IMPACT REPORT
Networking Sponsor

Industry leaders joined Mexico Health Summit 2022 to educate and share their experiences as the sector undergoes a digital transformation. After a complex 2021, the industry is ripe and ready to thrive in the digital era after overcoming challenges and transforming them into opportunities to improve operations, optimize costs and, most importantly, to adopt a patientcentric model.
This event gathered the expertise of multisectoral leaders of the health chain, allowing attendees to understand how tech and crisis created a novel, resilient industry that now offers the most innovative approaches to care provision to date.
To thrive in this new health sector, Mexico must integrate novel approaches to incoming challenges such as climate change, geriatrics, genetic diagnosis, chronic diseases, blood management and precision medicine. All these hurdles must be addressed with a limited budget and while still handling the COVID-19 pandemic, for which providers have stressed that public-private collaboration is fundamental.
Mexico’s long-time hurdles are still stopping the sector from reaching its full potential. The country has not yet overcome the medicine shortage crisis that began in 2019, to which providers in the private sector have been quick to offer solutions to bring medicines closer to patients.
Mexico Health Summit 2022 demonstrated that it is possible to move forward, innovate and prevent health emergencies despite existing barriers. Companies and organizations are now embracing technology to accelerate efforts and improve patient outcomes, promising an even stronger sector for 2022.
133 companies
286 conference participants
60 speakers
7 sponsors
1,455 visitors to the conference website
Breakdown by job title
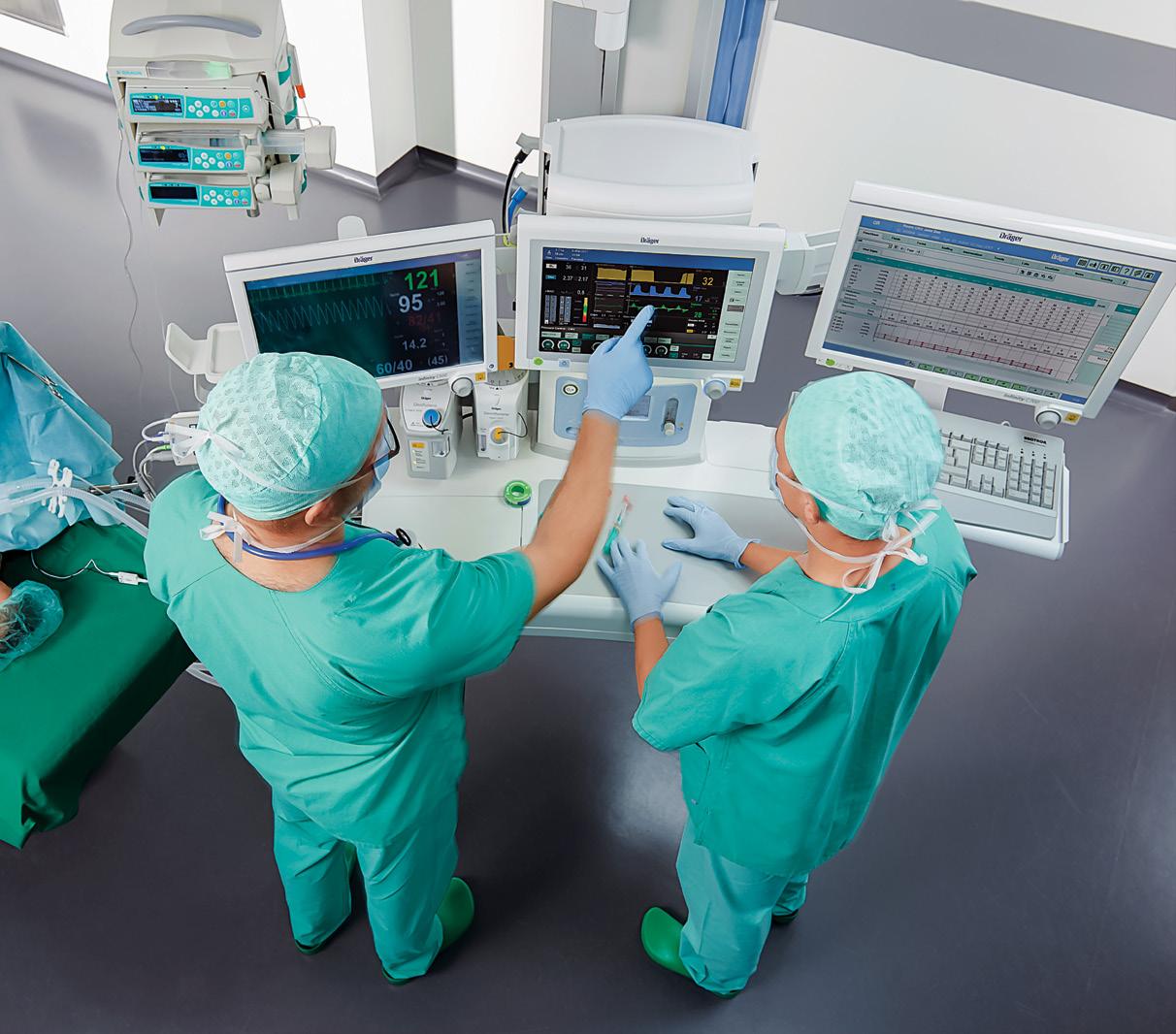
Mexico’s leading B2B conference organizer introduces the world’s leading event networking platform.
3,442 direct impressions during MHS
direct pre-conference LinkedIn impressions
3.19% click through rate during MHS 3.02% pre-conference click through rate 3.83% conference engagement rate
Delivering intent-based matchmaking powered by Artificial Intelligence that connects the right people. Network, no matter where you are.
193 participants
895 matchmaking communications
96 1:1 meetings conducted
Matchmaking intentions
1,865
• AbbVie
• Aidicare
• Alitea Life Science
• Alivia Clinica de Alta e specialidad
• AM eLAf, A.C.
• Amicis pharma
• AMID
• AMII f
• Anadim
• Apotex
• Arcus
• ArrOBA ING eNI erIA, SA D e CV
• Art Tecnica SA de CV
• asesoriaenfarmacias.com
• Asistensi Global Insurance
• Asociación Insurtech
• AS peN LABS
• AstraZeneca
• Avalon pharmaceutical
• Baker Mckenzie
• BioMarin
• Bobbinet
• Boston Scientific
• Brella
• British embassy
• Canifarma
• Cardinal Health Mexico 514 S de r L de CV
• C eI
• Centro de Investigación Sophia
• C eNTrO DIAGNÓSTICO HATVer
• Centro Médico ABC
• CHG-Meridian México
• Christus C eI
• CH rISTUS Center of e xcellence
• CH rISTUS e xcellence and Innovation Center
• CH rISTUS H e ALTH e XC eLLeNC e AND INNOVATION C eNTer LATAM
• Christus Muguerza
• CidVID
• CI rCUTO r México, Centro América y Caribe
• City Council
• CLINICA re S p ONSABLe O per ATIVA, S.C.
• Cold Chain Technologies
• Consejo mexicano de neurología
• Consultores Universales en Salud
• Crowdstrike
• Dalus Capital
• D eLeGACIÓN D e QU eB eC
• Deloitte
• Department for International Trade Mexico
• DHL Global forwarding
• DIAGNOSTICA MO reNO LABO r ATO rIO M eDICO
• DocInWay
• DocTour
• DocuSign
• Duppla
• DVA Health & Nutrition
• eC
• ecaresoft Inc.
• elipse
• eolis
• evonik Mexico S.A de C.V.
• farmacia paris S.A. de C.V.
• farmalisto
• fAr MApI eL
• frontier View
• Genomma Lab
• Geonomics england
• Global Health Intelligence
• Grünenthal
• Grupo Lister
• Grupo Médico rossano
• GS1 México
• Health Gorilla
• H e TerOD rUGS
• Holland House Mexico
• Hospital
• Hospital Infantil federico Gómez esta como HIM fG cambiarlo plis
• Imperial College London
• IMSS
• Indukern de México, S.A. de C.V.
• Instituto Nacional de Geriatría
• INTer NACIONAL fAr MAC eUTICA
• IQVIA
• King’s College London
• Klaver
• Laboratorios Alfasigma México SA de CV
• LABO r ATO rIOS GU errerO
• LM p
• Macrotech H e ALTH
• Mamotest
• Medartis Mexico
• MedCity
• Médica Sur
• Medical Vive
• M eDIC e Arzneimittel
• M eDINCAr
• Medisi America
• Medpacom
• MeetingDoctors
• Meraki smart solutions
• Mexican Council of Clinical pathology
• México Sin Alérgenos
• MexicoView
• MMM Holdings
• Netherlands embassy in Mexico
• NUBIX
• NU r A Health Science
• nutriADN
• OLArTe y AKLe
• Olivares & Cia.
• Omron
• Omron Healthcare
• Oxford Nanopore Technologies
• pharmaLinea Ltd.
• pragmatec
• prOA
• prOS periA
• p SQ r
• p yco Medical
• QbD Mexico
• randall Laboratories, S.A. de C.V.
• reckitt
• rGA reinsurance Company
• rossbach de México
S.A de C. V.
• Sánchez Devanny
• Sarstedt
• seca sistemas médicos de Medición
• Siemens Healthineers
• Silanes
• Sociedad Mexicana de Salud pública
• Sofía
• SSA
• Starmedica Aguascalientes
• Strategic Technology
Bioconsulting
• T5DC
• Tecnológico de Monterrey
• tecsalud
• Terapify
• Te VA pharmaAdvice
• Trifermed
• UDIM eB
• Ultragenyx pharmaceuticals
• Vitalmex
• Welbe
• Zenda.la
09:00 HEALTH AS A FUNDAMENTAL ISSUE FOR COP26
Speaker: Jon Benjamin, UK Ambassador to Mexico
09:45 MEXICO HEALTHCARE OVERVIEW
Speaker: Alec Lee, frontierView
10:15 REDEFINING HEALTHCARE: STATE OF THE SECTOR
Speaker: Alexandro Arias, Deloitte
11:15 MEXICAN HEALTHTECH ECOSYSTEM
Moderator: Cristina Raunich, Terapify
Panelists: Cristina Campero, prOS periA
Oscar de la Garza, Medpacom
Gustavo Rodríguez, nutriADN
Amiel Rosales, nubix
12:30 DIGITAL HEALTH REGULATION IN MEXICO: HITS AND OPPORTUNITIES
Moderator: Juan Luis Serrano Leets, Sánchez Devanny
Panelists: Víctor Sánchez, pragmatec
Fabiola Fajardo, Alitea
Andrea Arozamena, GS1
Gabriela Lerma Valencia, IQVIA
Christian López-Silva, Baker McKenzie
13:15 MEDICINE, DEVICES ACQUISITION PROCESSES THAT IMPROVE, GUARANTEE TREATMENT
Panelists: Ana Riquelme, AMID
Karla Báez, AMII f
Rafael Gual, CANI fAr MA
15:00 REDEFINING TECH SKILLS FOR HEALTH TALENT
Moderator: Nidia Garza, MMM Holdings
Panelists: Jorge Zita, CrowdStrike
Igor Renan Maciel da Costa, Docusign
Sonia Mayra Pérez Tapia, UDIBI-I pN
Jorge Valdéz, Tecnológico de Monterrey
15:45 MEXICO’S HEALTH BURDEN: CHRONIC DISEASE MANAGEMENT
Speaker: Omar Tomey, AbbVie
16:30 STRENGTHENING PRIMARY CARE ATTENTION THROUGH TECH
Moderator: Mario Aguillón, Zenda.la
Panelists: Guillermo Pepe, pragmatec
Andrés González-Silén, GS1
Carina Reverter, Meeting Doctors
Eduardo Medeiros, Welbe Care
17:15 THE IMPORTANCE OF DRUG, SUPPLY ACCESS
Moderator: Marcos Pascual, ANAfAr M e X
Panelists: Ignacio Merino, farmacia paris
Américo García, Apotex
Rodrigo Fernández, Te VA pharmaceuticals
09:00 DIAGNOSTIC TECHNOLOGIES FOR GENOMIC CAPABILITIES
Moderator: Ivana Poparic, MedCity
Panelists: Michael Johnson, Imperial College London
Katherine Melville, Oxford Nanopore Technologies Ltd.
Gerome Breen, King’s College Londone
Damian Smedley, Queen Mary University
09:45 PERSONALIZED, PRECISION MEDICINE AND DEVICES
Moderator: Sandra Sánchez, pharmaAdvice
Panelists: David López, BioMarin pharmaceuticals México
Jaen Velazquez, Siemens Healthineers
10:45 A ROADMAP TO A DIGITAL HOSPITAL
Moderator: Santiago Yeomans, Christus C eI
Panelists: Sandra García, Médica Sur
Jorge Camargo, ecaresoft
Juan Caceres, Aidicare
12:30 POPULATION’S HEALTH TRANSITIONING TRENDS
Panelists: Cristobal Thompson, AMII f
Luis Miguel Gutierrez Robledo, National Geriatrics Institute
Marlene Llópiz, C rO Mexicana
Vanessa Ballarte, Omron Health Care
13:15 TRACEABILITY AND DATA FOR HEALTH LOGISTICS
Moderator: Jaime Castro, QbD Mexico’s Office
Panelists: Miguel Angelo Ricchiuti, Apotex
Liliana Castillo Bautista, DHL Global forwarding México
15:00 VALUE AND IMPACT OF PATIENT BLOOD MANAGEMENT
Moderator: Arturo Vivas, Sarstedt
Panelists: Christa Seipelt, Sarstedt
Rafael Guerrero García, Mexican Council of Clinical pathology
Israel Parra Ortega, Mexico Children’s Hospital federico Gómez
15:45 INNOVATION, ITINERANT ARTICULATED SERVICES
Speakers: Ramon Mier, Vitalmex
Carlos Alcantara, Mexico Children’s Hospital federico Gómez
16:30 INNOVATION, WEB 3.0 & BLOCKCHAIN
Speaker: Andrew Ahachinsky, Bobbinet LATAM

