















In healthcare, we often assume that once we explain the science, fear will fade. Sometimes it does. But sometimes fear isn’t rooted in a lack of information, it’s rooted in stories.
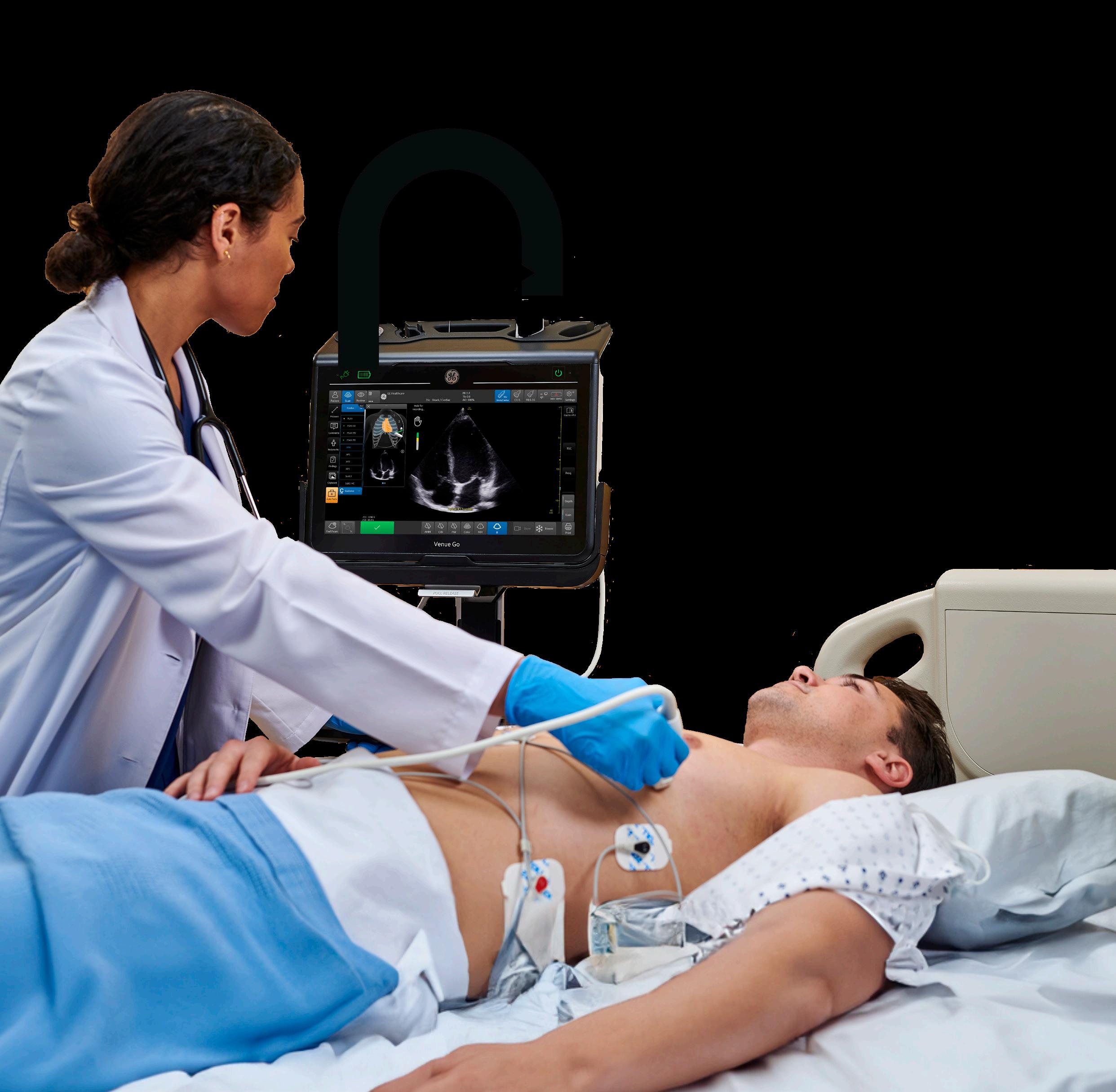
Ultrasound technology continues to advance at a rapid rate with benefits for a wide range of practices including pediatrics. Point-of-care
ultrasound, AI software and contrast-enhanced ultrasound continue to advance patient care.


Abbigail Dodson was as a medical assistant at a cardiology office when she discovered nuclear medicine.
MARCH 2026

Catch up on the latest news from around the diagnostic imaging world.



A look at some of the latest ultrasound systems and features.
EMOTIONAL INTELLIGENCE
Be willing to give up good things in your life if you want to achieve greater things.
President
Vice
Vice
Senior
Editorial
Beth
Kimberly
Megan
Art
Kristin
Webinars
Digital
Cindy
Accounting



Abbigail Dodson loves her job and plans to continue her career advancement and one day serve as a manager.
Lexington Medical Center Clinical Operations Supervisor in Nuclear Medicine and PET/CT Abbigail Dodson holds multiple degrees and certifications. She is also well thought of by her supervisors and peers. She was nominated as a Rising Star by Lexington Medical Center Director of Imaging Services and AHRA President Wesley Harden, CRA, FAHRA.
ICE Magazine Editor John Wallace recently found out more about Abbigail, her decision to work in imaging and what we can expect in the future.
Q: WHERE DID YOU GROW UP?
A: Culpeper, Virginia
Q: WHERE DID YOU RECEIVE YOUR IMAGING TRAINING/ EDUCATION? WHAT DEGREES/CERTIFICATIONS DO YOU HAVE?
A: I started my medical journey at ECPI University for Medical Assisting. I am a Certified Medical Assistant, Certified ECG Technician and Certified Phlebotomy Technician. I went to Midlands Technical College for nuclear medicine and became a Certified Nuclear Medicine Technologist.
Q: HOW DID YOU FIRST DECIDE TO START WORKING IN IMAGING?
A: I worked as a medical assistant at a cardiology office when I first moved to South Carolina and they performed in-house nuclear stress testing. The images they printed for the office visit were amazing and I wanted to learn more. Midlands Tech has the program in the state for nuclear medicine.
Q: WHAT IS THE MOST REWARDING ASPECT OF YOUR JOB?
A: Being a part of the patients’ journey, whether that be to diagnose, continue monitoring or finding solutions to their medical issues is extremely rewarding. I love every minute of it.
Q: WHAT DO YOU LIKE MOST ABOUT YOUR POSITION?
A: Knowing that I am making a difference. I am helping my staff thrive, therefore helping Lexington Medical Center succeed.
Q: WHAT INTERESTS YOU THE MOST ABOUT THE IMAGING FIELD?
A: In nuclear medicine specifically, we can test the function of organs, not just look at the anatomy. We are the only modality that does that, and it is very special.
Q: WHAT HAS BEEN YOUR GREATEST ACCOMPLISHMENT IN YOUR FIELD THUS FAR?
A: My greatest accomplishment thus far has been becoming supervisor. I have worked very hard to be able to put myself in a position that I can make a difference and grow not only myself, but Lexington Medical Center as well.
Q: WHAT GOALS DO YOU HAVE FOR YOURSELF IN THE NEXT 5 YEARS?
A: In the next 5 years, I hope that my departments of nuclear medicine and PET/CT will continue to thrive and be successful for the hospital. I would love for the chance to become a manager and be able to make even more of impact in the field of nuclear medicine. I love my job and want to be able to go as far as it will let me. •
FAVORITE HOBBY: Deer hunting with my husband and my boys. I also love reading.
FAVORITE SHOW: “The Ranch” and “Big Bang Theory”
FAVORITE FOOD: Steak Dianne, my husband makes the best
FAVORITE VACATION SPOT: Beaufort, South Carolina
1 THING ON YOUR BUCKET LIST: A chance to go to Ireland
SOMETHING YOUR CO-WORKERS DON’T KNOW ABOUT YOU: That I’ve been to 33 of the 50 states.

Di ana Radley, MBA, ARRT (R), CRT (M), is a wife, a mother, a student, an educator and the director of imaging services with MemorialCare Long Beach Medical Center and Miller Children’s & Women’s Hospital Long Beach. Each of her roles delivers responsibilities and opportunities, none more important than “the opportunity to impact lives.”
“I love my job because it allows me to serve both my team and our community in meaningful ways. I take care of my team so they can provide the best care possible to our patients. When caregivers feel supported, empowered, and valued, the quality of care naturally improves,” Diana says. “I strive to build genuine connections, fostering trust and partnership through transparency, encouragement, and a culture of safety and support.”
“What fulfills me most is the opportunity to impact lives, whether it’s guiding a team member toward their next career milestone or ensuring a patient receives timely, accurate imaging that supports their healing journey,” she continues. “This work is more than a job; it’s a calling. I’m honored to lead with heart, purpose and integrity.”
Diana is an accomplished imaging professional, but she says that her greatest accomplishments were achieved away from the workplace.
“While I’m proud of my professional accomplishments, my most outstanding achievement is my family,” Diana says. “My son is now in his third year of college, majoring in electrical engineering, mathematics and cybersecurity. My eldest daughter recently began her college journey to become a nurse practitioner. My youngest daughter, a high school junior, dreams of becoming a nurse.”
“Being a wife, a mother and a full-time professional while pursu-
ing my education has been the most rewarding challenge of my life. Balancing family, career and personal growth has shaped who I am today, and I wouldn’t trade that journey for anything,” she adds.
Speaking of her career, how did Diana begin her diagnostic imaging and leadership journey?
“I began my college journey in Michigan as a biology major on the pre-med track, with aspirations of becoming an OB-GYN. I’ve always had a strong passion for women’s health, and I was committed to pursuing a career in medicine, specifically in medical school,” Diana explains. “But after marrying my husband, Paul, and relocating to San Diego, I started to reconsider the demanding path of becoming a physician as we planned to start a family.”
“It was Paul, an MRI technologist, who encouraged me to explore medical imaging by volunteering at Sharp Memorial Hospital. That experience changed everything. I was introduced to a world where technology, precision and compassionate patient care came together in powerful ways,” she adds. “Inspired by what I saw, I shifted my career path to medical imaging, and I’ve never looked back.”
Her family and her career thrived in the years that followed.
“Shortly after my son was born, I completed X-ray school and began building my career in medical imaging at Sharp Healthcare. I earned my ARRT certification in radiography and my California mammography license. I later completed my bachelor’s degree while working full-time and advancing into leadership roles,” Diana says. “Most recently, I earned my MBA in healthcare administration, which has further solidified my role as director of imaging services at MemorialCare Long Beach Medical Center and Miller Children’s & Women’s Hospital.”
Diana is a leader on a mission to lead and serve.
“I lead with my heart. At my core, I’m a servant leader. I believe leadership is about lifting others, and standing beside them, not above them,” she says. “My job is to support my team, remove barriers, and create an environment where they feel safe, valued, and empowered to do their best work. When my team thrives, our patients receive the best care possible. That’s what drives me every day.”
“I also see myself as a transformational leader,” she adds. “I love inspiring people to grow, to think bigger, and to believe in their potential. I set high expectations, but I never ask my team to do anything that I wouldn’t do myself. I build trust through connection, consistency, and transparency, because authentic leadership starts with relationships.”
“For me, it’s not just about managing departments, it’s about creating a culture where people feel seen, supported and motivated to
DIANA RADLEY
MBA, ARRT (R), CRT (M), Director, Imaging Services, MemorialCare Long Beach Medical Center & Miller Children’s & Women’s Hospital
1. What book are you reading currently? “The Seven Spiritual Laws of Success” by Deepak Chopra, M.D.
2. Favorite movie? “Crazy Rich Asians”
3. What is something most of your coworkers don’t know about you? I am an artist at heart. Long before I was managing imaging departments and mentoring future leaders, I was sketching in notebooks, blending colors on canvas, and shaping clay with my hands. I draw, I paint, and I sculpt. Each medium offering a different kind of peace, a different kind of expression.
make a difference. That’s the kind of leader I strive to be,” Diana says. Her grandfather and uncle impacted her outlook and approach from an early age.
“I have always believed that mentorship is one of the most powerful tools we have as leaders. Not just to shape careers, but also to impact lives. I have been fortunate to have two incredible mentors who helped me become the person and leader that I am today: my great uncle, Robert ‘Bob’ Baird, and my grandfather, Roger Andersen,” Diana shares.
“Uncle Bob was once the CFO of Detroit Edison, and he showed me what it means to pursue excellence without sacrificing family. He even pursued law school while serving as CFO and being a husband and father of two daughters. Uncle Bob taught me that you do not have to choose between personal life milestones and professional growth. You can do both if you lead with intention and heart,” she continues. “He was also deeply involved in his community, even running for office in Ann Arbor, Michigan, and personally going door to door to connect with voters. Uncle Bob’s example taught me that leadership is service.”
“My grandfather, Roger, was a self-made entrepreneur who left high school to help support his family. He built a legacy in Brighton, Michigan, owning a restaurant, a snowmobile shop, co-owned a NASCAR truck race team, a real estate portfolio, among several other businesses,” Diana adds. “At 16, I begged my grandpa for a job at his restaurant, ‘Cheryl’s Place.’ I wanted to be a waitress; however, he started me as a busser and potato peeler in the prep kitchen. I eventually became the closing cook on the weekend. That experience gave me early leadership responsibilities and taught me the value of earning trust through hard work. Later, I worked as an office manager in the NASCAR world, where I learned about business operations and team dynamics, all lessons that serve me today.”
From the prep kitchen to the fast-track of NASCAR, Diana soaked up countless lessons from her experiences.
“Those experiences shaped my approach to leadership and mentorship. Throughout my career in imaging, I have mentored imaging professionals across southern California, and I absolutely love it,” Diana says.
In closing, Diana shares the importance mentors continue to have on her life and career.
“I carry the lessons of my Uncle Bob and Grandpa Roger with me every day. Their stories remind me that leadership is earned, not given, and that the most meaningful legacy we leave is one we build in others,” she says.•
4. Best advice you ever received? People come into and out of our lives to help form who we are. For some, their chapters in our lives may be very short, and some may last a lifetime. Either way, they come with a purpose, and we need them at the exact time they present themselves.
5. Who has had the biggest influence on your life? My faith and my family
6. What would your superpower be? To make everyone understand that we all have a very limited time on this earth. To appreciate how fragile life is. And to live with goodness and purpose.
7. What are your hobbies? I love planning parties.
8. What is your perfect meal? A home cooked meal with everyone that I love.

