PROVIDERS DIRECTLY ADDRESS RELATIONSHIP DYNAMICS EARLIER IN TREATMEN T

PLUS
Peers’ roles in treatment remain ill-defined
Professionals perpetuate patients’ shame












PROVIDERS DIRECTLY ADDRESS RELATIONSHIP DYNAMICS EARLIER IN TREATMEN T

PLUS
Peers’ roles in treatment remain ill-defined
Professionals perpetuate patients’ shame











Addiction is a battle that shouldn’t be fought alone. At Rogers Behavioral Health, patients have an ally every step of the way.
From withdrawal management and stabilization to residential and outpatient programs, adults and adolescents receive a continuum of care from leading clinicians specialized in addiction and co-occurring disorders.

Know someone who’s struggling?
Help them rediscover life worth living.
Make a referral at rogersbh.org/refer or call 800-767-4411.
 BY GARY A. ENOS
BY ALISON KNOPF
BY ROLAND REEVES, MD
JULIE MILLER
BY GARY A. ENOS
BY ALISON KNOPF
BY ROLAND REEVES, MD
JULIE MILLER
EDITORIAL
Editor in Chief Julie Miller jmiller@iabhc.com
Editor Gary A. Enos genos@iabhc.com
Senior Editor Tom Valentino tvalentino@iabhc.com
Associate Editor, Reader Engagement Megan Combs mcombs@iabhc.com
SALES
All inquiries please contact
Director of the Institute for the Advancement of Behavioral Healthcare
Douglas J. Edwards (216) 373-1201 • dedwards@iabhc.com
Traffic Manager Judi Zeng (212) 812-8976 • jzeng@vendomegrp.com
Please send IOs to: adtraffic@vendomegrp.com
All ad materials should be sent electronically to: https://vendome.sendmyad.com/
DESIGN
Creative Director Dave Villafañe
SUBSCRIPTIONS
Call: 1-888-244-5310, email to: VendomeHM@emailpsa.com, or visit: www.iadvancebehavioralhealthcare.com/subscribe
REUSE PERMISSIONS
Copyright Clearance Center info@copyright.com Ph: 978-750-8400
Fax: 978-646-8600
BY MICHAEL WEINER, PHD, MCAPADMINISTRATION
Chief Executive Officer Jane Butler
Chief Marketing Officer Dan Melore
Vice President, Finance Bill Newberry
Vice President, Custom Media Jennifer Turney
Director, Circulation Rachel Beneventi
BRIAN DUFFY, LMHC, LADC-I
Addiction Professional (ISSN: Print 1542-8435, Online 2168-460X) is published 4 times per year by Vendome Group, LLC, 237 West 35th Street, 16th Floor, New York, NY 10001-1905.
BY RACHAEL ZIMLICH, RN©2018 by Vendome Group. Addiction Professional is a trademark of Vendome Group, LLC. All rights reserved. No part of Addiction Professional may be reproduced, distributed, transmitted, displayed, published, or broadcast in any form or in any media without prior written permission of the publisher. To request permission to reuse this content in any form, including distribution in educational, professional, or promotional contexts or to reproduce material in new works, please contact the Copyright Clearance Center at info@copyright.com or 978.750.8400.
EDITORIAL: Addiction Professional is the addiction treatment and prevention field’s clinical resource that examines what works for individuals with addictive disorders. Articles and opinions published in Addiction Professional do not necessarily reflect the views of Vendome Group or the Editorial Advisory Board.
SUBSCRIPTIONS: For questions about a subscription or to subscribe, please contact us by phone: 888-244-5310, online: http://www.iadvance behavioralhealthcare.com/subscribe or email: VendomeHM@emailpsa.com.
Subscription rate per year: $140 domestic, $169 outside the US. Single copies and back issues: $20 Domestic, $32 outside the US.
POSTMASTER: Send changes of address to: Addiction Professional, PO Box 11404, Newark, NJ 07101-4014.
BY TOM VALENTINO




Since 1987, Brown Consulting, Ltd. has assisted hundreds of mental health and addictions treatment organizations in successfully reaching their goals.
We provide a full range of consulting services. Specialist in Regulatory Compliance. Give
East Meets West: Multiple Perspectives on Trauma & Addiction
https://vendome.swoogo.com/2018-Orange-County
The Opioid Crisis: Strategies for Treatment and Recovery
https://vendome.swoogo.com/2018-Chicago-Opioid-Summit
National Conference on Trauma, Addictions and Mindfulness:

https://vendome.swoogo.com/2018-Chicago
April 2-5, 2018
National Rx Drug Abuse & Heroin Summit
Atlanta
https://vendome.swoogo.com/2018-rx-summit
August 19-22, 2018
National Conference on Addiction Disorders
Anaheim, Calif.

https://vendome.swoogo.com/NCAD-2018
June 25-26, 2018
Summit for Clinical Excellence
The Opioid Crisis: The Clinician’s Role and Treatment Practices
Pittsburgh
https://vendome.swoogo.com/2018-Pitt-Opioid-Summit









ata in parts of the country continue to suggest a stealth re-emergence of stimulants, at a time when the opioid crisis still dominates communities’ attention. Though it remains too soon to tell whether we will see a reprise of the “cocaine cowboys” era, some treatment professionals are offering thoughts on how health professionals should prepare.

Our Fall 2017 issue cover story, “Stimulants: The Next Drug Crisis Looms,” left readers speculating on whether the field ever will see a “buprenorphine” for stimulant dependence—in other words, a medication that alters the course of treatment and creates new hope. Some also wonder whether a new category of medication treatment is even the answer.
Many professionals believe that another drug crisis inevitably will follow the opioid epidemic, although the significant presence of polysubstance use makes this issue less clear-cut. “A look at history would lead us to expect a stimulant epidemic following an opioid epidemic,” says Michael Weiner, PhD, a longtime director and researcher at Behavioral Health of the Palm Beaches. He traces this pattern back to the effects of opiate-focused anti-drug legislation in the early 20th century, “way back when cocaine was actually looked at as a cure for ‘morphinism.’ ”
Weiner’s comments that accompanied the online posting of our cover story included: “It’s about time that our profession becomes proactive rather than reactive. All of the data pointing to the next crisis is out there. Question is whether or not we’re going to pay attention.”
The lack of a “gold standard” medication treatment similar to what the agonist drugs methadone and buprenorphine have become for opioid addiction clearly is creating much of the anxiety about any resurgence in stimulant dependence. One reader, however, warns against placing too much stock in conventional responses.
“History is clear that there will always be a ‘next crisis’ in drug use,” says Richard Seitz. “Fighting fire with fire (drugs to combat drugs) is not effective in drug abuse and won’t do anything other than make the drug companies richer and soothe our feelings that we are doing ‘something.’ ”
Seitz favors a comprehensive prevention strategy, but one that employs methods more effective than what has been used historically in targeting youths. He cites as a farther-reaching approach the Good Behavior Game, which assists young people with goal orientation, self-regulation, delayed gratification and working in cooperation with peers to achieve goals. He points out that this approach has been shown to yield a variety of positive outcomes, from improved academic achievement to substantially reduced alcohol and drug use.

No matter what the next drug crisis looks like (and in recent interviews I’ve heard everything from benzodiazepines to marijuana mentioned as prime suspects), it will be important to apply any lessons learned from the opioid experience. Based on that, it would seem that earlier identification of trends, intervention at multiple entry points, and a compassionate rather than punitive approach should pay off.


Professionals are increasingly embracing couples therapy early in addiction treatment

 BY GARY A. ENOS
BY GARY A. ENOS
n cases where a couple in a committed relationship is affected by addiction in one or both partners, conventional wisdom has advised that healing the relationship should take a back seat to establishing a track record of stable recovery first. As the notion of addiction as a family disease has taken greater hold across the field, however, professionals and programs are breaking from that tradition and directly addressing relationship dynamics earlier in treatment.
What is resulting from this evolving mindset includes the establishment of defined treatment programs or tracks for couples in early recovery, including in residential facilities where in some cases couples will live together during their stay.

“My overall philosophy is they’re going to live together anyway, so let’s treat them the best way we can,” says FrediRuth Levitt, a program director at Behavioral Health of the Palm Beaches in South Florida. “These couples don’t know how to have a positive relationship—it has been more of an enabling relationship.”
Robert Navarra, PsyD, LMFT, a family therapist and consultant based in San Carlos, Calif., says that the addiction treatment field’s tendency to postpone addressing relationship dynamics until recovery is more fully established actually flies in the face of research evidence. Studies have demonstrated that satisfying family relationships constitute one of the greatest predictors of long-term recovery, Navarra says.
“There are the individual partner recoveries, and then there is relationship recovery,” says Navarra. “We work to create a language for the couple to talk about recovery in the relationship.”
Over the past year, the Addiction Reach luxury treatment program in Palm Beach County, Fla., has developed a track available to couples who want to share the experience of early recovery. “Our clients have researched couples programs countrywide and have not found any other integrated programs that let them support each other on their own terms,” says Addiction Reach CEO Sue Merklin.
Nicholas S. Aradi, PhD, oversees clinical care in Addiction
Reach’s couples program. Although a daily recovery contract that seeks to establish a few-week period of abstinence serves as a cornerstone of Addiction Reach’s work, relationship-focused intervention begins fairly early in treatment, Aradi says.
“When you do the relationship piece, there is a higher likelihood of success,” says Aradi. He saw the drawbacks of narrowly defined individual treatment during his time as a school psychologist, where he would see that children would regress after consistently being returned to a dysfunctional family system.
The level of trust declines to basically nothing in a relationship where one partner has a substance use disorder, says Aradi. He points out that the dynamic differs when both partners have a substance use problem. “The partners will con each other in that arrangement,” he says.
Developing better communication skills becomes critical during treatment. Aradi finds several therapeutic techniques to be useful here; one involves educating partners by employing videos of other couples talking. Another involves teaching couples to adopt a “7-to-1 ratio” pledge: agreeing to make seven positive comments or reactions to their significant other for every negative one. Because of the damage that negative acts or thoughts can inflict on the relationship, “you’ve got to have seven positives to neutralize one negative,” says Aradi.
Merklin says Aradi will see the couple up to five times a week while the partners are in the treatment setting. The goal becomes one of helping each partner express oneself in a respectful way, while being able to see things from the perspective of the other person. Problem solving strategies and negotiation of behavioral change agreements also are important components of the process.
It is also important to emphasize within couples treatment that the relationship did not cause the addiction, Aradi says.
More recently, Morningside Recovery in Orange County, Calif., announced in December that it has launched an inpatient center designed to treat couples in recovery. Hand in Hand Recovery combines individualized therapy and couples counseling, with an early goal of establishing autonomy for each partner, says Jennifer Friend, a primary therapist in Morningside’s residential detox program.
Couples admitted for treatment must be willing to work on their own issues separately as well, says Friend. The partners will be together during meals and recreational time at Morningside,
but they are housed in separate sleeping quarters, she says.
The latter is more in keeping with tradition in addiction treatment, with this approach used partly because of concerns that couples living together could contribute to triggering other patients in the treatment setting. But that is not a universally held view. Levitt says that at Behavioral Health of the Palm Beaches, couples in treatment are housed together but advised not to remain so close as to compromise the therapeutic environment. “We try to separate them in process group so that they each have different experiences,” Levitt says.
Friend says it is also important that the couple be committed to sobriety and to each other. “This is not a program for someone to do with someone they just met in [treatment],” she says.
Navarra emphasizes in his presentations to professionals on couples therapy that a relational approach to recovery has been a critical missing piece in substance use treatment. At a time
when a couple is most vulnerable as the result of damage caused by a partner’s addiction, the message from traditional treatment has been: “Now we’d like you not to talk to each other.”
Navarra is certified in the Gottman framework for couples therapy, an approach that focuses on enhancing friendship, managing conflict and creating shared meaning between partners. A therapeutic technique that Navarra himself developed is called Healing Emotions from Addiction and Recovery Trauma (HEART), which acknowledges that trauma is present in both addiction and the process of recovery, and that each partner is affected.

