

TABLE OF CONTENTS




Ticks
GCMS

Editor’s Note: All materials for the Journal must be submitted by the first of the month prior to publication.
Co-Editors:
Jim Blaine, MD
Minh-Thu Le, MD
Junior Co-Editor: Andrew K. Le
Managing Editor: Dalton Boyer
Editorial Committee:
Michael S. Clarke, MD
David Barbe, MD
Jaya LaFontaine, MD
Dalton Boyer
Andrew Le
Jean Harmison
Barbara Hover
SOCIETY OFFICERS
Melissa Ganies, MD, FACP, FAAHPM President
Vu Le, MD
Secretary
Jim Blaine, MD
Treasurer
James Rogers, MD Immediate Past President
Council Members:
Barbara Hover
James Rogers, MD
Melissa Gaines, MD
Rachelene Middleton, MD
Jim Blaine, MD
Sanjay Havaldar, MD
Jaya LaFontaine, MD
John Steinberg, MD
Taylor Brooks, MD Vu Le, MD
Managing Director: Jean Harmison
Executive Office: 4730 S. National Ave. Suite A1 Springfield, MO 65810 email: director@gcms.us
by Jim Blaine, MD
Happy Spring! This issue is dedicated to an amazing couple, Dr. David and Linda Brown. David and Linda retired and spent the next eight years golfing, traveling, and enjoying retirement life, but, then, they began engaging with homeless people who lived on the street near their downtown loft…..and they became friends. David and Linda’s story says a lot about the meaning of life and about humanitarianism.
Also in this issue is a wonderful companion article by former AMA President Dr. David Barbe who writes about “Gratitude, Faith and Giving”. We physicians are currently experiencing record numbers of burnout and much is blamed, by the AMA and others, on a decrease in autonomy. David poignantly points out that, when we give of ourselves, we regain a sense of agency and autonomy.
The fact that that both David Brown and David Barbe and their wives share strong religious convictions is not coincidental.

MSU Professor Emeritus Chris Barnhart is an expert on ticks and his timing is good to favor us with an article about my favorite arachnid to avoid and how to avoid their bites. I recently paid a visit my favorite endodontist, Dr. Stephen Raphael with the usual painless and professional results. Stephen agreed to share with us the mysteries of the root canal. He makes the lesson both informing and entertaining.
Finally, please consider joining GCMS members in Estes Park Colorado July 18-25. The condos are adjacent to the Rocky Mountain National Park. Your will receive 12 Cat. 1 CME hours.
GCMS welcomes three new Executive Council Members

S. Taylor Brooks, MD
Dr. S Taylor Brooks, MD, is a board certified internal medicine physician practicing in Springfield. He provides comprehensive care for adult patients, focusing on the prevention, diagnosis, and management of a wide range of medical conditions. His clinical interests include inpatient medicine, medical education, and the use of point-of-care ultrasound to support clinical decisionmaking. Dr. Brooks earned his medical degree from the University of Missouri School of Medicine in 2022 then did his residency training in internal medicine at Vanderbilt University in Nashville, Tennessee. After that he joined CoxHealth in Springfield, where he contributes to both patient care and physician training as a faculty physician working with residents.

John Steinberg, MD
Dr. John B. Steinberg, MD, is a board certified cardiothoracic surgeon based in Springfield with more than 40 years of experience treating complex heart and chest conditions. He specializes in procedures such as coronary artery bypass surgery, heart valve repair and replacement, and cardiac device implantation. Dr. Steinberg earned his medical degree from the University of Utah School of Medicine and completed surgical training at the University of Oklahoma Health Sciences Center and the University of Iowa Hospitals & Clinics. He has been affiliated with CoxHealth, providing advanced cardiovascular surgical care to patients throughout southwest Missouri.

Dr. Rachelene Middleton, MD, is a board certified family medicine physician who earned her degree from the University of Missouri-Kansas City School of Medicine in 2000 and completed residency at Baptist-Lutheran Hospital in Kansas City. She spent the last 21 years at Mercy Clinic Smith Glynn Callaway providing comprehensive primary care for patients of all ages. Dr. Middleton recently retired from Mercy Clinic and enjoys spending time with family, traveling, running, yoga, and lake time at Table Rock. She is passionate about the importance of primary care and has helped establish Volunteers in Medicine Christian County, a local free clinic where she volunteers as a family physician.
Rachelene Middleton, MD
PRESIDENT'S PAGE
By Melissa Gaines, MD, FACP, FAAHPM

As we move into the March–April season, I find myself thinking less about resolutions and more about preparation. Meaningful change in medicine rarely happens spontaneously. It requires thoughtful pre-work, collaboration, and a shared commitment to something larger than ourselves.
This spring, much of our energy is focused on preparing for GCMS Together aligning the Foundation, Council, and Alliance. The pre-work underway is intentional. We are listening carefully, identifying areas where physicians feel disconnected, and clarifying what would make engagement meaningful rather than just another obligation on a busy calendar. GCMS Together is not simply an event—it is a step toward cultivating belonging. If we are serious about strengthening physician resilience, we must first strengthen relationships and supporting physicians and their families.
At the same time, planning has already begun for the 2026 GCMS BASH. Last year’s inaugural event was a landmark moment for our organization, raising funds for the GCMS Foundation and demonstrating what is possible when we rally around a shared mission. The BASH was more than a fundraiser it was a celebration of community. As we look ahead, our goal is to build on that momentum with thoughtful planning, broader engagement, and a continued commitment to supporting the Foundation’s work in education and outreach.
In March, GCMS Council will gather for a strategic retreat focused on initiatives that foster a robust physician community. We will ask important questions: What does true physician resilience look like in our region? How do we create structures that promote mentorship, social connection, leadership development, and advocacy? How can GCMS serve not only as a professional society, but as a stabilizing force in a rapidly changing healthcare environment?
Resilience is often discussed as an individual trait something physicians must cultivate on their own. I believe it is far more communal than that. Community buffers burnout. Shared purpose restores meaning. Trusted colleagues provide perspective during difficult seasons. Our responsibility as a society is to intentionally
design opportunities where those connections can flourish.
The months ahead are about laying groundwork. Preparation may not always be visible, but it is powerful. If we invest wisely now by listening, planning, and building trust we will create a physician community capable of sustaining its members and serving our broader community with excellence.
Thank you for your continued engagement, your ideas, and your willingness to be part of something bigger than any one of us. The future of physician resilience in Greene County will not be built by accident. It will be built together.
Join or Renew Today


Bringing physicians together to improve the health of our community.

Tailored Tax, Wealth Management, and Family Office to help you prepare for what’s next.
The Physician’s Bounty: Gratitude, Faith, and the Practice of Giving
By David Barbe, MD

I. Introduction: The Clinical Case for Gratitude
In the modern landscape of medicine, we often find ourselves measuring our lives by metrics: RVUs, HCAHPS scores, and relentless documentation in the electronic health record. In this high-pressure environment, our perspective can become cynical. However, there is a potent, evidence-based "antidote" to the professional exhaustion that plagues our ranks. It is not a new pharmaceutical or management strategy, but an emotion native to the human heart: gratitude
By gratitude, I mean more than a polite "thank you." It is a mental and emotional state that recognizes the goodness in one's life and acknowledges that the source of that goodness lies, at least partially, outside oneself. When physicians move from a mindset of scarcity—not enough time, not enough staff, not enough reimbursement—to a mindset of gratitude, the result is a profound shift in our priorities and practices. This shift naturally culminates in a more outward focus and greater concern for others, leading one to look for opportunities for charitable giving, transforming a private feeling into a public good.
II. Ancient Wisdom: Giving as a Sacred Discipline
Physicians have long occupied a unique space in our communities, serving as both scientists and moral leaders. Our traditions of giving are deeply rooted in the faith practices that many of us follow in our personal lives and carry into our professional roles. As we reflect on our faith, we see that the world’s major religions do not view charity as an optional "extra," but as a fundamental requirement for a healthy soul and a just society.
• Christianity: The Sacrificial Giving of Lent
During the season of Lent, the Christian tradition emphasizes giving alongside prayer and fasting. This is not meant to be a comfortable donation of excess, but a generous or even sacrificial act. For physicians, this mirrors the daily sacrifices we make for patient care—the missed dinners, the lost sleep, the emotional weight of a difficult diagnosis. However, Lenten giving provides a different context for that sacrifice. It reminds us that our resources (time and wealth) are held in trust. By giving generously, we acknowledge that our professional success is a platform for service, not just a means for personal comfort.
• Islam: The Justice of Sadaqah and Sadaqah Jariyah
In the Islamic tradition, particularly during the holy month of Ramadan, the concept of Sadaqah (voluntary immediate or sustained charity) is elevated. Sadaqah is a gift given out of compassion, love, and generosity—a way to demonstrate the sincerity of one’s faith. For a Muslim physician, the physical experience of hunger during the fast provides a visceral reminder of the suffering of the poor, and that the health we treat is often tied to the socioeconomic realities we can help alleviate through our generosity.
• Judaism: The Duty of Tzedakah
In Judaism, the concept of Tzedakah is often translated as charity, but its root is Tzedek (justice). To give is not simply a gesture of kindness but a moral obligation based in fostering justice for individuals and the community. When we give to medical or community organizations, we are not merely helping; we are fulfilling divine expectations.
III. The Science of Generosity
While the spiritual benefits of charitable giving are clear, the neurobiological benefits are equally compelling. Research in positive psychology suggests that acts of giving trigger the areas in the brain that process reward and reinforcement—the same ancient pathways that facilitate human connection—releasing oxytocin and dopamine. For physicians, the positive and affirming feelings produced can be a vital defense against the negative impact of our frustrations and burnout.
In addition, when we give, we regain a sense of agency and autonomy. Burnout often stems from a feeling of losing these professional prerogatives and being just another "cog in the wheel." Generous giving allows us to step outside of the system and make a personal, intentional choice to positively impact another human life. It reinforces our identity as healers who have the power to influence the world beyond the walls of the exam room.
IV. The Grateful Patient: Stewarding the Impulse to Give
We cannot discuss gratitude without acknowledging the "Grateful Patient." Often, after a successful surgery or a compassionate end-of-life journey, patients feel a
profound need to give back. In the past, physicians may have felt awkward or ethically compromised by these gestures.
However, modern medical ethics increasingly recognizes that allowing a patient to express gratitude is, in itself, therapeutic. When a patient or family donates to a foundation or a research fund in your honor, they are closing the loop of their own healing. Our role is to provide a professional channel for that impulse—directing their gratitude toward a medical society’s foundation or local health initiative where it can do the most good without compromising the physician-patient relationship. We must see ourselves not just as recipients of their thanks, but as stewards of their desire to help others.
V. Conclusion: A Call to Healing for Our Communities— and Us
As members of the medical profession, we share a common bond that transcends our individual specialties and faiths. We are the stewards of our community’s
health. Whether we are inspired by the Lenten call to sacrifice, the Ramadan call to compassion, the Jewish call to justice, or a secular commitment to humanity, the conclusion remains the same: we are at our best when we give.
Charitable giving is the outward expression of a physician who has remained attuned to the privilege of their calling. It is a declaration that despite the frustrations of modern medicine, we still believe in the power of healing—not only the clinical care we provide at the bedside but the healing we bring to our broader community through our philanthropy.
I encourage you to look at your bounty—your skill, your time, your means, and your spirit—and make the conscious decision to share it. In exercising this native impulse to give, you may find that the person most healed by the gift is the one who gave it.