BY MATT SKOUFALOS
Long before he’d found his place in the imaging informatics world, Mac Beauchemin lived the life of a touring punk rocker. Growing up in Arnold, California, he was raised in the wilderness and the snow of the gold rush country between Yosemite and Tahoe. His mother, Suzanne, has been a piano teacher for 50 years; his dad, Mike, a welder who “played a little banjo and did a little singing.” Mac’s interest was rooted in the drums from an early age.
“My uncle, Bob Yater, played keyboard in a rock band that would play these [neighborhood] parties,” he recalled. “I would sit there at four or five years old and stare at Tommy Parker, their drummer. My parents eventually bought me a cheap drum set, and I started playing piano with my mom.”
Mac played in high school concert and marching bands, wrote parts for some marching competitions, and started a punk trio with his best friends, playing talent shows and then gigging at pizza joints in the Modesto and Stockton areas that would host shows on weekends.
“And then we all went to college, and that band split up,” he said.
Despite performing with a few replacement players through a couple years at Sonoma State University, Mac’s high-school band eventually re-formed. The performers socked away as much money as they could during the semester, working as valets and touring over winter and summer breaks. They called themselves Kalifornia Redemption; together, they released two records and completed four or five national tours between 1998 and 2003.
“We played all over the Midwest; the South, the West
coast,” Mac recalled. “Still to this day, I travel a lot for sales, but I saw a lot more of the country touring.”
During that time in music, the punk rock scene was thriving nationally thanks to the kinds of bands that Mac and his mates had formed. The late 1990s success of unsigned California acts like Sublime, which sold tens of thousands of tapes from the back of their van, and Green Day, which exploded on the strength of a vigorous touring schedule, were proving the doit-yourself (DIY) model had legs.
Of course, success is never guaranteed in the entertainment industry, and Kalifornia Redemption played “many a show for the bartender and the door person,” Mac said. Other bills were more remarkable. Among the many acts the band shared a stage with were The Mighty Mighty Boss Tones, No Means No, and Tilt, whose lead singer, Cinder Block, was an early punk ambassador in Mac’s life.
“In Petaluma, there’s a famous concert venue called the Phoenix Theater; we used to play it all the time because it was our local venue,” Mac said. “I got to meet Cinder Block and do soundchecks with them. I loved the Mighty Mighty Boss Tones, I love ska music; that was a star-struck moment. But [meeting] Tilt was the moment where I was at a loss of words. They were one of the first punk rock bands I’d ever heard.”
Kalifornia Redemption formed other friendships on the road, sometimes by pure chance. Mac recalled a moment driving down a Texas highway when another band full of punk rockers pulled up alongside their van, and screamed, “Who are you guys?”
“We yelled back and forth, traded CDs across the highway, and became very good friends with them,” Mac said. “They were from Indianapolis. We played a few shows on the way, booked in and around Indy, and we stayed in their house.”
“We also met a lot of good bands and formed good




relationships playing clubs; bands like Next to Nothing from New York City, with whom we toured south and east. Our first tour, we started in San Diego, jumped on with another band for 40 days all the way out to Florida, and played a bunch of shows on the way back.”
Today, the bandmates still get together a few times a month at their Oakland studio. Gigs are fewer and farther between, but Mac said there’s a new, 12-song record in the works. As the band Heater, they contributed a cover of the Operation Ivy song “Plea for Peace” for the compilation album Mooorree Than Just Another Comp from Lavasocks Records and Sell the Heart Records. (That track is available to stream on Spotify along with the Kalifornia Redemption catalogue.)
In the past 30 years, more than just time has changed the way that unsigned bands operate. Simply put, the methods they used to employ no longer offer the same opportunities. Websites like BYOFL.org (Book Your Own F---ing Life), which emerged from the magazine MAXIMUMROCKNROLL in 1992, helped self-funded touring acts compile a list of inexpensive resources to chart their courses on the road. Most performers are simply trying to earn enough money to reach the next destination and play again.
“Until we got a little bit of support from a small label and a booking agent, who was just a local guy, we used BYOFL,” Mac said. “We’d mail promoters a merch kit, and they’d call us back and say, ‘I’ve got a show for you.’ That’s how we did almost all our tours. It was all over the phone.”
“Nowadays, I feel like you need to either have serious finance, or you’ve got to know somebody,” he said. “The organizations that could help you from afar without requiring money – I don’t know that that exists anymore. You need to have financial backing, or know the right people to get your name out there, or you have to get lucky.”
“Even with a little bit of help, it seemed more hands-on and grassroots,” Mac said. “You could do it if you had the want and the dedication. You could make it pretty far. It wasn’t all fun, but if you had that dedication, if you were all really into it, I found it all quite rewarding.”
After his touring days ended, Mac was approached by a friend who worked for a staffing agency to fill a temporary receptionist position at a PACS company, so he put on a tie, sat at a desk, and made himself indispensable. It wasn’t long until he was hired on full-time, and then moved from PACS sales support, to lead development, and then to sales. He met Parag Paranjpe in the technical and development side of the business, and after Paranjpe left to found HealthLevel, he invited Mac to join the sales team, where he’s remained for years.
These days, Mac is focused more on passing along his love of playing and performing music to his daughter, Bailey. At 16, she’s already been to five or six times the number of shows he’d seen by that age; Mac chalks it up to living in the Bay Area instead of the mountains. But when she sits down behind the drum kit, nothing puts a bigger smile on his face. •
Techno-Aide is a Nashville, Tennessee-based medical imaging accessories manufacturer of Class 1 medical devices. It is an ISO certified company with certifications in ISO 9001:2015 for Quality Management Systems and ISO 13485:2016 for Medical Device Quality Management. Since 1977, Techno-Aide has been making a wide array of products to assist medical imaging personnel take better images safely.
Techno-Aide produces wearable radiation protection such as aprons, vests, skirts, and thyroid shields, as well as non-wearable radiation protection like mobile barriers and shields. Techno-Aide also manufactures a wide selection of positioning devices for patient comfort and image quality. With a variety of foam positioners for patients and DR panel holders for imaging personnel efficiency. Techno-Aide continues to live up to its desire to be a onestop-shop for medical imaging accessories.
ICE Magazine Editor John Wallace recently interviewed Techno-Aide Marketing & Design Coordinator Noah Lauck to find out more about the company and how it supports healthcare imaging professionals.
Q: HOW DOES YOUR COMPANY STAND OUT IN THE IMAGING SPACE?
LAUCK: Techno-Aide knows resilience and adaptation better than anyone. In March 2020, our facilities were destroyed by an EF-3 tornado that wiped out the company’s manufacturing facility and offices that had been home to
the business for 35 years. Techno-Aide’s team rallied in the wake of the tornado to remake the company for the future. Less than a year after the tornado, Techno-Aide moved into its new home, a 45,000-square-foot office and manufacturing facility in Whites Creek, Tennessee, just outside of Nashville.
Since then, we’ve expanded our business avenues to include medical contracting and metal fabrication and produced innovative products to the imaging world such as the world’s first remote controlled mobile panel positioner, The Sidekick. Where some might have seen the tornado as an obstacle too big to overcome, TechnoAide saw it as a chance to build something fresh and new. The ability to turn adversity into opportunity is what sets Techno-Aide apart.
Q: WHAT IS ON THE HORIZON FOR YOUR COMPANY? DO YOU HAVE ANY GOALS YOU WOULD LIKE TO ACHIEVE IN THE NEAR FUTURE?
LAUCK: We hold ourselves to a high standard at Techno-Aide and the goals we set for ourselves reflect that. Broadly speaking, our goal is to grow. We want to grow with our partnerships and industry presence. We also want to grow and develop our team so we can maintain the high standard we set for our business so when opportunities or obstacles present themselves, we’ll be ready. •
For more information, visit techno-aide.com.








In novatus Imaging’s Center of Excellence for Ultrasound Probe Repair was founded on a 40-year heritage leveraging the expertise and vision of Dennis Wulf, who remains on the Board of Directors today. Wulf pioneered ultrasound probe repair in the mid-1980s, years before others entered the industry. In those early days, many independent service organizations (ISOs) outsourced their repairs to Wulf’s facility in Tulsa, OK. Having performed over 195,000 repairs since 2000, Innovatus is recognized as the premier ultrasound probe repair provider and is a trusted partner of OEMs, ISOs, asset managers and healthcare facilities worldwide.
On a similar timeline began the legacy of Innovatus’ MRI Coil Center of Excellence. Once an FDA registered contract manufacturer and service center of MRI coils for multiple OEMs, the company expanded to include multi-vendor service of MRI coils. With over 50,000 coil repairs, Innovatus remains a service center for multiple OEMs. The organization brings an OEM standard of quality to the ISO market and supports healthcare organizations around the globe.
The company’s capstone is their Center of Excellence for Design and Manufacturing. The FDA-registered facility is a contract manufacturer of ultrasound probes and ultrasound related devices for several very prominent OEMs. The facility’s cGMP’s (Current Good Manufacturing Practices), engineering expertise, and acoustic testing lab assist to develop, verify and validate repair processes and materials for the Tulsa Ultrasound Repair Center of Excellence.
Q&A With Ted Lucidi, Director of Commercial Operations
WHAT IS THE MISSION AND VISION OF YOUR COMPANY?
Simply put, our goal is to assist healthcare organizations in realizing significant savings and improving upon the quality of patient care by restoring and extending the lifecycle of imaging devices. Our teams accomplish this by developing innovative solutions to meet our clients’ needs and strive to produce products and services of the highest quality and safety, while fulfilling all requirements - from customers, regulatory bodies, and industry standards.
WHAT MAKES YOUR COMPANY UNIQUE OR ESSENTIAL IN TODAY’S MARKET?
Innovatus Imaging is unique in that we are a true specialty organization. We may only provide 3 very specialized
services, yet we do them with extreme precision. In a time where more and more Independent Service Organizations (ISOs) are merging and being acquired by other ISOs to become one-stop-shops, Innovatus remains committed to providing the most comprehensive solutions on the products that we support. While many in our industry are currently focused upon providing replacement/exchange options, our efforts remain on repair/restoration. Our FDA registration and heritage make us uniquely qualified to restore your ultrasound probes and MRI coils back to OEM form, fit, function, safety and efficacy.
WHAT MILESTONES OR ACHIEVEMENTS HAS YOUR COMPANY REACHED?
What stands out is that some of the most prominent and well-respected OEMs have chosen to place their trust in our organization. OEMs choose to partner with us as we deliver consistent, high-quality solutions that meet the strict regulatory standards to which they are held accountable. That says a lot.
HOW HAS INNOVATUS GROWN AND ADAPTED TO REMAIN A LEADING PROVIDER IN SUCH A COMPETITIVE INDUSTRY?
We make investments. Investments in people, investments in engineering, and investments in tools and technology. Rather than be all things to all people, we ask: What are the most popular models, right now? Which of those are failing; AND, which are causing the most distress for our clients. Our teams determine how and why the devices are failing and determine what solutions can be developed to address the most-frequently encountered failures. We are always innovating and engineering new solutions. In the past year, we released full-repair capabilities on over 50 MRI coil models including the Philips dStream and GE Air coils. On the probe side, we recently released micro-technology repair solutions to our clients. This technology will make obsolete conventional probe repair processes, with regard to the cable harness, and Innovatus Imaging is first to market.
IS
For our teams, it’s all about honesty, integrity, transparency, and, ultimately, trust. Whether via email, phone, or live chat, our teams will inform on exactly what we can AND CANNOT do. If someone asks if we can repair model XYZ, and we cannot, they are informed, up-front. Inquirers will not encounter, “send it in and we’ll let you know.”
At Innovatus, our teams are driven to provide outstanding value to our clients in everything we do. We take pride in knowing that what we do is important, and that we are relied upon by countless healthcare professionals around the world. The source of our excellence is anchored in our honesty and integrity. We truly believe career satisfaction is realized through hard work, solving problems head-on with our teammates, and using new solutions to make ourselves, and the company, better for the future. By working together in this way, we build excellent business and technical judgement, a command of the facts, and the confidence to have a strong bias toward action. Our average tenure for employees exceeds 10 years, and some have over 20, indicating a strong sense of belonging, dedication and sense of mission.
CAN YOU SHARE SOME COMPANY SUCCESS STORIES WITH OUR READERS – A TIME THAT YOU “SAVED THE DAY” FOR A CUSTOMER?
Early last year, we released Next-Day MRI Coil Repair. Not every coil is a candidate, but if so, the repair time can be significantly accelerated. A few months ago, a local hospital experienced a failure on a newer-model, high-priority, specialized MRI coil. The HTM tech informed our team of their critical need, he hand-delivered the coil to our facility in the morning, and it was completed mid-day. The coil was placed back into service same day for a few thousand dollars versus the $75,000 replacement cost. Not only is that a success story, but it’s also a win-win-win scenario.
WHAT’S YOUR UNIQUE SELLING PROPOSITION?
A simple Internet search reveals that there are 50+ ISOs promoting probe repair or selling replacement probes; AND everyone uses the word “quality.” I like to ask potential clients, “How do you manage your risk?” How do you know that your chosen provider has the proper processes in-place, that qualified components are being used, and that their materials have undergone the appropriate testing? Non-conforming probes and coils will still function – but how do you know they meet the OEM intent? At Innovatus, the term compliance is very important. Our goal is to return every device to its original form, fit, function, and intended design, and do so at a fair, cost-effective price.
HOW DOES INNOVATUS MANAGE RISK?
As an OEM of ultrasound probes, acoustic arrays, and associated products, and with a legacy in MRI coil
manufacturing, our engineers possess a full understanding of the devices that we service. We approach service and repair with a manufacturing mindset.
Our approach to repair is consistent with that found in new product development manufacturing. Many of the processes and practices utilized in our manufacturing division are transferred to our repair divisions. For example, Innovatus will not perform repairs that have not undergone rigorous verification and validation processes which are required in new product development.
The engineers in our repair divisions utilize many of the same tools used in new product development. These include custom test fixtures, MRI scanner emulators, acoustic power measurement, pulse-echo testing, radiation force-balance testing, transducer face temperature testing, wiring light boxes, and cable and strain relief stress testing.
Release of new repair offerings include formal documentation of items such a schematic and wiring diagrams, bills of materials, component qualifications, material qualifications, biocompatibility testing (ISO 10993), as well as shipping package testing. All processes, test results, and documentation are captured within our ISO 13485:2016 certified quality management system.
Having a deep understanding of the technology we support and having all of the tools that are necessary to ensure that all of our products are fully qualified, gives a clinical engineer a high level of assurance that when that product is returned to the healthcare professional, that it is clinically safe and effective.
WHAT DOES PARTNERING WITH INNOVATUS MEAN FOR ME, MY BUDGET, MY CUSTOMERS, AND MY PATIENTS?
Clients who choose Innovatus, as a service partner for ultrasound probes and MRI coils have confidence in knowing that 1) The safety and performance of their devices has been entrusted to those with first-hand experience in manufacturing such devices, 2) The organization has a commitment to quality consistent with new device manufacturing and embraces practices to improve outcomes and lower costs, and 3) Is accountable to multiple OEMs, dozens of ISO partners and asset management organizations, hundreds of healthcare organizations, but, ultimately, each and every patient on which our repaired devices are used. •






iSono Health has announced the commercial launch of ATUSA, an FDA-cleared, wearable and automated 3D quantitative breast ultrasound platform. Designed to bring high-quality imaging into everyday clinics, ATUSA unlocks the $14 billion U.S. breast imaging market by eliminating reliance on hard-to-find skilled sonographers and cost-prohibitive equipment, according to a news release.
A graduate of Y Combinator and the Texas Medical Center Accelerator, iSono Health has gained significant industry recognition, including the HLTH 2025 Rising Star (Diagnostics) and the WISH 2024 Global Awards. Building on this commercial launch, the company has announced the opening of its Series A financing.
Standard mammography often fails the 40 million American women with dense breast tissue, creating a massive diagnostic gap where cancers can remain hidden, according to the release. It can be a painful experience and often exposes women to unnecessary X-ray radiation, leaving those of reproductive age with limited screening options. ATUSA can fundamentally change the economics and accessibility of breast health through a unique fusion of wearable hardware and cloud-based intelligence:
• Automated Scanning: Utilizing a wearable, hands-free accessory, ATUSA captures full 3D volumes in approximately two minutes per breast, roughly 10x faster than manual handheld ultrasound. This ensures consistent and repeatable images are generated, regardless of the operator’s skill level.
• Point-of-Care Integration: The system empowers OB/GYNs and primary care providers to offer specialistlevel imaging directly in their offices, generating standardized 3D whole-breast visualization directly at the point of care.

