

Medical Distribution Hall of Fame
Joe Grispo
Senior VP Sales, CSO
B. Braun Medical
Manny Losada
Jon Wells President/CEO
SAY AH!

SIMPLIFIED STREP A TESTING
ID NOW™ STREP A 2 TEST makes testing easy. Collect a single throat swab, test and provide treatment, all during the patient encounter.
• Actionable, reliable, molecular results in 2–6 minutes1
• 90% fewer false negatives than antigen tests*2
• No culture confirmation needed
NOW ™ RESPIRATORY ASSAY MENU

WE ARE HERE TO SUPPORT YOU AND YOUR CUSTOMERS. REACH OUT TO YOUR ABBOTT REPRESENTATIVE TODAY.


40 Primary Care at the Center of Obesity’s New Era
With GLP-1 medications, updated standards of care and growing awareness of weight bias, clinicians are navigating expanding treatment options — and rising expectations — in the fight against chronic disease.
47 Tailored Colorectal Cancer Care
How Dana-Farber’s Young-Onset CRC Center addresses the medical, emotional and practical needs of younger patients.
52 ChatGPT Health Signals a New Era of AI-Driven Patient Engagement
OpenAI’s latest platform aims to centralize medical records, wellness data and AI guidance in one place –raising both optimism about patient empowerment and concerns over accuracy, privacy and trust.
58 Using AI Tools Safely
Although AI chatbots have the potential to improve care, experts say guardrails are needed.
` ASCs
64 Focusing On Growth
NueHealth’s CEO discusses the reasons and goals behind a series of new partnerships.
` IDN INSIGHTS
68 Meaningful Medicine
How an Atrium Health initiative is tackling workforce gaps and expanding care access in North Carolina.
PEOPLE
Remembering Mike Carver
The med/surg community mourns the loss of a Hall of Famer whose mentorship, generosity and unwavering commitment to people left an incredible legacy.
Looking
Explore
Honoring the Steady Hands of Medical Distribution
Every industry has its version of a Hall of Fame. Baseball has the National Baseball Hall of Fame and Museum, where legends are immortalized in bronze. Rock & Roll has its shrine in Cleveland. And in the world of medical distribution – where the heroes wear polo shirts instead of pinstripes and spend their days in ASCs, physician offices, hospitals, distribution centers, boardrooms and trade shows – we have the Repertoire Medical Distribution Hall of Fame.

For nearly three decades, this recognition has celebrated people who quietly but profoundly shape the healthcare supply chain. It’s a Hall of Fame not for the loudest voices, but for steady hands – the people who make the ecosystem work a little better year after year. It is a place where inductees give not only to their organizations, but to the industry many of us proudly call home.
Take Joe Grispo of B. Braun. Over more than three decades, Joe built a reputation for combining classic sales discipline with a strategic understanding of the healthcare supply chain. He championed a distribution-first approach long before it became fashionable, strengthening relationships across GPOs, distributors, IDNs and government partners. In an industry that constantly evolves, Joe proved that steady leadership and long-term thinking still win the day.
To listen to Joe’s podcast with me scan the QR code.
Then there’s Manny Losada, whose career has been defined by one belief: the supply chain is really about people. Through leadership roles across manufacturing, distribution and representation – and through his work at MedPro / Optimal Healthcare Solutions
– Manny became known as a builder of organizations and relationships. In a business often measured by contracts and margins, Manny reminds us that trust and relationships are the real longterm investments. To listen to Manny’s podcast with me scan the QR code.
Finally, we honor Jon Wells of Midmark, whose career reflects a commitment to strengthening the bond between manufacturers and distribution. Jon championed what he often described as a “last-mile mindset,” ensuring products, processes and partnerships work where it matters most: at the point of care. Known for integrity and transparency, Jon helped guide his organization through major shifts in healthcare while keeping focus on the partnerships that make innovation possible. To listen to Jon’s podcast with me scan the QR code.
So let’s take a moment to congratulate Joe Grispo, Manny Losada and Jon Wells – three individuals whose careers remind us what excellence in medical distribution truly looks like.
editorial staff
editor Graham Garrison ggarrison@sharemovingmedia.com
editor-in-chief, Dail-eNews Jenna Hughes jhughes@sharemovingmedia.com
content creator Pete Mercer pmercer@sharemovingmedia.com
art director Brent Cashman bcashman@sharemovingmedia.com
circulation Laura Gantert lgantert@sharemovingmedia.com
sales executive Aili Casey acasey@sharemovingmedia.com (404) 625-9156
publisher Scott Adams sadams@sharemovingmedia.com (800) 536.5312 x5256
founder Brian Taylor btaylor@sharemovingmedia.com
Subscriptions www.repertoiremag.com/subscribe or (800) 536-5312 x5259
Repertoire is published monthly by Share Moving Media 350 Town Center Ave, Ste 201 Suwanee, GA 30024-6914 Phone: (800) 536-5312, FAX: (770) 709-5432; e-mail: info@sharemovingmedia.com; www.sharemovingmedia.com

When stress levels rise, the heart needs answers.
QuidelOrtho is your comprehensive cardiac partner, delivering clarity from the lab to the bedside and confidence in every result.




QUIDEL™ TRIAGE™ System cardiac testing menu










VITROS™ Systems cardiac testing menu
• hsTroponin I
• NT-proBNP
• Myoglobin
• D-dimer*
• Homocysteine
• Wide-range CRP*
• Apolipoprotein A
• Apolipoprotein B




• Cholesterol
• CK
• CK-MB
• Direct HDL
• Direct LDL
• Lipoprotein(a)*
• Triglycerides











What Do the Best POL Customers Have in Common?
Looking beyond revenue metrics, how defining your ideal physician office lab –and partnering with point-of-care leaders – can sharpen prospecting, strengthen relationships and drive long-term territory growth.
 From time to time, it is good to review our lab customers’ businesses, either formally in meetings with our manager or roundtables with management and other lab sales professionals. The focus is typically on performance: what does our lab customer revenue, margin and future business forecast look like?

By Jim Poggi



Don’t let symptoms get in the way of a clear picture.
In sexual health, symptoms often overlap, making it difficult to diagnose. That’s why comprehensive PCR testing isn’t just helpful — it’s essential.
At Cepheid, we deliver cutting-edge PCR diagnostics that look beyond the obvious, identifying infections at once with speed and accuracy. Because in sexual health, seeing the full picture means getting patients the right treatment, fast. Clear answers start here. Learn More about Cepheid’s Women’s & Sexual Health Portfolio.
These are important topics, but they stop short of asking the underlying question: what do our best POL customers have in common? In other words, how would we define our best customer?
Additionally, the exercise of identifying the traits our best customers have in common should help us identify our best few prospects to maintain and grow our lab business. The exercise of understanding what our best customers have in common is important and helps keep us sharp and productive as we manage our territories and deliver on customer and company expectations.
we consider what the best POL customers have in common is the input from others, particularly members of the IDN point-ofcare community. Most IDNs have a point-of-care coordinator (POCC) team in place to make sure POC testing is performed in compliance with the testing requirements of the IDN for quality of results and that POC testing does not duplicate testing done at the core lab location. This team is responsible for helping manage testing at every POC site, including the ER, the floors and the physician office labs that belong to the IDN.
Understanding that your job to identify what the best POLs have in common is a team job, it also makes sense to engage your trusted lab manufacturers to get their opinion and understanding.
No matter how often we conduct a customer review formally, we should conduct our personal customer review routinely and make sure we are managing our lab business optimally. In this column, I plan to outline the many characteristics our best customers have in common and to point out some red flags we need to be aware of as we qualify new prospects.
A full view of the customer
Customer qualification is yet another activity where we can and should obtain as much information from as many sources as possible. This helps us get a 360-degree view of our customers.
One source of information we sometimes forget or ignore as
I have had the opportunity in recent years to engage the POCC community through a series of webinars to understand their viewpoint on point-of-care testing, share my viewpoint that lab testing needs to be available to initiate or modify a patient treatment program, and to understand how closely aligned we were. I presented a series of lab webinars to the POCC community including topics like “Test standardization: some practical guidance” and “Point-of-care testing: cost vs. convenience.”
Since I am a known advocate for POL testing and my presentations make the point that POL testing is the best way to assure patients and care givers have results they can use to influence patient behavior for better health
outcomes, I was not sure what kind of reception I would receive. I found the POCC community surprisingly receptive.
My presentations depicted their role as counselor and expert colleague rather than the “police.” They mostly agreed that POC testing for the right reasons is important, and felt that they were frequently caught in the middle between their IDN responsibilities to manage POL practice performance and ensure most testing went to the core lab, and the POL viewpoint that the POCC were the police and were limiting their ability to test. Most members of the POCC community are looking for allies in their goal to have the POLs they manage perform testing at a high level and for these labs to be well organized and compliant with CLIA and other regulatory requirements.
If you engage them as allies and sources of information rather than the enemy, I am confident you will be able to work together in harmony to provide the highest level of service to their POLs. Given the fact that the majority of salespeople avoid the POCC coordinators, you should find a receptive audience looking for help. Can you get them to agree to migrate some testing to the POL location? Sometimes they will support this goal with IDN management if there is a compelling reason to do so. Overall, they agreed with the argument that “lab testing needs to be available to initiate or modify a patient treatment protocol.”
Through this lens, respiratory testing, glucose for chronic diabetic patients, hemoglobin A1C under similar conditions and other POL tests we would

TAKE THE FIGHT AGAINST CKM* TO THE POINT OF CARE (POC)
TAKE THE FIGHT AGAINST CKM* TO THE POINT OF CARE (POC)
TAKE THE FIGHT AGAINST CKM* TO THE POINT OF CARE (POC)
*Cardiovascular kidney metabolic (CKM) syndrome.
*Cardiovascular kidney (CKM) syndrome.
*Cardiovascular kidney metabolic (CKM) syndrome.
Cardiovascular kidney metabolic (CKM) syndrome is a serious health condition that requires early detection and intervention. POC testing for known risk factors, such as high HbA1c and cholesterol, is an important first step, allowing patients to receive immediate results and in-visit management planning.
Cardiovascular kidney metabolic (CKM) syndrome is a serious health condition that requires early detection and intervention. POC testing for known risk factors, such as high cholesterol, is an important first step, allowing patients to receive immediate results in-visit management planning.
Cardiovascular kidney metabolic (CKM) syndrome is a serious health condition that requires early detection and intervention. POC testing for known risk factors, such as high HbA1c and cholesterol, is an important first step, allowing patients to receive immediate results and in-visit management planning.
Check. K now. M anage.
K M anage.
With Afinion™ 2 and Cholestech LDX™ Analyzers, your customers can detect patient CKM risk factors within minutes. Both products offer: Results in 5 minutes or less
With Afinion™ 2 and Cholestech LDX™ Analyzers, your customers can detect patient CKM risk factors within minutes. Both products offer:
With Afinion™ 2 and Cholestech LDX™ Analyzers, your customers can detect patient CKM risk factors within minutes. Both products offer:
Results in 5 minutes or less
Results in 5 minutes or less
Small fingerstick sampling
Small fingerstick sampling Opportunity for immediate, in-visit coaching
Small fingerstick sampling
Opportunity for immediate, in-visit coaching
Opportunity for immediate, in-visit coaching


Easy to use in 3 simple steps
Easy to use in 3 simple steps
Zero required maintenance
Easy to use in 3 simple steps Zero required maintenance
Zero required maintenance
Afinion™ 2 Analyzer
Afinion™ 2 Analyzer
CLIA-waived Mod complex HbA1c Dx* and ACR* testing
CLIA-waived HbA1c testing, Mod complex HbA1c Dx* and ACR* testing
Cholestech LDX™ Analyzer Lipid testing
Cholestech LDX™ Analyzer
Lipid profile testing
Join the against CKM.
Join the fight against CKM.
Join the fight against CKM.
Contact your Abbott CM Account Executive or scan the QR code for more information.
Contact your Abbott CM Account Executive or scan the QR code for more information. Reference: 1.
1.
consider routine make sense to them. Since their ability to influence IDN management varies due to the policies and procedures of their IDN and the perceived quality of lab results in POL locations, you need to develop a relationship with them to understand the overall testing policies and procedures of their organization and the extent to which they are able to support POL testing.
To do this you need to establish trust and respect with them and to let them know that you will ensure any POL testing you establish or support in their IDN will adhere to the highest standards, and be compliant with IDN and regulatory requirements.
manufacturers to get their opinion and understanding. Aligning with their viewpoint on what the best POLs have in common will make your sales process more effective. Don’t be surprised if you receive a lead or two from a manufacturer who is confident your understanding of POL testing matches theirs. This is a long-term game and the relationships you develop now will bear fruit for years to come.
Commonalities among the best POLs
Now, let’s look at what the best POLs have in common. Simply stated, these are medical practices you would recommend to a family member. They are also practices
This may seem obvious, but a lab director who does not actively manage the lab is usually not a good sign. The lab director is the leader of the lab with responsibility for overall lab management, test selection, regulatory compliance and even the morale of the lab staff.
With an increasing number of physician practices under the ownership of IDNs, it is important to understand what the IDNs in your area also consider “the best POL.” I strongly recommend you develop relationships with your POCC teams. When they see you as an ally, they are more likely to help you put compliant POL testing in place and to help you identify POLs that need help from you and your trusted lab manufacturers.
Understanding that your job to identify what the best POLs have in common is a team job, it also makes sense to engage your trusted lab
you would consider as your personal medical practice.
I will be focused on the attributes of the lab, but there are more basic practice attributes to consider that also influence how the lab is run. Is the practice well organized? Is the front office staff polite and helpful? Does the practice staff have little to no turnover? Does the waiting room appear welcoming with patient-friendly information available? Is it obvious whether patient appointments are on time, or are there long waiting times?
From a POL viewpoint, the two most important factors in my opinion of whether they would
be on my list of “best POL” are whether the lab director is actively engaged with the lab, and the satisfaction and engagement level of the lab staff. This may seem obvious, but a lab director who does not actively manage the lab is usually not a good sign. The lab director is the leader of the lab with responsibility for overall lab management, test selection, regulatory compliance and even the morale of the lab staff. A key element of their job is to know and understand CLIA and other lab regulations, and to be able to communicate this information effectively to the lab staff.
Lack of active engagement by the lab director leads to a lack of direction for the staff and can lead to several adverse outcomes, including poor management of daily activities, the risk of poor lab results and even the possibility of a failed lab inspection.
Lack of engagement by their leader often leads to a lack of engagement and low morale by the lab staff. The lab staff needs to believe that their job is important to the overall health of the patients and work to create results that are high quality and delivered on time. The lab staff is responsible for the daily activities that result is a high-performance, well-organized lab. They need to believe their job is important and fundamental to help the practice achieve the goal of quality patient care.
From time to time, every lab will become aware of deficiencies they need to correct. The best customers correct deficiencies they uncover quickly and consider deficiencies as challenges to be met and conquered. They keep a few resources on hand, including you, your valued lab manufacturers, COLA and others to call on when
1 CBC/Day or

10,000 CBC/Day

Sysmex has the most reliable hematology solution for any lab.

3,000+
XN-L placements in the U.S.
26 years Sysmex has rated highest for System Reliability.*
1 hematology solution for all your customers.
XN-330™ Automated Hematology Analyzer
XN-9100™ Automated Hematology System
the need arises. They know that failure to assess staff competency every six months and failure of CLIA non-waived labs to enroll in and successfully complete proficiency testing surveys are the top two lab deficiencies, and they carefully manage their activities to ensure they are fully compliant. They put systems in place to list every CLIA requirement and permit them to create documentation to prove that they are compliant.
amount possible to be compliant. These customers tend to be the ones that frequently ask for better prices and are likely to shop your business for better deals.
The other book end customer is fascinated by the latest technology. They want the latest instrumentation and testing methods whether they have the specific patient need for it or not. Their problem is that they jump from one instrument to another
From the centrifuges to the rockers and rotators, every lab appliance has a label on it showing its current calibration date and the date the next one is due. They order reagents and lab supplies from you on time and on a routine basis, typically using your customer portal.
There are some excellent electronic lab management tools that make CLIA compliance easy. Using these tools is a great way to ensure they would pass an inspection, but, at a more fundamental level it creates a smooth-running lab that produces excellent results day after day.
The best POL labs are not “book end” customers. What is a book end customer? Book end customers are customers whose behavior is far from the mainstream.
One book end customer views the lab as nothing more than a cash cow. They look for the most highly reimbursed tests they can perform, often bringing in new equipment to perform these tests. They also tend to cut corners on lab personnel salaries and other areas of the lab. They view regulations as the enemy and do the least
as lab technology advances. If and when they depart from the practice, they leave a substantial challenge to return the lab to a well-managed condition with only the appropriate instruments in use for appropriate patient testing.
Administratively, the best POL customers shine, and you can recognize their labs the minute you walk in. The lab is neat and everything is in its place. The staff is cordial and not stressed. They may be busy but they have a workload they can handle and the right instruments and equipment to handle the work. Every element of the lab reflects this level of thoughtful organization. They know when their leases are due and have a plan for instrument upgrade or replacement as needed.
For the best POL customers, staff training, which is one of the
most frequently cited deficiencies by inspectors, is up to date and the training is put to good use by the staff. All the many lab appliances are calibrated and up to date. From the centrifuges to the rockers and rotators, every lab appliance has a label on it showing its current calibration date and the date the next one is due. They order reagents and lab supplies from you on time and on a routine basis, typically using your customer portal. They stay up to date on developments in new testing technology and use the philosophy of testing patients when needed to institute or amend their treatment program.
Maybe most importantly, they have a system in place to list every CLIA compliance requirement. They log their accomplishments against each requirement and always know when their next activity is due. Quality control and proficiency testing are taken seriously and are logged in the same electronic system that they use to manage their other CLIA requirements.
And they manage the lab for the benefit of the patients and care givers they serve. Their mission is clear and they perform their activities at a high level. While they may be busy, they respect you and your trusted lab manufacturers and make time for business reviews and lab reviews.
Being able to identify the best POL customers is a skill that takes years to develop and a commitment to ask others for their help and input. Once you identify the customers and prospects you would want to have yourself or a family member utilize, your territory will benefit. To be the best, identify the best and make sure they are your customers.
Engage, Elevate, Execute
Owens & Minor introduces new CCO and fresh strategic perspective at the company’s 2026 national sales meeting.
Courtesy of Owens & Minor
 While the theme of the Owens & Minor National Sales Meeting (NSM) in Dallas, Texas was ‘Engage, Elevate, Execute,’ this year’s conference offered attendees more than just an opportunity to learn and sharpen their skillsets. For the first time, commercial teammates heard from Owens & Minor’s new chief commercial officer (CCO), Dirk Benson, who shared his optimism and enthusiasm for the opportunities in store for Owens & Minor’s commercial organization.
“I could not be more excited to be at Owens & Minor right now. I’m energized not only by the strength of this commercial team, but by the possibilities Owens & Minor now has to make decisions more strategically, align itself for greater flexibility and double down on being more dynamic and responsive to customer needs,” said Benson.
Owens & Minor also hosted a number of its VIP industry partners, who provided perspectives on what defines a strong partnership: ` GPO discussion featuring Pamela Daigle and Anita Mouroutsos of Premier’s strategic sourcing and supplier engagement group ` Customer panel featuring senior supply chain leaders Mark Campbell of Tampa General Hospital, Deanna Loecker of Avera Health, Benn Sledge of Texas Health Resources and Kristin Komives of University of Michigan Health
In addition, commercial teammates received hands-on experience and held discussions with more than a dozen suppliers


from Owens & Minor’s branded product portfolio, including the company’s 2026 supplier
award winners B. Braun, Becton Dickinson and RJ Schinner.
The overall takeaway from this year’s NSM, says Christian Cook, interim CEO of Owens & Minor and Managing Director at Platinum Equity, is this:
“We believe this team – and this company – have the creativity, drive and determination to reimagine the Owens & Minor legacy and deliver a superior customer experience. I’m confident we are already well on our way and customers can expect great things from Owens & Minor in the days ahead.”
Dirk Benson
Antibiotic Stewardship with FebriDxTM
According to several World Health Organization studies conducted over the last 10 years, antimicrobial resistance, wherein germs build up resistance to antibiotics, is a significant threat to the health and safety of patients across the world. It’s considered one of the top 10 global health threats in the world, which makes the movement for antibiotic stewardship so important.
In a recent Repertoire podcast, host Scott Adams spoke to Tommy Hall, director of sales for Lumos Diagnostics, about the importance of antibiotic stewardship and how FebriDx can play a key role. Lumos announced the distribution partnership with Phase Scientific to exclusively distribute FebriDx within the United States.
What is antibiotic stewardship?
Antibiotic stewardship is the effort to ensure antibiotics are used only when necessary, with the correct drug, dose, and duration to improve patient outcomes. Rather than prescribing antibiotics empirically, providers are increasingly focused on targeted, appropriate use to reduce unnecessary exposure.
“The World Health Organization did a study in 2023 that showed if nothing was done to tackle it, by 2050 one person could die every three seconds from antimicrobial resistance,” Hall said, adding that it could become the leading cause of death worldwide.
A deeper review of World Health Organization data revealed the seriousness of the issue. Between 2016 and 2022, annual deaths linked to antimicrobial resistance increased from 700,000 to 1.2 million.
“People started to see those statistics and understand what was happening,” Hall said. “A light was shined on antimicrobial resistance as the next great epidemic. While more progress is needed, awareness has grown around the importance of using antibiotics properly.”
How FebriDx can help
FebriDx is a rapid point-of-care diagnostic test that uses a fingerstick blood sample to aid in the diagnosis of acute respiratory infection and differentiate bacterial from non-bacterial etiology. Understanding the difference can help providers make more informed treatment plans for their patients.
With a tool like FebriDx, providers can prove to their patients that they do not need an antibiotic for a non-bacterial infection with test results after 10 minutes. “When you look at a bacterial infection versus non-bacterial infection, the symptoms overlap. That makes it difficult on physicians and facilities to be able to dial in exactly what’s going on.”
FebriDx is helping to change the conversation about the necessity of antibiotics between providers and patients, as well as providing a way to ensure that unnecessary usage of antibiotics decreases. This is a huge shift towards a greater sense of antibiotic stewardship across the healthcare continuum.
“It’s a huge focus of being great stewards when we’re prescribing antibiotics, and informed patients who understand that we don’t have to demand those antibiotics for ourselves or for our kids. We need to be smart about when we’re taking them for our longterm health and longevity.”

