Mass in
Woman With History of Cysts



FROM THE DIRECTOR
Director
Nikki Kean
nikki.kean@haymarketmedia.com
Medical editor
Kristin Della Volpe
Assistant editor
Jeanelle Jacobs
Production editor Kim Daigneau
Group creative director
Jennifer Dvoretz
Senior production manager
Krassi Varbanov
Account executive
Guy Pawlak, 973.768.3907 guy.pawlak@haymarketmedia.com
Publisher
Kathleen Hiltz, 201.774.1078 kathleen.hiltz@haymarketmedia.com
Vice president, content, medical communications
Kathleen Walsh Tulley
Chief commercial officer Jim Burke, RPh
President, medical communications
Michael Graziani
Chairman & CEO, Haymarket Media, Inc.
Lee Maniscalco
All correspondence to:
The Clinical Advisor
275 7th Avenue, 10th Floor, New York, NY 10001
For advertising sales, call 646.638.6085.
For reprints/licensing requests, contact Customer Service at custserv@haymarketmedia.com.
Persons appearing in photographs in “Newsline,” “The Legal Advisor,” and “Features” are not the actual individuals mentioned in the articles. They appear for illustrative purposes only.
The Clinical Advisor® (USPS 017-546, ISSN 1524-7317), Volume 25, Number 5. Published 6 times a year, by Haymarket Media, Inc., 275 7th Avenue, 10th Floor, New York, NY 10001.
For Advertising Sales & Editorial, call 646.638.6000 (M–F, 9am–5pm, ET).
The Clinical Advisor is available on a paid subscription basis at the following annual rates: $75 USA, $85 Canada, $110 for all other foreign, in U.S. dollars, Single copy price: USA $20, Foreign $30. To order or update a paid subscription visit our website at www.ClinicalAdvisor.com or call 800.436.9269.
Periodicals postage rate paid at NewYork, NY, and additional mailing offices. Postmaster: Send changes of address to The Clinical Advisor, c/o Direct Medical Data, 10255 W. Higgins Rd., Suite 280, Rosemont, IL 60018.
All rights reserved. Reproduction in whole or in part without permission is prohibited.
Long-Term Psychological Effects of COVID-19
As a patient with long COVID, I am familiar with the symptoms of brain fog, migraines, and vertigo. And I am not alone. More research is being published about the long-term cognitive and mental health components of long COVID.

Prior to 2020, mental health disorders were among the leading causes of the global health-related burden, with depressive and anxiety disorders being the most disabling of these conditions. Since the start of the pandemic, rates of anxiety and depression among US adults were 4 times higher between April 2020 and August 2021 than in 2019.
To explore the mental health effects of COVID-19, Clinical Advisor invited a team of nurse practitioners to write a series of articles. The first in the series appeared in the July/ August 2022 issue and explored the rise in anxiety disorders among adults and children. In this issue, the authors focus on depression and COVID-19 and describe how to identify and treat this condition in a primary care setting (see page 6).
Although depression may be the natural result of isolation and increased stress faced during the COVID-19 pandemic, recent research also suggests that depression is one of the many symptoms of long COVID. As reported in this issue, depression was reported in 23% of 8591 people 1 year after their COVID-19 diagnosis.
Nurse practitioners and PAs can play an important role in screening for anxiety and depression and educating patients regarding the signs and symptoms of these conditions. September is Suicide Awareness Month and clinicians are reminded to focus on mental health, shift public perception of depression, and spread hope. Suicidal thoughts, although common, should not be considered normal and often indicate more serious issues, according to the National Alliance on Mental Health.
If you don’t ask the questions, you can’t help your patients.
Nikki Kean, Director The Clinical AdvisorFEATURES
Depression and COVID-19: Identifying and Treating in the Primary Care Setting
Rates of depression have risen 4-fold during the first 2 years of the COVID-19 pandemic: the causes may surprise you.

Salary Survey
Good news: salaries are up. Bad news: so is burnout!
Unusual Cause of Chest, Abdominal Pain in Teen Following ACL Repair


Patient has history of Helicobacter pylori infection, anterior cruciate ligament tear, and stress fracture of the right tibia.
Enlarging Breast Mass in 69-Year-Old Woman With History of Cysts
Rapidly growing breast mass discovered by patient during routine breast self-examination.
DEPARTMENTS
From the Director
Psychological
Roundup
of COVID-19
A summary of our most recent opinion, news, and multimedia content from ClinicalAdvisor.com.
on the
MORE WAYS TO FIND US!
EXCLUSIVE TO THE WEB AT
NEWS
ClinicalAdvisor.com
CLINICAL CHALLENGE
ClinicalAdvisor.com/News
Sleep Disturbances in Childhood May Predict Future Symptoms of ADHD
Parent-reported sleep disturbances predict increased symptomology of ADHD when the children grow older, according to study ndings.
Expert Panel Publishes Guides for Personalized Long-Term Acne Care
An expert panel provides recommendations to support comprehensive, personalized, long-term treatment strategies that address all presentations of acne and its current and potential future burden.
Safety of COVID-19 mRNA Vaccines in Pregnancy Proved in Large Study
The rate of postvaccination health events was lower among pregnant persons than among similarly aged, nonpregnant female individuals following COVID19 mRNA vaccinations.
Inappropriate Antibiotic Use for Uncomplicated Cystitis Still Occurs
Urologists appear more likely than other specialists to inappropriately treat uncomplicated cystitis with antibiotics, according to study ndings.
Diets High in Calcium and Potassium May Prevent Kidney Stones
Daily intake of 1200 mg of calcium may help prevent incident and recurrent kidney stones, study ndings show.
ClinicalAdvisor.com/Clinical-Challenge
Brady Pregerson, MD
Generalized Epigastric Pain and Syncope
A woman in her mid-50s presents to the emergency department with a history of nonradiating epigastric pain that began 36 hours ago. The patient notes that the pain has become more generalized. Can you make the diagnosis? See the full case at: clinicaladvisor.com/ case_september_october22

MY PRACTICE
ClinicalAdvisor.com/MyPractice

Kristin Della Volpe
Is It Time to End Medicare Indirect Billing for NPs and PAs?

Experts discuss the often hidden phenomenon of indirect billing for NP and PA services and whether the 85% reimbursement rate for APPs is equitable.
THE WAITING ROOM
Of cial Blog of The Clinical Advisor ClinicalAdvisor.com/WaitingRoom
Jim Anderson, MPAS, PA-C, DFAAPA
Rising Fentanyl Use Challenges

Current Methadone Induction Protocols
Jim Anderson, MPAS, PA-C, discusses strategies for adapting methadone induction protocols to meet the therapeutic needs of patients using fentanyl.
Advisor Dx
Interact with your peers by viewing the images and offering your diagnosis and comments. To post your answer, obtain more clues, or view similar cases, visit ClinicalAdvisor.com/AdvisorDx . Learn more about diagnosing and treating these conditions, and see how you compare with your fellow colleagues. Check out some of our latest cases below!
DERM DX
New Growth After Basal Cell Carcinoma
A 66-year-old man presents with several skin lesions. He has a history of basal cell carcinomas removed from his cheek and forehead. His medi cal history is also positive for hypertension, actinic keratoses, and stasis dermatitis. He works outdoors and has experienced several episodes of moderately severe sunburns throughout his life. Examination reveals multiple seborrheic keratoses and skin tags as well as a slightly erythema tous nodule with a hyperpigmented base located on his left shoulder.
CAN YOU DIAGNOSE THIS CASE?
• Basal cell carcinoma
• Nodular melanoma

• Dermal duct tumor
• Angiokeratoma
● See the full case at clinicaladvisor.com/dermdx_september_october22
ORTHO DX
Edema in Lower Leg
In partnership with TheJopa.org
A 65-year-old construction worker presents with complaints of right lower extremity edema. An emergency department visit ruled out deep vein thrombosis. He reports that the ultrasound showed a Baker cyst in the back of his knee. He has a history of a right total knee replace ment 13 years ago. On physical examination, knee effusion and pitting edema are observed in the right lower extremity. He has no edema in his left leg and his ankle pulses are strong in bilateral lower extremities.

CAN YOU DIAGNOSE THIS CASE?
• Infection
• Metallosis
Journal of Orthopedics for Physician Assistants
• Osteoarthritis
• Peripheral vascular disease
● See the full case at clinicaladvisor.com/orthodx_september_october22
Depression and COVID-19: Identifying and Treating in the Primary Care Setting
Depression was reported in 23% of patients 1 year after COVID-19 infection.