He explains that under the highly structured intervention, a partner will identify a pivotal event in the couple’s history and explain how that moment affected him/her. The other partner can ask questions related to the experience. Navarra’s role involves making sure that both partners are protected during this process—no blaming is allowed.
The session helps to demonstrate that addiction has affected
Treatment professionals interviewed for this article state that couples therapy is not indicated for every couple affected by a substance use disorder. These are some of the circumstances under which they say couples treatment would not be advised:
• A history of partner violence, creating an environment where one partner feels unsafe, means that this treatment could not unfold productively.
• Each partner must be able to communicate and hear accurately in this highly structured therapy, so this treatment is not effective when a psychotic disorder is present, says Addiction Reach’s Nicholas Aradi.
• Aradi adds that this treatment approach can become challenging in cases where treatment has been court-mandated. “The partners must be personally invested,” he says.
each partner as an individual, as well as affecting the couple relationship. Sometimes the partner who does not have the primary substance use issue will be left saying to the other, “It never occurred to me that you were traumatized by your own addiction,” he says.
Navarra adds, “The couples movement reflects a recalibration of how we’re approaching recovery.” He welcomes this, believing that “separating [partners] in treatment is a huge mistake.”
In fact, he would like programs to think in terms of at least three components of recovery for individuals in a committed relationship: each partner’s recovery individually; the relationship’s recovery; and the recovery of the entire family unit.
 Gary A. Enos is Editor of Addiction Professional.
Gary A. Enos is Editor of Addiction Professional.

Summer or winter, Skywood Recovery’s breathtaking Michigan landscape provides the space you need to heal. In our residential treatment program, each meeting, group and activity builds on the others to get to the root causes of addiction and address any co-occurring mental health issues. Patients learn healthy new habits to prepare them for lasting success.

• Integrated treatment for addiction and co-occurring depression, anxiety, bipolar, trauma, etc.
• Comprehensive addiction assessment and psychiatric evaluation
• Customized care plans focused on the unique needs of each individual
• Medication management directed by collaborating medical experts
• Intervention assistance, sober escort and travel support services
• Delicious, healthy meals prepared by an executive chef
• Year-round equine therapy along with ropes courses, yoga, adventure and art therapy
• Convenient Midwest location
For OUTPATIENT TREATMENT, choose from ...





