosocial Centre, 2018). PFA is designed to make individuals feel safe, connected, calm, and hopeful, which positively impacts long-term recovery after a crisis (Minihan et al., 2020).
Both PM+ and PFA are low-intensity and cost-effective interventions that can be delivered by trained nonspecialists: with brief training and appropriate supervision, individuals without a background in mental health can effectively implement these interventions (Dawson et al , 2015) This task-shifting approach can help reduce the need for high intensity psychological interventions, such as cognitive behavioral
therapy, for mild to moderate symptoms of depression and anxiety. It allows primary care doctors and other hospital staff to be the first line of support (Lange, 2021). This potentially reduces reliance on scarce specialists, making mental health services more accessible to individuals who present more severe medical conditions (Lange, 2021). Moreover, PM+ and PFA are transdiagnostic and easily adaptable interventions that target a wide range of common mental disorders e.g., depression, anxiety, etc (Dawson et al., 2015) They can also be adapted into different languages, cultures, and contexts to better serve various communities (Dawson et al., 2015).
Mental Health in College
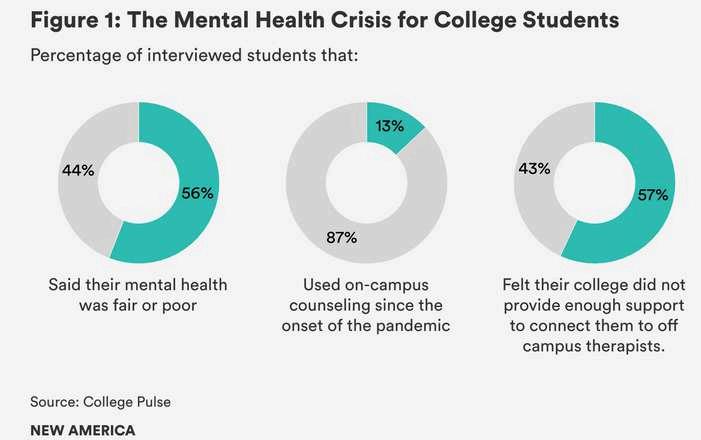
In a 2019 survey, 87% of college students reported feeling overwhelmed by their work, 85% felt mentally exhausted and 66% felt overwhelmingly anxious (Geary, 2022). Post-Covid-19 pandemic studies indicate
that these feelings of stress, anxiety, and isolation have reached unprecedented levels A March 2022 survey revealed that approximately 56% of respondents rated their mental health as fair or poor, only 13% had used on-campus counseling during the pandemic, and 57% felt their college did not provide adequate support to connect them to off-campus therapists (Geary, 2022).
Mental Health in Community College
Research suggests that community college students have greater mental health needs than their counterparts at four-year institutions, yet they often have access to fewer services Community colleges, typically, have much less funding and fewer services to address their students’ needs; and the Covid-19 pandemic exacerbated these challenges, straining already limited resources and increasing the difficulty of implementing and affording the costs of oncampus mental health interventions (Geary, 2022)
Many community college students come from low socioeconomic backgrounds. Over 70% of these students have household incomes of less than $30,000 a year, and they struggle to pay nontuition costs, such as books and transportation (Weissman, 2021) During the pandemic, nearly 40% of CUNY students lost their job, and 55% faced housing insecurities (GeringerSameth, 2020). Some reported experiencing hunger during their studies (Geringer-Sameth, 2020) Covid-19
Student Parents and First Generation College Students
In 2016, nearly half of CUNY students were first generation college students, and about 1 in 10 were parents or single parents (Geringer-Sameth, 2020). First generation college students and single student parents constitute a significant portion of the community college population and exhibit heightened mental health challenges (Geary, 2022). Additionally, a 2021 study by Ascend at the Aspen Institute and the Jed foundation found that approximately 43% of student parents in the United States experience extreme levels of stress, negatively impacting their educational success and mental health, with 38% considering dropping out in the last 30 days (2021). Major stressors include financial concerns and feelings of isolation on campus (Ascend Aspen Institute, 2021).

