A little bit of a problem
Annual Conference gets stuck in to the big issues for health

THE
THE MAGAZINE OF
ASSOCIATION OF SALARIED MEDICAL SPECIALISTS
Want to know more?
Find our latest resources and information on the ASMS website www.asms.org.nz or follow us on Facebook and Twitter.
Also look out for our ASMS Direct email updates.
This magazine is published by the Association of Salaried Medical Specialists and distributed by post and email to union members.
Executive Director: Sarah Dalton Magazine Editor: Andrew Chick Designer: Twofold
If you have any feedback on the magazine or contribution ideas, please get in touch at asms@asms.org.nz.
Prefer to read The Specialist online?
We have listened to your feedback and are aware that some members prefer not to receive hard copies of the magazine. If you want to opt out of the hard copy, just email asms@asms.org.nz and we can let you know via email when the next issue is available to read online.
ISSN (Print) 1174-9261
ISSN (Online) 2324-2787
The Specialist is produced with the generous support of MAS. The Specialist is printed on Forestry Stewardship Council® (FSC®) certified paper
issue
Inside this
ISSUE 133 | DECEMBER
03 Back and forth... 04 Tis the season... 05 Mind the gap 09 Five minutes with Liza Edmonds 10 Informed consent 12 “Savings” mean Dunedin’s going to pay 14 Annual Conference 2022 - better in person 16 Hitting the right note 18 Through the barriers 20 Never let the bullies grind you down 22 Working in an environment of resource constraints 25 South Canterbury first to take hard look at pay equity 25 "Too old to give up" 26 Research starting on fertility and doctors 26 In support of nurses 27 We can't rest 2 THE SPECIALIST | DECEMBER 2022
2022 Proposed position for FSC logo and text. Please align to bottom of this margin.
Back and forth…
Dr Julian Vyas | ASMS President

In May I described the DHBs’ convoluted approach to the MECA negotiations as a siege mentality. The last ever DHB MECA was signed by the employers on the 30th of June, three months after its stated term began which was, in turn, actually a whole year after the previous MECA had expired.
The next day Te Whatu Ora and Te Aka Whai Ora came into existence. The transitional provisions of the Pae Ora legislation moved our District Health Board members from working for 20 DHBs to having just one employer. With that came hope of an integrated, more equitable public health system, including more fair and equitable employment practises towards our members.
But, along with this optimism, was a realisation about the extreme complexity of integrating 20 DHBs into one organisation. As an example, across the DHBs’ financial systems, Te Whatu Ora identified 3.7 million unique cost codes that need consolidating.
For us, on the front line, decision-making that had happened locally in the past (however sub-optimally at times), became bogged down in disagreement about whether that authority now resided nationally, regionally or locally.
Again, the new national context helped us reach a nationally agreed winter rate for added SMO duties. Regrettably, the legacy of the DHB mindset meant that application of these rates at a local level was, at best, inconsistent. At its worst, some districts tried to pass the buck and/or skip out of their contractual obligations under the MECA entirely.
So, what of 2023?
When I emailed members before the indicative vote on the MECA this year I said we had “unfinished business.” For me that included two things in particular. The first is to make progress on fair and equitable shift work arrangements. Members will recall that the DHBs refused to even consider this in the MECA negotiations. ASMS has pursued - and achieved - pay improvement in several EDs. This work is still ongoing for other departments.
The second is to find a way to get out from under the Government’s unfair and provocative public sector pay restraint policy. Currently, we are some way from knowing if this will still be in place by the time we start bargaining. Electoral prospects and the wider political landscape will undoubtedly have an influence here too.
More broadly we must continue to work alongside Te Whatu Ora to help them “unlearn” the poor practises of the DHB era, and to develop an
organisational culture that enables them to be a better, more engaged employer. In November, I attended the first National JCC with Te Whatu Ora. I believe their national leadership team are genuinely looking for ways to make the system work better. At that meeting, we made it clear that long term recruitment strategies are important - but people “on the ground” are exhausted now. So we need Te Whatu Ora to find solutions now – not just offer tea and sympathy for how hard things are, and say “help is coming.”
“For us, on the front line, decisionmaking that had happened locally in the past, became bogged down in disagreement about whether that authority now resided nationally, regionally or locally.”
All districts have now had their first local JCC under the new system as well. Our plan is for at least two JCCs at a local level each year, and to then have interim “catch-up” meetings between a core group of industrial staff and local senior management. ASMS is consciously trying to change the tenor of the meetings to focus more on specific undertakings from local management, and to hold them to account for those commitments.
Lastly, as alluded to above, there will be a general election in 2023. The health system will undoubtedly be an election issue. A recent Ipsos poll found 33 per cent of New Zealanders think healthcare is one of the three most important issues currently facing the country. Only cost of living and housing were named more often.
What we really need from politicians is transparency about how much importance they really place on our public health system, including its workforce. That transparency is the foundation for a shared vision about how good our public health system can be. From that we can understand just what we can do to best help all our patients.
WWW.ASMS.ORG.NZ | THE SPECIALIST 3
Tis the season…
Sarah Dalton | Executive Director

On the day I wrote this column I also took domestic leave to support my mum. She was booked for day surgery for an eye problem. It was going so well - even down to finding a park - and she’d been handed her hospital bracelet, when…
Most of you can guess what happened. Her operation was cancelled to allow for an acute case.
It was fine – mum was even a bit relieved – and the booking clerk whose job it was to share the news was grateful we took it all in our stride.
But it also speaks to two key challenges within our health system - both of which featured heavily at this year’s Annual Conference.
The first is workforce. We don’t have enough clinicians out there – doctors, nurses, allied health staff. Or even support staff or IT liaison, let alone community-based aged residential care , GPs, dentists, midwives, or mental health workers.
It is a problem caused by active disinvestment in our health workforce. Inadequate funding over many years has been made worse by penny-pinching cultures, where balancing the books has trumped care for people (both staff and patients).
Te Whatu Ora’s arrival has now made it politically acceptable to admit to staffing shortages. Te Whatu Ora board members and senior staff all concede there are troubling gaps in our workforce. The Ministry of Health appears to agree. Perhaps this offers a tiny spark of hope.
“Te Whatu Ora’s arrival has now made it politically acceptable to admit to staffing shortages… perhaps this offers a tiny spark of hope.”
But troubling echoes of the old DHB cultures remain. Members still struggle to get basic entitlements and our industrial staff are busy supporting many services who continue to battle the ongoing culture of “no”.
I have met with district directors in various parts of the country, and I’ve been heartened they broadly agree we need a shift in attitude: to acknowledge people’s contribution, to listen first, to choose de-escalation
over aggressive HR-process-driven approaches. But there is much to do — and not enough resource to make rapid improvements.
There’s also a troubling tendency to fixate on overseastrained clinicians as the answer, while immigration processes remain swamped, unsympathetic and clunky; and everyone is aware Australia pays health workers a hell of a lot more than it appears NZ ever will.
I was talking to a group of psychiatry trainees earlier this week. Their diversity, passion and intelligence filled me with optimism. But they asked, quite reasonably, how can we continue to earn so much less than Australians, when both our Government and our employer know how stretched the international medical market is, and how hard it is to recruit?
The second key challenge is the larger question of what kind of health system we are prepared to fund? We commissioned Max Rashbrooke to write a discussion paper (available on our website) that tries to shape this critical question. Is it ok that we contribute so much less (as a proportion of GDP) than many other OECD countries? Can we keep pretending the current funding arrangements offer equitable access to care? Is designing a whole new health system without including how we fund it a tiny bit naïve?
While the coming year promises to be full of challenge, I hope that many of you will soon have a rest and some time to relax (and play) with whānau and friends. I am so grateful for your hard work and service to our communities over the last, very difficult, 12 months.
I would also like to thank the ASMS staff for their unstinting efforts on your behalves. They are a great crew and we are very lucky to have them. In particular, senior industrial officer, Lloyd Woods, begins his well-earned retirement in January. I know you have heaps of plans, Lloyd, and that you will have many projects on the go. Thank you, too, for all your years of hard work and service to Toi Mata Hauora, and to the union movement.
Ngā mihi o te Kirihimete me te Tau Hou.
4 THE SPECIALIST | DECEMBER 2022
Mind the gap
Matt Shand | Journalist
Christchurch City Council’s resistance to fluoridation is a case study in the ongoing battle for greater public dental health in Aotearoa New Zealand. How do gaps in political leadership lead to gaps in ratepayers’ wallets and their mouths?
Dentists say they used to be able to tell where a patient lived in Canterbury by their smile. Age groups who lived in areas where fluoride was added to the water had far less prominent dental decay and far fewer gaps.
Now Canterbury has been fluoride-free for many years and it is much harder to tell.
“We’ve normalised this idea of having bad teeth,” South Canterbury dentist Fraser Dunbar said.

