


Mission Statement
We, at Catholic Health, humbly join together to bring Christ’s healing mission and the mission of mercy of the Catholic Church expressed in Catholic health care to our communities.
St. Catherine of Siena Hospital Service Area
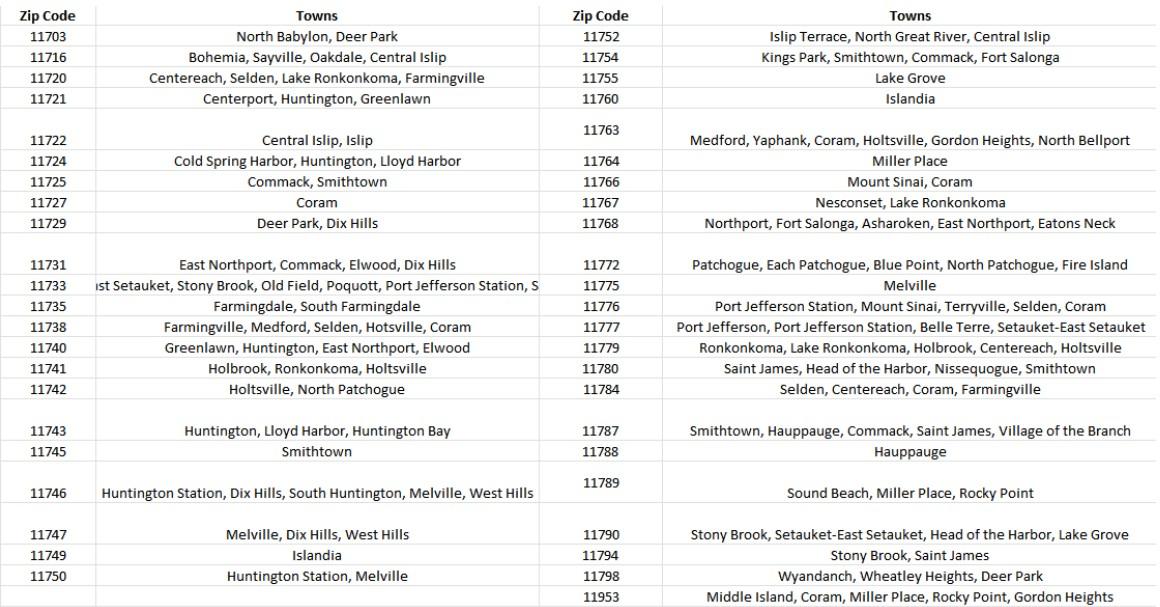
St. Catherine of Siena Hospital is a 265-bed, not-for-profit, community hospital and has served the residents of Smithtown for more than 50 years. St. Catherine of Siena Hospital’s primary service area is Suffolk County. The chart below defines the zip codes and municipalities (towns) comprising St. Catherine of Siena Hospital’s service area.
Demographics
Suffolk County’s total population as of 2024 was 1,525,465. Approximately 18% of Suffolk County was over 65 years old and approximately 20% was under 18 years old in 2024.1 The median age in Suffolk County in 2023 was 42.1 years. 2 In 2023, 50.4% if the population was female and 49.6% of the population was male in Suffolk County (2023 ACS, 1-year estimates). In 2024, 64.38% of the population was White, followed by 21.43% Hispanic, 7.89% Black, 4.79% Asian, 0.72% American Indian/Alaskan Native, and 0.12% Native Hawaiian/Pacific Islander.3
Geographic description
Suffolk County is 2,373 square miles and is the second largest county in New York. Catholic Health’s (CH) three hospitals in the county service this easternmost county in New Yok State and the county is divided into 10 towns: Babylon, Huntington, Islip, Smithtown, Brookhaven, Southampton, Riverhead, East Hampton, Shelter Island and Southold.2 Suffolk County is an area of growing diversity, cultures, and population characteristics.
