APRIL
11-14
2026




APRIL
11-14
2026


CLEANING CHEMISTRIES
INSTRUMENT & SCOPE REPROCESSING
CLEANING VERIFICATION
DETERGENT DELIVERY
PROTECTING PATIENTS
With effective instrument & scope cleaning solutions
HELPING MEDICAL PROFESSIONALS
With
DRIVING INNOVATION
With






Healthmark & Getinge believe by combining our strengths, we are positioned to better serve healthcare facilities moving forward into the future. We’re committed to providing innovative solutions, personalized implementation and best-in-class educational resources more than ever before. Together, we are striving to give you an unparalleled customer experience.
Scan to explore the bene ts of our partnership. Discover how we’re rede ning the customer experience to empower your facility.



Accreditation 360 is reshaping how hospitals are surveyed in 2026. Are your OR and SPD workflows ready?
On May 14th, this CE-eligible webinar will explore the most common — and often overlooked — compliance breakdowns between the operating room and sterile processing department. Learn how Accreditation 360 shifts the focus to continuous system reliability and what that means for IFUs, inspection standards, packaging decisions, and cross-department alignment.
Walk away with practical strategies to strengthen readiness — every day, not just before a survey.
Register Now!
Smoke capture mandate compliance made easy:
• Hands-free & flexible
• Unobstructed view
• Up to 2x the smoke capture1
• Shown in studies to remove infection-causing bioaerosols2,3



OR TODAY | Spring 2026
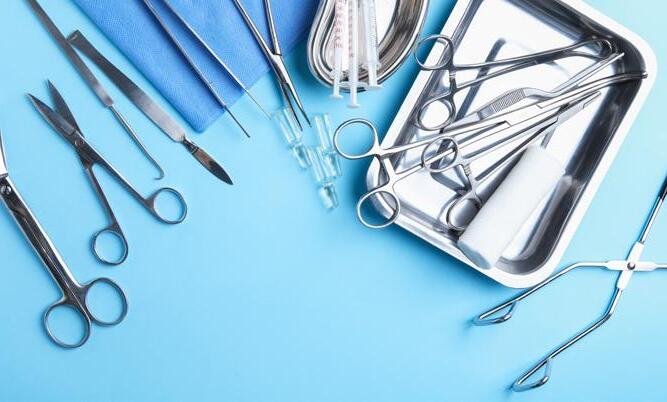
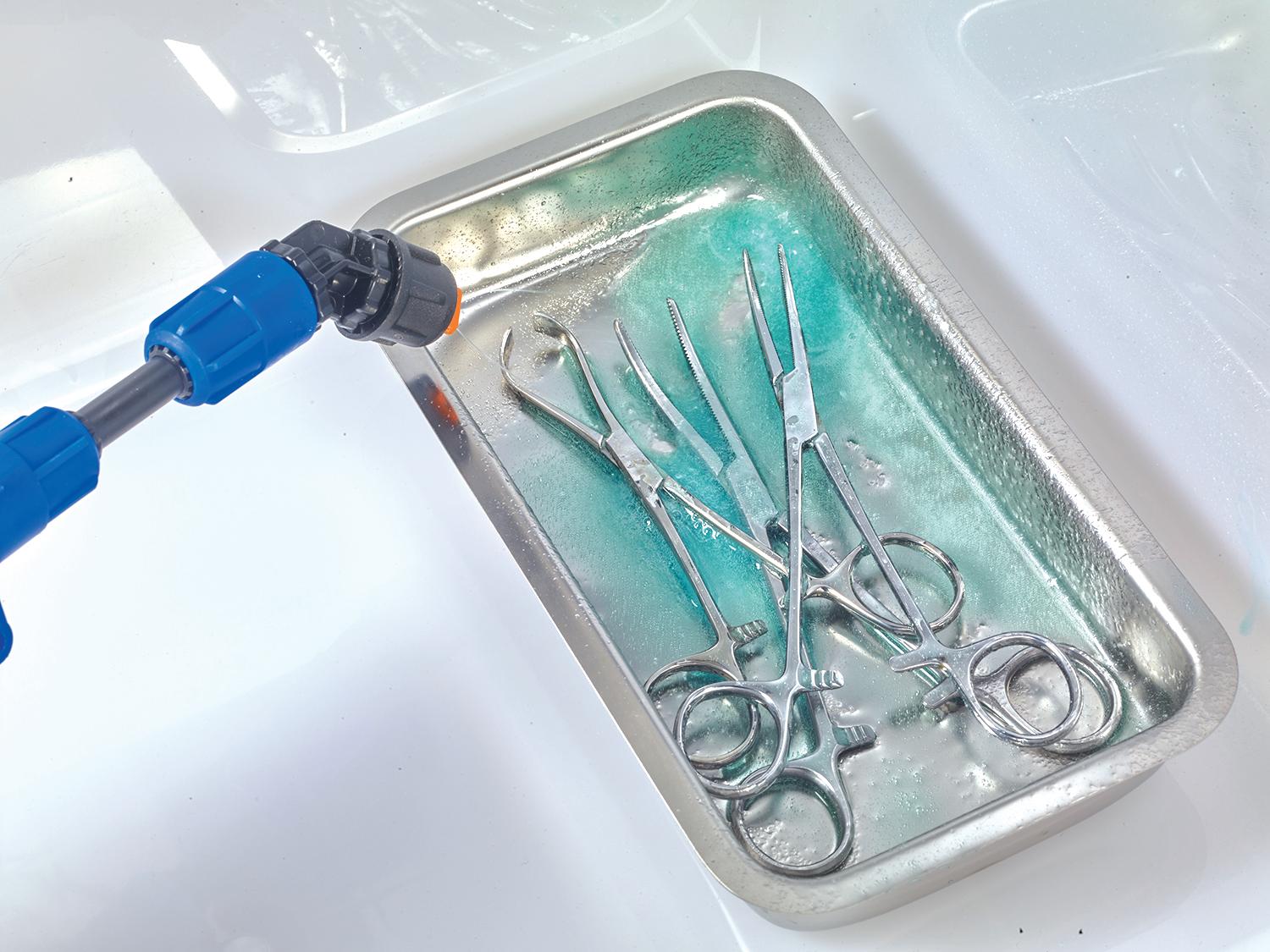
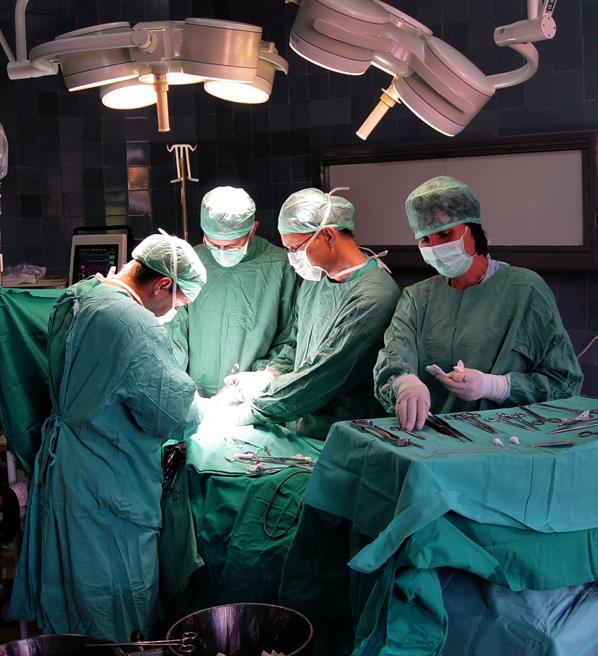
The global surgical equipment market is estimated to reach $31.58 billion by 2030. Check out some of the latest surgical tools.

When looking to strengthen one’s core, it is wise to go beyond the sixpack or flat abs image. The core is the foundation for all other movements.
Accreditation is one of the most important responsibilities of hospitals and ambulatory surgery centers (ASCs), helping ensure the highest levels of healthcare quality and patient safety.

Fiber may be having a cultural moment, but most Americans still aren’t getting enough of it – or fully understanding where it comes from.
OR Today (Vol. 26, Issue #2) Spring 2026 is published quarterly by MD Publishing, 1155 Senoia Road, Ste. 200 Tyrone, GA 30290. POSTMASTER: See address changes to OR Today at 1155 Senoia Road, Ste. 200 Tyrone, GA 30290. For subscription information visit www.ortoday.com. The information and opinions expressed in the articles and advertisements herein are those of the writer and/or advertiser, and not necessarily those of the publisher. Reproduction in whole or in part without written permission is prohibited. © 2026

PUBLISHER
John M. Krieg
john@mdpublishing.com
VICE PRESIDENT
Kristin Leavoy kristin@mdpublishing.com
VICE PRESIDENT OF BUSINESS DEVELOPMENT
Jayme McKelvey jayme@mdpublishing.com
EDITOR
John Wallace editor@mdpublishing.com
ART DEPARTMENT
Karlee Gower
Taylor Hayes
Alicia Brown
ACCOUNT EXECUTIVES
Megan Cabot
DIGITAL SERVICES
Cindy Galindo
Kennedy Krieg
EVENTS
Kristin Leavoy
Sydney Krieg
ACCOUNTING
Diane Costea WEBINARS
Linda Hasluem
EDITORIAL BOARD
Vangie Dennis, MSN, RN, CMLSO, CNOR, FAORN, FAAN Perioperative Consultants, LLC
Justin Fontenot, DNP, RN, NEA-BC, FAADN Associate Professor, Tulane University School of Medicine, New Orleans, LA
Natalie Lind, Education Director for the Healthcare Sterile Processing Association, HSPA
Pat Thornton, MSM, RN, CNOR Perioperative Consultant, RNFA Dermatology Institute
Dawn Whiteside, DNP, MSN, RN, CNOR, NPD-BC, RNFA, Director of Education, CCI
Julie Williamson, BA Director of Communications, HSPA



As National Volunteer Week (April 19-25) approaches, perioperative nurses nationwide are taking time to elevate their profession through service. For many, volunteering with the Competency & Credentialing Institute (CCI) is more than giving back – it’s a strategic path to developing leadership skills that support career growth and strengthen patient care (Journal of Applied Psychology).
Research consistently shows the connection between volunteerism and leadership development. A study published in the Journal of Applied Psychology found that 83% of professionals credited volunteer work with helping them gain or strengthen leadership competencies (Journal of Applied Psychology). For perioperative nurses, CCI’s structured volunteer pathways offer an ideal opportunity to build these capabilities while earning recertification points and contributing to the advancement of the specialty (Competency & Credentialing Institute, 2026).
CCI – the certifying body for perioperative nursing for more than 45 years
– has certified over 85,000 nurses worldwide. Its programs rely on volunteers to help develop certification exams, create educational resources, mentor peers and shape the future of perioperative practice (Competency & Credentialing Institute, 2026).
“Volunteering with CCI is a tremendous opportunity as a professional,” CCI Director of Credentialing Tabitha Kinlaw shares, “It’s a great way to earn recertification points but also a tremendous opportunity for professional growth.”
Deloitte research reinforces this: 92% of hiring managers believe volunteer experience reliably builds leadership competencies – skills increasingly essential in OR environments that demand team management, critical thinking and cross-functional collaboration (Deloitte, 2016).
CCI offers several volunteer opportunities designed to fit diverse interests, time commitments and career stages.
Certification Coaches mentor colleagues preparing for certification, earning 20 annual recertification points while building communication and motivational leadership skills. Test development committees engage volunteers in writing and
reviewing exam content through one- or two-year appointments. Educational content developers create webinars, podcasts, and practice questions, building instructional design and project management capabilities (Competency & Credentialing Institute, 2026).
Research from Markitects Inc. shows that volunteer work strengthens planning, time management, mentoring and cross-functional leadership (Markitects Inc.). CCI volunteers build strategic thinking through exam development, project management through content creation cycles and communication skill through coaching. Motivational leadership grows naturally as volunteers guide peers – skills that translate directly to OR practice.
Volunteer environments also support professional networking. Virgin Group research indicates that 85% of employment opportunities are filled through networking, and 28% of professionals have discovered new career roles through these connections (Virgin Group). CCI volunteers frequently build relationships with educators, managers and directors nationwide –expanding their career visibility.
CCI volunteer roles carry meaning-
ful recertification value. Committee volunteers earn 20 points annually, with certain test-development committees awarding 25-100 points depending on the role. Facility-based volunteering also counts, including precepting, committee service and clinical volunteer activities. The Bureau of Labor Statistics reports that 68% of volunteers work with more than one organization, making CCI a strong complement to other professional activities (Bureau of Labor Statistics).
Perioperative nurses can maximize leadership development by aligning volunteer roles with career goals, documenting accomplishments and applying new skills within their OR teams. According to the Corporation for National and Community Service, individuals with volunteer experience are 27% more likely to secure employment (Corporation for National and Community Service).
A phenomenological study of
volunteer leaders found that volunteer roles provide an environment for testing and refining leadership approaches, with skills transferring directly to professional practice. Approximately 45% of volunteers report being motivated by career advancement opportunities (VolunteerHub).
Over time, CCI volunteers help build a stronger perioperative leadership pipeline. Their contributions support certification advocacy, mentorship and surgical safety initiatives while upholding competency standards that reduce practice variation and strengthen patient outcomes. The Corporation for National and Community Service values volunteer work at $281.74 billion annually (Corporation for National and Community Service).
CCI offers volunteer roles for nurses at all career stages. Opportunities are available at info.cc-institute. org/volunteers.
References
1. Bureau of Labor Statistics. (n.d.). Volunteering in the United States.
2. Competency & Credentialing Institute. (2026). Certified Perioperative Nurse (CNOR) Handbook.
3. Corporation for National and Community Service. (n.d.). Volunteering and Civic Life in America.
4. Deloitte. (2016). The Deloitte Millennial Survey.
5. Journal of Applied Psychology. (n.d.). Study on volunteer service and leadership skills development.
6. Markitects Inc. (n.d.). Research on volunteer competencies.
7. Virgin Group. (n.d.). Research on networking and employment opportunities.
8. VolunteerHub. (n.d.). Career development research on professional networking.







In today’s operating rooms, the pressure is real. Nurses and surgical teams move efficiently, maintain compliance, protect patients and manage equipment, all while keeping cases on schedule. At the same time, hospitals must ensure that purchasing decisions support both clinical performance and responsible resource management. In this environment, value is measured not only by cost, but by reliability, support and the ability to prevent disruption before it occurs.
Innovative Medical Products (IMP) was founded on partnership. Its vision has always been to develop and deliver innovative solutions grounded in the practical realities of surgical patient positioning and supporting logistics. Ongoing engagement with orthopedic surgeons, leading companies and O.R. teams has informed the refinement of solutions that address universal positioning challenges while supporting consistent performance in the surgical environment.
IMP recognizes that dependable equipment is only part of the equation. Ongoing support, predictable service and long-term protection matter just as much to the teams who rely on that equipment every day. The MVP Program was developed from that understanding, an integrated partnership model designed to reinforce operational confidence and sustained value in demanding surgical environments.
Healthcare teams navigate a constant balance between clinical performance, workflow demands and responsible resource management. Those factors rarely operate independently. When equipment falls short of expectations or requires full replacement over a minor repair, the impact moves quickly through the department. Case preparation may take longer and planning becomes less predictable. Attention shifts toward troubleshooting rather than patient care. Over time, those disruptions accumulate in ways that are both operationally and financially significant.
Durability and life cycle support ultimately define the true value of any
equipment investment. Equipment selected for upfront savings may perform well initially, yet limited warranty coverage or restricted repair options can shift risk back to the facility. A single failed component may require full replacement. Over time, what seems minor in isolation can translate into unplanned capital expenses, added coordination and growing frustration among teams tasked with maintaining surgical flow. Support responsiveness also shapes the experience. When questions arise or service is needed, delays or unclear points of contact can extend disruption. Even well-designed equipment benefits from dependable guidance behind it. Without a support framework, staff members often shoulder the additional burden of navigating service logistics while maintaining their primary clinical responsibilities.
The common thread across these challenges is consistency. Teams seek equipment that performs predictably, service models that protect product lifespan and partnerships that reduce operational complexity. The focus extends beyond individual purchases toward sustained reliability in highdemand surgical environments.

The MVP (Most Valuable Partner) Program was developed to address the practical realities hospitals face long after an initial purchase is made. Rather than functioning as a traditional service add-on, MVP integrates protection, ongoing support and cost control into a comprehensive partnership model.
At its core, MVP protects long-term investment. Facilities receive a one-year warranty on new products, extended repair protection and a 10 percent discount on repairs. When equipment requires service, discounted repairs reduce unexpected maintenance costs and help extend product lifespan rather than forcing premature replacement. In cases where upgrades are needed, MVP provides complimentary product upgrades when applicable, ensuring that facilities are not left managing outdated configurations or incremental capital purchases.
Continuity of care remains equally important. Courtesy loaner equipment during repairs helps maintain surgical schedules without interruption. Loaner shipping support reduces administrative burden and associated costs, ensuring that service coordination does not become an added strain on already busy departments. For many facilities, maintaining workflow while equipment is serviced can be just as valuable as the repair itself.
The program also emphasizes guided support. MVP participants are supported by a dedicated IMP representative who remains accessible throughout implementation and ongoing service. This direct relationship simplifies communication, expedites coordination and reduces the time staff
spend navigating service channels. In high-demand surgical environments, clarity and responsiveness translate directly to efficiency.
Facilities qualify for the MVP Program through consistent use of IMP’s positioner-designed patient protective pads or by regularly incorporating IMP SteriBump into clinical workflow. Participation aligns naturally with practices already outlined in the IFU, reinforcing compliance while integrating products designed specifically for IMP positioning systems.
For facilities evaluating alternatives to traditional rolled towel preparation, processing requirements add another layer of consideration. Because AAMI standards require linens to be sterilized separately from medical instruments, additional sterilization cycles and transport logistics may be necessary. Even with careful preparation, variability in linen handling can introduce concerns regarding debris, contamination and cost.
IMP’s patient protective pads and SteriBump are engineered to promote safety, consistency and workflow efficiency. Through their routine use, facilities not only support patient protection and compliance standards, but also gain access to the service and financial protections built into the MVP Program.
Today, equipment partnerships are increasingly evaluated through the lens of life cycle stewardship rather than one-time acquisition. Purchasing decisions are no longer defined solely by acquisition cost, but by the full

life cycle of support that follows. Stewardship of resources now includes durability, service responsiveness and the ability to extend product value over time.
IMP’s approach recognizes that dependable partnership matters. As a focused organization dedicated to surgical positioning and logistics, IMP maintains direct relationships with the facilities it serves. Clear points of contact, accessible representatives and responsive communication are not layers within a large corporate structure, but integral parts of the partnership model. When questions arise or service is required, teams know who to call.
MVP formalizes that commitment. By aligning product usage with embedded service protections and guided support, the program reinforces a shared objective: sustaining performance while protecting institutional resources. It is not simply a purchasing program. It is a life cycle partnership designed to reduce disruption, extend investment value and support the people who rely on consistent equipment every day.
In demanding surgical environments, reliability is an expectation. The MVP Program was built to meet that expectation through partnership, responsiveness and long-term stewardship.
Visit us at impmedical.com or call 1-800-467-4944.