You Don’t Have a Sales Problem – You Have a Courage Problem
Explore how fear and avoidance – not lack of skill – keep top salespeople from closing deals.
By Brian Sullivan, CSP
 I’ve been in professional selling for 35 years. I’ve trained thousands of salespeople across medical distribution, manufacturing, healthcare, technology – you name it. And after all that time, I can tell you with absolute certainty that most struggling reps don’t have a skills problem. They don’t have a product knowledge problem. They don’t have a territory problem.

They have a courage problem. There. I said it. And I know it stings because it’s supposed to.
Let me paint a picture you’ll recognize. You’ve got a rep who knows the product catalog inside and out. They can quote GPO pricing in their sleep. They’ve been through every training module your company offers. They show up on time, fill out the CRM, and hit their call numbers. And yet – their results are flat. Quarter after quarter.
Why?
Because they keep calling on the same comfortable contacts, having the same comfortable conversations, and avoiding the same uncomfortable truths.
That’s not a skills gap. That’s a courage gap. Here’s what courage looks like in medical sales. It’s calling on the surgeon you’ve been avoiding because the last conversation didn’t go well. It’s walking past the friendly materials manager who
The industry’s only one-touch, silent mobility system has arrived.

A simple turn of a switch engages and disengages the EasyGlide Mobility System.
Introducing the Brewer EasyGlide™ Mobility System.
The first to offer a one-touch, whisper-quiet mobility system, Brewer makes it possible to reconfigure and clean exam rooms quickly and with zero disruption to patients and providers. Our advanced EasyGlide Mobility System is an available option on our Access® PLUS and FLEX™ PLUS Exam Tables.
Scan to explore Access PLUS with EasyGlide
loves to chat and has zero buying authority, and instead asking to speak with the VP of Supply Chain who intimidates you. It’s telling a prospect, “I don’t think this is the right fit for you,” when every fiber of your being wants to chase the deal. It’s asking the question you’re afraid to ask because the answer might be “no.”
I see this every single week. Salespeople trained to ask highvalue questions – but won’t. They know they should lead with something that hits – a Value Hook that earns attention or a Pain Hook that exposes a real problem – instead of “just checking in.” But they don’t. They understand that handling indecision is where deals are won or lost – yet fold the moment a buyer says, “Let me think about it.”
They’ve been taught disciplined questioning frameworks like CLEAR – to ask what’s Currently happening, what they’ve Looked At, what’s Effective, what they’d Alter, and who’s Responsible – but when the moment comes, they skip straight to the pitch because asking real questions takes courage.
They have the
tools. They lack the guts to use them.
And nobody fixes that with another webinar.
Before the sales managers reading this start nodding and pointing fingers at their teams, let’s talk about you for a second. Because courage isn’t just a rep problem. It’s a leadership problem. Do you have the courage to ride along with your reps and give them honest, direct feedback – even
Brian Sullivan,
when it’s uncomfortable? Or do you sit through a mediocre call and say, “Good job,” in the car afterward because you don’t want conflict? Do you have the courage to put underperformers on a plan – or do you let them coast because they’re “nice people”? Do you have the courage to sit in the front row of your own team’s training and fully participate – or do you introduce the trainer, disappear for three hours, and wonder why nothing changes?
the decision-maker directly: “What would need to change for you to move forward with us?”
And when they give you a vague answer, press a little further: “Help me understand what’s really holding this up.”
After three and a half decades, here’s what I know: the reps who win aren’t the smoothest talkers. They’re not the ones with the best territories or the most experience.
Do you have the courage to ride along with your reps and give them honest, direct feedback – even when it’s uncomfortable? Or do you sit through a mediocre call and say, “Good job,” in the car afterward because you don’t want conflict?
If you’re a sales leader who won’t do the hard stuff, don’t expect your people to do it either. Courage is cultural. It flows downhill.
So how do you build it?
You don’t wait for it to show up. Courage isn’t a feeling. It’s a decision repeated under discomfort. It’s doing the thing that makes your stomach tighten before you feel ready, before you feel confident, before the conditions are perfect. Start small.
Tomorrow morning, make the one call you’ve been avoiding. Not the easy one. The one that makes you hesitate.
Walk into the account where you got shut down last month and lead with a new hook. Ask
They’re the ones willing to walk toward the hard conversation instead of around it.
Most reps circle discomfort like it’s a pothole. Top reps drive straight through it.
That’s the difference.
You already have the skills. You already have the training. You already know what to do.
The only question left is whether you have the courage to actually do it.
Stop blaming your territory. Stop blaming the market. Stop blaming the GPO contracts, the economy, or the competition.
Look in the mirror.
That’s where your sales problem lives.
And that’s the only place it gets fixed.
is the founder of PRECISE Selling and author of PRECISE Selling: 20 Days to the Top. With 35 years of experience in healthcare and medical distribution sales, he delivers keynotes, bootcamps, and outsourced sales development for companies nationwide. Contact him at preciseselling.com.
CSP,
Giant-sized performance in the industry’s smallest footprint¹



















































CN-3000 and CN-6000 Systems
The CN-3000 and CN-6000 Systems were developed with the smart workflow features and compact size needed to help labs overcome today’s testing challenges.
Featuring a wide spectrum of testing methodologies including clotting, chromogenic, immunoassay, and aggregation these flexible systems enable testing consolidation in both mid- and high-volume labs.
siemens-healthineers.us
1. As of January 2024. Footprint compared to competitor systems in the same volume class as listed on https://www.captodayonline.com/ and in the COBAS T 511 and COBAS T 711 coagulation analyzers brochure, Roche, 2018, and sthemO 301 analyzer brochure, Stago, 2023.
The products/features/applications mentioned here are not commercially available in all countries and are subject to local regulations. Their future availability cannot be guaranteed.




























Scan here to see the CN in action.
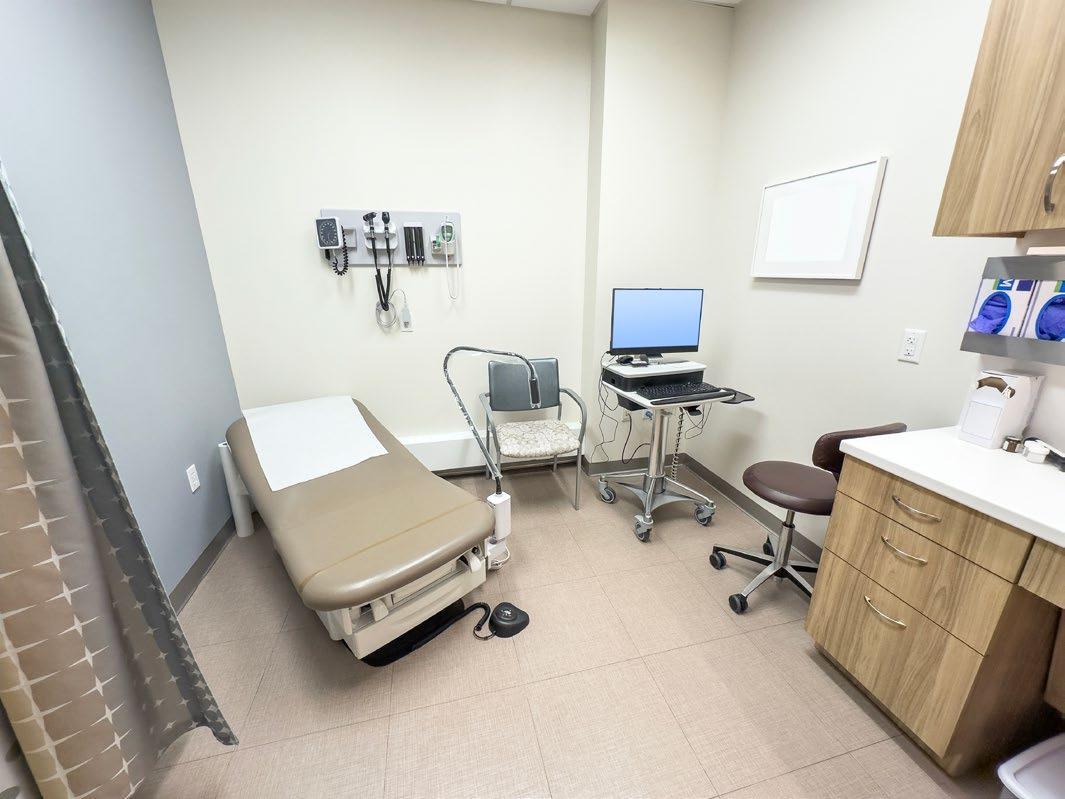
The Medical Distribution Hall of Fame recognizes individuals whose careers have gone beyond personal achievement to influence how the industry operates, collaborates and grows. This year’s inductees – Joe Grispo, Jon Wells, and Manny Losada – represent three distinct paths to leadership, united by a shared commitment to partnership, innovation and service to the healthcare community.
Across decades of transformation, each has helped redefine the relationships that power the healthcare supply chain. At B. Braun, Joe Grispo championed a distribution-first strategy and emphasized transparency and collaboration, helping strengthen supply chain resiliency during periods of unprecedented disruption. At Midmark, Jon Wells built a leadership philosophy rooted in trust and thoughtful design, reinforcing the importance of distribution as the critical “last mile” connecting strategy to patient care. Through MedPro Optimal, Manny Losada demonstrated the enduring value of relationships, mentorship and adaptability, balancing technological innovation with the belief that the handshake still matters.
Though their careers span different organizations and perspectives, common themes emerge: leadership grounded in trust, a willingness to embrace change, and a deep respect for the people who make healthcare distribution work every day. Their stories reflect an industry that succeeds not through transactions alone, but through collaboration among manufacturers, distributors and providers working toward shared outcomes.
In the following profiles, Repertoire Magazine celebrates Grispo, Wells and Losada not only for their individual accomplishments, but for the lasting impact they have made on the medical distribution community – and for the example they set for the next generation of industry leaders.
True leadership isn’t just about reaching the top — it’s about the path you pave for others to follow.
Today we join Repertoire in celebrating the visionaries, the disruptors, and the pioneers being inducted into the Medical Distribution Hall of Fame.
Joe Grispo B.Braun
Manny Losada Optimal MedPro
Jon Wells Midmark Corporation

Their dedication to excellence in healthcare distribution has helped shape our industry by improving the lives of patients and providers across the country.
Congratulations to this year’s inductees!


From Copy Machines to the Front Lines
Joe Grispo’s journey from grinding out copier sales to leading North American sales for B. Braun shows how foundational sales skills, strategic vision, and a willingness to leave the comfort zone can build a Hall of Fame career.
For Joe Grispo, the road to the Medical Distribution Hall of Fame didn’t begin with a high-level corporate strategy or a prestigious medical degree. It began with a stack of leads and the rhythmic hum of a fax machine.
When Grispo graduated from college, he knew exactly where he wanted to be: the med/surg industry. Influenced by family and friends already in the field, he saw the impact and stability of healthcare. However, breaking in proved difficult for a recent graduate. Rather than waiting for a door to open, Grispo decided to build his foundation elsewhere, taking a path familiar to many veterans of the trade – selling office equipment.
“I’m dating myself,” Grispo says with a laugh. “Fax machines were the brand-new cool thing when I was doing it.” In the high-pressure world of copier sales, Grispo learned the “sink or swim” reality of the business. It was here that he forged his work ethic, spending every day hunting for leads and honing the basic selling skills that would eventually serve as the bedrock of his career.
Finding the “corporate umbrella”
After four or five successful years in office equipment, Grispo finally cracked into the medical world at Carrington Laboratories, a wound and skincare company in Texas. It was here that his trajectory shifted. When he moved into the national accounts department, Grispo realized he had found his calling.
“I realized this is really what I want to do,” he explains. “I loved the corporate side of things.” To Grispo, “national accounts” wasn’t just a title; it was a massive umbrella covering GPOs, distribution, government sales, and eventually, the rise of IDNs. This multifaceted perspective became his specialty.
His expertise caught the attention of Bristol Myers Squibb (BMS), where he joined a new division focused on the burgeoning home healthcare market. When the market shifted and BMS folded
that division, Grispo transitioned to Convatec, further deepening his experience in managing the complex relationships between distributors and hospitals.
Connecting the dots at B. Braun
Twenty-four years ago, Grispo arrived at B. Braun with a specific mandate: take the company’s national account strategy to the next level. At the time, his focus was narrow, primarily managing GPO relationships. However, under the leadership of Manny Villafaña, the vision expanded.
Grispo and his leadership team began “connecting the dots,” realizing that GPOs, distributors, IDNs, and government sales were not siloed entities but parts of a singular, cohesive ecosystem. By folding these responsibilities together, Grispo helped B. Braun navigate a rapidly consolidating healthcare landscape.
In 2009, Grispo’s journey reached a new peak when he was named Chief Sales Officer. For the past 16 plus years, he has overseen
all sales in North America for the organization. From the grit of cold-calling office managers to leading the North America sales force of a global healthcare leader, Grispo’s career is a testament to the power of foundational sales skills and the ability to see the “big picture” in a complex industry.
One of the most defining chapters of Grispo’s tenure at B. Braun was his pivot toward a distribution-first strategy. When he arrived, the company’s relationship with distributors was largely transactional – an “afterthought” rather than a pillar of the business. Grispo recognized that B. Braun could not reach its full potential in the U.S. market without a fundamental shift in philosophy.
“My background said, no, this needs to be a core strategy,” Grispo recalls. To execute this vision, he brought in long-time colleague Tim Cokkinias to help re-engineer the organization’s approach. The results were transformative: today, approximately 95% of B. Braun’s
The honor of being inducted into the Medical Distribution Hall of Fame
“I am honored to be included in the long list of industry giants that came before me and that I have learned so much from. People like Mark Seitz, and the late John Sasen and Mike Carver. Each of these people taught me the lesson of leaving it better than you found it. They all poured into those around them and had a passion for this industry second to none.
“We recently lost Mike Carver, and I can say without hesitation, we lost a giant from our industry. He was a mentor, but he was also a friend who always made it his mission to make people feel good about themselves. He was a selfless leader, and I am better for knowing him. I will miss him every day.” – Joe Grispo
North American business flows through distribution.
This strategic shift was bolstered by B. Braun’s unique global structure. As a familyowned organization, the company operates with a “generational” lens rather than being tethered to the pressures of quarterly earnings. This longterm perspective allowed Grispo to build deep, enduring partnerships that go beyond simple logistics, ensuring that B. Braun remains a critical and stable fixture in the healthcare supply chain for decades to come.
Mentors and heroes
For Grispo, leadership was first modeled at home. He traces his professional “toughness” to his mother, a cancer survivor whose resilience left an indelible mark on his character. From his father, the son of an Italian immigrant and the first in his family to attend college, Grispo inherited a quintessential “bootstrap” work ethic. These foundational figures instilled the grit and honesty that would define his decades in medical distribution.
However, it was two specific industry giants who refined that raw potential into Hall of Fame leadership. Manny Villafaña, despite only managing Grispo for a single year, acted as a strategic catalyst. He challenged Grispo to move beyond tactical sales and embrace deep strategic thinking and the nuances of high-level partnership negotiation.
The final push came from former B. Braun CEO Caroll Neubauer. In a move that Grispo admits he didn’t see coming, Neubauer “forced” him out of his comfort zone. By

