Informed
A Guide for Critical Medical Decisions





This magazine was designed to help patients, families, and their advocates prepare for difficult and complex medical decisions. Doctors and healthcare staff do not always have what is best for the patient in mind. Therefore, it is important to have a plan in place before facing a medical crisis.
Historically, most governments, healthcare providers, and societies shared the presumption in favor of respecting and preserving life. Today, the increasing reports of negligence, abuse, and growing evidence of stealth euthanasia in healthcare settings are alarming. Some in the healthcare industry are pushing to legalize Physician Assisted Suicide and Euthanasia in the US and across the globe. This should be a red flag for everyone given the cost-cutting measures healthcare providers are being forced to make to comply with the Affordable Care Act and their employer’s demands. Human Life Alliance and the Healthcare Advocacy and Leadership Organization strive to create a culture in which every person’s life is respected and protected by healthcare providers, by law, and by society. We believe it is imperative that we all know our rights as patients and health care agents when faced with critical medical decisions.
The essential moral principle that guides us is clear:


“[L]ife is something before which we stand (or should stand) with reverence, awe, and grave respect–because it is beyond us and unfathomable…to regard life as sacred means that it should not be violated, opposed or destroyed, and, positively, that it should be protected, defended and preserved.”
(emphasis added)
(Leon
Kass, M.D., “Death With Dignity and the Sanctity of Human
Our objective is to help YOU become Informed. We hope you find this
informative guide, and that you will share this resource with your family, friends, and neighbors.
Informed is a joint offering from Human Life Alliance and the Healthcare Advocacy and Leadership Organization.


Being a Healthcare professional, legal guardian for my sister, and mother of eight children, I knew that it was important to have a person who could advocate for me in the event I was not able to communicate my needs. My husband and I decided that, as soon as each of our children turned 18, we would have them fill out a medical power of attorney so we could speak on their behalf when necessary. We realized the importance of that decision when two of our kids were in a very serious car accident on their way back to college from Thanksgiving break. We learned that, for whatever reason, we never had them fill out their forms and submit them to their health care providers. Since they were over 18, my husband and I were not notified where they would be taken.
My son was unable to communicate clearly at the scene. He was airlifted to one hospital while my daughter was taken to a different one.
Thankfully, my daughter was conscious, so she called us. She gave permission for the EMTs to talk to me and for my husband to go to the hospital where she was being transported.
The EMTs would not talk to me about my son because he could not give consent. However, my daughter was able to tell me the name of the hospital to which my son was being airlifted, so I drove two hours to be with him. Upon arrival at the hospital, the staff was not going to let me in or even acknowledge that he was a patient at the hospital because I did not have any documentation that gave me permission to see my son.
It did not matter that I was his mother.
Feeling so helpless, I just prayed for a miracle and that they would let me in. My phone rang. It was the nurse stating that my son had become alert and given his consent for me to see him and discuss his medical status. She was surprised that I was already at the hospital. I was then allowed into the emergency room. I discovered later that they were prepping him for surgery when he started asking for me.
My heart sinks to think of what would have happened had he not been able to give his consent. It is critically important to have a medical power of attorney on file with each of your healthcare providers so your legal representative can advocate for you in a medical crisis. It is easy to fill out.
I am so thankful it worked out for us, but the situation could have been so different had my son not been alert enough to give his consent.
~Paulette
Health care advance directives are legal documents by which competent adults express their wishes regarding medical treatment in the event of a future illness or injury. An advance directive goes into effect when the signer becomes incapable, either temporarily or permanently, of making health care decisions for himself or herself.
In general, state laws govern three types of advance directives: (1) the Living Will (a.k.a., Directive to Physicians), (2) the Medical Power of Attorney (a.k.a., Durable Power of Attorney for Health Care), and (3) Physician Orders for Life-Sustaining Treatment (POLST).
Every state’s advance directive law permits withholding or withdrawal of life-sustaining medical procedures—including food and fluids administered by tube or intravenously—even when their omission will directly cause a patient’s death.
A Living Will is a written document that includes details about the medical treatments you would and would not want to be used to keep you alive. This applies to an illness or injury you have in the future when you are unable to communicate your wishes to medical staff. You need to list as many possible end-of-life care decisions as possible because this is all the doctors have to go by. Living Wills can be dangerous because the medical staff treating you are usually strangers who may not accurately interpret your wishes, particularly if they do not share your values.

In a Medical Power of Attorney (MPA), you name a trusted person, usually a family member or friend, as your agent (a.k.a. proxy or surrogate) and instruct them on your wishes. Your agent can make medical decisions for you if you are unable to do so yourself, based on your values, current medical condition, and treatment options. You may appoint a second agent in case your primary agent is unreachable in a medical crisis.
The wording of an MPA is critically important, and idealy, it should comply with your state laws. Also, it should clearly state that no one, not even your agent, has the authority to approve any act or omission that will directly or intentionally end your life. This limitation protects you and also your agent from being pressured to approve any such decision.
Who you appoint as your agent is as important as the wording of your MPA. Choose someone you trust with your life. Your agent should be someone who is capable of making morally sound medical decisions, who will not be intimidated by medical professionals, and who will seek a second opinion or legal advice when necessary to protect you. Your next of kin may not be that person.
A life-affirming MPA is essential for everyone 18 years or older. Anyone, at any age, can become seriously ill or get injured. Filling out your MPA will take only a few minutes—a few minutes that could mean the difference between life and death.
Both HLA and HALO have life-affirming resources available at humanlife.org and halovoice.org


