



The Peer-Authored Management Source for Lab Professionals since 1969 MLO-online.com April 2024 Vol 56, No. 4 2024 LAB of the YEAR Salem Health Laboratories — Salem Health Hospitals & Clinics p.14 CE: Realizing the potential of digital pathology Page 8 LAB INNOVATOR Jessica DesLauriers, MBA, MLS (ASCP)CM Laboratory Director, Avera McKennan Hospital & University Health Center
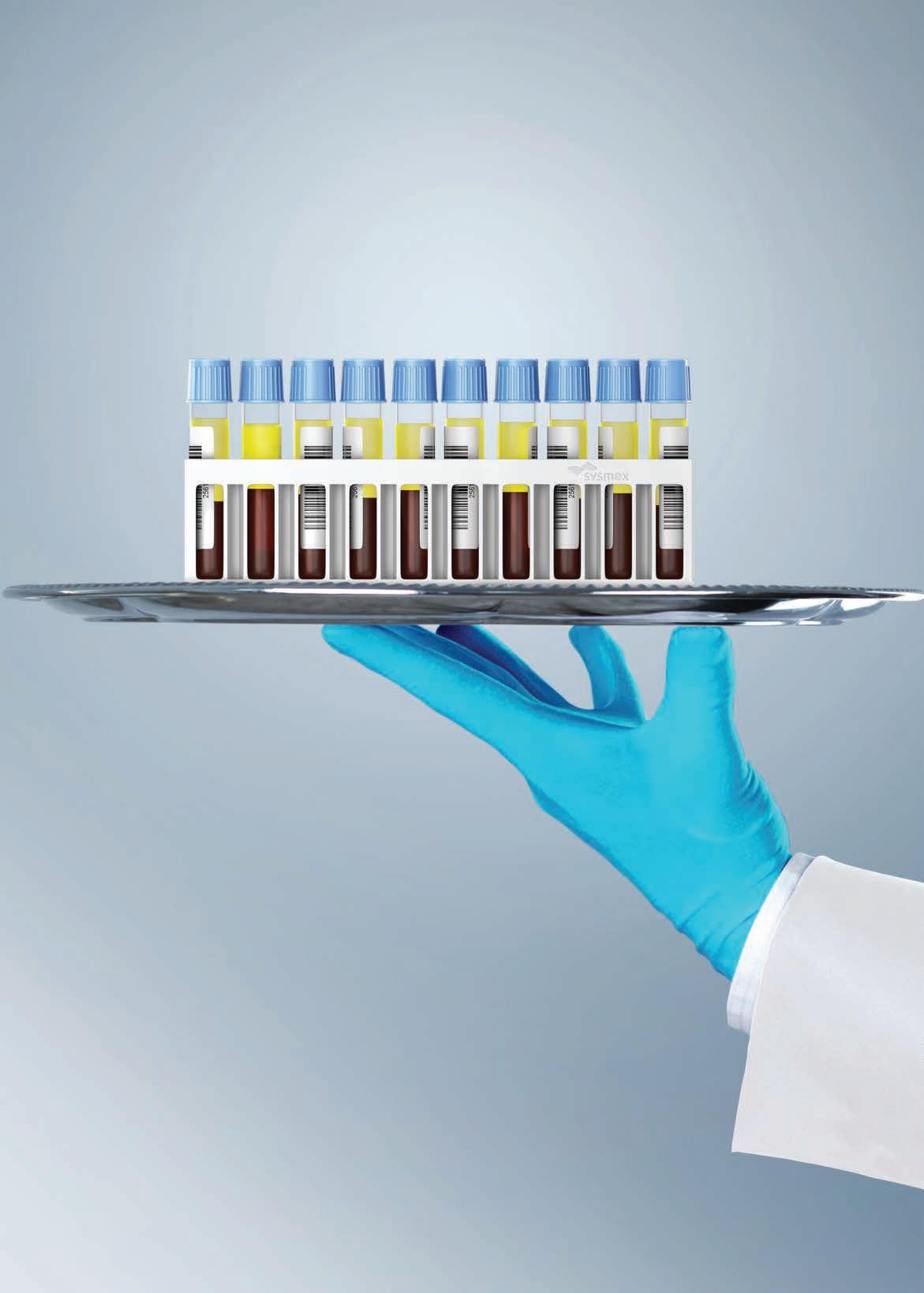
Venous Blood Collection
Designed for simple and safe blood collection.

Unistik® VacuFlip and Unistik® ShieldLock are engineered for intuitive blood collection, featuring easy to use safety mechanisms that can help reduce the risk of needlestick injuries. Unistik® Blood Collection devices are cost-effective and designed to not compromise quality or safety.










































BCAD23/OMI/0823/1/US For more information, call 1-800-421-6936 or visit owenmumford.com
AVAILABLE! Scan here to learn more!
NOW

Hemostasis. At your service.



The Sysmex CS-2500™ Automated Blood Coagulation Analyzer incorporates coagulation, chromogenic, immunoturbidimetric and aggregation** methodologies in full random access. Intelligent preanalytical sample checks provide confidence in first-pass results, without the need for manual sample handling.
A trusted reagent portfolio coupled with the service you expect from Sysmex is precisely what hemostasis laboratories have been waiting for.
* 2023 IMV ServiceTrak™ Annual Survey for Hematology
** For research use only, not for use in diagnostic procedures. RUO assays must be validated before use in clinical practice.
www.sysmex.com/us

Hemostasis solutions from the #1 trusted brand in hematology*
Sysmex supports the Sustainable Development Goals.



©2024 Sysmex America Inc.
Hematology • Hemostasis • Urinalysis • Flow Cytometry • Informatics
4





8
By Carolyn Pressman, PhD
12
14
By
20
22
By Erin Brady
Erin Brady
26
30



 By Alex
By Alex
2 | APRIL 2024 MLO-ONLINE.COM IN THIS ISSUE... FACEBOOK facebook.com//MLOMedicalLaboratoryObserver LINKEDIN linkedin.com /groups/2301731/ TWITTER twitter.com /MedicalLabMLO April 2024 | Vol. 56, No. 4 32 30 26 14 8
From the editor
The observatory CONTINUING EDUCATION
6
Realizing the potential of digital pathology
CLINICAL ISSUES
Neurofilament
chain: Unraveling the diagnostic and prognostic threads in neurological disorders
light
OF THE YEAR
By Dr. Thomas Kampfrath and Dr. Sascha Lange LAB
Salem Health Laboratories at
Hospitals and Clinics — Continuous and sustained commitment to excellence
Salem Health
OF THE YEAR — RUNNERS UP
Christina Wichmann LAB
Services
Southwest Transplant Alliance Laboratory
Diagnostic Laboratories
INFECTION DIAGNOSTICS
Wisconsin
By
Transforming infection detection with the CBC-Diff
EDUCATION
By Melissa Naiman, PhD, EMT-B and Ahmed Bentahar, MD, PhD
The role of training in error prevention
clinical laboratory professionals
BEST PRACTICES
How addressing bullying in medical labs will improve overall retention
for
By Stephen Bishop, MBA, MS, CLS, MLS(ASCP)CM, CPHQ
32
MOLECULAR DIAGNOSTICS
Molecular testing supports early, effective use of ESR1 -targeting therapies
Bittick PRODUCT FOCUS 38 Lab safety DEPARTMENTS
Index of advertisers LAB INNOVATOR
Jessica DesLauriers, MBA, MLS (ASCP) CM By Christina Wichmann ON THE COVER: Courtesy of Salem Health Laboratories
Mitchell
36
By Tom
39
40
SCALABLE SOLUTIONS FOR A BROAD RANGE OF LAB AUTOMATION NEEDS
Implementing changes to your automation system can be a complex and time-consuming process, potentially affecting your service delivery. However, with GLP systems Track, we’ve revolutionized the experience. Our solution has interlocking track components, standardized modules, and simplified software to allow you to change when you need to.


















In the United States, for the GLP systems Track, not all modules and features are commercially available and open connections to clinical analyzers/systems are under development. GLP systems Track is not approved for use in US blood donor and plasma testing laboratories.
AUTOMATION REINVENTED. FLEXIBILITY REDEFINED.

FREEDOM TO CHANGE
Customize tracks, clear pathways, and create personalized lab solutions.

NOW AVAILABLE!

SIMPLICITY THROUGH INTUITIVE DESIGN
Reduced track setup for efficient implementation, service and training.
CONTACT A REPRESENTATIVE FROM ABBOTT TODAY.

EXCELLENCE IN PERFORMANCE
Maximize uptime, optimize workflow, and decrease turnaround time.
GLP SYSTEMS TRACK
© 2023 Abbott. All rights reserved. All trademarks referenced are trademarks of either the Abbott group of companies or their respective owners. ADD-148123-USA-EN 12/23
Happy Medical Laboratory Professionals Week!
 By Christina Wichmann Editor in Chief
By Christina Wichmann Editor in Chief
This year, Medical Laboratory Professionals Week is celebrated April 14–20. This week highlights the vital role played by laboratory professionals and pathologists in diagnostic medicine. Lab Week is now in its 49 th year, and MLO would like to extend its appreciation for everything you do each day for the care and treatment of millions of patients.
To coincide with this celebration, MLO publishes its annual Lab of the Year award. This is my second year with MLO, and I am again extremely impressed by all the laboratory nominations I read. It is one of my favorite features in the magazine.Thank you so much to all the labs that submitted thoughtful nominations, and thank you tothe judgesfor yourtimereviewing and scoring the labs in the five categories: customer service, education and training, productivity, teamwork, and strategic outlook.
This year’s Lab of the Year award goes to Salem Health Laboratories at Salem Health Hospitals and Clinics in Salem, Oregon. The two runners-up are Southwest Transplant Alliance Laboratory Services in Dallas, Texas and Wisconsin Diagnostics Laboratories in Milwaukee, Wisconsin. We feature all three labs in this issue beginning on page 14. Some things you may find noteworthy about each winner include the following:
At Salem Health Laboratories, Lean management is used to support the overall laboratory quality management program, and all 226 employees lead and complete a process improvement project during the year. One laboratory project utilizing Lean tools improved on-time collections for inpatient morning rounds from 66% of the time to 98% of the time. On-time collections ensure that results are available to physicians first thing in the morning so that they can make treatment and discharge decisions. The laboratory’s work developing a tool to plan the next day’s morning rounds contributed to an overall reduction of 4.8% in average length of stay across the hospital over 12 months.
Innovations at Southwest Transplant Alliance Laboratory Services reduced organ donor infectious disease serology testing from an average of 7.67 hours to an average of 37 minutes. Previously, hands-on testing with a lot of manual pipetting was performed by staff, which is a high-pressure, time-consuming job. The biggest impact was the purchase of the Diasorin Liaison XL, an automated infectious disease analyzer. The ability to expedite a donor case and provide a recipient with a much-needed organ can make the difference between life and death, which this lab has done.
Wisconsin Diagnostic Laboratories (WDL) bolsters educational opportunities for its current employees, but it also does quite a bit of outreach to the community on laboratory professions. WDL visits local high schools to help teach students about the laboratory profession, and it partners with one high school to provide internship opportunities — these students got to work in specimen processing. WDL is also a sponsor of HOSA and provides a scholarship to an aspiring clinical laboratory student. WDL also supports students looking for clinical site opportunities to complete their MLS/MLT degrees, providing clinical spots to three area colleges/universities.
It is not an easy task choosing winners of this award, and something notable can truly be shared about each laboratory that applied. Thank you to all the laboratories that applied this year, and happy Medical Laboratory Professionals Week to all our readers!
I welcome your comments and questions — please send them to me at cwichmann@mlo-online.com.
Vo l.56, No. 4
PUBLISHER Chris Driscoll cdriscoll@endeavorb2b.com
EDITOR IN CHIEF Christina Wichmann cwichmann@mlo-online.com
MANAGING EDITOR Erin Brady ebrady@endeavorb2b.com
PRODUCTION MANAGER Edward Bartlett
ART DIRECTOR Kermit Mulkins
AUDIENCE DEVELOPMENT/LIST RENTALS
Laura Moulton | lmoulton@endeavorb2b.com
ADVERTISING SERVICES MANAGER
Karen Runion | krunion@endeavorb2b.com
ADVERTISING
DIRECTOR OF SALES
EAST COAST/MIDWEST SALES, CLASSIFIEDS
Carol Vovcsko (941) 321-2873 | cvovcsko@mlo-online.com
SOUTH/WEST COAST/ILLINOIS SALES
Lora Harrell (941) 328-3707 | lharrell@mlo-online.com
MLO EDITORIAL ADVISORY BOARD
John Brunstein, PhD, Biochemistry (Molecular Virology) President & CSO PathoID, Inc., British Columbia, Canada
Lisa-Jean Clifford, COO & Chief Strategy Officer Gestalt, Spokane, WA
Barbara Strain, MA, SM(ASCP), CVAHP Principal, Barbara Strain Consulting LLC, Formerly Director, Value Management, University of Virginia Health System, Charlottesville, VA
Jeffrey D. Klausner, MD, MPH Professor of Preventive Medicine in the Division of Disease Prevention, Policy and Global Health, Department of Preventive Medicine at University of Southern California Keck School of Medicine.
Donna Beasley, DLM(ASCP), Director, Huron Healthcare, Chicago, IL
Anthony Kurec, MS, H(ASCP)DLM, Clinical Associate Professor, Emeritus , SUNY Upstate Medical University, Syracuse, NY
Suzanne Butch, MLS(ASCP)CM, SBBCM, DLMCM Freelance Consultant, Avon, OH
Paul R. Eden, Jr., MT(ASCP), PhD, Lt. Col., USAF (ret.), (formerly) Chief, Laboratory Services, 88th Diagnostics/Therapeutics Squadron, Wright-Patterson AFB, OH
Daniel J. Scungio, MT (ASCP), SLS, CQA (ASQ), Consultant at Dan the Lab Safety Man and Safety Officer at Sentara Healthcare, Norfolk, VA
CORPORATE TEAM
CEO Chris Ferrell
PRESIDENT June Griffin
COO Patrick Rains
CRO Paul Andrews
CHIEF DIGITAL OFFICER Jacquie Niemiec
CHIEF ADMINISTRATIVE AND LEGAL

OFFICER Tracy Kane EVP CITY SERVICES & HEALTHCARE Kylie Hirko 30 Burton Hills Blvd., Suite 185 Nashville, TN 37215 800-547-7377 | www.mlo-online.com Medical Laboratory Observer USPS Permit 60930, ISSN 0580-7247 print, ISSN 2771-6759 online is published 10 times annually (Jan, Feb, Mar, Apr, May, Jul, Aug, Aug CLR, Sep, Nov) by Endeavor Business Media, LLC. 201 N Main St 5th Floor, Fort Atkinson, WI 53538. Periodicals postage paid at Fort Atkinson, WI, and additional mailing offices. POSTMASTER: Send address changes to Medical Laboratory Observer, PO Box 3257, Northbrook, IL 60065-3257. SUBSCRIPTIONS: Publisher reserves the right to reject non-qualified subscriptions. Subscription prices: U.S. $160.00 per year; Canada/Mexico $193.75 per year; All other countries $276.25 per year. All subscriptions are payable in U.S. funds. Send subscription inquiries to Medical Laboratory Observer, PO Box 3257, Northbrook, IL 60065-3257. Customer service can be reached toll-free at 877-382-9187 or at MLO@ omeda.com for magazine subscription assistance or questions. Printed in the USA. Copyright 2024 Endeavor Business Media, LLC. All rights reserved. No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including photocopies, recordings, or any information storage or retrieval system without permission from the publisher. Endeavor Business Media, LLC does not assume and hereby disclaims any liability to any person or company for any loss or damage caused by errors or omissions in the material herein, regardless of whether such errors result from negligence, accident, or any other cause whatsoever. The views and opinions in the articles herein are not to be taken as official expressions of the publishers, unless so stated. The publishers do not warrant either expressly or by implication, the factual accuracy of the articles herein, nor do they so warrant any views or opinions by the authors of said articles. 4 | APRIL 2024 MLO-ONLINE.COM FROM THE EDITOR

Fast Facts


Announcement of the re-approval of COLA under the Clinical Laboratory Improvement Amendments of 1988
The Centers for Medicare & Medicaid Services published a notice on March 6, 2024.
The notice announces the application of COLA for re-approval as an accreditation organization for clinical laboratories under the Clinical Laboratory Improvement Amendments of 1988 (CLIA) program for the following specialty and subspecialty areas under CLIA: Microbiology, including Bacteriology, Mycobacteriology, Mycology, Parasitology, and Virology; Diagnostic Immunology, including Syphilis Serology, and General Immunology; Chemistry, including Routine Chemistry, Toxicology, and Endocrinology; Hematology, including routine hematology and coagulation; Immunohematology, including ABO Group, D (Rho) typing, Unexpected Antibody Detection, Compatibility Testing, and Antibody Identification; Pathology, including Histopathology, Oral Pathology, and Cytology.


