october 2013
Best Practices
Some reasons for this failure will be familiar: heavy upfront investment in student loans, made worse by shrinking reimbursements and higher overhead. We have been promised new models of reimbursement focused around quality and efficiency, which would seem to favor primary care physicians in the medical landscape, but financial investments in patient-centered medical home (PCMH) have yet to pay off for many of us. Currently we are caught between two reimbursement paradigms, neither of which is sufficient to appeal to medical students tempted by more lucrative specialties. The situation is worse, however, because the doctors we have already trained and convinced to work in primary care may not be as productive as they used to be. Why? Technological requirements have reduced productivity for many of our physicians, who are never going to be as efficient with tools that are built around ease of reporting, not ease of documentation.
Primary care physician shortage
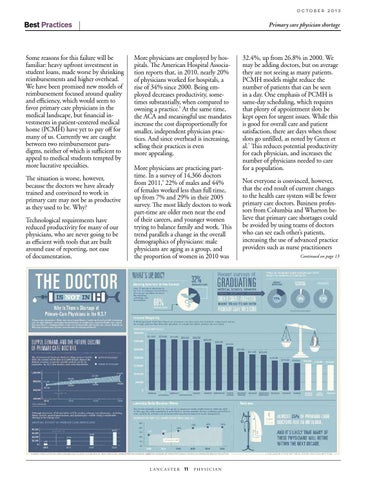
More physicians are employed by hospitals. The American Hospital Association reports that, in 2010, nearly 20% of physicians worked for hospitals, a rise of 34% since 2000. Being employed decreases productivity, sometimes substantially, when compared to owning a practice.5 At the same time, the ACA and meaningful use mandates increase the cost disproportionally for smaller, independent physician practices. And since overhead is increasing, selling their practices is even more appealing. More physicians are practicing parttime. In a survey of 14,366 doctors from 2011,6 22% of males and 44% of females worked less than full time, up from 7% and 29% in their 2005 survey. The most likely doctors to work part-time are older men near the end of their careers, and younger women trying to balance family and work. This trend parallels a change in the overall demographics of physicians: male physicians are aging as a group, and the proportion of women in 2010 was
LANCASTER
11
PHYSICIAN
32.4%, up from 26.8% in 2000. We may be adding doctors, but on average they are not seeing as many patients. PCMH models might reduce the number of patients that can be seen in a day. One emphasis of PCMH is same-day scheduling, which requires that plenty of appointment slots be kept open for urgent issues. While this is good for overall care and patient satisfaction, there are days when those slotsacgo unfilled, as noted by Green et al.7 This reduces potential productivity for each physician, and increases the number of physicians needed to care for a population.
o
a
-
Not everyone is convinced, however, , if thatyothe end result of current changes t to the health care system will be fewer primary care doctors. Business professors from Columbia and Wharton bey that primary care shortages could lieve be avoided by using teams of doctors who can see each other’s patients, increasing the use of advanced practice r providers such as nurse practitioners Continued on page 13