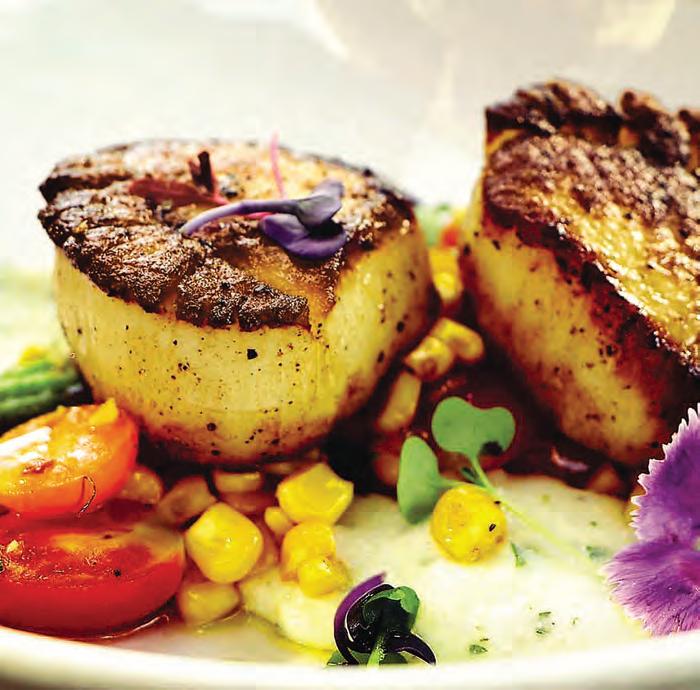CREATE THE PERFECT DINNER PARTY THIS SEASON SACMAG.COM NOVEMBER 2022 $4.95 THE GREAT RESIGNATION WHY LOCALS QUIT THEIR JOBS DAY TRIP: TRI-VALLEY FOOD, WINE, TRAILS WEDDING ROUNDTABLE COSTS AND TRENDS Autumn F east RECIPES − DÉCOR − SEATING PLAN − PLAYLIST − and more Plus: BE A GREAT GUEST! —


504 Pavilions Lane Sacramento, CA 95825 916-927-2300





































































































5220 DOUGLAS BLVD · GRANITE BAY, CA 95746 GraniteBayCosmetic.com · 916.436.5090 Granite Bay Cosmetic Surgery • BREAST AUGMENTATION • BREAST LIFT • BREAST REDUCTION • TUMMY TUCK • MOMMY MAKEOVER • LIPOSUCTION • BRAZILIAN BUTT LIFT • POST BARIATRIC OR POST WEIGHT LOSS BODY CONTOURING Dr. Orlando offers a full range of procedures for the breast & body including: @GraniteBayCosmeticSurgery @granitebaycosmetic MARC ORLANDO, MD • PLASTIC SURGEON






































www.ardenhills.club
You don’t need to leave town to leave the world behind.
Hosting an autumn gathering is a breeze with recipes and the right advice.










Table of Contents / Staff Box / Editor’s Note / Contributors
Some locals have rethought their relationship with employment.
 By Sasha Abramsky
By Sasha Abramsky
THE AU COURANT WEDDING Now that weddings are back on, experts talk trends—and costs.
By Angela Knight
)
A toast to fall and friends
SACMAG.COM November 2022 7
November
susan yee




8 SACRAMENTO MAGAZINE N ovember 2022 Contents 96 46 ON THE COVER The 916 20 DAY TRIPPER: TRI-VALLEY East Bay wine, food and trails 22 CHEERS TO CHURCHILL Book: booze with the British PM 23 DASH, THEN DINE Thanksgiving fun runs 23 SUSTAINABLE SAC Get rid of it the right way 53 Bravo 89 RED VOODOO BRINGS IT BACK Hard-rock band ) Taste 96 DO IT YOURSELF The Butterscotch Den 98 TACOS BY WAY OF NIGERIA Naija Boy 98 L AO TIME Hiso downtown restaurant 100 DINE Restaurant guide Reflect 106 SE W MUCH FUN! Katherine Kitchen class 20 susan yee Nest 63 IN THE DETAILS Making mid-mod modern Wedding trends ) When the workforce quits Wellness 27 ALL ABOUT FROZEN SHOULDER Ball-and-socket trouble Explore Tri-Valley ) Grill your own! )
At Kaufman & Davis Plastic Surgery we understand that making the decision to undergo cosmetic surgery is a big one, which is often associated with a little anxiety. We want you to feel warm and welcome, and will do anything we can to make you feel at home.

Our greatest asset at Kaufman & Davis Plastic Surgery is the dedicated team of caring professionals who make up our staff. Through this cohesive group we deliver meticulous, gentle, and compassionate care to our patients and strive to exceed their expectations.
FROM YOUR FIRST CALL, TO YOUR LAST POST-OPERATIVE VISIT… WE VOW TO TREAT YOU LIKE PART OF OUR FAMILY

TheNaturalResult.com EXPERIENCE THAT LEADS TO GREAT RESULTS
1841 Iron Point Road, Folsom, CA 95630 916.983.9895
Little Relics



Midtown owned and operated, Little Relics provides artisan and fine contemporary jewelry as well as custom and full-service repair. At the helm and leading the circus, Susan Rabinovitz, trained with Masters from around the world (over 1,000 hours with mentors) earned certified recognition as a Graduate Jeweler, Revere Academy of Jewelry Arts. Susan, also, had the esteemed privilege to be the only female competitor in Stuller’s International Battle of Benches, 2019. In an effort to continuously provide quality service, Susan is currently accepted and attending GIA, Graduate Gemologist Program (eta completion fall 2023). Wed–Fri. 11-5:30 • Sat & Sun 12-4

10 SACRAMENTO MAGAZINE November 2022 In this issue and online / November 2022
1111 24th St. #103 (Near K St. around the corner from Tres Hermanas) (916) 346-4615 • littlerelics.com
SACMAG.COM
ai166258468535_220907_TMPL_FallOutside_SacMag_2.25x4.875_PROD.pdf 1 9/7/2022 2:04:48 PM 2022 Top Dentists Special Section Featuring some of the region’s most notable dentists. See pages 68–85. SACMAG.COM/SPECIAL-SECTIONS
Certified & Repair Pearls
BIRTH DEFECT OF A WARRIOR

AUDREY PATIENT – HEART AND VASCULAR






By age 5, Audrey had undergone more than a dozen surgeries on her severely deformed heart, leaving her bedridden and unable to play outside. It was UC Davis Health pediatric cardiac interventionist Frank Ing and a team of specialists who were finally able to give Audrey back the life she deserved — one full of laughter, exploration and running around.
Find a UC Davis Health doctor you connect with today.

IT’S OPEN ENROLLMENT. CHOOSE THE CARE THAT CHANGES YOUR STORY.
ChooseHealth.ucdavis.edu
PUBLISHER

Dennis Rainey
EDITORIAL DIRECTOR
Krista Minard
ART DIRECTOR
Gabriel Teague
EDITORIAL MANAGING EDITOR

Darlena Belushin McKay
DINING EDITOR






Marybeth Bizjak






CONTRIBUTING WRITERS
Sasha Abramsky, Luna Anona, Mark Billingsley, Diana Bizjak, Cathy Cassinos-Carr, Ed Goldman, Dorsey Griffith, Jennifer Junghans, Angela Knight, Elena M. Macaluso, Reed Parsell, Kari L. Rose Parsell, Bill Romanelli, Thea Marie Rood, Nora Heston Tarte, Mari Tzikas Suarez, Catherine Warmerdam, Sara E. Wilson
ART GRAPHIC DESIGNER
Debbie Hurst CONTRIBUTING PHOTOGRAPHERS Kat Alves, Gary and Lisa Ashley, Mike Battey, Beth Baugher, Francisco Chavira, Debbie Cunningham, Wes Davis, Terence Duff y, Tim Engle, Kevin Fiscus, Aniko Kiezel, Ryan Angel Meza, Tyler Mussetter, Stephanie Russo, Rachel Valley, Susan Yee
12 SACRAMENTO MAGAZINE November 2022
ADVERTISING NATIONAL ACCOUNTS MANAGER Lisa Bonk ADVERTISING MANAGERS Duff y Kelly, Victor Obenauf, Carla Shults SENIOR ADVERTISING DESIGNER John Facundo MARKETING & WEB DIRECTOR OF MARKETING AND DIGITAL MEDIA Dan Poggetti CIRCULATION CIRCULATION MANAGER Barbie Baldwin PRODUCTION PRODUCTION DIRECTOR Stephen Rice SALES OFFICES SACRAMENTO 1610 R Street, Suite 300 Sacramento, CA 95811 info@sacmag.com M E R C E D E H S H E I K . C O M MERCEDEHSHEIK.COM @ S O L D B Y M E R C E D E H @SOLDBYMERCEDEH 9 1 6 . 7 4 1 . 2 3 4 4 916.741.2344 DRE 02047874 VotedBestRealtorinPlacerCounty
 CEO Stefan Wanczyk PRESIDENT John Balardo
CEO Stefan Wanczyk PRESIDENT John Balardo
FOR ISSUES OF THE MAGAZINE
SUBSCRIPTIONS To establish a subscription or make changes to an existing subscription, please call (866) 660-6247 or go to sacmag.com/subscribe.

SINGLE COPIES AND BACK ISSUES
To purchase back issues, please call (866) 660-6247.







































TO SUBMIT MATERIAL





STORY IDEAS Have you spotted something appropriate for editorial coverage in Sacramento Magazine? Please submit as much information as possible about the subject to Darlena Belushin McKay at darlena@sacmag.com. Keep in mind that we maintain a relatively strict local boundary— Sacramento, El Dorado, Placer and Yolo counties— and our lead times run long, with most issue lineups completed four months prior to publication.
WRITERS, PHOTOGRAPHERS
AND ILLUSTRATORS If you are interested in contributing to Sacramento Magazine, please send information to (writers) Krista Minard, krista@sacmag.com or (photographers and illustrators) Gabriel Teague, gabriel@sacmag.com. Include a cover letter, résumé and links to previously published work.
ADVERTISING Interested in advertising or a digital media package? Please visit sacmag.com/advertise
14 SACRAMENTO MAGAZINE November 2022
PUBLISHED BY SACRAMENTO MEDIA LLC
JOURNAL
A MEMBER OF CIRCULATION VERIFICATION COUNCIL
PRINTED BY
GRAPHICS
Woods
| SAR
Real Estate Group
Schultz As a consistent TOP PRODUCER for the past 16 years, I have successfully represented both sellers and buyers in all types of markets. I will help you navigate the process and will always be here for you. Team Up With Toddy!
| SAR
ALSO PUBLISHED BY SACRAMENTO MEDIA LLC:
Cynthia
Broker DRE# 01749720
Galster
(916) 743-6611 www.realestatesinger.com Toddy
DRE# 01483530
Lyon Real Estate (916) 342-3573 tschultz@golyon.com www.teamupwithtoddy.com
Fair Oaks Area Specialist









Harvest Feast
Icouldn’t resist: I made that goat cheese bacon concoction. The one on page 38, with the apples and dates and rosemary. It tasted like autumn on a cracker. (I used Trader Joe’s pita crackers in place of the recommended crostini—they’re what I had on hand.) It was so nuanced, with a bit of every flavor and texture, I could’ve eaten the whole pile of it by myself.
But the recipes in this issue are meant for gatherings, and that’s exactly what our advisers, Hannah Ray Flores and Lea Raymond of Hauste, told us how to do: Throw a dinner party. They gave us tips about such conundrums as how many people to invite, what to play as background music, and who to seat where, and they shared recipes for an approachable meal built around fall’s apple harvest. Perhaps best of all, our party happened outdoors in a beautiful backyard with a fire place—perfect for a Sacramento autumn evening, especially if you can pull up a few patio heaters.
The party theme continues this month, with writer Angela Knight’s roundtable discussion among wedding experts. While we’re not quite ready to say “post-pandemic,” at least weddings are actually happening now, so we wanted to find out what’s trending and how much it’s all costing. (In a word: lots.) This has become personally interesting in our family, as our daughter Anna and her guy, Travis, got engaged over the summer. What their wedding will entail remains to be seen, but as her dad and I celebrate our 30th anniversary this year, we consider ourselves living proof that the grandiosity of the wedding isn’t necessarily predictive of the strength of the union. For our wedding, family and close friends—50 people, tops—gathered at my sister and late brother-in-law’s house the first Satur day in December 1992. We partied in the garage—and we’re still going!
Also for this issue, writer Sasha Abramsky caught up with a few locals who recently quit their jobs, living examples of The Great Resignation that has swept the country during the pandemic. Sasha also talked with Patrick Mulvaney, one Sacramento restaurateur who lost a good portion of his workforce to this phenomenon. It all left me less mystified as to why restaurant service has been slower almost everywhere and why the shoe department at Target looked the way it did—the word ransacked came to mind—when we walked through there one Saturday evening this past summer. Fall has finally arrived. Let’s enjoy it.
KRISTA MINARD krista@sacmag.com


AND THERE’S MORE . . .
We are proud to produce the Visitors’ Guide for Visit Sacramento, and the fall issue is now out. With stories about the local music scene, Sacramento’s diversity, autumn dining, Little Saigon and more, it’s a reminder of many of our region’s greatest attributes, right here in town.

Sacramento Magazine’s free newsletter, The Daily Brief, goes to email subscribers every weekday. Catch the latest updates in dining, arts and entertainment, wine, recreation, health (including COVID case counts) and more. You’ll also find links to other community news and resources and social media posts that have caught our eye. Subscribe at sacmag.com/newsletters.
CONTRIBUTORS
Susan Yee

“I am a huge fan of dinner parties, so shooting this feature was a beautiful feast on the eyes and stomach!” says photographer Susan Yee. “The girls at Hauste created such an amazing menu and introduced me to new things, like the magic of whipped goat cheese with rosemary, honey, apples and dates (I definitely had more than one of these!), and brick chicken (so yummy!). I definitely need to re-create these for a future dinner party of my own.”

Ryan Angel Meza
“Learning of Erika Noon an and Adam Schmidt’s occupational journeys,” says Ryan Angel Meza, who photographed the resignation story, “I was humbly reminded of my own transition in 2014 from state-service employee into a full-time freelance creative entrepreneur. I remember all of the uncertainties, doubt, as well as optimism that went along with all the mixed emotions. However, [now] I’m a believer that when ‘forced’ change occurs, it is the universe pushing you closer to what you were meant to be doing.”
Angela Knight
“I was struck by the dedication, thoughtfulness and resiliency of the professionals I talked to,” says Angela Knight, a regular contributor to Sacramento Magazine; she wrote the wedding trends story for this issue. “The pandemic hit soon-to-be wed folks, their families and the people who make those weddings happen, hard. It was heartening to find out that couples are creating unique and playful ways to celebrate their love and commitment—it’s almost as if they’re making up for all that lost time.”
16 SACRAMENTO MAGAZINE N ovember 2022
Editor’s Note

We’re community-owned, not-for-profit.
SMUD employee, Tran





SMUD employees support the causes they care about through personal donations to local nonprofits. Giving back to our community is a key part of SMUD’s culture. And, we keep you at the heart of all we do.






Learn more at smud.org/Community Powering forward. Together.

Wonder
©SMUD 1053-9/22 ®A trademark/service mark of Sacramento Municipal Utility District, Reg. U.S. Pat. & Tm. Off. why our employees donated over $400,000 last year?
Wings of Change
Two 40-foot winged sculptures have risen in The River District, near Richards Boulevard and N. 12th Street. Titled “Uplift,” they’re the latest in the city of Sacramen to’s metamorphosis-themed public art project that includes seven murals along the N. 12th Street corridor. The sculptures, which will light up at night, were created by Seattle-based artist Vicki Scuri.

The 916
SACMAG.COM November 2022 19 inside: Visit Tri-Valley / Drinks With Winston / Dash & Dine / Throwing Stuff Out 11 22
gabriel teague
Day Tripper: Tri-Valley
VINEYARDS, BREWERIES, PARKS AND SEVERAL SWEET DOWNTOWNS ARE ENCOMPASSED WITHIN THIS EAST BAY REGION, A COMPILATION OF THREE VALLEYS. KRISTA MINARD






See the word Tri-Valley, and the next question comes quickly: What three valleys?
Answer: Amador, San Ramon and Livermore. This area is about 90 minutes from Sacramento and includes several towns off highways 580 and 680. We’ve all driven past Danville, Pleasanton, Livermore and Dublin on our way to other Bay Area destinations, but have you ever stopped? We did, and we discovered all kinds of treasures, including lovely downtown districts, a sprawling wine country tucked into California’s golden hills, lots of breweries, parks with trails, and plenty more. Some highlights:
DOWNTOWN LIVERMORE —About a dozen murals decorate the walls of downtown Livermore, a walkable district with plenty of Main Street charm— in this case on First Street. A prime gathering spot is the First Street Fountain, where an inviting array of market umbrellas sit outside a wine bar and several restaurants. Down the street, pop into Bar Quiote for mezcal, hot dogs and jukebox tunes (what a combo!) or pop into The Cheese Parlor for a little tasting. Off the main drag, Towne Center Books is tucked into a walkway adjacent to Bankhead Theater. Grab a coffee at Panama Bay or Story Coffee Co. A few blocks over, admire the Carnegie Building and the Centennial Park Totem Pole.
TRI-VALLEY BEER TRAIL —The TriValley tourism folks have teamed up with some 20 local craft breweries and alehouses to create a mobile-friendly passport for beer lovers. It’s a great way to get introduced to some wonderful taprooms and receive discounts, plus if you hit 10 or more, you can pick up a prize. (You don’t have to do all 10 in one day!) Some favorite stops include Beer Baron Whiskey Bar & Kitchen (Pleasanton); First Street Alehouse, Pennyweight and Shadow Puppet (Livermore); Three Sheets (Dublin); and Danville Brewing Co.
LIVERMORE WINE COUNTRY
Some 55 wineries line the roads not far from Livermore’s downtown. Two of the largest—and oldest—are Wente and Concannon, in operation since the 1880s. Visitors to either will learn all about Livermore’s viticultural history, including the story of Charles Wetmore, one of the California wine industry’s founding fathers. Livermore Valley is where the state’s cabernet sauvignon and chardonnay varietals were born. At Concannon, taste in the brick-and-wood tasting room or reserve a weekend spot at a library tasting, held in Concannon’s Historic Wine Library. At Wente, enjoy the sprawling compound, which includes beautiful indoor and outdoor tasting areas and an 18-hole golf course. The area is home to lots of boutique, small-batch wineries, and once S. Livermore Avenue turns into Tesla Road, you’re in the thick of it. Some notable wineries in the valley include Retzlaff (the only organic winery in the area), Las Positas, Garré, Darcie Kent and Fenestra, but the fun is in hitting the backroads and discovering some gems of your own.
SPEND THE NIGHT
The Purple Orchid Resort & Spa bed-and-breakfast inn sits among a rose garden, olive orchards and vineyards in the Livermore Valley, with 10 countrystyle suites, each with a fireplace. On-site spa services: facials, massage and other body treatments. Room rates include a full breakfast, and wine and olive oil tasting each evening.
The 916 20 SACRAMENTO MAGAZINE November 2022
The Cheese Parlor
Danville Brewing Co.
Wente
Retzlaff
MOUNT DIABLO STATE PARK Fall is a lovely time to hike Mount Diablo (near Danville), where summer’s heat can turn midday walks on the mountain into misery. From the summit (3,849-foot elevation), you can see all three of Tri-Valley’s valleys on a clear day, as well as (if you’re lucky) the Golden Gate Bridge and Farallon Islands, Mount Hamilton, Mount Loma Prieta, the Sacramento and San Joaquin valleys, and possibly Mount Saint Helena, Lassen Peak and parts of the Sierra. It’s worth the 7-mile out-and-back trek via the moderately challenging Summit Trail. (Lots of uphill!) Or you could drive up. Either way, the view is spectacular from the observation deck, and the visitor center will provide even more perspective, as well as maps to the numerous trails and destination points within the park.

DOWNTOWN DANVILLE —Duck into downtown Danville off highway 680 and you’ll find a collection of shops, restaurants, breweries and galleries. Some muststops include Danville Chocolates for a caramel apple or truffle or bark; Whim House, a delightful home décor shop; Lottie’s Creamery for a scoop of hand-crafted small-batch ice cream; and Bridges restaurant for a throwback to “Mrs. Doubtfire.” The late Robin Williams’ sweaty dinner scene, where he swapped between roles as a job interviewee and jealous middle-aged nanny, was filmed on location. Sideboard restaurant is a great spot for drinks and local farm-to-fork fare on the patio. Also in town: The Museum of the San Ramon Valley, which has plenty of worthy exhibits itself, and it’s also the shuttle pickup for tourgoers to the Eugene O’Neill National Historic Site. The Nobel Prize-winning playwright created his most memorable plays (think “The Iceman Cometh,” “Long Day’s Journey Into Night”) at Tao House, located behind a gate a couple of miles away, accessible only by reservation and the aforementioned shuttle.




DOWNTOWN PLEASANTON —On this inviting, pedestrian-friendly Main Street, start at Inklings coffeehouse, which pays homage to literary greats with wall art, bookshelves and a room called The Vault, where it’s common to see people (writers?) hunkered over laptops or books. Wander through Prim Boutique to see what’s on display in the curated clothing collection. Options for lunch and dinner are many and include the whitewashed Elia restaurant (Greek specialties on the menu: moussaka, hummus, avgolemono, grilled octopus, paella), Lokanta (Mediterranean and Turkish fusion), Blue Agave Club (seasonal for fall: chilies en nogada—picadillo-stuffed poblanos with walnut cream sauce and pomegranate arils), Gay Nineties Pizza and plenty of other eateries. Visit Museum on Main to learn the history of the area, and make sure and scoot down Neal Street to drive through Meadowlark Dairy—impossible to miss with its canopy of suspended rain umbrellas, “cattle crossing” and “milk” signage and a Holstein-centric mural. Drive over the wire to ding the bell and grab a soft-serve. (If pumpkin spice is still available, go for it.)
DEL VALLE REGIONAL
PARK—Anchored by a 5-mile-long lake, this park in Livermore includes some 4,300-plus acres for hiking, mountain biking and horseback riding. Kayakers and windsurfers take to the lake, while bird watchers and other nature lovers come out to enjoy the oak- and brush-dotted hillsides, tawny in the fall, brilliant with wildflowers in spring. It’s also the eastern gateway to the Ohlone wilderness, which includes 28 miles of trails.

SACMAG.COM November 2022 21
Whim House
Sideboard
Meadowlark Dairy
Cheers to Churchill
A new book limns the famous British PM through his favorite alcoholic beverages.
BY MARYBETH BIZJAK
It seems fitting that local author Jennifer Basye Sander and I should meet for cocktails at downtown’s Camden Spit & Larder to discuss her latest book: “Churchill: A Drinking Life.” (Skyhorse Publishing, $22.99) An oil painting of Britain’s legendary prime minister, Sir Winston Churchill, hangs on a wall at this British-inspired brasserie, and happy hour here is called “Winston’s Hour.” As we settle in at the table, Basye Sander tries to order Churchill’s favorite drink (Johnnie Walker Red and soda), but the server informs her he has only Johnnie Walker Black on hand. Keeping calm and carrying on, she agrees to the substitution.
Witty and well-researched, the Churchill book is filled with interesting historical tidbits, wild factoids (Churchill consumed more than 42,000 bottles of champagne in his lifetime) and gossipy anecdotes revolving around Sir Winston’s famed love for liquor. Basye Sander describes the book as “a drink with a side of history.” It is divided into chapters that look at what Churchill liked to drink, where and with whom. His favorite qua was a weak Scotch and soda, which he nursed all day long, but he also drank champagne (Pol Roger, to be precise), white wine with dinner and, when visiting FDR at the White House, martinis made by the president himself. He imbibed seemingly everywhere: hotels, racecourses, private clubs and stately homes; in 1929, on a trip to California, he drank a “wellchilled” Chablis at BV winery in Napa Valley. Churchill was the Zelig of the booze world: His illustrious drinking companions included kings (both Edward VIII and his brother, George VI), aristocratic pals like Lady Astor and the Duke of Westminster, media moguls such as William Randolph Hearst and plain old famous folk like Mark Twain and Greta Garbo.
According to Basye Sander, the Venn diagram of people who might enjoy this book includes World War II bu s, fans of Churchill and anyone who loves a good sti cocktail. It’s a handsome little tome that would not look out of place in a dimly lit, book-lined study, where it could be thoughtfully sipped from like a fi ne Mouton Rothschild Bordeaux. It would make the perfect stocking stu er for your favorite Anglophile.
I ask Basye Sander what a reader can expect to learn from reading her book. “How very human he was,” she replies. “This was a man who had many ups and downs in his career. But as the English would say, he just KBO: kept buggering on.”
She co-wrote the book under the “nom de cocktail” Gin Sander with her friend Roxanne Langer, a Carmel-based sommelier and wine judge. For material, they pored over memoirs and biographies of people whose lives intersected with the great man, and they conducted fi rst-person interviews with experts such as Sacramento’s own Darrell Corti, who taught them the ins and outs of cognac (one of Churchill’s favorite after-dinner drinks). The book concludes with a selection of recipes for “Churchill-inspired” cocktails such as Old Etonian (gin, Lillet Blanc and Crème de Noyaux) and Wallis Blue (a gin-forward nod to the Duchess of Windsor). And, of course, it wouldn’t be a book on Churchill without a recipe for Whisky and Soda, very weak, just the way he liked it.
On Nov. 30 (Winston Churchill’s birthday), Jennifer Basye Sander will be at Brasserie du Monde (1201 K St.) from 4 to 6 p.m. to share a few stories from her book over some of Churchill’s favorite libations.