By James X. Stobinski, Ph.D., RN, CNOR(E), CSSM(E), CNAMB(E)
I recently reviewed a number of articles on the evolution of Ambulatory Surgery including the recent thoughtprovoking article, “The ASC Surge”, in the Winter 2026 issue of OR Today.1 These articles prompted some reflection on the evolution of ambulatory surgery. When I began working in perioperative nursing in the mid-1980s our total joint cases, whether knees or hips, had a lengthy inpatient hospital stay. In comparison, total knee arthroplasties are now routinely scheduled as outpatient procedures for healthy patients and outpatient hip replacements are possible for some patients.
The prevalence of chronic disease such as osteoarthritis with an aging population that is living longer fuels the demand for surgery and stokes ASC volume. Industry reports inform us that 65% of surgeries performed in the U.S. are performed in an ASC.2 The projected market value of ASCs is estimated at $46.83 billion in 2025.3 New service lines in ASCs include spine, cardiology and total joints.4 The projected compound annual growth
rate (CAGR) for ASCs is projected at 4.1% to the year 2032 with a market value of $62.03 billion.3
The long-term trend of higher surgical volumes in ASCs is clear. We see a movement from inpatient to outpatient procedures but also a shift from outpatient surgeries performed in hospitals to these cases being done in ambulatory surgery centers. This has caused a change in case mix for hospitals as sicker patients are concentrated at hospitals for more complex surgeries. It appears that patients not suited for ASC care and those with lesser resources or less favored insurance status are being concentrated at hospitals which, by their mission, serve the wider community. In the hospital setting the revenue from surgical care as a percentage of total revenue may decrease as the payer mix changes.
The overarching factor in ASC growth is a desire to decrease healthcare costs. More favorable reimbursement policies favor the ASC setting. Commercial insurers, in search of cost savings, incentivize surgeons to increase ASC use. The CMS IPO list also continues a downward trend. According to Oakes, as reported by Catherman, “… we do know that when things come off the IPO list, they tend to
migrate to the outpatient setting.”(5) Catherman reports that when total knee replacements were removed from the IPO list in 2018 the inpatient volume for this surgery declined nearly 18% with that volume going to the ASC market.5
The ASC surge does have some headwinds. Prolonged staffing shortages in anesthesia providers, perioperative nurses and surgical techs are also felt in ASCs that lack the resources, such as nurse educators, to develop much needed staff. Consumer preference for new technology also compels hefty capital equipment purchases for surgical robots and advanced imaging equipment straining the thin profit margins of ASCs.1,4 Adding new service lines is costly and may require facility expansion and renovation. Some smaller ASCs may be limited in their response to the need for large capital expenditures.
Collectively, hospitals are not standing pat in response to the shifting markets for surgical care. To keep up with the shift in care settings, hospitals will invest in ASC capacity either in new construction or by merger and acquisition. Long term we may see a re-positioning of where surgical care is delivered in this country. For now, the
pendulum is swinging in favor of more surgical volume in ASCs, but that trend cannot continue exponentially. Surgery is a resource intensive process which necessitates innovation from stakeholders, The period of change in surgical care will continue for the near future and ASCs will surely figure prominently in that transition.
James X. Stobinski, Ph.D., RN, CNOR(E), CSSM(E), CNAMB(E), is a faculty member at Central Michigan University and director of hospital and ASC surgi cal education relationships with National Institute of First Assisting (NIFA).

H ow long do you hang your endoscopes after processing? In the latest episode of the Below the Hospital podcast, host Garland-Rhea Grisby Sr. sat down with Margaret Gilman, director of infection prevention in the department of quality and safety at Nemours Children’s Health to discuss her facility’s transition to a 14-day hang time and the research that backed it up.
In 2025, Gilman and her corresponding authors, Kwame Gyabaah, Katlyn Burr and Edna Gilliam, published Using a Risk Assessment to Transition to a 14Day Endoscope Hang Time in AAMI’s journal BI&T. The paper explores how evidence-based risk assessment can safely support longer endoscope storage intervals and is a great blueprint for sterile processing departments interested in producing their own studies.
Gilman explained that the study was prompted by a real-world challenge; supply shortages affecting endoscope reprocessing chemicals. As end users and sterile processing leaders at Nemours were thinking through possible countermeasures, the question of hang time came up. Many stakeholders, she noted, had not been present when Nemours previously reduced hang time from 14 days to seven, making it essential to revisit the decision using current evidence and guidance.
At the heart of the project was a comprehensive risk assessment aligned with ANSI/AAMI ST91:2021. “This was really probably the most important step in all of this,” she explained. “Those guidelines actually provide you all of the pieces [literature reviews, IFUs, internal quality controls, etc.] that you need to take into account when you’re performing this risk assessment.”
Following approval from the Infection Prevention and Control Committee, Nemours transitioned endoscope hang time from seven to 14 days and monitored outcomes over a threemonth period. Any scope that reached the full 14 days underwent quality testing upon return to sterile processing, with protein used as a marker for bioburden.
The results were clear.
“We had 72 scopes that hung for 14 days during that study period,” Gilman said. “And all of the 72 that came back, none of them returned as positive for protein on that initial quality testing.” Just as important, infection prevention surveillance showed no increase in endoscope-related infections during or after the study. “The change did not have any adverse patient safety outcomes,” she added.
Grisby, who has conducted similar hang time studies, underscored the importance of sharing this kind of data across the field.
“Folks need studies like yours so that they can look and perform their own
risk assessment,” he said.
Beyond safety, the study also examined cost implications. By extrapolating the findings over a full year, Nemours estimated more than $150,000 in annual savings, from reduced consumable use and 600 hours of saved sterile processing technician time. Still, Gilman was clear that financial benefits should never drive clinical decisions.
“Patient safety should always be our North Star,” she said. “Cost savings is very, very, important, but it should be a secondary metric when we’re talking about patient care.”
What should you do if your facility is considering a change in its hang time procedures? Gilman indicated that the decision-making process should involve infection prevention, sterile processing, end users, perioperative leadership and nursing leadership. “Don’t skip the risk assessment … Gather all of that information ahead of your trial to make sure you that don’t have any unintended consequences.”
Per Grisby, “a lot of times in our industry, there’s this fear of infection prevention, right?” However, sterile processing is a team sport, and “I learned years ago that infection prevention, we need you.”
Want more Below the Hospital? You can find the show on Spotify, Apple Podcasts, and on the AAMI YouTube channel.

By Bill Prentice
T he ASC Quality Collaboration (ASCQC) brings together leaders from across the ambulatory surgery center (ASC) community – such as associations like the Ambulatory Surgery Center Association (ASCA) and the Association of periOperative Registered Nurses (AORN), accrediting organizations, management companies and state associations – to advance patient safety and quality of care in surgery centers. Founded in 2006 to develop and support standardized quality measures, the mission of this independent, nonprofit organization is to serve as a resource for ASC quality and safety. It is governed by a board of directors and has an executive committee, a technical expert committee and several task forces that help drive its mission.
ASCQC maintains ASC benchmarking data and measure specifications on its website and provides quality improvement tools and resources pertinent to ASCQC measures. It also developed and maintains six ASC quality reporting (ASCQR) measures of the Centers for Medicare & Medicaid Services (CMS).
CMS currently requires surgery centers to report on 14 different quality measures to the government each year or be penalized 2 percent of the reimbursements that they receive for providing care to Medicare beneficiaries. Leaving aside the penalties, ASCA
supports these reporting requirements because they help policymakers, patients and payers see the high quality of care that surgery centers provide. In addition, the measures also help individual surgery centers compare their results to other centers and learn where there is room to improve.
ASCQC collects data from its members quarterly and provides benchmarking reports that represent more than 2.5 million encounters per quarter. On its website, the organization publishes those aggregate national results for nine measures. And because ASCQC reports are published quarterly, centers do not have to wait nearly two years like they do with CMS data.
Last year, ASCQC introduced a free safety and quality assessment tool that all surgery centers can use. It is a concise, 20-minute self-assessment tool that covers safety and quality practices such as governance, quality improvement, infection prevention and patient experience. ASCs receive a dashboard report showing how they compare nationally along with a certificate and a website badge to highlight their commitment to safety and quality. ASCs can share the report with interested payers, employers or other stakeholders. It is a credible ASC-specific quality comparison that can be used to build trust with patients, providers and payers while reinforcing the ASC value story for all of us.
The tool has a validation process to ensure that it has valid and reliable data.
Last year, which was the first year of the assessment, nearly 400 ASCs participated. The results were overwhelmingly positive and revealed strong safety and
quality practices across the centers with a few minor improvement opportunities.
This year, the assessment will open on May 1 and surgery centers will have until mid-June to enter their data. Once the submission window closes, ASCQC will validate the data in the next few weeks and prepare the dashboards with the national comparison. Participating surgery centers will get their results via email. All submissions are strictly confidential and results are never published.
This is a great opportunity for surgery centers to invest a few minutes and get powerful information back. Knowledge is power. The report ASCs get back shows how they are doing compared to others, as well as if there is an area where they are falling short and have an opportunity to improve. I strongly encourage every surgery center to use this tool every year. The aggregate can create great data that ASCA can use to advocate on behalf of surgery centers.
Led by Executive Director Nina Goins and Assistant Executive Director Becky Ziegler-Otis, the goal of ASCQC is to make it easy for surgery centers to report on quality measures that have been tested in surgery centers and make sense to the surgery center community. Goins and Ziegler-Otis regularly present and discuss quality and safety topics at conferences. Listen to an ASCA podcast with Goins: https://www.ascassociation.org/asca/news-and-publications/ podcast/episode-patient-safety-andquality-of-care-in-ascs. Access ASCQC’s annual report: https://ascquality.org/ wp-content/uploads/2026/01/ASCQC2025-Annual-Report.pdf.

By Rommie Johnson, MPH, PMP
A ccreditation surveys exist to strengthen organizations, not to catch them off guard. When ACHC surveyors identify areas for improvement, those findings become a roadmap for elevating patient safety and operational excellence.
ACHC’s latest analysis of surveys conducted between June 2024 and May 2025 highlights patterns worth examining – not as failures, but as opportunities. Understanding what surveyors observe most frequently gives your team a headstart on strengthening practices that protect patients and staff. Two infection prevention standards emerged as common areas where ASCs can focus their improvement efforts, before survey day arrives.
Building a robust infection prevention program
Approximately 29% of surveyed ASCs received findings related to infection control. The standard (05.00.02 Infection Prevention and Control Program Development) asks facilities to select nationally recognized guidelines, train staff consistently and maintain active surveillance. When
gaps appear, they typically fall into three predictable categories.
1. Policy alignment. Surveyors sometimes discover that infection control policies and procedures haven’t kept pace with current requirements. Missing elements might include:
• State-level notifiable disease reporting procedures.
• Personnel screening protocols.
• Clear authority structures for managing staff health concerns. A thorough policy audit can reveal these gaps before a surveyor does.
2. Training documentation. The intent behind training requirements is straightforward: Every team member should understand infection prevention principles and their role in maintaining a safe environment. When personnel files lack documentation of initial or annual training, it raises questions about whether that knowledge transfer actually occurred. Required training topics typically include:
• Hand hygiene and alcoholbased hand sanitizer use.
• Safe injection practices.
• Environmental cleaning and disinfection.
• Standard precautions.
• Bloodborne pathogen protocols. Systematic file audits help ensure documentation reflects the training your team has completed.
3. Practice consistency. Perhaps the most valuable survey observations involve real-time practices. Surveyors have noted instances where staff members exchanged gloves without performing hand hygiene between changes – a deviation from both policy and best practice. These observations aren’t meant to penalize. They’re meant to surface behaviors that training and reinforcement can address.
Proactive steps for your team
• Anchor your program in recognized guidelines. Whether your facility draws from AORN, APIC, CDC, SHEA or another source, that framework should be documented and visible throughout your policies.
• Audit personnel files with fresh eyes. Select a representative sample and verify that training documentation exists for each required topic. Treat gaps as an opportunity to strengthen onboarding and annual
education processes.
• Put monitoring data to work. If hand hygiene observations reveal inconsistencies, develop targeted training that addresses specific behaviors. Focused interventions tied to actual observations make a bigger difference than generic refreshers.
Maintaining a sanitary environment under daily pressure
Environmental sanitation findings appeared on 43% of surveys – making it the most frequently cited infection prevention standard (05.00.06 Sanitary Environment). Unlike documentation reviews, these findings stem entirely from direct observation. That’s actually encouraging news: What surveyors can see, your team can see, too. The physical environment of a busy ASC experiences constant stress. Equipment ages. Surfaces accumulate dust. High-touch areas show wear. The challenge lies in maintaining vigilance amid the pressure of daily operations.
Surveyor observations from the past year illustrate common environmental concerns:
• Dust accumulation on air vents and equipment surfaces.
• Floors with visible soil or inadequate cleaning.
• Fixtures in need of repair (detached faucets, non-functioning toilets).
• Storage practices that expose supplies to contamination.
• Rust on IV poles, tables, carts and casters.
• Debris from previous procedures remaining in ORs after turnover. One observation captures a tension navigated by many ASCs. The push
for efficient OR turnover can sometimes overshadow thorough betweencase cleaning. Surveyors have noted that actual cleaning practices did not match written protocols, for example, dry mopping replacing the required damp mopping with disinfectant. These aren’t “gotcha” moments. They’re insights into where operational pressures create risk, and where additional attention can make a meaningful difference.
Environmental awareness works best as a shared responsibility. When every team member feels empowered to identify and report concerns, issues are addressed promptly. Consider these strategies:
• Implement structured surveillance rounds. Regular walkthroughs focused specifically on environmental conditions help facilities stay ahead of accumulating issues. Engage all staff – not just housekeeping or infection preventionists – in observation-based rounding.
• Audit room turnover practices. Review between-case cleaning protocols and observe whether actual practice aligns with documented expectations. If policies specify damp mopping with appropriate contact time for disinfectants, verify that’s what happens when the clock is ticking.
• Build observational skills through training. “Spot the improvement opportunity” exercises during staff meetings sharpen awareness and reinforce that environmental quality belongs to everyone.
• Create clear reporting pathways. A chipped surface, a malfunctioning
fixture and dust on equipment are observations that should flow naturally into work orders and timely resolution.
The patterns revealed in this year’s data confirm something experienced leaders already understand. Most findings trace back to gaps between intention and execution. Policies exist but weren’t fully implemented. Training occurred but wasn’t documented. Cleaning protocols were established but adapted under time pressure. Accreditation surveys bring outside eyes that can see what daily familiarity sometimes obscures. ACHC’s role isn’t to identify problems and criticize organizations. Our role is to help identify opportunities for strengthening the practices that keep patients safe. To support that journey, ACHC offers resources at every stage:
• Expert guidance on common compliance challenges at https:// achc.org/articles/cat_-ambulatorysurgery-center/
• Free educational webinars and tools at achcu.com/ambulatorysurgery-center-webinars/. Your preparation starts now. ACHC is here to help.