One in eight people are now living with obesity
A new study released by the to by the World Health Organization shows the number of people worldwide living with obesity. The study also shows that even though the rates of undernutrition have dropped, it is still a public health challenge in many places, particularly in South-East Asia and subSaharan Africa. Countries with the highest combined rates of underweight and obesity in 2022 were island nations in the Pacific and the Caribbean and those in the Middle East and North Africa.
It was determined that COLA meets or exceeds the applicable CLIA requirements. The re-approval and grant COLA deeming authority for a period of 6 years was announced. This notice is effective from March 6, 2024, to March 6, 2030.
FDA clears over-the-counter continuous glucose monitor
The U.S. Food and Drug Administration cleared for marketing an over-the-counter (OTC) continuous glucose monitor (CGM).
The Dexcom Stelo Glucose Biosensor System is an integrated CGM (iCGM) intended for anyone 18 years and older who does not use insulin, such as individuals with diabetes treating their condition with oral medications, or those without diabetes who want to better understand how diet and exercise may impact blood sugar levels. Importantly, this system is not for individuals with problematic hypoglycemia (low blood sugar) as the system is not designed to alert the user to this potentially dangerous condition.

The Stelo Glucose Biosensor System uses a wearable sensor, paired with an application installed on a user’s smartphone or other smart device, to continuously measure, record, analyze and display glucose values in people 18 years and older that are not on insulin and who do not have problematic hypoglycemia. Users can wear each sensor up to 15 days before replacing with a new sensor. The device presents blood glucose measurements and trends every 15 minutes in the accompanying app. Users should not make medical decisions based on the device’s output without talking to their healthcare provider.
Data from a clinical study provided to the FDA showed that the device performed similarly to other iCGMs. Adverse events reported in the study included local infection, skin irritation and pain or discomfort.
Scientists develop a simple blood test to quickly diagnose sarcoidosis
A research project supported by the National Institutes of Health has developed a tool to rapidly and inexpensively diagnose sarcoidosis.
The tool, which uses a simple blood test, could allow for selective use of more invasive diagnostic tests often used to identify the disease. The findings published in the American Journal of Respiratory and Critical Care Medicine.
https://www.who.int/news/item/01-03-2024-onein-eight-people-are-now-living-with-obesity
To identify antigens and determine which might be linked to sarcoidosis, scientists collected lung fluid samples and blood cells from patients with pulmonary sarcoidosis, then
6 | APRIL 2024 MLO-ONLINE.COM
2X obese adults since 1990.
>1 billion people in the world are now living with obesity.
smartboy10/DigitalVision Vectors/Getty Images
43% of adults were overweight in 2022.
4X obese children and adolescents (5 to 19 years of age) since 1990.
Half of deaths in children under 5 years of age are by undernutrition and obesity can cause noncommunicable diseases such as cardiovascular diseases, diabetes and some cancers.
extracted the genetic material. Using a combination of molecular techniques, the researchers homed in on two newly described disease-specific antigen biomarkers that only bind to the antibodies of sarcoidosis positive patients.
They next designed a highly specific blood test, which only requires a small amount of blood, to determine if they could accurately detect sarcoidosis. To verify the test, researchers compared blood samples from 386 people, which included patients with sarcoidosis, patients with tuberculosis, patients with lung cancer, and healthy individuals. The researchers confirmed that their test was able to differentiate patients who had sarcoidosis from those with other respiratory diseases.
275 million new genetic variants identified in NIH precision medicine data
Researchers have discovered more than 275 million previously unreported genetic variants, identified from data shared by nearly 250,000 participants of the National Institutes of Health’s All of Us Research Program.
Half of the genomic data are from participants of non-European genetic ancestry. The unexplored cache of variants provides researchers new pathways to better understand the genetic influences on health and disease, especially in communities who have been left out of research in the past. The findings are detailed in Nature, along with three other articles in Nature journals.
Nearly 4 million of the newly identified variants are in areas that may be tied to disease risk.
To date, more than 90% of participants in large genomics studies have been of European genetic ancestry. NIH Institute and Center directors noted in an accompanying commentary article in Nature Medicine that this has led to a narrow understanding of the biology of diseases and impeded the development of new treatments and prevention strategies for all populations.
In a companion study published in Communications Biology, a research team led by Baylor College of Medicine, Houston, reviewed the frequency of genes and variants recommended by the American College of Medical Genetics and Genomics across different genetic ancestry groups in t he All of Us dataset. These genes and variants mirror those in the
program’s Hereditary Disease Risk research results offered to participants. The authors found significant variability in the frequency of variants associated with disease risk between different genetic ancestry groups and compared with other large genomic datasets.
In a separate study, investigators tapped the All of Us dataset to calibrate and implement 10 polygenic risk scores for common diseases across diverse genetic ancestry groups. These
scores calculate an individual’s risk of disease by taking into account genetic and family history factors. Without accounting for diversity, polygenic risk scores could cause false results that misrepresent a person’s risk for disease and create inequitable genetic tools. Using the diversity of the All of Us data, these polygenic risk scores are applicable to a broader population.
More than 750,000 people have enrolled in All of Us to date.






THE OBSERVATORY :: NEWS • TRENDS • ANALYSIS
Realizing the potential of digital pathology
By Carolyn Pressman, PhD
Advancements in whole slide imaging (WSI), also known as digital pathology, now support the ability of clinical laboratories to image large numbers of slides rapidly and at high resolution.1 Entire stained tissue sections from glass slides can be viewed by a pathologist on a computer monitor, where digital images can be magnified and visualized in a way that feels like standard microscopy. Similar to the transition in radiology from film to digital images, pathology labs feel the pressure to develop more efficient digital workflows and reduce the time to diagnosis. 2 Embracing digitization of slides has the potential to revolutionize the delivery of pathology services as labs face increasing volumes and complexity in the histopathology workload. 3
Digital pathology today

Digital pathology is a dynamic, imagebased environment that enables the acquisition, management, and interpretation of pathology information generated from a digitized glass slide.4 Common applications include primary diagnosis, review of immunohistochemistry (IHC) and/or special stains, intraoperative consultation, second opinion consultation, and presentation at a tumor board.2 To further clarify, primary diagnosis is the establishment of a final diagnosis solely by review of the hematoxylin and eosin (H&E) stain based on the histopathologic findings of the pathologist. In addition, slide digitization enables the use
Earning CEUs
See test online at https://ce.mlo-online.com/ courses/realizing-the-potentialof-digital-pathology/
Passing scores of 70 percent or higher are eligible for 1 contact hour of P.A.C.E. credit.
LEARNING OBJECTIVES
Upon completion of this article, the reader will be able to:

1. Describe how digital pathology works in the laboratory to support patient care.
2. Describe typical applications of digital pathology
3. Demonstrate an overall understanding of current technologies used in digital pathology
4. Describe key considerations for implementing digital pathology
of artificial intelligence (AI) derived algorithms for clinical decision support, which is perhaps the most exciting and rapidly advancing technology to be deployed in pathology. Examples include H&E image analysis for cancer detection and classification, and quantitative image analysis for IHC biomarkers like HER2 and PD-L1. WSI and AI image analysis will likely become integral to the practice of pathology and are already helping pathologists to improve workflow and turnaround times, support accurate and timely diagnosis, and may ultimately contribute to improved patient care.5,6,7
Digital pathology ecosystem
The digital pathology ecosystem is composed of three main parts — information systems, whole slide imaging systems (which include scanners, image management software, and monitors), and system tools such as native applications, third party applications, and image analysis.
Many labs may be familiar with the whole slide scanner and the digital image viewer. To truly harness the power of digital pathology, a full ecosystem needs to be implemented where the whole slide system is integrated with one or more of following systems: hospital information systems (HIS), picture archiving and communication systems (PACS), laboratory information systems (LIS), electronic medical record (EMR), and/or radiology information systems (RIS).
Digital pathology begins with a whole slide image (WSI) scanner that captures an entire glass slide in high-resolution images comparable to images seen under brightfield microscopes. Scanners can accommodate a broad range of stain or specimen types, including H&E, IHC, in situ hybridization (ISH), special stains, cytology, and frozen sections. Historically, whole slide imaging systems store image data in proprietary
8 | APRIL 2024 MLO-ONLINE.COM CONTINUING EDUCATION :: DIGITAL PATHOLOGY
Figure 1: Scanned H&E image for primary diagnosis, or comparison with IHC and/or special stains.
Scan code to go directly to the CE test.
file formats. While these systems allow interactive viewing, the proprietary nature of data formats and interfaces create vendor lock-in and impede data access.8 Other specialties, such as radiology, use Digital Imaging and Communications in Medicine (DICOM®) as the standard for the representation, storage, and communication of medical images and related information. While a DICOM file format for pathology has been defined, adoption by vendors is varied, limiting interoperability with other software solutions.8
Image quality, reliability, ease of use, and speed are all important considerations when choosing a whole slide imaging system. A tray-based system can reduce slide-handling errors, such as breakage, jams, and failure to pick up. Other considerations include capacity, with the flexibility to accommodate future growth of digital image interpretation, and built-in calibration to enhance accuracy.
Central to the digital pathology workflow is a dedicated software for pathologists, histologists, and administrators to view, organize, retrieve, and integrate digital images for a comprehensive review of disease status. Software systems that are intuitive, easy to use, and provide annotation tools can optimize user experience and workflow.
With the acceleration of personalized healthcare and increased test complexity, flexible software solutions that integrate third party vendor tools offer pathologists more choice and flexibility to adapt the digital workflow to their specific environment. For example, imagine how difficult it would be to operate a smartphone if an integrated app store did not include apps developed by third parties. This flexibility allows for faster innovation and improves access to the latest technologies with minimal disruption to the digital workflow.
Advantages of digital pathology
Compared with using glass slides and a microscope, digital pathology offers multiple advantages.
One operational benefit of WSI is the elimination of courier costs for transportation of physical glass slides to multiple locations.9 Instead of transporting slides to pathologists for diagnosis, slides are scanned at or near the point of collection. Scanning at or near the point of collection can reduce the risk of slides being lost, mislabeled, or damaged during physical transport, which impacts patient safety.3 Digitization also preserves the integrity and quality of the original slide by eliminating the risk of fading, stain degradation, or other changes to physical slides during storage or transport.3 Since whole slide images are delivered electronically, remote review is immediate and collaboration can take place across geographic regions, reducing time to results.9 Furthermore, a digital workflow may provide faster access to molecular and other ancillary testing.3
Digital pathology also enables a flexible and remote work environment that can increase recruitment and retention of pathologists, potentially prolonging careers of senior pathologists and providing a remote sign out option for locum tenens staff.3
Whole slide imaging can improve pathology service quality by streamlining access to archived images. For
example, direct comparison of digital H&E and IHC images from a former tumor biopsy with a current resected tumor from the same patient, may reduce additional costly immunohistochemical testing.3 To review a previous biopsy in the current glass slide workflow, slides must be pulled from the archive, potentially couriered/transported to the pathologists, then returned and refiled in the archive, all of which is time consuming to the pathologist and the ancillary staff. Digital pathology software permits synchronous analysis of multiple slides on a single screen, permitting faster and easier review.3 Access to on screen measurements tools make cancer staging more convenient and potentially more accurate and reproducible, with a clear audit trail of who has viewed the images and made annotations.3 For immunohistochemical analysis of biomarkers like HER2 and PD-L1 with targeted therapies, interobserver variability in manual scoring may impact patient treatment.10,11 The addition of biomarker quantitative image analysis (QIA) to the digital workflow offers a reproducible and objective method to decrease interobserver variability, improve therapy selection, and potentially lead to better patient outcomes.11,12
Regulatory and reimbursement considerations
The COVID-19 pandemic facilitated adoption of digital pathology for remote use in two ways. First, the Food and Drug Administration (FDA) issued guidance in April 2020, for the duration of the COVID-19 public health emergency, that allowed the marketing of new digital pathology devices that are intended for use in remote settings and that are not currently 510(k) cleared for any use.14 This guidance document expired in November 2023.15 Secondly, the Centers for Medicare & Medicaid Services (CMS) provide an updated memorandum in May 2023 pertaining to the continued use of remote digital image viewing: “To ensure the accuracy, reliability and timeliness of laboratory results, CMS will continue to exercise enforcement discretion to permit pathologists and other laboratory personnel to review laboratory digital data, digital results, and digital images (“digital materials”) remotely, without obtaining a separate CLIA certificate for the remote testing site, provided that the designated primary site or home base has such a certificate (using the address of

MLO-ONLINE.COM APRIL 2024 | 9 CONTINUING EDUCATION :: DIGITAL PATHOLOGY
Figure 2: Example of adjunctive quantitative image analysis tool for calculating HER2 gene amplification in breast cancer.
the primary site) and the work being performed at the remote testing site falls within the specialties/subspecialties under the primary site’s certificate.”16
Multiple WSI systems have submitted 510(k) premarket notifications and gained marketing authorization.Per the FDA, “The whole slide imaging system is an automated digital slide creation, viewing, and management system intended as an aid to the pathologist to review and interpret digital images of surgical pathology slides prepared from formalin-fixed, paraffin-embedded (FFPE) tissue. The system generates digital images that would otherwise be appropriate for manual visualization by conventional brightfield microscopy. The whole slide imaging system is not intended for use with slides prepared from frozen tissue, cytology, and non-FFPE hematopathology specimens. The whole slide imaging system consists of an image management system, a scanner and associated software, and a display monitor. The whole slide imaging system does not include any automated Image Analysis Applications that would constitute computer aided detection or diagnosis. Pathologists view and interpret scanned digital images, employing appropriate processes to ensure the validity of the interpretation.”17
Currently, there is only one on-market artificial intelligence tool that has marketing authorization as a software algorithm device to assist users in digital pathology. According to the FDA, “A software algorithm device to assist users in digital pathology is an in vitro diagnostic device intended to evaluate acquired scanned pathology whole slide images. The device uses software algorithms to provide information to the user about presence, location, and characteristics of areas of the image with clinical implications. Information from this device is intended to assist the user in determining a pathology diagnosis.”18
Reimbursement of digital pathology is evolving. Currently, the standalone process of whole slide imaging is not reimbursed. However, there are a small number of existing Current Procedural Terminology (CPT) Category I codes for IHC/ISH using computer-assisted technology that implicitly include reimbursement for digitization of whole slide images as part of the quantitative image analysis process.19 These Category l tissue codes have not been revalued in a decade, leading to suboptimal reimbursement for biomarker image analysis. In addition, there currently are no Category l tissue codes for other AI image analysis applications such as H&E.
The College of American Pathologists and the American Medical Association have been making strides in creating 43 digital pathology CPT Category III add-on codes to help close this gap. The use of these codes will inform the Centers for

Medicare & Medicaid Services when it is making reimbursement decisions for new services. Assuming that laboratories are diligent in consistently using them, which will establish an ongoing record that supports their value, the new codes could be seen as a step toward potential greater reimbursement in the future.
When digitized glass slides are used for consultations and second opinions, the appropriate Cat III add-on codes should be used.
Implementing digital pathology
As adoption of digital pathology gains momentum, the collective experience of early adopters provides a rich resource for institutions that are just beginning the planning process.20,21 Technical readiness, operational readiness, and cost are identified as the most significant challenges.21 A critical step in adopting digital pathology is to assemble a multidisciplinary implementation team to evaluate pathologists’ readiness for a transition to digital pathology, propose a budget, and evaluate resources needed for implementation, such as appropriate data storage and internet bandwidth.22
The initial assessment will lead to a better understanding of resources and infrastructure requirements than can then lead to a plan for execution, including definition of workflow, validation and delineation of SOPs, and training. To support labs in the implementation process, validation guidelines have been established to ensure whole slide digital images are acceptable for clinical diagnosis.23,24 Additionally, the National Society for Histotechnology has created an online Digital Pathology Certificate of Completion program to increase knowledge and improve competency in whole slide imaging.25
Given the complex, multifaceted nature of change management, it comes as no surprise that experts advocate a stepwise implementation, with the identification of one or two clinical needs as a starting point, adding additional applications over time.20
There are different perspectives to consider when implementing digital pathology. The first category encompasses tangible issues: acquisition costs of the digital pathology solution and personnel costs of planning and implementation, including validation, and new reimbursement strategies are just a few examples.22 The second category includes costs related to infrastructure updates and upgrades, notably in IT and training, personnel realignment with the new workflow, and the technical expertise and core competencies to support it.22 Last but not least is the human factor; change is difficult. As pathologists, lab personnel, IT, and other stakeholders learn new ways to work and collaborate, they develop the groundwork for a more efficient digital workflow.
REFERENCES

1. Zarella MD, Bowman D, Aeffner F, et al. A Practical Guide to Whole Slide Imaging: A White Paper from the Digital Pathology Association. Arch Pathol Lab Med. 2019;143(2):222-234. doi:10.5858/ arpa.2018-0343-RA.
2. Parwani AV. Digital pathology as a platform for primary diagnosis and augmentation via deep learning. Artificial Intelligence and Deep Learning in Pathology. Elsevier; 2021:93-118.
3. Williams BJ, Bottoms D, Treanor D. Future-proofing pathology: the case for clinical adoption of digital pathology. J Clin Pathol 2017;70(12):1010-1018. doi:10.1136/jclinpath-2017-204644.
10 | APRIL 2024 MLO-ONLINE.COM CONTINUING EDUCATION :: DIGITAL PATHOLOGY
Figure 3: Tray-based WSI scanner.
Scan code to go directly to the CE test.

