issn 1757-4625
New Free Student Membership

The Dangers of Non-Compliance: BDIA’s Adam Stanley In this issue: volume 19 issue 2 may 2026
volume 11 issue 4 november 2018 issn 1757-4625 the journal of the dental technologists association HOURS OF VERIFIED CPD

AI: Stupid But Fast, Spencer Kelly Why Don’t Dentists Get it? Mike Gregory
Boiling Frog Syndrome






Shape the future of dental technology
Dental Technology Showcase is the event where over 1,500 dental lab professionals meet to shape the future of dental technology. With 60+ exhibitors, 3 theatres, 50+ expert speakers and 40+ hours of free Enhanced CPD, this is the place to unite with your dental community. Embrace new ideas, explore the innovations of tomorrow and take your lab to the next level.





Editor: Derek Pearson
t: 07866 121597
Advertising: Rebecca Kinahan
t: 01242 461 931
e: info@dta-uk.org
DTA administration: Rebecca Kinahan Operations Coordinator
Address: PO Box 1318, Cheltenham GL50 9EA
Telephone: 01242 461 931
Email: info@dta-uk.org Web: www.dta-uk.org
Stay connected: @DentalTechnologists Association
@The_DTA @dentaltechnologists association
Dental Technologists Association (DTA)
DTA Council:
Joanne Stevenson President Chris Fielding
Deputy President Tony Griffin Treasurer Delroy Reeves DTA Liaison Delegate
Joanne Clark, James Green, Raya Karaganeva, Robert Leggett, and Jade Ritch.



DTA Column A DLN: Good, Safe, Oral, Health? A Boiling Frog Syndrome – Victoria Wilson A A Recipe for Health – Michael Sultan A Sticks and Stones – Dr Chris Turner
Editorial panel: Tony Griffin Joanne Stevenson
Editorial assistant: Dr Keith Winwood
The Technologist is published by the Dental Technologists Association and is provided to members as part of a comprehensive membership package. For details about how to join, please visit: www.dtauk.org or call 01242 461 931
AI: Stupid but Fast – Spencer Kelly and Sophie Lovett A Enhancing Digital Dentures Through Gingival Characterisation – Mia Harrison A Custom-made devices and the dangers of non-compliance – Adam Stanley A Why don’t dentists get it? – Mike Gregory A Dentists and Alcohol – Sandra Parker A Communication and collaboration with digital dentistry – Kristina Vaitelyte A The Importance of Disclosing CCJs, Convictions and Bankruptcy – UK Special Risks A Case Report: Management of a Labial Vertical Fracture – Dr Sandy Limerick
ISSN: 1757-4625
Views and opinions expressed in the publication are not
01634 862 525
Representing you PPP Free Student Membership
Exciting news for aspiring dental technicians! We are offering free membership to students training to become dental technicians. This initiative supports the next generation of dental technologists in building their
skills, knowledge, and career pathways. Invite your peers to join and take full advantage of the benefits. All current students have had their membership extended until their qualification year for free.

DTA Spring Council Meeting Held
We held our Spring Council Meeting on 28 February 2026 via Zoom, bringing together Council members, officers, and key contributors to review progress and discuss priorities for the year ahead.
Akey item of business was the election of officers. Both Joanne Stevenson (President) and Chris Fielding (Deputy President), having now
completed one year in office, were unanimously supported by Council to remain in their roles, ensuring continuity of leadership. The meeting highlighted the continued development of Digital Dental Technology CPD resources, planned to be a free benefit for members.
The DTA continues to engage regularly with regulators and key stakeholders, ensuring members remain informed and supported on current compliance requirements. This includes recent updates relating to MHRA
registration and associated fee changes. Council also reaffirmed its support for key industry events, including DTS and the BDIA Dental Showcase, recognising their importance in promoting innovation, collaboration, and professional engagement across the sector.
The meeting concluded with forward planning for upcoming activities and confirmation that the next Council meeting will take place in Autumn 2026.
Take part – a day in the life of a dental technologist

As part of its outreach and promotional work, the DTA is inviting members to get involved in creating a “day in the life” of a dental technologist.
This initiative aims to showcase the profession to school leavers, highlighting the diverse career pathways, training routes, and
exciting advancements within dental technology.
Make Your Summer Shine with Exclusive DTA Rewards Discounts
As the sun starts to shine, it’s the perfect time to plan your summer adventures! With DTA Rewards, your membership goes further than professional development — every day it helps you save on the things you love.
A Travel & Accommodation: Plan that long-awaited beach getaway or city escape with discounts on hotels, flights, and car rentals.
A Shopping: Stock up on summer
wardrobes, outdoor essentials, and festival gear.
A Lifestyle & Experiences: From theme parks to sporting events, enjoy exclusive offers on memorable outings.
A Insurance: Protect your adventures with discounted travel insurance.
Don’t miss out, make your summer brighter and more affordable. Explore deals by clicking on the DTA Rewards tab in your membership area.

A Click through from the rewards site to the online shop, browse, add to your basket, and enter the discount code at checkout.
Spotlight on DTS Speakers: Insight, Innovation and the Future of Dental Technology
As excitement builds for this year’s Dental Technology Showcase (DTS), we’re pleased to highlight just some of the outstanding speakers who will be taking to the stage, sharing real-world experience, regulatory insight and cutting-edge digital innovation.Once again, DTS promises a packed programme of expert-led sessions designed to support technicians at every stage of their careers. From complex prosthetic casework and evolving legislation to artificial intelligence in CAD design, these talks underline why DTS remains an unmissable date in the profession’s calendar, make a note 15th and 16th May at the NEC Birmingham.
Exploring Career Pathways in Dental Technology
Dental Technician Career Pathways: Progression, Technology and Future Challenges
Dr Raya Karaganeva BSc (Hons) PhD FHEA DCP, Senior Lecturer in Dental Technology,

University of Greater Manchester
Dr Nikolas Poulis, Head of Centre, University of Greater Manchester
Saturday 16 May, 15:45–16:30, DTA Slot DTA Council Member Dr Raya Karaganeva and Dr Nikolas Poulis will deliver a joint presentation exploring the evolving career pathways available to dental technicians. Their session will cover professional progression, the latest technological innovations in dental technology, and the future challenges that technicians may face in an ever-changing clinical and digital landscape.
Attendees can expect insights from both an academic and practical perspective, making

this talk essential for students, early-career technicians, and laboratory managers who want to understand how to navigate their professional development while keeping pace with technological advancement.
Developing Skills Through Real-World Prosthetics
Training into practice: early career learning through complex prosthetic case studies
Ella Cook, Prosthetic Dental Technician, University Hospitals Bristol & Weston NHS Foundation Trust
DTA Member Ella Cook will explore the vital transition from training into real-world clinical

practice. Drawing on complex prosthetic case studies from within an NHS setting, Ella’s session will provide valuable insight into the challenges faced by early-career technicians — and the learning opportunities that arise when theory meets reality.
This talk will be particularly relevant for students, newly qualified technicians and laboratory managers involved in mentoring and workforce development, offering practical takeaways on building confidence, competence and clinical judgement.
Navigating Regulation in a Changing Landscape
Custom-made medical device legislation: where are we following Brexit and COVID-19?
James Green, Maxillofacial and Dental Laboratory Manager, Great Ormond Street Hospital for Children NHS Foundation Trust
GDC
Regulation continues to be one of the most pressing topics facing dental laboratories. In this essential session, DTA Council Member James Green will examine the current position of custom-made medical device legislation in the wake of Brexit and the COVID-19 pandemic.
With his extensive experience of managing specialist services at Great Ormond Street Hospital, James will provide clarity on regulatory expectations, practical compliance considerations and what laboratories should be preparing for next, making this a must-attend for owners, managers and senior technical staff.
Exploring AI and Digital Dentistry
From pixels to patients: how AI is transforming CAD design and realworld cases
Kristina Vaitelyte, CAD/CAM Dental Technician, Avant Garde Dental Laboratory
Caroline Kirkpatrick, Clinical Dental Technician, OTS Dental Laboratory
Digital dentistry continues to evolve at pace, and this forward-looking session will showcase how artificial intelligence is already influencing everyday laboratory workflows.
DTA Member Kristina Vaitelyte and Caroline Kirkpatrick will take their audience on a journey from virtual design to clinical application, sharing real-world case examples that demonstrate how AI-driven CAD solutions are improving efficiency,
On 25 March, the GDC launched MyGDC, a new online portal replacing eGDC which is designed to modernise the way dental professionals and applicants interact with the GDC.
Existing dental professionals will now use MyGDC to manage their registration, complete their annual renewal, and submit and declare their continuing professional development (CPD) hours.
accuracy, and patient outcomes. For technicians keen to understand how emerging technologies can be integrated into their own laboratories, this talk promises both inspiration and practical insight.
These sessions represent just a snapshot of the rich educational programme awaiting visitors at DTS this year. With dozens of speakers, free CPD opportunities and access to the latest innovations from across the sector, the event offers unparalleled value for the entire dental technology community.
We encourage everyone to plan ahead, register early and join us at DTS, to learn, connect with peers and help shape the future of the profession.
A We look forward to seeing you there. Register for free via the QR code or through the website, visit https://www.the-dts.co.uk/

Existing users of eGDC will be able to access MyGDC using the email address they used to create their account.
They do not need to take any action now. When logging in to MyGDC for the first time, users will be asked to reset their password and complete multi-factor authentication (MFA) as part of the security process.
Supporting Dental Technologists Through the GDC Annual CPD Declaration
As the annual CPD declaration period approaches, we want to remind our members of their professional obligations under the GDC’s Enhanced CPD Scheme, and the wide range of technical CPD resources we provide to support you.
Your GDC CPD Responsibilities
As GDC-registered Dental Technologists, you are required to:
A Complete a minimum of 50 hours of verifiable CPD over a five-year cycle
A Undertake at least 10 hours within any consecutive two-year period (the “10/2 rule”)
A Submit an annual CPD declaration, even if no hours have been completed in that year.
In addition, you must maintain:
A A clear Personal Development Plan (PDP)
A A record of CPD activity with supporting evidence
A CPD that aligns with your scope of practice and GDC development outcomes
We encourage all members to review their current CPD status and ensure all their records are up to date well in advance of the declaration deadline.
CPD and the GDC Development Outcomes
The GDC’s Enhanced CPD Scheme requires that all CPD activities are mapped to at least one of the four development outcomes:
1. Outcome A — Effective Communication: Learning that improves the way you communicate with colleagues, stakeholders, or patients.
2. Outcome B — Effective Management: Development that enhances your ability
to manage yourself, contribute within a team, or lead effectively.
3. Outcome C — Maintenance & Development of Knowledge and Skills: The core technical and professional knowledge for your role as a Dental Technologist.
4. Outcome D — Professionalism and Ethical Practice: Learning that supports ethical behaviour, professional judgement, and safe practice.
While there are no specific hourly requirements per outcome, it is important that your CPD portfolio covers areas relevant to your professional practice. All DTA CPD resources reference one or more of these outcomes, making it straightforward to ensure your learning is aligned and verifiable.
Keeping CPD Relevant to Dental Technology
We recognise that CPD for Dental Technologists must be practical, technical, and directly applicable to laboratory practice. Don’t miss valuable and verifiable CPD which focuses on areas such as:
A From 3D Printing to 4D Innovation one-hour CPD
A Digital dentistry one-hour CPD
A Additive-manufactured ceramics for dental restorations: a systematic review one-hour CPD
A Occlusion and implants one-hour CPD.
How We Support Your CPD
We are committed to providing our members with accessible, high-quality, and relevant CPD opportunities to help you stay compliant and continue developing professionally.
Our key CPD resources include:
A The Technologist
Our flagship publication continues to deliver in-depth technical articles, case
studies, and expert insights tailored specifically to Dental Technologists. These articles are designed to support both foundational knowledge and advanced techniques within the laboratory environment.
A Articulate
Our digital CPD platform offers interactive, verifiable CPD content that allows you to learn flexibly and efficiently. It is particularly valuable for members looking to build or catch-up on their CPD hours in a structured way.
Together, these resources provide a strong foundation of technical CPD aligned to realworld dental technology practice.
Catching Up and Staying on Track
If you find yourself needing to catch up on CPD hours, whether to meet the 10/2 requirement or to complete your five-year cycle, we encourage you to make full use of the resources available to you as a member.
With flexible, on-demand content, you can:
A Work through CPD at your own pace
A Focus on areas most relevant to your role
A Align your learning with your PDP and professional goals
Even if you have completed minimal hours this year, submitting your declaration remains a requirement, and planning ahead will help avoid unnecessary pressure later in your cycle.
A If there are any topics that you would like to see in a future issue of The Technologist, or if you would like to contribute an article, please contact: info@dta-uk.org, or e-mail the editor, Derek Pearson, at derek.the.ed@gmail.com
50 years of National Smile Month
National Smile Month is a charity campaign dedicated to championing the benefits of good oral health and promoting the value of a healthy smile.
In 2026, the campaign is particularly significant as the Oral Health Foundation celebrates 50 years of National Smile Month, marking five decades of improving oral health awareness and education.
Running from 11th May to 11th June, the campaign continues to focus on helping the public understand the importance or prevention and their personal responsibility in maintaining good oral health, plus the positive impact it has on overall wellbeing.
Good oral health is shaped by everyday behaviours, access to education, and clear,

RECENT FAQS
Did you know?
Under the UK Medical Devices Regulations 2002 (as amended) and MHRA’s Custom-Made Devices Guidance, the manufacturer (in this case, the dental laboratory) is legally responsible for keeping all relevant technical documentation and the Statement of Manufacture for each custom-made device for at least 10 years after the device has been placed on the market (delivered to the dentist/patient). This requirement still applies even if the business ceases trading
reliable information. This year, National Smile Month highlights key oral health messages and encourages simple, positive actions that can make a lasting difference.
By supporting the campaign, we aim to empower individuals with the knowledge and confidence to take control of their oral health and contribute to healthier smiles across the nation.
A Take a look at the campaign resources and join us in making a positive difference to the oral health of millions of people, visit https://www.dentalhealth .org/ pages/site/national-smile-month

European Dental Technician’s Day
European Dental Technicians Day is an opportunity to highlight the expertise, craftsmanship, and medical responsibility that define the profession.
Through joint visibility across countries, associations, laboratories, and independent
dental technicians, we strengthen public awareness of the vital role technicians play in oral healthcare.
A Join us in celebrating this special day on Friday, 5 June and help raise awareness of the importance of what dental technician’s do behind the scenes
The regulations don’t include any exemption for closure. The principle is: There must remain a person or organisation responsible for holding those records for the required retention period.
So, if a lab closes three-years after delivering its last device, those records must still be securely held somewhere for another sevenyears (to reach the 10-year minimum).
Any confusion arises because, Under the previous Medical Devices Regulations 2002
(UK) Regulation 15(d) the manufacturer was required to keep the information “for a minimum period of five years” after the device had been placed on the market.
However, more recently under the EU-/UKaligned regulation framework (for custommade devices), the requirement is at least 10-years (for non-implantable custom-made devices) after the device has been placed on the market.
■ DLN: Good, Safe, Oral, Health?
At the Dental Leadership Network (DLN) meeting on 24th March teams from the audience were asked ‘How can we develop good safe oral health’?
Ben Atkins, Zaim Hameed, and Hazel Johnstone acted as adjudicators for a team of DLN members who were tasked with addressing the question ‘What gets in the way of providing good, safe oral care to people who are homeless or have housing insecurity?’ Nine groups of seven from every sector of the dental community brought some strong ideas to the table. What follows are The Technologist’s interpretations and notes from the discussion by just one of those teams, any errors or misunderstandings are ours.
When a person in need – in this case homeless, or in a state of housing insecurity – comes into an NHS practice, they are often seen and treated by a Vocational Trainee, the most cost-effective solution to the situation, that’s if they are treated at all. The problem is that at the current time there are not the funds to treat such patients based on clinical need. Minister of State (Department of Health and Social Care) Stephen Kinnock MP has stated that there is no new money to address the situation. This means that these people must rely on charities for their healthcare, which is a ridiculous situation for a first-world country in the twenty-first
century, let alone one of the richest countries in the world.
There is a need to make commissioned dental services based on the needs of the locality – for example in Hampshire an NHS practice is targeted to provide 8% of its activity as urgent care, but due to the demographic it can only effectively do 4%. Meanwhile in North Yorkshire an NHS practice is also targeted to provide 8% of its activity as urgent care but in fact the reality of demographic need is nearer to 16%. According to the team it becomes patently clear that there is a need for flexibility in commissioning; there is a need to reflect

Delroy Reeves
the reality of the practice’s community. An NHS practise cannot be a one-size fits all, one-stop shop, it exists in the real world.
We have spoken about emotional resilience elsewhere; in this case we understand that some dentists are terrified of coming faceto-face with homeless people, alcoholics, and substance abusers, unless those people have already been seen by other medical professionals and are free from infection, or possibly suffering from underlying medical conditions that might lead to complications and potential litigation.
The team also raised the question of who is best equipped to join the dental profession. Dentistry is a practical profession not an academic one. At one time the dental student would come out of education properly equipped to enter a practice as a dentist, there was no such thing as vocational training. Now a student will leave education having never practiced endodontics and having only ever placed a crown into a phantom head. It was also noted that all too often students are unable to take criticism or accept advice; what is needed here, the team opined, is a person with practical experience – not an ivory tower academic.