Hope and healing live right around the corner. Located in the heart of the Midwest, Foundations Detroit serves the unique needs of our neighbors in and around this historic city. Our comprehensive outpatient facility is filled with the support and resources needed to lay the foundation for a renewed life in recovery. As patients are equipped with new tools and create healthy habits, they rediscover joy along the way.
Located in the Loop, Foundations Chicago provides patients with an ideal setting for healing and renewal. Tucked away from the bustling city life outside, our comprehensive outpatient facility is a space for individuals to find support and encouragement for their personal goals. As patients learn to use new tools and create healthy habits, they lay the foundation for an energized life in recovery.
“At Skywood, we meet people right where they are and help them develop a greater clarity about the kind of life they want to live and how to pursue it.”
-David Pitts, Intake Coordinator
hether it is embracing the traditional 12 Steps or implementing medication in treatment, a majority of clinicians share a common mindset: If it works for the patient, run with it.
More than four out of five participants in Addiction Professional’s third annual Quality of Life Survey expressed a positive opinion on the 12 Steps, while nearly 90% of respondents shared favorable views on medication-assisted treatment (MAT).
BY TOM VALENTINO34.0% 15.7%
“I’ve come to decide that whatever is working for the individual, as long as it’s helpful and not causing harm, go for it,” says Jessica Holton, a licensed clinical social worker in private practice in Greenville, N.C., who participated in the 2017 survey.
Responses to questions regarding both the 12 Steps and MAT were mostly in line with results from the previous year’s survey.
The 2017 edition, which was conducted in September, drew responses from more than 650 clinicians. The survey is open to all clinicians in the field, and therefore, the individuals who have participated have varied from year to year.
A majority of clinicians who participated in the survey incorporate the 12 Steps into their treatment plans to at least some degree, as 48.1% said they feel it’s a key element at all levels of treatment and 34% said it was best for continuing care. Just 15.7% said it was time to phase out the Steps. Most notably,
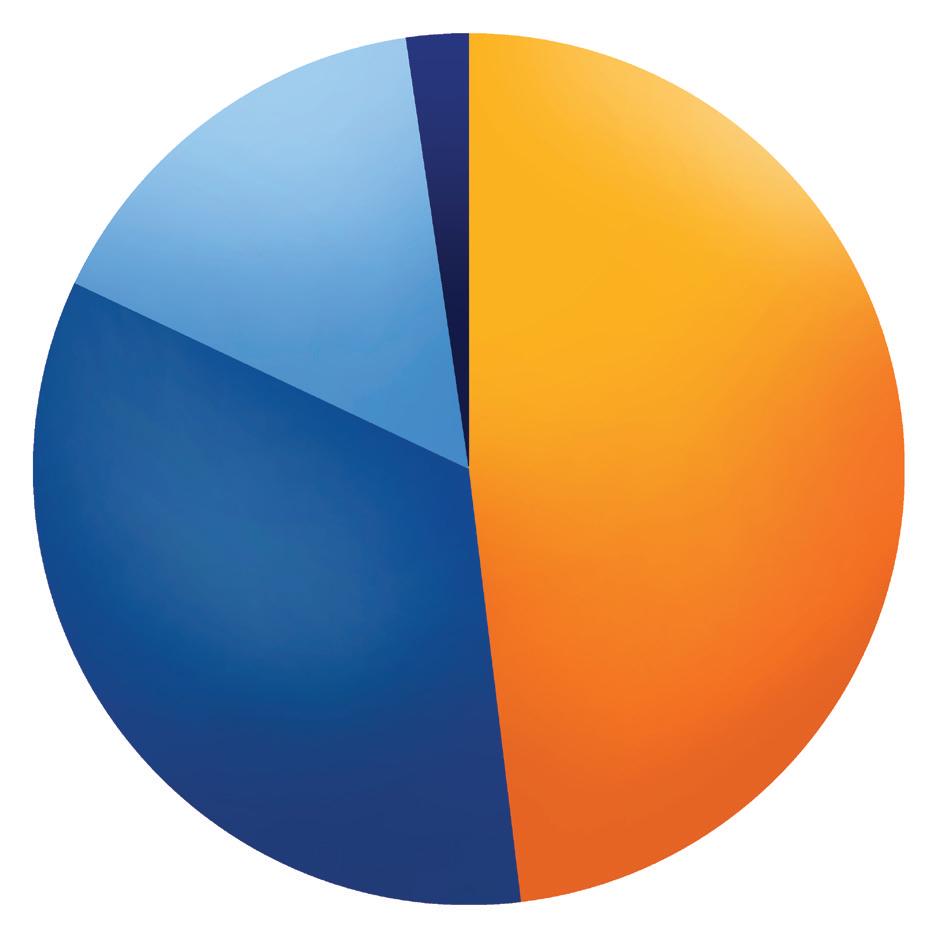
2.3% Key element at all levels of care Best for continuing care
48.1%
6% fewer participants said the 12 Steps are a key element at all levels of care compared to the previous year, but there was a 3% increase in those who felt the Steps were best for continuing care.
When applicants arrive at The Extension Recovery Services, they know from Day One that the 12 Steps are the basis of the Marietta, Ga.-based treatment center’s program, says Robert Jordan, CAC, director of The Extension’s men’s program.
“Coupled with the treatment we have, it gets them used to the part of the continuum of care once they transition out of treatment,” says Jordan, who has spent all nine years of his career at The Extension Recovery Services. “They’re set up, and they know the importance of having support.”
Lyle Fried, CAP, ICADC, CHC, co- founder and CEO of The Shores Treatment and Recovery in Port St. Lucie, Fla., says he finds value in implementing pieces of the Steps into a cognitive behavioral therapy approach.
“I ask people, ‘Do you think you need community or accountability in your life?’ ” says Fried. “Inevitably, they’ll say yes, and I’ll tell them, ‘Even if you believe nothing else that they teach there, they provide at least that.”
Fried, who is in long-term recovery after battling a polysubstance use addiction stemming from trauma, says he initially found little value in the Steps. Fried’s sponsor, his group leader and Fried himself all experienced a recurrence of their substance use, causing him to believe the Steps weren’t helpful at all. Fried’s feelings on the Steps evolved, however, once he found success with another faith-based approach to recovery. He reinvestigated the Steps and found that much of what worked for him was similar to the 12 Steps.
Fried says many of those in recovery who walk away from the 12 Steps do so because of the way some groups today interpret the fourth step.
“Nowadays, why do you think we have that 1-2-3 shuffle of people doing the first Steps, and then Step 4, it’s a daunting, shaming task, and they relapse in the process of it?” Fried says. “The original fourth step was just what it said it was: Searching and fearless moral inventory of ourselves. We use different words today. People early in their recovery aren’t ready for the guilt and shame that come with that.
“But, as a cognitive behavioral therapist, I would ask somebody what are their strengths and weaknesses, and how can we use these strengths to overcome these weaknesses?
That’s a normal process and why we include those kinds of questions in a bio-psycho-social evaluation.”
The 12 Steps, meanwhile, are not typically a focal point of discussions with clients for Holton, a practitioner for nearly 20 years. Holton says she recognizes the 12 Steps are important for some individuals in recovery, but that her work with clients focuses more on the neuroscience of addiction. Holton says she does have a few clients who attend 12 Step meetings.
“It’s been an interesting mix from the clients who do go to the 12 Step meetings,” Holton says. “They’ve shared that they don’t know of many people getting outpatient treatment and wish that some of them were. It’s almost a one-or-the-other scenario in my area.”
Holton says one client in particular shared an interesting observation: Those who seemed to benefit the most from the 12 Steps likely didn’t have guidance or mentoring throughout their lives.
“His vantage point was that for the folks who already have that moral compass in place, who have had good relationships and support, the 12 Steps don’t always feel as welcoming,” Holton says. A small percentage of survey respondents—2.1%—said they felt the 12 Steps seem like a cult. Fried says he can understand that perspective.
“Are there people who have taken basic tenets of it and turned it into a cult-like atmosphere and used it to weigh over people? Yes,” Fried says. “I liken it to any faith-based approach. There
“I liken it to any faithbased approach. There are synagogues, temples, churches and mosques that are abusive. But if you look at the core teachings of these faiths, they have good value. The same is true of the 12 Steps.”
— Lyle Fried, CAP, ICADC, CHC
are synagogues, temples, churches and mosques that are abusive. But if you look at the core teachings of these faiths, they have good value. The same is true of the 12 Steps.”
On the subject of abusing otherwise good parts of treatment, Fried, who has 16 years of experience in the field and has been full-time since 2008, expresses similar concern about medication-assisted treatment. He says he is concerned that doctors who prescribe buprenorphine to the full 275 patients for which they are licensed lack the capacity to devote themselves to other aspects of care.
“They have time to do a three-point checklist and send you on your way with another tab and another month’s prescription,” Fried says. “I believe MAT is a good thing, but not the way it’s practiced a lot in the world around me.
“It’s a disservice to tell someone that’s all they need. It’s supposed to be, according to SAMHSA, in conjunction with therapy so they can learn to live life eventually without it. If you start MAT without any vision or thoughts toward an endgame, you’re doing a disservice.”
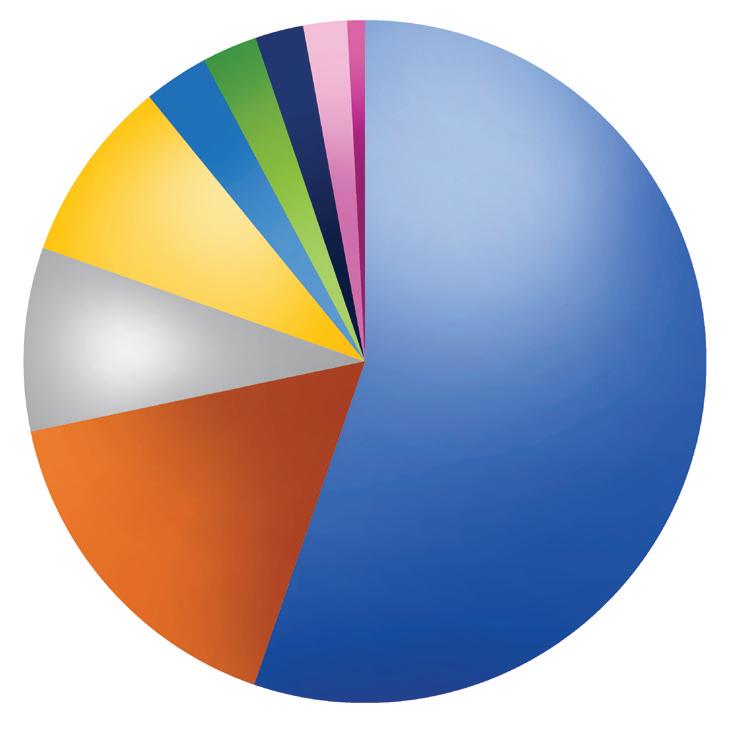
Fried’s views are in line with a strong majority of survey respondents: 75.9% say MAT is effective when it is provided in conjunction with counseling.
Jordan echoed Fried’s sentiments in that medicationassisted treatment offers a greater chance at quality longterm recovery—as long as the provider can get the patient stabilized to a point where they can eventually be weaned off the medication.
Holton says she does not have any clients using medicationassisted therapy and that early in her career, she was skeptical of MAT overall. Today, she says she remains on the fence as to whether MAT should be a first option in treatment for substance use disorders, but for those who have had several instances of recurrence, medication is worth trying to create a better foundation for recovery.
“I just want the field to be wise about how we’re using it and that we’re not exploiting people because of the money aspect of it,” she says.
Tom Valentino is Senior Editor of Addiction Professional.13.8% 8.4% 1.9%
75.9%
Of the 258 respondents to the Quality of Life Survey who said they have outstanding student loan debt, the median amount reported was $50,000, with more than 20% claiming debt of at least $100,000. This marked a significant jump from the previous year’s survey, in which the median amount of outstanding debt reported was $28,259.
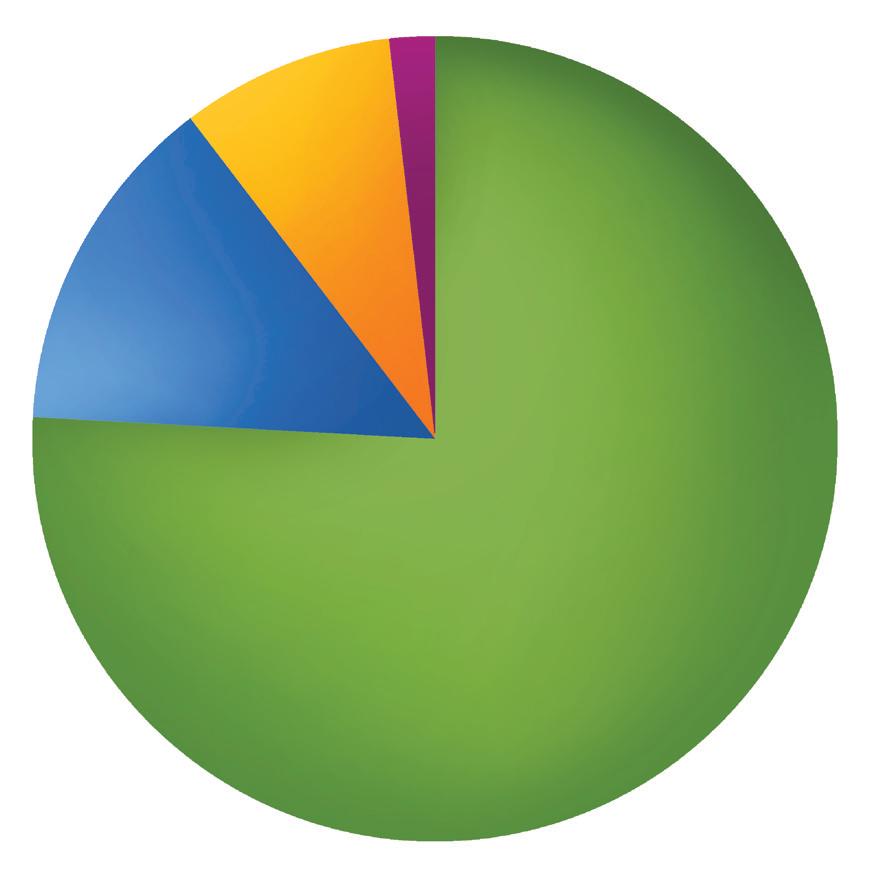
Of the clinicians who spoke with Addiction Professional for this story, Robert Jordan told the publication he has no outstanding debt, while Lyle Fried says he has $10,000 left to pay off. Jessica Holton, meanwhile, has nearly $25,000 to go. Holton says at one time she considered pursuing loan forgiveness programs through not-for-profit work arrangements, but ultimately found that few options existed in her area.
“The few times I did look into it, I didn’t meet the criteria,” she says.
Effective only with counseling in the primary role
Most essential component of successful recovery


When your patients are not responding to treatment, The Retreat at Sheppard Pratt can help. Our residential program offers individualized, compassionate and comprehensive care that empowers residents to manage even the most challenging mental health disorders. The Retreat is part of the Sheppard Pratt Health System, ranked among the nation’s top psychiatric hospitals by U.S. News & World Report for the past 27 years. For more information, visit our website or contact us.
retreat.sheppardpratt.org
410.449.2831
Industry leaders say the association is taking a bold step by requiring above-board business and clinical operations for membership
BY JULIE MILLERccording to a survey conducted last year by Behavioral Healthcare Executive, industry leaders believe that ethical standards should be enforced primarily by associations. The National Association of Addiction Treatment
Providers (NAATP) is starting off the year with an updated code of ethics as well as a new pledge to enforce it.
Executive Director Marvin Ventrell says that NAATP is taking a bold step by making ethical business and clinical operations requisites of membership for the first time.
“The preamble states clearly that members must comply with all elements of the code so there’s no confusion,” Ventrell says. “As a condition of membership, they agree to be removed if they do not comply.”
Of course, the goal is not to exclude organizations but rather to drive compliance across the industry with clear expectations. Ignorance is no longer an excuse for crossing the line on ethics.
“We might get smaller before we get larger,” says Doug Tieman, president and CEO of Caron Treatment Centers and one of the architects of the NAATP code.