Dunbar is at the front lines of the fight against dental decay in the Canterbury region, and it is a real fight. He works one day a week as a public dentist, where he sees an ever-growing parade of people unable to afford private dental care.
“It just breaks me. I could not do more than one day a week [at a public dental surgery],” he said.
“Most of the people I am giving full dental clearances [removing all their teeth] to are aged in their twenties and thirties.
“People gasp when I tell them that, but it is the reality of the state of our dental care system. They can’t afford to treat their teeth and they come to us when they get desperate.
“Every time I pull a tooth this pop of pus comes out. It feels good to be treating this patient but bad that they have been living this way.”
The Ministry of Health, under the direction of former director Dr Ashley Bloomfield, is directing councils to fluoridate their drinking water supplies in response to the growing health problems associated with bad teeth.
While some have started, Christchurch City Council has refused on the grounds it cannot afford to pay the estimated $55 million capital expenditure cost. This contrasts with the decision that it could afford an additional $150 million when the budget blew out on the $683 million Christchurch stadium project.
Councillors choosing not to spend money on dental care mirrors 40 per cent of New Zealanders who are unable to afford dental care due to its high cost. It will, however, further widen equity gaps for dental health. Those affected by the councillors’ decision will be at the lower end of the socio-economic scale where painkillers and denial are cheaper alternatives.
For most, dental intervention will only occur once pain becomes unbearable. A significant number will have to borrow money or go without some basic needs that week. In many cases, pliers will be reached for.

WWW.ASMS.ORG.NZ | THE SPECIALIST 5
“Frequently we are seeing more and more people turn up to emergency departments having pulled their teeth,” Dunbar said.
“They can have broken bits of teeth still in their gums. It’s devastating and depressing. It really hits you hard.”
New data produced by ASMS shows the private cost of dental care, for those who could afford it, was a staggering $896 million in 2021.
Canterbury residents contributed 12 per cent of that total with a spend of $108 million. The data is based on EFTPOS transactions and the national average per EFTPOS swipe at dental surgeries was $353 - about half the weekly pay of a person on the minimum wage.
Fluoride gap creates carious nights
Nights were the worst for Canterbury’s three-year-old Teuila (not her real name). Pain from her decayed teeth made sleep difficult, both for her and her family. Painkillers were used often to get her through but always the pain would return. She was referred to hospital dental services, like 8,605 other New Zealand children last year, requiring a general anaesthetic for dental health problems.
Canterbury saw 888 children put under for dental surgery last year, making up about 10 per cent of the national total. While costs are not easily recorded for these surgeries, it is estimated to be between $3,500 and $5,000 per procedure. This means Canterbury clocked up between $3.1 and $4.4 million last year in dental surgeries for children.
Going private was not a bill Teuila’s family could afford, so they had to wait. It took six months of sleep-deprived nights until Teuila would finally be able to rest easy after she made it through the clogged, public dental system. Teuila was lucky to receive assistance Navigators at E Tu Pasifika, a health provider, getting them access to dental care by making sure barriers, such as transport or other children, are taken care of.
“This child was in pain for six months before being seen,” Canterbury Dentist Tule Misa said.
“It’s not the hospital’s fault, they are doing all they can with what they have. Dental decay is preventable and we should make sure we prevent it before it reaches those stages that we need to treat under general anaesthesia.
“Oral health therapists are the main people working for community dental services treating children, which is great, but many of them are going to private practices because it pays better.
“After most oral health therapists graduate they come to work with the public health services for a year or two to build their confidence and competence and then leave to work in private practices.”
Misa says government needs to find a way to incentivise people to work within the public system. “With our dental care mostly privatised, and monetised, we need to find a way to incentivise people to work within the public system more, to keep good people here.”
Misa says part of the reason dentists leave public practices is due to working conditions. Some areas, like the West Coast, have no public dentists left to service the community. “I think we need to reward people for working in these
communities and providing basic health needs to rural communities,” she said.
Money gap speak volumes
Teeth are unique in our health system as they are treated separately. While healthcare is predominantly serviced by publicly funded organisations, nearly all dental work is performed by privately-owned dental practices in a user-pays model.