1 County Health Rankings https://www.countyhealthrankings.org/health-data/new-york/suffolk?year=2024
2 U.S. Census Bureau, 2023 American Community Survey, One-Year Estimates
3 County Health Rankings https://www.countyhealthrankings.org/health-data/new-york/suffolk?year=2024
Socioeconomic information
In Suffolk County, the median household income was $124,045 in 2023 with 62.2% of the population 16 years and older employed. In 2023, 25.2% of households made $200,000 or more. Followed by 19.8% made $100,000 to $149,999, 15.0% made $150,000 to $199,999, 10.6% made $50,000 to $74,999, 10.3% made $75,000 to $99,000, 6.2% made $35,000 to $49,000, 4.2% made $25,000 to $34,999, 3.9% made $15,000 to $24,999, 3.3% made less than $10,000, and 1.5% made $10,000 to $14,999. These estimates were inflation-adjusted. In 2023, among the population 16 years and older 62.2% were employed, 2.3% were unemployed, and 35.4% were not in the labor force4. In 2024, 3.12% of the population in Suffolk County was unemployed.5
According to research conducted by the United Way of New York’s ALICE report,6 Long Island residents are earning wages that do not cover life’s basic costs. As of 2024, 33% of Long Island households fall below the set income threshold needed to live and work, which equates to 184,307 households in Suffolk County that are struggling to afford these basic needs.
Suffolk County had a lower percent of the population in poverty at 6.8% compared to 14.2% in New York State in 2023. Individuals under 18 years old had the highest percent in poverty at 8.3% compared to 7.6% in those 65 years and older and 6.1% among those 18 to 64 years.7
Among the population 18 to 24 years old, 40.6% had some college or an associate’s degree, 33.7% were a high school graduate or equivalent, 18.6% had a Bachelor’s degree or higher, and 7.1% were less than a high school graduate in 2023. Higher educational attainment was achieved among Asian populations who 54.9% had a Bachelor’s degree or higher compared to 45.1% among White, 30.9% among Black, 20.4% among American Indian or Alaskan Native, 17.5% among some other race, 30.7% among two or more races, and 20.5% among Hispanic or Latino populations.8
Of the non-institutionalized population in Suffolk County, 11.2% had a disability in 2023.The percent with a disability was slighter higher among females at 11.6% compared to 10.8% among males. Individuals 75 years and over had the highest percent with a disability at 41.3%, followed by 22.4% among those 65 to 74 years, 8.8% among those 35 to 64 years, 5% among those 5 to 17 years and 0.3% among those under 5 years. Among disability types reported having an ambulatory difficulty was the highest being 5.9% of the percent with disability followed by having an independent living difficulty (5.2%), having a cognitive difficulty (4.4%), having a hearing difficulty (3.1%), having a self-care difficulty (2.4%), and having a vision difficulty (1.8%).
Suffolk County has a diverse population that speaks a variety of languages. In 2024, 3.80% of the population were non-English proficient.9 In 2023, among populations 5 years and older 25.8% reported speaking a language other than English at home.10 English only was reported as the type of language spoken at home by 74.2% of the population 5 years and older followed by Spanish at 16.6%, other Indo-European languages at 6.2%, Asian and Pacific Islander languages at 2.4% and other languages at 0.7% in 2023.
4 U.S. Census Bureau, 2023 American Community Survey, One-Year Estimates
5 County Health Rankings https://www.countyhealthrankings.org/health-data/new-york/suffolk?year=2024
6 ALICE 2024 (Asset Limited, Income Constrained, Employed) | United Way of Long Island
7 U.S. Census Bureau, 2023 American Community Survey, One-Year Estimates
8 U.S. Census Bureau, 2023 American Community Survey, One-Year Estimates
9 County Health Rankings https://www.countyhealthrankings.org/health-data/new-york/suffolk?year=2024
10 U.S. Census Bureau, 2023 American Community Survey, One-Year Estimates
Key Health Partners
Partnering with community-based organizations is the most effective way to determine how the health priorities will be addressed. As part of our collective impact strategies to promote health and well-being for residents in our communities, St. Catherine of Siena Hospital has strong relationships with local and regional community-based organizations, libraries, schools, faith-based organizations, the local health department, local fire departments and municipalities that support and partner with us to reduce chronic disease, mental health and substance misuse, and to promote health equity. Some of St. Catherine’s partners include: the LIHC, the Suffolk County Department of Human Services, Catholic Charities and Catholic Faith Network (CFN).
Public Participation
St. Catherine of Siena Hospital, along with Catholic Health’s other five hospitals, worked with the LIHC and the Suffolk County Department of Health Services (SCDOHS), and dozens of community-based organizations, libraries, schools and universities, local municipalities, and other community stakeholders to produce the CHNA. SCDOHS representatives offered input and consultation, when appropriate, regarding the data analyses conducted by the LIHC, DataGen, and Catholic Health. Top, high-level findings include a continued prevalence of chronic disease incidence, particularly heart disease, diabetes, obesity and cancer. Further, increasing rates of electronic cigarette (e-cigarette) use were found particularly among youth and consistent rates of food insecurity. In 2024, members of the LIHC reviewed extensive data sets selected from both primary and secondary data sources to identify and confirm New York State Prevention Agenda priorities for the 2025-2027 Community Health Needs Assessment cycle. Data analysis efforts were coordinated through the LIHC, which served as the centralized data return and analysis hub.