The 916 22 SACRAMENTO MAGAZINE November 2022
aniko kiezel
IT WOULD MAKE THE PERFECT STOCKING STUFFER FOR YOUR FAVORITE ANGLOPHILE.
Jennifer Basye Sander with a cognac at Camden Spit & Larder
Dash, Then Dine: Thanksgiving Day Fun Runs
Why sit around all morning waiting for the big meal when you can go outside, get some exercise and contribute to the common good? Thousands of folks, from weekend walkers to elite runners, ring in the holiday at festive races held around the region. Pre-register for a run, join in the fun, and you’re bound to feel good, maybe even virtuous—and a little less guilty as you gobble down that third slice of pie.
KARI ROSE PARSELL
Nov. 19
34TH ANNUAL DAVIS TURKEY TROT
Civic Center Park, Davis
• Half-marathon at 7:50 a.m. • 5K at 8:05 a.m.
• 2-mile “Dog Jog” at 8:25 a.m. • 10K at 9 a.m.
• Kids race events at 10:30 a.m.
A Change of Pace Foundation puts on this popular set of races, which this year benefits Yolo County SPCA and Cancer Champions. changeofpace.com/event/davis-turkey-trot-2
Nov. 24
ELK GROVE GOBBLE WOBBLE FAMILY 5K
8280LongleafDrive,ElkGrove
• Kids ¼-mile at 9 a.m. • 5K at 9:15 a.m.
The Elk Grove race benefits Chicks in Crisis, which supports teen parents in need. chicksincrisis.org
Nov. 24
FIFTH ANNUAL HUFFIN' FOR THE STUFFIN' TURKEY TROT
Twelve Bridges Park, Lincoln
• Kids Donut Dash at 8:15 a.m. • 5K at 8:30 a.m.
Lincoln’s fun run supports local parks and rec events and scholarships for kids. Click on “FindaRace”atrunsignup.com

Nov. 24
FOLSOM TURKEY TROT
Folsom City Lions Park, Folsom
• 10K run at 8:50 a.m. • 5K at 9 a.m.
Folsom’s family fun run benefits Twin Lakes Food Bank, Folsom Athletic Association Youth Financial Assistance and the Johnny Cash Trail. folsomturkeytrot.com
Nov. 24
10TH ANNUAL ROSEVILLE TURKEY TROT
VernonStreetTownSquare,DowntownRoseville
• 10K at 9 a.m. • 5K at 9:05 a.m.
Roseville’s road race funds programs for atrisk youth. rosevilletoday.com/event/rosevilleturkey-trot
Nov. 24
29TH ANNUAL RUN TO FEED THE HUNGRY
Sacramento State campus, East Sacramento
• 10K at 8:15 a.m. • 5K at 9 a.m.
This benefit for Sacramento Food Bank & Family Services is the largest Thanksgiving Day run in the country, attracting up to 28,000 participants each year. runtofeedthehungry.com

Nov. 24
THE WILD TURKEY (FORMERLY TURKEY’S REVENGE)
9704 Auburn Folsom Road, Granite Bay
• 10K at 9 a.m. • 5K at 9:15 a.m.
• Kids 1K at 10:30 a.m.
Folsom Lake is the backdrop for these challenging trail races. Click on “Find a Race” at runsignup.com
Get Rid of It the Right Way
BY REED PARSELL
ome of us—and count your blessings if this situation does not apply to you— hang onto used-up and no-longer-func tioning stuff because it contains chem icals (that might be toxic), metals or wires (that might be salvageable) or other components (that might be recyclable) because we don’t know how to properly dispose of whatever it is.
S
We would throw it in the trash and forget about it were we not inclined to feel a twinge of guilt for possibly wasting Earth’s limited resources, pol luting the environment or acting a bit entitled or lazy. So whatever it is gathers dust in a closet, is something we might trip over in the attic, or is embarrassingly out for all to see on a window ledge or atop some piece of furniture or large appliance.
We strongly suspect there is a responsible way to get rid of whatever it is, although we are wary that doing so might require some time and effort. (Lazy alert!)
If only there were a simple way to find out what to do with this guilt-inducing stuff. A magical source of instant information.
Well . . .
SACMAG.COM November 2022 23
SUSTAINABLE SAC
continued
next page
on
The city of Sacramento and Sacramento County are ready to grant you your wish. By visiting their recycling and solid waste webpages, you can say what problematical trash you have, and they can tell you exactly what to do with it.









On the city utilities site, the Waste Wizard takes questions 24/7. “Type the name of an item and we’ll tell you how to recycle or dispose of it,” the wizard instructs. Well, how about Styrofoam? The immediate answer is: “Put this item in your garbage container.”

Fluorescent light bulbs? “This item is a household hazardous waste.” Three drop-o locations are suggested, their street addresses (supplemented with a one-click “Directions” link) specified, in Sacramento, North Highlands and Elk Grove.
Mattresses? “This item is accepted for Household Junk Pickup.” A phone number is listed and website link provided to make an appointment.

The county o ers a very similar ask-and-answer feature, titled “How do I get rid of . . . .” I entered “ink cartridges” and was told, “Drop o this item for recycling. Always call ahead.”




The same three government-run waste-collection sites listed by the city pop up, as do a couple of others (in Sacramento and Roseville) and some private businesses.


What about bleach? Those same fi ve government-run drop-o sites.
Empty aerosol spray cans? “Put this item loose in your recycling cart. No bags!”
Which reminds me. Back to the city’s Waste Wizard I go to ask about a nagging item: Plastic bags. The answer:
“Tip: Some retailers take plastic bags for recycling. Take reusable shopping bags to stores.” With the additional insight: “Why do our facilities not accept plastic bags? Plastic bags regularly get loose from the recyclables and stuck in the sorting machinery. They also travel in the air throughout the facilities and contaminate other recycling. They need to be disposed of properly in the garbage or at a local recycler. Never bag recyclables in a plastic bag.”
Oh no. I have been guilty of doing the wrong thing with plastic bags. But ultimately, thanks to these very helpful recycling and solid waste websites, I overcame my laziness and found out the proper thing to do.
The 916 24 SACRAMENTO MAGAZINE November 2022 Turtle Bay Exploration Park McConnell Botanical Gardens 844 Sundial Bridge Drive • Redding, CA Festive food, drinks & gift shop Santaʼs Reindeer Kids ages 0-4 are FREE Free parking at Sundial Bridge turtlebay.org | 530-242-3123 Book your stay at our on-site Sheraton Hotel sheratonredding.com tickets & info Nov 18, 2022 - Jan 8, 2023 presented by C M Y CM MY CY CMY K 2022_GOL_SacMag.pdf 1 10/17/22 3:47 PM
The city of Sacramento and Sacramento County are ready to grant you your wish. By visiting their recycling and solid waste webpages, you can say what problematical trash you have, and they can tell you exactly what to do with it.







Always-onthe-go care.

























































This Open Enrollment, choose a plan that gives you access to Dignity Health.





















With more than 1,000 affiliated providers supporting our communities across more than 200 locations, we have you covered with care that best fits where you are and whatever your day brings. Learn more at DignityHealth.org/OpenEnrollment.

Wellness
1122
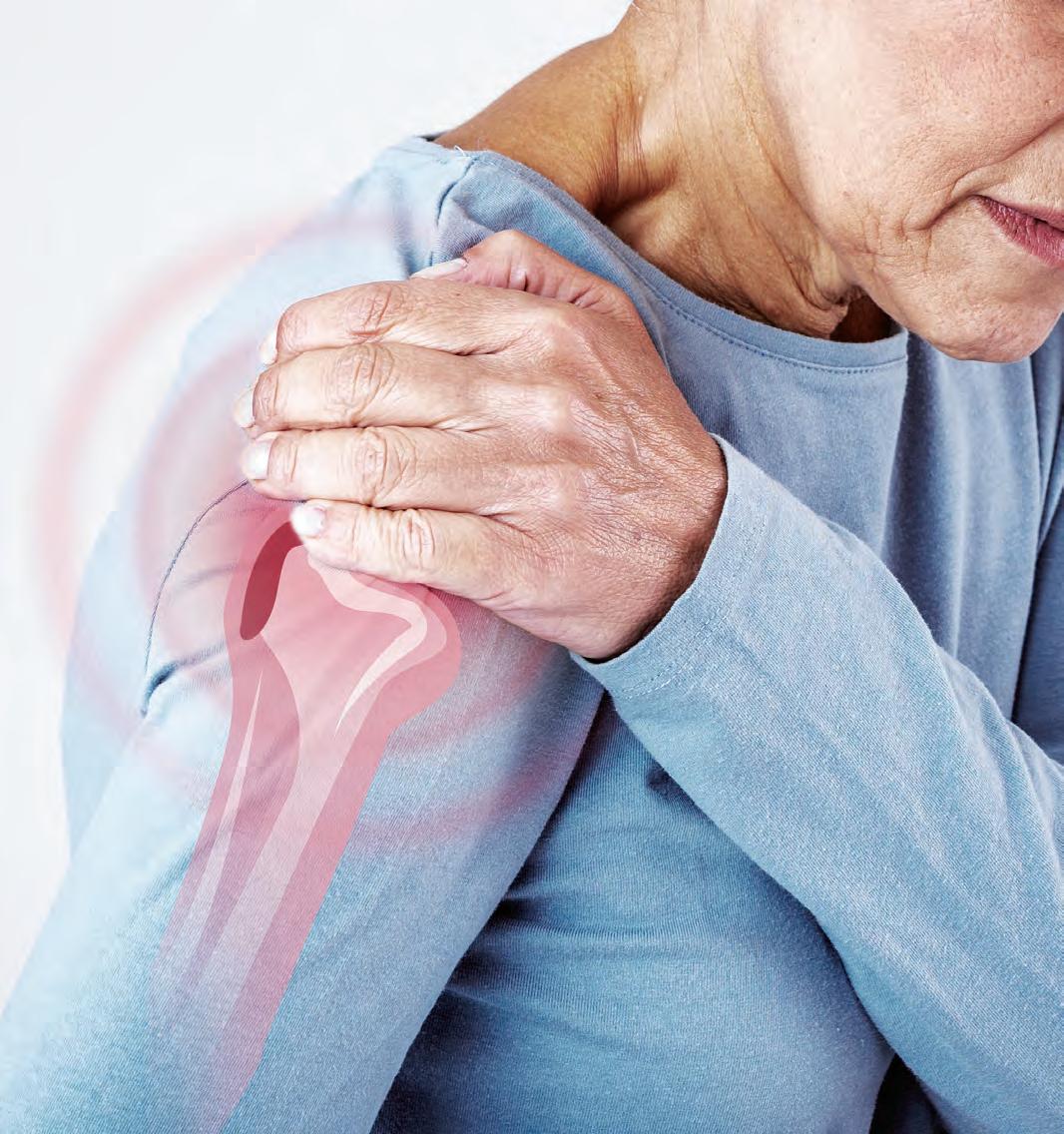
All About Frozen Shoulder
The puzzling, painful medical condition most often strikes women between the ages of 40 and 60.
SACMAG.COM November 2022 27
inside: Help for shoulder problems
BY CATHY CASSINOS-CARR
There are a lot of great unknowns about frozen shoulder, including the answer to the most basic question of all: Why does it happen?

If doctors puzzle over this (and they defi nitely do), imagine the frustration of being among the estimated 2 to 5% of the U.S. population affected by it, most of them never knowing why. When my own frozen shoulder saga began about a year ago, with a shooting pain in my upper arm that routinely woke me at 3 a.m., I racked my brain for a reason—and never found one. Was it the result of years of schlepping a heavy handbag over my left shoulder? I still don’t know. But now I know that not knowing is the norm.
Formally known as adhesive capsulitis, a reference to the thickening of the shoulder capsule and adhesions (bands of tissue) that develop, frozen shoulder is more than just painful: It is notoriously stubborn, sometimes taking up to two to three years to resolve. “It takes a long time, so there is a psychological aspect to that,” says orthopedic surgeon and sports medicine specialist Kent Sheridan, M.D., of Sutter Health Sacramento. Helping patients manage their frustration, he says, is part of the treatment process.
Kent Sheridan, M.D.

arm, there’s a block,” he says. That’s different from something like a rotator cu tear, in which only active range of motion is a ected, explains Bragg—a di erentiation that aids in diagnosis. A patient’s symptoms and exam fi ndings are typically all that’s needed to diagnose a frozen shoulder, Bragg says, though an X-ray or MRI may be used to rule out other issues. Primary care doctors are “really great” at diagnosing frozen shoulder, according to Bragg—so that’s where a patient should start.
What else do we know—and not know—about frozen shoulder? Local experts shared these eight takeaways.
STIFFNESS AND LIMITED RANGE OF MOTION ARE THE HALLMARKS. At the apex of my frozen shoulder journey, my range of motion was so limited I could barely raise my arm out to my side. Apply deodorant, shave under my arm or slide my hand into my back pocket? Fuggedaboudit.
This is all classic frozen shoulder, confi rms William Bragg, M.D., an orthopedic surgeon and shoulder surgery subspecialist for Dignity Health Mercy Medical Group in Sacramento. It’s kind of a double whammy, says Bragg, because frozen shoulder impacts not one but both types of range of motion: active, meaning the patient can’t fully raise the arm, and passive, meaning no one else can, either. “With frozen shoulder, when either the patient or the doctor tries to move the
“HUH?” THAT IS THE QUESTION . Most patients who show up at his door haven’t a clue how their frozen shoulder happened, says Sheridan. “‘I woke up and my shoulder really started hurting, and it keeps getting worse’ or ‘I’m getting an ice cream headache in my shoulder’ are a couple of the common descriptions I hear,” he says. But it doesn’t always seem to come out of nowhere; often, Sheridan says, a minor precipitating trauma (bumping against a shelf, for example) is identified, hinting at the possible trigger. While studies suggest systemic infl ammation and genetics also may play a role in the disease process, frozen shoulder is nonetheless considered idiopathic, according to Sheridan. “Exactly why it happens, we don’t know,” he says. “That’s frustrating to patients and to clinicians, too.” For that reason, he says, practitioners tend to focus on what to expect, the course of the disease (see item 4) and the timeline, instead of puzzling over causal factors.
WOMEN OF A CERTAIN AGE ARE HARDEST HIT. Scientists may not know why frozen shoulder hits, but they know who it most often strikes. Topping that list is women between the ages of 40 and 60, prompting this reporter to wonder if the shifting hormones of perimenopause and menopause play a role. “I’m sure there’s a link there,” Bragg says. “I would argue we don’t have the large-scale studies we need to answer that question.” Also at increased risk: People with endocrine disorders (diabetes, thy roid disease), Parkinson’s disease and cardiac disease. Immobilization of the shoulder, a common post-surgery or postinjury plight, can also set up the “freezing” process.
IT’S A THREE-ACT PLAY. Sheridan emphasizes the importance of under standing the disease’s three distinct stages: Stage 1, freezing, when pain and limited range of motion fi rst appear; Stage 2, frozen, when sti ness worsens and pain may start to fade; and Stage 3, thawing, when the shoulder gradually improves. It’s during Stage 1, when pain peaks, that most people call their doctors, says Sheridan, who prefers to label the phases “painful, sti ness and resolution.” But diagnosis is easiest to establish in Stage 2, he says, when the shoulder becomes sti . Duration of each stage is highly individual, but according to the American Academy of Orthopaedic Surgeons, average time frames look like this: Stage 1, six weeks to nine months; Stage 2, four to six months; and Stage 3, anywhere from five months to two years. Add
28 SACRAMENTO MAGAZINE November 2022 Wellness
1 2 3 4




















it up, and you’ll see just how long this process can take.
But most people aren’t willing to wait that long, as Bragg notes—and i n his opinion, there’s no reason why they should. “I tell my patients that progress is going to be slow, and you’re going to be frustrated. But we’re not going to let it take two years.” In the great majority of cases, a frozen shoulder will resolve with nonsurgical methods (or even nontreatment), but if a patient hasn’t seen results somewhere between six months and a year, Bragg says, he may suggest a surgical intervention. “When a shoulder issue is having a significant impact on a person’s mental health, their ability to function in leisure activities, their ability to do their job and be productive in society—at some point, you don’t just say, ‘Let’s wait longer.’ You make the choice to try to help them with an intervention.” Deciding whether to pull that trigger can be tricky, Bragg says, and it’s also a last resort. But in stubborn cases, manipulation under anesthesia (which stretches the shoulder capsule) and arthroscopy are options.
Bragg, M.D.

lifting weights, staying in shape, and suddenly I was having trouble trying to raise my arm over my head.” After about seven months of twice-weekly therapy sessions and regular stretching at home, Burk says, “I was out of pain and had my arm movement back.”
Eddy cautions that not all therapy is created equal; what matters, he says, is approach. In treating frozen shoulder, Eddy says, he and his sta typically use a combination of range-of-motion exercises, joint mobilization techniques and hands-on manual therapy, moving the shoulder in various directions “so that the shoulder, scapular region and the capsule itself frees up and gains mobility.” Early intervention, he stresses, is key. “I’ve found therapy is most useful early on,” says Eddy. “If you wait too long, you may be in a phase where it may not be beneficial.”

TO GET THE SHOULDER MOVING NORMALLY AGAIN, PHYSICAL THERAPY AND A WHOLE LOT OF STRETCHING ARE WIDELY CONSIDERED THE MOST ESSENTIAL TREATMENT TOOLS.
and one shot only. “Cortisone shots are overall safe and e ective,” Sheridan says. “But multiple injections, particularly in a short period of time, may have deleterious e ects on the soft tissues and the cartilage of the shoulder.” Timing, again, is key: According to the fi ndings of a large-scale study published in December 2020 in JAMA Network Open, corticosteroid use in patients who have had frozen shoulder for less than a year is associated with better outcomes. Coupling the treatment with a home exercise program maximizes chances for recovery, the study says.
5PHYSICAL THERAPY IS KEY. To get the shoulder moving normally again, physical therapy and a whole lot of stretching are widely considered the most essential treatment tools. “I’m a little biased,” says Mark Eddy, owner and president of Campus Commons Physical Therapy in Sacramento. “But I believe physical therapy can help a lot of people with this problem.” A practicing physical therapist for more than 25 years, Eddy says he can usually fi nd some reason behind a frozen shoulder if he asks enough questions. When working with client Jim Burk, the mild nature of the precipitating event took them both by surprise: After reaching behind his back to tie the strings of his apron, Burk felt a “twang” in his shoulder, and things got worse from there. “It was a very humbling experience,” says the 66-year-old Sacramentan. “I was used to going to the gym,
7 6

Bragg agrees timing is everything, noting physical therapy can be counterproductive if shoulder pain isn’t under control—so the fi rst step for most patients, he says, is anti-inflammatories.
TO GET THE SHOT, OR NOT? When frozen shoulder pain hits, most fi rst reach for the Advil (or other NSAID of choice) and an ice pack. But to attack pain and infl ammation more aggressively, a cortisone (steroid) injection, given directly into the shoulder joint, is commonly used. Should your primary care doctor do it? That is a matter of debate. Bragg, for one, recommends an image-guided injection, performed by a specialist, for best results.
Steroid use may not be for everyone. “Do you really want to put something into your body that could break down your tissues or have other harmful ramifications?” as Eddy asks. But most conventional clinicians agree that when used appropriately, the benefits outweigh the risks. The general rule of thumb? One shot,

MULTIMODAL WORKS BEST. As the foregoing suggests, a multimodal approach is often the best way to beat frozen shoulder. In my own case, nonsteroidal anti-infl ammatories and physical therapy got the engine started, but it was acupuncture that ultimately got me out of the woods. Jim Burk, who initially dodged the cortisone shot, made a di erent choice when he confronted a frozen shoulder in his other arm and says he’s glad he did. “It [the shot] was e ective almost immediately,” says Burk, who paired it with the at-home exercises he’d learned the fi rst time around. Burk’s “other arm” experience isn’t uncommon: A whopping 20 to 30% of frozen shoulder su erers are estimated to experience an occurrence in the opposite arm, according to the American Physical Therapy Association.
8
PREVENTION MAY BE POSSIBLE. Or is it? Experts say there’s no surefi re way to prevent a frozen shoulder. But keeping the shoulder moving might help, notes Bragg, directing his comment to those who have an injury or other shoulder issue, such as impingement. “Being immobile will just make you sti and potentially lead to frozen shoulder,” he says. “You don’t want to turn one problem into two.”
30 SACRAMENTO MAGAZINE November 2022 Wellness
Mark Eddy
William
Front: Vardenik “Rose” Khalatyan, MPH, CCRP, CEO and Founder.









THE FACES OF CLINICAL RESEARCH
in many specialties of medicine. True to our motto of “Bringing tomorrow’s treatments to patients today” and “Think outside the box”, DaVinci Research is leading the way in o ering state-of-theart treatments to under-represented segments of our communities, ensuring the integrity of the science behind all clinical trials. Research is a foundation of medicine and insuring diversity in research helps improve health inequality issues so important to our world today. Small, but mighty, we can, and we will make a di erence!

FAX
DAVINCI RESEARCH, LLC 5 MEDICAL PLAZA DRIVE SUITE 180 | ROSEVILLE, CA 95661 | 916.374.6730 MAIN | 916.596.4034
| WWW.DAVINCIRESEARCH.NET
DaVinci Research is a small, Sacramento-based company specializing in pharmaceutical and medical device phase 2/3 studies. Additionally, DVR conducts independent research and NIH-funded studies. DaVinci Research has led the country in many of its clinical trials with innovative companies such as ARRINEX and SPIROX (acquired by STRYKER), Intersect ENT (acquired by MEDTRONIC), Tusker Medical (acquired by SMITH and NEPHEW), Genentech and OPTINOSE. DVR is always interested in new studies and has qualified investigators ADVERTISEMENT
Back, from left to right: Marcy Adame, CCMA, CCRC, CPT; Claire Cinnamon BA/BS, CRC; Lilit Avetisyan, MBA, CRC; Elijah Cherkez, BS, CRC; Randall Ow, MD, President and Chief Medical O cer.


Let the Part y B egin






























HOSTING IS A BREEZE WITH THIS DINNER-PARTY HOW-TO FROM THE SISTERS BEHIND HAUSTE.
 BY MARYBETH BIZJAK PHOTOGRAPHY BY SUSAN YEE
BY MARYBETH BIZJAK PHOTOGRAPHY BY SUSAN YEE
34 SACRAMENTO MAGAZINE November 2022
As the evenings lengthen and the holidays approach, you may find yourself wanting to invite friends over for a cozy meal at home. But what if you’re not an absolute whiz in the kitchen, or you get stage fright at the thought of putting your entertaining skills in the spotlight? We turned to a pair of entertaining savants—sisters Hanna Ray Flores and Lea Raymond—for tips to help you pull o a perfectly simple, simply perfect autumn dinner party.
Hanna and Lea are the brains behind Hauste (pronounced host), which produces digital dinner party guides featuring easy-to-follow, 1-2-3 instructions that take the stress out of entertaining. The sisters come by their love of entertaining naturally: They were raised in Folsom by parents who hosted dinner parties nearly every weekend. “Some people have generational wealth,” Hanna jokes. “We have generational hosts.” As adults (Hanna is 31, Lea 22), they’ve made it their mission to instruct a new generation in the art of entertaining graciously.

For this autumnal dinner, they teamed up with local winemakers Sean and Nicole Minor, who supplied both the wine pairings and their beautiful backyard for the party. Hanna and Lea settled on an apple-forward menu, with apples featured as an ingredient in every course, from appetizer (a creamy whipped goat cheese spread topped with honey-glazed apples, dates and bacon) to dessert (an impressive-looking brown butter tarte tatin that’s a snap to make). For the main course, they chose brick chicken, also known as chicken under a brick: Roasted chicken legs are weighted down with a foil-wrapped brick and seared in a hot skillet for seductively crispy skin, then served with tarragon-scented beurre blanc and an apple thyme chutney that brings the apple theme home. They also made silky mashed potatoes, colorful roasted carrots and a shaved Brussels sprouts salad with apple cider vinaigrette.
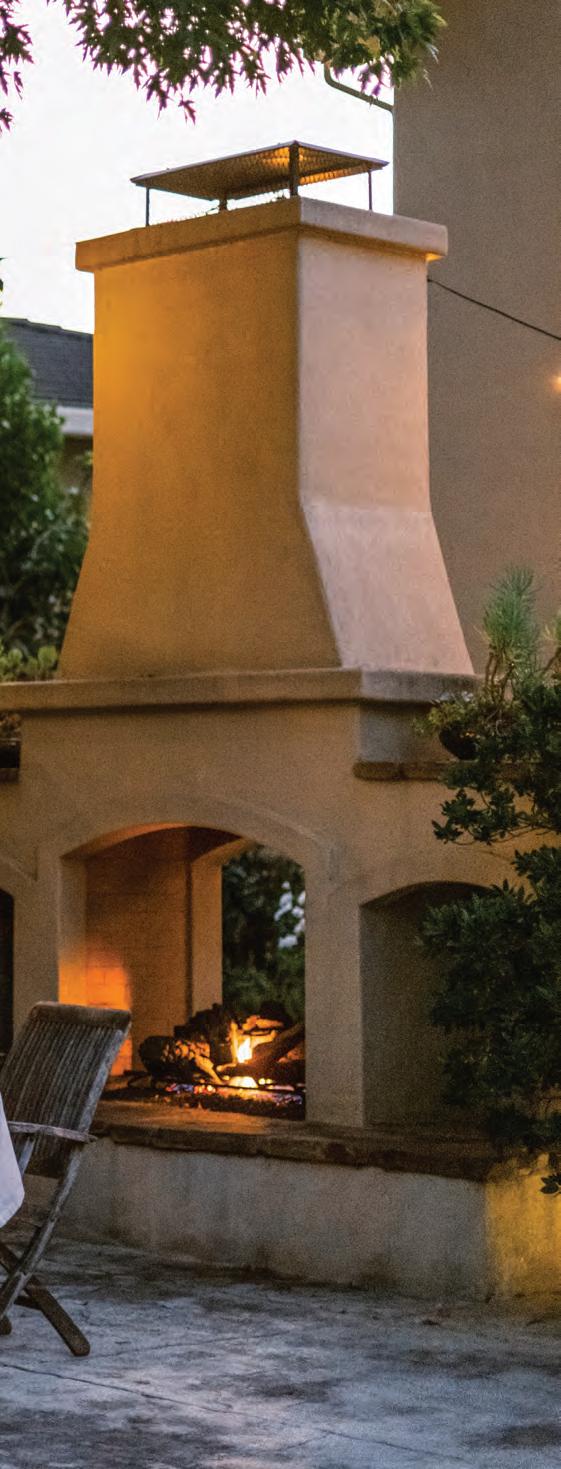
SACMAG.COM November 2022 35
Lea Raymond and Hanna Ray Flores
GETTING READY
According to Hanna and Lea, preparation is the key to a successful dinner party. Do whatever you can in the days leading up to the event so that you aren’t frazzled when your guests arrive. That way, you can enjoy your own party. Plan the menu and shop for g roceries at least a week in advance. Set your table the day before. Pro tip: Set out your serving pieces and label each with a Post-it note so you know what food goes where. You won’t want to have to scrounge around for a bowl at the last minute.
VINTAGE FINDS
Hanna and Lea are inveterate thrifters who frequently score beautiful glassware and serv ing pieces at Goodwill and secondhand shops. Mixing vintage with new ensures your table won’t ever look boring or basic.