HEALTH SYSTEMS TO BENEFIT FROM FIGHT AGAINST CLIMATE CHANGE
f ive years after the singing of the p aris Climate Agreement, the goal of limiting the increase in global warming below 2° C has not been reached. While healthcare is seldomly considered to be directly linked to climate change, the latter impacts numerous health indicators so it became one of the priority areas of the 26th UN Climate Change Conferenc e (CO p 26).
“Today, we are at a breaking point and immediate action is needed,” said Jon Benjamin, UK’s Ambassador to Mexico, during Mexico Health Summit 2022. Last November, the UK presided over CO p 26, which hosted over 200 countries from across the world to discuss best practices and work towards committing to limiting global warming to 1.5° C.
Climate change has a direct impact on public health because it affects air and water quality and food supply. In Mexico, for example, climate change has increased the number of areas where dengue fever has become endemic, affecting mainly the most disadvantaged communities and increasing health inequalities. As a commitment to these populations, every nation must adapt sustainable planning into its national healthca re system.
Benjamin discussed the responsibility countries worldwide have to implement sustainable practices as climate change is also a public health issue and must be addressed as such. Healthcare has been a fundamental value in the UK’s identity, explained Benjamin, as its national health service is considered one of the best worldwide. The country also is known for scientific breakthroughs in biomedical and health innovation. The incorporation of technology into the private or public national health system is fundamental but following CO p 26 these processes must be undertaken sustainably, said Benjamin.
A specific health program to support UN countries to strengthen these fronts through the adequate use of available resources was developed at COp26, including five campaign goals that aim to fight climate change and drive member countries closer to a zeroemission economy: adaptation and resilience, energy transition, clean transport, nature and ecosystems and green finance. This includes “Creating climate resilient health systems that support food and water sanitation ensuring a rapid transition to clean renewable energy for health’s facilities, promoting healthy and sustainable transport systems, protecting and restoring ecosystems to sustainable
livelihoods and inventing a climate-resilient health system with zero carbon emissions,” said Benjamin.
The WHO, in partnership with Healthcare Without Harm, the UN f CCC Climate Champions and the Global Climate and Health Alliance (GCHA), helped to develop the CO p 26 Health p rogram to enable transformational change in health systems globally. Governments need to commit to conducting a climate change and health vulnerability and adaptation assessment, develop a national adaptation plan and facilitate funding for climate change projects related to healthcare. Simultaneously, decarbonization is crucial to meet the committed goal of limiting global temperature increase to 1.5° C. The sooner these sustainable low carbon health systems
are developed, Benjamin said, the more cost effective they can be.
“The COVID-19 pandemic has shown the importance of having reliable and effective health systems as the main line of events to protect populations from emerging threats. It is essential for health systems to transform themselves to understand their vulnerabilities and to create the capacity to adapt to possible threats, all while being sustainable,” said the ambassador.
Governments will lead these commitments by promoting new policies and regulations that help prevent climate change and all countries can participate in the adaptation of these changes. As Benjamin said: “the benefits are evident and compelling, and our future generations and their healthcare depend on it.”
LIMITED BUDGETS, PRIMARY CARE TO AFFECT RECOVERY: FRONTIER VIEW
As COVID-19 cases decrease, Mexico’s healthcare sector faces numerous challenges in the form of budget restrictions, limited primary care and diagnostics, a pension deficit and the migration of medical professionals to the private sector, said Alec Lee, Director of Healthcare r esearch, f rontier View Strategy Group. Lee also discussed potential opportunities for Mexico’s healthcare sector.
Mexico’s macroeconomic growth has three main takeaways that will affect all sectors. Initially, “Mexico’s economic recovery will continue in 2022 mainly on the back of exports to the US but the country, alongside Argentina, will be one of the last to recover to pre-pandemic levels among Latin America’s top markets,” Lee said. Secondly, market players can expect consumer spending to
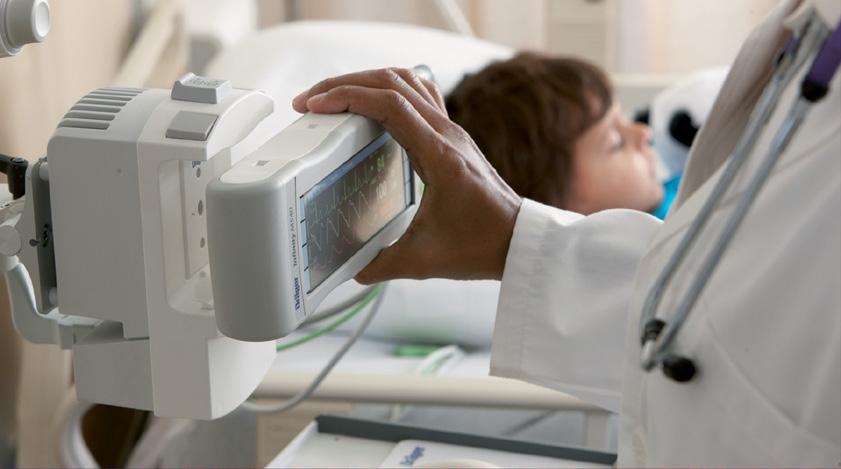

bounce back as a part of this recovery due to better Mexican labor market prospects and strong remittances. finally, firms in the country’s healthcare sector “will need to cope with inflationary pressures until 2023, mainly driven by faster-than-expected demand recovery and supply chain disruptions.”
frontier View forecasts that the economic recovery will continue this year despite the various downside risks laid out ahead but the expected economic stimulus will remain below 2 percent during 2022 based on export-led growth. In its forecasts, the firm considered the global COVID-19 outlook, Mexico’s COVID-19 environment, the international growth environment, economic stimulus, p resident Andrés Manuel López Obrador’s 2022 recall survey, Mexico-US relations and the infrastructure plan. frontier View’s pessimistic scenario forecasts a recovery in 2028, which is 20 percent likely. Its base scenario forecasts a recovery in 2023, which is 70 percent likely, and its optimistic scenario forecasts a recovery in 2022 that is 10 perce nt likely.
e ven though the government’s budget proposal for 2022 prioritizes health much more than in past years with an approved increase of MX$1.58 billion (US$77.5 million), Lee believes Mexico still has not reached an ideal financing for the sector because budget increases are lower than inflation. However,
the increased healthcare funding as a result of the pandemic is likely to continue as a trend for future years.
The approved budget for 2022 has notable increases for INSABI, vaccines and the healthcare industry as a whole. The Ministry of Health’s average budget totals by state are noticeably higher in Morena party affiliated states, where there has been an average 32 percent increase (including the nation’s capital) compared to 2 percent increase for states not associated with the party. Additionally, 37 percent of the year’s budget will go towards “subsidies and t ransfers.”
In the aftermath of the pandemic, which is seemingly in-sight as the explosive fourth wave continues to die down, primary care decreasing below pre-pandemic levels could result in many undiagnosed patients as screenings have decreased nationwide. However, private sector services and procedure volumes are expected to see a recovery sooner than those in the publ ic sector.
According to f rontier View’s analytics, challenges for a recovery of non-COVID-19 related treatments in the healthcare sector include IMSS’ pension deficit explosion in the last 12 months and the migration of medical professionals from the public to
the private sector even though less than three percent of the country’s population is covered by private health insurance. Additionally, patients will face difficulties in self-financing as the continued stockouts seen in hospitals will also play a role. f or
this Lee sees two possible key action steps: having private insurance facilitates access through low-cost premiums and digital health policy advancing access to insurance, which has been the case in Brazil’s successful teleheal th policy.
THE CHALLENGING PATH TOWARD INTEGRATED HEALTHCARE
The industry is moving toward new health delivery models, which are oriented around the patient rather than the provider.
The transition toward integral, integrated healthcare in Mexico will be filled with challenges, which are outweighed by the benefits to the economy and we llbeing..