Rommie Johnson, MPH, PMP, is program director for ambulatory surgery centers and office-based surgery settings at Accreditation Commission for Health Care (ACHC), where he leads a team of talented staff and surveyors.
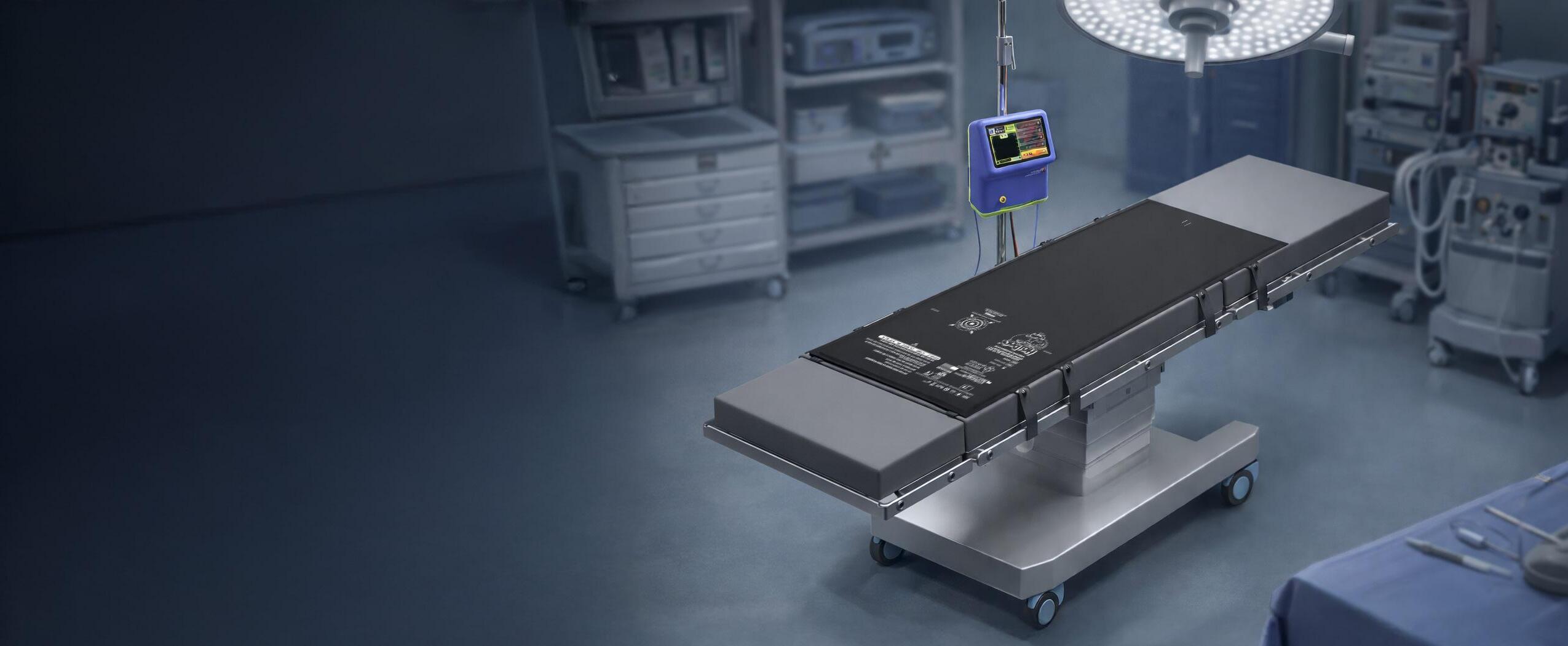
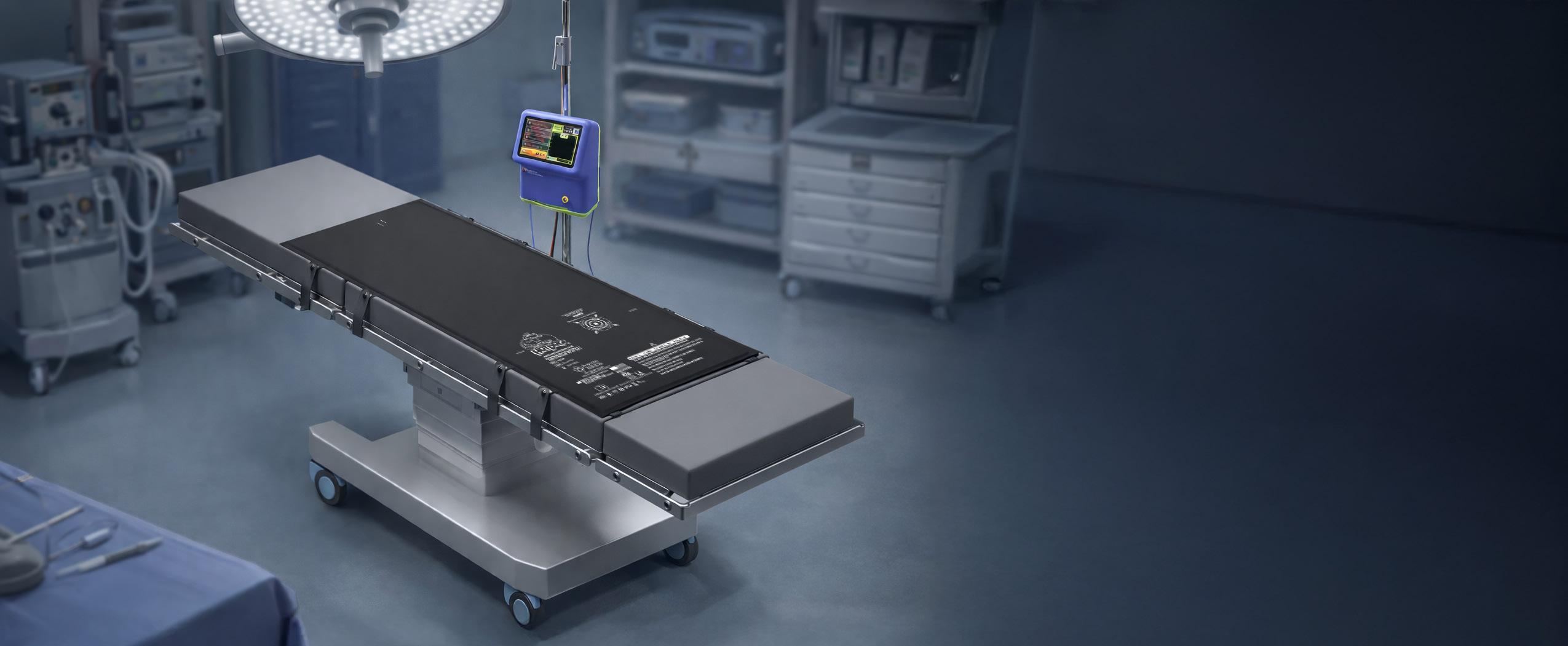


hile the stakes are undoubtedly higher in surgery, there are striking parallels between a high-performing kitchen and a well-run operating room. Every great chef will tell you that success relies on mise en place, having everything prepared, organized, and ready before the heat is even turned on.
W


hile the stakes are undoubtedly higher in surgery, there are striking parallels between a high-performing kitchen and a well-run operating room. Every great chef will tell you that success relies on mise en place, having everything prepared, organized, and ready before the heat is even turned on.
Although people thought it was impossible, Augustine Surgical has done just that! With Mega Soft® pads no longer available, many facilities are re-evaluating their approach to reusable grounding. This is the perfect moment for a "recipe update" that integrates active warming and grounding into one streamlined platform.
hile the stakes are undoubtedly higher in surgery, there are striking parallels between a highperforming kitchen and a well-run operating room. Every great chef will tell you that success relies on mise en place, having everything prepared, organized, and ready before the heat is even turned on.
In the OR, we depend on that same discipline: thoughtful setup, clear roles, and precise timing. But lately, the “kitchen” has become cluttered. In many facilities, patient warming and electrosurgical grounding exist as separate, bulky workflows, each requiring its own equipment, setup steps, and piles of disposables. It adds cost and complexity without necessarily improving the final “dish.”
In the OR, we depend on that same discipline: thoughtful setup, clear roles, and precise timing. But lately, the "kitchen" has become cluttered. In many facilities, patient warming and electrosurgical grounding exist as separate, bulky workflows, each requiring its own equipment, setup steps, and piles of disposables. It adds cost and complexity without necessarily improving the final "dish."
In the OR, we depend on that same discipline: thoughtful setup, clear roles, and precise timing. But lately, the "kitchen" has become cluttered. In many facilities, patient warming and electrosurgical grounding exist as separate, bulky workflows, each requiring its own equipment, setup steps, and piles of disposables. It adds cost and complexity without necessarily improving the final "dish."
For years, teams have asked, "What if grounding and warming could be combined into a single system?"
Although people thought it was impossible, Augustine Surgical has done just that! With Mega Soft® pads no longer available, many facilities are re-evaluating their approach to reusable grounding. This is the perfect moment for a "recipe update" that integrates active warming and grounding into one streamlined platform.
no longer available, many facilities are re-evaluating their approach to reusable grounding. This is the perfect moment for a “recipe update” that integrates active warming and grounding into one streamlined platform.
• HotDog Controller: The "brains" of the operation manages temperature delivery across all connected surfaces with quiet, air-free performance.
So, put away the hoses and the single-use grounding pads. Here is our new recipe for success in the OR, designed to deliver consistent, reliable outcomes every single time.
So, put away the hoses and the single-use grounding pads. Here is our new recipe for success in the OR, designed to deliver consistent, reliable outcomes every single time.
“The modern alternative for a streamlined workflow.”
So, put away the hoses and the single-use grounding pads. Here is our new recipe for success in the OR, designed to deliver consistent, reliable outcomes every single time.
return electrode integrated into the Mattress, simultaneously providing stable grounding and underbody conductive warming.
• HotDog Controller: The "brains" of the operation manages temperature delivery across all connected surfaces with quiet, air-free performance.
• HotDog Mattress: The foundation, this functions as a capacitive return electrode integrated into the Mattress, simultaneously providing stable grounding and underbody conductive warming.
• HotDog Mattress: The foundation, this functions as a capacitive return electrode integrated into the Mattress, simultaneously providing stable grounding and underbody conductive warming.
• HotDog® Blanket (Optional): The finishing touch, it adds overbody warming to increase total body surface area coverage, the key to maintaining normothermia ch bread or breadsticks, for serving
INSTRUCTIONS:
"The modern alternative for a streamlined workflow."
"The modern alternative for a streamlined workflow."
PREP TIME: 2 minutes
Prep Time < 2 Minutes
• HotDog Blanket (Optional): The finishing touch, it adds overbody warming to increase total body surface area coverage, the key to maintaining normothermia
• HotDog Blanket (Optional): The finishing touch, it adds overbody warming to increase total body surface area coverage, the key to maintaining normothermia
Prep Time < 2 Minutes
YIELD: Consistent Clinical Outcomes for thousands of Patients
Instructions
Instructions
Yield Consistent Clinical Outcomes for thousands of Patients
Yield Consistent Clinical Outcomes for thousands of Patients
INGREDIENTS:
1. Prepare the Surface: Place the HotDog Mattress directly on the OR table. Because it stays in continuous contact with the patient, warming begins immediately, no waiting for prep or draping. Early start warming significantly improves normothermia (Desai PLoS One, 2025)
For years, teams have asked, "What if grounding and warming could be combined into a single system?"
For years, teams have asked, “What if grounding and warming could be combined into a single system?” Although people thought it was impossible, Augustine Surgical has done just that! With Mega Soft® pads
• HotDog® Controller: The “brains” of the operation manages temperature delivery across all connected surfaces with quiet, air-free performance.
1. Prepare the Surface: Place the HotDog Mattress directly on the OR table. Because it stays in continuous contact with the patient, warming begins immediately, no waiting for prep or draping. Early start warming significantly improves normothermia (Desai PLoS One, 2025)
• HotDog® Mattress: The foundation, this functions as a capacitive
1. Prepare the Surface: Place the HotDog Mattress directly on the OR table. Because it stays in continuous contact with the patient, warming begins immediately, no waiting for prep or draping. Early start warming significantly improves normothermia (Desai PLoS One, 2025)
2. Connect the Controller: Plug the mattress (and Blanket, if using) into the Controller. The setup remains the same whether you are warming, grounding, or doing both.
2.Connect the Controller: Plug the mattress (and Blanket, if using) into the Controller. The setup remains the same whether you are warming, grounding, or doing both.
3. Enable Grounding: Skip the extra prep and disposable adhesive grounding pads. Plug the Mattress into your ESU. When the ESU is activated, current is dispersed across the large surface area. Stable grounding is provided to the patient simply by laying on the Mattress.
per-case costs become significantly lower and more predictable.
•Cost Savings: By eliminating single-use grounding pads and hoses, per-case costs become significantly lower and more predictable.
• Waste Reduction: This recipe uses ingredients that are 99.99% more environmentally friendly than other substitutions; fewer disposables are opened and discarded with every case.
From the Augustine Surgical Test Kitchen
From the Augustine Surgical Test Kitchen
3.Enable Grounding: Skip the extra prep and disposable adhesive grounding pads. Plug the Mattress into your ESU. When the ESU is activated, current is dispersed across the large surface area. Stable grounding is provided to the patient simply by laying on the Mattress.
4. Serve with Confidence: Monitor the quiet, consistent performance while the system works in the background, allowing the OR team to focus on the procedure rather than the equipment.
Chef’s Notes
4.Serve with Confidence: Monitor the quiet, consistent performance while the system works in the background, allowing the OR team to focus on the procedure rather than the equipment.
•Waste Reduction: This recipe uses ingredients that are 99.99% more environmentally friendly than other substitutions; fewer disposables are opened and discarded with every case.
• Consistency: Unlike traditional methods, this setup remains consistent from case to case, making training for new staff a breeze.
•Consistency: Unlike traditional methods, this setup remains consistent from case to case, making training for new staff a breeze.
Every great recipe starts with a master chef who understands the science behind the flavors. The HotDog system was developed by Dr. Scott Augustine, a world-renowned expert in patient temperature management. With a career dedicated to improving patient safety and clinical outcomes, Dr. Augustine envisioned a more efficient way to manage thermal care in the operating room.
Every great recipe starts with a master chef who understands the science behind the flavors. The HotDog system was developed by Dr. Scott Augustine, a world-renowned expert in patient temperature management. With a career dedicated to improving patient safety and clinical outcomes, Dr. Augustine envisioned a more efficient way to manage thermal care in the operating room.
• The Mega Soft Alternative: The HotDog System serves as a complete replacement for discontinued reusable pads while going further by integrating active warming.
“The integration of the grounding pad into the warming mattress has simplified our setup and reduced our waste by thousands of pounds.”
“The integration of the grounding pad into the warming mattress has simplified our setup and reduced our waste by thousands of pounds.”
- Operating Room Director
-Operating Room Director
By combining his background in medical device innovation with a commitment to simplifying complex surgical workflows, he created a “recipe” that removes the clutter of hoses and single-use disposables, allowing OR teams to focus on what matters most—the patient.
Chef’s Notes
• Cost Savings: By eliminating singleuse grounding pads and hoses,
•The Mega Soft Alternative: The HotDog System serves as a complete replacement for discontinued reusable pads while going further by integrating active warming.

“We stopped throwing money away on disposables. With HotDog, we’ve saved six figures while actually improving our normothermia rates.”
“We stopped throwing money away on disposables. With HotDog, we’ve saved six figures while actually improving our normothermia rates.”
- OR Charge Nurse
-OR Charge Nurse


By combining his background in medical device innovation with a commitment to simplifying complex surgical workflows, he created a "recipe" that removes the clutter of hoses and single-use disposables, allowing OR teams to focus on what matters most—the patient.



The recent OR Today webinar “Medical Laser Safety Officer Compliance: A Gateway to Certification” presented by Perioperative Consultants’ Vangie Dennis, MSN, RN, CNOR, CMLSO, FAORN, FAAN and AestheticMed Consulting International’s Patti Owens, MHA, BSN, RN, CMLSO, CNOR, FAORN, delivered tons of information.
The webinar is eligible for 1 CE credit. OR Today is approved and licensed to be a Continuing Education Provider with the California Board of Registered Nurses, License #16623. A recording of the webinar is available for on-demand viewing at ORTodayWebinars.live.
The webinar discussed the importance of medical laser safety officers. The presenters discussed the guidelines, standards and procedures required for the safe use of lasers in a practice. They also defined the roles and responsibilities of a laser safety officer.
Laser technology has transformed modern medicine and healthcare disciplines, utilizing lasers to perform precise procedures. These advances are risks to patients and professionals. The use of lasers in health care is associated
with a variety of hazards, such as eye exposure, misaligned laser beams, use of unfamiliar equipment, and improper handling, which can affect the safety of personnel and patients and are non-compliant with regulations and guidelines. The American National Standards Institute (ANSI)and the Association of PeriOperative Nurses (AORN) Lasers Guidelines has developed a series of standards for the safe use of lasers in the healthcare environment.
The ANSI Z136.3 standards and the AORN Guidelines require the designation of a laser safety officer (LSO), implementation of safety and engineering control measures, and trained authorized personnel. LSOs are responsible for enforcing hospital laser safety procedures. Healthcare facilities manage these risks by assigning safety duties to an LSO. These standards and guidelines are enforceable by the Occupational Safety and Health Administration (OSHA), Center for Medicare and Medicaid Services (CMS), national accreditation organizations, and numerous state regulatory statutes.
This webinar shared information about a live virtual course designed to provide operating room personnel with
a foundation of laser biophysics, tissue interaction, safety and administrative responsibilities. Technical aspects, as well as established best practices, will be reviewed on the multi-wavelength lasers. Laser safety protocols and documentation will be addressed according to the ANSI 136.3 – 2024 “Safe Use of Lasers in the Healthcare Facilities Standards,” and the AORN Laser Safety Guidelines 2020. Applicable national accreditation standards will be shared for laser safety program compliance. Instruction is accomplished through didactics and group discussion.
For more information about the course and becoming a laser safety officer, visit medicallasersafety.com/
Webinar attendees provided feedback via a survey that included the question, “How would you describe OR Today webinars to a colleague?”
“Practical and extremely informative,” said Dawn Yost, Clinical RN VI & Business Manager Surgical Services, West Virginia University Hospitals.

The OR Today webinar “New Year, New Momentum: 3 Red Flags Costing Hospitals
Time & Money (and How to Fix Them)” sponsored by Surgical Solutions is eligible for 1 CE credit. OR Today is approved and licensed to be a Continuing Education Provider with the California Board of Registered Nurses, License #16623.
Elizabeth “Betty” Casey, MSN, RN, CNOR, CRCST, CHL, senior vice president of clinical operations with Surgical Solutions was joined by Frank Majerowicz, a partner with FiberTech/Renovo to provide expert insights to webinar attendees.
This year, surgical services teams are under pressure to deliver predictable, efficient care while managing staffing constraints, rising case volume, and increasing costs tied to delays and equipment downtime.
The live webinar in January used the New Year as a reset moment: a practical “success plan” for OR and SPD leaders focused on equipment readiness and workflow reliability.
Attendees were guided through a set of high-impact strategies that work across hospitals nationwide, such as reducing avoidable delays, strengthening readiness processes, tracking the right KPIs, and preparing for survey readiness. Surgical Solutions partner Renovo/FiberTech was also featured to share what drives the most disruptive equipment failures like major scope repairs and how to prevent them, plus smart repair planning which helps reduce downtime when issues occur.
Almost 100 healthcare professionals registered for the webinar and Allison Leek, an ASC administrator with Grossnickle Eye Center in Indian, won an OR Today cooler lunchbox.
Attendees shared feedback via a survey that asked, “How will this webinar help you do your job better?”
“Instills that our processes are on track and allows for additional insight for new ideas,” shared Sandra Curatola, PAT Nurse/Circulator/Charge Nurse, Rochelle Community Hospital.
“Brought to light problems staff are facing,” said Dorothy Connell, Manager Medical Information, Baxter Healthcare.
“Handle scopes more carefully,” said Matt Blodgett, RN, West Penn Hospital.