A35-year-old woman presents to a primary care o ce complaining of depressed mood daily, some anxiety but not daily, not sleeping well, and overeating when she is “stressed.” She reports that she is not interacting much with friends and family and has not been exercising as she has in the past. The patient is a nurse in a medical-surgical unit at an urban hospital and has been caring for patients with COVID-19 over the last 2 years. She also reports having COVID-19 approximately 7 months ago. She was able to isolate and manage her symptoms on an outpatient basis.
The patient reports having had depressive symptoms in the past and that the symptoms decreased over time but returned over the last 6 months. She has been attending weekly individual therapy with a social worker for the last 6 weeks with minimal improvement. In the past, her symptoms were e ectively treated with paroxetine, but she gained weight and does not want to restart this agent. She also notes having trouble falling asleep and not feeling rested in the morning. She sleeps approximately 5 hours per night.
Her medical history is signi cant for hyperlipidemia; she does not currently take a lipidlowering medication. Her family history includes a mother with bipolar disorder (diagnosed at age 39 years) and sister with depression (diagnosed at age 28 years). No family history of suicide ideation or completion is reported.

A 35-year-old woman presents with depressed mood, fatigue, lack of interest in activities for the last 6 months after having COVID-19.
FEATURE: CHRISTY COOK-PERRY, DNP, PMHNP, ANP; JENNIFER ALLAIN, DNP, MSN, APRN, FNP-C; SHIRLEY GRIFFEY, DNP, PMHNP
Laboratory results are normal and do not show any abnormalities that may explain the current symptoms (Table 1).
Mental Status Examination
The patient is appropriately dressed and her body mass index falls in the overweight but not obese category. Her thoughts are organized and logical. She denies any hallucinations and does not appear to be attending to internal stimuli currently. She does not verbalize anything that could be considered delusional. She reports depressive symptoms for the last 6 months.
She describes her mood as sad and reports she is much more tearful than she has been in the past. She reports an increase in irritability and being easily frustrated. The patient appears to have a depressed mood. She is going to work as scheduled but then comes home and isolates herself until bedtime. She is not interacting much with her family or friends and has been declining invitations. She reports somatic complaints
such as headaches and stomachaches and uses these somatic complaints to avoid doing things. She reports anxiety at times, typically when someone is trying to get her to do something she does not want to do.
She denies suicidal and homicidal ideations and has not had these thoughts in the past. She denies any past hypomania or mania after being educated on the symptoms of these conditions and denies any current or past substance abuse. Her attention and judgment are intact and her speech is normal tone and rate, with no pressured speech. Her insight on depression is fair and she will benefit from additional education regarding disease process. The patient scored a 15 on the Patient Health Questionnaire (PHQ-9). She is diagnosed with recurrent major depressive disorder of moderate severity.
Discussion
The COVID-19 pandemic has had a severe effect on the mental health of people in the US and globally. In the first year of the COVID-19 pandemic, the prevalence of anxiety and depression increased by 25%, according to the World Health Organization.1
In 2020, an estimated 21.0 million US adults (or 8.4% of all US adults) had at least 1 major depressive episode.2 In approximately 14.8 million episodes, the impairment was severe. The prevalence of depressive disorder was approximately 4 times high in the first 2 quarters of 2022 compared to the second quarter of 2019 (24.3% vs 6.5%), according to findings from the Centers for Disease Control and Prevention (CDC).3 Although concern was raised that these numbers may have been exaggerated by the study method and the symptoms were not lasting, evidence suggests that the rate of depressive disorders increased with the onset of the COVID-19 pandemic.3
Data from the Household Pulse Survey conducted by the National Center for Health Statistics and the US Census Bureau (June 9-July 11, 2022) shows that 10% to 37% of Americans report symptoms of depressive disorder, with those aged 18 to 29 years showing the highest rates (Figure).4
In some cases, depression may be the result of isolation and increased stress faced during the COVID-pandemic. Research also suggests that depression is one of the many symptoms of long COVID.5
In a systematic review and meta-analysis of 1-year followup data from 8591 patients with COVID-19, depression was
The prevalence of depressive disorder was 4 times higher in the first 2 quarters of 2022 compared with the second quarter of 2019.
reported in 23%.6 In an observational study of 273 patients in India, 12% of patients developed depressive symptoms immediately (14-21 days) after a positive COVID-19 test and 5% of patients developed depressive symptoms approximately 3 months (90-97 days) after a positive test.7 A greater number of COVID-19 symptoms at the time of diagnosis and comorbid diabetes mellitus were associated with a greater risk for depression.7
Diagnosing Depression
The patient interview is an important element of the initial assessment for depression and should include patient history as well as current medical and mental status (Table 2, page 10).8 Assessment tools include the PHQ-2 and PHQ-9 for depressive symptoms, Columbia Suicide Severity Rating Scale for suicidal ideations and intent, Generalized Anxiety Disorder 7-item Scale (GAD-7) for anxiety, and CAGE for alcohol use disorder.9-12
When asking patients about sleep, it is important to clarify what “not sleeping well” means to the patient. Does she have trouble falling asleep, staying asleep, or both? What time does she go to bed? What time does she normally gets out of bed in the morning? Does she take any over-thecounter or prescribed medications for sleep or has she in the past? Does she drink alcohol or use any other substances
to help her sleep? Does she have a history of sleep apnea? If so, is she following the recommendations for sleep apnea treatment?
It is always important to assess for thoughts of suicide and past suicide attempts or thoughts. If a patient presents with suicidal ideation, ask if the patient has a plan. If the patient is actively having suicidal ideation with a viable plan, a safety plan must be made before the patient leaves the office. This may mean a transfer to an inpatient facility, so it is important to have a plan in advance. Is it appropriate to call 911, is there security in the building, and what are the policies to commit a patient against their will? It is important to have these details understood prior to an emergency. If a patient is not actively suicidal, has community resources, agrees to continue outpatient treatment, has family or social support, and does not verbalize intent then the patient may be treated on an outpatient basis.
In adults, the differential diagnosis should include hypothyroidism or hyperthyroidism; anemia; bipolar disorder and current episode depressed; and adjustment disorder with depressed mood. Routine laboratory studies should be completed to rule out hypothyroidism and any other medical conditions that could explain the current symptoms. Common symptoms of hypothyroidism are fatigue, depression, and weight gain.13 Common symptoms of hyperthyroidism
If a patient is having suicidal ideation with a viable plan, a safety plan must be made before the patient leaves the office.
TABLE 2. Signs and Symptoms of Major Depressive Disorder 8
Decreased interest in normal activities
Decreased concentration
Depressed mood
Fatigue
Feelings of worthlessness
Inappropriate guilt
Insomnia or hypersomnia
Psychomotor agitation or retardation
Recurrent thoughts of death and/or suicidal ideation
Significant unintentional weight loss
TABLE 3. Signs and Symptoms of Hypomania and/or Mania8
Decreased sleep or need to sleep
Elevated, expansive, or irritable mood
Flight of ideas or racing thoughts
Grandiosity
Hyperverbal or pressured speech
Increased activity in general
Increased risky behavior such as overspending, sexual indiscretions, or poor financial decisions
Poor concentration
Symptoms need to be present for at least 1 week and present most of the day to meet the criteria for mania
Symptoms need to be present for at least 4 consecutive days for most of the day to meet the criteria for hypomania
TABLE 4. Medications Used to Treat Depression
Among Adults in Primary Care
are increased anxiety, weight loss, and fatigue.14 Fatigue from anemia can be confused as depressive symptoms. Complete metabolic panel needs to be completed to rule out any electrolyte imbalances.
It is imperative to assess for any history of hypomania or mania (Table 3).8 Patients may have a history of bipolar disorder or an undiagnosed bipolar disorder and present with depressive symptoms. It is possible to induce mania or hypomania if an antidepressant is initiated in such patients.
Treatment of Depression
The American Psychological Association (APA) recommends that clinicians offer either psychotherapy or second-generation antidepressants as the first-line treatment of depression; a combination of these 2 strategies may also be used.15 Several medications are available for the treatment of depression in the primary care setting (Table 4).
The case patient had a positive response to paroxetine in the past but had significant weight gain. The patient should respond well to the other selective serotonin reuptake inhibitors (SSRI). She could also benefit from a serotoninnorepinephrine reuptake inhibitor (SNRI). Both SSRIs and SNRIs can decrease depressive symptoms as well as anxiety. Several SSRIs are weight neutral including fluoxetine, escitalopram, and sertraline.16
Nonpharmacologic Treatments for Adults With Depression
Effectiveness studies have shown similar effects across various forms of psychotherapy used to treat depression and the APA does not recommend one form over another.15 General models recommended by the APA include:
• Behavioral therapy
• Cognitive behavioral therapy (CBT) and mindfulness-based cognitive therapy
• Interpersonal psychotherapy
• Psychodynamic therapies
• Supportive therapy