4. About digital pathology. DPA. Accessed February 21, 2024. https:// digitalpathologyassociation.org/about-digital-pathology.
5. Vodovnik A. Diagnostic time in digital pathology: A comparative study on 400 cases. J Pathol Inform. 2016;29;7:4. doi:10.4103/2153-3539.175377.
6. Clarke E, Doherty D, Randell R, et al. Faster than light (microscopy): superiority of digital pathology over microscopy for assessment of immunohistochemistry. J Clin Pathol. 2023;76(5):333-338. doi:10.1136/ jclinpath-2021-207961.
7. Eloy C, Marques A, Pinto J, et al. Artificial intelligence-assisted cancer diagnosis improves the efficiency of pathologists in prostatic biopsies. Virchows Arch. 2023;482(3):595-604. doi:10.1007/s00428-023-03518-5.
8. Herrmann MD, Clunie DA, Fedorov A, et al. Implementing the DICOM Standard for Digital Pathology. J Pathol Inform. 2018 Nov 2;9:37. doi: 10.4103/jpi.jpi_42_18.
9. Guo H, Birsa J, Farahani N, et al. Digital pathology and anatomic pathology laboratory information system integration to support digital pathology sign-out. J Pathol Inform. 2016;4;7:23. doi:10.4103/2153-3539.181767.
10. Casterá Redal C, Bernet Vegué L. “HER2 immunohistochemistry inter-observer reproducibility in 205 cases of invasive breast carcinoma additionally tested by ISH” Answer to the statistical issue to avoid misinterpretation. Ann Diagn Pathol. 2020;48:151566. doi:10.1016/j.anndiagpath.2020.151566.
11. Brunnström H, Johansson A, Westbom-Fremer S, et al. PD-L1 immunohistochemistry in clinical diagnostics of lung cancer: inter-pathologist variability is higher than assay variability. Mod Pathol. 2017;30(10):1411-1421. doi:10.1038/modpathol.2017.59.
12. Gough M, Liu C, Srinivasan B, et al. Improved concordance of challenging human epidermal growth factor receptor 2 dual in-situ hybridisation cases with the use of a digital image analysis algorithm in breast cancer. Histopathology. 2023;83(4):647-656. doi:10.1111/ his.15000.
13. Haragan A, Parashar P, Bury D, Cross G, Gosney JR. Machine-learningbased image analysis algorithms improve interpathologist concordance when scoring PD-L1 expression in non-small-cell lung cancer. J Clin Pathol. 2024;18;77(2):140-144. doi:10.1136/jcp-2023-208978.
14. Regulations.Gov, Enforcement Policy for Remote Digital Pathology Devices During the Coronavirus Disease 2019 (COVID-19) Public Health Emergency Guidance for Industry, Clinical Laboratories, Healthcare Facilities, Pathologists, and Food and Drug Administration Staff. Accessed February 21, 2024. https://www.regulations.gov/document/ FDA-2020-D-1138-0078.
15. Withdrawn or expired guidance. U.S. Food and Drug Administration. Published December 18, 2023. Accessed February 21, 2024.
https://www.fda.gov/medical-devices/guidance-documentsmedical-devices-and-radiation-emitting-products/ withdrawn-or-expired-guidance.
16. CMS.gov. Accessed February 21, 2024. https://www.cms.gov/files/ document/qso-23-15-clia.pdf.
17. US Food and Drug Administration. Product classification. Accessed February 21, 2024. https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/ cfpcd/classification.cfm?id=5344.
18. US Food and Drug Administration. Product classification. Accessed February 21, 2024. https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/ cfpcd/classification.cfm?id=5349.
19. American Medical Association. AMA CPT® licensing overview. American Medical Association. Published May 31, 2023. Accessed February 21, 2024. https://www.ama-assn.org/practice-management/ cpt/ama-cpt-licensing-overview.
20. Evans AJ, Salama ME, Henricks WH, Pantanowitz L. Implementation of Whole Slide Imaging for Clinical Purposes: Issues to Consider from the Perspective of Early Adopters. Arch Pathol Lab Med 2017;141(7):944-959. doi:10.5858/arpa.2016-0074-OA.
21. Hartman DJ, Pantanowitz L, McHugh JS, et al. Enterprise Implementation of Digital Pathology: Feasibility, Challenges, and Opportunities. J Digit Imaging. 2017;30(5):555-560. doi:10.1007/s10278-017-9946-9.
22. Lujan G, Quigley JC, Hartman D, et al. Dissecting the Business Case for Adoption and Implementation of Digital Pathology: A White Paper from the Digital Pathology Association. J Pathol Inform. 2021;7;12:17. doi:10.4103/jpi.jpi_67_20.
23. Evans AJ, Brown RW, Bui MM, et al. Validating Whole Slide Imaging Systems for Diagnostic Purposes in Pathology. Arch Pathol Lab Med 2022;1;146(4):440-450. doi:10.5858/arpa.2020-0723-CP.
24. Bui MM, Riben MW, Allison KH, et al. Quantitative Image Analysis of Human Epidermal Growth Factor Receptor 2 Immunohistochemistry for Breast Cancer: Guideline from the College of American Pathologists. Arch Pathol Lab Med. 2019;143(10):1180-1195. doi:10.5858/ arpa.2018-0378-CP.
25. Digital pathology certificate of completion program. Nsh.org. Accessed February 21, 2024. https://elearn.nsh.org/products/ digital-pathology-certificate-of-completion-program.

Carolyn Pressman, PhD, Scientific Partner, Medical and Scientific Affairs, Roche Diagnostics, received her doctoral degree in Genes and Development from the University of Texas Health Science Center, at Houston. Her current work as part of the medical and scientific affairs team focuses on digital pathology and AI image analysis.
MLO-ONLINE.COM APRIL 2024 | 11 CONTINUING EDUCATION :: DIGITAL PATHOLOGY
Figure 4: Review of immunohistochemistry using digital pathology software.
Neurofilament light chain
Unraveling the diagnostic and prognostic threads
in neurological disorders
By Dr. Thomas Kampfrath and Dr. Sascha Lange
The pathological foundation of numerous acute and chronic neurological disorders, leading to enduring disability, lies in neuroaxonal damage and loss. The capability to easily identify and track such damage would offer significant advantages in evaluating disease activity, monitoring responses to treatment, and predicting prognosis. Neurofilaments are attracting growing interest as potential biomarkers for neuroaxonal injury. These abundant structural scaffolding proteins are exclusively present in neurons and show elevated levels in response to axonal damage in various conditions, including neurodegenerative, inflammatory, vascular, and traumatic diseases. Notably, this increase is observable not only in cerebrospinal fluid (CSF) but also in blood. The specificity of neurofilaments for neuronal cell damage and eventual cell death provides a distinct advantage over other potential biomarkers.
Alzheimer’s disease
The clinical diagnosis of Alzheimer’s disease relies on the cognitive decline or post-mortem diagnosis. Nonetheless, studies have shown that brain damage starts decades before the onset of clinical symptoms. NfL levels are significantly elevated in patients with mild cognitive impairment (MCI) and dementia stages when compared to the healthy population. Besides that, NfL can be used to predict cognitive decline and susceptibility in combination with other biomarkers. However, NfL is not able to predict the conversion from MCI within the disease spectrum.9
Amyotrophic lateral sclerosis (ALS)
ALS is characterized by the degeneration of both upper and lower motor neurons. Elevated NfL levels in the CSF or blood may therefore be indicative of motor neuron damage and can be used for assessing disease progression and prognosis.10 The FDA has accepted the use of NfL as a prognostic biomarker in ALS associated with a mutation in the superoxide dismutase 1 (SOD1) gene as a biomarker.11
Huntington’s disease
Huntington’s disease is characterized by an increased repeat of the CAG triplets in the Huntingtin gene (HTT) on chromosome 4 causing different neuronal symptoms. CAG triplets refer to a specific sequence of DNA nucleotides consisting of the bases cytosine (C), adenine (A), and guanine (G) repeated three times. The CAG triplet repeat expansion is a characteristic genetic feature of Huntington’s disease and is used in genetic testing to diagnose the condition or determine an individual’s risk of developing the disease. It has been shown that there is a correlation between prognosis and NfL levels as well as disease onset.12
Multiple sclerosis
Multiple sclerosis (MS) is an immune-mediated disorder characterized by neurodegeneration. In MS, NfL has been shown to predict susceptibility risk 13, as well as a marker for monitoring, treatment, and correlated prognosis of the disease.14
Neurofilaments are proteins classified as type IV of intermediate filaments (including the three neurofilament proteins) and are exclusively expressed in the cytoplasm of neurons. Together with microfilament and microtubules, neurofilaments form the neuronal cytoskeleton. As of today, there are five known neurofilament subunits that can be differentiated by their molecular mass. Besides neurofilament light (NfL), medium (NfM), and heavy (NfH) with molecular masses of approximately 68, 150 and 200 kiloDalton (kDa), peripherin and internexin with a molecular mass of 57 and 66 kDa exist.1 While NfL, NfM, and NfH are ubiquitously expressed in mature neurons, internexin is mainly found in central nervous system while peripherin is in the peripheral nervous system. Due to their stability and role in the neuronal structure, they gained interest in usage as markers for axonal damage. As the intermediate filaments always contain NfL, it was determined to be the optimal molecule for use as a biomarker. 2
Neurofilament light chain biomarkers: Which holds the diagnostic edge – blood or CSF?
Upon damage, neurofilaments leak into the interstitial space and eventually into CSF and blood (serum, plasma) where it can be quantified. While blood NfL concentration is at a lower level than CSF NfL concentration, there is a tight and strongly positive association between CSF NfL and blood NfL levels.3 CSF collections require lumbar punctures that are associated with more side effects such as headaches, backaches, nausea, or vomiting. In recent years, however, the development of improved assay technologies now allows for reliable NfL quantification in blood samples.4
How specific is neurofilament light chain as a clinical biomarker?
Any neuroaxonal damage or degeneration can lead to NfL release into the CSF and bloodstream. The clinical specificity of NfL as a biomarker can vary depending on the specific neurological disorder. It is crucial to emphasize that although increased levels of NfL are linked to neurodegeneration, they are not specific to a particular disease. In addition to increases due to clinical relapses in multiples sclerosis (MS), NfL levels can be influenced by age, comorbidities, and other diseases such as Alzheimer’s disease (AD), amyotrophic lateral sclerosis (ALS), Parkinson’s disease, as well as in stroke, traumatic brain injury (TBI), and epilepsy. Of these diseases, NfL is most strongly associated with MS.4 NfL appears to increase with age as well as show more variability. Studies have shown that NfL levels in the blood of healthy people can increase by 2.2% per year.5 These increases in the older population are likely partially explained by the higher prevalence of comorbidities such as diseases or stroke. Cardiovascular risk factors such as high body mass index (BMI), smoking and blood pressure, as well type 2 diabetes can also influence NfL levels, and careful interpretation is necessary in a clinical context.4
12 | APRIL 2024 MLO-ONLINE.COM CLINICAL ISSUES :: NEUROFILAMENT LIGHT CHAIN
Table 1. Disease states and application of NfL.
How does neurofilament light chain manifest across a spectrum of neurological disorders?
A recent publication analyzed blood NfL concentrations in 13 neurodegenerative diseases, Down syndrome, and depression.6 An increase in blood NfL levels was observed in all of them, confirming its role as a marker of neurodegeneration. Easy access to blood biomarkers such as NfL can play a significant role in the management of neurological disorders. It can be used as a rapid screening tool to identify or reject neurodegeneration as an underlying cause of cognitive symptoms for AD and beyond.7
Elevated NfL levels can also indicate non-disease-specific neuronal damage. Thus, interpretation of NfL results should always consider the overall clinical context and should be combined with a prior established disease diagnosis. Ongoing research continues exploring the utility of NfL as a biomarker in various neurological conditions, and its role in predicting risk and monitoring disease is continually evolving. A good overview regarding the use of NfL can be found in the review by Barro et al.7 and Khalil et al.8
Table 1 gives an overview of different diseases and the potential benefits for the use of NfL.
REFERENCES
1. Yuan A, Nixon RA. Neurofilament Proteins as Biomarkers to Monitor Neurological Diseases and the Efficacy of Therapies. Front Neurosci 2021;27;15:689938. doi:10.3389/fnins.2021.689938.
2. Mücke N, Kämmerer L, Winheim S, et al. Assembly Kinetics of Vimentin Tetramers to Unit-Length Filaments: A Stopped-Flow Study. Biophys J. 2018;22;114(10):2408-2418. doi:10.1016/j.bpj.2018.04.032.
3. Disanto G, Barro C, Benkert P, et al. Serum Neurofilament light: A biomarker of neuronal damage in multiple sclerosis. Ann Neurol. 2017;81(6):857-870. doi:10.1002/ana.24954.
4. Khalil M, Teunissen CE, Otto M, et al. Neurofilaments as biomarkers in neurological disorders. Nat Rev Neurol. 2018;14(10):577-589. doi:10.1038/s41582-018-0058-z.
5. Thebault S, Booth RA, Freedman MS. Blood Neurofilament Light Chain: The Neurologist’s Troponin? Biomedicines. 2020;21;8(11):523. doi:10.3390/biomedicines8110523.
6. Ashton NJ, Janelidze S, Al Khleifat A, et al. A multicentre validation study of the diagnostic value of plasma neurofilament light. Nat Commun. 2021;7;12(1):3400. doi:10.1038/s41467-021-23620-z.
7. Hampel H, O’Bryant SE, Molinuevo JL, et al. Blood-based biomarkers for Alzheimer disease: mapping the road to the clinic. Nat Rev Neurol 2018;14(11):639-652. doi:10.1038/s41582-018-0079-7.
8. Barro C, Chitnis T, Weiner HL. Blood neurofilament light: a critical review of its application to neurologic disease. Ann Clin Transl Neurol. 2020;7(12):2508-2523. doi:10.1002/acn3.51234.
9. Jung Y, Damoiseaux JS. The potential of blood neurofilament light as a marker of neurodegeneration for Alzheimer’s disease. Brain 2024;4;147(1):12-25. doi:10.1093/brain/awad267.
10. Abu-Rumeileh S, Vacchiano V, Zenesini C, et al. Diagnostic-prognostic value and electrophysiological correlates of CSF biomarkers of neurodegeneration and neuroinflammation in amyotrophic lateral sclerosis. J Neurol. 2020;267(6):1699-1708. doi:10.1007/s00415-020-09761-z.
11. Benatar M, Wuu J, Andersen PM, et al. Design of a Randomized, Placebo-Controlled, Phase 3 Trial of Tofersen Initiated in Clinically Presymptomatic SOD1 Variant Carriers: the ATLAS Study. Neurotherapeutics. 2022;19(4):1248-1258. doi:10.1007/s13311-022-01237-4.
12. Byrne LM, Rodrigues FB, Blennow K, et al. Neurofilament light protein in blood as a potential biomarker of neurodegeneration in Huntington’s disease: a retrospective cohort analysis. Lancet Neurol 2017;16(8):601-609. doi:10.1016/S1474-4422(17)30124-2.
13. Bjornevik K, Munger KL, Cortese M, et al. Serum Neurofilament Light Chain Levels in Patients With Presymptomatic Multiple Sclerosis. JAMA Neurol. 2020;1;77(1):58-64. doi:10.1001/jamaneurol.2019.3238.
14. Abdelhak A, Benkert P, Schaedelin S, et al. Neurofilament Light Chain Elevation and Disability Progression in Multiple Sclerosis. JAMA Neurol. 2023;1;80(12):1317-1325. doi:10.1001/jamaneurol.2023.3997.
15. Frank A, Bendig J, Schnalke N, et al. Serum neurofilament indicates accelerated neurodegeneration and predicts mortality in late-stage Parkinson’s disease. NPJ Parkinsons Dis. 2024;9;10(1):14. doi:10.1038/ s41531-023-00605-x.
Table 1 (continued). Disease states and application of NfL. Parkinson’s disease
The clinical course of Parkinson’s disease is categorized into different stages of the disease. While the first stages vary, the late stage is characterized by rapid clinical deterioration. Although NfL levels were described to be low in the early stages, a recent publication demonstrated that high levels of NfL not only correlate with clinical symptoms (e.g., disability) milestones but were also able to predict death within three years.15
Stroke
It has been shown that after the first days after stroke, the NfL level continuously increases and remains at a higher level for up to six months. In addition, a recent publication was able to correlate the infarct volume and long-term outcome with NfL levels. Although the study cohort was very small and not adjusted for age and other confounding factors, the results looked very promising for future evaluations.16
Traumatic brain injury (TBI)
TBI is caused by non-penetrating head trauma that leads to a damage of neurons. Consequently, NfL levels increase and can remain elevated for months, depending on the severity of the trauma. Therefore, in TBI NfL can be used to assess the severity of the injury and predict outcomes.17
HIV-associated neurocognitive disorders (HAND)
HIV can affect the central nervous system, leading to neurocognitive disorders. Elevated NfL levels may be associated with neuronal damage in HIV-infected individuals, providing insights into the risk of developing neurological complications.18
Coronavirus disease 2019 (COVID-19)
Although COVID-19 is a respiratory illness, it also has been linked to various neurological complications. The meta-analysis conducted by Huang et al. provides an overview regarding recent findings. In summary, COVID-19 patients showed elevated levels of NfL. While mild symptoms were no associated with significantly higher levels of NfL, moderate and severe cases showed not only elevated NfL levels but also were able to predict prognosis of COVID-19-related neurological injuries.19
16. Ahn JW, Hwang J, Lee M, et al. Serum neurofilament light chain levels are correlated with the infarct volume in patients with acute ischemic stroke. Medicine (Baltimore). 2022;30;101(39):e30849. doi:10.1097/ MD.0000000000030849.
17. Shahim P, Gren M, Liman V, et al. Serum neurofilament light protein predicts clinical outcome in traumatic brain injury. Sci Rep 2016;7;6:36791. doi:10.1038/srep36791.
18. Hagberg L, Edén A, Zetterberg H, Price RW, Gisslén M. Blood biomarkers for HIV infection with focus on neurologic complications-A review. Acta Neurol Scand. 2022;146(1):56-60. doi:10.1111/ane.13629.
19. Huang Z, Haile K, Gedefaw L, et al. Blood Biomarkers as Prognostic Indicators for Neurological Injury in COVID-19 Patients: A Systematic Review and Meta-Analysis. Int J Mol Sci. 2023;30;24(21):15738. doi:10.3390/ijms242115738.


