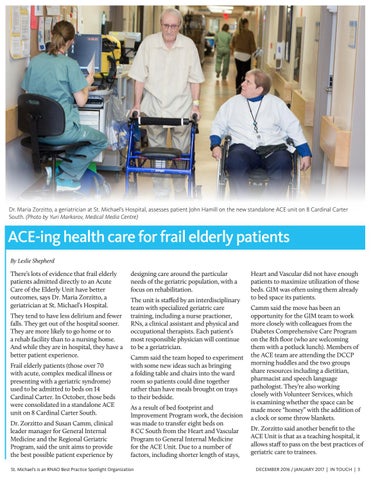
Dr. Maria Zorzitto, a geriatrician at St. Michael’s Hospital, assesses patient John Hamill on the new standalone ACE unit on 8 Cardinal Carter South. (Photo by Yuri Markarov, Medical Media Centre)
ACE-ing health care for frail elderly patients By Leslie Shepherd
There’s lots of evidence that frail elderly patients admitted directly to an Acute Care of the Elderly Unit have better outcomes, says Dr. Maria Zorzitto, a geriatrician at St. Michael’s Hospital. They tend to have less delirium and fewer falls. They get out of the hospital sooner. They are more likely to go home or to a rehab facility than to a nursing home. And while they are in hospital, they have a better patient experience. Frail elderly patients (those over 70 with acute, complex medical illness or presenting with a geriatric syndrome) used to be admitted to beds on 14 Cardinal Carter. In October, those beds were consolidated in a standalone ACE unit on 8 Cardinal Carter South. Dr. Zorzitto and Susan Camm, clinical leader manager for General Internal Medicine and the Regional Geriatric Program, said the unit aims to provide the best possible patient experience by
designing care around the particular needs of the geriatric population, with a focus on rehabilitation. The unit is staffed by an interdisciplinary team with specialized geriatric care training, including a nurse practioner, RNs, a clinical assistant and physical and occupational therapists. Each patient’s most responsible physician will continue to be a geriatrician. Camm said the team hoped to experiment with some new ideas such as bringing a folding table and chairs into the ward room so patients could dine together rather than have meals brought on trays to their bedside. As a result of bed footprint and Improvement Program work, the decision was made to transfer eight beds on 8 CC South from the Heart and Vascular Program to General Internal Medicine for the ACE Unit. Due to a number of factors, including shorter length of stays,
St. Michael’s is an RNAO Best Practice Spotlight Organization
Heart and Vascular did not have enough patients to maximize utilization of those beds. GIM was often using them already to bed space its patients. Camm said the move has been an opportunity for the GIM team to work more closely with colleagues from the Diabetes Comprehensive Care Program on the 8th floor (who are welcoming them with a potluck lunch). Members of the ACE team are attending the DCCP morning huddles and the two groups share resources including a dietitian, pharmacist and speech language pathologist. They’re also working closely with Volunteer Services, which is examining whether the space can be made more “homey” with the addition of a clock or some throw blankets. Dr. Zorzitto said another benefit to the ACE Unit is that as a teaching hospital, it allows staff to pass on the best practices of geriatric care to trainees. DECEMBER 2016 / JANUARY 2017 | IN TOUCH | 3