SETTING THE TABLE

Hanna and Lea decided on a palette of neutrals and naturals to let the food shine. They used a creamcolored linen tablecloth topped with a cream woven runner, along with rustic wood chargers, scalloped-edge plates in speckled oatmeal from World Market and delicate gauzy napkins tied with thin velvet ribbon. Tapers and tea lights provide a warm glow. And instead of florals, they opted for a bit of greenery. (You can purchase greens from Trader Joe’s or forage from your own backyard.) Pro tip: If your table isn’t big enough to seat everyone, Hanna and Lea recommend covering it with a larger sheet of plywood and topping it with a pretty tablecloth. No one will know the difference!

36 SACRAMENTO MAGAZINE N ovember 2022
SETTING THE MOOD



Sean
SACMAG.COM November 2022 37
Greet your guests with a cocktail, like this fruity sangria made with Pinot Noir. 1 orange, sliced 1 apple, cubed 1 bottle Sean Minor California Series Pinot Noir ⅓ cup apple brandy 2 cinnamon sticks 5 whole star anise Add apples and oranges to a pitcher and muddle with a spoon to release juices. Add wine and brandy and stir to combine. Add cinnamon sticks and star anise to the pitcher. Serve over ice, adding some fruit to each glass.
Minor Sangria
Whipped Goat Cheese With Rosemary Honey Bacon, Apples and Dates
6 slices bacon, chopped ⅓ cup honey
1 teaspoon brown sugar
2 tablespoons chopped fresh rosemary ½ teaspoon cayenne pepper (or to taste)
Preheat oven to 400 degrees. Line a baking sheet with parchment paper. Place the bacon on the sheet.
In a small bowl, combine honey, brown sugar, rosemary, cayenne and a pinch of salt. Drizzle half of the honey mixture over bacon and toss until coated.
Scatter dates and apples around the bacon. Bake for 10–12 minutes, until bacon is crisp.
Meanwhile, combine goat cheese, cream cheese, olive oil and a pinch of salt in a food
12 Medjool dates, pitted and torn into bite-size pieces

1 apple, cut into bite-size pieces
2 logs (16 ounces) creamy goat cheese, room temperature
processor and pulse until smooth and creamy.
Spoon goat cheese mixture into a serving bowl or onto a charcuterie board and top with warm bacon, apples and dates. Drizzle with the remaining honey mixture. Serve with crostini.

Make ahead: The goat cheese spread can be made 3 days ahead and kept in the fridge. Bring to room temperature before serving.
8 ounces cream cheese, room temperature
2 tablespoons extra-virgin olive oil
Sea salt Crostini
38 SACRAMENTO MAGAZINE N ovember 2022
KNOW YOUR PLACE
Where do I belong? That’s the dilemma guests face when the host calls everyone to the table. Lea and Hanna have an easy fi x for that: place cards. “We always do place cards,” says Hanna. “People are shy about seating themselves. This tells them where to go, and also helps introduce them to others at the table.” Adds Lea: “So much awkwardness—gone!” The sisters also like to leave a menu—either printed or handwritten—at every place setting. “It gets guests excited for what’s to come,” Hanna explains.

GUEST DUTIES

It’s not only the host who has responsibilities for making sure the party is a success; guests do, too. Here are Lea and Hanna’s tips for great guesting: First and foremost, be on time. Be respectful of your fellow guests. Ask questions and be open to conversation. We all know we’re not supposed to show up to a party empty-handed. But instead of bringing flowers (which may inconvenience your hosts as they search for a vase), bring a bottle of champagne or good whiskey. You can also have something delivered the next day: either flowers or something sweet, like chocolates from Ginger Elizabeth. And if you really want to endear yourself to the host, send over a housecleaner the day after a big party.
Brick Chicken
8 chicken leg quarters (extra fat and skin trimmed and patted dry)
¾ tablespoon dried rosemary ½ teaspoon salt
½ teaspoon freshly ground black pepper
2 lemons, sliced
2 tablespoons extra-virgin olive oil
Equipment : You will need 2 bricks wrapped in heavy-duty foil and a castiron skillet

Lay chicken leg quarters on a cookie sheet and season with dried rosemary, salt and pepper.
Preheat oven to 400 degrees. Place a cast-iron skillet (or heavy-bottomed pan) in the oven to heat.
Remove hot skillet, drizzle with olive oil and put seasoned chicken leg quarters in a skillet, skin side down, and top with lemon slices. Place foil-wrapped bricks on top of the chicken and put the skillet in the oven for 30 minutes. After 30 minutes, remove the skillet from the oven, turn the chicken over, remove juices from the pan, retop with bricks and return to the oven for 30 minutes, or until internal temperature of the chicken reaches 165 degrees. Remove from the oven. Place the skillet on the stovetop and cook the chicken on each side over high heat for a few minutes to crisp the skin.
SACMAG.COM November 2022 39
Nicole and Sean Minor
Silky Mashed Potatoes

THE RIGHT NUMBER


According to Hanna and Lea, six to eight people is the sweet spot for a dinner party. Fewer people and the conversation may lag. More and you’ll feel like a traffic controller. Consider inviting people who don’t know each other. “Who knows?” says Lea. “You could create a new friendship, or some one might meet their future husband.” Make sure to include at least one guest who likes to ask ques tions: That person will mix things up like the swizzle stick in a cocktail.
THE PLAYLIST
Don’t forget music; it sets the tone and puts guests at ease. For this dinner, Hanna and Lea came up with a jazzy playlist that leans heavily on ’70s standards from the likes of Fleetwood Mac, Billy Joel and The Beatles, plus music by Taylor Swift, Kasey Musgraves, Margie Rogers and others. For a link to the playlist, download the Spotify app and create a free account. Press the top-right camera icon in the search tab to scan the Spotify Code below.
40 SACRAMENTO MAGAZINE N ovember 2022
pounds
potatoes
ounces cream
room
1
3
Yukon Gold
4
cheese,
temperature
cup half-and-half 1 teaspoon salt White pepper Peel potatoes and boil until soft in heavily salted water, about 25 minutes. Drain the potatoes and mash with a hand mixer. Add half-and-half and cream cheese and mix until very smooth. Season with salt and white pepper.
Tarragon Beurre Blanc

2 shallots, peeled and roughly chopped
½ cup dry white wine
1 tablespoon white vinegar
1½ cups heavy whipping cream
½ cup (1 stick) unsalted butter, at room temperature
2 tablespoons fresh tarragon, finely chopped Juice from half lemon
Salt and white pepper to taste
In a heavy saucepan, boil shallots, wine and vinegar over high heat until liquid is syrupy and reduced by half, about 8 minutes. Turn heat down to medium, add cream and simmer 10 minutes. Drain liquid and discard solids.
Return liquid to saucepan over low heat. Whisk in 2 tablespoons of butter and the tarragon. Add remain ing butter a few pieces at a time, whisking constantly and adding new pieces before previous ones have completely liquefied. (The sauce should maintain consistency of hollandaise.) Lift the pan from heat occasionally to cool the mixture. Do not boil.
Remove from heat, add lemon juice and whisk until completely emulsified. Season to taste with salt and pepper. Serve warm with the chicken.
SACMAG.COM November 2022 41
Apple Thyme Chutney

1 tablespoon olive oil
1 large yellow onion, cut into ½-inch wedges
2 green apples, peeled, cored and cut into ½-inch dice ¼ cup cider vinegar
1 tablespoon brown sugar
½ teaspoon grainy mustard
½ teaspoon chopped fresh thyme
3 tablespoons unsalted butter
Salt and pepper to taste
In a large saucepan, heat oil over medium heat and add onions. Saute until trans lucent and starting to caramelize, about 10 minutes. Add apples, vinegar, brown sugar, mustard and thyme. Stir well to combine and cook until the apples soften, about 10–15 minutes. Add butter and season with salt and pepper. Serve the chutney alongside the chicken.
WINE TIME

Sean Minor Wines has winemaking operations both in Sonoma and on the Central Coast. But owners Sean and Nicole chose to raise their four children in Sacramento, where they do a lot of entertaining and hosting of their own—over Sean Minor Wines, of course. Their wines are sold in all 50 states as well as in 15 countries. Nicole supplied tasting notes for the wines paired with the meal:

SEAN MINOR CALIFORNIA SERIES SAUVIGNON BLANC 2021 : Vibrant and juicy with aromas of fresh ruby grapefruit, citrus and tropical fruit. On the palate, the combined flavors of lush melon, fig and lime are balanced perfectly to form a crisp, mouthwatering texture. A compelling finish leads to another sip. Serve with Whipped Goat Cheese With Rosemary Honey Bacon, Apples and Dates.
SEAN MINOR SIGNATURE SERIES PINOT NOIR 2021 : Leads with well-knit, rich flavors of cherry, plum, blueberry and hints of cedar bark. Elegant velvety texture; blood orange, dark cherry and earthy notes glide across the palate. Beautifully structured with sleek, bright acidity and a clean finish. Serve with Brick Chicken.

SEAN MINOR SIGNATURE SERIES CHARDONNAY 2021 : Merged flavors of baked green apple, soft rounded hints of lemon scone, and sweet cream finished with a hint of cardamom and spice. Serve with Brown Butter Apple Tarte Tatin.


42 SACRAMENTO MAGAZINE N ovember 2022
HoneyRoasted Carrots
2 pounds carrots, peeled and tops removed
3 tablespoons olive oil
½ teaspoon salt
½ teaspoon pepper
3 tablespoons honey
1½ tablespoons apple cider vinegar
2½ tablespoons chopped fresh parsley
2 teaspoons chopped fresh thyme leaves
Preheat oven to 400 degrees. Place carrots on a rimmed baking sheet. Drizzle with olive oil, season with salt and pepper, and toss to evenly coat. Spread into an even layer. Roast for 20 minutes, then remove from oven.
In a small bowl, stir together honey and apple cider vinegar. Drizzle carrots with honey mixture and toss well to evenly coat. Return to the oven and roast until tender, about 5 to 10 minutes longer. Remove from the oven, toss again and sprinkle with fresh parsley and thyme. Serve warm.


Shaved Brussels Sprouts and Pomegranate Salad
SALAD
1½ pounds Brussels sprouts, halved and thinly shaved
apple cider vinegar
tablespoon honey
teaspoon Dijon mustard
clove garlic, minced
Salt and pepper to taste
cup freshly chopped parsley
cup pomegranate seeds Shaved Parmesan
cup chopped almonds, lightly toasted
To make dressing, add ingredients to a jar with lid and shake until com bined. Set aside. To make salad, place Brussels sprouts, parsley and pomegranate seeds in a serving bowl. Toss with dressing. Add shaved Parmesan, top with toasted almonds and serve immediately.
SACMAG.COM November 2022 43
⅓
¼ cup
1
1
1
DRESSING
cup olive oil
¼
½
¼

44 SACRAMENTO MAGAZINE N ovember 2022
Brown Butter Apple Tarte Tatin
2 sheets frozen puff pastry, thawed 1 stick (8 tablespoons) salted butter
½ cup brown sugar
Equipment : You will need an oven-safe skillet
Preheat oven to 425 degrees.
1 teaspoon cinnamon
1 teaspoon vanilla
3 Honeycrisp apples, sliced into ½-inch rounds, seeds removed
On a lightly floured surface, press the 2 sheets of puff pastry together to make 1 large sheet. Trim to fit the size of the skillet you will be using for the tart. Wrap puff pastry dough in plastic wrap and refrigerate until ready to use.

Heat the skillet over low heat and brown the butter, about 10 minutes. Add brown sugar, cinnamon and vanilla and cook, stirring until the mixture is well combined. Remove pan from heat. Lay apple rounds in the pan, working from the outer edge in, fitting as many as possible.
Place skillet over medium heat and cook until the apples become golden brown, about 10 minutes. Flip over each apple round so the cooked edge faces up and the uncooked edge is face down in the mixture.
Place pastry over apples and press down gently, tucking the sides of the pastry under the apples as best you can. Make 3 small cuts in the center of the pastry. (If making ahead, wrap in plastic wrap and refrigerate until ready to use.) Place skillet on a baking sheet and bake for 20 minutes, or until the pastry is deep golden brown.
Remove from the oven. Let cool in the skillet for 15 minutes. Run a knife around the edge to loosen. Carefully invert onto a serving plate. If any apples fall out of place, just rearrange them. Serve warm topped with ice cream and sprinkled with flaky sea salt.
Vanilla bean ice cream for serving Flaky sea salt
HAUSTE: WHAT IS IT?
Hauste supplies downloadable party guides called Hauste Its. Each one in cludes a three-course menu, recipes, shopping list, prep schedule, wine and cocktail pairings, styling tips and cu rated playlist—everything you need to achieve your inner Martha. “We’re a steppingstone to those entertaining skills,” says Lea. Each party guide has a theme, an estimated cost per person and a difficulty level, from easy to pro. Cost: $16–$26. For more information, go to hauste.co.

SACMAG.COM November 2022 45
The Big Quit
BY SASHA ABRAMSKY PHOTOS BY RYAN ANGEL MEZA
The Sacramento region’s unemployment rate hit a low of 2.9% this past May, before rising slightly to 3.4% at the start of sum mer. Both numbers are among the lowest unemployment rate data in the city’s history.
As in so much of the country, however, the his torically low unemployment rate masks a more complicated truth. During the pandemic, huge num bers of people throughout California quit their jobs. In August 2021 alone, for example, 400,000 Califor nians left their place of employment. And in many months throughout 2020 and 2021, vast numbers of workers upped stakes and either opted out of the labor market altogether—which is partly why the unemployment rate is so low—or chose the moment to rethink their careers. As of this past summer, the labor force participation rate in California (the per centage of working-age adults either employed or actively looking for jobs) was just 61.7%; that com pares to 63.4% in February 2020, just before the pandemic hit, and 66% in 2008, just before the hous ing bubble burst.
As the economy recovered, jobs were there for the taking, but millions of Americans weren’t taking them. That presented a huge opportunity for those who didn’t like their jobs—were bored, tired, under paid or felt underappreciated—to leave those jobs and look for something better.
With the pandemic, some workers secondguessed their relationship with employment and moved on. Now what?
For a while, it became so hard for some business es to find staff that they had to reduce their hours—cafes would shut at 3 p.m., restaurants by 8:30 or 9 p.m.—or days of operation. In August, CNBC reported that three times as many businesses were offering signing bonuses to new employees as was the case pre-pandemic. Airports couldn’t find enough staff to get luggage from planes to terminals. Trans port systems struggled to find bus drivers. Hospitals ran short of nursing staff.
The Great Resignation, as commentators have dubbed it, affects people of all ages and all walks of life. Disproportionately, however, it has swept up younger workers, those with fewer family and finan cial responsibilities and more of an ability to take a chance, as well as middle-aged workers desperate for more stability and more reliable benefits. Many of those who left were service-sector workers— people who had either lost income during the pan demic or who saw a tight labor market as the economy rebounded from COVID shutdowns. They saw desperate employers willing to offer high wages and good starting perks to new employees, swallowed deeply and made the jump.
46 SACRAMENTO MAGAZINE N ovember 2022

SACMAG.COM November 2022 47
For restaurateur Patrick Mulvaney, the pandemic completely changed his workforce.
Iworked for Mulvaney’s [downtown restaurant] starting in ’06,” says 43-year-old Andrew Willsen. “I’ve been in restaurants about 21 years. Waiting tables in Sonoma, being a sommelier, a manager. I was working at Waterboy in March 2020, and then the restaurant closed for two years.”
Willsen had been looking for a career change for several years, as he found that being on his feet for hours at a stretch was too wearing on his middle-aged body. The restaurant business was exhilarating at times, he says, but it also led to “stress, repetitive strain injuries; you’re walking on cement or tile, walking 10 to 12 miles a day.”
At the start of the pandemic, many of Willsen’s friends quit the restaurant business. “They got into other sales jobs—tech, marketing—or in local govern ment, for the city or county. And once they did that, they decided to never go back to restaurants. They had downtime and got used to spending more time at home and with their families.” Many workers in what res taurants call the “back of the house”—the kitchen—quit, says Willsen, to start their own catering business, work for Amazon or take construction jobs.
For Patrick Mulvaney, one of Sacramento’s bestknown restaurateurs, the pandemic entirely changed his workforce at Mulvaney’s B&L. During the shut down, restaurants had to cut their staff down to the bare minimum, to the few needed to cook takeout orders, clean the kitchen, perhaps staff the front-ofthe-house food sales sites that many restaurants improvised, acting as gourmet markets while they tried to sell off their surplus produce. Then, as the economy stumbled toward reopening, Mulvaney’s had to grapple with chronic staffing shortages as large numbers of former employees had moved on to other forms of work. “People were saying, ‘I’m not sure if I want to work or where I want to work,’” Mulvaney says, recalling those difficult months. “We struggled, because we didn’t have the labor.”

“It was painful. We lost a lot of the institutional knowledge, the teachers who teach the next generation. I don’t know if there’s ever been a space where there just aren’t the middle- and upper-level folks. It’s something all of us in the industry talk about. Where are the folks we used to rely on and in some ways took for granted? We find ourselves in the trenches more. It’s more tiring, but it’s also invigorating.”—restaurateur
Patrick Mulvaney
To encourage workers to come back, Mulvaney, like many other restaurant owners, restructured his res taurant’s tipping policies, instituting tip sharing with back-of-the-house employees who in the past had often been left out of the process. Slowly, he was able to rebuild his fractured workforce, though even today it’s still not as large as it was prior to March 2020. (He estimates that, industrywide, the workforce is about 15% slimmer today than it was pre-pandemic.)
“It took eight months,” says Mulvaney. “It was pain ful. We lost a lot of the institutional knowledge, the teachers who teach the next generation. I don’t know
48 SACRAMENTO MAGAZINE N ovember 2022
Patrick Mulvaney
“
if there’s ever been a space where there just aren’t the middle- and upper-level folks. It’s something all of us in the industry talk about. Where are the folks we used to rely on and in some ways took for granted? We find ourselves in the trenches more. It’s more tiring, but it’s also invigorating.”
Willsen, who has asthma, hunkered down when the pandemic first hit. Then, he started to re-evalu ate his life. He had a teenage daughter, but she lived with her mom and stepdad. He’d been in a long-term relationship, but it had recently ended. He decided it was time to downsize and sold the house that he had shared with his ex-girlfriend.
He rented a 15-by-15-foot storage unit, kept what would fit in there and got rid of the rest of his pos sessions: couch, table, a bunch of other furniture, wine, many of his books, TV, even his computer. “I’m trying to have less things,” he reasoned, “a smaller footprint.” He decided to think of the COVID era as his “Great Reset.”
As the pandemic dragged on, Willsen started writ ing for blogs and other websites. He was interested in climate change and political extremism, and he wanted to explore why society was so good at ignor ing existential risks—such as deadly new viruses—until they literally threatened the social fabric. When the
lockdown lifted, rather than go back to the restau rant world, Willsen was ready to try something new. He began podcasting, started painting and made plans to head to the Mexican city of San Miguel de Allende for three months to write a book.
For Erika Noonan, a longtime hairstylist in a midtown salon, the pandemic crystallized all of her insecurities about employment, stable wages and access to benefits.
pandemic shifted the way I thought about life. There’s no security in hairdressing. The government can come in and say you can’t work. I feel like I’m one paycheck away from being homeless.”—stylist Erika Noonan
Noonan had always loved cutting hair, but she had two young kids, now 4 and 12. She was also in her 40s and had started to think about what she wanted her retirement years to look like. She knew that she wanted more reliable benefits,

SACMAG.COM November 2022 49
Erika Noonan
“The
and a secure paycheck that wasn’t at the mercy of inconvenient shutdowns.
Like Willsen, she had found her work taking a physical toll; standing all day long cutting hair was exhausting. When she was with a client, all was right in the world—she’d always loved shaping other peo ple’s hair and talking with them during their haircuts, rinses and head massages. But when she stopped at the end of the day, she was tired. Then, when the pandemic shut down her K Street salon, she felt deeply vulnerable.
“I realized the government can shut you down—and you’ve still got to feed your kids,” she says. It was something akin to a shattering realization. “The times are very unsettling, scary. The pandemic happened suddenly; things changed. I feel like things are more volatile. It’s always good to have stability.”
of politics that she had been immersed in for years. She wanted, she says, to do something toward im mediate, on-the-ground change.
“I was looking at where is power and where does power lie?” she says. “The answer is money. I don’t know if I believe in the political system [anymore]— which is an awful place to be if you’re working in it.”
She says she saw politicians free up large amounts of money for food assistance during the height of the pandemic, only to remove those benefits after the immediate emergency had passed, even though the poverty and the need remained.
“The pandemic showed me the hollowness of the system,” she says. “Things could be better. They are better in other countries and places.” She felt more and more disillusioned. “Why are we working?” she would ask her friends. “What does work mean? What is the impact on our health? Waking up depressed every day about work is not healthy.”
“The pandemic showed me the hollowness of the system,” says Amanda, who does social justice work. “Things could be better. They are better in other countries and places.” She felt more and more disillusioned. “Why are we working?” she would ask her friends. “What does work mean? What is the impact on our health? Waking up depressed every day about work is not healthy.”
Reluctantly, Noonan decided to apply for state employment. She got a job as a tax technician with the Franchise Tax Board. It was, she says, customer service work, helping answer taxpayers’ questions.
“Now we’ll get medical for sure, retirement at some point,” she explains, as if justifying a move she’s still not comfortable with. “You get sick pay and vacation pay and holiday pay.”
Without that, she says, her family would be reliant on Covered California or MediCal for their health insurance. She didn’t miss paying hundreds of dollars a month in health care premiums for herself and her two children. But she did miss the salon, so she has still been working there on weekends to supplement her income—and to get her fix talking with clients.
“The pandemic kind of shifted the way I thought about life. In terms of security, there’s no security for me in hairdressing, and no guarantee we’re going to be working,” says Noonan. “The government can come in and say you can’t work. I feel like I’m one paycheck away from being homeless.”
Amanda, a young woman who lives in midtown and worked at a large social justice organi zation near the Capitol (at her request, Sacramento Magazine is not using her real name or identifying her place of employment), says the past two years have involved lots of introspection.
For years, she felt she had been talking a good game about social justice. But as the pandemic wore on, increasingly she wanted to be more hands-on in crafting solutions rather than simply identifying problems. She became disillusioned with the world
She started craving community. “I think of tree roots, holding onto each other; in a storm they hold onto each other and sway. I think people are like that.”
This summer, after two years of struggling with her feelings, Amanda was offered the opportunity to do hands-on social justice work at a different orga nization. It better aligned with her new priorities. With a sense of relief, she quit her old job and pre pared for this new chapter in her life. “I’m in my mid-30s, have been an adult for a while. I want to go from talking about problems to solving problems.”
For Adam Schmidt, the crisis was less one of existential identity and more one of burn out. He was, quite simply, tired.
“I was in the restaurant industry for close to 20 years,” he says. “I started when I was 18, and I left the day before my 36th birthday. I toughed it out through the pandemic; it was about six months ago that I left. I wasn’t physically able to do it. I was a server in fine-dining atmospheres—at Mulvaney’s, then Allora, Ella and Localis.”
For years, Schmidt, who didn’t have a college de gree, wanted to leave the restaurant world behind. But when he applied for office jobs, he felt he wasn’t given a fair shake, perhaps because potential employ ers figured his skills wouldn’t translate easily to sedentary office work.
Then the pandemic hit, the Great Resignation kicked in, and an employment shuffle began. “I saw people making that leap,” says Schmidt. “So
50 SACRAMENTO MAGAZINE N ovember 2022
I decided to leap. People started to suddenly give me interviews.”
Within short order, Schmidt got his mortgage li cense and went to work as a mortgage loan officer. After six months, he quit that new job, and—at the urging of a friend who was already working for the company—took a new one as an insurance specialist at an electronic records startup. He works remotely from home helping clients having problems billing insurance companies.
“It’s much less demanding than the restaurant business, for sure,” he says. “I do miss being on my feet and being active. It was a big adjustment.”
Despite that nostalgia, the missing “going into battle every day” feeling, he has no regrets. “In terms of stability, in terms of my career, I can actually move up. The benefits are way better. I mean, you actually have benefits. I’d not had health insurance for I don’t know how long—since I was 26 and got kicked off my parents’ insurance. The ability to have paid time off is huge. In the restaurant industry, your vacation costs twice as much—because you’re not just spend ing $1,000; you’re also losing $1,000 by not working.”
Looking back on the pandemic, Schmidt thinks that, despite the horrors, he emerged in a better place. “It’s something my wife and I talk about. We met just before the pandemic and found it was a blessing for us. We were on unemployment. We made a ton of

money, saved up; we were able to buy a house.” His wife quit her corporate job and pursued her dreams as a freelance graphic designer. When a few restau rants began hosting outdoor dining again, he returned to work and, he says, raked in huge amounts of tips. Customers were suddenly treating staff more kindly. “Everything was shut down, nowhere to go, so what were you going to spend your money on?”
Then the pandemic hit, the Great Resignation kicked in, and an employment shuffle began. “I saw people making that leap,” says Schmidt. “So I decided to leap. People started to suddenly give me interviews.”
Moreover, he says, laughing, the pandemic clarified for people what they were willing to put up with and where they drew red lines. “People stopped tolerating things they used to tolerate,” he says, “such as rude management, inconsistent hours, the [different levels] of money people were making.”
For Schmidt, Sacramento’s Great Resignation was a once-in-a-lifetime opportunity. “When there are lots of jobs and not a lot of people who want to work them, it opens up doors for people like me,” Schmidt says. “People who don’t have college education but have a lot of skills.”
SACMAG.COM November 2022 51
Adam Schmidt





926 J STREET | SACRAMENTO, CA 95814 | THECITIZENHOTEL.COM | @ DINEGRANGE | @ THECITIZENHOTELSACRAMENTO
BUDTENDERS, DRONES AND SLINKY GOWNS ARE JUST A FEW OF TODAY’S HOTTEST BRIDAL TRENDS.