Cognitive behavioral therapy has been found to be as effective as medication in some cases. The focus of CBT is to change distorted thinking. Cognitive behavioral therapy improves a person’s mood by teaching appropriate and healthy coping mechanisms, increasing self-confidence, addressing fears instead of avoidance, and teaching patients to manage their stress independent of the therapist.17
Follow-up and Discussion
The patient continued with weekly individual therapy with a social worker and was initiated on fluoxetine 10 mg once
daily taken in the morning. She is asked to return to the clinic in 2 to 4 weeks.
At the follow-up appointment, the clinicians should assess for effectiveness of medication, current mental status, suicidal ideation, and sleep pattern. If the patient is not having any adverse effects from the selected medication but is still reporting symptoms, the medication dose can be increased until symptoms resolve or the patient has adverse effects.
If the patient cannot tolerate the first medication option, it is appropriate to change to another agent in the same class. If the patient fails 2 agents in the same class, it is appropriate to change to another class of medication such as an SNRI.18
Conclusion
The rising rates of depression stemming from the COVID-19 pandemic remain a major burden to overcome in the primary care setting. Screening for depressive symptoms can be part of the initial intake and subsequent visits in primary care. Education regarding the signs and symptoms of depression may be needed as people may not recognize their symptoms as those of depression.
Patients may present with insomnia and not verbalize that they are feeling more irritable or have been isolating. Primary care providers can provide appropriate treatment including prescribing medication, referrals to a therapist, or in some cases referral to a mental health provider.
The pandemic led many patients to be neglectful of regular medical appointments. Now, these patients may be seeking treatment for the first time in 2 years. Being alert to possible symptoms associated with depression in all patients will help improve overall care. ■
Christy Cook-Perry, DNP, PMHNP, ANP, is an assistant professor at Southeastern Louisiana University College of Nursing and Health Sciences. Jennifer Allain, DNP, MSN, APRN, FNP-C, is the NP program coordinator and master teacher of mental health psychiatric nursing at The LHC Group, Myers School of Nursing of the University of Louisiana at Lafayette College of Nursing and Health Sciences.
Shirley Griffey, DNP, PMHNP, is a psychiatric nurse practitioner at Baton Rouge General Medical Center and an instructor at Southeastern Louisiana University School of Nursing in Baton Rouge, Louisiana.
References
1. World Health Organization. Mental Health and COVID-19: Early evidence of the pandemic’s impact. Scientific brief. March 2, 2022. Accessed July 19, 2022. https://www.who.int/publications/i/item/ WHO-2019-nCoV-Sci_Brief-Mental_health-2022.1
2. Major depression. National Institute of Mental Health. Updated January 2022. Accessed July 20, 2022. https://www.nimh.nih.gov/health/statistics/ major-depression
3. Czeisler MÉ, Lane RI, Petrosky E, et al. Mental health, substance use, and suicidal ideation during the COVID-19 pandemic - United States, June 24-30, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(32):1049-1057.
4. Household Pulse Survey — anxiety and depression. Centers for Disease Control and Prevention, National Center for Health Statistics. Accessed August 1, 2022. http://www.cdc.gov/nchs/covid19/pulse/mentalhealth.htm
5. Centers for Disease Control and Prevention. Evaluating and caring for patients with post-covid conditions: interim guidance. Updated June 2021. Accessed April 28, 2022. https://www.cdc.gov/coronavirus/ 2019-ncov/hcp/clinical-care/post-covid-workup.html
6. Han Q, Zheng B, Daines L, Sheikh A. Long-term sequelae of COVID-19: a systematic review and meta-analysis of one-year follow-up studies on post-COVID symptoms. Pathogens. 2022;11(2):269.
7. Shah A, Bhattad D. Immediate and short-term prevalence of depression in COVID-19 patients and its correlation with continued symptoms experience. Indian J Psych. 2022;64(3):301-306.
8. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed, text revision. American Psychiatric Association; 2022.
9. Patient health questionnaire-9 (PHQ-9). Accessed July 20, 2022. https://www.apa.org/depression-guideline/patient-health-questionnaire.pdf
10. Interian A, Chesin M, Kline A, et al. Use of the Columbia-Suicide Severity Rating Scale (C-SSRS) to classify suicidal behaviors. Arch Suicide Res. 2018;22(2):278-294.
11. Spitzer RL, Kroenke K, Williams JB, Löwe B. A brief measure for assessing generalized anxiety disorder: the GAD-7. Arch Intern Med. 2006; 166(10):1092-1097.
12. CAGE substance abuse screening tool. Johns Hopkins Medicine. Accessed July 2, 2022. https://www.hopkinsmedicine.org/johns_hopkins_healthcare/ downloads/all_plans/CAGE%20Substance%20Screening%20Tool.pdf.
13. Hypothyroidism (underactive thyroid). Mayo Clinic. November 19, 2020. Accessed July 20, 2022. https://www.mayoclinic.org/diseases-conditions/ hypothyroidism/symptoms-causes/syc-20350284
14. Hyperthyroidism (overactive thyroid). Mayo Clinic. Accessed July 20, 2022. https://www.mayoclinic.org/diseases-conditions/hyperthyroidism/ symptoms-causes/syc-20373659
15. Guideline Development Panel for the Treatment of Depressive Disorders. Summary of the clinical practice guideline for the treatment of depression across three age cohorts. Am Psychol. 2021 Nov 29.
16. Gill H, Gill B, El-Halabi S, et al. Antidepressant medications and weight change: a narrative review. Obesity (Silver Spring). 2020;28(11): 2064-2072.
17. What is cognitive behavioral therapy? American Psychology Association. July 2017. Accessed July 23, 2022. https://www.apa.org/ptsd-guideline/ patients-and-families/cognitive-behavioral
18. Gelenberg AJ, Freeman MP, Rosenbaum J, et al. Practice guideline for the treatment of patients with major depressive disorder, 3rd Edition. American Psychiatric Association: 2010. https://psychiatryonline. org/pb/assets/raw/sitewide/practice_guidelines/guidelines/mdd.pdf
SALARY SURVEY
Salary Survey 2022: How Do You Compare to Your Peers?
The results from the ClinicalAdvisor 2022 Salary Survey are in. The good news is that many nurse practitioners (NPs) and PAs earned a higher salary this year compared with last year (48.6% and 38.9%, respectively), and nearly half of NPs and PAs reported that their income increased during the COVID-19 pandemic (49.5% and 40.4%, respectively). The average salary for NPs in 2022 was $117,054 compared with $112,979 last year. The average salary for PAs increased by $8,000, from $116,373 in 2021 to $124,182 in 2022.
Results of 2022
CLINICAL ADVISOR NP/PA SALARY SURVEY
The bad news is that 2.5 years into the COVID-19 pandemic, a large proportion of NPs and PAs reported experiencing burnout (66.2% and 62.6%, respectively). Work-related stress is a major contributor to burnout, with 41.4% of NPs reporting moderate stress, 35.6% high stress, and 15.1% extremely high stress. The picture is similar for PAs, with 41.7% experiencing moderate stress, 36.3% high stress, and 12.0% extremely high stress. Although internal medicine/family medicine/primary care
West 16.3% (n=152) $130,410 average salary
Midwest 25.3% (n=235) $111,150 average salary
Northeast 20.4% (n=189) $121,678 average salary
South 37.9% (n=352) $113,582 average salary
FIGURE 1. Average NP salary by geographic region
remains the top occupation for NPs and PAs, the number of clinicians working in this eld continues to decline as clinicians subspecialize. Last year, approximately 23.7% of NPs and 11.9% of PAs reported working in internal medicine/family medicine/ primary care and that percentage dropped to 15.4% of NPs and just 7.3% of PAs. For NPs, the next most common area of practice was adult care (8.8%); for PAs, orthopedic surgery came in second (5.8%).
Again this year, the majority of NP and PA respondents reported working in the South (37.9% and 32.6%, respectively). Similar to the ndings from the 2021 survey, both NPs and PAs in the West reported making the highest average salaries ($130,410 and $128.137) (see Figures). Most NPs reported working in urban areas (41.7%), followed closely by suburban areas (35.7%). For PAs, most respondents reported working in suburban areas (44.7%) with urban areas following closely behind (41.8%).
West 25.3% (n= 69) $128,137 average salary
Midwest 18.7% (n=51) $126,500 average salary
Northeast 23.4% (n= 64) $123,393 average salary
South 32.6% (n=89) $120,607 average salary
FIGURE 2. Average PA salary by geographic region
For a full recap of the 2022 Salary Survey, please visit ClinicalAdvisor.com/SalarySurvey2022.
Newsline
Depression Screening Increased in Primary Care
DEPRESSION screening increased after implementation of a general screening program in 2017, according to study findings published online in JAMA Network Open
Maria E. Garcia, MD, MPH, from the University of California in San Francisco, and colleagues examined depression screening rates among populations at risk for undertreatment of depression in electronic record data from 52,944 adults at 6 primary care facilities from September 1, 2017, to December 31, 2019. Depression screening rates were assessed after implementation of a general screening policy.
The researchers observed an increase in depression screening from 40.5% at rollout in 2017 to 88.8% in 2019. The
likelihood of being screened decreased with increasing age in 2018 (adjusted odds ratios: 0.89 and 0.75 for ages 45 to 54 years and 75 years and older, respectively, vs 18 to 30 years). Patients with limited English proficiency, except for Spanish-speaking patients, were less likely to be screened for depression than English-speaking White patients (adjusted odds ratios: 0.59 and 0.55 for Chinese language preference and other non-English preferences, respectively).
Depression screening rates increased for all at-risk groups by 2019 and disparities disappeared for most; lower odds of screening were still seen for men vs women (adjusted odds ratio: 0.87).
“Given well-documented depression care disparities for men, racial and
Depression screening increased among racial minorities after start of program.
ethnic minority individuals, patients with language barriers, older patients, and patients with public insurance, a focus on implementing depression screening and initial depression treatment in primary care may help to improve depression recognition and appropriate treatment for all patients,” the authors wrote.

