

ABOUT THE NEW ENGLAND RURAL HEALTH ASSOCIATION
For over 25 years the New England Rural Health Association (NERHA) has served as the state rural health association for the six New England states. We are a non-profit organization dedicated to advancing rural health. NERHA provides education, training, consulting, and advocacy in support of the rural health organizations and individuals in our region. We encourage future health professionals to practice rurally through scholarships for rural student internships. Headquartered in Vermont, the Association is governed by a Board of Directors and administered by an Executive Director.
With over 550 members and over 5,500 subscribers, we represent a wide range of rural health professionals, including hospitals, clinics, public health, and academic institutions. Key initiatives include strengthening the rural health workforce through student memberships, scholarships, and internships.
Join us in advancing rural health by becoming a member, serving on our committees or Board, or partnering with us. Learn more at NERHA.org.
RURAL ROOTS
Spring 2025 Vol. 2
Publishing
Dartmouth Printing
Planning & Design
New England Rural Health Association
Executive Editor: Andy Lowe
Design: Kiera Hight
E-mail: admin@newenglandrha.org
Read Rural Roots magazine online at the website: nerha.org
Copyright ©2025 New England Rural Health Association. All rights reserved.

FROM FIREPLACE TO WOOD STOVE: A PERSONAL JOURNEY
OF HOPE: SHANE’S JOURNEY WITH ANGEL FLIGHT EAST
Roots Locator STORIES FROM

Introduction
It’s Spring in New England! It was a good old cold, snowy winter, and now we get the prize for patiently enduring (and enjoying) that long spell of weather. Geese are winging back north to start their families. Green is the new order of the day. The sheer profusion of biomass reminds us of the overpowering abundance of life wrought by the simple magic of sun and rain. Fecundity is everywhere. Likewise, there is a veritable spring tide of good work going on in rural health. Need some examples? Just look inside and you’ll discover heroes in rural health all around our region. Read a tale of how rural communities refused to be held down by historic flooding, and how volunteerism benefits community and volunteer alike. Learn how rural health has shaped and been shaped by the life one Rhode Islander. How about heating with wood? Lots of us still do, but it’s important to understand the complex interplay of BTUs, wood smoke, and environmental impact. Stories of rural health and innovation are sprouting like new hay in the fields!
Featured In This Issue
“Mud dog” volunteers clad in Tyvek help communities dig out after flooding…
“Growing up in central New Hampshire, my dad taught me how to choose a large round log to place at the back of the fireplace…”
A training program with a unique twist helps build the community health workforce in rural Massachusetts…
“When I think about harm reduction, I think that is a rather fitting analogy…”
Other Highlights
Meet a Member: Gail Patry of Rhode Island shares what rural health has meant to her professionally and personally…
Tiffany Moreno of Berkshire Community College is honored with the Berkshire (MA) 40 Under 40 award…

Article by Andy Lowe
Photo by Terra Caballero
RISING ROOTS

AFTER THE STORM
On the morning I became a “mud-dog”, sleepy heads attentively nodded while given instruction: enter the crawlspace, scoop the mud, pass the bucket. Hurricane Helene had displaced hundreds and we were set on getting people home. Donned in Tyvek, head to toe, we began clearing the mud beneath the floorboards.
The only visible light shone through window panes, past floor joists. Our hands became trowels, scooping each five gallon plastic drum. Noxious mixtures of sludge, sewage, and flood water permeated through N-95 masks. Scoop the mud. Pass the bucket. Repeat.
To be rural Appalachian is to know resilience, ingenuity, and self reliance, but even mountain folk were not built for hurricanes. In its final report, NOAA identified Helene as the deadliest tropical cyclone in nearly twenty years since Katrina.
Six months following the storm, the healing process continues.
• Within 2 weeks, power was regained across 97% of North Carolinian residences.
• After 51 days, Asheville had running water again.
• Hot Springs (population 500) is considered a prominent stop along the Appalachian Trail. The town has welcomed back hikers with open arms — granted, with some modification.
• Further north, in Erwin, Tennessee, a new daily ferry service across the Nolichucky river is compensating for the loss of a significant bridge.


While things are seemingly normal on the surface, this can be taken at face value. Like mold creeping behind stone fireplaces and expensive finished floors, erosion isn’t always visible on the surface.
In December, Senate Bill 382, titled a “hurricane relief bill,” addressed only 13 of its 131 pages with storm damage. The rest reallocated officials’ responsibilities. The North Carolina Poor People’s Campaign called it a “disastrous bill for the disaster.” Of $227 million, none would fund immediate needs like rent, power, or temporary assistance.
In March, Duke Energy initiated a “storm clean up fee”. Users reported power bills exceeding $300 in counties like Macon, where the poverty status is higher than the national average (14.4% versus 12.4%).
This raises a critical question of the healing process: is a community healed when things are rebuilt or when enhanced? To explore this question, I turned toward another recent flood: Rumford, Maine.
RUMFORD: 15 MONTHS LATER
In December of 2023, Rumford and surrounding towns experienced flooding from the Androscoggin river. John, a Rumford local, explained that he and his family were trapped in their home’s upper level for two and a half days before the water level receded.
Debris washup along the French Board River