The orthopedic healthcare industry is moving forward on an ever-changing course, challenging sterile processing logistics in facilities performing orthopedic procedures for the first time, while also experiencing expanded adoption of advanced robotic technology in operating rooms around the globe. Specializing in surgical patient positioning, Innovative Medical Products, Inc., covers all these advancements. The positioning equipment provides another “pair of hands” to increase efficiency and convenience for the surgeon and surgical team.

Many ASCs and outpatient clinics report that the smaller autoclaves, limited storage space and smaller soak sinks present a variety of logistical and sterile processing challenges. While outpatient facilities are insisting on maintaining consistency in training and how they approach procedures, they need a new solution to overcome the limited resources in smaller facilities.

Container, the resulting smaller footprint allows the positioner to fit in smaller autoclaves typically found at Outpatient Centers. When disassembled, the Adapt2Fit’s reduced size also allows it to be fully submerged in standard sinks and cleaning vessels in a single pass, saving SPD valuable time, money, and resources.
The De Mayo Adapt2Fit™ Modular Knee Positioner, which solves these pain points with a two-piece baseplate that quickly separates the positioner down to half of its overall length, has created an instant impact in the OR, creating several benefits for the surgeon and their facility. When stored in its SteriPod Filtered Sterile

In effort to accommodate longer patient leg lengths and overcome the space constraints, IMP designed the Adapt2Fit to be the longest positioner on the market, when assembled. The result is that the Adapt2Fit is a full 2-7” longer than previous models. The increased positioner length provides more surface area for full flexion and extension of the knee, without moving the baseplate.
such as Stryker, Zimmer Biomet, Smith + Nephew, and CUREXO.
All De Mayo Knee Positioners use a boot to secure the leg to the positioner. The posterior side of the boot includes a distractor block for use with our De Mayo Universal Distractor to distract the knee joint via an external force applied to the underside of the patient’s thigh with the leg positioned at 90 degrees of flexion. The distractor is controlled by the operating surgeon in the sterile field, enabling controlled distraction via a lever to create an unobstructed view into the joint space between the posterior femur and proximal tibia.

The De Mayo Knee Positioner’s redesigned carriage and locking system delivers on both easy removal and improved holding power, helping to make knee surgeries easier for all types of cases, including bariatric. The patented ball and socket design provides the surgeon with more precise control of flexion, extension, tilt, and rotation.
Robotic Surgery Requires Improved Limb Stability and Access to the Knee Joint
The introduction of robotic-assisted knee replacement surgery offers greater value of the De Mayo Knee Positioner due to its ability to increase limb stability during total knee procedures, when used with robotic systems from companies
frames. In 1984, Innovative Medical Products became the gold standard with their original IMP McGuire Hip Positioner, many of which are still in use today. The McGuire Hip Positioner was then updated and is the current Universal Lateral Positioner, otherwise known as the ULP. The ULP provides stable lateral debubitus positioning and creates a reproducible point of reference for primary and revision hip arthroplasty. With removeable and independently adjustable anterior arms, it allows for more accurate contact with the iliac crests and accommodates various patient anatomies. Our patented hyperflexion plate allows up to 120 °of flexion

In the traditional use of the De Mayo Knee Positioner, the foot and ankle are secured in the boot. When the De Mayo Knee Positioner boot is locked into the traveling carriage, knee flexion/extension and varus/valgus motion are controlled in the surgical field. Research conducted by IMP investigated the use of the Universal Distractor to further stabilize the leg during the registration process employed by the surgeon during navigated or robotic-assisted knee reconstruction. The study results demonstrated that the combination of these two devices improved stability of the leg, over the Knee Positioner alone, to improve the reliability of the registration process supporting the knee reconstruction.
Redefining Rigid Patient
Patient positioning during reconstructive hip surgery was traditionally accomplished using various positioning aids, from bean bags to pegboards to rigid clamping
The IMP MorphBoard® surgical pegboard is a versatile and innovative solution for hip surgeries, designed to meet diverse patient needs. Its modular components allow for effortless adjustments to accommodate various BMIs and seamlessly adapt to any OR table. With multiple peg lengths, the system offers enhanced versatility and a secure fit for improved patient positioning. To ensure patient safety, foam pads and
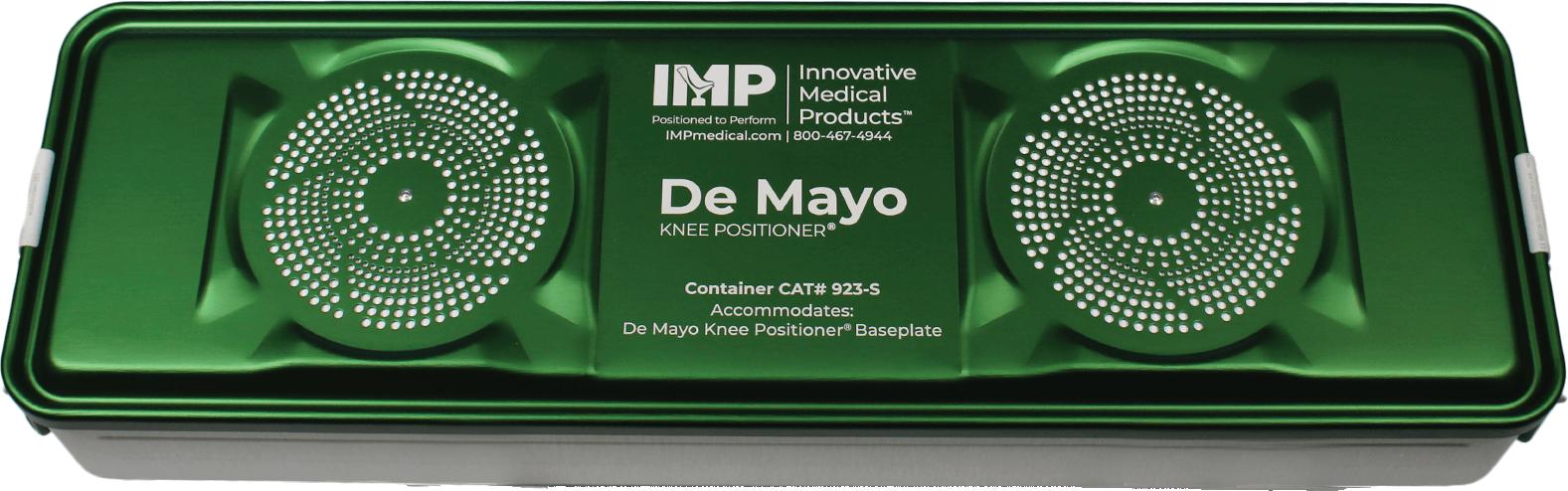

sleeves are available to provide protection against crosscontamination. Additionally, the PegDok Peg Stabilizer enhances stability by ensuring each peg is fully seated, delivering unmatched reliability during procedures.
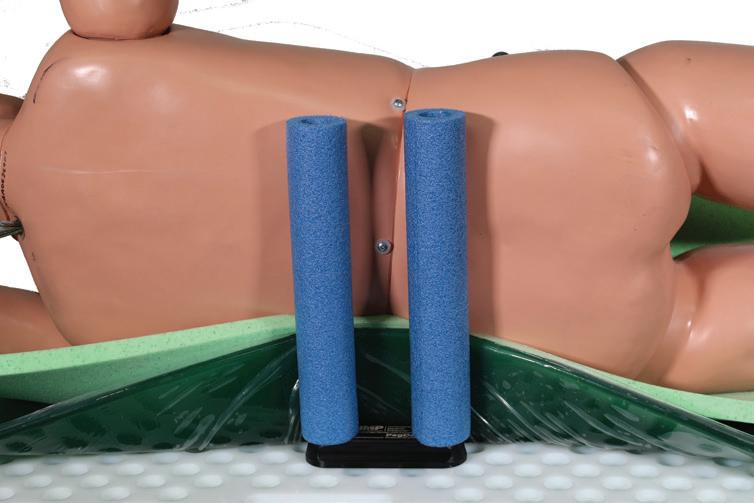
MVP: IMP’s Value-Added Commitment Transforms into the Most Valued Partnership
As part of IMP’s shared commitment to everyone, orthopedic facilities will now be able to gain special access to IMP’s premiere partnership level service and support by using genuine IMP patient protective pads for each procedure.
MVP, otherwise referred to as “Most Valuable Partner,” is a new program that helps facilities




maximize their initial investment. Discounted or complimentary upgrades, courtesy service loaners, repairs, and on-site training and education services are just a few of the benefits that facility administrators will find helpful in protecting their initial investment’s value.














IMP’s patient protective pads have been extensively tested during clinical trials to provide maximum patient protection from pressure sores and ulcers. By consistently using IMP’s premium patient protective pads, orthopedic healthcare providers may reduce liability by assuring that they meet AORN and AAMI standards for using the manufacturer’s recommended pad as defined in the IFU.
IMP’s vision for success has always been to collaborate with customers to design, manufacture, and distribute unique, innovative products where surgical patient positioning or supporting logistics has been problematic. IMP’s solutions to universal patient positioning challenges are developed through years of collaboration with busy orthopedic surgeons, marketleading orthopedic companies, and hands-on med/surg support teams. Ideas have been shared for product improvements with perceptive opinions on improving patient positioning in the surgical environment. Having completed ISO 13485 registration successfully in 2021 to expand IMP’s products outside of the US, the company is now supporting surgeries in global markets and the rapidly growing outpatient facility networks in the US.
Visit us at impmedical.com or call 1-800-467-4944.





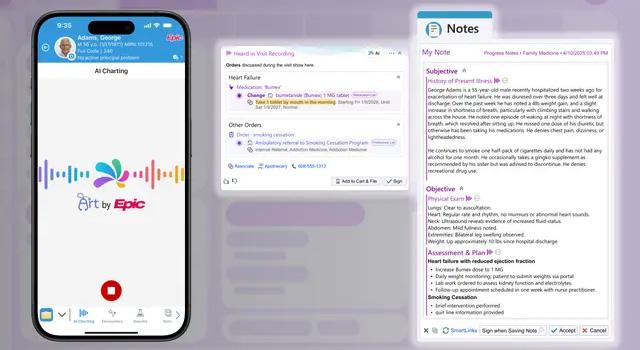
Epic has released AI Charting, a built-in feature that listens during patient visits, drafts the clinician’s note and queues up orders based on the conversation. Clinicians say that by handling documentation work in real time, Epic AI Charting helps them stay focused on the patient while capturing a more complete record of the visit – reducing work after the patient leaves the room and supporting stronger patient-clinician connections.
In a customer presentation, Epic highlighted a growing set of AI capabilities for clinicians, patients, and hospital operations, all built directly into Epic’s software.
AI Charting is part of Art, Epic’s AI for clinicians. In addition to drafting visit notes and suggesting orders based on the clinician-patient conversation, the initial release allows clinicians to personalize the structure of both current and future notes using voice commands, such as asking to format the history of present illness as a bulleted list.
“Our developers worked closely on site with physicians across many specialties as we created AI Charting,” Epic’s Corey Miller said. “Feedback has been very positive, and we’re iterating quickly based on what clinicians tell us works best.”
The release of AI Charting comes as overall adoption of Art continues to grow. For example, Art’s Insights feature, which brings together information from across the patient chart into a concise, easy-to-read summary to help clinicians prepare for visits, is now used over 16 million times each month – a nearly 3x increase in usage from November 2025.
For hospital operations and revenue cycle teams, Penny, Epic’s AI for operational workflows, continues to deliver
measurable results. More than 200 organizations now use Penny to automate professional billing coding, and many are seeing a more than 20% reduction in coding-related denials. Across organizations using Penny for medical necessity denial appeals, letters are created 23% faster.
Taken together, these features are helping organizations get paid more quickly for the care they provide.
The presentation highlighted continued expansion of Emmie, Epic’s AI for patients, which now provides conversational assistance within MyChart and over text message. Emmie helps patients schedule appointments, understand bills, make payments, set up payment plans, and generate detailed statements for reimbursement.
By pulling together relevant account details, Emmie can explain why patients owe what they owe. Across the Epic community, organizations are seeing sustained reductions in billing-related customer service messages – allowing staff to focus on the most complex cases that require human support. When needed, Emmie can escalate patients to a live chat with a staff member.
Epic also announced that MyChart Central, which provides patients with a single Epic ID they can use across all their Epic providers, is now live in all 50 U.S. states – making it easier for patients to log into MyChart and take advantage of Emmie’s capabilities in the secure MyChart environment.
Because these AI capabilities are built directly into Epic, they draw from information captured throughout the medical record – providing answers and insights grounded in a comprehensive understanding of the patient.
ZOLL, an Asahi Kasei company that manufactures medical devices and related software solutions, announced today that Zenix, the company’s most clinically advanced and easy-touse professional monitor/defibrillator, is approved under the European Union (EU) Medical Device Regulation 2017/745, commonly referred to as EU MDR.
The Zenix monitor/defibrillator is a groundbreaking device that redefines efficiency, clarity, and intelligence in both EMS and hospital settings. Built from years of feedback from customers, Zenix combines intuitive design with powerful functionality to enhance patient care and automate workflows for ease-of-use. Featuring a large, durable touchscreen, Zenix provides critical information when it’s needed. With on-thefly customization, healthcare professionals can make real-time adjustments, helping them stay in control during highpressure situations.
Equipped with ZOLL’s innovative Real BVM Help and exclusive Real CPR Help technology, Zenix gives healthcare providers real-time clinical feedback to improve ventilation quality and deliver high-quality CPR. The advanced technology of Zenix empowers EMS teams and hospital