If you haven’t attended a wedding in a while, be prepared: Things have changed. Thanks to supply-chain issues, inflation and changing mores and fashions, weddings are, let’s say, di erent than they used to be, with everything from smaller guest lists to bigger price tags. (Have you heard about the “new normal,” the $70,000 wedding?) We turned to three local bridal experts for the lowdown on the latest wedding styles and trends. Here is their report.
BY ANGELA KNIGHT
au courant we ing
SACMAG.COM November 2022 53
Susan Yee
The Experts
TALIA GONZALEZ: CEO, Talia Eliana Events

 SUSAN YEE: Photographer, Susan Yee Photography
JENN ROBIRDS: Event designer and coordinator, Jenn Robirds Events
SUSAN YEE: Photographer, Susan Yee Photography
JENN ROBIRDS: Event designer and coordinator, Jenn Robirds Events
Small weddings continue to be popular.
What are some pandemic-related changes to weddings?
TALIA GONZALEZ: Couples want to be intentional about everything they have for their wedding. They want it to feel like home, to feel inviting. A lot of that is because of COVID; so many people had to pivot because of the new restrictions. Destinations were popular before, but now everyone’s itching to get out.


SUSAN YEE: There’s more focus on families, and intimate weddings are more of a thing. Weekday weddings have carried over from the pandemic.
JENN ROBIRDS: People are more thoughtful about space utilization, as well as meal presentations. We saw a lot less bu ets, and even family style, this year, and people opting for plated dinners. That trend will probably continue, and it feels more elevated. We never left the trend of outdoor weddings, but we’re still seeing a huge push for outdoor ceremonies, cocktail hours and even receptions. I don’t see that slowing down.
What’s trending in venues and locations?
GONZALEZ: Couples are keeping the guest list small, 35 people and under, and planning destination weddings with a week or a weekend full of activities with their close ones.
YEE: Outdoor venues. That’s something that, especially since the pandemic, has carried over. I’ve shot a couple of weddings at Bear Flag Farm, which is a beautiful venue [in Winters]. People love to get married at lush places like that.
ROBIRDS: From warehouse to ballroom to tented wedding in Tahoe—I wouldn’t say that I’m seeing one more than the other. We’re doing more destination weddings in Napa and Sonoma, San Francisco, Carmel, and recently we’ve been busy in Lake Tahoe.

Describe some popular wedding styles or elements.
GONZALEZ: Boho weddings, where you have pampas grass, dried flowers, muted tones, with [printed materials in] a fi ne

54 SACRAMENTO MAGAZINE November 2022
Susan Yee
Talia Gonzalez
Jenn Robirds
Talia Gonzalez portrait: Miranda Rose Photography; Susan Yee portrait: Jasmine Fitzwilliam Photography; Jenn Robirds portrait: Yuliya Jul Photography; top ceremony: Susan Yee Photography; bottom ceremony: Sebastien Bicard (photo), Talia Gonzalez (event designer)
block font, and adding arches, half circles and asymmetric shapes into that. People are putting more intentionality into their weddings; they’re making it more themselves with pops of color. There are people who are not afraid to use color right now. There’s this other style—modern mini malist chic—where couples dive into Pinterest to get the colors, to get the pictures. The signage is in black and white, all the cutlery, linens, everything is black and white, and baby’s breath or some light greens as the accent.
YEE: What I’m seeing are silky dresses as opposed to princess or tulle dresses. Direct flash is becoming more prevalent, which creates a ’90s film look.
ROBIRDS: We started creating spaces with what we call cabanas or pavilions. It feels like you’re bringing the outdoors inside, through drap ing, height and drama. Personalization is king, meaning custom weddings are at the forefront. People don’t want cookie-cutter projects. They come to us and say, “I want something unique and a wow factor for my guests.” I’ve been having a lot of fun with seating charts; for a wedding in August, our escort display [seating chart] was designed like a vintage hotel concierge desk, and we had actors in bellhop attire. People thought that was fun because it’s rare you interact with somebody to get your seating assignment.
Let’s talk photography trends and ways of capturing images.

GONZALEZ: Most people want a drone if the venue allows it, their space allows it. But that means everything better be straight, because you need to focus on how it’s going to look from above, not just how it looks from the guests’ perspective. Semi-blurred inten tional action shots, they’re all the rage right now. People are hyped that they can create action and storytelling through photos, by having that movement in there.
Silky dresses (especially for bridesmaids) in neutrals and earth tones are a stylish trend.

SACMAG.COM November 2022 55
Bottom photo: The Indi Collective (photo), Talia Gonzalez (event designer)
Imperfect photos are a modern take on wedding photography.
Destination weddings are big. This one was in St. Helena.
Suits with custom linings, like this one from R. Douglas, are a fun, unexpected touch.

YEE: The whole ’90s vibe is back. Using a direct flash is part of wanting more imperfect photos. People want interesting photos that convey a feeling, like the blurry ones or something that might be out of focus.
ROBIRDS: Gone are the days of formal, super-posed photos. We’re seeing requests for beautiful, fun, candid shots, where the photographer is following the couple as the evening unfolds and capturing those moments. Natural light and film photog raphy continue to be a major trend. Couples want to look like themselves when they look at their album in 20 years.

Are $60,000 to $70,000 weddings the “new norm”? Who’s paying the bill?
GONZALEZ: If people have that budget, they can pretty much get what they want on a standard scale, with potentially 120 people. Makeup, floral and photography all play into that, and those costs have gone up. Most of my couples are paying 80 percent of the bill.
YEE: I don’t know how much people are spending overall, but the cost of everything’s gone up. I have three photography packages, depending on the hours and what they want to include—so average, I would say, around $5,000.
ROBIRDS: Our average client is eclipsing $100,000 very easily. The cost of raw materials has significantly increased from food to beverage to floral. That was one of the harderhit markets; we saw floral prices skyrocket because of supply and demand, and some wholesale growers didn’t make it through the pandemic. We see sometimes each family chip ping in 50-50. We’ve seen where each parent gives the couple $10,000 and then the couple pays the difference to the tune of a significant amount of money.
With inflation and supply-chain issues, how do you help your clients keep costs down?
GONZALEZ: We let everyone know why it’s important to have those conver sations in the beginning, so I know exactly how much money you have to work with. What are your must-haves? What’s your minimum on guests? If you take out 10 people, you’re taking out 10 plates of food, you’re taking out an entire table, so any linens, rentals that you have, a centerpiece, signage, it’s a small er seating chart, it’s less programs and less ceremony, chair rentals. It translates throughout the entire event, which is why guest counts have been decreasing as the costs are increasing.
YEE: If they can’t afford me, I will often see if there’s a way we can work together—even if that means paring down a photography package to some thing that works, where I can still cover it, even if it’s not the entire day or we’re not doing an engagement session or add-ons.
ROBIRDS: If we know your goal budget is $70,000, we’ll be able to tell you, “OK, this is the amount we should allocate for catering, this is the amount we should allocate for rentals, this is the amount that goes to floral.” The No. 1 way to save money on your wedding is to cut your head count.
Is the gift registry a relic?
GONZALEZ: If the couple is in a place where they don’t need any items, we still have them create a registry because people are expecting the registry and they will, espe cially older generations, be looking for one. If it’s things that are going toward your
56 SACRAMENTO MAGAZINE N ovember 2022
Couple: Rachel Artime (photo), Tre Posti (venue), Walnut and Main (florist), Talia Gonzalez (event designer); suit: Christopher Lombardo/Lyfe Captured Photography
honeymoon, your guests can pay for a ziplining excursion, for hotels, for a couple’s massage. People are likely to spend more if they know what it’s actually going toward versus just cash.
YEE: In the past, I’ve done a photography registry, but it’s not common. A lot of people do a honeymoon registry.
ROBIRDS: We’re seeing hybrid registries where a couple might still need a few things. Registries like Zola, where you can register for a vast array of di erent products across di erent retailers. Those are still popular.
What is the word or words that you’d use to describe your couples?
GONZALEZ: Adventurous.
YEE: Intentional.
ROBIRDS: Discerning, creative, fi nancially savvy. What’s your top FAQ?
GONZALEZ: A lot of people ask whether they should do a fi rst look. At least 75 percent of my couples choose to do it. On a logistics side, it’s amazing for the photographer because they can get those photos done earlier in the day.
YEE: If they hire a planner, especially if the planner is experienced, they’ll know what a photographer needs generally. That’s actually what I get most asked about: How should we fit in the photography schedule?
ROBIRDS: What is this going to cost me? What’s happening with food?
GONZALEZ: Stations and multiple types of food. We had a wedding where di erent food trucks showed up: late-night bites, taco stand, hot dog stand, In-N-Out Burger. Couples are focused on food people like and enjoy; it’s comfort food.
YEE: People have been expanding their food vocabulary. I had a wedding where they did Thai appetizers and a bubble tea station.
ROBIRDS: Beautiful, seasonal approaches. They still love family style; I think that’ll pick up again in the fall and into next year as people become more comfortable.


What clothing styles are popular for brides, grooms or their guests?
GONZALEZ: They’re wearing neutral formal: champagne, olive green, caramel, muted tones, lots of satins and linens. We send a mood board to guests so they know what the heck we’re talking about. We’re seeing [weddings where the guests are asked to wear] white—less so for weddings, unless it’s potentially a destination wedding, but more so for the welcome party, or post-brunch where everyone wears white.


YEE: There are places where men can get a special lining on the inside of their suits, a pattern or fabric that is unique and you can customize. When they open their jacket, you see this fun lining.
ROBIRDS: The ’80s might make a comeback in a unique way next year. I could see
Outside
SACMAG.COM November 2022 57
Trendy cabanas make the outdoors feel like inside.
Cabana: Carlie Statsky (photo), Jenn Robirds (event designer); bride: Lucas Mendes Photography
Boho weddings continue to be a popular style.
is in for ceremonies, cocktail hours and receptions.
Simple and modern, minimalist chic is a hot trend.
Semi-blurred action shots are all the rage right now.
Budtenders are the latest in wedding service personnel.

hats and gloves, or sleeves with bigger shoulder lines, in bridal attire. We’re going to see more playful and customized dresses in that brides have sleeves for the ceremony and then those snap o and the dress changes for the reception.

Are couples actively managing their wedding guests?
GONZALEZ: They’re managing their guests, but also managing their day based on the guests they’re choosing to invite. Are there a lot of smokers? Great. We’ll have a cigar station. We’ll have a smoking area. We have a wedding that’s having a budtender come in.
YEE: People are having unplugged weddings where guests don’t take any photos. I actually shot a wedding this weekend where they said you have one minute to take all the pictures you want with your phone right after the couple gets up the aisle. Then that’s it.


ROBIRDS: Absolutely. Wedding websites are a great way of communicating with guests the di erent events, expectations on attire, registry, transportation and experience information. It’s not uncommon for couples to put attire guidelines on their website, to the highest level of black tie, to dress for the cocktail hour, to “Hey, our venue is outdoors and it’s on grass, so avoid wearing stilettos.”
What’s the most interesting or unique wedding you’ve done recently?
GONZALEZ: This wedding in Palm Springs in October, their fi rst day is 15 people out at Joshua Tree, then a THC -infused fancy dinner; every course is dosed to that person’s tolerance. The next day it’s a tiki-style welcome party. We’re having hula dancers and fi re and karaoke. The next day is back to those neutral tones, earth tones, very intentional modern design, with a five-course plated dinner that’s wine paired. Then the budtenders come in and there’ll be a taco cart. They wanted things that people could only experience at their wedding and would be talking about forever. They have the budget to match, which is how they’re able to do all that.
YEE: I helped a friend of mine shoot a wedding in Palm Desert. They were all actors and actresses, including [the lead actor on the Netfl ix series] “Arrow.”
ROBIRDS: What really gets me excited is custom-curated weddings that are reflective of the couple. Every wedding we do is unique to the client.
If you had a crystal ball, what would you see?
GONZALEZ: Multiday events with fewer guests, like that Palm Springs wedding.
YEE: Intimate weddings focused on creating memories with the people you love as opposed to putting on this elaborate show.
ROBIRDS: Luxury, fun, engaging a airs, with a more intimate head count. There’ll always be a place for 300-person, 500-person weddings, but the majority are going to be cognizant and thoughtful about their guest lists. There are only so many dates and places that are available, so there is a big demand right now. That’s, of course, impacting supply and price.
58 SACRAMENTO MAGAZINE November 2022
Reception: Susan Yee Photography; couple: Maico Pereira Photography





702 Gold Lake Drive, Folsom CA 95630 | 916.932.2769 lakenatomainn.com ❦ weddings@lakenatomainn.com Photography by Holly D. Photography

In the Details
A ’70s kitchen gets a thoughtful redesign for the 21st century.

SACMAG.COM November 2022 63
kat alves
1122
inside: Making mid-mod modern again
Nest
BY CATHERINE WARMERDAM
There’s an old jazz ballad that posits that when it comes to love, “it’s the little things that mean so much.” The same can be said of kitchen design. Thoughtful details are often the difference between a kitchen that merely looks good and one that actually functions smoothly for daily living and is a joy to live in.
Take this kitchen in an iconic midcentury-modern home in Carmichael’s Del Dayo neigh borhood. When it needed a refresh, the team at Benning Design Construction focused on smart, subtle details both practical and beautiful—changes that enhance the home’s original architecture rather than interfere with it.
“The home was completely original, down to the ’70s appliances and the parquet flooring,” says principal Eric Benning, who credits lead designer Miche Victoria (who is no longer with Benning) for spearheading the transformation. “Our firm has become known for ‘restovating’ these types of homes by preserving the style while bringing them up to today’s standards. It’s a fun challenge to find that balance.”

Nest 64 SACRAMENTO MAGAZINE N ovember 2022
Opening page and below : A drop-down table was specially designed to hug the island. The V-shaped leg propping up the table allows ample legroom for three chairs and is an example of “the painstaking measures we go through to get details perfect,” says Eric Benning.

Opposite page: The continuous vertical grain of the cabinets gives the impression of being one piece of wood, adding to a sense of visual calm in the room. Rather than puncture the slatted ceiling in order to install canned lights, Benning and his team devised a clever solution: They carved a narrow channel in the beams and ran LED strip lights flush with the wood for an elegant, barely-know-they’re-there effect.
PRESERVING THE PARQUET FLOORS WAS A PRIORITY FOR THE DESIGN TEAM. “THEY WERE IN DECENT CONDITION AND THEY CONTINUE THROUGHOUT THE HOUSE, SO IT MADE SENSE NOT TO RIP THEM OUT,” SAYS ERIC BENNING. ABUNDANT NATURAL LIGHT, WHITE PAINT AND LIGHT COUNTERTOPS AND BACKSPLASH SERVE AS A COUNTERPOINT TO THE DARK FLOORS

SACMAG.COM November 2022 65
In a home with no crawl space or attic, great care was taken to upgrade the lighting, plumb ing and electrical systems without marring the original floors or ceiling. Understated fin ishes like the stacked tile backsplash and the streamlined hood allow other features—like the veined quartzite countertops and the wall of oversized windows—to steal the spotlight.

A lack of decorative molding and trim pieces helps preserve the spare lines of the architec ture. “In homes like these, the less the amount of material transition the better,” explains Benning. “It’s often harder to do something clean and simple, but it’s worth the effort.”
Above: By limiting open shelving to one small corner, the kitchen remains spare and tidy. “With those shelves, we were able to create some interest where the cabinetry meets the window while preserving the view and the natural light coming in from the window,” Benning says.
Nest 66 SACRAMENTO MAGAZINE N ovember 2022
DESIGNER/ CONTRACTOR: Benning Design Construction

















Subscriptions
subscription or
subscription,
Single Copies and Back Issues
purchase back issues, please
LET’S DO BRUNCH! 3 GREAT SPOTS THE OBSERVER SAC’S BLACK PRESS IN CASE OF FIRE LIFE UNDER THREAT RESTAURANTS • SHOPS • SERVICES • ENTERTAINMENT 229 WINNERS! SURVEY RESULTS PLACES THAT MAKE IT FROM SCRATCH ) FEEDING THE HUNGRY 4 LOCAL HELPERS SAC DESIGN INSPIRATION FOR YOUR HOME TAKING FLIGHT WINTER BIRDS TO WATCH 17 PRO TIPS AND HOLIDAY RECIPE plus Rhubarb-raspberry pie from Real Pie Company THE VIBE THE BOOZE AND MORE GREAT C OC KTAIL B AR S SMALL BUSINESS ENDURING THE PANDEMIC EXPLORE LOD WINE, FOOD, FUN ARTISAN HOME DECOR LOCAL MAKERS IT’S LIKE AN OWNER’S MANUAL FOR Enjoying The Sacramento Region !Delivered monthly for over 45 years!
To establish a
make changes to an existing
please call (866) 660-6247 or go to sacmag.com/subscribe
To
call (866) 660-6247
Your HEALTH and SAFETY is our top priority…













Many things have changed, but one thing has remained the same: our commitment to your safety. Infection control has always been a top priority for our practice. While we have always had high standards regarding infection control, we have incorporated additional CDC recommendations to keep our patients safe and healthy. The care and quality that our patients have come to appreciate remains a source of pride for our office.

Having loyally served the Sacramento community for the past 25 years, Doctors Amy Woo, Kristine Balcom, Kelly Brewer and Patricia Murphy look forward to continuing in our tradition of putting the health and safety of our patients first. ADA/CDA/CDC PPE COMPLIANT


Dr. Amy Woo Dental Care 2627 K Street, Sacramento 916.443.8955 www.DrAmyWoo.com HONORED AS ONE OF SACRAMENTO’S TOP DENTISTS*
Amy M. Woo, DDS
Hygiene Team
Administrative Team
Kristine E. Balcom, DDS
Kelly A. Brewer, DDS
Patricia Murphy, DDS
That’s the question Professional Research Services has asked thousands of dentists in order to determine who should be on the Top Dentists list.











Dentists and specialists were asked to take into consideration years of experience, continuing education, manner with patients, use of new techniques and technologies and physical results. The dentists’ names are checked against state dental boards for disciplinary actions to make sure they have an active license and are in good standing with the board.
Here are the top dental professionals in the seven specialties surveyed: endodontics, general dentistry, oral and maxillofacial surgery, orthodontics, pediatric dentistry, periodontics and prosthodontics.
“If you had a patient in need of a dentist, which dentist would you refer them to?”
ADVERTISING SECTION
A SPECIAL
ENDODONTICS
Aneet S. Bal
Endodontic Associates Dental Group Sacramento 916-485-6900
A. Rocklin Doms Doms Endodontics Davis 530-750-3636
John Fat Dr. Timothy Wong and Dr. John Fat Sacramento 916-427-2555
Cameron Fife Creekside Endodontics Folsom 916-983-3436

Philip J. Hankins
Capital Endodontics Sacramento 916-441-2366
Bruce M. Holt Bruce M. Holt, D.D.S., Inc. Roseville 916-781-3743
Homan Javaheri
Endodontic Associates Dental Group Sacramento 916-485-6900
David M. Keating
Endodontic Associates Dental Group Sacramento 916-485-6900
David P. Koehn
El Dorado Endodontics El Dorado Hills 916-941-9888
Gregory J. Kolber
Endodontic Associates Dental Group Sacramento 916-485-6900
Kevin M. O’Dea
Creekside Endodontics Roseville 916-786-3303
Sheri A. Opp
Endodontic Associates Dental Group Sacramento 916-485-6900
Steve E. Penn Steven E. Penn, DDS Davis 530-753-4530
Harkeet S. Sappal
Midtown Endodontics Sacramento 916-446-6143
Gina M. Savani
Endodontic Associates Dental Group Sacramento 916-485-6900
Fernando H. Solano Capital Endodontics Sacramento 916-441-2366
Loc Tran Elk Grove Endodontics Elk Grove 916-714-3636
Patrick Tsai Sacramento Endodontics Sacramento 916-929-3351
Clifford T. Wong
Aloha Endodontics Rocklin 916-435-9939
Timothy Wong Dr. Timothy Wong and Dr. John Fat Sacramento 916-427-2555
Mark Young Creekside Endodontics Folsom 916-983-7700

GENERAL DENTISTRY
Kristen Adams
Adams Dental Associates Sacramento 916-999-1302
Nima Aflatooni Gold River Smiles Gold River 916-635-9605 www.goldriversmiles. com
Todd B. Andrews
Todd B. Andrews, D.D.S. Sacramento 916-452-6772
Jenny Apekian
Midtown Dental Sacramento Sacramento 916-441-5800
Guillermo Arellano

Dental Excellence of Greenhaven Sacramento 916-293-0504
Kristine E. Balcom
Dr. Amy Woo Dental Care Sacramento 916-443-8955 www.DrAmyWoo.com
PAUL P. BINON DDS, MSD, FAO
PROSTHODONTIST
PRACTICE: Dr. Binon is a Prosthodontist, a dentist with three years of advanced training beyond dental school. His training focused on function and appearance and includes dental implants, crowns, bridges, veneers, dentures and partials. He graduated from Creighton University with a DDS and was inducted in Omicron Kappa Upsilon dental honor society. He received a three year National Institute of Health Fellowship to Indiana University and also completed a residency in Prosthodontics. Former academic appointments include Medical College of Georgia, Indiana University and as a research scientist at the University of California San Francisco. He is recognized as an authority on biomechanics and implant components. He has published some 50 articles involving research and clinical techniques. Dr. Binon trained under Dr. P.I. Branemark, the inventor of modern implant dentistry at U. of Washington in the early 1980s. He has also received additional implant surgical training at Montefiore Hospital in New York. He has the distinction of being the first recipient of the Academy of Osseointegration Certificate in Implant Dentistry. He currently has a private practice in Roseville that is focused on implant dentistry, aesthetic and functional complex dentistry. He is proud to be a Sacramento Magazine Top Dentist for 10 years in a row.
1158 Cirby Way, Ste A. Roseville, CA 95661 (916) 786-6676 • info.drbinon@gmail.com binondentalimplants.com
EXCELLENCE IN DENTISTRY 2022
EXCELLENCE IN DENTISTRY 2022
CAPITOL PERIODONTAL GROUP
FOCUS: For over 50 years, our surgical and implant specialists at Capitol Periodontal Group have been providing innovative periodontal and dental implant care for patients throughout Northern California.

