Services and Support Increasing
FOR LANCASTER COUNTY WOMEN FACING THE MULTI-FACETED CHALLENGES OF MENOPAUSE

OBSESSIVE-COMPULSIVE DISORDER BY

UNDERSTANDING PALLIATIVE AND HOSPICE CARE BY DEBRA VERMETTE, MD & COLLEEN HAZLETT-O’BRIEN, DO

FOR LANCASTER COUNTY WOMEN FACING THE MULTI-FACETED CHALLENGES OF MENOPAUSE

OBSESSIVE-COMPULSIVE DISORDER BY

UNDERSTANDING PALLIATIVE AND HOSPICE CARE BY DEBRA VERMETTE, MD & COLLEEN HAZLETT-O’BRIEN, DO

Our one-stop spine referral model guides your patients to the right provider, at the right time. Through a single point of entry, our specially trained registered nurse navigators clinically triage referrals to the appropriate level of care, supporting better outcomes. From referral to consultation, patients reach the specialist best suited to their condition and goals — f for timely, cost-effective care.

2025/2026 Board of Directors
Sarah E. Eiser, MD President
Penn Medicine Lancaster General Health Physicians Lancaster Physicians for Women
Stacey S. Denlinger, DO
Immediate Past President
UPMC Wound and Hyperbaric Center
Robin M. Hicks, DO President-Elect
UPMC Supportive Care & Palliative Medicine
Christopher R. Scheid, DO Vice President
UPMC Post-Acute and Senior Care Services
James M. Kelly, MD Treasurer
Penn Medicine Lancaster General Health Physicians Family Medicine Lincoln
David J. Gasperack, DO Secretary WellSpan Health
DIRECTORS
Lena Dumasia, MD
Laura H. Fisher, MD
Abby K. Geletzke, MD
Anna Goetze, DO | Resident
Logan Lawson, DO, MPH | Resident
Jessica Miller, MD | Resident
Karen A. Rizzo, MD, FACS
Daniel J. Schlegel, MD, MHA, FAAFP
Susanne E. Scott, MD, MPH
Danielle Rubinstein, DO
Osvaldo Zumba, MD
EDITORS
Dawn Mentzer
Bet h E. Gerber
Lancaster City &
Stacey S. Denlinger,
LancasterPhysicianis a publication of the Lancaster City & County Medical Society (LCCMS). The Lancaster City & County Medical Society’s mission statement: To promote and protect the practice of medicine for the physicians of Lancaster County so they may provide the highest quality of patient-centered care in an increasingly complex environment.



Personalized Treatment for Women Across the Care Continuum 10 Choosing the Safest and Most Effective Antiplatelet Therapy Through Genetic Testing: WellSpan Health’s Gene Health Project Provides Physicians with Lifesaving Insight
I hope everyone shoveled out of this winter okay! As always, we blinked and the spring season has arrived.
This issue of our magazine features the ever-popular topic of menopause and how Lancaster County health care systems are answering the demand for more support for this life transition.
We also include articles about OCD, hospice and palliative care, and insights about the CDC’s new vaccination recommendations, along with our regular segments about health system best practices, legislative updates, a member spotlight, restaurant review, a featured physician’s “passion outside of practice,” and more.
It is so great to hear the birds chirping again! Enjoy the gifts of the spring season.
Thank you,
Annual Dinner & Awards Celebration
Tuesday, June 16, 6 - 9 p.m. Inn at Leola Village
PAMED House of Delegates
Friday, October 23 - Sunday, October 25 Hershey Lodge (hybrid event) Holiday Social & Foundation Benefit Saturday, December 5, 6:30 - 10 p.m. Lancaster Country Club


Sarah Eiser, MD Penn Medicine Lancaster
General Health Physicians
Lancaster Physicians for Women
You’re proud to be a physician. Support the organization dedicated to serving you and your passion. United we are stronger and can work together to make a positive impact in Lancaster County medicine and beyond.
If you aren’t already a member, we hope you’ll consider a membership investment in LCCMS.
Scan the QR code below to learn more.

Pennsylvania General Assembly: 2026 Pennsylvania Legislative Outlook
The Pennsylvania General Assembly returned to session at the end of January. As PAMED looks ahead to the 2026 Pennsylvania legislative landscape, it is clear that it will be dominated by elections.
The gubernatorial election will take place this November, with Governor Shapiro and State Treasurer Stacy Garrity having already announced their candidacies. This is also year two of the 2025-2026 legislative session, and all 203 PA House seats and 25 of the 50 PA Senate seats will be contested.
Given this environment, the Republican-controlled Senate and the Democratic-controlled House can be expected to move a relatively large number of bills in 2026 that have no chance of passing the other chamber but are intended to send political messages to the electorate.
With that backdrop, PAMED is continuing to monitor and advocate on key issues, including:
• Midwives – Senate Bill 507 (Brown), a bill that would update provisions in the Medical Practice Act of 1985 regarding the practice of midwifery to include licensing certified midwives, passed the Senate in October 2025 and moved quickly in the House. It received final approval in the first quarter of 2026.
• Maternal Health – House Bill 1088 (Steele) and House Bill 1234 (Mayes), legislation requiring both private and government-provided health insurance to cover blood pressure monitors for pregnant or postpartum patients, passed the House and are awaiting consideration in the Senate.
• Private Equity – There has been significant legislative interest in getting something done on regulating the involvement of private equity in health care. Numerous bills have been introduced, and public hearings have been held on this issue in both the House and Senate. To date, only House Bill 1460 (Borowski) has moved, passing the House last summer. That bill was referred to the Senate Institutional Sustainability and Innovation Committee, which continues to work on the issue but does not appear ready to move legislation forward at this time.
• Scope of Practice – PAMED remains vigilant on all scope of practice legislation and continues to advocate for physician-led team-based care. Senate Bill 25 (Bartolotta) and House Bill (Guenst) on independent practice for nurse practitioners, House Bill 1000 (Frankel) on prescriptive authority for psychologists, and Senate Bill 197 (Brown) on physical therapist direct access are just some of the scope of practice bills on which we are actively engaged.
• Artificial Intelligence Use in Health Care – Various committees in both the House and Senate have already held, or will be holding in the near future, hearings on various aspects of the use of AI in health care. To date, no bills have been moved, but PAMED continues to monitor all developments on this issue.
On February 3, 2026, Governor Josh Shapiro delivered his annual budget address to the General Assembly, outlining his proposed Fiscal Year 2026–27. The proposal, totaling approximately $53 billion, will now be reviewed and negotiated by the General Assembly in the months ahead.
The budget proposes $260.3 million for health programs, reflecting a 0.3% increase over the prior fiscal year. Within the total budget, $2.019 million is proposed to maintain the Pennsylvania Immunization Electronic Registry System (PIERS), which supports statewide immunization reporting and public health surveillance.
The budget also proposes a $2.5 million increase for health promotion and disease prevention efforts, including expanded support for maternal health programs. Mental health remains a priority, with a 6.9% increase in funding for mental health services through the Department of Human Services, alongside a call to streamline credentialing for behavioral health providers. Several public health programs would see modest increases, including funding for state health care centers, the state laboratory, sexually transmitted disease screening and treatment, local health departments, and tuberculosis screening and treatment. At the same time, many programs are proposed to remain level-funded, including newborn screening, cancer screening services, AIDS programs and special pharmaceutical services, school district health services, maternal and child health services, regional poison control centers, and programs addressing sickle cell disease and Lyme disease.
In addition to funding proposals, the Governor reiterated support for several policy initiatives, including efforts to lower prescription drug costs by prohibiting copay accumulator programs, as well as proposals to increase the minimum wage and legalize adult-use marijuana.
PAMED will continue to monitor legislative events as they unfold.
For more information about any of the items mentioned above, please visit the Advocacy Section of PAMED’s web site at www.pamedsoc.org/advocacy
• Penn State Health Expands Women’s Cardiovascular Services in Lancaster County
• Choosing the Safest and Most Effective Antiplatelet Therapy Through Genetic Testing: WellSpan Health’s Gene Health Project Provides Physicians with Lifesaving Insight ALSO IN THIS SECTION