Physician Orders for Life-Sustaining Treatment (POLST) is an advance directive used extensively throughout the United States. While the acronyms and wording of POLST forms may differ, they generally encourage patients to refuse life-saving treatments and care, sometimes resulting in preventable deaths.
The form is brightly colored (usually neon pink, green or yellow) to make it highly visible in a patient’s medical chart, room, or home. This has replaced a Do Not Resuscitate (DNR) order in many cases. POLST forms reduce complicated medical decisions to a “check the box” format. A healthcare provider or other facilitator asks the patient questions and checks boxes indicating whether the patient does or does not want CPR, a ventilator, antibiotics, IV fluids, tube-feeding, and various other medical interventions. The way questions are phrased can manipulate patients’ responses. For example, a facilitator may ask, “Do you want us to focus on keeping you comfortable?” The patient says, “Yes of course,” not realizing that this answer may be interpreted to mean, “Stop efforts to treat my illness and only provide comfort measures.”
Once filled out, the POLST is signed by a doctor or other healthcare provider. This transforms it into medical orders that can go into effect immediately, even if the patient is still able to make medical decisions. Having a POLST may also keep your agent or loved ones from being able to protect you. Any treatments or care refused in a POLST form will not be provided. This is the case even if they could be beneficial and help the patient to recover.
The POLST usually overrides other medical decisions, even if the patient did not sign it. This is unique. To be legally valid, every other advance directive requires the patient’s signature. A POLST is the only kind that requires a healthcare provider’s signature.
According to the National POLST website, filling out a POLST form is always voluntary.1 When approached with a POLST form, do not allow anyone to push you into it. You can firmly state, “I have a Medical Power of Attorney for Health Care which will go into effect if I ever need my agent to make decisions for me. Until such time, I want to discuss my condition and treatment options with my attending physician as needed. Please respect my wishes.”

A Wisconsin attorney, Sara Buscher, Esq., reported: In 2012, a woman in her forties came to the ER at Ascension NE Wisconsin - St. Elizabeth Hospital. She was in such respiratory distress that she could not talk. While waiting for a doctor, she was approached by the unit clerk who wanted to complete a POLST with her. The nurse who brought her there intervened and stopped the POLST process. According to the clerk, it was hospital policy to do a POLST for anyone with respiratory problems. The woman was experiencing an allergic reaction to a new medication, and an Epi-Pen injection allowed her to breathe normally.


A bioethical misnomer, “futile care” has permeated the American, if not global, healthcare industry. The theory of “futile care” empowers physicians and hospitals to withhold or withdraw life-sustaining treatment that is desired by the patient or family. In many cases, it is the patient’s life that is deemed futile (i.e. useless) – not the medical care or treatment.
“Futile Care Theory” leads to euthanasia by omission.
Dr. Ezekiel Emanuel, chief architect of the Affordable Care Act (Obamacare), once predicted,
“Increasingly it will be our collective determination as to what lives are worth living that will decide how incompetent patients are treated.”1
In states and facilities with “futile care” policies, decisions to deny medical treatment are often made by a “hospital ethics committee.” When the committee decides that the patient’s life is futile, they can stop all medical treatment, often without notice to the patient. The patient then suffers a slow, imposed death. Worse yet, “futile care” policies have been crafted to undermine patients’ rights by shielding perpetrators from legal consequences for causing or hastening patients’ deaths.
One Texas family who fought a “futile care” decision stated:
“The battle for life is a difficult one even in the best of situations, but when a family is put through what we experienced at such a time, the saga was especially agonizing… We wish so much that we could have spent more time at our sister’s side when she was living and fighting for her life, rather than having to visit our attorney’s office, give interviews to radio and television stations to let the public know of the atrocity about to befall Andrea, and literally stand outside the hospital and beg them not to kill our sister.”2
It’s vital to research the medical futility laws or policies in your state and local hospitals. Know your rights as a patient before illness, injury, or hospitalization.
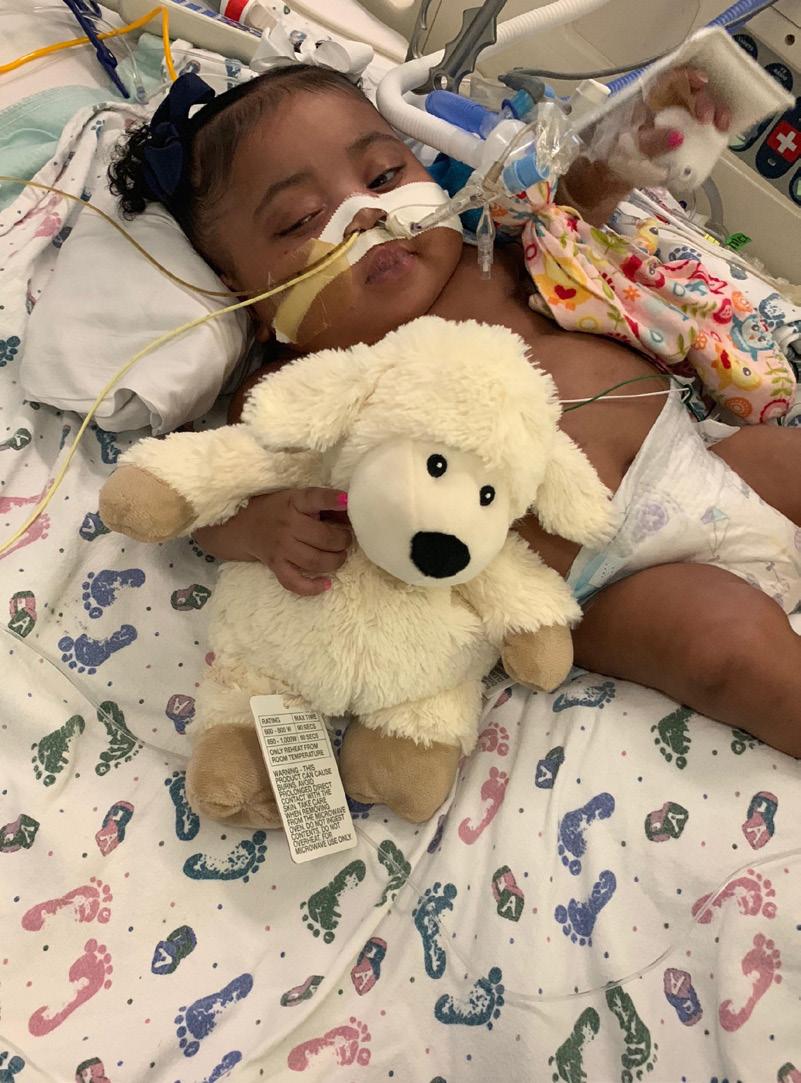