clinicians to make informed, confident decisions and ensure they are delivering exceptional patient care, every time.
“Whether you are a hospital clinician or an EMS professional, the ZOLL Zenix monitor/defibrillator is designed to work the way you work,” said Elijah White, president of ZOLL Acute Care Technology. “Zenix is our most advanced monitor/defibrillator, and yet it’s incredibly easy to use — virtually all functions of the device are accessible with three screen-touches or less. Along with the X Series, R Series and ZOLL M2, Zenix extends ZOLL’s leadership in professional monitors/defibrillators with unique features and intuitive design.”
Qventus, a provider of AI-based care operations automation software, recently announced strong results from its partnership with Erlanger, a nationally acclaimed, multihospital health system. With Qventus’ Surgical Growth Solution, the Tennessee-based health system serves more patients, helps surgeons to grow their practices and better supports dedicated staff.
Erlanger selected Qventus to drive surgical growth by filling ORs with high-value cases, maximizing robotics investments and strengthening referral patterns. Qventus is deeply embedded into Erlanger’s EHR system of record, serving as a system of action that creates OR capacity at scale.
Since going live in June 2025 across four sites, the health system has already realized positive returns on its initial spend and is on track to deliver an annualized 5x return on investment, according to a press release.
The partnership has delivered results across multiple OR performance metrics:
• 220 additional surgical cases per month compared to the same time last year
• Nearly 12 additional OR hours per room per month generated through intelligent block release nudges
• 10% higher growth rates for surgeons actively engaged with the Qventus solution compared to non-engaged surgeons
• More than a 25% increase in robotic surgical volume YoY for surgeons who engaged with marketed time
• Break-even achieved in less than 3 months, with the health system on track for 5x annualized ROI
The partnership, initially focused on expanding robotic surgery access and creating additional OR capacity, has delivered on its core objectives while establishing a foundation for continued operational excellence. The rapid implementation and outcomes demonstrate the ability to deliver immediate value while serving as a long-term strategic partner.
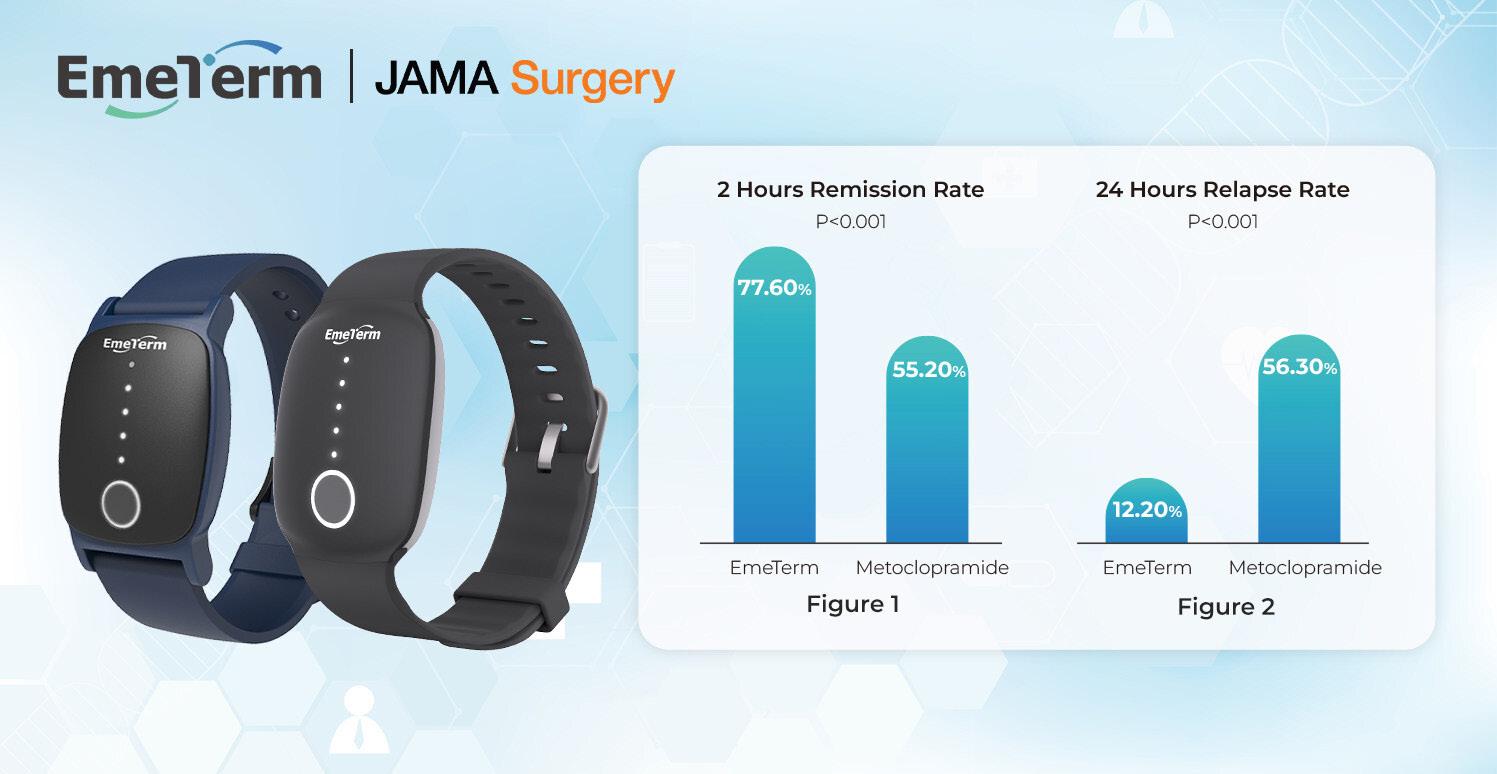
WAT Medical has announced the publication of a randomized clinical trial in “JAMA Surgery”. The study confirms that the EmeTerm wristband – a wearable device utilizing transcutaneous acupoint electrical stimulation –provides significantly better control of moderate to severe postoperative nausea and vomiting (PONV) compared to metoclopramide, a widely used antiemetic medication.
The patient-blinded, multicenter randomized clinical trial enrolled 232 female patients who developed moderate to severe PONV (numerical rating score [NRS] ≥4) following thyroidectomy or anterior cervical surgery under general anesthesia. Conducted across four leading hospitals, participants were randomized 1:1 to receive either active transcutaneous electrical acupoint stimulation (TEAS) via the EmeTerm wristband targeting the median nerve at acupoint PC6, or a control intervention consisting of a sham device combined with intravenous metoclopramide.
The primary endpoint was the 2-hour remission rate of PONV, while secondary endpoints included 24-hour relapse rates and crossover responses.
Key Findings
• 2-Hour Remission Rate: EmeTerm significantly improved PONV remission compared with metoclopramide (77.6% vs 55.2%, P < 0.001) (Figure 1).
• 24-Hour Relapse Rate: Patients treated with EmeTerm experienced significantly lower relapse rates than those treated with metoclopramide (12.2% vs 56.3%,
P < 0.001) (Figure 2).
• Safety: No device-related serious adverse events were reported.
These findings demonstrate that EmeTerm not only achieves superior and sustained symptom control compared with metoclopramide, but also offers a favorable safety and tolerability profile, according to a news release. The results highlight a shift toward non-pharmacological, patientcentered approaches in perioperative care – enhancing patient autonomy, minimizing drug-related side effects and improving overall recovery outcomes.
Developed by WAT Medical Enterprise Ltd., EmeTerm represents the company’s commitment to evidence-based innovation in neuromodulation for nausea management. The device has received multiple international regulatory clearances, including approvals from the U.S. FDA, Health Canada, and Australia’s TGA, affirming compliance with global safety and quality standards.
Publication in “JAMA Surgery” underscores the rigor and impact of the study, validating EmeTerm as an effective, non-drug therapeutic option for managing active PONV, the release adds. With a growing body of clinical evidence, EmeTerm is being increasingly adopted by clinicians and hospitals worldwide as a reliable solution for nausea control in perioperative settings.
Our legacy and advocacy is at the heart of perioperative nursing. Nurses find a calling to speak, act, and lead in ways that protect patients, support colleagues, and strengthen our profession.
Our legacy and advocacy celebrate the courage and commitment of nurses who transform challenges into opportunities for progress. From ensuring safe surgical environments to mentoring the next generation of leaders, perioperative nurses continue to raise the standard of excellence through every action of advocacy.
Perioperative nurses stand at the intersection of precision, protection, and advocacy. Our voices matter — in the policies that shape our practice, in the education that shapes the next generation, and in the compassion that shapes every patient’s journey.
In 2026 as we come together under the banner of The Power of Legacy and Advocacy, we honor those who lead

with purpose and passion — and we commit to advancing excellence and inspiring the future of surgical care.
Expectations are high and perioperative professionals are encouraged to visit https:// southeastperiop.com/ for more information and to sign up for the organization’s newsletter.



The Netherlands-based MedTech company UV Smart has officially received clearance from the United States Food and Drug Administration (FDA). With this 510(k) clearance, UV Smart is launching its UV-C technology for the high-level disinfection of TEE probes in the United States. The D60 is the first UV-C high-level disinfection device in the world to receive FDA clearance for this application, according to a news release.
What started as an innovative idea between two friends, has quickly grown into an international organization that is now active in 35 countries and is the market leader in its segment. With the support of investor Chris Oomen (founder of Optiver), UV Smart proves that Dutch innovation can make healthcare better and affordable worldwide.
The FDA clearance applies to the UV Smart D60: A system that disinfects medical TEE probes, sensitive medical instruments for heart examination used in cardiology, with UV-C light. Where current cleaning and disinfection with harsh chemicals can often take approximately two hours, the D60 achieves high-level disinfection in just two minutes using UV-C light. For healthcare providers, the D60 represents a significant improvement in efficiency and workflow; the D60 is the first device of its kind to receive FDA 510(K) clearance for high-level disinfection of TEE probes.
“This clearance will help fulfill the need in U.S. healthcare for validated options that reduce manual workload, improve safety and support more efficient clinical workflows,” says co-founder Thijs Kea.
“UV Smart is redefining hospital efficiency, seamlessly scaling facility capacity while fortifying safety for healthcare workers. Its equipment enables faster disinfection cycles, allowing more patients to be treated per day. In addition, the system eliminates the cost of chemicals and reduces wear and tear on costly cardiology equipment,” the release states.
“With its entry into to the United States, UV Smart is entering the next phase of its international growth strategy. UV Smart is demonstrating that chemical-free high-level disinfection can support both operational efficiency and long-term cost control in healthcare settings,” it adds.



Guide to AORN
Conference Provides Evidence-Based Education & Hands-On Learning


The 2026 AORN Global Surgical Conference & Expo returns April 11-14 in New Orleans, bringing together perioperative nurses at every career stage for immersive education, professional connection and practice-shaping dialogue.
Founded in 1949, AORN is the leading professional organization for perioperative nurses, supporting the practice of more than 200,000 perioperative nurses by providing evidence-based research, nursing education, standards and practice resources to enable optimal outcomes for patients undergoing operative and other invasive procedures.
The theme for the AORN Global Surgical Conference and Expo 2026 is Lighting the Pathway.
“This year’s theme, Lighting the Pathway, honors the legacy of Florence Nightingale. Carrying her lamp, she brought care and comfort to wounded soldiers, and the image of her walking through the wards remains a powerful symbol of hope and healing,” AORN President Darlene Murdock, MSN, BBA, RN, CNOR, CSSM, said. “It represents the enduring presence and unwavering dedication of nurses. At Expo 2026, perioperative nurses will carry forward Nightingale’s legacy, lighting the pathway with care, compassion, hope and guidance. Together, we’ll showcase the vital role of perioperative nursing in healthcare through insightful presentations and hands-on learning opportunities designed to strengthen practice and improve patient outcomes.”
The four-day conference features evidence-based education, handson engagement with emerging surgical technologies, and exclusive reveals that will help shape perioperative practice in the year ahead.
“The AORN Global Surgical Conference & Expo is where perioperative nurses engage with the latest surgical evidence, explore emerging technologies, and exchange ideas that actively shape practice and patient safety,” said David Wyatt, Ph.D., RN, NEA-BC, CNOR, FAORN, FAAN, AORN CEO and executive director. “It’s a dynamic space for learning and connection, where nurses step away from the daily intensity of the OR, challenge their thinking, learn from peers, and return to their teams energized, focused, and ready to lead.”
AORN Expo 2026 offers a practice-driven education experience built for perioperative professionals at every career stage. Education highlights include:
• Evidence-Based Clinical Education: Sessions grounded in the latest surgical evidence focus on infection prevention, surgical smoke safety, patient positioning, guideline implementation and emerging technologies shaping perioperative care.
• Hands-On and Applied Learning: Interactive formats – including Skill Studios, Learning Labs and case-based sessions –allow nurses to practice techniques, apply concepts and translate learning directly into day-to-day perioperative practice.
• Leadership Summit: A conference-within-the-conference designed for perioperative leaders, with sessions addressing workforce challenges, psychological safety, change management and strategies for leading teams through complexity.
• Ambulatory Surgery & ASC Hub Programming: Dedicated education for ambulatory surgery professionals, with sessions focused









“LIGHTING THE PATHWAY”

on applying AORN Guidelines in ASCs, improving workflows, strengthening policies and procedures, and supporting patient safety in outpatient settings.
• Educator Hub (new in 2026): A dedicated destination for perioperative educators, offering evidencebased teaching strategies, smarter training approaches, and practical tools to support onboarding, competency development and staff education across the perioperative continuum.
AORN Expo 2026 features built-in networking events and dedicated spaces designed to help attendees connect, exchange ideas and build relationships that support professional growth.
The Expo Hall is a central destination for exploring products, technologies and solutions shaping today’s surgical environment. With hundreds of exhibitors, attendees can engage in hands-on demonstrations, speak directly with product experts and evaluate innovations designed to support patient and staff safety in real-world perioperative settings.

“There’s nothing quite like the energy of Expo,” Wyatt said. “It’s where perioperative nurses reconnect with one another, share ideas face to face, and leave recharged – ready to take what they’ve learned back to their teams.”
For more information and to register, visit the AORN Expo website.
“This year’s theme, Lighting the Pathway, honors the legacy of Florence Nightingale. Carrying her lamp, she brought care and comfort to wounded soldiers, and the image of her walking through the wards remains a powerful symbol of hope and healing.”
Darlene Murdock AORN President
APRIL 11-14, 2026

Ambulatory Surgical Center Association ascassociation.org/home Booth #1461

Augustine Surgical augustinesurgical.com Booth #1507


Innovative Medical Products impmedical.com Booth # 328

Kapp Surgical kappsurgical.com Booth #1436
Ruhof ruhof.com Booth #219

C Change Surgical cchangesurgical.com Booth #737 Healthmark hmark.com


SurgiSmoke Solutions flamingofunnel.co Booth #651-OR1
Staff report
Grand View Research reports that the global surgical equipment market size was estimated at $18.37 billion in 2024 and is projected to reach $31.58 billion by 2030, growing at a CAGR of 9.54% from 2025 to 2030. Factors such as an increase in the incidence of lifestyle disorders that eventually require surgery, rising healthcare costs and large unmet surgical needs are mainly driving market growth.
Lowered hospital stays post-surgery and an increase in ambulatory surgical centers are projected to fuel the market growth during the forecast period. Furthermore, the increase in the prevalence of diseases like cardiovascular and cancer that necessitate surgeries is anticipated to propel industry growth. According to an article published by WebMD LLC in January 2024, open-heart surgery in the U.S. is the most common, with nearly 400,000 procedures done every year. Thus, the large number of surgical procedures conducted across developed and developing countries is anticipated to propel the demand for surgical equipment.
A growing geriatric population is a key factor contributing to market growth. Individuals that are aged 60 and above are at a higher risk of developing disorders that require surgery compared to the younger population.
BCC Research states that the global market for surgical equipment and
technologies was valued at $37.6 billion in 2023. This market is expected to grow from $40.0 billion in 2024 to $56.6 billion by 2029, at a compound annual growth rate (CAGR) of 7.2% from 2024 to 2029.
iHealthcareAnalyst reports that the global market for surgical instruments is estimated to reach $18.9 billion by 2033, growing steadily at a CAGR of 3.8% over the forecast period, driven by increasing surgeries coupled with advanced technologies such as smart instruments with integrated sensors.
Precedence Research reports that the global surgical equipment market size is calculated at $20.30 billion in 2025 and is predicted to increase from $22.25 billion in 2026 to approximately $50.14 billion by 2035, expanding at a CAGR of 9.46% from 2026 to 2035.
Technological advancements in the surgical equipment market feature robotics, imaging, 3D printing, smart devices and minimally invasive surgery (MIS). Robotics and AI technology are used in assisting surgery, helping in undertaking complex surgical procedures. The minimally invasive surgery (MIS) technique consists of the endoscope and laparoscopic instruments. This advancement helps in quick recovery and reduces trauma by discarding challenging complications. The imaging technologies include augmented reality and 3D virtualization. These features enable the availability of surgeons with solutions to complex surgeries. Smart devices and connectivity are a solution
to communications, supporting connection and in-time interaction across operating rooms.
The 3D printing introduces surgical tools, allowing customization of instruments and providing accurate treatment to individual patients. The advancement in the healthcare sector is encouraging medical providers to improve and advance their practice.
AI is significantly impacting the surgical equipment industry by transforming traditional tools into smart, integrated systems that enhance precision and outcomes. The technology powers advanced surgical robotics, which utilize machine vision and data analytics to assist with complex procedures and minimize human errors.
The global surgical equipment market is primarily driven by the growing prevalence of chronic diseases, growing geriatric population and rising number of road accident cases across the globe.
The rising awareness regarding the cost benefits associated with the early surgical intervention is an important factor that drives the demand for the surgeries among many patients. Technological advancements in surgery equipment and rising investments by market players is expected to provide growth opportunities in the foreseeable future. The demand for advanced and innovative surgical equipment is rising across the healthcare sector.
FDA-cleared in November 2025, the Francis Medical Vanquish Water Ablation System is a transurethral, ultrasound and electromagnetically guided, thermal water vapor device used to convectively ablate targeted prostate tissue. One in eight men will be diagnosed with prostate cancer in their lifetime. The majority of men with localized, low-to-intermediate risk prostate cancer will be presented with one of two options: whole prostate gland removal or radiation, which have a high potential for long-term side effects, or active surveillance, which allows them to maintain their quality of life. The Vanquish System offers a less invasive alternative for men looking for options that can help reduce the potential impact to their quality of life. The outpatient procedure harnesses the energy stored in water vapor (steam) to transfer energy to targeted tissue anywhere in the prostate, causing cell death. Vapor respects the natural boundaries of the prostate, minimizing or eliminating the potential for damage to structures outside the prostate. The Vanquish System includes capital, disposables and an informative user interface that displays recorded MRI images with realtime ultrasound and cystoscopy to support targeted ablation of prostate tissue.
IN THE OR product focus
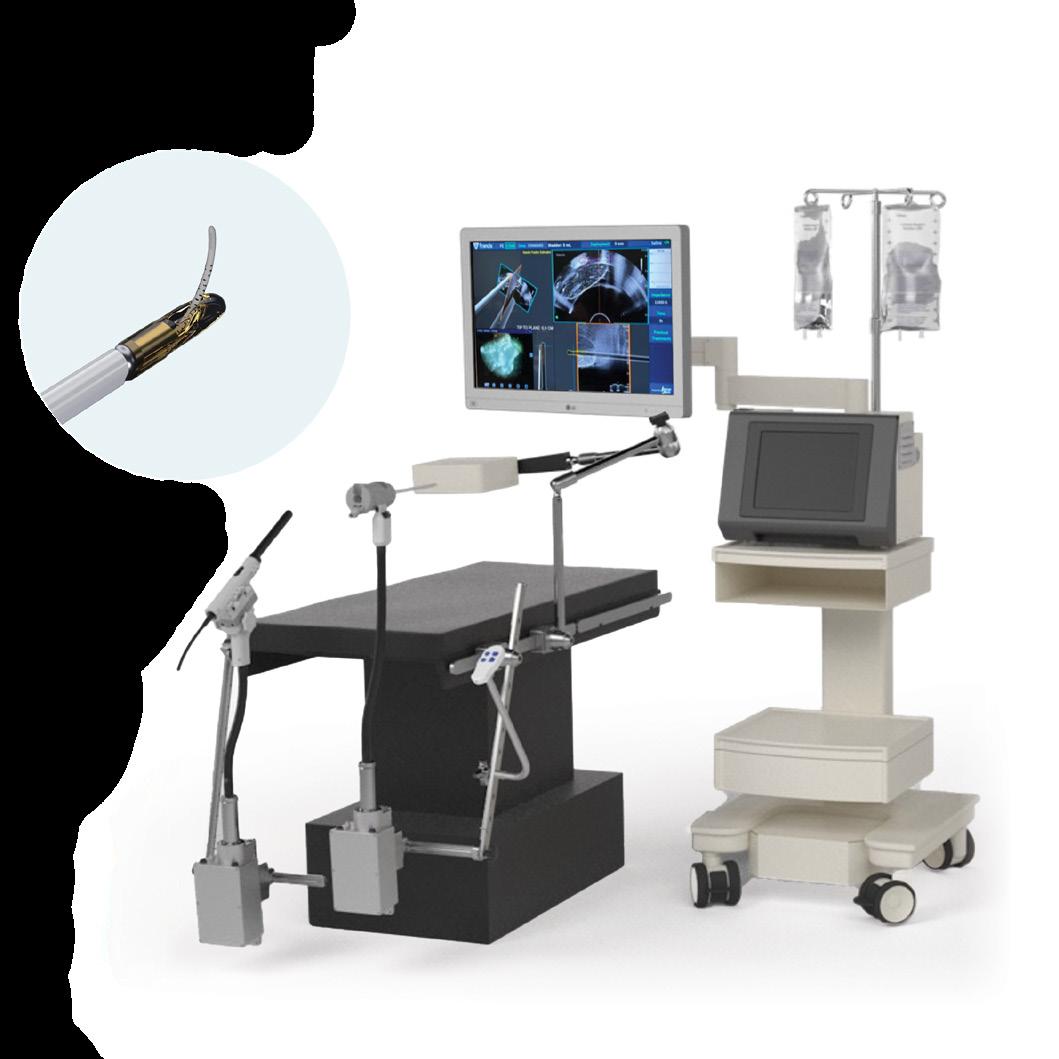
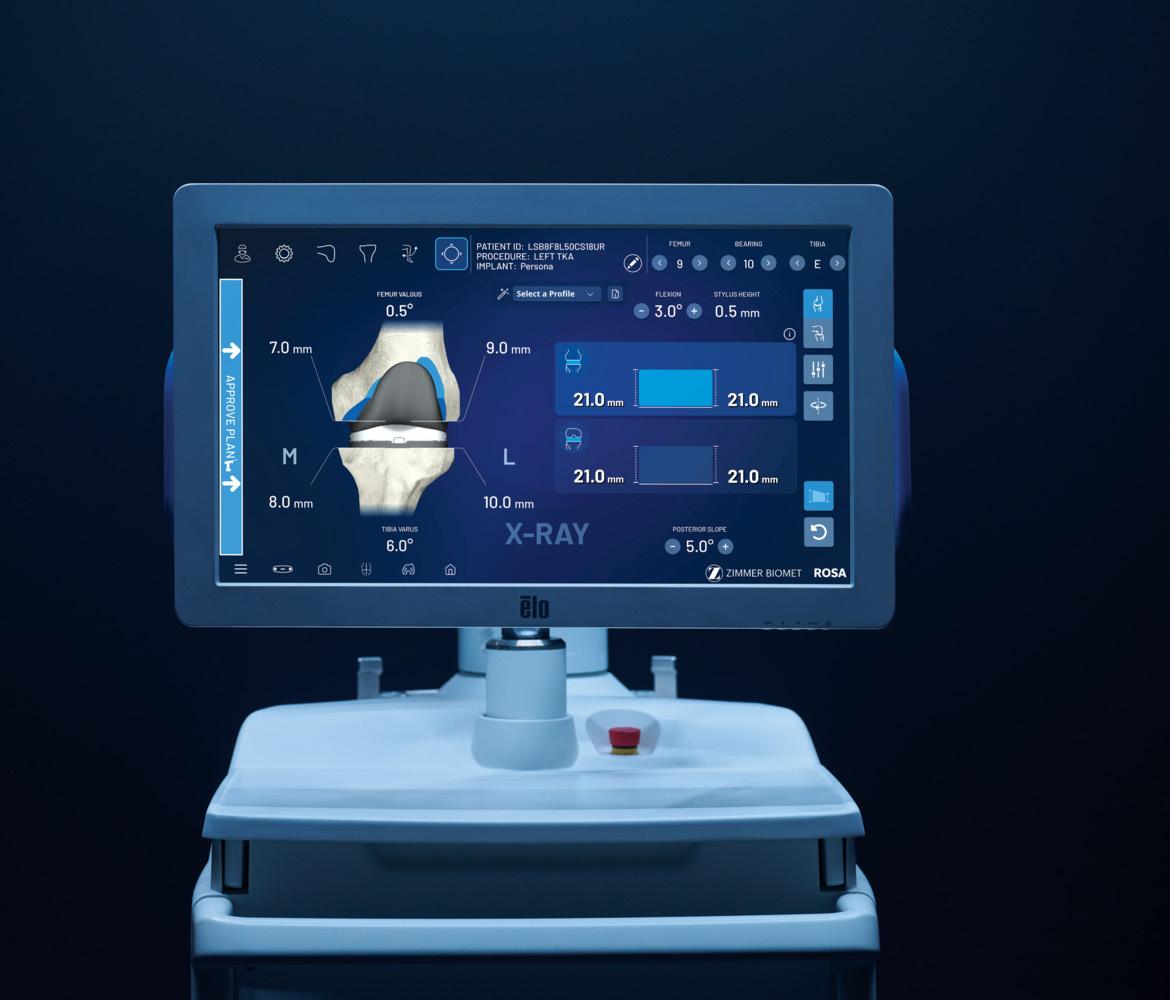