When a patient is hemorrhaging, minutes matter. Severe blood loss can cause irreversible shock and death within minutes, long before an ambulance can reach the trauma bay. To close that gap, Penn Medicine Lancaster General Health has established a breakthrough capability few health systems in the nation can offer: whole blood transfusions performed “in the field” by emergency physicians responding directly to the scene.
This innovative model is made possible through two highly coordinated assets—LG Health’s own Blood Donation Center and Penn Med One, the health system’s physician staffed emergency response vehicle. Together, they are delivering hospital level care when seconds count.
Penn Med One began offering whole blood transfusions in pre-hospital settings in 2023, joining a rapidly growing but still extremely limited national movement. Although the number of EMS agencies carrying whole blood has increased in recent years, just about 1% of EMS agencies nationwide currently provide this service—underscoring how uncommon and consequential LG Health’s capability is.
The rarity in Pennsylvania is even more pronounced. The state only authorized pre-hospital blood administration in late 2023, following new protocols developed by Penn Medicine, UPMC, and St. Luke’s physicians. Before that change, EMS crews were not legally able to transfuse blood en route to the hospital.
Penn Med One now responds with two units of low-titer O-positive whole blood—capable of being given to nearly any trauma patient—and can initiate transfusion before leaving the scene.
“The sooner we get patients blood products, the better we do,” said LG Health EMS Medical Director Brendan Mulcahy, DO.
One reason this model is so unusual: LG Health operates its own blood donation center, a capability “highly unusual these days,” according to Laboratory Operations Manager Lori Topper, MT (ASCP) SH.
Few hospitals maintain in house donor centers, making LG Health one of the rare systems able to collect, process, and supply whole blood locally—the key factor that made Penn Med One’s program feasible.
severe falls—and its ability to provide advanced therapies, including whole blood, has already made a measurable difference.
“I’d like to believe we’ve saved quite a few lives that would not have been saved through our efforts,” Mulcahy said.
With its clinician-led response model, rare in-house blood collection capacity, and expanding partnerships across Lancaster County, LG Health is redefining what pre-hospital emergency care can deliver. As Topper put it: “Minutes matter.”
And with whole blood now available at the scene, those minutes increasingly mean the difference between life and death.
Whole blood is difficult to obtain from outside sources due to donor eligibility restrictions, high demand, and its short 21-day shelf life. Yet between July 1, 2024, and September 30, 2025, LG Health collected 668 units of whole blood, an average of 45 usable units per month. During that same period, 15 patients received whole blood transfusions from Penn Med One in the field.
Building on Penn Med One’s impact, LG Health has expanded field-based blood availability through its partnership with New Holland EMS. Since May 2025, New Holland has been equipped with a unit of LG Health-supplied O-positive whole blood and a unit of packed red blood cells and plasma. This expansion strengthens the trauma response network across eastern Lancaster County and ensures more EMS crews have access to lifesaving blood products.
“Partnering with Penn Medicine and being able to bring blood products into rural Lancaster County—at the heart of the Amish community, where we see severe trauma across all ages—has been a game changer,” New Holland EMS Chief Darrell Fisher said. “In less than 10 months, we’ve administered more than 20 units to some of our most critically injured and ill patients.”
Since its launch, Penn Med One has responded to high risk calls—including crashes, cardiac arrests, industrial accidents, and




Cardiovascular disease remains the leading cause of death in women, yet it often goes unrecognized. Penn State Health cardiologists in Lancaster County offer a growing range of treatments to catch heart disease in women sooner and intervene before it progresses.
“Rather than meeting women for the first time after they’ve had a heart attack, a stroke, or artery disease, I would rather see them when we’re in a stage where we can prevent those events from happening,” says Dr. Audrey Damren, a cardiologist at Penn State Health Cardiology in Lancaster.
Many diagnostic procedures, including advanced imaging, can be scheduled within a week of the patient’s initial visit.
Staci Johnston, a nurse practitioner at Penn State Health Cardiology, often helps patients access expedited care. “If I’m
concerned about someone, I help them get the testing they need right away,” she says.
She recently experienced the practice’s efficient, personalized care as a patient herself. After waking up with an abnormal heart rhythm, she received an echocardiogram the same day. It showed she has a patent foramen ovale, a hole between the heart’s upper chambers.
Patients in Lancaster County have access to a comprehensive range of cardiovascular diagnostics and interventions at Penn State Health, including:
• Cardiac monitoring – Research published in JAMA Cardiology suggests women are more likely to develop arrhythmias than men of the same height. Classic Holter monitors required patients to strap bulky equipment to their chests to monitor irregular heartbeats. Now, lighter, more compact monitors enable continuous rhythm monitoring during patients’ routine daily activities, including exercising and showering.
• High-resolution cardiac computed tomography (CT) scans – Using coronary artery calcium scores and cardiac CT angiography, physicians map out a patient’s coronary arteries and look for calcium buildup or blockages. Findings guide preventive therapies such as statins or aspirin to keep arteries clear and reduce inflammation. These tests can also spot congenital arterial abnormalities and cardiomyopathies.
• Advanced imaging without radiation – Cardiac MRIs reveal heart structure and function without radiation exposure, making them an appealing alternative for younger patients or those who are pregnant. Using transesophageal echocardiograms, physicians can evaluate patients’ heart valves and plan for surgical interventions.
• Vascular care – Lancaster Medical Center has three cardiac catheterization labs to diagnose and treat certain heart conditions using catheterization or stents. Women often have smaller coronary vessels than men and can receive special, smaller stents.
• Hypertension management – Medications, exercise, and diet can keep high blood pressure in check. The evidence-based Dietary Approaches to Stop Hypertension diet works especially well in women, suggests research published in The American Journal of Cardiology. Doctors follow up frequently to monitor patients’ progress. “We work with women as teammates to develop a system that will help them maintain lifestyle changes,” Damren says.
Sharing the Message
During American Heart Month in February, Damren, Dr. Joy Cotton, a cardiologist at Penn State Health Cardiology in
“In the race to heart disease, men tend to develop conditions like coronary disease, electrical issues, myocardial infarctions, and stroke earlier, often in their early 30s. Once women have gone through menopause, their risk of these conditions within 10 years jumps ahead to match that of men their age.”
Lancaster, and Sandra Pasic, lead cardiac sonographer at Lancaster Medical Center, delivered a Wear Red Day presentation focused on preventing heart disease and stroke in women. The event, which was open to staff from all six Penn State Health hospitals, was also streamed virtually.
Their key message: To catch heart disease in women, you have to look for it. For many women, heart disease doesn’t show itself with heavy chest pain or symptoms of breathlessness. The symptoms can be subtle and easily missed or ignored.
“In the race to heart disease, men tend to develop conditions like coronary disease, electrical issues, myocardial infarctions, and stroke earlier, often in their early 30s,” Damren says. “Once women have gone through menopause, their risk of these conditions within 10 years jumps ahead to match that of men their age.”
Johnston is passionate about sharing this message, especially after her mother-in-law died from cardiac arrest in 2023. She’s following up on her own heart condition with additional tests at Penn State Health Milton S. Hershey Medical Center.
She encourages people to seek cardiology care if they have multiple risk factors, such as high blood pressure, high cholesterol, or uncontrolled type 2 diabetes, or if they just don’t feel right.
“If patients say they used to walk a mile and now they can barely walk down the street, that’s a red flag,” she says.