Dental disease is entirely preventable except in rare genetic cases, but what practical steps can be taken towards effective prevention? Some members of the
oralhealth
team – with a hint of frustration in their voices – suggested fluoridating the nation’s tap water, and, to avoid protest, don’t tell anyone you’re doing it. Plus, we are living longer; we need to bring aging into the conversation. We need more geriatricians to help cope with the needs of the elderly. The point was also raised that the need is not for flexible commissioning but adaptive. Rather than taking money from primary care where it is most needed the current funds should be used on the front line where they can do the most good. If primary care was properly funded there would be fewer cases of dental disease ending up in NHS hospitals which are already at breaking point.
There are different contract models for dental care in each of the four kingdoms, we need to stop talking about reforming NHS England as if it was the holy grail and start looking at the UK as a united whole.
And finally, prevention, prevention, prevention – prevention is the single most affordable facet of dental care but one size of preventive protocols does not fit all. The team suggested shared learning across the whole dental community in order to meet the demands of those most in need. Yes, that might include an effective skill mix for members of the dental team, and also

enhanced neighbourhood care supported by other front-line health professionals. They asked if there was an active role for private practices in the neighbourhood care model? From a clinical point of view shared care can be very effective.
At which point the discussion time was up.
Speaking after the discussions had been shared with the room, DTA Liaison Delegate Delroy Reeves said: “Some of those are strong opinions but it is the case that such things sometimes need to be said. Care for the patient must always come first, but effective team support and funding must also be in place to make the care practical. We can’t just cross our fingers and hope for the best. Effective dental care and education is a requirement in the modern UK society, but it is treated as an aspiration.”
Also, at DLN Sakina Needham spoke for five minutes
Sakina Needham, Dental Nurse, BADN Panel Representative and Community Oral Health Educator, delivered a five minute ‘Lightning Talk’ to the members of the GDC hosted DLN about the things the dental team needs to consider when delivering care to those most in need. In just five minutes she said a lot.
Sakina explained that she spoke first and foremost as an advocate for dental nurses. She observed that care for those most in need can be challenging, but that there is also an evident need to keep access to such care realistic. She highlighted the importance of oral health literacy, saying it is our duty to help improve general public understanding of the importance of maintaining oral health and hygiene. This might require overcoming language barriers, clarity of message, and keeping our communication simple.

We should provide practical advice that meets real life needs, providing oral health and hygiene education early enough that it becomes an embedded habit, a habit that stays with people into adulthood.
That might require more emotional resilience when dealing with some people. Those most in need might also be those most difficult to empathise with. We might need to see beyond alcoholism, substance abuse or homelessness to the person we want to help.
She concluded by saying that the parameters for the term ‘in need’ are changing. The number of people in what is described as ‘working poverty’ is increasing; housing costs and household bills are constantly rising, external global influences are playing their part, and pay for too many in the UK is not keeping pace with real world costs.
In fact, she added, there is a strong possibility that some lower-paid dental nurses might end up amongst those in economic need.
A See also the comment by Dr Helen Phillips, GDC Chair, at the conclusion of the event, pages 36 and 37 in this issue.
■ Boiling Frog Syndrome
Dental Therapist Victoria Wilson reveals a proven wellbeing model for dentistry
Alongside my role as a dental therapist, certified yoga instructor, functional breath coach and mental health first aider, I have been supporting a number of dental professionals over the past six years. As part of this I have been using a range of support networks to help improve access to multiple wellbeing resources for all members of dental teams.
Aims:
■ Effective communication across the dental team regarding stress and wellbeing
■ Effective management of self and others in the workplace to build healthy resilience
CPD Outcomes:
■ Raising concerns when a colleague demonstrates stress or difficulties
■ More effective practice management for wellness in the workplace
Development Outcomes: A & B

CPD OutcomesA&B 60minutes

This has given me the opportunity to witness how individuals make meaningful, positive changes in their lives, to achieve a healthier resilience. Knowing how to build healthy resilience amidst the continued stressors faced in the dental working environment is imperative if dental professionals are going to thrive in a long and healthy career.
In spite of this, I think that we should be careful not to be lulled into a false sense of security. Even when individuals are fully committed and determined to do everything it takes to prioritise their own wellbeing, keeping this sustainable might prove challenging if the environment is not set up to fully support this.
Qualitative studies1,2 of UK dental teams demonstrate that reactive, individualfocused approaches to managing stress are insufficient and contribute to burnout,
underscoring the need for systemic, practice-wide change rather than reliance on personal coping strategies alone. By this, I am referring to the implementation of a structured wellbeing framework embedded within the entire dental team or practice, designed to produce meaningful and sustained improvements in staff wellbeing.
Take the example of two people (let’s call them Mary and John) who both work in a dental practice and are incredibly motivated to make some life adjustments after recognising signs of burnout and mental fatigue.
Mary’s stance is to approach the practice owner to open up about feeling overwhelmed and running on empty. She also chooses to expand on the strategies she wants to put in place at work and at home to recharge. The collaboration helps Mary fine-tune the changes she wants to
boilingfrogsyndrome

make. She is left reassured and relieved that her employer validates her choices, knowing it will favourably impact on Mary’s performance in clinic.
John, on the other hand, decides to spend more time exercising as a means to switch off and recharge his battery. He is quite reserved and does not feel the need to let anyone know about his mental state and the detrimental impact it has on his work. John would benefit from gaining more breathing space if only his employer or colleagues were made aware of his stress triggers.
Instead, John worries about how he can fit everything in. He also feels anxious about how his peers might wrongly interpret the adjustments he has made at work. His gradual stress increases but John keeps soldiering on, all alone.
Although the prevalence of burnout in the profession is high,3 there is a lot we can do collaboratively to help. As it stands, there is no specific model which is followed to support wellbeing in dentistry. In the cases I cited, we have Mary who takes the initiative to discuss her issues with the principal and might get more support as a result; while John chooses to take a more personal approach, without any collaborative support. In both configurations, awareness of mental issues and repercussions at work depends entirely on the personality of the individual without touching on any robust framework to further support. That is where the need for change has been recognised. Across hospitals and the wider
healthcare sector,4 we observe consistent evidence that corporate, organisational wellbeing structure, culture, and peer support improves staff mental health and sometimes care quality.
What we need is a system which promotes an open culture around mental health to avoid what is known as the boiling frog syndrome. This already exists in other sectors. The boiling frog is an apologue describing a frog being slowly boiled alive. The premise is that if a frog is put suddenly into boiling water, it will jump out, but if the frog is put in tepid water which is then brought to a boil slowly, it will not perceive the danger and will be cooked to death. The story is often used as a metaphor for the inability or unwillingness of people to react to or be aware of threats that arise gradually rather than suddenly.
I recently partnered with an entity that specialises in corporate wellbeing interventions for multinationals banks, hospitals and the telecoms industry. Tapping into a proven structure and repurposing it specifically to the dental profession could really make headway in building a suitable model that would factor in the nuances and challenges faced by dental practices.
We ran a few pilots where we identified the key pain points and measured the impact of the interventions, working closely with practice principals, and all dental team members. Understanding and addressing these pain points via corporate training supports and builds healthy resilience in the
dental setting. We also ensured that every step was measured to appreciate the impact. The early findings appear to be really promising and will be investigated further.
The fact that the topic of mental health suffers less of a stigma nowadays is certainly helping but we need to do more as mental health statistics5 are alarming. At the same time, many practice principals are worried that increased awareness is often accompanied by higher levels of absenteeism and sickness absence. A structured approach to learning and ongoing support, embedded across the whole team, can help address these challenges. By equipping all team members with the right tools and understanding, fewer individuals are likely to be negatively affected, while issues can be identified and managed more proactively.
I am thankful of companies like Philips Oral Healthcare which has been very supportive of my wellbeing initiatives over the years. We need as much awareness as possible to ensure that this sector remains a safe and sustainable place for dental professionals now, and of course the next generations.
Professional Educator and Business Manager for Philips, Lauren Ward added: “Dentistry is an amazing profession. For me, it was a serendipitous discovery when I ended up assisting an orthodontist at just 15 years old, with hygiene therapy evolving into a true passion. Quite early in my career, I sustained a few injuries as a result of performing repetitive motions, and it was not always plain sailing.
“It is only natural to experience ups and downs in life, but what matters is how you deal with it and how you always prioritise your health. It is essential that we normalise wellbeing in dentistry and make it relatable and more relevant to the profession. Victoria’s work is highly commendable and we, at Philips, recognise the importance of integrating wellbeing tools to be able to thrive in dentistry”.
References:
1 Mills, I., Knights, J., Ellwood, F., Witton, R., & Young, L., 2025. Me, we, they: identifying the key stressors affecting the dental team. British Dental Journal, 239, pp. 197 - 203. https://doi.org/10.1038/s41415-0258645-z
2 Plessas, A., Paisi, M., Bryce, M., Burns, L., O’Brien, T., Hanoch, Y., & Witton, R., 2022. Mental health and
boilingfrogsyndrome
wellbeing interventions in the dental sector: a systematic review. Evidence-Based Dentistry, pp. 1 - 8. https://doi.org/10.1038/s41432-022-0831-0
3 https://pubmed.ncbi.nlm.nih.gov/37689455/
4 Brand, S., Coon, T., Fleming, L., Carroll, L., Bethel, A., & Wyatt, K., 2017. Whole-system approaches to improving the health and wellbeing of healthcare
Development Outcome A & B – 60 minutes
workers: A systematic review. PLoS ONE, 12. https://doi.org/10.1371/journal.pone.0188418
5 https://www.thegazette.co.uk/all-notices/content/ 103417
To complete your CPD, store your records and print a certificate, please visit www.dta-uk.org and log in using your member details.
Q1 Qualitative studies of UK dental teams regarding stress management demonstrate what?
A That women deal with stress better than men
B Stress is impacted by the situation at home
C Individual-focused approaches are insufficient
D Levels of alcohol abuse in the dental practice are rising
Q2 Rather than relying on personal coping strategies what do these studies recommend?
A A poster inviting staff to share their thoughts
B Systemic practice-wide change
C Weekly meetings and group hugs
D More social activities and team bonding
Q3 In the Mary and John examples what is Mary’s stance?
A She opened up to the practice owner about feeling overwhelmed
B She tells her partner that she is suffering at work
C She swims 10 laps every morning before going to work
D She takes prescribed sedatives and breathing exercises
Q4 In these examples what does John decide to do
A He visits the pub every day after work for a solitary pint or two
B He has joined a boxing club and pounds a punchbag
C Spends his time exercising to ‘switch off’
D He has taken up bird watching at weekends
Q5 How might John gain more breathing space
A Take time to pursue a new career
B Make his employer and colleagues more aware of his stress triggers
C Talk to his GP about therapy
D Get more competitive with his colleagues
Q6 Awareness of mental issues and repercussions at work depend entirely on what?
A Getting the work/life balance in order
B Getting the environment to be brighter and more welcoming
C The correct training for team leaders
D The personality of the individual
CPD OutcomesA&B 60minutes
Q7 Across hospitals and the wider healthcare sector, evidence has shown that what helped improve staff mental health?
A A corporate organisational wellbeing structure
B More flexible working hours
C A team reward scheme that recognises excellence
D Quiet classical music in the background
Q8 What is the ‘boiling frog’ syndrome
A Frogs are too stupid to realise they are in danger
B When frogs are plunged into boiling water they instantly pass out
C If the frog is placed into boiling water that is slowly brought to the boil it will be cooked
D A frog is highly sensitive to temperature change and will quickly climb out of the warming water
Q9 Understanding a person’s key pain points helps to build what?
A Healthy resilience in the dental setting
B Greater trust between colleagues
C A wariness regarding a colleagues mental health
D Caution about upsetting a colleague unwittingly
Q10 Many practice principals are worried that increased awareness of mental health issues is often accompanied by what?
A Avoidance of the individual affected
B Mockery behind the sufferer’s back
C Higher levels of absenteeism and sickness absence
D A negative impact on team professionalism and reduced patient care
■ Michael Sultan: A Recipe for Health
As dental professionals, we are tasked with helping people achieve better oral health. However, the mouth is not an isolated organ and, therefore, our remit is far broader than simply advising on how to maintain the teeth and gums.
Instead, we must consider the patient as a whole and offer comprehensive support where appropriate. For example, we know that diet can have a significant impact on a person’s dental and systemic health. Helping patients to assess their food and drink consumption, and make healthier decisions, will have a lasting effect on their mouth, body, and mind.
From the Mediterranean with love
There is some conflicting information online about which diets are best for health and wellbeing. However, a systematic review found a Mediterranean diet reduces the concentration of various inflammatory biomarkers – more so than a vegetarian or vegan diet.1 Often defined as a diet high in plant-derived foods like vegetables, fruits, whole grains, nuts, and seeds, as well as olive oil as the main fat

