














































































































































































































































o mask or not to mask is a valid question when visiting a Hamilton Healthcare System facility. While the facilities have unmasked, there may be times when masks are required. Per Centers for Disease Control guidelines, healthcare facilities must enforce universal masking based on COVID county transmission levels. "Think of it like a burn ban," said Infection Control Nurse Kim Edwards. When transmission levels are high, masking goes into effect. Edwards explains that transmission levels are based on many factors including vaccination statuses, COVID hospitalizations, community levels and county transmission. "It's not just how many in our community have it," she said. The best thing to do is be prepared and watch for the sign at the facility entrance. If it is green, masks are not required. If it is red or you have COVID symptoms, please wear a mask. Edwards asks visitors to remember that when masks are in effect, please comply to protect both healthcare workers and patients. "Who will take care of you if all of the employees are sick?" she said.



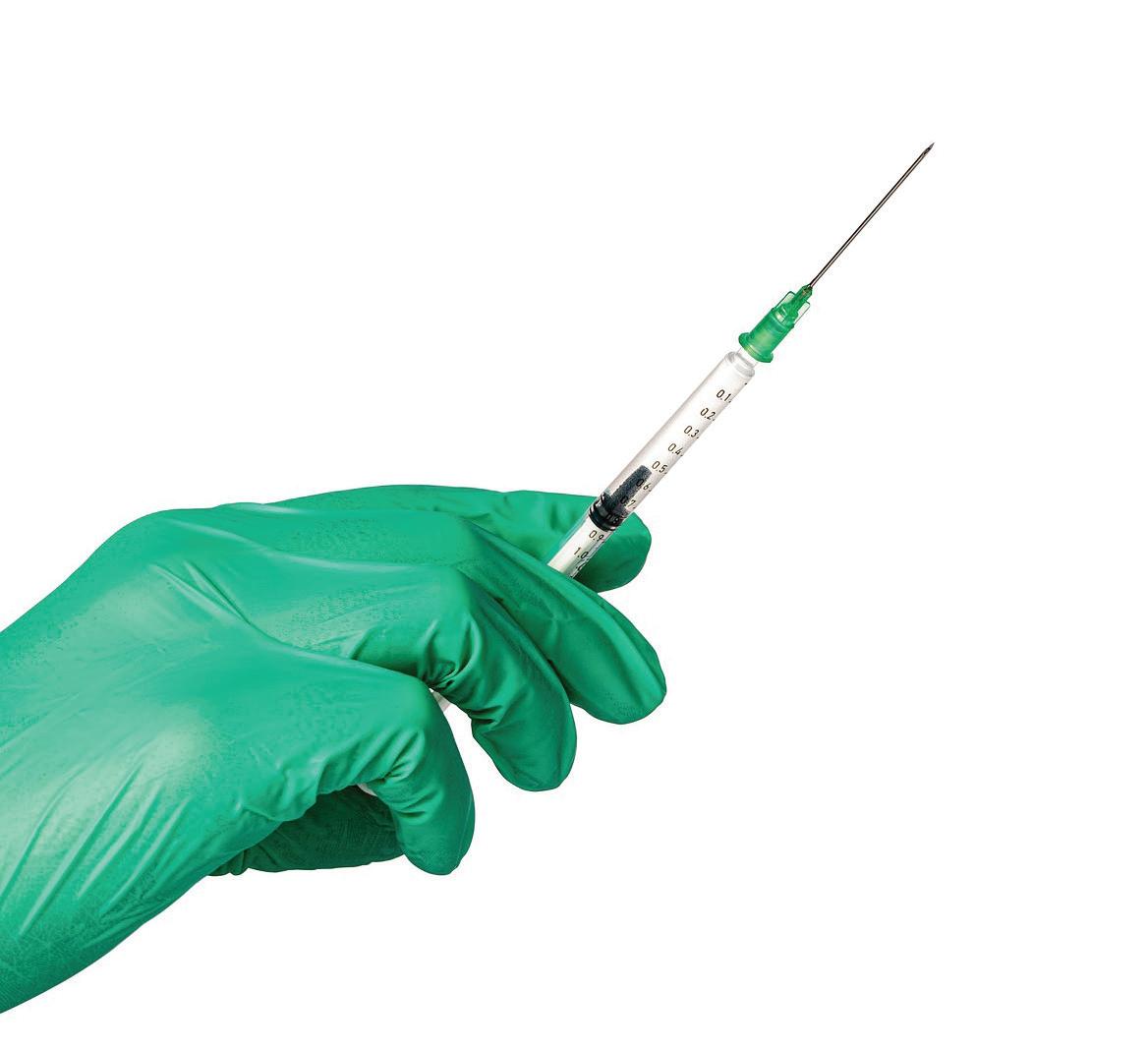
he Centers for Disease Control recommends an annual flu vaccine as the most important step in protecting against the flu this year. Flu vaccine can prevent flu or reduce the severity of illness in people who get vaccinated but still get sick.
The vaccine is recommended for everyone 6 months or older, especially caregivers, older adults, young children, pregnant women and those who have chronic health conditions. A higher dose or adjuvanted
influenza vaccine is recommeded for people age 65 and older.





The flu often begins in October and can continue as late as May, so the CDC recommends getting the flu shot by the end of October. However, it is not too late.
It takes about two weeks after receiving the flu shot to build immunity, so it is important to get the flu shot as soon as possible.
In many cases, health insurance covers 100% of the cost of the flu vaccine.


amilton Healthcare System Auxiliary Team offers installation services for Philips Lifeline, a round-the-clock monitoring system. With both at home and on-the-go options, Philips Lifeline medical alert services provide seniors independent living with peace of mind. At home, water-resistant buttons can be worn as a pendant or watch and offer two-way communication. On-thego options feature advanced GPS technology and include automatic fall detection that places a call for help in the event of a fall. Local installers are friendly faces that you know and trust. For more information, contact Kay Zschiesche at 254-485-9080 or Cindy Brooks at 512-618-0430.


ne in eight women will develop breast cancer in her lifetime.
According to the American Cancer Society, the good news is when breast cancer is detected early, and is in the localized stage, the 5-year relative survival rate is 99%.



Early detection includes regular clinical breast exams and mammograms.
Moncrief Cancer Institute works with Hamilton Healthcare System to provide breast cancer screening for the uninsured and underinsured in Hamilton County. Through Moncrief, patients can conveniently access the state-of-the-art 3D mammography services at Hamilton General Hospital.
According to a study in the Journal of American Medical Association, 3D mammography detects 41 percent more invasive breast cancers than a standard 2D mammogram and reduces the rate of false positives by up to 40 percent –leading to greater peace of mind.
To schedule a mammogram at Hamilton General Hospital call 254-386-1600. For more information about free mammography services through Moncrief Cancer Institute, call 800-405-7739 or visit moncrief.com.
laucoma is the leading cause of vision loss and blindness in the United States.

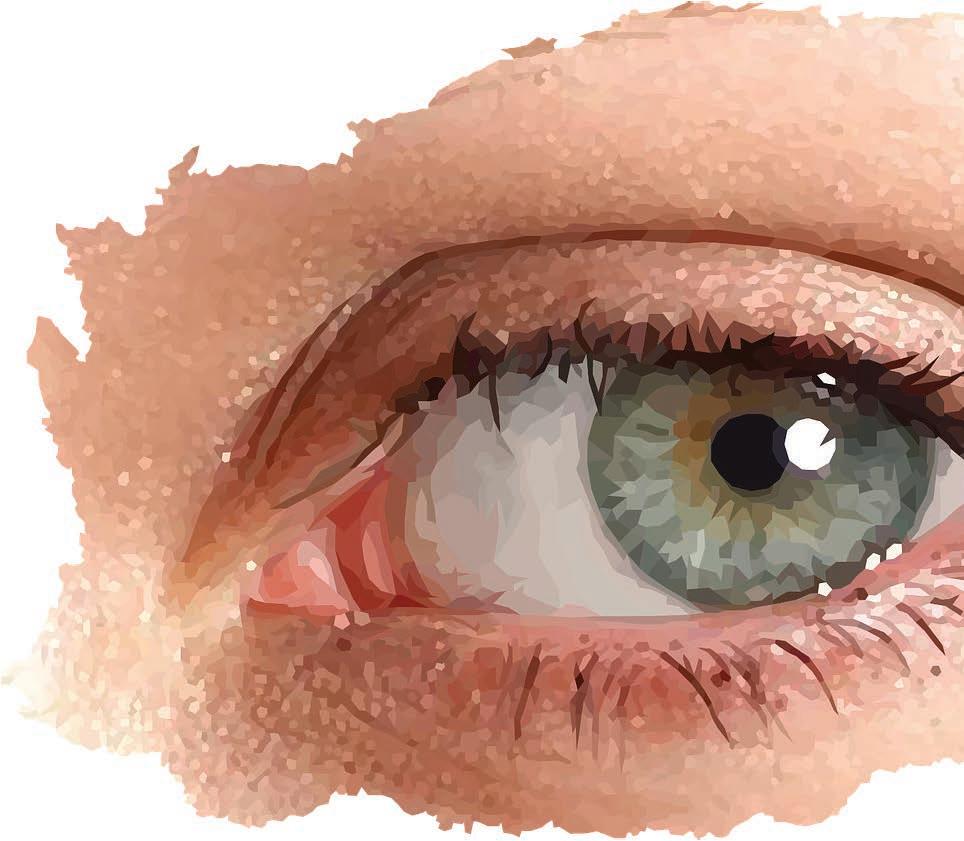


According to the National Eye Institute, nearly 3 million Americans have glaucoma. Half don’t know it.
Glaucoma often has no early warning signs. No pain. No discomfort. No blurry vision. Vision changes only occur during advanced stages.
African Americans over 40, adults over 60 - especially Hispanics/Latinos and people with a family history of glaucoma - are at higher risk. Getting a comprehensive dilated eye exam is the only way to find out if you have glaucoma.
There’s no cure for glaucoma, but early treatment can often stop the damage and protect vision. Call 325-648-2040 to schedule your eye exam.
1. How old are you?
Younger than 40 years (0 points) 40–49 years (1 point) 50–59 years (2 points) 60 years or older (3 points)
2. Are you a man or a woman? Man (1 point)•Woman (0 points)
3. If you are a woman, have you ever been diagnosed with gestational diabetes?