Plavix is the most commonly prescribed antiplatelet medication, yet it’s not effective for everyone. New research shows the reason: a genetic variant that affects how patients metabolize the drug. These patients face a much higher risk of recurrent cardiovascular events.
The American Heart Association (AHA) recently published new guidance recommending genetic testing before prescribing Plavix. The Gene Health Project at WellSpan Health is expanding access to this lifesaving testing to those in our community.
“The project makes genetic testing accessible to everyone. When patients get tested, it gives their providers critical information to guide their care,” says David Kann, MD, MPH, medical director of Precision Medicine at WellSpan Health. “Their genetic information will show, for example, whether Plavix is right for them or whether another antiplatelet medication would be safer.”
Why Plavix works for some patients and not others Plavix (clopidogrel) is a prodrug, which means it needs a specific enzyme (CYP2C19) to work in the body. About 30% of Americans have genetic variants that reduce or eliminate this enzyme’s activity.
As a result, they can’t activate Plavix effectively, even when they take it exactly as prescribed.
Choosing antiplatelet treatment based on genetic testing results
Genetic testing is a step forward in precision medicine, allowing providers to use patients’ genetic information to guide treatment decisions. Providers can choose antiplatelet therapy based on patients’ CYP2C19 genetic variant status:
• Brillinta (ticagrelor) and Effient (prasugrel) are among the safe, effective alternatives for patients with the genetic variants that inhibit Plavix metabolism.
• Patients who don’t have those genetic variants can take Plavix.
“Genetic testing helps us tailor antiplatelet therapy so patients get the medication that’s truly effective for them,” says Kate Cummins, PharmD, pharmacogenomics pharmacist at WellSpan Health. “That kind of precision can help prevent repeat heart attacks and strokes.”
New AHA guidance: Genetic testing before prescribing Plavix
In 2024, the AHA issued a scientific statement recommending CYP2C19 genetic testing for any patient who is taking or may need Plavix (Pereira et al. 2024). The goal is to help providers choose the antiplatelet therapy that will offer the strongest protection for each patient. A one-time genetic test can provide lifelong information to guide treatment decisions now and in the future.
How your patients can access no-cost genetic testing
Because genetic testing can be expensive and difficult to access, many patients don’t get tested, despite the AHA statement. WellSpan Health offers genetic testing for anyone over 18 years of age through The Gene Health Project.
The project reports on three hereditary conditions at no cost to participants: familial hypercholesterolemia, hereditary breast and ovarian cancer, and Lynch syndrome. But the genetic data offer much more—they can guide medication decisions for years to come.
“Once a patient is sequenced, we can use that data again and again,” says Dr. Kann. “It’s what we call ‘Sequence Once, Query Often,’ allowing us to revisit that genetic information as new therapies or questions come up.”
The initial testing includes full exome sequencing through WellSpan Health’s partner, Helix, a population genomics company. Helix stores patients’ results securely, and a patient’s authorized health care providers can access them when needed throughout the patient’s lifetime. When patients enroll, their genetic information becomes available for future medical decisions (at a small fee akin to a copayment)—beyond which blood thinner will work best.
“The project makes genetic testing accessible to everyone. When patients get tested, it gives their providers critical information to guide their care.”
— David Kann, MD, MPH
The Plavix finding is just one example of how genetic information can improve everyday prescribing decisions. WellSpan Health’s pharmacogenomics team is now expanding this work into other medication categories, such as behavioral health.
Gene-drug interactions with antidepressants, antipsychotics, and ADHD therapies can strongly influence side effects, dosing, and treatment response. That could mean months of trying different medications to find the right one. Genetic testing allows providers to identify the right medication from the start.
“Our goal is to support primary care and other specialties in getting patients tested ahead of time,” says Dr. Cummins. “When we have the genetic information up front, we can guide safer prescribing and help patients reach effective treatment faster.”
As more data become available, pharmacogenomics will continue to shape how we think about prescribing, not just for cardiology and behavioral health, but across many areas of medicine. By encouraging patients to join The Gene Health Project, providers gain a partner in WellSpan Health—and durable genetic insights they can use to guide safer, more personalized prescribing for years to come.
Reference
Pereira, Naveen L. et al. on behalf of the American Heart Association Professional/ Public Education and Publications Committee of the Council on Genomic and Precision Medicine; Council on Arteriosclerosis, Thrombosis and Vascular Biology; Council on Cardiovascular and Stroke Nursing; Council on Clinical Cardiology; Council on Peripheral Vascular Disease; and Stroke Council. “CYP2C19 genetic testing for oral P2Y12 inhibitor therapy: a scientific statement from the American Heart Association.” Circulation. 2024;150:e129–e150. doi: 10.1161/CIR.0000000000001257

Obsessive-compulsive disorder (OCD) is a chronic neuropsychiatric condition defined by intrusive obsessions and repetitive compulsions that cause significant distress and impairment. It affects 1–3% of the population, often begins in childhood or adolescence, and can persist without treatment. The pathophysiology involves dysregulation of cortico-striato-thalamo-cortical circuits, with contributions from serotonergic, glutamatergic, and dopaminergic systems, and a moderate genetic heritability. First-line treatments are exposure and response prevention (ERP) and selective serotonin reuptake inhibitors (SSRIs). For refractory cases, augmentation with antipsychotics, glutamatergic agents, or neuromodulation (transcranial magnetic stimulation [TMS], deep brain stimulation [DBS]) may be considered. Early diagnosis and evidence-based care improve outcomes, but many patients remain under-treated.
DEFINITION AND CLINICAL FEATURES
OCD is characterized by:
• Obsessions: Recurrent, intrusive thoughts, images, or urges that cause marked anxiety or distress.
• Compulsions: Repetitive behaviors or mental acts performed to reduce anxiety or prevent a feared event. These compulsions are usually not credibly connected to the thoughts.
• Insight: Patients often recognize their thoughts and behaviors as excessive or unreasonable, though insight varies.
• Impairment: It is important to note that symptoms are time-consuming and cause significant distress or functional impairment. It is not enough to just have symptoms; they must be severe enough to cause significant impairment in school, at work, or in relationships.
DIFFERENTIAL DIAGNOSIS
OCD should be distinguished from rumination of depression, preoccupations of mania, the delusions of psychosis, anxiety

symptoms associated with other anxiety disorders, normal avoidance of contamination or germs by washing or avoiding touching potentially infectious persons or items, and severe obsessive-compulsive personality disorder (OCPD): a rigid, perfectionistic personality type which is a separate disorder from OCD.
EPIDEMIOLOGY
OCD affects approximately 1–3% of the global population, with a lifetime prevalence of 2.3% in the United States. The disability caused by OCD is severe enough that the World Health Organization has listed OCD among the 10 medical illnesses most likely to cause disability. It typically begins in childhood or adolescence, with a bimodal age distribution (early childhood and late adolescence/early adulthood). The disorder is equally common in males and females, though males more often have an earlier onset. Late-onset OCD is relatively rare; OCD-like symptoms appearing for the first time in an older individual warrant a medical workup for a possible neurological cause.
PATHOPHYSIOLOGY
OCD arises from complex interactions among genetic, neurobiological, and environmental factors:
Neurocircuitry
The cortico-striato-thalamo-cortical (CSTC) circuit is central to OCD pathophysiology. Hyperactivity in the orbitofrontal cortex, anterior cingulate cortex, and striatum, coupled with impaired inhibitory control, drives repetitive thoughts and behaviors. Effective treatments normalize activity in these circuits.
Neurotransmitters
• Serotonin: SSRIs are first-line pharmacotherapy, indicating serotonergic dysregulation, though no consistent serotonergic abnormality has been identified.
• Glutamate: Emerging evidence implicates glutamatergic dysfunction; glutamate modulators (e.g., memantine, N-acetylcysteine) show promise in refractory cases.
• Dopamine: Antipsychotic augmentation targets dopaminergic hyperactivity in treatment-resistant OCD.
Genetics
OCD is moderately heritable (27–65%), with polygenic risk involving serotonergic, glutamatergic, and dopaminergic genes. No single gene accounts for a large proportion of risk, underscoring genetic complexity.
Environmental factors
Stressful life events, trauma, and infections (e.g., pediatric autoimmune neuropsychiatric disorders associated with streptococcal infections, PANDAS) may trigger or exacerbate OCD symptoms in susceptible individuals. Women are at particular risk of symptom exacerbation or new onset of symptoms during pregnancy and the postpartum period.
Psychotherapy
Exposure and response prevention (ERP) is the most effective psychotherapy, with large effect sizes and durable benefits. Patients are first exposed to stimuli that trigger their specific OCD symptoms. They then prevent themselves from responding to the stimuli as they usually would. As patients repeat their ERP exercises, both the amplitude of the anxiety and the time required for it to diminish will gradually decrease until patients become habituated to the stimuli. Cognitive-behavioral therapy (CBT) incorporating ERP is recommended as first-line treatment.
Pharmacotherapy
• SSRIs: First-line pharmacotherapy (e.g., fluoxetine, sertraline, fluvoxamine, paroxetine, citalopram, escitalopram).
• Clomipramine: A tricyclic antidepressant with robust efficacy, often used when SSRIs are ineffective.
• It is important that high doses be used with SSRIs and clomipramine because of higher response rates, and that patients are reminded that response may not be achieved until after 8-12 weeks of treatment.
• Augmentation strategies: Antipsychotics (e.g., risperidone, aripiprazole) for treatment-resistant cases; glutamatergic agents are under investigation.
• Transcranial magnetic stimulation (TMS): Non-invasive, non-medication neuromodulation procedure with emerging evidence for refractory cases. TMS was FDA-approved in 2018 for treatment-resistant OCD and is available in our county, although current insurance coverage is limited.
• Deep brain stimulation (DBS): Implanting electrodes to stimulate specific brain regions. Effective for severe, treatment-refractory OCD, targeting CSTC circuits.
Obsessive-compulsive disorder is a chronic neuropsychiatric condition characterized by intrusive obsessions and repetitive compulsions. It arises from complex interactions among genetic, neurobiological, and environmental factors, with CSTC circuit dysregulation playing a central role. Effective treatments include ERP, SSRIs, and neuromodulation for refractory cases, but many patients remain under-treated, highlighting the need for early diagnosis and comprehensive care. Nevertheless, recent data emphasize that long-term outcomes can be positive. Thus, patients should be encouraged to remain hopeful and to try a range of different evidence-based treatments.
References
1 Kaplan & Sadock’s Comprehensive Textbook of Psychiatry Wolters Kluwer, 2024
2 Textbook of Psychiatry The American Psychiatric Association Publishing, 2019
3 Obsessive-compulsive disorder Nature Reviews: Disease Primers, 2019
4 Obsessive-compulsive disorder: diagnosis, clinical features, nosology, and epidemiology The Psychiatric Clinics of North America, 2023
5 Obsessive-compulsive disorder in the world mental health surveys BMC Medicine, 2025
6 The heterogeneous course of OCD-A scoping review on the variety of definitions Psychiatry Research, 2020
7 Harmonizing the neurobiology and treatment of obsessive-compulsive disorder The American Journal of Psychiatry, 2021
8 Immunological causes of obsessive-compulsive disorder: is it time for the concept of an «autoimmune OCD» subtype? Translational Psychiatry, 2022
9 The genetic epidemiology of obsessive-compulsive disorder: a systematic review and meta-analysis Translational Psychiatry, 2023
10 Diagnosis and management of obsessive-compulsive disorder in the primary care setting American Family Physician, 2024