used in cooking, it also typically involves low amounts of red or processed meat and sweet items. It is believed that the diet helps to inhibit pro-inflammatory mediators, promote anti-inflammatory functions, and modulate cell-mediated immunity, among other potential functions.
There is also initial evidence to suggest that an anti-inflammatory diet such as this could support the management and treatment of mental disorders and neurodegenerative diseases.2 Once again, more research is required to confirm the full potential of dietary patterns on such conditions.
The same can be said of the link between the Mediterranean diet and oral health. A paper published in 2025 found that this anti-inflammatory dietary pattern, with lower red meat consumption, was also associated with reduced severity of periodontal disease.3 Larger scale studies are needed to confirm the relationship and mechanisms at play.
Of course, this is not the only way that food consumption affects oral health. Diet, and in particular, sugar intake, has also been linked to caries risk. The literature shows that when ≤10% of daily energy is consumed in free sugars, the risk of caries remains low.4 While this is not an absolute threshold, it does indicate a target for patients to aim for to protect their teeth from harm.
inflammation and periodontal diseases).7
The price of health
While all of this is important, and useful information to share with patients, we must remember that other barriers exist that prevent some from maintaining a healthy balanced diet.
The food environment in which patients live is one. At a time when cost of living remains high and many families are financially challenged, accessibility to healthy food may be reduced. A very interesting report published by The Food Foundation8 in 2025 found that, in general, healthier foods are more than twice as expensive per calorie as less healthy foods –the former group increased in price by almost double that of alternatives in the preceding two years.
Defining ‘healthy’ food according to its Nutrient Profile Modelling score category, it found that healthier options averaged £8.80 per 1,000 kcal, compared to £4.30 for other items. The same report calculated that the lowest income groups in the UK would have to spend a massive 45% of their disposable income just on food to meet the government-recommended diet. This figure increased even further to 70% for households with children.
■
■
Other ingredients that add to a balanced diet include cruciferous vegetables such as broccoli, cauliflower, kale, cabbage, Brussels sprouts, bok choy, arugula, radishes, turnip greens, and watercress, noted for their plaque-fighting properties,5 vitamin D for enamel strength and added protection from caries,6 and fibre for a reduced risk of
The situation is even worse for those with food allergies and dietary requirements. A report by Coeliac UK9 suggested that a gluten-free weekly food shop is costing an enormous 35% more than the glutencontaining equivalent – 77% of people affected struggled to afford the gluten-free products they needed. Higher costs are also associated with a lactose-free diet,10 with a Food Standards Agency report finding that household catering for any
food hypersensitivity or allergy also spend 11% more on meals when eating out or getting a takeaway.11
A matter of perspective
These are not barriers that dental professionals can overtly help affected patients to overcome. However, we can help the individuals we see to come up with practical options that might work for them and their families. We’re not striving for perfect, just a better diet for improved oral and systemic health. For some patients, this might be as simple as swapping a daily fizzy drink for water. Others might be interested in online recipes that promote healthy yet affordable meals. All it takes from us as healthcare professionals is to start the conversation and let people know that we are here to help support their wellbeing in any way that we can.
Author Specialist endodontist Michael Sultan is the founder and principal of endodontic referral practice EndoCare.
References:
1 Koelman L, Egea Rodrigues C, Aleksandrova K. Effects of Dietary Patterns on Biomarkers of Inflammation and Immune Responses: A Systematic Review and MetaAnalysis of Randomized Controlled Trials. Adv Nutr. 2022 Feb 1;13(1):101-115. doi: 10.1093/advances/nmab086. PMID: 34607347; PMCID: PMC8803482.
2 van Zonneveld SM, van den Oever EJ, Haarman BCM, Grandjean EL, Nuninga JO, van de Rest O, Sommer IEC. An Anti-Inflammatory Diet and Its Potential Benefit for Individuals with Mental Disorders and Neurodegenera tive Diseases—A Narrative Review. Nutrients. 2024; 16(16):2646. https://doi.org/10.3390/nu16162646
3 Mainas G, Grosso G, Di Giorgio J, et al. Relationship between Mediterranean diet and periodontal inflammation in a UK population: A cross-sectional study. J Periodontol. 2025; 1-12. https://doi.org/10.1002/jper.70016
4 Moynihan P. Sugars and Dental Caries: Evidence for Setting a Recommended Threshold for Intake. Adv Nutr. 2016 Jan 15;7(1):149-56. doi: 10.3945/an.115.009 365. PMID: 26773022; PMCID: PMC4717883.
5 Baruch Y, Golberg K, Sun Q, Yew-Hoong Gin K, Marks RS, Kushmaro A. 3,3’-Diindolylmethane (DIM): A Potential Therapeutic Agent against Cariogenic Streptococcus mutans Biofilm. Antibiotics (Basel). 2023 Jun 6;12(6):1017. doi: 10.3390/antibiotics12061017. PMID: 37370336; PMCID: PMC10295630.
6 Ziada, S., Wishahe, A., Mabrouk, N. et al. Vitamin D deficiency and oral health: a systematic review of literature. BMC Oral Health 25, 468 (2025). https://doi.org/10.1186/s12903-025-05883-w
7 Swarnamali H, Medara N, Chopra A, Spahr A, Jayasinghe TN. Role of Dietary Fibre in Managing Periodontal Diseases-A Systematic Review and MetaAnalysis of Human Intervention Studies. Nutrients. 2023 Sep 18;15(18):4034. doi: 10.3390/nu15184034. PMID: 37764817; PMCID: PMC10536522.
8 The Food Foundation. Broken Plate Report 2025. The state of the nation’s food system. https://foodfoundation .org.uk/sites/default/files/2025-01/TFF_The%20Broken %20Plate%202005%20FINAL%20DIGITAL.pdf
[Accessed December 2025]
9 Coeliac UK. Cost of living 2024 press release. People with coeliac disease paying up to 35% more for weekly food shop. June 2024. https://www.coeliac.org.uk/ document-library/9211-cost-of-living-2024-pressrelease/ [Accessed December 2025]
10 Taeger M, Thiele S. Additional costs of lactose-reduced diets: lactose-free dairy product substitutes are a cost-
effective alternative for people with lactose intolerance. Public Health Nutr. 2021 Sep;24(13):4043-4053. doi: 10.1017/S1368980021002779. Epub 2021 Jun 28. PMID: 34180787; PMCID: PMC10195326.
11 Food Standards Agency. Estimating financial cost to individuals with a food hypersensitivity. July 2022. https://www.food.gov.uk/research/food-hypersensitivity/ estimating-financial-cost-to-individuals-with-a-foodhypersensitivity?print=1 [Accessed December 2025]
Development Outcome B & C – 60 minutes
To complete your CPD, store your records and print a certificate, please visit www.dta-uk.org and log in using your member details.
Q1 Which diet is said to most reduce the concentration of various inflammation biomarkers?
A Vegetarian B Vegan C Mediterranean D High protein
Q2 What are the listed benefits of the diet in question?
CPD OutcomesB&C 60minutes
A Inhibits pro-inflammatory mediators B Promotes anti-inflammatory functions
C Modulates cell mediated immunity D All of the above
Q3 The diet in question is also said to reduce what?
A A bloated sensation at the end of the meal B Severity of periodontal disease
C The risk of halitosis D The risk of dental enamel wear
Q4 What percentage of free sugars should be consumed as the daily energy intake to keep the risk of caries low?
A No more than 25% B Less than 20% C Less than 10% D No more than 15%
Q5 Cruciferous vegetables are noted for what?
A Plaque-fighting propertie B Vitamin D for enamel strength
C Protection from caries D Reduced risk of inflammation, and all of the above
Q6 How much more expensive are healthier options compared to less healthy alternatives?
A 15% more expensive B Twice more expensive
C Three times more expensive D Shopped carefully they are the same price
Q7 How much of their disposable income would those in the UK’s lower income brackets have to spend to meet the cost of the government’s recommended diets?
A Over half B More than 60% C 28% D 45%
Q8 How much would that percentage of disposable income be for households with children in the lower income brackets wishing to meet government dietary recommendations?
A 70% B 92% C 80% D 67%
Q9 In percentage terms, how much more expensive is a gluten-free weekly food shop compared to a gluten-containing alternative?
A 60% B 45% C 35% D There is actually little difference
Q10 A household catering for any food hypersensitivities or allergies has to spend how much more in percentage terms when eating out or ordering a takeaway?
A 11% B 23% C 32% D 7%
■ Sticks and Stones
Dr Chris Turner, MSc,BDS,MDS,FDSRCS, FCGDent, QDR Specialist in Restorative Dentistry (Rtd), Bath.

I used to give a lecture entitled ‘Sticks and Stones’ during which I looked at the significant improvement in retention that air abrasion, the stones, gave by creating a low energy surface prior to the cementation of all the dental restorations that I fitted. It was especially useful in cementing veneers and in cleaning, at the chairside, cement from both teeth and Maryland type etch-retained bridges rather than having to post those bridges to yourselves in the dental labs. Many patients would not wait for a day or two and always seemed to claim that they had something important to do, or somewhere to be, and they “couldn’t do it looking like this”.
The Stick relates to ‘Stick’, the Finnish invention of treated fibreglass reinforcement for composite restorations and acrylic dentures. I had the privilege to be the first British dentist invited to Turku in 1999 to evaluate the product – which was made behind both closed doors and a very definite NO ENTRY sign – to see how the first polymer coated reinforcement material was manufactured. Using ‘Stick’ changed my thinking about restorative dentistry.
expensive than a removeable acrylic partial denture, but in the longer term this is unlikely to be the case when the costs of repairs, replacements and orthodontics are taken into account, PLUS, and this is important, the added costs of surgery time, laboratory time and more materials.
CPD Outcomes:
■
■
I am on record that in the 21st century no child who loses a single maxillary central incisor through trauma should ever be subjected to wearing an acrylic partial denture. They break, become lost and when they are not worn the space between the retained central incisor and the opposite lateral incisor closes quickly, making aesthetic and size-balanced restoration some years in the future much more difficult.
My solution, a reinforced composite veneer on the sound central incisor with a cantilevered pontic for the missing tooth has already been described for you. The point about labial bonding is that it is far more secure than palatal bonding, does not get dislodged during eating, and lasts for years. Yes, I know that the cost of the initial prescription for this restoration is more
However, if you are asked to repair an acrylic denture there is now the option of reinforcement with StickNET. Stick and StickNET are, respectively, unidirectional and net-shaped polymer coated glass fibre reinforcement materials developed by GC Europe to strengthen, repair, and reinforce composite and acrylic materials in dentistry.
These products use a patented Interpenetrating Polymer Network (IPN) structure, which allows the fibres to create a strong, durable, and aesthetic bond with dental composites and acrylics, often providing a metal-free alternative to traditional dental restorations.
The use of a wire strengthener, as used to be an additional NHS fee, is contraindicated; it’s actually better described as a wire weakener.
Stick is also an excellent material for reinforcing maxillary complete dentures. It is more aesthetic than carbon fibre. Additionally, it is easier to make an ideal
cupid’s bow, effective post dam without the difficulties that arise when using a cobalt chromium base, unless the design is modified with tags to hold acrylic along the posterior border.
When my patients wanted a more aesthetic restoration than amalgam, I turned to making Stick reinforced composite inlays made indirectly in the laboratory as a more satisfactory restoration than packing and curing composite (except for very small cavities) at the chairside because any shrinkage during curing had already occurred and all I needed to do was etch the cavity walls and cement in place with flowable composite.
My restorations were therefore much stronger because of the reinforcement and I did not have to spend chairside time adjusting the occlusion or making sure that there was an adequate contact point.
Stick came into its own when I wanted to splint teeth. The most frequent position was for mobile mandibular incisors following
emergingtechnologies

Stick: Fibre reinforcement – providing a strong, aesthetic and profitable solution for strengthening composites and acrylics
periodontal treatment. My technician made a lingual splint, reinforced to reduce fracture, and extending from canine to canine. Additionally, had any incisors been extracted a pontic could be built up. This made for a far better tolerated appliance than the traditional acrylic tissue supported partial denture, the gum stripper. You will appreciate I tried to avoid these wherever I could after my visit to Turku.
Some of my patients presented with badlyfitting crowns with overhangs, deficiencies, or both that were plaque traps and needed removal as part of periodontal treatment. I found that composite crowns reinforced with StickNET made an ideal intermediate restoration while periodontal treatment took place. They often lasted for several
years and gave time for patients to prove that their plaque control merited more expensive crowns such as porcelain fused to metal or zirconium oxide reinforced.
Let’s look at another case, one I had to look after some years ago. This lady presented with a broken down maxillary central incisor and had been advised that it needed to be extracted and replaced with a partial denture for about six months before she could have a conventional bridge carried on crowns on her other central and a lateral, and that it would make sense to crown the other, intact, lateral to get a better result. She had declined my colleague’s treatment plan, did not want unnecessary crowns and would not wear a denture.

emergingtechnologies
Talk about a challenge! I proposed to make her an immediate bridge in reinforced composite, palatally bonded because the occlusion allowed that, with the proviso that there would be recession under the pontic, and the bridge would need to be replaced, perhaps with the same procedure between six- and nine-months in the future. The next challenge was how I could ensure an accurate fit of the central incisor pontic once the tooth had been extracted. I recognise how skilled many of you are in sectioning models for such cases. However, even a slight error could prevent the bridge seating properly after the extraction. I dread to think what would have been said if I had
had to send this lady away with a gap while I waited for a remake.
The answer here was to do as follows: I booked the work in with my technician for return after one week rather than the usual two and agreed to pay for guaranteed next day delivery both ways.
I then cleared the contact points on the tooth to be extracted using an air turbine so there could be no doubt regarding the exact space available, then I took an elastomeric impression.
In order to prevent space loss, I acid etched the sides of the above tooth and added a
Development Outcome C – 60 minutes
light-cured composite to recreate the contact points. Shade taking followed the usual methods.
One week later the broken-down tooth was extracted and the bridge fitted under rubber dam. I was relieved my method worked, and have used this technique for other patients. My suggestion is, if you are presented with an impression where you have to trim for contact points for an immediate restoration that you suggest the above method to my colleagues.
To complete your CPD, store your records and print a certificate, please visit www.dta-uk.org and log in using your member details.
Q1 In which country was Stick invented?
A United State B Japan C Finland D France
Q2 In what year did the author evaluate the product?
A 2002 B 1999 C 2012 D 1995
Q3 What is Stick?
A A polymer coated glass fibre reinforcement material
B A biomimetic monomer reinforcement
C A malleable nylon bridge material
D A carbon fibre reinforcement material
Q4 What does the author say is amongst the problems with acrylic partial dentures?
A They break B They quickly discolour
C They lack the translucency of natural dentition
D They become plaque traps
Q5 What is described as the ‘point’ about labial bonding?
A It is far more secure than palatal bonding
B It is initially more cost-effective
C Does not get dislodged when eating
D Lasts for years and a) and c) only
Q6 If you are asked to repair an acrylic denture what does the author suggest as the best reinforcement?
A StickNET glass fibre B Wire strengthener
C Carbon fibre paste D Silicon dental cement
Q7 What did the author use instead of amalgam?
A Gold reinforced ceramic
B Chrome reinforced ceramic inlays
C Stick reinforced composite inlays
D Glass ionomer filler
CPD OutcomeC 60minutes
Q8 What was the most frequent position when the author wanted to splint teeth, when he said ‘Stick came into its own’.
A Maryland bridge B Crown supported pontic
C Mobile mandibular incisors following periodontal treatment
D Mobile anterior canines following trauma
Q9 Why did the author say composite crowns reinforced with StickNET make an ideal intermediate restoration while periodontal treatment took place?
A Instant placement
B The patient likes the aesthetic qualities
C A rapid and cost-effective chairside restoration solution
D They often lasted several years and gave the patient time to prove their plaque control
Q10 What was the answer when the patient refused a partial denture and unnecessary crowns?
A An immediate placed dental implant
B Pontic cemented to adjoining dentition
C Palatally bonded immediate bridge
D Single denture with a lingual splint
■ AI: Stupid but Fast
Spencer Kelly and Sophie Lovett discuss AI matters
On the main stage during BDIA Dental Showcase science innovation
TV presenter Spencer Kelly and Sophie Lovett, International Account Manager for dental diagnostic AI software company Pearl (known as Hello Pearl in the UK) discussed the connection between broader AI-driven technologies and those designed specifically for dentistry. The Technologist was there to take notes, and join the laughter.