Integration of PM+ and PFA at CUNY Community Colleges
Incorporating PM+ and PFA at CUNY community colleges offers numerous benefits. PM+ equips students with effective strategies to think critically, address and cope with personal challenges such as interpersonal conflict and unemployment. PM+ can be especially beneficial for first generation and first year college students as they transition into college life by providing strategies to better process and manage stress and burnout. The implementation of PM+ into first year programming a program typical of both community and four-year colleges for new students can contribute to their academic success and meet their mental health needs. Moreover, PFA serves as a supportive tool for those experiencing psychological crises. Community college students trained in PFA would learn how to identify signs of distress, how to listen actively and how to connect peers to additional resources when necessary. Given the heightened demand for mental health services at community colleges, interventions such as PFA and PM+ can serve as the first line of support and guidance for those in need. Their adaptability and the fact that they can be administered by trained nonspecialists ensure that implementing these strategies does not require extensive resources
Overall, integrating and implementing problem management plus (PM+) and psychological first aid (PFA) at CUNY community colleges offers a promising approach to addressing the rising mental health challenges among community college students. These interventions provide accessible and cost-effective strategies for managing stress and mild symptoms of anxiety and depression. By equipping students with the tools to navigate personal and academic challenges, PM+ and PFA can potentially enhance their overall well-being and academic success.
Engers Polanco Tejada

Acknowledgments
Our sincere thanks to all the individuals and organizations who contributed to the CFMDE Summer Program. Your generous sharing of insights on global mental health and forced migration, as well as discussions on current challenges and innovative initiatives for future change have been invaluable
















2024 Bern Study Abroad Organizing Committee

Principal Investigator / Program Lead
Professor of Psychology at The New School
Adam Brown brownad@newschool.edu
Program Coordinator
Mental Health & Psychosocial Support
Technical Specialist at The New School
Alesha Cid Vega cidva377@newschool.edu
Program Coordinator
Research Coordinator at The New School
Linda Kim (Han) kims5@newschool.edu
Program Coordinator
Research Associate at The New School
Janus Wong wongj1@newschool.edu

Sarah Lawrence College
Enhancing Mental Health Services at Welcome Corps
kakhalbedashvili@gm slc edu

Bard College
Integrating PFA into Existing Health Care Services at Bard College
nb3745@bard.edu

Bard College
Integrating PFA into Existing Health Care Services at Bard College
mg0995@bard.edu
Bennington College
Telenovelas and Latinx immigrant communities
Karinagonzalezperez@bennington edu

Bennington College
Psychological Intervention Project: Grace Church– Houston, TX
andreamorantes@bennington.edu

Sarah Lawrence College
Evaluating the Potential Benefits of Integrating PM+ and PFA...