“This situation impacts directly on the general economy. The money used for health expenses is replacing other expenses that people used to make ”
Alexandro Arias
Partner - Life Sciences & Heath Care Leader S-Latam | Deloitte
This layer can be built around workplaces, schools, hospitals, clinics, retail stores and community facilities, taking advantage of digital tools.
“Monitoring and diagnostics are crucial for silent diseases. An early diagnosed disease is better treated and reduces system costs. Being [Mexico’s] a disintegrated system, there is not enough information to treat patients. This is one of the greatest opportunities in the sector. With enough data, patients will be treated more efficiently, both in-person or virtually,” said Arias.
The current state of health delivery focuses primarily on physical health, with models oriented around the provider offering fragmented and analog experiences that have negative consequences both for the patient’s health and for the country’s economy, said Alexandro Arias, p artner - Life Sciences and Heath Care Leader S-Latam, Deloitte. “There are cost overruns when information is lost between doctors, in time between appointments and non-attachment to treatments, causing patients to have a decline, which will translate to a greater cost for the health system and the economy in general.”
The future of health delivery models is patient-centric, taking into account the spiritual, emotional, financial, social, mental and physical conditions when discussing wellness or illness, said Arias. for this integral approach, “we must create a layer around” patients that includes education, counseling, monitoring, diagnostics, insights, behavioral nudges, intervention and treatment, he added.
Among the aspects taken into account for patients’ wellbeing, the pandemic did not only impact the physical side of the patients, it also affected their mental and financial health. Lockdowns and mourning impacted mental health, which has not been addressed with the importance it deserves, said Arias. The financial side was also affected during the pandemic.
In Mexico, over 50 percent of health expenditure comes from the public sector, 40.7 percent is paid out of pocket and 7.3 percent is paid by private insurers, reported MBN. Out-of-pocket expenditure increased during the pandemic due to people’s unwillingness to visit hospitals. “This situation impacts directly on the general economy. The money used for health expenses is replacing other expenses that people used to make,” said Arias.
Integrated care is whole-person, team-based care that provides access to affordable, evidence-based care at a population level and across the care continuum, said Arias. With the patient at the center, there are four key areas where actors across diverse
sectors converge. One of these key areas is the primary care team, which includes health generalists, social workers, nursing staff, pharmacists, nutritionists and health coaches. Then, the specialist care team includes all non-primary care members involved in the patient’s healthcare, such as surgeons, endocrinologists or cardiologists. The other two key areas, said Arias, are social-community support and digital care tools such as telehealth, remote patient monitoring or digital therapeutics and selfmanagement tools.
A patient-centric, integrated healthcare improves the patient’s experience, which translates to general benefits that include decreased hospitalization and readmission, lower rates of avoidable healthcare utilization, improved quality of work atmosphere, better communication and lower burnout rates among healthcare professionals, said Arias. “During the peaks of the pandemic, healthcare professionals’ burnout was impressive. They worked 24-hour, 36-hour shifts.” Integral, team-based healthcare for chronic patients reduces hospitalization by 18.6 percent, which translates into cost savings, according to a comparative study.
An integrated care model design must be grounded in all three foundational components to effectively operate, said Arias. These components are: data, which needs
the core technology capabilities that enable cross-functional stakeholders to capture and access it; wellbeing and care delivery, which are the physical and virtual care facilities that provide the care services; and care enablement, which involves the clinical operational and financial factors and services that promote access to care.
“Today, there are unique opportunities to reform the underlying structures of public health. However, there are also extreme challenges, such as a decades-long backlog of funding needs, a global pandemic, ongoing preventable chronic disease epidemics and pervasive inequities that threaten our health, longevity and trust in government and its leadership,” said Arias.
The Mexican healthcare system, with lag, “is preparing to become more flexible, grow and reduce its size according to its needs,” said Arias. He added that the 15.2-percent increase in the public spending on health “is one of the most important in the last years.”
While the path toward integrated healthcare will be challenging, multiple players are already transforming their health delivery models, creating a positive ecosystem to boost patient-centric care. Overcoming the challenges will represent important benefits for Mexicans’ health and the country’s economy as a whole.

“There
ENTREPRENEURS WORK TO CREATE A MEXICAN HEALTHTECH ECOSYSTEM
As the digital transformation permeates the health sector, creating a complete healthtech ecosystem has become the goal of industry providers. Healthtech has proven to be a bridge for care provision and as local companies further develop solutions, results show more precise outcomes.
In Mexico, “medtech companies share the common goal of closing the tech gap that exists in health and propel a digital advancement for the country,” said Cristina Campero, C eO, pr OS per iA. Local health developments have a unique focus and thus, unique outcomes. They are created for Mexico’s population profile and target the needs of a fragmented system that depends almost entirely on the patient’s chosen treatment and provider, according to Amiel rosales, CeO, Nubix.

is a gray area where we have to guess and try to communicate with COFEPRIS to create a regulatory pathway. PROSPERiA, for instance, has an endorsement from COFEPRIS where it acknowledges there is no regulation for us but for investors it is still a gray are ”
Cristina Campero CEO | PROSPERiA
the economic stability relies on healthcare, especially on health professionals, who are the ones we are targeting to support with novel tech developments.”
Innovation goes beyond ideas and imagination, “it requires a technological base and must respond to a current trend to succeed,” explains Gustavo rodríguez, CeO, nutriADN. To date, technology adoption has been favored by the limitations caused by the pandemic, which was a watershed that made embracing technology a natural process, said rodríguez.
Moreover, as digital health has been more open and receptive, it has promoted a culture of prevention. “Users have adopted a new social behavior based on tech for daily life activities, including through healthcare apps,” said rodriguez.
Another pivotal part of success are healthcare professionals: “they must understand the added value of our solutions. The doctor is the first implementer, giving credibility and supporting our developments. If this fails, achieving a true impact is difficult,” said de la Garza.
To date, entrepreneurs consider Mexico to be in the golden age to launch healthcare technology. “We are making life easier for users in terms of operations, practices, administration, costs, mobility and health. Based on competitiveness, if a tech solution is not disruptive, it does not have a good future,” said Oscar de la Garza, CeO, Medpacom.
De la Garza explains that in this digital age and transformation, many startups have consolidated business models that have proven their effectiveness and capacity for regional expansion. “But to further expand our services, the country needs to accept that
There are several ways to approach doctors, but based on Medpacom’s experience, approaching recognized institutions and schools that doctors respect and trust is an effective way to introduce these new technologies. “even so, introducing healthtech subjects to these institutions is difficult, as there are actors who trust foreign solutions more than with Mexican ones. This is why it has been more effective for us to approach the new generations of doctors to promote our solutions,” de la Garza said.
entrepreneurs have learned that lack of trust from healthcare providers is a barrier to succeed in this market. “Health services have been working the same way for decades, with a traditional and paternal dynamic from the physician. However, delegating
responsibility to other actors has also proven to be effective,” explains Campero.
Tech will help professionals provide a higher quality of diagnosis and consultations. “By generating confidence in the solution and understanding that tech is here to cooperate and not to replace, providers will be creating a harmony that will break the challenge of interoperability,” said rosales.
Novel solutions can create an ecosystem that supports intercommunication so these integrated platforms allow patients to be guided in their health journey, while informing them which solutions they can access, how they can access them and what benefits they will gain from them, said Campero.
In their journey to position their solutions in the market and in standard medicine practice, education for providers and patients has been essential, said Cristina raunich, CMO, Terapify. “There is not much education pertaining to topics such as genetics, for example,” r odriguez said, “so creating training and courses on topics that were not addressed in education or included in awareness campaigns is important to facilitate adoption of tech and prevention.”
Apart from education and evangelization, entrepreneurs have also pioneered in regulation and regulatory initiatives, as Mexico lacks clear regulations for innovation or new developments. “There is a gray area where we have to guess and try to communicate with
CO fepr IS to create a regulatory pathway. prOSperiA, for instance, has an endorsement from COfeprIS where it acknowledges there is no regulation for us but for investors it is still a gray area,” said Campero.
entrepreneurs also shared that investment, especially from local sources, has also been challenging. The IMf estimates that low and middle-income countries will decrease their health budgets, leading to a need for local enterprises to play a larger role by contributing to the reduction of diseases. By supporting these developments, investors are helping to reduce governmental underinvestment.
Investment in healthcare is low in comparison to areas like fintechs because “for investors [fintech] is exciting, it is booming,” said de la Garza. However, he explained that health is indispensable and investors should be looking for options to democratize health. “Tech saves costs, supports diagnosis and is essential to change the system. Investing US$1 in health saves you US$6. Investing in health is profitable and brings long-term results, which is why it takes time to make profit but it is undoubtedly profitable,” de la Garza said.
While investment in health exists, it is focused on medicines, surgeries and devices, said rodriguez. “I invite investors to look back to our biological origins and reconsider if we need more of that innovation or if we need to invest in innovation that drives a change that avoids health events.”


DIGITAL HEALTH REGULATION IN MEXICO: HITS, OPPORTUNITIES
Mexico has an urgent need for regulation in the healthcare sector after the pandemic exacerbated digitalization and the adoption of new technological innovations, agreed industry experts during the panel “Digital Health r egulation in Mexico: Hits and Opportunities.”
Digihealth is in a unique position as it combines tech and healthcare to give Mexican citizens access to health services and digital technologies, said Juan Luis Serrano Leets, p artner- Life Sciences, Sánchez Devanny. However, despite the significant impact it has on companies, medics and patients, regulation is lacking, he added.
Because digihealth merges health and information, its regulation must not only focus on health regulation but also on information technologies to avoid skipping important steps such as technological neutrality, said Christian López-Silva, p artner, Head of p harmaceuticals and Life Sciences, Baker Mckenzie. To do so, regulation identifies sanitary risks and prepares for potential eventualities.
regulation in digital health also brings different concerns at different levels. In mobile apps, for example, companies and regulators must distinguish between medical purposes and wellbeing purposes. These small distinctions
require smart regulation and different levels of intervention depending on circumstances. Mexico usually relies on authorizations and notifications but the system must realize that not everything requires an authorization. A modern regulatory framework that follows risk analysis can determine what actually requires authorization and what does not.
r egulatory concerns are increasingly prominent considering that digital health is expected to grow 10 percent in the next five years in Mexico due to greater access to mobile devices and the pandemic’s acceleration of technology, said Víctor Sánchez, CeO, pragmatec. This phenomenon is creating new ways of providing healthcare that were previously not even imagined. Under these circumstances, regulation will impact not only the final user but also doctors who trust that the technologies have passed regulations and companies who invest in the health sector. Technological innovations brought by Industry 4.0, AI, big data, IOT and digihealth must be addressed federally as well as by state.
Sanitary regulation also promotes innovation, said Sánchez, but it must arrive at the right time. Setting regulations too early can break the cycles of generation of new knowledge. But if set too late, new applications can run into issues with formerly developed
technologies. Therefore, regulation should be considered in intermediary steps once prototypes are ready and readjustments can be made, said Sánchez.
regulation is a necessity because digihealth is here to stay, said fabiola fajardo, Strategic Consultant, Alitea. But digihealth is only a tool and as such it needs to be regulated. Digihealth will impact companies by affecting the interoperability between the public and private sector, the capacity of reimbursement with insurance companies and the impact perceived by investors. for doctors, digihealth will mean a temporary workload increase that has long-term benefits and increases demand for services at decentralized clinical practices..

