

Recommended Treatment Plan for Relapsed Orthodontic Patient


Cover: Patients
12 Resolution of Severe Lateral Open Bite with Surgically Enhanced Orthodontic and Myofunctional Therapies
Daniel Kuncio, D.D.S.; Maria Karpov, D.M.D.
The patient presented with severe lateral open bite and complained of problems chewing on his right side. Previous orthodontic treatment with fixed orthodontic appliances and vertical elastics proved to be unstable. Authors offer alternative treatment plan with surgically assisted rapid palatal expansion, surgically facilitated orthodontic therapy and myofunctional therapy.
18 Laser-Assisted New Attachment Procedure
A Review
Divya Khanna, B.D.S., M.D.S.
Lasers have proved to be an effective tool by providing myriad of benefits and advantages while eliminating many of the negative sequelae historically associated with conventional pocket-elimination surgery.
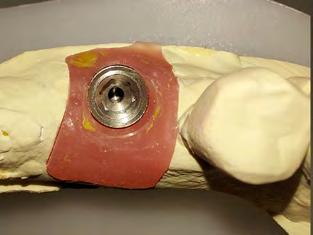
24 Restoration of Dental Implants with Screw-Retained Crowns Optimizing Contact Area Geometry to Prevent Food Impaction
John Mamoun, D.M.D.
Errors of contact plane geometry for screw-retained restoration may be due to restoration not having optimal path of placement to follow for insertion into implant. Author defines path of placement and optimal contact area geometry of screw-retained implant crown restoration and describes how dentist can contour interproximal tooth surfaces to facilitate path of placement.

in the Dental Office
What to do when you no longer recognize the patient you’ve treated for years.
Dementia is a debilitating syndrome that is estimated to affect over five million Americans. A recent study by Fang M. et al., found the projected lifetime risk of developing dementia “after age 55 years was 42%.”[1] In 2022, dementia took the lives of 288,436 American adults over 65 years old.[2]
Statistics show that once diagnosed with dementia, most people decline rapidly, with men who were diagnosed at 65 years old living on average 5.7 years, and women 8 years. Men diagnosed at 85 years old lived another 2.2 years, and women another 4.5 years. Thirty-five percent of dementia patients were admitted to nursing homes three years after being diagnosed, and 57% were admitted after five years.[3]
As the U.S. population ages, dentists can expect to see more patients in various stages of dementia. It is important that they recognize the signs and symptoms, to help in providing care and, perhaps, discovering it before their patients are even aware that they are exhibiting the symptoms.
Multiple Causes
Dementia includes a host of signs and symptoms that can be caused by multiple diseases. These include memory loss, poor problem solving, getting lost, decline of communication skills, inability to get organized, inability to perform complex tasks, easily confused and disoriented, noticeable personality changes, acting inappropriately, uncaring, becoming anxious, experiencing paranoia and hallucinations. Of the several diseases that can precipitate dementia, Alzheimer’s is the leading cause. Other conditions that may be accompanied by dementia-like symptoms are vascular dementia, Lewy body dementia, frontotemporal dementia, Parkinson’s disease, Huntington’s disease, multiple sclerosis, chronic traumatic encephalopathy, and Creutzfeldt-Jakob disease. People who have syphilis, HIV/AIDS and Lyme disease may also develop dementia-like symptoms.[4]
In one of my recurrent hospital lectures that I present every year to PGY-1 and 2 residents, I include the case of a dear patient. For over 20 years, Ms. Star was extremely thank-
ful for being able to keep her front teeth despite 90% bone loss. She agreed to allow me to discuss her situation with the residents and to show them her dental records. She even volunteered to go to the hospital to show her dentition and tell her story. I never took her up on it. Looking back now, I wish I had.
Not long ago, Ms. Star started missing her appointments. Not only was she a no-show, but when we called to see what had happened, she said she didn’t remember she had an appointment. My staff was upset because they knew she had done this before and called her multiple times to remind her. During each call, she confirmed she would be keeping her appointment, yet she still did not show up. Some days, Ms. Star would show up unexpectedly and say she had an appointment, even though she didn’t.
One of my secretaries informed me of the ongoing situation, suggesting Ms. Star was breaking her appointments purposely, which I couldn’t believe. Something was very wrong. I called Ms. Star, and we spoke about her oral health and history at my practice and even about how the hospital residents learned so much from her mouth. During the conversation, I noticed Ms. Star did not remember a lot of her own health history. I referred her to a neurologist, explaining that I had noticed some memory problems in our conversations and wanted her to be evaluated.
Three months later, Ms. Star again didn’t show up for her appointment despite being confirmed. That was when I had a very important realization: you cannot refer a patient with memory problems to another doctor, because they simply won’t remember to go! I asked Ms. Star if she had any children or family whom I could call. She initially didn’t want to give me her daughter’s phone number, but after further discussion of its importance, she relinquished. Fortunately, her daughter brought her to her physician and a neurologist, and she was later diagnosed with dementia. Sadly, I never saw her again.
Memory Failed Him
Another of my patients, Dr. Know, would repeatedly ask me to explain the same thing. Then at his follow-up a week later, when I mentioned our previous conversation, he denied I ever gave him that information, and made me repeat it all over again.
Dr. Know is extremely intelligent; however, he seemed to forget most of our discussions. Five years ago, I referred him to a neurologist after calling his wife, with his permission, and reviewing my recommendations. His wife seemed hesitant to agree with my assessment and didn’t want to upset her husband. Dr. Know was unhappy with me when I next saw him. He said he went to the neurologist, who ran
EDITOR
Stuart L. Segelnick, D.D.S., M.S.
MANAGING EDITOR
Mary Grates Stoll
ADVERTISING/SPONSORSHIP MANAGER
Jeanne DeGuire
ART DIRECTOR
Ed Stevens
EDITORIAL REVIEW BOARD
Frank C. Barnashuk, DDS. Past Clinical Assistant Professor, Department of Restorative Dentistry, University at Buffalo School of Dental Medicine, Buffalo, NY.
David A. Behrman, DMD. Chief, Division Dentistry/OMS, Associate Professor of Surgery, New York-Presbyterian Hospital, Weill Cornell Medicine, New York, NY.
Michael R. Breault, DDS. Periodontic/Implantology. Private Practice. Schenectady, NY.
David Croglio, DDS. Clinical Assistant Professor, University at Buffalo School of Dental Medicine, Buffalo, NY. Private Practice (retired), Amherst, NY.
Jennifer Frustino, DDS, PhD. Director, Oral Cancer Screening and Diagnostics, Division Oral Oncology and Maxillofacial Prosthetics, Department of Dentistry, Erie County Medical Center, Buffalo, NY.
Michael F. Gengo, DDS. Board-certified Endodontist, Clinical Assistant Professor, Department of Endodontics, University at Buffalo School of Dental Medicine, Buffalo, NY. Private Practice, Hamburg, NY.
G. Kirk Gleason, DDS. General Dental Practice (retired), Clifton Park, NY.
Kevin Hanley, DDS. Orthodontic Private Practice, Buffalo, NY.
Stanley M. Kerpel, DDS. Diplomate, American Board Oral and Maxillofacial Pathology, Associate Director, Oral Pathology Laboratory, Inc. Attending, Section of Oral Pathology, New York-Presbyterian, Queens, NY.
Mohini Ratakonda, DDS, Clinical Assistant Professor, University at Buffalo School of Dental Medicine, Buffalo, NY. Endodontics.
Joseph Rumfola, DDS. Clinical Assistant Professor, AEGD Program Director, University at Buffalo School of Dental Medicine, Buffalo, NY. Private Practice, Springville, NY.
Jay Skolnick, DMD. Board-certified Pediatric Dentist. Attending dentist, Rochester General Hospital. Private Practice, Webster, NY.
Lisa Marie Yerke, DDS, MS. Diplomate, American Board Peiodontology, Clinical Associate Professor, Director Advanced Education Program in Periodontics, University at Buffalo School of Dental Medicine Department Periodontics & Endodontics, Buffalo, NY. Private Practice, East Amherst, NY.
PRINTER
Fort Orange Press, Albany

NYSDJ (ISSN 0028-7571) appears two times a year in print: January and June/July. The March, April, August/September and November issues are available online only at www.nysdental.org. The Journal is a publication of the New York State Dental Association, 20 Corporate Woods Boulevard, Suite 602, Albany, NY 12211. In February, May, October and December, members have online access to the NYSDA News. Subscription rates for nonmembers: $75 per year or $12 per issue, U.S. and Canada; $135 per year foreign or $22 per issue. Editorial and advertising offices are at Suite 602, 20 Corporate Woods Boulevard, Albany, NY 12211. Telephone (518) 465-0044. Email info@nysdental.org. Website www.nysdental.org.
some tests and said his memory was fine, though he found a cyst in the brain that may have been congenital.
He kept returning for his periodontal maintenance appointments, each time asking me questions that I had previously answered. Dr. Know was also getting traumatic ulcers interproximally by his papilla, which I attributed to his repeated cleansing of the area with a Proxabrush, that could have been exacerbated by his forgetting he had already cleaned the area. A biopsy of the area verified my diagnosis, and it was further confirmed by his wife, who said he spent inordinate time performing oral hygiene. About a year ago, he told me that he went to his neurologist again, who told him his memory was deteriorating and advised him to write down important instructions he receives from his medical and dental providers. Many times, I have noticed the patient and their family are in denial.[5,6]
Last week, Dr. Know came in with literature on laser treatments that he had read online and wanted to know if he needed to find another dentist to see if laser treatments would help him. I explained he was very well-maintained, with a healthy but moderately reduced periodontium and did not need any laser treatment. Dr. Know became agitated and didn’t seem convinced. This may have been my fault for giving a complex answer instead of simply saying his gums were healthy. Stating simple facts without talking down to someone with dementia is vital.
I called his wife, who said he was now taking medication to help with his memory and that he is having difficulty differentiating between his dreams and reality. He has an upcoming appointment with his doctor for further testing. Subsequent to my last visit with Dr. Know, he was diagnosed with Alzheimer’s disease.
Positive Intervention
Important protocols should be implemented to ensure that patients you suspect have dementia receive the care they need. First, direct the patient to a neurologist for an official diagnosis as soon as you notice signs or symptoms. “Geriatric psychiatrists, neuropsychologists and geriatricians may also be able to diagnose dementia.”[7]
Prior to each dental appointment, be sure to contact a family member or caregiver to update the patient’s medical history and identify who is the health proxy, if appropriate. Regarding informed consent for treatment in dementia patients, Dr. Paul Palo in a JADA “Ethical Moment” says, “taking into account that patients who are possibly in the early stages of dementia may still be capable of making their own treatment decisions, it would be prudent to first seek consultation with the patient’s treating physician in regard to their mental state” and “no treatment recommendations
should be made” or treatment rendered until the patient is evaluated and diagnosed.
Many of us may have had a parent, grandparent or loved one suffer from dementia and know the stressful effects it has on your own mental health. Dementia patients are at increased risk of having caries, periodontal disease, denture problems and xerostomia. Strategies for treating dementia patients, depending on the stage of their disease, include having a caregiver help brush their teeth, timely scheduling, anti-anxiety medications, proper communication, helping direct the course of the dental visit, including comfortable dental chair seating, possible sedation during treatment and more frequent dental visits.[9] As dementia progresses, it will be more difficult for the patient to care for their oral health, and they may be unable to go to the dentist. Thankfully, there are dentists who are experienced in caring for people with dementia in hospitals, nursing homes and the homebound.
Recognizing dementia can be a critical first step in patients’ dental management and overall health.

D.D.S., M.S.
REFERENCES
1. Fang M, Hu J, Weiss J, Knopman DS, Albert M, Windham BG, Walker KA, Sharrett AR, Gottesman RF, Lutsey PL, Mosley T, Selvin E, Coresh J. Lifetime risk and projected burden of dementia. Nat Med 2025 Mar;31(3):772-776. doi: 10.1038/s41591-024-03340-9. Epub 2025 Jan 13.
2. https://www.cdc.gov/nchs/data/hestat/dementia/E-Stat-Dementia-Mortality.pdf.
3. Brück CC, Mooldijk SS, Kuiper LM, Sambou ML, Licher S, Mattace-Raso F, Wolters FJ. Time to nursing home admission and death in people with dementia: systematic review and metaanalysis. BMJ 2025 Jan 8;388:e080636. doi: 10.1136/bmj-2024-080636.
4. https://www.mayoclinic.org/diseases-conditions/dementia/symptoms-causes/syc-20352013
5. https://www.alzheimers.org.uk/get-support/help-dementia-care/when-family-friends-carers-denial-about-dementia
6. Wollney EN, Armstrong MJ, Bedenfield N, Rosselli M, Curiel-Cid RE, Kitaigorodsky M, Levy X, Bylund CL. Barriers and best practices in disclosing a dementia diagnosis: a clinician interview study. Health Serv Insights 2022 Dec 5;15:11786329221141829.
7. https://www.nia.nih.gov/health/alzheimers-and-dementia/what-dementia-symptomstypes-and-diagnosis#:~:text=Who%20can%20diagnose%20dementia?%20Visiting%20a%20 primary,%E2%80%94%20are%20often%20consulted%20to%20diagnose%20dementia
8. Palo P. Ethical obligations treating a patient with questionable decision-making capacity. J Am Dent Assoc 2023 Aug;154(8):771-772. doi: 10.1016/j.adaj.2023.05.008.
9. https://dimensionsofdentalhygiene.com/article/strategies-patients-alzheimer-disease/