• USaaS Business Model: A scalable “Ultrasound-as-a-Service” model that combines the wearable hardware, cloud-based AI, and consumables to create a recurring revenue stream while lowering the barrier to entry for local clinics.
• Advanced “Sentient” AI: iSono Health is working to move beyond simple detection toward a “sentient partner” model, where the system utilizes acoustic biomarkers and machine learning to sense patient-specific needs and provide real-time diagnostic support.
“ATUSA is a system-wide upgrade for women’s breast health,” said Neda Razavi, CEO of iSono Health. “We are putting the power of a world-class radiology suite into the hands of local clinicians, replacing slow, manual workflows with real-time diagnostic images at the point of care.”
FUJIFILM Healthcare Americas Corporation recently issued a news release to announce a strategic partnership with Voicebrook Inc., a leader in pathology reporting solutions, to integrate Voicebrook’s VoiceOver PRO reporting platform with Fujifilm’s Synapse Pathology, a comprehensive pathology PACS that streamlines case management through proprietary advances in image digitization. This collaboration brings together comprehensive digital-pathology capabilities and voice-driven reporting workflows to help laboratories modernize operations, reduce manual steps and accelerate pathology turnaround.
With the integration, pathologists using Synapse Pathology will be able to seamlessly shift from reviewing whole-slide images to generating reports that are compliant with College of American Pathologists (CAP) standards and structured data capture, all by voice control. By eliminating slide-to-report context switching and minimizing manual entry, the combined solution enables more fluid case review, enhanced diagnostic focus and greater operational throughput.
“Fujifilm is committed to bringing digital pathology into the enterprise-imaging mainstream – enabling pathologists to collaborate, review and report with the same agility as radiology,” said Dr. Mark Lloyd, vice president of digital pathology, FUJIFILM Healthcare Americas Corporation. “By integrating with Voicebrook, we’re enriching the slide-to-report workflow with a voice-first reporting paradigm that meets labs where they are and takes them where they’re going.”
The partnership leverages key strengths of both companies:
• Seamless Integration: Direct connection between Synapse Pathology and VoiceOver PRO enables smooth movement from digital slide review to report creation within one environment.
• Voice-Driven Efficiency: Pathologists can dictate findings, navigate slides and complete CAP eCP protocols hands-free, reducing manual steps and maintaining diagnostic focus.
• Vendor-agnostic, workflow-centric design: Synapse Pathology supports multi-scanner inputs, DICOM and proprietary formats, cloud or on-premises deployment, and enterprise imaging integration.
• Enterprise readiness: Both products are designed to support high-volume labs, multi-site deployments, and complex workflows, aligning with the vision of digitized pathology as a core part of enterprise imaging.
“Pathologists are under mounting pressure to deliver accurate diagnoses more efficiently,” said Filipe Carreira, chief operating officer, Voicebrook. “By integrating VoiceOver PRO with Synapse Pathology’s open, vendor-agnostic architecture, we’re offering labs a voice-enabled workflow that aligns with the future of digital pathology.”
The joint solution is available now to clinical and reference laboratories seeking to enhance diagnostic workflows with a fully integrated digital-pathology and reporting platform.

Radiology is under pressure. Imaging volumes continue to rise while specialists face increasing workload and staff shortages. Many healthcare organizations see the promise of AI but struggle with complex integrations and uncertain value. A partnership between Konica Minolta Healthcare Americas Inc. and deepc, a provider of the healthcare AI infrastructure operating system deepcOS, aims to change that reality by making AI practical, trusted and seamlessly part of everyday work across hospitals and imaging centers in North America, according to a news release.
Through this collaboration, deepcOS will connect directly with Konica Minolta’s Exa Platform, which includes Exa PACS|RIS, Exa Enterprise and Exa Teleradiology. This creates a single, unified environment where hospitals and clinics can access a rigorously validated library of AI tools within their existing workflows. It eliminates the need for separate systems or extensive IT projects and allows radiology teams to benefit from AI support where it matters most, in their daily practice.
Radiologists experience a smoother reading flow as AI insights appear within their familiar viewer, turning routine image review into faster, more focused decision-making. IT teams gain simplicity through se-
cure, cloud-native deployment that strengthens data protection and keeps compliance effortless. Together, these improvements create tangible value for hospitals: consistent performance across sites, lower technical burden, and a scalable foundation for clinical AI. Ultimately, patients feel the difference in faster results and more confident diagnoses.
“At deepc, we focus on what happens after AI reaches the clinic,” said Alex King, chief revenue officer at deepc. “By joining forces with Konica Minolta, we can bring validated, ready-to-use AI directly to Konica Minolta customers. Together, we are giving radiology teams the confidence to work smarter and the freedom to focus on what matters most: the patient in front of them.”
“At Konica Minolta, our Healthcare IT AI strategy is to provide our customers with a single source and single platform to utilize the power of AI-enabled insights. The Exa Platform integrates with deepcOS, providing radiologists a unified, seamless experience. We’re thrilled to partner with deepc to bring the value of an integrated AI platform to our shared customers,” stated Kevin Chlopecki, COO, Konica Minolta HCIT.
Two medical ultrasound organizations recently announced their endorsement of expanded training in contrast enhanced ultrasound (CEUS) under the newly updated National Education Curriculum (NEC) for sonography programs.
“CEUS has transformed how we diagnose and monitor disease, and expansion of CEUS training for sonography students is a critical step forward in ensuring broader patient access to one of the most innovative and patient friendly advances in diagnostic imaging,” according to a joint statement issued by the International Contrast Ultrasound Society (ICUS) and Inteleos.
The NEC is a consensus-based curriculum guide developed by a coalition of sonography professional organizations as a framework for sonography training programs across the United States. This guide can also be used by sonographers who are preparing for credentialing examinations.
The new NEC updates follow the recent expansion of the sonographer scope of practice to include a more active role for trained sonographers in the administration of CEUS examinations. The “Scope of Practice and Clinical Standards for the Diagnostic Medical Sonographer” was updated in 2024 by the Society of Diagnostic Medical Sonography (SDMS).
“Expanded CEUS training will help prepare the next generation of sonographers to deliver safer, more effective and more patient-centered care,” according to Maria


Stanczak, a member of the ICUS board who was instrumental in developing the new CEUS content for general imaging concentrations.
The earlier version of the NEC, adopted in 2016, contained little CEUS training information, which helped slow the adoption of CEUS in the United States compared to Europe and Asia, according to Dr. Jordan Strom, associate professor of medicine at Harvard Medical School, director of the echocardiography laboratory at Beth Israel Deaconess Medical Center, and an officer of ICUS. Strom played a leading role in developing the new CEUS content for cardiac concentrations.
UCAs do not contain iodine or gadolinium, and have not been shown to have an effect on thyroid or renal function, he said.
In addition, CEUS does not expose patients or staff to ionizing radiation, and CEUS exams provide highly accurate clinical information in real time so that appropriate therapy can be initiated without delay.
“Training in CEUS during formal sonography education enables students to graduate with the knowledge and skills necessary to meet the evolving demands of modern healthcare,” said Hannah Simmons, director of global business growth at Inteleos.
Artificial intelligence (AI) chatbots in healthcare top the 2026 list of the most significant health technology hazards. The report is prepared annually by ECRI, an independent, nonpartisan patient safety organization.
Chatbots that rely on large language models (LLMs) – such as ChatGPT, Claude, Copilot, Gemini and Grok –produce human-like and expert-sounding responses to users’ questions. The tools are not regulated as medical devices nor validated for healthcare purposes but are increasingly used by clinicians, patients and healthcare personnel. More than 40 million people daily turn to ChatGPT for health information, according to a recent analysis from OpenAI.
ECRI says that chatbots can provide valuable assistance, but they can also provide false or misleading information that could result in significant patient harm. Thus, ECRI advises caution whenever using a chatbot for information that can impact patient care. Rather than truly understanding context or meaning, AI systems generate responses by predicting sequences of words based on patterns learned from their training data. They are programmed to sound confident and to always provide an answer to satisfy the user, even when the answer isn’t reliable.
“Medicine is a fundamentally human endeavor. While chatbots are powerful tools, the algorithms cannot replace the expertise, education and experience of medical professionals,” said Marcus Schabacker, MD, Ph.D., president and chief executive officer of ECRI. “Realizing AI’s promise while protecting people requires disciplined oversight, detailed guidelines and a clear-eyed understanding of AI’s limitations.”
ECRI experts say that chatbots have suggested incorrect diagnoses, recommended unnecessary testing, promoted subpar medical supplies and even invented body parts in response to medical questions while sounding like a trusted expert. For example, one chatbot gave dangerous advice when ECRI asked whether it would be acceptable to place an electrosurgical return electrode over the patient’s shoulder blade. The chatbot incorrectly stated that placement was appropriate – advice that, if followed, would leave the patient at risk of burns.
The risks of using chatbots for healthcare decisions could become an even greater concern as higher healthcare costs and hospital or clinic closures reduce access to care, leading more patients to rely on them as a substitute for professional medical advice.
Chatbots can also exacerbate existing health disparities, according to ECRI’s experts. Any biases embedded in the data used to train chatbots can distort how
the models interpret information, leading to responses that reinforce stereotypes and inequities.
“AI models reflect the knowledge and beliefs on which they are trained, biases and all,” Schabacker said. “If healthcare stakeholders are not careful, AI could further entrench the disparities that many have worked for decades to eliminate from health systems.”
ECRI’s report offers recommendations for using chatbots more wisely. Patients, clinicians and other chatbot users can reduce risk by educating themselves on the tools’ limitations and always verifying information obtained from a chatbot with a knowledgeable source. For their part, health systems can promote responsible use of AI tools by establishing AI governance committees, providing clinicians with AI training and regularly auditing AI tools’ performance.
The Top 10 Health Technology Hazards for 2026 in ranked order are:
• Misuse of AI chatbots in healthcare
• Unpreparedness for a “digital darkness” event, or a sudden loss of access to electronic systems and patient information
• Substandard and falsified medical products
• Recall communication failures for home diabetes management technologies
• Misconnections of syringes or tubing to patient lines, particularly amid slow ENFit and NRFit adoption
• Underutilizing medication safety technologies in perioperative settings
• Inadequate device cleaning instructions
• Cybersecurity risks from legacy medical devices
• Health technology implementations that prompt unsafe clinical workflows
• Poor water quality during instrument sterilization
Now in its 18th year, ECRI’s Top 10 Health Technology Hazards report identifies critical healthcare technology issues. ECRI follows a rigorous review process to select topics, drawing insight from incident investigations, reporting databases and independent medical device testing. Since its creation in 2008, the report has supported hospitals, health systems, ambulatory surgery centers, and manufacturers in mitigating risks.
An executive brief of the Top 10 Health Technology Hazards report is available for download. The full report is accessible to ECRI members and includes detailed steps that organizations and industry can take to reduce risk and improve patient safety.
To learn more, visit ECRI.org.
Profound Medical Corp., a commercial-stage medical device company that develops and markets AI-powered, MRI-guided, incision-free therapies for the ablation of diseased tissue, recently announced that Mount Sinai Hospital has successfully treated its first prostate cancer patient with the TULSA-PRO system.
The TULSA Procedure represents an advancement in prostate care and is used by physicians to treat prostate cancer and benign prostatic hyperplasia (BPH, also known as an enlarged prostate), according to a news release. Robotically controlled directional ultrasound is delivered from inside the urethra to precisely and gently heat prostate tissue to “kill temperature” (55-57°C), while protecting surrounding nerves and anatomy. Real-time MRI thermography enables continuous visualization and autonomous temperature adjustment throughout the procedure. This level of precision allows physicians to tailor therapy to each patient, resulting in no procedural blood loss, no overnight hospital stay, and a quicker return to everyday life, while minimizing side effects typically associated with surgery or radiation, such as urinary incontinence and/or erectile dysfunction.
Mount Sinai Health System doctors recently col-
laborated to perform the health system’s first TULSA Procedure, with the patient responding well to the treatment and being discharged the same day.
“With this milestone, Mount Sinai continues to establish itself as a leader in robotic surgical care, becoming the first health system in the New York Metro Area to offer the innovative, AI-driven, MRI-guided, and incision-free TULSA Procedure to prostate disease patients,” said Arun Menawat, Profound’s CEO and Chairman.
“This unique collaboration between the Department of Urology and the Department of Interventional Radiology at Mount Sinai will pave the way for future studies and guidelines in prostate cancer and BPH using TULSA-PRO. Patients will have another option for best-in-class treatment of these complex conditions,” said Ash Tewari, MD, MBBS, MCh, Surgeon-in-Chief Tisch Cancer Hospital & System, Chair of Urology and Professor at the Mount Sinai Health System.




Innovative Radiology, founded in 2016, recently celebrated the grand opening of its new location in Gallatin, Tennessee.
Innovative Radiology, founded in 2016, recently celebrated the grand opening of its new location in Gallatin, Tennessee.
“It was a long work in progress getting to here, growing our team, growing the organization, working with the various customers and vendors in our space forming relationships and trust which led us to this moment,”
“It was a long work in progress getting to here, growing our team, growing the organization, working with the various customers and vendors in our space forming relationships and trust which led us to this moment,” Co-CEO Josh Glas said. “We’re just grateful and proud of our new space here.”
Co-CEO Kyle Hall agreed.
Co-CEO Josh Glas said. “We’re just grateful and proud of our new space here.”
Co-CEO Kyle Hall agreed.
“It’s been exciting to open up this location,” Hall said. “We already have a location in Conyers, just outside of Atlanta. Here in Gallatin, we were able to expand a little bit. We started out in a 3,000-square-foot warehouse about two years ago and we’ve added personnel, added capabilities and systems and testing so now the warehouse that we have here is about 10,000 square feet. We’ve been able to triple our space of occupancy in the past two years.”
“It’s been exciting to open up this location,” Hall said. “We already have a location in Conyers, just outside of Atlanta. Here in Gallatin, we were able to expand a little bit. We started out in a 3,000-square-foot warehouse about two years ago and we’ve added personnel, added capabilities and systems and testing so now the warehouse that we have here is about 10,000 square feet. We’ve been able to triple our space of occupancy in the past two years.”
Gallatin’s 10,000-square-feet is a perfect complement to Innovative Radiology’s 45,000-square-foot facility in Conyers Georgia, Hall added.
Gallatin’s 10,000-square-feet is a perfect complement to Innovative Radiology’s 45,000-square-foot facility in Conyers Georgia, Hall added.
Innovative Radiology provides high-quality imaging equipment and parts through a commitment to rigorous testing, sourcing, and service, ensuring healthcare facilities experience minimal downtime. With a culture
Innovative Radiology provides high-quality imaging equipment and parts through a commitment to rigorous testing, sourcing, and service, ensuring healthcare facilities experience minimal downtime. With a culture
built on integrity, collaboration, and excellence, the team takes an innovative approach to delivering reliable solutions and outstanding service. Hospitals and clinics can depend on Innovative Radiology for quality, speed and value.
built on integrity, collaboration, and excellence, the team takes an innovative approach to delivering reliable solutions and outstanding service. Hospitals and clinics can depend on Innovative Radiology for quality, speed and value.
The Gallatin space focuses on mammography and women’s health. The facility tests detectors for patient care to ensure they are fully functional when they leave.
The Gallatin space focuses on mammography and women’s health. The facility tests detectors for patient care to ensure they are fully functional when they leave.
The commitment to service and quality was apparent at the grand opening celebration as several customers were on hand and expressed excitement about Innovative Radiology’s growth.
The commitment to service and quality was apparent at the grand opening celebration as several customers were on hand and expressed excitement about Innovative Radiology’s growth.
Kristen Miller from Legendary Supply Chain, who has worked with Innovative Radiology for three years, stated that they are “one of our best partners” and expressed excitement for their 2026 growth.
Kristen Miller from Legendary Supply Chain, who has worked with Innovative Radiology for three years, stated that they are “one of our best partners” and expressed excitement for their 2026 growth.
Kim Roland from RSTI, a vendor and supporter of Innovative Radiology, expressed excitement for the turnout and the company’s expansion, particularly in mammography and other modalities.
The grand opening was also used as an opportunity to recognize “high achievers” and people who stand out, since “our people ... make IR successful,” Glas added. •
Kim Roland from RSTI, a vendor and supporter of Innovative Radiology, expressed excitement for the turnout and the company’s expansion, particularly in mammography and other modalities.
The grand opening was also used as an opportunity to recognize “high achievers” and people who stand out, since “our people ... make IR successful,” Glas added. •
For more information, visit innovative-radiology.com/
Scan the QR code to cast your vote


