















































































The Next Generation Of Contamination Monitoring Technology
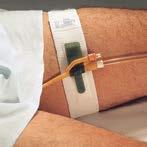
For the cleaning verification of surgical instruments, endoscopes, and surfaces, ATP Complete 2 by Ruhof a cloud-based cleaning monitoring system used to help hospitals and other healthcare organizations achieve optimal standardized cleaning levels.






















CONTENTS > JULY 2024
































Sourcing & Logistics
8 > Inventory Control vs. Inventory Management: An Important Distinction
ASHLEA SOUFFROU
36 > UDI Gets a Collaborative Kickstart
KAREN CONWAY
Surgical/Critical Care
12 > Educating Workers on Sharps Safety
MATT MACKENZIE
Infection Prevention
14 > AHE Director of Education Shares Insights into New EVS Training Program
JANETTE WIDER
Sterile Processing
18 > 10 Key Considerations in Instrument Reprocessing Site Selection
KARA NADEAU
28 > Tips for a New Sterile Processing Technician BY
ARTHUR HENDERSON
32 > Progressive Discipline in the SPD: When & Why? BY
DAVID TAYLOR AND KRISTINA PIROLLO-KETCHUM
34 > Under Pressure: PSI and “Instrument Air” Drying
STEPHEN M. KOVACH
Departments
4 > Three Cheers for EVS
6 > What’s on the Web, Advertiser Index



DETECTO manufactures more unique models for each clinical product category than any other medical scale company. Giving you better choices means you never have to settle for a product that isn’t the right fit for your application.
DETECTO: A true vertically-integrated medical scale manufacturer – family owned and privately held – with factory and headquarters in Webb City, MO.

Best Choice is the One That Gives

BY JANETTE WIDER, EDITOR-IN-CHIEF
Last edition I wrote my editorial about the fine folks in sterile processing. This month, I want to say a few words about those who work in environmental services (EVS).
EVS teams are often thought of as housekeepers or janitorial staff, not as a line of defense against bacteria and viruses. Training and education are often inadequate, time consuming, and not up to par for these departments. One might simply think that you could pluck a housekeeper from a hotel and put them into a hospital with little training, but this is not the case.
I spoke with Monika Berrier, EdD, PMP, director, Association for the Health Care Environment (AHE) Education (page 14) about a new training subscription program for EVS called Skill.Set.Go. The program is from the American Hospital Association (AHA) and led by AHE. There are details of what comes with the program in the article, but what stood out most to me was the notion that all departments in the hospital should be learning. This mindset, I think, is very often overlooked by those in leadership roles.

This is understandable due to the day-to-day getting in the way of taking meaningful time for education—which my article this month also touches on.
And speaking of time constraints, in my experience across this brand and the other healthcare brands at Endeavor Business Media ( Healthcare Innovation and Medical Laboratory Observer), I’ve noted one of the major pain points from those I’ve interviewed over the years is that “there just isn’t enough time in the day.” Thanks to programs like Skill. Set.Go. from AHE, education can be done on-demand.
Now, back to those working in EVS. I wouldn’t describe the job as glamorous by any means, but individuals in these positions should be praised for being on what I would consider the front line in the fight against microorganisms that are lurking in hospitals. And I believe we should celebrate these individuals by investing in their education and training to ensure their continued success and commitment to what is truly most important: patient safety.
So, let’s have a round of applause for our EVS teams!
VP & Market Leader
Healthcare and Dental
Chris Driscoll
cdriscoll@endeavorb2b.com | 978-880-8345
Editor-in-Chief
Janette Wider jwider@hpnonline.com
Associate Editor Matt MacKenzie
mmackenzie@endeavorb2b.com
Senior Contributing Editor Kara Nadeau knadeau@hpnonline.com
Advertising Sales
East & West Coast
Kristen Hoffman khoffman@endeavorb2b.com | 603-891-9122
Midwest & Central
Brian Rosebrook brosebrook@endeavorb2b.com | 918-728-5321
Advertising & Art Production
Production Manager | Ed Bartlett
Art Director | Tracy Arendt
Advertising Services
Karen Runion | krunion@endeavorb2b.com
Audience Development Laura Moulton | lmoulton@endeavorb2b.com
Endeavor Business Media, LLC
CEO Chris Ferrell | President June Griffin
COO Patrick Rains
CRO Paul Andrews
Chief Digital Officer Jacquie Niemiec
Chief Administrative & Legal Officer Tracy Kane
EVP Medical & Healthcare Technology Kylie Hirko
EVP Endeavor Business Intelligence Paul Mattioli
Healthcare Purchasing News USPS Permit 362710, ISSN 1098-3716 print, ISSN 2771-6716 online is published 11 times annually with an additional issue in November - Jan, Feb, Mar, Apr, June, Jun, Jul, Aug, Sep, Oct, Nov, Nov IBG, by Endeavor Business Media, LLC. 201 N Main St 5th Floor, Fort Atkinson, WI 53538. Periodicals postage paid at Fort Atkinson, WI, and additional mailing offices. POSTMASTER: Send address changes to Healthcare Purchasing News, PO Box 3257, Northbrook, IL 60065-3257. SUBSCRIPTIONS: Publisher reserves the right to reject non-qualified subscriptions. Subscription prices: U.S. $160.00 per year; Canada/Mexico $193.75 per year; All other countries $276.25 per year. All subscriptions are payable in U.S. funds. Send subscription inquiries to Healthcare Purchasing News, PO Box 3257, Northbrook, IL 600653257. Customer service can be reached toll-free at 877-382-9187 or at HPN@omeda.com for magazine subscription assistance or questions.
Printed in the USA. Copyright 2024 Endeavor Business Media, LLC. All rights reserved. No part of this publication June be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopies, recordings, or any information storage or retrieval system without permission from the publisher. Endeavor Business Media, LLC does not assume and hereby disclaims any liability to any person or company for any loss or damage caused by errors or omissions in the material herein, regardless of whether such errors result from negligence, accident, or any other cause whatsoever. The views and opinions in the articles herein are not to be taken as official expressions of the publishers, unless so stated. The publishers do not warrant either expressly or by implication, the factual accuracy of the articles herein, nor do they so warrant any views or opinions by the authors of said articles.



































































































































According to a press release from the American Heart Association, total costs related to cardiovascular disease conditions are likely to triple by 2050, according to projections from the association. Further, at least six in 10 U.S. adults (61%), which equates to more than 184 million people, are expected to have a type of CVD within the next 30 years. The association says that this reflects a disease prevalence that will have a $1.8 trillion price tag in direct and indirect costs. Read on: hpnonline.com/55056142
Introducing Healthcare Hodgepodge with Healthcare Purchasing News, featuring interviews and article reads. The podcast features topics from the publication’s many verticals including supply chain, infection prevention, sterile processing, surgical/ critical care, healthcare IT, EVS, and more. Learn more: https://healthcarehodgepodge.podbean.com/e/introducing-healthcarehodgepodge/

The FDA has released a list of seven tips to assist in charging medical devices correctly in order to avoid overheating, which can cause fires and injury. Specifically, these tips concern “devices that use a USB charger including hearing aids, glucose monitors, [and] insulin pumps.” Chief among the tips is to “read, understand, and follow the manufacturer’s directions for the use and care of your device.” It is also vital to use “the charging accessories provided by the manufacturer.”
Read on: hpnonline.com/55039600

Jimmy Chung, MD, MBA, FACS, FABQAURP, CMRP, Chief Medical Officer, Advantus Health Partners and Bon Secours Mercy Health, Cincinnati, OH
Joe Colonna, Chief Supply Chain and Project Management Officer, Piedmont Healthcare, Atlanta, GA; Karen Conway, Vice President, Healthcare Value, GHX, Louisville, CO
Dee Donatelli, RN, BSN, MBA, Senior Director Spend symplr and Principal Dee Donatelli Consulting LLC, Austin, TX
J.Hudson Garrett Jr., PhD, FNAP, FSHEA, FIDSA, Adjunct Assistant Professor of Medicine, Infectious Diseases, University of Louisville School of Medicine
Melanie Miller, RN, CVAHP, CNOR, CSPDM, Value Analysis Consultant, Healthcare Value Management Experts Inc. (HVME) Los Angeles, CA
Dennis Orthman, Consulting, Braintree, MA
Janet Pate, Nurse Consultant and Educator, Ruhof Corp.
Richard Perrin, CEO, Active Innovations LLC, Annapolis, MD
Jean Sargent, CMRP, FAHRMM, FCS, Principal, Sargent Healthcare Strategies, Port Charlotte, FL