Dr. Thomas Kampfrath is a board-certified clinical chemist and medical officer for Siemens Healthineers Dr. Sascha Lange is a biochemist and serves as director of Clinical Sciences for Siemens Healthineers
MLO-ONLINE.COM APRIL 2024 | 13 CLINICAL ISSUES :: NEUROFILAMENT LIGHT CHAIN

14 | APRIL 2024 MLO-ONLINE.COM LAB MANAGEMENT :: LAB OF THE YEAR
Courtesy of Salem Health Laboratories
Salem Health Laboratories at Salem Health Hospitals and Clinics
Continuous and sustained commitment to excellence
By Christina Wichmann
Medical Laboratory Observer’s 2024 Lab of the Year is the Salem Health Laboratories at Salem Health Hospitals and Clinics. Salem Health Laboratories employs 226 people and handles 1.6 million test requests at its three high-complexity laboratories; the laboratories also support and oversee all point-of-care testing across its health system. The health system includes Salem Hospital, a 502-bed, level II trauma center in Salem, Oregon and West Valley Hospital, a 25-bed critical access hospital in Dallas, Oregon. The health system also includes Salem Health Medical Group, which provides primary care and specialty services throughout the health system’s five-county service area.
MLO received many outstanding nominations for the 2024 Lab of the Year. However, Salem Health Laboratories’ sustained commitment to improving laboratory quality and services made it stand out. Lean management is used to support the overall laboratory quality management program, and all 226 employees lead and complete a process improvement project during the year. The laboratory staff believe that if they have good processes and well-designed systems, they will consistently achieve high-quality outcomes.

Laboratories partners with anatomic pathologists, who are an independent practice. The new LIS upgraded the interoperability between the pathologists and Salem Health Laboratories by integrating rich format pathology reports and images, whereas previously, the lab was only able to capture unformatted textual data. This has improved the useability of the pathology reports by clinicians throughout the health system.
Previously, in Oregon, state law limited a laboratory’s ability to provide results directly to patients. The patient’s provider was primarily responsible for sharing results with patients. With the implementation of the 21 st Century Cures Act, the Oregon law was amended to allow all laboratory results to be available directly to patients. In 2023, the number of patients electronically interacting with their laboratory results reached 80%. Now, patients and their providers can see results together, which improves outcomes and allows patients to be full partners in their care. As Salem Health Laboratories continues its work to increase patient engagement with the laboratory, it is now exploring methods to allow patients to pre-schedule lab visits and complete insurance verification prior to arriving in the laboratory.
Lab of the Year nominations are judged on achievements across five categories: customer service, productivity, teamwork, education and training, and strategic outlook. Salem Health Laboratories’ achievements in each of these categories follows.
Customer service
In January 2023, the laboratory went live on Epic Beaker. The multi-year project to replace the legacy laboratory information system (LIS) resulted in full integration of laboratory services with Salem Health’s Epic medical record. This integration improved communication of orders to the laboratory, useability of pathology reports by clinicians, and distribution of results to clinicians and patients.
While the full integration of the LIS with Salem Health’s medical record has improved workflows and provided a complete patient record, the new LIS has improved access to laboratory results to everyone in the community. Prior to the conversion, none of the providers in the laboratory’s community were able to submit orders electronically to the LIS — each order had to be hand entered. Test results were made available electronically to only 16% of the clinics the laboratory served. The remainder of results were issued via facsimile, which is still very common in laboratory outreach.
The new LIS also improved useability of anatomic pathology reports. Like many health systems, Salem Health
Productivity
This past year, Salem Health Laboratories participated in two significant performance improvement initiatives. The first was to improve on-time collections for inpatient morning rounds. The second was to reduce medically unnecessary testing in preoperative patients.
The laboratory’s work to improve on-time collections for morning rounds contributed to the overall goal to improve patient length of stays post-pandemic in the Salem Hospital.

MLO-ONLINE.COM APRIL 2024 | 15 LAB MANAGEMENT :: LAB OF THE YEAR
Courtesy of Salem Health Laboratories
Salem Health Regional Lab staff.

On-time collections ensure that results are available to physicians first thing in the morning so that they can make treatment and discharge decisions. By working with its partners throughout the medical center, the lab discovered that if results posted to a patient chart after the physician had already seen the patient, it could delay care and discharge decisions by up to six hours. At baseline, the laboratory was performing on-time collection of morning rounds only 66% of the time.
Utilizing Lean process improvement to review this process, the phlebotomy teams identified three drivers that were key to successful on-time collections. The first driver was the number of patients hospitalized during morning rounds. The second driver was the number of patients under isolation precautions. And the third driver was the availability of team members to collect specimens.
Through job breakdown analysis, the team identified the amount of time needed to perform collections, how many minutes the amount of time increased when caring for patients with isolation precautions, and how many collections a phlebotomist could do to determine an appropriate workforce to perform these collections. With a clear understanding of the process, the team created a predictive tool based on these drivers. Each afternoon, the phlebotomy teams across the organization assess the number of hospitalized patients and evaluate the staffing for the next shift, including unplanned absences, etc. The tool informs the team if they have enough resources to complete rounds on time and allows them to react the day prior to ensure that collections can be performed on time and results available when physicians are on the unit with their patients. Now, utilizing this tool, the lab has been able to increase on-time collection of morning rounds to 98% of the time. And, on the rare occasion where they have not met their goal, they have reduced the amount of time they were late from an average of 62 minutes to only 16 minutes. This work contributed to an overall reduction of 4.8% in average length of stay across the hospital over 12 months.
In the second project, the laboratory medical director and one of the laboratory managers participated in Salem Health’s Physician Leadership Institute (PLI). As part of the lab leaders’ participation in PLI, they completed a quality improvement project, setting a goal to reduce preoperative Type and Screen testing by 50% by December 31, 2023, in patients undergoing vascular surgery. By reviewing current performance, the team identified that preoperative blood bank testing for open
carotid vascular surgery patients was unnecessary 91% of the time. The team estimated that the cost to each patient of this unnecessary testing was between $274–$368 per episode. Additionally, unnecessary testing diverts laboratory resources that can be utilized to improve patient care. Through review of current literature, the team discovered that presurgical type and screen was frequently obtained, because the surgical procedure was considered an intermediate risk for blood loss. However, current literature also showed that patients require transfusion only 1.7% of the time, and in a single institution study with a cohort of over 1,500 patients, transfusion was used less than 5% of the time for patients undergoing this procedure. This knowledge allowed the team to challenge assumptions that presurgical type and screen testing was essential to the care of these patients.
The team developed a simplified algorithm, that classified patients with a hematocrit below 30% as at risk. Patients that had a presurgical hematocrit above 30% were more likely to tolerate the procedure successfully, without transfusion. During their study period, the team also monitored the use of emergency release or urgent transfusion in patients who did not have a preoperative type and screen. Zero patients required emergency release or urgent transfusion when their preoperative hematocrit was above 30%.
As a result of their work, the team surpassed their initial goal and reduced unnecessary preoperative transfusion testing by 73%, with an estimated annual savings of over $13,000.
Teamwork
In 2023, 100% of laboratory staff led and completed a Lean process improvement project, calling this work, “Lean to the Front Line.”This front-line commitment to improvement and the empowerment of employees to be in control of their work sets Salem Health Laboratories apart. To achieve sustainable improvement, employees must work together as a team. Some of the improvement projects are laboratory centric and affect a small team. Other projects stretch across the health system, involving multiple teams and many people.
An example of this work was partnering with two other clinical departments to improve communication and teamwork. Microsoft Teams chat was implemented to assist with communication. With the pharmacy team, the lab targeted improving the environmental cultures process. Before this work, the lab was successful in completing cultures only 10% of the time. With the improved communication on when cultures were being started and completed, the lab improved completion to 100%, with no failures.


16 | APRIL 2024 MLO-ONLINE.COM LAB MANAGEMENT :: LAB OF THE YEAR
Blood draw at West Valley Hospital.
Photos Courtesy of Salem Health Laboratories
Salem Health Laboratory staff at Salem Hospital.

Sexual health testing for every body.
Our STI portfolio empowers you with accuracy and trust. So you can serve diverse patient populations and meet your lab’s changing needs – while making the most of your resources.
Learn more and contact your Roche representative, today. usinfo.roche.com/STI
With the infusion and wound clinic, the lab was struggling to ensure that blood product was ready and available for transfusion when the patient had a scheduled appointment. The lab identified that everything was ready for patient care only 70% of the time. Using Teams chat to improve communication, the lab was successful in getting blood products ready for patient appointments 100% of the time. And, while there is a quality component to these projects, they also had a financial impact. All staff quality projects combined saved Salem Health Laboratories over $4 million last year.
Education and training
In 2023, 82% of the laboratory’s leadership positions were filled with internal candidates. Not only does this practice promote career growth within the organization but builds stronger teams. Each new leader on the laboratory’s team participates in a formal leadership training pathway. They receive training in the Lean management system and participate in laboratoryspecific training on the strategic plan, future planning, financial management tools, and high-reliability culture. They also receive support on developing their personnel and how to lead in an area where they may not be the subject matter expert. The outcome of this work is that leaders can successfully support their teams. Leaders that have gone through this process have an easier transition into leadership and they feel supported in their development. As they apply what they learn, their teams experience a better transition without experiencing a significant decline in support because of a new leader.
In 2023, Salem Health Laboratories launched an internal development pathway for all its employees. While some of employees are enrolled in local programs, the lab has leveraged online Medical Laboratory Science programs to help its employees have another pathway for career growth. Employees apply to be part of the formal program, which includes support for flexible scheduling to allow them to attend online classes. It also ensures a place to complete their clinical rotations, as the laboratories partner as a clinic site with the online program. Additional support is given with an assigned mentor, so the student has someone to help them and encourage them to complete their program. The hospital provides test proctoring services, so students can participate in exams. Last fall, the lab welcomed its first three employees into this program.
In addition, all of Salem Health Laboratories routinely host students from local medical laboratory education programs. By rotating them among the laboratories, students see how the different-sized laboratories function similarly and differently. This program also includes preceptor support. Laboratory staff meet with students regularly to get their feedback and to support them as they complete their rotations. Salem Health Laboratories has employed 100% of the students upon completion of their degrees.
Strategic outlook
Improvements in the laboratory are not possible without a strong strategic outlook. As the Salem Health laboratory staff worded it,“We believe it is critical for laboratory staff to know who they are, what they want to become, and to do it well and have fun.” The two primary goals of the strategic plan are to deliver a consistent and highly reliable patient and provider experience that is aligned with and supports the strategic goals for Salem Health Hospitals and Clinics and to develop a team of staff and leaders who have the skillset to support the future of laboratory services.

The laboratory’s strategic plan is built on a foundation of the following characteristics:
• Al igned leadership
• Sta ndard procedures
• Al igned instruments
• Training and competency
• Sha red accreditation
• St aff recruitment and well-being
• St udent program and career pathway
This past year, Salem Health Laboratories realigned all laboratory functions under one leadership structure and all locations now operate together as a single laboratory system, bringing quality and regulatory oversight together. Bringing all laboratory operations together into one structure allowed them to review policies and procedures and align them with shared best practices — spreading these best practices throughout the organization.
This alignment of operations required cooperation. The laboratory leadership team meets weekly to discuss issues and initiatives and to benefit from the combined experience of every member of the team when moving forward. The regular meetings ensure protected time each week to work towards strategic goals. Sometimes they meet for less than 30 minutes and other times longer. This regular forum has become a place for innovation and partnership.
Closing
Medical Laboratory Observer is proud to award the 2024 Lab of the Year to Salem Health Laboratories. Its commitment to providing high-quality laboratory services, continuous improvement, and fostering a culture of teamwork is very impressive and inspiring. When we shared the news with the laboratory, its leadership expressed the following sentiments about this hard-working laboratory in Oregon:
Director, Laboratory Services — Jamie Rouse, MBA-HM, MT(ASCP) — “I am deeply humbled and honored for our lab to be recognized as the 2024 MLO Lab of the Year. This achievement is a testament to the unwavering dedication and hard work of our team. Despite how busy we are, we remain resilient and committed to delivering the highest quality services. I am incredibly proud of each member of our team, and I am grateful for the opportunity to lead such an exceptional group of individuals.”
System Director, Clinical Support Operations — Karl Kamper, MBA, MT(ASCP), FACHE — “I am so proud of the commitment to continuous improvement by our laboratory team. They are excellent. This honor recognizes their hard work, their commitment to our patients and their contributions to Salem Health.”

18 | APRIL 2024 MLO-ONLINE.COM LAB MANAGEMENT :: LAB OF THE YEAR
Salem Health Laboratory staff at Salem Hospital.
Courtesy of Salem Health Laboratories
One big family.
From our extended family of products to your lab family, Happy Lab Week!

Share your lab family photo and get a cell poster.
Scan QR code to upload your photo and find Lab Week ideas and downloads. Sysmex.com/LabWeek

You work together. You laugh together. You’re like family. As you continue to make important contributions to healthcare, take a moment to acknowledge how great (and sometimes weird) your lab family is. And while you’re at it, send us a photo! During Lab Week — and every day — we celebrate everything you do. #LabWeek2024.
©2024 Sysmex America Inc.
Hematology • Hemostasis • Urinalysis • Flow Cytometry • Informatics

2024 Lab of the Year Runner Up Southwest Transplant Alliance Laboratory Services
By Erin Brady
Southwest Transplant Alliance (STA) Laboratory Services is one of MLO’s 2024 Lab of the Year Runner Ups! STA is one of the largest federally designated organ procurement organizations in the United States.
Located in Dallas, Texas, STA’s service area includes 10 hospital transplant centers, over 270 hospitals, 89 Texas counties, and one Arkansas county. They serve a population of more than 10.5 million people, honoring heroic donors, courageous donor families, and those on the transplant waiting list. Over the last 50 years, STA has recovered more than 35,000 organs and saved more than 100,000 people. The laboratory provides timely testing for donors giving the gift of life, including a variety of clinical testing on viability of organs, any infectious diseases, and compatibility testing.
STA’s mission is to save lives through donation. They operate 24 hours a day, 365 days a year and perform over 66,000 specialized tests annually. The laboratory specializes in infectious disease/ serology for organ and tissue donors, chemistry, hematology, urinalysis, coagulation, special chemistry, molecular, NAT, histocompatibility (HLA and ABO), histology, and microbiology. The organization is regulated by Clinical Laboratory Improvement Amendments (CLIA), College of American Pathologists (CAP), Food and Drug Administration (FDA), American Association of Tissue Banks (AATB), and Eye Bank Association of America (EBAA).
Opportunities
STA saw opportunities for improvement in these categories: Discarded organs: Of the 25 expedited cases for 2022 that were reviewed, 92 organs were unable to be transplanted due to time restraints. This resulted in many missed opportunities and discarded organs.