“We have a health care system, but our dental health care system is too disconnected from it,” Otago University Professor Jonathan Broadbent said.
“Oral health conditions have severe consequences for well-being, both physical and mental. We need good teeth in order to be healthy overall.”
Broadbent says dental health has not been taken seriously in New Zealand for a long time and, as a result, dental decay, and a culture of pulling teeth has become a norm again.
“WHO have just released their Global Oral Health Status Report, which calls for universal health coverage for oral health by 2030,” Broadbent said.
“The WHO report discusses how health conditions are treated like an expensive non-essential healthcare issue, but this should not be the case.
“We need universal coverage for basic oral health services – no New Zealander should have to experience dental pain or disfigurement and be unable to receive quality care”
Dental treatments can cost in the thousands of dollars should they get out of hand and there are only a few public ways to receive help in New Zealand
The first is a $300 grant from the Ministry of Social Development. The second is a Dental Treatment Advance from the Ministry, which needs to be repaid. The figure for the grant has not increased in 30 years but will be moving up to $1000 before the end of 2022.
Demonstrating the growing need for financial assistance is the fact that the amount granted for dental care by the Ministry has doubled in the past five years, from $23 million to $48 million per year.
Christchurch City had the second highest number of applications with 6,678 people seeking financial assistance last year.
6 THE SPECIALIST | DECEMBER 2022
Broadbent says we need to create rules about how the additional MSD money can be spent to ensure it is used efficiently.
“MSD should set a price list for what procedures cost and health providers should not refuse service to anyone seeking MSD-funded care,” he said.
“There is also a need for more salaried positions for junior dentists to work in the public sector to provide basic dental care services.
“This will help fill gaps in our healthcare system and allow people to visit the dental offices closest to them and be sure that these limited funds are being used in the most efficient way possible.”
Leadership and thinking gap
Earlier this year Christchurch City councillors voted not to pay a cent towards the price of fluoridating their water supply. Fluoridation has been a major debating point within council chambers around the country. Many councils breathed a sigh of relief when the decision to fluoridate was placed under the jurisdiction of the Ministry of Health.
Now the Ministry has decided fluoridation should go ahead and it is up to local government to follow central government’s directive.
Recently Christchurch City Councillor Pauline Cotter, who retained her seat by 16 votes, told Stuff.co.nz “Firstly [councillors] unanimously agreed that this is actually a health issue. So it’s not a city council issue, it’s a health issue, therefore the Ministry [of Health] should fund it.”
“Have they ever had a swollen face and been unable to sleep night after night or watched their children crying because their teeth are sore and there is nothing they can do?”
Juliet Gray
“And secondly, Christchurch, we’re quite different and special. I like to say we’re special because we have a multitude of wells and therefore it’s going to be very, very expensive.”
Funds have been made available by the Ministry of Health, but Christchurch’s estimate is more than five times the total that has been put aside.
Te Whatu Ora Waitaha dental public health specialist Martin Lee said the council cannot just shrug off its responsibilities to the government and the needs of its people.
“Fluoridation makes a big difference to the population of a city,” Lee said. “We’ve seen this time and time again and the science is very well proven now.
“I’m unsure why Christchurch thinks it can get off scotfree without any cost. The Council has been difficult to engage with and we have never managed to engage with the mayor on dental health over the last two decades.”
Tule Misa says, “It could make a world of difference. Fluoride helps everyone, it is an equitable treatment.”
Like many local authorities, Christchurch has adopted a Health in all Policies (HiAP) approach. Christchurch
has even gone further by establishing a regional HiAP partnership, where it has embedded health experts working alongside decisions makers. Though it is sometimes not immediately obvious, many policies made at a local council level have far reaching health implications, such as rubbish collection, housing zoning laws or alcohol policies.
“Councils play a big part in public health,” public health physician and co-lead of the Health in all Policies team in Christchurch Anna Stevenson said.
“However, they often don’t immediately recognise themselves as being big health players.
“We’ve been working with them to help grow understanding of the direct health outcomes and wider well-being of certain decisions and get them to understand their actions have public health responsibilities.”
The partnership, including Christchurch City and Te Whatu Ora Canterbury, has been running for 15 years to ensure future decisions factored in health outcomes.
“One example is the decision to improve air quality,” Stevenson said. “If you simply removed all the log burners you get cold people who will eventually get sick.
“Our team worked with ECan staff on a health impact assessment of the clean air policy. Two outcomes were the employment of healthy homes coordinators by ECan and the development of a low interest loan scheme ratepayers could use to access heating and insulation. This means we were able to improve air quality and ensure people were able to stay warm in their homes.
“It’s this change of thinking that allows for excellent health outcomes.”
Unfillable gaps in dental health
Gaps are growing when it comes to dental equity and decisions need to be made to ensure they do not widen further. Like everything, costs of dental care in the private sector are increasing year on year.
ASMS data shows a more than $185 million increase in spending at private dental facilities in the last five years, rising from $701 million in 2017 to $896 million in 2021.
With a privatised dental system there needs to be more incentive for dentists to pick up work in the public dental space.
Special care dental specialist Juliet Gray says the challenge with decision making around dental health is that most people making the decisions have not had to live with the consequences of or equity issues arising from poor health outcomes.
“Have they ever had a swollen face and been unable to sleep night after night or watched their children crying because their teeth are sore and there is nothing they can do?
“Every time I pull a tooth this pop of pus comes out. It feels good to be treating this patient but bad that they have been living this way.”
WWW.ASMS.ORG.NZ | THE SPECIALIST 7
Fraser Dunbar
“The people who make these decisions [about fluoridation and public dental funding] haven’t typically lived this life.”
There are other innovative solutions being considered in Christchurch. One is using school dental clinics after hours as walk-in clinics for adults after work. A similar idea has been employed in South Africa and has seen a big jump in dental equity. It works with dentists donating some of their time to public health and running a two-hour per week time for walk-ins.
In another, the University of Canterbury partnered with Ilam Dental and Moriarty Dental to offer 50 per cent subsidies for their students up to the value of $210. This service has been so popular it ran through its allotted funding well before the year was out.
The biggest gap to overcome remains funding. Public dentists require money. Fluoridation requires money. But as anyone who has been to the dentist after ignoring the pain for a while knows, you never really save money. You simply delay spending it and it often ends up costing more, financially and physically, in the long run.
Auckland City Mission knows 96 per cent of people needing their service have significant dental needs due to a lack of access to dental care.
They have taken steps towards meeting this need by setting up a dental clinic at their new HomeGround facility. But, as yet, they have been unable to find the funding to staff or equip it.
“Some reported to pulling their own teeth out with a wrench to remove a bad tooth causing severe pain,” Missioner – Manutaki Helen Robinson said.
“Others said they did not go to a dentist because they cannot afford it, while barriers to free dental services are hampered by a lack of transport and lengthy wait times.” So the room stands ready, missing only its chair and a dentist to staff it.
But, as brushing and flossing can prevent cavities, good public investment prevents decaying equity.

ASMS’ Tooth be told report uses treasury data to show that for each $1 invested in public access to dental care it should save $1.6 dollars in return. For each dental surgery
prevented by fluoridation or education resources, it is another $3,500 to $5,000 of public health money saved.
“It’s time somebody put on their big boy pants and made this a cross-party, political issue,” Fraser Dunbar said. “Whatever colour your tie is you should know people suffering is not good politics. We need more public dentists. It’s common sense really.”
ASMS has released the Tooth be told report which makes the case for universal dental care in New Zealand. Forty-two per cent of New Zealanders report having unmet dental need. Predictably the proportion rises with socio-economic deprivation. Publicly funded dental hospitalisations have risen by a third in the last decade. The report marks the beginning of a campaign seeking political commitments to greater public funding of dental.
The key recommendations include:
1. Extending subsidised basic dental care for children to adults. 2. Urgently developing a workforce plan which includes strategies to ensure services are fairly distributed nationally. 3. Make options available for dentists to be employed on salary as part of the public health system. 4. Increase the oral health learning component in the medical curricula. 5. Routinely collect and report data on the state of dental health 6. Fully implement recommendations from the 2019 Welfare Expert Advisory Group.
8 THE SPECIALIST | DECEMBER 2022
with Liza Edmonds FIVE MINUTES
Liza Edmonds is a paediatrician working in Dunedin. She is also Southern branch Vice-President and has been closely involved in developing ASMS' Te Roopū Māori.
What inspired you to get into your field of medicine?
My whānau and the whānau I care for alongside the child health teams I work with. I just fitted in, and the holistic medicine provided was what I believe might make a difference.

What are some of the challenging aspects of your job?
The sheer volume of mahi to be done can feel almost overwhelming, especially when it feels like nothing is changing. Alongside racism (in its various forms) –that adds to the challenge and how you address and deconstruct this within the health environment is a huge challenge.
What do you find rewarding about your job?
The whānau I care for and get to meet provide us with so much aroha and I always learn so much from them. It makes me smile as they often feel we give them so much and rather they give us so much. It’s such a privilege.
What do you see as the biggest challenge facing the health system?
I think the major structural changes have such great potential, to change a system that only privileges some (based on health outcomes) and instead redistribute health care to the greatest need. However, this will require resourcing and some real bravery to make these changes. Will we be brave enough?
What keeps you happy outside of work?
My whānau keep me happy, they ground me, keep me in line and remind me of what I really value in life.
Why did you become involved in ASMS?
I believe that ASMS is well placed to support our mahi. It is a challenging environment and the foundations they provide allow us to do the mahi and advocate for our teams and whānau.
WWW.ASMS.ORG.NZ | THE SPECIALIST 9
The whānau I care for and get to meet provide us with so much aroha and I always learn so much from them.