Celebrating a Career. Honoring a Legacy.
Congratulations to our own Joe Grispo, 2026 inductee into the Medical Distribution Hall of Fame.
insisting that Grispo interview for the Chief Sales Officer role – a position he wasn’t seeking –Neubauer fundamentally altered the trajectory of Grispo’s life. This mentorship of “pushing” rather than just “pulling” is what Grispo credits for his evolution from a successful specialist into a transformational leader.
Resilience in the face of the unforeseen
Since Grispo stepped into the role of Chief Sales Officer in 2009, the healthcare industry has navigated a gauntlet of challenges. From the implementation of the Affordable Care Act and medical device taxes to the volatility of global tariffs, Grispo thought he had seen it all. Then came 2020.
company’s communication with distributors grew exponentially. They moved beyond spreadsheets to real-time collaboration, identifying “hotspots” and directing bolus shipments of life-saving products exactly where patient need was greatest.
When the world was upended by a “brand new, off-the-charts” crisis like COVID-19, Grispo realized that past experience alone wouldn’t suffice. Leadership in a vacuum of precedent requires a specific, disciplined process.
For Grispo, that process begins with radical prioritization. “We can’t be everything to everybody,” he notes. “What are the top three or four things that we need to deal with that we have in our control?” By stripping away the noise and focusing
While inspirational leaders can rally a crowd, transformational leaders elevate the entire ecosystem.
“I don’t like giving COVID credit for anything because it was awful,” Grispo admits. Yet he acknowledges that the pandemic served as a massive catalyst for institutional growth, forcing the industry to evolve in ways that are now mission-critical for the future of patient care.
The most vital lesson was the absolute necessity of supply chain resiliency. When borders snapped shut at the onset of the pandemic, the vulnerability of global logistics became a glaring reality. For B. Braun, the answer was a renewed focus on domestic strength and end-to-end visibility. Under Grispo’s leadership, the
on the controllable variables, Grispo and his team were able to stabilize and drive the focus needed by his organization. He leaned into a war room mentality, fostering a culture of constant communication and total transparency. This wasn’t just internal and took a cross-functional team approach. It extended to weekly, senior-level dialogues with distribution and government partners, to sync what B. Braun was seeing with what was happening on the front lines.
Building a resilient system requires better communication and physical infrastructure. Grispo highlights B. Braun’s
more than $1 billion investment in domestic production redundancy as a key differentiator. By establishing two major IV plants – one on each coast – the company created a safety net against more than just viral outbreaks. Whether facing a global pandemic or a localized natural disaster like a hurricane, B. Braun’s decentralized manufacturing ensures that the flow of critical supplies remains uninterrupted.
“That redundancy’s really important regardless of what the situation is,” Grispo notes. It is a strategic hedge against a world that has become increasingly unpredictable.
A culture of rising to the occasion
Beyond the logistics and the manufacturing plants, what Grispo finds most rewarding is the human element of the industry. His work with the Health Industry Distributors Association (HIDA) and his partnerships across the supply chain have reinforced his pride in the medical distribution community.
When the world slowed down, the med/surg industry accelerated. “We see the problem and we step in,” Grispo says. “What we do has to keep moving. It can’t just stop.” This collective “rise to the occasion” spirit – a seamless collaboration between manufacturers, distributors, and providers – is what Grispo believes sets this industry apart.
One of Grispo’s most profound management insights is the importance of context. In high-pressure situations, leaders often issue directives without explanation, leading to






confusion or pushback. Grispo believes that explaining the “why” is the bridge to total organizational alignment.
“Most people, when they know the why, will get on board and really give that effort that they need,” he explains. Without
that detail, even the most talented professionals can waste valuable energy questioning a strategy they don’t fully understand. For Grispo, leadership isn’t just about making the right call; it’s about ensuring the people making decisions across
Advice to the next generation
If Joe Grispo could send a message back to the young sales rep selling copiers in the early 1990s, the advice would be remarkably simple: Get out of your comfort zone.
For Grispo, the greatest danger in a successful career isn’t failure – it’s stagnation. Before 2009, he was the master of national accounts. He loved the work, he was good at it, and he assumed he would finish his career there. It wasn’t until he was asked to step into the role of Chief Sales Officer that he realized he had become “stale.”
“I did not realize how much there was to learn,” he admits. Moving from a specialized corporate role to overseeing hundreds of people across North America was an immediate jolt to the system. Yet he credits this period of intense discomfort as the most transformative learning phase of his life.
Grispo also observes a unique challenge for the modern, remote-first workforce. While tools like Teams and Zoom offer efficiency, they often eliminate the “hallway discussions” – those serendipitous, post-meeting interactions where institutional knowledge is shared and relationships are cemented.
“When you’re on a Teams meeting, it’s over and you’re off the screen,” Grispo notes. For the younger generation, he suggests that getting out of the comfort zone today means:
` Mastering the digital impression: Ensuring your “on-screen” presence – lighting, audio, and engagement – is as professional as a face-to-face meeting.
` Seeking the “in-between” moments: Actively creating opportunities for informal mentorship and networking that don’t happen naturally in a remote setting.
` Embracing the learning curve: Recognizing that while digital fluency is a strength, the foundational “people skills” of the past still carry immense value.
Grispo remains optimistic, noting that while the medium has changed, the drive of the new generation will likely take the industry to “new heights” – provided they are willing to step away from the familiar.
the business have the full picture to execute with confidence.
Inspirational vs. transformational leadership
When reflecting on the qualities that define the Hall of Famecaliber leaders in his industry, Grispo draws a distinction between being inspirational and being transformational. While inspirational leaders can rally a crowd, transformational leaders elevate the entire ecosystem.
“Transformational leaders go a level further,” Grispo says. “They look to elevate the entire organization and the people in it.” These are the leaders who take calculated risks and “pour into” their subordinates, helping them grow while simultaneously pushing the boundaries of what the company can achieve. It is this willingness to do things differently – combined with a highly motivated, great team – that separates a good leader from a great one.
The balance of tenure and drive
While many industries see high turnover, Grispo finds inspiration in the veterans who have been with the organization for 30 or 40 years.
To him, the mark of a healthy culture isn’t just how long people stay, but how hard they continue to work. He points to those decades-long veterans who are still hitting their biggest numbers and achieving their highest goals as the ultimate proof of a thriving organization. In Grispo’s world, leadership is about creating an environment where a 40-year career doesn’t end in a slow fade, but in a continued pursuit of excellence.
May 4, 2026!






Join Us To Be Inspired, Empowered, and Equipped To Create Your Own Breakthrough Open to Women & Men From All Career Levels – Aspiring Leaders to C-Suite Executives.
Gain actionable takeaways through our PWH Leadership Insights,, empowering keynote speakers, engaging panel discussions, workshops & breakout sessions that cover a host of topics around pressing leadership issues.
PWH® 2026 Summit Breakout Sessions





Work Smarter: Building Careers and Connections with AI Amie Rafter, Founder, Hbird

Communicate to Connect: Adapting Your Communication Style to Lead More Effectively Vicky Lyle, Founder, Coach Lyle
Grow Revenue, Get Respect: How Sales & Marketing Leaders Use Finance to Level Up Allison Therwhanger, Vice President of Corporate Sales, Innovia Medical
The Power of Us Therese Gopaul-Robinson, Performance Strategist & Professional Speaker, TGR


True Brand Meaning: Creating a Personal Brand That’s Invigorating Kaycee Kalpin, CMO, Premier



How to BE the Talent Your Company Needs Rosina Racioppi, President & CEO, AscentPoint Leadership
Why Mattering Matters: Why Feeling Seen Changes Everything for Women at Work Karen Dutton, Senior Director of Culture & Belonging Integration, Sodexo

Appreciative Inquiry: Ignite the Leader Within Lisa Ramsey & Amy Nelson, Senior Learning Experience Designers, Midmark
The Stories We Release, The Lives We Create Dr. Christina Bowen, Chief Well-Being Officer & Nickie Dixon, Program Manager, Provider Well-Being, Engagement & Retention, ECU Health
Thank you to our 2026 Leadership Summit Sponsors
Additional sponsorships still available! Contact Michelle Rydberg at mrydberg@mypwh.org to learn more.






Last chance to register to attend the industry’s only conference completely dedicated to inclusive leadership development.
Registration at mypwh.org/summit

Member Non-Member




Jon Wells: Trust, Tenacity, Transformation
Hall of Fame inductee Jon Wells reflects on the relationships, mentors, and leadership lessons that have guided him through decades of change in healthcare and distribution.
Jon Wells never planned on a career in healthcare. A graduate of The Ohio State University with a degree in architecture, he was drawn instead to the satisfaction of creating something lasting – designs that moved from concept to construction and ultimately served people for years. “What drove me was being part of something that built meaningful things,” Wells, president and CEO of Midmark, recalls. That instinct to build would become the throughline of a career that eventually led him to Midmark and, this year, to induction into the Medical Distribution Hall of Fame.
Wells’ entry into healthcare came almost by accident, but it didn’t take long for the industry’s real-world impact to capture his attention. Early in his Midmark career, he worked closely with architects across the country, traveling extensively and seeing firsthand how thoughtfully designed clinical environments could influence care. The work, he says, was far from abstract. “It really affects clinicians, patients and healthcare,” he explains. Later, as a sales representative in Atlanta, Wells gained a deeper appreciation for the role of distribution. “It’s more than moving products,” he says. “It’s relationships, trust from distributors, trust from clinicians … that last mile matters.”
Across decades with Midmark, Wells has continued to follow that
same builder’s mindset, shaping products, teams and partnerships that support better care delivery. His Hall of Fame recognition reflects a career defined by thoughtful design in its many forms – from physical spaces to the systems and relationships that help healthcare run more effectively.
Designing for the “last mile”
For Midmark, innovation doesn’t end when a product leaves the factory floor – it’s tested in the hands of healthcare stakeholders every day. Wells says that reality has shaped the company’s approach to product development for decades. “Distribution is the front line of Midmark,” he explains. “It’s where strategy and execution meets reality.” From early design conversations to
post-sale support, the company considers how products will be delivered, installed and serviced through its distribution partners, who he calls “truly an extension of Midmark.”
That emphasis on the “last mile” has helped the company refine products and processes based on real-world feedback. Distributors provide insight into everything from workflow challenges to installation barriers, and that input loops back into future designs. “It amplifies who Midmark is to thousands of customers each and every day,” Wells says. “The feedback from distributors because of that last mile is critically important to us.” In an industry where small inefficiencies can ripple into patient care delays, he adds, seamless implementation and reliable support are just as important as the product itself.
Wells’ leadership perspective has also been shaped by the industry’s constant state of change. Over the course of his career, he has navigated the rise of managed care in the 1990s, waves of consolidation among providers and distributors, the shift from promotion-driven sales to contract-based purchasing, and more recently, the disruption of COVID-19 and global supply chain challenges. Each era, he says, forced leaders to rethink how they operate.
A guiding influence has been the concept of a growth mindset – the belief that challenges strengthen organizations rather than weaken them. Wells credits that philosophy with helping Midmark weather the pandemic, when dental practices temporarily shut down and uncertainty gripped the industry. The experience
reinforced the value of a strong leadership team and deep distributor relationships. “We can’t predict what the next Black Swan will be,” he says. “The best way to manage Black Swan events is having a really strong leadership team.”
Balancing the long view with the front line
For Wells, leadership at Midmark means constantly toggling between two timelines: the realities of today’s distribution environment and the investments that will shape the company years from now. To keep both in focus, Midmark relies on a five-year rolling strategy – a framework that allows leaders to evaluate present-day decisions through a longer lens while still executing against annual goals. “We used to be very one-year, twoyear focused,” Wells says. “Now, that five-year rolling strategy helps us understand decisions we’re making today and how they’ll impact us two and three years out.”
set of strategic priorities. Wells says the key to making that balance work is honesty – an unvarnished look at what’s happening in the field. “You really need to be very open and honest and taking in all of this information, and kind of a brutal reality of what’s real and what’s not,” he explains. Much of that real-time insight comes from distributors, whose feedback helps inform both monthly adjustments and longer-term investments, from production capacity to product line decisions.
The planning process itself is internal, built over time as the leadership team gained confidence in long-range forecasting. In a capital-intensive industry with factories, facilities and large product lines, those decisions carry significant weight. “You have to develop some confidence with it over time,” Wells says. As leaders began to see multi-year plans materialize as expected, that
Wells emphasizes the need to ask more questions than feels comfortable, to truly understand the client’s perspective, and to work alongside them to solve problems.
“Once they see the results of that work, then you become much more of an asset for them.”
The structure is both disciplined and flexible. The first three years of the plan are mapped in detail, while the later years remain directional, allowing the organization to adjust as market conditions change. Annual budgets and tactical plans still drive day-to-day operations, but those actions are guided by a broader mission and
confidence grew, enabling the company to invest more decisively while remaining cautious about where to double down or pull back. The ability to shift resources across product lines and sales channels, he adds, has become a strategic advantage.
Wells’ own leadership style has evolved alongside that planning
discipline. One of his biggest lessons, he says, was learning to slow down and empower others to make decisions. Early in his career, he prided himself on decisiveness and speed. Over time, he realized that moving too quickly could leave teams without the confidence or experience to lead on their own. “I needed to work through them and have them make more decisions, and support them,” he says. Today, he measures success by how well a team functions in his absence – a shift that reflects a deeper focus on trust, development and long-term strength.
Built on trust, strengthened by transparency
For Wells, the relationship between manufacturers and distributors has always been rooted in trust – but what that trust looks like has changed dramatically over time. Earlier in his career, he says, trust was often measured by responsiveness and reliability: returning calls quickly, meeting ship dates and delivering consistent quality. Those fundamentals still matter, but the expectations on both sides of the partnership have expanded.
Today, transparency and collaboration are just as critical. “The partnership and the transparency on what we’re going through as companies and in the industry,” Wells says, “to be able to share those things and help each other move forward and support our customers – that’s what’s evolved.”
The past decade, and especially the last five years, have tested those relationships in new ways. Distributors have been asked to manage unprecedented complexity, from pandemicdriven surges in PPE and vaccine
HONORING LEADERS



distribution to shifting capital spending and supply chain volatility. Wells notes that navigating those changes has required closer communication and a shared understanding of challenges on both sides. “Distributors manage so much more complexity than they used to,” he says. In response, Midmark has worked to maintain open lines of communication, even when the news isn’t always positive. “We’re always here for our distributors. We’ll listen,” he says. “Sometimes the news isn’t great for us or for them, but they know that we’re here, and we’ll always pick up the phone, and we’ll work through it the best we can, and we always land on the other side.”
That commitment to partnership extends across the Midmark medical, dental and veterinary businesses, where Wells sees continued opportunity for deeper collaboration in the years ahead. As the industry grows more complex, he believes strong channel relationships will be essential to helping providers navigate change and deliver care effectively.
When asked what he hopes his legacy will be, Wells points less to specific accomplishments and more to the values that guided his career. A strong work ethic and integrity, he says, have always been central. “Always take the high road,” he notes, emphasizing sincerity and consistency in every interaction. He also points to empathy – not only in leadership, but in design. Understanding the needs of clinicians, distributors and customers has shaped how he approaches both product development and partnerships. “It’s really how I worked with others and listened
and earned trust,” he says. “Stayed focused on building things … and just keep moving forward.”
Wells credits that mindset to a network of mentors who influenced him at every stage of his life and career, from his father’s work ethic to colleagues and leaders within Midmark and across the industry. Each, he says, helped shape his approach to leadership and relationships. Taken together, those influences reflect a career defined by steady progress, collaboration and a belief that trust – earned over time and reinforced daily – remains the foundation of lasting partnerships in healthcare distribution.
The project is the product
Looking ahead, Wells sees the next five years as an opportunity to expand Midmark’s impact beyond individual products to entire ecosystems of care. For him, it’s not about tables, sterilizers, or any single piece of equipment – it’s about making workflows function seamlessly and supporting clinicians in the environments where they deliver care. “The project is the product,” Wells explains. “Getting that practice up and running and getting it running in a good functional way is important.” This perspective requires sales and distribution teams to think holistically, to understand the clinician’s daily challenges, and to offer solutions that make work easier and more efficient.
Central to this approach is collaboration and trust. Wells emphasizes the need to ask more questions than feels comfortable, to truly understand the client’s perspective, and to work alongside them to solve problems. “Once they see the results of that work, then you become much more of
an asset for them,” he says. In essence, the value isn’t just in the equipment sold, but in helping practices and hospitals operate better, smarter, and more seamlessly. This mindset is shaping the next generation of salespeople at Midmark, reinforcing the company’s legacy of thoughtful design, attentive service, and proactive problem-solving.
Wells’ Hall of Fame induction offers a moment to reflect on that legacy, but he is quick to redirect praise to the broader community. “It isn’t about me. It’s really Midmark, reflective of Midmark and the people and the history and the distribution partners, and customers that I’ve had the privilege to work with for so many years,” he says. For Wells, the honor represents the collective effort of countless professionals committed to advancing healthcare. At the same time, he views it as a responsibility – to mentor, guide, and support the next generation so they, too, can innovate and build trust in a rapidly evolving industry. Through decades of navigating change, from technological shifts to global crises, Wells’ career has been defined by the same principle that drives his vision for the future: build thoughtfully, collaborate intentionally, and keep moving forward. In his view, success is less about individual accolades and more about creating environments where teams, partners, and clinicians can thrive. As he continues to shape Midmark’s journey, Wells embodies a philosophy that’s as forward-thinking as it is grounded: in healthcare, the project truly is the product, and the people involved are the heart of its success.

Honoring Jon Wells 2026 Medical
Distribution
Hall of Fame Inductee
Congratulations on your induction into the Medical Distribution Hall of Fame. Your leadership and vision continue to strengthen the collaboration between manufacturers and distributors— helping Midmark deliver solutions that improve the experience at the point of care.

“The most value for all of us is in taking the time to listen to our customers and working together with them to design their best way forward.”
- Jon Wells President and CEO