Beneficial Effects of Salt Substitutes on Blood Pressure
THE BENEFICIAL effects of salt substitutes on blood pressure were consistent across geographies and populations, according to a review published online in Heart
Xuejun Yin, from the George Institute for Global Health at the University of New South Wales in Newtown,Australia, and colleagues conducted a systematic review to examine the effects of salt substitutes on outcomes to understand the likely generalizability of the results of the Salt Substitute and Stroke Study, which reported blood pressure-mediated benefits of a potassium-enriched
salt substitute. Data were included from 21 trials with 31,949 participants; 19 reported effects on blood pressure, and 5 reported effects on clinical outcomes.
The overall reduction of systolic and diastolic blood pressure was -4.61 and -1.61 mm Hg, respectively. Consistent reductions in blood pressure were seen across geographical regions and population subgroups defined by age, sex, hypertension history, body mass index, baseline blood pressure, and baseline 24-hour urinary sodium and potassium. Each 10% lower proportion of sodium chloride in the salt substitute was
associated with -1.53 and -0.95 mm Hg greater reduction in systolic and diastolic blood pressure, respectively. Protective effects were seen for salt substitutes on total mortality, cardiovascular mortality, and cardiovascular events (risk ratios, 0.89, 0.87, and 0.89, respectively).
“These findings are unlikely to reflect the play of chance and support the adoption of salt substitutes in clinical practice and public health policy as a strategy to reduce dietary sodium intake, increase dietary potassium intake, lower blood pressure, and prevent major cardiovascular events,” the authors wrote.
© LAYLABIRD / GETTY IMAGESAppendectomy vs Antibiotics: Which Is Best for Acute Appendicitis?
did not differ between the antibiotic group and the appendectomy group (0.85; 95% CI, 0.66-1.11). Six of the 8 trials did not find statistically significant differences in the primary outcome between the antibiotic and appendectomy groups. One study reported a statistically significant benefit with surgical treatment, while another showed that antibiotic treatment was superior to appendectomy.
Higher ADHD Scores Seen for Children Born Early Term

CHILDREN WITH early-term birth have increased hyperactivity scores and attention-deficit/hyperactivity disorder (ADHD) scores, according to study findings published online in The Journal of Pediatrics.
Antibiotics may be preferred over surgery in uncomplicated appendicitis.
FOR ACUTE uncomplicated appendicitis, is nonoperative management with antibiotics as safe as surgery? When nonoperative management is compared with appendectomy, treatment success or likelihood of major complications are similar, according to findings published in JAMA Surgery. However, nonoperative management is linked to a longer length of hospital stay and a higher rate of recurrent appendicitis compared with appendectomy.
The findings are based on a systematic review and meta-analysis of 8 randomized clinical trials.The primary outcome was treatment success at 30 days (or the longest period of follow-up when different time points were reported) as defined in the individual trials, which included resolution of abdominal pain, no complications, and improvement of inflammatory markers.
Previous studies have shown that antibiotic treatment of appendicitis is a safe alternative to appendectomy; however, a wide range of treatment failure rates (7% to 39%) was found with nonoperative management.
The overall risk ratio (RR) for successful treatment of appendicitis at follow-up
A meta-analysis of the 6 trials that reported rates of major adverse effects at 30 days showed that antibiotic treatment was associated with a nonsignificant trend toward lower rates of major adverse effects compared with appendectomy (RR, 0.72; 95% CI, 0.29-1.79). One study reported significant superiority of antibiotic treatment, while another reported superiority of operative treatment.The other 4 trials showed no statistically significant difference in major adverse effects between the groups. Mortality was low in both groups and across trials.
In a meta-analysis of findings from the 3 trials that reported total hospital length of stay, operative treatment was associated with a significantly shorter length of hospital stay (RR, 1.48; 95% CI, 1.26-1.70).
According to data from the largest trial in the meta-analysis, the CODA collaborative trial (N=1552), the median rate of rehospitalization for appendicitis was 18%.
The study authors emphasized the need to consider local infrastructure conditions when selecting antibiotic treatment and for close monitoring of patients using serial physical examinations and round-the-clock availability of imaging, interventional radiology, laboratory testing, and rehospitalization, as well as the flexibility to change treatment approach if needed.
Researchers examined the associations between gestational age and teacher-reported ADHD-related symptom patterns at age 9 years in a secondary analysis involving approximately 1400 children in the Fragile Families and Child Wellbeing study born at term (37 to 41 weeks). Teachers evaluated their students at age 9 years using the Conners Teacher Rating Scale-Revised Short Form that included subscales for symptoms of hyperactivity, ADHD, oppositional behavior, and cognitive problems/ inattention, noted Geethanjali Lingasubramanian, MD, from Rutgers University in New Brunswick, New Jersey, and colleagues.
Each week of gestational age at term was associated with lower hyperactivity scores, ADHD scores, and cognitive problems/inattention scores (adjusted incidence rate ratios [IRR]: 0.94, 0.95, and 0.95, respectively). Increased hyperactivity scores and ADHD scores were seen in association with early-term birth (37 to 38 weeks) compared with birth at 39 to 41 weeks (adjusted IRR: 1.23 and 1.17, respectively) as well as an increase in the odds of scoring 1.5+ standard deviations above the sample mean for hyperactivity (adjusted odds ratio: 1.51). No significant associations were seen between gestational age and oppositional behavior scores. ■
Unusual Cause of Chest, Abdominal Pain in Teen Following ACL Repair
A17-year-old Black woman presents to a family medicine clinic with a 1-day history of acute-onset chest discomfort, palpitations, and abdominal pain.The patient denies aggravating or alleviating factors as well as shortness of breath, activity intolerance, hematemesis, or melena. Two weeks prior, she was prescribed naproxen 500 mg twice daily for knee pain that was precipitated by squatting exercises at physical therapy (PT). She was completing PT after a right anterior cruciate ligament (ACL) repair several months prior. The family medicine provider who prescribed naproxen instructed her to take it with food and to avoid all other nonsteroidal anti-in ammatory drugs (NSAIDs). She was not taking any other known gastric mucosa irritants.
Since sustaining the ACL tear, the patient took 3 separate courses of ibuprofen and naproxen without incident. She experienced improved mobility and denied any additional trauma to the right knee. Up until the PT visit, the patient had been well managed with nonpharmacologic pain treatments.The care for this patient occurred over several visits; a timeline of the progression of care is shown in Figure (page 20).
History
The patient is a refugee from South Sudan and moved to the United States in 2017. She is currently enrolled at a local high school. She denies alcohol, tobacco, or drug use and is not participating in any organized sports. The patient has