Results of Community-Wide Survey
Primary data was obtained from a community health needs assessment sent to individuals and a similar survey to community-based organization leaders.11 Additionally, we looked at results from two qualitative studies to round out our primary data.12 Secondary data was derived from publicly-available data sets curated by DataGen into its proprietary data analytics platform, CHNA Advantage ™, offering 200 plus metrics to determine health issues within Suffolk County.13 As such, priorities selected for the 2025-2027 cycle are different from the 2022-2024 cycle except for a focus on prevention of chronic disease. The selected health disparities in which partners are focusing their efforts rests on the inequities experienced by those in historically underserved communities and communities of color.
11 Community Health Assessment Survey (CHAS) assessing responses from individuals, summary report and survey instrument (Appendix A) CBO Survey Analysis 2024, assessing responses from community-based organization leader, summary report and survey instrument (Appendix B)
12 Qualitative Analysis of Key Informant Interviews Conducted Among Community-Based Organization Leaders (Appendix C) Catholic Health Listening Session Summary Report (Appendix D)
13Statewide Planning and Research Cooperative System (SPARCS), New York State Prevention Agenda dashboard, Behavioral Risk Factor Surveillance System (BRFSS), , New York State Community Health Indicators by Race/Ethnicity Reports, Community Health Indicator Reports, Prevention Quality Indicators, CDC Places, and U.S. Census Bureau. The CHNA Advantage™ data analytics platform includes these and other state and national level indicators.
Community Health Priorities for 2025-2027
Chronic disease, tobacco/e-cigarette use, and nutrition insecurity were identified as priority areas for 2025-2027. Adult obesity contributes to chronic disease and was identified as a health disparity in primary and secondary research. According to the Robert Wood Johnson Foundation’s 2024 County Health Rankings for Suffolk County, the prevalence of obesity was 29.7% in Suffolk County. The prevalence increased from 27.60% in 2023. In 2019, The New England Journal of Medicine studied projected adult obesity in the United States by 2030 based on today’s obese and overweight adult populations.14 By 2030, the obesity epidemic is projected to impact nearly 1 in 2 adults.
According to the Suffolk County Department of Health, obesity is a condition in which an individual has too much body fat and increases the risk for many diseases including high blood pressure, heart disease, type 2 diabetes, stroke, and cancer.15 The prevalence of obesity is persistent in Suffolk County and the United States. From 2017March 2020, 41.9% of U.S. adults 20 years and older (more than 100 million people) were obese. Nationally, disparities in obesity prevalence exist with the highest prevalence of obesity being in non-Hispanic Black adults (49.9%), Hispanic (45.6%), non-Hispanic White (41.4%) and non-Hispanic Asian (16.1%) from 2017-March 2020. In the U.S. obesity is more prevalent in U.S. adults with a high school diploma or some college education (46.4%) and those with less than a high school diploma (40.1%) compared to those with a college degree or above (34.2%). Obesity is serious as it increases risk for chronic diseases. 16
Nationally, communities of color experience higher rates of chronic disease. Using diabetes as an example, the American Indian/Alaska Native population represents 13.6% percent of adults who are diagnosed with diabetes followed by Black, non-Hispanic at 12.1% and Hispanic overall at 11.7% in the United States. Asians and Whites experience the disease at 9.1% and 9.1% respectively.17 Chronic diseases are preventable conditions sensitive to lifestyle (diet/physical activity) habits but hampered by the obstacles presented by SDOH - income/employment, race/ethnicity, food access, housing/neighborhood location, and level of education. The county and hospitals identified in this report through collaborative efforts and facility-specific programming acknowledge and address these determinants regularly.
Nutrition security or food insecurity has also been identified as a priority area. The cost of food has been rising with food costs in the New York City Metropolitan area rising by 56.2% from 2012-2013 to 2022-2023.18 Although the food share of income for the average household in the New York Metropolitan area as remained around the national average, lower-income households may be particularly impacted by the rise in food prices and are more likely to face food insecurity. In 2024, 5.20% of the population in Suffolk County was food in secure. This decreased from 6.60% in 2023. In 2024, 34.27% of children were on free or reduced lunch in school.
