







Balancing a busy work schedule?

Find time for continuing education with AVA!

Check out all the educational courses & continuing education credits offered:
Free CEs for AVA Members!
Procedural courses: Ultrasound Guided
Peripheral Intravenous Catheter
Insertion, Intro to Midline Catheters using MST

PIV Curriculum - 6 CEs available for PIV Essentials Bundle!
Previous ISAVE that Line webinar events and AVA Conference Presentations. & many more!
Complete a short quiz in AVA Academy to earn JAVA CE credit




GulfVAN proudly welcomed members of the Gulfcoast Infusion Nurses Society (INS) to our network in September, and October marked our first joint meeting as one unified community. It was inspiring to see our communities come together so seamlessly. This milestone reflects our shared commitment to advancing best practices and improving patient outcomes.
The meeting presentation, “Reduce CVAD Infections and Improve Outcomes: Optimizing Device Securement and Dressing Adherence,” was led by Matt Gibson, RN, CRNI, CPUI, VA-BC, and was sponsored by Eloquest Healthcare. Thank you to all who attended and contributed to this important discussion—the conversation, case pearls, and collegial energy were exactly what we hoped for (and the food didn’t hurt either!).
Our next meeting will be held virtually on December 9th, featuring presentations from our scholarship recipients on what they learned at the AVA Scientific Meeting

President David Markle, RN, VA-BC™
Treasurer Amanda Pierce BSN, RN, VA-BC™ Presidential Advisor Meagan Capen, APRN, CPNP-AC, MSN, VA-BC™
The 2025 AVA Annual National Scientific Meeting in Orlando, Florida presented the opportunity for collaboration and exchange of ideas with Vascular Access Specialists from around the world! This

2025 at Orlando Regional Medical Center in Orlando, Florida provided 5 CEs, community and collaboration for our members and guests! Malachi LeVeilee presented The Role of Vessel Assessment in Vessel Health, Victor Lange discussed Needleless Connector Design: The impact on intraluminal occlusion and associated
infection risk, Kirsotpher Hunter presented 555, A Call to Action. Hospital Onset Bacteremia (HOB), Jennifer Ballar discussed Enhancing Vascular Access Safety: The Role of Tissue Adhesives in Infection Prevention, and Vance Clement discussed The Effect of External Forces on PIVs and the Use of a Break-away Device to Improve IV Care. We were able to give away many door prizes to our attendees thanks to our sponsors and vendor partners! PLATINUM sponsor: ORMC, GOLD sponsor: BD, SILVER sponsor: Solventum, Vendor partners: B.Braun, Lineus Medical, H.B. Fuller, Teleflex, Eloquest, AccuVein, Merit Medical, Kurin, RyMed, and IVAccess. HUGE thanks to our GulfVAN partners Kristin Jacobs and Sandra Mehner! Attendees enjoyed food, community, education, chair massages, and the exhibit hall! We were also able to support the AVA Foundation through donations from attendees!





For more FLAVAN news and upcoming events please visit our website by clicking the link FLAVAN and don’t forget to like and follow us on Facebook!
The AVA Education Department truly enjoyed connecting with so many of you at the 2025 Annual Scientific Meeting in Orlando. Your enthusiasm, participation, and commitment to advancing vascular access education continue to inspire our team. Planning is already underway for AVA’s 40th Annual Scientific Meeting, to be held in Grapevine, Texas, in October 2026. We look forward to reviewing an exciting array of new presentations and topics that will shape next year’s program. Don’t forget—the Call for Topics and Presentations close January 4, 2026. Submission details are available: Click here.