Cultural


References
A Guide to Psychological First Aid for Red Cross and Red Crescent Societies, IFRC Reference Centre for Psychosocial Support, Copenhagen, 2018. American College Health, 57(2), 173–182. https://doi.org/10.3200/JACH.57.2.173- 182 American families. Adversity and Resilience Science, 3(3), 233-245. American student mental health. Community Mental Health Journal, 57, 1001-1009. AmeriCorps. (2024). Eleven States Launch New Initiative to Address America’s Youth Mental Health Crisis. AmeriCorps.
Ascend Aspen Institute. (2021, May 26). New Study: Student Parents in College Experience Unique Mental Health Challenges but Lack Access to Support on Campus. https://ascend.aspeninstitute.org/new-study-student-parents-in-college-experienceunique-mental-health-challenges-but-lack-access-to-support-on-campus/
Asian American Federation. (2024). Bridging the gap: policy recommendations for improving Asian American mental health services. Asian American Federation. https://www.aafederation.org/wp-content/uploads/2024/04/Mental-HealthRoundtable-Policy-Brief_FINAL.pdf
Ayón, C., Nieri, T., & Gurrola, M. (2020). Latinx immigrant health and mental health. In Encyclopedia of Social Work. Bard CCE Community Partners. (n.d.). Bard Center for Civic Engagement. Retrieved July Bard EMS. (n.d.). Bard College. Retrieved July 25, 2024, from https://www.bard.edu/campus/departments/bems/ Bard Health-Counseling-Wellness. (n.d.). Health, Counseling, and Wellness at Bard College. Retrieved July 26, 2024, from https://hcw.bard.edu/ Bard Institute for International Liberal Education. (2022, January 25). Bard Institute for International Liberal Education. Retrieved July 26, 2024, from https://iile.bard.edu/afghanistan/
Bernal G, Bonilla J, Bellido C. Ecological validity and cultural sensitivity for outcome research: issues for the cultural adaptation and development of psychosocial treatments with Hispanics. J Abnorm Psychol. 1995;23(1):67-82.
Bitsko RH, Claussen AH, Lichstein J, Black LI, Jones SE, Danielson ML, Hoenig JM, Davis Jack SP, Brody DJ, Gyawali S, Maenner MJ, Warner M, Holland KM, Perou R, Crosby AE, Blumberg SJ, Avenevoli S, Kaminski JW, Ghandour RM; Contributor. Mental Health Surveillance Among Children - United States, 20132019. MMWR Suppl. 2022 Feb 25;71(2):1-42. doi: 10.15585/mmwr.su7102a1. PMID: 35202359; PMCID: PMC8890771.
BRAVE Menu. (n.d.). Bard College. Retrieved July 25, 2024, from https://www.bard.edu/brave/ Crisis Support. (n.d.). Red Hook Village, NY. Retrieved July 29, 2024, from https://www.redhookvillage.org/218/Crisis-Support
Brown, Adam D., M. Claire Greene, Manaswi Sangraula, Annie Bonz, Diany Castellar, Valeria Merino, Jennifer Diaz, Marcela Venegas, Camilo Ramirez, Maria Cristobal, Luisa Morales, Ana Maria Trejos, Ana Maria Chomorro Coneo. (2023). Adapting Group Problem Management Plus (Group PM+) for Venezuelan Refugees and Migrants in Colombia. Final Report. Long-term Assistance and Services for Research - Partners for University-Led Solutions Engine (LASER PULSE Consortium).
Brown, F.L., Taha, K., Steen, F. et al. Feasibility randomized controlled trial of the Early Adolescent Skills for Emotions psychological intervention with young adolescents in Lebanon. BMC Psychiatry 23, 131 (2023). https://doi.org/10.1186/s12888-02304571-9
Bureau, U. S. C. (2024.). Explore census data. https://data.census.gov/profile/Houston_city,_Texas?g=160XX00US4835000
Cai, J., & Lee, R. M. (2022). Intergenerational communication about historical trauma in Asian call for task-sharing interventions. SSM-Mental Health, 1, 100006.
Castañeda, M. (2020). Television and its impact on Latinx communities. The Oxford handbook of Latino studies, 462.
Centers for Disease Control and Prevention. (2022, February 24). Mental health surveillance among children - United States, 2013–2019. Centers for Disease Control and Preventionhttps://www.cdc.gov/mmwr/volumes/71/su/su7102a1.htm? trk=public_post_comment-text#suggestedcitation