10 THE SPECIALIST | DECEMBER 2022
Health and Disability Commissioner Morag McDowell
Informed consent
Matt Shand | Journalist

Since her appointment in late 2020, Commissioner Morag McDowell has seen a steady rise in the Health and Disability Commission’s public profile. That is bringing more issues to their attention.
Complaints to the Health and Disability Commissioner are on the increase with a 25 per cent rise in complaints over the last 12 months and a 14 per cent increase in 2021.
Commissioner Morag McDowell says one of the common reasons medical professionals can find themselves subject to a complaint is when there is a breakdown of informed consent between patient and practitioner.
“Informed consent is very much at the heart of the Code of Health and Disability Services Consumers’ Rights,” McDowell said. “It forms about 15 per cent of our complaints and that number has remained steady over the years.
“It is important to think about informed consent as a process rather than a tick box. It is the right to make an informed choice to give informed consent and that consent must be freely given. It is the right to receive reasonable information and have that communicated effectively.”
“Communication regarding health information can be complex, so does require consideration of how this is being heard. Communication can be more challenging for providers when engaging with people who are distressed, who have difficulties processing information or who are from different cultures or speak different languages. So additional considerations need to be taken into account.
“Practitioners need to be attuned to signs a person may not be understanding,” she said.
“A good process is to ask the patient to explain back to you what it is they understood about the information they have been given.
“Consent is an interactive process and it’s not a single moment in time. There needs to be ongoing discussions if things change.”
To assist people in their understanding of informed consent the HDC launched an e-learning module on November 17, Aotearoa Patient Safety Day, to provide education resources and methods to ensure effective communication.
The three modules cover topics such as understanding the purpose of the Code, applying it to practice, ensuring informed consent is gained, and understanding the right to complain. Each module can be completed in about 30 minutes.
“Understanding responsibilities under the Code helps improve the quality of care and avoids complaints,” McDowell said.
“I do acknowledge the stress that being on the receiving end of a complaint can cause.”
The HDC is looking into its processes in a bid to make the complaints process more people centric, both for consumers and for providers.
Resolving complaints in a timely manner is also a key priority. “Last year we managed to close 71 per cent of complaints within three months, 78 per cent within six months and 87 per cent within 12 months.
“Complaints can be serious and highly complex," she said. There are often multiple providers, and we need to gather clinical notes and other information.
“We are focused on fairness in our process and ensure the provider and consumer have the opportunity to be heard. Sometimes in the case of an investigation this process can take time to resolve sometimes more than two years.”
“Early resolution is the best resolution. Robust internal practices can prevent complaints making it to us in the first place, as the consumer has their needs met.”
With the healthcare system becoming overstretched and under resourced there is more pressure on the health workforce. McDowell says her office factors in this additional pressure when ruling on cases and looks for systemic issues that can be resolved.
“We have a wide jurisdiction,” she said. “We can look at systemic issues and use our data to raise concerns immediately. If we are seeing, for example, a group of complaints coming from a particular service we can go to Te Whatu Ora to ask what is going on.
“If it is a matter of concern, we can escalate that immediately.” McDowell says the best course of action for people who find themselves on the receiving end of a complaint is to treat it as a chance to learn and look for opportunities for early resolution.
“Early resolution is the best resolution,” she said. “Robust internal practices can prevent complaints making it to us in the first place, as the consumer has their needs met. It’s good for a provider to identify what concerns the consumer has and take the action needed. If it can be managed, then it is more effective than waiting months or years for resolution.
“Most complainants want what happened to them to not happen to someone else. Look at what remedial options you can put in place to address the issue at hand. If it escalates to a formal process, it is important to engage with requests for information and seek professional personal support if you need it.”
WWW.ASMS.ORG.NZ | THE SPECIALIST 11
“Savings” mean Dunedin’s going to pay
Matt Shand | Journalist

Plans to shave $100 million off the price tag of the $1.4 billion New Dunedin Hospital (NDH) project put the entire project at risk of failure and represent a “broken promise” to the community.

Several months ago people involved in the four-year project to plan the New Dunedin Hospital were told to trim $100 million from the budget. Now a report from Te Whatu Ora Southern has revealed doing so will result in “significant reputational, operational and clinical risk.”
The proposed cuts and changes are known as Option 4.2. A 50-page report written by Te Whatu Ora Southern concluded Option 4.2 had potential risks still yet unidentified.
The report said, “Any change in the size or scope of NDH, and any demand for significant redesign with accompanying consultant costs and demands on clinical staff’s time, will have a widespread negative effect on
the reputation and expectations of the NDH project and facility.”
Another passage referenced the proposed changes as a “broken promise” to the community and a reputational risk for the Minister of Health.
Most of the proposed cuts come from clinical services. These include inpatient, surgical and mental health beds, operating theatres, workspaces for doctors, the PET-CT scanner and pathology services.
“Everyone is frustrated,” ASMS Southern Industrial Officer Kris Smith says.
12 THE SPECIALIST | DECEMBER 2022
“The delivery of the new hospital has been promised for years. Then there was nothing. Then there were plans and more plans and failed promises.”
Smith says changes to the hospital may save on capital costs but will inflate operational costs, as staff must work around poor design.
“Staff are concerned oncology will not be included in the new building,” she said. “Someone receiving cancer treatment will need to be taken from that building, transferred in an ambulance with a nurse alongside them, and brought to radiology for treatment.
“The costs of doing so, and returning the patient, will balloon out.”
Former elected Southern District Health Board member Dr John Chambers was aware, towards the end of his board tenure, pressure was being put on to make significant savings in the project but understood that efforts would be made to ensure that these did not involve clinical areas.
"Early in the planning process there had already been a process of reducing the number of beds,” he said.
“The reasoning for this was that ‘new models of care’ would develop, shifting elements of secondary care into the primary sector/community. Perhaps basing future calculations on carrying on with ‘business as usual’ could result in oversizing the new hospital."
Chambers considered this approach is not evidencebased and at best wishful thinking.
"To propose making cuts to the clinical area of NDH would surely be false economy and lead to problems of service delivery,” he said.
“It is not surprising that clinical leaders have questioned such a proposal.

"The NDH is not planned to replace all services in 2028. For example, the current cancer treatment facility will not be replaced for another few years which might surprise the public."
"A very current issue is the difficulty of meeting acute demand while continuing to provide elective procedures and surgery in the same building/theatre suite."
Chambers calls for the building of a sperate planed procedure hospital on the Wakari site. It is of note
that one of the 101 recommendations (number 100 on the list) of the recent Connolly report on addressing waiting lists was to consider developing separate elective facilities."
Smith says there is real concern the costs involved in attempting to save the $100 million could cost more than the cut savings.
“Those costs will include architect’s fees, workshopping sessions, staff time and changes to construction prices,” Smith said.
“It also creates a loss in terms of the opportunity cost of the previous four years work setting the model of care and design fine tuning from clinical staff. They did all that work and we understand staff were largely happy with the proposal. To have that changed in the last few months seems improper.”
There are concerns Option 4.2 will ‘take the heart’ out of the hospital and the removal of 35 beds will mean the hospital can only cater for acute cases instead of elective cases.
“Patients will likely have their surgeries delayed and will eventually present as an acute when things worsen,” Smith said.
We need to leave the design the way it is and find a way to locate the money.
“Any savings will be gone in a few years as operational costs increase.”
ASMS shared the report and concerns about the NDH project with Te Whatu Ora CEO Margie Apa.
ASMS executive director Sarah Dalton said the people of Dunedin deserve to have a hospital that is fit for purpose and will serve the needs of the communities, now and into the future.