Ticks and tick-borne disease in the Ozarks
By Chris Barnhart, PhD, MSU Professor Emeritus
Ticks are the most significant vectors of infectious disease in the Ozarks. By feeding on blood from multiple hosts, ticks can transmit pathogens, including the causative agents of Rocky Mountain spotted fever, ehrlichiosis, tularemia, Lyme disease, anaplasmosis, Southern tick–associated rash illness (STARI), Heartland virus disease, and Bourbon virus disease. Tick bites can also cause allergic reactions including alpha-gal syndrome, and in rare cases, whole body paralysis. Some of these illnesses are potentially fatal and some lack effective treatment, but all are preventable. Ticks are not dramatic, but they are a ubiquitous and complex health hazard that deserves attention. This article focuses on tick biology, life history, and transmission dynamics as they relate to disease risk in the Ozarks. A second article will address diagnosis, clinical features, and treatment considerations.
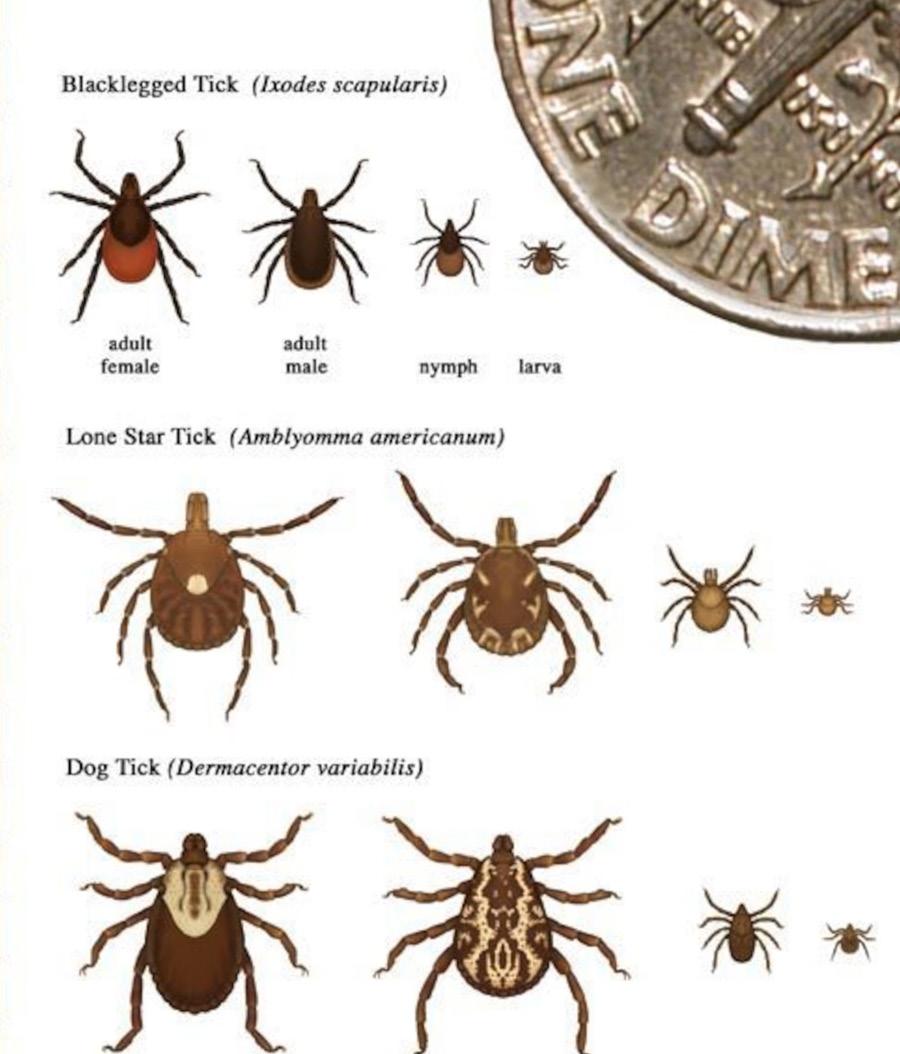
IDENTIFICATION. Ticks are arachnids, related to spiders and mites rather than insects. Like other arachnids, adult ticks possess eight legs and lack a defined head and antennae. They feed on the blood of vertebrate hosts. The medically
important tick species in our area all belong to the family Ixodidae, the “hard ticks,” which are characterized by a rigid dorsal shield or scutum. These are the Lonestar tick, American dog tick, and Black-legged tick. Our discussion refers primarily to these three species. Several other tick species are also present but are less likely to bite humans and transmit disease.