ROSA Knee with OptimiZe is a next generation robotic-assisted solution designed to support surgeon control, streamline workflow and enhance consistency in total knee arthroplasty. The system builds on the ROSA platform with intelligent planning tools, realtime tracking, and a simplified user interface that prioritizes efficiency and reproducibility. As the most significant update to the ROSA Knee System since its launch in 2019, key features include OptimiZe Planning, which enables surgeons to create personalized balancing profiles and reduce preoperative planning time by 46%. OptimiZe Landmarking and OptimiZe Tracking help minimize variability even when the leg moves, giving surgeons confidence in delivering accurate and reproducible outcomes. ROSA Knee with OptimiZe is the only robotic system to offer automated Kinematic Alignment planning, resurfacing the knee to its prearthritic position and restoring native joint lines. For surgeons who prefer Functional Alignment, customizable profiles balance the knee based on patient anatomy and surgeon preference, supporting a wide range of surgical philosophies. The system connects with ZB Edge Analytics to transform intraoperative data into actionable insights, reflecting the broader industry shift toward digital visualization and datadriven decision support. This connectivity allows surgeons to evaluate performance, refine technique and enhance overall workflow.
HypoHolder is an innovative needle safety device designed to reduce needlestick injuries during hypodermic needle handling in the operating room. Developed by surgical clinicians with decades of firsthand OR experience, HypoHolder addresses the highest-risk moments of hypodermic needle handling, including uncapping, recapping and temporary stabilization during procedures. HypoHolder enables secure, one-handed needle handling by stabilizing the hypodermic needle cap within a dedicated holding device. Despite widespread adoption of safety-engineered needles, many needlestick injuries continue to occur during manual handling steps, when the needle remains exposed during procedures. By providing a consistent location for needle management, HypoHolder minimizes hand-to-needle contact, helps eliminate unsafe two-handed recapping and enhances safety without disrupting surgical flow. HypoHolder is designed as a flexible needle safety device with
both reusable and disposable configurations intended for sterile surgical environments. Both versions integrate seamlessly into established OR workflows, require minimal training, and support compliance with sterile field protocols and regulatory expectations in high-acuity surgical settings. Compatible with a wide range of hypodermic needles, HypoHolder complements existing sharps safety devices by addressing risks that occur before disposal. By improving safety at the point of use, HypoHolder supports staff protection, workflow efficiency and reduced costs associated with needlestick injuries.
Come see us at AORN Booth #2109. Learn more at hypoholder.com/safety
SurgiSmoke Solutions is pioneering the future of operating room air safety through its hands-free smoke and bioaero sol capture technology. The Flamingo Funnel family of devices outperforms traditional smoke evacuation pens – removing nearly twice as much smoke –while offering a hands-free, non-obstructive footprint optimized for modern surgical work flows. The SurgiSmoke Solutions mission is to deliver cleaner air, clearer vision and safer operating rooms, while helping facilities comply with smoke evacuation mandates and standards (AORN, OSHA, state-level requirements). SurgiSmoke Solutions is flocking to the AORN Global Surgical Conference & Expo in New Orleans!
Come see us at AORN Booth #651-OR1. Find out more at flamingofunnel.co


As an industry leader in sterile processing and operating room solutions, Aesculap continues to raise the bar with its next generation of bone punches, SQ.line KERRISON Bone Punches. Designed specifically to meet the demands of spinal and cranial neurosurgery, SQ.line KERRISON Bone Punches help to ensure the surgeon and staff are equipped with a dependable and comfortable instrument. SQ.line KERRISON Bone Punches are designed to be consistent, comfortable, clean and convenient. With a handle designed for comfortable forward and backhand punching, users can experience more punches until repair/blunt with less jamming compared to the predecessor. SQ.line KERRISON Bone Punches offer time savings in the operating room and sterile processing department with assembly/ disassembly designed to be intuitive and easy to clean.
Customized ProcedurePak Trays can reduce surgical preparation time by up to 40%, giving healthcare teams more time to focus on patients and supporting smoother, more predictable operations. Mölnlycke’s customised ProcedurePak Trays are assembled to contain all the singleuse components required for a particular surgical intervention, replacing numerous individually packaged items. This tailored approach helps generate significant savings in time, cost and waste across both major and minor procedures.
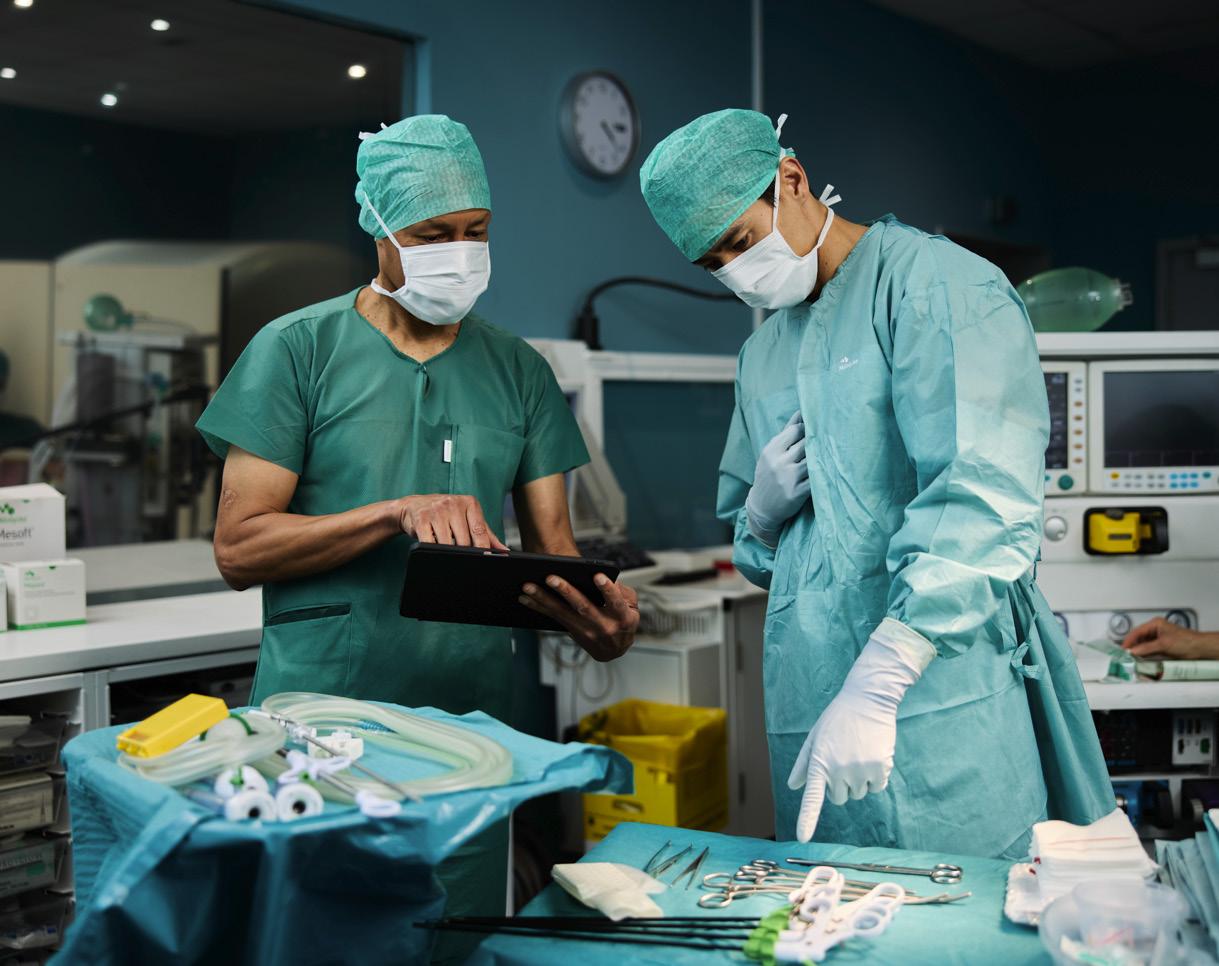

The VISERA ELITE III Imaging Platform is a compact, multispecialty imaging platform designed for laparoscopic diagnosis, treatment and video observation. Co-developed by SONY Olympus Medical Joint Venture, the Visera Elite III Platform integrates advanced imaging technologies into a software-driven platform that supports minimally invasive surgery in a wide range of specialties,
including arthroscopy, colorectal, ENT, bariatric, thoracic, gynecological, urological, HPB transplant and general surgery. Advanced features include True 4K and 3D imaging, Continuous Auto Focus (CAF), Narrow Band Imaging (NBI) technology, Yellow Enhancement (YE), ENDOEYE rigid and flexible videoscopes, and Fluorescence-Guided Surgery (IR/ICG) – now in full 4K White Light and high contrast Magenta Mode. All these features are now available in a single system that may improve workflow and clinical decision support.
The Cosgrove® Retractor is a unique heart retractor designed and proven specifically for heart valve surgery. It provides surgeons with the greatest visualization of the operative field, plus exceptional and consistent exposure of the right and left atrium, tricuspid valve and mitral valve, for surgical repair or replacement, while reducing the need for surgical assistance.
• Readily detachable, self-retaining atrial retractor requires placement only during the intracardiac portion of the procedure
• Universally adjustable atrial retractor blades are made of durable, malleable surgical stainless steel
• Several styles and sizes of retractor blades are available
• Kapp provides the Cosgrove® Retractor System mounted on a Cooley sternum retractor or custom mounted on any other sternum retractor, on request.
For more information, visit https://kappsurgical.com/productcategory/cosgrove/
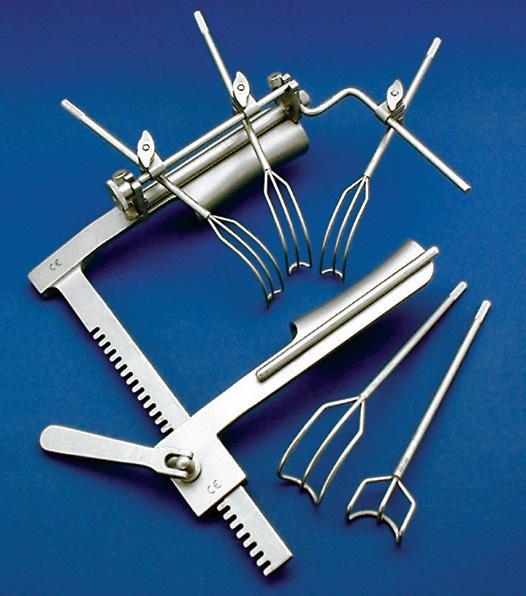