SPONSORED BY: INNOVATUS IMAGING

As ultrasound departments face rising exam volumes, increasingly complex patient populations, and heightened expectations around efficiency and staff well-being, the definition of a “best-in-class” system is evolving fast. For this Director’s Circle roundtable, ICE Magazine asked industry leaders to discuss what truly matters when evaluating ultrasound technology in 2026 — from image quality and AI assistance to ergonomics, serviceability and long-term value. Joining the conversation are:
• AdventHealth Ambulatory Imaging Center Clinical Manager of Ambulatory Imaging Services Lillian McGrier;
• Hartford Hospital/Bone & Joint Institute Ultrasound Manager Ashley Burke;
• Innovatus Imaging Vice President Sales and Marketing Matt Tomory; and
• University Hospitals Cleveland Medical Center Radiology Manager Jackie Knotek.
Q: WHEN EVALUATING ULTRASOUND SYSTEMS TODAY, WHAT FEATURES OR CAPABILITIES ARE TRULY “MUSTHAVES,” AND HOW HAS THAT CHANGED OVER THE PAST FEW YEARS?
MCGRIER: From a front-line ultrasound tech perspective, “must-have” features today are the ones that directly impact image quality, exam efficiency, patient comfort and tech ergonomics. Image quality that works on real patients, not just the ideal ones. We scan a lot more difficult patients than we used to: higher BMIs, sicker patients and limited mobility. Systems must deliver strong penetration, good contrast resolution and consistent performance across body types without forcing us to constantly fight the knobs. Advanced beamforming and AI assisted opti-
mization are helpful when they’re reliable, but only if they don’t slow us down or override our control.
Time pressure has increased everywhere. A must-have system today must be able to boot quickly, have customizable presets that actually stay saved, minimize keystrokes and menu digging, and use auto measurements and auto labeling without sacrificing accuracy. One of the biggest changes is there seems to be more awareness of sonographer injuries, and newer systems should support safer scanning. They should be lightweight, have well-balanced transducers, flexible monitor arms and adjustable height consoles. They should also use touchscreens or simplified controls to reduce the strain of repetition. If a system causes shoulder or wrist pain by the end of a shift, it’s not acceptable anymore, no matter how good the images look. Society of Diagnostic Medical Sonography (SDMS) emphasizes the importance of these considerations.
Probes take a beating. Must-haves include clear imaging without drop-out and cables that hold up over time and clean easily without destroying a probe. Frontline staff feel it immediately when a system is unreliable. Crashes, freezing or long service delays are dealbreakers. A must-have system is one we can trust in a full schedule with no backup room available. Connectivity with PACS, reporting systems and EMRs is expected. We shouldn’t have to enter patient data, fix mislabeled studies or chase missing images. Anything that creates rework ends up falling back on the tech. There is a change from “image quality first” to “workflow efficiency and ergonomics.” Five to ten years ago, image quality alone could win the conversation. Today, how the system fits into our day
matters just as much. With higher volumes and staffing challenges, ease of use and exam speed are no longer “nice to have,” they’re essential.
Automation and AI are now expected – but with caution. Automeasurements, view recognition, and AI assistance weren’t common before; now they’re expected baseline features. That said, frontline techs want tools that assist, not replace judgment. We trust automation when it’s consistent and transparent – and ignore it when it’s not. There’s more recognition of MSK injuries and burnout among techs. Systems are increasingly evaluated through the lens of “Can I scan on this for 8-10 hours a day, year after year?” That way of thinking is much stronger than it used to be. Older systems often required deep technical knowledge and heavy manual input. Today’s expectation is simplicity without sacrificing control.
The “must-have” ultrasound system today is one that: Produces reliable diagnostic images on real-world patients, helps us work faster without rushing patient care, protects our bodies and reduces fatigue, integrates cleanly into the clinical workflow, holds up under daily, high-volume use. If it doesn’t make a tech’s day easier, safer, or more efficient, it’s not truly a must-have anymore, no matter how advanced it looks on paper.
BURKE: Image quality has improved dramatically compared to even five years ago, and the top-performing systems are now much more comparable. Because of this, it’s increasingly important to evaluate the additional features and tools each system offers. For example, at our facility we perform a growing number of contrast-enhanced exams, and the quality varies significantly among vendors. When evaluating equipment, consider not only the exams you currently perform but also the services you may want to offer in the future. The technology available today can help expand your capabilities, elevate patient care and open the door to new clinical opportunities. In turn, this can support a more profitable department and enhance the care you provide to your community.
TOMORY: AI has certainly come a long way and is now standard on contemporary ultrasound systems. From exam flow to anatomy identification and analysis, it improves scan accuracy and speed while reducing the sonographer interactions with the controls. From a service perspective, I see access to diagnostics and service documentation as a must-have. Healthcare providers should have service options beyond the warranty period outside of the manufacturer if they choose to perform the service in-house or outsource to an independent service organization.
KNOTEK: The scan assistant is a great feature that we have on our GE machines. This aligns the tech to scan within the protocol parameters and in compliance with ACR guidelines. Another great tool is the use of contrast enhanced ultrasounds and elastography for specialty cas-
es. From an interventional radiology perspective, contrast and fusion ultrasound is a highly used tool that has been very beneficial to our patients and performance of our intricate procedures.
Q: FROM YOUR PERSPECTIVE, WHERE DO CURRENT ULTRASOUND SYSTEMS FALL SHORT? ARE THERE WORKFLOW, PERFORMANCE OR RELIABILITY CHALLENGES YOUR TEAM REGULARLY ENCOUNTERS?
MCGRIER: Color doppler is an area where more optimizations can be made. The use of AI while helpful still needs some improvement. From the front-line ultrasound tech perspective, current ultrasound systems have improved in many ways, but there are still clear gaps between how the systems are designed and how they’re used in real clinical environments. Many systems are called “workflow optimized,” yet there are too many important functions buried in menus, presets that don’t always stay customized the way we set them, and switching between exam types, patients or probes can be clunky. When schedules are full and add ons are constant, even small inefficiencies add up. If a system requires extra steps to do basic things like labeling, measuring, or adjusting depth and gain, the tech absorbs that time pressure, not the system.
AI-assisted measurements, auto optimization and view recognition are improving, but they’re not always reliable. Auto measurements may be off in technically difficult patients. As a result, many techs end up doublechecking or redoing the work, which cancels the time savings. Automation helps when it’s consistent, but when it’s not, it becomes another thing we must manage while scanning.
Current systems still struggle at times with higher BMI patients, patients who can’t hold their breath or follow instructions, and limited mobility exams. Even high-end systems can lose penetration or contrast in these situations, forcing us to compensate with longer scan times, more patient repositioning or repeated scans. The expectation hasn’t changed, though, we’re still expected to deliver diagnostic images within the same time slot.
While ergonomics have improved, many systems still fall short for techs scanning 8-12 hours a day. Not all consoles adjust easily once positioned; monitors don’t always rotate or lower far enough for seated scanning, and some controls require repetitive wrist or shoulder movements. These issues contribute directly to fatigue and musculoskeletal strain. Over time, that affects not just comfort, but career longevity, something frontline techs are increasingly vocal about.
One of the biggest frustrations is software freezes or lag, unexpected boots, and slow bootup times at the start of the day or between patients. When a system goes down, it immediately impacts patient flow, delays exams and increases stress. In many departments, especially outpatient imaging, there’s little to no buffer or backup room, so reliability is just as important as image quality. Probes remain at a pain point due to cable failures, intermittent signal dropout, and lengthy turnaround times for replacements. Even a single


probe issue can disrupt an entire day’s schedule.
The current ultrasound systems are powerful, but they’re still often designed with ideal workflows and ideal patients in mind. Front-line techs work in the opposite reality: high volume, staffing shortages, physically demanding exams and constant time pressure. From our perspective, the biggest opportunity for improvement isn’t adding more features; it’s making the existing ones work seamlessly, intuitively and sustainably for the people who use them all day, every day.
BURKE: We have identified several limitations in the vascular imaging performance of our current units. Visualizing slow flow is particularly difficult. Achieving consistent color flow and reliable spectral Doppler remains challenging even with optimized settings and support from our clinical applications teams. Additionally, penetration is insufficient for many patients with larger body habitus. While not all patients are ideal ultrasound candidates, there is a significant opportunity to improve image quality for this population.
TOMORY: Modern ultrasounds have come an exponentially long way in image quality, features, probe design and reliability – especially when compared to other imaging technologies. As mentioned previously, AI or as General Electric calls it, Intelligent Assist reduces sonographer repetitive motions which is critical for sonographer safety and career longevity. Probes are also getting lighter and more ergonomic which is a trend I would like to see continuing – again for sonographer health and safety.
KNOTEK: Our current ultrasound machines are highly functional and utilized for every need that we see in a Level 1 trauma facility. Workflow issues tend to fall under the volume within the department and triaging the ED, ICU and outpatient exams. This is when it is very important to have a strong team like the one at CMC to come together and do what is best for our patient care.


Q: IMAGE QUALITY HAS ALWAYS BEEN CRITICAL, BUT WHAT OTHER FACTORS NOW CARRY EQUAL OR GREATER WEIGHT IN PURCHASING DECISIONS, SUCH AS SERVICE SUPPORT, UPTIME, SOFTWARE UPGRADES OR TOTAL COST OF OWNERSHIP?
MCGRIER: Service support and quality in timely responses, upgrades included in original cost and transparency in pricing all impact purchasing decisions. Workflow efficiency and ease in use should be considered. Systems need to help us work faster without forcing more advanced critical thinking on the tech’s part. Ergonomics and tech safety are major issues to be considered. We recommend techs look at console height and monitor adjustments, weight of probes, controls that decrease repetitive wrist movements and shoulder strain, and the ability to be seated and other scanning positions. Systems must be reliable under real-world, high-demand conditions. Other considerations should include solid integration into PACS, EHR, minimal data entry, and accurate data/demographic transfer. We now assume there will be AI and automations, but they need to be transparent and consistent. Patient variability such as BMI, mobility issues, patients who cannot hold their breath, and inconsistent penetration and contrast directly affect scan time and image quality. From an ultrasound tech’s perspective, does the system make their day easier, safer and efficient every time we use it? If the system doesn’t meaningfully improve the tech’s daily work, it’s no longer considered a strong purchase decision.
BURKE: We are fortunate to have an exceptional onsite biomedical team that is highly knowledgeable about our equipment and understands the importance of rapid turnaround times. Clinical application support is equally essential. We rely heavily on our clinical applications specialist to help us optimize our imaging and ensure we are consistently producing the highest quality images possible. This collaboration involves ongoing feedback and feedforward communication, which strengthens our ability to troubleshoot and improve performance. While I strive to be well versed in the functionality of our units
so I can make necessary adjustments onsite, having accessible, responsive support remains critical. This level of support is not only necessary during installation of new systems but also whenever new challenges arise or updated software becomes available. Additionally, cost considerations cannot be overlooked. It is important that software upgrades and probe replacements are built into our contracts to ensure we remain fully covered and operational without unexpected financial burdens.
TOMORY: Contemporary ultrasound systems are all excellent in many areas and there is almost a parity when it comes to image quality. What is critical to look at are long-term features needed, service and probe repair support, and software support. Here we need to differentiate between software updates and upgrades. Updates are critical to system reliability, safety and cyber protection and need to be provided by the OEM regardless of warranty or contract status. Upgrades are added features that are optional but can be very expensive post sale so plan ahead on what you need now and down the road. Regarding service, HTM departments are becoming more involved in purchasing decisions due to their unique perspective. The availability of diagnostics, service manuals, “magic decoder rings” to access service software and probe repair support are all critical when evaluating the total cost of ownership. Probe repair capabilities are also critical. The OEMs continue to change the technology in their probes. One example is the new micro-connector and micro-coax that GE, Philips and Siemens started using. This technology will obsolete current probe repair service models. We at Innovatus have developed exclusive processes and instruments on these seemingly impossible probes to repair.
Q: HOW DO YOU APPROACH TRAINING AND ADOPTION WHEN NEW ULTRASOUND TECHNOLOGY IS INTRODUCED, AND WHAT ROLE DO VENDORS PLAY IN MAKING THAT TRANSITION SUCCESSFUL OR UNSUCCESSFUL?
MCGRIER: Hands-on, exam-based training is more effective than classroom overview or feature demonstration. If we can’t immediately translate what we’re seeing in training to a live patient schedule, adoption may be slower. It is an advantage to introduce new systems while full patient load volumes continue, in parallel with on-site vendor support. Techs learn best from each other. Having a super-user and/or subject matter expert in addition to vendor support helps by sharing practical tips that vendors may not have highlighted and help translate features into how it helps the tech finish the exam on time. Vendors who focus on everyday exams and do not showcase features, address difficult patients (high BMI, limited mobility, poor breath hold) and explain when NOT to use certain features, earn credibility with techs. Vendors should be avail-
able beyond the go-live date. They should return within weeks and months when issues arise. They should be expected to assist in optimizing presets after clinical use and continue providing ongoing education. Also critical is listening to tech feedback such as what is slowing them down and what features they are ignoring and why.
What vendors do that make an unsuccessful install are training each location as if it is the same as all other settings and companies, having limited support after golive, excessive focus on features versus workflow impact, slow response to software or equipment issues, and restricting customization.
BURKE: With our high exam volumes and the varying schedules of our technologists, coordinating training can be challenging, but it is essential. We make sure every staff member receives adequate one-on-one time with the clinical applications specialist. On training days, we adjust room assignments to support technologists’ learning and ensure they have the time and space to focus. I also ask that my lead technologist be present for nearly every exam during applications training so they can continue developing as a subject matter expert and superuser. Additionally, I request that the vendor hold a brief huddle with the team at the start of the day, or during lunchtime, to provide background information, reinforce key updates, and answer any immediate questions. We ensure that there are multiple days of training and that we schedule follow-ups to cover any lingering questions or concerns.
TOMORY: A good applications specialist is critical to training when purchasing a new ultrasound platform or adding features to an existing one. My wife, a highly credentialed sonographer and ultrasound social media star (www.sonoeyesultrasound.com), was recently hired as a GE applications specialist and the training is very rigorous. Passion and extensive knowledge from the OEMs are critical to maximize the performance and usability of a new ultrasound system.
KNOTEK: Vendors and application specialists play a very important role for training. They allow for multiple days and make sure that all techs are properly trained to feel comfortable.
MCGRIER: The implementation of AI will impact patient care and departmental efficiency; however, it is important for new grads to still understand how to optimize without the use of AI, and to have an understanding of physics. As AI expands, the impact will depend on consistency and trust in the product. We need more accurate auto-measurements and auto-labeling on technically difficult pa-
tients. AI should adapt to high BMI, poor breath holds and limited mobility. The ability to override AI should be available. Exam times can expect to decrease under reliable AI. We should expect more consistent studies across all tech experience levels. New techs will still need to understand physics and image optimization. Small fixes in repetitive workflow pain points will help techs have a cleaner exam from start to finish with fewer steps for labeling, measurements and reporting. When the schedule is packed, saving 30-60 seconds per exam adds up. Less work means fewer delays, corrections and stress on the techs.
We should expect to see improvements with stronger penetration and contrast in high BMI patients, more stable color Doppler and spectral Doppler under difficult conditions, and better image quality when patients are unable to follow instructions. This means patients can expect fewer scans, shorter exam times and less patient repositioning and discomfort.
Over the next 2-3 years, the biggest impact will come from technology that aids techs in working faster without rushing patient care, performs consistently on patients, protects the tech and reduces burnout, is integrated seamlessly into daily workflow and supports clinical judgement, not replace it.
BURKE: With our high exam volumes and the varying schedules of our technologists, coordinating training can be challenging, but it is essential. We make sure every staff member receives adequate one-on-one time with the clinical applications specialist. On training days, we adjust room assignments to support technologists’ learning and ensure they have the time and space to focus. I also ask that my lead technologist be present for nearly every exam during applications training so they can continue developing as a subject matter expert and superuser. Additionally, I request that the vendor hold a brief huddle with the team at the start of the day, or during lunchtime, to provide background information, reinforce key updates, and answer any immediate questions. We ensure that there are multiple days of training and that we schedule follow-ups to cover any lingering questions or concerns.
TOMORY: AI will continue to evolve to the point where a system will perform sweeps through anatomy and then dissect for diagnoses and analysis. This does not mean a highly trained and credentialed/registered sonographer will be replaced by the system, but it will assist to improve exam accuracy, speed and sonographer safety.
Q: IF YOU COULD OFFER ONE PIECE OF ADVICE TO PEERS EVALUATING OR UPGRADING ULTRASOUND EQUIPMENT IN 2026, WHAT WOULD IT BE?
MCGRIER: Be open to doing a lot of research and making decisions based on the consistency of the vendors. Hav-
ing a clinical ultrasound team member and radiologist involved in the decision can help with cost savings in purchasing the technology that will be used. I recommend evaluating the system under real clinical conditions and listening to the technologists who will use it every day. Decisions should be made based on how the system works in the hands of the ultrasound techs and the physicians reading the exams. If you trust the ultrasound tech’s feedback and evaluate the system under real conditions, your decision should hold up long after installing.
BURKE: Be critical. When trialing new units, ask detailed questions, test them on challenging patients, and know the image quality standards you expect. Stay open to vendors you haven’t worked with before, you may even find value in having multiple manufacturers represented within your department. Even if you decide not to move forward with a purchase, your honest, constructive feedback helps advance the field and pushes vendors to continue improving. Remember, they want your business, make them earn it.
TOMORY: Plan on supporting the new system for an average of seven years – what do you need to support the system and probes after the warranty expires? Probe repair for high technology probes and service options for the platform are critical.
KNOTEK: It is important to think outside of the box with new technology and future state for the department. Ultrasound is always advancing and although you may not see a need for the technology presented at the time, it is a great opportunity to advance not only the skills of the techs but also broaden the department and increase patient experience. •
This month’s article was sponsored by Innovatus Imaging. For more information on this company, visit innovatusimaging.com.