Spencer and Sophie
Spencer explained that as the lead presenter for ‘Click’ he has been exploring the interaction between tech and humans for over two decades. AI has been around since the 1950s but when most people talk about AI (artificial intelligence) these days they are thinking of innovations such as ChatGPT, software that can be used to create essays and forms of
Aims:
■ Look at where AI fits into the dental workflow
■ Gain a better understanding of AI benefits and drawbacks
CPD Outcomes:
■ Clinical and technical areas of study
■ Knowledge and skill within your field of study
Development Outcome: C
literature, and help students cheat in their dissertations.
We hear of AI actors, deep fake images, AI music parroting copyrighted material, but these are just a fraction of the technology’s uses. AI can learn to think for itself, and steer self-driving cars, although, hmm, note the recent complete system breakdown of
self-driving taxis in Wuhan, China causing traffic mayhem.
AI is now actually doing what it was predicted to do in science fiction stories written by visionaries such as Isaac Asimov decades ago.
And yet it is only over the last ten years that AI has become normalised. But wait, here’s a question, how do we draw the line between intelligent machine innovation and technology evolution? Good question. In a way AI is like a biological organism because it uses what are known as neural networks – a form of algorithmic technology able to learn and remember what it has learned – but we don’t actually quite know how it works. When we look at AI through modern eyes, we now realise that in fact it is both innovation and evolution.


Spencer described technology as following a specific acceptance arc into society. When mechanisms are new, they are expensive and very few people know how to use them. Then, as the innovation matures, it becomes less expensive and simpler to operate so more people use it. For example, look at smartphones. The technology has evolved from a bulky brick of a quote ‘mobile’ phone that needed a briefcase to cart it around in, to a slim super computer that barely bulges our pockets and contains every facet of our lives.
But, people ask, won’t AI replace our jobs? Frankly, yes, but how and which jobs? Robots replaced blue collar workers in car production lines but other jobs remained in the automotive industry – is AI’s intelligence now coming into the workforce so very different to the mechanised muscle that replaced car workers? Perhaps AI will replace white collar workers with its ability to sort and find links and connections between different types of data, make economic predictions, forecast the weather, work out what the White House will do next... or, perhaps not.
Let’s take a look at some examples of the way some innovations are used, and ask can we trust it? Spencer posited that we tend to put our trust in the wrong things, consider how we believe the claims made in social media. Antivaxxers are a fine example of people believing and acting on misinformation entering the public awareness through sources such as X, Instagram, and Facebook.
Social media is cheap and easy to use, but in the wrong hands it can be dangerous. It can

drive away trust. For example, forget taxis in Wuhan for a minute, driverless cars are often safer than vehicles in human hands – but selfdriving cars will sometimes do weird things. The media focuses on the weird to the exclusion of the technology’s safer features and so impresses us with a fear of the innovation. We lose our trust, and once the trust has been lost it can be hard to regain.
Transparency and honesty is essential in accepting any innovation/evolution, but there are a lot of snake oil salesmen out there with promoters making improbable AI promises – but wait, we’re getting ahead of ourselves. We need to understand what AI is and how it works, and here we are, already talking about it as if it’s an old and well understood friend. Let’s have a quick lesson in AI dynamics. Let’s play a game called ‘Spot the Fuggler!’ Yes, Spencer said ‘Fuggler’, a toothy creature that consumes humans from the feet up leaving the brain ‘til last.
He showed his audience an image of a Fuggler, pointing out its salient features. It is
a squat, bug-eyed monster with human teeth, and Spencer asked his audience if they could tell the difference between the monster and, for example, a cat or a puppy. We humans can spot the Fuggler after seeing just a few examples, but a computer can’t, it needs to see millions. It is paradoxically a very slow learner but also fantastically quick.
Technology like the software created by Pearl has access to millions of medical images, x-rays and scans through which it can learn to recognise dental problems such as tumours, caries, and periodontal disease. The human brain is faster. A human can sit in a class and learn to recognise tumours and accept the spoken word from a teacher while the computer can’t. To the computer images are just pixels, we might quickly learn to recognise those pixels as representations of a cat, a dog, or a Fuggler, but the computer can’t.
But it will learn. Spencer reiterated, at heart computers are dumb. They learn by trial

and error – but when they get things wrong, they remember, and when they get it right, they remember – and they never forget. After multiple trials they make very few mistakes, and they can make connections between what they’ve learned and other relevant data they know to be correct to make valuable correlations that the human mind might easily miss.
Pearl technology uses AI; it has been trained to support the diagnosis of a dental problem. Computers are dumb but they can learn to spot problems very quickly, but even so you still need the human cognisance. You cannot completely replace a human healthcare specialist like a dentist with AI, no, said Spencer, don’t do that, but you can use AI to support and aid what the human does. AI can augment the human’s diagnosis not replace it. It is important to vet everything AI does, AI offers a second opinion but the human eye remains essential in truly understanding what the patient’s needs are.
Killer robots
How are other countries using AI? Here’s a fun example. In both South Korea and Japan, the workforce is shrinking by some 700,000 people per annum, largely due to the low birth rate, and many manufacturing processes are now fully roboticized. In Korea they attach technology to just about everything. For example, they are using technology to solve South Korea’s biggest problem, and no it isn’t North Korea. It’s jellyfish, translucent floating creatures with a sting in their tails but also endowed with an alien elegance. Unfortunately these are creatures that get into pipes and ducts and pumping systems and cause billions of dollars of damage every year.
The Koreans have now devised jellyfish killer robots that use image recognition technology to track down the jellyfish and chop them to pieces with whirling razorsharp blades then pump the mush safely away. Don’t worry, the jellyfish don’t have a nervous system and don’t experience pain,

CPD OutcomeC 60minutes
just keep your fingers out of the way while the blades are spinning. (Image from YouTube KAIST Urban Robotics Lab 2013).
Another example; in India the innovative population will use technology to do whatever they need. That doesn’t mean they will use a smartphone to drive in a nail, but in one remote village the inhabitants have lashed an LED board to a tree. Why? Because young people from the village move away to find work and villagers can use the device to contact their distant family members to ensure they’re alright and prospering. They can also get the latest weather reports and news.
Advances in AI healthcare are driven by the huge volume of training material available, but, Spencer stressed, although it is not yet about the technology doing the clinician’s job – it can help them understand the situation a bit easier, it can also help inform the patient with clear imagery. The patient can see what, why and where they need treatment, aiding informed consent. We must make it clear that there is a lot of hype and exaggeration out there regarding what AI can do, and the people who develop the technology need investment so they play it big on the world’s stage. But

that is not the case with diagnostic AI which is purely based on experience and proven facts.
In conclusion, Spencer said, we are entering an era of transition (and perhaps in some cases delusion) regarding AI, but we are not yet at the destination. AI will change the world through its ability to analyse and find links in big data; it will mean incredible technology working on behalf of health diagnosis and – through systems like Pearl –offering a second opinion. Think of it as a support tool, a second pair of eyes.
The clinician makes a choice based on all the available data, while the Pearl system works with the practice’s existing technology (such as Dentally) with no transitional downtime and no change to the workflow. It benefits the clinician and the patient, and at the end of the day it is the patient who comes first. As with Align’s ClinCheck and the gamut of intraoral scanners on the market the Pearl technology allows the patient to make a more fully informed consent, and that doesn’t need artificial intelligence to recognise the benefits.
Development Outcome C – 60 minutes

Last words, Sophie asked Spencer if he had any advice for young people facing a future with AI in it, will it mean driving harder for academic attainment? Talking of his own children Spencer said he just wants them to be happy, but that in the future critical thinking and depth of education will prove essential.
To complete your CPD, store your records and print a certificate, please visit www.dta-uk.org and log in using your member details.
Q1 How long has AI been around?
A Two decades B Since the 1980s
C Since the 1970s D Since the 1950s
Q2 Which specific science fiction author is described as a ‘visionary’
A Jules Verne B Isaac Asimov
C H G Wells D Robert Heinlein
Q3 What are neural networks?
A The links between computers on the internet
B Fine crystal fibres used by engineers to build AI systems
C A form of algorithmic technology
D The biological system used by human synapses and mimicked by AI
Q4 Is AI the result of innovation or evolution
A Both B Innovation C Evolution
D Neither, it is self-designed by computers and humans don’t understand it
Q5 To demonstrate how AI works Spencer Kelly introduced the game of ‘Spot the...’ what?
A Kitten B Puppy C Fuggler D Wally
Q6 Can a computer instantly learn how to recognise something?
A Yes if it has first been described in detail in word form
B No, it needs to see millions of examples
C No, it needs to study images in detail for hours
D Yes, if the images are at the right size in enough detail
Q7 Can AI replace the human in dental diagnosis?
CPD OutcomeC 60minutes
A Yes, it can even spot incipient caries not visible to the naked eye
B Yes, if it has been given sufficient examples to work from
C No, the subject is yet too complex and AI goes into stasis
D No, it offers a second opinion but the human eye remains essential
Q8 Approximately how many members of the workforce are Japan and South Korea each losing every year?
A 200,000 B 700,000
C 500,000 D 1.2 million
Q9 What is cited as South Korea’s biggest problem?
A Sourcing rare minerals for computer manufacture
B North Korea
C Jellyfish clogging pipes and pumps
D A rapidly aging population
Q10 What is the benefit of providing the patient with AI enhanced imagery of their oral situation?
A They are more likely to accept an expensive procedure
B It aids informed consent
C They are more likely to follow a more effective at-home hygiene regime
D Very little, they prefer to leave things in the hands of the specialist
Enhancing Digital Dentures Through Gingival Characterisation
Mia Harrison, BSc (Hons) RDH, FdSc RDT
Mia is a registered Dental Hygienist and second-generation Dental Technician at Bespoke Denture Clinic, with a combined passion for digital prosthodontics and periodontal health.

In the ever-evolving field of dentistry, current workflows have become increasingly integrated with digital technologies. Clear benefits can be seen whilst using this technology, such as improved accuracy, efficiency and reproducibility. However, the materials used in digitally manufactured dentures –whether it be milled or 3D printed – do not alone achieve the level of realism required for a truly lifelike prosthesis.
Characterisation therefore is a crucial step in digital prosthetic workflow, allowing technicians to replicate natural variations found within the oral cavity. Psychologically, the impact of monochromatic “block pink” dentures has been widely discussed. Raj et al. (2022) reported that gingival characterisation and staining can improve patient acceptance and make adaptation to denture use easier.
CPD OutcomeC 30minutes
interdental papilla. Whilst the aim of prosthetic work is not to replicate unhealthy tissue, observing these variations is useful when aiming to avoid the artificial appearance of a uniform denture base and instead replicate realistic gingival aesthetics.
Histologically, healthy gingiva can be divided broadly into three different sections: the free gingiva, attached gingiva and the alveolar mucosa. The free and attached gingiva consist of keratinised tissue, which is a collagen-dense structure that creates a protective barrier between the oral environment and the periodontium (Zhang et al., 2023) and is therefore notably more resilient (Poul et al., 2024).
Aims:
■ Understanding the aesthetic importance of natural characterisation in the manufacture of dentures
■ Gain insight into the way characterisation can lead to improved acceptance and adaptation to denture use
CPD Outcomes:
■ Maintenance and development of knowledge and skill within your field of practice
■ CPD specific for your daily role
■ Clinical and technical areas of study
Development Outcome: C
Therefore, adapting one’s skillset to include gingival characterisation when finishing the prosthesis is critical for patient satisfaction when using digital workflows, ensuring overall confidence and that patient satisfaction remains at a high standard (Sony et al., 2021).
Natural gingiva varies with each patient in colour, texture and vascular appearance. Healthy gingiva is notably described as a coral pink colour, with increased vascularity partially at the alveolar mucosa contributing to deeper red tones. The interdental papillae often appear in knife-edged triangular form. Surface texture may also be present with stippling.
In contrast, gingival tissue which is not at optimal health may present with deeper red tones alongside swelling of the
This is in contrast with the alveolar mucosa, which is non keratinised. It is softer and thinner in texture and often darker in appearance due to its increased vascular visibility.
Variations in tissue contribute to the natural gradient often seen within the oral cavity which contrasts with the monochromatic denture bases commonly produced in prosthetic workflows. Gradual transitions of pinks, browns and reds can be observed as the tissue transitions naturally between the attached gingiva and the alveolar mucosa.

