TOWARDS AN EQUAL AUSTRALIA: ADVOCATING FOR HEALTH AND GENDER EQUITY
INSIDE
ANZAC DAY:
Remembering our wartime nurses: The incredible story of Vivian Bullwinkel and her accomplishments post-war
International Day of the Midwife and International Nurses Day: No limits – The achievements of inspirational nurses and midwives
World first: Australasian Nursing and Midwifery Clinical Trials Network set to boost clinical research for nurse and midwife researchers

A PUBLICATION OF THE AUSTRALIAN NURSING AND MIDWIFERY FEDERATION VOLUME 27, NO.11 APR–JUN 2023



FOR WORK. Take your health career to South Australia and discover work-life balance at its best. Visit sahealth.sa.gov.au/forworkforlife FOR life.
Adding to a raft of new reforms set to improve the quality and safety in the aged care sector, the Fair Work Commission recently ruled to lift the Award wages of low-paid aged care workers by 15% from 30 June this year.
This was a meaningful step in recognising workers’ true value, and after years of neglect, the sector can start to retain and recruit nurses and carers if the wage increase is passed on in full. Disappointingly, however, we know of some providers who plan to withhold the government-funded increase from workers.
Recently, the ANMF Victorian Branch filed a bargaining dispute Application with the Fair Work Commission against two aged care providers with these intentions. In response, the providers said they were prepared to start cancelling agreements and move to modern awards, absolving them from paying allowances and penalties to workers.
This is undoubtedly the tip of the iceberg, given the lack of transparency aged care providers have shown in the past.
The ANMF will work with the federal government to guarantee providers pass on the funding in pay rises to aged care workers.
Despite the many inroads made in the sector, it is abundantly clear by this example and others that we still have much work to do. The ANMF, however, remains committed to achieving a better aged care system, including better conditions for aged care workers.
On top of our work in aged care, much of ANMF’s efforts are improving conditions for members and, more broadly, building a better healthcare system.
One of these initiatives includes a new national enterprise to support nurses, midwives and students with sensitive health issues related to mental health, substance use, family violence, or anything affecting their health and wellbeing across the country.
The Albanese Government has invested $25.2 million to establish and run the new National Nurse and Midwife Health Service, which the ANMF is implementing.
When fully up and running early next year, the service will employ RNs, ENs, nurse practitioners and midwives to offer free, independent advice, support, information, treatment, and specialist referrals.
The ANMF is thrilled to be rolling out the program nationwide. The health and wellbeing of nurses and midwives are crucial, making this program essential and invaluable to so many of our members. More details about the service can be found on page 40.
Special mention in this editorial goes out to nurses and midwives also making significant advancements in care and research within their specialities.
Leading the way in delivering quality care is the promising establishment of the Nursing and Midwifery Clinical Trials Network, founded by nursing academics and run by the Rosemary Bryant AO Research Centre in Adelaide.

Detailed on page 30 of the ANMJ, the world’s first Network brings together academic institutions to facilitate and support nurse or midwife-led clinical research and translating evidence into practice. Additionally, the Network provides a platform to accelerate growth in nurse and midwife-led trials across Australasia and collaboration among nursing and midwifery clinical researchers.
This initiative is significant for the future of our professions. Nurses and midwives have immense potential to contribute to advancing science and knowledge in all aspects of healthcare. We comprise 60% of the healthcare workforce but are often unrepresented in the leadership of large-scale clinical research projects and clinical trials. With the rollout of this network, we look forward to this changing. In acknowledgment of International Day of the Midwife on 5 May and International Nurses’ Day on 12 May, the ANMJ has highlighted remarkable nurses and midwives whose work makes a significant difference in healthcare and our society.
These include Nurse Practitioner Lynette Byers, who has worked across remote Aboriginal communities in the APY lands for the past two decades and Midwife Melanie Briggs, who works at Waminda South Coast Aboriginal Women’s Health and Welfare Corporation and is also the manager of the Minga Gudjaga Birthing on Country program.
Their stories are just a few examples of how nurses, midwives and carers make a difference to influence positive change for patients, communities, and the professions. There are many of you doing the same and I commend you for the invaluable difference you make.
That being said, I wish you a happy International Day of the Midwife and International Nurses’ Day, as we celebrate the wonderful professions we belong to together.
Follow me on Twitter
@AbutlerAnnie
Annie Butler
EDITORIAL Apr–Jun 2023 Volume 27, No. 11 1
ANMF Federal Secretary
DIRECTORY
ANMF FEDERAL & ANMJ
Level 1, 365 Queen Street, Melbourne Vic 3000 anmffederal@anmf.org.au
To contact ANMJ: anmj@anmf.org.au
FEDERAL SECRETARY
Annie Butler
FEDERAL ASSISTANT SECRETARY
Lori-Anne Sharp


ACT
BRANCH SECRETARY
Matthew Daniel
NT
BRANCH SECRETARY
Cath Hatcher

SA
BRANCH SECRETARY
Elizabeth Dabars
VIC
BRANCH SECRETARY
Lisa Fitzpatrick





OFFICE ADDRESS
2/53 Dundas Court, Phillip ACT 2606
POSTAL ADDRESS
PO Box 4, Woden ACT 2606
Ph: 02 6282 9455
Fax: 02 6282 8447 anmfact@anmfact.org.au
NSW
BRANCH SECRETARY
Shaye Candish
OFFICE ADDRESS
16 Caryota Court, Coconut Grove NT 0810
POSTAL ADDRESS
PO Box 42533, Casuarina NT 0811
Ph: 08 8920 0700
Fax: 08 8985 5930 info@anmfnt.org.au
QLD
BRANCH SECRETARY
Beth Mohle
OFFICE ADDRESS
191 Torrens Road, Ridleyton SA 5008
POSTAL ADDRESS PO Box 861 Regency Park BC SA 5942
Ph: 08 8334 1900
Fax: 08 8334 1901 enquiry@anmfsa.org.au
TAS
BRANCH SECRETARY
Emily Shepherd
OFFICE ADDRESS 535 Elizabeth Street. Melbourne Vic 3000
POSTAL ADDRESS PO Box 12600, A’Beckett Street.
Melbourne Vic 8006
Ph: 03 9275 9333 / Fax: 03 9275 9344
MEMBER ASSISTANCE anmfvic.asn.au/memberassistance
WA
BRANCH SECRETARY
Janet Reah
OFFICE ADDRESS
50 O’Dea Avenue, Waterloo NSW 2017
Ph: 1300 367 962
Fax: 02 9662 1414
gensec@nswnma.asn.au
OFFICE ADDRESS 106 Victoria Street West End Qld 4101
POSTAL ADDRESS GPO Box 1289
Brisbane Qld 4001
Phone 07 3840 1444
Fax 07 3844 9387 qnmu@qnmu.org.au
OFFICE ADDRESS 182 Macquarie Street


Hobart Tas 7000
Ph: 03 6223 6777
Fax: 03 6224 0229
Direct information
1800 001 241 toll free enquiries@anmftas.org.au
OFFICE ADDRESS 260 Pier Street, Perth WA 6000
POSTAL ADDRESS PO Box 8240
Perth BC WA 6849
Ph: 08 6218 9444
Fax: 08 9218 9455
1800 199 145 (toll free) anf@anfwa.asn.au
Front cover
RN Emma Murphy

Image by Dylan Crawford
Editorial
Editor: Kathryn Anderson
Journalist: Robert Fedele
Journalist: Natalie Dragon
Production Manager: Cathy Fasciale
Level 1, 365 Queen Street, Melbourne Vic 3000 anmj@anmf.org.au
Advertising Heidi Hosking heidi@anmf.org.au
0499 310 144
Design and production
Graphic Designer: Erika Budiman instagram.com/pixels_and_paper_studio
Printing: IVE Group
Distribution: D&D Mailing Services
The Australian Nursing & Midwifery Journal is delivered free quarterly to members of ANMF Branches other than New South Wales, Queensland, Western Australia and ACT. Subscription rates are available via anmjadmin@anmf.org.au. Nurses and midwives who wish to join the ANMF should contact their state or territory branch. The statements or opinions expressed in the journal reflect the view of the authors and do not represent the official policy of the Australian Nursing & Midwifery Federation unless this is so stated. Although all accepted advertising material is expected to conform to the ANMF’s ethical standards, such acceptance does not imply endorsement. All rights reserved. Material in the Australian Nursing & Midwifery Journal is copyright and may be reprinted only by arrangement with the Australian Nursing & Midwifery Journal
Note: ANMJ is indexed in the cumulative index to nursing and allied health literature and the international nursing index ISSN 2202-7114
Online: ISSN 2207-1512
Moving state.
Transfer your ANMF membership
If you are a financial member of the ANMF, QNMU or NSWNMA, you can transfer your membership by phoning your union branch. Don’t take risks with your ANMF membership – transfer to the appropriate branch for total union cover. It is important for members to consider that nurses who do not transfer their membership are probably not covered by professional indemnity insurance.
ANMJ is printed on A2 Gloss Finesse, PEFC accredited paper. The journal is also wrapped in biowrap, a degradable wrap.
The ANMJ acknowledges the Traditional Owners and Custodians of this nation. We pay our respects to Elders past, present and emerging. We celebrate the stories, culture and traditions of Aboriginal and Torres Strait Islander Elders of all communities. We acknowledge their continuing connection to the land, water and culture, and recognise their valuable contributions to society.
REGULAR COLUMNS 1 Editorial 2 Directory 4 News Bites 6 Lori-Anne 14 Environment & Healthcare 18 ANZAC Day 20 International Days 25 Research & Policy 26 James 28 Issues 30 Innovation I 32 Innovation II 34 Professional 39 Legal 40 Wellbeing 42 Industrial 56 Healthy Eating FEATURE 8 Towards an equal Australia: Advocating for health and gender equity CLINICAL UPDATE 36 Optimising patients discharge processes to enhance patient experience GUEST EDITORIAL 44 Nurse practioners transforming healthcare FOCUS 46 Men’s/Women’s & Sexual health
8 APR–JUN 2023 VOLUME 27, NO.11 @ANMJAUSTRALIA ANMJ.ORG.AU
CONTENTS
FINAL-YEAR CLINICAL PLACEMENT HELPS RECRUIT TO AGED CARE SECTOR
A novel final-year university placement in aged care is helping nursing students transition work-ready into the sector on graduation.
One of the first in Australia, the University of the Sunshine Coast (UniSC) and aged care provider Lutheran Services have expanded a pilot final-year placement program to three aged care sites across South East Queensland. UniSC aged care specialist

Dr John Rosenberg says the ‘Transition to Practice’ program provided Bachelor of Nursing Science students with a genuine interest in careers in aged care with a final placement that incorporates hands-onlearning of clinical aspects vital to improving quality of life for elderly residents.
“The curriculum includes dementia, falls prevention, wound management and end-of-life care to prepare students for careers as
registered nurses in aged care. “It’s a great way of harnessing the passion of our up-and-coming nursing students and providing an easier pathway into such a rewarding area as aged care,” CEO of Lutheran Services Nick Ryan said.
Some of the students involved in the pilot have been employed as RNs at Lutheran Services, which operates 11 aged care sites across Queensland. Wendy Williams, one of the graduating students who secured a role with Lutheran Services, chose aged care for her final placement instead of a clinical hospital setting.
“Aged care, particularly palliative care, was a career goal when I began my studies. It requires a lot of critical thinking to put your practices and education together to work out the optimal care for residents with complex needs –and that is ultimately hugely rewarding,” she said.
Interventions needed to curb ‘high-risk’ drinking among Australian nurses
Tailored interventions are urgently needed to address growing alcohol consumption among Australian nurses, with booze levels within the profession now rivalling high-risk industries such as mining and construction, according to a new paper.
A national survey of 1,159 nurses, conducted from June to October 2021, found Australian nurses were drinking more than previously reported, with the COVID-19 pandemic emerging as a leading contributing factor.

The overall prevalence of risky drinking among Australian nurses who took part in the study, conducted in partnership with the Nursing and Midwifery Health Program Victoria (NMHPV), was 37%. More than a quarter drank at risky or hazardous levels, 5.6% at a high-risk or harmful level, and 5.3% at a high-risk, almost certainly dependent level.
SHIFT WORKERS EAT MORE AND FACE HIGHER ILLNESS RISK THAN DAY WORKERS

Rotating shift workers eat more kilojoules, snack more on junk food and consume fewer nutritious foods, increasing their risk of dietrelated illness.
A Monash University-led systematic review of dietary habit and energy intake studies found rotating shift workers ate on average 264 more kilojoules than regular day workers. An increase of just 100 kilojoules each day can lead to a 0.5 kilogram weight gain over a year.
Shift workers also reported unhealthier dietary patterns, including irregular meals, more snacking or eating at night, less core food consumption and more eating of discretionary foods.
Nurses working in Emergency Departments drank the most, followed by medical/surgical wards, ICU and mental health. Participants were also asked about upsurges in their alcohol consumption since the beginning of the COVID-19 pandemic, with almost 40% saying that their drinking had increased “a little” or “a lot”.
Given the “currently vulnerability” in the nursing workforce due to the COVID-19 pandemic, researchers argue that action is now urgently required to help reduce high-risk alcohol consumption among the workforce.
For the first time, the study found rotating shift workers may be eating more kilojoules with a large proportion at night, helping to explain why they face increased risk of chronic diseases. PhD candidate and Research Dietitian, Angela Clark, at Monash University’s SWIFt Study (Shifting weight in night shift workers), said while the disruption that shift work causes could not be changed, improving diets and eating patterns could make a difference. The study found the diets of rotational workers tended to contain less protein and carbohydrates, and more fat than day workers. Monash University, in collaboration with the University of South Australia, is trialling three weight loss strategies for night shift workers. Funded by the NHMRC, the SWIFt Study considers the complexities of circadian rhythms and meal timing on weight-loss success. The research was published in journal Advances in Nutrition
NEWS BITES 4 Apr–Jun 2023 Volume 27, No. 11
Alarming bias among healthcare students could impact future care
Healthcare students often hold negative attitudes and beliefs towards people living with obesity, which could lead to poor clinical care and outcomes, according to new Curtin University-led research.
The study, which surveyed 900 healthcare students across 39 Australian universities, found students held explicit and implicit weight-biased attitudes and beliefs, were fearful of ‘gaining weight’ and lacked confidence in clinical settings when helping patients living with obesity.
Students surveyed believed obesity was within a person’s control and that they lacked willpower, while some expressed dislike towards people living with obesity. Male students were more likely to explicitly state their bias towards these groups, and while females expressed greater empathy for these patients, they held a greater fear of ‘gaining weight’ themselves.

Lead researcher and PhD student Ravisha Jayawickrama, from the Curtin School of Population Health, said individuals around the
world who were on the receiving end of weight bias or discrimination had a 60% greater risk of mortality and were 2.5 times more likely to experience mental health disorders, such as anxiety.
“Our study found the level of weight bias exhibited in Australian healthcare students was alarming and has the potential to negatively impact the care that people living with obesity receive, contributing to poor health outcomes and quality of life,” Mr Jayawickrama said.
Researchers are calling for educators and universities to play a key role in reducing the stigma and weight bias exhibited by some healthcare students by providing greater support and skill development.
TAKE 15 MINUTES TO LEARN ABOUT A VOICE TO PARLIAMENT
Australians are being encouraged to get behind the ‘Yes’ vote in the referendum on constitutional recognition for Aboriginal and Torres Strait Islander people.
The First Nations groups campaigning for a Voice to Parliament have created educational resources, including an interactive digital learning platform, produced in partnership by From the Heart and the Uluru Dialogues, designed to help answer questions.

The content covers the key points and takes 15 minutes.
In May 2022, Prime Minister Anthony Albanese made a commitment to establish an Indigenous Voice to Parliament that is guaranteed by the Australian Constitution. This commitment represents the recognition sought in the Uluru Statement From the Heart and will involve every Australian voter in a referendum to change the constitution.
To access the course, visit: fromtheheart.com.au/education
For more information on the Yes campaign, visit: yes23.com.au
New mobile app helps patients access My Health Record
The Australian Digital Health Agency has launched a new mobile app, my health, to make it easier for Australians to instantly access key health information contained in My Health Record.
Offering users greater autonomy over their health journey, from the home screen users can quickly see medicines information history, check pathology results, view vaccination history, look over hospital discharge summaries, and share documents with others.
According to The Agency, My Health Record views increased
by 292% in the last financial year, prompting design of the app to empower consumers to take even greater ownership of their healthcare.
“One of the things we have learned from the surge in use of My Health Record is that around 75% of interactions between the system and users occurred on mobile devices,” Agency CEO Amanda Cattermole said.
“The accessibility of a consumerfacing app will further enhance the way people engage with their health and equips users with a simplified way to efficiently see, store, and share documents.”
NEWS BITES Apr–Jun 2023 Volume 27, No. 11 5
Lori-Anne Sharp ANMF Federal Assistant Secretary

Support a YES vote for a Voice to Parliament, the beginning of a fairer Australia
Later this year, our country will have the opportunity to make history by voting YES in a referendum to enshrine an Aboriginal and Torres Strait Islander Voice to Parliament.
Some in the community may ask what this means and what it will achieve. In short, it is a meaningful first step that will seek to improve the lives of Aboriginal and Torres Strait Islander peoples by changing the constitution, allowing for an Aboriginal and Torres Strait Islander permanent voice to Parliament. This will mean that Aboriginal and Torres Strait Islander Peoples will have a say on policies and issues that directly affect their lives.
Aboriginal and Torres Strait Islanders Peoples are one of the world’s oldest surviving cultures with 65,000 years of continuous connection to the land and water. Since the invasion and European settlement, there has been a long trail of failed government policies and broken promises that have had devastating and longlasting impacts on the lives of Aboriginal and Torres Strait Islander Peoples.
These policies have contributed to the enduring theft and destruction of lands, forced separation of children and families, generational trauma, high child mortality rates, inadequate compensation for labour, excessive incarceration and deaths in custody, denial of rights to language and culture, overt and casual racism and, ultimately a reduced life expectancy. At present, there is no systemic way that Aboriginal and Torres Strait Islander Peoples can have their say and provide their views on decisions and legislation directly impacting their lives. A YES vote in the upcoming referendum to enshrine an Aboriginal and Torres Strait Islander voice in our 122-year-old constitution will change that. The first element is a Voice to Parliament with treaty and truth, the next steps as defined in the Uluru Statement from the Heart.
There is no doubt that progress has been frustratingly slow for Aboriginal and Torres Strait Islander Peoples in this country. Now, with an opportunity for a positive and meaningful change, it will require the nation to unite and vote for constitutional change. This will be a crucial first step in working to close health, education and life expectancy gaps and achieving a more equitable nation.
It is important to note that the Australian constitution cannot be changed without the approval of the Australian people. Since Federation, 44 proposals for constitutional change have been put to the Australian electorate, and only eight have been successful. A referendum is run like an election in that it is a direct vote that is compulsory. A referendum is only passed if it achieves a double majority meaning it must have a majority of voters across the nation and a majority of states (at least four of the six States). Territory voters are counted in the national majority. The Australian public overwhelmingly voted YES to the 1967 referendum giving the Federal Parliament the power to make laws about Aboriginal and Torres Strait Islander Peoples, some 56 years later, it’s well time to take the next step.
Nurses, midwives, carers and the broader union movement will play a part in the success of the YES campaign. ANMF members will also be acutely aware of their professional responsibility to have culturally safe and respectful conversations, appreciating that conversation and discussion on the issue will potentially impact the mental health of Aboriginal and Torres Strait Islander communities.
I encourage all ANMF members to get behind the YES campaign, and where informed and comfortable, start the important conversations with peers, family and community to assist in educating people to understand the significance a YES vote will have on the future lives of Aboriginal and Torres Strait Islander Peoples. ANMF will be running free webinars in May and September to assist in educating members on the Voice to Parliament. Keep a look out on our social media sites for the registration details in the coming weeks.

LORI -ANNE 6 Apr–Jun 2023 Volume 27, No. 11
 Slip resistant oil/fuel liquids
Slip resistant oil/fuel liquids
@skechersaustralia /skechersaustralia SKECHERS.COM.AU
Air cooled memory foam Leather upper with mesh panelling
Towards an equal Australia: Advocating for health and gender equity
Australian nurses, midwives and carers are starting to see meaningful reforms, particularly in aged care. The Australian Nursing and Midwifery Federation is celebrating these hardfought wins after years of lobbying. On the back of this momentum, the union is forging ahead in campaigning for further advancements in aged and healthcare as well as gender equity.
NATALIE DRAGON reflects on the union’s achievements and its plans over 2023 to improve conditions and fairness for all.