WHAT IS PERIODONTICS: Periodontics is a dental specialty that involves the prevention, diagnosis and treatment of diseases of the supporting and surrounding tissues of the teeth or their substitutes and the maintenance of the health, function and esthetics of these structures and tissues.
WHAT SETS YOU APART: We offer evidence-based and research proven comprehensive care, utilizing the latest technology, such as 3-D Cone beam computed tomography (or CBCT, 3-D imaging) for patients. Our Periodontists work closely with your general dentists and other specialists to develop an individualized treatment plan to treat periodontal disease, maintain natural teeth and replace lost teeth with permanent replacements through dental implants. We specialize in providing long term solutions for single or multiple lost teeth with dental implants.
DR. THERESA WORSHAM, DR. KEVIN CHEN, DR. ROBERT W. PRETEL, DR. P. PAUL TOWFIGHI, DR. ANEEL NATH, DR. NIDHI JAIN, DR. KHALID RASHEED AND DR. ROSEMARY WU
Sacramento | Elk Grove | Roseville | Folsom | Davis • 916-236-3131 • www.capitolperiodontal.com A Special
Section
Advertising
Garry J. Barone
Garry J. Barone DDS Sacramento 916-443-1905
Ronald T. Blanchette
Ronald T. Blanchette, D.D.S. Sacramento 916-392-7373
Damon Boyd
Damon W. Boyd DDS Sacramento 916-500-3200



Steven J. Brazis
Steven J. Brazis, DDS Sacramento 916-731-5151
Christopher J. Cantrell
Sutter Terrace Dental Group Sacramento 916-736-6750
Michael S. Casagrande
Casagrande Dental Sacramento 916-441-0655
Shareen Char-Fat Kenneth F. Fat, DDS & Shareen Char-Fat, DDS Sacramento 916-925-9222
Nikki Chauhan
Nikki Chauhan, D.D.S. Sacramento 916-392-7110
James W. Childress
James W. Childress D.D.S. Davis 530-756-7400
Sonney L. Chong Sonney L. Chong DMD Sacramento 916-421-3057
Christopher Cooper A+ Dental Care Rocklin 916-312-6902
Miguel Cortez

Miguel A. Cortez Dental Corporation Sacramento 916-514-0489
Monica Crooks Dr. Monica Crooks, DDS Sacramento 916-922-2027

Jerome J. Daby
Daby Dental Sacramento 916-443-8908
Binh Dao
Douglas Dental & Orthodontics Roseville 916-783-4888
Stella Dariotis J Street Dental Group Sacramento 916-443-5677
Elisabeth de Gaust, DDS Sutter Terrace Dental Group (916) 447-6453
Barry Dunn
East Sac Dental Sacramento 916-452-7874 www.eastsacdental. com
Shellie A. Edwards
Edwards Everhart Dental El Dorado Hills 916-939-9912
Ryan J. Everhart
Edwards Everhart Dental El Dorado Hills 916-939-9912
Kenneth F. Fat
Kenneth F. Fat, DDS & Shareen Char-Fat, DDS Sacramento 916-925-9222
Ronald G. Fong
Ronald G F ong & Kimberly A Fong Sacramento 916-424-0760
Sandra Fouladi
Elk Grove Family Dentistry Elk Grove 916-685-2105 www.elkgrovedds. com

Douglas A. Gedestad
Douglas A. Gedestad, DMD, Inc. Sacramento 916-448-1444
Stephen A. Genus
Stephen A. Genus, DMD Sacramento 916-427-8900
Eric Grove Eric Grove, DDS and Kendall Homer, DMD Sacramento 916-363-9171
Steven Higashi
Steven Higashi DDS Sacramento 916-428-7713
Ryan B. Higgins
Higgins Family Dentistry Folsom 916-984-9933
Russell G. Hirano
Russell G. Hirano, DDS Sacramento 916-486-1322
Steven Holm
Courtyard Dental Care Auburn 530-823-2568
Kendall D. Homer Eric Grove, DDS and Kendall Homer, DMD Sacramento 916-363-9171 www. grovehomerdentists. com
Dick C. Huang
Dr. Dick C. Huang, DMD West Sacramento 916-372-5757
Terrence W. Jones Terrence W. Jones D.D.S. Sacramento 916-929-6631
Ashley Joves Smile & Co. Folsom 916-500-4577
Darcy L. Kasner Artisan Dentistry Sacramento 916-452-2002
Sean Khodai Enhanced Dental Concepts Roseville 916-791-2907
Merlin Lai Arena Family Dental Care Sacramento 916-515-1764
Julie L. Leaverton Julie L. Leaverton, DDS El Dorado Hills 916-933-2010
Ronald C. Lee
Ronald C. Lee, DDS Sacramento 916-928-9212
Y. Samantha Lee Y. Samantha Lee, DDS Sacramento 916-483-5100
Jesan Liu Comfort Dental Sacramento 916-421-4790
Maylene Luc
Luc Dental Care Elk Grove 916-684-1922
Jeffrey Ma
Jeffrey J. Ma DDS Sacramento 916-452-5264
Daniel G. Mazza
Mazza Dental Care Winters 530-795-2222
Timothy E. Mickiewicz
Timothy E. Mickiewicz, D.D.S Sacramento 916-469-9178 www.drmickdds.com
Michael A. Miyasaki
Miyasaki Dental Sacramento 916-442-8911
Charles Newens
Charles Newens, DDS., Inc. Carmichael 916-332-9240
Novan Nguyen
Blossom Dental Wellness Sacramento 916-422-399
Michael R. O’Brien
Michael R. O’Brien, DDS Sacramento 916-391-9200
Gregory H. Owyang
Gregory Owyang, DDS & Deborah Owyang, DDS Sacramento 916-454-2919
Alan C. Pan
Alan C. Pan, DDS Roseville 916-781-6688
Upen J. Patel
Upen J. Patel, DDS, MAGD & Associates Sacramento 916-621-2116
Viren R. Patel
Viren R. Patel, DDS, APC Folsom 916-988-3402
Paul Phillips
East Sac Dental Sacramento 916-452-7874 www.eastsacdental. com
Christy RollofsonK.
Elk Grove Family Dentistry Elk Grove 916-685-2105 www.elkgrovedds. com
Sean A. Roth
Dr. Sean A. Roth Folsom 916-983-1114
Matthew Ryan
Dr. Matthew Ryan Sacramento 916-486-8255
Stephanie Sandretti
Galleria Smile Designs Roseville 916-532-1635
Sahil Sethi
Sutter Terrace Dental Group Sacramento 916-736-6750
Edwin J. Sims
Edwin J. Sims, DDS Sacramento 916-447-1731
ROHINI RATTU, DDS DIMPLES PEDIATRIC DENTAL

PEDIATRIC DENTISTRY
FOCUS: Pediatric Dentistry EDUCATION: Dr. Rohini obtained her B.S. from UC Davis and went on to graduate from Columbia Univer sity School of Dental Medicine and completed her Pediatric Dental training at Boston University Goldman School of Dental Medicine. She is a Board Certified Diplomate with the American Board of Pediatric Dentistry. WHAT SETS US APART: Dr. Rohini’s practice is a solo practice, so you will always get the Doctor’s personal at tention. For the more apprehensive children or those with special needs, we offer Nitrous Oxide, in-house sedation with an Anesthesiologist, and sedation in a Surgery Center. IF YOU COULD GIVE ANY ADVICE TO PARENTS, WHAT WOULD IT BE? Think pre vention! Bring your child in to see us on his or her first birthday so we can prevent any issues before they begin.
1665 Creekside Drive, Suite #103, Folsom, CA 95630 (916) 260-5127 info@dimplespd.com dimplespd.com
DAMON P. SZYMANOWSKI, D.M.D.
SZYMANOWSKI ORTHODONTICS
FOCUS: Each person’s smile is unique and invaluable and de serves the best in expert and personalized care. Our team at Szymanowski Orthodontics is committed to giving you the smile you’ve always wanted and deserve. Dr. Szymanowski and his team work seamlessly to ensure that all patients receive superior care in a professional, friendly and comfortable setting. We offer compre hensive orthodontic treatment at our state-of-the art facility for patients of all ages.
• As an Invisalign Top 1% Diamond Plus Provider, we are highly experienced in Invisalign treatment for teens and adults!

• We remain dedicated to continuing education in order to bring the latest innovative techniques and highest level of orthodontic treatment to the Sacramento community.
• Whether it’s through donations or providing treatment for those less fortunate, we love our community and give back whenever we can!
99 Scripps Drive, Suite 201, Sacramento, CA 95825 (916) 993-4171 drdamonsmiles.com
EXCELLENCE IN DENTISTRY 2022
EXCELLENCE IN DENTISTRY 2022
Aashima S. Vaid
Chirag R. Vaid, DDS Sacramento 916-444-2957
Chirag R. Vaid
Chirag R. Vaid, DDS Sacramento 916-444-2957
Gary Vedenoff
Dr. Gary Vedenoff, D.D.S. Sacramento 916-489-1720
Harry M. Viani
Harry M. Viani DDS Sacramento 916-929-4546
Shivani Vohra
Sacramento Community Clinics–Del Paso Dental Sacramento 916-642-1890
Wayne E. Walters
Wayne E. Walters, D.D.S. Sacramento 916-929-5544

Nancy Welch
Nancy S. Welch DDS Sacramento 916-929-3115
Joel Whiteman
Smile Art Dental Sacramento 916-446-0203
Jill D. Whitney
Jill D. Whitney, D.D.S. Sacramento 916-427-3003
Edward Wiggins II
D2O Dental Sacramento 916-442-7000 d2odental.com
Ryan Wilgus
Dr. Ryan Wilgus Dentistry Sacramento 916-457-7710
Amy M. Woo
Dr. Amy Woo Dental Care Sacramento 916-443-8955 www.DrAmyWoo.com

Lynn Yamamoto
Yamamoto & Lee Family Dentistry Roseville 916-783-5241
Kenneth T. Yasuda
Howe Dental Care Sacramento 916-929-8928
Bianca Yee
Complete Health Dentistry of Sacramento Sacramento 916-482-7886
Agnes S. Yumiaco
Agnes S. Yumiaco, DMD, Inc. Sacramento 916-929-0248
Karl M. Zander III
Karl M. Zander, III, DDS Sacramento 916-391-4848
ORAL & MAXILLOFACIAL SURGERY

Craig X. Alpha
Heise & Alpha OMS Sacramento 916-442-1882
Dale L. Alto
Capital Oral & Maxillofacial Surgery Sacramento 916-483-4379
Alexander V. Antipov
Galleria Oral & Maxillofacial Surgery Roseville 916-783-2110
Nanlin Chiang Valley Oral & Maxillofacial Surgery Sacramento 916-283-8818
Reza Fouladi Sacramento Oral Surgery Sacramento 916-423-4092
Louis Gallia
Scripps Oral Surgery Sacramento 916-570-3088
Gregory Hailey
Gregory Hailey DDS, Inc. Fair Oaks 916-723-1111
Brian C. Harris
Sierra Foothills Oral & Maxillofacial Surgery Roseville 916-786-3930

CHRISTOPHER MYERS, DDS
ORTHODONTICS
FOCUS: Dr. Christopher Myers and his team offer a friendly and family-ori ented atmosphere where you are welcomed by name. Our goal is to provide each patient with a customized plan for an amazing smile and balanced bite. By doing this we hope to establish long-lasting oral health for our patients. Combining advanced orthodontic techniques and technologies with personalized care, we ensure you achieve your best smile: efficiently and comfortably, with beautiful results! We create radiant, healthy smiles for all ages, offering: Airway orthodontics, Inbrace lingual (behind the teeth) braces, traditional metal and clear braces, clear aligners for teens and adults, palatal expanders and early treatment for children, digital impressions, craniofacial orthodontics, dentofacial orthopedics, and setup for corrective jaw surgery.
New Element Orthodontics
2525 K St #106, Sacramento, CA 95816 • (916)-441-3925 10425 Fair Oaks Blvd., Fair Oaks, CA 95628 • (916)-966-1751 www.newelementortho.com

MICHAEL B. GUESS, DDS, MS, MA
ORTHODONTICS
FOCUS: Anyone from six to ninety-six years old can utilize aligners or tradi tional braces to correct “crooked” teeth. We believe aligned teeth and jaws create a great, confident smile. We think that aligned and functioning teeth translate to self-confidence. After the exam, a 5 to 7-page outline of the pro posed treatment is presented for your review. Treatment appointments are booked 6-12 months in advance to ensure treatment efficiency. In addition, Dr. Guess and the staff utilize dental acupuncture, botox, and sleep apnea appliances. Call and come in to talk about your smile!
Natomas Ortho
1966 Del Paso Rd Ste 150, Sacramento CA 95834 (916) 392-5670
www.natomasortho.com
TIMOTHY MICKIEWICZ, DDS MICKIEWICZ DENTAL

CORP.
PRESIDENT, DENTIST TMJ THERAPY/ DENTAL SLEEP MEDICINE
PRACTICE: Over the past 30 years, Dr. Mickiewicz has developed a comprehensive practice that truly integrates medicine and dentistry. Creating a “clinic without walls,” Dr. Mickiewicz has partnered with major medical groups in Northern California to treat complex facial pain and sleep issues, often as the doctor of last resort.
EXPERIENCE: He is a pioneer in the use of oral appliances for treating sleep apnea and other breathing disorders. Known throughout the medical and dental community for his vast, evidence-based knowledge, he is called upon to testify as an expert, render second opinions and to be an educator for both physicians and dentists. Decades spent as a restorative dentist strengthen his resolve to provide patients with the most conservative treatment, while embracing and enhancing cutting edge, Facial Pain, Airway, Sleep Medicine and Orthodontic Therapies.
SPARE TIME: Dr. Mick’s spare time is devoted to family and local philanthropic endeavors focused on health care innovations including Botox Techniques, Migraine Therapy, Tinnitus research, stabilization of Arthritic Joints and incorporation of Neuroscience and Artificial Intelligence advances to improve clinical outcomes.
930 Alhambra Blvd., Suite 110, Sacramento (916) 469-9178 drmickdds.com
EXCELLENCE
DENTISTRY
A Special Advertising Section
IN
2022
Jagdev Heir
Sacramento Surgical Arts, PC Sacramento 866-930-5837
Gregory J. Heise
Heise & Alpha OMS Sacramento 916-442-1882
Greggory Irving
Kids Care Dental & Orthodontics Sacramento 916-391-2101 www.kidscaredental.com
Loche M. Johnson
Capital Oral & Maxillofacial Surgery Sacramento 916-483-4379
Don Kim
Serenity Oral Surgery & Implant Center Roseville 916-787-1515
Grace Lee Valley Oral & Maxillofacial Surgery Sacramento 916-283-8818
Donald R. Liberty
Golden Foothills Oral & Facial Surgery Center El Dorado Hills 916-941-9860
Daniel A. Martin
Placer Oral & Dental Implant Surgery Roseville 916-773-1188
Gregory G. Olsen
Folsom Oral Surgery and Implant Center Folsom 916-983-6637
Michael S. Phelps
Capital Oral & Maxillofacial Surgery Sacramento 916-483-4379
Gregory S. Pluckhan

Gregory S. Pluckhan, DDS Roseville 916-772-2228
Michael H. Preskar
Sacramento Oral Surgery Sacramento 916-482-3444
Esther Rhee

Sacramento Oral Surgery Roseville 916-782-6868
Voltaire Sambajon
The Oral & Facial Surgery Center Folsom 916-817-8000
Itien Emily Shaw
Sacramento Surgical Arts, PC Sacramento 866-788-2420
Jason A. Straw
True Oral, Facial & Dental Implant Surgery Placerville 530-626-3300
J. Alex Tomaich
Tomaich Oral Surgery Davis 530-753-0550
David Trent Kids Care Dental & Orthodontics Sacramento 916-391-2101 www.kidscaredental.com
Kingsley Wang
Woodland Oral Surgery Woodland 530-207-5288
Kenneth Wong
King Oral Surgery & Dental Implant Center Rocklin 916-797-2700
ORTHODONTICS
Crystal Anderson
Folsom Lake Orthodontics Folsom 916-983-0525
Steven D. Anderson
Dr. Steven D. Anderson, DDS Sacramento 916-929-5991
Thais Booms
Giannetti & Booms
Orthodontic Specialists Sacramento 916-452-3584
Chuen Chiang
Kids Care Dental & Orthodontics Sacramento 916-344-1000 www.kidscaredental. com
DR. DONALD P. ROLLOFSON, D.M.D KIDS CARE DENTAL Kids Care Dental is proud to recognize Dr. Rollofson as one of Sacramento’s Top Dentists! Learn more about him at KidsCareDental.com (844) 616-5437 EXCELLENCE IN DENTISTRY 2022

DR. ERIN CARSON, DR. DAVID TRENT, DR. COLLEEN BUEHLER, DR. KEVIN VO, DR. STACY SILVA, DR. DAVID STEINBERG, AND DR. CHUEN CHIANG. DR. REGINALD FULFORD (NOT PICTURED) KIDS CARE DENTAL & ORTHODONTICS DENTISTRY, ORTHODONTICS AND ORAL SURGERY 15 Northern California Practices Near You • (916) 827-1454 • kidscaredental.com EXCELLENCE IN DENTISTRY 2022 FOCUS: Dentistry, Orthodontics and Oral Surgery for Kids WHAT SETS YOU APART: At Kids Care Dental & Orthodontics, we’re fanatical about creating a lifetime of happy smiles. That’s why we’re a practice for kids. We believe when kids grow up enjoying the dentist, healthy teeth and gums will follow.
set up
differ
of dental practice that delivers fun,
giggly smiles. PROFESSIONAL MEMBERSHIPS/AFFILIATIONS: ADA, AAO, AAOMS, AMA, CMA, CDA, SDDS CHARITABLE WORK: Smiles for Kids, Operation Backpack, Valentine’s Day Cards for Kids, and Candy Buy Back ONE PIECE OF ADVICE TO READERS IS: Take your child to see the dentist by their first birthday or when their first tooth erupts.
We’ve
a
ent kind
not fear. So your kids get stress free dental visits—and beautiful,
Brian Crawford
Crawford Orthodontics Lincoln 916-408-8688
David Datwyler
Datwyler Orthodontics El Dorado Hills 916-939-2330
Andrea B. DeLurgio
DeLurgio Orthodontics Citrus Heights 916-966-5517
Jennifer Drew
Kids Care Dental & Orthodontics Roseville 916-780-6300 www.kidscaredental.com
J. Patrick Dunbar
Dunbar Orthodontics Folsom 916-983-2434
Marc Dunn Dunn Orthodontics Roseville 916-788-0202
Jeff Elenberger
Elenberger Orthodontics Rocklin 916-774-6006 www.elenberger orthodontics.com
Gregory W. Evrigenis
Evrigenis Orthodontics Sacramento 916-575-9990
Scott Favero Favero Orthodontics Roseville 916-782-2332

Reginald Fulford
Kids Care Dental & Orthodontics Elk Grove 916-683-7645 www.kidscaredental.com
Kelly Giannetti
Giannetti & Booms Orthodontic Specialists Sacramento 916-452-3584
Michael B. Guess
Dr. Michael B. Guess
El Dorado Hills 916-933-0123 www.natomasortho. com
Daniel Haberman


Daniel Haberman DDS MS Sacramento 916-428-1354

Mark H. Holt Holt Orthodontics Folsom 916-245-7181 www.bracesbyholt. com
Douglas Jaul Chapa-De Indian Health Auburn 530-887-2800
Stephen Kineret Kineret Orthodontics Rocklin 916-772-5832
Laski Kung Kung Orthodontics Fair Oaks 916-288-8408
Jeffrey Kwong
Jeffrey Kwong Orthodontics
El Dorado Hills 916-933-0532
Seth Lucas Lucas Orthodontics Folsom 916-461-5465
David Markham Markham Orthodontics Sacramento 916-665-0894
Brandon D. Alexander & Martin Orthodontics 916-630-0306 ambraces.com
Matthew Molitor
Matthew Molitor DDS, MS Davis 530-758-6420
KENDALL HOMER, D.M.D. ERIC GROVE, D.D.S.

DENTISTS
FOCUS: General Dentistry, including cosmetics, implant resto ration, and emergency dental care. EDUCATION:Dr. Homer com pleted his B.A. at Sacramento State and earned his Doctorate of Medical Dentistry from Washington University. Dr. Grove received a B.S. from Pacific Union College and a Doctorate of Dental Sur gery from Loma Linda University. PROFESSIONAL MEMBERSHIPS: Drs. Homer and Grove belong to the ADA/CDA/SDDS. Dr. Grove is also an active participant in the SDDS. WHAT SETS THEM APART: Dr. Homer’s and Dr. Grove’s patients’ apprecia tion is evident in client loyalty, with 40-year plus patients bringing their children and grandchildren in for treatment. CHARITABLE WORK: Dr. Homer supports Save Ourselves, an organization that provides counseling and peer support to people living with breast cancer. Dr. Grove has participated in overseas dental mission trips and also participates in the Smiles for Big Kids program in Sacra mento. FREE ADVICE: Studies have linked diabetes, heart dis ease and stroke to gum disease. Oral health is a significant part of overall well-being.
9216 Kiefer Blvd., Suite 5, Sacramento (916) 363-9171
dentist@grovehomerdentists.com grovehomerdentists.com
EXCELLENCE IN DENTISTRY 2022
EXCELLENCE IN DENTISTRY 2022
ALEXANDER & MARTIN ORTHODONTICS

FOCUS: Certified Orthodontic Specialists - Braces & Invisalign (Top 1%) for Children & Adults
EDUCATION: Dr. Martin received his training at UCSF and the U. of Maryland. Dr. Quach went to Harvard for her DDS degree followed by UCLA for her Orthodontic Speciality certificate. Dr Alexander attended UCSF for both of his degrees.
WHAT SETS US APART: You deserve to Love. Your Smile. We want to partner with you to give you a lifetime of renewed confidence. Utilizing the best materials, techniques, and training in the industry - our team strives to give predictable results. To top it off, we hope we can listen to some good music, terrible jokes, and have fun along your journey.
REPUTATION: The team at AMO is known for exceptional results, honesty, and giving back to the awesome community that has trusted us over the years.
CONSULTATIONS: No referral needed, No pressure, Awesome technology! We use 3-D technology to scan your teeth to generate a virtual simulation of your smile in a few minutes. Together, we tailor your treatment to your unique needs. And don’t worry - we won’t recommend treatment unless it is needed (not all 8 year-olds need braces). We offer flexible in-house financing where you get to pick your down-payment and payment terms. Consultations are complimentary.
ADVICE: Retainers are night-time for a life-time. But don’t panicwe have very reasonable replacement options. You don’t even have to get impressions - digital scanning and 3-D printers are great!
BRANDON D. MARTIN, DDS, MS; ALISON J. QUACH, DMD, MS; ROBERT M. ALEXANDER, DDS, MS
Locations in Sacramento,
and
(916) 630-0306 • ambraces.com
Rocklin,
Roseville.
Christopher
New Element Orthodontics Sacramento 916-441-3925 www.newelement
Jack C. Oates
Smart Choice Orthodontics Sacramento 916-444-7844
Michael H. Payne
American River Orthodontics Sacramento 916-486-4233
Paolo A Poidmore Poidmore Orthodontics Orangevale 916-988-1744
Richard Portalupi Portalupi Orthodontics Woodland 530-662-9191
Donald Rollofson Kids Care Dental & Orthodontics Vacaville 707-455-7001
Benton Runquist
Benton Runquist, DDS Davis 530-756-0220
Matthew Sanders Sunrise Orthodontics Elk Grove 916-512-3600
Matthew Sandretti
Elk Grove Orthodontics Elk Grove 916-685-2164
Steven Scott Markham Orthodontics Sacramento 916-665-0894
Stacy Silva
Kids Care Dental & Orthodontics Sacramento 916-391-2101 www.kidscaredental. com Damon Szymanowski Szymanowski Orthodontics Sacramento 916-848-5651 www.drdamonsmiles. com
Richard D. Talbot
Richard D. Talbot, DMD, MS, Inc. Citrus Heights 916-965-8026
Alan C. Tan
Tan Orthodontics Woodland 530-662-5240
Garri Tsibel
Olympus Pointe Orthodontics Roseville 916-789-1100
Melvin Walters
Evrigenis Orthodontics Sacramento 916-575-9990
Peter Worth
Peter W. Worth, D.D.S., INC Roseville 916-782-3161
Jamson Wu Laguna Creek Orthodontics Elk Grove 916-392-1885
PEDIATRIC DENTISTRY
Jessica Alt
Rocklin Pediatric Dentistry Rocklin 916-435-9100
John C. Birch
Sac Kids Dental Sacramento 916-929-5534
Colleen Buehler
Kids Care Dental & Orthodontics Sacramento 916-575-7701 www.kidscaredental. com
Erin Carson Kids Care Dental & Orthodontics Elk Grove 916-683-7645 www.kidscaredental. com
Mark Choi
Mark Choi, DDS Pediatric Dentistry & Orthodontics Woodland 530-662-3915
DAVID WESTERHAUS, DDS



MOBILE ANESTHESIA AND SEDATION FOR DENTISTRY

SPECIALTY: I am a residency trained dentist anesthesiologist who provides mobile anesthesia and sedation. I am blessed to have these skills as an anesthesiologist that allow dental patients, regardless of their fear and anxiety, to complete their dental treatment and “wake up with a smile!”
EDUCATION: Bachelor of Arts: Wheaton College, Wheaton, IL. Doctor of Dental Surgery: Loma Linda University Health, Loma Linda, CA. Residency in Anesthesiology: Loma Linda University Health, Loma Linda, CA.

PROFESSIONAL MEMBERSHIPS: American Dental Society of Anesthesiology, California Dental Society of Anesthesiology, California Dental Association, Sacramento District Dental Society and Diplomate of the National Dental Board of Anesthesiology.
8359 Elk Grove Florin Road, Ste. 103-340, Sacramento, CA 95829 david@sleeptosmile.com • (916) 827-0046 www.sleeptosmile.com
JEFFREY ELENBERGER DDS
ELENBERGER ORTHODONTICS

FOCUS: Serving the Sacramento community for over 30 years, Dr. Elen berger continues to help patients transform their happy, healthy smiles. Dr. E mentions, “My patients are incredible, I have had the honor to meet and care for amazing people. I love hearing about their lives, hobbies, and everything else. They keep me constantly learning, motivated, and ener gized. I love coming to work every day because of those interactions.” Dr. E is pleased to be voted top orthodontist. He and his staff look forward to continuing their great work for many years to come.