In collaboration with AVA’s Beyond Acute Care Special Interest Group (BACSIG) and our partners at Mighty Well, the Education Department is pleased to introduce the Mighty Well Shower Guide. This brochure was designed to help patients with vascular access devices safely manage daily hygiene at home. It includes practical guidance for protecting various types of vascular access devices during showering, key “dos and don’ts” to maintain dressing integrity, and recommendations for protective products that minimize the risk of infection. Attendees of AVASM25 received a copy in their conference swag bag. To access a copy of the Mighty Well Shower Guide, please visit the AVA website and navigate to the Resources tab.
Finally, we extend our sincere appreciation to everyone who participated in the public review of AVA’s Clinical Practice Guidelines for Adult Vascular Access. Your thoughtful comments and suggestions are invaluable. Each submission is being carefully reviewed for inclusion in either the forthcoming first edition or consideration in the second edition, based on the established parameters of the publication protocol. We are thrilled to be nearing publication of this first edition and are already preparing to begin work on the next.
If you are passionate about evidence-based practice and would like to contribute as an author for the second edition, we encourage you to complete the AVA Volunteer Form: click here. Together, we can ensure that these guidelines continue to reflect the highest standards of vascular access care and support our global community of clinicians.
MATHEUS F.P.T. VAN RENS, MAANP, RN, KEVIN HUGILL, RN, PHD, GIOVANNI BARONE, MD, ROBIN VAN DER LEE, MD, FIAMMETTA PIERSIGILLI, MD, PHD
Since the mid 1990’s smart infusion pumps with their embedded drug libraries and dose error reduction software have become the trusted workhorses of infusion therapy. They beep, they calculate, and they reassure us with their digital readouts of drug and fluid delivery. We tend to believe them without question. But here’s the catch: being ‘smart’ doesn’t always mean being ‘precise’. Patients are put at risk due to inappropriate use, human factors, and the intrinsic limitations of these systems.1 Risks especially amplified when it comes to the low flow rates and multi-infusion setups that typically characterize neonatal and pediatric care.
THE HIDDEN CHALLENGE
Infusion tubing compliance swallows up flow, startup delays and flow resistance leads to inaccurate delivery and nothing reaching the baby for minutes; and when an occlusion resolves, a surprise bolus sneaks through. Pumps inline alarms may not be triggered early enough, or sometimes not at all, leaving the consequences of partial kinks and slowdowns invisible until the patient shows clinical signs. It doesn’t stop there. Multi-infusion setups bring their own chaos: drugs mixing in Y-infusion sets, backflow into other syringes, and dead space that delays delivery.
Ask a smart pump to deliver 3 microgram/Kg/ min at 0.3 mL/hr of Dopamine while sharing a line with a Prostaglandin analogue infusion at 5 nanogram/Kg/minute, with additional fluids, and things quickly get complicated. In these situations, even the choice of syringe, length, diameter, or vertical height of infusion tubing can change the flow profile. What looks like a smooth 0.3 mL/hr on the pump display can
arrive at the patient as a stuttering pattern of stop-and-go delivery. For a neonate receiving critical lifesaving drugs, even these small variations can be clinically destabilizing in moments.2
Now imagine being able to see those invisible fluctuations as they happen. That’s where new MEMS-based (Micro-Electro-Mechanical Systems) flow sensor technology comes in. Using silicon micro-devices, no bigger than a grain of sand, these sensors transform the invisible into visible, measuring what really moves through the infusion line in real-time.3
Instead of assuming that ‘programmed equals delivered,’ clinicians can get direct feedback: has the infusion started, is there a pause, is a bolus creeping through? The sensor doesn’t replace the pump, but it makes the system truly smarter.
MEMS stands for Micro-Electro-Mechanical Systems. Imagine microscopic machines carved into silicon, smaller than a grain of sand, yet powerful enough to sense the tiniest movements of fluid. They’re the same hidden devices that trigger your car’s airbag or tell your cell phone when to flip the screen.
Now this technology is moving into IV therapy. The new sensor is clip-on, non-invasive, and simple to use, no line changes, no extra complexity. By attaching it to the outside of the tubing, clinicians can finally see what smart pumps can’t: the real flow, in real time. Tiny chips, massive safety potential.
For fragile neonates, ‘almost right’ isn’t good enough. Unwarranted variability in infusion delivery translates into swings in blood pressure, oxygenation, or glucose. In critically ill neonates where highly concentrated infusions are required to minimize fluid overload, even tenths of a milliliter can significantly alter the delivered drug dose, potentially leading to clinically relevant changes in the baby’s condition. In practice, this can mean the difference between a baby being stable or spiraling into crisis. By challenging the ‘smartness’ of smart pumps, real-time flow sensing equips clinicians with the information they need to act early, and to trust that every milliliter is truly reaching the patient.
Advancing practice and supporting vascular access developments to protect patients and save lives are key ambitions of the AVA. In this light maybe it’s time to redefine what is ‘smart infusion.’ It’s not just pumps that can calculate dose and infusion rates that are needed, but systems that can prove they’re delivering them.4 Real-time flow data also opens the door to the next step in infusion safety: closed-loop infusion therapy, where pumps adjust automatically based on measured flow, much like automated oxygen control systems that continuously adapt inspired oxygen to target saturations in neonates. As highlighted in recent neonatal research, realtime monitoring transforms an invisible risk into actionable data, making precision therapy truly possible at the bedside.4
• ��Smart pumps aren’t always that smart at low flow rates.
• ��Multi-infusion adds hidden variability: mixing, backflow, dead space, delays.
• ��Alarms may come too late, or not at all.
• ��Real-time flow sensing could make safety critical infusion therapy safer.
• ��For neonates, every milliliter, every microgram, and every nanogram matters
References
1. Weiss M, van der Eijk A, Lönnqvist PA, Lucchini A, Timmerman A. 10 clinical tips for advancing patient safety when using syringe pump systems for microinfusion intravenous drug therapy. Eur J Anaesthesiol 2023;40(6):387-90. doi:10.1097/EJA.0000000000001839
2. van der Eijk AC, van Rens RM, Dankelman J, Smit BJ. A literature review on flow-rate variability in neonatal IV therapy. Paediatr Anaesth 2013;23(1):9-21. doi:10.1111/pan.12039
3. Zhang L, Yang Y, Bertos GA, Liu C, Hu H. Bio-inspired micromachined volumetric flow sensor with a big dynamic range for intravenous systems. Sensors (Basel) 2022;23(1). https://doi.org/10.3390/s23010234
4. van Rens M, van der Lee R, Barone G, Piersigilli F. Innovation in neonatology - Authors’ reply. Lancet Child Adolesc Health 2025;9(11):e21. doi:10.1016/S2352-4642(25)00267-6
December 2, 2025

AVA offers connection. Perhaps it offered you a mentor or provided a resource that help you navigate a decision or promotion. Maybe a conversation opened a new door AVA is a place where knowledge, purpose, and community come together. It’s a movement. Now it’s your turn to give back on Giving Tuesday on December 2, 2025.
The AVA Foundation invites you to help us continue that mission. Your donation will support our shared vision: To build interprofessional leaders in vascular access who advance knowledge, practice, advocacy, and collaboration to improve outcomes.
With your support, we can reach more clinicians, provide more resources, and foster a future where every vascular access professional feels empowered, equipped, and connected.

Consider the reflection of a recent scholarship recipient, Erin Reed:
“Attending the AVA Conference had a profound impact on me both professionally and personally. Networking with experts from around the world and learning from their techniques, knowledge, and experience enhanced my own skill set and elevated the care I provide to my patients. The opportunity to exchange contact information and share experiences continues to serve as an invaluable resource in my daily practice.
It was also encouraging to realize that vascular access professionals everywhere face many of the same challenges, regardless of setting. Exploring new products and bringing back innovative solutions to my organization was especially rewarding. The AVA Foundation Scholarship made this experience possible and meant so much to me; it truly refueled my passion for advocating for better outcomes and advancing vascular access care.”
KRISTY LYNNE POINDEXTER