“In one short night, everything we owned was underwater,” he explained. Relief and aid came from a mission group based out of Cincinnati. Moved by this effort, John made the choice to assist in clean up following Helene. “We had a great team come and help us from Ohio. Not only did they [help us with the] mud out, but also touched our hearts. I felt it was my calling to help others in the same way,” John said.
Catherine, a pharmacist, shared her experience and what she sees now.
Moving to the area in 2015, rural living was an appropriate option for her family. Smaller class sizes facilitated a personalized education for her son, allowing him to excel in Rumford, compared to Minneapolis.
Most were unaware of the impending flood severity. The December flood caused road wash-outs, trapping several people; the scars remain in sink holes along county roads today.
“In the winter, the ground will freeze, and the water doesn’t have anywhere else to go,” she said, “we were warned of a winter-rain, but that was it.” Two community members lost their lives in the flood and the community came together to host a memorial service.
Waterlogged debris from a home flooded by Hurricane Helene
Catherine mentioned a lack of access to healthcare services, as a continued result of these events. Last year, she was able to start seeing a psychiatrist. However, the appointment took over six months. A friend recently sought similar treatment, but the waitlist was now over a year. Many locals rely on transporting to Portland or Boston for services. In urgent situations, often the only option is to seek out emergency care and risk excessive financial burden.
BUILDING RESILIENT COMMUNITIES
With consideration to weather related disasters, a critical component to ensuring community resilience is through education.
Nikki, a current disaster relief volunteer, spoke about her experiences. Today, programs in Western North Carolina have transitioned toward rebuilds. After four months stationed in Asheville, Nikki was sent to Allen, Kentucky to tend to the February floods.


Neighborhood in Western North Carolina after the flood waters receeded
Swannanoa River, Asheville, NC


Significant budget constraints inhibited her team’s ongoing presence.
“[Our international non-profit] signed onto a year in North Carolina, but we were given two weeks in Kentucky…Many people, even those in the big cities, look down their noses at little towns like Allen.” Before leaving, Nikki’s team trained some of Allen’s 200 residents how to sanitize, providing them with kit and donating 150 industrial fans.
“Often, people don’t know the first step. All people in flood zones are susceptible, but need to know their options when something happens. We need to bring awareness to those who are vulnerable.”
Article by Terra Caballero
Terra making a heart in the appalachians
Sunrise in the Blue Ridge Mountains, North Carolina
Photos by Terra Caballero
ANNOUNCING THE 2025 RURAL HEALTH LEADERSHIP INITIATIVE!

Are you a current rural health professional interested in building your leadership skills?
The New England Public Health Training Center and NERHA announce the 2025 Rural Health Leadership Institute (RHLI). Building on the success of the 2024 RHLI, this year’s program will accept a limited number of applicants for an all-new, two-month program designed to prepare them to lead in the changing world of rural public health and primary care.
RHLI is designed to be fast-paced, interactive, and tailored to trainee interests, featuring a combination of short virtual classes and two exciting in-person events where students will work with a team of peers on real challenges confronting rural health leaders. Emphasis will be on team-based learning to develop real-world approaches and problem-solving solutions. You will learn effective techniques for communicating data and qualitative information to build support for growth in community-based and interprofessional settings.
Be sure you are on our mailing list and watch for an announcement coming soon with course details and application instructions. We hope you will join the 2025 RHLI to prepare yourself to lead in tomorrow’s rural health settings!
In each edition of Rural Roots we feature one or more of our amazing rural health members to celebrate the diverse paths they have followed in their rural practice. We think you will be as inspired as we are by these incredible, experienced rural practitioners.
This month, we invite you to meet Gail Patry, a former NERHA Board Member and newly retired from Healthcentric Advisors!
State: Rhode Island
Role: Recently retired from my position as the Senior Vice President of Quality Programming
Org: Healthcentric Advisors

GAIL PATRY
Can you please tell us a little about yourself and your work in rural health?
Greetings from Rhode Island! It’s a beautiful sunny day and looks like we’ve turned the weather corner.
My name is Gail Patry and I served on the NERHA board until the end of February when I retired from my position at Healthcentric Advisors.
Healthcentric Advisors is a respected healthcare quality improvement organization and has proudly served all 6 New England states for over 10 years. Prior to 2014, our work was primarily anchored in Rhode Island so I had a lot to learn about rural health, its strengths, challenges, and the residents it serves. I can confidently say that I have had great teachers including many of the leaders of NERHA. When Healthcentric Advisors opened our Maine office, I was fortunate enough to have Ann Marie Day, Michael Pancook and Jenn McCarthy on our team. I hope that they can remember those days as fondly as I do and that we played a small part in their healthcare journey.
I was completely unfamiliar with critical access hospitals and now am in awe of the tremendous role they play in serving our rural neighbors. As a native Rhode Islander, it was almost a foreign concept to understand people having to travel so far to receive healthcare services (as a reminder, RI is a little smaller than Disney World) and how challenging that can be in snowy winters in northern New England. In today’s reality, where all healthcare providers are struggling to recruit and retain staff, these rural providers have even more obstacles to overcome.
Gail Patry, former NERHA Board member, hiking