The patient has a history of Helicobacter pylori infection, anterior cruciate ligament tear, and stress fracture of the right tibia.
Patient’s vitals are notable for tachycardia and hypertension.
FEATURE: AMALIA GEDNEY-LOSE, DNP, ARNP, FNP-C
regular menstrual cycles that last 5 to 6 days and are moderately heavy for 2 to 3 days.
The patient’s medical history includes Helicobacter pylori infection, an isolated episode of syncope with negative cardiology workup, ACL tear of the right knee, and stress fracture of the right tibia. Her medical history is limited by lack of documentation prior to 2017. Her family history is notable for maternal hypertension and diabetes.The patient has no known coagulation disorders, liver disease, or other chronic conditions.
Physical Examination
Physical examination findings are normal except for tachycardia (112 beats/min) and hypertension (142/82 mm Hg and 134/74 mm Hg upon recheck); other vital signs are stable. Abdominal examination is normal with active bowel sounds, no tenderness to palpation, guarding, rigidity, organomegaly, masses, or costovertebral angle tenderness. Blood work for complete blood cell count (CBC) and comprehensive metabolic panel (CMP) is taken and electrocardiography is ordered.
The patient is instructed to discontinue naproxen immediately and begin omeprazole 20 mg once daily. She is scheduled for a follow-up visit in 5 days to discuss the laboratory results.
Laboratory Evaluation and Follow-Up Visit
Findings from CBC show various abnormalities consistent with anemia (Table 1). Her CMP results are within normal limits except for a glucose level of 103 mg/dL and carbon dioxide of 19 mmol/L. The patient did not present to the local medical center to have the electrocardiography completed.
During the first follow-up visit, the patient denies symptoms; however, when a more specific review of systems is taken, the
patient notes exercise intolerance and shortness of breath when participating in her physical education class. She also experiences dizziness that she attributes to not “drinking enough water.” The patient has improved abdominal pain following naproxen discontinuation. Currently, she is not experiencing syncope or near syncope, appetite changes, sleep changes, nose bleeds, melena, or hematuria. However, she does report melena associated with episodes of abdominal pain earlier in the week.
Her vitals are somewhat improved with a heart rate of 98 beats per minute and blood pressure of 128/72 mm Hg; other vital signs are stable. A physical examination reveals generalized abdominal tenderness and is otherwise normal with no tachycardia, respiratory abnormalities, organomegaly, or changes to bowel sounds. Because of the patient’s recent hemoglobin of 9.0 g/dL, blood work is ordered to recheck CBC and evaluate iron studies including ferritin, iron, total iron binding capacity (TIBC), and reticulocyte count (Table 2). Fecal occult studies, H pylori antibodies, and hematopathology smear review are also ordered (Table 3).
The differential diagnosis includes gastrointestinal (GI) bleed, peptic ulcer disease, H pylori infection, acute gastritis, coagulopathy, and angiodysplasia. Considering the recent naproxen use and anemia, omeprazole 20 mg daily is continued to treat acute gastritis and suspected GI bleeding.
Treatment
The day 5 laboratory evaluation confirms that the patient has anemia. The patient’s low mean corpuscular volume (MCV) indicates smaller than usual red blood cell (RBC) size and low mean corpuscular hemoglobin concentration (MCHC) indicates decreased hemoglobin concentration within the RBC (Table 2).
TABLE 1. Complete Blood Count by Day
Measure
Hematocrit, %29.5
Reference
13.0-17.7 MCH,
Hemoglobin, g/dL9.0
MCHC, g/dL
MCV,
Platelets, x10E3/µL300
RBC, x 10E6/µL4.12
RDW,
WBC, x 10E3/µL6.9
3.4-10.8 MCH
Iron Studies by Day
Other Laboratories Studies by
The ndings indicate microcytic hypochromic anemia.The differential diagnosis for a patient with microcytic hypochromic anemia suggest iron-de ciency anemia, anemia of chronic disease, thalassemia, lead poisoning, and x-linked sideroblastic anemia.1
The elevated reticulocyte count indicates that the patient is producing immature RBCs to compensate for acute blood loss. The low iron saturation indicates that the body is depleting iron stores too quickly through blood loss. The total iron binding capacity, unsaturated iron binding capacity, iron, and serum ferritin levels are all within normal limits. Additionally, acute blood loss from the GI tract is con rmed by the 3 positive fecal occult blood tests.
The hematopathologist’s review con rms the presence of microcytic hypochromic anemia with anisocytosis most likely representing iron-de ciency anemia.
The patient is started on ferrous sulfate 325 mg daily and continues omeprazole 20 mg once daily

After further discussion with the patient’s mother regarding the results, she reports that the patient had previously been treated for an H pylori infection. It is unsure if a test of cure was completed. If this information was available during the initial workup, it would have been preferred to order the H pylori fecal antigen test to evaluate for active infection as serologic levels do not di erentiate between active and past infection.2 A breath test would not be appropriate as the patient had already been started on a proton pump inhibitor (PPI) and this may cause false-negative results.2
A consultation is scheduled with a pediatric GI provider at a local academic medical center. In the meantime, the patient continues to experience intermittent symptoms of dizziness, shortness of breath, and dark tarry stools.
At the time of the pediatric GI consultation, her symptoms have stabilized on omeprazole therapy and iron supplementation. After consultation, the plan is to continue treating the microcytic anemia that is suspected to be caused by an NSAID-induced upper GI bleed. The shortness of breath and tarry stools have resolved. The pediatric GI provider orders repeat CBC with di erential (Table 1, Day 17) and adds erythrocyte sedimentation rate and C-reactive protein. The CBC shows improving anemia with hemoglobin and hematocrit trending upward.The in ammatory markers are within normal limits.
The patient and her mother are counseled on avoidance of over-the-counter or prescription NSAIDs including aspirin, ibuprofen, and naproxen because of their suspected role in this patient’s GI bleed. The omeprazole dose is increased to
40 mg daily on an empty stomach 20 minutes prior to breakfast to help suppress acid production and allow for healing of the gastric mucosa. No additional imaging or procedures are completed at this time because of the improvement in the patient’s status.
Outcome and Discussion
Overall, the patient stabilized well after an acute GI bleed. However, she will require close monitoring and follow-up with both her primary care provider and pediatric GI provider. Approximately 2 months after identi cation of GI bleeding, elimination of the cause and initiation of ferrous sulfate led to an increase in hemoglobin to 11.9 g/dL and hematocrit to 40.8%. She is asymptomatic and has no abnormal ndings on physical examination. The patient has a repeat laboratory evaluation 7 months later, which shows stable levels. However, the patient continues to have microcytic hypochromic anemia and requires ongoing ferrous sulfate supplementation.
If this patient had shown hemodynamic instability, including a hemoglobin less than 7 mg/dL, possible interventions would have included inpatient hospitalization, administration of blood products, uid resuscitation, urgent endoscopy after stabilization, vasopressors, intravenous acid suppression, and trending of CBC.3 Depending on the severity of bleeding, more invasive procedures including arterial embolization, balloon tamponade, and surgical intervention may be necessary.3
The patient notes exercise intolerance, shortness of breath in gym class. She also reports dizziness that she attributes to not drinking enough water.
Lessons Learned
Most NSAIDs work by nonselectively blocking cyclooxygenase (COX) 1 and COX 2, which play integral factors in blocking pain signals to the brain and inhibiting the synthesis of prostaglandins.4 NSAIDs work to inhibit prostaglandin synthesis in the pain pathway, while concurrently blocking prostaglandin synthesis in the stomach where COX 1 provides gastric mucosal protection.5 This may lead to NSAID-induced GI bleeding, which is caused by a breakdown in the gastrointestinal lining secondary to nonselective COX inhibition in the gastric mucosa.4
Ibuprofen is a more commonly used NSAID in pediatric patients for management of pain and fevers. In this patient’s case, naproxen was appropriately initiated for management of musculoskeletal knee pain but resulted in GI bleeding. One study found that the median time between NSAID initiation and onset of GI bleeding was 4 days.6 Therefore, practitioners prescribing or recommending NSAID medications should be aware that adverse effects and significant complications are not limited to long-term use.
One study suggests that 36% of upper GI bleeds in children were secondary to NSAID use.7 While GI side effects are a well-known risk of NSAID use in children, management techniques for GI bleeding often stem from those used in the management of adult GI bleeding.8 In the setting of upper GI bleeding, acid suppression with the use of higher doses of a PPI at 1 to 3 mg/kg/d in children or 40 mg twice daily in adults is recommended as initial PPI management.8 No significant benefit is found in choosing one PPI over another and PPI therapy has shown to be more beneficial than histamine 2 antagonists.8 Initially, this patient was started on omeprazole 20 mg daily; because the patient weighed 80 kg, the care team could have initiated omeprazole at up to 80 mg per day.
This case also demonstrated that H pylori can precipitate peptic ulcer disease, gastric and duodenal ulcerations, and gastritis with an unexplained link between H pylori infection and iron-deficiency anemia.2 Testing for H pylori should be considered in the workup.2
The patient remained hemodynamically stable but if her status had deteriorated, she would have required additional intervention for stabilization and consideration of procedural interventions such as endoscopy.4 Continued counseling of patients and parents on the risks associated with short-term use of NSAIDs is essential, as well as the signs and symptoms they should monitor for. Although this patient was a young, healthy female, she experienced a significant adverse reaction
to NSAIDs that may not typically be expected. Providers should continue to use caution and close monitoring when prescribing NSAIDs to any population, especially children. ■
Amalia Gedney-Lose, DNP, ARNP, FNP-C, is a clinical assistant professor and family nurse practitioner at the University of Iowa College of Nursing and University of Iowa Hospitals and Clinics in Iowa City, Iowa.
References
1. Chaudhry HS, Kasarla MR. Microcytic hypochromic anemia. In: StatPearls [Internet]. StatPearls Publishing; 2022 Jan. Updated May 2, 2022. Accessed July 29, 2022. https://www.ncbi.nlm.nih.gov/books/NBK470252/
2. Saleem N, Howden CW. Update on the management of Helicobacter pylori infection. Curr Treat Options Gastroenterol. 2020;18(3):476-487.
3. Al Duhailib Z, Dionne JC, Alhazzani W. Management of severe upper gastrointestinal bleeding in the ICU. Curr Opin Crit Care. 2020;26(2):212-218.
4. Qureshi O, Dua A. COX Inhibitors. In: StatPearls [Internet]. StatPearls Publishing; 2022 Jan-. Updated April 29, 2022. Accessed July 29, 2022. https://www.ncbi.nlm.nih.gov/books/NBK549795/
5. Flower RJ. The development of COX 2 inhibitors. Nat Rev Drug Discov. 2003;2(3):179-191.
6. Cardile S, Martinelli M, Barabino A, et al. Italian survey on non-steroidal anti-inflammatory drugs and gastrointestinal bleeding in children. World J Gastroenterol. 2016;22(5):1877-1883.
7. Grimaldi-Bensouda L, Abenhaim L, Michaud L, et al. Clinical features and risk factors for upper gastrointestinal bleeding in children: a case-crossover study. Eur J Clin Pharmacol. 2010;66(8):831-837.
8. Romano C, Oliva S, Martellossi S, Miele E, et al. Pediatric gastrointestinal bleeding: perspectives from the Italian Society of Pediatric Gastroenterology. World J Gastroenterol. 201;23(8):1328-1337.
More Ways
Find Us
The patient’s elevated reticulocyte count means she is producing immature red blood cells to compensate for acute blood loss.
Enlarging Breast Mass in 69-Year-Old Woman With History of Cysts