STAFF REPORT
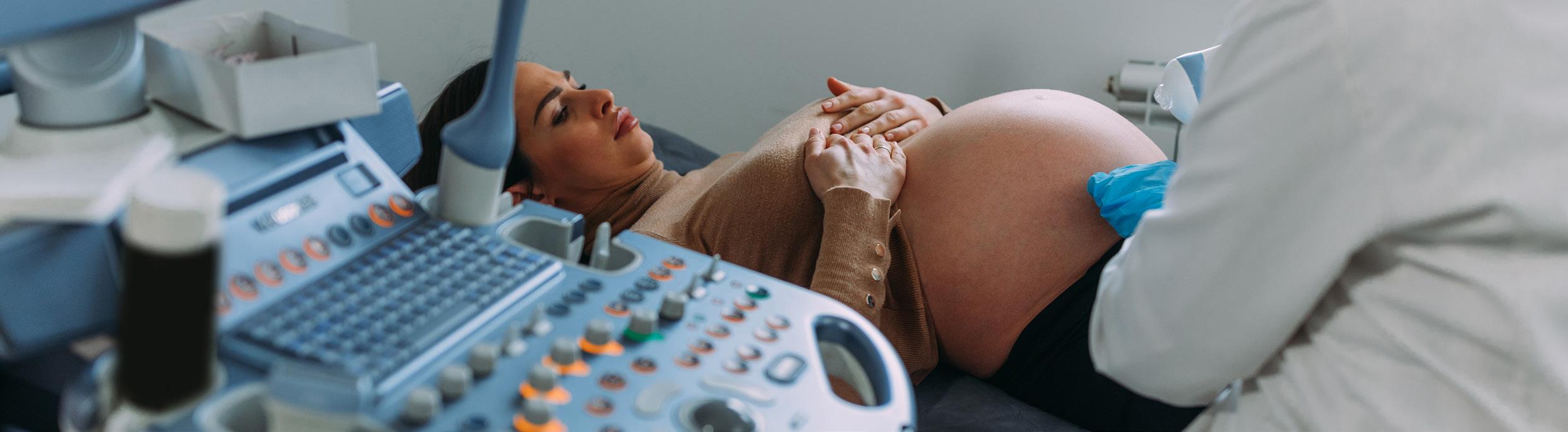
Th e ultrasound devices market will grow at a CAGR of 6.2% during the forecast period 2024-2031, according to DataM Intelligence report.
The report highlighted recent industry developments in the United States, including:
• In October 2025, GE HealthCare expanded its U.S. portable ultrasound production with the new Vscan Air SL featuring AI-powered cardiac and lung assessment, partnering with major hospitals to improve point-of-care diagnostics by 22% in emergency departments.
• In September 2025, Philips launched the EPIQ Elite ultrasound system with advanced 3D/4D imaging certified for obstetrics, targeting women’s health clinics via e-commerce platforms amid rising demand for high-resolution fetal monitoring.
• In August 2025, Butterfly Network introduced the Butterfly iQ3 handheld ultrasound with extended battery life and cloud connectivity, compliant with FDA guidelines and distributed through Amazon for remote and telemedicine applications.
In addition, the report states that “the global ultrasound devices market is thriving” because of surging demand for non-invasive, real-time imaging amid rising chronic diseases, expanding applications in obstetrics, cardiology, radiology, and point-of-care diagnostics, and increasing awareness around early detection and portable solutions. Key trends mentiond in the report include innovation in technologies (e.g., AI-powered image enhancement, wireless handheld probes, 3D/4D imaging), growth in portable and compact formats (point-of-care ultrasound for emergency and rural settings), and increasing adoption in emerging markets (affordable color Doppler for maternal health). The rise of telemedicine, premiumization in advanced imaging, and regulatory pushes for safety and accessibility (FDA 510(k), CE marking) are significantly accelerating market expansion amid shifting healthcare preferences for efficient, cost-effective and high-resolution ultrasound solutions.
The market is moderately consolidated among North American, European, and Asia-Pacific producers, with intense
competition in AI integration, portability and image quality.
Precedence Research reports that the global ultrasound market size was calculated at $10.06 billion in 2024 and is predicted to increase from $10.80 billion in 2025 to approximately $20.21 billion by 2034, expanding at a CAGR of 7.23% from 2025 to 2034. The rise in the number of diagnostic centers and hospitals is driving the growth of the ultrasound market.
It also states that the U.S. ultrasound market size was exhibited at $3.30 billion in 2024 and is projected to be worth around $6.78 billion by 2034, growing at a CAGR of 7.47% from 2025 to 2034.
North America dominated the ultrasound market in 2024. The market growth is generally driven by the rising prevalence of target diseases, the growing trend of cosmetic surgeries, and increased healthcare spending by the private and public sectors. Moreover, new research developments and innovations in the medical field, along with new approvals from the United States Food and Drug Administration and the launch of new products by key market players such as Mindray, Butterfly, GE, Medtronic, Siemens and others.
In North America, the U.S. led the market owing to the growing adoption of point-of-care ultrasound along with ongoing technological innovations. Also, heavy private investments in healthcare infrastructure and government funding are major factors contributing to the country’s growth. Major market players in the U.S. are Siemens Healthineers AG, GE HealthCare, Koninklijke Philips N.V., and Canon Medical Systems.
Grand View Research reports that the global ultrasound devices market size was estimated at $9.79 billion in 2023 and is anticipated to reach $13.07 billion by 2030, growing at a CAGR of 4.24% from 2024 to 2030. The market growth is poised to be driven by the rising usage of ultrasound equipment for diagnostic imaging and treatment, along with the increasing prevalence of chronic and lifestyle disorders.
The global point of care ultrasound market was valued at $4.2 billion in 2025 and is projected to grow from $4.5 billion in 2026 to $8.4 billion by 2035, expanding at a CAGR of 7.2%, according to the latest report published by Global Market Insights Inc. The steady growth of the market is driven by the increasing prevalence of chronic diseases, advancements in point-of-care ultrasound technology and a growing geriatric population base. •
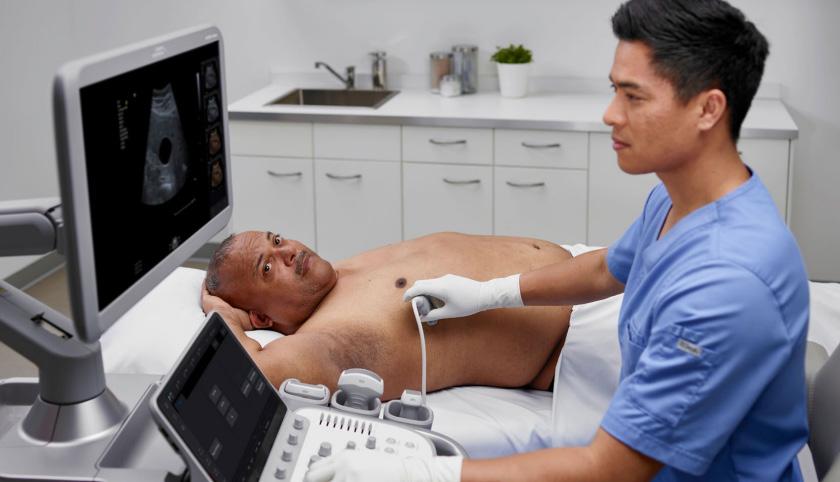
The latest release of ACUSON Juniper, a Siemens Healthineers ultrasound system, now features the ACUSON Liver Suite to enable early detection and routine monitoring, making it suitable for population-level MASLD screening. With ACUSON Juniper, clinicians can make fast, non-invasive assessments in just one minute.1 Integrated UDFF and pSWE technologies give reliable, actionable insights to identify and monitor liver disease early –enabling proactive, efficient care for every patient.
Clinically validated ultrasound solutions give healthcare providers the confidence to see more, act sooner and deliver better outcomes. ACUSON Juniper delivers consistency and confidence in every result with a portfolio of imaging tools for liver care including:
• Ultrasound-derived fat fraction (UDFF) to quantify hepatic fat
*Disclaimer: Products are listed in no particular order.
in good agreement with MRI-PDFF for MASLD screening
• pSWE to quantify liver stiffness to assess chronic liver disease
• Contrast-enhance ultrasound (CEUS) for enhanced lesion characterization
• Needle visualization for safe, precise targeting during liver biopsies and interventions
• Single crystal transducers for improved penetration with high resolution
With ACUSON Juniper clinicians can detect steatosis and assess its progression – non-invasively, at low cost and at scale, unlocking the potential to reverse liver disease and improve global health.
1 Data on file
Canon Medical Systems offers a complete line of ultrasound systems, including its ultra-premium Aplio i-series Prism Edition systems. Built on a common architectural platform, the Apio i-series line offers industry leading imaging depth and detail, matrix array transducers, and “smart” workflows and HealthySonographer ergonomics for a confident and efficient imaging experience.
Key features of the Aplio i-series Prism Edition line include:
• Imaging depths up to 50cm (transducer specific)
• Ultra-high resolution detail with high frequency transducers, including 24 & 33MHz
• iBEAM+ parallel processing beamforming
• Advanced imaging with Full Focus, Panoramic, Ultra Wide View, SMI, Smart 3D and Reference Imaging
• Smart workflow with Protocols, Smart 3D, Reference Imaging, advanced breast and quantitative liver tools packages
• HealthySonographer ergonomics, lightweight probes an enhanced mobility
• Advanced communication tools ApliGate and ApliCam for remote viewing, teaching and service