Richard W. Schule, MBA, BS, FAST, CST, FCS, CRCST, CHMMC, CIS, CHL, AGTS, Senior Director Enterprise Reprocessing, Cleveland Clinic, Cleveland, OH
Barbara Strain, MA, CVAHP, Principal, Barbara Strain Consulting LLC, Charlottesville, VA
Deborah Petretich Templeton, RPh, MHA,Chief Administrative Officer (Ret.), System Support Services, Geisinger Health, Danville, PA
Ray Taurasi, Principal, Healthcare CS Solutions, Washington, DC
LOGIQUIP ............................... 9 Intelli-Flip.com Medline Industries ............... 7 medline.com Medtrica 24 Medtrica.com MIRION TECHNOLOGIES | DOSIMETRY SERVICES DIVISION ........... 17 instadose.com OMNICELL 33 Omnicell.com/XTAmplify Owen Mumford 19 owenmumford.com Ruhof Corporation ............. C2 ruhof.com
Uline ...................................... 25 uline.com

BY ASHLEA SOUFFROU, FOUNDER AND CEO, SXANPRO
The healthcare supply chain has started embracing advanced digital inventory management systems, especially in the perioperative and procedural areas, where manual processes and workarounds are becoming costly endeavors. While automation is looming on the horizon—with AI solutions promising complete information transparency, including everything from end-to-end inventory management and real-time demand planning—a comprehensive solution isn’t simple to implement. Procedural areas are much more complex than standard linear supply chain methodologies, and they require a dynamic approach to solve the entire workflow problem. Linear solutions solve one problem while creating another: Inventory
management systems allow hospitals to check products in and out and thus manage their inventories, but they do not enable the healthcare supply systems to conduct inventory control to identify expired or recalled products that are still on the shelves. Hospitals that rely solely on inventory management systems face risk in terms of patient safety, under-utilization, and over-spending.
Most large hospitals have an inventory management system, and many now are moving toward enterprise resource planning (ERP) platforms to integrate entire healthcare systems. These supply chain systems are being integrated to ensure the

facilities have the supplies they need based on demand, consumption schedule, and supply costs. While time-consuming to implement and very expensive, these inventory management solutions present a relevant and valuable tool for managing supplies.
However, while inventory management systems are a key tool in the hospital’s purchasing structure and practice, inventory management alone falls short of eliminating waste and ensuring access to safe pharmaceuticals, devices, and instruments. Challenges include the following: • Inventory management systems do not allow the hospital to identify areas of excessive buying due to, for example, physician preference changes, over-aggressive PAR













Save over 50 minutes per PAR location per day
Clinicians, simply pull down the Flipper when you access supplies from the back bin when the front bin is empty. That’s it!
Supply Techs manage supplies from the Intelli-Flip web based portal.
Fully automate your ordering process by integrating Intelli-Flip with your ERP system.
To learn more or to request a demo, go to Intelli-Flip.com.



levels, or trunk stock coming in from sales representatives.
• Inventory management systems do not “look into supply rooms” to identify supplies that have “fallen through the cracks” or are squirreled away in secret stash locations or in specialty carts. And make no mistake—there is a lot of this happening in the average hospital supply room.
• A lot of information is left out of inventory management systems, some of which is critical to the proper and safe use of medical supplies: Product expiration dates, lot numbers, and recall notifications are not included in data processed and stored by the typical inventory management system.
These gaps left by inventory management systems are severe and costly to the bottom line, to the point that they could be driving the facility to operate in the red. Hospitals have significant amounts of expired products on their shelves, and an inventory control audit will identify these, as well as worrisome amounts of recalled products and a LOT of excess inventory that can be transferred to other network facilities, returned back to the manufacturer, or sold in markets for surplus devices, etc.
In short, hospital inventory management (“I know what I log in and what I log out”) does not mean “I know what I have and what I can use.” This probably sounds odd to someone not familiar with healthcare purchasing, but wastefulness and risk associated with hospital supplies are substantial.
Moving from management to control
So how do you conduct inventory control to supplement your inventory management system to reduce risk and financial waste? In most hospitals, the solution is manual counts, during which clinical or material staff
work with pen and paper to register items in supply rooms. This method is inherently inaccurate, costs the hospitals lots of money in labor, and does not capture key pieces of data, such as recalls, expiration dates, etc. In short, this form of inventory control may capture on-hand inventory variances, but it does not constitute data registration that allows for corrective actions or proactive directives to drive safer and less wasteful outcomes.
Fortunately, there are now digital tools available for inventory control. Medical devices must be equipped with a Unique Device Identifier (UDI) that contains information about lot number and expiration date, for instance.. These identifiers unlock the potential for significant advances in inventory control.
In an inventory control audit recently conducted at a Southwest U.S. healthcare system, hospital staff registered 60,000 items across three sites in just six days, using UDI scanning. Each scan of a UDI barcode registers the item and vital product information, such as batch and lot numbers, expiration dates, GTIN number, and other significant data.
During this audit, 1,112 expired items were identified, and 369 recalled items were removed from supply rooms. The 369 recalled products were linked to 17 recalls. Over half of these recalls were urgent product removals, and 23 percent involved implantable products, representing significant patient risk. Most of these recalls were initiated more than six months prior to the inventory scan date, with two recalls dating back over two years. Excluding outliers, patients were at risk for an average of 8.2 months.
For the identified recalled products, patient risk was effectively mitigated, and the health system received $107,000 in credits from product manufacturers. Additionally, $413,768 worth of devices with
short shelf life were transferred to other facilities within the system where the devices were in demand. Finally, $401,000 worth of supplies were identified as no-move items that could be removed from PAR locations.
These numbers are staggering and paint a picture of the massive amounts of waste hospital systems create— even hospitals that are otherwise efficiently run. It also points to the risk of inventories that are not regularly controlled for the presence of expired and recalled items—items that might end up implanted in patients.
Findings from facilities with inventory management systems show the magnitude of the problem: There is a need for systems to be supplemented by manual or low-tech inventory control systems that can:
• Identify expired/recalled products and direct staff to exactly where they are located on the shelf
• Provide insights for hospitals to change their PAR levels and stop auto replenishment ordering on slow- and low-use products
• Identify products that should be returned to the manufacturer
• Identify products that can be transferred within the health system network to areas of greater demand
An inventory management system needs to be complemented by inventory controls that capture expired and recalled products (inventory safety) and excess inventory that is simply aging on the shelves (inventory currency). An inventory control system adds to the hospital’s inventory management efforts to reduce risk and free financial resources that can be applied toward patient care improvement initiatives. HPN
Ashlea Souffrou is a highly experienced medical device industry veteran with a passion for developing sustainable and cost-effective healthcare solutions. As the founder and CEO of SxanPro, she has successfully digitized inventory processes throughout the hospital supply chain.

TrapMore ® Disposable Dusting Sheets from Contec Professional leave others in the dust.
Regular dusting is an important part of good cleaning and disinfecting protocols.
TrapMore® Disposable Dusting Sheets quickly collect, trap, and remove dirt, dust, and other small debris. And because the dusting sheets are single-use, TrapMore® helps reduce cross-contamination and improve outcomes.

TrapMore Disposable Dusting Sheets are preforated for customizable lengths and can also be used with Contec’s ZeroGravity™ suite of cleaning hardware.
For more information, visit contecprofessional.com/products



BY MATT MACKENZIE, ASSOCIATE EDITOR
In healthcare settings, clinicians and other workers have a whole lot to be mindful of when it comes to protecting their patients and themselves. For instance, sharps are a constant in hospitals and other healthcare settings, and they can cause myriad problems, from the simple risk of being stuck with a needle to harboring bloodborne pathogens that can infect patients and workers alike if exposed.
Healthcare Purchasing News had the opportunity to speak with Amanda Hessels, PhD, MPH, RN, CIC, FAPIC, FAAN, assistant professor of Nursing at Columbia University School of Nursing, about sharps safety and how workers across multiple disciplines can share knowledge to help one another stay safe. Hessels authored a
study in the April 2023 edition of the American Journal of Infection Control entitled “Impact of patient safety climate on infection prevention practices and healthcare worker and patient outcomes,” which comprehensively observed over 5,200 standard precautions and collected over 450 surveys across 43 hospital units.
First, could you tell our readers about your background?
I’ve been a nurse for 20 years and in that time, I have worked in adult critical care nursing, epidemiology, and infection prevention spaces. I worked in acute care nursing and public health nursing early in my career before taking a broader approach as nurse epidemiologist and communciable disease director before becoming an infection preventionist Infection preventionists
are skilled personnel who are so typically under-recognized within healthcare systems, or at least they were, and now they’re becoming more broadly known in these settings as the people who really have their feet on the ground, and they keep the pulse in the hospital of who’s doing what to help prevent infections.
Do you have any background that you’d like to share on the Needlestick Safety and Prevention Act of 2001?
What was quite striking about that report was that we haven’t moved the needle (no pun intended). When I was a clinical nurse in an ICU years ago, you would see so many novice nurses get pricked by a needle. I don’t think we have a true handle on the burden of these needle sticks. Along with the needle stick comes the potential