For 38 years, I have depended on parenteral nutrition (PN). That means one thing above all else: reliable central venous access is my lifeline. Over the decades, I’ve had multiple catheters, but one stood out—my Hickman catheter that lasted an incredible 22 years.
For clinicians, such longevity is almost unheard of. For me, it was my everyday reality. This article offers my perspective as a patient: what it meant to live with one line for over two decades, how I knew it was time to replace it, the emotional process of letting it go, and the care practices that helped it last so long. My hope is that my story can help inform and inspire clinicians caring for patients who rely on central access as much as I do.
I was eight years old when I began home parenteral nutrition (HPN) in 1988—one of the youngest patients at the time to do so. At that point, my doctors predicted I wouldn’t survive past age eleven. Thirty-eight years later, PN remains my bridge to life.
Clinicians know the risks: catheter-related bloodstream infections (CRBSIs), thrombosis, mechanical failure, and loss of access sites. For patients like me, each line is precious. Central access is not temporary—it is lifelong. Protecting each catheter means protecting my future.
Living with a line for 22 years transforms your relationship with it. My Hickman was not “just a catheter”—it was part of me.
• Every dressing change, flush, and hookup became second nature.
• Psychologically, I viewed it as an extension of my body.
• That perspective shaped my behaviors—I respected and protected it as if it were a vital organ.
For clinicians, this emotional bond is important to recognize. A central line is not just a piece of silicone; for patients, it can feel like a literal lifeline.
After more than two decades, my line began to show its age. The signs were subtle at first:
• Sluggish flushing/aspiration: I often used Cathflo (Alteplase) when the lumen grew resistant, but over time, it became less effective.
• Changes in flow: Infusions felt different—slower, less predictable.
• Patient intuition: After 22 years of daily use, I could sense it wasn’t going to last.
Clinical takeaway: Patients who live with their lines every day often detect early functional changes before they are measurable. Trust their instincts and investigate concerns, even if initial tests appear normal.
When it became clear the Hickman needed to be replaced, I was flooded with emotions:
• Gratitude for a line that had carried me through two decades without major complication.
• Anxiety about the unknown—would the new line last as long? Would my body adjust?
• Grief, because it felt like saying goodbye to a body part.
Clinical takeaway: Replacing a long-standing line isn’t just a procedure. It can feel like a loss. Acknowledging the emotional impact helps patients feel validated and supported.
My new line is a double-lumen catheter. From a clinical standpoint, it offers flexibility—one lumen for PN, the other for labs or medications.
But for me, the adjustment was more than clinical. It felt foreign, noticeable with every movement. After years with one familiar line, this new one required learning new habits, new securement strategies, and a new routine. Over time, I’ve adapted, but the sense of comfort and familiarity takes time to build.

So, how did my Hickman last 22 years? I believe it came down to four main practices:
1.Aseptic technique, every single time
• Every access was treated as high-stakes.
• Hand hygiene and maintaining an aseptic field were non-negotiable. While I don’t routinely wear a mask at home, I do during new line care or early dressing changes, and I always insist hospital staff wear one when accessing or handling my line.
• Even when tired or rushed, I never cut corners.
2.Repair instead of replace
• Small cracks or damages were repaired when possible.
• Catheter repair kits and skilled nurses allowed me to preserve the line rather than replace it prematurely.
3.Listening to my body
• I trusted my instincts when something felt off.
• I advocated for interventions (Cathflo, evaluations) before issues became emergencies.
4.Respect for the line
• I avoided unnecessary blood draws or extra manipulations.
• I positioned and taped it carefully, protecting it during sleep, movement, and daily activities.
Clinical takeaway: Reinforcing aseptic technique in patient training is critical. Patients need to understand not just the steps, but the mindset that every access is an opportunity to protect their line.
• Meticulous hand hygiene before every contact.
• Changing dressings consistently—never pushing past the recommended interval.
• Using sterile caps/connectors and replacing them as directed.
• Scrub the hub, every single time—I wipe the connection with alcohol before and between every flush, med pass, hookup, and disconnect. Even if it feels repetitive, it’s the habit that protects my line.
• Changing claves: I replace the needleless connector every dressing change, and also after each blood draw.
• Speaking up immediately about fever, chills, or unexplained malaise.
I credit these habits—especially the repetition of scrubbing hubs and changing connectors—with keeping my line safe for so long.
While every institution has its own blood draw protocols, this is the approach I was taught decades ago and have consistently followed:
1. Prepare the setup with blood vials, saline flushes, alcohol wipes, and a new clave.
2. Wear gloves, scrub the clave end with alcohol, attach saline, flush, then draw back 8–10 mL to discard.
3. Attach the vacutainer and fill the lab vials.
4. Remove vacutainer, scrub clave, then flush with 10 mL saline.
5. Clamp the catheter, remove the clave, scrub the hub with alcohol, place a new clave, then flush with another 10 mL saline.
6.At that point, the line is ready to clamp or hook up for infusion
This process became second nature for me, and I credit it as one reason my line lasted so long.
Clinical takeaway: While my exact method worked well for me, it’s important to emphasize that patients should always follow the most current institutional policies and protocols. What matters most is consistency, aseptic technique, and connector replacement.
Many patients don’t realize repairs are possible. My Hickman survived multiple small repairs over 22 years. Each one bought me more time.
• Repair kits, when used correctly, maintained catheter integrity.
• Skilled vascular nurses and IR teams played a critical role in preserving the line.
Clinical takeaway: Educating patients and clinicians about repair options can extend the life of a line and protect limited venous access.
• Patient insight is invaluable: Patients often notice changes first.
• Longevity is possible: With vigilant care and partnership, central lines can last far longer than expected.
• Partnership improves outcomes: Trust grows when clinicians respect the patient’s expertise in their own body.
My 22-year Hickman catheter was more than a device—it was a lifeline, a companion, and a symbol of resilience. For clinicians, I hope my story underscores the importance of patient-clinician partnership, education, and respect for central lines as more than just medical tools. By listening to patients, supporting their instincts, and emphasizing careful technique, we can help more lines last, more patients thrive, and more lives continue with stability and dignity.
Insights from 38 years on PN and a Hickman catheter that lasted 22 years
Aseptic Technique
• Treat every access as high-stakes. Hand hygiene and maintaining an aseptic field are non-negotiable.
Scrub the Hub
• Wipe the connection with alcohol before and between every flush, med pass, hookup, and disconnect.
• Repetition protects the line—it’s never “too much.”
Clave/Connector Changes
• Change the needleless connector at every dressing change.
• Always replace the clave after blood draws.
• Prepare fully before starting.
• Discard 8–10 mL, collect samples, flush, then always replace the clave.
• Note: This was my longstanding personal protocol. Patients should always follow current institutional policies.
• Small cracks or damage can often be repaired instead of replacing the entire catheter.
• Avoid unnecessary access or manipulation.
• Secure it carefully during sleep, movement, and daily activities.
Hi!MynameisJaydenStarke,andI’m22yearsold.I’vebeenlivingwith chronichealthchallengesmywholelifethatbecamemoreprominentin
senioryearofhighschool,Ineededmyfirstfeedingtube.Afterawhile, In2020,IhadmyfirstPICClineplaced,andafterhavingoneonandoff