The next evolution of the Venue family introduces artificial intelligence (AI)-enabled and digital tools designed to boost confidence and efficiency at the point of care. Among these tools is Nerveblox, an AI-enabled feature that automatically labels anatomical landmarks in ultrasound images, designed to help clinicians feel confident during the peripheral nerve block procedure and streamline the workflow. The latest Venue family ultrasound systems also feature advanced imaging modes, and AI-enabled and digital tools that aim to simplify the scanning process, enhance speed and accuracy during assessments and decision making, including:
• Contrast Enhanced Ultrasound, an advanced imaging mode that enables dynamic bedside evaluation of abdominal inju-
ries and lesions and supports cardiac assessments.
• Automated Function Imaging provides objective analysis of myocardial strain across heart chambers. In addition to the existing Caption Guidance AI-enabled software, which provides turn-by-turn, on-screen guidance to help expert and non-expert users capture diagnostic-quality cardiac ultrasound images.
• Auto Bladder Volume, which simplifies urinary bladder volume measurement from two views, reducing exam clicks. This feature is also now available on the wireless Vscan Air CL probe that can also connect to the Venue family systems.
• Gastric Measurement to calculate the gastric cross-sectional area, volume and the volume-to-weight ratio.
The ARIETTA 750 DeepInsight (DI) ultrasound system is designed to provide superior image quality, excellent noise reduction, stable penetration and high spatial resolution. The DeepInsight cognitive technology powering ARIETTA 750 DI provides improved clarity at depth, making it easier to visualize structures even in a difficult body habitus. The ARIETTA 750 DI combines the advanced Variable Beamformer with a suite of novel features designed to improve resolution and reduce noise at all depths. In addition, a variety of efficiency tools based on automated image analysis and protocol-based operation accelerate the scanning process, automatically performing routine actions, so the sonographer does not have to. For example, the system’s eFocusing focal-free scanning provides homogenous image quality and improves sensitivity for both near and far field screening. Tissue structure clarity is further enhanced through Carving Imaging, based on Fujifilm’s advanced image processing technology. Together, these technologies ensure high image quality and consistency for both routine and complex examinations, ultimately contributing to faster diagnoses. Supporting a large selection of probes for both diagnostic scanning and therapeutic guidance, the ARIETTA 750 DI can help take provider’s ultrasound capabilities to the next level.
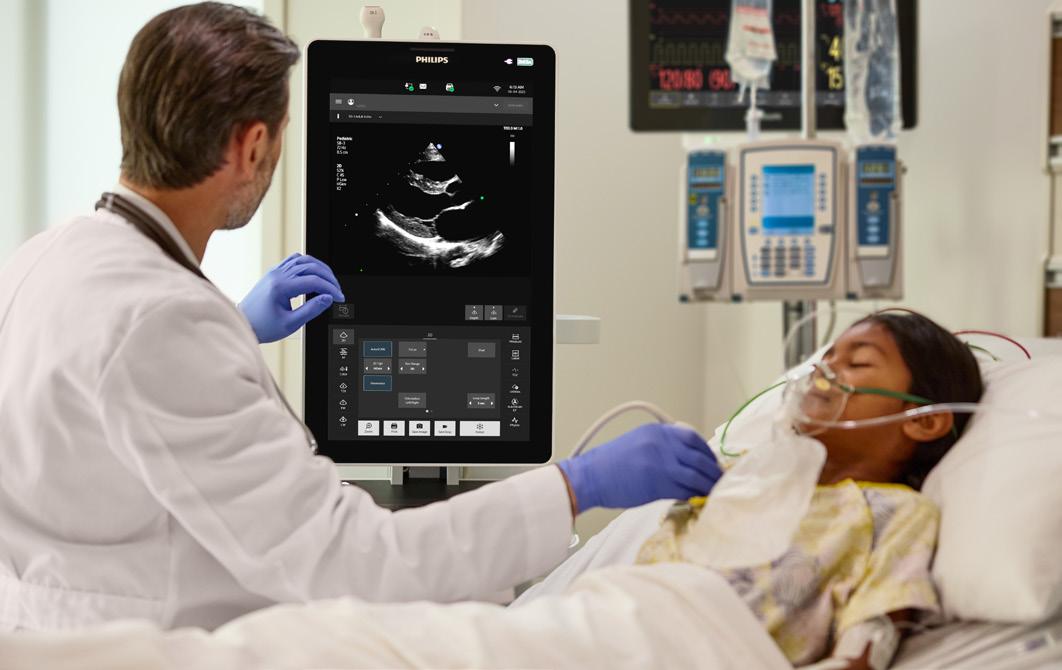
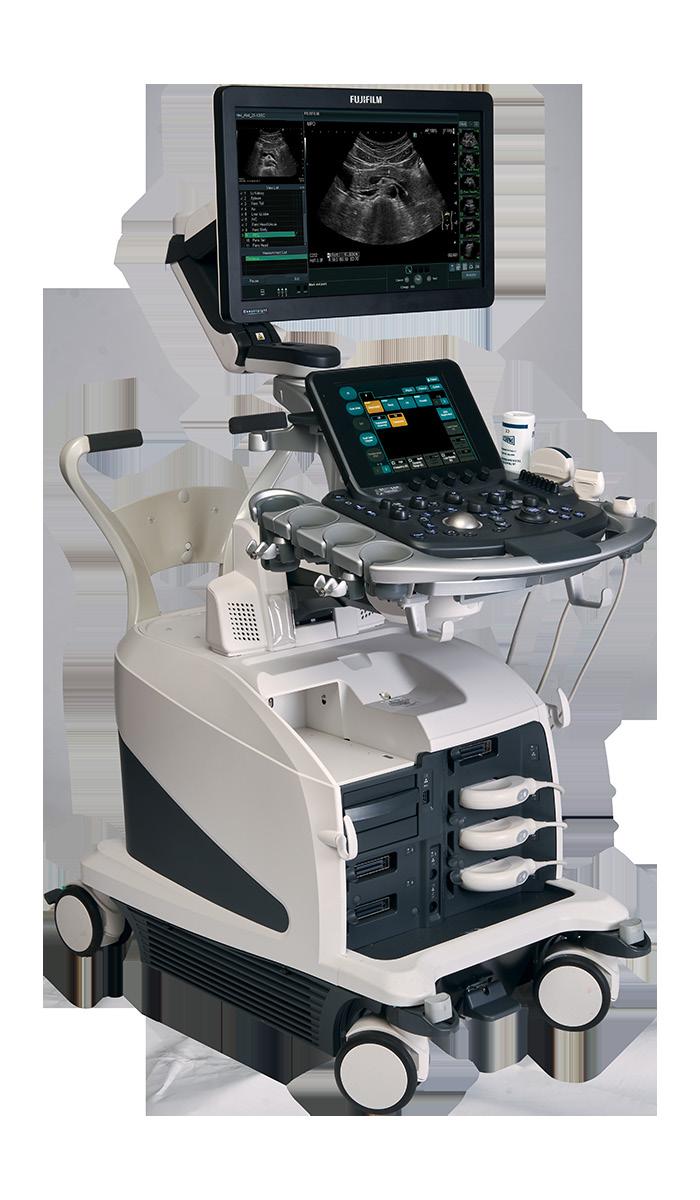
The Flash Ultrasound System 5100 POC is a breakthrough point-of-care (POC) ultrasound system engineered for the fast-moving needs of anesthesia, critical care, emergency medicine and musculoskeletal imaging. Built on Philips’ established foundation of cardiology and general imaging ultrasound technology, Flash 5100 POC combines exceptional image clarity, smart automation and intuitive touchscreen controls in a highly portable system that supports rapid, confident decision-making for users of all experience levels. Its encounter-based workflow enables clinicians to perform and document exams in real time, without waiting for formal orders, making it ideal for high-pressure environments like the ER, ICU and trauma units. As healthcare systems face mounting pressure from staff shortages, rising patient volumes, and the need for faster, more flexible care delivery, pointof-care ultrasound is increasingly vital.
The Philips Flash 5100 POC is designed for precisely these environments, where time, clarity and precision can make all the difference. Combining high performance with true portability and seamless interoperability, the system enables clinicians to make confident decisions at the bedside or on the move. With built-in support for Philips tele-ultrasound solution, Collaboration Live, clinicians can also connect with remote colleagues in real-time, sharing screens, images and guidance instantly. The new Flash 5100 POC system marks a bold step forward in meeting the growing demand for fast, agile, high-performance POC ultrasound imaging in POC settings.
The Universal Probe from Vave Health is the world’s first wireless, handheld, whole-body ultrasound powered by a single PZT transducer. It is designed to be simple, portable, affordable, and patient-centric, enabling imaging at the point of care for timely and accurate diagnoses. The Vave ecosystem enables clinicians to capture high-quality ultrasound images, share them instantly through a secure cloud platform and collaborate efficiently. This approach supports faster decision-making, streamlined workflows and improved access to care. Built for versatility, the Universal Probe supports multiple scanning applications, including cardiac, abdominal, lung, bladder, OB/GYN, musculoskeletal, vascular, and soft tissue imaging, across a range of clinical settings. Advanced imaging technology ensures clarity and consistency across applications, while AI-driven features assist with interpretation, enhance diagnostic confidence and reduce variability in care. These innovations aim to make ultrasound more accessible for clinicians and patients in diverse environments, from routine exams to critical care situations. By combining wireless portability, multi-application capability and intelligent tools, the Universal Probe simplifies ultrasound delivery and supports better outcomes for clinicians and patients. •


• A niche job board for the HTM and imaging communities powered by TechNation.
• 3,800+ actively looking biomedical and imaging professionals.
» Completely free and confidential registration and application process.

Featured Employers: Agiliti, Block Imaging, Intelas Health, Renovo Solutions, TRIMEDX, and more!
htmjobs@mdpublishing.com for posting inquiries htmjobs.com to register today
• The fastest growing HTM talent network in the country.
• 350+ open opportunities throughout the United States.
» A variety of posting options ranging from single-job postings to 12-month unlimited memberships.

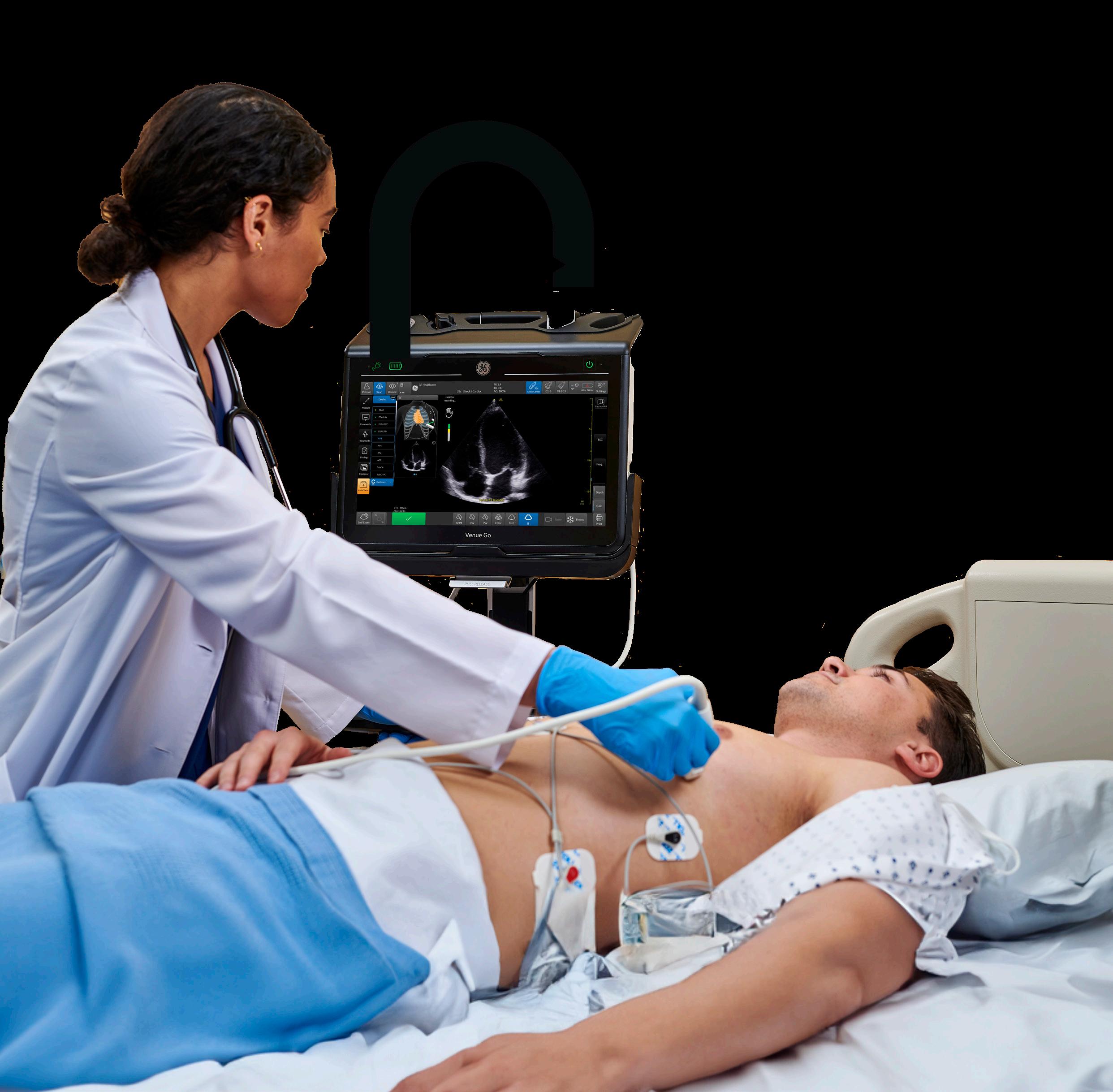
BY MATT SKOUFALOS
With study volumes continuing to climb – along with wait times in patient scheduling and staffing shortfalls that don’t show signs of self-correction – health systems are seeking more and different ways to increase access to medical imaging services without dramatically elevating costs. In the past decade-plus, diagnostic ultrasound has emerged as a fairly ubiquitous, low-barrier option with an increasing number of use cases. As the medical imaging industry works to address its capacity issues, practitioners are finding that ultrasound represents a versatile firstread option for more and different care environments.
Kassa Darge, radiologist-in-chief and chair at Children’s Hospital of Philadelphia (CHOP) and a professor of radiology and surgery at the Perelman School of Medicine at the University of Pennsylvania, said ultrasound technology is particularly suited to pediatric patients in ways that other modalities may not be.
For a start, it helps parents and practitioners avoid exposing their children to the ionizing radiation of computed tomography (CT) scanners, the requirement to hold a specific position that magnetic resonance imaging (MRI) demands, or exposure to sedation or anesthesia as a condition of such studies. Unlike either of those modalities, parents can sit with their children for an ultrasound, and even help to position them under the guidance of a sonographer. Pediatric institutions like
CHOP even warm the transducer gel before applying it to the patient for an added level of comfort, Darge said — a step that’s not typically taken in caring for adult patients.
When a study does call for the use of contrast agents, recent implementation of contrast-enhanced ultrasound has mitigated the potential of contrast adverse events in children, and is even safe to be used in patients with reduced kidney function.
“It has opened new doors for ultrasound that make it possible to diagnose many issues without MR and CT, sedation, radiation and less safer contrast agents,” Darge said. “Additional advanced ultrasound modalities enhance our possibilities, including being able to measure organ stiffness or fat content; things that were done with MRI before.”
In addition to those applications, computing processes powered by artificial intelligence (AI) support automated organ measurement and volumetric calculations, as well as workflow enhancements that im prove repetitive processes and make
“For pediatrics, this enhancement is not just measuring an organ, but making the study faster –which, in the case of a restless child, is really a positive.”
KASSA DARGE
enhancement is not just measuring an organ, but making the study faster –which, in the case of a restless child, is really a positive,” he said. “Some
manufacturers have added pathology-recognizing AI applications; having such an application for a child that’s crying and moving is a huge additional advantage.”
Tele-ultrasound can offer new options for practices that are expanding. CHOP’s pediatric radiology services are available at 12 sites in New Jersey and Pennsylvania, with future expansions planned into Delaware. Additional ultrasound studies from those remote sites hit the workflow queues at CHOP, and there’s less oversight over how they’re conducted from the centralized radiology department.
The promise of tele-ultrasound would allow radiologists to see the images in real-time during the scan, and even speak directly with the sonographer – advantages that can be consolidated further with the addition of a robotic scanner arm that can be directed remotely by an offsite practi

multisite radiology operations in a way that that will reduce the impact of the skilled labor shortage in the imaging field at present.
“It’s very hard to put a pediatric radiologist in every satellite site where there are pediatric patients,” Darge said, “but you do need experienced personnel; the machine will not do it all alone.”
Point-of-care ultrasound (POCUS) remains a growth area throughout the field, including at CHOP, allowing for bedside imaging without the need for a large, wired, scanning device. Its continued advancement, which is being driven at the point of clinical education from whitecoat ceremonies to specialized sonography training, allows patients to get their initial ultrasounds “right where they need it,” Darge said, whether for procedural or diagnostic purposes.
“In low-resource countries, the impact of ultrasound is much more significant,” Darge said. “Access to CT and MR is very limited, so radiologists maximize the use of ultrasound. That’s something we should not forget: every advancement of ultrasound that we do here has a global impact.”
Hannah Simmons is director of product for Inteleos, the non-profit organization that oversees the American Registry for Diagnostic Medical Sonography (ARDMS) the Alliance for Physician Certification & Advancement (APCA), and the Point-of-Care Ultrasound Certification Academy.

