





: 9/1/2024 to 8/31/2025









: 9/1/2024 to 8/31/2025



Spot
PerkSpot
TripBeat:
Active&Fit
Liberty
iThink
Wellcard
Dell
International
Verizon
The
Invite
Cigna
Compliance


At Magnit, we prioritize our employees’ well-being and are committed to offering a robust benefits program to promote Vitality within our workforce. Vitality is a person’s ability to live life with health, strength, and energy. In the workplace, it equates to high-performing, motivated and healthy employees.
To achieve this goal, our benefits program is built on the 8 Pillars of Wellness. We believe in a holistic approach to well-being, recognizing that health extends beyond physical and mental states. While health is commonly defined as the absence of illness, this definition overlooks a broader perspective. Evaluating your holistic health and wellness involves considering multiple factors beyond mere disease prevention.
At Magnit, we are dedicated to support our employees on their vitality journey, by equipping them with necessary tools to incorporate the 8 Pillars of Wellness into their daily lives.
These dimensions collectively contribute to a person’s overall vitality and well-being, promoting a balanced and fulfilling life.
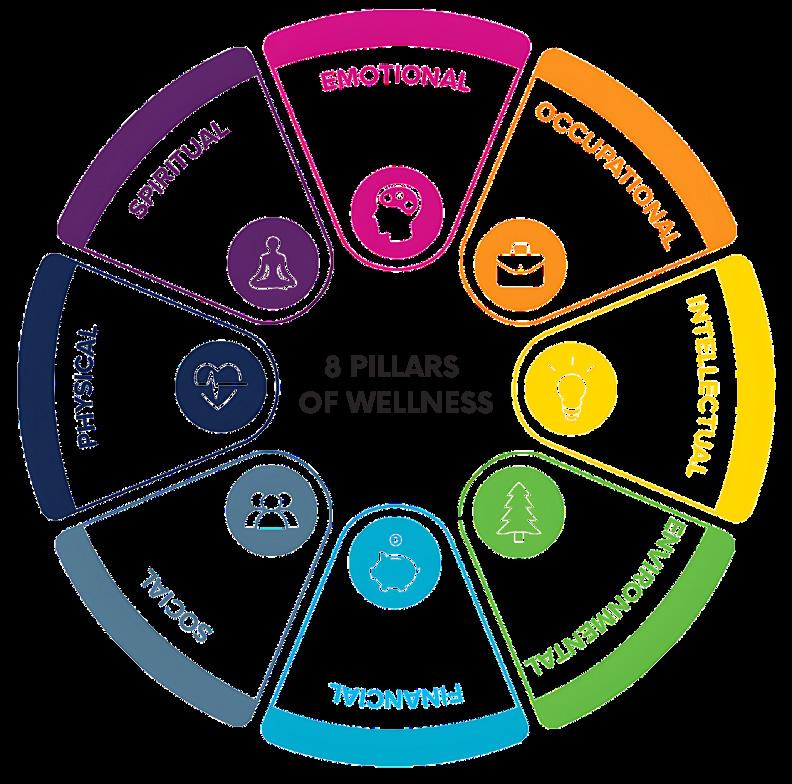
















Physical Wellness: Focuses on maintaining a healthy body through exercise, nutrition, and rest.
Spiritual Wellness: Centers on finding meaning and purpose in life, exploring personal beliefs and values, and achieving inner peace.
Emotional Wellness: Involves understanding and managing emotions effectively, fostering resilience, and achieving overall mental well-being.
Occupational Wellness: Focuses on finding satisfaction and fulfillment in one’s work, maintaining a healthy work-life balance, and achieving career goals.
Intellectual Wellness: Involves engaging in lifelong learning, expanding knowledge and skills, and stimulating intellectual curiosity.
Environmental Wellness: Involves respecting the environment, promoting sustainability, and making choices that contribute to a healthier planet.
Financial Wellness: Involves effectively managing finances, planning for the future, and reducing financial stress.
Social Wellness: Centers on building positive relationships, fostering a sense of belonging, and contributing to the community.
For more information about the benefits outlined in this guide, you can visit your Virtual Benefits Fair via your Employee Portal, HRconnection. Within this portal, you will find a series of valuable resources including detailed plan summaries, carrier brochures, provider links, and an extensive video library, offering education on a series of topics and specific plan offerings.
Click Here to visit HRconnection
US Guest Key: Sourcingcontractors1



You are eligible to participate in our health and ancillary benefits on the first of the month, following 30 days of full-time (30+ hours per week) employment. Elections must be made by the last day of your eligibility month. Late enrollments will be retroactive to the 1st of the month. Missed contributions will be collected in arrears. If you enroll, you must maintain full-time (30+ hours per week) status. If your status changes to part-time your benefits may be subject to cancelation. A monthly hours audit is conducted to ensure compliance of the eligibility policy. If your status has changed to part-time you will be notified prior to cancellation to confirm that change is due to a reduction of work hours. If you are missing time due to sick leave or personal time off, please complete the Supplemental Payroll Deduction (SPD) Form and submit to the Global Support Center . Sick leave and personal time off is not considered when determining status, only reductions in work hours are considered.
You can enroll in any combination of medical, dental, and/or vision plans based on your needs. For example, you can enroll in the company medical and dental plan and decline the vision plan.
You can also enroll in a combination of coverage options. For example, you can enroll only yourself in the company medical and vision and enroll your spouse in the dental plan. The only requirement is that you must elect coverage for yourself in order to elect any dependent coverage.
Medical, Dental, and Vision
Company employees may enroll qualified dependents, as defined by the IRS, into the healthcare coverage. The Dependent Policy requires that proof of dependency be submitted for each dependent enrolling, to ensure compliance with IRS guidelines. If proof is not provided by the last day of your eligibility month, the dependent will be removed from coverage.
Eligible dependents include:
• Your legal spouse
• Your domestic partner
• You or your spouse’s children (including birth children, step-children, legally adopted children, children placed for adoption or children for whom you or your spouse are the legal guardian) as follows:
• Up to age 26 regardless of student or marital status (30 for Cigna Medical)
• Unmarried children age 26 or over who are incapable of self-support because of a total physical or mental disability
• Retirement (401k)*
• Employee Assistance Program (EAP)
• Employee Discounts & Memberships
*Not available to Contractors based in Puerto Rico
First of month following
30 days of full-time employment
• Medical, Dental, and Vision
• Life: Employee, Spouse and Child
• Short and Long Term Disability
• Legal and Identity Theft
• Ancillary and Supplemental Benefits
• Benefits Eligibility and Coverage ends on last day of employment.
• If you are enrolled in medical, dental and vision, Cobra documents will be sent within 30 days of termination.
Coverage Options Include:
Employee Only
Employee + 1 Dependent Family
Make sure you have the Social Security Numbers and birth dates of your dependents. You won’t be able to enroll your dependents without this information!
Please Note: Under Magnit’s Dependent Policy, dependent proof is required for all dependents enrolled in healthcare coverage. To complete the enrollment of your dependents, documentation is needed to show they are valid dependents under IRS guidelines. Failure to provide valid dependent proof, by the last day of your eligibility period, will result in the dependent’s removal from coverage. The cancellation will be backdated to your coverage effective date.
Section 125 defined: Under a cafeteria, or Section 125 plan, you pay for your employer-sponsored benefits with pretax dollars. Your employer deducts your payments from your wages before withholding certain taxes. Your employer doesn’t include your pretax payments in your taxable wages on your annual W-2.

Plans renew on September 1st every year and are subject to coverage and rate changes.
The plan year runs from September 1st to August 31st. Each August, during Open Enrollment, you will have the opportunity to make changes to your benefit elections for yourself and your covered dependents. Outside of Open Enrollment, you must experience a qualifying event that satisfies federal regulations outlined below:
• Gain or Loss of health coverage
• Marriage, legal separation or divorce
• Birth or adoption of a child
• Becoming a U.S. Citizen
• Moving
• Death of a dependent family member
• Dependents no longer eligible to be a named dependent on a parent’s plan
You will need to submit supporting documentation to process your life event.

• Remember, you have until the last day of your eligibility month to enroll.
• If you do not enroll within this time frame, you will have 100% employer-paid benefits only.
• Outside of Open Enrollment, you must experience a qualifying event that satisfies federal regulations in order to enroll at a later date.

It’s important to read over the benefit descriptions for the plans offered. Additionally, make sure you understand all the terms and definitions used in the descriptions—this guide can help. Not knowing something now could cost you later in the year.
Do you need healthcare, financial, or ancillary benefits for you or your family? Ask yourself:
• Do you or your dependents have any chronic health conditions?
• Are you saving enough for retirement or college?
• How much healthcare coverage and what type of care do you need this year?
• Do you expect your needs to change in the near future?
• Do you prefer to pay less from your paycheck or less out of your pocket when you need care?
• If something happened to you and you couldn’t work – could you still pay your bills?
Answering these questions will help you determine what coverage you need.
Have You Considered a High Deductible Health Plan?*
High deductible health plans have lower premiums and may result in lower annual medical costs. These plans offer several advantages to reward you for taking an active role in your health care spending.
• Lower paycheck costs – allowing you to keep control over more of your money
• Tax-advantaged savings account – enrolling in a Health Savings Account (HSA) helps you pay your deductible and out-of-pocket costs
• Comparable benefits – these plans use the same networks that other plans offer, and in-network preventive care is still 100% covered
*Not available to contractors based in Hawaii and Puerto Rico
Are you interested in a high-deductible plan with a lower premium? You may want additional coverage that pays benefits directly to you to help cover deductibles and out-of-pocket expenses.
Consider combining your medical coverage with supplemental insurance. These plans are a great complement to your medical plan choice and can help reduce the financial risk associated with illness and injury.
Depending on your situation, you may be able to save money by purchasing a lower-cost medical plan and adding one or more supplemental plans to achieve effective protection at a lower plan cost. Refer to the supplemental insurance section on page 24 for more information.