Hi! My name is Jayden Starke, and I’m 22 years old. I’ve been living with chronic health challenges my whole life that became more prominent in middle school. Over the years, things have progressed, and by my senior year of high school, I needed my first feeding tube. After a while, my body could no longer be sustained by tube feedings, and I transitioned to TPN (Total Parenteral Nutrition, a way of receiving essential nutrients via the bloodstream).
Hi!MynameisJaydenStarke,andI’m22yearsold.I’vebeenlivingwith chronichealthchallengesmywholelifethatbecamemoreprominentin middleschool.Overtheyears,thingshaveprogressed,andbymy senioryearofhighschool,Ineededmyfirstfeedingtube.Afterawhile, mybodycouldnolongerbesustainedbytubefeedings,andI transitionedtoTPN(TotalParenteralNutrition,away ofreceiving essentialnutrientsvia the bloodstream).
fluids,andmedications.Fromtheverybeginning,Istruggledwithskin reactionstothedressingsandadhesives.I’vealwayshadsensitiveskin,whenIwasyounger, dn’tgetalongwithbandaids.Overtime, that sensitivity becamemorechallengingtomanage.IwastoldthatskinirritationwassimplysomethingI’d havetodealwithassomeonewhoreliesonlong-termcentrallines.Ididn’tlikethatanswer,but forawhile,Ididn’tknowwhatotheroptionsexisted.
Hi!MynameisJaydenStarke,andI’m22yearsold.I’vebeenlivingwith chronichealthchallengesmywholelifethatbecamemoreprominentin middleschool.Overtheyears,thingshaveprogressed,andbymy senioryearofhighschool,Ineededmyfirstfeedingtube.Afterawhile, mybodycouldnolongerbesustainedbytubefeedings,andI transitionedtoTPN(TotalParenteralNutrition,away ofreceiving essentialnutrientsvia the bloodstream).

In2020,IhadmyfirstPICClineplaced,andafterhavingoneonandoff fortwoyears,aHickmanlinewasplacedin2022toinfuseTPN,IV fluids,andmedications.Fromtheverybeginning,Istruggledwithskin reactionstothedressingsandadhesives.I’vealwayshadsensitiveskin,whenIwasyounger, weusedtojokethatmyskinjustdidn’tgetalongwithbandaids.Overtime, that sensitivity becamemorechallengingtomanage.IwastoldthatskinirritationwassimplysomethingI’d havetodealwithassomeonewhoreliesonlong-termcentrallines.Ididn’tlikethatanswer,but forawhile,Ididn’tknowwhatotheroptionsexisted.

In 2020, I had my first PICC line placed, and after having one on and off for two years, a Hickman line was placed in 2022 to infuse TPN, IV fluids, and medications. From the very beginning, I struggled with skin reactions to the dressings and adhesives. I’ve always had sensitive skin, when I was younger, we used to joke that my skin just didn’t get along with band aids. Over time, that sensitivity became more challenging to manage. I was told that skin irritation was simply something I’d have to deal with as someone who relies on long-term central lines. I didn’t like that answer, but for a while, I didn’t know what other options existed.
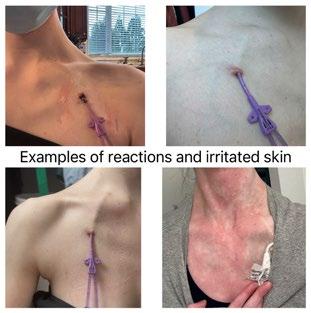
In2020,IhadmyfirstPICClineplaced,andafterhavingoneonandoff fortwoyears,aHickmanlinewasplacedin2022toinfuseTPN,IV fluids,andmedications.Fromtheverybeginning,Istruggledwithskin reactionstothedressingsandadhesives.I’vealwayshadsensitiveskin,whenIwasyounger, weusedtojokethatmyskinjustdidn’tgetalongwithbandaids.Overtime, that sensitivity becamemorechallengingtomanage.IwastoldthatskinirritationwassimplysomethingI’d havetodealwithassomeonewhoreliesonlong-termcentrallines.Ididn’tlikethatanswer,but forawhile,Ididn’tknowwhatotheroptionsexisted.
LaterIswitchedtoasilicone-baseddressingwithoutacrylic themselveswerealso Ihadred,circularmarksexactlywherethe discssat,alongwithincreaseditching,skinbreakdown,and evengranulationtissue.Assomeonemanagingmultiple chronicconditions,smalldiscomfortsinadditiontochronic paincanbecomeoverwhelming.Notonlywasmyskin integritybeingcompromised,Iwasuncomfortableand constantlyitchingorrubbingmyskin.Whenmyskin breaksdownunderthedressing,the riskofinfectionincreasessignificantly.
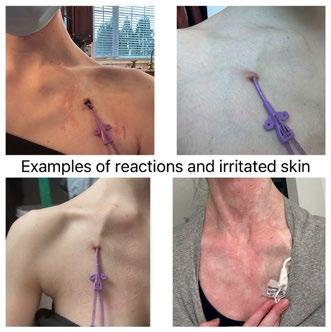
Later I switched to a silicone-based dressing without acrylic and I realized that the CHG discs themselves were also irritating my skin. I had red, circular marks exactly where the discs sat, along with increased itching, skin breakdown, and even granulation tissue. As someone managing multiple chronic conditions, small discomforts in addition to chronic pain can become overwhelming. Not only was my skin integrity being compromised, I was uncomfortable and constantly itching or rubbing my skin. When my skin becomes irritated or breaks down under the dressing, the risk of infection increases significantly.
LaterIswitchedtoasilicone-baseddressingwithoutacrylic andIrealizedthattheCHGdiscs themselveswerealso Ihadred,circularmarksexactlywherethe discssat,alongwithincreaseditching,skinbreakdown,and evengranulationtissue.Assomeonemanagingmultiple chronicconditions,smalldiscomfortsinadditiontochronic paincanbecomeoverwhelming.Notonlywasmyskin integritybeingcompromised,Iwasuncomfortableand constantlyitchingorrubbingmyskin.Whenmyskin breaksdownunderthedressing,the riskofinfectionincreasessignificantly.
LaterIswitchedtoasilicone-baseddressingwithoutacrylic andIrealizedthattheCHGdiscs themselveswerealso irritatingmy skin. Ihadred,circularmarksexactlywherethe discssat,alongwithincreaseditching,skinbreakdown,and evengranulationtissue.Assomeonemanagingmultiple chronicconditions,smalldiscomfortsinadditiontochronic paincanbecomeoverwhelming.Notonlywasmyskin integritybeingcompromised,Iwasuncomfortableand constantlyitchingorrubbingmyskin.Whenmyskin becomesirritated or breaksdownunderthedressing,the riskofinfectionincreasessignificantly.
Finding alternative products is hard when you don’t know what other options are available. I had known about silver dressings from prior experiences with them for surgical wound care but had never thought of trying to find an option for my central lines. Once I tried the silver plated Silverlong disc, I noticed improvements with my skin within a few weeks, something that felt like such a relief after years of irritation.
Findingalternativeproductsishardwhenyoudon’tknowwhatotheroptionsareavailable.Ihad
Findingalternativeproductsishardwhenyoudon’tknowwhatotheroptionsareavailable.Ihad knownaboutsilverdressingsfrompriorexperienceswiththem forsurgicalwoundcarebuthadneverthoughtoftryingtofind anoptionformycentrallines.OnceItriedthesilverplated Silverlongdisc,I noticed improvementswithmyskinwithina fewweeks,somethingthatfeltlikesuchareliefafteryearsof irritation.
Findingalternativeproductsishardwhenyoudon’tknowwhatotheroptionsareavailable.Ihad knownaboutsilverdressingsfrompriorexperienceswiththem forsurgicalwoundcarebuthadneverthoughtoftryingtofind anoptionformycentrallines.OnceItriedthesilverplated Silverlongdisc,I noticed improvementswithmyskinwithina fewweeks,somethingthatfeltlikesuchareliefafteryearsof irritation.
BecauseIlivewithintestinalfailureandrelyonTPNasmy solesourceofnutrition,keepingmylinesafeandmyskin healthyisabsolutelyessential.Havingproductsthatareboth effectiveandgentleonmyskinmakesallthedifferencein maintaining myhealthandcomfort.
Because I live with intestinal failure and rely on TPN as my sole source of nutrition, keeping my line safe and my skin healthy is absolutely essential. Having products that are both effective and gentle on my skin makes all the difference in maintaining my health and comfort.
BecauseIlivewithintestinalfailureandrelyonTPNasmy solesourceofnutrition,keepingmylinesafeandmyskin healthyisabsolutelyessential.Havingproductsthatareboth effectiveandgentleonmyskinmakesallthedifferencein maintaining myhealthandcomfort.
Outsideofall themedicalstuff,Ilovetoread,bake,andspend timewithfriends.Thesemomentsremindmethatevenwhile managingcomplexmedicalconditionsthere’sstillsomuchlife toenjoy.
Outside of all the medical stuff, I love to read, bake, and spend time with friends. These moments remind me that even while managing complex medical conditions there’s still so much life to enjoy.