A69-year-old woman presents to the clinic with complaints of a large right breast mass that has grown rapidly over the past 2 weeks. The patient reports she was in the shower conducting a routine breast self-examination when she noticed a firm, nontender, moveable hard mass. She states there was no nipple discharge. The mass has greatly increased in size since first being felt just a couple of weeks ago and is palpable at the 10-o’clock position. The patient reports she previously had several “breast cysts” so she was not overly concerned until this mass grew at an alarming rate.
History
The patient has a history of diabetes, hypertension, hypothyroidism, diverticulitis, osteoarthritis, glaucoma, migraines, rheumatic heart disease with murmur, breast cysts, and breast adenomas. The patient breastfed her 2 children. The patient has glaucoma and recently underwent a failed eye stent procedure that resulted in 95% blindness in her left eye.
The patient’s current medications include levothyroxine, triamterene, atenolol, pioglitazone, losartan, bupropion XL, long-acting insulin glargine, and acetazolamide. The patient is also taking several prescription eye drops and a laxative.
The patient is allergic to morphine and hydromorphone, which caused migraines; prochlorperazine caused angioedema. She is up to date on
The patient first noticed a firm, nontender, moveable hard mass while conducting a routine breast self-examination in the shower.
The patient reports a history of breast cysts.
Vital Signs
all immunizations and annual screenings. She is a nonsmoker, rarely drinks alcohol, and follows a diabetes-friendly diet. The patient’s family history is significant for hypertension, liver failure, and coronary artery disease.
Physical Examination
On presentation, the patient appears well but anxious (Table 1). The patient’s HEENT (head, eyes, ears, nose, and throat) examination is unremarkable except for a cloudy right pupil.
Lungs are clear anteriorly and posteriorly. Her heart has regular rhythm and rate with soft murmur grade (grade I/VI) audible at the midclavicular line fifth intercostal space. Right breast
has a firm, movable mass at the 10-o’clock position measuring 10 cm × 10 cm. No nipple retraction from either breast or peau d’orange appearance is noted; positive retraction of the mass is observed but no further breast abnormality.
Discussion
Phyllodes tumor of the breast, or cystosarcoma phyllodes, are rare tumors that begin in the stromal tissue of the breast.1 They make up 0.3% to 1% of all breast tumors.2 Phyllodes tumors generally appear in the fourth or fifth decade of life but can occur at any age.3
Benign phyllodes tumors will appear like fibroadenomas on radiologic and cytologic examination. They are fast growing but rarely spread outside the breast. The underlying cause of phyllodes is unknown.4 Rosen et al first subclassified the tumors histologically as benign, borderline, or malignant according to features such as tumor margins, stromal overgrowth, tumor necrosis, cellular atypia, and number of mitosis per high power field (Table 2).2,5,6
Many phyllodes tumors are benign (35%-64%) and can be treated with local excision. The remainder of tumors are divided between borderline and malignant (25%).1,2 The fastest growing tumors tend to be malignant, are more likely to metastasize to other areas, and are more likely to recur after treatment.1
Patients most often present with skin stretched taunt over a rapidly growing tumor. The median size of phyllodes tumors is approximately 4 cm.7 Twenty percent of tumors can grow larger than 10 cm, termed giant phyllodes, with some reaching 20 cm to up to 40 cm. Nipple retraction and ulceration are rarely seen. The tumors are most commonly found in the upper quadrant of either the right or left breast and rarely occur bilaterally.7 Positive lymph nodes occur in less than 1% of cases. Patients with phyllodes tumors commonly have a history of fibroadenomas.7-9
On mammography, phyllodes tumors appear to be large, round masses with smooth, polylobulated well-defined borders (Figure, page 27). Ultrasonography findings of the breast tumor may mimic that of fibroadenomas; the tumors are usually well circumscribed with smooth margins with fluid-filled clefts in a sold mass. A core needle biopsy of the tumor often reveals stromal cells but can also contain cells from the ducts and lobules.7,8
tumor classification is to have the tumor surgically excised. Patients diagnosed with benign and borderline phyllodes tumors are considered cured after local excision.8-10 With such an approach, local recurrence and 5-year survival rates of 4% and 96%, respectively, have been reported for benign phyllodes tumors.7
The only accurate way to diagnose the
FIGURE . Normal bilateral mediolateral oblique digital screening mammogram in 66-year-old woman (left) and findings from the case patient (right).

Diagnosis and Treatment
A team consisting of a general surgeon, oncologist, primary care provider, and reconstructive plastic surgeon was brought together in consultation for this patient’s mastectomy with a wide excision. The pathology report in this case demonstrated “spindle” cells, which caused greater concern for a malignant process.