Lone star tick is the most aggressive and abundant tick in the Ozarks. It prefers wooded and brushy habitats as well as pastures and is associated with ehrlichiosis, STARI, and alpha-gal syndrome. Abundance and active host-seeking behavior make it the major cause of tick bites in the Ozarks. American dog tick is the primary vector of Rocky Mountain spotted fever. It is slightly larger than the Lone Star and favors open fields and edge habitats. Adults are commonly encountered and frequently attach to dogs and humans. Blacklegged tick is the primary vector of Lyme disease in the Northeast states. This small tick is less abundant in the Ozarks but is present and transmits Lyme and anaplasmosis. Bites are likely to go unnoticed because of its small size.
LIFE CYCLE. Ticks develop in 4 stages: egg, larva, nymph, and adult. Maturation requires 1-2 years, yet a tick feeds only three times, once as a larva, again as a nymph, and finally as an adult. Each meal requires several days of attachment, during which the tick inflates tremendously beyond its unfed size. After feeding the tick leaves the host for 1-3 months to digest the meal, grow and molt the exoskeleton, after which another host must be acquired. Each host is an opportunity for pathogen acquisition or transmission. After the final blood meal, the engorged female, as large as a pea or small grape, drops to the ground. She later deposits a single mass of several hundred to several thousand eggs. The eggs hatch 1-2 months later, depending on temperature.
TIMING. Lone star ticks overwinter primarily as nymphs in leaf litter and tolerate temperatures down to 0°F (-18°C). Questing occurs mainly between 45-85°F (7-29°C). Dog ticks and Black-legged ticks are more likely to overwinter as adults. They are active at lower temperature (40°F) (4°C) and appear earlier in the spring. Tick activity is stimulated after rain and suppressed by low humidity and high temperature. Most egg laying occurs in May–June and hatching in late June–July. A host unlucky enough to pause beside a
hatching egg mass may acquire a swarm of dozens or even hundreds of hungry larvae (“seed ticks”), an experience not soon forgotten.
PATHOGEN TRANSMISSION. Transmission occurs only during feeding. Unlike biting insects, hard ticks attach securely and feed for up to several days. Attachment involves insertion of barbed mouthparts and secretion of an adhesive protein to bind the tick in place. Anticoagulant, vasodilatory, and anti-inflammatory saliva secretions flow into the wound to facilitate blood flow and minimize irritation to the host. Pathogens residing in the tick migrate to the salivary glands during feeding. Therefore, transmission risk increases significantly after 24–48 hours of attachment, and prompt removal is important.
LIFE STAGE RISK. All life stages potentially carry pathogens. The proportion of infective ticks increases from larva to nymph to adult. On the other hand, larvae and nymphs are more likely to attach and feed unnoticed, which increases the risk of transmission. Groups of seed ticks can trigger inflammation and alpha-gal syndrome. Unlike immatures and adult females, which engorge and leave the host after feeding, adult males may take several small meals and move about on the host to seek females for mating. These behaviors may enhance both irritation and disease transmission.
COMPETENT HOSTS. Mammals are hosts of ticks, and both ticks and mammals are hosts of pathogens. Competent hosts of a pathogen become infective after infection. That is, a competent host “can take it, and can dish it out”. Cattle are important hosts for ticks but are generally not competent hosts for tick-borne disease. Dogs and cats are also tick hosts and may become infected with the human pathogens and others, `but do not usually pass the diseases on to other ticks that bite them. The most abundant competent hosts are rodents and white-tail deer. Cycles of rodent abundance following mast years have been correlated with Lyme disease outbreaks in the Northeast. In our area the abundance of white-tail deer correlates with abundance of ticks, and the increase in deer populations over recent decades is one likely cause of the increased incidence of ticks and tickborne disease.
HOST CONTACT. Like fishermen, ticks meet hosts by a combination of strategy and luck. A characteristic behavior is known as questing—climbing vegetation, extending the forelegs, and waiting for the approach of a host. Ticks have poor eyesight but possess sensitive chemosensory organs on the front pair of legs that detect carbon dioxide, heat, and host-associated odors. These signals alert the tick and can trigger movement toward the source. Adult Lone star ticks
are relatively mobile and can move several meters toward a host within hours. Questing is not continuous. It is most common in mid-morning through early afternoon in the spring. During summer heat, activity shifts toward morning and late afternoon, and is stimulated after rain.
PREVENTION. Consider the risk factors and take precautions when and where ticks are likely to be present. Dress for success-- ticks must contact the skin to attach and clothes can prevent contact. Fabrics should be tightly woven. Most socks are too porous to block seed ticks. Pantlegs should be taped or tucked into boots or socks, and shirt tails tucked in. For extreme protection, lightweight, full body ‘tick suits’ are available to wear under clothing. DEET repellents are effective against ticks and can be applied to the skin on ankles and waistline as well as on clothes. Permethrin sprays are available to treat clothing and remain active through multiple wash cycles. After outdoor activity it is very important to bathe thoroughly, make a full body check and remove ticks as soon as possible. Pay careful attention to any stray itch that develops. Seed ticks can be removed with duct tape. Attached nymphs and adults should be grasped with fine point forceps, as close to the skin as possible, and slowly pulled free with steady pressure. Beware of any rash that develops.
Ticks are more than a nuisance but less than an emergency. The risk of tick encounter is generally low but rises sharply in wildlife habitat and wildlife-adjacent adjacent yards of homes. Many locals know others who have been diagnosed with a tick-related illness, and a restaurant specializing in alpha-gal free foods recently opened in Springfield. Ticks are dynamic participants in pathogen ecology. Their multi-host life cycle connects wildlife reservoirs, domestic animals, and humans in a shared transmission network. The next article will examine the major tick-borne diseases encountered in the Ozarks, including their clinical presentation, diagnostic considerations, and treatment approaches.
RESOURCES
Missouri Extension. https://extension.missouri.edu/publications/ipm1032 US Centers for Disease Control and Protection. https://www.cdc.gov/ticks/site.html#gen
Chris Barnhart is Distinguished Professor emeritus at Missouri State University. He taught parasitology for many years and has had his share of tick bites and doxycycline.
GCMS Rocky Mountain Medicine 2026
President Melissa Gaines has chosen Estes Park Colorado and the Rocky Mountain National Park as our site for the GCMS Rocky Mountain Medicine site for 2026; July 18 through 25, 2026. CME meetings will be July 20,21, and 23. CME will qualify as AMA Cat I. Tuition will be $250 for GCMS members and $300 for non members.
We have reserved a block of condos at the Estes Park Condos. These units are only a mile from the famous Rocky Mountain National Park (RMNP) entrance. The RMNP Fall River is stocked with Rainbow trout and runs directly out of the park and in front of our condos. There is a community hot tub, but many of the condos have their own private hot tub as designated by the (HT) on their number. We have reserved a total of 25 condos. We have 4 one bedroom condos and 11 two bedroom condos in Creekside Suites which are closest to the Fall River meeting room and the community hot tub. We have also 5 one bedroom and 5 two bedroom condos in the Bugle Point A suites; many of these have private hot tubs. That gives us 25 condos reserved for 60 days, but any non reserved condos will be released to the public after the 60 days.

Please check out the web site https://estesparkcondos.com/ and select your condo from the following list we have reserved:
• Creekside Suites: 2 Bed 1 Bath: 2,3,4,5,9,10,11,18,19,20, and 21(HT)
• Creekside Suites: 1 Bed 1 Bath: 1,12,16, and 22
• Bugle Pointe A: 2 Bed 2 Bath: A9(HT), A10, A11, A12, A14, A15
• Bugle Pointe A: 1 Bed 1 Bath: A2(HT), A5(HT), A13(HT), A16(HT)
Please check out the site map on the web site to see the location of the condos and their proximity to the community hot tub and Fall River meeting room.

When you have made your choice, call the number on the web site, identify yourself as a Greene County Medical Society attendee and reserve your condo choice (you will receive a 10% discount).
Once you have made your reservation, please report your reservation to this email (jimblaine@aol.com) and we will remove your condo from the available condo list.
We plan to be approved for 12 hours of AMA Cat I CME. Attendees are encouraged, but not mandated to do a 45 minute presentation with an additional 10 minutes for question and answer.
Please let us know if you have any questions Melissa Gaines and Jim Blaine, co-chairs 417 861-9286

The Stanley Hotel (Estes Park, CO): The famous hotel where Harry and Lloyd stay, including the bar where Lloyd waits for Mary from the film Dumb and Dumber..
Turn Tax Season: Pain Point or Planning Opportunity
By Carlee Lynn, CFP® and Justin Stockam, CPA

‘Tis the season! Tax season, that is. For some, this can be a frustrating time faced with unwanted payments due or outsized refunds not preferred. Year-round proactive tax planning might help alleviate some of these outcomes, especially when coordinated with your specific goals. While taxes likely cannot be eliminated entirely, here are some opportunities to consider implementing to help improve your tax outlook for 2026.
Charitable giving strategy review: Make your already highimpact gifts to others have a tax impact for yourself.
• If charitable giving is a priority for you, review your methods for tax efficiency. Consider a charitable bunching strategy, use a donor-advised fund (DAF), or give appreciated stocks held longer than one year rather than cash. These changes could have a notable tax impact if planned.
Get the most from employer retirement plans: Pre-tax payroll deductions placed into employer retirement plans may decrease your taxable income.
• For 2026, the limit is $24,500 for employee deferrals into an employer plan. If your payroll deduction amount is not currently set to max out this limit by or before year-end, consider adjusting it. This is a step in building your foundational savings habits toward retirement and helps ensure you don’t miss out on the tax deduction available.
• Important change in 2026 from SECURE Act 2.0: For employees 50 and older, any catch-up contributions must be made into a Roth account and will not count toward tax-deductible income.
Health savings accounts (HSAs): Utilize, maximize, and invest in these potential investment accounts.
• HSAs can be a powerful tool for tax-free healthcare funds. If eligible, elect a healthcare coverage plan that qualifies you to save into an HSA account. Then, contribute the annual maximum amount ($4,400 for individuals/$8,750 for families) for 2026, and invest the funds for growth rather than spending them on today’s healthcare costs. The contributions made today are tax deductible from your income, and the proceeds grow without being taxed if used for qualified medical expenses. Long-term investment growth of these funds can add up to use tax-free on potentially higher healthcare costs in retirement.
Portfolio management: Use asset location and tax-loss harvesting as a strategy.
• Portfolio management strategies can support taxefficient investing by utilizing asset location and tax-loss harvesting. Asset location refers to the placement of assets across different account types to mitigate taxes.


Tax-loss harvesting is another investment strategy to reduce the amount of realized gains you pay tax on in your portfolio without reducing the actual returns of your portfolio. These are strategic investment decisions your investment advisor should be able to help implement.
Tax professional: Get the support you need if your 2025 tax situation wasn’t what you hoped.
• If the recent tax filing season left you wondering if there’s something you should have done differently, it may be time to find a new tax professional. Tax planning throughout the year and attention to the goals unique to your family and financial situation are key parts of a relationship with your CPA. If it’s time for a change, make the switch while there’s time left for it to impact 2026.
The information set forth in this article contains the analysis and conclusions of the authors based upon their research and analysis of industry information and legal authorities. Such analysis and conclusions should not be deemed opinions or conclusions by Forvis Mazars or the author(s) as to any individual situation, as situations are fact-specific. The reader should perform their own analysis and form their own conclusions regarding any specific situation. Further, the author(s)’ conclusions may be revised without notice with or without changes in industry information and legal authorities.
Forvis Mazars Private Client services may include investment advisory services provided by Forvis Mazars Wealth Advisors, LLC, an SEC-registered investment adviser, and/or accounting, tax, and related solutions provided by Forvis Mazars, LLP. The information contained herein should not be considered investment advice to you, nor an offer to buy or sell any securities or financial instruments. The services, or investment strategies mentioned herein, may not be available to, or suitable, for you. Consult a financial advisor or tax professional before implementing any investment, tax or other strategy mentioned herein. The information herein is believed to be accurate as of the time it is presented and it may become inaccurate or outdated with the passage of time. Past performance does not guarantee future performance. All investments may lose money.

WE TAKE PRIVATE BANKING PERSONALLY.
With Private Banking at Central Bank, you have exclusive access to a host of financial services and products, where we take care of the details across the full spectrum of the bank. You will have access to higher deposit rates, custom credit solutions and home financing, as well as individualized guidance with your investments. Our main goal is to help you maximize your money seamlessly. You have complex needs. We have the concierge level solutions you want.