Turnaround time: Lab average turnaround time in 2022 for infectious disease serologies was 7.67 hours, up from an average of 4–6 hours. If there were any repeats, it could take up to 12 hours.
Staff stress: The STA staff performed a lot of hands-on testing with a good deal of manual pipetting, which complicated processes dictated by timers.
User errors: There were user errors due to manual entry of results and lots of paperwork tracking each step.
High costs: For the volume of testing, staffing and reagent costs were high. Several test kits would only have a small part used, resulting in over 400 tests being discarded after two weeks.
2023 accomplishments
STA’s laboratory aims to minimize the testing turnaround time, providing more opportunities to save lives through organ donation. In 2023, they accomplished that goal by improving turnaround time (TAT) and confidence in the lab’s TAT. They decreased the stress on their staff resulting in improvements in staff satisfaction. This led to reduced costs and errors.
20 | APRIL 2024 MLO-ONLINE.COM LAB MANAGEMENT :: LAB OF THE YEAR
STA LAB Team. Photos Courtesy of STA


Specifically, STA validated the following specialties:
• Human leukocyte antigens (HLA) typing
• Hematology
• Coagulation
• D iasorin Liaison brought in and validated 9 assays
• Epredia Cryostat validated for frozen sections
• Chagas blood test
• 3 new EPOC blood gas analyzers validated for use in the donor care unit
• M icrobiology - blood cultures validated to reduced TAT and recipient outcomes
STA said the implementation of the Diasorin Liaison XL made the biggest impact in their laboratory. STA was doing all testing manually and wanted a platform that could perform all their organ serology testing needs.
Southwest Transplant Alliance saved $297,000 in 2023 on reagents and hands-on tech time after switching to an automated platform. An additional $110,000 was saved by internalizing coagulation, hematology, and microbiology.
Three of STA’s strategic goals are to create a culture of joy, act as a catalyst for donation, and be a center of excellence. They achieved CAP accreditation in 2023. They lowered organ donor serology testing from 7.67 hours to about 37 minutes! To accomplish this, they separated organ donor testing from tissue donor testing. Doing this resulted in the opportunity to save more lives.
Employee training and updates to policies reduced sample hold times down to 15 in November versus more than 50, 3% holds versus an average of 16%. To remove identical orders, an LIS rule was written. Another improvement was made to the ABO subtyping workflow, allowing for better outcomes for transplant recipients. To decrease errors, the report structure


was changed to match documentation formatting in the donor record. Three new IQCPs were put into action, resulting in cost savings and increased staff satisfaction. In addition, employee engagement action plans were implemented, increasing engagement scores in nearly every category.
Teamwork
STA has five core values: passionate, selfless, trustworthy, collaborative, and creative. The following departments collaborated to accomplish STA’s 2023 goals: Finance, Leadership, Project Management, Facilities, Quality, Education, Information Technology, Clinical, and the external LIS Admin teams.
To help create a culture of joy, they introduced a new automated platform to replace manual testing. STA said, “The burden on the staff has been significantly reduced, allowing them to focus on other critical areas in the laboratory. This has not only resulted in increased efficiency, but also mitigated the risk of human error. Manual testing requires extensive attention to detail, concentration, and dexterity. The pressure to avoid errors and ensure accurate results can be overwhelming, causing high stress levels that can impede productivity and even compromise the quality of testing. The new platform has successfully eliminated much of the burden faced by the staff. As a result, the staff can allocate their time and expertise to other crucial aspects of the laboratory operations.”
STA saved $142,598.82 on their annual reagent costs and had a 92% turnaround time improvement on their infectious disease assays. The decrease in turnaround time led to staff confidence, which leads to employee satisfaction and retention. In addition, these improvements open doors to countless opportunities for hope and healing.
MLO-ONLINE.COM APRIL 2024 | 21 LAB MANAGEMENT :: LAB OF THE YEAR
Skills Fair 2024.
Southwest Transplant Alliance Dallas, TX.
The campus was designed around a 100-year-old oak tree that anchors the donor memorial garden. The memorial garden is a tribute to every donor, their family, and every transplant recipient.
STA COO Doug Butler, with Lab Director Selena Warden and CEO Brad Adams.
Photos Courtesy of STA


2024 Lab of the Year Runner Up Wisconsin Diagnostic Laboratories
By Erin Brady
Wisconsin Diagnostic Laboratories (WDL) is one of the recipients of MLO’s 2024 Lab of the Year Runner Up Awards! WDL is located in the Milwaukee Regional Medical Center but operates independently while being owned by Milwaukee-based organization, Froedtert Health. They are the main laboratory for this 735-bed teaching hospital and the only Level-1 adult trauma center in Southeastern Wisconsin. They perform over 6.5 million tests each year.
Customer service
WDL uses the My MOMENT and AIDET customer service guidelines. Each department is accountable for their customer service, but the WDL Client Services department handles over 100,000 customer calls a year and provides 24/7/365 support to Froedtert Health. Client Services launched the “Epic Cheers Customer Relations Management (CRM) system.” This system optimizes workflow by documenting customer calls and concerns in a more formalized, standardized, and centrally captured way. It was designed by WDL staff and will help improve customer experience by identifying issues.
Other notable customer service achievements from different departments at WDL included:
• I n the past year, over 240,000 specimens were collected by the Phlebotomy and Long-Term Care Services Department.
• M aking sure multiple locations have adequate staff.
• Resolving conflict the first time.
Another example of WDL’s customer service is their Anatomic Pathology department introducing oncology panels. Now, patients with advanced disease have the chance to get novel molecularly targeted treatments.
One of WDL’s valued customers, Froedtert’s Cancer Center and Transplant Services, said,“Without our partnership with WDL we would be unable to provide our essential services to the community.”
Productivity and teamwork
The WDL team achieved ISO 15189 Accreditation through the College of American Pathologists in June 2023. WDL says one of the keys to their success in productivity is,“That every department has a Leadership Team with the authority and support to manage their own resources and the flexibility of decentralized decision-making. This structure has led to consistent and numerous operational achievements, which are then presented by each Department Leader at the annual Operational Excellence meeting.”
The Anatomic Pathology department expanded its IHC menu by 35 new strains. They also grew the number of stains within Histology cases by 40%. This led to a turnaround time decrease of 25 hours! Their Blood Bank also reduced turnaround time by bringing in Grifols antisera. The Chemistry and Toxicology Departments also got a technology upgrade. They replaced the Roche Cobas 6000 modular system with the Roche Cobas Pro. This reduced instrument maintenance.


22 | APRIL 2024 MLO-ONLINE.COM LAB MANAGEMENT :: LAB OF THE YEAR
Courtesy of WDL
WDL all staff photo.
Always one step ahead.
• Liquid, ready-to-use
• Superior stability
• Fast, reliable results



Enhance efficiency with our robust liquid, ready-to-use reagents. Central to Werfen’s total Hemostasis testing solution, our comprehensive line of HemosIL reagents deliver superior onboard stability and fewer manual steps—from routine to specialty testing. Other key components include ACL TOP® Family 50 Series systems with automated pre-analytical sample integrity checks, and HemoCell Specialized Lab Automation, designed specifically for the automation of Hemostasis testing. Rely on HemosIL reagents for improved laboratory efficiency—for better patient care.
Simply efficient.
For more information, contact your local Werfen representative. werfen.com
Hemostasis Innovation is Here.
ACL, ACL AcuStar, ACL TOP, HemosIL, ReadiPlasTin, RecombiPlasTin, SynthAFax and SynthASil are trademarks of Instrumentation Laboratory Company and/or one of its subsidiaries or parent companies and may be registered in the United States Patent and Trademark Office and in other jurisdictions. The Werfen logo is a trademark of Werfen and may be registered in the Patent and Trademark Offices of jurisdictions throughout the world. ©2021 Instrumentation Laboratory. All rights reserved.

When faced with supply shortages, an Inventory Specialist was hired for Microbiology and Molecular Diagnostics. The Cytogenetics department reduced staff shortages and burnout by modifying workflows. Impressively, the Billing Team recovered over $430,000 in lost revenue.
Other 2023 team accomplishments:
• Internal audit program administered to track risks and prevent failures.
• MediaLab was launched to monitor nonconforming events.
• Ac ross all laboratory services, key performance metrics were reviewed and standardized.
• Th rough the launch of new policies and procedures, noncompliant documents in the lab were significantly reduced, including those in PolicySTAT.
• Flow Cytometry went from 8-color to 12- color antibody panels reducing reagent costs, the amount of sample needed, and processing time.
work in specimen processing. WDL visits local high schools to help teach students about the laboratory profession. One of WDL’s laboratory members, Clinical Laboratory Utilization Specialist, Kathryn Golab, MLS(ASCP)CMSH(ASCP) CM, is also a board member at large at the Healthcare Career Academy with Menomonee Falls High School. WDL said, “This allows laboratory input into the curriculum for high school students who plan to go into a healthcare related field after high school. Upon her integration into the board, several graduating senior students have declared an MLS/MLT major going into college.”
For students completing their MLS/MLT degrees, WDL provided clinical site opportunities for the University of Wisconsin-Milwaukee, Marquette University, and the Milwaukee Area Technical College. In fall of 2023, WDL offered ten clinical spots to students, following thirteen in fall of 2022.
To combat staffing shortages, WDL Executive Director, Mike Baron, created a virtual WDL Laboratory Collaborative. The collaborative connects laboratories, so they can share their strategies for staff recruitment. Baron also initiated another way for individuals to complete certification. Specifically, the Anatomic Pathology Department incorporated an apprenticeship opportunity where Laboratory Technical Assistants (LTA) work to obtain eligibility for histology certifications. In 2023, three staff members achieved certification and more will be eligible to take the exam in 2024.

• Long Term Care and Phlebotomy Services simplified the management of their vehicle fleet with eMV. The new electronic system gives WDL a direct connection to the DMV for automated notifications regarding vehicle registration renewal. WEX fuel cards were allotted to each vehicle’s VIN so team members could use different vehicles.
• The Chemistry Team and the Beaker team worked together to introduce 158 IT improvements, including auto-verification for blood gases and a new generation of AST and ALT that prevents falsely low enzyme activity in patients with Vitamin B deficiency.
• The WDL 6 Reference Testing Team and the MCW Department of Pathology Medical Section Directors conduct a yearly review of all reference testing, resulting in patients saving more than $90,000.
Education and training
WDL endorses the education of their employees and community, raising awareness of jobs in the laboratory. Last academic year, they partnered with Cristo Rey High School to provide internship opportunities for their students. Five students participated in the internship program last year and got to
Strategic outlook
Department managers at WDL develop “operational excellence plans” for their teams. Some of the goals include improving customer service, employee wellness, teamwork, quality, and supporting technical advancement. They plan to expand on programs already implemented, like their Education Collaborative, their non-conforming event process, and Atalan- an Access-to-Access Lab Network.
Matthew Long, Third Shift Laboratory Operations Manager, Wisconsin Diagnostic Laboratories said, “While labs across the nation are struggling to keep their doors open, WDL Team Members have found a way to normalize excellence…to make the extraordinary feel ordinary.”












Management OF DUSTRY ta ta NNOV Bork aging meriP 24 | APRIL 2024 MLO-ONLINE.COM LAB MANAGEMENT :: LAB OF THE YEAR
WDL Anatomic Pathology Technologist examining specimen.
WDL 3rd Shift Team.
ISO Quality Team- Lauren Otter, Alyssa Thomaschek, Mike Baron, Kate Jacoby, Gilberto Cruz, Titi Tieu.
Photos Courtesy of WDL














































































































































Management Source for Lab Professionals since 1969 No 3 OF DUSTRY VATOR owski MD and Medical Director ath, Central Florida of Excellence PLUS Qualit d control merging FREE MAGAZINE SUBSCRIPTION! 9 Issues Plus the annual Clinical Laboratory Reference guide. WEBSITE mlo-online.com MAGAZINE mlo-online.com/subscribe NEWSLETTERS Sign up for monthly updates FACEBOOK MLOMedicalLaboratoryObserver X (FORMERLY TWITTER) @MedicalLabMLO LINKEDIN medical-laboratory-observer Scan Here to Subscribe to our FREE Magazine