Although no longer working with the rural provider community, I am looking forward to continuing my vacation jaunts to the woods of northern New England. My husband and I feel tremendous peace when we are there. The people are warm, the food is spectacular and the vistas are second to none.
I am in the enviable position of having had a rewarding career surrounded by stellar professionals and thank the folks at NERHA for allowing me to play a small part in supporting rural healthcare communities.
What does
being a member of the New England Rural Health Association mean for you?
I have the opportunity to meet interesting dedicated professionals. I applaud NERHA for starting their student initiatives and exposing our future healthcare professionals to the rewarding world of rural health, not to mention the beauty of the New England landscape. Seeing how warmly the students are welcomed at the annual NERHA conference gives me hope that the future of care in rural areas of New England will be in good hands. Speaking of the conference…I have been to more conferences than I can count in the last 25 years and honestly can say that the NERHA conference is the very best. The sessions are always varied and thought provoking and have exposed me to information that I would not have had the opportunity to learn otherwise.
At last year’s conference, I had an opportunity to talk with Michael for a bit. He went out of his way, as busy as he was, to talk with me about my perspective on other ways that the NERHA can grow across the continuum of care. Being an old long term care nurse, I never miss an opportunity to
Spring in Newport County, Rhode Island
Gail Patry
promote organizations being inclusive of skilled nursing facilities, or SNFs, which at times are underrepresented in discussions. Supporting rural SNFs is critical to enhancing safe and timely care transitions and providing necessary services such as physical therapy so that individuals can successfully return to their homes. Additionally, many require longer term care for dementia or other conditions and deserve to receive that in a warm, safe environment. These care facilities have experienced unprecedented challenges in the last several years and many have had to close, making care options limited for the most vulnerable among us. There is actually one county in Maine that does not have a single SNF, making it impossible for people to get the care they need close to their home. Bringing them into the mix and having providers from all settings participating in the conference can only enhance the relationships between the hospitals, SNFs and outpatient services. I was and remain thankful to Michael for being curious enough to ask and for taking the time to thoughtfully listen.
What does rural health mean to you?
A couple of things come to mind. First, I would say that in many ways, rural health goes way beyond a narrow description of healthcare. I think that the provider community serves a much broader role than what people often put in the box they call care. Many residents of these rural communities can become isolated and can be challenged with being able to get out into the community, especially during the long winters. Rural health often serves the critical role in identifying what services or supports that people need to achieve their highest level of wellness.
The second thing I think of is the dedication and resilience of the professionals working in rural health. They face challenges often not experienced by those working in the “big city” but strive to find solutions and support those they serve in the best way possible.

Gail Patry, first row (left), and the NERHA Board members at the NERHA annual conference, 2024