Outsideofall themedicalstuff,Ilovetoread,bake,andspend timewithfriends.Thesemomentsremindmethatevenwhile managingcomplexmedicalconditionsthere’sstillsomuchlife toenjoy.



Don't miss the opportunity to lead with knowledge, improve care quality, and elevate the role of vascular access in every healthcare setting! AVA Clinical Practice Guidelines (CPGs) are evidence-based recommendations that offer practical, multidisciplinary guidance for bedside caregivers, vascular access teams, educators, and facilities without specialists.
active?

Standardization of Vascular Access Practice - Provides an evidence-based framework to reduce variability in assessment, insertion, and management, improving consistency across diverse care settings in conjunction with previously established and published guidance.
Patient-Centered Care - Emphasizes individualized assessment of physiologic, psychosocial, and environmental factors to guide device selection , optimize outcomes, and minimize complications.
Complication Prevention and Management - Offers practical, evidence-driven strategies to reduce device-related risks. Renew your AVA Membership Today! Not an AVA Member? www.joinAVAnow.com

1 Nursing and Midwifery Research Centre, Royal Brisbane and Women’s Hospital, Herston, Queensland, Australia
2 School of Nursing, Midwifery and Social Work, University of Queensland, Brisbane, Queensland, Australia
3 School of Nursing and Midwifery, Griffith University, Nathan Campus, Brisbane, Queensland, Australia
With years of critical care nursing experience, our team has seen firsthand how central venous catheters (CVCs) are essential for delivering life-saving treatments. But here’s the catch, while CVCs are indispensable, they’re also incredibly vulnerable. One of the most stubborn challenges we face is keeping the dressing, the protective barrier that secures the catheter to the skin, intact. Over time, adhesives weaken, securements loosen, and what starts as a small disruption can quickly spiral into a serious complication.
Globally, millions of CVCs are inserted in intensive care units (ICUs) each year, and about one in four will fail prematurely, frequently due to poor attachment to the skin.1-4 Jugular CVCs are the most difficult to manage. With constant neck movement, limited space for dressings, and the tug of multiple infusion lines, keeping these catheters secure is a daily battle. Frequent dressing disruptions don’t just compromise care, they open the door to central line-associated bloodstream infections (CLABSIs), which can cost U.S. healthcare systems anywhere from $33,696 to $71,443 per episode.5-7 And that’s not all. A poorly secured catheter can irritate the vessel wall, increasing the risk of thrombosis and CVC dislodgement.
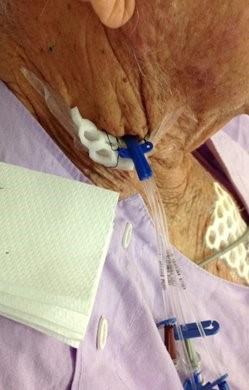
After witnessing countless dressing failures and the complications they trigger, our team knew we needed a solution that went beyond the basics, something that could truly support long-term dressing integrity. Because when a dressing fails, everything else is at risk. Infection, dislodgement, thrombosis, the cascade of consequences is real, and it starts with a simple peel at the dressing edge. That’s why we turned our attention to Mastisol, a medical liquid adhesive (MLA) which is a nonwater-soluble gum mastic derived from the resin of the Pistacia lentiscus tree. After antisepsis, it’s applied to the skin where the dressing border will sit, creating a tacky, secure foundation that helps dressings stay in place longer.
So, we launched the STICKY Trial, a multi-site, randomised controlled study across four metropolitan ICUs in Australia. Between September 2021 and February 2023, we enrolled 160 participants with the aim of determining whether the use of a MLA (in conjunction with standard care), could outperform standard care alone in preventing dressing failure for jugular CVCs. The results were compelling - MLA use was associated with a significant reduction in dressing failure (Odds Ratio 0.39; 95% CI, 0.20–0.76) and fewer dressing changes (incidence rate ratio, 0.74; 95% CI, 0.55–0.99). Jugular CVC dressings with MLA dwelled longer (59hrs vs 24hrs) and used fewer dressings (64 vs 124) than standard care alone.
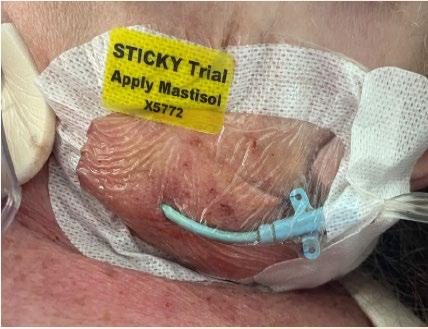
Beyond dressing durability, we wanted to know if Mastisol could reduce microbial growth underneath the dressing. To explore this, we conducted a microbiological sub-study that included a convenience sample of 20 patients (10 per arm). We found that the MLA group samples had growth for 4 out of 10 swabs (40%), with only 1 swab exceeding 100 colony-forming units (CFU). In contrast, the standard care group was higher with 8 out of 10 swabs (80%) showing growth, and 4 swabs had ≥100 CFU. Each patient’s swab revealed between 1 to 9 different colony types, and the species identified were consistent with commensal skin flora. It’s worth noting that chlorhexidine dressings weren’t used in either group for this sub-study, so the differences observed were likely influenced by the adhesive itself.
We were also aware that when it comes to patient care, every dollar counts, especially in high pressure environments like the ICU. So alongside clinical outcomes, we looked at the financial costs of using MLA. In our cost analysis we found that the estimated expected cost per participant was $310 for the MLA group and $321 for the standard care group. That is a saving of $11 per participant, with a 95% credible interval ranging from $13.96 to $8.08. While it may seem modest at first glance, these savings add up, especially when multiplied by thousands of patients. And when paired with better dressing integrity, fewer dressing changes, and reduced infection risk, MLA appears a smart investment in both care and cost.
Our work was published in Critical Care Medicine in early 2025 (doi: 10.1097/ CCM.0000000000006533), where it was selected as an Editor’s Choice article and featured on the journal’s website.
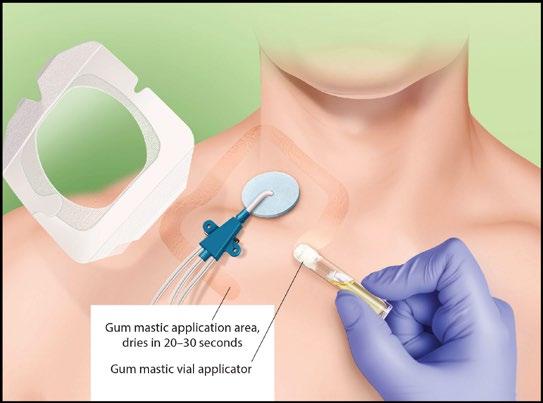