Transforming infection detection with the CBC-Diff
By Melissa Naiman, PhD, EMT-B and Ahmed Bentahar, MD, PhD
In a world overpopulated by pathogens, the human immune system has evolved to protect against pathogens that are, themselves, continually evolving. Host immune response to infection refers to the dynamic process that maintains the delicate balance between effective pathogen clearance and minimizing damage to the host tissues that allows the body to recognize and fight infections. However, when the system becomes dysregulated, overreacting to invaders, it can lead to sepsis, septic shock, and ultimately death.
With nearly 50 million yearly global cases of sepsis and 11 million sepsis-related deaths,1 the need for diagnostic tests that quickly identify infection and immune dysregulation is obvious. This clinical need has inspired significant innovations over the past decade, which are now emerging as regulatory-cleared diagnostic products and solutions.
Innate immunity diagnostics:
Targeting the first line of defense
The host immune response is a diverse, complex, and dynamic defense system that plays a crucial role in protecting the body against infectious agents. When an infection occurs, the immune system is activated to identify and eliminate the pathogen. This response involves coordinated efforts between innate and adaptive immune components, as well as various immune cells, molecules, and signaling pathways, working together for an effective defense.
Each of these components, to varying degrees, could serve as diagnostic targets for the presence of infection and/or indicate infection severity. Based on these diagnostic targets, multiple tests have been developed, such as those in Table 1
One of the challenges in implementing these tests is that they require an additional order when there is diagnostic
26 | APRIL 2024 MLO-ONLINE.COM INFECTION DIAGNOSTICS :: COMPLETE BLOOD COUNT WITH DIFFERENTIAL
Photo: Beckman Coulter
uncertainty or suspicion of sepsis. However, many patients present to the emergency department (ED) with vague signs and symptoms that do not align with sepsis screening criteria. In a study of over 2,100 ED patients that ultimately developed sepsis within 12 hours of presentation, 33% did not meet SIRS criteria and 88% did not meet qSOFA criteria.2 Accordingly, for these tests to aid in sepsis management, they would need to be performed routinely during triage and provide useful insights to support clinical decisions. For example, MeMed BV rapidly and accurately discerns bacterial from viral infections in suspected sepsis patients,3 potentially leading to earlier initiation of appropriate care in the ED. One of the challenges in implementing these tests, however, is that they require an additional order when there is diagnostic uncertainty or suspicion of sepsis.
One of the first and most commonly ordered tests in the ED is the complete blood count with differential (CBC-diff).
One of the first and most commonly ordered tests in the ED is the complete blood count with differential (CBC-diff).4–6 Significant advances in hematology analyzers have expanded its capabilities so that the tried-and-true technique can be applied to enhance severe infection screening.
White blood cell activation
The automated differential is a cornerstone of modern medicine. In the context of host immune response, an abnormal white blood cell count is among the first signals of infection and immune dysregulation in many clinical scenarios. Absolute count and percentages of the five normal blood cell types provide a wealth of clinical insights. High band counts (immature neutrophils) and elevated immature granulocyte levels can signal severe infection. The neutrophil to lymphocyte ratio (NLR) is recognized as a marker for infection and inflammatory stress indicative of severe illness. Absolute count and percentages of metamyelocytes, myelocytes, and promyelocytes suggest immune response to bacterial illness.
More recently, some hematology analyzers have introduced enhanced volume measurements, permitting automated assessment of morphological characteristics. For example, monocyte distribution width (MDW) is a regulatory-cleared
TestMeasures
MeMed
BV® C-Reactive Protein (CRP), Tumor Necrosis Factor (TNF)-Related Apoptosis-Inducing Ligand (TRAIL), and Interferon Gamma-Induced Protein 10 (IP-10) levels
FebriDx®CRP and Myxovirus Resistance Protein A (MxA)
hematological parameter that measures variation in monocyte size.7 MDW values of ≥20 (K2EDTA) or ≥21.5 (K3EDTA) are associated with a higher risk of developing sepsis within the first 12 hours of hospital admission. MDW elevation is pathogen agnostic,8 meaning that it will respond similarly to bacterial, viral, and fungal agents. Interpreting MDW in the context of other leukocyte parameters can enhance diagnostic accuracy. For example, many studies have demonstrated strong diagnostic performance of elevated MDW and abnormal WBC as compared with any single leukocyte parameter.9–11 In one study, patients with elevated MDW, abnormal WBC count, and elevated NLR were 12 times more likely to develop sepsis and 9.3 times more likely to develop septic shock.12
Sepsis, like many serious conditions, often presents with vague symptoms, but without prompt treatment, septic patients can rapidly deteriorate. Thus, identifying and validating novel biomarkers to assist in accurate disease diagnosis is important to help in early sepsis detection and timely treatment. Using MDW, abnormal WBC count, and NLR in combination has shown superior diagnostic performance over any single parameter, including among patients who presented to the ED without overt sepsis symptoms.13,14
Maximize clinical insight, minimize microscopy
Like monocytes, each white blood cell type undergoes specific morphological and functional changes during the host immune response. Neutrophils increase in number and, in some severe infections, can present cytoplasmic toxic granules and vacuoles, eosinophils show increased cytoplasmic vacuolization, and monocytes, in addition to changing in size, show large coalescing cytoplasmic vacuoles that can be visualized under light microscopy.15,16 However, conducting a manual review to identify these features is too time consuming for routine clinical screening or as part of emergent care.15,16 The advent of digital hematology systems have provided the power to review, detect, and identify cells in full context with AI-powered image recognition and clinical decision support technology without reverting to the microscope.17,18
Differentiates
Bacterial (and bacterial co-infections) from viral infections
Automated hematology analyzers will never fully replace manual slide review. Manual review is still required to fully characterize cell abnormalities and establish whether these abnormalities are likely associated with infection or some other cause. However, recent advances in digital hematology will minimize microscope time and enable streamlined slide review. And hematology automation innovations introduced by companies such as Scopio® provide integrated hardware and software solutions to streamline the transition from automatic differential to manual review.
Bacterial infections from non-bacterial infections
SeptiCyte® Four genes using real time RT-qPCRSIRS from sepsis in critically ill adults
The next generation of digital pathology imaging incorporates larger fields of view in high resolution, as well as AI decision support and off-site reviews. For example, the Scopio Lab Full-Field Peripheral Blood Smear ®
MLO-ONLINE.COM APRIL 2024 | 27 INFECTION DIAGNOSTICS :: COMPLETE BLOOD COUNT WITH DIFFERENTIAL
Table 1. Tests that differentite infection and infection severity.
application provides a view of all clinically relevant areas of the blood smear, including the monolayer and feathered edge, at 100X magnification. This configuration supported remote viewing for a tertiary medical center hematology division that reduced turnaround time while maintaining overall workload and clinical quality. Retrospective analysis of 10,704 peripheral blood smear samples were analyzed pre- and post-implementation over a 5-month period. Incorporating effective remote viewing, where pathologists were able to conduct satisfactory peripheral blood smear slide review from home, resulted in an overall 15.8% reduction in turnaround time for the entire lab.
These capabilities could provide a new opportunity to evaluate additional aspects of white blood cells to determine the presence and severity of infection. As AI cell typing matures, the opportunities for assistance in cell classification, disease identification, and response to therapies will grow.19,20
Conclusion
Continued study of the intricacies of the host response to infection is facilitating novel diagnostic strategies to identify disease presence and severity using results from the CBC-diff and other blood biomarkers. These advances are changing diagnostics, providing opportunities to improve routine clinical care and give clinicians valuable tools to quickly identify infections and immune dysregulation, leading to improved patient outcomes. Diagnostic tests that measure host immune response biomarkers have shown promise for earlier sepsis detection as well as in differentiating between bacterial and viral infections. Additionally, advances in hematology analyzers, including enhanced volume measurements and AI-powered image recognition, allow for more accurate and efficient blood analysis. The integration of AI support in digital hematology imaging with CBC-diff results and other patient information holds great potential for further advancements in cell classification and disease identification— all with less than 0.5 mL of blood.
By leveraging these evolving complementary technologies, discovering how they can be combined and protocolized and adopting future innovations as they become available, healthcare professionals can effectively triage, detect, and intervene, to deliver a higher standard of care in the battle against infections, from common colds to septic shock.
REFERENCES
1. Sepsis. Who.int. Accessed March 4, 2024. https://www.who.int/ health-topics/sepsis.
2. Crouser ED, Parrillo JE, Martin GS, et al. Monocyte distribution width enhances early sepsis detection in the emergency department beyond SIRS and qSOFA. J Intensive Care. 2020;5;8:33. doi:10.1186/ s40560-020-00446-3
3. Angel A, Eden E, Avioz NZ, Gottlieb T, Navon R. 161 A host response test (MMBV) for differentiating between bacterial and viral infection has potential to improve antibiotic stewardship in patients with suspected sepsis. Ann Emerg Med. 2023;82(4):S72-S73. doi:10.1016/j. annemergmed.2023.08.183.
4. Young GP. CBC or not CBC? That is the question. Ann Emerg Med 1986;15(3):367-371. doi:10.1016/s0196-0644(86)80587-x.
5. Rui P, Kang K. National Hospital Ambulatory Medical Care Survey: 2017 Emergency Department Summary Tables. U S Census Bureau 2017;2017(37).
6. Barnes PW, McFadden SL, Machin SJ, Simson E, international consensus group for hematology. The international consensus group for hematology review: suggested criteria for action following automated CBC and WBC differential analysis. Lab Hematol. 2005;11(2):83-90. doi:10.1532/LH96.05019.
7. Crouser ED, Parrillo JE, Seymour C, et al. Improved early detection of sepsis in the ED with a novel monocyte distribution width biomarker. Chest. 2017;152(3):518-526. doi:10.1016/j.chest.2017.05.039.
8. Piva E, Zuin J, Pelloso M, et al. Monocyte distribution width (MDW) parameter as a sepsis indicator in intensive care units. Clin Chem Lab Med. 2021;59(7):1307-1314. doi:10.1515/cclm-2021-0192.
9. Crouser ED, Parrillo JE, Seymour CW, et al. Monocyte distribution width: A novel indicator of Sepsis-2 and Sepsis-3 in high-risk emergency department patients. Crit Care Med. 2019;47(8):1018-1025. doi:10.1097/CCM.0000000000003799.
10. Hausfater P, Robert Boter N, Morales Indiano C, et al. Monocyte distribution width (MDW) performance as an early sepsis indicator in the emergency department: comparison with CRP and procalcitonin in a multicenter international European prospective study. Crit Care 2021;25(1):227. doi:10.1186/s13054-021-03622-5.
11. Poz D, Crobu D, Sukhacheva E, et al. Monocyte distribution width (MDW): a useful biomarker to improve sepsis management in Emergency Department. Clin Chem Lab Med. 2022;60(3):433-440. doi:10.1515/cclm-2021-0875.
12. Malinovska A, Hinson JS, Badaki-Makun O, et al. Monocyte distribution width as part of a broad pragmatic sepsis screen in the emergency department. J Am Coll of Emerg Physicians Open 2022;3(2):e12679. doi:10.1002/emp2.12679.
13. Hinson JS, Sarani N, Smith A, et al. A-155 Unlocking the complete blood count: derivation of a single-panel laboratory test that includes monocyte distribution width to create a universal sepsis screening tool. Clin Chem. 2023;69(Supplement_1). doi:10.1093/clinchem/ hvad097.140.
14. Hinson J, Sarani M, Smith A, Badaki-Makun L, Malinovska A, Levin S. Unlocking the CBC: Derivation of a Single-Panel Laboratory Test That Includes Monocyte Distribution Width to Create a Universal Sepsis Screening Tool. In: Wiley; 2023. Accessed December 13, 2023. https:// onlinelibrary.wiley.com/toc/15532712/2023/30/S1.
15. Zonneveld R, Molema G, Plötz FB. Analyzing neutrophil morphology, mechanics, and motility in sepsis: options and challenges for novel bedside technologies. Crit Care Med. 2016;44(1):218-228. doi:10.1097/ CCM.0000000000001266.
16. Pozdnyakova O, Connell NT, Battinelli EM, et al. Clinical significance of CBC and WBC morphology in the diagnosis and clinical course of COVID-19 infection. Am J Clin Pathol. 2021;155(3):364-375. doi:10.1093/ ajcp/aqaa231.
17. Katz B-Z, Benisty D, Sayegh Y, Lamm I, Avivi I. Remote digital microscopy improves hematology laboratory workflow by reducing peripheral blood smear analysis turnaround time. Appl Clin Inform 2022;13(5):1108-1115. doi:10.1055/a-1957-6219.
18. Katz B-Z, Feldman MD, Tessema M, et al. Evaluation of Scopio Labs X100 Full Field PBS: The first high-resolution full field viewing of peripheral blood specimens combined with artificial intelligence-based morphological analysis. Int J Lab Hematol. 2021;43(6):1408-1416. doi:10.1111/ijlh.13681.
19. Walter W, Pohlkamp C, Meggendorfer M, et al. Artificial intelligence in hematological diagnostics: Game changer or gadget? Blood Rev 2023;58:101019. doi:10.1016/j.blre.2022.101019.
20. Walter W, Haferlach C, Nadarajah N, et al. How artificial intelligence might disrupt diagnostics in hematology in the near future. Oncogene 2021;40(25):4271-4280. doi:10.1038/s41388-021-01861-y.

Melissa Naiman, PhD, EMT-B serves as a Medical Director for Sepsis and Host Response at Beckman Coulter Diagnostics . She holds a Master of Science in Forensic Science and a PhD in Public Health from the University of Illinois at Chicago. Prior to coming to Beckman Coulter, Dr. Naiman spent most of her career in an academic research center for science and technology developing medical devices and diagnostics, including identifying novel biomarkers for military health applications.

Ahmed Bentahar, MD, PhD is a clinical pathologist with more than 30 years of experience in the fields of hematology and laboratory medicine. For the past 33 years, he served as a hematology product specialist, hematology product manager, staff applications scientist, senior manager of global scientific marketing, and Medical Director at Beckman Coulter. Dr. Bentahar received his MD and PhD from État de Liège University, Belgium. Dr. Bentahar has earned international recognition as a respected thought leader and uniquely qualified facilitator of hematology industry seminars, workshops, and congresses.
28 | APRIL 2024 MLO-ONLINE.COM INFECTION DIAGNOSTICS :: COMPLETE BLOOD COUNT WITH DIFFERENTIAL
Find the right test, for the right patient, at the right time with our FDA-cleared assays and expanding test menu.

Healthcare-Associated Infections
Simplexa® Candida auris Direct Kit (In Development)1
Simplexa® C. difficile Direct Kit
Respiratory
Simplexa® Bordetella Direct Kit
Simplexa® COVID-19 Direct Kit FDA Cleared
Simplexa® COVID-19 & Flu A/B Direct Kit FDA Cleared
Simplexa® Flu A/B & RSV Direct Gen II Kit
Simplexa® Group A Strep Direct Kit
Simplexa® SARS-CoV-2 Variants Direct Kit (RUO)2


Herpes Viruses
Simplexa® HSV 1 & 2 Direct Kit (Swab)
Simplexa® VZV Swab Direct Kit
Meningitis/Encephalitis
Simplexa® HSV 1 & 2 Direct Kit (CSF)
Simplexa® VZV Direct Kit (CSF)
Women’s/Neonatal Health
Simplexa® Congenital CMV Direct Kit
Simplexa® GBS Direct Kit
Test VERIGENE® Gram-Negative Blood Culture Test
VERIGENE® Gram-Positive Blood Culture Test
VERIGENE® Respiratory Pathogens Flex Test
and syndromic molecular solutions for clinical utility based
your
Targeted
on
patient testing
Enteric Pathogens
VERIGENE®
For In Vitro Diagnostic Use. Products are region specific and may not be approved in some countries/regions. 1. This assay is under development and not currently FDA cleared for IVD use. 2. RUO - This product is for Research Use Only. Not for use in diagnostic procedures. Simplexa, LIAISON MDX, and the associated logos are all trademarks or registered trademarks of DiaSorin Molecular LLC, or its affiliate, in the U.S. and/ or other countries. VERIGENE is a trademark of Luminex Corporation, registered in the US and other countries. ©2024 DiaSorin Molecular LLC. All rights reserved. ©2024 Luminex Corporation. All rights reserved. To learn more, please visit us at bit.ly/diasorin-molecular-diagnostics PRTA681702.0124
w: diasorin.com e: cs.molecular@diasorin.com MOLECULAR SOLUTIONS

The role of training in error prevention for clinical laboratory professionals
By Stephen Bishop, MBA, MS, CLS, MLS(ASCP)CM, CPHQ
Every day, clinical laboratory professionals stand at the vanguard of patient safety by ensuring that errors in laboratory testing are either prevented or identified and managed. Errors in the clinical laboratory testing process can have serious consequences. The ramifications in delayed interventions for sepsis patients and stroke patients can be devastating. Inappropriate treatments can cause undue harm and expense, and not just from a financial position — some expenses cannot be measured, such as decreased trust in the health system. Regardless of the scenario, errors in laboratory testing can compromise the reliability of diagnostic information, leading to erroneous conclusions or ineffective therapeutic interventions. Clinical laboratory leaders can enhance error prevention by strengthening their team’s onthe-job training through elevating personnel competency and cultivating a culture of continuous improvement.
Competency assessment versus attainment
Clinical laboratory leaders should be acquainted with the CLIA (Clinical Laboratory Improvement Amendments) guidelines for competency assessment for laboratory personnel. Initially, competency must be assessed upon hiring or assignment to new testing procedures. This typically occurs after initial “on the job” training. Ongoing assessment is required
at six months for new personnel, and then subsequently, competency is assessed annually for all employees. Additionally, competency assessments should occur whenever significant changes in laboratory procedures, methodologies, or instrumentation take place. Furthermore, prompt assessment is necessary if performance problems or errors are identified. These guidelines ensure that laboratory personnel remain competent and proficient in their roles, promoting the quality and reliability of laboratory testing processes.
Regardless of the interval (initial, six months, etc.), the six elements of the CLIA competency assessment must be present. Firstly, direct observation of routine patient test performance ensures personnel can proficiently conduct testing procedures correctly. Secondly, monitoring the recording and reporting of test results verifies adherence to standard operating procedures and regulatory requirements. Thirdly, reviewing test results, proficiency testing performance, and quality control records assesses personnel’s ability to manage results and maintain quality standards. Fourthly, direct observation of instrument maintenance and function checks confirms personnel’s competence in instrument upkeep and troubleshooting. Fifthly, assessment of problem-solving skills evaluates personnel’s ability to identify and resolve issues effectively. Finally, evaluating basic knowledge through written exams or
30 | APRIL 2024 MLO-ONLINE.COM EDUCATION :: COMPETENCY ASSESSMENT
Hispanolistic/E+/Getty Images
oral assessments ensures personnel possess the foundational understanding required for safe and competent performance. These elements collectively provide a baseline framework for assessing the competency of laboratory personnel.
Attaining competency encompasses the acquisition of skills and knowledge, while assessing competency involves evaluating the extent to which those skills and knowledge have been acquired and can be effectively applied. Clinical laboratory leaders are now faced with a challenge because current CLIA standards for competency assessment do not necessarily address the complexities of clinical decision making. CLIA merely defines how competency should be assessed, as opposed to how competency should be attained. The CLIA six elements do not provide laboratory leaders with a roadmap for attaining competency, which is a crucial aspect of error prevention. Complexities in clinical decision making are ever more present, so every laboratory professional, regardless of their role, should attain competencies that address the intricacies associated with their particular work.
Elevating personnel competency
Methods for attaining competency should be a joint effort from the laboratory medical director, administrative leaders, and technical leaders in the laboratory. It also takes significant input from experienced team members from all roles. Engagement and collaboration from all are essential. Clinical laboratory personnel should be taught and trained to analyze situations critically by recognizing patterns and identifying deviations from expected results that may indicate an error. Additionally, they should learn how to troubleshoot problems systematically, employing logical approaches to isolate and address the root causes of errors.
Phlebotomists and pre-analytic staff should be trained to think critically about various tests and the requirements of those tests. For example, during my phlebotomy training program, my clinical instructor required students to know which tests could be performed on corresponding tube types based on the anticoagulant present in the tube. Various tests would be listed off by the instructor, and the students needed to know if the hepatitis panel could be performed on the same specimen as the CMP (comprehensive metabolic panel). This of course corresponded to the tests and specimen types that were validated on the instrument, so this was laboratory specific to an extent. On the surface, this may appear to be a great deal of work, but ultimately, the phlebotomist becomes empowered to make appropriate decisions regarding use of tubes, which can minimize errors where specimens are received and accessioned into the laboratory for analysis.
One way that the testing personnel can attain competency is through the use of scenario-based training. This is especially true in trauma and emergency blood banking situations. Once baseline blood banking competency has been attained, laboratory leaders can create scenarios to mimic the pressures of real-life situations to better equip the trainees. For instance, the blood bank can call a mock trauma, using the phones and/or alarms, and run through scenarios such as preparing and modifying blood products while timing the trainees. Time standards can be set for the completion of coolers or trauma packs.
While performing the tasks necessary to complete the cooler, the trainees may also be given “unknown” factors, such as repeated phone calls asking for the status of the blood products, or a notification that the ED is unable to send a runner to pick up the blood. These types of scenarios can allow trainees to develop
critical thinking skills under pressure, where the likelihood of errors occurring increases. Following the training scenario, it is important to debrief each scenario with the trainee, offering both positive and constructive feedback on their performance. In every case, and for every role, laboratory leaders can deploy scenario-based training as a means to prevent errors, especially when personnel are under pressure.
Leading the change to job integration
The relationship between training and a culture of continuous improvement is essential to error prevention in the clinical laboratory. Routine training not only equips laboratory personnel with the necessary knowledge and skills to perform their duties accurately and efficiently, but also instills a culture of continuous improvement. In a culture of continuous improvement, laboratory personnel are enabled to seek out opportunities for growth, actively participate in training programs, and apply new insights and best practices to their work. This continuous cycle of learning, feedback, and adaptation enhances personnel competency, promotes critical thinking and problem-solving skills, and fosters a proactive approach to quality assurance. Personnel who are supported with tools and resources to continuously improve are better equipped to identify and mitigate potential sources of error, which enhances the reliability and integrity of the laboratory testing process.
However, shifting the mindset of training from a single event to a fully integrated aspect of one’s job demands focused planning and execution. Leaders play a crucial role in communicating the value of continuous learning, emphasizing its importance in achieving organizational objectives and its role in error reduction. By aligning training initiatives with the laboratory’s strategic goals, leaders provide employees with a clear understanding of how their learning efforts contribute to overall success. Integration of training into daily work processes is essential and is achieved through methods such as incorporating training modules into onboarding processes or scheduling regular learning sessions. Through these efforts, laboratory leaders can cultivate a culture of continuous improvement, driving error reduction in laboratory operations.
Final remarks
The consequences of errors in the total testing process can be severe and the complexities of clinical decision making create more opportunities for errors to occur. As a means to prevent errors, laboratory professionals should be trained to think critically, especially under pressure. This luxury can empower the laboratory team to provide clarity in the midst of complexity. Additionally, laboratory leaders should work to empower their personnel to continuously improve their skills. Training is a cornerstone of continuous improvement and clinical laboratory leaders can cultivate team members that are vigilant, responsive, and committed to error prevention. By enriching personnel competency attainment and fostering a culture of continuous improvement, clinical laboratory leaders can strengthen their laboratory’s error prevention efforts and amplify the integrity of the laboratory testing process.