STEVE GASSEL
Senior Vice President - Director of Private Banking | NMLS # 554828
3333 S. National Ave., Springfield, MO 65807
Phone: (417) 841-4213
Steve.Gassel@centralbank.net
KARA TURNER
Vice President - Private Banking | NMLS # 1833785
3333 S. National Ave., Springfield, MO 65807
Phone: (417) 841-4253
Kara.Turner@centralbank.net
JOYCE WONG-HSU
Officer - Private Banking | NMLS # 1239617
3333 S. National Ave., Springfield, MO 65807
Phone: (417) 841-4214
Joyce.Wong-Hsu@centralbank.net
The Future of Rural Medicine
By Brian Biggers, MD
Recently, I had the distinct honor of receiving an invitation to the White House to represent my state and medical community. While such an invitation may carry political connotations, my purpose in attending was not partisan. Rather, it was an opportunity to serve as a voice for our patients, particularly those in rural communities.
I grew up on a dairy farm in Marshfield, a rural community close to Springfield, Missouri. Rural communities are close-knit; neighbors know one another and look out for each other. Yet despite the strength of these communities, geography remains a powerful determinant of health. It was striking to learn that a patient’s ZIP code can significantly influence life expectancy in the United States. Data consistently demonstrates disparities in health outcomes between rural and urban populations. In my own practice, this disparity is evident in the advanced-stage malignancies more frequently diagnosed among patients from rural areas.
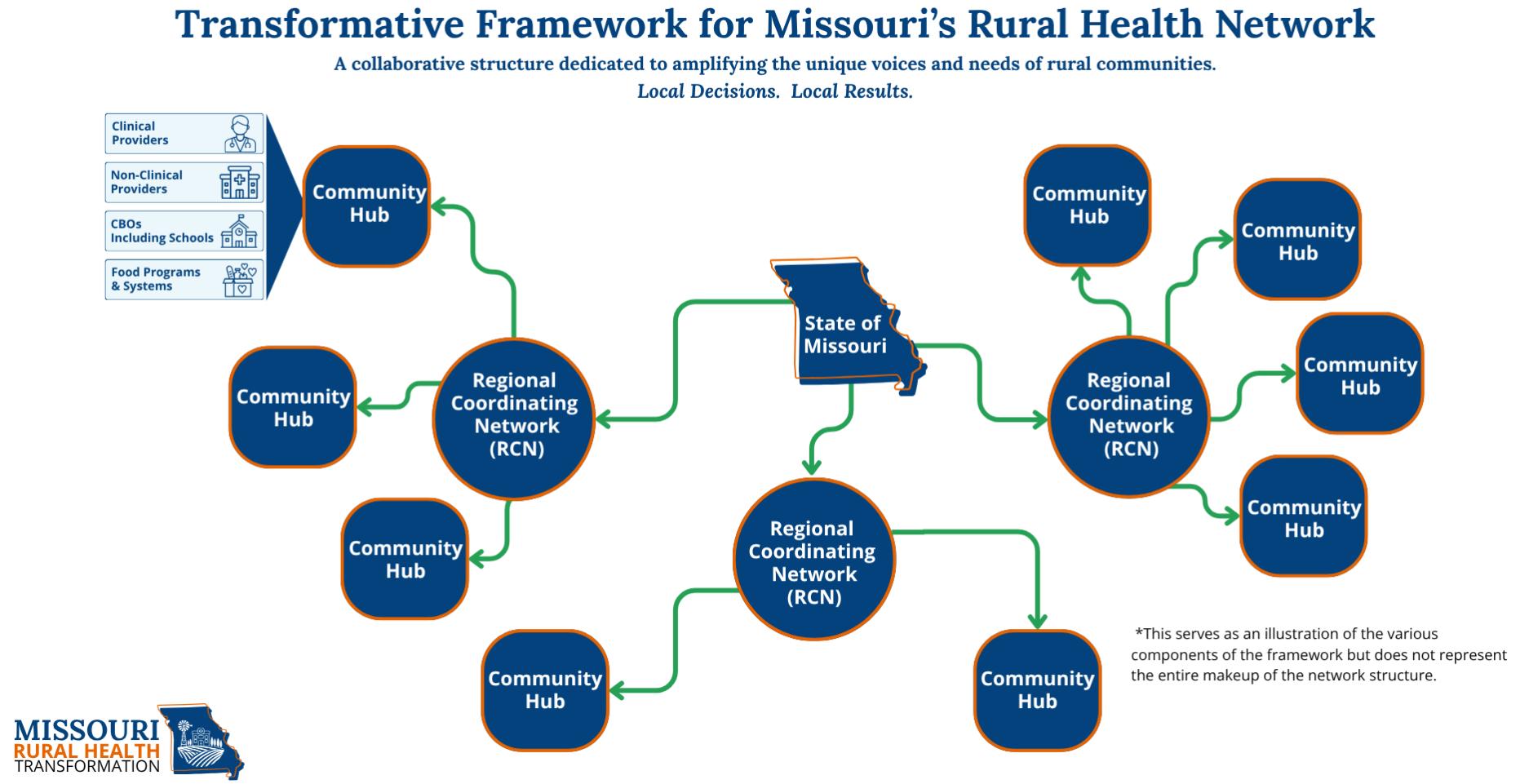
My visit to Washington, D.C., centered on participation in discussions surrounding the Rural Health Transformation Program. Missouri is among the top ten states selected to receive funding through this initiative—$214 million in the first year and up to $1 billion over five years. These funds are intended to strengthen rural health systems and improve clinical outcomes. Importantly, allocation strategies will vary by state, reflecting differences in infrastructure, workforce capacity, population needs, and geographic challenges. Tailored implementation is essential; what works in Missouri may not mirror the needs of states such as Wyoming. The responsibility now rests with state leadership to ensure that these resources are deployed effectively and equitably.
Preserving access to care remains central to any rural health strategy. Critical access hospitals serve as lifelines in many Missouri communities. Yet numerous small hospitals across our state—and nationwide—are struggling financially, with some
forced to close. Each closure widens the gap in access to essential services. Expanding scope of practice alone will not resolve systemic access challenges if the underlying infrastructure continues to erode.

At the same time, improving outcomes requires careful consideration of volume-outcome relationships. For example, data suggests that cancer outcomes are often superior at highvolume centers. Reconciling this evidence with the need for local access presents a complex challenge. Potential solutions may include the development of satellite clinics affiliated with tertiary centers, expansion of telemedicine services, and strategic regional partnerships that allow patients to receive specialized expertise closer to home while maintaining high standards of care.
Emerging technologies will also shape the future of rural medicine. Artificial intelligence (AI) has the potential to enhance diagnostic accuracy, optimize resource allocation, and expand specialty consultation through decision-support tools. However, the medical community has yet to fully define its applications, limitations, and governance structures within clinical practice. Thoughtful integration—grounded in evidence, ethics, and patient safety—will be necessary to ensure that technology narrows, rather than widens, existing disparities.
Regardless of political perspective, we now face a meaningful opportunity to improve patient outcomes across our state. Rural health transformation requires bipartisan commitment, data-driven decision-making, and sustained collaboration among clinicians, administrators, and policymakers. Missouri is known as the “Show-Me State.” This is our opportunity to demonstrate—through measurable improvement in access, quality, and outcomes—what thoughtful investment in rural health can achieve.
Thank You Dr. Pat Dix
(Reprinted with permission of Kevin Agee, CoxHealth Internal & Corporate Communications Coordinator)
In 1946, two unexpected twins were born prematurely at a Catholic hospital in Chicago. One weighed 2 pounds, 10 ounces. Her sister, 1 pound, 13 ounces. Their parents were told to go home, as the twins’ survival was unlikely.
Instead, the twins were transferred to Chicago’s Michael Reese Hospital – one of the nation’s earliest special-care baby units –and survived.
But not only did they live, they thrived. And that 2-pound, 10-ounce baby – Dr. Patricia Dix – recently retired from CoxHealth after a 50-year career (including 37 years at CoxHealth), caring for the same high-risk pregnancies that she once embodied herself.
“I went from being a preemie to delivering preemies. I’ve told that story to so many families: I’m the proof,” Dr. Dix says. “Not only did I survive, but I’m the doctor they’re talking to. So have hope.”
Dr. Dix earned a biology degree at Alverno College, received her medical degree from the University of Illinois Chicago, and later specialized in maternal-fetal medicine.
“My maternal-fetal medicine fellowship at Bowman Gray School of Medicine was where I really learned how to take care of
families, not just patients,” she says. “It confirmed I was exactly where I was supposed to be.”
That experience led to a decades-long career that included delivering thousands of babies – a total she estimates around 5,000, including close to 3,000 at CoxHealth.
“I love delivering babies. It’s so much fun,” she says. “For me, it’s never been a job. I’m just doing what I love to do.”
Dr. Dix moved to Springfield with her husband, Tom, and started her career at CoxHealth as a contract doctor in 1988 before going full-time. She had a demanding career and a strong marriage that Dr. Dix fondly remembers.
“Tom bragged about me all the time, and I bragged about him,” Dr. Dix says. “He never, ever, ever, ever, ever complained about me not being home. Not ever.”
That time at the hospital involved leadership roles, too. In addition to her core job where she consistently cared for highrisk pregnancies, she also served as director of the Regional Perinatal Center for many years and spent 25 years as a member of the CoxHealth Board of Directors.
It’s a legacy that will persist, says Kayla Miller, Clinic Manager of Maternal and Fetal Health in Springfield.