periodontalhealth
Case Study
A case was presented at Bespoke Denture Clinic requiring maxillary and mandibular complete dentures. The patient requested an aesthetic prosthesis that avoided the appearance of conventional monochromatic denture bases. A digital workflow was utilised for denture design and manufacturing, followed by gingival composite characterisation to enhance realism.
With clinical work carried out by CDT Richard Harrison RCS, the prosthesis was then designed using CAD software, with the digital workflow and gingival characterisation undertaken by the author. The dentures were initially 3D printed to produce a try-in prosthesis, before the final design was sent away to be milled. Prior to characterisation, the denture base was prepared to ensure optimal bonding of the composite materials via sandblasting and a suitable bonding agent.
Gingival composite stains were applied in multiple layers to recreate the natural variations seen within oral tissues. Lighter tones were placed within the attached gingiva, whilst deeper red and brown tones were used to replicate the vascular appearance of the alveolar mucosa. The
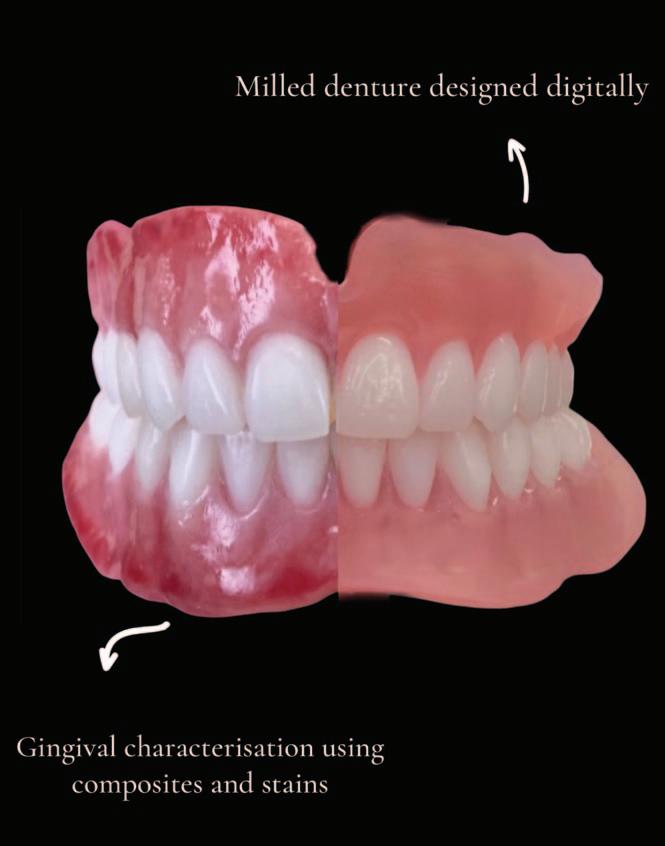
materials were then cured following the manufacturer’s guidelines.
The final prosthesis demonstrated a more natural gingival appearance when compared to conventional monochromatic denture bases, resulting in greater patient and clinician satisfaction. A comparison between the monochromatic milled denture and the characterised prosthesis is shown in Figure 1 (below).
This case reinforces the role of gingival characterisation in elevating digital dentures, ensuring that advancements in technology are matched by equally high standards in aesthetic realism.
References:
– Raj, N., et al., 2022. Aesthetic perception of conventional and characterised dentures. Journal of Prosthodontic Research.
– Sony, M., et al., 2021. Patient satisfaction and aesthetic outcomes in denture prosthetics. Journal of Prosthetic Dentistry.
– Zhang, X., et al., 2023. Structural characteristics of keratinised gingival tissues. Journal of Periodontal Research.
– Poul, J., et al., 2024. Histological differences between gingiva and alveolar mucosa. Oral Biology Research.
Development Outcome C – 30 minutes
To complete your CPD, store your records and print a certificate, please visit www.dta-uk.org and log in using your member details.
Q1 According to the article what might specifically improve patient acceptance and make patient adaptation to denture use easier?
CPD OutcomeC 30minutes
A Using digital imagery to explain what their new smile will look like
B Gingival characterisation and staining
C Giving the prosthesis a higher gum line for a bigger smile
D Using natural acrylic restorations for a more cost-effective outcome
Q2 What colour is healthy gingiva?
A Rose pink B Blood red C Coral pink
D It varies according to the patients natural skin colour
Q3 With regards to colour, what does increased vascularity partially at the alveolar mucosa contribute to?
A Deeper red tones B Brown shading
C Enhanced plumpness and lighter pink
D Slight blueish tint to the pink, purplish red
Q4 How do interdental papillae often appear?
A Plump and rounded B In what is described as stubby projections
C Varies according to the size and proximity of the dentition
D Knife-edged triangular form
Q5 What can be observed as the tissue transitions naturally between the attached gingiva and alveola mucosa?
A Variations in tissue striations
B Transitions between pinks, browns and reds
C Very little variations in healthy tissue
D Tissue translucency in the alveola mucosa increases
■ Custom-made devices and the dangers of non-compliance
Adam Stanley, is the Policy & Public Affairs Manager at BDIA

From the cars we drive to the food we eat, the aircraft we travel in and the buildings where we live and work, these industries are backed up by regulations to ensure that products are appropriate, safe and effective. The world of medical devices is no different and, like all of these industries, the materials and processes involved in manufacturing of custom-made devices in dental laboratories are crucial to ensuring compliance. Unfortunately, that compliance is far from universal and it’s imperative to ensure that you understand the requirements, the risks associated with using non-compliant products and materials and the actions you should take.
Why does regulation matter?
Something that the BDIA, as an industry body, has been working to highlight to the dental team is the need to understand the regulatory implications of chairside manufacturing activity. We have seen significant growth of, and interest in, in-surgery use of CAD/CAM and 3D printing technologies, and this is a trend that is likely to continue.
What has been slower to develop, however, is an awareness of the regulatory implication of these activities. An understanding that the production of custom-made medical devices within the practice brings with it manufacturer responsibilities, including registration with the Medicines and Healthcare products Regulatory Agency (MHRA), is sometimes lacking.
As we continue to promote awareness of, and compliance with, these regulatory requirements for dental practices it is vital to ensure that dental laboratories are also compliant. While dental technicians may have a greater level of familiarity, on average, with the requirements surrounding the manufacture of custom-made devices than other members of the dental team, we have nonetheless seen some concerning instances of non-compliance.
For Dental Technicians and Clinical Dental Technicians registered with the General Dental Council (GDC) there is a clear and direct link between the regulations and their professional registration. The GDC’s own Standards for the Dental Team highlights the importance of regulation in a professional context: “Standard 1.9.1 – You must find out about, and follow, laws and regulations affecting your work”. This obligation places the onus on those purchasing, using and manufacturing medical devices to be vigilant and to ensure that the products are compliant.
Even for non-registrants working in a laboratory setting (such as laboratory managers or others with responsibility for purchasing, trainees or process workers) awareness of and compliance with these requirements is hugely important. First and foremost, the patient safety implications of non-compliant products being used are the same whether or not the individual manufacturing them is a registrant. Beyond this, there is also the reputational risk for
customdevices&compliance
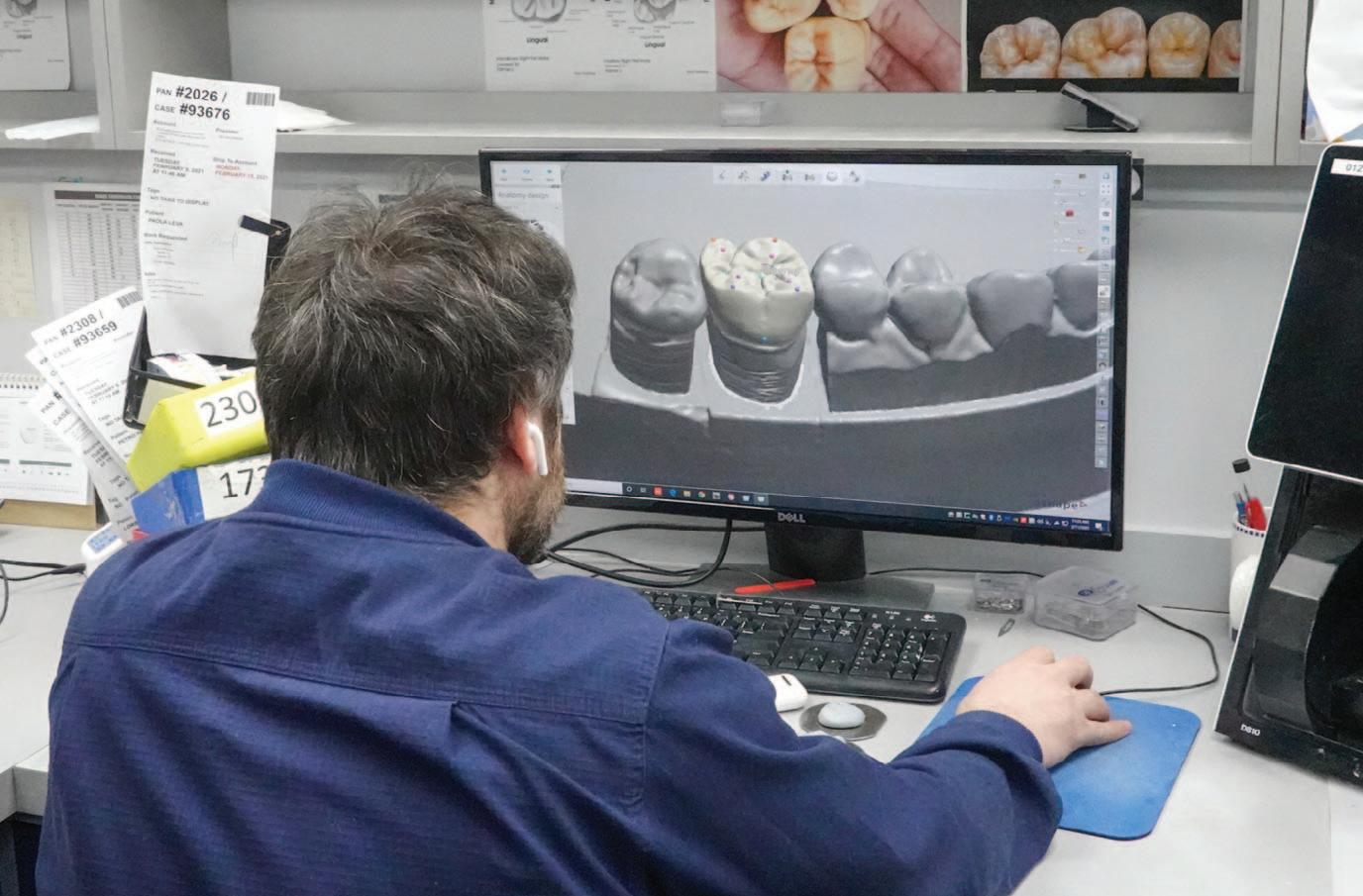
dental laboratories should their usage of non-compliant products and materials lead to a patient safety incident or enforcement action by the MHRA.
While discussions of compliance surrounding custom-made devices have tended to focus on manufacturer registration requirements, we are also aware of the usage of non-compliant products in dental laboratories, whether as a result of a lack of awareness of the regulations and how they apply or through attempts to circumvent the costs associated with legal, compliant products.
While the custom-made device – whether it be a crown, denture or orthodontic appliance – is the end product and what is ultimately registered with the MHRA, the materials used in their manufacture are also subject to stringent requirements and regulation.
What is (and isn’t) a medical device?
The key test of whether medical device certification is required is the intended purpose of the product as defined by their manufacturer. Where products such as resins and powders are used for the manufacture of a medical device which is not custom made for an individual patient, then they would be regarded as raw materials and would not require to be CE/UKCA marked. However, if the products are intended by their manufacturer to be used for the production of custom-made devices, they will need to be appropriately certified.
In the BDIA’s engagement with the regulator, the MHRA has made it clear that products such as 3D printing resins, laser sintering powders, zirconia blocks or other materials used for the manufacture of custom-made medical devices are considered to be medical devices in their own right and must be properly certified as such – which means
having been granted either CE or UKCA certification as a medical device.
Nonetheless, a significant range of uncertified products are available on the market and are making their way into UK dental laboratories for the production of custom-made devices. In turn, these custom-made devices are then being supplied to dental practices and ultimately being fitted in patients mouths.
What are the risks?
For more than a decade, the European Union (and subsequently United Kingdom) medical device regulatory frameworks have been through a fundamental overhaul. Following years of drafting and development, the EU Medical Device Regulation (EU MDR) was introduced in 2017 and replaced the previous EU Directive from 1992. This overhaul was driven in large part by serious patient safety concerns following a number of highprofile scandals that revealed gaps and inadequacies in the approval and oversight of medical devices, including incidents involving Poly Implant Prothèse (PIP) breast implants, metal-on-metal hip implants and vaginal mesh implants.
While a link between silicone breast implants and custom-made dental devices may not be immediately apparent, there is a parallel to some of the non-compliant products we see in use in the dental sector that should give both their manufactures and the laboratories that may be using them cause for concern. The PIP implants

were manufactured using non-medical grade industrial silicone, producing a medical device implanted into patients that utilised materials that were uncertified and not fit for purpose.
The result was a product that was prone to failure and that put thousands of patients at risk. As well as the harm caused to patients, the scandal caused reputational damage and undermined confidence in the healthcare sector and broader medical device regulatory system, prompting the development of the new regulations.
Given the sheer number of custom-made dental devices being produced, the potential exists for a widespread safety issue should uncertified or non-compliant products be used in their manufacture. Dentists and patients may only see the finished product, but the materials being used in the production of a custom-made device can have serious safety and efficacy implications. As the products are uncertified, their safety and efficacy have not been proven, potentially putting patients at risk.
Requirements for medical devices under the regulations
cover:
A The choice of materials and substances used and considerations such as toxicity
A The compatibility between these materials and substances, taking into account the intended purpose of the device
A The mechanical properties of the material(s) used, taking into account properties such as strength, fracture resistance, wear resistance and fatigue resistance
A Minimising any patient risk from contaminants, including wear debris, degradation products and processing residues.
Without these checks, it’s impossible to know how the materials may interact with the human body once the resulting custom-made device is fitted, with the
customdevices&compliance
potential for adverse reactions to take place. On top of these types of safety concerns, there is also the risk that uncertified materials will simply be of a poor quality and fail to behave as expected or as advertised, resulting in poor performance or premature failure.
Certification of a product as a medical device comes at a cost and, unfortunately, some companies will choose to ignore these requirements in order to save money and offer their product at a lower cost. Unfortunately, that decision comes at the expense of safety.
Where are non-compliant products supplied from?
Products must be appropriately certified regardless of where they are supplied from, and while most of the non-compliant products that we see are supplied from outside of the UK this is by no means always the case, with illegal product imported into the country available for purchase online from UK-based sellers.
It is important to note that personal direct importation of medical devices is not permitted under the UK regulations –importation is strictly regulated and importing a medical devices from outside of Great Britain comes with a set of legal requirements and obligations.
Devices may only be imported by the manufacturer’s designated UK Responsible Person (UKRP) or another importer whose details have been notified to the MHRA via the manufacturer’s UKRP.
Just because a device is available for sale online and can be shipped to you in the UK it does not mean that the device is compliant with UK requirements or that it has been legally placed on the market. You should always check that a manufacturer and its products have been registered with the MHRA – you can search for these details on the MHRA’s Public Access Registration Database (PARD).