The STICKY Trial provides clinical staff a practical solution to CVC dressing securement. Our encouraging results showed adding Mastisol (MLA) to jugular CVC dressings reduces dressing disruption and cuts down on dressing changes. That’s not just a win for workflow; it’s a meaningful step forward for patient safety and cost savings.
1. 1. Napalkov P, Felici DM, Chu LK, Jacobs JR, Begelman SM. Incidence of catheter-related complications in patients with central venous or hemodialysis catheters: a health care claims database analysis. BMC Cardiovasc. Disord. 2013;13(1):86.
2. 2. Rickard C, Edwards M, Spooner A, et al. A 4-arm randomized controlled pilot trial of innovative solutions for jugular central venous access device securement in 221 cardiac surgical patients. J. Crit. Care 2016;36:35-42.
3. 3. Ullman AJ, Marsh N, Mihala G, Cooke M, Rickard CM. Complications of central venous access devices: a systematic review. Pediatrics 2015;136(5):e1331-e44.
4. 4. Gunther SC, Schwebel C, Hamidfar-Roy R, et al. Complications of intravascular catheters in ICU: definitions, incidence and severity. A randomized controlled trial comparing usual transparent dressings versus new-generation dressings (the ADVANCED study). Intensive Care Med. 2016;42(11):1753-65 doi: 10.1007/s00134-016-4582-2 [published Online First: 2016/10/21].
5. 5. Goudie A, Dynan L, Brady PW, Rettiganti M. Attributable cost and length of stay for central line-associated bloodstream infections. Pediatrics 2014;133(6):e1525-32 doi: 10.1542/peds.2013-3795 [published Online First: 20140505].
6. 6. Dimick JB, Pelz RK, Consunji R, Swoboda SM, Hendrix CW, Lipsett PA. Increased resource use associated with catheter-related bloodstream infection in the surgical intensive care unit. Arch. Surg. 2001;136(2):229-34 doi: 10.1001/archsurg.136.2.229.
7. 7. Zhang Y, Wang Y, Sheng Z, et al. Incidence Rate, Pathogens and Economic Burden of Catheter-Related Bloodstream Infection: A Single-Center, Retrospective Case-Control Study. Infect Drug Resist 2023;16:3551-60 doi: 10.2147/IDR.S406681 [published Online First: 20230605].
Join Dr. Nicole Marsh for “The STICKY Solution: Preventing Dressing Disruption in Central Line Care,” an exclusive AVA webinar on Tuesday, November 18, 2025, at 7:00 p.m. ET.
SUBMITTED BY: AMANDA HOUCK
Situation Midwest, Level II Trauma Teaching Hospital with 13 CLASBIs in 2022 and 10 CLASBIs in 2023.
Background Majority of CLASBIs were from Central Lines in the Critical Care Unit. Infection Prevention and previous Vascular Access Team Leadership were not having success with their initial solution: mandating that PICC lines can only be placed within 24-48 hours of discharge.
Assessment In all documented CLASBIs the identified problem was linked to lack of device maintenance, not insertion.
Intervention In June of 2024, Vascular Access Team Leadership rolled out a mandatory “Nursing “FUN”damental s” class, focusing on Central Line care and maintenance to all Critical Care Nurses. The class was 2 hours long - the 1st hour was dedicated to lecture, and the 2nd hour was dedicated to hands on sterile dressing changes.
The lecture focused on a combination of skill review, and purpose refocusing. Discussions included Mortality Rate associated with CLASBIs, Nurse Burnout and accountability, and best practice review.
To address the remaining CLASBIs coming from the step-down and rehab floors, the Vascular Access Team created a position that’s sole purpose is to round throughout the hospital auditing all IV’s and providing real-time intervention and bedside education to both nurses and patients.
Outcomes
Since the completion of the Nursing “FUN”damentals classes, there have been ZERO CLASBIs from the Critical Care Unit - we are going on 17 months.
Since the addition of the Vascular Access Auditor Position in January 2025, there have been 3 CLASBIs. 2024 ended with 7 CLASBIs and 2025 is trending to end with 3-4.
Conclusions Basic principles exist for a reason: they provide the framework for safe and effective clinical practice. Intentional education and consistent reinforcement of vascular access fundamentals foster a culture of accountability and enhance bedside nurse confidence. Patient safety and high-quality care are best achieved when nurses possess strong clinical competence and operate within environments that actively support evidencebased best practices.
Submissions accepted until January 4, 2026
AVA is a not-for-profit multidisciplinary professional organization uniquely positioned as the leader in vascular access education and research. Its mission is to build interprofessional leaders in vascular access to advance knowledge, practice, advocacy, and collaboration to improve outcomes.
AVA’s membership includes clinicians from many disciplines including nursing, medicine, radiology, respiratory therapy, pharmacy, as well as consumers, professionals from industry, education, research, and others with an interest or specialization in vascular access and related fields.
Meeting attendees come from many countries and include professionals from: Interventional Radiology • Oncology • Surgery • Education and Training • Critical Care • Home Care • Home Infusion • Hematology • Radiology • Pediatrics and Neonatology • Nephrology and Dialysis • Anesthesiology • Infectious Disease • Infection Prevention • Vascular Access • Research and Development • Sales and Marketing • Engineering
2026 marks AVA’s 40th Annual Scientific Meeting with at least 1,300 attendees, which include 60–70 industry partners. The meeting site is Gaylord Texan Resort and Convention Center. AVA demonstrates its leadership role in the art and science of vascular access. This three-day conference (October 3–5, 2026) provides attendees with opportunities to participate in educational sessions, hands-on training, facilitated discussion, and networking.
GENERAL SESSIONS focus on development of the vascular access specialty, clinical research, professional development, technological advances, and evidence-based practice.
BREAKOUT SESSIONS will offer small group presentations emphasizing subjects of interest for the vascular access specialist and related disciplines; abstract and poster presentations allow participants to share original research, education projects and clinical innovations.