Trinity Lewis gave birth to a sweet baby girl whom she named Tinslee on February 1, 2019. She was born with a rare congenital heart defect. The 22-member ethics committee at Cook Children’s Medical Center (Fort Worth, TX) unanimously voted against continuing life-saving measures when Tinslee was nine months old. Her mother disagreed, and a long legal battle ensued.3 HALO, with a diverse group of organizations and individuals, submitted an amicus brief to the Texas Supreme Court defending Tinslee’s right to life.4 After a long struggle, Tinslee and her mother finally won the case!
Tinslee celebrated six years of life in February 2025.5
The decision to accept or forgo a treatment belongs to the patient or agent, not to the physician or healthcare team. Ventilators and cardio-pulmonary resuscitation (CPR) are two treatments that many people have questions about. Here are some honest answers.
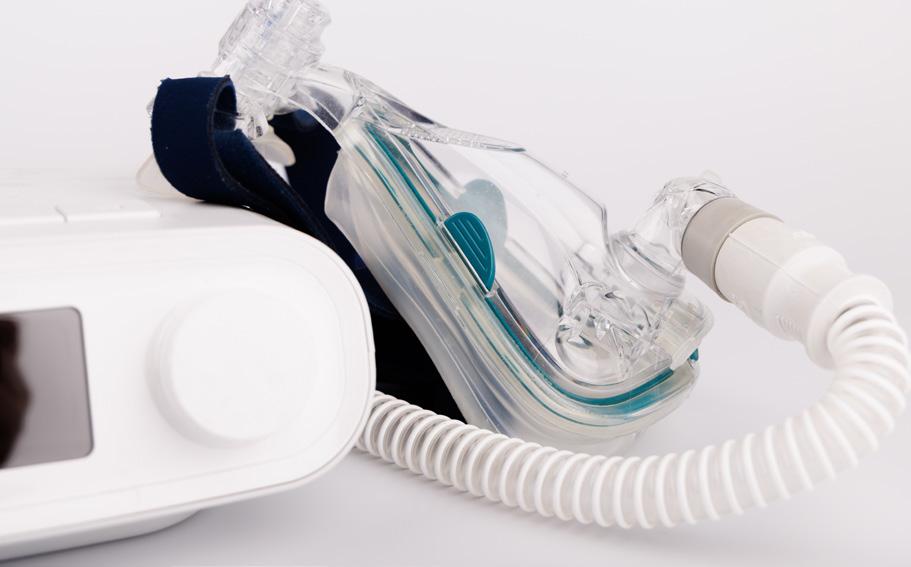
Ventilators provide breathing assistance to patients whose respiratory functions are impaired. A ventilator is typically for short-term help, like in cases of severe pneumonia. For patients with lung cancer, using a ventilator may reduce the need for morphine or sedation during the end-stage of life. There are even people with disabilities or chronic conditions who can live at home and go to work with portable ventilators.
There are many types of respiratory assistance, but most questions concerning ventilators are about intubation and tracheostomies.
• Intubation: the insertion of an endotracheal tube through the mouth or nose. This is usually a short-term measure.
• Tracheostomy: a small incision in the neck where a breathing tube may be inserted. This is used for long-term breathing assistance.
Either of these breathing tubes can be connected to various machines such as oxygen tanks, ventilators, and airway pressure machines.
Many people mistakenly think a ventilator causes respiration: the exchange of oxygen and carbon dioxide that occurs in the lungs and body tissues. In reality, the sole function of a ventilator is to push air into the lungs. Respiration can occur only when the respiratory and circulatory systems are intact and functioning. A ventilator supports life; it cannot keep a corpse alive.