“But if set too late, new applications can run into issues with formerly developed technologies. Therefore, regulation should be considered in intermediary steps once prototypes are ready and readjustments can be made ”
Victor Sánchez CEO | Pragmatec
Arozamena, Healthcare Linkage Leader, GS1. Not having a clear regulation opens the door to products without assurance and security, but the regulation process should flow in the same direction as the operation, said Arozamena. GS1 has observed poor communication between the government and the industry. Uniting efforts and following international examples facilitate the flexibility to innovate by allowing demonetization, democratization and dematerialization in access to digihealth.
This technology brings numerous benefits to the sector such as empowerment and increased accessibility geographically, said Gabriela Lerma Valencia, Contract Sales & Medical Solutions BU Director, IQVIA. However, it is necessary for patients and doctors to have guarantees regarding the use of their data. It is also necessary to have a regulation that ensures all players are well informed regarding regulated markets, telemedicine, prescriptions and digital file management, among ot her areas.
A regulatory framework will bring benefits not only for innovation in digihealth but also in the infrastructure of telecommunications, according to fajardo. Germany’s 2019 Digital Healthcare Act, considered a pioneer in the matter, provides an example to follow with fast-track evaluation to show its effect in the sector.
Digihealth must be regulated to guarantee its quality and efficiency, said Andrea
Challenges in the road to implement digihealth include the cultural transformation to adopt these digital solutions, poor interoperability, lack of information regarding the use of these technologies, literalizing digital information and limited accessibility due to the discrepancy between the public and private sectors. for patients in the public sector, there are other types of challenges: problems related to storage, data property and security. However, the implementation of further technologies such as AI can be a strong tool in overpassing thes e hurdles.
PUBLIC-PRIVATE DIALOGUE IS CRUCIAL TO GUARANTEE MEDICAL SUPPLIES
public medicine and medical device supply has been one of the main issues for the health industry since the Acquisition Law was changed. A path to improve and guarantee treatment for patients will only be possible if the public and private sectors have open dialogue and work together on
planning, processes and monitoring, agreed industry experts.
“ p ublic-private collaboration is required to have conversations regarding inventory control and institutional strengthening. The pharmaceutical industry is a strong, important
sector for the country and all actors involved in the value chain have the need to work with legal certainty. We all share the same end goal, which is to deliver medical supplies to the patient,” said Karla Báez Ángeles, Director of Access to Innovation, AMIIf
An early sign of inconsistencies with public medicine supply came with changes to the Acquisition Law for medicines and medical supplies, as reported by MBN. The new regulations involved a consolidated purchasing model that would centralize operations through INSABI. The move was meant to bring savings and support the current federal administration’s austerity and anti-corruption policies, as a single institution would be acquiring medicines for all states.
However, the federal government removed distribution companies from the equation and, as a result, each public institution and state had to send its own orders. The complexity of this change drove the government to implement new adjustments, leading the Mexican government and UNO p S to sign a “technical assistance” agreement for the administration and management of projects and the acquisition of goods and services. Later, on July 31, 2021, INSABI and UNO pS signed a new agreement, called “Acquisition of medicines and healing materials,” which empowered the UN-backed organization to carry out the bidding procedures to supply medicines to the Mexican health system between 2021 and 2024.
The industry’s main worry with the transition to these new models is that while “the international scheme places us in a healthy competition, which can bring benefits,” large transitions and process modifications usually are difficult and take time to absorb, said Báez. Although the government has said that the healthcare system is saving money while guaranteeing supplies, the media reported several medicine shortages at public institutions during the past two years.
“The results [of the changes to the Acquisition Law] have been frankly bad. The processes carried out by UNO p S have also not been
positive. The lack of planning has led to shortages. We have an enviable industry in Mexico, with the capacity to supply the entire market. for instance, 97 percent of allocations given by UNOpS were previously handled by companies established in the country,” said rafael Gual, Director General, CANIfArMA.
The main catalyst to work toward securing medicine supply is to collaborate as a sector with effective, permanent communication channels with the government, said Báez. “We need planning, clarity of processes, certainty of times and traceability to enable this monitoring of supplies reaching the end goal, which in turn will create a virtuous circle to allow correct, strategic planning.”
Although communication is key for successful planning, the public sector is not considering the private sector in the conversation, said Gual. “[At CANI fA r MA] every six years we elaborate a development program for the pharmaceutical industry. We play a crucial role within the health ecosystem and unfortunately, we were excluded from the conversation. There must be a dialogue in which we can contribute with our knowledge and experience to have a win-win situation between the private and public sectors.”
Mexico is fertile Ground for Clinical research, Innovation
Open dialogue between the public and private sectors must include innovative initiatives, such as clinical research, to attract investment to Mexico. While the country has potential to become the top research hub in Latin America, Mexico is not taking advantage of it, agreed industry experts.
Logistic chains across the world are experiencing severe problems and North America is facing challenges to supply certain pharmaceutical chemicals due to its dependence on the Asian market, said Gual. “We are not exploiting the potential of the country in the research field. We are promoting the production of pharmaceutical chemicals in Mexico to avoid depending on the Asian production chains and taking
advantage of the US’s need to boost collaboration between the two countries.”
Mexico has all the needed ingredients to attract investment to the country to foster innovation and clinical research, from researchers to facilities and well-designed processes, said Báez.
With its large population, closeness to the US, well-trained physicians, large network of public hospitals and responsive regulatory entity, Mexico looks on paper as an ideal destination for clinical trials, reported MBN. Moreover, the country is the largest exporter of medical devices in Latin America and the eighth largest in the world. Mexico is also the leading exporter of pharmaceutical products in Latin America and the second-largest market for pharmaceuticals in the region. However, only 1.1 percent of all clinical trials done in the world were carried out in Mexico. Although this figure seems to be consistent
with Mexico’s population, which represents 1.6 percent of the total world population, the US has only 4.2 percent of the population and 40 percent of all clinical trials in the world.
The path to solve medicine supply shortages and guarantee treatment for Mexican patients must start with communication, planning and certainty, said Ana riquelme, executive Director, AMID. “We are all in the same boat. everyone is susceptible to becoming a patient and we must work together with authorities to find solutions. If we do not achieve this in the following three years, we will continue experiencing problems.”
Improving acquisition processes and guaranteeing treatment for patients will need all actors to get involved. The life sciences industry, both medicine and medical devices, must be seen by the government as part of the solution rather than the problem to advance toward a better healthcare system.
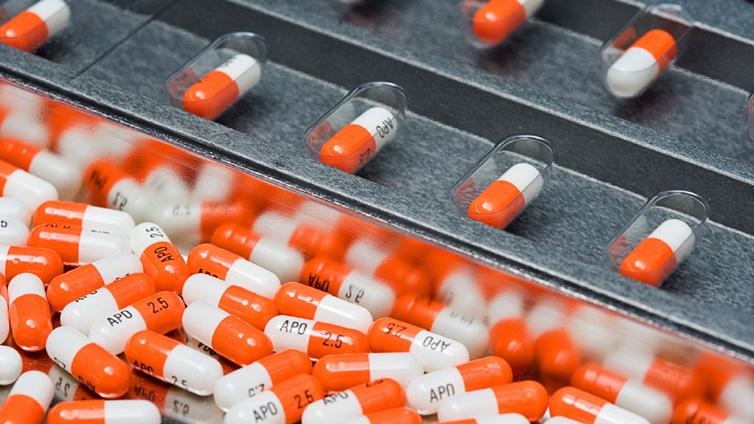
TECHNOLOGY TO MANAGE CHRONIC DISEASES
Although the COVID-19 pandemic has taken the spotlight in health, chronic diseases continue being one of the largest crises populations worldwide are facing, said Omar Tomey, Medical Director, AbbVie Mexico, during Mexico Health Summit 2022. Worldwide, chronic diseases cause 71 percent of deaths and are the primary
cause of disability. In Mexico, 80 percent of deaths pre-pandemic were caused by a chronic disease and in 2021, over 1.5 million new cases were reported between January and June. The prevalence of chronic diseases is greatly influenced by overweight and age. In Mexico, 75 percent of the population is overweight or obese and the percentage of
the population over 60 is expected to reach 30 percent by 2050 as life expectancy rises to 83 years. In 2019, obesity cut 2.1 percent of Mexico’s GDp through chronic diseases and its impact on the economy is only expected to keep increasing, according to the World Obesity federation and the research Triangle Institute.
Those who suffer from a chronic disease have to face challenges at every step of dealing with their disease. Delays in diagnostics range between seven and 10 years and Mexico has insufficient mechanisms for a timely referral among health institutions to collaborate in the diagnosis. Additionally, patients have to wait 4.3 years on average to access innovative medicines and have to spend large amounts of money as Mexicans spend 43 percent of their budgets on medical attention. These limitations only exacerbate the psychological and physical suffering patients are subjected to.
Although healthcare funding has greatly increased in the last two years, most of the money has been allocated to the fight against COVID-19. Meanwhile, Mexican healthcare still has to address historic problems. There are only 2.1 medics per 1,000 habitants and only 3 percent of the country’s hospitals are of high specialty. Additional challenges include the differences in the care provided by the public and private sectors and geographical barriers
preventing 21 percent of the population from receiving healthcare.
Under these circumstances, many health experts consider preventive measures one of the best tools for managing chronic diseases and reduce the percentage of the population that will develop a chronic illness in their lifetime.
Technology can be a great asset in preventing diseases and managing care. But health systems benefit from interoperability, which in turns is based on predictive analysis, data management, virtual resource access, secure information availability, remote follow-ups and multidisciplinary teams. Technology can support sustainable healthcare centered around a patient using telemedicine, direct messaging tools, remote monitoring and digital platforms for medicine management, resulting in better health systems.
f urthermore, digital transformations in diagnostics and therapy systems reflect the adaptations to a changing world. AbbVie foresees an increase in remote primary care and diagnostics, AI incorporation for remote monitoring, the continued adaptation of telemedicine as the pandemic demonstrated its efficiency and an increased use of mobile device apps to improve treatment of many patients, said Tomey. By 2025, 40 percent of the hyperconnected innovation will follow social, sanitary and environmental objectives.