SYMPOSIA, VA TALKS, and EXHIBITS afford participants, industry partners, and exhibitors the opportunity to learn from one another in order to design and apply new technologies, science, and techniques in the most effective ways.
With separate registration fees, an additional day of Pre-Meeting Workshops (October 2, 2026) offers in-depth exploration of topics of critical importance to the vascular access community.
The Call for Topics seeks submissions from:
1) Professionals who wish to submit a topic for presentation.
2) Recommendations for speakers and/or topics to be included in the Scientific Meeting.
• Participation and submission of topic suggestions is NOT limited to AVA members.
• Topics should address the general or specific interests of AVA members and meeting participants keeping in mind that AVA is an organization of clinicians, healthcare specialties, and industry/corporate professionals involved in vascular access and related fields.
• Presentations must avoid any semblance of commercialism.
• General Sessions are limited to 60 minutes in length.
• Breakout Sessions may be scheduled from 30 to 60 minutes in length at the discretion of the selection committee.
• Hands-On Workshops may be scheduled for a full day (8 hours) or for a half day (4 hours).
• You may submit more than one topic, but please note that each speaker may be limited to presenting at only one invited session and one poster/ oral abstract as the principal author.
• AVA values diversity, inclusion, and professional mentoring among its membership and promotes these values in its topic and speaker selection processes.
• AVA reserves the right to solicit additional and/or new speakers for any proposed topic.
The information listed below is required to complete the submission process. Each submission is reviewed by program committee members who score the key elements based on how closely the given criteria are met.
Presentation Title:
Use key words that describe the specific topic and content of the abstract. Catch phrases can be used but need to include a reference to the topic. For example, “Making a Difference” may get attention but does not suggest what the abstract is about. By adding a specific reference to the abstract subject matter, the abstract title becomes clearer; i.e., “Making a Difference: Ace Inhibitors in Hypertensive Patients.”
Target Audience:
What population is this session designed to benefit most?
Level of experience of the target audience: Basic, Intermediate, Advanced
What type of presentation is this?
General Session
Breakout Session* Hands-On Workshop
*Breakout Sessions may be scheduled from 30 to 60 minutes in length at the discretion of the selection committee.
Prerequisite:
Include the minimum knowledge and/or skills required to most benefit from this session.
Purpose/Goals:
This statement should be the most important primary information you want to convey for the abstract. This should be one or two sentences. The title should not be repeated.
Has this presentation been given before? Where?
Minimum of three objectives are required. Provide three to five outcomes that complete the statement: “By the end of this session, the participant will be able to...” DO NOT type this statement in the text box when entering each of your outcomes.
Content Description:
The content description should be concise yet comprehensive. Ask yourself as you are reading the session description, “As an attendee, do I know what this abstract is about and would I want to attend?” Ask a colleague to read it as well while considering the same question. (max. 1,000 characters including spaces)
Additional Text:
Any additional text that expands the content description to be used for the review process. This narrative is your opportunity to provide a convincing overview of the value of your proposed session. If the reviewers cannot clearly understand what this session is about, your odds of having your abstract selected are greatly reduced. Expansion of the content description must be written in a brief, wellorganized, and focused manner. In one paragraph the potential speaker should have written a narrative that:
1 Identifies the key topics that will be addressed 2 . Describes any special learning activities, such as case study analysis, audience participation, or interactive discussion.
Speaker Contact Information, CV/Resume, Presentation Experience, and Availability Over Meeting Dates.
Contracts are signed only with the primary presenter. Only the Primary Presenter may be eligible for any speaker incentives. All presenters must be aware that this application is being submitted.
21
Some applicants will be contacted by an AVA 2026 Annual Meeting Design Team for a phone interview between January–February 2026 to discuss. Please try to return messages promptly. The interview is an integral part of the submission review process. Failure to participate, or be available for an interview may result in the elimination of the submission from the review process.
The program will be selected by early March 2026. Applicants will receive notice by email.
SUSAN KACACHOS
I have returned from this year’s AVA scientific meeting inspired by all the great presentations, for example, Navigating an Innovative Nursing Research Fellowship to Tackle Outdated Port Beliefs, Perceptions & Practices, presented by Guadalupe Ordaz-Nielsen, BSN, VA-BC.
My vascular access specialty team (VAST) was able to use the knowledge gained to put into our facilities’ practices the use of the existing patients’ Porta Cath instead of adding device placement of a peripherally inserted central catheter (PICC) by siting the slide from the PowerPoint using evidence based knowledge, such as, The INS 2021 & 2024 SOP recommends using ports unless contraindicated (e.g., existing complications with the device) as the preferred IV route of an additional VAD
Our VAST used secure chat (encrypted communication channels for interprofessional communications) to collaborate with the care team for the patient to advocate the use of the patient’s existing Port instead of placing another central line that supported a “call to action aligns with our vascular access policies with INS SOP to improve patient outcomes. “