8 Apr–Jun 2023
27, No. 11 FEATURE
RN Emma Murphy Credit: Dylan Crawford
Volume
Witha new government at the helm, a raft of historic changes have occurred across various landscapes, including industrial relations and the health and aged care sectors. Promisingly, there are also advances towards gender equity and a more accessible universal healthcare system in Australia.
INDUSTRIAL RELATIONS
The Albanese Government’s landmark Secure Jobs, Better Pay Bill passed Federal Parliament on 2 December 2022, giving nurses and aged care workers better access to a collective bargaining system for wage growth and increasing gender equity across workplaces.
While existing bargaining may have been successful in larger, male-dominated industries, workers in fragmented, female-dominated industries, like aged care and the primary healthcare sector, were unable to achieve any real wage growth, Ms Butler said.
“Many of our members have been ‘lockedout’ under the existing bargaining system and haven’t had a proper wage rise in years. It is a crisis that has been deepening over the last decade but has now become acute with the impacts of COVID and escalating costs of living hitting workers extremely hard, especially female workers in femaledominated industries.”
Victorian nurse Sam Read told a Senate Inquiry into the Bill, with a decline in wages, she’d had to leave several general practice settings, and community care where she worked.

“Often GPs and general practice community care business owners are unclear about
which wages and conditions to follow. This means that, for me on the ground, I’m there trying to advocate for myself on my own for a better wage to support the community that I’m working with, often in a community at risk.”
Other improvements under the new legislation include putting gender pay equity at the heart of the Fair Work Act, banning pay secrecy clauses holding back women’s wages, expanding access to flexible rostering arrangements, limiting the use of fixed-term contracts, and giving the Fair Work Commission (FWC) more powers to arbitrate industrial disputes. The federal government is expected to deliver a second tranche of workplace relations reforms this year to close the loopholes undermining job security and wage growth.
The ANMF, along with other unions and the ACTU, will continue to advocate to ensure implementation of the new laws occurs as intended and work to the benefit, and not disadvantage its members and all Australian workers.
Key focus areas the ANMF will lobby in for further industrial relations reform include creating less burdensome threshold requirements for taking protected industrial action; advocating for permanent employment and only limited use of fixedterm contracts; and keeping pressure on employers to comply with flexible working arrangement obligations rather than relying on casual work arrangements.
AGED CARE
New reforms to improve the quality of the aged care sector, many of which the ANMF had advocated for, have also been enacted.
The Aged Care Amendment (Implementing Care Reform) Bill 2022, passed in Parliament on 27 October 2022, includes the requirement of a registered nurse on duty 24/7 in all aged care homes and residents to receive a mandated minimum of 215 minutes of care time per day (including 44 minutes of care time with a registered nurse by 2024). Further, the legislation includes a new funding model for residential aged care, the introduction of star ratings, and a new Code of Conduct for staff and providers.
“While implementation of these crucial reforms will take some time and will need to be phased in over the next two years, it marks the first real step towards actually fixing the aged care sector,” Australian Nursing and Midwifery Federation (ANMF) Federal Secretary Annie Butler said.
However, Ms Butler said the ANMF will be watching how the aged care industry responds to the incoming legislative changes in aged care. Some providers have already looked at adjustments to their staffing models, including substituting enrolled nurses with personal care workers in response to the federal government’s mandated minimum care minutes in nursing homes.
“Instead of implementing the Royal Commission’s recommendations to increase care minutes for residents, they’re reducing frontline EN positions, replacing them with lower-paid personal care workers – and putting extra workloads on to already burnt-out RNs,” Ms Butler said.
Following the passing of the Bill, the Fair Work Commission handed down its decision as part of the landmark Work Value case granting a 15% pay increase in minimum wages for aged care workers on an award.
In February this year, the Commission ruled the increase would start 30 June 2023. The ANMF, which was heavily involved in the Fair Work proceedings, said the outcome represented a significant achievement, but emphasised that the increase must be passed on in full to aged care workers.

“It has given us some real hope that after a decade of neglect the industry can finally start to retain and recruit nurses and carers. But this will only be achieved if the full wage increase, as determined by the FWC and supported by the federal government, is passed on in full to all aged care workers,” said Ms Butler.
Ms Butler said the ANMF is calling on the government to ensure transparency and accountability around the new funding to ensure the full 15% pay increase goes to workers.
“Many of our members have been ‘locked-out’ under the existing bargaining system and haven’t had a proper wage rise in years. It is a crisis that has been deepening over the last decade but has now become acute with the impacts of COVID and escalating costs of living hitting workers extremely hard, especially female workers in femaledominated industries.”
ANMF Federal Secretary Annie Butler
FEATURE Apr–Jun 2023 Volume 27, No. 11 9
(left) with Victorian nurse Sam Read
Ms Butler said the ANMF was already aware of some aged care providers not only refusing to pass on the wage increase but were also threatening to cancel their Enterprise Agreements (EA) with aged care workers. Some members had also reported that some employers were rushing to lock them into new EAs offering wage increases that would not pass on the full amount of additional funding set by the Fair Work Commission to cover wage increases.
“If these providers proceed to cancel agreements, it means nurses and care workers could potentially lose a whole range of allowances and entitlements, such as penalty rates; paid parental leave (PPL); personal leave, professional development leave and qualification allowances. It’s a disgrace that yet again some providers fail to recognise the true value of their workforce. This attitude will do little to grow the workforce so desperately needed to address the aged care crisis,” Ms Butler said.
Queensland nurse Emma Murphy, who was heavily involved in campaigning for changes in aged care, said offering
competitive wages to work in the sector in the current economy should be at the forefront of recruiting and retaining staff in aged care.
“There’s such a disparity in wages between Queensland Health and aged care,” she said.
Emma, who started her career as an agency nurse in aged care, submitted to the Aged Care Royal Commission in 2019 and subsequently flew to Perth to give evidence alongside three other aged care workers. At that time she singled out the lack of staffing ratios in aged care as the main barrier to providing person-centred care.
“I’ve worked throughout various aged care facilities and I’ve seen, on a daily basis, the neglect that our residents face due to the lack of ratios.
With the passing of the Aged Care Amendment (Implementing Care Reform) Bill 2022, Emma says she is excited about what these changes will mean for residents.
“Put simply, it cannot not help to improve the sector. It will make a difference, but there’s still a long way to go in terms of
attraction and retention in aged care,” said Emma.
Emma, who has now left the aged care sector, said it took months to secure employment in a tertiary hospital.
“It speaks volumes to the perception of how the aged care experience is valued. Yet despite this, what I am often commended on is my assessment skills, which ironically, I gained in aged care.
“You can have 100 people to care for [in aged care]. It’s your responsibility to recognise the deterioration and make the decision to either call an ambulance or continue to monitor them.
“The ability to notice the deteriorating patient and quickly intervene has been particularly relevant since my transition to work in the ED which I attribute to my experience working in aged care.

The experience of campaigning for aged care has ignited Emma’s passion for the union and shaped the course of her future. She has since been elected to the Queensland Nurses and Midwives’ Union (QNMU, ANMF Qld Branch) Branch

“It has given us some real hope that after a decade of neglect the industry can finally start to retain and recruit nurses and carers. But this will only be achieved if the full wage increase, as determined by the FWC and supported by the federal government, is passed on in full to all aged care workers.”
10 Apr–Jun 2023 Volume 27, No. 11 FEATURE
RN Emma Murphy Credit: Dylan Crawford
Council, was part of a delegation that went to Canberra lobbying in Parliament and was involved in QNMU’s recent enterprise bargaining agreement (EA) in Queensland. “It’s lit a fire in me that’s not going away. My personal fight against injustice is not just in aged care but for every sector of nursing.
“I am in such a fortunate position to be able to advocate, which I’m grateful for. It can be simple as having those conversations; it’s about having a safe and supported workplace.”
GENDER INEQUITY AND LINK TO HEALTH
Supporting women’s workforce participation and advancing gender equity were prioritised in the Albanese Government’s first budget. Several provisions were made for better-paid parental leave entitlements, access to childcare, and paid family domestic violence leave.
The ANMF continues to call on the federal government for a national plan for gender equality. Australian women lag considerably behind their male counterparts in income, labour force engagement and health. At current rates, it will take 70 years for Australian women to reach full-time employment equality with men, and more than 200 years to reach income equity, according to the first Australian Women’s Health and Wellbeing Scorecard: Towards equity for women released last December.
“Women disproportionately have lower income and less engagement in the labour force, which drives poorer health, even in a high-income country like Australia,” said
report co-author, Monash Centre for Health Research and Implementation Director Professor Helena Teede.
In 2020, there was a 19-percentage point gap in full-time employment, a $23,767 annual income gap and a $44,746 superannuation gap between men and women.
“Removing the structural barriers that prevent equality is an urgent priority to prevent the declining health of women in Australia. Urgent action is required to address women’s health and wellbeing through a women-centred, evidence-based approach – focused on achieving real change for women,” Professor Teede said.
The Australian Government has established a National Women’s Health Advisory Council to address sex and gender differences in the health system and the disparate health outcomes for women and girls.

A key role for the new Council, chaired by Ged Kearney, Assistant Minister for Health and Aged Care and former ANMF Federal Secretary, will be to guide how the government delivers on the National Women’s Health Strategy 2020-2030.

“The many existing inequities in the system are only exacerbated by the extraordinary things we’ve experienced recently, like pandemics and, particularly in our regions, natural disasters like floods. From delayed diagnosis, overprescribing, dismissal of pain or other symptoms, there are unique challenges that women and girls face that lead to poorer health outcomes. Women and girls deserve tailored and targeted healthcare that recognises and reflects their experiences and concerns,” Ms Kearney said.
Figures show that menopause results in lost earnings and superannuation costs for Australian women in the billions of dollars each year. The Australian Institute of Superannuation Trustees has called on the federal government to look at how menopause affects women’s employment, retirement decisions and superannuation. While women’s average superannuation balances increased from 2001-2020, women continue to have less superannuation than men. Many women live their final years in poverty, with the next generation of women also at risk. The ANMF is pushing for super reform, including mandatory superannuation requirements on all periods of parental leave, the introduction of a benchmark on retirement adequacy that does not disadvantage women, and a fair share of super tax concessions for women. New laws have seen greater protections for women come into play. New legislation, which provides access to 10 days of paid family and domestic violence (FDV) leave, came into effect in February 2023. The legislation results from years of tireless advocacy and campaigning by the ANMF, the ACTU and the broader union movement. Statistics show that one woman is killed by a partner, former partner or a family member every 10 days in Australia.
“Nurses and midwives are too often at the coalface of the FDV crisis in this country, identifying and caring for women who are experiencing abuse and violence – and it’s why this entitlement is a significant gain for the ANMF and its members,” ANMF Federal Assistant Secretary Lori-Anne Sharp said.
Members of the National Women’s Health Advisory Council
FEATURE Apr–Jun 2023 Volume 27, No. 11 11
“Women disproportionately have lower income and less engagement in the labour force, which drives poorer health, even in a high-income country like Australia.”
NEW OPPORTUNITIES
ANMF Federal Secretary Annie Butler said the union welcomed the opportunity to work collaboratively with the federal government to ensure effective implementation of the landmark reforms and commitments of 2022.
Additional projects for 2023 include the rollout of a new national support service for Australia’s nurses and midwives. The federal government has invested $25.2 million to establish and run a national nurse and midwife health service to provide peer-to-peer counselling, case management and referrals due to years of lobbying by the ANMF.



The ANMF federal office is leading the national rollout framework in consultation with the Australian and state and territory governments, key service providers and nursing and midwifery peaks. The project team kicked off on 23 January 2023, with the new National Nurse and Midwife Health Service anticipated to be operational in early 2024.
Other promising opportunities on the horizon, include the prospect of increasing the implementation of nurse practitionerled models in aged care, Ms Butler said. The government’s Strengthening Medicare Taskforce final report released in February recommended additional funding to allow frontline nurses, midwives and allied health professionals to deliver care in primary health settings as part of a new model of multi-disciplinary care for patients. The report recommended new blended funding models integrated with the existing fee-for-service model, allowing teams of GPs, nurses, midwives and allied health professionals to work together to deliver the care people need.
Ms Butler, who sat on the Taskforce, said the Albanese government and state and territory leaders must work together and ‘not waste this historic opportunity for reform’. “Highly-qualified healthcare professionals, such as nurses, midwives, nurse practitioners (NPs) and other health professionals, who up until now, have been unable to fully work to their full capacity, expertise and skill must be central to the reform of Australia’s universal healthcare system,” Ms Butler said.
ACT Palliative Care NP Juliane Samara said outdated funding models remained one of the most significant barriers to increasing
the number of NPs in aged care. “If I went in as a private nurse practitioner, with the current MBS rebates, there’s no way I could make enough money to earn a wage in residential aged care.”
Ms Samara considers real change is possible under the current federal Labor government. “There’s so much work to do in aged care. It’s hard to know where to start, but finally we are getting some progress. I’m hopeful that it will be a continuing process and that it won’t just stop when we get a wage rise and nurses 24/7; I’m hopeful that there’ll be a continuous reform approach.”
“Highly-qualified healthcare professionals, such as nurses, midwives, nurse practitioners (NPs) and other health professionals, who up until now, have been unable to fully work to their full capacity, expertise and skill must be central to the reform of Australia’s universal healthcare system.”
Nurses meet with Ged Kearney, Assistant Minister for Health and Aged Care at Parliament House
FEATURE 12 Apr–Jun 2023 Volume 27, No. 11
ACT Palliative Care Nurse Practitioner Juliane Samara

Organised by the International Council of Nurses NURSES TOGETHER: A FORCE FOR GLOBAL HEALTH REGISTER NOW! In partnership with the Canadian Nurses Association #ICN Congress #ICN2023 @ICN urses
CREATING MOMENTUM TOWARDS A GREENER HEALTHCARE SYSTEM
By Kathryn Anderson
Health service delivery in Australia currently contributes 7% to our nation’s emissions. Fortunately, the response to climate change is increasingly being recognised as a healthcare priority across the sector.
While there is growing concern about healthcare’s carbon footprint, the havoc extreme climate events and increasing incidents of bushfires and heatwaves is having on health is also detrimentally affecting providers in managing healthcare needs.
Correspondingly, many healthcare providers are ramping up their efforts to pursue sustainable healthcare.
According to a Review of Sustainable Healthcare, developed by the Climate and Health Alliance (CAHA) and Monash Sustainable Development Institute, around a third of all Australian hospitals are now
part of the Global Green and Healthy Hospitals (GGHH) network. The GGHH network has assisted these hospitals to actively work on a range of sustainability goals areas, such as energy, waste, leadership, procurement, and others, as per their sustainable goals.1

Over 80 countries, including Australia and New Zealand joined the (GGHH) network. Australian health institutions are part of the Pacific regional network of GGHH, founded and managed by CAHA.1
ANMF Vic Branch’s Sustainability Officer

Ros Morgan welcomes this momentum and hopes it will encourage local champions to persevere, knowing they are part of a larger movement. Environmental sustainability needs to be embedded at every level of health service, Ros says, from supporting and enabling local champions, to governance accountabilities. This includes health services monitoring, measuring
and reporting emissions, with targeted improvements.
Ros says while there is a growing global movement to measure the emissions profile in healthcare, there is a lack of standardised processes and metrics for monitoring and improvement. The Review of Sustainable Healthcare states nearly half (45%) of surveyed healthcare services for their review were unsure about the implications of sustainability activities on safety and quality of care.1
Ultimately, healthcare needs re-evaluation to find better ways to implement sustainable practices. This includes reducing low-value care, unwarranted variation and a reduction of large amounts of waste to improve the safety and quality of care, equity to access and decrease healthcare’s sizable carbon footprint.1,2
Nurses and midwives are key players in leading action on climate change to protect our health. Let’s educate, support and encourage each other to achieve a sustainable future.
14 Apr–Jun 2023 Volume 27, No. 11 ENVIRONMENT & HEALTHCARE
A US study quantified solid waste and greenhouse gas emissions from inpatient stays at a large US hospital. The results showed that a regular inpatient acute care unit generates 5.5kg of solid waste and 45kg CO2-e per hospitalisation day. The ICU generated 7.1kg of solid waste and 138kg CO2-e per bed day.
Over one year, an estimated 656,000kg of CO2-e and 80,000kg of solid waste were generated from acute care. An estimated 349,000kg of CO2-e and 18,100kg of solid waste each year from intensive care. This is equivalent to the GHG emissions from 139 passenger vehicles and 74 vehicles driven for one year, respectively.
The study suggested that most emissions originated from the purchase of consumable goods, building energy consumption, purchase of capital equipment, food services, and staff travel.2 Within this list there are things that we can influence says Ros.
There are lots of moving parts in this jigsaw, Ros argues. For example, currently, preventive health is allocated less than 2% of Commonwealth, state and territory health expenditures. There are now calls to increase that amount to 5%.2
Yet, Ros believes this sum is still inadequate, considering preventative health’s many benefits.
Education, early recognition and trained intervention can often mean both complications and admission are avoided, Ros observes.
“An avoidable admission is an avoidable emission. It’s ethical, it’s compassionate, and it’s attainable.”
Resourcing sectors such as aged care and mental health adequately, will also reduce
unnecessary admissions, resulting in improved quality and safety of care and lessen healthcare’s carbon footprint, Ros suggests. “For example, it could be argued that even ANMF’s Aged Care Campaign has sustainability implications,” she says. “If [the residents] were getting the care they needed because they had adequate staff numbers, then they wouldn’t need escalating to a hospital admission. They would have early assessment and intervention in place, delivered by trained staff. It’s a win for everyone as well as our emissions profile.”
GOVERNMENT LEADERSHIP IN SUSTAINABILITY

Sustainable healthcare policies and programs now exist in most states and territories, including the creation of sustainable units. Yet many are in the early stages of implementation and not incorporated at the level of individual service.1
Nevertheless, state and territory governments have committed to achieving net zero emissions for the public health sector. The ACT Government has committed to zero emissions by 2040, and the NSW Government by 2050, and halve emissions by 2030. The NT has an emissions reduction target of net zero by 2050, while the WA government recently announced 2030 emission reduction targets of 80% below 2020 levels.
Currently there are no policies that support sustainable healthcare at the Commonwealth level. However, the Albanese Government has recognised the need for leadership in this area and has committed $3.4 million in its 2022-23 Federal Budget to fund Australia’s first National Health and Climate Strategy and a National
Health Sustainability and Climate Unit to better prepare the health system for the challenges of climate change.
“As well as adapting to the new challenges of climate-related health issues, it’s important that our health system is included as part of the climate solution by reducing its own carbon footprint,” Assistant Minister for Health and Aged Care Ged Kearney MP said when speaking about the strategy.
Other relevant activities include the Australian Health Protection Principal Committee (AHPPC), which has identified climate change as a health protection priority. There is also the Healthy Environments and Lives (HEAL) research network funded by the National Health and Medical Research Council to strengthen the Australian health system’s resilience, preparedness, and responsiveness to climate change.1
Recognising that improving sustainability can improve the safety and quality of care, the Australian Commission on Safety and Quality in Health Care has drafted a Sustainable Healthcare Module for healthcare providers.

The ANMF Vic Branch suggests the module would ensure health services consider their vulnerability to climate change and how they contribute. It would provide a recognised framework for the many sustainability activities nurses, and midwives undertake, embedding them into a safety and quality in health service delivery. The module, developed with the guidance of a Sustainable Environment Advisory Group of industry experts will be for health service organisations. It is anticipated that the module will be voluntary and can be assessed as part of the organisation’s routine accreditation.
The module has undergone recent public consultation, and a revised draft module is currently being reviewed by the Commission’s Sustainable Healthcare Advisory Committee.
References
1. Wyns A, Bragge P, Armstrong F, Carino, S, Dolker D, Lennox A, Tsering D, A review of sustainable healthcare policy, practice, and research with a focus on safety and quality. Monash Sustainable Development Evidence Review Service, BehaviourWorks Australia, Monash University, and Climate and Health Alliance, Melbourne, June 2022. Accessed Feb 2023 safetyandquality.gov.au/publications-and-resources/ resource-library/review-sustainable-healthcare
2. PHAA Pre-Budget submission for the 2022-23 Commonwealth Budget. Accessed Feb 2023 treasury.gov.au/sites/default/ files/2022-03/258735_public_health_association_of_ australia.pdf
3. Prasad PA, Joshi D, Lighter J. et al. Environmental footprint of regular and intensive inpatient care in a large US hospital. Int J Life Cycle Assess 27, 38–49 (2022). doi.org/10.1007/s11367-02101998-8 Accessed Feb 2023
ENVIRONMENT & HEALTHCARE Apr–Jun 2023 Volume 27, No. 11 15
Healthcare sustainability tips and hints


The ANMJ was asked:
“Many nurses are embarrassed by the amount of waste they generate at work but locating the correct bin, pulling apart items to sort components is not easy in an acute environment. Any knowledge of processes and resources that would make the process simple and effective would be greatly appreciated.”