Dental Offices Subject to New Legal Mandates
Recently enacted laws put onus on dentist employers to add to employee protections.
Lance Plunkett, J.D., LL.M.
Several new workplace laws, applicable to dental practices, have been enacted, as New York continues its aggressive push in the employment law arena.
First up is the newly minted Section 27-f of the New York State Labor Law. It requires offices subject to first aid requirements under the federal Occupational Safety and Health Act of 1970 (OSHA) have an opioid antagonist available for use in providing first aid or emergency treatment at the workplace. Dental offices, and many other settings (including NYSDA) are subject to OSHA first aid requirements. The law takes effect on Dec. 12. The bill was A.9453 (Paulin) / S.8770 (Fernandez) and was signed by Gov. Hochul as Chapter 17 of the Laws of 2026.
The law defines an employer as any person, corporation, limited liability company or association employing any individual in any occupation, industry, trade, business or service. It excludes the state, political subdivision of the state, public authority, or any other governmental agency or instrumentality thereof.
An opioid antagonist is defined consistent with Section 3309 of the New York State Public Health Law as a drug approved by the United States Food and Drug Administration that, when administered, negates or neutralizes in whole or in part the pharmacological effects of an opioid in the body. It is limited to naloxone and other medications approved by the New York State Department of Health for such purpose.
Administering an opioid antagonist pursuant to Section 27-f of the Labor Law is first aid or emergency treatment shielded under Section 3000-a of the Public Health Law as emergency medical treatment.
The Commissioner of Labor will promulgate regulations, in coordination with the Commissioner of Health, to address the appropriate number of opioid antagonists for workplaces based on the size of the workplace; the training of personnel and use of such opioid antagonists; and any other matter deemed necessary by the commissioner to effectuate the law.
The Legislature noted that the term “opioid” refers to a variety of substances, including both prescription medications and illegal drugs. Opioids are highly addictive and carry transversal risks, which can damage an individual’s health status. In New York State, opioid overdose deaths have increased more than 360%, from 1,074 deaths in 2010 to 5,017 deaths in 2021, with a sharp increase of 70.7% from 2,939 deaths in 2019. Additionally, workplace surveys highlight that over 70% of employers have found opioids to be detrimental to the working environment. Indeed, opioid misuse or abuse can lead to work-related injuries or illnesses, chronic medical conditions, over-prescription in employee health services or health plans, and over-prescription in Workers’ Compensation medical care.
In September 2024, California enacted a law requiring that state’s Division of Occupational Safety and Health (Cal/OSHA) to submit a draft regulation demanding that first aid kits in the workplace contain the nasal spray naloxone hydrochloride. While New York often does not care what other states do legislatively, the Legislature noted that New York’s growing opioid epidemic underscores the need for protective measures like the California bill and promoted the new Section 27-f of the Labor Law as crucial for enhancing workplace and community safety in New York.
Dental offices should review their current first aid procedures and ensure the addition of an appropriate opioid antagonist to office supplies. Dental offices should also prepare to update internal first aid protocols, including training staff on storage, access and proper use of opioid antagonists. Keep in mind that this is a Labor Law requirement aimed at protecting employees, not a law aimed at patients.
Nix on Credit History
Another new law is Section 380-b(d)(1) of the New York State General Business Law, which was amended to add provisions modeled after a law that New York City
NYSDA Directory
OFFICERS
Maurice Edwards, President 30 East 60th St., #1401, New York, NY 10022
Amarilis Jacobo, President-Elect 824 East 181st St., Bronx, NY 10460
Lynn Stacy, Vice President 7504 East State St., Lowville, NY 13367
Paul Leary, Secretary-Treasurer 80 Maple Ave., Ste 206, Smithtown, NY 11787
William Karp, Speaker of the House 4500 Pewter Ln., Bldg 6, Manlius, NY 13104
BOARD OF TRUSTEES
Prabha Krishnan, Immediate Past President 11045 Queens Blvd., Ste 108, Forest Hills, NY 11375
Brendan Dowd, ADA Trustee 3435 Main St., Squire Hall, Room 235G, Buffalo, NY 14214
NY – James E. Jacobs 10 East 53rd St., Ste 2500, New York, NY 10022
2 – John P. Demas 8814 Fort Hamilton Pkwy, Brooklyn, NY 11209
3 – Geoffrey Gamache 24 Eastview Rd., Averill Park, NY 12018
4 – Adrienne L. Korkosz 1309 Union St., Schenectady, NY 12308
5 – Steven Stacey 6702 Buckley Rd., Ste 120, Syracuse, NY 13212
6 – Louis Giordano 864 Hooper Rd., Endwell, NY 13760
7 – David Ramjattansingh 71 King Arthurs Ct., Rochester, NY 14626
8 – Raymond G. Miller 122 Covington Rd., Buffalo, NY 14216
9 – Gary M. Scharoff 1255 North Ave., Ste A1H, New Rochelle, NY 10804
N – Donald R. Hills 5 Willow Rd., Old Bethpage, NY 11804
Q – Mitchell S. Greenberg 11966 80th Rd., #1A, Kew Gardens, NY 11415
S – Martin Dominger 5225 Nesconset Hwy., Suite 57, Port Jefferson Station, NY 11776
B – Jacqueline J. Samuels 120 Alcott Place, Bronx, NY 10475
New Dentist – Kathryn Rothas 920 Lark Dr., Albany, NY 12207
COUNCIL CHAIRPERSONS
Dental Benefit Programs Joseph A. Craddock 3325 East Main St., Attica, NY 14011
Dental Education
Dental Health Planning
Robert M. Peskin
601 Franklin Ave. #225, Garden City, NY 11530
Maria Maranga
8 Rolling Meadow Ln., Northport, NY 11768
Dental Practice Mina Kim 2 West 46th Street, #501, Bryant Park Dental Assoc., New York, NY 10036
Ethics
Governmental Affairs
Julie A. Connolly 115 East 61st Street, Fl. 8, New York, NY 10065
Radha Sachdeva-Munk 203 Smithtown Blvd., Nesconset, NY 11767
Membership & Communications Christopher W. Calnon 3220 Chili Ave., Rochester, NY 14624
Nominations
Peer Review
OFFICE
Prabha Krishnan 11045 Queens Blvd., Ste 108, Forest Hills, NY 11375
Lawrence J. Lehman 7303 197th St., Fresh Meadows, NY 11366
Suite 602, 20 Corporate Woods Blvd., Albany, NY 12211 (518) 465-0044 | (800) 255-2100
Michael Herrmann Executive Director
Lance R. Plunkett General Counsel/Director Governmental Affairs
Mary Grates Stoll Managing Editor
Jenna Bell Director Meeting Planning
Jacquie Donnelly Director Dental Practice Support
Heather Relation
Director Outreach Membership & Engagement
Stacy McIlduff Executive Director NYS Dental Foundation
had adopted first. It prohibits using a person’s credit history in making employment decisions. The law took effect on April 18. It makes it an unlawful discriminatory practice for an employer, labor organization, employment agency or any agent of such entities to request or to use for employment purposes the consumer credit history of an applicant for employment or of an employee.
Neither can an employer otherwise discriminate against an applicant or employee regarding hiring, compensation or the terms, conditions or privileges of employment based on the credit history of the applicant or employee. There are limited exceptions to the new law, such as for employment related to national security, but none is relevant to dental offices.
The law was adopted because there is little to no evidence of a correlation between credit history and job performance. However, in today’s job market, the majority of large employers are now using credit checks as part of their hiring process and in how they treat their existing employees. In addition to lacking any such meaningful correlation, the Federal Trade Commission released a study indicating that as many as one-in-four consumers may have a material error in their credit reports. At a public hearing on the accuracy and use of consumer credit reports, both the credit reporting industry and numerous consumer advocates testified that millions of Americans have errors in their credit reports that put them in a lower credit risk tier, whether they are aware of any such errors or not.
Many New Yorkers, through no fault of their own, have less than ideal credit histories that may stem from issues completely unrelated to their job performance or capabilities. These consumers were disadvantaged because employers were using credit reports to determine if an applicant or employee is worthy of a job or a promotion. The new law puts an end to this practice. The bill was A.9475 (Dinowitz) / S.8789 (Sanders) and was signed by Gov. Hochul as Chapter 71 of the Laws of 2026.
Retirement Mandate
Finally, New York employers who do not offer a retirement plan now have a mandate to do so—the New York State Secure Choice Savings Program. The new law took effect on March 16 for larger employers (30 or more employees) but has a rolling effective date for smaller employers: May 15 for employers with 15 to 29 employees; and July 15 for employers with 10 to 14 employees. The bill was A.8508 (Stirpe) / S.8087 (Gounardes) and was signed into law by Gov. Hochul as Chapter 20 of the Laws of 2024.
The program was first created in 2018 as part of the New York State Budget, but has been substantially amend-
ed over time and is only now taking effect for all employers in 2026 and requiring employers to automatically enroll their employees in a state-facilitated Roth IRA through payroll deductions.
The New York State Secure Choice Program (Secure Choice) applies to private-sector employers, whether for-profit or not-for-profit, that are located in New York State, have been in business for at least two years, have employed 10 or more employees in New York State in the past 12 months, and do not already offer a qualified retirement plan to their employees, such as a 401(k), 403(b) or similar arrangement. Employers cannot drop an existing qualified plan to participate in Secure Choice instead. And covered employers must automatically enroll eligible employees in the program, although employees may opt out from participation or change their contribution rate or investment option at any time. Eligible employees are those age 18 or older who receive taxable wages from a covered employer.
Covered employers should take the following steps:
• Automatically enroll eligible employees in the program.
• Facilitate payroll deductions at the default contribution rate of three percent (3%) of gross wages.
• Remit contributions to the program.
• Provide required informational materials and disclosures to employees upon commencement of the program and upon hire.
Employees can opt out of the program entirely or they can alter the 3% contribution rate at their discretion subject to normal Roth IRA contribution limits set by the Internal Revenue Service.
Employers may not themselves contribute to employee Secure Choice accounts other than through remitting the required payroll deductions. Employers also are not fiduciaries under the program and bear no liability for employees’ participation choices, investment decisions or outcomes. The program is overseen by the New York State Secure Choice Savings Program Board, which has the fiduciary responsibility to act in the best interests of participants.
The Secure Choice Savings Program Board is authorized to enforce any penalties for employer noncompliance. The Board has established a comprehensive website with information for both employers and employees. Employers should check the website at www.securechoice.ny.gov to keep up to date on the program’s requirements and Board guidance.
The Secure Choice program chose to establish Roth IRAs for participating employees, meaning contributions are made on an after-tax basis. Depending on the timing
of any withdrawals, qualified distributions may be tax-free. Accounts are portable, allowing employees to keep their savings if they change jobs.
Dental employers should take the following steps now:
• Determine whether your practice is subject to Secure Choice by confirming your number of employees and whether you offer a different qualifying retirement plan.
• If you determine you are covered under Secure Choice, register with the Secure Choice Board at: www.NewYorkSecureChoice.com.
• Prepare payroll systems to handle automatic deductions and remittances.
• Develop a process to distribute required informational materials and disclosures to employees.
• Consider whether establishing your own employersponsored qualifying retirement plan, which would exempt you from the Secure Choice program, would better serve your practice. As always, consult a knowledgeable attorney and your accountant on what options would work best for your practice.
New York is not unique among states in establishing a mandatory retirement savings program for private sector
employees, but there is still a minority of states that have taken this path. However, New York continues to push proemployee legislation and more may well come in 2026. Let’s hope that New York is as active in pursuing dental insurance reform this year.
The material contained in this column is informational only and does not constitute legal advice. For specific questions, dentists should contact their own attorney.

Association Activities

Introduction to NYSDA
IN MARCH, NYSDA President-Elect Amarilis Jacobo hosted component presidents-elect at orientation meeting held to acquaint them with each other and workings of state Association. Photographed during break in meeting at NYSDA headquarters are, from left: Jennifer Frustino, Eighth District; Devin Klein, Suffolk County; Phyllis Merlino, Second District; Jemima Louis, Bronx County; Egidio Farone, New York County; Dr. Jacobo; Clair Kiehl, Fourth District; NYSDA Executive Director Michael Herrmann; Michael Smith, Ninth District; Dennis Mitchell, dean, Faculty Dental Medicine, Columbia University, guest speaker; Katayoon Noroozi Leibowitz, Nassau County; Sandra Popelka, Seventh District; Christopher Arena, Third District.
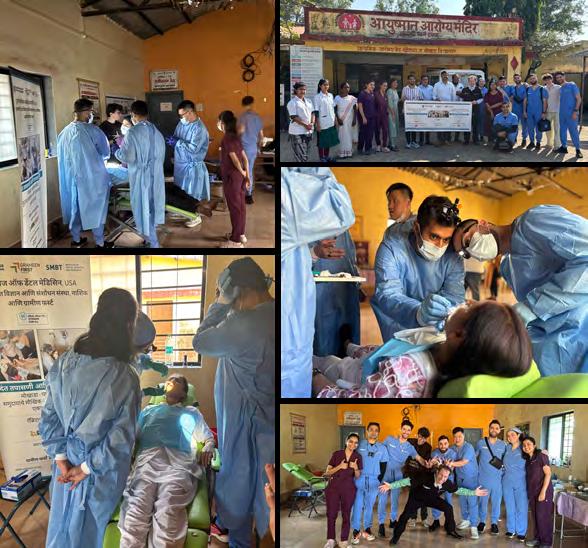
Student Mission Delivers Needed Care
THIS PAST DECEMBER, six third-year dental students from Touro College of Dental Medicine New York and New Mexico campuses traveled to Mukata Maharashtra, India, a remote area north of Mumbai, to deliver dental care to an underserved population, most of whom were receiving care for the first time. Working out of a temporary clinic in an unused building, the team performed 120 oral exams, 80 extractions and 30 cleanings over three days. Students carried out their mission under supervision of Touro faculty member Dr. Robert Weber and in partnership with local NGO Gabriel Project Mumbai.
Association Activities
Council on Nominations Approves Officer Slate
The NYSDA Council on Nominations meeting in March via Zoom approved the following slate of officers, which if confirmed by NYSDA House in June, will lead the Association in 2026-2027:
• Dr. Amarilis Jacobo of Bronx County, currently serving as president-elect, was advanced to the office of president.
• Dr. Lynn A. Stacy of the Fifth District, currently serving as vice president, was nominated for the office of president-elect.
• Dr. Michael Shreck of Nassau County was nominated for the office of vice president.
• Dr. Paul R. Leary of Suffolk County was nominated to continue in the office of secretary-treasurer. In one additional action, the council nominated William Karp of the Fifth District to continue in the office of speaker of the House.
In Memoriam
SECOND DISTRICT
Thomas Dennison
New York University ‘66 250 Ridgedale Ave., #M6
Florham Park, NJ 07932
December 21, 2025
Harold Weiss
New York University ‘59
134 Mariner Lane
Bay Shore, NY 11706
March 21, 2026
SIXTH DISTRICT
Alan Hinkley
University at Buffalo ‘66 1932 Falling Waters Road, #247 Knoxville, TN 37922
March 10, 2026
EIGHTH DISTRICT
Brian Cushing
University at Buffalo ‘65 20 Schimwood Court Getzville, NY 14068
March 4, 2026
TCDM Students Take First Prize in National Contest
WINNERS of the 2025 Dental Student Health Literacy Video Contest sponsored by the ADA and National Advisory Committee on Health Literacy in Dentistry are from Touro College of Dental Medicine: second-year student Faith Nguyen and fourth-year student Kwadwo Ampofo. Their winning entry, “X-Ray Vision: Inside Your Smile,” was a creative solution for responding to patient questions about oral healthcare and recommended dental treatment.
Winners of the contest, which is also sponsored by Colgate, shared a $2,000 prize for their first-place finish.
NINTH DISTRICT
Walter Lipson
New York University ‘58 101 Gedney Street, #5B Nyack, NY 10960
May 22, 2024
SUFFOLK COUNTY
Carl Girolamo
New York University ‘83
18 Elizabeth Drive
Syosset, NY 11791
July 29, 2023
Resolution of Severe Lateral Open Bite with Surgically Enhanced Orthodontic and Myofunctional Therapies
Daniel Kuncio, D.D.S.; Maria Karpov, D.M.D.
ABSTRACT
Patients often present to our practices with dental relapse of previous orthodontic treatment. Many times, the underlying skeletal and/or functional problems leading to the malocclusion were not addressed, causing the teeth to revert to their initial positions, even with good retainer wear. This patient presented with a severe lateral open bite and complained of problems chewing on his right side.
Previous orthodontic treatment with fixed orthodontics appliances and vertical elastics proved to be unstable. We recommended a treatment plan with surgically assisted rapid palatal expansion (SARPE)[1] to correct the skeletal maxillary constriction and provide more tongue space, followed by surgically facilitated orthodontic therapy (SFOT),[2,3] with myofunctional therapy to address the lateral tongue thrust most likely contributing to relapse.[4,5,6]
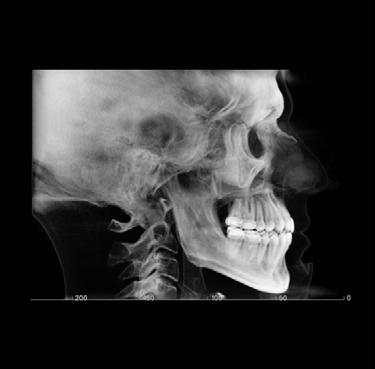
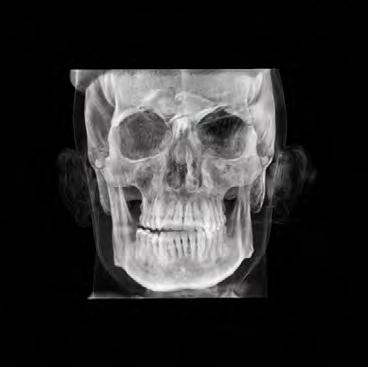
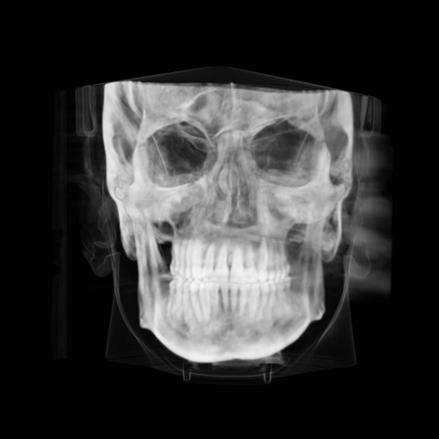
Clinical evaluation showed a mild Class III skeletal pattern with a constricted maxilla, mildly dolichofacial and straight
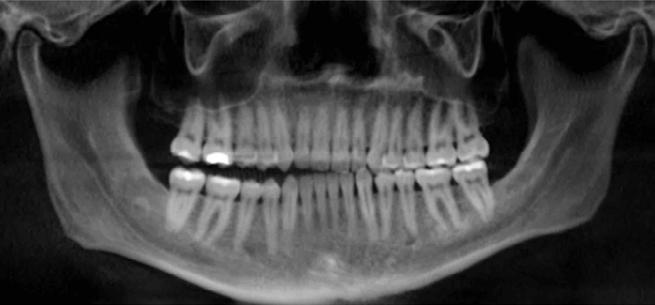
profile (Figure 1). Full adult dentition was present with all third molars extracted. Maxillary and mandibular incisors were normoclined. The maxillary midline coincided with the facial midline, and the mandibular midline was 2 mm to the right of the facial midline. There was a 2 mm to 5 mm lateral open bite on the right side from the second molar to the lateral incisor, and the maxillary occlusal plane was canted to the left of the interpupillary line. A lateral tongue thrust into the open bite was noted on swallow.
The right side was in posterior crossbite and there was an edge-to-edge anterior bite with wear on the maxillary central incisors. Mild gingival recession was noted, but soft tissue was generally within normal limits. CBCT analysis found no radiographic evidence of osteoarthritis in the TMJ joints, nor osseous or apical pathology involving the maxillary or mandibular teeth. His airway was not constricted. Initial report from the myofunctional therapist indicated that the patient never developed a mature swallow sequence and had a bilateral posterior tongue thrust.
The treatment objectives were to correct the midlines and coordinate the dental arches, close the lateral open bite, correct the posterior crossbite and provide adequate tongue space, level the occlusal cants and address the tongue-thrusting habit. To achieve these goals, the following treatment plan was recommended.
• Surgically assisted rapid palatal expander (SARPE), along with mandibular self-ligating fixed appliances to level, align and upright the mandibular dentition during maxillary expansion.
• After expansion, place maxillary self-ligating fixed appliances to level and align the maxillary arch.
• Switch to SureSmile custom wires for more accurate posterior occlusion.
• Refer to oral surgeon for a partial SFOT procedure on the maxillary and mandibular right segments for skeletal correction of the lateral open bite.
• Refer to myofunctional therapist to correct the lateral tongue-thrust habit.
Estimated treatment time is 20 to 24 months. Eight 30-minute myofunctional therapy sessions were recommended to address the resting, chewing, swallowing and speaking functions.
Treatment Progress
Palatal mini-implants were placed by a periodontist, followed by placement of the rapid palatal expander (RPE) and bonding of the mandibular arch with self-ligating Damon clear braces. Patient had SARPE surgery performed by the oral surgeon three weeks later (Figure 2), and the expander was turned once a day for three weeks (Figure 3). The maxillary arch was then bonded. Both archwires were incremen-