able to translate in their day-to-day practice,” she said.
“There’s no technology for the sake of technology only. It must expand access to care outside the hospital, and improve the standard of care.”
Simmons said that her organization sees a lot of global growth for POCUS in less-regulated, less-standardized spaces. The challenge from there remains finding the best ways to integrate this newer tool within established institutional and societal protocols.
JOCELYNE
MEKONTSO
Adding contrast-enhanced ultrasound to the national sonography curriculum is one example of the industry finding ways to build processes that support existing use cases, Simmons said. Most hospitals can offer contrast-enhanced ultrasound, but break up the responsibilities for administering contrast agents, capturing images and reading studies across multiple professionals’ roles. Advanced credentialing must accompany meaningful changes to adjusted scopes of practice in day-to-day operations to help maximize patient access to such services. Some of these shortfalls can be overcome by technology, but Simmons pointed out that many of them can be addressed interpersonally, too.
“As we have more people using ultrasound, clear competency expectations can help translate training into practice as hospitals adapt workflows to support broader ultrasound use. It’s one thing to incorporate into sonography training programs, but it’s quite another thing to have hospitals shift their workflows to accommodate these skills that practitioners are acquiring,” Simmons said.
“We can provide this up-skilled certificate program, but it’s not as important to practitioners to do this in a formal way until it’s going to be
“Hands-on training is easy to come by in hospitals, and that’s what we find a lot of people are doing,” she said. “AI support is still evolving, but technology in general helps to make it so that we don’t need the expert right beside you. You could message your mentor, your colleague, while out in the field; mentor-mentee relationships help to close that diagnostic gap with complicated cases.”
Along with the expanded access to services that POCUS and broader adoption of ultrasound applications provides, healthcare institutions must also help provide the capacity to support action on study findings. These
“It’s so important that the whole patient care is considered. People have to have the ability to act on the right technology, resources, safety and health regulations.”
HANNAH SIMMONS
challenges may be more pronounced in rural and distributed areas, where, if a study identifies something that must be resolved, the institution must have the capacity to address it.
“You need to make sure that you have the capacity, the resources, even the workflow in place to act on that,” Simmons said. “It’s so important that the whole patient care is considered. People have to have the ability to act on the right technology, resources, safety and health regulations.”
Patient access to ultrasound will always be contingent upon practitioners’ access to meaningful, standards-based training, and in the push to ramp up trained sonographers to address increased study volumes, Inteleos is working to deliver supplemental training through virtual reality (VR) and augmented reality (AR) education.
“It sounds counter-intuitive, but if we want to continue to provide good, strong education, and people aren’t seeing certain cases, this is a way to get more people trained in ultrasound,” Simmons said. “We’re not only using AI and new technologies for procedural assistance, but
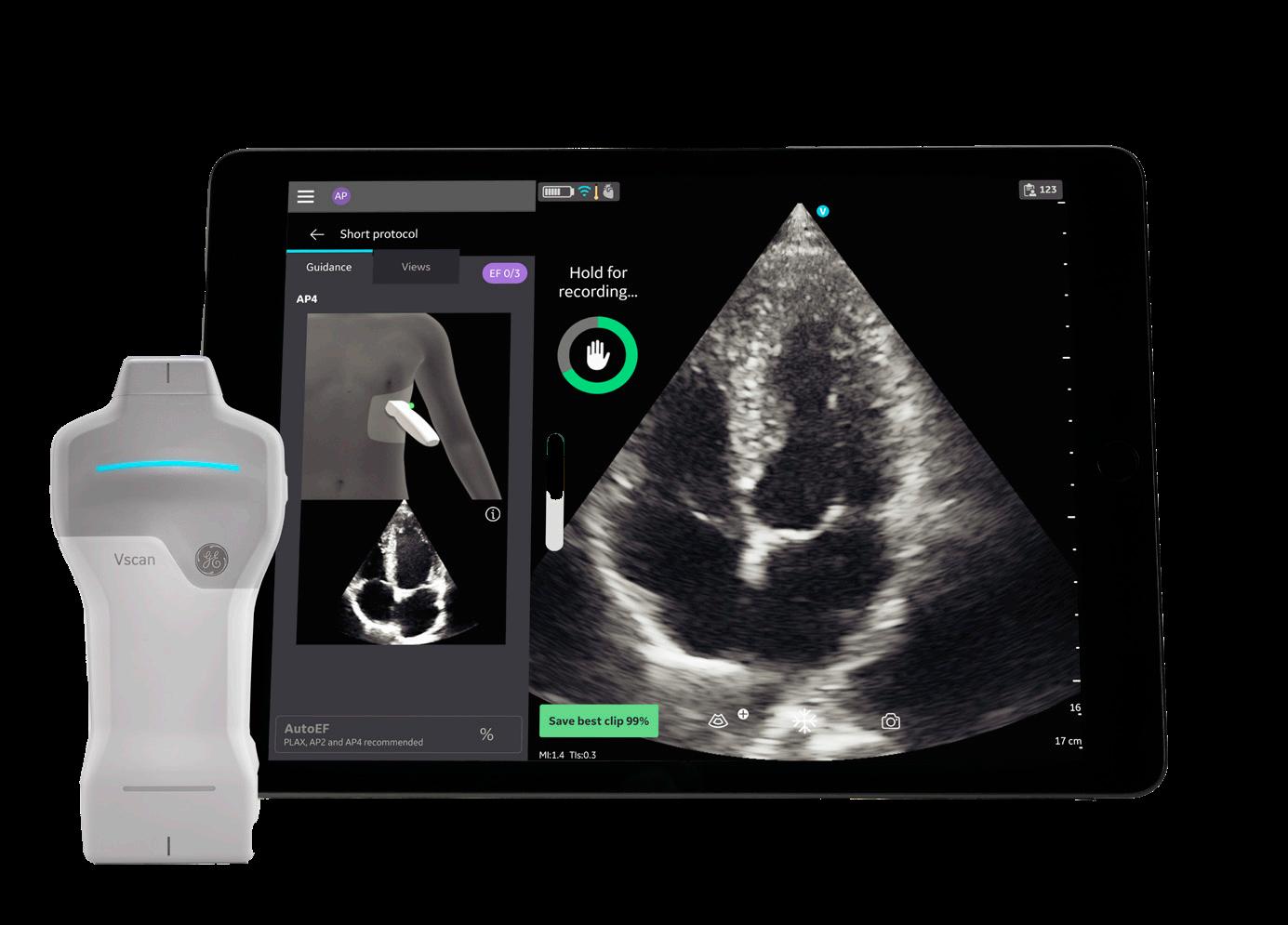
also to make education and training more scalable, so more practitioners or students are able to see different types of things in the field.
“We all care about patient safety,” she said. “That peer-to-peer mindset gets increasingly more important as we learn things here around the globe. Making sure that our findings are shared globally is so important; connecting people with regional health hubs across the world. The more partners we can have to improve patient care, the better it will be.”
As president and chief commercial officer of ultrasound probe manufacturer Vave Health of San Jose, California, Timothy Kartisek is bullish on the growth potential of POCUS, particularly when paired with AI-powered technologies and in global market settings.
Since its soft launch in the spring of 2025, Vave Health has sought to make inroads at some of the lowest levels of direct patient care with its universal probe. Kartisek described prospective customers in emergency medical services (EMS), sports medicine, rural healthcare, and
sub-acute settings, all the way up to medical-surgical areas and frontline medicine in developing markets.
“Our organization was designed to create a device that offers a universal approach to imaging: whole-body ultrasound,” Kartisek said. “We’re using transducers made from PZT crystals, and designing this product to be used in the front lines of healthcare.”
Companies like Vave are looking to compete in the spaces between those filled by larger competitors by building an ultrasound device that doesn’t rely upon wired networks, cart-based systems or physicians’ credentials. It’s designed to be high-quality but low-cost, “scalable without adding a ton of friction to the places it’s being deployed,” Kartisek said.
“We’re excited that more and more people are getting trained on how to use this technology to provide a frontline level of care,” Kartisek said. “We’re creating very specialized workflows dictated to us from the providers. We’re talking to users on the front lines of Africa, Asia, on the battlefield – places that are not typically a customary spot for ultrasound to be done – and layering AI on top of it.”
Kartisek wants Vave to help practitioners to “deliver a first look through ultrasound,” addressing “speed to care” through AI-managed data sets that source study data across health systems to help build workflows that trigger protocols based upon users’ real-time results.
“We’re increasing throughput because we’re able to scale patients, rank the levels of how quickly they need care, and drive down costs,” he said. “We’re really trying to help the health system, help the provider, learn what’s going on with the patient so they can discharge the patient or get them care quicker.”
“The winners in this are not going to be the people with the flashiest demo or the biggest number of sales reps out there,” Kartisek said. “They’re going to be the guys that can take POCUS and make it deployable at scale inside health systems and ministries of health around the world at the lowest cost possible. Our goal is that 10 years from now, we have advanced POCUS so far that if you see a monitor in a room that provides patient care, you see an ultrasound device bolted to the side of it.”
Jocelyne Mekontso, head of diagnostic ultrasound at Siemens Healthineers, said that her company has been most focused on closing gaps in access to diagnostic imaging by automating mundane operational tasks with practical AI. Such technologies can improve conditions for clinicians that frees them up to focus on patients’ needs, whether by reducing operators’ hand movements to cut back on stress-related injuries and minimize repetitive tasks, or by automating workflow to improve the speed and ease of exams.
In addition to serving clinicians, however, diagnostic imaging inno vations continue to represent a vital component of improved patient care, Mekontso said. Advanced ultrasound solutions particularly support in creased patient access to care not only through diagnostic applica tions, but also through interventional means, whether guiding biopsies, delivering other therapies or support ing follow-up care.
“I can now see diagnostic treat ment in the middle of intervention,”

“Our goal is that 10 years from now, we have advanced POCUS so far that if you see a monitor in a room that provides patient care, you see an ultrasound device bolted to the side of it.”
TIMOTHY KARTISEK

she said. “If we can shorten that cycle for patients, make sure we provide the right care, I think ultrasound will allow us to really be part of the full continuum of care for the patient, depending on the disease state that the patient is being evaluated for.”
Another major policy change supporting expanded use of contrast-enhanced ultrasound – which Mekontso said she’s anticipated for two decades – involves the recent doubling of the CMS reimbursement rate for non-cardiac, contrast-enhanced ultrasound.
“This is also where the policymakers are seeing how beneficial ultrasound could be,” she said; “how economically viable for institutions and also the patient.”
Most of all, ultrasound — like any imaging modality — is only as significant as the ways in which it’s deployed, and the skill with which its operator employs it, Mekontso said.
“There’s no technology for the sake of technology only,” she said. “It must expand access to care outside the hospital, and improve the standard of care.” •



BY NICOLE DHANRAJ
In the first article, we talked about why onboarding needs to be treated as a long-term engagement strategy, not a one-week administrative task. See the first article at theicecommunity.com/?p=76971
This guide builds on that by offering a practical structure you can apply right away, even in a busy, high-pressure department.
If you’ve ever had a great hire leave within the first few months, there’s a good chance the issue wasn’t the job it was how the job started. This 90-day guide is designed to help you change that.
It’s simple, sustainable and built for real-world imaging teams where time is tight and support has to be intentional.
Orientation gets someone in the door. Onboarding helps them stay.
Research (and experience) shows that what happens in the first 90 days has a major impact on whether a new employee becomes a longterm contributor or starts looking elsewhere. That’s why this guide focuses on creating a consistent experience across three phases:
Phase Timeframe Focus
Phase 1 Days 1-14
Foundation: tools, expectations, introductions
Phase 2 Days 15-45 Integration: clinical learning, workflow support, team connection
Phase 3 Days 46-90 Growth: independence, confidence, retention touchpoints
Let me show you the specifics.
In this phase you are looking to lay the groundwork. Make sure the basics are in place and the new hire feels welcomed and supported, not just informed.
Key actions include:
• Assign a point person (lead tech, supervisor or peer mentor)
• Confirm access to all systems: PACS, RIS, EMR, protocols, shift communications
• Review basic expectations: shift flow, documentation, communication norms
• Share a simple 90-day onboarding roadmap
• Introduce them across shifts and teams, not just who they’ll work with today
• Schedule weekly check-ins starting now Check-In Focus:
• First impressions and early questions
• Any missing tools or access issues
• Comfort level with initial tasks and shift expectations
• Identify one or two small early wins to build momentum
(DAYS 15-45)
In Phase 2, you will support skill-building, clarify workflow expectations and create meaningful connections with peers and leaders.
Key actions include:
• Keep weekly check-ins going (short, focused, predictable)
• Provide real-time feedback during shifts, reinforce good work and clarify expectations
• Track progress on clinical and workflow milestones
• Invite to team meetings or huddles, even if they’re not presenting
• Encourage cross-training or observation with
other modalities
• Schedule a midpoint leadership touchpoint Check-In Focus:
• What’s becoming more comfortable?
• Where are they still uncertain?
• Do they feel like they know who to go to for help?
• Recognize effort and visible progress
The goal here is to support the shift from learning to ownership. Reinforce confidence, team connection and readiness for longer-term goals.
Key actions include:
• Gradually reduce oversight (based on performance and comfort)
• Confirm readiness for solo workflow, call coverage (if applicable) and shift independence
• Invite feedback from peers they’ve worked with
• Schedule a final onboarding review: highlight wins, gather input, discuss development goals
• Ensure they’re included in the rhythm of the department (communications, initiatives, informal culture) Check-In Focus:
• What do they feel most confident about now?
• Any remaining gaps or questions?
• Feedback on the onboarding experience – what helped, what was missing
• Talk through what comes next in their growth (cross-training, leadership interest, etc.)
SAMPLE 90-DAY ROADMAP
Week 1 Shadow core modality Learn downtime & safety protocols
Week 2 Assist on common procedures Document in EMR with support
Intro to staff across shifts
Join huddles or team chats
Week 4 Run basic scans independently Navigate workflow without reminders Build peer relationships
Week 6 Cross-train or rotate Manage full shift workload Leadership touchpoint
Week 8 Operate independently Ready for oncall or weekends (if relevant)
Week 12 Fully integrated Performance review + growth discussion
Feedback from peers
Included in team communications
This onboarding approach doesn’t require a complex system or hours of extra time. What it does require is consistency, follow-through and a department-wide expectation that onboarding is part of leadership, not just HR. When new hires are supported beyond the first week, they get up to speed faster, stay longer and become contributors to a stronger department culture.
The 90-day mark isn’t the end of the journey; it’s the handoff to long-term engagement. By this point, new employees should be clinically independent and culturally integrated. But they still need continued check-ins, development opportunities and recognition.
Here are a few ways to maintain momentum:
• Monthly 1:1s: Transition from weekly check-ins to monthly development conversations.
• Professional goals: Revisit growth areas discussed during onboarding – cross-training, certification or project work.
• Peer involvement: Encourage them to support the next new hire, reinforcing their sense of contribution.
• Leadership visibility: Keep senior leaders connected through informal touchpoints or ongoing check-ins.
The transition from onboarding to long-term engagement should feel seamless not like the support suddenly disappears. Maintaining that connection keeps retention high and morale strong.
If you’d like to connect or share what’s working in your department, I’d love to hear from you. Reach out anytime: nicoledhanraj@gmail.com. •
Nicole Dhanraj, Ph.D., SHRM-SCP, PMP, GPHR, CPSS, CRA, R.T(R)(CT)(MR), is an experienced imaging director.

BY MARK WATTS
Editor’s Note: The four-part series on FDA post deployment requirements for Software as a Medical Device will continue in April.
Iwrote my first article for Imaging Community Exchange (ICE) Magazine, “Will AI Replace Radiologist” for the January 1, 2020, issue. I am reviewing it today, more than 5 years later. The recent paper “The Effect of AI on the Radiologist Workforce: A Task-Based Analysis” by Curtis P. Langlotz, MD, Ph.D., a professor of radiology, medicine, and biomedical data science at Stanford University, is a summary of the task-based analysis.
For nearly a decade, a shadow of uncertainty has loomed over the field of radiology. High-profile experts once predicted that machine learning would soon displace the human doctors who interpret our X-rays and MRIs. Yet, as we move into 2025, the conversation has shifted from “if” AI will be used to exactly “how it will reshape the daily grind” of the medical workforce. The study by Langlotz provides a groundbreaking, quantitative look at this transformation, moving past the hype to analyze the specific tasks that make up a radiologist’s day.
This research matters because it serves as a “canary in the coal mine” for other highly skilled professions. By looking at radiology – a field where three-quarters of new FDA-cleared AI devices are already concentrated – we can catch a glimpse of how innovation might alter the workflow of any job that relies on expert data analysis. The study utilizes a “task-based analysis,” an approach favored by labor economists, which breaks down a job into individual units of activity to see which specific pieces AI can handle better or faster than a human.
The findings are striking: the model predicts a 33% reduction in the total hours worked by radiologists over the next five years. While that number might sound like the beginning of the end for the profession, the sources suggest a more nuanced reality. Most of this time savings comes from streamlining the
most repetitive and tedious parts of the job, such as drafting reports and filtering out “normal” scans that don’t actually need a human’s expert eye.
To understand how we get to that 33% figure, we first have to look at how these doctors spend their time. Research shows that while roughly 67% of their day is spent interpreting images, the rest is a mix of “protocoling” (deciding which specific test a patient needs), communicating with other doctors and explaining results to patients. AI isn’t just a single tool; the study identifies 15 different types of AI applications that target these specific moments in the workday, from the second a doctor orders a test to the moment the patient reads their report.
One of the biggest “productivity boosters” identified is automated report drafting. Instead of a doctor starting from a blank page for every patient, AI can now produce a high-quality initial draft describing the findings. This alone could increase productivity by up to 20% for complex scans like CTs and MRIs. It functions similarly to having a digital medical resident who does the heavy lifting of documentation, allowing the senior doctor to focus on verification and high-level diagnosis.
Another major shift involves “imaging study delegation.” In fields like mammography and chest X-rays, a huge portion of scans are “normal.” The study suggests that AI is now capable of identifying these unremarkable cases and pulling them out of the human queue entirely. In fact, the model assumes AI could handle up to 50% of screening mammograms and 40% of outpatient X-rays without human intervention. By putting the radiologist “out of the loop” for routine cases, the remaining workforce can focus on the patients who actually need help.
However, innovation isn’t always a time-saver. The study introduces the concept of “opportunistic screening,” where AI finds things the doctor wasn’t even looking for – like hidden signs of bone loss or heart calcium on a standard chest scan. While this is great for patient health, it actually increases the
radiologist’s workload because they now must validate and document these extra findings. It’s a classic example of how technology can solve one problem while creating more work in another area.
Beyond the images themselves, AI is poised to act as a digital assistant for communication. New tools can summarize a patient’s messy medical history into a quick “cheat sheet” for the doctor or translate dense medical jargon into plain English for patients. This reduces the time spent on “non-routine communication,” such as playing phone tag with other clinicians or answering confused messages from patients about their results.
If AI is cutting work hours by a third, why aren’t radiologists losing their jobs? The answer lies in the explosion of medical imaging. Over the past decade, the number of scans performed has nearly doubled, while the number of radiologists has remained relatively flat. The sources argue that AI’s productivity gains will simply help doctors keep their heads above water as demand continues to rise. Instead of job loss, we are looking at a quality-of-life improvement where AI takes over the “needle-ina-haystack” tasks that doctors find less interesting.
While the study’s quantitative approach is a major strength, it does have limitations. Much of the data is “U.S.-centric” and based on academic hospitals, which might not reflect how a small community clinic operates. Furthermore, because some of these technologies are so new, the researchers had to rely on their own expert judgment to fill in the gaps where published evidence was missing.
Critically, the study assumes that hospitals will adopt all
these AI tools rapidly, which might not happen because of high costs or “resistance to adoption” regarding AI-only interpretations. There is also the unmodeled “AI governance” work – the time doctors must spend monitoring the AI itself to make sure it hasn’t developed errors or biases over time. Outside of the sources, it is worth noting that the legal responsibility for a misdiagnosis still rests on the human doctor, which may limit how much they are willing to “delegate” to a machine.
Looking ahead, the significance of this work is clear: AI is a partner, not a replacement. The transition will likely mirror the move from physical film to digital “PACS” systems years ago – a change that made radiologists much faster but didn’t make them obsolete. For students eyeing a career in medicine or tech enthusiasts imagining the future of work, the lesson is that innovation usually shifts the type of work we do rather than the amount.
In the end, the most important outcome of this AI revolution might not be efficiency, but “better care.” By automating the mundane, we give human experts more time for complex cases and meaningful patient interaction. As we move toward a future where AI handles the routine, the human radiologist’s role will likely evolve from a high-speed “image reader” into a high-level diagnostic consultant, ensuring that technology serves the patient, rather than the other way around.•
Mark Watts is an experienced imaging professional who founded an AI company called Zenlike.ai.