“Dr. Dix has been a foundational leader in the high-risk obstetrics community in southwest Missouri,” Miller says. “Her dedication to patient care and the profound impact she has had on countless families will remain. We will deeply miss her, and we’re excited for her as she embarks on this next chapter: One that allows her to enjoy time beyond the hospital and discover new passions.”
In retirement, Dr. Dix says she has no plans to slow down. After a short break in March, you can find her volunteering locally and teaching residents and doulas.
“I’m planning to hit the ground running,” she says. “I can’t imagine sitting around doing nothing. I’ll be busy as long as I’m able.”
So after a long career that touched thousands of lives, Dr. Dix steps away with gratitude and knowledge of a job well done.
The premature baby born in Chicago became an awardwinning doctor who’s given hope and joy to so many.
“I came full circle,” Dr. Dix says. “It’s been a great 37 years.”
From Pat Dix herself: "From the beginning of my practice at The Regional Perinatal Center until my retirement I have been supported by amazing staff, colleagues snd L&D, postpartum nurses. It was always a team effort and a two way street. My thanks to all of you".
Root Canals
By Stephen Rafael, DDS, Diplomate, American Board of Endodontics
Hi, my name is Steven, and everyone hates me. Let me back up a sec — 'cause, I know, that sounds bad. But to be honest, I get it. It’s not personal. I'm an endodontist, you see — the kind of dentist that specializes in root canals, or, as they're more commonly known to patients: "I have to get a WHAT?!"
Now, no one especially likes having dental work in the first place — but root canals? They're in a whole other stratosphere. These things have a reputation for being roughly akin to medieval torture.
To make matters worse, in this day and age, there's so much nonsense being spread on the internet that it's hard for even the most well-intentioned patients to separate fact from fiction and figure out just how frightened they ought to be. Far from the painful ordeal of myth, though, modern root canal treatment is a routine procedure no more invasive than a simple filling. When performed by a skilled professional, it is highly successful and relatively pain-free, and it's a critical tool in maintaining long-term oral health and function.
So, what does root canal treatment mean? Let’s start with some basic dental anatomy. The way I explain it to patients is by comparing a tooth to an ice cream cone: The scoop is the part in your mouth that you see, the cone is the root that extends below the surface, and the ice cream is soft tissue called the dental pulp. The pulp contains nerves, blood vessels, and connective tissue. In the simplest possible terms, then, root canal treatment means taking the ice cream out of the cone. (See? That doesn't sound so bad!) Why would
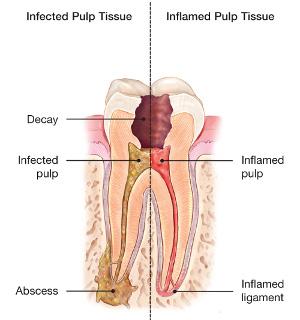
we need to do this, you might be wondering? The most common reason is untreated dental decay —a.k.a. a cavity — that slowly works its way into the pulp.

As estimated 20 billion bacteria live in the human mouth. When kept in balance by proper oral hygiene, they're mostly harmless. However, they produce acid as a byproduct of metabolism. And that means if they're left on teeth for too long, that acid eats away at tooth structure. Ergo...the cavity. If undetected and untreated, a cavity continues to erode away tooth structure until it reaches the pulp. The bacteria causes an inflammatory reaction and, eventually, necrosis and infection. Sometimes, that results in horrible pain and swelling. Other times, it’s a silent infection that leads to localized bone loss.
While tooth decay is the primary etiology, it’s not the only one. I often use the “straws on a camel’s back” analogy: Anything that irritates and damages the pulp is like a “straw.” That includes decay, restorations, trauma, cracks, and parafunctional habits like grinding. Eventually, when the “camel’s back” breaks, the pulp responds with inflammation, necrosis, and infection. So back to the actual treatment itself: Like any medical procedure, the first step of a root canal is proper diagnosis and treatment planning, which includes patient history, twodimensional and three-dimensional radiographs and a clinical evaluation.
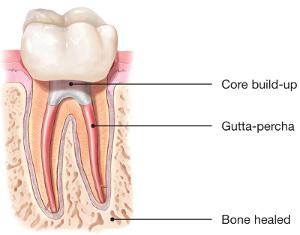
After this comes the dreaded “shot,” or local anesthetic. Once we're sure the patient is numb, we use a rubber dam to isolate the tooth. The procedure itself involves carefully maneuvering a drill to remove decay and expose the pulp. We
then locate all canals that branch from the pulp chamber. We measure the length of each canal with a machine that relies on electrical impedance to identify where the root canal ends and the periodontal ligament begins. With a series of highly specialized metal instruments, we remove the dental pulp and a little dentin circumferentially to create an optimal shape for disinfection and filling. The space is then disinfected thoroughly and filled with an inert rubber material and a cement that helps to seal, kill any residual bacteria and prevent reinfection. This should ideally be followed by placement of a restoration and a crown to protect the tooth.

It is most certainly a sign of the times that I feel the need to address a common misconception about root canals. Surveys from the American Association of Endodontists have shown that nearly half of young adults and almost three-fourths of teens look to social media for health advice. And, unfortunately, there’s a lot of bad information floating around, just waiting to be ingested. Most of the misinformation about root canal treatment seems to circle back to the same obsolete and conclusively disproven theory — the “focal infection theory,” first proposed in the early 1900s. In short, it suggests that localized “focal infections,” which includes healthy root canal treated teeth, can disseminate bacteria and toxins into the body and cause systemic diseases.
Over a century ago, the theory led to a frightening era of patients having teeth, tonsils, and other organs removed pointlessly. In the years since, it has been conclusively and repeatedly disproven. In fact, modern evidence shows the
exact opposite is true: Successful root canal treatment can actually help with systemic inflammation, glucose regulation, and lipid metabolism.
Nevertheless, since the advent of social media, it feels like the focal infection theory makes a return every few years under a different name. Modern online platforms are optimized for engagement, not accuracy. The more sensational the claim, the faster it spreads. And, let's face it: “Root canals cause cancer” is a much more titillating headline than “Root canals save teeth.” As is typically the case, the truth is much more mundane. When done properly by a trained professional, root canal treatment is a highly researched, safe, and effective way to save teeth. Studies consistently show success rates in the 90-95% range or higher. Root canal offers patients an effective, comfortable, and long-lasting solution to maintaining their smile, health, and ability to enjoy food without pain — and that's a reality I'll eagerly explain to anyone, even if they still hate me a little when I'm done.

Eden Village: An Interview with David Brown
By Jim Blaine, MD
Jim: Hi David. Thanks for taking the time to do this interview! You and I sure spent a lot of enjoyable time together in the ED over the years when you were the orthopedist on call. What years were you practicing in Springfield? Didn’t you sub- specialize at some point?
David: I sub-specialized a little more over the course of the 30 years (1969-99). Orthopedics is such a huge field that you've got to focus on certain areas and not try to do it all. So, over time, I did sub-specialize. I love to take care fractures, and I did a lot of arthroscopic surgery. I did the first arthroscopic knee surgery in Springfield, and I did a lot of hip and knee replacement surgeries.
Jim: So your involvement in Eden Village was not a surprise to me because I knew that you are compassionate, but you've gone above and beyond with this one. When did you first conceive the plan?
David: Well my wife Linda has had a curiosity about homeless people for a long time, way before we even started into this. But what really triggered this was in 2010 when I was 11 years into retirement. In fact, when I first retired, I didn't do anything for eight years other than travel, play golf, and read, and after those eight years, I realized I'm still really healthy, and I've got a lot of knowledge in my head, particularly orthopedic knowledge. So, I found an occupational medicine clinic that was looking for a part time doctor. I was 69 at the time, and I started working part time in an occupational medicine clinic. If you think about it, in occupational medicine, we take care of people who get hurt on a job. Probably 90% of those injuries are orthopedic in nature, and most of the primary care doctors that run those clinics are a little uneasy about taking care of what I would call routine orthopedic injuries that don't require surgery or manipulation. So, I filled a gap in the occupational medicine clinic.
Jim: Wow, one day a week!
David: That was at Cox Occupational Medicine, and it was a pretty easy job and they went on my schedule! Talking about retirement, we let so much talent go to waste when people completely retire too early. Most people, when they retire, fully retire. It would be better, in my opinion, to allow them to set up a schedule that they would like to do, and that's what I got to do. Cox let me do what I wanted to, and when I wanted to, and I filled in a gap for them.
Jim: That's a great idea, and a win/win!
David: It was a very good opportunity for those of us that are kind of in the twilight of our years. Getting to do it at my pace; I loved that! I always loved seeing patients but having all the time I needed to deal with the patients, that was special! I tell people if I was starting all over in this world today, I would be an orthopedist. Yeah! I would do it all over again!
Jim: Was there ever a day that you regretted going to work?
David: Never!

Jim: Me neither; we were very lucky! So, what year did the Eden Village vision come to fruition?