Tobacco and e-cigarette use have also been identified as a health need in the region. Tobacco use is a risk factor for several chronic diseases. Smoking causes cancer, cardiovascular disease and lung disease while the use of smokeless tobacco increases the risk for cancers of the mouth, esophagus and pancreas. Tobacco use is the leading cause of preventable disease and death in the U.S. with 49.2 million people reporting current tobacco product use in 2022.19
14 https://www.nejm.org/doi/full/10.1056/NEJMsa1909301
15 Obesity Prevention
16 Adult Obesity Facts | Obesity | CDC
17 Diabetes in America: Prevalence, Statistics, and Economic Impact
18 report-2-2026.pdf
19 Current Cigarette Smoking Among Adults in the United States |
In New York State, 12.5% of adults were current smokers in 2022 (age adjusted). On Long Island, 8.7% of the adult population were smokers with a slightly higher percent of adults in Suffolk County compared to Nassau County. In 2022 7.5% of the adult population were smokers in Nassau County and 9.7% in Suffolk County.20
According to the County Health Rankings, the percent of smokers in Suffolk County has decreased in 2024 to 12.50%.
Electronic cigarettes (e-cigarettes) are other vapor products are high addictive nicotine products and are not Food and Drug Administration (FDA) approved smoking cessation products. They are classified and regulated as a tobacco product. The long-term health risks of e-cigarettes are still unknown and are currently being studied. Exposure to nicotine is highly addictive and can harm brain development among adolescents into early adulthood. There has been dramatic increases in e-cigarette use among youths. In 2019, there was an outbreak of vaping product use-associated lung injury (EVALI). E-cigarettes are included in the Clear Indoor Air Act in New York State which means they are not allowed to be used in places where smoking tobacco is prohibited. With the rise of smoking and e-cigarette use particularly among younger populations, there is a need to focus on this as a priority area to reduce the prevalence of smoking/e-cigarette use and prevent e-cigarette use.21
In 2021, 5.3% of the adult population in NYS used e-cigarettes this was lower than the national average of 6.6% of adults. In NYS, e-cigarette use was highest among individuals age 18-24 (15.1%), current smokers (14.1%), adults with frequent mental distress (11.4%), and adults with Medicaid (8.5%) in 2021. In Nassau County the prevalence of e-cigarette use among adults was 5.5% in 2021. In Nassau County the prevalence of e-cigarette use among adults was 6.0% in 2021
These are the main health challenges and contributing causes affecting residents of the county, especially in low-income communities of color. That these social determinants of health are predictors of chronic disease is well documented.22 23 24 Health care access issues are mostly tied to economics (quality of health insurance, employment, and cost of living).
St. Catherine of Siena Hospital’s Priorities, Interventions and Strategies
Priority Number One: Preventive Services for Chronic Disease Prevention & Control
Interventions, Strategies and Activities:
1. St. Catherine of Siena Hospital will host its annual community health fair in fall 2026 and offer free glucose screenings.
2. At a system level, Catholic Health will host its annual community health fair in 2026 and offer free glucose screenings.
3. Catholic Health’s mobile clinic unit offers free glucose screenings.
20 https://apps.health.ny.gov/public/tabvis/PHIG_Public/chirs/reports/#state
21 https://www.health.ny.gov/statistics/brfss/reports/docs/2023-14_brfss_electronic_cigarette.pdf
22 Cockerham WC, Hamby BW, Oates GR. The Social Determinants of Chronic Disease. Am J Prev Med. 2017 Jan;52(1S1):S5-S12. https://doi.org/10.1016%2Fj.amepre.2016.09.010 PMID: 27989293; PMCID: PMC5328595.
23 Pantell MS, Prather AA, Downing JM, Gordon NP, Adler NE. Association of Social and Behavioral Risk Factors With Earlier Onset of Adult Hypertension and Diabetes. JAMA Netw Open. 2019;2(5):e193933. Https://doi:10.1001/jamanetworkopen.2019.3933
24 Vennu, V., Abdulrahman, T.A., Alenazi, A.M. et al. Associations between social determinants and the presence of chronic diseases: data from the osteoarthritis Initiative. BMC Public Health 20, 1323 (2020) https://doi.org/10.1186/s12889-020-09451-5
4. Long Island Health Collaborative Digital Lifestyle Medicine Awareness Campaign "Live Better": Digital awareness campaign about chronic disease prevention and self-management.
Priority Number Two: Nutrition Security
Interventions, Strategies and Activities:
1. All patients seen in St. Catherine’s Emergency Department will be screened for insecurity. Those identified as food insecure will be offered a Long Island Cares food to go bag, contact information for Long Island Cares, and SNAP enrollment information.