The final diagnosis of phyllodes tumor with malignancy was determined with excision of the tumor down to the muscle wall.The literature suggests that a 1-cm negative margin be used in malignant phyllodes tumors.10 Axillary node involvement is rare with malignant phyllodes tumors.9 A positron emission tomography (PET) scan was performed and demonstrated no metastases at the time of surgery. This case was presented at the hospital’s Tumor Board by the oncologist and the plan was to treat after surgical excision with radiation and then chemotherapy.
The American Cancer Society reports that malignant phyllodes are different than other types of breast cancers and are treated more like sarcomas.1 Follow-up is recommended every 6 months for 2 years after treatment and then annually.10 In patients diagnosed with malignancy, chest surveillance with computed tomography (CT) scans should be performed following the guidelines for treatment of sarcomas instead of breast cancers. ■
Deborah L. Hopla, DNP, APRN-BC, FAANP, FAAN, is an associate professor and director of DNP/MSN/FNP Programs in the Department of Nursing at Francis Marion University in Florence, South Carolina. Dr Hopla is a family nurse practitioner at Hope Health, a federally qualified health care clinic.
References
1. Phyllodes tumors of the breast. The American Cancer Society. Accessed August 2, 2022. https://www.cancer.org/cancer/breast-cancer/non-cancerousbreast-conditions/phyllodes-tumors-of-the-breast.html
2. Zhang Y, Kleer CG. Phyllodes tumor of the breast: histopathologic features, differential diagnosis, and molecular/genetic updates. Arch Pathol Lab Med. 2016;140(7):665-671.
3. Phyllodes tumors of the breast. Breast360.org. The American Society of Breast Surgeons Foundation. Accessed August 2, 2022. https://breast360.org/ topic/2020/03/02/phyllodes-tumors-of-the-breast/
4. Phyllodes tumor of the breast. Genetic and Rare Diseases Information Center. National Institutes of Health. Accessed August 2, 2022. https:// rarediseases.info.nih.gov/diseases/9514/phyllodes-tumor-of-the-breast
5. Rosen PP. Rosen’s Breast Pathology. 2nd edition. Lippincott William Wikins; 2001.
6. Limalem F, Kashyap S. Phyllodes tumor of the breast. StatsPearls StatPearls [Internet]. Updated June 5, 2022. Accessed August 4, 2022. https:// www.statpearls.com/ArticleLibrary/viewarticle/20225
7. Mishra SP, Tiwary SK, Mishra M, Khanna AK. Phyllodes tumor of breast: a review article. ISRN Surg. 2013;2013:361469.
8. Aydo˘ gan F, Tas¸çı Y, Sagara Y. Phyllodes tumors of the breast. In: Aydiner A, Igci A, Soran A, eds. Breast Disease: Management and Therapies, Vol 2. 2nd Ed. Springer; 2019;25:365-369.
9. Tan BY, Acs G, Apple SK, et al. Phyllodes tumours of the breast; a consensus review. Histopathology. 2016; 68(1):5-21.
10. Grau AM, Chakravarthy AB. Chug R. Phyllodes of the breast. UpToDate. Accessed August 2, 2022. https://uptodate.com/contents/ phyllodes-tumors-of-the-breast
Dermatology Clinic
CASE Skin Thickening Around Fingers, Forearms, and Face
SARAH FRISKE, BBA;TARA L. BRAUN, MDA 47-year-old otherwise healthy woman presents to the clinic with several concerns. Over the past several months, she has experienced thickening of her skin around her hands, forearms, and face. Her fingers turn blue and then pale when she is exposed to cold. Additional recent symptoms include fatigue and gastroesophageal reflux. She takes no medications and has no family history of autoimmune disease. On physical examination, the patient has skin thickening on the hands, forearms, and face. She also has hypopigmented macules on the hands and lower legs.
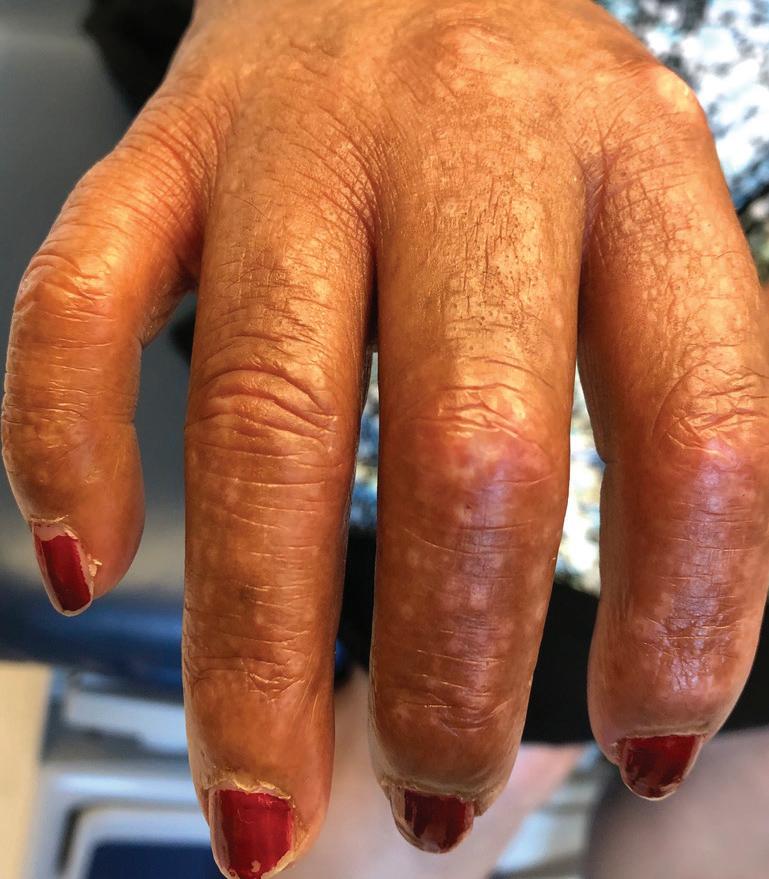
DIAGNOSIS
Systemic Sclerosis
Systemic sclerosis (SSc), also known as scleroderma, is an autoimmune connective tissue disease affecting multiple organ systems.1,2 Systemic sclerosis was first recognized as a clinical entity in the mid-19th century.The first description of the pathologic features of scleroderma occurred in 1861 when skin from an autopsy was noted to be “markedly thickened by proliferation of connective tissue.”2 In 1894, Paul Gerson Unna, a German dermatopathologist, described the condition as “mainly hypertrophy of preexisting collagen bundles which affects all parts of the dermis.”2
Patients with SSc with skin involvement can be grouped into 2 subtypes: limited cutaneous SSc and diffuse cutaneous SSc.The primary targets of autoantibodies for limited cutaneous SSc are centromere proteins, and the autoantibodies associated with diffuse cutaneous SSc target topoisomerase I and RNA polymerase III.3
Limited cutaneous SSc manifests clinically with distal skin fibrosis (limited to the distal extremities and face), sclerodactyly (skin fibrosis of the fingers), telangiectasia, and calcinosis cutis. Compared with diffuse cutaneous SSc, the disease course of
limited cutaneous SSc is characterized by a slower progression of skin fibrosis and later development of internal organ involvement, which includes pulmonary arterial hypertension and severe gut disease. Patients may have a long history of Raynaud phenomenon (reversible vasospasm of digital arteries) prior to development of SSc.3,4
Diffuse cutaneous SSc clinically manifests as proximal skin fibrosis up to the elbows and knees, including the trunk.These patients are more likely to experience tendon friction rubs. Compared with limited cutaneous SSc, diffuse cutaneous SSc is characterized by rapidly progressive skin fibrosis and early occurrence of internal organ complications. Interstitial lung disease and scleroderma renal crisis are more common in patients with diffuse disease than in patients with limited disease.3
Systemic sclerosis is estimated to affect 17.6 in 100,000 people globally.5 Although the frequency varies depending on case definition, the prevalence of SSc is consistently higher in the US and Australia compared with Japan and Europe.5 Systemic sclerosis is much more common in women suggesting that hormonal or pregnancy-related factors are involved in the pathogenesis
of SSc.1,3-5 Ethnicity may play a role in SSc, with Black patients presenting at a younger mean age than White patients and more likely to have antibodies against topoisomerase I and less likely to have antibodies that are centromere-specific.6 Familial clustering is also significant with a 13- to 14-fold increase in the relative risk for a first-degree relative as well as various HLA class II alleles influencing disease susceptibility.1,3-6 In addition, environmental exposures associated with an increased risk for SSc include silica dust, silicone breast implants, certain chemotherapy drugs, solvents, chemicals, and infectious agents.6
The pathogenesis of SSc is described as an interaction between an environmental event and genetically susceptible individuals that triggers vascular alterations, autoinflammation, and fibrosis. Activated endothelial cells from the microvascular injury upregulate expression of adhesion molecules, inflammatory mediators, and chemokines leading to recruitment of inflammatory cells.Type 2 T-helper cells secrete transforming growth factor beta β (TGF-β), interleukin (IL)-13, and IL-4. Recruited B cells then lead to overproduction of a variety of autoantibodies including anti-topoisomerase I, anti-RNA polymerase III (anti-RNAP III), anti-U3 RNP, anti-centromere, anti-Th/To, and anti-U1 RNP antibodies. Macrophages further increase the amount of TGF-β leading to a profibrotic state.3,7,8
The diagnosis of SSc is made via history, physical examination, and fulfillment of the 2013 American College of Rheumatology and European Alliance of Associations for Rheumatology (formerly European League Against Rheumatism) criteria for the classification of SSc (Table).3,4,9
Localized skin-thickening diseases that can appear similar to SSc include morphea and stiff-skin syndrome. Diseases that cause diffuse skin thickening include eosinophilic fasciitis, graft-vs-host disease, deposition diseases (scleredema, scleromyxedema, amyloidosis, nephrogenic systemic fibrosis), and metabolic syndromes (eg, hypothyroidism).These diseases can be differentiated from SSc via clinical history, distribution of skin involvement, autoantibody testing, and findings on skin biopsy.10 Differential diagnosis of vascular findings include other causes of peripheral vascular disorders, especially vasculitis, as well as other causes of Raynaud phenomenon including isolated Raynaud phenomenon.4 Also on the list of diseases to eliminate are other immune-mediated connective tissue diseases including lupus, arthritis, and myositis.4
Histologically, SSc has increased epidermis to subcutis thickness, thickened and sclerotic dermal collagen bundles, loss of periadnexal fat and hair follicles, compression of pilosebaceous units, and little infiltration of plasma cells and lymphocytes. Scleromyxedema, which mimics SSc, presents with histologic patterns of mucin deposition, fibroblast proliferation, and increased collagen density. Furthermore, scleredema is differentiated histologically from SSc by swelling of collagen
TABLE. 2013 ACR and EULAR Classification of Systemic Sclerosis3,4,9
Clinical Findings Points
Proximal skin involvement including skin thickening of the fingers on both hands that extends from the proximal to the metacarpophalangeal joints
Puffy fingers
Raynaud phenomenon
Sclerodactyly of the fingers
Fingertip ulcers
Fingertip pitting scars
Telangiectasia
Abnormal nail fold capillaries
Pulmonary arterial hypertension
Interstitial lung disease
Systemic sclerosis-related antinuclear antibodies including anticentromere, anti-topoisomerase I, and anti-RNAP III
, American College of Rheumatology; anti-RNAP III, anti-RNA polymerase III; EULAR, European Alliance of Associations for Rheumatology
fibers, thickening of reticular dermis, and mucin deposition without fibroblast proliferation.4,11
Because of the diverse systemic complications of SSc, treatment of the disease is multidisciplinary and focuses on reducing morbidity and mortality. In the case patient, management will focus on treatment of skin-associated complications, which consist of several immune-modulating treatments. Methotrexate and mycophenolate mofetil have shown clinical benefit in several clinical trials, while cyclophosphamide is used for more severe skin involvement.4 Injection of botulism toxin has been found effective to avert Raynaud phenomenon.7 Lung function and skin thickening complications have been successfully addressed through B-cell depletion with rituximab. Fresolimumab, a neutralizing antibody that targets TGF-β dermal myofibroblasts,
Dermatology Clinic
reduces skin fibrosis and dermal myofibroblasts.4,7 The anti-IL6 receptor antibody tocilizumab has also been shown to reduce skin thickening, though not significantly when compared with placebo.4 Pigment alterations in skin including increased skin tone and postinflammatory hyperpigmentation may cause cosmetic concerns for the patient but, unfortunately, few treatments are available for these concerns.4
For the patient in this case, punch biopsy of the arm was consistent with scleroderma and, given the clinical findings,
References
1. Asano Y. Systemic sclerosis. J Dermatol. 2018;45(2):128-138.
2. Medsger TA, Benedek TG. History of skin thickness assessment and the Rodnan skin thickness scoring method in systemic sclerosis. J Scleroderma Relat Disord. 2019;4(2):83-88.
3. Allanore Y, Simms R, Distler O, et al. Systemic sclerosis. Nat Rev Dis Primers 2015;1:15002.
4. Denton CP, Khanna D. Systemic sclerosis. Lancet. 2017;390(10103): 1685-1699.
5. Bairkdar M, Rossides M, Westerlind H, Hesslestrand R, Arkema EV, Homqvist M. Incidence and prevalence of systemic sclerosis globally: a comprehensive systematic review and meta-analysis. Rheumatol. 2021;60(7):3121-3133.
6. Nikpour M, Stevens WM, Herrick AL, Proudman SM. Epidemiology of systemic sclerosis. Best Pract Res Clin Rheumatol. 2010;24(6):857-869.
7. Furue M, Mitoma C, Mitom H, et al. Pathogenesis of systemic sclerosis— current concept and emerging treatments. Immunol Res. 2017;65(4):790-797.
the patient was diagnosed with diffuse SSc. The patient was seen in conjunction with rheumatology and has been put on a trial of methotrexate, then mycophenolate mofetil, and more recently she was started on tocilizumab. ■
Sarah Friske, BBA, is a medical student at Baylor College of Medicine; Tara L. Braun, MD, is a dermatologist at Elite Dermatology in Houston,Texas.
8. Derk CT, Jimenez SA. Systemic sclerosis: current views of its pathogenesis. Autoimmun Rev. 2003;2(4):181-191.
9. Van Den Hoogen F, Khanna D, Fransen J, et al. 2013 classification criteria for systemic sclerosis: an American College of Rheumatology/European League against Rheumatism collaborative initiative. Arthritis Rheum. 2013;65(11):2737-2747.
10. Tyndall A, Fistarol S. The differential diagnosis of systemic sclerosis. Curr Opin Rheumatol. 2013;25(6):692-699.
11. Showalter K, Gordon JK. Skin histology in systemic sclerosis: a relevant clinical biomarker. Curr Rheumatol Rep. 2020;23(1):3.
Statement of Ownership, Management, and Circulation
Total Number of Copies (Net
Paid and/or Requested Circulation
run) [i] 101,462 [ii]
Paid/Requested Outside—County Mail Subscriptions Stated on Form 3541 [i] 62,844 [ii] 51,245
Paid In-County Subscriptions Stated on Form 3541 [i] 0 [ii]
Sales Through Dealers and Carriers, Street Vendors, Counter Sales, and Other Non-USPS Paid Distribution [i] 0 [ii]
Other Classes Mailed Through the USPS [i] 6 [ii]
Paid and/or Requested Circulation [i] 62,849 [ii] 51,248
Free Distribution by Mail
Outside-County as Stated on Form 3541 [i] 38,182 [ii] 49,625
In-County as Stated on Form 3541 [i] 0 [ii] 0
Nonrequested Copies Distributed Through the USPS by Other Classes of Mail [i] 0 [ii] 0
Nonrequested Copies Distribution Outside the Mail [i] 262 [ii]
Nonrequested Distribution [i] 38,444 [ii] 49,887
Distribution [i] 101,292 [ii] 101,135
Copies not Distributed [i] 170 [ii] 152
[i] 101,462 [ii] 101,277
Paid and/or Requested Circulation [i] 62.05% [ii] 50.67%
or Owner: Tracie Palmer, Sr. Director Business Media Marketing & Audience 09/29/2022
certify that all information furnished on this form is true and complete. I understand that anyone who furnishes false or misleading information on this form or who omits material or information requested on the form may be subject to criminal sanctions (including fines and imprisonment) and/or civil sanctions (including civil penalties).
The pathogenesis of SSc is described as an interaction between an environmental event and genetically susceptibility.
LEGAL ADVISOR
Injured Wife Brings Suit Against NP
BY ANN W. LATNER, JDIn 2001, Mr R began having numerous episodes of syncope. In 2002, he was diagnosed with swallow syncope, which is associated with intense vagal afferent activation from esophageal stimulation. A pacemaker was implanted to remedy the situation and Mr R did not have a passing out episode again until 2016.
A month earlier, Mr R began to experience episodes of dizziness and lightheadedness when he got up from bed. The episodes did not occur if Mr R stood, sat still, or swallowed liquids.They only occurred in the morning and not throughout the day. To have this checked out, Mr R went to a cardiology practice where he was seen by Ms N, a nurse practitioner, and Dr I, an internal medicine resident.
During the visit, Dr I performed a physical examination and took a medical history. He noted in the appointment progress report that Mr R received a pacemaker in 2002, but no mention was made of why the pacemaker was installed. Ms N ordered a pacemaker interrogation to evaluate how well the leads were working and to determine if the patient was having arrhythmias.
The report indicated that the patient had not experienced any arrhythmias and that the pacemaker’s right ventricular lead was not being used to pace his heart. Ms N was aware that the report showed an elevated number for impedance of the pacemaker’s right ventricular lead, and she attempted to determine whether the dizzy episodes were related to this. In light of the patient’s report that the dizziness lasted minutes to hours, occurred when he moved his head, and that the symptoms were lessened by the medication meclizine, Ms N believed that Mr R’s dizziness was caused by an inner ear problem. Ms N referred Mr R to an otolaryngologist, instructed him to stop taking his blood pressure medications, and asked him to return for a follow-up visit in 6 months. The cardiologist at the practice did not see or treat Mr R, but he signed off on the progress report of the appointment that Ms N prepared.
Cases presented are based on actual occurrences. Names of participants and details have been changed. Cases are informational only; no specific legal advice is intended. Persons pictured are not the actual individuals mentioned in the article.