We reached out to nurses and midwives for their suggestions.
Sustainability tips or questions

We don’t need to reinvent the wheel to find ways to reduce our impact on the planet.
Ask a question or share your sustainable practices at work and at home with the ANMJ so nurses and midwives nation-wide can do their bit to save the planet. Together we will make a difference. One lucky contributor will also receive a $50 e-voucher from Koala Eco. Email ANMJ with your tip or question at:
ClimateActionForHealth@ anmf.org.au
“I would say that time poor nurses need the hospitals to help. Hospitals need to make it just as easy to recycle as it is to throw things in landfill bins. Set up recycling stations with very clear signage, educate on induction and regularly throughout the year and hospital recognition of departments doing well from audit results.”
Jacqui Dunn
“Easy to view pictures of what is accepted in each bin. Helps take the stress out of remembering what waste is accepted in which bin. Have separate bins in shared areas. Educate ALL staff, nurses, cleaners, doctors, allied health on waste streams and sustainability projects.”
Marj Garcia
“Make it easy as possible for many people to participate by having good systems in place thus saving everyone’s time.”
Linda Cunningham
“I am time poor being a full time clinician but I have just persevered. I think the key to success is just that constant ongoing attempt to create change and engage people in that change process through knowledge and information transfer and also education. It’s a hard task but it’s something I am very grateful that I persisted with. Don’t let someone tell you that it can’t be done. Work on how to work around those problems even if that’s a different – way of approaching things.”
Darren Bradbrook
More resources to help make sustainability easier can be found at: anmfvic.asn.au/healthenvironmental sustainability
Do you live in Victoria and want to learn new ways to reduce waste, promote sustainability and improve your community?
Join a growing movement of health professionals who are changing the way we deliver health and striving to improve our work, home and wider environments at the ANMF Vic Branch Health and Environmental Sustainability conference on Thursday 27 April 2023.
TO REGISTER VISIT: anmfvic.asn.au/events-and-conferences/2023/04/27/ health-and-environmental-sustainability-conference

ENVIRONMENT & HEALTHCARE 16 Apr–Jun 2023 Volume 27, No. 11
Sustainability in health champion
Anaesthetic nurse Darren Bradbrook has been on a sustainability crusade to reduce hospital waste at one of Adelaide’s largest hospitals.

Through his efforts he has single handily forged a path with contractors within the public health sector in South Australia to divert hospital waste from land fill.
Initially, Darren set up recycling streams for PVC, low and high grade plastics, cardboard, paper and later aluminium, at the 593 bed major public tertiary hospital, resulting in a 60-70% diversion of its operating room waste from landfill.
“Flinders [Medical Centre] was the first hospital in South Australia to pick up any of these initiatives.”
Darren says since then there has been significant progress in reducing landfill.
“Our contractors are now able to receive more diverse range of product.

“We have now amalgamated low grade plastics to a dry material stream which has enabled our processes to be more streamlined. It enables our processes to have more capability for land fill diversion which really has given people a bit more encouragement with regards to feeling like they are contributing to a cause that started off so strong but has now been endorsed by so many more people at the other end of the supply chain.”
Through his efforts Darren is now well known and recognised in hospital waste reduction in South Australia and interstate. He is also influential with hospital management, attending strategic
meetings to help better improve service delivery in the hospital.
“I really get listened to and I’ve got the Director of Nursing at Flinders very much on board [to continue working towards sustainability].”
Darren says the hospital has been working hard towards some big infrastructure changes in regards to business plans. These include compactors on site which primarily deals with bi-product, where previously waste was trucked off the grounds. This has resulted in improved safety, storage and processes.
An initiative Darren is working on at the moment is the development of an intranet page- focussing on all things sustainable.
“This is a very large piece of work but it’s been well received and is very much supported by the executive body of the hospital. That will hopefully give our local staff and people who have access to that intranet an opportunity to look at what we are doing, what we are planning on doing and what targets we are aiming for.”
The site also intends to encourage people to get involved in recycling processes. “We hope that when we have this intranet formed it will snowball into the other health networks in our state.”

Each issue we will be highlighting a sustainability in health champion. To nominate yourself or someone else, contact the ANMJ at ClimateActionForHealth @anmf.org.au
Signs and prompts can help colleagues remember to follow organisational ‘norms’ or expectation that support positive sustainable behaviour. The Planet Ark Business Recycling website suggests tips that can make signs as effective as possible:
MAKE IT NOTICEABLE:
Make it stand out with bright colours or an eye-catching image. Once a sign has been in the same place for a few weeks people stop noticing it so changing the colour or moving it around a bit will ensure people keep on noticing it.

MAKE IT SELF-EXPLANATORY:
If you want people to switch off the lights when they leave a room, make sure that’s exactly what the sign says. Something like “Please switch off the lights when you leave the room,” is more likely to be effective than one like “Save the planet, turn me off.”
PUT IT AS CLOSE TO THE ACTION AS POSSIBLE:
If you want people to use the correct recycling bin, put the sign on the lid of the bin, or just above it. You can create an association between the desirable action and the location where it happens.
MAKE IT POSITIVE:
“Don’t” isn’t a nice word and most people become resentful being told not to do something. So whenever possible, make your signs positive. Words like “Thanks for turning your computers off at night,” is much more likely to be effective than ‘Don’t leave your computers on overnight.” And because it’s a nicer message and makes people feel good about the actions they have undertaken, it increases the likelihood that the actions will be carried out in the future.
For more information go to: businessrecycling. com.au/research/ right-signs.cfm
Darren Bradbrook
ENVIRONMENT & HEALTHCARE Apr–Jun 2023 Volume 27, No. 11 17
I saw the sign!
Nursing war hero Vivian Bullwinkel’s legacy burns brightly



 By Chloe Horrabin
By Chloe Horrabin
AN
18 Apr–Jun 2023 Volume 27, No. 11
z AC DAY
While Nurse Vivian Bullwinkel is remembered for her heroic actions during WWII, it was her ongoing leadership and service to others including preserving the memory of fallen nurses that is now her legacy.
In February 1942, Vivian was amongst 65 Australian Army Nurses, wounded servicemen and civilians on the Australian navy ship SS Vyner following a Japanese onslaught in Singapore. Despite their escape the ship was bombed by Japanese aircraft and was sunk. Some survivors of the sinking ship managed to reach Bangka Island, east of Sumatra, in the Dutch East Indies, including 22 of the nurses. However, Japanese forces also occupied Bangka Island and captured those who made it to shore. Held on the beach, the Japanese soldiers gathered the surviving servicemen and brutally executed most of them. Any survivors were placed in prisoner-of-war camps on the island.
The Japanese soldiers then proceeded to rape the 22 nurses and marched them into the water at Banka beach. Knowing the soldiers’ intentions, Matron Irene Drummond shouted to her sisters, “Chin up girls! I’m proud of you all, and I love you!”
The women were ‘thigh deep’ in the water when massacred. All of the nurses perished, bar Vivian who survived after being shot in the hip and feigning her death. After spending 12 days hiding, she surrendered and was imprisoned in a Japanese camp. Under barbaric conditions she spent the next three years in captivity and was liberated at the end of WWII, where she returned to Australia in 1945.
Vivian bravely testified before the Tokyo War Crimes Tribunal in 1947, describing the horrors she witnessed. She likened the day to a scene from a movie, stating, “When we were thigh deep in the surf, they opened up a murderous fire, mowing us down like a scene I saw in a film as a child. The women around me shrieked, stiffened, and sank. I was hit here, in the left side, under the ribs, falling unconscious in the water.”
Back in Australia, Vivian and fellow veteran nurse Betty Jeffrey were inspired to open a centre where veteran nurses could congregate and, most importantly, preserve the memory of fallen Australian Veteran nurses.
With the support of their colleagues, Vivian and Betty visited every hospital in
Victoria to explain their vision of their ‘living memorial’.
The nurses fundraised to achieve their goal, and in March 1949, the Australian Nurses Memorial Centre (ANMC) was opened.
ANMC Historian and Past President Arlene Bennett said the centre’s current goals are two-pronged.
“One is that we remember what happened to the nurses, and we commemorate that at our ANZAC day service,” she said. “The other prong is the scholarships which is a very important part of keeping the story alive.”
On top of being a living memorial, ANMC awards scholarships to nurses and hosts lectures to continue the professional development of nurses through education.
The ANMC is one of the largest nursing scholarship contributors in Australia.

After successfully setting up ANMC, Vivian returned to nursing. In 1959 she became the Director of Nursing at Fairfield Infectious Diseases Hospital in Victoria.
During this time, Vivian was involved in many nursing-related ventures that included the positions of President of the College of Nursing Australia and member of Council for the Australian War Memorial.
During her tenure at the Fairfield Infectious Diseases Hospital, Vivian was known for her “… compassion and the deep concern she had for everyone,” as described by Dr Olga Kanitsaki AM, who was a colleague at the Fairfield Infectious Diseases Hospital.
“She kept an eye on you … she wanted the staff to be healthy,” she said.
Vivian was also known for treating her staff with the utmost respect, which was rare amongst most hospital matrons at the time. Dr Kanitsaki reiterated, “She was an extraordinary woman, really.”
After the withdrawal of forces signalling the end of the Vietnamese war in 1975, Vivian volunteered to join a mission to move orphaned children out of Saigon to Melbourne. Out of the many nurses that applied, Vivian was chosen for her tenure and experience with infectious diseases and medivac nursing. Vivian, who was instrumental in the mission, was fondly nicknamed ‘Operation Babylift’.
In September 1977, Vivian married Colonel Francis (Frank) Statham and moved to
Perth. Post-war, Vivian continued to be a consistent and powerful voice within the veteran community, including attending ANZAC Day parades. Vivian was awarded an Order of Australia Decoration, the Florence Nightingale Medal, the Royal Red Cross Medal, and a Member of the British Empire for her bravery in the war and her post-war services to Australia.
In 1993, Vivian bravely and triumphantly returned to Bangka Island to erect a memorial for her fallen sisters and those prisoners of war in Bangka Island camps. In 2000, Vivian passed away peacefully from natural causes.
Vivian’s memory is commemorated in the Australian War Memorial with a portrait of her with her Florence Nightingale Medal displayed proudly.
Since her passing, Vivian has been remembered with many memorials. The Australian War Memorial in Canberra recently announced the erection of a statue in her memory.
“Sister Bullwinkel’s harrowing story of dedication, compassion, survival, and bravery will be commemorated in bronze at the Australian War Memorial … Vivian Bullwinkel should be a household name,” War Memorial Director Matt Anderson declared.
“The Memorial will commemorate this inspirational Australian and her legacy as a proud nurse and a brave leader.”
The bronze statue will feature a life-sized portrait of Vivian in a standing pose in her summer uniform with her hands gently clasped. The sculpture will also include a series of discs representing the women killed in the Banka Island massacre. The discs will be arranged at the base of the sculpture as a reflection of the stars that would have been visible in the night sky on 16 February 1942.
Vivian Bullwinkel’s legacy shines brightly upon the landscape of nursing in Australia. She will never be forgotten.
Memberships at ANMC provide funding to update the centre and its facilities while furthering the education of nurses. For more information, go to: australiannursesmemorialcentre.org.au
LEFT: Sister (Sr) Vivian Bullwinkel and former prisoners.
AN z AC DAY Apr–Jun 2023 Volume 27, No. 11 19
RIGHT: Vivian Bullwinkel (front) at the party held for the closing of the Fairfield Hospital. Both pictures courtesy of the Australian War Memorial
Celebrating International Nurses Day and International Day of the Midwife
By Robert Fedele
Each year, the International Council of Nurses (ICN) and the International Confederation of Midwives (ICM) lead global celebrations for International Nurses Day (12 May) and International Day of the Midwife (5 May).
ICN’s theme for IND 2023 is: Our Nurses. Our Future, with ICN looking ahead to the future in order to address global health challenges and improve health for all.
Meanwhile, this year’s IDM theme is ‘Together again: from evidence to reality’, with ICM acknowledging its upcoming 33RD

ICM Triennial Congress, where the global midwife community will come together for the first time in more than five years. The theme also honours the efforts of midwives and professional associations to action critical evidence such as the State of the World’s Midwifery (SoWMy) 2021 report,
which can lead towards meaningful change for the profession and women and families. To celebrate the International Days, the ANMJ shines the spotlight on inspirational nurses and midwives making a difference across the country.
INTERNATIONAL DAYS 20 Apr–Jun 2023 Volume 27, No. 11
NURSES
LYNETTE BYERS
For over two decades, Lynette Byers has worked across remote Aboriginal communities in central Australia as a Nurse Practitioner, remote area nurse (RAN) and registered midwife, to improve health.
“It’s the broadest scope of practice that you’ll ever have,” says Lynette.

“I look after patients from birth. I look after babies that are born unexpectedly, right through to palliative care patients that are dying. You have to look after people across the lifespan and be creative and innovative.”
Nganampa Health Council runs six clinics, all on remote Aboriginal land. Lynette travels from clinic to clinic as needed, the closest a four-hour drive. In this unique role, limited supplies and medicines, and the often-unpredictable weather, pose a constant challenge.
“This is the sickest population in Australia, the remote Aboriginal population, and they are entitled to the best care we can give. Therefore, we want really good health workers working out here; we want nurses, Aboriginal health workers, and doctors at the top of the tree.”

For Lynette, recipient of the 2022 Aurora Award as CRANAplus’ Remote and Isolated Health Professional of the Year, the ongoing challenge continues to drive her work and advocacy to improve remote healthcare.
Her advice to the future generation of nurses and midwives looking to work out bush is to hone up on their history taking and physical assessment skills.
“It’s not all about emergencies. The bulk of our work is really about being able to take a good history and examination to work out what is wrong with the person and what they need.”
PETER JENKIN Specialist Palliative Care Nurse Practitioner

Peter Jenkin was the first Specialist Palliative Care Nurse Practitioner employed by an aged care provider, Resthaven, in Australia. His role aimed to improve or maintain the quality of life of residents through the prevention and relief of suffering using an innovative model of care. Underpinning it was appropriate advanced care planning, improved processes for end-of-life care, and recognising the signs of early deterioration.
“We were able to demonstrate that the quality of end-oflife care from the perspective of families and residents was overwhelmingly positive. Importantly, the symptom management reduced presentations to hospital and emergency departments in the last weeks and months of life.”
Peter, who recently moved to the ACT to work in a similar role across Calvary’s residential aged care facilities, has been involved in clinical, research and education roles within palliative care for more than 25 years. He suggests his advanced scope as an NP has allowed him to make a real difference in aged care by providing timely access to healthcare for residents, along with mentoring staff.
“I always try and emphasise the fact that I’m a nurse, I’m a specialist nurse who has some added skills; I’m not a mini doctor.
Clinical Nurse Consultant with Nganampa Health Council in the APY Lands, SA
“This is the sickest population in Australia, the remote Aboriginal population, and they are entitled to the best care we can give. Therefore, we want really good health workers working out here; we want nurses, Aboriginal health workers, and doctors at the top of the tree.”
“I always try and emphasise the fact that I’m a nurse, I’m a specialist nurse who has some added skills; I’m not a mini doctor. I bring my knowledge and expertise and the art of nursing to what I do first.”
INTERNATIONAL DAYS Apr–Jun 2023 Volume 27, No. 11 21
Lynette Byers ( left)
I bring my knowledge and expertise and the art of nursing to what I do first,” says Peter.
“This is intimate work, it’s physically hard work, and it’s psychologically and emotionally difficult but also very rewarding. You need skills to engage with people at their most vulnerable times and the education around aged care and palliative care is still substandard.”
On top of his work with Resthaven, Peter has been instrumental during the COVID-19 pandemic, where he was an active member of the National COVID-19 Clinical Evidence Taskforce: Care of Older People and Palliative Care expert panel. He was responsible for two national webinars early in the pandemic, giving practical advice for aged and palliative care frontline staff to plan for the potentially devastating effects of COVID-19 in residential and community settings.
“It is incredibly rewarding work. I’ve never felt depressed from it. I have on many occasions felt terribly sad, and that’s ok. We’re all going to die, it’s going to happen for everyone and I think the more we can talk about death and dying the less scary it becomes.”
Back then, in 2007, information, resources and support for health and environmental sustainability was limited. Yet, as she became more conscious of the links between healthcare and the environment, Roslyn began making gradual changes on her ward, like waste recycling.
Her sustainability and activism eventually led to taking up her current role as Environmental Health Officer with the ANMF (Vic Branch).
More than a decade ago, at the 2012 Delegates’ Conference, members passed a resolution calling on their union to become more involved in environmental sustainability and climate change action.
The branch acted swiftly, implementing a host of initiatives in under a year. They included establishing an Environment Committee and joining Global Green and Healthy Hospitals, an international network of hospitals, healthcare facilities, systems and organisations dedicated to reducing their environmental footprint.
By 2013, the first ANMF (Vic Branch) Health and Environmental Sustainability Conference was held.
“I looked around that room and there were 150 people and I went, ‘I’m not alone’.”
Environmental Health Officer, ANMF (Victorian Branch)
Roslyn Morgan’s awareness and passion for creating opportunities for sustainable healthcare practices traces back to working as a nurse on the ICU ward.
“We recycle at home, we should recycle at work. What can we recycle at work?” she recalls thinking.

“That was the platform from which my awareness and engagement grew.”

As the branch’s Environmental Health Officer, Roslyn leads a variety of internal and external projects geared towards improving sustainability in healthcare.
For members, her work includes building an ever-growing suite of supportive resources and opportunities to help them take action in the workplace via a one-stop-shop that sits on the ANMF (Vic Branch) website. These include a Green nurses and midwives Facebook group to share ideas and connect health professionals passionate about sustainability in healthcare; online CPD that teaches members how to start a Green Team in their workplace; and Nursing for the Environment – Intensive, a practical course designed to strengthen advocacy and leadership around climate mitigation and environmentally sustainable workplace practice.
Collectively, Roslyn says the aim is to provide support, resources and education to drive cultural change and make environmental sustainability part of “business as usual” in the workplace. “We give them a platform and applaud their work and that gives other members ideas of what they can take back to their workplaces. It’s part of that cultural shift and a better way of doing things where you can still deliver the same quality of care but with that lower emissions profile.”
ROSLYN MORGAN
INTERNATIONAL DAYS 22 Apr–Jun 2023 Volume 27, No. 11
“I looked around that room and there were 150 people and I went, ‘I’m not alone’.”
MIDWIVES
MELANIE BRIGGS
Senior Midwife at Waminda South Coast Aboriginal Women’s Health and Welfare Corporation and manager of the Minga Gudjaga Birthing on Country program
A descendant of the Dharawal and Gumbaynggirr people, midwife Melanie Briggs runs the Minga Gudjaga (Mother and Baby) child and maternal health program and Birthing on Country at Waminda. The first endorsed Aboriginal midwife in NSW and a BOC advocate, she developed the first Aboriginal-led maternity model of care in Australia.
As an early career midwife, she began working in the community with Aboriginal families.
“I wanted better outcomes for our mothers and babies and you achieve that by providing good quality services that the women will access and want to access,” Melanie recalls.
Aboriginal-led and community controlled, Melanie is the heart of the maternity services offered by Waminda. Birthing on Country is a continuation of thousands of years of knowledge and practice, which provides holistic maternal, child and family healthcare that embeds cultural integrity and safety during pregnancy, labour, birth and postnatal care.
Last October, the federal budget granted Waminda funding to undertake a landmark project to build Australia’s first Indigenous Birthing on Country centre in Nowra.