Yes (1 point) • No (0 points)
4. Do you have a mother, father, sister, or brother with diabetes? Yes (1 point) •No (0 points)
5. Have you ever been diagnosed with high blood pressure?
Yes (1 point) •No (0 points)
6. Are you physically active? Yes (0 points)•No (1 point)
7. What is your weight category? (See chart below)
Height Weight (lbs.)
4'10" 119-142 143-190 191+
4'11" 124-147 148-197 198+ 5'0" 128-152 153-203 204+




5'1" 132-157 158-210 211+
5'2" 136-163 164-217 218+
5'3" 141-168 169-224 225+ 5'4" 145-173 174-231 232+ 5'5" 150-179 180-239 240+ 5'6" 155-185 186-246 247+
5'7" 159-190 191-254 255+
5'8" 164-196 197-261 262+
5'9" 169-202 203-269 270+ 5'10" 174-208 209-277 278+
5'11" 179-214 215-285 286+
6'0" 184-220 221-293 294+
6'1" 189-226 227-301 302+
6'2" 194-232 233-310 311+ 6'3" 200-239 240-318 319+ 6'4" 205-245 246-327 328+ 1 Point 2 Points 3 Points You weigh less than the 1 Point column (0 points)
If you scored 5 or higher... You are at increased risk for having prediabetes and are at high risk for type 2 diabetes. However, only your doctor can tell for sure. Talk to your doctor to see if additional testing is needed.

iabetes is a long-lasting, chronic disease that affects how your body turns food into energy. When the body breaks food down into sugar, the pancreas releases insulin to allow the blood sugar into the cells for energy. With diabetes, the body doesn’t produce enough insulin or utilize it efficiently so sugar remains in the blood stream where it can cause serious problems like heart disease, vision loss and kidney disease.
There is no cure for diabetes; however, it can be managed through medication and healthy lifestyle changes.
There are three main types of diabetes: Type 1, Type 2, and gestational diabetes. Type 2 is the most common type of diabetes.
Before developing Type 2 diabetes, many people develop prediabetes, elevated blood sugar that is not yet high enough for a diabetes diagnosis. According to Centers for Disease Control, prediabetes is really common – 96 million US adults have it, though more than 80% of them don’t know they do.



Prediabetes can be reversed.
Take these steps to prevent diabetes:
• Create a starting point. Pinpoint the motivation for this journey and keep it in focus.
• Set a weight loss goal. If you are overweight and have prediabetes, shedding just 5% of your weight can help lower A1C and reverse prediabetes.
• Make a healthier eating plan. Whether it is cutting back on sugar, eating more protein, adding extra fruits or vegetables or reducing portion sizes, eating better not only helps shed pounds, it helps you feel and think better.
• Move. Set an activity goal and gradually work up to moderate intensity exercise, like a brisk walk, at least 150 minutes per week - that’s 30 minutes five days per week.
• Track your progress. Research shows that people who keep track of their food, activity and weight reach their goals more often than people who don’t.
• Prepare for the long run. Share your goals with your friends, family and medical team. Having their support and encouragement can help you stay on track.
Hamilton Healthcare System offers comprehensive diabetes education led by certified diabetes care and education specialists. Through individual sessions or televisits, patients learn daily selfmanagement through healthy food choices, physical activity, blood sugar monitoring, medication management and insulin pump training in an American Diabetes Association-accredited program.





















Diabetes can be hard on vision creating problems like macular edema and retinopathy that can lead to vision loss.
Hamilton Healthcare System offers Diabetic Retinal Screening through Intelligent Retinal Imaging Systems. Closely monitoring the retina through screenings can catch changes early before symptoms are present and slow the progress of vision loss.


Gain the guidance and support you need to embark on a healthier lifestyle. A registered dietitian tailors a meal plan unique to your goals. The program includes education in healthy choices, portion control, nutrition labels, heart-healthy fats, complex carbohydrates, plant-based proteins and meal planning. If you have Medicare Part B or a BMI greater than 30, insurance may cover the cost of the program.
Diabetes can make wounds detrimental. Hamilton Healthcare System’s Wound Care Clinic offers a comprehensive outpatient program designed to provide ongoing medical management of problematic wounds. Knowledgeable professionals take steps to ensure that a wound such as a foot ulcer heals correctly.


















































































































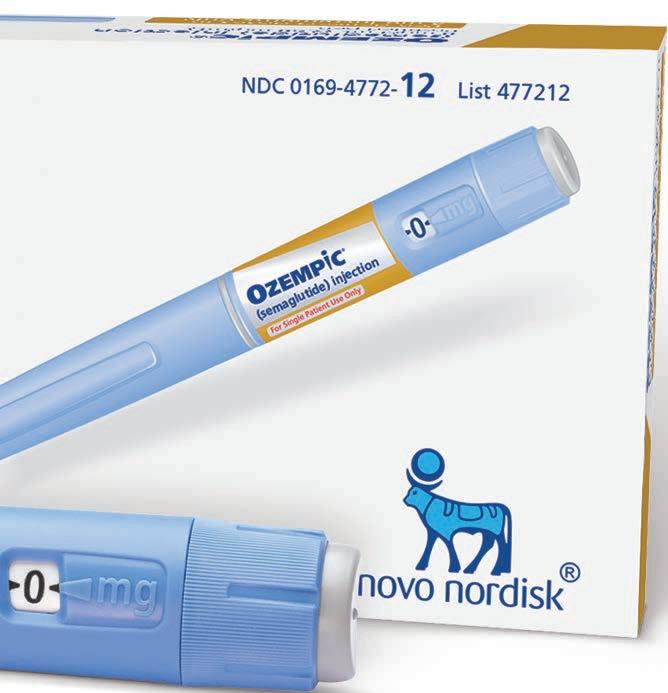
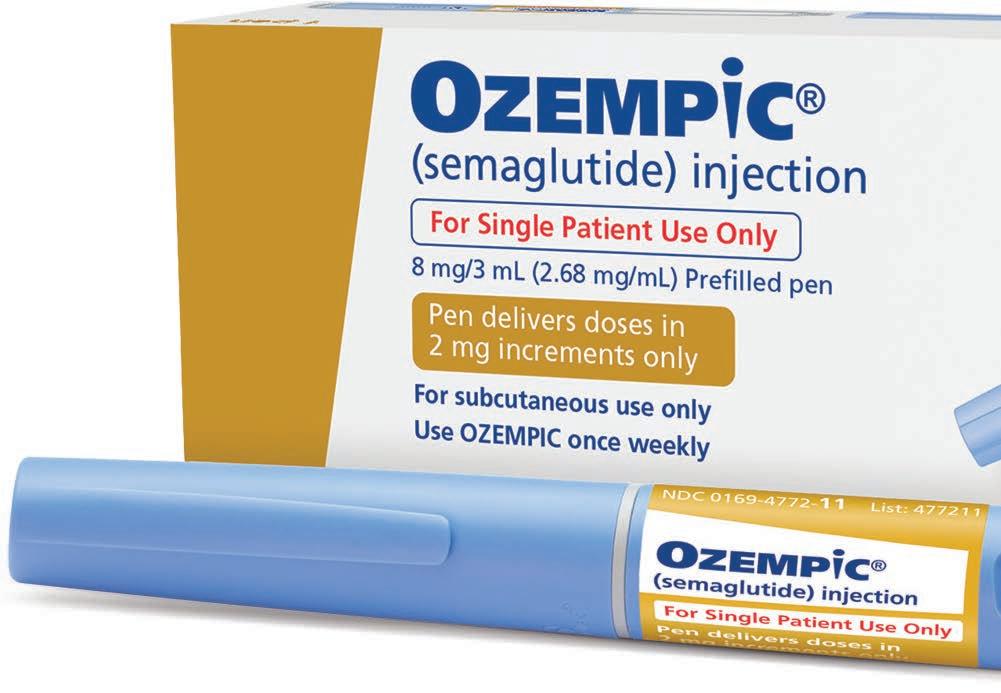
or many central Texans the struggle to manage blood sugar levels and lose weight is an ongoing battle. Local physician Shalor Craig, MD, has seen some promising results in the treatment of Type 2 diabetes and weight loss with a new injectable medication called Ozempic®.








Semaglutide, the active ingredient in Ozempic®, Victoza® and Wegovy®, was invented in 2012, went into clinical trials in 2015, and Ozempic® was approved for medical use in the U.S. in Dec. 2017.
How does Ozempic® work?