Cerdeña, J. P., Rivera, L. M., & Spak, J. M. (2021). Intergenerational trauma in Latinxs: A scoping review. Social Science & Medicine, 270, 113662.
Chavez-Najera, R. (2023). Necesito Un Psicólogo” A Behavioral Activation Telenovela Intervention for Depressed Latinas (Doctoral dissertation, University of Nevada, Reno).
Dawson, Deborah & Bird, Susannah & Horsburgh, Gavin & Ball, Alex. (2015). Dawson et al. 2015 Supplementary File 1 Enhanced bird markers.
Dawson, K. S., Bryant, R. A., Harper, M., Kuowei Tay, A., Rahman, A., Schafer, A., & van Ommeren, M. (2015). Problem Management Plus (PM+): a WHO transdiagnostic psychological intervention for common mental health problems. World Psychiatry, 14(3), 354–357. https://doi.org/10.1002/wps.20255
Dawson, K. S., Watts, S., Carswell, K., Shehadeh, M. H., Jordans, J. D., Bryant, R. A., Miller, K. E., Malik, A., Brown, F. L., & Servili, C. (2019). Improving access to evidence-based interventions for young adolescents: Early Adolescent Skills for Emotions (EASE). World Psychiatry, 18(1), 105-107. https://doi.org/10.1002/wps.20594
De Graaff, A. M., Cuijpers, P., Acarturk, C., Bryant, R., Burchert, S., Fuhr, D. C., Huizink, A. C., de Jong, J., Kieft, B., Knaevelsrud, C., McDaid, D., Morina, N., Park, A. L., Uppendahl, J., Ventevogel, P., Whitney, C., Wiedemann, N., Woodward, A., & Sijbrandij, M. (2020). Effectiveness of a peer-refugee delivered psychological intervention to reduce psychological distress among adult Syrian refugees in the Netherlands: study protocol. European journal of psychotraumatology, 11(1), 1694347.
Engage in the Halls. (n.d.). Bard College. Retrieved July 25, 2024, from https://www.bard.edu/reslife/residencehalls/engage/ Fancourt, D., Bhui, K., Chatterjee, H., Crawford, P., Crossick, G., DeNora, T., & South, J. (2021). Social, cultural and community engagement and mental health: crossdisciplinary, co-produced research agenda. BJPsych Open, 7(1), e3. doi:10.1192/bjo.2020.133
Ferrer-Wreder L, Sundell K, Mansoory S. Tinkering with perfection: theory development in the intervention cultural adaptation field. Child Youth Care Forum. 2012;41(2):14971.
Gao, C., Cho, L. L., Dhillon, A., Kim, S., McGrail, K., Law, M. R., ... & Barbic, S. (2024). Understanding the factors related to how East and Southeast Asian immigrant youth and families access mental health and substance use services: A scoping review. Plos one, 19(7), e0304907.
Geary, Chris. (2022, May 3). The Growing Mental Health Crisis in Community Colleges. New America. https://www.newamerica.org/education-policy/edcentral/the-growingmental-health-crisis-in-community-colleges/ Geringer-Sameth, Ethan. (2020, June 11). Challenges, Uncertainty Abound for CUNY System and Its Students, Faculty and Staff. Gotham Gazette. https://www.gothamgazette.com/state/9483-challenges-uncertainty-cuny-schoolsstudents-faculty-staff coronavirus#:~:text=URL%3A%20https%3A%2F%2Fwww.gothamgazette.com% 2Fstate%2F9483,100
Gonzalez, F., & Benuto, L. T. (2022). ¡ yo no estoy loca! A behavioral health telenovela style entertainment education video: Increasing mental health literacy among latinas. Community mental health journal, 58(5), 850-861.
Griner, D., & Smith, T. B. (2006). Culturally adapted mental health intervention: A metaanalytic review. Psychotherapy: Theory, Research, Practice, Training, 43(4), 531–548. https://doi.org/10.1037/0033-3204.43.4.531
Hansen, P. (2018). A Guide to Psychological First Aid for Red Cross and Red Crescent Societies (L. Vinther-Larsen & N. Wiedemann, Eds.). IFRC Reference Centre for Psychosocial Support.
Heim, E., & Kohrt, B. A. (2019). Cultural adaptation of Scalable Psychological Interventions: A new conceptual framework. Clinical Psychology in Europe, 1(4). https://doi.org/10.32872/cpe.v1i4.37679