The company is committed to offering you a competitive benefits program that offers the flexibility to select coverage that best fits your needs and your budget. The company coverage is in compliance with the ACA affordability guidelines. You will be responsible for any remaining costs for the benefits you select, which will be provided as you enroll in the Employee Hub.
Employees eligible for medical insurance and all other benefits will receive a system generated email from Dayforce during their onboarding process offering them the opportunity to elect coverage, once their access is established.
Enrollment for most health and financial benefits is completed in Dayforce Click here for more information and training resources on how to access and use Dayforce. If you have not setup your Dayforce account access, you will need to setup your security access first. Security access is completed on Okta. Click here for Okta registration instructions.
Enrollment for 401(k)*, 529 plan, Wellness, Voluntary Whole Life, Long Term Care, and employee perks are handled directly with the provider. Enrollment details are listed in the benefits guide.
All new hires and conversions are required to complete enrollment, even if they are waiving all coverage.
If you are an active employee and do not enroll in benefits during the annual open enrollment period your current benefit elections will automatically carry over to the next plan year, excluding any plans no longer offered. This feature is designed to make the enrollment process as easy as possible for employees who want to keep current coverage for another year. However, we will require you to complete an annual confirmation or declination of coverage to ensure you have reviewed the new plan year offering.
*The 401(k) plan is not available to contractors based in Puerto Rico


• Click Here to view
• Click Here to view
• If there is a conflict between the guide and carrier summary plan description, the carrier document will be the ruling document.
• Alternative rates with restrictive abortion coverage available for employees located in TX, OK, and MO.
• The information on the following pages reflects what the covered individual/family will be required to pay out-of-pocket, until the Annual Out-of-Pocket Maximum (OOPM) is reached. This handout is provided as an overview of medical benefits offered. For specific coverage information, please refer to the full Plan Summaries and documentation located on HRconnection
** Employee +1 or Family tier coverage for any HSA compatible plan will not have individual limits for Deductible or Out-of-Pocket Maximum. Covered members must meet the family deductible and out-of-pocket maximum, not to exceed $6,900 In-Network per covered individual. Please note out of network coverage is limited to customary and reasonable charges and out-of-pockets expenses are not protected by contract limits.
For those enrolled in a Cigna Medical Plan

Resources that are designed to help you make smarter choices to improve your whole health

Register on myCigna.com to access your digital ID cards and activate all available programs. That way you’re ready to go whenever you need to find in-network health care providers, estimate costs or use My Health Assistant. Scan the QR Code or Click Here to Register
Get the right care, at the right time, at the right place for you and your family.
Click Here to learn which type of care is best for your situation!
Schedule Your Preventive Care
Preventive care, such as check-ups, biometric screenings and wellness screenings, are available at no additional cost to you. It’s even available virtually for maximum convenience.
Conveniently connect with board-certified physicians for your Urgent Care needs. MDLive also offers virtual access to Primary Care Doctors, Behavioral Health Specialists and Dermatologists. Customer cost share for MDLIVE Cigna Appointments vary. Click here to register and learn more.
Cigna offers access to Convenience Care Clinics nationwide matching the Physician Copay/Cost on the plan you are enrolled in. Click Here to learn more.
Call the Cigna 24/7
Speak with a clinician who can help you choose the right care, whenever you need it – late nights, holidays and more.
Prioritize Behavioral
• 115K+ virtual providers, the largest network of its kind in the country
• 285K+ mental health and substance use providers
Click Here to view the Cigna Preventive Care Drug List
Cigna Formulary List
Click Here to view the Cigna Healthcare Standard 4-tier Prescription Drug List
Simplify With Home Delivery Medications
Express Scripts® Pharmacy, your home delivery pharmacy, is a convenient option when you’re taking a medication on a regular basis. It’s simple and safe – and saves you trips to the pharmacy.
Click Here to view the detailed Home Delivery flyer
Complex medical conditions can be overwhelming. The Cigna trained teams can help you coordinate care, understand benefits and reach goals through online coaching.
Cigna Knowledge Center
Looking for Health Insurance 101?
Visit the Cigna Knowledge Center to gain a detailed understanding of the terms used throughout this guide and a deeper understanding of your overall benefits program. Click Here to access.
myCigna® and One Guide can help you stay in-network, maximize savings and avoid any surprises. To access directory, click below.
www.cigna.com/hcpdirectory
Plan Name: Open Access Network w/o Carelink

For those enrolled in a Cigna Medical Plan

Your Cigna Plan offers Personalized Support to Help You Get and Stay Well
100% Coverage for In-Network Preventive Care
This includes well visits, screenings, and routine immunizations.
Personal Health Coaching
Available at NO additional charge, to help you:
• Analyze and understand your health assessment results
• Get started with Health Improvement program and services available to you

• Learn ways to better manage health issues like lower back pain, high blood pressure, and high cholesterol
• Understand treatment options so you and your provider can make decisions that work best for you
• Answer questions about your health, health coverage, and how to get the best value when you seek care
myCigna Tools and Resources Make it Easy to Manage Your Plan
• View your HSA balance and transactions (When enrolled in a Cigna
• Track expenses and pay bills online
• Estimate your medical expenses
• Find an In-network provider
• Compare provider cost and quality information
• Get instant, real-time health and plan information
Tips For When Enrolled in a Cigna High Deductible Health Plan
Shop for Procedures
You might ask yourself, “how much do x-rays cost?” When it comes to medical procedures—like x-rays or surgery—prices can vary from one facility to another. If your physician suggests a costly test or procedure, you can shop around for the best deal, even if they refer you to a specific location. Before you agree to a medical cost, contact comparable facilities in your area to receive a quote for services.
Remember, it is most cost effective to stay in your health plan’s network when looking for a physician or facility, as you are protected by contracted rates.
Prescriptions can be expensive. If you’re prescribed a costly medication, ask your doctor if there is a generic version you can try instead. Often, generic alternatives are provided at lower costs.
If a replacement is not available, take some time to contact pharmacies in your area and compare prices. Sometimes, you’ll find the same prescription available at a lower cost.
When enrolling in an HSA eligible medical plan that is eligible to be paired with a Health Savings Account (HSA), an HSA will automatically be opened for you when your medical enrollment is complete. You may choose to contribute or not, but the account is established if you choose to contribute at any time.
Did you know that most major medical plans cover certain preventative services at no cost to you? These services include certain vaccinations and health screening tests. To learn what may be available under your specific plan, review your policy documents or contact your employer.
Taking advantage of these tips can help you manage the costs associated with your high-deductible health plan.


A Health Savings Account (HSA) is a powerful savings tool. You can start setting aside money in a tax-free account to save for future qualified healthcare expenses.
Health Savings Accounts are administered by HSA Bank
Eligibility
You are eligible to open and contribute to a Health Savings Account if:
• You are enrolled in a company High Deductible Medical Plan
• You are not covered by your spouse/domestic partner’s health plan, health care flexible spending account or health reimbursement account
• You are not eligible to be claimed as dependent on someone else’s tax return
• You are not enrolled in Medicare or TRICARE
Benefits of an HSA
• You choose how much to set aside for healthcare expenses - start, stop or change your contributions at any time
• Reduces taxable income - your HSA is deducted from your paycheck, so the tax benefits are immediate
• Grows tax-free - you can invest excess balances over $2,000 into mutual funds and the earnings are tax-free
• If you switch to a non-HDHP you can continue to use your HSA to pay for eligible medical expenses, you just won’t be able to make any more contributions
• Your HSA is portable if you change jobs
• At age 65, distributions from your HSA on non-qualified medical expenses are taxed as income with no penalty
You can always use your HSA for any contributions towards your deductible, but did you know you can use your HSA for expenses that are not covered by insurance?
Click here to check out the full list of eligible expenses.
Once you’ve enrolled in a Health Savings Account, HSA Bank will mail you a debit card that you can use to pay for your eligible expenses or you can continue to pay upfront for expenses and file for reimbursement. You can use the accounts to pay for your own expenses or those of an eligible dependent. In general, an eligible dependent under this plan is anyone you list as a dependent on your federal income tax return. This includes immediate family members, a close relative or other person whose primary residence is your home and for whom you provide over 50% support.
HSA Bank will never ask you for any records or receipts, but the IRS could. Make sure you keep all of your records! If you take a distribution from your HSA for non-eligible expenses there is a 20% excise tax plus any applicable income taxes.
Click Here to learn more!
Click Here to view your HSA Guide!
Email: askus@hsabank.com
Phone: (800)357.6246
Fax Number: (877)851.5274
UnitedHealthcare FlexWork Limited Medical (MEC) Package Plans are designed to provide affordable benefits that are easy to access and simple to use, so you can manage your health and well-being with confidence. The plans cover Minimum Essential Coverage preventive services at no member cost, as well as many of the most frequently utilized health care services. Package plans include Enhanced Hospital Indemnity (EHIPP) benefits to provide additional financial protection and reduce your total cost of care. Please note, this is not traditional Major Medical Coverage, this is a Limited Medical plan.
**Outpatient mental health and substance use coverage includes partial hospitalization program, intensive outpatient treatment
Key Features:
• No pre-existing condition exclusions
• COBRA coverage continuation is available if you leave your employer (restrictions apply)
• No annual or lifetime dollar limits
• Pretax payroll deductions may reduce your cost of coverage
FlexWork plans have limitations and exclusions that may not make them suitable for everyone.
and Wellness Resources provided when enrolled in the United Healthcare FlexWork plan
Once your FlexWork plan becomes active, you’ll have access to a variety of Wellness Programs & Heath Support Services with United Healthcare at no additional cost outside of your weekly payroll deduction outlined on page 12.