David: 2010. My wife Linda and I had lived in 10 different places in Springfield over our forty years of marriage. But we finally moved into a loft downtown. 1500 square feet, 2 bedrooms, and a really nice place. What happens when you live downtown, if you ever walk the street, you start running into our friends that live on the street. And you can avoid them, which I did most of my life. Or you can engage. And after a while, we began engaging. We also began meeting with a small group from our church in mid 2010, and one of the guys said, "you know, we've been meeting for several years and talking; why don't we do something?" And so, the "do something" was a decision to open an evening drop-in center, right in the heart of downtown Springfield. November 2010, we opened an evening dropin center for three hours, and we just did one night a week to start with, but over a couple years period, we got more and more people interested in helping us, and we eventually had it open five nights a week. Then, we moved to a different location because the people in the businesses around us didn't like us very well. But we were able to maintain and found a location that worked out close to downtown, and it was a place where people would get off the street and have a few hours of rest. A real compliment for us would be if somebody would line up two or three chairs against the wall, lay down, and sleep for those
David Brown
three hours because it was the safest place they could sleep. We did that till 2018 (8 years). But about halfway through, I think it was sometime in 2015, we were leaving the drop-in center, and it was cold and dreary, and our homeless friends were going off into the woods to sleep. My wife was the one that had the vision before I did, and she said, "you know, this isn't solving the problem, and this is not the solution. It's necessary what we're doing, but it's not solving the problem for the homeless." And out of that began the idea of Eden Village, which is where we are today. Unfortunately, in the beginning, we had the idea, but didn't have the knowledge of how to do it. But soon, God sent us a man, by the name of Nate Schlueter, who had been working in Austin, Texas in a place similar to ours, but much bigger. He had the expertise, and he was a former Springfieldian, and he moved back to Springfield, and hooked up with us. So, with our connections here in Springfield, and with Nate's know-how, we started Eden Village. We're currently housing 57 people in Springfield in 2 villages.
At first, Linda and I thought that we would need to buy a big piece of property, and Nate said, "no, let's start small." And his wisdom "starting small" made this work. Nate's project in Austin is large and amazing, but it's a nightmare to run. By contrast, we've got a very compact village that's easy to run.
Jim: You know, I found that with other projects too. It's always best to start small and get it right.
David: That's what we did. So that's how it started. We started the idea in early 2016 and that's when we met Nate. By the summer of 2016, in August, we signed a contract on a piece of property with a 90-day stipulation that mandated that, if we could raise the funds in 90 days, we could buy it. So, the closing was 90 days away, and our first donor gave us $50,000! So, here we are trying to sell an idea that nobody's done, and trying to raise money on it, and we're trying to raise money from the community, not from the government. We don't do any government funding. It's all private finance by individuals and businesses and foundations. We do get grants, but not government grants. Our grants are from foundations. Oh, gosh. We visited the Community Foundation of the Ozarks a lot.
Jim: What is the acreage for Eden Village?
David: It's about four and half acres for this Eden Village at 2801 E Division. Then there is Eden Village 2 at 3155 W Brower Street, which is over on the west side of town with about the same acreage and it has 24 houses. We are also under construction of Eden Village 3, which is in the northwest part of town, and it also has around four and a half acres.
I would like to point out that our model works, and it can be replicated. So we have 12 cities across the country that we have licensed to build Eden Villages. Three of them are open. One of them is in Wilmington, North Carolina. One of them is in Tulsa, Oklahoma, and one of them is in Kansas City, Kansas. There is an Eden Village in Mesa, Arizona that just broke ground. We license them, give them all of our information, counsel them, and help them get going. We don't run them. They run them, and they are their own entity. And that's been amazing, but we started little fires and they just took off!
Jim: That is wonderful! Our community needs to be proud of what you guys are doing. Your wife must be special.
David: Yeah, she is. I'm here because of Linda. She's the one that had the idea. She had the dream way before I did.
Jim: Tell me a bit about her background. Where did she grow up?
David: She grew up in Miami, Oklahoma. She came here to attend Burge Nursing School and graduated in 1967. She then helped us in surgery. My first wife passed away in 1985, and, about a year later, I married Linda, and we are coming up on our 40th anniversary. We have a lot of commonalities. I'm on the introvert side of neutral, and she's just the opposite. She can talk to a wall, you know, and she's out there. She has a passion to understand homelessness. And I can tell you that my perception of homelessness and probably yours initially was totally wrong, and probably the average American's perception is wrong. It's not what you think it is, you know?
Jim: Tell us what you thought it was and what you have discovered.
David: Well, first, I never talked to homeless people. Talking to them is the key to understanding homeless people, but nobody talks to them! The people who do talk at them and tell them what they need rather than asking them what they need. There's a huge difference. What I saw happening was many people saying, "why don't you go get a job?" I used to have similar thoughts, and I thought, well, they're drunk or alcoholic, and obviously losers. What I have come to realize is that it's exact opposite! When I speak to groups or to you, I would say that I bet you if I sat with you, and we looked at your family or extended family, we would find somebody that was homeless or would have been homeless if it hadn't been for the family. And I tell people, we have a son who would have been homeless a portion of his live if it hadn't been for us. That's the only difference. It is so situational! Yeah, when you do that, people then say, “oh, I never thought of it that way”. Yep. And it's not the drugs, and not the alcohol. Those come later. Usually, a lot of it has to do with mental illness, and a lot of it has to do with one third of kids coming out of foster care ending up homeless. One third. Because of that situation. That's a horror, and that system could be great, but there's a lot of bad stories to come out of that too. But because they get shifted around so much and maybe in 2 or 3 or 4 foster homes in different schools and they just leave, they go out on their own. At 18, they're off on their own. So, there is a lot being done to try to correct that now. And I think it's one of those areas that would help reduce homelessness if we could improve the foster care, and what we do for those kids! You don't turn them loose at 18, they're not ready! Our own kids weren't ready. We still took care of them and sent them to college or whatever. Or get them off to trade school. That's the thing to do these days.
Jim: OTC?
David: Yes, OTC! Yes! You know, we're losing the trades. I was 31 years old when I started practice. So, first third of my life, I was growing up and getting educated. The thing I talk about now, in our book, is the middle part of my life, I practiced medicine. I'm now in the last third of my life. I'm in the 28th year of retirement
Jim: How old are you?
David: I’ll be 88 in June. Oh my gosh! And I think a third of my lifetime is in retirement, what's my purpose in life? My purpose was growing up, getting educated, and my purpose was relevant! What's my purpose in retirement? I thought about the financial aspects of it, but not my purpose. And actually going back to work and working part time was a purpose. Now Eden Villge, our purpose. So, we have a purpose every day. We have a reason to get up and get going and get out. And every day is different. Yep. And it's so much fun to see what today's going to be like. Yeah. You know? Yeah, so many in our age range now are depressed because they're waiting for the finale. Social isolation is a huge problem in this country. It is even more common with older people. Yes. We get socially isolated. If you don't try to keep contact, you get more and more isolated. And our young kids are getting socially isolated because of the internet and the media and the cell phones. They don't sit down like you and I and talk anymore. If you and I were two kids, we'd probably be looking at phone, even though we're sitting next to each other, and that’s social isolation. It is. Yeah. It's a real problem. That's a real problem for us elders too! It's so easy to drift into, just kind of pull back and pull back, and you start losing your peers, you know, they die off.
Jim: So, you guys have been doing this since 2016. Have you had chance to look back and evaluate what happened?
David: We've got some sad stories, and we've got some great stories. We have had many people with successes, but we've had some failures too, so I can't tell you it's all been roses. But what makes this work is having a house. Obviously, to solve homelessness, you got to have a home first. But you also must have a community. Again, social isolation is the concern. Our homeless friends get socially isolated. too, and so having community is what makes this really work. We know that the

solution to solving homelessness is permanent, supportive housing. So that's what we have here; permanent housing. They can live here the rest of their life. It's not transient housing. We bring support to them; whatever they need and are willing to accept we'll get that for them. We don't force anything on anybody. If they want to isolate themselves in their house, they can do that, but we have services offered to them if they need them. And a lot of them take us up on it, and a lot of their lives have changed for the better. You talk to many people living in Eden Village, and they'll say, "this place saved my life". So, we've got the great success stories. Well, we've also got failures. The biggest thing that gets you in trouble here is having drugs on the property. We're not naive to think you have got to be clean drug-wise or alcohol-wise. If that were the case, we probably wouldn't have any residents. But if you're a good neighbor and don't cause problems, even if you do drink alcohol, or even if you use drugs off the property, but don't cause a problem on the property, then we can live with that. Because in your own neighborhood, you have no idea who uses drugs in your neighborhood. It's the same thing here. But if they spill out into the community or if they have drugs on the property, then that becomes a problem. We then must have an intervention and we have to give them either a chance to either go get help or leave. one of the two. That's the most common reason that somebody will have to leave here is they have drugs on the property.
This house we are in is our show house. So, when we do tours, we get to show somebody what a house looks like. It's not too common for people to come here, get improved, and then leave. We're dealing mostly with people that probably can't survive on their own, and most of it has to do with mental illness. They just can't quite function if they get out in a community. One of the things that happens to them, if you give them section 8 housing, is that they get a house or an apartment, and the first thing that happens is their friends on the streets show up, and they can't say no to them. So, then they're living there. After a while, they all get evicted. So, some of our tenants have said, We don't have to say no anymore. You guys are saying it for us. Because that gate up there is to protect them, not to keep them in. They can come and go anytime they want. It's there only to protect them. And, of course, we have security cameras and we are able to watch those from home anytime I want to. And so, we kind of nipped all that in the bud. Everybody knows you can't do that here now.
Jim: I suspect that Springfield Police Department is supportive.
David: Very supportive! Yeah, the whole police department. They love what we're doing. They said, “don't ever hesitate to call us to come out here if you need us”. They love what we're doing. I love what Desmond Tutu, said that, "We need to stop pulling people out of the river. We need to go upstream and see why they're falling in".
Jim: Who will be the next David and Linda?
David: No one for now; Nate Schluete and Linda and I are the cofounders of this, and we started together. The three of us started the Eden Village. We call Nate the Chief Visionary Officer, which is really the CEO. So, he runs the village, and he also runs our
A Book written by David Brown