“It’s not only maternity, it’s everything that encompasses the woman and that baby in the first 1,000 days of life,” says Melanie.
“It’s pre-conception, pregnancy and up to school age. It’s everything to make sure that that woman has the best possible health before she even becomes pregnant and then when she is pregnant receives the best quality care by a known midwife in community. That then sets that baby up for a long, healthy, thriving life. Born into a wealth of health.”
“It connects you to the land. It’s about power and strength. It’s also about incorporating language and practices. What that does is it sets up not only that baby for connection to country but connection to mother and family. It’s so important for our people.”
PAULA WELLS Clinical Midwife, King Edward Memorial Hospital, WA

In 2016, Paula Wells helped establish a hospital- based Midwifery Group Practice (MGP) model at the King Edward Memorial Hospital in Western Australia.
A Clinical Midwife and MGP Team Leader, Paula has a full-time caseload of 40 women per year and provides antenatal, intrapartum and postnatal care.
Her greatest passion is Midwifery Continuity of Care (CoC), where midwives play a central and reassuring role throughout the journey. “Women are allocated a primary midwife and get to know that midwife throughout their pregnancy. The midwife is on call for the labour and birth and then follows up with postnatal care when they go home,” explains Paula.
While midwives remain on call, they cannot be available 24/7, which is where the unique group model steps in.
“It’s a small group of midwives that work together. On the days that I’m not working, I have a backup midwife. My client would have met my backup midwife and other midwives within the team, so if they do labour and birth when I’m on a day off or if something comes up; it’s still quite often with a midwife they’ve met before.”
According to Paula, women with access to the model have a 70–80% chance of having a familiar face with them for their labour and birth experience. Benefits include increased satisfaction with pregnancy care, higher vaginal birth rates, and lower complications throughout pregnancy.
Melanie says the Birthing on Country model embedded within Waminda’s broader model of care is helping improve maternal, infant and child health, and empowering Indigenous women to have more control over the birth of their babies.
In her leadership role, Paula also provides support to early career midwives undergoing their graduate program, and new staff who join the team. She describes the dual nature of the workload, led by caring for women and families throughout their journey, as incredibly rewarding.
Named the 2022 Australian College of Midwives (ACM) Midwife of the Year for her commitment and passion for the profession, Paula remains a strong advocate for wider access to Midwifery Group Practice so that all women have the opportunity to receive continuity of care, especially those with risk factors.
“I wanted better outcomes for our mothers and babies and you achieve that by providing good quality services that the women will access and want to access.”
INTERNATIONAL DAYS Apr–Jun 2023 Volume 27, No. 11 23
Paula Wells (right)
Melanie Briggs (right)
PROFESSOR
Co-Program Director Maternal, Child and Adolescent Health, Burnet Institute, and Chair of the Council of the National Health and Medical Research Council (NHMRC)
One of the world’s leading midwifery researchers, Professor Caroline Homer has more than 30 years of experience as a clinician, educator, researcher and leader.

At the Burnet Institute, her role focuses on improving the quality of midwifery care and health outcomes for women and babies.
Last October, she received a NHMRC Investigator Grant to carry out a five-year project aiming to reduce maternal and newborn deaths and stillbirths by strengthening midwifery in the Asia-Pacific region by supporting improved education, regulation and leadership. Key countries will include Papua New Guinea, Cambodia and Pakistan.
“In Australia and across the world, we talk a lot about the need to strengthen midwifery leadership,” Professor Homer explains.
“But what is that, and how would you do it? And what would a strengthened midwifery leader look like, and what could they do?”
The other big aim of the Investigator Grant is developing an investment case for why countries should invest in midwives.
“All the global documents say invest in midwives,” Professor Homer says.
“But if I’m a Ministry of Health in a country and I’ve got $10 million, what’s the best bang for my buck to improve maternal health? How much should I put into midwifery and midwives, and how much should I put into something else? If we don’t know that, we can’t help governments make those sorts of policy decisions; what do you need to spend to actually strengthen midwifery?”
Professor Homer’s work reflects the global strategy for maternal, child and adolescent health –survive, thrive and transform.
“I’m really interested in mothers and babies surviving, so less stillbirths, less neonatal deaths, less maternal deaths. I’m interested in thriving; it’s not good enough to just survive childbirth, you actually have to do well. We want healthy mothers, thriving midwifery communities, as well as strong midwives that can transform the capacity of women and communities.”
Closer to home, Professor Homer considers the state of midwifery in Australia an “exciting space” with strong recognition of the value of midwives and the need to support education and regulation. Yet, challenges remain, including strengthening the role and flexibility of midwives to provide continuity of midwifery care.
“The two to three years of COVID-19 have put a big strain on the sector. Midwives are tired and they’re burnt out in many settings and they don’t feel as valued as they should be so we really need to spend the next few years rebuilding, refocusing and re-energising the sector.”
Professor Homer’s advice to early career midwives and nurses looking to pivot into research is to be brave, jump in, and importantly, find good mentors. “Find good people who back you along the way,” she says.
“My other piece of advice is don’t give up the clinical. I only stopped working clinically three or four years ago. Doing clinical, even a tiny bit all the time, is really important because it enables you to see the real world and always keeps your feet on the ground to what the reality is.”
 CAROLINE HOMER
CAROLINE HOMER
We want healthy mothers, thriving midwifery communities, as well as strong midwives that can transform the capacity of women and communities.”
INTERNATIONAL DAYS 24 Apr–Jun 2023 Volume 27, No. 11
References
1. Nursing and Midwifery Board of Australia (NMBA). Nursing and Midwifery Board of Australia registrant data reporting period: 1 January 2022 to 31 March 2022. Online: NMBA. 2022. Available: nursingmidwifery.gov.au/ About/Statistics.aspx
2. Nursing and Midwifery Board of Australia (NMBA). Nurse and Midwife registrant data: December 2012. Online: NBA. 2013. Available: nursingmidwiferyboard. gov.au/About/Statistics.aspx
The importance of enrolled nurses in Australian healthcare
Australia, like many nations, faces current and future nursing shortages. These shortages have been exacerbated by the pandemic and ongoing pressure in aged care, however signs of the impending shortfall have precedent.
While nurses represent the largest group of healthcare professionals in Australia, some sectors will be disproportionally challenged to ensure a suitably sized and skilled future workforce including aged care, mental health, disability care, and primary health. The risk of shortages are particularly serious in regional and remote areas and areas of socioeconomic disadvantage. While nursing workforce shortages include (registered nurses) RNs and (enrolled nurses) ENs, the role and contribution of ENs to the operation of the health and associated sectors is often overlooked.
With an ageing population more people have complex care needs including chronic disease, mental health, and disability. Infectious diseases and climate change also influence healthcare demand. The workforce needs the right number of staff with the right education and skills to care for a diverse population with a range of clinical needs and preferences. While ENs and RNs have quite different scopes of practice, roles, and functions, there can be confusion regarding these differences. ENs work with RNs and other staff in roles where they can be delegated to provide both clinical and non-clinical tasks. ENs use their skills to interpret information and provide skilled, timely nursing care that promote patients’ independence and decision–making. ENs are responsible and accountable for their own practice but must work under direct or indirect supervision of RNs.
Ensuring articulation between different workforce groups is critical to a sufficiently sized and skilled workforce. Ways for assistants in nursing and care workers to upskill and be educated as ENs is an important step. Likewise, ensuring that ENs can, if desired, become RNs is also important for career progression and linked to workforce attraction and retention. Endeavours to support ENs must also focus on education. While RN education largely left the hospital and is now delivered in the university sector, ENs are chiefly educated in the Vocational Education and Training (VET) sector.
There are suggestions to enhance compatibility and articulation between EN and RN qualifications including educating ENs in universities via an Associate Degree, however concerns exist that this might have detrimental impacts on the diversity and sustainability of the workforce, particularly in regional areas.

Without the right number and skills mix of nurses, care can be delayed, rushed, or missed especially overnight when staffing levels and skills mix are lowest. This is a common problem in Australian nursing homes where staff shortages are prevalent. Unregulated workers rely on both RNs and ENs to provide guidance, support, and clinical care. Without ENs, many tasks and activities that cannot be safely or legally done by assistants in nursing and care workers. Despite the contribution of ENs, their numbers are unlikely to be sufficiently increasing, especially compared to growing numbers of assistants in nursing and care workers.
Assistants in nursing and care workers are also tremendously important to Australia’s health and wellbeing, however as an unregulated workforce with very different education and training pathways and requirements, they are not substitutable for ENs.
Recent figures from the Nursing and Midwifery Board of Australia report 74,969 ENs with general registration (about 16% of the total nursing workforce) not including nurses registered as both an EN and an RN and non-practicing and provisionally registered ENs.1 This is 15,861 higher than 2012 figures.2 Workforce de-professionalisation replaces more highly educated, regulated health professionals with staff who are less highly educated in healthcare, cheaper to employ, and not accountable regulatory standards and oversight. To dwell briefly on the aged care sector, where around 13% of ENs work, the Royal Commission into Aged Care Quality and Safety heard that by 2050, the provision of best-practice nursing home care will require another 13,250 ENs and as noted above, the EN role represents an important step in career pathways for assistants in nursing and care workers, which is related to ensuring better workforce recruitment and retention rates.
The ANMF is stalwart in its support of ENs and is active in advocating for greater official recognition of their roles and ensuring that their work and the profession is sustained and valued in the future. While specific research regarding the contribution of ENs is urgently needed, the Australian health workforce needs ENs, and the ANMF will be tireless in its work with Governments, education providers, employers, and other stakeholders to ensure ENs continue to occupy respected, well-rewarded roles in every setting.
Dr Micah DJ Peters
INTERNATIONAL DAYS Apr–Jun 2023 Volume 27, No. 11 25
Dr Micah DJ Peters is the Director of the ANMF National Policy Research Unit (Federal Office) and Senior Research Fellow in the Rosemary Bryant AO Research Centre, UniSA Clinical & Health Sciences, University of South Australia
James Lloyd ANMF Vice President

Assisted dying: Ethical considerations
Voluntary assisted dying (VAD) in Australia is a controversial topic that has been widely debated in recent years. At its core, the issue revolves around whether individuals should have the right to end their own lives if suffering from a terminal illness that causes significant pain and suffering.
~ Martin Luther
In all jurisdictions within Australia, VAD can be considered only if the individual will die within 6–12 months. Some nurses accept that VAD fits ethically within the patient-centred nursing care model, whereas others believe it conflicts with the ‘Do no harm’ ethos of our profession. Nurses, midwives, and carers are central to the discussion and implementation of VAD in Australia.
VAD has been legislated in all Australian states; currently, it is available in Victoria, Western Australia, Tasmania, South Australia, and Queensland. In New South Wales, laws for VAD will begin late 2023. In the ACT and the Northern Territory, the Restoring Territory Rights Bill 2022 will now allow those territories to pass VAD legislation in their respective parliaments. Other than Switzerland, the Northern Territory was the first government in the world to introduce a legal VAD scheme in 1995, but it was soon overruled by the then current federal Liberal/National coalition under pre-existing federal and territory laws. VAD is termed assisted suicide or euthanasia in other countries. Consequently, how their laws are applied and who is eligible varies.
VAD in Australia is a well-defined process involving numerous steps. It can only be considered if the individual is over 18 years old, has a terminal illness, likely to die within 12 months (or six months for neurological conditions) and has the capacity to make that decision. Most state legislations on VAD are very similar: to see the VAD laws in your state go to –tinyurl.com/VADAUST
Opponents of VAD argue that it is morally and ethically wrong to take a human life, regardless of the circumstances. They argue that there is a danger of abuse and coercion, particularly for vulnerable individuals who may feel pressured to end their lives to alleviate the burden on their loved ones. Additionally, opponents argue that there is a risk of medical professionals becoming desensitised to death and losing the ability to provide adequate palliative care to patients in their final stages of life. Opponents further contend that good palliative care should control symptoms, including pain and distress; therefore, people who consider ending their lives may change their minds when symptoms are properly controlled. Some nurses and midwives raise concerns that VAD may affect the overall nurse-patient relationship, trust may be eroded, and the therapeutic relationship affected.
Researching this article, I consistently came across themes that nurse and midwives felt VAD goes against the core values of their profession, ‘Do no harm’. In one academic article, an RN expressed their fear, “Every day, I am assisting patients to live, regain their health and leave the hospital. I also help patients during their last days when illness becomes too much. I have a great love for this part of my job, it is a beautiful thing to make my patients comfortable and happy in their final hours … the act of assisting them in suicide rocks me to my core.”1
References
1. Manag. 2022 Jun 1;11(6):777785. Introducing Voluntary Assisted Dying: Staff Perspectives in an Acute Hospital. Int J Health Policy Digby R, McDougall R, Gold M, Ko D, O’Driscoll L, Bucknall T.
2. Snir J.T., Ko D.N., Pratt B., McDougall R. 2022Anticipated impacts of voluntary assisted dying legislation on nursing practice, Nursing Ethics, Vol. 29(6) 1386–1400,
3. Tasmanian House of Assembly – Hansard 3/3/2021 –tinyurl.com/yckkvw3j, Accessed 14/2/23
Proponents of VAD argue that this is a compassionate and humane option for those suffering and have no chance of recovery. One of the main arguments in favour of VAD is that it alleviates suffering and improves the quality of life for individuals who are in the final stages of a terminal illness or chronic condition. Persons who choose VAD ultimately have control over the timing and manner of their death. Many proponents argue that allowing individuals to have this control can help them to die with dignity and peace, rather than suffering through a prolonged and painful death. Proponents say that the safeguards that are entrenched into the various state legislations, ensures that all patients are fully informed, can make conscious decisions and no patient can be exploited. Proponents further state that palliative care still plays an important role in the journey of a terminally ill patient, but sometimes palliative care treatments such as pain relief are unable to relieve the suffering of a terminally ill patient.
Alternatively, in other journal articles, nurses expressed the view that VAD was congruent to the professional obligation to alleviate patient suffering. They viewed VAD a preferred option for the patient (if they so choose) rather than prolong life with treatments that prolonged suffering. “There is no point lying to a person, providing them unnecessary and often painful treatments to facilitate an extra few weeks of life.”2 During debate in the Tasmanian Parliament, many referred to VAD as not being a choice between life and death, but rather a choice between two deaths.3
Voluntary assisted death is a complex and controversial issue that raises a wide range of ethical, moral, and practical concerns. While there are valid arguments on both sides, it is vital to consider the potential benefits and harms associated with this practice, and to ensure that any regulations or laws regarding assisted death are carefully considered.
Every man must do two things alone; he must do his own believing and his own dying.
JAMES 26 Apr–Jun 2023 Volume 27, No. 11
AusCAPPS is an NHMRC funded national online community of practice developed in partnership with the APNA, RACGP, RANZCOG, PSA, and other key stakeholders interested in increasing women's access to long-acting reversible contraception (LARC) and early medical abortion (EMA) services.

We support nurses, general practitioners and pharmacists to provide LARC and EMA in primary care. This free multidisciplinary online community of practice is designed to help AHPRA verified clinicians to connect with peers, experts and resources for support, knowledge and information.
Connect with nurses, GPs and community pharmacists who have an interest in providing LARC and/or EMA services in Australia

Discuss case studies and chat with expert clinicians

Find providers near you and build local networks



Keep up to date with education and training opportunities related to LARC and EMA






Get access to the latest evidence-based resources, guidelines, webinars and podcasts
" I love hearing about the things that pop up in other peoples work and how they resolve these issues. I aim to prioritise time in my week to make the most of this amazing resource. "
AusCAPPS member














ADVERTISING P R O J E C T P A R T N E R S
AusCAPPS trial@monash edu 1 SCAN TO SCAN TO JOIN JOIN Register for a free Medcast account 2 Sign up to AusCAPPS Network with your AHPRA number 3 HOW TO JOIN AUSCAPPS AusCAPPS
https://medcast com au/ communities/auscapps
W H A T C A N A U S C A P P S M E M B E R S D O ?
H O W W I L L A U S C A P P S H E L P M Y P R A C T I C E ? W H A
T I S A U S C A P P S ?
A u s t r a l i a n C o n t r a c e p t i o n a n d A b o r t i o n P r i m a r y C a r e P r a c t i t i o n e r S u p p o r t N e t w o r k The Department of Health and Aged Care is an official partner of AusCAPPS The Department of Health and Aged Care is an official partner of AusCAPPS
prepare nursing and midwifery students for work in a climate emergency
By Aletha
With increasing frequency, droughts, floods, fire, and air pollution, resulting in respiratory disease, vector-borne disease, death, physical injuries, and mental health deterioration, are having a detrimental impact on health.1
Although a global issue, climate change effects are felt uniquely at a local level, requiring diverse responses within each context of clinical practice.2 Furthermore, a paradox exists whereby the healthcare industry looks after those most vulnerable to climate change impacts while contributing 7% of Australia’s overall carbon emissions.3
When preparing nursing and midwifery students to transition to practice, educators must equip these students with knowledge of climate change impacts on health and
environmentally sustainable healthcare services and the skill to actively participate in addressing this threat.
As nurses and midwives are at the forefront of providing care to those affected by climaterelated extreme weather events, they must be able to identify and mitigate ever-fluid climaterelated risks.4


Natural disasters can impact healthcare infrastructure by damaging facilities, cutting access to supplies, equipment, and medications, and requiring mass patient evacuations.5
Thus, nursing and midwifery students transitioning to the workforce must be equipped with the skill and knowledge to help build climate-resilient and environmentally sustainable healthcare services adaptable to planning and responding
to complex impacts of natural disasters on healthcare systems and communities.
Health services also produce large amounts of clinical and non-clinical waste exacerbated by the COVID-19 pandemic, a significant contributor to healthcare’s carbon emissions, driven largely by singleuse supplies to maintain infection control.6 Nursing and midwifery students must be aware of and advocate for sourcing sustainable options for clinical supplies, responsible use and waste reduction, and sustainable energy and water usage.7 Educating the emerging workforce to be environmentally responsible by considering what they ‘need’ to perform a task, only using required supplies and considering alternative
Educators must step up to
Ward, Gavin Carson and Zerina Lokmic-Tomkins
Climate change is not a ‘future’ problem – it is impacting the health and wellbeing of the community now.
28 Apr–Jun 2023 Volume 27, No. 11 ISSUES
Dr Aletha Ward
resource usage is essential in environmentally sustainable practice.8
Professional standards of practice for nurses and midwives mandate our responsibility to provide patient education.9
In the context of climate change, this includes managing chronic health conditions, having an adequate supply of medications, means of resupply, or backup options to store medicines requiring refrigeration during power outages. Awareness of this role starts with educating and empowering nursing and midwifery students with knowledge and skills to communicate the impacts of climate change on health and help prime community members to be resilient and prepared for a climate changedriven environment.
As Australia further experiences extreme weather events, student nurses and midwives transitioning to practice will be left to respond to the climate crisis. Educators have a duty of care to prepare these students to respond well. Students themselves are supportive of climate change science integration within the nursing curriculum.10 Now, it is up to nursing educators to step up and deliver as a matter of urgency.
Authors
Dr Aletha Ward PhD, MBA, BNurs, RN, GAICD MACN, is a Lecturer at the University of Southern Queensland, Ipswich Qld Australia
Gavin Carson is a Student Nurse at the University of Southern Queensland, Ipswich Qld Australia
Associate Professor Zerina LokmicTomkins PhD, MNSc, BAppSci, BAppSc, GradCert, RN, MACN, is Affiliate Research Fellow at Monash University, Clayton, Victoria Australia
References
1. United Nations. 2022. Climate action fast facts. Retrieved 3 Oct 2022 at un.org/en/climatechange/science/ key-findings
2. Butterfield P, Leffers J, & Díaz Vasquez M. 2021. Nursing’s pivotal role in global climate action. BMJ: British Medical Journal, 373. doi:10.1136/bmj. n1049

3. Malik A, Lenzen M, McAlister S, & McGain F. 2018. The carbon footprint of Australian health care. The Lancet Planetary Health, 2(1), e27-e35
4. Australian College of Nursing. 2021a. Position Statement – Ethical leadership in emissions reduction. acn.edu.au/wp-content/uploads/ position-statement-ethicalleadership-in-emissions-reduction. pdf (Accessed 11 November 2021)
5. Attorney-General’s Department. 2020. Royal Commission into national natural disaster arrangements report October 2020. Chapter 15. naturaldisaster. royalcommission.gov.au/ publications/html-report/chapter-15
6. Rivas ML, Albion I, Bernal B, Handcock RN, Heatwole SJ, Parrott ML, Piazza KA, & Deschaseaux E. 2022. The plastic pandemic: COVID-19
has accelerated plastic pollution, but there is a cure. Science of The Total Environment, 847, 157555. dx.doi. org/10.1016/j.scitotenv.2022.157555
7. Kallio H, & Kangasniemi M. 2020. Environmental responsibility in nursing in hospitals: A modified Delphi study of nurses’ views. Journal of Clinical Nursing, (29),4045–4056. doi:10.1111/jocn.15429
8. Ward A, Heart D, Richards C, Bayliss L, Holmes M, Keogh S, Best O. Reimagining the role of nursing education in emissions reduction. Teaching and Learning in Nursing [Internet]. 2022: Available from: doi. org/10.1016/j.teln.2022.02.003
9. Nursing and Midwifery Board of Australia. 2017. Registered nurse standards for practice. nursingmidwiferyboard.gov.au/ Codes-Guidelines-Statements/ Professional-standards/registerednurse-standards-for-practice.aspx
10. Álvarez-Nieto C, Richardson J, Navarro-Perán MÁ, Tutticci N, Huss N, Elf M, Anåker A, Aronsson J, Baid H, & López-Medina IM. 2022. Nursing students’ attitudes towards climate change and sustainability: A cross-sectional multisite study. Nurse Education Today, 108, 105185-105185. doi.org/10.1016/j. nedt.2021.105185
Apr–Jun 2023 Volume 27, No. 11 29
When preparing nursing and midwifery students to transition to practice, educators must equip these students with knowledge of climate change impacts on health and environmentally sustainable healthcare services and the skill to actively participate in addressing this threat.
ISSUES
Promising new Network set to boost nursing and midwifery research
Kathryn Anderson
The recently formed Australasian Nursing and Midwifery Clinical Trials Network (ANMCTN) is set to elevate and support nursing and midwifery research across Australasia.
The world first Network, formed in 2020, brings together academic institutions to enhance, support and facilitate nurse or midwife-led clinical research.