Cardio-pulmonary resuscitation (CPR) may save a person’s life in the event of cardiac arrest (the moment a person’s heart stops beating and breathing becomes impaired). However, if you have concerns, you can ask a physician about the effectiveness of CPR in a given patient’s case. Be wary. A DNR order may be misinterpreted.
A Do Not Resuscitate (DNR) order means that, in the event of cardiac arrest, the person will not be given chest compressions, electrical shock to the heart, resuscitative drugs, intubation, or mechanical ventilation. Medical experts recommend that patients and agents refuse blanket DNR orders; instead, be specific. For instance, if a frail patient is concerned about chest compressions possibly breaking ribs, he or she can refuse chest compressions but still request other life-saving care.1
There is a tendency to reduce other kinds of treatment and medical attention when a patient has a DNR. The patient, family, and agent should clearly inform the physician that their refusal of CPR does not limit any other form of care. You can include this information in the patient’s Medical Power of Attorney form.
Physician Assisted Suicide is called Medical Aid in Dying or MAID by some. This practice is when someone, often a medical professional, assists a patient to kill him or herself.1 This is usually done by prescribing a lethal dose of drugs but sometimes can involve simply providing the information needed to kill oneself.
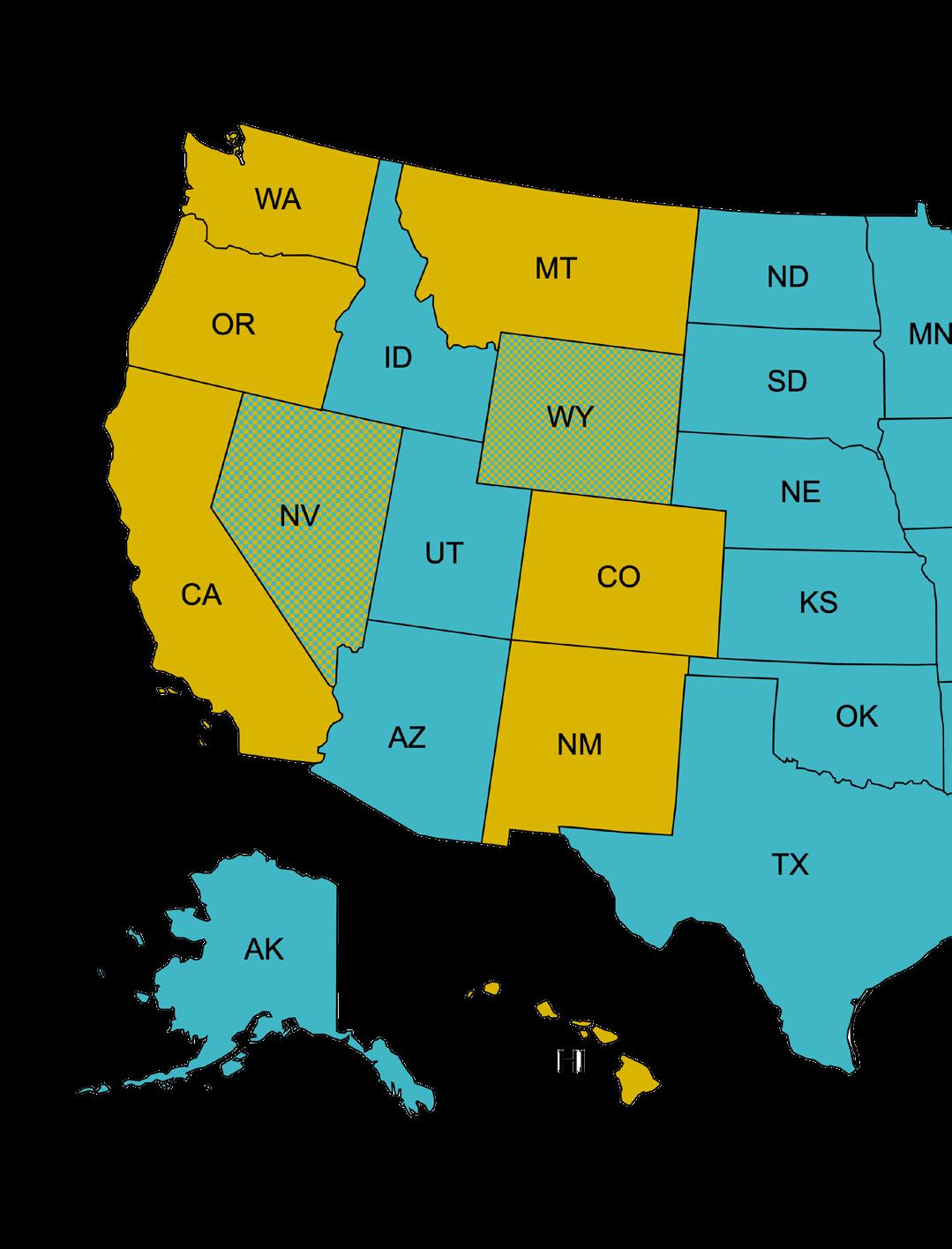
The person is supposed to self-administer the drugs, but since witnesses are not required, it is impossible to rule out abuse of this system. It is also impossible to know if the patient was coerced to prematurely end his or her life. Legalizing Assisted Suicide gives doctors a license to kill. As of January 2026, this practice is legal in 13 states and the District of Columbia.2