exposure to a potentially infectious pathogen. We’ve now adopted and developed different mechanisms for voluntary event reporting to create a non-punitive environment to encourage healthcare workers to report when these events occur. I think another issue is that most of the work that’s published is really on these percutaneous, not mucotaneous, exposures. If you were to get a needlestick and there’s a splash, it may land in your eyes, nose, or mouth. The risk of exposure has only grown since the act was passed 20 years ago.
How much education and training do healthcare workers receive when it comes to sharps safety?
You have classroom training where you’re educated on what to do, and you have procedural training where you’re educated on how and what to do with regards to administering medication using sharps safety. I’m really pleased to see we have advanced our modalities by which we educate learners, for instance with simulation training. That allows us to not have to train clinicians giving their first-ever injection to a patient in a hospital, and it allows them to practice their skills to gain confidence and competence to allow them to do things correctly every time.
The issue arises after they’re licensed and they’re out in the care delivery space — how often they have the opportunity to practice these skills. Some sites and institutions may do an annual basic training and others will continue to do psychomotor-based training, so that you have to demonstrate that you can still competently conduct this skill when needed.
Do you think there should be more explicitly coming from leadership when it comes to sharps safety?
I think that leaders should encourage the principles of high reliability and
safety throughout their organization. Many are, but if they’re not, then yes, more should happen. I think there is literature emerging on the influential power of organizational leadership from the unit level to the department level, and to the entire system. Having leaders who understand the complexity and who have a handle on what healthcare workers are doing is key.

Amanda Hessels
It’s not just coming from the top down, but also having a culture that embraces transparency and using true collaboration to get to the point where you can make meaningful decisions and interventions is important. Leadership should be able to identify nuances across different personnel settings and engage across those settings purposefully.
Could you elaborate on the risk of bloodborne pathogens?
Each one of us is alive because we have blood circulating. When you go into the healthcare setting, they’re going to often want samples of that, and you’re going to have needles and tubes and other devices inserted. Depending on the nature of that, whether it’s a surgical procedure or a childbirth or you’re having an IV, there’s going to be different volumes of and types of blood that could expose that healthcare worker, and the healthcare workers who interact with certain populations of patients are going to vary. That’s not even taking into account the risks of different patient populations who are being treated for known infectious diseases. Unfortunately, healthcare workers often bring into their decision-making of whether to don and doff PPE factors of patients’ condition, diagnosis, age, race, ethnicity, etc. So, they may say for a 7-year-old going in for a concussion, “Oh, it’s just a 7- year- old. I don’t have to worry about this kid’s
blood.” But then, if you have an HIV-positive patient who comes into your department, suddenly everyone’s donning and doffing. But we don’t know what’s in whose blood when we’re exposed to it. That’s one thing that drives my program of research — trying to understand what that risk assessment is that providers are making, this sort of occupational psychology of whether they do or don’t adopt different safety practices.
What associations or organizations are trying to get the word out there about sharps safety?
The Association of Occupational Health Professionals (AOHP) has been a tremendous supporter and partner in looking at the intersection between occupational and patient safety. I was also a past research committee chair of the Association for Professionals in Infection Control and Epidemiology, who are also beginning to look at this. The American Nurses Association has also been doing work on this, as has the CDC and the National Institute of Occupational Safety and Health (NIOSH). I also helped to develop a safety curriculum within the CDC where we could explore some of these issues and opportunities regarding safety to put the tools in the hands of the organization so they could then educate their healthcare workers.
Is there anything else you’d like to share with our readers?
We need to continue to focus on the interdisciplinary nexus in sharps safety — sharps are sharps are sharps. We can collaborate to generate priority areas across different settings and put them together to develop and innovate solutions we may not have thought of viewed through our own professional lens. HPN
Skill.Set.Go is an educational subscription program now available to EVS teams for on-demand training
BY JANETTE WIDER, EDITOR-IN-CHIEF
Environmental Services (EVS) teams are imperative to the day-to-day functions of a hospital. Therefore, training and education of EVS teams should be of utmost importance. Sometimes it seems like the industry has forgotten about this extremely important
department, yet there are resources out there for getting these teams in one’s organization up to snuff.
One such resource is Skill.Set.Go, a skills-driven training subscription designed for EVS teams. Powered by a team of experienced environmental service leaders


































The role of supply chain has expanded, and your importance to health system operations is more critical than ever. The Allergan Aesthetics portfolio of market leading products delivers the value you expect from the industry leader.1,2,*




The combined use of the plastic and regenerative medicine portfolio of products has not been studied.

Choose the inventory solution that works best for you, and our team will help manage it through consignment, provisional stock, or direct purchase.
We’re here to help. Field sales, reimbursement experts, customer service professionals, and an experienced medical team are all standing by to assist every step of the way.
*Based on surgeon survey data. Natrelle® (n = 516); AlloDerm™ (n = 203); Keller Funnel (n = 299); REVOLVE™ System (n = 98); STRATTICE™ (n = 147).1,2
References: 1. Data on file, Allergan Aesthetics, March 2024; Plastic Surgery Aesthetic Monthly Tracker. 2. Data on file, Allergan Aesthetics, July 2023; Surgical Scaffold AU Surgeon Perceptions 2023. 3. Data on file, Allergan Aesthetics, January 2022; Allergan Plastic Surgery Order Form. 4. Data on File, Allergan Aesthetics, January 2023; AlloDerm SELECT Ordering Information. 5. Data on file, Allergan Aesthetics, July 2023; Artia Ordering Sheet. 6. Data on file, Allergan Aesthetics, January 2023; STRATTICE Ordering Information.

Allergan Aesthetics products offer a wide range of SKUs tailored to meet surgeons’ diverse needs.3-6
Your trusted partner from start to finish.
Follow us on LinkedIn and stay up to date on all things Allergan Aesthetics.
Learn more about partnering with us. Call 1.800.367.5737 or Email PRMorder@allergan.com
and state-of-the-art designers, supported by American Hospital Association (AHA) and led by the Association for the Health Care Environment (AHE), Skill.Set.Go is a new resource for training, transforming, and retaining EVS teams.
To get more information on this new training series, Healthcare Purchasing News spoke with Monika Berrier, EdD, PMP, director, AHE Education. Berrier works at the Association for the Health Care Environment of the American Hospital Association. This non-profit organization makes every effort to establish and maintain care environments free of environmental surface contamination and support safety, service, and efficient and effective operations. As a director of education at AHE, Berrier manages a team of education specialists and instructional designers who develop and deliver in-person and virtual educational offerings, including publications, certifications, workshops, conferences, and on-demand content delivery. She also leads the delivery of the AHA’s learning management system (LMS). Before joining AHE, Berrier was part of the American Society for Health Care Engineering (ASHE), also part of the AHA, working as an instructional design manager, managing ASHE’s extensive portfolio of in-person and virtual offerings similar to AHE’s. Berrier originally started her career in graphic design. She worked on large brands designing catalogs and books for companies like Staples, Kohl’s, True Value, and McGraw-Hills. She always worked as a designer and trainer, eventually leading to her career switch to instructional design and education. Berrier holds a Doctor of Education (EdD) degree and a Master of Science in Educational Media Design and Technology. Both degrees significantly strengthened Berrier’s ability to deliver education strategy and helped her become a visionary leader in various areas of education. She continues to search for new ways to provide education to adult learners and constantly seeks new technologies to improve learner engagement.
Let’s start with a 40,000-foot view. Why are environmental services important to hospital systems? And why do we need to educate these folks?
In many healthcare organizations, environmental services are just cleaning people who come in, clean, and remove trash. What we’re really trying to change is the notion that you can take a person that does the same job in a hotel or another non-healthcare facility and bring them into healthcare. Individuals who work in healthcare settings need to know how to prevent infection with detailed knowledge of how bacteria and viruses thrive and exist in the environment, and that is driven by the knowledge rather than what we see. For example, cleaning and
disinfection—using different agents for different areas is driven by the knowledge of the chemicals they use and their reaction. Essentially, what the bacteria, viruses, and microorganisms respond to in order to properly clean and disinfect the areas—areas like patient rooms and hallways. But then, when you’re single OR, you really need to have that knowledge to make sure that the next patient that gets that room is thoroughly clean of all microorganisms that could be left behind.
Somebody who is not skilled in this particular job is really an environmental technician vs. facility housekeeping because of that extra level of knowledge that they need to make sure that the places that they leave behind are really cleaned and disinfected and are free of any microbial organisms.
And why is education important? It’s not only important for technicians to know how to properly treat microorganisms and how to bring agents back to the clean areas from the dirty areas. It is also important for managers, supervisors, and directors to realize how important their job is. And then invest in training technicians and themselves [managers, directors, supervisors] to have a certain level of knowledge. CEOs of organizations should also be aware of this and consider investing in training to get their staff at the right level of education.
Can you tell us a little bit about the training subscription program?
Managers, directors, and supervisors have found the need to educate their team. They need to stay compliant, and technicians need to be trained. So, we came up with the subscription model for Skill.Set.Go. It gives the supervisors the ability to control training of the teams. They can buy one subscription that comes with two free seats (additional seats are also available for purchase).
For example, if I have a team of 10, and I have two technicians to clean the floor and two that are brand new coming up, I can, as a supervisor of the team, preview all the training because I do have those two [seats] free. They were designed to come with those [seats], so then the managers can preview what their technicians will be accessing as far as content. And then they have the ability to purchase additional seats and the ability to use the seats within the year. And then, they also not only have access to a dashboard where they can assign the trainers to technicians, but they can also upload the entire team in one click and create their accounts for them.
It seems like the subscription model is a new concept for the industry. Is this accurate? Yes, I agree with that. I also want to point out that most training is pushed toward the supervisors and managers
of these teams, which lowers the overall team productivity because they need to train. Having this subscription that is based on micro learning and very small bites allows the team to do the training in between tasks. For example, they can take 10 minutes at lunch and do some. Managers have to take people on the floor and allocate a trainer, and other training often has pages and pages of reading. And when teams are being trained this way, with binders of information, the information may not stick. Our model is making it accessible via an online portal that is available on the go. Our model also eases up the training on the manager and supervisor side who in the past would have had to train their team without software and, as we all know, they have many more responsibilities than to just teach the basics to their team.