Ozempic® blocks glucogen receptors. Glucogen works the opposite of insulin to make blood sugar go up. When we block glucogen, it prevents blood sugar from going high. Ozempic® also slows GI motility, which makes people stay full longer.
Is it designed for short-term or long-term use? Long-term to treat Type 2 diabetes



What results have you seen in your patients?


Dramatic improvement in diabetes control in most patients. The advertisement for Ozempic® says it decreases A1C by 2.0. I’ve seen cases higher than that. I’ve seen people lose a significant amount of weight – 10-20 percent of their body weightdepending on many factors: how hard they work, their dosage and other things.
What are advantages to taking it?
• Typically, significant improvement in blood sugar control.
• Weight loss.
• Once-a-week dosing versus multiple times per day of insulin.
• Decreased risk of cardiac events like stroke and heart attack.

What are disadvantages?
I have to stress the cost. If insurance won’t cover it, Ozempic® cost anywhere from $800 to $1000 per month. If you are diabetic, there’s a pretty good chance insurance will cover it, but a lot of plans don’t cover it. Compared to gastric bypass, it's not as expensive or life changing; you can always stop taking this, but you can’t reverse gastric bypass.


Are there any side effects?
• One side effect is nausea. It’s usually tolerable. Sometimes we’ll give patients Zofran. It’s usually after an increase in dosage and happens a day or two after the injection, not immediately. If you stick with it, it gets better.

• Some patients have reported constipation.

• Some have reported acid reflux, but that is usually tolerable.

Should it be the first option for someone trying to manage diabetes?
Normally, we try Metformin first. Most insurance companies make patients try Metformin. It’s common that diabetes is not controlled by Metformin alone; then we try Ozempic® especially for those patients who are overweight and have a desire to lose weight.

Who is the ideal candidate for Ozempic? Type 2 diabetic is overweight with blood sugar not under control with Metformin or can’t tolerate Metformin.
Is it approved for kids?
No. It is not approved for kids or adolescents. There are similar medications,






– Victoza® and Trulicity®.

Trials are currently underway for both managing diabetes and weight loss.
Is it safe to use for weight loss?
I think it is very safe for weight loss for those who are not diabetic. The down side is the cost. The main hold up there is whether patients can afford it. There is some hope that after the first of the year insurance might start covering it better. Wegovy® is the same thing but was released for overweight patients. We hope to see more availability.
Is it FDA approved?
Yes, for weight loss and Type 2 diabetes.
Does it work alone or should you continue to incorporate exercise, a healthy diet and other diabetes management/weight loss practices?
It certainly works better if combined with exercise and a healthy diet. You typically feel full with less food. Like if I normally order a sliced barbecue sandwich and eat the whole thing, I might feel very full. With Ozempic® I might eat only half that
sandwich and feel fuller longer.
Does the body build resistance to it?
The body will build some resistance as far as weight loss goes. Even after the 10 to 20 percent body weight loss, Ozempic® still helps control appetite.
Are there alternatives that work as well?



There are several similar drugs on the market. This is the one I’ve had the best experience with and am most confident using.
If someone thinks this might be a fit for them, what should they do?
Make an appointment with one of our providers.

A Hamilton native, Dr. William Shalor Craig received his M.D. from the University of Texas Health Science Center Houston in 2005 and specializes in family medicine. Dr. Craig is the Hico Clinic Medical Director and sees patients in Hamilton, too. He and his wife, Melissa, live in Hamilton with their three boys.

No matter what the loss, most of us will experience the following sequential stages of grief, although these can certainly vary in some people. Remember these stages are not always the same with all people. Don’t think that you are wierd just because you are not experiencing all stages.

The emotional shock of losing someone or something dear to us is really no different than the state of shock after physical trauma, in both we shut down. Shock protects our bodies/psyches from what we are not yet ready to feel, a protective “timeout.” Shock is of short duration, measured in hours, days.




We tell ourselves this can’t be true, can’t be happening, can’t be real, there must be some mistake. Denial, like shock, is usually of short duration.













Often, we tell ourselves that if we just do this or that, we won’t have to suffer this horrible loss, feel this pain. Bargaining is usually a relatively short grief stage unless we get stuck there by telling ourselves we can do something to avoid the pain of the next stages of grief.


We may get angry at the doctors who could not save our loved one, angry at God, angry at ourselves for not doing something that might have prevented this loss, even angry at the one who died for leaving us. We may even displace our anger onto some innocent friend or family member. In anger, we often utter the words, WHY ME? The anger stage is not normally a lengthy process.



We may not be able to sleep, have changes in appetite, not want to engage in activities with others, have no energy, have overwhelming feelings of sadness, cry a lot and sometime even feel hopeless. Depression is usually the longest and most difficult stage of grief. Ironically, what brings us out of our depression is finally allowing ourselves to experience our very deepest sadness.

Finally, we come to the place where we accept the loss, make some meaning of it for our lives and are able to move on. If we have lost a loved one, we often transition from a physical relationship to a spiritual one with that person and are able to remember and be thankful for the good times. If there has been a tragic loss, either from some horrible disease or an accident, people often find a way to reach out to others who are experiencing the same type of loss and give help and comfort. In this way we are able to make meaning of the loss for our lives.
rief is part of life, an emotional process we all experience after a significant loss.
It can be triggered by the death of a loved one, isolation, job loss, divorce, empty nest, death of a pet or even the COVID-19 pandemic.
Hamilton nurse Alicia Saldana-Stephens said she looked up one day and it seemed everyone was grieving. She also was grieving, so she wanted to do something about it. So, she started a grief support group. It meets on the second Wednesday of every month at noon at the Hamilton Community Center.
Alicia explains that an event in January 2020 caused the loss of a relationship in her life.
“A divorce can be similar to losing a person, and with that came a loss of relationship with family and friends,” she says. “I found myself all of a sudden mostly alone with only a few people standing with me.
“At that moment, I began to experience grief. I didn’t know what it was at first, but I knew it made me start having emotions I was not used to feeling.”
a new state and all of a sudden they were working from home and therefore unable to make new friends and plug into their local community.
“Because of COVID and the devastating effects of the illness, many people lost loved ones. They lost contact with loved ones. They couldn’t go see family. We missed Thanksgiving and Christmas, birthdays, weddings, births, many life events.
“And there was just this sense of grief everywhere.
“I’m a nurse,” says Alicia, who works for Solaris Hospice. “Being a nurse, I encounter people, and people everywhere were hurting and there wasn’t an outlet for it.
“Grief demands a witness. People can’t go through grief by themselves. You have to have community; you have to have people.
“So I got this bright idea to start a grief support group in my home.”
Alicia held the meetings in her living room, which she felt was a neutral space for folks who didn’t want to go to a church or a healthcare setting or worry about being judged.
Alicia Saldana-StePHensAt that point, COVID-19 had become a pandemic, and Alicia felt isolation and depression.

“When I looked up, life no longer looked the same as it used to,” she says. “Going through COVID, I encountered many people that were having the same experience but maybe their experience looked different from mine. They lost a job. They moved to
“It was just my living room, comfortable and friendly,” she says. “People came. Most of the time just one at a time, but it was beautiful to have the one-onone experiences with the people who came in.”
As the group progressed, Alicia got calls
"Grief demands a witness. People can’t go through grief by themselves. You have to have community; you have to have people."
grieving
Do not try to self-medicate your emotional pain away. Do not avoid the pain you feel. Do not hide yourself away from friends and family. Do not focus on regrets, choices you’ve made or past actions you’ve taken. Do not make major, life-changing decisions.
drjeffcaster.com





about people who wanted to come but maybe didn’t have a ride, or maybe they were homebound and could go to the Hamilton Community Center but really couldn’t get out otherwise.

“In my community, people are hurting,” she says. “Caregivers struggle with caregiver’s strain and stress and compassion fatigue. People struggle with grief over the loss of a loved one or a job relationship. All of these create that same overwhelming sad, confusing emotion that we call grief.”
Grief can cause a variety of effects on the body including increased inflammation, joint pain, headaches and digestive problems, according to the National Council on Aging. It can lower your immunity, making you more susceptible to illness. Grief also can contribute to cardiovascular problems, difficulty sleeping and unhealthy coping mechanisms.





“Grief causes chemical reactions in our body,” Alicia says. “Anxiety, fear and depression all can have negative impacts on our health.”

Depression is usually the longest and most difficult stage of grief, according to the NCA. Ironically, what brings us out of our depression is finally allowing ourselves to experience our very deepest

sadness. We come to the place where we accept the loss, make some meaning of it for our lives and are able to move on.

“Grief is normal,” says Alicia. “Grief is part of life. It means that somewhere along the way you have loved and you have cared.”
Alicia felt compelled to do something about all the hurting people she encountered, and the support group was born.

She reached out to chaplains, mentors and other people she knew who had a knack for connecting other folks and asked them what they thought was the most important thing for a grief support group.
“The answers were mostly the same,” she says. “It’s not the program, not the place, it’s just people with something in common in a safe place to talk about it.”
Alicia is using Griefshare to give the meetings structure, but mostly facilitates discussion.
“We’re all on this journey together,” she says. “Mostly it’s just a safe place for people to share. Grief demands a witness; we need people. Grief is normal, and it’s OK. Our journeys look different but if we can be here together, we can all come out on the other side OK.”