DEBRA VERMETTE, MD Vice President, Chief Medical Officer, Choices Healthcare

COLLEEN HAZLETT-O’BRIEN, DO Medical Director, In-Home Palliative Care, Choices Healthcare
As physicians, we routinely care for patients living with serious illness—advanced cancer, congestive heart failure, COPD, dementia, Parkinson’s disease, and other progressive conditions. While many of these illnesses can be treated and slowed, they cannot be cured. They progress over time and often impose increasing symptom burden, functional decline, and caregiver strain.
Understanding the distinction between palliative and hospice care—and when to refer—can significantly improve quality outcomes for both patients and the healthcare system.
Palliative Care: An Added Layer of Support
Palliative care is specialized medical care for people living with serious life-limiting illnesses. Its focus is relief from symptoms and improvement in quality of life, regardless of diagnosis, stage, or prognosis. Serious illnesses carry a high risk of mortality and negatively impact daily function and quality of life. Without intentional support, patients may experience uncontrolled symptoms, fragmented care, and repeated hospitalizations.
Palliative care addresses these gaps by providing:
• Expert symptom management (pain, dyspnea, nausea, fatigue, anxiety)
• Clarification of goals of care
• Advance care planning
• Education about disease trajectory
• Caregiver support
• Coordination across care settings
Importantly, palliative care is delivered alongside disease-directed treatment. It
does not replace the primary care or specialty physician. Rather, it strengthens the care plan by working collaboratively with a patient’s care team and aligning treatment decisions with what matters most to the patient and their care partners.
Consider a patient with cardiac amyloidosis, a progressive condition leading to restrictive cardiomyopathy and worsening heart failure. Despite advanced cardiac interventions and optimized medical therapy, he developed increasing fatigue, fluid retention, dyspnea, and declining functional status. Medication adjustments became more frequent, and hospital visits increased. His family felt overwhelmed by navigating complex decisions.
Initially hesitant, the patient associated additional support with “giving up.” After engagement with a palliative care provider, symptom management improved, care coordination became more streamlined, and structured conversations clarified goals of care. The cardiology plan remained intact, but it was strengthened by anticipatory guidance and longitudinal support.
With better symptom control and reduced uncertainty, hospital utilization decreased, and the patient was able to focus more fully on time with family. This is the role of palliative care: improving quality of life while ongoing treatment continues.
Palliative care can be delivered in hospitals, outpatient clinics, or in the home. Early integration—often at the time of diagnosis of a serious illness—has been shown to improve symptom control, patient and caregiver satisfaction, and in some populations, survival.
According to the Center to Advance Palliative Care, palliative care programs reduce avoidable utilization and spending across settings, including reductions in hospital readmissions, emergency department visits, and total healthcare costs. These outcomes align with value-based care initiatives and population health strategies.
All hospice care is palliative care, but not all palliative care is hospice care.
Hospice is designed for patients who are likely in the last six months of life if their disease follows its expected course. At that point, the focus shifts from curative treatment to comfort-oriented care.
Hospice care:
• Recognizes dying as a normal part of living
• Affirms life and neither hastens nor postpones death
• Prioritizes quality of life for patients and families
• Provides interdisciplinary, person- and family-centered care
Hospice services involve a robust interdisciplinary team framework that includes physicians, nurse practitioners, RN case managers, skilled nursing, hospice aides, social work, chaplain support, volunteer services, and bereavement support. Hospice also covers any medications, durable medical equipment, and supplies that are related to the patient’s terminal diagnosis with a focus on comfort and quality of life.
The hospice team develops and manages an individualized plan of care, addresses physical symptoms, attends to psychosocial and spiritual needs, educates caregivers, and advocates for patient goals. Care is delivered wherever a patient calls “home”—private residences, nursing facilities, assisted living communities, hospitals, hospice units, and other community settings.
Studies consistently demonstrate that hospice care improves symptom management and patient and family satisfaction while reducing high-intensity interventions such as ICU stays, emergency department visits, and CPR in the final weeks of life.
Approximately one-third of health care expenditures in the United States occur in the last year of life. Yet roughly one-quarter of hospice patients enroll in the final seven days of life, limiting the full benefit of interdisciplinary support.
Timely referral matters.
A Collaborative Extension of Good Medicine
Palliative and hospice care are sometimes
misunderstood as signaling therapeutic failure. In reality, they represent an evolution of care—one that integrates symptom management, communication, and goal alignment into routine medical practice.
They allow us to treat suffering with the same diligence with which we treat disease.
Early, appropriate referral does not diminish the physician’s role; it reinforces it. By integrating palliative care earlier and hospice care at the appropriate time, we ensure that patients receive comprehensive, coordinated, and compassionate care throughout the trajectory of serious illness.
In an era increasingly defined by value, quality metrics, and patient-centered outcomes, palliative and hospice services are not ancillary—they are essential.
When Should I Consider a Referral?
When caring for a patient with a life-limiting illness…
Consider Palliative Care if:
• You would not be surprised if the patient died within the next year
• There are recurrent hospitalizations or ED visits
• Symptom burden is increasing
• Functional decline is evident
• Caregivers demonstrate strain
• The patient expresses uncertainty about ongoing treatment decisions
Consider Hospice if:
• Prognosis is likely six months or less if the disease runs its normal course
• Disease-directed therapies no longer provide meaningful benefit
• The burdens of treatment outweigh potential gains
• The patient prioritizes comfort and quality of life

Dr. Wu at the podium during the 2025 “Wishes Among the Stars Gala,” a fundraising event benefiting Share of Lancaster. The organization supports Lancaster County families as they grieve and recover from the loss of a baby.
Would you briefly describe your passion outside of practice for those who might be unfamiliar with it?
One of my passions outside of practice and work is volunteering for Share of Lancaster and Walking Forward Together. These organizations deal with families that have the unfortunate experience of an adverse pregnancy outcome, such as stillbirth, miscarriage, interruption of pregnancy for medical and fetal reasons, second-trimester pregnancy loss, incompatible fetal birth differences leading to perinatal palliative care and hospice, congenital birth differences, or neonatal death.
These organizations offer services at no cost to families in need. They include bi-monthly burial assistance, a 24-hour hotline, counseling services, bereavement resources, and educational materials for local hospitals and organizations. Annual memorial events, such as the Walk to Remember/Wave of Light Remembrance, are organized to honor families and friends. In addition, they host various family-oriented activities, including afternoons at the ballpark, parent date afternoons, and a holiday train ride with Santa on the Strasburg Railroad.
These organizations also prioritize education. They have coordinated a national conference offering Continuing Medical Education (CME) credit, along with seminars and outreach programs directed at local and regional organizations and healthcare facilities.
How did you develop an interest in your passion outside of practice?
As a specialist in maternal-fetal medicine, I address a wide range of pregnancy-related concerns, with an emphasis on managing high-risk cases. My responsibilities encompass the evaluation of maternal medical factors, pregnancy complications, and fetal issues. A critical aspect of my role involves the interpretation of ultrasounds, through which I often serve as the initial photographer and storyteller for the unborn child.
Regrettably, I am also tasked with delivering difficult news, such as explaining structural differences in fetal development or informing families that their baby has no detectable heartbeat. Such moments signify profound loss—specifically, the loss of expectations and significant milestones, including first smiles, first words, first steps, and first birthdays.
It’s our pleasure to highlight a Lancaster City & County Medical Society member’s “passion outside of practice” in each issue of Lancaster Physician. Beyond their commitment to health care, LCCMS members have many other talents, skills, and interests that might surprise you. In this issue, we’re thrilled to feature Serena Wu, MD, and her passion outside of practice.
The silence following such announcements can be profound, overshadowing the condolences offered and the physical recovery from pregnancy. The loss of a child, particularly one who has not lived beyond the womb, is an experience that is both devastating and often difficult to comprehend.
I firmly believe that providing support to families and mothers as they navigate the multifactorial and nuanced journey of welcoming a rainbow baby and managing subsequent pregnancies is of paramount importance. As a maternal-fetal medicine specialist, I endeavor to offer compassionate care to facilitate their ongoing journey of healing and hope. I believe that taking care of families and moms for their rainbow baby and pregnancy is of utmost importance.
How long have you been participating in this activity?
I have participated in this activity for 10 years since moving to Lancaster. However, my husband and I have been involved in this activity for over 15 years.
Why is this pursuit special to you?
Pregnancy loss occurs in one of four pregnancies. It represents a profound loss that many do not anticipate. This unexpected journey introduces parents to a community of those who have experienced similar grief, allowing for mutual understanding and support. Together, we traverse a path that, while challenging, is marked by shared experiences.
This mission is special to me because I want to support parents and families. No one should have to walk alone or feel isolated in their grief. I am here to validate their pregnancy, to honor their journey, and to acknowledge and affirm that we are all parents—despite the outcome.
What else would you like readers to know about this passion?
Healing from grief takes many forms, and the journey is never a straight path. While each person navigates their own unique experience, we are ultimately walking together. Every day, I learn from my patients, striving to be a better physician and to understand their experiences by trying to walk a mile in their shoes.