Monika Berrier
How can managers or supervisors get c-suite or leadership support for EVS training?
It is important to invest in a training program like this and education for your staff. I think of EVs almost as unsung heroes. We need them, but I don’t think we really focus on
the needs of education and growing their careers in the hospital system enough. It comes down to changing the mind of leadership. Leadership really needs to realize that they have to be a learning organization and that’s how they get every department to participate and contribute to patient safety. It can start with simple moves like changing the titles of the housekeeping and janitorial department to EVS.
This department is usually the underdog, not being recognized as doing more than just cleaning. It needs to be understood that this team prevents infection; they really clean and disinfect so the next patient can enter into the room free of microorganisms.
Overall, I think the c-suite and all the leaders of organizations need to understand the why behind it. And then have the concept of a learning organization in mind— every department needs learning every day. Departments need to have that investment in training because it is going to make the hospital better. It is going to increase customer satisfaction rates and if you have happy customers in your organization then you are going to have a better business. HPN

BY KARA NADEAU, SENIOR CONTRIBUTING EDITOR
U.S. health systems and hospitals continue to be challenged financially and operationally by ongoing staffing shortages, rising equipment and supply costs, growing surgical volumes, and increasing instrument and device complexity. All this impacts the engine driving effective, efficient, and safe surgical procedures – the sterile processing (SP) department.
When asked to describe the state of SP departments today, multiple experts used the term “pressured.”
“The demand for surgical procedures is on the rise and continues to grow, putting pressure on sterile processing departments that are not equipped to handle the increased volume,” said Matthew Thell, CHL, CRCST, program manager, Highlevel Disinfection and Sterilization Practice, M Health Fairview. “This is a common challenge faced by many healthcare facilities, especially considering the financial constraints faced within the healthcare industry.”
“The Sterile Processing Department (SPD) is under a lot of pressure,” said


Lars Thording, VP of Marketing and Public Affairs at Innovative Health. “This is where the hospital typically performs its reprocessing of reusable devices like cables, accessories, and many OR instruments. The SPD is

Designed for simple and safe blood collection.

Unistik® VacuFlip and Unistik® ShieldLock are engineered for intuitive blood collection, featuring easy to use safety mechanisms that can help reduce the risk of needlestick injuries. Unistik® Blood Collection devices are cost-effective and designed to not compromise quality or safety.









































tasked with ensuring that devices are reprocessed to the device’s specifications and returned to the many different departments of the hospital that utilize reusable devices.”
“As hospitals struggle with limited space and resources, navigating this issue becomes increasingly complex,” Thell added. “Centralized models have been trending over the years and have proven to be effective in other industries to reduce waste.”
Whether it is driven by the need to consolidate reprocessing in response to low staffing levels and/or cost restraints, expand SP department capacity to meet growing surgical volume, improve the effectiveness and efficiency of SP processes, or another factor, some healthcare organizations are centralizing SP to a single hospital, an offsite reprocessing location, or outsourcing this function to a third party.
with a sterile processing consultant can provide invaluable expertise in evaluating your current landscape and determining the viability of an offsite processing model.”
According to Thell, physician buyin is important. He stated:
“The idea of instrument sets having to travel from one location to their destination can make people feel uneasy about their cases. Helping physicians understand that quality monitoring will be the same offsite as it would be onsite is essential to build trust. Nobody wants to have their case canceled or delayed due to instruments not arriving on time or arriving with quality defects.”
While on the surface it seems logical that those individuals performing instrument and device reprocessing – the organization’s SP professionals – would take a leading role in any type of change, Randalyn Harreld,
other stakeholders as well, including representatives from facilities management to provide expertise on infrastructure, along with those from supply chain, infection control, environmental services (EVS), and risk or quality management.
As a subject matter expert in centralized SP offsite reprocessing concepts, Kimberly Jones, managing partner, KJ Staffing Solutions, which specializes in staffing and workflow optimization, education and project management, stresses the need to put people at the top of the consideration list.
“Staffing is tricky for administrators to understand, because many incorrectly assume that the offsite reprocessing center (ORC) can be staffed using a ‘lift and shift’ model with existing sterile processing full-time employees (FTE),” said
“As hospitals struggle with limited space and resources, navigating this issue becomes increasingly complex. Centralized models have been trending over the years and have proven to be effective in other industries to reduce waste.”
MATTHEW THELL, CHL, CRCST, PROGRAM MANAGER, HIGH-LEVEL DISINFECTION AND STERILIZATION PRACTICE, M HEALTH FAIRVIEW
HPN reached out to SP professionals and providers of SP department products, equipment, and services to ask, “What factors must a healthcare organization take into consideration when considering a change in their reprocessing strategy/location?”
This article summarizes their responses (in no specific order of criticality).
“When considering a change in your sterile processing operations, it is crucial to engage the appropriate stakeholders to aid in the decision-making process,” said Thell. “Seeking input from vendors or an analysis performed
national clinical education manager, Belimed, said this is not always the case, stating:
“Because health systems and hospitals come to us with ideas and lean on us as experts, we hear a broad range of proposed reprocessing strategies. Often the idea for change in the SP department comes from someone who is not operational, such as a VP or surgeon. And it makes sense that these initiatives would originate from physicians because they want to grow, maybe take on a new specialty, which means additional capacity in SP. But they must have an SP expert at the table.”
Harreld recommends proposed changes in reprocessing should involve
Jones. “Many organizations base FTE allocation for sterile processing departments on number of surgical cases performed. We know in sterile processing that volume does not equal volume. The number of trays allocated for a complex orthopedic case varies greatly to the number of instrument sets needed to perform a basic general surgery case.”
“When the organization grows in surgical volume in a complex instrument heavy service line, this is almost never translated to the need to increase staffing for sterile processing,” she added. “When preparing to open an ORC, these fluctuations in volume as they relate to the long-term


growth plan of the organization need to be realized.”
Throughout her career, Jones has toured as well as assisted in the development of ORCs across the country. Jones shared an example of one healthcare organization that allocated only 8 net new SP FTEs to open a new offsite reprocessing center.
“While on paper it appeared the surgical set volume would just relocate to the ORC as would the staff, this allocation proved to be inadequate,” Jones explained. “Unfortunately, the assumption in this case is all too common. Many organizations planning to operationalize an ORC assume among administrators that the organization can move 60%-80% of their SP staff to the offsite location, but that rarely happens right out of the gate. Especially in the beginning, the organization will need to maintain SP operations onsite as well to manage fluctuations in the surgery schedule, preference card inaccuracies, and reprocessing of trays that stay in the home locations due to low quantities of inventory.”
As Harreld noted, not all SP professionals from the current reprocessing site will have the desire or ability to move to an offsite location.
“Logistically, you might think, ‘we’re just going to build this new location and all our people will move there.’ I worked for an organization that believed this would be the case and we lost 16 staff members with the offsite move. Some were reliant on public transit and there was no way for them to get to the offsite location, which was 30 minutes outside the city.”
“Additionally, an offsite location might require a completely different work schedule, perhaps molding two shifts into six shifts to accommodate a new layout and workflows,” she added. “This might not work for your current team members. I don’t think managers always put a lot of thought
into staff accommodations during the planning stage.”
While there are barriers to successfully launching an offsite reprocessing center, according to Jones, a move to offsite reprocessing forces constant communication between the SP and operating room (OR) teams because there is no longer the convenience of residing in the same building.
“Increasing the distance between SP and the OR forces accountability of both teams and opens lines of communication, specifically related to physician preference card updates and surgical scheduling,” said Jones. “The OR must inform the ORC of any preference card changes prior to the instrument sets being prepared and shipped proactively. Having a solid cut off time in place for add on cases and room changes on the surgery schedule will enable SP to be successful in meeting their goal of timely delivery of instrumentation. Without a strict cut off time, SP staff are working at a disadvantage that is out of their control.”
“Standardization of a singular instrument tracking system as well as a standard naming convention for instruments and devices is also crucial when there are multiple surgery locations that the offsite SP team supports,” she added.
Sufficient instrument and device inventory was cited by many of those interviewed as a key consideration when planning an offsite move, including Hannah Schroeder, BSHA, CRCST, CHL, CIS, CER, clinical education specialist, Pure Processing, who stated:
“Inventory is a substantial component of success when it comes to centralizing reprocessing practices and updating strategies. Take the time to analyze and understand the