The defendants makes a motion to dismiss the malpractice claim by the spouse, asserting that she had no patient-physician relationship with the clinician.
Is a clinician liable for misdiagnosis of a patient that results in injury to a third party?
The following month, Mr R was driving with his wife. He took a sip of co ee and had a feeling similar to his prior experiences before passing out. Mr R pulled o the road but was unable to stop the truck and he crashed into a tree, injuring himself and his wife. Following the accident, Mr R was hospitalized and underwent a right ventricular lead revision. In January 2017, the cardiologist signed a letter indicating that the patient had su ered a syncopal episode caused by “malfunction of his right ventricular lead of his previously placed pacemaker” while driving that led to the automobile accident. The letter advised that the malfunction was corrected and that Mr R was able to resume driving without restrictions.
Two years later, Mr R and his wife sued the cardiology practice and the cardiologist for medical malpractice. The complaint alleged that the cardiologist owed a duty to the
such a claim, the third party must establish that the physician owed a duty to the third party. Generally, duty is based on a relationship between the parties. According to the court, “a duty of reasonable care may arise when one stands in a special relationship with either the victim or the person causing the injury.” Although the determination of duty is generally an issue of law,“the facts and circumstances of a special relationship may give rise to an issue for resolution by the jury,” noted the court, particularly in cases of a dangerous medical condition. Ultimately the court refused to dismiss the case and sent it back to the lower court for a trial.
Protecting Yourself
Both the nurse practitioner and physician failed to get enough information to determine whether Mr R was a danger to himself or others. Notably, Ms N ordered a pacemaker interrogation and the results determined that it was not functioning properly. Despite this, no further testing of the pacemaker was ordered, no e orts were made to x it, and the patient was not warned about the abnormality with the pacemaker or that he could faint while driving. He was not told that he should not drive.
wife, as a foreseeable passenger, to properly treat Mr R and that the physician breached this duty by failing to:
• Take a speci c history to determine the pattern, frequency, and duration of the episodes
• Determine if there was a correlation between the dizzy episodes and the pacing of the right ventricular lead in the pacemaker
• Implement a plan to repair or replace the right ventricular lead
• Advise Mr R not to drive
The defendants made a motion to dismiss the medical malpractice claim by the wife, asserting that she had no patientphysician relationship with the cardiologist or the practice and, thus, they owed no duty to her. The trial court denied the motion and the physician appealed.
Legal Decision
On appeal, the defendants alleged that the wife was not owed a duty under the law and that it was not foreseeable that Mr R would have a swallow syncope episode while driving. The appeals court disagreed. “The duty owed by the health care professional arises from the health care professional’s relationship with the patient,” noted the court, “however, it does not follow that only a patient may bring a malpractice claim or that a physician never owes a duty to third parties.”
To the contrary, the court noted that other courts have sometimes recognized malpractice claims by a third party despite the lack of a doctor-patient relationship. To maintain
Additionally, neither Ms N nor Dr I asked why Mr R had the pacemaker installed. Had they known about Mr R’s history of swallow syncope, they might have handled his treatment di erently. Information is power — gather as much of it as possible to make the best, most informed decisions. ■
Ann W. Latner, JD, a former criminal defense attorney, is a freelance medical writer in Port Washington, New York.
Case Study Library
Check out all of our case studies in obesity, diabetes, and other important topics in primary care — along with our clinical challenges — by visiting us at: ClinicalAdvisor.com/Case-Study
The court argued that it does not follow that “a physician never owes a duty to third parties.”
