Transforming Pediatric Environments Through Sensory Inclusive Design
A Case Study on Collaboration with Dr. Alessandro Morganti, MUSC, and LS3P
LS3P’s Design In-Kind program encourages team members to dedicate up to 1% of their time to high impact pro bono work that strengthens communities. Through this initiative, LS3P partnered with Dr. Alessandro Morganti, M.D., PhD and the Medical University of South Carolina (MUSC) on a pioneering research and design project focused on creating more inclusive pediatric healthcare environments.
This ongoing project integrates evidence-based design strategies from Dr. Morganti’s Design Toolkit for Autism
Friendly Healthcare Spaces and applies them within MUSC Children’s Health Developmental Behavioral Services Clinic. The effort represents a significant step towards understanding and improving the healthcare experience for neurodivergent patients and their families.
The Context
According to a 2025 study by the Centers for Disease Control (CDC), about 1 in 31 children is diagnosed with Autism Spectrum Disorder (ASD) i ASD is one form of neurodivergence, which also includes differences such as dyslexia and attention deficit hyperactive disorder (ADHD). Neurodivergent people may experience stimuli such as sounds, smells, and textures differently from their neurotypical peers, and their experiences in a healthcare setting may profoundly impact their diagnosis and treatment.
For example, sitting in a waiting room can be an uncomfortable experience for all of us. We aren’t sure when we’ll be called, or what will happen once we’re in the room with the doctor, or whether it will hurt. The room might be
crowded, or the chair might be too hard, or it might be uncomfortably chilly. There may be a blaring television or harsh antiseptic smells.
While adults may have learned coping strategies to make this situation easier, many children have not; for children with ASD or other types of neurodivergence, this sensory overload in a new situation could cause agitation or an emotional response. The clinical room, likewise, might be filled with distracting sounds or smells and unfamiliar equipment. If a child with ASD begins a clinical appointment distressed, it may be difficult for the medical team to assess and treat the patient effectively. This unpleasant experience now has medical consequences.
The Research Foundation
Dr. Morganti conducted his doctoral research with Design & Health Lab at Politecnico di Milano and the Autism Center at Stanford University. This research involved:
• Systematic literature reviews
• Clinical scale integrated surveys
• Co design workshops with caregivers, patients, and clinical staff
• Data from 1845 caregivers and 1035 adults with autism across Italy and the U.S.
This extensive data driven process resulted in a validated toolkit of 73 design strategies for autism friendly outpatient facilities. This toolkit, the Design Toolkit for Autism friendly Healthcare Spaces, provided the foundation for this research project.
The Methodology
Before implementing the design interventions at MUSC Children’s Developmental Clinic Dr. Morganti conducted a six month survey of patients, families, and caregivers to assess user experience barriers, sensory challenges, and clinical indicators related to patient well being and behavior. He collected insights through multilingual UX surveys, clinical staff workshops, and evidence based evaluation tools. After evaluating the data, Dr. Morganti prioritized design strategies most likely to improve wayfinding, sensory comfort, waiting and transition experiences, and privacy and de-escalation needs. LS3P collaborated with MUSC staff and Dr. Morganti to adapt selected strategies to the constraints and opportunities of the existing facility.
The Objectives
1
Apply the evidence based design strategies from the Design Toolkit within a functioning pediatric clinical environment.
Design Interventions
The project focused on adapting three primary clinic spaces and improving wayfinding.
2
Improve the patient experience and well being for autistic children and their families.
3
Identify benefits to non autistic patients using the same adapted spaces.
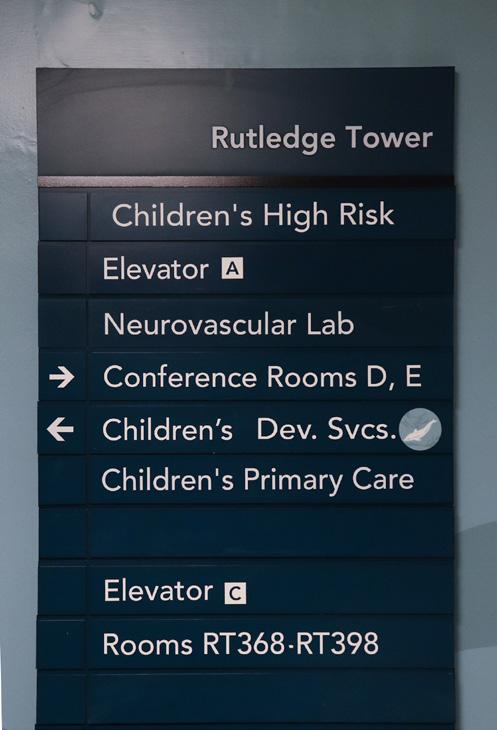



WAYFINDING IMPROVEMENTS
4
Refine design strategies for broader use by architects, designers, and healthcare decision makers.
5
Conduct pre- and post-intervention research to validate the impact of design adaptations.
To address confusing circulation from parking to the clinic, the team introduced dolphin and turtle “breadcrumb” icons for children to find, and experiential graphics that orient patients and families within the space while reducing anxiety triggers.
WAITING ROOM ADAPTATIONS
Changes to the waiting areas addressed sensory comfort, noise reduction, and flexibility. New furniture offers varied seating and play zones, and acoustical seals on toilet room doors prevent disruptive flushing sounds. A soft flooring “fin wall” play space creates a defined calming zone.
SENSORY ROOM ADDITION
An office adjacent to the waiting room was converted into a sensory friendly decompression space featuring soft beanbag seating, patient-controlled color changing LED lighting, three available channels of original audio sounds and music, and a variety of sensory toys.
OBSERVATION ROOM
ADAPTATION
An exam room was modified to support observation by removing medical shelving and clutter and creating a simplified, calming spatial environment.
By reducing sensory overload, enhancing comfort, and engaging the patients with an autism-friendly environment, these interventions help to get clinical visits started on the right food to support a better, more effective therapeutic journey.
Ongoing Research & Evaluation
At the time of this report, the design interventions have been implemented, and Dr. Morganti is conducting postadaptation experience surveys over a 10 month period. These surveys will assess:
• Well being and emotional regulation
• Satisfaction among autistic and nonautistic patient groups, and
• Clinical process efficiencies
Data will be shared with MUSC Children’s Health, submitted for publication in peer-reviewed journals, and used to refine the Design Toolkit for Autism-Friendly Spaces as appropriate.
Project Significance
This MUSC pilot project contributes to a growing movement toward neuroinclusive healthcare design. This ongoing work exemplifies how design and clinical science can merge to address significant gaps in healthcare accessibility for neurodivergent populations. As post occupancy evaluation continues, the findings will help shape scalable guidelines for autism friendly healthcare design impacting not only this clinic but the broader landscape of pediatric health environments.
Findings are anticipated to shed light on sensory barriers in clinical environments, anxiety and behavioral challenges during visits, caregiver stress, and healthcare provider safety and efficiency. This work will advance knowledge by providing a real world
test case for evidence based autism friendly strategies; measurable data on patient experience improvements; and replicable model for future clinics, hospitals, and specialty care settings.
The collaboration between Dr. Morganti, MUSC, and LS3P demonstrates the potential of evidence driven architectural interventions to improve the patient experience, empower families, and result in better healthcare outcomes.
Conclusions
This report will be updated with conclusions when data collection is complete. Stay tuned for results in late 2026 or early 2027!