appropriate inventory pars needed to not only meet usage rates, but also reprocessing and maintenance times, transportation, and available real estate for storage. All are crucial to the success of both the end user and the sterile processing department.”
Speaking to specific inventory issues related to reprocessing for clinics, Amy DeGraw, BSHA, CRCST, CHL, sterile processing education coordinator, Ambulatory, Froedtert Health, commented:
“Often instruments are not well maintained in the clinic setting or there is an abundance of single-use instruments that have been placed into rotation. These issues should be addressed prior to transitioning offsite, and clinics should have a sufficient instrument inventory to facilitate patient care while instruments are reprocessed.”
“Also, understanding how increased volumes will affect your hospital SPD may lead you to decide to open a separate ambulatory reprocessing location to offset the workload,” she added.
“Overall conversations we’re having with customers regarding sterilization processing are how to drive better cost efficiencies,” said Sean O’Hara VP, Distribution & Customer Operations, Zimmer Biomet. “Several pricing factors that must be evaluated are advancements in facility scalability, reprocessing technology requiring additional compliance updates, and increasing equipment costs.”
As Thell points out, centralized sterile processing does not always


Sean O’Hara Terry Hahn
remove the need for site-based operations, and sometimes a hybrid option is optimal to balance the workload.
“Many situations arise where having access to a sterile processing department on-site is needed, whether that is immediate use steam sterilization or reprocessing of complex instrumentation,” he stated.
A multi-site reprocessing approach adds costs, which Harreld said sometimes flies under the radar during offsite planning:
“If you plan to maintain some level of reprocessing in your current SPD space — for example, reprocessing of loaner trays or endoscopes — there are additional costs associated with maintaining operations in multiple sites. Supply expenses will increase as the locations will require items such as blue wrap and biologics.”
“To budget for what will be needed, compile a list of everything, including consumables,” she added. “Because you might get a big pool of funds to buy capital equipment, but there are so many additional costs to consider.”
Terry Hahn, field operations manager, Zimmer Biomet, spoke to considerations around integrating new and old equipment:
“When considering whether you should keep sterile processing onsite that services one or multiple facilities, understand the overall compatibility of the current equipment with new sterilizers because it may be necessary to acquire new equipment. Consider if there is enough space to house the sterilizers plus
the increased number of instrument trays. Lastly, can the utilities support the expansion?”
“When purchasing all new equipment, consider consolidating your purchase with a single vendor capable of meeting your needs,” said Jones. “This can present substantial
contract savings opportunities, such as bulk pricing, and the ability to negotiate more favorable service contract terms.”
When outfitting an old SPD space with new equipment, Jones cautions stakeholders to assess and budget for any potential roadblocks.


“One challenge in older facilities when installing new equipment is outdated plumbing,” she explained. “It’s like doing home repair. Once you get the equipment in there and try to hook it up, you may find your facility needs $15k worth of plumbing upgrades to accommodate it. At this point, organizations begin to ask the questions around feasibility and sustainability of maintaining several older sites or looking at consolidating to an ORC.”
7. Risk mitigation and quality control
“Initiate your first steps by engaging with key stakeholders for input, determining a budget, and conducting a risk assessment,” said Hahn. “Within the risk assessment, note the current processes/protocols, equipment, staffing, and the overall environment.”
Schroeder emphasized the need for quality control management when planning a reprocessing site, noting the importance of specialized and governed processes for success. She offered the examples of cleaning verification for medical devices and added visual inspection using borescopes.
“Having specialized teams and consolidated work allows patient-facing staff to focus on direct care, while putting reprocessing back into the hands of trained technicians,

where we can centralize the time requirements and resources to achieve compliance,” she stated.

B. Raymond
“Regardless of where reprocessing is completed, the same standards should be met to ensure patients are receiving the same quality of care,” said DeGraw. “In terms of ambulatory clinics, there is a general lack of education and oversight leading to gaps and failures in the process that drives the decision to change where reprocessing is performed.”
“The decision to centralize ambulatory clinic reprocessing should include a risk assessment similar to those conducted in a hospital-based SPD and should look at items such as workflow, space requirements, adherence to IFUs, and competencies,” DeGraw continued. “There should also be a thorough assessment of the instrument quality and volume.”
Tracy B. Raymond, BS, MS, CRCST, CIS, CER, CHL, manager of Training and Education, Vested Medical, spoke to some of the reasons as to why facilities may look to move instrument processing off-site:
“A facility might need to expand surgical suites or revenue producing services and the facility is landlocked; their SPD and equipment is old, and it is too costly to renovate or add space, again the facility and/or department is landlocked with nowhere to expand to; they are expanding and building ASCs and a centralized SPD can support many locations.”
“You’ll want to understand the local and national regulatory requirements,” said Melanie Towery Prevost, associate director marketing, ASC Solutions, Zimmer Biomet. “Is the location centrally positioned for reliable logistics? If the SPD is being built within an existing infrastructure, is there enough capacity and capability to handle reprocessing requirements efficiently? Lastly, consider water lines, supplies, staffing, and regular training to maintain the highest integrity and sterility of instruments.”
When the SP department is in the same building as the OR, while last minute requests for surgical instruments can be tricky in terms of turnaround, the transport of trays between floors is manageable. But when the reprocessing takes places miles away from the procedural site, even scheduled tray requests can be complicated by the distance.
That’s why Harreld stresses the importance of location when it comes to the selection of an offsite reprocessing site, commenting on potential challenges that must be considered and overcome to keep surgical schedules on track.

“Geographically, think about traffic patterns between the site of reprocessing and the facilities served,” she stated. “If you are planning to have trucks on the road transporting trays at 7:30 a.m. and the route to the care sites encompasses five elementary schools, you will have problems delivering on time.”
“Another factor to consider when transitioning to offsite reprocessing is how instruments will be transported,” said DeGraw. “Depending on the number of locations and the instrument volume, transportation needs may strain your current services.”
Raymond spoke to the considerations on how trays are transported - rigid containers or blue wrap, case carts, racks, and instrument tracking systems (ITS), stating:
“Best practices in this area include the use of sealed case carts and rigid containers for transportation as sealed case carts do not allow anything to go into or out of the cart. Blue wrap is prone to holes, therefore rigid containers is the preferred method for transportation. Use of temperature and humidity-controlled vehicles for transportation because outside environmental conditions would potentially render the tray unsterile and risk quality patient care.”
Harreld noted how “moving things from point A to point B opens up a new can of worms for problems.” She explained that when she worked for a healthcare organization that moved reprocessing offsite, there was the assumption that the truck drivers transporting dirty instruments to the offsite and clean instruments to the care sites would use mobile scanners to document this movement in the organization’s instrument tracking system (ITS). But Harreld said they missed the mark on education and training, stating:
“Everybody’s got some form of ITS, right? But does that really work in the truck? We implemented mobile device scanners and assumed our drivers would do the scanning, but they were couriers, not experts in instrument tracking. If you plan to leverage transport professionals in the tracking process, you must educate and train them.”
Then there are the federal and state requirements related to transporting dirty instrumentation, which Schroeder further commented on:
“Whether within the same building or across town, departments will want to have sound policies and procedures on how biohazardous and sterile medical devices are being transported that will encourage safety, compliance and integrity.”
Jones commented on staffing challenges with regards to instrument transport:
“Moving reprocessing offsite begs the question, ‘do you need additional FTEs for transport to load trays onto the case carts and onto the trucks, as well as remove the case carts off the trucks at the care site?’ That raises the question, ‘where do you place the responsibility for moving carts? Do you need to increase staff hours at the offsite location or at the delivery sites?’”
In Jones’ experience, some healthcare organizations create and employ new job codes at the care sites to receive trays from the offsite reprocessing center and station them.
“Throughout the day, if there are any additions or cancellations in the surgery schedule, this individual is accountable to communicate changes to someone from SP, to keep the lines of communication open, and provide efficiency for the clinical teams in having the proactive communication with the ORC,” she explained.
Acknowledging how many SP departments are understaffed and under immense pressure to be efficient, Thording said some hospital leaders are turning to third parties for reprocessing assistance.