Monk fruit naturally contains mogrosides, an antioxidant responsible for the sweet taste of this treat. Manufacturers extract this antioxidant to produce a sugar-free sweetener that does not contain calories and does not affect blood sugar levels.

The leaves of the Stevia rebaudiana plant are harvested and processed into fine crystals to create this sweetner. Stevia is low in calories and retains its flavor when heated, making it an ideal sweetener for baking or hot drinks.




A sugar alcohol derived from the fermentation of cornstarch or wheat, erythritol has few calories and no impact on blood sugar. Sugar alcohols are notorious for causing upset stomach, but erythritol is less likely to do so. Start with small amounts and discontinue if it causes discomfort.
Fresh fruit can be a great way to naturally sweeten recipes, as fruits contain fiber that helps slow down sugar absorption and thus reduce the impact on blood sugar levels. Try using mashed bananas, unsweetened applesauce or date paste in your next recipe.
Is sugar bad for you?
A high sugar diet can support weight gain and may increase the risk for cavities, type two diabetes, high blood pressure and fatty liver disease.
How much sugar is too much?
The American Heart Association recommends no more than 36 grams of added sugar for men and no more than 25 grams of added sugar for women daily. For comparison, one 12 oz. can of soda has about 40 grams of added sugar.
When reading food labels, what sugary ingredients should be watched for? Sugar has many different names so navigating the ingredients list can be tricky. Some common names for sugar are sucrose, lactose, glucose and high fructose corn syrup. The ingredients are listed by weight in descending order, meaning that ingredients present in larger amounts are listed first on food labels.
Are some sugars worse than others?
It’s important to recognize the difference between natural sugars and added sugars. The negative health effects of too much sugar are linked to processed foods and sugary drinks. Fruits and vegetables contain natural sugars but they’re also rich in vitamins, minerals, and fibers.
Are natural sugars like honey, molasses, and fruit juices healthier than refined cane sugar?



Honey and molasses have antiinflammatory benefits and contain some vitamins and minerals but are still high in calories from sugar and may cause blood sugars to rise depending on how much is consumed. I don’t recommend processed fruit juices; it’s more nutritious to eat fruits in their whole form.
Which is worse – sugar or artificial sweeteners?
When compared to sugar, artificial sweeteners have a significantly less impact on blood sugars, have negligible calories and are better for oral health.
Do artificial sweeteners pose any health concerns?
The FDA has approved the use of several sugar alternatives, such as Sucralose and Stevia. Research suggests these nonnutritive sweeteners may have health benefits but could also come with a downside. Sugar alternatives have the potential to cause GI issues and heighten cravings for sugary foods.
What are some healthy ways to reduce sugar intake?
Cut the sodas out first and foremost! They are usually the number one culprit for excessive added sugars in the diet. To reduce sugar intake, eat more whole foods and limit processed foods.
How can a dietitian help those needing to reduce sugar intake to manage diseases like diabetes?

By teaching healthier preparation or substitutions in recipes and how to build balanced meals to meet individualized nutrition needs and support weight management goals.
When you want something sweet, what are your favorite low-sugar or sugar-free treats?
One of my usual sweet snacks is cream cheese strawberries because it’s easy to make and not loaded with sugar. Mix 1/4 c. low fat cream cheese, 1/4 c. light Greek yogurt, 1 tsp. vanilla extract and 2 tsp. Stevia. Slice up some strawberries, layer with the mixture and crumble a little graham cracker on top.


INGREDIENTS:
1 whole wheat pie crust

1 can 15 oz pureed pumpkin or 2 cups fresh pumpkin
½ cup milk (I used 1% milk)


4 beaten eggs
½ tsp salt



2 tsp vanilla extract
2 tsp pumpkin spice or mix together nutmeg, cinnamon, cloves
1 tsp vanilla liquid stevia
INSTRUCTIONS:
Prepare whole wheat crust.
Preheat oven to 350 degrees.
Lay aluminum foil over the pie crust and add pie weights or raw dry beans, about 2 pounds. Spread beans over the bottom of the pie on foil.
Place pie plate onto a baking sheet. Bake the crust for 10 minutes, remove the foil and beans and bake another 10 minutes.
While the crust is baking, mix filling ingredients in a bowl.
Pour filling mixture into the crust. Bake for 45 minutes -1 hour or until center is set.
Cool to room temperature on wire rack.
Refrigerate until ready to serve.

2 ¾ -3 cups whole wheat pastry flour
1 tsp salt
½ cup oil
1 cup milk
INSTRUCTIONS:

Mix flour and salt together in a bowl.

Pour milk and oil into a bowl, do not stir. Add all at once to flour. If using whole wheat pastry flour and dough is sticky, add ¼ cup more flour.
Stir until mixed and shape into 2 flat balls. Wrap in plastic wrap and chill for ½ an hour.

Lay one dough onto plastic wrap,

sprinkle some flour on plastic wrap and on top of dough and lay another piece on top. Roll out with a rolling pin as large as your pie dish.
Spray your pie plate with nonstick cooking spray, take the top piece off and flip over into the pie dish, pressing dough all around.
Prick the bottom of the dough with a fork. Cut off the excess so the crust is flush with the rim.

Save your second dough in the refrigerator wrapped in plastic wrap to use within a few days or roll out into a pie dish following same procedure as above and freeze in a Ziploc freezer bag for another day

Per serving:191 calories
5+ Weight Watcher points 26 g carbohydrates, 6 g protein, 7 g total fat, 71 mg cholesterol, 231 mg sodium, 5 g fiber, 1 g sugar.
Krista Lindley has worked as a registered dietitian and certified diabetes educator since 2012 at Hamilton Healthcare System. In addition to diabetes education, Krista also conducts nutrition and weight loss counseling. If you have a BMI of greater than 30, insurance may cover the cost of the program. For more information, call Krista at 254-386-1894.


Packed with antioxidants, this decadent brownie recipe is a heart healthier version of it store-bought cousins with less fat, sodium and carbohydrates and more fiber.

Serves 16

1 cup black beans, drained and rinsed
¼ cup canola oil


3 ounces prune puree (find this in the baby food aisle)
1/3 cup sugar
1 tsp vanilla extract
1 large egg




2 egg whites
¼ cup unsweetened cocoa powder
⅓ cup semi-sweet chocolate baking bits (mini chips work best)
½ cup white whole wheat flour ½ tsp baking powder ½ tsp sea salt ¾ cup pomegranate seeds

INSTRUCTIONS:
1. Preheat oven to350 degrees F. Spray 9x9 inch square pan with cooking spray. In a blender, puree the beans with the oil and prune puree. Add the eggs, cocoa powder, sugar and vanilla extract.
2. Melt half the chocolate chips in the microwave in a microwave-safe bowl. Add to the blender. Blend on medium high until smooth.
3. In a small bowl whisk together the flour, baking powder and salt. Add to the blender and pulse until just incorporated.
4. Stir half the pomegranate seeds into the batter. Pour batter into the prepared pan.
5. Sprinkle with the remaining chocolate chips and pomegranate seeds. Bake for 20 to 25 minutes or until a toothpick inserted comes out clean. Sprinkle brownies with ¼ teaspoon sea salt.
6. Cool for at least 15 minutes before cutting.
Per serving:130 calories, 6 g total fat, 1 g saturated fat, 10 mg cholesterol, 120 mg sodium, 18 g carbohydrate, 2 g dietary fiber, 10 g sugars, 3 g protein, 20 mg calcium, 1 mg iron, 136 mg potassium.




Pomegranates are juicy, sweet fruits with edible seeds called arils packed tightly inside. They’re rich in fiber, vitamins and minerals and even contain some protein. They’re also full of antioxidants and anti-inflammatory compounds such as punicalagins. These have been studied for their protective benefits for heart, urinary, brain, digestive and prostate health.






Pomegranates are rich in antioxidants and polyphenolic compounds, which may boost exercise endurance. There is evidence that fruits rich in polyphenolic compounds, such as pomegranate, may benefit heart health.



Studies have found that pomegranate extract may help reduce the formation of kidney stones, a benefit that’s largely attributed to its antioxidant activity. Pomegranate compounds may help fight harmful microorganisms such as certain types of bacteria, fungi and yeast.


Pomegranates contain compounds called ellagitannins, which act as antioxidants and reduce inflammation in the body. As such, they also offer protective benefits for your brain against conditions that are influenced by inflammation and oxidative stress. Some studies have found that ellagitannins may help protect the brain from developing Alzheimer’s disease and Parkinson’s disease by reducing oxidative damage and increasing the survival of brain cells.
Chili peppers (Capsicum annuum) are the fruits of Capsicum pepper plants, notable for their hot flavor. Many varieties exist and are primarily used as a spice. They can be cooked or dried and powdered. Powdered, red chili peppers are known as paprika. Capsaicin is the main bioactive plant compound in chili peppers, responsible for their unique, pungent taste and many of their health benefits.


Heat level: None!
Green, yellow or red, bell peppers are chiles that are never spicy and can be sweet and fruity when ripe. They score a zero on the



Heat level: A little spicy
These deep green peppers are a key ingredient in chile relleno. When picked red, they can be dried and sold as ancho peppers. These relatively mild peppers score less than 1,000 on the Scoville scale.
Heat level: A little spicy
These long, smooth peppers are typically light green. They are generally similar in spiciness to poblanos, at around 1,000 SHUs, but some species can get to 3,000 SHUs.