Once your plan becomes active, you’ll be able to reach Member Services by calling the number on your health plan ID card, plus you’ll have access to the member portal at FlexWork.UHC.com .
Save time and money with virtual doctor visits for diagnosis of non-emergency medical conditions, personal care plans, and some prescriptions. Register at Healthiestyou.com or call
Click Here to view a high-level summary of health care reform mandated preventive benefitscovered at 100% of the allowed amount with $0 copays, network only.
The Limited Medical Plans include OptumRx for pharmacy benefit management services. The Limited Pharmacy Plan provides coverage for medications as described in the FlexWork limited Benefit Prescription Drug List (PDL). Specialty drugs are not covered.
Click Here to learn more
Access additional savings for most FDA-approved medications not covered by your pharmacy plan.
When life gets stressful, the Employee Assistance Program (EAP) support line is just a phone call away. Care coordinators are available 24/7 for confidential conversations and referrals to expert care and services.
Find ways to stay healthy and enjoy thousands of negotiated prices on items such as health and wellness, apparel, auto, beauty, personal care, cell phone, virtual learning, electronics, entertainment, everyday savings, flowers, and food. Visit FlexWork.UHC.com for details.
Have fun and get healthier with Rally. Take a health survey to see how you’re doing in key areas like nutrition and fitness, get personalized recommendations that fit your lifestyle, track your progress on your dashboard and earn Rally coins that can be redeemed for rewards.
UnitedHealthcare Hearing offers access to hundreds of name-brand and private-label hearing aids at significant savings. You’ll also get convenient ordering options and personalized care.
If you’re enrolled in a medical and supplemental health plan, you’ll be notified of claims that may qualify for benefits.

This year, the company is excited to announce the addition of Lyric Telehealth benefits. Employees and their dependents can have access to telehealth services for wellness, urgent care, mental health counseling and dermatology for only $10 per month. Lyric Health is an award-winning virtual care service provider that powers access to modern remote care, reducing costs and improving satisfaction and outcomes.
Head-to-toe healthcare that fits in your pocket!
Schedule Consultation: Call, Click, or Tap to schedule your consultation
Talk to a Provider: A doctor will call you directly or join on video from the website or Lyric app
Access your Treatment Plan: See your diagnoses, prescriptions, and doctors’ notes as directed
Feel Better: Stay healthier! Use the app to keep track of your personal health records anytime from anywhere
Comprehensive suite of Virtual Care services.
Urgent Care - $0 Copay
24/7/365 on-demand access to licensed physicians to help with non-emergency needs.
Primary Care - $0 Copay
Get ongoing, personalized care from a provider comitted to your complete health.
Virtual Counseling - $0 Copay
Virtual visits with caring mental health professionals.
Dermatology - $0 Copay
Get a treatment plan for Acne, Eczema, or other conditions.
Advanced Mental Healthcare Available - $100 Copay
Visit with an advanced mental healthcare pro for depression, anxiety, and other concerns.


Consult with Doctors in English or Spanish!
Download the Lyric app and get instant access to integrated virtual care designed to treat the complete you.
Website: GetLyric.com Phone: 1.866.223.8831
Guidance and Navigation to make healthcare easy to access, understand, and use.
Virtual MSK
Physical therapists deliver care plans proven to prevent injuries and guide members to pain relief.
Labs
Leveraging data to determine potential risk factors in order to manage special conditions.
Get a quick and easy specialist referral for any condition your doctor can’t treat.


Access Your Virtual Urgent Care
Doctors can be hard to reach, illnesses can occur in the middle of the night, and sometimes you just have a question. Get on-demand care when you need it.
Healthcare Cost Savings: Redirecting unnecessary doctor, urgent and ER visits can reduce healthcare spending significantly.
Productivity: A typical doctors appointment can take half of the work day. Lyric gives employees easy access to a physician wherever they are located.
Access Your Virtual Behavioral Health
Therapy from the privacy of your home or office
In some cases, a visit to the doctor’s office can be avoided, saving time and money.
• Flu Symptoms
• Ear infection
• Urinary Tract Infection
• Pink eye
• Rashes
• Acne
• Sinus Problems
• Allergies
• Nausea
• Stomach Viruses
• Sore Throat
• and Much More...
Whether it’s stress, anxiety, depression, or sudden loss, we can help. Speak with a licensed therapist anytime from anywhere.
The Lyric suite of mental health services includes:
Virtual Counseling - $0 Copay
Consult with a Master-level therapist/counselor. The amount of counseling sessions will be clinically appropriate based on the issue.
• Substance Abuse
• Relationship Issues
Virtual Psychologist - $100 Copay
• Depression
• Stress and Anxiety
• Death of a loved one
• Parenting Issues
Speak with a licensed psychologist, one-on-one, to assess your symptoms and evaluate your medical, psychological, and family history to determine a productive treatment plan.
• Depression
• Life changes
Virtual Psychiatrist - $100 Copay
• Addiction
• Grief and Loss
• Stress Management
• Relationship
Connect with a U.S. based, board-certified Psychiatrist who can diagnose, treat and prescribe medications for a range of mental health disorders, as necessary.
• Anxiety
• Panic Disorders
Required notices for Lyric Health
• Depression
• Bipolar Disorder
• Trauma & PTSD
• Addictive Behaviors
Emergency Services Notice: Client understands and will inform members that if in the providers sole medical judgement, the consult involves a life threatening emergency, provider may direct the member to the nearest emergency facility.
Provider/Patient Relationship: Client understands and will inform members that in order to receive any services, member is required to complete the necessary steps to create a provider/patient relationship via telephone or video, in accordance with applicable state and federal laws. Those steps include:
1. Completing a medical history disclosure, within the member’s health portal or by telephone with a designated care coordinator, 2. Agreement to informed patient consent and release form confirming an understanding that the provider is not obligated to accept the member as a patient, and that the member’s participation in the program may be cancelled at any time without recourse by the member; and,
3. Acknowledgement and understanding of additional MTM policies and disclosures.


Not only does good dental hygiene prevent tooth decay, gum disease and bad breath - it can also prevent more serious health consequences such as heart disease and stroke. To provide employees and their families with the most suitable coverage, the company offers dental coverage through Cigna.
The Cigna Dental plans offer you the option to enroll in a DPPO or DHMO. Plan coverage includes preventive services covered at 100%, including routine cleanings twice a year. All plans are linked to a national network of providers.
With the Dental Preferred Provider Organization plan (DPPO), you can see any licensed dentist or specialist. You do not have to choose a primary care dentist or get specialist referrals. Preventive Services are covered at 100%. Two levels of coverage are available with either $2,000 or $1,000 in annual coverage, once a small deductible is met.
• You choose a licensed dentist for routine, preventive, diagnostic, and emergency care. You’ll pay less for many covered services if you use in-network dentists. Out-of-network services will cost you more.
• When you meet your annual deductible and satisfy any waiting periods, you pay a coinsurance (a portion of covered charges), and the plan pays the rest (up to the yearly dollar limit of the plan).
The Cigna Dental Care (DHMO) plan requires you to select a general dentist for routine, preventive, diagnostic, and emergency care. They will refer you to specialists as needed.
• This plan covers preventive services at 100%.
• Cigna Dental Care (DHMO) plans do not have a deductible or a yearly dollar limit.
• No coverage waiting period.
• This plan includes orthodontia for adults & children.
• This plan does not cover out-of-network services.
Easily search for Cigna DPPO or DHMO network providers in the directory on cigna.com or mycigna.com.
*The Cigna DHMO plan is not available to contractors based in Puerto Rico
Dental Plan Comparison







Available to all contingent workers & their families

Your EAP has great online information at your fingertips!
Log on and Learn! Check out the Unum online offerings such as trainings, articles, webinars, courses and more to help make your job and life easier and less stressful.
Log onto your member website at Unum.com/lifebalance and click on “Access Your EAP Benefits” to access these EAP + Work/Life resources.
Here are just a few ways you can take advantage of your Employee Assistance Program:
Financial Information
Topics covering Contracts, Bankruptcy, Divorce, Custody, Real Estate, Wills & Estates, and more. Get access to some of the most commonly used financial forms.
Parenting Resources
Information for personal development, managing work and family, communicating effectively, and more! View topics covering Adoption, Bullying, Child care and development, children with disabilities, and more!
Relationships
We offer a variety of resources to help you improve your relationships with friends, family, coworkers, and spouses/partners; further improving your communication skills, personal and professional development, leadership, and interpersonal skill.
Education
Webinars from leading experts on a host of Work/Life topics.
Counseling Support
HealthAdvocate can connect you to the right confidential counseling support. Explore the virtual therapy program allowing you to focus on your mental health from anywhere!
Virtual Therapy Flyer



Turn to us, when you don’t know where to turn.
Toll-free 24/7 access to EAP and Work/Life Balance
Phone: 1.800.854.1446
Website: Unum.com/lifebalance
Up to 3 sessions per issue per year are available to you and your household members.

Help when you need it most!
With your Employee Assistance Program and Work/Life Balance Services, confidential assistance is as close as your phone or computer.
Employee Assistance Program (EAP)
Your EAP is designed to help you lead a happier and more productive life at home and at work. Call for confidential access to a Licensed Professional Counselor* who can help you.
A Licensed Professional Counselor can help with:
• Stress, Depression, Anxiety
• Relationship issues, Divorce
• Job stress, Work conflicts
• Family and Parenting Problems
• Anger, Grief, and Loss
• and more
*The counselors must abide by federal regulations regarding duty to warn of harm to self or others. In these instances, the consultant may be mandated to report a situation to the appropriate authority.
Work/Life Balance
You can also reach out to a specialist for help with balancing work and life issues. Just call and one of Unum’s Work/Life Specialists can answer your questions and help you find resources in your community.
Ask Unum Work/Life Specialists about:
• Child care
• Elder care
• Legal questions
• Identity Theft
• Financial Services, Debt Management
• Even reducing your Medical/Dental Bills!
• and more
If you experienced a medical emergency while traveling (business or personal), would you know who to call? Whenever you travel 100 miles or more from home — to another country or just another city — be sure to pack your worldwide emergency travel assistance phone number found below! Travel assistance speaks your language, helping you locate hospitals, embassies and other “unexpected” travel destinations. Add the number to your cell phone contacts, so it’s always close at hand! Just one phone call connects you and your family to medical and other important services 24-hours a day.
Within the US: 1.800.872.1414
Outside the US: +16099861234
Preparing a will doesn’t have to be complicated or expensive. Your employee assistance program includes simple tools that can help you create a basic will in no time.
Always by your side
• Expert Support 24/7
• Convenient Website
• Short-term Help
• Referrals for additional care
• Monthly Webinars
• Medical Bill Saver
Who is covered?
Unum’s EAP services are available to all eligible employees, their spouses or domestic partners, dependent children, parents and parents-in-law.
Help is easy to Access.
• Online Support
• Phone Support
• In-Person Support
Medical Bill Saver is one more way the Unum Employee Assistance Program helps employees manage the stresses of modern life.
When a covered employee has a medical or dental bill totaling over $400 in out-of-pocket costs, Unum’s skilled negotiating team works with the provider(s) to get a discount. Successful negotiations can save employees hundreds, and sometimes thousands of dollars.
Unum experts can also show employees how to keep bills lower in the future — for example, by using in-network providers.
By helping reduce employees’ out-of-pocket costs, Medical Bill Saver can make consumer-driven health plans (CDHPs) more attractive — and more effective.