Tieman says the high road might
not be easy and might lead to legal snarls along the way, but NAATP is prepared to defend its position. The hope is that members removed will ultimately comply and become members reinstated.
The most significant updates in the code address marketing tactics. For example, standards expressly forbid patient brokering or any form of remuneration for referrals. “There is no buying and selling of leads—that needs to be said,” Ventrell says.
Guidelines for marketing also demand transparency about the center’s identity in terms of name, location, services, licensing, accreditation and staff credentials. Online directories, for example, must include each featured center’s direct phone number.
“There are sites that pose as directories or resources, when in fact they are feeder sites to a particular organization,” Ventrell says. “It’s not clear to the consumer because the center’s name isn’t even on the page. They think it’s a clinical resource that leads to the best treatment.”
Similarly, transparency extends to statements made about licensing. Centers must be clear about what type of treatment they are licensed for and in which states. According to Ventrell, the specificity is important for consumer protection, and it's no longer acceptable for treatment centers to gloss over their licensing details on websites and in marketing materials.
Tieman says too often treatment centers are justifying their own actions as ethical while judging their competitors as unethical. Now the code creates a common definition for marketing standards.
“The beauty of this is that we lay out ethical marketing behavior instead of allowing everybody to interpret it for themselves,” he says.
Using a patient’s testimonial, image or identity as a marketing tool while the patient is still in treatment also is prohibited by NAATP. Testimonials are usually appropriate further along the recovery path—with the patient’s written consent—and many centers use them in their marketing strategies.
However, Ventrell notes that some popular television talk shows are known to follow individuals in crisis and might ask a treatment center to cooperate with
the show producers. NAATP members must avoid any situation that would exploit a patient for what is essentially entertainment, however, upholding ethics as they relate to media interaction might be evaluated on a case-by-case basis, he says. And clearly, the show shouldn’t have any financial ties to the treatment center.
“There’s nothing wrong with Dr. Phil or anyone referring someone to a center for assessment and treatment as long as there’s no payment for that referral,” he says.
NAATP is planning to offer in-person and online training sessions for members, according to Tieman. In time, the association also will compile a list of

providers that have completed training and pledge to follow the ethics code. That list could be valuable to third-party payers looking to contract with the best quality providers.
“You’ve got a built-in advantage because you can say you’re doing things the right way,” Tieman says.
In his experience, payers are skeptical of most providers because they all claim to be high quality but have no way to verify it. Tieman anticipates that NAATP membership could serve as that verification and ultimately offer a competitive advantage in the market.
eers have been involved in alcohol and drug use disorder treatment for decades. They started as volunteers who had personally experienced addiction and recovery, helping new patients learn the 12 Steps and cope with life’s challenges. More recently, peers have started to gain a professional aura, with credentialing and insurance reimbursement available.
In particular, peers are being used to help on the front end of the opioid crisis. Their work can begin immediately after someone has been rescued from an overdose, to help the individual get through the next few hours and days and in many cases to help engage the person in treatment. This is a desperately needed function, not only for humane purposes (people recovering from a naloxone rescue are confused, sick and unable to think clearly about what has just happened to them), but also because there simply is not enough professional staff to go around.
Addiction Professional spoke with several experts in the recovery movement to examine the current status of peers.
“Peer support is the process of giving and receiving nonclinical assistance so that people can achieve long-term recovery,” says Tom Coderre, senior advisor for behavioral health at the Altarum Institute, a health systems research and consulting organization.
Coderre, who worked on recovery issues as senior advisor to the assistant secretary at the Substance Abuse and Mental Health Services Administration (SAMHSA) from 20142017, and before that as national field director for Faces &
Voices of Recovery, emphasizes that a peer is not the same as a treatment professional. In fact, the person who is being assisted ultimately might not want to go to treatment, but it is the peer’s job to help the person follow through on the best path to recovery for that individual.
For peers to be most effective in responding to the opioid overdose epidemic, they need to be in places where people show up, says Coderre. “That’s why you’re seeing them in police departments,” he says, with first responders often being the ones providing the dose of naloxone that rescues people.
In Rhode Island, the most active peer program in the country has a foothold in emergency departments and in outreach. “They don’t wait for people to show up,” Coderre says of the Anchor ED program.
There are thousands of peers working through recovery community organizations (RCOs), says Patty McCarthy Metcalf, executive director of Faces & Voices of Recovery. About 100 of the RCOs are part of Faces & Voices. The model is for the RCO to provide training to peers, and for peers to work through the RCO. The RCO itself may have a contract with an emergency department, drug court, police department or other organizations, with the peers assigned by the RCO.
The peer has an experiential knowledge of addiction. But some organizations want peers to be in recovery for a set period of time before working with clients. Two years generally has been the standard, with this originally having been based on when it was believed to be personally safe for a person to share publicly that he/she was in recovery.
“It’s a state-by-state decision in terms of recruiting peers to participate in the training of a recovery support worker,” Metcalf says of the sobriety period.
She adds that despite the dire need for more assistance to combat the opioid crisis, she would not recommend relaxing the two-year sobriety period “because we need to protect the integrity of peer services. And we need to build capacity and infrastructure to meet the demand.”
Peers are not sponsors, as in Alcoholics Anonymous (AA), and they are not counselors—or in fact any type of clinical professional. But the precise scope of what they do is still being worked out and depends largely on where they are working.
Rachel Witmer, assistant director of the International Certification and Reciprocity Consortium (IC&RC), which offers a peer recovery credential, explains that many issues with peers involve the newness of the work. Definitions vary from state to state and organization to organization. “What Faces & Voices calls a recovery coach, some people call a peer recovery specialist,” Witmer says.
In some jurisdictions, the peers must themselves be in recovery from a substance use disorder. In others, a peer can be a family member or friend of someone with a substance use disorder, Witmer says.
Even though the title and credential are new, the presence of peers is as old as the drug and alcohol treatment field itself, says Witmer. “Peers were very much about the origins of treatment before it was more regulated,” she says. “Now they’re cycling back in.” But because the concept of peers as professionals is so new, there are still problems defining the scope of their work, she says.
The purpose of a credential is to develop expertise in a field, says Witmer. “Both a credential and a license are indicators of a certain amount of experience and training,” she says. The IC&RC peer recovery credential is developed to include basic concepts for both substance use and mental health disorders. “It’s a combined credential,” Witmer explains. “It’s pliable.” There are now about 2,000 IC&RC-certified peers in the United States.
Credentialing, for the most part, is used to establish reimbursement for peers. “This is a growing trend,” says Coderre. Ten years ago, reimbursement was rare, mostly coming from grants. “Now we’re actually seeing insurance companies and Medicaid reimburse for peer services,” he says.
Credentialing is needed in most states in order for a peer support worker to be paid. The International Certification and Reciprocity Consortium (IC&RC) offers a peer recovery credential, now available in 26 states. Individual state boards can determine the length of sober time required. Here are the minimum requirements for the credential:
Education: High school diploma or jurisdictionally certified high school equivalency.
Training: 46 hours specific to a number of domains, with 10 hours each in the three domains of advocacy; mentoring and education; and recovery/wellness support and 16 hours in the domain of ethical responsibility.
Experience: 500 hours of volunteer or paid work experience specific to the domains.
Supervision: 25 hours of supervision specific to the domains. Supervision must be provided by an organization’s documented and qualified supervisory staff per job description.
Examination: Applicants must pass the IC&RC Peer Recovery Examination.
Code of Ethics: The applicant must sign a code of ethics statement or affirmation that the applicant has read and will abide by the code of ethics.
Recertification: 20 hours of continuing education earned every two years, including six hours in ethics.
Coderre believes licensing is not a good idea for peers, however. “My worry is that if you license peers, you start to take them away from the non-professional experiential model and you put them more into a professional class, and that defeats the entire purpose of what a peer is supposed to do,” he says.
Peers should be paid salaries, not just a stipend, says Metcalf. “They’re not volunteers in RCOs,” she says. “They’re moving into the workforce, and they go through just as much training as a community health worker.”
In RCOs, peers are paid at least $15 an hour, says Metcalf. They may be full- or part-time, depending on the funding source. They may have the title of certified recovery coach, or recovery support specialist, she says.
But the definition of their role remains blurry at times. In some cases, treatment programs send peers—sometimes graduates of the programs—into hospital emergency departments to help steer patients back to the program. “That’s not the role of the peer,” says Metcalf, adding that this practice is unethical.
“The peer has to work with clients on all the options— whether it’s residential or outpatient, all of that is information that the peer worker explores” with the patient, Metcalf says. The peer worker then helps to engage the patient in whatever path the patient chooses, she says. “The RCOs don’t have an obligation to send people to a particular treatment program,” she says.
She adds, “Recovery support workers help people with the things that sponsors don’t. If I’m a recovery coach, I would
When Faces & Voices of Recovery’s Patty McCarthy Metcalf hears about programs in police departments that are enrolling peers to help with the overdose epidemic, such as the growing Police Assisted Addiction Recovery Initiative that started in Gloucester, Mass., she is supportive in part. For example, when there is a structure, it works, she says. “But peers need to be with other peers,” Metcalf says. “It’s tokenism if you put [only] one peer in an environment” such as a police department, she says. Another potential problem is “role drift,” in which peers end up being assigned other roles that are not intended for them.
Ultimately, using peers the wrong way, for the wrong purposes, will destroy the integrity of peer recovery, says Metcalf. “Our whole movement is in jeopardy,” she says.
look at things like cleaning up your criminal record, getting a job, looking for education if you need it, cleaning up your family relationships. The peer can say, ‘It was hard for me to get jobs because of my criminal record,’” and thus can empathize, she says.
When peers help engage people who have been rescued from an overdose, the message they convey is one of hope, says Metcalf. The patient needs to have a relationship with someone who is “not an authority or a treatment provider, but someone who can sit with them while they’re going through this experience,” she says. “They can say, ‘I’m with you, I overdosed four times, now I’m four years in recovery. Life will get better.’ ”
In general, first responders and even healthcare workers can be judgmental. The patient may need support, even if he or she has decided to go to treatment. For instance, there might be a wait of three days before admission. At that point, the peer might say, “Let’s talk about what you’re going to do for the next three days.”
In 2007, when state Medicaid directors were first told that peer support is an evidence-based practice for both substance use and mental health disorders, it was asked why this wasn’t made a reimbursable service. This is an even more pressing question now, says Metcalf. “This is the time to do it—it’s an all-hands-on-deck moment,” she says.
One of the more controversial suggestions is for money for peers to come from the treatment side of the equation, even though funding for treatment is already strained. “We aren’t pointing fingers at treatment—treatment programs are our allies,” says Metcalf. But the problem is that eventually, treatment ends, and that’s where recovery support starts.
Metcalf says an infrastructure for peer support can be put in place in every state in one of two ways. One is by ensuring that Medicaid will reimburse peer recovery services. But Faces & Voices would prefer a second option: a 20% set-aside in the federal Substance Abuse Prevention and Treatment Block Grant, administered by SAMHSA. But with 20% of this grant already set aside for prevention, an additional 20% would take a huge bite out of treatment.
“In no way do we want to take away money from treatment or prevention,” says Metcalf. “It’s time to put more money [overall] into the block grant.”
One of the best peer programs in the addiction field is Medication Assisted Recovery Services (MARS), a peerinitiated program sponsored by the National Alliance for Medication Assisted Recovery. Founded in 2005 with a SAMHSA grant and run out of the Albert Einstein College of Medicine, MARS trains peers who are in medication-assisted treatment with methadone to help others access treatment.