2204 Plaza Drive #140, Rocklin CA 95765 ( 916) 774-6006
www.elenbergerorthodontics.com
HOLT ORTHODONTICS
MARK H. HOLT, D.D.S., M.S., INC. TYLER HOLT, D.D.S., M.S. MIRIAM BEHPOUR, D.M.D., MBA

FOCUS: Invisalign or braces are not the same at every office–the doctors you choose matter. Dr. Holt has been a specialist in orthodontics for over 30 years and is the leading provider of Invisalign for teens and adults in the Sacramento Region. He is both a Top 1% Provider and AlignTech Faculty member, having taught classes to other doctors in over 40 cities across the country. Holt Orthodontics has proudly achieved the status of #1 Private Practice Invisalign Provider in California for Teens and Adults. Along with Dr. Holt, Dr. Tyler Holt and Dr. Miriam Behpour, are excellent orthodontists who have the expertise, craft and passion to transform the lives of patients by creating beautiful and confident Winning Smiles.
2605 Eastern Ave #3, Sacramento, CA 95821 With Offices in Roseville, Rocklin and Folsom (916) 481-6424
bracesbyholt.com
CHRISTY ROLLOFSON PORRINO, DDS SANDRA FOULADI, DDS
ELK GROVE FAMILY DENTISTRY SCRIPPS FAMILY DENTAL
VALUES: We are two female dentists who share a common set of core values and high standards in the way we practice. Our goal is to deliver the best quality dental health care to our patients.

PRACTICE: We balance the joys of raising our families with the satisfaction of practicing clinical dentistry. We deliver exceptional customer service by treating our patients like family. Our practice thrives by making teamwork and relationship building a priority and meets the highest standards in infection control. Find happi ness in whatever you do.
Elk Grove Family Dentistry
9727 Elk Grove-Florin Road, Suite 270 Elk Grove, CA 95624 (916) 685-2105 www.elkgrovedds.com
Scripps Family Dental 103 Scripps Drive, Suite 8 Sacramento, CA 95825 (916) 929-1156 www.scrippsfamilydental.com
IN DENTISTRY 2022
EXCELLENCE
EXCELLENCE IN DENTISTRY 2022
Richard Keilson Sac Kids Dental
Rosemary Wu Capitol Periodontal
916-786-6585
capitolperiodontal.
Academy for Reconstructive Periodontics and Implant
The
PROSTHODONTICS
Paul Binon
Paul Binon, DDS, MSD




916-786-6676 binondentalimplants.
Clark Jefferson Clark DDS MS Sacramento 916-800-1878
Brock E. Hinton
Prosthodontic Dental Group Fair Oaks 916-596-3313
Y. Vinny Huang Marconi Dental Group Carmichael 916-589-6462


Ronald R. Larsen
Ronald R. Larsen, DDS Sacramento 916-484-0000
Jeffrey G. Light
Sacramento Prosthodontics Sacramento 916-451-9400

Michael Mikitka

Alhambra Dental Plaza Sacramento 916-455-3247
Jeffrey Y. Nordlander
Prosthodontic Dental Group Fair Oaks 916-596-3313



DR. PAUL PHILLIPS, DR. BARRY DUNN AND DR. SUZANNE SAIDI
EAST SAC DENTAL

FOCUS: When you visit East Sac Dental, we want to change your mind about dentistry. Our entire team is dedicated to providing you with the personalized, gentle care that you deserve. In our prac tice, you will experience all that modern dentistry has to offer. We thrive in creating comfortable dental experiences for patients of all ages. It is our personal mission to assist each patient in achieving and maintaining long term dental health and a beautiful, confident smile. We accomplish this by living our philosophy, “We don’t treat teeth, we treat patients.”
1273 32nd St., Sacramento CA 95816 (916) 452-7874 www.eastsacdental.com
NIMA AFLATOONI, DDS
GOLD RIVER SMILES

GENERAL AND COSMETIC DENTISTRY
PRACTICE: Patients don’t care how much you know, until they know how much you care.” These are words that guided Dr. Nima Aflatooni throughout his education at the prestigious University of the Pacific Arthur A. Dugoni School of Dentistry and these are the values that we, at Gold River Smiles, uphold today. MISSION: We are a group of friendly, enthusiastic, and highly skilled dental professionals who are truly passion ate about our patients and improving their oral health in a non-judgmental and compassionate environment. Taking care of our community’s oral health is a team mission we take seriously. INNOVATIONS: By investing in the latest technology, protocols and continuing education, Dr. Nima and his team strive to stay in the forefront of the dental profession. Our goal is to educate you on your oral health and how it relates to your overall health, and help you achieve your goals. Creating beautiful healthy smiles is our passion!
11230 Gold Express Dr.,
(916) 635-9605 • goldriversmiles.com
DENTISTRY
Ste. 301, Gold River •
EXCELLENCE IN
2022
EXCELLENCE IN DENTISTRY 2022
The professionals listed herein were selected by their peers in a survey conducted by Professional Research Services Company of Troy, Michigan. Professionals may be screened and selected through the verification of licensing wand review of any infractions through various applicable boards, agencies, and rating services. For further information visit prscom.com or email PRS at sshevin@hour-media.com. To purchase Top Dentists plaques, please see prsawards.com
JOSE JUAREZ, D.D.S.
SMILE KINGDOM DENTAL

FOCUS: Dentistry for Infants, Children and Teens

WHAT SETS US PART: Smile Kingdom Dental is a fun themed dental office dedicated to alleviate children’s fears of going to the dentist. We implement creative methods in effort to treat the spe cial needs of infants, children and teens, one smile at a time. It is our mission to provide quality pediatric dental care in a warm, caring, educational and most of all, fun environment!
PHILOSOPHY: Smile Kingdom strives to make every child’s visit to the dentist an enjoyable one. Our staff is highly trained and skilled in treating children of all ages. Because every child is unique, we customize each appointment based on your child’s age, needs, and cooperation level. Our philosophy is to not push children be yond their ability to cooperate, but rather apply techniques to gain their trust and establish a good rapport.
CHARITABLE WORK: Smiles for Kids, Give Kids a Smile, Hallow een Candy Buy Back.
2340 Sunrise Blvd, Suite 25, Rancho Cordova (916) 852-8510 smilekingdom.com
EXCELLENCE IN DENTISTRY 2022
DR. EDWARD WIGGINS II, DDS
D2O DENTAL
FOCUS: At D2O Dental, Dr. Wiggins and his team work together to deliver the ultimate patient experience.

WHAT SETS YOU APART: Patients can enjoy a five star concierge experience and relax knowing they are being served by a team of highly skilled and trained professionals who understand the anxiety most people feel when seeing a dentist.
EDUCATION: Dr. Wiggins is a graduate of the University of California, San Francisco and is the only dentist in Sacramento to complete the rigorous nine-course advanced curriculum in restorative, aesthetic and implant dentistry at the Kois Center in Seattle, Washington.
REPUTATION: Together with a team of dedicated professionals, Dr. Wiggins combines evidence-based dentistry and advanced technology to provide even the most high-risk, fearful patients a place where they can receive care in a safe and spa-like environment.
LOCATION: Dr. Wiggins provides restorative, cosmetic, implant and sedation services at D2O Dental in Midtown Sacramento.
EXCELLENCE IN DENTISTRY 2022
1816 L Street, Sacramento, CA 95811 • (916) 442-7000 • d2odental.com
This December, Sacramento Magazine is presenting a list of physicians who were all chosen through a formal process similar to the informal peer-to-peer process doctors themselves use to connect their patients to the right specialists. Professional Research Services, LLC conducted our survey, verifying each doctor’s credentials and specific areas of expertise.


To learn more about the selection process, go to prscom.com

2023 FIVE STAR be named? Who will Find out in a special section inside the March issue. Wealth Managers TO LEARN MORE ABOUT OUR RESEARCH PROCESS, GO TO: fivestarprofessional.com/public/research




PBS VIDEO APP Stream the best of PBS on any device Download today & start watching for free kvie.org/app

Red Voodoo Brings It Back
Lead vocalist Dino McCord, drummer Andy Nathan, guitarist Davin Loiler and bassist Andrew Edwards comprise Red Voodoo, a hard-rockin’ Sacramento band that’s captured the attention of Sammy Hagar.

SACMAG.COM November 2022 89
Bravo 11 22
Davin Loiler, Dino McCord, Andy Nathan and Andrew Edwards
inside: All about the band
kevin graft
BY MARK BILLINGSLEY
Soon after the drums thunder and the iconic opening guitar riff to Montrose’s “Rock Candy” blasts from the speakers, Dino McCord lets loose a guttural yell of “Lord, yeah” that sounds like it could have come from Sammy Hagar circa 1973, when the tune first hit the airwaves. McCord and his bandmates in Sacramento’s rising rock group Red Voodoo wouldn’t be born for another 30 years, but their rendition of “Rock Candy” not only showcases their talents but pays homage to the Red Rocker. Hagar has become a sort of mentor for the group and invited them to play three nights in October at his Cabo Wabo Cantina nightclub in Cabo San Lucas, Mexico. The gig for the group, whose oldest member is just 21, came during Hagar’s weeklong 75th birthday celebration.
“When you think about the grand scope of things and how young we are, not many bands get to go play the Cabo Wabo. Plus it’s Sammy’s birthday, so we thank our lucky stars that we can do this, that we get to play our music and do this and have fun with it,” says McCord, who turned 20 in Sep tember. “When I went down two years ago and met Sammy for his birthday bash, it was seven days after Eddie Van Halen had died. So I got to not only honor Sammy on his birthday, but also honor Eddie. We sang “Eagles Fly” and “Finish What Ya Started,” and that was the best moment, so far, in my life. I was trembling in my boots.”
This time, the entire band was onstage at Cabo Wabo and played originals off its nine-song debut album, called “Bring It Back,” which was produced by Tesla’s lead guitarist Frank Hannon, himself once a rock ’n’ roll wunderkind.

Red Voodoo is named after the Sammy Hagar solo album that came out in 1999, two years before the band’s oldest member, drummer Andy Nathan, was born.
Before Tesla broke out of playing Sacramento rock clubs and released its platinum-selling debut, the band was known as City Kidd. When City Kidd formed in 1982, Hannon was just 15—the same age as McCord when he started Red Voodoo—and Tesla bassist Brian Wheat was 20. The now-defunct Oasis Ballroom was City Kidd’s home base, just as Roseville’s Opera House Saloon or Folsom’s Powerhouse Pub is home for Red Voodoo.
“I can see some parallels, because we changed our name, too,” says Red Voodoo lead guitarist Davin Loiler. “We were Teazer. But we knew we needed another name. With Sammy being such a big influence, we looked at the album ‘Red Voodoo.’ That title fit the idea and motif of the band, and what we were doing. Sammy himself said that’s an awesome name.”
Wheat and Hannon changed from City Kidd to Tesla during the recording of their debut album, “Mechanical Resonance,” which went platinum in 1989. They also got help from Ronnie Montrose, who hired Sammy Hagar in 1972.

Now Hannon is helping the next generation.
“When COVID -19 hit and shut everything down, I had a refueled interest in helping local Sacramento artists learn and produce music in
Bravo 90 SACRAMENTO MAGAZINE N ovember 2022
the recording studio,” Hannon says. “My band, Tesla, has been blessed to work with many great producers and songwriters over the past 35 years and make many contacts. I wanted to help and pass that experience forward to young local musi cian kids as a coach.”
Hannon helped Red Voodoo write, record, pro duce and promote a song about the COVID -19 lockdown called “Rise Up!” The song was played on radio stations coast to coast and on many streaming sites.

Fast-forward 50 years since Hagar recorded “Rock Candy” and 35 years since Hannon and Tesla released “Mechanical Resonance” and Red Voodoo is bringing the 1970s and ’80s hard rock back with “Bring It Back.” The title track features a throaty “Oh, yeah” roar from McCord that’s in credibly similar to the one that opens “Rock Candy.” The lyrics, too, are emblematic for Red Voodoo.
Here’s a sample of the lyrics from “Bring It Back”: Rock ’n’ roll it ain’t old / It’s for a new age / We’re gonna bring it back / To a new generation
And here’s a line from “Rock Candy”: W hen you’re 17 / Reachin’ for your dreams / But don’t let no one reach ’em for you / Pull up your pants / Stretch out take a chance / Now if it can be done, well you can do it
Red Voodoo is still unsigned by a record label, and touring oppor tunities have yet to materialize. But that hasn’t stopped the band from taking gigs wherever and whenever, winning over rock fans of all ages by bringing it back. McCord is the band’s de facto man ager and was working at his day job at Skip’s Music this past Sep tember when the manager for 1990s rock stalwart Everclear called to say its opening act had suffered a COVID -19 outbreak and asked if Red Voodoo could fill in on 72 hours’ notice.

The boys loaded up the van and off they went to Rolling Hills Casino in Corning. It’s gigs like that, and at Cabo Wabo last month, where the band will likely make a connection with an industry bigwig who will then guide the band to its next, higher step. The band is preparing new material and reworking some songs from “Bring It Back” to record at San Fran cisco’s famous Hyde Street Studios with producer Jaimeson Durr. Durr has worked with Hagar in the past, Nathan says, extending that connection.
“For a young band, we’re doing pretty good for
SACMAG.COM November 2022 91
ourselves, but we’re putting everything back into the band,” says Nathan, who joined the band just six months ago after a stint in a psychedelic indie rock band and attempting to make it big in the Los Angeles rock scene. “I was moving back from LA and Dino sent me a message on Instagram and asked if I wanted to audition,” Nathan recalls. “I said, ‘Yeah, I’ve never heard of you guys, but I’m moving back and I want to keep playing.”
McCord heard about Nathan from J.T. Loux, who played with Nathan in Tonic Zephyr, the psychedelic indie rock group. Hannon also pro duces Loux’s solo effort, which is more straight-ahead, bluesy rock ’n’ roll.
“I heard Davin and, damn, this kid can play Eddie Van Halen so well,” Nathan says. “My dad’s favorite band is Van Halen, the David Lee Roth version. The fact that they do all these songs and had such a high level of technicality, I had a lot of respect from the get-go.”
A ndrew Edwards, the bassist, an swered a Craigslist ad posted by McCord. Edwards was a guitar player when his father told him about a Van Halen tribute band holding a tryout.

“When I joined, we didn’t have any originals and I had 36 cover songs to learn,” Edwards says. “I took a month to practice and then we started booking shows. We wrote ‘Bring It Back’ first, like three years ago. The song sounded a lot different back then. We dabbled writing originals, and as time went
on, we started writing more and more and got better and better.”
The band still holds down day jobs because payments for downloads from streaming sites and local gigs are not enough to make them fulltime musicians.
Yet.
McCord works at Skip’s Music; Edwards works at Del’s Family Pizza in Fair Oaks; Nathan is an instructor at Rocklin’s Bach to Rock music school, and Loiler works for his father’s Ione-based gutter installation company.
“Putting up gutters keeps me humble,” Loiler says. “It keeps me active, but I’d rather be out on the road. We’re out here paying our dues because we all gotta start somewhere. Slowly but surely the shows are starting to get bigger and the num bers are growing on our socials (media) as we’re honing our craft.”
Nathan says each member has supportive par ents and the band is growing at a pace everyone is happy with, so there’s not as much pressure to be signed as there might be with older groups with family commitments and mortgages to pay. The band hasn’t given itself a deadline. “We haven’t hit a block where we’re all like, ‘We gotta pay these bills,’” he says.
“This is a conversation that a lot of musicians have with themselves: ‘When am I a professional musician?’ It’s not just when you make money because you can get $20 to play at a bar for an hour,” Nathan says. “For me, I feel successful when it feels like there’s a connection with the audience and people are really getting something from our music. Sharing that experience with people I may have never met is special.”
The band, to a member, says they can feel the momentum building and as long as they stay true to the music and each other, the call from a highpowered agent with a big-name record company will happen. They’re still young, still hungry, and the music they play is timeless.

In the meantime, it’s back to the grind—in their day jobs and on local stages.
“They still need time to mature as a band,” Hannon says. “All the guys in the Red Voodoo band are extremely talented musically. And if they continue to develop, they will have a suc cessful career. I know they are paying their dues and doing a lot of local shows. I wish them the best of luck and hope they can stick it out. It’s a long way to the top ”
If you wanna rock ’n’ roll.
Bravo 92 SACRAMENTO MAGAZINE N ovember 2022
“I FEEL SUCCESSFUL WHEN IT FEELS LIKE THERE’S A CONNECTION WITH THE AUDIENCE AND PEOPLE ARE REALLY GETTING SOMETHING FROM OUR MUSIC,” SAYS ANDY NATHAN.
Events
Totally Irreverent
Leave it to the creators of Comedy Central’s darkly satirical “South Park” to craft a raucous musical comedy about two mismatched Latter-day Saints mis sionaries assigned to a remote Ugandan vil lage—and make it a huge Broadway hit! Winner of nine Tonys (including for best musical), “The Book of Mormon” comes to the SAFE Credit Union PAC stage on national tour. broadwaysacramento.com

Hero Worship
Treat the family to Disney on Ice: Find Your Hero, where your kids’ favorite Disney charac ters come to life on the ice. Join Mickey, Minnie and friends as they meet up with Moana and Maui, Anna and Elsa, Belle and the Beast, Ariel, Rapun zel and more, and share their tales of bravery and adventure. At Golden 1 Center. disneyonice.com

Motown Megastar
With a career spanning more than six decades and including such iconic R&B hits as “Shop Around,” “The Tracks of My Tears” and “I Second That Emotion,” Detroit singersongwriter Smokey Robinson is a living legend of American mu sic and, at 82, still going strong. Catch his per formance at Hard Rock Hotel & Casino in Wheatland. hardrock hotelsacramento.com


Big

Bird—
It’s a sure sign of autumn: elegant formations of sandhill cranes flying high over head, singing their haunt ingly beautiful bugle call. Every year, thousands of these large migratory birds winter in area wet lands—and every year, they’re celebrated at the Lodi Sandhill Crane Festival . Now in its 24th year, the free fest offers tours, exhibits, art and more at Hutchins Street Square in Lodi. lodisand hillcrane.org
Get Funky—
John Natsoulas Center for the Arts in Davis presents California Funk to Figu ration: A New Narrative Mythology, an exhibition of paintings, sculpture and works on paper by such leading West Coast Funk artists as Roy De Forest, Maija PeeplesBright, Robert Arneson and David Gilhooly. Funk art, which emerged in the rebellious 1960s, embraced color, absur dity, irony and humor. natsoulas.com
SACMAG.COM November 2022 93
NOV. 2–13 THROUGH JAN. 7 NOV. 3 6 NOV. 5 NOV.
“Tea
5 6 Bottom right:
Party” by M. Louise Stanley
NOVEMBER



















Tower of Power
What’s more impressive than a tow ering platter of fresh seafood? Not much. At the new OYSTER BAR in Natomas, you can order a seafood tower in one of three sizes, evoca tively named The Teaser ($58), Getting Wet ($108) and Getting Lucky ($169). The last one comes with eight scallops and clams, a dozen oysters, mussels and shrimp, two lobster tails, a whole crab and a quarter pound of King crab. Put us down for wanting to get lucky. 4261 Truxel Road; (916) 468-6989; oysterbarsacramento.com

SACMAG.COM November 2022 95
11 22
inside:
Thai Taste
francisco chavira
Cheffing It Up / Nigerian-Mexican Fusion / Beyond
Do It Yourself
You’re the chef at The Butterscotch Den, where you grill your own steak.
 BY MARYBETH BIZJAK
BY MARYBETH BIZJAK
Arestaurant where you cook your own steak: What could go wrong?
A lot, actually. You could overcook it or underseason it or simply not cook it as well as a professional chef, which is why most of us go to restaurants in the first place. You could burn yourself. You could give yourself food poisoning. All of these thoughts ran through my head as I entered The Butterscotch Den, a sortof-new, sort-of-old restaurant in Oak Park where you do, indeed, cook your own steak, as well as your own hamburger, hot dog, vegetables and garlic bread on a roaring gas grill in the middle of the dining room.
But as it turned out, a lot could, and did, go right when I ate at The Butterscotch Den. Dining here is a weirdly fun and entertaining experience, even if it is a bit of a busman’s holiday for people like myself who make dinner at home most nights. Here, you’re completely in charge of your own meal and your own entertainment. Think of it as a cross between The Melting Pot and Benihana.
There’s something charmingly endear ing about the place. The servers are friendly and helpful, and the diners en thusiastically throw themselves into the experience. The night I visited, a group of eight crowded around the grill, drinks in
hand, appearing to be having a blast as they flipped their burgers with commer cial-style spatulas. They acted like friends in someone’s backyard, not a restaurant.
Irish Hospitality Group took over the restaurant a few months ago from its previous owner. Back then, it was known as Arthur Henry’s Supper Club, and with its crowd-around-the-grill concept, it no doubt suffered even more than most res taurants during COVID’s social distanc ing era.
Walking in the front door, I briefly found myself wishing I had a miner’s headlamp. But my eyes quickly adjusted to the inky lighting in the bar, where you can order an ice-cold martini or a fun cocktail. When it comes to drinks, Irish Hospitality Group knows what it’s doing; it owns The Snug and Ro Sham Beaux, respectively one of the city’s top cocktail bars and one of its original natural wine bars.
My friend and I moved into the adjoin ing dining room, sat down in a roomy booth and ordered like we hadn’t eaten in a week: prawn cocktail (luckily already prepared by the kitchen, so we didn’t have to shell our own shrimp or whip up our own cocktail sauce), two steaks (a rib-eye and a feather blade, a cut I’d never heard of; it’s a small, flat steak from the shoul der), a vegetable skewer, a piping-hot baked potato in an aluminum foil jacket, and garlic bread. The steaks came to the table neatly wrapped in butcher paper and ready for us to season and throw on the grill.
The grill is equipped with long-handled barbecue tongs and spatulas, along with seasonings such as salt, pepper and house-
made steak seasoning, and add-ons like chimichurri and A.1. Sauce. Years ago, a local chef showed me how to correctly season a steak: You want to coat every square millimeter of the meat with salt. Use a heavy hand.
My companion and I had a friendly little competition to see who could make the better steak. The fire was nice and hot at one end of the grill, and we were able to get a good sear on both pieces of meat while cooking them to a perfect medium rare in just a couple of minutes. Everything else we ordered from the vaguely retro menu was tasty, es pecially the baked potato, served with butter, sour cream and chives.
THE FIRE WAS NICE AND HOT AT ONE END OF THE GRILL, AND WE WERE ABLE TO GET A GOOD SEAR ON BOTH PIECES OF MEAT WHILE COOKING THEM TO A PERFECT MEDIUM RARE IN JUST A COUPLE OF MINUTES.
Prices here are exceedingly gentle for both food and alcohol. Cocktails hover around the $10 mark, and you can get a steak—in this case, top sirloin— for as little as $10.50. At $34, the 12ounce rib-eye is the most expensive thing on the menu; by comparison, Morton’s 16-ounce rib-eye will set you back $68.

Just so you know, The Butterscotch Den is not The Palm or Charlie Palmer. It’s fun dining, not fine dining. But some times, fun is what you want. And as it turns out, cooking your own steak in a restaurant can be really fun.
THE BUTTERSCOTCH DEN
3406 Broadway; thebutterscotchden.com
Taste 96 SACRAMENTO MAGAZINE N ovember 2022
kevin fiscus





SACMAG.COM November 2022 97
Tacos By Way of Nigeria
Sacramento chef Rasheed Amedu knows it takes some moxie to open a fusion restaurant. That’s because some consider fusion to be the f-word of the restaurant world, a concept that can dilute or even disrespect the very cultures it purports to celebrate. Yet others (Amedu and celebrity chef David Chang among them) have come to embrace how a mash-up of distinctive cuisines can result in some spectacularly good dishes.

At Naija Boy Tacos in the Mansion Flats neighborhood, Amedu ingeniously marries the Nigerian dishes he ate at home in his native Chicago with the Mexican food that was ubiquitous in his boyhood neighborhood. By serving tortillas made with plantains, a starchy staple in Nigeria, and filling them with his mother’s chicken stew recipe or curry goat, Amedu is reimagining what a taco can be while also bringing West African cuisine to new audiences.
“It made sense in my head to fuse the two because the flavor profiles aren’t too far off,” says Amedu. “And the proteins are similar, with goat being prevalent in both cuisines. Most importantly, it was an easy way for people to begin to understand African cuisine. Once there’s a point of reference, then we can show the actual dish that we’re drawing inspiration from.”
Housed in a mobile structure, Naija Boy Tacos is part popup, part temporary restaurant, part food truck. Currently, it sits on a parcel of land that will be developed into housing next year. Eventually, says Amedu, it will find a permanent home on that land.
What allows fusion cooking to be successful, according to Amedu, is understanding a food’s origins from the outset. Before launching Naija Boy, Amedu read up on regional Mexican cooking, comparing and contrasting it with the ingredients and flavors of his upbringing. The Nigerian elements of Naija Boy’s menu can be traced directly back to his mother’s kitchen. “The rice and beans is literally my mom’s stewed beans. The chicken stew, the beef stew, everything came from her. It’s everything I grew up eating,” Amedu says. “The whole menu is a love letter to my mom.” 628 15th St.; (916) 2964525; naijaboytacos.com—CATHERINE WARMERDAM

Lao Time
California is home to the country’s largest Laotian American population, yet Lao restaurants have never enjoyed the ubiquity that Thai and Vietnamese eateries have. Three Sacramento women aim to change that with the opening of Hiso, an impressive Lao and Thai restaurant that opened this past December in the heart of downtown.
Laisa Yabaki and two friends from her days at John F. Kennedy High School, sisters Annie and Alina Manikhong, had worked in kitchens across the city since their teens. Now in their 20s, they wanted to start a business of their own. “We had a lot of experience and were waiting for a good opportunity to get into the industry,” says Yabaki.
When a space became available downtown, they rolled up their sleeves and got to work making it theirs. “We built the bar ourselves. We painted the ceiling,” says Yabaki, adding that the three knew their way around power tools, having fi xed up a house they bought together just three or so years out of high school. “We actually love going to Home Depot. We’re really hands-on and very driven.”