Manny Losada: Leading with Trust in Medical Distribution
Hall of Fame inductee Manny Losada shares lessons on growth, innovation and the enduring power of relationships across the healthcare supply chain.
For Manny Losada, a career in medical distribution has always been about more than products, contracts or market share. It has been about people – the partners, mentors and colleagues who have shaped the industry and the patients ultimately served by the work behind the scenes. Over decades, Losada has never lost sight of the relationships that make the business run.
“I think people will believe first a friend,” he says of the legacy he hopes to leave. That perspective has guided him from his earliest days in the field through the growth of MedPro Optimal Healthcare Solutions and into a leadership role that has touched nearly every corner of the healthcare supply chain.
In advance of his induction into the Medical Distribution Hall of Fame, Losada reflected on the partnerships, lessons and sense of purpose that have defined his journey, and on the industry family that continues to inspire him.
Seizing an opportunity
Losada’s healthcare career journey has included sales and marketing positions for Procter & Gamble and Johnson & Johnson. He was appointed Vice President
of Corporate Special Markets for Henry Schein, Inc. following the acquisition of Microbiomedics where he served as Vice President of acute care. He held the position of Senior Vice President and Chief Sales Officer for the U.S. commercial business of medical device manufacturer B. Braun Medical. He also served as Executive Vice President of publicly traded Medical Action Industries Inc.
Since June 2009, Losada has been the President and CEO of Optimal, successfully completing an acquisition by now parent Keralty, a multinational, global company, and serves as the President and General Partner of MedPro Associates, one of the nation’s largest national manufacturer’s representation organizations.
Losada traces the origins of MedPro Optimal to a long-standing
partnership and a clear market opportunity. More than a decade ago, he and industry veterans Bill Sparks and Parker Bigley began doing early work representing government business for Optimal. From that collaboration came the idea of bringing complementary capabilities together more strategically. “There was a need – and still is a need – in the industry to fill gaps with national sales coverage while also providing logistics solutions for manufacturers,” Losada says.
MedPro Optimal was designed to sit squarely in that space, supporting both manufacturers and distributors with expanded reach and operational support. “Our mission is really to provide that coverage and be able to support partners logistically. I don’t think there’s another organization out there doing it quite like this.”
A key differentiator has been the addition of government services, an area many manufacturers find difficult to enter. By outsourcing to partners with deep industry knowledge, Losada says companies can scale more effectively.
Acting as an extension
As MedPro and Optimal have grown, maintaining the agility that defines independent manufacturer reps has required a deliberate shift in how the organizations operate. For Losada, scaling relationships and responsiveness starts with investing in the right infrastructure. “Scale is never easy,” he says. “And in today’s world, it just can’t be done manually anymore.” To sustain growth without sacrificing flexibility, both organizations have leaned heavily into advanced CRM and ERP platforms supported by AI.
“AI isn’t leading,” Losada explains, “but it’s providing us with a backbone of information and efficiency that we’ve never seen before.”
That technology investment allows the team to act as an extension of its manufacturer and distribution partners, using data to forecast growth and improve service. “Data is key,” he says. “We become an extension of our trading partners.” Even so, Losada keeps a sense of humor about the future, joking that the only thing that worries him is “an AI bot of Sparky” someday replacing trusted colleague Bill Sparks.
the purchasing and supply chain landscape. From reimbursement pressures to labor shortages and the growing influence of private equity, the forces affecting providers and suppliers are complex – and, at times, unsettling. “I’m not a great sleeper,” he admits with a laugh, before turning serious. “At a high level, how do you sustain delivery of care at the level we’re supposed to be at here in the U.S. as a world-class healthcare system?”
Among the biggest concerns, he says, are the mounting challenges facing clinicians. Rising costs, workforce shortages and
“This business connects you not only to the rewards and challenges of the business side, but it also gives you a connection to purpose.”
Despite the focus on technology, Losada emphasizes that leadership fundamentals remain unchanged. “Do what you say you’re going to do, develop the people around you, listen before you speak,” he says. “The handshake and the visit still matter.”
Encouraging innovation across a large, independent sales force requires balance. New ideas bring energy and opportunity, but also risk. “It’s exciting to see the next generation coming in with new ways to do things,” Losada says. “Without encouraging innovation, you’re standing still – and when you’re standing still, someone just walked past you.”
A shared commitment
As healthcare continues to evolve, Losada sees both opportunity and uncertainty shaping
reimbursement constraints all ripple through the supply chain. “You see the challenges with doctors being able to afford to be a doctor, nurses with labor shortages – if you look at the forecasts over the next 10 years, it’s alarming,” Losada says. Product innovation brings promise, but also cost pressures tied to insurance coverage and reimbursement models. At the same time, private equity has reshaped the distribution and manufacturing landscape, introducing new capital and perspectives but also new expectations. “There are concerns, but at the same time, it’s exciting because it’s a new view,” he explains. “You can’t replace experience, but you have to be open to other thoughts.” What gives him confidence is the industry’s collective willingness to
collaborate. Across manufacturers, distributors, providers, group purchasing organizations and trade associations, Losada sees a shared commitment to solving problems. “There’s nobody in the industry that knows our business better than ourselves,” he says. “We spend a lot of time – personal time – trying to tackle these issues and make sure our voices are heard.”
Over decades in the industry, Losada has prioritized trust, loyalty and mentorship. He takes pride in the number of colleagues who have grown into leadership roles after working alongside him and in maintaining a reputation for honesty. “My handshake out there is solid,” he says. “I’m not afraid to make mistakes and keep smarter people around me. I don’t know it all, and I’m learning so much from others, especially our younger next generation.”
Known for speaking his mind, Losada also emphasizes the importance of positivity and service. “As long as I’ve impacted somebody in a positive way, that to me is personal success,” he says. He describes the healthcare supply chain as an “industry family,” one he has remained fiercely loyal to throughout his career. At the same time, he credits his own family for supporting the long hours and extensive travel that come with that commitment. “I’m forever grateful to my wife and my four children for allowing me to serve the industry for as long as I have,” he says.
“This business connects you” For Losada, the most important message to young sales reps entering medical distribution is to recognize the deeper purpose behind
In healthcare, what gets measured gets improved. And true leadership leaves a lasting mark.
DETECTO is proud to celebrate this year’s Medical Distribution Hall of Fame inductees –leaders whose vision and dedication continue to move our industry forward.
Joe Grispo
B. Braun
Jon Wells Midmark Corporation
And an extra special congratulations to long-time DETECTO partner
Manny Losada Optimal MedPro
Thank you for raising the standard and shaping the future of healthcare distribution.
Congratulations on this well-deserved honor.
the work. While the industry offers the familiar rewards and challenges of business, he believes it also provides something harder to find elsewhere – a direct connection to patient care. “This business connects you not only to the rewards and challenges of the business side,” he says, “but it also gives you a connection to purpose.”
people here will welcome you with open arms.”
A career filled with gratitude
For Losada, induction into the Medical Distribution Hall of Fame is both a personal milestone and a moment of deep reflection on the relationships that have defined his career. When he received
Often described as an extended family, the medical distribution community tends to rally together when challenges arise. For those considering a career in the field, Losada’s advice is simple: there is opportunity and support waiting. “Come on down.”
That purpose comes from knowing that every product delivered, relationship built and contract secured ultimately supports clinicians and impacts patient outcomes. At some point, Losada notes, everyone will have a family member or friend facing a health issue. Understanding that your role helps make care possible adds meaning to the day-to-day grind. “Knowing you played a role in helping others heal gives you passion and compassion at the same time,” he says.
He also points to the industry’s resilience and culture. Healthcare is essential, and the relationships within it run deep. Often described as an extended family, the medical distribution community tends to rally together when challenges arise. For those considering a career in the field, Losada’s advice is simple: there is opportunity and support waiting. “Come on down,” he says. “There’s a need for you, and
the invitation, he admits he was momentarily speechless. “It was completely unexpected,” he says. “I’m really never at a loss for words, and at that moment I was.”
Losada has long admired the Hall of Fame from the audience, even participating in roasts honoring industry legends such as the late John Sasson and his longtime partner Bill Sparks. Now, standing alongside those he once celebrated feels surreal. “Being on the receiving side of that company and all the other members of the Hall of Fame, it’s just very humbling,” he says. “I consider this a lifetime achievement award, and I’m grateful to be sticking around long enough to have been part of this.”
Sharing the honor with fellow inductees makes the moment even more meaningful. He points to Joe Grispo, a trusted colleague from his B. Braun days, and Jon Wells of Midmark, whose steady leadership and thoughtful
counsel left a lasting impression. “Jon taught me to be a listener,” Losada says. “Early on his words of wisdom and approach – I have a lot of respect for him.”
When asked about mentors, Losada’s answer spans decades. He begins with his father, an immigrant from Spain whose work ethic and independence shaped his outlook. “He told me, ‘I get up every morning, put my two feet on the ground and don’t owe anyone where I’m going,’” Losada recalls – advice that guided early career decisions. From there came industry figures who helped shape his professional path: Marvin Caligor, who modeled relationship-driven leadership; Bruce Haber, who instilled financial discipline and confidence; and Mark Mlotek and Brad Connett, who taught him the art of negotiation and growth. He credits Dave Meyers, Allison Therwhanger and Gina Marchese in keeping his balance throughout difficult times both personally and professionally.
Later in his career, partners and colleagues such as Bill Sparks and trusted advisor Mark Seitz continued to influence his perspective. “I’m a little bit of all of them,” Losada says. “There are so many people who have shaped me into the person I have become today.”
As he prepares for the ceremony, Losada returns to a familiar theme: gratitude. Surrounded by family, friends and industry peers, he views the honor not as an endpoint but as a celebration of shared effort and enduring relationships. “It’s humbling and numbing at the same time,” he says. “I’m looking forward to spending the evening with both my family and industry family. I couldn’t be more blessed.”
Our clinically trained, HIDA AMS-accredited sales professionals are strategically located throughout the country, delivering expert, in-person support to providers and streamlined execution for manufacturers and distributors alike.

www.mproassociates.com
CaviCide HP
1-Min Hydrogen Peroxide Surface Disinfectant
The power of CaviWipes™ HP now available in ready-to-use liquid
1-Minute universal contact time for all listed pathogens
Effective disinfection against 70 pathogens including MDRO and Candida auris
Hydrogen Peroxide with no signal word –no PPE required*
1-Step cleaning/disinfection*


Ordering Information
Part No. Item Description
16-1024 CaviCide HP 24 oz spray bottle
16-1000 CaviCide HP 1 gal bottle
and PPE instructions

Primary Care at the Center of Obesity’s New Era
With GLP-1 medications, updated standards of care and growing awareness of weight bias, clinicians are navigating expanding treatment options — and rising expectations — in the fight against chronic disease.
 Obesity care is undergoing a profound shift – from a narrow focus on weight loss to a more comprehensive, chronic-disease approach that spans prevention, treatment and long-term support. Across primary care clinics, specialty organizations and patient advocacy groups, clinicians are increasingly recognizing obesity as a complex medical condition that intersects with diabetes, cardiovascular disease and a host of other health risks. That evolution is reshaping everything from care delivery models to the products and therapies used to support patients.
Family physicians are often on the front lines of that change.
Dr. Brent Smith, a family physician and member of the American Academy of Family Physicians’ Board of Directors, said the past five years have brought a stronger emphasis on addressing obesity as a root cause of many chronic conditions.
“Family physicians play a key role in helping patients get to a healthy weight and reduce risks for related health concerns,” he notes. Today, care teams are combining lifestyle counseling, behavioral health strategies, medications such as GLP-1s and, when appropriate, bariatric surgery – an approach echoed by experts from

the American Diabetes Association and the Obesity Action Coalition, who stress that effective obesity care requires coordinated, patient-centered support across the continuum.
New options, greater expectations
As new therapies and care models reshape obesity treatment, family physicians are finding themselves at the center of a rapidly expanding set of options – and expectations. From counseling patients on nutrition and physical activity to prescribing advanced medications and coordinating referrals, primary care practices are navigating a broader, more complex treatment landscape than ever before.
Dr. Smith said that shift is both encouraging and challenging. For years, family physicians have treated the chronic conditions associated with obesity, such as Type 2 diabetes, hypertension and cardiovascular disease. Now, they are increasingly able to target obesity itself as a root
cause. “We have always known that reducing a patient’s weight might prevent, lessen or eliminate these chronic conditions altogether,” he explained. “We are just now gaining the tools to more effectively act on the need to combat obesity.”
The emergence of GLP-1 medications and other antiobesity drugs has been particularly transformative. While these therapies build on medications long used in diabetes care, they represent a new era in which pharmacotherapy can significantly affect weight. Family physicians weigh a range of factors when considering these treatments, including patients’ existing conditions, risk profiles and ability to manage potential side effects. At the same time, access remains uneven. Coverage for obesity medications and behavioral interventions varies widely across public and private payers, often lagging behind clinical evidence and patient demand. As a result, physicians frequently must help patients navigate benefit limitations, affordability concerns and the risks associated with unregulated or counterfeit weight-loss drugs.
In this evolving environment, team-based care has become essential. Dietitians, behavioral health specialists, pharmacists and, when appropriate, bariatric surgeons all play a role in helping patients achieve and maintain healthier weights. Yet Dr. Smith emphasized that the family physician remains the central coordinator. As the patient’s medical home, primary care brings together medical history, ongoing conditions and treatment goals to ensure that interventions –whether lifestyle changes, medications or surgery – are aligned
and sustainable. That coordinated approach, he said, offers the best chance of improving long-term outcomes in a condition that is both chronic and deeply interconnected with overall health.
A patient’s point of view
For many patients living with obesity, the primary care office can be either a gateway to effective treatment or a place that reinforces long-standing stigma. Joe Nadglowski, president and CEO of the Obesity Action Coalition (OAC), said that historically, too many patients have experienced the latter. “For many years, patients didn’t see their PCP as a trusted source for information on obesity,” he said. Conversations about weight were often framed in ways that felt judgmental or dismissive, leaving patients feeling shamed rather than supported. Those early negative encounters can linger, making individuals less likely to seek follow-up care or engage in future discussions about their health.
Yet Nadglowski noted that the landscape is beginning to change. Greater clinical understanding of obesity as a chronic disease, along with the emergence of more effective treatments, has prompted a shift in how some primary care practices approach care. He pointed to his own recent experience with a new physician as an example: a visit marked by empathy, privacy and thoughtful accommodations such as appropriate seating and respectful weighing procedures. “Progress is possible,” he said, but it requires both intentional actions by clinicians and institutional changes that make healthcare environments more inclusive for people with larger bodies.
Weight bias, however, remains a persistent barrier. It can surface in subtle ways – language choices, assumptions about patient behavior or treatment decisions – as well as in the physical environment of a practice. Waiting rooms without sturdy, armless chairs; exam rooms without properly sized gowns or blood pressure cuffs; and weighins conducted without privacy all send signals that patients with obesity are not fully considered. These experiences erode trust and can lead to delayed or avoided care. According to Nadglowski, patients who encounter stigma are less likely to pursue preventive services such as cancer screenings, vaccinations or mental health care, and more likely to cancel appointments or avoid new providers altogether. Even when patients find a skilled and compassionate primary care physician, access to treatment can be complicated by insurance requirements. Coverage for antiobesity medications, behavioral counseling and multidisciplinary support varies widely, often requiring extensive documentation, step-therapy protocols or referrals to specific programs. For patients who have already overcome fear or embarrassment to seek help, these hurdles can feel discouraging. Nadglowski said improving outcomes will require not only empathetic clinical care but also more consistent coverage policies and stronger support systems that make evidence-based obesity treatment accessible and sustainable.
Setting a standard
As obesity care evolves, new clinical standards are seeking to reshape both how patients are treated and what treatment looks like in practice.
Last May, the American Diabetes Association’s Obesity Association released the first installment of new Standards of Care in Overweight and Obesity, offering comprehensive, evidencebased guidance aimed at improving treatment and reducing weight stigma in healthcare settings. The recommendations call for clinician training on bias, more inclusive clinical environments, respectful, person-centered communication and shared decision-making that prioritizes outcomes beyond weight alone. Developed with input from multiple medical organizations, the standards are designed to help clinicians deliver compassionate, effective care and recognize obesity as a complex chronic disease. Leaders say the guidance represents a broader effort to improve access, quality and dignity for people living with overweight and obesity.
public: one focused on weight bias and stigma, and another on pharmacologic treatment. Together, they emphasize that patients with overweight or obesity should expect respectful care and clinical environments that accommodate people of all sizes. “People with obesity should expect to be treated with respect in healthcare settings and clinics should have equipment and furniture that accommodates all individuals,” Dr. Gudzune said.
The pharmacologic chapter highlights the growing role of medications in obesity management. Today’s treatments can lead to meaningful health benefits – such as improved blood sugar control, lower blood pressure and weight reduction – but are typically intended for long-term use. Patients should work with clinicians to determine the most
“ Obesity still impacts a significant number of people across the U.S., although the prevalence is typically higher in the South and Midwest regions among both adults and children.”
Kimberly Gudzune, MD, MPH, FTOS – co-chair of the Standards of Care in Overweight and Obesity “Pharmacologic Treatment of Obesity in Adults” section and chair of the American Diabetes Association’s Professional Practice Committee on obesity – said the recently published guidelines send a clear message: obesity is a chronic condition that deserves comprehensive, evidence-based care delivered with dignity.
The current standards include two chapters most relevant to the
appropriate therapy based on their medical history and undergo a comprehensive evaluation before a prescription is written. Medication, she added, should be paired with guidance on nutrition and physical activity, along with regular follow-up to monitor progress and address challenges.
Beyond individual treatment decisions, the standards aim to influence the broader healthcare ecosystem. By grounding expectations in scientific evidence, they provide a roadmap for clinicians
and a reference point for insurers and policymakers considering coverage for obesity care. “Having standards may also help policymakers … when evaluating eligibility for and benefits coverage of obesity care services,” Dr. Gudzune noted.
Dr. Gudzune also pointed to persistent disparities in obesity prevalence across the United States. “Obesity still impacts a significant number of people across the U.S., although the prevalence is typically higher in the South and Midwest regions among both adults and children,” she said. “Obesity prevalence continues to be higher among low-income individuals.” These patterns underscore the role that social and economic conditions play in both the development of obesity and access to treatment.
Addressing those conditions will be essential to improving outcomes. “They are critically important when thinking about obesity, as these factors impact a person’s risk of developing obesity as well as their ability to access and engage in treatment,” Dr. Gudzune said, referring to determinants such as food access, housing and economic inequality. She highlighted insurance coverage as a particularly pressing barrier: “One of the most critical factors currently impacting treatment access is insurance coverage for obesity care. Many people’s insurance plans do not include coverage of nutritional counseling, obesity medications or metabolic-bariatric surgery –and other people who previously had coverage are discovering that their plans no longer cover the treatments that had been working for them. This is happening
Don’t Just Sell an ADA Scale. Partner with the ADA Scale Experts.
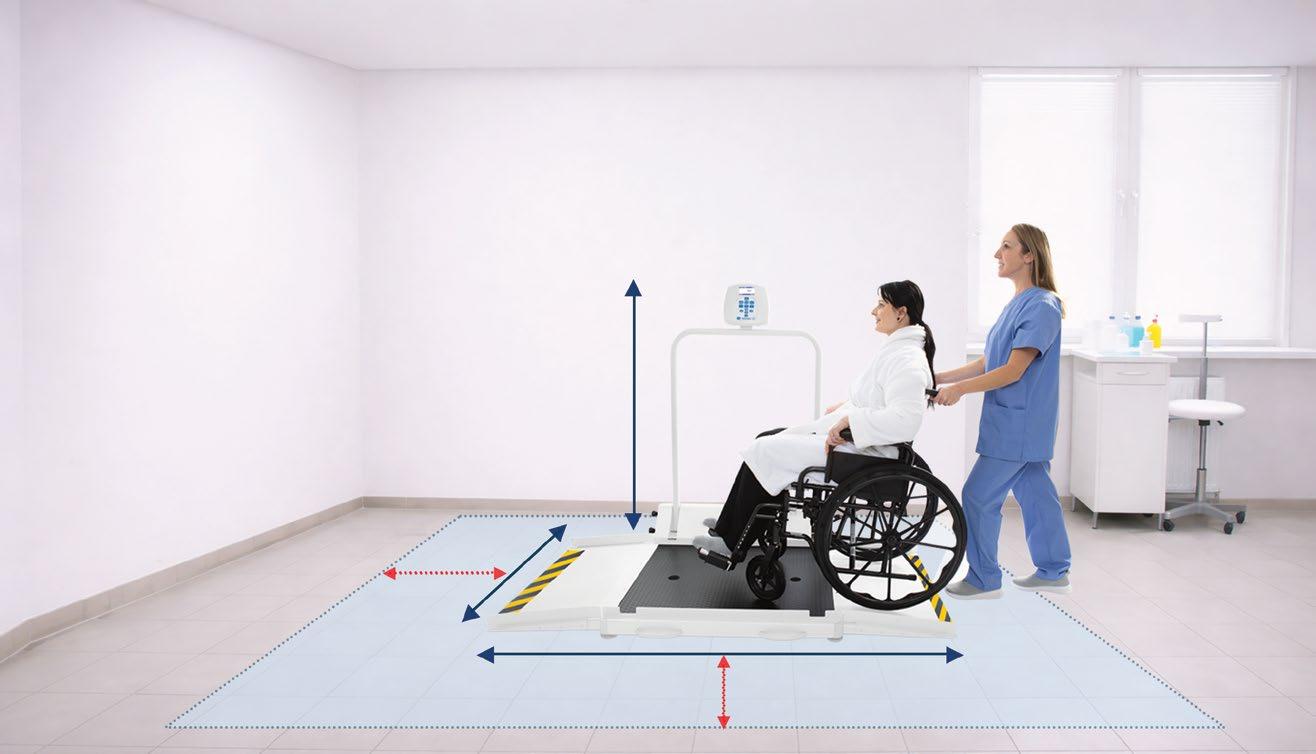
ADA compliance isn’t optional, and recommending the wrong scale can lead to workflow disruptions, safety concerns, compliance risks, and costly returns.
Health o meter® Professional Scales delivers more than certified ADA Compliant products. We deliver the expertise and support to help you sell with confidence and protect your customer relationships.
Why Distribution Partners Choose Us:






Expert guidance to recommend the right ADA scale the first time
In-depth knowledge of evolving ADA requirements
Space, layout, and mobility planning support
Certified, trusted medical scales
Installation and post-sale support
Ongoing partnership that extends well beyond the sale

We help you reduce risk, avoid costly replacements, and strengthen your credibility with healthcare customers. From evaluating facility needs to ensuring compliant installation, our team supports you every step of the process. When accessibility, accuracy, and compliance matter, your reputation matters too.