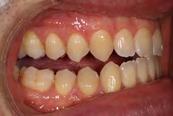
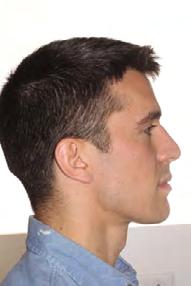
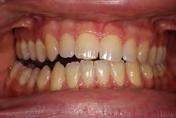
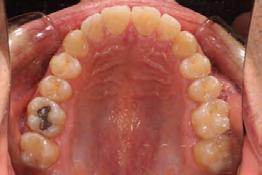
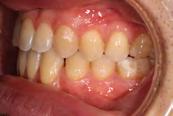
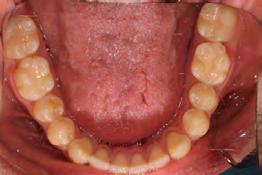
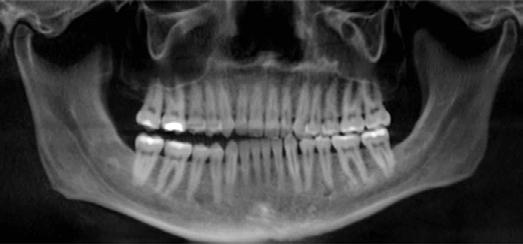
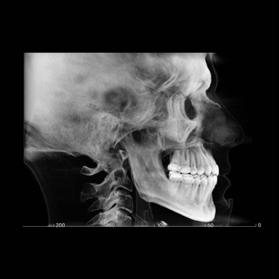
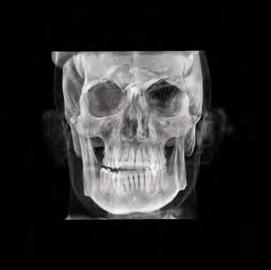
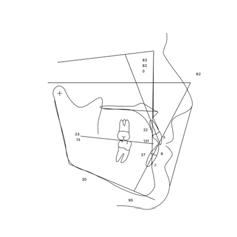
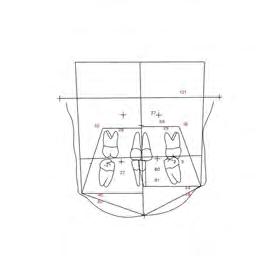
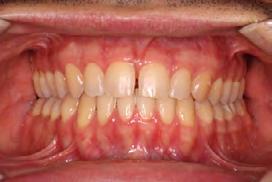
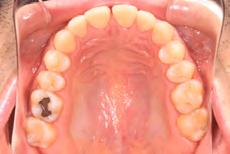
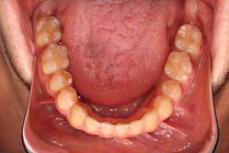
Figure 1. Initial records.
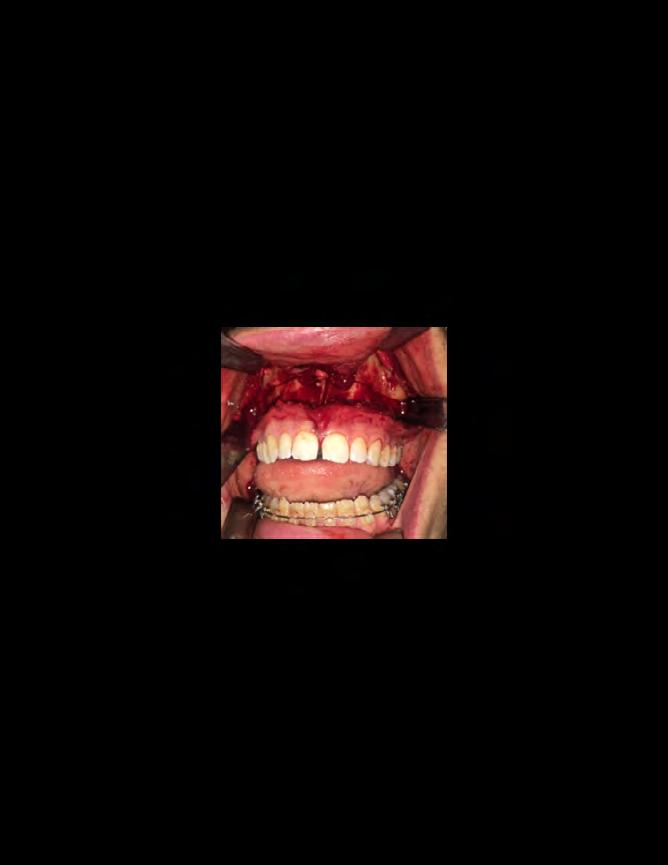
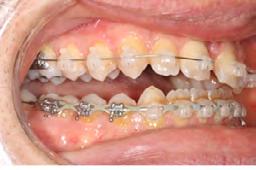
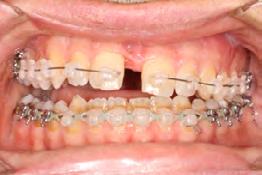
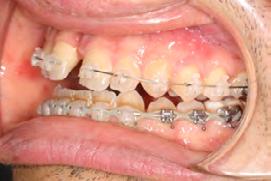
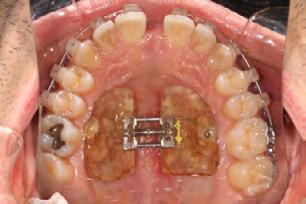
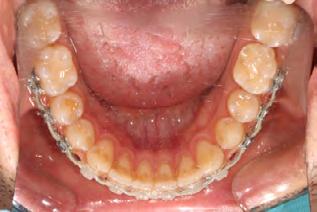
tally upgraded to an 18 x 25 NiTi wire, and the patient was placed on vertical elastics on the right side. With enough space for the tongue, the lateral open bite began to close.
Approximately six months after insertion of the RPE, digital scans were taken for SureSmile custom wires and the patient was scheduled for the SFOT procedure with the oral surgeon. The RPE was removed, SureSmile wires inserted and segmental corticotomies performed, immediately followed by further vertical elastics on the right side (Figure
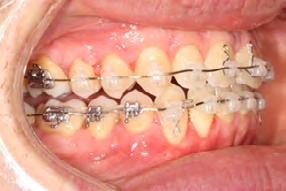
4). Archwires were upgraded incrementally into 19 x 25 SS. Once the bite was completely closed, the patient was referred to the myofunctional therapist to begin treatment. Eight sessions of myofunctional exercises were performed, focusing on muscle building, toning, synchronicity and awareness. Improvement in correct chewing, swallowing and resting postures of the lip and tongue were addressed. All appliances were removed 21 months after initial insertion (Figure 5), and the patient was referred to a re-
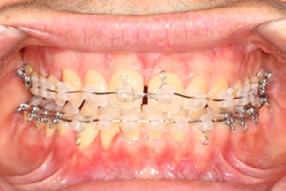
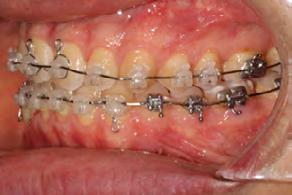
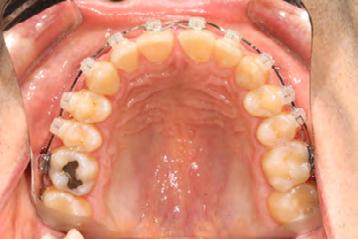
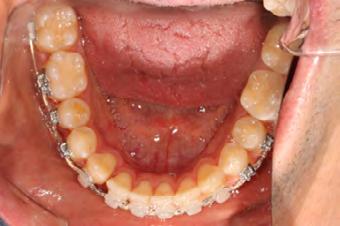
Figure 4. Post-corticotomy, with SureSmile custom wires.



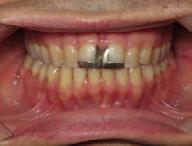
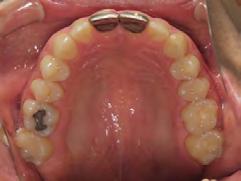
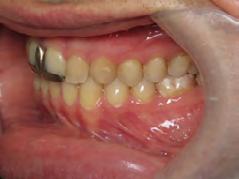
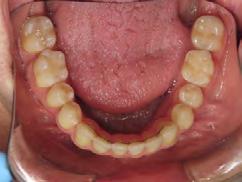
storative dentist for veneers on the maxillary central incisors; the patient opted for gold veneers (Figure 6). Clear removable retainers were inserted with a fixed mandibular retainer canine-to-canine.
Treatment Results
The patient finished with Class I occlusion, ideal overbite and overjet. The arches are co-
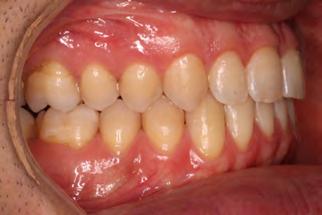
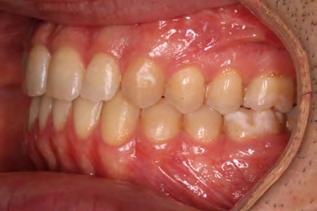
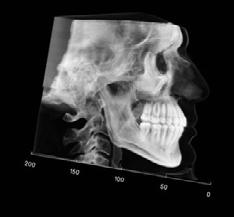
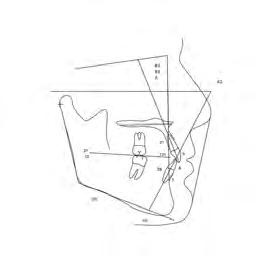
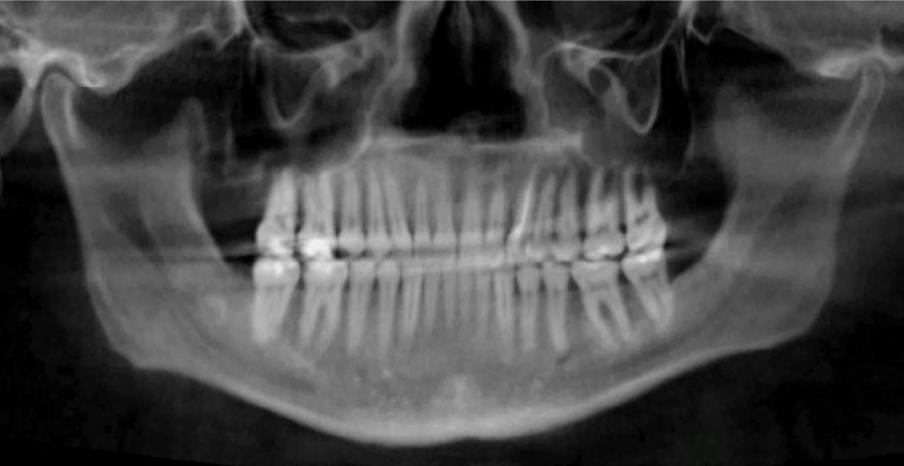
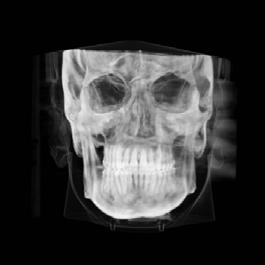
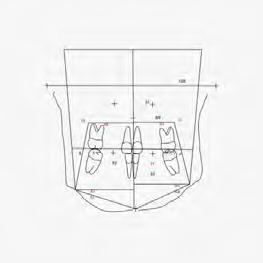
Figure 5. Final records.