Located on the west side of Lancaster along Rohrerstown Road, just south of Marietta Avenue, Ida’s Cafe is a true neighborhood gem. For nearly two decades, this family-owned breakfast and lunch spot has quietly built a loyal following since opening in 2008. For my family, it has been our Saturday morning tradition—at least when I’m not on weekend call or covering office hours.
Owners Lisa and Jim Nudy, together with their sons Augustine and Anthony, have created something special. Jim helms the kitchen (with Anthony’s help), while Lisa orchestrates the front of the house alongside Augustine and an exceptional wait staff. The result is an atmosphere that feels as welcoming as it is efficient—no small feat on a bustling Saturday morning.
The menu offers something for everyone, from traditional comfort fare to lighter, more contemporary options. As a Midwest farm boy at heart, I gravitate toward the
Rise and Shine Omelet, paired with fresh-cut fruit and multigrain toast—with hot sauce on the side (a habit acquired during military service—veterans will understand). All baked goods come from a small family-run bakery in South Philadelphia and are excellent. The multigrain bread is outstanding—think of a close cousin to the “Sensational” loaf at Whole Foods Market.
My wife, Mary, prefers the more adventurous side of the menu: crepes, pancakes, or waffles topped with fresh fruit. In the winter, the baked oatmeal is a favorite. Our son Mitchell—now in law school in Ohio—has ordered the same breakfast for nearly 18 years: creamed chipped beef on biscuits, a bowl of chicken soup (yes, for breakfast), and two glasses of milk. The staff knows it by heart. Our daughter Emily, a local CRNP, opts for the egg white vegetable omelet with multigrain toast. Coffee and iced tea are brewed fresh throughout the day; while I defer to Mary on the coffee, her repeat orders speak for themselves.
Lunch is equally strong, with freshly-made soups prepared daily, along with sandwiches, wraps, salads, and quesadillas. Mary’s choice is the turkey club on multigrain toast; mine is the spinach quesadilla with fresh guacamole and salsa.
Beyond the food, Ida’s reflects the fabric of Lancaster itself. Retirees, young families, students from nearby Millersville University, and professionals—often including a few familiar medical colleagues—fill the dining room. Conversations flow in multiple languages, and it is not unusual to see regulars offering recommendations to visitors seeking local attractions.
In an era of chain restaurants and constant turnover, Ida’s Cafe remains a steady presence—a family-run institution grounded in hospitality, quality, and community. If you find yourself free on a Saturday morning, I hope you will stop in. You will not be disappointed.
Ida’s Cafe
507 Rohrerstown Rd. Lancaster, PA 17603 717-293-1311 idascafe.com
Over the last several months, many different initiatives have been released regarding vaccines, causing understandable confusion. The Centers for Disease Control (CDC), historically seen as the authority on vaccine policy, has made many changes in a short amount of time. The Pennsylvania Medical Society (PAMED) strongly supports vaccination and other evidence-based practices and has significant concerns about recent changes to several different authoritative organizations on their vaccine policies and recommendations.
Vaccines, in one form or another, have been used for hundreds of years to protect people from the worst outcomes of
certain diseases. As they exist today, they are one of the safest preventive tools available for multiple illnesses. When enough people in a population are vaccinated against a disease, they can reach what is called “herd immunity.” This means that enough people are immune to a disease, which in turn indirectly helps to protect others in the population who are not immune or are at higher risk of contracting that illness.
In order to prevent outbreaks and put people in a population at risk, the vaccination process begins early in life, and experts determine the vaccination schedule. Recently, the CDC has revised their child vaccination schedule recommendations. These changes include the removal of several “mandatory” vaccines and downgrading them to a “recommended” status, encouraging families and individuals to make their own decisions. Downgraded vaccinations include the annual COVID-19 vaccine and Hepatitis B vaccine, including the birth dose.
PAMED maintains that the longstanding, evidence-based approach used to review and provide guidelines for childhood immunizations remains the most reliable way to keep children healthy and prevent serious infections that often lead to serious complications and hospital stays. For decades, immunologists, pediatricians, and other leading health experts have carefully evaluated new data as part of this process, helping to ensure that newborns, infants, and children are protected from infectious diseases they may encounter as they grow.
The CDC’s recent decision is based on a brief review of practices in other countries. It was not reviewed by national subject matter experts, it lacks public input, and it disrupts the deliberate and time-tested scientific framework for effective population health. For the best guidance on vaccination schedules for children, PAMED recommends following the guidance of the American Academy of Pediatrics (AAP). The CDC has also rolled back its previous stance that vaccines do not cause autism and has taken a more ambivalent stance.
Back in October 2025, and in response to these changes, Governor Josh Shapiro signed an executive order (Executive Order 2025-02) ensuring access to vaccines in the state. Part of this order ensures continued coverage of vaccines downgraded to “recommended” status by private insurance companies and Medicaid. This order also requires state agencies to align with trusted medical experts like the AAP.
In addition to sudden changes in policy, there are also more subtle changes in language and recommendations around vaccines, sowing doubt and causing hesitancy.
The measles vaccine, as it exists now, was created in 1971. It was com bined with the mumps and rubella vaccines to create the MMR vaccine, a routine immunization in the United States today. In the year 2000, after a pro-vaccination campaign, the measles disease was considered officially eradicated in America. In order to achieve eradication status, there cannot be an outbreak of a specific disease for over 12 months across the country. However, increased vaccine hesitancy has caused the measles vaccination rate to fall. As a result, increased measles outbreaks are occurring, and the disease’s eradication status is being called into question.
Outbreaks have been occurring more frequently in recent years across the country. Pennsylvania has been among the states with confirmed measles cases, and Lancaster County has had multiple confirmed cases this year. As these cases become more common, PAMED encourages patients to speak with their physicians to make informed decisions for themselves and their families based on trusted medical expertise.
PAMED’s “Facts Not Fear” webpage has been updated to reflect the recent vaccine recommendation changes. PAMED started this campaign in 2024 as a resource to physicians and patients on the facts and questions to ask surrounding immunizations. From practical Q&As on navigating patient conversations to straightforward explanations on herd immunity and how vaccines are shaped, this resource is built to support confident and informed dialogue.
Visit pamedsoc.org/FactsNotFear and join PAMED in strengthening vaccine understanding across Pennsylvania. As always, PAMED will continue to advocate for evidence-based care and work to protect Pennsylvanians from vaccine-preventable diseases.










Suppor t the Tools That Make Independence Possible.
Behind every home at Friendship Community is essential equipment that helps adults with Intellectual Disabilities and Autism live safely and independently in a family home, not a facility
Adaptive lifts, accessible beds, safety supports, and mobility equipment are everyday necessities These critical items are costly and rarely fully covered by insurance
Your support provides the tools our residents need to thrive at home and in their communities



SUSAN SHELLY Writer
Menopause is a natural process that signals the end of the female reproductive years, affecting about half of the worldwide population. And yet for decades, menopause—which occurs in a woman when she has not experienced a menstrual period in a full year—has been misunderstood and largely undertreated.
Fortunately, that situation is changing as awareness about menopause is on the rise, and women are increasingly looking for relief from symptoms that can be bothersome and disruptive. “There’s definitely a lot more attention being given to menopause and the women experiencing it than there was five or 10 years ago,” noted Dr. Cynthia Chuang, a women’s health and internal medicine physician at Penn State Health, which recently started a virtual menopause clinic program.
Menopause treatment has been inconsistent in the United States since the 1960s, due primarily to controversy surrounding hormone replacement therapy (HRT). Although HRT has proven to be the most effective menopause treatment available to date, its use has increased and decreased sharply for decades as research produced varying results concerning its role in either preventing or contributing to cancer, heart disease, osteoporosis, dementia, and other conditions.
The first HRT was approved in the 1940s, and—despite fluctuating rates of popularity— hormones were widely prescribed for decades, according to Chuang. During the 1990s, in fact, estrogen-based menopausal therapy was the most often-prescribed treatment in the country. However, the popularity of HRT plunged dramatically in 2002 after the