Professor Marion Eckert, Director of the Rosemary Bryant AO Research Centre (RBRC) at University of South Australia, said the idea was born in 2019 when a group of nurses in academia discussed how nursing and midwifery research was ‘falling behind’ and failing to get funding in favour of other projects.
“We were wanting to know how to get on the bus basically, around breaking the profile that nurses and midwives actually do research. The academics concluded that they wanted to build focus on bringing awareness and support for nurse and midwife researchers.
Instigated and coordinated from the RBRC, the group of enthusiastic academics from across the country formed, pledging to take on the project on top of what they were already doing because they could see the benefits.
Seeking funding to set up ANMCTN from the Council of Deans, the group argued their case by identifying the gaps in nursing and midwifery research.
They reasoned that nurses and midwives, who, despite making up 60% of the healthcare workforce, were often underrepresented in the leadership of large-scale clinical research projects and clinical trials. Further, they argued, nurses and midwives received little of the pool of clinical research funding yet had tremendous potential to be influential by contributing to advancing science and knowledge in all aspects of healthcare.
“We needed a strategy because essentially nursing and midwifery is in every gamut of healthcare and therefore has a huge ability to contribute to evidence-based practice,” said Professor Eckert.
Ultimately, the group believed the work of the Network could retain nurses and midwives in the professions, offer sustainable career pathways, elevate the profile of nurse and midwife-led research, foster the next
generation of healthcare research leaders and develop new industry partnerships.
After putting a prospectus together, which included a value proposition to improve patient care, advance clinical care and improve the efficiency of the healthcare system, the group brought 10 Universities on board as foundation members.
“This was just enough funding to get the Network started,” Professor Eckert said. Since then, the Network has grown to 25 universities from across all states and territories, including all five Universities from New Zealand.
The association has also expanded to invite professional organisations.
“We are trying to encourage as many membership groups to join as possible,” Professor Eckert said.
Network membership also extends to individual nurses and midwives who work anywhere in health. Professor Eckert said she would like to attract people interested
INNOVATION 30 Apr–Jun 2023 Volume 27, No. 11
Photos courtesy of the Australasian Nursing and Midwifery Clinical Trials Network and its Network Partners
in evidence-based practice or who want to understand more about research.
“It’s those people we want to hear from too.”
A key focus of the Network is building infrastructure and strategy to support people when they apply for grants.
Professor Eckert said that as grant tender submissions are highly competitive, the ANMCTN can strengthen nurse and midwife research applications. Additionally, she suggests when clinical research is conducted across networks, it attracts a more significant proportion of competitive funding.
“This is something we are building on at the moment because now we have moved through the governance structure, the brand, the membership and the funding, we are moving into, ‘let’s support people to get their grants’.
“When people send their application for a clinical trial, we will assist and guide them if they want to submit a grant. We are happy to review the grant, and we are happy to endorse it” Professor Eckert said.
Currently, there is a lack of sufficient supporting structures for nurses and midwives interested in clinical research.
“So if we could become that trusted party, and build network support, then that would be brilliant,” Professor Eckert said.
“It doesn’t matter if they are in Mt Gambier or Mt Isa; we would hope that they would engage with the Network.”
The Network is also moving into the stage where similar interest group members are being connected to build collaboration among nursing and midwifery clinical researchers and provide opportunities for sharing resources.

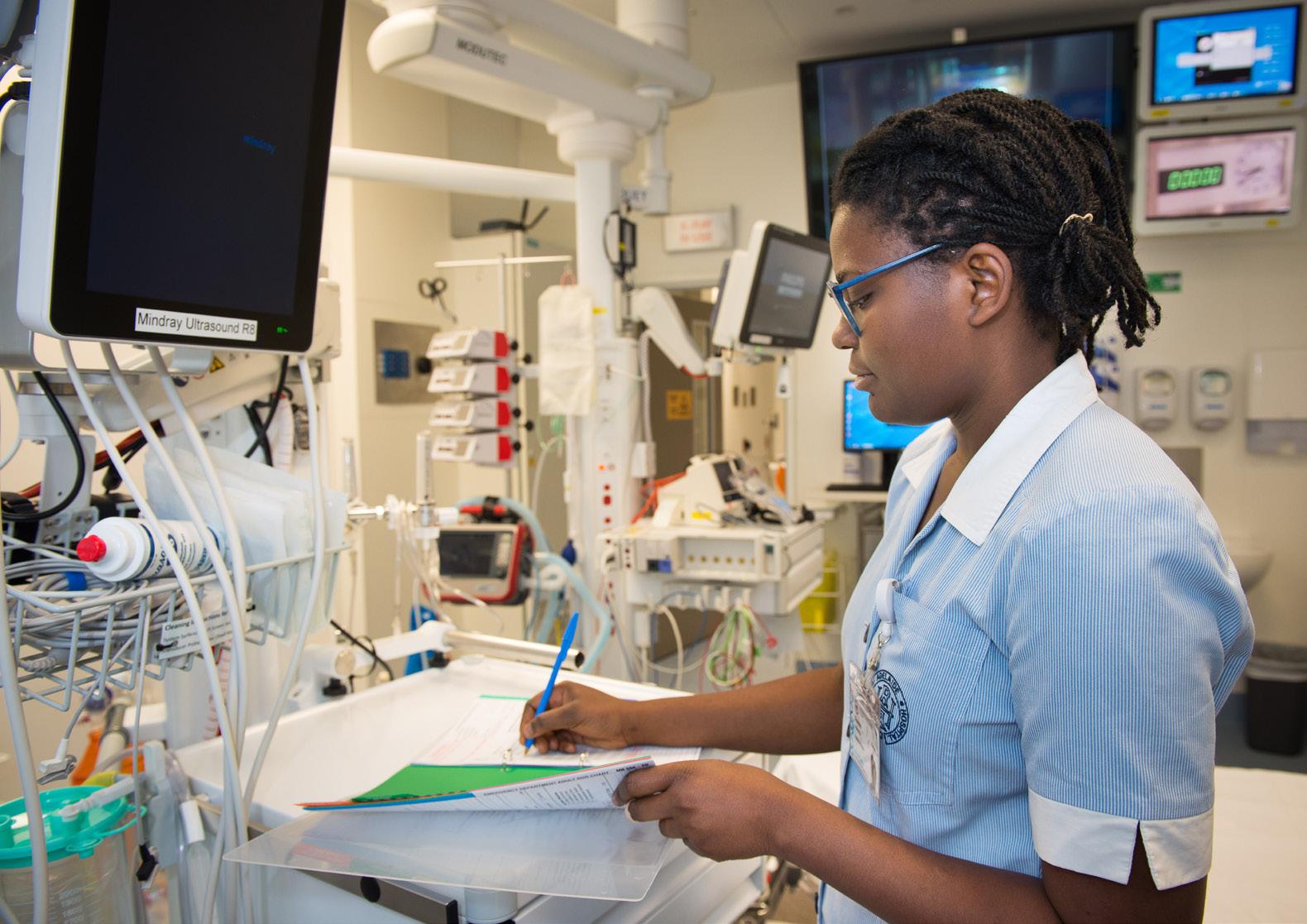
“We may have people working on [similar] informal projects in other states that we can put together, and when they are linked, they can build on what they have been working on.” Professor Eckert said.
The Network also plans to facilitate new education pathways.
“We are in the process of developing a strategy for a suite of online platforms for
getting started and understanding research. We are also running some seminars.”
Professor Eckert is not aware of any similar nursing and midwifery network like the Australasian Nursing and Midwifery Clinical Trials Network in the world.

“In other disciplines, there are networks, but they focus on diseases like musculoskeletal, cancer and cardiac, stroke and things like that. We focus on the profession and bringing the profession together.”
To find out more and sign up for the Network, go to: anmctn.com.au
“When people send their application for a clinical trial, we will assist and guide them if they want to submit a grant. We are happy to review the grant, and we are happy to endorse it.”
INNOVATION Apr–Jun 2023 Volume 27, No. 11 31
“We needed a strategy because essentially nursing and midwifery is in every gamut of healthcare and therefore has a huge ability to contribute to evidence-based practice.”
CoNNMO: Australia’s nursing and midwifery alliance influencing healthcare across the lifespan
Natalie Dragon
Australia’s national coalition of nursing and midwifery organisations ( CoNNMO) has secured renewed funding from the federal government, including for the first time, sitting fees for member attendance, recognising the inherent value of the alliance.

“This is significant recognition of the value of nurses, midwives and CoNNMO that makes a big difference to the vast majority of members. Most representatives work for health services and they represent their specialty not their workplace so they need to take leave to attend. Now they will be remunerated for the time they spend at CoNNMO,” said Australian Nursing and Midwifery Federation (ANMF) Federal Senior Professional Officer Julianne Bryce.
The Coalition of National Nursing and Midwifery Organisations (CoNNMO) currently represents 61 Australian nursing and midwifery organisations – diverse in function, size and structure.
“Our strength is our diversity; it’s a coming together of people with expert knowledge
of nursing and midwifery with shared objectives,” said Ms Bryce.
“Some coalitions or alliances speak with one voice. In that sense, we don’t. We discuss matters of shared importance, and it’s a way to navigate in to the nursing and midwifery professions and to learn from that expert knowledge and opinion.”
The Coalition, which started out as an informal forum sponsored by the ANMF in 1991, is now supported with funding from the Australian Government Department of Health and Aged Care and, ANMF as the secretariat, is responsible for day to day operations.
“The key role for the forum is for the specialty nursing organisations to communicate, to network. It’s a conduit
for information, where people can communicate,” said former CoNNMO Chair (2018-2022) Marian Linnane.
“We provide support and assist where there are challenges; putting members in touch with organisations or inviting guest speakers who can help with whatever challenge they are facing, whether that be governance, sustainability, business continuity, membership attraction and retention,” said Ms Linnane, also former Chair of Nursing Informatics Australia (now Nursing & Midwifery Digital Health Network). CoNNMO provides an opportunity for smaller organisations to get an audience with national stakeholders, such as the Australian Department of Health and Aged Care, Chief Nursing and Midwifery Officer, Nursing and Midwifery Board of Australia, Australian Nursing and Midwifery Accreditation Council (ANMAC), Australian Digital Health Agency and the Australian Commission on Safety and Quality in Health Care, said Ms Bryce.
“Specialty organisations/groups are often very much focused on their clinical practice and it gives them a chance to have a voice on both local and national policy and professional issues.”
Likewise, CoNNMO facilitates access to its membership, for example enabling the Australian Department of Health and Aged Care to tap into a broader nursing and midwifery perspective on matters such as the new National Nursing and Midwifery Strategies.
The Coalition includes groups with diverse organisational structures, including colleges, associations, universities; societies, councils, confederations, a federation, congress, networks and institutes.
Some are set up to be principally networks for dissemination of information; others have a broader remit including professional representation; education; advice and/or
CoNNMO members at the 2019 meeting
INNOVATION 32 Apr–Jun 2023 Volume 27, No. 11
advocacy; scholarships; collegial support; research; policy development; professional standards; new healthcare initiatives; and/ or enhancing clinical expertise.
In 2007, a new governance structure was determined which included the name change to the Coalition of National Nursing Organisations (CoNNO) followed by the election of an inaugural Council in 2008. The establishment of the governance framework represented a new, more formalised phase in the life of the Coalition.
“CoNNMO is driven by the feedback from members and ideas brought to the table by Council for discussion and debate,” Ms Bryce said.
“CoNNMO members meet under their individual autonomy, and each organisation has intrinsic value in its own right as part of the Coalition.
While many discussions do not require agreement, two of the issues that have reached consensus at CoNNMO are: the importance of undergraduate Bachelor
VISION
The vision of the Coalition of National Nursing & Midwifery Organisations is to be an authoritative alliance influencing healthcare across the lifespan, for the Australian community, through the professions of nursing and midwifery.
of Nursing and Midwifery education remaining in the university sector; and Aboriginal and Torres Strait Islander health, history and culture incorporation into the undergraduate curriculum (which is now embedded in the ANMAC standards).
CoNNMO hosts a variety of speakers, including recently a session on contemporary ethics following the global pandemic and a panel discussion involving nurses from various specialties, talking about their experiences of COVID. Other topics addressed include social media, governance models, auditing, lobbying, advocacy, workforce, rural and remote practice, new graduates, national safety and quality standards, digital health, positive practice environments, electronic health records, medicines management, even marriage equality and the associated plebiscite.
“Many of us work deeply in our specialty areas, so when we come to CoNNMO we get to listen to the challenges of others, learn about different initiatives, and understand
the broader issues relevant to our profession/s and that is advantageous and, to me, a privilege,” Ms Linnane said.
“To have 60-80 members in a room and facilitate a successful meeting with many diverse opinions but with one key focus –improved person-centred care – that manages to keep us on track. This is why we do what we do for as long as we do it, whether that be in management, leadership, education, clinical or research, that’s the whole point of it.”

A key highlight for Ms Linnane was the formal addition of midwifery into the title of CoNNO to become CoNNMO in 2017. CoNNMO’s success is evident in the ongoing interest and applications from new or existing groups to join every year, she said.
“These groups have either recently heard of CoNNMO, or are newly established sub-specialty groups. We have three new additions from our last meeting – the Cosmetic Nurses Association, the National Enrolled Nurses Advisory Council and the Gerontological Alliance of Nurses Australia.”
Tracey Nicholls, Deputy Chair of CoNNMO and immediate past President of the Otorhinolaryngology, Head and Neck Nurses Group concurs. She considers the value of CoNNMO is its accessibility and networking opportunities, and as a sounding board for knowledge and advice.
“It’s a really good platform for the smaller nursing specialty groups to be seen and heard. The bonds and relationships made are invaluable and we are able to contact one another with ongoing challenges we face in our professional groups.
“There’s knowledge that comes from everybody, including from nursing organisations that I never knew existed. It helps us to keep abreast of what’s happening beyond our individual specialties.”
Co NNMO OBJECTIVES
• Promote recognition of nursing and midwifery as essential to the health and wellbeing of the Australian community
• Provide leadership in the national debate on health and public policy
• Be a forum for discussion and consultation on professional matters
• Facilitate communication between member organisations and other stakeholders
• Be a recognised conduit for access within and to the nursing and midwifery professions
• Assist the development of governance and capacity of member organisations
• Ensure CoNNMO remains robust using the principles of good governance
INNOVATION Apr–Jun 2023 Volume 27, No. 11 33
Julie Reeves ANMF Federal Professional Officer
Aged care – Change is afoot
Nurses and care workers working in aged care understand firsthand the desperate need for change within the sector to improve care delivery and working conditions.
The ANMF has been campaigning for decades to improve the visibility of the long-standing issues in aged care and improve care delivery. The Royal Commission into Aged Care Quality and Safety publically reinforced these issues and made many recommendations. Two years on and what has really changed? Here’s a snapshot of the significant changes made to date and reform still to come.
CHANGES IMPLEMENTED
AN-ACC – on 1 October 2022, a new funding model was introduced for residential care. The evidence based Australian National Aged Care Classification model (AN-ACC) provides funding to aged care providers based on an independent assessment of an older person’s health needs and requirements.
IHACPA – the former Independent Hospital Pricing Authority who sets the funding price for hospitals in the country was expanded to include aged care. The Independent Health and Aged Care Pricing Authority (IHACPA) now has the responsibility of providing independent advice to Government about the costs of care for future funding. IHACPA has recently commenced a large costing study for residential aged care.
Medication management – The Department of Health and Aged Care released their Guiding Principles for Medication Management in Residential Aged Care Facilities late last year. The guiding principles provide evidence based parameters and procedures for medicine management in aged care facilities. It describes 15 principles and outlines the roles and responsibilities in medication management to achieve quality use of medicines. Guiding principle 15: Administration of medicines by nurses detail the essential role nurses undertake in administration of medicines and specifically states that ‘registered nurses and enrolled nurses, are responsible for the administration of medicines in RACFs’.1 Translation of these principles into practice is the next step.
Code of Conduct for Aged Care – the Aged Care Quality and Safety Commission implemented the Code of Conduct for Aged Care on 1 December 2022. Its intention is to improve safety for people receiving care. It consists of eight behaviour statements that

are expected of aged care workers, including nurses and those governing aged care services. Concerns about a workers conduct who may not be meeting the expectations of the Code will be managed by the Commission and for nurses could also involve the Nursing and Midwifery Board of Australia. An Aged Care register of banning orders was also implemented with the Code.
Pay increase – The ANMF along with the HSU made applications to the Fair Work Commission (FWC) and sought a 25% pay increase for all classifications including nurses and care workers. On 4 November 2022, the FWC decided that more work needed to be done but in the interim granted a 15% increase for all direct care workers to be implemented from 30 June 2023. The union is concerned the full increase will not be passed on by some aged care providers and is urging the Albanese Government to ensure that the pay rise is passed on to aged care workers.
CHANGES TO COME
Registered nurses 24/7 – from 1 July 2023 nursing homes must have a registered nurse on site and on duty 24 hours per day.
Care minutes – from 1 October 2023, nursing homes will have to ensure that there is an average of 200 care minutes (registered nurse, enrolled nurse and care workers time) per day, per resident, which will include a minimum of 40 minutes of registered nurse time. From October 2024, this will increase to an average of 215 care minutes, with a minimum of 44 minutes of registered nurse time.
Other changes to come include the review of the Aged Care Act, a new home care delivery model and the implementation of the new quality standards.
We have achieved significant reform in aged care and when fully implemented, it will improve care delivery and working conditions but there is still much to do. The ANMF will continue to lobby strongly to ensure that we have a leading voice in influencing the extensive reform agenda and that the implemented changes make a real difference to care and to you. For more information on the work of the ANMF in aged care head to the ANMF Federal Office website.
Reference
1. Commonwealth of Australia
(Department of Health and Aged Care) Medication management in residential aged care facilities – Guiding Principles, 2022.
PROFESSIONAL 34 Apr–Jun 2023 Volume 27, No. 11
Nurse & Midwife Support o ers free, confidential and 24/7 health and wellbeing support to nurses, midwives and students across Australia.