Heat level: Pretty spicy!
Typically found green, jalapenos are closely related to bell peppers but can be quite hot at 2,500–10,000 SHUs. A chipotle is a fully ripe, red jalapeño that’s smoked and dried, with a spiciness similar to that of a green jalapeño.



Heat level: Likely to be hot!
Although closely related, serranos can score much higher on the Scoville scale, from jalapeños’ upper limit of 10,000 SHUs all the way up to 25,000 SHUs.
Heat level: Scorching!
Shaped like little lanterns, habaneros are some of the world’s spiciest peppers with scores 100,000–400,000 SHUs. Aside from the spice, they have a sweet, fruity flavor .


Red chile and pork come together with hominy to warm the belly and palate in this traditional Mexian stew. Serve with tortillas or corn bread.


INGREDIENTS: 2 Tbsp olive oil 1lb pork shoulder cubed 1 onion, diced
guajillo or ancho peppers, diced 2 cloves garlic
tsp dried oregano 1 tsp cumin
tsp black pepper 2 cups low sodium chicken broth 1 15-oz can golden or white hominy, drained 1 4-oz can diced green chilies
1. Wash your hands and clean your cooking area. In a large saucepan, heat olive oil on high heat. Add pork and sear on all sides. Continue to cook pork until internal temperature reaches at least 160 degrees.

2. Add onion, peppers, garlic, oregano, cumin and black pepper. Cook until the onions are translucent.
3. Add chicken broth. When broth starts to boil, turn down the heat and simmer for 30 minutes.
4. Stir in hominy and green chilies; cook until pork meat is tender and stew thickens, about 30 more minutes.
5. Serve soup hot with garnishes.
Vitamin C
Chili peppers are very high in this powerful antioxidant, which is important for wound healing and immune function.
Vitamin B6
A family of B vitamins, B6 plays a role in energy metabolism.
Vitamin K1
Also known as phylloquinone, vitamin K1 is essential for blood clotting and healthy bones and kidneys..


An essential dietary mineral that serves a variety of functions, potassium may reduce your risk of heart disease when consumed in adequate amounts..
Often lacking in the Western diet, copper is an essential trace element, important for strong bones and healthy neurons.
Vitamin A
Red chili peppers are high in beta carotene, which your body converts into vitamin A.
etting kids involved in meal preparation is not only a great way to teach kitchen safety and food preparation skills but also a wonderful time to create family memories and establish healthy nutrition habits.
Try these tips for cooking safely with children: Always supervise kids in the kitchen. While younger, inexperienced children need direct assistance, it’s still a good practice to know when more experienced, independent children are cooking and be available nearby.

Teach good kitchen hygiene. Remind kids that clean hands are a big part of food safety. Wash hands with soap and water often. Tie back long hair. Wear shoes to help avoid burns, spills and wounds from dropped items.

Start with clean surfaces and cooking tools and wipe up spills immediately. Avoid contamination by keeping surfaces clean. Teach kids that spills are a part of working in the kitchen but it is important to clean up messes as soon as possible.

Explain safe food handling.
Rinse produce. Handle raw meat and eggs with special care to avoid cross contamination. Teach kids the importance of cooking certain foods to proper temperatures. Food handling continues through storage. Explain the dangers of leaving food on the counter too long and demonstrate proper ways to store ingredients and leftovers.

Following instructions, listening and reading through the recipe are important life skills to reinforce in the kitchen. Gather ingredients and tools before getting started to set children up for success.
It’s hard not to lick fingers or spoons while cooking, but to prevent illnesses from uncooked foods and spreading germs, children must learn to resist the urge to lick.
Teach knife, appliance and stove safety.


Knife safety – Beginners can learn to slice, chop and dice first with a plastic knife on softer foods like a peeled banana or watermelon. Teach kids to peel away from themselves, keep knuckles clear of the grater and use the bear claw method to avoid cutting fingers. Progress to adult knives as children gain experience and motor control.

Appliance safety – Model small appliance safety for children. Start by allowing them to push buttons with your supervision. As they gain experience and demonstrate safe operation, allow more operating freedom. Don’t forget to teach them how to use electrical plugs safely and unplug appliances after use.

Stove safety – With proper supervision, children can learn to use the stovetop and oven safely. Strict lessons on turning burners on and off, adjusting heat and properly putting food in the oven are a must. Remind children to point handles to the side or back. Use mittens for hot pots and pans. Make sure the stovetop and oven are off when cooking is complete.


Clean up! Cooking isn’t complete until the kitchen is clean. Teach kids to put away ingredients, load the dishwasher or wash tools, wipe down counters, sweep and mop floors, unplug and store appliances and double check that the stove is off.

















Spin Group Mon. & Wed. 4:45 a.m.
Body Works Tues. & Thur. 4:45 a.m.
Arthritis Aerobics (aquatic) Mon., Wed. & Fri. 8:00 a.m.
Aqua Fitness Mon., Wed. & Fri. 9:00 a.m.
Tai Chi Tues., Wed. & Thur. 10:00 a.m.

Arthritis Exercise Program
Tues. & Thur. 11:00 a.m.
Yoga Mon., Wed. & Fri. 12:00 p.m.
Clogging Mon. & Thur. 1:00 p.m.
Clogging Mon.-Fri. 2:00 p.m.
Aqua Aerobics Mon. & Wed. 4:30 p.m.
Aqua Aerobics Mon. & Wed. 5:30 p.m.
Body Works Tues. & Thur. 5:30 p.m.
BY KYMBIRLEE JESCHKEamilton Wellness Center is excited to add aqua aerobics and bodyworks classes to their fitness class lineup.
Instructor Jessica Rushing, who also serves the system as Employee Fitness Coordinator, is vivacious and energetic.
She began teaching fitness classes in 2018 after an instructor at LA Fitness picked her out of class and encouraged her to get her group fitness certification.
“She told me, ‘you’ve got something; you’d inspire people,’” said Jessica, who began teaching classes in aqua aerobics, kick boxing, bodyworks and Pilates.
She brings her energy and excitement for fitness to her classes.
Aqua aerobics is offered on Mondays and Wednesdays at 4:30 p.m. and 5:30 p.m., and bodyworks classes are Tuesdays and Thursdays at 4:45 a.m. and 5:30 p.m.
“Classes are upbeat, positive, challenging and fun,” said Jessica, who encourages attendees to make the workout their own through modifications.
“I guide the class and show how to modify for your limitations. Maybe it is slowing down the movement or shortening the range of motion. When you are ready to intensify, we can add weight, noodles or a board.”
Aqua aerobics is in the heated fitness pool in the Wellness Center. The pool is kept at a


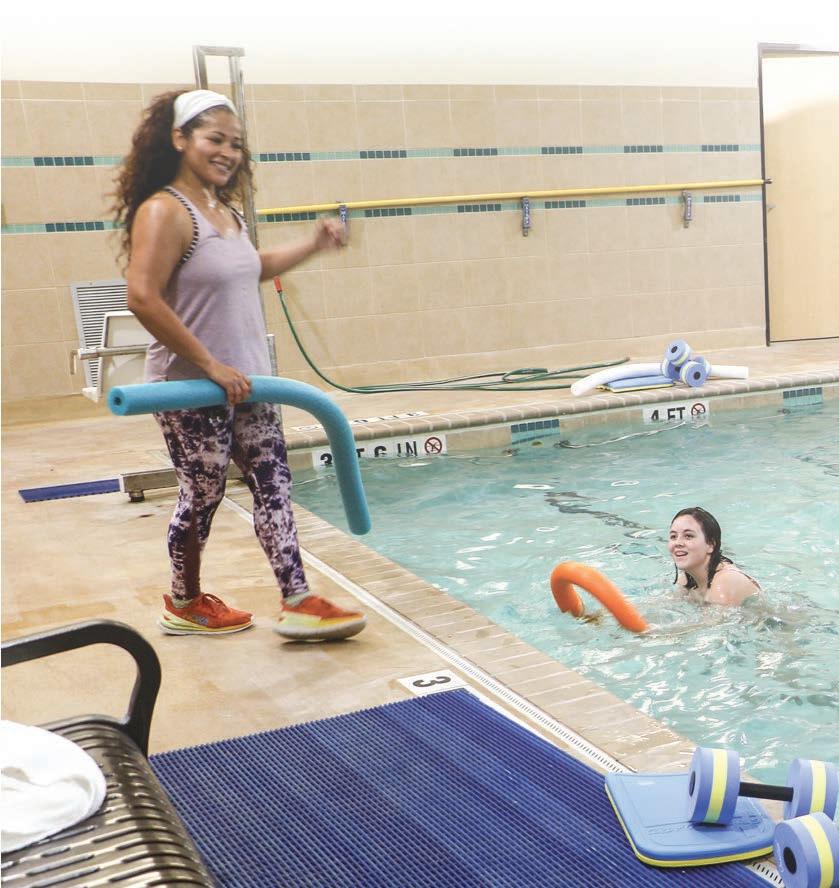
comfortable 86 degrees year-round.
Water creates its own resistance, which makes it great for toning and building strength.
It supports the body, lessening the impact on joints and making aqua aerobics an ideal activity for those managing arthritis, joint injuries or just getting started on their fitness journey.