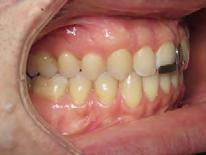

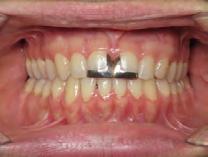
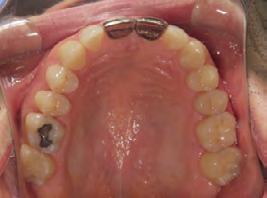

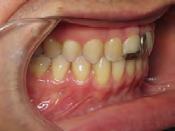

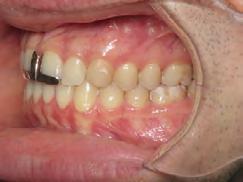
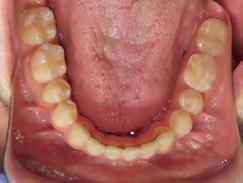


ordinated, lateral open bite closed and occlusal cants leveled. From the frontal cephalometric tracings, maxillary width increased from 58 mm to 69 mm. From the lateral cephalometric tracing, the incisor angulations remained unchanged. The final report from the myofunctional therapist indicated the patient eliminated the bilateral posterior tongue-thrust swallowing pattern with saliva, liquid and solid swallows. Correct swallowing mechanics were demonstrated while sipping/gulping liquids from a cup. His day and nighttime tongue-resting postures were reported to be on his incisive papilla, with lateral margins lightly suctioned into the upper arch. Lips were closed and competent diurnally and nocturnally.
Most recent records are two years after removal of the orthodontic appliances, demonstrating the stability of the results (Figure 7).
Clinical orthodontic work completed by Dr. Maria Karpov; SARPE and SFOT performed by Dr. Sherrill Fay; myofunctional therapy performed by Dana Hockenbury. Queries about this article can be sent to Dr. Karpov at mariakarpov@yahoo.com.
REFERENCES
1. Suri L, Taneja P. Surgically assisted rapid palatal expansion. Am J Ortho Dentofacial Orthopedic 2008 Feb;133(2):290-302.
2. Brugnami F, Caiazzo A, Mehra P. Can corticotomy (with or without bone grafting) expand the limits of safe orthodontic therapy? J Oral Biol Craniofac Res 2018;8:1-6.
3. Kuncio D, Karpov M, Fay S. Surgically enhanced orthodontic treatment. NY State Dental J 2017 June/July;83(4):31-3.
4. Cabrera MdC, Cabrera CAG, deFreitas KMS, Janson G, deFreitas MR. Lateral open bite: treatment and stability. Am J Ortho Dentofacial Orthopedic 2010 May;137(5):701-1.
5. Alexander RG. The role of occlusal forces in open-bite treatment. J Clin Orthod 2000 January;34:23-9.
6. Shah SS, Nankar MY, Bendgude VD, Shetty BR. Orofacial myofunctional therapy in tongue thrust habit: a narrative review. Int J Clin Pediatr Dent 2021 Mar/April;14(2):298-303.


Daniel Kuncio, D.D.S., is an orthodontist in private practice in New York City. He is former assistant professor and clinical attending at Montefiore Medical Center, Albert Einstein College of Medicine and BronxCare Health System, Icahn School of Medicine at Mount Sinai.
Maria Karpov, D.M.D., is an orthodontist in private practice in New York City. She is a former assistant professor and clinical attending at the School of Dental Medicine at the University of Pennsylvania.
Figure 6. Post-restorative work.
Figure 7. Two years post-debond.
Dr. Kuncio Dr. Karpov

Laser-Assisted New Attachment Procedure A Review
Divya Khanna, B.D.S., M.D.S.
ABSTRACT
Periodontal treatment modalities have evolved substantially to evidence-based minimally invasive treatment options. Lasers have proved to be an effective tool by providing a myriad of benefits and advantages while eliminating many of the negative sequelae that have been historically associated with conventional pocket elimination surgery. Laser-assisted new attachment procedure (LANAP) is a welldefined treatment protocol that has been validated with human histology and has demonstrated both short- and long-term success. LANAP has proven to be an effective, safe and predictable treatment option for achieving regeneration and new attachment formation, leading to favorable clinical outcomes, improved patient compliance and acceptability.
Dental therapeutics have evolved tremendously over the past few decades to the benefit of both the clinician and the patient. Newer materials and technologies are being researched and introduced every day, which not only improves efficiency but the predictability of treatment modalities as well.
Light amplification by stimulated emission of radiation (LASER) today forms an inevitable tool in the spectrum of possible medical, dental and periodontal therapies. Everyday clinicians are discovering myriad applications of lasers for various treatment options. Lasers not only increase patient comfort, they reduce surgical time, provide bloodless field and sterile operating site and greatly enhance patient acceptance of treatment, thereby increasing compliance as well.[1] One such technique being utilized more in clinical dentistry is the laser-assisted new attachment procedure (LANAP).[3] The concept of LANAP took hold in 1989 with Dr. Robert Gregg and Dr. Del McCathy. They encountered patients who refused to undergo traditional surgery and tooth extraction. This led them to develop LANAP. The LANAP protocol eventually achieved United States FDA clearance in 2004 (FDA 510k clearance K030290), after which it opened a multitude of avenues for research in the field of periodontology.
Nd:YAG (Neodymium
Yttrium Aluminium Garnet) Lasers Since its discovery at Bell Labs in 1964, Nd:YAG laser has undergone an enormous evolution. It mainly consists of a semi-organic nonlinear crystal and is employed in multiple applications in material processing, such as coating, welding, polishing, drilling and processing of metallic thin films; in medicine as a treatment modality, drug adminis-
tration, etc.; and in various other fields, like semiconductor nano-technology, plasma spectroscopy and laser-induced breakdown spectroscopy.[5,6,7]
Diode lasers and carbon dioxide lasers are also known for their selective absorption in pigmented tissues, but the Nd:YAG laser selectively and intensely gets absorbed by diseased tissue and has bactericidal effect on pigmented bacteria. The Nd:YAG’s capacity to function at extremely high peak powers with longer pulse widths in short timeframes, enables it to have deeper penetration and more noticeable thermal effects, both of which are essential for achieving disinfecting and preventing collateral damage,[2,8,9] making them an ideal choice for LANAP.[3]
Achieving true regeneration or reconstitution has been an elusive goal for periodontists globally. Hence, a great deal of present clinical research in periodontology is directed at achieving this goal.
In 1996 at the World Workshop in Periodontics, a specific histologic criterion for proof of regeneration was established.[10]It states that experimental teeth must have periodontitis-related loss of CTA (connective tissue attachment) and AB (alveolar bone). Regeneration is evidenced by the presence of new CEM (cementum), PDL (periodontal ligament) and AB coronal to the apical extent of the notch, which is marked presurgically, prior to attempting any regenerative procedure.[11] Similarly, proof of new attachment is demonstrated by new CEM and CTA formation.[10]
Laser-Assisted New Attachment Procedure
In concept, the LANAP protocol is simple, safe and rather predictable, when compared to conventional periodontal procedures. Healing with LANAP is mainly reported to be either true regeneration, new attachment formation or by long junctional epithelium.[10,11,12]
The FDA[4] approved it as “cementum-mediated periodontal ligament new attachment to the root surface in absence of long junctional epithelium” because of its benefits and impact on the pocket’s soft-tissue wall, which led to a reduction in the size of the pocket. LANAP biologically regenerates the tooth-supporting structures, CEM and PDL without relying on less ideal tissue healing by long junctional epithelium and leads to a measurable improvement in reduction of pocket depth, thus indicating not just healing, but also true periodontal regeneration. LANAP with laser sulcular debridement received approval initially for carbon dioxide laser and Nd:YAG laser.[4,13]
Critical probing depth is explained as the baseline PD (probing depth) value, above which the outcome of therapy will result in attachment gain, and below which outcome of therapy will result in attachment loss. Lindhe and So-
cransky, in 1982, proposed the critical probing depth for scaling and root planing to be 2.9 mm and for periodontal flap surgery as 4.2 mm. Critical PD for LANAP therapy was suggested as 4.88 mm by Nevins et al., in 2014.[14] LANAP has a specified protocol of well-researched and proven operating specifications that was granted FDA clearance in 2004.[4,13,15] The steps involved in LANAP protocol are listed below.
1. Periodontal probing around the affected teeth to determine pocket depth and identify calculus deposits subgingivally. After administration of local anaesthesia at the surgical site, bone sounding around each affected tooth is carried out to determine the areas of osseous defects that cannot be seen radiographically.
2. An optic fibre tip measuring 0.3-0.4μ is placed parallel to the root surface. First pass laser is used to dissipate energy, at 4.0 W (mean power), free running 100 milliseconds pulse duration at 20 Hz. It travels laterally and apically, paralleling the root surface, from the gingival margin to the pocket base. The aim of doing this is to remove only the diseased pocket epithelium and, simultaneously, decontaminate the pocket by affecting the bacteria and their thermo-labile toxins, which lead to periodontal disease. Thermo-labile toxins are bacterial proteinaceous toxins that are heat-sensitive in nature and lose their toxic properties when exposed to elevated temperatures, typically around 60°C or higher. These toxin proteins are inactivated by denaturation when heated. It also increases the vascular access to the wound (inflamed periodontal pocket wall) and causes the tissues to relax for easy insertion of the instruments for scaling and root planing.
3. Calculus on the root surfaces is removed using piezo scalers. After the laser energy interacts with the calculus, it is simpler to remove, due to tissue relaxation and formation of mini flap after the use of lasers.
4. Laser application is done for the second time with variation in parameters, energy dissipation at 4.0 W, 650 milliseconds pulse duration at 20 Hz from the apical extent of defect to the gingival margin. To improve the ability to create a fibrin clot to seal the mini flap and disinfect the site again, the parameters are changed. The fibrin clot is essential to promote healing in the initial 14 days, hence should remain stable in the initial phases of wound healing. It seals the sulcus against bacterial infiltration and prevents epithelial downgrowth into the sulcus, preventing healing through the formation of long junctional epithelium.
5. Compression of the fibrin clot to seal any dead space and remove any exudates improves the healing process
and promotes closer approximation to enhance the healing.
6. Refining the occlusion is essential, followed by patient education, motivation and follow-up.
It is crucial to note that periodontal probing is not done until sulcus becomes completely epithelized and stable with no signs of inflammation or suppuration. The junctional epithelium undergoes repair and reattachment, which can take up to four to six weeks. Early probing can traumatize healing tissues, potentially disrupt new attachment or lead to false pocket readings.
Several authors, including Yukna et al., Nevins et al., McAllister, Brown and Harris et al., and McCawley et al., used this methodology in their main research investigations, yielding unambiguous favorable results for LANAP. [10,14,16-19]
Discussion
Laser dentistry is new technology that helps to treat patients with a high degree of precision and accuracy. For proper utilization of lasers, the clinician should have exact knowledge of the characteristics and effects of each laser system and its applications, tissue characteristics and interaction between the two, as well as a full understanding of the conventional treatment procedures and, finally, should exercise appropriate caution during use.
Diseased pocket epithelium removal has been the basis or foundation of subgingival curettage, the excisional new attachment procedure (ENAP) that would result in a favorable environment for new CTA, which is the hallmark of regeneration.[20-22] However, elimination of pocket epithelium by conventional procedures like curettage and ENAP appears nearly impossible.[22,23] Laser is an effective and advanced technology to overcome the limitations of various traditional treatment modalities. Lasers offer multiple advantages, like complete access and disinfection during the treatment of periodontal pockets, bactericidal effect, detoxification effect, and removal of the epithelium lining and granulation tissue.[1,2,5-7]
In a study by McCawley et al. in 2014, LANAP protocol was also proven to immediately bring about a suppression in the red and orange complex periodontal pathogens below culture detection limits in periodontal pockets >6mm deep.[19]
In the largest human histology research, Yukna et al. conducted and reported that LANAP therapy produced positive results in comparison to traditional periodontal therapy. The results were very promising, showing that 100% of the teeth treated with LANAP formed new attachment as opposed to 0% of the control teeth.[3,10] A split-mouth, randomized multi-center trial guided by Harris et al. in 2014, advocated that LANAP protocol could produce a systemic
effect on subgingival wound healing and minimal postoperative discomfort to the patient.[18]
McAllister in a 2009 study reported apparent clear radiographic bone regeneration after LANAP, thus demonstrating the definitive favorable effects of LANAP employing the Nd:YAG laser for the treatment of moderate-to-severe adult periodontitis. He concluded that LANAP unveils a less invasive approach and shows better patient compliance.[16]
Nevins et al. carried out another significant landmark human block research in 2012, demonstrating that individuals with severe periodontitis who received LANAP had positive and successful outcomes.[11] Moreover, in 2014, Nevins et al. conducted another prospective LANAP clinical study with a nine-month follow-up on eight patients with advanced periodontitis and achieved a 73% reduction in PD and 58% gain in CAL.[13]
Mayfield and Trombelli, in 2002, reported significant CAL gain and PD reduction in pockets >6mm after open-flap debridement.[24] Similar results were reported by Philstrom et al. in 1983.[25] LANAP studies have shown comparable and promising results in short-term evaluations.[14,26] Initial studies indicate promising results with LAPIP. Schwarz & Harris conducted a retrospective analysis of clinical outcomes of 437 implants diagnosed with per-implantitis and treatment with LAPIP protocol. A 94% survival rate was recorded after 13 months follow-up from the diseased implants analyzed.[27]
Conclusion
LANAP as an adjunctive treatment option provides greater control of inflammation and positive clinical results. Hence, it can be considered a valid alternative for treatment of periodontal disease. Since no adverse effects to this treatment modality have been reported in the literature, it’s a safe and promising alternative to surgical pocket-reduction techniques.
LANAP offers the advantage of being a minimally invasive, predictable, cost- and time-effective method to achieve pocket reduction and regenerative outcomes. Currently, LAPIP (laser-assisted peri-implant procedure), which is still in its infancy, is being researched for the treatment of peri-implantitis.
Future Perspective
There is a need for multi-centric, randomized controlled clinical trials with a larger sample size and longer followup time for comparison and to check the efficacy of LANAP with various conventional surgical and nonsurgical treatment modalities. Further, there is a need for evaluation of true regeneration histologically, achieved by LANAP protocol and LAPIP in peri-implantitis cases.
The author has declared no conflict of interest nor potential conflict of interest relevant to this article. Neither has she received any funding support. Queries about this article can be sent to Dr. Khanna at drdivyakhanna31@gmail.com.
REFERENCES
1. Lin Z, Rios HF, Cochran DL. Emerging regenerative approaches for periodontal reconstruction. A systematic review. J Periodontal 2015;Feb 86(2):S134-S152.
2. Convissar RA. Principles and practice of laser dentistry. AAP (The American Academy of Periodontology). Lasers in Periodontics (position paper). Chicago: AAP, 1991:1–5.
3. Yukna RA, Evans GH, Vastardis S, Carr RF. Human periodontal regeneration following the laser assisted new attachment procedure. J Dent Res 2004; 83(Special issue A): Abstract 2411.
4. US Food and Drug Administration. 510(k)s Final Decisions Rendered for July 2004 (PerioLaseMVP-7, 510(k) numberK030290). Available at: http://www.accessdata.fda.gov/cdrh_docs/ pdf3/k030290.pdf. Accessed: August 16, 2012.
5. George R. Lasers in dentistry—review. Int J of Dent Clin 2009;1(1):13-19.
6. Rossmann JA, Cobb CM. Lasers in periodontal therapy. Periodontol2000 1995;(9):150-164.
7. Lasers in periodontics. J Periodontol 2002 73:1231-1239.
8. Lasers in periodontics (position paper). AAP (The American Academy of Periodontology). J Periodontol 1996; 67: 826–830.
9. Quadri T, Poddani P, Javed F, Turner J, Gustafsson A. Short term evaluation of Nd:YAG laser as an adjunct to scaling and root planing in the treatment of periodontal inflammation. J Periodontol 2010;81:1161-1166.
10. Yukna RA, Carr RL, Evans GH. Histologic evaluation of an Nd:YAG Laser–assisted new attachment procedure in humans. Int J Periodontics Restorative Dent 2007;27:577–587.
11. Nevins ML, Camelo M, Schupbach P, Kim SW, Kim DM, Nevins M. Human clinical histological evaluation of LANAP. Int J Periodontics Rest Dent 2012;32:497-507.
12. Yukna RA, Carr RL, Evans GH. Histological evaluation of Nd: YAG laser- assisted new attachment procedure in humans. Int J Periodontics Rest Dent 2014;27:577-587.
13. Robert HG. Introduction to the LANAP protocol for the treatment of periodontitis. C.E. article_ LANAP procedure. https://www.lanap.com/site/wp-content/uploads/2016/08/ Dr.Gregg-CE-article-Laser-2012.pdf.
14. Nevins M, Kim SW, Camelo M, Martin IS, Kim D, Nevins M. A prospective 9-month human clinical evaluation of laser assisted new attachment procedure therapy. Int J Periodontics Restorative Dent 2014;34:21-27.
15. Jha A, Gupta V, Adinarayan R. LANAP, periodontics and beyond: a review. J Lasers Med Sci 2018;9(2):76-81.
16. McAllister J. A high-tech approach to managing periodontal disease: case reports. Compend Contin Educ Dent 2009;30(4):228-230, 232-223.
17. Brown S. Current advances in the use of lasers in periodontal therapy: a laser-assisted new attachment procedure case series. Clin Adv Periodontics 2013;3:96-104.
18. Harris DM, Nicholson DM, McCarthy D, et al. Change in clinical indices following laser or scalpel treatment for periodontitis: a split-mouth, randomized, multi-center trial. Proc SPIE Int Soc Opt Eng 2014;8929:89290G-1.
19. McCawley TK, McCawley MN, Rams TE. LANAP immediate effects in vivo on human chronic periodontitis microbiota. J Dent Res 2014;93(Special A):428.
20. Yukna RA, Bowers GM, Lawrence JJ, Fedi PF Jr. A clinical study of healing in humans following the excisional new attachment procedure. J Periodontol 1976;47:696–700.
21. Echeverria JJ, Caffesse RG. Effects of gingival curettage when performed 1 month after root instrumentation. A biometric evaluation. J Clin Periodontol 1983;10: 277–286.
22. Ramfjord SP, Caffesse RG, Morrison EC, Hill RW, Kerry GJ, Appleberry EA, Nissle RR, Stults DL. Four modalities of periodontal treatment compared over 5 years. J Clin Periodontol 1987;14:445–452.
23. Litch JM, O’Leary TJ, Kafrawy AH. Pocket epithelium removal via crestal and subcrestal scalloped internal bevel incisions. J Periodontol 1984;55:142–148.
24. Heitz-Mayfield LJ, Trombelli L, Heitz F, Needleman I, Moles D. A systematic review of the effect of surgical debridement vs non-surgical debridement for the treatment of chronic periodontitis. J Clin Periodontol 2002;29 (Suppl 3):92-102.
25. Philstrom BL, McHugh RB, Oliphant TH, Ortiz-Campos C. Comparison of surgical and nonsurgical treatment of periodontal disease. A review of current studies and additional results after 6 1/2 years. J Clin Periodontol 1983 Sep;10(5):524-41.
26. Kimmel D. Laser-assisted new attachment procedure (LANAP). Laser 2011;3:6-9.
27. Schwarz GM, Harris DM. Laser-assisted treatment of peri-implantitis: a retrospective cohort study. Gen Dent 2020; 68(3):18-25.