quite commonly with coverage of obesity medications.”
At the same time, the treatment landscape is evolving quickly.
“In the last few years, we have had multiple new obesity medications come to market and there will likely be more medications approved in the next few years,” Dr. Gudzune said. “These represent important treatment advancements as having more medications that work in different ways will give clinicians more tools; we can find the medications that work best for each patient.” She also pointed to emerging opportunities in behavioral care: “It will be exciting to see how AI might influence behavioral interventions. There is already work demonstrating that an AI version of the Diabetes Prevention Program achieved just as well as the traditional human-led program that is typically based in the community.”
Primary care and preventive health systems will play a central role in putting the standards into practice, but only if clinicians and clinics are equipped to do so. Before beginning to treat obesity, Dr. Gudzune said primary care and preventive health systems should determine whether their clinicians have:
1. Training in obesity care as appropriate knowledge and skills are needed,
2. Have adequate time in their schedules dedicated to obesity care,
3. Have resources in place to support obesity treatment such as access to experts that can address questions that may arise or staff available to assist with prior authorizations, and
4. The clinic environment supports a non-stigmatizing care
experience for people with obesity (e.g., furniture and equipment appropriate for all body sizes)
“For clinics without these resources, they can consider referring their patients to obesity medicine physicians or other clinical settings that have these requirements in place.”
A cultural shift
Even as treatment options expand, family physicians say one of the most important shifts in obesity care is cultural: recognizing obesity as a chronic disease while confronting the stigma that still surrounds it. Dr. Smith noted that family medicine has
resources in rural or underserved communities can make comprehensive obesity care difficult to deliver. Conversations about weight can be sensitive, leading both patients and clinicians to avoid them altogether. Expanding access to dietitians, behavioral health support, medications and structured weight-management programs could help bridge those gaps.
The AAFP sees continued emphasis on holistic, team-based care as the path forward. Treating obesity as part of a broader fight against chronic cardiovascular disease – rather than as a personal failing – can improve outcomes and reduce stigma. As new therapies such as
Many patients celebrate what advocates call “non-scale victories” – better blood sugar or blood pressure control, increased energy, the ability to play with children or grandchildren, or simply greater comfort in everyday activities like traveling.
long approached obesity through a whole-person lens, even before it was formally classified as a chronic disease in 2013. Yet weight bias and fear of judgment continue to create barriers. Patients who feel shamed are less likely to trust providers or stick with care plans, making the exam room environment critical. Family physicians, he said, must create safe, supportive spaces where patients feel heard rather than judged.
Practical challenges remain. Time constraints during routine visits, uneven access to specialists and programs, and limited
GLP-1s evolve, Dr. Smith said physicians will be watching longterm effects, coverage and affordability closely. “No matter how a patient chooses to move forward with their care plan,” he added, “we have their backs and want the best for them.”
From the patient perspective, the rapid expansion of obesity treatment options is bringing something that has long been in short supply: hope. Nadglowski said that for years many people felt they had to manage obesity on their own, cycling through do-it-yourself approaches with limited support from the
healthcare system. Newer medications, more informed primary care providers and the growth of telehealth services are beginning to change that dynamic. “The new treatment options … have given many with obesity new hope that they might find an option that works for them,” he said. For some who had previously given up on seeking care, the availability of effective therapies and more compassionate clinical conversations is prompting a return to the healthcare system.
Importantly, patients are redefining what success looks like. While weight loss may be an initial goal, Nadglowski

emphasizes that long-term engagement is often driven by improvements in health, mobility and quality of life. Many patients celebrate what advocates call “non-scale victories” – better blood sugar or blood pressure control, increased energy, the ability to play with children or grandchildren, or simply greater comfort in everyday activities like traveling. These outcomes, he noted, are powerful motivators that reinforce sustained treatment and healthier behaviors.
Looking ahead, Nadglowski believes two changes could dramatically improve the patient
experience in primary care. First, consistent insurance coverage for evidence-based obesity treatment – including medications, counseling and multidisciplinary support – would remove one of the biggest barriers to care. “We need to stop making people earn obesity care and treat obesity just like every other chronic disease,” he said. Second, continued education and training for primary care and other healthcare professionals can further reduce stigma and improve clinical confidence. Together, those shifts could help ensure that more patients not only seek care, but stay engaged in it for the long term.




Looking Beyond the Sticker Price
The true life cycle cost of a healthcare scale.
When healthcare providers evaluate scales, the conversation often starts — and ends — with purchase price. This is especially true in large RFPs, where high volumes and tight budgets can push decisions toward the lowest upfront cost. But focusing only on the sticker price overlooks a much bigger financial picture. Like most capital equipment, scales carry a full life cycle cost, and many of the most impactful expenses don’t appear until after the scale is in use.
For distributor reps, understanding total cost of ownership helps shift the conversation from price to value — and helps customers avoid unexpected costs.
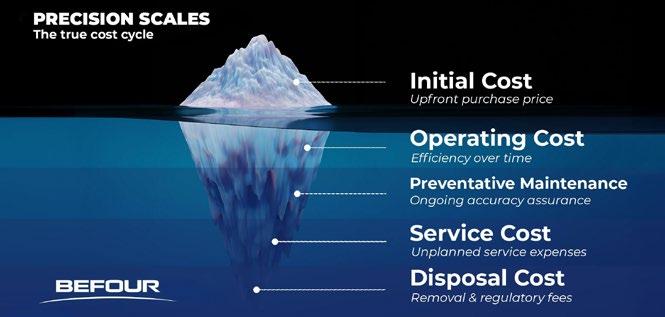
Initial Cost: More Than the Sticker Price
The initial cost of a scale goes beyond the number on the quote. Assembly time, add-on features, and replacement parts can quickly add to the total. Befour scales arrive fully assembled or require minimal setup, saving staff time immediately. Key features such as active handrails, MotionLock® technology, and LB/KG lockout are included — not optional upgrades. Built with durable, USA-made materials, Befour scales are engineered for a life expectancy of up to 20 years, positioning them as a long-term investment rather than a disposable purchase.
Operating Cost: Designed for Efficiency
Operating costs often show up as lost time. Complicated interfaces, inconsistent displays, and slow readings can disrupt workflows. Befour uses the same simple, seven-button display console across its scale portfolio, reducing training time and eliminating retraining as staff move between departments. Faster, more accurate readings — especially for unsteady patients — mean clinicians spend less time reweighing and more time on patient care.
Preventive Maintenance Cost: Fewer Headaches
Some scales require regular recalibration or frequent adjustments,
adding ongoing maintenance costs. Befour scales arrive fully calibrated and are designed to maintain accuracy without routine recalibration. Their robust construction supports demanding healthcare environments, helping minimize maintenance over the life of the scale.
Service Cost: Planning Ahead
Service and repair costs are another often-overlooked factor. Befour scales include a three-year warranty and complimentary troubleshooting support for the life of the product. Their future-proof design allows customers to add wireless connectivity or lock into kilograms later — without purchasing a new scale. Battery life also matters: Befour scales use a single set of non-hazardous alkaline batteries that can last more than 100,000 weight readings — approximately two years — reducing battery changes and biomed involvement.
Disposal Cost: The Final Consideration
Disposal costs can add up, particularly for equipment with short life spans. Befour scales are made with more than 90% recyclable materials and designed to last significantly longer than typical replacement cycles. A local supply chain and longer battery life further reduce environmental impact.
Looking Below the Surface
At Befour, the message is simple: purchase price is just the tip of the iceberg. Beneath it are operating, maintenance, service, and disposal costs that shape the true cost of ownership. For distributor reps and healthcare providers alike, evaluating the full life cycle cost of a scale leads to smarter decisions and greater long-term value.
Tailored Colorectal Cancer Care
How Dana-Farber’s Young-Onset CRC Center addresses the medical, emotional and practical needs of younger patients.
 Thejus (TJ) Jayakrishnan, MD, a gastrointestinal oncologist at Dana-Farber Cancer Institute, wasn’t surprised by a recent American Cancer Society study showing that while overall cancer mortality among Americans under 50 has declined, colorectal cancer rates have risen. In fact, colorectal cancer incidence has steadily increased since 2005 and, by 2023, became the leading cause of cancer death among Americans under 50.
“The increase in colorectal cancer among younger adults is something we’ve been noticing over the last several years,” said Dr. Jayakrishnan, who treats patients at Dana-Farber’s YoungOnset Colorectal Cancer (CRC) Center, led by Dr. Kimmie Ng. “The creation of a dedicated center reflects how urgently this trend needs focused clinical care and research.”
The reasons behind the surge in cases are still largely unknown, though researchers have identified several potential contributing factors. One pattern, known as a “birth cohort effect,” suggests that successive generations face higher risks of developing colorectal cancer before age 50. “Because this increase is happening over generations, it’s likely related to environmental exposures – changes in diet and lifestyle,” Dr. Jayakrishnan said. Studies have linked risk to factors such as consumption of sugar-sweetened beverages, ultra-processed foods, obesity, sedentary lifestyles, alcohol use, and smoking.
Yet these known factors don’t tell the whole story. “I see patients who are physically fit and lead active lifestyles, and they still develop young-onset colorectal cancer,” Dr. Jayakrishnan said. Other potential contributors, including exposure to microplastics and pollution, are still under investigation, and the complex ways these environmental factors may interact remain unclear.
Emerging research also points to differences in the gut microbiome between younger and older patients with colorectal cancer, though how these changes affect disease progression and treatment
is not fully understood. “We are beginning to see that young-onset colorectal cancer often presents more aggressively and may not respond to treatments as well as cancers diagnosed at the typical age of onset,” Dr. Jayakrishnan said. “We don’t yet know why this is, which makes it a critical area for research.”
For now, the rise of colorectal cancer in younger adults underscores the need for vigilance, awareness and continued investigation. Physicians and researchers hope that by identifying the underlying causes, from lifestyle factors to environmental exposures and microbiome differences, they can develop more effective prevention strategies and treatment options for this vulnerable population.
the unique challenges faced by patients under 50, a population often confronting not only cancer but complex personal, professional, and psychosocial issues.
“When Dr. Kimmie Ng developed the Young-Onset CRC Center, the team conducted a study to understand patients’ experiences and needs,” said Dr. Jayakrishnan. “Through the study we learned that younger patients face challenges ranging from navigating careers and financial pressures to fertility concerns and long-term treatment toxicity. Therefore, the center was designed with a mission to address all of these factors.”
A hallmark of the center is its multidisciplinary approach. Patients meet with medical oncologists, surgeons and radiation oncologists
“ Younger adults are often at a stage of life where they’re establishing careers, raising families, or may lack insurance coverage. Colonoscopy requires time off work, and many people in this age group haven’t had major hospitalizations, so awareness of personal risk can be limited.”
“Ultimately, we need more research to understand the disease and design better treatments for younger patients,” Dr. Jayakrishnan said. “The goal is to improve outcomes and, hopefully, prevent these cancers from developing in the first place.”
Addressing the full spectrum of young-onset CRC
At the Dana-Farber Young-Onset CRC Center, care goes far beyond treating the disease itself. The center was designed to address
who specialize in young-onset CRC. Genetic counseling is also a key component, as younger patients are more likely to have inherited cancer syndromes than older individuals. “Even though most patients do not have a genetic predisposition, we make sure those who do – and their families – receive appropriate screening and guidance,” Dr. Jayakrishnan explained.
Fertility preservation is another focus. Patients receive consultations with reproductive health specialists to explore
options for having children in the future and provide counseling regarding sexual health. Dedicated social workers help patients manage psychosocial stressors, from mental health concerns to the emotional toll of cancer during a formative stage of life.
Research and clinical trials are integrated into the care model.
“Many young patients are motivated to participate in research. We provide access to studies that explore risk factors, biomarkers, and response to treatment, as well as opportunities to enroll in clinical trials,” Dr. Jayakrishnan said.
By addressing the medical, emotional and practical aspects of cancer care, the Dana-Farber Young-Onset CRC Center is setting a new standard for treating younger patients. “Our approach ensures patients aren’t just treated for cancer – they’re supported as individuals navigating a complex and challenging life stage,” Dr. Jayakrishnan said.
Early screening: Promises and barriers for young adults
The U.S. Preventive Services Task Force (USPSTF) made headlines in 2021 when it lowered the recommended age for colorectal cancer screening from 50 to 45. While the move was widely seen as a proactive step, the impact on outcomes is still emerging.
“It may be too early to see a measurable effect,” said Dr. Jayakrishnan. “Adherence to screening is still not 100%, and the benefits of colonoscopy take years to manifest. Research is ongoing to determine whether this change will help reduce rates of advanced colorectal cancer through early detection.”
International data provide some optimism. Countries such
dukal.com

as Austria and Italy which have implemented early-onset colorectal cancer screening programs, have reported improvements in early detection and a decline in incidence of young-onset CRC. In the U.S., similar population-level effects are still being studied.
For younger adults, however, barriers to screening remain significant. “Younger adults are often at a stage of life where they’re establishing careers, raising families, or may lack insurance coverage,” Dr. Jayakrishnan explained. “Colonoscopy requires time off work, and many people in this age group haven’t had major hospitalizations, so awareness of personal risk can be limited.”
The consequences of these barriers can be severe. Dr. Jayakrishnan has seen patients diagnosed at stage four – sometimes with minimal symptoms –during their first screening. “Early screening can make a difference, but awareness and access are critical. Overcoming logistical, financial, and educational barriers is key to ensuring more young adults get screened in time,” he said.
As the medical community continues to study the effects of earlier screening, experts emphasize that education and access may be just as important as lowering the screening age itself. Awareness campaigns and patient outreach could help ensure that the promise of early detection translates into tangible outcomes for younger adults at risk.
Technology, innovation, and awareness
As colorectal cancer continues to rise among adults under 50, researchers and clinicians are exploring how technology and
innovation can change the trajectory of the disease. For Dr. Jayakrishnan, the next five to ten years hold both promise and challenges.
“One area that’s generating a lot of discussion is whether the screening age should be lowered even further,” Dr. Jayakrishnan said. “On an individual level, expanding screening may seem intuitive, as it would allow more people to be tested. However, there are important considerations regarding cost-effectiveness at the population level, and this remains an active area of evaluation within health policy.”
To address these concerns, Dana-Farber and other institutions are engaged in research that may inform risk-stratified screening, which uses machine learning and artificial intelligence (AI) to
to identify molecules produced by microorganisms that may drive cancer development. The goal is to develop interventions that can block these mechanisms and potentially prevent disease.”
Advances in targeted therapies are also encouraging. Recent clinical studies presented at gastrointestinal oncology conferences have demonstrated new treatments that attack specific molecular targets in colorectal tumors. These approaches may reduce side effects compared with traditional chemotherapy while providing more effective disease control.
“These innovations are promising for all patients with colorectal cancer, including younger adults,” Dr. Jayakrishnan said.
Despite the promise of technology, Dr. Jayakrishnan
“ We are beginning to see that young-onset colorectal cancer often presents more aggressively and may not respond to treatments as well as cancers diagnosed at the typical age of onset. We don’t yet know why this is, which makes it a critical area for research.”
identify individuals at higher risk. By analyzing environmental exposures, diet, lifestyle factors, microbiome characteristics, and genetic markers, these tools aim to pinpoint who may benefit from earlier screening, rather than screening everyone in a broad age group.
“AI is also helping us study biomarkers and molecular characteristics more efficiently,” Dr. Jayakrishnan explained. “For example, we’re analyzing the microbiome of patients with youngonset colorectal cancer, intending
emphasizes that awareness and timely evaluation remain critical. Many young-onset colorectal cancers are detected only after symptoms appear, such as blood in the stool, persistent abdominal pain, or changes in bowel habits. “Patients and primary care physicians need to take these symptoms seriously,” he said. “Early evaluation can make a major difference in outcomes.”
The Dana-Farber YoungOnset CRC Center cares for patients who have already been
diagnosed with colorectal cancer and provides education about risk assessment and prevention for family members. Patients and their relatives are advised to discuss appropriate screening options with their primary care providers, including alternative screening technologies, such as stool-based tests like Cologuard, which detect tumor-related DNA, and emerging blood-based multi-cancer detection tests that can trigger colonoscopy when abnormalities are found. These tools expand options for early detection and may play an increasing role in identifying cancers before they progress.
The Dana-Farber YoungOnset CRC Center offers comprehensive, multidisciplinary
care to individuals diagnosed with this type of cancer. Patients can access specialists in medical oncology, surgery, radiation, reproductive health, and psychosocial support. Fertility preservation consultations, genetic counseling, and guidance on long-term treatment effects are integrated into patient care. Clinical trials across medical, surgical and radiation oncology are also available, allowing patients to explore innovative treatments.
“The Young-Onset Center is one of the first of its kind in the world and remains one of the few dedicated to this population,” Dr. Jayakrishnan said. “Even patients receiving treatment elsewhere can benefit from second

YOUR GO-TO PARTNER FOR IMAGING TABLES
From ultrasound to C-arm tables, Oakworks delivers the quality, reliability, and support your customers expect, so you can sell with confidence.
Dependable delivery and support
Trusted by leading health systems
One partner for all your needs
opinions, and consultations, and have access to opportunities for enrollment in clinical trials. Addressing the unique challenges of younger patients — medical, emotional, and practical – is at the heart of our approach.”
As research advances and new tools become available, Dr. Jayakrishnan remains cautiously optimistic. “We’re making progress in detection, treatment, and understanding the biology of young-onset colorectal cancer. But awareness, timely screening, and multidisciplinary care are just as important as technology. For anyone under 50 experiencing persistent symptoms, seeking evaluation promptly can save lives.”



ChatGPT Health Signals a New Era of AI-Driven Patient Engagement
OpenAI’s latest platform aims to centralize medical records, wellness data and AI guidance in one place – raising both optimism about patient empowerment and concerns over accuracy, privacy and trust.
By Pete Mercer
 In January, OpenAI announced the launch of ChatGPT Health, which is an extension of the AI chatbot that will act as a hub where people can connect their wellness apps and medical records, allowing ChatGPT to help individuals better understand and interpret any recent test results, prepare for upcoming doctor appointments, navigate differentiating insurance options, and advise on diet and workout plans.