FROM
FIREPLACE TO WOOD STOVE: A PERSONAL JOURNEY
Growing up in central New Hampshire, my dad taught me how to choose a large round log to place at the back of the fireplace so that there would still be coals in the morning. He called it an “all nighter log.” It seemed to work.
I looked up to my dad as a fountain of not just knowledge, but wisdom passed down through the generations. Turns out, some of this was not good advice and was not good for our health. “All nighter logs” were designed to smolder through the night and open fireplaces are notorious for leaking smoke into the home.
Early fascination with wood stoves
My dad also made me chop and stack wood far more than I wanted to as I kid. Once I was old enough to realize how much I loved that activity, I got to experience the challenge of getting my son to do it with me!
I remember a friend once telling me I smelled like wood smoke after I came out of my house. It didn’t really disturb me at the time, but in retrospect it should have. As I went through my teens I was drawn to Nichols Hardware, down the hill from where we lived. In the basement they had dozens of models of wood stoves, and for some reason I just liked being around them. In the late 1970s and 1980s they were so popular the Nichols family could barely keep them in stock. But the idyllic little New England towns, like mine, located in valleys soon became filled with wood smoke.
In my twenties, when I began paying my own utility bills, the benefit of wood heating hit home. Wood is the people’s fuel, and if you don’t want to go out and get it yourself, there is likely someone down the road who sells it. It is never controlled by some corporate giant that adds any number of taxes and fees to their monthly bills.
History of wood heat in New England
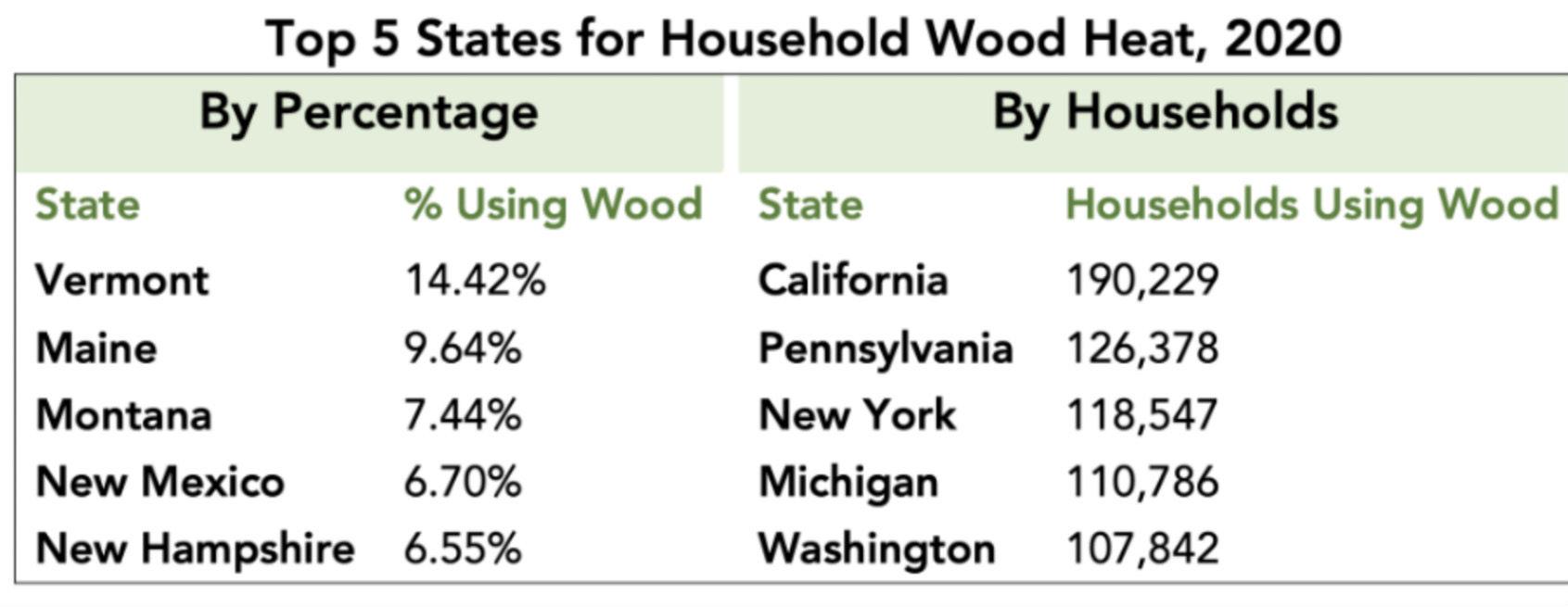
In the mid-1800s every house in New England heated with wood and we had clearcut the land for sheep, building and energy. The Troy, New York area was for woodstoves what Detroit would become for cars. By 1940, 23% of the country still heated with wood, falling to a low point in 1970 when only 1.3% did. But New England states held on to wood, with 36% of New Hampshire homes heating with it, and 33% coal.
In 1972, before the Arab Oil embargo, a woman from Maine named Eva Horton was the first American to popularize modern wood stove designs by importing Jotul stoves from Norway. They used less wood and made less smoke, a dual advantage. Vermont Castings didn’t start until 1975 but soon dominated the market and built a cult-like following.
Regulation of wood stoves
But the rush for wood stoves in the aftermath of the Arab Oil Embargo led to far too much wood smoke, especially in the Pacific Northwest where trade winds created terrible inversions in valleys, trapping all the wood smoke. When wood smoke gets that bad, it’s like a nearby wildfire, and the smoke seeps into everyone’s home, regardless of whether you heated with wood or not.
States put pressure on the EPA to regulate wood stoves and as of 1988, they must meet basic emission regulations. This helped a lot, as did a declining number of people heating with wood. Today ambient outdoor wood smoke, especially in the Northeast is far better and the biggest health threat is usually
not from outdoor ambient smoke, but smoke from your own stove, leaking into your home.
Choosing a career promoting wood stoves
I moved away from New Hampshire, pursued a career and family, and in my mid-50s, I needed a career shift. After being an armchair wood stove aficionado, I decided to start a non-profit, the Alliance for Green Heat, dedicated to cleaner and more efficient wood stoves. With all the interest in renewable energy, I thought there was an opening because wood stoves were in about 10% of American homes, whereas in 2010, not even 1% had solar panels, much less electric cars. I scraped by earning somewhat of a living for 15 years, finding that foundations, governments and the public regarded wood stoves with some suspicion, even though they are a lifeline to millions of rural households.
Part of that suspicion is well-founded in that stoves can create unhealthy indoor air, but that does mean all stoves lead to bad indoor air quality. And the rise of uncertified outdoor wood boilers which create more smoke than heat gave wood heating a bad name during a crucial decade when we were seeking to show wood stoves had promise. Vermont took the lead to regulate them and then ban them unless they were for homes with virtually no neighbors.

John Ackerly and his father and child
My passion was to computerize the wood stove, and we got grants from New York state and the Department of Energy to hold wood stove design challenges to get manufacturers to add sensors, and combustion fans so people would only have to load the wood, then let modern technology shoot just the right amount of air, at the right time, to the right part of the firebox.
Our group also got funding from the US Forest Service and support firewood banks all over the country, and especially in New England. The Trump administration is cutting funding for them now, as they are to local food banks.
Environmental and health impacts of wood heat today
Firewood is a very low-carbon heating fuel assuming its harvested sustainably, which is not a problem today in New England. Homes heated with wood or pellets do not contribute to the devastating impact that fossil