Divya Khanna, B.D.S., M.D.S., is senior consultant periodontist, laser specialist and implantologist, AGM Clove Dental, New Delhi, India.

Endorsed Vendor Updates
NYSDA Membership Has it Perks: Exclusive Discounts for You
Did you know your NYSDA membership includes offers from a curated network of trusted, vetted vendors who understand the needs of dental professionals? Don’t miss out.
From everyday essentials to practice-enhancing services, these member-only discounts are one more way your NYSDA is working behind the scenes to support your success and help you get more value from your membership.
Taking advantage of these partnerships is an easy way to maximize your return on membership— delivering tangible benefits that go beyond education and advocacy.
Start exploring your member discounts today and see how these trusted partnerships can support both your practice and your bottom line.

Endorses Key Bank for Student Loan Refinancing Tackle student loan debt with an expert guide. As a NYSDA member, you can get personalized, one-on-one guidance and help understanding all your student loan options —including how to qualify for forgiveness—by scheduling your free consultation with a KeyBank student loan specialist. A student loan consultation can help you:
• Understand your repayment or forgiveness options, such as, Public Service Loan Forgiveness (PSLF),1 Income-Driven Repayment (IDR), or refinancing
• Get an exclusive 0.30% rate discount 2 on refinancing for NYSDA members
• Develop a personalized plan to manage student loan debt
• Go to KeyBank and schedule your 30-minute consultation to get started. 833.427.2265


Endorsed Vendor Updates

Webinar for NYSDA Members
Social media shouldn’t feel like another full-time job. In the on-demand webinar, “Using Social Media to Maximize Patient Engagement with NYSDA-endorsed ProSites,” you’ll learn how to simplify your strategy, stay consistent, and turn online engagement into real patient appointments without adding more to your plate—all in under 30 minutes. Watch it on demand today.
Shipping Discounts for
NYSDA Members
The world moves fast–and your ADA UPS® Savings Program has the tools you need to help your dental practice move even faster. They’re here to help you push envelopes and ride the edge of what’s possible. They’ll be right by your side with everything you need to keep blazing forward. Let UPS® help make your practice unstoppable. Members enjoy the following savings every time they ship:
• 65% off Domestic Next Day
• 42% off Ground
• 65% off International













Sign up for a new account or enroll your existing account. Already have an ADA UPS® Savings Program account? Re-enroll by calling 1-800Members (1-800-6362377) and give them your ADA number. Ask for Greg Brown, our dedicated Member Benefits Consultant (if possible).



Restoration of Dental Implants with Screw-Retained Crowns
Optimizing Contact Area Geometry to Prevent Food Impaction
John Mamoun, D.M.D.
ABSTRACT
A single-unit, screw-retained fixed partial denture or crown, made for a dental implant, may show food impaction between the screw-retained crown and an inter-proximal tooth surface. This restorative error may be due to an open contact or a large interproximal embrasure space volume between the screwretained prosthesis and an interproximal tooth surface. Food impaction may also occur due to the contact plane of the restoration being parallel with the contact plane of the neighboring tooth instead of a more correct contact plane geometry where both interproximal contact planes converge slightly towards each other to form a “triangular” embrasure space. These errors of contact plane geometry for a screw-retained restoration may be due to the screwretained restoration not having an optimal path of placement to follow for insertion into the implant.
This article defines the path of placement and the optimal contact area geometry of a screw-re-
tained implant crown restoration and describes how a dentist can contour interproximal tooth surfaces to facilitate an optimal path of placement for the screw-retained crown that will be made for a dental implant, to allow a dental laboratory technician to fabricate a fixed partial denture with an optimal contact area geometry. The article also shows how microscope-level magnification and coaxial illumination facilitate visualizing and optimizing the path of insertion for a screw-retained crown.
The path of placement of a fixed partial denture is a set of imaginary parallel axes, such that every atom (or mass element) of the fixed partial denture travels along an axis that is parallel to this set of imaginary axes, while the fixed partial denture is being seated onto its abutment. To prevent food impaction around a fixed partial denture made for an abutment, the plane of the interproximal surface of each tooth that neighbors the fixed partial denture should converge slightly towards the set of imaginary parallel axes that form the path of placement of the fixed partial denture. This slight convergence of the neighboring tooth interproximal surface to the axes of the fixed partial denture path of placement
permits fabricating a fixed partial denture that follows a specific path of placement, such that the resulting prosthesis will have interproximal contact planes with a tiny angle of convergence with neighboring interproximal tooth surfaces and minimal embrasure space volume between the prosthesis and the neighboring teeth. This may result in minimal or no food impaction at the interproximal contact areas.[1,2]
There are minimal evidence-based criteria that define what constitutes an ideal interproximal contact plane geometry that will minimize food impaction between a fixed partial denture and a neighboring tooth.[3-15] The author suggests that an optimal contact area geometry has three components. First, the interproximal surfaces of the fixed partial denture and a neighboring tooth should slightly converge towards one another. Second, the embrasure space volume between the two surfaces should be minimal. Third, the contact between the two interproximal surfaces should consist of a contact area, instead of a contact line consisting of the occlusal-interproximal line angle.
The cylinder-shaped intaglio surface and volume of an implant will rigidly define the path of placement of a screwretained fixed partial denture that will be made for that implant. The circular perimeter, and the relatively cylindrical three-dimensional shape of an implant intaglio volume, form the dimensions of an imaginary cylinder. The set of imaginary parallel axes that form this imaginary implant intaglio cylinder forms the set of imaginary parallel axes of the path of placement of the future screw-retained prosthesis made for this implant.
For a laboratory technician to be able to fabricate a screw-retained restoration for an implant that features an optimal contact area geometry, the interproximal surface of each tooth neighboring the future screw-retained prosthesis should converge slightly towards the set of imaginary parallel axes that form the cylindrical path of placement of the future screw-retained prosthesis. This slight convergence allows the laboratory technician to fabricate a screwretained prosthesis that can follow the path of placement defined by the cylindrical shape of the implant intaglio surface and that also has interproximal surfaces that can slightly converge towards the interproximal surfaces of the neighboring teeth (Figure 1).
This slight convergence of interproximal surfaces between the screw-retained prosthesis interproximal surface and a neighboring tooth interproximal surface will result in a screw-retained prosthesis with minimal embrasure space volume between the prosthesis and a neighboring tooth at a specific interproximal contact area. The less volume the embrasure space has, the less food that hypothetically might impact into the embrasure space (Figure 2).
If the plane of a neighboring tooth interproximal surface is slightly divergent relative to the set of imaginary axes that form the path of placement of the screw-retained restoration, then the laboratory technician will be forced to fabricate a screw-retained prosthesis such that the contact
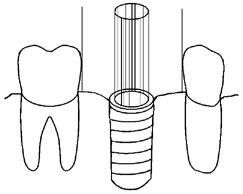
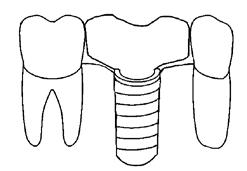
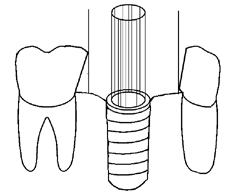
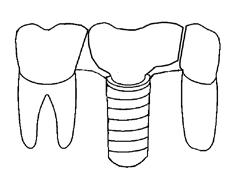
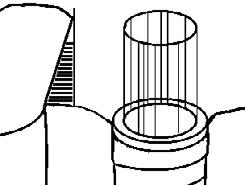
Figure 1. Diagram shows optimal interproximal contact plane geometry, where neighboring teeth interproximal contact planes converge by tiny angle towards set of imaginary parallel axes that form imaginary cylinder-shaped path of placement determined by cylinder-shaped intaglio volume of implant.
Figure 2. Diagram shows screw-retained crown placed with optimal interproximal contacts, resulting in small interproximal volume space with both neighboring teeth, thanks to slightly convergent interproximal surfaces of neighboring teeth.
Figure 3. Diagram shows two examples of nonoptimal interproximal contact plane geometries. Neighboring molar interproximal surface converges at wide angle towards set of imaginary parallel axes that form imaginary cylinder-shaped path of placement that is determined by cylinder-shaped intaglio volume of implant. Neighboring premolar interproximal surface diverges from path of placement axes.
Figure 4. Diagram shows screw-retained crown placed with nonoptimal interproximal contacts, resulting in “teepee” contact with large interproximal volume space with neighboring molar, and a noncontacting interproximal crown surface that is parallel with, but not contacting, divergent premolar interproximal surface.
Figure 5. Imaginary plane shown parallel with axes that form path of placement of future screw-retained crown and also intersects occlusal-interproximal line angle of tooth neighboring implant. Linear bars at each vertical height point along neighboring tooth interproximal surface show distance between interproximal surface and imaginary plane at different vertical height points. Laboratory technician cannot shape crown interproximal surface material to be closer to tooth interproximal surface than distance between imaginary plane and interproximal surface at various vertical height points.
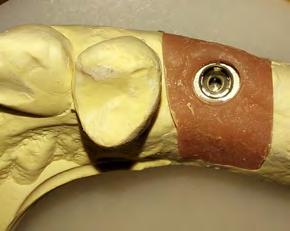
6. Model shows optimal, interproximal contact plane on premolar neighboring implant. Only superior line angle of interproximal surface is visible when implant is viewed such that entire intaglio surface volume of implant is visible, which corresponds with viewing axis parallel with set of imaginary parallel axes that form cylinder-shaped path of placement of implant.
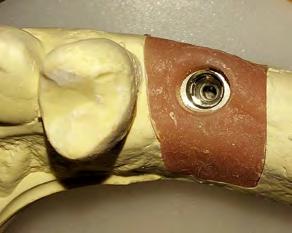
Figure 7. Same implant in Figure 6, now viewed with viewing axis that is shifted by tiny angle, such that viewing axis is slightly nonparallel with axes of path of placement. Slight reduction of visibility of implant intaglio surface proves viewing angle is only slightly off parallel with axes of the path of placement formed by the implant intaglio volume. Inferior line angle of interproximal contact is barely visible in this slightly off-parallel viewing axis, which proves interproximal surface has optimal, tiny tilt angle slightly convergent towards path of placement axes.
plane of the prosthesis is parallel with the contact plane of that divergent interproximal tooth surface and the parallel interproximal surfaces cannot contact each other. A divergent tooth interproximal surface is one where the superior aspect of the interproximal surface is more distal from the implant compared to the inferior aspect of that interproximal surface (Figure 3).
If the plane of a neighboring tooth interproximal surface converges at a large angle (Figure 3) towards the set of imaginary parallel axes that form the cylindrical path of placement of the future screw-retained prosthesis, the laboratory technician will be forced to design a screw-retained prosthesis with a large embrasure space volume at that interproximal contact (Figure 4).
Embrasure Space Geometry
An imaginary plane can be envisioned that is parallel to the axes that form the path of placement of the future screw-retained crown. This plane can be visualized as intersecting the occlusal-interproximal line angle of a tooth neighboring the future screw-retained crown. The interproximal surface of that neighboring tooth, and the imaginary plane, form an imaginary three-dimensional triangle. The volume of this imaginary triangle will be the maximum volume of the interproximal embrasure space between that tooth and the future screw-retained crown made for that implant. The larger the angle at which the interproximal surface converges towards the imaginary axes of the path of placement of that future screw-retained crown, the larger the volume of that imaginary triangle will be, and the larger the volume of the resulting interproximal embrasure space at that interproximal contact will be.
8. Model shows nonoptimal, divergent, interproximal contact plane on premolar neighboring implant. Both superior and inferior line angles of interproximal surface are visible when implant is viewed such that entire intaglio surface volume of implant is visible, which corresponds with viewing axis parallel with set of imaginary parallel axes that form the cylindershaped path of placement of implant.
At each vertical height point along the interproximal surface of a tooth neighboring the future screw-retained crown, there is a specific quantity of linear distance between that point and the imaginary plane (Figure 5). This specific distance, at each vertical point along the neighboring tooth interproximal surface, forms an imaginary linear distance boundary. When a laboratory technician fabricates a screw-retained crown that follows the path of placement that is defined by the cylinder-shaped intaglio surface of the implant for that crown, the technician cannot form crown interproximal surface material any closer towards the interproximal tooth surface than the distance limit formed by this boundary.
Put another way, the technician cannot form crown interproximal surface material any closer to the interproximal tooth surface than the distance formed between the interproximal surface and the imaginary plane that is both parallel to the path of placement axes of the screwretained crown and that also intersects the occlusal-interproximal line angle of that tooth neighboring the future screw-retained crown. Such crown material would be obstructed by the interproximal surface of the neighboring tooth while the screw-retained crown was being inserted along the implant-determined path of placement. Hence, an interproximal tooth surface that converges at a “tiny angle” towards the imaginary path of placement of the future screw-retained implant will allow a technician to make a screw-retained crown that shows minimum embrasure space volume at that interproximal tooth surface.
Interproximal Surface Contouring
A dentist may need to contour the interproximal surface of a neighboring tooth to reduce the angle at which the surface
Figure
Figure
converges towards the imaginary path of placement axes, from a large convergence angle to a small convergence angle. To determine how much to contour the interproximal surfaces of a tooth neighboring a future screw-retained implant crown, a dentist must identify a visual axis that allows the dentist to see the entire intaglio surface of the implant. This visual axis will then be parallel with the set of imaginary parallel axes that form the cylinder-shaped path of placement of the future screw-retained restoration. Typically, the dentist must identify such a parallel visual axis while observing the implant intaglio surface indirectly through an intraoral mirror. The dentist must then precisely move the mirror such that the visual axes provided by the mirror remain parallel with the set of imaginary axes that form the implant intaglio surface cylinder shape, until the dentist can observe an interproximal tooth surface with the mirror.
If the dentist can observe the superior aspect of the neighboring tooth interproximal surface, but not the inferior aspect, while viewing that interproximal surface with a viewing axis that is parallel with the set of imaginary axes
of the cylinder-shaped path of placement defined by the implant intaglio volume, then the interproximal surface is convergent with the set of imaginary parallel axes that form the path of placement of the future screw-retained restoration (Figure 6). At this position, if the dentist, by shifting the mirror by a tiny angle of perhaps 10 degrees or less, can see the inferior aspect of the interproximal surface of the neighboring tooth, then the interproximal tooth surface will be slightly convergent towards the set of imaginary parallel axes that form the path of placement of the future screw-retained restoration (Figure 7).
However, if instead, the dentist must shift the mirror at a relatively large angle of perhaps greater than 10 degrees to be able to see the inferior aspect of the neighboring tooth interproximal surface, then this interproximal surface converges with a relatively large angle towards the set of imaginary parallel axes that form the path of placement of the future screw-retained restoration. The dentist would need to trim the superior aspect of that heavily convergent neighboring tooth interproximal surface until that surface was slightly convergent with the set of imaginary parallel