The idea is that your medical records and data from the health apps would work to inform ChatGPT Health’s answers to any questions, centralizing this information to make it accessible to the user. Any questions you ask ChatGPT Health will be “grounded in your own health information,” according to a statement from the company.
According to the release, ChatGPT worked with 260 licensed physicians across 60 countries of practice to evaluate model performance using real clinical scenarios to test and train the platform. This physician-led training built a foundation for ChatGPT Health, testing more than 600,000 model outputs spanning 30 areas of focus. With this input from providers and other benchmarks in place to make the platform more reliable, ChatGPT and OpenAI

are working to “ensure that AI benefits all of humanity.”
This is a significant development, and it could indicate a huge shift in the delivery of healthcare.
Depending on how you feel about the emergence of artificial intelligence and the intersection of data and healthcare, this is either exciting or a big red flag.
AI in Healthcare: Promise and Peril
As platforms like ChatGPT Health expand the role of artificial intelligence in patient engagement, healthcare leaders are weighing both the opportunities and the risks. Here’s a quick look at where AI could help, and where caution is still warranted.
Three Potential Positives
1. Greater patient understanding AI tools can help translate complex medical language into plain terms, allowing patients to better understand test results, diagnoses and treatment options between provider visits.
2. Improved access to information
With millions already turning to AI for health questions, these platforms offer on-demand guidance that can help patients prepare for appointments, navigate insurance decisions and track long-term health trends.
3. More empowered patients
By centralizing medical records and wellness data, AI may give patients a clearer picture of their health over time, encouraging more informed conversations with clinicians and stronger engagement in care decisions.
Three Potential Pitfalls
1. Risk of inaccurate information
AI systems can still produce incorrect or misleading responses. In healthcare contexts, even small errors could lead to confusion, delayed care or harmful decisions if users rely too heavily on AI guidance.
2. Privacy and data security concerns
Uploading sensitive medical records to third-party platforms raises questions about data ownership, confidentiality and how health information could be used beyond its original purpose.
3. Overreliance on technology
Experts caution that AI tools are meant to supplement – not replace – medical professionals. Patients who treat AI as a provider rather than a support tool may develop false confidence in automated advice.
Using AI for health consultations
The idea of using ChatGPT for health questions is certainly not a new one. Axios reported that “more than 40 million people globally turn to ChatGPT daily for health information,” viewing the platform “as an ally in navigating their health care, according to analysis of anonymized interactions with ChatGPT and a survey of ChatGPT users by the AI-powered tool Knit.”
Patients are already using ChatGPT to ask questions about healthcare, whether it’s to get information about symptoms, ask questions about navigating health insurance, or seek “deeper” context about any of their healthcare issues. It makes sense that OpenAI and ChatGPT would take advantage of a huge opportunity to provide an extra service for their users, but it also comes with its fair share of challenges.
The use of AI in these scenarios is still largely divisive, which is in no small part due to the fact that ChatGPT can give the wrong information out to its users. A study published by the BBC and EBU in October 2025 found that “around 45% of AI news queries to ChatGPT, MS Copilot, Gemini, and Perplexity produce errors.” Worse than that, the information could even turn out to be deadly.
A report from The Transparency Coalition, an organization devoted to ensuring that AI technologies are developed to prioritize safety and transparency, found that seven new lawsuits were filed against OpenAI in November 2025. These suits included various allegations like wrongful death and assisted
You shouldn’t have to choose between clinical precision and safety. With Terumo’s innovative SurTract™ hypodermic line, you don’t have to.
Engineered with an automatic retraction mechanism. The needle withdraws inside the syringe barrel the moment the injection is complete – reducing the risk of needlestick injuries.*
Call your Terumo representative at: 1.800.888.3786 or visit www.TerumoTMP.com
suicide after several notable cases of suicides of individuals who were heavily engaging with the platform. The argument is that these mental health crises were triggered by the contents of the conversations people were having with the chatbot.
How does this factor into ChatGPT Health? While this new feature to the platform might add a certain level of convenience and even a better understanding of complex patient information, it shouldn’t be treated as a provider. In fact, OpenAI and ChatGPT both argue that this new feature is not designed or intended to replace providers.
ChatGPT said the following in the announcement for ChatGPT Health: “[ChatGPT] Health is designed to support, not replace, medical care. It is not intended for
user’s sensitive health records. This new addition to ChatGPT exists in its own space, where any conversations, connected apps, or files that you have previously used are kept separate from the Health component of the platform.
While the healthcare conversations you have in the platform will stay contained within the context and confines of the Health space, the bot can use context from your non-Health chats, like any recent lifestyle changes to make the conversation more relevant. ChatGPT said in the media release, “Due to the sensitive nature of health data, Health builds on this foundation with additional, layered protections – including purpose-built encryption and isolation – to keep health conversations protected
“ I feel that anything that further empowers patients will actually be helpful given a focus on patient safety throughout my career. That is, patients will have access to expertise that continues to improve and (should in the future) well exceed a random internet-based search engine.”
diagnosis or treatment. Instead, it helps you navigate everyday questions and understand patterns over time – not just moments of illness – so you can feel more informed and prepared for important medical conversations.”
Security and privacy concerns
One of the biggest obstacles to launching a product that uses an AI platform is any anxieties over the security and privacy of the
and compartmentalized. Conversations in Health are not used to train our foundation models.”
Time Magazine spoke to Dr. Danielle Bitterman, a radiation oncologist and clinical lead for data science and AI at Mass General Brigham Digital, about the launch of ChatGPT Health. While she wasn’t surprised by the announcement, she did urge users to exhibit caution when using the platform: “The most conservative approach is to
assume that any information you upload into these tools, or any information that may be in application you otherwise link to the tools, will no longer be private.”
Dr. David Liebovitz, codirector of the Institute for Artificial Intelligence in Medicine’s Center for Medical Education in Data Science and Digital Health at Northwestern University Feinberg School of Medicine, has a positive outlook on the utility of the platform, but he’s also aware of the challenges with security and confidentiality.
He said, “Privacy and security and confidentiality guarantees are not covered when a consumer, no longer a patient with protected health information, but a consumer uploads information to a third party. So those issues need to be carefully reviewed and addressed. There are ways in the meantime to give snippets for assessment as opposed to comprehensive records. It remains a concerning aspect in terms of secondary use of this data that’s outside the control of the consumer who uploaded this information.”
Is this a good thing?
The big question here is whether any of this is a good idea. It’s a fair question – even with all of the security and privacy measures, it will be hard for some people to trust the platform with their sensitive, personal information. Despite the risks, Dr. Liebovitz thinks that ChatGPT Health is going to be a beneficial tool for patient safety.
“I feel that anything that further empowers patients will actually be helpful given a focus on patient safety throughout my
career,” he said. “That is, patients will have access to expertise that continues to improve and (should in the future) well exceed a random internet-based search engine. This parallels the development and application of rules and now machine learning algorithms leading to generative AI supporting the workflow of physicians with tools and efficiency gains by providing expertise here for patients to assist with understanding their medical care.”
The reality is that platforms like this are a huge opportunity for patients to develop a better understanding of test results or a diagnosis, especially in those moments when the physician is unavailable to communicate. For Dr. Liebovitz, this is
an inevitable step towards the democratization of healthcare. “We’ll wonder about the time we used to practice when we didn’t have additional safeguards throughout all steps of care.”
As for the scenarios where people are given inaccurate information from AI platforms, Dr. Liebovitz pointed out that the uploaded medical records of the patient provide an extra layer of context that can help to inform the answers provided by ChatGPT Health.
“In terms of a balance between empowering patients and avoiding false confidence or misinformation, this is incredibly tricky. False information can easily arise, and a recent study suggested that some answers
from chatbots in a test group of patients were no greater than using a search engine. However, part of this is often that the full context of the medical record is not available, or the values of the patient that a clinician could take time to understand.”
In a perfect world, users would treat ChatGPT as a supplemental service, not a trusted healthcare professional. That’s a huge expectation to have for millions of people using this platform every day, which is an interesting dilemma for the modern age. While it’s only another step in the evolution of AI, it’s a huge shift for patients and providers who will likely have to work together to navigate these murky waters.
NEVER CHANGE BATTERIES

Using AI Tools Safely
Although AI chatbots have the potential to improve care, experts say guardrails are needed.
By Jenna Hughes
 Artificial Intelligence (AI) technology is transforming the healthcare industry rapidly – and the advent of AI chatbots such as ChatGPT, Claude, Copilot, Gemini and Grok are significantly changing the way providers deliver care and patients seek medical advice.
Many users – both providers and the people they serve – now rely on AI chatbots for answers to common health questions. In fact, more than 40 million people turn to ChatGPT daily for health information, according to a recent analysis from OpenAI.
Family members may use chatbots to check on their own symptoms or their families’ symptoms, while physicians may use these tools for help




One Partner. Two Disciplines. No Compromise.
One Partner. Two Disciplines. No Compromise.
Complete Lab Coverage
Complete
Micros 60 Hematology Analyzer: Compact, reliable 3-part differential
Lab Coverage
One Partner. Two Disciplines. No Compromise.
Micros 60 Hematology Analyzer: Compact, reliable 3-part differential
Pentra C400 Chemistry Analyzer: Compact benchtop, broad chemistry menu, no special electrical or water system required
Lite : Consolidated data management, LIS/EMR connectivity
Pentra C400 Chemistry Analyzer: Compact benchtop, broad chemistry menu, no special electrical or water system required
Complete Lab Coverage
Lite : Consolidated data management, LIS/EMR connectivity
Micros 60 Hematology Analyzer: Compact, reliable 3-part differential
Efficiency That Scales
Efficiency That Scales
Pentra C400 Chemistry Analyzer: Compact benchtop, broad chemistry menu, no special electrical or water system required
Automated sample processing & data transfer reduces manual steps
Lite : Consolidated data management, LIS/EMR connectivity
Seamless integration for small-to-mid volume labs → fewer errors, faster TAT
Automated sample processing & data transfer reduces manual steps
Seamless integration for small-to-mid volume labs → fewer errors, faster TAT
Efficiency That Scales
Confidence in Every Result
Automated sample processing & data transfer reduces manual steps
Confidence in Every Result
HORIBA provides 30+ years of chemistry and hematology excellence
Standardized, reproducible results across disciplines
Seamless integration for small-to-mid volume labs → fewer errors, faster TAT
HORIBA provides 30+ years of chemistry and hematology excellence
Smart QC + data traceability with Lite ensure CLIA compliance
Standardized, reproducible results across disciplines
Smart QC + data traceability with Lite ensure CLIA compliance DM
Confidence in Every Result
HORIBA provides 30+ years of chemistry and hematology excellence
Standardized, reproducible results across disciplines
Smart QC + data traceability with Lite ensure CLIA compliance
Empower every site to deliver better patient care.
Empower every site to deliver better patient care.
Built with value-based design to ensure long-term reliability.
Built with value-based design to ensure long-term reliability.
Scan the QR code to contact a HORIBA Rep Today!
Scan the QR code to contact a HORIBA Rep Today!
Empower every site to deliver better patient care.
Built with value-based design to ensure long-term reliability.
Scan the QR code to contact a HORIBA Rep Today!
writing a report or for more information on general medical questions.
Indeed, a growing majority of physicians report using AI tools in practice. Surveys show that about two-thirds (66%) of U.S. physicians now use AI tools at least weekly or daily for tasks ranging from documentation to clinical support, and adoption of AI has doubled in a single year, from around 38% to 66% in 2024.
Despite how reliable and truthful chatbots may seem to the user, when it comes to medical purposes, chatbots are not considered medical devices – and they’re not approved for medical use by the Food and Drug Administration (FDA). When these tools are used by physicians and their patients incorrectly, chatbots can produce false or misleading health information.
How do chatbots work?
When something feels definitive and helpful in healthcare, it is common for providers and patients to develop over-reliance. While chatbots can certainly provide valuable assistance, they can also give false or misleading information that has the potential to result in significant patient harm, according to ECRI.
Chatbots are designed to produce confident answers that are satisfying to the user – even when information is missing, incorrect or biased.
“This can result in responses that appear credible but are false or misleading, embedded biases, and sycophancy (telling users what they want to hear),” said Christie Bergerson, PhD, Biomedical Engineer and AI subject matter expert at ECRI.
“ Chatbots can be powerful tools, but without disciplined implementation, their current design makes misinformation or poor decision making based on prompt responses not just possible, but unfortunately, likely.”
For this reason, AI chatbots in healthcare top the 2026 list of the most significant potential health technology hazards, according to a report prepared annually by ECRI.
ECRI lists chatbots as a number one concern going into this year, not because they recently became dangerous, but because they have become normalized –everyone has been using them for everything, without fully understanding how these AI tools work or the potential risks.
Chatbots rely largely on Large Language Models (LLMs) to get their information. LLMs organize and process massive amounts of text (books, media, etc.) to produce expert-sounding responses to users’ questions. Chatbots can explain ideas, answer questions and create new ideas for its users.
“Specifically, chatbots’ inherent design characteristics create risks that are fundamentally different from traditional health IT tools”, said Dr. Bergerson. “General-use LLMs are typically
designed to generate fluent, contextually plausible responses, not to do things like verify facts, weigh clinical risk, or ensure consistency, any and all of which can be critical in healthcare settings.”
Some new medical devices may have embedded LLMs that assist with clinical processes –however the chatbots that everyone has access to, such as online and cellphone apps, are ECRI’s main concern.
“Chatbots generate responses probabilistically. From the patient or physician’s prompt, the LLMs gather words which are commonly present in conversations on that topic and then organize them into sentences based on patterns in their training data,” said Dr. Bergerson. “This means they can produce answers that sound authoritative even when they are incomplete, outdated or incorrect. In a clinical or operational environment, fluency can easily be mistaken for reliability.”
The inherent design of chatbot technology significantly increases its potential to make mistakes, and incorrect guidance in medicine can be as serious as life and death for a patient.
In fact, patients following the advice of LLMs without consulting a doctor have resulted in harm including incorrect diagnoses, recommendations for unnecessary testing, promotion of subpar medical supplies, and even invented body parts in response to medical questions while sounding like a trusted expert, according to ECRI.
“For ECRI, this underscores several key concerns: these tools are not regulated medical devices, they have not been validated for clinical decision support and
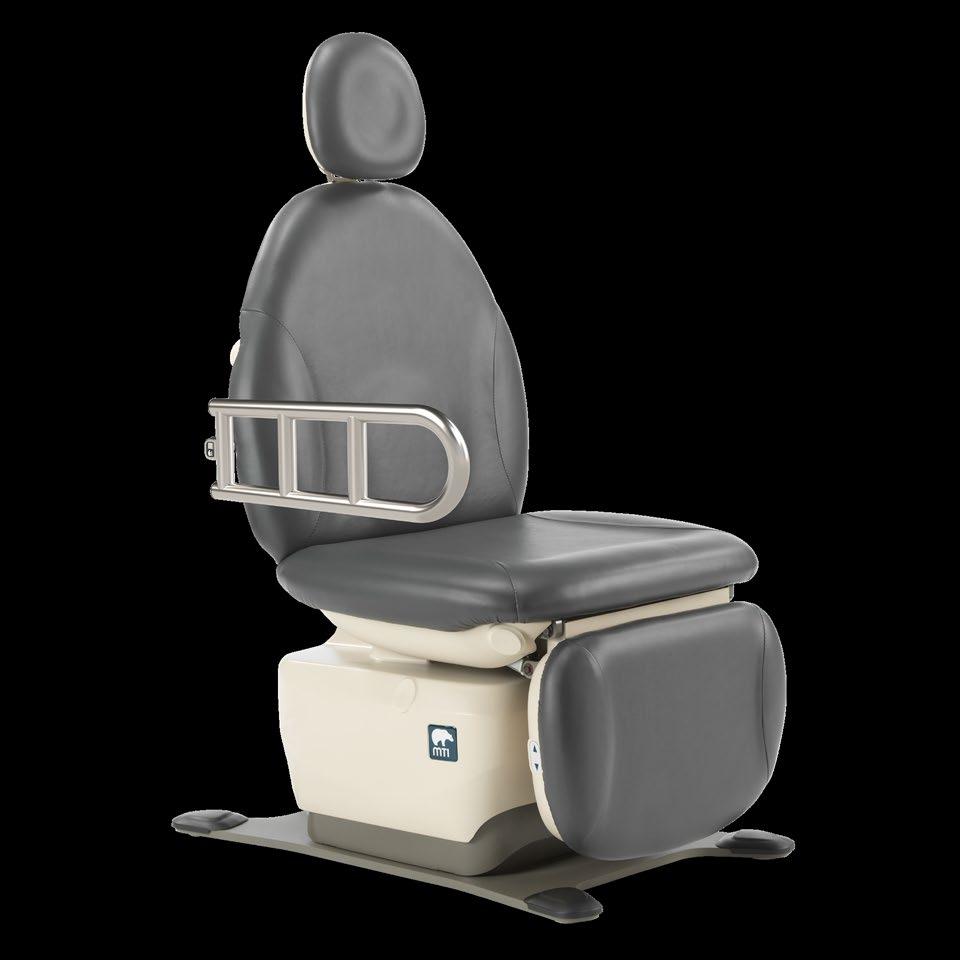
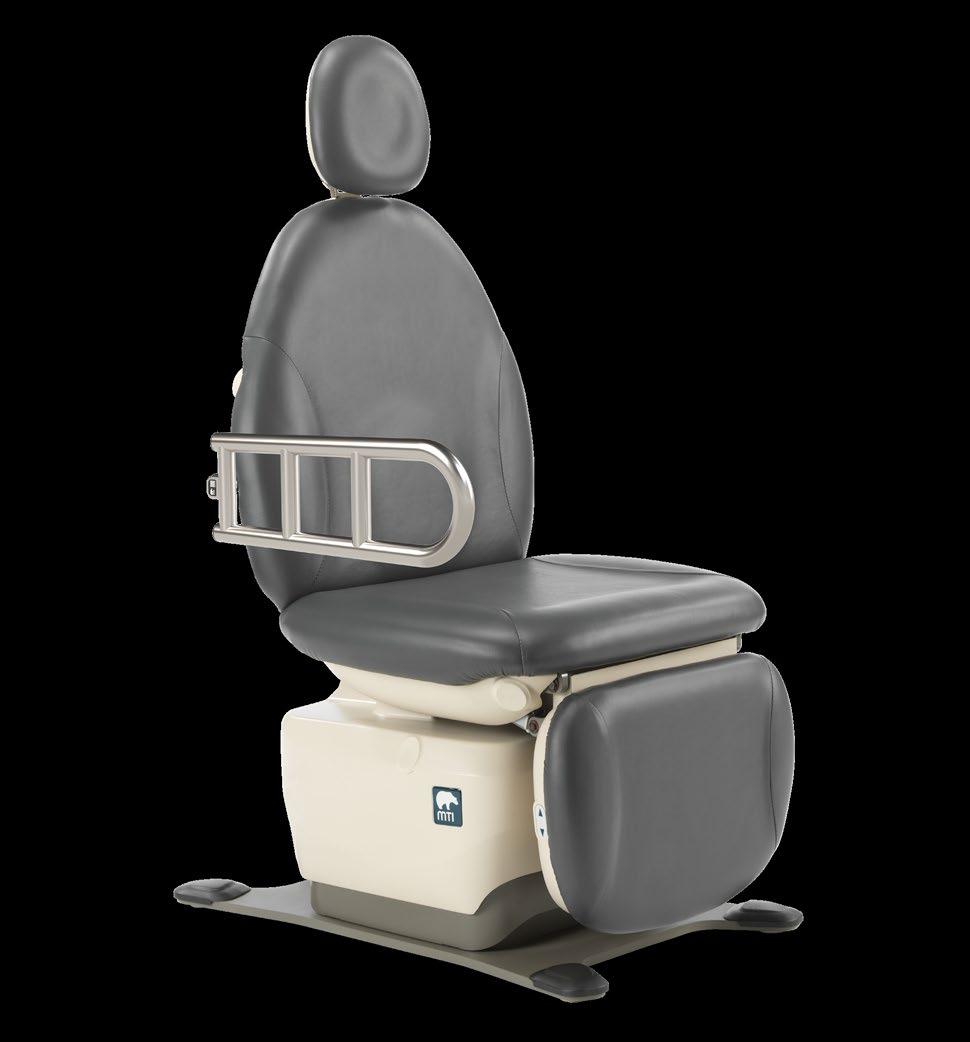
their widespread use – especially without oversight, training or integration into safe workflows –can amplify misinformation, variability and risk in real-world care settings,” said Dr. Bergerson.
How AI tools can be used safely
There are, however, many benefits to the use of AI chatbots in a clinical context, if used with appropriately and with caution.
Clinicians may use chatbots as a rapid information support tool (similar to a search engine) to do things like review differential diagnoses, clarify medication mechanisms, summarize clinical guidelines, or generate patientfriendly explanations. They may also use chatbots for educational support practices such as drafting research outlines, summarizing literature, preparing presentations or creating teaching materials.
For patients, chatbots can explain difficult medical topics in a way that is easier to understand. Patients often substitute medical chatbot advice for a physician’s due to the technology’s accessibility, convenience and perceived usefulness, said Dr. Bergerson.
Dr. Bergerson recommends a few strategies to get the best possible and most reliable answer out of AI, such as giving careful thought to the wording that is used, not asking AI to do things it has no business doing (such as making a definitive medical diagnosis), and always double checking with an expert on any medical advice chatbots provide. Patients should never attempt treatment without a medical professional’s opinion.
Advocating for chatbot guardrails
There is significant potential for beneficial use of chatbot tools in healthcare, but ECRI emphasizes that they must be used, designed and regulated responsibly.
Some safeguards that healthcare organizations can implement that allow for the use of its benefits without compromising safety, according to Dr. Bergerson, include clear use-case definition (no diagnostic or treatment substitution), mandatory human review and sign-off for clinical documentation, transparent labeling of AI-generated content, monitoring for and reporting errors/unintended consequences
AI chatbot safeguards
Dr. Bergerson noted some safeguards that healthcare organizations can implement that allow for the use of its benefits without compromising safety include:
` Clear use-case definition (no diagnostic or treatment substitution)
` Mandatory human review and sign-off for clinical documentation
` Transparent labeling of AI-generated content
` Monitoring for and reporting errors/unintended consequences
` Governance oversight defining where/how AI use is appropriate and where it is not
and governance oversight defining where/how AI use is appropriate and where it is not.
“Chatbots can be powerful tools, but without disciplined implementation, their current design makes misinformation or poor decision making based on prompt responses not just possible, but unfortunately, likely,” said Dr. Bergerson. “From ECRI’s perspective, these design characteristics underscore the need for structured governance, human oversight, real-world usability testing, and clearly defined use cases before integrating chatbots into clinical or operational workflows.”
Advocating for clear, enforceable criteria to regulate AI chatbots capable of giving medical advice will push regulators to require evidence of safe performance in interactive use with humans (not just exam-style benchmarks), according to Dr. Bergerson, and emphasize the development of trustworthy AI along with responsible use in health contexts.
“From ECRI’s perspective, healthcare organizations should push for risk-based guardrails that treat patient-facing and clinically used chatbot functions more like other high-risk health technologies, with evidence, transparency, and accountability requirements that match the potential for harm,” said Dr. Bergerson. “ECRI believes the most effective policy asks are the ones that convert chatbot risk from an individual user judgment problem into system requirements – clear intended-use boundaries, validated performance, auditability, monitoring, and truthful claims, so governance can be operationalized and users can use this powerful tool reliably.”