Women’s Health Initiative (WHI) ended an HRT trial three years before its scheduled completion date and published findings pointing to increased risks for breast cancer, heart disease, and stroke among trial participants.
Those findings, explained Dr. Dorothy May, an obstetrics and gynecology physician (OB/GYN) with Penn Medicine Lancaster General Health, stopped many providers from prescribing any type of HRT treatment. “The whole study was stopped, and there was a panic,” May said. “Everyone went off hormone replacement therapy, and people were afraid.”
Without HRT—which, before the release of the trial results, was the gold standard for treating menopause symptoms—treatment of any type for menopausal women was reduced to a trickle. “For a long time, we
really didn’t treat women because of those concerns,” May said.
A closer look at the WHI study, however, revealed that the average age of women in the HRT trial was mid-60s, and many had been menopausal for more than a decade. Re-analyses of data from the trial showed that while HRT did result in risks for older patients, it is much safer for younger women. “So, we were comparing results for women in their 60s versus those in their 40s or 50s,” said Dr. Kristine Leaman, an OB/GYN with WellSpan Health. “We weren’t comparing apples to apples.”
Since then, HRT has regained traction as physicians recognize that younger patients can safely take hormones, which have been shown to result in a 75% improvement in symptoms on average. “We’re much more comfortable now with prescribing hormones as it’s appropriate,” said Chuang.
Also, according to Dr. Sameera Syed, medical director of obstetrics and gynecology services in Lancaster County for UPMC Magee-Womens, in November, the Food and Drug Administration (FDA) removed the “black box” warning from menopause hormone therapy products, increasing the willingness of providers to prescribe them and of women to use them. Increased use of HRT, coupled with improved knowledge and demand for menopause treatment from patients, has resulted in a significant increase in menopause care, including in Lancaster County.
Lancaster Physician reached out to health care systems serving Lancaster County residents to find out what their patients are looking for regarding menopause care and their efforts to meet patients’ needs.

Dr. Cynthia Chuang works with Lancaster County patients from Penn State Health’s Menopause Clinic, which opened in July in Hershey, but serves most patients virtually. “I see about 80% of patients on virtual visits,” she said. “Virtual care works well for
this population because most of what we do doesn’t require extensive exams or anything.”
Chuang, who is also a professor of medicine in Penn State College of Medicine’s Department of Medicine, became interested in having a dedicated menopause clinic within Penn State Health after observing that while some providers offered menopause care, others shied away from it. “I think they were trying to avoid dealing with questions that remained over hormone treatments,” she said. “I noticed there were women who weren’t getting much care in this area.”
Chuang began educating herself about menopause and last year was certified as a Menopause Society Certified Practitioner. The Menopause Society is an Ohio-based nonprofit founded in 1989 to raise awareness and provide resources for health care professionals. With cooperation from other Penn State Health staff and administrators, the clinic opened and has been very well received. It is staffed by Chuang and another internal medicine physician.
For patients who prefer in-person appointments, Dr. Laura Hunter, an OB/GYN, provides menopause care in her Lancaster office. Many primary care physicians and OB/GYNs also treat menopausal patients and can work in conjunction with the menopause clinic.
While the average age for a woman to enter menopause is 51, many younger women can experience a range of symptoms associated with perimenopause, a transitional period that marks the early stages of menopause and that can last for years. “Perimenopause can start in the early 40s and can be very confusing for women who don’t recognize its symptoms,” Chuang said. Those symptoms can include irregular periods, weight gain, sleep changes, hot flashes, vaginal and bladder problems, mood changes, bone density changes, and others.
Sometimes, explained Chuang, patients are confused by the symptoms they’re having because they don’t associate them with menopause. “It can be a very confusing time,” she said. “We’re always happy to talk to anyone
who might have questions or concerns about how they’re feeling or any symptoms they’re experiencing.”
Patients can be referred to the clinic by a Penn State Health provider or can self-refer.

Dr. Dorothy May, who runs Penn Medicine Menopause Care
Centerville, has witnessed the shifts in menopause treatment during her 30-year-plus career. The Women’s Health Initiative study, she said, was detrimental to women because providers who pulled back from providing HRT treatments often had little else to offer their patients. “It’s not that the medical field overlooked this population; it’s just that there weren’t a lot of treatments other than HRT available,” May said.
She is encouraged, however, by recent attention that’s been given to menopause and women who are actively learning about it and seeking care to manage symptoms. “I think there is significant interest in menopause and the need for care,” she said. “Women are educating themselves and looking to get the care they need.”
Kristen Schaefer, Reproductive Endocrinology and Infertility program manager, said women have responded very positively to the health system’s menopause center, which opened in November. “The referrals have been flowing in,” Schaefer noted. “It’s clear that there’s a need for this type of care.”
Interest in menopause has increased recently due to several factors, including celebrities speaking out about it and an abundance of information, advice, and product offerings available on social media platforms. May noted that while social media has helped raise awareness about menopause—a good thing— it also shares information and misinformation that can be confusing. “I think the clinic is so popular because it addresses that confusion and clarifies the correct information from a medical standpoint,” she said. A Menopause Society Certified Practitioner, May urged
Continued on page 22
women to seek medical advice rather than relying on information they encounter online.
While HRT is a viable treatment for many menopausal women, it is not for everyone. Women with certain medical conditions, such as a history of blood clots or certain types of cancer, may not be candidates for HRT, but can be directed toward alternative medications and other types of care. May partners with a range of health care providers, including mental health professionals, nutritionists, pharmacists, urologists, gynecologists, and others, to effectively treat each patient.
The clinic works alongside Penn Medicine Lancaster General Health’s Health Weight Management program to assist patients struggling with menopause-related weight gain. “We’ve really tried to find partners within the system who can support the needs of all our patients,” she said. May meets with patients during an initial consultation, conducts an assessment, and develops a treatment plan. A nurse navigator helps coordinate care and facilitate appointments. “And then we follow through with a multi-disciplinary team,” May said.
May is the only provider with the menopause clinic at this point and sees patients there just two days a week. Plans to expand clinic hours are underway, as more women seek care. “We’ve been busy since we opened and haven’t had a single negative review,” Schaefer said. “The clinic is off to a great start.”

A Menopause Society Certified Practitioner who practices in Lancaster County, Dr. Kristine Leaman is sought out by women seeking treatment for menopause-related conditions. She is one of 12 practitioners throughout the WellSpan system certified by the Menopause Society, enabling patients to find providers who specialize in menopause care and can provide personalized treatment based on their symptoms, circumstances, and needs. “At WellSpan, we really want to make sure the experience is what the patient is expecting,” Leaman said. The health care system provides menopause treatment through its Midlife Health and Wellness centers, which operate in
several locations. A nurse navigator is available to guide patients through the process of locating providers and setting up appointments.
The most common concerns of patients include hot flashes, night sweats, trouble sleeping, joint pain, weight gain, bleeding issues, and skin and hair concerns—all common symptoms of menopause and perimenopause. Typically, Leaman described, she will meet with a patient to discuss symptoms, conduct a period history, and review medical history. Once she thoroughly understands the patient’s condition, concerns, and needs, they discuss treatment options and decide on a plan.
Patients who elect HRT schedule another appointment in two months so they can be assessed and the treatment evaluated, Leaman explained. Most patients who qualify for HRT do very well on it, she said, with some continuing the treatment for long periods of time. Patients who are not candidates for HRT can receive alternative treatments, such as non-hormonal drugs that can reduce hot flashes and ease other symptoms.
WellSpan menopause specialists also confer with patients about the importance of sleep, exercise, nutrition, stress control, and other factors that may help reduce the severity of menopause symptoms. Specialists often work with primary care providers who consult with them on behalf of their patients who are looking for menopause care, Leaman said. “We’ll consult with PCPs and make recommendations, which enables patients to continue care with a doctor they know and eliminates the need for them to see someone new,” she explained. “There’s a group of people at WellSpan who have really worked to streamline the process and make it easier for patients who are looking for care.”