CLINICAL UPDATE 36 Apr–Jun 2023 Volume 27, No. 11
Optimising patients’ discharge processes to enhance patient experience
By Thelma De Lisser-Howarth, Hazel Maxwell and Elizabeth Cummings
This discussion is an exploration of hospital discharge planning from the view of a multidisciplinary team (MDT) working from an interdisciplinary perspective.
Differing perspectives regarding discharge planning are unpacked from the viewpoint of registered nurses, visiting medical officers (VMOs), physiotherapists and occupational therapists. These clinicians provide an in-depth understanding of the factors affecting the MDT, working collaboratively to improve preparing patients for discharge home. Using an Improvement Science Framework to explore and answer the research question: How can the MDT work collaboratively to streamline patient discharge in a private hospital? This research provides an example of nurses taking the lead to facilitate and conduct quality improvement research, as indicated by (Flynn et al. 2017).2
OVERVIEW OF ISSUE
Evidence-based practices must be adopted by healthcare organisations, hospitals, and educational institutions to enhance the discharge planning practices of MDTs and the discharge outcomes of patients. There must be an emphasis on interprofessional education and practice change that focuses on individual health professional roles and functions when involved in the discharge planning process. Consideration of how each professional role interacts will provide the foundations to promote cohesiveness and accountability of the MDT when preparing patients for discharge. Ideally, education relating to discharge planning should commence in university curricula for nursing, medicine and allied health professionals training and consolidated practical learning occurring in the clinical area.
PROJECT OUTLINE
The research is based on the premise that the MDT coordinate, collaborate and communicate effectively to address as many aspects of care as possible to provide the best discharge experience for patients. Patients’ circumstances can change at any time, so the flexibility of the MDT when
approaching patients’ care is vital. Previous research suggests the discharge experience of patients is impacted negatively when the MDT fail to collaborate effectively to meet their discharge planning needs.3,4
A two-phase study was adopted to examine which factors inhibit the MDT from working collaboratively to streamline patients’ discharge.5 The Exploratory Phase and the Improvement Phase provided the best opportunity to address the research question methodically and systematically. A mixed-methods study design was adopted, underpinned by an Improvement Science Framework, utilising Plan-Do-Study-Act (PDSA) cycles.6 Qualitative and quantitative data were obtained through surveys, a focus group and PDSA cycles.
Descriptive statistics7 were used to analyse the quantitative data, and thematic analysis8,9 was used to analyse the qualitative data. The Tasmania Human Research Ethics Committee approved this research, and a clear governance structure was put in place to mitigate risk and ensure that the most appropriate people were available to support the research. The project governance consisted of a Guidance Team, Project Team, and the Multidisciplinary Team (MDT), which were purposely recruited.
RESULTS
The Project Team focused on strategies to enhance communication using a communication board as a tool, and these were developed over five PDSA cycles. The communication board facilitated a discussion about discharge planning between the MDT and patients and their families and/or carer regarding decisions about patients’ discharge plans. This, in turn, influenced patient outcomes and empowered the MDT to create an environment of quality improvement linked to everyday clinical practice.
Four themes were derived from the data obtained from the online survey and focus group, and these were: communication
breakdown, discharge date, medication list, and resources. The theme “communication breakdown” involves the MDT not providing timely and appropriate written and verbal information to each other, patients and their families/carers, and GPs. The theme “discharge date” relates to a lack of documentation and minimal discussion of estimated discharge dates with patients by the MDT. The theme “medication list” involved issues relating to documenting discharge medications in an appropriate timeframe and format. The theme “resources” was derived from the MDT identifying a lack of supplies and hospital processes which impacted their efficiency.
The MDT expressed that a lack of education and poor understanding of the discharge planning process impacted their ability to work collaboratively to streamline patients’ discharge effectively. Furthermore, hierarchical and occupational boundaries were found to impede their clinical practice. For example, the registered nurses (RNs) and physiotherapists perceived that the action of preparing patients for discharge home was beyond their control. Hence they were unable to optimise the discharge process for patients. The factors that contributed to placing the RNs and physiotherapists into this vulnerable position include the actions of VMOs, patient activities, and hospital processes. For example, to involve the discharge planning team to assist with the discharge preparation of complex patients, members of the MDT had to seek permission from VMOs prior to making a referral. The findings validate the need to continue to focus on rigorous methods that create MDT improvements in clinical practice and patient safety related to discharge planning.
OPPORTUNITIES TO ADDRESS –AIMS/NURSING/MIDWIFERY
A key recommendation is that solid partnerships between MDTs, academics and consumers are established before initiating

CLINICAL UPDATE Apr–Jun 2023 Volume 27, No. 11 37
quality improvement research in healthcare. This step will assist in breakdown silos and promote mutual respect. It is recommended that hospitals implement discharge protocols and policies to support MDTs in the discharge planning process. Policies and protocols must clearly define roles for MDTs so that there is no ambiguity concerning decision-making that focuses on streamlining patients’ discharge.
The discovery of hierarchical and occupational boundaries extends to previous research.10 Professional boundaries added to complications in the discharge planning process, and this paper extends this argument. Notably, anecdotal comments by patients negotiating their discharge times with VMOs affords new knowledge and insights into how the MDT are impeded from proactively streamlining patients’ discharge.
The authority of the private VMO was dominant as other members of the MDT required and valued clinical direction and permission from VMOs to commence the discharge planning process. The evidence presented suggests that VMOs’ authoritarian status in patient discharge-related decisions could specifically be related to the structure of the private hospital system, and this argument develops from the findings of previous research.11
This research generates new understandings, such as the importance of involvement in interprofessional education for MDTs. Encouragement of education focusing on each MDT role and how each role interacts and impacts each other may enhance decision-making, communication and team collaboration when preparing patients for discharge home. Education

should commence in all health and medicine-related undergraduate degree courses such as nursing, doctor, physiotherapy, and occupational therapy. Consideration must be given to undergraduate courses to enhance learning for students through theory and practice. This approach to learning must be integrated into the curricula with measurable outcomes. Government and regulatory bodies responsible for legislation related to health and medical training and education should support hospitals and educational organisations to embrace interprofessional education in the discharge planning process.
CONCLUSION
The aim is for all MDTs to work in an interprofessional manner to streamline patients’ discharge preparation and the discharge planning process effectively and proactively. Achieving enhanced and positive discharge planning outcomes for patients whilst improving MDTs’ skills and knowledge in the discharge planning process is vital.
Authors
Dr Thelma De Lisser-Howarth RN, DrHlth, BSc(Hons), Grad Dip HE, Manager Consumer and Patient Experience, Northern Sydney Local Health District Clinical Governance Unit, Royal North Shore Campus, St Leonards, NSW Australia and University of Tasmania, School of Nursing, Hobart Tasmania Australia Dr Hazel Maxwell PhD, MA, BA (Hons), Senior Lecturer School of Health Sciences, College of Health and Medicine, University of Tasmania, Rozelle Campus, Sydney NSW Australia Associate Professor Elizabeth Cummings RN, PhD BA, BIS(Hons), Adjunct Associate Professor, School of Nursing, University of Tasmania, Hobart Tasmania Australia
REFERENCES
1. Jeffers AM. Safe transitions from the hospital to home: A review of the pediatric hospitalist’s discharge workflow. Current Problems in Pediatric and Adolescent Health Care 2021;51(5):101021.
2. Flynn R, Scott SD, Rotter T, Hartfield D. The potential for nurses to contribute to and lead improvement science in health care. Journal of Advanced Nursing 2017;73(1):97-107.
3. Okoniewska B, Santana MJ, Groshaus H, Stajkovic S, Cowles J, Chakrovorty D, et al. Barriers to discharge in an acute care medical teaching unit: a qualitative analysis of health providers’ perceptions. Journal of Multidisciplinary Healthcare 2015;8:83.
4. Armor BL, Wight AJ, Carter SM. Evaluation of adverse drug events and medication discrepancies in transitions of care between hospital discharge and primary care follow-up. Journal of Pharmacy Practice 2016;29(2):132-7.
5. DeLisser-Howarth T, Maxwell H, Cummings E & Walker K. An exploration of the barriers that influence the patient discharge experience: a multidisciplinary team perspective. Enhancing Practice Conference 2022; Sage Hotel, Wollongong, NSW, Australia 2022.
6. Langley GJ, Moen RD, Nolan KM, Nolan TW, Norman CL, Provost LP. The improvement guide: a practical approach to enhancing organizational performance: John Wiley & Sons; 2009.
7. Cohen L, Manion L, Morrison K. Research methods in education: routledge; 2002.
8. Braun V, Clarke V, Rance N. How to use thematic analysis with interview data (process research). 2014.
9. Riger S, Sigurvinsdottir R. 33Thematic Analysis. In: Jason LA, Glenwick DS, editors. Handbook of methodological approaches to communitybased research: qualitative, quantitative, and mixed methods: Oxford University Press; 2015. p. 0.
10. Waring J, Bishop S, Marshall F, Tyler N, Vickers R. An ethnographic study comparing approaches to interprofessional knowledge sharing and learning in discharge planning and care transitions. Journal of Health Organization and Management. 2019.
11. Peet J, Theobald K, Douglas C. Strengthening nursing surveillance in general wards: a practice development approach. Journal of Clinical Nursing. 2019;28(15-16):2924-33.

CLINICAL UPDATE 38 Apr–Jun 2023 Volume 27, No. 11
A preventable death in custody
The Coroners Court is an independent investigation of reportable deaths undertaken to determine the cause and circumstances surrounding a death. A broader purpose is the contribution that the findings and recommendations made from the investigation can make to reduce preventable deaths.
The findings in the Inquest into the death of Veronica Nelson (2023), a proud Gunditjmara, Dja Dja Wurrung, Wiradjuri and Yorta Yorta woman, highlight not only the tragic circumstances of this woman’s death but the continued risk First Nations people face in custodial settings and the need for health practitioners (and others) to be competent in delivering culturally safe and respectful care. This case also demonstrates the risks when health professionals fail to act as advocates and allow stigma to influence their judgement in decision making. This risk is heightened in custodial settings where there is tension between care vs custody and healthcare can become more punitive than preventative and where the environment lacks adequate policy to support good communication amongst all divisions within the organisation.
This was a death in custody. More specifically, a preventable death of an Aboriginal woman in an environment that was legally required to provide the equivalent standard of care that could be expected in the community. The Coroner found many missed opportunities to intervene, that could have prevented Veronica’s death, in both the health and justice systems following her admission to the prison where she was noted to be extremely unwell and withdrawing from opioids. Evidence given revealed that Veronica used the intercom 49 times to request assistance or complain of her worsening cramp and vomiting during the 36 hours she was held in the women’s prison before her death –alone and unattended.
Evidence identified poor working relationships between correctional and clinical staff leading to limited information exchange between the two –this disconnect and the gaps in communication compromised Veronica’s care as not all information received by the prison officers through these intercom connections was conveyed to the healthcare team and vice versa. In addition to this it was noted that many correctional and clinical staff failed to take their obligations to provide adequate care to prisoners seriously. This was evident through their normalisation of a prisoners experience of withdrawal, with staff desensitised to the suffering experienced which in this case blinded them to Veronica’s clinical deterioration and her need for urgent medical care.
As with many cases before the Coroners Court, there were issues regarding a failure to communicate, failure to undertake adequate/accurate health
assessments and a failure to document clinical findings by medical and nursing staff. This established not only a breach of duty but also a failure to observe and adhere to established professional standards and codes of conduct – particularly around cultural practice and respectful relationships.

The Coroner found that Correct Care Australia (CCA) lacked clear polices and processes that would enable the safe medical management of patients in their care. Stigma was inherent in the policies that governed treatment of opioid dependence with guidelines taking a punitive approach in the provision of opioid therapy preventing any clinical discretion in either dose or type of therapy. The restricted access to pharmacotherapy, denying the patient the equivalent care to that available in the community for someone with an opioid disorder was described as cruel and inhumane treatment.
This highlights the practitioners need to advocate and intervene on behalf of their patients to ensure that policies associated with the delivery of healthcare do not breach human rights and enable them to practice in accordance with current standards. Where this is not the case practitioners must work with the organisation to secure change and ensure that patient rights are protected.
Whilst the Coroner noted that the psychiatric assessment and care provided by Forensicare was reasonable and appropriate, this was not the case for some of the medical and nursing care provided. The Coroner found that the care provided by one medical practitioner was a significant departure from reasonable standards of care and diligence expected in medical practice through the failure to undertake adequate assessments, develop ongoing care plans and maintain accurate records. The Coroner described a registered nurse’s conduct as lazy, unprofessional, and not in keeping with the standards of care one would reasonably expect, through their failure to provide adequate assessment, treatment or care. Overall, the Coroner concluded that Veronica was culturally isolated, did not receive culturally competent or culturally-specific care or support at any time during her incarceration and that the care she did receive by both correctional and healthcare staff was influenced by drug use stigma. All of these failings and the failure to transfer Veronica to hospital causally contributed to her death. A death that was preventable. A number of recommendations were made focusing on the improvement of providing culturally safe care, better governance and targeted education around alcohol and other drugs.
Linda Starr
LEGAL Apr–Jun 2023 Volume 27, No. 11 39
An expert in the field of nursing and the law Associate Professor Linda Starr is in the School of Nursing and Midwifery at Flinders University in South Australia
Rollout begins on new national nurse and midwife health service
A project team has been appointed and work is afoot on the rollout of a new national support service for Australia’s nurses and midwives.
 Natalie Dragon and Robert Fedele
Natalie Dragon and Robert Fedele
40 Apr–Jun 2023 Volume 27, No. 11 WELLBEING
NNMHS Director Heather Pickard
The Albanese Government has invested $25.2 million to establish and run a national nurse and midwife health service to provide peer-to-peer counselling, case management and referrals after years of lobbying by the Australian Nursing and Midwifery Federation (ANMF).
The project team kicked off on 23 January, with the new National Nurse and Midwife Health Service (NNMHS) anticipated to be operational in early 2024.
Newly-appointed NNMHS Director Heather Pickard, a registered nurse (RN) and founding CEO of the Nursing and Midwifery Health Program Victoria (NMHPV), said she was delighted that funding had been secured for this “incredibly invaluable service”.
“This will make a real difference in individuals’ lives. The strong wellness focus offers a compassionate response to sensitive health issues,” Ms Pickard said.
“Approximately 10% of the community experiences an episode/episodes of mental illness and/or substance use challenges, and nurses and midwives are no different. What is different is that they can be resistant to getting treatment due to the high regulatory framework they work in and the culture within nursing and midwifery of being the helper.
“The free, confidential and independent service will provide holistic case management for complex health issues and the provision of health information.”
The ANMF Federal Office is leading the national rollout framework in consultation with the Australian and state and territory governments, key service providers and nursing and midwifery peaks.
ANMF Federal Assistant Secretary
Lori-Anne Sharp welcomed the federal government’s commitment to a national program to care for the health and wellbeing of nurses and midwives.
“Nurses and midwives have carried us through the pandemic and they’re continuing to support the community in the ongoing response. This service will be vital in offering support across the professions, and it’s fantastic that we have an established framework and the experience and solid success of the Nursing and Midwifery Health Program Victoria to guide us along.”
The new national service committed in the 2022-23 Federal Budget is modelled on the NMHPV, which has been operating since 2006. The NMHPV is a free, independent and confidential nurse-midwife-led service for Victorian nurses, midwives and students
who experience sensitive health issues related to mental health, substance use, family violence, or anything affecting their health and wellbeing.
Glenn Taylor, CEO of the NMHPV since 2008 and an RN, said the program was unique in that it provided a safe place for any nurse or midwife, or student to come and speak to one of their own who has experience working in the profession and quite often has a lived experience with issues like stress and anxiety.
“We can help them navigate a path through the challenge they’re experiencing in a safe way and really challenge the fear and stigmas associated with being a nurse who isn’t quite right, or is struggling for a period of time.”
The new national service aims to help Australia’s nurses and midwives, including students, to better manage their health and wellbeing with counselling and case management services. The support aims to reduce increasing rates of fatigue, stress and burnout, which have escalated since the start of the pandemic.
“Our nurses and midwives contribute so much to our communities, and it’s imperative that we support them to manage their health in a way that works for them. Expanding this program nationally is about providing that support in a welcoming, accessible way,” said Federal Assistant Minister for Health and Aged Care, Ged Kearney.
“This is about providing a familiar front door for nurses and midwives to be able to talk about their mental health concerns to their peers who just get it,” said Ms Kearney, also an RN and former ANMF Federal Secretary. The point of difference of the new national service from most EAPs is that it is designed and run by nurses, enabling unparalleled connection and providing unlimited sessions.
The stigma-free entry point offers tailored counselling and case management, and specialist referrals to respond to mental health issues requiring additional services for nurses and midwives with a range of health issues. Registered nurses, midwives, and nurse practitioners will offer free, confidential and independent counselling, case management, health information and specialist referrals. Telehealth counselling will also form a significant part of the service, making it more accessible to nurses and midwives in regional and rural locations. The service will operate through four central hub locations, including Victoria-Tasmania, New South Wales-Australian Capital Territory, South Australia-Western Australia, Queensland-Northern Territory, and additional regional offices. A stakeholder consultation process will ensure that the Victorian model is localised to suit each state’s and territory’s needs.
The NNMHS will help to keep more nurses and midwives healthy, supported, and retained in the workforce, said Deputy Director of the NNMHS Mark Aitken. An RN for more than 30 years, he has worked at the NMHPV and was part of the team who set up Nurse & Midwife Support (national phone service).
“This case management health service will be an additional complimentary service and potential referral pathway from Employee Assistance Programs (EAP) and Nurse & Midwife Support, the national 24/7 support service that provides brief interventions, counselling and referral pathways and treatment providers,” Mr Aitken said.
For more information on the national service, contact Heather Pickard, Director: hpickard@anmf.org.au, or Mark Aitken, Deputy Director: maitken@anmf.org.au
For contact with the NMHP Victoria visit nmhp.org.au
KEY POINTS
The new national Nurse and Midwife Health Service:
Plans to help Australia’s nurses and midwives, including students, to better manage their health and wellbeing with counselling and case management services.
Aims to reduce increasing rates of fatigue, stress and burnout, which have escalated since the start of the pandemic. Will operate through four central hubs, Victoria–Tasmania, New South Wales–Australian Capital Territory, South Australia–Western Australia, Queensland–Northern Territory, and additional regional offices. Service operational in early 2024
WELLBEING Apr–Jun 2023 Volume 27, No. 11 41
Kristen Wischer ANMF Senior Federal Industrial Officer
Australia’s gender pay gap in 2023 –its causes and promising reforms

Australia’s national gender pay gap (GPG) across public and private sector employers sits at 22.8%, the same as in 2021. This means women earn, on average, $263.90 less than men each week.
The ANMF’s membership is predominantly female, with 89% of the nursing profession identifying as women. Measures to eliminate the gender pay gap are vital for our members to enjoy a healthier working life and retirement. There are many reasons for the GPG, and in the last year, a number of measures have been introduced to tackle the problem.
CARING RESPONSIBILITIES
Women take parental leave, some of which is paid, but most will have a period of unpaid work or be paid at a lower rate than their usual income. Over this period, it is rare for employers to pay superannuation on the paid component of leave and even more so for the unpaid period. This means that women experience reduced income while on parental leave and lose vital contributions to their super balance. The Commonwealth Government has recently increased the period of government-funded parental leave from 18 weeks to 26. This is a positive step forward, but the rate is set at the minimum weekly wage rather than actual income. In addition, we are still fighting to ensure superannuation is paid on Government funded leave.
LACK OF FLEXIBLE WORK
After returning to work, women also lose income –it may be necessary to reduce availability to work to meet caring responsibilities. Rosters that require night shift and weekend work may be impossible due to a lack of childcare options outside of weekday times. This can lead to women either leaving the profession or cutting back on work hours. Women also bear the greatest responsibility over their working lives for caring for elderly family members, or loved ones with a chronic illness or disability. As nurses, women are even more likely to take on unpaid caring roles.
There have been welcome legislative changes to address this problem. New provisions now require employers to provide more consultation and information in response to a request for a flexible work arrangement to accommodate caring responsibilities. Employees will soon be able to challenge an employer’s refusal of a flexible work arrangement to test whether there really is a ‘reasonable business ground’ for the refusal.
HISTORIC UNDERVALUATION
More insidious and harder to identify is the historic undervaluation of female-dominated work. As a caring profession, nursing is particularly affected by historical bias and ongoing unconscious bias. Wage rates set decades ago were discounted based on the nature of the work performed, being caring and as secondary to the primary breadwinner. In addition, the level of skill required of caring work has long been underestimated, considered ‘inherent’, and therefore undervalued.
New legislation to improve job security and achieve gender equality has created promising avenues to address the problem at Australia’s industrial tribunal, the Fair Work Commission. The tribunal must now consider whether any decision it makes contributes to achieving gender equality and job security. For example, when setting minimum rates of pay under awards, these two objective factors must be taken into consideration. The ANMF is currently using these provisions to increase wages for nurses and care workers.
JOB SECURITY
Obtaining secure work is important for ensuring women are not vulnerable to the disadvantages of precarious employment. The rise of the gig economy, while offering some flexibility, does not promote secure work and can undermine wages and conditions. Casual work also impacts working women in that entitlements such as annual and sick leave do not accrue. This means any time off work for sickness or holidays is not paid.
There are new measures in the industrial legislation that will help tackle the problems of insecure work, such as converting casual employment to permanent, limiting the use of contract work and allowing clauses in enterprise agreements to make special provisions for gender equality.
The above are just some of the measures introduced into legislation in Australia in 2023. The ANMF is working to make the most of each opportunity to eliminate the gender pay gap.
INDUSTRIAL 42 Apr–Jun 2023 Volume 27, No. 11