Studies show that behavioral problems, such as depression, can contribute to heart disease.1 Many physical conditions can worsen with stress, substance use and other behavioral health issues. The Cigna Total Behavioral Health® program can help.
The Cigna whole-person approach
If you or a loved one has been diagnosed with a behavioral health condition, we are here for you. Cigna’s comprehensive program provides help with life events, dedicated support, lifestyle coaching, and online tools. You can call us anytime, any day. We’re here 24/7 to assist you with your routine or urgent needs. We can also help you find a provider with confirmed appointment availability.
Virtual behavioral care
You can talk to a licensed psychiatrist or counselor by phone or video with MDLIVE2’³ or the Behavioral Health network. With MDLIVE you can schedule phone and video appointments online. With the Behavioral Health network, you can find a provider and start video counseling by going to MyCigna.com, Find Care & Costs.
You can also access online therapy through Talkspace,2 via private messaging or live video session. Refer to your plan documents for costs and details of coverage. We also include Ginger behavioral health coaching via text-based chats, self-guided learning activities and content, and, if needed, video-based therapy and psychiatry.2’³ myCigna.com guided navigation
This digital portal includes guided navigation that provides you with personalized, convenient care options to help you along your journey. Care options include digital, coaching, virtual and in person options.
On-demand coaching and personalized learning with iPrevail offered through Cigna2
Learn how to boost your mood and improve mental health with on-demand coaching 24/7. After completing a brief assessment, you receive a program tailored to your needs that includes interactive lessons and tools. You get access to a peer coach who is matched based on your symptoms. You can also join support communities focused on stress, anxiety, depression and more. iPrevail also includes a caregiver support program designed to help you cope with stress, improve resilience and enhance your overall health and well-being.
We offer provider search and match support, in-the-moment appointment scheduling, and new online scheduling options.7
At no additional charge to you, you can receive face-to-face sessions4 with a licensed mental health professional in the Employee Assistance Program network.5 You also get online, on-demand seminars, as well as community resources and referrals on a range of topics, including:
• Child care
• Adoption
• Senior care
• Pet care
• Legal and financial consultation services6
• Identity theft support
• Summer camps
• Parenting
• Convenience services
Take control of your health with extra support.
Lifestyle management programs
Get help to reach your goals like losing weight, quitting tobacco or lowering your stress level. Each program offers support with phone and online coaching.
Behavioral awareness webinars
We offer free monthly seminars on autism, eating disorders, substance use and behavioral health awareness for children and families. The seminars are taught by industry experts and offer tips, tools and helpful information.
Visit myCigna.com or use the myCigna® app to access on-demand support, including:
• Information about your benefits, in-network providers and treatment options
• Health and well-being articles
• Self-assessment, stress management and mindfulness podcasts and tools

The Cigna team will take time to talk through your issue and get you to the right resource or licensed clinician based on your needs.7
100% follow up
After your initial consult, we’ll check in with you digitally or telephonically to see if your needs are being met or provide additional assistance if needed.7
Science-based activities and games for stress and worries, with Happify offered through Cigna2
Everyday stressors can impact your relationships, work, health and emotional well-being. But you can change your outlook — and the way you see the world — with Happify. Happify’s activities and games are designed to help you overcome life’s challenges and can be accessed at any time.
Behavioral coaches provide dedicated support for a broad range of conditions including:
• Autism spectrum disorder
• Intensive behavioral case management
• Substance use
• Eating disorders
• Opioid and pain management
We also provide coaching and support for parents and families, which empowers individuals to be effective advocates for their family member or their own mental health needs. The team can help for as long as needed (you must stay covered under your plan to continue service).
They can help you:
• Understand a behavioral diagnosis
• Learn about treatment choices and how your choices can affect what you’ll pay out of pocket
• Identify and manage triggers that affect your condition
• Find a health care professional or facility in-network geared to your needs. The Cigna network includes a Centers of Excellence (COE) program.8 COE facilities have earned a top ranking for quality and cost-effective care. With nationwide locations for adult mental health, child and adolescent mental health, eating disorder and substance use treatment, help is available and closer than you think.
• Find community resources and programs near you
• Get referrals to other wellness and lifestyle programs available to you
Coaching and Support services include a digital interface through Vela.2 Your Coach will help you acquire the app which features secure two-way messaging, ability to share resources, as well as appointment tracking on a shared calendar.
1. CDC. “Heart Disease and Mental Health Disorders.” https://www.cdc.gov/heartdisease/mentalhealth.htm.
2. Program services are provided by independent companies/entities and not by Cigna. Programs and services are subject to all applicable program terms and conditions. Program availability is subject to change. These programs do not provide medical advice and are not a substitute for proper medical care provided by a physician. Information provided should not be used for self-diagnosis. Always consult with your physician for appropriate medical advice. References to third-party organizations and/or their products, processes or services, doesn’t mean Cigna endorses them.
3. Cigna provides access to virtual care through national telehealth providers as part of your plan. This service is separate from your health plan’s network and may not be available in all areas or under all plans. Referrals are not required. Video may not be available in all areas or with all providers. Refer to plan documents for complete description of virtual care services and costs.
4. Three face-to-face visits per issue per year. Some restrictions apply, please check with your employer to confirm services included in your plan.
5. Employee assistance program services are in addition to, not instead of, your health plan benefits. These services are separate from your health plan benefits and do not provide reimbursement for financial losses. Program availability may vary by plan type and location, and are not available where prohibited by law.
6. Customers are required to pay the entire discounted charge for any discounted legal and/or financial services. Legal consultations related to employment matters are excluded. Additional restrictions may apply.
7. Available beginning 1/1/24.
8. The Cigna Center of Excellence designation is a partial assessment of quality and cost-efficiency and should not be the only basis for decision-making (as such measures have a risk of error). Individuals are encouraged to consider all relevant factors and talk with their physician about selecting a health care facility. Quality designations and ratings found in Cigna’s online provider directories are not a guarantee of the quality of care that will be provided to individual patients. Providers are solely responsible for any treatment provided and are not agents of Cigna.

The company offers all benefits eligible employees with Voluntary Term Life Insurance, up to a maximum of $500,000, with Term Life and Accidental Death & Dismemberment benefits through Unum. This coverage provides financial protection during your working years. Your spouse and children are also eligible for coverage.
Voluntary Term Life and AD&D insurance gives you the opportunity to purchase additional life insurance for you and your eligible dependents, if you are enrolled.
Evidence of Insurability (EOI) is required when electing coverage over the guaranteed issue amount. Coverage will not become effective until your EOI is approved by Unum. You choose the coverage that’s right for you and your beneficiary(ies). And you keep that coverage for a set period of time or “term”.
To get an accurate representation of your payroll deduction, click here to utilize the rate calculator.

Disability insurance protects your income in the event of a short-term or long-term illness or injury. The company offers short-term and long-term disability coverage through Unum. Disability coverage is voluntary for all benefit eligible employees. Both plans are established so you can use the money however you choose; to help pay for rent or mortgage, groceries, out of pocket medical expenses and more.
That’s why having disability insurance is so important. Our disability plans are designed to help protect your financial security by providing replacement income if you are ever disabled due to a non-work-related injury or illness.
Please review your plan information brochure for further coverage details.
The Unum Voluntary STD and LTD Insurance are only available to those enrolled in a Cigna Medical Plan. If you are not enrolled in a Unum Medical Plan and still are interested in these types of programs you may consider the options available with Unum Benefits. For more information and rates on the Unum Benefits offerings you can call 1.800.346.3620.
When you are unable to work for a period of time due to a disabling illness or injury, short term disability insurance can replace a percentage of your lost income (up to a maximum weekly benefit) for a period of time as defined by the policy.
When you are unable to work for an extended period of time due to a disabling illness or injury, long term disability insurance can replace a percentage of your lost income (up to a maximum monthly benefit) for a period of time as defined by the policy.

The company is offering Supplemental benefits from Unum. These benefits are Guaranteed Issue at initial eligibility, late entries will be subject to evidence of insurability. Take a moment to learn how these benefits can help protect your finances when you need it most. This information below will help guide you through the benefits Unum has to offer as well as important information to keep in mind while making your selections.
Click Here to learn more about these benefits.
Accident Insurance pays a set benefit amount based on the type of injury you have and the type of treatment you need. It covers accidents that occur on and off the job. And it includes a range of incidents, from common injuries to more serious events.
Why is this coverage so valuable?
It can help you with out-of-pocket costs that your medical plan doesn’t cover, like copays and deductibles. You’ll have base coverage without medical underwriting. The cost is conveniently deducted from your paycheck. You can keep your coverage if you change jobs or retire. You’ll be billed directly.
Click Here to view the detailed Accident Insurance flyer.
Hospital Insurance helps covered employees and their families cope with the financial impacts of a hospitalization. You can receive benefits when you’re admitted to the hospital for a covered accident, illness or childbirth.
Why is this coverage so valuable?
• The money is paid directly to you — not to a hospital or care provider. The money can also help you pay the out-of-pocket expenses your medical plan may not cover, such as coinsurance, copays and deductibles.
• You get affordable rates when you buy this coverage at work.
• The cost is conveniently deducted from your paycheck.
• The benefits in this plan are compatible with a Health Savings Account (HSA).
• You may take the coverage with you if you leave the company or retire, without having to answer new health questions. You’ll be billed directly.
• Wellness Benefit Available
Click Here to view the detailed Hospital Insurance flyer.
You: If you’re actively at work
Your Spouse*:
Can get coverage as long as you have purchased coverage for yourself.
Your Children*:
Dependent Children from birth until their 26th birthday, regardless of marital or student status.
*Employee must purchase coverage for themselves in order to purchase spouse or child coverage.