Changing what’s possible in sterilization assurance
















Streamline your sterilization process with our latest innovations:


















1
2
3M™ Attest™ eBowie-Dick Test System
Get quick, definitive pass/fail results of your steam sterilizer in less than five seconds.
3M™ Attest™ Super Rapid Vaporized Hydrogen Peroxide Clear Challenge Pack











3
No assembly required — save time and reduce potential error.
3M™ Attest™ Super Rapid Steam Clear Challenge Packs
Inspect the BI and the CI before and after processing without opening the pack.

It’s all part of how we never stop solving for you and your patients
Contact us to learn more
Focusing On Growth
NueHealth’s CEO discusses the reasons and goals behind a series of new partnerships.
By Pete Mercer
 Earlier this year, NueHealth announced four new partnerships across Missouri and New Jersey, expanding its national footprint with four distinct and diverse partnerships. NueHealth provides physician-aligned management services for ambulatory surgery centers, working with these facilities to improve the efficiency, clinical outcomes and economic performance for their partners.
Repertoire Magazine recently spoke to Michael Sheerin, CEO of NueHealth, about these partnerships, their business intelligence platform and the biggest challenges facing ASCs right now.
Repertoire Magazine : What’s the most exciting thing for you about these new partnerships and how does it play into the overall mission and vision of NueHealth for 2026?
Michael Sheerin: We are focused on growth and value-based care in 2026 and beyond. It’s always exciting to announce a new partnership – let alone four new partnerships. What excites me even more about these deals is the diversity in their deal structure. In one agreement


we are managing a center without equity while in another we are manager and minority equity partner. One of the deals is a de novo development and management project, and another is with a major health system partner.
Many of our competitors have a “boilerplate” approach to deal structure that often requires
both a management contract and equity in the center. We adopted a philosophy of meeting customers where they are in their ASC journey as long as it still makes financial sense to NueHealth. It’s that diversity and approach that excites me as it illustrates our commitment and ability to adapt to the needs of our partners.
Michael Sheerin
Microstream™ Luer sampling lines
Capture CO2 not compromise
Reliable.
Flexible. Ready for your ASC.
Intubated and non-intubated patients Uni-junction™ technology captures from both nares and mouth1-4
Delivers O2 without diluting CO2 readings2
Compatible with most sidest monitors
Smarter CO2 monitoring starts here
Scan the QR code for more information


1 Based on internal report D006122, Report for evaluation testing against Welch Allyn products for
2 Based on internal report D005886, Evaluation Testing with the New Version of the Adult/Intermediate Smart CapnoLine Plus, an Injection Molded, One-Piece Cannula (Appendix 5.3 and 5.4 relate to accuracy even with up to 5 Lit/min O2).
3 Based on internal report D005655, Clinical Validation Test -CO2 Oral Nasal FilterLine, Adult, Intermediate, and Pediatric -Healthy Patients (Protocol, See Objectives Chapter 3).
4 Based on internal report D05658, Clinical Validation Test -CO2 Oral Nasal FilterLine, Adult, Intermediate, and Pediatric -Healthy Patients (Report, See Conclusions, Chapter 3.1 and Analysis of Results, Chapter 5).
The Microstream™ capnography monitoring system should not be used as the sole basis for diagnosis or therapy and is intended only as an adjunct in patient assessment.
©2025 Medtronic Medtronic, Medtronic logo, and Engineering the extraordinary are trademarks of Medtronic All other brands are trademarks of a Medtronic company 10/2025 – US-PM-2500443 –[WF#19766474]
Repertoire: What kind of management services does NueHealth provide?
Sheerin: If the project is a new center, whether “greenfield” or “brownfield,” we offer a full array of development services to include project management, engaging an architect, construction managers, etc. We facilitate syndication documents, financial/ cap ex planning, banking, etc.
In addition to new development deals, we offer HR services, policy and procedure manuals, operating agreement(s) and contract completion. NueHealth manages general operations of the ASC; the “blocking and tackling,” licensure readiness, insurance services, payor contracting and revenue cycle management.
episode where we collectively take the risk for the total cost of care. While not for everyone, for the right center and the right group, it’s a nice value add.
Repertoire: What kind of company culture are you looking for in a partnership?
Sheerin: We look for partners aligned in quality and value. Partners that are aligned around best clinical, operational and financial practices. Quality and safety must always “trump” financial gain. We are very interested in our potential partner’s “why.” Our “why” around ASCs is that we believe many patients can receive highestquality care and have a great experience in a lower cost facility – facilities where the surgeon is in
We are very interested in our potential partner’s “why.” Our “why” around ASCs is that we believe many patients can receive highest-quality care and have a great experience in a lower cost facility –facilities where the surgeon is in control. That’s the ideal partnership; one based on quality and service. When we have that, financial profitability will follow.
In addition to what most might consider standard in the industry, we have invested heavily in robust business analytics focused on managing key performance indicators that are financially, operationally and clinically focused. NueHealth has developed a value-based care platform that enables a surgery center to contract with the payer and take risk for a prospective episodic bundle; a fixed price for the entire
control. That’s the ideal partnership; one based on quality and service. When we have that, financial profitability will follow.
Repertoire: What are the most common challenges facing ASCs today and how does NueHealth work to navigate those challenges?
Sheerin: What we’re seeing is that a lot of ASCs today are struggling with staffing challenges. They’re competing with health systems
who often pay a little more and may have better benefit plans. To offset this, we’ve instituted gain sharing programs at many of the centers that we manage where the staff also benefit when the centers perform well financially. This allows the employee to share in the success of the center.
We’re also seeing a lot of surgery centers struggling with rising anesthesia costs. Surgery centers subsidizing anesthesia losses (net of what they bill for services) is becoming more common. We are seeing significant consolidation and PE backed mergers in anesthesia. In certain regions we have let requests for proposals that have creative funding and subsidy models around staffing and anesthesia coverage.
Supply costs also continue to rise, cutting into center margins. Group purchasing agreements are key. Many standalone, self-managed ASCs just don’t have the buying power that others get from GPOs that can pass along the benefits of economies of scale.
Finally, the costs associated with robotic surgery has become challenging for ASCs of late. Many of those coming out of surgical training programs with significant emphasis on robotics struggle with transitioning to ASCs without robotics. The robots and disposable costs associated with a case are very expensive and once again cut into already thin margins. We’ve been focused on creative capital deals with these robotic companies where we can pay down the cost of the robot with volume. The surgeons get what they need, and we also are able to protect the bottom line of the center.
Repertoire : What is the Insights business intelligence platform? How does it help to deliver results?
Sheerin: Most traditional ASC EMRs collect the minimum information needed to provide surgical care. We felt it was important to collect data and have the ability to query multivariate data to not only understand what is happening but develop actionable strategies for improvement. That is the essence of Insights platform. Our analytics help surgery centers understand and take action to improve operational efficiency, profitability, patient satisfaction, surgeon satisfaction, etc.
Repertoire: Is there a strategy for scaling these partnerships, while trying to preserve the local leadership and physician autonomy?
Sheerin: It starts with identifying and aligning around common goals. What are the surgeons looking for? If there’s a health system, what are they looking for? If we can’t establish common ground or alignment, then perhaps we need to walk away from the deal before getting into a “bad marriage.” That’s a tough discipline – nobody wants to walk away from new business. But in the long run it is much easier to never enter a misaligned partnership than to get out of it later.
Some partnerships start out great, but the players change over time. When new leaders come in, sometimes the priorities change. We need to be OK with recognizing when this is the case making a change if we don’t have the right fit. Surgeon autonomy begins with them having control over their environment to ensure safe and highest quality care. This includes the use of protocols and evidence-based pathways. Our strategy for partnerships and surgeon autonomy focuses on goal alignment, recognizing when partners are not aligned and focusing on safety, quality and satisfaction.



Meaningful Medicine
How an Atrium Health initiative is tackling workforce gaps and expands care access in North Carolina.
 As North Carolina’s health care system wrestles with widening access gaps and a shrinking workforce, Atrium Health is betting that the two challenges can be solved together. Through a recent initiative, the health system is reimagining how care is delivered – and who gets to deliver it – by bringing services, opportunity and career pathways directly into the communities that need them most.


CPR Depth Gauge
Actively measures the depth of every CPR compression.

Real-Time Feedback
AHA-driven guidelines help deliver high-quality CPR.

Integrated Pediatric Rescue
CPR Uni-Padz® enable a single solution for adult and pediatric victims.

The health system’s Meaningful Medicine program – launched with a landmark $10 million, five-year grant from Bank of America – is delivering measurable progress through innovative partnerships and communitycentered programs.
Introduced in 2022, Meaningful Medicine was born out of a clear and urgent reality: tremendous health inequities persist across the Charlotte region, even as the city continues to experience rapid growth, said Pooja Palmer, MS, portfolio strategy and special projects manager, impact evaluation and grants management, National Center for Clinical and Community Impact.
a full spectrum of integrated, community-centered care through Meaningful Medicine.”
Meaningful Medicine brings together two highly collaborative pillars: Meaningful Access and Meaningful Connections –uniting innovation across health care delivery, social impact, and workforce development. The goal has always been to address health inequities at their root, not in silos, Palmer said. “This investment serves a dual purpose: expanding access to care for our most vulnerable communities while creating clear pathways into health care careers, helping disrupt cycles of intergenerational poverty.”
If there is a single lesson that stands out, Palmer said it would be “engagement is everything.” The success of Meaningful Medicine is directly tied to the unprecedented level of collaboration among public sector, education, and community partners.
“From the beginning, we recognized that growth presented both a challenge and an opportunity – a chance to rethink how care is delivered to communities that have historically faced barriers to access,” she said. “We recognize that health is shaped by the structural conditions in which people live, and that improving outcomes requires bringing care, resources, and opportunity directly into communities. In response, our clinical and operational teams came together to design an innovative, interconnected model for delivering
Defining meaningful access
Since its inception, the program has achieved notable success. It has brought school-based virtual care to 115 Charlotte-Mecklenburg schools, facilitating more than 13,000 visits and helping keep students and staff healthy and present in classrooms. Mental wellness services through school-based virtual therapy have supported hundreds of students with more than 11,000 visits to date. Nearly 300 high school students have engaged in workforce development and training opportunities that aim to guide them toward careers in nursing and other high-demand health fields.
“From the outset, we defined meaningful access as care that is timely, trusted, convenient and connected to a broader system of support,” Palmer said. “Our initial focus was on delivering services in high-need communities and Title I schools, where barriers to access were most pronounced.”
Meaningful Medicine’s holistic model operates through six core initiatives – including virtual primary care, suicide prevention training, and social health screening – in collaboration with partners such as Charlotte-Mecklenburg Schools, Central Piedmont Community College, Mecklenburg County Public Health and local community organizations.
“During early implementation we learned that significant need existed more broadly across the Charlotte-Mecklenburg Schools footprint, prompting an evolution in our approach,” Palmer said. Meaningful access is no longer about geography alone, but about meeting people wherever the need exists, in alignment with Atrium Health’s For All mission. This philosophy has guided program expansion beyond our original footprint and informed the design of care models that are flexible, scalable and responsive to community-identified needs.
Atrium Health leadership highlights the importance of cross-sector collaboration in scaling impact. By weaving job training with accessible care, the program not only improves health outcomes but also builds economic mobility and nurtures the next generation of healthcare professionals in the region.
“Meaningful access means removing barriers that inhibit

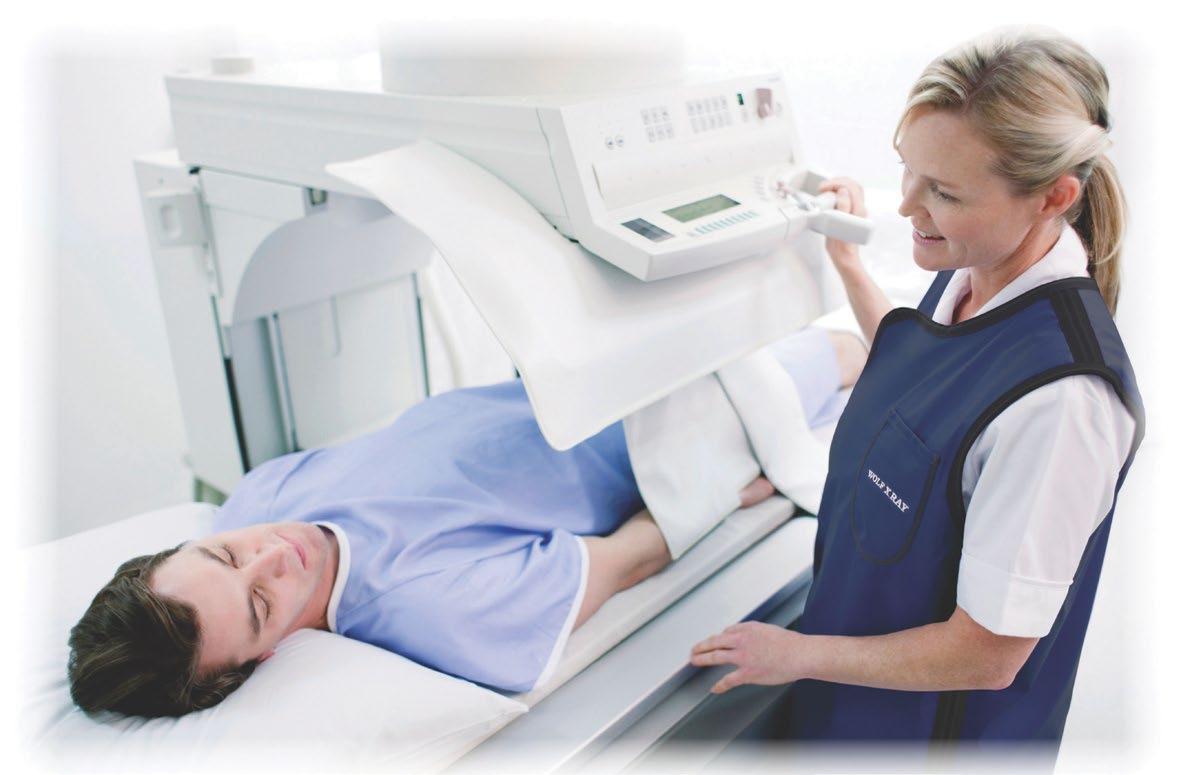
Only Wolf delivers with the broadest line of aprons and accessories that exceed radiation requirements of your hospital, clinic and practice customers... while providing the most professional look to their patients.
` Available in standard lead, lightweight lead and lead-free
` All sizes, from pediatric and small to XX large
` Collars, apronettes, lumbar support belt, and scoliosis stole also available

` Convenient breast pocket for pens, papers, clips, etc.
` Custom sizes available upon request
` Custom embroidery and logos available
` Available in a host of colors and patterns
accessibility – whether that’s transportation, cost, time away from school or work, or lack of trust – while ensuring that care is high-quality, approachable, integrated and sustainable when and where it is accessed,” Palmer noted.
Metrics and measurements
Atrium Health is tracking dozens of operational, clinical and engagement metrics to continuously improve the program, “but our success is ultimately measured by something broader: our ability to deliver whole-person care,” Palmer said.
Meaningful Medicine is intentionally designed to go beyond episodic, acute care. In addition to addressing immediate health needs, stakeholders are focusing on connecting individuals to a medical home, screening for social drivers of health, providing mental health resources, and linking families to community health workers and local resources. At the same time,
they are investing in the future by helping build the next generation of health care workers.
“Metrics such as attendance, utilization, return to class rates, and student engagement matter – but they are all in service of a larger objective: creating sustainable pathways to better health, stability, and opportunity,” Palmer said.
If there is a single lesson that stands out, Palmer said it would be “engagement is everything.”
The success of Meaningful Medicine is directly tied to the unprecedented level of collaboration among public sector, education, and community partners. “In particular, our sustained partnership with Bank of America has gone far beyond the initial philanthropic investment, serving as a true collaboration that has shaped strategy, strengthened execution, and reinforced shared accountability to community impact,” she said.
Rather than duplicating efforts, Meaningful Medicine
Building the future workforce
Workforce development has been a core pillar of Atrium Health’s Meaningful Medicine program since its launch, recognizing health care careers as a driver of both community health and economic mobility. Through partnerships with schools and community organizations, the program introduces students early to real-world health care settings, offering career exploration, internships and mentorship. These pathways extend beyond clinical roles to include non-clinical opportunities, highlighting the breadth of sustainable careers available in health care. By pairing access to care with access to opportunity, Meaningful Medicine strengthens individual well-being while helping build a resilient future health care workforce.
organizers focused on filling gaps, sharing resources, and leveraging each partner’s unique strengths. “That mutual trust allows us to move faster, design smarter solutions, and remain accountable to the communities we serve,” Palmer noted. “Our partners aren’t just stakeholders – they are co-creators. That mindset has been our secret sauce.”
Long-term goals
One of the initiative’s most important long-term goals is to create a proven, scalable blueprint that can be sustained through ongoing operational workflows and replicated in other regions. “From the beginning, we approached Meaningful Medicine not as a one-off program, but as a learning laboratory for what’s possible when health care, education and community partners are deeply aligned,” Palmer said. “Wherever possible, we are using the demonstrated success of this model to advocate for ongoing system investment.”
Organizers are actively developing expansion strategies with a particular focus on rural areas, where access challenges can be even more complex. Just as importantly, Palmer said, they are using lessons learned from Meaningful Medicine to reimagine and strengthen existing Atrium Health programs, redesigning them to be more integrated, more equitable and more impactful.
“Success for us means that the most impactful elements of this work continue through our broader operational strategies and we continue to influence how care is delivered well beyond the initial funding period.”
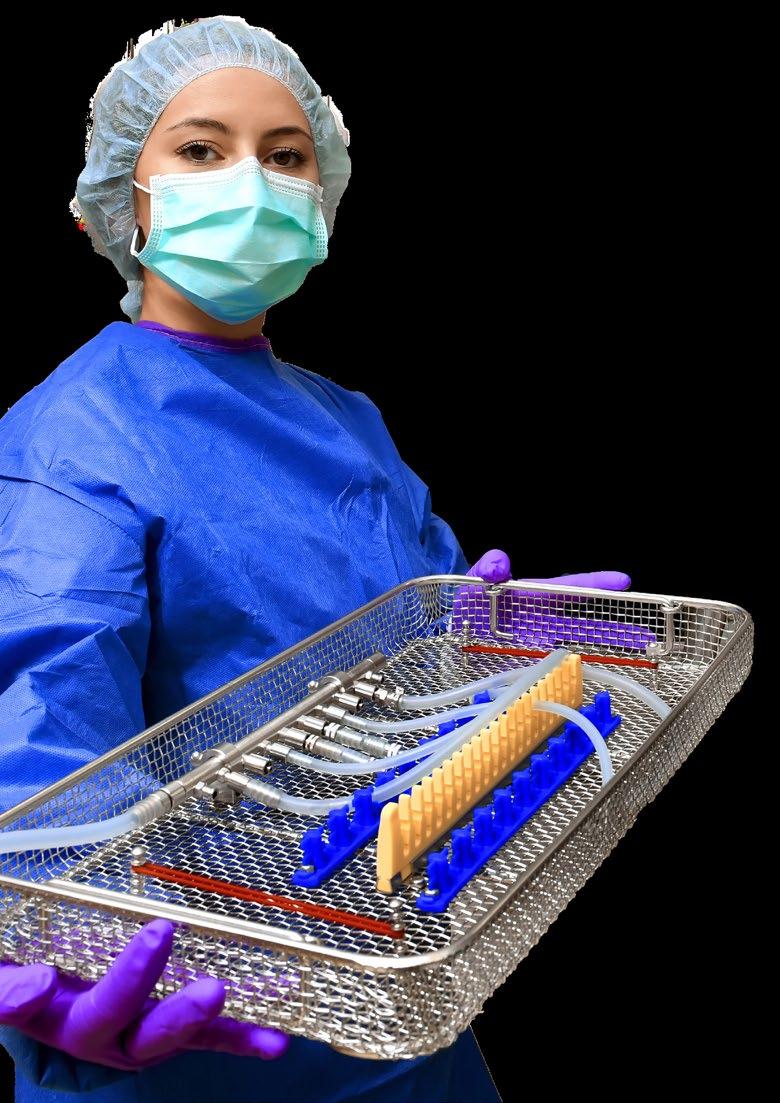








Remembering Mike Carver
The med/surg community mourns the loss of a Hall of Famer whose mentorship, generosity and unwavering commitment to people left an incredible legacy.