But there is what Coderre calls the “eternal stigma” of addiction, which is heightened for people treated with methadone. In this situation, peers are even more important, as medication-assisted treatment has been shown in research to be the most effective type of care for opioid use disorders.
“People need to tell their stories of how they are in recovery using medications,” says Coderre. “We rarely hear those stories.”
Last fall, an initiative funded by the Office of National Drug Control Policy (ONDCP) released a $2 million grant for an effort that will fund nine programs. One gives $135,000 to The Providence Center, which operates the Anchor ED program in Rhode Island, for implementing Safe Stations, a program in which fire department personnel will respond to people with opioid disorders who walk into fire stations. The project will support on-call recovery coaches to provide peer-based recovery support services. Coderre hopes such programs will continue to surface in 2018.
e seem to be constantly trying to change the public’s perception of substance use disorders and of people who have them. At best, progress is slow. The terms “stigma” and “shame” both apply. Stigma may be what is inflicted upon us by others. Shame is what we carry.
We have been trying to change the world. That’s hard to do. It’s easier to “have the courage to change the things we can.” Is it possible that we create at least some of the shame that feeds the stigma? I believe so.
What we do is treat a chronic disease with a series of episodic interventions (an acute-care model), and then we can’t understand why people feel like a failure (shame) when the symptoms of the disease become active. We leave our patients with the belief that the only measure of success is lifelong abstinence, so when a “relapse” (another word that evokes shame) occurs, they need to start over. This leaves people with a drawer full of white chips and several “walks of shame.” This is also the image we present to the public.
Maybe we have to change.
Chronic diseases require monitoring over the course of a lifetime. It is recognized that symptoms might become active at any point in time, and shame is not attached to the recurrence of symptoms. People with hypertension are not shamed when their blood pressure becomes unstable.
The word “relapse” is not applied to the recovery process for any other chronic disease. “Relapse” is a word shrouded in shame.
As William White wrote in a 2016 blog, “The lapse/relapse language in the alcohol and drug problems arena emerged during the temperance movement and was linked in the public mind to lying, deceit, and low moral character—a product of sin rather than sickness.”
We treat patients with substance use disorders intensely for about a month and then they “graduate.” Let’s say that we treat patients with an average age of 30 to 35. They can generally expect to live another 30 to 35 years. The only measure of success that we give them is lifespan abstinence. So we set up an expectation that a person with a chronic disease will be symptom-free for the 30 to 35 years he/she will spend in recovery. Does that even make sense?
And when symptoms do recur, we start the process all over again, only this time with the patient carrying even more shame. We treat another acute episode. This is another way we create failure.
Episodic care leads patients to say things such as, “I’ve been to treatment three times.” Doesn’t that sound like, “I’ve failed three times”? I’ve stopped asking patients how many times they’ve been in treatment. I simply ask for a history.
We continually send messages. Sometimes they convey that the patient had better get well fast—and in the way in which we want it to happen. We have made statements such as, “Come back when you’re ready,” or, “You need to do more research.” These messages imply, “You’re not worth my time right now.”
Similarly, I’ve often heard a professional say, “I’m not going to work harder on your recovery than you are.” On the other hand, we generally expect a patient to be ambivalent about recovery. So we expect a patient who is ambivalent and probably doesn’t want to be in treatment in the first place to work hard? We can’t have it both ways.
We also allow patients to diminish themselves. Have you ever heard people in treatment or recovery refer to themselves as “convicts” or “inmates”? I have, and too often I have just ignored it. This disease already beats them down. We don’t have to help it. Today I intervene in the conversation.
For the patient, there is a fine line between being humble and feeling shame. Does a person have to surrender and say he/she is an alcoholic/addict? Using labels may depend upon the mutual support group that a person prefers. Labels are more regularly used in 12-Step recovery meetings than at SMART Recovery meetings. I suggest giving patients the option between the two.
Many people, including professionals who work very hard to help others, perceive that treatment for substance use disorders is not very effective. Among people in recovery, it appears that failure is expected as well. It may be argued that minimizing stigma and shame will result in better outcomes. But there we go again. Chronic diseases do not have outcomes. Treatments for acute conditions have outcomes. Treating a cold makes it go away. It’s over. Chronic diseases hang around. When we measure the effectiveness of treatment by looking at the status of the disease over time, we measure up very well.
Maybe we got here because we are all part of a culture that shaped our thinking. Are we over the temperance movement hangover yet? We may have accepted the stigma and shame far too easily. On the surface, the changes we need to make do not seem that difficult, but changing how we’ve been shaped takes time, effort and practice.
Michael Botticelli, former director of the Office of National Drug Control Policy (ONDCP), recommended changes in the language we use, in order to minimize stigma and allow for better communication with the medical community. Simple changes, such as using “recovery management” instead of “aftercare” and “recurrence” instead of “relapse,” are steps in the right direction.

Stigma and shame keep people from coming to treatment—and keep people from coming back if they need to. I suspect some still will say that we can’t help people until they are willing to change. A better question might be, “Are we willing to change?” Do we have the courage to change the things we can?
Michael Weiner, PhD, MCAP, has held faculty positions at the University of North Carolina and the Rochester Institute of Technology. He has been a director and researcher for Behavioral Health of the Palm Beaches since 1999. He is also in private practice at Veritas Palm Beach.
We set up an expectation that a person with a chronic disease will be symptom-free for the 30 to 35 years he/ she will spend in recovery. Does that even make sense?
s a vascular surgeon, I learned to care for an extremely complex disease. More often than not, by the time I saw a patient with a vascular problem, the disease was fairly advanced. A clot or a blockage in a vessel was causing severe symptoms that needed treatment.
Complex interactions between inflamed vessel linings and body reactions culminate in symptoms that must be addressed. Clots are removed, blockages are repaired, or a substitute artery is used. Relief is provided and recovery can now begin. After the repair, aftercare instructions are given to the patient in the hope of avoiding recurrent episodes, but the suggestions may not be faithfully followed.
Many people are more willing to have a surgical repair of the problem once symptoms can no longer be ignored than to adhere to a longer process addressing diet, stress or lifestyle. A timely and expedient bypass graft has saved the day, but it has done nothing for the underlying disease of atherosclerosis that led to the problem. Medicines are used to help recovery and prevention,
and they do help. Patients are better than they were before treatment with these medicines, but not as well as they could be if they followed suggestions. The disease process is relentless and progressive.
We follow this same pathway with addiction treatment. Symptoms eventually crescendo into some unacceptable situation demanding stabilization. Actions are taken and medicines are used, in the hope of replacing a substance or blocking it. Today we call this medication-assisted treatment (MAT). We have named the use of medicines for addiction as if this use is unique in disease treatment. Later, aftercare suggestions are given and variably followed. MAT improves the complications and ramifications of addiction, similar to what a vascular graft does for vascular disease. These are beneficial treatments, and no one is suggesting they not be used. Worse problems are averted, and function improves. New bandages are placed on the underlying disease, giving hope that it will not happen again. The disease still smolders, however.
What exactly is this disease of addiction that we are acutely treating? An excellent review of this brain disease was provided in a 2016 article in the New England Journal of Medicine by Volkow et al., “Neurobiologic Advances
From the Brain Disease Model of Addiction.” The article underscores the complexity of the disease of addiction, a complexity matching or exceeding that of vascular disease. Changes in the brain leading to the symptoms of the disease
The progression of addiction and other diseases is relentless unless treatment takes a comprehensive and long-range approach
“I would not be alive today if it weren’t for Sierra Tucson. I believe that every person who enters those front doors by that beautiful fountain is a blessed miracle, just like me.” -Andrew S., Scottsdale, AZ.
NO ONE KNOWS WHAT DESPERATION FEELS LIKE UNLESS YOU’VE BEEN THERE.
It renders you hopeless. Whether you are suffering from depression, anxiety, or PTSD, we are here to help you heal.
Call us to help your clients take the next step on their journey of change.

844-202-7373 | SierraTucson.com
We work with most insurance.
go far beyond the oft-quoted dopamine problem given in standard neurobiology lectures.
The article describes important areas of the midbrain and frontal cortex that are affected. Many areas of the brain that once allowed rational thinking and reasoned behaviors are changed. The same survival part of the brain that mandates breathing and drinking water has now elevated a substance to being just as important as air and water. “Flow” in the brain progresses unimpeded from bottom up, acting as a gas pedal to the part of the brain that makes us human: the cortex.
The frontal cortex contains what has been called the executive functioning center of the brain, with the name alone suggesting its roles and importance. While motivation, or “gas,” is flowing toward the cortex, the balancing flow from the cortex back down is “blocked.” All gas and no brake. No steering, either. The frontal cortex that normally promotes moderation, attunement, creativity and other human things has become impotent. Structural changes in wiring occur. Chemical changes, such as an altered glutamate system in specific areas of control, are present. Decisions are now made by a brain with imbalanced wiring and chemistry. The journal article goes into much more detail, but ultimately harmonious brain balance has become chaotic.
You get the picture. Addiction is very complex, and our underestimation of this complexity has led to answers that are partial or temporary. Today’s treatments are helpful and have benefits, but they often are inadequate to address the disease process. MAT and a few weeks of treatment are to addiction what an acute repair is to vascular disease. Things are better, but real problems remain.
To treat this complex brain disease successfully, the brain must be changed. The brain wires itself using a process called neuroplasticity. Needed connections form in response to the environment. Neuroplasticity is how an unwired newborn becomes a musician or a teacher. It is also how this same musician or teacher later dies of an overdose. Treatment must use methods to harness this natural process of neuroplasticity to rewire the brain again, restoring health and harmony.
Practices that actively seek the things lost in addiction will strengthen wiring in areas of brain that have been short-circuited
Practices that restore awareness, reason, discovery, connection and choice actually change the brain. Some would call these spiritual or mindful practices. Others would use behavioral or biological definitions. They are all correct, and they are necessary to change the brain.
MAT is spoken of today almost as a holy grail for addiction treatment. This is not because it restores a normal brain, but rather because it is affordable and expedient and provides relief just like a bypass for vascular disease. Yes, we should use these things. They decrease loss of life and complications. They are only bandages, though, for the underlying disease process. We must not be lulled into believing that these medicines are the answer. Addiction is far too complex.
Roland Reeves, MD, is the Medical Director of Destin Recovery and South Walton Medical Center in Destin, Fla.
Today’s treatments are helpful and have benefits, but they often are inadequate to address the disease process.
by addiction.
To help build on your success and increase your chance for long-term recovery, Ashley Addiction Treatment offers a 60-day Young Adult Extended Care Program for males 18 to 25. Through treatment plans that focus on identifying underlying factors contributing to addiction, training in life-skills, and participation in on and off-campus recreational activities designed to integrate fun, we help young men find a new path toward a life of connection and fulfillment.
Our programs offer:
• Integrated team of counselors, therapists, family therapists, psychologists, and clinical technicians