If you’re diagnosed with an illness that is covered by this insurance, you can receive a lump sum benefit payment. You can use the money however you want.
Why is this coverage so valuable?
• The money can help you pay out-of-pocket medical expenses, like copays and deductibles.
• You can use this coverage more than once. Even after you receive a payout for one illness, you’re still covered for the remaining conditions and for the reoccurrence of any critical illness with the exception of skin cancer. The reoccurrence benefit can pay 100% of your coverage amount. Diagnoses must be at least 180 days apart or the conditions can’t be related to each other.
• Wellness Benefit Available
Why should I buy coverage now?
• It’s more affordable when you buy it through your employer and the premiums are conveniently deducted from your paycheck.
• Coverage is portable. You may take the coverage with you if you leave the company or retire. You’ll be billed at home.
Click Here to view the detailed Critical Illness Insurance Flyer.
Choose $10,000, $20,000 or $30,000 of coverage with no medical underwriting to qualify if you apply during this enrollment.
Your Spouse:
Spouses can only get 50% of the employee coverage amount as long as you have purchased coverage for yourself.
Your Children:
Children from live birth to age 26 are automatically covered at no extra cost. Their coverage amount is 50% of yours. They are covered for all the same illnesses plus these specific childhood conditions: cerebral palsy, cleft lip or palate, cystic fibrosis, Down syndrome and spina bifida. The diagnosis must occur after the child’s coverage effective date.

This qualified, pre-tax program allows for immediate enrollment with no waiting period for all company employees, regardless of status. Auto-enrollment occurs on the 45th day of full-time employment. Auto-enrollment can be waived by calling Principal at 800.986.3343 or online at www.principal.com.
• Enroll, change, or cease contribution at anytime
• Contribute up to 70% of your earnings, up to the IRS annual mandate or HCE limitations
• Catch-up benefit available for employees over 50
• Comprehensive fund portfolio
Principal
Note: Employees defined as Highly Compensated Employees (HCE) under IRS regulations will be restricted to $10,000 in annual contributions due to plan testing requirements. Magnit uses a “look-back” year to determine HCE status. HCE status is reviewed annually. HCEs that are 50 years old or older are still eligible for the Catch-up contribution and their annual limit will be increased accordingly. Learn more about HCE status by clicking here .
*The 401(k) plan is not available to contractors based in Puerto Rico
529 Plans - Offered by College America
A 529 plan is a tax-advantaged investment vehicle in the United States designed to encourage saving for the future higher education expenses of a designated beneficiary. Beneficiary can attend any school nationwide. For more information contact John Fischer at john.fischer@wealthbfinancial.com for an individual consultation. Your employer’s education savings plan is here to help, Click Here to learn more.
Enjoy life with fewer worries with legal insurance from ARAG, available to company employees via a simple payroll deduction! Legal insurance provides its members a place to turn for help when facing life’s unexpected legal and financial issues. Two plan options are available to select from to best suit your needs. Click Here to learn more about Legal Insurance from ARAG, and view a comparison of the two plans available to you!

Phone: Website: Access Code: 800.247.4184 ARAGLegal.com/myinfo 18294mag
The company offers permanent, and portable whole life insurance to all of our benefits eligible employees, provided by Unum. This product also includes a long-term care rider!
You can purchase from $10,000 up to $300,000 of coverage. This plan is portable with coverage that does not decrease. Individual coverage for your spouse and your children is available even if you don’t purchase coverage for yourself. Please refer to your plan information for more details.
Please note: You may only enroll in the Unum Whole Life benefit at the time of hire or during the annual Open Enrollment period. Guarantee issue limits are only available to employees at the time of hire. All other employees will need to complete an Evidence of Insurability form.
Have questions, or need more information on the offerings by Unum?
Reach out to our call center at 1.800.346.3620 or Click Here to enroll!

Do you know who would provide care if you needed extended assistance with everyday activites like bathing and dressing because of an accident, chronic illness, or due to aging? Where would the money to pay for that care come from? Long Term Care insurance can play an important role in addressing your own and your family’s long-term care needs.
Click Here to access the Genworth Portal or Call 800.416.3624 , Monday - Friday 7am-7pm, Central Time. Reference Group Policy number: 18640
• Reduced/limited medical review for eligible employees.*
• Coverage available up to a lifetime maximum benefit pool of $288,000
• Coverage is available for employees and their family members at group rates, including spouses, parents, and others.
• Fully portable; Coverage goes with you when your employment ends.
*Eligible Full-time Employees 65 and under during their new hire enrollment period, excluding Alaska residents.
The insurance program is underwritten by Genworth Life Insurance Company with Administrative Offices in St. Paul, MN. Coverage under this plan is not available to residents of Vermont. Insurance is provided under a group policy 18640 issued to Magnit Global Solution Inc. using policy forms 7053POL-CA and 7053CRT-CA. Coverage is intended to be tax qualified under IRS code 7702(B).
Identity
Proprietary technology monitors for fraudulant use of your Social Security Number, Name, Address, and date of birth in applications for credit and services.
Device Security
Multi-layered, advanced security helps protect devices against existing and emerging malware threats, including ransomware.
Parental Control
Employees can take action to monitor their child’s online activity and identify potential dangers to help keep children safe when exploring online.
Online Privacy
Protect devices on vulnerable connections through bank-grade encryption to keep information private.
This benefit is subject to closed enrollment.
Click Here to learn more about Norton LifeLock benefit plans.
A will is essential for ensuring that your assets are distributed according to your wishes, that your loved ones are taken care of, and that potential conflicts are minimized. It’s a proactive step that offers both legal protection and peace of mind. So, whether enrolled in a ARAG Legal Plan or, taking advantage of the “Free” SImple Will Service with your UNUM EAP, we encourage you to complete this process as part of your overall financial plan. For more information, visit the UNUM Legal Resource Center by clicking here .

Travel Guard for Business Travel - Administered by AIG
Traveling requires attention to a number of unique details. A study from the Travel Leaders Corporate survey shows that travelers’ top concerns are travel logistics. You are covered with business travel accident insurance along with travel assistance services to help you with travel mishaps or emergencies during your trip. This insurance coverage is provided by your employer. Whether it’s a medical emergency, flight delay or lost luggage, we are here 24 hours a day, 7 days a week to support you. For support with the U.S., just call 1.877.244.6871, or outside of the U.S., call +1.715.346.0859 (Collect/Reverse Charge call).
Click Here to access the AIG Portal; Your policy number is 9155849.
Click Here to view the AIG Business Travel Summary
Medical Assistance
• Medical evacuation and repatriation assistance
• Out-of-Country Medical Coverage up to $200,000
• Hospital and provider assistance
• Emergency prescription replacement assistance
• Assistance with the renting and/or replacement of medical equipment
Travel Assistance
• Lost/stolen baggage assistance
• Lost passport/travel documents assistance
• ATM locator
• Emergency telephone interpretation coordination
• Legal/bail bond referrals
• Embassy and consulate information
Concierge Services
• Restaurant referrals and reservations
• Event ticketing
• Ground transportation coordination
• Wireless device assistance
Identity Theft Assistance**
• Account activity monitoring assistance
• Financial account investigation assistance
• Credit review and fraud detector assistance
• Social Security personal earnings and benefits statement assistance
• Collaborate with law enforcement
Assistance Website and Mobile App
• Travel Security Awareness Training - online instruction modules
• Country reports
• Travel alerts
Security Assistance
• Security evacuation assistance with on-the-ground physical response
• Security and safety advisories
• 24-hour response services to assist employees and their families during an incident
• Online access to up-to-date security intelligence
**Identity theft services are not available for residents in New York or outside the United States.



https://spotpet.link/magnit



PerkSpot is a one-stop-shop for exclusive discounts at many of your favorite national and local merchants. It is completely free and optimized for use on any device: desktops, tablets and phones. Enjoy access to thousands of discounts in dozens of categories, updated daily. Take advantage of online offers from popular national retailers, and discover discounts in your neighborhood with PerkSpot’s streamlined Local Map. Filter your map results by categories like restaurants, health and fitness, retail and more.
Opt in to PerkSpot’s weekly email to receive a curated selection of discounts. Each week’s email features both new and popular deals, as well as seasonal and thematic groupings of offers. The PerkSpot weekly email is a particularly great resource for your holiday shopping.
Start saving today by signing up or logging in at: MagnitGlobal .PerkSpot.com
PerkSpot’s customer service team works tirelessly to help you access your Discount Program and redeem deals easily. Below are some important details regarding customer service availability.
Hours: 9am - 6pm, Monday - Friday
Phone: 866.606.6057
Email: cs@perkspot.com
Support*: support.perkspot.com
*If you’ve still got some questions, visit support.perkspot.com to submit a request. PerkSpot’s bilingual Customer Service team will reach out and can answer any questions in both English and Spanish.
Join Tripbeat, Save Big, and Travel the World!
We are delighted to announce that Tripbeat is now available to all Magnit employees.
Magnit has partnered with Tripbeat, powered by Travel + Leisure Co., to bring you exclusive access to incredible savings on your future travels. Tripbeat is easy-to-use online platform that offers a wide range of travel deals, from savings on resorts and hotels to car rentals and tours, all at incredible prices. TripBeat brings you unparalleled savings and benefits. Whether you are dreaming of relaxing on breathtaking beaches, indulging in delicious cuisine, or delving into rich historical landmarks, the platform has you covered. Magnit is providing all employees a complimentary 12-month premium membership. You will have access to the deepest discounts on the website, allowing you to save in time for your upcoming summer travels.
HOTELS: Deeper discounts on 600,000+ hotels worldwide at up to 60% off*
RESORTS: $389 week-long resort stays
CAR RENTALS: Up to 20% off at major rental companies
AIRFARE: Book popular airlines for domestic and international flights
ACTIVITIES: Access to 345,000+ tours and activities
CRUISES:
Premium Member Exclusive – Sail away with up to $1,500 in onboard credits
VACATION HOMES: Premium Member Exclusive – Rentals with special member pricing
TICKETS: Premium Member Exclusive – Enjoy special member pricing on theme parks, concerts, movie tickets, and more
After the 12-months, the company will provide employees a complimentary standard membership. Employees may maintain their premium membership for $9.95 per month. Consider signing up today, and begin booking hotels, resorts, car rentals, cruises and more.
Click Here to sign up for FREE today with activation code: Magnit12