Improving technological infrastructure will be a main priority during the next three years that associations such as medical information companies can promote.
Multiple digital tools can empower patients to make wiser decisions regarding their own health by following specialists’ advice. One of which is patients Like Me, a platform that redefined medical attention around the patient’s experience that has over 300,000 users dealing with more than 2,300 diseases. This high participation has led to the collection of valuable data that could further advance other medical products.
Advancements in scientific and technological innovation to treat chronic diseases due to general pharmaceutical advancements in the last two years present a unique opportunity to better the lives of chronic disease patients. These should be joined with further advancements in health devices and inpatient infrastructure and a strengthening of clinical research and its connectivity to patients. There are three focus steps for future digital transformation: telemedicine, IT collaboration and AI. These technological advancements must be pushed in the education of future and current doctors to bring the best health practices for their patients in the next 15 years.
REDEFINING TECH SKILLS FOR HEALTH TALENT
While technology is already used daily in healthcare, increasing its penetration could further benefit their profession and the patient, said health professionals. But despite its great promise, most health professionals feel insufficiently trained to deal with the digital revolution, according to a survey by the eU Health parliament.
“We need to acknowledge that tech must be integrated into medical education and first train educators to pass on that information,” said Jorge Valdez, Dean of the Medicine and Health Sciences f aculty (TecSalud), Tecnológico de Monterrey. education could benefit the profession but training should be continuous throughout the medical professional’s entire career. Training should also be practical and hands-on to directly benefit the patient..

“The industry must be aware that on this training, there are different levels of required skills ”
Sonia Mayra Pérez Executive Director | UDIBI-IPN
“The industry must be aware that on this training, there are different levels of required skills,” said Sonia Mayra p érez, e xecutive Director, UDIBI-IpN. Tech is highly dynamic, thus, staying updated on specialized
competencies in health is a demanding job.
“As care providers and educators, we must consider the basic, specific and superior levels of competences we are going to learn and teach and to whom we must teach them. Once this is defined, updating the knowledge becomes the challenge.”
Basic competences to begin with that can updated easily, according to Valdez, include:
+ Providing clinical digital skills and a minimum degree of literacy in digital health.
+ Having good information management and knowledge on how to manage databases.
+ Providing knowhow to communicate in different environments, such as doctorpatient or colleague to colleague.
+ Using digital solutions in an intelligent and hybrid way.
+ Creating digital content and transferring data from paper to digital.
+ Including tech in management as it is a guide to navigate sudden changes, such as a pandemic.
Tech can be the ultimate solution to many of the health and life sciences professionals’ problems because it aims to be an ally on diagnosis, management and growth.
“Automation in the health sector has reflected on greater productivity and time management, which is easy to measure because projects in this sector always have a certain level of urgency and a direct impact on people’s lives,” said Igor renan da Costa, Latam Account executive, Docusign.
Healthcare generates a large number of documents, which is one of the most urgent processes to automate to increase efficiency. “I worked on a project where an initial acquisition process took 30 days. We automated the process, reducing the acquisition process first to three days and then to seven hours. When talking about medicine delivery, the difference is significant,” da Costa said.
The benefits of the digital transformation are undeniable but so are its risks as it continues to expand. “Many companies and institutions worked on-site, accustomed to their IT department protecting their internal information. But as working processes become remote and more data is generated, users become more exposed,” explained Jorge Zita, r egional Sales Manager GH e , CrowdStrike.

“Many companies and institutions worked on-site, accustomed to their IT department protecting their internal information. But as working processes become remote and more data is generated, users become more expose”
Jorge Zita Regional Sales Manager GHE | CrowdStrike
Web browsing and fake emails are the most common means of attacks because they are highly used and receive little attention as they are considered safe activities in general. “These two means are the most common causes of theft and information ransoming. This implies that health professionals working with delicate, private information must be educated on how to protect it to avoid having to pay to recover the data or losing it completely,” Zita said.
Moreover, misused data can lead to an inhouse mistake or a cyberattack, according to Nidia Garza, Vice president Talent Management, MMM Holdings. “It is important to inform professionals of these dangers to make sure they are aware of what a poor understanding of tech can cause,” Garza said.
f or companis or institutions in which the final user is not the patient, “safe access to information and data protection is fundamental, so it supports decision making regarding the application of tech on daily work and r &D,” said p érez. Mexico has poor data protection practices for science and technology and it is even worse in data collaboration, even after the COVID-19 vaccine development made clear the importance of digital coll aboration.
Health professionals also need to be made aware of how these tools will provide a higher quality of care. “This will boost the correct use of these technologies, because they will be seen as a medical tool rather than a lifestyle tool, taking the solution as serious as it is,” sa id Valdez.
When the entire sector has experienced the benefits of technology, it will be used for the greater good, for example by generating reliable health data about the Mexican health sector. “The US, for example, generates a lot of health data that is highly useful and serves to make an impact on health and social matters,” according to Valdez. The task right now is to avoid a regressive trend to paper and non-tech practices, he added. “Now that the pandemic seems to be coming to an end, we need to identify our gains with the use of tech and recognize it would be counterproductive to let the achieve ments go.”
Changing the mindset to permanently adopt technology is key, said da Costa. “ p roviders and users have experienced the benefits of tech and how it does change possibilities, now we need to use the mindset so that the solutions can permeate.”
This mindset seeks to establish data responsibility by following the three fundamental pillars of data: it needs to be reliable, integrated and available. But data also needs to be open to be used in collaboration to generate better results, said Zita.
TECHNOLOGY TO STRENGTHEN, DEMOCRATIZE PRIMARY HEALTHCARE
Technology has played an important role as an enabler and paradigm-shifter in multiple industries. Although the Mexican health sector is far from reaching its full technological potential due to diverse barriers, technology will break paradigms and democratize primary healthcare (pHC) and insurance culture in the country, agreed industry experts.
“The low penetration of medical insurance in Mexico is astonishing. Technology offers great advantages regarding pHC, both for patients and for healthcare providers. patients save time and do not need to be exposed, while healthcare providers have a more efficient model, which takes advantage of technologies such as telemedicine,” said Carina reverter, CeO, Meeting Doctors.
p HC comprises most of the healthcare services a person might receive in their lifetime. It is also the most inclusive, equitable, cost-effective and efficient approach to enhance people’s physical and mental health, as well as social wellbeing. Because of this, pHC is being highly encouraged and strengthened in health systems globally, as reported by MBN. pHC encompasses three interrelated and synergistic components: comprehensive and integrated health services that embrace primary care and public health goods and function as central pieces; multisectoral policies and actions to address the
upstream and wider determinants of health; and the engagement and empowerment of individuals, families and communities for increased social participation and enhanced self-care and self-reliance in health, according to WHO.
There are several players boosting the implementation of technology in the Mexican health ecosystem. f or example, Mexican insurtech Sofía aims to foster prevention by managing the different stages of a health journey from first contact with a doctor to serious accidents.
“Access to pHC is the foundation for good healthcare. Combining pHC with insurance, which could cover long-term diseases, is key. prevention and timely detection of serious diseases allow us to subsidize the cost of providing p HC. This combination links the financial incentive with people being healthier,” said Arturo Sánchez, CeO, Sofía.
Technology focused on improving pHC has also penetrated the Mexican B2B market, with companies such as Welbe Care offering a comprehensive wellbeing ecosystem that integrates artificial intelligence and human contact to ensure the physical and mental health of employees. “Twenty-one million from the 29 million Mexican employees only have access to public health. We aim


to increase access and raise the quality of healthcare. Although in Mexico developing an integrated ecosystem will take time, we are empowering doctors and users, allowing the latter to track and access their medical data,” said eduardo Medeiros, Co- founder and CeO, Welbe Care.
p HC, which covers prevention, treatment, rehabilitation and palliative care, is the base of a health system’s structural transformation, according to the World Bank. To be effective, pHC should engage and empower individuals, families and communities for enhanced selfcare and self-reliance in health, adds WHO.
Technology itself may not be enough to boost p HC in Mexico, said Mario Aguillón, Board of Members, AIM and Co- founder, Zenda.la. “The question here is what do we need for our solutions to be adapted and adopted to Mexicans’ lifestyles.”
Another insurtech that has been working with telemedicine and digital healthcare solutions is Asistensi, a platform for emergency insurance and immediate medical assistance. Led by doctors, the company specializes in health and insurance plans and services with a commitment to generate value and quality of life for its users.
The way to foster pHC is through incentives, said Andrés González-Silén, e xecutive Chairman and Co- f ounder, Asistensi.
“Medical emergencies are unexpected and usually cause a health and financial disaster when they happen. Through technology, we can offer telemedicine and home healthcare, besides other services. We foster p HC, which allows a greater admissibility to our insurance, that is now available for people up to 85 years,” he said.
Technology plays a key role in the democratization of healthcare services, by making them more accessible both by distance and financial issues. for instance, Mamotest, the first tele-mammogram network in Latin America, uses technology to promote social impact, aiming to drastically reduce breast cancer mortality.
“Technology is an enhancer of democratization, not only to healthcare access but to quality services. It allows us to become more efficient and lower costs. We seek the demonetization of services, such as mammograms, which would be able to reach millions of women if they are available at a very low cost,” said Guillermo p epe, C eO, Mamotest.
Although the benefits of implementing technology in the health ecosystem are clear, companies face several barriers to do so in Mexico. Two of the main problems are the country’s disintegrated system and a cultural resistance from Mexicans to delve into their own health, said Medeiros.
In addition, regulations in Mexico are not keeping up with companies and the market in general, said reverter. While technology in the health sector has not penetrated as
fast as it has in other industries in Mexico, it will break paradigms and democratize pHC in the near future, shifting the way people get access to healthcare in the country.
THE ROLE OF PHARMACIES IN MEDICINE ACCESS
Health access in Mexico has been compromised by medicine shortages, poor infrastructure, long waiting times and high out-of-pocket expenditures. e xperts in the private sector try to fight these problems to guarantee the right to health.
Medicine access depends on many actors. The first are manufacturers of generics and innovative medicines. The second is the distributor, which is responsible for bringing the products to all pharmacies while overcoming the logistical challenges in efficiency and cost. The final actors are pharmacies. “ p rivate sector pharmacies ensure supplies meet the highest quality standards in accordance with the law, while respecting the prescription,” said Ignacio Merino, Director General, farmacia paris.
The entire health chain intervenes so patients can access medicines and health treatments. “We cannot fail to see how the public and private sectors can be complementary in improvingthe health of Mexicans. Trained health personnel, adequate infrastructure, medical devices and medications should be available at both sectors, so their collaboration is fundamental,” said Américo
García, Vice president and General Manager LATAM, Apotex.
Both sectors play equal but complementary roles throughout the entire health chain to supply medications. But regulators also play a key role in ensuring access to medications. In the case of generics, authorities need to work faster so generic drugs can reach the population on time, said García, which will furtherpromote a “framework that will propel quick access to new medications.”
In the case of specialized medication, access becomes more critical. “Bringing highly specialized drugs to the country in the private and public sectors can be facilitated by effective health authorities and regulations that readily authorize medicines for common and rare diseases,” said rodrigo fernández, LATAM Head and General Manager, Te VA pharmaceuticals. pharmaceuticals must also help the industry “go beyond the prescription, help detect diseases and collaborate with medical professionals to support them in making the diagnosis more efficient.”
Mexico’s limited access to healthcare services has seen a short-term solution in the form

of p harmacy-Adjacent Medical Offices ( pAMOs), which are equally used by those who have access to public health services and those who do not. “The primary reasons why pAMOs are the top choice is because they offer low-prices, immediate attention, high schedule availability and the opportunity to obtain an immediate prescription,” sai d Merino.
Only 12 percent of those who use pAMOs could satisfy their ambulatory health needs through public health services, found a study called “The responsibility of the state in the access of health ser vices.” .