HISO’S DISHES ARE FULL OF THE SPICY, SALTY, PUNGENT (AKA FUNKY) FLAVORS THAT LAO CUISINE IS KNOWN FOR.
The Manikhong sisters, who were born in Laos and run Hiso’s kitchen, grew up eating many of the recipes on the restaurant’s menu. The trio made a decision early on to o er Lao cuisine beside more familiar Thai dishes in order to attract a wider dining audience. “The Thai food is just to get them in the door,” says Yabaki with a laugh. “Once they get here, we recommend all the Lao dishes. One thing I love about our customers is that they’re so openminded. They love the Lao food and they keep coming back for it.”
With good reason. Hiso’s well-executed dishes are full of the spicy, salty, pungent (Yabaki calls it “funky”) flavors that Lao cuisine is known for. While it shares much in common with Thai cuisine, food from Laos tends to make greater use of fermented ingredients, especially padaek, a traditional Lao fi sh sauce.
Standout dishes at Hiso include mee kati, ground pork in a rich, stewlike sauce served alongside rice noodles and crunchy vegetable and herb condiments; tender, chewy pork ribs accompanied by jeow bong, a Lao chili paste, and traditional sticky rice; and khao piak, a hearty chicken noodle soup that Yabaki says is popular at Saturday morning brunch as a hangover cure.
“A lot of our Laotian customers tell us that our food tastes like their mom’s food, and I love that compliment,” says Yabaki. “That’s exactly the reaction we want.” 524 12th St.; (916) 603-8309; hisosac.com—CATHERINE
WARMERDAM
Taste 98 SACRAMENTO MAGAZINE November 2022
Below: Aniko Kiezel; above: Bryant and Jenn Nguyen
Rasheed Amedu of Naija Boy Tacos
Salmon bite
Crab fried rice
Sacramento’s favorite ice cream parlour for 35+ years. Our award-winning ice cream and sauces are made fresh daily and served in generous portions. We also offer a large variety of delicious sandwiches–from our specialty crab sandwich to great burgers. Leatherby’s is the perfect old fashioned ice cream parlour for families, friends, large groups or parties.












Sun–Thur: 11 a.m.–11 p.m.



Fri–Sat: 11 a.m.–12 a.m.

Sacramento | Arden Way | 916-920-8382

Citrus Heights | Antelope Road | 916-729-4021
Elk Grove | Laguna Blvd | 916-691-3334 www.leatherbys.net
FAMILY CREAMERY WWW.SACMAG.COM/DIGITAL-EDITION GET THE DIGITAL EDITION NOW AVAILABLE ONLINE OR VIA THE APP
LEATHERBY’S
Carla Layton DRE# 01395619 | PCAR Coldwell Banker Realty (916) 580-8018 carla.layton@cbrealty.com
American River Conservancy preserves 35 miles of trails that are open to the public for education, recreation & volunteer opportunities.
www.HomeGirlPlacerCounty.com
Dine
As a reader service, Sacramento Magazine offers the following list of noteworthy restaurants in the Sacramento region. This is not intended to be a complete directory, and not all restaurants profiled appear every month. Before heading to a restaurant, call or check its website to make sure it’s open.

ARDEN ARCADE
BENNETT’S AMERICAN COOKING This neighbor hood hangout has an approachable menu and a familiar, “Cheers”-like ambience. The food is like homemade, only better: things like braised short rib with mashed potatoes, lasagna Bolognese and chicken enchiladas. There’s seemingly something for every taste and diet, from avocado toast, available all day long, to prime rib (weekends only). The lengthy menu features dishes that are vegetarian, heart healthy, nut-free or “gluten-free friendly.” 2232 Fair Oaks Blvd.; (916) 515-9680; bennettsameri cancooking.com. L-D-Br. American. $$$
CAFE VINOTECA Located in Arden Town Center, Cafe Vinoteca serves some of the loveliest Italian-inspired cuisine in the city. 3535 Fair Oaks Blvd.; (916) 4871331; cafevinoteca.com. L–D. Italian. $$$
DUBPLATE KITCHEN & JAMAICAN CUISINE One of the few places in Sacramento where you can get Caribbean food, this restaurant serves Jamaican specialties such as curry goat and jerk chicken. 3419 El Camino Ave.; (916) 339-6978; dubplatekitchen cuisine.com. L–D. Jamaican. $$
THE KITCHEN Part supper club, part theatrical production, part cocktail party: This is like no other restaurant in Sacramento, and it’s Michelin starred. You need to make reservations months in advance for the multi-course dinner. The food is complex and mind-blowingly creative. 2225 Hurley Way; (916) 568-7171; thekitchenrestaurant.com. D. American. $$$$
LEATHERBY’S FAMILY CREAMERY Go for the ice cream, all made on the premises and used in shakes, malts and towering sundaes. 2333 Arden Way; (916) 920-8382; leatherbys.net. L–D. Sandwiches/ice cream. $
BROADWAY
ANDY NGUYEN VEGETARIAN RESTAURANT This bastion of Buddhist-inspired vegetarian cuisine serves food that is fresh and flavorful. 2007 Broad way; (916) 736-1157; andynguyenvegetarian.com. L–D. Vegetarian/Asian. $
REAL PIE COMPANY At this homey pie shop, you’ll find the pies of your dreams, made with all-butter crusts and seasonal fruit sourced from local farms. In addition to dessert pies such as jumbleberry and butterscotch banana cream, you can order savory pot pies, shepherd’s pies and dishes like mac and cheese, all available to eat in or take out. 2425 24th St.; (916) 838-4007; realpiecompany.com. L–D. American. $
SELLAND’S MARKET-CAFE Choose from an array of appetizers and hot items along with crowd-pleas ing side dishes and pizza. This high-quality takeout food can be a real lifesaver on nights when you’re too busy to cook. 915 Broadway; (916) 732-3390; sellands.com. L–D–Br. Gourmet takeout. $$
TOWER CAFE This place is a hot spot on weekend mornings. Regulars swear by the New Mexico blue berry cornmeal pancakes and the thick-cut, custardy French toast. Breakfast is all-American, but lunch and dinner have a global flavor. 1518 Broadway; (916) 441-0222; towercafe.com. B–L–D. World fu sion. $$
CAPAY
ROAD TRIP BAR & GRILL This family-friendly joint serves up classic roadhouse fare, from salads and burgers to chops. 24989 State Highway 16; (530) 796-3777; roadtripbg.com. B–L–D. American. $–$$
CITRUS HEIGHTS
LEATHERBY’S FAMILY CREAMERY For description, see listing under “Arden Arcade.” 7910 Antelope Road; (916) 729-4021; leatherbys.net. L–D. Sand w iches/ice cream. $
SAM’S CLASSIC BURGERS At this drive-up burger shack, the shakes are great and the burgers wonder fully straightforward. 7442 Auburn Blvd.; (916) 723-7512. L–D. Burgers. $
CURTIS PARK
PANGAEA BIER CAFE While it’s known as a beer cafe and bottle shop, this casual spot also serves up tasty bar food, including a burger that has taken home top honors more than once at Sacramento Burger Battle. 2743 Franklin Blvd.; (916) 454-4942; pangaeabiercafe.com. L–D. American. $$
DIXON
CATTLEMENS This Western steakhouse serves up slabs of prime rib, porterhouse, T-bone and cowboy steaks, plus all the trimmings: shrimp cocktail, po tato skins, fried onions and more. 250 Dorset Court; (707) 678-5518; cattlemens.com. D. Steakhouse. $$$
100 SACRAMENTO MAGAZINE N ovember 2022
The Ward 8 cocktail from Paul Martin’s American Bistro
DOWNTOWN
BAWK! CHICKEN & BAR Along with crispy chicken coated with a red spice mix that kicks it up a notch, you can order salads, oysters on the half shell and collard greens. 1409 R St.; (916) 465-8700; bawk friedchicken.com. L–D–Br. Southern. $$
BRASSERIE DU MONDE This beautifully designed restaurant is based on a traditional French bras serie. The menu hits the high points of the brasserie canon, everything from onion soup to steak frites. 1201 K St.; (916) 329-8033; brasseriedumonde.com. L–D. French. $$–$$$
CAFE BERNARDO The menu offers straightforward fare guaranteed to please just about everyone. Breakfast includes huevos rancheros and eggs Ber nardo, drizzled with housemade hollandaise sauce. Lunch and dinner feature chewy-crusted pizzas, burgers, sandwiches and substantial entrées such as pan-seared chicken breast with mashed potatoes. 1431 R St.; (916) 930-9191; cafebernardo.com. B–L–D. New American. $
CAMDEN SPIT & LARDER Highly regarded chef Oli ver Ridgeway opened this swank brasserie in a mod ern, glass-walled building near the Capitol. It appeals to lobbyists, lawyers and legislators with its ginforward cocktails (martini, anyone?) and a menu that’s an interesting mash-up of British chop-house classics, English schoolboy favorites and elevated pub fare. 555 Capitol Mall; (916) 619-8897; camden spitandlarder.com. L–D. Steakhouse. $$$–$$$$
ECHO & RIG Located in the lobby of The Sawyer hotel, this outpost of a Vegas steakhouse is sleek and un stuffy. Prices are considerably gentler than at most other steakhouses, but the quality of the meat is high.
In addition to standard cuts like filet, NY steak and rib-eye, you’ll find butcher cuts such as hanger, ba vette, skirt and tri-tip. 500 J St.; (877) 678-6255; echoandrig.com. B–L–D–Br. Steakhouse. $$$
ELLA This stunning restaurant (owned by the Selland family and designed by award-winning European architects) is an elegant oasis compared to the gritty hustle and bustle outside. From the open kitchen, the staff turns out innovative dishes and old favorites. The emphasis is on seasonal, local and artisanal. 1131 K St.; (916) 443-3772; elladining roomandbar.com. L–D. New American. $$$$
FRANK FAT’S Downtown Sacramento’s oldest res taurant, Fat’s is a favorite of the Capitol crowd. The restaurant is well known for its steaks—especially Frank’s Style New York Steak—and its brandy-fried chicken. This is Chinese cuisine at its most sophis ticated. 806 L St.; (916) 442-7092; frankfats.com. L–D. Chinese. $$$
GRANGE RESTAURANT & BAR Located in The Citizen Hotel, Grange proves that a hotel restaurant doesn’t have to be pedestrian. The menu changes frequently and spotlights some of the area’s best producers. At dinner, the ambience in the stunning dining room is seductive and low-lit. 926 J St.; (916) 492-4450; grangerestaurantandbar.com. B–L–Br. Californian/American. $$$$
KODAIKO RAMEN & BAR Partly owned by Kru’s Billy Ngo, this below-ground ramen shop takes the Jap anese noodle soup to a whole new level. Ingredients are organic, and almost everything is made in-house. For a fun experience, sit at the six-person ramen counter and chat with the chefs. 718 K St.; (916) 426-8863; kodaikoramen.com. L–D–Br. Japanese/ ramen. $$–$$$
MAGPIE CAFE This restaurant has a casual, unas suming vibe, and its hallmark is clean, simple fare that tastes like the best version of itself. 1601 16th St.; (916) 452-7594; magpiecafe.com. B–L–D. Cali fornian. $$
MAS TACO BAR Tasty little tacos are the headliners at this eatery. They come with all sorts of delicious fillings: braised short rib, Korean fried chicken, banh mi shrimp and, for veg heads, roasted cauliflower and butternut squash. You can also get Latin-flavored rice bowls, salads and fun starters. 1800 15th St.; mastacobar.com. L–D–Br. Mexican. $$
MIKUNI JAPANESE RESTAURANT AND SUSHI BAR
This hip sushi bar serves its sushi with a side of sass. There are three sushi bars and a dense menu of ap petizers, rice bowls, bento boxes and sushi rolls. 1530 J St.; (916) 447-2112; mikunisushi.com. L–D. Japanese/sushi. $$

MORTON’S THE STEAKHOUSE From cozy, candlelit booths and stunning, glass-enclosed wine room to the crisply outfitted chefs, Morton’s oozes Special Occasion. Red meat is the star here. 621 Capitol Mall; (916) 442-5091; mortons.com/sacramento. D. Steakhouse. $$$$
NASH & PROPER The owners first rocked Sacra mento’s food scene with a food truck featuring Nashville-style hot chicken sandwiches. Now, they have two brick-and-mortar locations serving their famous sandwiches, along with quarter and half birds, impressive sides and chicken and waffles (weekends only). You pick the heat level for your fowl, ranging from naked (no heat) to cluckin’ hot. 1023 K St.; (916) 426-6712; nashandproper.com. L. Fried chicken sandwiches and plates. $
THE 7TH STREET STANDARD Located inside the Hyatt Centric, this is an unabashedly big-city res taurant: chic, stylish, urban, sophisticated, serious. Heading up the kitchen is Ravin Patel, a Sacra mento native with an impressive fine-dining pedi gree. (He worked for Danny Meyer in New York, later for Randall Selland in Sac.) His menu has a modern California sensibility, using fresh ingredi ents, classic French techniques and a healthy dash of South Indian flavors. 1122 Seventh St.; (916) 3717100; the7thstreetstandard.com. B-L-D. Modern American. $$$
SHADY LADY SALOON The charming faux speakeasy is an excellent place to meet up with friends for a round of cocktails and a first-rate meal. Bordelloinspired wallpaper and dim lighting set an alluring stage for the robust and flavorful food. 1409 R St.; (916) 231-9121; shadyladybar.com. L–D. American/ Southern. $$
URBAN ROOTS
BREWING & SMOKEHOUSE
At this brewery, a massive smoker turns out succulent meats—brisket, ribs, turkey and sausage—in the tradition of the great barbecue houses of Texas, Louisiana and Tennessee. Sides include collard greens, mac and cheese, yams and poblano cheese grits. Sit indoors or out at long picnic tables. 1322 V St.; (916) 706-3741; urbanrootsbrewing.com. L–D. Barbecue. $$
EAST SACRAMENTO
ALLORA Modern Italian fare with a heavy seafood bent is the focus at this sophisticated eatery. Tasting menus come in three, four and five courses, with caviar service and in-season truffles offered at an additional cost. The menu changes with the seasons, but you’ll always find fresh pasta and balsamicglazed polpo (octopus). Extensive vegetarian and vegan options are also available, along with a wine list weighted with classic Italian wines and new-
SACMAG.COM November 2022 101
Wood-fired oysters from Ella
world expressions of Italian varieties. 5215 Folsom Blvd.; (916) 538-6434; allorasacramento.com. D. Italian. $$$$
CANON With Michelin-starred chef Brad Cecchi at the helm, this breezily chic restaurant offers an ambitious menu of globally inspired sharable plates. Much of the menu is vegetarian, vegan or gluten free, but you can also order from a small selection of hearty meat, poultry and fish dishes. 1719 34th St.; (916) 469-2433; canoneastsac.com. Global/New American. D–Br. $$$–$$$$
KRU Long considered one of Sacramento’s best res taurants, chef/owner Billy Ngo produces high cali ber, exciting Japanese fare. The restaurant has a craft cocktail bar, outdoor patios and an omakase bar. (An omakase cocktail pairing is also available.) 3135 Folsom Blvd.; (916) 551-1559; krurestaurant. com. L-D. Japanese. $$$-$$$$
MATTONE RISTORANTE When Sacramento’s famed Biba restaurant closed its doors, a few alums struck out on their own to open this Italian eatery. It’s a worthy successor to Biba, serving freshly made pasta and classic Italian fare such as calamari fritti, veal marsala and chicken cooked under a brick. 5723 Folsom Blvd.; (916) 758-5557; mattonesac.com. L-D. Italian $$$–$$$$
THE MIMOSA HOUSE This local chain offers a com prehensive lineup of breakfast fare: omelets, Bene dicts, crepes, waffles, burritos and, of course, mi mosas. The rest of the menu is similarly broad, with burgers, salads, grilled sandwiches and Mexican “street food.” 5641 J St.; (916) 400-4084; mimosa house.com. B–L. American. $$
OBO’ ITALIAN TABLE & BAR This casual Italian eat ery is beautifully designed and efficiently run. There are hot dishes and cold salads behind the glass cases, ready for the taking. But the stars of the menu are the freshly made pastas and wood-oven pizzas. There’s also a full bar serving Italian-theme craft cocktails. 3145 Folsom Blvd.; (916) 822-8720; oboitalian.com. L–D. Italian. $$
ONESPEED Chef Rick Mahan, who built his stellar reputation at The Waterboy in midtown, branched out with a more casual concept at his East Sac eat ery. The open bistro has a tiled pizza oven that cranks out chewy, flavorful pizzas. 4818 Folsom Blvd.; (916) 706-1748; onespeedpizza.com. B–L–D. Pizza. $$
ORIGAMI ASIAN GRILL This fast-casual eatery serves Asian-flavored rice bowls, banh mi sandwiches, sal ads and ramen, along with killer fried chicken and assorted smoked-meat specials from a big smoker on the sidewalk. 4801 Folsom Blvd.; (916) 400-3075; origamiasiangrill.com. L–D. Asian fusion. $–$$
SELLAND’S MARKET-CAFE For description, see list ing under Broadway. 5340 H St.; (916) 736-3333; sellands.com. L–D–Br. Gourmet takeout. $$
EL DORADO HILLS
AJI JAPANESE BISTRO This casually elegant res taurant offers an innovative menu of Japanese street food, interesting fusion entrees, traditional dishes such as teriyaki and tempura and—yes—sushi. There’s a short, approachable wine list, sakes and a full bar serving handcrafted cocktails. 4361 Town Center Blvd.; (916) 941-9181; aji-bistro.com. L-D. Japanese/sushi. $-$$
ALMIGHTY FOOD CO. This all gluten-free restaurant has a large menu that includes salads, sandwiches, tapas and small plates, large plates and lots of meat less options. You’ll find bluefin tuna poke, baby kale Caesar salad, avocado toast on an everything bagel,
grass-fed burgers, short ribs, falafel, shiitake beans & rice—a tremendous variety for every dietary need. Happy hour includes bubbly and sangria and bargain bites such as $8 focaccia toasts to share. 4355 Town Center Blvd.; (916) 510-1204; almightyeats.com. L–D–Br. Gluten-free global. $$