What are your obligations?
As a manufacturer of custom-made devices, while your responsibilities begin before production takes place with the selection of materials, they don’t end with the completion of the manufacturing stage; you have post-market obligations including the maintenance of a post-market surveillance (PMS) system and reporting of incidents relating to the device.
While many dental custom-made devices are exempted from requirements such as implant cards relating to the information that is provided to the patient, these devices are nonetheless items that will be fitted into patients for long-term usage and unsafe products could pose serious risks. Before purchasing and using a substandard product, it is worth asking whether you would be comfortable sharing the details of the products that have been used in the creation of the custom-made device with the patient. Patients naturally have the right to expect that the products associated with their treatment are safe, compliant and effective.
What should be done?
Before purchasing a device, make sure that you are undertaking appropriate checks and precautions:

customdevices&compliance
A Only purchase from reputable suppliers, such as BDIA members
A Consider the price – if it looks too good to be true, it probably is
A Is the manufacturer registered with the MHRA? Try checking the MHRA’s registration database, visit https://pard .mhra.gov.uk/manufacturer-search/. If the manufacturer isn’t registered, the device is being supplied illegally
A Ask the manufacturer or supplier whether they can provide details of the device’s certification.
If you encounter a device that you suspect could be counterfeit or non-compliant:
A Do not use the device – doing so could put patients, your professional registration and your business at risk
A Report the device to the MHRA using the Yellow Card reporting scheme: https://yellowcard.mhra.gov.uk/
A Report a suspicious online seller of medical devices to the MHRA
https://report-or-check-suspiciousactivity.mhra.gov.uk/report
Development Outcome C – 60 minutes
A The BDIA has developed a series of FAQ explainer documents aimed at the dental team looking at the dangers of counterfeit and non-compliant devices, importation requirements for medical devices and chairside manufacturing requirements, as well as a short video addressing key topics which can be accessed at https://bdia.org.uk/whatwe-do/device-regulation-faqs/
To complete your CPD, store your records and print a certificate, please visit www.dta-uk.org and log in using your member details.
Q1 What registration is required for custom-made medical devices, even when manufactured chairside in the dental practice?
A Registration with BDIA
B None, registration is covered by the CAD-CAM device manufacturer
C None, dentists are exempt
D Registration with MHRA is compulsory, even for dentists
Q2 Which GDC Standard for the Dental Team highlights the importance of regulation in a professional context?
A 1.9.1 B 2.5.1 C 1.7.2 D 2.1.1
Q3 Does this registration affect non-GDC registrants in the dental laboratory?
A No, like dentists non-registrants are exempt
B Yes, for laboratory managers
C Yes for those with a responsibility for purchasing
D Yes for trainees and process workers and b) and c) only
Q4 MHRA has made it clear that product such as 3D printing resins, laser sintering powders, and zirconia blocks must be properly certified, how?
A As ISO 6040
B As manufactured by a member of the BDIA
C CE or UKCA certification as a medical device
D As provided by a manufacturer in the UK or EU
Q5 When was the EU Medical Device Regulation (EUMDR) introduced?
A 1995 B 2017 C 2022 D 2005
Q6 What medical device scandals are cited as driving the overhaul of the EUMDR?
A PIP breast implants
B Silicon cement used in bone grafting
C Metal on metal hip implants
CPD OutcomesA,C&D 60minutes
D Vaginal mesh implants and a) and c) only
Q7 What was actually wrong with the PIP breast implants?
A They leaked
B They very quickly became distorted and looked unnatural
C They were manufactured using non-medical grade industrial silicon
D The manufacturer followed a ‘one-size-fits-all’ manufacturing model
Q8 What is not a requirement for medical devices under MHRA regulations
A Choice of material used and toxicity
B Must be signed off by a GDC registrant
C Mechanical properties of the materials used
D Compatibility between materials and substances
Q9 What is a UKRP
A UK Registered Practitioner B UK Registrant in Practice
C UK Regulated Product D UK Responsible Person
Q10 What is a PMS system?
A Post-Market Surveillance system
B Post-Manufacturing Satisfaction system
C Pre-Manufacture compliance Spot-Check system
D Prior to Manufacture Surveillance system
■ Why don’t dentists get it?

I’ve spent more than 50 years in dentistry, and I’ve had the unusual privilege of seeing the profession from both sides - first as a dental technician, and then as a dentist. That dual perspective has shaped the way I think about dentistry, and in particular, the relationship between the clinic and the laboratory.
It’s a relationship that has always been essential, but not always easy. And if I’m honest, it’s one that still frustrates many of us today.
That’s exactly what I’ll be exploring in my session at the Dental Technology Showcase in May. But before anything else, I want to make one thing very clear: this isn’t just a talk for technicians. If you can, bring your dentist. Because the issues we’re dealing with don’t belong to one side or the other, they exist in the space between us.
My journey
I didn’t take a conventional route into dentistry. I left school at 16, and I certainly wasn’t academic. What I did enjoy was making things such as model aircraft or anything that involved working with my hands.
It was my mother who suggested I try spending some time with a dental technician. I didn’t know much about the profession at the time, but it didn’t take
Mike Gregory has been both a dental technician and a dentist, here he shares his thoughts from a dual perspective before his talk at DTS this coming May.
There are few people in dentistry who can genuinely claim to understand both sides of the clinician/technician divide. Mike Gregory is one of them. In this insightful feature ahead of Dental Technology Showcase (DTS), he shares his thoughts on bridging the gap between clinics and labs plus why technicians should bring their dentists to DTS.
long before I realised I’d found something that suited me perfectly.
It felt like model-making, but with a purpose. There was a real sense of craft involved: precision, attention to detail, and the satisfaction of creating something that would ultimately help someone else. I trained at what is now Barts and The London, and from there moved into a production laboratory before going on to teach. For eight years, I taught dental students the laboratory side of prosthetics, something I’m still passionate about today.
Interestingly, it was the students who encouraged me to take the next step. They kept asking why I wasn’t doing dentistry myself. Eventually, I listened.
I retrained in my 30s, qualified as a dentist, and later returned to teaching, this time on the clinical side. That journey gave me a perspective that I don’t think I could have gained any other way. I’ve experienced the pressures, challenges, and frustrations of both roles. And that’s why I feel so strongly about the disconnect that still exists between them.
Understanding changes everything
When I was working as a technician, I remember looking at impressions coming into the lab and thinking, why are these so
poor? It was easy to assume that the clinician hadn’t taken enough care or hadn’t really tried. But everything changes when you step into the surgery yourself. You quickly realise that being a dentist is incredibly demanding. You’re dealing with patients who may be anxious, uncomfortable, or unable to tolerate certain procedures. You’re working under time pressure. You’re making decisions in real time. Perhaps most importantly, you start to recognise that you may not have been taught the best way to do things in the first place.
In my view, so much of the frustration between technicians and clinicians comes down to assumptions. Technicians assume dentists don’t care. Dentists assume technicians will fix things. In reality, most people are doing their best, but without a full understanding of what the other side is dealing with. And that lack of understanding is where problems often begin.
The frustration with impressions
If there’s one topic that consistently comes up when you talk to technicians, it’s impressions. Poor impressions are a major source of frustration and rightly so. But again, context matters. From the clinical side, I can tell you that taking a good impression isn’t always straightforward. Patients gag, they move, conditions aren’t
dualperspective
ideal. You’re working within constraints that aren’t always visible to the technician receiving the case. That doesn’t excuse poor work, of course. But it does explain some of it.
The real issue is what happens next. If a technician believes that the dentist hasn’t made much of an effort, they’re less likely to go the extra mile. That’s human nature.
Once that mindset sets in, the quality of the final result can suffer. It becomes a cycle, frustration on one side leading to disengagement on the other and ultimately, it’s the patient who pays the price.
The importance of communication
One of the most surprising things about modern dentistry is how little we still communicate with each other, despite having more tools than ever. We can instantly share images, ask questions, clarify instructions and yet many clinicians still send lab tickets with minimal information. Sometimes it’s just a single line: ‘make a denture.’
That’s not enough. If you want a good result, you need to provide detail. What are

you trying to achieve? What does the patient want? What challenges did you encounter? I like to compare it to cooking. If you tell someone to make a beef stew, they need a recipe. They need to know the ingredients, the method, the desired outcome. Otherwise, they’re guessing and dentistry shouldn’t be about guessing.
When clinicians provide clear, detailed instructions, and ideally images, it not only
improves the technical outcome, it also builds trust. It shows that they’re engaged in the process. And that makes a real difference to how technicians approach the work.
Opportunity and limitation
There’s no doubt that digital dentistry has transformed the way we work. In many cases, it offers speed, consistency, and efficiency that simply weren’t possible before. But we must be careful about how we use it. There’s a tendency to see digital as a solution to everything, to assume that because something can be done digitally, it should be. But that’s not always the case.
For standardised work, digital can be excellent. But when you’re trying to create something with individuality, something that looks natural and suits the patient, that’s where skill, communication, and experience come into play.
Patients don’t want something that looks manufactured. They want something that looks like them. And achieving that requires collaboration between clinician and technician. Technology can support that process, but it can’t replace it.
Working together, not apart
We need to break down the barriers between clinic and lab. We need to create opportunities for shared learning and mutual understanding. One of the simplest ways to do that is to attend courses together. If you’re a dentist, take your technician. If you’re a technician, encourage your clinician to come along. Why do we learn in isolation when our work is so interconnected? When clinicians and technicians learn together, they develop a shared language. They understand each other’s challenges and that leads to better outcomes. It also fosters respect, something that is essential if we’re going to improve the way we work.
Two-way feedback
Another important aspect of collaboration is feedback. Technicians should feel able to provide constructive feedback to clinicians - not just rejecting work, but explaining what’s needed and why. At the same time, clinicians need to be open to receiving that feedback.
That’s not always easy. No one likes being told that their work could be improved. But if we’re serious about delivering the best possible care, we must be willing to have those conversations.
It’s not about criticism. It’s about improvement.
When communication breaks down, the consequences go beyond frustration. There are real costs involved for clinicians, technicians, and patients.
From a clinical perspective, retaking impressions or remaking appliances takes time. It may mean another appointment, additional chair time, and lost revenue. For technicians, it often means rework that isn’t always compensated.
Ultimately for patients, it means inconvenience, discomfort, and sometimes a loss of confidence in the treatment

process. Getting things right the first time isn’t just more efficient, it’s better for everyone involved.
Looking ahead at DTS
When I speak at the Dental Technology Showcase, I’m not aiming to provide all the answers. What I do want to do is start a conversation. I want people to reflect on how they work, how they communicate, and how they can improve. Most importantly, I want to bring people together. If we can get technicians and clinicians in the same room, listening to the same discussion, we’ve already taken a step in the right direction.
It’s also important to recognise we are all learning. What you’ve been doing for years might not be as good as it could be and that’s fine, as long as you’re open to change.
That applies to technicians, dentists and all of us! Because ultimately, we’re working towards the same goal — providing the best possible care for our patients and the only way we can do that consistently is by working together.
So, if you’re coming to DTS, please don’t just come on your own. Bring your dentist. Bring your technician. Start the conversation. It’s long overdue.

■ Dentists and Alcohol Alcohol, the hidden epidemic
Sober coach Sandra Parker, of “Just the Tonic coaching”, https://justthetoniccoaching.com/, explains how dentists use alcohol to manage what their training never taught them.
The profession doesn’t want to talk about it, but dentists are quietly using alcohol to cope with a level of pressure most people don’t understand. Not occasionally - daily.
This isn’t about moral failing or lack of discipline. It’s the predictable outcome when a profession demands emotional control, sustained precision, and constant decisionmaking without ever teaching clinicians how to actually process the pressure.
Over the years supporting high-achieving professionals who’ve lost control of their drinking, I’ve noticed dentists appear in my client base more than any other healthcare profession. These clinicians present perfectly - successful practices, happy families, respected in their communitiesyet behind closed doors, they’re drinking a bottle or more of wine every night just to feel normal.
While the profession talks about stress management and mental health, it rarely addresses what’s actually happening: alcohol
has become the primary coping mechanism for managing professional pressure.
Most dentists try the usual strategiescutting back, taking breaks, setting limits. These don’t work because they’re addressing the wrong problem.
Why Dentistry Creates the Perfect Storm
Dentistry isn’t just stressful - it’s a particular type of stress that makes alcohol especially appealing.
For hours, you’re working in isolation, making irreversible decisions about people’s bodies while they’re anxious and vulnerable. Risk accompanies every procedure. Each patient interaction demands you absorb their fear while projecting calm confidence.
Between patients? There’s no team to decompress with, no time to process. The accumulated tension in your body carries straight into the next appointment.


Then the business side hits: managing staff conflicts, navigating insurance complications, chasing payments, handling patient dissatisfaction. Even after the last patient leaves, the administrative burden never ends.
By day’s end, hours of unprocessed stress sit lodged in your nervous system. Your mind won’t stop, your body stays tight, and you’re emotionally depleted yet mentally wired.
Alcohol promises instant relief. Except it doesn’t deliver what it promises.
The Illusion of Relief
That first glass? It creates the sensation of relaxation. Mental noise drops, physical tension seems to ease.
For approximately twenty minutes. My clients call this the twenty-minute high. Then the rest of the bottle beckons. Just one more, you tell yourself. The evening blurs, conversations become less coherent, and you’re not truly present with your family - instead, you’re in an alcohol-
dentists&alcohol
induced haze, numbing out rather than genuinely relaxing.
Reality sets in when disrupted sleep hits, followed by 3am wakefulness staring at the ceiling, morning brain fog, and reduced emotional regulation. Despite being in bed for hours, you wake feeling unrested. Your patience thins, your concentration takes longer to engage.
Here’s the cruel irony: the very things you’re using alcohol to manage - stress, anxiety, sleep quality - actually deteriorate. Alcohol doesn’t process stress; it delays and increases it.
Artificially sedating your nervous system prevents the natural discharge of accumulated pressure, which over time creates more anxiety, worse sleep quality, and diminished resilience.
When your profession demands precision, emotional stability, and sustained concentration, even small reductions in mental clarity compound quickly.
Yet because dentists are high-achieving and conscientious, you push through and maintain standards. You deliver quality care. That’s precisely why the habit escalatesthe job keeps demanding more while alcohol delivers progressively less.
Why Willpower Strategies Fail
When drinking starts feeling problematic, most reach for willpower-based solutions: Dry January, cutting back to weekends only, rules about when to start drinking, taking a month off.
These approaches share a fatal flaw –they focus on trying not to drink without addressing why you’re drinking in the first place.
Consider this: if alcohol creates your boundary between work mode and home mode, discharges accumulated pressure,

and manages difficult emotions, then simply trying to stop doesn’t solve the underlying need. The pressure persists. Emotions remain unprocessed. The need for an off-switch has not gone away.
So, you rely on willpower, count days, and white-knuckle through cravings. It feels like deprivation because nothing has replaced what alcohol was doing for you.
You haven’t learned to actually discharge professional pressure or developed tools to process emotions. Genuine ways to transition from work to rest without wine?
Still missing
Eventually, you return to drinking – not because you’re weak, but because the fundamental problem was never addressed.
What High-Functioning Professionals Actually Need
A completely different approach is what high-functioning professionals need. Not another test of willpower. Not generic programmes designed for people who’ve hit rock bottom and lost everything.
What works is support that recognises you’re still performing at a high level while addressing why alcohol became essential in the first place.
Real control? It comes from replacing the function alcohol serves, not just removing the substance.
Learning to discharge pressure rather than suppress it. Processing emotions rather than carrying them in your body. Creating genuine boundaries between work and rest that don’t depend on a glass of wine - this is what creates lasting change.
Challenging fundamental beliefs matters too: that you deserve alcohol as a reward, that you need it to unwind, that life without it would be dull or unbearable.
That’s when genuine change occurs - not forced abstinence, but because the need has gone.
The Professional Reality
Daily drinking isn’t a character flaw - it’s evidence that professional pressure has exceeded available coping strategies. Another temporary challenge? You don’t need it. Labels? Not necessary. Waiting until things get worse? Absolutely not. A fundamental mindset transformation is what you need - seeing alcohol for what it actually is. Not your reward, not your relaxation tool, not your friend. It’s the substance actively creating the problems it claims to solve.
With the right approach, you can reach a place where control isn’t about resisting temptation. Instead, you’re simply not interested.
That’s where real freedom exists – and it’s absolutely achievable with the right framework and support.
■ Communication and collaboration with digital dentistry
Kristina Vaitelyte is an internationally-recognised digital dental technician who is passionate about helping colleagues utilise the capabilities of the modern digital workflow. Here she considers what she feels are the main challenges faced by dentists and dental technicians when introducing digital dentistry into their processes. Kristina is the ADI Technical Representative – and the first female in the role.