Hopkins Tanne J. (2002). Patients are more satisfied with care from doctors of same race. BMJ : British Medical Journal, 325(7372), 1057. https://americorps.gov/newsroom/press-release/eleven-states-launch-newinitiative-addre ss-americas-youth-mental-health https://doi.org/10.1080/20008198.2019.1694347
IFRC Psychosocial Centre. (2018). A Guide to Psychological First Aid. https://pscentre.org/resource/a-guide-to-psychological-first-aid-for-red-cross-redcrescent-societies/
Jordans, M. J. D., Kohrt, B. A., Sangraula, M., Turner, E. L., Wang, X., Shrestha, P., Ghimire, R., Van't Hof, E., Bryant, R. A., Dawson, K. S., Marahatta, K., Luitel, N. P., & van Ommeren, M. (2021). Effectiveness of Group Problem Management Plus, a brief psychological intervention for adults affected by humanitarian disasters in Nepal: A cluster randomized controlled trial. PLoS medicine, 18(6), e1003621. https://doi.org/10.1371/journal.pmed.1003621
Jordans, M. J., Brown, F. L., Kane, J., Taha, K., Steen, F., Ali, R., Elias, J., Meksassi, B., Aoun, M., Greene, C. M., Malik, A., Akhtar, A., Van Ommeren, M., Sijbrandij, M., & Bryant, R. (2023). Evaluation of the Early Adolescent Skills for Emotions (EASE) intervention in Lebanon: A randomized controlled trial. Comprehensive Psychiatry, 127, 152424. https://doi.org/10.1016/j.comppsych.2023.152424
Jorrin, C. (n.d.). Trustee Leader Scholar Program. Bard Center for Civic Engagement. Retrieved July 29, 2024, from https://cce.bard.edu/student-leadership/tls/ Kajiyama, B., Fernandez, G., Carter, E. A., Humber, M. B., & Thompson, L. W. (2017). Helping Hispanic dementia caregivers cope with stress using technology-based resources. Clinical Gerontologist, 41(3), 209–216. https://doi.org/10.1080/07317115.2017.1377797
Kim, J. M., Kim, S. J., Hsi, J. H., Shin, G. H. R., Lee, C. S., He, W., & Yang, N. (2021). The “let’s talk!” Conference: A culture-specific community intervention for Asian and Asian American student mental health. Community Mental Health Journal, 57, 1001-1009.
Kormendi, N. M., & Brown, A. D. (2021). Asian American mental health during COVID-19: a call for task-sharing interventions. SSM-Mental Health, 1, 100006. Lange, K. W. (2021). Task sharing in psychotherapy as a viable global mental health approach in resource-poor countries and also in high-resource settings. Global Health Journal, 5(3), 120–127. https://doi.org/10.1016/j.glohj.2021.07.001
Leong, F.T.L., Tang, M. (2002). A Cultural Accommodation Approach to Career Assessment with Asian Americans. In: Kurasaki, K.S., Okazaki, S., Sue, S. (eds) Asian American Mental Health. International and Cultural Psychology Series. Springer, Boston, MA. https://doi.org/10.1007/978-1-4615-0735-2_18
McBride, O., Butter, S., Murphy, J., Hartman, T. K., McKay, R., Hyland, P., Shevlin, M., Bennett, K. M., Stocks, T. V. A., Lloyd, A., Gibson-Miller, J., Levita, L., Mason, L., Martinez, A. P., Vallières, F., Karatzias, T., & Bentall, R. P. (2022). Tracking the psychological and socio-economic impact of the COVID-19 pandemic in the UK: A methodological report from Wave 5 of the COVID-19 Psychological Research Consortium (C19PRC) Study. International journal of methods in psychiatric research, 31(4), e1928. https://doi.org/10.1002/mpr.1928
Minihan, E., Gavin, B., Kelly, B. D., & McNicholas, F. (2020). COVID-19, mental health and psychological first aid. Irish Journal of Psychological Medicine. https://doi.org/10.1017/ipm.2020.41
Moitra, M., Owens, S., Hailemariam, M., Wilson, K. S., Mensa-Kwao, A., Gonese, G., Kamamia, C. K., White, B., Young, D. M., & Collins, P. Y. (2023, June 27). Global Mental Health: Where we are and where we are going - current psychiatry reports. SpringerLink. https://link.springer.com/article/10.1007/s11920-023-01426-8
Patel, S. G., Bouche, V., Thomas, I., & Martinez, W. (2023). Mental health and adaptation among newcomer immigrant youth in United States educational settings. Current Opinion in Psychology, 49, 101459.