Imposed Death is an act or an omission which, with or without the person’s permission, ends his or her life for any purpose. Euthanizing a person for the purpose of eliminating suffering, rationing medical resources, cost-containment, obtaining vital organs for transplantation, etc., denies the fundamental right to life. The term “Imposed Death” does not distinguish between what are commonly called “active euthanasia” and “passive euthanasia,” both of which are morally and ethically wrong.
Stealth Imposed Death means intentionally causing a person’s death by neglect or over-medicating while pretending to provide appropriate end-of-life care.
The harmful effects of a clinical overdose of opioids, sedatives, and anti-anxiety medications conveniently—for the perpetrator—mimic some of the signs of the end-stage of a terminal illness, making a cover-up easy.
Doctors and other healthcare providers who do not recognize the sanctity and dignity of every human life cannot be trusted to safely treat you or your loved ones. Therefore, if you ever feel that something is not right and you or a loved one may be in danger, it is crucially important to carefully examine the advice, orders, and actions of healthcare providers.
Note: The legality of Assisted Suicide and Euthanasia is on a state-by-state basis.


Logically, the legalization and normalization of Assisted Suicide will lead to Imposed Death, otherwise known as Euthanasia.















February 9th, 2026 | humanlife.org



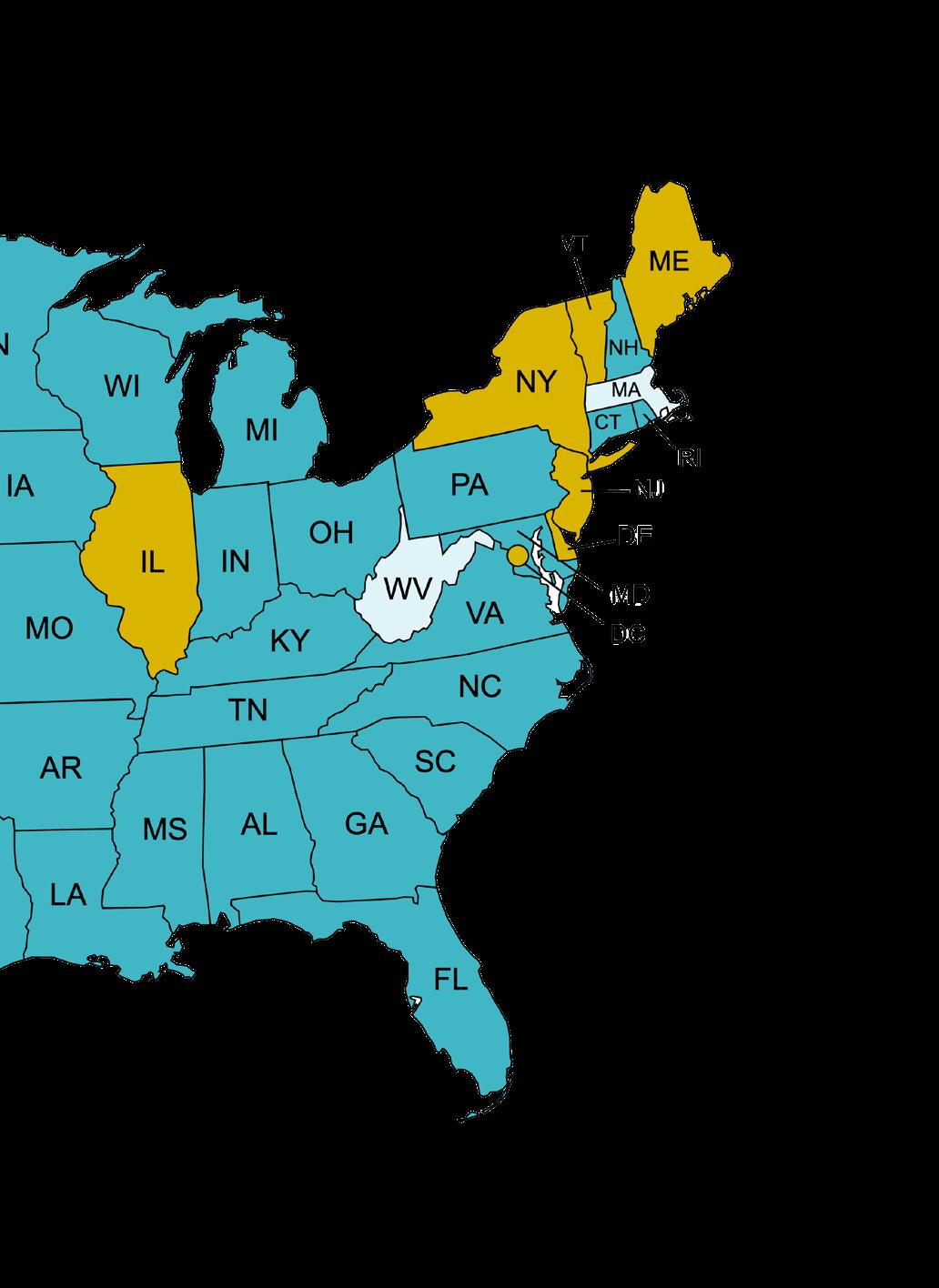

Legal In:
Australia
Austria
Belgium
Canada
Columbia
Cuba
Ecuador
Germany
Italy
Luxenburg
New
Zealand
Portugal
Spain
Switzerland
The Netherlands3
HLA’s Executive Director testified in January of 2024 against a proposed bill to legalize Assisted Suicide in Minnesota. Here are some excerpts.
I’ve experienced the pain and suffering that cancer and other incurable diseases can cause a family, firsthand. But make no mistake, begging a doctor to kill someone that you love, or a complete stranger that you think has no value to society, is not compassionate.1
MAID, “medical assistance in dying,” exploits the suffering and preys on the vulnerable. […] Financial burdens and outside pressures will also drive many requests for assisted suicide.2 Just over a year ago, professionals at a MAID seminar in Canada acknowledged that they have patients who are seeking death simply because they are poor.3
Depression is another clear sign of vulnerability. Oregon, the first US state to legalize physician assisted suicide, has a suicide rate 40% higher than other states.4 More importantly, in Oregon, 98% of those seeking physician assisted suicide weren’t even referred for psychological evaluation.5
This isn’t compassion, it’s a dark message from our society that some lives just aren’t worth caring for. Needing care and assistance from others does not mean that a person no longer has dignity or value. […]