Since the fitness pool at the Wellness Center is 4’6” at its deepest, participants don’t have to be swimmers.
“The good news is your feet can touch the ground,” said Rushing, who adds that the class is great for core stability, which translates to improved balance.
Aqua aerobics classes are limited to 10 people but signup is available at the front desk a week in advance.
Rushing’s bodyworks classes focus on light weight and high repetition.
“The class is intense, but I make it fun with music and energy,” she said.
In addition to getting fit while having fun, Rushing says she loves that her classes build confidence.
Attendees start to notice toner muscles, an increase in range of motion and speed. She says these are great motivators and build self-esteem.
Participants in Rushing’s classes range in age from 28 to 86.
“In Austin, my oldest was 86, and she killed it,” said Rushing.
Originally from California, she and husband Kenneth moved to Hamilton from Austin.
400 N. Brown • Hamilton, TX 254-386-1670



Monday -Thursday 7 a.m. - 6 p.m. Friday 7 a.m. - 4 p.m.
24-hour access for members





"There have been lots of changes in that big city, but I’ve always been a small-town girl at heart,” she said.
Aqua aerobics and bodyworks join instructor-led tai-chi, clogging, yoga and arthritis exercise program classes offered throughout the week at the Wellness Center. A group spin class meets Mondays and Wednesdays at 4:45 a.m.



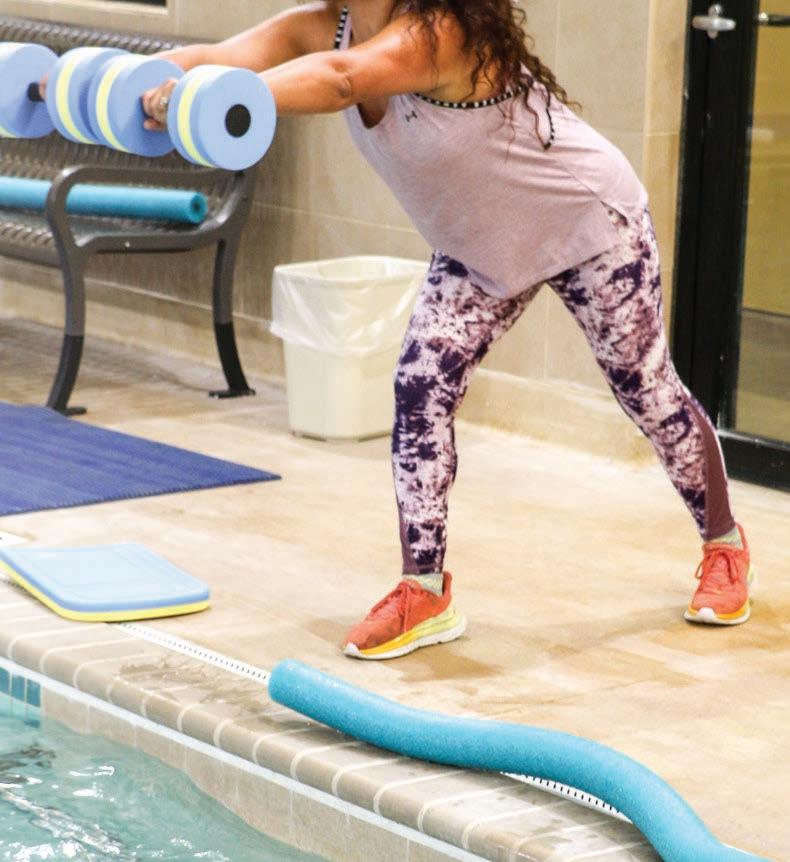


Fitness on Demand offers all types of virtual workouts 24/7 in a wide range of levels and durations.
All classes are included in Wellness Center memberships. Daily passes are available for $5.

Free or discounted memberships are available through SilverSneakers and Silver & Fit.





n October, Hamilton Wellness Center announced new challenges. With a focus on strength building, the 500-pound and 1000-pound clubs acknowledge the physical achievement and dedication of fitness center members.




To complete a challenge and become a club member, lifters must perform one successful squat, bench press and deadlift. The total of the three successful lifts must be at least 500 pounds or 1000 pounds.

Heavy Lifting Club members receive a T-shirt, certificate and their successful lift archived on the board at the Wellness Center.
On October 4, Nik Adams, a sophomore at Hamilton High School, became the first member of
















With the barbell horizontal across the shoulders and hands gripping the bar, bend the knees and lower the body until the top surface of the legs at the hip joint is level to the top of the knees. Power up through the glutes to a standing position.




the 1000-pound club. Adams bench pressed 225 pounds., squatted 405 poumds. and deadlifted 405 pounds for a total lift of 1035 pounds.
On October 31, Darryl Moore, a veteran and retired law enforcement officer, became the first member of the 500-pound club.
"I'm older and this is a great way to stay in shape," said Moore, who uses strength training to manage stress and heal an injury. "I want to challenge my veteran buddies out there to up their game. Even though we are retired we can still take care of ourselves."



MacKenzie Suggs became the first woman on the board in November with a total lift of 705 pounds.

To participate, members should call Joey Richardson at 254-386-1670.









Lie on the back with head, shoulders and buttocks in contact with the bench. Feet flat on the floor. With the bar overhead at arms length distance, grip the bar by wrapping the thumbs around. Lower the bar to the chest then press the bar back to straight arm length.


With the barbell laid horizontally at the lifter's feet, assume a shoulder width stance. Squat and grip the barbell so the inner forearms touch the outside of thighs and shins lightly touch the bar. Push through the feet to standing, bringing the bar and weight to about the midway position of the upper thigh.






ccording to research, an estimated 70 percent of adults in the United States have experienced a traumatic event at least one time in their lives. Of these people, up to 20 percent go on to develop Post-Traumatic Stress Disorder (PTSD), but what is it?
The stress caused by a traumatic event can often affect a person mentally, emotionally and physically. Research suggests that extended trauma may even interrupt and change the brain’s chemistry. A traumatic event can often change a person’s views about themselves and the world around them, which may increase the likelihood of developing PTSD.

Understanding typical responses to traumatic events can help you cope effectively with your feelings, thoughts and behaviors, and help you along the path to recovery.
Common responses can be:
• Intense or erratic feelings.
• Changes to thoughts and behaviors.
• Sensitivity to noises, smells and environmental factors that can be a reminder of the traumatic event.
• Strained relationships with others
• Stress-related physical symptoms.
• Re-living the event through nightmares or other disturbing images.
• Avoiding reminders of the event or talking about the event.
• Being on guard or hyper-aroused.
Luckily, research also shows that most people are resilient and are able to bounce back from a traumatic event over time.
Immediately after a trauma, most people experience stress.
Within a few weeks or months, most people are able to continue functioning as they did before the trauma.
Thankfully, resilience and recovery are
the norm, not prolonged distress.

There are several steps you can take to build emotional resilience and regain a sense of control following a traumatic event including:
• Give yourself time to adjust.
• Ask for support from people who care about you and who will listen and empathize with you.
• Attend local or online support groups led by appropriately trained and experienced professionals.

• Engage in healthy lifestyle choices to enhance your ability to cope with excessive stress.
• Establish or reestablish routines in your daily life.
• Avoid making major life decisions during times of stress.

If symptoms continue for one month or longer or reappear over time, it could be a sign to seek professional help.
According to research compiled by the National Center for PTSD, several types of psychotherapies have been proven to help decrease or eliminate PTSD symptoms including, Eye Movement Desensitization and Reprocessing (EMDR), Prolonged Exposure (PE) and Cognitive Processing Therapy (CPT). You may also choose to consult your physician, because medication can be an effective option, however, therapies have been proven to be more effective than medications.

Consider your mental health to be just as important as your physical health. You would get help with heart issues, a broken bone, diabetes, etc., but often choose not to get help for PTSD. Choosing to get help for PTSD symptoms is important, because only a small percentage people who choose to do nothing about their PTSD symptoms end up eliminating PTSD symptoms. Since PTSD is linked to extremely high rates of medical and mental health costs and it is possibly the highest per-capita cost of any psychological condition, it is important to seek help from trained professionals.