axes that form the path of placement of the future screw-retained restoration. The dentist can use a thin, pointy, coneshaped aluminum oxide polishing bur to trim the superior line angle of the interproximal contact in a direction that is distal from the implant. The dentist trims the superior line angle of the interproximal surface until only a tiny tilt of a mouth mirror visual axis, which was previously parallel with the axes of the imaginary path of placement cylinder, will permit the dentist to see both the inferior and superior line angles of that interproximal tooth surface.
If the dentist can observe both the superior and inferior line angles of the interproximal tooth surface while viewing that interproximal surface with a viewing axis that is parallel with the set of imaginary axes of the cylinder-shaped path of placement defined by the implant intaglio volume, then the surface plane will be divergent with the set of imaginary parallel axes that forms the path of placement of the future screw-retained restoration (Figure 8). It may be difficult or impossible to contour a surface to convert a divergent interproximal tooth surface angle to a convergent angle.
Extreme visual precision is needed to visualize the imaginary cylinder of the path of placement formed by the intaglio volume of the implant and to determine if a visual axis used to observe an interproximal tooth surface is exactly parallel with the set of imaginary axes that form the path of placement of the future screw-retained prosthesis. The dentist needs extreme visual precision to determine if a tooth interproximal surface converges at a tiny angle (perhaps 10 degrees or less) towards the imaginary parallel axes of the projected path of placement of the future screw-retained crown. Microscope-level magnification of 6x to 8.0x or greater, combined with shadow-free, co-axial illumination, helps a dentist verify these characteristics with microscopic precision and to verify that contouring interproximal tooth surfaces have created more optimal interproximal contact plane geometries.
Conclusion
Prior to making impressions or a scan of an implant that will receive a screw-retained fixed partial denture,[16,17] the dentist should verify that the interproximal surfaces of teeth that will neighbor the future screw-retained crown are slightly convergent in angle with the set of imaginary axes that define the implant-dictated, cylinder-shaped path of placement of that future screw-retained implant prosthesis and contour interproximal surfaces, as needed, to achieve this slightly convergent angle. This slight angular convergence of the interproximal tooth surface will allow a laboratory technician to fabricate a screw-retained
prosthesis that will follow the implant-determined path of placement, such as to form an optimally shaped contact area with each neighboring tooth, which will help prevent future food impaction between the screw-retained crown and the neighboring interproximal surface(s).
Queries about this article can be sent to Dr. Mamoun at mamounjo@gmail.com
REFERENCES
1. Mamoun JS. The path of placement of a removable partial denture: a microscope-based approach to survey and design. J Adv Prosthodont 2015;7:76–84. doi: 10.4047/jap.2015.7.1.76.
2. Mamoun J. Preparing fixed partial denture abutments such that they provide a path of placement free of undercuts. Gen Dent 2012;60:519-525.
3. Abduo J, Lau D. Proximal contact loss between implant prostheses and adjacent natural teeth: a qualitative systematic review of prevalence, influencing factors and implications. Heliyon 2022 Aug 1;8(8):e10064. doi: 10.1016/j.heliyon.2022.e10064.
4. Bompolaki D, Edmondson SA, Katancik JA. Interproximal contact loss between implantsupported restorations and adjacent natural teeth: a retrospective cross-sectional study of 83 restorations with an up-to-10-year follow-up. J Prosthet Dent 2022 Mar;127(3):418-424. doi: 10.1016/j.prosdent.2020.09.034. Epub 2020 Dec 17.
5. Cheng Y, Wang Z, Shi Y, Guo Q, Li Q, Chai R, Wu F. Research on the characteristics of food impaction with tight proximal contacts based on deep learning. Comput Math Methods Med 2021 Nov 5;2021:1000820.
6. Chopra Aditi & Sivaraman, Karthik & Narayan, Aparna & Balakrishnan, Dhanasekar. Etiology and classification of food impaction around implants and implant-retained prosthesis. Clin Implant Dent Relat Res 2019;21:391–397.
7. French D, Naito M, Linke B. Interproximal contact loss in a retrospective cross-sectional study of 4325 implants: distribution and incidence and the effect on bone loss and periimplant soft tissue. J Prosthet Dent 2019;122:108–114.
8. Gasser TJW, Papageorgiou SN, Eliades T, Hämmerle CHF, Thoma DS. Interproximal contact loss at implant sites: a retrospective clinical study with a 10-year follow-up. Clin Oral Implants Res 2022 May;33(5):482-491. doi: 10.1111/clr.13908. Epub 2022 Mar 1.
9. Ghasemi S, Oveisi-Oskouei L, Torab A, Salehi-Pourmehr H, Babaloo A, Vahed N, Abolhasanpour N, Taghilou S, Ghasemi A. Prevalence of proximal contact loss between implant-supported fixed prosthesis and adjacent teeth and associated factors: a systematic review and meta-analysis. J Adv Periodontol Implant Dent 2022 Nov 12;14(2):119-133. doi: 10.34172/ japid.2022.023.
10. Greenstein G, Carpentieri J, Cavallaro J. Open contacts adjacent to dental implant restorations: etiology, incidence, consequences, and correction. J Am Dent Assoc 2016;147:28–34.
11. Jeong JS, Chang M. Food impaction and periodontal/peri-implant tissue conditions in relation to the embrasure dimensions between implant-supported fixed dental prostheses and adjacent teeth: a cross-sectional study. J Periodontol 2015 Dec;86(12):1314-20. doi: 10.1902/ jop.2015.150322. Epub 2015 Aug 13.
12. Kim JH, Yi YJ. Factors influencing proximal contact loss between fixed implant prostheses and adjacent natural teeth: a retrospective study. J Korean Assoc Oral Maxillofac Surg 2025 Feb 28;51(1):26-32. doi: 10.5125/jkaoms.2025.51.1.26.
13. Manicone PF, De Angelis P, Rella E, Papetti L, D’Addona A. Proximal contact loss in implantsupported restorations: a systematic review and meta-analysis of prevalence. J Prosthodont 2022 Mar;31(3):201-209. doi: 10.1111/jopr.13407. Epub 2021 Aug 5.
14. Wang J, Lin J, Chen Y, Wu X. Analysis of the risk of interproximal contact loss between adjacent teeth and implant-supported fixed prostheses: a retrospective cross-sectional study. J Prosthet Dent 2025; Mar 27:S0022-3913(25)00195-7. doi: 10.1016/j.prosdent.2025.02.047. Epub ahead of print. PMID: 40155260.
15. Yen J-Y, Kang L, Chou I-C, et al. Risk assessment of interproximal contact loss between implant-supported fixed prostheses and adjacent teeth: a retrospective radiographic study. J Prosthet Dent 2022;127:86–92.
16. Assaf M, Abu Gharbyeh AZ. Screw-retained crown restorations of single implants: a step-bystep clinical guide. Eur J Dent 2014;8:563-70.
17. Fiorillo L, D’Amico C, Ronsivalle V, Cicciù M, Cervino G. Single dental implant restoration: cemented or screw-retained? A systematic review of multi-factor randomized clinical trials. Prosthesis 2024;6:871–886. https://doi.org/ 10.3390/prosthesis6040063.

John S. Mamoun, D.M.D., is in private practice in Manalapan, NJ.
NEWS General
Kids Most in Need of Dental Care Least Likely to Benefit from School Programs
CHILDREN WHO DON’T GO to the dentist are less likely to participate in school-based cavity prevention programs, according to research published in JAMA Network Open.
“Our study suggests that children who may need these services the most are the ones least likely to receive them,” said health economist and study author Shulamite Huang, an assistant professor of epidemiology and health promotion at NYU College of Dentistry.
In addition, the study found that improving participation in statewide school dental programs to reach those at high risk for tooth decay could yield significant savings for state Medicaid programs and healthcare systems, averting up to $2.4 million in emergency department charges annually in New York State.
Children miss more than 34 million hours of school each year to receive emergency dental care. In recent years, hospitals have seen a sharp increase in emergency room visits for pediatric dental issues.
To prevent tooth decay and the related pain and infections that land kids in the ER, some schools offer cavity prevention programs. New York State recently announced a $10-million initiative to expand access to school-based dental programs and improve children’s oral health.
Research shows that school dental programs, which use noninvasive treatments like sealants, are effective at preventing cavities. But parents must opt in for their kids to receive care in school, and it’s unclear if these programs reach those who are most in need.
Dr. Huang and her colleagues evaluated data from more than 63,000 children living in the Bronx and covered by Medicaid, including more than 1,000 children who participated in school-based cavity prevention programs in local elementary schools. They looked at Medicaid claims data to see whether children had visited a dentist outside of school or received emergency dental care.

The researchers found that kids who already had a history of dental care were more likely to participate in schoolbased cavity prevention programs. In contrast, children with no prior dental visits were 18 percent less likely to participate in these programs. Children with a history of dental emergencies (and probably at high risk for tooth decay) were also less likely to participate in school-based programs. The researchers then calculated the potential cost savings of expanding school-based dental care across New York State and improving participation among the children most at risk for tooth decay. They estimate that optimizing recruitment to enroll high-need children in school programs could save the state up to $2.4 million annually in dental-related emergency department costs (not including dental care related to accidents or injuries).
“This has staggering implications for Medicaid costs,” said Dr. Huang. “As New York expands access to school-based dental care, improving recruitment strategies and reorienting outreach to high risk-children could save the state millions and offset some of the costs of expanding care.”
Additional study authors include Ryan Richard Ruff of the University of Pennsylvania School of Dental Medicine, Heather Gold of NYU Grossman School of Medicine and Scarlett Wang of NYU Wagner School of Public Service.
UB Study Shows Key Protein Can Slow Aging Process
THE UNITED STATES is a rapidly aging country. By the year 2050, nearly one in four Americans will be 65 or older, and many will live into their 90s and beyond. This leads to healthcare and social support concerns and also begs the question: What is the quality of life in those later years?
Despite advances in medicine and the eradication of many diseases, it’s hard to escape the downfalls of advanced age: lower immunity and increased chronic inflammation, which can result in arthritis, fatigue, weaker bones and decreased strength, among other maladies.
This chronic activation of inflammation associated with aging has been coined “inflammaging,” says Keith Kirkwood, D.D.S., Ph.D., senior associate dean for research and Centennial Endowed Chair in the Department of Oral Biology in the University at Buffalo School of Dental Medicine.
“These age-related changes, known as immunosenescence, lead to a decline in immune resilience and an increased susceptibility to age-related chronic inflammatory diseases,” he explains.
Dr. Kirkwood led a lengthy study looking into a way to decrease age-
NEWS General
related frailty in mice. He and his team, which includes two top geriatric experts, focused on tristetraprolin (TTP), an RNA-binding protein that essentially puts the brakes on inflammation. As people age, TTP levels drop, especially in immune cells, leading to more inflammation.
The team genetically manipulated one group of elderly mice so that TTP was stabilized. Their findings — that these mice had reduced physical frailty scores compared with control mice — were published in the January 2026 issue of Aging and Disease.
“This protein really targets RNA for rapid degradation,” says, Dr. Kirkwood, who has focused his decades-long research on the role of obesity and aging in myeloid cell biology as it relates to oral inflammation in periodontal disease and oral cancer progression. “Most pro-inflammatory mediators have a very short half-life, meaning they only last for minutes, not hours.”
Funded by a $2.1-million grant from the National Institutes of Health, the study took place over the past six years at both UB’s South and Downtown campuses.
“In the United States, the prevalence of frailty in the non-nursing home population ages 65 and older is about 15%,” Dr. Kirkwood says. “Therefore, understanding the mechanisms connecting inflammaging, immune system alterations, bone health and frailty is essential for developing targeted interventions to improve the quality of life in aging populations.”
He created the study with longtime collaborators Bruce Troen, M.D.,
professor and chief of geriatric medicine and director of the Landon Center on Aging at the University of Kansas School of Medicine, who previously taught in UB’s Jacobs School of Medicine and Biomedical Sciences, and Perry Blackshear, M.D., Ph.D., a now retired investigator with both the Department of Biochemistry and Medicine at Duke University Medical Center and the Molecular and Cellular Biology Laboratory at the National Institute of Environmental Health Science in the Research Triangle Park.
The mice, which were 22 months old, were tested on grip strength, gait speed, treadmill endurance and energy levels. The frailty score was significantly lower in the male mice with the TTP increase and somewhat lower in the female mice compared with the controls.
“The increase in TTP resulted in better grip strength, better walking, endurance and overall physical performance,” Dr. Kirkwood explains. “These mice had healthier bones and reduced bone breakdown. They exhibited a more youthful-looking immune profile.”
Female mice with increased TTP didn’t fare quite as well as their male counterparts. Dr. Kirkwood attributes this to their smaller physical size and estrogen declines, which may restrict tissue responsiveness to anti-inflammatory modulation. However, he says that both sexes with the enhanced TTP expression had stronger bones.
While this study shows amazing results in mice, Dr. Kirkwood points out that clinical trials for humans are a long way off.