HLA believes pain and suffering needs answers, love, and care, not suicide. True compassion offers healing, support, and hope.
You can find the video link, written testimony, and more info on our blog post: humanlife.org/inform/opposing-physician-assisted-suicide

America has a dark past that included Eugenics—a movement aimed at eradicating persons deemed “unfit for society.” Is prenatal testing coupled with induced abortion a resurgence of that practice?
Parents used to hope for ten fingers and toes. Now, modern technology makes it possible for parents to know more about their pre-born babies than ever before. The blessing of medical advancements is that prenatal treatments and surgeries are available to enhance babies’ lives. The curse is that, when tests indicate genetic abnormalities or adverse health conditions, abortion is frequently offered to families as the only solution. Misinformation, fear, and intimidation are used to coerce a family into aborting their child.
Often, families are told that ending the lives of their children is the most loving choice. The support group Prenatal Partners for Life helped a family who had been told,
“We recommend that you compassionately dissolve your pregnancy. This would be the best course of action for you and your family.”
Many parents say they are not informed of the option to continue the pregnancy and embrace the life of their child. And, even if families resist the pressure to abort, they may have to fight for treatment. After their child is born, the risk of stealth euthanasia (a.k.a., imposed death) is an ever-present danger. Conversations about the child’s quality of life, projected life expectancy, or resources may occur. Parents may be told, “Wrap your baby up in a blanket and let him go.” The negative and sometimes hostile attitude toward those who choose to keep their babies and help them reach their full potential is a shock to these families.
This eugenic mentality is increasingly common as medical professionals become more concerned about rationing resources to contain costs than preserving and enhancing their patients’ lives. This is a “futile care” approach to medicine, and it is a danger to all of us.
Thankfully, many support groups now exist so families need not feel alone. Prenatal Partners for Life (PPFL) offers life-affirming support, information, and encouragement to help families choose life for their babies with adverse diagnoses. PPFL also supports them in raising their special needs children. Furthermore, a ministry within PPFL called Lumen Caeli (Light of Heaven) offers support for families who experience miscarriage, stillbirth, and early infant death.
In addition to advocating for both parents and their babies, PPFL strives to educate and inform the world about the unique blessings and gifts children and adults with disabilities bring to their families and society, and the gift that all life is.