 Mike Carver, whose warmth, wit, and unwavering mentorship left an indelible mark on the healthcare industry, passed away recently. Known for his infectious enthusiasm and genuine kindness, Carver shaped not only the careers of those around him but also the culture of every team he touched.
Carver spent more than four decades in medical distribution and manufacturing, building businesses, mentoring colleagues and, above all, forming relationships. Over 43 years in the industry, he worked on both the
distributor and manufacturer sides, holding leadership roles and helping launch territories, companies and programs.
Born in Huntington, West Virginia, Carver was introduced early to the profession by his
father, a medical supply salesman. He graduated from the University of Tennessee in 1973 and began his career at Baxter Travenol Laboratories, gaining foundational experience selling through distribution channels.
He later joined Skyland Hospital Supply (now Concordance Healthcare Solutions), where he built a territory from the ground up and eventually helped establish a Knoxville branch that quickly became the company’s top-performing location.
An entrepreneur at heart, Carver co-founded Southland Medical Supply in the early 1990s, expanding it into a 16-location distribution network focused on home care and known for early adoption of technology such as barcode inventory scanning and direct-to-patient shipping. After selling the company, he moved into manufacturing roles and in 2003 joined GOJO Industries, where he helped build meaningful relationships between the company and medical distributors during a critical period for infection prevention and hand hygiene in healthcare.
Throughout his career, Carver emphasized that success in medical sales began with people. He often said that “meaningful relationships remain the priority for success,” a philosophy that shaped how he worked with customers, colleagues and competitors alike. Those who knew him describe a leader driven by passion and results but grounded in empathy, generosity and a desire to give back. He helped organize industry charitable events for years and was known for showing up personally to support customers and friends in times of need.
Inducted into the Medical Distribution Hall of Fame in 2017, Carver was widely respected not only for what he accomplished but for how he accomplished it. He believed deeply in the healthcare community and the
people in it, once reflecting that the industry was filled with “the most honest and compassionate and kindest and hardest-working people in the world.”
Beyond his professional accomplishments, those who knew Carver say his life was guided by a simple set of priorities: faith, family, friendship and helping others. He was remembered as a humble, thankful and generous man who made it a point to lift people up and make them feel valued – whether they were customers, colleagues or friends.
His faith was central to his life. An active member of NewLife Gathering Church in Knoxville, Carver dedicated time and resources to mission work and community outreach. He was especially devoted to FISH Hospitality Pantry, where he volunteered and
only for his long and successful career, but for the way he treated people along the way. He built companies, partnerships and programs, but more importantly, he built relationships. In an industry driven by trust, reliability and service, he set a standard that colleagues and friends say will endure long after his passing.
“Mike embodied what it means to be a mentor, a true friend, and a trusted colleague,” recalls Joel Rich, Vice President at GOJO/PURELL Healthcare.
“His influence across the industry was remarkable, but it was his humanity that made his impact unforgettable. His compassion and drive inspired all of us to reach further and believe in what once felt impossible.”
Rich shares a vivid memory of meeting Carver nearly two decades ago at a long-term care
“ His influence across the industry was remarkable, but it was his humanity that made his impact unforgettable. His compassion and drive inspired all of us to reach further and believe in what once felt impossible.”
supported fundraising efforts for more than two decades, helping provide food and assistance to those in need. Colleagues say this commitment to service reflected the same spirit he brought to his professional life – a belief that success meant little if it wasn’t used to help others.
‘One-of-a-kind’
For many in medical distribution, Carver will be remembered not
advisory board dinner in Akron. Between toasts and laughter, Carver predicted Rich would one day join GOJO – a prophecy fulfilled nearly a decade later.
“I’m genuinely grateful that I had the opportunity to join Mike and become part of #TeamGOJO,” Rich says.
“Calling Mike a one-of-a-kind colleague hardly does him justice,” Rich continued. “Every text or call from him was its own
adventure – you never knew what topic he’d bring up, but you could always count on the conversation ending the same way: with his genuine encouragement, a ‘you’re a star,’ and a reminder that this is ‘why we win.’ His presence and positivity made a real difference.”
Carver was a friend in the truest sense of the word, said Tim Cokkinias, Corporate VP at B. Braun Medical. Cokkinias recalls that his relationship with Mike began around 1990 through business, but it quickly grew into a deep personal bond. “We shared many values around faith and family,” Cokkinias says. “When you became friends with Mike, you became friends with his entire family, and your family became his. He was the king of building a network of real friends.”
assessing a business opportunity,” Cokkinias says. “He had a way of getting you out of your comfort zone to achieve more than you ever thought possible, while making you feel like the most important person in the world –genuinely. Some of the best ideas for building relationships with our distributor partners came from hours-long discussions between Mike and me.”

“ Mike was the absolute king of relationship building. He believed that relationships always have and always will be the most important part of building a business.”
Carver’s personality was infectious. He loved to laugh, and his humor could brighten any room. He had a fearless intellect and a drive to succeed – whether at work, in family life, or through charitable efforts with FISH Hospitality Pantry. He demanded loyalty, but he gave it in equal measure. One of his favorite sayings, “I always want to know the final score before the game even starts,” reflected his relentless preparation and determination. Working with Carver was equally inspiring. “Nothing was impossible when Mike was
Cokkinias emphasizes that having Carver as a friend was a gift: “He made you a better person and always wanted to make you look good. I was lucky to be in that elite group. I already miss my friend.”
A true Hall of Famer
Industry colleagues were deeply affected by Carver’s passing. During a recent Repertoire podcast, Manny Losada of MedPro Optimal Healthcare Solutions reflected, “We lost a dear colleague, a bigger-than-life person in our industry …he’s touched so many lives, including mine.”
Repertoire publisher Scott Adams added, “Mike was an unbelievable individual. The time he gave back to FISH, the charity we’re donating to this year at the Hall of Fame dinner, was remarkable. Even in retirement, his presence affected all of us dramatically. When I found out, it just hurt my heart.” Losada noted the profound impact Mike had on the community: “Everybody stopped … you’re going to know where you were when you heard the news of Mike Carver because it hits home.”
Carver’s legacy in the healthcare industry will forever be defined by his unmatched ability to build relationships and bring people together. Cokkinias reflects, “Mike was the absolute king of relationship building. He believed that relationships always have and always will be the most important part of building a business. He was also a big believer that doing business could be fun, and the folks we worked with every day at our mutual distributors also became our friends. Our annual distribution summit and charity golf outing was always called ‘Friends of Healthcare,’ and through it, we built true lifetime friendships.”
Rich adds, “Mike had a remarkable gift for making every customer interaction feel like the most important moment in the world. Whether it was a simple rep call, a tradeshow presentation, or even a Mediterranean cruise with customers, his ability to genuinely connect with people was energizing and unforgettable. His presence didn’t just elevate the experience – it made everyone around him feel truly valued.”
They Won’t Sell It.


We take training seriously.
Distributor sales reps are chasing $67B in Med-Surg sales every year.
The manufacturers who win are the ones who train them.
Our 2-Minute Game Plan videos give distributor reps the quick product education they need to confidently introduce your solution to customers.
And reps are using them.
` 75+ products currently available for training in the RepConnect app
` 40,000+ total video views last year
` 87% of Repertoire readers are more likely to talk about a product when they’ve been trained on it
Because when reps understand your product, they sell it.

Product Data: The Hidden Barrier to E-Commerce Growth in Healthcare Distribution
 Digital commerce in healthcare distribution runs on product data. And like a lot of foundational infrastructure, it tends to get attention only when it falls short – an image that won’t render, an attribute that’s missing, a new item that takes weeks to onboard instead of days. Few companies have the bandwidth to tackle it, and no single company could solve it alone. It’s the kind of challenge that requires the whole industry to move together.
Without a shared standard for how product information is structured and exchanged, manufacturers and distributors have each built their own workarounds.
Manufacturers field different data requests from different partners and reformat the same information multiple times over. Distributors piece together what they need to get products live on their digital channels. It’s time-consuming on both sides, and it’s become an accepted cost of doing business.
In February 2026, HIDA launched a pilot program with 33 member companies to test a Product Data Exchange (PDX) – a centralized, standardized way to share product descriptions, images, attributes, and
marketing content across trading partners.
The idea is straightforward: manufacturers build a strong product data set once, and it flows reliably to distributor partners in a format that’s ready to use.
The benefits are tangible on both sides of the transaction. Faster new item setup. Cleaner e-commerce listings. Less manual work on both sides of the transaction. And over time, a supply chain where product information is something companies can depend on rather than constantly chase down.
The PDX pilot is an early step, but it reflects something the industry has been ready for: a better way to share the data that makes digital commerce work.

By Kelley Taft, Senior Vice President for Membership, Health Industry Distributors Association

With healthcare supply chain decision-makers. In private, pre-scheduled business meetings. Partnerships that move your business forward.



Where The Industry Meets
Three
Scan to explore #StreamliningHealthcare26 and see what’s planned.


Industry News
CDC reports low respiratory illness levels; flu activity remains elevated
The Centers for Disease Control (CDC) released an update midMarch on nationwide respiratory virus activity as of March 6, 2026. The amount of acute respiratory illness causing people to seek health care is now low. Seasonal influenza activity remains elevated nationally. Influenza A activity is decreasing in most areas of the country while trends in influenza B activity vary by region, according to the CDC. RSV activity has started later than expected in most regions of the United States, though severity is not higher compared with recent seasons, per the CDC. This atypical season indicates that higher levels of RSV activity may continue into April in many regions. Emergency department visits and hospitalizations for RSV are highest among infants and children less than 4 years old. Additionally, COVID-19 activity is decreasing nationally but remains elevated in some areas of the country.
Cardinal Health named one of America’s Best Large Employers of 2026
Cardinal Health has been recognized as one of America’s Best Large Employers of 2026
by Forbes, according to a recent LinkedIn post. The annual rankings are based on survey responses from U.S. employees. According to Cardinal Health, “We are committed to creating a workplace where all employees can be themselves and do their best work to deliver products and solutions that improve the lives of people every day.”
B. Braun announces significant reduction of greenhouse gas emissions through Renewable Electricity Purchase Agreements
B. Braun Medical Inc. announced the purchase of renewable electricity for its operations in the U.S., leading to a significant reduction of greenhouse gas emissions and furthering B. Braun’s dedication to protecting people and the planet by reducing environmental impact. This action will result in a greater than 30% reduction of B. Braun’s scopes 1 & 2 CO2e emissions in North America and represents a significant investment in renewable energy deployment. The purchase agreements are part of B. Braun’s commitment to reducing CO2e emissions 50% by 2030 and will result in all of the company’s U.S. based manufacturing facilities, affiliated distribution centers and locations in Pennsylvania being matched with
100% renewably sourced electricity from 2026 onwards. B. Braun is also taking additional steps to invest in alternative energy technologies, including the installation of a fuel cell microgrid at B. Braun’s 710,000 sq. ft. IV fluid and generic pharmaceutical manufacturing facility in Irvine, California.
Henry Schein unveils new Dallas Discovery Center
Henry Schein, Inc. celebrated the grand opening of its new Dallas Discovery Center (DDC)—an 8,300-square-foot, state-of-the-art training facility designed to bring health care education, technology, and innovation together under one roof. The center marks Henry Schein’s first integrated dental and medical training facility, reinforcing the company’s commitment to advancing integrated, systemic models of health care delivery.
“Our goal with the Dallas Discovery Center is to create a collaborative space where clinicians, supplier partners, and our Team Schein Members can learn from one another and see what’s possible in health care,” said Ty Ford, Vice President and General Manager, Henry Schein U.S. Medical Sales. “By bringing medical and dental training together, we’re helping build a more integrated, patient-centric future.”
Midmark is the first and only manufacturer in the market to have both a procedure chair and an examination chair that comply with the US Access Board Standard.
Getting to know the standard
01 Seat Height: 17" or lower and 25" or higher
02 Transfer Surface: 21" wide and 17" deep
03 Base Clearance: 26" wide or less
04 Transfer Supports: Compliant to the US Access Board Standard
05 Leg Supports: Support the patient’s thigh, knee and calf
Learn more at: midmark.com/accessible-care

Source: US Access Board. (2024, July 25). Standards for accessible medical diagnostic equipment. Federal Register, 89(143), 47823-47839. https://www.federalregister.gov/documents/2024/07/25/2024-16266/standards-for-accessible-medical-diagnostic-equipment © 2026 Midmark Corporation, Versailles, Ohio USA
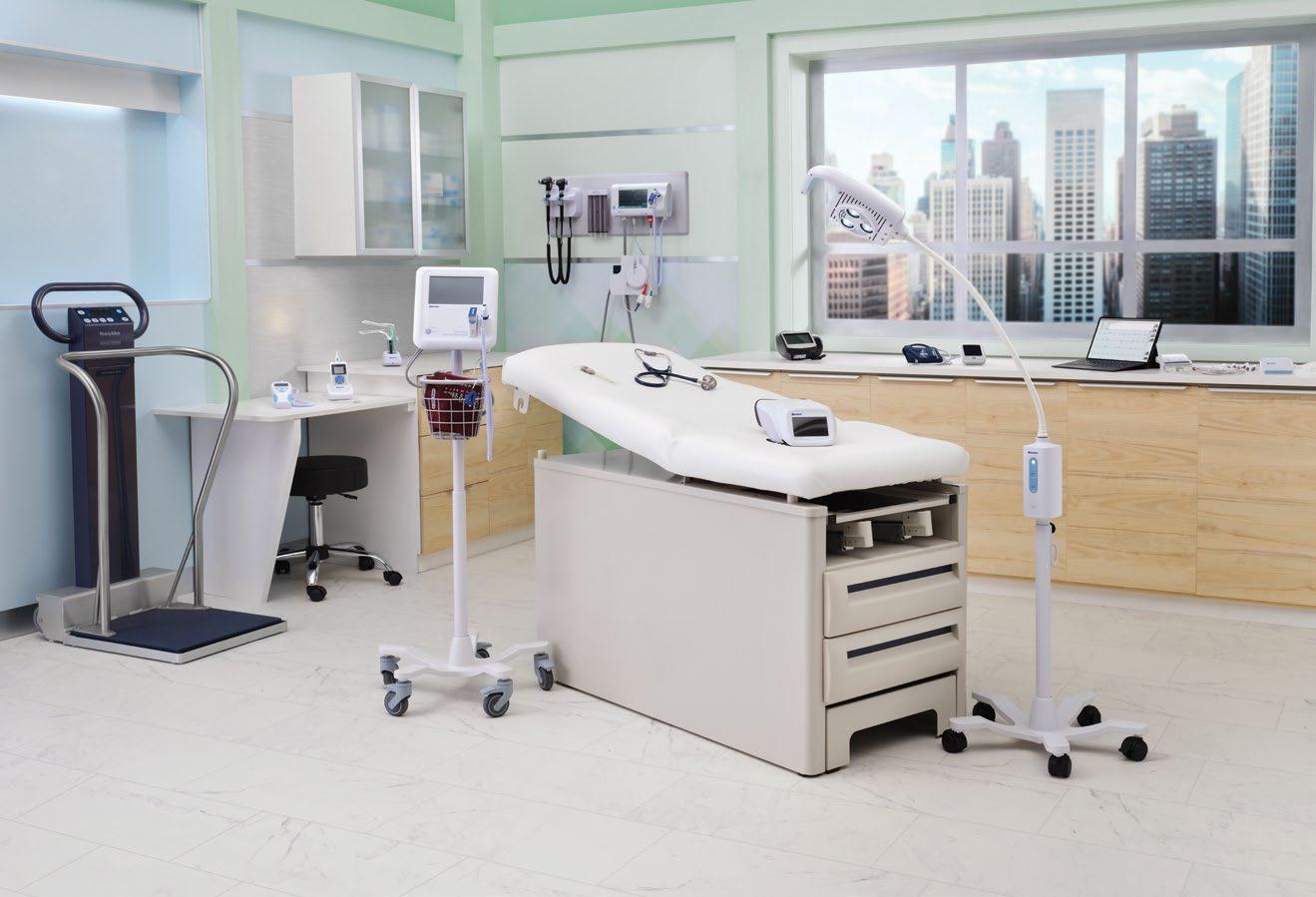
Check-up on Device Health During Your Next Off ice Visit
Connect with us and review the latest Baxter and Welch Allyn technology empowering patient exams. ON SPOTLIGHT THIS MONTH:
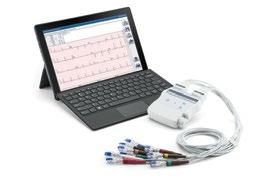
Welch Allyn Diagnostic Cardiology Suite

















Welch Allyn Integrated Wall Systems

Welch Allyn RetinaVue 700










Welch Allyn Spot 4400 Vital Signs Device


< Scan To View Our Current Promotions
Rx Only. For safe and proper use of the product mentioned here, please refer to the appropriate Operator’s Manual or Instructions for Use.
Baxter, Hillrom and Welch Allyn are trademarks of Baxter International Inc. or its subsidiaries.
US-FLC45-260004 (v1.0) 02/2026