• Individual and group counseling services, art therapies, equine therapy, and mindfulness activities


• Innovative programming designed to help young men overcome obstacles to recovery and successfully navigate life
Everything for recovery because recovery is everything.
800.799.HOPE




 BY BRIAN DUFFY, LMHC, LADC-I
BY BRIAN DUFFY, LMHC, LADC-I
uch has been written about people being addicted to a chaotic lifestyle. This article, however, is not influenced by formal research. These are merely my own observations and experiences dealing with clients who seem to choose (or create) a chaotic environment. For simplicity’s sake, I’ll divide “chaos addicts” into two groups.
Here, we’re talking about those whose family of origin was riddled with uncertainty. In these families, rules were always changing, anger and depression were omnipresent, and adults were emotionally unavailable. Coming from this environment, people learn that anger, tears, noise and threats can be useful to get one’s needs met. To compete with all the distractions in the household, one must demand attention—even if it means acting out in a negative way. Understandably, this
lifestyle becomes their “normal.” They can’t imagine what a more stable home life would feel like.
Many people come from this type of dysfunction and never develop a substance use disorder or any other problematic behavior. If they seek treatment, it probably will be later in life, when they begin experiencing problems with relationships, career or serenity. By this time in the life cycle, they are heavily invested in their coping strategies, making it difficult to break old habits that used to work but are now creating unwanted consequences.
These individuals become addicted to chaos as a result of their relationship with drugs. Chances are, many from Group 1 will end up in Group 2.
Many individuals with addictions grew up in stable homes with a strong work ethic and a socially responsible set of values. But they quickly learned that lying, conning, scamming, cheating and stealing became easy and necessary to continue a “using” lifestyle. The consequences of these behaviors became acceptable over time. Most people with addiction never thought they’d be prostituting themselves or breaking the law, but addiction reprioritized their brains and made bad behavior the norm. With these learned behaviors come consequences and chaos.
Unfortunately, the person with an addiction becomes adept at settling for less, justifying his behavior in countless ways. It’s the disease of denial. Although he probably won’t see it when actively using, a bit of sobriety might allow him to begin to connect the dots.
In early sobriety, a patient might recognize himself as the frog in a pot of room-temperature water. You know the frog: It continues to swim around, although jumping out is an option. When heat is gradually applied, the frog won’t notice its worsening situation and will ultimately die. Our clients don’t fully recognize the amount of chaos they’ve created—the depths to which they’ve sunk.
Most of those in recovery from substance use disorders will miss their drugs because there certainly were some good times associated with use. Many also will miss the criminality—the thrill of scoring on the street, the rush produced by jumping over the counter to rob a convenience store, or the subtler excitement of manipulating others to behave in a certain way. In short, chaos often becomes an attractive switched addiction.
Whereas people from Group 1 might adopt a persona of victimhood, blaming others for their circumstances, Group 2 is populated by individuals who (if honest) ultimately will blame themselves for their predicaments. In my experience, the most painful consequence of addiction is selfloathing: “I want to stop the madness, but I keep screwing up. I’m a loser. I have no will power.”
A medical doctor might ask a patient, “Where does it hurt?” Addiction professionals need to ask the same question, from a psychological perspective:
• What is the nature of the pain?
• When is it worse?
• What are its triggers?
• Are we making realistic assumptions?
Bottom line: Can we connect the dots, and discover the causes, benefits and consequences of the chaos habit? Can we learn if there ever has been sober time and, if so, how it was achieved? Most important, we need to explore how our client is going to have fun in the future, without the drugs and without the chaos. Let’s assume our patient is at least in
Can we connect the dots, and discover the causes, benefits and consequences of the chaos habit? Can we learn if there ever has been sober time and, if so, how it was achieved?
the contemplative stage, ready to examine her thinking and maybe even make some behavioral changes. We might use cognitive-behavioral therapy as well as motivational interviewing, looking at the thinking habits as well as the behaviors. To address cognitions, we help patients to challenge their assumptions, to identify when they’re “catastrophizing,” to remember that feelings are not facts.
Living life one day at a time is a skill learned over time, and the good old Serenity Prayer is always useful, stressing the importance of accepting things beyond our understanding. I use the Serenity Prayer liberally in my practice, treating mood, anxiety,
psychotic and, of course, substance use disorders. Relaxation techniques, including meditation, guided imagery and expressive arts, also can help keep our patient in the here and now.

Although addressing thinking habits is an important component of treatment, I believe behavioral modification offers the strongest opportunity for long-term success. But breaking the chaos habit can be slow going. The unproductive behaviors probably have been on board for many years, so we must be patient and ready to applaud even the smallest steps in the right direction.
Whereas anger and impulsive behavior are common threads of a

chaotic lifestyle, we work with the patient to distinguish between anger (a normal feeling) and aggressiveness, which is usually unproductive and a manifestation of the chaos habit. We also examine the patient’s exercise habits, nutritional needs, and participation in social activities, community service or spiritual fellowships.

As with any addiction, we must identify and avoid high-risk situations that could trigger a relapse to chaotic behavior (or to the original drug of choice). And if there is a situation that cannot be avoided, we will devise a relapse prevention plan, which might include asking for help or practicing self-soothing exercises.


As addiction professionals, we understand the challenges of helping people break any habit, whether it’s a substance or a behavior. But the process remains the same: The patient must examine the pros and cons of the addiction, agree that change is necessary, learn new ways to view the world, associate with safe, sober people, and learn to be comfortable with (and have fun in) a non-chaotic environment. No one ever said it was going to be easy.


eople with substance use problems don’t usually return home to sit by the phone when they’ve been denied immediate treatment. In fact, they often return to what brought them to seek help in the first place. The federal government estimates that overall, around 90% of the people who need treatment for substance use never receive it.
King County, Wash., has embarked on an ambitious effort to reverse the trend. The county Health and Recorder Division oversees a network of 30 providers furnishing addiction and mental health services. County officials have partnered with the Ballmer Group and Third Sector Capital Partners, along with MTM Inc., to find a way to offer patients same-day access to these providers. The program, dubbed “Pay for Success,” directs $1.4 million per year to behavioral health providers who offer treatment on demand to the 22,000 low-income King County residents who will be eligible for the program.
mental health services. Patients who don’t get access to the treatment and care coordination they need when they need it most end up having poor outcomes and are more likely to die prematurely as a result, Vollendroff says.
A 2006 report published in the Journal of Drug Issues highlighted this problem through narratives. The study followed 52 individuals with substance use disorders, reporting on their experiences in seeking treatment. More than 45% went to rehabilitation intake centers of their own accord, 21% were court-ordered to do so, nearly 12% were referred by another provider, around 10% were sent by family members or friends, and about 12% were referred by homeless shelters or children’s services. Only about one-third of the patients who reported to the intake unit received an appointment within 24 hours, according to the report, with 11.5% having to wait more than a week to get help. The average wait time to enter a treatment program after initial contact with a provider was 42.5 days. These, Vollendroff says, are the types of delays King County is working to avoid with the new program, which has been modeled after the National Council for Behavioral Health’s same-day access initiative. “One of the things that we found as we looked into this is, the earlier you access care, the better the outcome,” he says.
Jim
Vollendroff,director of the county Behavioral Health and Recovery Division, tells Addiction Professional that it’s critical for the county to be able to offer timely access to addiction and
The county is rolling out the program with a small group of outpatient providers and will increase the number of participants and the financial incentives offered over time. Debra Srebnik, a quality improvement specialist with the county, says providers who participate are offered a front-end
incentive payment simply for implementing a rapid access program, in order to recognize them for the resources they have spent in developing these systems.
“We really wanted to recognize those first six months,” says Srebnik. With the submission of a plan and the results of patient satisfaction monitoring, the providers are getting six months of incentives without having to undergo a performance review. “After six months, incentives will be based on their ability to meet the metrics,” says Srebnik.
There are three metrics the program will use to measure performance and to award incentives, Srebnik says:
• The first is the amount of time it takes from a patient’s request for service to when intake is offered. The target is zero to one days, and the goal is to have 85% of patients covered in that range, she says, adding that half of the incentive payment will be based on this metric alone.
• The second metric is the time elapsed from when a service was requested until actual intake occurs. Srebnik says that ideally, an appointment would take place no more than four days from the initial request or offer, and 80% of patients would fall under this.
• Finally, providers will be incentivized based on the time it takes for patients to move from their first appointment to a routine or follow-up visit. The target is within seven days, based on a national benchmark, Srebnik says.
This move toward better outcomes is ambitious, Vollendroff says, because many challenges complicate the effort to offer same-day services in addiction and mental health.
“We’re rolling out a number of projects in which we are moving to a value-based system and paying providers a number of incentives to reach certain outcomes,” he says. “It’s a challenge for providers from a staffing standpoint,” which he sees as the most pressing issue for participating organizations.
Vollendroff says King County is working on a legislative strategy for improving reimbursement for addiction and mental healthcare as a way to attract more providers to the field, alleviating workforce shortages.
Initially, six agencies signed on to the King County program, says Srebnik. Now, 23 of 29 outpatient providers are participating. Although the effort is still in its pilot phase, Srebnik says metric-based incentive payments will start later in 2018. Program leaders report early successes, based on
anecdotal reports.
“I hear a lot of feedback, and I hear a lot of phone calls from family members,” Vollendroff says. “Just having the conversation with our providers has heightened their awareness and commitment.”
Beratta Gomillion, executive director of the Center for Human Services, says the provider agency has worked with the county and MTM to implement same-day access and that it has been a “win-win-win” for patients, the organization and clinicians.
“The consumer benefits because it eliminates long wait times for an assessment. It allows us to strike while the iron is hot and provide services when the consumer wants it,” Gomillion says. “Clinicians love it because it eliminates no-shows, freeing up their time to do other tasks. Our management loves it because it improves clinicians’ productivity. My only wish is that we had implemented this years ago.”
“The consumer benefits because it eliminates long wait times for an assessment. It allows us to strike while the iron is hot and provide services when the consumer wants it.”
— Beratta Gomillion
The Institute is a trusted educational resource that helps address daily challenges. Our conferences convene thought leaders that share clinical best practices, discuss how to effectively and ef ciently operate a behavioral healthcare organization, and strategize solutions for addressing the opioid epidemic. Join us at an upcoming event to network with peers and take home valuable tools. Learn more about us and how we can help you at www. iadvancebehavioralhealthcare.com.