2. During Lent, hospital staff will participate in a Meals of Hope food packing event, assembling soup packages to be distributed to local parishes and shelters.
3. Catholic Health mobile clinical units traverse LI assisting/screening underserved communities, providing food to go bags and referrals to Long Island Harvest and food pantries.
4. Catholic Health Healthy Sundays are held in underserved communities, providing food to go bags and referrals to Long Island Cares/LI Harvest and food pantries.
5. Catholic Health Physician Partners practices will screen patients for income/food insecurity, providing referrals and food.
6. Catholic Health and St. Catherine’s will partner with Catholic Charities HUD Housing Program and Senior Services to screen for food insecurity.
7. Catholic Health collaborates with Catholic schools on annual food drives to supply food to students and families in need, during summer months.
8. Catholic Health/St. Catherine of Siena Hospital, partners with Smile Farms to build a cooperative garden on its campus, to address food insecurity on Long Island. Produce from the garden will be distributed to local parishes.
9. LI Harvest/Partnership with Catholic Health: Program aimed at improving health and decreasing the risk of chronic disease for low, income individuals and families.
10. Long Island Health Collaborative Nutrition Security/Healthy Eating Digital Awareness Campaign: Components and messaging will amplify LIHC members' community nutrition/food program offerings.
Priority Number Three: Tobacco/E-cigarette Use -
Interventions, Strategies and Activities:
1. In collaboration with the Suffolk County Department of Health, we will offer smoking cessation education. The program will offer referrals for appropriate supportive pharmaceuticals. Also, we will refer to New York State Quit Line.
2. Each patient is screened for smoking upon hospital admission. Upon discharge, patients connected with smoking cessation referral sources, including Suffolk County Department of Health, St. Francis Hospital’s
DeMatteis Center, and the St. Catherine’s Lung Cancer Screening Program. We will also provide referrals to the New York State Quit Line.
3. Catholic Health’s community outreach buses screen and collects data on smoking status and makes referrals to smoking cessation programs.
4. Catholic Health hosts a Healthy Sundays program at local parishes and collects data on smoking status and makes referrals to smoking cessation programs.
5. St. Catherine of Siena Hospital will educate the community about the harms of tobacco and the benefits of tobacco-free treatment.
6. Catholic Health Physician Partners screens patients and collects data on smoking status and makes referrals to smoking cessation programs. Data will be collected in EPIC EMR.
7. Long Island Health Collaborative Tobacco Cessation Digital Awareness Campaign: tobacco cessation and education messaging via digital media outlets and traditional media outlets when applicable. Messaging will amplify LIHC members' smoking cessation offerings and programs.
Living the Mission
The CH mission is the driving force behind all community outreach activities. In addition to the interventions summarized above, St. Francis Hospital, along with the overall system and including skilled nursing facilities, Catholic Health Home Care and Good Shepherd Hospice, provide additional outreach programs that promote the health care ministry of the Catholic Church and address social determinants of health.
Interventions, Strategies and Activities:
1. Virtual education series streaming on YouTube, that provides short videos on various topics
2. Broadcast health-related television shows for the public in collaboration with Catholic Faith Network provide education and prevention lectures to improve knowledge related to specific diseases and conditions, preventive care, and up-to-date treatment options.
3. Promotion of all programs, events, and education is on the CH website and all CH social media outlets, including Facebook, Twitter, Instagram, and LinkedIn.
4. Lectures in Catholic schools, local libraries, and other community organizations.
5. Community Outreach Screening Buses
6. Healthy Sundays
Dissemination of the Plan to the Public
The St. Catherine of Siena Hospital Community Service Plan will be posted on the hospital’s website at https://www.chsli.org/st-catherine-siena-hospital/about/community-health. Copies will be available at local free health screenings and can be mailed upon request.
By encouraging friends and neighbors to complete the LIHC Wellness Survey online or at local screenings, the Community Health Needs Assessment will help St. Catherine Hospital continue to develop ways to best serve our community.
Conclusion
The Community Service Plan is intended to be a dynamic document. Utilizing the hospital’s strengths and resources, St. Catherine’s, along with community partners, will work to continue to best address health disparities and needs. The hospital will strive to improve the overall health and well-being of individuals and families by expanding free health promotion and disease prevention/education screenings and programs in communities where they are most needed. St. Catherine of Siena Hospital is committed to continue to develop ways to best serve the community.