BY NICOLE DHANRAJ
hen you work in healthcare long enough, certain things start to feel routine. Procedures become familiar. Risks feel manageable. You know what’s safe, what’s common and what’s done every single day.
Patients don’t always experience it that way.
Recently, my husband went in for surgery. In a conversation beforehand, he said something that made me laugh at first. “You know, long ago they used to say not many people came back from anesthesia.”
I chuckled and said, “Yeah, that was long ago.” and responded the way many of us would. I told him that anesthesia today is used all the time, that it’s closely monitored, and that it’s very safe.
It caught my attention. I asked him if he was nervous, and he said yes. I reassured him that honestly everything would be fine. And, I believed that reassurance completely.
But after surgery, when he said, “I made it back,” it stopped me.
That comment wasn’t about the outcome. It was about what he had been carrying with him the entire time.
In healthcare, we often assume that once we explain the science, fear will fade. Sometimes it does. But sometimes fear isn’t rooted in a lack of information, it’s rooted in stories. Things people have heard growing up. Family experiences. Cultural beliefs. Old warnings that linger long after medicine has changed.
For clinicians, anesthesia is routine. For patients, it can feel like handing over control. And those fears don’t always show up as clear questions. They show up sideways in a comment, a joke or a passing remark we might easily brush past if we’re not listening closely.
What this experience reminded me is that even when we ask, “Are you nervous?” and even when we reassure patients appropriately, that underlying fear doesn’t always disappear. Trust and fear can exist at the same time.
This isn’t about patients believing myths. It’s about recognizing that people bring beliefs and stories into healthcare spaces whether we ask about them or not. And if we don’t make room for those conversations, we may never hear what’s really sitting underneath the surface.
Sometimes it only takes a gentle follow-up to open the door:
• “Have you heard anything about this procedure that stuck with you?”
• “Are there stories you’ve been carrying into this?”
• “Is there anything about this that’s been worrying you, even if it’s hard to explain?”
These questions don’t slow care down. They help us connect with patients in a more honest way.
Patients don’t walk into procedures as blank slates. They walk in with history, belief and fear already in place. When we learn to listen for those quiet cues, we meet patients where they actually are not just where we assume they should be.
What stayed with me most is that this came from someone I know well and someone I talk to about healthcare all the time.
It was a reminder of how easy it is to overlook the deeper meaning behind what sounds like a simple comment, even when we think we’re listening. •
Nicole Dhanraj, Ph.D., SHRM-SCP, PMP, GPHR, CPSS, CRA, R.T(R)(CT)(MR), is an experienced imaging director.






Many people are good at what they do, yet struggle to find the time or energy for the bigger things they dream about. The biggest obstacle is rarely laziness or lack of ability; it’s being too busy doing good things.
Think of it this way: When your calendar is filled with worthy activities, there’s no room left for extraordinary accomplishments. Breaking free requires abandoning some of the good to achieve the great. Good things aren’t bad things, but if we do only good things, there won’t be time for great things.
Author Jim Collins addresses this in his book, “Good to Great.” He says:
“We don’t have great schools, principally because we have good schools. We don’t have great government, principally because we have good government. Few people attain great lives, primarily because it is easy to settle for a good life. The vast majority of companies never become great precisely because they become quite good – and that is their main problem.”
I saw this firsthand with a friend I’ll call Sarah. She worked in marketing and she served on three nonprofit boards. She also volunteered at her kids’ school and helped organize community events.
Everything Sarah did was worthwhile and everyone loved her contributions, but she had a dream that wasn’t being fulfilled – she wanted to start her own consulting firm. She’d been “planning to get to it” for five years, but every time we spoke, she’d sigh and say, “I’m just too busy right now.”
One day I shared with her an analogy an executive once told me. He said, “Picture yourself holding huge stacks of $20 bills in both hands. Those are good things. Then imagine someone placing stacks of $100 bills on a table and
saying you can have as many as you want.”
Sarah understood the analogy right away. To pick up the $100 bills, she first needed to put down the $20s. We talked about how hard it can be to set aside things that have value, even when the things being offered to you have even more value.

BY DANIEL BOBINSKI
Soon Sarah acted on her new understanding. Within two months, she stepped down from two of the three boards she was on, plus she reduced her volunteer hours at the school. A few months later she launched her consulting firm.
Today, Sarah runs a thriving business, and she still serves on the one board she’s most passionate about.
I’ve seen this pattern repeatedly in my consulting work. A client whom I’ll call Tom worked as an IT manager at a mid-sized company. He was excellent at solving problems and mentoring junior staff, and his bosses loved that he kept systems running smoothly. But Tom dreamed of moving into executive leadership. He wanted to shape company strategy, not just implement it. The problem? He spent every spare moment being the go-to person for technical issues. People would bypass the help desk and come straight to Tom because he always said yes.
When we analyzed Tom’s schedule, we found he was spending roughly 15 hours each week on tasks that could be handled by others. Was Tom good at those tasks? Absolutely. But those good things were blocking his path to developing the skills he needed for executive roles.

To make time for classes on executive development, Tom started delegating more. He also scheduled meetings with senior leaders to discuss his goals. Within a year he was promoted to director. A year after that he became a vice president. The lesson here is that being content with doing good things can easily become a subtle form of procrastination that keeps us from reaching our potential.
In his book, “The Dip,” author Seth Godin says the idea that “winners never quit” is false. He says winners quit all the time –they quit doing good things to make room for great things.
What about you? Do you have great things you want to accomplish but can’t find the drive to say no to all the good things you’re doing? Here are some suggestions that may help: Get together with a trusted friend, family member or co-worker and create a list of benefits you’ll get by accomplishing your bigger dreams. This should not be an academic exercise. Dig deep into the positive ripple effects that will come by achieving your dream.
Once you identify the benefits, get emotionally connected to each one. The stronger your emotional connection to your core values, the more likely you are to act on your dreams.
Take it to the next level. For each benefit you identified, think of a “benefit of getting that benefit.” Then get deeply connected to those benefits, as well.
In other words, get a deep sense of what resonates within you as you imagine yourself achieving your greater goals and dreams. Once you have identified these things, choose one or two to serve as your main motivators. Then put tasks

on your calendar that lead to your greater goals. Set up regular meetings with an accountability partner – or even two. These should be people who want to see you succeed. Ask them to help you stay on track for achieving your goals.
At the same time, know that procrastination can still be a problem, even if you have accountability partners. Here are a few ways to create conditions for better success:
1. Divide overwhelming tasks into small ones. For example, if you want to write a 200-page book, write two pages daily and you’ll finish in just over three months.
2. Attach a “by when” to every action item. With a clearly identified completion time you have a goal. Without one you have only an idea.
3. Choose one task as your day’s priority. Little things accomplished steadily over time create big things.
Bottom line: Be willing to give up good things in your life if you want to achieve greater things. Make the tough decisions and then work with accountability partners to help you succeed. Otherwise, good things might forever be the obstacles to the great things you can do. •
Daniel Bobinski, who has a doctorate in theology, is a best-selling author and a popular speaker at conferences and retreats. For more than 30 years he’s been working with teams and individuals (1:1 coaching) to help them achieve excellence. He was also teaching Emotional Intelligence since before it was a thing. Reach him by email at DanielBobinski@ protonmail.com or 208-649-6400.
Image One Medical is the only Engineer-Owned medical equipment service group that is fully dedicated to Florida’s amazing base of Imaging Centers, Hospitals, and Cancer Treatment Centers.
We have a mission: Self perform on every aspect of our business. Specialize on specific modalities: Pet CT, CT & MRI, and Focus in a key geographic region.
Fort Myers I Fort Lauderdale I Tampa I Orlando
FLORIDA BASED
Dealer and servicer of PET CT, CT and nuclear medicine
• Equipment service: full coverage plans
• Equipment sales: installation, relocation and project management
• Mobile coach construction, refurbishment, maintenance and management


CHICAGO – Using a deep learning AI model, researchers identified the first-of-its-kind biomarker of chronic stress detectable through routine imaging, according to research presented at the annual meeting of the Radiological Society of North America (RSNA).
Chronic stress can affect both physical and psychological well-being, causing a variety of problems including anxiety, insomnia, muscle pain, high blood pressure and a weakened immune system, according to the American Psychological Association. Research shows that chronic stress can contribute to the development of major illnesses, such as heart disease, depression and obesity.
The study’s lead author, Elena Ghotbi, M.D., a postdoctoral research fellow at Johns Hopkins University School of Medicine in Baltimore, Maryland, developed and trained a deep learning model to measure adrenal gland volume on existing CT scans.
Each year, tens of millions of chest CT scans are performed in the United States alone.
“Our approach leverages widely available imaging data and opens the door to large-scale evaluations of the biological impact of chronic stress across a range of conditions using existing chest CT scans,” Ghotbi said. “This AI-driven biomarker has the potential to enhance cardiovascular risk stratification and
guide preventive care without additional testing or radiation.”
Senior author Shadpour Demehri, M.D., professor of radiology at Johns Hopkins, said chronic stress is a prevalent condition or complaint that many adults deal with on a daily basis.
“For the first time, we can ‘see’ the long-term burden of stress inside the body, using a scan that patients already get every day in hospitals across the country. Until now, we haven’t had a way to measure and quantify the cumulative effects of chronic stress, other than questionnaires, surrogate serum markers like chronic inflammation, and cortisol measurement, which is very cumbersome to obtain.” Demehri said.
Unlike single cortisol measurements, which provide a momentary snapshot of stress levels, adrenal volume acts like a biological barometer of chronic stress.
In the study, the researchers obtained data on 2,842 participants (mean age 69.3; 51% women) from the Multi-Ethnic Study of Atherosclerosis, a comprehensive study combining chest CT scans, validated stress questionnaires, cortisol measures and markers of allostatic load – the cumulative physiological and psychological effects of chronic stress on the body. This rare integration of imaging, biochemical and psychosocial data made it the optimal, and likely only, cohort for developing an imaging biomarker of chronic stress.
The researchers retrospectively applied their deep learning model to the CT scans to segment and calculate the volume of
the adrenal glands. Adrenal Volume Index (AVI) was defined as volume (cm³) divided by height² (m²). Salivary cortisol was collected eight times per day over two days. Allostatic load was based on body mass index, creatinine, hemoglobin, albumin, glucose, white blood count, heart rate and blood pressure.
Statistical associations were assessed between AVI and cortisol, allostatic load, and psychosocial stress measures, including depression and perceived stress questionnaires. The researchers found that AI-derived AVI correlated with validated stress questionnaires, circulating cortisol levels and future adverse cardiovascular outcomes.
Higher AVI was associated with greater cortisol, peak cortisol and allostatic load. Participants with high perceived stress had higher AVI compared to those with low stress. AVI was also associated with a higher left ventricular mass index. Each 1 cm³/m² increase in AVI was linked to greater risk of heart failure and mortality.
“With up to 10-year follow-up data on our participants, we were able to correlate AI-derived AVI with clinically meaningful and relevant outcomes,” Ghotbi said. “This is the very first imaging marker of chronic stress that has been validated and shown to have an independent impact on a cardiovascular outcome, namely, heart failure.”
“For over three decades, we’ve known that chronic stress can wear down the body across multiple systems,” said Teresa

E. Seeman, Ph.D., study co-author and professor of epidemiology at UCLA and a pioneering researcher in stress and health. “What makes this work so exciting is that it links a routinely obtained imaging feature, adrenal volume, with validated biological and psychological measures of stress and shows that it independently predicts a major clinical outcome. It’s a true step forward in operationalizing the cumulative impact of stress on health.”
Demehri said that by linking an easily measurable imaging feature with multiple validated indicators of stress and downstream disease, this research introduces an entirely new, practical way to quantify chronic stress.
“The key significance of this work is that this biomarker is obtainable from CTs that are performed widely in United States for various reasons,” Demehri said. “Secondly, it is a physiologically sound measure of adrenal volume, which is part of the chronic stress physiologic cascade.”
The researchers said the imaging biomarker could be used in a variety of diseases that are associated with chronic stress in middle-aged and older adults.
Other co-authors are Roham Hadidchi, Seyedhouman Seyedekrami, Quincy A. Hathaway, M.D., Ph.D., Michael Bancks, Nikhil Subhas, Matthew J. Budoff, M.D., David A. Bluemke, M.D., Ph.D., R. Graham Barr and Joao A.C. Lima, M.D. •



“What you do makes a difference, and you have to decide what kind of difference you want to make.”
– Jane Goodall,









Espin Medical www.espinmedical.com • (206) 755-1768
ImageOne Medical image1group.com • 877-304-9000 55
Innovative Radiology innovative-radiology.com • (888) 909-9894 53
KEI Medical Imaging Services keimedicalimaging.com • 512-477-1500 53
LASO Imaging Solutions lasoimaging.com • 800-674-5276 57 Metropolis International, LLC Metropolismedical.com • 718-371-6026 62
Radon Medical radonmedicalimaging.com • 866-723-6698 25 Ray-Pac
843-767-8090
Maull Biomedical Training maullbiomedical.com • 440-724-7511 27 Diagnostic Imaging
Brandywine
Innovatus Imaging innovatusimaging.com
•
•
•
•
•





•