Stephen Bishop, MBA, MS, CLS, MLS(ASCP)CM, CPHQ is currently the Director of Laboratory Services at Dignity Health California Hospital Medical Center, located in downtown Los Angeles, CA. Stephen is passionate about healthcare leadership, clinical laboratory education, and process improvement.
MLO-ONLINE.COM APRIL 2024 | 31 EDUCATION :: COMPETENCY ASSESSMENT
How addressing bullying in medical labs will improve overall retention
By Alex Mitchell
It is well established that medical laboratories continue to face an unprecedented staffing crisis that is putting a strain on patient care and healthcare systems across the country. While this shortage is being driven by several factors, including an aging workforce, a lack of training programs, and a significant demand for lab services, these factors are also combining to create increasing anecdotal reports of bullying.
“This issue of bullying or creating less than welcoming work environments in healthcare is not unique to labs, but it is a problem we’re hearing more and more about from the professionals we work with and is something we feel has been underreported,” said Jon Harol, President of Lighthouse Lab Services, a Charlotte, North Carolina–based laboratory management, recruiting, and consulting firm.
Last fall, Harol and Lighthouse conducted an informal poll inviting lab professionals to weigh in on whether they’ve ever witnessed or personally experienced bullying in the lab during their careers.
Out of 341 total respondents, 75 percent said bullying in the lab is a real concern. Just 14 percent said they have never experienced bullying, while the remaining 11 percent said they were unsure. See Figure 1.
This response, combined with continued reports of burnout and dissatisfaction, is an obvious thorn in the efforts of labs to increase the long-term recruitment pipeline while improving the retention of their existing employees. However, by acknowledging and addressing these concerns head-on, labs can be part of the solution to building a more sustainable future for the patients they serve.

Existing concerns
As part of Lighthouse’s 2023 annual survey of wages and morale among laboratory professionals, the dual issues of limited staffing and stagnating compensation routinely were cited by respondents as the chief reasons for dissatisfaction with their careers. But a majority of the 1,062 respondents (52 percent) also said they are overworked relative to the responsibilities of their role, which in turn creates friction between bench-level employees and managers.
The hierarchical structure of labs and healthcare systems in general contributes to the prevalence of bullying, according to some survey respondents who chose to leave follow-up comments. Subordinates may be afraid to report incidents due to concerns about retaliation, damaging their career prospects, or simply not being taken seriously. The culture of silence surrounding instances of bullying perpetuates the problem, allowing it to fester and persist.
“It’s very difficult to get decent supervisors who will work the bench, which helps with morale,” reported one season tech, who asked to remain anonymous. “A bad manager can take a good staff and destroy it, causing the best employees to flee and the remainder to lose all motivation.”
Others cited a lack of communication from their managers regarding administrative changes that caused their working relationships to deteriorate.
“Our managers don’t relay anything from management or nursing and that fails to create a harmonious spirit,” another lab professional responded.
Another form of bullying cited by some lab professionals is lateral violence, which involves colleagues attacking each other, most often with verbal or emotional abuse. This behavior can manifest in various ways, from condescending remarks and gossip to workplace sabotage and exclusion.
However, while such behaviors are a concern in medical labs and must be addressed, many are quick to point out that these problems exist across the spectrum in healthcare settings and are not unique to the laboratory setting. According to a 2021 Joint Commission report, 44 percent of nursing staff members report having been bullied in a healthcare setting.
Rick Panning, Senior Healthcare Consultant for ARUP Laboratories, said in response to the Lighthouse poll that while he believes bullying exists in labs, those examining the issue must be careful not to generalize or overstate the problem.
“I think a lot of the issue has to do with the example set by leadership,” Panning said. “I really don’t believe we can generalize on this topic.”
Addressing bullying to improve retention and morale
Addressing the issue of bullying in medical labs in order to improve overall morale and retention will require a multifaceted approach that begins with cultivating a working culture of openness and support. Encouraging employees to report incidents without fear of reprisal is crucial in dismantling the walls of silence surrounding bullying. Establishing confidential reporting mechanisms, such as hotlines or anonymous surveys, can also provide an avenue for victims to share their experiences.
Education also plays a vital role in preventing bullying. Healthcare professionals should undergo training to recognize the signs of bullying and learn effective strategies to address and prevent such behavior. Leadership training is equally essential to ensure that those in supervisory positions understand their role in fostering a positive and respectful workplace culture.


Yes 75% No 14% Unsure 11% 32 | APRIL 2024 MLO-ONLINE.COM BEST PRACTICES :: WORKPLACE BULLYING
Figure 1. Have you ever seen or experienced bullying in a medical laboratory?








API DataDirect The process is simple INNOVATIVE SOLUTIONS. TECHNICAL EXCELLENCE. 800-333-0958 api-pt.com DataDirect@api-pt.com
entry of proficiency testing results is a time-consuming process and prone to errors. DataDirect utilizes the ability of your LIS to run a report and create a data file which is then uploaded onto API’s website. This process removes the need for manual entry, saves time, and elimates the number one cause of proficiency testing failures, clerical errors! Register PT samples in your LIS Order and complete testing Export PT data & save in a file Upload the file to API Review & submit results API DataDirect is the future of proficiency testing, eliminating clerical errors in data entry to help you focus on the work that really matters. Learn More Not an API Customer? Take API for a Test Drive. Call a Key Accounts Specialist at 800-333-0958 or email KeyAccounts@api-pt.com & sign up to receive FREE Chemistry PT samples and CE credits for your entire lab. COUNTLESS CLERICAL ERRORS AVOIDED 7 MILLION RESULTS UPLOADED 80 HOURS SAVED EACH YEAR
Manual
But, as mentioned previously, bullying is often a symptom of other pervasive issues such as staffing constraints and stagnating compensation, which in turn can create increased stress that leads to workplace conflicts. With that in mind, here are proactive steps labs can take to improve overall morale and employee retention within their labs.
Create clear growth paths
Establishing a well-defined growth path for employees in your medical lab is vital in retaining top talent and ensuring they feel like a part of your organization’s future, Harol notes. This can be done by:
• Outlining promotion criteria: C learly outline the criteria for promotions to various roles within the lab. For example, achieving specific performance targets or obtaining new certifications may be goals on career ladders you create for your employees.

employees to gain a better understanding of their perception of your lab’s benefits and compensation.
• Non-CLIA-designated roles: Develop supervisor or manager positions that offer advancement opportunities beyond just CLIA-designated roles. This is key to making employees feel they have something to progress toward instead of being stuck on a hamster wheel with little hope of advancement.
Invest in professional development and training
Promoting employee growth and development is essential for their career progression and overall engagement. By investing in skill training, employees can grow alongside your lab and take on new responsibilities. This can be achieved as follows:
• Mentorship programs: Create a mentorship program within the lab where experienced managers and supervisors can train newer employees and facilitate their skill development.
• Industry-wide welcome: Welcome individuals from non-traditional pathways into the industry and offer training in specialized areas to enhance their skill set.
Harol noted that many new techs joined the industry during the pandemic through pathways that didn’t involve graduating from two- or four-year laboratory-centric programs. While their knowledge may be specialized in certain lines of testing, these individuals also should be viewed as a boon to the workforce who can be retrained to remain in the industry long term.
“Treat new employees well to help make sure they want to stay in the industry,” Harol said. “Investing in them early on will show that you care about their growth and their career in general.”
Stay competitive in the job market
Labs should regularly evaluate and adjust compensation, benefits, and growth opportunities to remain competitive with other employers. Consider the following:
• Ma rket analysis: Examine what competitors offer in terms of salary, benefits, and professional development opportunities to stay competitive.
• Internal review: Continuously assess the benefits package for current employees to ensure it remains attractive compared to external offers. You can also survey
“You have to stay competitive, or you will see your top talent jump to competitors,” says Joe Kessler, Director of Recruiting for Lighthouse Lab Services.“The days of pizza parties being an acceptable reward or bonus are long over.”
Prioritize employee engagement
Engaged employees outperform their disengaged counterparts by as much as 28 percent, Harol noted, making employee engagement a priority. Lab managers and leadership should:
• Be present and listen: Regularly engage with employees, attend to their concerns, and actively listen to their feedback to make them feel valued.
• Pr ovide transparent leadership: Keep employees informed about the company’s performance, goals, and plans to instill a sense of investment in the organization’s future.
Looking ahead
By addressing bullying in laboratories head-on, the industry and its stakeholders not only improve the well-being of the professionals who dedicate their lives to providing accurate test results but also enhance patient outcomes. Promoting a culture of respect and support while also working to improve overall working conditions and morale can contribute to a more positive and effective lab environment, where benchlevel techs and managers alike can thrive. By shining a light on this issue and talking about its impact openly, we can collectively pave the way for a healthier future in healthcare.
REFERENCES
1. Quick Safety 24: Bullying has no place in health care (Updated June 2021). Jointcommission.org. Accessed February 28, 2024. https://www.jointcommission.org/resources/ news-and-multimedia/newsletters/newsletters/quick-safety/ quick-safety-issue-24-bullying-has-no-place-in-health-care/ bullying-has-no-place-in-health-care/.

Alex Mitchell is Marketing Communications Manager at Lighthouse Lab Services . He works to keep the team and their clients abreast of industry news and changes that could impact their operations or revenue. Alex also manages Lighthouse’s educational content, including monthly webinars, blogs, and industry newsletters.

34 | APRIL 2024 MLO-ONLINE.COM BEST PRACTICES :: WORKPLACE BULLYING
Photo 51948846
© Pat Olson | Dreamstime.com

Efififi fifififi fififififififi fifififi fifififififififi
fififi fififififififififi fififi fifififififi fifififi fifififififi
fififififififififi fifi fifififififi
fififififififififi fifi fi fifififi fififififififififififi
















Yfifi fifififi
fififififi fififififi
fififi Pfifififififi
fififififififififi
Nfifi
fifififififififififi
KfifiSfifififi

Rfifififififififi

fifi fififififififi
fifififififi
fifi fifi fififi
fifififififi fififififi


1.877.251.9246 Serving laboratories since 2002 | Contact us for literature and sales information Afififififififififififi fififi fififififi fifififi fififififi fififi fi fififififififi fifi fifififififififi fififififi Lfififififififififi fifififififi & Pfififififififififififi Ffififi fififi fifififififi fifi fififififififififi fififififififififi fififi fififififififififi fififififififififi fififi fififififififififi
SAFE SOLUTIONS
RECAPPING
DEC APPING
Make your goal ZERO repetitive stress injuries Vfifififi fififi fififififififi fififi fifififififififififi fififififififififififi fififififififififififififififififififififi
Molecular testing supports early, effective use of ESR1 -targeting therapies
By Tom Bittick