1 Find your perfect gym from 12,500+ options nationwide including:
• 24 Hour Fitness®
• EōS Fitness®
• Crunch Fitness®
• Blink Fitness®
• Anytime Fitness®
• Chuze Fitness®
• and more.
2 Enroll online in minutes, with no long-term contracts or annual fees.
3 Start working out today! Your membership also includes 1:1 well-being coaching! PLUS
• 8,500+ premium gym options including FIT4MOM®, Pure Barre®, Club Pilates®, Row House®, and more with 20% - 70% discounts at most locations1
• Membership options for your spouse2
• Get Fit at Home™ for Free with 12,000+ on-demand workout videos before you enroll! Just create an account.
Register today! The access link can be found in Dayforce under the Benefits Overview Page. Click here to login to Dayforce.
Click Here to Chat With Active & Fit or call

Noom works for weight loss
Powered by psychology, Noom Weight uses evidence based techniques to empower behavior change. It’s a personalized, mind-first approach that combines technology and human support to create healthier daily habits that lead to long-lasting results.
• Techniques that teach people the why behind their habits and how to change them
• Daily lessons tailored to each person’s goals
• One-on-one coaching and peer support to help improve outcomes
• GLP-1 Companion delivers a holistic treatment plan powered by behavior change for members who utilize GLP-1 medication.
• Noom Move in partnership with FitOn Health, offers thousands of fitness videos, and all users get a daily recommended class. Within GLP-1 Companion, there is a special fitness track known as MuscleDefense with curated workouts that help support lean muscle mass.
• Macro monitoring supports quality and balanced meals,
• 3D body scan aids early detection of health risks.
Magnit is proud to offer Noom at a discount!
Enrollment is Easy.
1. Visit Noom.com
2. Use Code: NOOM20
HelloFresh Benefit - America’s #1 Meal Kit
As a Magnit Global employee, you have access to an exclusive discount to get started with HelloFresh.
1st Box: 60% Off + Free Shipping (as low as $25!)
2nd - 5th Box: 20% Off
How HelloFresh Works!
1. Pick a Plan
Choose a plan to match your lifestyle. Modify or skip a week with ease.
2. Get Your Delivery
Receive weekly deliveries with step-by-step recipes and pre-measured ingredients.
3. Cook, Eat, Enjoy
Welcome to a world where dinner is always planned, simple, and delicious.
How can you begin ordering?
Click Here, or Create a hellofresh.com account using code MAGNIT2024 for your automatic discount. Call HelloFresh Customer Service at 646.362.3066 if you need help or have questions!

Liberty Mutual has partnered with the company to offer employees special savings on quality auto and home insurance and with benefits such as Multi-Policy Discount, Personal Property Replacement, and 24-Hour Claims Assistance, you’ll worry less and save more. Call 800.699.4378 or visit LibertyMutual.com/magnitglobal to learn more or get a free quote.
Financial services include:
•No-fee checking
•Online banking
•No-fee VISA credit cards
•Financial planning services
•Auto and consumer loans
•Mortgages and home equity loans
•IRAs and money market accounts
Click Here to learn more about iThink Financial. Click here to learn how to join iThink Financial today.
Save up to 65% on prescription medication costs and wide range of other health services.
Click Here for more information.
Now available to Magnit Employees Exclusive Savings on Dell products and services. Click here to learn more or go to www.dell.com/mpp/magnit to access the savings.
International Travel Insurance by Patriot Travel
Traveling abroad is an exciting experience, but unpredictable illnesses and accidents can happen. Most travelers assume that they are already covered by their standard medical plan – but that is not always the case. Chose a Patriot Travel plan to provide safety solutions for:
·Physical Health
·Financial Protection
·Crisis Support
·Personal Property
Click here to quote and apply for coverage today!
Employees can receive a 15% discount on wireless services from Verizon, additionally, the Disney bundle is now included with select Unlimited Plans.*
Click Here for more information and *Terms
Reasons to choose The Learning Experience as your childcare provider include: Curriculum that develops the whole child, Expert Guidance, State-of-the-Art Facilities, Health and Safety Protocols.
Click Here to learn more!
•Fitness discount store with Invite Fitness Use Code: msg23
• Cigna Wellness Webinars , for those enrolled in medical
For information on the discounts listed above, please visit the Global Support Center , or visit HRconnection


This notice is being provided to ensure that you understand your right to apply for group health insurance coverage. You should read this notice even if you plan to waive coverage at this time.
If you are declining coverage for yourself or your dependents (including your spouse) because of other health insurance or group health plan coverage, you may be able to enroll yourself and your dependents in this plan if you or your dependents lose eligibility for that other coverage (or if the employer stops contributing toward your or your dependents’ coverage).
However, you must request enrollment within 30 days after your or your dependents other coverage ends (or after the employer stops contributing toward the other coverage).
Example: You waived coverage because you were covered under a plan offered by your spouse’s employer. Your spouse terminates their employment. If you notify your employer within 30 days of the date coverage ends, you and your eligible dependents may apply for coverage under our health plan.
If you or your dependent(s) lose coverage under a state Children’s Health Insurance Program (CHIP) or Medicaid, you may be able to enroll yourself and your dependents. However, you must request enrollment within 60 days after the loss of CHIP or Medicaid coverage.
If you or your dependent(s) become eligible to receive premium assistance under a state CHIP or Medicaid, you may be able to enroll yourself and your dependents. However, you must request enrollment within 60 days of the determination of eligibility for premium assistance from state CHIP or Medicaid.
If you have a new dependent as a result of a marriage, birth, adoption or placement for adoption, you may be able to enroll yourself and your dependents. However, you must request enrollment within 30 days after the marriage, birth, adoption, or placement for adoption.
Group health plans and health insurance issuers generally may not, under Federal law, restrict benefits for any hospital length of stay in connection with childbirth for the mother or newborn child to less than 48 hours following a vaginal delivery, or less than 96 hours following a cesarean section.
However, Federal law generally does not prohibit the mother’s or newborn’s attending provider, after consulting with the mother, from discharging the mother or her newborn earlier than 48 hours (or 96 hours as applicable). In any case, plans and issuers may not, under Federal law, require that a provider obtain authorization from the plan or the insurance issuer for prescribing a length of stay not in excess of 48 hours (or 96 hours).
The Genetic Information Nondiscrimination Act of 2008 (“GINA”) protects employees against discrimination based on their genetic information. Unless otherwise permitted, your Employer may not request or require any genetic information from you or your family members. Click Here for the entire disclosure notice.
A Summary of Benefits Coverage (SBC) for each of the employer-sponsored medical plans is available on your portal at HRconnection.com

Under the Women’s Health and Cancer Rights Act, group health plans must make certain benefits available to participants of health plans who have undergone a mastectomy. In particular, a plan must offer mastectomy patients benefits for:
• Reconstruction of the breast on which the mastectomy was performed;
• Any necessary surgery and reconstruction of the other breast to produce a symmetrical appearance;
• Prostheses;
• Treatment of physical conditions related to the mastectomy including lymphedema.
Our medical plans comply with these requirements. Benefits for these items are similar to those provided under the plan for similar types of medical plan services and supplies.
The privacy provisions of the Health Insurance Portability and Accountability Act of 1996 (HIPAA) help to ensure that your healthcare-related information stays private. New employees will receive a Privacy Practice notice which outlines the ways in which the medical plan may use and disclose protected health information (PHI). The notice also describes your rights. For more information, please visit the Global Support Center .
The Medical Plan will cover eligible dependent children of an employee to age 26 regardless of student status, marital status, residence or financial dependence on the employee, if not eligible to access coverage through his/her employer’s plan.
The Mental Health Parity and Addiction Equity Act of 2008 generally requires group health plans and health insurance issuers to ensure that financial requirements (such as copays and deductibles) and treatment limitations (such as annual visit limits) applicable to mental health or substance use disorder benefits are no more restrictive than the predominant requirements or limitations applied to substantially all medical/surgical benefits. For information regarding the criteria for medical necessity determinations made under the plan with respect to mental health or substance use disorder benefits, please visit the Global Support Center .