Perera, C., Salamanca-Sanabria, A., Caballero-Bernal, J., Feldman, L., Hansen, M., Bird, M., … & Vallières, F. (2020). No implementation without cultural adaptation: a process for culturally adapting low-intensity psychological interventions in humanitarian settings. Conflict and health, 14, 1-12.
Pérez Villacís, L. A. (2013). Análisis de los discursos y contenidos de las narco novelas y el impacto que estas han tenido en los niños de 15 a 17 años que habitan en el sur de Quito (Bachelor's thesis).
Shultz, J. M., & Forbes, D. (2013). Psychological First Aid: Rapid proliferation and the search for evidence. Disaster health, 2(1), 3–12. https://doi.org/10.4161/dish.26006 Social, educational and health impacts. Ethnic and Racial Studies, 46(3), 391-419. Sponsorship Essentials for the Welcome Corps, 2023. https://learn.sponsoressentials.org/#/course/144392/lesson/529255/screen/7
Suh, H. N., Nelson, B. M., Goergen, J. L., Clinton, L., & Osborne, A. (2023). The role of model minority stereotype on general self-efficacy and depressive symptoms. The Counseling Psychologist, 51(1), 62-83.
The National Child Traumatic Stress Network (NCTSN). (n.d.). About PFA. https://www.nctsn.org/treatments-and-practices/psychological-first-aid-and-skillsfor-psychological-recovery/about-pfa
United Nations High Commissioner for Refugees. (2024, June 13). UNHCR warns against apathy and inaction amid spike in forced displacement. UNHCR. Retrieved July 29, 2024, from https://www.unhcr.org/news/press-releases/unhcr-warnsagainst-apathy-and-inaction-amid-spike-forced-displacement
United Nations Refugee Agency. (n.d.). Refugee Statistics. USA for UNHCR. Retrieved July 29, 2024, from https://www.unrefugees.org/refugee-facts/statistics/ United States Department of State. (2024, January 19). One-Year Anniversary of the Welcome Corps - United States Department of State. State Department. Retrieved July 29, 2024, from https://www.state.gov/one-year-anniversary-of-the-welcomecorps/ Walton, J., & Truong, M. (2023). A review of the model minority myth: understanding the Wang, L., Norman, I., Edleston, V., Oyo, C., & Leamy, M. (2024). The Effectiveness and Implementation of Psychological First Aid as a Therapeutic Intervention After Trauma: An Integrative Review. Trauma, Violence, & Abuse, 0(0). https://doi.org/10.1177/15248380231221492
Weissman, Sara. (2021, July 1). Nontuition Costs Burden CUNY Community College Students. Inside Higher Ed. https://www.insidehighered.com/news/2021/07/02/nontuition-costs-burden-cunycommunity-college-students
Welcome Corps. (n.d.). Welcome Corps: Home. Retrieved July 29, 2024, from https://welcomecorps.org/
Welcome Corps - United States Department of State. (n.d.). State Department. Retrieved July 29, 2024, from https://www.state.gov/welcome-corps/
World Health Organization. (2016). Problem Management Plus (PM+): Individual psychological help for adults impaired by distress in communities exposed to adversity (No. WHO/MSD/MER/16.2). World Health Organization.
World Health Organization. (2018, January 1). Problem management plus (PM+): individual psychological help for adults impaired by distress in communities exposed to adversity. World Health Organization (WHO). Retrieved July 29, 2024, from https://www.who.int/publications/i/item/WHO-MSD-MER-18.5
World Health Organization. (2021). Self help plus (SH+): A group-based stress management course for adults.
World Health Organization. (2022). World Mental Health Report: Transforming Mental Health for All. World Health Organization.
World Health Organization. (2024). Mental health. World Health Organization. https://www.who.int/health-topics/mental-health#tab=tab_2
Yorgason, J. B., Linville, D., & Zitzman, B. (2008). Mental Health Among College Students: Do Those Who Need Services Know About and Use Them? Journal of
2024 CFMDE BERN