IN PHARMACY NU M B I NG CR EAM #1 SCAN QR CODE TO APPLY
an Aged Care locum for the Rural Locum Assistance Program (Rural LAP), you’ll have the opportunity to travel, meet new people, develop new skills and work in some of the most beautiful places, from the countryside to Outback Australia. You’ll receive an hourly wage, a $150 incentive allowance per working day and $100 meal allowance per day plus we also arrange and pay for your travel and accommodation. Join our team
As
Leanne Boase BN MN(NP) MHSc(Ed) FACNP President, Australian College of Nurse Practitioners

Nurse Practitioners transforming healthcare
Projects to develop the Nurse Practitioner role began in Australia in the 1990s, with the first two Nurse Practitioners approved in 2000. Now in 2023, we have around 2,500 nurse practitioners. So how far have we travelled in 23 years?
While estimates on the number of Nurse Practitioners needed in Australia vary, most agree that we should have 10,000-15,000 by now. Although our growth has been slow, there are a number of positive aspects to how our role has been implemented, and a lot of much needed change on the horizon.
Australia, like every other country in the world, has its unique challenges in relation to healthcare. The remoteness of parts of our country makes equitable access to care extraordinarily difficult, and we need every health professional working to their full abilities. As nurses we all develop our practice to address the healthcare needs of our populations, it has always been this way. Constantly evolving scopes of practice are essential to continue meeting healthcare needs, especially as they become more complex, and nurses do this exceptionally well.
It is in remote parts of Australia where those first projects to explore the Nurse Practitioner role began. Nurses were already working independently to meet the needs of the community, with little support or formal preparation. This was recognised, and the work began to ensure they could continue this work, and expand their scope of practice even further. While there is still considerable frustration amongst Nurse Practitioners in Australia around our barriers to practice, there is now a significant amount of work being done to remove them. Nurse Practitioners are very poorly funded, patients often have to duplicate consultations with doctors, or their healthcare is simply too expensive. Additionally, there are barriers to Nurse Practitioners referring for mental healthcare and for chronic disease management, which has a direct impact on the health of individuals, and communities, where there is often no alternative healthcare practitioner available.
In 2020, a government-led wide ranging review of how healthcare is funded in Australia resulted in no recommendations to improve access to Nurse Practitioners, despite an abundance of robust evidence presented to support the recommendations made by its own reference group.
The Australian College of Nurse Practitioners, astounded at the ignorance of the most evidence based response to this review, approached all of the other lead nursing organisations, and healthcare organisations in Australia, and formed a new and united leadership group in response to this. With combined lobbying, the government at the time rapidly agreed to draft a 10 year plan to address the issues with the Nurse Practitioner role, and significantly increase and enable the workforce.
In 2022, a new government was elected, reinvigorating this plan, with even more enthusiasm, commitment, and resources. The plan is now called ‘increasing access to health and aged care: a strategic plan for the nurse practitioner workforce’. This is now in the final stages of drafting, and we expect implementation of the first of the outcomes in 2023, with many more to follow in the next few years.
What this plan will achieve, along with allowing Nurse Practitioners to work to full scope of practice, is better access to healthcare for Australian people. Like many other parts of the world, people struggle to access timely medical care, especially in rural and remote areas. People living at disadvantage are even more severely affected, in all geographical locations. While it has taken some time to reach this crucial juncture in Australia, there are a lot of positives in the way the Nurse Practitioner role has been implemented. The regulation of Nurse Practitioners is through a national system, and is therefore consistent across Australia, and both Practice Standards and Education Standards are in place. While some of our work is governed by jurisdictional legislation, such as prescribing, our practice standards underpin the way, and at what level, we work. Our educational standards (Master’s level) are extensive, and support diagnosis and prescribing at an advanced level, across the lifespan.
Importantly, Nurse Practitioners in Australia are authorised to work independently and autonomously, which means that we are in control of our own scope of practice development, supported by a decision making framework. This means the Nurse Practitioner can develop their practice continuously to meet areas of need. The Nurse Practitioner title is protected, only those authorised by our regulator can use it.
While there has been a lot of opposition to the Nurse Practitioner role in Australia, largely based on fear of
GUEST EDITORIAL 44 Apr–Jun 2023 Volume 27, No. 11
It is in remote parts of Australia where those first projects to explore the Nurse Practitioner role began. Nurses were already working independently to meet the needs of the community, with little support or formal preparation.
competition, or ‘turf protection’, these attitudes are no longer considered by our government to be an acceptable reason to continue holding the Nurse Practitioner workforce back. The arguments frequently put forward in opposition to our role are not evidence based, and they directly support retention of practice barriers that prevent people from accessing healthcare.
The need for better access to healthcare is seen by the current government as the far greater need. This has also led to a much greater role in development of policy for the Australian College of Nurse Practitioners, now considered an important stakeholder, not only in relation to the Nurse Practitioner role, but in health. While most of the opposition to our role comes from medical groups, medical practitioners in Australia generally have no issue working with Nurse Practitioners, and many highly value our work, knowledge and experience. We currently have a significant number of Nurse Practitioners, estimated at 30%, working in other nursing roles, or underemployed, and this is directly related to the practice and funding barriers that we have. Already with the recent changes, including the Nurse Practitioner Plan, we have seen a significant increase in enrolments to Nurse Practitioner Master’s courses around the country. In five years we expect our workforce to double, along with the jobs available, as the private and primary care sectors become viable, and Nurse Practitioners can work to their full scope of practice. It has taken over 20 years, but in Australia, we now have confidence that the role of the Nurse Practitioner is about to be fully enabled, and implemented.
Author
Leanne Boase BN MN (NP), MHSc (Ed), MAICD, FACNP is a practising Nurse Practitioner, endorsed since 2009, now working in her own primary care practice, and has been the President of The Australian College of Nurse Practitioners since September 2018. She is also the Executive Director of Nursing and Clinical Services for Luminar Health and Fullarton Clinic. She has over 25 years’ experience working in a wide range of hospital and private health settings, including metropolitan and regional areas, and primary care.

GUEST EDITORIAL Apr–Jun 2023 Volume 27, No. 11 45
The plan is now called ‘increasing access to health and aged care: a strategic plan for the nurse practitioner workforce’. This is now in the final stages of drafting, and we expect implementation of the first of the outcomes in 2023, with many more to follow in the next few years.
Nurse Practitioner Jo Perks
Photo credit: Michael Amendolia
FOCUS
MEN’S/WOMEN’S & SEXUAL HEALTH

with general practice
By Ruth Mursa, Elizabeth Halcomb, Christopher Patterson and Gemma McErlean
One in two Australian males have at least one chronic condition.
Current estimates indicate that some 75% of males in Australia are affected by overweight or obesity.1 Males are more likely to smoke, consume fewer fruits and vegetables, drink too much alcohol, and be less physically active than females.3 Over a third of the disease burden in males is potentially preventable through lifestyle risk factor reduction.2
Most Australians’ first point of contact with the health system is in general practice.4 Beyond managing acute episodes of illness, the multidisciplinary general practice team supports individuals and families to maintain their physical and mental wellbeing and to prevent future ill health by proactive screening and risk reduction. Robust general practice systems reduce health inequality, decrease the need for hospital admission, and improve overall population health.5
Our recent review of the literature identified that men can find general practice unwelcoming and unaccommodating. Men were also found to predominantly view the general practice as a source of acute healthcare without a clear understanding of its role in preventive healthcare and advice. Review findings identified a gap in the knowledge in relation to the impact of gender on the effective utilisation of general practice to its full capacity.
These review findings, together with many years of clinical practice, motivated Ruth Mursa to undertake a PhD project to further explore men’s help-seeking and engagement with general practice.
Ruth is enrolled in the School of Nursing at the University of Wollongong and is supervised by Professor Liz Halcomb, Dr Christopher Patterson, and Dr Gemma McErlean.
The Doctoral project uses a sequential mixed methods approach to address the research aims. To reach a defined group of men with varying education levels, demographic characteristics, health status, and the geographical distribution across metropolitan and regional/rural areas, the study is being undertaken in partnership with the New South Wales Rural Fire Service (NSW RFS).
The initial quantitative phase used an online survey to explore men’s adoption of and relationships between health literacy, lifestyle risk and engagement in preventive care.
Survey data has been collected and is currently undergoing analysis. This will be followed by semistructured telephone interviews to deeply explore men’s experiences engaging with general practice for preventive healthcare and explain the survey data in more detail.
Findings can potentially inform policy and practice in supporting change, reducing access barriers, and enhancing men’s health outcomes.
The findings of this project generate new knowledge to build on the review findings. In addition, the partnership with the NSW RFS will mean that findings can immediately be used to inform and create evidence-based workplace health strategies around men’s health.

Authors
Ruth Mursa, PhD Candidate, RN NP MN(NP) is in the School of Nursing, Faculty of Science, Medicine & Health, University of Wollongong, NSW Australia
Dr Elizabeth Halcomb RN PhD FACN, is Professor of PHC Nursing, School of Nursing, Faculty of Science, Medicine & Health, University of Wollongong, NSW Australia
Dr Christopher Patterson RN PhD MN(MH) is Senior Lecturer, School of Nursing, Faculty of Science, Medicine & Health, University of Wollongong, NSW Australia
Dr Gemma McErlean RN PhD MPH (Health Promotion) is Senior Lecturer, School of Nursing, Faculty of Science, Medicine & Health, University of Wollongong, NSW Australia
References
1. Australian Bureau of Statistics. Health conditions prevalence 2020-21 [Available from: abs.gov.au/ statistics/health/health-conditionsand-risks/health-conditionsprevalence/latest-release.
2. Australian Institute of Health and Welfare. Australia’s health 2022: in brief Canberra: AIHW; 2022 [Available from: aihw.gov. au/reports/australias-health/ australias-health-2022-in-brief.
3. Fetherston H, Craike M. Australia’s gender health tracker technical appendix.australian health policy collaboration: Mitchell Institute Victoria University 2020 [Available from: vu.edu.au/sites/default/ files/australias-gender-healthtracker-2020.pdf.
4. The Royal Australian College of General Practitioners. RACGP aged care clinical guide (Silver Book-part B) 2020 [Available from: racgp.org.au/clinicalresources/clinical-guidelines/ key-racgp-guidelines/view-allracgp-guidelines/silver-book/silverbook-part-b/collaboration-andmultidisciplinary-team-based-car.
5. Swerissen H, Duckett S, Moran G. Mapping primary care in Australia: Grattan Institute. 2018 [Available from: grattan.edu.au/ report/mapping-primary-care-inaustralia/
6. Mursa R, Patterson C, Halcomb
E. Men’s help seeking and engagement with general practice: an integrative review. Journal of Advanced Nursing. 2022;78(7):1938-53.
Australian men’s helpseeking and engaging
FOCUS Apr–Jun 2023 Volume 27, No. 11 47
Prostate cancer survivors living with sexual dysfunction and loneliness: A role

for nurses
By Chantal Hunter, Stephen Brown and Peter ‘Kevin’ O’Shaughnessy
Sexual dysfunction is the most common long-term adverse quality of life outcome following prostate cancer treatment.1–3 This impacts men, partners and their relationships.1–5
Australian men are living longer following their diagnosis and treatment of prostate cancer but not necessarily better.6-7 Healthcare professionals, including nurses, need to address the unmet needs of this population.2-6
Prostate cancer is the most reported cancer diagnosis for men in Australia.8 With each prostate cancer treatment choice, there are potential adverse outcomes. The two main adverse physical events are sexual dysfunction and urinary incontinence.3,5,9,10 These two adverse outcomes are common to all active treatment options and can potentially be lifelong, although symptoms are often reduced over time.10 These physical complications of prostate cancer
treatment can potentially lead to changes in masculinity and psychological status.3,11,12 Men often bottle up concerns and are unwilling to discuss them with others, leaving them feeling less masculine, vulnerable, and at risk of social isolation and loneliness.3,11,12
Social isolation and loneliness can lead to poor mental and physical health outcomes.13-14 Prostate cancer is mostly a disease of older males. Coyle & Duggan note the health risks associated with loneliness and social isolation are particularly severe for older adults.13 In Australia, a gender gap in loneliness exists across all ages and backgrounds.14-15 Men appear to be consistently lonelier than women from early adulthood to old age.14 Flood & Flood identified men’s social networks vary from women’s. There are differences in the number of social contacts, composition, homogeneity, geographic dispersion and frequency.14 Social isolation for men is modifiable. Thus there is an opportunity for creative programs and nurse-led interventions to foster social connections for older men.15
Prostate cancer survivors feel they can solve problems on their own, potentially excluding their significant others within the decision.16 This, in turn, can lead to changes in marital stress and relationship challenges.12,17 It is also common for men to feel like they are unable to communicate their concerns about the physical changes they are experiencing to their spouse or loved ones.5,12,17 Men can be apprehensive when seeking health-
related advice regarding sexual dysfunction due to cultural factors, embarrassment or threats to masculinity.18 The value of understanding psychological needs and providing appropriate psychological care is integral to supportive care in oncology.19 Men need guidance in understanding their own personal agency, improving their selfassessment, and accessing help.18,20
During COVID-19, social connections for vulnerable communities, such as older men, have been disrupted.21-22 Many older adults face barriers in understanding how to implement telehealth services, potentially leading to further isolation.23 Fortunately, community nurses have been identified as potential conduits to empower older adults regarding self-care in the time of COVID-19.24 Nurses have a unique patient–client relationship and are often in a position to identify prostate cancer survivors at risk. For example, those men who are vulnerable due to post-treatment side effects and provide counsel to these men and their families regarding these sensitive issues.
Authors
Chantal Hunter BN, RN, is a Registered Nurse in the Emergency Department at Lyell McEwin Hospital, Northern Adelaide Local Health Network, South Australia
Dr Stephen Brown MD Hon.BMSc, is a senior Registrar in the Emergency Department at Lyell McEwin Hospital, Northern Adelaide Local Health Network, South Australia
Dr Peter ‘Kevin’ O’Shaughnessy, PhD, BHSc (Hons), BN, RN, is a lecturer at the University of South Australia Clinical Health Sciences and is a member of the Rosemary Bryant AO Research Centre in South Australia
References
1. Litwin MS, Tan HJ. The diagnosis and treatment of prostate cancer: a review. Jama. 2017 Jun 27;317(24):2532-42.
2. Albaugh JA, Sufrin N, Lapin BR, Petkewicz J, Tenfelde S. Life after prostate cancer treatment: a mixed methods study of the experiences of men with sexual dysfunction and their partners. BMC urology. 2017 Dec;17(1):1-9.
3. O’Shaughnessy PK, Ireland C, Pelentsov L, Thomas LA, Esterman AJ. Impaired sexual function and prostate cancer: a mixed method investigation into the experiences of men and their partners. Journal of Clinical Nursing. 2013 Dec;22(2324):3492-502.
4. Wittmann D, Mehta A, McCaughan E, Faraday M, Duby A, Matthew A, Incrocci L, Burnett A, Nelson CJ, Elliott S, Koontz BF. Guidelines for sexual health care for prostate cancer patients: recommendations of an international panel. The Journal of Sexual Medicine. 2022 Oct 1.
5. O’Shaughnessy PK, Laws TA, Esterman AJ. The prostate cancer journey: results of an online survey of men and their partners. Cancer Nursing. 2015;38(1):E1-2.
6. Ralph N, Ng SK, Zajdlewicz L, Lepore SJ, Heathcote P, Kneebone A, Dunn JC, Chambers SK. Ten-year quality of life outcomes in men with prostate cancer. Psycho-oncology. 2020 Feb 1;29(2):444-9.
7. Chambers SK, Ng SK, Baade P, Aitken JF, Hyde MK, Wittert G, Frydenberg M, Dunn J. Trajectories of quality of life, life satisfaction, and psychological adjustment after prostate cancer. Psycho-oncology. 2017 Oct;26(10):1576-85.
FOCUS 48 Apr–Jun 2023 Volume 27, No. 11
8. Australian Institute of Health and Welfare. Cancer in Australia, Cancer series no 133. Canberra: AIHW; 2021 [cited 2023 Jan 13]. AIHW cat. no. CAN 144. Available from: aihw. gov.au/getmedia/0ea708eb-dd6e-4499-9080-1cc7b5990e64/ aihw-can-144.pdf.aspx?inline=true
9. Shabataev V, Saadat SH, Elterman DS. Management of erectile dysfunction and LUTS/incontinence: the two most common, long-term side effects of prostate cancer treatment. Can J Urol. 2020 Feb 1;27(Suppl 1):17-24.
10. Marzorati C, Monzani D, Mazzocco K, Pavan F, Cozzi G, De Cobelli O, Monturano M, Pravettoni G. Predicting trajectories of recovery in prostate cancer patients undergone Robot-Assisted Radical Prostatectomy (RARP). PLoS One. 2019 Apr 4;14(4):e0214682.
11. Ettridge KA, Bowden JA, Chambers SK, Smith DP, Murphy M, Evans SM, Roder D, Miller CL. “Prostate cancer is far more hidden”: Perceptions of stigma, social isolation and helpseeking among men with prostate cancer. European Journal of Cancer Care. 2018 Mar;27(2):e12790.
12. O’Shaughnessy PK, Laws TA, Esterman AJ. Love, faith and hope–a secondary analysis of prostate cancer survivors and their partners. Contemporary Nurse. 2015 May 4;50(23):149-68.
13. Coyle CE, Dugan E. Social isolation, loneliness and health among older adults. Journal of Aging and Health. 2012 Dec;24(8):1346-63
14. Flood M, Flood M. Mapping loneliness in Australia. Discussion Paper 76. Canberra: Australia Institute; 2005 Feb 28. Coyle CE, Dugan E. Social isolation, loneliness and health among older adults. Journal of Aging and Health. 2012 Dec;24(8):1346-63.
15. Franklin A, Barbosa Neves B, Hookway N, Patulny R, Tranter B, Jaworski K. Towards an understanding of loneliness among Australian men: gender cultures, embodied expression and the social bases of belonging. Journal of Sociology. 2019 Mar;55(1):124-43.
16. Manne SL, Kashy DA, Kissane D, Zaider T, Heckman CJ, Penedo FJ, Myers S. Relationship intimacy processes during treatment for couple-focused interventions for prostate cancer patients and their spouses. Journal of Psychosocial Oncology Research and Practice. 2019 Sep 1;1(2):e7.
17. Collaço N, Wagland R, Alexis O, Gavin A, Glaser A, Watson EK. The experiences and needs of couples affected by prostate cancer aged 65 and under: a qualitative study. Journal of Cancer Survivorship. 2021 Apr;15(2):358-66.
18. Hyde MK, Zajdlewicz L, Wootten AC, Nelson CJ, Lowe A, Dunn J, Chambers SK. Medical help-seeking for sexual concerns in prostate cancer survivors. Sexual Medicine. 2016 Mar 1;4(1):e7-17.
19. Grassi L, Watson M, IPOS Federation of Psycho-Oncology Societies’ co-authors. Psychosocial care in cancer: an overview of psychosocial programmes and national cancer plans of countries within the International Federation of Psycho-Oncology Societies. Psycho-oncology. 2012 Oct;21(10):1027-33.
20. Crawford-Williams F, March S, Goodwin BC, Ralph N, Galvao DA, Newton RU, Chambers SK, Dunn J. Interventions for prostate cancer survivorship: a systematic review of reviews. Psycho-oncology. 2018 Oct;27(10):2339-48.
21. Wilson-Genderson M, Heid AR, Cartwright F, Collins AL, Pruchno R. Change in loneliness experienced by older men and women living alone and with others at the onset of the COVID-19 pandemic. Research on Aging. 2022 May;44(56):369-81.
22. Rodrigues NG, Han CQ, Su Y, Klainin-Yobas P, Wu XV. Psychological impacts and online interventions of social isolation amongst older adults during COVID-19 pandemic: a scoping review. Journal of Advanced Nursing 2022 Mar;78(3):609-44.
23. James S, Ashley C, Williams A, Desborough J, Mcinnes S, Calma K, Mursa R, Stephen C, Halcomb EJ. Experiences of Australian primary healthcare nurses in using telehealth during COVID-19: a qualitative study. BMJ open. 2021 Aug 1;11(8):e049095.
24. Yi X, Jamil NA, Gaik IT, Fee LS. Community nursing services during the COVID-19 pandemic: the Singapore experience. British Journal of Community Nursing. 2020 Aug 2;25(8):390-5.
25. Collaço N, Wagland R, Alexis O, Gavin A, Glaser A, Watson EK. The experiences and needs of couples affected by prostate cancer aged 65 and under: a qualitative study. Journal of Cancer Survivorship. 2021 Apr;15(2):358-66.
Call to improve
airport
screening
for women wearing a breast prosthesis
Women wearing a breast prosthesis after a mastectomy are being insensitively treated during airport security screening, including being asked to remove their prosthesis, according to Breast Cancer Network Australia (BCNA).
The Network, which is Australia’s leading voice for those affected by breast cancer, has had more than 10 women contact its Helpline this year, distressed at their treatment.
The number of women who have had a similar experience but have not contacted BCNA is believed to be higher.
BCNA Director Policy, Advocacy & Support Services Vicki Durston has called on Australian airports to be aware of their obligations and to ensure staff know how to sensitively interact with travellers wearing a breast prosthesis following a mastectomy associated with breast cancer.
Airport staff should only conduct a pat down over a person’s clothes and never touch or remove a prosthesis. Travellers should be allowed to have the pat down in a private area and by an officer of the same gender.
Ms Durston welcomed training on breast prostheses and security screening processes delivered by Cancer Council ACT to security staff at Canberra Airport in November and calls on all airports to do the same.
In 2018 the Australian Government mandated airports across Australia move from metal detector scanners to full body scanners. Most major airports have already installed the new scanners.