When you get emergency care or get treated by an out-of-network provider at an in-network hospital or ambulatory surgical center, you are protected from surprise billing or balance billing.
What is “balance billing” (sometimes called “surprise billing”)?
When you see a doctor or other health care provider, you may owe certain out-of-pocket costs, such as a copayment, coinsurance, and/or a deductible. You may have other costs or have to pay the entire bill if you see a provider or visit a health care facility that isn’t in your health plan’s network.
“Out-of-network” describes providers and facilities that haven’t signed a contract with your health plan. Out-of-network providers may be permitted to bill you for the difference between what your plan agreed to pay and the full amount charged for a service. This is called “balance billing.” This amount is likely more than in-network costs for the same service and might not count toward your annual out-of-pocket limit.
“Surprise billing” is an unexpected balance bill. This can happen when you can’t control who is involved in your care—like when you have an emergency or when you schedule a visit at an in-network facility but are unexpectedly treated by an out-of-network provider.
You are protected from balance billing for: Emergency services
If you have an emergency medical condition and get emergency services from an out-of-network provider or facility, the most the provider or facility may bill you is your plan’s in-network cost-sharing amount (such as copayments and coinsurance). You can’t be balance billed for these emergency services. This includes services you may get after you’re in stable condition, unless you give written consent and give up your protections not to be balanced billed for these post-stabilization services.
When you get emergency care or are treated by an out-of-network provider at an in-network hospital or ambulatory surgical center, you are protected from balance billing. In these cases, you shouldn’t be charged more than your plan’s copayments, coinsurance and/or deductible.
Certain services at an in-network hospital or ambulatory surgical center
When you get services from an in-network hospital or ambulatory surgical center, certain providers there may be out-of-network. In these cases, the most those providers may bill you is your plan’s in-network cost-sharing amount. This applies to emergency medicine, anesthesia, pathology, radiology, laboratory, neonatology, assistant surgeon, hospitalist, or intensivist services. These providers can’t balance bill you and may not ask you to give up your protections not to be balance billed.
If you get other services at these in-network facilities, out-of-network providers can’t balance bill you, unless you give written consent and give up your protections. You’re never required to give up your protections from balance billing. You also aren’t required to get care out-of-network. You can choose a provider or facility in your plan’s network. When balance billing isn’t allowed, you also have the following protections:
• You are only responsible for paying your share of the cost (like the copayments, coinsurance, and deductibles that you would pay if the provider or facility was in-network). Your health plan will pay out-of-network providers and facilities directly.
• Your health plan generally must:
o Cover emergency services without requiring you to get approval (prior authorization) for services in advance.
o Cover emergency services by out-of-network providers.
o Base what you owe the provider or facility (cost-sharing) on what it would pay an in-network provider or facility and show that amount in your explanation of benefits.
o Count any amount you pay for emergency services or out-of-network services toward your deductible and out-of-pocket limit.
If you believe you’ve been wrongly billed, you may contact the No Surprises Helpdesk, operated by the U.S. Department of Health and Human Services, at 1.800.985.3059
Click Here for more information about your rights under federal law.

If you or one of your dependents experience a COBRA qualifying event resulting in a loss of coverage under one of the company’s group health insurance plans, you and your eligible dependents may have the right to continue your medical, dental, or vision coverage through COBRA for at least 18 months or more at your (or your dependents’) expense.
Examples of COBRA qualifying events include but are not limited to:
• Termination of employment with the company for reasons other than gross misconduct
• Reduction in hours resulting in the loss of group health coverage
• Divorce or Legal Separation
• Dependent child ceases to be dependent child under the group health plan
The United States Department of Labor Wage and Hour Division Leave Entitlements
Eligible employees who work for a covered employer can take up to 12 weeks of unpaid, job protected leave in a 12-month period for the following reasons:
• The birth of a child or placement of a child for adoption or foster care;
• To bond with a child (leave must be taken within 1 year of the child’s birth or placement);
• To care for the employee’s spouse, child, or parent who has a qualifying serious health condition;
• For the employee’s own qualifying serious health condition that makes the employee unable to perform the employee’s job;
• For qualifying exigencies related to the foreign deployment of a military member who is the employee’s spouse, child, or parent.
An eligible employee who is a covered servicemember’s spouse, child, parent, or next of kin may also take up to 26 weeks of FMLA leave in a single 12-month period to care for the servicemember with a serious injury or illness.
An employee does not need to use leave in one block. When it is medically necessary or otherwise permitted, employees may take leave intermittently or on a reduced schedule.
Employees may choose, or an employer may require, use of accrued paid leave while taking FMLA leave. If an employee substitutes accrued paid leave for FMLA leave, the employee must comply with the employer’s normal paid leave policies.
While employees are on FMLA leave, employers must continue health insurance coverage as if the employees were not on leave.
Upon return from FMLA leave, most employees must be restored to the same job or one nearly identical to it with equivalent pay, benefits, and other employment terms and conditions.
An employer may not interfere with an individual’s FMLA rights or retaliate against someone for using or trying to use FMLA leave, opposing any practice made unlawful by the FMLA, or being involved in any proceeding under or related to the FMLA.

General FMLA Notice (Continued)
Eligibility Requirements
An employee who works for a covered employer must meet three criteria in order to be eligible for FMLA leave. The employee must:
• Have worked for the employer for at least 12 months;
• Have at least 1,250 hours of service in the 12 months before taking leave;* and
• Work at a location where the employer has at least 50 employees within 75 miles of the employee’s worksite.
*Special “hours of service” requirements apply to airline flight crew employees.
Requesting Leave
Generally, employees must give 30-days’ advance notice of the need for FMLA leave. If it is not possible to give 30-days’ notice, an employee must notify the employer as soon as possible and, generally, follow the employer’s usual procedures.
Employees do not have to share a medical diagnosis, but must provide enough information to the employer so it can determine if the leave qualifies for FMLA protection. Sufficient information could include informing an employer that the employee is or will be unable to perform his or her job functions, that a family member cannot perform daily activities, or that hospitalization or continuing medical treatment is necessary. Employees must inform the employer if the need for leave is for a reason for which FMLA leave was previously taken or certified.
Employers can require a certification or periodic recertification supporting the need for leave. If the employer determines that the certification is incomplete, it must provide a written notice indicating what additional information is required.
Once an employer becomes aware that an employee’s need for leave is for a reason that may qualify under the FMLA, the employer must notify the employee if he or she is eligible for FMLA leave and, if eligible, must also provide a notice of rights and responsibilities under the FMLA. If the employee is not eligible, the employer must provide a reason for ineligibility. Employers must notify its employees if leave will be designated as FMLA leave, and if so, how much leave will be designated as FMLA leave.
Enforcement
Employees may file a complaint with the U.S. Department of Labor, Wage and Hour Division, or may bring a private lawsuit against an employer. The FMLA does not affect any federal or state law prohibiting discrimination or supersede any state or local law or collective bargaining agreement that provides greater family or medical leave rights.
The Magnit Global Solutions, Inc. Plan generally allows the designation of a primary care provider. You have the right to designate any primary care provider who participates in our network and who is available to accept you or your family members. For information on how to select a primary care provider, and for a list of the participating primary care providers, contact:
Jennifer Brancazio
110 Front St, Suite 353 Jupiter, FL 33477
1-800-813-7946
For children, you may designate a pediatrician as the primary care provider.

The purpose of this notice is to advise you that the prescription drug coverage listed under the Magnit medical plans is expected to pay out, on average, at least as much as the standard Medicare prescription drug coverage will pay in the plan year. This is known as “creditable coverage.”
Please read this notice carefully and keep it where you can find it. This notice has information about your current prescription drug coverage with Rightsourcing, Inc. and about your options under Medicare’s prescription drug coverage. This information can help you decide whether or not you want to join a Medicare drug plan. If you are considering joining, you should compare your current coverage, including which drugs are covered at what cost, with the coverage and costs of the plans offering Medicare prescription drug coverage in your area. Information about where you can get help to make decisions about your prescription drug coverage is at the end of this notice.
There are two important things you need to know about your current coverage and Medicare’s prescription drug coverage:
1. Medicare prescription drug coverage became available in 2006 to everyone with Medicare. You can get this coverage if you join a Medicare Prescription Drug Plan or join a Medicare Advantage Plan (like an HMO or PPO) that offers prescription drug coverage. All Medicare drug plans provide at least a standard level of coverage set by Medicare. Some plans may also offer more coverage for a higher monthly premium.
2. Magnit Global has determined that the prescription drug coverage offered by the 2023-2024 Plan Year is, on average for all plan participants, expected to pay out as much as standard Medicare prescription drug coverage pays and is therefore considered Creditable Coverage. Because your existing coverage is Creditable Coverage, you can keep this coverage and not pay a higher premium (a penalty) if you later decide to join a Medicare drug plan.
You can join a Medicare drug plan when you first become eligible for Medicare and each year from October 15th to December 7th.
However, if you lose your current creditable prescription drug coverage, through no fault of your own, you will also be eligible for a two (2) month Special Enrollment Period (SEP) to join a Medicare drug plan.
If you decide to join a Medicare drug plan, your current Rightsourcing, Inc. coverage will not be affected. Medicare eligible employees who are on the benefit plan, will have the same access as non-Medicare employees.
If you do decide to join a Medicare drug plan and drop your current Rightsourcing, Inc. coverage, be aware that you and your dependents will be able to get this coverage back.
You should also know that if you drop or lose your current coverage with Rightsourcing, Inc. and don’t join a Medicare drug plan within 63 continuous days after your current coverage ends, you may pay a higher premium (a penalty) to join a Medicare drug plan later.
If you go 63 continuous days or longer without creditable prescription drug coverage, your monthly premium may go up by at least 1% of the Medicare base beneficiary premium per month for every month that you did not have that coverage. For example, if you go nineteen months without creditable coverage, your premium may consistently be at least 19% higher than the Medicare base beneficiary premium. You may have to pay this higher premium (a penalty) as long as you have Medicare prescription drug coverage. In addition, you may have to wait until the following October to join.