Component
Second District cont.
FOURTH DISTRICT
Women’s Night Out
The Fourth District wrapped up 2025 with one of its annual events, the 17th Women Dentists Meeting. Chair Dr. May Hwang organized a dinner lecture with guest speaker Dr. Amrita Patel lecturing on “Effective Patient Communication.” Her presentation was filled with interesting, funny and practical advice for every stage of a dentist’s professional life.
Members save the date for this yearly get-together, as it is a great social outlet to reconnect with peers, seek mentorship and enjoy a relaxing night out.
Officers Installed
January brought a changing of the guard, as the Fourth District installed its 2026 officers on a beautiful, cold and snowy evening. We welcomed: President Edmund Wun, an oral surgeon with Empire Oral and Maxillo-

FOURTH DISTRICT
facial Surgery; President-Elect Claire Kiehl, Adirondack Dental Group; Vice President Katherine Guilfoyle, Lake Periodontal; Secretary Crystal ArpeiMcHugh, Arpei-McHugh Family Dentistry; and Treasurer Rachel Hargraves, Dr. Rachel Hargraves Dental.
The district wishes all its officers a successful year and thanks them for their commitment to organized dentistry.
Educational Opportunities
Our continuing education program is off and running for the year. We hosted local periodontists Dr. Katherine Guilfoyle, Dr. Mahogany Miles and Dr. Linda Lam for an informative and engaging morning lecture. We appreciate the value of having local specialists be our experts. In March, we heard from Dr. Priya Tirumalasetty.
Dr. Peter Auster (perio), Dr. Jacob Dent (inclusive dentistry) and RDH JoAnne Jones will be presenters at the Saratoga Dental Congress on May 20 and 21. And we have arranged for Binghamton University to do a live, in-person Child Reporting Addendum in Saratoga on the evening of May 20. Looking further ahead, Compliance Day is set for Sept. 25, with Dr. Rubinstein (HIPPA) and Matt Altman (OSHA). Also coming up are our annual new dentist and women dentists fall meetings.
Thank You
Thank you in advance to all the volunteers who signed up for the RAM event in Schuylerville and the oral cancer screening at the CR Wood Cancer Center in Glens Falls, both taking place in April.
NASSAU COUNTY
Neither Rain nor Snow
Eugene Porcelli, D.D.S. Executive Director
It was an exceptionally snowy 2026 for us here in Nassau County, but that didn’t stop us from having several important
Attendance at Annual Women Dentists Meeting was large and enthusiastic.
Newly installed officers are, from left, Secretary Crystal Arpei-McHugh, Vice President Katherine Guilfoyle, Treasurer Rachel Hargraves, President-Elect Clair Kiehl, President Edmund Wun.
Nassau County cont.
events take place. On Jan. 31, we had our President’s Gala and Officer Installation at the Crest Hollow Country Club in Woodbury. Dr. Maureen Tredwell was installed as 2026 President, along with line officers, President-Elect Katayoon Noroozi-Leibowitz, Vice President Edward Perlow, Secretary John Gaeta and Treasurer Howard Baylarian.
During the event, Dr. David Grossman received the NCDS Humanitarian Award, and Executive Director Dr. Gene Porcelli received the Herbert L. Taub Distinguished Service Award. We were pleased to have in attendance the dean of Stony Brook School of Dental Medicine, Dr. Patrick Lloyd, along with 10 Stony Brook dental students and 20 residents from local hospital programs.
Treatment, Treats and Fun
Close on the heels of our Gala was our 2026 Give Kids A Smile event on Feb. 6 at the Cradle of Aviation Museum in Garden City. This year, 1,250 children from 13 local schools were seen by 360 volunteers. The children received dental exams, fluoride treatments and sealants, oral hygiene instruction and nutritional counseling, as well as eye screenings provided by the Lion’s Club.
For the first time, we had a book reading by local author Christine LaSpina, who has written a series of children’s dental books called “Tooth Adventures.” The children enjoyed listening to “Toothkins: The Dentist Is Your Friend.” All the children went home with a backpack filled with goodies, including an oral hygiene kit supplied by HealthFirst; a dental coloring book; oral hygiene instructions; and a toy. They also received an insulated lunch bag filled with several containers



NASSAU COUNTY
Leading NCDS in 2006 are, from left, President Maureen Tredwell, President-Elect Katayoon Noroozi-Leibowitz, Vice President Edward Perlow, Secretary John Gaeta, Treasurer Howard Baylarian.
David Grossman, right, recipient of NCDS Humanitarian Award, with Treasurer Baylarian.
Executive Director Gene Porcelli receives Herbert L. Taub Distinguished Service Award from Treasurer Baylarian.
of milk and an apple supplied by Farm Fresh Dairy. All the children, as well as the volunteers, received a voucher for a free basketball game at the Veterans Memorial Coliseum courtesy of the Long Island Nets organization.
Planning for next year’s staging of GKAS has already begun in preparation for NCDS hosting the ADA national kickoff event for 2027, Give Kids A Smile’s 25th Anniversary.
Attention Getters
Kudos to our own Dr. Doug Schildhaus, who represented NYSDA when being interviewed on Feb. 28 by Albany News 13 for an extended piece on Children’s Dental Health Month. And we were pleased to learn that our New Dentist/ Resident Seminar & Social Event Series for 2026 was awarded an ADA ARC Grant.
A Leader Passes
On a sadder note, we mourned the passing of our friend and colleague Dr. Sandy Klein on Jan. 16, just shy of his 96th birthday. He was a NYSDA past president and an active member of our Board of Directors right up to the end.
We Keep on Learning
The weather didn’t stop our CE courses. Over a dozen courses were in session in the first three months of the year. And speaking of CE, the Greater Long Island Dental Meeting takes place April 26-27, a Sunday and Monday, at the Huntington Hilton in Melville. It will feature a diverse selection of 30 courses for dentists, hygienists and staff. All mandated courses are being given, including the Pain Control and Addiction course due again in 2026.
Meals are included with all course registrations as a bonus. To register, go to www.GLIDM.org.



NASSAU COUNTY
Past presidents were special guests at January installation. They are, from left, Drs. Hills, Baylarian, Schildhaus, Shreck, Fitzgerald, Patrella, Porcelli, Miller, Bofsky, Akseizer, Verma.
Children are warmly received to Give Kids A Smile Event in Garden City in February by Elmo and Bingo.
Young attendees at GKAS event benefit from free dental exams, fluoride treatments and sealants.
Component
SECOND DISTRICT
Hospital Residents Guests at Membership Meeting
Sejndi (Sandy) Rusi, D.D.S.
The Second District Dental Society hosted a successful, well-attended general membership meeting on March 12 at the historic Dyker Beach Golf Course. The meeting’s featured lecture, “Pediatric Dental Trauma Essentials: From Guidelines to Chairside Application,” was presented by Dr. Meeta Grewal. Dr. Grewal is a pediatric dentist and associate program director at NYU Langone Brooklyn, who maintains a thriving private practice in New Jersey.
The meeting was a valuable opportunity for hospital residents to engage with SDDS and its Board members, hear about the benefits of organized dentistry and learn how to get involved. Residents from the following programs were in attendance: Brookdale, Kings County, Maimonides, NY-Presbyterian Brooklyn Methodist Hospital, NYU Langone Brooklyn, Staten Island University Hospital Northwell and Woodhull Hospital.

SECOND DISTRICT
The evening ended with a wonderful dinner and new connections having been made between seasoned dentists and residents.
Staten Island Hospital Hosts Give Kids A Smile
Staten Island University Hospital welcomed and cared for 22 children in a successful Give Kids A Smile event on Feb. 21. The outing was a welcoming and educational experience for children and their parents, especially for those without a dental home.
Volunteers focused on oral hygiene, diet education and other daily habits that influence the oral health of both children and their caregivers. The children were entertained with cartoons, magic tricks and interactive activities, including a learning board. They left with goody bags filled with dental supplies and educational materials, reinforcing the lessons learned and encouraging healthy habits moving forward.
This GKAS event was a meaningful opportunity to connect families with dental care and promote long-term oral health.

Attendees at March General Membership Meeting included residents from eight area hospital programs.
Free Shredding Events
SDDS hosted two free shredding events for members, on Friday, April 10, at District Headquarters, and Friday April 17, at the Hilton Garden Inn in Staten Island. This is a member-benefit service and an opportunity to securely dispose of old documents and dental records. Participants received a certificate of destruction.
Dr.
Irving E. Gruber Memorial Lecture
On March 13, SDDS hosted the Gruber Memorial Lecture, “Full Mouth Rehabilitation and Changing Lives: Aesthetics, Implants and Occlusion,” with renowned clinician Dr. Dean C. Vafiadis. Dr. Vafiadis, a prosthodontist, is director of the full-mouth rehabilitation continuing education course at NYUCD and an associate professor of prosthodontics. He is founder of the New York Smile Institute. His lecture focused on practical, applicable techniques for fullmouth rehabilitation, occlusal analysis and the keys to provisionalization. Dr. Louis DeSantis, RCDS Past President, was presiding chair of the event.
QUEENS COUNTY
C.K. Reddy, President
Queens County Dental Society’s newest elected leader is President Chiran K. Reddy, D.D.S., a dental practitioner with over three decades of clinical experience and humanitarian service

NYSDA Endorsed Services
BANKING
Bank of America
800-932-2775
800-497-6076
FINANCIAL SERVICES
CareCredit
800-300-3046 (#5)
Altfest Personal Wealth Management
888-525-8337
Best Card
877-739-3952
Key Bank
833-427-2265
INSURANCE SERVICES
MLMIC
800-683-7769
888-263-2729
888-744-6729
Arthur Gallagher
888-869-3535
Long-term Care
844-355-2596







OTHER
Henry Schein Electronic Prescribing 800-734-5561
ProSites


888-932-3644 Solutions www.prosites.com/nysda
Mercedes
Vehicles 866-628-7232
Lands’ End Apparel for Staff 800-490-6402
UPS
800-636-2377
The Dentists Supply Company
888-253-1223
Volvo

Vehicles 800-550-5658 ada.org/volvo
OnDiem
Staffing hub.ondiem.com

Practice Mojo Patient Communications
888-932-3644 practicemojo.com


For further information about NYSDA Endorsed Programs, call Jeanne DeGuire at 800.255.2100
Dr. Reddy
Component
Queens County cont.
who has dedicated himself to advancing oral health and access to care across diverse populations.
Founder and principal dentist with Reddy Dental Associates in Queens, Dr. Reddy received his D.D.S. Degree from New York University College of Dentistry in 1991 and Bachelor of Dental Surgery Degree (B.D.S.) from Raja Muttiah Dental College & Hospital, Annamalai University, India, in 1988.
As organizer and lead dentist with Guyana Watch Inc., Dr. Reddy has provided free dental care to underserved communities in Guyana, South America, for the past 20 years. For his service, Guyana presented him with a Humanitarian Award.
Volunteering with St. Raphael’s Roman Catholic Church and St. Thomas Moore Church on Long Island, Dr. Reddy has led community outreach programs, providing free oral health screenings, hygiene instruction and preventive care to underserved families in the community. And he helped organize oral health education workshops for children, seniors and immigrant families. At the same time, he has mentored youth and student volunteers interested in healthcare careers.
Dr. Reddy previously organized and led mobile dental units to rural areas in India as a member of the Indian Dental Association.
QCDS congratulates Dr. Reddy on his installation as president and applauds him for his commitment to learning, ethical service and advancing global oral health.
SEVENTH DISTRICT
Educating the Next Generation of Dentists
Becky Herman, Executive Director
The Monroe County Dental Society’s Careers in Dentistry Program held two additional events for area high school and college students interested in pursuing a career in dentistry. In early March, students heard from Drs. Jolly Caplash and Thomas Helfst from Rochester Regional Health’s Oral Surgery Program, who shared their insights and expertise about the rewards and challenges of a career in oral surgery and academic dentistry.
Mid-month, students toured the University at Buffalo School of Dental Medicine. Thank you to Dr. John Bi-
alkowski, who participated in the Careers in Dentistry Program four years ago and is now a D3 dental student at UB, for sharing his journey as a dental student and offering advice about the application process and what to expect in dental school.
By the Book
“The New Dentist/Resident Playbook: What They Didn’t Teach You in Dental School” was the title of the Mentorship & Leadership Development Program put on by the Seventh District on March 24. Held in a Jeopardy game-style format, with hosts attorneys Matthew Feldman and Al Anthony Mercado from Feldman Kieffer, the event was fun and interactive. It brought together


SEVENTH DISTRICT
Enjoying luau and learning are, from left, Drs. Sanel Sadibasic, Madelyn Sadibasic, Shaughna Winslow, Andrew Winslow.
February CE program featured Hawaiian theme. Seen during break in program are, from left, NYS Dental Foundation
Executive Director Stacy McIlduff, spirited sign holder, Executive Director Becky Herman, Drs. David Reed and Jay Skolnick.
members of all ages to learn about legal topics, including risk management, social media, patient complaints, insurance and practice management. Thank you to program sponsors Empire Dental Administrators, Kuraray, Ultradent, Vision Financial and Walsh Insurance.
A Fun Way to Learn
Members from the 7th District and surrounding area attended the New York State Dental Foundation’s CE Luau in Rochester in late February. Thank you to Stacy McIIduff, NYSDF Executive Director and members of the NYSDF Board for planning a fun day of learning and fellowship. A shoutout to event sponsors Align Technology and Liberty Endodontics.
NEW YORK COUNTY
Celebrating Black History Month
Jaskaren
Randhawa, D.M.D.
The New York State Dental Association hosted a Black History Month celebration on Feb. 25 at the New York County Dental Society headquarters. The event, titled “Rooted in Excellence,” explored how collaboration, culture and clinical mastery continue to shape modern dentistry. Attendees enjoyed authentic Jamaican cuisine while connecting with colleagues before the evening lecture
began. The panel featured three accomplished dentists, Drs. Emma Guzman, Chanelle Small and Ashley Lofters. Each speaker shared insights from her professional journey and experiences, leaving the audience inspired.
General Membership Meeting
The New York County Dental Society hosted its April General Membership Meeting on Monday, April 13. The evening’s professional program was led by Marcus Johnson, D.D.S., M.S.D. He presented “Minimally Engaging Endodontics: Navigating Anatomical Challenges and MB2.”
This meeting was a great opportunity to connect with fellow members while earning one complimentary CE credit.
Are You Ready to Sell Your Practice and Retire?
Join us on April 22 at the New York County Dental Society for a timely program designed to help dental professionals navigate the path toward selling a practice and planning for retirement with greater clarity.
This updated course reflects today’s evolving market and provides a clear look at the sales process, along with practical insights you can apply right away. You will hear directly from experienced professionals who guide these transitions every day, including Mark


Epstein, Epstein Practice Brokerage, LLC; David J. Goodman CPA, MST; and Mitchell Brill, JD, MSFS, CFP, CAP. Whether your timeline is near or still taking shape, thoughtful planning today can help you move forward with confidence.
Restorative Dentistry Explained
A two-part lecture on restorative dentistry with Dr. Marc Geissberger on April 17 introduced participants to several new materials and techniques in restorative dentistry designed to simplify clinical practice and yield predictable, problemfree restorations. Treatment planning, designing and managing complex restorative and esthetic cases were discussed. Course participants earned six CE credits.
Dr. Christensen Comes to NYCDS
Renowned dental expert Dr. Gordon Christensen will appear in person May 1 at NYCDS to deliver “The Christensen Bottom Line,” a fast-moving course that looks at the areas of dentistry with the most activity and change in any given year. Course material is easily understood and includes summaries that help attendees interpret the ongoing advancements in the profession.
The course, which will run from 8:30 a.m.-3:30 p.m., encourages audience participation with interactive questions and answers and is presented in an engaging and enjoyable way.
Continuing Education & Special Events
• April 22 6:30-8:30 p.m. Ready to Sell Your Practice and Set Your Sights on Retirement? (In-Person)
• April 23 1:30-4:30 p.m. TMD Talking Points, with Drs. Donald Tanenbaum, John E. Dinan and Aimee Werfel. (In-Person)
• May 1 8:30 a.m.-3:30 p.m. The Christensen Bottom Line, with Dr. Gordon Christensen. (In-Person)
• May 6 9:30 a.m.-1:30 p.m. Basic Life Support/-CPR Certification Course. (In-Person)
• May 13 9:30 a.m.-12:30 p.m. Implant Interactions in Orthodontics, with Dr. Frank Celenza (In-Person)
New York County cont.
• May 13 7-9 p.m. OSHA-Mandated Update for Dentists and Staff: What You Need to Know to Comply with the Law, with Dr. Peter Mychajliw. (Zoom)
• May 18 9:30 a.m.-12:30 p.m. Effective Management of TMJ Disorders, with Nojan Bakhtiari. (In-Person)
• May 21 6-8 p.m. Grow Your Practice: One Tooth, One Quadrant & One Arch at a Time, with Dr. Steve Katz (Zoom)
• June 3 9:30 a.m.-4:30 p.m. Two-Part Lecture on Laser Dentistry, with Dr. Robert Convissar. (In-Person)
• June 9 9 a.m.-4:30 p.m. Contemporary Insights into Orthodontic Practice: Investigational Studies Relating to How and Why We Do What We Do (In-Person)
• June 17 9:30 a.m.-4:30 p.m. Innovations in Aesthetic Dentistry: Everything You Need to Know About Veneers, with Dr. Ghalili. (In-Person)

• June 18 9:30 a.m.-4:30 p.m. Hands on Veneers Workshop, with Dr. Ghalili. (In-Person)
• June 23 6-8 p.m. Harmony in the OP: Top Tips for Hygienists & Dentists to Work Smart Together, with Debbie Seidel. (Zoom)
New courses are added regularly, so be sure to visit www.nycdentalsociety.org for the latest course schedule.
SUFFOLK COUNTY Research Symposium
Devin J. Klein, D.D.S., M.S.
We were honored to be present for the Leo and Mickey Sreebny Research Symposium and the ASDA Spring Vendor Fair March 3 at the Stony Brook School of Dental Medicine.
Officer Installation/Celebration
On March 7, we celebrated our 2026 officers with a gala brunch at the Watermill in Smithtown.
The honorees included: President Natalia Elson, D.D.S.; President-Elect Devin J. Klein, D.D.S., M.S.; Vice-President Alan Berman, D.D.S.; Treasurer Steven Feigelson, D.D.S.
Off to a Good Start
Seminar number one in our series on March 25 was a fantastic event, with Dr. Joshua Austin lecturing on modern materials. It was informative, educational, engaging and very entertaining. Feedback has been great from attendees and sponsors alike.