“We cannot fail to see how the public and private sectors can be complementary in improvingthe health of Mexicans. Trained health personnel, adequate infrastructure, medical devices and medications should be available at both sectors, so their collaboration is fundamental”
Américo García Vice President and General Manager LATAM | Apotex
In Mexico, social security provided by IMSS, ISSSTe and peM e X is conditional to formal employment. “However, being affiliated to these services does not guarantee access,” highlights García. He shares that in 2018 there were 32,000 pharmacies but in 2021 this number grew to 37,500. This growth increases attention and relieves pressure from the public health system. Moreover,
despite their inability to address the most complex diseases, pAMOs are convenient, fast and in expensive.
In Mexico, 49.1 percent of medical care was obtained at a private healthcare provider and a large percentage of it financed by the poorest segment of the population. “ p rior to the pandemic, homes in rural areas of the country with seniors and young children were the ones with the highest expenditure on health,” explained Sergio Bautista, r esearcher, CISS-INS p Those with chronic diseases also had some of the highest health exp enditures.
The private sector mostly relieves the public sector in the treatment of acute illnesses, according to García. “Mexico lives with acute and chronic illnesses and the pharmacy has been instrumental in covering these acute illnesses that represent urgency to the public sector.”
To date, Mexico has 18,000 p AMOs employing a total of 36,000 doctors, said Marcos p ascual, Commercial Director, ANA f A r M e X. “Through these offices, we offer almost 400,000 appointments per day. Doctors at pAMOs are treating mild COVID-19 cases and directing complex cases to specialists. Aware of the importance of increasing health access, we are allying with CC e and the government of Mexico City to strengthen our health provision and our role as the primary health contact with the patient.”
GENOMICS IS TAKING DIAGNOSTICS TO THE NEXT LEVEL
p ersonalized medicine has long been considered an opportunity to overcome the limitations of traditional medicine, with the industry and academia now able to make more precise decisions thanks to human genome sequencing. Genomics is making it possible to predict, diagnose and treat diseases more precisely than ever, so it is necessary to continue expanding this practice across the world, agreed industr y experts.

“Drug development is costly and inefficient. There is a 90 percent overall failure rate from pre-clinical to p hase II/III trials. for example, there is a 99.6 percent failure rate for Alzheimer’s drug trials. The most common reason for failure is lack of efficacy and the most common reason for it is inadequate target validation,” said Michael Johnson, p rofessor of Neurology and Genomic Medicine, Imperial Colle ge London.
Genetics studies genes and their roles in inheritance to understand the way certain traits or conditions are passed down from one generation to the next. Genomics, a more recent term, describes the study of all of a person’s genes, including the interactions of those genes with each other and with the person’s environment, according to the National Human Genome research Institute. Genomics has found applications in the study of complex diseases such as heart disease, asthma, diabetes and cancer, which are typically caused by the combination of genetic and environmental factors..

“Although the genomics studies continue moving forward, there is a shortage of talent supply. Professionals with good education in other sectors, physics, mathematics and computer sciences”
Ivana Poparic, Head of Life Sciences Cluster Development | MedCity
Several countries across the world are working on genomics projects, which offer new possibilities for therapies and treatments for some complex diseases as well as new diagnostic methods. for example, in Dec. 2012, former UK p rime Minister David Cameron announced the creation of “The 100,000 Genomes p roject” to sequence the whole genomes of 100,000 individuals with rare inherited diseases and cancers. The project aimed to return new diagnoses to National Health Service (NHS) patients, build research infrastructure, capability and skills,
generate inward investment and “to lead the world in the application of genomic medicine across national healthcare systems,” said Damian Smedley, professor in Computational Genomics, Queen Mary University and Director of Genomic Interpretation, Genomics e ngland. In May 2016, Genomics england opened a new Sequencing Center, which reached the goal of sequencing 100,000 genomes in Dec. 2018, added Smedley.
Genomics e ngland collaborates with 3,580 researchers and 413 academic institutions worldwide, said Smedley. The UK-owned company is present in North America, including Mexico. Since July 2017, Genomics e ngland has worked with the industry through its Discovery forum, which provides a platform for collaboration and engagement between Genomics england, industry partners, academia, the NHS and the wider UK genomics landscape, according to the company.
p rimarily funded by the UK Medical research Council, Johnson’s research at the Imperial College London uses single-cell transcriptomics of the human brain, single-cell Mendelian randomization for causal inference and integrative multi-model genomics. from the 216 new drugs entering the German market between 2011 and 2017, 160 showed no quantifiable benefit over existing licensed therapies, said Johnson. The Mendelian randomization helps for better drug target validation, resulting in drugs with improved efficacy, he added.
Despite the complexity of genomics studies, there are efforts to decentralize them and make them accessible to more professionals worldwide. for example, Oxford Nanopore Diagnostics, a new subsidiary of Oxford Nanopore Technologies, was established to facilitate the development of a new generation of DNA/rNA sequencing technology for diagnostic applications through collaborations with clinical and industry partners.
Oxford Nanopore Technologies offers devices that “suit all throughput needs and work
environments,” and has a large and rapidly growing customer base, with sequencers in over 100 countries and presence in key global institutes, said Katherine Melville, Diagnostic Testing Solutions Manager, Oxford Nanopore Technologies. “We intend to deliver products that make the benefits of genomics accessible to all. Our vision is to transform healthcare through real-time genomics,” she added.
Although the genomics studies continue moving forward, there is a shortage of talent supply. professionals with good education in other sectors, physics, mathematics and computer sciences, could always contribute, said Ivana p oparic, Head of Life Sciences Cluster Development, MedCity. “Bringing people from other sectors into genomics to provide new talent can provide a solution to the shortage of talent supply in the field.”
Multidisciplinary teams enrichen the work and are important for Oxford Nanopore Technologies. “We have people hired from many different backgrounds, such as machine learning and material science,” said Melville.
In Mexico, genomic medicine research is led by the National Institute of Genomic Medicine (INM eG e N). Created in 2004 in response to a revolution in biological sciences and in experimental biology at the time, INMeGeN is the eleventh National Institute of Health. It was created as a result of the p romoter Consortium of the Institute of Genomic Medicine, integrated by UNAM, the Ministry of Health’s National Council of Science and Technology and the Mexican f oundation for Health. INM eG e N aims to incorporate much of the biomedical research and molecular oriented research into the Mexican healthcare sector.
PERSONALIZED MEDICINE: A GROWING OPPORTUNITY
In the past three to four years, the onceconsidered distant personalized or precision medicine and medical devices have become a reality for global healthcare systems. Mexico is no exception but to continue advancing this revolutionary technology, the country needs continued participation, said industry experts during the “ personalized, precision Medicine and Devices” panel of Mexico Health Summit 2022.
Applications are numerous as therapies tailored to a patient’s genetic makeup can even prevent diseases. The sector has become one of the industry’s fastest growing areas and its current market value of US$52 billion is expected to quadruple by 2028 with a steady annual growth of 10 percent, explained Sandra Sánchez, president and CeO, pharmaAdvie.
There is a growing shift from reactive to preventive medicine in Mexico, particularly as chronic diseases continue rising, making personalized medicine even more attractive. However, this technology will have to face several challenges in the coming years, including complicated regulation due to ambiguous frameworks, lack of knowledge,
limited accessibility (as true accessibility is defined by at least 80 percent of a product being available to the greater population), data privacy and synchronicity within industry players, amongst others.
A primary issue, as far as regulation and understanding of this technology is concerned, is its broad scope. f rom pharmaceuticals to medical devices, many evolving technologies fall into the category of personalized medicine. Currently, the f DA has approved 22 genetic treatments for use worldwide but their use will depend on national regulations and developmental projects. To move forward, health experts suggest looking to neighboring countries as examples.
The US’ chronic disease management research model has been successful because of the union between universities and the industry, as 95 percent of large projects come from institutions of higher learning. Mexico should take this model as an example, said David López, Country Managing Director, BioMarin pharmaceuticals Mexico. However, there may not be enough researchers in
the field despite the large number of young people in the country studying healthcare.
To improve regulations, López suggests contacting legislative bodies as regulation efforts start with them. “Connecting scientific research done in Mexico with industry interests is one of the great opportunities for drug development… We need a strong alliance between the industry and the legislative branch, since much of the regulation emanates from there. There must be political will to regulate and promote innovation in healthcare,” López said.
Mexico is considered one of the Top 5 Latin American countries with the best conditions to integrate and promote personalized medicine according to the Latin American personalized Medicine Index. The country made great strides in the field of orphan medicine, which often relies on personalized medicine, by explaining the technology to local authorities. These efforts show that legislative bodies can be open to learning about this technology, said López, so there is a pressing need to contact and collaborate with them to advance personalized medicine.
The technological revolution facilitated by the pandemic greatly benefited personalized medicine. The personalized aspect of the
devices and pharmaceuticals, as of most revolutionary technologies, relies on the collection of large amounts of personal data. Continuous monitoring diagnostic equipment and wearables such as smart watches already collect health data of their users, making them useful tools for the development of preventive personalized technology, said Jaen Velazquez, Director Business Development Mexico and Innovation Latin America, Siemens Healthineers. “ precision medicine requires data. AI and digital health are very promising sources to meet this requirement,” Velazquez said.
for the continued evolution of this science, patient participation is needed, agreed Velazquez, Sánchez and López. Timely diagnoses have the potential to change the framework of the Mexican healthcare ecosystem. The continuous participation and empowerment of patients in Mexico has historically shaped and driven efforts for breakthroughs in treatments of a broad range of diseases from HIV to diabetes. There has been an explosion of investment into personalized medicine in countries such as the US and Ireland, which have opened seven new biomedicine plants recently. Mexican advancement in the sector will require participation from all players, from patients to doctors to the federal government.
THE ROADMAP TO A DIGITAL HOSPITAL IS NOT COMPLEX
The hospital of the future may look quite different than the hospital of today. Already, a growing number of inpatient health care services are being pushed to the home and to outpatient ambulatory facilities but there are still complex cases who will continue to need acute inpatient services.
A hospital is made up of several areas working together to make care provision possible, from management, supply chain and financing to clinical practices and diagnosis. In this dynamic, tech came to support management operations and medical professionals in their daily practice. As such, tech in a hospital impacts the patient and its experience in and out the facility.
“The overall targets of hospital technology are to help it operate better, take better care of patients and reach more people at a better cost. A digital hospital breaks the paradigm of quality versus quantity because it can provide attention to more people with an improved service,” said Jorge Camargo, CeO, ecaresoft. Moreover, hospitals do not need to switch face-to-face attention for virtual care as they can offer both with equal quality.
from a medical perspective, digitalization at a hospital has five pivotal targets: reduce inefficiency, improve accessibility, reduce long-term cost by saving on materials and times, increase quality and deliver personalized medical outcomes.
“Additionally, the data it generates must provide better communication and better diagnostic support for them, aside from fomenting transparency,” said Sandra García, Cardiologist, Médica Sur.
Digital hospitals have an implementation challenge that varies depending on the country, their size and the population target, explained Santiago yeomans, Health r esearch and Innovation Director, Christus CeI.
While the benefits are numerous, integrating new software can be challenging because everyone at the hospital may be used to traditional practices. Thus, “tech providers must realize that the goal is not to modify the clinical path of a hospital. If technology is going to enter, we must look for tools that do not disrupt the clinical way of working,” said Juan Caceres, C eO, Aidicare. He stressed that tech companies must add value to their processes without trying to change them because “that is not technology’s area of expertise.”
Nonetheless, a hospital should not be dogmatic in its processes. “Hospitals need to analyze, from their principles, how tech can help and support them in their operations,” said Camargo. He recommends tech companies begin with smart targets to have quick wins that will then allow them to continue the digital transformation. “Learn
from the hospital and its advances to know when and how they may be ready for another change,” Camargo explained.
Apart from considering the areas of adoption, tech providers should also take into account the groups of professionals ready to adopt tech. “ for example, Mexican nurses know how to use computers and smartphones but they are still skeptical about tech. residents, however, have a greater adoption of tech, so training for them is much simpler,” said García.
Hospitals such as Médica Sur recommend a transition that begins with management to then progress to clinical areas. “With Aidicare, we began with management and then expanded to the hospitalization areas. Now, we are transitioning the therapy and emergency areas,” García said. More importantly, it is key to find a perfect match between the tech provider and the hospital. “The chosen tech provider must have a clear path and answers to incoming questions, and provide personalized training if possible,” said García.
Transitional implementation has been well received because professionals perceive how tasks on their daily work have improved. Thus, they are willing to integrate other solutions that will do the same, said Caceres. “furthermore, we need to break the paradigm that tech is about “being fancy” because it is not, it is a matter of being efficient.”