“Unfortunately, there is a trade-off between patient safety (proper cleaning and sterilization handling) and efficiency,” he commented. “When the pressure is on to run hundreds of instruments through sterilization, some cleaning procedures may be cut short, sterilization parameters may be slightly altered to allow for more instruments to go in fewer loads, and the counting of prescribed number of uses may be skipped. Despite the commitment and professionalism of SPD staff, in the SPD, unfortunately, efficiency always beats patient safety.”
“This has led some hospital executives to move the reprocessing of particularly delicate and high-risk devices from the SPD to third-party reprocessors with the appropriate standards and procedures to ensure patient safety and operational quality,” he added.
Raymond says facilities may look to private third parties offsite to take some of the burden off their small or short staffed SPDs especially for smaller ASCs.
“More and more surgeries are being moved over to ASCs and they do not have the space, capacity, or the staffing to meet the large number of trays, especially loaner trays for total joints or spine cases,” she explained.
Thording noted how singleuse device reprocessors operate under tight U.S. Food and Drug Administration (FDA) supervision and handle devices that are more complex than those typically reprocessed in the SPD.
Case in point: Necessity drives offsite reprocessing decision Health systems and hospitals turn to offsite reprocessing for instruments and devices for a variety of reasons. Sterile processing subject matter expert Sharon Greene Golden, BA, CRCST, CER, SME, FCS, president & CEO, Central Service Patient Advocate, shared her story of an offsite move driven by necessity.
As Greene Golden described, the healthcare organization with one large hospital had merged with a smaller hospital, which did not have the needed or correct equipment to care for any instruments above small trays.
While the sterile processing (SP) department team in the smaller hospital was reprocessing instrument trays for total joint procedures, they had only two small immediate use steam sterilization (IUSS) sterilizers, one sink in a small room, no ultrasonic machine, no washer decontaminator, and a humidifier blowing all day.
“Needless to say, we had to make drastic immediate changes in the processing of major total joint instruments right away,” Greene Golden explained. “They were able to get a washer decontaminator, but the actual processing of instruments had to be addressed as a patient safety issue.”
According to Greene Golden, the healthcare organization assembled a multi-task team comprised of SP, infection control, and administrators. They decided the larger hospital would become an offsite processing department for the smaller one.
“We had to set up delivery of the instruments to our department where we processed them as if they were for our patients,” said Greene Golden. “Once cooled, we would package the trays in dust covers and place them in containers. We had to set up a specific truck for delivery of the clean, processed instruments to the smaller hospital for patient use.”When asked for her advice to healthcare organizations considering a change in reprocessing location, Greene Golden stated:
“It is imperative that any hospital or surgery center contemplating an offsite reprocessing program do their fiduciary duty to their patients. You must study standards, regulations and the actual process while including all players at the table. Know what is needed and why, while all the time knowing your decisions can impact a patient’s life. What we do matters every day and choices have consequences.”
As Thell pointed out, SP departments designed and built years or decades ago often cannot accommodate the growing demand for reprocessing reusable medical devices. He believes this squeeze for space is one factor that will continue to drive the move to offsite reprocessing.
“I foresee more healthcare systems exploring this model in the future, but it must have a return on investment,” said Thell. “Offsite is not a one-sizefits-all solution. Deciding what will be processed onsite and offsite will be critical to the success of implementing an offsite reprocessing model.” HPN
“It is imperative that any hospital or surgery center contemplating an offsite reprocessing program do their fiduciary duty to their patients. ... Know what is needed and why, while all the time knowing your decisions can impact a patient’s life. What we do matters every day and choices have consequences.”
SHARON GREENE GOLDEN, BA, CRCST, CER, SME, FCS, PRESIDENT & CEO, CENTRAL SERVICE PATIENT ADVOCATEAND STERILIZATION PRACTICE, M HEALTH FAIRVIEW
Scan here, and toggle the calculator based on your own data.












It’s been proven time and again that the more efficient surgical workflows are, the sooner cases are completed. By addressing one surgeon’s procedures with ONE TRAY® and EZ-TRAX™, we’ve seen five-year cost savings in the range of $80,000 to nearly half a million dollars a year. Imagine the impact of scaling that across multiple surgeons. Based on this kind of analysis, it becomes easier to make investment decisions.”
-Mark Copeland, VP of Sales at 3T Medical Systems




BY ARTHUR HENDERSON, RN, BA, CNOR, CRCST, CHL, GTS, SENIOR CLINICAL EDUCATION SPECIALIST, STERIS CORPORATION
Starting a new job is stressful. Learning thousands of instruments and thoroughly cleaning and preparing each for patient use can be overwhelming. Before jumping in to learn all the details, the Clinical Education veterans at STERIS have some pointers for the Sterile Processing Technicians just starting out.
“You want to go home in the same condition that you came in for your shift.”
Manon LaFlame Clinical Education Specialist Canada Operation Processing used surgical instrumentation and medical devices exposes technicians to many potential hazards and dangers. Here are some hazards to be aware of.
• Bloodborne pathogens and infectious microorganisms can hide in and on used instrumentation.
• Chemicals used to remove surgical soils and kill microorganisms can be toxic, corrosive, and irritating.
1. List safety considerations that a new technician should know
2. Describe the items and organizations that can help a new technician learn the complex tasks of sterile processing
3. Create a proactive plan to learn department dynamics and culture
Contributed by:

Manual Cleaning
Changing drums of cleaning chemistries
Tray Assembly
Steam Sterilization
Vaporized Hydrogen Peroxide Sterilization
• Bending, lifting, and twisting to move trays of instruments upwards of 25 pounds/11 kilograms can strain backs and cause injuries.
• Standing in one spot for extended periods of time can cause fatigue.
Always wear personal protective equipment (PPE) right for the task at hand. Preventing exposure of dangerous materials to skin, nose, mouth, and airways is the best way to protect oneself and others. Table 1 lists the PPE requirements typically associated with sterile processing activities. A common error made by many new technicians is improper wearing of the face mask. Face masks should cover the nose and mouth. The mask should be adjusted to ensure that it contacts the skin, leaving no gaps. Nose bands can be bent to form a seal at the bridge of the nose. Elastic band or ties should be positioned on the head to prevent puckering along the sides of the mask. Not covering the nose or having side puckers in the masks allow unfiltered potentially contaminated air to enter the lungs which could lead to infection.
Facility provided scrubs, fluid resistant face mask, face shield, fluid-resistant gown, general purpose utility gloves, fluid resistant shoe covers, and hair cover
Facility provided scrubs, fluid resistant face mask, face shield, fluid-resistant gown, general purpose utility gloves, fluid resistant shoe covers, hair cover, steel toe shoes
Facility provided scrubs with long sleeves, gloves when handling manually cleaned but not disinfected items
Facility provided scrubs with long sleeves, thermal protective gloves, shoe covers, hair cover
Facility provided scrubs with long sleeves, chemical resistant gloves, shoe covers, hair cover
Table 1: List of common personal protective equipment for sterile processing activities.
A second common error is donning of general-purpose gloves. Typically, technicians first don disposal gloves with long cuffs. The gloves are pulled over the sleeve. Next, a general-purpose glove is worn over the disposable gloves and sleeve. The general-purpose glove prevents cleaning solution from reaching the technicians’ hands and sleeves. The internal disposable gloves help prevent fluid contact if the general-purpose glove is cut or punctured during cleaning.
Decontamination technicians wear shoe covers and bouffant hair covers to protect themselves from splashes during manual cleaning and drips from carrying wet medical devices. It is important to remove these potentially contaminated items before leaving the department.
Familiarize yourself with the location and use of room safety equipment. Learn how to work it before an emergency. Emergency showers, eye wash stations, fire extinguishers, and chemical spill kits should have clear instructions. If instructions are not immediately available, ask for them. This education should be covered in your orientation to the department.
Locate emergency stop buttons or cords on equipment prior to use. Emergency stops work faster than canceling a cycle and could be the difference between serious and fatal injuries. This is especially true when staff clean or service equipment.
Cart washers pose a particular safety concern of individuals being trapped within the cart washer during a cleaning cycle. Internal kill cords allow trapped staff members to shut off the washer from the inside preventing bodily harm from hot water and cleaning chemistries. Find kill cord locations and ensure that they
are within reach when entering a cart washer.
Read the safety data sheets of the chemicals you work with. Safety data sheets (SDS) have valuable information about the chemical and potential harm it can cause. It lists PPE needed to protect oneself from chemical exposures. It also lists the fi rst aid steps to take if an exposure to the chemical occurs.
Take steps to reduce ergonomic injuries and fatigue. Have experienced colleagues or supervisors show ergonomic lifting techniques. Some facilities may employ their occupational therapist to assess the sterile processing area for potential ergonomic injuries and help with fi nding solutions. Ask for antifatigue mats at stations where stationary standing occurs for extended periods of time. Consider sweat wicking under garments and compression socks to help reduce discomfort and fatigue when working within the decontamination space.