APRIL 2-5, 2018 | ATLANTA, GA
Be part of the discussion at the largest national gathering of stakeholders working together to address the opioid crisis. Prevention, treatment, law enforcement, public health, and many others exchange best practices and hear from state and federal of cials at the annual Rx Summit.
www.nationalrxdrugabusesummit.org

AUGUST 19-22, 2018 | DISNEYLAND, CA
Addiction professionals annually convene at NCAD to share what’s working: Clinicians hear from thought leaders on delivering treatment, while executives of behavioral healthcare organizations learn how to run more effective, more ef cient, and ethically minded businesses. www.ncadcon.com
NOVEMBER 12-14, 2018 | FORT LAUDERDALE, FL
The opioid crisis is making headlines, but another category of drugs continues to devastate communities: stimulants. Join other stakeholders to explore how to address and treat stimulant use.
www.stimulantsummit.com


DECEMBER 10-12, 2018 | SCOTTSDALE, AZ
Senior executives of treatment centers, and those investing in these enterprises, discuss growth strategies and market dynamics at this exclusive, three-day educational and networking event.
www.treatmentcenterretreat.com
APRIL 30-MAY 2, 2018 | HILTON HEAD, SC
TCEM provides CEOs, CFOs, COOs, directors, senior marketing/business development/ admissions leaders, and other executives with the tools they need to effectively and ethically grow their services in a rapidly changing market. www.executiveandmarketingretreat.com
Interested in attending an event? Contact Ellen Kelley at ekelley@iabhc.com or 216-373-1223.
Photography: Pete Winkel GPA President Obama addressed Institute attendees in 2016. Matt Bevin, Governor of Kentucky, addressed Institute attendees in 2017.CE Credits
The Summits for Clinical Excellence bring together thought leaders on cutting-edge topics in multi-day national and regional conferences. Summits on mindfulness, trauma, process addiction, and shame appeal particularly to private practice behavioral healthcare professionals. Other Summits address the national opioid crisis from a regional perspective and engage a diverse group of stakeholders. Many Summits offer treatment ethics continuing education credits.
• PHOENIX, AZ February 14-16, 2018
The Opioid Crisis: The Clinician’s Role and Treatment Practices - Featuring the 2nd Annual Arizona Opioid Summit www.arizonaopioidsummit.com
• ORANGE COUNTY, CA March 1-2, 2018
East Meets West: Multiple Perspectives on Trauma and Addictions www.iabhc.com/orangecounty2018
• CHICAGO, IL March 7-8, 2018
The Opioid Crisis: Strategies for Treatment and Recovery www.chicagoopioidsummit.com
• CHICAGO, IL March 7-10, 2018
The National Conference on Trauma, Addictions, and Mindfulness: Where Freud Meets Buddha www.iabhc.com/chicago2018
• PITTSBURGH, PA June 25-26, 2018
The Opioid Crisis: The Clinician’s Role and Treatment Practices www.pittsburghopioidsummit.com
• ATLANTA, GA October 18-21, 2018
Brain Matters: Shame, Trauma, and Process Addictions www.iabhc.com/atlanta2018
• NEW ENGLAND November 8-9, 2018
The Opioid Crisis: Strategies for Treatment and Recovery www.newenglandopioidsummit.com

CE Credits
WEBINARS
The National Conference on Addiction Disorders convenes panel discussions across the country in a lunch’n’learn format. Clinicians hear about treatment practices, while those on the business side of the field share strategies for managing and marketing behavioral healthcare organizations. www.iabhc.com/local
Upcoming events:
Hear from experts on clinical, managerial, and other topics in our frequent, free-to-attend Webinars. www.iabhc.com/webinars
CE Credits
Contact Ellen Kelley at ekelley@iabhc.com or 216-373-1223.
he next time you feel overcome with anger over underfunding and the treatment gap in substance use services, take solace (or get more outraged) in these comparative numbers regarding services for gambling disorders:
• Substance use disorders in the U.S. are 3.8 times more common than gambling disorders, but public funding for substance use treatment is a whopping 330-plus times greater than public funding for problem gambling services.
• While traditionally around 10% of people who need substance use treatment receive it, the comparative statistic in gambling disorder treatment was around one-quarter of 1% in 2016.
• 10 states and the District of Columbia provide absolutely no public funding for problem gambling services, even though only two states in the entire country offer no government-sanctioned gambling.
The data come from the newly released 2016 Survey of Problem Gambling Services in the United States, and illustrate the significant challenge that treatment and prevention advocates face in elevating the negative effects of gambling to a front-burner issue in state policy discussions. The periodic survey, which had been last released for 2013, is coproduced by the Association of Problem Gambling Service Administrators (APGSA), representing the state government administrators of public funds for problem gambling services, and the National Council on Problem Gambling, a policy and program development organization.
APGSA president Terri Sue Canale-Dalman, who heads the California Office of Problem Gambling within the state Department of Public Health, says that while virtually no one would contend that substance use treatment services are sufficiently funded, the comparatively more disappointing
data for gambling services still startle her every time she refers to them.
Some incremental progress has been made at the state level, the latest survey indicates. The total number of states with publicly funded problem gambling services increased to 40 in 2016; the number had been 35 in 2006 and 39 at the time of the previous survey in 2013. Twenty-five states increased funding levels for gambling-related services from 2013 to 2016, but nine saw cuts in funding. Arkansas eliminated all public funding for problem gambling services, according to the report.
Data on per-capita spending in the states shed significant light on the underfunding issue. The average per-capita spending in the 40 states that have publicly funded services for problem gambling is only 37 cents, with a range from a low of one penny in South Carolina to a high of $1.46 in Delaware. If all states, including those with no public funding, are counted in this analysis, per-capita spending drops to an average of 23 cents.
Canale-Dalman says that in general, growth in legalized gambling opportunities in a state is the factor that ends up spurring interest in initiating or expanding publicly funded treatment. The survey found that increased state funding for problem gambling services was associated with a number of variables, including state spending and revenue from gambling, the estimated number of adult problem gamblers within a state, and the number of problem gamblers treated.
However, Canale-Dalman says this tends to create a scenario in which states are consistently trying to play catch-up while government-sanctioned gambling options relentlessly expand.
For example, she says, Massachusetts moved forward with its first dedicated state funding for problem gambling services on the occasion of the development of the state’s first casino, which of course was not the state’s first foray into sanctioned gambling.
“We need to get out ahead of the gambling growth,” says Canale-Dalman.
The 2016 survey also illustrated a lack of uniformity in the types of problem gambling services that receive government funding support in each state. Problem gambling awareness programs remain the most commonly supported service, followed by counselor training, gambling helplines and problem gambling treatment. The researchers reported that higher spending on problem gambling services was associated with increases in gambling treatment utilization.
Twenty-three states reported providing gambling prevention services in 2013, with
problem identification and referral the most prominent of the services. Research spending, including for prevalence studies and risk behavior analyses, appears to be very low in the surveyed government agencies and nonprofit organizations.
Canale-Dalman says APGSA has traditionally prioritized the need to integrate problem gambling and substance use disorder efforts at the state level. Respondents to the latest survey listed improved integration of problem gambling into behavioral health services as the most pressing need in their state’s problem gambling system, followed by the need

for federal guidance on how to address various forms of Internet-based gambling.
In times of budget uncertainty, the substance use treatment and problem gambling service communities must look for ways to collaborate and leverage resources, Canale-Dalman suggests.
For a substantial number of state governments, it remains challenging to maintain consistent attention to issues around problematic gambling at all. According to the latest survey, only 17 states funded a full-time position devoted to administering problem gambling initiatives, as in what Canale-Dalman is dedicated to in California.
More than 70% of high school seniors say they don’t view regular marijuana smoking as harmful
Although nearly two-thirds of adolescents polled for the 43rd annual Monitoring the Future survey said they disapprove of regular marijuana use, the study finds that usage of the drug among students in 10th and 12th grades is up for the first time in seven years.
A total of 43,703 students in grades 8, 10 and 12 from 360 public and private schools from across the country participated in the survey, which was conducted by the National Institute on Drug Abuse (NIDA) and the University of Michigan.
71% of high school seniors said they do not view regular marijuana smoking as harmful,
although 64.7% said they disapprove of regular marijuana use.
39.9 %
37.1%
of 12th graders have used marijuana within the past year, a year-over-year increase of 1.5%.
Overall, 24 % of students surveyed in the three grades overall have used marijuana within the past year, a 1.3 % increase from the previous year.
5.9%
of 12th graders use marijuana daily, overtaking daily use of cigarettes (4.2%).
of high school seniors said they have used an illicit drug within the past year, up from 38.3% in 2016. Excluding marijuana use, however, illicit drug use among the same population is down 1% year-over-year (13.3% vs. 14.3%)
SOURCE: monitoringthefuture.org
Northern Kentucky University is the proud Platinum Sponsor of Education and Community for the 2018 National Rx Drug Abuse & Heroin Summit. When we come together, we can uncover breakthrough solutions to our society’s most challenging population health problems. We are excited to carry this mission forward when our Health Innovation Center opens this fall.