Dentistry is a team effort, requiring the skills and expertise of various individuals in order to deliver exceptional outcomes for each patient. The advent and advancement of digital solutions has elevated workflows and afforded a number of additional benefits for professionals and patients alike. Collaboration and communication between dentists and dental technicians are crucial for success.
Communication is key when migrating systems to digital software, but it can be difficult to adapt processes and behaviours that have been unchanged for what could be decades. Our job as technicians is to use the written and visual aids provided to create the right restoration for the patient –this requires a good level of detail from the clinician to ensure it translates effectively into a physical product. This communication must be strong throughout the ‘golden triangle’, which consists of the dentist, the dental technician and the patient. All three need to be clear in what they require. We are treating people, not just solving problems, and being able to enhance someone’s quality of life is very powerful.
Looking at implantology more specifically, it’s important to accept that this is a complex field that takes time to accomplish. Don’t be afraid to dive in, to give things a try and to learn from mistakes. Digital dentistry is changing rapidly, so it’s important to seek guidance from the equipment manufacturers and to work well with the rest of the dental team. It’s a very exciting field, with the chance to increase the predictability of patient care, but it is a team sport! You need a village to complete a case.
It’s crucial to research any technology before investing. This should include a conversation with the manufacturer and speaking to other users or pilot testers – they could save you time in making a decision and help you select the right product. Be wary of marketing and exciting headlines – they shouldn’t be relied on alone and must be backed up by honest feedback from other technicians or clinicians.
Despite the advancements in digital, it is fundamental for professionals to retain a proper understanding of analogue techniques. You need to know how procedures work in order to correctly apply them to cases. In addition, you need to be able to verify and sense-check digital plans and guides – none of us can rely on
technology entirely; our skills and expertise are still crucial.
I presented at BDIA Dental Showcase from within the dedicated ADI Implantology Theatre at 16:15 on Friday 13th March, during which I talked about how to apply strategies for effective digital diagnostics and treatment planning in prostheticallydriven workflows, as well as how to integrate digital workflows into different teams. It’s not just about replacing each analogue step with a digital one, the sequence needs to change in some circumstances. I also explored how planning tools can reduce the clinician’s time and improve patient outcomes with increased predictability and accuracy.
Events like the BDIA Dental Showcase 2026 allow us to access the largest amount of product, clinical and technical information in one place. I think London is a really convenient location for Showcase and I was very excited to be visiting. Thanks to the ADI Implantology Theatre and Zone, we were able to expand the dental implant community and create new opportunities for everyone. I believe this session sparks great conversation, and can’t wait to see where it goes from here.
■ The Importance of Disclosing CCJs, Convictions and Bankruptcy
The team at UK Special Risks explains the vital importance of legal disclosure
When applying for insurance, it is crucial to disclose any county court judgments (CCJs), criminal convictions or bankruptcy proceedings. Failing to do so can have serious consequences, including policy invalidation and denied claims.
As an insurance broker we work for you as our customer and we are not here to cast judgement, we are here to advise on and arrange the right insurance cover for you so that it will protect you and respond if and when called upon. We also understand that in the dental industry liquidations and CCJs do occur and not always through any direct fault of the business.

Why Disclosure Matters
Insurance providers assess risk based on the information you provide. Non-disclosure of material facts, such as financial difficulties or criminal history, can lead insurers to believe they were misled. This perception may result in the cancellation of your policy or refusal to pay out on a claim.
CCJs and Bankruptcy
A CCJ is a court order that a person must pay a debt. If unpaid, it remains on your credit record for six years. Bankruptcy, a legal process for individuals unable to repay outstanding debts, this affects your credit history. Both can influence an insurer’s decision to offer coverage and at what cost.
Criminal Convictions
Under the Rehabilitation of Offenders Act 1974, unspent convictions must be disclosed when applying for insurance. These convictions remain unspent for
varying periods, depending on the sentence. While spent convictions don’t legally need to be disclosed, some insurers may still request this information.
Consequences of Non-Disclosure
A Policy Invalidation: Insurers may cancel your policy if they discover undisclosed information.
A Claim Denial: Any claims made could be refused if the insurer finds out about non-disclosure.
A Legal Repercussions: In severe cases, non-disclosure can be considered fraudulent, leading to legal action.
A Future Insurance Difficulties: Non-disclosure can make it harder and more expensive to obtain insurance in the future.
Best Practices
A Be Transparent: Always disclose CCJs, convictions and bankruptcy when asked by insurers.
A Seek Advice: If unsure about what to disclose, consult with an insurance broker or legal advisor.
A Keep Records: Maintain documentation of all disclosures made to insurers.
Conclusion
Honesty in insurance applications is not just a legal obligation but also a means to ensure you receive the coverage you need without future complications.
Always provide accurate information to protect yourself and your assets.

■ Dr Sandy Limerick: Case Report: Management of a Labial Vertical Fracture in a Bruxing Patient with Class III Incisor Relationship
Dr Sandy Limerick is an award-winning Dental Implant and General Restorative Surgeon, caring for patients from her boutique dental practice, Cottage Dental, in Sandbach, Cheshire.
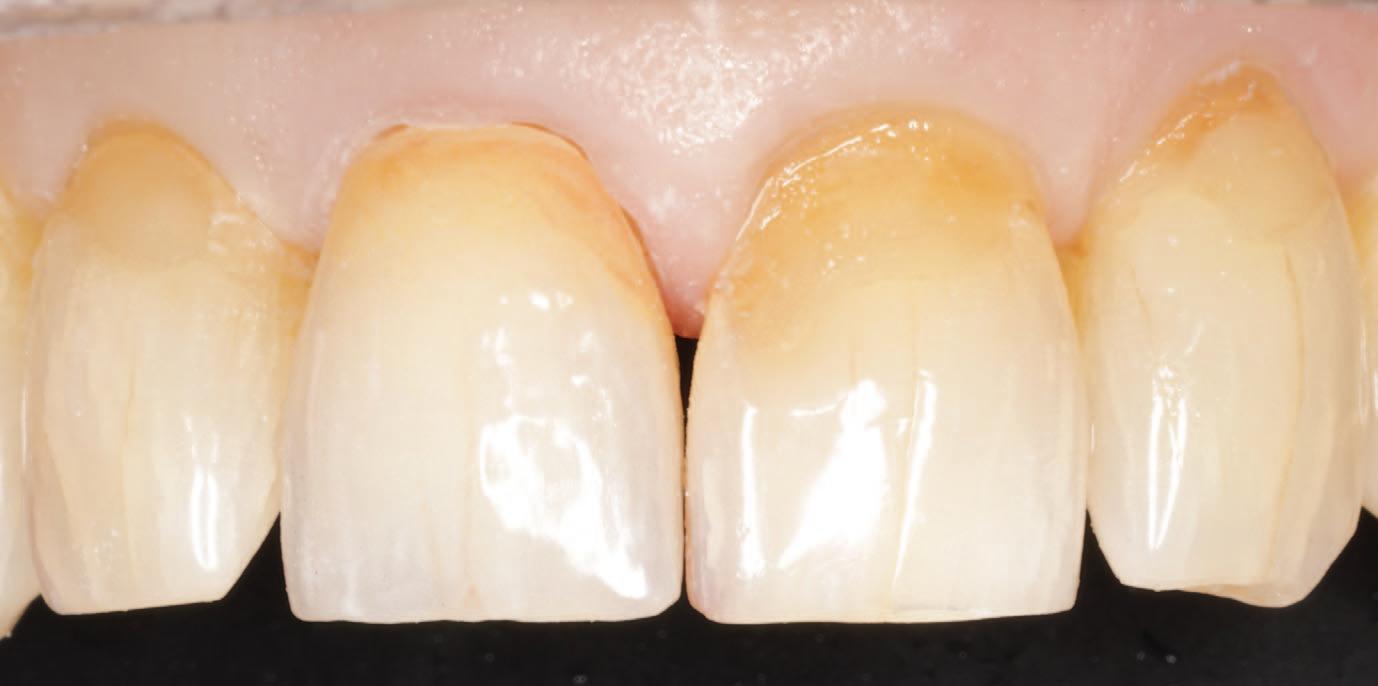