heating fuels have had. Wood heating also has a major health benefit because the exercise of chopping and stacking wood is not to be underestimated.
But it also comes with a significant health threat - air pollution - that many of us like my father, don’t take seriously enough.
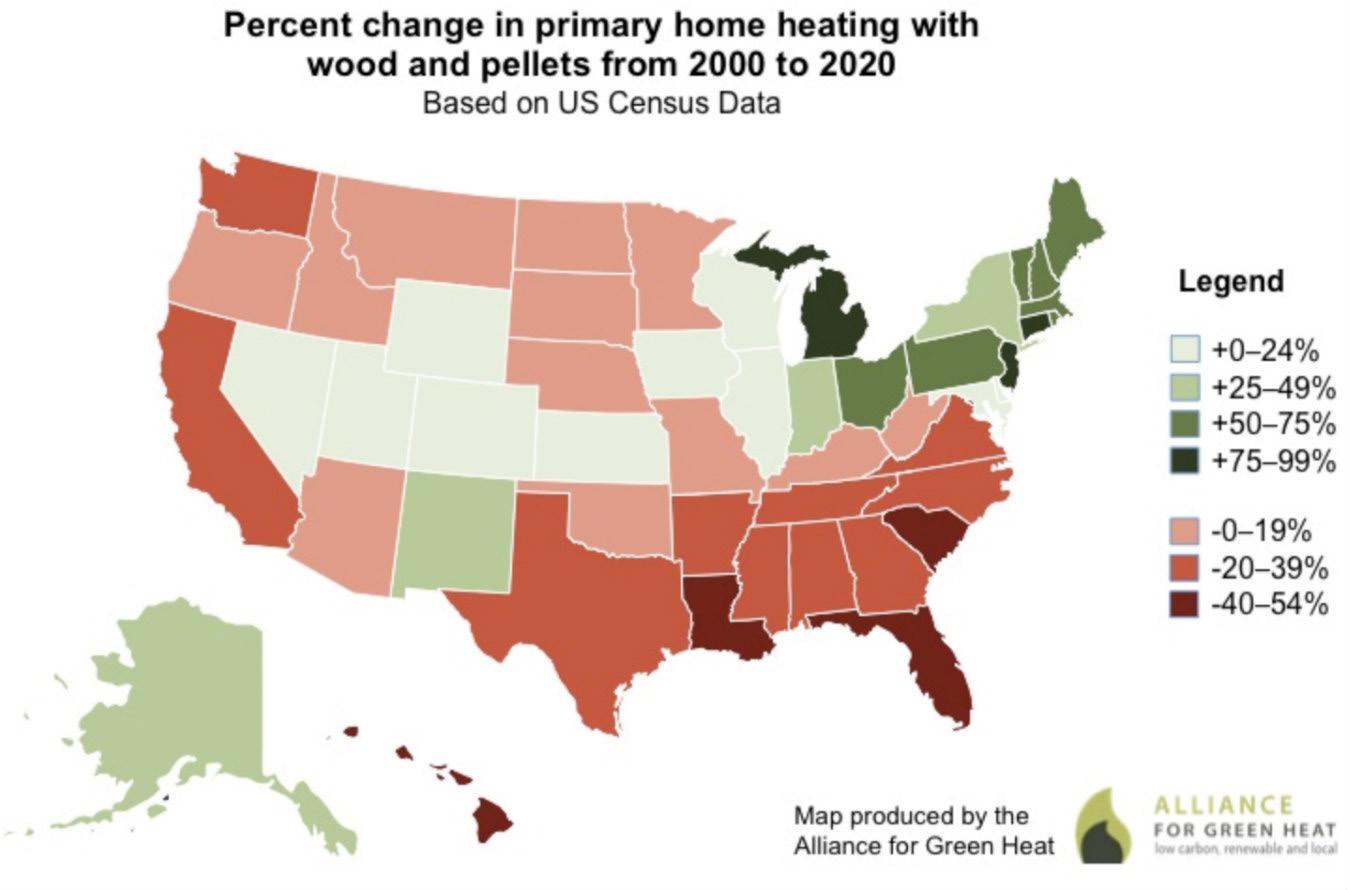
Map of changes in home heating from 2000 to 2020

Bottom line: if you regularly smell wood smoke in your home, the safest thing to do is to call a chimney sweep and see if they can help figure out what is going wrong. Often, it’s from a poorly installed stove that doesn’t have a strong enough draft. Sometimes, it is prevailing wind that blows smoke down your chimney and can be fixed with a special chimney cap. Or you may be burning unseasoned wood. Whatever you do, don’t ignore it.
Getting to the source of the problem is important, but using HEPA air filters can help. You can even make a low-cost effective air filter from a box fan and a furnace filter. Children and the elderly are most susceptible to poor indoor air quality.
Intergenerational knowledge is extremely important and rural New Englanders tend to understand the importance of securing firewood at least a year in advance and seasoning it well. Burning extra dry wood (15-20% moisture content) in a modern, EPA certified wood stove, and not letting your stove smolder is the best thing you can do to reduce wood smoke for your family and your neighbors. My dad passed away a few years ago and would laugh if he knew I was writing about his bad advice. Most of it was good and I will always treasure that.
Article by John Ackerly
Photos by John Ackerly
Freshly cut wood pile