This lesson was developed by STERIS. Lessons are administered by Endeavor Business Media.
After careful study of the lesson, complete the examination online at educationhub.hpnonline.com. You must have a passing score of 80% or higher to receive a certificate of completion.
The Certification Board for Sterile Processing and Distribution has pre-approved this in-service unit for one (1) contact hour for a period of five (5) years from the date of original publication. Successful completion of the lesson and post-test must be documented by facility management and those records maintained by the individual until recertification is required. DO NOT SEND LESSON OR TEST TO CBSPD. www.cbspd.net.


Sterile Processing Association, myhspa.org, has pre-approved this in-service for 1.0 Continuing Education Credits for a period of three years, until June 5, 2027.
For more information, direct any questions to Healthcare Purchasing News editor@hpnonline.com.
Quiz Answers: 1. D, 2. D, 3. D, 4. A, 5. A, 6. B, 7. D, 8. C, 9. B, 10. B

“Rome was not built in a day, and neither will your skill mix for the position. Relax, take a deep breath, and enjoy the journey. You will be amazed at how much knowledge you build every day.”
Delores O’Connell Senior Clinical Education Specialist Pacific Northwest U.S.
The first week can be overwhelming when starting in sterile processing. Thousands of instruments; multiple cleaning, disinfection, and sterilization instructions; and a general fear of not delivering what was promised at the interview can overwhelm even the most confident new technician. No one is expected to know everything the first week.
Learning takes time and repetition. Read all policies and procedures. Follow the manufacturer’s instructions for use and work instructions each time. If you cannot find them, ask! Do not fear asking sterile processing supervisors and other experienced sterile processing staff members for help.
Sterile processing is a complex ever-changing industry. Keep up on the latest best practices by asking for and reading the standards followed by the facility. Standards often give the why behind what the facility requires staff to do.
Establishing a network helps new technicians expand their pool of experts to ask questions and gain valuable education. Networks can include external and internal people. Becoming a member of a local sterile processing association and attending meetings will accelerate the learning curve.
Many organizations have networking software, such as Microsoft Teams, which allows staff from different facilities within the same healthcare organization to reach out to each other. Ask to join internet teams and shared education sites.
Technicians should consider certification, even if they have attended a trade school for sterile processing. Certification shows commitment but also opens a great deal of education opportunities and resources provided by their certifying organization.
The Healthcare Sterile Processing Association (HSPA) and The Certification Board of Sterile Processing and Distribution (CBSPD) are sterile processing certification organizations which provide online education lesson plans, publications, and a host of resources including career development, reference guides, and sample documents to name a few.
Join a local chapter of a national professional organization that supports sterile processing professionals. Often, these organizations provide education during chapter meetings and a platform to meet others within your profession. Take advantage of all opportunities that these organizations can provide.
“Talk to your colleagues and be proactive. Never be afraid to ask a question.”
Arthur Henderson Senior Clinical Education Specialist Southeast U.S. Sterile processing is a profession, and technicians are professionals. Establishing a professional relationship with colleagues is important. Make time to talk to colleagues. Ask them about the department’s culture. What makes the department tick? Why do people stay? Do not be afraid to ask colleagues how to succeed and what tips they may have for someone new to sterile processing.
Avoid the rumor mill. Rumors are nonproductive and could leave colleagues with a negative fi rst impression. Excuse yourself or change the subject when rumors creep into a conversation. If unavoidable, do not agree or disagree with the rumor. Stay neutral.

Learn the sterile processing department’s team dynamics. This requires conversations. Learn how colleagues communicate and their work styles. Some colleagues may come in and immediately organize their workspace. Others may seek information on priorities and problems prior to settling in to work. Understanding preferences and communication styles can aid the new technician when trying to fit in.

Discover what happens at shift change. Make note of what is reported and how it is reported. Communication styles, department resources, and key names, such as the vendor service technician, can be golden nuggets learned during shift change communications.
Being proactive is more than starting a task without being told. Proactive technicians arrive early and are never late. They take stock of the environment and look for opportunities to contribute. Once an opportunity is found they jump right in. Willingness to help is key when developing the trust of colleagues.
It is also important to ask for help. Though it may be true that anything can be “figured out” given time, it is not the most productive way to manage it. Knowing when to ask for help is an important part of being proactive. Never be afraid to ask a question or to be shown the correct way to complete a task. Learning the right way is the best way. Planning is a critical part of any endeavor. New technicians should have an onboarding plan ready and waiting
on the first day, but this is not always the case. If a facility does not have an onboarding plan or has left the new technician with more questions than answers, work with the supervisor to develop an education plan. Working together to develop the plan contributes to the technician-supervisor relationship and provides clear direction. Share the plan with colleagues, even those without direct responsibility for training. The entire department helps guide the education of the new technician and can help them when they themselves are unaware of missed steps or improper activities.
Sterile processing is an exciting profession with many opportunities. Take time to learn and cultivate connections. Discover the best career path as you grow into the sterile processing professional you will become. HPN
Visit https://www.hpnonline.com/55055784 for references.
1. Which are potential hazards for sterile processing technicians?
A. Blood borne pathogens
B. Cleaning chemistries
C. Bending and lifting
D. All of the above
2. Which personal protective equipment is often worn incorrectly?
A. Shoe Covers
B. Fluid resistant gown
C. Hair covers
D. Face masks
3. What can enter the lungs if the nose is not covered by the face mask?
A. Cigarette smoke
B. The odor of blood
C. Splashes
D. Potentially contaminated air
4. Why should shoe covers and bouffant be removed prior to leaving the department?
A. They may be contaminated
B. They may cause a slip
C. They are not needed
D. They do not have to be removed
5. When is the best time to learn how to use safety equipment?
A. Prior to an emergency or exposure
B. When there is a chemical spill
C. When the fire alarm sounds
D. During an emergency
6. What is a kill cord?
A. A cord used to trap insects
B. An emergency shut off found within the cart washer
C. A cord used to shut off the electricity
D. A cord used prevent the use of damaged equipment
7. What should new technicians read?
A. Facility Policies
B. Standards followed by the facility
C. Facility work instructions
D. All of the above
E. A and B only
All CEU quizzes must be taken online at: educationhub.hpnonline.com. The cost to take the quiz is $10.
8. What can a technician’s network do?
A. Provide promotions
B. List the latest best practices
C. Give answers to questions
D. Gives employee reviews
9. Which organization does not provide sterile processing certifications?
A. Healthcare Sterile Processing Association (HSPA)
B. Centers for Disease Control and Prevention (CDC)
C. Certification Board of Sterile Processing and Distribution (CBSPD)
D. All of the above
10. Why should discussions of rumors be avoided?
A. Job termination
B. Gives a negative impression
C. Disrupts the workflow
D. d. They are harmless




BY DAVID L. TAYLOR, PRINCIPAL, RESOLUTE ADVISORY GROUP LLC AND KRISTINA PIROLLO-KETCHUM
Patient safety is the cornerstone of quality healthcare, and sterile processing (SP) technicians play a crucial role in its delivery. Every patient should expect and receive the highest standard of care, which includes the provision of properly processed medical and surgical devices. When deficiencies or errors occur, the degree of action depends on the underlying issue. For example, if the core cause is unrelated to equipment, resources, or education, behavioral or productivity issues could be to blame. In such cases, SP leaders must determine the cause of the error and devise a plan to prevent its recurrence.
Every SP technician is a behindthe-scenes caregiver for patients. Although they may not have direct interactions with patients, their work significantly influences the quality of care provided. Therefore, they must consistently strive for excellence, acknowledging that there is no room for error when it comes to safety. But when technicians fail to meet these high professional standards, disciplinary measures are warranted. Disciplinary action typically involves a structured process that addresses behavioral and performance issues in a gradual manner. The objective is to offer employees an opportunity to rectify deficiencies and enhance their performance while ensuring they are aware of the possible outcomes and repercussions if the concerns persist.
Progressive discipline is typically a sequence of steps, although managers can take appropriate action on a case-by-case basis. Certain situations, such as an egregious or deliberate flouting of policies, procedures, and best practices, may warrant immediate termination. Still, the intent of discipline is not to terminate an employee but to mentor and strengthen their performance. Progressive discipline should be fair and structured and give employees an opportunity to address mistakes and shortcomings before they face harsher consequences.
A verbal warning is an initial step in employee discipline. It involves SP leadership communicating concerns with the employee and listening with an intent to understand. A verbal warning should clearly and concisely outline the behavior or performance that requires correction, the steps necessary to be successful, and a reasonable timeframe for the employee to be successful. SP leaders should also document the incident so they can reference it as appropriate. If the issue persists, the next step is a written warning, a formal disciplinary method. It is important to give the employee an opportunity to give their perspective about the problem to shed light on underlying issues that leaders may have overlooked. When warranted, it is also essential that the employee understands their failure to improve their behavior or performance may result in further
discipline, which can include termination. Having a witness present during the meeting can be beneficial, as can gathering signatures to ensure all parties understand the issue and any determined next steps.
If unsatisfactory performance continues despite a verbal and initial written warning, a final written warning can be issued. The same process (witness, signatures, etc.) will still be in place; however, it must be stressed that this is the final opportunity for the employee to improve their behavior or performance. Suspension or termination would be the next step.
Suspension without pay can occur if there is no improvement after warnings were issued and steps were taken to correct the problem. Suspension usually precedes termination, the final resort in progressive discipline. The decision to suspend or terminate depends on the error’s severity and frequency as well as facility policy. Often, managers have the flexibility to address each situation and escalate disciplinary action according to the unique circumstances and the resulting risks.
Discipline is a necessary part of effective management. It can improve understanding and performance and help employees more clearly recognize their contributions to patient safety. Appropriate, consistent disciplinary steps also demonstrate to employees that patient safety and service quality always remain the utmost priorities. HPN




























