Avery important change in the breast cancer treatment landscape has made it necessary to expand access to routine testing for acquired genetic variants in patients: the availability of new drugs to address mutations associated with treatment resistance.
Patients diagnosed with hormone receptor-positive (HR+) breast cancer are typically treated with first-line endocrine therapies designed to reduce estrogen levels in the body. A common outcome of these treatments is the development of mutations in the ESR1 gene, seen in up to 40% of patients.1 These acquired variants are specific to patients undergoing endocrine therapies, particularly aromatase inhibitors; they are very rarely seen in treatment-naïve patients.
Of the many variants that have been documented in the ESR1 gene, a certain subset can confer treatment resistance. Such mutations actually eliminate the tumor’s need for estrogen, turning on the biological pathway that is usually only active in the presence of estrogen and once again giving the cancer the ingredients it uses to grow. The endocrine therapies blocking the activation of estrogen cease being effective, and the cancer can relapse.
There are a few approved therapies targeting ESR1 mutations (fulvestrant, elacestrant) that can be used to render those tumors susceptible to treatment again. And positive data from ongoing clinical trials indicates that more effective ESR1-targeting treatments may be on the way.
In light of these developments, it has become essential for clinical laboratories to perform routine monitoring for ESR1 variants in patients with HR+ metastatic breast cancer who are being treated with endocrine therapies. Recently, guidelines from the American Society of Clinical Oncology were updated; they now include a recommendation for frequent ESR1 monitoring to detect emerging mutations during the course of treatment for patients who have been diagnosed with estrogen receptor-positive metastatic breast cancer.2 Clinical data clearly demonstrates that intervening early — as soon as a new mutation is detected — gives patients better outcomes.
In some cases, monthly testing may be appropriate to catch mutations as early as possible.
Clinical trials that are underway have shown promising interim results to support the idea of using ESR1-targeting therapies to overcome treatment resistance in cancers that previously responded well to endocrine therapies. One major trial has been evaluating a currently available therapy, while another has been assessing a candidate therapy not yet approved by the FDA.
The multi-center, randomized, phase 3 PADA-1 trial has been going on for about seven years. It is testing the outcomes of incorporating an ESR1-targeting therapy for patients who develop an ESR1 mutation. The trial includes about 1,000 patients diagnosed with HR+ metastatic breast cancer, all of whom began on a conventional endocrine therapy.3 Patients in one arm of the trial are monitored with bi-monthly ESR1 genetic testing, and the detection of a relevant mutation triggers a shift to fulvestrant, a treatment that has shown good results when used for cancers with ESR1 mutations. Other patients can be switched to fulvestrant if their regular imaging scans reveal growth of the tumor, indicating that the cancer was no longer responding to the endocrine therapy. The PADA-1 trial is scheduled for completion in 2025, but already, reported results have been promising. While patients who were switched to fulvestrant due to imaging-based detection of tumor progression received little benefit, the patients who made the switch earlier — when ESR1 mutations were first detected by genetic testing — had a significant change in outcome.4,5 For the latter group, median progression-free survival was more than twice that of a control group that stayed on aromatase inhibitor therapy.
A candidate ESR1-targeting therapy from AstraZeneca also appears to be performing well in clinical trials. The SERENA series of trials is evaluating the new therapy, camizestrant, in patients with breast cancer.6 In a phase 2 trial, results demonstrated that patients with ESR1 mutations experienced almost three times as much progression-free survival when
36 | APRIL 2024 MLO-ONLINE.COM MOLECULAR DIAGNOSTICS :: ESR1 GENE
45895879 © 9nongphoto | Dreamstime.com
using the candidate treatment compared to standard of care.7 A phase 3 trial known as SERENA-6 is now underway, but expectations are that camizestrant will be effective against a broad range of ESR1 mutations for patients whose cancers become resistant to endocrine therapy.
How to test for ESR1 mutations
For clinical laboratories interested in expanding their test menu with ESR1 monitoring, there are a number of options. Due to differences in technology availability and other factors, though, not all approaches will be right for all labs. Before considering any individual method, it is worth reviewing the key attributes of any ESR1 test.
Sensitivity: ESR1 mutations will first emerge at very low levels against a significantly larger wild-type. Any testing platform must be sensitive enough to identify a clinically relevant mutation that may be present at vanishingly small volumes.
Accuracy: While a test must be sensitive enough to detect ESR1 mutations, it must also be accurate enough not to lead to false-positive results. Most molecular detection technologies that have the required sensitivity will also have the necessary specificity, but it is important to confirm this in any platform evaluation.
Easy access: Clinical trials have proven that shifting patients to an ESR1-targeting therapy as soon as possible is the best way to improve health outcomes. Consequently, ESR1 monitoring must be performed frequently — maybe even monthly — for HR+ metastatic breast cancer patients taking endocrine therapies. Given the need for such frequent testing, an easily accessible sample such as a liquid biopsy is preferable.
With increasing demand for ESR1 testing, an in-house test is likely to be faster and more cost-effective than a send-out test. Here’s a quick look at the different technology platforms available for this application.
Droplet digital PCR: This is the technology used in the PADA-1 clinical study, with demonstrated sensitivity for detecting ESR1 mutations. Digital PCR is highly sensitive and can be used with blood samples. However, there is limited availability of digital PCR platforms in clinical laboratories because of their high cost and complex setup. For ESR1 mutations, there is the added drawback of having to run several different reactions to test the full range of clinically relevant variants.
Next-generation sequencing: This widely available technology is also sensitive enough to detect ESR1 mutations amid a background of non-tumor DNA from virtually any sample
What are exosomes?
Exosomes are part of the vast communication network among cells. These small particles are shed by cells — by all cells, every day, by the thousands — and they carry molecular cargo of DNA, RNA, and/or proteins used to convey biological messages to other cells. By intercepting these molecular data packets and analyzing their contents, clinical labs can identify valuable signals and infer key information about the cells from which these exosomes came. Because exosomes are released by all cells, they can be accessed in all biological fluids. Exosome analysis has already been used to distinguish high-grade from low-grade prostate cancer, identify neurological biomarkers typically blocked by the blood-brain barrier, and more.
type. Unfortunately, most NGS platforms are not designed for cost-effective analysis of single genes. Clinical labs with very high demand for ESR1 mutation testing might have sufficient sample volume to run an NGS-based test affordably, but most labs will find it too expensive to deploy a modern sequencer for this purpose.
qPCR: Unlike the prior two techniques, qPCR instrumentation does not typically meet the sensitivity threshold for ESR1 variant detection. But a new method may allow clinical lab teams to use this affordable, widely available technology for ESR1 monitoring. Scientists have successfully paired circulating tumor DNA (ctDNA) with exosomal RNA analysis to produce highly sensitive ESR1 mutation detection on a standard qPCR instrument. The idea is to use a liquid biopsy approach, capturing both the low-abundance ctDNA and the high-abundance exosomes shed by a tumor. Either signal on its own may be undetectable with qPCR, but combining them into a single assay overcomes that issue. In a presentation at last year’s annual meeting of the Association for Molecular Pathology, scientists reported the development of a single workflow identifying allele-specific ESR1 mutations from ctDNA and exosomal RNA, achieving the sensitivity required for clinical monitoring.8
Going forward, clinical lab teams may find that one of the approaches above is a good fit for incorporating ESR1 monitoring. With ESR1-targeting therapies available today, and more on the horizon, routine variant testing will be a useful way to spot the signs of treatment resistance among HR+ breast cancer patients undergoing endocrine therapy.
REFERENCES
1. Hermida-Prado F, Jeselsohn R. The ESR1 Mutations: From Bedside to Bench to Bedside. Cancer Res. 2021;1;81(3):537-538. doi:10.1158/0008-5472.CAN-20-4037.
2. Burstein HJ, DeMichele A, Somerfield MR, et al. Testing for ESR1 Mutations to Guide Therapy for Hormone Receptor-Positive, Human Epidermal Growth Factor Receptor 2-Negative Metastatic Breast Cancer: ASCO Guideline Rapid Recommendation Update. J Clin Oncol. 2023;20;41(18):3423-3425. doi:10.1200/JCO.23.00638.
3. National Library of Medicine. PAlbociclib and Circulating Tumor DNA for ESR1 Mutation Detection (PADA-1). Available at https://clinicaltrials. gov/study/NCT03079011. Accessed February 28, 2024.
4. Bidard FC, Hardy-Bessard AC, Dalenc F, et al. Switch to fulvestrant and palbociclib versus no switch in advanced breast cancer with rising ESR1 mutation during aromatase inhibitor and palbociclib therapy (PADA-1): a randomised, open-label, multicentre, phase 3 trial. Lancet Oncol. 2022;23(11):1367-1377. doi:10.1016/S1470-2045(22)00555-1.
5. Helwick C. PADA-1 Trial: With Early Identification of ESR1 Mutation, Switch to Fulvestrant in Metastatic Breast Cancer. October. 2022;10.
6. National Library of Medicine. Phase III Study to Assess AZD9833+ CDK4/6 Inhibitor in HR+/HER2-MBC With Detectable ESR1m Before Progression (SERENA-6) (SERENA-6). Available at https://www. clinicaltrials.gov/study/NCT04964934. Accessed February 28, 2024.
7. Camizestrant significantly delayed disease progression in advanced ER-positive breast cancer, adding at least 3.5 months benefit versus Faslodex. Astrazeneca.com. Published December 8, 2022. Accessed March 4, 2024. https://www.astrazeneca.com/media-centre/ press-releases/2022/camizestrant-significantly-delayed-diseaseprogression-in-advanced-er-positive-breast-cancer.html.
8. Thibert JR. Development of a Novel Exosome-Based, Multiplexed RT-qPCR Technology for Rapid and Accurate Detection of Circulating Tumor Acquired Resistance Variants in ESR1 at ≤ 0.1% Frequency. Poster Presented at the Annual Meeting of the Association for Molecular Pathology.; 2023.

Tom Bittick serves as senior product manager for oncology in the molecular diagnostics division at Asuragen, a Bio-Techne brand. He has 30 years of experience in the life sciences, with prior positions at Sigma-Aldrich, Ambion, and Thermo Fisher. He holds a master’s degree in microbiology and immunology from LSU Medical Center and a bachelor’s degree in biology from Louisiana State University.
MLO-ONLINE.COM APRIL 2024 | 37 MOLECULAR DIAGNOSTICS :: ESR1 GENE

Safer, more gentle blood collection
Greiner Bio-One’s VACUETTE EVOPROTECT SAFETY
Implement a laboratory safety program
CLSI GP17 was written for laboratorians who are responsible for developing and implementing a safety program. Aspects of a safety program addressed in this guideline include:
• Maintenance and inspection.
• Personal safety.
• Warning signs and labels.
• F ire prevention.
• E lectrical and radiation safety.
CLSI
Store flammables, even in confined spaces

National Fire Protection Association-approved cabinet (17696) is made of double-wall steel with insulating air space and includes dual vents with flame arresters to protect against fire hazards. An adjustable shelf directs spills to the bottom of the leak-proof sump to minimize adverse reactions. Lockable handle includes 2 keys.
Health Care Logistics
Blood Collection Set is a winged needle with semiautomatic safety mechanism designed for onehanded, in-vein activation and improved protection from risk of needlestick injuries. EVOPROTECT is available in several configurations of needle gauge, tubing length and attachment for flexibility in blood collection and infusion.
Greiner Bio-One

Safety product for laboratories

Bench-top automated recapper
KapSafe Recapper model #3101-1102-LS is a bench top 24” x 24” footprint for the automatic recapping of sample tubes, of various heights, at a throughput of 700 Tubes/Hour. KapSafe serves to eliminate exposure to repetitive stress injury during manual recapping. Uses muti-tier caps to fit various tube diameters. Other models available.
LGP Consulting
The Safety Station is a multi-purpose drench shower, eye/face wash and safety supply storage cabinet. It is for laboratories where persons may be exposed to potentially hazardous chemicals. Safety Stations are fully assembled and ready for installation to water supply. Call 816-796-2900 or visit HEMCO.
HEMCO

38 | APRIL 2024 MLO-ONLINE.COM PRODUCT FOCUS :: LAB SAFETY






















































































































2404MLO_HealthCareLogistics.indd 1 2/23/24 11:08 AM e for Lab Professionals since 1969 RY e for Pro essionals sin MA rector id Excellen e WEBSITE mlo-online.com MAGAZINE mlo-online.com/subscribe NEWSLETTERS Sign up for monthly updates FACEBOOK MLOMedicalLaboratoryObserver X (FORMERLY TWITTER) @MedicalLabMLO LINKEDIN medical-laboratory-observer Quali ce 19 RCH 2 and Scan Here to Subscribe to our FREE Magazine FREE MAGAZINE SUBSCRIPTION! 9 Issues 2403MLO_House_Subscription_14v.indd 1 2/8/24 8:58 AM MLO-ONLINE.COM APRIL 2024 | 39 INDEX OF ADVERTISERS This index is provided as a service. The publisher does not assume liability for errors or omissions. Abbott Diagnostics diagnostics.abbott C3 Abbott Diagnostics ........................................................diagnostics.abbott ...................................................................................... 3 American Proficiency Institute (API) ............................api-pt.com ................................................................................................. 33 Asuragen bit.ly/48aZ2ac 5 Cygnus Medical cygnusmedical.com....................................................................................7 Diasorin diasorin.com 29 Health Care Logistics .....................................................GoHCL.com ............................................................................................... 39 LGP Consulting ..............................................................lgpconsulting.com .................................................................................... 35 Owen Mumford owenmumford.com C2 Roche Diagnostics Corporation usinfo.roche.com/STI 17 Roche Diagnostics Corporation diagnostics.roche.com C4 Sysmex America sysmex.com/us 1 Sysmex America ............................................................Sysmex.com/LabWeek ............................................................................. 19 Werfen (Instrumentation Laboratory) - Hemostasis werfen.com 23 Advertiser .......................................................................Web ....................................................................................................... Page
LABORATORY INNOVATOR

Jessica DesLauriers, MBA, MLS (ASCP) CM is a laboratory professional with a successful career of delivering efficiency and standardization and maintaining CAP ISO 15189 and Six Sigma quality management systems. She is the Laboratory Director for Avera McKennan Hospital & University Health Center in Sioux Falls, SD and oversees four laboratories and over 200 employees. Avera McKennan Laboratory consists of the core lab as well as several specialty departments including genetics, HLA, molecular, cellular therapy, and flow cytometry. Jessica is responsible for ensuring services are provided in a safe, efficient, and cost-effective manner that enhances patient, staff, and physician satisfaction in collaboration with interdisciplinary team members. She also serves as the Quality and Compliance Functional Leader for Avera’s Laboratory Service Line as well as volunteers her time as a member of the Quality Expert Panel for CLSI.
Avera McKennan’s Department of Pathology and Laboratory Medicine was MLO’s 2023 Lab of the Year. One thing that set your lab apart was your use of data analytics to improve laboratory operations. Could you share a recent example(s) of how your lab is utilizing data to improve?
Avera McKennan Laboratory is harnessing the power of data analytics to drive continuous improvement and enhance key metrics within the lab, such as reducing blood culture contamination rates and optimizing other laboratory initiatives. By collecting and analyzing data on blood culture contamination incidents, the laboratory can identify patterns, root causes, and trends that
Directing a winning lab
By Christina Wichmann
contribute to contamination events. This data-driven approach enables Avera McKennan Laboratory to implement targeted interventions, such as staff training, process improvements, and workflow modifications, to reduce contamination rates and improve the accuracy of blood culture results. Through real-time monitoring and analysis of data, the laboratory can proactively identify areas for improvement, track progress over time, and drive sustainable quality enhancements in blood culture testing processes.
Furthermore, Avera McKennan Laboratory is leveraging data analytics to optimize various laboratory initiatives and performance metrics, such as turnaround times, test accuracy, and resource utilization. By collecting and analyzing data on testing processes, equipment performance and staff productivity, the laboratory can identify opportunities for efficiency gains, workflow enhancements and cost savings. This data-driven approach empowers Avera McKennan Laboratory to make informed decisions, set performance targets, and monitor key metrics to drive operational excellence and deliver high-quality patient care. Through a culture of continuous improvement and data-driven decision-making, the laboratory can achieve greater efficiency, accuracy, and patient satisfaction.
What are some of your goals
for the Avera McKennan Laboratory this year?
In line with the health care system’s commitment to innovation, Avera McKennan Laboratory also seeks to enhance its testing capabilities by adopting cutting-edge technologies and expanding its test menu to meet the growing demand for specialized tests. By staying abreast of technological advancements and industry best practices, the laboratory aims to offer a comprehensive range of diagnostic services to support clinical decision-making and patient care.
Avera McKennan Laboratory is also navigating the growing needs of the rapid population growth of Sioux Falls, S.D., while also serving as a reference lab for our rural regions. Our goal is to ensure that the laboratory can scale its operations effectively to meet the growing demand, while maintaining high standards of quality and efficiency. Our
goals involve strategic planning for infrastructure, workforce optimization, and technology integration to enhance the laboratory’s capacity and ability to serve a larger patient population effectively. Furthermore, we aim to collaborate with educational institutions, professional organizations, and industry partners to cultivate a pipeline of future MLS professionals and address the long-term sustainability of the laboratory workforce.
What measures does your laboratory take to prevent staff burnout?
Avera prioritizes the well-being of its staff and implements strategies to prevent burnout. One approach is to foster a supportive and collaborative work environment that encourages open communication, teamwork, and mutual respect. The laboratory has developed a Culture Committee that has staff representation from various departments and shifts. The committee is completely run by the staff who work hard to put on events and activities throughout each month. They do an incredible job at fostering a fun, educational, and collaborative environment. The team hosts events that range from continuing education and community volunteer opportunities, to themed potlucks and games. Occasionally, they will plan competitions with traveling trophies that add a lot of fun and camaraderie throughout the lab. Additionally, Avera offers wellness programs, mental health resources, and professional development opportunities to help employees manage stress, maintain work-life balance, and enhance their overall well-being.
What is the most exciting new technology currently being used in your laboratory?
One of the exciting new technologies being utilized in our lab is the Liquid Chromatography Mass Spectrometry (LC-MS) system in our special chemistry department. The LC-MS system offers unparalleled sensitivity and specificity in detecting and quantifying a wide range of compounds in biological samples. This advanced technology allows for precise analysis of complex molecules, such as drugs, metabolites, and proteins, with high accuracy and efficiency.

40 | APRIL 2024 MLO-ONLINE.COM

If

hospital performs one
tests per year
loses one in 1,400 tubes at a cost of $400-600 per tube, then the annual cost could be as much as $428K – not to mention the burden on patients and hospital1.




•
Avoid lost samples and save thousands with Indexor. PRE-ANALYTICS, POWERED BY INDEXOR DIGITAL HEALTH SOLUTIONS © 2024 Abbott. All rights reserved. All trademarks referenced are trademarks of either the Abbott group of companies or their respective owners. Indexor trademarks are owned by Isens-Electronica, LDA. The Indexor system is manufactured by Isens Electronica, LDA and is available in select countries. ADD-148277-USA-EN 1/24 1. Wiwanitkit, V. Types and frequency of preanalytical mistakes in the first Thai ISO 9002:1994 certified clinical laboratory, a 6 – month monitoring. BMC Clin Pathol 1, 5 (2001). SEE HOW INDEXOR STREAMLINES AND AUTOMATES SAMPLE TRACKING FOR BETTER RESULTS.
Trace samples from patient draw to arrival in the lab
Monitor key quality indicators
•
•
Automate to save time and improve service levels AT PHLEBOTOMY SITES DURING TRANSPORT IN THE LAB HELP MINIMIZE ERRORS AND ADVANCE THE QUALITY OF HEALTHCARE SERVICES
INDEXOR CAN INTEGRATE WITH YOUR LIS FOR MAXIMUM POTENTIAL BENEFITS
a
million
and

Primary vials.
Primary screening.
Primary solution.
The Roche cobas® 5800 System is built to offer a fully automated workflow that encompasses primary vial handling for cervical and sexual health samples, transfer and preparation, amplification and detection, result calculation and delivery to the laboratory information system (LIS).
Designed to bring efficiency, flexibility and simplicity to laboratories of all sizes, enabling greater patient access.
Learn more and contact your Roche representative, today.






























































 By Alex
By Alex


















 By Christina Wichmann Editor in Chief
By Christina Wichmann Editor in Chief






































































































































































































