Elizabeth Bays completed her Master’s degree in Counseling Psychology from Tarleton State University. She has been a member of the Solutions Behavioral Health team since 2015 and serves as clinical director while seeing a wide range of client populations. Her passion and expertise are working with survivors of trauma. She uses an eclectic approach to therapy and utilizes a blend of cognitive behavioral therapy, solution focused, reality based, and psycho-education. She has also been trained in Eye Movement Desensitization and Reprocessing (EMDR). Elizabeth is invested in an approach emphasizing a more integrative, dynamic and holistic approach to mental health. She is particularly concerned with the impact of trauma and improving intervention to support trauma recovery for better emotional, physical and relationship health.
Solutions Behavioral Health offers therapy and treatment for PTSD call 254-386-1800 to begin healing today.






of













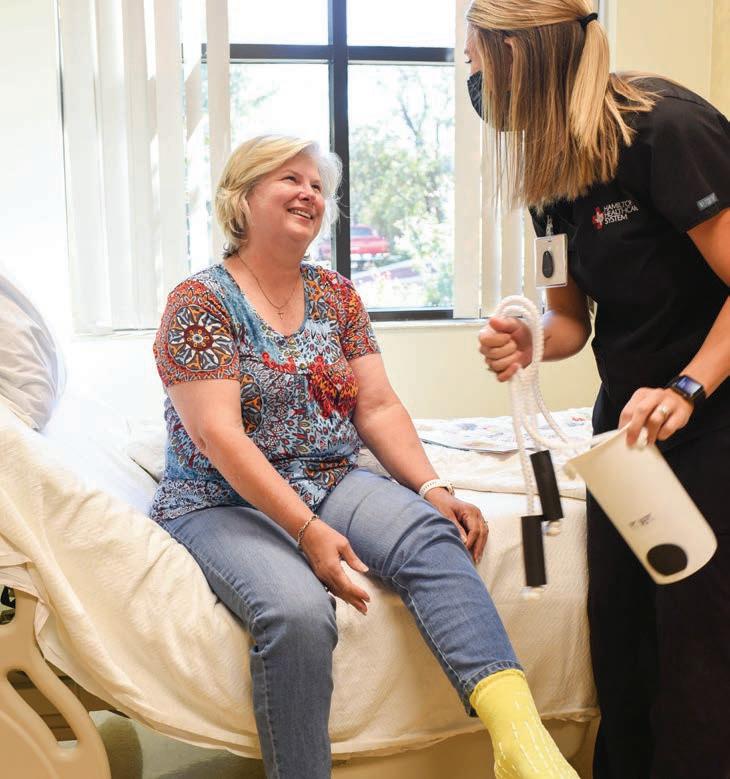
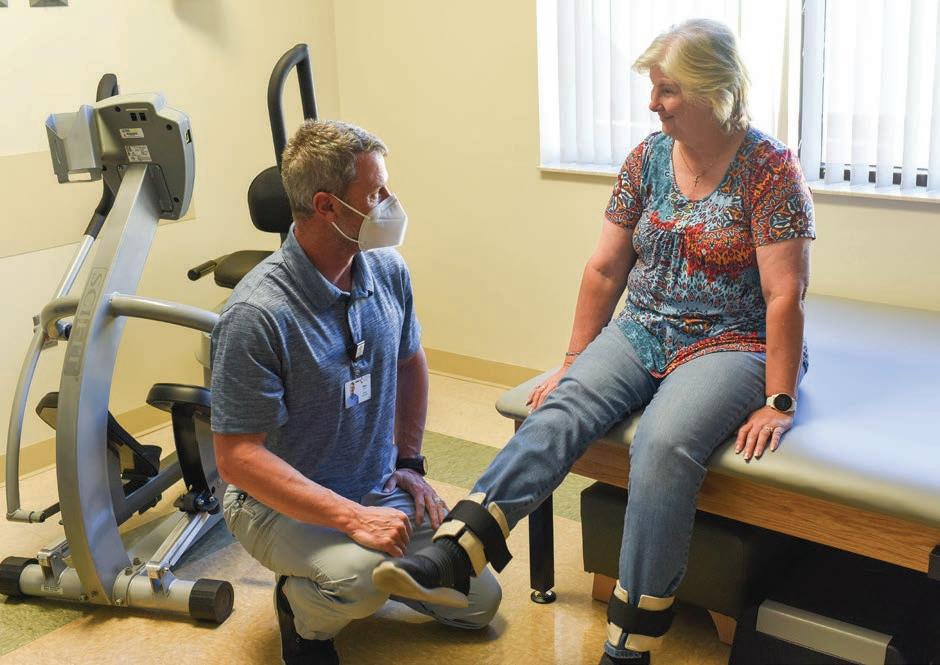
ou never know when illness will strike or just how hard the blow will be.
Lucy Lee was both fascinated and terrified when she had a stroke in October.



On that morning, she was working at her computer in her dining room when she heard trucks in her driveway. Workers were coming to restore the power in her barn after an electrical fire.
It was about 8:15 when she heard Justin Cozby in her driveway. She rushed to her room to get dressed and had a little trouble putting on her pants and shirt.

“As a nurse, I was thinking, ‘This is so cool.’ I was wobbling and hitting the wall,” she says. “I felt clumsy.”
She thrust her feet into her shoes and went into the bathroom for lipstick.
“I couldn’t get my hand to go to my lips,” she says. She knew then she was having a stroke.
“I was observing and experiencing it on two different levels,” Lucy says. “As a


nurse, that’s really cool.”
She wobbled to the door and in a slurred voice asked Justin to take her to Hamilton General Hospital.

“When she came to the door, I was a little freaked out,” Justin said. “She said, ‘I’m having a stroke.’
“I said, ‘Sh--!’ We piled into her car and headed to town.”
“I felt totally normal by 9 a.m.,” Lucy says. “I could tell it was resolving.

“Justin is such a thoughtful person. He stayed there with me and even ran my errands while I was in the emergency room.”
Lucy was home by noon and is now doing well.
Her three sons, Chris, Michael and Jason, called and texted, worried about their mom. Chris was on a flight from Geneva to New York but called as soon as he landed.
“He is on the board at Baylor College of Medicine and emailed a contact and got me an appointment with a neurologist.









“Michael is in Round Rock and took me to Houston to Jason’s, and the next day I saw the doctor and had an MRI and MRA.

“My first thought was, my mom had a stroke at 69.”
Lucy learned her brain had shrunk a little, and there were signs of ischemia. She also has developed a non-essential tremor, but other than that, there are no after-effects.”
No medication?
“Baby aspirin,” she says with a smile. “And my sons wanted me to get one of those necklaces so I could push the button if it happens again. But instead, I got this cool Apple watch.”
“Talk about perfect timing,” Justin says. “I’m glad she is all right.”
“It definitely made me thankful for my village,” Lucy says. “A lot of people have been there for me. God is love, and my experiences have been perfect examples of that love.”
or many years, rural central Texans have relied on the services of Central Texas Urology. Dr. Mark Story saw many patients at Hamilton’s Family Practice Rural Health Clinic. With his retirement this summer, Hamilton Healthcare System is excited to welcome Tyler Stewart, M.D. to its team of courtesy specialists.
Dr. Stewart joined Central Texas Urology in August after completing his training in July. He finished his undergraduate degree at Texas A&M and completed his surgical internship and urologic specialization at the top of his class at the UT Health Science Center in San Antonio.

Dr. Stewart grew up in Lorena and has always wanted to become a urologist.
“My mom found a kindergarten project where I drew a picture of a doctor and said, ‘I want to be a bladder doctor,’” said Stewart. “My dad is also a urologist. I joined his practice. It’s fun to practice with my dad and his partners.”

Stewart is enjoying learning from the experienced doctors that he has known for much of his life and sharing the latest techniques with them.
At the forefront of technology, Dr. Stewart is trained in robot-assisted surgery, which gives surgeons more precision, flexibility and control and results in smaller incisions and faster recovery times for patients.

“We are just starting in Waco,” he said.
For those with non-cancerous enlarged prostate, Dr. Stewart offers Rezum, water vapor therapy, instead of resection.

“We inject steam that allows the tissue to dissolve over time without removing tissue with a knife,” he said.
The procedure take less than 10 minutes with fairly long-term results.
Dr. Stewart sees patients twice per month at Hamilton Rural Health Clinic, where he performs clinical exams, small clinic procedures and has surgical privileges at Hamilton General Hospital.
As a general urologist, he treats patients

experiencing kidney stones, incontinence or urinary difficulties, urological cancers of the kidneys, prostate and bladder and provides prostate screening.
Dr. Stewart sees adults and children.
“There is no one I won’t see,” he said.
“I love hearing people’s stories and love teaching people about their body. Urological subjects can make us feel alone or isolated. If you live long enough, you will need a urologist. I can help you feel better.”
Some of the most common ailments that urologists in Central Texas see are kidney stones, incontinence and urinary tract infections.
“Central Texas is ripe for kidney stones,” said Dr. Stewart. “We are actually in a stone belt.”

For those who live long enough and/ or have multiple children, incontinence is a common issue, but one that doesn’t necessarily require surgery, says Dr. Stewart.
Pelvic floor therapy and devices are treatment options as is a minimally invasive outpatient surgery.

Dr. Stewart says there are a lot of new cases of prostate and kidney cancers probably due to gaps in screenings during the COVID pandemic.
He stresses the importance for men ages 50 to 75 to have a PSA blood test every two years through their family doctor or more frequently for those with family history.
While Dr. Stewart is happy to accept referrals from family doctors, patients can call and make an appointment without a referral.
He looks forward to continuing to serve Hamilton and its surrounding communities.
“I’m a small town guy. I love Hamilton and its people. When patients come to see me, they can expect to talk to someone a lot like them,” said Dr. Stewart, who loves hunting, fishing and the great outdoors.
When he’s not working, he enjoys spending time with his wife and children, being outside or watching football.
When you refer your patients to Texas Oncology, you can be confident they’re getting leading edge cancer care, right here in Waco. Our physicians provide compassionate, comprehensive care, offer the latest treatment innovations, and share one goal: to make sure every Texan can receive recognized cancer care — and stay close to loved ones.