Learn more about NKU’s Health Innovation Center and our work to understand – and address – challenges to health and wellness.


Stop by Booth 802 during the conference in Atlanta April 2-5 or visit us online at
NKU.EDU/HICINFO
Kentucky’s drug death rate has risen 33% in the past five years and the state is ranked as having the 2nd highest number of deaths.
(America’s Health Rankings® Annual Report)
high-profile sexual abuse cases sparking more patients to open up, providers focus on ways to facilitate productive discussions in treatment
BY TOM VALENTINOrom Hollywood executives and actors to politicians to members of the media, high-profile stories of sexual harassment and sexual assault have continually made national headlines in recent months. The #MeToo movement 1 has drawn attention to the pervasive nature of such abuse, igniting conversations and challenging previously
held perceptions.
Statistics bear out the degree to which sexual assault and sexual harassment have plagued American culture, particularly in the workplace. According to an ABC News/Washington Post survey2 released in October:

• 54% of women say they have experienced unwanted sexual advances;
• 30% say they have had such experiences in the workplace; and
• 23% say they have experienced an unwanted sexual
advance from someone who had influence over their work situation.
If the #MeToo movement has a lasting impact—and the continued proliferation of cases coming to light seems to indicate that is a real possibility—mental health treatment professionals will play a key role in answering one critical question as more victims feel empowered to open up: What now?
“I don’t know if anything has been put out there well in terms of solutions,” says Jamie Marich, PhD, a trauma therapy specialist based in Ohio, who is also a contributing writer for Addiction Professional.
The lack of solutions is what concerns Marich the most.
“It’s great the conversation is happening, and I don’t think it’s going away,” she continues. “But the next logical place the conversation has to shift to is what we do about it now. It’s similar to recovery: Once you know you have a problem, what are you going to do about it?”
Marich and other clinicians contacted by Addiction Professional shared some key points for treatment professionals to keep in mind moving forward.
Stories in the news can often trigger trauma response for others who have shared similar experiences—although not always—notes Stephanie S. Covington, PhD, co-director of both the Institute for Relational Development and the Center for Gender and Justice. Managing such triggers is a critical component of treatment.

“For a trauma survivor, triggers are everywhere, and they don’t know when and where they may happen,” Covington says. “That’s why one of the primary things we do when we work with survivors is help them have grounding techniques and skills they can use when they are triggered. They understand what a trigger is, they can identify it, and they can do something
about how to manage their emotions.”
When patients are willing to open up, clinicians need to be able to validate their stories as “legitimate grist for the clinical mill,” Marich says.
“I really hate it when clinicians or people in recovery say, ‘Oh my gosh, it’s not going on in their real life. They’re just being a bunch of babies,’ ” Marich says. “A solid clinician needs to be able to work with what’s happening in current events and understand how it’s impacting clients.”
Julie Hergenrather, PhD, a clinical psychologist who specializes in women’s issues at Geisinger in Pennsylvania, says the #MeToo movement isn’t only empowering victims to speak out,
ISBN: 978-1-942094-56-2

E-book: 978-1-942094-57-9
230 pages • $17.95 • 6 x 9 centralrecoverypress.com
A far-ranging examination of how the eff ects of addiction and trauma in the family can reverberate for generations.
“An excellent and accessible book that elucidates both the path of illness and that of recovery.”
ÑTian Dayton, PhD , author of The ACoA Trauma Syndrome and Emotional Sobriety




it is also opening the door for issues previously discussed between patients and therapists to be re-examined.

“These are experiences they might have heard about from their clients in the past, but not necessarily labeled them as such,” Hergenrather says. “Perhaps both patients and clinicians will view past harassment experiences as more important and more impactful than previously since there seems to be a growing acceptance that sexual harassment happens frequently, and it actually is problematic, upsetting and even life-altering for the victim.”
According to the ABC News/Washington Post poll, just 42% of women who say they have experienced unwanted sexual advances in the workplace have reported it to a supervisor. And this occurs despite the fact that 83% say they’re angry about the experience, 64% say it made them feel intimidated and 52% say they were humiliated.
Marich says many victims choose to stay quiet for years out of fear of being chastised, ridiculed or simply not believed.
“One of the dumbest things I’ve heard from some male politicians through all of this was, ‘Now, everybody is coming out of the woodwork,’ ” Marich says. “Well, there’s a very good reason for that. When
Just 42% of women who say they have experienced unwanted sexual advances in the workplace have reported it to a supervisor.

CleanSlate Centers offers hope for patients and families battling addiction, but we can’t do it alone.

Join our team by visiting us at CleanSlateCenters.com



Physician anesthesiologists are key to reduced opioid use during surgery and postoperative non-opioid pain control


• Ensure a physician anesthesiologist is involved in your pain care plan when undergoing surgery
• Regional anesthesia and analgesia with a multimodal approach is key to opioid free surgery; physician anesthesiologists have specialized training in these techniques and can assist with non-opioid postsurgical pain control
• Interventional therapies can be used to treat chronic pain and therefore prevent addiction to opioids
Contact your physician anesthesiologist when preparing for surgery asahq.org/resources
any kind of survivor is empowered to believe they’re not alone, you see more people coming forward.”
When working with victims of sexual abuse, Covington says it is beneficial for clinicians to explore a patient’s history, but to still understand that patients might not open up completely, either leaving out parts of their experience intentionally or just not remembering. She adds that it’s critical to recognize that similar experiences can have different effects on different patients.
“Trauma impacts different people differently, and we have to be open to that range and not have tunnel vision about it,” Covington says.
Group therapy environments can bring their own challenges. Marich says she has observed group settings where those who speak up about inappropriate behavior have been made to feel uncomfortable.
“Part of the cultural change has to be about us calling each other out when we see behaviors that are victimizing,” she says. “I think now there’s an attitude going forward where hopefully this won’t be tolerated anymore. We shall see.”
Tom Valentino is Senior Editor of Addiction Professional.References
1. http://fortune.com/2017/10/16/ me-too-facebook-alyssa-milano/

2. http://www.langerresearch.com/wp-content/uploads/1192a1SexualHarassment.pdf


The National Rx Drug Abuse & Heroin Summit is where solutions are formulated, stakeholders convene, and change begins. Be part of the international discussion on addressing the opioid crisis by attending the 2018 Summit.

Who Attends:
• Clinicians, counselors, social workers, therapists, psychologists, interventionists
• Physicians, psychiatrists, nurses, pharmacists, dentists
• Advocates, families, and people in recovery
• Law enforcement personnel
• Public health and prevention officials
• Federal, state, and local officials and lawmakers
• Education specialists and researchers
• Treatment center owners and operators
• Lawyers
www.NationalRxDrugAbuseSummit.org
ubstance use took the promising BMX career of Tony Hoffman off course, but a spiritual journey in recovery has him back on the bike, both figuratively and literally, and he’s now riding in new directions as a coach and motivational speaker.
By his senior year of high school, Hoffman was nationally ranked in BMX. He appeared on magazine covers and had endorsement deals for sunglasses, shoes and more. But in spite of his burgeoning fame, Hoffman says he struggled with depression, anxiety and low self-esteem, issues that had plagued him since junior high.

“Those were the underlying factors that led me to my experimentation with smoking marijuana,” says Hoffman, 34, who resides in Clovis, Calif. “Once I got into smoking weed, that felt good, and I liked it. I wanted to experiment with other things as they came along. When you get involved in something like that, you think, ‘It will never be something else. It will just be this.’ But then, the more parties you go to, you start to see other things and friends start trying things. Then, you find out, ‘Wow, this drug works better than the weed does.’ ”
Hoffman says he moved on to cocaine and then prescription painkillers. His substance use helped with his feelings of anxiety and depression, if only temporarily, but they also led to him eventually being kicked out of a friend’s home where he was staying in 2006. The first night Hoffman spent on the street homeless was his lowest moment, he says.
On Jan. 21, 2007, Hoffman says he was welcomed into a church and was told by a pastor that God would forgive his transgressions. Still, that night, Hoffman broke into an empty house. The next day, real estate agents found him passed out on the floor of the home. The break-in was a parole violation—Hoffman previously was convicted on charges of home invasion and robbery in 2005—and he was sentenced to four-and-a-half years in prison, where, he says, his spiritual journey began.
“God told me four directions in which He wanted me to take my life,” Hoffman says. “One, get back on my bicycle
and race BMX. Two, He was going to take me to the Olympics. Three, He wanted me to become a public speaker. And four, He wanted me to start a program for kids using my bike.”
Hoffman was released on Dec. 13, 2008, and by the following May, he was competing in a lower level professional BMX class. He won five races in 2009, despite having not touched a bike in seven years. Hoffman began speaking publicly in 2010. In 2012, he launched the Freewheel Project, a not-for-profit youth action sports initiative.
Hoffman’s BMX riding career ended in 2011 with a knee injury, but he transitioned into coaching, working with several BMX athletes before guiding racing cyclist Brooke Crain to the Olympics in 2016.
Hoffman, meanwhile, has maintained his sobriety by staying disciplined, developing microprocesses to complete tasks—“master a lot of little things that, over time, would become big things that created successful moments like going to the Olympics,” he says.
“Meetings are important. Church is important. Meditation is important. Giving back is important. Admitting when you’re wrong is important. Not always needing to be right is important,” he says. “Simple things.”
Tom Valentino is Senior Editor
of Addiction Professional.Hear more about Tony Hoffman’s journey in recovery when he speaks at the National Conference on Addiction Disorders, Aug. 19-22 in Anaheim, Calif. Register at: vendome.swoogo.com/ncad-2018
Once derailed by substance use, former phenom Tony Hoffman has flourished as a coach and motivational speaker
A 207-bed, state-of-the-art facility supporting all phases of treatment in a campus environment.


Our fully-licensed, caring and compassionate staff are passionate about helping people to successfully recover. ARC is dedicated to changing the way the world views treatment by providing all levels of care in one ergonomically balanced system – all in one location.
47-Bed Medical Detox







160-Bed Residential Program
Partial Hospitalization Treatment

Intensive Outpatient Treatment

Programs for Military Personnel

First Responders and Public Service Programs

Sober Living Program