Artificially administered nutrition and hydration (ANH) is provided through a tube or an intravenous (IV) line.
• When ANH is needed short-term, a naso-gastric (NG) tube is inserted through the nose into the stomach.
• When needed long-term, a percutaneous endoscopic gastrostomy (PEG) tube is surgically inserted into the stomach.
These are both low-risk procedures that sustain people whose digestive systems function, but who are unable to eat or drink by mouth.
The widespread medical and legal support of denying food and water to patients with a “low quality of life” makes many people uneasy, and rightly so.
Seriously ill or disabled individuals still need food and water. Withholding sustenance often makes their condition worse and can create serious complications. Depriving a person of all food and fluids will also speed up or cause death, usually within a week or two.
Sometimes, a doctor may decrease or withdraw nutrition if it exacerbates the patient’s condition. For example, a patient with severe congestive heart failure may not be able to tolerate fluids for a period, or a patient who has abdominal cancer may not be able to tolerate tube-feeding. Even so, that patient should still receive hydration.
When the body is no longer able to absorb nutrition or hydration, there is a legitimate medical reason to stop administering them while still caring for the patient’s comfort. In such cases, the cause of death will be the patient’s disease or injury, not starvation and dehydration.
ANH accomplishes the exact purpose for which it is given–sustaining life. It is not futile care.
Death by starvation and dehydration is typically NOT chosen by the patient. However, some people check a box rejecting “life-sustaining procedures” in their Advance Directive, or someone else indicates this “on behalf of the patient.”
Some people do choose to refuse food and fluids to cause or hasten their own death, for whatever reason. This is called VSED (Voluntary Stopping of Eating or Drinking). VSED is legal in every state. It is also suicide. When a healthcare provider gives “comfort care” to ease the suffering caused by VSED, the ethical concerns are the same as for Assisted Suicide.
Beware: In hospice and palliative care settings, patients are often too medicated to eat, drink, swallow, or complain of thirst and hunger.
As the patient naturally approaches death, the body requires less fluids and food. However, as long as he or she can swallow appropriately:
• Sips of fluid and ice or popsicle chips can sustain hydration.
• A few bites of pudding, yogurt, or ice cream can be all the nutrition needed. Dehydration is miserable—even for folks who are near death.
For more information about ANH, visit: halovoice.org/nutrition-and-hydration
The services provided by one hospice may be very different from those provided by another. So, patients, families, and healthcare agents should investigate any hospice agency, ask questions, and get the answers before agreeing to use their services.
What Questions Should You Ask?
1. What is the “mission” or “business statement” of the hospice?
2. Is the hospice non-profit or for profit?1
3. Is the hospice licensed by the state?
4. Is the hospice Medicare certified?
5. Has the hospice ever committed insurance fraud?2
6. How many counties does the hospice serve?3
7. Can I meet or speak by phone with the hospice administrator prior to hospice admission?
8. Can I meet the staff who will be providing care prior to admission?
9. What types of services are provided and how often?
10. Can I receive IV fluids and tube feedings?
11. Will services be provided by the same individuals throughout the course of my care?
12. What kinds of support are available to my family/caregivers?
13. How are services provided after hours? What is the response time?
14. What do hospice volunteers do? Am I eligible for volunteer services?
15. Can the hospice provide care in a nursing home or personal care home/assisted living?
16. Do you require a family member or friend to be with me at all times?
17. Must I commit to a DNR (Do Not Resuscitate) status?
18. Is the hospice pro-life? Is this evidenced on the website, in brochures, mission, etc.
19. What is the hospice’s position regarding Terminal Sedation (also called Palliative Sedation)?
20. Will I receive a bill for expenses not covered by insurance?
21. What should I do first if I am having a problem with the care my hospice is providing?
22. What should I do if I feel the hospice hasn’t addressed my concerns adequately?
1. Most hospices caught for insurance fraud are for-profit companies. Many for-profits are governed by shareholders concerned about returns on their investments. However, many non-profits also follow a business model. So, asking about a hospice agency’s business status is as important as asking about profit status. Any hospice that keeps saying, “We don’t provide that,” is not enhancing life and is most likely cutting costs at the bedside in order to enrich investors and pay executives’ salaries.
2. “Stop Hospice Fraud.” HALO, 22 March 2025, halovoice. org/hospice-palliative-care. Accessed 21 January 2026.
3. Hospice agencies often serve many counties from a single office. The on-call nurse may have difficulty reaching you quickly in an emergency as he/she may be several hours away.


Every person in the United States is asked to be an organ donor when applying for or renewing a driver’s permit or license, even teenagers. However, the form does not provide the information they need to give informed consent at the DMV.
The American College of Physicians (ACP) stated that the ACP, “emphasizes the importance of truly informed consent for organ donation and advocates for prioritizing equity and transparency in transplantation processes.”1
“Our findings show that hospitals allowed the organ procurement process to begin when patients showed signs of life, and this is horrifying,” Health and Human Services Secretary Robert F. Kennedy, Jr. asserted in a press release July 21, 2025. “…The entire system must be fixed to ensure that every potential donor’s life is treated with the sanctity it deserves.”2
The following should be provided to individuals before asking them to be organ donors.
• If you choose to be an organ donor, irrevocable organ procurement policies are set in motion to ensure your desire to be a donor is honored. Your healthcare agent, spouse, and family members cannot stop this process.
• After you are declared dead, your organs will be surgically removed and prepped for transplantation. Most transplantable vital organs come from patients who are declared “brain dead.”3
• A person declared “brain dead” is not biologically dead. The heart still beats, the lungs aerate with the help of a ventilator, and vital body systems, controlled by the brain stem, continue to function.
• The apnea test, which is required when determining “brain death,” can worsen a brain injury and cause serious complications, including cardiac arrest.
• In preparation for the organ removal surgery, you will likely be given paralyzing drugs to prevent you from moving.
• During the surgery, you are not guaranteed anesthesia to treat signs of bodily distress (e.g., muscle tensing, heart rate elevations, and blood pressure increases).
• People who are declared legally dead before their vital organs are removed are certainly dead afterwards.
• Some people have recovered after being declared legally dead, when given appropriate medical treatment.
This article is endorsed by Heidi Klessig, MD, a retired anesthesiologist and pain management specialist. Dr. Klessig writes and speaks on the ethics of organ donation and transplantation. She is the author of “The Brain Death Fallacy.” Her work may be found at respectforhumanlife.com.

In 2007, 21-year-old Zack Dunlap was diagnosed “brain dead” after a catastrophic brain injury. He was saved from having his organs harvested when a relative used the blunt side of a pocketknife to check his foot reflexes. Zack jerked his foot away. Just months later, he was walking and talking. He recalled hearing a doctor say he was dead and being “mad” but unable to move or scream. Zack is now a husband and father.4
You can watch Zack’s story here: https://youtu.be/6_TUF3hEZXw?si=-AD9nT4LGhiVXv3C start at 34:50.