MILESTONE This unstuffy eatery serves great takes on comfort-food classics like pot roast and fried chicken. It’s straightforward, without pretense or gimmickry. The setting is like a Napa country porch, and the service is warm and approachable. 4359 Town Center Blvd.; (916) 934-0790; milestoneedh. com. L–D–Br. New American. $$–$$
THE MIMOSA HOUSE For description, see listing under East Sacramento, 2023 Vine St.; (916) 9340965; mimosahouse.com. B–L–D. American. $$
SELLAND’S MARKET-CAFE For description, see list ing under “East Sacramento.” 4370 Town Center Blvd.; (916) 932-5025; sellands.com. L–D–Br. Gour met takeout. $$
SIENNA RESTAURANT A luxurious Tuscan interior features a large bar. The menu includes a playful melange of global cuisine, including fresh seafood, hand-cut steaks, stone hearth pizzas, inventive ap petizers and a stacked French dip sandwich. Sunday brunch includes a made-to-order omelet bar and unlimited mimosas. 3909 Park Drive; (916) 941-9694; siennarestaurants.com. L–D–Br. Global. $$–$$$
ELK GROVE
BOULEVARD BISTRO Located in a cozy 1908 bun galow, this bistro is one of the region’s best-kept dining secrets. Chef/owner Bret Bohlmann is a pas
sionate supporter of local farmers and winemakers, and his innovative food sings with freshness and seasonality. 8941 Elk Grove Blvd.; (916) 685-2220; blvdbistro.com. D–Br. New American. $$–$$$
JOURNEY TO THE DUMPLING This Elk Grove eatery specializes in Shanghai-style dumplings (try the soup-filled xiao long bao), along with Chinese dish es such as green onion pancakes, garlic green beans a nd salt-and-pepper calamari. 7419 Laguna Blvd.; (916) 509-9556; journeytothedumpling.com. L–D. Chinese. $$
LEATHERBY’S FAMILY CREAMERY For description, see listing under “Arden Arcade.” 8238 Laguna Blvd.; (916) 691-3334; leatherbys.net. L–D. Sandwiches/ ice cream. $
MIKUNI JAPANESE
RESTAURANT AND
SUSHI BAR For description, see listing under “Downtown.” 8525 Bond Road; (916) 714-2112; mikunisushi.com. L–D. Japanese/sushi. $$
NASH & PROPER For description, see listing under Downtown. 9080 Laguna Main St.; (916) 897-8437; nashandproper.com. L. Fried chicken sandwiches and plates. $
THAI CHILI This plain restaurant offers an entire menu just for vegetarians, plus interesting meat and fish dishes. 8696 Elk Grove Blvd.; (916) 7143519; thaichilielkgrove.net. L–D. Thai. $$
FOLSOM
BACK BISTRO A warm pocket of coziness and urban sophistication in a retail center, this place offers an appealing menu of casual nibbles and swankier en
Dine 102 SACRAMENTO MAGAZINE N ovember 2022
Meatball sandwich from OBO ’ Italian Table & Bar
trées. But it’s the wine program that really knocks this charming little bistro out of the park. 230 Pal ladio Parkway, Suite 1201; (916) 986-9100; backbis tro.com. D. New American/Mediterranean. $$–$$$
CHICAGO FIRE Oodles of melted cheese blanket the pizzas that fly out of the kitchen of this busy res taurant. Here, you get to choose between thin-crust, deep-dish and stuffed pizzas. 310 Palladio Parkway; (916) 984-0140; chicagofire.com. L –D. Pizza. $
FAT’S ASIA BISTRO AND DIM SUM BAR The menu focuses on Asian cuisine, from Mongolian beef and Hong Kong chow mein to Thai chicken satay served with a fiery curry-peanut sauce. 2585 Iron Point Road; (916) 983-1133; fatsasiabistro.com. L–D. Pan-Asian. $$
LAND OCEAN The menu hits all the steakhouse high notes: hand-cut steaks, lobster, seafood and rotisserie, entrée salads and sandwiches. 2720 E. Bidwell St.; (916) 983-7000; landoceanrestaurants. com. L–D–Br. New American/steakhouse. $$$
THE MIMOSA HOUSE For description, see listing under East Sacramento, 25075 Blue Ravine Road; (916) 293-9442; mimosahouse.com. B–L. Ameri can. $$
SCOTT’S SEAFOOD ROUNDHOUSE This restaurant offers a solid menu of delicious seafood, from crab cakes and calamari to roasted lobster tail. 824 Sutter St.; (916) 989-6711; scottsseafoodround house.com. L–D. Seafood. $$$–$$$$
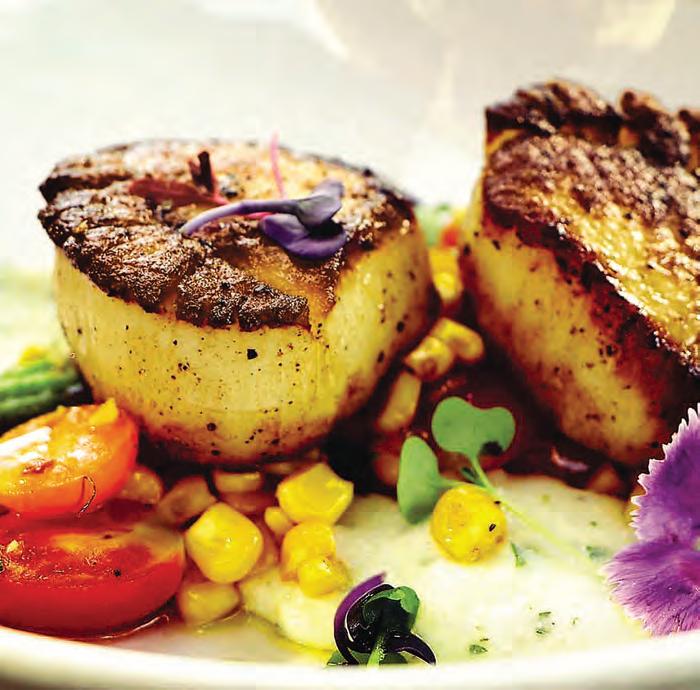
THAI PARADISE Standouts on the extensive menu include spring rolls, tom kha koong (coconut milk soup with prawns), green curry, spicy scallops and pad thai. Try the fried banana with ice cream for
dessert. 2770 E. Bidwell St.; (916) 984-8988; thai paradisefolsom.com. L–D. Thai. $$
GARDEN HIGHWAY
CRAWDADS ON THE RIVER This riverfront restau rant draws crowds looking for a great place to party on the water during warm-weather months. Boats pull up to the restaurant’s deck, where you can sip a cocktail, and roll-up doors blur the line between indoors and out. The Cajun-inspired menu includes fish tacos and several fun entrées. 1375 Garden Highway; (916) 929-2268; saccrawdads.com. L–D–Br. Cajun/American. $$
GRANITE BAY
HAWKS One of Placer County’s best restaurants, Hawks is known for its elegant cuisine and beautiful interior. The dining room has clean lines, soothing colors, and crisp white tablecloths. Framed photos of farmscapes remind diners of owners Molly Hawks and Michael Fagnoni’s commitment to locally sourced ingredients. The seasonal menu is full of delicious surprises, such as seared scallop and sea urchin. 5530 Douglas Blvd.; (916) 791-6200; hawksrestaurant. com. L–D–Br. New American/French. $$$–$$$$
GREENHAVEN/POCKET
CACIO This tiny sliver of a restaurant has only a handful of tables—and more than a handful of people who want to dine here. The fare is highquality Italian comfort food, with an emphasis on pasta. Service is warm and homey, prices are gentle, and reservations (even at lunch) are a must. 7600
Greenhaven Drive; (916) 399-9309; caciosacra mento.com. L–D. Italian. $$
SCOTT’S SEAFOOD ON THE RIVER Located in The Westin Sacramento, Scott’s has a patio and a view of the river. Breakfast dishes include crab cake Bene dict, and lunch entrées range from petrale sole to a prawn Caesar salad. For dinner, splurge on a lobster tail or choose a more modestly priced grilled salm on. 4800 Riverside Blvd.; (916) 379-5959; scotts seafoodontheriver.com. B–L–D. Seafood. $$$–$$$$
MIDTOWN
BEAST + BOUNTY The beating heart of this chic restaurant is its open hearth, where meats and veg etables are roasted over a wood fire. The meaty rib-eye, served over potatoes roasted in the meat’s fat, is meant to be shared. So is the pizza, thin, flat and seductively charred from the wood-burning pizza oven. 1701 R St.; (916) 244-4016; eatbeastand bounty.com. L–D–Br. American. $$$
58 DEGREES & HOLDING CO. This wine bar show cases an astonishing number of wines by the glass— all available in 3- and 6-ounce pours. There’s also an abbreviated menu of small plates designed to complement and enhance the wines. 1217 18th St.; (916) 442-5858; 58degrees.com. L–D. Wine bar. $$
THE GOLDEN BEAR Remember the adage “Don’t judge a book by its cover”? Keep it in mind when you come here. You may have to wave cigarette smoke away from your face as you cross the patio, and you might even have to dodge a leashless dog to get in the door. But once inside the dim bar, you’ll find a surpris ingly sophisticated menu. 2326 K St.; (916) 441-2242; goldenbear916.com. L–D–Br. Gastropub. $$
HAWKS PROVISIONS & PUBLIC HOUSE This sophis ticated gastropub is the latest offering from the owners of Granite Bay’s upscale Hawks. The food is rustic Mediterranean, with beautifully executed dishes like country pate and baked rigatoni. The pastas are made in-house, and even the burger is top-notch: Wagyu beef is ground in the walk-in fridge, and it’s served on a house-made brioche bun with hand-cut French fries. In addition to the res taurant (the “public house”), there’s a casual takeout shop next door serving coffee, pastries and sand wiches (the “provisions”). 1525 Alhambra Blvd.; (916) 588-4440; hawkspublichouse.com. L-D-Br. Mediter ranean gastropub. $$$
HOOK & LADDER MANUFACTURING COMPANY Lo cated in a Quonset hut, this restaurant is both hip and cozy. Despite the barlike ambience, Hook & Lad der is serious about food. All the pastas and desserts are made in-house. 1630 S St.; (916) 442-4885; hook andladder916.com. L–D–Br. Californian. $$
MULVANEY’S BUILDING & LOAN Distinctive and cozy, this topflight restaurant exudes the generous affability of its owner, chef Patrick Mulvaney. It’s housed in a brick firehouse from the late 1800s, and the lush patio is a popular spot in warm months. The menu changes frequently and is focused on locally sourced, seasonal ingredients. 1215 19th St.; (916) 441-6022; mulvaneysbl.com . L–D. Califor nian. $$$
PARAGARY’S This legendary restaurant focuses on elegant, Mediterranean-inspired cuisine. 1401 28th St.; (916) 457-5737; paragarys.com. L–D–Br. New American/Californian. $$–$$$
THE RED RABBIT KITCHEN & BAR The menu is a playful jumble of dishes, some robustly American, others with an Asian, Latin or Mediterranean influ ence. 2718 J St.; (916) 706-2275; theredrabbit.net. L–D–Br. New American. $$
SACMAG.COM November 2022 103
Susan Yee
Scallops from 58 Degrees & Holding Co.
RICK’S DESSERT DINER This diner has a playful ’50s vibe, with red booths and a jukebox. The ever-pres ent line of customers in front of the display case can make it difficult to see the mind-boggling assort ment of sweets. 2401 J St.; (916) 444-0969; ricks dessertdiner.com. Dessert. $
THE RIND At this cheese-centric bar, you can savor cheese in a number of ways. The menu includes variations on macaroni and cheese, cheese boards and creative grilled cheese sandwiches. 1801 L St.; (916) 441-7463; therindsacramento.com. L–D. American. $$
SAIGON ALLEY KITCHEN + BAR This hip restaurant and bar serves modern versions of Vietnamese street food, such as a “Pho-rench” dip (a French dip with pho flavors) and a “banh mi” burger (a rib-eye burg er garnished with pickled daikon and carrot on a baguette). A big draw is the $3 happy hour, featuring snacks like banh mi taco, fish sauce chicken wings, and taro fries and sugarcane shrimp. 1801 L St.; (916) 758-6934; saigonalley.com. L–D. Vietnamese. $$
TANK HOUSE This midtown ’cue joint offers a lim ited menu of ribs, brisket and sides along with a thoughtful selection of craft beers. 1925 J St.; (916) 431-7199; tankhousebbq.com. L–D. Barbecue. $
TAPA THE WORLD At this dark space, the best seats are along the windows that look out onto J Street— perfect for people-watching as you savor classic tapas along with a Spanish cava or tempranillo from the lengthy, exciting wine list. 2115 J St.; (916) 4424353; tapatheworld.com. L–D. Spanish/tapas. $$
THE WATERBOY This Mediterranean-inspired res taurant produces perhaps the finest cooking in the region. Chef/owner Rick Mahan honors local farm ers with his commitment to simply prepared, highcaliber food. You can’t go wrong if you order one of the lovely salads, followed by the gnocchi, ravioli or a simple piece of fish, finished with butter and fresh herbs. You’ll also find French classics such as veal sweetbreads and pomme frites. 2000 Capitol Ave.; (916) 498-9891; waterboyrestaurant.com. L–D. Mediterranean. $$$$
ZELDA’S ORIGINAL GOURMET PIZZA Zelda’s is leg endary for the greatness of its pizza and its attitude. But that’s part of Zelda’s charm, along with the dark, dingy atmosphere. It’s all about the food: old-school, Chicago-style deep-dish pizza that rou tinely wins “best pizza” in local polls. 1415 21st St.; (916) 447-1400; zeldasgourmetpizza.com. L–D. Pizza/Italian. $$
ZÓCALO This Mexican restaurant is one of the best places to while away an evening with friends over margaritas. The restaurant is high-ceilinged, with a wood bar and roomy booths, and the wraparound sidewalk patio is one of the most popular spots in town. . 1801 Capitol Ave.; (916) 441-0303; zocalo sacramento.com. L–D–Br. Mexican. $$
OAK PARK
FIXINS SOUL KITCHEN This bustling place, partly owned by former mayor Kevin Johnson, serves up friendly Southern hospitality along with delicious Southern fare, including chicken and waffles, gumbo, fried catfish, and shrimp and grits. 3428 Third Ave.; (916); 999-7685. fixinssoulkitchen.com. B–L–D–Br. Southern. $$
LA VENADITA This inviting, casual taqueria has a concise menu that includes inventive street tacos, a brightly flavored ceviche and an enchilada with rich mole sauce. It also boasts a full bar and an enticing menu of craft cocktails. 3501 Third Ave.; (916) 4004676; lavenaditasac.com. L–D. Mexican. $$
OLD SACRAMENTO
THE FIREHOUSE Since opening in 1960, this has been Sacramento’s go-to restaurant for romantic atmosphere and historic charm. Located in a 1853 firehouse, it’s white tablecloth all the way, with crys tal wine glasses and top-notch service. The outdoor courtyard is one of the prettiest in town, and its canopy of trees sparkles at night with tiny lights. The food is special-occasion worthy, and the wine list represents more than 2,100 labels. 1112 Second St.; (916) 442-4772; firehouseoldsac.com. L–D. Californian/American. $$$$
RANCHO CORDOVA
CATTLEMENS This classic Western steakhouse serves up big slabs of prime rib, porterhouse, T-bone and cowboy steaks, plus all the trimmings: shrimp cocktail, loaded potato skins, deep-fried onions and more. 12409 Folsom Blvd.; (916) 985-3030; cattle mens.com. D. Steakhouse. $$$
J.J. PFISTER RESTAURANT & TASTING ROOM In ad dition to a tasting room where you can sample lo cally made premium gin, vodka and rum, this fam ily-owned distillery also operates a restaurant serving lunch and dinner. The all-day menu features salads, sandwiches and tacos, along with the whim sical “Adult Lunchable”—an assortment of cheeses, deli meats and accompaniments. Desserts get the boozy treatment: Order cheesecake topped with bourbon caramel and whipped cream, or fudge clus ters made with Pfister’s Navy Strength rum. 9819 Business Park Drive; (916) 672-9662; jjpfister.com. L–D. Casual American. $$
THE MIMOSA HOUSE For description, see listing under East Sacramento, 3155 Zinfandel Drive; (916)
970-1761 and 2180 Golden Centre Lane; (916) 8224145; mimosahouse.com. B–L. American. $$
ROSEVILLE
CATTLEMENS This classic Western steakhouse serves up big slabs of prime rib, porterhouse, T-bone and cowboy steaks, plus all the trimmings: shrimp cocktail, loaded potato skins, deep-fried onions and more. 2000 Taylor Road; (916) 782-5587; cattlemens. com. D. Steakhouse. $$$

CHICAGO FIRE For description, see listing under “Folsom.” 500 N. Sunrise Ave.; (916) 771-2020; chi cagofire.com. L–D. Pizza. $
FAT’S ASIA BISTRO AND DIM SUM BAR For descrip tion, see listing under “Folsom.” 1500 Eureka Road; (916) 787-3287; fatsasiabistro.com. L–D. Pan-Asian. $$
LA PROVENCE RESTAURANT & TERRACE This el egant French restaurant offers some of the region’s loveliest outdoor dining. The seasonal menu features items such as bouillabaisse and soupe au pistou. 110 Diamond Creek Place; (916) 789-2002; laprovence roseville.com. L–D–Br. French. $$$–$$$$
MIKUNI JAPANESE RESTAURANT AND SUSHI BAR For description, see listing under “Downtown.” 1565 Eureka Road; (916) 797-2112; mikunisushi.com. L–D. Japanese/sushi. $$
THE MIMOSA HOUSE For description, see listing under East Sacramento, 761 Pleasant Grove Blvd.; (916) 784-1313; mimosahouse.com. B–L. American. $$
PAUL MARTIN’S AMERICAN GRILL The bustling,
Dine 104 SACRAMENTO MAGAZINE N ovember 2022
Scott’s Seafood Roundhouse’s filet Oscar steak with Dungeness crab
comfortable restaurant is a local favorite. The kitchen offers a great list of small plates and robust, approachable entrées. 1455 Eureka Road; (916) 783-3600; paulmartinsamericangrill.com. L–D–Br. New American. $$–$$$

P.F. CHANG’S CHINA BISTRO The extensive menu offers dishes whose origins spring from many re gions in China but that reflect a California sensibil ity. 1180 Galleria Blvd.; (916) 788-2800; pfchangs. com. L–D. Chinese. $$
RUTH’S CHRIS STEAK HOUSE This swanky dinner house serves some of the tastiest meat in town. Expertly cooked steaks are seared at 1,800 degrees. Don’t miss the cowboy rib-eye or the fork-tender filet mignon. 1185 Galleria Blvd.; (916) 780-6910; ruthschris.com. D. Steakhouse. $$$$
THE MIMOSA HOUSE For description, see listing under “East Sacramento.” 761 Pleasant Grove Blvd., Roseville; (916) 784-1313; mimosahouse.com. B–L–D. American. $$
SIERRA OAKS
CAFE BERNARDO AT PAVILIONS For description, see listing under “Downtown.” 515 Pavilions Lane; (916) 922-2870; cafebernardo.com. B–L–D. New American. $
ETTORE’S This bakery is a convivial spot for a ca sual meal. It’s hard to take your eyes off the dessert c ases long enough to choose your savory items. But you’ll soon discover the kitchen’s talent extends to the wonderful pizzas, cooked in a wood-burning oven, hearty sandwiches and burgers, and fresh salads. 2376 Fair Oaks Blvd.; (916) 482-0708; ettores. com. B–L–D. Bakery/New American. $–$$
RUTH’S CHRIS STEAK HOUSE For description, see listing under “Roseville.” 501 Pavilions Lane; (916) 286-2702; ruthschris.com. L (Fridays only)–D. Steakhouse. $$$$
WILDWOOD RESTAURANT & BAR Owned by the Haines brothers of 33rd Street Bistro fame, this chic restaurant serves New American and global cuisine, with naan, ahi poke, pancetta prawns and rock shrimp risotto sharing the menu with an allAmerican burger. The spacious patio is a great place to grab a drink and listen to live music. 556 Pavil ions Lane; (916) 922-2858; wildwoodpavilions.com. L–D–Br. American/global fusion. $$$
SOUTHSIDE PARK
BINCHOYAKI Small plates of grilled meats, fish and vegetables are the stars at this izakaya-style restau rant. But you can also order ramen, tempura and other Japanese favorites, as well as a variety of sake. 2226 10th St.; (916) 469-9448; binchoyaki.com. L–D. Japanese. $$–$$$
TAHOE PARK
BACON & BUTTER Lively and delightfully urban, the place is packed with fans of chef Billy Zoellin’s homey flapjacks, biscuits and other breakfasty fare. 5913 Broadway; (916) 346-4445; baconandbutter sac.com. B–L. Breakfast/American. $–$$
MOMO’S MEAT MARKET This family-run business serves simply first-rate barbecue, smoked over wood in huge drums in the parking lot. Sides include pepper Jack mac ’n cheese, cornbread and deepfried cabbage. 5780 Broadway; (916) 452-0202. L–D. Barbecue. $$
WEST SACRAMENTO
DRAKE’S: THE BARN Located in a stunningly mod ern indoor-outdoor structure along the river, Drake’s serves excellent thin-crust pizzas, along with a few salads and appetizers. You can get table service indoors or on the patio. But if you prefer something more casual, grab a folding lawn chair, find a spot at the sprawling outdoor taproom and order a pizza to go. It’s fun galore, with kids, dogs, fire pits and a tap trailer serving beer. 985 River front St.; (510) 423-0971; drinkdrakes.com. L–D. Pizza. $$
FRANQUETTE This contemporary French café from the owners of Canon is an open-all-day, drop-infor-a-glass-of-wine kind of place. You can order a freshly baked croissant or tartine at breakfast, a salad, quiche or jambon sandwich on a baguette for lunch, and something a little more filling—say, duck meatballs or a crock of boeuf bourguignon—at din ner. It’s grandma food—or, in this case, grandmère food: warm, satisfying and homey. 965 Bridge St.; hellofranquette.com. B-L-D. French. $$–$$$
Subscription rates: $19.95 for one year, U.S. only. All out-of-state subscribers add $3 per year. Single copies: $4.95. Change of address: Please send your new address and your old address mailing label. Allow six to eight weeks’ advance notice. Send all remittances and requests to Sacramento Magazine, 5750 New King Drive, Suite 100, Troy, MI 48098. Customer service inquiries: Call (866) 660-6247. Copyright 2022 by Sacramento Media LLC. All rights reserved. Reproduction in whole or part without written permission from the publisher is prohibited. Prices quoted in advertisements are subject to change without notice. Sacramento Magazine (ISSN 0747-8712) Volume 48, Number 11, November 2022. Sacramento Magazine (ISSN 0747-8712) is published monthly by Sacramento Media, LLC, 1610 R St., Suite 300, Sacra mento, CA 95811. Periodical postage paid at Troy, MI and additional offices. Postmaster: Send change of address to Sacramento Magazine, 5750 New King Dr., Suite 100, Troy, MI 48098
SACMAG.COM November 2022 105
(All Periodicals Publications Except Requester Publications) SACRAMENTO MAGAZINE 3 6 9 0 Addr 1: City, State ZIP: City, State ZIP: Addr 1: Addr 2: City, State ZIP: Name: Addr 1: Addr 2: City, State ZIP: Name: Addr 1: Addr 2: City, State ZIP: 10. Owner (Do not leave blank. the publication is owned by a corporation, give the name and address of the corporation immediately followed by the names and addresses of all stockholders owning or holding 1 Percent or more of the total amount of stock. If not owned by a corporation, give the names and addresses of all the individual owners. If owned by a partnership or other unincorporated firm, give it's name and address as well as those of each individual owner. If the publication is published by nonprofit organization, give it's name and address.) 11. Known Bondholders, Mortgagees and Other Security Holders Owning or Holding 1 Percent or more of Total Amount of Bonds, Mortgages, or Other Securities. If none, check box X 12. Tax Status (For completion by nonprofit organizations authorized to mail at nonprofit rates) (Check one) The purpose, function, and nonprofit status of this organization and the exempt status for federal income tax purposes: X Has Not changed During Preceding 12 Months Has Changed During Preceding 12 Months (Publisher must submit explanation of change with this statement below) PS Form 3526 July 2014 5750 NEW KING DR STE 100, TROY,MI 48098-2696 Complete Mailing Address 7. Complete Mailing Address of Known Office of Publication (Not printer) (Street, city, county, state, and ZIP+4) 1610 R STREET STE 300 1610 R STREET STE 300 Telephone SACRAMENTO, CA 95811 KRISTA MINARD 8. Complete Mailing Address of Headquarters or General Business Office of Publisher (Not Printer) TROY, MI 48098-2696 9. Full Names and Complete Mailing Addresses of Publisher, Editor and Managing Editor (do not leave blank) Publisher (Name and complete mailing address) DENNIS RAINEY SACRAMENTO, CA 95811 Editor (Name and complete mailing address) 1610 R STREET STE 300 Statement of Ownership, Management and Circulation 3. Filing Date SACRAMENTO, CA 95811 Managing Editor (Name and complete mailing address) DARLENA BELUSHIN MCKAY SACRAMENTO, CA 95811 Full Name Complete Mailing Address 5750 NEW KING DR STE 100, TROY,MI 48098-2696 5750 NEW KING DR STE 100, TROY,MI 48098-2696 09/30/2022 4. Issue Frequency 5. Number of Issues Published Annually 6. Annual Subscription Price MONTHLY 12 $19.95 Full Name STEFAN WANCZYK JOHN BALARDO STEFAN WANCZYK Average No. Copies Each Issue During Preceding 12 Months 27,000 PS Form 3541 (Include paid distribution above nominal Form 3541 (Include paid distribution above nominal Through Dealers and Carriers, Street Vendors, Counter d. Free or Nominal Rate Outside-County Copies Included on PS Form 3541 Free or Nominal In-County Copies Included Free or Nominal Rate Copies Mailed at Other Classes Through the USPS (e.g. First-Class Mail) Free or Nominal Rate Distribution Outside the Mail (Carriers or other means) 9,074 f. 25,004 1,996 h. 27,000 i. 63.71% * if you are claiming electronic copies, go to line 16 on page 3. If you are not claiming electronic copies, skip to line 17 on page 3. 16. Electronic copy Circulation If present, check box 0 15,929 25,004 63.71% certify that 50% of all my distribution copies (electronic and Print) are paid above a nominal price X Publication required. Will be printed in the 11/01/2022 issue of this publication. Publication not required 18. Signature and Title of Editor, Publisher, Business Manager, or Owner PUBLISHER 09/22/2022 certify that all information furnished on this form is true and complete. understand that anyone who furnishes false or misleading information on this form or who omits material or information requested on the form may be subject to criminal sanctions (including fines and imprisonment) and/or civil sanctions (including civil penalties) PS Form 3526 July 2014 38 0 16,553 9,037 0 0 8,387 0 0 SACRAMENTO MAGAZINE 10/01/2022 No. Copies of Single Issue 0 Requested rate, advertiser's proof copies, and exchange copies) Extent and Nature of Circulation Published Nearest to filing Date a. Total Number of Copies (Net press run) 27,000 (1) Mailed Outside-County Paid Subscriptions Stated on 15,066 15,736 rate, advertiser's proof copies, and exchange copies) (2) Mailed In-County Paid Subscriptions Stated on PS 0 Circulation (3) Paid Distribution Outside the Mails Including Sales 863 817 Sales ,and Other Paid Distribution Ouside USPS Paid Distribution by Other Classes of Mail Through 0 c. Total Paid Distribution 15,929 (4) 0 (2) (3) (1) Free or Nominal (By Mail and Outside the Mail) (4) Total Free or Nominal Rate Distribution (Sum of 15d. (1), (2), (3) and (4)) 8,387 Total Distribution (Sum of 15c. and 15e.) 24,940 Copies not Distributed (See Instructions to Publishers #4 (page #3)) 2,060 Total (Sum of 15f. and g.) 27,000 Percent Paid (15c. Divided by 15f. Times 100) 66.37% 24,940 0 16,553 Dennis Rainey 66.37%
The Firehouse’s rack of lamb
Sew Much Fun!
Starting in 1934, The Sacramento Bee ran a household hints column for decades called “Katherine Kitchen.” Katherine Kitchen wasn’t the name of a real woman ; the column was written by Bee staffers. The Bee also published cookbooks and hosted cooking and home-ec classes under the Katherine Kitchen name. In late October or early November of 1947, The Bee and KFBK held a Katherine Kitchen sewing class for “business and professional women” in the newspaper’s auditorium at 716 I St.—DARLENA BELUSHIN MCKAY

106 SACRAMENTO MAGAZINE N ovember 2022 Center for Sacramento History, Sacramento Bee Collection, 1983/001/09433
Reflect
Seated at sewing machines, left to right: Lois Hepworth, Ethel Frey, Margaret Moore and Sally Martin























































































































































 By Sasha Abramsky
By Sasha Abramsky






























 CEO Stefan Wanczyk PRESIDENT John Balardo
CEO Stefan Wanczyk PRESIDENT John Balardo





































































































































































































 BY MARYBETH BIZJAK PHOTOGRAPHY BY SUSAN YEE
BY MARYBETH BIZJAK PHOTOGRAPHY BY SUSAN YEE

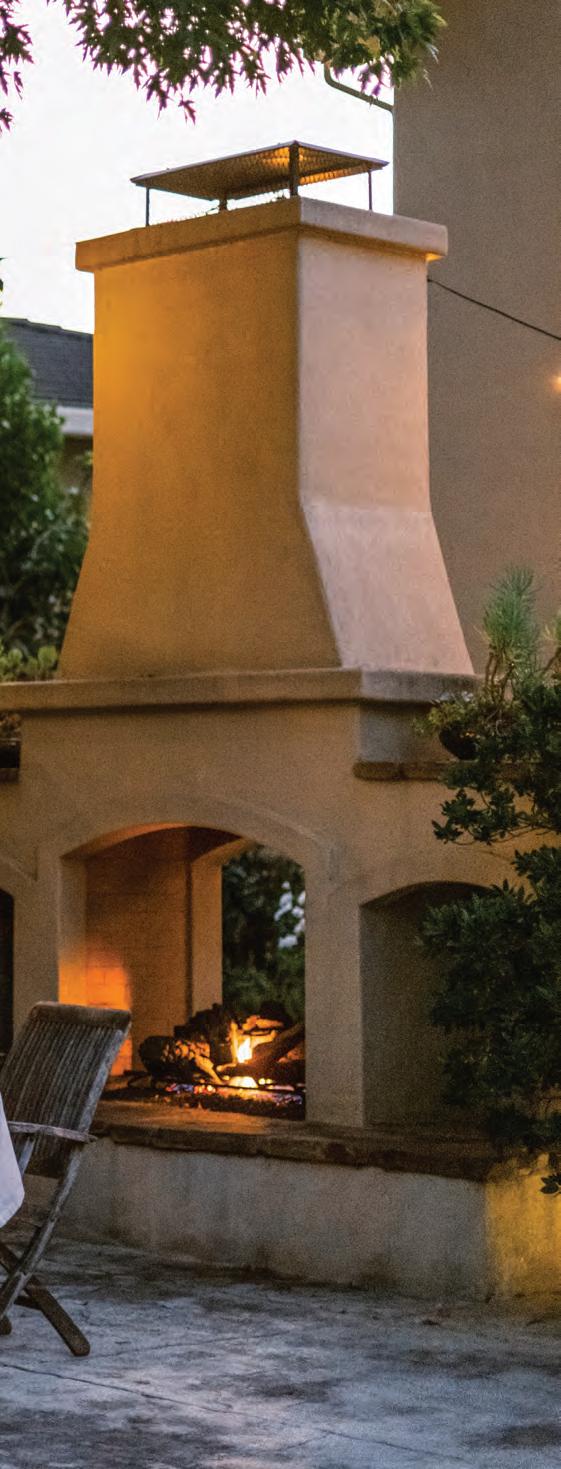








































 SUSAN YEE: Photographer, Susan Yee Photography
JENN ROBIRDS: Event designer and coordinator, Jenn Robirds Events
SUSAN YEE: Photographer, Susan Yee Photography
JENN ROBIRDS: Event designer and coordinator, Jenn Robirds Events




























































































































































 BY MARYBETH BIZJAK
BY MARYBETH BIZJAK