BY STEPHEN M. KOVACH, BS, CFER, CLINICAL EDUCATOR EMERITUS, HEALTHMARK INDUSTRIES
Q“What psi is used for drying instruments in the decontamination area of Sterile Processing?”
A“Instrument air” is used in the decontamination area to “blow out” debris and in the prep and packaging area to help dry lumened devices and wet sets. Items should be dried for steam and low-temperature sterilization methods, unless otherwise directed by the sterilizer manufacturer/medical device manufacturer’s instructions for use (IFU).
The Association for the Advancement of Medical Instrumentation (AAMI) introduced the term “instrument air” in standard ST79:2017. This air should be used to dry instruments. “Using methods other than instrument air for drying can adversely affect the device or contaminate it.”1
If the device (e.g., semi-rigid endoscope) manufacturer recommends drying, refer to the IFU to see if there is specific pressure to prevent damaging the device.
I recommend installing a pressure gauge on the hose to monitor the pressure of the air or water. I also recommend having a set of adapters to fit various sizes of lumens. Therefore, instrument air should be available to blow out and dry lumens and any residual moisture on sets or individual medical devices.
AAMI does not give any psi setting, so technicians must read their IFU and use the settings the device manufacturers give. That is why I recommend a gauge to monitor for proper pressure.
Sterile Processing Professionals (SPP) should remember (whether psi is given for air or water pressure) they need to use critical thinking to find safe pressure to clean/dry that specific medical device with the proper cleaning devices (i.e., air/water pistol/gun). Some IFU might state to use a syringe to dry or irrigate for cleaning.
Examples of various manufacturers’ IFU details:
No pressure advice. Just use a water gun: “Use a soft towel, a plastic brush, or a water gun for cleaning.”2
Pressure minimum: “For cleaning: Cold water [50–77°F (10–25°C), potable or better as defined in TIR34:2007] pressurized at a minimum of 30 psi [pressure gauge and regulator recommended].”3
Use a dry cloth and pressurized air but no psi given: “Instruments must be thoroughly dried with a clean, soft cloth. The use of pressurized air is recommended to aid in drying, especially in the crevices of the instrument. Residual moisture may contain waterborne pathogens and must be removed prior to sterilization. Additionally, any remaining moisture, especially in the internal areas, may result in corrosion that can cause the instrument to bind up and shorten the life of the instrument.”4
Very specific pressure requirements: “When aerating or irrigating the endoscope channels, the air or water pressure must not exceed 0.5 MPa (5 kgf/ cm2, 71 psig). Higher pressures may cause damage to the endoscope.”5
Options on what to use: “Rinse device using DI or PURW. Use a syringe,

pipette, or water pistol to flush lumens, channels, and other hard-toreach areas. Actuate joints, handles, and other movable device features in order to rinse thoroughly under running water.”6
Because SPP work in a dynamic environment, the IFU are always in what I call a “flux mode—ever changing.” Make sure you are using the most up-to-date version of the IFU for your medical devices (when understanding what pressures to use for air or water).
I also recommend each department have a policy in place and document how they have arrived at setting pressure on devices when the manufacturers give vague guidance on what pressure to use. Also, if an IFU states use of a syringe and you substitute the use of something else, you need to provide sound reasoning for this divergence.
Lastly, staff need proper training for safety precautions in using pressurized air/water gun/pistols within the department. This could even be a “core competency” staff must review yearly.
Here is an earlier HPN article I wrote titled “Instrument Air and A° Validation”7 that may be helpful with more background. HPN
References
1. AAMI (2017). ANSI/AAMI ST79:2017 Comprehensive guide to steam sterilization and sterility assurance in health care facilities. Arlington, VA: Association for the Advancement of Medical Instrumentation.
2. Mizuho Corporation. (2020, October 23). MES-CK09259-01EN-0 Instructions for Use: Bulldog clamp, Version 2. (p. 1). https://www.mizuho.co.jp/ifu/wp-content/uploads/ifu/ CK09-259-01EN-0.pdf
3. Intuitive Surgical, Inc. (2016, March). PN 1004943-US da Vinci Xi® Surgical System Readiness Guide, Rev. G 03/16. (p. 6). http://mplusmedtech.com/16001/pdf/11687.pdf
References continue online at https://www.hpnonline.com/55055190




BY KAREN CONWAY, CEO, VALUEWORKS
Recently, several colleagues have asked me if I think healthcare will ever fully adopt unique device identifiers. I can certainly understand their skepticism - after all it has been more than a decade since the U.S. FDA UDI rule was published with relatively little uptake beyond what was required by regulation - but I do not share their pessimism. There are just too many agreed upon healthcare priorities, such as improved supply continuity, post market surveillance, and demand planning, that UDI is key to achieving.
My optimism is supported by a new collaboration between two trade associations – AHRMM and SMI – that is based on their shared commitment to work with the FDA to maximize “implementation and use of the Unique Device Identifier (UDI) as a means to enhance patient safety, inform medical research through the use of real-world evidence, improve supply chain efficiency, and reduce costs.” Together, the associations plan to bring together multiple stakeholders from across the supply chain and clinical worlds to develop resources to advance the use of UDI in their respective settings.
During the most recent SMI Forum, providers and suppliers came together to discuss the new collaboration and consider the two primary pathways to UDI implementation (see image at hpnonline.com/55055116). One is focused on clinical improvement and regulatory compliance, while the other

looks to support supply chain efficiency, but both require coordination and collaboration between providers and suppliers. Further, advancements in supply chain adoption of UDI can play an important role in supporting the clinical use cases for the standard identifiers. For example, supply chain as the keeper of the system of record for product information can ensure UDIs are included in the item master and other ERP supported systems, which in turn supports capture of UDIs in electronic health records. Knowing which devices were used on which patients is foundational to clinical research to understand the role of products in delivering better quality care and financial research to understand the true costs of care delivery, both of which were identified as key benefits of UDI by the forum participants.
Use of standard product identifiers can also play an important role in supporting inventory management, demand planning, and supply continuity. For example, during the pandemic, if providers had reported their burn rate and inventory levels of critical products using UDIs and if manufacturers, distributors, and the U.S. Strategic National Stockpile had used UDIs to manage inventory and logistics, we may have been able to better ensure products in short supply were delivered where they were needed most.
Those attending the UDI session also listed lack of a clear ROI for UDI as the biggest barrier to broader adoption. This is where the disconnect between UDI and its role in achieving other strategic objectives presents a problem. There is no real ROI for UDI adoption in and of itself. Instead, value is derived from using the UDI for things like measuring the cost per case, responding faster to recalls, and improving inventory management and demand planning.

Once this relationship is better understood, providers and suppliers can incorporate UDI into business cases and work plans to achieve those broader objectives. Along the way, the new collaboration between SMI and AHRMM plans to develop quick start guides to help providers and suppliers with the various steps, such as incorporating UDI in item masters and ERP systems, in EDI transaction sets, and in inventory management and contracting systems. HPN







Unwrap the future of sterile supply management. With features that help streamline processes and reduce the possibility of wet sets, Aesculap’s next generation rigid container is everything you’d expect from the market leader.
Visit aesculapusa.com/aicon to learn more about how this breakthrough technology can help your SPD Operate With Greater Precision.
Healthmark’s SST Tray Systems are containers that provide safe handling and transportation of soiled medical supplies in compliance with OSHA Guidelines.
SST Tray Systems include three parts: a solid base tray, a drain basket and a cover. Each SST Tray System varies in size, style, material compatibility and accessory options - such as latches and drain ports.















Healthmark offers the removable 4x4 “Clean” label to conceal and cover the biohazard symbol when transporting clean instruments.
Other options include the Transportation Identification Tag. This 2-in-1 removable label allows the user to remove the perforated “Clean” portion of the label to reveal a biohazard symbol when transporting hazardous instruments.