“Any savings will be gone in a few years as operational costs increase.”
the doctors and nurses who will work in the new facility deserve the best workplace we can provide. With health resources already stretched thin we need the hospital design to cater to the needs of staff and patients - not work against them.
“There is a real risk the new hospital will not be fit for purpose. I urge Te Whatu Ora to stick with the original plan.”
“Likewise,
"To propose making cuts to the clinical area of NDH would surely be false economy and lead to problems of service delivery.”
Dr John Chambers
“Someone receiving cancer treatment will need to be taken from that building, transferred in an ambulance with a nurse alongside them, and brought to radiology for treatment.”
WWW.ASMS.ORG.NZ | THE SPECIALIST 13
Kris Smith
Annual Conference 2022 – better in person
A commitment to greater representation for Māori was made at the 34th ASMS Annual Conference held in Wellington, November 24-25.


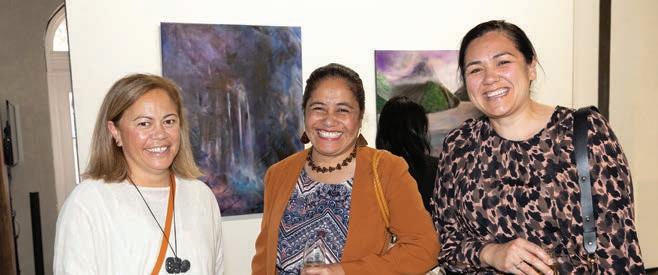



Two remits that will see changes made to ASMS’ constitution. The first sees a commitment to Te Tiriti o Waitangi and Mātauranga Māori added to the Association’s objectives. The second enables two members to represent the Association’s Māori membership on National Executive. Both received more than the 70 per cent support required, and work will begin to undertake a membership consultation about the consequent changes to the Constitution.
“The constitutional remits signal an exciting next step for Toi Mata Hauora,” Executive Director Sarah Dalton said. “There will be an ongoing consultation process with members about the constitutional changes leading up to next year’s Conference.”

More than 150 members attended Conference, with many having questions for Minister of Health Andrew Little who addressed the room on day two.

Tanya Wilton outlined the “insane” conditions staff were working in at Hutt Hospital and said the workforce is at “breaking point”.
He was told about 10-hour waits in emergency departments, patients piling up in corridors waiting for treatment and ambulances unable to unload due to wait times.

Little was asked when the Government will admit the healthcare system is in a crisis but refused to label it as such and pointed to the lack of long-term workforce planning as a key factor behind the issues.
“It’s pretty evident, if there was workforce planning, it wasn’t done well,” he said.
“I repeatedly acknowledge the incredibly challenging circumstances that we’re in. The challenge for me is to work with the people I work alongside to address those challenges and find fixes to the problems.”
Given the popularity of this year’s event, ASMS is looking at securing a larger venue for Annual Conference in 2023.
14 THE SPECIALIST | DECEMBER 2022
A medical expression

The second annual doctors and dentists’ art exhibition took place to coincide with ASMS' Annual Conference. With $10,000 in prizes up for grabs, Best Overall Artwork was won by Counties Manukau anaesthetist Catherine Francis for her photorealistic work Wings and Water. Francis admitted to feeling “a bit shaky” when she got the phone call saying she’d won.







Tauranga psychologist Bronwyn Copeland picked up Best Artwork for a First Time Exhibitor for Castle Rock Pointillism and shared the People’s Choice prize for Fly Away Masks (pictured) - a work constructed from N95 surgical masks. “Last year I chickened out,’ said Copeland. “So this year I challenged myself”.
 Bronwyn Copeland
Bronwyn Copeland
WWW.ASMS.ORG.NZ | THE SPECIALIST 15
A close-up of Wings and Water by Catherine Francis
Hitting the right note
Matt Shand | Journalist

For the past 11 years Tim Wilkinson has been organising the New Zealand Doctors Orchestra, putting on concerts across New Zealand and giving doctors a much-needed creative outlet and a chance to swap medical instruments for musical ones.
“I play the double bass, my wife Lynette plays the violin, and our son Tom plays the trumpet,” Tim said.
“We started the New Zealand Doctors Orchestra after being part of the Christchurch Artist Doctor Concert and wanted to see if there were enough players across New Zealand.
“It turns out a lot of doctors are very talented musicians. Our soloist this year, Louise Webster, won a national concerto competition. We have a mix of those that played professionally before becoming doctors and some that played a long time ago and want to pick it up again.”
The Orchestra's first concert was held in Nelson and it sold out with all proceeds going to the local hospice. Since then, they have travelled around the country putting on shows once a year and raised more than $61,000 in donations for various hospice around New Zealand.
 The Wilkinsons are a family of doctors who have orchestrated their love of music into a symphony of healing sound for New Zealand.
Left to right: Tim, Lynette and Tom Wilkinson
The Wilkinsons are a family of doctors who have orchestrated their love of music into a symphony of healing sound for New Zealand.
Left to right: Tim, Lynette and Tom Wilkinson
16 THE SPECIALIST | DECEMBER 2022
The logistics of organising 60 to 70 musicians every year and a time when everyone’s schedules will be free is a challenge for Tim. He combats this by doing the rehearsal, the conducting and concert all on one weekend of the year.

“We look for a space with good rehearsal facilities and work around that,” Tim said. “It’s hard, as we must select the orchestra and we have started to have a bit of a wait list. We’re lucky in that people self-select when they are available, and everyone knows we give priority to those that missed out last year.
“The music breaks down barriers between people and helps remove some of the hierarchy from our profession. We can have medical students playing next to senior surgeons and sharing knowledge.”
“We meet up one weekend, begin practicing immediately with the conductor, have a dinner on the Saturday night and put the concert on Sunday afternoon. It’s always great to see the mix of people attending. It gives people a nudge to play instruments again and meet people they didn’t know before.”
Lynette says the “crazy idea of Tim’s” swept the whole family along with it but their passion for music is shared by many in the medical profession and it is needed to help cope with the day-to-day stresses of the job.
“I picked up my violin again in my forties,” she said. “I guess I needed something creative and something completely different to medicine. I think it was for my personal wellbeing and work-life balance. Music is an important gateway for that.
“I look forward to meeting people at the weekend practices and old friends who have been coming along for years. It’s great to have this shared purpose
Doctor’s Orchestra in 2023
and most people are too busy to talk shop. It’s all about music.
“The music breaks down barriers between people and helps remove some of the hierarchy from our profession. We can have medical students playing next to senior surgeons and sharing knowledge. We are all working together to achieve the same goal."
Harpist Vanessa Souter says the orchestra is a great way for doctors to support other doctors.
Souter had a lengthy career as a professional harpist in Australia before studying medicine. She has played the harp for more than 40 years now. She was inspired to study medicine by her late husband.
“Music is a powerful thing,” she said. “It expresses emotions and connects us all. As doctors we all see a particular amount of grief and we deal with people suffering. You need a creative outlet and a way to ground yourself. At a time when New Zealand doctors are doing it tough it is great to be able to look forward to and rehearse for the concert. Everyone plays together and, when playing music, if you make a mistake no one dies.
“Tim is a bit of a legend for organising us all and giving us that.”
In 2023 the NZDO will be in New Plymouth 20-23 July, 2023. Mark Hodgkinson will be the conductor and the repertoire will include Shostakovich’s Symphony No 5. Organisers are adding an extra day for rehearsals (so, starting on the Thursday) to allow more time to work on the symphony. Enrolments open in February. If you are interested in finding out more visit www.nzdo.org.nz or email enquiries@nzdo.org.nz

WWW.ASMS.ORG.NZ | THE SPECIALIST 17
Through the barriers
Matt Shand | Journalist
Doctors and specialists listening to disabled people will play a critical role in ensuring quality of life and equity for disabled people and whānau, newly appointed chief executive of Whaikaha Paula Tesoriero says.
Her success on the bike as a Paralympian, winning gold in the 2008 Beijing games, is matched by success in the legal sector and now the public sector - becoming the first person who identifies as a disabled person to be appointed as a chief executive for a public service agency in New Zealand.
“At a full chief executive meeting last week, I did sit there and realise the significance of having a disabled person at the table along with the others responsible for delivering public services to New Zealand,” she said.