Women in Lancaster County can receive treatment for menopause-related conditions from Dr. Sameera Syed, who is an OB/ GYN and a certified menopause practitioner through The Menopause Society. She, along with other board-certified physicians and certified nurse midwives, is available to care for women with menopause symptoms through
UPMC Magee-Womens in Annville, Lititz, Lancaster, and Elizabethtown.
Syed urged women to start thinking about menopause before they develop symptoms and to empower themselves by learning the most evidence-based knowledge regarding treatments for symptoms. Once they’ve educated themselves, women can consult with their health care providers, who will discuss potential treatment options and help patients understand their risk factors if they’re considering HRT.
There are also non-hormonal treatments available, including selective serotonin reuptake inhibitors, serotonin-norepinephrine reuptake inhibitors, antiepileptics, gabapentin, oxybutynin, and other centrally acting drugs.
Syed issued a warning regarding custom-compounded bioidentical hormone therapy, which employs formulations prepared by mixing hormones with inactive ingredients in pill, gel, or cream form. Marketing for custom-compounded bioidentical hormone therapy describes it as a customized approach to HRT in which hormone dosages and formulations are based on a patient’s specific lab results, symptoms, and health profile, and it implies that the products are derived from all-natural ingredients. Many postmenopausal women are turning to custom-compounded bioidentical hormone therapy because they have safety concerns about conventional hormone preparations, Syed explained. However, she stressed that these products are not FDA-approved, and noted that expert groups, including the Menopause Society, American College of Obstetricians and Gynecologists, and the Endocrine Society, have issued scientific statements advising against their use.
She urged women to discuss all menopause treatments with their providers and consider various options for FDA-approved hormone therapies, including oral, transdermal, topical gels and lotions, and vaginal rings. “Patients should understand that research and evidence are the strongest tools we have to guide management of their symptoms and relief from their suffering,” Syed wrote.

Lancaster Skin Center, PC has been providing dermatologic care to the Lancaster community since 1997. Founded by William Andersen, MD, the practice serves patients from throughout Lancaster County and the surrounding region.
The office is located at 190 North Pointe Boulevard, Suite 1, in Lancaster, just off Oregon Pike, a convenient location for patients traveling from across the county. Over the years, the location has become familiar to many patients through referrals and long-standing relationships within the community.
Dr. Andersen is quadruple board-certified in dermatology, anatomic pathology, dermatopathology, and Mohs micrographic surgery, and he remains actively involved in daily patient care. Rather than shifting focus away from the practice, he continues to see patients regularly, emphasizing careful evaluation, clear communication, and long-term management of skin conditions.
Over the years, Lancaster Skin Center has evolved alongside advances in dermatology. Patients are seen for a broad range of needs, including routine skin examinations, chronic dermatologic conditions, and the diagnosis and treatment of skin cancer. Dr. Andersen also provides cosmetic dermatologic procedures, offering patients options to improve the appearance and health of their skin while maintaining the same
thoughtful, individualized approach that has defined the practice for decades. New techniques and treatments have been incorporated thoughtfully, with attention to what best serves patients in a community-based practice.
Patients are seen by Dr. Andersen and Molly Casey, CRNP, the practice’s other primary provider. Molly Casey has been with Lancaster Skin Center for 13 years. Before becoming a nurse practitioner, she served as Director of Nursing for six years and completed her nurse practitioner training alongside Dr. Andersen. Her long-standing presence allows patients to receive consistent, coordinated care and fosters a sense of familiarity and trust throughout every visit.
Supporting the clinical team is an experienced group of staff members who help ensure the office operates smoothly from check-in through follow-up care. Many patients return to the practice year after year, often seeing the same providers and staff members at each visit.
In a community where personal connections remain important, Lancaster Skin Center has remained grounded in its original mission— providing reliable, high-quality dermatologic care close to home. The practice’s longevity reflects both its connection to the Lancaster community and its commitment to consistent, patient-focused care.
Longest Tenured LCCMS Member— Continuous Membership Since 1959
Silas Kendrick Eshleman III died peacefully at the age of 97 on December 21, 2025, at Landis Homes, Lititz, PA. He was born in Gainesville, Florida, the son of Silas Kendrick Eshleman, Jr. and Aileen Hope McClamrock Eshleman. Ken’s father was a professor at the University of Florida, and the family resided in Florida during the school year, returning to Lancaster County each summer.
Ken’s lifelong interest in science was evident at an early age, when he was a student at the P.K. Yonge Lab School in Gainesville, where he was allowed to have a weather station on the roof, provided he gave a daily weather forecast.
He graduated from the University of Florida, Gainesville, with a B.S. in Biology with high honors and Phi Beta Kappa. He did much field research on the flora and fauna of Florida during his undergraduate years, with an emphasis on freshwater sponges. After college, he attended the University of Pennsylvania School of Medicine, Philadelphia, PA, and graduated with his M.D. in 1953.
In his third year of medical school, he met Judith Wills Cooper, R.N., and they married in 1954.
He served in the U.S. Army Medical Corps, with the rank of Captain, and was in charge of the psychiatric wards at the U.S. Army Hospital in Fort Knox, Kentucky.
In 1959, he and Judy moved to Lancaster, PA, where he established his private psychiatric medical practice (until retiring in July 1997). He was a member of the medical staff at the former St. Joseph Hospital and Lancaster General Hospital. At St. Joseph Hospital, he helped establish the psychiatric unit, which was one of the first in PA. He was also the Chairman of the Department of Psychiatry for many years. Additionally, he served as a consultant in psychiatry at the Veterans Administration Hospital in Lebanon, PA, and was a consultant at the Lancaster County Family and Children’s Service.
He is survived by a daughter, Diane Eshleman Djordjevic, her husband Milic, granddaughter Tatiana, and many cousins. He was preceded in death by his wife of nearly 60 years, Judith Wills Cooper Eshleman, and a brother, John Martin Slaymaker Eshleman.


BARTON L. HALPERN, MD President-Emeritus, Lancaster Medical Heritage Museum
If you haven’t been to the Lancaster Medical Heritage Museum recently, please come prepared to be amazed!
Founded in 1981 by the Lancaster City & County Medical Society, local physicians, and concerned citizens, the Lancaster Medical Heritage Museum preserves the rich medical history of Lancaster County.
The museum was originally incorporated with the name Edward Hand, a Lancaster County physician, general in George Washington’s army, politician, and owner of land now known as the Rock Ford Estate. The museum was recently renamed the Lancaster Medical Heritage Museum, in keeping with its diverse collection of medical artifacts donated by local hospitals and retired Lancaster physicians. Thanks to the extraordinary generosity of Penn Medicine Lancaster General Health, the museum was given space and funding, which allowed it to open to the public in December 2022.
Currently, the museum has an estimated 11,000 medical artifacts, 8,000 square feet of space, and a growing number of exhibits. The museum has added a public education aspect to its mission—interns have written numerous papers, and staff as well as volunteers have lectured at retirement communities, held public seminars, and hosted programs for homeschooled students.
The Lancaster Medical Heritage Museum welcomes volunteers and gratefully accepts artifacts and financial donations to allow it to maintain Lancaster County’s fascinating medical history. Anyone interested in learning more about the evolution of medicine in our area is encouraged to visit and see all that the museum has to offer. If you would like to support the museum, visit lancastermedicalheritagemuseum.org, and click on “Support Us” at the top of the home page.
Art Exhibit
Our exhibit includes Scherenschnitte art and posters in our pharmacy exhibit; a wall including approximately 100-year-old original scrolls of human anatomy; reproductions of classic art documenting topics in medicine; a wall of Lancaster history expressed in art; and posters documenting medicine in ancient times. It has been updated to include reproductions of letters between former President James Buchanan and his Lancaster physician, Dr. Henry Carpenter.
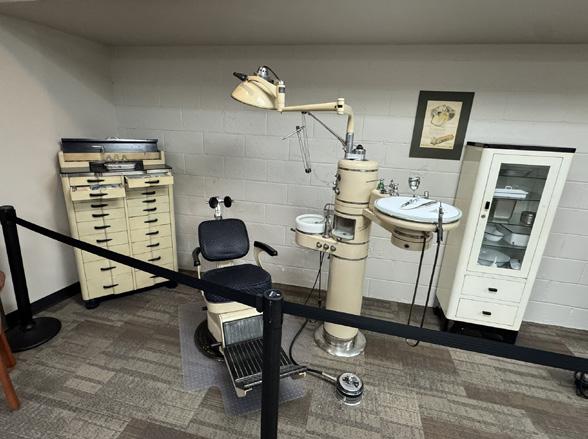
Dental Exhibit
The dental exhibit showcases dental offices, one circa 1900 and one circa 1950.
This exhibit has been expanded to include educational lectures (on topics including the iron lung and polio) and experiences for homeschooled students. Exhibits focus on the doctor’s skills of history taking, inspection, palpation, percussion, and auscultation. A functioning interactive medical mannequin is also available to study.

This updated exhibit shows an in-home family doctor’s office circa the early 1900s.
This new exhibit showcases battlefield medicine with artifacts from the Civil War to World War II.
This new exhibit features an early 1900’s operating room, showcasing the advances in infection prevention and instrument sterilization.

The museum boasts one of the most extensive ophthalmology collections around and showcases a typical early 1900’s eye doctor’s office.