1700 W. State Hwy. 6 Waco, TX 76712 • 254-399-0741



Texas Oncology–Horizon Circle 6520 Horizon Circle Waco, TX 76712 • 254-755-4460
















Additional locations in Clifton, Gatesville, Groesbeck, Hamilton, Hillsboro and Mexia.
 Carl G. Chakmakjian, D.O., FACP • Tyler W. Snedden, M.D. • Thomas J. Harris, M.D. • Rachel Ramsey, NP, AOCNP Carlos A. Encarnación, M.D., FACP • Ofobuike N. Okani, M.D., FACP • Katie Bone, MSN, APRN, FNP-BC Dawn Turner, RN, FNP-C, AOCNP • Justin W. Wray, M.D., Ph.D.
Carl G. Chakmakjian, D.O., FACP • Tyler W. Snedden, M.D. • Thomas J. Harris, M.D. • Rachel Ramsey, NP, AOCNP Carlos A. Encarnación, M.D., FACP • Ofobuike N. Okani, M.D., FACP • Katie Bone, MSN, APRN, FNP-BC Dawn Turner, RN, FNP-C, AOCNP • Justin W. Wray, M.D., Ph.D.
 BY KYMBIRLEE JESCHKE
BY KYMBIRLEE JESCHKE
or more than a year, Anjenette Juracek has been part of the Hamilton Healthcare System psychiatry team at Solutions Behavioral Health.
A board-certified psychiatric mental health nurse practitioner, Juracek works with doctors and therapists to develop patient treatment plans that promote healthy behavior and healing in the lives of her patients.

She began her healthcare journey as a nurse. While working with patients in the emergency room, surgery and trauma, she began to notice a very real need for mental health resources and providers.
“It doesn’t matter what you do in nursing, you are going to run into some aspect of












mental health, and there are not enough people to provide it,” said Juracek.
















With this realization, she went back to school to become a mental health nurse practitioner.

“All of us have someone in our life – a friend, family member or both – that suffers from mental health issues,” said Juracek.

At Solutions Behavioral Health, Juracek’s expertise is in medication management. She works with patients of all ages but her favorite populations are children and adolescents.


“Kids tell you exactly what they are thinking,” she said. “They don’t hold anything back. They want to have friends, be happy and not be in trouble all the time – which is what anyone wants.”
Juracek works closely with therapist Kayelen Helton, even traveling regularly to Goldthwaite to treat patients.



“Often with kids, we use therapy before medication,” she said.



Juracek says children express their needs differently than adults.
Clues that a child may need treatment include mood disturbances over a long period of time, drastic changes, experiencing a traumatic event – even if they are acting like they are doing OK, expressing suicidal thoughts, increased anger or instability, disruptive relationships at home or school and dropping grades.
“One of the most important things we can do is normalize treatment for mental health,” said Juracek. “It is just as important as physical health. When left untreated, it leads to chronic medical conditions.”
Through Solutions Behavioral Health, rural central Texans have access to mental health resources including individual counseling, an intensive outpatient program for seniors, couples and family counseling, suicide risk assessment and reduction, PTSD treatment, play therapy for children and psychiatric medication management.

Juracek is impressed by the resources available through Solutions Behavioral Health and says in many other areas mental health resources like these are hard to access.
“People come from Waco, Marble Falls, Brownwood, even Arlington and the Fort Worth area to get care here,” she said. “It’s hard to find the psychiatric model we have here. It’s a pretty big deal.”

In addition to doctors and therapists who specialize in different modalities, Juracek praises the great support staff that helps patients navigate the process.
“People get overwhelmed and don’t know where to start,” she said. “A friendly voice on the phone greets them and guides them through the steps.
“I’m proud to work here.”
When she’s not working, Juracek enjoys spending time with her children, dogs and enjoys rucking, hiking with weighted backpacks.
"One of the most important things we can do is normalize treatment for mental health."











amilton General Hospital Healthcare Foundation hosted Celebration '22 on Sept. 14 at J. Waddy Bullion Pavilion at Texas Botanical Gardens in Goldthwaite.



The celebration was the Foundation's first fundraiser since Celebration '19 and was met with much enthusiasm with approximately 220 people in attendance.
Attendees enjoyed a fajita dinner catered by Diamond R, auction, wine pull, stretch drawing and dancing to the Tejas Brothers.
The main fundraiser for the Foundation, Celebration '22 raised more than $68,000 for healthcare services in Hamilton and Mills counties.
"We appreciate everyone who came


President Robert Witzsche. "Your support helps with projects like purchasing 3D mammography equipment to improve the healthcare services for our families, friends and neighbors in Hamilton, Hico and Goldthwaite."
Now more than ever, Central Texans are reminded of how grateful we are to have outstanding healthcare professionals and facilities in Hamilton, thanks to the foresight, tenacity and stewardship of many of our citizens over the years.
The Hamilton General Hospital Healthcare Foundation, 501(c)3 organization, maintains the legacy of ensuring vital healthcare services now and for the future for Hamilton County and surrounding areas.







Thanks to the generosity of our donors, the Foundation has been instrumental in providing grants for needed equipment and services like the new 3D digital mammography machine and annual community health fair.
As you plan your end-of-the-year gifts, please consider the Hamilton General Hospital Healthcare Foundation.













Providing excellence in rural healthcare











P.O. Box 788 • Hamilton, Texas 76531 Donate online at hamiltonhospital.org/hghh-foundation


Give a gift that makes a difference.
amilton General Hospital has been awarded the prestigious honor of Top 20 Critical Access Hosptial in Patient Satisfaction from the National Rural Health Association.
Of the 1360 critical access hospitals in the United States, HGH was the only Texas hospital to receive the award, which was based on Hospital Consumer Assessment of Healthcare Providers and Systems information gathered through patient satisfaction surveys.
“It’s important to fill out the survey and give us feedback,” said Director of Quality Tracey Karasek, MSN, RN. “The more surveys we receive, the better perspective we get. We want the positive as well as the didn’tgo-as-well-as-we-wanted answers.”


Surveys are collected and tabulated by a third party vendor then uploaded to the Centers for Medicare and Medicaid Services to ensure patient confidentiality.



HGH strives to maintain a 5-star overall rating for patient satisfaction from CMS.












“We are competitive within ourselves,” said Karasek. “We have a volunteer committee made up of frontline, staff and directors that closely monitor quality. We set quarterly goals and send a weekly score update to staff. ”
Critical Access Hospital in Patient Satisfaction



In addition to being named a Top 20 Critical Access Hospital, HGH has also been recognized with a 2022 Performance Leadership Award for excellence in Outcomes and Perspective.
Compiled by The Chartis Center for Rural Health, the Performance Leadership Awards honor top quartile performance among rural hospitals in Quality, Outcomes and Patient Perspective.


In a rural community, the caregivers and patients know one another.
“We have a close connection with our patients,” said Karasek. That connection is the driving force for providing the best patient care.


















General Assistance
211 Texas Help finding services/resources www.211texas.org
211 or 1-877-541-7905
Crisis Text Line www.crisistextline.org
Text HOME to 741741 to connect with a Crisis Counselor Free 24/7 support at your fingertips
Mental Health & Developmental Disabilities Central Counties Services 254-386-8179
7

9




FOCUSED CARE 254-386-3171 fpacp.com

Texas Health & Human Services Office Medicaid, Food Stamps, Medicare Savings Programs (254) 386-8965
Hamilton Co. United Care Help w/ food & clothing 254-206-7371
Hamilton Community Center Daily free lunches 254-784-3358
Hill Country Community Action 1-866-372-5167
Hamilton TX Helping Hands find them on Facebook
Aged & Disabled, Veterans
Texas Health & Human Services
Long Term Care Services 1-855-937-2372
Crisis Hotline 1-800-888-4036 • • • Adult Substance Abuse Texas Health & Human SvcsBluebonnet Trails 1-800-841-1255 (Crisis) 1-844-309-6385 (Main) • • •
Women
Women & Children
Texas Health Steps
Services for Pregnant Women, Children on Medicaid Birth-20 yrs 1-877-THSTEPS (1-877-847-8377)


Texas WIC Women, Infants, Children 1-866-907-0080 TexasWIC.org 254-216-9211 Hamilton
14
15
27
TEXAS ONCOLOGY 888-864-4226 TexasOncology.com

CAREFLITE 877-DFW CARE (membership) careflite.org
Area Agency on Aging | Aging & Disability Resource Center Services, Info & Referral for Aged, Disabled & Veterans 254-770-2330 or 1-800-447-7169
Hico Senior Center 254-796-4488
Mills County Senior Center 325-648-3122 • • •
Transportation
Texas Medicaid Transportation 1-877-MED-TRIP (1-800-633-4227)
The Hop Rural Transit 254-933-3700 ext. 5005 or 1-800-791-9601 ext. 5005 • • •
Mental Health
Texas Health & Human Services

COVID 19 Mental Health Support Line 1-833-986-1919
Early Childhood Intervention 254-773-6787

Hamilton Early Head Start 254-386-8936 • • •
Domestic Violence
4 WACO CARDIOLOGY ASSOCIATES 254-399-5400 wacocardiology.com SERVICES ADVERTISERS directory Be a part of the Spring issue of Thr ve Health and Wellness Magazine for Rural Central Texans Call Kym at Hamilton Herald-News 254-386-3145 or kym@hhnpaper.com Sign up at carterbloodcare.org
5 We’re coming to Hamilton! Jan. 5 • March 16 12-6 p.m. @ HGH Parking Lot February 7 @ Hamilton High SChool
HOPE – Tri-Rivers Domestic Violence Emergency Shelter Emergency Shelter & Assistance for DV Survivors 254-865-2151