“It really crystallised to me the importance of Whaikaha in implementing change across this level of government.
“It’s significant to me personally but it’s significant for our entire community. We have this entity and role now to transform and make the changes many people with disabilities have been fighting for.”
Whaikaha is a new ministry with a difficult task ahead of it. Coinciding with the recent reforms to the health system, Whaikaha aims to remove the barriers that prevent disabled people and their whānau from achieving ordinary life outcomes.
Previously, a fragmented approach with multiple eligibility criteria for different services with different agencies has made the system difficult to navigate and services hard to access.
Top of Whaikaha’s mandate is removing traditional barriers that have blocked access or locked people out from accessing support. Tesoriero says disabled people have been calling for changes and improvements in the areas of education and access to health for a long time now.
“Disabled people face different access barriers,” she says. “There are barriers around cost, around transport and to quality of health care as a result.”
“The New Zealand Health Survey really crystallises information about these barriers. Things like 16 per cent of disabled adults have not visited a GP - which is twice the number of non-disabled adults.”
Tesoriero says another major barrier is a lack of understanding and empathy towards a person’s disability from medical professionals.
“No one really knows their impairment better than a disabled person themselves,” she said.
“It’s important to listen, to respect disabled people when they talk about the effect on them. This has a real impact. The stories I have heard when things have not gone well stem from a perceived idea about the impact an impairment has on a person’s life.
“Taking the time to listen is where I have seen things flourish. Medical professionals have to set out to understand the individual and try to support them getting access to a wide range of things they need.
“Doctors and the medical profession have a huge role to play and can be wonderful allies.”
A key change Whaikaha advocates for, is giving disabled people greater say in how services are provided to them.
“Instead of deciding how it will be done, we will work with people to ask what help they believe will make a difference and find ways to help fund that,” Tesoriero said.
“Many, many disabled people have fought for the development of our agency and we’re finally here and we have a lot of work to do building the organisation and starting to deliver some change.”
Inaugural chief executive of the new Whaikaha - Ministry of Disabled People Paula Tesoriero shares insight into the new agency and the significance of her appointment.
“Many, many disabled people have fought for the development of our agency and we’re finally here and we have a lot of work to do building the organisation and starting to deliver some change.”
18 THE SPECIALIST | DECEMBER 2022

WWW.ASMS.ORG.NZ | THE SPECIALIST 19
Chief Executive of Whaikaha - Ministry of Disabled People Paula Tesoriero
Never let the bullies grind you down
Matt Shand | Journalist

After 50 years in the unions, 14 of them at ASMS, Senior

January leaving behind an anti-bullying legacy.
Exactly 14 years to the day of walking into ASMS' offices to start work as an industrial officer, Lloyd Woods will be walking out for the last time and retiring from a lifetime of union work.
“I like things to be neat and tidy,” he said about the timing. “It seemed right.”
Lloyd has spent much of his working life involved in the union movement, starting as a delegate at a glass factory before working at a polytechnic and becoming involved in the Association of Staff in Tertiary Education (ASTE) when he was teaching automotive engineering.
“I eventually became Vice President of that union and then President from 2003 to 2007,” he said.
This long history in union positions opened doors for Lloyd to take up a role at ASMS.
“It was a bit different as I did not have a law degree which was the previous standard for industrial officers. I did have a lot of experience and had worked at a national level.
“I have always described this work as being on the side of the angels. That is not to say the employers are devils, but it is work towards the good and it is important.
“Doctors are humans and can make mistakes. I always view us as guardians of the process. It is not for us to determine guilt, assess a medico-legal issue or defend the indefensible, just to make sure the process is fair throughout.”
Bullying prevention is a particular focus for Lloyd.
“I’ve had a horror of it since I was a kid, while I never really suffered from it, it’s not something I put up with and I really hate it,” he said.
Industrial Officer Lloyd Woods is retiring in
20 THE SPECIALIST | DECEMBER 2022
Lloyd Woods will retire after 14 years at ASMS
“I have always described this work as being on the side of the angels. That is not to say the employers are devils, but it is work towards the good and it is important."
“Growing up with parents from Liverpool we had strong accents which required some speech training to resolve. I remember being bullied over that a little bit, but I stood up to every kid that gave it and I would not put up with it.
“All my years in unions have been to ensure people are given a fair go, not subject to bullying, and I remember those lessons from my childhood.”
Along with Deborah Powell from the New Zealand Residents Doctors Association, Lloyd was involved in an anti-bullying taskforce.
“I think we can both claim we got the ball rolling on that front,” Lloyd said.
“We still have issues with doctors being bullied as well as allegations against doctors. When you look at the training of doctors its still very much an apprenticeship model. The whole idea of a senior doctor yelling at a registrar was not unknown and, given many people teach the way
they were taught, certainly this went through the ranks in the past. But this is no longer acceptable. It required a cultural change.”
Over the past 14 years he has seen changes at ASMS first hand. “We used to only have 3,500 members and there were just two industrial officers plus Henry Stubbs as senior. We have recruited heavily since then.
“The other change is the number of non-DHB doctors getting collective agreements through our services. Former Deputy Executive Director Angela Belich got this going and handed the baton to me about 12 years ago. I think I can claim to have made a difference through my non-DHB work. It is a green field for our union.”
“We now have 22, soon to be 25, collective employment agreements covering doctors throughout New Zealand working outside of what is now Te Whatu Ora."
After 50 years in the workforce, Lloyd says he is looking forward to retirement. “I am not going to miss working. I have done 50 years of it. But I will miss the colleagues and people I have met and helped along the way. I intend to keep up with people wherever I can and my partner Sheryl and I will host our annual barbecue with all invited.
“It’s been a privilege to work with our members who are an extraordinary group of people. I now look forward to spending more time with my grandkids.”

WWW.ASMS.ORG.NZ | THE SPECIALIST 21
Spending time with family, and the project car, are Lloyd's retirement goals
Working in an environment of resource constraints
Dr Lucy Gibberd | Medicolegal Consultant at Medical Protection