The objective and motive for administering pain medication must be to relieve a patient’s pain, NOT to hasten or cause death.
Why is pain control important?
Pain can lead to adverse effects on appetite, sleep, energy, mood, ability to work, and relationships. Fear of uncontrollable pain is common for chronically and terminally ill people. The Assisted Suicide lobby claims that Assisted Suicide is a solution for “unbearable pain.”
What if my physician cannot control my pain?
Pain treatment is a specialized field of medicine. Not all physicians have the skills with analgesic medications to maximize their benefits while minimizing their side effects. If your pain is not being effectively controlled, find a physician or healthcare facility that focuses on pain management.
What is the “best way” to control pain?
Whatever works best for you is the “best way.” Most pain can be relieved by drugs administered orally or by other routes. Nerve blocks are performed in certain situations, and for tumors, reducing their size with chemotherapy and radiation therapy often results in pain relief.
There are also nonpharmacological pain control methods—ice, heat, elevation, immobilization, rest, relaxation techniques, or meditation—that can be utilized in any pain management plan.
A realistic goal should not be zero pain but a tolerable level of pain that allows for optimal physical and emotional functioning while preserving the patient’s alertness and ability to interact with others.
Will I become addicted to pain medication?
When opioids (such as morphine) are given to relieve physical pain, addiction (a psychological drug dependency) is not likely to occur. However, the ability of a given dose to relieve the same amount of pain decreases over time, so it may be necessary to gradually increase the dosage. Pain control needs may also change as an illness progresses.
Will pain medications cause me to sleep a lot?
Pain may cause poor sleep. Effective pain control will help you catch up on lost sleep, and soon you should be able to do normal activities. Prolonged sleepiness is usually caused by other medications such as tranquilizers and anti-anxiety drugs.
At times, it is not possible to treat pain or other symptoms effectively without sacrificing the patient’s awareness and ability to communicate. However, good physicians treat with the objective of maintaining that ability.

We can’t help everyone, but everyone can help someone.”
– President Ronald Reagan
A patient advocate is a relative, friend, volunteer, or healthcare provider who strives to safeguard the welfare of a vulnerable patient. As a visible ally of a seriously ill, elderly, or disabled patient, an advocate is a witness that this patient is worthy of care and protection. Even more importantly, a devoted advocate is a sign to the patient that he or she is valued and loved.
A patient advocate may be the agent authorized in an MPA to make medical decisions for the patient or may simply work with the agent. The agent can give permission for the advocate to speak to medical personnel about the patient’s condition, care, and wishes.
Administrators and some staff members of hospitals, longterm care, and hospice facilities may see occupied beds, not patients. The faster they can discharge a patient, the sooner they can clear the bed. This mentality can lead to prematurely discharging patients or even withholding care to hasten their deaths. Even on Medicare, a patient or agent has the right to refuse being discharged if the patient is not ready.
A major difficulty in making healthcare decisions is the overwhelming and confusing amount of information and options. Trustworthy healthcare providers will clearly explain a patient’s condition and all the available medical options. Unprincipled healthcare providers tend to push the most profitable or easiest options, not what is best for the patient.
A patient and his or her agent have the right to review the patient’s medical records and consult with another doctor. A patient advocate can support them by using reputable sources to research prognoses and treatment options.
HALO’s primary mission is to be a voice for the medically vulnerable. We offer tools to help you become a highly effective patient advocate. Check out the “Patient Advocacy” and “Resources” pages on HALO’s website: halovoice.org.
If you need to talk to an experienced patient advocate: Call the HALO Helpline 1(888)221-4256
Or the Terri Schiavo Life & Hope Network’s 24/7 National Crisis Lifeline 1(855)-300-4673

During an in-person doctor visit, an advocate’s essential role is to help the patient and doctor communicate well. The advocate can write a list of the patient’s symptoms and questions, make certain that these are answered clearly, and also take notes so the patient can review the doctor’s advice later. The essence of patient advocacy is to be in solidarity with our weakest and most vulnerable human beings, even sacrificing ourselves for their sake. Most of us will have opportunities to serve as patient advocates. This magazine is meant to be a tool to help you prepare to be a caring and effective advocate for your loved ones.

Human Life Alliance promotes awareness of the inherent dignity and personhood of human life, born and preborn, without exception or compromise. Human Life Alliance (HLA) proclaims and defends a culture of life and chastity through education, social and political awareness, and life-affirming alternatives to abortion, infanticide, assisted suicide, and euthanasia. HLA accomplishes its mission in a spirit of prayer and non-violence.
Over the years, HLA has established an extraordinary record of service—an unrelenting commitment and dedication to developing respect for all human life. Since 1977, HLA has served the pro-life community around the world by pioneering educational initiatives, working with policymakers, assisting unwed mothers, reaching teens, and saving the lives of young women and their babies. HLA supports life-affirming alternatives to infanticide, euthanasia, assisted suicide, and the so-called “safer-sex” myths to change hearts and save lives every day.
Since its first printed educational campaigns in 1990, HLA has reached over 240 million people in all 50 States, 88 different countries, and all 7 continents.
To order copies of Informed, please visit humanlife.org/informed or call 651-484-1040.
All sources available at humanlife.org/sources
Human Life Alliance 1614 93rd Lane NE, Blaine, MN 55449 feedback@humanlife.org | 651-484-1040 Learn more at humanlife.org