EMPOWERING MASSACHUSETTS’ RURAL COMMUNITIES: WORKFORCE TRAINING PROGRAM
TACKLES HEALTH WORKFORCE
CHALLENGES
Rural Public Health Workforce Training Network Program a Major Success, Surpassing Project Expectations by Training Over 100 in First Two Years
The New England Rural Health Association (NERHA) proudly announces the success of its transformative Rural Public Health Workforce Training Network (RPHWTN) initiative in Massachusetts. Funded by the Health Resources and Services Administration (HRSA) Federal Office of Rural Health Policy and led by NERHA, this three-year program addresses critical workforce shortages and advances health access in rural communities across the state.
Through a collaborative effort spanning three rural Area Health Education Center regions—the Cape & Islands, Franklin County, and Berkshire County—this program is creating a pipeline of skilled Community Health Workers (CHWs) to meet the growing healthcare needs of the state’s rural communities. By leveraging resources across the state and working with key clinical and educational partners, the program equips current and future CHWs with the tools they need to deliver essential services while fostering a workforce to provide services across many languages and cultures.
Students speaking togther at the annual NERHA conference, 2024

“Community Health Workers are the backbone of community-based healthcare delivery,” said Stephen McLeod, Director of Cape & Islands Area Health Education Center. “This program is breaking down barriers to care. It’s creating access to health care education, expanding career pathways, and increasing local job opportunities for individuals who are too often overlooked. It’s not just about healthcare—it’s about economic development and making a meaningful impact on the communities and residents we serve, one neighborhood at a time.”
Since its launch, the program has exceeded expectations, training more than 100 students annually and enhancing healthcare access across rural Massachusetts. Partners, including Outer Cape Health Services, Baystate Franklin Medical Center, Community Health Programs of Berkshire County, Volunteers in Medicine, and Outer Cape Community Solutions, have been instrumental in tailoring the program to meet local community needs.
“This initiative is a game-changer for rural healthcare in Massachusetts,” said Ann Marie Day, Chief Operating Officer of NERHA. “By building capacity and addressing workforce gaps, we’re ensuring that the most vulnerable among us have increased access to compassionate, highquality care.”

Berkshire County, Massachusetts
Cape & Islands, Massachusetts

Key Highlights of the RPHWTN Program:
Targeted Training: Cape Cod Community College and Berkshire Community College have developed flexible, multilingual training curricula, offering both in-person and distance learning opportunities. Courses include cross-training in billing and coding, electronic health record support, service coordination, peer recovery support, and more.
Innovative Recruitment: The program recruits trainees from non-traditional communities, including tourism, agriculture, fishing, and other rural industries. These efforts not only diversify the workforce but also ensure that services reach those most isolated by language, culture, and economic barriers.
Comprehensive Support: All trainees, including those still learning the English language, are eligible for financial scholarships, which reduce economic barriers and incentivize program completion.
Ongoing Workforce Development: In addition to training new CHWs, the program provides upskilling opportunities for current workers, strengthening the existing healthcare workforce and creating clear pathways for career advancement.


With the program’s overwhelming success over the first two years, the RPHWTN program is poised to serve as a model for rural health workforce development across New England. By the time the funding period ends in July 2026, the program plans to expand operations by working with a broader group of community partners and pursuing new funding avenues from public and private foundation sources.
For more information about this program or to learn about opportunities to participate, please contact Kiara Badillo at kiara@newenglandrha. org.

Article by
Kiara Badillo
Photos by Various
Franklin County, Massachusetts
Ezekiel Baskin (NERHA), Michael Fallahkhair (FORHP) and Leo Blandford, Outer Cape Health Services, discuss rural health networks in Provincetown


NOT JUST SAFER - SEEN: WHAT HARM REDUCTION REALLY
OFFERS
I was driving home recently on a dark and gloomy day. I was feeling so very tired, as it had been a week or so with no sun in the sky. It wasn’t exactly raining, but the clouds seemed to have sunken down into the street. The world was grey, dim, and not as beautiful of a day as maybe one would hope. I was struck by the thought however, that the gloomy, rainy weather was giving life and energy to what would become the green grasses and brightly colored flowers that we all love so much in April and May. I was reminded that sometimes what we actually need in life isn’t always beautiful in the typical way.
When I think about harm reduction, I think that is a rather fitting analogy. Harm reduction on face value might not sound like or even look like its helping. For many, who maybe haven’t gotten to give it as much thought, it could look like enabling, condoning drug use, or letting people stay stuck in their ways. To put it simply, however, that’s incorrect.
Harm reduction just downright works. In Litchfield County back in 2020 (per the Department of Public Health), we had an overdose death rate of 39.4 per 100,000. As a result of the integration of harm reduction services across the region, that rate is now the lowest in our state—down to 15.1 per 100,000.
Rural Feature
IT’S HOW WE LOOK AT THE PROBLEM
Organizations across the county have banded together for the last 10 years under the Litchfield County Opiate Task Force (LCOTF). From that collaboration, we have reduced the silos that so often occur between behavioral health treatment, first responders, and hospitals. We come together for shared learnings, community responses, and so much more. For the last five years, we have been connecting folks to harm reduction services.
Partnership alone has not been the biggest factor— it’s how we look at the problem.