The result, VAST organizational support to standardize the use of patients Port was initiated by the expert VAST champions plus the multidisciplinary team members, for example, the case managers set up the use of the port at the aftercare facility thereby avoiding the use of a port by inserting another VAD that would increase the risk of infection and support the VAST organization by using the patients existing Port for outpatient antibiotics.
The physician trusted the VAST expert advice, and the patient was able to be discharged without being poked and charged for an additional line, therefore preserving veins and decreasing the risk of infection and complications associated with another device and portal of entry for infection, care, and maintenance for an additional device.
Sincerely,
Susan Kacachos MSN-ED, RN, VA-BCTM
Houston Methodist Baytown Hospital
Radiology-Vascular Access, PICC Team 4401 Garth Road, Unity 5, Office # 5972
Baytown, Texas 77521
Work Phone: (346) 292-2047
Skacachos@houstonmethodist.org
NISHA GUPTA, BSC, MSC, PHD MONICA KOEHLER, BS
Healthcare is an ever-changing landscape, especially with the introduction of new quality measures that aim to expand the current scope of reporting requirements. One such measure, Hospital-Onset Bacteremia and Fungemia (HOB), significantly expands bloodstream infection (BSI) reporting beyond central lines to include infections from all organisms and devices. In the face of these changes and increasing complexity, the need for innovative, targeted solutions to address the pathogens most responsible for BSIs has never been more critical.
Chlorhexidine (CHX) is a clinically proven broad-spectrum antimicrobial agent.1 With the rise of Candida auris as a multidrug resistant fungal pathogen,2 the present study was conducted to evaluate the effectiveness of Chlorhexidine against this pathogen by determining the Minimum Inhibitory and Minimum Bactericidal Concentrations (MIC/MBCs).
Minimum Inhibitory Concentration (MIC): Two-fold dilutions of a CHX stock solution were prepared to produce a concentration range of 0.03-512 μg/mL. Broth cultures of nineteen clinically isolated Candida auris strains were matched to a 5.0 McFarland Standard and diluted to 105-6 CFU/mL. Each Chlorhexidine dilution was mixed with inoculum and nutrient broth in micro titer plates, then incubated at 37oC for 18-24 hours before spectrophotometric analysis. Test controls were utilized to ensure proper microbial growth, sterility and complete solubilization of chlorhexidine.
Minimum Bactericidal Concentration (MBC): Aliquots from each MIC well were grown for 24-48 hours on neutralizing agar plates at 37oC. Growth was confirmed via colony counting.
CHX MIC: Chlorhexidine inhibited all nineteen isolates of Candida auris. MIC concentrations ranged from 8-128 μg/mL. Two isolates, CA-1097/23 and CA-1101/26, were the most susceptible with an MIC range of 8-16 μg/mL. Six isolates, CA- 0381/01, 0383/03, 0385/05, 0386/06, 1100/25, and 1102/27 had an MIC range of 16-32 μg/mL. Almost half of the Candida auris strains, CA-0382/02, 0384/04, 0388/08, 0389/09, 0390/10, 0931/21, 1099/24, 1103/28, and 1104/29 were inhibited by 32-64 μg/mL. CA-0387/07 and 1105/30 were the most tolerant with an MIC range of 64-128 μg/ mL.
CHX MBC: All isolates were killed within 128 μg/mL of Chlorhexidine. Eleven of the nineteen isolates had the same MIC and MBC value. Six isolates, CA-0381/01, 0389/09, 0390/10, 0931/21, 1103/28 and 1101/26 had an increase in the MBC value over the higher end of the MIC range by 1-2fold. One isolate, CA-1104/29, had a slightly lower MBC value than MIC (16-32 μg/mL compared to 32-64 μg/mL).
Candida auris is emerging as a nosocomial multi-drug resistant pathogen of international concern. As new threats to healthcare continue to develop and focus expands beyond central lines through the quality measure HOB, technologies must meet the need of delivering lifesaving solutions. Although Chlorhexidine has been used for decades in a variety of clinical settings, its antimicrobial effectiveness continues to hold true.
The present study demonstrated that this broad-spectrum antiseptic agent is not only inhibitory, but cidal against the fungal pathogen, Candida auris.
Disclosure Statement and Limitations
Study was funded by and authors are employed by Teleflex Incorporated. Chlorhexidine based antimicrobial technologies are manufactured by Teleflex. Study was conducted with sample size of 3 for each of the 19 strains so statistical analysis was not performed. Data on file at Teleflex. In Vitro study may not be indicative of clinical performance.
Future Directions
Further characterization of the effects of Chlorhexidine against C. auris will include determinization of the Kill Time and the Minimum Biofilm Eradication concentration.
References
1.KS Lim and PCA Kam. Chlorhexidine –pharmacology and clinical applications. Anesthesia and Intensive Care, Vol. 36, No. 4, July 2008.
2.JF Meis and A Chowdhry. Candida auris: a global fungal public health threat. The Lancet Infectious Diseases. Vol. 18, issue 12, 1298-1299, Dec 2018.



INTRAVASCULAR QUARTERLY (IQ)


AVA's mission is to build interprofessional leaders in vascular access to advance knowledge, practice, advocacy, and collaboration to improve outcomes.
AVA’s exclusive quarterly enewsletter, delivering the latest updates on vascular access directly to members’ inboxes. Stay informed, stay connected!

Peer-reviewed quarterly journal available in both print and online, providing trusted insights and research at your fingertips!

Tune in on all major streaming platforms for expert insights, industry trends, & real conversations about vascular access. Stay informed, get inspired, & elevate your practice—anytime, anywhere!


Your resource to ace the VABC exam, then keep as your go-to reference for success throughout your career!

Unlock learning on your schedule! Access ondemand CE courses, including procedural training, webinar recordings, & past conference sessions—free or discounted for AVA members. Stay ahead in vascular access, anytime!