Introduction
Vertical fractures in anterior teeth present a restorative challenge, particularly in patients with parafunctional habits and complex occlusal relationships. This case outlines the conservative management of a vertically fractured maxillary anterior tooth in a bruxing patient with a Class III incisor relationship.
Case Presentation
A 76-year-old male presented with a stained vertical fracture line on the labial surface of the upper right central incisor. The patient had a long-standing bruxism habit and a skeletal Class III incisor relationship, increasing the risk of fracture propagation.
Clinical examination revealed a heavily stained vertical crack line extending close to the cemento-enamel junction (CEJ), with no signs of mobility, tenderness, or swelling. A periapical radiograph (Figure 1) confirmed the absence of periapical pathology.
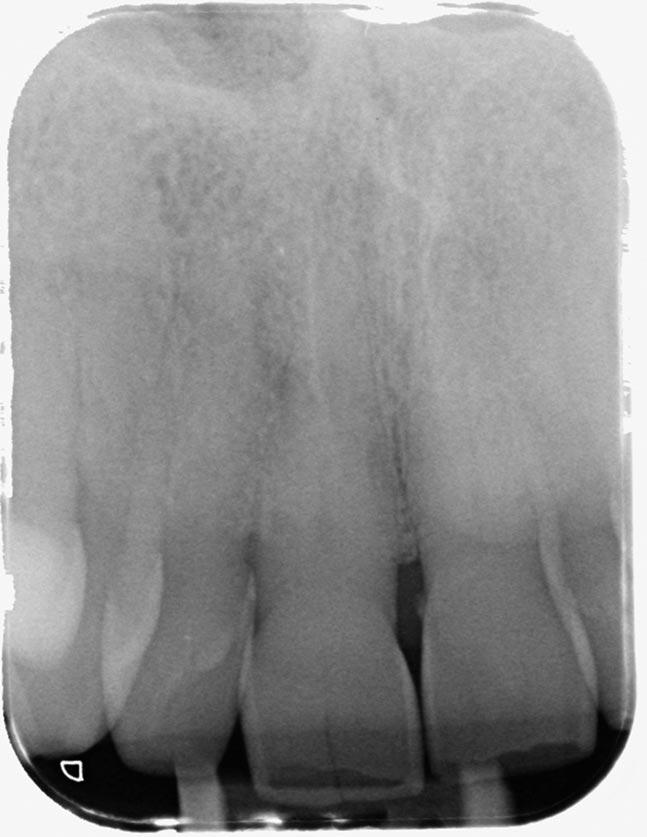
Treatment
Initial shade matching was carried out at the beginning of the appointment to ensure accurate colour selection (Figure 2).
A 3D scan of the fractured tooth (Figure 3) was taken to aid in documenting the crack morphology and designing the definitive restoration.
The tooth was prepared with a traditional full-coverage crown design (Figure 4), incorporating appropriate axial reduction and taper to ensure optimal mechanical retention and resistance form.
A zirconia monolithic crown with buccal porcelain layering was fabricated for optimal aesthetics and strength.
Due to the depth and location of the fracture, and the patient’s occlusal risk factors, a full-coverage crown was proposed to limit further structural compromise.
The patient agreed to proceed.
To promote soft tissue health and biological integration, a narrow marginal band of highly polished monolithic zirconia was designed at the cervical margin. This approach supports epithelial cell
attachment and reduces bacterial plaque accumulation.
The final restoration showed excellent shade integration with the adjacent teeth (Figure 5).
Outcome and Follow-Up
The crown was cemented with adhesive resin cement. The patient reported no postoperative sensitivity or discomfort.
Small occlusal adjustment was performed to minimize functional loading during protrusive and lateral excursions.
Discussion
Vertical fractures in anterior teeth are often multifactorial. In this case, bruxism and the Class III incisal relationship likely contributed to structural fatigue.
Early intervention with a crown helped preserve tooth vitality and function. Digital tools, including 3D scans, provided enhanced diagnostic and restorative precision.
Conclusion
Full-coverage restoration proved to be a predictable option for managing vertical labial fractures in patients with high occlusal risk. Accurate diagnosis, shade control, and minimally invasive preparation were key to success.
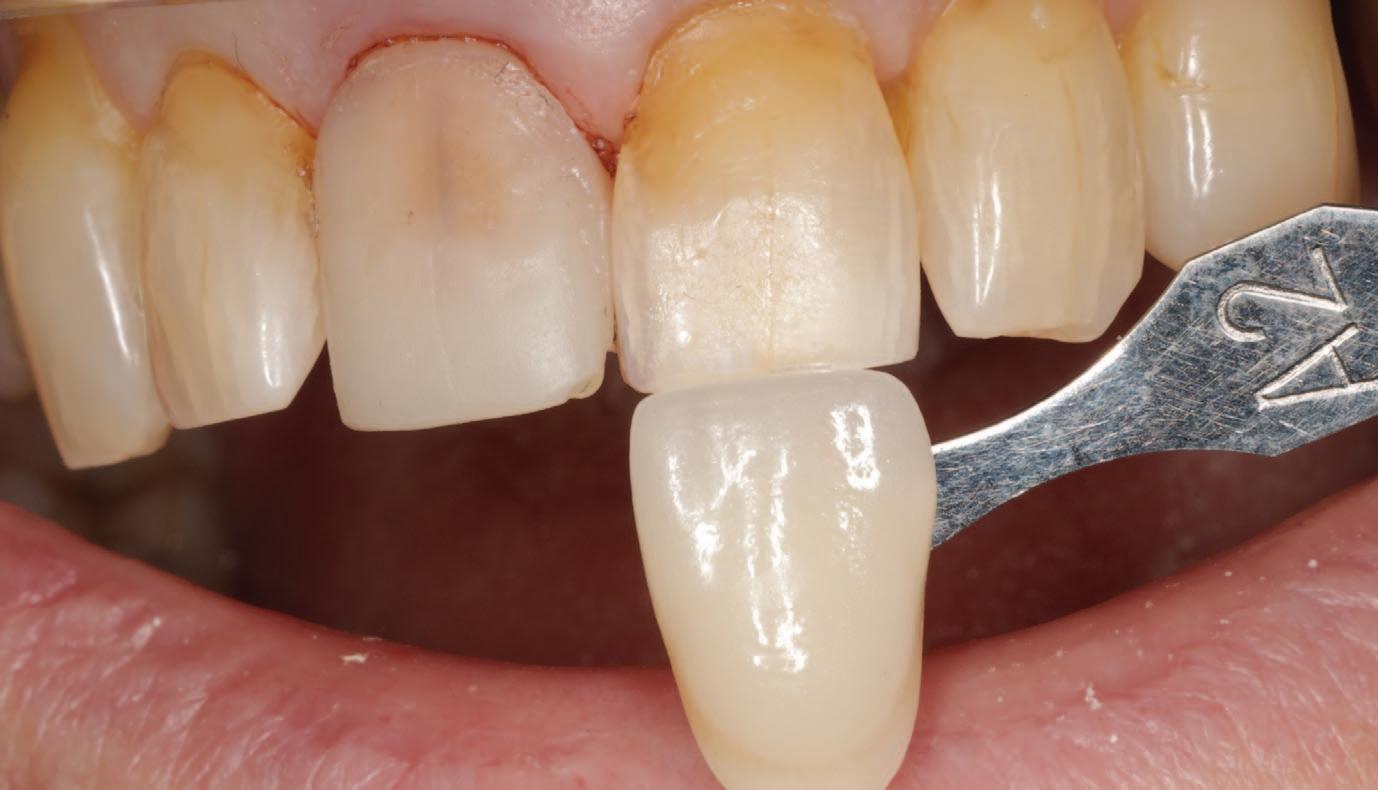
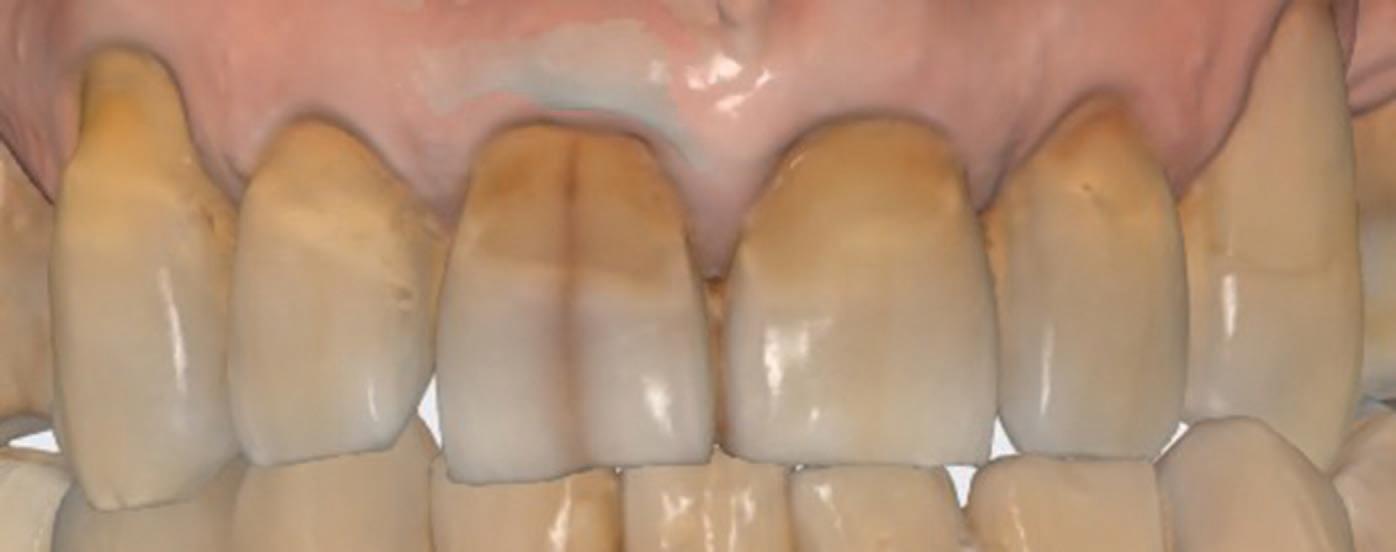
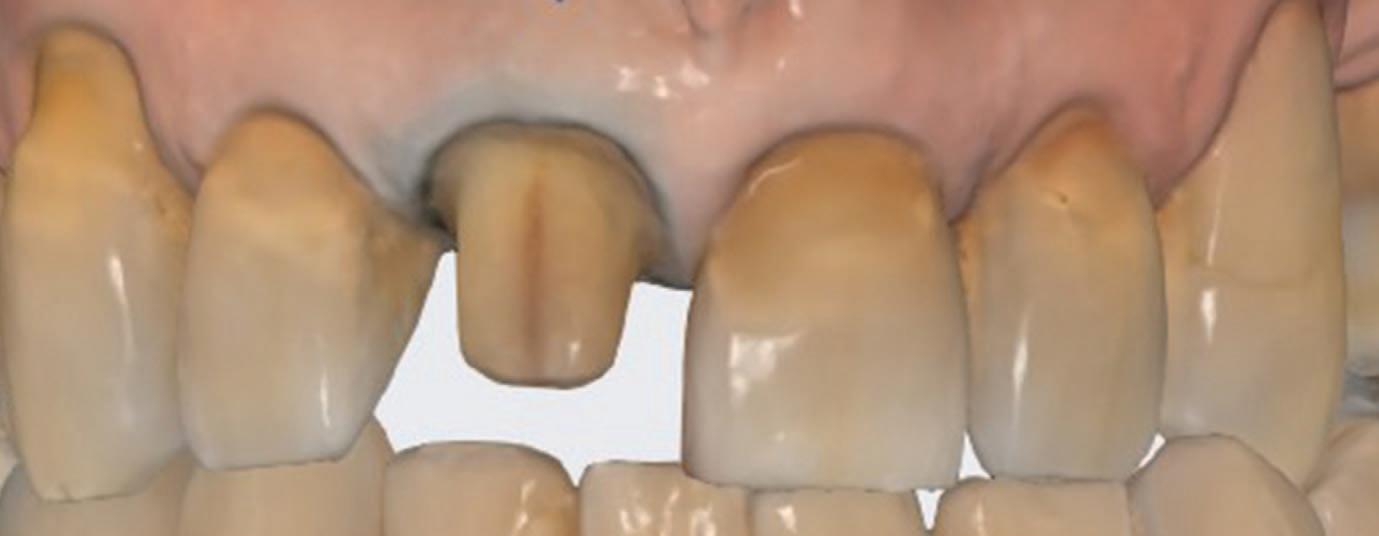
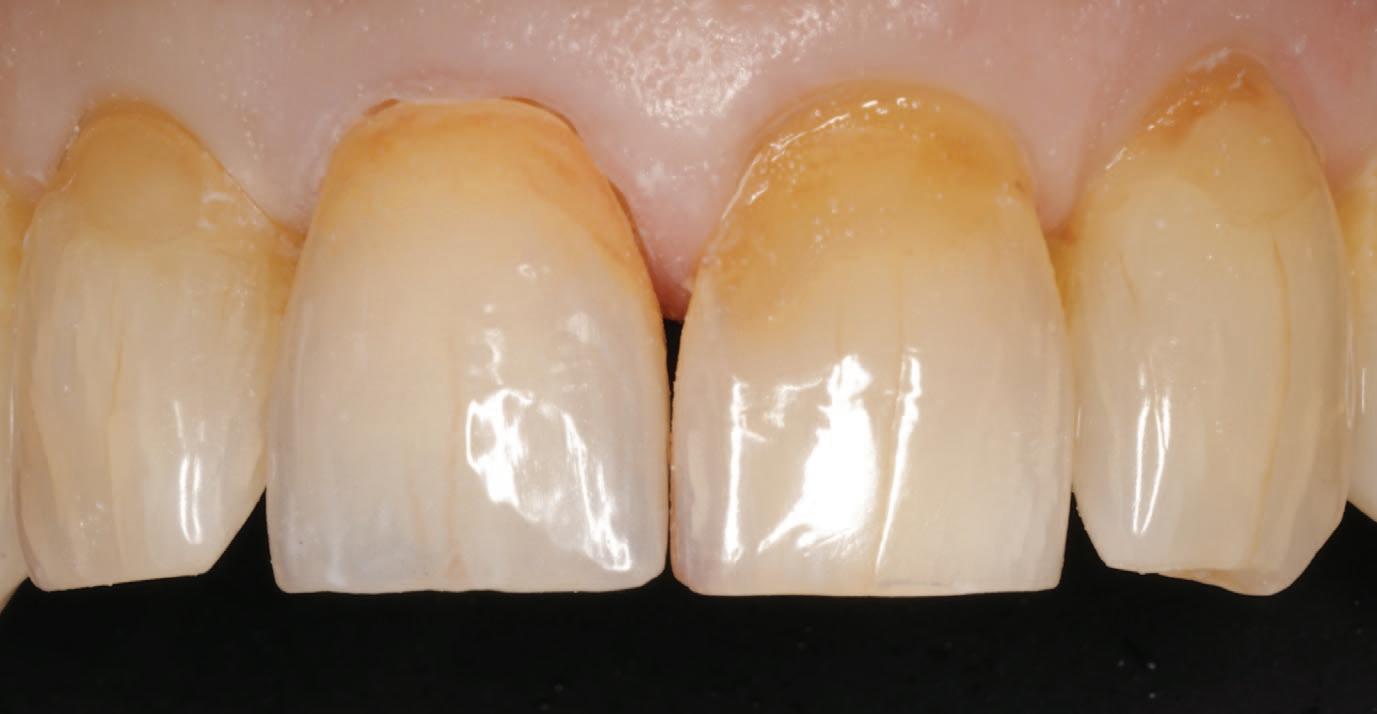
■ The value of the Dental Leadership Network (DLN)
Dr Helen Phillips, Chair, General Dental Council (GDC), was speaking at the Dental Leadership Network. What follows has not been checked against delivery but it accords with what The Technologist heard during the event.

Ihave really enjoyed my first DLN today – thank you for the warm welcome – it has been a pleasure to meet so many of you in person. Thank you for your warmth and for your candid insights. For those who I have not yet managed to speak with, I am Helen Phillips, I was appointed Chair of the GDC in October last year.
Like many of us here, I have spent time in a variety of organisations and roles. Mine include 35 years in professional standards and regulation, in the health, environment, insurance and legal services sectors.
As Chair of an NHS Trust for nine years, and now as Chair of NHS Professionals, I see the challenges of large-scale workforce planning, recruitment and retention. The imperative to wrap the team around the patient, and for all members of the team to work to the top of their licence. Not just in pursuit of access targets but in the interest of patient safety and improved patient
experience. There are obvious parallels in dentistry.
This network certainly lives up to its reputation as a place where leaders can share information, build relationships and collaborate. It’s definitely an important date in the dental calendar and I can see why Minister Kinnock took the opportunity to speak at your last meeting. Speaking of which, apologies that I missed that event which would have been my first on being appointed Chair. I had recently returned from the Middle East and I was suffering from a bad dose of Manama Malady!
Thank you to today’s speakers –Today’s theme has been ‘Delivering safe and effective oral health for those most in need’.
A prescient topic – I thank the speakers and panellists for doing it justice, and everyone in the room for the thoughtful workshop discussion too.
It is essential that we spend time thinking about those most in need – people with housing insecurity, older adults living in care homes, people living in areas with low levels of NHS dentistry, patients with physical disabilities and those who are neurodivergent.
Rakhee set the scene so well. Matt and Harriett made the case for an evidence-led approach. Sakina’s perspective as both a dental nurse and community oral health educator was illuminating. Fiona was as persuasive as she was succinct. Eloise from the Single Homeless Project really brought to life what oral health means for people with housing insecurity. I thank the panel – Natalie, Jyoti, Nicola and John – for sharing what safe and effective oral healthcare means for special care and community dentistry.
The strong theme continued into the afternoon, with the workshop expertly facilitated by Ben, Zain and Hazel. You
reminded us, if any reminder was necessary, that patients and the public are at the heart of everything we all do.
Thank you, speakers, panellists and facilitators, for a superb day.
Early reflections as Chair of the GDC
I’ll say a little about my early reflections as Chair of the GDC. It was certainly an interesting time to join – arriving just as Council was approving our strategy for the next three years.
I wasn’t the only new arrival to Council in October – Mike Driver and Bill Gunnyeon were appointed as lay members, both with significant experience in government and regulation. Joining an experienced Council of lay and registrant members and working with a talented and committed group of Executives, has been a real pleasure. Fellow Council colleagues, Serbjit Kaur, Simon Morrow and Laura Simons are here today.
There is still some work to do in communicating our strategy, narrating what all the actions we have committed to delivering over the next three years will mean practically for those we serve; patients, registrants, the public – including those who have difficulty accessing dental services. Our ability to influence this wider agenda is dependent on us meeting our own targets and the expectations of the PSA as the oversight regulator, notably on fitness to practice and EDI.
Transparency is an essential ingredient of good governance. We shall keep any Council deliberations in private to a bare minimum and we shall invite first hand testimony from our key stakeholders at Council meetings. The BDA joined us in February. Please let us know if your organisation would like to speak with Council.
At the centre of our strategy, our vision is to be a trusted and effective regulator,
supporting dental professionals to provide safe and effective care for their patients.
Barely three months in, we are already well into delivery.
We announced this month changes we are making to the Overseas Registration Examination (ORE) which could result in a five-fold increase in the number of internationally qualified dentists joining the register via the ORE route. More ORE places is great news for the dental workforce and, in turn, patients and the public and this has been a top priority for the GDC.
On 25 March, we launch our new online registration service, called MyGDC. This marks a significant step forward in our commitment to modernising our services. Last year, we received around 13,000 new applications to join the registers.
The new service means that people can upload supporting documents online - no more sending original documents by post. People will be able to verify their identity using facial recognition technology and track progress or actions online. This will be a more modern and user-centred experience.
Growth of the dental workforce is obviously a priority. Making it easier for them to register, while maintaining the high standards required, is a very good thing that we are very keen to support.
And a further sign of progress is our support for trainee dental nurses to move into formal training more quickly. From June this year all new trainee dental nurses must start a recognised training programme within 12 months of starting work. We are pleased to support this drive for greater professionalism in what is a vital role in dentistry – the dental nurse.
These are just some of our priorities –expect to hear more about others in future,
and we welcome you to hold us to account to deliver them.
Motivated by collaboration and supporting professions
Everyone here knows that no single intervention will increase the NHS dental workforce nor add capacity in regions that are currently underserved. We need to work together to tackle this.
One of the things that motivates me is collaboration – finding ways to work together to tackle the challenges. We have a shared interest in making dentistry work across the UK, and we all have a role to play.
I’m also motivated by supporting professions – because you put your specialised knowledge to work in the service of others. In a world that is increasingly automated, accelerated, and transactional, you remain one of the few last great face-to-face professions, where skill, compassion and judgement cannot be downloaded or outsourced.
Professionalism in dentistry isn’t just about meeting standards; it is about holding yourselves to a purpose. It is the quiet courage of doing the right thing for the patient in front of you, the commitment to continual learning, and the pride of belonging to a community that safeguards the nation’s oral health. This is what sets you apart — not just as clinicians, but as professionals in the truest sense of the word.
With rights, in this case to practise, come responsibilities and you should rightly be proud of the role you play in society – we at the GDC will play our part in supporting you in every way we can to deliver on your responsibilities.
UK PROFESSIONAL DENTAL TECHNOLOGIST
● are individually registered with the GDC to be able to use the titles that relate to our role in the UK
● maintain our own lifelong learning through relevant continuous professional development (as provided free to the Dental Technologists Association [DTA] members)
● ensure that we are covered by specific indemnity insurance related to our dental laboratory custom-made dental device manufacturing work, and if necessary, related clinical work and/or extended roles
● work within the GDC Scope of Practice for our registered role, along with other extended areas as confirmed by further additional training
● are, as a current GDC registered dental technologist, able to sign-off custom-made dental devices under MHRA/MDR regulations, indicating that such appliances are fit for purpose as stated on the Statement of Manufacture
● maintain and develop our dental team networks to enhance patient care