This thinking goes in line with the misconception that tech is complex and hard to understand and adapt. “Applications must be intuitive, as easy as delivery for rappi is. That must be our benchmark: intuitive enough so that implementation has the smallest amount of hand-holding,” said Camargo.
One of the pivotal parts of a successful digital hospital is its ability to interconnect with other areas and devices. “At Médica Sur we have interconnected nursing sheets with measurements of vital signs. We also used our robots to interconnect different specialties of the hospital. This takes digitalization from a commodity to a necessity for competitiveness,” Garcia
said. “In an ideal world, everyone should be interconnected to access the patient’s clinical file and provide better care and follow-up,” she added.
An interconnected system is the core of a value-based healthcare model, which has been called to be the ultimate goal of the sector. “To achieve this, tech providers and hospitals must be passionate about providing security and services,” said Caceres. Moreover, hospitals need to have a futuristic view of their reach and “think beyond the walls of the hospital, which allows them to operate beyond its infrastructure to remotely service new and recurring patients remotely,” said Camargo.
INNOVATION, COLLABORATION ARE CRUCIAL FOR HEALTHY AGING
Diverse factors, including science and technology, have allowed people to live longer. The global population is aging at an accelerated pace, with over 1 billion people aged 60 years and older. While this active phenomenon presents considerable financial challenges for countries across the world, it also opens opportunities for several actors including healthcare, agreed industry experts.
“We saw a large evolution in the last 20 years. Living longer carries enormous financial challenges to countries. f or example, by 2025, pensions will represent 6.4 percent of Mexico’s GD p. In addition, staying healthy and improving quality of life are important challenges, which in turn present the opportunity for the health industry to collaborate and offer solutions,” said Cristobal Thompson, executive Director, AMIIf
By 2050, the proportion of the world’s population over 60 years is forecasted to nearly double from 12 percent to 22 percent, according to WHO. Countries are facing major challenges to ensure that their health and social systems are prepared for the demands and opportunities of this demographic shift. In Mexico, between 1990 and 2020, the 60 year and older population went from 5 million to 15.1 million people, now making up 12 percent of the total population, according to IN eGI.
Twenty percent of those over 60 years old are not affiliated to any healthcare institution.
Seniors are common targets of stigmatization and discrimination, said Luis Miguel Gutiérrez, Director General, National Geriatrics Institute. But healthy and independent seniors contribute to the well-being of families and communities. It is a myth to portray them as passive recipients of social or health services, points pAHO, which promotes public policies and alliances toward healthy aging in the Americas. “The fact that old age is coming increasingly later offers opportunities. In Mexico, less than 5 percent of those aged 60 years or older fully rely on their families [for care and economic support],” said Gutiérrez.
Although the shift in the distribution of a country’s population toward older ages started in high-income countries, such as Japan, where 30 percent of the population is already over 60 years old, currently low and middle-income countries are experiencing the greatest change, according to WHO.
The private sector is also contributing to healthy ageing. “In Japan, similarly to Mexico, one out of every three people suffer arterial hypertension. Omron created the first home blood pressure monitor, aiming to reach zero cardiovascular events,” said Vanessa Ballarte,

e xecutive Director Corporate Strategy and Digital Health for Latin America, Omron Health Care. Japanese-based medical devices company Omron specializes in blood pressure monitors, nebulizers, electrotherapy T e NS2 devices and other innovative products and services.
Health monitoring is essential to prevention because the early detection of diseases can reduce suffering and medical costs. While remote monitoring was already advanced in certain countries, the pandemic boosted its penetration in Mexico and Latin America, said Ballarte. “It is important to educate patients so they can monitor themselves at home and raise awareness on the importance of mo nitoring.”
Working toward healthy ageing requires the participation of the public sector, civil society, academia and the private sector. However, care for seniors is still framed around chronic disease management rather than in the person, said Gutiérrez. “Seniors are usually excluded from clinical trials due to their complexity, but they still are part of the real world. Clinical trials are an important area of opp ortunity.”
Technology continues to play an important role as an enabler and paradigm-shifter within the health industry. When it comes to the implementation of digital tools, it is important that patients of all ages understand how to use them but this becomes crucial with products targeted at seniors, said Ballarte.
Digital tools are not adopted in the same way by people of different ages and socioeconomical situations, said Thompson. “We have to work toward greater equity in the use of technology. (Digital tools) must become massive, patient-centric and inclusive. We will adopt simple technology but for more complex tools we must all educate ourselves, from the medical community to people in general.” Technology adoption requires collaboration between public and private actors to make a real impact, he added.
To democratize and massify technology in Mexico, regulations play a key role, said Ballarte. “Currently, there is not enough regulation regarding telemedicine and remote monitoring. Software is not considered as medical equipment yet. In terms of data security, companies work under high-standard security schemes but it is important to have a clear regulatory
framework for the entire industry to benefit.”
Globally, the growth of the share of the population aged 60 years and older is a reality. The multiple challenges and
opportunities that this paradigm shift has brought must be tackled jointly by all actors involved, from the general public to private and public sectors, taking advantage of technology adv ancements.
DATA, TRACEABILITY SUPPORT HEALTH LOGISTICS

The pandemic transformed the logistics industry by changing client expectations regarding delivery times, which were made possible thanks to the fast adaptation of logtech advancements improving communication with freight forwarders.
The pharmaceutical logistics industry is no different. Industry insiders discussed recent and future innovations for the industry through the increased incorporation of traceability and big data technology during Mexico Health Summit 2022.
The implementation of these technologies brought forward major changes and benefits to the transportation of health supplies. from a freight forwarder’s perspective, technology improved distribution practices through the implementation of smart sensors to measure temperature, light, security and geographical location in real time to provide better information to clients.
following the pandemic, the medical industry is catching up in the implementation of
technology as the sector had not capitalized in this area, said Andrés posada, Supply Chain Manager Mexico and Central America, Boston Scientific. The pandemic forced the sector to be even more flexible. Some hospitals in Latin America that might have been registering processes by hand adopted new technologies and processes following the outbreak.
freight forwarders are not staying behind.
“Within the medical devices industry, the implementation of blockchain and AI is being explored to improve logistics distribution,” said posada.
Many logistics partners of medical companies are using logtech developments to provide better services. DHL’s DHLi, for example, allows customers to exchange information with companies to optimize their logistics, said Liliana Castillo Bautista, Head of Life Sciences and Chemicals Sales, DHL Global forwarding México. This information is then readily available for customers in real time, as DHL does not only provide basic geographic
information but also data regarding the temperature, light and security of products en-route. These traceability processes are made possible through the collection of big data, making DHL not only a service provider but a business partner of their clients.
“Logistic distributors work hand in hand with laboratories to ensure the best distribution practices for drugs and medical equipment,” Bautista said in reference to one of the many ways freight forwarders collaborate with clients to ensure best practices.
Big data expedited the optimization of routes by logistics companies worldwide but in Mexico additional regulation regarding this development and other technologies are needed, said Miguel Angelo r icchiuti, Operations and Supply Chain Director Mexico and LATAM, Apotex. Industry 4.0 has arrived but Mexico is still behind countries such as Brazil and Argentina in digitalization, serialization and regulation, necessary tools for industry players to ensure that their technologies are sound proof and their products cannot be replicated.
Once these hurdles are overcome, there are infinite opportunities in the sector, said ricchuiti. AI is one of these, as even though it is usually thought of only in aspects of robotization and automatization, it has the potential to bring benefits to all individuals in the industry. IoT and AI technology will not replace human labor, ricchuiti said, but lower demand for human labor to manage simple tasks, smoothen out transportation processes and reduce overall costs.
Interconnection between clients and suppliers through blockchain systems is another innovation that could continue to optimize in-real-time traceability, benefitting all players. p harmaceutical companies, in particular, use less warehouse space to store higher-value products that need more technological security and information about their geological location. The industry was not prepared for the challenges the pandemic brought but with the increased incorporation of technological advancements, it seems to be better prepared for whatever may come in the future.
VALUE, IMPACT OF PATIENT BLOOD MANAGEMENT
p atient Blood Management ( p BM), a multimodal and multidisciplinary approach to limit the use and the need for blood transfusions in at-risk patients, arrives in Mexico to improve clinical outcomes. p BM encompasses all aspects of the transfusion decision-making process, beginning with the initial patient evaluation and continuing through clinical management, explained Christa Seipelt, International p roduct Manager Diagnostics, Sarstedt AG&Co.KG.