Important Notice from Magnit Global About Your Prescription Drug Coverage and Medicare (Continued)
For More Information About This Notice or Your Current Prescription Drug Coverage
For further information, visit the Global Support Center
NOTE: You’ll get this notice each year. You will also get it before the next period you can join a Medicare drug plan, and if this coverage through Rightsourcing, Inc. changes. You also may request a copy of this notice at any time.
For More Information About Your Options Under Medicare Prescription Drug Coverage
More detailed information about Medicare plans that offer prescription drug coverage is in the “Medicare & You” handbook. You’ll get a copy of the handbook in the mail every year from Medicare. You may also be contacted directly by Medicare drug plans.
For more information about Medicare prescription drug coverage:
· Visit www.medicare.gov
· Call your State Health Insurance Assistance Program (see the inside back cover of your copy of the “Medicare & You” handbook for their telephone number) for personalized help
· Call 1.800.MEDICARE (1.800.633.4227). TTY users should call 1.877.486.2048
If you have limited income and resources, extra help paying for Medicare prescription drug coverage is available. For information about this extra help, visit Social Security on the web at www.socialsecurity.gov, or call them at 1.800.772.1213 (TTY 1-800-325-0778).
Remember: Keep this Creditable Coverage notice. If you decide to join one of the Medicare drug plans, you may be required to provide a copy of this notice when you join to show whether or not you have maintained creditable coverage and, therefore, whether or not you are required to pay a higher premium (a penalty).
Premium Assistance Under Medicaid and the Children’s Health Insurance Program (CHIP)
If you or your children are eligible for Medicaid or CHIP and you’re eligible for health coverage from your employer, your state may have a premium assistance program that can help pay for coverage, using funds from their Medicaid or CHIP programs. If you or your children aren’t eligible for Medicaid or CHIP, you won’t be eligible for these premium assistance programs but you may be able to buy individual insurance coverage through the Health Insurance Marketplace. For more information, visit www.healthcare.gov.
If you or your dependents are already enrolled in Medicaid or CHIP and you live in a State listed below, contact your State Medicaid or CHIP office to find out if premium assistance is available.
If you or your dependents are NOT currently enrolled in Medicaid or CHIP, and you think you or any of your dependents might be eligible for either of these programs, contact your State Medicaid or CHIP office or dial 1.877.KIDS.NOW or www.insurekidsnow.gov to find out how to apply. If you qualify, ask your state if it has a program that might help you pay the premiums for an employer-sponsored plan.
If you or your dependents are eligible for premium assistance under Medicaid or CHIP, as well as eligible under your employer plan, your employer must allow you to enroll in your employer plan if you aren’t already enrolled. This is called a “special enrollment” opportunity, and you must request coverage within 60 days of being determined eligible for premium assistance. If you have questions about enrolling in your employer plan, contact the Department of Labor at www.askebsa.dol.gov or call 1-866-444-EBSA (3272).
If you live in one of the states on the following pages, you may be eligible for assistance paying your employer health plan premiums. The following list of states is current as of January 31, 2023. Contact your State for more information on eligibility –

Alabama - Medicaid
Website: http://myalhipp.com/
Phone: 1-855-692-5447
Alaska - Medicaid
The AK Health Insurance Premium Payment Program
Website: http://myakhipp.com/
Phone: 1-866-251-4861
Email: CustomerService@myakhipp.com
Medicaid Eligibility: https://health.alaska.gov/dpa/Pages/default.aspx
Arkansas - Medicaid
Website: http://myarhipp.com/
Phone: 1-855-692-7447
California - Medicaid
Health Insurance Premium Payment (HIPP) Program
Website: http://dhcs.ca.gov/hipp
Phone: 916-445-8322
Fax: 916-440-5676
Email: hipp@dhcs.ca.gov
Colorado - Health First Colorado (Colorado’s Medicaid Program) & Child Health Plan Plus (CHP+)
Health First Colorado Website: https://www.healthfirstcolorado.com/
Health First Colorado Member Contact Center: 1-800-221-3943/ State Relay 711
CHP+: https://hcpf.colorado.gov/child-health-plan-plus
CHP+ Customer Service: 1-800-359-1991/ State Relay 711 Health Insurance Buy-in Program (HIBI): https://www.mycohibi.com/ HIBI Customer Service: 1-855-692-6442
Florida - Medicaid
Website:
https://www.flmedicaidtplrecovery.com/flmedicaidt plrecovery.com/hipp/index.html
Phone: 1-877-357-3268
Georgia - Medicaid
GA HIPP Website: https://medicaid.georgia.gov/health-insurance-premium-payment-program-hipp
Phone: 678-564-1162, press 1
GA CHIPRA Website: https://medicaid.georgia.gov/programs/third-party-lia bility/childrens-health-insurance-program-reauthori zation-act-2009-chipra
Phone: 678-564-1162, press 2
Indiana - Medicaid
Healthy Indiana Plan for low-income adults 19-64
Website: http://www.in.gov/fssa/hip/ Phone: 1-877-438-4479
All other Medicaid Website: https://www.in.gov/medicaid Phone: 1-800-457-4584
Iowa - Medicaid and Chip (Hawki)
Medicaid Website: https://hhs.iowa.gov/programs/welcome-iowa-medicaid
Medicaid Phone: 1-800-338-8366
Hawki Website: http://dhs.iowa.gov/hawki
Hawki Phone: 1-800-257-8563
HIPP Website: https://hhs.iowa.gov/programs/welcome-iowa-medicaid/ fee-service/hipp
HIPP Phone: 1-888-346-9562
Kansas - Medicaid
Website: https://www.kancare.ks.gov/
Phone: 1-800-792-4884
HIPP Phone: 1-800-766-9012
Kentucky - Medicaid
Kentucky Integrated Health Insurance Premium Payment Program (KI-HIPP) Website: https://chfs.ky.gov/agencies/dms/member/Pages/ kihipp.aspx
Phone: 1-855-459-6328
Email: KIHIPP.PROGRAM@ky.gov
KCHIP Website: https://kidshealth.ky.gov/pages/index.aspx
Phone: 1-877-524-4718
Kentucky Medicaid Website: https://chfs.ky.gov
Louisiana - Medicaid
Website: www.medicaid.la.gov or www.ldh.la.gov/lahipp
Phone: 1-888-342-6207 (medicaid hotline) or 1-855-618-5488 (LaHIPP)
Maine - Medicaid
Enrollment Website: https://www.mymaineconnection.gov/benefits
Phone: 1-800-442-6003
TTY: Maine Relay 711
Private Health Insurance Premium Webpage: https://www.maine.gov/dhhs/ofi/applications-forms
Phone: 1-800-977-6740
TTY: Maine relay 711
Massachusetts - Medicaid and CHIP
Website: https://www.mass.gov/masshealth/pa
Phone: 1-800-862-4840
TTY: 617-886-8102
Minnesota - Medicaid
Website:
https://mn.gov/dhs/people-we-serve/children-and-families/health-care/health-care-programs/ programs-and-services/other-insurance.jsp
Phone: 1-800-657-3739
Missouri - Medicaid
Website: http://www.dss.mo.gov/mhd/participants/pages/hipp.htm
Phone: 573-751-2005
Montana - Medicaid
Website:
http://dphhs.mt.gov/MontanaHealthcarePrograms/HIPP
Phone: 1-800-694-3084
Email: HHSHIPPProgram@mt.gov
Nebraska - Medicaid
Website: http://www.ACCESSNebraska.ne.gov
Phone: 1-855-632-7633
Lincoln: 402-473-7000
Omaha: 402-595-1178
Nevada - Medicaid
Medicaid Website: http://dhcfp.nv.gov
Medicaid Phone: 1-800-992-0900
New Hampshire - Medicaid
Website: https://www.dhhs.nh.gov/programs-services/ medicaid/health-insurance-premium-program
Phone: 603-271-5218
Toll Free Number for the HIPP program: 1-800-852-3345, ext. 5218
New Jersey - Medicaid and CHIP
Medicaid Website: http://www.state.nj.us/humanservices/dmahs/clients/ medicaid/
Medicaid Phone: 609-631-2392
CHIP Website: http://www.njfamilycare.org/index.html
CHIP Phone: 1-800-701-0710
New York - Medicaid
Website: https://health.ny.gov/health_care/medicaid/ Medicaid Phone: 1-800-541-2831
North Carolina - Medicaid
Website: https://medicaid.ncdhhs.gov/ Phone: 919-855-4100
North Dakota - Medicaid and CHIP
Website: http://www.nd.gov/dhs/services/medicalserv/medicaid/ Phone: 1-844-854-4825
Oklahoma - Medicaid and CHIP
Website: http://www.insureoklahoma.org Phone: 1-888-365-3742
Oregon - Medicaid
Website: http://healthcare.oregon.gov/Pages/index.aspx http://www.oregonhealthcare.gov/index-es.html Phone: 1-800-699-9075
Pennsylvania - Medicaid and CHIP
Website: https://www.pa.gov/en/agencies/dhs.html
Phone: 1-800-692-7462
Chip Website: https://www.pa.gov/en/services/dhs/apply-for-childrens-health-insurance-program-chip.html
CHIP Phone: 1-800-986-KIDS (5437)
Rhode Island - Medicaid and CHIP
Website: http://www.eohhs.ri.gov/ Phone: 1-855-697-4347, or 401-462-0311 (Direct Rite Share Line)
South Carolina - Medicaid
Website: https://www.scdhhs.gov Phone: 1-888-549-0820
South Dakota - Medicaid
Website: http://dss.sd.gov Phone: 1-888-828-0059
Texas - Medicaid
Website: http://gethipptexas.com/ Phone: 1-800-440-0493
Utah - Medicaid and CHIP
Medicaid Website: https://medicaid.utah.gov/ CHIP Website: https://chip.utah.gov/ Phone: 1-877-543-7669
Vermont - Medicaid
Website: https://dvha.vermont.gov/members/medicaid/ hipp-program
Phone: 1-800-250-8427
Virginia - Medicaid and CHIP
Website: https://www.coverva.org/en/famis-select https://www.coverva.org/en/hipp
Medicaid/CHIP Phone: 1-800-432-5924
Washington - Medicaid
Website: https://www.hca.wa.gov/ Phone: 1-800-562-3022
West Virginia - Medicaid and CHIP
Website: https://dhhr.wv.gov/bms/ http://mywvhipp.com/
Medicaid Phone: 304-558-1700
CHIP Toll-free phone: 1-855-MyWVHIPP (1-855-699-8447)
Wisconsin - Medicaid and CHIP
Website: https://www.dhs.wisconsin.gov/badgercareplus/p-10095.htm
Phone: 1-800-362-3002
Wyoming - Medicaid Website: https://health.wyo.gov/healthcarefin/medicaid/programs-and-eligibility/ Phone: 1-800-251-1269
For more information on special enrollment rights, you can contact one of the below resources:
U.S. Department of Labor Employee Benefits Security Administration www.dol.gov/ebsa
1.866.444.EBSA (3272)
U.S. Department of Health and Human Services Center for Medicare and Medicaid Services www.cms.hhs.gov
1.877.267.2323, Menu Option 4, Ext. 61565