organization. Linda and I purposely have stepped out of any role that depends on us because of our age. We want Eden Village to continue forever and so the way it's set up, it should keep on going just like the Kitchen has. Sister Lorraine's gone, but the kitchen keeps going. And that's what we want. We want to leave a legacy.
Jim: If someone wanted to participate in that legacy, and fund a house do you have a program where that can happen?
David: Yeah, we do. Right now, we have all our houses sponsored, even Eden Village 3. However, we really want to be able to build at least 2 more Eden Villages here in Springfield.
We hope that we'll be able to get these future projects built and running. Financially, we're relying on community support, not the government, and unfortunately, the government has said they're transitioning their funding to transient housing instead of permanent supportive housing. That is even though the National Alliance to End Homelessness says that permanent supportive housing is the best solution. We're sideways with a lot of things the administration's doing right now. However, we do have naming opportunities for people. They just need to contact us so we can tell them what's available. It would be great to help us now. We will be using robotic 3D concrete printers making our houses sometime in the near future; they are safer and last a very long time. We charge $325 a month rent for our houses. No lease, no down payment, no nothing. Most of the homeless receive SDI or SSI of up to $1200 per month. These houses would rent for $1,000 on the open market currently so this is very affordable for them. The nonprofit Eden Village is a project of the Gathering Tree. So many wonderful people helped us along the way!
Jim: Those anonymous donors are wonderful! Former Health Director Harold Bengsch has always said that "It is amazing what you can accomplish if you do not care who gets the credit".
David: Absolutely! Linda and I talked to a group today at lunch. That's what we like to do. We like to go tell our story and talk to a group, but I quit expecting when I go in a group that you automatically get donations. I remember in our early years talking to a group with several wealthy individuals in attendance and thought they would donate. That didn’t happen however, a lady stepped up after the meeting and said, "My mom died last year, and I want to do a house in her honor". I was shocked. So, I am going to quit predicting. However, the Community Foundation has been very helpful. Back in 2016, Brian Fogle was our sounding board over the years. Our motto is #No one sleeps outside.
Several people predicted that we would never reach our goal. My answer is, "If you have a goal you can accomplish, you don't have a big enough goal!” We don’t have that problem.
Jim: You had mentioned earlier that “This is God's project?”
David: Yes. And there's no doubt that this project is God's doing! He is using us. That's what He does. It's his idea and his plan, but he needs us to carry it out. He makes it happen and he makes everything we need. And I can’t tell you how many times I have
worried, but I quit worrying a long time ago because I trust now. How many times have I said “0h man, what are we going to do”, and then the next day it shows up. What God does is He gives it to us when we need it, not when we think we need it. And there's no doubt about it. We're not cramming God down anybody's throat. We made no bones about Who we believe in and Who we believe has made this happen. And our philosophy is to show and tell. And I think sometimes religion gets it backward to try to tell before they show. And we try to show who Jesus is, but we bring no bones about that. One of the questions a homeless person asked me one time was kind of related to this. They said, “why are you doing this?” And I started to go into kind of a religious answer. And they said, “no, no, why do you love us?” That must have been obvious to them, and that’s exactly what we said. We need to show them that God is love. Linda and I are putting our name on it. We had to be here. We had to be boots on the ground. Fortunately, we had a fairly good reputation in the community and the people knew us, and so they would stop and listen to us. I think if we just came in here from the outside to do this, it probably would have never gotten done. Our friends on the street have also been part of this community, but hardly anyone talks to them or listens to them. People at least listen to us. It takes you a while to get there. That's when Linda tells our story, and the way we started our drop-in center for two purposes. One of them was to get them off the street for a few hours. They had no place to go in the evening, but the second one, we wanted to get to know how to build relationships, and that's how we got to understand the root causes of homelessness and what we're supposed to say and our understanding of the people and to see them, the way Jesus sees them. I use the medical analogy of a surgeon that if I look at an audience, everybody looks different. But as a surgeon, as soon as I cut you open, we're all the same inside. I said, that's where God looks. He doesn't look at the exterior. Unfortunately, we do. He looks at the inside and that's how we see, our friends. We look at this as well. And then that’s what we're doing, and I would say it is easy because we know God's in charge of this, and if we have a challenge, we know Who's going to fix it one way or another. Maybe not the way we want it fixed, but the way God wants it fixed. And so, hey, we're not going to complain about that.
Jim: Cool. Good. I'm glad we got that.



Smart Practices for Reviewing Trust and Estate Plans
By : Chad Brueckner, Arvest Trust Officer
Change is constant – as life shifts, so do families, finances, priorities and tax laws. For high earners like medical professionals, periodically reviewing their trust and estate plans helps ensure these documents reflect how they want their assets to be handled in the future.
Knowing where to start when figuring out how to posthumously protect and provide for loved ones can be difficult, so here are six recommendations to follow to get the most out of regular trust and estate plan reviews.
#1 : Significant life events, such as births, marriages, divorces or deaths, can alter family structures, necessitating new beneficiary designations or other changes in a trust or will.
#2 : Ambiguous or outdated estate documents can cause family disputes, while regular reviews can bring clarity about a person’s intentions and avoid confusion.
#3 : Trust and estate plans should reflect current portfolios and recent changes in financial situation, such as acquiring property, selling investments, starting a business or receiving an inheritance.
#4 : Annual reviews help high earners adjust to recent estate-planning changes, including the One Big Beautiful Bill Act, which permanently raises the federal estate, gift and GST tax exemption to $15 million per person starting in 2026. Even with the higher federal exemption, strategic gifting and regular planning are valuable for shifting future asset growth out of someone’s estate and limiting exposure in states that impose their own estate taxes.
#5 : Review the following items.
• Beneficiary designations - Are all beneficiaries correct, and do they still align with current wishes?
• Trustees, executors and powers of attorney - Are the chosen people still willing, able and the best fit for these roles?
• Asset coverage - Does the plan cover all significant assets, including recently acquired ones?
• Healthcare directives – Are medical personnel and power-holders up to date with preferred values and preferences?
• Tax considerations – Are adjustments needed due to
changes in estate tax thresholds or state-specific laws?

#6 : Use these tips to help alleviate stress and avoid confusion when discussing trust and estate plans with loved ones.
• Choose the right time and place. Plan a calm, uninterrupted setting outside of a high-stress occasion to discuss future intentions. If a family member is only available during holiday gatherings, consider scheduling some time with them before or after the main family activity.
• Frame it as care for the family. Emphasize intentions to make things easier for loved ones by removing uncertainty and avoiding disputes.
• Be selective about details. Share broad goals and choices rather than itemizing every aspect to provide clarity without overwhelming or creating tension.
• Engage a professional. In addition to an experienced attorney, a trust officer can be helpful in filling in some of the blanks and answering common questions.
Reviewing trust and estate plans at least once a year is one of the most meaningful ways people can protect their loved ones, and high-earning medical professionals can save their families time, stress and unnecessary conflict in the future. Clear, up-to-date documents and open communication can help these earners better protect their assets, maximize available financial and tax advantages and ensure their wishes are honored after their passing.
Chad Brueckner is a vice president and trust officer with Arvest. He can be reached at rbrueckner@arvest.com.