What are some of the medicolegal implications for individual medical specialists working in an environment of significant workforce and resource shortages?
It’s 5 pm in a rural hospital emergency department and you are due to finish your shift, but the roster is blank for the next shift and no one has come to replace you and there are five patients in the waiting room.
You have 42 acute medical in-patients under your care and you are worried that you are not on top of what is happening with all of them.
You have been asked to ‘cull’ the outpatient waiting list based on the initial referrals letter which the GPs sent more than 6 months ago – you are worried that you will miss someone who may have cancer.”
Over the past few months, the Medical Protection advice line has received many calls like these from doctors who are concerned about their medicolegal risk when working in areas of resource constraint. Common scenarios include hospitals where the workload exceeds the capacity of the doctors available, being asked to triage patients who need care but who are not offered timely appointments, covering for colleagues, where the clinician may be acting on the edge of their scope, and the ever-increasing paperwork burden.
Where the care of patients may be compromised by resource constraints, doctors feel vulnerable as they are worried that they will ultimately be held responsible when things go wrong. These concerns are not unreasonable, although the professional standard you should be held to, should only be that of any of your peers in the same circumstances.
The Health and Disability Commissioner (HDC) is charged with upholding the Consumers Code of Rights, but in so doing the Commissioner is obliged to take into account the circumstances in which the care was provided:
Code of Health and Disability Services Consumers' Rights - Provider compliance
(1) A provider is not in breach of this Code if the provider has taken reasonable actions in the circumstances to give effect to the rights, and comply with the duties, in this Code.
(2) The onus is on the provider to prove that it took reasonable actions.
(3) For the purposes of this clause, the circumstances means all the relevant circumstances, including the consumer's clinical circumstances and the provider's resource constraints.”
Considering the above, the question is what would be considered ‘reasonable actions’ and how can you prove that you took them? The Medical Council of New Zealand’s statement on Safe practice in an environment of resource limitation lays out the professional standards that doctors will be held to, should there be a criticism about their professional conduct. I would urge clinicians to read this statement in full, but its essence is that resources should be allocated in an equitable, and sustainable way, upholding the best interests of the whole community. It outlines that any decisions made about resource allocation should be transparent and your reasoning should be well documented. The statement also advises:
“If you are unable to provide services that are safe for yourself and your patients, you should bring your concerns to the attention of the management in your workplace or your Primary Health Organisation (PHO), and should seek advice from an appropriate agency such as a peer, your College, specialty societies, New Zealand Resident Doctors’ Association, Association of Salaried Medical Specialists, the Rural GP Network, or your medical indemnity insurer.”
This last point is particularly important, because if you raise those concerns with your employer by email, you will then have an email trail which can be used as proof that you took reasonable actions to address the concern (as required by the HDC).
22 THE SPECIALIST | DECEMBER 2022
ASMS membership adds another dimension to addressing resource constraints
The issues raised in this article are primarily considered from a specific medicolegal perspective. But that is only part of the story - and the solutionfor ASMS members.
•
If you feel you are being systematically limited in the quality of care you can provide, the ASMS MECA provides a number of contractual provisions to support you:
• An SMO’s hours of work and job size must “be mutually agreed and shall objectively reflect the requirements of the service and the time reasonably required for the employee to complete their agreed duties and responsibilities, as set out in their job description.” – Clause 13
• The employer must “take reasonable and timely steps to fill actual vacancies… including vacancies or gaps on after-hours call rosters, as soon as they occur or are reasonably foreseen, except where the employer and affected employees reach agreement over satisfactory alternative arrangements.” – Clause 47

• Where a locum cannot be sourced “alternative arrangements for service delivery shall be made and/or appropriate compensation for increased workload or work pressure shall be negotiated with the employee(s) affected”. – Clause 47
• “Managers will support employees to provide leadership in service design, configuration and best practice service delivery.” – Clause 2
“In particular the employer undertakes to be a good employer and will provide the resources and support reasonably necessary to enable the employees to discharge their obligations under this Agreement” – Clause 9
• “In recognition of the rights and interests of the public in the health service, the employer respects and recognises the right of its employees to comment publicly and engage in public debate on matters relevant to their professional expertise and experience. In exercising this provision employees shall, prior to entering into such public debate and dialogue, where this is relevant to the employer, have advised and/or discussed the issues to be raised with the employer” – Clause 40
•
“Employees who have serious concerns over actual or potential patient safety risks shall make every reasonable effort to resolve them satisfactorily with the employer”, “Where either the Association or the employer believes that the serious concerns remain unresolved, they shall develop a process for resolution of these concerns” – Clause 41
If your service is under pressure and is struggling with current demand, contact your industrial officer for advice and assistance.

WWW.ASMS.ORG.NZ | THE SPECIALIST 23
A radiologist, Dr A, is working in a department where several colleagues have recently retired and not been fully replaced. They are concerned that there is a backlog of plain films which have not been reported and that the delay in reporting could lead to patient harm.
Medical Protection would suggest that Dr A writes an email to the hospital management outlining the workload issue and specifying the risks to patients. Dr A should advise management of what additional resources they consider are required to perform the work safely. Then, as a group, the radiologists, should suggest a plan to their management to provide the safest possible care, with the resources that are currently available. It is better to do this as a group because then the responsibility for any resource allocation decisions can be shared. The radiology department should consider notifying the providers who use their service regarding a possible delay in receiving reports and ask them to contact the department with any specific concerns.
Respiratory medicine outpatient wait times have become unacceptable and the hospital management has asked the Head of Department, Dr B, to re-prioritise any referral that is more than four months old and determine which patients are to be offered an appointment in the next two months. Dr B is concerned that information in the referrals is now four months old and that, while doing the triage process, they may miss someone who later turns out to have a malignancy and they will be held accountable.
Medical Protection would suggest that Dr B should formalise the process of how triage will be done and what criteria will be used to decide which patients will be offered an appointment. They should try to get a consensus with colleagues regarding this process and should keep minutes of any meetings held/email trails where this is agreed. The process should include that any patient whose appointment has been delayed would be given clear written information on this, on when they may be expected to be seen and that they should return to their GP if their condition has changed. It would be important to also let the GP know, as this may impact their service and may encourage the GP to review the case and provide updated clinical information. Dr B should make sure there is written communication with management about the risks to patient safety and any ideas they may have about how these could be mitigated.
Dr C is working in a rural hospital emergency department. At end of their shift, the next doctor did not arrive to take over and Dr C was informed that there was no one rostered on as Dr X was on leave and they had been unable to fill the shift. There are two unwell patients in the department and six patients waiting in the queue. Can Dr C go home?
The answer is, probably not, if the care of the acutely unwell patients would be compromised. The Medical Council outlines a doctor’s obligation to assist in an emergency and this situation could be considered an emergency. Dr C cannot leave them unattended without making some alternative arrangement for their care. Dr C should urgently notify management of the issue and ask them to find a solution and then should arrange triage of the patients in the waiting rooms and see if they can be directed elsewhere.
It should be considered whether the unwell patients could safely be transferred elsewhere, but while they are there, Dr C has an ethical obligation to stay, if their care would be compromised if he left.
However, if Dr C becomes so exhausted that they are not safe to practice and are a risk to themself and the patients, they should inform management and leave. The decision to leave should not be taken lightly, should be discussed with colleagues and management and any actions possible to mitigate the risk of harm to the patient should be considered.


24 THE SPECIALIST | DECEMBER 2022
brief
South Canterbury first to take hard look at the gender pay gap
When it comes to addressing the gender pay gap, South Canterbury district has led the way. “Management at South Canterbury have been very open and transparent with us,” ASMS industrial officer Kris Smith says, “They were the first to provide ASMS with a comprehensive and useable set of data, after the request to all districts in February of 2022”.
The data allowed a first scan for gender pay concerns. “It was our initial view that there looked like a number of staff who were not on the right step,” Kris says.
Following discussion at a JCC, a working group was set up with union, SMO and HR representatives. First, the group looked at what qualifications SMOs had and when they received them, along with the date of vocational registration. Then they looked at CVs and each SMO's initial letter of appointment.
From there the group took a more detailed look at some examples. A common factor was parental leave, particularly when SMOs took leave relative to completing their fellowship or receiving their vocational registration. Staff who changed jobs and had their anniversary date changed were also found to have problems.
Not all the cases looked at in detail identified issues. But, with just over 50 SMOs in South Canterbury, the audit did find a significant number with errors.