By integrating harm reduction into every level of care and ensuring best practices, our community has continued to heal.
In the last few years doing direct work as a harm reductionist, I’ve thought a lot about what would happen to the people we serve if this work wasn’t being done. We hear often, “people need to hit rock bottom to recover,” and while it’s catchy, those implications are serious. Rock bottom right now is not what it used to be. The ever changing, incredibly volatile street drug supply has made rock bottom not just being at your lowest, but six feet under the ground. Rock bottom now is death. So no, we cannot wait for rock bottom.
In my little corner of Connecticut, as everywhere else, substance use is heavily stigmatized. What that means for people who use drugs, is that they don’t feel like they can outwardly share about it. Not doing so puts people at greater risk of an overdose, adverse health conditions, and at a minimum, keeps them isolated.
Some of the outreach folks at a local harm reduction site
Kyle at a harm reduction site with the harm reduction rover and naloxone

Shame is crippling, and this shame is deeply embedded into every facet of our society. Every time a person in a movie, on the sidewalk, in an office, or any other setting uses the term “junkie,” it is inadvertently telling people who use drugs, they’re garbage. Imagine being defined by such a fractional aspect of your life. All your hobbies, your desires and passions, your humanity, boiled down to the term “junkie” or any other term like it for that matter. Imagine knowing your loved ones think of people like you in that way. Would you tell anyone? This shame isn’t just crippling, it’s deadly - and we have lost people because of it.
A photo from the recent Save a Life Day - 231 Naloxone kits were passed out in response to an uncharacteristic spike in overdoses during the month of February.
The task force had 16 pop-up Naloxone sites everywhere from local grocery stores, soup kitchen, ambulance service center, and more


Harm reduction isn’t just about the materials that we pass out that allow people to slow the compounding negative health effects drugs have on their bodies. It’s quality of life. Every time a harm reduction participant comes to see one of us, we become an access point. Sometimes, it’s to treatment, and others it’s to safer use supplies, food, or a jacket. Above everything else however, is access to human connection without condition. To step into a space where someone, even a total stranger, can see you not for what you do in your free time, but for your humanity— to say it’s beautiful is an understatement.
As a society, we see the devastation and often think that something drastic needs to be done. We see the calls for “cracking down on drug use.” Harsh punishments, mandatory minimum sentences, and forced treatment have been the recommended responses. For decades we have done this, and spent more money than we can count with very little progress. So, why isn’t that working? I have found that the best antidote for this is often a little bit of curiosity.
Why do people use drugs? It’s not a surprising answer really—drugs work! Stay with me – they work to help folks cope – at least for a time. They dull the sharp edges
Litchfield County Opiate Task Force includes about 60 organizations - pictured is a mix of police, behavioral health, local hospital, rural health, and health district staff
The overdose awareness symbol, that people are able to sign every year in memory of those they have lost. Last year it travelled around Litchfield County to raise awareness and get to those who couldn’t make it to the vigil
HARM REDUCTION OFFER AN ALTERNATE SOLUTION
of traumatic memories, act as a form of liquid courage, a social lubricant, or change an experience in one way or another. To normalize this idea, we need only look to alcohol. It is normalized by society, regulated, and what many turn to after a bad day at work, at a wedding before a nerveracking speech, or at a party just because.
The difference with alcohol is acceptance and regulation. Imagine if that beer or seltzer you had with dinner one night wasn’t the typical 5% but was really 90-proof, and you couldn’t taste the difference until it was too late. If that little relief from the strains of life, a normalized coping mechanism, simply wasn’t regulated, the outcome would be vastly different.
Imagine that using a substance is your only coping skill, or even just the one you most often turn to. Compounding issues such as declining health, homelessness, likelihood of violence, shame, overwhelm, and so many more crescendo to a deafening roar that simply feels inescapable.
However, you know that the one thing that dulls that roar to a manageable whisper might also kill you. Then imagine someone asking, “Why can’t you just stop?” You can see how terribly ineffective this approach is to someone in that situation. Harm reduction offers an alternate solution.
Harm reduction philosophy values the idea that we can support people and offer practical safety strategies without condoning or shaming their usage. By doing so, we are giving people a space to talk about themselves without fear of judgment. The use of harm reduction supplies gives people a higher likelihood to avoid issues like abscesses, HIV/ AIDS, and gives them a more sanitary option to the ones they would have without. It also increases accessibility to life saving Naloxone, wound care, and to treatment should they ever desire it. The services as a whole, when put together, put simply, save lives.
Article by Kyle Fitzmaurice

Photos by Kyle Fitzmaurice
BERKSHIRE’S 40 UNDER 40
TIFFANY MORENO
The New England Rural Health Association is proud to congratulate Tiffany Moreno of Berkshire Community College (BCC) for being one the Berkshire’s 40under40! Tiffany Moreno is the Instructional Program Manager: Health & Social Services at BCC and is one of the core partners in our Massachusetts Rural Public Health Workforce Training Network (RPHWTN). Tiffany has been working diligently with MA RPHWTN to create and deliver trainings for new and incumbent community health workers (CHWs) in rural areas of MA. In addition to Tiffany’s professional contributions, her perspective and enthusiastic dedication to this work has been instrumental in our program’s success. Tiffany is a champion for this project and for her community. Congratulations Tiffany!
If you would like to learn more about the MA RPHWTN, please visit our website at nerha.org or email Kiara Badillo at kiara@newenglandrha.org
Article by Name Here
Article by
Article by Kiara Badillo & Tiffany Moreno
Photos by Name Here
Kiara Badillo & Tiffany Moreno