By Don Sadler
Accreditation is one of the most important responsibilities of hospitals and ambulatory surgery centers (ASCs), helping ensure the highest levels of healthcare quality and patient safety. There are three main independent accrediting bodies: The Joint Commission, the Accreditation Association for Ambulatory Health Care (AAAHC) and QUAD A (formerly known as the AAAASF).
These accrediting bodies are similar but also different in several key respects, says perioperative consultant Patti Owens, MHA, BSN, RN, CMLSO, CNOR, FAORN.
“Deciding which one to work with depends on the type of facility (hospital or ASC), type of services offered, goals of the organization and whether CMS deemed status is desired,” Owens explains.
According to Owens, QUAD A is often chosen for office-based or procedural practices needing strong surgeon credentialing and safety transparency while The Joint Commission is preferred for organizations requiring broad national recognition. “AAAHC is commonly selected by ambulatory-only providers seeking a quality-improvement focused, peer-driven model,” she says.
All three organizations conduct onsite surveys performed by trained healthcare professionals. They all award accreditation on a multiyear cycle (typically three years) with expectations for ongoing compliance and offer Medicare-deemed status, which allows eligible organizations to meet CMS requirements without separate federal surveys.
“In addition, all three use published standards and evidence-based practices in covering patient safety, quality of care, governance, credentialing, infection control and risk management,” says Owens.
While they are similar in some ways, there are important differences that should be considered when choosing an accrediting body, says Elethia Dean, RN, BSN, MBA, Ph.D., the CEO of consulting firm ASC Compliance.
“For example, The Joint Commission also focuses on environment of care and national patient safety goals
while AAAHC includes a chapter on administration, which is different from leadership/governance, and QUAD A includes standards that focus on prevention of drug diversion,” says Dean.
Owens says The Joint Commission survey is the most rigorous and formal, with highly structured tracers tied to National Patient Safety Goals. “AAAHC is known as educational and collegial with a peer-based, educational survey style,” she says. “And QUAD A is clinically strict but operationally narrower in focus.”
Here are some of the main things you should know about each major accrediting organization, along with tips to help you prepare for accreditation surveys.
“THE JOINT COMMISSION
ACCREDITATION IS CONSIDERED THE ‘GOLD STANDARD’ BY MANY IN THE INDUSTRY. “
- BEVERLY KIRCHNER
The largest and most widely recognized healthcare accrediting body in the U.S., The Joint Commission accredits more than 23,000 healthcare organizations, including hospitals and ASCs. “The Joint Commission sets national benchmarks for quality, patient safety and performance improvement,” says Owens.
Beverly Kirchner, MSN, RN, CNOR, CNAMB, vice president, compliance with SurgeryDirect, says The Joint Commission accreditation is considered the “gold standard” by many in the industry. “I view them as a marketing opportunity for ASCs,” she says. “I can tell my patients and doctors that our center follows the same regulations and standards of care as hospitals and hospital-owned ASCs.”
Here are a few unique characteristics of Joint Commission accreditation surveys:
• Usually unannounced and highly structured, with outcomes-driven standards.
• Focus on patient-centered culture of safety.
• Feature strong integration with CMS Conditions of Participation (CoP).
• Recognized by most states for licensure and Medicare/Medicaid eligibility.
• Recognized by third-party payers and investors.
Lindsey Fujimoto-Mullica, CST, administrator with SurgeryDirect, was part of the facility’s Joint Commission accreditation process last year.
“One of the most important lessons I learned is that Joint Commission accreditation is not about ‘passing a survey’ – it’s about building a culture of patient safety and continuous improvement,” she says. “The process reinforced the importance of standardized workflows, clear accountability and consistent, ongoing staff education.”
Fujimoto-Mullica was pleasantly surprised at how collaborative and educational The Joint Commission surveyors were during the process.
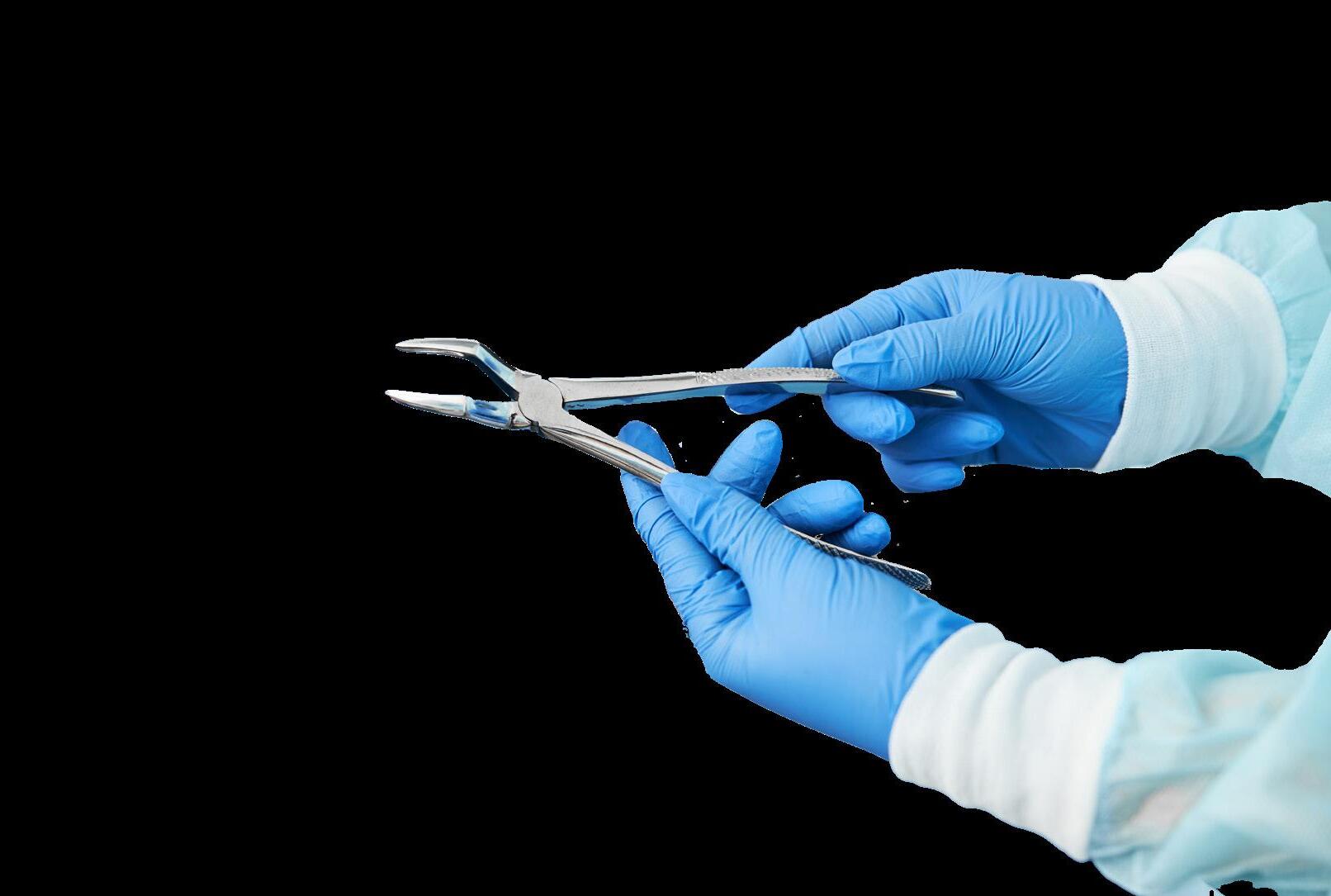
surveyors love to share their knowledge, including how they have seen regulations met in other facilities. I find them easy to work with and more consistent in their survey process.”
Even though they are seen by some as more difficult, Kirchner believes The Joint Commission is fair and consistent with the survey process. “They educate the whole team as they survey and their website is also very educational, which help ASCs stay survey-ready,” she says.
Dean says that success during a Joint Commission survey can be achieved by maintaining an ASC that mimics the setup of hospitals. “Over the past year, The Joint Commission has decreased their standards by 50 percent,” she says. “The impact of these changes is still yet to be determined.”
Owens lists several new Joint Commission developments to watch out for this year. These include Accreditation 360 for hospitals and critical access hospitals, National Patient Safety Goals and National Performance Goals, survey reporting and benchmarking improvements (SAFER), and Survey Process Guides, which will replace Survey Activity Guides.
The AAAHC focuses exclusively on accreditation for ASCs. “The AAAHC is widely known for promoting continuous quality improvement (QAIP) rather than one-time compliance,” says Owens. “They focus on the 1095 Strong, Quality Every Day model during the entire accreditation cycle with a strong emphasis on patient
widely used by independent and physician-owned centers,” says Kirchner, who has completed 13 AAAHC accreditation surveys in the past two years. “The organization is aligned with CMS ASC Conditions for Coverage and surveyors tend to have extensive ASC experience.”
When preparing for an AAAHC survey, Kirchner focus on credentialing and privileging, QAIP integration into the center’s care practice, infection prevention, governance and patient rights. “Infection prevention is a big focus because without great infection prevention practices, the center’s care is not safely provided,” she says.
AAAHC surveyors like to meet with the medical director and board members to make sure they understand their responsibilities for all operational practice. “I find the surveyors to be collaborative throughout the survey process,” says Kirchner. “They share their knowledge freely with all center team members.”
“While AAAHC surveyors are fair, they tend to bring more of their opinion to the survey than Joint Commission surveyors,” adds Kirchner.
“What I like most about AAAHC is that they offer a supportive survey approach and do not come in heavy handed,” says Jamie Ridout, CNOR, NEA-BC, CASC, system vice president, perioperative nursing practice at Geisinger Health System. “The sense I’ve always gotten is that the surveyors want you to be successful, offering consultative instruction and things to consider for future surveys.”
AAAHC seems to be more commonly used by larger, free-standing, multi-specialty ASCs, says Ridout.
“While their requirements can seem vague at times, I’ve always felt it’s not impossible to keep my ASC continually
ready for survey compliance.”
According to Dean, the AAAHC prides itself on being “not prescriptive. In this methodology, facilities can interpret standards and implement compliance measures. What I am seeing is that sometimes surveyors interpret the standards differently from the facility and the facility receives deficiencies based on the surveyor’s interpretation.”
Owens lists several new AAAHC developments to watch out for this year. These include v44 Standards becoming fully effective, making 2026 the first full survey year under v44, an expanded focus on data collection and outcomes, greater alignment of standards with state scope of practice rules, and integration of survey outcomes with Quality Roadmap reports.
QUAD A is a physician-founded accreditation organization created in 1980 with a strong focus on patient safety, procedural quality and provider qualifications, particularly in outpatient and office-based procedural settings. “Initially, they were primarily focused on office-based plastic surgery centers,” says Kirchner. “QUAD A is considered to be very physician friendly.”
Dean prefers QUAD A as an accrediting organization. “Their standards are clear, objective and have very few gray areas for interpretation. The standards are free on the QUAD A website (quada.org) which represents a cost saving for all facilities. In 2025, QUAD A also included an interpretative guidelines section in the standards manuals to close any gaps
“MY ADVICE IS SIMPLE: BE PREPARED. FAMILIARIZE YOURSELF WITH THE STANDARDS AND PROVIDE THE EVIDENCE TO SUPPORT YOUR COMPLIANCE WITH THEM.” - JAMIE RIDOUT
that may exist in the standards.”
Dean stresses that QUAD A requires 100 percent compliance with all of its standards for QUAD A facilities. “This is something that can be achieved with clear, concise and objective standards. Without this information, it’s a guessing game and often facilities guess incorrectly; hence deficiencies are cited.”
Owens lists several new AAAHC developments to watch for this year. These include revised standards for 2026 that supersede all past interpretive guidance and newsletters, updated anesthesia classification and monitoring requirements, and a stronger emphasis on leadership awareness of updated requirements.
Margaret Vargas, BSN, RN, nursing accreditation officer with Refreshed Aesthetic Surgery in Aliso Viejo, Calif., participated in her first QUAD A survey last year. “I would say the most important things I learned are the importance of being organized and staying up to date,” she says. “This proved crucial as the surveyor reviewed everything from patient charts and policies to sterilization and narcotic logs.”
The surveyor was also present in the OR during patient timeouts and checked the crash cart, including medication lists, supplies and expiration dates. “Regular monitoring of medications, supplies and their expiration dates, along with maintaining a thorough log, assured that everything was up to date and resulted in a successful survey,” says Vargas.
Vargas was surprised at how friendly and thorough the surveyor was in discussing her role in the survey process. “This allowed our team to perform with confidence while maintaining patient safety and quality of care as the primary goal,” she says. “She told us that while having standards, policies and protocols in place is important, every member following them is what makes the biggest difference in a positive survey outcome.”
Vargas’ main advice for centers that are preparing for a QUAD A survey? “Conduct regular meetings in which everyone is encouraged to provide feedback on whether current policies, standards and protocols are being met. I would also advise having logs and records regularly audited to make sure they’re up to date because our surveyor was very thorough in reviewing these.”
“While the survey experience may seem stressful and intimidating, our surveyor made it easy and informative,” Vargas adds. “Our
team feels confident and prepared for our next survey!”
Regardless of which accreditation body you choose, Kirchner recommends learning its regulations inside-out. “Don’t argue during the survey because you have options to address anything you thought was not fair or not accurate afterward,” she says. “Be prepared to write an appeal letter that quotes the organization’s regulations, how you addressed them and why you addressed them this way.”

“My advice is simple: Be prepared,” says Ridout. “Familiarize yourself with the standards and provide the evidence to support your compliance with them. I believe my center has been successful in our surveys because we treat compliance as part of our daily operations so when the survey comes, it’s business as usual.”
Owens recommends that hospitals and ASCs make sure staff is well-educated on the specific accreditation body’s standards and understands their role in the survey process. “Take advantage of seminars, workshops and educational tools associated with your accreditation organization,” she says. “Take a deep breath and use this survey as a learning opportunity.”
Dean says ASCs that achieve success in accreditation surveys usually have a mock survey completed by an individual or consultant with expertise in the chosen accrediting body.
“Each facility must search throughout the industry to find the individual who knows the most about the standards and regulations they will be measured by,” Dean says. “Then choose someone who can objectively measure your compliance and provide a report with recommendations.”
“My advice is to prepare every day, not just in the months leading up to the survey,” says Fujimoto-Mullica. “While the process is rigorous, it ultimately strengthens operations, improves outcomes and reinforces trust with the patients and communities we serve. I view accreditation not as an obligation, but as an opportunity to continuously elevate the care we provide.”
“WHILE THE PROCESS IS RIGOROUS, IT ULTIMATELY STRENGTHENS OPERATIONS, IMPROVES OUTCOMES AND REINFORCES TRUST WITH THE PATIENTS AND COMMUNITIES WE SERVE. I VIEW ACCREDITATION NOT AS AN OBLIGATION, BUT AS AN OPPORTUNITY TO CONTINUOUSLY ELEVATE THE CARE WE PROVIDE.”
- LINDSEY

By Don Sadler
W hen Colleen Becker was offered the opportunity to work as the Director of Perioperative Education for the Association of periOperative Registered Nurses (AORN) in 2021, this fulfilled a passion for surgical education that had grown throughout her four-decade nursing career.
“I’ve always believed that people took the time to teach me how to take excellent care of patients early in my career, so I believe it’s my responsibility to provide that kind of education to new colleagues in the profession,” says Colleen. “It’s very gratifying when you teach people something and you can see them grasp the concept and be able to implement it in practice.”
During her last year of nursing school, Colleen selected the operating room as an elective. “This is where I first developed a love for taking care of patients and their families during the surgical process,” she says. “One of my instructors infused a love for the operating room in me and I’ve had it ever since.”
After graduation, Colleen went to work in critical care “because you couldn’t go directly into the operating room back then,” she says. From here, she moved into hospital leadership and management roles, eventually becoming the director of perioperative services for a large academic medical center.
“I was responsible for 80 operating rooms, two ambulatory centers, 150 PACU bays and five sterile processing departments,” Colleen says.
In her current role as the senior director of perioperative education, Colleen oversees development, design and dissemination of all AORN educational content. This includes perioperative staff education, clinical tools and resources, and career and leadership development guidance, all based on the evidence-based “Guidelines for Perioperative Practice.”
“We provide education in many different formats, including online, on demand, in written form and face to face,” says Colleen. “We also host webinars and the annual AORN Global Surgical Conference & Expo.” This year’s conference will be held April 11-14 in New Orleans. (See Page 34)
The most gratifying part of her job, says Colleen, is helping touch so many lives by educating AORN members about evidence-based practice and research surrounding perioperative nursing. Meanwhile, the most challenging part is not being able to communicate directly

with all AORN members to find out what they want and need. “Our members are national and international so it’s hard to stay in communication with all of them,” she says.
Throughout her career, Colleen says she’s been fortunate to witness a lot of new technology and innovation in the OR. “When I was in nursing school, and I’m dating myself, a gallbladder surgery required a large incision on the right side of your body,” she says. “Now this surgery is done minimally invasive. Innovations and technology improve patients’ quality of life and allow them to spend more time with their loved ones.”
In addition to AORN, Colleen has been actively involved in a number of other professional nursing organizations throughout her career. These include the American Association of Critical Care Nurses; the Emergency Nurses Association; the Association of Women’s Health, Obstetric and Neonatal Nurses; and the American Society of Perianesthesia Nurses (ASPEN).
“I believe that involvement in these kinds of organizations is critical to professional development,” Colleen says. “In addition, we integrate with other types of nurses to take better care of surgical patients.”
Looking ahead, Colleen expects technology to continue playing a major role in patient care delivery. “Robotics, virtual reality, artificial intelligence … they’re

already here now, but they will continue to improve the way we care for patients,” she says. “The OR nurse’s voice needs to be heard to ensure that technology is implemented for the bet terment of patient care.”
Colleen believes that new technology will also present new career opportunities for nurses, such as informatics. This emerging field of nursing integrates nursing science, computer science and information science to better manage and communicate patient data and enhance the clinical experience.
Colleen and her husband, Scott, own two Australian sheep dogs “who still think they’re puppies,” she says, “so they keep us busy. We just enjoy being outside, whether it’s gardening, hiking or bike riding.” They recently returned from a snowmobiling trip to Vail, Colorado.
Healthcare runs in the Becker family. Colleen’s oldest daughter, Brit, is an OR assistant nurse manager and her youngest daughter, Jenn, is an emergency medicine physician. In addition, her husband is a perfusionist, her sister-in-law is a doctor and her brother is a pharmacist. “We could pretty much open a hospital,” she says.

“I’ve always believed that people took the time to teach me how to take excellent care of patients early in my career, so I believe it’s my responsibility to provide that kind of education to new colleagues in the profession.”