For those SMOs it is now a matter of resolution. “One sticking point is back pay. While the district has agreed to correct a number of salary steps, they don’t yet accept they were at fault and so don’t consider back pay relevant,” Kris says. “Also, with the arrival of Te Whatu Ora, there are concerns about getting ahead of any national approach.”
"Too old to give up"
The initial results from ASMS’ 2022 Future Intentions survey show senior doctors and dentists are less sure about staying put than they were six years ago.
The proportion of members intending to leave medicine in the next five years has not shifted dramatically. In 2016, when the survey was last run, 16.2 per cent felt likely or extremely likely to leave. In 2022 the figure is 18 per cent.
However, at the other end of the scale, uncertainty has grown. In 2016, nearly half of respondents (47.2 per cent) indicated they were extremely unlikely to leave. But, in 2022, this has fallen to 39.3 per cent.
As one respondent noted, “as service demands go up in public, my hard work is being less valued by management, I’m losing all my non-clinical time, and the more dissatisfied I am with my current FTE. There’s just too much pressure”. On the other hand, another commented, “I’m too old to give up”.
Full results from the 2022 Future Intentions survey, including specific question for IMGs, will be published in 2023.
How likely are you to leave medicine or dentistry in the next five years?
In
2022 2016 Extremely Likely (%) Likely (%) Unsure (%) Unlikely (%) Extremely Unlikely (%) 7.76 9.08 9.93 7.11 13.16 10.04 29.8 26.53 39.35 47.24 WWW.ASMS.ORG.NZ | THE SPECIALIST 25
Research starting on fertility and doctors
Orthopaedic Trainee at Waikato Hospital Dr Alexandria Gibson is conducting a research project to investigate the impact of medical career choice on fertility for New Zealand doctors. The research is under the supervision of Dr Jillian Lee at Waikato Hospital and University of Auckland Associate Professor Joseph Baker. “Dr Lee and I noticed that 90 per cent of the women in our department were currently, or had recently experienced difficulties with fertility, pregnancy loss and complications,” Gibson says. “This was usually suffered alone and in silence. We wanted to open a dialogue about these important issues.”
The project involves a short online survey about fertility, pregnancy and post-natal experiences of female doctors. Gibson is keen for as many doctors as possible to complete the survey - it is anonymous and intends to highlight the issues that come with having and raising a family whilst working as a doctor.
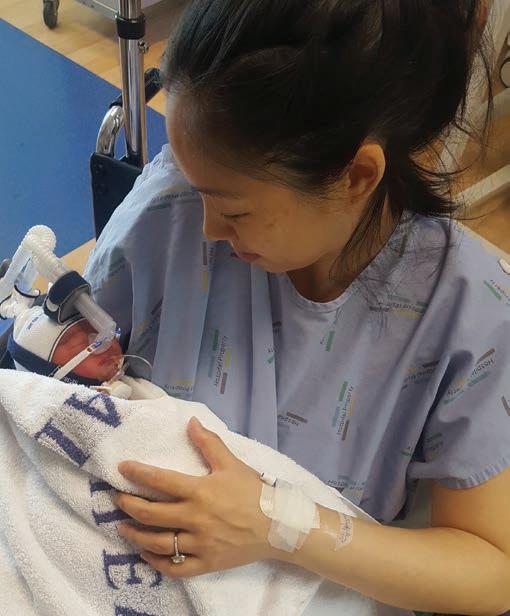
It is open until the end of the year and can be found at https://www.surveymonkey.com/r/N95FB98 Any other questions or feedback can also be sent to alexandria.gibson@waikatodhb.health.nz
Note: This research is approved by the Auckland Health Research Ethics Committee for three years. Reference number AH24523.
In support of nurses


On 27 October New Zealand Nurses Organisation members covered by the Primary Health Care MECA – including nurses working in GP practices, after hours emergency clinics, Plunket and Healthcare NZ – went on strike. They held rallies up and down the country and ASMS was there to show our support. Nurses in these areas are paid less than their colleagues working directly for Te Whatu Ora. You can add your name to the petition calling on Minister Little to fund that pay difference at https://maranga-mai.nzno.org.nz/equal_pay_for_primary_health_care_nurses

26 THE SPECIALIST | DECEMBER 2022
Meri kirihimete
Everyone at ASMS – your National Executive and National Office staff – want to wish you and your whanau a very Merry Christmas and a happy holiday season
Our National Office will close on Friday 23 December and reopen again on Monday 9 January. For any queries during this period please email asms@asms.org.nz – this address will be monitored over the closedown.
ASMS staff
Executive Director
Sarah Dalton Communications
Andrew Chick
Journalist
We can't rest
In June 2020, The Specialist ran a story on the state of overnight accommodation at our public hospitals. The findings weren’t flash and, even then, there had been services raising the problem for over a decade.
Since then, in JCC meetings up and down the country, it’s remained a constant source of frustration for members.
So, two years on we want to take a visual review of what progress – if any –has been made. We are after a photo from every hospital in the country of what is currently available in terms of overnight accommodation. Email your pics to ac@asms.nz. Then we’ll see what the New Zealand public thinks.

Matt Shand
Industrial
Senior Industrial Officer
Steve Hurring
Senior Industrial Officer
Lloyd Woods
Senior Industrial Officer
Ian Weir-Smith Industrial Officer David Kettley Industrial Officer George Collins Industrial Officer
ASMS services to members
As a professional association, we promote:
• the right of equal access for all New Zealanders to high quality health services
• professional interests of salaried doctors and dentists
• policies sought in legislation and government by salaried doctors and dentists.
As a union of professionals, we:
• provide advice to salaried doctors and dentists who receive a job offer from a New Zealand employer
• negotiate effective and enforceable collective employment agreements with employers. This includes the collective agreement (MECA) covering employment of senior medical and dental staff in DHBs, which ensures minimum terms and conditions for more than 5,000 doctors and dentists, nearly 90% of this workforce
• advise and represent members when necessary
• support workplace empowerment and clinical leadership.
ASMS job vacancies online
Check out jobs.asms.org.nz a comprehensive source of job vacancies for senior medical and dental specialists/ consultants within New Zealand hospitals and health services.
Contact us
Association of Salaried Medical Specialists Level 9, The Bayleys Building, 36 Brandon St, Wellington Postal address: PO Box 10763, The Terrace, Wellington 6140
P 04 499 1271
E asms@asms.org.nz W www.asms.org.nz
Follow us
facebook.com/asms.nz twitter.com/ASMSNZ
Have you changed address or phone number recently?
Please email any changes to your contact details to: asms@asms.org.nz
If you have reason or need to seek a reduction or waiver to your annual subscription, please write to us. Our constitution allows for this in certain circumstances. Emails should be addressed to sarah.dalton@asms.org.nz
Kris Smith Industrial Officer Georgia Choveaux Industrial Officer
Jenny Chapman Industrial Officer
Tanja Bristow Industrial Officer Georgia Bates Industrial Officer Greg Lloyd
PO Box 10763, The Terrace Wellington 6140, New Zealand
+64 4 499 1271 asms@asms.org.nz



Senior Communications Advisor
| Communications Advisor
Policy & Research
Director of Policy and Research
Harriet Wild Policy Advisor
Services
Services
Mary Harvey Health Policy Analyst Lyndon Keene Support
Manager Support
Sharlene Lawrence Finance and Technical Support Advisor Vanessa Wratt
Membership Officer
Saasha Mason Support Services Administrator Cassey van Riel
WWW.ASMS.ORG.NZ | THE SPECIALIST 27
Our insurance is choice.
There’s a reason our House, Contents and Car insurance policies have been voted Consumer People’s Choice for six years running. Find out why at mas.co.nz

6






























 Bronwyn Copeland
Bronwyn Copeland

 The Wilkinsons are a family of doctors who have orchestrated their love of music into a symphony of healing sound for New Zealand.
Left to right: Tim, Lynette and Tom Wilkinson
The Wilkinsons are a family of doctors who have orchestrated their love of music into a symphony of healing sound for New Zealand.
Left to right: Tim, Lynette and Tom Wilkinson






