“PBM encompasses all aspects of the transfusion decision-making process, beginning with the initial patient evaluation and continuing through clinical management”
Christa Seipelt, International Product Manager Diagnostics | Sarstedt
pBM “is fundamental because, for example, for the most vulnerable patients such as children, the elderly or the chronically ill, taking frequent and numerous blood samples weakens them and might force them to receive foreign blood, which is a benefit but does not strengthen vulnerable patients when their blood was already weak,” sai d Seipelt.
Laboratories need to consider many aspects before drawing blood, including the patients’ conditions and medical records and blood extraction guidelines, said rafael Guerrero García, Vice president of the Board of Directors, Mexican Council of Clinical p athology. Laboratories must also take into account that they must extract the smallest possible quantities to avoid affecting the patient and potentially causing or aggravating anemia, which could further complicate the patient’s condition.

“Blood extraction implies a responsible request for studies and the use of methodologies that would sustain the patient as long as possible,” said Guerrero. In a regular blood extraction patients may lose up to 25 percent of their hemoglobin, which is not always necessary, said Seipelt.

“Diagnostic studies need to be requested more thoughtfully and take into account the patient’s record by establishing protocols and awareness”
Arturo Vivas, Product Diagnostic Specialist | Sarstedt
This loss of hemoglobin is more alarming in pediatric patients because their total blood volume is much less than an adult’s, said Israel p arra Ortega, Head of the Clinical Laboratory Department, Mexico Children’s Hospital f ederico Gómez. “In fact, there are studies that require that the patient has not received a transfusion,” he said. f or pediatric patients, less blood volume handled means less risk of an infection, making p BM even more important. “ p BM means patient safety and the efficiency of analytical and laboratory processes. Such benefits must be shared to make this practice a standard process in the health system,” p arra said.
Despite its importance, p BM has not been widely applied in Mexico neither in adults or infants, impacting health outcomes and increasing costs. “Only 2-3 percent of laboratories in Mexico take optical blood management measures,” said Guerrero.“Although there are already clear guidelines to be able to establish p BM, we have not been able to adopt them,” said parra. e xperts recommend that the effective way to standardize p BM is through regulation. Some of the best pBM practices are used in Germany and other eU countries that have proved that pBM can be standardized in a healthcare system.
“While it has not been greatly adopted in Mexico, professionals are showing interest in p BM,” said Seipelt. Those professionals, alongside the public health sector, generated the clinical practice guidelines for patient blood management of public institutions, which is proof of the interest and is a first step to expand its impact, she added.
Transitioning to p BM implies avoiding extracting unnecessary blood samples and having reserve samples. “Diagnostic studies need to be requested more thoughtfully and take into account the patient’s record by establishing protocols and awareness,” said Arturo Vivas, product Diagnostic Specialist, Sarstedt.
Common practices include taking 800 ml of blood for a serum clinical chemistry, but “the truth is that that amount is not really necessary,” said Seipelt.
p roper use of blood extraction and management tools is also important, said parra, because some procedures require the extraction of more blood than others. even when the volume extracted is small, it is still a loss for the patient. However, laboratories need to ensure to have a large enough sample to avoid compromising the study, said parra.
BIG DATA TO DRIVE HEALTHCARE 3.0
As the healthcare industry continues realizing the value of big data, the question of access and storage becomes a pressing issue.
During Mexico Health Summit 2022, Andrew Ahachinsky, president and C eO, Bobbinet LatAm, explained what the Canadian company is doing to drive big data efforts forward in healthcare through innovation, Web 3.0 and blockchain, as well as why the region presents unique opportunities.
Under a Health 2.0 application centric approach, multiple apps request patients’ data as each manages it for its own monitoring purpose. This outdated and disconnected model discourages patient participation. A switch to 3.0 would give patients an increased role in the collection, distribution and storage
“I would like to see more work and scientific information made by and for Mexicans, because that is important to standardize the practice and recognize limitations and opportunities of the system,” he said.
Awareness forums for laboratories and professionals regarding pBM are necessary for these concepts to permeate to all professionals. But most importantly, p BM “should be included in the Mexican Official Norm and mandated in the functions of the health professional,” said Guerrero.
of their own data, said Ahachinsky. To do so, Bobbinet envisions a patient subscription system that provides transparency over where patient data is going and how it helps others. This can then result in a situation where not only patients benefit but also pharmaceutical companies create better products and health services maximize their accessibility to data, potentially sharing information regarding rare diseases that might be of greater value to pharma companies to look at.
At its core, Bobbinet provides a way for blockchain to safely decentralize healthcare, consumer and patient data, while giving the patient better control and understanding of where their data is going and how it is used, said Ahachinsky. It even allows them to share

data with third parties and organizations. Using anonymous records, patients can keep all their healthcare and data materials in one place, allowing the Latin American healthcare system to maximize development, access and participation, he added. Latin America is an ideal market for this technology as it has had 25 percent of global clinical trials and annually spends US$50 billion in pharmaceuticals annually.
North American and e U governments have cracked down on these efforts and prohibited their development, so Latin America could become the next largest opportunity market for this type of development, particularly as 30 percent of the population does not have access to health services because of economic reasons. Mexico in particular has a large discrepancy between its public and private health sectors and its urban-centered health facilities leave many in rural areas witho ut access.
The data accumulated by these efforts will be large and have great quality, said Ahachinsky. It will allow patients and consumers to become data stakeholders with the benefits this carries, as 60 percent of generated data comes from patients (30 percent is genomic and 10 percent is clinical).
Another possible solution to increase patient data sharing could come through the use of non-fungible tokens (NfT), said Ahachinsky. This proposal would add patient data into the blockchain through smart contracts to provide further control, security and management access, he said. Under this proposed model, patients could earn money by providing it to third parties with a clear understanding of who owns and who uses the data, said Ahachinsky.
The healthcare Metaverse could also bring potential solutions by decentralizing health profiles and providing anonymity and live access to a digital extension in the coming metaverse where digital human as a service may soon take place, said Ahachinsky. particularly as by 2026, the average person is expected to spend at least one hour within the Metaverse, he added.
The company is also looking at enabling patient permissions within existing health education research models already used in hospitals to create a more patient centric approach within existing environments. These efforts look to improve outcomes in terms of cost savings, optimizing the doctor’s work and empowering patients within the medical data revolution as the incorporation of technological advancements continues becoming a social determinant of health.
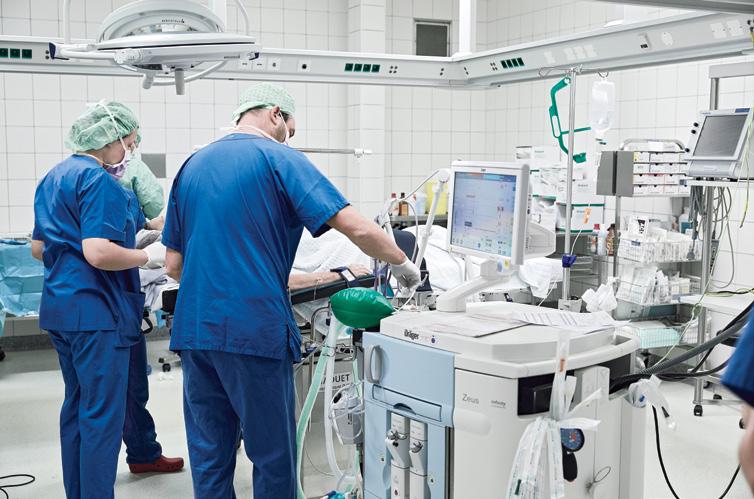
INNOVATIVE, ITINERANT ARTICULATED SERVICES FOR HEART SURGERIES
Technology and healthcare continue evolving amid several challenges and crises such as the COVID-19 pandemic, which forced healthcare professionals and companies to become more creative and innovative to solve non-COVID-19 issues, such as cardiovascular surgeries.
As some hospitals focused exclusively on COVID-19 cases during the pandemic’s peaks, several non-urgent procedures were postponed. However, some medical specialties still needed urgent treatment. f or these cases, Vitalmex innovated within its renowned articulated services to start offering its new itinerant articulated services, which work on an on-demand basis and help carry out procedures in different sites.
Vitalmex is a leading provider of surgical support services to some of Mexico’s largest public and private hospitals. The company’s activities range from surgical technician services and inventory management to medical technology and equipment management. “Our main goal is to support institutions and healthcare professionals in every aspect of their work, from supplies and equipment to technology and expert personnel, allowing them to focus on what they do best: taking care of patients,” said ramón Mier, Commercial Director, Vitalmex.
Ten years ago, Vitalmex increased its footprint beyond Mexico after acquiring Germany’s Gimmi, a company focused on manufacturing surgical instruments, which it sells to over 60 countries. In addition, Vitalmex began implementing its articulated services in the US market, where the company already is present in 10 states.
Since 1993, Vitalmex has been characterized for its articulated services for the clinicalsurgical, administrative-operational, technological and financial areas of the health sector, said Mier. These services are configurable, adaptable and flexible both for patients and healthcare professionals.
The itinerant articulated service is an alternative to the traditional services. Under this scheme, Vitalmex assists healthcare professionals and institutions on-demand to carry out heart and minimally invasive surgeries. “Usually 5 days before the surgery, hospitals or healthcare professionals call us to request the service. Our personnel have a meeting with the hospital and we get everything prepared as requested, from medical supplies to instruments and equipment to help them perform the surgery,” said Mier. Itinerant articulated services offer several benefits, such as collaborative work, state-of-the-art technology, high-quality supplies, workflow improvement, prestige and qualified, well-trained personnel, he added.