The scanners detect foreign items worn on the body, under clothing. For people who have had a mastectomy, they have found that new scanners have picked up their breast prostheses. This requires them to undertake an additional secondary screening process, which may include a pat-down or screening using a handheld security device. Sue, who lives in Perth, had two bad experiences when she travelled from Perth to Melbourne and returned in October.
Leaving Perth, she was patted down in public and leaving Melbourne. She was also patted down in public and taken to a private room, where she was asked to remove her prosthesis.
“I was travelling alone and so distressed, I rang my husband. This was more than four years after my mastectomy and wearing a breast prosthesis – I can only imagine how much more traumatic it would be for women who are travelling only months after surgery and wearing a prosthesis,” Sue said.
“Although the staff were not blatantly rude, they seemed to lack sensitivity and compassion to my situation. It took me by surprise, and I didn’t know I could ask to be patted down in a private room, and they didn’t offer.”
BCNA is calling for all people travelling with breast prostheses to have their rights respected.
FOCUS Apr–Jun 2023 Volume 27, No. 11 49
Anal cancer: A women’s health issue
By Mary Hayes
Anal cancer is a rare disease affecting less than 1% of the world’s population each year.1
In Australia, rates among women are consistently higher than men since the first available case numbers in 1982.2
Well-known celebrities in the United States such as Marcia Cross and Farrah Fawcett have used their platforms to work towards destigmatising the disease for years. They have critically supported campaigns raising awareness about the human papillomavirus (HPV), a leading risk factor for the disease. Despite their efforts, anal cancer as a threat to women’s health remains unheard of to most.
In the clinical setting, anal cancer among women is often characterised by feelings of stigma and shame. Although the literature is scarce, some studies found that women felt socially isolated because of their disease and/or treatment.3 This has been shown to have subsequent impacts on psychosocial wellbeing amounting to increased suffering and loneliness.4
Despite high cure rates, patient-reported outcomes suggest that chemotherapy and radiotherapy contribute to life-long adverse consequences which negatively impact quality of life. 4,5
Symptoms affecting sexual interaction such as vaginal dryness, pain, and stenosis are increasingly common,6 threatening irreversible damage if left untreated. Healthcare professionals are disinclined to discuss these symptoms with their patients,5 while several studies found women significantly under-reported their symptoms.7 As a result, appropriate supports such as counselling, therapy, and medication, are not in place, posing a serious threat to the psychosexual wellbeing of females recovering from the disease.

Nurse-led research into the effects of anal cancer treatment on female sexuality and intimacy is about to get underway at St Vincent’s Hospital, Sydney. Female survivors of the disease will be offered the opportunity to share their experience and describe their sexual and intimacy concerns. Findings will be used to inform holistic and dignified supportive care pathways for women and will contribute to the global conversation focused on reducing the barriers and taboos around anal cancer.
Author
Mary Hayes Bachelor of Science in General Nursing (Hons.), Master of Science in Cancer and Haematology Nursing, PhD candidate is Medical Oncology Clinical Nurse Consultant at the The Kinghorn Cancer Centre, Darlinghurst, NSW Australia
References
1. Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics
2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71(3):209-49.
2. Australian Institute of Health and Welfare. Australian Cancer Incidence and Mortality (ACIM) books: Anal cancer. Canberra; 2021.
3. Canty J, Stabile C, Milli L, Seidel B, Goldfrank D, Carter J. Sexual Function in Women with Colorectal/ Anal Cancer. Sex Med Rev 2019;7(2):202-22.
4. Benedict C, Philip EJ, Baser RE, Carter J, Schuler TA, Jandorf L, et al. Body image and sexual function in women after treatment for anal and rectal cancer. Psycho-Oncology. Vol.25(3), 2016, pp. 316-323.; 2016.
5. Corrigan KL, Rooney MK, De B, Ludmir ED, Das P, Smith GL, et al. Patient-reported sexual function in long-term survivors of anal cancer treated with definitive intensity-modulated radiotherapy and concurrent chemotherapy. Pract Radiat Oncol. 2022.
6. Jensen PT, Froeding LP. Pelvic radiotherapy and sexual function in women. Translational Andrology and Urology. 2015;4(2):186-205.
7. Sterner A, Derwinger K, Staff C, Nilsson H, Angenete E. Quality of life in patients treated for anal carcinoma-a systematic literature review. International Journal of Colorectal Disease 2019;34(9):1517-28.w
FOCUS 50 Apr–Jun 2023 Volume 27, No. 11




MAKE YOUR IMPACT IN NURSING AND MIDWIFERY 3 Buffalo Court Berwick VIC info@safe-super.com.au INVEST IN YOUR FUTURE N V E S T S A F E L Y ACH OUT TO LEARN MORE Select 4-bedroom property investments are more stable and profitable than investments in shares. ( 0 3 ) 9 7 0 2 2 5 9 5 HIRING URSES C, & NT MAKE YOUR NEXT CAREER MOVE Why Choose Altaira? Opportunities for further career advancements Job security and free training 24/7 clinical support and family friendly culture Access to mental health and wellness initiatives
Long diagnostic delays in cases of endometriosis
Some cases of endometriosis in Australia take up to eight years to diagnose, prompting guidance for clinicians to increase awareness and avoid the long diagnostic delays that many women experience.

The report, ‘Endometriosis – easily missed’, details the research findings and guidance, and was published in the British Medical Journal (BMJ)
Endometriosis is a progressive, chronic condition where tissue that lines the uterus (the endometrium) grows in other parts of the body. This most commonly occurs in the pelvis and can affect other parts of the body.
The report revealed that the average worldwide diagnostic delay had been reported as seven years from when symptoms start to a definitive diagnosis, compared to eight years in the UK and Australia. Using a population-based survey in Australia in 2021, approximately 6.3% of women aged 40-44 have clinically confirmed endometriosis.
Further analysis in the UK showed that one-third of patients had consulted their GP six times or more before referral, with 39% having two or more gynaecological referrals before receiving a definitive diagnosis, with diagnostic delay even more common in adolescents.
The report offers new advice about specific questions to ask patients about their symptoms and how best to investigate them to confirm the diagnosis. However, the reports also recognises that the lack of a reliable non-invasive test for endometriosis and some patients’ reluctance or difficulty in reporting symptoms may contribute to delays in diagnosis.
“I am encouraging clinicians to ask their patients about painful periods and pelvic pain. Sometimes, the age of the patient influences what questions are asked, but these questions need to be asked no matter the age,” Professor Martha Hickey from the University of Melbourne, Department of Obstetrics and Gynaecology and the Royal Women’s Hospital is one of the authors of the report.
Professor Hickey also advises when clinicians should refer patients to specialised care.
The long-term consequences of endometriosis include poor quality of life, anxiety, depression, and self-harm.
“We know that delays in diagnosis can cause considerable suffering, distress, economic hardship and reduced workforce participation. Despite increased public awareness and clinical education, early recognition of endometriosis remains uncommon, and we need to listen to patients who are experiencing symptoms,” Professor Hickey said.
FOCUS 52 Apr–Jun 2023 Volume 27, No. 11
Program equips nurses to support sex assault survivors
An innovative online training program has helped prepare Queensland nurses and midwives to support survivors of sexual assault.
Developed in partnership between Queensland Health and CQUniversity, the Sexual Assault Nurse Examiner (SANE) microcredential program has trained nearly 100 nurses and midwives across regional Queensland, improving knowledge and skills to deliver care to directly responds to community demand for personcentred forensic examination following sexual assault.
Launched in April 2021, the training was thoroughly tested and scaled by CQUniversity’s Centre for Professional Development (CPD) and developed around person-centred care principles.
CQUniversity CPD Manager Deb Friel said the program’s success was mainly due to the hyperflexible format that accommodates nurses’ work routines and availability for study.
“The program has been carefully developed using a combination of asynchronous e-learning and a face-to-face workshop,” she said.
“After completing the online modules, nurses participate in a workshop with Queensland Health’s Senior Forensic Physicians to test their competence using simulated scenarios.
“CQU’s ongoing support and commitment to its industry partners and regions have ensured the success of this partnership, enabling nurses and midwives to provide more accessible healthcare for sexual assault survivors in their communities.”
“The co-designed program delivery showcases innovation via online learning, technology and co-design to work together to deliver better access to and quality of training supporting quality local jobs for regionally-based nurses and midwives, which in turn delivers better outcomes for Queensland by having this support service available regionally for victims of sexual assault.
“The SANE program has further flow-on effects advancing positive social outcomes for Queensland, via potential improvements to the extremely low rates of reporting of (and convictions for) sexual assault by providing better local support and forensic services needed to help regional victims report and gather evidence.”
It’s estimated that 75% of sexual assaults in Australia are never reported. In July 2019, Queensland Health introduced a process for adults who experience sexual assault to access a forensic examination without reporting to the police in case they decide to make a police report at a later time.

FOCUS
Men’s health
By Michael Whitehead
Men’s health simply refers to the state of physical, psychological and social wellbeing experienced by boys and men.1
Men’s health awareness within the international space has been steadily developing over the past few decades, with recognised organisations such as the Movember Foundation and the Men’s Shed movement progressing the unmet biopsychosocial needs of men. Men’s life expectancy is lower than those of females across every nation on Earth, with evidence supporting other contributing mortality factors separate from biology alone.2 The overall health and wellbeing of boys and men within Australia are comparable to other developed nations.3
However, there are biological and lifestyle issues that require purposeful attention. Within the Australian context, prostate cancer has surpassed breast cancer as the most diagnosed cancer,4 75% of suicides are men,5 men are more likely to be homeless6 and have a life expectancy approximately five years less than females.7 The most disadvantaged population group within Australia are Aboriginal and Torres Strait Islander men.8
Men, compared to women, have lower participation rates in preventative health initiatives (eg. National Bowel Cancer Screening Program) and attend fewer GP consultations. However, to assume that men are ambivalent about their health is presumptive. So, what low-cost strategies can health planners embed into practice that could positively affect change for boys and men.
START AT THE FRONT DOOR
An observational study examining health promotion in hospitals, general practice and community health waiting rooms revealed that only 3% of displayed health material was male-specific (compared to 15% for females).9 Gender, as a determinant of health, requires

promotional strategies that recognise differences in health responses by men and women.10 The purposeful allocation of readily available resources such as magazines, posters, and digital messaging that speaks to men’s health issues is achievable and requires minimal, or zero cost outlays. Beginning at the front door is a visible signal to men that their health needs have been considered and acknowledged.
APPLY A MEN’S-LENS
Research supports the view that men will participate in healthcare strategies when a gendered lens is applied.11 For example, a study in the UK reported that mental health programs that promoted male-positive values and language elicited greater levels of trust and engagement from male participants.12 Whilst acknowledging that men are diverse and not homogenous, broad approaches can be deployed that increase reach to boys and men. For example, if there is low engagement by men in particular outpatients’ settings (eg. diabetes clinic), or conversely, higher rates of men with a particular preventative condition, consider developing a male consumer engagement group (with clinicians) to inform practice on areas to strengthen service delivery. This approach is lowcost, with potentially high-yield results in both partnering with consumers and also shaping a nuanced, proactive men’slens direction to care.
Nurses are uniquely positioned to be champions and advocates for healthcare reform, social advocacy and new models of care. From its inception under Nightingale, nursing has progressed the development of evidence-based care and innovation in healthcare design.13 The delivery of targeted health initiatives to boys and men requires the nuance and dexterity that nursing retains within its existing workforce. The solutions to begin this re-focus in gendered healthcare delivery requires subtle changes that could impact healthcare engagement, behaviour and outcomes.
Author
Michael Whitehead RN, B. Nursing, M. Clinical Nursing, Grad. Cert. Clinical Redesign is Men’s Health Clinical Nurse Consultant at St Vincent’s Hospital Sydney, NSW Australia
FOCUS 54 Apr–Jun 2023 Volume 27, No. 11
References
1. Houman JJ, Eleswarapu SV, Mills JN. Current and future trends in men’s health clinics. Translational Andrology and Urology. 2020 Mar;9(Suppl 2):S116. ncbi.nlm.nih.gov/pmc/articles/PMC7108990/>.
1. Thornton J. WHO report shows that women outlive men worldwide. BMJ: British Medical Journal (Online). 2019 Apr 5;365.

2. Organisation for Economic Co-operation and Development. Health at a glance 2017: OECD indicators [Internet].
3. Australian Institute of Health and Welfare. 2022. Cancer in Australia. aihw.gov.au/reports/ australias-health/cancer>.
4. Australian Institute of Health and Welfare. 2022. Suicide and self-harm monitoring. aihw.gov.au/ suicide-self-harm-monitoring/data/suicide-selfharm-monitoring-data.
5. Australian Institute of Health and Welfare. 2021. Homelessness and homelessness services. aihw. gov.au/reports/australias-welfare/homelessnessand-homelessness-services>.
6. Australian Institute of Health and Welfare. 2022. Australia’s health 2022: in brief. aihw.gov.au/ reports/australias-health/australias-health-2022-inbrief/summary>.
7. Blashki G, Brown A. Indigenous male health disadvantage: linking the heart and mind. Australian Family Physician. 2005 Oct;34(10).
8. Whitehead M, Chok HN, Whitehead C, Luck L. Men’s health promotion in waiting rooms: an observational study. International Journal of Men’s Social and Community Health. 2021 Feb 10;4(1):e17-27.
9. Östlin P, Eckermann E, Mishra US, et al. Gender and health promotion: A multisectoral policy approach. Health Promot Int 2006;21(Suppl_1):25–35..
10. Oliffe JL, Rossnagel E, Kelly MT, Bottorff JL, Seaton C, Darroch F. Men’s health literacy: a review and recommendations. Health Promot Int. 2020 Oct;35(5):1037-51. ncbi.nlm.nih.gov/pmc/articles/ PMC7585483/>.
11. Robertson S, Gough B, Hanna E, Raine G, Robinson M, Seims A, White A. Successful mental health promotion with men: the evidence from ‘tacit knowledge’. Health Promot Int. 2018 Apr 1;33(2):334-44. academic.oup.com/heapro/ article/33/2/334/2555433? login=false>.
12. McEnroe N. Celebrating Florence Nightingale’s bicentenary. The Lancet. 2020 May 9;395(10235): 1475-8. ncbi.nlm.nih.gov/pmc/articles/ PMC7252134/>.
FOCUS Apr–Jun 2023 Volume 27, No. 11 55
Welcome to Healthy Eating
Each issue we will be featuring a recipe from Maggie Beer’s Foundation, which ensures research, education and training will lead to better outcomes and the delivery of nutritious and flavoursome meals to our ageing population in nursing homes. Maggie’s vision is not only to improve nutrition and wellbeing for the aged, but also for all who enjoy good wholesome food.

Loaded LCM bars
Packed with protein and so versatile, these loaded LCM bars are sure to be a hit.

Preparation 10 mins
Cooking 10 mins
Makes 16 slices
INGREDIENTS
1 1/3 cup Rice Bubbles
1/3 cup desiccated coconut
1/3 cup sunflower seeds
1/3 cup pepitas
1/3 cup sultanas
1/3 cup cranberries
1/3 cup dried peaches, chopped into thin strips
1/3 cup dark chocolate chips (min 70%)
1/2 cup hulled tahini
1/4 cup honey pinch of salt
METHOD
1. Preheat oven to 180°C.
2. Line a 20 cm x 20 cm tray with baking paper and set aside.
3. Combine all the dry ingredients except salt in a bowl and set aside.
4. In a saucepan on the stove, warm the honey until runny, then combine with the tahini and a pinch of salt.
5. Allow the sauce to cool for a few minutes.
6. Fold the wet and dry ingredients together until well combined.
7. Then with damp hands press into the prepared baking tray.
8. Place into the oven on 180°C for 8 to 12 min and bake until golden.
We invite you to try and make Maggie’s recipe. Send a photo of you and your creation from this issue, and in a sentence, let us know what you liked about It. If we pick your entry, we’ll publish it in the next ANMJ and reward you with a $50 Maggie Beer voucher. Send your entry to: healthyeating@anmf.org.au Angela Wylie, good job on making Maggie’s peaches stuffed with ginger and almonds, published last issue. We hope you enjoy your $50 Maggie Beer voucher.
“Thank you Maggie; these peaches stuffed with ginger and almonds were delicious! I baked them in my IXL wood oven ‘Cindy’, and swapped out the cream with yoghurt. My elderly mother will love these peaches, especially with the ginger surprise!” says Angela Wylie
9. Leave to cool in the baking tray and refrigerate for one hour before slicing.

HEALTHY EATING 56 Apr–Jun 2023 Volume 27, No. 11
Food styling and photo by Erika Budiman © instagram.com/pixels_and_paper_studio
If her iron is causing constipation, try the one more women are moving to.
Move to Maltofer
Maltofer contains iron as iron polymaltose. Healthcare professionals should review the full product information before recommending, which is available from Vifor Pharma on request. For more information visit maltofer.com.au


^Australia’s no.1 selling therapeutic oral iron IQVIA MAT October 2022.


*In a meta-analysis of 6 trials comparing Maltofer to ferrous sulfate in patients with iron deficiency, Maltofer resulted in significantly fewer incidents of upper digestive troubles, including nausea, diarrhoea, and constipation.1
†In a study comparing iron polymaltose with ferrous sulfate in iron deficient pregnant patients. n=80.2
References: 1. Toblli JE & Brignoli R. Arzneimittelforschung 2007;57:431–38. 2. Ortiz R et al. J Matern Fetal Neonatal Med 2011;24:1–6. 3. Jacobs P et al. Hematology 2000;5:77–83. Maltofer is for the treatment of iron deficiency in adults and adolescents where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate. For the prevention of iron deficiency in adults and adolescents determined by a medical practitioner to be at high-risk, where the use of ferrous iron supplements is not tolerated, or otherwise inappropriate. Maltofer® is a registered trademark of Vifor (International) Inc used under licence by Aspen Pharmacare Australia Pty Ltd. For medical and product enquiries, contact Vifor Pharma Medical Information on 1800 202 674. For sales and distribution enquiries, contact Aspen Pharmacare customer service on 1300 659 646. AU-MAL-1900004. November 2022.
Ferrous sulfate
Maltofer 2 Adapted from Ortiz R et al. 2011.2
Maltofer
23 % 2%
of patients of patients
restores iron levels with better treatment compliance and significantly fewer GI side effects vs. ferrous sulfate:*1-3 It’s the reason Maltofer has become Australia’s No.1 selling oral iron!^
Less constipation in pregnant women†2
ADVERTISING


























 Slip resistant oil/fuel liquids
Slip resistant oil/fuel liquids

























 By Chloe Horrabin
By Chloe Horrabin





















































 Natalie Dragon and Robert Fedele
Natalie Dragon and Robert Fedele