professional
To Advertise in this directory call Jean Harmison at the Society office: 417-887-1017.
Please Note: Changes to ads will be made quarterly and must be submitted in writing. H Denotes GCMS Membership “A” Denotes GCMS Applicant GCMS Member Ad Rates: $10.00 per 2” sq. • Non-Member Ad Rates: $13.75 per 2”sq.
Statement
Dermatology, Procedural
MICHAEL H. SWANN, MD
ELIZABETH SPENCERI, MD
MICHAEL KREMER, MD
JOHN CANGELOSI, MD
AUTUMN BERTHOLDI, PA-C
PATSY DUGGAN, PA-C
LORI MILLER, NP-C
HANNAH LEE, FNP-BC
BROOKLYN FORT, FNP-C
3850 S. National Ave, Suite 705 Springfield, MO 65807 (Located inside Hulston Cancer Building-7th floor)
1240 E. Independence Springfield, MO 65804
Phone: 417-888-0858 • Fax: 417-889-0476 www.swanndermatology.com
Hollister Location 590 Birch Rd, Ste 2c Hollister, MO 65672
PH. 417-690-3858 Fax 417-690-3862
Monett Satellite Location (Inside CoxHealth Urgent Care) 2200 E. Cleveland Ave Monett, MO 65708
Phone: 417-888-0858 • Fax: 417-889-0476
Lebanon Location 331 Hospital Drive Suite C Lebanon, MO 65536
Phone : 417-344-7200 Fax : 417-344-7299
Direct Primary Care
ASCENT DIRECT PRIMARY CARE, LLC
MATTHEW GREEN, DO H
Family Medicine www.ascentdpc.com 417-595-0956
413 N McCroskey, Ste 2 Nixa, MO 65714
Eye Surgery/Ophthalmology
EYE SURGEONS OF SPRINGFIELD, INC.
C. BYRON FAULKNER, MD H Comprehensive Cataract Ophthalmology
JUDD L. McNAUGHTON, MD H Comprehensive Cataract Ophthalmology Diplomates, American Board of Ophthalmology
1330 E. Kingsley St. • Springfield, MO 65804 Phone 417-887-1965 • Fax 417-887-6499 417eyecare.com
Eye Surgery/Ophthalmology
MATTAX • NEU • PRATER
EYE CENTER
JAMES B. MATTAX, JR., MD, FACS H American Board of Ophthalmology
LEO T. NEU III, MD, FACS H American Board of Ophthalmology
DAVID NASRAZADANI, MD
DREW A. YOUNG, MD
THOMAS PRATER, MD, FACS H American Board of Ophthalmology
JACOB K. THOMAS, FACS, MD H American Board of Ophthalmology
BENJAMIN P. HADEN, MD H American Board of Ophthalmology
MICHAEL S. ENGLEMAN, OD
MARLA C. SMITH, OD
MATTHEW T. SMITH, OD
1265 E. Primrose Springfield, MO 65804 417-886-3937 • 800-995-3180
Family Medicine
COXHEALTH
FAMILY MEDICINE RESIDENCY
FAMILY MEDICAL CARE CENTER
3800 S National Ste 700 Springfield, MO 65807 (417) 269-8817
AmericAn BoArd of fAmily medicine
Marc Carrigan, MD
Cameron Crymes, MD
Kristin Crymes, DO
Kristen Glover, MD
Kyle Griffin, MD
Shelby Hahn, MD
Laura Isaacson, DO
Evan Johnson, MD
Katie Davenport-Kabonic, DO
Michael Kabonic, DO Jessica Standeford, MD
Gynecology
WOMAN’S CLINIC www.womansclinic.net
Leaders in Minimally Invasive Gynecology & Infertility
DONALD P. KRATZ, MD, FACOG H American Board of Obstetrics and Gynecology
AMY LINN, FNP-BC American Academy of Family Nurse Practitioners
ANGIE JONES, WHNP-BC 1135 E. Lakewood, Suite 112 Springfield, MO 65810
Located inside Tri-Lakes Family Care 1065 Hwy 248 Branson, MO 65616
Phone 417-887-5500
Fax 883-8964 or toll free 877-966-2607 Monday-Thursday 8am-4:30pm Friday 8am-12pm
Internal Medicine
MERCY CLINIC–INTERNAL MEDICINE WHITESIDE
RAJ ANAND, MD
JAMES T. ROGERS, JR. MD, FACP H Board Certified in Internal Medicine
MARIA DELA ROSA, MD
NELSON DELA ROSA, MD
AMANDA MCALISTER, MD
ALEJANDRA ROA, MD
KELLY TRYGG, MD
GABBY BONNER, NP
STEVEN BOWLIN, MD Board Certified in Internal Medicine
STEPHANIE HOVE, NP
CARRIE KUGLER, PA COURTNEY WEATHERFORD, PA
JENNIFER WHITE, PA
VICTOR GOMEZ, MD
Board Certified in Internal Medicinee 2115 S. Fremont, Suite 2300 Springfield, MO 65804
Phone 417-820-5600 Fax 417-820-5606
Urology
MERCY CLINIC UROLOGY (FREMONT)
ERIC P. GUILLIAMS, MD, FACS H American Board of Urology
ROBERT D. JOHNSON, MD, FACS H American Board of Urology
TYRUN K RICHARDSON, MD American Board of Urology
Phone 417-820-0300
Fax 417-882-9645
1965 S Fremont, Ste. 370 Springfield, MO 65804
ADULT MEDICINE & ENDOCRINOLOGY
JONBEN D. SVOBODA, MD, FACE, ECNU
American Board of Endocrinology
JAMES T. BONUCCHI, DO, ECNU, FACE
American Board of Endocrinology
NICOLA W. GATHAIYA, MD, ECNU, FACE, CCD
American Board of Internal Medicine
American Board of Endocrinology
STEPHEN M. REEDER, MD, FACP
American Board of Internal Medicine
ANA MARCELLA RIVAS MEJIA, MD, CCD
American Board of Internal Medicine
American Board of Endocrinology
JACQUELINE L. COOK, FNP-BC, CDCES, CCD
KELLEY R. JENKINS, FNP-C, CDCES
ALINA CUMMINS, PA-C
STACY GHOLZ, FNP-C
SHELLEY L. CARTER, DNP
JESSICA A. CROUCH, FNP-C
Phone (417) 269-4450
960 E. Walnut Lawn, Suite 201 Springfield, MO 65807
Nephrology

SPRINGFIELD NEPHROLOGY ASSOCIATES, INC.
1911 South National, Suite 301 Springfield, MO 65804
Phone 417-886-5000 • Fax 417-886-1100 www.springfieldnephrology.com
STEPHEN E. GARCIA, MD H
American Board of Internal Medicine
American Board of Nephrology
ETHAN T. HOERSCHGEN, MD
American Board of Internal Medicine
American Board of Nephrology
GISELLE D. KOHLER, MD H
American Board of Internal Medicine
American Board of Nephrology
DAVID L. SOMMERFIELD, MD
American Board of Internal Medicine
American Board of Nephrology
SUSAN A. WOODY, DO H
American Board of Internal Medicine
American Board of Nephrology
Neurosurgery
SPRINGFIELD
NEUROLOGICAL AND SPINE INSTITUTE
CoxHealth Jared Neuroscience
West Tower • 3801 S National, Ste 700 Springfield, MO 65807 • 417-885-3888
Neurosurgery:
VYACHESLAV MAKLER, DO
EDWIN J. CUNNINGHAM, MD
MAYUR JAYARAO, MD
J. CHARLES MACE, MD, FACS H
CHAD J. MORGAN, MD
MICHAEL L. MUMERT, MD
SALIM RAHMAN, MD, FACS
ANGELA SPURGEON, DO
ROBERT STRANG, MD
Interventional Neuroradiology
MICHAEL J. WORKMAN, MD
Physiatry:
TED A. LENNARD, MD
KELLY OWN, MD
JESSE STOKKE, DO
Physician Assistants:
JOSHUA BARBIERI, PA-C
MARK BROWN, PA-C
ERIC CHAVEZ, PA-C
KEVIN STOKES, PA-C
HEATHER TACKETT, PA-C
Nurse Practitioner:
EMILY CROUSE, NP-C
MINDY GRANT, NP-C
ROZLYN MCTEER, FNP
BRANDON RUBLE, ACNP-AG
ALYSSA CHASTAIN, FNP
Obstetrics/Gynecology
COXHEALTH
PRIMROSE OB/GYN
MARCUS D. MCCORCLE, MD, FACOG
Diplomate, American Board of Obstetrics and Gynecology
THOMAS M. SHULTZ, MD, FACOG
Diplomate, American Board of Obstetrics and Gynecology
GREGORY S. STAMPS, MD, FACOG
Diplomate, American Board of Obstetrics and Gynecology
P. MICHAEL KIDDER, DO, FACOOG
Diplomate, American Osteopathic Board of Obstetrics & Gynecology
Phone 882-6900
1000 E. Primrose • Suite 270 Springfield, MO 65807
Obstetrics/Gynecology
SPRINGFIELD OB/GYN, LLC
MATTHEW H. TING, MD, FACOG H
American Board of Obstetrics & Gynecology
909 E. Montclair, Suite 120 Springfield, MO 65807
Phone 417/882-4466 • Fax 417/890-5631
Oncology/Hematology
ONCOLOGYHEMATOLOGY
ASSOCIATES OF SPRINGFIELD, MD, P.C.
WILLIAM F. CUNNINGHAM, MD, FACP
American Board of Internal Medicine
American Board of Medical Oncology
JIANTAO DING, MD H
American Board of Internal Medicine
American Board of Hematology
American Board of Medical Oncology
ROBERT J. ELLIS, MD, FACP
American Board of Internal Medicine
American Board of Hematology
American Board of Medical Oncology
BROOKE GILLETT, DO
American Board of Internal Medicine
American Board of Medical Oncology
V. ROGER HOLDEN, MD, PhD
American Board of Hematology
American Board of Medical Oncology
DUSHYANT VERMA, MD, FACP
American Board of Internal Medicine
American Board of Hematology
American Board of Medical Oncology
Springfield Clinic 3850 S. National, Ste. 600 Springfield, Missouri 65807
Monett Clinic 802 US Hwy 60 Monett, Missouri 65708
Phone 882-4880 Fax 882-7843
Visit our website: www.ohaclinic.com
MERCY CLINIC–EAR, NOSE & THROAT
BENJAMIN L. HODNETT, MD, PHD H
ERICH D. MERTENSMEYER, DO, FAOCOO
AARON R. MORRISON, MD
RAJEEV MASSON, MD
MARK J. VAN ESS, DO, FAOCOO
Diplomates, American Board of Otolaryngology
SHELBY BRITT, PA
MELISSA COONS, FNP
TAHRA LOCK, NP
ELIZABETH (BETSY) MULLINGS, FNP
PAUL STRECKER, FNP
Audiology
JASON BOX, AuD, CCC-A
MAMIE JAYCOX, AuD, CCC-A
JENNIFER PLOCH, AUD
ALLISON WHITE, AUD, CCC-A
Phone 417-820-5750 Fax 417-820-5066
1229 E. Seminole, Ste. 520 Springfield, MO 65804
Plastic Surgery
MERCY CLINIC–FACIAL PLASTIC SURGERY
MATTHEW A. KIENSTRA, MD, FACS
American Board of Facial Plastic & Reconstructive Surgery
American Board of Otolaryngology
Phone 417-887-3223
1965 S. Fremont, Ste. 120 Springfield, MO 65804 facialplasticsurgeon.com
Psychiatry
JAMES E. BRIGHT, MD H Diplomate, American Board of Psychiatry & Neurology.
Practice Limited to: Adult Psychiatry
Phone 882-9002
1736 E. Sunshine, Ste. 400 Springfield, MO 65804

chAnge Service requeSted