SUFFOLK COUNTY
Don’t Miss a Thing
We continue to make a significant push to better communicate and connect with our members in methods that more easily integrate with their lifestyle. You can find us on Facebook, X, Instagram, LinkedIn and Spotify, in addition to our traditional www.SuffolkDental.Org presence.
BRONX COUNTY
Donation Does Good

Many thanks to Align, GC America, Pearl, Equitable, DDSMatch, CareCredit, Pulpdent and Henry Schein for their support. Don’t miss our next seminar on May 13, with Dr. Kyle Reeves.
It’s Coming and it’s Huge
NEW YORK COUNTY
The Greater Long Island Dental Meeting, the largest dental event on Long Island, takes place April 26 and 27 at the Huntington Hilton. Register before April 23 at www.glidm.org. ADA members save 50% on registrations.

sive medical, dental and behavioral health services to an underserved population.
Ashley Lofters shares insights from her professional journey with audience at “Rooted in Excellence” event, celebration of Black History Month.
Seen at NYSDA Black History Celebration are, from left, NYCDS Past President Mina Kim; Emma Guzman, event speaker; Immediate Past President Vera Tang; NYSDA President Maurice Edwards.
Newly installed officers are, from left, President Natalia Elson, President-Elect Devin Klein, VicePresident Alan Berman, Treasurer Steven Feigelson.
First seminar of the year featured presentation by Joshua Austin on latest dental materials.
Bronx County Treasurer Don Safferstein, third from left, with representatives of Healthfirst and Morris Heights Health Center following announcement that Healthfirst had donated $10,000 to support charitable works of BCDS. A portion of that donation will go to Morris Heights, a federally qualified health center that provides comprehen-
FOR SALE
QUEENS: Jackson Heights. Dental office coop for sale or rent. Located at 37-30 73rd Street. Two minutes from train station (E,F,R#7). Street level. Please inquire by email: conciergesmile@gmail.com; or call: (347) 678-7662.
QUEENS: Long-time established practice offered for sale by original owner. Practice fully renovated and features all new interior finishes, mechanicals, cabinetry, plumbing/ heating & cooling and dental equipment throughout. Office occupies 3 floors (4,828 square feet) and features 1st floor entrance, waiting room & reception area; 2 lavatories & 5 fully equipped operatories with A-Dec chairs, Vatech X-Rays, wall-mounted monitors, data wiring and custom cabinetry with Quartz countertops. Spare room ready for sixth operatory and separate dedicated room with Vatech Green X CBCT/PANO/CEPH. Busy dental office centrally located in Queens (recently redeveloped) in exceptionally high-traffic area, only a minute’s walk from subway and bus stops on same block. Location serves primarily as FFS practice with no Medicaid or State insurance. Sale is confidential; serious inquiries only. Please email: officeforsale2026@gmail.com
NASSAU COUNTY: South Shore dental practice for sale after 20+ years serving community. Owner exploring all transition options, including sale or partnership, with focus on continuity of care. Desirable submarket within NYC metro area. Established general practice operates from freestanding building with five operatories and real estate available. 1,825 active patients and 10 new patients per month. Practice generates approximately $880K collections over just 180 working days producing $482K true take-home income. Reduced hours create clear upside. Learn more by contacting Bailey, Headwaters Transition by email: bailey@headwaterstransition.com; or call (719) 694-8320. Reference #HNY21126. View online at: www.headwaterstransition. com/places/nassau-county-ny-dental-practice-for-sale/
BROOKLYN: Central Brooklyn 35-year general practice for sale. Strong community presence and consistent patient demand. Owner exploring all transition options and plans to retire within six months. Recently updated office features three operatories in multi-tenant building, with real estate available. Nearly 2,000 active patients and 20-25 new patients per month generated with minimal advertising. Practice collects approximately $800K and produces $390K true take-home income. Learn more by contacting Bailey, Headwaters Transition by email: bailey@headwaterstransition. com; or call (719) 694-8320. Ref #HNY32625. View online at: www.headwaterstransition.com/places/brooklyn-ny/
CENTRAL NEW YORK: Established general dental practice offers strong community ties, consistent demand and long-term stability. Owner doctor practicing more than 15 years and seeks partnership. Recently updated office features nine operatories with additional expansion space available for lease. Operating just four days per week. Practice supports 2,815 active patients and generates $2.248M collections with $815K in EBITDA. Minimal advertising and steady word-of-mouth referrals create meaningful growth potential. Learn more by contacting Bailey, Professional Transition Strategies by email: bailey@ professionaltransition.com; or call (719) 694-8320. Ref #NY112625. Online here: www. professionaltransition.
CLASSIFIED
Online Rates for 60-day posting of 150 words or less — can include photos/images online: Members: $200. Nonmembers: $300. Corporate/Business Ads: $400. Classifieds will also appear in print during months when Journal is mailed: Jan and July.
com/places/general-dental-practice-for-sale-in-centralnew-york/
CENTRAL NJ: Thriving periodontal practice for sale. Established, highly regarded practice, exceptional location. Strong hygiene program. Services balanced across periodontal procedures, hygiene and robust 17% implant component. Four equipped operatories in leased space. Revenue of $2M. Solid referrals and growth potential. For more information, contact Donna Costa by phone: (609) 304-0652; or email: donna.costa@henryschein. com. #NJ4591.
CENTRAL NJ: Surgery practice for sale. Turnkey, 5-op, recently constructed 2,900-square-foot office in prestigious, high-demand area. $800K average revenue; 80% FFS; strong growth potential. Excellent visibility with prominent signage. Real estate available. For more information, please contact Donna Costa by phone (609) 304-0652; or email: donna.costa@henryschein.com. #NJ4210.
HAMPTONS: Established FFS general practice on Long Island’s South Fork. $1.685M collections and $340K EBITDA. Recently remodeled freestanding building with four operatories and space available to add fifth. Real estate also available for purchase, offering strong long-term investment opportunity. 915 active patients; 15 to 20 new patients each month. Strong patient loyalty, high household incomes and consistent demand for quality dental care. Area attracts families and professionals seeking balanced lifestyle, with access to beaches, parks, outdoor recreation and top local amenities. Both owner doctors ready to transition and will support smooth handoff. Rare opportunity to acquire modern, profitable FFS practice in highly desirable South Fork community. Contact Bailey, Professional Transition Strategies by email: bailey@professionaltransition.com for more information. Reference #NY112025.
TRIBECA: Cosmetic dentistry practice available for merger, buyout, sale, associate-to-own or strategic partnership. Distinguished Manhattan practice. Strong presence in esthetic dentistry, offering flexible pathways, including associate-to-own, merger or full buyout/sale. Ideal for clinician interested in cosmetic dentistry and comprehensive care who values supportive transition and practice with strong community roots. Structure and timeline flexible for right fit. Inquiries by email; first send CV or brief background to: Patmoez@gmail.com; then call (917) 392-0506.
LONG ISLAND CITY: Rare opportunity to own thriving dental practice in Long Island City, one of New York City’s fastest-growing neighborhoods. Modern, fully equipped office produces over $1M annual revenue, with strong patient retention and steady new-patient flow. State-ofthe-art operatories, digital technology and efficient layout designed for both comfort and productivity. High-traffic,
rapidly developing area surrounded by new residential and commercial projects. Practice perfectly positioned for continued growth. Excellent lease terms and well-established brand make this ideal turnkey opportunity for solo practitioner or group looking to expand. Don’t miss this chance to acquire profitable, well-managed dental office in one of NYC’s most dynamic communities. Serious inquiries only. Confidential information available upon request. Email: ianmapes@gmail.com
GLENS FALLS, QUEENSBURY: Beautiful 5,800-squarefoot, 8-chair office for sale or lease. Large lab, library, conference room, 2 private offices, staff lounge, surgery suite, X-ray and sterilization rooms. Office liquidation, including office furniture and equipment, CBCT/PAN, 8 chairs/ units, extensive instruments and supplies, including periodontal surgery and preventive maintenance, oral surgery, endodontics, implants, C&B and restorative. Dual motor air compressor and suction pump. Very nicely decorated; immaculate. Call (518) 793-5908 to leave message; or email: robertsharpdds@adirondackdentalimplantcenter.com
WATERTOWN/THOUSAND ISLANDS: Dental practice for sale in beautiful Northern NY. Desirable location approximately 1 hour north of Syracuse in close proximity to Thousand Islands and Canadian border. Modern, well-designed, attractive, standalone building with ample parking. 3,395 square feet. Main floor offers 9 ops with digital X-ray, CBCT, Eaglesoft, Schick Sensors, 3D printing and CEREC. Finished 1,500-square-foot basement includes conference room, laundry/locker room, kitchen and 2 additional offices. Building available for sale or lease. Reputable practice can run 1-2 dentists with gross revenue in excess of $1M annually on 4-day week. Experienced, highly motivated team of 8 willing to remain after sale. Owner retiring and willing to help with transition. Contact Robert Schonfield, DDS, by phone: (315) 771-4012; or email: rob@docschonfield.com
FOR RENT
CAPITAL DISTRICT: Dental office for rent in Latham. Located at hub of the Tri-Cities, right on heavily traveled Route 9; short distance to exit 6 of Northway and Route 7. Office available June 1, 2026. Dental office with 4 functional operatories, large lab, private office with bathroom, reception, business and staff areas; 1,300 square feet with heat and hot water included. Tenant pays electric and trash removal. Large private parking lot of 18 spaces. Renovations are at tenant’s expense. Contact Stephen Conway, D.D.S., by phone (518) 542- 7932; or email: SJConway97@gmail.com
GLENS FALLS, QUEENSBURY: Beautiful 5,800-squarefoot, 8-chair office for sale or lease. Large lab, library, conference room, 2 private offices, staff lounge, surgery suite, X-ray and sterilization rooms. Office liquidation, including office furniture and equipment, CBCT/PAN, 8 chairs/ units, extensive instruments and supplies, including periodontal surgery and preventive maintenance, oral surgery, endodontics, implants, C&B and restorative. Dual motor air compressor and suction pump. Very nicely decorated; immaculate. Call (518) 793-5908 to leave message; or email: robertsharpdds@adirondackdentalimplantcenter.com
ADVERTISERS
QUEENS: Jackson Heights. Dental office coop for sale or rent. Located at 37-30 73rd Street. Two minutes from train station (E, F, R, #7). Street level. Please inquire by email: conciergesmile@gmail.com; or call: (347) 678-7662.
ROCKLAND COUNTY: Turnkey practice with three ops. Recently constructed. Exceptional location; easy access to major highways. Excellent opportunity for new dentists or satellite office. Extremely low overhead. Rent only $1,600 per month. Eaglesoft software and ScanX digital system. Extensive instruments and supplies. Asking: $100K. Contact to learn more: (203) 979-1970; or email: mzdds2000@ yahoo.com
EQUIPMENT FOR SALE
Retiring dentist has equipment to sell including: Dentsply Sirona Prime Scan, four (4) operatories (two (2) hygiene, two (2) dental units) with LED lights and stools, two (2) X-ray units (Belmont and Focus), Mid Mark M9 Steam Autoclave and Orthophos XG3 Digital Panorex. Other equipment also available. Interested parties should contact: (315) 468-3327; or email: info@danaherdental.com
OPPORTUNITIES AVAILABLE
SARATOGA: Sitwell Dental, leading family practice with locations in Albany, Clifton Park, Malta and Saratoga Springs, seeks full-time General Dentist to join our Saratoga Springs team. We provide compassionate, patient-first care with services ranging from preventive and restorative dentistry to implants, cosmetic, orthodontics, and emergency care--all in modern, supportive environment. What we offer: Competitive base salary, health/dental/vision benefits, 401(k) match, malpractice coverage, paid CE, mentorship, and access to state-of-the-art technology. No practice management responsibilities. Responsibilities: Deliver preventive, restorative, cosmetic, implant, pediatric, and emergency dentistry. Lead treatment planning, collaborate with team members, and provide Invisalign® and other orthodontic care. Requirements: DDS/DMD from accredited school, active NYS license, DEA certification, 2+ years experience preferred. Proficiency in restorative, preventive, cosmetic, and implant dentistry required. Strong communication skills and commitment to CE; Invisalign®/ Six Month Smiles® experience preferred. For more information, please call or email Meredith Brown-Parsons at Meredith.brown-parsons@saltdentalpartners.com; or call (859) 613-3029.
BUFFALO: Nuvia Dental Implant Center, growing dental implant center, seeks Prosthodontist or General Dentist with full-arch, fixed experience to join our new location. We provide dental implants and full-mouth restorations to patients, literally changing their lives. An exceptional patient experience for every patient is our top priority. At Nuvia, our Restorative Doctors are adaptable and have an eagerness to learn and grow. Ideal candidate would have extensive knowledge of dental implants, along with fixed and removable prosthodontic background. Strong interpersonal
skills with patients and team are crucial. Full-time hours Monday-Friday, 8 am-5 pm. Compensation is base salary plus percentage of production. Our Restorative Doctors make $300-500K/year. See full job description and apply here: Dentist | Nuvia Dental Implant Center Careers
SULLIVAN COUNTY: Seeking passionate part-time general dentist to join thriving children’s dental program. Role offers two-day-per-week commitment with convenient daytime hours, making it an excellent opportunity for dentists seeking flexibility—including early-career dentists looking to gain experience and those who are semi-retired and interested in continuing to practice. Ideal candidate will have at least two years of clinical experience and genuine interest in working with children. Provide preventive and basic restorative care in fully equipped mobile dental clinic, supported by experienced staff who handle scheduling and logistics—so you can focus on patient care. Competitive daily compensation and opportunity to be part of missiondriven organization dedicated to improving children’s oral health. To apply, email resume to: prasad@prasad.org; or call (845) 434-0376.
CENTRAL NEW YORK: Seeking associate dentist for Phoenix, NY, practice. Growing area, 10 minutes from Micron Technologies in Clay and just 15 minutes from Syracuse. Starting $750 guaranteed per diem with monthly 40% production bonuses. Health insurance, 401K and other benefits available. Please phone or email to learn more: elopez4024@gmail.com; or (315) 460-0616.
BASSETT HEALTHCARE NETWORK: Bassett Healthcare Network, progressive, academic health system in Central New York, major teaching affiliate of Columbia University, seeking Dentist to join staff. Join established group of general dentists, hygienists and oral surgeon. Applicants must possess outstanding communication and documentation skills, be able to function independently and as part of team and be competent in all aspects of general dentistry, including behavior management for children and special needs patients. Minimal evening and weekend phone call shared among network dentists Salary Range: $174,736 - $189,785. Sign-On Bonus up to $100,000 Group Employed Model. Please contact Jennifer Hulse, Medical Staff Recruitment by phone: (607) 547-6982; or email: jennifer.hulse@bassett.org