With a focus on the history of pandemics and the importance of vaccines, this exhibit showcases the Marietta Vaccine Farm and Lancaster’s important contributions to smallpox vaccine development and distribution. The polio portion of the exhibit includes a recently refurbished, fully functional iron lung machine courtesy of Lancaster General Hospital.
This new exhibit includes a neonatal incubator plus unique artifacts such as a murder bottle, birthing chair and anti-thumb sucking infant gloves.
This new exhibit features pseudo-medical treatments.
This new exhibit features a historic Coolidge X-ray machine as well as X-ray viewing boxes featuring changeable X-ray images of the human body.
Medical Society Foundation to Make Awards to Students with Lancaster County Connections
The Lancaster Medical Society Foundation (LMSF) has opened its application process for the 20262027 academic year. Each year, the Foundation presents scholarships to support students who are pursuing MD or DO medical degrees.
The annual scholarship awards help offset the continually rising cost of medical school. Thanks to generous donations from the Lancaster County medical community, including local hospitals/health systems, group practices, individual Lancaster City & County Medical Society members, various businesses, and individuals, The Foundation has provided more than $323,000 in funds since its establishment in 1991. In 2025, LMSF awarded a total of $15,000 in scholarships to six deserving students.
This year’s awards will be made to medical students with a strong connection to Lancaster County. Eligible applicants will:
• demonstrate academic achievement, motivation, and leadership;
• show an interest in meeting societal needs; and
• share a desire to potentially serve Lancaster County residents as a future physician.
In addition to a completed application, interested students must also submit a one-page essay describing why they have chosen medicine as a career and their anticipated contribution to Lancaster County as a physician; a transcript from their undergraduate, postgraduate, and medical school institutions (as applicable); and a current CV.
For more information or to obtain an application, please visit lancastermedicalsociety.org or contact Lancaster City & County Medical Society at 717.393.9588. Applications must be received by July 1, 2026, for consideration.

Penn Medicine LG Health Physicians Thoracic Surgery
Where do you practice and why did you settle in your present location or community?
I am an employed physician of the University of Pennsylvania Health System, and I practice at Penn Medicine Lancaster General Hospital and at the Ann B. Barshinger Cancer Institute. Before my current position, I spent the first 23 years of my professional career in the Chicago area as an accomplished thoracic and cardiovascular surgeon in a 35-surgeon single specialty private practice group. The group practiced at 28 hospitals that spanned multiple health care systems as well as a large university practice. Throughout my career, I had been offered career opportunities outside of the Chicago area. However, my wife and I, as well as both of our families, are Chicago-based, and we were quite comfortable being at home. Although we have no family in Pennsylvania (and to be honest, we had never even visited Pennsylvania other than a stopover at the Philadelphia airport), I accepted an invitation to explore a career opportunity in Lancaster. During my initial visit, it became instantly apparent that health care delivery in Lancaster is patient-focused and that providers and practitioners have a deep commitment to serve the community by providing passionate and cutting-edge care. Eight years later, that initial impression continues to resonate and hold true.
What do you like best about practicing medicine?
Practicing medicine is a unique and rewarding career. We all begin at a very similar starting point by learning basic science and timidly interacting with our first patients as we begin clinical rotations. We learn from our mentors, and we develop clinical interests that shape our future career pathways. Somehow, we then amazingly transform into practitioners who are entrusted to care for others. As we mature, we repeat the process and train the next generation of physicians. This journey is an addictive and fulfilling process that yields great satisfaction. I could not have chosen a more fluid and rewarding career.
Are you involved in any community, non-profit, or professional organizations? If so, please list the groups. I am a member of numerous professional organizations, including the American College of Surgeons and the Society of Thoracic Surgeons.
What are your hobbies and interests when you’re not working?
I enjoy spending time with my wife and our married children. College football is a fall-time passion. Travel (although not frequent enough) is always a great experience. My wife and I also enjoy taking on new cooking challenges and eating our creations.
For what reason(s) did you become a member of the Lancaster City & County Medical Society, and what do you value most about your membership?
I have always been a member of local and county medical societies when I practiced in Illinois, so it was a natural desire for me to join the Lancaster City & County Medical Society. Initially, it was an opportunity for me as a new addition to the community to meet and network with colleagues from across all of our local health care systems. More recently, it has also become a passionate opportunity to support scholarships for our local students who are pursuing healthcare studies.



Frontline Practice Groups have made a 100% membership commitment to LCCMS and PAMED. We thank them for their unified support of our efforts in advocating on your behalf and facilitating an environment for physicians to work collaboratively for the benefit of the profession and patients.
Avalon Primary Care
BestFit Virtual Health + Wellness, PLLC
Carter MD Aesthetics
Community Anesthesia Associates
Community Services Group
Conestoga Eye
Dermasurgery Center, PC
Dermatology Associates of Lancaster, Ltd
Dermatology Physicians, Inc
DermDox Dermatology Centers, PC – Leola
Eye Associates of Lancaster Ltd
Family Eye Group
Family Practice Center, PC – Elizabethtown
Glah Medical Group
The Heart Group of Lancaster General Health
Hospice & Community Care
Hypertension & Kidney Specialists
Lancaster Arthritis & Rheumatology Care
Ayesha S. Ali, MD
Jerome Barron, DO Penn Medicine Lancaster General Health Physicians Sports Medicine
Monodeep Biswas, MD UPMC Heart & Vascular InstituteLancaster
Martin T. Brown, MD FACTS About Fertility
Patricia Carr Reese, MD Penn Medicine Lancaster General Health Physicians Comprehensive Care
Rachel L. Angstadt, DO Penn Medicine Lancaster General Health Physicians Palliative Care
Rodney E. Brenneman, MD Orthopedic Associates of Lancaster, Ltd
Anna C. Catalano, DO Penn Medicine Lancaster General Health Physicians Family Medicine Norlanco
Marguerite R. Duane, MD
FACTS About Fertility
Lex J. Gardner, MD

Lancaster Cancer Center, Ltd
Lancaster Family Allergy
Lancaster Radiology Associates, Ltd
Lancaster Skin Center, PC
LNC Oculoplastics
Luz Medicine
Manning Rommel & Thode Associates
Nemours duPont Pediatrics Lancaster
Patient First – Lancaster
Penn Medicine Lancaster General Health Care Connections
Penn Medicine Lancaster General Health
Physicians Family Medicine Lincoln
Penn Medicine Lancaster General Health
Physicians Family Medicine Manheim
Penn Medicine Lancaster General Health
Physicians Family Medicine Norlanco
Penn Medicine Lancaster General Health
Physicians Thoracic Surgery
Simone Hughes, MD Clinic for Special Children
Julia A. Goroff, DO Clinic for Special Children
Joseph M. Kontra, MD
Weston P. Shertzer, DO Penn Medicine Lancaster General Health Physicians Anesthesiology
Autumn R. Vogel, MD Union Community Care – Duke St
Stephen I. Warren, MD The Heart Group of Lancaster General Health
Kayla Williams, DO Union Community Care – KinzerChurch St
Kristen Wong, MD The Heart Group of Lancaster General Health
Kerolos R. Yousef, DO Penn Medicine Lancaster General Health Physicians Anesthesiology
Ashley A. Kempsell, MD Penn Medicine Lancaster General Health Physicians Family Medicine Lincoln
Janine Kiernan, Practice Administrator UPMC Heart & Vascular Institute –Lancaster
Agnieszka E. Mochon, MD WellSpan Cardiology – Lancaster
Jonathan Musyt, MD Penn Medicine Lancaster General Health Physicians Family Medicine Lincoln
Tuyet-Nga Q. Vu, DO Union Community Care – New Holland Ave
Wen Y. Helena Wu-Chen, MD Lancaster General Health Physicians Neurology
Jennifer C. Zampogna, MD Lancaster General Health Physicians Behavioral Health
Nicole D. Zimmerman, DO Penn Medicine Lancaster General Health Physicians Family Medicine Lincoln
Penn State Health Lancaster Medical Center –Palliative Medicine
Pennsylvania Specialty Pathology
Retina Associates of Lancaster
Union Community Care – Duke Street
Union Community Care – Hershey Avenue
Union Community Care – Kinzer-Church Street
Union Community Care – New Holland Avenue
Union Community Care – Water Street
UPMC Breast Health Associates
UPMC Ephrata Primary Care
UPMC Heart & Vascular Institute – Lancaster
UPMC Lititz Wound and Hyperbaric Center
WellSpan Family Health – Georgetown
WellSpan Family Medicine – West Main St
WellSpan Interventional Radiology at Ephrata
WellSpan Physiatry – Ephrata Hospital
Lancaster City & County Medical Society (LCCMS) is your home to help you deal with local and regional health care issues. When you join LCCMS, to network, learn, share ideas and advocate locally, you also join Pennsylvania Medical Society (PAMED), the voice of Pennsylvania’s physicians, advancing quality patient care, the ethical practice of medicine, and advocating for the patients they serve. PAMED works with the LCCMS to promote physician leadership, education, professional satisfaction, practice sustainability, and the public’s health. To join or renew your LCCMA/PAMED membership, contact PAMED at 800.228.7823 or visit them online at www.pamedsoc.org/join.