T he effect of obesity on brain health may depend not only on how much fat is in the body, but also on the areas of the body where fat is stored, according to a study published in Radiology, the flagship journal of the Radiological Society of North America (RSNA).
Researchers at The Affiliated Hospital of Xuzhou Medical University in Xuzhou, China described two previously unidentified fat distribution types on MRI that show the strongest associations with adverse brain and cognitive outcomes: a “pancreatic predominant” type, which shows a markedly high concentration of fat in the pancreas compared with other areas of the body, and a “skinny fat” type,
which has a high fat burden despite not fitting the typical patterns of high obesity.
While previous research has established a link between obesity and brain/ cognitive health, particularly in people with higher ratios of visceral fat, this new study focuses on the specific risks associated with specific fat distribution patterns, explained study coauthor Kai Liu, M.D., Ph.D., an associate professor in The Affiliated Hospital’s Department of Radiology.
“Our work leveraged MRI’s ability to quantify fat in various body compartments, especially internal organs, to create a classification system that’s data-driven instead of subjective,” Liu said. “The data-driven classification unexpectedly discovered two previously
undefined fat distribution types that deserve greater attention.”
The researchers used data from 25,997 individuals in the UK Biobank database, which houses anonymized medical imaging measurements alongside volunteers’ physical measurements, demographics, disease biomarkers, medical history and answers to lifestyle questionnaires. This allowed the team to compare brain health outcomes with patterns of body fat distribution.
Of the body fat profiles the team identified, “pancreatic-predominant” and “skinny fat” profiles were most associated with extensive gray matter atrophy, accelerated brain aging, cognitive decline and increased risk of neurological disease. These risks were present in both men and women, with
nuanced variations between the sexes.
Individuals with “pancreatic-predominant” distribution patterns showed a proton density fat fraction – an MRI marker that provides a precise estimation of fat concentration in tissue – of around 30 percent in the pancreas.
“This level is about two to three times higher than that of other fat distribution categories, and it can be up to six times higher than that of lean individuals with low overall fat,” Liu said. “Additionally, this group tends to have a higher BMI and overall body fat load.”
Interestingly, however, these individuals didn’t have significantly pronounced liver fat compared to those with other profiles. High pancreatic fat accompanied by relatively low liver fat emerges as a distinct, clinically overlooked phenotype, Liu noted.
“In our daily radiology practice, we often diagnose ‘fatty liver,’” Liu said. “But from the perspectives of brain structure, cognitive impairment and neurological disease risk, increased pancreatic fat should be recognized as a potentially higher-risk imaging phenotype than fatty liver.”
Individuals with “skinny fat” profiles show the highest fat burden in nearly all areas except the liver and pancreas. Unlike a balanced “high obesity” profile, “skinny fat” tends to be more concentrated in the abdomen.
“Most notably, this type does not fit the traditional image of a very obese person, as its actual average BMI ranks only fourth among all categories,” explained Liu.
“The increase is perhaps more in fat proportion. Therefore, if one feature
best summarizes this profile, I think, it would be an elevated weight-to-muscle ratio, especially in male individuals.”
In this study, the research team focused specifically on the neurological and brain cognitive risks associated with different fat distribution patterns. As for risks in other areas, such as cardiovascular or metabolic health, Liu noted that more research is needed to determine how these patterns could be related.
Understanding the risks associated with specific fat distribution patterns can help healthcare providers guide more personalized treatment and help patients keep their brains healthier. As Liu explained, “Brain health is not just a matter of how much fat you have, but also where it goes.”
The SEITZ SOLUTION ® Upper Extremity Implant Systems

Radial Head Implants

Ulnar Head Implants
• Off-the-Shelf Consignment
• Patented Spacer to Adjust Osteotomy
• Custom Orders Available
• EN ISO 13485:2016 Cert.
• US Patent #8,353,965


New and Improved
• New - wider backing for easy removal
• Keeps sterile tethered appliances on the surgical field from falling to the floor with 4 hook & loop closures
• Latex free self adhesive back for attachment to the surgical field
• Economical - Saves pre-op time
• Sterile shelf life 2 years
• New Users call for FREE SAMPLES
• Patented


/ Fax 216-587-0411 / 800-282-5277 www.kappsurgical.com / info@kappsurgical.com EN ISO 13485: 2016 Cat #SC5000-4Y
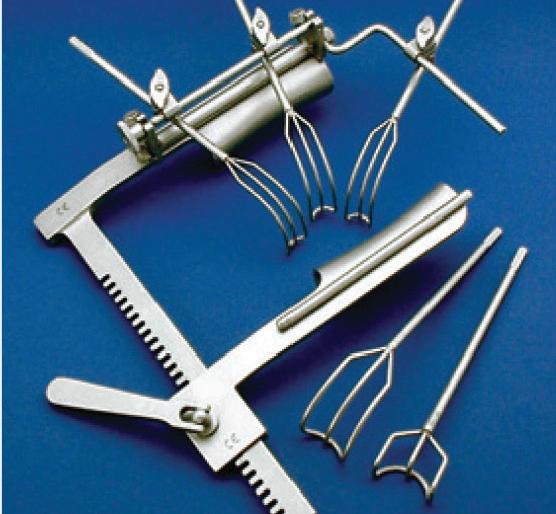
Original
• Universal Self-retaining Heart Retractor
• Mitral Valve Repair or Replacement Surgery
• Exceptional Exposure for Right & Left Atrium

Visit Kapp Surgical at AORN Conference Booth #1436 800-282-5277


By Miguel J. Ortiz
W hen looking to strengthen one’s core, it is wise to go beyond the six-pack or flat abs image. A six-pack is the result of building a strong core. When it comes to fitness, the core deserves much more attention. The core is the foundation for all other movements.
You wouldn’t buy a house if it had a severely cracked foundation! Would you buy a house or add to it if it had the same problem? No and the reason is because before you add to it you need to reinforce or strengthen it. Also, primal core strength will yield distal joint strength. Since the core muscles are the foundation for all movement, it is vital that a workout includes exercise to start strengthening it. The workout can start with a beginner movement and work up to an advanced movement.
This first suggested core strengthening movement is known as a “Bird Dog” or bi-lateral raise. This move will start to strengthen the core muscles
because, as simple as it looks, it serves as a fantastic progression movement to many other patterns – like crawling and advanced planks. This exercise will help expose imbalances in the hips and shoulders because to raise the opposite arm and leg requires greater core stabilization in order to move those joints and muscles. It is important to focus on more control. Do not focus on trying to do faster reps. Make the movements in a slow and steady manner. You want to be as smooth as possible to get the most control as possible.
The second exercise is very similar. The active quadruped shoulder taps movements is not exactly the same with a hidden benefit. The difference is that you must be able to place more weight on your hands and shoulders because your knees need to be lifted off the floor enough to keep a neutral spine. Taking your knees off the floor increases core activation and makes knee and shoulder stability more difficult. You have to shift your weight without rotating out of position and losing control and that is where some of the benefits to this movement come into play.
The last exercise is a side Copenhagen plank with a knee drive. There are regressions to this movement, but when mastered it is sure to challenge one’s core. This movement will also help increase hip and shoulder strength. This can be done without the knee drive, but it is important to hold that knee up for at least 1 full second to exhibit control at the top of the motion with quality posture.
I would like to point out that each of these movements has some level of shoulder and hip mobility and/or strength. The point is that with core strength you are helping other joints. Your core strength is something that your joints can build upon, so train wisely.
Miguel J. Ortiz is a personal trainer in Atlanta, Georgia. He is a Master Trainer for Pain-Free Performance and a Certified Nutritional Consultant. You can find videos of the exercises mentioned in this column at tinyurl. com/ORTfitness.


Healthmark & Getinge believe by combining our strengths, we are positioned to better serve healthcare facilities moving forward into the future. We’re committed to providing innovative solutions, personalized implementation and best-in-class educational resources more than ever before. Together, we are striving to give you an unparalleled customer experience.
Scan to explore the bene ts of our partnership. Discover how we’re rede ning the customer experience to empower your facility.

iber may be having a cultural moment, but most Americans still aren’t getting enough of it – or fully understanding where it comes from. A new IFIC Spotlight Survey: Americans’ Perceptions of Fiber & Whole Grains finds that two-thirds of Americans say they either fall short on fiber or don’t know how much they consume, even as “fibermaxxing” trends across TikTok and Instagram, and experts forecast fiber as the “new protein.”
The findings come just weeks after the release of the Dietary Guidelines for Americans, 2025-2030 (DGA) which notably feature fruits, vegetables, and whole grains in a different position in the New Food Pyramid, yet stop short of offering explicit daily fiber targets for consumers.
“Fiber is suddenly everywhere in the wellness conversation – yet our data show most Americans still don’t know how much they need or where to get it,” said IFIC President & CEO Wendy Reinhardt Kapsak, MS, RDN. “There’s a real disconnect between cultural hype and everyday understanding and action.”
According to the survey, nearly three in 10 Americans (29%) report consuming less than 20 grams of fiber per day – well below recommended levels – while 37% don’t know their intake at all. In reality, fewer than 10% of women and just 3% of men meet fiber recommendations, and more than 95% of U.S. adults fall short on whole grains.
Yet interest is not the problem. Zero percent of respondents said they don’t want or need more fiber, signaling broad motivation – but limited clarity.
“As someone who regularly analyzes consumer data, that zero percent really stands out,” said Kris Sollid, RD, IFIC Senior Director of Research & Consumer Insights. “It suggests that Americans realize the importance of fiber in the diet and believe they would likely benefit from consuming more, which is encouraging.”
While many Americans correctly associate fiber with fruits, vegetables, and grains, there are signals that Americans could use a refresher on fiber – nearly one in four (24%) selected meat/seafood as a best source of fiber and 19% say the same about dairy. Neither source inherently contains dietary fiber.
Knowledge of fiber sources is just one hurdle to increase intake. The survey illuminates other barriers, including:
• Not knowing which foods contain fiber (30%)
• Cost (27%)
• Taste (26%)
• Inconvenience (17%)
“It’s clear people want to eat healthier, but we’re in a moment where the rhetoric can be confusing. Fiber is praised while carbohydrates are often demonized, but people don’t realize that many carbohydrate-rich foods are good sources of fiber. Oats/oatmeal, bran cereal, whole wheat pasta, and whole grain breads are good sources of dietary fiber, and legumes such as lentils and black beans are
also excellent sources. Ultimately, eating a varied diet that includes fruits, vegetables, legumes, and whole-grain based cereals and breads is a satisfying and nutrient-dense way to achieve your daily fiber goals,” Amburn said.
“This is where healthcare professionals, including registered dietitians, play a critical role in helping connect those dots and translating muddled guidance into practical, realistic choices,” Amburn added.
Despite years of low-carb narratives, Americans are twice as likely to say carbohydrate-rich foods can be part of a healthy diet than to say they cannot. Still, confusion remains: one in three are unsure which foods even count as carbohydrate-rich.
While 70% view whole grains as healthy, fewer than half feel the same about refined carbohydrates.
“The conversation around carbs, fiber and whole grains
has become overly polarized,” said Amburn. “What’s missing is nuance – and trusted voices to help people make sense of it.”
The survey also shows Americans rely more on front-ofpackage claims like “100% Whole Grain” or “Good Source of Fiber” than on the Nutrition Facts label itself – suggesting that messages with meaning, not just metrics, shape behavior.
As fiber takes center stage in wellness culture and as dietary guidance evolves, IFIC’s findings point to a growing need for healthcare professionals, registered dietitians and science communicators to step in.
“Fiber doesn’t need to be a trend – it can become a habit,” said Reinhardt Kapsak. “The communications landscape is ripe for clear, consistent and actionable guidance Americans can use to improve their health and wellbeing every day.”


By Daniel Bobinski
Here’s something I’ve observed countless times. The most reliable person on a team carries way more weight than anyone realizes and eventually burns out. But nobody notices until it’s too late.
One could call it the “reliable employee syndrome.” To me, it’s one of the most insidious problems in the modern workplace. Think about it. These are the people who always say yes. They consistently deliver quality work, and they always step up during a crisis. These are the people managers lean on when deadlines are tight or when something absolutely, positively must be done with solid attention to detail.
And that’s exactly the problem: it’s almost always that one quiet, reliable employee.
Let me paint a picture. Sarah is your goto person. She’s been with the company seven years, knows the systems inside and out, and rarely complains. When a project needs help, Sarah gets the call. When a difficult client needs handling, Sarah can fix it. When someone’s out sick, Sarah covers. Over time, her workload has grown, but nobody notices. After a while, Sarah is doing the work of two people while getting paid for one.
Here’s what makes this particularly destructive. The reliable ones typically
have a strong work ethic and a personal pride that prevents them from saying no. They worry that declining work might look like weakness or lack of commitment. Meanwhile, management thinks everything’s fine because Sarah keeps delivering. It’s a silent agreement that benefits everyone – except Sarah.
The breakdown doesn’t happen overnight. First comes subtle changes. Quality might slip ever so slightly, and response times might get a little longer. The reliable person seems tired or stressed but still produces.
Why are these early signs easy to miss? Because the reliable one is still performing better than average, even while struggling.
Then one day, without warning, they quit. Or worse, they stay but become a shadow. The extra effort stops and their passion is gone.
Smart leaders understand something fundamental about human capacity, and that just because someone can handle extra work doesn’t mean they should keep doing it indefinitely. They also know recovering from burnout can take months or even years.
Additionally, they know that preventing burnout isn’t complicated, but it requires intentional action and good management practices.
First, managers must look at the workload distribution across their team. If
their best people are consistently carrying significantly more than others, that’s a yellow flag. Evaluating everyone’s workload takes time, but it’s part of being a manager.
Second, managers initiate honest conversations about capacity and create an environment in which saying, “I’m at my limit.” isn’t career suicide.
Third, managers redistribute work proactively before burnout happens, not after.
Bottom line, an organization’s most reliable employees are their most valuable assets. If those employees’ needs get overlooked, they’ll eventually burn out and become invisible. They may even leave. Therefore, it’s a core management responsibility to openly recognize the contributions of their reliable employees and ensure their workloads don’t become unsustainable.

Daniel Bobinski, who has a doctorate in theology, is a bestselling author and a popular speaker at conferences and retreats. For more than 30 years he’s been working with teams and individuals (1:1 coaching) to help them achieve excellence. He was also teaching Emotional Intelligence since before it was a thing. Reach him by email at DanielBobinski@ protonmail.com or 208-649-6400. OUT OF THE OR
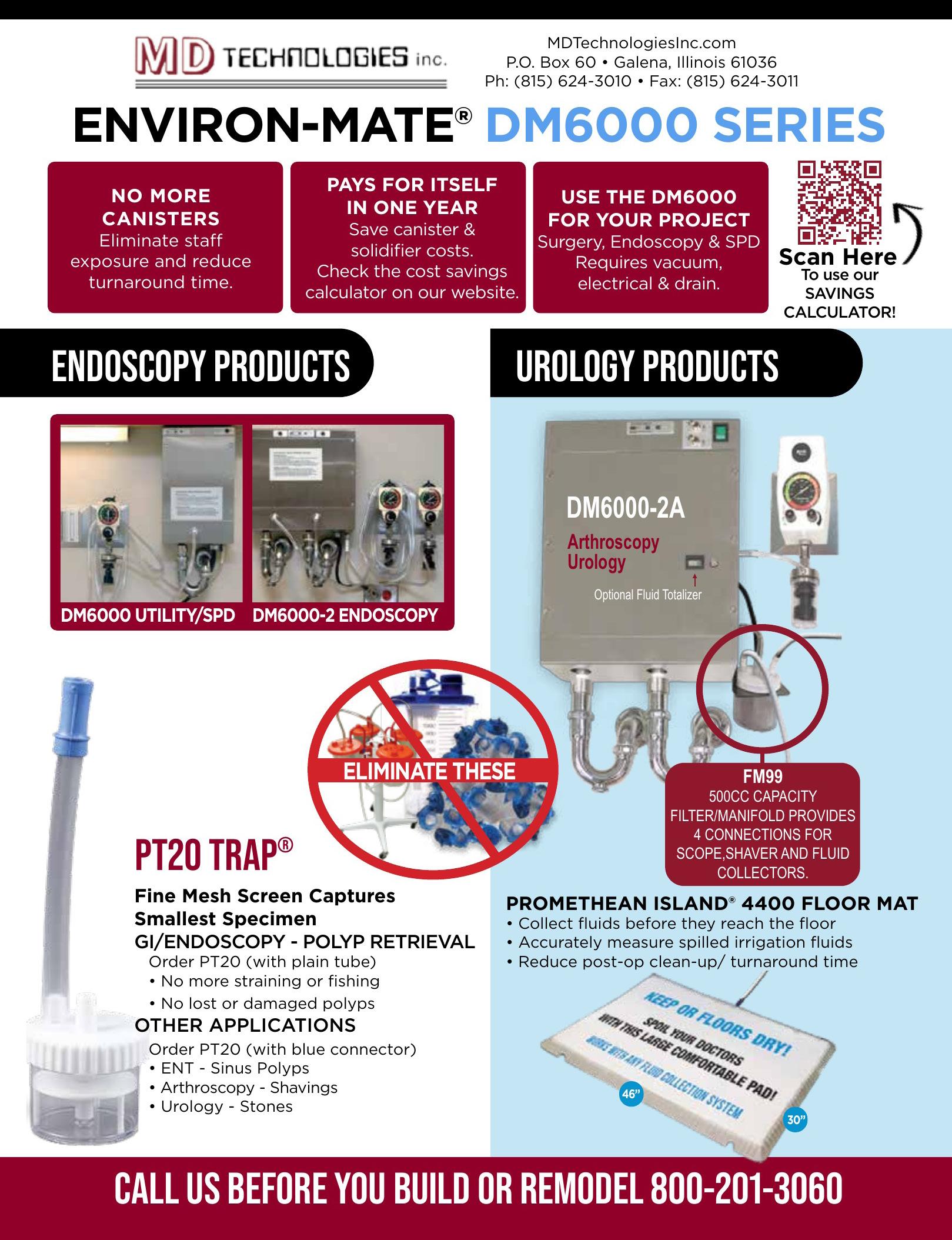
• 1 pound ground beef
• 1 pound spaghetti noodles
• 1 jar (16 ounces) alfredo sauce
• 1 jar (24 ounces) marinara sauce
• 2 tablespoons garlic powder
• 2 tablespoons onion powder
• salt, to taste
• pepper, to taste
• 2 cups shredded cheese
• French bread or breadsticks, for serving

By family features

OUT OF THE OR recipe
B
ecause this time of year can be crazy busy, drive-thru meals can easily become the norm. While fast-food burgers may do the trick once in a while, they can get old quick if your family is eating them every other night. This quick and easy Baked Spaghetti can bring everybody back to the table and it won’t break the bank either..
Find more weeknight dinner inspiration at Culinary.net.
Baked Spaghetti
Recipe courtesy of “Cookin’ Savvy”
Servings: 4-6
1. Heat oven to 350 F.
2. Brown and drain ground beef. Cook noodles according to package instructions. Drain noodles; add alfredo sauce and mix well.
3. Add marinara sauce, garlic powder and onion powder to ground beef. Season with salt and pepper, to taste.
4. Place noodles in 9-by-13-inch baking dish. Spoon beef mixture on top but do not mix in. Cover with shredded cheese then cover with foil and bake 30-40 minutes.
5. Serve with French bread or breadsticks.
Smoke capture mandate compliance made easy:
• Hands-free & flexible
• Unobstructed view
• Up to 2x the smoke capture1
• Shown in studies to remove infection-causing bioaerosols2,3




Everyone likes FREE stuff and we want to hear from our readers! It is a win-win! Please take a moment to tell us what you like about OR Today magazine.
You could win a $25 gift card! Simply go to ORToday.com/ Contest and fill out the short form for your chance to win!



THIS MONTH'S WINNER Quatisha Ashley ECHN MemorialManchester Hospital
“From a Sterile Processing Technician’s perspective, OR Today serves as a valuable resource for teaching and professional development. It provides current information on surgical practices, sterile processing, and perioperative care, offering real-world examples that help connect learning to actual OR environments. The magazine also supports discussion, critical thinking, and staying up to date with industry standards, making it a practical tool for guiding and inspiring learners.”
– Quatisha Ashley