“During my time at Berkshire Community College, I have had the privilege of addressing workforce gaps in Berkshire County by collaborating with organizations like New England Rural Health Association, MassHire, County Ambulance, and Berkshire AHEC. Together, we’ve developed training programs such as the EMT Training Program, Community Health Worker certification, and Registered Behavioral Technician training. These initiatives are designed to meet the needs of local residents while building a stronger, more skilled workforce.
In addition to my professional work, I serve as a mentor for Latinas413, supporting Latina women in achieving their educational and career aspirations. As a member of the Board of Directors for Berkshire United Way, I contribute to initiatives that enhance community well-being and strengthen connections between residents and local employers. Through these roles, I am committed to creating positive change, fostering collaboration, and inspiring individuals to reach their goals, all while helping to build a more vibrant and resilient community.”
-TiffanyMoreno

WINGS OF HOPE:
SHANE’S JOURNEY WITH ANGEL FLIGHT EAST
Every community has its stories of resilience, and for many families, those stories are filled with struggles and triumphs in the face of adversity. For Shane and his family, the road to essential medical care has been long and difficult, made even harder by the distance between them and the treatment they needed. Angel Flight East became a beacon of hope during one of their toughest times. This is their story - a reminder of the difference that kindness, community, and a helping hand can make when it’s needed most.
SHANE & PHYLECIA MARTIN’S STORY
My 9-year-old son Shane was diagnosed with Early Onset Infantile Scoliosis at 12 months old. Since his diagnosis, WVU Medicine and Shriner’s Medical Center Lexington have seen and treated him. He started casting at 17 months and has been in over 20 Mehta casts and 5 TLSO braces. We found out in December 2022 that the braces were no longer controlling the curvature of his spine and that he would need surgery to have Magec Rods placed along his spine to help maintain and straighten out his curvature.
We live 4 hours away from Lexington, KY where he is currently being treated and has been for the last six years. Going back and forth for castings, brace appointments and regular check-ups has not been easy.


Shane Martin getting ready for his



It has caused quite a few financial hardships trying to make it payday to payday. When we learned about Shane’s upcoming surgery for his rod placement, we were concerned about the best way to get him home. If we made the drive, we would have to get out so Shane could walk every hour- almost doubling the travel time. My husband and I also worried about the pain he would be in for having to sit up for that long of a trip home.
That is when we learned about Angel Flight East. I called them and got the ball rolling to get my son home safely and quickly after his surgery. Angel Flight East worked with me to inform the medical team of what was available and how we could make this work for our son in so much pain.
The day we flew home was when we met our pilot, JJ. We got lost because we were dropped off at the wrong airport. JJ helped us get a shuttle to the correct airport since there was no way Shane could have been able to walk that far. JJ made sure they took us all the way
to the plane to make it the most comfortable for my little boy.
We are excited to fly for his 3-month post-op in the next few weeks. We can never thank Jessica, David, and JJ from Angel Flight East for everything they did for us and continue to do for us. Thank you, Angel Flight East, for helping Shane have this opportunity during his most significant times of need.
- Phylecia Martin, Shane’s Mother
Together, let’s continue to make a difference, one flight at a time.
Shane’s journey with Angel Flight East is just one of many that reminds us of the power of human connection. With over 400 volunteer pilots, this network of caring individuals continues to change lives by offering not just a flight, but a path to healing, dignity, and hope.
For families like Shane’s, these flights aren’t just about getting from one place to anotherthey are about restoring peace of mind, easing the burden of travel, and making medical care accessible when it feels impossible. If you or someone you know is facing similar challenges, or if you’re inspired to offer your support, there are ways to get involved. Sometimes, a small act of kindness can be the thing that makes all the difference.


Article by
Jessica Ames, Angel Flight East & Phylecia Martin, Shane’s Mother
Photos by Angel Flight East



JOIN US IN SUPPORTING RURAL HEALTH IN NEW ENGLAND!
The New England Rural Health Association is dedicated to improving the health and well-being of rural communities across our region. Access to quality healthcare shouldn’t depend on your zip code — yet many rural areas face significant challenges, including limited resources, healthcare provider shortages, and transportation barriers.

Dollar Makes a Difference.
Help us ensure that every rural New Englander has access to the care they deserve. Together, we can bridge the healthcare gap and create a brighter future for all. Your donation can help us bring essential healthcare services to those who need them most. Together, we can build healthier, more resilient rural communities.














The New England Rural Health Association (NERHA), established in 1997, is the largest regional rural health association in the U.S., serving all six New England states. As a non-profit governed by a Board of Directors, we provide advocacy, education, technical assistance, and program support to improve rural health.


NERHA Rural Roots uses eco-friendly paper that looks at environment safety and the future of humanity


